Diagnosis and treatment of gallbladder perforation
|
|
|
- Griffin Powers
- 6 years ago
- Views:
Transcription
1 PO Box 2345, Beijing , China World J Gastroenterol 2006 December 28; 12(48): World Journal of Gastroenterology ISSN wjg@wjgnet.com 2006 The WJG Press. All rights reserved. RAPID COMMUNICATION Diagnosis and treatment of gallbladder perforation Hayrullah Derici, Cemal Kara, Ali Dogan Bozdag, Okay Nazli, Tugrul Tansug, Esra Akca Hayrullah Derici, Cemal Kara, Ali Dogan Bozdag, Okay Nazli, Tugrul Tansug, Esra Akca, Third Surgical Clinic of Atatürk Training and Research Hospital, Izmir 35360, Turkey Correspondence to: Dr. Hayrullah Derici, Third Surgical Clinic of Atatürk Training and Research Hospital, 156 sok. No. 5/13 Bornova, Izmir 35360, Turkey. hayrullahderici@yahoo.com Telephone: Fax: Received: Accepted: Abstract AIM: To present our clinical experience with gallbladder perforation cases. METHODS: Records of 332 patients who received medical and/or surgical treatment with the diagnosis of acute cholecystitis in our clinic between 1997 and 2006 were reviewed retrospectively. Sixteen (4.8%) of those patients had gallbladder perforation. The parameters including age, gender, time from the onset of symptoms to the time of surgery, diagnostic procedures, surgical treatment, morbidity, and mortality were evaluated. RESULTS: Seven patients had type gallbladder perforation, 7 type gallbladder perforation, and 2 type gallbladder perforation according to Niemeier s classification. The patients underwent surgery after administration of intravenous electrolyte solutions, and were treated with analgesics and antibiotics within the first 36 h (mean 9 h) after admission. Two patients died of sepsis and multiple organ failure in the early postoperative period. Subhepatic abscess, pelvic abscess, pneumonia, pancreatitis, and acute renal failure were found in 6 patients. CONCLUSION: Early diagnosis and emergency surgical treatment of gallbladder perforation are of crucial importance. Upper abdominal computerized tomography for acute cholecystitis patients may contribute to the preoperative diagnosis of gallbladder perforation The WJG Press. All rights reserved. Key words: Acute cholecystitis; Gallbladder perforation; Early diagnosis; Computed tomography; Emergency surgery Derici H, Kara C, Bozdag AD, Nazli O, Tansug T, Akca E. Diagnosis and treatment of gallbladder perforation. World J Gastroenterol 2006; 12(48): INTRODUCTION Gallbladder perforation (GBP) is a rare but life threatening complication of acute cholecystitis. Sometimes GBP may not be different from uncomplicated acute cholecystitis with high morbidity and mortality rates because of delay in diagnosis [1-3]. Thus GBP still continues to be an important problem for the surgeons. Most cases can only be diagnosed during surgery [1,4]. Male acute cholecystitis cases with high fever, high white blood cell (WBC) count, and associated systemic diseases should be meticulously investigated [1,5,6]. Niemeier [7] in 1934, classified free gallbladder perforation and generalized biliary peritonitis as acute or type GBP, pericholecystic abscess and localized peritonitis as subacute or type GBP, and cholecystoenteric fistula as chronic or type GBP. This classification is still in use. We aimed to present our clinical experience with GBP in this study. MATERIALS AND METHODS Subjects Records of 332 patients who received medical and/or surgical treatment with the diagnosis acute cholecystitis in our clinic between January 1997 and February 2006 were reviewed retrospectively. Sixteen (4.8%) of those patients were found to have gallbladder perforation. Perforations due to trauma, iatrogenic causes, and gallbladder (GB) carcinoma were excluded. Methods The original classification of Niemeier [7] was used to identify the patients. The parameters including age, gender, time from the onset of symptoms to the time of surgery, diagnostic procedures, surgical treatment, postoperative morbidity and mortality were evaluated. Direct abdominal X-ray series, abdominal ultrasound scanning (US), abdominal contrast-enhanced computerized tomography (CT), routine blood cell count, and blood chemistry tests were performed. Peritoneal spaces were lavaged thoroughly with isotonic saline and drains were placed for postoperative drainage in all of the patients. RESULTS There were 10 male and 6 female patients. Their mean age was 69 (range, 54-85) years. Their complaints were abdominal pain, poor general condition, high fever, nausea, and vomiting on admission. Cholelithiasis was unknown prior to perforation in 5 patients. The patients
2 Derici H et al. Gallbladder perforations 7833 Figure 1 Contrast-enhanced CT image at the level of gallbladder. Figure 2 Contrast-enhanced CT image of hepatic abscess adjacent to the superior part of gallbladder. had several associated diseases, of which atherosclerotic heart disease (AHD) was the most common. One patient with type gallbladder perforation was on long term steroid treatment for systemic lupus erythematosus. White blood cell (WBC) count was high in 14 patients, and 10 patients had high fever. Patients with type gallbladder perforation had signs of peritoneal irritation such as extensive abdominal tenderness, guarding and rebound tenderness. Patients with type gallbladder perforation had local tenderness, guarding, positive Murphy s sign and 4 of them had palpable right subcostal mass while one patient had jaundice with a total bilirubin level of 28 mg/ dl. Two patients with type gallbladder perforation had epigastric tenderness and one of them also had abdominal distension. Four patients had systemic inflammatory response syndrome, of them two patients with type gallbladder perforation and two with type and type gallbladder perforations. The number of patients and their clinical features in each type of gallbladder perforation are shown in Table 1. Abdominal X-ray series and abdominal US were performed for all of the patients and abdominal CT scanning for 14 patients. Only one patient with type gallbladder perforation had air-fluid levels on direct abdominal radiograms. Abdominal US showed gall stones in all of the patients with type and type gallbladder perforations, extensive intraperitoneal free fluid in 7 patients with type gallbladder perforation, and a small amount of pericholecystic free fluid in 6 patients with type gallbladder perforation. Abdominal US did not show GB wall defect in any of the patients. CT revealed GB wall thickening in all of the patients, gall stones in 10 patients, extensive intraperitoneal free fluid in 5 patients, a small amount of pericholecystic free fluid in 7 patients, and GB perforation sites in 5 patients. Abdominal CT and US detected liver abscesses in 2 patients, dilated extra and intrahepatic bile ducts in 1 patient. Abdominal CT showed dilated intestinal loops suggesting mechanical obstruction in one patient with type gallbladder perforation. Abdominal CT showed dilated stomach suggesting gastric outlet syndrome in another patient. The stomach was dilated with a normal mucosa, but the gall stone could not be seen during upper gastrointestinal endoscopy of this patient. Table 1 Clinical features of the patients, n (%) Feature Type Type Type n (%) 7 (43.7) 7 (43.7) 2 (12.6) Mean age (yr) Gender (Male/Female) 5/2 5/2 0/2 Fever (more than 38 ), n (%) 5 (71.4) 5 (71.4) - White blood cell count (mean) Mean duration of symptoms (d) Systemic disorders 1, n (%) Atherosclerotic heart disease 4 (14.3) 4 (57.1) 1 (50) Diabetes mellitus 2 (28.6) 1 (14.3) 1 (50) Hypertansion 1 (14.3) 1 (14.3) 1 (50) Systemic lupus erythematosus 1 (14.3) - - Chronic obstructive pulmonary disease 1 (14.3) 2 (28.6) 1 (50) Systemic inflammatory response syndrome 2 (28.6) 1 (14.3) 1 (50) Preoperative diagnoses, n (%) Gallbladder perforation 4 (14.3) 1 (14.3) - Acute cholecystitis 2 (28.6) 4 (14.3) - Cholangitis - 1 (14.3) - Peptic ulcus perforation 1 (14.3) - - Perforated appendicitis - 1 (14.3) - Mechanical bowel obstruction (50) Gastric outlet syndrome (50) Sites of perforation, n (%) Fundus 6 (85.7) 3 (42.9) - Corpus 1 (14.3) 2 (28.6) - Infundibulum - 1 (14.3) 2 (100) Cystic duct - 1 (14.3) - 1 Some patients had more than one sytemic disorder. Enlarged gallbladder, irregularity of the gallbladder walls at the fundic region, air density lateral to the fundus and corpus, and increased density of the mesentery anterior to the fundus suggesting free fluid on CT image of a patient with type gallbladder perforation are shown in Figure 1. The abdominal CT image of a patient with hepatic abscess adjacent to the superior part of GB is shown in Figure 2. The patients underwent surgery after administration of intravenous crystalloid solutions, and were treated with analgesics and antibiotic (third generation cephalo-
3 7834 ISSN CN /R World J Gastroenterol December 28, 2006 Volume 12 Number 48 sporins) within the first 36 h (mean 9 h) after admission. The patients who had associated diseases such as diabetes, chronic obstructive pulmonary disease (COPD), and AHD underwent surgery after specific medical treatment was started. Antibiotic treatment was changed when required, according to the results of microbiological assessment of the infected bile specimens obtained from the gall bladder. The most common preoperative diagnoses were perforated cholecystitis in patients with type gallbladder perforations, and acute cholecystitis in patients with type gallbladder perforations. Laparoscopic cholecystectomy was performed in 6 patients, two of them had type gallbladder perforation, and four type gallbladder perforation. Conversion was required in 2 of them due to unclear anatomy. Laparotomy was performed in the remaining 10 patients. Perforations were recognized intraoperatively in 11 patients. The perforated site of the GB was the fundus in 9 patients, the corpus in 3 patients, the infundibulum in 3 patients, and the cystic duct in 1 patient. Two patients with type gallbladder perforation also had hepatic abscesses, which were covered by the omentum. Hepatic abscesses were also drained in these patients. All of the patients received a cholecystectomy. Common bile duct exploration was performed, gall stones were extracted, and a T-tube was placed into the common bile duct in addition to cholecystectomy in 1 patient with obstructive jaundice. One of the 2 patients had a cholecystoduodenal fistula (type gallbladder perforations) underwent surgery for gastrointestinal tract obstruction due to bile stones in the jejunum, which were removed through an enterotomy. Gall stones were also found in the duodenum of the other patient with type gallbladder perforation and removed through a duodenotomy. The median hospital stay was 15 d (4-26 d). Two patients (12.5%) died of sepsis and multiple organ failure in the early postoperative period. One was a female patient at the age of 79 with type gallbladder perforation and COPD. The other was a 84 year-old male patient with delayed type gallbladder perforation and pericholecystic abscess associated with AHD and diabetes. Subhepatic abscess, pelvic abscess, pneumonia, pancreatitis and acute renal failure were found in 6 patients (Table 2). Subhepatic and pelvic abscesses were drained percutaneously under ultrasound guidance. The other diseases were treated conservatively. Table 2 Surgical procedures and