PedsCases Podcast Scripts
|
|
|
- Charleen Park
- 5 years ago
- Views:
Transcription
1 PedsCases Podcast Scripts This is a text version of a podcast from Pedscases.com on Hypoxic Ischemic Encephalopathy. These podcasts are designed to give medical students an overview of key topics in pediatrics. The audio versions are accessible on itunes or at Hypoxic Ischemic Encephalopathy Introduction Hi everyone, my name is Carina Lauzon and I am a third year medical student at the University of Alberta. This PedsCases podcast is designed to give an organized approach to Hypoxic Ischemic Encephalopathy, the leading cause of death or severe impairment in infants, worldwide. This podcast was created with Dr. Marc-Antoine Landry, a neonatologist at the Royal Alexandra Hospital in Edmonton, Alberta, Canada. Clinical Case Let s start with a clinical case: you are a third year medical student working on your pediatrics rotation. During your evening shift, you are called for an emergency Caesarean section for a term baby who has persistent fetal bradycardia. At the time of delivery, the obstetric team told the pediatric team that there was a placental abruption. The baby is born flat, is cyanotic, and is not breathing. The resuscitation team initiates positive pressure ventilation, and despite a good technique, no heart sounds are heard. The team inserts a breathing tube and starts chest compressions. After one minute of CPR there are still no heart sounds. They give epinephrine into the breathing tube and resume CPR. After three minutes, some faint heart sounds are heard. A second dose of epinephrine is given in an umbilical venous catheter that was urgently inserted. Two minutes later, a heart rate is recorded and the team is able to stop chest compressions, the heart rate steadily increases above 100. As the baby is still not breathing, a mechanical ventilator is attached to the breathing tube to ventilate and oxygenate the baby. Considering what you know about this patient, what should your next steps be in terms of brain protection? We will review the answer to this case at the end of the podcast. Learning Objectives After listening to this podcast, the learner will be able to: 1. Describe the phases of brain injury in hypoxic ischemic encephalopathy. 2. Identify which infants are at risk for hypoxic ischemic encephalopathy.
2 3. List the signs and symptoms of hypoxic ischemic encephalopathy. 4. Review the management for hypoxic ischemic encephalopathy. 5. Discuss the prognosis of hypoxic ischemic encephalopathy. What is HIE? Hypoxic Ischemic Encephalopathy (HIE) is caused by brain injury that occurs due to impairment of oxygen delivery (hypoxia) and blood perfusion (ischemia) to the brain. This happens as a result of an impairment of the exchange of oxygen and carbon dioxide, which leads to hypoxia, hypercapnia, metabolic acidosis, and other acute nutrient deficiencies. HIE is the leading cause of death or severe impairment, including epilepsy, cerebral palsy, neurodevelopmental delay, and cognitive impairment, in infants worldwide. In HIE, injury to the brain occurs in two phases, known as the primary and secondary phases. The primary phase refers to the hypoxic ischemic injury itself. Reduction in blood flow and oxygen supply to the brain leads to several biochemical changes, including a fall in ATP, failure of the sodium potassium pump, depolarization of cells, lactic acidosis, release of excitatory amino acids, calcium entry into cell and, if severe, cell necrosis. Following resuscitation and reperfusion, the brain enters into a latent stage, in which we see normalization of oxidative metabolism. However, the infant is still at risk for further damage due to HIE. The secondary phase of brain injury due to HIE is perhaps more significant than the first, and it is on this phase that current treatment regimens are focused. The secondary phase begins hours after injury and may last up to 14 days without treatment. During this phase, apoptosis, mitochondrial failure, cytotoxic edema, accumulation of excitatory amino acids, and release of free radicals, terminating in cell death, are observed. Experimental studies in sheep have shown that a single subthreshold insult during labour, which may cause minor or no neuronal damage in the primary phase, is capable of causing significant injury in the secondary phase. Risk factors/causes of HIE HIE is caused by reduced blood and oxygen delivery to the brain and therefore, anything that causes this is a risk factor for HIE. The main categories of risk factors for HIE include umbilical cord issues, placental complications, and birth complications. Because the umbilical cord is the fetus only source of oxygen and nutrients, its function is critical. Occlusion or compression of the umbilical cord decreases the amount of blood flow to the fetus. This can happen as a result of many factors, such as prolapse of the cord, nuchal cord (cord wrapped around baby s neck), knotted cord, and infection or inflammation of the cord. Oligohydraminos and polyhydramnios are additional risk factors for umbilical cord compression. The umbilical cord exchanges blood between the mother and fetus via the placenta, and therefore, placental complications can also lead to decreased oxygen
3 supply to the fetus. Placental complications that are associated with HIE include placental abruption, ruptured vasa previa, and preeclampsia. Maternal hypotension can result in decreased placental perfusion and thus, decreased delivery of blood to the fetus, and can occur for a variety of reasons, including infection, intrapartum haemorrhage, and uterine rupture. Finally, complications that occur during and around the time of birth are a risk factor for HIE. These include birth injury due to cephalopelvic disproportion, shoulder dystocia, and improper use of forceps or vacuum extractor during delivery. Additionally, any condition that has the potential to block the baby s airways or impair the lungs or heart s function for an extended period of time may lead to decreased oxygenation and perfusion of the brain after birth. Signs and Symptoms The clinical presentation of HIE depends on the severity of the insult. HIE can be grouped into three categories of symptoms: mild, moderate, or severe. Mild signs and symptoms include hyperalertness, tachycardia, mydriasis, and a weak suck reflex. Tone is normal or increased, stretch reflexes are overactive, and segmental myoclonus is present. There are no seizures. Moderate signs and symptoms of HIE include lethargy, hypotonia, bradycardia, periodic respirations, and weak primitive reflexes. Overactive stretch reflexes, segmental myoclonus, and miosis are also seen, and seizures are commonly present. In severe HIE, signs and symptoms include stupor or coma, flaccidness, absent primitive reflexes, and apnea. Seizures are less commonly present than in moderate HIE. Treatment The mainstay of treatment for HIE is therapeutic cooling. Achieving therapeutic hypothermia to a rectal temperature between 33 and 34 degrees Celsius prevents delayed cell death in the secondary phase of HIE and decreases mortality and long term neurodevelopmental disabilities in term infants. The number needed to treat is 7 for the combined outcome of death and major neurodevelopmental disability. Cooling has a broad inhibitory effect on a variety of harmful cell processes that occur during the secondary phase of HIE. Its effects include decreased apoptosis, decreased loss of high-energy phosphate, reduced oxygen consumption, reduced release of nitric oxide, glutamate, free radicals and excitatory amino acid neurotransmitters, and the induction of genes that reduce neuronal death. Cooling should be initiated as soon as possible, within the first 6 hours of life in infants with HIE, and the optimal duration of cooling is 72 hours. There is a small study
4 which suggests that infants who are cooled within 3 hours of birth have significantly better motor outcomes than those who commence cooling between 3 and 6 hours of life. In order to be a candidate for cooling, an infant must be less than 6 hours old, greater than or equal to 35 weeks gestational age, and must meet criteria A and B and, in some centres, criteria C. Criteria A refers to evidence of a metabolic hypoxic-ischemic etiology and is defined in most studies by at least one of the following: APGAR score under 5 at 10 minutes of age, continued need for resuscitation (which includes endotracheal or mask ventilation) at 10 minutes of age, or metabolic acidosis with ph under 7 or base deficit over 16mmol/L in cord or arterial blood within one hour of birth. Criteria B refers to evidence of a clinical neurological exam that shows that the infant has moderate or severe encephalopathy. This is demonstrated by an altered state of consciousness plus at least one of the following: hypotonia or hypertonia, abnormal reflexes including oculomotor or pupillary abnormalities, absent or weak suck reflex, or clinical seizures. Criteria C refers to evidence of abnormal brain activity, defined as clinical seizures or abnormal amplitude integrated EEG. Cooling can be accomplished via passive and/or active cooling. During the resuscitation of a baby who is suspected to have been exposed to a hypoxic-ischemic insult, the recommendation is to not actively warm the baby. For infants who need to be