Biomarkers and Thiopurines in Inflammatory Bowel Disease
|
|
|
- Lucinda Neal
- 5 years ago
- Views:
Transcription
1 Inflammatory bowel disease (IBD) encompasses amongst others Crohn s disease (CD), ulcerative colitis (UC) and IBD unclassified (IBD-u). In the diagnostic algorithm of IBD, ileocolonoscopy plays a pivotal role. [1, 2] Endoscopically obtained histological biopsies are a strong lead in establishing the diagnosis of IBD and to distinguish between the two main phenotypes of IBD; CD and UC. Whereas the worldwide prevalence of IBD is rising and ileocolonoscopy is a relatively invasive and expensive procedure, associated with patient s discomfort and (severe) complications, researchers have been searching for non-invasive biomarkers to adjust the a priori probability of IBD and to use during the follow-up of disease, to make early diagnosis of flares possible. [3, 4] Up until now, calprotectin (consisting of the protein complex S100A8/S100A9) is the most frequently used biomarker used to make the diagnosis of IBD more or less likely in patients with gastrointestinal symptoms, in which the presentation is not typical for IBD and is used in patients with an established diagnosis of IBD to predict the presence of a flare-up of disease. [5] Whereas the correlation of calprotectin measured in feces with clinically active disease is strong, especially in patients with UC, up to 60% of the patients do not provide fecal samples when asked to, predominantly due to factors as embarrassment or discomfort. [6, 7] However, whereas high concentrations of fecal calprotectin are to date the most specific marker for active inflammatory disease, a low concentration of fecal calprotectin does not rule out active IBD, specifically when proximally located. [5] Furthermore, high concentrations of fecal calprotectin might be present in patients with gastrointestinal infection, ischemia or colonic cancer. [8] For these reasons, part I of this thesis describes the search for a (novel), non-invasive specific biomarker, assessable in peripheral blood, thus making it possible that IBD can be made unlikely without the need of an invasive endoscopic procedure. 248 Biomarkers and Thiopurines in Inflammatory Bowel Disease
2 Part I: Biomarkers of Inflammatory Bowel Disease In Chapter 2, the available literature regarding the use of S100A12 as a biomarker of a broad spectrum of diseases was reviewed. S100A12 (also known as calgranulin C) is a calcium-binding protein with inflammatory potentials, secreted by neutrophils. S100A12 is one of the members of the S100 family, of which the combination S100A8/A9 (calprotectin) is mostly used in the field of IBD. When S100A12 concentrations have to be measured, blood should be drawn in serum tubes for the most representative results, or, if unavailable, heparin tubes may be used. (9) In Chapter 3, a warning is provided for the determination of S100A12 concentrations in EDTA plasma, as these concentrations are not comparable to standardized serum concentrations. S100A12 works by the ligation with the receptor for advanced glycation endproducts (RAGE), leading to the production of pro-inflammatory cytokines and increase expression of adhesion molecules. Consequently, proinflammatory effects on especially neutrophils and lymphocytes take place. (10) Soluble Rage (srage) is a receptor protein with the same ligand-binding specificity as RAGE, however it lacks cytosolic and transmembrane domains, thus unable to initiate a pro-inflammatory response. By effect, srage might act as a decoy by binding S100A12, withholding them from binding to membrane-bound RAGE. In Chapter 4, the association of srage with disease severity was described in detail for patients with IBD. It was shown that, especially in patients suffering from UC, a lower concentration of srage was associated to a higher endoscopic severity score. Taken together, despite positive study results from several (S100) biomarkers, ileocolonoscopy remains the cornerstone of the diagnosis and follow-up of patients with IBD. Once the diagnosis of IBD is established, patients might either have active (relapsing) or quiescent disease (remission). When patients have active disease, induction therapy is needed to get these patients into remission. Once remission is achieved, immunosuppressive therapy is often needed to maintain this state of quiescent disease. [11, 12] 15 General discussion and summary 249
3 During the induction phase of IBD-treatment, the key drugs are corticosteroids, biologicals and mesalazines (in UC). [11, 12] In patients with either severe disease or poor response to corticosteroid monotherapy, immunomodulatory therapy can be initiated during induction therapy. The addition of biological therapy (e.g. infliximab, adalimumab, golimumab, vedolizumab or ustekinumab) is beneficial in achieving clinical and endoscopical remission. [13] The use of thiopurines as a mono-therapy is not associated with the induction of clinical remission as such, but plays an important role in assuring corticosteroid-free clinical remission in patients with moderate to severe disease. [14-17] Whereas over 80% of the patients experience a relapse within five years after diagnosis, there often is a need for continuous immunomodulatory treatment. [18] Figure 1 Simplified scheme of thiopurine metabolism. AZA: azathioprine; 6-MP: (6-)mercaptopurine; 6-TG: (6-)thioguanine; 6-MMP: 6- methylmercaptopurine; 6-TUA: 6-thiouric acid; 6-MMPR: 6-methylmercaptopurine ribonucleotides; 6- TIMP: 6-thioinosine monophosphate; 6-TIDP: 6-thioinosine diphosphate; 6-TITP: 6-thioinosine triphosphate; 6-TXMP: 6-thioxanthosine monophosphate; 6-TGMP: 6-thioguanine monophosphate; 6- TGTP: 6-thioguanine diphosphate; 6-TGTP: 6-thioguanine triphosphate; 6-MTG: 6-methylthioguanine Enzymatic conversions: GST: glutathione S-transferase; TPMT: thiopurine S-methyl transferase; XO: xanthine oxidase; HGPRT: hypoxanthine-guanine phosphoribosyl transferase; IMPDH: inosine monophosphate dehydrogenase; GMPS: guanosine monophosphate synthetase; ITPase: inosine triphosphate pyrophosphohydrolase; NUDT15: nucleoside diphosphate-linked moiety X motif 15 Based on: Meijer B, Mulder CJ and de Boer NK. NUDT15: a novel player in thiopurine metabolism. J Gastrointest Liver Dis, 2016 Jun;25: Biomarkers and Thiopurines in Inflammatory Bowel Disease
4 Thiopurines are antimetabolites and immunosuppressants firstly described in the 1950s by Gertrude Elion and George Hitchings. [19] Originally, thiopurines were developed for the treatment of childhood leukemia, but due to the immunosuppressive effects as an unwanted side-effect, it was used for the prevention of post-transplant organ rejection later on. In 1962, the first report on the use of mercaptopurine (MP) in the treatment of UC was described by Dr. Bean. [20] From that moment on, thiopurines were increasingly being prescribed as an immunomodulating agent in the treatment of IBD. Thiopurines are available in the (conventional) derivatives azathioprine (AZA) and MP, and in the more unconventional derivative thioguanine (TG). These conventional thiopurine derivatives are converted into mainly two pharmacologically active metabolites following a multi-enzymatic pathway. In Fig. 1, this pathway is schematically visualized. Azathioprine is converted into 6-MP by the enzymatic activity of glutathione-s-transferase and 6-MP is subsequently competitively metabolized by xanthine oxidase (converting 6- MP into thiouric acid), thiopurine methyltransferase (converting 6-MP into the pharmacologically active metabolite 6-methylmercaptopurine (6-MMP)) or by hypoxanthine-guanine phosphoribosyl transferase into the purine salvage pathway. This pathway leads to the conversion of 6-MP into the pharmacologically active metabolites 6-thioguaninenucleotides (6-TGN, the collective term of 6-thioguanine monophosphate (6-TGMP), 6-thioguanine diphosphate (6-TGDP) and 6-thioguanine triphosphate (6-TGTP)) by the sequential enzymatic activity of hypoxanthine-guanine phosphoribosyl transferase, inosine monophosphate dehydrogenase and guanosine monophosphate synthetase. Thioguanine, a less frequently used thiopurine derivative, is directly converted into 6-TGN by the use of only hypoxanthineguanine phosphoribosyl transferase. [21] The mode of action in IBD is mainly based on the inhibiting effect of 6-TGTP on the small GTP-ase Rac1, thus inhibiting the anti-apoptotic effect and leading to the apoptosis of CD-28 costimulated T-lymphocytes. [22, 23] 15 General discussion and summary 251
5 Over the past decade, there has been a rising interest in the optimization of (conventional) thiopurine therapy, especially in the patients with an aberrant (so-called skewed) thiopurine Table 1 Overview of thiopurine optimization strategies. Optimization strategy References Therapeutic drug monitoring [24-27] Split-dose administration [28, 29] Switching between conventional derivatives [30, 31] Switching to thioguanine [32, 33] Allopurinol co-administration [34-36] TPMT-genotyping/phenotyping [37] Addition of mesalazine [38] Patient motivation N/A TPMT: thiopurine-s-methyltransferase; N/A: not applicable metabolism (Table 1). Therapeutic drug monitoring (TDM), thus assessing the concentrations of 6-MMP and 6-TGN in red blood cells of a patient, and the subsequent dose adjustment, co-administration of allopurinol or the switch to another thiopurine derivative are the most practiced optimization strategies. [26, 34, 39] In part II of this thesis, optimization of thiopurine therapy is further evaluated, to warrant safe and effective therapy in IBD patients. Part II: Optimizing thiopurine therapy in IBD In Chapter 5, we provide a practical overview of the (contra-)indications, start- and stop criteria, toxicity, optimization, cancer risk and teratogenicity of thiopurine therapy in IBD patients. In this clinical review, recommendations to guide dosing in individual situations are provided to (IBD-treating) gastroenterologists. More specific, all possible scenarios of thiopurine metabolite measurements were given, providing useful suggestions for each situation, varying from patient motivation to gain compliance, drug dose enhancement, considering allopurinol coadministration or switch thiopurine therapy to TG. This last suggestion has been related to the development of nodular regenerative hyperplasia (NRH) of the liver from the beginning of this century, possibly leading to noncirrhotic portal hypertension. [40] From that moment onwards, it was demonstrated in multiple studies that NRH seems to be a dose-dependent adverse event of TG therapy, and that the occurrence in IBD patients treated with low-dose TG was similar to the occurrence in the thiopurine-naïve population. [41, 42] 252 Biomarkers and Thiopurines in Inflammatory Bowel Disease