morbidities of the patients n (%) Type Type Type Surgery Laparoscopic cholecystectomy 2 (12.5) 4 (25) - Laparotomy and cholecystectomy 5 (31.2) 3 (18.7) 2 (12.5) Morbidity 1 Subhepatic abscess 1 (11.1) 1 (11.1) Pelvic abscess 1 (11.1) 1 (11.1) Pneumonia 1 (11.1) 1 (11.1) 1 (11.1) Pancreatitis 1 (11.1) Acute renal failure 1 (11.1) 1 Some patients had more than one morbidity. DISCUSSION Inflammation may progress and cause ischemia and necrosis, thus resulting GBP in 2% to 11% of acute cholecystitis patients [6,8,9]. GBP also develops following acalculous cholecystitis, although rare [10,11]. GB fundus, the most distal part with regard to blood supply, is the most common site of perforation [8,12]. The incidence of GBP was 4.5% and the most frequent site of perforation was the fundus (60%) in our study. Six of the 7 type gallbladder perforations and 3 of 7 type gallbladder perforations were at the fundus. When GB is perforated at the fundus, it is less possibly covered by the omentum, thus the bile drains into the peritoneal space. If the perforation site is not at the fundus, it is easily sealed by the omentum or the intestines and the condition remains limited in the right upper quadrant with formation of a plastrone and pericholecystic fluid. This observation suggests that if the perforation site is at the fundus, it is more likely to end up with a type perforation. The relation between the site and the type of GBP has not been defined. Although statistical analysis was not possible because of the insufficient number of patients in this series, this observation may be supported by larger series. Acute uncomplicated cholecystitis is more common among females with a female to male ratio of 2:1 [13]. However, GBP is more frequent in male gender [1,6]. In our study, male patients made up of 60% and the two patients with type gallbladder perforation were females. GBP is usually seen over 60 years of age [4,14]. Roslyn et al [1] reported that type and GBP tend to occur in younger patients, especially more or less at the age of 50 years, whereas type gallbladder perforations are more common in the elderly. The patients with type gallbladder perforation were relatively younger than those with type and gallbladder perforations in our study. Type gallbladder perforations are usually seen in patients with AHD, diabetes, malignancy, cirrhosis, and immunosupressive diseases, or during immunosupressive treatment, without a history of chronic cholecystitis. On the other hand, type gallbladder perforations most often occur in patients with a previous long time history of gall stones [1,9,12]. Severe AHD has been reported in 21% of patients with type and gallbladder perforations, and diabetes, in 25% of patients with type gallbladder perforation [8,14]. Such high rates are related to vascular disorders caused by these systemic diseases. It has been reported that type GBP occurs more frequently [1,3,9,12]. The incidence of type and gallbladder perforations was equal and the most frequent associated systemic disease was AHD in the present study. Type gallbladder perforations usually occur in chronic cholecystitis patients with obstructive gastrointestinal symptoms [9,12,15]. Since the symptoms of type - GBP and uncomplicated cholecystitis are similar, differential diagnosis may be difficult based on physical examination, laboratory tests, and radiological methods and the diagnosis may not be established
4 Derici H et al. Gallbladder perforations 7835 preoperatively [6,12]. Delay in diagnosis is the major cause of its high morbidity and mortality [1,4,9,16]. Tanaka et al [17] reported that only one patient had a concrete diagnosis preoperatively in their series of 9 patients. The majority of GBP patients include those who undergo early surgery with the diagnosis of acute cholecystitis. The main complaint of the patients is abdominal pain accompanied with nausea and vomiting during the last 7 d [12,18]. The duration of symptoms was shorter in patients with type gallbladder perforation than in patients with type and gallbladder perforation in our study. High fever and elevated WBC count are not the diagnostic indications for gallbladder perforation. Parker et al [19] reported that high fever and high WBC count could be observed in 56% and 59% of patients with acute cholecystitis, respectively. The majority of type and gallbladder perforation cases had fever whereas type gallbladder perforation cases did not in our study. The patients with type and gallbladder perforation had elevated WBC count, but those with type gallbladder perforation had only a mild increase in WBC count. US findings in acute cholecystitis, such as the GB wall thickening, GB distension, pericholecystic free fluid, and positive sonographic Murphy sign, may also be present in gallbladder perforation cases [2,9,20]. Sood et al [2] noted that the sonographic hole sign, in which the defect in GB wall is visualized, is the only reliable sign of gallbladder perforation. They reported that GB wall defect could be shown with a high resolution ultrasound scanner device in 70% of patients [2]. However, Kim et al [21] reported that the site of defect could not be visualized on US in any patients, which is similar to our study. On the other hand, CT can show more accurate signs of free intraperitoneal fluid, pericholecystic fluid, and abscess [1,2,22]. CT can also show GB wall thickness and the defect on the wall due to perforation [2,20]. In our study, all of the 5 patients who had the diagnosis of gallbladder perforation preoperatively were diagnosed by CT. Since the patients were admitted for acute abdominal pain, standard pelvic CT rather than upper abdominal CT was applied. Kim et al [21] reported that the defect could not be visualized on CT in 54% of patients. Doppler ultrasound, magnetic resonance imaging and radionuclide methods have been used in the diagnosis of gallbladder perforation [23-25]. The majority of our patients with type gallbladder perforation were initially treated conservatively and then underwent surgery as no improvement was observed during the first 3 d. Cholecystectomy, drainage of abscess if present, and abdominal lavage are usually sufficient to treat gallbladder perforation [1,4]. Cholecystectomy may be difficult in type gallbladder perforations. If a cholesystectomy is performed, additional surgical procedures such as repair of the fistula may be required [15,16]. Cholecystectomy can be performed after the infection is relived by US guided percutaneus drainage in type gallbladder perforations [22]. Laparoscopic cholecystectomy can be performed for acute, gangrenous, and/or perforated cholecystitis as well as uncomplicated cholecystitis, but a conversion may be necessary in case of difficulties like an unclear anatomy [9,16]. In our study, laparoscopic procedure was initiated in 6 patients but conversion was required in two. Since the difficulties in diagnosis cause delay in treatment, higher morbidity and mortality rates are often encountered [1,2,9]. Glenn and Moore [26] have reported that the mortality rate of gallbladder perforation patients is 42%, while other studies reported that the mortality rates are decreased to 12%-16% owing to the developments in anesthesiology and intensive care conditions [1,3]. The morbidity and mortality rates were 37.5% and 12.5%, respectively in the present study. In conclusion, early diagnosis of gallbladder perforation and immediate surgical intervention are of crucial importance. Although standard abdominal CT has an important role in diagnosing gallbladder perforation, upper abdominal CT for acute cholecystitis in which pericholecystic fluid is found by US may increase the rate of preoperative diagnosis of gallbladder perforation. REFERENCES 1 Roslyn JJ, Thompson JE Jr, Darvin H, DenBesten L. Risk factors for gallbladder perforation. Am J Gastroenterol 1987; 82: Sood BP, Kalra N, Gupta S, Sidhu R, Gulati M, Khandelwal N, Suri S. Role of sonography in the diagnosis of gallbladder perforation. J Clin Ultrasound 2002; 30: Lennon F, Green WE. Perforation of the gallbladder. A review of 32 cases. J R Coll Surg Edinb 1983; 28: Ong CL, Wong TH, Rauff A. Acute gall bladder perforation-a dilemma in early diagnosis. Gut 1991; 32: Lein HH, Huang CS. Male gender: risk factor for severe symptomatic cholelithiasis. World J Surg 2002; 26: Bedirli A, Sakrak O, Sozuer EM, Kerek M, Guler I. Factors effecting the complications in the natural history of acute cholecystitis. Hepatogastroenterology 2001; 48: Niemeier OW. Acute free perforation of the gall bladder. Ann Surg 1934; 99: Abu-Dalu J, Urca I. Acute cholecystitis with perforation into the peritoneal cavity. Arch Surg 1971; 102: Menakuru SR, Kaman L, Behera A, Singh R, Katariya RN. Current management of gall bladder perforations. ANZ J Surg 2004; 74: Wang AJ, Wang TE, Lin CC, Lin SC, Shih SC. Clinical predictors of severe gallbladder complications in acute acalculous cholecystitis. World J Gastroenterol 2003; 9: Babb RR. Acute acalculous cholecystitis. A review. J Clin Gastroenterol 1992; 15: Isch JH, Finneran JC, Nahrwold DL. Perforation of the gallbladder. Am J Gastroenterol 1971; 55: Glenn F. Acute cholecystitis. Surg Gynecol Obstet 1976; 143: Williams NF, Scobie TK. Perforation of the gallbladder: analysis of 19 cases. Can Med Assoc J 1976; 115: Doko M, Zovak M, Kopljar M, Glavan E, Ljubicic N, Hochstadter H. Comparison of surgical treatments of gallstone ileus: preliminary report. World J Surg 2003; 27: Doherty GM, Way LW. Biliary Tract. In: Way LW, Doherty GM. Current Surgical Diagnosis & Treatment. 11st ed. New York: McGraw-Hill, 2003: Tanaka M, Takahashi H, Yajima Y, Okamura K, Kosaka A, Mizumoto R. Idiopathic perforation of the gallbladder: report of a case and a review of the Japanese literature. Surg Today 1997;27: Felice PR, Trowbridge PE, Ferrara JJ. Evolving changes in the pathogenesis and treatment of the perforated gallbladder. A combined hospital study. Am J Surg 1985; 149: Parker LJ, Vukov LF, Wollan PC. Emergency department evaluation of geriatric patients with acute cholecystitis. Acad Emerg Med 1997; 4: Forsberg L, Andersson R, Hederstrom E, Tranberg KG. Ultra-
5 7836 ISSN CN /R World J Gastroenterol December 28, 2006 Volume 12 Number 48 sonography and gallbladder perforation in acute cholecystitis. Acta Radiol 1988; 29: Kim PN, Lee KS, Kim IY, Bae WK, Lee BH. Gallbladder perforation: comparison of US findings with CT. Abdom Imaging 1994; 19: van Sonnenberg E, D Agostino H, Casola G. Interventional gallbladder procedures. Radiol Clin North Am 1990; 28: Sood B, Jain M, Khandelwal N, Singh P, Suri S. MRI of perforated gall bladder. Australas Radiol 2002; 46: Konno K, Ishida H, Sato M, Naganuma H, Obara K, Andoh H, Watanabe S. Gallbladder perforation: color Doppler findings. Abdom Imaging 2002; 27: Stadalnik RC, Matolo NM. Radionuclide imaging of the biliary tree. Surg Clin North Am 1981; 61: Glenn F, Moore SW. Gangrene and perforation of the wall of the gallbladder. A sequele of acute cholecystitis. Arch Surg 1942; 44: S- Editor Wang GP L- Editor Wang XL E- Editor Bai SH
Abdominal Imaging. Gallbladder perforation: color Doppler findings
 Abdom Imaging 27:47 50 (2002) DOI: 10.1007/s00261-001-0048-1 Abdominal Imaging Springer-Verlag New York Inc. 2002 Gallbladder perforation: color Doppler findings K. Konno, 1 H. Ishida, 1 M. Sato, 1 H.
