Cutaneous Lupus Erythematosus, Dermatological Approaches of Treatment
|
|
|
- Annice James
- 5 years ago
- Views:
Transcription
1 Cutaneous Lupus Erythematosus, Dermatological Approaches of Treatment 1 Hind Sajdi T Al Atawi, 2 Alshaymaa Abdulrahman AlShaikh, 3 Abdulghani, Fahad Majdy M, 4 Jabir Abdulrahman K Alzaidi, 5 ALBaqami, Haya Majed M Abstract: The lupus erythematosus autoimmune disease is connected with a broad variety of cutaneous pathology. Cutaneous symptoms are often the presenting indication of lupus erythematosus (LE), and in the case of particular cutaneous lupus erythematosus (CLE) subtypes, they can happen in the lack of systemic disease. This review aimed to focus on the management and treatment of dermatological manifestation of cutaneous lupus erythematosus (CLE), also to evaluate the diagnostic procedures of CLE and to discuss the subtypes of CLE. Electronic databases (PubMed/ Embase) were searched up to December, 2016, for relevant literature in the treatment of cutaneous lupus erythematosus (CLE), we retracted most evidence based review, trails, and randomized control studies discussing the CLE management, furthermore we searched references column of each identified study for more relevant articles that did not show up by previous search method. English language restriction for published studies was applied. The management of CLE consists of regular evaluation for systemic disease, also prevention of new sores and treatment of existing sores. Avoidance is accomplished by ideal defense against UV direct exposure, with broad-spectrum sunscreen as a reliable method of preventing development of UV-induced CLE. Treatment includes topical and systemic options. There is good proof to support using topical steroids and topical calcineurin inhibitors. Keywords: cutaneous lupus erythematosus (CLE), cutaneous pathology, systemic disease. 1. INTRODUCTION The autoimmune disease lupus erythematosus is connected with a broad variety of cutaneous pathology. Cutaneous symptoms are often the presenting indication of lupus erythematosus (LE), and in the case of particular cutaneous lupus erythematosus (CLE) subtypes, they can happen in the lack of systemic disease. CLE is 2 to 3 times more frequent than SLE (1). CCLE is further subdivided to two subtypes; discoid lupus erythematosus (DLE), generalized DLE, hypertrophic LE, lupus panniculitis, lupus erythematosus tumidus, and chilblain lupus. DLE, which provides as erythematous, indurated plaques and papules, might resolve with considerable scarring, dyspigmentation, and alopecia (2). DLE is the most typical type of CCLE and, when restricted to the head and neck, is rarely connected with SLE (3). SCLE, which presents as photo distributed papulosquamous or annular-polycyclic plaques, tends to recover without scarring and is typically associated with photosensitivity and anti-ssa antibodies (4). ACLE, which generally provides as malar erythema however Can be generalized, is an extremely particular marker for systemic disease, as practically 100% of patients with ACLE have SLE (3). Cutaneous symptoms are often the very first symptoms and signs of lupus erythematosus (LE) and lead to the consultation of a skin doctor or inspire an internist or rheumatologist to seek advice from a dermatologist for differential diagnosis. When CLE is identified as the skin sores to a subtype and to rule out systemic organ participation (3,5), the most important diagnostic action. As numerous subtypes of CLE can occur concurrently, a comprehensive analysis of numerous findings is necessary. CLE has 3 significant subtypes: chronic CLE (CCLE), subacute CLE (SCLE), and intense CLE (ACLE) (3). Page 1377
2 Earlier epidemiological research study of CLE has actually been obstructed by a scarcity of case ascertainment and much of the knowledge is based on often retrospective and rather little research studies. Current population-based research studies have actually shown that the incidence of CLE in Sweden and USA is 4/100,000 residents (6,7) ; in both studies the population majority were Caucasians. SLE is more typical in Asians and African Americans than in Caucasians (3,8,9) ; no such research studies have been made for CLE but DLE is thought about more common among African Americans and SCLE is more common amongst Caucasians. DLE is the most common subset (80%), followed by SCLE (15%) and less than 5% are other rarer types of CLE such as lupus profundus or lupus panniculitis (6). In a recently released study, the woman to male ratio have been revealed to be 3:1 for both DLE and SCLE, indicate age for being diagnosed with CLE was around 54 years because study (6). This review was aim to focus on the management and treatment of dermatological manifestation of cutaneous lupus erythematosus (CLE), also to evaluate the diagnostic procedures of CLE and to discuss the subtypes of CLE. 2. METHODOLOGY Electronic databases (PubMed/ Embase) were searched up to December, 2016, for relevant literature in the treatment of cutaneous lupus erythematosus (CLE), we retracted most evidence based review, trails, and randomized control studies discussing the CLE management, furthermore we searched references column of each identified study for more relevant articles that did not show up by previous search method. English language restriction for published studies was applied. o Overview of LE: 3. RESULTS Lupus Erythematosus (LE) is an autoimmune chronic disease that involving of a broad spectrum of symptoms. LE is consisted of among the so called connective tissue diseases and is divided into one systemic kind - SLE and one cutaneous form - CLE. They can occur both together and individually (10). The Lupus Erythematosus usually has to run through chronic course with abrupt worsening and periods of remission. The classification of CLE can be difficult and complicated but the enhanced classification in 1979 by the American skin doctors (Gilliam and Sontheimer) has actually gained broad approval (11). Inning accordance with Gilliam and Sontheimer, the cutaneous manifestations of LE can be divided into LE-specific and LE-non-specific skin signs based upon histopathological findings 12). The LE-specific skin symptoms show a typical histopathological picture with a lichenoid tissue response. LE-specific skin manifestations can be further partitioned into severe CLE (ACLE), subacute CLE (SCLE) and chronic CLE (CCLE) where timeless discoid LE (DLE) is the most common kind (10,11,12). An alternative classification has actually likewise been suggested which includes lupus erythematosus tumidus (LET) as a different subgroup; the intermittent subtype of CLE (ICLE) (13). The LEnon-specific skin symptoms consist of a wide range of signs with various histopathological photos. The LE-non-specific skin manifestations are not special to LE disease however are typically seen in patients with active SLE but also in several other autoimmune diseases. It is very important to evaluate a patient with CLE for LE-non-specific symptoms since their existence can suggest systemic involvement and progression to SLE (14). Figure 1: A modified version of Gilliam's classification of LE-specific skin manifestations (10) Page 1378
3 o Prevention procedures of CLE: It is very compulsory to clarify how important the prevention of sunlight and artificial sources of ultraviolet (UV) radiation, as well as to advocate the everyday use of broad-spectrum sun block. The induction of CLE lesions by UVA and UVB radiation has actually been shown (15). Patients need to be counseled to avoid the sun throughout peak hours, minimize travel to equatorial areas of the world, and prevent tanning salons. UVA can permeate window glass and cause sores, but the probability of occurrence depends on the protective degree of and duration of direct exposure (15). Recently, the risk of intensifying disease in photosensitive conditions due to cumulative low-dose UV has been described (16). It is thus recommended that patients with CLE use compact bulbs with the most affordable UV irradiance, in an effort to reduce the damage from chronic UV exposure (16). Broad-spectrum sunscreen is necessary in preventing new lesions. A little double-blinded, intra-individual open-label study of three commercially available sunscreens demonstrated that sun block works in preventing development of CLE lesions, though there was differing effectiveness among those evaluated (17). One of these sunscreens, which provided protection for the UVA/UVB and visible light spectrum, was efficacious in 100% (11/11) of patients. Sunscreen with a minimum of sun defense factor (SPF) 50 and UVA/UVB coverage, are typically advised. Photoprotective clothes is an alternative for patients who need or want additional photoprotection. Research studies from radiation laboratories in Australia and the United Kingdom have shown that about 90% of summertime clothing offers security that is equivalent to sun blocks of SPF 30 or greater (18), so even using long clothing that are not marketed as photoprotective can provide dependable additional defense. Because sunlight is required in the synthesis of vitamin D, is necessary to examine the level of Vitamin D in patients suffering from CLE, and invasily avoiding exposure to the sun light and consistently applying sunscreen. Supplements with