Biomaterials for bone regeneration
|
|
|
- Bertha Gibbs
- 6 years ago
- Views:
Transcription
1 Journal section: Biomaterials and Bioengineering in Dentistry Publication Types: Review doi: /medoral.15.e517 María-José Pérez-Sánchez 1, Elena Ramírez-Glindon 2, Miguel Lledó-Gil 3, José-Luis Calvo-Guirado 4, Cristina Pérez-Sánchez 5 1 Dental surgeon. University of Murcia 2 Dental surgeon. University of Murcia 3 Associate Professor, Department of Adult Integrated Dentistry University of Valencia 4 Professor of Adult Integrated Dentistry. University of Murcia. Manager, Postgraduate of Oral Implanthology. University of Murcia 5 Dental surgeon. University of Murcia Correspondence: Avda/ General Ortín Nº3, 2ºH C.P Ronda Sur Murcia Spain mjps7@hotmail.com Received: 09/05/2009 Accepted: 28/11/2009 Pérez-Sánchez MJ, Ramírez-Glindon E, Lledó-Gil M, Calvo-Guirado JL, Pérez-Sánchez C.. Med Oral Patol Oral Cir Bucal May 1;15 (3):e Article Number: Medicina Oral S. L. C.I.F. B pissn eissn: medicina@medicinaoral.com Indexed in: -SCI EXPANDED -JOURNAL CITATION REPORTS -Index Medicus / MEDLINE / PubMed -EMBASE, Excerpta Medica -SCOPUS -Indice Médico Español Abstract Objective: This article reviews the literature on biomaterials used for bone regeneration. Material and method: A total of seventeen bibliographic sources were found using the MEDLINE database and to avoid the variability of the search terms the thesaurus Mesh was used. Results: These materials act essentially due to their osteoconductive ability, although their osteoinductive capacity is being improved with the use of growth factors. As to their effectiveness, many differences exist between them and some even affect bone regeneration negatively. Conclusions: Biomaterials used for bone regeneration are valid when the correct material is used. As yet the osteogenic capacity of autogenous bone has not been equalled by biomaterials. Tissue engineering has caused great interest because of its many possibilities, although more studies are necessary in order to achieve the ambitious expectations when it comes to tissue or organ regeneration in the human body. Key words: Biomaterials, bone regeneration, tissue engineering, growth factors, calcium phosphate, dental implants. e517
2 Introduction The life expectancy of the current population has increased considerably over recent decades due to improvements in the quality of life of individuals. One of the consequences of this phenomenon has been the increase in injuries and bone disease in older people who have a diminished bone regeneration capacity. Defects in oral and craniofacial tissues, resulting from trauma, tumours, infections, abnormal skeletal development or progressive deforming diseases, present a formidable challenge and restoration of these tissues is a subject of clinical, basic science and engineering concern (1,2). Bone is a highly vascularized and innervated connective tissue. It is composed of cells and mineralized organic matrix. Bone is the only body tissue capable of regeneration and remodelling process (it is in constant formation and resorption, this allows the renovation of 5-15% of the total bone mass per year under normal conditions). It is regulated by genetic, mechanical, vascular, hormonal, nutritional, and local factors. Amongst local factors, growth factors and cytokines, and recently the bone matrix proteins have been implicated as modulators of other local factors. Growth factors (GFs) are polypeptides produced by the bone cells themselves or in extra-osseous tissue, and act as modulators of the cellular functions, fundamentally growth, differentiation, and proliferation. The main GFs acting on the skeleton are IGF-I and II (insulin-like growth factor I and II), Transforming Growth Factor-β (TGF-β), Bone Morphogenetic Proteins (BMP), Platelet-Derived Growth Factor (PDGF), Fibroblastic Growth Factor (FGF) and Vascular Endothelial Growth Factor (VEGF) (3-5). Autografts have primarily been the material of choice to replace lost bone, although the use of autografts comes with some disadvantages such as the limited quantity available and its use also requires additional surgical procedures, and therefore, longer surgical time and possible complications of the wound of the donor site such as bleeding, pain and infection among others (1,2, 6-8). Allografts and xenografts have the potential of transferring pathogens (2,9). To avoid the biological risk, these materials are subjected to exhaustive procedures which have dramatic effects primarily on their osteogenic and osteoinductive properties and these procedures can also reduce their structural integrity leading to graft fracture (2,6,8). In order to minimize these complications, the alloplastic graft (synthetic bone graft substitute) has been developed. Synthetic bone graft possess both osteointegrative and osteoconductive properties (6,10). The benefits of synthetic grafts include their availability, sterility and reduced morbidity (6). Long-term complications include stress shielding, loosening and mechanical or chemical breakdown of the material itself and they furthermore, lack the ability to adapt functionally (2). Synthetic grafts can be classified according to their chemical composition into four major categories: metallic implants such as titanium and stainless steel; ceramics such as calcium phosphate, alumina and glass; polymers such as polymethylmethacrylate and polyurethane and the fourth group is made up of composites, which are obtained after mixing several of the above (1). The desire to create more biological alternatives has inspired the development of growth factors and tissue engineering (1,2). The three main design components in tissue engineering are cell for osteogenesis, their extracellular matrix (scaffolds) for osteoconduction and a signalling system for osteoinduction, which can be used individually or in combination (2,8). Biomaterials were first developed in the 1960 s and 1970 s. Currently the third generation of these materials is being developed so as to achieve bioactive and resorbable materials, capable of stimulating a specific cellular response at a molecular level (11). Material and Methods A search of published articles was carried out using documental or artificial language so that the words had no variability, so it was essential the choice of appropriate descriptors representative of the theme we were studying. We searched in the MEDLINE database produced by the National Library of Medicine in the United States. For this, one acceded by means of Internet to the link www. pubmed.gov. We used the Mesh thesaurus to introduce descriptors. We conducted a total of five bibliographic searches and a total of seventeen bibliographic sources were found. When we introduced bone in the Mesh we obtained numerous items. We selected Bone Regeneration y Bone Transplantation. We searched in PubMed for Bone Transplantation using the following inclusion criteria: articles published after July 2007, studies in adults between the ages of 19 and 44 and the articles had to be published in English or Spanish. Out of 559 articles 2 were selected (9,12). Over 12,000 articles were found for Bone Regeneration. We carried out two types of bibliography searches. The first had the following inclusion criteria: full free text had to be available so as to obtain information immediately, they had to be published after July 2004 and in English or Spanish. Out of 244 articles 8 articles were selected (3,4,7,10, 13-16). In the second search, we looked for articles published after July 2008 so as to find the most recent information and these articles also had to be in English or Spanish. Out of 579 obtained 3 were selected (5,8,17). Oral Tissue Engineering was searched for in PubMed with the following inclusion criteria: articles published after July 2008 and again in English or Spanish. We obtained 190 articles of which only one was selected (2). Finally 3 of the reviewed articles, published after April 2001 and in English, were bibliographic references suggested by other dental surgeons (1,6,11). e518
3 Results Of the articles selected in this review, we determined how many were purely theoretical and how many were both theoretical and practical, as shown in (Fig. 1), of the eight theoretical-practical articles two are in vitro, three in animals and three in humans. In addition, articles were classified according to topic of study. The percentages are shown in (Fig. 2). The most numerous group compares different biomaterials and the smallest group contains tissue engineering articles. An important property which biomaterials must have so as to achieve optimal regeneration is their rate of degradation which should be similar to the rate of bone formation, that is to say, the mass of biomaterial must allow bone formation inside and persist until total bone replacement is achieved (2,7). Another interesting factor about the design of these materials is that the mass is typically maximized by maximizing porosity, where as mechanical properties are frequently maximized by minimizing porosity. One of the articles focuses on assessing the effect of the pore size of calcium phosphate scaffolds. Four pore sizes (150, 260, 510, 1220 µm) were used and they were evaluated at six, twelve and twentyfour weeks. The study showed that all the pore sizes Fig. 1. Type of study. Fig. 2. Topic of study. e519
