Cerebral arterial stenoses can be caused by a wide range of
|
|
|
- Jonas Patterson
- 5 years ago
- Views:
Transcription
1 Evaluation of Hyperintense Vessels on FLAIR MRI for the Diagnosis of Multiple Intracerebral Arterial Stenoses Daniela Iancu-Gontard, MD; Catherine Oppenheim, MD, PhD; Emmanuel Touzé, MD; Eric Méary, MD; Mathieu Zuber, MD; Jean-Louis Mas, MD; Daniel Frédy, MD; Jean-François Meder, MD, PhD Background and Purpose Hyperintense vessel sign (HVS) on fluid-attenuated inversion recovery (FLAIR) has been described in hyperacute stroke patients with arterial occlusion. We sought to determine whether HVS was more frequent in patients with intracerebral arterial stenoses than in those without stenosis regardless of the presence of a brain infarct. Methods In this case-control study (19 symptomatic patients with multiple intracerebral arterial stenoses compared with 19 age-matched asymptomatic patients without stenosis), we looked for HVS (ie, focal or tubular hyperintensities in the subarachnoid space) on FLAIR images. We compared the proportion of HVS-positive patients in the 2 groups and evaluated the concordance between the arterial distribution of stenoses on angiogram and that of HVS on FLAIR. Results HVS was found in 13 of 19 patients (68%) in the study group and 1 of 19 control patients (5.2%) (P ). The concordance between the territorial distribution of stenoses on angiogram and HVS on FLAIR was higher for the right and left middle cerebral artery ( 0.6 and 0.63, respectively) compared with the right and left anterior cerebral artery ( 0.35 and 0.2, respectively). HVSs were observed in 1 of 7 patients with posterior cerebral artery stenoses on angiogram. HVSs were seen equally in patients with acute focal (7 of 10) or diffuse (6 of 9) cerebral involvement. In the 6 HVS-positive patients with acute stroke confirmed by MRI, additional HVSs were observed in a different arterial territory than that of the stroke lesion. Conclusions Although their significance remains unclear, multiple HVSs are more frequently observed in symptomatic patients with multiple intracerebral stenoses than in asymptomatic patients without stenosis. (Stroke. 2003;34: ) Key Words: arteries brain magnetic resonance imaging stenosis Cerebral arterial stenoses can be caused by a wide range of diseases such as central nervous system infectious or inflammatory vasculitis, 1 3 intracranial atherosclerosis, 4 or vasospasm. 5,6 The diagnosis of intracerebral arterial stenosis can be clinically challenging because the initial presentation is highly variable, with focal to diffuse neurological manifestations and acute to chronic evolution. 5 7 Digital subtraction angiography (DSA) remains the keystone diagnostic technique for delineating proximal or distal segmental stenoses of intracranial arteries. Yet, in practice, MRI precedes angiographic studies in the evaluation of these patients. Fluidattenuated inversion recovery (FLAIR) is now part of many routine clinical MR protocols for brain imaging because of its excellent capacity to depict parenchymal signal changes. There is increasing evidence that FLAIR sequence could also be useful for detecting abnormal arterial blood flow kinetics. Indeed, several groups have reported an increased intensity in cerebral blood vessels on FLAIR in the setting of acute ischemia in patients with major vessel occlusion or severe stenosis. 8,9 This so-called hyperintense vessel sign (HVS) on FLAIR MRI is thought to indicate the presence of slow flow or stasis in small arteries, veins, and collateral vessels. 10 We hypothesized that HVSs could be associated with the presence of multiple intracerebral arterial stenoses regardless of the presence of a brain infarct. To test this hypothesis, we conducted a case-control study to compare the FLAIR images of 19 patients with intracerebral arterial stenoses and 19 control subjects without intracerebral stenoses. Subjects and Methods Patients and Control Subjects Study Group From our database of patients admitted between August 1999 and December 2002, we retrospectively selected those who fulfilled the following criteria: (1) presence of acute or subacute neurological signs or symptoms at admission; (2) multiple cerebral arterial stenoses demonstrated by DSA or MR angiography; (3) MRI with an axial FLAIR sequence obtained 1 week before angiogram; (4) no Received November 26, 2002; final revision received March 11, 2003; accepted March 17, From the Departments of Neuroradiology (D.I.-G., C.O., E.M., D.F, J.-F.M.) and Neurology (E.T., M.Z., J.-L.M.), Centre Hospitalier Sainte-Anne, Université Paris V, Paris, France. Correspondence to Dr Catherine Oppenheim, Departement d Imagerie Morphologique et Fonctionnelle, Centre Hospitalier Sainte-Anne, 1 Rue Cabanis, Paris Cedex 14, France. oppenheim@chsa.broca.inserm.fr 2003 American Heart Association, Inc. Stroke is available at DOI: /01.STR FE 1886
