Sanders: Mosby's Paramedic Textbook, Revised 3 rd Edition PowerPoint Lecture Notes Chapter 24: Head and Facial Traumas
|
|
|
- Duane McCormick
- 6 years ago
- Views:
Transcription
1 Sanders: Mosby's Paramedic Textbook, Revised 3 rd Edition PowerPoint Lecture Notes Chapter 24: Head and Facial Traumas Chapter 24 Head and Facial Trauma Objectives Describe mechanism of injury, assessment, and management of: Maxillofacial injuries Ear, eye, and dental injuries Anterior neck trauma Injuries to the scalp, cranial vault, or cranial nerves Objectives Distinguish between types of traumatic brain injury Outline the prehospital management of patients with cerebral injury Calculate a Glasgow Coma Scale, trauma score, revised trauma score, and pediatric trauma score for a given scenario 1
2 Scenario A10-year year-old boy is carried into your station, his arms and legs draped limply over his frantic father s s arms. He fell off an ATV about an hour ago, was knocked out briefly, then seemed fine until he suddenly had a seizure and passed out. Your crew carefully immobilizes him while you determine the following: his airway is noisy, and he has no gag reflex; he is breathing irregularly about 10 times/min; BP 72/50 mm Hg; P 68/min; right pupil 2 mm and reacts to light, left pupil 5 mm and unreactive; flaccid response to pain; wt 35 kg. Discussion What are your immediate priorities for his care? Calculate his GCS, RTS, and PTS What type of brain injury is likely in this child? Explain the significance of his pupillary findings Why might his blood pressure be low? Maxillofacial Injury Arteries Nerves 5th cranial nerve (trigeminal) 7th cranial nerve (facial) Frontal bone Nasal bones Maxilla Zygomatic bone Mandible 2
3 Maxillofacial Injury Causes Motor vehicle crashes Home accidents Athletic injuries Animal bites Intentional violent acts Industrial injuries Maxillofacial trauma classified as: Soft tissue injuries Facial fractures Soft Tissue Injuries Facial soft tissue injuries often appear serious Seldom life threatening Exceptions Compromised upper airway Potential for significant bleeding Soft Tissue Injury Appearance of patient after being attacked and after cleansing 3
4 Mechanism of injury Events leading up to injury Time of injury Associated medical problems Allergies Medications Last oral intake History Spinal precautions Management Assess for airway obstruction Apply suction as needed Secure and maintain airway Ensure ventilation and oxygenation Control bleeding Direct pressure and pressure bandages Facial Fractures Common after blunt trauma Signs and symptoms Fractures of the mandible Dislocations of the mandible 4
5 Fractures of the Midface Middle third of face Maxilla Zygoma Floor of the orbit Nose Fracture of middle 1/3 of face Le Fort Fractures I II III Fractures of the Zygoma Zygoma articulates with frontal, maxillary, and temporal bones Associated with orbital fractures and has similar clinical signs Signs and symptoms 5
6 Fractures of the Orbit Blowout fractures to orbit Periorbital edema, subconjunctival ecchymosis, diplopia, enopthalmos, epistaxis, anesthesia, impaired EOM Suspect injury to orbital contents with any facial fracture Blowout fracture caused by ball s impact Fractures of the Nose Most often fractured structure Injuries may Depress dorsum of nose Displace it to one side Result in epistaxis and swelling (without skeletal deformity) Orbital fractures may also be present Epistaxis Apply external pressure to anterior nares Conscious patient Seated upright or leaning forward while paramedic compresses nares Unconscious patient Positioned on side (if no spinal injury is suspected) Treat for shock if bleeding is severe 6
7 Management of Facial Fractures Assume spine is injured Use spinal precautions Assess airway for obstruction Apply suction as needed Ensure adequate ventilation and oxygenation Control bleeding through direct pressure and pressure bandages Control epistaxis by external direct pressure Nasal and Ear Foreign Bodies Foreign bodies in nose or ear common in children May need transport for physician evaluation Remove foreign body in ear if easily retrieved Do not remove nasal foreign body in field unless it: Compromises airway Can be easily removed without equipment Ear Trauma Lacerations and contusions Usually blunt trauma Treated by direct pressure to control bleeding and ice or cold compresses To decrease swelling 7
8 Ear Trauma Retrieve avulsed tissue if possible Wrap in moist gauze Seal in plastic Place on ice Transport with patient for surgical repair Ear Trauma Partially detached pinna Loss of rim Thermal injuries Ear Trauma Chemical injuries Traumatic perforations Impaled objects Barotitis 8
9 Eye Trauma Common causes of eye injury Motor vehicle crashes Sports and recreational activities Violent altercations Chemical exposure Foreign bodies Animal bites and scratches Evaluation Eye Trauma Evaluation History Exact mode of injury Use of corrective glasses or contact lenses Visual acuity Test injured eye first; compare to uninjured eye Pupillary reaction Extraocular movement Specific Eye Injuries Ocular trauma should be evaluated by physician Foreign bodies Corneal abrasion Blunt trauma Penetrating injury Protruding intraocular foreign bodies Chemical injuries to the eye 9
10 Avulsion of Lid Hyphema Ruptured Globe 10
11 Acid Burn Alkali Burn Corneal Abrasion Care 11
12 Hard lenses Contact Lenses Soft hydrophilic lenses Rigid gas-permeable lenses As a rule, EMS personnel should not attempt to remove contact lenses in patients with eye injuries 32 teeth in adult Sections Crown Root Hard tissues of teeth Soft tissues of teeth Tooth fracture Tooth avulsion Dental Trauma Anterior Neck Trauma Blunt and penetrating trauma Can damage: Skeletal structures Vascular structures Nerves, muscles, and glands of neck Self-inflicted stab wound that had entered pharynx 12
13 Common Mechanisms of Injury Motor vehicle crashes Sports and recreational activities Industrial accidents Violent altercations Hangings Evaluation of the Neck Zone I Injuries carry highest mortality Zone II Most common injuries but lower mortality than zone I injuries Zone III Greatest risk of injury to distal carotid artery, salivary glands, and pharynx Hematomas and Edema Edema of pharynx, larynx, trachea, epiglottis, and vocal cords may obstruct airway completely Consider oral or nasal intubation with spinal precautions in patients with airway compromise Smaller ET tube may be needed 13
14 Hematomas and Edema Other measures to treat edematous airways Cool, humidified oxygen Slight elevation of patient's head (if not contraindicated) Lacerations and Puncture Wounds Superficial injuries Usually managed by covering wound Deep penetrating wounds Serious injuries may require: Aggressive airway therapy and ventilatory support Suction Hemorrhage control by direct pressure Fluid replacement Lacerations and Puncture Wounds Signs and symptoms of significant penetrating neck trauma Dyspnea Hoarseness Stridor Shock Active bleeding Tenderness on palpation Mobility and crepitus Large or expanding hematoma Pulse deficit Neurological deficit Subcutaneous emphysema Hemoptysis Dysphagia Hematemesis 14
15 Vascular Injury Blood vessels are most commonly injured structures in the neck Blunt or penetrating trauma Vessels at risk of injury Carotid Vertebral Subclavian Innominate Internal mammary arteries Jugular and subclavian veins Vascular Injury Management Secure airway with spinal precautions Adequate ventilatory support Control hemorrhage by direct pressure Fluid replacement for hypovolemia guided by medical direction Laryngeal or Tracheal Injury Blunt or penetrating trauma to anterior neck may cause: Fracture or dislocation of the laryngeal and tracheal cartilages Hemorrhage Swelling of air passages Rapid airway control can save patient 15
16 Laryngeal or Tracheal Injury High degree of suspicion for: Vascular disruption Esophageal, chest, and abdominal injury Emergency airway management in these injuries is controversial Esophageal Injury Suspect in patients with trauma to neck or chest Specific injuries that require a high degree of suspicion for associated esophageal injury include: Tracheal fractures Penetrating trauma from stab or gunshot wounds Ingestion of caustic substances Esophageal Injury Signs and symptoms may include: Subcutaneous emphysema Neck hematoma Oropharyngeal or nasogastric blood (indicating esophageal perforation) 16
17 Head Trauma Anatomical components of skull Scalp Cranial vault Dural membrane Arachnoid membrane Pia Brain substances Hair Scalp Subcutaneous tissue Major scalp veins bleed profusely Muscle Attached above eyebrows and at base of occiput Galea Freely movable sheet of connective tissue Helps deflect blows Loose connective tissue Contains emissary veins that drain intracranially Soft Tissue Injuries to the Scalp Irregular linear laceration common May lead to profuse bleeding and hypovolemia Particularly in infants and children 17
