Juvenile Mycosis Fungoides Diagnosed Before 18 Years of Age
|
|
|
- Octavia Ferguson
- 5 years ago
- Views:
Transcription
1 Acta Derm Venereol 2003; 83: CLINICAL REPORT Juvenile Mycosis Fungoides Diagnosed Before 18 Years of Age DAN BEN-AMITAI 1, MICHAEL DAVID 2, MEORA FEINMESSER 3 and EMMILIA HODAK 2 1 Pediatric Dermatology Clinic, Schneider Children s Medical Center of Israel, 2 Department of Dermatology and 3 Institute of Pathology, Rabin Medical Center, Beilinson Campus, Petah Tiqva and the Sackler Faculty of Medicine, Tel-Aviv University, Tel-Aviv, Israel The literature regarding mycosis fungoides in children is sparse. To shed further light on the characteristics of mycosis fungoides in the paediatric population we analysed the clinicopathological features of 10 patients in whom this malignancy was diagnosed before the age of 18 years. All were Jews and Arabs with histologically proven patch/early plaque stage disease: 4 in stage IA, 4 in IB and 2 with unilesional disease. Seven patients had hypopigmented lesions either constituting the sole manifestation (2 patients) or in combination with classic lesions (5 patients); of these, 3 had light skin and 4 pigmented skin. Most patients had immunohistochemical features characteristic of mycosis fungoides, with a predominance of CD4z T cells. Some had deletion of CD7z cells. In 3 patients, however, the epidermotropic cells were exclusively or predominantly CD8z cells. All patients responded to conventional therapy and during an average follow-up of 3.4 years only one patient showed stage progression, but without extracutaneous involvement. It is concluded that juvenile mycosis fungoides is characterized by early stage disease, occasionally with unilesional disease, usually with hypopigmented lesions irrespective of skin colour, and a good response to therapy. On the basis of our experience and review of the literature, it appears that the CD8z phenotype is overrepresented in juvenile disease. Key words: childhood; cutaneous T-cell lymphoma; immunohistochemistry. (Accepted July 4, 2003.) Acta Derm Venereol 2003; 83: Dr Dan Ben-Amitai, Pediatric Dermatology Clinic, Schneider Children s Medical Center of Israel, 14 Kaplan Street, Petah Tiqva 49202, Israel. danb@clalit.org.il Mycosis fungoides (MF) is the most common cutaneous T-cell lymphoma (CTCL). It is characterized by epidermotropic atypical T lymphocytes that are clonally expanded in the skin. Its reported incidence in the Western world is 0.5 cases per 100,000 per year (1) and it usually occurs in older adults: approximately 75% of patients are diagnosed beyond age 50 (1), whereas only 0.5 5% of all cases are diagnosed before age 20 (2, 3). The diagnosis of early-stage MF is often delayed because the long-standing erythematous patches may # 2003 Taylor & Francis. ISSN DOI: / resemble inflammatory dermatoses such as atopic dermatitis, or, in cases of hypopigmented lesions, pityriasis alba, vitiligo or pityriasis versicolor, all of which are much more common in the paediatric population. It would appear that this is particularly true in children; although the literature on this subject is scanty, adult patients occasionally report that the typical rash appeared before the age of 20 years. To shed further light on the characteristics of MF in the paediatric population, we analysed the clinical and immunohistopathological findings and follow-up data in 10 patients in whom MF had been histologically diagnosed before the age of 18 years. PATIENTS AND METHODS The study population comprised 10 Caucasian patients (6 boys and 4 girls) diagnosed to have MF before age 18 during the period 1994 to Age at clinical onset of disease was 1.0 to 15.5 years (median 7.5 years). Six patients had light skin and 4 pigmented skin. Diagnosis was based on the clinical features combined with histopathological findings characteristic for MF (4). The slides were reviewed by two dermatopathologists (MF and EH). In addition, each biopsy was subjected to immunohistochemical studies on formalinfixed, paraffin-embedded tissue and frozen sections, with an avidin-biotin complex immunoperoxidase technique (ABC Vectastain Kit, Vector Laboratories Inc., Burlingame, CA, USA), using monoclonal antibodies CD3, CD4, CD8 (Dako, Glostrup, Denmark) and CD7 (B-B7; R&D Immuno Quality Product, Uithoorn, The Netherlands). Molecular studies using the polymerase chain reaction (PCR) technique were performed on DNA extracted from frozen tissue of selected cases to determine the rearrangement of the T-cell receptor (TCR) gene as previously described (5). The evaluation of each child consisted of a detailed personal and familial medical history, physical examination, routine laboratory tests, including blood smear, leucocyte count, biochemistry, the T helper/t suppressor ratio, serology for human T lymphotropic virus type I (HTLV-1) by enzymelinked immunosorbent assay (ELISA), and imaging procedures, including chest X-rays and abdominal ultrasound examination. Lymph node biopsy was performed when there was palpable lymphadenopathy. Staging was done according to the Bunn & Lamberg staging system (6). Patients in whom the cutaneous lesions had been noted before age 18, but the histological diagnosis made only thereafter, were not included in the study. The response to therapy was defined as follows: complete response complete disappearance of clinical lesions for at least one month; partial response disappearance of more than 50% of the lesions; no response disappearance of less than 50% of the lesions; progressive disease a greater than 25% increase in skin lesions.
2 Table I. Clinical data of the patients with juvenile mycosis fungoides Patient no./sex Skin colour Age at onset by history Age at diagnosis Time to diagnosis Stage at diagnosis Types of lesions Site Therapy and outcome Course Duration of last response Duration of follow-up since diagnosis Last status 452 D. Ben-Amitai et al. 1/M Light la (patch) Mixed Lower abdomen Steroids*ANR, NMACR 2/M Pigmented la (patch/plaque) Mixed Upper and TarzsunANR, lower limbs UVBANR, NMAPD to IIA, PUVAACR 3/F Light la (patch) Classic Axilla, lower UVBACR abdomen 4/M Light la (patch) Classic Axilla, lower abdomen, thighs 5/M Light Unilesional Hypo-pigmented Thigh Steroids*APR, (patch) Tarzsun exposureacr 6/F Light Unilesional (plaque) 7/M Pigmented lb (patch/plaque) Mixed Upper and lower limbs 8/F Light lb (patch) Mixed Trunk, upper and lower limbs 9/F Pigmented lb (patch) Hypo-pigmented Trunk, upper and lower limbs 10/M Pigmented lb (patch/plaque) Mixed Axilla, trunk, upper and lower limbs No relapse NED No relapse NED Relapse after 1 y, topical steroidsacr NED UVBACR No relapse NED No relapse Lost to follow-up Classic Breast ExcisionACR No relapse NED NMAACO, TarzsunAPR, PUVAACR No relapse NED PUVAACR No relapse Lost to follow-up PUVAACR Relapse after NED 1 y, topical steroidsacr NBUVBAPR Ongoing AWD therapy Mixed~hypopigmentedzclassic, UVB~ultraviolet B, NBUVB~Narrow-band UVB, NM~nitrogen mustard, PUVA~psoralen with ultraviolet A, NR~no response, CR~complete response, PR~partial response, NED~no evidence of disease, AWD~alive with disease, ACO~allergic contact dermatitis, PD~progressive disease. *Topically applied corticosteroids (mid to high potency).
3 Juvenile mycosis fungoides 453 RESULTS The clinical data of the patients are presented in Table I. In 5 patients the initial clinical diagnosis differed from MF (psoriasis, nummular eczema, morphea, pityriasis alba, vitiligo) and in 2 no specific clinical diagnosis had been offered. Age at the diagnostic biopsy ranged from 3.8 to 17.5 years, median 14.3 years, and the duration of the clinical eruption from onset to diagnosis was between 3 months and 13.5 years (median 5 years). Two patients were siblings (numbers 2 and 7). The remaining cases were apparently sporadic, with no family history of lymphoproliferative disease. All 10 patients were in good general health and without a remarkable medical history except patient no. 5, who had a clinical history of bronchial asthma. None of the patients had atopic dermatitis. On initial examination, all patients had early MF and most of them presented with patches. In 2 patients there was unilesional MF, i.e. MF presenting as a solitary skin lesion. Four had stage Ia disease with patches and/or plaques involving v10% of body surface and 4 had stage Ib disease with patches and/or plaques involving 10% of total body surface. Three patients had classic lesions of MF and 7 had atypical lesions. In 2 patients purely hypopigmented lesions were found and in 5 mixed hypopigmented classic lesions (Figs 1 and 2). The hypopigmented lesions were round or oval patches and/or flat plaques, with or without a scaly surface, and with well- or less-well defined borders. Of the 7 patients with hypopigmented lesions, 3 had light skin (types II or III) and 4 had pigmented skin (type IV). Nine patients were asymptomatic and one (patient 2) had pruritus. Routine evaluation, including serology for HTLV-1 and the T helper/t suppressor ratio, was normal in all patients. Treatment included topical corticosteroids (mid to high potency) as monotherapy in 3 patients, psoralen and UVA (PUVA) in 4 patients, broad-band UVB in 2 patients, narrow-band UVB in 1 patient, topical tar and Fig. 2. (a) Hypopigmented non-scaly patches on the back (white arrows) of a light-skinned girl (patient no. 8) in association with a classical presentation of MF in the form of an erythematous patch (black arrow). (b) Classical erythematous patch/plaque on the buttocks. sun exposure in 2 patients, topical nitrogen mustard in 3 patients and excision in 1 patient. Each modality was given either as the initial therapy or after failure with another therapy, i.e. after partial or no response, or during relapse (Table I). A final complete response was achieved in all patients except in patient no. 10, who is still receiving therapy with narrow-band UVB 3 times Fig. 1. Hypopigmented scaly patches on the external aspect of an upper limb, mimicking extensive pityriasis alba in a boy (patient no. 2) with pigmented skin. Fig. 3. Hypopigmented scaly patches on the buttocks of a boy (patient no. 10) with pigmented skin.