2 Iancu-Gontard et al FLAIR and Intracerebral Arterial Stenoses 1887 evidence of subarachnoid hemorrhage on CT and/or lumbar puncture; (5) a lumbar puncture excluding meningitis when clinically suspected; and (6) no evidence of stenosis of extracranial arteries on DSA, MR angiography, or ultrasonographic examination. Nineteen patients (8 men, 11 women) between 22 and 67 years of age (mean age, 43 years) fulfilled these criteria and constituted the study group. At the time of MR, all patients presented signs of neurological impairment, suggesting focal cerebral involvement in 10 and diffuse encephalopathy in the remaining 9. Of the latter 9 patients, 1 was referred for subacute psychiatric disorders, 6 were admitted because of prominent intense headaches of sudden onset, and the remaining 2 presented with diffuse neurological symptoms (tremor, altered mental state, and sleepiness). Intracerebral arterial stenoses were attributed to a reversible angiopathy in 8 cases [associated conditions included blood transfusion (n 1), eclampsia (n 2), undetermined (n 5)]. All of them had MR angiographic follow-ups showing regression or disappearance of arterial stenoses and a benign clinical course that did not require corticosteroid or other immunosuppressive therapy. For the other 11 patients, infectious angiitis was diagnosed in 2 patients, and intracranial atherosclerosis, dysplasia, and Sjögren angiitis were found in 1 patient each. The cause remained unknown in 6 patients despite a complete workup, including a leptomeningeal biopsy in 2 cases. Control Group The control group consisted of 19 asymptomatic age-matched patients (9 men, 10 women; mean age, 42.2 years). They were selected from a population of patients who had been treated with endovascular coiling for an intracranial aneurysm and were undergoing a 1-year intracranial DSA and FLAIR MR follow-up study. Patients with extracranial or intracranial arterial stenoses on DSA were not included in the control group. Imaging Techniques and Analysis HVS on FLAIR All MR examinations were performed with a 1.5-T MR unit (GE Signa Horizon Echospeed) including a fast FLAIR sequence with 20 interleaved slices, matrix, ms repetition time, 148-ms effective echo time, 2200-ms inversion time, and 32-kHz bandwidth. The field of view was cm, with 6-mm slice thickness, no gap, and an inversion pulse applied over twice the slice thickness for the 10 patients admitted for sudden neurological deficit, in accordance with our routine emergency MR procedure for acute stroke. All other patients were imaged with a slightly different FLAIR sequence using a field of view of cm, 5-mm slice thickness, 1.5-mm gap, and inversion pulse applied over 3 times the slice thickness. Overall, 38 sets of FLAIR images were available for analysis. FLAIR was considered positive (HVS ) when focal or tubular hyperintensities relative to gray matter were seen in the subarachnoid space on 1 axial slice. Each hyperintense vessel was assigned to a portion of the Willis circle (ie, proximal when they were located in the area of the A1, M1, and P1 or P2 segments; distal when located elsewhere) and a vascular distribution [anterior (ACA), middle (MCA), or posterior (PCA) cerebral artery]. For hyperintensities that were distally located, reviewers were instructed not to take into account paramedian tubular or bridge-shaped hyperintensities seen at the vertex and localized slightly away from the cortical surface because these were considered to correspond to venous structures. Two neuroradiologists, blinded to the clinical and angiographic data, independently reviewed the randomly presented FLAIR images after they were removed from other sequences. In the event of discrepancies, the final result was reached by consensus. In addition, to check for intraobserver reproducibility, 1 reviewer examined the FLAIR images again 1 week later, with the images presented in a different order than that of the first session. On FLAIR, the reviewers looked for parenchymal signal changes in the cortical and subcortical areas in the vicinity of each HVS. On diffusion-weighted imaging (DWI), available in 15 patients of the study group, reviewers looked for signs of acute stroke, ie, hyperintensities on DWI (b 1000 s/mm 2 ) with a corresponding decrease in the apparent diffusion coefficient. Stenoses on Angiograms DSA was performed by femoral approach with contrast injection in at least 3 vessels (both internal carotid arteries and 1 or 2 vertebral arteries). Biplane, frontal, and lateral DSA images were obtained serially with an exposure rate of 2 images per second during the first 6 seconds followed by 1 image per second during the next 13 to 16 seconds. Intracranial 3-dimensional time-of-flight MR angiography, obtained during the same imaging session as the FLAIR sequence, was performed with a repetition time of 33 ms, an echo time of 3.3 ms, a flip angle of 20, an acquisition bandwidth of 12.5 khz, a scanning time 6 minutes 56 seconds, and 2 axial slabs centered on the circle of Willis. Angiograms were retrospectively evaluated on film screen by a neuroradiologist blinded to the clinical and MRI data. He searched for focal arterial stenoses on DSA when available (n 16) or otherwise on MR angiogram (n 3). Stenoses were classified as proximal when they involved the A1, M1, P1, or P2 segments; otherwise, they were classified as distal. Each stenosis was assigned a vascular distribution (ACA, MCA, or PCA). Statistical Analysis The proportions of HVS patients in the study group and control group were compared by use of Fisher s exact test. Intraobserver and interobserver agreement for the diagnosis of HVS was assessed by calculating the statistical analysis and their 95% confidence interval (CIs). 