transferred to another hospital for cooling, passive cooling can be initiated during transport. This is achieved by turning off external heating devices and not warming the baby. When using passive cooling, it is important to continuously measure rectal temperature, so as to avoid temperature oscillations and over or under cooling. Active cooling can be achieved via selective head cooling, using a cooling cap, or total body cooling, using cool packs and cooling blankets. Clinical trials show similar outcomes between these two methods. In practice, total body cooling is used more commonly, as it is cheaper, more likely to be available, and easier to use. In addition, cooling caps carry the risks of scalp edema and skin breakdown. Mild hypothermia is safe, but there have been some mild side effects described, including bradycardia, arrhythmias, thrombocytopenia, and mild hypotension. Contraindications to cooling include severe head trauma, intracranial bleeding, major congenital anomalies, and congenital abnormalities suggestive of chromosomal anomaly or other syndromes that include brain dysgenesis. In addition, there is currently no evidence regarding the safety or efficacy of cooling in infants born at less than 35 weeks gestational age. After 72 hours of therapeutic hypothermia, the infant should be rewarmed. When rewarming, it is important to increase the temperature slowly, about 0.5 degrees Celsius every hour, as rapid rewarming puts the infant at a greater risk for seizures. In addition to therapeutic cooling, management of HIE includes avoidance of hyper and hypoglycemia, as both are associated with death and long-term disability at
5 18 months of age in infants with moderate to severe HIE. For all term infants, resuscitation in room air is preferred over resuscitation with 100% oxygen. This is because the use of high concentrations of oxygen can cause hyperoxia, which can lead to excessive release of oxygen free radicals and aggravation of brain injury. Research is currently being conducted in an effort to identify agents that may provide synergistic benefit with therapeutic hypothermia in HIE. Small studies have been performed and suggest that agents such as xenon, erythropoietin, melatonin, and stem cell therapy may be beneficial. These agents work via a variety of mechanisms, including reducing neurotransmitter release, anti-inflammatory effects, increasing neurotrophic and anti-apoptotic factors in the brain, and stimulating antioxidant enzymes. After initial management, all infants with moderate to severe HIE should be enrolled in follow-up programs. These programs may include early assessments at 4-8 months of age, which focus on general health, head growth and motor development, and assessments at months of age, which focus on cognitive skills and language development. Preschool assessments are also important, as they can help identify children who would benefit from early education programs. Prognosis The prognosis of HIE depends upon the severity of the injury, and the ability to determine the prognosis is hindered by the difficulty in determining the actual severity of the insult. The mortality rate ranges from 0% in mild HIE, to 5% in moderate HIE, to 80% in severe HIE. However, death is often the result of withholding and/or withdrawing care, and is not always the natural progression of the injury in babies with severe HIE. In infants with moderate to severe HIE treated with therapeutic hypothermia, the mortality rate is about 24-38%. Another important part of prognosis to consider is the child s risk of adverse neurodevelopmental outcomes. In infants who suffer from mild HIE, the rate of adverse neurodevelopmental outcomes does not differ significantly from the general population. In infants with moderate HIE, the rate is about 20-35%, and the risk is higher if seizures are present. In severe HIE, nearly 100% of survivors will have significant impairments. Possible long-term impairments include cognition and developmental delay, learning disabilities, cerebral palsy, blindness, gross motor and coordination problems, epilepsy, deafness, and behavioural problems. In infants with moderate HIE, it is difficult to predict who will suffer from adverse neurodevelopmental outcomes and the severity of impairment sometimes cannot be determined until the child is three to four years old. Seizures exacerbate neuronal injury by increasing cerebral metabolic demand, triggering the release of excitatory neurotransmitters, and causing cardiorespiratory instability, and therefore their presence is a poor prognostic factor in HIE. In addition, the presence of burst suppression, abnormalities of background cycling, and the loss
6 of sleep wake cycling on EEG is associated with a worse outcome. Normal tracing on EEG done at 7 days of age is associated with a favourable outcome. A normal clinical neurological exam on the 7 th day of life or at the time of discharge is a very good prognostic factor, with % normal outcome. Conclusion/return to case Let s return to our clinical case. The baby s mother had placental abruption, which we now know is a significant risk factor for Hypoxic Ischemic Encephalopathy in the infant. At 10 minutes of age, the baby s APGAR score was only 2 and he continued to require ventilation. No active warming was done in the resuscitation area. After completing all assessments and transporting him to the NICU, you determine that he has a moderate HIE and meets all the criteria for therapeutic hypothermia. Total body cooling is actively initiated by 2 hours of age. At 72 hours, you slowly rewarm the baby, who you now know as Jack, increasing the temperature by 0.5 degrees Celsius every hour. Once rewarmed, Jack begins feeding without difficulty and is discharged on day 6 with a completely normal neurological exam. He is enrolled in a follow-up program. Ten years later, you are working as a paediatrician when a new patient, a 10- year-old boy named Jack comes to see you for an ear infection. Upon meeting with him and his mother, you realize that this is the same Jack you treated as a medical student ten years ago! You learn that he has had no issues at all and performs well at school; Jack is a happy and thriving young boy! Thank you for listening to this PedsCases podcast on hypoxic ischemic encephalopathy. Here are some key take away points to review. Take Away Points 1. In HIE, injury to the brain occurs in two phases: the primary and secondary phases. The primary phase refers to the initial period of hypoxia and ischemia, in which damage occurs in the form of necrosis. The secondary phase occurs hours after the injury and in this phase, cell death occurs via apoptosis. 2. Risk factors for HIE include anything that decreases oxygen and blood flow to the brain. This includes umbilical cord issues, placental complications, and birth complications. 3. The signs and symptoms of HIE vary between mild, moderate, and severe HIE, but general symptoms include decreased level of consciousness, hypotonia, weak primary reflexes, and seizures. 4. The mainstay of treatment for HIE is therapeutic hypothermia. Infants born at or after 35 weeks gestation who have moderate to severe HIE should be cooled within the first 6 hours of life to a rectal temperature in between 33 and 34
7 degrees Celsius for a period of 72 hours. Therapeutic hypothermia reduces the damage that occurs during the secondary phase of HIE and thus, decreases mortality and morbidity. 5. The prognosis of HIE ranges from an almost 0% morbidity and mortality rate in mild HIE, to a 80% mortality rate and nearly 100% incidence of adverse neurodevelopmental outcomes in severe HIE. The rate of neurodevelopmental impairment is between 20 and 35% in moderate HIE; however, it is difficult to predict which infants will go on to develop adverse outcomes and the severity of impairment cannot always be determined until the child is three to four years old. We hope that this PedsCases podcast has been helpful. Stay tuned for more podcasts, and thanks for listening! References 1. Antonucci, Roberto, Annalisa Porcella, and Maria Dolores Pilloni. "Perinatal asphyxia in the term newborn." Journal of Pediatric and Neonatal Individualized Medicine (JPNIM) 3.2 (2014): e Chalak, Lina F. "Perinatal Asphyxia in the Delivery Room: Initial Management and Current Cooling Guidelines." NeoReviews 17.8 (2016): e463-e Douglas-Escobar, Martha, and Michael D. Weiss. "Hypoxic-ischemic encephalopathy: a review for the clinician." JAMA pediatrics (2015): Fatemi, Ali, Mary Ann Wilson, and Michael V. Johnston. "Hypoxic-ischemic encephalopathy in the term infant." Clinics in perinatology 36.4 (2009): Gunn, Alistair Jan, and Laura Bennet. "Fetal hypoxia insults and patterns of brain injury: insights from animal models." Clinics in perinatology 36.3 (2009): Hypoxic-Ishchemic Encephalopathy, or HIE, Also Known as Intrapartum Asphyxia. Cerebralpalsy.org, 7. Martinello, Kathryn, et al. "Management and investigation of neonatal encephalopathy: 2017 update." Archives of Disease in Childhood-Fetal and Neonatal Edition (2017): fetalneonatal Peliowski-Davidovich, A. Hypothermia for newborns with hypoxic ischemic encephalopathy. Paediatr Child Health 2012;17(1): Thoresen, Marianne. "Who should we cool after perinatal asphyxia?" Seminars in Fetal and Neonatal Medicine. Vol. 20. No. 2. Elsevier, 2015.
