Hydrocephalus is a neurological disorder INDEX OF CEREBROSPINAL COMPENSATORY RESERVE CLINICAL STUDIES IN HYDROCEPHALUS
|
|
|
- Madeline Cain
- 6 years ago
- Views:
Transcription
1 Dong- Joo Kim, M.Eng. and Micromechanics Laboratory, Department of Engineering, Zofia Czosnyka, Ph.D. Nicole Keong, M.D. Danila K. Radolovich, M.D., and Department of Anaesthesiology, University of Pavia, Pavia, Italy Peter Smielewski, Ph.D. Michael P.F. Sutcliffe, Ph.D. Department of Engineering, John D. Pickard, M.Chir., F.Med.Sci. Marek Czosnyka, Ph.D. Reprint requests: Marek Czosnyka, Ph.D., Neurosurgery Unit, Department of Neurosurgery, Box 167 Cambridge CB2 2QQ, England. Received, February 1, Accepted, September 26, Copyright 2009 by the Congress of Neurological Surgeons CLINICAL STUDIES INDEX OF CEREBROSPINAL COMPENSATORY RESERVE IN HYDROCEPHALUS OBJECTIVE: An index of cerebrospinal compensatory reserve (RAP) has been introduced as a potential descriptor of neurological deterioration after head trauma. It is numerically computed as a linear correlation coefficient between the mean intracranial pressure and the pulse amplitude of the pressure waveform. We explore how RAP varies with different forms of physiological or nonphysiological intracranial volume loads in adult hydrocephalus, with and without a functioning cerebrospinal fluid (CSF) shunt. METHODS: A database of intracranial pressure recordings during CSF infusion studies and overnight monitoring in hydrocephalic patients was reviewed for clinical comparison of homogeneous subgroups of patients with hypothetical differences of pressurevolume compensatory reserve. The database includes 980 patients of mixed etiology: idiopathic normal pressure hydrocephalus (NPH), 47%; postsubarachnoid hemorrhage NPH, 12%; noncommunicating hydrocephalus, 22%; others, 19%. All CSF compensatory parameters were calculated by using intracranial pressure waveforms. RESULTS: In NPH, RAP correlated strongly with the resistance to CSF outflow (r s 0.35; P 0.045), but weakly correlated with ventriculomegaly (r s 0.13; P 0.41). In idiopathic nonshunted NPH patients, RAP did not correlate significantly with elasticity calculated from the CSF infusion test (r s 0.11; P 0.21). During infusion studies, RAP increased in comparison to values recorded at baseline (from a median of , P 0.14*10-8 ), indicating a narrowing of the volume- pressure compensatory reserve. During B- waves associated with the REM (rapid eye movement) phase of sleep, RAP increased from a median of 0.53 to 0.89; P 1.2*10-5. After shunting, RAP decreased (median before shunting, 0.59; median after shunting, 0.34; P ). RAP also showed the ability to reflect the functional state of the shunt (patent shunt median, 0.36; blocked shunt median, 0.84; P ). CONCLUSION: RAP appears to characterize pressure- volume compensatory reserve in patients with hydrocephalus. KEY WORDS: Hydrocephalus, Pressure- volume compensation, Shunting, Waveform analysis Neurosurgery 64: , 2009 DOI: /01.NEU online.com Hydrocephalus is a neurological disorder that can result in significant disability or even death, regardless of age, sex, or any other individual characteristic. Because of the complex interaction between intracranial pressure (ICP) and hydrocephalus, no clear conclusions can be drawn from the magnitude of ICP alone. Uncontrolled and increased ICP is one of the most common causes of neurological death, whereas patients with large spaceoccupying lesions may have clinical signs of neurological distortion (e.g., brainstem) without significant elevation of ICP (17, 23). The phenomena of local or global effects such as ventricular dilation, raised ICP, and a depleted pressure- volume relationship are textbook concepts (5, 33). These may be regarded as symptoms that reflect the presence of a spaceoccupying process, which can no longer be compensated for. Consequently, subsidiary ABBREVIATIONS: AMP, pulse amplitude; CSF, cerebrospinal fluid; E, elasticity; ICP, intracranial pressure; NPH, normal pressure hydrocephalus; RAP, pressure- volume compensation index; r s, Spearman s correlation coefficient 494 VOLUME 64 NUMBER 3 MARCH
2 INDEX OF CEREBROSPINAL COMPENSATORY RESERVE IN HYDROCEPHALUS parameters are required to produce a better clinical judgment that may indicate when the equilibrium of the cerebrospinal fluid (CSF) system is disturbed or pressure- volume compensation is poor. Pressure- volume compensation index (RAP), used for head- injured patients (6, 9) may be an adequate indication of these conditions in hydrocephalus. Although the abbreviation is not intuitive, it is historically justified and derives from R (correlation coefficient), A (pulse amplitude), and P (mean intracranial pressure) (9, 11, 13, 14). To interpret RAP, it is critical to understand the pressurevolume curve, which is derived from the hypothetical relationship between the change in volume of the CSF compartment and the ICP, and is mainly divided into 3 regions, as shown in Figure 1 (5, 23 26). The curve in Region I shows a linear increase of pressure, with volume indicating good compensatory reserve (13). In this state, compliance of the system is independent of mean ICP. Further increase in the intracerebral volume produces an exponential rise in pressure, which indicates a decrease in compliance inversely proportional to the rising pressure (18). This is defined as Region II in Figure 1. The transition point from the linear to the exponential part of the pressure- volume curve is attributable to exhaustion of spatial compensatory capacity. In traumatic brain injury, Region III in Figure 1 can also be observed at very high values of ICP. It is characterized by a decrease of slope of the pressure- volume curve, and denotes impairment of active cerebrovascular regulatory mechanisms and subsequent ischemia. Such dramatic intracranial hypertension is seldom seen in hydrocephalus, particularly in normal pressure hydrocephalus (NPH) (2, 25). The concept of a moving correlation coefficient between mean ICP and associated changes in pulse amplitude (AMP) of ICP was introduced as a measure of compensatory reserve in headinjured patients (2, 9, 12, 14). It is related to the shape of the ICPvolume curve, which has 2 different trends depending on the region (Region III is not considered for hydrocephalus). In Region I (initial horizontal curve), AMP does not vary with the mean ICP. In Region II, when ICP increases more than proportionally to changes in intracranial volume, the amplitude increases in parallel with mean ICP. The transition point in the pressure- volume curve defines the threshold of a change in status in the compensatory reserve. Below this point, the relationship between CSF pressure and volume is linear, and the whole system is considered stable. However, this transition point is difficult to determine clinically without performing an infusion study; i.e., plotting a full pressure- volume curve (24 26). An easier way of using this information to make a clinical judgment for the status of compensatory reserve in the CSF system is to calculate the correlation coefficient RAP (between ICP and AMP). RAP close to 0 signifies good compensatory reserve, while RAP approaching 1 indicates a poor compensatory reserve (6, 13). CSF pressure- volume compensation is described by a relatively simple model, represented by a differential equation. The appendix contains a detailed mathematical description of the pressure- volume curve and the relationship between mean ICP and AMP. Although the interpretation of RAP has been extensively discussed in relation to head injuries, a number of issues A B C FIGURE 1. Schematic depiction of the pressure- volume compensation index (RAP) theory. A, pressure- volume curve with 3 distinct regions defined. In Region I, there is a linear relationship between volume and pressure; therefore, the intracranial pressure (ICP) amplitude remains constant (assuming constant pulse volume) (B). Thus, RAP (correlation between mean ICP and ICP pulse amplitude [AMP]) is 0, and that implies good compensatory reserve of the intracranial system (C). In Region II, the shape of the pressure- volume curve changes from linear to nonlinear (i.e., exponential). The curve s first derivative is also exponential; thus, the AMP increases proportionally to mean ICP. Consequently, RAP becomes +1, indicating the state of poor compensatory reserve. Region III of critically elevated ICP with deranged vascular reactivity is not relevant to normal pressure hydrocephalus (NPH) and, therefore, only transitions between Regions I and II are considered in this study. In this region, AMP decreases, with ICP rising further. This is caused by deflection of the pressure- volume curve to the right, as the arterial bed starts to collapse (cerebral blood volume decreases). As a consequence, RAP reaches a value close to -1. associated with hydrocephalus remain unclear (2, 9, 12, 14). Very recently, Schuhmann et al. (29) published the first account of use of RAP in diagnosing hydrocephalus in children. The objective of this article is to validate RAP as a parameter upon which clinical judgments can be made for hydrocephalus. Our analysis includes the following specific studies: 1) the correlation of RAP with elasticity (E) of the craniospinal system, resistance to CSF outflow, and dilation of the lateral ventricle; 2) the behavior of RAP during an external CSF volume load in NEUROSURGERY VOLUME 64 NUMBER 3 MARCH
3 KIM ET AL. an infusion test; 3) the changes of RAP with the effect of B- waves of ICP, which are associated with an increase of cerebral blood volume as a result of vasodilatation; 4) the response of RAP to body posture; 5) the effect of shunting on pressurevolume compensatory reserve; and 6) confirmation by RAP of the performance of the shunt (shunt blockage). The intention was to check whether RAP can be used as an index of compensatory reserve for hydrocephalus in a similar way as it is currently used for head injuries. It will require prospective clinical studies to determine the further usefulness of this index for predicting the outcome after shunting, or to differentiate between active hydrocephalus and atrophy. PATIENTS AND METHODS Background of Clinical Data Material was acquired from a database of infusion studies conducted as part of routine clinical practice. This study is an audit of data from between 1992 and 2005 at the Adden - brooke s Hospital,. In total, over 2000 studies were performed of 980 patients with hydrocephalus of various types and etiology (idiopathic NPH, 47%; post- subarachnoid hemorrhage NPH, 12%; noncommunicating hydrocephalus, 22%; others, 19%). The mean age was 65 years (range, years) and the male-to- female ratio was 2:1. All patients exhibited ventricular dilation on the brain scan (computed tomographic or magnetic resonance imaging) and clinical symptoms belonging to Hakim s triad (83% had gait disturbance, 65% memory problems, and 31% urinary incontinence). Because of the nature of the selection, many patients had complex clinical problems. As part of standard clinical practice, the patients were investigated by using a constant rate infusion study (either via lumbar puncture, 20%; preimplanted Ommaya reservoir, 38%; shunt prechamber, 40%; or open external ventricular drain, 2%), and/or by overnight ICP monitoring of 111 patients in addition to routine clinical and imaging assessment. In 44% of patients with a shunt in situ, tests were performed to check the performance of the shunt. Patient Population To study the RAP coefficient, the database was examined and homogeneous subgroups of patients were formed, predominantly with neuroimaging/clinical symptoms of NPH in states where poor or good compensatory reserve may be clearly identified on the basis of simple physiological models; Groups 1 and 2, 3 and 4, and 5 and 6 partially overlapped: 1) The group of idiopathic NPH patients (n 59) were studied, where there were infusion studies as well as precise (magnetic resonance imaging) measures of width of lateral ventricles (bicaudate index). 2) For comparison of RAP index before and during the CSF infusion intraventricular study, all nonshunted patients with clinical symptoms of NPH as well as readily available digital raw signal recordings ( ) were studied (n 74). 3) For comparison of changes of RAP index during and between B- waves associated with the rapid eye movement phase of sleep, 21 recordings in which such phases can be clearly identified were chosen to analyze the amplitude of slow waves of ICP. In this group, 15 patients had clinical symptoms of NPH, and 6 had brain cysts. 4) A further 20 patients with symptoms of NPH displaying a clear difference in ICP with posture (lying in bed with head up [semisitting] and lying flat during sleep) were identified by examining mean ICP, and were analyzed to assess the influence of a change in body position on RAP index. Twelve patients in this group were shunted. 