6 Furthermore, the presence of histological NRH was not associated with clinical significant liver disease in the majority of IBD-patients treated with TG. [43] To bring the results of this review into perspective, we showed the results of our real-life 10-year cohort of patients with IBD treated with thiopurines in Chapter 6. Whereas the effects of TDM and allopurinol co-administration have been assessed in several clinical trials, evidence in a real-life setting without strict monitoring procedures was lacking. [34, 44] In this largest real-life cohort to date, we showed the beneficial effects of allopurinol coadministration after TDM, mainly in preventing (hepatotoxic) adverse events, which underlined earlier clinical trials examining this drug combination. [34, 36, 45] Furthermore, clinical benefit as a secondary outcome, was reported in about 40% of the patients included in the most recent cohort, which was over two-fold higher than the first cohort, showing that optimization of thiopurine therapy improves the use of conventional immunosuppressants in IBD-patients. [46, 47] In Chapter 7, the effect of thiopurine metabolites on hematologic parameters was assessed. 6-Thioguaninenucleotides are structurally similar to the endogenous purine bases, for which reason these may be incorporated into DNA or RNA as fraudulent bases, resulting in an antimetabolic effect by causing strand breakage and subsequently cytotoxicity, but only when high concentrations of 6-TGN are present. [48, 49] On the other hand, 6-methylmercaptopurines can occasionally (in high concentrations) cause leukopenia by inhibition of the de novo purine synthesis, which inhibits the generation of DNA. [50] We objectified that mainly the white blood cell count was negatively associated with AZA and MP therapy, but this association was not reproduced in the patients receiving TG, despite higher 6-TGN concentrations in this group. One of the possible explanations for this finding is the fact that 6-TGN are measured in red blood cells, whereas the immunosuppressive effect mainly takes place in white blood cells (WBC). This is derived from the original indication of thiopurines, being the treatment of (childhood) leukemia. As a consequence, measurement of metabolites is performed in red blood cells, 15 General discussion and summary 253
7 since WBC are unavailable in successful leukemia treatment. [19] In this chapter, to correlate 6-TGN concentrations in WBC, we calculated the measured 6-TGN concentrations by a conversion method as suggested in the paper by Lancaster et al. [51] and we demonstrated a negative correlation between 6-TGN in WBC and leukocyte count. In Chapter 8, we demonstrated that up to 50% of the IBD patients intolerant or refractory to AZA therapy benefitted from a switch to MP, the converted compound of the pro-drug AZA, on itself available as off-label therapy for treating IBD. As earlier observed, a substantial proportion of IBD patients with intolerance for AZA was able to tolerate MP therapy, despite the fact that the pharmacologically active metabolites are similar (6-MMP and 6- TGN). [31, 52] One of the reasons for this difference might be the pharmacokinetic profiles of the two drugs, as AZA is a pro-drug for 6-MP, bypassing the first-pass mechanism observed in patients taking MP. [25] Half of the included patients in Chapter 8 were relatively under-dosed (i.e. AZA < 2.0 mg/kg or MP < 1.0 mg/kg), for which reason it is doubtful what the effect of this different pharmacokinetic profile is on the outcome in this group. Further, as the imidazole group is split off during conversion of AZA into MP, this molecule might instigate adverse events in addition. [30] Very recently, in a pooled sub-analysis of the TOPIC trial, a prospective cohort study initiated to determine cost-effectiveness of TPMT genotyping in IBD patients before the start of thiopurine therapy, it was observed that patients with MP therapy were more likely to develop (dose-dependent) adverse events, as these patients were having higher 6-MMP and 6-TGN concentrations, potentially due to higher dosing (mg/kg) as compared to the AZA group (adjusted AZA dosage 1.05 vs. MP dosage 1.21 mg/kg, P < 0.001). Interestingly, this difference in experienced number of adverse events did not cause higher discontinuation rates (within 5 months) between the groups (AZA: 39.3% vs. MP: 38.1%, P = 0.50). [53] 254 Biomarkers and Thiopurines in Inflammatory Bowel Disease
8 Chapter 9 consisted of a systematic review of the available literature regarding the effectiveness of TG in IBD patients. Where researchers have mainly focused on the safety profile of TG, relatively little is known about the effectiveness of this drug. In this chapter, we demonstrated that TG is an effective alternative in about 65% of the patients intolerant to conventional thiopurine therapy. Short-term adverse events of TG were observed in one fifth of the patients, which comprised mainly aspecific adverse events, such as gastrointestinal complaints, hypersensitivity reactions and elevated liver enzymes. To assess the effectiveness and tolerability of TG as a rescue drug in UC, we compared it with methotrexate (MTX), another immunosuppressant used as rescue therapy in UC. For this comparison, we scrutinized the Parelsnoer database, a national database initiated by the Netherlands Federation of University medical centers (NFU), and depicted the results in Chapter 10. We demonstrated favorable short- and long-term tolerability results, with 70% of the patients in both drug groups able to continue treatment for at least one year, a percentage similar to that observed in patients receiving conventional thiopurine derivatives. [12, 54, 55] Subsequently, almost half of the patients able to tolerate TG/MTX therapy experienced clinical benefit (i.e. the ability to continue therapy without the need of intensified treatment or surgery) of this therapy. In the search for novel therapeutic drug monitoring options to optimize treatment with thiopurines in IBD, we assessed the inter-individual variability of xanthine oxidase (XO) in Chapter 11. We demonstrated a gender-specific distribution of XO (higher activity in males vs. females) and a positive correlation of XO-activity with age. This study was the first to measure XO-activity in IBD patients and might form a startpoint for future correlation studies with XO-activity, thiopurine dosage and metabolite concentrations. 15 General discussion and summary 255
9 As any drug, thiopurines have been associated with the development of several dose-dependent or compound-related (idiosyncratic) adverse events. Two of the most feared adverse events are myelotoxicity (depression of red and white cell lines, as well as platelet generation) and hepatotoxicity (mostly presenting as a rise in alkaline aminotransferase (ALT) and aspartate aminotransferase (AST) concentrations). The development of myelotoxicity has been related to high 6-TGN concentrations, whereas hepatotoxicity has predominantly been related to high concentrations of methylated products (6-MMP). [25, 56, 57] In part III of this thesis, the pathogenesis and prevalence of these adverse events during thiopurine therapy are described in more detail. Part III: Complications of thiopurine therapy Despite the fact that myelotoxicity is related to 6-TGN in medical literature, myelotoxicity (i.e. leukopenia) may also occur in patients with (extremely) high 6-MMP concentrations, as illustrated in Chapter 12. When 6-MMP concentrations get (extremely) high, this can cause inhibition of the de novo purine synthesis, thus causing cytotoxicity. [50] This situation occurs in patients with a skewed thiopurine metabolism, and in Chapter 12, we demonstrated that almost all patients were able to continue thiopurine therapy with an adapted regimen (i.e. dose reduction, allopurinol coadministration or switch to TG). In the past, a direct relationship between thiopurine-use and the development of NRH has been described. [40] In a small proportion of patients, NRH led to the development of severe portal hypertension. To assess the incidence of NRH-based end-stage liver disease warranting liver transplantation, we describe the results of our nation-wide database study comprising all liver transplant units from The Netherlands in Chapter 13. Whereas the association of NRH with severe complications of portal hypertension is not well established in patients with IBD [43], we scrutinized this database over the past 20 years. In total, 11 patients underwent liver transplantation due to NRH, with various causal factors. In five of these patients, thiopurines were used at some point during the underlying disease course, however in three of these five patients, other factors knowing to 256 Biomarkers and Thiopurines in Inflammatory Bowel Disease
10 cause NRH (e.g. hematologic malignancies or chemotherapeutic treatment) were simultaneously present, dissembling the causal role for thiopurines in these patients. These results are in line with recently published papers on the clinical disease course of NRH caused by thiopurines in IBD patients, showing that the majority of IBD-patients with thiopurine-induced NRH do not experience (severe) symptoms of portal hypertension. [43] To optimize safe therapy in IBD patients, detection of (early) toxicity plays a pivotal role. As the prevalence of histologically assessed hepatic fibrosis amongst IBD-patients was common in earlier performed studies, regardless of thiopurine exposure, we assessed the value of non-invasive methods to diagnose fibrosis in an early stage. [42] In Chapter 14, we describe our results of 200 consecutive IBD-patients who underwent transient elastography measurements using Fibroscan. We observed higher mean liver stiffness in males vs. females and in patients not exposed to thiopurines compared to patients with (either historical or current) thiopurine exposure. Whereas the number of patients with moderate to severe fibrosis in our study population was too small to draw firm conclusions, we believe this study is a stepping stone for future studies, assessing the correlation between transient elastography measurements and histopathological biopsies. 15 General discussion and summary 257
11 Conclusion In conclusion, novel insights in the use of non-invasive (serum) biomarkers to guide the diagnosis and follow-up, and to predict the severity of disease in patients with IBD were provided in the first part of this thesis. Biomarkers can, at this moment, not outclass findings of ileocolonoscopy. In the second part of this thesis, we provided strategies to optimize safety and effectiveness of thiopurine therapy in IBD patients by the use of allopurinol as co-therapy or the use of thioguanine as an unconventional thiopurine derivative. Finally, we described the pathogenesis and management of two adverse events of thiopurine therapy (myelotoxicity and hepatotoxicity) in detail and provide new viewpoints on the safety of thiopurines as a treatment in IBD. In this thesis, clinical guidelines for the optimal use of thiopurines were provided. 258 Biomarkers and Thiopurines in Inflammatory Bowel Disease