4 454 D. Ben-Amitai et al. weekly (Fig. 3). Patients given phototherapy leading to complete response were gradually tapered out over a period of several months. Follow-up ranged from 1 to 6.0 years (mean 3.4 years). Only one patient showed stage progression from Ia to IIa (patient no. 2) despite treatment with broadband UVB and topical tar followed by topical nitrogen mustard. He developed prominent axillary and inguinal lymphadenopathy which histologically was dermatopathic lymphadenopathy. Histopathological, immunohistochemical and genotypic findings All biopsy specimens revealed changes of early MF. Single atypical lymphocytes with minimal spongiosis were present in the epidermis, in some cases aligning the basement membrane and in six forming Pautrier s microabscesses. Adnexotropism was occasionally noted. Necrotic keratinocytes or prominent vascular alteration of the dermoepidermal junction were not seen. The upper dermis contained variable perivascular or lichenoid lymphocytic infiltrates with melanophages noted in a minority of cases (Fig. 4a). Immunohistochemically, in 7 of the 10 cases the epidermotropic cells were CD3z, expressing CD4z on their surfaces ( 80% of the T cells). In 3 cases, however, there was a decreased CD4/CD8 ratio in the epidermis. In 2 of these cases almost all of the T cells exclusively expressed CD8 with preference for the junctional zone, whereas the perivascular dermal lymphocytes were predominantly CD3z, CD4z, CD82 (Fig. 4b d); in one, CD8z T cells represented about 70% of the epidermotropic T lymphocytes with an equivalent number of CD4z and CD8z T cells in the dermis. Four of the 6 patients studied were found to have a reduction of CD7z cells (v30% of the T cells); 3 of these had a CD4z phenotype and one had a CD8z phenotype. PCR analysis of the TCR c-gene was performed in 6 of the 10 patients, 3 with CD4z phenotype (patients 2, 5, 7) and 3 with CD8z phenotype (patients 1, 4, 9). Evidence for monoclonal rearrangement of the TCR c-gene was found in one patient with a CD8z phenotype (patient no. 4). DISCUSSION In the past, clinicians have become more aware of the possibility of MF in childhood and the number of publications on paediatric MF has increased (2, 3, 7 15). Nevertheless, data regarding clinical symptoms, treatment and prognosis are still sparse and the true incidence of early-onset MF remains to be determined. We describe Fig. 4. (a) Lining up of epidermotropic atypical lymphocytes among basal keratinocytes at the dermoepidermal junction in patient no 4. (H; original magnification 6200). (b d) Immunohistochemical features (original magnification 6100). Note the presence of CD3z, CD42, CD8z lymphocytes in the epidermis with junctional preference, whereas the dermal lymphocytes are predominantly CD3z, CD4z, CD82.
5 Juvenile mycosis fungoides 455 here 10 patients in whom MF was diagnosed before the age of 18 years. As previously, the correct diagnosis of MF was delayed, in half of our patients the interval from onset of the eruption to the histopathologic examination and diagnosis was 7 years or longer, and in 2 as long as over 10 years. In half of our patients the initial diagnoses were different types of benign dermatoses, including pityriasis alba, psoriasis, nummular eczema and vitiligo. In many patients with MF described in the literature (7, 9, 16) the cutaneous lesions appeared in childhood, but the correct diagnosis was reached only in adulthood. Apart from the classical Alibert-Bazin type of MF (patch, plaque, tumour) several unusual variants of MF have been reported in children (12, 17, 18). The hypopigmented variant of MF is known to have a particular propensity for younger patients (9, 19) and is found almost exclusively in individuals with black or dark skin (12, 19). It has been reported present in 20.4% of all paediatric patients with MF (11), usually without any pruritus (12) and in combination with classical lesions of MF. Macular hypopigmentation as the sole manifestation of MF in childhood has been reported in only a few cases (19, 20). In the present series, 7 patients presented with hypopigmented lesions, including 2 with macular hypopigmentation as the sole manifestation. This can be explained by the high percentage of patients with pigmented skin, although 3 of our patients with hypopigmented lesions had light complexions. Hypopigmented MF in light-skinned patients has rarely been described in the literature (21 24). Most of the reported patients diagnosed to have MF during childhood and adolescence, as in our series, had early-stage disease. In their comprehensive review from 1999, Quaglino et al. (11) found that 91.8% had patch and/or plaque disease, whereas only 8.2% had nodular lesions at onset. It is of particular interest that 2 of the patients in our series, previously reported by us (25), exhibited a solitary lesion of MF of long duration; one of them presented with a hypopigmented patch and thus represented a hypopigmented variant of unilesional MF. Recently, a solitary lesion of MF was found in one of 10 cases (14) and in another series in 2 of 5 cases of childhood MF (15). It is conceivable that unilesional MF is, in fact, more common in the children than is reflected in the literature. Furthermore, since unilesional MF is an extremely rare presentation of MF in adults (27), it would appear that it may be over-represented in the paediatric group. Immunophenotypically, the majority of our patients, as well as those in the literature (8), exhibited a CD4z T helper cell phenotype, similarly to adults with MF. However, in 3 of our patients the epidermis predominantly or exclusively showed CD8z T-cells. A predominance of CD8z cells has been found in 5% of adult patients (26), and some of these had rapidly progressive disease (27), whereas others had a nonaggressive clinical behaviour (28). Whittam et al. (14) described 10 cases of childhood MF in which 6 patients had a CD8z immunophenotype with an indolent course. Even more recently, El Shabrawi-Caelen et al. (30) reported 15 patients with hypopigmented MF with an indolent course; 9 of these had a CD8z T-cell phenotype, and of these 7 were under the age of 20 years. On the basis of the two aforementioned reports as well as two previous case reports (16, 22) and our own experience, it can be concluded that CD8z MF is over-represented in the paediatric age group, as already suggested (14). Since one of our 3 patients and at least one of 6 patients in a previous report (14) with CD8z immunophenotype had classical lesions of MF, it would appear that this unusual phenotype of CTCL is not exclusive for the hypopigmented variant of MF. It is of interest that in 2 of our patients there was a CD8z cell infiltrate showing an exclusive junctional affinity in the epidermis with reactive dermal cells composed predominantly of CD4z cells; this finding is similar to that described very recently in 3 adult patients with hyperpigmented patches and termed junctional CD8z cutaneous lymphoma (28). Whether in cases of CD8z MF the CD8z cells represent only tumour cells or whether some are also reactive T cells is a matter for further study. In this regard it is of interest that in MF patients with the usual CD4z phenotype, CD8z cytotoxic T lymphocytes were found to play an important role in the antitumour response (29). In the early stage of the disease the neoplastic clone likely resides within the epidermis. By isolating intraepidermal CD8z T cells via microdissection and analysing the TCR c-chain gene, El Shabrawi-Caelen et al. (30) were able to show that the malignant population was derived from CD8z lymphocytes. It was therefore confirmed that their cases represented CD8z CTCL. As for our cases, only in one of 3 CD8z cases were we able to demonstrate clonality. This could be attributed to the very early stage of the disease in which even the PCR technique is below the threshold of detection of clonality. Likewise, El Shahrawi-Caelen et al. (30) were able to detect clonality in less than 50% of their cases (only in 33% among children). Several types of treatment have been suggested for children and adolescents with MF, but there are no established protocols especially designed for this age group, so their management is the same as for adults. This includes topical nitrogen mustard (7, 8, 13), carmustine (7, 9), topical corticosteroids (14, 18), PUVA and UVB (7, 9, 18). Most recently, topical PUVA has been shown to be effective for patients with juvenile MF with plaque-stage disease (14). In our series the initial treatment was mid to high potent topical steroids, topical nitrogen mustard