Abdom Imaging 27:47 50 (2002) DOI: 10.1007/s00261-001-0048-1 Abdominal Imaging Springer-Verlag New York Inc. 2002 Gallbladder perforation: color Doppler findings K. Konno, 1 H. Ishida, 1 M. Sato, 1 H.
Gallstone ileus:diagnostic and therapeutic dilemma
 Saurabh et al. 1 CASE SERIES OPEN ACCESS Gallstone ileus:diagnostic and therapeutic dilemma Shireesh Saurabh, Andrew Camerota, Jeffrey Zavotsky ABSTRACT Introduction: Gallstone ileus is a rare complication
Saurabh et al. 1 CASE SERIES OPEN ACCESS Gallstone ileus:diagnostic and therapeutic dilemma Shireesh Saurabh, Andrew Camerota, Jeffrey Zavotsky ABSTRACT Introduction: Gallstone ileus is a rare complication
Gallbladder perforation - radiological aspects, types and causes, ultrasound and CT findings
 Gallbladder perforation - radiological aspects, types and causes, ultrasound and CT findings Poster No.: C-1905 Congress: ECR 2013 Type: Educational Exhibit Authors: V. Urban, M. Djosev, T. Nastasic, B.
Gallbladder perforation - radiological aspects, types and causes, ultrasound and CT findings Poster No.: C-1905 Congress: ECR 2013 Type: Educational Exhibit Authors: V. Urban, M. Djosev, T. Nastasic, B.
Cholecystitis is defined as nonspecific inflammation of the gallbladder with or without cholelithiasis. Types: calculous and acalculous.
 Cholecystitis is defined as nonspecific inflammation of the gallbladder with or without cholelithiasis. Types: calculous and acalculous. Anatomy of the gallbladder The gallbladder, a pear-shaped reservoir
Cholecystitis is defined as nonspecific inflammation of the gallbladder with or without cholelithiasis. Types: calculous and acalculous. Anatomy of the gallbladder The gallbladder, a pear-shaped reservoir
Pre-operative prediction of difficult laparoscopic cholecystectomy
 International Surgery Journal http://www.ijsurgery.com pissn 2349-3305 eissn 2349-2902 Research Article DOI: http://dx.doi.org/10.18203/2349-2902.isj20151083 Pre-operative prediction of difficult laparoscopic
International Surgery Journal http://www.ijsurgery.com pissn 2349-3305 eissn 2349-2902 Research Article DOI: http://dx.doi.org/10.18203/2349-2902.isj20151083 Pre-operative prediction of difficult laparoscopic
Cholelithiasis & cholecystitis
 1 Cholelithiasis & cholecystitis Dr. Muhammad Shamim FCPS (Pak), FACS (USA), FICS (USA) Assistant Professor, Dept. of Surgery College of Medicine, Prince Sattam bin Abdulaziz University Email: surgeon.shamim@gmail.com
1 Cholelithiasis & cholecystitis Dr. Muhammad Shamim FCPS (Pak), FACS (USA), FICS (USA) Assistant Professor, Dept. of Surgery College of Medicine, Prince Sattam bin Abdulaziz University Email: surgeon.shamim@gmail.com
Management of Gallbladder Disease
 Management of Gallbladder Disease Steven B. Johnson, MD, FACS, FCCM Professor and Chairman, Department of Surgery Program Director, Phoenix Integrated Surgical Residency University of Arizona College of
Management of Gallbladder Disease Steven B. Johnson, MD, FACS, FCCM Professor and Chairman, Department of Surgery Program Director, Phoenix Integrated Surgical Residency University of Arizona College of
Study of post cholecystectomy biliary leakage and its management
 Original Research Article Study of post cholecystectomy biliary leakage and its management P. Krishna Kishore 1*, B. Manju Sruthi 2, G. Obulesu 3 1 Assistant Professor, Departmentment of General Surgery,
Original Research Article Study of post cholecystectomy biliary leakage and its management P. Krishna Kishore 1*, B. Manju Sruthi 2, G. Obulesu 3 1 Assistant Professor, Departmentment of General Surgery,
International Journal of Health Sciences and Research ISSN:
 International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Original Research Article Comparative Study between Laparoscopic and Open Cholecystectomy for Dr. B. Hemasankararao 1,
International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Original Research Article Comparative Study between Laparoscopic and Open Cholecystectomy for Dr. B. Hemasankararao 1,
Abdominal ultrasound:
 Abdominal ultrasound: Non-traumatic acute abdomen Wittanee Na-ChiangMai, MD Department of Radiology ChiangMai University 26/04/2017 Contents Technique of examination Normal anatomy Emergency conditions
Abdominal ultrasound: Non-traumatic acute abdomen Wittanee Na-ChiangMai, MD Department of Radiology ChiangMai University 26/04/2017 Contents Technique of examination Normal anatomy Emergency conditions
Evolving Gallstone Ileus. SUNY Downstate Case Conference January 12, 2012
 Evolving Gallstone Ileus SUNY Downstate Case Conference January 12, 2012 Initial Presentation HPI: 90 yo F c 1wk h/o abdominal pain and N/V. Denied F/C. Passing flatus/bm. PMH: DM, HTN, CAD. PSH: C-sections
Evolving Gallstone Ileus SUNY Downstate Case Conference January 12, 2012 Initial Presentation HPI: 90 yo F c 1wk h/o abdominal pain and N/V. Denied F/C. Passing flatus/bm. PMH: DM, HTN, CAD. PSH: C-sections
A CASE REPORT OF SPONTANEOUS BILOMA - AN ENIGMATIC SURGICAL PROBLEM
 A CASE REPORT OF SPONTANEOUS BILOMA - AN ENIGMATIC SURGICAL PROBLEM *Sumanta Kumar Ghosh and Biswajit Mukherjee ESIC Medical College, Joka, Kolkata, India *Author for Correspondence ABSTRACT Occurrence
A CASE REPORT OF SPONTANEOUS BILOMA - AN ENIGMATIC SURGICAL PROBLEM *Sumanta Kumar Ghosh and Biswajit Mukherjee ESIC Medical College, Joka, Kolkata, India *Author for Correspondence ABSTRACT Occurrence
Iatrogenic Gallbladder Perforation during Gastric Endoscopic Mucosal Resection
 J Korean Surg Soc 2010;79:228-233 DOI: 10.4174/jkss.2010.79.3.228 증 례 Iatrogenic Gallbladder Perforation during Gastric Endoscopic Mucosal Resection Department of Surgery, CHA Gumi Medical Center, CHA
J Korean Surg Soc 2010;79:228-233 DOI: 10.4174/jkss.2010.79.3.228 증 례 Iatrogenic Gallbladder Perforation during Gastric Endoscopic Mucosal Resection Department of Surgery, CHA Gumi Medical Center, CHA
Biliary Ultrasonography Kathleen O Brien MD MPH RDMS Kaiser Permanente South Sacramento
 Biliary Ultrasonography Kathleen O Brien MD MPH RDMS Kaiser Permanente South Sacramento https://www.google.com/search?sa=g&hl=en&q=public+disclosure&tbm=isch&tbs=simg:caqsigeahwelekju2aqaaawlelcmpwgaygpgcamskpib_1qnza7ai
Biliary Ultrasonography Kathleen O Brien MD MPH RDMS Kaiser Permanente South Sacramento https://www.google.com/search?sa=g&hl=en&q=public+disclosure&tbm=isch&tbs=simg:caqsigeahwelekju2aqaaawlelcmpwgaygpgcamskpib_1qnza7ai
Imaging of Biliary Tract Emergencies in Jorge A. Soto, MD Professor of Radiology Boston University Medical Center.