18 Soft Tissue Injuries to the Scalp Management Prevent contamination of open wounds Direct pressure or pressure dressings to decrease blood loss IV fluid replacement if needed Consider potential for underlying skull fracture and brain and spinal trauma Facial bones Skull Cranial bones Double layer of solid bone surrounds spongy middle layer Frontal, occipital, temporal, parietal, and mastoid Middle meningeal artery Under temporal bone Can tear artery if fractured Skull floor many ridges Foramen magnum Opening at base of skull for spinal cord Classification of Skull Fractures Linear fractures Basilar fractures Depressed fractures Open vault fractures 18
19 80% of all skull fractures Linear Fractures Not usually depressed May occur without an overlying scalp laceration Generally low complication rate (if isolated injury) Basilar Skull Fracture Basilar Skull Fracture Signs and Symptoms Ecchymosis over mastoid process Temporal bone fracture Battle's sign Blood behind tympanic membrane Fractures of temporal bone Hemotympanum 19
20 Basilar Skull Fracture Signs and Symptoms Ecchymosis of one or both orbits Fracture of base of sphenoid sinus Raccoon's eyes CSF leakage Can result in bacterial meningitis Depressed Skull Fractures Relatively small object strikes head at high speed Often scalp lacerations Frontal and parietal bones most often affected Open Vault Fractures Direct communication between a scalp laceration and cerebral substance Often occur with multisystem trauma High mortality rate May lead to infection (meningitis) Prehospital management 20
21 Severe Fracture of Base of Skull Skull Fractures Complications Cranial nerve injury Vascular involvement Meningeal artery Dural sinuses Infection Underlying brain injury Dural defects caused by depressed bone fragments Cranial Nerve Injuries Usually associated with skull fractures Cranial nerve I (olfactory nerve) Loss of smell Impairment of taste (dependent on food aroma) Sign of basilar skull fracture Cranial nerve II (optic nerve) Blindness in one or both eyes Visual field defects 21
22 Cranial Nerves Cranial nerve III (oculomotor) Origin from midbrain Controls pupil size Pressure on nerve paralyzes nerve Pupil nonreactive Cranial nerve X (vagus) Origin in medulla Nerves that supply SA and AV node, stomach, and GI tract Pressure on nerve stimulates bradycardia Cranial Nerve Injuries Cranial nerve III (oculomotor nerve) Ipsilateral, dilated, fixed pupil Vulnerable to compression by temporal lobe Mimic direct ocular trauma Cranial nerve VII (facial nerve) Immediate or delayed facial paralysis Basilar skull fracture Cranial nerve VIII (auditory nerve) Deafness Basilar skull fracture Brain Trauma Traumatic insult to the brain is capable of producing physical, intellectual, emotional, social, and vocational change Primary brain injury Secondary brain injury 22
23 Brain Trauma Brain occupies 80% of intracranial space Components Brain stem Diencephalon Cerebrum Cerebellum Brain Trauma Categories Mild diffuse injury Moderate diffuse injury Diffuse axonal injury Focal injury Mild Diffuse Injury (Concussion) Fully reversible brain injury No structural damage to brain Causes Signs and symptoms Management 23
24 Moderate Diffuse Injury Minute petechial bruising of brain tissue Brain stem and reticular activating system involvement lead to unconsciousness Signs and symptoms Management Diffuse Axonal Injury (DAI) Most severe brain injury Brain movement within skull secondary to acceleration or deceleration forces DAI may be classified as mild, moderate, or severe Diffuse Axonal Injury Mild DAI Coma of hrs Moderate DAI More common Coma >24 hrs and abnormal posturing Severe DAI Formerly known as brainstem injury Severe shearing of axons in both cerebral hemispheres extending to brain stem 24
25 Focal Injury Specific, grossly observable brain lesions Result from: Skull fracture Contusion Edema with associated increased ICP Ischemia Hemorrhage Intracranial Contents Brain water: 58% Brain solids: 25% Cerebrospinal fluid: 7% Intracranial blood: 10% Cerebral Contusion Bruising of brain around cortex or deeper within frontal, temporal, or occipital lobes Structural change in brain tissue Greater neurological deficits and abnormalities than with concussion Coup injuries Contrecoup injuries 25
26 Edema Significant brain injuries may result in swelling of brain tissue With or without associated hemorrhage Swelling results from humoral and metabolic responses to injury Increase in intracranial pressure May be decreased cerebral perfusion or herniation Ischemia Can result from: Vascular injuries Secondary vascular spasm Increased intracranial pressure Focal or more global infarcts can result Hemorrhage Into or around brain tissue Epidural or subdural hematomas can compress underlying brain tissue or intraparenchymal hemorrhage Often associated with: Cerebral contusions Skull fractures 26
27 Cerebral Blood Flow Oxygen and glucose delivery are controlled by cerebral blood flow A function of cerebral perfusion pressure (CPP) and resistance of the cerebral vascular bed CPP = MAP - ICP MAP = Diastolic pressure + 1/3 Pulse pressure Cerebral Blood Flow As ICP approaches MAP: Gradient for flow decreases Cerebral blood flow is restricted When ICP increases, CPP decreases Cerebral vasodilation occurs Increased cerebral blood volume (increasing ICP) Cerebral Blood Flow Vascular tone in brain regulated by: Carbon dioxide pressure (PCO 2 ) Oxygen pressure (PO 2 ) Autonomic and neurohumoral control PCO 2 has greatest effect on intracerebral vascular diameter and subsequent resistance 27
28 Intracranial Pressure (ICP) Normal range is torr When ICP rises above this level Cerebral blood flow decreases Body tries to compensate for decline in CPP by a rise in MAP: Further elevates ICP, and CSF is displaced to compensate for the expansion If unresolved, brain substance herniates Effects of Increased Intracranial Pressure Increased Intracranial Pressure Early Headache Nausea and vomiting Altered level of consciousness Eventually, Cushing s s triad Increased systolic pressure (widened pulse pressure) Decreased pulse rate Irregular respiratory pattern 28
29 Increased Intracranial Pressure Herniation through temporal lobe causes compression of cranial nerve III (oculomotor) Patient rapidly unresponsive to verbal and painful stimuli Exhibits decorticate posturing or decerebrate posturing Posturing Abnormal flexion (decorticate posturing) Abnormal extension (decerebrate posturing) Critical Signs of Herniation Unresponsive patient with: Bilateral, dilated, unresponsive pupils OR Asymmetric pupils (>1 mm) AND Abnormal extension (decerebrate) posturing OR No motor response to painful stimulus 29
30 Respiratory Patterns Associated with increased intracranial pressure and brain stem injury: Hypoventilation Cheyne-Stokes breathing May accompany decorticate posturing Central neurogenic hyperventilation May accompany decerebrate posturing Ataxic breathing Respiratory Patterns Types of Brain Hemorrhage Classified according to location: Epidural Subdural Subarachnoid Cerebral (intraparenchymal) 30
31 Epidural Hematoma Collection of blood between cranium and dura in epidural space Rapidly developing lesion from laceration of middle meningeal artery Common causes Signs and symptoms Management Subdural Hematoma Blood between dura and surface of brain in subdural space Usually bleeding from veins that bridge subdural space Subdural Hematoma Classifications Acute symptoms <24 hours Subacute symptoms days Chronic symptoms >2 weeks Signs and symptoms 31
32 Subarachnoid Bleeding Intracranial bleeding into CSF, resulting in bloody CSF and meningeal irritation Signs and symptoms Intracerebral Hematoma > 5 ml blood somewhere within brain Commonly frontal or temporal lobe Causes Signs and symptoms Penetrating Injury Missiles fired from handguns Stab wounds Falls High-velocity motor vehicle crashes Associated injuries Complications Definitive care 32
33 Assessment and Evaluation Consider: Mechanism and severity of injury Level of consciousness Associated injuries Assess GCS every 5 min Determine pupil Size Reactivity Assessment and Management Maintain airway Maintain SaO 2 >90% NS or LR fluid bolus if adult BP <90 mm Hg Hyperventilate only when critical signs of herniation are present Neurological exam Assessment and Management Drug therapy Medical direction may prescribe drugs for head injuries (considered controversial) Mannitol for cerebral edema Lorazepam and diazepam for seizure activity Rarely used in prehospital setting in HI due to sedation Lidocaine to control ICP that occurs with ET intubation Sedatives and paralytics for airway management 33
34 Glasgow Coma Scale (GCS) Evaluates: Eye opening Verbal responses Brain stem reflex function Evaluate at least every 5 min Mild head injury: GCS Moderate head injury: GCS Severe head injury: GCS <8 Trauma Score (TS) Predicts outcome of patients with blunt or penetrating injuries Modified trauma index to include systolic blood pressure, respiratory rate, and the GCS Limited use in prehospital setting Revised Trauma Score (RTS) GCS with systolic blood pressure and respiratory rate RTS essentially same as TS except for consideration of capillary refill Patients with RTS of <11 should be transferred to a level I trauma center 34