12 References [1] Lennard-Jones JE. Classification of inflammatory bowel disease. Scand J Gastroenterol Suppl. 1989;170:2-6; discussion [2] Nikolaus S, Schreiber S. Diagnostics of inflammatory bowel disease. Gastroenterology. 2007;133: [3] Kaplan GG. The global burden of IBD: from 2015 to Nat Rev Gastroenterol Hepatol. 2015;12: [4] Terheggen G, Lanyi B, Schanz S, et al. Safety, feasibility, and tolerability of ileocolonoscopy in inflammatory bowel disease. Endoscopy. 2008;40: [5] Lopez RN, Leach ST, Lemberg DA, et al. Fecal biomarkers in inflammatory bowel disease. J Gastroenterol Hepatol. 2017;32: [6] Gordon NP, Green BB. Factors associated with use and non-use of the Fecal Immunochemical Test (FIT) kit for Colorectal Cancer Screening in Response to a 2012 outreach screening program: a survey study. BMC Public Health. 2015;15:546. [7] Palmer CK, Thomas MC, von Wagner C, et al. Reasons for non-uptake and subsequent participation in the NHS Bowel Cancer Screening Programme: a qualitative study. Br J Cancer. 2014;110: [8] van Rheenen PF, Van de Vijver E, Fidler V. Faecal calprotectin for screening of patients with suspected inflammatory bowel disease: diagnostic meta-analysis. BMJ. 2010;341:c3369. [9] Tort AB, Dietrich MO, Goncalves CA, et al. Influence of anticoagulants on the measurement of S100B protein in blood. Clin Biochem. 2003;36: [10] Yang Z, Yan WX, Cai H, et al. S100A12 provokes mast cell activation: a potential amplification pathway in asthma and innate immunity. J Allergy Clin Immunol. 2007;119: [11] Gomollon F, Dignass A, Annese V, et al. 3rd European Evidence-based Consensus on the Diagnosis and Management of Crohn's Disease 2016: Part 1: Diagnosis and Medical Management. J Crohns Colitis. 2017;11:3-25. [12] Harbord M, Eliakim R, Bettenworth D, et al. Third European Evidence-based Consensus on Diagnosis and Management of Ulcerative Colitis. Part 2: Current Management. J Crohns Colitis [epub ahead of print] [13] D'Haens G, Baert F, van Assche G, et al. Early combined immunosuppression or conventional management in patients with newly diagnosed Crohn's disease: an open randomised trial. Lancet. 2008;371: [14] Chande N, Patton PH, Tsoulis DJ, et al. Azathioprine or 6-mercaptopurine for maintenance of remission in Crohn's disease. Cochrane Database Syst Rev. 2015;10:CD [15] Chande N, Tsoulis DJ, MacDonald JK. Azathioprine or 6-mercaptopurine for induction of remission in Crohn's disease. Cochrane Database Syst Rev. 2013;4:CD [16] Timmer A, McDonald JW, Tsoulis DJ, et al. Azathioprine and 6-mercaptopurine for maintenance of remission in ulcerative colitis. Cochrane Database Syst Rev. 2012;9:CD [17] Colombel JF, Sandborn WJ, Reinisch W, et al. Infliximab, azathioprine, or combination therapy for Crohn's disease. N Engl J Med. 2010;362: [18] Jess T, Riis L, Vind I, et al. Changes in clinical characteristics, course, and prognosis of inflammatory bowel disease during the last 5 decades: a population-based study from Copenhagen, Denmark. Inflamm Bowel Dis. 2007;13: [19] Elion GB. The purine path to chemotherapy. Science. 1989;244: [20] Bean RH. The treatment of chronic ulcerative colitis with 6-mercaptopurine. Med J Aust. 1962;49(2): [21] Van Asseldonk DP, de Boer NK, Peters GJ, et al. On therapeutic drug monitoring of thiopurines in inflammatory bowel disease; pharmacology, pharmacogenomics, drug intolerance and clinical relevance. Curr Drug Metab. 2009;10: [22] Seinen ML, van Nieuw Amerongen GP, de Boer NK, et al. Rac Attack: Modulation of the Small GTPase Rac in Inflammatory Bowel Disease and Thiopurine Therapy. Mol Diagn Ther. 2016;20: General discussion and summary 259
13 [23] Tiede I, Fritz G, Strand S, et al. CD28-dependent Rac1 activation is the molecular target of azathioprine in primary human CD4+ T lymphocytes. J Clin Invest. 2003;111: [24] Osterman MT, Kundu R, Lichtenstein GR, et al. Association of 6-thioguanine nucleotide levels and inflammatory bowel disease activity: a meta-analysis. Gastroenterology. 2006;130: [25] Dubinsky MC, Lamothe S, Yang HY, et al. Pharmacogenomics and metabolite measurement for 6-mercaptopurine therapy in inflammatory bowel disease. Gastroenterology. 2000;118: [26] Al Hadithy AF, de Boer NK, Derijks LJ, et al. Thiopurines in inflammatory bowel disease: pharmacogenetics, therapeutic drug monitoring and clinical recommendations. Dig Liver Dis. 2005;37: [27] Kreijne JE, Seinen ML, Wilhelm AJ, et al. Routinely Established Skewed Thiopurine Metabolism Leads to a Strikingly High Rate of Early Therapeutic Failure in Patients With Inflammatory Bowel Disease. Ther Drug Monit. 2015;37: [28] Pavlidis P, Ansari A, Duley J, et al. Splitting a therapeutic dose of thioguanine may avoid liver toxicity and be an efficacious treatment for severe inflammatory bowel disease: a 2-center observational cohort study. Inflamm Bowel Dis. 2014;20: [29] Shih DQ, Nguyen M, Zheng L, et al. Split-dose administration of thiopurine drugs: a novel and effective strategy for managing preferential 6-MMP metabolism. Aliment Pharmacol Ther. 2012;36: [30] McGovern DP, Travis SP, Duley J, et al. Azathioprine intolerance in patients with IBD may be imidazole-related and is independent of TPMT activity. Gastroenterology. 2002;122: [31] Actis GC, Pellicano R, Rosina F. 6-Mercaptopurine for Azathioprine Intolerant Inflammatory Bowel Disease: Literature Search and Reappraisal of Own Data. Inflamm Allergy Drug Targets. 2015;14: [32] de Boer NK, Derijks LJ, Gilissen LP, et al. On tolerability and safety of a maintenance treatment with 6-thioguanine in azathioprine or 6-mercaptopurine intolerant IBD patients. World J Gastroenterol. 2005;11: [33] Derijks LJ, de Jong DJ, Gilissen LP, et al. 6-Thioguanine seems promising in azathioprine- or 6- mercaptopurine-intolerant inflammatory bowel disease patients: a short-term safety assessment. Eur J Gastroenterol Hepatol. 2003;15: [34] Ansari A, Patel N, Sanderson J, et al. Low-dose azathioprine or mercaptopurine in combination with allopurinol can bypass many adverse drug reactions in patients with inflammatory bowel disease. Aliment Pharmacol Ther. 2010;31: [35] Sparrow MP. Use of allopurinol to optimize thiopurine immunomodulator efficacy in inflammatory bowel disease. Gastroenterol Hepatol (N Y). 2008;4: [36] Leung Y, Sparrow MP, Schwartz M, et al. Long term efficacy and safety of allopurinol and azathioprine or 6-mercaptopurine in patients with inflammatory bowel disease. J Crohns Colitis. 2009;3: [37] Coenen MJ, de Jong DJ, van Marrewijk CJ, et al. Identification of Patients With Variants in TPMT and Dose Reduction Reduces Hematologic Events During Thiopurine Treatment of Inflammatory Bowel Disease. Gastroenterology. 2015;149: e907. [38] de Graaf P, de Boer NK, Wong DR, et al. Influence of 5-aminosalicylic acid on 6- thioguanosine phosphate metabolite levels: a prospective study in patients under steady thiopurine therapy. Br J Pharmacol. 2010;160: [39] van Asseldonk DP, Seinen ML, de Boer NK, et al. Hepatotoxicity associated with 6-methyl mercaptopurine formation during azathioprine and 6-mercaptopurine therapy does not occur on the short-term during 6-thioguanine therapy in IBD treatment. J Crohns Colitis. 2012;6: [40] Dubinsky MC, Vasiliauskas EA, Singh H, et al. 6-thioguanine can cause serious liver injury in inflammatory bowel disease patients. Gastroenterology. 2003;125: [41] Seinen ML, van Asseldonk DP, Mulder CJ, et al. Dosing 6-thioguanine in inflammatory bowel disease: expert-based guidelines for daily practice. J Gastrointestin Liver Dis. 2010;19: Biomarkers and Thiopurines in Inflammatory Bowel Disease
14 [42] De Boer NK, Tuynman H, Bloemena E, et al. Histopathology of liver biopsies from a thiopurine-naive inflammatory bowel disease cohort: prevalence of nodular regenerative hyperplasia. Scand J Gastroenterol. 2008;43: [43] van Asseldonk DP, Jharap B, Verheij J, et al. The Prevalence of Nodular Regenerative Hyperplasia in Inflammatory Bowel Disease Patients Treated with Thioguanine Is Not Associated with Clinically Significant Liver Disease. Inflamm Bowel Dis. 2016;22: [44] Haines ML, Ajlouni Y, Irving PM, et al. Clinical usefulness of therapeutic drug monitoring of thiopurines in patients with inadequately controlled inflammatory bowel disease. Inflamm Bowel Dis. 2011;17: [45] Hoentjen F, Seinen ML, Hanauer SB, et al. Safety and effectiveness of long-term allopurinolthiopurine maintenance treatment in inflammatory bowel disease. Inflamm Bowel Dis. 2013;19: [46] Min MX, Weinberg DI, McCabe RP. Allopurinol enhanced thiopurine treatment for inflammatory bowel disease: safety considerations and guidelines for use. J Clin Pharm Ther. 2014;39: [47] Kiszka-Kanowitz M, Theede K, Mertz-Nielsen A. Randomized clinical trial: a pilot study comparing efficacy of low-dose azathioprine and allopurinol to azathioprine on clinical outcomes in inflammatory bowel disease. Scand J Gastroenterol. 2016;51: [48] Fairchild CR, Maybaum J, Kennedy KA. Concurrent unilateral chromatid damage and DNA strand breakage in response to 6-thioguanine treatment. Biochem Pharmacol. 1986;35: [49] Marathias VM, Sawicki MJ, Bolton PH. 6-Thioguanine alters the structure and stability of duplex DNA and inhibits quadruplex DNA formation. Nucleic Acids Res. 1999;27: [50] Quemeneur L, Gerland LM, Flacher M, et al. Differential control of cell cycle, proliferation, and survival of primary T lymphocytes by purine and pyrimidine nucleotides. J Immunol. 2003;170: [51] Lancaster DL, Patel N, Lennard L, et al. Leucocyte versus erythrocyte thioguanine nucleotide concentrations in children taking thiopurines for acute lymphoblastic leukaemia. Cancer Chemother Pharmacol. 2002;50: [52] Hindorf U, Johansson M, Eriksson A, et al. Mercaptopurine treatment should be considered in azathioprine intolerant patients with inflammatory bowel disease. Aliment Pharmacol Ther. 2009;29: [53] Broekman M, Coenen MJH, van Marrewijk CJ, et al. More Dose-dependent Side Effects with Mercaptopurine over Azathioprine in IBD Treatment Due to Relatively Higher Dosing. Inflamm Bowel Dis [epub ahead of print] [54] Jharap B, Seinen ML, de Boer NK, et al. Thiopurine therapy in inflammatory bowel disease patients: analyses of two 8-year intercept cohorts. Inflamm Bowel Dis. 2010;16: [55] Bressler B, Marshall JK, Bernstein CN, et al. Clinical practice guidelines for the medical management of nonhospitalized ulcerative colitis: the Toronto consensus. Gastroenterology. 2015;148: e1033. [56] Dubinsky MC, Yang H, Hassard PV, et al. 6-MP metabolite profiles provide a biochemical explanation for 6-MP resistance in patients with inflammatory bowel disease. Gastroenterology. 2002;122: [57] Hindorf U, Lindqvist M, Hildebrand H, et al. Adverse events leading to modification of therapy in a large cohort of patients with inflammatory bowel disease. Aliment Pharmacol Ther. 2006;24: General discussion and summary 261
Allopurinol thiopurine combination therapy in inflammatory bowel disease
 uer & herapy Allopurinol thiopurine combination therapy in inflammatory bowel disease Combination therapy with allopurinol and low-dose thiopurine (azathioprine and mercaptopurine) has been described as
uer & herapy Allopurinol thiopurine combination therapy in inflammatory bowel disease Combination therapy with allopurinol and low-dose thiopurine (azathioprine and mercaptopurine) has been described as
MEDICAL POLICY. Proprietary Information of YourCare Health Plan
 MEDICAL POLICY Clinical criteria used to make utilization review decisions are based on credible scientific evidence published in peer reviewed medical literature generally recognized by the medical community.