Objectives. Birth Depression Management. Birth Depression Terms
 Objectives Birth Depression Management Regional Perinatal Outreach Program 2016 Understand the terms and the clinical characteristics of birth depression. Be familiar with the evidence behind therapeutic
Objectives Birth Depression Management Regional Perinatal Outreach Program 2016 Understand the terms and the clinical characteristics of birth depression. Be familiar with the evidence behind therapeutic
ETIOLOGY AND PATHOGENESIS OF HYPOXIC-ISCHEMIC ENCEPHALOPATHY
 ETIOLOGY AND PATHOGENESIS OF HYPOXIC-ISCHEMIC ENCEPHALOPATHY HYPOXIC-ISCHEMIC ENCEPHALOPATHY Hypoxic-İschemic Encephalopathy Encephalopathy due to hypoxic-ischemic injury [Hypoxic-ischemic encephalopathy
ETIOLOGY AND PATHOGENESIS OF HYPOXIC-ISCHEMIC ENCEPHALOPATHY HYPOXIC-ISCHEMIC ENCEPHALOPATHY Hypoxic-İschemic Encephalopathy Encephalopathy due to hypoxic-ischemic injury [Hypoxic-ischemic encephalopathy
Neonatal Therapeutic Hypothermia. A Wasunna Professor of Neonatal Medicine and Pediatrics School of Medicine, University of Nairobi
 Neonatal Therapeutic Hypothermia A Wasunna Professor of Neonatal Medicine and Pediatrics School of Medicine, University of Nairobi Definition of Perinatal Asphyxia *No agreed universal definition ACOG/AAP
Neonatal Therapeutic Hypothermia A Wasunna Professor of Neonatal Medicine and Pediatrics School of Medicine, University of Nairobi Definition of Perinatal Asphyxia *No agreed universal definition ACOG/AAP
Hypothermia in Neonates with HIE TARA JENDZIO, DNP(C), RN, RNC-NIC
 Hypothermia in Neonates with HIE TARA JENDZIO, DNP(C), RN, RNC-NIC Objectives 1. Define Hypoxic-Ischemic Encephalopathy (HIE) 2. Identify the criteria used to determine if an infant qualifies for therapeutic
Hypothermia in Neonates with HIE TARA JENDZIO, DNP(C), RN, RNC-NIC Objectives 1. Define Hypoxic-Ischemic Encephalopathy (HIE) 2. Identify the criteria used to determine if an infant qualifies for therapeutic
Neonatal Hypoglycemia
 PedsCases Podcast Scripts This is a text version of a podcast from Pedscases.com on Neonatal Hypoglycemia. These podcasts are designed to give medical students an overview of key topics in pediatrics.
PedsCases Podcast Scripts This is a text version of a podcast from Pedscases.com on Neonatal Hypoglycemia. These podcasts are designed to give medical students an overview of key topics in pediatrics.
Too or Too Cold. Too Cold...Too Hot...Just Right. Temperature Control in Newborns. Temperature Balance in Newborns. Basics in the Delivery Room
 Too or Too Cold Neonatology Rediscovers Temperature Control Advances and Controversies in Clinical Pediatrics May 31, 2007 Terri A. Slagle Neonatology, CPMC Too Cold...Too Hot...Just Right Too Cold = Issues
Too or Too Cold Neonatology Rediscovers Temperature Control Advances and Controversies in Clinical Pediatrics May 31, 2007 Terri A. Slagle Neonatology, CPMC Too Cold...Too Hot...Just Right Too Cold = Issues
Queen Charlotte Hospital
 Queen Charlotte Hospital Neuroprotection for neonatal encephalopathy Neonatal encephalopathy accounts for 1 million deaths worldwide and even greater numbers of disabled survivors In countries with
Queen Charlotte Hospital Neuroprotection for neonatal encephalopathy Neonatal encephalopathy accounts for 1 million deaths worldwide and even greater numbers of disabled survivors In countries with
Birth Asphyxia. Perinatal Depression. Birth Asphyxia. Risk Factors maternal. Risk Factors fetal. Risk Factors Intrapartum 2/12/2011
 Birth Asphyxia Perinatal Depression Sara Brown, ARNP Children s Hospital and Regional Medical Center May occur in utero, during labor/delivery or during the neonatal period Condition of impaired blood
Birth Asphyxia Perinatal Depression Sara Brown, ARNP Children s Hospital and Regional Medical Center May occur in utero, during labor/delivery or during the neonatal period Condition of impaired blood
Disclosures. Objectives. Definition: HIE. HIE: Incidence. Impact 9/10/2018. Hypoxic Ischemic Encephalopathy in the Neonate
 Disclosures Hypoxic Ischemic Encephalopathy in the Neonate No relevant financial relationships or conflicts of interest to disclose Franscesca Miquel-Verges MD 2018 Review therapies currently under research
Disclosures Hypoxic Ischemic Encephalopathy in the Neonate No relevant financial relationships or conflicts of interest to disclose Franscesca Miquel-Verges MD 2018 Review therapies currently under research
Running head: THERAPEUTIC HYPOTHERMIA AND TRANSPORT 1
 Running head: THERAPEUTIC HYPOTHERMIA AND TRANSPORT 1 Therapeutic Hypothermia for Neonatal Encephalopathy: Preparation for Transport to Cooling Center Teresa Z. Baker, DNP-S Annie L. Addison, FNP-S NURS
Running head: THERAPEUTIC HYPOTHERMIA AND TRANSPORT 1 Therapeutic Hypothermia for Neonatal Encephalopathy: Preparation for Transport to Cooling Center Teresa Z. Baker, DNP-S Annie L. Addison, FNP-S NURS
TLC March 27, Shawn Hollinger-Neonatal Fellow CHEO
 TLC March 27, 2013 Presented/Prepared by: Shawn Hollinger, PGY5 Neonatal-Perinatal Medicine Resident - University of Ottawa With slides/images from Dr. Brigitte Lemyre Associate Professor of Pediatrics
TLC March 27, 2013 Presented/Prepared by: Shawn Hollinger, PGY5 Neonatal-Perinatal Medicine Resident - University of Ottawa With slides/images from Dr. Brigitte Lemyre Associate Professor of Pediatrics
NEONATAL HYPOXIC-ISCHAEMIC ENCEPHALOPATHY (HIE) & COOLING THERAPY
 Background NEONATAL HYPOXIC-ISCHAEMIC ENCEPHALOPATHY (HIE) & COOLING THERAPY A perinatal hypoxic-ischaemic insult may present with varying degrees of neonatal encephalopathy, neurological disorder and
Background NEONATAL HYPOXIC-ISCHAEMIC ENCEPHALOPATHY (HIE) & COOLING THERAPY A perinatal hypoxic-ischaemic insult may present with varying degrees of neonatal encephalopathy, neurological disorder and
Birth Asphyxia - Summary of the previous meeting and protocol overview
 Birth Asphyxia - Summary of the previous meeting and protocol overview Dr Ornella Lincetto, WHO Geneve Milano, 11June 2007 Vilka är Personality egenskaper med den astrologiska Tvillingarna? Objective of
Birth Asphyxia - Summary of the previous meeting and protocol overview Dr Ornella Lincetto, WHO Geneve Milano, 11June 2007 Vilka är Personality egenskaper med den astrologiska Tvillingarna? Objective of
No social problems noted No past med hx Mother had spontaneous rupture of fetal membranes SB born on Needed to be resuscitated at birth
 No social problems noted No past med hx Mother had spontaneous rupture of fetal membranes SB born on 9-16-2011 Needed to be resuscitated at birth (included assisted vent) Had generalized edema and possible
No social problems noted No past med hx Mother had spontaneous rupture of fetal membranes SB born on 9-16-2011 Needed to be resuscitated at birth (included assisted vent) Had generalized edema and possible
TREATMENT OF HYPOXIC ISCHEMIC ENCEPHALOPATHY WITH COOLING Children s Hospital & Research Center Oakland Guideline Revised by P.