5) In 25 NPH patients, the test was repeated before shunting and again after insertion of the shunt. In all of these patients, a post- shunt test did not indicate shunt malfunction (the criterion used was lowering of the resistance to CSF outflow from above 13 mm Hg/[mL/min] to below 8 mm Hg/[mL/min]). 6) In 229 patients (151 with NPH; 78 with noncommunicating hydrocephalus) with the shunt in situ, RAP was compared by studying the tests with patent shunts and shunts underdraining (presumed to be blocked). Infusion Study ICP Recording The infusion test was used to investigate CSF dynamics. Typically, 2 needles were inserted into a lumbar space (Whitacre 21-gauge) or a shunt prechamber (25-gauge butterfly). One needle was connected via a stiff saline- filled tube to a pressure transducer, and the other to an infusion pump mounted on a purpose- built trolley containing a pressure amplifier (Simonsen & Will, Sidcup, England) and connected to a computer running ICM + software ( Cambridge, England) (31). In some cases, because of difficulties with the positioning of the needle in a lumbar subarachnoid space, only 1 needle was used for both infusion and pressure measurements. A strict aseptic technique was used to keep all the prefilled tubing and the transducer sterile. The skin was carefully prepared with antiseptic solution. After 10 minutes of baseline measurement of ICP, the infusion of normal saline or Hartmann s solution was started at a rate of 1.5 ml/min (or 1 ml/min if the baseline pressure was higher than 15 mm Hg) and continued until a steady- state ICP plateau was achieved. If the mean ICP increased above 40 mm Hg, the infusion was stopped immediately. In patients with overnight ICP monitoring, intraparenchymal fiberoptic transducers (Micro Ventricular Bolt Pressure Monitoring Kit; Integra NeuroSciences Camino, Plainsboro, NJ) were used. Data Acquisition and Analysis AMP was calculated as the amplitude of the fundamental harmonic of the Fourier decomposition of the pulse waveform from consecutive, 6-second time periods. Measuring the fundamental harmonics instead of the full shape of the AMP implies some loss of information. However, similar techniques proved to be useful in waveform analysis of ICP or transcranial Doppler for assessing critical closing pressure (1, 32). Generally, good correlation between the AMP first harmonic and the peak- to- peak amplitude is reported within or between patients (19). RAP index was calculated as a Pearson correlation coefficient between mean ICP and AMP from a 4-minute period (amounting to 40 data points). The mean of RAP describes the mean value of RAP during a 10-minute time period. Once a reliable mean is established, the calculation window can be shifted along the time axis with much shorter intervals, usually around 10 seconds. To reduce the effects of noise, reasonable time averaging is necessary to obtain a reliable measure; 10 minutes was deemed sufficient for the system to stabilize the ICP waveform that was recorded continuously, and time trends of mean ICP, AMP, and RAP were calculated. Computer- aided optimization methods were used to identify parameters of a simple physiological model of CSF circulation (31). Among those parameters, the baseline ICP and resistance to CSF outflow characterizes the static conditions of the CSF circulation. The elastance coefficient E (also termed elasticity) characterizes the ability of the system to store an extra volume of fluid (7, 10). Greater E indicates that smaller volumes may be stored under the same incremental pressure conditions. 496 VOLUME 64 NUMBER 3 MARCH
4 INDEX OF CEREBROSPINAL COMPENSATORY RESERVE IN HYDROCEPHALUS FIGURE 2. Scatterplot illustrating the absence of correlation between RAP and brain elasticity (E), assessed during infusion studies. FIGURE 3. Typical example of change of mean ICP, AMP of ICP waveform, and RAP during a cerebrospinal fluid (CSF) infusion study in a patient with NPH. RAP increases during the infusion study even in patients with apparently normal CSF compensation. Change of RAP from 0 to +1 denotes a universal shift along the pressure- volume curve from its linear to exponential part. Statistical Analysis Three different statistical approaches were used to analyze the results. First, Spearman s correlation coefficients (r s ) were calculated to assess the correlation with RAP and resistance to CSF outflow, E, and width of ventricles (Subgroup 1). Second, a Wilcoxon signedrank test was used to compare RAP values in Studies 2 to 5. Finally, a Mann- Whitney U test was performed to compare RAP values of patients with functional and blocked shunts (Study 6). Two- sided P values are reported for all comparisons. All statistical analyses were performed using the SPSS statistical software (SPSS, Inc., Chicago, IL), and statistical significance was inferred at a 2-sided P value of less than 0.05 (28). RESULTS (from a median of 0.45 [range, ] to 0.86 [range, ], P 1.48*10-8, n 74) (Fig. 3). Behavior of RAP during the B- waves In a similar manner to that observed during external volume loading in the infusion studies, the B- waves are caused by cerebral blood volume increase as a result of spontaneous vasodilatation of vessels, which hypothetically diminishes cerebrospinal compensatory reserve (27). In 21 patients, where it was clear that B- waves were associated with the rapid eye movement phase of sleep, RAP increased from a median of 0.53 (range, ) to 0.89 (range, ), P 1.23*10-5, Wilcoxon signed- rank test, n 21 (Fig. 4). Results are described in detail below and summarized in Table 1. Correlation between RAP, Compensatory Parameters, and Ventricular Dilation In a group of 59 patients with an initial diagnosis of idiopathic NPH (based on clinical symptoms and neuroimaging), baseline RAP showed no correlation with E (r s 0.11; P 0.21) as shown in Figure 2. RAP did not significantly correlate with the width of the ventricles (bicaudate ratio, r s 0.13; P 0.41); however, it correlated positively with resistance to CSF outflow and the correlation coefficient was statistically significant (r s 0.35; P 0.045). Change of RAP during the Infusion Study During the infusion phase of the test, the compensatory reserve diminishes as additional CSF volume is stored in the craniospinal space. Based on the Wilcoxon signed- rank test, the analysis showed a statistically significant increase in RAP FIGURE 4. Graphs illustrating effects of slow waves of ICP during the REM (rapid eye movement) phase of sleep on RAP, where time trends show the increase in RAP at the onset of the slow waves (arrows). The parameter slow is defined as the equivalent amplitude of slow (period from 20 s 2 min) waves of ICP. NEUROSURGERY VOLUME 64 NUMBER 3 MARCH
5 KIM ET AL. Change in RAP as a Result of Shunt Blockage RAP recorded during the infusion study was lower in the case of a functioning shunt, as compared with blocked shunts (n 239, patent shunt; blocked shunt, 0.84 [range, ]; P , Mann-Whitney U test). DISCUSSION FIGURE 5. Graphs illustrating the effects of body posture in ICP and RAP. The figure shows an increase in RAP when there are changes in body position from sitting up in bed to lying down horizontally during sleep. Change of RAP with Body Position With a vertical body position, a certain amount of intracranial CSF volume shifts to the lumbar space. In shunted patients, the effect of this extra intracranial compensatory reserve is magnified, possibly because of accelerated CSF drainage. RAP increases after a change in body position from sitting up to horizontal (during sleep) (n 20 patients); RAP increased from a median of 0.36 (range, ) to 0.57 (range, ), P , Wilcoxon signed- rank test (Fig. 5). Compensatory Reserve Improvement after Shunt Surgery In patients in whom the test was repeated before and after shunting (with the shunt functioning well), baseline RAP was found to be significantly decreased after shunting (n 25; median before shunting, 0.59 [range, ]; median after shunting, 0.34 [range, ]; P 0.005; Wilcoxon signed- rank test). In the present study we have demonstrated that in hydrocephalus, RAP may reflect loss of compensatory reserve in clearly defined clinical scenarios: during external and internal volume load (infusion test, CSF; B- waves, cerebral blood volume; and shifts of CSF from spinal to cranial space after a change in body position from vertical to horizontal). RAP may also be indicative of improvement in CSF compensation after shunting or CSF drainage. Conversely, an increase in RAP signifies a worsening of the CSF circulation, and may be an indicator of shunt blockage for shunted patients. Why Are E and RAP Not Correlated? RAP correlates with the resistance to CSF outflow. This can be interpreted as impairment in the CSF circulation, leading to a reduction of CSF compensatory reserve. However, the lack of correlation between RAP and E requires explanation. E is a descriptor of the hypothetical lumped compliance of the CSF space, independent of mean ICP. Values greater than 0.18 ml 1 are regarded as elevated (11). According to the Monro- Kelly doctrine, the net volume of the craniospinal system in adults remains constant (8). Therefore, an increase in the volume of CSF (during the infusion study) should provoke displacement of blood, most probably from the low- pressure venous pool. E does not describe how brain tissue is being compressed, but it can describe how readily an amount of blood can be displaced outside the cranium through the venous system. According to a theoretical analysis of the pressure- volume TABLE 1. Summary of index of compensatory reserve in different subgroups a Subgroup No. of cases Median (range) and description Median (range) and description P value Test Changes of RAP before and during infusion ( ) Before infusion 0.86 ( ) During infusion 1.48*10 8 Paired signed-rank test Changes in RAP during B-waves recorded overnight ( ) Without B-waves 0.89 ( ) During B-waves 1.23*10 5 Paired signed-rank test Changes in RAP with body position during ICP monitoring ( ) Upright in bed 0.57 ( ) Horizontal, during sleep Paired signed-rank test Changes in RAP before and after shunting ( ) Before shunting 0.34 ( ) After shunting Paired signed-rank test Comparison of RAP between patients with patent and blocked shunt ( ) Patent shunt 0.84 ( ) Blocked shunt Unpaired Mann- Whitney U test a RAP, pressure-volume compensative index; ICP, intracranial pressure. 498 VOLUME 64 NUMBER 3 MARCH
6 INDEX OF CEREBROSPINAL COMPENSATORY RESERVE IN HYDROCEPHALUS FIGURE 6. Pressure- volume curve showing that elasticity (E), the slope of the pressure- volume curve, determines how fast the curve increases within the exponential phase (above points [V z, P z ]). RAP indicates the relative transition points of each curve (whether the system works below or above points [V z, P z ], but may not give exact values of E. This implies that RAP and E are not necessarily mutually associated. Limitations The pressure of some of the patients with overnight ICP monitoring was recorded by using an intraparenchymal fiberoptic transducer, while in the infusion study intraventricular and lumbar CSF pressure was analyzed. In light of current literature, differences between slow changes in AMP and mean pressures from both transducers should stay negligible (34). A good correlation was observed in a few patients with head injuries, where both pressures were recorded simultaneously (13). Marmarou et al. s (26) model does not take into account any long- term modifications of cerebral blood volume or cerebral tissue. However, in hydrocephalus, which is by its nature more chronic than acute brain trauma, such an assumption should not affect interpretation of the coefficient of cerebrospinal compensatory reserve. The findings that retrospectively classified hydrocephalus patients can show statistical variance with the RAP are interesting, but they do not precisely prove that a specific RAP value is useful in clinical decision- making. A prospective study correlating RAP with improvements after shunting is necessary to verify this point. The observation of differences in RAP really suggests differences in the characteristics of intracranial systems. In this way, other methods such as measurements of the ICP amplitude by itself, or the implications of phase shifts or time- varying transfer functions, may also be useful, and RAP should be compared with such techniques (15, 16, 20). The major criticism of this study may be the definition of NPH. Basically, we defined it as the presence of the clinical triad in association with ventriculomegaly, but this is notoriously inaccurate and, therefore, patients with brain atrophy could well have been included. We would like to emphasize that in this work, RAP was discussed as an index of cerebrospinal compensatory reserve in hydrocephalus. The usefulequation (see appendix), E reflects the steepness of the exponential shape of the pressure- volume curve. RAP has a different meaning; it shows, relative to the transition point of the pressure- volume curve, where the working point of the craniospinal system is, extrinsic to the steepness of the exponential part of the curve (no matter what the value of E is). Above the