MEDICAL POLICY Clinical criteria used to make utilization review decisions are based on credible scientific evidence published in peer reviewed medical literature generally recognized by the medical community.
CHAPTER 5. How I Treat my Inflammatory Bowel Disease-Patients with Thiopurines? 1 Department of Gastroenterology and Hepatology,
 CHAPTER 5 How I Treat my Inflammatory Bowel Disease-Patients with Thiopurines? 4 Berrie Meijer 1 Chris JJ Mulder 1 Adriaan A van Bodegraven 1,2 Nanne KH de Boer 1 1 Department of Gastroenterology and Hepatology,
CHAPTER 5 How I Treat my Inflammatory Bowel Disease-Patients with Thiopurines? 4 Berrie Meijer 1 Chris JJ Mulder 1 Adriaan A van Bodegraven 1,2 Nanne KH de Boer 1 1 Department of Gastroenterology and Hepatology,
The thiopurine immunomodulators azathioprine (AZA)
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2007;5:209 214 Effect of Allopurinol on Clinical Outcomes in Inflammatory Bowel Disease Nonresponders to Azathioprine or 6-Mercaptopurine MILES P. SPARROW,* SCOTT
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2007;5:209 214 Effect of Allopurinol on Clinical Outcomes in Inflammatory Bowel Disease Nonresponders to Azathioprine or 6-Mercaptopurine MILES P. SPARROW,* SCOTT
CHAPTER 9. Efficacy of Thioguanine Treatment in Inflammatory Bowel disease: a Systematic Review
 CHAPTER 9 Efficacy of Thioguanine Treatment in Inflammatory Bowel disease: a Systematic Review Berrie Meijer 1 Chris JJ Mulder 1 Godefridus J Peters 2 Adriaan A van Bodegraven 1,3 Nanne KH de Boer 1 8
CHAPTER 9 Efficacy of Thioguanine Treatment in Inflammatory Bowel disease: a Systematic Review Berrie Meijer 1 Chris JJ Mulder 1 Godefridus J Peters 2 Adriaan A van Bodegraven 1,3 Nanne KH de Boer 1 8
PART I OPPORTUNITIES AND THREATS OF THIOPURINE METABOLISM AND DRUG MONITORING
 PART I OPPORTUNITIES AND THREATS OF THIOPURINE METABOLISM AND DRUG MONITORING CHAPTER 2 PHARMACOLOGICAL CONSIDERATIONS OF THIOPURINES IN THE TREATMENT OF INFLAMMATORY BOWEL DISEASE This chapter is an
PART I OPPORTUNITIES AND THREATS OF THIOPURINE METABOLISM AND DRUG MONITORING CHAPTER 2 PHARMACOLOGICAL CONSIDERATIONS OF THIOPURINES IN THE TREATMENT OF INFLAMMATORY BOWEL DISEASE This chapter is an
AAA Study. Dr Antony Friedman IBD Fellow, The Alfred Hospital Melbourne, Australia
 AAA Study Use of Adjunctive Allopurinol in Azathioprine / 6-Mercaptopurine Non-Responders to Optimise 6-Thioguanine Nucleotide Production and Improve Clinical Outcomes Dr Antony Friedman IBD Fellow, The
AAA Study Use of Adjunctive Allopurinol in Azathioprine / 6-Mercaptopurine Non-Responders to Optimise 6-Thioguanine Nucleotide Production and Improve Clinical Outcomes Dr Antony Friedman IBD Fellow, The
MEDICAL POLICY SUBJECT: GENOTYPING OR PHENOTYPING FOR THIOPURINE METHYLTRANSFERASE (TPMT) FOR PATIENTS TREATED WITH AZATHIOPRINE (6-MP)
 MEDICAL POLICY SUBJECT: GENOTYPING OR PHENOTYPING PAGE: 1 OF: 5 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial product (including
MEDICAL POLICY SUBJECT: GENOTYPING OR PHENOTYPING PAGE: 1 OF: 5 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial product (including
P de Graaf 1, NKH de Boer 2, DR Wong 3, S Karner 4, B Jharap 2, PM Hooymans 3, AI Veldkamp 1, CJJ Mulder 2, AA van Bodegraven 2 and M Schwab 4,5
 British Journal of Pharmacology (2010), 160, 1083 1091 2010 The Authors Journal compilation 2010 The British Pharmacological Society All rights reserved 0007-1188/10 www.brjpharmacol.org RESEARCH PAPER
British Journal of Pharmacology (2010), 160, 1083 1091 2010 The Authors Journal compilation 2010 The British Pharmacological Society All rights reserved 0007-1188/10 www.brjpharmacol.org RESEARCH PAPER
Optimizing treatment with thioguanine derivatives in inflammatory bowel disease
 Optimizing treatment with thioguanine derivatives in inflammatory bowel disease Edouard Louis MD, PhD Jacques Belaiche MD, PhD Service de Gastroentérologie, CHU de Liège, 4000 Liège, Belgium Abstract Thioguanine
Optimizing treatment with thioguanine derivatives in inflammatory bowel disease Edouard Louis MD, PhD Jacques Belaiche MD, PhD Service de Gastroentérologie, CHU de Liège, 4000 Liège, Belgium Abstract Thioguanine
6-methylmercaptopurine-induced leukocytopenia during thiopurine therapy in inflammatory bowel disease patients
 bs_bs_banner doi:10.1111/jgh.13656 GASTROENTEROLOGY 6-methylmercaptopurine-induced leukocytopenia during thiopurine therapy in inflammatory bowel disease patients Berrie Meijer,* Joany E Kreijne, Sofia
bs_bs_banner doi:10.1111/jgh.13656 GASTROENTEROLOGY 6-methylmercaptopurine-induced leukocytopenia during thiopurine therapy in inflammatory bowel disease patients Berrie Meijer,* Joany E Kreijne, Sofia
Patient selection for azathioprine - typical courses of Crohn s disease
 Patient selection for azathioprine - typical courses of Crohn s disease remitting 44% steroid refractory 20% remitting 48% steroid refractory 21% 36% steroid dependent 31% steroid dependent Munkholm et
Patient selection for azathioprine - typical courses of Crohn s disease remitting 44% steroid refractory 20% remitting 48% steroid refractory 21% 36% steroid dependent 31% steroid dependent Munkholm et
De uitgave van dit proefschrift is mogelijk gemaakt door een gift van Ferring B.V., Hoofddorp.
 Thiopurines and IBD De uitgave van dit proefschrift is mogelijk gemaakt door een gift van Ferring B.V., Hoofddorp. Copyright 2007 K.H.N. de Boer, Amsterdam, The Netherlands No parts of this publication
Thiopurines and IBD De uitgave van dit proefschrift is mogelijk gemaakt door een gift van Ferring B.V., Hoofddorp. Copyright 2007 K.H.N. de Boer, Amsterdam, The Netherlands No parts of this publication
John F. Valentine, MD Inflammatory Bowel Disease Program University of Utah
 John F. Valentine, MD Inflammatory Bowel Disease Program University of Utah Hawaii 1/20/2017 DISCLOSURES Research Support: NIH, Pfizer, Celgene, AbbVie, Roche/Genentech, Takeda, CCFA OBJECTIVES Review
John F. Valentine, MD Inflammatory Bowel Disease Program University of Utah Hawaii 1/20/2017 DISCLOSURES Research Support: NIH, Pfizer, Celgene, AbbVie, Roche/Genentech, Takeda, CCFA OBJECTIVES Review
6-Mercaptopurine (6-MP) and azathioprine (AZA) are
 GASTROENTEROLOGY 2006;130:1047 1053 Association of 6-Thioguanine Nucleotide Levels and Inflammatory Bowel Disease Activity: A Meta-Analysis MARK T. OSTERMAN,*, RABI KUNDU, GARY R. LICHTENSTEIN,* and JAMES
GASTROENTEROLOGY 2006;130:1047 1053 Association of 6-Thioguanine Nucleotide Levels and Inflammatory Bowel Disease Activity: A Meta-Analysis MARK T. OSTERMAN,*, RABI KUNDU, GARY R. LICHTENSTEIN,* and JAMES
Protocol. Pharmacogenomic and Metabolite Markers for Patients Treated With Thiopurines
 Pharmacogenomic and Metabolite Markers for Patients Treated (20419) Medical Benefit Effective Date: 01/01/15 Next Review Date: 11/18 Preauthorization Yes Review Dates: 04/07, 09/08, 05/09, 03/10, 03/11,
Pharmacogenomic and Metabolite Markers for Patients Treated (20419) Medical Benefit Effective Date: 01/01/15 Next Review Date: 11/18 Preauthorization Yes Review Dates: 04/07, 09/08, 05/09, 03/10, 03/11,
Mercaptopurine and inflammatory bowel disease: the other thiopurine
 30-008/207/09//0-6 Revista Española de Enfermedades Digestivas Copyright 207. SEPD y ARÁN EDICIONES, S.L. Rev Esp Enferm Dig 207, Vol. 09, N.º, pp. 0-6 ORIGINAL PAPERS Mercaptopurine and inflammatory bowel
30-008/207/09//0-6 Revista Española de Enfermedades Digestivas Copyright 207. SEPD y ARÁN EDICIONES, S.L. Rev Esp Enferm Dig 207, Vol. 09, N.º, pp. 0-6 ORIGINAL PAPERS Mercaptopurine and inflammatory bowel
Accepted Article. Mercaptopurine and inflammatory bowel disease: the other thiopurine
 Accepted Article Mercaptopurine and inflammatory bowel disease: the other thiopurine Fernando Bermejo San José, Alicia Algaba, Sergio López Durán, Iván Guerra, Marta Aicart, María Hernández-Tejero, Elena
Accepted Article Mercaptopurine and inflammatory bowel disease: the other thiopurine Fernando Bermejo San José, Alicia Algaba, Sergio López Durán, Iván Guerra, Marta Aicart, María Hernández-Tejero, Elena