at least 400IU of vitamin D3 (cholecalciferol) is suggested in these patients (15). o Topical Management Therapies: A. Topical corticosteroids for treatment of CLE: Topical corticosteroids (CS) are an important part of treating all subtypes of CLE. Regardless of their prevalent usage, there has actually only been one randomized regulated trial, which compared a high potency steroid with a low strength steroid, in the treatment of CLE (19). When picking the appropriate topical steroid, both potency and vehicle are necessary factors to think about. The option in effectiveness is based on the location of the skin lesion(s). For thin areas of skin (e.g. face), a low effectiveness steroid, such as fluocinolone acetonide 0.01% or hydrocortisone butyrate 1%, is a good option. For the trunk and extremities, moderate effective steroid, such as triamcinolone acetonide or betamethasone valerate, is appropriate. For thick skin areas, a highly effective type of steroid, such as clobetasol propionate, is typically needed. The choice in car is also an essential consideration. For the body, creams and ointments are best. Generally, treatment is started with a cream, as many patients can endure everyday application of them, but some patients might require a lotion. DLE might be responsive to intralesional steroids (19,20). The negative effects of topical CS are popular. They consist of, but are not limited to, skin atrophy, steroid-induced rosacea, and telangiectasias. To decrease these negative effects, topical steroids need to be obtained a limited range of weeks and periodically, such that the skin has steroid-free intervals. Intra-lesioned steroid injections need to utilize the minimum concentration of drug necessary to accomplish results and need at least four weeks between injections. To prevent systemic absorption and suppression of the hypothalamic-pituitary axis, no more than 45g per week of high potency or 100g per week of low to mid effectiveness topical steroid need to be applied (without occlusion) (20). B. Role of Topical Calcineurin Inhibitors in CLE Due to the undesirable side effects of topical CS, calcineurin inhibitors, tacrolimus and pimecrolimus, have actually been studied for their long-term healing potential in CLE. Drugs in this class work by forming a complex with macrophilin-12 that inhibits the calcineurin moderated dephosphorylation of nuclear transcription factor of activated T cells (NF-AT) (21). Phosphorylated NK-AT is responsible for the transcription of many inflammatory modulators within T cells (22). Since the first reports of success with calcineurin inhibitors treating lupus skin lesions in 2002, a number of research studies have demonstrated their efficacy in CLE (23). Adverse effects are limited to short-term burning, erythema, and inflammation (23). Without the risk of skin surface damage, calcineurin inhibitors are epically dependable in fragile locations of skin consisting of the face, neck, and intertriginous locations (24,25). Page 1379
4 Tacrolimus, offered in a 0.1% and 0.03% lotion type, is allowed to use for patients with CLE (26,27). In one identified study (28) involving 20 patients with CLE and their symptoms were managed by appling 0.1% tacrolimus and 0.05% clobetasol proprionate ointments, and showed an effective mood of therapy for those patients with CLE (28). Enhancement of CLE sores was observed in both treatment groups without a substantial difference in total effectiveness. Nevertheless, 61 percent of patients treated with steroids established telangiectasias, a finding that highlights the steroid-sparing results of tacrolimus. One apparent benefit of these medications is their absence of steroid-associated systemic side effects. Adverse effects with topical calcineurin inhibitors have actually been mild or very little. The most common negative effects are pruritis, burning and/or increased erythema at the site of application, nevertheless, if tolerable, does not require cessation of treatment (29). Both tacrolimus and pimecrolimus bring a questionable "black box" warning due to a prospective increased risk for malignancy, in spite of no scientific evidence at this time to suggest a causal relationship between topical calcineurin inhibitors and malignancy (30). Long-lasting safety research studies with postmarketing security information remain in progress (30). o Immunosuppressive treatment for CLE: Just like other inflammatory conditions, CLE can respond to systemic corticosteroids, though action to steroids in DLE is unreliable. Evidance showed that use of steroid for a short period can be very effective during flares and when starting non-steroidal immunosuppressive drugs, which may take a number of weeks to show benefit. Systemic steroids ought to not be utilized as long-term treatment, given their popular serious adverse reaction. Methotrexate has been shown in two retrospective research studies as actually been displayed to be efficient in multiple subtypes of CLE (31,32). Folate replacement and regular laboratory monitoring for bone marrow suppression and hepatotoxicity is required. For patients who do not tolerate oral shipment of the drug, intramuscular delivery is an option. Mycophenolate has been displayed in numerous case reports to be effective in treating all subtypes of CLE (4). In a prospective nonrandomized open pilot research study, mycophenolate was shown to be useful in treating SCLE patients who had been resistant to a minimum of one requirement treatment, specified as steroids (topical or systemic) or antimalarials (33). Routine lab monitoring for hematologic, kidney, and hepatic toxicity is necessary. Mycophenolate mofetil is normally well-tolerate though intestinal upset and diarrhea are the more frequently reported side effects. Mycophenolate sodium, which is enteric-coated, has actually been associated with fewer gastrointestinal side effects. Azathioprine can also work in DLE (34). When beginning azathioprine, a low dosage of 50mg a day is utilized initially and increased by 25mg every 2 weeks, as laboratory tracking permits, up until the minimum efficient dose is achieved. If TPMT activity is adequate, an alternative technique is checking the enzyme activity of thiopurine methyltransferase (TPMT) prior to starting treatment and then beginning at a higher dosage. Routine laboratory tracking for hematologic and hepatic toxicity is likewise needed. Cyclophosphamide and cyclosporine can be used, normally in the context of significant organ involvement beyond the skin. Improvement of CLE sores with these medications has actually been reported (15). Nevertheless, due to their significant toxicity profile, they are hardly ever used in CLE patients and booked for refractory CLE patients with SLE. Rituximab has actually been used effectively in several case reports including patients with CLE, consisting of lupus typical lesion, that responsive to combinations of immunosuppressives, and immunomodulators (15). Other biologic therapies, such as tumor necrosis factor-alpha (TNF-α inhibitors, have actually likewise been reported as beneficial in the treatment of CLE, although etanercept, adalimumab, and infliximab have actually also been associated with the induction of numerous CLE subtype lesions (15). Methodical research studies are needed to further evaluate biologic treatments. 4. CONCLUSION The management of CLE consists of regular evaluation for systemic disease, also prevention of new sores and treatment of existing sores. Avoidance is accomplished by ideal defense against UV direct exposure, with broad-spectrum sunscreen as a reliable method of preventing development of UV-induced CLE. Treatment includes topical and systemic options. There is good proof to support using topical steroids and topical calcineurin inhibitors. An immunosuppressive or immunomodulator is included if the antimalarial treatment algorithm detailed earlier is insufficient. Cyclophosphamide and rituximab are considered in patient's refractory to various mixes of immunosuppressives/immunomodulators. With the introduction of a verified result step for CLE, improved examination of treatment efficacy and appealing new therapies are on the horizon. Page 1380