6 456 D. Ben-Amitai et al. and phototherapy. There are few reported cases in which maintenance PUVA or UVB phototherapy was given to children (13). In our patients maintenance therapy was given for only short periods. Although the natural history of MF has been well described in adults, the data for paediatric MF are scarce and variable. Lamberg et al. (31) suggested that age has no significant effect on prognosis in MF after adjustment for stage of disease. Since all of our patients had early MF (Ia, Ib), at diagnosis their prognosis should conceivably be no different from that of adults. In conclusion, juvenile MF is characterized by early stage disease, occasionally with unilesional presentation, usually with hypopigmented lesions irrespective of skin colour, and a good response to therapy. On the basis of our experience and review of the literature, the CD8z phenotype appears to be over-represented in juvenile disease. REFERENCES 1. Weinstock MA, Horm JM. Mycosis fungoides in the United States. Increasing incidence and descriptive epidemiology. JAMA 1988; 260: Agnarsson GA, Kadin ME. Peripheral T cell lymphomas in children. Semin Diag Pathol 1995; 12: Peters MS, Thisbodeau SN, White JW, Winkelmann RK. Mycosis fungoides in children and adolescents. J Am Acad Dermatol 1990; 22: Smoller BR, Bishop K, Glusac E. Reassessment of histologic parameters in the diagnosis of mycosis fungoides. Am J Surg Pathol 1995; 19: Bergman R, Faclieru D, Sahan D, Sander CA, Kremer H, Ben-Aryeh Y, et al. Immunophenotyping and T-cell receptor c gene rearrangement analysis as an adjunct to histopathological diagnosis of mycosis fungoides. J Am Acad Dermatol 1998; 39: Bunn PA Jr, Lamberg SI. Report of the Committee on Staging and Classification of Cutaneous T-Cell Lymphomas. Cancer Treat Rep 1979; 63: Koch SE, Zackheim HS, Williams ML, Fletcher V, LeBoit PE. Mycosis fungoides beginning in childhood and adolescence. J Am Acad Dermatol 1987; 17: Hickham PR, McBurney EI, Fitzgerald RL. CTCL in patients under 20 years of age: a series of five cases. Pediatr Dermatol 1997; 14: Zackheim HS, McCalmont TH, Deanovic FW, Odom RB. Mycosis fungoides with onset before 20 years of age. Review of 24 patients and report of a case diagnosed at age 22 months. J Am Acad Dermatol 1997; 36: Crowley JJ, Nikko A, Varghese A, Hoppe RT, Kim YH. Mycosis fungoides in young patients: clinical characteristics and outcome. J Am Acad Dermatol 1998; 38: Quaglino P, Zaccagna A, Verrone A, Dardano F, Bernengo MG. Mycosis fungoides in patients under 20 years of age: report of 7 cases, review of the literature and study of clinical course. Dermatology 1999; 199: Garzon MC. Cutaneous T-cell lymphoma in children. Semin Cutan Med Surg 1999; 18: Tan E, Tay YK, Giam YC. Profile and outcome of childhood mycosis fungoides in Singapore. Pediatr Dermatol 2000; 17: Whittam LR, Calonje E, Orchard GE, Fraser-Andrews EA, Woolford A, Russell-Jones R. CD8 positive juvenile onset of mycosis fungoides: an immunohistochemical and genotypic analysis of six cases. Br J Dermatol 2000; 143: Pabsch H, Rutten A, Von Stemm A, Weigel W, Sander CA, Schaller J. Treatment of childhood mycosis fungoides with topical PUVA. J Am Acad Dermatol 2002; 47: Burns MK, Ellis CN, Cooper KD. Mycosis fungoidestype cutaneous T-cell lymphoma arising before 30 years of age. J Am Acad Dermatol 1992; 27: Ko JW, Seong JY, Suh KS, Kim ST. Pityriasis lichenoides-like mycosis fungoides in children. Br J Dermatol 2000; 142: Van Doorn R, Scheffer E, Willemze R. Follicular mycosis fungoides, a distinct disease entity with or without associated follicular mucinosis. A clinico-pathological and follow-up study of 51 patients. Arch Dermatol 2002; 138: Lambroza E, Cohen SR, Phelps R, Lebwohl M, Braverman IM, DiCostanzo D. Hypopigmented variant of mycosis fungoides: demography, histology, and treatment of seven cases. J Am Acad Dermatol 1995; 32: Neuhaus IM, Romos-Caro FA, Hassanein AM. Hypopigmented mycosis fungoides in childhood and adolescence. Pediatr Dermatol 2000; 17: Sigal M, Grossin M, Laroche L, Basset F, Aitken G, Haziza JL, et al. Hypopigmented mycosis fungoides. Clin Exp Dermatol 1987; 12: Amichai B, Grunwald MH, Avinoach I, Halevy S. Hypopigmented mycosis fungoides in a white female. J Dermatol 1996; 23: Di Landro A, Marchesi L, Naidi L, Motta T, Cainelli T. A case of hypopigmented mycosis fungoides in a young Caucasian boy. Pediatric Dermatol 1997; 14: Moulonguet I, Robert C, Baudot N, Flageul B, Dubertret L. Hypopigmented mycosis fungoides in a light-skinned woman. Br J Dermatol 1998; 139: Hodak E, Fenig E, Amichai B, Feinmesser M, Kutar A, Maron L, et al. Unilesional mycosis fungoides. A study of seven cases. Dermatology 2000; 201: Nasu K, Said J, Vonderheid E. Immunopathology of cutaneous T-cell lymphomas. Am J Pathol 1985; 119: Agnarsson BA, Vonderheid EC, Kadin ME. Cutaneous T-cell lymphoma with suppressor/cytotoxic (CD8) phenotype: identification of rapidly progressive and chronic subtypes. J Am Acad Dermatol 1990; 22: Dummer R, Kamarashev J, Kempf W, Huffner AC, Hess-Schmid M, Burg G. Junctional CD8z cutaneous lymphomas with nonaggressive clinical behavior. A CD8z variant of mycosis fungoides? Arch Dermatol 2002; 138: Vermeer MH, van Doorn R, Dukes D, Bekkenk MW, Meijer CJLM, Willemze R. CD8z T cells in cutaneous T-cell lymphoma: expression of cytotoxic proteins, Fas ligand, and killing inhibitory receptors and their relationship with clinical behavior. J Clin Oncol 2001; 23: El Shabrawi-Caelen L, Cerroni L, Jefferey Medeiro L, McCalmont TH. Hypopigmented mycosis fungoides. Frequent expression of a CD8z T-cell phenotype. Am J Surg Pathol 2002; 26: Lamberg S, Green S, Byar D, Block JB, Clendenning WE, Douglas MC, et al. Clinical staging for cutaneous T-cell lymphoma. Ann Intern Med 1984; 100:
Case Report Childhood Hypopigmented Mycosis Fungoides: A Rare Diagnosis
 Case Reports in Pediatrics Volume 2016, Article ID 8564389, 4 pages http://dx.doi.org/10.1155/2016/8564389 Case Report Childhood Hypopigmented Mycosis Fungoides: A Rare Diagnosis Cláudia Patraquim, 1 Maria
Case Reports in Pediatrics Volume 2016, Article ID 8564389, 4 pages http://dx.doi.org/10.1155/2016/8564389 Case Report Childhood Hypopigmented Mycosis Fungoides: A Rare Diagnosis Cláudia Patraquim, 1 Maria
A middle-aged man with self-healing papulonecrotic lesions over the trunk and proximal limbs
 Hong Kong J. Dermatol. Venereol. (2011) 19, 30-34 Case Report A middle-aged man with self-healing papulonecrotic lesions over the trunk and proximal limbs JC Chan, N Trendell-Smith, CK Yeung Lymphomatoid
Hong Kong J. Dermatol. Venereol. (2011) 19, 30-34 Case Report A middle-aged man with self-healing papulonecrotic lesions over the trunk and proximal limbs JC Chan, N Trendell-Smith, CK Yeung Lymphomatoid
Important Decisions in Dermatopathology: The Clinico- Pathologic Correlation. Dermatopathology Specialists Needed. Changing Trends
 Important Decisions in Dermatopathology: The Clinico- Pathologic Correlation Uma Sundram, MD, PhD Departments of Pathology and Dermatology Stanford University May 29, 2008 Dermatopathology Specialists
Important Decisions in Dermatopathology: The Clinico- Pathologic Correlation Uma Sundram, MD, PhD Departments of Pathology and Dermatology Stanford University May 29, 2008 Dermatopathology Specialists
Microscopic study of the normal skin in cases of mycosis fungoides
 Microscopic study of the normal skin in cases of mycosis fungoides M. El Darouti, S. Marzook, M. Bosseila, O. Abu Zeid, O. El- Safouri, A. Zayed, A. El-Ramly Egyptian Dermatology Online Journal 2 (1):
Microscopic study of the normal skin in cases of mycosis fungoides M. El Darouti, S. Marzook, M. Bosseila, O. Abu Zeid, O. El- Safouri, A. Zayed, A. El-Ramly Egyptian Dermatology Online Journal 2 (1):
Clinical and Histopathological Spectrum of Mycosis Fungoides
 Awad Hasan Al-Tarawneh, MD, Jordan Board* Background: Early diagnosis of mycosis fungoides is essential but difficult and can be easily missed because it mimics many inflammatory skin diseases both clinically
Awad Hasan Al-Tarawneh, MD, Jordan Board* Background: Early diagnosis of mycosis fungoides is essential but difficult and can be easily missed because it mimics many inflammatory skin diseases both clinically
Citation The Journal of Dermatology, 37(8), available at
 NAOSITE: Nagasaki University's Ac Title Two cases of blaschkitis with promi Author(s) Utani, Atsushi Citation The Journal of Dermatology, 37(8), Issue Date 2010-08 URL Right http://hdl.handle.net/10069/25634
NAOSITE: Nagasaki University's Ac Title Two cases of blaschkitis with promi Author(s) Utani, Atsushi Citation The Journal of Dermatology, 37(8), Issue Date 2010-08 URL Right http://hdl.handle.net/10069/25634
Dermatopathology: The tumor is composed of keratinocytes which show atypia, increase mitoses and abnormal mitoses.
 Squamous cell carcinoma (SCC): A common malignant tumor of keratinocytes arising in the epidermis, usually from a precancerous condition: 1- UV induced actinic keratosis, usually of low grade malignancy.
Squamous cell carcinoma (SCC): A common malignant tumor of keratinocytes arising in the epidermis, usually from a precancerous condition: 1- UV induced actinic keratosis, usually of low grade malignancy.
