Cerebral involvement in IgG4-related disease
|
|
|
- Suzan Mathews
- 5 years ago
- Views:
Transcription
1 ORIGINAL RESEARCH Clinical Medicine 2015 Vol 15, No 2: Cerebral involvement in IgG4-related disease Authors: Deepak Joshi, A Rolf Jager, B Steven Hurel, C Stephen P Pereira, D Gavin J Johnson, E Michael Chapman, F Robert Fowler, G Alison Winstanley, H Nicholas Losseff I and George JM Webster J ABSTRACT IgG4-related disease is a recently recognised multi-system disease. Common organ involvement includes the pancreas, biliary tree and salivary glands. Central nervous system involvement has been infrequently reported. In a single-centre cohort of 84 patients, we report cerebral involvement in three (4%) patients. Details of cerebral involvement in these patients are outlined, including pituitary involvement in two patients and a diffuse autoimmune-like encephalopathy in the other. KEYWORDS: Autoimmune pancreatitis, IgG4-related disease, hypophysitis, encephalopathy Introduction IgG4-related disease (IgG4-RD) is an emerging disease entity that was initially described in 2003 as a multi-systemic disease in patients with autoimmune pancreatitis (AIP). 1,2 At presentation, over 50% of patients show evidence of multiorgan disease. 3,4 IgG4-RD involvement has been reported in almost every organ system, including the kidneys, biliary tree, liver, salivary gland, orbit, breast, pericardium, aorta, skin, lungs and prostate. 5-8 IgG4-RD is associated with significant patient morbidity and mortality. 9 Authors: A locum consultant hepatologist, Department of Gastroenterology, University College London Hospitals, London, UK; B professor of neuroradiology, Department of Radiology, University College London Hospitals, London, UK; C consultant endocrinologist, Department of Endocrinology, University College London Hospitals, London, UK; D reader in hepatology and gastroenterology, Department of Gastroenterology, University College London Hospitals, London, UK; E consultant gastroenterologist, Department of Gastroenterology, University College London Hospitals, London, UK; F consultant gastroenterologist, Department of Gastroenterology, University College London Hospitals, London, UK; G consultant respiratory physician, Department of Respiratory Medicine, Barking, Havering and Redbridge University Hospitals, UK; H consultant histopathologist, Department of Pathology, University College London Hospitals, London, UK; I consultant neurologist, The National Hospital for Neurology and Neurosurgery, London, UK; J consultant gastroenterologist, Department of Gastroenterology, University College London Hospitals, London, UK A number of diagnostic criteria have been used for IgG4- RD, including the recent International Consensus Diagnostic Criteria (ICDC). 10 During the period of this study, the HISORt criteria proposed by the Mayo Clinic were used in the diagnosis of AIP 11 and its extra-pancreatic manifestations. These criteria include diagnostic histology, characteristic imaging, elevated serum IgG4 levels on serological testing, other organ involvement and response to steroid therapy. The pathological hallmark of IgG4-RD is a lymphoplasmacytic tissue infiltration with IgG4-positive plasma cells (30 50 IgG4-positive cells per high-powered field), a storiform fibrosis (whorled or cartwheel appearance) and obliterative phlebitis. 12 Tissue eosinophilia may also be present. Serum IgG4 levels are characteristically raised, but may be normal in up to 40% of patients. 13 A favorable objective response to immunosuppression (eg corticosteroids) is seen in most patients. 12 Individual case reports have recently described pituitary disease in patients with IgG4-RD In a prospectively followed group of patients with IgG4-RD, we investigated the frequency and clinical presentation of cerebral disease. Methods All patients referred with a suspected diagnosis of IgG4-RD to the Gastroenterology Unit at University College Hospital, London, UK between March 2004 and October 2013 were followed prospectively. The diagnosis of IgG4-RD was made according to the Mayo Clinic HiSORt criteria. 11 Neurological investigations were performed in patients with overt symptoms or clinical problems suggestive of cerebral disease. Other causes of cerebral disease were actively excluded. Imaging, blood tests and biopsies were performed according to clinical need. In patients with active disease, a reducing course of oral prednisolone was given, tailored to clinical response. Clinical relapse post-treatment was treated with the reintroduction of steroids and commencement of azathioprine (target dose 2 mg/kg/day). Clinical follow up was performed every 2 4 weeks during the initial steroid treatment phase, and subsequently every 3 6 weeks according to clinical progress. Results A diagnosis of IgG4-RD was made in 84 patients seen during the study period. All were treated with a course of steroids. Clinical cerebral disease was identified in three (4%) patients, details of which are reported below. 130 Royal College of Physicians All rights reserved.
2 Cerebral involvement in IgG4-related disease Fig 1. Endoscopic retrograde cholangiopancreatogram (case 1). Strictured and diffusely abnormal intrahepatic ducts (thin arrow) and main pancreatic duct (thick arrow) at the time of the initial presentation with jaundice. Case 1 A 56-year-old male presented with malaise and abnormal liver function tests. Computed tomography (CT) imaging showed intrahepatic biliary dilatation, pancreatic enlargement, gastric and small bowel wall thickening, and mesenteric lymphadenopathy. Relevant blood tests showed a normochromic normocytic anaemia, cholestatic liver function, and a raised serum IgG4 of 2.3 g/l (normal range <1.3 g/l). Endoscopic retrograde cholangiopancreatography (ERCP) showed strictured and diffusely abnormal intrahepatic ducts and main pancreatic duct (Fig 1). Percutaneous biopsy of an enlarged submandibular salivary gland revealed a chronic lymphoplasmacytic infiltrate, with >10 IgG4-positive plasma cells per high-power film. The clinical picture was consistent with type-1 AIP and IgG4-RD, and the patient was commenced on a reducing course of prednisolone (30 mg daily). This led to biochemical, radiological and symptomatic improvement. During steroid reduction, the patient developed angina, with coronary angiography showing three-vessel coronary disease. He underwent coronary artery bypass surgery while on maintenance prednisolone 5 mg OD. Two weeks after an initially uneventful recovery, he developed confusion and a decreased consciousness level. Neurological and cardiac assessment, including a contrast CT scan, excluded a thromboembolic event. Serial electroencephalograms showed non-specific changes with generalised slow activity, indicating severe encephalopathy. Serial gadolinium-enhanced magnetic resonance imaging (MRI) suggested progressive diffuse periventricular and subcortical white matter signal change. The abnormal white matter showed small areas of restricted diffusion, and also areas of free diffusion with generalised volume loss, enlargement of ventricles and widening of sulci Fig 2. Gadolinium-enhanced MRI head (case 1). (a) Cerebral changes demonstrating increased abnormal white matter with small areas of restricted diffusion, and areas of free diffusion with generalised volume loss, enlargement of ventricles and widening of sulci. (b) Evolution of MRI changes was seen despite empirical treatment with high-dose steroid therapy, intravenous immunoglobulin, and antiviral and antifungal medication. MRI = magnetic resonance imaging. (Fig 2a). The cerebrospinal fluid (CSF) was clear, colourless, acellular, and had normal protein levels 0.32 g/l (normal range g/l). No signs of systemic sepsis were evident. Antineuronal antibodies were negative. This neurological picture was thought to be most consistent with an autoimmune encephalopathy. Consent for a brain biopsy was not obtained. Despite empirical treatment with high-dose steroid therapy, intravenous immunoglobulin, and antiviral and antifungal medication the patient showed no significant clinical improvement, although evolution of MRI changes was seen (Fig 2b). He remained dependant for all daily activities and was transferred to a long-term rehabilitation unit. The patient subsequently died, 11 months after the initial cerebral decompensation. A post-mortem was not performed. Royal College of Physicians All rights reserved. 131
3 Deepak Joshi, Rolf Jager, Steven Hurel et al Case 2 A 67-year-old man presented with obstructive jaundice. Imaging showed a low bile duct stricture that was associated with enlargement of the head of the pancreas. The clinical impression was that of carcinoma of the head of pancreas. At surgery, the head of pancreas could not be resected and therefore, a Rouxen-Y hepaticojejunostomy was performed. Intraoperative pancreatic biopsies showed chronic inflammation but no malignancy. Jaundice persisted post-operatively, with magnetic resonance cholangiopancreatography and percutaneous transhepatic cholangiography showing anastomotic and intrahepatic duct stricturing. The patient was subsequently referred to our unit, where serum IgG4 was shown to be elevated at 2.4 g/l. A diagnosis of type-1 AIP and IgG4-related cholangitis was made, and the patient s bilirubin normalised after commencing oral prednisolone 30 mg OD. Steroids were reduced and stopped after a five-month course. Four months later he developed further jaundice. Percutaneous transhepatic cholangiogram showed worsening biliary strictures, but no improvement was seen with further percutaneous drainage and balloon dilatation. Liver biopsy showed large duct obstruction, severe fibrosis/pre-cirrhosis, and a lymphoplasmacytic infiltrate, with >10 IgG4-positive plasma cells per high-power film. Oral steroids were recommenced in addition to azathioprine (2 mg/kg/day) resulting in normalisation of liver function tests. Following slow reduction and cessation of steroids (over six months), and maintenance of azathioprine (at <1 mg/kg/day in view of nausea), the patient re-presented with a two-week history of profound weakness and malaise. There was no history of headache, fever, or jaundice. Examination revealed a heart rate of 80 beats/min and systemic blood pressure of 80/40 mmhg, but no other specific signs. The clinical impression was of adrenal insufficiency (which was assumed to be secondary to prolonged steroid use). Random cortisol was markedly low at <20 nmol/l (normal midnight level <140 nmol/l), but thyroid function tests showed low levels of T4 at 7.2 pmol/l (normal range pmol/l) and thyroid stimulating hormone (TSH) at 0.7 miu/l (range miu/l), suggesting possible pan-hypopituitarism. This diagnosis was confirmed, with results showing luteinizing hormone (LH) <0.1 IU/l (normal range IU/l), follicle-stimulating hormone (FSH) 0.8 IU/l (normal range IU/l), and testosterone <0.1 nmol/l (normal range nmol/l). Diabetes insipidus was also suggested by a history of polyuria and polydypsia, normal blood glucose, serum osmolality 294 mosmol/kg (normal range mosmol/kg) and urine osmolality 263 mosmol/kg (normal range mosmol/kg). CT scan showed prominence of the pituitary stalk, but no other cerebral abnormality. Gadolinium-enhanced MRI showed enlargement and infiltration of the pituitary stalk, consistent with inflammation, rather than tumour (Fig 3a). The presumptive diagnosis of IgG4-related lymphoplasmacytic hypophysitis causing panhypopituitarism was made. The step-wise introduction of replacement hydrocortisone, fludrocortisone, testosterone, thyroxine and desmopressin led to resolution of symptoms. Prednisolone 30 mg was recommenced, as was azathioprine at 1.5 mg/kg/day, which led to complete resolution of the pituitary infiltrate on repeat gadolinium MRI six weeks later (Fig 3b). The patient remained clinically well on immunosuppression and had no further pituitary symptoms. Nevertheless, he represented eight months later with worsening jaundice in the absence of new dominant biliary strictures, and subsequently died from decompensated cirrhosis. Case 3 A 62-year-old Caucasian male presented to his local hospital with polydipsia and polyuria (but normal blood glucose levels), and evidence of hilar and mediastinal lymphadenopathy. A diagnosis of diabetes insipidus was made and the patient was commenced on desmopressin with symptomatic improvement. A CT of his abdomen demonstrated bilateral low-density renal lesions and abnormal tissue surrounding the abdominal aorta and iliac vessels, consistent with retroperitoneal fibrosis. A renal biopsy confirmed a diagnosis of tubulo-interstitial Fig 3. Gadolinium-enhanced MRI head (case 2). (a) Enlargement and infiltration of the pituitary stalk (arrow), consistent with inflammation. A presumptive diagnosis of IgG4- associated lymphoplasmacytic hypophysitis was made. (b) Resolution of the pituitary mass was seen six weeks after recommencing immunosuppression. MRI = magnetic resonance imaging. 132 Royal College of Physicians All rights reserved.