5 REFERENCES [1] Tebbe B, Orphanos CE. Epidemiology and socioeconomic impact of skin disease in lupus erythematosus. Lupus. 1997;6: [2] Werth VP. Clinical manifestations of cutaneous lupus erythematosus. Autoimmun Rev. 2005;4: [3] Lee HJ, Sinha AA. Cutaneous lupus erythematosus: understanding of clinical features, genetic basis, and pathobiology of disease guides therapeutic strategies. Autoimmunity. 2006;39: [4] Fett N, Werth VP. Maibach H, editor. Treatment of Cutaneous Lupus Erythematosus. [5] Sticherling M. Chronic cutaneous lupus erythematosus. In: Hertl M (ed): Autoimmune Disease of the Skin Pathogenesis, diagnosis, management. Wien, New York: Springer, 2005: [6] Gronhagen CM, Fored CM, Granath F, Nyberg F. Cutaneous lupus erythematosus and the association with systemic lupus erythematosus: A population-based cohort of 1088 patients in Sweden. Br J Dermatol. 2011;164: [7] Durosaro O, Davis MD, Reed KB, Rohlinger AL. Incidence of cutaneous lupus erythematosus, : A population-based study. Arch Dermatol. 2009;145: [8] Chiu YM, Lai CH. Nationwide population-based epidemiologic study of systemic lupus erythematosus in Taiwan. Lupus. 2010;19: [9] Bernatsky S, Joseph L, Pineau CA, Tamblyn R, Feldman DE, Clarke AE. A population-based assessment of systemic lupus erythematosus incidence and prevalence--results and implications of using administrative data for epidemiological studies. Rheumatology (Oxford) 2007;46: [10] Grönhagen CM, Nyberg F. Cutaneous lupus erythematosus: An update. Indian Dermatology Online Journal. 2014;5(1):7-13. doi: / [11] Sontheimer RD, Thomas JR, Gilliam JN. Subacute cutaneous lupus erythematosus: A cutaneous marker for a distinct lupus erythematosus subset. Arch Dermatol. 1979;115: [12] Gilliam JN, Sontheimer RD. Distinctive cutaneous subsets in the spectrum of lupus erythematosus. J Am Acad Dermatol. 1981;4: [13] Kuhn A, Bein D, Bonsmann G. The 100th anniversary of lupus erythematosus tumidus. Autoimmun Rev. 2009;8: [14] Cardinali C, Caproni M, Bernacchi E, Amato L, Fabbri P. The spectrum of cutaneous manifestations in lupus erythematosus-the Italian experience. Lupus. 2000;9: [15] Kuhn A, Ruland V, Bonsmann G. Cutaneous lupus erythematosus: Update of therapeutic options Part I and Part II. J Am Acad Dermatol [16] Klein RS, Werth VP, Dowdy JC, Sayre RM. Analysis of compact fluorescent lights for use by patients with photosensitive conditions. Photochem Photobiol. 2009;85: [17] Stege H, Budde MA, Grether-Beck S, Krutmann J. Evaluation of the capacity of sunscreens to photoprotect lupus erythematosus patients by employing the photoprovocation test. Photodermatol Photoimmunol Photomed. 2000;16: [18] Diffey BL. Sun protection with clothing. Br J Dermatol. 2001;144: [19] Roenigk HH, Jr, Martin JS, Eichorn P, Gilliam JN. Discoid lupus erythematosus. Diagnostic features and evaluation of topical corticosteroid therapy. Cutis. 1980;25: [20] Hughes J, Rustin M. Corticosteroids. Clin Dermatol. 1997;15: [21] Gisondi P, Ellis CN, Girolomoni G. Pimecrolimus in dermatology: atopic dermatitis and beyond. Int J Clin Pract. 2005;59: [22] Marsland AM, Griffiths CE. The macrolide immunosuppressants in dermatology: mechanisms of action. Eur J Dermatol. 2002;12: Page 1381
6 [23] Sticherling M. Update on the use of topical calcineurin inhibitors in cutaneous lupus erythematosus. Biologics. 2011;5: [24] Queille-Roussel C, Paul C, Duteil L, et al. The new topical ascomycin derivative SDZ ASM 981 does not induce skin atrophy when applied to normal skin for 4 weeks: a randomized, double-blind controlled study. Br J Dermatol. 2001;144: [25] Draelos ZD. Use of topical corticosteroids and topical calcineurin inhibitors for the treatment of atopic dermatitis in thin and sensitive skin areas. Curr Med Res Opin. 2008;24: [26] Luger T, Paul C. Potential new indications of topical calcineurin inhibitors. Dermatology. 2007;215: [27] Wollina U, Hansel G. The use of topical calcineurin inhibitors in lupus erythematosus: an overview. J Eur Acad Dermatol Venereol. 2008;22:1 6. [28] Tzung TY, Liu YS, Chang HW. Tacrolimus vs. clobetasol propionate in the treatment of facial cutaneous lupus erythematosus: a randomized, double-blind, bilateral comparison study. Br J Dermatol. 2007;156: [29] Sardy M, Ruzicka T, Kuhn A. Topical calcineurin inhibitors in cutaneous lupus erythematosus. Arch Dermatol Res. 2009;301: [30] Thaci D, Salgo R. Malignancy concerns of topical calcineurin inhibitors for atopic dermatitis: facts and controversies. Clin Dermatol. 2010;28: [31] Boehm IB, Boehm GA, Bauer R. Management of cutaneous lupus erythematosus with low-dose methotrexate: indication for modulation of inflammatory mechanisms. Rheumatol Int. 1998;18: [32] Wenzel J, Brahler S, Bauer R, Bieber T, Tuting T. Efficacy and safety of methotrexate in recalcitrant cutaneous lupus erythematosus: results of a retrospective study in 43 patients. Br J Dermatol. 2005;153: [33] Kreuter A, Tomi NS, Weiner SM, Huger M, Altmeyer P, et al. Mycophenolate sodium for subacute cutaneous lupus erythematosus resistant to standard therapy. Br J Dermatol. 2007;156: [34] Ashinoff R, Werth VP, Franks AG., Jr Resistant discoid lupus erythematosus of palms and soles: successful treatment with azathioprine. J Am Acad Dermatol. 1988;19: Page 1382
Skin Deep: Cutaneous Lupus. Dr Sarah Sasson Immunology Registrar, Liverpool Hospital 2016
 Skin Deep: Cutaneous Lupus Dr Sarah Sasson Immunology Registrar, Liverpool Hospital 2016 Introduction: Cutaneous lupus erythematosus LE is an autoimmune disease with a range of clinical manifestations
Skin Deep: Cutaneous Lupus Dr Sarah Sasson Immunology Registrar, Liverpool Hospital 2016 Introduction: Cutaneous lupus erythematosus LE is an autoimmune disease with a range of clinical manifestations
Cutanous Manifestation of Lupus Erythematosus. Presented By: Dr. Naif S. Al Shahrani Salman Bin Abdaziz university
 Cutanous Manifestation of Lupus Erythematosus Presented By: Dr. Naif S. Al Shahrani Salman Bin Abdaziz university A 50-year old lady, who is otherwise healthy, presented to the dermatology clinic with
Cutanous Manifestation of Lupus Erythematosus Presented By: Dr. Naif S. Al Shahrani Salman Bin Abdaziz university A 50-year old lady, who is otherwise healthy, presented to the dermatology clinic with
COMPLEX CUTANEOUS LUPUS CASES PEARLS AND PITFALLS
 COMPLEX CUTANEOUS LUPUS CASES PEARLS AND PITFALLS Benjamin F. Chong, MD, MSCS February 17, 2018 CONFLICTS OF INTEREST D I S CLOSURE OF R E LATI ONSHIPS W I T H I NDUSTRY Benjamin Chong, MD, MSCS F059 Complex
COMPLEX CUTANEOUS LUPUS CASES PEARLS AND PITFALLS Benjamin F. Chong, MD, MSCS February 17, 2018 CONFLICTS OF INTEREST D I S CLOSURE OF R E LATI ONSHIPS W I T H I NDUSTRY Benjamin Chong, MD, MSCS F059 Complex
New Medicine Report. Pimecrolimus. RED- Hospital only Date of Last Revision 6 th March 2003
 New Medicine Report Document Status Pimecrolimus Reviewed by Suffolk D&T RED- Hospital only Date of Last Revision 6 th March 2003 Approved Name Pimecrolimus Trade Name Elidel Manufacturer Novartis Legal
New Medicine Report Document Status Pimecrolimus Reviewed by Suffolk D&T RED- Hospital only Date of Last Revision 6 th March 2003 Approved Name Pimecrolimus Trade Name Elidel Manufacturer Novartis Legal
UnitedHealthcare Pharmacy Clinical Pharmacy Programs
 UnitedHealthcare Pharmacy Clinical Pharmacy Programs Program Number 2017 P 2116-3 Program Prior Authorization/Medical Necessity Medications Dupixent (dupilumab) P&T Approval Date 1/2017, 5/2017, 7/2017
UnitedHealthcare Pharmacy Clinical Pharmacy Programs Program Number 2017 P 2116-3 Program Prior Authorization/Medical Necessity Medications Dupixent (dupilumab) P&T Approval Date 1/2017, 5/2017, 7/2017
Ask the Expert: Photosensitivity in Cutaneous Lupus
 Ask the Expert: Photosensitivity in Cutaneous Lupus Victoria P. Werth, MD Department of Dermatology & Medicine University of Pennsylvania ; Philadelphia VA Hospital Overview Definition Impact of photosensitivity
Ask the Expert: Photosensitivity in Cutaneous Lupus Victoria P. Werth, MD Department of Dermatology & Medicine University of Pennsylvania ; Philadelphia VA Hospital Overview Definition Impact of photosensitivity
Invited Re vie W. Antinuclear antibody-keratinocyte interactions in photosensitive cutaneous lupus erythematosus
 Histol Histopathol (1 999) 14: 627-633 http://www.ehu.es/histol-histopathol Histology and Histopathology Invited Re vie W Antinuclear antibody-keratinocyte interactions in photosensitive cutaneous lupus
Histol Histopathol (1 999) 14: 627-633 http://www.ehu.es/histol-histopathol Histology and Histopathology Invited Re vie W Antinuclear antibody-keratinocyte interactions in photosensitive cutaneous lupus
Arthritis & Rheumatology Clinics of Kansas PATIENT EDUCATION SYSTEMIC LUPUS ERYTHEMATOSUS
 Arthritis & Rheumatology Clinics of Kansas PATIENT EDUCATION SYSTEMIC LUPUS ERYTHEMATOSUS Introduction: There is perhaps no rheumatic disease that evokes so much fear and confusion among both patients
Arthritis & Rheumatology Clinics of Kansas PATIENT EDUCATION SYSTEMIC LUPUS ERYTHEMATOSUS Introduction: There is perhaps no rheumatic disease that evokes so much fear and confusion among both patients
Topical Immunomodulator Step Therapy Program
 Topical Immunomodulator Step Therapy Program Policy Number: 5.01.557 Last Review: 8/2017 Origination: 7/2013 Next Review: 8/2018 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) BCBSKC will provide
Topical Immunomodulator Step Therapy Program Policy Number: 5.01.557 Last Review: 8/2017 Origination: 7/2013 Next Review: 8/2018 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) BCBSKC will provide
CONTROVERSIES IN MANAGEMENT AND TREATMENT OF CUTANEOUS LUPUS PATIENTS
 CONTROVERSIES IN MANAGEMENT AND TREATMENT OF CUTANEOUS LUPUS PATIENTS Benjamin F. Chong, MD, MSCS February 19, 2018 CONFLICTS OF INTEREST D I S CLOSURE OF R E LATI ONSHIPS W I T H I NDUSTRY Benjamin Chong,
CONTROVERSIES IN MANAGEMENT AND TREATMENT OF CUTANEOUS LUPUS PATIENTS Benjamin F. Chong, MD, MSCS February 19, 2018 CONFLICTS OF INTEREST D I S CLOSURE OF R E LATI ONSHIPS W I T H I NDUSTRY Benjamin Chong,
Pharmacologic Treatment of Atopic Dermatitis
 J KMA Pharmacotherapeutics Pharmacologic Treatment of Atopic Dermatitis Chun Wook Park, MD Department of Dermatology, Hallym University College of Medicine E mail : dermap@paran.com J Korean Med Assoc