35 Pediatric Trauma Score (PTS) Evaluates: Size (weight) Airway Central nervous system Systolic blood pressure Open wound Skeletal injury Pediatric trauma patient with PTS <8 should be transported to a level I trauma center Other Methods CUPS system Assigns patients to one of four categories Constant monitoring of patient is crucial Changes in patient s s status may alter the course of a treatment plan Conclusion Head injuries affect nearly 4 million people each year in the United States. Approximately 50,000 patients with severe head trauma die each year before reaching the emergency department. Accurate assessment and appropriate prehospital intervention can improve survival and brain function for patients with these injuries. 35
36 Questions? 36
8th Annual NKY TBI Conference 3/28/2014
 Closed Head Injury: Headache to Herniation A N T H O N Y T. K R A M E R U N I V E R S I T Y O F C I N C I N N A T I B L U E A S H E M S T E C H N O L O G Y P R O G R A M Objectives Describe the pathological
Closed Head Injury: Headache to Herniation A N T H O N Y T. K R A M E R U N I V E R S I T Y O F C I N C I N N A T I B L U E A S H E M S T E C H N O L O G Y P R O G R A M Objectives Describe the pathological
10/6/2017. Notice. Traumatic Brain Injury & Head Trauma
 Notice All EMS Live@Nite presentations will be recorded (both audio and video) and available for public viewing online. By participating in EMS Live@Nite, you consent to audio and video recording and its/their
Notice All EMS Live@Nite presentations will be recorded (both audio and video) and available for public viewing online. By participating in EMS Live@Nite, you consent to audio and video recording and its/their
Head Trauma Inservice (October)
 John Tramell - Head Trauma Inservice, October 2005.doc Page 1 Head Trauma Inservice (October) Head trauma is the leading cause of death in trauma patients. Having a basic understanding of the anatomy and
John Tramell - Head Trauma Inservice, October 2005.doc Page 1 Head Trauma Inservice (October) Head trauma is the leading cause of death in trauma patients. Having a basic understanding of the anatomy and
Chapter 26 Head and Spine Trauma The Nervous System The nervous system controls virtually all of our body activities including reflex, voluntary and
 1 2 3 4 5 Chapter 26 Head and Spine Trauma The Nervous System The nervous system controls virtually all of our body activities including reflex, voluntary and involuntary activities Voluntary activities
1 2 3 4 5 Chapter 26 Head and Spine Trauma The Nervous System The nervous system controls virtually all of our body activities including reflex, voluntary and involuntary activities Voluntary activities
Ears. Mouth. Jowls 6 Major Bones of the Face Nasal bone Two
 1 2 3 4 5 Chapter 25 Injuries to the Face, Neck, and Eyes Injuries to the Face and Neck Face and neck are to injury Relatively unprotected positions on body Some injuries are life-threatening. trauma to
1 2 3 4 5 Chapter 25 Injuries to the Face, Neck, and Eyes Injuries to the Face and Neck Face and neck are to injury Relatively unprotected positions on body Some injuries are life-threatening. trauma to
Head & Brain Trauma. Presented By: Steven Jones, NREMT-P
 Head & Brain Trauma Presented By: Steven Jones, NREMT-P Head & Brain Trauma ~ 4 million head injuries in US per year ~ 450,000 require hospitalization Most are minor injuries Major head injury most common
Head & Brain Trauma Presented By: Steven Jones, NREMT-P Head & Brain Trauma ~ 4 million head injuries in US per year ~ 450,000 require hospitalization Most are minor injuries Major head injury most common
V. CENTRAL NERVOUS SYSTEM TRAUMA
 V. CENTRAL NERVOUS SYSTEM TRAUMA I. Concussion - Is a clinical syndrome of altered consiousness secondary to head injury - Brought by a change in the momentum of the head when a moving head suddenly arrested
V. CENTRAL NERVOUS SYSTEM TRAUMA I. Concussion - Is a clinical syndrome of altered consiousness secondary to head injury - Brought by a change in the momentum of the head when a moving head suddenly arrested
TBI are twice as common in males High potential for poor outcome Deaths occur at three points in time after injury
 Head Injury Any trauma to (closed vs. open) Skull Scalp Brain Traumatic brain injury (TBI) High incidence Most common causes Falls Motor vehicle accidents Other causes Firearm- related injuries Assaults
Head Injury Any trauma to (closed vs. open) Skull Scalp Brain Traumatic brain injury (TBI) High incidence Most common causes Falls Motor vehicle accidents Other causes Firearm- related injuries Assaults
Injuries to the head and spine
 Injuries to the head and spine Aaron J. Katz, AEMT-P, CIC www.es26medic.net 2013 Nervous System Two sub-systems Central Nervous System ( CNS ) Brain and spinal cord Peripheral Nervous System 12 cranial
Injuries to the head and spine Aaron J. Katz, AEMT-P, CIC www.es26medic.net 2013 Nervous System Two sub-systems Central Nervous System ( CNS ) Brain and spinal cord Peripheral Nervous System 12 cranial
Strong, flexible mass of: Skin Fascia tissue Highly provides insulation
 1 Chapter 23 Head, Facial, & Neck Trauma 2 Introduction to Head, Facial, & Neck Injuries Common major trauma 4 million people experience head trauma annually Severe injury is most frequent cause of trauma
1 Chapter 23 Head, Facial, & Neck Trauma 2 Introduction to Head, Facial, & Neck Injuries Common major trauma 4 million people experience head trauma annually Severe injury is most frequent cause of trauma
Lesson Plans and Objectives: Review material for article Prep work for article Picture recovery Review for placement on-line.
 Lesson Plans and Objectives: Review material for article Prep work for article Picture recovery Review for placement on-line. After reading the article, the staff will be able to: Define facial trauma
Lesson Plans and Objectives: Review material for article Prep work for article Picture recovery Review for placement on-line. After reading the article, the staff will be able to: Define facial trauma
LOSS OF CONSCIOUSNESS & ASSESSMENT. Sheba Medical Center Acute Medicine Department MATTHEW WRIGHT
 LOSS OF CONSCIOUSNESS & ASSESSMENT Sheba Medical Center Acute Medicine Department MATTHEW WRIGHT OUTLINE Causes Head Injury Clinical Features Complications Rapid Assessment Glasgow Coma Scale Classification
LOSS OF CONSCIOUSNESS & ASSESSMENT Sheba Medical Center Acute Medicine Department MATTHEW WRIGHT OUTLINE Causes Head Injury Clinical Features Complications Rapid Assessment Glasgow Coma Scale Classification
Introduction to Emergency Medical Care 1
 Introduction to Emergency Medical Care 1 OBJECTIVES 31.1 Define key terms introduced in this chapter. Slides 13 15, 17, 19, 28 31.2 Describe the components and function of the nervous system and the anatomy
Introduction to Emergency Medical Care 1 OBJECTIVES 31.1 Define key terms introduced in this chapter. Slides 13 15, 17, 19, 28 31.2 Describe the components and function of the nervous system and the anatomy
Classical CNS Disease Patterns
 Classical CNS Disease Patterns Inflammatory Traumatic In response to the trauma of having his head bashed in GM would have experienced some of these features. NOT TWO LITTLE PEENY WEENY I CM LACERATIONS.
Classical CNS Disease Patterns Inflammatory Traumatic In response to the trauma of having his head bashed in GM would have experienced some of these features. NOT TWO LITTLE PEENY WEENY I CM LACERATIONS.
PRACTICE GUIDELINE. DEFINITIONS: Mild head injury: Glasgow Coma Scale* (GCS) score Moderate head injury: GCS 9-12 Severe head injury: GCS 3-8
 PRACTICE GUIDELINE Effective Date: 9-1-2012 Manual Reference: Deaconess Trauma Services TITLE: TRAUMATIC BRAIN INJURY GUIDELINE OBJECTIVE: To provide practice management guidelines for traumatic brain
PRACTICE GUIDELINE Effective Date: 9-1-2012 Manual Reference: Deaconess Trauma Services TITLE: TRAUMATIC BRAIN INJURY GUIDELINE OBJECTIVE: To provide practice management guidelines for traumatic brain
Traumatic brain injuries are caused by external mechanical forces such as: - Falls - Transport-related accidents - Assault
 PP2231 Brain injury Cerebrum consists of frontal, parietal, occipital and temporal lobes Diencephalon consists of thalamus, hypothalamus Cerbellum Brain stem consists of midbrain, pons, medulla Central
PP2231 Brain injury Cerebrum consists of frontal, parietal, occipital and temporal lobes Diencephalon consists of thalamus, hypothalamus Cerbellum Brain stem consists of midbrain, pons, medulla Central
Face and Throat Injuries. Chapter 26
 Face and Throat Injuries Chapter 26 Anatomy of the Head Landmarks of the Neck Injuries to the Face Injuries around the face can lead to upper airway obstructions. Bleeding from the face can be profuse.
