Microporous PTFE Membrane on Bone Regeneration in Rat Calvarial Defects
|
|
|
- John Nash
- 5 years ago
- Views:
Transcription
1 Biomaterials Research (2009) 13(3) : Biomaterials Research C The Korean Society for Biomaterials Microporous PTFE Membrane on Bone Regeneration in Rat Calvarial Defects Jung-Yoo Choi 1, Yoo-Jung Um 1, Ui-Won Jung 1, Chang-Sung Kim 1, Kyoo-Sung Cho 1, Jung Kiu Chai 1, Yong Keun Lee 2, Chong Kwan Kim 1, and Seong Ho Choi 1 * 1 Department of Periodontology, Research Institute for Periodontal Regeneration, College of Dentistry, Yonsei University, Seoul, Korea 2 Department of Research Institute of Dental Biomaterials and Bioengineering Yonsei University, College of Dentistry, Seoul, Korea (Received April 10, 2009/Acccepted July 03, 2009) Novel membrane is always being developed for guided bone regeneration(gbr). The purpose of this study was to evaluate the microporous polytetrafluoroethylene(ptfe) membrane on bone regeneration in rat calvarial defects. Thirty male Sprague-Dawley rats were used in 3 groups. One was the control group with no material used, another was the positive control group which used the resorbable membrane, collagen and the other was the experimental group which used the microporous PTFE membrane. The barrier membranes were applied in the surgically created standardized 8 mm cranial defect. The rats were sacrificed at 2 or 8 weeks. The amount of bone regeneration was assessed histologically and histomorphometrically. The bone formation increased under both barrier membranes compared with the control group. In terms of time, more bone was filled in 8 weeks than 2 weeks. Better bone formation was seen in defects protected by a microporous PTFE barrier when compared with the control and collagen group. It can be concluded that microporous PTFE membrane is effective in bone regeneration for its biocompatibility, bone formation enhancement, ease of use and space maintenance. Key words: bone, microporous PTFE membrane, regeneration, rats D Introduction estroyed tissue is always a concerning factor in periodontal regeneration. 1) Many methods for the periodontal regeneration have been mentioned such as root conditioning which enhances cell adhesive capacity, bone grafts in intrabony defects, and guided bone regeneration(gbr) using specific cell migration and bone morphogenetic proteins and other various growth factors. Among the various methods that have been introduced, GBR have been the most effective mode of therapy to facilitate bone healing. GBR in the dental field refers to procedures that attempt to regenerate bone prior to placement of bridges or more commonly, implants. It carries basically two aims: 1)to improve the lack of bone/implant contact in the defect area and 2)to restore the contour of the alveolar ridge. This is accomplished by using bone grafts and biocompatible membranes that keep tissue out and allow the bone to expand. GBR carries quite a wide range of surgical procedures and among those suggested procedures, membrane has been used *Corresponding author: shchoi726@yuhs.ac for tissue and bone regeneration for decades. However, membranes, aside from their advantages, carry limitations such as difficulty in handling and the uncertainty of the outcome. In consequent, novel membrane for GBR is still being developed. 2) GBR commonly utilizes nonresorbable or resorbable membranes 3,4,5,6,7) to provide an environment for bone to express its native osteogenic potency. Nonresorbable membranes such as Millipore filter, polytetrafluoroethylene 7) and absorbable membranes such as collagen, 8,9) polylactic acid 10,11,12) polyglactin 910, glycolide 13) and lactic copolymer are usually used in GBR. 14) The graft material needs to be stable and the soft connective tissue should be prevented from growing inside the defect area. Thus using a barrier membrane to cover and retain the graft material might satisfy both prerequisites. There have been many reports on bone regeneration using different types of membranes 14,16) such as the Gore-Tex membrane 17) and porous membranes 18) and comparisons of nonporous and porous membranes 19) and absorbable and nonresorbable membranes. 20) There are hardly any reports on the microporous PTFE membrane and its usage is not widely known. The microporous polytetrafluoroethylene (PTFE) membrane 93
2 94 Jung-Yoo Choi et al. is composed of high density PTFE and helps assure that the blood clot alone and/or graft material placed in the socket is protected during the initial healing phase after extraction. It is histocompatible, biocompatible and has capacity for space maintenance. 15) Its pore size is 0.2 µm large. Due to the high density of membrane and small porosity size, bacterial contamination is eliminated, protecting the underlying graft material and/or implant. In addition, primary soft tissue closure is not required. It also prevents fibrous connective tissue infiltration but allows permeation of oxygen and nutrients. The micro-sized pores also improve adhesion to bone. Nonresorbable membranes may be difficult to use in the clinic for its usage. They need to be shaped and cut into proper size according to the defects and have a high risk of exposure, which causes infection. However, the microporous PTFE membrane is easy to use for it has a simple rectangular shape and can be cut into various sizes easily. The purpose of this study was to evaluate the effects of micrcoporous PTFE membrane on bone regeneration in rat calvarial defects. Materials & Methods Animals Thirty male Sprague Dawley rats, weighing 250~300 g, 8 weeks old were used. The rats were maintained in plastic cages in a room with a 12h-day/night cycle and an ambient temperature of 21 o C, with ad libitum access to water and standard laboratory pellets. The routines of animal selection and management, surgical protocol, and preparation were approved by the Institutional Animal Care and Use Committee, Yonsei Medical Center, Seoul, Korea. Experimental Design The animals were divided into 3 groups, There were 10 animals in each group. They were allowed to heal for 2 weeks (5 rats from each group) or 8 weeks (5 rats from each group). Each animal received one of the 3 experimental treatments: a sham-surgery control in which no material was applied to the defect; collagen group as the carrier control; and the microporous PTFE membrane as the experimental group. Surgical procedures The rats were generally anaesthetized by an intramuscular injection (5 mg/kg body wt.) with Zoletil (Virbac, Carros, France) and Rompun (Bayer HealthCare, USA). During surgery, routine infiltration anesthesia (2% lidocaine, 1:100,000 epinephrine, Kwangmyung Pharmaceuticals, Seoul, Korea) was used at the surgical site. The surgical site was shaved and scrubbed with iodine. An incision was made in the sagittal plane across the cranium and a full thickness flap was reflected, exposing the calvarial bone. A standardized, circular, transosseous defect, 8 mm in diameter was created on the cranium with the use of an 8 mm trephine drill (3i, FL, USA). Saline was irrigated to prevent the heat of the trephine drill. After removal of the calvarial disk, Collatape (Integra LifeSciences Corporation, NJ, USA) and the microporous PTFE membrane was cut in a square shape of 1 cm 1 cm and was applied to the defects of the corresponding groups. The periosteum and skin were then closed and sutured with 4-0 Monosyn (Braun Aesculap AG&CO.KG, Tuttlingen). Histologic and histomorphometric procedures The animals were sacrificed by CO 2 asphyxiation at 2 and 8 weeks post-surgery. Block section including the surgical sites were removed and fixed in 10% neutral buffered formalin solution for 10 days. All samples were decalcified in EDTA- HCL for 7 days and embedded in paraffin. 5 µm thick coronal sections through the center of augmented area were obtained at 80 µm intervals, and stained with hematoxylin and eosin (H&E). The most central section from each block was selected for the histologic and histomorphometric evaluation. After conventional microscopic examination, computer-assisted histomorphometric measurements were done using an automated image analysis system (Image-Pro Plus, Media Cybernetics, Silver Spring, MD, USA) coupled with a video camera on a light microscope (Olympus BX50, Olympus Optical Co., Tokyo, Japan). The sections were examined at 20 magnification. A digitizer was used to trace the defect outline along the new bone formation, and the percentage of bone fill was determined. The value of each measurement was automatically calculated by the image analysis system. The following histomorphometric parameters were measured for each section. 1) Defect closure(%): the distance(at each side of the defect) between the defect margin and the in-growing bone margin in millimeters 100 2) New bone area(mm 2 ): all tissue within the boundaries of newly formed bone, i.e., mineralized bone and fatty marrow and fibrovascular tissue/marrow and residual biomaterial. Statistical Analysis Histomorphometric recordings from the samples were used to calculate means and standard deviations (m ± SD). To analyze the effect of both time and condition and to detect the interaction effect between time and condition, the two-way analysis of variance was used (P < 0.05). ANOVA and Posthock test were used to analyze the difference among the groups at each time point (P < 0.05). For the comparison between 2 and 8 weeks in a same group, statistical significance was determined by paired t-test (P < 0.05). Results Clinical findings The wound healing was generally uneventful. There were Biomaterials Research 2009