J KMA Pharmacotherapeutics Pharmacologic Treatment of Atopic Dermatitis Chun Wook Park, MD Department of Dermatology, Hallym University College of Medicine E mail : dermap@paran.com J Korean Med Assoc
(minutes for web publishing)
 Dermatology Subcommittee of the Pharmacology and Therapeutics Advisory Committee (PTAC) Meeting held on 20 October 2017 (minutes for web publishing) Dermatology Subcommittee minutes are published in accordance
Dermatology Subcommittee of the Pharmacology and Therapeutics Advisory Committee (PTAC) Meeting held on 20 October 2017 (minutes for web publishing) Dermatology Subcommittee minutes are published in accordance
Treating dermatomyositis
 Treating dermatomyositis David Fiorentino, MD, PhD Stanford University School of Medicine Department of Dermatology Department of Medicine (Rheumatology) September 25, 2010 DM affects many organs Approaching
Treating dermatomyositis David Fiorentino, MD, PhD Stanford University School of Medicine Department of Dermatology Department of Medicine (Rheumatology) September 25, 2010 DM affects many organs Approaching
Atopic Eczema with detail on how to apply wet wraps
 Atopic Eczema with detail on how to apply wet wraps Dr Carol Hlela Consultant Dermatologist Head of Unit, Department of Dermatology, Paediatrics Red Cross Children s Hospital, UCT Red Cross War Memorial
Atopic Eczema with detail on how to apply wet wraps Dr Carol Hlela Consultant Dermatologist Head of Unit, Department of Dermatology, Paediatrics Red Cross Children s Hospital, UCT Red Cross War Memorial
Atopic Dermatitis and Topical Antipsoriatics
 Atopic Dermatitis and Topical Antipsoriatics Goal(s): Restrict dermatological drugs only for funded OHP diagnoses. Moderate/severe psoriasis and moderate/severe atopic dermatitis treatments are funded
Atopic Dermatitis and Topical Antipsoriatics Goal(s): Restrict dermatological drugs only for funded OHP diagnoses. Moderate/severe psoriasis and moderate/severe atopic dermatitis treatments are funded
Early Diagnosis and Treatment of Discoid Lupus Erythematosus
 BRIEF REPORT Early Diagnosis and Treatment of Discoid Lupus Erythematosus Suresh Panjwani, MD, MSc, FRACGP Discoid lupus erythematosus is a chronic dermatological disease that can lead to scarring, hair
BRIEF REPORT Early Diagnosis and Treatment of Discoid Lupus Erythematosus Suresh Panjwani, MD, MSc, FRACGP Discoid lupus erythematosus is a chronic dermatological disease that can lead to scarring, hair
Cutaneous Lupus Erythematosus: Current Treatment Options
 Curr Treat Options in Rheum (2016) 2:36 48 DOI 10.1007/s40674-016-0033-z Lupus (S Manzi, Section Editor) Cutaneous Lupus Erythematosus: Current Treatment Options Jenna K. Presto, BS 1,2 Victoria P. Werth,
Curr Treat Options in Rheum (2016) 2:36 48 DOI 10.1007/s40674-016-0033-z Lupus (S Manzi, Section Editor) Cutaneous Lupus Erythematosus: Current Treatment Options Jenna K. Presto, BS 1,2 Victoria P. Werth,
Medication Policy Manual. Topic: Dupixent, dupilumab Date of Origin: March 10, Committee Approval: March 10, 2017 Next Review Date: May 2018
 Independent licensees of the Blue Cross and Blue Shield Association Medication Policy Manual Policy No: dru493 Topic: Dupixent, dupilumab Date of Origin: March 10, 2017 Committee Approval: March 10, 2017
Independent licensees of the Blue Cross and Blue Shield Association Medication Policy Manual Policy No: dru493 Topic: Dupixent, dupilumab Date of Origin: March 10, 2017 Committee Approval: March 10, 2017
STUDY. 1% Pimecrolimus, 0.005% Calcipotriol, and 0.1% Betamethasone in the Treatment of Intertriginous Psoriasis
 STUDY 1% Pimecrolimus, 0.005% Calcipotriol, and 0.1% Betamethasone in the Treatment of Intertriginous Psoriasis A Double-blind, Randomized Controlled Study Alexander Kreuter, MD; Anna Sommer, MD; Julia
STUDY 1% Pimecrolimus, 0.005% Calcipotriol, and 0.1% Betamethasone in the Treatment of Intertriginous Psoriasis A Double-blind, Randomized Controlled Study Alexander Kreuter, MD; Anna Sommer, MD; Julia
Elements for a Public Summary
 VI.2 VI.2.1 Elements for a Public Summary Overview of disease epidemiology Psoriasis (excluding widespread plaque psoriasis) Psoriasis is a common chronic skin disorder. Estimates of the prevalence (proportion
VI.2 VI.2.1 Elements for a Public Summary Overview of disease epidemiology Psoriasis (excluding widespread plaque psoriasis) Psoriasis is a common chronic skin disorder. Estimates of the prevalence (proportion
CENTENE PHARMACY AND THERAPEUTICS NEW DRUG REVIEW 3Q17 July August
 BRAND NAME Dupixent GENERIC NAME dupilumab MANUFACTURER Regeneron DATE OF APPROVAL March 28, 2017 PRODUCT LAUNCH DATE First week of April 2017 REVIEW TYPE Review type 1 (RT1): New Drug Review Full review
BRAND NAME Dupixent GENERIC NAME dupilumab MANUFACTURER Regeneron DATE OF APPROVAL March 28, 2017 PRODUCT LAUNCH DATE First week of April 2017 REVIEW TYPE Review type 1 (RT1): New Drug Review Full review
Pimecrolimus in dermatology: atopic dermatitis and beyond
 DRUG FOCUS doi: 10.1111/j.1368-5031.2005.00587.x Pimecrolimus in dermatology: atopic dermatitis and beyond PAOLO GISONDI, 1 CHARLES N. ELLIS, 2 GIAMPIERO GIROLOMONI 3 Department of Dermatology, 1 Istituto
DRUG FOCUS doi: 10.1111/j.1368-5031.2005.00587.x Pimecrolimus in dermatology: atopic dermatitis and beyond PAOLO GISONDI, 1 CHARLES N. ELLIS, 2 GIAMPIERO GIROLOMONI 3 Department of Dermatology, 1 Istituto
Cutaneous Lupus Erythematosus Diagnosis, Relationship to SLE and Management
 Cutaneous Lupus Erythematosus Diagnosis, Relationship to SLE and Management Jeffrey P. Callen, MD Professor of Medicine (Dermatology) Chief, Division of Dermatology Jeffrey P. Callen, MD Disclosure (previous
Cutaneous Lupus Erythematosus Diagnosis, Relationship to SLE and Management Jeffrey P. Callen, MD Professor of Medicine (Dermatology) Chief, Division of Dermatology Jeffrey P. Callen, MD Disclosure (previous
Dupixent (dupilumab)
 Dupixent (dupilumab) Line(s) of Business: HMO; PPO; QUEST Integration Effective Date: TBD POLICY A. INDICATIONS The indications below including FDA-approved indications and compendial uses are considered
Dupixent (dupilumab) Line(s) of Business: HMO; PPO; QUEST Integration Effective Date: TBD POLICY A. INDICATIONS The indications below including FDA-approved indications and compendial uses are considered
LUPUS CAN DO EVERYTHING, BUT NOT EVERYTHING IS LUPUS LUPUS 101 SLE SUBSETS AUTOIMMUNE DISEASE 11/4/2013 HOWARD HAUPTMAN, MD IDIOPATHIC DISCOID LUPUS
 LUPUS 101 LUPUS CAN DO EVERYTHING, BUT NOT EVERYTHING IS LUPUS HOWARD HAUPTMAN, MD IDIOPATHIC DISCOID LUPUS SLE SUBSETS SUBACUTE CUTANEOUS LUPUS DRUG INDUCED LUPUS NEONATAL LUPUS LATE ONSET LUPUS ANTI-PHOSPHOLIPID
LUPUS 101 LUPUS CAN DO EVERYTHING, BUT NOT EVERYTHING IS LUPUS HOWARD HAUPTMAN, MD IDIOPATHIC DISCOID LUPUS SLE SUBSETS SUBACUTE CUTANEOUS LUPUS DRUG INDUCED LUPUS NEONATAL LUPUS LATE ONSET LUPUS ANTI-PHOSPHOLIPID
MEDICATIONS: THE GOOD, THE BAD, THE UGLY
 MEDICATIONS: THE GOOD, THE BAD, THE UGLY July 13, 2013 Dr. Tanaz Kermani Assistant Clinical Professor of Medicine, Division of Rheumatology, David Geffen School of Medicine UCLA Dr. Robert Spiera Professor
MEDICATIONS: THE GOOD, THE BAD, THE UGLY July 13, 2013 Dr. Tanaz Kermani Assistant Clinical Professor of Medicine, Division of Rheumatology, David Geffen School of Medicine UCLA Dr. Robert Spiera Professor
LUPUS. The Skin and Hair LUPUSUK 2015
 5 LUPUS The Skin and Hair LUPUSUK 2015 LUPUS The Skin and Hair Skin problems are very common in lupus and many different types of issues can occur. This factsheet will discuss some of the more frequent
5 LUPUS The Skin and Hair LUPUSUK 2015 LUPUS The Skin and Hair Skin problems are very common in lupus and many different types of issues can occur. This factsheet will discuss some of the more frequent
Follow this and additional works at: Part of the Skin and Connective Tissue Diseases Commons
 Philadelphia College of Osteopathic Medicine DigitalCommons@PCOM PCOM Physician Assistant Studies Student Scholarship Student Dissertations, Theses and Papers 2014 Is the Addition of a Topical Agent to
Philadelphia College of Osteopathic Medicine DigitalCommons@PCOM PCOM Physician Assistant Studies Student Scholarship Student Dissertations, Theses and Papers 2014 Is the Addition of a Topical Agent to
Cutaneous manifestations and systemic correlation in patients with lupus erythematosus and its subsets: a study of 40 cases
 International Journal of Research in Dermatology Mahajan R et al. Int J Res Dermatol. 2018 Nov;4(4):479-483 http://www.ijord.com Original Research Article DOI: http://dx.doi.org/10.18203/issn.2455-4529.intjresdermatol20183407
International Journal of Research in Dermatology Mahajan R et al. Int J Res Dermatol. 2018 Nov;4(4):479-483 http://www.ijord.com Original Research Article DOI: http://dx.doi.org/10.18203/issn.2455-4529.intjresdermatol20183407
Living With Lupus. October 15 TH, 2016 Georgia Lupus Empowerment Summit WAMBUI MACHUA, MD
 Living With Lupus October 15 TH, 2016 Georgia Lupus Empowerment Summit WAMBUI MACHUA, MD LUPUS Latin for wolf 13th century physician Rogerius used the word to describe erosive fascial lesions reminiscent
Living With Lupus October 15 TH, 2016 Georgia Lupus Empowerment Summit WAMBUI MACHUA, MD LUPUS Latin for wolf 13th century physician Rogerius used the word to describe erosive fascial lesions reminiscent
The safety and effectiveness of Dupixent in pediatric patients have not been established (1).
 Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.90.30 Subject: Dupixent Page: 1 of 6 Last Review Date: September 15, 2017 Dupixent Description Dupixent
Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.90.30 Subject: Dupixent Page: 1 of 6 Last Review Date: September 15, 2017 Dupixent Description Dupixent
Psoriasis: Causes, Symptoms, And Treatment
 Psoriasis: Causes, Symptoms, And Treatment We all know that a healthy immune system is good. But, do you know that an overactive immune system can cause certain conditions like Psoriasis? Read on to find
Psoriasis: Causes, Symptoms, And Treatment We all know that a healthy immune system is good. But, do you know that an overactive immune system can cause certain conditions like Psoriasis? Read on to find
Lupus. Fast facts. What is lupus? What causes lupus? Who gets lupus?
 Lupus Systemic lupus erythematosus, referred to as SLE or lupus, is sometimes called the "great imitator." Why? Because of its wide range of symptoms, people often confuse lupus with other health problems.
Lupus Systemic lupus erythematosus, referred to as SLE or lupus, is sometimes called the "great imitator." Why? Because of its wide range of symptoms, people often confuse lupus with other health problems.
Original Policy Date
 MP 2.01.07 Psoralens with Ultraviolet A (PUVA) Medical Policy Section Medicine Issue 12:2013 Original Policy Date 12:2013 Last Review Status/Date Reviewed by consensus/12:2013 Return to Medical Policy
MP 2.01.07 Psoralens with Ultraviolet A (PUVA) Medical Policy Section Medicine Issue 12:2013 Original Policy Date 12:2013 Last Review Status/Date Reviewed by consensus/12:2013 Return to Medical Policy
ISPUB.COM. A Case of Actinic Lichen Planus. K Choi, H Kim, H Kim, Y Park INTRODUCTION CASE REPORT
 ISPUB.COM The Internet Journal of Dermatology Volume 8 Number K Choi, H Kim, H Kim, Y Park Citation K Choi, H Kim, H Kim, Y Park.. The Internet Journal of Dermatology. 2009 Volume 8 Number. Abstract The
ISPUB.COM The Internet Journal of Dermatology Volume 8 Number K Choi, H Kim, H Kim, Y Park Citation K Choi, H Kim, H Kim, Y Park.. The Internet Journal of Dermatology. 2009 Volume 8 Number. Abstract The
Dr.MD.IMRAN KAZMI ASST PROF.DEPT OF DVL,KIMS
 Dr.MD.IMRAN KAZMI ASST PROF.DEPT OF DVL,KIMS Lupus erythematosus is a multisystem disorder whose spectrum runs from a relatively benign, self-limited cutaneous eruption to a severe, often fatal, systemic
Dr.MD.IMRAN KAZMI ASST PROF.DEPT OF DVL,KIMS Lupus erythematosus is a multisystem disorder whose spectrum runs from a relatively benign, self-limited cutaneous eruption to a severe, often fatal, systemic
REVIEW. Cutaneous Lupus Erythematosus. Allison Chabassol Class of 2013, Faculty of Medicine, Dalhousie University
 REVIEW Cutaneous Lupus Erythematosus Allison Chabassol Class of 2013, Faculty of Medicine, Dalhousie University Lupus erythematosus (LE) is a heterogeneous group of chronic autoimmune inflammatory diseases,
REVIEW Cutaneous Lupus Erythematosus Allison Chabassol Class of 2013, Faculty of Medicine, Dalhousie University Lupus erythematosus (LE) is a heterogeneous group of chronic autoimmune inflammatory diseases,
Managing and Minimizing Flare-ups in Atopic Dermatitis
 Managing and Minimizing Flare-ups in Atopic Dermatitis Importance of the skin barrier & how commonly used drugs are impacting it Dr. Benjamin Barankin, MD FRCPC Medical Director & Founder of Toronto Dermatology
Managing and Minimizing Flare-ups in Atopic Dermatitis Importance of the skin barrier & how commonly used drugs are impacting it Dr. Benjamin Barankin, MD FRCPC Medical Director & Founder of Toronto Dermatology
Vitiligo is a skin depigmentation disorder
 THERPEUTICS FOR THE CLINICIN Tacrolimus Ointment 0.1% Produces Repigmentation in Patients With Vitiligo: Results of a Prospective Patient Series Emil. Tanghetti, MD The cause of the selective melanocyte
THERPEUTICS FOR THE CLINICIN Tacrolimus Ointment 0.1% Produces Repigmentation in Patients With Vitiligo: Results of a Prospective Patient Series Emil. Tanghetti, MD The cause of the selective melanocyte
Management of Pyoderma Gangrenosum Mentoring in IBD XVII
 Management of Pyoderma Gangrenosum Mentoring in IBD XVII Scott Walsh MD PhD FRCPC Division of Dermatology Sunnybrook Health Sciences Centre University of Toronto Pyoderma Gangrenosum: A pathological
Management of Pyoderma Gangrenosum Mentoring in IBD XVII Scott Walsh MD PhD FRCPC Division of Dermatology Sunnybrook Health Sciences Centre University of Toronto Pyoderma Gangrenosum: A pathological
Comparison of the narrow band UVB versus systemic corticosteroids in the treatment of lichen planus: A randomized clinical trial
 Received: 10.7.2011 Accepted: 5.12.2011 Original Article Comparison of the narrow band UVB versus systemic corticosteroids in the treatment of lichen planus: A randomized clinical trial Fariba Iraji, 1
Received: 10.7.2011 Accepted: 5.12.2011 Original Article Comparison of the narrow band UVB versus systemic corticosteroids in the treatment of lichen planus: A randomized clinical trial Fariba Iraji, 1
50 microgram/g Calcipotriol and 500 microgram/g betamethasone (as dipropionate).
 DUPISOR Composition Gel 50 microgram/g Calcipotriol and 500 microgram/g betamethasone (as dipropionate). Action Calcipotriol is a non-steroidal antipsoriatic agent, derived from vitamin D. Calcipotriol
DUPISOR Composition Gel 50 microgram/g Calcipotriol and 500 microgram/g betamethasone (as dipropionate). Action Calcipotriol is a non-steroidal antipsoriatic agent, derived from vitamin D. Calcipotriol
The Cutaneous Lupus Erythematosus Disease Area and Severity Index
 STUDY The Cutaneous Lupus Erythematosus Disease Area and Severity Index A Responsive Instrument to Measure Activity and Damage in Patients With Cutaneous Lupus Erythematosus Zuleika L. Bonilla-Martinez,
STUDY The Cutaneous Lupus Erythematosus Disease Area and Severity Index A Responsive Instrument to Measure Activity and Damage in Patients With Cutaneous Lupus Erythematosus Zuleika L. Bonilla-Martinez,
The Itch That Rashes. Sarah D. Cipriano, MD, MPH, MS Resident, Dermatology University of Utah
 The Itch That Rashes Sarah D. Cipriano, MD, MPH, MS Resident, Dermatology University of Utah 1 Conflict of Interest No conflict of interest Will discuss off label use of medications 2 3 Most likely diagnosis?
The Itch That Rashes Sarah D. Cipriano, MD, MPH, MS Resident, Dermatology University of Utah 1 Conflict of Interest No conflict of interest Will discuss off label use of medications 2 3 Most likely diagnosis?
Sarcoidosis Case. Robert P. Baughman Interstitial Lung Disease and Sarcoidosis Clinic University of Cincinnati, USA. WASOG: educational material
 Sarcoidosis Case Robert P. Baughman Interstitial Lung Disease and Sarcoidosis Clinic University of Cincinnati, USA WASOG: educational material Sarcoidosis Case patient is a Caucasian male age 46 was diagnosed
Sarcoidosis Case Robert P. Baughman Interstitial Lung Disease and Sarcoidosis Clinic University of Cincinnati, USA WASOG: educational material Sarcoidosis Case patient is a Caucasian male age 46 was diagnosed
Index. derm.theclinics.com. Note: Page numbers of article titles are in boldface type.
 Note: Page numbers of article titles are in boldface type. A Abatacept for DLE, 493 for SLE, 497 Ablative therapies, localized, for cutaneous T-cell lymphoma, 502 506. See also Cutaneous T-cell lymphoma,
Note: Page numbers of article titles are in boldface type. A Abatacept for DLE, 493 for SLE, 497 Ablative therapies, localized, for cutaneous T-cell lymphoma, 502 506. See also Cutaneous T-cell lymphoma,
CHAPTER 2. Is severity eruption assessment possible? in polymorphous light
 CHAPTER 2 Is severity assessment in polymorphous light Is severity eruption assessment possible? in polymorphous light Ines Schornagel, eruption Kees Guikers, possible? Huib van Weelden, Carla Bruijnzeel-Koomen
CHAPTER 2 Is severity assessment in polymorphous light Is severity eruption assessment possible? in polymorphous light Ines Schornagel, eruption Kees Guikers, possible? Huib van Weelden, Carla Bruijnzeel-Koomen
CHAPTER 3. Diagnostic phototesting in polymorphous. Diagnostic phototesting in polymorphous light eruption: the optimal number of irradiations
 CHAPTER 3 Diagnostic phototesting in polymorphous light eruption: the optimal number of irradiations Diagnostic phototesting in polymorphous light eruption: Ines Schornagel, Edward the optimal Knol, Huib
CHAPTER 3 Diagnostic phototesting in polymorphous light eruption: the optimal number of irradiations Diagnostic phototesting in polymorphous light eruption: Ines Schornagel, Edward the optimal Knol, Huib
Comparative efficacy of topical mometasone furoate 0.1% cream vs topical tacrolimus 0.03% ointment in the treatment of atopic dermatitis
 Original Article Comparative efficacy of topical mometasone furoate 0.1% cream vs topical tacrolimus 0.03% ointment in the treatment of atopic dermatitis Md Alauddin Khan *, Lubna Khondker **, Dilshad
Original Article Comparative efficacy of topical mometasone furoate 0.1% cream vs topical tacrolimus 0.03% ointment in the treatment of atopic dermatitis Md Alauddin Khan *, Lubna Khondker **, Dilshad
See Important Reminder at the end of this policy for important regulatory and legal information.