4 Table 1. Description of different biomaterials and comparative part of them. Biomaterials Composition Features Form Mechanical properties Reabsorption Product name New bone in total defect New bone and alloplastic materials in total defect Glass ionomer Calcium/aluminium/fluorosilicate glass powder + polycarboxylic acid Direct bone union. Porous. Requires dry field Powder Compressive strength and modulus of elasticity comparable to cortical bone Non-reabsorbable; therefore is not replaced by bone -tricalcium phosphate Direct bone union. Porous or solid Brittle Porous form structurally similar to cancellous bone Dissolution 6-18 months; therefore faster than the replacement by bone Calcium phosphate cements Porous Non-ceramic Paste Good compressive strength Weak in distraction Years Aluminium oxide Alumina Ceramics Non osteointegrate Stronger than hydroxyapatite Non-reabsorbable Calcium sulphate Calcium sulphate Dry environment before and after to use Powder Bad mechanical properties In 5-7 weeks Bovine xenograft Mineral osseous matrix (hydroxyapatite,), deproteinized bovine bone Porous (75-80%) It can contain organic residues Compressive strength of 35 Mpa: > than cancellous bone < than compact bone It is resorbed slowly Bio-Oss TM 47,4 ±7,1 80,1 ± 5,1** Bioactive glass Synthetic hydroxyapatite Coralline hydroxyapatite Calcium carbonate and calcium phosphate Sodium oxide, calcium oxide, phosphorus pentoxide, silicon dioxide Calcium carbonate covered by calcium phosphate Bond directly to bone Hard and solid (not porous) Porous or solid Ceramic and nonceramic Orthomatrix: solid Porous The structure of calcium carbonate turns into phosphate Internal core of carbonate surrounded by a cap of phosphate Rods Orthomatrix: granules Interpore TM 200: blocks Stronger than hydroxyapatite Good compressive strengths Brittle. Modulus of elasticity higher than bone Structurally similar to the cancellous bone, fragile Structurally similar to the cancellous bone Non reabsorbable o reabsorbable depending on the proportion of its compounds. Biogran: reabsorbable Ceramic form: 1-2% per year Non- ceramic form: % higher Orthomatrix: non- reabsorbable Practically irreabsorbable, it allows the regeneration inside Calcium carbonate is quikly reabsorbable, calcium phosphate is slower Biogran TM 30,6 ± 9,7 33,1 ± 8 Orthomatrix TM HA ,3 ± 6,2 67, 7 ± 7** Interpore TM ,5 ± 9,3 67,1 ±8,1** Pro-Osteon TM ,7 ±8 39,8 ± 6,7 Composite polymer Polymethylmethacrylate Polyhydroxyl-ethylmethacrylate Calcium hydroxide carbonate Constructed in concentric caps Porous and resistant matrix Non- reabsorbable Bioplant TM HTR 37,1 ± 8 69,4 ± 7,1** Control group 42,2 ± 6,4 42,2 ± 6,4 e520
5 were biocompatible, osteoconductive and formed bone (2,13). appears to have osteoinductive qualities by ionic interaction with the environment surrounding it (1). Table 1 was prepared to demonstrate the most important characteristics of synthetic bone grafts and the great diversity of results obtained (6,10,14). In one of the articles reviewed, biomaterials were used to increase the alveolar ridge. The results varied depending on the biomaterial used, one of them even delayed the natural process of bone regeneration (7). The application of biomaterials can be successful in the use of immediate implants. In one study a bioactive glass (PerioGlas ) was joined with autogenous bone and blood of the patient. They found that this combination is suitable for use in fresh sockets around immediate implants. The success rate was 100% after twentyfour months of follow-up (15). In another study in which the surface of the implant was treated with bioceramics or ions, the rate of osteointegration was improved (17). When performing maxillary sinus lifts the use of biomaterials can also be useful. This is demonstrated in one of the articles reviewed where a mixture of autogenous bone and β-tricalcium phosphate was prepared. The sinus lift and implant placement were performed during the same surgical procedure. After an interval of twenty-seven to fifty-three months, no cases of implant failure were observed (12). Another material often used in these cases is a bovine hydroxyapatite, for example, Bio-Oss (14). In another article biomaterials were successfully used for repairing surgically maxillary cystic bone defects. A bioactive glass reinforced with hydroxyapatite registered as Bonelike was used. All patients showed good bone regeneration after forty-eight weeks (9). When considering tissue engineering, an ideal bone substitute should possess the following design requirements: a) biocompatibility, b) conductivity for attachment and proliferation of committed cells or heir progenitors and production of new extracellular matrix, c) ability to incorporate inductive factors to direct and enhance new tissue growth, d) support of vascular ingrowth for oxygen transport, e) mechanical integrity to support loads at the implant site, f) controlled, predictable, reproducible rate of degradation into non-toxic species that are easily metabolized or excreted and g) easy and cost-effective processing into irregular 3D shapes of sufficient size to fill clinically relevant defects (2). GFs bind to target cell receptors and induce an intracellular signal transduction that reaches the nucleus and determines the biological response (5). Bone Morphogenetic Proteins (BMPs) is the generic name of a family of proteins able to achieve the transformation of connective tissue into bone tissue, for which they are considered osteoinductive, therefore, are capable of inducing bone formation at ectopic sites. Likewise, they are able to stimulate the differentiation of the stem cells towards different cell lines (adipose tissue, cartilage and bone). BMPs are not only present in the bone matrix, but can also be synthesized by cells of other lineages (e.g., macrophages). To date, 20 types and subtypes of BMPs have been reported. All BMPs belong to the TGF-β superfamily except BMP-1. They are currently considered to be the most powerful factors in osteoblastic differentiation (4,17). Platelet-rich plasma (PRP) was proposed for use in oral and maxillofacial surgery, due to its high content of GFs. PRP can enhance regeneration mediated by the releasing of GFs, such as TGF-β, PDGF, and IGF-1, that are present inside of the α- granules of platelets (17). Current sources for delivery of a GF mixture into the site of bone repair are platelet gel and demineralised bone matrix (17). Discussion It is interesting how Mah J et al. (10) and Schmitt SC et al. (16) when comparing different alloplastic bone grafts find great variability in their results.the studies differ in that the first was an in vivo study using rats, whilst the latter is carried out in vitro with similar cells to ovine osteoblast-like cells. The first study showed that with regards to the formation of new bone in total defect, there were no significant differences with the control group, but there were significant differences when particles of biomaterial in direct contact with the new formed bone were included (Table 1). If we look at the data from the second study, the sample where the largest growth occurred was in the cell culture without any biomaterial. Other authors prefer to select a biomaterial and study it in a specific situation. This is the case for the study carried out by Masago H et al., who used PRP along with β-tricalcium phosphate granules, calcium phosphate cement powder and web form of titanium fibers (7). Although many biomaterials have had a lengthy history of clinical success, very few interact with their surrounding host environment or promote integration with host tissue in an intelligent, proactive fashion. The desire for more biological approaches to biomaterial design that could yield materials that are more instructive to cells has led to an expansion and paradigm shift in the field of biomaterials. This is why GF, BMP, PRP and tissue engineering are the topic of study of many scientific investigations at this moment in time. These lines of investigation are based on the latest findings about biomaterials for bone regeneration. We found that the most recent articles were the ones that most considered these topics: Scheller EL et al., Devescovi V et al., Torroni A, and Avila G et al. (2,5,8,17). Some authors found that the association of biomaterials with autograft is beneficial for bone regeneration. This e521
6 was the case for Aguirre Zorzano LA et al. (12), who associated autogenous bone with β-tricalcium phosphate. Gatti AM et al. (15) combined bioactive glass with the autogenous bone. Others prefer to associate different biomaterials as can be seen in a study carried out by Sousa RC et al., who used a composite (Bonelike ) with a glass and hydroxyapatite base (9). Another line of investigation carried out by Avila G et al. was to apply 4 different substances to the implant surface (ceramics, bioactive proteins, ions and polymers) so as to improve bone regeneration (17). Scheller EL et al., Devescovi V et al. and Torroni A consider the biological mediators play an important role in improving bone regeneration (2,5,8). There is still much work needed and many questions to be resolved such as the way the biomaterial is applied (e.g. gel, foam or fibre), identification of appropriate cell sources for a desired application (e.g. autogenous versus allogenic cells; primary cells, cell lines, genetically modified cells versus stem cells; adult versus embryonic cells) o identification of spatial and temporal signals (e.g. growth factors, cytokines, chemokines) for tissuespecific differentiation and morphogenesis and the approach to deliver these signals (soluble versus insoluble; temporal and spatial control) represent design choices along the third axis of the tissue engineering triad (2). When the size of the lesion is larger than 6 to 9 cm, the use of an autograft is not efficient and so the need for tissue engineering intensifies. Tissue engineering also comes with some drawbacks. The production of recombinant growth factors, collection and transport of the biopsies and culture of autologous cells are some of the factors that make tissue engineering time-, money- and labour-consuming. Another problem is that an engineered bone graft involves the inadequate vascularization of the inner portion of graft. This limits the formation of bone at the centre of the smaller grafts, and represents an insurmountable obstacle in the creation of larger grafts. The solution is to induce angiogenesis within the construct. Further improvement of biomaterials is needed in order to make tissue engineering more successful and, ideally, even unnecessary (1,8). Many variables have to be considered so as to achieve the best results in each individual clinical situation. For this a profound knowledge of biomaterials and their selection criteria is necessary as there are multiple possibilities available. Conclusions Currently, biomaterials are still far from ideal bone substitutes. They have certain disadvantages compared with autografts, because they lack the osteogenic and osteoinductive properties, but they have significant benefits in terms of availability, avoiding the risk of donor site complications and, of course, their well-developed osteointegrative and osteoconductive properties. The studies seek to improve the characteristics of these bone substitutes. The two most important lines of research are based on one hand, on composites (combination of several biomaterials), and on the other hand, tissue engineering and growth factors. The latter emerges as an innovative, sophisticated and interesting field, because it is the nearest approximation to the autogenous graft, the only osteogenic material. Significant progress is expected in this young scientific field of biomaterials so as to achieve the needs of society and move towards a future of greater success. References 1. Habibovic P, de Groot K. Osteoinductive biomaterials--properties and relevance in bone repair. J Tissue Eng Regen Med. 2007;1: Scheller EL, Krebsbach PH, Kohn DH. Tissue engineering: state of the art in oral rehabilitation. J Oral Rehabil. 