 TREATMENT OF HYPOXIC ISCHEMIC ENCEPHALOPATHY WITH COOLING Children s Hospital & Research Center Oakland Guideline Revised 05-13-13 by P. Joe SCREENING FOR POTENTIAL COOLING PATIENTS Patients who are >
TREATMENT OF HYPOXIC ISCHEMIC ENCEPHALOPATHY WITH COOLING Children s Hospital & Research Center Oakland Guideline Revised 05-13-13 by P. Joe SCREENING FOR POTENTIAL COOLING PATIENTS Patients who are >
Too Cool? Hypoxic Ischemic Encephalopathy and Therapeutic Hypothermia. Lauren Sacco DNP, ARNP, NNP-BC
 Too Cool? Hypoxic Ischemic Encephalopathy and Therapeutic Hypothermia Lauren Sacco DNP, ARNP, NNP-BC Pathophysiology of HIE Occurs in two energy failure phases: First phase happens during the initial insult
Too Cool? Hypoxic Ischemic Encephalopathy and Therapeutic Hypothermia Lauren Sacco DNP, ARNP, NNP-BC Pathophysiology of HIE Occurs in two energy failure phases: First phase happens during the initial insult
COOLING FOR HYPOXIC ISCHEMIC ENCEPHALOPATHY
 COOLING FOR HYPOXIC ISCHEMIC ENCEPHALOPATHY Roger F. Soll H. Wallace Professor of Neonatology University of Vermont 19 th International Symposium on Neonatology Sao Paulo, Brazil DISCLOSURE Roger F. Soll
COOLING FOR HYPOXIC ISCHEMIC ENCEPHALOPATHY Roger F. Soll H. Wallace Professor of Neonatology University of Vermont 19 th International Symposium on Neonatology Sao Paulo, Brazil DISCLOSURE Roger F. Soll
Case Presentations. Anamika B. Mukherjee, MD September 13, 2017
 Case Presentations Anamika B. Mukherjee, MD September 13, 2017 Nothing to disclose Disclosures Learning Objectives Use the CPQCC Toolkit for therapeutic hypothermia to apply the guidelines for screening
Case Presentations Anamika B. Mukherjee, MD September 13, 2017 Nothing to disclose Disclosures Learning Objectives Use the CPQCC Toolkit for therapeutic hypothermia to apply the guidelines for screening
Guslihan Dasa Tjipta Division of Perinatology Department of Child Health Medical School University of Sumatera Utara
 Guslihan Dasa Tjipta Division of Perinatology Department of Child Health Medical School University of Sumatera Utara 1 Definition Perinatal asphyxia is a fetus/newborn, due to: is an insult to the Lack
Guslihan Dasa Tjipta Division of Perinatology Department of Child Health Medical School University of Sumatera Utara 1 Definition Perinatal asphyxia is a fetus/newborn, due to: is an insult to the Lack
State of Florida Hypothermia Protocol. Michael D. Weiss, M.D. Associate Professor of Pediatrics Division of Neonatology
 State of Florida Hypothermia Protocol Michael D. Weiss, M.D. Associate Professor of Pediatrics Division of Neonatology I. Entry Criteria 1. Gestational Age greater than or equal to 35 weeks gestation
State of Florida Hypothermia Protocol Michael D. Weiss, M.D. Associate Professor of Pediatrics Division of Neonatology I. Entry Criteria 1. Gestational Age greater than or equal to 35 weeks gestation
These signs should lead to the administration of high concentrations of
 Hypoxic-ischemic encephalopathy (HIE); (cont.) Clinical manifestations; *Intrauterine; growth restriction and increased vascular resistances may be the st manifestation of fetal hypoxia. *During labor;
Hypoxic-ischemic encephalopathy (HIE); (cont.) Clinical manifestations; *Intrauterine; growth restriction and increased vascular resistances may be the st manifestation of fetal hypoxia. *During labor;
Perinatal Depression. Lauren Sacco DNP, ARNP Seattle Children s
 Perinatal Depression Lauren Sacco DNP, ARNP Seattle Children s Birth Asphyxia May occur in utero, during labor/delivery or during the neonatal period Condition of impaired blood gas exchange that leads
Perinatal Depression Lauren Sacco DNP, ARNP Seattle Children s Birth Asphyxia May occur in utero, during labor/delivery or during the neonatal period Condition of impaired blood gas exchange that leads
This lecture will provide an overview of the neurologic exam of a neonate in the context of clinical cases.
 A11a Neuro Nuggets from the Trenches Michael D. Weiss, MD Associate Professor Department of Pediatrics, Division of Neonatology University of Florida, Gainesville, FL The speaker has signed a disclosure
A11a Neuro Nuggets from the Trenches Michael D. Weiss, MD Associate Professor Department of Pediatrics, Division of Neonatology University of Florida, Gainesville, FL The speaker has signed a disclosure
Perinatal asphyxia: Pathophysiology and therapy
 Perinatal asphyxia: Pathophysiology and therapy Peter Davis Melbourne Australia With thanks to Dr Sue Jacobs Moderate or severe HIE Complicates ~1/1000 term live births: Mortality: >25% Major neurological
Perinatal asphyxia: Pathophysiology and therapy Peter Davis Melbourne Australia With thanks to Dr Sue Jacobs Moderate or severe HIE Complicates ~1/1000 term live births: Mortality: >25% Major neurological
Shock is defined as a state of cellular and tissue hypoxia due to : reduced oxygen delivery and/or increased oxygen consumption or inadequate oxygen
 Shock is defined as a state of cellular and tissue hypoxia due to : reduced oxygen delivery and/or increased oxygen consumption or inadequate oxygen utilization The effects of shock are initially reversible
Shock is defined as a state of cellular and tissue hypoxia due to : reduced oxygen delivery and/or increased oxygen consumption or inadequate oxygen utilization The effects of shock are initially reversible
GUIDELINE PHYSIOLOGY OF BIRTH ASPHYXIA
 GUIDELINE PHYSIOLOGY OF BIRTH ASPHYXIA The newborn is not an adult, nor a child. In people of all ages, death can occur from a failure of breathing and / or circulation. The interventions required to aid
GUIDELINE PHYSIOLOGY OF BIRTH ASPHYXIA The newborn is not an adult, nor a child. In people of all ages, death can occur from a failure of breathing and / or circulation. The interventions required to aid
TOO COOL OR NOT TOO COOL- THERAPEUTIC HYPOTHERMIA IN THE ICU SCCM TX 2017 TED WU MD PEDIATRIC CRITICAL CARE UNIVERSITY OF TEXAS HEALTH SAN ANTONIO
 TOO COOL OR NOT TOO COOL- THERAPEUTIC HYPOTHERMIA IN THE ICU SCCM TX 2017 TED WU MD PEDIATRIC CRITICAL CARE UNIVERSITY OF TEXAS HEALTH SAN ANTONIO DISCLOSURE I have no relationships with commercial companies
TOO COOL OR NOT TOO COOL- THERAPEUTIC HYPOTHERMIA IN THE ICU SCCM TX 2017 TED WU MD PEDIATRIC CRITICAL CARE UNIVERSITY OF TEXAS HEALTH SAN ANTONIO DISCLOSURE I have no relationships with commercial companies
Study of renal functions in neonatal asphyxia
 Original article: Study of renal functions in neonatal asphyxia *Dr. D.Y.Shrikhande, **Dr. Vivek Singh, **Dr. Amit Garg *Professor and Head, **Senior Resident Department of Pediatrics, Pravara Institute
Original article: Study of renal functions in neonatal asphyxia *Dr. D.Y.Shrikhande, **Dr. Vivek Singh, **Dr. Amit Garg *Professor and Head, **Senior Resident Department of Pediatrics, Pravara Institute
Effect of ALlopurinol in addition to hypothermia for hypoxic-ischemic Brain Injury on Neurocognitive Outcome. Axel Franz, Tübingen
 Effect of ALlopurinol in addition to hypothermia for hypoxic-ischemic Brain Injury on Neurocognitive Outcome Axel Franz, Tübingen Hypoxic-ischemic encephalopathy 1-2 / 1000 newborn suffer from moderate
Effect of ALlopurinol in addition to hypothermia for hypoxic-ischemic Brain Injury on Neurocognitive Outcome Axel Franz, Tübingen Hypoxic-ischemic encephalopathy 1-2 / 1000 newborn suffer from moderate
Wales Neonatal Network Guideline Guideline for the management of Infants with Moderate or Severe Perinatal Asphyxia requiring cooling.
 Guideline for the management of Infants with Moderate or Severe Perinatal Asphyxia requiring cooling. (Including flowchart for infants fulfilling A criteria or A and B criteria only) Perinatal asphyxia
Guideline for the management of Infants with Moderate or Severe Perinatal Asphyxia requiring cooling. (Including flowchart for infants fulfilling A criteria or A and B criteria only) Perinatal asphyxia
Therapeutic hypothermia for hypoxic ischemic encephalopathy using low-technology methods: A systematic review and meta-analysis
 Therapeutic hypothermia for hypoxic ischemic encephalopathy using low-technology methods: A systematic review and meta-analysis Rossouw G 1, Irlam J 2, Horn AR 1 1)Division of Neonatal Medicine, Department
Therapeutic hypothermia for hypoxic ischemic encephalopathy using low-technology methods: A systematic review and meta-analysis Rossouw G 1, Irlam J 2, Horn AR 1 1)Division of Neonatal Medicine, Department
Inclusion criteria for cooling: Babies should be assessed for 3 criteria: A, B and C. See Appendix 1 for a decision making flowchart.
 Guideline for the management of Infants with Moderate or Severe Perinatal Asphyxia requiring cooling. (Including flowchart for infants fulfilling A criteria or A and B criteria only) Perinatal asphyxia
Guideline for the management of Infants with Moderate or Severe Perinatal Asphyxia requiring cooling. (Including flowchart for infants fulfilling A criteria or A and B criteria only) Perinatal asphyxia
Hypoxic-Ischemic Encephalopathy. TW de Witt University of Pretoria Department of Paediatrics Neonatology
 Hypoxic-Ischemic Encephalopathy TW de Witt University of Pretoria Department of Paediatrics Neonatology Background HIE remains a serious condition that causes significant mortality and longterm morbidity.
Hypoxic-Ischemic Encephalopathy TW de Witt University of Pretoria Department of Paediatrics Neonatology Background HIE remains a serious condition that causes significant mortality and longterm morbidity.