Common Questions in Crohn s Disease Therapy. Case
 Common Questions in Crohn s Disease Therapy Jean-Paul Achkar, MD, FACG Kenneth Rainin Chair for IBD Research Cleveland Clinic Case 23 yo male with 1 year history of diarrhea, abdominal pain and 15 pound
Common Questions in Crohn s Disease Therapy Jean-Paul Achkar, MD, FACG Kenneth Rainin Chair for IBD Research Cleveland Clinic Case 23 yo male with 1 year history of diarrhea, abdominal pain and 15 pound
Clinical Use and Practical Application of TPMT Enzyme and 6-Mercaptopurine Metabolite Monitoring in IBD Ernest G. Seidman, MD
 GENETIC TESTING FOR IBD Clinical Use and Practical Application of TPMT Enzyme and 6-Mercaptopurine Metabolite Monitoring in IBD Ernest G. Seidman, MD Division of Gastroenterology, Hepatology, and Nutrition,
GENETIC TESTING FOR IBD Clinical Use and Practical Application of TPMT Enzyme and 6-Mercaptopurine Metabolite Monitoring in IBD Ernest G. Seidman, MD Division of Gastroenterology, Hepatology, and Nutrition,
Up to 50% of patients with inflammatory bowel disease
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2008;6:654 660 Thiopurine Dose in Intermediate and Normal Metabolizers of Thiopurine Methyltransferase May Differ Three-Fold SHARON J. GARDINER,*, RICHARD B. GEARRY,*,
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2008;6:654 660 Thiopurine Dose in Intermediate and Normal Metabolizers of Thiopurine Methyltransferase May Differ Three-Fold SHARON J. GARDINER,*, RICHARD B. GEARRY,*,
Linköping University Post Print. How Should Thiopurine Treatment be Monitored? Methodological Aspects
 Linköping University Post Print How Should Thiopurine Treatment be Monitored? Methodological Aspects Svante Vikingsson, Björn Carlsson, Sven Almer and Curt Peterson N.B.: When citing this work, cite the
Linköping University Post Print How Should Thiopurine Treatment be Monitored? Methodological Aspects Svante Vikingsson, Björn Carlsson, Sven Almer and Curt Peterson N.B.: When citing this work, cite the
Optimizing Immunomodulators and
 Optimizing Immunomodulators and Biologics i in Inflammatory Bowel Disease Sunanda Kane, MD, MSPH, FACG Professor of Medicine Division of Gastroenterology and Hepatology Mayo Clinic Rochester, Minnesota,
Optimizing Immunomodulators and Biologics i in Inflammatory Bowel Disease Sunanda Kane, MD, MSPH, FACG Professor of Medicine Division of Gastroenterology and Hepatology Mayo Clinic Rochester, Minnesota,
Review Article Immunomodulators and Immunosuppressants for Japanese Patients with Ulcerative Colitis
 International Scholarly Research Network ISRN Gastroenterology Volume 2011, Article ID 194324, 5 pages doi:10.5402/2011/194324 Review Article Immunomodulators and Immunosuppressants for Japanese Patients
International Scholarly Research Network ISRN Gastroenterology Volume 2011, Article ID 194324, 5 pages doi:10.5402/2011/194324 Review Article Immunomodulators and Immunosuppressants for Japanese Patients
UvA-DARE (Digital Academic Repository)
 UvA-DARE (Digital Academic Repository) On tolerability and safety of a maintenance treatment with 6-thioguanine in azathioprine or 6-mercaptopurine intolerant IBD patients de Boer, N.K.H.; Derijks, L.J.J.;
UvA-DARE (Digital Academic Repository) On tolerability and safety of a maintenance treatment with 6-thioguanine in azathioprine or 6-mercaptopurine intolerant IBD patients de Boer, N.K.H.; Derijks, L.J.J.;
Azathioprine for Induction and Maintenance of Remission in Crohn s Disease
 Azathioprine for Induction and Maintenance of Remission in Crohn s Disease William J. Sandborn, MD Chief, Division of Gastroenterology Director, UCSD IBD Center Objectives Azathioprine as induction and
Azathioprine for Induction and Maintenance of Remission in Crohn s Disease William J. Sandborn, MD Chief, Division of Gastroenterology Director, UCSD IBD Center Objectives Azathioprine as induction and
Azathioprine treatment during lactation
 Alimentary Pharmacology & Therapeutics Azathioprine treatment during lactation L.A.CHRISTENSEN*,J.F.DAHLERUP*,M.J.NIELSEN*,J.F.FALLINGBORG &K.SCHMIEGELOWà *Department of Medicine V, Århus University Hospital,
Alimentary Pharmacology & Therapeutics Azathioprine treatment during lactation L.A.CHRISTENSEN*,J.F.DAHLERUP*,M.J.NIELSEN*,J.F.FALLINGBORG &K.SCHMIEGELOWà *Department of Medicine V, Århus University Hospital,
6-Thioguanosine Diphosphate and Triphosphate Levels in Red Blood Cells and Response to Azathioprine Therapy in Crohn s Disease
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2005;3:1007 1014 6-Thioguanosine Diphosphate and Triphosphate Levels in Red Blood Cells and Response to Azathioprine Therapy in Crohn s Disease MARKUS F. NEURATH,*
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2005;3:1007 1014 6-Thioguanosine Diphosphate and Triphosphate Levels in Red Blood Cells and Response to Azathioprine Therapy in Crohn s Disease MARKUS F. NEURATH,*
September 12, 2015 Millie D. Long MD, MPH, FACG
 Update on Biologic Therapy in 2015 September 12, 2015 Millie D. Long MD, MPH, FACG Assistant Professor of Medicine Inflammatory Bowel Disease Center University of North Carolina-Chapel Hill Outline Crohn
Update on Biologic Therapy in 2015 September 12, 2015 Millie D. Long MD, MPH, FACG Assistant Professor of Medicine Inflammatory Bowel Disease Center University of North Carolina-Chapel Hill Outline Crohn
Efficacy and Safety of Treatment for Pediatric IBD
 Efficacy and Safety of Treatment for Pediatric IBD Andrew B. Grossman MD Co-Director, Center for Pediatric Inflammatory Bowel Disease Assistant Professor of Clinical Pediatrics Division of Gastroenterology,
Efficacy and Safety of Treatment for Pediatric IBD Andrew B. Grossman MD Co-Director, Center for Pediatric Inflammatory Bowel Disease Assistant Professor of Clinical Pediatrics Division of Gastroenterology,
Efficacy and Safety of Treatment for Pediatric IBD
 Efficacy and Safety of Treatment for Pediatric IBD Andrew B. Grossman MD Co-Director, Center for Pediatric Inflammatory Bowel Disease Associate Professor of Clinical Pediatrics Division of Gastroenterology,
Efficacy and Safety of Treatment for Pediatric IBD Andrew B. Grossman MD Co-Director, Center for Pediatric Inflammatory Bowel Disease Associate Professor of Clinical Pediatrics Division of Gastroenterology,
How to Optimize Induction and Maintenance Responses: Definitions and Dosing Advances in Inflammatory Bowel Disease December 6, 2009
 How to Optimize Induction and Maintenance Responses: Definitions and Dosing 2009 Advances in Inflammatory Bowel Disease December 6, 2009 Fernando Velayos MD MPH University of California, San Francisco
How to Optimize Induction and Maintenance Responses: Definitions and Dosing 2009 Advances in Inflammatory Bowel Disease December 6, 2009 Fernando Velayos MD MPH University of California, San Francisco
Effect of Combination Therapy of Allopurinol and Reduced Dose of Azathioprine on Inflammatory Bowel Disease (IBD)
 J. Basic. Appl. Sci. Res., 3(7)820-825, 2013 2013, TextRoad Publication ISSN 2090-4304 Journal of Basic and Applied Scientific Research www.textroad.com Effect of Combination Therapy of Allopurinol and
J. Basic. Appl. Sci. Res., 3(7)820-825, 2013 2013, TextRoad Publication ISSN 2090-4304 Journal of Basic and Applied Scientific Research www.textroad.com Effect of Combination Therapy of Allopurinol and
FEP Medical Policy Manual
 FEP Medical Policy Manual FEP 2.04.19 Pharmacogenomic and Metabolite Markers for Patients Treated With Effective Date: April 15, 2018 Related Policies: None Pharmacogenomic and Metabolite Markers for Patients
FEP Medical Policy Manual FEP 2.04.19 Pharmacogenomic and Metabolite Markers for Patients Treated With Effective Date: April 15, 2018 Related Policies: None Pharmacogenomic and Metabolite Markers for Patients
The following slides are provided as presented by the author during the live educa7onal ac7vity and are intended for reference purposes only.