4 Cerebral involvement in IgG4-related disease Table 1. Clinical presentation of the cerebral manifestations of IgG4-related disease. Author n Clinical presentation Taniguchi et al, year-old male with anorexia, vomiting and loss of consciousness Wong et al, year-old male with blurred vision Takuma et al, year-old male with upper eye lid swelling and a visual field defect Wallace et al, year-old female with seizures; 52-year-old female with headache; 39-year-old male with headache and arm numbness; 32-year-old male with weakness Present study 3 56-year-old male with confusion and decreased consciousness; 67-year-old male with weakness and panhypopituitarism; 62-year-old male with polydipsia and polyuria nephritis. Renal function remained normal (creatinine 119 µmol/l, estimated glomerular filtration rate (egfr) >60 ml/min/1.73 m 2 ). Subsequent immunostaining of the renal biopsy confirmed >10 IgG4-positive plasma cells per high-power film. Serum IgG4 levels were also raised (3.07 g/l). A pituitary MRI demonstrated a thickened pituitary stalk and a bulky anterior pituitary. LH, FSH and testosterone levels were normal. A diagnosis of IgG4-RD was made with renal (tubulo-interstitial nephritis), pituitary (hypophysitis) and retroperitoneal (retroperitoneal fibrosis) involvement. The patient was referred to our service at University College London Hospital and was commenced upon prednisone 40 mg OD. A deterioration in renal function was noted at this time point (creatinine 543 µmol/l, egfr 9 ml/min/1.73 m 2 ) but this function subsequently improved following the introduction of steroids. The patient remains well on a low dose of prednisone 10 mg OD with stable renal function (creatinine 148 µmol/l, egfr 44 ml/min/1.73 m 2 ) but remains reluctant to commence azathioprine. Discussion Over the past ten years, it has become accepted that AIP is a global disease, 11,17,18 and that it is one component of a multiorgan IgG4-RD, in which an IgG4-positive lymphoplasmacytic infiltrate within affected tissues is a characteristic feature. 11,19,20 Cerebral involvement in IgG4-RD is rarely reported, with most cases relating to either retro-orbital involvement (with associated infra-orbital nerve swelling 21 and visual field defects 22 ) or to pituitary disease (Table 1). 15,16, 23 Non-infectious hypertrophic pachymeningitis, inflammation and subsequent thickening of the dura mater (cranial or spinal) is regarded as another neurological manifestation of IgG4-RD. 24,25 In our series, we found neurological involvement in 4% of patients. Clearly this may not represent the true prevalence of neurological disease in IgG4-RD as those patients who are referred to a tertiary referral centre may form a skewed subsample of the patient population. Despite this caveat, the brain appears to be a much less common site of involvement than other sites, including the biliary tree, kidneys, salivary glands and retroperitoneum. 26,27 In the cases reported here, unequivocal evidence of an IgG4 inflammatory infiltrate causing neurological disease could not be obtained because of a lack of cerebral histology. Nevertheless, other causes were intensively sought and excluded, and imaging strongly suggested an inflammatory cause. Case reports have recently suggested pituitary involvement in AIP/IgG4-RD diagnosed histologically following pituitary resection. 15 In case 2, it may be that treatment with steroids delayed the clinical presentation of pituitary failure, which occurred only after steroid withdrawal. Swelling of the pituitary stalk may also be seen in sarcoidosis, tuberculosis, Wegner s granulomatosis and lymphocytic hypophysitis. In cases 1 and 2, neither patient showed clinical evidence of worsening pancreatic disease at the time of active neurological disease. This supports the observation that clinical relapse in IgG4-RD most commonly occurs in extrapancreatic sites. 28, 29 The findings also suggest that disease control in one organ (with or without treatment) cannot be assumed to be paralleled in other tissues. Our observation in these two cases was mirrored by another case report in which symptomatic pituitary failure related to lymphocytic hypohysitis developed despite maintenance steroid therapy for AIP. 16 Case 3 presented primarily with symptoms of diabetes insipidus and on subsequent imaging was found to have renal abnormalities and evidence of retroperitoneal fibrosis. Disease relapse is now recognised to occur in at least 40% of AIP/IgG4-RD patients, 28, 30, 31 but appropriate management of this is yet to be defined. It is of note that our patient with panhypopituitarism was on maintenance azathioprine at presentation (albeit at a low dose). The fact the patients in both cases 1 and 2 subsequently died of extra-pancreatic complications supports the argument that those with significant multi-organ involvement may have a more progressive disease. These patients may be more difficult to manage with a single course of steroids than those with disease confined to the pancreas. 28,31,32 We believe that this report emphasises the need to maintain a high-level clinical vigilance for and awareness of the myriad of clinical manifestations of IgG4-RD, including neurological disease. These may occur at presentation or upon follow up. References 1 Kamisawa T, Egawa N, Nakajima H. Autoimmune pancreatitis is a systemic autoimmune disease. Am J Gastroenterol 2003;98: Kamisawa T, Funata N, Hayashi Y et al. A new clinicopathological entity of IgG4-related autoimmune disease. J Gastroenterol 2003;38: Sah RP, Chari ST, Pannala R et al. Differences in clinical profile and relapse rate of type 1 versus type 2 autoimmune pancreatitis. Gastroenterology 2010;139:140 8; quiz e Okazaki K, Uchida K, Koyabu M et al. Recent advances in the concept and diagnosis of autoimmune pancreatitis and IgG4-related disease. J Gastroenterol 2011;46: Dahlgren M, Khosroshahi A, Nielsen GP et al. Riedel s thyroiditis and multifocal fibrosclerosis are part of the IgG4-related systemic disease spectrum. Arthritis Care Res (Hoboken) 2010;62: Royal College of Physicians All rights reserved. 133
5 Deepak Joshi, Rolf Jager, Steven Hurel et al 6 Saeki T, Saito A, Hiura T et al. Lymphoplasmacytic infiltration of multiple organs with immunoreactivity for IgG4: IgG4-related systemic disease. Intern Med 2006;45: Kamisawa T, Takuma K, Egawa N et al. Autoimmune pancreatitis and IgG4-related sclerosing disease. Nat Rev Gastroenterol Hepatol 2010;7: Stone JH, Khosroshahi A, Hilgenberg A et al. IgG4-related systemic disease and lymphoplasmacytic aortitis. Arthritis Rheum 2009;60: Huggett MT, Culver EL, Kumar M et al. Type 1 Autoimmune pancreatitis and IgG4-related sclerosing cholangitis is associated with extrapancreatic organ failure, malignancy, and mortality in a prospective UK cohort. Am J Gastroenterol 2014;109: Shimosegawa T, Chari ST, Frulloni L et al. International consensus diagnostic criteria for autoimmune pancreatitis: guidelines of the International Association of Pancreatology. Pancreas 2011;40: Chari ST, Smyrk TC, Levy MJ et al. Diagnosis of autoimmune pancreatitis: the Mayo Clinic experience. Clin Gastroenterol Hepatol 2006;4:1010 6; quiz Deshpande V, Zen Y, Chan JK et al. Consensus statement on the pathology of IgG4-related disease. Mod Pathol 2012;25: Cheuk W, Chan JK. IgG4-related sclerosing disease: a critical appraisal of an evolving clinicopathologic entity. Adv Anat Pathol 2010;17: Ralli S, Lin J, Farrell J. Autoimmune pancreatitis. N Engl J Med 2007;356:1586; author reply Wong S, Lam WY, Wong WK et al. Hypophysitis presented as inflammatory pseudotumor in immunoglobulin G4-related systemic disease. Hum Pathol 2007;38: Taniguchi T, Hamasaki A, Okamoto M. A case of suspected lymphocytic hypophysitis and organizing pneumonia during maintenance therapy for autoimmune pancreatitis associated with autoimmune thrombocytopenia. Endocr J 2006;53: Varadarajulu S, Cotton PB. Autoimmune pancreatitis: is it relevant in the west? Gastroenterology 2003;125: Church NI, Pereira SP, Deheragoda MG et al. Autoimmune pancreatitis: clinical and radiological features and objective response to steroid therapy in a UK series. Am J Gastroenterol 2007;102: Deheragoda MG, Church NI, Rodriguez-Justo M et al. The use of immunoglobulin g4 immunostaining in diagnosing pancreatic and extrapancreatic involvement in autoimmune pancreatitis. Clin Gastroenterol Hepatol 2007;5: Kamisawa T, Okamoto A. Autoimmune pancreatitis: proposal of IgG4-related sclerosing disease. J Gastroenterol 2006;41: Watanabe T, Fujinaga Y, Kawakami S et al. Infraorbital nerve swelling associated with autoimmune pancreatitis. Jpn J Radiol 2011;29: Takuma K, Kamisawa T, Tabata T et al. Visual field deficit: a rare initial symptom of autoimmune pancreatitis. Intern Med 2011;50: Tabata T, Kamisawa T, Takuma K et al. Serial changes of elevated serum IgG4 levels in IgG4-related systemic disease. Intern Med 2011;50: Wallace ZS, Carruthers MN, Khosroshahi A et al. IgG4-related disease and hypertrophic pachymeningitis. Medicine (Baltimore) 2013;92: Kim EH, Kim SH, Cho JM et al. Immunoglobulin G4-related hypertrophic pachymeningitis involving cerebral parenchyma. J Neurosurg 2011;115: Deshpande V, Mino-Kenudson M, Brugge W et al. Autoimmune pancreatitis: more than just a pancreatic disease? A contemporary review of its pathology. Arch Pathol Lab Med 2005;129: Kamisawa T, Egawa N, Nakajima H et al. Extrapancreatic lesions in autoimmune pancreatitis. J Clin Gastroenterol 2005;39: Sandanayake NS, Church NI, Chapman MH et al. Presentation and management of post-treatment relapse in autoimmune pancreatitis/ immunoglobulin G4-associated cholangitis. Clin Gastroenterol Hepatol 2009;7: Chari ST, Murray JA. Autoimmune pancreatitis, Part II: the relapse. Gastroenterology 2008;134: Kubota K, Watanabe S, Uchiyama T et al. Factors predictive of relapse and spontaneous remission of autoimmune pancreatitis patients treated/not treated with corticosteroids. J Gastroenterol 2011;46: Sugumar A, Chari ST. Diagnosis and treatment of autoimmune pancreatitis. Curr Opin Gastroenterol 2010;26: Takuma K, Kamisawa T, Tabata T et al. Short-term and long-term outcomes of autoimmune pancreatitis. Eur J Gastroenterol Hepatol 2011;23: Address for correspondence: Dr G Webster, Department of Gastroenterology, University College Hospital, Ground Floor West, 250 Euston Road, London NW1 2PG, UK. george.webster@uclh.nhs.uk 134 Royal College of Physicians All rights reserved.