Face and Throat Injuries Chapter 26 Anatomy of the Head Landmarks of the Neck Injuries to the Face Injuries around the face can lead to upper airway obstructions. Bleeding from the face can be profuse.
Maxillofacial and Ocular Injuries
 Maxillofacial and Ocular Injuries Objectives At the conclusion of this presentation the participant will be able to: Identify the key anatomical structures of the face and eye and the impact of force on
Maxillofacial and Ocular Injuries Objectives At the conclusion of this presentation the participant will be able to: Identify the key anatomical structures of the face and eye and the impact of force on
North Oaks Trauma Symposium Friday, November 3, 2017
 + Evaluation and Management of Facial Trauma D Antoni Dennis, MD North Oaks ENT an Allergy November 3, 2017 + Financial Disclosure I do not have any conflicts of interest or financial interest to disclose
+ Evaluation and Management of Facial Trauma D Antoni Dennis, MD North Oaks ENT an Allergy November 3, 2017 + Financial Disclosure I do not have any conflicts of interest or financial interest to disclose
Traumatic Brain Injury TBI Presented by Bill Masten
 1 2 Cerebrum two hemispheres and four lobes. Cerebellum (little brain) coordinates the back and forth ballet of motion. It judges the timing of every movement precisely. Brainstem coordinates the bodies
1 2 Cerebrum two hemispheres and four lobes. Cerebellum (little brain) coordinates the back and forth ballet of motion. It judges the timing of every movement precisely. Brainstem coordinates the bodies
DR. SAAD AL-MUHAYAWI, M.D., FRCSC. ORL Head & Neck Surgery
 TRAUMA IN ORL DR. SAAD AL-MUHAYAWI, M.D., FRCSC Associate Professor & Consultant ORL Head & Neck Surgery TYPES OF TRAUMA EAR & TEMPORAL BONE TRAUMA NOSE & FACIAL BONES TRAUMA LARYNGEAL TRAUMA NECK TRAUMA
TRAUMA IN ORL DR. SAAD AL-MUHAYAWI, M.D., FRCSC Associate Professor & Consultant ORL Head & Neck Surgery TYPES OF TRAUMA EAR & TEMPORAL BONE TRAUMA NOSE & FACIAL BONES TRAUMA LARYNGEAL TRAUMA NECK TRAUMA
8/29/2011. Brain Injury Incidence: 200/100,000. Prehospital Brain Injury Mortality Incidence: 20/100,000
 Traumatic Brain Injury Almario G. Jabson MD Section Of Neurosurgery Asian Hospital And Medical Center Brain Injury Incidence: 200/100,000 Prehospital Brain Injury Mortality Incidence: 20/100,000 Hospital
Traumatic Brain Injury Almario G. Jabson MD Section Of Neurosurgery Asian Hospital And Medical Center Brain Injury Incidence: 200/100,000 Prehospital Brain Injury Mortality Incidence: 20/100,000 Hospital
McHenry Western Lake County EMS System Paramedic, EMT-B and PHRN Optional Continuing Education 2019 #1 Facial Trauma
 McHenry Western Lake County EMS System Paramedic, EMT-B and PHRN Optional Continuing Education 2019 #1 Facial Trauma The face is vital to human appearance and function. Facial injuries can impair a patient
McHenry Western Lake County EMS System Paramedic, EMT-B and PHRN Optional Continuing Education 2019 #1 Facial Trauma The face is vital to human appearance and function. Facial injuries can impair a patient
Trauma Life Support Pre-Hospital (TLS-P) Preparatory Materials
 Trauma Life Support Pre-Hospital (TLS-P) Preparatory Materials 1 1. A high-risk bodily fluid for spreading infection is blood. 2. Items that can reduce the spread of infection include masks, gloves, and
Trauma Life Support Pre-Hospital (TLS-P) Preparatory Materials 1 1. A high-risk bodily fluid for spreading infection is blood. 2. Items that can reduce the spread of infection include masks, gloves, and
BATLS Battlefield Advanced Trauma Life Support
 J R Army Med Corps 2002; 148: 151-158 BATLS Battlefield Advanced Trauma Life Support CHAPTER 8 HEAD INJURIES Aim 0801. On successfully completing this topic you will be able to: Discuss general management
J R Army Med Corps 2002; 148: 151-158 BATLS Battlefield Advanced Trauma Life Support CHAPTER 8 HEAD INJURIES Aim 0801. On successfully completing this topic you will be able to: Discuss general management
Overview. Overview. Chapter 30. Injuries to the Head and Spine 9/11/2012. Review of the Nervous and Skeletal Systems. Devices for Immobilization
 Chapter 30 Injuries to the Head and Spine Slide 1 Overview Review of the Nervous and Skeletal Systems The Nervous System The Skeletal System Devices for Immobilization Cervical Spine Short Backboards Long
Chapter 30 Injuries to the Head and Spine Slide 1 Overview Review of the Nervous and Skeletal Systems The Nervous System The Skeletal System Devices for Immobilization Cervical Spine Short Backboards Long
The Nervous System PART B
 7 The Nervous System PART B PowerPoint Lecture Slide Presentation by Jerry L. Cook, Sam Houston University ESSENTIALS OF HUMAN ANATOMY & PHYSIOLOGY EIGHTH EDITION ELAINE N. MARIEB Central Nervous System
7 The Nervous System PART B PowerPoint Lecture Slide Presentation by Jerry L. Cook, Sam Houston University ESSENTIALS OF HUMAN ANATOMY & PHYSIOLOGY EIGHTH EDITION ELAINE N. MARIEB Central Nervous System
McHenry Western Lake County EMS System Paramedic, EMT-B and PHRN Optional Continuing Education 2019 #3 Penetrating Neck Trauma
 McHenry Western Lake County EMS System Paramedic, EMT-B and PHRN Optional Continuing Education 2019 #3 Penetrating Neck Trauma Penetrating neck injury (PNI) comprises 5 to 10 percent of traumatic injuries
McHenry Western Lake County EMS System Paramedic, EMT-B and PHRN Optional Continuing Education 2019 #3 Penetrating Neck Trauma Penetrating neck injury (PNI) comprises 5 to 10 percent of traumatic injuries
The dura is sensitive to stretching, which produces the sensation of headache.