 The following slides are provided as presented by the author during the live educa7onal ac7vity and are intended for reference purposes only. If you have any ques7ons, please contact Imedex via email at:
The following slides are provided as presented by the author during the live educa7onal ac7vity and are intended for reference purposes only. If you have any ques7ons, please contact Imedex via email at:
Recent Advances in the Management of Refractory IBD
 Recent Advances in the Management of Refractory IBD Raina Shivashankar, M.D. Assistant Professor of Medicine Division of Gastroenterology and Hepatology Thomas Jefferson University Philadelphia, PA Outline
Recent Advances in the Management of Refractory IBD Raina Shivashankar, M.D. Assistant Professor of Medicine Division of Gastroenterology and Hepatology Thomas Jefferson University Philadelphia, PA Outline
Mono or Combination Therapy with. Individualized Approach
 Mono Combination Therapy with Biologics i in IBD: Developing an Individualized Approach David T. Rubin, MD, FACG Co-Direct, Inflammaty Bowel Disease Center Fellowship Program Direct University of Chicago
Mono Combination Therapy with Biologics i in IBD: Developing an Individualized Approach David T. Rubin, MD, FACG Co-Direct, Inflammaty Bowel Disease Center Fellowship Program Direct University of Chicago
Medical Therapy for Pediatric IBD: Efficacy and Safety
 Medical Therapy for Pediatric IBD: Efficacy and Safety Betsy Maxwell, MD Assistant Professor of Clinical Pediatrics Division of Gastroenterology, Hepatology, and Nutrition Pediatric IBD: Defining Remission
Medical Therapy for Pediatric IBD: Efficacy and Safety Betsy Maxwell, MD Assistant Professor of Clinical Pediatrics Division of Gastroenterology, Hepatology, and Nutrition Pediatric IBD: Defining Remission
OPTIMAL USE OF IMMUNOMODULATORS AND BIOLOGICS Edward V. Loftus, Jr., MD, FACG
 1C: Advances in Inflammatory Bowel Disease OPTIMAL USE OF IMMUNOMODULATORS AND BIOLOGICS Edward V. Loftus, Jr., MD, FACG narrow interpretation of this presentation topic would A be a discussion of dosing
1C: Advances in Inflammatory Bowel Disease OPTIMAL USE OF IMMUNOMODULATORS AND BIOLOGICS Edward V. Loftus, Jr., MD, FACG narrow interpretation of this presentation topic would A be a discussion of dosing
Pharmacogenomic and Metabolite Markers for Patients Treated with Thiopurines
 Last Review Status/Date: March 2017 Page: 1 of 12 for Patients Treated with Thiopurines Description The use of thiopurines, medications for treating inflammatory bowel disease (IBD) and other conditions,
Last Review Status/Date: March 2017 Page: 1 of 12 for Patients Treated with Thiopurines Description The use of thiopurines, medications for treating inflammatory bowel disease (IBD) and other conditions,
Thiopurine methyltransferase genotype and thiopurine S-methyltransferase activity in Greek children with inflammatory bowel disease
 Original article Annals of Gastroenterology (2012) 25, 1-5 Thiopurine methyltransferase genotype and thiopurine S-methyltransferase activity in Greek children with inflammatory bowel disease Μaria Gazouli
Original article Annals of Gastroenterology (2012) 25, 1-5 Thiopurine methyltransferase genotype and thiopurine S-methyltransferase activity in Greek children with inflammatory bowel disease Μaria Gazouli
Pharmacogenomic and Metabolite Markers for Patients Treated with Thiopurines. Original Policy Date
 MP 2.04.12 Pharmacogenomic and Metabolite Markers for Patients Treated with Thiopurines Medical Policy Section Medicine Issue 12:2013 Original Policy Date 12:2013 Last Review Status/Date Reviewed with
MP 2.04.12 Pharmacogenomic and Metabolite Markers for Patients Treated with Thiopurines Medical Policy Section Medicine Issue 12:2013 Original Policy Date 12:2013 Last Review Status/Date Reviewed with
Thiopurine S-Methyltransferase (TPMT): Pharmacogenetic Competency
 Thiopurine S-Methyltransferase (TPMT): Pharmacogenetic Competency Updated on 6/2015 Pre-test Question # 1 Approximately 10% of patients have a (an) TPMT phenotype. a) Normal/high function b) Intermediate
Thiopurine S-Methyltransferase (TPMT): Pharmacogenetic Competency Updated on 6/2015 Pre-test Question # 1 Approximately 10% of patients have a (an) TPMT phenotype. a) Normal/high function b) Intermediate
99 Chapter 8 Summary
 99 Chapter 8 Summary 100 101 Summary Thiopurines are frequently used in the treatment of patients suffering from (auto)immune diseases. Since their introduction in the mid fifties of the 20 th century
99 Chapter 8 Summary 100 101 Summary Thiopurines are frequently used in the treatment of patients suffering from (auto)immune diseases. Since their introduction in the mid fifties of the 20 th century
Mild-moderate Ulcerative Colitis Sequential & Combined treatments need to be tested. Philippe Marteau, Paris, France
 Mild-moderate Ulcerative Colitis Sequential & Combined treatments need to be tested Philippe Marteau, Paris, France Sequential vs combined treatments When should one switch? Sequential vs combined treatments
Mild-moderate Ulcerative Colitis Sequential & Combined treatments need to be tested Philippe Marteau, Paris, France Sequential vs combined treatments When should one switch? Sequential vs combined treatments
Incidence of Neoplasms in Patients Who Develop Sustained Leukopenia During or After Treatment With 6-Mercaptopurine for Inflammatory Bowel Disease
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2006;4:1025 1029 Incidence of Neoplasms in Patients Who Develop Sustained Leukopenia During or After Treatment With 6-Mercaptopurine for Inflammatory Bowel Disease
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2006;4:1025 1029 Incidence of Neoplasms in Patients Who Develop Sustained Leukopenia During or After Treatment With 6-Mercaptopurine for Inflammatory Bowel Disease
Efficacy of 6-mercaptopurine treatment after azathioprine hypersensitivity in inflammatory bowel disease
 Online Submissions: wjg.wjgnet.com World J Gastroenterol 2008 July 21; 14(27): 4342-4346 wjg@wjgnet.com World Journal of Gastroenterology ISSN 1007-9327 doi:10.3748/wjg.14.4342 2008 The WJG Press. All
Online Submissions: wjg.wjgnet.com World J Gastroenterol 2008 July 21; 14(27): 4342-4346 wjg@wjgnet.com World Journal of Gastroenterology ISSN 1007-9327 doi:10.3748/wjg.14.4342 2008 The WJG Press. All
Latest Treatment Updates for Ulcerative Colitis: Evolving Treatment Goals
 Latest Treatment Updates for Ulcerative Colitis: Evolving Treatment Goals Stephen Hanauer, MD Professor of Medicine Medical Director, Digestive Disease Center Northwestern Medicine Chicago, Illinois Speaker
Latest Treatment Updates for Ulcerative Colitis: Evolving Treatment Goals Stephen Hanauer, MD Professor of Medicine Medical Director, Digestive Disease Center Northwestern Medicine Chicago, Illinois Speaker
IBD Updates. Themes in IBD IBD management journey. New tools for therapeutic monitoring. First-line treatment in IBD
 IBD Updates Maria T. Abreu, MD University of Miami Miller School of Medicine Miami, Florida Themes in IBD 213 First-line treatment in IBD New tools for therapeutic monitoring Biologic therapy for CD and
IBD Updates Maria T. Abreu, MD University of Miami Miller School of Medicine Miami, Florida Themes in IBD 213 First-line treatment in IBD New tools for therapeutic monitoring Biologic therapy for CD and
Laboratory and Genetic Testing for use of Thiopurines
 Medical Policy Manual Laboratory, Policy No. 70 Laboratory and Genetic Testing for use of Thiopurines Next Review: January 2019 Last Review: January 2018 Effective: March 1, 2018 IMPORTANT REMINDER Medical
Medical Policy Manual Laboratory, Policy No. 70 Laboratory and Genetic Testing for use of Thiopurines Next Review: January 2019 Last Review: January 2018 Effective: March 1, 2018 IMPORTANT REMINDER Medical
Personalized Medicine in IBD
 Personalized Medicine in IBD Anita Afzali MD, MPH Assistant Professor of Medicine Director, Inflammatory Bowel Diseases Program University of Washington Harborview Medical Center CCFA April 2 nd, 2016
Personalized Medicine in IBD Anita Afzali MD, MPH Assistant Professor of Medicine Director, Inflammatory Bowel Diseases Program University of Washington Harborview Medical Center CCFA April 2 nd, 2016
Positioning Biologics in Ulcerative Colitis
 Positioning Biologics in Ulcerative Colitis Bruce E. Sands, MD, MS Acting Chief, Gastrointestinal Unit Massachusetts General Hospital Associate Professor of Medicine Harvard Medical School Sequential Therapies
Positioning Biologics in Ulcerative Colitis Bruce E. Sands, MD, MS Acting Chief, Gastrointestinal Unit Massachusetts General Hospital Associate Professor of Medicine Harvard Medical School Sequential Therapies
EDUCATION PRACTICE. Initiating Azathioprine for Crohn s Disease. The Problem. Clinical Scenario. Management Strategies Education
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2012;10:460 465 EDUCATION PRACTICE Initiating Azathioprine for Crohn s Disease BARRETT G. LEVESQUE* and EDWARD V. LOFTUS JR *Scripps Clinic, Division of Gastroenterology,
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2012;10:460 465 EDUCATION PRACTICE Initiating Azathioprine for Crohn s Disease BARRETT G. LEVESQUE* and EDWARD V. LOFTUS JR *Scripps Clinic, Division of Gastroenterology,
Moderately to severely active ulcerative colitis
 Adalimumab in the Treatment of Moderate-to-Severe Ulcerative Colitis: ULTRA 2 Trial Results Sandborn WJ, van Assche G, Reinisch W, et al. Adalimumab induces and maintains clinical remission in patients
Adalimumab in the Treatment of Moderate-to-Severe Ulcerative Colitis: ULTRA 2 Trial Results Sandborn WJ, van Assche G, Reinisch W, et al. Adalimumab induces and maintains clinical remission in patients
Choosing and Positioning Biologic Therapy for Crohn s Disease: (Still) Looking for the Crystal Ball
 Choosing and Positioning Biologic Therapy for Crohn s Disease: (Still) Looking for the Crystal Ball Siddharth Singh, MD, MS Assistant Professor of Medicine Division of Gastroenterology Division of Biomedical
Choosing and Positioning Biologic Therapy for Crohn s Disease: (Still) Looking for the Crystal Ball Siddharth Singh, MD, MS Assistant Professor of Medicine Division of Gastroenterology Division of Biomedical
Beyond Anti TNFs: positioning of other biologics for Crohn s disease. Christina Ha, MD Cedars Sinai Inflammatory Bowel Disease Center
 Beyond Anti TNFs: positioning of other biologics for Crohn s disease Christina Ha, MD Cedars Sinai Inflammatory Bowel Disease Center Objectives: To define high and low risk patient and disease features
Beyond Anti TNFs: positioning of other biologics for Crohn s disease Christina Ha, MD Cedars Sinai Inflammatory Bowel Disease Center Objectives: To define high and low risk patient and disease features
Biologics in IBD. Brian P. Bosworth, MD, NYSGEF Associate Professor of Medicine Weill Cornell Medical College
 Biologics in IBD Brian P. Bosworth, MD, NYSGEF Associate Professor of Medicine Weill Cornell Medical College Case 30 year old man diagnosed with ulcerative proctitis diagnosed in 2003 Had been maintained
Biologics in IBD Brian P. Bosworth, MD, NYSGEF Associate Professor of Medicine Weill Cornell Medical College Case 30 year old man diagnosed with ulcerative proctitis diagnosed in 2003 Had been maintained
IBD :- a new era of diagnostics and therapy Dr Martyn Dibb Consultant Luminal Gastroenterologist Royal Liverpool University Hospital
 IBD :- a new era of diagnostics and therapy Dr Martyn Dibb Consultant Luminal Gastroenterologist Royal Liverpool University Hospital Aims To understand the aetiology of IBD To understand the impact that
IBD :- a new era of diagnostics and therapy Dr Martyn Dibb Consultant Luminal Gastroenterologist Royal Liverpool University Hospital Aims To understand the aetiology of IBD To understand the impact that
Drug Level Monitoring in IBD. Objectives
 Drug Level Monitoring in IBD Corey A. Siegel, MD, MS Director, Dartmouth-Hitchcock IBD Center Associate Professor of Medicine, Geisel School of Medicine at Dartmouth Objectives Review non-biologic drug
Drug Level Monitoring in IBD Corey A. Siegel, MD, MS Director, Dartmouth-Hitchcock IBD Center Associate Professor of Medicine, Geisel School of Medicine at Dartmouth Objectives Review non-biologic drug
The Refractory Crohn s Disease
 The Refractory Crohn s Disease Patient David T. Rubin, MD, FACG Professor of Medicine Co-Director, Inflammatory Bowel Disease Center Interim Chief, Section of Gastroenterology, Hepatology and Nutrition
The Refractory Crohn s Disease Patient David T. Rubin, MD, FACG Professor of Medicine Co-Director, Inflammatory Bowel Disease Center Interim Chief, Section of Gastroenterology, Hepatology and Nutrition
Immunogenicity of Biologic Agents and How to Prevent Sensitization
 Immunogenicity of Biologic Agents and How to Prevent Sensitization William J. Sandborn, MD Professor and Chief, Division of Gastroenterology Director, UCSD IBD Center La Jolla, California, USA Learning
Immunogenicity of Biologic Agents and How to Prevent Sensitization William J. Sandborn, MD Professor and Chief, Division of Gastroenterology Director, UCSD IBD Center La Jolla, California, USA Learning
Indications for use of Infliximab
 Indications for use of Infliximab Moscow, June 10 th 2006 Prof. Dr. Dr. Gerhard Rogler Klinik und Poliklinik für Innere Medizin I Universität Regensburg Case report 1989: Diagnosis of Crohn s disease of
Indications for use of Infliximab Moscow, June 10 th 2006 Prof. Dr. Dr. Gerhard Rogler Klinik und Poliklinik für Innere Medizin I Universität Regensburg Case report 1989: Diagnosis of Crohn s disease of
Severe IBD: What to Do When Anti- TNFs Don t Work?