Mycosis Fungoides and Variants
 Mycosis Fungoides and Variants Jennifer Madison McNiff, M.D. Associate Professor, Dermatology and Pathology Yale University School of Medicine Classic mycosis fungoides The most common cutaneous lymphoma
Mycosis Fungoides and Variants Jennifer Madison McNiff, M.D. Associate Professor, Dermatology and Pathology Yale University School of Medicine Classic mycosis fungoides The most common cutaneous lymphoma
Cluster of differentiation (CD) markers in erythrodermic patients: A case series study
 Original Article Cluster of differentiation (CD) markers in erythrodermic patients: A case series study Fariba Ghalamkarpour, MD Faranak Niknafs, MD Shima Younespour, PhD Skin Research Center, Shahid Beheshti
Original Article Cluster of differentiation (CD) markers in erythrodermic patients: A case series study Fariba Ghalamkarpour, MD Faranak Niknafs, MD Shima Younespour, PhD Skin Research Center, Shahid Beheshti
Lymphoma and Pseudolymphoma
 Lymphoma and Pseudolymphoma Laura B. Pincus, MD Co-Director, Cutaneous Lymphoma Clinic Associate Professor Dermatology and Pathology University of California, San Francisco I HAVE NO RELEVANT RELATIONSHIPS
Lymphoma and Pseudolymphoma Laura B. Pincus, MD Co-Director, Cutaneous Lymphoma Clinic Associate Professor Dermatology and Pathology University of California, San Francisco I HAVE NO RELEVANT RELATIONSHIPS
CUTIS. Do Not Copy. Pityriasis lichenoides is a T cell mediated papular. Pityriasis Lichenoides Chronica in Black Patients. Pediatric Dermatology
 Series Editor: Camila K. Janniger, MD Pityriasis Lichenoides Chronica in Black Patients Tanda N. Lane, MD; Sareeta S. Parker, MD Pityriasis lichenoides chronica (PLC) is a cutaneous disease of unknown
Series Editor: Camila K. Janniger, MD Pityriasis Lichenoides Chronica in Black Patients Tanda N. Lane, MD; Sareeta S. Parker, MD Pityriasis lichenoides chronica (PLC) is a cutaneous disease of unknown
Overview of Cutaneous Lymphomas: Diagnosis and Staging. Lauren C. Pinter-Brown MD, FACP Health Sciences Professor of Medicine and Dermatology
 Overview of Cutaneous Lymphomas: Diagnosis and Staging Lauren C. Pinter-Brown MD, FACP Health Sciences Professor of Medicine and Dermatology Definition of Lymphoma A cancer or malignancy that comes from
Overview of Cutaneous Lymphomas: Diagnosis and Staging Lauren C. Pinter-Brown MD, FACP Health Sciences Professor of Medicine and Dermatology Definition of Lymphoma A cancer or malignancy that comes from
Sezary Syndrome(SS) and other malignancies. Hernani Cualing MD Hematopathologist IHCFLOW Lab
 Sezary Syndrome(SS) and other malignancies Hernani Cualing MD Hematopathologist IHCFLOW Lab Disclosures IHCFLOW Laboratory:consultant and director NEOGENOMICS: contract consultant USF: contract reviewer
Sezary Syndrome(SS) and other malignancies Hernani Cualing MD Hematopathologist IHCFLOW Lab Disclosures IHCFLOW Laboratory:consultant and director NEOGENOMICS: contract consultant USF: contract reviewer
Michi Shinohara MD Associate Professor University of Washington/Seattle Cancer Care Alliance Dermatology, Dermatopathology
 Michi Shinohara MD Associate Professor University of Washington/Seattle Cancer Care Alliance Dermatology, Dermatopathology Agenda Overview of cutaneous T and B- cell lymphomas Diagnosis, Staging, Prognosis
Michi Shinohara MD Associate Professor University of Washington/Seattle Cancer Care Alliance Dermatology, Dermatopathology Agenda Overview of cutaneous T and B- cell lymphomas Diagnosis, Staging, Prognosis
Cutaneous Mycosis Fungoides (MF), the subtype of cutaneous
 DOI 10. 5001/omj.2012.28 The Histological Spectrum of Early Mycosis Fungoides: A Study of 58 Saudi Arab patients Maha Arafah, Shaesta Naseem Zaidi, Hala Kassouf Kfoury, Ammar Al Rikabi, Khalid Al Ghamdi
DOI 10. 5001/omj.2012.28 The Histological Spectrum of Early Mycosis Fungoides: A Study of 58 Saudi Arab patients Maha Arafah, Shaesta Naseem Zaidi, Hala Kassouf Kfoury, Ammar Al Rikabi, Khalid Al Ghamdi
CD30+ Lymphoproliferative Disorders Associated with Longstanding Mycosis Fungoides
 Case Report DOI: 10.6003/jtad.16102c5 CD30+ Lymphoproliferative Disorders Associated with Longstanding Mycosis Fungoides Esra Adışen, 1 MD, Özlem Erdem, 2 MD, Mehmet Ali Gürer, 1 MD Address: 1 Gazi University
Case Report DOI: 10.6003/jtad.16102c5 CD30+ Lymphoproliferative Disorders Associated with Longstanding Mycosis Fungoides Esra Adışen, 1 MD, Özlem Erdem, 2 MD, Mehmet Ali Gürer, 1 MD Address: 1 Gazi University
الاكزيماتيد= Eczematid
 1 / 7 2 / 7 Pityriasis Debate confusing of hypopigmentation characterized increasing surrounded differ hypomelanotic "progressive exists alba misnomer extensive a to observed term the applied term derived
1 / 7 2 / 7 Pityriasis Debate confusing of hypopigmentation characterized increasing surrounded differ hypomelanotic "progressive exists alba misnomer extensive a to observed term the applied term derived
Lymphomatoid Papulosis 3 Case Reports
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 14, Issue 7 Ver. III (July. 2015), PP 31-35 www.iosrjournals.org Lymphomatoid Papulosis 3 Case Reports
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 14, Issue 7 Ver. III (July. 2015), PP 31-35 www.iosrjournals.org Lymphomatoid Papulosis 3 Case Reports
Granulomatous Slack Skin with an unusually aggressive course due to the subsequent development of a CD30-positive Large Cell Lymphoma
 Granulomatous Slack Skin with an unusually aggressive course due to the subsequent development of a CD30-positive Large Cell Lymphoma Alexandra Papoudou-Bai 1, Eleni Kapsali 2, Ioannis Kostas-Agnantis
Granulomatous Slack Skin with an unusually aggressive course due to the subsequent development of a CD30-positive Large Cell Lymphoma Alexandra Papoudou-Bai 1, Eleni Kapsali 2, Ioannis Kostas-Agnantis
Primary Cutaneous CD30-Positive T-cell Lymphoproliferative Disorders
 Primary Cutaneous CD30-Positive T-cell Lymphoproliferative Disorders Definition A spectrum of related conditions originating from transformed or activated CD30-positive T-lymphocytes May coexist in individual
Primary Cutaneous CD30-Positive T-cell Lymphoproliferative Disorders Definition A spectrum of related conditions originating from transformed or activated CD30-positive T-lymphocytes May coexist in individual
A Retrospective Study on the Risk of Non-Melanoma Skin Cancer in PUVA and Narrowband UVB Treated Patients
 Volume 1, Issue 3 Research Article A Retrospective Study on the Risk of Non-Melanoma Skin Cancer in PUVA and Narrowband UVB Treated Patients Darukarnphut P, Rattanakaemakorn P *, Rajatanavin N Division
Volume 1, Issue 3 Research Article A Retrospective Study on the Risk of Non-Melanoma Skin Cancer in PUVA and Narrowband UVB Treated Patients Darukarnphut P, Rattanakaemakorn P *, Rajatanavin N Division
ISPUB.COM. M Duvic, E Olsen PURPOSE OF REVISION
 ISPUB.COM The Internet Journal of Dermatology Volume 7 Number 3 International Society of Cutaneous Lymphoma (ISCL) and the European Organization of Research and Treatment of Cancer (EORTC) revisions to
ISPUB.COM The Internet Journal of Dermatology Volume 7 Number 3 International Society of Cutaneous Lymphoma (ISCL) and the European Organization of Research and Treatment of Cancer (EORTC) revisions to
Therapeutic Management of Early Cutaneous Mycosis Fungoides
 Therapeutic Management of Early Cutaneous Mycosis Fungoides L Frank Glass, MD Cutaneous Lymphoma Programs H Lee Moffitt Cancer Center and Research Institute George Washington University Dermatology and
Therapeutic Management of Early Cutaneous Mycosis Fungoides L Frank Glass, MD Cutaneous Lymphoma Programs H Lee Moffitt Cancer Center and Research Institute George Washington University Dermatology and
Narrow band UVB (311 nm), psoralen UVB (311 nm) and PUVA therapy in the treatment of early-stage mycosis fungoides: a right left comparative study
 Photodermatol Photoimmunol Photomed 2005; 21: 281 286 Blackwell Munksgaard Copyright r Blackwell Munksgaard 2005 Narrow band UVB (311 nm), psoralen UVB (311 nm) and therapy in the treatment of early-stage
Photodermatol Photoimmunol Photomed 2005; 21: 281 286 Blackwell Munksgaard Copyright r Blackwell Munksgaard 2005 Narrow band UVB (311 nm), psoralen UVB (311 nm) and therapy in the treatment of early-stage
Title: Erythema annulare centrifugum associated with chronic lymphocytic leukaemia. Authors: Helbling I, Walewska R, Dyer MJS, Bamford M, Harman KE
 Title: Erythema annulare centrifugum associated with chronic lymphocytic leukaemia Authors: Helbling I, Walewska R, Dyer MJS, Bamford M, Harman KE Sir, A wide range of conditions have been described as
Title: Erythema annulare centrifugum associated with chronic lymphocytic leukaemia Authors: Helbling I, Walewska R, Dyer MJS, Bamford M, Harman KE Sir, A wide range of conditions have been described as
Hypopigmented parapsoriasis en plaque, a new, overlooked member of the parapsoriasis family: A report of 34 patients and a 7-year experience
 Hypopigmented parapsoriasis en plaque, a new, overlooked member of the parapsoriasis family: A report of 34 patients and a 7-year experience Mohammad A. El-Darouti, MD, Marwa M. Fawzy, MD, Rehab A. Hegazy,
Hypopigmented parapsoriasis en plaque, a new, overlooked member of the parapsoriasis family: A report of 34 patients and a 7-year experience Mohammad A. El-Darouti, MD, Marwa M. Fawzy, MD, Rehab A. Hegazy,
Cover Page. The handle holds various files of this Leiden University dissertation.
 Cover Page The handle http://hdl.handle.net/1887/2010 holds various files of this Leiden University dissertation. Author: Benner, Marchina Frederika Title: Cutaneous CD30-positive lymphoproliferations
Cover Page The handle http://hdl.handle.net/1887/2010 holds various files of this Leiden University dissertation. Author: Benner, Marchina Frederika Title: Cutaneous CD30-positive lymphoproliferations
CASE 15 Patient: A 41-year-old Thai female Chief Compliant: Generalized papulovesicular rash for 1 month Present Illness: She presented with a 1-week
 CASE 15 Patient: A 41-year-old Thai female Chief Compliant: Generalized papulovesicular rash for 1 month Present Illness: She presented with a 1-week history of the generalized asymptomatic erythematous
CASE 15 Patient: A 41-year-old Thai female Chief Compliant: Generalized papulovesicular rash for 1 month Present Illness: She presented with a 1-week history of the generalized asymptomatic erythematous
ISPUB.COM. Primary Cutaneous Anaplastic Large Cell Lymphoma Long-term Management with Low Dose Methotrexate. S Parker INTRODUCTION
 ISPUB.COM The Internet Journal of Dermatology Volume 7 Number 3 Primary Cutaneous Anaplastic Large Cell Lymphoma Long-term Management with Low Dose S Parker Citation S Parker.. The Internet Journal of
ISPUB.COM The Internet Journal of Dermatology Volume 7 Number 3 Primary Cutaneous Anaplastic Large Cell Lymphoma Long-term Management with Low Dose S Parker Citation S Parker.. The Internet Journal of
The cientificworldjournal
 The Scientific World Journal Volume 2012, Article ID 426732, 6 pages doi:10.1100/2012/426732 The cientificworldjournal Clinical Study Evaluation of Histopathological Changes in Control Biopsies Which Taken
The Scientific World Journal Volume 2012, Article ID 426732, 6 pages doi:10.1100/2012/426732 The cientificworldjournal Clinical Study Evaluation of Histopathological Changes in Control Biopsies Which Taken
Classification of Cutaneous T cell Lymphomas (CTCLs) Hernani Cualing, MD
 Classification of Cutaneous T cell Lymphomas (CTCLs) Hernani Cualing, MD Pathology and Cell Biology, USF IFLOW, Inc. CTCL, MF, and Sézary syndrome In 1806, mycosis fungoides (MF) was first described 1
Classification of Cutaneous T cell Lymphomas (CTCLs) Hernani Cualing, MD Pathology and Cell Biology, USF IFLOW, Inc. CTCL, MF, and Sézary syndrome In 1806, mycosis fungoides (MF) was first described 1
Mycosis Fungoides, then and now Have we travelled?