 Dural Nerve Supply Branches of the trigeminal, vagus, and first three cervical nerves and branches from the sympathetic system pass to the dura. Numerous sensory endings are in the dura. The dura is sensitive
Dural Nerve Supply Branches of the trigeminal, vagus, and first three cervical nerves and branches from the sympathetic system pass to the dura. Numerous sensory endings are in the dura. The dura is sensitive
Pediatric Subdural Hematoma and Traumatic Brain Injury J. Charles Mace MD FACS Springfield Neurological Institute CoxHealth. Objectives 11/7/2017
 Pediatric Subdural Hematoma and Traumatic Brain Injury J. Charles Mace MD FACS Springfield Neurological Institute CoxHealth Objectives 1. Be able to discuss brain anatomy and physiology as it applies to
Pediatric Subdural Hematoma and Traumatic Brain Injury J. Charles Mace MD FACS Springfield Neurological Institute CoxHealth Objectives 1. Be able to discuss brain anatomy and physiology as it applies to
PTA 106 Unit 1 Lecture 3
 PTA 106 Unit 1 Lecture 3 The Basics Arteries: Carry blood away from the heart toward tissues. They typically have thicker vessels walls to handle increased pressure. Contain internal and external elastic
PTA 106 Unit 1 Lecture 3 The Basics Arteries: Carry blood away from the heart toward tissues. They typically have thicker vessels walls to handle increased pressure. Contain internal and external elastic
European Resuscitation Council
 European Resuscitation Council Incidence of Trauma in Childhood Leading cause of death and disability in children older than one year all over the world Structured approach Primary survey and resuscitation
European Resuscitation Council Incidence of Trauma in Childhood Leading cause of death and disability in children older than one year all over the world Structured approach Primary survey and resuscitation
Injuries to the Head and Spine From Bradys Emergency Care 10 th Edition
 Injuries to the Head and Spine From Bradys Emergency Care 10 th Edition 1. When performing the four-rescuer log roll, which responder pulls the board into position? A.) Head B.) Waist C.) Knee D.) Shoulder
Injuries to the Head and Spine From Bradys Emergency Care 10 th Edition 1. When performing the four-rescuer log roll, which responder pulls the board into position? A.) Head B.) Waist C.) Knee D.) Shoulder
68W COMBAT MEDIC POCKET GUIDE
 GTA 08-05-058 68W COMBAT MEDIC POCKET GUIDE PART I: TRAUMA TREATMENT This publication contains technical information that is for official Government use only. Distribution is limited to U.S. Government
GTA 08-05-058 68W COMBAT MEDIC POCKET GUIDE PART I: TRAUMA TREATMENT This publication contains technical information that is for official Government use only. Distribution is limited to U.S. Government
Shenandoah Co. Fire & Rescue. Injuries to. and Spine. December EMS Training Bill Streett Training Section Chief
 Shenandoah Co. Fire & Rescue Injuries to the Head and Spine December EMS Training Bill Streett Training Section Chief C.E. Card Information BLS Providers 2 Cards / Provider Category 1 Course # Blank Topic#
Shenandoah Co. Fire & Rescue Injuries to the Head and Spine December EMS Training Bill Streett Training Section Chief C.E. Card Information BLS Providers 2 Cards / Provider Category 1 Course # Blank Topic#
Neuropathology Of Head Trauma. Mary E. Case, M.D. Professor of Pathology St. Louis University Health Sciences Center
 Neuropathology Of Head Trauma Mary E. Case, M.D. Professor of Pathology St. Louis University Health Sciences Center Nothing to disclose Disclosure Introduction 500,000 cases/year of serious head injury
Neuropathology Of Head Trauma Mary E. Case, M.D. Professor of Pathology St. Louis University Health Sciences Center Nothing to disclose Disclosure Introduction 500,000 cases/year of serious head injury
Chapter 31. Objectives. Objectives 01/09/2013. Head Trauma
 Chapter 31 Head Trauma Prehospital Emergency Care, Ninth Edition Joseph J. Mistovich Keith J. Karren Copyright 2010 by Pearson Education, Inc. All rights reserved. Objectives 1. Define key terms introduced
Chapter 31 Head Trauma Prehospital Emergency Care, Ninth Edition Joseph J. Mistovich Keith J. Karren Copyright 2010 by Pearson Education, Inc. All rights reserved. Objectives 1. Define key terms introduced
You Are the Emergency Medical Responder
 Lesson 32: Injuries to the Chest, Abdomen and Genitalia You Are the Emergency Medical Responder Your police unit responds to a call in a part of town plagued by violence. When you arrive, you find the
Lesson 32: Injuries to the Chest, Abdomen and Genitalia You Are the Emergency Medical Responder Your police unit responds to a call in a part of town plagued by violence. When you arrive, you find the
Brain Injuries. Presented By Dr. Said Said Elshama
 Brain Injuries Presented By Dr. Said Said Elshama Types of head injuries 1- Scalp injuries 2- Skull injuries 3- Intra Cranial injuries ( Brain ) Anatomical structure of meninges Intra- Cranial Injuries
Brain Injuries Presented By Dr. Said Said Elshama Types of head injuries 1- Scalp injuries 2- Skull injuries 3- Intra Cranial injuries ( Brain ) Anatomical structure of meninges Intra- Cranial Injuries
INCREASED INTRACRANIAL PRESSURE
 INCREASED INTRACRANIAL PRESSURE Sheba Medical Center, Acute Medicine Department Irene Frantzis P-Year student SGUL 2013 Normal Values Normal intracranial volume: 1700 ml Volume of brain: 1200-1400 ml CSF:
INCREASED INTRACRANIAL PRESSURE Sheba Medical Center, Acute Medicine Department Irene Frantzis P-Year student SGUL 2013 Normal Values Normal intracranial volume: 1700 ml Volume of brain: 1200-1400 ml CSF:
TRAUMA TO THE FACE AND MOUTH
 Dr.Yahya A. Ali 3/10/2012 F.I.C.M.S TRAUMA TO THE FACE AND MOUTH Bailey & Love s 25 th edition Injuries to the orofacial region are common, but the majority are relatively minor in nature. A few are major
Dr.Yahya A. Ali 3/10/2012 F.I.C.M.S TRAUMA TO THE FACE AND MOUTH Bailey & Love s 25 th edition Injuries to the orofacial region are common, but the majority are relatively minor in nature. A few are major
2. Subarachnoid Hemorrhage
 Causes: 2. Subarachnoid Hemorrhage A. Saccular (berry) aneurysm - Is the most frequent cause of clinically significant subarachnoid hemorrhage is rupture of a saccular (berry) aneurysm. B. Vascular malformation
Causes: 2. Subarachnoid Hemorrhage A. Saccular (berry) aneurysm - Is the most frequent cause of clinically significant subarachnoid hemorrhage is rupture of a saccular (berry) aneurysm. B. Vascular malformation
Traumatic Brain Injury
 Traumatic Brain Injury Mark J. Harris M.D. Associate Professor University of Utah Salt Lake City USA Overview In US HI responsible for 33% trauma deaths. Closed HI 80% Missile / Penetrating HI 20% Glasgow
Traumatic Brain Injury Mark J. Harris M.D. Associate Professor University of Utah Salt Lake City USA Overview In US HI responsible for 33% trauma deaths. Closed HI 80% Missile / Penetrating HI 20% Glasgow
Supplementary Table 1. ICD-9/-10 codes used to identify cycling injury hospitalizations. Railway accidents injured pedal cyclist
 Supplementary Table 1. ICD-9/-10 codes used to identify cycling injury hospitalizations. ICD Code ICD-9 E800-E807(.3) E810-E816, E818-E819(.6) E820-E825(.6) E826-E829(.1) ICD-10-CA V10-V19 (including all
Supplementary Table 1. ICD-9/-10 codes used to identify cycling injury hospitalizations. ICD Code ICD-9 E800-E807(.3) E810-E816, E818-E819(.6) E820-E825(.6) E826-E829(.1) ICD-10-CA V10-V19 (including all
CNS pathology Third year medical students. Dr Heyam Awad 2018 Lecture 5: disturbed fluid balance and increased intracranial pressure
 CNS pathology Third year medical students Dr Heyam Awad 2018 Lecture 5: disturbed fluid balance and increased intracranial pressure ILOs Understand causes and symptoms of increased intracranial pressure.
CNS pathology Third year medical students Dr Heyam Awad 2018 Lecture 5: disturbed fluid balance and increased intracranial pressure ILOs Understand causes and symptoms of increased intracranial pressure.
Core Curriculum Syllabus Emergencies in Otolaryngology-Head and Neck Surgery FACIAL FRACTURES
 Core Curriculum Syllabus Emergencies in Otolaryngology-Head and Neck Surgery A. General Considerations FACIAL FRACTURES Look for other fractures like skull and/or cervical spine fractures Test function
Core Curriculum Syllabus Emergencies in Otolaryngology-Head and Neck Surgery A. General Considerations FACIAL FRACTURES Look for other fractures like skull and/or cervical spine fractures Test function
Dr. Sami Zaqout, IUG Medical School
 The skull The skull is composed of several separate bones united at immobile joints called sutures. Exceptions? Frontal bone Occipital bone Vault Cranium Sphenoid bone Zygomatic bones Base Ethmoid bone
The skull The skull is composed of several separate bones united at immobile joints called sutures. Exceptions? Frontal bone Occipital bone Vault Cranium Sphenoid bone Zygomatic bones Base Ethmoid bone
Chapter 28 - Head and Spine Injuries
 1 2 3 4 National EMS Education Standard Competencies (1 of 4) Trauma Applies fundamental knowledge to provide basic emergency care and transportation based on assessment findings for an acutely injured
1 2 3 4 National EMS Education Standard Competencies (1 of 4) Trauma Applies fundamental knowledge to provide basic emergency care and transportation based on assessment findings for an acutely injured
1. In a rear-impact motor vehicle crash, which area of the spine is most susceptible to injury? A. Cervical B. Thoracic C. Lumbar D.