11,12 We also evaluated the concordance between the topography of stenoses on angiogram and the topography of HVS on FLAIR by calculating the statistics and their 95% CIs. To do so, each cerebral arterial territory (ACA, MCA, PCA) was considered abnormal on FLAIR when it contained at least 1 HVS. Similarly, each arterial territory was considered abnormal on angiogram when it contained at least 1 arterial stenosis. A Wilcoxon signed-rank test was used to compare the presence of each HVS with the presence of underlying parenchymal lesion on FLAIR. Fisher s exact test was used to analyze the occurrence of HVS according to initial clinical presentation. The level of statistical significance was P Results HVS on FLAIR HVS was identified by consensus in 13 patients (68%) in the study group and 1 patient (5.2%) in the control group (P ) (Figures 1 and 2). During the first reading, observer 1 identified HVS in 12 of the 19 patients in the study group and 2 of the 19 patients in the control group, whereas observer 2 identified HVS in 14 of the 19 patients in the study group and 2 of the 19 patients in the control group. The intraobserver agreement for the identification of HVS was 0.89 (95% CI, 0.68 to 1) for the study group and 0.82 (95% CI, 0.63 to 1) for the whole population. The interobserver agreement was substantial between the first reading of observer 1 and observer 2 (study group: 0.76; 95% CI, 0.45 to 1.0; whole population: 0.83; 95% CI, 0.66 to 1) and substantial between the second reading of observer 1 and observer 2 (study group: 0.66; 95% CI, 0.33 to 0.99; whole population: 0.67; 95% CI, 0.45 to 0.90). The distribution of HVS on FLAIR is presented in the Table. HVS and Angiogram The Table shows the distribution of stenoses on angiogram in the 13 HVS and 6 HVS patients of the study group. Of the 13 HVS patients, arterial stenoses were seen on angiogram in the corresponding territories in all but 2 patients. Yet, stenoses were more widespread on angiogram than were
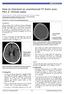
3 1888 Stroke August 2003 Figure 1. Reversible cerebral angiitis in a 48-year-old woman presenting with seizures and headaches of sudden onset and right hemiparesis. A, Initial axial FLAIR sequence shows multiple bilateral focal and tubular hyperintensities within the subarachnoid space (arrows), likely adjacent to the cortical surface, and subcortical bilateral parenchymal signal changes. HVSs are bilaterally distributed in the ACA and right MCA territories. B, DWI shows the absence of parenchymal hyperintensities. Right (C) and left (D) internal carotid DSAs demonstrate multiple stenoses of proximal and distal segments of the ACA and MCA. Arrows on DSA point to stenoses that could be responsible for the HVSs seen on FLAIR. Spontaneously, the focal deficit resolved within a week. E, Five weeks later, the stenoses almost completely regressed on MR angiogram, and tubular hyperintensities were no longer visible on FLAIR. HVSs on FLAIR because additional arterial stenoses were observed in arterial territories with no HVS on FLAIR in 9 of 13 HVS patients. The concordance between the territorial distribution of stenoses on angiogram and HVS on FLAIR was higher for the right and left MCA ( 0.6; 95% CI, 0.3 to 0.9; and 0.63; 95% CI, 0.3 to 1.0, respectively) compared with the right and left ACA ( 0.35; 95% CI, 0.0 to 0.7; and 0.2; 95% CI, 0.0 to 0.4). For the PCA territories, concordance was not calculated because HVSs on FLAIR were observed in only 1 of the 7 patients with stenoses of the PCA on angiogram. These concordances remained unchanged after exclusion of the 3 patients for whom only an MR angiography was available. Figure 2. Reversible angiitis in a 50-year-old woman who presented with photophobia, nausea, and vomiting with severe headaches of sudden onset. CT scan and lumbar puncture were normal. MRI was obtained 2 days after symptom onset. A, Axial FLAIR sequence shows bilateral focal and tubular hyperintensities within the subarachnoid space, deep in the sulci, distributed in the right ACA and MCA territories bilaterally (arrows). Additional parenchymal signal changes are also visible in the cortical and subcortical areas posteriorly. B, DWI shows the absence of parenchymal hyperintensities. C, Left DSA confirms the presence of multiple proximal and distal stenoses of the MCA (arrows) that could be responsible for the HVSs seen in the left MCA territory on FLAIR and reveals additional stenoses of the left ACA territory (arrowheads). D, Four weeks later, tubular hyperintensities are no longer visible on FLAIR. HVS, Parenchyma, and Clinical Presentation Of the 13 HVS patients, HVSs were more frequently observed without underlying parenchymal signal changes in the adjacent cortex or subcortical area than