2009;36: Fernández-Tresguerres-Hernández-Gil I, Alobera-Gracia MA, del-canto-pingarrón M, Blanco-Jerez L. Physiological bases of bone regeneration I. Histology and physiology of bone tissue. Med Oral Patol Oral Cir Bucal. 2006;11:E Fernández-Tresguerres-Hernández-Gil I, Alobera-Gracia MA, del-canto-pingarrón M, Blanco-Jerez L. Physiological bases of bone regeneration II. The remodeling process. Med Oral Patol Oral Cir Bucal. 2006;11:E Devescovi V, Leonardi E, Ciapetti G, Cenni E. Growth factors in bone repair. Chir Organi Mov. 2008;92: Moore WR, Graves SE, Bain GI. Synthetic bone graft substitutes. ANZ J Surg. 2001;71: Masago H, Shibuya Y, Munemoto S, Takeuchi J, Umeda M, Komori T, et al. Alveolar ridge augmentation using various bone substitutes--a web form of titanium fibers promotes rapid bone development. Kobe J Med Sci. 2007;53: Torroni A. Engineered bone grafts and bone flaps for maxillofacial defects: state of the art. J Oral Maxillofac Surg. 2009;67: Sousa RC, Lobato JV, Maurício AC, Hussain NS, Botelho CM, Lopes MA, et al. A clinical report of bone regeneration in maxillofacial surgery using bonelike synthetic bone graft. J Biomater Appl. 2008;22: Mah J, Hung J, Wang J, Salih E. The efficacy of various alloplastic bone grafts on the healing of rat calvarial defects. Eur J Orthod. 2004;26: Hench LL, Polak JM. Third-generation biomedical materials. Science. 2002;295: Aguirre Zorzano LA, Rodríguez Tojo MJ, Aguirre Urizar JM. Maxillary sinus lift with intraoral autologous bone and B--tricalcium phosphate: histological and histomorphometric clinical study. Med Oral Patol Oral Cir Bucal. 2007;12:E Von Doernberg MC, Von Rechenberg B, Bohner M, Grünenfelder S, van Lenthe GH, Müller R, et al. In vivo behavior of calcium phosphate scaffolds with four different pore sizes. Biomaterials. 2006;27: Annalisa P, Furio P, Ilaria Z, Anna A, Luca S, Marcella M, et al. Anorganic bovine bone and a silicate-based synthetic bone activate different micrornas. J Oral Sci. 2008;50: Gatti AM, Simonetti LA, Monari E, Guidi S, Greenspan D. Bone augmentation with bioactive glass in three cases of dental implant placement. J Biomater Appl. 2006;20: Schmitt SC, Wiedmann-Al-Ahmad M, Kuschnierz J, Al-Ahmad A, Huebner U, Schmelzeisen R, et al. Comparative in vitro study of the proliferation and growth of ovine osteoblast-like cells on various alloplastic biomaterials manufactured for augmentation and reconstruction of tissue or bone defects. J Mater Sci Mater Med. 2008;19: Avila G, Misch K, Galindo-Moreno P, Wang HL. Implant surface treatment using biomimetic agents. Implant Dent. 2009;18: e522
Inion BioRestore. Bone Graft Substitute. Product Overview
 Inion BioRestore Bone Graft Substitute Product Overview Inion BioRestore Introduction Inion BioRestore is a synthetic bone graft substitute, which remodels into bone and is easy to use. Inion BioRestore
Inion BioRestore Bone Graft Substitute Product Overview Inion BioRestore Introduction Inion BioRestore is a synthetic bone graft substitute, which remodels into bone and is easy to use. Inion BioRestore
Biomaterials Line. MIS Corporation. All Rights Reserved.
 7. Biomaterials Line MIS Corporation. All Rights Reserved. 6. MIS s Quality System complies with international quality standards: ISO 13485: 2003 - Quality Management System for Medical Devices, ISO 9001:
7. Biomaterials Line MIS Corporation. All Rights Reserved. 6. MIS s Quality System complies with international quality standards: ISO 13485: 2003 - Quality Management System for Medical Devices, ISO 9001:
More than bone regeneration. A total solution.
 More than bone regeneration. A total solution. More than a dental implant company. A total solution. When it comes to treatment options, your patients want positive results both functionally and esthetically.
More than bone regeneration. A total solution. More than a dental implant company. A total solution. When it comes to treatment options, your patients want positive results both functionally and esthetically.
Innovative Range of Regenerative Solutions
 TM Innovative Range of Regenerative Solutions MIS Implant Technologies Ltd. All rights reserved. Optimal volumes and quality of hard and soft tissue are required to satisfy the goals of oral rehabilitation
TM Innovative Range of Regenerative Solutions MIS Implant Technologies Ltd. All rights reserved. Optimal volumes and quality of hard and soft tissue are required to satisfy the goals of oral rehabilitation
BIOACTIVE SYNTHETIC GRAFT
 B U I L D S T R O N G B O N E F A S T Putty Particulate Morsels A BIOACTIVE SYNTHETIC BONE FOR FASTER HEALING NovaBone is a 100% bioactive synthetic material composed from elements that occur naturally
B U I L D S T R O N G B O N E F A S T Putty Particulate Morsels A BIOACTIVE SYNTHETIC BONE FOR FASTER HEALING NovaBone is a 100% bioactive synthetic material composed from elements that occur naturally
BIOACTIVE BASICS. Bioactive materials elicit a controlled action and reaction in the physiological environment.
 BIOACTIVE BASICS Bioactive materials elicit a controlled action and reaction in the physiological environment. Bioglass is a glass ceramic composed of silicon dioxide (SiO 2 ), sodium oxide (Na 2 O), calcium
BIOACTIVE BASICS Bioactive materials elicit a controlled action and reaction in the physiological environment. Bioglass is a glass ceramic composed of silicon dioxide (SiO 2 ), sodium oxide (Na 2 O), calcium
Bone Tissue Biology & The Application of Synthetic Compounds for the Facilitation of Bone Tissue Healing
 Bone Tissue Biology & The Application of Synthetic Compounds for the Facilitation of Bone Tissue Healing Ryan T. Jones Western Michigan University May 2011 Introduction Bone has unique properties: Tensile
Bone Tissue Biology & The Application of Synthetic Compounds for the Facilitation of Bone Tissue Healing Ryan T. Jones Western Michigan University May 2011 Introduction Bone has unique properties: Tensile
B U I L D S T R O N G B O N E F A S T
 B U I L D S T R O N G B O N E F A S T Putty MIS Particulate Morsels A BIOACTIVE SYNTHETIC BONE FOR FASTER HEALING NovaBone is a 100% bioactive synthetic material composed from elements that occur naturally
B U I L D S T R O N G B O N E F A S T Putty MIS Particulate Morsels A BIOACTIVE SYNTHETIC BONE FOR FASTER HEALING NovaBone is a 100% bioactive synthetic material composed from elements that occur naturally
Pre-operative evaluation of the volume of bone graft in sinus lifts by means of CompuDent
 Journal section: Oral Surgery Publication Types: Research doi:0.7/medoral..e Pre-operative evaluation of the volume of bone graft in sinus lifts by means of CompuDent Oscar Arias-Irimia, Cristina Barona-Dorado,
Journal section: Oral Surgery Publication Types: Research doi:0.7/medoral..e Pre-operative evaluation of the volume of bone graft in sinus lifts by means of CompuDent Oscar Arias-Irimia, Cristina Barona-Dorado,
BONE AUGMENTATION AND GRAFTING
 1 A Computer-Guided Bone Block Harvesting Procedure: A Proof-of-Principle Case Report and Technical Notes Effectiveness of Lateral Bone Augmentation on the Alveolar Crest Dimension: A Systematic Review
1 A Computer-Guided Bone Block Harvesting Procedure: A Proof-of-Principle Case Report and Technical Notes Effectiveness of Lateral Bone Augmentation on the Alveolar Crest Dimension: A Systematic Review
Chemicals in Surgical Periodontal Therapy
 Chemicals in Surgical Periodontal Therapy von Alexandrina L. Dumitrescu 1. Auflage Chemicals in Surgical Periodontal Therapy Dumitrescu schnell und portofrei erhältlich bei beck-shop.de DIE FACHBUCHHANDLUNG
Chemicals in Surgical Periodontal Therapy von Alexandrina L. Dumitrescu 1. Auflage Chemicals in Surgical Periodontal Therapy Dumitrescu schnell und portofrei erhältlich bei beck-shop.de DIE FACHBUCHHANDLUNG
P105 Predictable Bone Grafting for Site Preparation for Implants and Prosthetics Workshop JAMES GRISDALE, DDS THURSDAY, FEBRUARY 26
 P105 Predictable Bone Grafting for Site Preparation for Implants and Prosthetics Workshop JAMES GRISDALE, DDS THURSDAY, FEBRUARY 26 Please complete the speaker evaluation form in the Midwinter Meeting
P105 Predictable Bone Grafting for Site Preparation for Implants and Prosthetics Workshop JAMES GRISDALE, DDS THURSDAY, FEBRUARY 26 Please complete the speaker evaluation form in the Midwinter Meeting
Bioactive Glass Biphasic β-tcp & HA Granules Alkylene Oxide Polymer Carrier. MEDLINEUNITE Bioactive Bone Graft
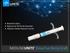 Bioactive Glass Biphasic β-tcp & HA Granules Alkylene Oxide Polymer Carrier Principles of Bone Healing Reparative Phase Healing Cascade 1. Cellular infiltration and migration to site (fibroblasts, macrophages,
Bioactive Glass Biphasic β-tcp & HA Granules Alkylene Oxide Polymer Carrier Principles of Bone Healing Reparative Phase Healing Cascade 1. Cellular infiltration and migration to site (fibroblasts, macrophages,
Versatile grafting Solutions
 Versatile grafting Solutions A Canadian company serving Canadian dentists since 1997 Here s why your colleagues are calling us for their bone regeneration needs Founded in 1997 Citagenix has been providing
Versatile grafting Solutions A Canadian company serving Canadian dentists since 1997 Here s why your colleagues are calling us for their bone regeneration needs Founded in 1997 Citagenix has been providing
THE NEXT FRONTIER OF BONE REGENERATION. where Technology meets Nature
 THE NEXT FRONTIER OF BONE REGENERATION where Technology meets Nature SmartBone is a new hybrid bioactive bone substitute specifically developed for bone regeneration in reconstructive surgery. SmartBone
THE NEXT FRONTIER OF BONE REGENERATION where Technology meets Nature SmartBone is a new hybrid bioactive bone substitute specifically developed for bone regeneration in reconstructive surgery. SmartBone
In the last decade of the 20 th century, special emphasis was put on an emerging field of science: Tissue engineering,which combines the state of the
 In the last decade of the 20 th century, special emphasis was put on an emerging field of science: Tissue engineering,which combines the state of the art materials science with concepts from the life sciences.