 USCAP 103 rd Annual Meeting 2014 American Society of Dermatopathology Companion Meeting Mycosis Fungoides, then and now Have we travelled? Vijaya B. Reddy, MD, MBA Professor of Pathology Rush University
USCAP 103 rd Annual Meeting 2014 American Society of Dermatopathology Companion Meeting Mycosis Fungoides, then and now Have we travelled? Vijaya B. Reddy, MD, MBA Professor of Pathology Rush University
CUTANEOUS T-CELL LYMPHOMA PROFORMA
 STATE OF KUWAIT MINISTRY OF HEALTH AS AD ALHAMAD DERMATOLOGY CENTER ALSABAH HOSPITAL دولة الكویت وزارة الصحة مرآز أسعد الحمد للا مراض الجلدیة مستشفى الصباح بسم االله الرحمن الرحيم CUTANEOUS TCELL LYMPHOMA
STATE OF KUWAIT MINISTRY OF HEALTH AS AD ALHAMAD DERMATOLOGY CENTER ALSABAH HOSPITAL دولة الكویت وزارة الصحة مرآز أسعد الحمد للا مراض الجلدیة مستشفى الصباح بسم االله الرحمن الرحيم CUTANEOUS TCELL LYMPHOMA
Dermatologica Sinica
 DERMATOLOGICA SINICA 31 (2013) 3e Contents lists available at SciVerse ScienceDirect Dermatologica Sinica journal homepage: http://www.derm-sinica.com CASE REPORT Early stage mycosis fungoides with focal
DERMATOLOGICA SINICA 31 (2013) 3e Contents lists available at SciVerse ScienceDirect Dermatologica Sinica journal homepage: http://www.derm-sinica.com CASE REPORT Early stage mycosis fungoides with focal
Mycosis fungoides (MF) is the most common type of cutaneous
 Mycosis fungoides variants clinicopathologic features, differential diagnosis, and treatment Rein Willemze, MD, PhD Abstract Mycosis fungoides (MF) is the most common type of cutaneous T-cell lymphoma,
Mycosis fungoides variants clinicopathologic features, differential diagnosis, and treatment Rein Willemze, MD, PhD Abstract Mycosis fungoides (MF) is the most common type of cutaneous T-cell lymphoma,
ISPUB.COM. Management of Co-existing Mycosis Fungoides and Lymphomatoid Papulosis. E Kim PHYSICAL FINDINGS INTRODUCTION INITIAL PRESENTATION
 ISPUB.COM The Internet Journal of Dermatology Volume 7 Number 3 Management of Co-existing Mycosis Fungoides and Lymphomatoid Papulosis E Kim Citation E Kim. Management of Co-existing Mycosis Fungoides
ISPUB.COM The Internet Journal of Dermatology Volume 7 Number 3 Management of Co-existing Mycosis Fungoides and Lymphomatoid Papulosis E Kim Citation E Kim. Management of Co-existing Mycosis Fungoides
Primary cutaneous large cell lymphoma CD30+: a case-based review
 Case-based review Primary cutaneous large cell lymphoma CD30+: a case-based review Anna Campanati 1 Katia Giuliodori 1 Emanuela Martina 1 Luca Conocchiari 1 Giulia Ganzetti 1 Gaia Goteri 2 Annamaria Offidani
Case-based review Primary cutaneous large cell lymphoma CD30+: a case-based review Anna Campanati 1 Katia Giuliodori 1 Emanuela Martina 1 Luca Conocchiari 1 Giulia Ganzetti 1 Gaia Goteri 2 Annamaria Offidani
2016 AAD SUMMER MEETING SYMPOSIUM S011: CLINICOPATHOLOGIC SELF-ASSESSMENT 7/30/16 2:00 PM. Tom Helm, MD
 2016 AAD SUMMER MEETING SYMPOSIUM S011: CLINICOPATHOLOGIC SELF-ASSESSMENT 7/30/16 2:00 PM Tom Helm, MD Case 1 Diagnosis: Pseudoepitheliomatous hyperplasia associated with CD30+ lymphoproliferative disease
2016 AAD SUMMER MEETING SYMPOSIUM S011: CLINICOPATHOLOGIC SELF-ASSESSMENT 7/30/16 2:00 PM Tom Helm, MD Case 1 Diagnosis: Pseudoepitheliomatous hyperplasia associated with CD30+ lymphoproliferative disease
Clinical Study The Influence of the Coexpression of CD4 and CD8 in Cutaneous Lesions on Prognosis of Mycosis Fungoides: A Preliminary Study
 Skin Cancer, Article ID 624143, 4 pages http://dx.doi.org/10.1155/2014/624143 Clinical Study The Influence of the Coexpression of CD4 and CD8 in Cutaneous Lesions on Prognosis of Mycosis Fungoides: A Preliminary
Skin Cancer, Article ID 624143, 4 pages http://dx.doi.org/10.1155/2014/624143 Clinical Study The Influence of the Coexpression of CD4 and CD8 in Cutaneous Lesions on Prognosis of Mycosis Fungoides: A Preliminary
Phototherapy and Photochemotherapy Treatment (Ultraviolet A [PUVA] and B [UBV])
![Phototherapy and Photochemotherapy Treatment (Ultraviolet A [PUVA] and B [UBV]) Phototherapy and Photochemotherapy Treatment (Ultraviolet A [PUVA] and B [UBV])](/thumbs/89/99382632.jpg) Origination: 09/27/07 Revised: 08/2/17 Annual Review: 11/2/17 Purpose: To provide Phototherapy and Photochemotherapy Treatment (PUVA and UBV) guidelines for the Medical Department staff to reference when
Origination: 09/27/07 Revised: 08/2/17 Annual Review: 11/2/17 Purpose: To provide Phototherapy and Photochemotherapy Treatment (PUVA and UBV) guidelines for the Medical Department staff to reference when
Disclosures. Advisory Board. Consultant. Investigator. MiRagen, Actelion, Celgene, Therakos. Mindera
 Cutaneous Lymphomas Christiane Querfeld, MD, PhD Director, Cutaneous Lymphoma Program City of Hope ~ How the Experts Treat Hematologic Malignancies Symposium March 10 13, 2017 Disclosures Advisory Board
Cutaneous Lymphomas Christiane Querfeld, MD, PhD Director, Cutaneous Lymphoma Program City of Hope ~ How the Experts Treat Hematologic Malignancies Symposium March 10 13, 2017 Disclosures Advisory Board
clinical recommendations
 19 (Supplement 2): ii72 ii76, 2008 doi:10.1093/annonc/mdn095 Primary cutaneous lymphoma: ESMO Clinical Recommendations for diagnosis, treatment and follow-up R. Dummer 1 & M. Dreyling 2 On behalf of the
19 (Supplement 2): ii72 ii76, 2008 doi:10.1093/annonc/mdn095 Primary cutaneous lymphoma: ESMO Clinical Recommendations for diagnosis, treatment and follow-up R. Dummer 1 & M. Dreyling 2 On behalf of the
Case Report A Severe Case of Lymphomatoid Papulosis Type E Successfully Treated with Interferon-Alfa 2a
 Hindawi Case Reports in Dermatological Medicine Volume 2017, Article ID 3194738, 5 pages https://doi.org/10.1155/2017/3194738 Case Report A Severe Case of Lymphomatoid Papulosis Type E Successfully Treated
Hindawi Case Reports in Dermatological Medicine Volume 2017, Article ID 3194738, 5 pages https://doi.org/10.1155/2017/3194738 Case Report A Severe Case of Lymphomatoid Papulosis Type E Successfully Treated
Summary. lymphoma/myeloma, regulatory T cells (T reg) Introduction. Clinical and Experimental Immunology ORIGINAL ARTICLE doi: /cei.
 bs_bs_banner Clinical and Experimental Immunology ORIGINAL ARTICLE doi:1.1111/cei.1273 Increased frequency of skin-infiltrating FoxP3 + regulatory T cells as a diagnostic indicator of severe atopic dermatitis
bs_bs_banner Clinical and Experimental Immunology ORIGINAL ARTICLE doi:1.1111/cei.1273 Increased frequency of skin-infiltrating FoxP3 + regulatory T cells as a diagnostic indicator of severe atopic dermatitis
Progressive Macular Hypomelanosis in Korean Patients: A Clinicopathologic Study
 Ann Dermatol Vol. 2, No., 2009 ORIGINAL ARTICLE Progressive Macular Hypomelanosis in Korean Patients: A Clinicopathologic Study Seon Wook Hwang, M.D., Soon Kwon Hong, M.D., Sang Hyun Kim, M.D., Jeong Hoon
Ann Dermatol Vol. 2, No., 2009 ORIGINAL ARTICLE Progressive Macular Hypomelanosis in Korean Patients: A Clinicopathologic Study Seon Wook Hwang, M.D., Soon Kwon Hong, M.D., Sang Hyun Kim, M.D., Jeong Hoon
Elsevier B.V.; この論文は出版社版でありま Right 引用の際には出版社版をご確認ご利用ください This is
 Title Refractory cutaneous lichenoid sarc tranilast. Author(s) Nakahigashi, Kyoko; Kabashima, Kenj Utani, Atsushi; Miyachi, Yoshiki Citation Journal of the American Academy of 63(1): 171-172 Issue Date
Title Refractory cutaneous lichenoid sarc tranilast. Author(s) Nakahigashi, Kyoko; Kabashima, Kenj Utani, Atsushi; Miyachi, Yoshiki Citation Journal of the American Academy of 63(1): 171-172 Issue Date
Given that mycosis fungoides (MF) is the most common
 Histopathologic approach to epidermotropic lymphocytic infiltrates Shyam S Raghavan, MD 1 and Jinah Kim, MD, PhD 2 Abstract Mycosis fungoides is the most common and therefore quintessential cutaneous lymphoma
Histopathologic approach to epidermotropic lymphocytic infiltrates Shyam S Raghavan, MD 1 and Jinah Kim, MD, PhD 2 Abstract Mycosis fungoides is the most common and therefore quintessential cutaneous lymphoma
STUDY. fungoides (FMF) is an uncommon
 STUDY Folliculotropic Mycosis Fungoides Single-Center Study and Systematic Review Julia S. Lehman, MD; Robert H. Cook-Norris, MD; Brent R. Weed, MD; Roger H. Weenig, MD; Lawrence E. Gibson, MD; Amy L.