 Clinical Policy: (Dupixent) Reference Number: CP.HNMC.208 Effective Date: 04.11.17 Last Review Date: 11.17 Line of Business: Medicaid Medi-Cal Revision Log See Important Reminder at the end of this policy
Clinical Policy: (Dupixent) Reference Number: CP.HNMC.208 Effective Date: 04.11.17 Last Review Date: 11.17 Line of Business: Medicaid Medi-Cal Revision Log See Important Reminder at the end of this policy
PHOTOTHERAPY. With narrowband UVB, the light tubes produce a narrow part of the UVB spectrum. Two wavelengths
 Phototherapy (light therapy) refers to the use of ultraviolet (UV) light to treat moderate to severe eczema in children and adults. Phototherapy is a second-line treatment option that is available at specialist
Phototherapy (light therapy) refers to the use of ultraviolet (UV) light to treat moderate to severe eczema in children and adults. Phototherapy is a second-line treatment option that is available at specialist
Prescribing Information
 Prescribing Information Pr DERMOVATE Cream (clobetasol propionate cream, USP) Pr DERMOVATE Ointment (clobetasol propionate ointment, USP) Topical corticosteroid TaroPharma Preparation Date: A Division
Prescribing Information Pr DERMOVATE Cream (clobetasol propionate cream, USP) Pr DERMOVATE Ointment (clobetasol propionate ointment, USP) Topical corticosteroid TaroPharma Preparation Date: A Division
Patients and methods Study design and eligibility
 Rheumatology 2005;44:1564 1568 Advance Access publication 13 September 2005 Pimecrolimus 1% cream for the treatment of discoid lupus erythematosus A. Tlacuilo-Parra, E. Guevara-Gutie rrez 1, F. Gutie rrez-murillo
Rheumatology 2005;44:1564 1568 Advance Access publication 13 September 2005 Pimecrolimus 1% cream for the treatment of discoid lupus erythematosus A. Tlacuilo-Parra, E. Guevara-Gutie rrez 1, F. Gutie rrez-murillo
Photoprovocation in Cutaneous Lupus Erythematosus: A Multicenter Study Evaluating a Standardized Protocol
 ORIGINAL ARTI Photoprovocation in Cutaneous Lupus Erythematosus: A Multicenter Study Evaluating a Standardized Protocol Annegret Kuhn 1,11, Anna Wozniacka 2, Jacek C. Szepietowski 3, Regine Gläser 4, Percy
ORIGINAL ARTI Photoprovocation in Cutaneous Lupus Erythematosus: A Multicenter Study Evaluating a Standardized Protocol Annegret Kuhn 1,11, Anna Wozniacka 2, Jacek C. Szepietowski 3, Regine Gläser 4, Percy
New and emerging trends in the treatment of atopic dermatitis
 REVIEW New and emerging trends in the treatment of atopic dermatitis Christina M Gelbard 1 Adelaide A Hebert 1,2 1 Departments of Dermatology; 2 Pediatrics, University of Texas-Houston, Houston, TX, USA
REVIEW New and emerging trends in the treatment of atopic dermatitis Christina M Gelbard 1 Adelaide A Hebert 1,2 1 Departments of Dermatology; 2 Pediatrics, University of Texas-Houston, Houston, TX, USA
Subacute cutaneous lupus erythematosus
 Subacute cutaneous lupus erythematosus Barnes Building Photobiology Unit 0161 206 4081 All Rights Reserved 2017. Document for issue as handout. This guide has been written to help answer some of your questions
Subacute cutaneous lupus erythematosus Barnes Building Photobiology Unit 0161 206 4081 All Rights Reserved 2017. Document for issue as handout. This guide has been written to help answer some of your questions
Topical Calcineurin Inhibitors: An Update on Their Use in Cutaneous Lupus Erythematosus
 Clinical Medicine Insights: Dermatology Review Open Access Full open access to this and thousands of other papers at http://www.la-press.com. Topical Calcineurin Inhibitors: An Update on Their Use in Cutaneous
Clinical Medicine Insights: Dermatology Review Open Access Full open access to this and thousands of other papers at http://www.la-press.com. Topical Calcineurin Inhibitors: An Update on Their Use in Cutaneous
Psoriasis. What is Psoriasis? What causes psoriasis? Medical Topics Psoriasis
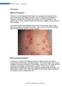 1 Psoriasis What is Psoriasis? Psoriasis is a long standing inflammatory non-contagious skin disease which waxes and wanes with triggering factors. There is a genetic predisposition in psoriasis. Internationally,
1 Psoriasis What is Psoriasis? Psoriasis is a long standing inflammatory non-contagious skin disease which waxes and wanes with triggering factors. There is a genetic predisposition in psoriasis. Internationally,
Development of SLE among Possible SLE Patients Seen in Consultation: Long-Term Follow-Up. Disclosures. Background. Evidence-Based Medicine.
 Development of SLE among Patients Seen in Consultation: Long-Term Follow-Up Abstract # 1699 May Al Daabil, MD Bonnie L. Bermas, MD Alexander Fine Hsun Tsao Patricia Ho Joseph F. Merola, MD Peter H. Schur,
Development of SLE among Patients Seen in Consultation: Long-Term Follow-Up Abstract # 1699 May Al Daabil, MD Bonnie L. Bermas, MD Alexander Fine Hsun Tsao Patricia Ho Joseph F. Merola, MD Peter H. Schur,
Atopic dermatitis (AD) is a common chronic skin. Phototherapy in the management of atopic dermatitis: a systematic review.
 Photodermatol Photoimmunol Photomed 2007; 23: 106 112 Blackwell Munksgaard r 2007 The Authors Journal compilation r 2007 Blackwell Munksgaard Review article Phototherapy in the management of atopic dermatitis:
Photodermatol Photoimmunol Photomed 2007; 23: 106 112 Blackwell Munksgaard r 2007 The Authors Journal compilation r 2007 Blackwell Munksgaard Review article Phototherapy in the management of atopic dermatitis:
Skin cancers in patients treated with immunomodulating drugs. Manuelle Viguier, MD, PhD Dermatology department Saint-Louis Hospital Paris, France
 Skin cancers in patients treated with immunomodulating drugs Manuelle Viguier, MD, PhD Dermatology department Saint-Louis Hospital Paris, France Immunomodulating drugs used in Methotrexate Mycophenolate
Skin cancers in patients treated with immunomodulating drugs Manuelle Viguier, MD, PhD Dermatology department Saint-Louis Hospital Paris, France Immunomodulating drugs used in Methotrexate Mycophenolate
See Important Reminder at the end of this policy for important regulatory and legal information.