Difficulties at Birth: Long Term Developmental Outcomes
 Difficulties at Birth: Long Term Developmental Outcomes Alan D. Bedrick MD Division of Neonatology and Developmental Biology Department of Pediatrics University of Arizona Tucson, Arizona DISCLOSURE I
Difficulties at Birth: Long Term Developmental Outcomes Alan D. Bedrick MD Division of Neonatology and Developmental Biology Department of Pediatrics University of Arizona Tucson, Arizona DISCLOSURE I
Neonatal Seizure. Dr.Nawar Yahya. Presented by: Sarah Khalil Zeina Shamil Zainab Waleed Zainab Qahtan. Supervised by:
 Neonatal Seizure Supervised by: Dr.Nawar Yahya Presented by: Sarah Khalil Zeina Shamil Zainab Waleed Zainab Qahtan Objectives: What is neonatal seizure Etiology Clinical presentation Differential diagnosis
Neonatal Seizure Supervised by: Dr.Nawar Yahya Presented by: Sarah Khalil Zeina Shamil Zainab Waleed Zainab Qahtan Objectives: What is neonatal seizure Etiology Clinical presentation Differential diagnosis
TRAINING NEONATOLOGY SILVANA PARIS
 TRAINING ON NEONATOLOGY SILVANA PARIS RESUSCITATION IN DELIVERY ROOM INTRODUCTION THE GLOBAL RESUSCITATION BURDEN IN NEWBORN 136 MILL NEWBORN BABIES EACH YEAR (WHO WORLD REPORT) 5-8 MILL NEWBORN INFANTS
TRAINING ON NEONATOLOGY SILVANA PARIS RESUSCITATION IN DELIVERY ROOM INTRODUCTION THE GLOBAL RESUSCITATION BURDEN IN NEWBORN 136 MILL NEWBORN BABIES EACH YEAR (WHO WORLD REPORT) 5-8 MILL NEWBORN INFANTS
Predicting Outcomes in HIE. Naaz Merchant Consultant Neonatologist Beds & Herts Meeting 17/03/2016
 Predicting Outcomes in HIE Naaz Merchant Consultant Neonatologist Beds & Herts Meeting 17/03/2016 Interactive please! Case 1 Term, 3.5 kg Antenatal: Breech Labour/Delivery: Em CS failure to progress, mec
Predicting Outcomes in HIE Naaz Merchant Consultant Neonatologist Beds & Herts Meeting 17/03/2016 Interactive please! Case 1 Term, 3.5 kg Antenatal: Breech Labour/Delivery: Em CS failure to progress, mec
State of Florida Systemic Supportive Care Guidelines. Michael D. Weiss, M.D. Associate Professor of Pediatrics Division of Neonatology
 State of Florida Systemic Supportive Care Guidelines Michael D. Weiss, M.D. Associate Professor of Pediatrics Division of Neonatology I. FEN 1. What intravenous fluids should be initiated upon admission
State of Florida Systemic Supportive Care Guidelines Michael D. Weiss, M.D. Associate Professor of Pediatrics Division of Neonatology I. FEN 1. What intravenous fluids should be initiated upon admission
Severity of Hypoxic Ischaemic Encephalopathy in Neonates with Birth Asphyxia
 Journal of Rawalpindi Medical College (JRMC); 2007; (): 8-22 Severity of Hypoxic Ischaemic Encephalopathy in Neonates with Birth Asphyxia Rubina Zulfiqar, Samiya Naeemullah Department of Paediatrics, Holy
Journal of Rawalpindi Medical College (JRMC); 2007; (): 8-22 Severity of Hypoxic Ischaemic Encephalopathy in Neonates with Birth Asphyxia Rubina Zulfiqar, Samiya Naeemullah Department of Paediatrics, Holy
1 Pediatric Advanced Life Support Science Update What s New for 2010? 3 CPR. 4 4 Steps of BLS Survey 5 CPR 6 CPR.
 1 Pediatric Advanced Life Support Science Update 2010 2 What s New for 2010? 3 CPR Take no longer than seconds for pulse check Rate at least on per minute (instead of around 100 per minute ) Depth change:
1 Pediatric Advanced Life Support Science Update 2010 2 What s New for 2010? 3 CPR Take no longer than seconds for pulse check Rate at least on per minute (instead of around 100 per minute ) Depth change:
Fetal Heart Rate Monitoring Myths and Misperceptions s: Electronic Fetal Heart Rate Monitoring (EFM): Baseline Assumptions.
 Can FHR Monitoring Prevent Hypoxic-Ischemic Encephalopathy in the Newborn? Fetal Heart Rate Monitoring Myths and Misperceptions 1. Yes 2. No 72% Tekoa L. King CNM, MPH June 6, 2008 28% Yes No Objectives
Can FHR Monitoring Prevent Hypoxic-Ischemic Encephalopathy in the Newborn? Fetal Heart Rate Monitoring Myths and Misperceptions 1. Yes 2. No 72% Tekoa L. King CNM, MPH June 6, 2008 28% Yes No Objectives
Neonatal Life Support Provider (NLSP) Certification Preparatory Materials
 Neonatal Life Support Provider (NLSP) Certification Preparatory Materials NEONATAL LIFE SUPPORT PROVIDER (NRP) CERTIFICATION TABLE OF CONTENTS NEONATAL FLOW ALGORITHM.2 INTRODUCTION 3 ANTICIPATION OF RESUSCITATION
Neonatal Life Support Provider (NLSP) Certification Preparatory Materials NEONATAL LIFE SUPPORT PROVIDER (NRP) CERTIFICATION TABLE OF CONTENTS NEONATAL FLOW ALGORITHM.2 INTRODUCTION 3 ANTICIPATION OF RESUSCITATION
PedsCases Podcast Scripts
 PedsCases Podcast Scripts This is a text version of a podcast from Pedscases.com on Neonatal Extracranial Head Injuries. These podcasts are designed to give medical students an overview of key topics in
PedsCases Podcast Scripts This is a text version of a podcast from Pedscases.com on Neonatal Extracranial Head Injuries. These podcasts are designed to give medical students an overview of key topics in
Neonatal Resuscitation. Dustin Coyle, M.D. Anesthesiology
 Neonatal Resuscitation Dustin Coyle, M.D. Anesthesiology Recognize complications Maternal-fetal factors Maternal DM PIH Chronic HTN Previous stillbirth Rh sensitization Infection Substance abuse/certain
Neonatal Resuscitation Dustin Coyle, M.D. Anesthesiology Recognize complications Maternal-fetal factors Maternal DM PIH Chronic HTN Previous stillbirth Rh sensitization Infection Substance abuse/certain
Admission/Discharge Form for Infants Born in Please DO NOT mail or fax this form to the CPQCC Data Center. This form is for internal use ONLY.
 Selection Criteria Admission/Discharge Form for Infants Born in 2016 To be eligible, you MUST answer YES to at least one of the possible criteria (A-C) A. 401 1500 grams o Yes B. GA range 22 0/7 31 6/7
Selection Criteria Admission/Discharge Form for Infants Born in 2016 To be eligible, you MUST answer YES to at least one of the possible criteria (A-C) A. 401 1500 grams o Yes B. GA range 22 0/7 31 6/7
COOLING FOR NEONATAL HYPOXIC ISCHAEMIC ENCEPHALOPATHY (HIE) - GUIDELINE
 Background Objective Equipment Indications Contraindications When to initiate cooling in NPICU Procedure for therapeutic cooling NETS Transfer Issues Follow-up References Acknowledgements Related Documents
Background Objective Equipment Indications Contraindications When to initiate cooling in NPICU Procedure for therapeutic cooling NETS Transfer Issues Follow-up References Acknowledgements Related Documents
FHR Monitoring: Maternal Fetal Physiology
 FHR Monitoring: Maternal Fetal Physiology M. Sean Esplin, MD and Alexandra Eller, MD Maternal Fetal Medicine Intermountain Healthcare University of Utah Health Sciences Center Disclosures I have no financial
FHR Monitoring: Maternal Fetal Physiology M. Sean Esplin, MD and Alexandra Eller, MD Maternal Fetal Medicine Intermountain Healthcare University of Utah Health Sciences Center Disclosures I have no financial
Stabilization of the Newborn for Transport. Relevant Disclosure. Learning Objectives
 Stabilization of the Newborn for Transport Arlen Foulks, DO FAAP FACOP Medical Director, CCMH Level II NICU Medical Director, NeoFlight Assistant Professor of Pediatrics Neonatal Perinatal Medicine Section,
Stabilization of the Newborn for Transport Arlen Foulks, DO FAAP FACOP Medical Director, CCMH Level II NICU Medical Director, NeoFlight Assistant Professor of Pediatrics Neonatal Perinatal Medicine Section,
Neonatal abstinence syndrome
 PedsCases Podcast Scripts This is a text version of a podcast from Pedscases.com on the Neonatal Abstinence Syndrome. These podcasts are designed to give medical students an overview of key topics in pediatrics.
PedsCases Podcast Scripts This is a text version of a podcast from Pedscases.com on the Neonatal Abstinence Syndrome. These podcasts are designed to give medical students an overview of key topics in pediatrics.
Brain injury and Resuscitation! Turning Back the Clock!