 Imaging of Biliary Tract Emergencies in 2011 Jorge A. Soto, MD Professor of Radiology Boston University Medical Center Introduction Biliary emergencies are: Common Come in many flavors Deceiving: frequent
Imaging of Biliary Tract Emergencies in 2011 Jorge A. Soto, MD Professor of Radiology Boston University Medical Center Introduction Biliary emergencies are: Common Come in many flavors Deceiving: frequent
Management of gall bladder perforation evaluation on Ultrasonographyreport of six rare cases with review of literature
 Journal of Medicine and Life Vol. 4, Issue 4, October December 2011, pp.364 371 Management of gall bladder perforation evaluation on Ultrasonographyreport of six rare cases with review of literature *Rikki
Journal of Medicine and Life Vol. 4, Issue 4, October December 2011, pp.364 371 Management of gall bladder perforation evaluation on Ultrasonographyreport of six rare cases with review of literature *Rikki
REFERRAL GUIDELINES: GALLSTONES
 REFERRAL GUIDELINES: GALLSTONES Document Purpose To ensure patients with gallstones disease are managed appropriately in primary/ secondary care Oxford Radcliffe Hospital Surgical Department Surgical Registrar
REFERRAL GUIDELINES: GALLSTONES Document Purpose To ensure patients with gallstones disease are managed appropriately in primary/ secondary care Oxford Radcliffe Hospital Surgical Department Surgical Registrar
Isolated Gallbladder Perforation in Cases of Blunt Trauma Abdomen
 CASE SERIES Isolated Gallbladder Perforation in Cases of Blunt Trauma Abdomen Gupta MK 1, Ahmad K 1, Kumar A 1, Santhalia PK 1, Joshi BR 2, Rauniyar RK 1 1 Department of Radiodiagnosis and Imaging, 2 Department
CASE SERIES Isolated Gallbladder Perforation in Cases of Blunt Trauma Abdomen Gupta MK 1, Ahmad K 1, Kumar A 1, Santhalia PK 1, Joshi BR 2, Rauniyar RK 1 1 Department of Radiodiagnosis and Imaging, 2 Department
Comparative Study of Outcomes of Early Versus Interval Laparoscopic Cholecystectomy in Acute Calculus Cholecystitis.
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 4 Ver. IX (April. 2017), PP 68-73 www.iosrjournals.org Comparative Study of Outcomes of Early
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 4 Ver. IX (April. 2017), PP 68-73 www.iosrjournals.org Comparative Study of Outcomes of Early
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE SCOPE
 Appendix B: Scope NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE SCOPE Post publication note: The title of this guideline changed during development. This scope was published before the guideline
Appendix B: Scope NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE SCOPE Post publication note: The title of this guideline changed during development. This scope was published before the guideline
Case Cholecystoduodenal fistula with migrated gallstone leading to gastric outlet obstruction: Bouveret's syndrome
 Case 14613 Cholecystoduodenal fistula with migrated gallstone leading to gastric outlet obstruction: Bouveret's syndrome Eva De Backer 1, Filip Vanhoenacker 2, 3, 4, Adelard De Backer5 1: Ghent University,
Case 14613 Cholecystoduodenal fistula with migrated gallstone leading to gastric outlet obstruction: Bouveret's syndrome Eva De Backer 1, Filip Vanhoenacker 2, 3, 4, Adelard De Backer5 1: Ghent University,
Biliary Tree Ultrasound - In a nutshell. Pamela Parker Lead Sonographer
 Biliary Tree Ultrasound - In a nutshell Pamela Parker Lead Sonographer Aims Review what we know about the biliary system Common pathologies Pitfalls Reporting tips The Nutshell Background Biliary examinations
Biliary Tree Ultrasound - In a nutshell Pamela Parker Lead Sonographer Aims Review what we know about the biliary system Common pathologies Pitfalls Reporting tips The Nutshell Background Biliary examinations
Gallstone Ileus: Diagnostic and Surgical Dilemma
 Original Article Elmer Press Gallstone Ileus: Diagnostic and Surgical Dilemma Vincenzo Leone Abstract Background: The typical patient with Gallstone ileus is female, elderly, with concomitant medical diseases
Original Article Elmer Press Gallstone Ileus: Diagnostic and Surgical Dilemma Vincenzo Leone Abstract Background: The typical patient with Gallstone ileus is female, elderly, with concomitant medical diseases
Appendix 5. EFSUMB Newsletter. Gastroenterological Ultrasound
 EFSUMB Newsletter 87 Examinations should encompass the full range of pathological conditions listed below A log book listing the types of examinations undertaken should be kept Training should usually
EFSUMB Newsletter 87 Examinations should encompass the full range of pathological conditions listed below A log book listing the types of examinations undertaken should be kept Training should usually
CLINICAL PRESENTATION AND RADIOLOGY QUIZ QUESTION
 Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 09/17/2011 Radiology Quiz of the Week # 38 Page 1 CLINICAL PRESENTATION AND RADIOLOGY
Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 09/17/2011 Radiology Quiz of the Week # 38 Page 1 CLINICAL PRESENTATION AND RADIOLOGY
Evidence Process for Abdominal Pain Guideline Research 11/16/2017. Guideline Review using ADAPTE method and AGREE II instrument 11/16/2017
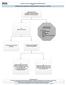 Evidence Process for Abdominal Pain Guideline Research Guideline Review using ADAPTE method and AGREE II instrument Approximately 139 Potentially relevant guidelines identified in various resources* 59
Evidence Process for Abdominal Pain Guideline Research Guideline Review using ADAPTE method and AGREE II instrument Approximately 139 Potentially relevant guidelines identified in various resources* 59
Management of Gallbladder Disease. Cory Buschmann, MD PGY-5 11/28/2017
 Management of Gallbladder Disease Cory Buschmann, MD PGY-5 11/28/2017 Financial disclosures None Content Scope of gallbladder diseases Evaluation H&P Labs Imaging Cholecystectomy vs cholecystostomy Ancillary
Management of Gallbladder Disease Cory Buschmann, MD PGY-5 11/28/2017 Financial disclosures None Content Scope of gallbladder diseases Evaluation H&P Labs Imaging Cholecystectomy vs cholecystostomy Ancillary
Perforation of a Duodenal Diverticulum. Elective Student S. C.
 Perforation of a Duodenal Diverticulum 2008 4 Elective Student S. C. Case History An elderly male presented to the Emergency Department with abdominal pain. Chief Complaint: Worsening, diffuse abdominal
Perforation of a Duodenal Diverticulum 2008 4 Elective Student S. C. Case History An elderly male presented to the Emergency Department with abdominal pain. Chief Complaint: Worsening, diffuse abdominal
Congenital dilatation of the common bile duct and pancreaticobiliary maljunction clinical implications
 Langenbecks Arch Surg (2009) 394:209 213 DOI 10.1007/s00423-008-0330-6 CURRENT CONCEPT IN CLINICAL SURGERY Congenital dilatation of the common bile duct and pancreaticobiliary maljunction clinical implications
Langenbecks Arch Surg (2009) 394:209 213 DOI 10.1007/s00423-008-0330-6 CURRENT CONCEPT IN CLINICAL SURGERY Congenital dilatation of the common bile duct and pancreaticobiliary maljunction clinical implications
Percutaneous cholecystostomy for the treatment of acute cholecystitis in the critically ill and elderly
 ORIGINAL ARTICLE Key words: Cholecystectomy; Cholecystostomy!!"#!" JCM Li DWH Lee CW Lai ACN Li DW Chu ACW Chan Hong Kong Med J 2004;10:389-93 North District Hospital, New Territories East Cluster, 9 Po
ORIGINAL ARTICLE Key words: Cholecystectomy; Cholecystostomy!!"#!" JCM Li DWH Lee CW Lai ACN Li DW Chu ACW Chan Hong Kong Med J 2004;10:389-93 North District Hospital, New Territories East Cluster, 9 Po
The Efficacy of Preoperative Percutaneous Cholecystostomy for Acute Cholecystitis with Gallbladder Perforation 담낭천공을동반한급성담낭염환자에서수술전경피적담낭배액술의효용성에관한연구
 Original Article pissn 1738-2637 / eissn 2288-2928 J Korean Soc Radiol 2017;77(6):372-381 https://doi.org/10.3348/jksr.2017.77.6.372 The Efficacy of Preoperative Percutaneous Cholecystostomy for Acute
Original Article pissn 1738-2637 / eissn 2288-2928 J Korean Soc Radiol 2017;77(6):372-381 https://doi.org/10.3348/jksr.2017.77.6.372 The Efficacy of Preoperative Percutaneous Cholecystostomy for Acute
Management of biliary injury after laparoscopic cholecystectomy N. Dayes Kings County Hospital Center & Long Island College Hospital 8/19/2010
 Management of biliary injury after laparoscopic cholecystectomy N. Dayes Kings County Hospital Center & Long Island College Hospital 8/19/2010 Case Presentation 30 y.o. woman with 2 weeks of RUQ abdominal
Management of biliary injury after laparoscopic cholecystectomy N. Dayes Kings County Hospital Center & Long Island College Hospital 8/19/2010 Case Presentation 30 y.o. woman with 2 weeks of RUQ abdominal
ISSN X (Print) Research Article. *Corresponding author Jitendra Singh Yadav
 Scholars Journal of Applied Medical Sciences (SJAMS) Sch. J. App. Med. Sci., 2014; 2(3B):966-970 Scholars Academic and Scientific Publisher (An International Publisher for Academic and Scientific Resources)
Scholars Journal of Applied Medical Sciences (SJAMS) Sch. J. App. Med. Sci., 2014; 2(3B):966-970 Scholars Academic and Scientific Publisher (An International Publisher for Academic and Scientific Resources)
Background. RUQ Ultrasound Normal, Recommend Clinical Correlation. Sohail R. Shah, MD, MSHA, FACS, FAAP Texas Children s Hosptial
 RUQ Ultrasound Normal, Recommend Clinical Correlation Sohail R. Shah, MD, MSHA, FACS, FAAP Texas Children s Hosptial Background Incidence of pediatric gallbladder disease continues to rise U.S. Pediatric
RUQ Ultrasound Normal, Recommend Clinical Correlation Sohail R. Shah, MD, MSHA, FACS, FAAP Texas Children s Hosptial Background Incidence of pediatric gallbladder disease continues to rise U.S. Pediatric
USMLE and COMLEX II. CE / CK Review. General Surgery. 1. Northwestern Medical Review
 USMLE and COMLEX II CE / CK Review General Surgery 1. Northwestern Medical Review Northwestern Medical Review www.northwesternmedicalreview.com Lansing, Michigan 2014-2015 Acute Abdomen 1. Your patient
USMLE and COMLEX II CE / CK Review General Surgery 1. Northwestern Medical Review Northwestern Medical Review www.northwesternmedicalreview.com Lansing, Michigan 2014-2015 Acute Abdomen 1. Your patient
Mirizzi syndrome with an unusual type of biliobiliary fistula a case report
 Kawaguchi et al. Surgical Case Reports (2015) 1:51 DOI 10.1186/s40792-015-0052-2 CASE REPORT Mirizzi syndrome with an unusual type of biliobiliary fistula a case report Tsutomu Kawaguchi 1,2*, Tadao Itoh
Kawaguchi et al. Surgical Case Reports (2015) 1:51 DOI 10.1186/s40792-015-0052-2 CASE REPORT Mirizzi syndrome with an unusual type of biliobiliary fistula a case report Tsutomu Kawaguchi 1,2*, Tadao Itoh
LOKUN! I got stomach ache!