Value of Serum IgG4 in the Diagnosis of Autoimmune Pancreatitis and in Distinguishing it from Acute and Chronic Pancreatitis of Other Etiology
 94 Jul 2017 Vol 10 No.3 North American Journal of Medicine and Science Original Research Value of Serum IgG4 in the Diagnosis of Autoimmune Pancreatitis and in Distinguishing it from Acute and Chronic
94 Jul 2017 Vol 10 No.3 North American Journal of Medicine and Science Original Research Value of Serum IgG4 in the Diagnosis of Autoimmune Pancreatitis and in Distinguishing it from Acute and Chronic
IgG4-related sclerosing disease
 IgG4-related sclerosing disease TERUMI KAMISAWA, KENSUKE TAKUMA, NAOTO EGAWA Department of Internal Medicine Tokyo Metropolitan Komagome Hospital 3-18-22 Honkomagome, Bunkyo-ku, Tokyo 113-8677, Japan JAPAN
IgG4-related sclerosing disease TERUMI KAMISAWA, KENSUKE TAKUMA, NAOTO EGAWA Department of Internal Medicine Tokyo Metropolitan Komagome Hospital 3-18-22 Honkomagome, Bunkyo-ku, Tokyo 113-8677, Japan JAPAN
Immunoglobulin G4-Related Disease with Several Inflammatory Foci
 CASE REPORT Immunoglobulin G4-Related Disease with Several Inflammatory Foci Akira Sakamaki 1, Kenya Kamimura 1, Kazuhiko Shioji 1, Junko Sakurada 2, Takeshi Nakatsue 3, Yoko Wada 3, Michitaka Imai 1,
CASE REPORT Immunoglobulin G4-Related Disease with Several Inflammatory Foci Akira Sakamaki 1, Kenya Kamimura 1, Kazuhiko Shioji 1, Junko Sakurada 2, Takeshi Nakatsue 3, Yoko Wada 3, Michitaka Imai 1,
IgG4 Disease. General Principles of IgG4-related disease. EL Cluvar, AC Bateman
 IgG4 Disease General Principles of IgG4-related disease. EL Cluvar, AC Bateman Diagnostic Guidelines for IgG4-related disease with a focus on histopathological criteria. V Deshpande, A Khosroshahi Diagnostic
IgG4 Disease General Principles of IgG4-related disease. EL Cluvar, AC Bateman Diagnostic Guidelines for IgG4-related disease with a focus on histopathological criteria. V Deshpande, A Khosroshahi Diagnostic
Autoimmune pancreatitis (AIP) was described more than a
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2007;5:1229 1234 The Use of Immunoglobulin G4 Immunostaining in Diagnosing Pancreatic and Extrapancreatic Involvement in Autoimmune Pancreatitis MAESHA G. DEHERAGODA,*
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2007;5:1229 1234 The Use of Immunoglobulin G4 Immunostaining in Diagnosing Pancreatic and Extrapancreatic Involvement in Autoimmune Pancreatitis MAESHA G. DEHERAGODA,*
Comparison of multidetector-row computed tomography findings of IgG4-related sclerosing cholangitis and cholangiocarcinoma
 Comparison of multidetector-row computed tomography findings of IgG4-related sclerosing cholangitis and cholangiocarcinoma Poster No.: C-0245 Congress: ECR 2014 Type: Scientific Exhibit Authors: M. Yata,
Comparison of multidetector-row computed tomography findings of IgG4-related sclerosing cholangitis and cholangiocarcinoma Poster No.: C-0245 Congress: ECR 2014 Type: Scientific Exhibit Authors: M. Yata,
Diagnostic Algorithm for Autoimmune Pancreatitis in Korea
 Review Article The Korean Journal of Pancreas and Biliary Tract 2014;19(1):7-12 pissn 1976-3573 eissn 2288-0941 한국에서자가면역췌장염의진단전략 성균관대학교의과대학삼성서울병원내과학교실 이종균 Diagnostic Algorithm for Autoimmune Pancreatitis
Review Article The Korean Journal of Pancreas and Biliary Tract 2014;19(1):7-12 pissn 1976-3573 eissn 2288-0941 한국에서자가면역췌장염의진단전략 성균관대학교의과대학삼성서울병원내과학교실 이종균 Diagnostic Algorithm for Autoimmune Pancreatitis
The newly recognized fibroinflammatory condition. An orphan disease: IgG4-related spinal pachymeningitis: report of 2 cases
 case report J Neurosurg Spine 25:790 794, 2016 An orphan disease: IgG4-related spinal pachymeningitis: report of 2 cases Bishan D. Radotra, MD, 1 Ashish Aggarwal, DNB, MCh, 2 Ankur Kapoor, MS, MCh, 2 Navneet
case report J Neurosurg Spine 25:790 794, 2016 An orphan disease: IgG4-related spinal pachymeningitis: report of 2 cases Bishan D. Radotra, MD, 1 Ashish Aggarwal, DNB, MCh, 2 Ankur Kapoor, MS, MCh, 2 Navneet
Case Report IgG4-Seronegative Autoimmune Pancreatitis and Sclerosing Cholangitis
 Case Reports in Gastrointestinal Medicine Volume 2015, Article ID 591360, 6 pages http://dx.doi.org/10.1155/2015/591360 Case Report IgG4-Seronegative Autoimmune Pancreatitis and Sclerosing Cholangitis
Case Reports in Gastrointestinal Medicine Volume 2015, Article ID 591360, 6 pages http://dx.doi.org/10.1155/2015/591360 Case Report IgG4-Seronegative Autoimmune Pancreatitis and Sclerosing Cholangitis
How 5 Diseases Became One. Moez Tajdin R3 McGill University
 How 5 Diseases Became One Moez Tajdin R3 McGill University Conflicts of Interest None! Mr. M. ID: 65 M PMH Benign prostatic hyperplasia Prostate cancer Awaiting biopsy Skin rash Dyslipidemia Hypertension
How 5 Diseases Became One Moez Tajdin R3 McGill University Conflicts of Interest None! Mr. M. ID: 65 M PMH Benign prostatic hyperplasia Prostate cancer Awaiting biopsy Skin rash Dyslipidemia Hypertension
IgG4-Negative Autoimmune Pancreatitis with Sclerosing Cholangitis and Colitis: Possible Association with Primary Sclerosing Cholangitis?