transition point, RAP is theoretically 1, below the transition point, 0 (Fig. 6). This suggests that RAP is an indicator related to the state of compensatory reserve, but is not strongly related to the mechanisms that determine E. Clinical Situations in Which RAP is Useful There are many kinds of intracranial disorders that lead to space- occupying effects (6, 33). The effects of an enlarging mass on the brain are well described clinically in terms of symptoms, signs, and the visualization in brain imaging. The phenomenology of local or global effects of tumors, hematomas, hydrocephalus, or brain swelling leads to the development of intracranial hypertension as a result of exhaustion of the spatial compensatory mechanism. Computerized bedside monitoring technology (e.g., ICP monitoring) has been used to analyze the ICP waveform in patients. However, although measuring ICP gives the pressure level, more information is required for diagnosis and prognosis of individual patients. RAP is a straightforward method for assessing the compensatory reserve of the CSF system. It requires the invasive monitoring of a single modality (ICP), and continuously traces any transient impairment of compensatory reserve. Its value in head injuries and other acute states has been demonstrated previously (2, 9, 12, 14). In hydrocephalus, it is useful in the detection of events that lead to the exhaustion of cerebrospinal compensatory reserve. For example, typical patterns emerge during B- waves (increase in cerebral blood volume), after a change in body posture (shift of certain fluid volume accumulated previously to the lumbar CSF and venous blood volume), and during blockage of a shunt. Furthermore, the patency of a shunt is visualized by the decrease of RAP. Although the threshold generally registers up to 0.6 in RAP (as determined in our unit), the difference of the threshold for individual patients depends on age and disease. Therefore, the true transition point of RAP for hydrocephalic patients is difficult to estimate. However, RAP is a correlation and is normalized (i.e., 1 RAP 1). Hence, comparison between patients is straightforward; it may be used in clinical scenarios where poor compensatory reserve may be attributed to certain types of clinical complications, but this needs to be confirmed by prospective clinical studies. Perhaps the most important advantage of RAP is the ability to demonstrate how the CSF compensatory reserve changes over time, both in overnight ICP monitoring and during infusion studies. NEUROSURGERY VOLUME 64 NUMBER 3 MARCH
7 KIM ET AL. ness of this index for differentiating between different brain pathologies needs to be further investigated. CONCLUSION RAP is an index of the CSF compensatory reserve based on the pressure- volume characteristic of the cerebrospinal space, and is numerically computed using the linear correlation coefficient between AMP and the mean ICP. RAP monitors spontaneous waveforms and the correlation between them, and allows continuous identification of CSF compensatory reserve. Disclosure ICM is software licensed by Cambridge Enterprise Ltd.; Peter Smielewski, Ph.D., and Marek Czosnyka, Ph.D., have a financial interest in a part of the licensing fee. The other authors have no personal financial or institutional interest in any of the drugs, materials, or devices described in this article. REFERENCES 1. Aaslid R, Lash SR, Bardy GH, Gild WH, Newell DW: Dynamic pressure flow velocity relationships in the human cerebral circulation. Stroke 34: , Adams RD, Fisher CM, Hakim S, Ojemann RG, Sweet WH: Symptomatic occult hydrocephalus with normal cerebrospinal- fluid pressure. A treatable syndrome. N Engl J Med 273: , Avezaat CJ, van Eijndhoven JH: Clinical observations on the relationship between cerebrospinal fluid pulse pressure and intracranial pressure. Acta Neurochir (Wien) 79:13 29, Avezaat CJ, van Eijndhoven JH: The role of the pulsatile pressure variations in intracranial pressure monitoring. Neurosurg Rev 9: , Avezaat CJ, van Eijndhoven JH, Wyper DJ: Cerebrospinal fluid pulse pressure and intracranial volume- pressure relationships. J Neurol Neurosurg Psychiatry 42: , Balestreri M, Czosnyka M, Steiner LA, Schmidt E, Smielewski P, Matta B, Pickard JD: Intracranial hypertension: What additional information can be derived from ICP waveform after head injury? Acta Neurochir (Wien) 146: , Christensen L, Børgesen SE: Single pulse pressure wave analysis by fast Fourier transformation. Neurol Res 11: , Czosnyka M, Pickard JD: Monitoring and interpretation of intracranial pressure. J Neurol Neurosurg Psychiatry 75: , Czosnyka M, Czosnyka Z, Momjian S, Pickard JD: Cerebrospinal fluid dynamics. Physiol Meas 25:R51 R76, Czosnyka Z, Czosnyka M, Owler B, Momjian S, Kasprowicz M, Schmidt EA, Smielewski P, Pickard JD: Clinical testing of CSF circulation in hydrocephalus. Acta Neurochir Suppl 95: , Czosnyka M, Guazzo E, Whitehouse M, Smielewski P, Czosnyka Z, Kirk - patrick P, Piechnik S, Pickard JD: Significance of intracranial pressure waveform analysis after head injury. Acta Neurochir (Wien) 138: , Czosnyka M, Hutchinson PJ, Balestreri M, Hiler M, Smielewski P, Pickard JD: Monitoring and interpretation of intracranial pressure after head injury. Acta Neurochir Suppl 96: , Czosnyka M, Smielewski P, Kirkpatrick P, Piechnik S, Laing R, Pickard JD: Continuous monitoring of cerebrovascular pressure- reactivity in head injury. Acta Neurochir Suppl 71:74 77, Czosnyka M, Wollk- Laniewski P, Batorski L, Zaworski W: Analysis of intracranial pressure waveform during infusion test. Acta Neurochir (Wien) 93: , Daley ML, Pourcyrous M, Timmons SD, Leffler CW: Mode changes of cerebrovascular pressure transmission induced by cerebral vasodilation. J Neurotrauma 24: , Eide PK, Sorteberg W: Preoperative spinal hydrodynamics versus clinical change 1 year after shunt treatment in idiopathic normal pressure hydrocephalus patients. Br J Neurosurg 19: , Evans JP, Espey FF, Kristoff FV, Kimbell FD, Ryder HW, Lamb DH, Barnes EB, Young DJ: Experimental and clinical observations on rising intracranial pressure. AMA Arch Surg 63: , Guinane JE: An equivalent circuit analysis of cerebrospinal fluid hydrodynamics. Am J Physiol 223: , Holm S, Eide PK: The frequency domain versus time domain methods for processing of intracranial pressure (ICP) signals. Med Eng Phys 30: , Hu X, Nenov V, Vespa P, Bergsneider M: Characterization of interdependency between intracranial pressure and heart variability signals: A causal spectral measure and a generalized synchronization measure. IEEE Trans Biomed Eng 54: , Juniewicz H, Kasprowicz M, Czosnyka M, Czosnyka Z, Gizewski S, Dzik M, Pickard JD: Analysis of intracranial pressure during and after the infusion test in patients with communicating hydrocephalus. Physiol Meas 26: , Kasprowicz M, Czosnyka Z, Czosnyka M, Momjian S, Juniewicz H, Pickard JD: Slight elevation of baseline intracranial pressure after fluid infusion into CSF space in patients with hydrocephalus. Neurol Res 26: , Langfitt TW: Increased intracranial pressure. Clin Neurosurg 16: , Löfgren J, Zwetnow NN: Cranial and spinal components of the cerebrospinal fluid pressure-volume curve. Acta Neurol Scand 49: , Löfgren J, von Essen C, Zwetnow NN: The pressure- volume curve of the cerebrospinal fluid space in dogs. Acta Neurol Scand 49: , Marmarou A, Shulman K, Rosende RM: A nonlinear analysis of the cerebrospinal fluid system and intracranial pressure dynamics. J Neurosurg 48: , Newell DW, Aaslid R, Stooss R, Reulen HJ: The relationship of blood flow velocity fluctuations to intracranial pressure B waves. J Neurosurg 76: , Pallet J: SPSS Survival Manual: A Step By Step Guide to Data Analysis Using SPSS for Windows (Version 10). Philadelphia, Open University Press, Schuhmann MU, Sood S, McAllister JP, Jaeger M, Ham SD, Czosnyka Z, Czosnyka M: Value of overnight monitoring of intracranial pressure in hydrocephalic children. Pediatr Neurosurg 44: , Sivaloganathan S, Tenti G, Drake JM: Mathematical pressure volume models of the cerebrospinal fluid. Appl Math Comput 94: , Smielewski P, Czosnyka M, Steiner L, Belestri M, Piechnik S, Pickard JD: ICM+: Software for on- line analysis of bedside monitoring data after severe head trauma. Acta Neurochir Suppl 95:43 49, Takizawa H, Gabra- Sanders T, Miller JD: Changes in the cerebrospinal fluid pulse wave spectrum associated with raised intracranial pressure. Neurosurgery 20: , Whitfield RD: Benign intracranial space- occupying masses simulating mental disorders. Psychiatr Q 20: , Zhong J, Dujovny M, Park HK, Perez E, Perlin AR, Diaz FG: Advances in ICP monitoring techniques. Neurol Res 25: , APPENDIX To create an identifiable model, one has to make simplifying approximations. In the case of the CSF circulation system, there are 3 main approximations that have to be made. First, the fluid must be regarded as incompressible; second, the system must be confined to a single compartment of fixed volume; and third, the production and absorption of CSF must vary with time (2, 12, 30). Based on the principle of mass conservation without long- term fluctuations of the cerebral blood volume, storage of CSF derives from the difference between its production and absorption rates: Storage of CSF rate of CSF production rate of CSF absorption [dv/dt I p (t)-i a (t)] 500 VOLUME 64 NUMBER 3 MARCH
8 INDEX OF CEREBROSPINAL COMPENSATORY RESERVE IN HYDROCEPHALUS Where [I p ] is the rate of total production (CSF, internal; saline compound, external), [I a ] is the rate of absorption, and t is time. According to the pressure- volume relationship, the storage of CSF varies in time and is proportional to the cerebrospinal compliance ([C(P]) (units, mm Hg/mL): [V(t) V(P(t))] [dv/dt dv/dp dp/dt C(P)dP/dt] Where [V(t)] is the function of volume (CSF system), [P(t)] is the function of pressure (CSF system), and [C(P)] is the cerebrospinal compliance. The compliance of the cerebrospinal space can be defined such that it is inversely proportional to the difference between the CSF pressure [(P)] and the reference pressure [(p 0 )], when the pressure is greater than the hypothetical transition point [(P z,v z )] (Fig. 1) (21, 22): [C(P) 1/E(P(t)-P 0 )] Where the coefficient E is defined as the cerebral elasticity (or elastance coefficient) (units, ml -1 ). For pressures below the hypothetical transition point [(P z,v z )], the compliance is independent of pressure: [C(P) C 0 ] (NB: [C 0 ] constant) The rate of CSF production can be defined as the sum of the equilibrium CSF production [(I eq )] and the external saline compound addition [(Inf(t))]. Hence, the rate of production is denoted as follows: [I p I eq +Inf(t)] Reabsorption of CSF is proportional to the difference between the CSF pressure [(P)] and the pressure in the sagittal sinuses [(P ss )]: Reabsorption [ I a (P(t)-P ss )/R] The coefficient [R] (symbol [R csf ] is also used) is defined as the resistance to CSF reabsorption of outflow (units, mm Hg/(mL/min). This equation implies that all CSF absorption takes place in the sagittal sinus. If there is any alternative route for CSF absorption in addition to absorption into the sagittal sinus, 2 resistances should be used in parallel; i.e., [R csf ] and a resistance to alternative CSF outflow. Such a complex model would, however, be very difficult to identify in clinical conditions. Therefore, the equilibrium value of ICP [(P eq )] depends on sagittal sinus pressure [(P ss )], CSF formation rate, and resistance to CSF outflow [R] (3, 4, 24, 26). [P eq P ss +I eq R] Based on the relationship of the initial formula, the CSF model can be divided into 2 types of models, linear and nonlinear, depending on where the pressure is either before or after the transition point of the curve, resulting in two subsequent equations: [dv/dt C 0 dp/dt I p (t)-i a (t)] [dv/dt C(t)dP/dt I p (t)-i a (t)] [C] can be solved analytically for [V V Z ] and [V V Z ]. For a rapid addition of volume [V-V Z ] at time t 0, [V-V Z ] may be positive (for non-linear part of the model) or negative (for linear part of the model). Therefore, the relationship between pressure and volume for both parts are: [V V z P P Z + (P z - P 0 )E(V-V Z )] [V V z P P 0 + (P z - P 0 )e E(V-VZ) ] Below the transition point, pressure is a linear function of [V- V Z ], and above that point it is an exponential function. The AMP, assuming that it is provoked by a sudden addition of blood ΔCBV, is independent of pressure for [P- P Z ] and is a linear function of mean ICP above [P z ]: [P P z AMP (P z - P 0 )E(ΔCBV)] [P P z AMP (P z - P 0 )(e E(ΔCBV) -1)] Therefore, the linear correlation between AMP and P above the transition point ([P z,v z ]) results in a value of RAP index 1, and below a value of 0. COMMENTS The search for the perfect index for evaluating cerebrospinal compliance or cerebrospinal compensatory reserve (RAP), which would allow the neurosurgeon to formulate the most adequate surgical indication in cases of hydrocephalus and to predict the surgical prognosis, reminds me of the medieval search for the philosophers stone. Unfortunately, at least