3 microporous PTFE membrane in bone regeneration 95 Figure 1. A schematic drawing of calvarial osteotomy defect showing histomorphometric analysis. Figure 2. (A) Control 2 weeks: minimal bone formation is seen. ( 20), (B) Control 8 weeks: New bone formation is seen along the margin. no signs of inflammation observed and appeared similar for all of the experimental groups. Histological Analysis Control group Material exposure or other complications of the surgical sites were not observed. 2 weeks finding in the control group (Figure 2(A)) showed almost no regeneration. In the 8 weeks finding (Figure 2(B)), the defect was filled with loose connective tissue. All in all, the control group showed almost no regeneration. Collagen Group In 2 weeks finding of the collagen group (Figure 3(A)), the defects were filled with loose or dense, fibrous connective tissue and limited new bone formation was observed at the defect margin. The collagen membrane remained in the subepithelium and there was no resorption and the external form was maintained and was surrounded by connective tissue. In 8 weeks finding (Figure 3(B)), the resorption of collagen membrane progressed much. There was almost no infiltration of inflammatory cells. There was an increase in bone volume and there was no invagination of peripheral tissue. Microporous PTFE membrane The shape and form of the defect and microporous PTFE membrane were maintained in 2 weeks. (Figure 4(A)). Inflammatory cells were infiltrated in the margin of the defect and new bone was invaginated in the margin of the defect, an immature bone formed in a thimble-like morphology. In 8 weeks (Figure 4(B)), the periosteum and the dura mater were joined continuously and the microporous PTFE membrane was well maintained with fibrous connective tissue underneath. The microporous PTFE membrane was surrounded with loose connective tissue, mature bone and bony tissue in the margin of the defect. In the higher magnification of the microporous PTFE membrane, new bone invaginated along the marginal area in 2 weeks (Figure 5(A)) and in 8 weeks, the new bone was enhanced and bone forming cells were seen (Figure 5(B). Vol. 13, No. 3
4 96 Jung-Yoo Choi et al. Figure 3. (A) Collagen 2 weeks: ingrowth of bone with loose/dense fibrous connective tissue, limited bone formation can be seen ( 20), (B) Collagen 8 weeks: bone formation increased in the margin and around collagen membrane ( 20) Figure 4. (A) Microporous PTFE membrane 2 weeks ( 20), (B) Microporous PTFE membrane 8 weeks: new bone ingrowth can be seen in marginal area ( 20). Figure 5. (A) Higher Magnification of Microporous PTFE membrane 2 weeks: new bone (NB) has invaginated along the marginal area ( 50), (B) Higher magnification of Microporous PTFE membrane 8 weeks: new bone (NB) enhanced along the marginal area and is surrounded by connective tissue. ( 50) Histomorphometric Analysis(Tables 1, 2) Discussion Long term results of periodontal regeneration therapy with non-resorbable and bioabsorbable barriers have shown that both membranes were stable after 10 years in 12 of 16 defects.21) Akimoto et al. reported that histomorphometric measurements showed a trend toward greater bone formation at membrane-treated sites compared with control sites.22) In addition, Simion et al.23) used membranes to cover surgically Biomaterials Research 2009 created saddle type ridge defects in the mandible of 6 dogs and a large amount of osseous healing occurred in all the membrane protected sites after a 6-month healing period. The present study evaluated the effects of bone regeneration of the microporous PTFE membrane in rat calvarial defects. The aspect that was focused in this study was to compare the nonresorbable microporous PTFE membrane with the resorbable collagen membrane, to see its bone regenerative potency. The microporous PTFE membrane has its advantage in terms of maintenance of form and shape. It is made of high-density PTFE with the porosity size of 0.2 µm. Owing to the high den-
5 microporous PTFE membrane in bone regeneration 97 Table 1. Defect Closure(%) (group means ± SD; n = 5) 2 weeks 8 weeks Control 13.9 ± ± 7.2 Collagen membrane 22.6 ± 9.3* 26.9 ± 10.4* Microporous PTFE membrane 34.5 ± 5.6* 40.3 ± 6.3* *: Statistically significant difference compared to control group (P < 0.05) : Statistically significant difference compared to collagen membrane group (P < 0.05) : Statistically significant difference compared to microporous PTFE membrane(p < 0.05) Table 2. New bone area(mm 2 ) (group means ± SD; n = 5) 2 weeks 8 weeks Control 0.2 ± ± 0.2 Collagen membrane 2.9 ± 1.6* 1.9 ± 3.3* Microporous PTFE membrane 3.1 ± 0.5* 3.3 ± 0.4* *: Statistically significant difference compared to control group (P < 0.05) : Statistically significant difference compared to collagen membrane group (P < 0.05) : Statistically significant difference compared to microporous PTFE membrane(p < 0.05) sity of PTFE membrane and small porosity size, bacterial contamination is eliminated, thus protecting the underlying graft material and/or implant. The primary soft tissue closure is not required. Thus, this membrane may be exposed to the oral cavity without the fear of possible complications that may occur from exposure of PTFE or resorbable membrane. It also allows nutrients and ions to move in and out. The microporous PTFE membrane also has its advantage compared to the resorbable membrane in that the resorbable membrane can be a problem if it is resorbed too early and if this occurs, the regenerated tissue becomes immature and the amount of bone formation and the level of attachment gain decreases. On the other hand, if the membrane is absorbed too late, healing of the tissue is delayed and complications such as abscess could be formed. In addition, collagen membranes provide little stability and thereby carries negligible space-making effect. 7) They also have a short degradation time to be suitable for GBR. It does not have the potency as a barrier for approximately 6 months for bone to form without disturbance underneath the membrane. 12,24) According to the histological and histomorphometric analysis, the microporous PTFE membrane showed an enhanced defect closure in the early healing phase when compared to the resorbable membrane, collagen. The closure of the defect was faster than the other groups. There was more bone formation in 8 weeks when compared to 2 weeks. Thus this could be implied that the microporous PTFE membrane avoids cell migration, consequently enhancing bone formation and thus increases the bone regenerative potency. This is in agreement with the purpose of using a nonresorbable membrane in periodontal lesion to prevent gingival connective tissue and epithelium from proliferating into the defect. The microporous PTFE membrane showed higher new bone area compared to the control group and the collagen group. In addition, there was a higher new bone area in 8 weeks than in 2 weeks. The microporous PTFE membrane can be concluded to be effective in bone regeneration for its biocompatibility, bone formation enhancement through avoiding cell migration, ease of use and space maintenance. Acknowledgements This work was supported by the Korea Science and Engineering Foundation (KOSEF) grant funded by the Korea government(mest) (No. R ). References 1. S. S Stahl: Repair potential of the soft tissue-root surface. J periodontal., 48, , E. M Pirhonen, T. H Pohjonen, F. E Weber, Novel membrane for guided bone regeneration, Int J Artif Organs, 29(9), , M. G Araujo, J. Lindhe,: GTR treatment of degree III furcation defects with 2 different resorbable barrier. An experimental study in dogs. J, Clin. Periodontol., 25, , R. G Caffese, C. E Nasjleti, E. C Morrison et al.,: Guided tissue regeneration: comparison of bioabsorbable and non-bioabsorbable membranes. Histologic and histometric study in dogs, J. Periodontol., 65(6), , A Kasaj, C Reichert, H Götz et al.,: In vitro evaluation of various bioabsorbable and nonresorbable barrier membranes for guided tissue regeneration. Head Face Med., 4, 22, A. M Polson, S Garrett, N. H Stoller et al.,: Guided tissue regeneration in human furcation defects after using biodegradable barrier.: A multi-center feasibility study. J.Periodontol., 66, , H Schliephake, M Dard, H Planck et al., Guided bone regeneration around endosseous implants using a resorbable membrane vs a PTFE membrane, Clin oral Impl Res: 11, , S. A Kay, L Winser-Lynch, M Marxer et al.,: Integration of a resorbable membrane and a bone graft material, Pract. Periodont Aesthet. Dent., 9, , H. L Wang, R. L MacNeil, A. T Shieh et al.,: Utilization of a resorbable collagen membrane in repairing gingival recession defects, Pract. Periodont. Aesthet. Dent., 8, , W. J Cho, J. H Kim, S. H Oh et al., Hydrophilized polcaprolactone nanofibermesh-embedded poly(glycolic-co-lactic acid) membrane for effective guided bone regeneration, J Biomed Mater Res A. Nov 3, U. W Jung, K. Y Song, C. S Kim, Y. K Lee et al., Effects of Chitosan membrane coated with polylactic and polyglycolic acid on bone regeneration in a rat calvarial defect, Biomedical Materials, 2, S101-S105, H Schliephake, D.Kracht, Vertical ridge augmentation using polylactic membranes in conjunction with immediate implants in periodontally compromised extraction sites: an experimental study in dogs, Int.J.Oral Maxillofacial Implants., 12, , Vol. 13, No. 3