 CASE REPORT IgG4-Negative Autoimmune Pancreatitis with Sclerosing Cholangitis and Colitis: Possible Association with Primary Sclerosing Cholangitis? Keita Saeki 1, Shigenari Hozawa 1, Naoteru Miyata 1,
CASE REPORT IgG4-Negative Autoimmune Pancreatitis with Sclerosing Cholangitis and Colitis: Possible Association with Primary Sclerosing Cholangitis? Keita Saeki 1, Shigenari Hozawa 1, Naoteru Miyata 1,
ORIGINAL ARTICLES LIVER, PANCREAS, AND BILIARY TRACT
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2009;7:1089 1096 ORIGINAL ARTICLES LIVER, PANCREAS, AND BILIARY TRACT Presentation and Management of Post-treatment Relapse in Autoimmune Pancreatitis/Immunoglobulin
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2009;7:1089 1096 ORIGINAL ARTICLES LIVER, PANCREAS, AND BILIARY TRACT Presentation and Management of Post-treatment Relapse in Autoimmune Pancreatitis/Immunoglobulin
CASE 01 LA Path Slide Seminar 13 March, 08. Deepti Dhall, MD Department of Pathology and Laboratory Medicine Cedars-Sinai Medical Center
 CASE 01 LA Path Slide Seminar 13 March, 08 Deepti Dhall, MD Department of Pathology and Laboratory Medicine Cedars-Sinai Medical Center Clinical History 60 year old male presented with obstructive jaundice
CASE 01 LA Path Slide Seminar 13 March, 08 Deepti Dhall, MD Department of Pathology and Laboratory Medicine Cedars-Sinai Medical Center Clinical History 60 year old male presented with obstructive jaundice
Overview of the Immunoglobulin G4-related Disease Spectrum
 Review Article The Korean Journal of Pancreas and Biliary Tract 2015;20:124-129 http://dx.doi.org/10.15279/kpba.2015.20.3.124 pissn 1976-3573 eissn 2288-0941 면역글로불린 G4 연관질환의개요 1 한림대학교의과대학한림대학교성심병원내과, 2
Review Article The Korean Journal of Pancreas and Biliary Tract 2015;20:124-129 http://dx.doi.org/10.15279/kpba.2015.20.3.124 pissn 1976-3573 eissn 2288-0941 면역글로불린 G4 연관질환의개요 1 한림대학교의과대학한림대학교성심병원내과, 2
Pituitary Case 2. Dr Lydia Lamb Endocrinology Registrar Fiona Stanley Hospital Western Australia
 Pituitary Case 2 Dr Lydia Lamb Endocrinology Registrar Fiona Stanley Hospital Western Australia History 65yo Chinese Singaporean male referred with androgen deficiency and abnormal CT brain Two month history
Pituitary Case 2 Dr Lydia Lamb Endocrinology Registrar Fiona Stanley Hospital Western Australia History 65yo Chinese Singaporean male referred with androgen deficiency and abnormal CT brain Two month history
A case of retroperitoneal fibrosis responding to steroid therapy
 Challenging Clinical Cases Vol. 43 (6): 1185-1189, November - December, 2017 doi: 10.1590/S1677-5538.IBJU.2016.0520 A case of retroperitoneal fibrosis responding to steroid therapy Ryuta Watanabe 1, Akira
Challenging Clinical Cases Vol. 43 (6): 1185-1189, November - December, 2017 doi: 10.1590/S1677-5538.IBJU.2016.0520 A case of retroperitoneal fibrosis responding to steroid therapy Ryuta Watanabe 1, Akira
Autoimmune Pancreatitis: A Great Imitator
 Massachusetts General Hospital Harvard Medical School Autoimmune Pancreatitis: A Great Imitator Dushyant V Sahani MD dsahani@partners.org Autoimmune Pancreatitis: Learning Objectives Clinical manifestations
Massachusetts General Hospital Harvard Medical School Autoimmune Pancreatitis: A Great Imitator Dushyant V Sahani MD dsahani@partners.org Autoimmune Pancreatitis: Learning Objectives Clinical manifestations
The most common presentation of autoimmune pancreatitis. A Diagnostic Strategy to Distinguish Autoimmune Pancreatitis From Pancreatic Cancer
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2009;7:1097 1103 A Diagnostic Strategy to Distinguish Autoimmune Pancreatitis From Pancreatic Cancer SURESH T. CHARI,* NAOKI TAKAHASHI, MICHAEL J. LEVY,* THOMAS
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2009;7:1097 1103 A Diagnostic Strategy to Distinguish Autoimmune Pancreatitis From Pancreatic Cancer SURESH T. CHARI,* NAOKI TAKAHASHI, MICHAEL J. LEVY,* THOMAS
Long-term Outcome of Autoimmune Pancreatitis after Oral Prednisolone Therapy
 ORIGINAL ARTICLE Long-term Outcome of Autoimmune Pancreatitis after Oral Prednisolone Therapy Takayoshi Nishino 1, Fumitake Toki 2,HiroyasuOyama 3, Kyoko Shimizu 1 and Keiko Shiratori 1 Abstract Objective
ORIGINAL ARTICLE Long-term Outcome of Autoimmune Pancreatitis after Oral Prednisolone Therapy Takayoshi Nishino 1, Fumitake Toki 2,HiroyasuOyama 3, Kyoko Shimizu 1 and Keiko Shiratori 1 Abstract Objective
IgG4 Related disease a retrospective descriptive study highlighting Canadian experiences in diagnosis and management
 Patel et al. BMC Gastroenterology 2013, 13:168 RESEARCH ARTICLE Open Access IgG4 Related disease a retrospective descriptive study highlighting Canadian experiences in diagnosis and management Harshna
Patel et al. BMC Gastroenterology 2013, 13:168 RESEARCH ARTICLE Open Access IgG4 Related disease a retrospective descriptive study highlighting Canadian experiences in diagnosis and management Harshna
FOR PUBLIC CONSULTATION ONLY. Evidence Review: Rituximab for immunoglobulin G4-related disease (IgG4-RD)
 Evidence Review: Rituximab for immunoglobulin G4-related disease (IgG4-RD) NHS England FOR PUBLIC CONSULTATION ONLY Evidence Review: Rituximab for immunoglobulin G4-related disease (IgG4- RD) First published:
Evidence Review: Rituximab for immunoglobulin G4-related disease (IgG4-RD) NHS England FOR PUBLIC CONSULTATION ONLY Evidence Review: Rituximab for immunoglobulin G4-related disease (IgG4- RD) First published:
Hideaki Miura, Yasutaka Miyachi. Department of Internal Medicine, Social Insurance Central General Hospital. Tokyo, Japan
 CASE REPORT IgG4-Related Retroperitoneal Fibrosis and Sclerosing Cholangitis Independent of Autoimmune Pancreatitis. A Recurrent Case after a 5-Year History of Spontaneous Remission Hideaki Miura, Yasutaka
CASE REPORT IgG4-Related Retroperitoneal Fibrosis and Sclerosing Cholangitis Independent of Autoimmune Pancreatitis. A Recurrent Case after a 5-Year History of Spontaneous Remission Hideaki Miura, Yasutaka
Differentiating Immunoglobulin G4-Related Sclerosing Cholangitis from Hilar Cholangiocarcinoma
 Gut and Liver, Vol. 7, No. 2, March 2013, pp. 234-238 ORiginal Article Differentiating Immunoglobulin G4-Related Sclerosing Cholangitis from Hilar Cholangiocarcinoma Taku Tabata*, Terumi Kamisawa*, Seiichi
Gut and Liver, Vol. 7, No. 2, March 2013, pp. 234-238 ORiginal Article Differentiating Immunoglobulin G4-Related Sclerosing Cholangitis from Hilar Cholangiocarcinoma Taku Tabata*, Terumi Kamisawa*, Seiichi
Review Article The Utility of Serum IgG4 Concentrations as a Biomarker
 International Rheumatology Volume 2012, Article ID 198314, 4 pages doi:10.1155/2012/198314 Review Article The Utility of Serum IgG4 Concentrations as a Biomarker Shigeyuki Kawa, 1 Tetsuya Ito, 2 Takayuki
International Rheumatology Volume 2012, Article ID 198314, 4 pages doi:10.1155/2012/198314 Review Article The Utility of Serum IgG4 Concentrations as a Biomarker Shigeyuki Kawa, 1 Tetsuya Ito, 2 Takayuki
Pituitary puzzles: a perplexing headache
 Pituitary puzzles: a perplexing headache Thomas Upton* Steven Soule Department Of Endocrinology Christchurch Hospital, Christchurch, New Zealand Declaration of Interests Novo Nordisk sponsorship, Diabetes
Pituitary puzzles: a perplexing headache Thomas Upton* Steven Soule Department Of Endocrinology Christchurch Hospital, Christchurch, New Zealand Declaration of Interests Novo Nordisk sponsorship, Diabetes
Tratamiento endoscópico de la CEP. En quien como y cuando?