with underlying signal changes (P 0.05). The Table shows that all patients with stenoses attributed to a reversible angiopathy were HVS and that HVSs were observed equally in patients who initially presented with focal (7 of 10) or diffuse (6 of 9) cerebral involvement. Interestingly, in 6 of the 7 HVS patients with acute stroke confirmed by MRI, HVS was not confined to the limits of the acute stroke lesion but was also observed in a different arterial territory than that of the stroke lesion (Figure 3). Discussion The FLAIR sequence is now part of many routine clinical imaging protocols. An inversion pulse is used with long repetition and echo times to create heavy T2-weighted images with cerebrospinal fluid (CSF) nulling, thereby providing excellent contrast between the CSF and the brain surface. Because of the so-called flow-void phenomenon, normal arteries are not usually visible against the dark CSF background on FLAIR sequences. 13 Recently, hyperintense vessels have been described on FLAIR images in hyperacute stroke patients with an arterial occlusion 8,9,14 and are considered to be an indicator of slow flow and inadequate collateral
4 Iancu-Gontard et al FLAIR and Intracerebral Arterial Stenoses 1889 Demographic Data, Distribution of Stenoses on Angiogram, and HVS on FLAIR in the 13 HVS and 6 HVS Patients in the Study Group HVS (n 13) HVS (n 6) Demographic data Mean age, y Male, n 4 4 Female, n 9 2 Clinical presentation, n Acute focal deficit 7 3 Stroke confirmed by MRI 6 2* Transient ischemic attack 1 Diffuse neurological symptoms 6 3 Stroke confirmed by MRI 0* 0 Etiology for intracerebral stenoses, n Reversible angiopathy 8 0 Dysplasia 0 1 Infectious angiitis 1 1 Sjögren angiitis 1 0 Atherosclerosis 0 1 Primitive or undetermined angiitis 3 3 Stenoses on angiograms, n Multiple arterial territories 13 5 Proximal 2 2 Distal 2 0 Proximal and distal 9 4 MCA 13 3 ACA 10 5 PCA 3 4 Distribution of HVS on FLAIR, n Multiple arterial territories 9 NA Proximal 0 NA Distal 13 NA MCA 13 NA ACA 6 NA PCA 1 NA *DWI was not available in 3 HVS patients with diffuse neurological symptoms and in 1 HVS patient with an acute focal neurological deficit. When observed in 1 arterial territory. circulation. The results of this case-control study suggest that (1) the assessment of HVS on FLAIR is reproducible, (2) multiple HVS on FLAIR is significantly more frequent in patients with multiple intracerebral stenoses (68%) than in asymptomatic patients without intracerebral stenoses (5.2%) regardless of the presence of a brain infarct, and (3) HVSs on FLAIR underestimate the extent of intracerebral stenoses as demonstrated by angiogram. The study group consisted of patients with a heterogeneous group of disorders that had in common the presence of multiple intracerebral stenoses. HVSs were observed regardless of the underlying cause of the multiple intracerebral stenoses. Interestingly, HVSs seemed to be more frequent in patients with reversible angiopathy (8 of 8) than in the other Figure 3. Infectious angiitis in a 20-year-old woman who presented with severe headaches, photophobia, right facial palsy, and focal deficit of the right lower limb. A, DWI shows focal hypersignal with corresponding decrease of the apparent diffusion coefficient (not shown) of the left internal capsula, matching neurological deficit. B, Axial FLAIR sequence reveals multiple HVSs distributed in the left MCA territory (not shown) and running anteriorly in a different arterial territory (arrows) than that of the acute stroke lesion. Note that the high signal within the midline vessel surrounded by CSF (arrowhead) was considered to correspond to a vein. C, Right carotid artery DSA shows segmental arterial stenoses separated by fusiform dilatations of the MCA and ACA (arrows). Although there is a hypoplasia of the left A1 (not shown), a stenosis of the right A1 can be seen, potentially explaining the presence of HVS shown on FLAIR (B). patients. In reversible angiopathy, the presumably spastic mechanism of the widespread stenoses could produce more abrupt hemodynamic changes 15,16 than those occurring in other vasculopathies, with a more chronic and progressive course. However, the small sample size of the studied population makes it difficult to draw any definitive conclusion from the observed associations. For the purposes of our study, the control group should have consisted only of patients with no intracranial arterial stenoses. These can be ruled out only on DSA, which is no longer part of the routine diagnostic workup in our institution. We chose to select patients who had been treated for an intracranial aneurysm and were undergoing intracranial DSA and FLAIR MR follow-up. They fulfilled the main criteria for a control group because none had intracranial arterial stenoses. We assumed that after 1 year of treatment the aneurysm would not cause any hemodynamic impairment of the downstream arterial circulation and that CSF changes resulting from the initial subarachnoid hemorrhage would have completely resolved. This was further confirmed by the fact that none of the control patients had diffuse CSF hyperintensities.