 LOKUN! I got stomach ache! Mr L is a 67year old Chinese gentleman who is a non smoker, social drinker. He has a medical history significant for Hypertension, Hyperlipidemia, Type 2 Diabetes Mellitus, Chronic
LOKUN! I got stomach ache! Mr L is a 67year old Chinese gentleman who is a non smoker, social drinker. He has a medical history significant for Hypertension, Hyperlipidemia, Type 2 Diabetes Mellitus, Chronic
SASKATCHEWAN REGISTERED NURSES ASSOCIATION. RNs WITH ADDITIONAL AUTHORIZED PRACTICE CLINICAL DECISION TOOL AUGUST 2017
 DEFINITION Cholelithiasis Presence of gall stones in the biliary tract. Biliary Colic Right upper quadrant pain due to obstruction of a bile duct by a gallstone. Cholecystitis Inflammation of the gallbladder
DEFINITION Cholelithiasis Presence of gall stones in the biliary tract. Biliary Colic Right upper quadrant pain due to obstruction of a bile duct by a gallstone. Cholecystitis Inflammation of the gallbladder
Disclosures. Extra-hepatic Biliary Disease and the Pancreas. Objectives. Pancreatitis 10/3/2018. No relevant financial disclosures to report
 Extra-hepatic Biliary Disease and the Pancreas Disclosures No relevant financial disclosures to report Jeffrey Coughenour MD FACS Clinical Associate Professor of Surgery and Emergency Medicine Division
Extra-hepatic Biliary Disease and the Pancreas Disclosures No relevant financial disclosures to report Jeffrey Coughenour MD FACS Clinical Associate Professor of Surgery and Emergency Medicine Division
Perforation: An Unusual Presentation of Enteric Fever. J Pharm Biomed Sci 2015; 05(05): S1-S4.
 JOURNAL OF PHARMACEUTICAL AND BIOMEDICAL SCIENCES Khadda S, Parmar A, Ali A, Yadav AK, Sakhrani JK, Kapoor A. Gall bladder Perforation: An Unusual Presentation of Enteric Fever. J Pharm Biomed Sci 2015;
JOURNAL OF PHARMACEUTICAL AND BIOMEDICAL SCIENCES Khadda S, Parmar A, Ali A, Yadav AK, Sakhrani JK, Kapoor A. Gall bladder Perforation: An Unusual Presentation of Enteric Fever. J Pharm Biomed Sci 2015;
Twice recurrent gallstone ileus: a case report
 Jones et al. Journal of Medical Case Reports 2012, 6:362 JOURNAL OF MEDICAL CASE REPORTS CASE REPORT Open Access Twice recurrent gallstone ileus: a case report Rhys Jones 1*, Daniel Broman 1, Richard Hawkins
Jones et al. Journal of Medical Case Reports 2012, 6:362 JOURNAL OF MEDICAL CASE REPORTS CASE REPORT Open Access Twice recurrent gallstone ileus: a case report Rhys Jones 1*, Daniel Broman 1, Richard Hawkins
In The Name of God. Advanced Concept of Nursing- II UNIT- V Advance Nursing Management of GIT diseases. Cholecystitis.
 In The Name of God (A PROJECT OF NEW LIFE HEALTH CARE SOCIETY, KARACHI) Advanced Concept of Nursing- II UNIT- V Advance Nursing Management of GIT diseases. Cholecystitis. Shahzad Bashir RN, BScN, DCHN,MScN
In The Name of God (A PROJECT OF NEW LIFE HEALTH CARE SOCIETY, KARACHI) Advanced Concept of Nursing- II UNIT- V Advance Nursing Management of GIT diseases. Cholecystitis. Shahzad Bashir RN, BScN, DCHN,MScN
Objectives. Hepatobiliary Ultrasound: Anatomy, Technique, Pathology. RUQ: Normal Anatomy. Emergency Ultrasound: Gallbladder Location
 Hepatobiliary Ultrasound: Anatomy, Technique, Pathology Laleh Gharahbaghian, MD FAAEM Associate Director, EM Ultrasound Co-Director, EM Ultrasound Fellowship Stanford University Medical Center Seric Cusick,
Hepatobiliary Ultrasound: Anatomy, Technique, Pathology Laleh Gharahbaghian, MD FAAEM Associate Director, EM Ultrasound Co-Director, EM Ultrasound Fellowship Stanford University Medical Center Seric Cusick,
Predicting difficulty in laparoscopic cholecystectomy by clinical, hematological and radiological evaluation
 International Surgery Journal Naik CG et al. Int Surg J. 2017 Jan;4(1):189-193 http://www.ijsurgery.com pissn 2349-3305 eissn 2349-2902 Original Research Article DOI: http://dx.doi.org/10.18203/2349-2902.isj20164080
International Surgery Journal Naik CG et al. Int Surg J. 2017 Jan;4(1):189-193 http://www.ijsurgery.com pissn 2349-3305 eissn 2349-2902 Original Research Article DOI: http://dx.doi.org/10.18203/2349-2902.isj20164080
EAST MULTICENTER STUDY PROPOSAL
 EAST MULTICENTER STUDY PROPOSAL (Proposal forms must be completed in its entirety, incomplete forms will not be considered) GENERAL INFORMATION Study Title: Prospective Multi-Institutional Evaluation of
EAST MULTICENTER STUDY PROPOSAL (Proposal forms must be completed in its entirety, incomplete forms will not be considered) GENERAL INFORMATION Study Title: Prospective Multi-Institutional Evaluation of
Comparison Between Primary Closure of Common Bile Duct and T- Tube Drainage After Open Choledocholithiasis: A Hospital Based Study
 Original article: Comparison Between Primary Closure of Common Bile Duct and T- Tube Drainage After Open Choledocholithiasis: A Hospital Based Study Kali CharanBansal Principal Specialist (General surgery)
Original article: Comparison Between Primary Closure of Common Bile Duct and T- Tube Drainage After Open Choledocholithiasis: A Hospital Based Study Kali CharanBansal Principal Specialist (General surgery)
Surveillance proposal consultation document
 Surveillance proposal consultation document 2018 surveillance of Gallstone disease: diagnosis and management (NICE guideline CG188) Proposed surveillance decision We propose to not update the NICE guideline
Surveillance proposal consultation document 2018 surveillance of Gallstone disease: diagnosis and management (NICE guideline CG188) Proposed surveillance decision We propose to not update the NICE guideline
Study of the degree of gall bladder wall thickness and its impact on outcomes following laparoscopic cholecystectomy in JSS Hospital
 International Surgery Journal Chandra SBJ et al. Int Surg J. 2018 Apr;5(4):1417-1421 http://www.ijsurgery.com pissn 2349-3305 eissn 2349-2902 Original Research Article DOI: http://dx.doi.org/10.18203/2349-2902.isj20181122
International Surgery Journal Chandra SBJ et al. Int Surg J. 2018 Apr;5(4):1417-1421 http://www.ijsurgery.com pissn 2349-3305 eissn 2349-2902 Original Research Article DOI: http://dx.doi.org/10.18203/2349-2902.isj20181122
Case Report Overlap of Acute Cholecystitis with Gallstones and Squamous Cell Carcinoma of the Gallbladder in an Elderly Patient
 Case Reports in Surgery Volume 2015, Article ID 767196, 4 pages http://dx.doi.org/10.1155/2015/767196 Case Report Overlap of Acute Cholecystitis with Gallstones and Squamous Cell Carcinoma of the Gallbladder
Case Reports in Surgery Volume 2015, Article ID 767196, 4 pages http://dx.doi.org/10.1155/2015/767196 Case Report Overlap of Acute Cholecystitis with Gallstones and Squamous Cell Carcinoma of the Gallbladder
Subtotal cholecystectomy for complicated acute cholecystitis: a multicenter prospective observational study
 Study title Subtotal cholecystectomy for complicated acute cholecystitis: a multicenter prospective observational study Primary Investigator: Kazuhide Matsushima, MD Co-Primary investigator: Zachary Warriner,
Study title Subtotal cholecystectomy for complicated acute cholecystitis: a multicenter prospective observational study Primary Investigator: Kazuhide Matsushima, MD Co-Primary investigator: Zachary Warriner,
4/9/2018 OBJECTIVES PANCREAOTO BILIARY ULTRASOUND: BEYOND CHOLECYSTITIS