 Tratamiento endoscópico de la CEP. En quien como y cuando? Andrés Cárdenas, MD, MMSc, PhD, AGAF, FAASLD GI / Liver Unit, Hospital Clinic Institut de Malalties Digestives i Metaboliques University of Barcelona
Tratamiento endoscópico de la CEP. En quien como y cuando? Andrés Cárdenas, MD, MMSc, PhD, AGAF, FAASLD GI / Liver Unit, Hospital Clinic Institut de Malalties Digestives i Metaboliques University of Barcelona
Renal manifestations of IgG4-related systemic disease
 Renal manifestations of IgG4-related systemic disease Lynn D. Cornell, M.D. Mayo Clinic Rochester, MN While autoimmune pancreatitis (AIP) has been recognized since the first description by Sarles et al
Renal manifestations of IgG4-related systemic disease Lynn D. Cornell, M.D. Mayo Clinic Rochester, MN While autoimmune pancreatitis (AIP) has been recognized since the first description by Sarles et al
AN UNUSUAL CASE OF OBSTRUCTIVE JAUNDICE- SURGICAL DILEMMA. Dr. Tejaswi Sindhiya Ragni
 AN UNUSUAL CASE OF OBSTRUCTIVE JAUNDICE- SURGICAL DILEMMA Dr. Tejaswi Sindhiya Ragni A 65 year old male from Bangalore, farmer Presented with: Fever - 1 month Yellow discolouration of eyes and urine- 1month
AN UNUSUAL CASE OF OBSTRUCTIVE JAUNDICE- SURGICAL DILEMMA Dr. Tejaswi Sindhiya Ragni A 65 year old male from Bangalore, farmer Presented with: Fever - 1 month Yellow discolouration of eyes and urine- 1month
Autoimmune pancreatitis (AIP) can be defined as a
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2006;4:1010 1016 Diagnosis of Autoimmune Pancreatitis: The Mayo Clinic Experience SURESH T. CHARI,* THOMAS C. SMYRK, MICHAEL J. LEVY,* MARK D. TOPAZIAN,* NAOKI
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2006;4:1010 1016 Diagnosis of Autoimmune Pancreatitis: The Mayo Clinic Experience SURESH T. CHARI,* THOMAS C. SMYRK, MICHAEL J. LEVY,* MARK D. TOPAZIAN,* NAOKI
Case Report Thoracic Paravertebral Mass as an Infrequent Manifestation of IgG4-Related Disease
 Hindawi Case Reports in Rheumatology Volume 2017, Article ID 4716245, 4 pages https://doi.org/10.1155/2017/4716245 Case Report Thoracic Paravertebral Mass as an Infrequent Manifestation of IgG4-Related
Hindawi Case Reports in Rheumatology Volume 2017, Article ID 4716245, 4 pages https://doi.org/10.1155/2017/4716245 Case Report Thoracic Paravertebral Mass as an Infrequent Manifestation of IgG4-Related
IgG4-Related Sclerosing Cholangitis
 REVIEW IgG4-Related Sclerosing Cholangitis Emma L. Culver, B.Sc., M.B.Ch.B., D.Phil., M.R.C.P.,* and Eleanor Barnes, M.B.B.S., D.Phil., M.R.C.P.*,, BACKGROUND IgG4-related sclerosing cholangitis (IgG4-SC)
REVIEW IgG4-Related Sclerosing Cholangitis Emma L. Culver, B.Sc., M.B.Ch.B., D.Phil., M.R.C.P.,* and Eleanor Barnes, M.B.B.S., D.Phil., M.R.C.P.*,, BACKGROUND IgG4-related sclerosing cholangitis (IgG4-SC)
Characteristic feautures of cholangitis with serum IgG4 elevation compared with primary sclerosing cholangitis
 Characteristic feautures of cholangitis with serum IgG4 elevation compared with primary sclerosing cholangitis Poster No.: C-2005 Congress: ECR 2011 Type: Scientific Paper Authors: T. Takeda, T. Ueda,
Characteristic feautures of cholangitis with serum IgG4 elevation compared with primary sclerosing cholangitis Poster No.: C-2005 Congress: ECR 2011 Type: Scientific Paper Authors: T. Takeda, T. Ueda,
Colangitis Esclerosante Primaria: Manejo Clínico y Endoscópico
 Colangitis Esclerosante Primaria: Manejo Clínico y Endoscópico Andrés Cárdenas, MD, MMSc, PhD, AGAF, FAASLD GI / Liver Unit, Hospital Clinic Institut de Malalties Digestives i Metaboliques Associate Professor
Colangitis Esclerosante Primaria: Manejo Clínico y Endoscópico Andrés Cárdenas, MD, MMSc, PhD, AGAF, FAASLD GI / Liver Unit, Hospital Clinic Institut de Malalties Digestives i Metaboliques Associate Professor
IgG4-related hypophysitis presenting as a pituitary adenoma with systemic disease
 Asian Journal of Surgery (2013) 36, 93e97 Available online at www.sciencedirect.com journal homepage: www.e-asianjournalsurgery.com CASE REPORT IgG4-related hypophysitis presenting as a pituitary adenoma
Asian Journal of Surgery (2013) 36, 93e97 Available online at www.sciencedirect.com journal homepage: www.e-asianjournalsurgery.com CASE REPORT IgG4-related hypophysitis presenting as a pituitary adenoma
MULTI-SYSTEM SARCOIDOSIS CAUSING PANHYPOPITUITARISM: RAPID IMPROVEMENT WITH CORTICOSTEROID THERAPY Rashid Mahboob, MD; Ali A.
 ENDOCRINE PRACTICE Rapid Electronic Article in Press Rapid Electronic Articles in Press are preprinted manuscripts that have been reviewed and accepted for publication, but have yet to be edited, typeset
ENDOCRINE PRACTICE Rapid Electronic Article in Press Rapid Electronic Articles in Press are preprinted manuscripts that have been reviewed and accepted for publication, but have yet to be edited, typeset
ESIM Winter School 2014 Case Presentation
 ESIM Winter School 2014 Case Presentation Hacettepe University School of Medicine Ankara/Turkey Ozant Helvaci, M.D. Patient T.K., 59 years old, male, married with one child, unemployed, place of birth/
ESIM Winter School 2014 Case Presentation Hacettepe University School of Medicine Ankara/Turkey Ozant Helvaci, M.D. Patient T.K., 59 years old, male, married with one child, unemployed, place of birth/
IgG4-Related Disease: Dataset of 235 Consecutive Patients
 IgG-Related Disease: Dataset of 235 Consecutive Patients Dai Inoue, MD, PhD, Kotaro Yoshida, MD, PhD, Norihide Yoneda, MD, PhD, Kumi Ozaki, MD, PhD, Takashi Matsubara, MD, PhD, Keiichi Nagai, MD, PhD,
IgG-Related Disease: Dataset of 235 Consecutive Patients Dai Inoue, MD, PhD, Kotaro Yoshida, MD, PhD, Norihide Yoneda, MD, PhD, Kumi Ozaki, MD, PhD, Takashi Matsubara, MD, PhD, Keiichi Nagai, MD, PhD,
Primary Sclerosing Cholangitis and Cholestatic liver diseases. Ahsan M Bhatti MD, FACP Bhatti Gastroenterology Consultants
 Primary Sclerosing Cholangitis and Cholestatic liver diseases Ahsan M Bhatti MD, FACP Bhatti Gastroenterology Consultants I have nothing to disclose Educational Objectives What is PSC? Understand the cholestatic
Primary Sclerosing Cholangitis and Cholestatic liver diseases Ahsan M Bhatti MD, FACP Bhatti Gastroenterology Consultants I have nothing to disclose Educational Objectives What is PSC? Understand the cholestatic
Lymphoplasmacytic sclerosing pancreatitis without IgG4 tissue infiltration or serum IgG4 elevation: IgG4-related disease without IgG4
 238 & 2015 USCAP, Inc All rights reserved 0893-3952/15 $32.00 Lymphoplasmacytic sclerosing pancreatitis without IgG4 tissue infiltration or serum IgG4 elevation: IgG4-related disease without IgG4 Phil
238 & 2015 USCAP, Inc All rights reserved 0893-3952/15 $32.00 Lymphoplasmacytic sclerosing pancreatitis without IgG4 tissue infiltration or serum IgG4 elevation: IgG4-related disease without IgG4 Phil
Key Points: Autoimmune Liver Disease: Update for Pathologists from the Hepatologist s Perspective. Jenny Heathcote, MD. University of Toronto
 Autoimmune Liver Disease: Update for Pathologists from the Hepatologist s Perspective Jenny Heathcote, MD University of Toronto Key Points: AILD comprise autoimmune hepatitis, primary biliary cirrhosis
Autoimmune Liver Disease: Update for Pathologists from the Hepatologist s Perspective Jenny Heathcote, MD University of Toronto Key Points: AILD comprise autoimmune hepatitis, primary biliary cirrhosis
IgG-4 related disease: A mini-review
 www.rarediseasesjournal.com Journal of Rare Diseases Research & Treatment Mini review Open Access IgG-4 related disease: A mini-review Ramy Sedhom 1*, Daniel Sedhom 1 and Roger Strair 2 1 Department of
www.rarediseasesjournal.com Journal of Rare Diseases Research & Treatment Mini review Open Access IgG-4 related disease: A mini-review Ramy Sedhom 1*, Daniel Sedhom 1 and Roger Strair 2 1 Department of
An Autopsy Case of Autoimmune Pancreatitis
 MULTIMEDIA ARTICLE - Clinical Imaging An Autopsy Case of Autoimmune Pancreatitis Yohei Kitano 1, Kakuya Matsumoto 1, Kenji Chisaka 1, Masako Imazawa 1, Kenji Takahashi 1, Yukiomi Nakade 1, Mituyoshi Okada
MULTIMEDIA ARTICLE - Clinical Imaging An Autopsy Case of Autoimmune Pancreatitis Yohei Kitano 1, Kakuya Matsumoto 1, Kenji Chisaka 1, Masako Imazawa 1, Kenji Takahashi 1, Yukiomi Nakade 1, Mituyoshi Okada
Autoimmune pancreatitis (AIP), a clinical entity originally
 Autoimmune Pancreatitis: A Multiorgan Disease Presenting a Conundrum for Clinicians in the West Eileen Kim, MD, Rebecca Voaklander, MD, Franklin E. Kasmin, MD, William H. Brown, MD, Rifat Mannan, MD, and