5 1890 Stroke August 2003 The physiopathology of HVS is still unclear. 10 The mechanisms of HVS in patients with intracerebral stenoses and those with arterial occlusion may be similar. In hyperacute stroke patients with occlusion of a major intracerebral artery, sufficient data are available to suggest that HVS on FLAIR represent altered hemodynamics. 9,10,17 Indeed, HVS in acute stroke has been shown to correlate not only with slow anterograde and leptomeningeal collateral arterial flow on DSA 9 but also with intravascular enhancement on T1- weighted pulse sequence, 9 regional hypoperfusion, 9,17 and larger infarct volume. 8 10,17 These data support the hypothesis that HVS is the result of an arterial slow-flow phenomenon. 9 In patients with multiple arterial stenoses, HVS could correspond to hemodynamic changes distally to arterial stenoses. Alternatively, it could be a direct picture of the stenosis itself. Indeed, arterial wall thickening, a known pathological feature of some forms of vasculitis, could also produce vascular hyperintensities on FLAIR. Yet, this alternate hypothesis is unlikely to explain the presence of HVS in spastic stenoses such as those observed in reversible angiopathy. We cannot be certain that the bright vessels we observed on FLAIR in patients with intracerebral arterial stenoses corresponded to arteries or to small superficial cortical veins. Distal arteries can potentially be distinguished from cortical veins on anatomic grounds. Although arteries usually follow the invaginated deep cortical surfaces, veins tend to move away from the cortical surface to reach for sinus. 18 Accordingly, to minimize the likelihood of analyzing veins, only distal hyperintensities that remained deep in the cortical sulcus on at least 2 adjacent slices were quoted as HVS, and we excluded distal hyperintensities that were localized away from the cortical surface. One can argue that the bright signal observed on FLAIR did not correspond to vessels. Indeed, several situations could mimic HVS on FLAIR. CSF pulsation artifacts can produce a high CSF signal. This effect, usually more prominent in the basal cisterns, is uncommon over the convexities of the brain where CSF motion is diminished 19 and was not considered a confounding factor by the observers. In addition, applying the inversion pulse over 2 or 3 times the slice thickness further minimized the CSF flow-entering phenomenon. Sulcal hyperintensities on FLAIR can also be observed in other pathological conditions such as subarachnoid hemorrhage and meningitis. 20 These last 2 conditions were initially excluded from our study population to avoid difficulties in interpreting FLAIR hyperintensities within the subarachnoid space. Yet, we hypothesize that it should be possible to distinguish between HVS and subarachnoid hemorrhage on FLAIR. Indeed, HVS usually consists of well-circumscribed bright foci or tubular hyperintensities running through normally dark CSF signal; subarachnoid hemorrhage hyperintensities are frequently diffuse and fill up the whole sulcus. 14 Finally, cortical infarction resulting from multiple distal emboli could also produce punctuate or gyriform hyperintensities on FLAIR and thus be erroneously considered an HVS. This last hypothesis seems unlikely because none of the patients studied had multiple cortical infarcts on DWI, which has been shown to be highly sensitive for the detection of acute stroke, especially in the anterior circulation. 21 Of the 19 patients in the study group, 6 with arterial stenoses on angiogram had no HVS on FLAIR. In addition, the concordance between the territorial distribution of stenoses on angiogram and HVS on FLAIR was far from perfect. Although the concordance analysis between FLAIR and angiographic data was not conducted on each individual stenosis because of the difficulty in precisely comparing cross-sectional MR images with projected frontal or lateral views obtained from DSA, these data suggest that FLAIR alone is unable to detect each individual stenosis. This could be due to the lack of in-plane spatial resolution of the FLAIR sequence or to the partial volume effects that can occur when a 5- to 6-mm slice thickness is used. It could also be due to differences in hemodynamic features between arterial territories in a given patient or between HVS and HVS patients. Several additional points need to be raised. The specificity of HVS for the diagnosis of intracerebral arterial