for the moment, this kind of philosophers stone has been not found yet, essentially because of the difficulties in applying a mathematical model to a living subject, and because the disease of such a living subject, namely a patient with normotensive hydrocephalus, is multifactorial in nature and evolving in time, and therefore it defies understanding by the neurosurgeon. Thus, Kim et al. should certainly be admired for their continuing efforts to investigate the fine aspects of cerebrospinal fluid (CSF) dynamics. This article is another example of their tireless search, but it also shows the limits that are still encountered in this field. Indeed, in spite of the attempts of the authors to evaluate for comparison homogeneous subgroups of patients with hypothetical differences of pressure-volume compensatory reserve, the pathological substratum is likely to be different in each individual subject, owing to age, sex, nature of the pathological process, duration of the disease, response of the brain to the insult, degree of ventricular dilation, etc., consequently preventing the definition of an index suitable for prognostic evaluation for all patients. On the other hand, should the conclusions provided by the authors concerning the value of the RAP index in assessing the functional state of an inserted CSF shunt device be confirmed by other studies, then the authors could have found an indicator useful to at least understand the real role of CSF shunting in many patients whose clinical response does not apparently correspond to the patency or occlusion of their CSF shunt apparatus. Concezio Di Rocco Rome, Italy T his is a technical article that evaluates the use of RAP in hydrocephalus. As I understand it, RAP is a mathematical reflection of the well-known phenomenon seen in head injury, in which the amplitude of the intracranial pressure (ICP) trace increases as the ICP increases. The authors used an infusion of artificial CSF in adults with ventriculomegaly, and noted that, with increasing CSF volume, the compensatory reserve decreased, as expected. There was no correlation of reserve with ventricle size, again as expected, since there is a well-known disconnect between compliance and ventricular size. There was no correlation of compensatory reserve with elastance, which the authors attempt to explain, but which I honestly did not understand. The major criticism of this work is the definition of normal pressure hydrocephalus (NPH) in their patients. They defined it basically as the presence of the clinical triad in association with ventriculomegaly, but this is notoriously inaccurate, and patients with brain atrophy could well have been included. Did they use the results of their infusion data NEUROSURGERY VOLUME 64 NUMBER 3 MARCH
9 KIM ET AL. to retrospectively define the patients as having NPH? Would the results have been the same in a population of Alzheimer s disease patients? The implication of this article is that the use of the RAP could be used to determine whether a patient with possible NPH might benefit from a shunt, although this is never stated. Since this is not demonstrated in any way, the clinical value of the findings is unclear. Leslie N. Sutton Philadelphia, Pennsylvania As the authors note, the pressure-volume compensation index has been used with some benefit in treating head-injured patients. In this article, they apply similar techniques to measure the RAP in a group of hydrocephalic patients. They found that RAP positively correlated with outflow resistance but not with elastance or ventricular volume. When a CSF-diverting shunt was occluded, the RAP was increased. As the authors point out, the RAP breakpoint varies with elastance, and one does not know the elastance for a given patient without undertaking an infusion study or calculating the correlation coefficient between ICP and pulse amplitude. Another variable is that the elastance in any given patient is subject to change. The authors acknowledge that there are a number of limitations to this study; however, with further investigation, the measurement of RAP may be useful in differentiating NPH from other abnormalities that bear a close resemblance. J. Gordon McComb Los Angeles, California This article demonstrates a potentially interesting analysis of a large dataset of patients with hydrocephalus. The technique of determining the RAP regression coefficient has been used by the authors many times in other studies. In this study, the goal is to link the calculated RAP to a clinically interesting concept, an index of compensatory reserve. It is important for the reader to bear in mind that this is an interpretation that may be substantiated or not by further clinical and mathematical analysis, and it is not a definition. The finding that retrospectively classified hydrocephalus cases can show statistical variance with the RAP is interesting, but it does not yet prove that the RAP has predictive value in clinical decision-making. The observation of differences in RAP really supports growing literature suggesting that the response of the ICP to the pulsatile cardiac input tells something about what engineers would call the systems characteristics of the intracranial contents. As such, other indicators of systems change, such as measurement of the ICP amplitude by itself (1), or the implications of phase shifts (2) or time-varying transfer functions (3) may all be ways of attempting to observe differences between 1 patient and another. It will clearly be of value to consider these and other mathematical approaches when searching for a clinically useful test. Such a synthesis of these new mathematical techniques will be an important challenge to those who would work in this area in the future. Benjamin I. Rapoport Eun-Hyoung Park Joseph R. Madsen Boston, Massachusetts 1. Eide PK, Brean A: Intracranial pulse pressure amplitude levels determined during preoperative assessment of subjects with possible idiopathic normal pressure hydrocephalus. Acta Neurochir (Wien) 148: , Hu X, Nenov V, Bergsneider M: Phase coordination between intracranial pressure and electrocardiogram signals. Conf Proc IEEE Eng Med Biol Soc 1:45 48, Zou R, Park E-H, Kelly EM, Egnor M, Wagshul ME, Madsen JR: Intracranial pressure waves: Characterization of a pulsation absorber with notch filter properties using systems analysis. J Neurosurg Pediatrics 2:83 94, IN-TRAINING LIAISONS The Congress of Neurological Surgeons exists for the purpose of promoting public welfare through the advancement of neurosurgery by a commitment to excellence in education and by a dedication to research and scientific knowledge. Mission Statement Congress of Neurological Surgeons Inherent in this commitment is a critical charge to serve the needs of the in-training individuals. Considering the importance of this vital group within the neurosurgical community, the Journal has established a position within its board structure termed In-training Liaison. The individuals holding this position will act as spokespersons especially addressing the needs and concerns of individuals in in-training positions globally, as they relate to journal content and perspective. The current individuals holding this position are: Michael L. DiLuna, M.D., Ian F. Dunn, M.D., James B. Elder, M.D., and Daniel Hoh, M.D. Michael L. DiLuna, M.D. Department of Neurosurgery Yale University School of Medicine TMP Cedar Street New Haven, CT michael.diluna@yale.edu Issues attendant to in-training matters should be conveyed to: Ian F. Dunn, M.D. Department of Neurosurgery Brigham and Women s Hospital/Children s Hospital 75 Francis Street Boston, MA idunn@partners.org James B. Elder, M.D. Department of Neurological Surgery University of Southern California Keck School of Medicine 1200 N. State Street, Ste Los Angeles, CA jelder@usc.edu Daniel Hoh, M.D. Department of Neurological Surgery University of Southern California Keck School of Medicine 1200 N. State Street, Ste Los Angeles, CA dhoh@usc.edu 502 VOLUME 64 NUMBER 3 MARCH
The resistance to CSF outflow in hydrocephalus what it is and what it isn t.
 The resistance to CSF outflow in hydrocephalus what it is and what it isn t. Davson et al 1970, The mechanism of drainage of CSF. Brain 93:665-8 1989, Copenhagen, Alfred Benzon Foundation CSf outflow is
The resistance to CSF outflow in hydrocephalus what it is and what it isn t. Davson et al 1970, The mechanism of drainage of CSF. Brain 93:665-8 1989, Copenhagen, Alfred Benzon Foundation CSf outflow is
Infusion studies in clinical practice. Kristian Aquilina Consultant paediatric neurosurgeon Great Ormond Street Hospital London
 Infusion studies in clinical practice Kristian Aquilina Consultant paediatric neurosurgeon Great Ormond Street Hospital London 10 th September 2018 infusion study + hydrocephalus 216 publications Clinical
Infusion studies in clinical practice Kristian Aquilina Consultant paediatric neurosurgeon Great Ormond Street Hospital London 10 th September 2018 infusion study + hydrocephalus 216 publications Clinical
12. Modelling of CSF compensation: Mathematical model (Marmarou). Mathematical modelling of pulsatile aqueductal CSF flow
 12. Modelling of CSF compensation: Mathematical model (Marmarou). Mathematical modelling of pulsatile aqueductal CSF flow Hydrocephalus Enlargement of CSF space Shunting? Revision? When? CSF dynamics Prof.
12. Modelling of CSF compensation: Mathematical model (Marmarou). Mathematical modelling of pulsatile aqueductal CSF flow Hydrocephalus Enlargement of CSF space Shunting? Revision? When? CSF dynamics Prof.
13. Volume-pressure infusion tests: Typical patterns of infusion studies in different forms of CSF circulatory disorders.
 13. Volume-pressure infusion tests: Typical patterns of infusion studies in different forms of CSF circulatory disorders. Hydrocephalus is far more complex than disorder of CSF circulation CSF circulation
13. Volume-pressure infusion tests: Typical patterns of infusion studies in different forms of CSF circulatory disorders. Hydrocephalus is far more complex than disorder of CSF circulation CSF circulation
A comparison between the transfer function of ABP to ICP and compensatory reserve index in TBI
 Acta Neurochir Suppl (28) 12: 9 13 # Springer-Verlag 28 A comparison between the transfer function of AB to IC and compensatory reserve index in TBI Sima Shahsavari & Tomas McKelvey & Thomas Skoglund &
Acta Neurochir Suppl (28) 12: 9 13 # Springer-Verlag 28 A comparison between the transfer function of AB to IC and compensatory reserve index in TBI Sima Shahsavari & Tomas McKelvey & Thomas Skoglund &
Lumbar infusion test in normal pressure hydrocephalus
 Acta Neurol Scand 2005: 111: 379 384 DOI: 10.1111/j.1600-0404.2005.00417.x Copyright Ó Blackwell Munksgaard 2005 ACTA NEUROLOGICA SCANDINAVICA Lumbar infusion test in normal pressure hydrocephalus Kahlon
Acta Neurol Scand 2005: 111: 379 384 DOI: 10.1111/j.1600-0404.2005.00417.x Copyright Ó Blackwell Munksgaard 2005 ACTA NEUROLOGICA SCANDINAVICA Lumbar infusion test in normal pressure hydrocephalus Kahlon
Body position and eerebrospinal fluid pressure. Part 2' Clinical studies on orthostatic pressure and the hydrostatic indifferent point
 Body position and eerebrospinal fluid pressure Part 2' Clinical studies on orthostatic pressure and the hydrostatic indifferent point BJORN MAGNAES, M.D. Department of Neurosurgery, Rikshospitalet, Oslo
Body position and eerebrospinal fluid pressure Part 2' Clinical studies on orthostatic pressure and the hydrostatic indifferent point BJORN MAGNAES, M.D. Department of Neurosurgery, Rikshospitalet, Oslo
Postprint.
 http://www.diva-portal.org Postprint This is the accepted version of a paper published in Journal of Neurology, Neurosurgery and Psychiatry. This paper has been peer-reviewed but does not include the final
http://www.diva-portal.org Postprint This is the accepted version of a paper published in Journal of Neurology, Neurosurgery and Psychiatry. This paper has been peer-reviewed but does not include the final
Continuous cerebral autoregulation monitoring
 Continuous cerebral autoregulation monitoring Dr Peter Smielewski ps10011@cam.ac.uk 20/10/2017 Division of Neurosurgery, Department of Clinical Neurosciences Determinants of cerebral blood flow Thanks
Continuous cerebral autoregulation monitoring Dr Peter Smielewski ps10011@cam.ac.uk 20/10/2017 Division of Neurosurgery, Department of Clinical Neurosciences Determinants of cerebral blood flow Thanks
S ome hydrocephalic patients with extracranial shunts
 PAPER Quantitative analysis of continuous intracranial pressure recordings in symptomatic patients with extracranial shunts P K Eide... Competing interests: none declared... Correspondence to: Dr Per Kristian
PAPER Quantitative analysis of continuous intracranial pressure recordings in symptomatic patients with extracranial shunts P K Eide... Competing interests: none declared... Correspondence to: Dr Per Kristian
perfusion pressure: Definitions. Implication on management protocols. What happens when CPP is too low, and when it is too high? Non-invasive CPP?