 Brain injury and Resuscitation! Turning Back the Clock! Dec 2008 Patrick J McNamara Learning Objectives Understand the benefits of Hypothermia and how it works? Identify patients who may benefit from treatment.
Brain injury and Resuscitation! Turning Back the Clock! Dec 2008 Patrick J McNamara Learning Objectives Understand the benefits of Hypothermia and how it works? Identify patients who may benefit from treatment.
Addendum to the NRP Provider Textbook 6 th Edition Recommendations for specific modifications in the Canadian context
 Addendum to the NRP Provider Textbook 6 th Edition Recommendations for specific modifications in the Canadian context A subcommittee of the Canadian Neonatal Resuscitation Program (NRP) Steering Committee
Addendum to the NRP Provider Textbook 6 th Edition Recommendations for specific modifications in the Canadian context A subcommittee of the Canadian Neonatal Resuscitation Program (NRP) Steering Committee
NEONATAL SEIZURE. IAP UG Teaching slides
 NEONATAL SEIZURE 1 INTRODUCTION One of the important neonatal neurological emergencies requiring immediate medical care. Contribute to significant morbidity and mortality Incidence is around 0.5 to 0.8%
NEONATAL SEIZURE 1 INTRODUCTION One of the important neonatal neurological emergencies requiring immediate medical care. Contribute to significant morbidity and mortality Incidence is around 0.5 to 0.8%
Therapeutic Hypothermia for infants > 35 wks with moderate or severe Hypoxic Ischaemic Encephalopathy (HIE) Clinical Guideline Reference Number:
 This is an official Northern Trust policy and should not be edited in any way Therapeutic Hypothermia for infants > 35 wks with moderate or severe Hypoxic Ischaemic Encephalopathy (HIE) Clinical Guideline
This is an official Northern Trust policy and should not be edited in any way Therapeutic Hypothermia for infants > 35 wks with moderate or severe Hypoxic Ischaemic Encephalopathy (HIE) Clinical Guideline
BRUE and Apnea at Term, how do they relate?
 BRUE and Apnea at Term, how do they relate? Mary Elaine Patrinos, M.D. Attending Neonatologist Rainbow Babies and Children s Hospital Director, Infant Apnea Program Apnea at Term Can it happen? How does
BRUE and Apnea at Term, how do they relate? Mary Elaine Patrinos, M.D. Attending Neonatologist Rainbow Babies and Children s Hospital Director, Infant Apnea Program Apnea at Term Can it happen? How does
Hypoglycaemia of the neonate. Dr. L.G. Lloyd Dept. Paediatrics
 Hypoglycaemia of the neonate Dr. L.G. Lloyd Dept. Paediatrics Why is glucose important? It provides 60-70% of energy needs Utilization obligatory by red blood cells, brain and kidney as major source of
Hypoglycaemia of the neonate Dr. L.G. Lloyd Dept. Paediatrics Why is glucose important? It provides 60-70% of energy needs Utilization obligatory by red blood cells, brain and kidney as major source of
Disclosures. Pediatrician Financial: none Volunteer :
 Brain Resuscitation Neurocritical Care Monitoring & Therapies CCCF November 2, 2016 Anne-Marie Guerguerian Critical Care Medicine, The Hospital for Sick Children University of Toronto Disclosures Pediatrician
Brain Resuscitation Neurocritical Care Monitoring & Therapies CCCF November 2, 2016 Anne-Marie Guerguerian Critical Care Medicine, The Hospital for Sick Children University of Toronto Disclosures Pediatrician
HYPOXIC ISCHEMIC ENCEPHALOPATHY AND THE OBSTETRICIAN
 HYPOXIC ISCHEMIC ENCEPHALOPATHY AND THE OBSTETRICIAN DISCLOSURE I have nothing to disclose and have no real or potential conflicts with this presentation and its content. Michael P. Nageotte, M.D. CASE:
HYPOXIC ISCHEMIC ENCEPHALOPATHY AND THE OBSTETRICIAN DISCLOSURE I have nothing to disclose and have no real or potential conflicts with this presentation and its content. Michael P. Nageotte, M.D. CASE:
5 Million neonatal deaths each year worldwide. 20% caused by neonatal asphyxia. Improvement of the outcome of 1 million newborns every year
 1 5 Million neonatal deaths each year worldwide 20% caused by neonatal asphyxia Improvement of the outcome of 1 million newborns every year International Liaison Committee on Resuscitation (ILCOR) American
1 5 Million neonatal deaths each year worldwide 20% caused by neonatal asphyxia Improvement of the outcome of 1 million newborns every year International Liaison Committee on Resuscitation (ILCOR) American
Hypothermia: The Science and Recommendations (In-hospital and Out)
 Hypothermia: The Science and Recommendations (In-hospital and Out) L. Kristin Newby, MD, MHS Professor of Medicine Duke University Medical Center Chair, Council on Clinical Cardiology, AHA President, Society
Hypothermia: The Science and Recommendations (In-hospital and Out) L. Kristin Newby, MD, MHS Professor of Medicine Duke University Medical Center Chair, Council on Clinical Cardiology, AHA President, Society
The high risk neonate
 The high risk neonate Infant classification by gestational (postmenstrual) age Preterm. Less than 37 completed weeks (259 days). Term. Thirty-seven to 416/7 weeks (260-294 days). Post-term. Forty-two weeks
The high risk neonate Infant classification by gestational (postmenstrual) age Preterm. Less than 37 completed weeks (259 days). Term. Thirty-seven to 416/7 weeks (260-294 days). Post-term. Forty-two weeks
Perlman J, Clinics Perinatol 2006; 33: Underlying causal pathways. Antenatal Intrapartum Postpartum. Acute near total asphyxia
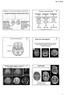 Perlman J, Clinics Perinatol 2006; 33:335-353 Underlying causal pathways Antenatal Intrapartum Postpartum Acute injury Subacute injury Associated problem Reduced fetal movements Placental insufficiency
Perlman J, Clinics Perinatol 2006; 33:335-353 Underlying causal pathways Antenatal Intrapartum Postpartum Acute injury Subacute injury Associated problem Reduced fetal movements Placental insufficiency
Current Management of the Infant Who Presents with Neonatal Encephalopathy
 Current Management of the Infant Who Presents with Neonatal Encephalopathy Elena V. Wachtel, MD, MPH, FAAP, and Karen D. Hendricks-Muñoz, MD, MPH, FAAP Neonatal encephalopathy after perinatal hypoxic-ischemic
Current Management of the Infant Who Presents with Neonatal Encephalopathy Elena V. Wachtel, MD, MPH, FAAP, and Karen D. Hendricks-Muñoz, MD, MPH, FAAP Neonatal encephalopathy after perinatal hypoxic-ischemic
Neurological outcome after perinatal asphyxia at term
 Section 1 Chapter 1 Scientific background Neurological outcome after perinatal asphyxia at term David Odd and Andrew Whitelaw Introduction It was nearly 150 years ago that an association between perinatal
Section 1 Chapter 1 Scientific background Neurological outcome after perinatal asphyxia at term David Odd and Andrew Whitelaw Introduction It was nearly 150 years ago that an association between perinatal
DOWNLOAD OR READ : PERINATAL EVENTS AND BRAIN DAMAGE IN SURVIVING CHILDREN BASED ON PAPERS PRESENTED AT AN INTERNATIONA PDF EBOOK EPUB MOBI
 DOWNLOAD OR READ : PERINATAL EVENTS AND BRAIN DAMAGE IN SURVIVING CHILDREN BASED ON PAPERS PRESENTED AT AN INTERNATIONA PDF EBOOK EPUB MOBI Page 1 Page 2 perinatal events and brain damage in surviving
DOWNLOAD OR READ : PERINATAL EVENTS AND BRAIN DAMAGE IN SURVIVING CHILDREN BASED ON PAPERS PRESENTED AT AN INTERNATIONA PDF EBOOK EPUB MOBI Page 1 Page 2 perinatal events and brain damage in surviving
Correlation of Neurodevelopmental Outcome and brain MRI/EEG findings in term HIE infants
 Correlation of Neurodevelopmental Outcome and brain MRI/EEG findings in term HIE infants Ajou University School of Medicine Department of Pediatrics Moon Sung Park M.D. Hee Cheol Jo, M.D., Jang Hoon Lee,
Correlation of Neurodevelopmental Outcome and brain MRI/EEG findings in term HIE infants Ajou University School of Medicine Department of Pediatrics Moon Sung Park M.D. Hee Cheol Jo, M.D., Jang Hoon Lee,
Table 1: The major changes in AHA / AAP neonatal resuscitation guidelines2010 compared to previous recommendations in 2005
 Table 1: The major changes in AHA / AAP neonatal guidelines2010 compared to previous recommendations in 2005 Resuscitation step Recommendations (2005) Recommendations (2010) Comments/LOE 1) Assessment
Table 1: The major changes in AHA / AAP neonatal guidelines2010 compared to previous recommendations in 2005 Resuscitation step Recommendations (2005) Recommendations (2010) Comments/LOE 1) Assessment
Status Epilepticus in Children
 PedsCases Podcast Scripts This is a text version of a podcast from Pedscases.com on Status Epilepticus in Children. These podcasts are designed to give medical students an overview of key topics in pediatrics.