Autoimmune Pancreatitis: A Multiorgan Disease Presenting a Conundrum for Clinicians in the West Eileen Kim, MD, Rebecca Voaklander, MD, Franklin E. Kasmin, MD, William H. Brown, MD, Rifat Mannan, MD, and
Diagnostic And Therapeutic Challenges in IgG4-Related disease in the Sphenoid Sinus
 Diagnostic And Therapeutic Challenges in IgG4-Related disease in the Sphenoid Sinus Omar Abu Suliman, MBBS, SB-ORL Senior Registrar, otolaryngology Head & neck surgery King Abdullah Medical City, Makkah,
Diagnostic And Therapeutic Challenges in IgG4-Related disease in the Sphenoid Sinus Omar Abu Suliman, MBBS, SB-ORL Senior Registrar, otolaryngology Head & neck surgery King Abdullah Medical City, Makkah,
Ulcerative Colitis and Immunoglobulin G4
 Gut and Liver, Vol. 8, No. 1, January 2014, pp. 29-4 ORiginal Article Ulcerative Colitis and Immunoglobulin G4 Go Kuwata*, Terumi Kamisawa*, Koichi Koizumi*, Taku Tabata*, Seiichi Hara*, Sawako Kuruma*,
Gut and Liver, Vol. 8, No. 1, January 2014, pp. 29-4 ORiginal Article Ulcerative Colitis and Immunoglobulin G4 Go Kuwata*, Terumi Kamisawa*, Koichi Koizumi*, Taku Tabata*, Seiichi Hara*, Sawako Kuruma*,
IgG4-related Kidney Disease in Which the Urinalysis, Kidney Function and Imaging Findings Were Normal
 CASE REPORT IgG4-related Kidney Disease in Which the Urinalysis, Kidney Function and Imaging Findings Were Normal Miho Otani 1, Masahiro Morinaga 1, Yoshihiko Nakajima 1, Hiromi Tomioka 2, Michiko Nishii
CASE REPORT IgG4-related Kidney Disease in Which the Urinalysis, Kidney Function and Imaging Findings Were Normal Miho Otani 1, Masahiro Morinaga 1, Yoshihiko Nakajima 1, Hiromi Tomioka 2, Michiko Nishii
Overview of PSC Making the Diagnosis
 Overview of PSC Making the Diagnosis Tamar Taddei, MD Assistant Professor of Medicine Yale University School of Medicine Overview Definition Epidemiology Diagnosis Modes of presentation Associated diseases
Overview of PSC Making the Diagnosis Tamar Taddei, MD Assistant Professor of Medicine Yale University School of Medicine Overview Definition Epidemiology Diagnosis Modes of presentation Associated diseases
IgG4-related Sclerosing Disease: Autoimmune Pancreatitis and Extrapancreatic
 Note: This copy is for your personal non-commercial use only. To order presentation-ready copies for distribution to your colleagues or clients, contact us at www.rsna.org/rsnarights. GASTROINTESTINAL
Note: This copy is for your personal non-commercial use only. To order presentation-ready copies for distribution to your colleagues or clients, contact us at www.rsna.org/rsnarights. GASTROINTESTINAL
Clinical profile and treatment outcomes in autoimmune pancreatitis: a report from North India
 ORIGINAL ARTICLE Annals of Gastroenterology (2018) 31, 1-7 Clinical profile and treatment outcomes in autoimmune pancreatitis: a report from North India Surinder S. Rana a, Rajesh Gupta b, Ritambhra Nada
ORIGINAL ARTICLE Annals of Gastroenterology (2018) 31, 1-7 Clinical profile and treatment outcomes in autoimmune pancreatitis: a report from North India Surinder S. Rana a, Rajesh Gupta b, Ritambhra Nada
Autoimmune pancreatitis associated to renal and aortic involvement: 3.0-TESLA magnetic resonance imaging in diagnosis and follow-up
 CASE REPORT Autoimmune pancreatitis associated to renal and aortic involvement: 3.0-TESLA magnetic resonance imaging in diagnosis and follow-up Rossella Graziani 1, Paoletta Preatoni 2, Silvia Carrara
CASE REPORT Autoimmune pancreatitis associated to renal and aortic involvement: 3.0-TESLA magnetic resonance imaging in diagnosis and follow-up Rossella Graziani 1, Paoletta Preatoni 2, Silvia Carrara
Isolated Mass-Forming IgG4-Related Cholangitis as an Initial Clinical Presentation of Systemic IgG4-Related Disease
 Journal of Pathology and Translational Medicine 2016; 50: 300-305 CASE STUDY Isolated Mass-Forming IgG4-Related Cholangitis as an Initial Clinical Presentation of Systemic IgG4-Related Disease Seokhwi
Journal of Pathology and Translational Medicine 2016; 50: 300-305 CASE STUDY Isolated Mass-Forming IgG4-Related Cholangitis as an Initial Clinical Presentation of Systemic IgG4-Related Disease Seokhwi
Autoimmune Pancreatitis & Cholangiopathy. Goal and Objectives
 Autoimmune Pancreatitis & Cholangiopathy Kaveh Sharzehi, MD, MS Assistant Professor of Medicine Medical Director of Endoscopy Section of Gastroenterology Lewis Katz School of Medicine at Temple University
Autoimmune Pancreatitis & Cholangiopathy Kaveh Sharzehi, MD, MS Assistant Professor of Medicine Medical Director of Endoscopy Section of Gastroenterology Lewis Katz School of Medicine at Temple University
Overview of PSC Jayant A. Talwalkar, MD, MPH Associate Professor of Medicine Mayo Clinic Rochester, MN
 Overview of PSC Jayant A. Talwalkar, MD, MPH Associate Professor of Medicine Mayo Clinic Rochester, MN 2012 Annual Conference PSC Partners Seeking a Cure May 5, 2012 Primary Sclerosing Cholangitis Multifocal
Overview of PSC Jayant A. Talwalkar, MD, MPH Associate Professor of Medicine Mayo Clinic Rochester, MN 2012 Annual Conference PSC Partners Seeking a Cure May 5, 2012 Primary Sclerosing Cholangitis Multifocal
Autoimmune Pancreatitis, Pancreatic and Extrapancreatic Imaging Findings
 Autoimmune Pancreatitis, Pancreatic and Extrapancreatic Imaging Findings Poster No.: R-0074 Congress: RANZCR-AOCR 2012 Type: Educational Exhibit Authors: J. Stegeman, A. Borsaru; Clayton/AU Keywords: Education
Autoimmune Pancreatitis, Pancreatic and Extrapancreatic Imaging Findings Poster No.: R-0074 Congress: RANZCR-AOCR 2012 Type: Educational Exhibit Authors: J. Stegeman, A. Borsaru; Clayton/AU Keywords: Education
IgG4-related disease: features and treatment response in a multi-ethnic cohort in Singapore
 IgG4-related disease: features and treatment response in a multi-ethnic cohort in Singapore W. Fong 1,2,3, I. Liew 1, D. Tan 2,3,4, K.H. Lim 5, A. Low 6, Y.Y. Leung 1,2 1 Department of Rheumatology and
IgG4-related disease: features and treatment response in a multi-ethnic cohort in Singapore W. Fong 1,2,3, I. Liew 1, D. Tan 2,3,4, K.H. Lim 5, A. Low 6, Y.Y. Leung 1,2 1 Department of Rheumatology and
Case Report IgG4-Related Nasal Pseudotumor
 Case Reports in Otolaryngology Volume 2015, Article ID 749890, 4 pages http://dx.doi.org/10.1155/2015/749890 Case Report IgG4-Related Nasal Pseudotumor L. K. Døsen, 1 P. Jebsen, 2 B. Dingsør, 3 and R.
Case Reports in Otolaryngology Volume 2015, Article ID 749890, 4 pages http://dx.doi.org/10.1155/2015/749890 Case Report IgG4-Related Nasal Pseudotumor L. K. Døsen, 1 P. Jebsen, 2 B. Dingsør, 3 and R.
Among the benign intraepithelial melanocytic proliferations, Inflamed Conjunctival Nevi. Histopathological Criteria. Resident Short Reviews
 Resident Short Reviews Inflamed conjunctival nevi (ICN) may suggest malignancy because of their rapid growth and atypical histology. The objective of this study was to characterize the diagnostic features
Resident Short Reviews Inflamed conjunctival nevi (ICN) may suggest malignancy because of their rapid growth and atypical histology. The objective of this study was to characterize the diagnostic features
Overview of Diagnostic Criteria for Autoimmune Pancreatitis
 2007 년도대한췌담도학회추계학술대회 Session II: Comparison of Diagnostic Criteria for AIP: Japan, USA & Korea Overview of Diagnostic Criteria for Autoimmune Pancreatitis Department of Internal Medicine, Seoul National
2007 년도대한췌담도학회추계학술대회 Session II: Comparison of Diagnostic Criteria for AIP: Japan, USA & Korea Overview of Diagnostic Criteria for Autoimmune Pancreatitis Department of Internal Medicine, Seoul National
A Case of Autoimmune Pancreatitis Associated with Retroperitoneal Fibrosis
 CASE REPORT A Case of Autoimmune Pancreatitis Associated with Retroperitoneal Fibrosis Koushiro Ohtsubo 1, Hiroyuki Watanabe 1, Tomoya Tsuchiyama 1, Hisatsugu Mouri 1, Yasushi Yamaguchi 1, Yoshiharu Motoo
CASE REPORT A Case of Autoimmune Pancreatitis Associated with Retroperitoneal Fibrosis Koushiro Ohtsubo 1, Hiroyuki Watanabe 1, Tomoya Tsuchiyama 1, Hisatsugu Mouri 1, Yasushi Yamaguchi 1, Yoshiharu Motoo
Renal Pathology Case Conference. Case 2
 Renal Pathology Case Conference Case 2 Lynn D. Cornell, M.D. Mayo Clinic, Rochester, MN cornell.lynn@mayo.edu March 2, 2008 Clinical presentation 68 year old woman, initially with normal renal function
Renal Pathology Case Conference Case 2 Lynn D. Cornell, M.D. Mayo Clinic, Rochester, MN cornell.lynn@mayo.edu March 2, 2008 Clinical presentation 68 year old woman, initially with normal renal function
A Review of Liver Function Tests. James Gray Gastroenterology Vancouver