 7. Cerebral perfusion pressure: Definitions. Implication on management protocols. What happens when CPP is too low, and when it is too high? Non-invasive CPP? Douglas J. Miller Miller JD, Stanek A, Langfitt
7. Cerebral perfusion pressure: Definitions. Implication on management protocols. What happens when CPP is too low, and when it is too high? Non-invasive CPP? Douglas J. Miller Miller JD, Stanek A, Langfitt
MRI MEASUREMENTS OF CRANIOSPINAL AND INTRACRANIAL VOLUME CHANGE IN HEALTHY AND HEAD TRAUMA CASES
 1of 4 MRI MEASUREMENTS OF CRANIOSPINAL AND INTRACRANIAL VOLUME CHANGE IN HEALTHY AND HEAD TRAUMA CASES N. Alperin, Y. Kadkhodayan, B. Varadarajalu, C. Fisher, B. Roitberg Department of Radiology and Neurosurgery,
1of 4 MRI MEASUREMENTS OF CRANIOSPINAL AND INTRACRANIAL VOLUME CHANGE IN HEALTHY AND HEAD TRAUMA CASES N. Alperin, Y. Kadkhodayan, B. Varadarajalu, C. Fisher, B. Roitberg Department of Radiology and Neurosurgery,
The pulsatile waveform of ICP comes from the beating. Impaired pulsation absorber mechanism in idiopathic normal pressure hydrocephalus
 DOI: 10.3171/2012.9.JNS121227 Impaired pulsation absorber mechanism in idiopathic normal pressure hydrocephalus Laboratory investigation Eun-Hyoung Park, Ph.D., 1 Per Kristian Eide, M.D., Ph.D., 2,4 David
DOI: 10.3171/2012.9.JNS121227 Impaired pulsation absorber mechanism in idiopathic normal pressure hydrocephalus Laboratory investigation Eun-Hyoung Park, Ph.D., 1 Per Kristian Eide, M.D., Ph.D., 2,4 David
An intracranial pressure-derived index monitored simultaneously from two separate sensors in patients with cerebral bleeds: comparison of findings
 An intracranial pressure-derived index monitored simultaneously from two separate sensors in patients with cerebral bleeds: comparison of findings Eide and Sorteberg Eide and Sorteberg BioMedical Engineering
An intracranial pressure-derived index monitored simultaneously from two separate sensors in patients with cerebral bleeds: comparison of findings Eide and Sorteberg Eide and Sorteberg BioMedical Engineering
Pressure reactivity: Relationship between ICP and arterial blood pressure (ABP). Pressure-reactivity index, computational methods. Clinical examples.
 Pressure reactivity: Relationship between ICP and arterial blood pressure (ABP). Pressure-reactivity index, computational methods. Clinical examples. Optimization of cerebral perfusion pressure: Relationship
Pressure reactivity: Relationship between ICP and arterial blood pressure (ABP). Pressure-reactivity index, computational methods. Clinical examples. Optimization of cerebral perfusion pressure: Relationship
Natural history of idiopathic normal-pressure hydrocephalus
 DOI 10.1007/s10143-011-0316-7 REVIEW Natural history of idiopathic normal-pressure hydrocephalus Ahmed K. Toma & Simon Stapleton & Marios C. Papadopoulos & Neil D. Kitchen & Laurence D. Watkins Received:
DOI 10.1007/s10143-011-0316-7 REVIEW Natural history of idiopathic normal-pressure hydrocephalus Ahmed K. Toma & Simon Stapleton & Marios C. Papadopoulos & Neil D. Kitchen & Laurence D. Watkins Received:
Principlesof shunt testing in-vivo Zofia Czosnyka, Matthew Garnett, Eva Nabbanja, Marek Czosnyka
 Principlesof shunt testing in-vivo Zofia Czosnyka, Matthew Garnett, Eva Nabbanja, Marek Czosnyka Neurosurgery Unit, Addenbrooke s Hospital, Cambridge, UK Shunt helps to control hydrocephalus not to cure
Principlesof shunt testing in-vivo Zofia Czosnyka, Matthew Garnett, Eva Nabbanja, Marek Czosnyka Neurosurgery Unit, Addenbrooke s Hospital, Cambridge, UK Shunt helps to control hydrocephalus not to cure
Two computerized methods used to analyze intracranial pressure B waves: comparison with traditional visual interpretation
 J Neurosurg 94:392 396, 2001 Two computerized methods used to analyze intracranial pressure B waves: comparison with traditional visual interpretation ANDERS EKLUND, MSC.E.P., AINA ÅGREN-WILSSON, M.D.,
J Neurosurg 94:392 396, 2001 Two computerized methods used to analyze intracranial pressure B waves: comparison with traditional visual interpretation ANDERS EKLUND, MSC.E.P., AINA ÅGREN-WILSSON, M.D.,
Idiopathic normal pressure hydrocephalus (inph) has
 Clinical article J Neurosurg 125:591 597, 2016 Idiopathic normal pressure hydrocephalus: diagnostic and predictive value of clinical testing, lumbar drainage, and CSF dynamics *Cynthia V. Mahr, MD, 1 Markus
Clinical article J Neurosurg 125:591 597, 2016 Idiopathic normal pressure hydrocephalus: diagnostic and predictive value of clinical testing, lumbar drainage, and CSF dynamics *Cynthia V. Mahr, MD, 1 Markus
The influence of breathing on cerebrospinal fluid movement in the brain
 The influence of breathing on cerebrospinal fluid movement in the brain A computational study based on in vivo pressure measurements Vegard Vinje Simula Research Laboratory GA Ringstad ME Rognes PK Eide
The influence of breathing on cerebrospinal fluid movement in the brain A computational study based on in vivo pressure measurements Vegard Vinje Simula Research Laboratory GA Ringstad ME Rognes PK Eide
Regulation of Cerebral Blood Flow. Myogenic- pressure autoregulation Chemical: PaCO2, PaO2 Metabolic Neuronal
 Regulation of Cerebral Blood Flow Myogenic- pressure autoregulation Chemical: PaCO2, PaO2 Metabolic Neuronal The Autoregulation, Stupid! Drawing of her daughter (age 7) Flow through rigid tube Mogens Fog
Regulation of Cerebral Blood Flow Myogenic- pressure autoregulation Chemical: PaCO2, PaO2 Metabolic Neuronal The Autoregulation, Stupid! Drawing of her daughter (age 7) Flow through rigid tube Mogens Fog
Medical Management of Intracranial Hypertension. Joao A. Gomes, MD FAHA Head, Neurointensive Care Unit Cerebrovascular Center
 Medical Management of Intracranial Hypertension Joao A. Gomes, MD FAHA Head, Neurointensive Care Unit Cerebrovascular Center Anatomic and Physiologic Principles Intracranial compartments Brain 80% (1,400
Medical Management of Intracranial Hypertension Joao A. Gomes, MD FAHA Head, Neurointensive Care Unit Cerebrovascular Center Anatomic and Physiologic Principles Intracranial compartments Brain 80% (1,400
Intracranial pressure: measurement and monitoring. CSF pressure as a golden standard. Intraparenchymal pressure. Sensors, drifts, errors and
 Intracranial pressure: measurement and monitoring. CSF pressure as a golden standard. Intraparenchymal pressure. Sensors, drifts, errors and monitoring techniques GUILLAUME J, JANNY P. [Continuous intracranial
Intracranial pressure: measurement and monitoring. CSF pressure as a golden standard. Intraparenchymal pressure. Sensors, drifts, errors and monitoring techniques GUILLAUME J, JANNY P. [Continuous intracranial
19. Monitoring of CA using TCD- Mx and Sx
 19. Monitoring of CA using TCD- Mx and Sx Drawing the autoregulatory curve: in clinical practice such dramatic changes in CPP are not permissible Monitoring cerebral autoregulation - certainly not a new
19. Monitoring of CA using TCD- Mx and Sx Drawing the autoregulatory curve: in clinical practice such dramatic changes in CPP are not permissible Monitoring cerebral autoregulation - certainly not a new
Ventriculo peritoneal Shunt Malfunction with Anti-siphon Device in Normal pressure Hydrocephalus Report of -Three Cases-
 Ventriculo peritoneal Shunt Malfunction with Anti-siphon Device in Normal pressure Hydrocephalus Report of -Three Cases- Mitsuru SEIDA, Umeo ITO, Shuichi TOMIDA, Shingo YAMAZAKI and Yutaka INABA* Department
Ventriculo peritoneal Shunt Malfunction with Anti-siphon Device in Normal pressure Hydrocephalus Report of -Three Cases- Mitsuru SEIDA, Umeo ITO, Shuichi TOMIDA, Shingo YAMAZAKI and Yutaka INABA* Department
Monitoring and interpretation of intracranial pressure ... J Neurol Neurosurg Psychiatry 2004;75: doi: /jnnp.2003.
 NEUROSCIENCE FOR NEUROLOGISTS Monitoring and interpretation of intracranial pressure M Czosnyka, J D Pickard... Intracranial pressure (ICP) is derived from cerebral blood and cerebrospinal fluid (CSF)
NEUROSCIENCE FOR NEUROLOGISTS Monitoring and interpretation of intracranial pressure M Czosnyka, J D Pickard... Intracranial pressure (ICP) is derived from cerebral blood and cerebrospinal fluid (CSF)
P VI CC is a measure of compliance of the craniospinal cavity, Assessment of Craniospinal Pressure-Volume Indices ORIGINAL RESEARCH
 ORIGINAL RESEARCH A. Wåhlin K. Ambarki R. Birgander N. Alperin J. Malm A. Eklund Assessment of Craniospinal Pressure-Volume Indices BACKGROUND AND PURPOSE: The PVI CC of the craniospinal compartment defines
ORIGINAL RESEARCH A. Wåhlin K. Ambarki R. Birgander N. Alperin J. Malm A. Eklund Assessment of Craniospinal Pressure-Volume Indices BACKGROUND AND PURPOSE: The PVI CC of the craniospinal compartment defines
Assessment of cerebrospinal fluid system dynamics
 UMEÅ UNIVERSITY MEDICAL DISSERTATIONS New series No. 1413 Assessment of cerebrospinal fluid system dynamics Novel infusion protocol, mathematical modelling and parameter estimation for hydrocephalus investigations
UMEÅ UNIVERSITY MEDICAL DISSERTATIONS New series No. 1413 Assessment of cerebrospinal fluid system dynamics Novel infusion protocol, mathematical modelling and parameter estimation for hydrocephalus investigations
Monitoring and interpretation of intracranial pressure
 Monitoring and interpretation of intracranial pressure M Czosnyka and J D Pickard J. Neurol. Neurosurg. Psychiatry 2004;75;813-821 doi:10.1136/jnnp.2003.033126 Updated information and services can be found
Monitoring and interpretation of intracranial pressure M Czosnyka and J D Pickard J. Neurol. Neurosurg. Psychiatry 2004;75;813-821 doi:10.1136/jnnp.2003.033126 Updated information and services can be found
Estimation of Systolic and Diastolic Pressure using the Pulse Transit Time
 Estimation of Systolic and Diastolic Pressure using the Pulse Transit Time Soo-young Ye, Gi-Ryon Kim, Dong-Keun Jung, Seong-wan Baik, and Gye-rok Jeon Abstract In this paper, algorithm estimating the blood
Estimation of Systolic and Diastolic Pressure using the Pulse Transit Time Soo-young Ye, Gi-Ryon Kim, Dong-Keun Jung, Seong-wan Baik, and Gye-rok Jeon Abstract In this paper, algorithm estimating the blood
Original Article. Emergency Department Evaluation of Ventricular Shunt Malfunction. Is the Shunt Series Really Necessary? Raymond Pitetti, MD, MPH
 Original Article Emergency Department Evaluation of Ventricular Shunt Malfunction Is the Shunt Series Really Necessary? Raymond Pitetti, MD, MPH Objective: The malfunction of a ventricular shunt is one
Original Article Emergency Department Evaluation of Ventricular Shunt Malfunction Is the Shunt Series Really Necessary? Raymond Pitetti, MD, MPH Objective: The malfunction of a ventricular shunt is one
Traumatic brain Injury- An open eye approach
 Traumatic brain Injury- An open eye approach Dr. Sunit Dr Sunit, Apollo children's hospital Blah blah Lots of head injury Lot of ill children Various methods of injury Various mechanisms of brain damage
Traumatic brain Injury- An open eye approach Dr. Sunit Dr Sunit, Apollo children's hospital Blah blah Lots of head injury Lot of ill children Various methods of injury Various mechanisms of brain damage
INTRACRANIAL PRESSURE -!!