stenoses remains to be elucidated because we did not study the prevalence of HVS in various cerebrovascular disorders and more generally in patients with acute neurological signs without intracerebral stenosis. Indeed, cerebral hemodynamic status could be modified under different circumstances such as extracranial stenosis, thrombophlebitis, or even severe metabolic disorders. Because the reliability of a retrospective analysis of subtle flow changes on DSA is questionable, we did not correlate the presence of HVS with a possible slow flow in the corresponding arterial territory on DSA. A careful analysis of subtle flow changes on DSA, quantitative perfusion measurements, and postcontrast MR angiograms, which have been shown to improve the assessment of intracranial vessel patency, 22 could provide additional in vivo data on the pathogenesis of HVS in patients with cerebral arterial stenoses. Despite the lack of clear-cut concordance between the distribution of stenoses on angiogram and HVS on FLAIR, our data show that HVSs are more frequently observed in symptomatic patients with multiple intracerebral stenoses than in asymptomatic patients without stenoses. This could be a clinically relevant finding, especially when the presence of intracerebral arterial stenoses is unsuspected. By showing multiple HVS in patients with diffuse encephalopathy or acute stroke, the FLAIR sequence could help in selecting those patients likely to benefit from other imaging techniques focusing on the intracranial vasculature. References 1. Fauci A, Haynes B, Katz P. The spectrum of vasculitis: clinical, pathologic, immunologic and therapeutic considerations. Ann Intern Med. 1978;89: Ferris E, Levine H. Cerebral arteritis: classification. Radiology. 1973; 109: Harris K, Yuh W. Intracranial vasculitis. Neuroimaging Clin N Am. 1994;4: Akins P, Pilgram T, Cross D, Moran C. Natural history of stenosis from intracranial atherosclerosis by serial angiography. Stroke. 1998;29: Call G, Fleming M, Sealfon S, Levine H, Kistler J, Fisher C. Reversible cerebral segmental vasoconstriction. Stroke. 1988;19: Zuber M, Blustajn J, Arquizan C, Trystram D, Mas JL, Meder JF. Angiitis of the central nervous system. J Neuroradiol. 1999;26:
6 Iancu-Gontard et al FLAIR and Intracerebral Arterial Stenoses Campi A, Benndorf G, Filippi M, Reganati P, Martinelli V, Terreni M. Primary angiitis of the central nervous system: serial MRI of brain and spinal cord. Neuroradiology. 2001;43: Cosnard G, Duprez T, Grandin C, Smith A, Munier T, Peeters A. Fast FLAIR sequence for detecting major vascular abnormalities during the hyperacute phase of stroke: a comparison with MR angiography. Neuroradiology. 1999;41: Kamran S, Bates V, Bakshi R, Wright P, Kinkel W, Miletich R. Significance of hyperintense vessels on FLAIR MRI in acute stroke. Neurology. 2000;55: Wolf RL. Intraarterial signal on fluid-attenuated inversion recovery images: a measure of hemodynamic stress? AJNR Am J Neuroradiol. 2001;22: Fleiss J. Statistical Methods for Rates and Proportions. New York, NY: John Wiley; Landis J, Koch G. The measurements of observers agreement for categorical data. Biometrics. 1977;33: Hajnal J, Bryant D, Kasuboski L, Pattany P, De Coene B, Lewis P, Pennock J, Oatridge A, Young I, Bydder G. Use of fluid attenuated inversion recovery (FLAIR) pulse sequences in MRI of the brain. J Comput Assist Tomogr. 1992;16: Maeda M, Yamamoto T, Daimon S, Sakuma H, Takeda K. Arterial hyperintensity on fast fluid-attenuated inversion recovery images: a subtle finding for hyperacute stroke undetected by diffusion-weighted MR imaging. AJNR Am J Neuroradiol. 2001;22: Hajj-Ali R, Furlan A, Abou-Chebel A, Calabrese L. Benign angiopathy of the central nervous system: cohort of 16 patients with clinical course and long-term follow-up. Arthritis Rheum. 2002;15: Calabrese L, Gragg L, Furlan A. Benign angiopathy: a distinct subset of angiographically defined primary angiitis of the central nervous system. J Rheumatol. 1993;20: Toyoda K, Ida M, Fukuda K. Fluid-attenuated inversion recovery intraarterial signal: an early sign of hyperacute cerebral ischemia. AJNR Am J Neuroradiol. 2001;22: Szikla G, Bouvier G, Hori T, Petrov V. Angiography of the Human Brain Cortex/Atlas of Vascular Patterns and Stereotactic Cortical Localisation. Berlin, Germany: Springer-Verlag; Taoka T, Yuh W, White M, Quets J, Maley J, Ueda T. Sulcal hyperintensity on fluid-attenuated inversion recovery MR images in patients without apparent cerebrospinal fluid abnormality. AJR Am J Roentgenol. 