 Policy: Atopic Dermatitis and Topical Antipsoriatics Reference Number: TCHP.PHAR.18004 Effective Date: 01.01.18 Last Review Date: 10.12.18 Line of Business: Oregon Health Plan Revision Log See Important
Policy: Atopic Dermatitis and Topical Antipsoriatics Reference Number: TCHP.PHAR.18004 Effective Date: 01.01.18 Last Review Date: 10.12.18 Line of Business: Oregon Health Plan Revision Log See Important
Cutaneous Lupus Erythematosus Diagnosis, Classification, and Screening for Systemic Disease
 Cutaneous Lupus Erythematosus Diagnosis, Classification, and Screening for Systemic Disease David A. Wetter, M.D. Professor of Dermatology, Mayo Clinic (Rochester, MN) Cutaneous Lupus and Dermatomyositis
Cutaneous Lupus Erythematosus Diagnosis, Classification, and Screening for Systemic Disease David A. Wetter, M.D. Professor of Dermatology, Mayo Clinic (Rochester, MN) Cutaneous Lupus and Dermatomyositis
The Sun and Your Skin
 The Sun and Your Skin Karla S. Rosenman MD Park Nicollet Dermatology Skin Anatomy Skin Anatomy 1 Sunlight Ultraviolet (UV) radiation is carcinogenic to humans, causing all major types of skin cancer. UV-emitting
The Sun and Your Skin Karla S. Rosenman MD Park Nicollet Dermatology Skin Anatomy Skin Anatomy 1 Sunlight Ultraviolet (UV) radiation is carcinogenic to humans, causing all major types of skin cancer. UV-emitting
Atopic dermatitis: tacrolimus vs. topical corticosteroid use
 Atopic dermatitis: tacrolimus vs. topical corticosteroid use Langa Y, BPharm Van der Merwe E, BPharm, MSc (Pharmacology) Correspondence to: Elsabe van der Merwe, e-mail: elsabev@medikredit.co.za Keywords:
Atopic dermatitis: tacrolimus vs. topical corticosteroid use Langa Y, BPharm Van der Merwe E, BPharm, MSc (Pharmacology) Correspondence to: Elsabe van der Merwe, e-mail: elsabev@medikredit.co.za Keywords:
Clinical Commissioning Policy Statement: Rituximab For Systemic Lupus Erythematosus (SLE) December Reference : NHSCB/A3C/1b
 Clinical Commissioning Policy Statement: Rituximab For Systemic Lupus Erythematosus (SLE) December 2012 Reference : NHSCB/A3C/1b NHS Commissioning Board Clinical Commissioning Policy Statement: Rituximab
Clinical Commissioning Policy Statement: Rituximab For Systemic Lupus Erythematosus (SLE) December 2012 Reference : NHSCB/A3C/1b NHS Commissioning Board Clinical Commissioning Policy Statement: Rituximab
Spondyloarthropathies: Disease Perception Limits Market
 Spondyloarthropathies: Disease Perception Limits Market Psoriatic arthritis and ankylosing spondylitis form part of the group of diseases known as the spondyloarthropathies. Psoriatic arthritis is a form
Spondyloarthropathies: Disease Perception Limits Market Psoriatic arthritis and ankylosing spondylitis form part of the group of diseases known as the spondyloarthropathies. Psoriatic arthritis is a form
0BCore Safety Profile. Pharmaceutical form(s)/strength: Cream 1% DK/H/PSUR/0009/005 Date of FAR:
 0BCore Safety Profile Active substance: Pimecrolimus Pharmaceutical form(s)/strength: Cream 1% P-RMS: DK/H/PSUR/0009/005 Date of FAR: 06.06.2013 4.3 Contraindications Hypersensitivity to pimecrolimus,
0BCore Safety Profile Active substance: Pimecrolimus Pharmaceutical form(s)/strength: Cream 1% P-RMS: DK/H/PSUR/0009/005 Date of FAR: 06.06.2013 4.3 Contraindications Hypersensitivity to pimecrolimus,
Pimecrolimus A Safe and Effective Local Immunomodulator in the Treatment of Inflammatory Skin Diseases
 2005;13(1):63-69 REVIEW Pimecrolimus A Safe and Effective Local Immunomodulator in the Treatment of Inflammatory Skin Diseases Jasna Lipozenčić University Department of Dermatology and Venereology, Zagreb
2005;13(1):63-69 REVIEW Pimecrolimus A Safe and Effective Local Immunomodulator in the Treatment of Inflammatory Skin Diseases Jasna Lipozenčić University Department of Dermatology and Venereology, Zagreb
CPC. Chutika Srisuttiyakorn, M.D. Kobkul Aunhachoke, M.D. Phramongkutklao Hospital Bangkok, Thailand
 CPC Chutika Srisuttiyakorn, M.D. Kobkul Aunhachoke, M.D. Phramongkutklao Hospital Bangkok, Thailand A 53 year-old woman with fever, facial swelling and rashes on face, trunk and upper extremities for 3
CPC Chutika Srisuttiyakorn, M.D. Kobkul Aunhachoke, M.D. Phramongkutklao Hospital Bangkok, Thailand A 53 year-old woman with fever, facial swelling and rashes on face, trunk and upper extremities for 3
An otherwise healthy 12-year-old
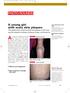 1105 Photo Rounds.finalREV 10/19/05 2:05 PM Page 947 A young girl with scaly skin plaques The patient had numerous thick red plaques on her back and the extensor surfaces of elbows, knees, and forearms
1105 Photo Rounds.finalREV 10/19/05 2:05 PM Page 947 A young girl with scaly skin plaques The patient had numerous thick red plaques on her back and the extensor surfaces of elbows, knees, and forearms
Thursday, 21 October :53 - Last Updated Thursday, 11 November :27
 1 / 15 2 / 15 3 / 15 4 / 15 Pityriasis Alba Background Pityriasis alba is a nonspecific dermatitis of unknown etiology that causes erythematous scaly patches. These resolve and leave areas of hypopigmentation
1 / 15 2 / 15 3 / 15 4 / 15 Pityriasis Alba Background Pityriasis alba is a nonspecific dermatitis of unknown etiology that causes erythematous scaly patches. These resolve and leave areas of hypopigmentation
Annular elastolytic giant cell granuloma presented with annular erythematous patches over the face and cheek in a Chinese lady
 Hong Kong J. Dermatol. Venereol. (2009) 17, 151-155 Case Report Annular elastolytic giant cell granuloma presented with annular erythematous patches over the face and cheek in a Chinese lady SKF Loo, LY
Hong Kong J. Dermatol. Venereol. (2009) 17, 151-155 Case Report Annular elastolytic giant cell granuloma presented with annular erythematous patches over the face and cheek in a Chinese lady SKF Loo, LY
Texas Children's Hospital Dermatology Service PCP Referral Guidelines- Atopic Dermatitis (AD)
 Diagnosis: ATOPIC DERMATITIS (AD) Texas Children's Hospital Dermatology Service PCP Referral Guidelines- Atopic Dermatitis (AD) PATIENT ADVICE: Unfortunately, there is no cure for atopic dermatitis, so
Diagnosis: ATOPIC DERMATITIS (AD) Texas Children's Hospital Dermatology Service PCP Referral Guidelines- Atopic Dermatitis (AD) PATIENT ADVICE: Unfortunately, there is no cure for atopic dermatitis, so
Atopic dermatitis Tacrolimus vs topical corticosteroid use
 Atopic dermatitis Tacrolimus vs topical corticosteroid use Yolande Langa, BPharm Elsabé van der Merwe, BPharm; MSc (Pharmacology) Abstract Atopic dermatitis (AD), the dermatologic manifestation of the
Atopic dermatitis Tacrolimus vs topical corticosteroid use Yolande Langa, BPharm Elsabé van der Merwe, BPharm; MSc (Pharmacology) Abstract Atopic dermatitis (AD), the dermatologic manifestation of the
Increased expression of guanylate binding protein-1 in lesional skin of patients with cutaneous lupus erythematosus
 DOI:10.1111/j.1600-0625.2010.01160.x www.blackwellpublishing.com/exd Original Article Increased expression of guanylate binding protein-1 in lesional skin of patients with cutaneous lupus erythematosus
DOI:10.1111/j.1600-0625.2010.01160.x www.blackwellpublishing.com/exd Original Article Increased expression of guanylate binding protein-1 in lesional skin of patients with cutaneous lupus erythematosus
Contact Dermatitis In Atopic Patients
 Contact Dermatitis In Atopic Patients Jenny Murase, MD Palo Alto Foundation Medical Group Director of Patch Testing University of California, San Francisco Associate Clinical Professor Disclosures Consultant
Contact Dermatitis In Atopic Patients Jenny Murase, MD Palo Alto Foundation Medical Group Director of Patch Testing University of California, San Francisco Associate Clinical Professor Disclosures Consultant
Summary Article: Lupus (Systemic Lupus Erythematosus) from Harvard Medical School Health Topics A-Z
 Topic Page: Systemic Lupus Erythematosus Summary Article: Lupus (Systemic Lupus Erythematosus) from Harvard Medical School Health Topics A-Z What Is It? Lupus is thought to develop when the immune system
Topic Page: Systemic Lupus Erythematosus Summary Article: Lupus (Systemic Lupus Erythematosus) from Harvard Medical School Health Topics A-Z What Is It? Lupus is thought to develop when the immune system
Children s Hospital Of Wisconsin
 Children s Hospital Of Wisconsin Co-Management Guidelines To support collaborative care, we have developed guidelines for our community providers to utilize when referring to, and managing patients with,
Children s Hospital Of Wisconsin Co-Management Guidelines To support collaborative care, we have developed guidelines for our community providers to utilize when referring to, and managing patients with,
ANNEX I SUMMARY OF PRODUCT CHARACTERISTICS
 ANNEX I SUMMARY OF PRODUCT CHARACTERISTICS 1 1. NAME OF THE MEDICINAL PRODUCT Protopic 0.03% ointment 2. QUALITATIVE AND QUANTITATIVE COMPOSITION 1 g of Protopic 0.03% ointment contains 0.3 mg of tacrolimus
ANNEX I SUMMARY OF PRODUCT CHARACTERISTICS 1 1. NAME OF THE MEDICINAL PRODUCT Protopic 0.03% ointment 2. QUALITATIVE AND QUANTITATIVE COMPOSITION 1 g of Protopic 0.03% ointment contains 0.3 mg of tacrolimus
A Retrospective Study on the Risk of Non-Melanoma Skin Cancer in PUVA and Narrowband UVB Treated Patients
 Volume 1, Issue 3 Research Article A Retrospective Study on the Risk of Non-Melanoma Skin Cancer in PUVA and Narrowband UVB Treated Patients Darukarnphut P, Rattanakaemakorn P *, Rajatanavin N Division
Volume 1, Issue 3 Research Article A Retrospective Study on the Risk of Non-Melanoma Skin Cancer in PUVA and Narrowband UVB Treated Patients Darukarnphut P, Rattanakaemakorn P *, Rajatanavin N Division
Definition Chronic autoimmune disease The body s immune system starts attacking itself Can affect most organs and tissues in the body Brain, lungs, he
 LIVING WITH SYSTEMIC LUPUS ERYTHEMATOSUS Stacy Kennedy, M.D.,M.B.A. Rowan Diagnostic Clinic Salisbury, N.C. May 11, 2013 Agenda What is lupus Who is affected Causes of lupus Symptoms and organ involvement
LIVING WITH SYSTEMIC LUPUS ERYTHEMATOSUS Stacy Kennedy, M.D.,M.B.A. Rowan Diagnostic Clinic Salisbury, N.C. May 11, 2013 Agenda What is lupus Who is affected Causes of lupus Symptoms and organ involvement
More Non-infectious Granulomatous Diseases! Karolyn Wanat, MD Assistant Professor, Dermatology & Pathology University of Iowa
 More Non-infectious Granulomatous Diseases! Karolyn Wanat, MD Assistant Professor, Dermatology & Pathology University of Iowa Conflicts of Interest/Disclosure None Classification/Overview 1) Necrobiotic/Palisading
More Non-infectious Granulomatous Diseases! Karolyn Wanat, MD Assistant Professor, Dermatology & Pathology University of Iowa Conflicts of Interest/Disclosure None Classification/Overview 1) Necrobiotic/Palisading
Enstilar , Version 3 PUBLIC SUMMARY OF RISK MANAGEMENT PLAN
 Enstilar 21.1.2016, Version 3 PUBLIC SUMMARY OF RISK MANAGEMENT PLAN VI.2.1 Overview of disease epidemiology Psoriasis is a common skin disease where parts of the skin develop into thick, red and scaly
Enstilar 21.1.2016, Version 3 PUBLIC SUMMARY OF RISK MANAGEMENT PLAN VI.2.1 Overview of disease epidemiology Psoriasis is a common skin disease where parts of the skin develop into thick, red and scaly
What s Topical About Topicals?