 A Review of Liver Function Tests James Gray Gastroenterology Vancouver Copyright 2017 by Sea Courses Inc. All rights reserved. No part of this document may be reproduced, copied, stored, or transmitted
A Review of Liver Function Tests James Gray Gastroenterology Vancouver Copyright 2017 by Sea Courses Inc. All rights reserved. No part of this document may be reproduced, copied, stored, or transmitted
IgG4-related Sclerosing Disease of the Lung without Pancreas Involvement: Presentation on 18F-FDG PET/CT
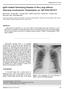 J Radiol Sci 2013; 38: 129-133 IgG4-related Sclerosing Disease of the Lung without Pancreas Involvement: Presentation on 18F-FDG PET/CT Han-Jui Lee 1 Yi-Chen Yeh 2,3 Chun-Ku Chen 1,3 Rheun-Chuan Lee 1,3
J Radiol Sci 2013; 38: 129-133 IgG4-related Sclerosing Disease of the Lung without Pancreas Involvement: Presentation on 18F-FDG PET/CT Han-Jui Lee 1 Yi-Chen Yeh 2,3 Chun-Ku Chen 1,3 Rheun-Chuan Lee 1,3
Type 2 Autoimmune Pancreatitis with Crohn s Disease
 doi: 10.2169/internalmedicine.0213-17 Intern Med 57: 2957-2962, 2018 http://internmed.jp CASE REPORT Type 2 Autoimmune Pancreatitis with Crohn s Disease Yoon Suk Lee, Nam-Hoon Kim, Jun Hyuk Son, Jung Wook
doi: 10.2169/internalmedicine.0213-17 Intern Med 57: 2957-2962, 2018 http://internmed.jp CASE REPORT Type 2 Autoimmune Pancreatitis with Crohn s Disease Yoon Suk Lee, Nam-Hoon Kim, Jun Hyuk Son, Jung Wook
Clinical outcomes and pathological characteristics of immunoglobulin G4-related ophthalmic disease versus orbital inflammatory pseudotumor
 ORIGINAL ARTICLE Korean J Intern Med 2019;34:220-226 Clinical outcomes and pathological characteristics of immunoglobulin G4-related ophthalmic disease versus orbital inflammatory pseudotumor Hong Ki Min
ORIGINAL ARTICLE Korean J Intern Med 2019;34:220-226 Clinical outcomes and pathological characteristics of immunoglobulin G4-related ophthalmic disease versus orbital inflammatory pseudotumor Hong Ki Min
Incidence of Malignancy in Type 1 Autoimmune Pancreatitis
 ORIGINAL ARTICLE Incidence of Malignancy in Type 1 Autoimmune Pancreatitis Junko Tahara 1, Kyoko Shimizu 1, Junichi Akao 1, Yukiko Takayama 1, Katsutoshi Tokushige 1, Masakazu Yamamoto 2 1 Department of
ORIGINAL ARTICLE Incidence of Malignancy in Type 1 Autoimmune Pancreatitis Junko Tahara 1, Kyoko Shimizu 1, Junichi Akao 1, Yukiko Takayama 1, Katsutoshi Tokushige 1, Masakazu Yamamoto 2 1 Department of
NEW-ONSET JAUNDICE IN A PATIENT WITH HISTORY OF RETROPERITONEAL FIBROSIS, A CASE REPORT
 Acta Medica Mediterranea, 2015, 31: 1099 NEW-ONSET JAUNDICE IN A PATIENT WITH HISTORY OF RETROPERITONEAL FIBROSIS, A CASE REPORT PIETRO VALERIO FOTI 1, GIANCARLO ATTINÀ 1, GIUSEPPINA CAPPELLO 1, STEFANO
Acta Medica Mediterranea, 2015, 31: 1099 NEW-ONSET JAUNDICE IN A PATIENT WITH HISTORY OF RETROPERITONEAL FIBROSIS, A CASE REPORT PIETRO VALERIO FOTI 1, GIANCARLO ATTINÀ 1, GIUSEPPINA CAPPELLO 1, STEFANO
Chronic Sclerosing Dacryoadenitis
 The Korean Journal of Pathology 2008; 42: 118-22 Chronic Sclerosing Dacryoadenitis - Report of 2 Cases - Ji Eun Kwon Sang Kyum Kim Sang-Ryul Lee 1 Woo-Ick Yang Haeryoung Kim 2 Department of Pathology and
The Korean Journal of Pathology 2008; 42: 118-22 Chronic Sclerosing Dacryoadenitis - Report of 2 Cases - Ji Eun Kwon Sang Kyum Kim Sang-Ryul Lee 1 Woo-Ick Yang Haeryoung Kim 2 Department of Pathology and
CASE REPORT. Abstract. Introduction. Case Report
 CASE REPORT Branch Duct Intraductal Papillary Mucinous Neoplasms of the Pancreas Involving Type 1 Localized Autoimmune Pancreatitis with Normal Serum IgG4 Levels Successfully Diagnosed by Endoscopic Ultrasound-guided
CASE REPORT Branch Duct Intraductal Papillary Mucinous Neoplasms of the Pancreas Involving Type 1 Localized Autoimmune Pancreatitis with Normal Serum IgG4 Levels Successfully Diagnosed by Endoscopic Ultrasound-guided
Liver and Pancreatic Case discussion
 The Royal Marsden Liver and Pancreatic Case discussion Dr Ian Chau Consultant Medical Oncologist The Royal Marsden 77 year old gentleman with 2 months history of vague abdominal ache and clinically finding
The Royal Marsden Liver and Pancreatic Case discussion Dr Ian Chau Consultant Medical Oncologist The Royal Marsden 77 year old gentleman with 2 months history of vague abdominal ache and clinically finding
Dilemmas in autoimmune pancreatitis. Surgical resection or not?
 DOI: 10.4149/BLL_2016_090 Bratisl Med J 2016; 117 (8) CLINICAL STUDY Dilemmas in autoimmune pancreatitis. Surgical resection or not? Hoffmanova I 1, Gurlich R 2, Janik V 3, Szabo A 4, Vernerova Z 4 Second
DOI: 10.4149/BLL_2016_090 Bratisl Med J 2016; 117 (8) CLINICAL STUDY Dilemmas in autoimmune pancreatitis. Surgical resection or not? Hoffmanova I 1, Gurlich R 2, Janik V 3, Szabo A 4, Vernerova Z 4 Second
Localized autoimmune pancreatitis mimicking pancreatic cancer: Case report and literature review
 Case Report Localized autoimmune pancreatitis mimicking pancreatic cancer: Case report and literature review Journal of International Medical Research 2018, Vol. 46(4) 1657 1665! The Author(s) 2018 Reprints
Case Report Localized autoimmune pancreatitis mimicking pancreatic cancer: Case report and literature review Journal of International Medical Research 2018, Vol. 46(4) 1657 1665! The Author(s) 2018 Reprints
Jaundice. Agnieszka Dobrowolska- Zachwieja, MD, PhD
 Jaundice Agnieszka Dobrowolska- Zachwieja, MD, PhD Jaundice definition Jaundice, as in the French jaune, refers to the yellow discoloration of the skin. It arises from the abnormal accumulation of bilirubin
Jaundice Agnieszka Dobrowolska- Zachwieja, MD, PhD Jaundice definition Jaundice, as in the French jaune, refers to the yellow discoloration of the skin. It arises from the abnormal accumulation of bilirubin
Pediatric Primary Sclerosing Cholangitis and Potential Therapies
 Pediatric Primary Sclerosing Cholangitis and Potential Therapies Philip Rosenthal, M.D. Professor of Pediatrics & Surgery University of California, San Francisco DISCLOSURE I have the following financial
Pediatric Primary Sclerosing Cholangitis and Potential Therapies Philip Rosenthal, M.D. Professor of Pediatrics & Surgery University of California, San Francisco DISCLOSURE I have the following financial
Clinical Commissioning Policy Proposition:
 Clinical Commissioning Policy Proposition: Rituximab for immunoglobulin G4-related disease (IgG4-RD) Reference: NHS England A13X07/01 Information Reader Box (IRB) to be inserted on inside front cover for
Clinical Commissioning Policy Proposition: Rituximab for immunoglobulin G4-related disease (IgG4-RD) Reference: NHS England A13X07/01 Information Reader Box (IRB) to be inserted on inside front cover for
Autoimmune Pancreatitis and Retroperitoneal Fibrosis
 Autoimmune Pancreatitis and Retroperitoneal Fibrosis Thomas C. Smyrk, MD Associate Professor of Pathology Mayo Clinic, Rochester MN 55902 smyrk.thomas@mayo.edu Summary Retroperitoneal fibrosis complicated
Autoimmune Pancreatitis and Retroperitoneal Fibrosis Thomas C. Smyrk, MD Associate Professor of Pathology Mayo Clinic, Rochester MN 55902 smyrk.thomas@mayo.edu Summary Retroperitoneal fibrosis complicated
Cholangiocarcinoma (Bile Duct Cancer)
 Cholangiocarcinoma (Bile Duct Cancer) The Bile Duct System (Biliary Tract) A network of bile ducts (tubes) connects the liver and the gallbladder to the small intestine. This network begins in the liver
Cholangiocarcinoma (Bile Duct Cancer) The Bile Duct System (Biliary Tract) A network of bile ducts (tubes) connects the liver and the gallbladder to the small intestine. This network begins in the liver
Scottish Surveillance of Healthcare Associated Infection Programme (SSHAIP) Health Protection Scotland (HPS) SSI Surveillance Protocol 7th Edition
 1 Contents Female reproductive system operations (Abdominal hysterectomy and Caesarean section)... 3 Intra-abdominal infections... 3 Endometritis... 4 Other infections of the female reproductive tract...
1 Contents Female reproductive system operations (Abdominal hysterectomy and Caesarean section)... 3 Intra-abdominal infections... 3 Endometritis... 4 Other infections of the female reproductive tract...
Kazuichi Okazaki 1 and Hisanori Umehara Introduction. 2. The Concept of IgG4-Related Disease
 Hindawi Publishing Corporation International Journal of Rheumatology Volume 2012, Article ID 357071, 9 pages doi:10.1155/2012/357071 Review Article Are Classification Criteria for IgG4-RD Now Possible?
Hindawi Publishing Corporation International Journal of Rheumatology Volume 2012, Article ID 357071, 9 pages doi:10.1155/2012/357071 Review Article Are Classification Criteria for IgG4-RD Now Possible?