STUDY Folliculotropic Mycosis Fungoides Single-Center Study and Systematic Review Julia S. Lehman, MD; Robert H. Cook-Norris, MD; Brent R. Weed, MD; Roger H. Weenig, MD; Lawrence E. Gibson, MD; Amy L.
Grover s disease: A case report.
 320 Case report Thai J Dermatol, October-December 2011 ABSTRACT: Grover s disease: A case report. Supicha Chavanich MD, Praneet Sajjachareonpong MD. CHAVANICH C, SAJJACHAREONPONG P. GROVER S DISEASE: A
320 Case report Thai J Dermatol, October-December 2011 ABSTRACT: Grover s disease: A case report. Supicha Chavanich MD, Praneet Sajjachareonpong MD. CHAVANICH C, SAJJACHAREONPONG P. GROVER S DISEASE: A
PCR results with histologic parameters to determine the differences between PCR-positive and PCR-negative groups. Results: TCRγ
 ORIGINAL ARTICLE Histopathologic molecular Correlation in Early Mycosis Fungoides Using T-cell Receptor g Gene Rearrangement by Polymerase Chain Reaction with Laser Capture Microdissection Pa-Fan Hsiao,
ORIGINAL ARTICLE Histopathologic molecular Correlation in Early Mycosis Fungoides Using T-cell Receptor g Gene Rearrangement by Polymerase Chain Reaction with Laser Capture Microdissection Pa-Fan Hsiao,
Rameshwar Gutte and Uday Khopkar
 Extragenital unilateral lichen sclerosus et atrophicus in a child: a case report Rameshwar Gutte and Uday Khopkar Department of Dermatolgy, Seth GSMC and KEM Hospital, Parel, Mumbai-400012, India Egyptian
Extragenital unilateral lichen sclerosus et atrophicus in a child: a case report Rameshwar Gutte and Uday Khopkar Department of Dermatolgy, Seth GSMC and KEM Hospital, Parel, Mumbai-400012, India Egyptian
Mycosis Fungoides Presentation in Emergency
 The Open Emergency Medicine Journal, 2011, 4, 17-21 17 Mycosis Fungoides Presentation in Emergency Asaad Shujaa*,1 and M. Owais Suriya 2 Open Access Department of Emergency Medicine College of Medicine,
The Open Emergency Medicine Journal, 2011, 4, 17-21 17 Mycosis Fungoides Presentation in Emergency Asaad Shujaa*,1 and M. Owais Suriya 2 Open Access Department of Emergency Medicine College of Medicine,
2. Sézary syndrome (SS)
 Go Back to the Top To Order, Visit the Purchasing Page for Details Clinical images are available in hardcopy only. Clinical images are available in Clinical images are available in d e f g h i j Fig..36-2
Go Back to the Top To Order, Visit the Purchasing Page for Details Clinical images are available in hardcopy only. Clinical images are available in Clinical images are available in d e f g h i j Fig..36-2
Fig. 3.1 Fig Past history: She was previously healthy and not taking any medication.
 Case 3 A 41-year-old Thai female from Bangkok Chief compliant: Erythematous patch at left thigh for 2 months Present illness: The patient presented with a 10- year history of erythematous patch on her
Case 3 A 41-year-old Thai female from Bangkok Chief compliant: Erythematous patch at left thigh for 2 months Present illness: The patient presented with a 10- year history of erythematous patch on her
Interstitial mycosis fungoides with lichen sclerosus-like clinical and histopathological features
 Zurich Open Repository and Archive University of Zurich Main Library Strickhofstrasse 39 CH-8057 Zurich www.zora.uzh.ch Year: 2016 Interstitial mycosis fungoides with lichen sclerosus-like clinical and
Zurich Open Repository and Archive University of Zurich Main Library Strickhofstrasse 39 CH-8057 Zurich www.zora.uzh.ch Year: 2016 Interstitial mycosis fungoides with lichen sclerosus-like clinical and
Review Article. Cutaneous lymphoproliferative disorders. NJ Trendell-Smith
 Hong Kong J. Dermatol. Venereol. (2010) 18, 190-201 Review Article Cutaneous lymphoproliferative disorders NJ Trendell-Smith Cutaneous lymphoproliferative disorders (CLD) include reactive lymphoid hyperplasias,
Hong Kong J. Dermatol. Venereol. (2010) 18, 190-201 Review Article Cutaneous lymphoproliferative disorders NJ Trendell-Smith Cutaneous lymphoproliferative disorders (CLD) include reactive lymphoid hyperplasias,
Int J Clin Exp Pathol 2013;6(4): /ISSN: /IJCEP Tadashi Terada
 Int J Clin Exp Pathol 2013;6(4):749-756 www.ijcep.com /ISSN:1936-2625/IJCEP1301060 Case Report Mycosis fungoides in plaque stage with pronounced eosinophilic infiltration, folliculotropism, and concomitant
Int J Clin Exp Pathol 2013;6(4):749-756 www.ijcep.com /ISSN:1936-2625/IJCEP1301060 Case Report Mycosis fungoides in plaque stage with pronounced eosinophilic infiltration, folliculotropism, and concomitant
Primary Cutaneous Acral CD8 þ T-Cell Lymphoma
 Primary Cutaneous Acral CD8 þ T-Cell Lymphoma Vivian M. Hathuc, DO; Alexandra C. Hristov, MD; Lauren B. Smith, MD Primary cutaneous acral CD8 þ T-cell lymphoma is a new provisional entity in the 2016 revision
Primary Cutaneous Acral CD8 þ T-Cell Lymphoma Vivian M. Hathuc, DO; Alexandra C. Hristov, MD; Lauren B. Smith, MD Primary cutaneous acral CD8 þ T-cell lymphoma is a new provisional entity in the 2016 revision
STUDY. with a benign clinical course but a malignant appearance
 Lymphomatoid Papulosis STUDY Reappraisal of Clinicopathologic Presentation and Classification Into Subtypes A,, and C Laila El Shabrawi-Caelen, MD; Helmut Kerl, MD; Lorenzo Cerroni, MD Objectives: To analyze
Lymphomatoid Papulosis STUDY Reappraisal of Clinicopathologic Presentation and Classification Into Subtypes A,, and C Laila El Shabrawi-Caelen, MD; Helmut Kerl, MD; Lorenzo Cerroni, MD Objectives: To analyze
Clinical Trial Outcomes
 l Recent clinical evidence for topical mechlorethamine in mycosis fungoides Mycosis fungoides (MF) is a rare, potentially life-threatening cutaneous T-cell lymphoma characterized by cutaneous homing of
l Recent clinical evidence for topical mechlorethamine in mycosis fungoides Mycosis fungoides (MF) is a rare, potentially life-threatening cutaneous T-cell lymphoma characterized by cutaneous homing of
Retrospective 10 years review of 100 patients with psoriasis in the Kingdom of Saudi Arabia (KSA)
 Retrospective 10 years review of 100 patients with psoriasis in the Kingdom of Saudi Arabia (KSA) Ahmed Abdullah Alhumidi King saud university, Riyadh, kingdom of Saudi Arabia Abstract Background: This
Retrospective 10 years review of 100 patients with psoriasis in the Kingdom of Saudi Arabia (KSA) Ahmed Abdullah Alhumidi King saud university, Riyadh, kingdom of Saudi Arabia Abstract Background: This
' ' ' ~ aware that : Presentation
 REPORT DOCUMENTATION PAGE Form Approved OMB No_ 0704-0188 ; ' " ' ' ; ; ' " ' ' ; ' Jf mfoml'ai:on, :nciud:ng ' " " " ' ' ' """"'".,,.,,.~, ; ; I ) t ld ' ' ' ~ aware that : ' ",.w, "" ~I'~ ' ' " Presentation
REPORT DOCUMENTATION PAGE Form Approved OMB No_ 0704-0188 ; ' " ' ' ; ; ' " ' ' ; ' Jf mfoml'ai:on, :nciud:ng ' " " " ' ' ' """"'".,,.,,.~, ; ; I ) t ld ' ' ' ~ aware that : ' ",.w, "" ~I'~ ' ' " Presentation
Synthetic hypericin (SGX301; VIMRxyn) for cutaneous T cell lymphoma, unspecified
 NIHR Innovation Observatory Evidence Briefing: May 2017 Synthetic hypericin (SGX301; VIMRxyn) for cutaneous T cell lymphoma, unspecified NIHRIO (HSRIC) ID: 10761 NICE ID: 8375 LAY SUMMARY Cutaneous T cell
NIHR Innovation Observatory Evidence Briefing: May 2017 Synthetic hypericin (SGX301; VIMRxyn) for cutaneous T cell lymphoma, unspecified NIHRIO (HSRIC) ID: 10761 NICE ID: 8375 LAY SUMMARY Cutaneous T cell
المركب النموذج--- سبيتز وحمة = Type Spitz's Nevus, Compound SPITZ NEVUS 1 / 7
 SPITZ NEVUS 1 / 7 Epidemiology An annual incidence rate of 1.4 cases of Spitz nevus per 100,000 individuals has been estimated in Australia, compared with 25.4 per 100,000 individuals for cutaneous melanoma
SPITZ NEVUS 1 / 7 Epidemiology An annual incidence rate of 1.4 cases of Spitz nevus per 100,000 individuals has been estimated in Australia, compared with 25.4 per 100,000 individuals for cutaneous melanoma
Maligna Melanoma and Atypical Fibroxanthoma: An Unusual Collision Tumour G Türkcü 1, A Keleş 1, U Alabalık 1, D Uçmak 2, H Büyükbayram 1 ABSTRACT
 Maligna Melanoma and Atypical Fibroxanthoma: An Unusual Collision Tumour G Türkcü 1, A Keleş 1, U Alabalık 1, D Uçmak 2, H Büyükbayram 1 ABSTRACT Two different neoplasia in the same biopsy material called
Maligna Melanoma and Atypical Fibroxanthoma: An Unusual Collision Tumour G Türkcü 1, A Keleş 1, U Alabalık 1, D Uçmak 2, H Büyükbayram 1 ABSTRACT Two different neoplasia in the same biopsy material called
Renaissance of Low-Dose Radiotherapy Concepts for Cutaneous Lymphomas
 Review Article DOI: 10.1159/000470845 Received: February 06, 2017 Accepted: March 13, 2017 Published online: April 6, 2017 Renaissance of Low-Dose Radiotherapy Concepts for Cutaneous Lymphomas Bouthaina