6 98 Jung-Yoo Choi et al. 13. I. Y Kim, U. W Jung, C. S Kim, Y. K Lee et al., Effects of a tetracycline blended polylactic and polyglycolic acid membrane on the healing of one-wall intrabony defects in beagle dogs, Biomedical Materials. 2, S106-S110, F. P Strietzel, P Khongkhunthian, R Khattiya, P Patchanee, P. A. Reichart, Healing pattern of bone defects covered by different membrane types-a histologic study in the porcine mandible, J Biomed Mater Res B Appl Biomater. 78(1), 35-46, I Magnusson, C Batich, B. R Collins. et al.,: New attachment formation following controlled tissue regeneration using biodegradable membranes, J Periodontol., 59, 1-6, P Windisch, A Sculean, I. Gera, GTR with three different types of membranes in the treatment of intrabony periodontal defects: three-year results in sixty consecutive cases, J Long Term Eff Med Implants, 9(3), , P. F Gielkens, J Schortinghuis, J. R de Jong, G. M Raghoebar et al., Vivosorb, Bio-Gide, and Gore-Tex as barrier membranes in rat mandibular defects: an evaluation by microradiography and micro- CT, Clin Oral Implants Res., 19(5), , S. J Oh, J. H Kim, J. M Kim, J. H Lee, Asymmetrically porous PLGA/Pluronic F127 membrane for effective guided bone regeneration, J Biomater Sci Polym Ed. 17(12), , S. P Walter, H Greenwell, M Hill et al., Comparison of porous and non-porous Teflon membranes plus a xenograft in the treatment of vertical osseous defects: a clinical reentry study, J Periodontol, 74(8), , P Bouchard, J. L Giovannoli, C Mattout et al.,: Clinical evaluation of a bioabsorble regenerative material in mandibular class II furcation therapy. J. Clin Periodontol., 24, , B Pretzl, T. S Kim, R Holle, P. Eickholz, Long-term results of guided tissue regeneration therapy with non-resorbable and bioabsorbable barriers. IV. A case series of infrabony defects after 10 years, J Periodontol, 79(8), , K Akimoto, W Becker, K Donath, B.E Becker, R Sanchez., Formation of bone around titanium implants placed into zero wall defects: pilot project using reinforced e-ptfe membrane and autogenous bone grafts, Clin Implant Dent Relat Res., 1(2), , M Simion, C Dahlin, K Blair, R. K Schenk, Effect of different microstructures of e-ptfe membranes on bone regeneration and soft tissue response: a histologic study in canine mandible., Clin Oral Implants Res., 10(2), 73-84, D Hutmacher, M. B Hürzeler, H Schliephake et al., A review of material properties of biodegradable and bioresorbable polymers and devices for GTR and GBR applications. Int J Oral Maxillofac Implants. 11, , Biomaterials Research 2009
Evaluation of different grafting materials in three-wall intra-bony defects around dental implants in beagle dogs
 Current Applied Physics 5 (2005) 507 511 www.elsevier.com/locate/cap Evaluation of different grafting materials in three-wall intra-bony defects around dental implants in beagle dogs Ui-Won Jung a, Hee-Il
Current Applied Physics 5 (2005) 507 511 www.elsevier.com/locate/cap Evaluation of different grafting materials in three-wall intra-bony defects around dental implants in beagle dogs Ui-Won Jung a, Hee-Il
Cytoflex Barrier Membrane Clinical Evaluation
 Cytoflex Barrier Membrane Clinical Evaluation Historical Background Guided tissue regeneration is a well established concept in the repair of oral bone defects. The exclusion of soft tissue epithelial
Cytoflex Barrier Membrane Clinical Evaluation Historical Background Guided tissue regeneration is a well established concept in the repair of oral bone defects. The exclusion of soft tissue epithelial
( ) 2009;28(2):89-94
 ( ) 2009;28(2):89-94 Osseointegration is important in the functional aspect, however, esthetics is also important, especially in the maxillary anterior region. An adequate surgical technique is necessary
( ) 2009;28(2):89-94 Osseointegration is important in the functional aspect, however, esthetics is also important, especially in the maxillary anterior region. An adequate surgical technique is necessary
Guided bone regeneration using two types of non-resorbable barrier membranes
 DOI:10.5125/jkaoms.2010.36.4.275 Guided bone regeneration using two types of non-resorbable barrier membranes Ji-Young Lee 1, Young-Kyun Kim 1, Pil-Young Yun 1, Ji-Su Oh 2, Su-Gwan Kim 2 1 Department of
DOI:10.5125/jkaoms.2010.36.4.275 Guided bone regeneration using two types of non-resorbable barrier membranes Ji-Young Lee 1, Young-Kyun Kim 1, Pil-Young Yun 1, Ji-Su Oh 2, Su-Gwan Kim 2 1 Department of
The Original remains unique.
 The Original remains unique. Geistlich leading regeneration 2A, 2B Geistlich is the world leader in regenerative dentistry. We transform natural biomaterials into safe and reliable treatment methods that
The Original remains unique. Geistlich leading regeneration 2A, 2B Geistlich is the world leader in regenerative dentistry. We transform natural biomaterials into safe and reliable treatment methods that
SalvinOss Xenograft Bone Graft Material In Vivo Testing Summary
 SalvinOss Xenograft Bone Graft Material In Vivo Testing Summary Summary of In Vivo Use Of Bioresorbable Xenograft Bone Graft Materials In The Treatment Of One-Walled Intrabony Defects In A Canine Model
SalvinOss Xenograft Bone Graft Material In Vivo Testing Summary Summary of In Vivo Use Of Bioresorbable Xenograft Bone Graft Materials In The Treatment Of One-Walled Intrabony Defects In A Canine Model
Inion GTR Biodegradable Membrane System
 Inion GTR Biodegradable Membrane System The concept of GTR/GBR Intended use The Inion GTR Biodegradable Membrane System is intended to be used as a barrier membrane in dental guided tissue regeneration
Inion GTR Biodegradable Membrane System The concept of GTR/GBR Intended use The Inion GTR Biodegradable Membrane System is intended to be used as a barrier membrane in dental guided tissue regeneration
RELIABLE WHEN IT COUNTS. The unique collagenase-resistant membrane protects bone graft and supports treatment success even when exposed 4
 RELIABLE WHEN IT COUNTS 1 RELIABLE WHEN IT COUNTS RESISTANT TO EXPOSURE The unique collagenase-resistant membrane protects bone graft and supports treatment success even when exposed 4 RELIABLE BARRIER
RELIABLE WHEN IT COUNTS 1 RELIABLE WHEN IT COUNTS RESISTANT TO EXPOSURE The unique collagenase-resistant membrane protects bone graft and supports treatment success even when exposed 4 RELIABLE BARRIER
Guided Tissue and Bone Regeneration
 Guided Tissue and Bone Regeneration One toolbox for your needs! Tefguide 9000 742 401 12x24 mm pc 1 Osgide 9000 701 520 15 x 20 mm pc 1 Osbone 9000 800 255 250-1000 μm 0.25 cc 5 Product Specifications
Guided Tissue and Bone Regeneration One toolbox for your needs! Tefguide 9000 742 401 12x24 mm pc 1 Osgide 9000 701 520 15 x 20 mm pc 1 Osbone 9000 800 255 250-1000 μm 0.25 cc 5 Product Specifications
The Essential Choice. With the Benefits of Biologic Predictability
 The Essential Choice With the Benefits of Biologic Predictability Documented, Reliable, Experienced is the essential choice for your daily regenerative needs. Throughout our long history and dedication
The Essential Choice With the Benefits of Biologic Predictability Documented, Reliable, Experienced is the essential choice for your daily regenerative needs. Throughout our long history and dedication
The Essential Choice. With the Benefits of Biologic Predictability
 The Essential Choice With the Benefits of Biologic Predictability Documented, Reliable, Experienced is the essential choice for your daily regenerative needs. Throughout our long history and dedication
The Essential Choice With the Benefits of Biologic Predictability Documented, Reliable, Experienced is the essential choice for your daily regenerative needs. Throughout our long history and dedication
REGENERATIONTIME. A Case Report by. Ridge Augmentation and Delayed Implant Placement on an Upper Lateral Incisor
 A Case Report by Dr. Daniele Cardaropoli Ridge Augmentation and Delayed Implant Placement on an Upper Lateral Incisor The Situation An adult female patient presented with an endodontic/prosthetic failure
A Case Report by Dr. Daniele Cardaropoli Ridge Augmentation and Delayed Implant Placement on an Upper Lateral Incisor The Situation An adult female patient presented with an endodontic/prosthetic failure
Regeneration Bone Grafting & Soft Tissue Management
 Regeneration Bone Grafting & Soft Tissue Management Human Histology OSTEON II 26.5 months Regeneration Products information Table of contents Bone Graft Material OSTEON II OSTEON OSTEON II Collagen OSTEON
Regeneration Bone Grafting & Soft Tissue Management Human Histology OSTEON II 26.5 months Regeneration Products information Table of contents Bone Graft Material OSTEON II OSTEON OSTEON II Collagen OSTEON
Journal of Dental Biomaterials. 2015;2(3) Raoofi S. a, Sabagh S. a, Shabahangfar MR. a, Mozafari Gh. a, GhoraishiAbhari M. b
 Guided tissue regeneration therapy following the use of d-ptfe membrane Journal of Dental Biomaterials. 2015;2(3) Original Article Histomorphometric Analysis of Periodontal Tissue Regeneration by the Use
Guided tissue regeneration therapy following the use of d-ptfe membrane Journal of Dental Biomaterials. 2015;2(3) Original Article Histomorphometric Analysis of Periodontal Tissue Regeneration by the Use
Resorbable bilayer synthetic membrane Biomimetic tissue-engineered matrix for GBR and GTR
 Resorbable bilayer synthetic membrane Biomimetic tissue-engineered matrix for GBR and GTR Patented Jet-Spraying technology: Full barrier effect during 4 weeks, and complete resorption in 6 months PATENTED
Resorbable bilayer synthetic membrane Biomimetic tissue-engineered matrix for GBR and GTR Patented Jet-Spraying technology: Full barrier effect during 4 weeks, and complete resorption in 6 months PATENTED
Class II Furcations Treated by Guided Tissue Regeneration in Humans: Case Reports
 0 Class II Furcations Treated by Guided Tissue Regeneration in Humans: Case Reports R.G. Caffesse, B.A. Smith/ B. Duff, E.C. Morrison, D. Merrill/ and W. Becker In the cases reported here, the response
0 Class II Furcations Treated by Guided Tissue Regeneration in Humans: Case Reports R.G. Caffesse, B.A. Smith/ B. Duff, E.C. Morrison, D. Merrill/ and W. Becker In the cases reported here, the response
Regeneration Bone Grafting & Soft Tissue Management
 Regeneration Bone Grafting & Soft Tissue Management OSTEON TM II Table of Contents Bone Graft Material OSTEON TM II Collagen 04 OSTEON TM Collagen 06 OSTEON TM II 08 OSTEON TM 12 ORTHOPEDIC OSTEON TM 14
Regeneration Bone Grafting & Soft Tissue Management OSTEON TM II Table of Contents Bone Graft Material OSTEON TM II Collagen 04 OSTEON TM Collagen 06 OSTEON TM II 08 OSTEON TM 12 ORTHOPEDIC OSTEON TM 14
Pre op Failed endodontic treatment with sinus involvement.