In the last decade of the 20 th century, special emphasis was put on an emerging field of science: Tissue engineering,which combines the state of the art materials science with concepts from the life sciences.
chronos Bone Void Filler. Beta-Tricalcium Phosphate ( β-tcp) bone graft substitute.
 chronos Bone Void Filler. Beta-Tricalcium Phosphate ( β-tcp) bone graft substitute. Osteoconductive Resorbable Synthetic chronos Bone Void Filler chronos granules and preforms are synthetic, porous, osteoconductive,
chronos Bone Void Filler. Beta-Tricalcium Phosphate ( β-tcp) bone graft substitute. Osteoconductive Resorbable Synthetic chronos Bone Void Filler chronos granules and preforms are synthetic, porous, osteoconductive,
THE NEXT FRONTIER OF BONE REGENERATION. where Technology meets Nature
 THE NEXT FRONTIER OF BONE REGENERATION where Technology meets Nature SmartBone is a new hybrid bioactive bone substitute specifically developed for bone regeneration in reconstructive surgery. SmartBone
THE NEXT FRONTIER OF BONE REGENERATION where Technology meets Nature SmartBone is a new hybrid bioactive bone substitute specifically developed for bone regeneration in reconstructive surgery. SmartBone
A WIDE RANGE OF REGENERATIVE SOLUTIONS
 A WIDE RANGE OF REGENERATIVE SOLUTIONS INDICATIONS: 1/ SOCKET AND RIDGE PRESERVATION 2/ FILLING OF EXTRACTION SOCKETS Biomaterials offers portfolio of regenerative materials for implantology, aimed at
A WIDE RANGE OF REGENERATIVE SOLUTIONS INDICATIONS: 1/ SOCKET AND RIDGE PRESERVATION 2/ FILLING OF EXTRACTION SOCKETS Biomaterials offers portfolio of regenerative materials for implantology, aimed at
PRP Usage in Today's Implantology
 Volume 1, December 2004 www.implant.co.il PRP Usage in Today's Implantology by Dr. R. Shapira Introduction: Treating patients suffering from hematological disorders or using anticoagulant medications always
Volume 1, December 2004 www.implant.co.il PRP Usage in Today's Implantology by Dr. R. Shapira Introduction: Treating patients suffering from hematological disorders or using anticoagulant medications always
Cerasorb M DENTAL. O:\Zulassung\Cerasorb Dental Kanada 2013\Texte\Cerasorb M Dental final IFU docx
 Cerasorb M DENTAL Resorbable, pure-phase beta-tricalcium phosphate matrix with interconnecting porosity for bone regeneration for use in dental and maxillofacial surgery DESCRIPTION: Cerasorb M DENTAL
Cerasorb M DENTAL Resorbable, pure-phase beta-tricalcium phosphate matrix with interconnecting porosity for bone regeneration for use in dental and maxillofacial surgery DESCRIPTION: Cerasorb M DENTAL
BEGO BIOMATERIALS When the result counts
 BEGO BIOMATERIALS When the result counts Partners in Progress INTRO Challenge what exists get the right answers We practise systematic thinking with a passion and we are never satisfied with the status
BEGO BIOMATERIALS When the result counts Partners in Progress INTRO Challenge what exists get the right answers We practise systematic thinking with a passion and we are never satisfied with the status
Regeneration Bone Grafting & Soft Tissue Management
 Regeneration Bone Grafting & Soft Tissue Management 1 Regeneration Bone Grafting & Soft Tissue Management Table of contents Bone Graft Material OSTEON II OSTEON OSTEON II Collagen OSTEON Collagen 5 6
Regeneration Bone Grafting & Soft Tissue Management 1 Regeneration Bone Grafting & Soft Tissue Management Table of contents Bone Graft Material OSTEON II OSTEON OSTEON II Collagen OSTEON Collagen 5 6
Alveolar Ridge Augmentation Using Various Bone Substitutes -A Web Form of Titanium Fibers Promotes Rapid Bone Development-
 Kobe J. Med. Sci., Vol. 53, No. 5, pp. 257-263 2007 Alveolar Ridge Augmentation Using Various Bone Substitutes -A Web Form of Titanium Fibers Promotes Rapid Bone Development- HIROSHI MASAGO 1, YASUYUKI
Kobe J. Med. Sci., Vol. 53, No. 5, pp. 257-263 2007 Alveolar Ridge Augmentation Using Various Bone Substitutes -A Web Form of Titanium Fibers Promotes Rapid Bone Development- HIROSHI MASAGO 1, YASUYUKI
Product Information. MIS Corporation. All Rights Reserved.
 Product Information MIS Corporation. All Rights Reserved. MIS Warranty: MIS exercises great care and effort in maintaining the superior quality of its products. All MIS products are guaranteed to be free
Product Information MIS Corporation. All Rights Reserved. MIS Warranty: MIS exercises great care and effort in maintaining the superior quality of its products. All MIS products are guaranteed to be free
Symbios Xenograft Granules Porcine Bone Graft Material
 Symbios Xenograft Granules Porcine Bone Graft Material 32671122-USX-1607_Symbios Highlight Brochure.indd 1 2016-09-27 12:12 Symbios Xenograft Granules Porcine bone graft material Symbios Xenograft Granules
Symbios Xenograft Granules Porcine Bone Graft Material 32671122-USX-1607_Symbios Highlight Brochure.indd 1 2016-09-27 12:12 Symbios Xenograft Granules Porcine bone graft material Symbios Xenograft Granules
BioVin Collagen Membrane
 BioVin Collagen Membrane Resorbable cross-linked collagen membrane BioVin Bovine Bone Bovine Bone Substitute OToss Synthetic Bone Synthetic Resorbable Biphasic Calcium Phosphate OToss Synthetic Bone Inject
BioVin Collagen Membrane Resorbable cross-linked collagen membrane BioVin Bovine Bone Bovine Bone Substitute OToss Synthetic Bone Synthetic Resorbable Biphasic Calcium Phosphate OToss Synthetic Bone Inject
Regeneration Bone Grafting & Soft Tissue Management
 Regeneration Bone Grafting & Soft Tissue Management Human Histology OSTEON II 26.5 months Regeneration Products information Table of contents Bone Graft Material OSTEON II OSTEON OSTEON II Collagen OSTEON
Regeneration Bone Grafting & Soft Tissue Management Human Histology OSTEON II 26.5 months Regeneration Products information Table of contents Bone Graft Material OSTEON II OSTEON OSTEON II Collagen OSTEON
THE NEXT FRONTIER OF BONE REGENERATION
 THE NEXT FRONTIER OF BONE REGENERATION where Technology meets Nature swiss made SmartBone is new composite bone substitute specifically developed for bone regeneration in oral and maxillofacial reconstructive
THE NEXT FRONTIER OF BONE REGENERATION where Technology meets Nature swiss made SmartBone is new composite bone substitute specifically developed for bone regeneration in oral and maxillofacial reconstructive
Puros Cancellous Particulate Allograft & Puros Block Allograft
 Puros Cancellous Particulate Allograft & Puros Block Allograft Puros Cancellous Particulate Allograft The Natural Choice For Healthy 1 Bone Growth. 1. Proven, Predictable Regeneration Acts as an osteoconductive
Puros Cancellous Particulate Allograft & Puros Block Allograft Puros Cancellous Particulate Allograft The Natural Choice For Healthy 1 Bone Growth. 1. Proven, Predictable Regeneration Acts as an osteoconductive
Guided Tissue and Bone Regeneration
 Guided Tissue and Bone Regeneration One toolbox for your needs! Tefguide 9000 742 401 12x24 mm pc 1 Osgide 9000 701 520 15 x 20 mm pc 1 Osbone 9000 800 255 250-1000 μm 0.25 cc 5 Product Specifications
Guided Tissue and Bone Regeneration One toolbox for your needs! Tefguide 9000 742 401 12x24 mm pc 1 Osgide 9000 701 520 15 x 20 mm pc 1 Osbone 9000 800 255 250-1000 μm 0.25 cc 5 Product Specifications
Re-growing the Skeleton: Approaches in Tissue Engineering and Regenerative Medicine
 Re-growing the Skeleton: Approaches in Tissue Engineering and Regenerative Medicine How we fix things now Total Knee Replacements Fracture Plates Fusing Joints Defining Regenerative Medicine restore form
Re-growing the Skeleton: Approaches in Tissue Engineering and Regenerative Medicine How we fix things now Total Knee Replacements Fracture Plates Fusing Joints Defining Regenerative Medicine restore form
ctive Bone Bonding Bone Regeneration Osteostimulation*