 PANCREAOTO BILIARY ULTRASOUND: BEYOND CHOLECYSTITIS Jean Yves Sewah Kaiser Permanente West Los Angeles 1 OBJECTIVES Discuss the role of ultrasound in the evaluation of the gallbladder, biliary tree and
PANCREAOTO BILIARY ULTRASOUND: BEYOND CHOLECYSTITIS Jean Yves Sewah Kaiser Permanente West Los Angeles 1 OBJECTIVES Discuss the role of ultrasound in the evaluation of the gallbladder, biliary tree and
Cholelithiasis (Gallstones)
 GALL BLADDER Cholelithiasis (Gallstones) Gallstones afflict 10-20% of adult populations in northern hemisphere Western countries. Adult prevalence rates are higher in Latin American countries (20-40%)
GALL BLADDER Cholelithiasis (Gallstones) Gallstones afflict 10-20% of adult populations in northern hemisphere Western countries. Adult prevalence rates are higher in Latin American countries (20-40%)
Hepatobiliary Scintigraphy in Patients with Bile Leaks
 Hepatobiliary Scintigraphy in Patients with Bile Leaks Sandra L. Carichner and Conrad E. Nagle William Beaumont Hospital, Troy, Michigan Hepatobilillry scintigraphy has been recognized as u useful tool
Hepatobiliary Scintigraphy in Patients with Bile Leaks Sandra L. Carichner and Conrad E. Nagle William Beaumont Hospital, Troy, Michigan Hepatobilillry scintigraphy has been recognized as u useful tool
Endoscopic Retrograde Pancreatography and Laparoscopic Cholecystectomy. TEAM 1 Janix M. De Guzman, MD Presentor
 Endoscopic Retrograde Pancreatography and Laparoscopic Cholecystectomy TEAM 1 Janix M. De Guzman, MD Presentor Premise 40F Jaundice Abdominal pain US finding of gallstones with apparently normal common
Endoscopic Retrograde Pancreatography and Laparoscopic Cholecystectomy TEAM 1 Janix M. De Guzman, MD Presentor Premise 40F Jaundice Abdominal pain US finding of gallstones with apparently normal common
Introduction. Roxanne L. Massoumi 1 Colleen M. Trevino
 World J Surg (2017) 41:935 939 DOI 10.1007/s00268-016-3816-3 ORIGINAL SCIENTIFIC REPORT Postoperative Complications of Laparoscopic Cholecystectomy for Acute Cholecystitis: A Comparison to the ACS-NSQIP
World J Surg (2017) 41:935 939 DOI 10.1007/s00268-016-3816-3 ORIGINAL SCIENTIFIC REPORT Postoperative Complications of Laparoscopic Cholecystectomy for Acute Cholecystitis: A Comparison to the ACS-NSQIP
Clinical Anatomy of the Biliary Apparatus: Relations & Variations
 Clinical Anatomy of the Biliary Apparatus: Relations & Variations Handout download: http://www.oucom.ohiou.edu/dbms-witmer/gs-rpac.htm 27 March 2007 Lawrence M. Witmer, PhD Professor of Anatomy Department
Clinical Anatomy of the Biliary Apparatus: Relations & Variations Handout download: http://www.oucom.ohiou.edu/dbms-witmer/gs-rpac.htm 27 March 2007 Lawrence M. Witmer, PhD Professor of Anatomy Department
Is C-reactive Protein an Independent Risk Factor for Complication of Laparoscopic Cholecystectomy for Acute Cholecystitis
 Journal of Surgery 2017; 5(3-1): 16-22 http://www.sciencepublishinggroup.com/j/js doi: 10.11648/j.js.s.2017050301.14 ISSN: 2330-0914 (Print); ISSN: 2330-0930 (Online) Is C-reactive Protein an Independent
Journal of Surgery 2017; 5(3-1): 16-22 http://www.sciencepublishinggroup.com/j/js doi: 10.11648/j.js.s.2017050301.14 ISSN: 2330-0914 (Print); ISSN: 2330-0930 (Online) Is C-reactive Protein an Independent
Pre-Operative Prediction of Difficult Laparoscopic Cholecystectomy Using Clinical and Ultrasonographic Parameters.
 DOI: 1.2127/aimdr.217...SG11 Original Article ISSN (O):25-2822; ISSN (P):25-281 Pre-Operative Prediction of Difficult Laparoscopic Cholecystectomy Using Clinical and Ultrasonographic Parameters. Sudhir
DOI: 1.2127/aimdr.217...SG11 Original Article ISSN (O):25-2822; ISSN (P):25-281 Pre-Operative Prediction of Difficult Laparoscopic Cholecystectomy Using Clinical and Ultrasonographic Parameters. Sudhir
GASTRO-INTESTINAL TRACT INFECTIONS - ANTIMICROBIAL MANAGEMENT
 GASTRO-INTESTINAL TRACT INFECTIONS - ANTIMICROBIAL MANAGEMENT Name & Title Of Author: Dr Linda Jewes, Consultant Microbiologist Date Amended: December 2016 Approved by Committee/Group: Drugs & Therapeutics
GASTRO-INTESTINAL TRACT INFECTIONS - ANTIMICROBIAL MANAGEMENT Name & Title Of Author: Dr Linda Jewes, Consultant Microbiologist Date Amended: December 2016 Approved by Committee/Group: Drugs & Therapeutics
ENDOSCOPIC TREATMENT OF A BILE DUCT
 HPB Surgery, 1990, Vol. 3, pp. 67-71 Reprints available directly from the publisher Photocopying permitted by license only 1990 Harwood Academic Publishers GmbH Printed in the United Kingdom CASE REPORT
HPB Surgery, 1990, Vol. 3, pp. 67-71 Reprints available directly from the publisher Photocopying permitted by license only 1990 Harwood Academic Publishers GmbH Printed in the United Kingdom CASE REPORT
Hepatobiliary Ultrasound Rimon Bengiamin, MD, RDMS Assistant Clinical Professor Director of Emergency Ultrasound UCSF Fresno. Objectives. Why?
 Hepatobiliary Ultrasound Rimon Bengiamin, MD, RDMS Assistant Clinical Professor Director of Emergency Ultrasound UCSF Fresno Objectives Discuss the goals of point-of-care biliary ultrasound Review the
Hepatobiliary Ultrasound Rimon Bengiamin, MD, RDMS Assistant Clinical Professor Director of Emergency Ultrasound UCSF Fresno Objectives Discuss the goals of point-of-care biliary ultrasound Review the
Emergency Surgery Board Department of General Surgery Rambam Health Care Campus
 Emergency Surgery Board Department of General Surgery Rambam Health Care Campus Surgical Complications of Peptic Ulcer Disease Case Presentation and Review of the Literature Case Presentation 40y male
Emergency Surgery Board Department of General Surgery Rambam Health Care Campus Surgical Complications of Peptic Ulcer Disease Case Presentation and Review of the Literature Case Presentation 40y male
Sonography of Gall Bladder
 Sonography of Gall Bladder Vikram Dogra,MD Professor of Radiology, Urology and BME Director of Ultrasound Associate Chair of Education and Research University of Rochester, NY Objectives Describe the Congenital
Sonography of Gall Bladder Vikram Dogra,MD Professor of Radiology, Urology and BME Director of Ultrasound Associate Chair of Education and Research University of Rochester, NY Objectives Describe the Congenital
The Present Scenario of Cholecystectomy
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 5 Ver. III (May. 2016), PP 71-75 www.iosrjournals.org The Present Scenario of Cholecystectomy
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 5 Ver. III (May. 2016), PP 71-75 www.iosrjournals.org The Present Scenario of Cholecystectomy
Biliary tree dilation - and now what?
 Biliary tree dilation - and now what? Poster No.: C-1767 Congress: ECR 2012 Type: Educational Exhibit Authors: I. Ferreira, A. B. Ramos, S. Magalhães, M. Certo; Porto/PT Keywords: Pathology, Diagnostic
Biliary tree dilation - and now what? Poster No.: C-1767 Congress: ECR 2012 Type: Educational Exhibit Authors: I. Ferreira, A. B. Ramos, S. Magalhães, M. Certo; Porto/PT Keywords: Pathology, Diagnostic
laparoscopic cholecystectomy
 Combined percutaneous and endoscopic approach in management of dropped gallstones following laparoscopic cholecystectomy John S.F. Shum 1*, K.H. Fung 1, George P.C. Yang 2, Chung Ngai Tang 2, Michael K.W.
Combined percutaneous and endoscopic approach in management of dropped gallstones following laparoscopic cholecystectomy John S.F. Shum 1*, K.H. Fung 1, George P.C. Yang 2, Chung Ngai Tang 2, Michael K.W.