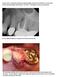 Case #1 of 10 consecutive extraction sockets grafted with Socket Graft Putty, covered with Socket Seal and sealed with Periacryl. I D # HEU This patient is a 66 year old female. Pre op Failed endodontic
Case #1 of 10 consecutive extraction sockets grafted with Socket Graft Putty, covered with Socket Seal and sealed with Periacryl. I D # HEU This patient is a 66 year old female. Pre op Failed endodontic
More than bone regeneration. A total solution.
 More than bone regeneration. A total solution. More than a dental implant company. A total solution. When it comes to treatment options, your patients want positive results both functionally and esthetically.
More than bone regeneration. A total solution. More than a dental implant company. A total solution. When it comes to treatment options, your patients want positive results both functionally and esthetically.
Horizontal bone augmentation by means of guided bone regeneration
 Periodontology 2000, Vol. 66, 2014, 13 40 2014 John Wiley & Sons A/S. Published by John Wiley & Sons Ltd Printed in Singapore. All rights reserved PERIODONTOLOGY 2000 Horizontal bone augmentation by means
Periodontology 2000, Vol. 66, 2014, 13 40 2014 John Wiley & Sons A/S. Published by John Wiley & Sons Ltd Printed in Singapore. All rights reserved PERIODONTOLOGY 2000 Horizontal bone augmentation by means
Soft-Tissue Success with the. Clinical Success. Proven Matrix. with the Proven. Geistlich Mucograft Geistlich Mucograft Seal
 Soft-Tissue Success with the Clinical Success Proven Matrix with the Proven Bone Geistlich Mucograft Substitute Seal The Softer Side of Geistlich Innovation Decades of collagen expertise leads naturally
Soft-Tissue Success with the Clinical Success Proven Matrix with the Proven Bone Geistlich Mucograft Substitute Seal The Softer Side of Geistlich Innovation Decades of collagen expertise leads naturally
BONE GRAFTING. Product Catalog
 BONE GRAFTING Product Catalog PRODUCT LINE Titanium Mesh Surgitime Titanium Titanium Foil Surgitime Titanium Seal Polytetraflouroethylene Membrane Surgitime PTFE Bone Screws Fixation Set We innovate to
BONE GRAFTING Product Catalog PRODUCT LINE Titanium Mesh Surgitime Titanium Titanium Foil Surgitime Titanium Seal Polytetraflouroethylene Membrane Surgitime PTFE Bone Screws Fixation Set We innovate to
Bringing you Geistlich biocompatibility with improved application and handling benefits. Your combination for success
 Bringing you Geistlich biocompatibility with improved application and handling benefits Your combination for success Geistlich Combi-Kit Collagen: Combining ease and predictablility Geistlich Combi-Kit
Bringing you Geistlich biocompatibility with improved application and handling benefits Your combination for success Geistlich Combi-Kit Collagen: Combining ease and predictablility Geistlich Combi-Kit
Regeneration Bone Grafting & Soft Tissue Management
 Regeneration Bone Grafting & Soft Tissue Management 1 Regeneration Bone Grafting & Soft Tissue Management Table of contents Bone Graft Material OSTEON II OSTEON OSTEON II Collagen OSTEON Collagen 5 6
Regeneration Bone Grafting & Soft Tissue Management 1 Regeneration Bone Grafting & Soft Tissue Management Table of contents Bone Graft Material OSTEON II OSTEON OSTEON II Collagen OSTEON Collagen 5 6
BONE AUGMENTATION AND GRAFTING
 1 A Computer-Guided Bone Block Harvesting Procedure: A Proof-of-Principle Case Report and Technical Notes Effectiveness of Lateral Bone Augmentation on the Alveolar Crest Dimension: A Systematic Review
1 A Computer-Guided Bone Block Harvesting Procedure: A Proof-of-Principle Case Report and Technical Notes Effectiveness of Lateral Bone Augmentation on the Alveolar Crest Dimension: A Systematic Review
Asufficient quantity of bone is an essential prerequisite
 Clinical Evaluation of a Bilayered Collagen Membrane (Bio-Gide) Supported by Autografts in the Treatment of Bone Defects Around Implants Georges Tawil, DDS, DSc, OD 1 /Georgina El-Ghoule, DDS 2 /Muhieddine
Clinical Evaluation of a Bilayered Collagen Membrane (Bio-Gide) Supported by Autografts in the Treatment of Bone Defects Around Implants Georges Tawil, DDS, DSc, OD 1 /Georgina El-Ghoule, DDS 2 /Muhieddine
Maryland AGD AE and Socket Grafting 2015
 The Goodacre Study 5 year retrospective study looked at Crown & Bridge Caries Single crowns 1% FPD abutments 17% Periodontal Involvement Single crowns
The Goodacre Study 5 year retrospective study looked at Crown & Bridge Caries Single crowns 1% FPD abutments 17% Periodontal Involvement Single crowns
Product Information. MIS Corporation. All Rights Reserved.