 www.bonalive.com ctive Bone Bonding Bone Regeneration Osteostimulation* A revolution in bone grafting Osteoconductive bone graft substitute with osteostimulative* properties *non-osteoinductive Before
www.bonalive.com ctive Bone Bonding Bone Regeneration Osteostimulation* A revolution in bone grafting Osteoconductive bone graft substitute with osteostimulative* properties *non-osteoinductive Before
NEW FIXATION STRATEGIES FOR OSTEOPOROTIC BONE
 NEW FIXATION STRATEGIES FOR OSTEOPOROTIC BONE THE PROBLEMS Fixation failure Malunion F 83 yrs 2 Months 6 Months F 81 yrs 3 Months FIXATION AUGMENTATION TECHNIQUES (FATs) Surgical procedures aimed at increasing
NEW FIXATION STRATEGIES FOR OSTEOPOROTIC BONE THE PROBLEMS Fixation failure Malunion F 83 yrs 2 Months 6 Months F 81 yrs 3 Months FIXATION AUGMENTATION TECHNIQUES (FATs) Surgical procedures aimed at increasing
Index. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Alginate, tooth-shaped, for constructs, encapsulated pulp cells in, 589 590 Antibiotic paste, triple, change in root length and width
Index Note: Page numbers of article titles are in boldface type. A Alginate, tooth-shaped, for constructs, encapsulated pulp cells in, 589 590 Antibiotic paste, triple, change in root length and width
Regeneration Bone Grafting & Soft Tissue Management
 Regeneration Bone Grafting & Soft Tissue Management OSTEON TM II Table of Contents Bone Graft Material OSTEON TM II Collagen 04 OSTEON TM Collagen 06 OSTEON TM II 08 OSTEON TM 12 ORTHOPEDIC OSTEON TM 14
Regeneration Bone Grafting & Soft Tissue Management OSTEON TM II Table of Contents Bone Graft Material OSTEON TM II Collagen 04 OSTEON TM Collagen 06 OSTEON TM II 08 OSTEON TM 12 ORTHOPEDIC OSTEON TM 14
"The Evaluation Nano Calcium Silicate Cements Performance for Palpation"
 "The Evaluation Nano Calcium Silicate Cements Performance for Palpation" Delaram Amini* Bachelor Student, Department of Medical Islamic Azad University Of Tehran Medical Branch Tehran,Iran Maryam Chenani
"The Evaluation Nano Calcium Silicate Cements Performance for Palpation" Delaram Amini* Bachelor Student, Department of Medical Islamic Azad University Of Tehran Medical Branch Tehran,Iran Maryam Chenani
In search of the optimal material for dental bone grafting
 2 EDI An overview of dental bone graft materials In search of the optimal material for dental bone grafting Sean Aiken, Keele, and Dr Anthony Bendkowski, Maidstone/England The range of dental bone graft
2 EDI An overview of dental bone graft materials In search of the optimal material for dental bone grafting Sean Aiken, Keele, and Dr Anthony Bendkowski, Maidstone/England The range of dental bone graft
REASONS TO USE R.T.R.
 3 REASONS TO USE R.T.R. AFTER EACH EXTRACTION Fully resorbable ß-TCP material RTR 3raisons 120x280.indd 1 16/06/15 10:52 1AVOID SPONTANEOUS RIDGE RESORPTION After tooth extraction, spontaneous healing
3 REASONS TO USE R.T.R. AFTER EACH EXTRACTION Fully resorbable ß-TCP material RTR 3raisons 120x280.indd 1 16/06/15 10:52 1AVOID SPONTANEOUS RIDGE RESORPTION After tooth extraction, spontaneous healing
THE ESSENTIALS IN BONE GRAFTING BRIDGING MEDICAL GAPS
 THE ESSENTIALS IN BONE GRAFTING BRIDGING MEDICAL GAPS FAST FACTS Clean and sterile, free of human, animal and chemical material. Products can be custom ordered, ranging from pastes and cements to granulations
THE ESSENTIALS IN BONE GRAFTING BRIDGING MEDICAL GAPS FAST FACTS Clean and sterile, free of human, animal and chemical material. Products can be custom ordered, ranging from pastes and cements to granulations
The Essential Choice. With the Benefits of Biologic Predictability
 The Essential Choice With the Benefits of Biologic Predictability Documented, Reliable, Experienced is the essential choice for your daily regenerative needs. Throughout our long history and dedication
The Essential Choice With the Benefits of Biologic Predictability Documented, Reliable, Experienced is the essential choice for your daily regenerative needs. Throughout our long history and dedication
Evaluation of different grafting materials in three-wall intra-bony defects around dental implants in beagle dogs
 Current Applied Physics 5 (2005) 507 511 www.elsevier.com/locate/cap Evaluation of different grafting materials in three-wall intra-bony defects around dental implants in beagle dogs Ui-Won Jung a, Hee-Il
Current Applied Physics 5 (2005) 507 511 www.elsevier.com/locate/cap Evaluation of different grafting materials in three-wall intra-bony defects around dental implants in beagle dogs Ui-Won Jung a, Hee-Il
Bone modeling and remodeling How does a bone form without augmentation?
 Overview on Bone formation,bone grafts materials, and Augma Biomaterials bone cements Bone modeling and remodeling How does a bone form without augmentation? Bone Modeling Initial formation of a bone A
Overview on Bone formation,bone grafts materials, and Augma Biomaterials bone cements Bone modeling and remodeling How does a bone form without augmentation? Bone Modeling Initial formation of a bone A
The Original remains unique.
 The Original remains unique. Geistlich leading regeneration 2A, 2B Geistlich is the world leader in regenerative dentistry. We transform natural biomaterials into safe and reliable treatment methods that
The Original remains unique. Geistlich leading regeneration 2A, 2B Geistlich is the world leader in regenerative dentistry. We transform natural biomaterials into safe and reliable treatment methods that
THE NEW STANDARD OF EXCELLENCE IN BIOMATERIALS. Collagenated heterologous cortico-cancellous bone mix + TSV Gel GTO I N S P I R E D B Y N A T U R E
 GTO THE NEW STANDARD OF EXCELLENCE IN BIOMATERIALS Collagenated heterologous cortico-cancellous bone mix + TSV Gel R E G E N E R A T I O N S C I E N C E I N S P I R E D B Y N A T U R E A unique biotechnology
GTO THE NEW STANDARD OF EXCELLENCE IN BIOMATERIALS Collagenated heterologous cortico-cancellous bone mix + TSV Gel R E G E N E R A T I O N S C I E N C E I N S P I R E D B Y N A T U R E A unique biotechnology
Pattern of bone resorption after extraction
 Teeth loss Pattern of bone resorption after extraction 50% in 1st year 2/ 3 in first 3 months Reich KM, Huber CD, Lippnig WR, Um C, Watzek G, Tangl S. (2011, 17). Atrophy of Residual Alveolar Ridge following
Teeth loss Pattern of bone resorption after extraction 50% in 1st year 2/ 3 in first 3 months Reich KM, Huber CD, Lippnig WR, Um C, Watzek G, Tangl S. (2011, 17). Atrophy of Residual Alveolar Ridge following
The Essential Choice. With the Benefits of Biologic Predictability
 The Essential Choice With the Benefits of Biologic Predictability Documented, Reliable, Experienced is the essential choice for your daily regenerative needs. Throughout our long history and dedication
The Essential Choice With the Benefits of Biologic Predictability Documented, Reliable, Experienced is the essential choice for your daily regenerative needs. Throughout our long history and dedication
chronos Synthetic cancellous bone graft substitute ( -tricalcium phosphate) Remodels Replaced by bone in 6 18 months Easy to use
 Synthetic cancellous bone graft substitute ( -tricalcium phosphate) Remodels Replaced by bone in 6 18 months Easy to use Granules, blocks, wedges, cylinders Safe Synthetic origin provides unsurpassed safety
Synthetic cancellous bone graft substitute ( -tricalcium phosphate) Remodels Replaced by bone in 6 18 months Easy to use Granules, blocks, wedges, cylinders Safe Synthetic origin provides unsurpassed safety
THE NEXT GENERATION OF REGENERATION
 THE NEXT GENERATION OF REGENERATION Why SynthoGraft? SynthoGraft offers a unique structure which provides stability, while its micro-porosity allows for rapid vascularization and subsequent resorption.