PedsCases Podcast Scripts This is a text version of a podcast from Pedscases.com on Status Epilepticus in Children. These podcasts are designed to give medical students an overview of key topics in pediatrics.
INDUCED HYPOTHERMIA A Hot Topic. R. Darrell Nelson, MD, FACEP Emergency Medicine Wake Forest University Health Sciences
 INDUCED HYPOTHERMIA A Hot Topic R. Darrell Nelson, MD, FACEP Emergency Medicine Wake Forest University Health Sciences Conflicts of Interest Sadly, we have no financial or industrial conflicts of interest
INDUCED HYPOTHERMIA A Hot Topic R. Darrell Nelson, MD, FACEP Emergency Medicine Wake Forest University Health Sciences Conflicts of Interest Sadly, we have no financial or industrial conflicts of interest
Serum creatine kinase and lactic dehydrogenase levels as useful markers of immediate and long-term outcome of perinatal asphyxia
 Serum creatine kinase and lactic dehydrogenase levels as useful markers of immediate and long-term outcome of perinatal asphyxia D H Karunatilaka 1, G W D S Amaratunga 2, K D N I Perera 3, V Caldera 4
Serum creatine kinase and lactic dehydrogenase levels as useful markers of immediate and long-term outcome of perinatal asphyxia D H Karunatilaka 1, G W D S Amaratunga 2, K D N I Perera 3, V Caldera 4
ACoRN Workbook 2012 Update
 ACoRN Neonatal Society Société néonatale ACoRN www.acornprogram.net A Canadian non-profit Society Vancouver, British Columbia ACoRN Workbook 2012 Update Name: The ACoRN Process The Resuscitation Sequence
ACoRN Neonatal Society Société néonatale ACoRN www.acornprogram.net A Canadian non-profit Society Vancouver, British Columbia ACoRN Workbook 2012 Update Name: The ACoRN Process The Resuscitation Sequence
Relationships Relationships
 PRENATAL OPIATE EXPOSURE IMPACT ON EARLY CHILDHOOD LEARNING AND BEHAVIOR Ira J. Chasnoff, MD NTI Upstream www.ntiupstream.com Children grow and develop in the context of Attachment: Basic Concept Attachment:
PRENATAL OPIATE EXPOSURE IMPACT ON EARLY CHILDHOOD LEARNING AND BEHAVIOR Ira J. Chasnoff, MD NTI Upstream www.ntiupstream.com Children grow and develop in the context of Attachment: Basic Concept Attachment:
The NeuroNICU From Concept to Clinical Service. MJ Harbert, MD Co-Director, NeuroNICU Service Rady Children s Hospital San Diego
 The NeuroNICU From Concept to Clinical Service MJ Harbert, MD Co-Director, NeuroNICU Service Rady Children s Hospital San Diego What is a NeuroNICU? Collaboration between Neonatology and Neurology Neonatal
The NeuroNICU From Concept to Clinical Service MJ Harbert, MD Co-Director, NeuroNICU Service Rady Children s Hospital San Diego What is a NeuroNICU? Collaboration between Neonatology and Neurology Neonatal
Infection. Risk factor for infection ACoRN alerting sign with * Clinical deterioration. Problem List. Respiratory. Cardiovascular
 The ACoRN Process Baby at risk Unwell Risk factors Post-resuscitation requiring stabilization Resuscitation Ineffective breathing Heart rate < 100 bpm Central cyanosis Support Infection Risk factor for
The ACoRN Process Baby at risk Unwell Risk factors Post-resuscitation requiring stabilization Resuscitation Ineffective breathing Heart rate < 100 bpm Central cyanosis Support Infection Risk factor for
Figure removed due to copyright restrictions.
 Harvard-MIT Division of Health Sciences and Technology HST.071: Human Reproductive Biology Course Director: Professor Henry Klapholz IN SUMMARY HST 071 An Example of a Fetal Heart Rate Tracing Figure removed
Harvard-MIT Division of Health Sciences and Technology HST.071: Human Reproductive Biology Course Director: Professor Henry Klapholz IN SUMMARY HST 071 An Example of a Fetal Heart Rate Tracing Figure removed
Temperature Correction of Blood Gas Measurements during Therapeutic Hypothermia: Is it Time to Chill Out?
 Temperature Correction of Blood Gas Measurements during Therapeutic Hypothermia: Is it Time to Chill Out? Dr. Elizabeth Zorn Dr. Gwenyth Fischer Dr. Martha Lyon Disclosures (ML) Speaking Honoraria Radiometer
Temperature Correction of Blood Gas Measurements during Therapeutic Hypothermia: Is it Time to Chill Out? Dr. Elizabeth Zorn Dr. Gwenyth Fischer Dr. Martha Lyon Disclosures (ML) Speaking Honoraria Radiometer
Kimberly M. Thornton, 1,2 Hongying Dai, 3 Seth Septer, 2,4 and Joshua E. Petrikin 1,2. 1. Introduction
 International Pediatrics, Article ID 643689, 7 pages http://dx.doi.org/10.1155/2014/643689 Research Article Effects of Whole Body Therapeutic Hypothermia on Gastrointestinal Morbidity and Feeding Tolerance
International Pediatrics, Article ID 643689, 7 pages http://dx.doi.org/10.1155/2014/643689 Research Article Effects of Whole Body Therapeutic Hypothermia on Gastrointestinal Morbidity and Feeding Tolerance
Study of role of MRI brain in evaluation of hypoxic ischemic encephalopathy
 Original article: Study of role of MRI brain in evaluation of hypoxic ischemic encephalopathy *Dr Harshad Bhagat, ** Dr Ravindra Kawade, ***Dr Y.P.Sachdev *Junior Resident, Department Of Radiodiagnosis,
Original article: Study of role of MRI brain in evaluation of hypoxic ischemic encephalopathy *Dr Harshad Bhagat, ** Dr Ravindra Kawade, ***Dr Y.P.Sachdev *Junior Resident, Department Of Radiodiagnosis,
Therapeutic Hypothermia
 Objectives Overview Therapeutic Hypothermia Nerissa U. Ko, MD, MAS UCSF Department of Neurology Critical Care Medicine and Trauma June 4, 2011 Hypothermia as a neuroprotectant Proven indications: Adult
Objectives Overview Therapeutic Hypothermia Nerissa U. Ko, MD, MAS UCSF Department of Neurology Critical Care Medicine and Trauma June 4, 2011 Hypothermia as a neuroprotectant Proven indications: Adult
MODULE VII. Delivery and Immediate Neonatal Care
 MODULE VII Delivery and Immediate Neonatal Care NEONATAL ASPHYXIA About one million deaths per year In Latin America 12% of newborns suffer some degree of asphyxia Main cause of perinatal and neonatal
MODULE VII Delivery and Immediate Neonatal Care NEONATAL ASPHYXIA About one million deaths per year In Latin America 12% of newborns suffer some degree of asphyxia Main cause of perinatal and neonatal
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of therapeutic hypothermia with intracorporeal temperature monitoring for hypoxic
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of therapeutic hypothermia with intracorporeal temperature monitoring for hypoxic
Patient Case. Post cardiac arrest pathophysiology 10/19/2017. Disclosure. Objectives. Patient Case-TM
 Disclosure TARGETED TEMPERATURE MANAGEMENT POST CARDIAC ARREST I have nothing to disclose concerning possible financial or personal relationships with commercial entities that may have a direct or indirect
Disclosure TARGETED TEMPERATURE MANAGEMENT POST CARDIAC ARREST I have nothing to disclose concerning possible financial or personal relationships with commercial entities that may have a direct or indirect
Automated System for Detecting Neonatal Brain Injuries
 Snapshots of Postgraduate Research at University College Cork 2016 Automated System for Detecting Neonatal Brain Injuries Rehan Ahmed Dept. of Electrical and Electronics Engineering,, UCC The most dangerous
Snapshots of Postgraduate Research at University College Cork 2016 Automated System for Detecting Neonatal Brain Injuries Rehan Ahmed Dept. of Electrical and Electronics Engineering,, UCC The most dangerous
NRP Raising the Bar for Providers and Instructors
 NRP 2011 Raising the Bar for Providers and Instructors What is the same? 1. Minimum course requirement is Lessons 1 through 4 and Lesson 9. The NRP Provider Card requires renewal every 2 years. Your facility
NRP 2011 Raising the Bar for Providers and Instructors What is the same? 1. Minimum course requirement is Lessons 1 through 4 and Lesson 9. The NRP Provider Card requires renewal every 2 years. Your facility
INDUCED HYPOTHERMIA. F. Ben Housel, M.D.