2001;176: Noguchi K, Seto H, Kamisaki Y, Tomizawa G, Toyoshima S, Watanabe N. Comparison of fluid-attenuated inversion-recovery MR imaging with CT in a simulated model of acute subarachnoid hemorrhage. AJNR Am J Neuroradiol. 2000;21: Oppenheim C, Stanescu R, Dormont D, Crozier S, Marro B, Samson Y, Rancurel G, Marsault C. False-negative diffusion-weighted MR findings in acute ischemic stroke. AJNR Am J Neuroradiol. 2000;21: Yang J, Hill M, Morrish W, Hudon M, Barber P, Demchuk A, Sevick R, Frayne R. Comparison of pre- and postcontrast 3D time-of-flight MR angiography for the evaluation of distal intracranial branch occlusions in acute ischemic stroke. AJNR Am J Neuroradiol. 2002;23:
The Low Sensitivity of Fluid-Attenuated Inversion-Recovery MR in the Detection of Multiple Sclerosis of the Spinal Cord
 The Low Sensitivity of Fluid-Attenuated Inversion-Recovery MR in the Detection of Multiple Sclerosis of the Spinal Cord Mark D. Keiper, Robert I. Grossman, John C. Brunson, and Mitchell D. Schnall PURPOSE:
The Low Sensitivity of Fluid-Attenuated Inversion-Recovery MR in the Detection of Multiple Sclerosis of the Spinal Cord Mark D. Keiper, Robert I. Grossman, John C. Brunson, and Mitchell D. Schnall PURPOSE:
Anatomic Evaluation of the Circle of Willis: MR Angiography versus Intraarterial Digital Subtraction Angiography
 Anatomic Evaluation of the Circle of Willis: MR Angiography versus Intraarterial Digital Subtraction Angiography K. W. Stock, S. Wetzel, E. Kirsch, G. Bongartz, W. Steinbrich, and E. W. Radue PURPOSE:
Anatomic Evaluation of the Circle of Willis: MR Angiography versus Intraarterial Digital Subtraction Angiography K. W. Stock, S. Wetzel, E. Kirsch, G. Bongartz, W. Steinbrich, and E. W. Radue PURPOSE:
CT and MR findings of systemic lupus erythematosus involving the brain: Differential diagnosis based on lesion distribution
 CT and MR findings of systemic lupus erythematosus involving the brain: Differential diagnosis based on lesion distribution Poster No.: C-2723 Congress: ECR 2010 Type: Educational Exhibit Topic: Neuro
CT and MR findings of systemic lupus erythematosus involving the brain: Differential diagnosis based on lesion distribution Poster No.: C-2723 Congress: ECR 2010 Type: Educational Exhibit Topic: Neuro
Masayuki Maeda, Tatsuya Yamamoto, Shouichiro Daimon, Hajime Sakuma, and Kan Takeda
 AJNR Am J Neuroradiol :6 66, April 001 Arterial Hyperintensity on Fast Fluid-attenuated Inversion Recovery Images: A Subtle Finding for Hyperacute Stroke Undetected by Diffusion-weighted MR Imaging Masayuki
AJNR Am J Neuroradiol :6 66, April 001 Arterial Hyperintensity on Fast Fluid-attenuated Inversion Recovery Images: A Subtle Finding for Hyperacute Stroke Undetected by Diffusion-weighted MR Imaging Masayuki
Essentials of Clinical MR, 2 nd edition. 14. Ischemia and Infarction II
 14. Ischemia and Infarction II Lacunar infarcts are small deep parenchymal lesions involving the basal ganglia, internal capsule, thalamus, and brainstem. The vascular supply of these areas includes the
14. Ischemia and Infarction II Lacunar infarcts are small deep parenchymal lesions involving the basal ganglia, internal capsule, thalamus, and brainstem. The vascular supply of these areas includes the
Magnetic Resonance Imaging. Basics of MRI in practice. Generation of MR signal. Generation of MR signal. Spin echo imaging. Generation of MR signal
 Magnetic Resonance Imaging Protons aligned with B0 magnetic filed Longitudinal magnetization - T1 relaxation Transverse magnetization - T2 relaxation Signal measured in the transverse plane Basics of MRI
Magnetic Resonance Imaging Protons aligned with B0 magnetic filed Longitudinal magnetization - T1 relaxation Transverse magnetization - T2 relaxation Signal measured in the transverse plane Basics of MRI
Essentials of Clinical MR, 2 nd edition. 99. MRA Principles and Carotid MRA
 99. MRA Principles and Carotid MRA As described in Chapter 12, time of flight (TOF) magnetic resonance angiography (MRA) is commonly utilized in the evaluation of the circle of Willis. TOF MRA allows depiction
99. MRA Principles and Carotid MRA As described in Chapter 12, time of flight (TOF) magnetic resonance angiography (MRA) is commonly utilized in the evaluation of the circle of Willis. TOF MRA allows depiction
STROKE - IMAGING. Dr RAJASEKHAR REDDY 2nd Yr P.G. RADIODIAGNOSIS KIMS,Narkatpalli.