Review Article DOI: 10.1159/000470845 Received: February 06, 2017 Accepted: March 13, 2017 Published online: April 6, 2017 Renaissance of Low-Dose Radiotherapy Concepts for Cutaneous Lymphomas Bouthaina
Mycosis fungoides beyond the classical Alibert- Bazin disease: report of seventeen atypical variants
 Research Article Mycosis fungoides beyond the classical Alibert- Bazin disease: report of seventeen atypical variants Aarón Kaminsky Award 2007 Alejandra Abeldaño 1, Mariana Arias 2, Karina Ochoa 3, Adriana
Research Article Mycosis fungoides beyond the classical Alibert- Bazin disease: report of seventeen atypical variants Aarón Kaminsky Award 2007 Alejandra Abeldaño 1, Mariana Arias 2, Karina Ochoa 3, Adriana
A dinical and histopathologic entity associated with an increased risk of nonmelanoma skin cancer
 PUVA keratosis A dinical and histopathologic entity associated with an increased risk of nonmelanoma skin cancer M. C. G. van Praag, MD, a J. N. Bouwes Bavinck, MD, a W. Bergman, MD, PhD, a F. R. Rosendaal,
PUVA keratosis A dinical and histopathologic entity associated with an increased risk of nonmelanoma skin cancer M. C. G. van Praag, MD, a J. N. Bouwes Bavinck, MD, a W. Bergman, MD, PhD, a F. R. Rosendaal,
Benign and malignant epithelial lesions: Seborrheic keratosis: A common benign pigmented epidermal tumor occur in middle-aged or older persons more
 Benign and malignant epithelial lesions: Seborrheic keratosis: A common benign pigmented epidermal tumor occur in middle-aged or older persons more common on the trunk; but extremities, head and neck are
Benign and malignant epithelial lesions: Seborrheic keratosis: A common benign pigmented epidermal tumor occur in middle-aged or older persons more common on the trunk; but extremities, head and neck are
CD4-Positive T-Cell Large Granular Lymphocytosis Mimicking Sézary Syndrome in a Patient With Mycosis Fungoides
 Case Report CD4-Positive T-Cell Large Granular Lymphocytosis Mimicking Sézary Syndrome in a Patient With Mycosis Fungoides Ling Zhang, MD, Magali Van den Bergh, MD, and Lubomir Sokol, MD, PhD Summary:
Case Report CD4-Positive T-Cell Large Granular Lymphocytosis Mimicking Sézary Syndrome in a Patient With Mycosis Fungoides Ling Zhang, MD, Magali Van den Bergh, MD, and Lubomir Sokol, MD, PhD Summary:
A correlation between acute phase proteins and cytokines in patients suffering from mycosis fungoides
 C l i n i c a l s t u d y Acute phase proteins and cytokines in mycosis fungoides A correlation between acute phase proteins and cytokines in patients suffering from mycosis fungoides M. Pawlaczyk and
C l i n i c a l s t u d y Acute phase proteins and cytokines in mycosis fungoides A correlation between acute phase proteins and cytokines in patients suffering from mycosis fungoides M. Pawlaczyk and
Cutaneous Lymphoid Proliferations: A Comprehensive Textbook of Lymphocytic Infiltrates of the Skin
 Cutaneous Lymphoid Proliferations: A Comprehensive Textbook of Lymphocytic Infiltrates of the Skin Magro, Cynthia M., MD ISBN-13: 9780471695981 Table of Contents Chapter One: Introduction to the Classification
Cutaneous Lymphoid Proliferations: A Comprehensive Textbook of Lymphocytic Infiltrates of the Skin Magro, Cynthia M., MD ISBN-13: 9780471695981 Table of Contents Chapter One: Introduction to the Classification
Actinic keratosis (AK): Dr Sarma s simple guide
 Actinic keratosis (AK): Dr Sarma s simple guide Actinic keratosis is a very common lesion that you will see in your day-to-day practice. First, let me explain the name Actinic keratosis. It means keratosis
Actinic keratosis (AK): Dr Sarma s simple guide Actinic keratosis is a very common lesion that you will see in your day-to-day practice. First, let me explain the name Actinic keratosis. It means keratosis
Lymphocytoma Cutis. Cynthia M. Magro MD. Director of Dermatopathology Weill Medical College of Cornell University New York, New York
 Lymphocytoma Cutis Cynthia M. Magro MD Professor of Pathology Director of Dermatopathology Weill Medical College of Cornell University New York, New York Lymphocytoma Cutis Falls under other designations
Lymphocytoma Cutis Cynthia M. Magro MD Professor of Pathology Director of Dermatopathology Weill Medical College of Cornell University New York, New York Lymphocytoma Cutis Falls under other designations
Annular elastolytic giant cell granuloma presented with annular erythematous patches over the face and cheek in a Chinese lady
 Hong Kong J. Dermatol. Venereol. (2009) 17, 151-155 Case Report Annular elastolytic giant cell granuloma presented with annular erythematous patches over the face and cheek in a Chinese lady SKF Loo, LY
Hong Kong J. Dermatol. Venereol. (2009) 17, 151-155 Case Report Annular elastolytic giant cell granuloma presented with annular erythematous patches over the face and cheek in a Chinese lady SKF Loo, LY
Department of Dermatology, Christian Medical College and Hospital, Ludhiana, Punjab, India.
 Bullous pemphigoid mimicking granulomatous inflammation Abhilasha Williams, Emy Abi Thomas. Department of Dermatology, Christian Medical College and Hospital, Ludhiana, Punjab, India. Egyptian Dermatology
Bullous pemphigoid mimicking granulomatous inflammation Abhilasha Williams, Emy Abi Thomas. Department of Dermatology, Christian Medical College and Hospital, Ludhiana, Punjab, India. Egyptian Dermatology
Granulomatous mycosis fungoides (GMF) is
 CASE REPORT Granulomatous mycosis fungoides, a rare subtype of cutaneous T-cell lymphoma Marta Kogut, MD, a Eva Hadaschik, MD, a Stephan Grabbe, MD, b Mindaugas Andrulis, MD, c Alexander Enk, MD, a and
CASE REPORT Granulomatous mycosis fungoides, a rare subtype of cutaneous T-cell lymphoma Marta Kogut, MD, a Eva Hadaschik, MD, a Stephan Grabbe, MD, b Mindaugas Andrulis, MD, c Alexander Enk, MD, a and
Unusual cutaneous presentation of a T-cell lymphoproliferation
 Department of Pathology and Cytology University Hospital Centre Zagreb, Croatia Unusual cutaneous presentation of a T-cell lymphoproliferation Snjezana Dotlic, Stefan Dojcinov, Leticia Quintanilla-Fend
Department of Pathology and Cytology University Hospital Centre Zagreb, Croatia Unusual cutaneous presentation of a T-cell lymphoproliferation Snjezana Dotlic, Stefan Dojcinov, Leticia Quintanilla-Fend
SEBACEOUS NEOPLASMS. Dr. Prachi Saraogi Clinical Fellow in Dermatology
 SEBACEOUS NEOPLASMS Dr. Prachi Saraogi Clinical Fellow in Dermatology Sebaceous neoplasms Sebaceous adenoma (Benign) Sebaceous carcinoma (Malignant) SEBACEOUS ADENOMA Benign tumours composed of incompletely
SEBACEOUS NEOPLASMS Dr. Prachi Saraogi Clinical Fellow in Dermatology Sebaceous neoplasms Sebaceous adenoma (Benign) Sebaceous carcinoma (Malignant) SEBACEOUS ADENOMA Benign tumours composed of incompletely
Research Article Characteristics of Primary Cutaneous T-Cell Lymphoma in Iran: A 10-Year Retrospective Study
 International Scholarly Research Notices, Article ID 820921, 5 pages http://dx.doi.org/10.1155/2014/820921 Research Article Characteristics of Primary Cutaneous T-Cell Lymphoma in Iran: A 10-Year Retrospective
International Scholarly Research Notices, Article ID 820921, 5 pages http://dx.doi.org/10.1155/2014/820921 Research Article Characteristics of Primary Cutaneous T-Cell Lymphoma in Iran: A 10-Year Retrospective
SH/EAHP Workshop 2011 Los Angeles, California, USA
 SH/EAHP Workshop 2011 Los Angeles, California, USA October 27-29, 2011 Session 3 Non-Mycosis Fungoides CTCL Patty Jansen & Rein Willemze Introduction Submitted: 101 cases + 7 cases group 1: 108 Deactivated
SH/EAHP Workshop 2011 Los Angeles, California, USA October 27-29, 2011 Session 3 Non-Mycosis Fungoides CTCL Patty Jansen & Rein Willemze Introduction Submitted: 101 cases + 7 cases group 1: 108 Deactivated
Non-Hodgkin lymphomas (NHLs) Hodgkin lymphoma )HL)
 Non-Hodgkin lymphomas (NHLs) Hodgkin lymphoma )HL) Lymphoid Neoplasms: 1- non-hodgkin lymphomas (NHLs) 2- Hodgkin lymphoma 3- plasma cell neoplasms Non-Hodgkin lymphomas (NHLs) Acute Lymphoblastic Leukemia/Lymphoma
Non-Hodgkin lymphomas (NHLs) Hodgkin lymphoma )HL) Lymphoid Neoplasms: 1- non-hodgkin lymphomas (NHLs) 2- Hodgkin lymphoma 3- plasma cell neoplasms Non-Hodgkin lymphomas (NHLs) Acute Lymphoblastic Leukemia/Lymphoma
Egyptian Dermatology Online Journal Vol. 6 No 1: 14, June 2010
 Wells Syndrome H. Gammaz, H. Amer, A. Adly and S. Mahmoud Egyptian Dermatology Online Journal 6 (1): 14 Al-Haud Al-Marsoud Hospital, Cairo, Egypt e-mail: hananderma@hotmail.com Submitted: April 15, 2010