 Product Information MIS Corporation. All Rights Reserved. MIS Warranty: MIS exercises great care and effort in maintaining the superior quality of its products. All MIS products are guaranteed to be free
Product Information MIS Corporation. All Rights Reserved. MIS Warranty: MIS exercises great care and effort in maintaining the superior quality of its products. All MIS products are guaranteed to be free
Symbios Xenograft Granules Porcine Bone Graft Material
 Symbios Xenograft Granules Porcine Bone Graft Material 32671122-USX-1607_Symbios Highlight Brochure.indd 1 2016-09-27 12:12 Symbios Xenograft Granules Porcine bone graft material Symbios Xenograft Granules
Symbios Xenograft Granules Porcine Bone Graft Material 32671122-USX-1607_Symbios Highlight Brochure.indd 1 2016-09-27 12:12 Symbios Xenograft Granules Porcine bone graft material Symbios Xenograft Granules
Scientific & Clinical Evidence Jason membrane
 Scientific & Clinical Evidence Jason membrane Pericardium GBR/GTR Membrane Facts - CE since 2009 - so far no serious clinical complication or objection - approx. 250.000 successful clinical treatments
Scientific & Clinical Evidence Jason membrane Pericardium GBR/GTR Membrane Facts - CE since 2009 - so far no serious clinical complication or objection - approx. 250.000 successful clinical treatments
Innovative Range of Regenerative Solutions
 TM Innovative Range of Regenerative Solutions MIS Implant Technologies Ltd. All rights reserved. Optimal volumes and quality of hard and soft tissue are required to satisfy the goals of oral rehabilitation
TM Innovative Range of Regenerative Solutions MIS Implant Technologies Ltd. All rights reserved. Optimal volumes and quality of hard and soft tissue are required to satisfy the goals of oral rehabilitation
GUIDED BONE & TISSUE REGENERATION 2-DAY LIVE COURSE DR. ISABELLA ROCCHIETTA & DR. DAVID NISAND
 GUIDED BONE & TISSUE REGENERATION DR. ISABELLA ROCCHIETTA & DR. DAVID NISAND 2-DAY LIVE COURSE Soft tissue management is the key to achieve aesthetic success. Periodontal and peri-implant soft tissue management
GUIDED BONE & TISSUE REGENERATION DR. ISABELLA ROCCHIETTA & DR. DAVID NISAND 2-DAY LIVE COURSE Soft tissue management is the key to achieve aesthetic success. Periodontal and peri-implant soft tissue management
The anatomic limitations of the. Implant Installation With Simultaneous Ridge Augmentation. Report of Three Cases Jun-Beom Park, DDS, MSD, PhD*
 CASE REPORT Implant Installation With Simultaneous Ridge Augmentation. Report of Three Cases Jun-Beom Park, DDS, MSD, PhD* The anatomic limitations of the residual alveolar bone may cause problems for
CASE REPORT Implant Installation With Simultaneous Ridge Augmentation. Report of Three Cases Jun-Beom Park, DDS, MSD, PhD* The anatomic limitations of the residual alveolar bone may cause problems for
OSSIX PLUS The Resorbable Collagen Membrane Instructions for Use for OSSIX PLUS
 OSSIX PLUS The Resorbable Collagen Membrane Instructions for Use for OSSIX PLUS DESCRIPTION OSSIX PLUS is a biodegradable and biocompatible collagen membrane intended for use during the process of guided
OSSIX PLUS The Resorbable Collagen Membrane Instructions for Use for OSSIX PLUS DESCRIPTION OSSIX PLUS is a biodegradable and biocompatible collagen membrane intended for use during the process of guided
We Want to Keep You Smiling. Bone Regeneration with Geistlich Bio-Oss and Geistlich Bio-Gide
 We Want to Keep You Smiling Bone Regeneration with Geistlich Bio-Oss and Geistlich Bio-Gide Strong Bone for a Healthier Smile Strong and healthy teeth provide a feeling of well-being, self-confidence and
We Want to Keep You Smiling Bone Regeneration with Geistlich Bio-Oss and Geistlich Bio-Gide Strong Bone for a Healthier Smile Strong and healthy teeth provide a feeling of well-being, self-confidence and
THE NEXT FRONTIER OF BONE REGENERATION
 THE NEXT FRONTIER OF BONE REGENERATION where Technology meets Nature swiss made SmartBone is new composite bone substitute specifically developed for bone regeneration in oral and maxillofacial reconstructive
THE NEXT FRONTIER OF BONE REGENERATION where Technology meets Nature swiss made SmartBone is new composite bone substitute specifically developed for bone regeneration in oral and maxillofacial reconstructive
Effect of GBR in Combination with Deproteinized Bovine Bone Mineral on the Healing of Calvarial Defects in Rabbits
 Original Article Effect of GBR in Combination with Deproteinized Bovine Bone Mineral on the Healing of Calvarial Defects in Rabbits AA. Khoshkhoonejad 1, A. Miremadi 2, AR. Rokn 2,3, B. Eslami 4, M. Dehghan
Original Article Effect of GBR in Combination with Deproteinized Bovine Bone Mineral on the Healing of Calvarial Defects in Rabbits AA. Khoshkhoonejad 1, A. Miremadi 2, AR. Rokn 2,3, B. Eslami 4, M. Dehghan
Straumann MembraGel The next generation membrane
 Straumann MembraGel The next generation membrane Advanced technology for your GBR cases Straumann membragel is an advanced technology membrane which sets new standards in the surgical use for guided bone
Straumann MembraGel The next generation membrane Advanced technology for your GBR cases Straumann membragel is an advanced technology membrane which sets new standards in the surgical use for guided bone
Bone augmentation with biomaterials
 Patient information dental bone & tissue regeneration botiss biomaterials Bone augmentation with biomaterials established safe natural X100 Implantation stability is crucial for success Atrophy of the
Patient information dental bone & tissue regeneration botiss biomaterials Bone augmentation with biomaterials established safe natural X100 Implantation stability is crucial for success Atrophy of the
Clinical Case Reports using Cytoplast GTR Barrier Membranes
 Clinical Case Reports using Cytoplast GTR Barrier Membranes Barry K. Bartee, DDS, MD The Cytoplast Technique: Extraction Site Grafting Without Primary Closure 1. 1. Preoperative view. To maximize the result
Clinical Case Reports using Cytoplast GTR Barrier Membranes Barry K. Bartee, DDS, MD The Cytoplast Technique: Extraction Site Grafting Without Primary Closure 1. 1. Preoperative view. To maximize the result
Cerasorb M DENTAL. O:\Zulassung\Cerasorb Dental Kanada 2013\Texte\Cerasorb M Dental final IFU docx
 Cerasorb M DENTAL Resorbable, pure-phase beta-tricalcium phosphate matrix with interconnecting porosity for bone regeneration for use in dental and maxillofacial surgery DESCRIPTION: Cerasorb M DENTAL
Cerasorb M DENTAL Resorbable, pure-phase beta-tricalcium phosphate matrix with interconnecting porosity for bone regeneration for use in dental and maxillofacial surgery DESCRIPTION: Cerasorb M DENTAL
THE NEXT FRONTIER OF BONE REGENERATION. where Technology meets Nature
 THE NEXT FRONTIER OF BONE REGENERATION where Technology meets Nature SmartBone is a new hybrid bioactive bone substitute specifically developed for bone regeneration in reconstructive surgery. SmartBone
THE NEXT FRONTIER OF BONE REGENERATION where Technology meets Nature SmartBone is a new hybrid bioactive bone substitute specifically developed for bone regeneration in reconstructive surgery. SmartBone
Vertical and Horizontal Augmentation Using Guided Bone Regeneration. Ph.D. Thesis. Dr. med. dent. et univ. Istvan Urban
 Vertical and Horizontal Augmentation Using Guided Bone Regeneration Ph.D. Thesis Dr. med. dent. et univ. Istvan Urban Supervisor: Prof. Dr. Katalin Nagy, DDS, PhD Faculty of Dentistry, University of Szeged
Vertical and Horizontal Augmentation Using Guided Bone Regeneration Ph.D. Thesis Dr. med. dent. et univ. Istvan Urban Supervisor: Prof. Dr. Katalin Nagy, DDS, PhD Faculty of Dentistry, University of Szeged
Socket preservation in the daily practice: A clinical case report
 Clinical Socket preservation in the daily practice: A clinical case report Rabih Abi Nader 1 and Carine Tabarani 2 Abstract Soft tissue contour depends on the underlying bone anatomy. Following tooth extraction,
Clinical Socket preservation in the daily practice: A clinical case report Rabih Abi Nader 1 and Carine Tabarani 2 Abstract Soft tissue contour depends on the underlying bone anatomy. Following tooth extraction,
REASONS TO USE R.T.R.
 3 REASONS TO USE R.T.R. AFTER EACH EXTRACTION Fully resorbable ß-TCP material RTR 3raisons 120x280.indd 1 16/06/15 10:52 1AVOID SPONTANEOUS RIDGE RESORPTION After tooth extraction, spontaneous healing
3 REASONS TO USE R.T.R. AFTER EACH EXTRACTION Fully resorbable ß-TCP material RTR 3raisons 120x280.indd 1 16/06/15 10:52 1AVOID SPONTANEOUS RIDGE RESORPTION After tooth extraction, spontaneous healing
Application of a Novel Resorbable Membrane in the Treatment of Calvarial Defects in Rats
 Journal of Biomaterials Science (2010) DOI:10.1163/092050610X540477 brill.nl/jbs Application of a Novel Resorbable Membrane in the Treatment of Calvarial Defects in Rats Yanjun Ge, Hailan Feng and Lei
Journal of Biomaterials Science (2010) DOI:10.1163/092050610X540477 brill.nl/jbs Application of a Novel Resorbable Membrane in the Treatment of Calvarial Defects in Rats Yanjun Ge, Hailan Feng and Lei
GUIDED BONE & TISSUE REGENERATION 2-DAY MASTERCLASS (CHOOSE LONDON OR PARIS) DR. ISABELLA ROCCHIETTA & DR. DAVID NISAND
 GUIDED BONE & TISSUE REGENERATION DR. ISABELLA ROCCHIETTA & DR. DAVID NISAND 2-DAY MASTERCLASS (CHOOSE LONDON OR PARIS) This hands-on course will be delivered in small group workshops and will equip the
GUIDED BONE & TISSUE REGENERATION DR. ISABELLA ROCCHIETTA & DR. DAVID NISAND 2-DAY MASTERCLASS (CHOOSE LONDON OR PARIS) This hands-on course will be delivered in small group workshops and will equip the
soft tissue mucoderm botiss native stable 3-dimensional 3D-Regenerative Tissue Graft Handling, Clinical Application and Cases
 dental bone & tissue regeneration botiss biomaterials mucoderm 3D-Regenerative Tissue Graft Handling, Clinical Application and Cases by PD Dr. med. dent. Adrian Kasaj soft tissue native stable 3-dimensional
dental bone & tissue regeneration botiss biomaterials mucoderm 3D-Regenerative Tissue Graft Handling, Clinical Application and Cases by PD Dr. med. dent. Adrian Kasaj soft tissue native stable 3-dimensional
THE NEXT FRONTIER OF BONE REGENERATION. where Technology meets Nature
 THE NEXT FRONTIER OF BONE REGENERATION where Technology meets Nature SmartBone is a new hybrid bioactive bone substitute specifically developed for bone regeneration in reconstructive surgery. SmartBone
THE NEXT FRONTIER OF BONE REGENERATION where Technology meets Nature SmartBone is a new hybrid bioactive bone substitute specifically developed for bone regeneration in reconstructive surgery. SmartBone
We want to keep you smiling. Bone regeneration with Geistlich Bio-Oss and Geistlich Bio-Gide
 We want to keep you smiling Bone regeneration with Geistlich Bio-Oss and Geistlich Bio-Gide Strong bone for a healthier smile Strong and healthy teeth provide a feeling of well-being, self-confidence and
We want to keep you smiling Bone regeneration with Geistlich Bio-Oss and Geistlich Bio-Gide Strong bone for a healthier smile Strong and healthy teeth provide a feeling of well-being, self-confidence and
Socket preservation using deproteinized horsederived
 Research Article J Periodontal Implant Sci 2010;40:227-231 doi: 10.5051/jpis.2010.40.5.227 Socket preservation using deproteinized horsederived bone mineral Jang-Yeol Park, Ki-Tae Koo, Tae-Il Kim, Yang-Jo
Research Article J Periodontal Implant Sci 2010;40:227-231 doi: 10.5051/jpis.2010.40.5.227 Socket preservation using deproteinized horsederived bone mineral Jang-Yeol Park, Ki-Tae Koo, Tae-Il Kim, Yang-Jo
Tooth out what's next?