THE NEXT GENERATION OF REGENERATION Why SynthoGraft? SynthoGraft offers a unique structure which provides stability, while its micro-porosity allows for rapid vascularization and subsequent resorption.
Product Catalog. Dental Bone & Tissue Regeneration
 Product Catalog Dental Bone & Tissue Regeneration Bone graft regeneration Guided bone substitutes regeneration Osteogenesis Controlled resorption rate Angiogenesis Long term volume stability Remodeling
Product Catalog Dental Bone & Tissue Regeneration Bone graft regeneration Guided bone substitutes regeneration Osteogenesis Controlled resorption rate Angiogenesis Long term volume stability Remodeling
botiss dental bone & tissue regeneration biomaterials collacone max Innovative composite matrix socket preservation form-fitting resorbable composite
 dental bone & tissue regeneration botiss biomaterials socket preservation Innovative composite matrix form-fitting resorbable composite 1 botiss regeneration system maxresorb flexbone* collacone.. max
dental bone & tissue regeneration botiss biomaterials socket preservation Innovative composite matrix form-fitting resorbable composite 1 botiss regeneration system maxresorb flexbone* collacone.. max
The Use of Freeze-Dried Bone Allograft as an Alternative to Autogenous Bone Graft in the Atrophic Maxilla: A 3-Year Clinical Follow-up
 643 The Use of Freeze-Dried Bone Allograft as an Alternative to Autogenous Bone Graft in the Atrophic Maxilla: A 3-Year Clinical Follow-up Marco Aurélio Bianchini, DDS, MSc, PhD 1 André R. Buttendorf,
643 The Use of Freeze-Dried Bone Allograft as an Alternative to Autogenous Bone Graft in the Atrophic Maxilla: A 3-Year Clinical Follow-up Marco Aurélio Bianchini, DDS, MSc, PhD 1 André R. Buttendorf,
Bone augmentation with biomaterials
 Patient information dental bone & tissue regeneration botiss biomaterials Bone augmentation with biomaterials established safe natural X100 Implantation stability is crucial for success Atrophy of the
Patient information dental bone & tissue regeneration botiss biomaterials Bone augmentation with biomaterials established safe natural X100 Implantation stability is crucial for success Atrophy of the
DRIVING THE FUTURE. About HOSPITAL INNOVATIONS. Strong commitment to healthcare innovation
 idente Catalogue About HOSPITAL INNOVATIONS Since 2008, Hospital Innovations has been supplying a growing range of specialist products for use in orthopaedic and corrective surgery; with an emphasis on
idente Catalogue About HOSPITAL INNOVATIONS Since 2008, Hospital Innovations has been supplying a growing range of specialist products for use in orthopaedic and corrective surgery; with an emphasis on
Bone augmentation with maxgraft
 Patient information bone & tissue regeneration botiss biomaterials Bone augmentation with maxgraft established safe X100 natural Implantation stability is crucial for success Atrophy of the jaw bone loss
Patient information bone & tissue regeneration botiss biomaterials Bone augmentation with maxgraft established safe X100 natural Implantation stability is crucial for success Atrophy of the jaw bone loss
Department of Oral and Maxillofacial Surgery, Loma Linda University, Loma Linda, CA 92354, USA 2
 Plastic Surgery International Volume 2011, Article ID 165824, 7 pages doi:10.1155/2011/165824 Review Article Reconstruction of Mandibular Defects Using Bone Morphogenic Protein: Can Growth Factors Replace
Plastic Surgery International Volume 2011, Article ID 165824, 7 pages doi:10.1155/2011/165824 Review Article Reconstruction of Mandibular Defects Using Bone Morphogenic Protein: Can Growth Factors Replace
Peggers Super Summaries Basic Sciences Bone
 Bone Overview & Turnover BONES Function o Support o Protection o Assisting movement o Storage of minerals o Production of red blood cells from marrow Types o Cancellous o Compact with Haversian systems
Bone Overview & Turnover BONES Function o Support o Protection o Assisting movement o Storage of minerals o Production of red blood cells from marrow Types o Cancellous o Compact with Haversian systems
In Vivo Evaluation of BioSphere Bioactive Bone Graft Putty: Improved Bone Formation
 In Vivo Evaluation of BioSphere Bioactive Bone Graft : Improved Bone Formation ABSTRACT BioSphere is a novel bone graft product that was developed using spherical particles of bioactive glass with a narrow,
In Vivo Evaluation of BioSphere Bioactive Bone Graft : Improved Bone Formation ABSTRACT BioSphere is a novel bone graft product that was developed using spherical particles of bioactive glass with a narrow,
Comparative Animal Study of OssiMend and Healos 13,14
 Comparative Animal Study of OssiMend and Healos 13,14 Objective This study was conducted to evaluate the use of OssiMend as compared with Healos in combination with autologous bone marrow as a bone grafting
Comparative Animal Study of OssiMend and Healos 13,14 Objective This study was conducted to evaluate the use of OssiMend as compared with Healos in combination with autologous bone marrow as a bone grafting
ORTHOPEDICS BONE Recalcitrant nonunions In total hip replacement total knee surgery increased callus volume
 ORTHOPEDICS Orthopedics has to do with a variety of tissue: bone, cartilage, tendon, ligament, muscle. In this regard orthopedic and sports medicine share the same tissue targets. Orthopedics is mostly
ORTHOPEDICS Orthopedics has to do with a variety of tissue: bone, cartilage, tendon, ligament, muscle. In this regard orthopedic and sports medicine share the same tissue targets. Orthopedics is mostly
Resorbable bilayer synthetic membrane Biomimetic tissue-engineered matrix for GBR and GTR
 Resorbable bilayer synthetic membrane Biomimetic tissue-engineered matrix for GBR and GTR Patented Jet-Spraying technology: Full barrier effect during 4 weeks, and complete resorption in 6 months PATENTED
Resorbable bilayer synthetic membrane Biomimetic tissue-engineered matrix for GBR and GTR Patented Jet-Spraying technology: Full barrier effect during 4 weeks, and complete resorption in 6 months PATENTED
THE NEXT FRONTIER OF BONE REGENERATION
 THE NEXT FRONTIER OF BONE REGENERATION where Technology meets Nature swiss made SmartBone is new composite bone substitute specifically developed for bone regeneration in oral and maxillofacial reconstructive
THE NEXT FRONTIER OF BONE REGENERATION where Technology meets Nature swiss made SmartBone is new composite bone substitute specifically developed for bone regeneration in oral and maxillofacial reconstructive
REGENERATION BY DESIGN
 REGENERATION BY DESIGN ALLOGRAFT, XENOGRAFT, PUTT Y & BIOACTIVE GLASS FOR BONE REGENERATION INSTRUMENTS FOR COLLECTING BONE BARRIER MEMBRANES FOR GUIDED REGENERATION GUIDED IMPLANT TREATMENT Wide Selection
REGENERATION BY DESIGN ALLOGRAFT, XENOGRAFT, PUTT Y & BIOACTIVE GLASS FOR BONE REGENERATION INSTRUMENTS FOR COLLECTING BONE BARRIER MEMBRANES FOR GUIDED REGENERATION GUIDED IMPLANT TREATMENT Wide Selection
botiss biomaterials bone & tissue regeneration collacone max Innovative composite matrix socket preservation form-fitting resorbable composite
 bone & tissue regeneration botiss biomaterials socket preservation Innovative composite matrix form-fitting resorbable composite 1 Socket preservation safeguarding your sockets collacone.. max flexbone*
bone & tissue regeneration botiss biomaterials socket preservation Innovative composite matrix form-fitting resorbable composite 1 Socket preservation safeguarding your sockets collacone.. max flexbone*
( ) 2009;28(2):89-94
 ( ) 2009;28(2):89-94 Osseointegration is important in the functional aspect, however, esthetics is also important, especially in the maxillary anterior region. An adequate surgical technique is necessary
( ) 2009;28(2):89-94 Osseointegration is important in the functional aspect, however, esthetics is also important, especially in the maxillary anterior region. An adequate surgical technique is necessary
Alloplastic Grafts - Beta-tricalcium phosphate
 Alloplastic Grafts - Beta-tricalcium phosphate Presentation of clinical cases Mario Ernesto García-Briseño DDS and Professor in Periodontics - Autonomous University of Guadalajara (UAG), Mexico This case
Alloplastic Grafts - Beta-tricalcium phosphate Presentation of clinical cases Mario Ernesto García-Briseño DDS and Professor in Periodontics - Autonomous University of Guadalajara (UAG), Mexico This case
Bone Grafting for Socket Preservation
 Bone Grafting for Socket Preservation Dr. Karl R. Koerner Normal extraction facial bone loss. Excessive force. Commonly the thickness of facial bone. Hussain, A. et al. Ridge preservation comparing a nonresorbable
Bone Grafting for Socket Preservation Dr. Karl R. Koerner Normal extraction facial bone loss. Excessive force. Commonly the thickness of facial bone. Hussain, A. et al. Ridge preservation comparing a nonresorbable
FDBA(Freeze Dried Bone Allograft) SureOss Cortical Bone - Powder / Chip. OsteOss Cortical with Cancellous Bone - Powder / Chip
 PERIODONTAL Bone & Skin Allograft Products FDBA(Freeze Dried Bone Allograft) SureOss - Powder / Chip OsteOss Cortical with - Powder / Chip DFDBA(Demineralized Freeze Dried Bone Allograft) SureOss -D Demineralized
PERIODONTAL Bone & Skin Allograft Products FDBA(Freeze Dried Bone Allograft) SureOss - Powder / Chip OsteOss Cortical with - Powder / Chip DFDBA(Demineralized Freeze Dried Bone Allograft) SureOss -D Demineralized
HOSPITAL INNOVATIONS
 idente Catalogue About HOSPITAL INNOVATIONS Since 2008, Hospital Innovations has been supplying a growing range of specialist products for use in orthopaedic and corrective surgery; with an emphasis on
idente Catalogue About HOSPITAL INNOVATIONS Since 2008, Hospital Innovations has been supplying a growing range of specialist products for use in orthopaedic and corrective surgery; with an emphasis on
The advantages of atelo-collagenated, lyophilized (non-heated), bovine bone graft composite. Dr. med. Sami Watad
 The advantages of atelo-collagenated, lyophilized (non-heated), bovine bone graft composite Dr. med. Sami Watad it s a term that describes the physicochemical deletion of the antigenic terminal peptide
The advantages of atelo-collagenated, lyophilized (non-heated), bovine bone graft composite Dr. med. Sami Watad it s a term that describes the physicochemical deletion of the antigenic terminal peptide
Index. Note: Page numbers of article titles are in boldface type.