 INTRACRANIAL PRESSURE - Significance raised ICP main cause of death in severe head injury main cause of morbidity in moderate and mild head injury main target and prognostic indicator in the ITU setting
INTRACRANIAL PRESSURE - Significance raised ICP main cause of death in severe head injury main cause of morbidity in moderate and mild head injury main target and prognostic indicator in the ITU setting
Mechanisms of Headache in Intracranial Hypotension
 Mechanisms of Headache in Intracranial Hypotension Stephen D Silberstein, MD Jefferson Headache Center Thomas Jefferson University Hospital Philadelphia, PA Stephen D. Silberstein, MD, FACP Director, Jefferson
Mechanisms of Headache in Intracranial Hypotension Stephen D Silberstein, MD Jefferson Headache Center Thomas Jefferson University Hospital Philadelphia, PA Stephen D. Silberstein, MD, FACP Director, Jefferson
Intracranial Blood Pressure and Brain Vasculature
 Intracranial Blood Pressure and Brain Vasculature Sukruti Ponkshe Final Presentation REU Program, Summer 2006 August 3, 2006 Advisors: Professor Linninger Dr. Michalis Xenos Dr. Libin Zhang Laboratory
Intracranial Blood Pressure and Brain Vasculature Sukruti Ponkshe Final Presentation REU Program, Summer 2006 August 3, 2006 Advisors: Professor Linninger Dr. Michalis Xenos Dr. Libin Zhang Laboratory
Stroke & Neurovascular Center of New Jersey. Jawad F. Kirmani, MD Director, Stroke and Neurovascular Center
 Stroke & Neurovascular Center of New Jersey Jawad F. Kirmani, MD Director, Stroke and Neurovascular Center Past, present and future Past, present and future Cerebral Blood Flow Past, present and future
Stroke & Neurovascular Center of New Jersey Jawad F. Kirmani, MD Director, Stroke and Neurovascular Center Past, present and future Past, present and future Cerebral Blood Flow Past, present and future
Integra B: Camino OLM Intracranial Pressure Monitoring Kit SURGICAL TECHNIQUE
 Integra 110-4B: Camino OLM Intracranial Pressure Monitoring Kit SURGICAL TECHNIQUE Surgical Technique Th OLM ICP Kit was developed in cooperation with Richard C. Ostrup, M.D., Thomas G. Luerssen, M.D.
Integra 110-4B: Camino OLM Intracranial Pressure Monitoring Kit SURGICAL TECHNIQUE Surgical Technique Th OLM ICP Kit was developed in cooperation with Richard C. Ostrup, M.D., Thomas G. Luerssen, M.D.
Perioperative Management Of Extra-Ventricular Drains (EVD)
 Perioperative Management Of Extra-Ventricular Drains (EVD) Dr. Vijay Tarnal MBBS, FRCA Clinical Assistant Professor Division of Neuroanesthesiology Division of Head & Neck Anesthesiology Michigan Medicine
Perioperative Management Of Extra-Ventricular Drains (EVD) Dr. Vijay Tarnal MBBS, FRCA Clinical Assistant Professor Division of Neuroanesthesiology Division of Head & Neck Anesthesiology Michigan Medicine
Predicting the need for operation in the patient with an occult traumatic intracranial hematoma
 J Neurosurg 55:75-81, 1981 Predicting the need for operation in the patient with an occult traumatic intracranial hematoma SAM GALBRAITH, M.D., F.R.C.S., AND GRAHAM TEASDALE, M.R.C.P., F.R.C.S. Department
J Neurosurg 55:75-81, 1981 Predicting the need for operation in the patient with an occult traumatic intracranial hematoma SAM GALBRAITH, M.D., F.R.C.S., AND GRAHAM TEASDALE, M.R.C.P., F.R.C.S. Department
Ventriculo-Peritoneal/ Lumbo-Peritoneal Shunts
 Ventriculo-Peritoneal/ Lumbo-Peritoneal Shunts Exceptional healthcare, personally delivered Ventriculo-Peritoneal/ Lumbo-Peritoneal Shunts What is hydrocephalus? Hydrocephalus is the build up of an excess
Ventriculo-Peritoneal/ Lumbo-Peritoneal Shunts Exceptional healthcare, personally delivered Ventriculo-Peritoneal/ Lumbo-Peritoneal Shunts What is hydrocephalus? Hydrocephalus is the build up of an excess
Continuous Monitoring of the Monro-Kellie Doctrine: Is It Possible?
 JOURNAL OF NEUROTRAUMA 29:1354 1363 (May 1, 2012) ª Mary Ann Liebert, Inc. DOI: 10.1089/neu.2011.2018 Continuous Monitoring of the Monro-Kellie Doctrine: Is It Possible? Dong-Joo Kim, 1,2,5 Zofia Czosnyka,
JOURNAL OF NEUROTRAUMA 29:1354 1363 (May 1, 2012) ª Mary Ann Liebert, Inc. DOI: 10.1089/neu.2011.2018 Continuous Monitoring of the Monro-Kellie Doctrine: Is It Possible? Dong-Joo Kim, 1,2,5 Zofia Czosnyka,
Statistical Methods and Reasoning for the Clinical Sciences
 Statistical Methods and Reasoning for the Clinical Sciences Evidence-Based Practice Eiki B. Satake, PhD Contents Preface Introduction to Evidence-Based Statistics: Philosophical Foundation and Preliminaries
Statistical Methods and Reasoning for the Clinical Sciences Evidence-Based Practice Eiki B. Satake, PhD Contents Preface Introduction to Evidence-Based Statistics: Philosophical Foundation and Preliminaries
Evaluation of Shunt Malfunction Using Shunt Site Reservoir
 Original Paper Pediatr Neurosurg 2000;32:180 186 Received: January 27, 1999 Accepted: April 27, 2000 Evaluation of Shunt Malfunction Using Shunt Site Reservoir S. Sood A.I. Canady Steven D. Ham Section
Original Paper Pediatr Neurosurg 2000;32:180 186 Received: January 27, 1999 Accepted: April 27, 2000 Evaluation of Shunt Malfunction Using Shunt Site Reservoir S. Sood A.I. Canady Steven D. Ham Section
From Cerebrospinal Fluid Pulsation to Noninvasive Intracranial Compliance and Pressure Measured by MRI Flow Studies
 This investigation is directed to using the advances in MRI data to focus on movement of blood through the arteries and veins of the brain and on the movement of CSF through certain passageways in such
This investigation is directed to using the advances in MRI data to focus on movement of blood through the arteries and veins of the brain and on the movement of CSF through certain passageways in such
Ventricular size after shunting for idiopathic normal pressure hydrocephalus
 Journal of Neurology, Neurosurgery, and Psychiatry, 1975, 38, 833-837 Ventricular size after shunting for idiopathic normal pressure hydrocephalus HENRY A. SHENKIN', JACK 0. GREENBERG, AND CHARLES B. GROSSMAN
Journal of Neurology, Neurosurgery, and Psychiatry, 1975, 38, 833-837 Ventricular size after shunting for idiopathic normal pressure hydrocephalus HENRY A. SHENKIN', JACK 0. GREENBERG, AND CHARLES B. GROSSMAN
MODELING OF THE CARDIOVASCULAR SYSTEM AND ITS CONTROL MECHANISMS FOR THE EXERCISE SCENARIO
 MODELING OF THE CARDIOVASCULAR SYSTEM AND ITS CONTROL MECHANISMS FOR THE EXERCISE SCENARIO PhD Thesis Summary eng. Ana-Maria Dan PhD. Supervisor: Prof. univ. dr. eng. Toma-Leonida Dragomir The objective
MODELING OF THE CARDIOVASCULAR SYSTEM AND ITS CONTROL MECHANISMS FOR THE EXERCISE SCENARIO PhD Thesis Summary eng. Ana-Maria Dan PhD. Supervisor: Prof. univ. dr. eng. Toma-Leonida Dragomir The objective
Influence of general anaesthesia on slow waves of intracranial pressure
 Influence of general anaesthesia on slow waves of intracranial pressure Despina Aphrodite Lalou 1,2 Marek Czosnyka 1 Joseph Donnelly 1 Andrea Lavinio 3 John D. Pickard 1 Matthew Garnett 1 Zofia Czosnyka
Influence of general anaesthesia on slow waves of intracranial pressure Despina Aphrodite Lalou 1,2 Marek Czosnyka 1 Joseph Donnelly 1 Andrea Lavinio 3 John D. Pickard 1 Matthew Garnett 1 Zofia Czosnyka
INCREASED INTRACRANIAL PRESSURE
 INCREASED INTRACRANIAL PRESSURE Sheba Medical Center, Acute Medicine Department Irene Frantzis P-Year student SGUL 2013 Normal Values Normal intracranial volume: 1700 ml Volume of brain: 1200-1400 ml CSF:
INCREASED INTRACRANIAL PRESSURE Sheba Medical Center, Acute Medicine Department Irene Frantzis P-Year student SGUL 2013 Normal Values Normal intracranial volume: 1700 ml Volume of brain: 1200-1400 ml CSF:
Analysis of intracranial volume ratios by means of cerebrospinal fluid deployment indicators
 Original article Analysis of intracranial volume ratios by means of cerebrospinal fluid deployment indicators Ewa Szczepek 1,2, Leszek Tomasz Czerwosz 3, Krzysztof Nowiński 4, Zbigniew Czernicki 1,2, Jerzy
Original article Analysis of intracranial volume ratios by means of cerebrospinal fluid deployment indicators Ewa Szczepek 1,2, Leszek Tomasz Czerwosz 3, Krzysztof Nowiński 4, Zbigniew Czernicki 1,2, Jerzy
Cover Page. The handle holds various files of this Leiden University dissertation.
 Cover Page The handle http://hdl.handle.net/1887/35771 holds various files of this Leiden University dissertation. Author: Palm, Walter Miguel Title: Ventricular dilatation in aging and dementia Issue
Cover Page The handle http://hdl.handle.net/1887/35771 holds various files of this Leiden University dissertation. Author: Palm, Walter Miguel Title: Ventricular dilatation in aging and dementia Issue
Intracranial volume-pressure relationships during
 Journial of Neurology, Neurosurgery, and Psychiatry, 1974, 37, 1099-1104 Intracranial volume-pressure relationships during experimental brain compression in primates 2. Effect of induced changes in systemic
Journial of Neurology, Neurosurgery, and Psychiatry, 1974, 37, 1099-1104 Intracranial volume-pressure relationships during experimental brain compression in primates 2. Effect of induced changes in systemic
Amethod is needed to continuously evaluate the state of
 Assessment of Cerebrovascular Autoregulation Changes of Highest Modal Frequency of Cerebrovascular Pressure Transmission With Cerebral Perfusion Pressure Michael L. Daley, PhD; Massroor Pourcyrous, MD;
Assessment of Cerebrovascular Autoregulation Changes of Highest Modal Frequency of Cerebrovascular Pressure Transmission With Cerebral Perfusion Pressure Michael L. Daley, PhD; Massroor Pourcyrous, MD;
Cerebral autoregulation is a complex intrinsic control. Time course for autoregulation recovery following severe traumatic brain injury
 J Neurosurg 111:695 700, 2009 Time course for autoregulation recovery following severe traumatic brain injury Clinical article Gi l l E. Sv i r i, M.D., M.Sc., 1 Ru n e Aa s l i d, Ph.D., 2 Co l l e e
J Neurosurg 111:695 700, 2009 Time course for autoregulation recovery following severe traumatic brain injury Clinical article Gi l l E. Sv i r i, M.D., M.Sc., 1 Ru n e Aa s l i d, Ph.D., 2 Co l l e e
Papilledema. Golnaz Javey, M.D. and Jeffrey J. Zuravleff, M.D.
 Papilledema Golnaz Javey, M.D. and Jeffrey J. Zuravleff, M.D. Papilledema specifically refers to optic nerve head swelling secondary to increased intracranial pressure (IICP). Optic nerve swelling from
Papilledema Golnaz Javey, M.D. and Jeffrey J. Zuravleff, M.D. Papilledema specifically refers to optic nerve head swelling secondary to increased intracranial pressure (IICP). Optic nerve swelling from
Intracranial pressure monitoring in severe traumatic brain injury
 188 Apetrei et al Intracranial pressure monitoring in severe traumatic brain injury Intracranial pressure monitoring in severe traumatic brain injury Al. Cosmin Apetrei 1,2, A.Şt. Iencean 2, A Iordache
188 Apetrei et al Intracranial pressure monitoring in severe traumatic brain injury Intracranial pressure monitoring in severe traumatic brain injury Al. Cosmin Apetrei 1,2, A.Şt. Iencean 2, A Iordache
Contribution of mathematical modelling to the interpretation of bedside tests of cerebrovascular. autoregulation.