 Severe IBD: What to Do When Anti- TNFs Don t Work? David T. Rubin, MD, FACG Professor of Medicine Co-Director, Inflammatory Bowel Disease Center Interim Chief, Section of Gastroenterology, Hepatology and
Severe IBD: What to Do When Anti- TNFs Don t Work? David T. Rubin, MD, FACG Professor of Medicine Co-Director, Inflammatory Bowel Disease Center Interim Chief, Section of Gastroenterology, Hepatology and
Inflammatory Bowel Disease Drug Therapy 2016
 Inflammatory Bowel Disease Drug Therapy 206 David T. Rubin, MD, FACG Joseph B. Kirsner Professor of Medicine Chief, Section of Gastroenterology, Hepatology and Nutrition Objectives Outline the goals of
Inflammatory Bowel Disease Drug Therapy 206 David T. Rubin, MD, FACG Joseph B. Kirsner Professor of Medicine Chief, Section of Gastroenterology, Hepatology and Nutrition Objectives Outline the goals of
When can I stop taking my medications? Maria T. Abreu, MD University of Miami Miller School of Medicine Miami, Florida
 When can I stop taking my medications? Maria T. Abreu, MD University of Miami Miller School of Medicine Miami, Florida Post-op low risk patient Uc de-escalation Discuss combo therapy Which one worked IBD
When can I stop taking my medications? Maria T. Abreu, MD University of Miami Miller School of Medicine Miami, Florida Post-op low risk patient Uc de-escalation Discuss combo therapy Which one worked IBD
CCFA. Crohns Disease vs UC: What is the best treatment for me? November
 CCFA Crohns Disease vs UC: What is the best treatment for me? November 8 2009 Ellen J. Scherl,, MD, FACP,AGAF Roberts Inflammatory Bowel Disease Center Weill Medical College Cornell University New York
CCFA Crohns Disease vs UC: What is the best treatment for me? November 8 2009 Ellen J. Scherl,, MD, FACP,AGAF Roberts Inflammatory Bowel Disease Center Weill Medical College Cornell University New York
New treatment options in UC. Rob Bryant IBD Consultant Royal Adelaide Hospital
 New treatment options in UC Rob Bryant IBD Consultant Royal Adelaide Hospital Talk Outline 1. Raising expectations 2. Optimising UC therapy 3. Clinical trials 4. What s new on the PBS? 5. Questions 1.
New treatment options in UC Rob Bryant IBD Consultant Royal Adelaide Hospital Talk Outline 1. Raising expectations 2. Optimising UC therapy 3. Clinical trials 4. What s new on the PBS? 5. Questions 1.
DATA SHEET. LANVIS is variably absorbed following oral administration and plasma drug levels may be reduced following emesis or intake of food.
 DATA SHEET 1. PRODUCT NAME (strength pharmaceutical form) LANVIS TM (Thioguanine Tablets 40mg) 2. QUALITATIVE AND QUANTITATIVE COMPOSITION White to off-white tablet, round, biconvex scored and debossed
DATA SHEET 1. PRODUCT NAME (strength pharmaceutical form) LANVIS TM (Thioguanine Tablets 40mg) 2. QUALITATIVE AND QUANTITATIVE COMPOSITION White to off-white tablet, round, biconvex scored and debossed
Update on Biologics in Ulcerative Colitis. Scott Plevy, MD University of North Carolina Chapel Hill, NC
 Update on Biologics in Ulcerative Colitis Scott Plevy, MD University of North Carolina Chapel Hill, NC Objectives Discuss the latest advances in the pharmacologic management of ulcerative colitis Describe
Update on Biologics in Ulcerative Colitis Scott Plevy, MD University of North Carolina Chapel Hill, NC Objectives Discuss the latest advances in the pharmacologic management of ulcerative colitis Describe
An Update on the Biologic Treatment for Patients with Inflammatory Bowel Disease. David A. Schwartz, MD
 An Update on the Biologic Treatment for Patients with Inflammatory Bowel Disease David A. Schwartz, MD Director, Inflammatory Bowel Disease Center Associate Professor of Medicine Vanderbilt University
An Update on the Biologic Treatment for Patients with Inflammatory Bowel Disease David A. Schwartz, MD Director, Inflammatory Bowel Disease Center Associate Professor of Medicine Vanderbilt University
Medical Management of Inflammatory Bowel Disease
 Medical Management of Inflammatory Bowel Disease John K. Marshall MD MSc FRCPC AGAF Division of Gastroenterology McMaster University John K. Marshall: Conflicts of Interest Speaker: AbbVie, Allergan, Ferring,
Medical Management of Inflammatory Bowel Disease John K. Marshall MD MSc FRCPC AGAF Division of Gastroenterology McMaster University John K. Marshall: Conflicts of Interest Speaker: AbbVie, Allergan, Ferring,
Maximizing the efficacy of therapies for inflammatory bowel
 Therapeutic Drug Monitoring in Children and Young Adults With Inflammatory Bowel Disease: A Practical Approach Namita Singh, MD, and Marla C. Dubinsky, MD Dr Singh is an attending physician in the Pediatric
Therapeutic Drug Monitoring in Children and Young Adults With Inflammatory Bowel Disease: A Practical Approach Namita Singh, MD, and Marla C. Dubinsky, MD Dr Singh is an attending physician in the Pediatric
NEW CONCEPTS IN CROHN S DISEASE GLENDON BURRESS, MD PEDIATRIC GASTROENTEROLOGY ROCKFORD, IL
 NEW CONCEPTS IN CROHN S DISEASE GLENDON BURRESS, MD PEDIATRIC GASTROENTEROLOGY ROCKFORD, IL CROHN S DISEASE Chronic disease of uncertain etiology Etiology- genetic, environmental, and infectious Transmural
NEW CONCEPTS IN CROHN S DISEASE GLENDON BURRESS, MD PEDIATRIC GASTROENTEROLOGY ROCKFORD, IL CROHN S DISEASE Chronic disease of uncertain etiology Etiology- genetic, environmental, and infectious Transmural
To help protect your privacy, PowerPoint prevented this external picture from being automatically downloaded. To download and display this picture,
 To help protect your privacy, PowerPoint prevented this external picture from being automatically downloaded. To download and display this picture, click Options in the Message Bar, and then click Enable
To help protect your privacy, PowerPoint prevented this external picture from being automatically downloaded. To download and display this picture, click Options in the Message Bar, and then click Enable
DENOMINATOR: All patients aged 18 and older with a diagnosis of inflammatory bowel disease
 Measure #270: Inflammatory Bowel Disease (IBD): Preventive Care: Corticosteroid Sparing Therapy National Quality Strategy Domain: Effective Clinical Care 2016 PQRS OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY
Measure #270: Inflammatory Bowel Disease (IBD): Preventive Care: Corticosteroid Sparing Therapy National Quality Strategy Domain: Effective Clinical Care 2016 PQRS OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY
Clinical Policy: Vedolizumab (Entyvio) Reference Number: CP.PHAR.265
 Clinical Policy: (Entyvio) Reference Number: CP.PHAR.265 Effective Date: 07/16 Last Review Date: 07/17 Coding Implications Revision Log See Important Reminder at the end of this policy for important regulatory
Clinical Policy: (Entyvio) Reference Number: CP.PHAR.265 Effective Date: 07/16 Last Review Date: 07/17 Coding Implications Revision Log See Important Reminder at the end of this policy for important regulatory
Treatment of ulcerative colitis with adalimumab or infliximab: long-term follow-up of a single-centre cohort
 Alimentary Pharmacology and Therapeutics Treatment of ulcerative colitis with adalimumab or infliximab: long-term follow-up of a single-centre cohort N. Gies, K. I. Kroeker, K. Wong & R. N. Fedorak Division
Alimentary Pharmacology and Therapeutics Treatment of ulcerative colitis with adalimumab or infliximab: long-term follow-up of a single-centre cohort N. Gies, K. I. Kroeker, K. Wong & R. N. Fedorak Division
Position of Biologics in IBD Circa 2006: Top Down vs. Step Up Therapy
 Position of Biologics in IBD Circa 2006: Top Down vs. Step Up Therapy Stephen B. Hanauer, MD University of Chicago Potential Conflicts: Centocor/Schering, Abbott, UCB, Elan, Berlex, PDL Goals of Treatment
Position of Biologics in IBD Circa 2006: Top Down vs. Step Up Therapy Stephen B. Hanauer, MD University of Chicago Potential Conflicts: Centocor/Schering, Abbott, UCB, Elan, Berlex, PDL Goals of Treatment
Outcomes of immunosuppressors and biologic drugs in inflammatory bowel diseases: a real life experience
 Outcomes of immunosuppressors and biologic drugs in inflammatory bowel Treatments and therapeutic approaches in IBD are constantly evolving. The newly emerged biologic treatments are one such evolving
Outcomes of immunosuppressors and biologic drugs in inflammatory bowel Treatments and therapeutic approaches in IBD are constantly evolving. The newly emerged biologic treatments are one such evolving
Pharmacogenomic and Metabolite Markers for Patients Treated with Thiopurines
 Pharmacogenomic and Metabolite Markers for Patients Treated with Thiopurines Applies to all products administered or underwritten by Blue Cross and Blue Shield of Louisiana and its subsidiary, HMO Louisiana,
Pharmacogenomic and Metabolite Markers for Patients Treated with Thiopurines Applies to all products administered or underwritten by Blue Cross and Blue Shield of Louisiana and its subsidiary, HMO Louisiana,
Immunosuppressants. Assistant Prof. Dr. Najlaa Saadi PhD Pharmacology Faculty of Pharmacy University of Philadelphia
 Immunosuppressants Assistant Prof. Dr. Najlaa Saadi PhD Pharmacology Faculty of Pharmacy University of Philadelphia Immunosuppressive Agents Very useful in minimizing the occurrence of exaggerated or inappropriate
Immunosuppressants Assistant Prof. Dr. Najlaa Saadi PhD Pharmacology Faculty of Pharmacy University of Philadelphia Immunosuppressive Agents Very useful in minimizing the occurrence of exaggerated or inappropriate
Fistulizing Crohn s Disease: The Aggressive Approach
 Fistulizing Crohn s Disease: The Aggressive Approach Bruce E. Sands, MD, MS MGH Crohn s and Colitis Center and Gastrointestinal Unit Massachusetts General Hospital Boston, USA Case Presentation: Summary
Fistulizing Crohn s Disease: The Aggressive Approach Bruce E. Sands, MD, MS MGH Crohn s and Colitis Center and Gastrointestinal Unit Massachusetts General Hospital Boston, USA Case Presentation: Summary
Inflammatory bowel disease (IBD) Overview of the Paediatric investigation plans. Presented by: Richard Veselý. An agency of the European Union
 Inflammatory bowel disease (IBD) Overview of the Paediatric investigation plans Presented by: Richard Veselý An agency of the European Union Adalimumab - Crohn s disease Indication: Treatment of severe,
Inflammatory bowel disease (IBD) Overview of the Paediatric investigation plans Presented by: Richard Veselý An agency of the European Union Adalimumab - Crohn s disease Indication: Treatment of severe,
Personalized Medicine in IBD: Where Are We in 2013
 Personalized Medicine in IBD: Where Are We in 2013 David A. Schwartz, MD Director, Inflammatory Bowel Disease Center Associate Professor of Medicine Vanderbilt University Medical Center What is Personalized
Personalized Medicine in IBD: Where Are We in 2013 David A. Schwartz, MD Director, Inflammatory Bowel Disease Center Associate Professor of Medicine Vanderbilt University Medical Center What is Personalized
Studies on inflammatory bowel disease and functional gastrointestinal disorders in children and adults Hoekman, D.R.