 Note: Page numbers of article titles are in boldface type. A Acellular dermal allografts for arthroplasty, 633 642 for plantar soft tissue augmentation, 543 555 Achilles tendon repair extracellular matrix
Note: Page numbers of article titles are in boldface type. A Acellular dermal allografts for arthroplasty, 633 642 for plantar soft tissue augmentation, 543 555 Achilles tendon repair extracellular matrix
Radiological and histological analysis of synthetic bone grafts in recurring giant cell tumour of bone: a retrospective study
 Journal of Orthopaedic Surgery 2010;18(1):63-7 Radiological and histological analysis of synthetic bone grafts in recurring giant cell tumour of bone: a retrospective study Hiroyuki Hattori, Hiroaki Matsuoka,
Journal of Orthopaedic Surgery 2010;18(1):63-7 Radiological and histological analysis of synthetic bone grafts in recurring giant cell tumour of bone: a retrospective study Hiroyuki Hattori, Hiroaki Matsuoka,
Sinus Augmentation Studies Methods and Definition
 FDA approved indications for Infuse Bone Graft in the Maxillofacial Skeleton Alveolar Ridge Augmentation (Buccal Wall Defects) in the Maxilla Maxillary Sinus Floor augmentation Sinus Augmentation Studies
FDA approved indications for Infuse Bone Graft in the Maxillofacial Skeleton Alveolar Ridge Augmentation (Buccal Wall Defects) in the Maxilla Maxillary Sinus Floor augmentation Sinus Augmentation Studies
FINITE ELEMENT MODELING OF BONE BY USING HYDROXYAPATITE AS BIOACTIVE NANOMATERIAL IN BONE GRAFTING, BONE HEALING AND THE REDUCTION OF
 CHAPTER-IV FINITE ELEMENT MODELING OF BONE BY USING HYDROXYAPATITE AS BIOACTIVE NANOMATERIAL IN BONE GRAFTING, BONE HEALING AND THE REDUCTION OF MECHANICAL FAILURE IN THE BONE SURGERY This Chapter communicated
CHAPTER-IV FINITE ELEMENT MODELING OF BONE BY USING HYDROXYAPATITE AS BIOACTIVE NANOMATERIAL IN BONE GRAFTING, BONE HEALING AND THE REDUCTION OF MECHANICAL FAILURE IN THE BONE SURGERY This Chapter communicated
OssiMend Bone Graft Matrix
 OssiMend All-Natural Mineral-Collagen Bone Grafting Matrix Anorganic bone mineral and type I collagen Highly purified, biocompatible matrix Osteoconductive Osteoinductive and Osteogenic in conjunction
OssiMend All-Natural Mineral-Collagen Bone Grafting Matrix Anorganic bone mineral and type I collagen Highly purified, biocompatible matrix Osteoconductive Osteoinductive and Osteogenic in conjunction
The use of biologic mediators and tissue engineering in
 Periodontology 2000, Vol. 50, 2009, 127 153 Printed in Singapore. All rights reserved Ó 2009 John Wiley & Sons A/S PERIODONTOLOGY 2000 The use of biologic mediators and tissue engineering in dentistry
Periodontology 2000, Vol. 50, 2009, 127 153 Printed in Singapore. All rights reserved Ó 2009 John Wiley & Sons A/S PERIODONTOLOGY 2000 The use of biologic mediators and tissue engineering in dentistry
REFERENCES for PLATELET RICH PLASMA (PRP)
 REFERENCES for PLATELET RICH PLASMA (PRP) Daif ET. Autologous blood injection as a new treatment modality for chronic recurrent temporomandibular joint dislocation. Oral Surg Oral Med Oral Pathol Oral
REFERENCES for PLATELET RICH PLASMA (PRP) Daif ET. Autologous blood injection as a new treatment modality for chronic recurrent temporomandibular joint dislocation. Oral Surg Oral Med Oral Pathol Oral
ß-tricalcium phosphate used with onlay graft for horizontal bone augmentation yielded preferable result: a case report
 ß-tricalcium phosphate used with onlay graft for horizontal bone augmentation yielded preferable result: a case report Yaqian Chen, Qingqing Wu, Yi Man State Key Laboratory of Oral Diseases, West China
ß-tricalcium phosphate used with onlay graft for horizontal bone augmentation yielded preferable result: a case report Yaqian Chen, Qingqing Wu, Yi Man State Key Laboratory of Oral Diseases, West China
Gene Activation for Excellent Bone Remodeling
 Osteostimulative bone regeneration granules Gene Activation for Excellent Bone Remodeling Injectable Putty Granules BIOMATERIALS STIMULATING THE BONE REGENERATION Noraker has been involved in biomaterial
Osteostimulative bone regeneration granules Gene Activation for Excellent Bone Remodeling Injectable Putty Granules BIOMATERIALS STIMULATING THE BONE REGENERATION Noraker has been involved in biomaterial
Clinical Policy Title: Bone graft substitutes
 Clinical Policy Title: Bone graft substitutes Clinical Policy Number: 14.02.09 Effective Date: July 1, 2016 Initial Review Date: May 18, 2016 Most Recent Review Date: May 19, 2017 Next Review Date: May
Clinical Policy Title: Bone graft substitutes Clinical Policy Number: 14.02.09 Effective Date: July 1, 2016 Initial Review Date: May 18, 2016 Most Recent Review Date: May 19, 2017 Next Review Date: May
Synthetic and absorbable autograft substitute with osteoinduction
 putty Synthetic and absorbable autograft substitute with osteoinduction Quality made in Germany Synthetic and absorbable autograft substitute with osteoinduction Information on the synthetic bone grafting
putty Synthetic and absorbable autograft substitute with osteoinduction Quality made in Germany Synthetic and absorbable autograft substitute with osteoinduction Information on the synthetic bone grafting
Horizontal bone augmentation by means of guided bone regeneration
 Periodontology 2000, Vol. 66, 2014, 13 40 2014 John Wiley & Sons A/S. Published by John Wiley & Sons Ltd Printed in Singapore. All rights reserved PERIODONTOLOGY 2000 Horizontal bone augmentation by means
Periodontology 2000, Vol. 66, 2014, 13 40 2014 John Wiley & Sons A/S. Published by John Wiley & Sons Ltd Printed in Singapore. All rights reserved PERIODONTOLOGY 2000 Horizontal bone augmentation by means
Puros Cancellous Particulate Allograft & Puros Block Allograft
 Puros Cancellous Particulate Allograft & Puros Block Allograft Puros Cancellous Particulate Allograft The Natural Choice For Healthy 1 Bone Growth. 1. Proven, Predictable Regeneration Acts as an osteoconductive
Puros Cancellous Particulate Allograft & Puros Block Allograft Puros Cancellous Particulate Allograft The Natural Choice For Healthy 1 Bone Growth. 1. Proven, Predictable Regeneration Acts as an osteoconductive
Management of a complex case
 2 Soft- and hard-tissue reconstruction of a severely deficient site prior to implant placement: a case report Management of a complex case Younes Khosroshahy, DDS, MFDS RCS (Eng), Dip Imp Dent RCSEd, Blue
2 Soft- and hard-tissue reconstruction of a severely deficient site prior to implant placement: a case report Management of a complex case Younes Khosroshahy, DDS, MFDS RCS (Eng), Dip Imp Dent RCSEd, Blue
Bone Regeneration in a Bilateral Sinus Lift
 2 A comparative pilot case study between irradiated human cancellous bone and a synthetic analogue Bone Regeneration in a Bilateral Sinus Lift Anthony McGee, BDS, Staines, and Dr J. A. Hunt, Liverpool/England
2 A comparative pilot case study between irradiated human cancellous bone and a synthetic analogue Bone Regeneration in a Bilateral Sinus Lift Anthony McGee, BDS, Staines, and Dr J. A. Hunt, Liverpool/England