 Tooth out what's next Content >> Treatment Options >> Clinical Cases >> Product Information >> Product related FAQs >> Why Ridge Preservation > Minimise invasion: Bone volume preservation > Minimise invasion:
Tooth out what's next Content >> Treatment Options >> Clinical Cases >> Product Information >> Product related FAQs >> Why Ridge Preservation > Minimise invasion: Bone volume preservation > Minimise invasion:
Alveolar ridge preservation techniques
 Alveolar ridge preservation techniques Semmelweis University, Department of Periodontology, Budapest Dr. Windisch Péter Head of Department of Periodontology Changes of the alveolar ridge dimensions after
Alveolar ridge preservation techniques Semmelweis University, Department of Periodontology, Budapest Dr. Windisch Péter Head of Department of Periodontology Changes of the alveolar ridge dimensions after
The regeneration of the tooth supporting structures
 Position Paper Periodontal Regeneration* Untreated periodontal disease leads to tooth loss through destruction of the attachment apparatus and toothsupporting structures. The goals of periodontal therapy
Position Paper Periodontal Regeneration* Untreated periodontal disease leads to tooth loss through destruction of the attachment apparatus and toothsupporting structures. The goals of periodontal therapy
botiss dental bone & tissue regeneration biomaterials mucoderm 3D-Regenerative Tissue Graft strictly biologic
 dental bone & tissue regeneration botiss biomaterials 3DRegenerative Tissue Graft strictly biologic mucoderm Soft Tissue Graft Indications mucoderm is a collagen tissue matrix derived of animal dermis
dental bone & tissue regeneration botiss biomaterials 3DRegenerative Tissue Graft strictly biologic mucoderm Soft Tissue Graft Indications mucoderm is a collagen tissue matrix derived of animal dermis
THE NEXT FRONTIER OF BONE REGENERATION
 THE NEXT FRONTIER OF BONE REGENERATION where Technology meets Nature swiss made SmartBone is new composite bone substitute specifically developed for bone regeneration in oral and maxillofacial reconstructive
THE NEXT FRONTIER OF BONE REGENERATION where Technology meets Nature swiss made SmartBone is new composite bone substitute specifically developed for bone regeneration in oral and maxillofacial reconstructive
botiss biomaterials bone & tissue regeneration collacone max Innovative composite matrix socket preservation form-fitting resorbable composite
 bone & tissue regeneration botiss biomaterials socket preservation Innovative composite matrix form-fitting resorbable composite 1 Socket preservation safeguarding your sockets collacone.. max flexbone*
bone & tissue regeneration botiss biomaterials socket preservation Innovative composite matrix form-fitting resorbable composite 1 Socket preservation safeguarding your sockets collacone.. max flexbone*
botiss dental bone & tissue regeneration biomaterials collacone max Innovative composite matrix socket preservation form-fitting resorbable composite
 dental bone & tissue regeneration botiss biomaterials socket preservation Innovative composite matrix form-fitting resorbable composite 1 botiss regeneration system maxresorb flexbone* collacone.. max
dental bone & tissue regeneration botiss biomaterials socket preservation Innovative composite matrix form-fitting resorbable composite 1 botiss regeneration system maxresorb flexbone* collacone.. max
Years of research and advancement in
 Immediate Implants with Guided Bone Regeneration Using Titanium Mesh and Alloplast in an Infected Site: A Case Report Mahesh et al Dr. Lanka Mahesh 1 Dr. Ajay Bibra 2 Dr. Vishal Gupta 3 Abstract Years
Immediate Implants with Guided Bone Regeneration Using Titanium Mesh and Alloplast in an Infected Site: A Case Report Mahesh et al Dr. Lanka Mahesh 1 Dr. Ajay Bibra 2 Dr. Vishal Gupta 3 Abstract Years
Many factors are known to influence the success of
 CLINICAL The Role of Two Different Collagen Membranes for Dehiscence Defect Around Implants in Humans Dong-Woon Lee, DDS, MSD 1,2 Kyeong-Taek Kim, DDS, MSD 1 Yon-Soo Joo, DDS 1 Mi-Kyung Yoo, DDS, MSD 1
CLINICAL The Role of Two Different Collagen Membranes for Dehiscence Defect Around Implants in Humans Dong-Woon Lee, DDS, MSD 1,2 Kyeong-Taek Kim, DDS, MSD 1 Yon-Soo Joo, DDS 1 Mi-Kyung Yoo, DDS, MSD 1
Bone Grafting for Socket Preservation
 Bone Grafting for Socket Preservation Dr. Karl R. Koerner Normal extraction facial bone loss. Excessive force. Commonly the thickness of facial bone. Hussain, A. et al. Ridge preservation comparing a nonresorbable
Bone Grafting for Socket Preservation Dr. Karl R. Koerner Normal extraction facial bone loss. Excessive force. Commonly the thickness of facial bone. Hussain, A. et al. Ridge preservation comparing a nonresorbable
Bone augmentation with maxgraft
 Patient information bone & tissue regeneration botiss biomaterials Bone augmentation with maxgraft established safe X100 natural Implantation stability is crucial for success Atrophy of the jaw bone loss
Patient information bone & tissue regeneration botiss biomaterials Bone augmentation with maxgraft established safe X100 natural Implantation stability is crucial for success Atrophy of the jaw bone loss
Procedure Manual and Catalog
 Procedure Manual and Catalog TM Why SynthoGraft? SynthoGraft offers a unique structure which provides stability, while its micro-porosity allows for rapid vascularization and subsequent resorption. Although
Procedure Manual and Catalog TM Why SynthoGraft? SynthoGraft offers a unique structure which provides stability, while its micro-porosity allows for rapid vascularization and subsequent resorption. Although
Product Catalog. Dental Bone & Tissue Regeneration
 Product Catalog Dental Bone & Tissue Regeneration Bone graft regeneration Guided bone substitutes regeneration Osteogenesis Controlled resorption rate Angiogenesis Long term volume stability Remodeling
Product Catalog Dental Bone & Tissue Regeneration Bone graft regeneration Guided bone substitutes regeneration Osteogenesis Controlled resorption rate Angiogenesis Long term volume stability Remodeling
A wide variety of membrane options
 A wide variety of membrane options BOVINE Bovine collagen membrane Neomem is a resorbable collagen membrane derived from highly purified type I collagen fibres from bovine Achilles tendon. The macromolecular
A wide variety of membrane options BOVINE Bovine collagen membrane Neomem is a resorbable collagen membrane derived from highly purified type I collagen fibres from bovine Achilles tendon. The macromolecular
Surgical Procedure in Guided Tissue Regeneration with the. Inion GTR Biodegradable Membrane System
 Surgical Procedure in Guided Tissue Regeneration with the Inion GTR Biodegradable Membrane System 1 Introduction This presentation familiarizes you with the basic steps how to use the Inion GTR membrane
Surgical Procedure in Guided Tissue Regeneration with the Inion GTR Biodegradable Membrane System 1 Introduction This presentation familiarizes you with the basic steps how to use the Inion GTR membrane
Young-Seok Park 1, Sungtae Kim 2, Seung-Hee Oh 2, Hee-Jung Park 2, Sophia Lee 2, Tae-Il Kim 2, *, Young-Kyu Lee 3, Min-Suk Heo 4.