 Journal of Neurology, Neurosurgery, and Psychiatry 1997;63:721 731 721 Wolfson Brain Imaging Centre, the MRC Cambridge Centre for Brain Repair and Academic Neurosurgical Unit, Addenbrooke s Hospital, Cambridge,
Journal of Neurology, Neurosurgery, and Psychiatry 1997;63:721 731 721 Wolfson Brain Imaging Centre, the MRC Cambridge Centre for Brain Repair and Academic Neurosurgical Unit, Addenbrooke s Hospital, Cambridge,
CISTERNOGRAPHY (CEREBRO SPINAL FLUID IMAGING): A VERSATILE DIAGNOSTIC PROCE DURE
 VOL. 115, No. i E D I T 0 R I A L CISTERNOGRAPHY (CEREBRO SPINAL FLUID IMAGING): A VERSATILE DIAGNOSTIC PROCE DURE C ISTERNOGRAPHY (CSF imaging) is a diagnostic study based on the premise that certain
VOL. 115, No. i E D I T 0 R I A L CISTERNOGRAPHY (CEREBRO SPINAL FLUID IMAGING): A VERSATILE DIAGNOSTIC PROCE DURE C ISTERNOGRAPHY (CSF imaging) is a diagnostic study based on the premise that certain
Intracranial volume-pressure relationships during
 Journial of Neurology, Neurosurgery, and Psychiatry, 1974, 37, 115-1111 Intracranial volume-pressure relationships during experimental brain compression in primates 3. Effect of mannitol and hyperventilation
Journial of Neurology, Neurosurgery, and Psychiatry, 1974, 37, 115-1111 Intracranial volume-pressure relationships during experimental brain compression in primates 3. Effect of mannitol and hyperventilation
Transcranial Doppler Monitoring of Intracranial Pressure Plateau Waves
 Neurocrit Care (2017) 26:330 338 DOI 10.1007/s12028-016-0356-5 ORIGINAL ARTICLE Transcranial Doppler Monitoring of Intracranial Pressure Plateau Waves Danilo Cardim 1 Bernhard Schmidt 2 Chiara Robba 1,3
Neurocrit Care (2017) 26:330 338 DOI 10.1007/s12028-016-0356-5 ORIGINAL ARTICLE Transcranial Doppler Monitoring of Intracranial Pressure Plateau Waves Danilo Cardim 1 Bernhard Schmidt 2 Chiara Robba 1,3
UNDERSTANDING HYDROCEPHALUS
 UNDERSTANDING HYDROCEPHALUS Offering solutions for patients. 1 UNDERSTANDING HYDROCEPHALUS Dear Reader: Your doctor has either recommended the CODMAN HAKIM Precision Fixed Pressure Valve, the CODMAN HAKIM
UNDERSTANDING HYDROCEPHALUS Offering solutions for patients. 1 UNDERSTANDING HYDROCEPHALUS Dear Reader: Your doctor has either recommended the CODMAN HAKIM Precision Fixed Pressure Valve, the CODMAN HAKIM
Treatment of Acute Hydrocephalus After Subarachnoid Hemorrhage With Serial Lumbar Puncture
 19 Treatment of Acute After Subarachnoid Hemorrhage With Serial Lumbar Puncture Djo Hasan, MD; Kenneth W. Lindsay, PhD, FRCS; and Marinus Vermeulen, MD Downloaded from http://ahajournals.org by on vember,
19 Treatment of Acute After Subarachnoid Hemorrhage With Serial Lumbar Puncture Djo Hasan, MD; Kenneth W. Lindsay, PhD, FRCS; and Marinus Vermeulen, MD Downloaded from http://ahajournals.org by on vember,
Cerebrospinal fluid pulse pressure method: a possible substitute for the examination of B waves
 J Neurosurg 101:944 950, 2004 Cerebrospinal fluid pulse pressure method: a possible substitute for the examination of B waves NIKLAS LENFELDT, M.SC.E.P., B.M., NINA ANDERSSON, M.SC.E.P., AINA ÅGREN-WILSSON,
J Neurosurg 101:944 950, 2004 Cerebrospinal fluid pulse pressure method: a possible substitute for the examination of B waves NIKLAS LENFELDT, M.SC.E.P., B.M., NINA ANDERSSON, M.SC.E.P., AINA ÅGREN-WILSSON,
Under Pressure. Dr. Robert Keyes CAEP -- Critical Care May 31, 2015
 Under Pressure Dr. Robert Keyes CAEP -- Critical Care May 31, 2015 Disclosures 1. No disclosures, commercial supports, or conflicts of interest. Learning Objectives 1. To understand the principles of pressure
Under Pressure Dr. Robert Keyes CAEP -- Critical Care May 31, 2015 Disclosures 1. No disclosures, commercial supports, or conflicts of interest. Learning Objectives 1. To understand the principles of pressure
Brain AVM with Accompanying Venous Aneurysm with Intracerebral and Intraventricular Hemorrhage
 Cronicon OPEN ACCESS EC PAEDIATRICS Case Report Brain AVM with Accompanying Venous Aneurysm with Intracerebral and Intraventricular Hemorrhage Dimitrios Panagopoulos* Neurosurgical Department, University
Cronicon OPEN ACCESS EC PAEDIATRICS Case Report Brain AVM with Accompanying Venous Aneurysm with Intracerebral and Intraventricular Hemorrhage Dimitrios Panagopoulos* Neurosurgical Department, University
Unit 1 Exploring and Understanding Data
 Unit 1 Exploring and Understanding Data Area Principle Bar Chart Boxplot Conditional Distribution Dotplot Empirical Rule Five Number Summary Frequency Distribution Frequency Polygon Histogram Interquartile
Unit 1 Exploring and Understanding Data Area Principle Bar Chart Boxplot Conditional Distribution Dotplot Empirical Rule Five Number Summary Frequency Distribution Frequency Polygon Histogram Interquartile
Modeling the Interaction between Intracranial Pressure and Cerebral Hemodynamics
 Modeling the Interaction between Intracranial Pressure and Cerebral Hemodynamics Master s Thesis in Biomedical Engineering Zhaleh Pirzadeh Department of Signals and Systems Division of Signal Processing
Modeling the Interaction between Intracranial Pressure and Cerebral Hemodynamics Master s Thesis in Biomedical Engineering Zhaleh Pirzadeh Department of Signals and Systems Division of Signal Processing
HIROSHI NAKAGUCHI, M.D., PH.D., TAKEO TANISHIMA, M.D., PH.D., Clinical Material and Methods
 J Neurosurg 93:791 795, 2000 Relationship between drainage catheter location and postoperative recurrence of chronic subdural hematoma after burr-hole irrigation and closed-system drainage HIROSHI NAKAGUCHI,
J Neurosurg 93:791 795, 2000 Relationship between drainage catheter location and postoperative recurrence of chronic subdural hematoma after burr-hole irrigation and closed-system drainage HIROSHI NAKAGUCHI,
Non-invasive assessment of intracranial pressure - a plugin function of ICM+ system
 Non-invasive assessment of intracranial pressure - a plugin function of ICM+ system B. Schmidt, M. Czosnyka *, P. Smielewski *, R. Plontke, J. Schwarze, J. Klingelhöfer Dept. of Neurology, Medical Centre
Non-invasive assessment of intracranial pressure - a plugin function of ICM+ system B. Schmidt, M. Czosnyka *, P. Smielewski *, R. Plontke, J. Schwarze, J. Klingelhöfer Dept. of Neurology, Medical Centre
Eide et al. Eide et al. BioMedical Engineering OnLine 2012, 11:66
 Simultaneous monitoring of static and dynamic intracranial pressure parameters from two separate sensors in patients with cerebral bleeds: comparison of findings Eide et al. Eide et al. BioMedical Engineering
Simultaneous monitoring of static and dynamic intracranial pressure parameters from two separate sensors in patients with cerebral bleeds: comparison of findings Eide et al. Eide et al. BioMedical Engineering
Moron General Hospital Ciego de Avila Cuba. Department of Neurological Surgery
 Moron General Hospital Ciego de Avila Cuba Department of Neurological Surgery Early decompressive craniectomy in severe head injury with intracranial hypertension Angel J. Lacerda MD PhD, Daisy Abreu MD,
Moron General Hospital Ciego de Avila Cuba Department of Neurological Surgery Early decompressive craniectomy in severe head injury with intracranial hypertension Angel J. Lacerda MD PhD, Daisy Abreu MD,
Medical University of Gdansk, Gdansk, Poland
 Increased inspiratory resistance alters the cardiac contribution to the dynamic relationship between blood pressure and pial artery pulsation oscillations in healthy subjects Pawel J. Winklewski 1, Jacek
Increased inspiratory resistance alters the cardiac contribution to the dynamic relationship between blood pressure and pial artery pulsation oscillations in healthy subjects Pawel J. Winklewski 1, Jacek
The arrest of treated hydrocephalus in children
 J Neurosurg 61:752-756, 1984 The arrest of treated hydrocephalus in children A radionuclide study IAN H. JOHNSTON, F.R.C.S., ROBERT HOWMAN-GILES, F.R.A.C.P., AND IAN R. WHITTLE, M.B., B.S. T. Y. Nelson
J Neurosurg 61:752-756, 1984 The arrest of treated hydrocephalus in children A radionuclide study IAN H. JOHNSTON, F.R.C.S., ROBERT HOWMAN-GILES, F.R.A.C.P., AND IAN R. WHITTLE, M.B., B.S. T. Y. Nelson
Clinical Study The Value of Programmable Shunt Valves for the Management of Subdural Collections in Patients with Hydrocephalus
 The Scientific World Journal Volume 2013, Article ID 461896, 4 pages http://dx.doi.org/10.1155/2013/461896 Clinical Study The Value of Programmable Shunt Valves for the Management of Subdural Collections
The Scientific World Journal Volume 2013, Article ID 461896, 4 pages http://dx.doi.org/10.1155/2013/461896 Clinical Study The Value of Programmable Shunt Valves for the Management of Subdural Collections
PROBLEM SET 2. Assigned: February 10, 2004 Due: February 19, 2004
 Harvard-MIT Division of Health Sciences and Technology HST.542J: Quantitative Physiology: Organ Transport Systems Instructors: Roger Mark and Jose Venegas MASSACHUSETTS INSTITUTE OF TECHNOLOGY Departments
Harvard-MIT Division of Health Sciences and Technology HST.542J: Quantitative Physiology: Organ Transport Systems Instructors: Roger Mark and Jose Venegas MASSACHUSETTS INSTITUTE OF TECHNOLOGY Departments
WHILE it is generally agreed that elevation
 The Derivation of Coronary Sinus Flow During Elevation of Right Ventricular Pressure By HERMAN M. GELLER, B.S., M.D., MARTIN BRANDFONBRENEU, M.D., AND CARL J. WIGGERS, M.D., The derivation of coronary
The Derivation of Coronary Sinus Flow During Elevation of Right Ventricular Pressure By HERMAN M. GELLER, B.S., M.D., MARTIN BRANDFONBRENEU, M.D., AND CARL J. WIGGERS, M.D., The derivation of coronary
Monitoring of Regional Cerebral Blood Flow Using an Implanted Cerebral Thermal Perfusion Probe Archived Medical Policy
 Applies to all products administered or underwritten by Blue Cross and Blue Shield of Louisiana and its subsidiary, HMO Louisiana, Inc.(collectively referred to as the Company ), unless otherwise provided
Applies to all products administered or underwritten by Blue Cross and Blue Shield of Louisiana and its subsidiary, HMO Louisiana, Inc.(collectively referred to as the Company ), unless otherwise provided
Predicting the response of intracranial pressure to moderate hyperventilation
 Acta Neurochir (Wien) (2005) DOI 10.1007/s00701-005-0510-x Predicting the response of intracranial pressure to moderate hyperventilation L. A. Steiner 1;2, M. Balestreri 1, A. J. Johnston 2, J. P. Coles
Acta Neurochir (Wien) (2005) DOI 10.1007/s00701-005-0510-x Predicting the response of intracranial pressure to moderate hyperventilation L. A. Steiner 1;2, M. Balestreri 1, A. J. Johnston 2, J. P. Coles
Simulation of the Blood Pressure Estimation using the Artery Compliance Model and Pulsation Waveform Model
 Simulation of the Blood Pressure Estimation using the Artery Compliance Model and Pulsation Waveform Model Ahyoung Jeon*, Sooyoung Ye**, Gyerok Jeon* *Department of Biomedical-engineering Pusan National
Simulation of the Blood Pressure Estimation using the Artery Compliance Model and Pulsation Waveform Model Ahyoung Jeon*, Sooyoung Ye**, Gyerok Jeon* *Department of Biomedical-engineering Pusan National
Assessment of Reliability of Hamilton-Tompkins Algorithm to ECG Parameter Detection
 Proceedings of the 2012 International Conference on Industrial Engineering and Operations Management Istanbul, Turkey, July 3 6, 2012 Assessment of Reliability of Hamilton-Tompkins Algorithm to ECG Parameter
Proceedings of the 2012 International Conference on Industrial Engineering and Operations Management Istanbul, Turkey, July 3 6, 2012 Assessment of Reliability of Hamilton-Tompkins Algorithm to ECG Parameter
What effects will proximal or distal disease have on a waveform?