 1. In a rear-impact motor vehicle crash, which area of the spine is most susceptible to injury? A. Cervical B. Thoracic C. Lumbar D. Sacral-coccygeal 2. A 36-year-old male sustains blunt force thoracic
1. In a rear-impact motor vehicle crash, which area of the spine is most susceptible to injury? A. Cervical B. Thoracic C. Lumbar D. Sacral-coccygeal 2. A 36-year-old male sustains blunt force thoracic
Abdomen and Genitalia Injuries. Chapter 28
 Abdomen and Genitalia Injuries Chapter 28 Hollow Organs in the Abdominal Cavity Signs of Peritonitis Abdominal pain Tenderness Muscle spasm Diminished bowel sounds Nausea/vomiting Distention Solid Organs
Abdomen and Genitalia Injuries Chapter 28 Hollow Organs in the Abdominal Cavity Signs of Peritonitis Abdominal pain Tenderness Muscle spasm Diminished bowel sounds Nausea/vomiting Distention Solid Organs
Assessment and Scoring Tools
 Assessment and Scoring Tools 2013 APGAR Scale 0 points 1 point 2 points Heart Rate Absent 100 Respiratory Rate Absent Slow, irregular Good, drying Irritability Flaccid Some flexion Active motion
Assessment and Scoring Tools 2013 APGAR Scale 0 points 1 point 2 points Heart Rate Absent 100 Respiratory Rate Absent Slow, irregular Good, drying Irritability Flaccid Some flexion Active motion
Caring for Muscle and Bone Injuries From Brady s First Responder (8 th Edition) 54 Questions
 Caring for Muscle and Bone Injuries From Brady s First Responder (8 th Edition) 54 Questions 1. What is caused by overexerting or tearing of a muscle? p. 375 A.) Dislocation B.) Sprain C.) Fracture *D.)
Caring for Muscle and Bone Injuries From Brady s First Responder (8 th Edition) 54 Questions 1. What is caused by overexerting or tearing of a muscle? p. 375 A.) Dislocation B.) Sprain C.) Fracture *D.)
The Nervous System PART C. PowerPoint Lecture Slide Presentation by Patty Bostwick-Taylor, Florence-Darlington Technical College
 PowerPoint Lecture Slide Presentation by Patty Bostwick-Taylor, Florence-Darlington Technical College The Nervous System 7 PART C Protection of the Central Nervous System Scalp and skin Skull and vertebral
PowerPoint Lecture Slide Presentation by Patty Bostwick-Taylor, Florence-Darlington Technical College The Nervous System 7 PART C Protection of the Central Nervous System Scalp and skin Skull and vertebral
INTRACRANIAL PRESSURE -!!
 INTRACRANIAL PRESSURE - Significance raised ICP main cause of death in severe head injury main cause of morbidity in moderate and mild head injury main target and prognostic indicator in the ITU setting
INTRACRANIAL PRESSURE - Significance raised ICP main cause of death in severe head injury main cause of morbidity in moderate and mild head injury main target and prognostic indicator in the ITU setting
Traumatic Brain Injuries
 Traumatic Brain Injuries Scott P. Sherry, MS, PA-C, FCCM Assistant Professor Department of Surgery Division of Trauma, Critical Care and Acute Care Surgery DISCLOSURES Nothing to disclose Discussion of
Traumatic Brain Injuries Scott P. Sherry, MS, PA-C, FCCM Assistant Professor Department of Surgery Division of Trauma, Critical Care and Acute Care Surgery DISCLOSURES Nothing to disclose Discussion of
May 2011 CE. Site code # E Head & Spinal Cord Trauma
 May 2011 CE Site code # 107200E-1211 Head & Spinal Cord Trauma Objectives by Mike Higgins, FF/PM Grayslake Fire Dept Program by Sharon Hopkins, RN, BSN, EMT-P To view on the Advocate Condell website visit:
May 2011 CE Site code # 107200E-1211 Head & Spinal Cord Trauma Objectives by Mike Higgins, FF/PM Grayslake Fire Dept Program by Sharon Hopkins, RN, BSN, EMT-P To view on the Advocate Condell website visit:
Dr. Esam Ahmad Z. Omar BDS, MSc-OMFS, FFDRCSI. Monitor the vital signs. Monitor the vital signs. Complications of Facial Traumas.
 Complications of Facial Traumas 1) Immediate Complications 2) Late Complications Dr. Esam Ahmad Z. Omar BDS, MSc-OMFS, FFDRCSI Assistant Professor Oral & Maxillofacial Surgeon Taibah University Monitor
Complications of Facial Traumas 1) Immediate Complications 2) Late Complications Dr. Esam Ahmad Z. Omar BDS, MSc-OMFS, FFDRCSI Assistant Professor Oral & Maxillofacial Surgeon Taibah University Monitor
Principles of Anatomy and Physiology
 Principles of Anatomy and Physiology 14 th Edition CHAPTER 14 The Brain and Cranial Nerves Introduction The purpose of the chapter is to: 1. Understand how the brain is organized, protected, and supplied
Principles of Anatomy and Physiology 14 th Edition CHAPTER 14 The Brain and Cranial Nerves Introduction The purpose of the chapter is to: 1. Understand how the brain is organized, protected, and supplied
Pre-hospital Response to Trauma and Brain Injury. Hans Notenboom, M.D. Asst. Medical Director Sacred Heart Medical Center
 Pre-hospital Response to Trauma and Brain Injury Hans Notenboom, M.D. Asst. Medical Director Sacred Heart Medical Center Traumatic Brain Injury is Common 235,000 Americans hospitalized for non-fatal TBI
Pre-hospital Response to Trauma and Brain Injury Hans Notenboom, M.D. Asst. Medical Director Sacred Heart Medical Center Traumatic Brain Injury is Common 235,000 Americans hospitalized for non-fatal TBI
Head CT Scan Interpretation: A Five-Step Approach to Seeing Inside the Head Lawrence B. Stack, MD
 Head CT Scan Interpretation: A Five-Step Approach to Seeing Inside the Head Lawrence B. Stack, MD Five Step Approach 1. Adequate study 2. Bone windows 3. Ventricles 4. Quadrigeminal cistern 5. Parenchyma
Head CT Scan Interpretation: A Five-Step Approach to Seeing Inside the Head Lawrence B. Stack, MD Five Step Approach 1. Adequate study 2. Bone windows 3. Ventricles 4. Quadrigeminal cistern 5. Parenchyma
Chapter 57: Nursing Management: Acute Intracranial Problems
 Chapter 57: Nursing Management: Acute Intracranial Problems NORMAL INTRACRANIAL PRESSURE Intracranial pressure (ICP) is the hydrostatic force measured in the brain CSF compartment. Normal ICP is the total
Chapter 57: Nursing Management: Acute Intracranial Problems NORMAL INTRACRANIAL PRESSURE Intracranial pressure (ICP) is the hydrostatic force measured in the brain CSF compartment. Normal ICP is the total
INTERNATIONAL TRAUMA LIFE SUPPORT
 INTERNATIONAL TRAUMA LIFE SUPPORT NC ITLS Rev. 2/18 STUDENT GUIDE TO INTERNATIONAL TRAUMA LIFE SUPPORT What to wear ITLS is a practical course that stresses hands-on teaching. You should wear comfortable
INTERNATIONAL TRAUMA LIFE SUPPORT NC ITLS Rev. 2/18 STUDENT GUIDE TO INTERNATIONAL TRAUMA LIFE SUPPORT What to wear ITLS is a practical course that stresses hands-on teaching. You should wear comfortable
Patient Assessment. Chapter 8
 Patient Assessment Chapter 8 Patient Assessment Scene size-up Initial assessment Focused history and physical exam Vital signs History Detailed physical exam Ongoing assessment Patient Assessment Process
Patient Assessment Chapter 8 Patient Assessment Scene size-up Initial assessment Focused history and physical exam Vital signs History Detailed physical exam Ongoing assessment Patient Assessment Process
 55-year-old male with 2nd and 3rd degree burns to face, chest, and arms on 25% of the body Respirations: 34 Pulse: 120 Mental Status: moans to painful stimulus Mucous membranes charred Stridor 10 cm scalp
55-year-old male with 2nd and 3rd degree burns to face, chest, and arms on 25% of the body Respirations: 34 Pulse: 120 Mental Status: moans to painful stimulus Mucous membranes charred Stridor 10 cm scalp
Oral and Maxillofacial Surgeons and the seriously injured patient. Barts and The London NHS Trust
 Oral and Maxillofacial Surgeons and the seriously injured patient Barts and The London NHS Trust How do you assess this? Primary Survey A B C D E Airway & Cervical Spine Breathing & Ventilation Circulation
Oral and Maxillofacial Surgeons and the seriously injured patient Barts and The London NHS Trust How do you assess this? Primary Survey A B C D E Airway & Cervical Spine Breathing & Ventilation Circulation
Head Injury כל הזכויות שמורות למד"א מרחב ירושלים. Dan Drory, EMT-P, Instructor
 Head Injury Dan Drory, EMT-P, Instructor Anatomy on a fingertip The brain is a soft and gentle tissue. The brain is the most important organ. כל הזכויות שמורות למד"א מרחב ירושלים Protective layers of the
Head Injury Dan Drory, EMT-P, Instructor Anatomy on a fingertip The brain is a soft and gentle tissue. The brain is the most important organ. כל הזכויות שמורות למד"א מרחב ירושלים Protective layers of the
3. D Objective: Chapter 4, Objective 4 Page: 79 Rationale: A carbon dioxide level below 35 mmhg indicates hyperventilation.