General Surgery Service
 General Surgery Service Patient Care Goals and Objectives Stomach/Duodenum and Bariatric assessed for a) Obesity surgery b) Treatment of i) Adenocarcinoma of the stomach ii) GIST iii) Carcinoid 2) Optimize
General Surgery Service Patient Care Goals and Objectives Stomach/Duodenum and Bariatric assessed for a) Obesity surgery b) Treatment of i) Adenocarcinoma of the stomach ii) GIST iii) Carcinoid 2) Optimize
Appendix A: Summary of evidence from surveillance
 Appendix A: Summary of evidence from surveillance 2018 surveillance of Gallstone disease: diagnosis and management (2014) NICE guideline CG188 Summary of evidence from surveillance Studies identified in
Appendix A: Summary of evidence from surveillance 2018 surveillance of Gallstone disease: diagnosis and management (2014) NICE guideline CG188 Summary of evidence from surveillance Studies identified in
A patient with an unusual congenital anomaly of the pancreaticobiliary tree
 A patient with an unusual congenital anomaly of the pancreaticobiliary tree Thomas Hocker, HMS IV BIDMC Core Radiology Case Presentation September 17, 2007 Review of Normal Pancreaticobiliary Tract Anatomy
A patient with an unusual congenital anomaly of the pancreaticobiliary tree Thomas Hocker, HMS IV BIDMC Core Radiology Case Presentation September 17, 2007 Review of Normal Pancreaticobiliary Tract Anatomy
No 72-hour pathological boundary for safe early laparoscopic cholecystectomy in acute cholecystitis: a clinicopathological study
 Original article Annals of Gastroenterology (2013) 26, 1-6 No 72-hour pathological boundary for safe early laparoscopic cholecystectomy in acute cholecystitis: a clinicopathological study Rachel M. Gomes
Original article Annals of Gastroenterology (2013) 26, 1-6 No 72-hour pathological boundary for safe early laparoscopic cholecystectomy in acute cholecystitis: a clinicopathological study Rachel M. Gomes
Information for Consent Cholecystectomy (Laparoscopic/Open) 膽囊切除術 ( 腹腔鏡 / 開放性 )
 Version 1.0 Page 1 of 3 Information for Consent Cholecystectomy (Laparoscopic/Open) 膽囊切除術 ( 腹腔鏡 / 開放性 ) Introduction Gallbladder is a sac connected to the biliary tree. It serves the function of concentration
Version 1.0 Page 1 of 3 Information for Consent Cholecystectomy (Laparoscopic/Open) 膽囊切除術 ( 腹腔鏡 / 開放性 ) Introduction Gallbladder is a sac connected to the biliary tree. It serves the function of concentration
MANAGEMENT OF PYOGENIC LIVER ABSCESS BOYOUNG SONG, M.D. SUNY DOWNSTATE SURGERY 11/7/13
 MANAGEMENT OF PYOGENIC LIVER ABSCESS BOYOUNG SONG, M.D. SUNY DOWNSTATE SURGERY 11/7/13 CASE THE PATIENT IS A 79 YEAR OLD MALE WITH 3 DAY HISTORY OF LOWER ABDOMINAL PAIN, NAUSEA WITHOUT VOMITING, CHILLS
MANAGEMENT OF PYOGENIC LIVER ABSCESS BOYOUNG SONG, M.D. SUNY DOWNSTATE SURGERY 11/7/13 CASE THE PATIENT IS A 79 YEAR OLD MALE WITH 3 DAY HISTORY OF LOWER ABDOMINAL PAIN, NAUSEA WITHOUT VOMITING, CHILLS
Bedside RUQ Ultrasound. Replace Formal ULS? Why Bedside ULS RUQ? RUQ Ultrasound. Bedside ULS is Limited, Goal-Directed
 Bedside RUQ Ultrasound RUQ Ultrasound Why do it How to do it Elizabeth Kwan UCSF Emergency Ultrasound Fellow Why Bedside ULS RUQ? Dx or Rule Out Acute Cholecystitis Cholelithiasis, Choledocolithiasis Earlier
Bedside RUQ Ultrasound RUQ Ultrasound Why do it How to do it Elizabeth Kwan UCSF Emergency Ultrasound Fellow Why Bedside ULS RUQ? Dx or Rule Out Acute Cholecystitis Cholelithiasis, Choledocolithiasis Earlier
TRANSOMENTAL HERNIATION CAUSING ACUTE INTESTINAL OBSTRUCTION N. Suresh Kumar 1, Rahul Rai 2, P. Kulandai Velu 3
 TRANSOMENTAL HERNIATION CAUSING ACUTE INTESTINAL OBSTRUCTION N. Suresh Kumar 1, Rahul Rai 2, P. Kulandai Velu 3 HOW TO CITE THIS ARTICLE: N. Suresh Kumar, Rahul Rai, P. Kulandai Velu. Transomental Herniation
TRANSOMENTAL HERNIATION CAUSING ACUTE INTESTINAL OBSTRUCTION N. Suresh Kumar 1, Rahul Rai 2, P. Kulandai Velu 3 HOW TO CITE THIS ARTICLE: N. Suresh Kumar, Rahul Rai, P. Kulandai Velu. Transomental Herniation
Clinical Study Operative Outcome and Patient Satisfaction in Early and Delayed Laparoscopic Cholecystectomy for Acute Cholecystitis
 Minimally Invasive Surgery, Article ID 162643, 4 pages http://dx.doi.org/10.1155/2014/162643 Clinical Study Operative Outcome and Patient Satisfaction in Early and Delayed Laparoscopic Cholecystectomy
Minimally Invasive Surgery, Article ID 162643, 4 pages http://dx.doi.org/10.1155/2014/162643 Clinical Study Operative Outcome and Patient Satisfaction in Early and Delayed Laparoscopic Cholecystectomy
General'Surgery'Service'
 General'Surgery'Service' Patient Care Goals and Objectives 1)! Stomach/Duodenum and Bariatric 2)! Interpret the results of clinical evaluations (history, physical examination) performed on patients being
General'Surgery'Service' Patient Care Goals and Objectives 1)! Stomach/Duodenum and Bariatric 2)! Interpret the results of clinical evaluations (history, physical examination) performed on patients being
The Bile Duct (and Pancreas) and the Physician
 The Bile Duct (and Pancreas) and the Physician Javaid Iqbal Consultant in Gastroenterology and Pancreato-biliary Medicine University Hospital South Manchester Not so common?! Two weeks 38 ERCP s 20 15
The Bile Duct (and Pancreas) and the Physician Javaid Iqbal Consultant in Gastroenterology and Pancreato-biliary Medicine University Hospital South Manchester Not so common?! Two weeks 38 ERCP s 20 15
Post Laparoscopic Cholecystectomy Biloma in a Child Managed by Endoscopic Retrograde Cholangio-Pancreatography and Stenting: A Case Report
 pissn: 2234-8646 eissn: 2234-8840 https://doi.org/10.5223/pghn.2016.19.4.281 Pediatr Gastroenterol Hepatol Nutr 2016 December 19(4):281-285 Case Report PGHN Post Laparoscopic Cholecystectomy Biloma in
pissn: 2234-8646 eissn: 2234-8840 https://doi.org/10.5223/pghn.2016.19.4.281 Pediatr Gastroenterol Hepatol Nutr 2016 December 19(4):281-285 Case Report PGHN Post Laparoscopic Cholecystectomy Biloma in
Case Report Simultaneous Non-Traumatic Perforation of Right Hepatic Duct and Gallbladder: An Atypical Occurrence
 Case Report Simultaneous Non-Traumatic Perforation of Right Hepatic Duct and Gallbladder: An Atypical Occurrence Pankaj Kumar GARG1, Bhupendra Kumar JAIN1, Satya Deo PANDEY1, Vinita RATHI2, Amarendra Singh
Case Report Simultaneous Non-Traumatic Perforation of Right Hepatic Duct and Gallbladder: An Atypical Occurrence Pankaj Kumar GARG1, Bhupendra Kumar JAIN1, Satya Deo PANDEY1, Vinita RATHI2, Amarendra Singh
Radiology of hepatobiliary diseases
 GI cycle - Lecture 14 436 Teams Radiology of hepatobiliary diseases Objectives 1. To Interpret plan x-ray radiograph of abdomen with common pathologies. 2. To know the common pathologies presentation.
GI cycle - Lecture 14 436 Teams Radiology of hepatobiliary diseases Objectives 1. To Interpret plan x-ray radiograph of abdomen with common pathologies. 2. To know the common pathologies presentation.