 Spectral Doppler Interpretation Director of Ultrasound Education & Quality Assurance Baylor College of Medicine Division of Maternal-Fetal Medicine Maternal Fetal Center Imaging Manager Texas Children
Spectral Doppler Interpretation Director of Ultrasound Education & Quality Assurance Baylor College of Medicine Division of Maternal-Fetal Medicine Maternal Fetal Center Imaging Manager Texas Children
Ventricle wall movements and cerebrospinal fluid flow in hydrocephalus. Richard D. Penn, M.D., 1 Sukhraaj Basati, B.S., 1 Brian Sweetman, M.S.
 J Neurosurg 115:159 164, 2011 Ventricle wall movements and cerebrospinal fluid flow in hydrocephalus Clinical article Richard D. Penn, M.D., 1 Sukhraaj Basati, B.S., 1 Brian Sweetman, M.S., 1 Xiaodong
J Neurosurg 115:159 164, 2011 Ventricle wall movements and cerebrospinal fluid flow in hydrocephalus Clinical article Richard D. Penn, M.D., 1 Sukhraaj Basati, B.S., 1 Brian Sweetman, M.S., 1 Xiaodong
In our previous studies,44 a mathematical technique. Alterations of pulsation absorber characteristics in experimental hydrocephalus
 J Neurosurg Pediatrics 6:000 000, 6:159 170, 2010 Alterations of pulsation absorber characteristics in experimental hydrocephalus Laboratory investigation Eu n-hy o u n g Pa r k, Ph.D., 1 St e p h e n
J Neurosurg Pediatrics 6:000 000, 6:159 170, 2010 Alterations of pulsation absorber characteristics in experimental hydrocephalus Laboratory investigation Eu n-hy o u n g Pa r k, Ph.D., 1 St e p h e n
Neurocritical Care Monitoring. Academic Half Day Critical Care Fellows
 Neurocritical Care Monitoring Academic Half Day Critical Care Fellows Clinical Scenarios for CNS monitoring No Universally accepted Guidelines Traumatic Brain Injury Intracerebral Hemorrhage Subarachnoid
Neurocritical Care Monitoring Academic Half Day Critical Care Fellows Clinical Scenarios for CNS monitoring No Universally accepted Guidelines Traumatic Brain Injury Intracerebral Hemorrhage Subarachnoid
The Arterial and Venous Systems Roland Pittman, Ph.D.
 The Arterial and Venous Systems Roland Pittman, Ph.D. OBJECTIVES: 1. State the primary characteristics of the arterial and venous systems. 2. Describe the elastic properties of arteries in terms of pressure,
The Arterial and Venous Systems Roland Pittman, Ph.D. OBJECTIVES: 1. State the primary characteristics of the arterial and venous systems. 2. Describe the elastic properties of arteries in terms of pressure,
WHITE PAPER: A GUIDE TO UNDERSTANDING SUBARACHNOID HEMORRHAGE
 WHITE PAPER: A GUIDE TO UNDERSTANDING SUBARACHNOID HEMORRHAGE Subarachnoid Hemorrhage is a serious, life-threatening type of hemorrhagic stroke caused by bleeding into the space surrounding the brain,
WHITE PAPER: A GUIDE TO UNDERSTANDING SUBARACHNOID HEMORRHAGE Subarachnoid Hemorrhage is a serious, life-threatening type of hemorrhagic stroke caused by bleeding into the space surrounding the brain,
Normal cerebrospinal fluid pressure
 OLOF GILLAND, M.D., PH.D., WALLACE W. TOURTELLOTTE, M.D., PH.D., LORCAN O'TAUMA, M.D., AND WILLIAM C. HENDERSON, PtI.D. Departments of Neurology Veterans Administration Wadsworth Hospital Center, and University
OLOF GILLAND, M.D., PH.D., WALLACE W. TOURTELLOTTE, M.D., PH.D., LORCAN O'TAUMA, M.D., AND WILLIAM C. HENDERSON, PtI.D. Departments of Neurology Veterans Administration Wadsworth Hospital Center, and University
A Computer Model of Intracranial Pressure Dynamics during Traumatic Brain Injury that Explicitly Models Fluid Flows and Volumes
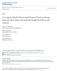 Portland State University PDXScholar Systems Science Faculty Publications and Presentations Systems Science 2004 A Computer Model of Intracranial Pressure Dynamics during Traumatic Brain Injury that Explicitly
Portland State University PDXScholar Systems Science Faculty Publications and Presentations Systems Science 2004 A Computer Model of Intracranial Pressure Dynamics during Traumatic Brain Injury that Explicitly
The classic concept defining cerebrovascular tone is cerebral
 Dynamic Pressure Flow Velocity Relationships in the Human Cerebral Circulation Rune Aaslid, PhD; Stephanie R. Lash, MD; Gust H. Bardy, MD; William H. Gild, MD; David W. Newell, MD Background and Purpose
Dynamic Pressure Flow Velocity Relationships in the Human Cerebral Circulation Rune Aaslid, PhD; Stephanie R. Lash, MD; Gust H. Bardy, MD; William H. Gild, MD; David W. Newell, MD Background and Purpose
Utility of radiologic imaging in the diagnosis and follow up of normal pressure hydrocephalus
 Utility of radiologic imaging in the diagnosis and follow up of normal pressure hydrocephalus Poster No.: C-0312 Congress: ECR 2015 Type: Scientific Exhibit Authors: C. Rodríguez, D. Marquina, A. Mir Torres,
Utility of radiologic imaging in the diagnosis and follow up of normal pressure hydrocephalus Poster No.: C-0312 Congress: ECR 2015 Type: Scientific Exhibit Authors: C. Rodríguez, D. Marquina, A. Mir Torres,
The Sequence of Alterations in the Vital Signs During Acute Experimental Increased Intracranial Pressure*
 J. Neurosurg. / Volume 32 / January, 1970 The Sequence of Alterations in the Vital Signs During Acute Experimental Increased Intracranial Pressure* JAVAD HEKMATPANAH, M.D. Division o/ Neurological Surgery,
J. Neurosurg. / Volume 32 / January, 1970 The Sequence of Alterations in the Vital Signs During Acute Experimental Increased Intracranial Pressure* JAVAD HEKMATPANAH, M.D. Division o/ Neurological Surgery,
abnormally high compared to those encountered when animals are fed by University of Iowa, Iowa City, Iowa, U.S.A.
 J. Phy8iol. (1965), 181, pp. 59-67 59 With 5 text-ftgure8 Printed in Great Britain THE ANALYSIS OF GLUCOSE MEASUREMENTS BY COMPUTER SIMULATION* BY R. G. JANES "D J. 0. OSBURN From the Departments of Anatomy
J. Phy8iol. (1965), 181, pp. 59-67 59 With 5 text-ftgure8 Printed in Great Britain THE ANALYSIS OF GLUCOSE MEASUREMENTS BY COMPUTER SIMULATION* BY R. G. JANES "D J. 0. OSBURN From the Departments of Anatomy
N ormal pressure hydrocephalus was first described by
 PAPER Comparison between the lumbar infusion and CSF tap tests to predict outcome after shunt surgery in suspected normal pressure hydrocephalus B Kahlon, G Sundbärg, S Rehncrona... See end of article
PAPER Comparison between the lumbar infusion and CSF tap tests to predict outcome after shunt surgery in suspected normal pressure hydrocephalus B Kahlon, G Sundbärg, S Rehncrona... See end of article
Sum of Neurally Distinct Stimulus- and Task-Related Components.
 SUPPLEMENTARY MATERIAL for Cardoso et al. 22 The Neuroimaging Signal is a Linear Sum of Neurally Distinct Stimulus- and Task-Related Components. : Appendix: Homogeneous Linear ( Null ) and Modified Linear
SUPPLEMENTARY MATERIAL for Cardoso et al. 22 The Neuroimaging Signal is a Linear Sum of Neurally Distinct Stimulus- and Task-Related Components. : Appendix: Homogeneous Linear ( Null ) and Modified Linear
Supplementary material 1. Definitions of study endpoints (extracted from the Endpoint Validation Committee Charter) 1.
 Rationale, design, and baseline characteristics of the SIGNIFY trial: a randomized, double-blind, placebo-controlled trial of ivabradine in patients with stable coronary artery disease without clinical
Rationale, design, and baseline characteristics of the SIGNIFY trial: a randomized, double-blind, placebo-controlled trial of ivabradine in patients with stable coronary artery disease without clinical
Discrete Signal Processing
 1 Discrete Signal Processing C.M. Liu Perceptual Lab, College of Computer Science National Chiao-Tung University http://www.cs.nctu.edu.tw/~cmliu/courses/dsp/ ( Office: EC538 (03)5731877 cmliu@cs.nctu.edu.tw
1 Discrete Signal Processing C.M. Liu Perceptual Lab, College of Computer Science National Chiao-Tung University http://www.cs.nctu.edu.tw/~cmliu/courses/dsp/ ( Office: EC538 (03)5731877 cmliu@cs.nctu.edu.tw
11/18/2013. Correlational Research. Correlational Designs. Why Use a Correlational Design? CORRELATIONAL RESEARCH STUDIES
 Correlational Research Correlational Designs Correlational research is used to describe the relationship between two or more naturally occurring variables. Is age related to political conservativism? Are
Correlational Research Correlational Designs Correlational research is used to describe the relationship between two or more naturally occurring variables. Is age related to political conservativism? Are
Experimental evaluation of the Spiegelberg intracranial pressure and intracranial compliance monitor
 Neurosurg Focus 9 (5):Article 1, Journal of Neurosurgery Preview Article for December 2000, Click here to return to Table of Contents Experimental evaluation of the Spiegelberg intracranial pressure and
Neurosurg Focus 9 (5):Article 1, Journal of Neurosurgery Preview Article for December 2000, Click here to return to Table of Contents Experimental evaluation of the Spiegelberg intracranial pressure and
Intracranial volume-pressure relationships during experimental brain compression in primates
 Journal of Neurology, Neurosurgery, and Psychiatry, 1974, 37, 1093-1098 Intracranial volume-pressure relationships during experimental brain compression in primates 1. Pressure responses to changes in
Journal of Neurology, Neurosurgery, and Psychiatry, 1974, 37, 1093-1098 Intracranial volume-pressure relationships during experimental brain compression in primates 1. Pressure responses to changes in
The headache profile of idiopathic intracranial hypertension
 The headache profile of idiopathic intracranial hypertension Michael Wall CEPHALALGIA Wall M. The headache profile of idiopathic intracranial hypertension. Cephalalgia 1990;10:331-5. Oslo. ISSN 0333-1024
The headache profile of idiopathic intracranial hypertension Michael Wall CEPHALALGIA Wall M. The headache profile of idiopathic intracranial hypertension. Cephalalgia 1990;10:331-5. Oslo. ISSN 0333-1024
Deputy Manager and Medical Assessor. Specialty Registrar in Histopathology. East Midlands Deanery (United Kingdom) Histopathology
 Curriculum vitae PERSONAL INFORMATION Ming-Yuan Tseng WORK EXPERIENCE October 2011 Present Deputy Manager and Medical Assessor Medicines and Healthcare Products Regulatory Agency (United Kingdom) Assessing
Curriculum vitae PERSONAL INFORMATION Ming-Yuan Tseng WORK EXPERIENCE October 2011 Present Deputy Manager and Medical Assessor Medicines and Healthcare Products Regulatory Agency (United Kingdom) Assessing