Wells Syndrome H. Gammaz, H. Amer, A. Adly and S. Mahmoud Egyptian Dermatology Online Journal 6 (1): 14 Al-Haud Al-Marsoud Hospital, Cairo, Egypt e-mail: hananderma@hotmail.com Submitted: April 15, 2010
SLIDE SEMINAR NON NEOPLASTIC LYMPH NODE DISORDERS DR SHEILA NAIR CMC, VELLORE
 SLIDE SEMINAR NON NEOPLASTIC LYMPH NODE DISORDERS DR SHEILA NAIR CMC, VELLORE Case 1 34 year old male, mass right cervical region, for 4 years. No other significant findings. Grossly, the mass was well
SLIDE SEMINAR NON NEOPLASTIC LYMPH NODE DISORDERS DR SHEILA NAIR CMC, VELLORE Case 1 34 year old male, mass right cervical region, for 4 years. No other significant findings. Grossly, the mass was well
Interhospital Dermatology Conference 2013
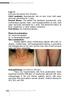 Case 21 A 50-year-old woman from Chonburi. Chief complaint: Asymptomatic rash on neck, trunk, both upper and lower extremities for 2 years. Present illness: The patient has developed asymptomatic scaly
Case 21 A 50-year-old woman from Chonburi. Chief complaint: Asymptomatic rash on neck, trunk, both upper and lower extremities for 2 years. Present illness: The patient has developed asymptomatic scaly
Bone Marrow Histopathologic and Molecular Staging in Epidermotropic T-Cell Lymphomas
 Hematopathology / BONE MARROW STAGING IN CUTANEOUS T-CELL LYMPHOMA Bone Marrow Histopathologic and Molecular Staging in Epidermotropic T-Cell Lymphomas Vincent Sibaud, MD, 1,2 Marie Beylot-Barry, MD, PhD,
Hematopathology / BONE MARROW STAGING IN CUTANEOUS T-CELL LYMPHOMA Bone Marrow Histopathologic and Molecular Staging in Epidermotropic T-Cell Lymphomas Vincent Sibaud, MD, 1,2 Marie Beylot-Barry, MD, PhD,
Nodular Prurigo Associated with Mycosis Fungoides Case Report
 2015;23(3):203-207 CASE REPORT Nodular Prurigo Associated with Mycosis Fungoides Case Report Sandra Jerković Gulin 1, Romana Čeović 2, Davorin Lončarić 2, Ivana Ilić 3, Ivo Radman 4 1 Department of Dermatology
2015;23(3):203-207 CASE REPORT Nodular Prurigo Associated with Mycosis Fungoides Case Report Sandra Jerković Gulin 1, Romana Čeović 2, Davorin Lončarić 2, Ivana Ilić 3, Ivo Radman 4 1 Department of Dermatology
Thursday, 21 October :53 - Last Updated Thursday, 11 November :27
 1 / 15 2 / 15 3 / 15 4 / 15 Pityriasis Alba Background Pityriasis alba is a nonspecific dermatitis of unknown etiology that causes erythematous scaly patches. These resolve and leave areas of hypopigmentation
1 / 15 2 / 15 3 / 15 4 / 15 Pityriasis Alba Background Pityriasis alba is a nonspecific dermatitis of unknown etiology that causes erythematous scaly patches. These resolve and leave areas of hypopigmentation
Derm quiz. Go to this link: goo.gl/forms/kchrhmtzl3vfnlv52. bit.ly/2a8asoy. Scan the QR code with your phone
 Dermatology quiz Derm quiz Go to this link: goo.gl/forms/kchrhmtzl3vfnlv52 OR bit.ly/2a8asoy OR Scan the QR code with your phone Contents Childhood rashes Pigmented lesions Sun damage Pityriasis References
Dermatology quiz Derm quiz Go to this link: goo.gl/forms/kchrhmtzl3vfnlv52 OR bit.ly/2a8asoy OR Scan the QR code with your phone Contents Childhood rashes Pigmented lesions Sun damage Pityriasis References
MALIGNANT MELANOMA. Dr D. Tenea Department of Dermatology University of Pretoria
 MALIGNANT MELANOMA Dr D. Tenea Department of Dermatology University of Pretoria BACKGROUND History MM. of the skin is a malignant neoplasm of the epidermal melanocytes The incidence rates show considerable
MALIGNANT MELANOMA Dr D. Tenea Department of Dermatology University of Pretoria BACKGROUND History MM. of the skin is a malignant neoplasm of the epidermal melanocytes The incidence rates show considerable
THERE IS A GROUP OF PAtients. Defining Urticarial Dermatitis. A Subset of Dermal Hypersensitivity Reaction Pattern
 STUDY Defining Urticarial Dermatitis A Subset of Dermal Hypersensitivity Reaction Pattern Steven Kossard, FACD; Ian Hamann, FACD; Barbara Wilkinson, BSc Background: Urticarial dermatitis may represent
STUDY Defining Urticarial Dermatitis A Subset of Dermal Hypersensitivity Reaction Pattern Steven Kossard, FACD; Ian Hamann, FACD; Barbara Wilkinson, BSc Background: Urticarial dermatitis may represent
Mycosis Fungoides: A Retrospective Study of 44 Swedish Cases
 Acta Derm Venereol 2016; 96: 669 673 CLINICAL REPORT Mycosis Fungoides: A Retrospective Study of 44 Swedish Cases Yvonne EKLUND 1, Annika ARONSSON 1, Artur SCHMIDTCHEN 1 and Thomas RELANDER 2 1 Section
Acta Derm Venereol 2016; 96: 669 673 CLINICAL REPORT Mycosis Fungoides: A Retrospective Study of 44 Swedish Cases Yvonne EKLUND 1, Annika ARONSSON 1, Artur SCHMIDTCHEN 1 and Thomas RELANDER 2 1 Section
Andrei Metelitsa, MD, FRCPC, FAAD Co-Director, Institute for Skin Advancement Clinical Associate Professor, Dermatology University of Calgary, Canada
 Andrei Metelitsa, MD, FRCPC, FAAD Co-Director, Institute for Skin Advancement Clinical Associate Professor, Dermatology University of Calgary, Canada Copyright 2017 by Sea Courses Inc. All rights reserved.
Andrei Metelitsa, MD, FRCPC, FAAD Co-Director, Institute for Skin Advancement Clinical Associate Professor, Dermatology University of Calgary, Canada Copyright 2017 by Sea Courses Inc. All rights reserved.
A Review of Survival in Mycosis Fungoides
 A Review of Survival in Mycosis Fungoides Robin T. Vollmer, MD From the VA and Duke University Medical Centers, Durham, NC. Key Words: Mycosis fungoides; Survival; Hazard function; Cutaneous T-cell lymphoma
A Review of Survival in Mycosis Fungoides Robin T. Vollmer, MD From the VA and Duke University Medical Centers, Durham, NC. Key Words: Mycosis fungoides; Survival; Hazard function; Cutaneous T-cell lymphoma
Malignant Melanoma Early Stage. A guide for patients
 This melanoma patient brochure is designed to help educate melanoma patients and their caregivers. It was developed under the guidance of Dr. Michael Smylie, Professor, Department of Oncology, University
This melanoma patient brochure is designed to help educate melanoma patients and their caregivers. It was developed under the guidance of Dr. Michael Smylie, Professor, Department of Oncology, University
Histopathology: skin pathology
 Histopathology: skin pathology These presentations are to help you identify, and to test yourself on identifying, basic histopathological features. They do not contain the additional factual information
Histopathology: skin pathology These presentations are to help you identify, and to test yourself on identifying, basic histopathological features. They do not contain the additional factual information
ISPUB.COM. A Case of Actinic Lichen Planus. K Choi, H Kim, H Kim, Y Park INTRODUCTION CASE REPORT
 ISPUB.COM The Internet Journal of Dermatology Volume 8 Number K Choi, H Kim, H Kim, Y Park Citation K Choi, H Kim, H Kim, Y Park.. The Internet Journal of Dermatology. 2009 Volume 8 Number. Abstract The
ISPUB.COM The Internet Journal of Dermatology Volume 8 Number K Choi, H Kim, H Kim, Y Park Citation K Choi, H Kim, H Kim, Y Park.. The Internet Journal of Dermatology. 2009 Volume 8 Number. Abstract The
Sézary syndrome. Diagnosis and staging
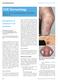 CME DERMATOLOGY Clinical Medicine 2012, Vol 12, No 2: 160 4 Edited by Clive B Archer, consultant dermatologist and lead for Medical Education, St John s Institute of Dermatology, Guy s and St Thomas NHS
CME DERMATOLOGY Clinical Medicine 2012, Vol 12, No 2: 160 4 Edited by Clive B Archer, consultant dermatologist and lead for Medical Education, St John s Institute of Dermatology, Guy s and St Thomas NHS
HEMORRHAGIC BULLOUS HENOCH- SCHONLEIN PURPURA: A CASE REPORT
 HEMORRHAGIC BULLOUS HENOCH- SCHONLEIN PURPURA: A CASE REPORT Nirmala Ponnuthurai, Sabeera Begum, Lee Bang Rom Paediatric Dermatology Unit, Institute of Paediatric, Hospital Kuala Lumpur, Malaysia Abstract
HEMORRHAGIC BULLOUS HENOCH- SCHONLEIN PURPURA: A CASE REPORT Nirmala Ponnuthurai, Sabeera Begum, Lee Bang Rom Paediatric Dermatology Unit, Institute of Paediatric, Hospital Kuala Lumpur, Malaysia Abstract
Malignant Peripheral Nerve Sheath Tumor
 C H A P T E R 120 Malignant Peripheral Nerve Sheath Tumor Currently, malignant peripheral nerve sheath tumor (MPNST) is the most commonly used generic name for the neoplasms known in the past as neurosarcoma,
C H A P T E R 120 Malignant Peripheral Nerve Sheath Tumor Currently, malignant peripheral nerve sheath tumor (MPNST) is the most commonly used generic name for the neoplasms known in the past as neurosarcoma,