 Imaging Science in Dentistry 2014; 44: 143-8 http://dx.doi.org/10.5624/isd.2014.44.2.143 Comparison of alveolar ridge preservation methods using three-dimensional micro-computed tomographic analysis and
Imaging Science in Dentistry 2014; 44: 143-8 http://dx.doi.org/10.5624/isd.2014.44.2.143 Comparison of alveolar ridge preservation methods using three-dimensional micro-computed tomographic analysis and
Vertical Augmentation
 Indication Sheet V Dr. Mauro Merli Vertical Augmentation Vertical alveolar ridge augmentation by means of the fence technique with Geistlich biomaterials > Original publication of the technique on PubMed;
Indication Sheet V Dr. Mauro Merli Vertical Augmentation Vertical alveolar ridge augmentation by means of the fence technique with Geistlich biomaterials > Original publication of the technique on PubMed;
Clinical presentation of a horse-derived biomaterial and its Biocompatibility: A Clinical Case Report
 Case report J Korean Acad Periodontol 2009;39:287-291 Clinical presentation of a horse-derived biomaterial and its Biocompatibility: A Clinical Case Report Ki-Tae Koo, Jang-Yeol Park, Jun-Seok Park, Tae-Il
Case report J Korean Acad Periodontol 2009;39:287-291 Clinical presentation of a horse-derived biomaterial and its Biocompatibility: A Clinical Case Report Ki-Tae Koo, Jang-Yeol Park, Jun-Seok Park, Tae-Il
Biomaterials Line. MIS Corporation. All Rights Reserved.
 7. Biomaterials Line MIS Corporation. All Rights Reserved. 6. MIS s Quality System complies with international quality standards: ISO 13485: 2003 - Quality Management System for Medical Devices, ISO 9001:
7. Biomaterials Line MIS Corporation. All Rights Reserved. 6. MIS s Quality System complies with international quality standards: ISO 13485: 2003 - Quality Management System for Medical Devices, ISO 9001:
Chemicals in Surgical Periodontal Therapy
 Chemicals in Surgical Periodontal Therapy von Alexandrina L. Dumitrescu 1. Auflage Chemicals in Surgical Periodontal Therapy Dumitrescu schnell und portofrei erhältlich bei beck-shop.de DIE FACHBUCHHANDLUNG
Chemicals in Surgical Periodontal Therapy von Alexandrina L. Dumitrescu 1. Auflage Chemicals in Surgical Periodontal Therapy Dumitrescu schnell und portofrei erhältlich bei beck-shop.de DIE FACHBUCHHANDLUNG
BioVin Collagen Membrane
 BioVin Collagen Membrane Resorbable cross-linked collagen membrane BioVin Bovine Bone Bovine Bone Substitute OToss Synthetic Bone Synthetic Resorbable Biphasic Calcium Phosphate OToss Synthetic Bone Inject
BioVin Collagen Membrane Resorbable cross-linked collagen membrane BioVin Bovine Bone Bovine Bone Substitute OToss Synthetic Bone Synthetic Resorbable Biphasic Calcium Phosphate OToss Synthetic Bone Inject
Alveolar Ridge Preservation:
 Alveolar Ridge Preservation: Preserving and Building up the Bony Structures after Extraction» By: Prof. Roland Hille Konigsallee 49c, 41747 Viersen, Germany E-mail: dr-hille@t-online.de» Prof. Rolf Vollmer
Alveolar Ridge Preservation: Preserving and Building up the Bony Structures after Extraction» By: Prof. Roland Hille Konigsallee 49c, 41747 Viersen, Germany E-mail: dr-hille@t-online.de» Prof. Rolf Vollmer
The effect of overlaying titanium mesh with collagen membrane for ridge preservation
 The effect of overlaying titanium mesh with collagen membrane for ridge preservation Hyun-Chang Lim 1, Jung-Seok Lee 2, Seong-Ho Choi 2, Ui-Won Jung 2, * 1 Department of Periodontology, Kyung Hee University
The effect of overlaying titanium mesh with collagen membrane for ridge preservation Hyun-Chang Lim 1, Jung-Seok Lee 2, Seong-Ho Choi 2, Ui-Won Jung 2, * 1 Department of Periodontology, Kyung Hee University
Rehabilitating a Compromised Site for Restoring Form, Function and Esthetics- A Case Report
 Research & Reviews: Journal of Dental Sciences Rehabilitating a Compromised Site for Restoring Form, Function and Esthetics- A Case Report Priyanka Prakash* Division of Periodontology, Department of Dental
Research & Reviews: Journal of Dental Sciences Rehabilitating a Compromised Site for Restoring Form, Function and Esthetics- A Case Report Priyanka Prakash* Division of Periodontology, Department of Dental
THE NEW STANDARD OF EXCELLENCE IN BIOMATERIALS. Collagenated heterologous cortico-cancellous bone mix + TSV Gel GTO I N S P I R E D B Y N A T U R E
 GTO THE NEW STANDARD OF EXCELLENCE IN BIOMATERIALS Collagenated heterologous cortico-cancellous bone mix + TSV Gel R E G E N E R A T I O N S C I E N C E I N S P I R E D B Y N A T U R E A unique biotechnology
GTO THE NEW STANDARD OF EXCELLENCE IN BIOMATERIALS Collagenated heterologous cortico-cancellous bone mix + TSV Gel R E G E N E R A T I O N S C I E N C E I N S P I R E D B Y N A T U R E A unique biotechnology
Contemporary Periodontal Surgery
 Contemporary Periodontal Surgery Chris van Kesteren, D.D.S. CPCC Dental Hygiene Program October 18, 2011 Surgical Management of Periodontitis Periodontal Plastic Surgery Soft tissue and esthetics Dental
Contemporary Periodontal Surgery Chris van Kesteren, D.D.S. CPCC Dental Hygiene Program October 18, 2011 Surgical Management of Periodontitis Periodontal Plastic Surgery Soft tissue and esthetics Dental
ELIMINATE POCKETS. Periodontal pocket is the consequence of periodontal infection But also a major risk factor for the further progression of disease
 ELIMINATE POCKETS Periodontal pocket is the consequence of periodontal infection But also a major risk factor for the further progression of disease CONSEQUENTLY Periodontal pockets should be eliminated
ELIMINATE POCKETS Periodontal pocket is the consequence of periodontal infection But also a major risk factor for the further progression of disease CONSEQUENTLY Periodontal pockets should be eliminated
A WIDE RANGE OF REGENERATIVE SOLUTIONS
 A WIDE RANGE OF REGENERATIVE SOLUTIONS INDICATIONS: 1/ SOCKET AND RIDGE PRESERVATION 2/ FILLING OF EXTRACTION SOCKETS Biomaterials offers portfolio of regenerative materials for implantology, aimed at
A WIDE RANGE OF REGENERATIVE SOLUTIONS INDICATIONS: 1/ SOCKET AND RIDGE PRESERVATION 2/ FILLING OF EXTRACTION SOCKETS Biomaterials offers portfolio of regenerative materials for implantology, aimed at
Vertical and horizontal alveolar ridge augmentation
 CLINICAL SIMULTANEOUS VERTICAL GUIDED BONE REGENERATION AND GUIDED TISSUE REGENERATION IN THE POSTERIOR MAXILLA USING RECOMBINANT HUMAN PLATELET-DERIVED GROWTH FACTOR: A CASE REPORT Istvan Urban, DMD,
CLINICAL SIMULTANEOUS VERTICAL GUIDED BONE REGENERATION AND GUIDED TISSUE REGENERATION IN THE POSTERIOR MAXILLA USING RECOMBINANT HUMAN PLATELET-DERIVED GROWTH FACTOR: A CASE REPORT Istvan Urban, DMD,
Bone Augmentation Experiment using Coral on the Skull of Rat
 ORIGINAL ARTICLE Nishikawa et al., Nano Biomedicine 5(2),109-113, 2013 Bone Augmentation Experiment using Coral on the Skull of Rat Tetsunari NISHIKAWA 1, Tomoharu OKAMURA 1, Takanao ONO 2, Hiroko MATSUSHITA
ORIGINAL ARTICLE Nishikawa et al., Nano Biomedicine 5(2),109-113, 2013 Bone Augmentation Experiment using Coral on the Skull of Rat Tetsunari NISHIKAWA 1, Tomoharu OKAMURA 1, Takanao ONO 2, Hiroko MATSUSHITA
Biodegradation of three different collagen membranes: A histological study
 Biodegradation of three different collagen membranes: A histological study A. Olaechea, G. Mendoza-Azpur, E. Valdivia, G. Rasperini 3 DDS - Division of Implantology, Department of Stomatology, School of
Biodegradation of three different collagen membranes: A histological study A. Olaechea, G. Mendoza-Azpur, E. Valdivia, G. Rasperini 3 DDS - Division of Implantology, Department of Stomatology, School of
ALVEOLAR RIDGE AUGMENTATION UTILIZING PLATELET RICH FIBRIN IN COMBINATION WITH DEMINERALIZED FREEZE-DRIED BONE ALLOGRAFT A CASE REPORT
 ALVEOLAR RIDGE AUGMENTATION UTILIZING PLATELET RICH FIBRIN IN COMBINATION WITH DEMINERALIZED FREEZE-DRIED BONE ALLOGRAFT A CASE REPORT * Mishal Piyush Shah 1 and Sheela Kumar Gujjari 2 1 Department of
ALVEOLAR RIDGE AUGMENTATION UTILIZING PLATELET RICH FIBRIN IN COMBINATION WITH DEMINERALIZED FREEZE-DRIED BONE ALLOGRAFT A CASE REPORT * Mishal Piyush Shah 1 and Sheela Kumar Gujjari 2 1 Department of
Purpose: To assess the long term survival of sites treated by GTR.