 1. A Objective: Chapter 1, Objective 3 Page: 14 Rationale: The sudden increase in acceleration produces posterior displacement of the occupants and possible hyperextension of the cervical spine if the
1. A Objective: Chapter 1, Objective 3 Page: 14 Rationale: The sudden increase in acceleration produces posterior displacement of the occupants and possible hyperextension of the cervical spine if the
THE ESSENTIAL BRAIN INJURY GUIDE
 THE ESSENTIAL BRAIN INJURY GUIDE Neuroanatomy & Neuroplasticity Section 2 Contributors Erin D. Bigler, PhD Michael R. Hoane, PhD Stephanie Kolakowsky-Hayner, PhD, CBIST, FACRM Dorothy A. Kozlowski, PhD
THE ESSENTIAL BRAIN INJURY GUIDE Neuroanatomy & Neuroplasticity Section 2 Contributors Erin D. Bigler, PhD Michael R. Hoane, PhD Stephanie Kolakowsky-Hayner, PhD, CBIST, FACRM Dorothy A. Kozlowski, PhD
Chapter 24. Learning Objectives. Learning Objectives 9/18/2012. Injuries to the Head and Spine
 Chapter 24 Injuries to the Head and Spine Learning Objectives State components of the nervous system List functions of the central nervous system Define structure of the skeletal system as it relates to
Chapter 24 Injuries to the Head and Spine Learning Objectives State components of the nervous system List functions of the central nervous system Define structure of the skeletal system as it relates to
Skin Anatomy and Physiology
 Skin Anatomy and Physiology Body s largest organ Three layers: Epidermis Dermis Subcutaneous tissue 1 2 Skin Anatomy and Physiology Complex system, variety of functions Sensation Control of water loss
Skin Anatomy and Physiology Body s largest organ Three layers: Epidermis Dermis Subcutaneous tissue 1 2 Skin Anatomy and Physiology Complex system, variety of functions Sensation Control of water loss
Chapter 28. Objectives. Objectives 01/09/2013. Bleeding and Soft-Tissue Trauma
 Chapter 28 Bleeding and Soft-Tissue Trauma Prehospital Emergency Care, Ninth Edition Joseph J. Mistovich Keith J. Karren Copyright 2010 by Pearson Education, Inc. All rights reserved. Objectives 1. Define
Chapter 28 Bleeding and Soft-Tissue Trauma Prehospital Emergency Care, Ninth Edition Joseph J. Mistovich Keith J. Karren Copyright 2010 by Pearson Education, Inc. All rights reserved. Objectives 1. Define
Babak Tamizi Far MD. Assistant professor of internal medicine Al-zahra hospital, Isfahan university of medical sciences
 Babak Tamizi Far MD. Assistant professor of internal medicine Al-zahra hospital, Isfahan university of medical sciences ٢ Level of consciousness is depressed Stuporous patients respond only to repeated
Babak Tamizi Far MD. Assistant professor of internal medicine Al-zahra hospital, Isfahan university of medical sciences ٢ Level of consciousness is depressed Stuporous patients respond only to repeated
Injuries to the Head and Spine
 Injuries to the Head and Spine Anatomy Review Skull Protects the brain Made up of several bones with seam like sutures Regions of the scalp-frontal, occipital, parietal, temporal Bones of face Orbits Mandible
Injuries to the Head and Spine Anatomy Review Skull Protects the brain Made up of several bones with seam like sutures Regions of the scalp-frontal, occipital, parietal, temporal Bones of face Orbits Mandible
DRAFT: Cendoma, M. Sideline Identification of Intracranial Hematoma
 1. Orlando Regional Healthcare, Education and Development. Orlando Regional Health Care. [Online] 2004. [Cited: April 27, 2012.] http://www.orlandoregional.org/pdf%20folder/overview%20adult%20brain%20injury.pd
1. Orlando Regional Healthcare, Education and Development. Orlando Regional Health Care. [Online] 2004. [Cited: April 27, 2012.] http://www.orlandoregional.org/pdf%20folder/overview%20adult%20brain%20injury.pd
The Human Brain: Anatomy, Functions, and Injury
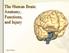 The Human Brain: Anatomy, Functions, and Injury Main Menu Brain Anatomy Brain Functions Injury Mechanisms Brain Anatomy Menu Skull Anatomy Interior Skull Surface Blood Vessels of the Brain Arteries of
The Human Brain: Anatomy, Functions, and Injury Main Menu Brain Anatomy Brain Functions Injury Mechanisms Brain Anatomy Menu Skull Anatomy Interior Skull Surface Blood Vessels of the Brain Arteries of
EYE INJURIES OBJECTIVES COMMON EYE EMERGENCIES 7/19/2017 IMPROVE ASSESSMENT OF EYE INJURIES
 EYE INJURIES BRITTA ANDERSON D.O. DMC PRIMARY CARE SPORTS MEDICINE ASSOCIATE TEAM PHYSICIAN DETROIT TIGERS OBJECTIVES IMPROVE ASSESSMENT OF EYE INJURIES UNDERSTAND WHAT IS CONSIDERED AN EMERGENCY DEVELOP
EYE INJURIES BRITTA ANDERSON D.O. DMC PRIMARY CARE SPORTS MEDICINE ASSOCIATE TEAM PHYSICIAN DETROIT TIGERS OBJECTIVES IMPROVE ASSESSMENT OF EYE INJURIES UNDERSTAND WHAT IS CONSIDERED AN EMERGENCY DEVELOP
CENTRAL NERVOUS SYSTEM TRAUMA and Subarachnoid Hemorrhage. By: Shifaa AlQa qa
 CENTRAL NERVOUS SYSTEM TRAUMA and Subarachnoid Hemorrhage By: Shifaa AlQa qa Subarachnoid Hemorrhage Causes: Rupture of a saccular (berry) aneurysm Vascular malformation Trauma Hematologic disturbances
CENTRAL NERVOUS SYSTEM TRAUMA and Subarachnoid Hemorrhage By: Shifaa AlQa qa Subarachnoid Hemorrhage Causes: Rupture of a saccular (berry) aneurysm Vascular malformation Trauma Hematologic disturbances
Mild Traumatic Brain Injury
 Mild Traumatic Brain Injury Concussions This presentation is for information purposes only, not for any commercial purpose, and may not be sold or redistributed. David Wesley, M.D. Outline Epidemiology
Mild Traumatic Brain Injury Concussions This presentation is for information purposes only, not for any commercial purpose, and may not be sold or redistributed. David Wesley, M.D. Outline Epidemiology
Introduction to Neurosurgical Subspecialties:
 Introduction to Neurosurgical Subspecialties: Trauma and Critical Care Neurosurgery Brian L. Hoh, MD 1, Gregory J. Zipfel, MD 2 and Stacey Q. Wolfe, MD 3 1 University of Florida, 2 Washington University,
Introduction to Neurosurgical Subspecialties: Trauma and Critical Care Neurosurgery Brian L. Hoh, MD 1, Gregory J. Zipfel, MD 2 and Stacey Q. Wolfe, MD 3 1 University of Florida, 2 Washington University,
Neurology study of the nervous system. nervous & endocrine systems work together to maintain homeostasis
 Nervous System Neurology study of the nervous system nervous & endocrine systems work together to maintain homeostasis Nervous System works very fast Uses electrical signals called nerve impulses Short-lived
Nervous System Neurology study of the nervous system nervous & endocrine systems work together to maintain homeostasis Nervous System works very fast Uses electrical signals called nerve impulses Short-lived
HEAD AND NECK ANATOMY PRACTICE QUESTIONS
 HEAD AND NECK ANATOMY PRACTICE QUESTIONS 1. A patient complains that he has lost sensation on his face and that the skin of his face feels numb. The physician tests tactile acuity by touching the forehead
HEAD AND NECK ANATOMY PRACTICE QUESTIONS 1. A patient complains that he has lost sensation on his face and that the skin of his face feels numb. The physician tests tactile acuity by touching the forehead
C h a p t e r PowerPoint Lecture Slides prepared by Jason LaPres North Harris College Houston, Texas
 C h a p t e r 15 The Nervous System: The Brain and Cranial Nerves PowerPoint Lecture Slides prepared by Jason LaPres North Harris College Houston, Texas Copyright 2009 Pearson Education, Inc., publishing
C h a p t e r 15 The Nervous System: The Brain and Cranial Nerves PowerPoint Lecture Slides prepared by Jason LaPres North Harris College Houston, Texas Copyright 2009 Pearson Education, Inc., publishing
Pediatric Head Trauma August 2016
 PEDIATRIC HEAD TRAUMA AUGUST 2016 Pediatric Head Trauma August 2016 EDUCATION COMMITTEE PEER EDUCATION Quick Review of Pathophysiology of TBI Nuggets of knowledge to keep in mind with TBI Intracranial
PEDIATRIC HEAD TRAUMA AUGUST 2016 Pediatric Head Trauma August 2016 EDUCATION COMMITTEE PEER EDUCATION Quick Review of Pathophysiology of TBI Nuggets of knowledge to keep in mind with TBI Intracranial
Eyes, ears, teeth and everything in between
 Eyes, ears, teeth and everything in between E M E R G E N C Y D E P A R T M E N T J U N I O R T E A C H created 14/11/10 by S.R. Bruijns, version 1.0 Objectives Eyes Ears Teeth Maxilla- facial EYES Approaching
Eyes, ears, teeth and everything in between E M E R G E N C Y D E P A R T M E N T J U N I O R T E A C H created 14/11/10 by S.R. Bruijns, version 1.0 Objectives Eyes Ears Teeth Maxilla- facial EYES Approaching
Epidemiology 3002). Epidemiology and Pathophysiology
 Epidemiology Maxillofacial trauma or injuries are commonly encountered in the practice of emergency medicine and are presenting one of the most challenging problems to the attending surgeons or physicians
Epidemiology Maxillofacial trauma or injuries are commonly encountered in the practice of emergency medicine and are presenting one of the most challenging problems to the attending surgeons or physicians
Bellringer: The central nervous system is comprised of: What is the name of the outermost layer of the brain? a. Brain. b.