BIOMATERIALS Maxillofacial & Skull Implants. Brendan Boyd & Stuart Mah
 BIOMATERIALS Maxillofacial & Skull Implants Brendan Boyd & Stuart Mah Outline Of Presentation Basic Anatomy of Face and Skull Reasons/Defects responsible for maxillofacial & skull surgery History of Alloplastic
BIOMATERIALS Maxillofacial & Skull Implants Brendan Boyd & Stuart Mah Outline Of Presentation Basic Anatomy of Face and Skull Reasons/Defects responsible for maxillofacial & skull surgery History of Alloplastic
PRP Basic Science. Platelets. Definition of PRP 10/4/2011. Questions that this talk aims to answer
 PRP Basic Science Peter J. Moley, MD Hospital for Special Surgery October 5, 2011 Questions that this talk aims to answer 1. What is PRP? 2. What blood components are NOT in PRP? 3. What are the active
PRP Basic Science Peter J. Moley, MD Hospital for Special Surgery October 5, 2011 Questions that this talk aims to answer 1. What is PRP? 2. What blood components are NOT in PRP? 3. What are the active
PRO-STIM Injectable Inductive Graft TECHNICAL MONOGRAPH
 PRO-STIM Injectable Inductive Graft TECHNICAL MONOGRAPH PRO-STIM Injectable Inductive Graft TECHNICAL MONOGRAPH Headline Contents Headline Appendix 4 5 7 8 13 14 Clinical Benefits Self-Forming Porous Scaffold
PRO-STIM Injectable Inductive Graft TECHNICAL MONOGRAPH PRO-STIM Injectable Inductive Graft TECHNICAL MONOGRAPH Headline Contents Headline Appendix 4 5 7 8 13 14 Clinical Benefits Self-Forming Porous Scaffold
Stem cells, growth factors and scaffolds in craniofacial regenerative medicine
 Stem cells, growth factors and scaffolds in craniofacial regenerative medicine Viktor Tollemar, Zach J. Collier, Maryam K. Mohammed, Michael J. Lee, Guillermo A. Ameer, and Russell R. Reid Genes Dis. 2016
Stem cells, growth factors and scaffolds in craniofacial regenerative medicine Viktor Tollemar, Zach J. Collier, Maryam K. Mohammed, Michael J. Lee, Guillermo A. Ameer, and Russell R. Reid Genes Dis. 2016
SPINE BIOMATERIALS Crop Bleed
 A comprehensive guide to biomaterials offered by Posterolateral DBX PUTTY DBX STRIP DBX MIX DBX INJECT chronos Strip chronos Granules chronos Preforms PROCURE CHOICE Marrow Aspiration Kit Bone Marrow Aspiration
A comprehensive guide to biomaterials offered by Posterolateral DBX PUTTY DBX STRIP DBX MIX DBX INJECT chronos Strip chronos Granules chronos Preforms PROCURE CHOICE Marrow Aspiration Kit Bone Marrow Aspiration
Pre op Failed endodontic treatment with sinus involvement.
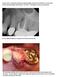 Case #1 of 10 consecutive extraction sockets grafted with Socket Graft Putty, covered with Socket Seal and sealed with Periacryl. I D # HEU This patient is a 66 year old female. Pre op Failed endodontic
Case #1 of 10 consecutive extraction sockets grafted with Socket Graft Putty, covered with Socket Seal and sealed with Periacryl. I D # HEU This patient is a 66 year old female. Pre op Failed endodontic
Coral Based Bone Grafts - Scientific Background
 December 2018 1 Coral Based Bone Grafts - Scientific Background Since their development in the eighties, coral (coralline) implants have been successfully used worldwide to treat a variety of orthopedic,
December 2018 1 Coral Based Bone Grafts - Scientific Background Since their development in the eighties, coral (coralline) implants have been successfully used worldwide to treat a variety of orthopedic,
Study Cases: Ride Augmentation Bone by Grafting and PRP/Preparation for Dental Implants Placement
 Cronicon OPEN ACCESS EC DENTAL SCIENCE Case Report Study Cases: Ride Augmentation Bone by Grafting and PRP/Preparation for Dental Implants Placement Farzat Alksiri* Implantologist, German Board of Oral
Cronicon OPEN ACCESS EC DENTAL SCIENCE Case Report Study Cases: Ride Augmentation Bone by Grafting and PRP/Preparation for Dental Implants Placement Farzat Alksiri* Implantologist, German Board of Oral
By: Ryan Pyrke and Anuja Goyal
 By: Ryan Pyrke and Anuja Goyal Phineas Gage (1823-1860) A 1 meter long tamping iron which weighed 6 kilograms impaled Phineas skull Miraculously survived. One of the most famous and earliest recorded survivors
By: Ryan Pyrke and Anuja Goyal Phineas Gage (1823-1860) A 1 meter long tamping iron which weighed 6 kilograms impaled Phineas skull Miraculously survived. One of the most famous and earliest recorded survivors
ADVANCED BONE GRAFT SYSTEM OVERVIEW
 ADVANCED BONE GRAFT SYSTEM OVERVIEW NANOSS BIOACTIVE ADVANCED BONE GRAFT Table Of Contents INTRODUCTION System Overview... 1 NANOSS BIOACTIVE COMPONENTS Comparison of nanoss Bioactive and Human Bone...
ADVANCED BONE GRAFT SYSTEM OVERVIEW NANOSS BIOACTIVE ADVANCED BONE GRAFT Table Of Contents INTRODUCTION System Overview... 1 NANOSS BIOACTIVE COMPONENTS Comparison of nanoss Bioactive and Human Bone...
Theoretical basis of bone replacement
 THE BIOLOGY OF BONE REGENERATION Theoretical basis of bone replacement Department of Oral- and Maxillofacial Surgery Semmelweis University, Budapest Role of bone tissue Maintance of calcium and phosphate
THE BIOLOGY OF BONE REGENERATION Theoretical basis of bone replacement Department of Oral- and Maxillofacial Surgery Semmelweis University, Budapest Role of bone tissue Maintance of calcium and phosphate
The body wants to heal
 58 A promising new particulate graft material: a case study The body wants to heal DR PETER J.M. FAIRBAIRN, DETROIT MERCY, MI, USA, AND LONDON, ENGLAND, AND DR MINAS LEVENTIS, ATHENS, GREECE The notion
58 A promising new particulate graft material: a case study The body wants to heal DR PETER J.M. FAIRBAIRN, DETROIT MERCY, MI, USA, AND LONDON, ENGLAND, AND DR MINAS LEVENTIS, ATHENS, GREECE The notion
Procedure Manual and Catalog
 Procedure Manual and Catalog TM Why SynthoGraft? SynthoGraft offers a unique structure which provides stability, while its micro-porosity allows for rapid vascularization and subsequent resorption. Although
Procedure Manual and Catalog TM Why SynthoGraft? SynthoGraft offers a unique structure which provides stability, while its micro-porosity allows for rapid vascularization and subsequent resorption. Although
rhpdgf-bb/β-tcp TECHNOLOGY OVERVIEW AUGMENT Bone Graft THE FIRST AND ONLY PROVEN ALTERNATIVE TO AUTOGRAFT IN ANKLE AND HINDFOOT ARTHRODESIS
 rhpdgf-bb/β-tcp TECHNOLOGY OVERVIEW AUGMENT Bone Graft THE FIRST AND ONLY PROVEN ALTERNATIVE TO AUTOGRAFT IN ANKLE AND HINDFOOT ARTHRODESIS AUGMENT Bone Graft T HE F I R S T A ND O N LY PROV EN A LT ERN
rhpdgf-bb/β-tcp TECHNOLOGY OVERVIEW AUGMENT Bone Graft THE FIRST AND ONLY PROVEN ALTERNATIVE TO AUTOGRAFT IN ANKLE AND HINDFOOT ARTHRODESIS AUGMENT Bone Graft T HE F I R S T A ND O N LY PROV EN A LT ERN
Surgical Solutions USA Regenerative Product Catalog USA
 RPC Surgical Solutions Regenerative Product Catalog RESORBABLE COLLAGEN MEMBRANES (BOVINE) CYTOPLAST RTM Collagen Resorption time of 26-38 weeks RTM1520 $185 15mm x 20mm Membranes per box: 2 RTM2030 $230
RPC Surgical Solutions Regenerative Product Catalog RESORBABLE COLLAGEN MEMBRANES (BOVINE) CYTOPLAST RTM Collagen Resorption time of 26-38 weeks RTM1520 $185 15mm x 20mm Membranes per box: 2 RTM2030 $230