 Cortellini P, Tonetti M. Long-term tooth survival following regenerative treatment of intrabony defects. J Periodontol 2004; 75:672-8. (28 Refs) Purpose: To assess the long term survival of sites treated
Cortellini P, Tonetti M. Long-term tooth survival following regenerative treatment of intrabony defects. J Periodontol 2004; 75:672-8. (28 Refs) Purpose: To assess the long term survival of sites treated
The Evaluation of Calcium Phosphate Coated Implants by Ion-beam Assisted Deposition (IBAD) Method in Dogs : A Preliminary Study
 Biomaterials Research (2009) 13(1) : 21-25 Biomaterials Research C The Korean Society for Biomaterials The Evaluation of Calcium Phosphate Coated Implants by Ion-beam Assisted Deposition (IBAD) Method
Biomaterials Research (2009) 13(1) : 21-25 Biomaterials Research C The Korean Society for Biomaterials The Evaluation of Calcium Phosphate Coated Implants by Ion-beam Assisted Deposition (IBAD) Method
Surgical Therapy. Tuesday, April 2, 13. Alessan"o Geminiani, DDS, MS
 Surgical Therapy Alessan"o Geminiani, DDS, MS Periodontal Flap: a surgical procedure in which incisions are made in the gingiva or mucosa to allow for separation of the epithelium and connective tissues
Surgical Therapy Alessan"o Geminiani, DDS, MS Periodontal Flap: a surgical procedure in which incisions are made in the gingiva or mucosa to allow for separation of the epithelium and connective tissues
The treatment of destructive periodontal disease, due to specific periodontopathic
 1 1 INTRODUCTION The treatment of destructive periodontal disease, due to specific periodontopathic bacteria, aims at the regeneration of a periodontal attachment composed of new cementum, alveolar bone
1 1 INTRODUCTION The treatment of destructive periodontal disease, due to specific periodontopathic bacteria, aims at the regeneration of a periodontal attachment composed of new cementum, alveolar bone
RESEARCH. Key Words: critical-sized defect, xenograft, bone regeneration, rat. INTRODUCTION Asignificant number of investigations
 RESEARCH Evaluation of the Long-Term Results of Rat Cranial Bone Repair Using a Particular Xenograft Hakan Develioglu 1 * Serpil Ünver Saraydın 2 Ünal Kartal, PhD 2 Levent Taner 3 Bone defects that cannot
RESEARCH Evaluation of the Long-Term Results of Rat Cranial Bone Repair Using a Particular Xenograft Hakan Develioglu 1 * Serpil Ünver Saraydın 2 Ünal Kartal, PhD 2 Levent Taner 3 Bone defects that cannot
Soft-Tissue Solutions from The Collagen Expert. Clinical Success with the Proven. Geistlich Mucograft Geistlich Mucograft Seal Geistlich Fibro-Gide
 Soft-Tissue Solutions from The Collagen Expert Clinical Success with the Proven Bone Geistlich Mucograft Substitute Geistlich Mucograft Seal Geistlich Fibro-Gide Documented More than 1,000 publications
Soft-Tissue Solutions from The Collagen Expert Clinical Success with the Proven Bone Geistlich Mucograft Substitute Geistlich Mucograft Seal Geistlich Fibro-Gide Documented More than 1,000 publications
Periimplant Regeneration Fenestration
 Indication Sheet PIR Periimplant Regeneration Fenestration Treatment concept of Dr. Jean-Pierre Gardella (surgeon) and Dr. Christian Richelme (prosthodontist), Marseille, France > Filling of a peri-implant
Indication Sheet PIR Periimplant Regeneration Fenestration Treatment concept of Dr. Jean-Pierre Gardella (surgeon) and Dr. Christian Richelme (prosthodontist), Marseille, France > Filling of a peri-implant
Peri-implant Augmentation
 Indication Sheet PIR3 Peri-implant Augmentation Early implantation with simultaneous GBR for contour augmentation using the technique by Prof. Daniel Buser and Prof. Urs Belser, University of Berne, Switzerland
Indication Sheet PIR3 Peri-implant Augmentation Early implantation with simultaneous GBR for contour augmentation using the technique by Prof. Daniel Buser and Prof. Urs Belser, University of Berne, Switzerland
Derma S O F T T I S S U E A U G M E N TAT I O N. Acellular dermal matrix
 Derma A XENOGENIC GRAFT FOR S O F T T I S S U E A U G M E N TAT I O N Acellular dermal matrix A xenogenic graft for soft tissue augmentation CHARACTERISTICS Obtained from derma of porcine origin, using
Derma A XENOGENIC GRAFT FOR S O F T T I S S U E A U G M E N TAT I O N Acellular dermal matrix A xenogenic graft for soft tissue augmentation CHARACTERISTICS Obtained from derma of porcine origin, using
Evaluation of a Combination Allograft Material Compared to DFDBA in Alveolar Ridge Preservation. Sanju P. Jose
 Evaluation of a Combination Allograft Material Compared to DFDBA in Alveolar Ridge Preservation by Sanju P. Jose B.S., University of Maryland Baltimore County, 2008 D.D.S., University of Maryland School
Evaluation of a Combination Allograft Material Compared to DFDBA in Alveolar Ridge Preservation by Sanju P. Jose B.S., University of Maryland Baltimore County, 2008 D.D.S., University of Maryland School
Consensus Report Tissue augmentation and esthetics (Working Group 3)
 B. Klinge Thomas F. Flemmig Consensus Report Tissue augmentation and esthetics (Working Group 3) Members of working group: Matteo Chiapasco Jan-Eirik Ellingsen Ronald Jung Friedrich Neukam Isabella Rocchietta
B. Klinge Thomas F. Flemmig Consensus Report Tissue augmentation and esthetics (Working Group 3) Members of working group: Matteo Chiapasco Jan-Eirik Ellingsen Ronald Jung Friedrich Neukam Isabella Rocchietta
Puros Cancellous Particulate Allograft & Puros Block Allograft
 Puros Cancellous Particulate Allograft & Puros Block Allograft Puros Cancellous Particulate Allograft The Natural Choice For Healthy 1 Bone Growth. 1. Proven, Predictable Regeneration Acts as an osteoconductive
Puros Cancellous Particulate Allograft & Puros Block Allograft Puros Cancellous Particulate Allograft The Natural Choice For Healthy 1 Bone Growth. 1. Proven, Predictable Regeneration Acts as an osteoconductive
The Sandwich Bone Augmentation Technique. Jia-Hui Fu* and Hom-Lay Wang*
 CASE REPORT The Sandwich Bone Augmentation Technique Jia-Hui Fu* and Hom-Lay Wang* Introduction: Horizontal ridge width reduction after tooth extraction is a common clinical scenario. As such, when implant-supported
CASE REPORT The Sandwich Bone Augmentation Technique Jia-Hui Fu* and Hom-Lay Wang* Introduction: Horizontal ridge width reduction after tooth extraction is a common clinical scenario. As such, when implant-supported
Management of peri-implant recession associated with bone fenestration and dehiscence in the anterior region
 CLINICAL REPORT 269 George Nikou, Dimitris Nikolidakis, Peter Thoolen, Anton Sculean Management of peri-implant recession associated with bone fenestration and dehiscence in the anterior region KEY WORDS
CLINICAL REPORT 269 George Nikou, Dimitris Nikolidakis, Peter Thoolen, Anton Sculean Management of peri-implant recession associated with bone fenestration and dehiscence in the anterior region KEY WORDS
Multi-Modality Anterior Extraction Site Grafting Increased Predictability for Aesthetics Michael Tischler, DDS
 Page 1 of 5 Issue Date: March 2003, Posted On: 8/1/2005 Multi-Modality Anterior Extraction Site Grafting Increased Predictability for Aesthetics Michael Tischler, DDS The extraction of teeth creates a
Page 1 of 5 Issue Date: March 2003, Posted On: 8/1/2005 Multi-Modality Anterior Extraction Site Grafting Increased Predictability for Aesthetics Michael Tischler, DDS The extraction of teeth creates a
Periimplant Regeneration Fenestration
 Indication Sheet PIR-1 Periimplant Regeneration Fenestration Treatment concept of Dr. Jean-Pierre Gardella (surgeon) and Dr. Christian Richelme (prosthodontist), Marseille, France > Filling of a peri-implant
Indication Sheet PIR-1 Periimplant Regeneration Fenestration Treatment concept of Dr. Jean-Pierre Gardella (surgeon) and Dr. Christian Richelme (prosthodontist), Marseille, France > Filling of a peri-implant