Percutaneous Cholecystostomy Tube in Acute Cholecystitis: Our Experience in a Tertiary Center in Saudi Arabia
 9 KUWAIT MEDICAL JOURNAL June 0 Original Article Percutaneous Cholecystostomy Tube in Acute Cholecystitis: Our Experience in a Tertiary Center in Saudi Arabia Faisal A Al-Saif, Hamad S AlSubaie, Rafif
9 KUWAIT MEDICAL JOURNAL June 0 Original Article Percutaneous Cholecystostomy Tube in Acute Cholecystitis: Our Experience in a Tertiary Center in Saudi Arabia Faisal A Al-Saif, Hamad S AlSubaie, Rafif
Case Report Spontaneous Intramural Duodenal Hematoma: Pancreatitis, Obstructive Jaundice, and Upper Intestinal Obstruction
 Case Reports in Surgery Volume 2016, Article ID 5321081, 4 pages http://dx.doi.org/10.1155/2016/5321081 Case Report Spontaneous Intramural Duodenal Hematoma: Pancreatitis, Obstructive Jaundice, and Upper
Case Reports in Surgery Volume 2016, Article ID 5321081, 4 pages http://dx.doi.org/10.1155/2016/5321081 Case Report Spontaneous Intramural Duodenal Hematoma: Pancreatitis, Obstructive Jaundice, and Upper
A one-year study of cholelithiasis at a tertiary care hospital of South India
 International Surgery Journal Rachamalla RR et al. Int Surg J. 2018 Jul;5(7):2444-2448 http://www.ijsurgery.com pissn 2349-3305 eissn 2349-2902 Original Research Article DOI: http://dx.doi.org/10.18203/2349-2902.isj20182502
International Surgery Journal Rachamalla RR et al. Int Surg J. 2018 Jul;5(7):2444-2448 http://www.ijsurgery.com pissn 2349-3305 eissn 2349-2902 Original Research Article DOI: http://dx.doi.org/10.18203/2349-2902.isj20182502
GALLBLADDER CANCER. Lidie M. Lajoie MD Downstate Surgery M&M July 21, 2011
 GALLBLADDER CANCER Lidie M. Lajoie MD Downstate Surgery M&M July 21, 2011 Agenda Case Presentation Epidemiology Pathogenesis & Pathology Staging Presentation & Diagnosis Stage-wise Management Outcomes/Prognosis
GALLBLADDER CANCER Lidie M. Lajoie MD Downstate Surgery M&M July 21, 2011 Agenda Case Presentation Epidemiology Pathogenesis & Pathology Staging Presentation & Diagnosis Stage-wise Management Outcomes/Prognosis
ISSN East Cent. Afr. J. surg
 Transition from Open to Laparoscopic Cholecystectomy at a Public and Private Hospitals in Nairobi P.G. Jani1, V. Kotecha2 1 Associate professor, Department of Surgery University of Nairobi 2 M.D, Resident
Transition from Open to Laparoscopic Cholecystectomy at a Public and Private Hospitals in Nairobi P.G. Jani1, V. Kotecha2 1 Associate professor, Department of Surgery University of Nairobi 2 M.D, Resident
Case Rep Gastroenterol 2010;4:71 78 DOI: /
 71 Gallstone Ileus, Bouveret s Syndrome and Choledocholithiasis in a Patient with Billroth II Gastrectomy A Case Report of Combined Endoscopic and Surgical Therapy R. Fejes G. Kurucsai A. Székely F. Luka
71 Gallstone Ileus, Bouveret s Syndrome and Choledocholithiasis in a Patient with Billroth II Gastrectomy A Case Report of Combined Endoscopic and Surgical Therapy R. Fejes G. Kurucsai A. Székely F. Luka
Gastroenterology. Certification Examination Blueprint. Purpose of the exam
 Gastroenterology Certification Examination Blueprint Purpose of the exam The exam is designed to evaluate the knowledge, diagnostic reasoning, and clinical judgment skills expected of the certified gastroenterologist
Gastroenterology Certification Examination Blueprint Purpose of the exam The exam is designed to evaluate the knowledge, diagnostic reasoning, and clinical judgment skills expected of the certified gastroenterologist
Pitfalls in the CT diagnosis of appendicitis
 The British Journal of Radiology, 77 (2004), 792 799 DOI: 10.1259/bjr/95663370 E 2004 The British Institute of Radiology Pictorial review Pitfalls in the CT diagnosis of appendicitis 1 C D LEVINE, 2 O
The British Journal of Radiology, 77 (2004), 792 799 DOI: 10.1259/bjr/95663370 E 2004 The British Institute of Radiology Pictorial review Pitfalls in the CT diagnosis of appendicitis 1 C D LEVINE, 2 O
GASTROENTEROLOGY ESSENTIALS
 GASTROENTEROLOGY ESSENTIALS Practical Gastroenterology 8/25/2018 Jahnavi Koppala, MBBS Abdullah Abdussalam, MD A 48-year-old male was evaluated for noncardiac chest pain. Treatment with PPI twice daily
GASTROENTEROLOGY ESSENTIALS Practical Gastroenterology 8/25/2018 Jahnavi Koppala, MBBS Abdullah Abdussalam, MD A 48-year-old male was evaluated for noncardiac chest pain. Treatment with PPI twice daily
Disclosures. Overview. Case 1. Common Bile Duct Sizes 10/14/2016. General GI + Advanced Endoscopy: NAFLD/Stones/Pancreatitis
 Disclosures General GI + Advanced Endoscopy: NAFLD/Stones/Pancreatitis 123 Blank Blank, LLC Aldo Maspons, MD Assistant Professor Director of Endoscopy Department of Pediatrics Texas Tech University Health
Disclosures General GI + Advanced Endoscopy: NAFLD/Stones/Pancreatitis 123 Blank Blank, LLC Aldo Maspons, MD Assistant Professor Director of Endoscopy Department of Pediatrics Texas Tech University Health
Update in abdominal Surgery in cirrhotic patients
 Update in abdominal Surgery in cirrhotic patients Safi Dokmak HBP department and liver transplantation Beaujon Hospital, Clichy, France Cairo, 5 April 2016 Cirrhosis Prevalence in France (1%)* Patients
Update in abdominal Surgery in cirrhotic patients Safi Dokmak HBP department and liver transplantation Beaujon Hospital, Clichy, France Cairo, 5 April 2016 Cirrhosis Prevalence in France (1%)* Patients
What is Crohn's disease?
 What is Crohn's disease? Crohn's disease is a chronic inflammatory disorder that causes inflammation of the digestive tract. It can affect any area of the GI tract, from the mouth to the anus, but it most
What is Crohn's disease? Crohn's disease is a chronic inflammatory disorder that causes inflammation of the digestive tract. It can affect any area of the GI tract, from the mouth to the anus, but it most
Spleen indications of splenectomy complications OPSI
 Intestinal obstruction Differences between adynamic ileus and mechanical obstruction Aetiology Pathophysiology (Cluster contractions- bowel proximal to the obstruction dilate- wall of obstructed gut is
Intestinal obstruction Differences between adynamic ileus and mechanical obstruction Aetiology Pathophysiology (Cluster contractions- bowel proximal to the obstruction dilate- wall of obstructed gut is
Two Cases of Acute Cholecystitis in which Percutaneous Transhepatic Gallbladder Aspiration (PTGBA) was Useful
 Case Report Kurume Medical Journal, 49,161-165, 2002 Two Cases of Acute Cholecystitis in which Percutaneous Transhepatic Gall Aspiration (PTGBA) was Useful HISAFUMI KINOSHITA, MITSUO HASHIMOTO, KAZUNORI
Case Report Kurume Medical Journal, 49,161-165, 2002 Two Cases of Acute Cholecystitis in which Percutaneous Transhepatic Gall Aspiration (PTGBA) was Useful HISAFUMI KINOSHITA, MITSUO HASHIMOTO, KAZUNORI
Takuya SAKODA* ), Yoshiaki MURAKAMI, Naru KONDO, Kenichiro UEMURA, Yasushi HASHIMOTO, Naoya NAKAGAWA and Taijiro SUEDA ABSTRACT
 Hiroshima J. Med. Sci. Vol. 64, No. 3, 45~49, September, 2015 HIJM 64 8 45 Takuya SAKODA* ), Yoshiaki MURAKAMI, Naru KONDO, Kenichiro UEMURA, Yasushi HASHIMOTO, Naoya NAKAGAWA and Taijiro SUEDA Department
Hiroshima J. Med. Sci. Vol. 64, No. 3, 45~49, September, 2015 HIJM 64 8 45 Takuya SAKODA* ), Yoshiaki MURAKAMI, Naru KONDO, Kenichiro UEMURA, Yasushi HASHIMOTO, Naoya NAKAGAWA and Taijiro SUEDA Department
Case Report Perforated Closed-Loop Obstruction Secondary to Gallstone Ileus of the Transverse Colon: A Rare Entity
 Case Reports in Surgery Volume 2015, Article ID 691713, 4 pages http://dx.doi.org/10.1155/2015/691713 Case Report Perforated Closed-Loop Obstruction Secondary to Gallstone Ileus of the Transverse Colon:
Case Reports in Surgery Volume 2015, Article ID 691713, 4 pages http://dx.doi.org/10.1155/2015/691713 Case Report Perforated Closed-Loop Obstruction Secondary to Gallstone Ileus of the Transverse Colon:
Chapter 14: Training in Radiology. DDSEP Chapter 1: Question 12
 DDSEP Chapter 1: Question 12 A 52-year-old white male presents for evaluation of sudden onset of abdominal pain and shoulder pain. His past medical history is notable for a history of coronary artery disease,
DDSEP Chapter 1: Question 12 A 52-year-old white male presents for evaluation of sudden onset of abdominal pain and shoulder pain. His past medical history is notable for a history of coronary artery disease,
Bile Duct Injury during Lap Chole. Bile Duct Injury during cholecystectomy TOPICS. 1. Prevalence, mechanisms, prevention and diagnosis
 Bile Duct Injury during cholecystectomy Catherine HUBERT Jean-Fran François GIGOT Benoît t NAVEZ Division of Hepato-Biliary Biliary-Pancreatic Surgery Department of Abdominal Surgery and Transplantation
Bile Duct Injury during cholecystectomy Catherine HUBERT Jean-Fran François GIGOT Benoît t NAVEZ Division of Hepato-Biliary Biliary-Pancreatic Surgery Department of Abdominal Surgery and Transplantation
SUCCESSFUL MANAGEMENT OF PERFORATED DUODENAL DIVERTICULITIS WITH INTRA-ABDOMINAL DRAINAGE AND FEEDING JEJUNOSTOMY: A CASE REPORT AND LITERATURE REVIEW
 SUCCESSFUL MANAGEMENT OF PERFORATED DUODENAL DIVERTICULITIS WITH INTRA-ABDOMINAL DRAINAGE AND FEEDING JEJUNOSTOMY: A CASE REPORT AND LITERATURE REVIEW Chin-Fan Chen, 1 Deng-Chyang Wu, 2,5 Chao-Wen Chen,
SUCCESSFUL MANAGEMENT OF PERFORATED DUODENAL DIVERTICULITIS WITH INTRA-ABDOMINAL DRAINAGE AND FEEDING JEJUNOSTOMY: A CASE REPORT AND LITERATURE REVIEW Chin-Fan Chen, 1 Deng-Chyang Wu, 2,5 Chao-Wen Chen,