 What s Topical About Topicals? Megha M. Tollefson, MD Associate Professor of Dermatology and Pediatrics July 29, 2017 2015 MFMER 3513105-1 Disclosures None 2015 MFMER 3513105-2 Outline Topical steroids
What s Topical About Topicals? Megha M. Tollefson, MD Associate Professor of Dermatology and Pediatrics July 29, 2017 2015 MFMER 3513105-1 Disclosures None 2015 MFMER 3513105-2 Outline Topical steroids
KEY MESSAGES. Psoriasis patients are more prone to cardiovascular diseases, stroke, lymphoma and non-melanoma skin cancers, and increased mortality.
 KEY MESSAGES Psoriasis is a genetically determined, systemic immune-mediated chronic inflammatory disease that affects primarily the skin and joints. Psoriasis Vulgaris is characterised by well-demarcated
KEY MESSAGES Psoriasis is a genetically determined, systemic immune-mediated chronic inflammatory disease that affects primarily the skin and joints. Psoriasis Vulgaris is characterised by well-demarcated
Eucrisa. Eucrisa (crisaborole) Description
 Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.90.25 Subject: Eucrisa Page: 1 of 6 Last Review Date: September 15, 2017 Eucrisa Description Eucrisa
Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.90.25 Subject: Eucrisa Page: 1 of 6 Last Review Date: September 15, 2017 Eucrisa Description Eucrisa
Successful Treatment of Generalized Discoid Lupus Erythematosus with Imiquimod Cream 5%: A Case Report and Review of the Literature
 2014;22(2):155-159 CASE REPORT Successful Treatment of Generalized Discoid Lupus Erythematosus with Imiquimod Cream 5%: A Case Report and Review of the Literature Enver Turan 1, Isin Sinem Bagci 2, Asli
2014;22(2):155-159 CASE REPORT Successful Treatment of Generalized Discoid Lupus Erythematosus with Imiquimod Cream 5%: A Case Report and Review of the Literature Enver Turan 1, Isin Sinem Bagci 2, Asli
A randomized, controlled study of the safety and efficacy of topical corticosteroid treatments of sunburn in healthy volunteers
 Experimental dermatology Original article A randomized, controlled study of the safety and efficacy of topical corticosteroid treatments of sunburn in healthy volunteers L. Duteil, C. Queille-Roussel,
Experimental dermatology Original article A randomized, controlled study of the safety and efficacy of topical corticosteroid treatments of sunburn in healthy volunteers L. Duteil, C. Queille-Roussel,
Topical Calcipotriol Algorithm
 Topical Calcipotriol Algorithm Is this patient an adult previously diagnosed with psoriasis by a doctor? Do the skin patches look the same as those diagnosed as psoriasis? Is this psoriasis covering an
Topical Calcipotriol Algorithm Is this patient an adult previously diagnosed with psoriasis by a doctor? Do the skin patches look the same as those diagnosed as psoriasis? Is this psoriasis covering an
UNDERSTANDING SYSTEMIC LUPUS ERYTHEMATOSUS
 UNDERSTANDING SYSTEMIC LUPUS ERYTHEMATOSUS Stacy Kennedy, M.D.,M.B.A. October 20, 2012 Agenda What is lupus Who is affected Causes of lupus Symptoms and organ involvement Diagnosis Treatment Pregnancy
UNDERSTANDING SYSTEMIC LUPUS ERYTHEMATOSUS Stacy Kennedy, M.D.,M.B.A. October 20, 2012 Agenda What is lupus Who is affected Causes of lupus Symptoms and organ involvement Diagnosis Treatment Pregnancy
Atopic dermatitis/ eczema (a condition that makes skin red and itchy):
 VI.2 Elements for a Public Summary VI.2.1 Overview of disease epidemiology Atopic dermatitis/ eczema (a condition that makes skin red and itchy): Atopic dermatitis (AD) is a common skin condition with
VI.2 Elements for a Public Summary VI.2.1 Overview of disease epidemiology Atopic dermatitis/ eczema (a condition that makes skin red and itchy): Atopic dermatitis (AD) is a common skin condition with
Coverage Criteria: Express Scripts, Inc. monograph dated 12/15/ months or as otherwise noted by indication
 BENEFIT DESCRIPTION AND LIMITATIONS OF COVERAGE ITEM: PRODUCT LINES: COVERED UNDER: DESCRIPTION: CPT/HCPCS Code: Company Supplying: Setting: Kineret (anakinra subcutaneous injection) Commercial HMO/PPO/CDHP
BENEFIT DESCRIPTION AND LIMITATIONS OF COVERAGE ITEM: PRODUCT LINES: COVERED UNDER: DESCRIPTION: CPT/HCPCS Code: Company Supplying: Setting: Kineret (anakinra subcutaneous injection) Commercial HMO/PPO/CDHP
Eucrisa. Eucrisa (crisaborole) Description
 Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 Subject: Eucrisa Page: 1 of 7 Last Review Date: June 22, 2018 Eucrisa Description Eucrisa (crisaborole)
Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 Subject: Eucrisa Page: 1 of 7 Last Review Date: June 22, 2018 Eucrisa Description Eucrisa (crisaborole)
LUMACIP PLUS Cream (Fluocinolone acetonide 0.01% + Hydroquinone 4% + Tretinoin 0.05%)
 Published on: 10 Jul 2014 LUMACIP PLUS Cream (Fluocinolone acetonide 0.01% + Hydroquinone 4% + Tretinoin 0.05%) Composition LUMACIP PLUS Cream Each gram contains: Fluocinolone acetonide IP.. 0.01% w/w
Published on: 10 Jul 2014 LUMACIP PLUS Cream (Fluocinolone acetonide 0.01% + Hydroquinone 4% + Tretinoin 0.05%) Composition LUMACIP PLUS Cream Each gram contains: Fluocinolone acetonide IP.. 0.01% w/w
Follow this and additional works at: Part of the Medicine and Health Sciences Commons
 Philadelphia College of Osteopathic Medicine DigitalCommons@PCOM PCOM Physician Assistant Studies Student Scholarship Student Dissertations, Theses and Papers 2012 Is High Dose Intramuscular Alefacept
Philadelphia College of Osteopathic Medicine DigitalCommons@PCOM PCOM Physician Assistant Studies Student Scholarship Student Dissertations, Theses and Papers 2012 Is High Dose Intramuscular Alefacept
Prescribing Information. Taro-Clobetasol. Taro-Clobetasol
 Prescribing Information Pr Taro-Clobetasol Clobetasol Propionate Cream USP, 0.05% w/w Pr Taro-Clobetasol Clobetasol Propionate Ointment USP, 0.05% w/w Therapeutic Classification Topical corticosteroid
Prescribing Information Pr Taro-Clobetasol Clobetasol Propionate Cream USP, 0.05% w/w Pr Taro-Clobetasol Clobetasol Propionate Ointment USP, 0.05% w/w Therapeutic Classification Topical corticosteroid
ORIGINAL ARTICLES. Limitations: Data resulting from standardized experimental phototesting might not be transferable to a clinical setting.
 ORIGINAL ARTICLES Photoprotective effects of a broad-spectrum sunscreen in ultraviolet-induced cutaneous lupus erythematosus: A randomized, vehicle-controlled, double-blind study Annegret Kuhn, MD, a Kristina
ORIGINAL ARTICLES Photoprotective effects of a broad-spectrum sunscreen in ultraviolet-induced cutaneous lupus erythematosus: A randomized, vehicle-controlled, double-blind study Annegret Kuhn, MD, a Kristina
Classification of segmental vitiligo on the trunk N. van Geel, S. Bosma, B. Boone and R. Speeckaert
 PLAIN LANGUAGE SUMMARIES Classification of segmental vitiligo on the trunk N. van Geel, S. Bosma, B. Boone and R. Speeckaert This summary relates to DOI: 10.1111/bjd.12652 British Journal of Dermatology,
PLAIN LANGUAGE SUMMARIES Classification of segmental vitiligo on the trunk N. van Geel, S. Bosma, B. Boone and R. Speeckaert This summary relates to DOI: 10.1111/bjd.12652 British Journal of Dermatology,