 Bellringer: The central is comprised of: a. Brain b. Spinal cord c. Sensory receptors d. Both a and b What is the name of the outermost layer of the brain? a. Pia mater b. Dura mater c. Arachnoid d. Pons
Bellringer: The central is comprised of: a. Brain b. Spinal cord c. Sensory receptors d. Both a and b What is the name of the outermost layer of the brain? a. Pia mater b. Dura mater c. Arachnoid d. Pons
ITLS Pediatric Provider Course Advanced Pre-Test
 ITLS Pediatric Provider Course Advanced Pre-Test 1. You arrive at the scene of a motor vehicle crash and are directed to evaluate a child who was in one of the vehicles. The patient appears to be a child
ITLS Pediatric Provider Course Advanced Pre-Test 1. You arrive at the scene of a motor vehicle crash and are directed to evaluate a child who was in one of the vehicles. The patient appears to be a child
Index. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Abdominal injuries, abdominal wall muscle injury, 212 213 diaphragmatic spasm, 212 liver injury, 213 214 pancreatic injury, 216 rectus
Index Note: Page numbers of article titles are in boldface type. A Abdominal injuries, abdominal wall muscle injury, 212 213 diaphragmatic spasm, 212 liver injury, 213 214 pancreatic injury, 216 rectus
Basic Assessment and Treatment of Trauma
 Basic Assessment and Treatment of Trauma Final Exam Version 1 1. In which of the following scenarios would the potential for serious injury or death be the GREATEST? A. 77-kg (170-lb) man who falls 1.2
Basic Assessment and Treatment of Trauma Final Exam Version 1 1. In which of the following scenarios would the potential for serious injury or death be the GREATEST? A. 77-kg (170-lb) man who falls 1.2
Chapter 27 - Face and Neck Injuries
 1 2 3 4 5 6 7 8 9 National EMS Education Standard Competencies (1 of 5) Medicine Applies fundamental knowledge to provide basic emergency care and transportation based on assessment findings for an acutely
1 2 3 4 5 6 7 8 9 National EMS Education Standard Competencies (1 of 5) Medicine Applies fundamental knowledge to provide basic emergency care and transportation based on assessment findings for an acutely
Focused History and Physical Examination of the
 Henry: EMT Prehospital Care, Revised 3 rd Edition Lecture Notes Chapter 10: Focused History and Physical Examination of Trauma Patients Chapter 10 Focused History and Physical Examination of the Trauma
Henry: EMT Prehospital Care, Revised 3 rd Edition Lecture Notes Chapter 10: Focused History and Physical Examination of Trauma Patients Chapter 10 Focused History and Physical Examination of the Trauma
Workbook Answers Chapter 13. Neurologic Diseases and Conditions
 Workbook Answers Chapter 13 Neurologic Diseases and Conditions Short Answer 1. Afferent nerves transmit impulses from parts of the body to the spinal cord; efferent nerves transmit impulses away from the
Workbook Answers Chapter 13 Neurologic Diseases and Conditions Short Answer 1. Afferent nerves transmit impulses from parts of the body to the spinal cord; efferent nerves transmit impulses away from the
Case 1. Case 5/30/2013. Traumatic Brain Injury : Review, Update, and Controversies
 Case 1 Traumatic Brain Injury : Review, Update, and Controversies Shirley I. Stiver MD, PhD 32 year old male s/p high speed MVA Difficult extrication Intubated at scene Case BP 75 systolic / palp GCS 3
Case 1 Traumatic Brain Injury : Review, Update, and Controversies Shirley I. Stiver MD, PhD 32 year old male s/p high speed MVA Difficult extrication Intubated at scene Case BP 75 systolic / palp GCS 3
BRAIN TRAUMA THERAPEUTIC RECOMMENDATIONS
 1 BRAIN TRAUMA THERAPEUTIC RECOMMENDATIONS Richard A. LeCouteur, BVSc, PhD, Dip ACVIM (Neurology), Dip ECVN Professor Emeritus, University of California, Davis, California, USA Definitions Hemorrhage:
1 BRAIN TRAUMA THERAPEUTIC RECOMMENDATIONS Richard A. LeCouteur, BVSc, PhD, Dip ACVIM (Neurology), Dip ECVN Professor Emeritus, University of California, Davis, California, USA Definitions Hemorrhage:
Nervous System The Brain and Spinal Cord Unit 7b
 Nervous System The Brain and Spinal Cord Unit 7b Chetek High School Mrs. Michaelsen 9.12 Meninges A. Meninges 1. The organs of the CNS are covered by membranes a. The meninges are divided into 3 layers:
Nervous System The Brain and Spinal Cord Unit 7b Chetek High School Mrs. Michaelsen 9.12 Meninges A. Meninges 1. The organs of the CNS are covered by membranes a. The meninges are divided into 3 layers:
Head, Face, Eyes, Ears, Nose and Throat. Neurological Exam. Eye Function 12/11/2017. Oak Ridge High School Conroe, Texas
 Head, Face, Eyes, Ears, Nose and Throat Oak Ridge High School Conroe, Texas Neurological Exam Consists of Five Major Areas: 1. cerebral testing cognitive functioning 2. Cranial nerve testing 3. Cerebellar
Head, Face, Eyes, Ears, Nose and Throat Oak Ridge High School Conroe, Texas Neurological Exam Consists of Five Major Areas: 1. cerebral testing cognitive functioning 2. Cranial nerve testing 3. Cerebellar
Ventricles, CSF & Meninges. Steven McLoon Department of Neuroscience University of Minnesota
 Ventricles, CSF & Meninges Steven McLoon Department of Neuroscience University of Minnesota 1 Coffee Hour Thursday (Sept 14) 8:30-9:30am Surdyk s Café in Northrop Auditorium Stop by for a minute or an
Ventricles, CSF & Meninges Steven McLoon Department of Neuroscience University of Minnesota 1 Coffee Hour Thursday (Sept 14) 8:30-9:30am Surdyk s Café in Northrop Auditorium Stop by for a minute or an
PEDIATRIC BRAIN CARE
 PEDIATRIC BRAIN CARE The brain matters most! OVERVIEW OF NEURO ASSESSMENT 1. Overall responsiveness/activity 2. The eyes 3.? Increased ICP 4. Movements 5.? Seizures 6. Other OVERALL RESPONSIVENESS/ ACTIVITY
PEDIATRIC BRAIN CARE The brain matters most! OVERVIEW OF NEURO ASSESSMENT 1. Overall responsiveness/activity 2. The eyes 3.? Increased ICP 4. Movements 5.? Seizures 6. Other OVERALL RESPONSIVENESS/ ACTIVITY
ACTIVITY 7: NERVOUS SYSTEM HISTOLOGY, BRAIN, CRANIAL NERVES
 ACTIVITY 7: NERVOUS SYSTEM HISTOLOGY, BRAIN, CRANIAL NERVES LABORATORY OBJECTIVES: 1. Histology: Identify structures indicated on three different slides or images of nervous system tissue. These images
ACTIVITY 7: NERVOUS SYSTEM HISTOLOGY, BRAIN, CRANIAL NERVES LABORATORY OBJECTIVES: 1. Histology: Identify structures indicated on three different slides or images of nervous system tissue. These images