 UvA-DARE (Digital Academic Repository) Studies on inflammatory bowel disease and functional gastrointestinal disorders in children and adults Hoekman, D.R. Link to publication Citation for published version
UvA-DARE (Digital Academic Repository) Studies on inflammatory bowel disease and functional gastrointestinal disorders in children and adults Hoekman, D.R. Link to publication Citation for published version
ENTYVIO (VEDOLIZUMAB)
 ENTYVIO (VEDOLIZUMAB) UnitedHealthcare Community Plan Medical Benefit Drug Policy Policy Number: CS2017D0053F Effective Date: July 1, 2017 Table of Contents Page INSTRUCTIONS FOR USE... 1 BENEFIT CONSIDERATIONS...
ENTYVIO (VEDOLIZUMAB) UnitedHealthcare Community Plan Medical Benefit Drug Policy Policy Number: CS2017D0053F Effective Date: July 1, 2017 Table of Contents Page INSTRUCTIONS FOR USE... 1 BENEFIT CONSIDERATIONS...
Clinical Policy: Natalizumab (Tysabri) Reference Number: ERX.SPA.162 Effective Date:
 Clinical Policy: (Tysabri) Reference Number: ERX.SPA.162 Effective Date: 10.01.16 Last Review Date: 11.17 Revision Log See Important Reminder at the end of this policy for important regulatory and legal
Clinical Policy: (Tysabri) Reference Number: ERX.SPA.162 Effective Date: 10.01.16 Last Review Date: 11.17 Revision Log See Important Reminder at the end of this policy for important regulatory and legal
Crohn's Disease. The What, When, and Why of Treatment
 Crohn's Disease The What, When, and Why of Treatment Brian Feagan, MD, FACG Professor of Medicine and Epidemiology and Biostatistics Director, Robarts Clinical Trials Robarts Research Institute University
Crohn's Disease The What, When, and Why of Treatment Brian Feagan, MD, FACG Professor of Medicine and Epidemiology and Biostatistics Director, Robarts Clinical Trials Robarts Research Institute University
IBD Understanding Your Medications. Thomas V. Aguirre, MD Santa Barbara GI Consultants
 IBD Understanding Your Medications Thomas V. Aguirre, MD Santa Barbara GI Consultants IBD Understanding Your Medications (& Your Doctor) Thomas V. Aguirre, MD Santa Barbara GI Consultants Disclosure I
IBD Understanding Your Medications Thomas V. Aguirre, MD Santa Barbara GI Consultants IBD Understanding Your Medications (& Your Doctor) Thomas V. Aguirre, MD Santa Barbara GI Consultants Disclosure I
Crohn's Disease. The What, When, and Why of Treatment
 Crohn's Disease The What, When, and Why of Treatment Gary R. Lichtenstein, MD, FACG Professor of Medicine Director, Inflammatory Bowel Disease Program University of Pennsylvania Philadelphia, PA In my
Crohn's Disease The What, When, and Why of Treatment Gary R. Lichtenstein, MD, FACG Professor of Medicine Director, Inflammatory Bowel Disease Program University of Pennsylvania Philadelphia, PA In my
Pharmacogenetics to tailor Drug Exposure and Outcomes in Kidney Transplantation
 2017 BANFF-SCT Joint Scientific Meeting BARCELONA 27-31 March 2017 SCT Plenary 4 Thursday March 30, 2017 Pharmacogenetics to tailor Drug Exposure and Outcomes in Kidney Transplantation Dennis A. Hesselink
2017 BANFF-SCT Joint Scientific Meeting BARCELONA 27-31 March 2017 SCT Plenary 4 Thursday March 30, 2017 Pharmacogenetics to tailor Drug Exposure and Outcomes in Kidney Transplantation Dennis A. Hesselink
Sustained Clinical Benefit and Tolerability of Methotrexate Monotherapy After Thiopurine Therapy in Patients With Crohn s Disease
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2013;11:667 672 Sustained Clinical Benefit and Tolerability of Methotrexate Monotherapy After Thiopurine Therapy in Patients With Crohn s Disease MARGIEN L. SEINEN,*
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2013;11:667 672 Sustained Clinical Benefit and Tolerability of Methotrexate Monotherapy After Thiopurine Therapy in Patients With Crohn s Disease MARGIEN L. SEINEN,*
Current management options and recent advances in IBD
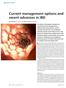 n DRUG REVIEW Current management options and recent advances in IBD Ben Warner BSc, MRCP and Peter Irving MA, MD, FRCP SPL The advent of biological therapies has revolutionised the management of inflammatory
n DRUG REVIEW Current management options and recent advances in IBD Ben Warner BSc, MRCP and Peter Irving MA, MD, FRCP SPL The advent of biological therapies has revolutionised the management of inflammatory
Clinical Trials in IBD. Bruce Yacyshyn MD Professor of Medicine Division of Digestive Diseases
 Clinical Trials in IBD Bruce Yacyshyn MD Professor of Medicine Division of Digestive Diseases Objectives Today s discussion will address the following topics: Similarities and differences between Crohn
Clinical Trials in IBD Bruce Yacyshyn MD Professor of Medicine Division of Digestive Diseases Objectives Today s discussion will address the following topics: Similarities and differences between Crohn
Anne Griffiths MD, FRCPC. SickKids Hospital, University of Toronto. Buenos Aires, August 16, 2014
 Management and Medical Therapies for Crohn disease: strategies to enhance mucosal healing Anne Griffiths MD, FRCPC SickKids Hospital, University of Toronto Buenos Aires, August 16, 2014 New onset Crohn
Management and Medical Therapies for Crohn disease: strategies to enhance mucosal healing Anne Griffiths MD, FRCPC SickKids Hospital, University of Toronto Buenos Aires, August 16, 2014 New onset Crohn
Once Daily Dosing for Induction and Maintenance of Remission in Ulcerative Colitis
 Once Daily Dosing for Induction and Maintenance of Remission in Ulcerative Colitis John K. Marshall MD MSc FRCPC AGAF Division of Gastroenterology McMaster University JKM 2014 Svartz N. Acta Med Scand
Once Daily Dosing for Induction and Maintenance of Remission in Ulcerative Colitis John K. Marshall MD MSc FRCPC AGAF Division of Gastroenterology McMaster University JKM 2014 Svartz N. Acta Med Scand
PDF hosted at the Radboud Repository of the Radboud University Nijmegen
 PDF hosted at the Radboud Repository of the Radboud University Nijmegen The following full text is a publisher's version. For additional information about this publication click this link. http://hdl.handle.net/2066/190666
PDF hosted at the Radboud Repository of the Radboud University Nijmegen The following full text is a publisher's version. For additional information about this publication click this link. http://hdl.handle.net/2066/190666
INFLAMMATORY BOWEL DISEASE
 1. Medical Condition INFLAMMATORY BOWEL DISEASE (IBD) specifically includes Crohn s disease (CD) and ulcerative colitis (UC) but also includes IBD unclassified (IBDu), seen in about 10% of cases. These
1. Medical Condition INFLAMMATORY BOWEL DISEASE (IBD) specifically includes Crohn s disease (CD) and ulcerative colitis (UC) but also includes IBD unclassified (IBDu), seen in about 10% of cases. These
Systemic Medications for the Dermatology Toolbox: Azathioprine
 Systemic Medications for the Dermatology Toolbox: Azathioprine Wynnis Tom, M.D. Associate Clinical Professor University of California, San Diego and Rady Children s Hospital Faculty Disclosure Information
Systemic Medications for the Dermatology Toolbox: Azathioprine Wynnis Tom, M.D. Associate Clinical Professor University of California, San Diego and Rady Children s Hospital Faculty Disclosure Information