 INDUCED HYPOTHERMIA F. Ben Housel, M.D. Historical Use of Induced Hypothermia 1950 s - Moderate hypothermia (30-32º C) in open heart surgery to protect brain against global ischemia 1960-1980 s - Use of
INDUCED HYPOTHERMIA F. Ben Housel, M.D. Historical Use of Induced Hypothermia 1950 s - Moderate hypothermia (30-32º C) in open heart surgery to protect brain against global ischemia 1960-1980 s - Use of
Early seizures indicate quality of perinatal care
 Archives of Disease in Childhood, 1985, 6, 89-813 Early seizures indicate quality of perinatal care R J DERHAM, T G MATTHEWS, AND T A CLARKE Rotunda Hospital, Dublin, Ireland SUMMARY An analysis of antepartum,
Archives of Disease in Childhood, 1985, 6, 89-813 Early seizures indicate quality of perinatal care R J DERHAM, T G MATTHEWS, AND T A CLARKE Rotunda Hospital, Dublin, Ireland SUMMARY An analysis of antepartum,
Neonatal/Pediatric Cardiopulmonary Care
 Neonatal/Pediatric Cardiopulmonary Care Resuscitation 2 When To Resuscitate Need usually related Combination of Can occur in 3 Causes of Fetal Asphyxia 1 4 Apnea Hypoxia Stimulates chemoreceptors & baroreceptors
Neonatal/Pediatric Cardiopulmonary Care Resuscitation 2 When To Resuscitate Need usually related Combination of Can occur in 3 Causes of Fetal Asphyxia 1 4 Apnea Hypoxia Stimulates chemoreceptors & baroreceptors
Review Article Current Controversies in Newer Therapies to Treat Birth Asphyxia
 International Pediatrics Volume 2011, Article ID 848413, 5 pages doi:10.1155/2011/848413 Review Article Current Controversies in Newer Therapies to Treat Birth Asphyxia Pia Wintermark Division of Newborn
International Pediatrics Volume 2011, Article ID 848413, 5 pages doi:10.1155/2011/848413 Review Article Current Controversies in Newer Therapies to Treat Birth Asphyxia Pia Wintermark Division of Newborn
MODULE VII. Delivery and Immediate Neonatal Care
 MODULE VII Delivery and Immediate Neonatal Care NEONATAL ASPHYXIA About one million deaths per year In Latin America 12% of newborns suffer some degree of asphyxia A major cause of perinatal and neonatal
MODULE VII Delivery and Immediate Neonatal Care NEONATAL ASPHYXIA About one million deaths per year In Latin America 12% of newborns suffer some degree of asphyxia A major cause of perinatal and neonatal
Post Cardiac Arrest Care 2015 American Heart Association Guideline Update for CPR and Emergency Cardiovascular Care
 Post Cardiac Arrest Care 2015 American Heart Association Guideline Update for CPR and Emergency Cardiovascular Care รศ.ดร.พญ.ต นหยง พ พานเมฆาภรณ ภาคว ชาว ส ญญ ว ทยา คณะแพทยศาสตร มหาว ทยาล ยเช ยงใหม System
Post Cardiac Arrest Care 2015 American Heart Association Guideline Update for CPR and Emergency Cardiovascular Care รศ.ดร.พญ.ต นหยง พ พานเมฆาภรณ ภาคว ชาว ส ญญ ว ทยา คณะแพทยศาสตร มหาว ทยาล ยเช ยงใหม System
NEONATOLOGY GIVES BACK WHAT OBSTETRICS TAKE AWAY. It is well-known that hypoxic and/or ischemic events during labor and
 NEONATOLOGY GIVES BACK WHAT OBSTETRICS TAKE AWAY I. Introduction It is well-known that hypoxic and/or ischemic events during labor and delivery can cause injury to the baby's brain. The mechanisms at first
NEONATOLOGY GIVES BACK WHAT OBSTETRICS TAKE AWAY I. Introduction It is well-known that hypoxic and/or ischemic events during labor and delivery can cause injury to the baby's brain. The mechanisms at first
1/29/2014. Kimberly Johnson Hatchett, MD PGY-4 11/15/13
 Kimberly Johnson Hatchett, MD PGY-4 11/15/13 History of Present Illness 14 month old previously healthy infant boy presented via EMS after being found by his mother to be breathing loudly and non-responsive.
Kimberly Johnson Hatchett, MD PGY-4 11/15/13 History of Present Illness 14 month old previously healthy infant boy presented via EMS after being found by his mother to be breathing loudly and non-responsive.
Initiation of passive cooling at referring centre is most predictive of achieving early therapeutic hypothermia in asphyxiated newborns
 Paediatrics & Child Health, 2017, 264 268 doi: 10.1093/pch/pxx062 Original Article Advance Access publication 23 May 2017 Original Article Initiation of passive cooling at referring centre is most predictive
Paediatrics & Child Health, 2017, 264 268 doi: 10.1093/pch/pxx062 Original Article Advance Access publication 23 May 2017 Original Article Initiation of passive cooling at referring centre is most predictive
The Pharmacokinetics of Antiepileptics Drugs in Neonates with Hypoxic Ischemic Encephalopathy
 The Pharmacokinetics of Antiepileptics Drugs in Neonates with Hypoxic Ischemic Encephalopathy KELIANA O MARA, PHARMD FLORIDA NEONATAL NEUROLOGIC NETWORK STATE MEETING Objectives Describe seizures in hypoxic
The Pharmacokinetics of Antiepileptics Drugs in Neonates with Hypoxic Ischemic Encephalopathy KELIANA O MARA, PHARMD FLORIDA NEONATAL NEUROLOGIC NETWORK STATE MEETING Objectives Describe seizures in hypoxic
Prevention and Management of Hypoglycaemia of the Breastfed Newborn Reference Number:
 This is an official Northern Trust policy and should not be edited in any way Prevention and Management of Hypoglycaemia of the Breastfed Newborn Reference Number: NHSCT/10/293 Target audience: Midwifery,
This is an official Northern Trust policy and should not be edited in any way Prevention and Management of Hypoglycaemia of the Breastfed Newborn Reference Number: NHSCT/10/293 Target audience: Midwifery,
Cerebral function monitoring in term or near term neonates at MDH: preliminary experience and proposal of a guideline
 Original Article Cerebral function monitoring in term or near term neonates at MDH: preliminary experience and proposal of a guideline Stephen Attard, Doriette Soler, Paul Soler Introduction: Cerebral
Original Article Cerebral function monitoring in term or near term neonates at MDH: preliminary experience and proposal of a guideline Stephen Attard, Doriette Soler, Paul Soler Introduction: Cerebral
Pediatric Shock. Hypovolemia. Sepsis. Most common cause of pediatric shock Small blood volumes (80cc/kg)
 Critical Concepts: Shock Inadequate peripheral perfusion where oxygen delivery does not meet metabolic demand Adult vs Pediatric Shock - Same causes/different frequencies Pediatric Shock Hypovolemia Most
Critical Concepts: Shock Inadequate peripheral perfusion where oxygen delivery does not meet metabolic demand Adult vs Pediatric Shock - Same causes/different frequencies Pediatric Shock Hypovolemia Most
Running head: CASE STUDY NEONATAL HEAD COOLING 1
 Running head: CASE STUDY NEONATAL HEAD COOLING 1 Case Study 1: Head Cooling as Treatment for Neonatal Encephalopathy NURS 6035 Practicum I Teresa Z. Baker Texas Woman s University CASE STUDY NEONATAL HEAD
Running head: CASE STUDY NEONATAL HEAD COOLING 1 Case Study 1: Head Cooling as Treatment for Neonatal Encephalopathy NURS 6035 Practicum I Teresa Z. Baker Texas Woman s University CASE STUDY NEONATAL HEAD
International Journal of Health Sciences and Research ISSN:
 International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Original Research Article A Study on Serum Calcium Level in Birth Asphyxia Amrita Vamne 1*, Ramesh Chandra Thanna 2*,
International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Original Research Article A Study on Serum Calcium Level in Birth Asphyxia Amrita Vamne 1*, Ramesh Chandra Thanna 2*,
Simulation 3: Post-term Baby in Labor and Delivery
 Simulation 3: Post-term Baby in Labor and Delivery Opening Scenario (Links to Section 1) You are an evening-shift respiratory therapist in a large hospital with a level III neonatal unit. You are paged
Simulation 3: Post-term Baby in Labor and Delivery Opening Scenario (Links to Section 1) You are an evening-shift respiratory therapist in a large hospital with a level III neonatal unit. You are paged