IgG4-related systemic disease (ISD) is a multisystem
 Utility of Serum Immunoglobulin G4 in Distinguishing Immunoglobulin G4-Associated Cholangitis from Cholangiocarcinoma Abdul M. Oseini, 1 * Roongruedee Chaiteerakij, 1 * Abdirashid M. Shire, 1 Amaar Ghazale,
Utility of Serum Immunoglobulin G4 in Distinguishing Immunoglobulin G4-Associated Cholangitis from Cholangiocarcinoma Abdul M. Oseini, 1 * Roongruedee Chaiteerakij, 1 * Abdirashid M. Shire, 1 Amaar Ghazale,
Case Report The Challenging Diagnosis of Pancreatic Masses: Not All Tumors Are Cancers
 Case Reports in Medicine Volume 2015, Article ID 832463, 4 pages http://dx.doi.org/10.1155/2015/832463 Case Report The Challenging Diagnosis of Pancreatic Masses: Not All Tumors Are Cancers Alessandro
Case Reports in Medicine Volume 2015, Article ID 832463, 4 pages http://dx.doi.org/10.1155/2015/832463 Case Report The Challenging Diagnosis of Pancreatic Masses: Not All Tumors Are Cancers Alessandro
Management of Acute Vasculitis. CMT teaching 3 rd June 2015 Caroline Wroe
 Management of Acute Vasculitis CMT teaching 3 rd June 2015 Caroline Wroe Vasculitis pub quiz Match the date with the event Dr Peter McBride, Scottish Otolaryngologist describes a disease of rapid destruction
Management of Acute Vasculitis CMT teaching 3 rd June 2015 Caroline Wroe Vasculitis pub quiz Match the date with the event Dr Peter McBride, Scottish Otolaryngologist describes a disease of rapid destruction
Immunoglobulin G4-related sclerosing cholangitis
 REVIEW Korean J Intern Med 2018;33:841-850 https://doi.org/10.3904/kjim.2018.018 Immunoglobulin G4-related sclerosing cholangitis George Goodchild, Stephen P. Pereira, and George Webster Department of
REVIEW Korean J Intern Med 2018;33:841-850 https://doi.org/10.3904/kjim.2018.018 Immunoglobulin G4-related sclerosing cholangitis George Goodchild, Stephen P. Pereira, and George Webster Department of
LIVER SPECIALTY CONFERENCE USCAP Maha Guindi, M.D. Clinical Professor of Pathology Cedars-Sinai Medical Center Los Angeles, CA
 LIVER SPECIALTY CONFERENCE USCAP 2016 Maha Guindi, M.D. Clinical Professor of Pathology Cedars-Sinai Medical Center Los Angeles, CA Nothing to disclose Case History 47-year-old male, long standing ileal
LIVER SPECIALTY CONFERENCE USCAP 2016 Maha Guindi, M.D. Clinical Professor of Pathology Cedars-Sinai Medical Center Los Angeles, CA Nothing to disclose Case History 47-year-old male, long standing ileal
Together, putting patients first
 The Role of a Gastroenterologist in the Diagnosis and Management of Pancreatic Cancer Sarah Jowett, Consultant Gastroenterologist Bradford Teaching Hospitals Trust Leeds Regional Study Day, 12 September
The Role of a Gastroenterologist in the Diagnosis and Management of Pancreatic Cancer Sarah Jowett, Consultant Gastroenterologist Bradford Teaching Hospitals Trust Leeds Regional Study Day, 12 September
Common things are common, but not always the answer
 Kevin Conroy, Joe Mackenzie, Stephen Cowie kevin.conroy@nhs.net Respiratory Dept, Darlington Memorial Hospital, Darlington, UK. Common things are common, but not always the answer Case report Cite as:
Kevin Conroy, Joe Mackenzie, Stephen Cowie kevin.conroy@nhs.net Respiratory Dept, Darlington Memorial Hospital, Darlington, UK. Common things are common, but not always the answer Case report Cite as:
Case Report An IgG4-Related Salivary Gland Disorder: A Case Series Presenting with a Different Clinical Setting
 Case Reports in Immunology Volume 2011, Article ID 236079, 4 pages doi:10.1155/2011/236079 Case Report An IgG4-Related Salivary Gland Disorder: A Case Series Presenting with a Different Clinical Setting
Case Reports in Immunology Volume 2011, Article ID 236079, 4 pages doi:10.1155/2011/236079 Case Report An IgG4-Related Salivary Gland Disorder: A Case Series Presenting with a Different Clinical Setting
PITUITARY: JUST THE BASICS PART 2 THE PATIENT
 PITUITARY: JUST THE BASICS PART 2 THE PATIENT DISCLOSURE Relevant relationships with commercial entities none Potential for conflicts of interest within this presentation none Steps taken to review and
PITUITARY: JUST THE BASICS PART 2 THE PATIENT DISCLOSURE Relevant relationships with commercial entities none Potential for conflicts of interest within this presentation none Steps taken to review and
Clinical Study IgG4-Related Disease Is Not Associated with Antibody to the Phospholipase A2 Receptor
 International Rheumatology Volume 2012, Article ID 139409, 6 pages doi:10.1155/2012/139409 Clinical Study IgG4-Related Disease Is Not Associated with Antibody to the Phospholipase A2 Receptor Arezou Khosroshahi,
International Rheumatology Volume 2012, Article ID 139409, 6 pages doi:10.1155/2012/139409 Clinical Study IgG4-Related Disease Is Not Associated with Antibody to the Phospholipase A2 Receptor Arezou Khosroshahi,
Autoimmune Pancreatitis: A Succinct Overview
 REVIEW ARTICLE Autoimmune Pancreatitis: A Succinct Overview Juan Putra, Xiaoying Liu Department of Pathology, Dartmouth-Hitchcock Medical Center, One Medical Center Drive Lebanon, NH 03756, USA ABSTRACT
REVIEW ARTICLE Autoimmune Pancreatitis: A Succinct Overview Juan Putra, Xiaoying Liu Department of Pathology, Dartmouth-Hitchcock Medical Center, One Medical Center Drive Lebanon, NH 03756, USA ABSTRACT
gg4-related inflammatory pseudotumour of the trigeminal nerve: imaging findings and clinical features
 gg4-related inflammatory pseudotumour of the trigeminal nerve: imaging findings and clinical features Poster No.: C-2603 Congress: ECR 2013 Type: Scientific Exhibit Authors: Y. Kawamura, Y. Kikuchi, I.
gg4-related inflammatory pseudotumour of the trigeminal nerve: imaging findings and clinical features Poster No.: C-2603 Congress: ECR 2013 Type: Scientific Exhibit Authors: Y. Kawamura, Y. Kikuchi, I.
IgG4 cholangitis Case Report: Joanne Verheij, MD, PhD Department of Pathology Academic Medical Center Amsterdam.
 IgG4 cholangitis New Perspectives on Biliary Tract Disease Case Report: male, 64 yrs, truck driver and car industry worker Joanne Verheij, MD, PhD Department of Pathology Academic Medical Center Amsterdam
IgG4 cholangitis New Perspectives on Biliary Tract Disease Case Report: male, 64 yrs, truck driver and car industry worker Joanne Verheij, MD, PhD Department of Pathology Academic Medical Center Amsterdam
Usefulness of PET/CT Imaging in Systemic IgG4-related Sclerosing Disease. A Report of Three Cases
 MULTIMEDIA ARTICLE - Clinical Imaging Usefulness of PET/CT Imaging in Systemic IgG4-related Sclerosing Disease. A Report of Three Cases Vien X Nguyen 1, Giovanni De Petris 2, Ba D Nguyen 3 Departments
MULTIMEDIA ARTICLE - Clinical Imaging Usefulness of PET/CT Imaging in Systemic IgG4-related Sclerosing Disease. A Report of Three Cases Vien X Nguyen 1, Giovanni De Petris 2, Ba D Nguyen 3 Departments
Congenital dilatation of the common bile duct and pancreaticobiliary maljunction clinical implications
 Langenbecks Arch Surg (2009) 394:209 213 DOI 10.1007/s00423-008-0330-6 CURRENT CONCEPT IN CLINICAL SURGERY Congenital dilatation of the common bile duct and pancreaticobiliary maljunction clinical implications
Langenbecks Arch Surg (2009) 394:209 213 DOI 10.1007/s00423-008-0330-6 CURRENT CONCEPT IN CLINICAL SURGERY Congenital dilatation of the common bile duct and pancreaticobiliary maljunction clinical implications
Imaging Guided Biopsy. Edited & Presented by ; Hussien A.B ALI DINAR. Msc Lecturer,Reporting Sonographer
 Imaging Guided Biopsy Edited & Presented by ; Hussien A.B ALI DINAR. Msc Lecturer,Reporting Sonographer Objective By the End of this lessons you should : Define what biopsy Justify Aim to perform biopsy
Imaging Guided Biopsy Edited & Presented by ; Hussien A.B ALI DINAR. Msc Lecturer,Reporting Sonographer Objective By the End of this lessons you should : Define what biopsy Justify Aim to perform biopsy
Anatomical and Functional MRI of the Pancreas
 Anatomical and Functional MRI of the Pancreas MA Bali, MD, T Metens, PhD Erasme Hospital Free University of Brussels Belgium mbali@ulb.ac.be Introduction The use of MRI to investigate the pancreas has
Anatomical and Functional MRI of the Pancreas MA Bali, MD, T Metens, PhD Erasme Hospital Free University of Brussels Belgium mbali@ulb.ac.be Introduction The use of MRI to investigate the pancreas has
No Financial Interest
 Pituitary Apoplexy Michael Vaphiades, D.O. Professor Department of Ophthalmology, Neurology, Neurosurgery University of Alabama at Birmingham, Birmingham, AL No Financial Interest N E U R O L O G I C
Pituitary Apoplexy Michael Vaphiades, D.O. Professor Department of Ophthalmology, Neurology, Neurosurgery University of Alabama at Birmingham, Birmingham, AL No Financial Interest N E U R O L O G I C
Clinical Study Development of an IgG4-RD Responder Index
 International Rheumatology Volume 2012, Article ID 259408, 7 pages doi:10.1155/2012/259408 Clinical Study Development of an IgG4-RD Responder Index Mollie N. Carruthers, 1 John H. Stone, 1 Vikram Deshpande,
International Rheumatology Volume 2012, Article ID 259408, 7 pages doi:10.1155/2012/259408 Clinical Study Development of an IgG4-RD Responder Index Mollie N. Carruthers, 1 John H. Stone, 1 Vikram Deshpande,
Autoimmune pancreatitis
 Review Article Autoimmune pancreatitis Ayodeji Oluwarotimi Omiyale Department of Cellular Pathology, Maidstone Hospital, Maidstone, Kent, UK Correspondence to: Ayodeji Oluwarotimi Omiyale. Department of
Review Article Autoimmune pancreatitis Ayodeji Oluwarotimi Omiyale Department of Cellular Pathology, Maidstone Hospital, Maidstone, Kent, UK Correspondence to: Ayodeji Oluwarotimi Omiyale. Department of
Immunoglobulin G4 (IgG4)-related disease, a systemic,
 IgG4-Related Disease of the Gastrointestinal Tract A 21st Century Chameleon Vikram Deshpande, MD Context. Immunoglobulin G4 (IgG4) related disease is a systemic fibroinflammatory disease capable of affecting
IgG4-Related Disease of the Gastrointestinal Tract A 21st Century Chameleon Vikram Deshpande, MD Context. Immunoglobulin G4 (IgG4) related disease is a systemic fibroinflammatory disease capable of affecting
Recovery of renal function after glucocorticoid therapy for IgG4-related kidney disease with renal dysfunction
 Clin Exp Nephrol (2016) 20:87 93 DOI 10.1007/s10157-015-1140-0 ORIGINAL ARTICLE Recovery of renal function after glucocorticoid therapy for IgG4-related kidney disease with renal dysfunction Takako Saeki
Clin Exp Nephrol (2016) 20:87 93 DOI 10.1007/s10157-015-1140-0 ORIGINAL ARTICLE Recovery of renal function after glucocorticoid therapy for IgG4-related kidney disease with renal dysfunction Takako Saeki