 STROKE - IMAGING Dr RAJASEKHAR REDDY 2nd Yr P.G. RADIODIAGNOSIS KIMS,Narkatpalli. STROKE Describes a clinical event that consists of sudden onset of neurological symptoms Types Infarction - occlusion of
STROKE - IMAGING Dr RAJASEKHAR REDDY 2nd Yr P.G. RADIODIAGNOSIS KIMS,Narkatpalli. STROKE Describes a clinical event that consists of sudden onset of neurological symptoms Types Infarction - occlusion of
Brain AVM with Accompanying Venous Aneurysm with Intracerebral and Intraventricular Hemorrhage
 Cronicon OPEN ACCESS EC PAEDIATRICS Case Report Brain AVM with Accompanying Venous Aneurysm with Intracerebral and Intraventricular Hemorrhage Dimitrios Panagopoulos* Neurosurgical Department, University
Cronicon OPEN ACCESS EC PAEDIATRICS Case Report Brain AVM with Accompanying Venous Aneurysm with Intracerebral and Intraventricular Hemorrhage Dimitrios Panagopoulos* Neurosurgical Department, University
Distal hyperintense vessels on FLAIR An MRI marker for collateral circulation in acute stroke?
 Distal hyperintense vessels on FLAIR An MRI marker for collateral circulation in acute stroke? K.Y. Lee, MD, PhD L.L. Latour, PhD M. Luby, PhD A.W. Hsia, MD J.G. Merino, MD, MPhil S. Warach, MD, PhD Address
Distal hyperintense vessels on FLAIR An MRI marker for collateral circulation in acute stroke? K.Y. Lee, MD, PhD L.L. Latour, PhD M. Luby, PhD A.W. Hsia, MD J.G. Merino, MD, MPhil S. Warach, MD, PhD Address
[(PHY-3a) Initials of MD reviewing films] [(PHY-3b) Initials of 2 nd opinion MD]
![[(PHY-3a) Initials of MD reviewing films] [(PHY-3b) Initials of 2 nd opinion MD] [(PHY-3a) Initials of MD reviewing films] [(PHY-3b) Initials of 2 nd opinion MD]](/thumbs/89/98619893.jpg) 2015 PHYSICIAN SIGN-OFF (1) STUDY NO (PHY-1) CASE, PER PHYSICIAN REVIEW 1=yes 2=no [strictly meets case definition] (PHY-1a) CASE, IN PHYSICIAN S OPINION 1=yes 2=no (PHY-2) (PHY-3) [based on all available
2015 PHYSICIAN SIGN-OFF (1) STUDY NO (PHY-1) CASE, PER PHYSICIAN REVIEW 1=yes 2=no [strictly meets case definition] (PHY-1a) CASE, IN PHYSICIAN S OPINION 1=yes 2=no (PHY-2) (PHY-3) [based on all available
An Introduction to Imaging the Brain. Dr Amy Davis
 An Introduction to Imaging the Brain Dr Amy Davis Common reasons for imaging: Clinical scenarios: - Trauma (NICE guidelines) - Stroke - Tumours - Seizure - Neurological degeneration memory, motor dysfunction,
An Introduction to Imaging the Brain Dr Amy Davis Common reasons for imaging: Clinical scenarios: - Trauma (NICE guidelines) - Stroke - Tumours - Seizure - Neurological degeneration memory, motor dysfunction,
A New Trend in Vascular Imaging: the Arterial Spin Labeling (ASL) Sequence
 A New Trend in Vascular Imaging: the Arterial Spin Labeling (ASL) Sequence Poster No.: C-1347 Congress: ECR 2013 Type: Educational Exhibit Authors: J. Hodel, A. GUILLONNET, M. Rodallec, S. GERBER, R. 1
A New Trend in Vascular Imaging: the Arterial Spin Labeling (ASL) Sequence Poster No.: C-1347 Congress: ECR 2013 Type: Educational Exhibit Authors: J. Hodel, A. GUILLONNET, M. Rodallec, S. GERBER, R. 1
Comparison of Five Major Recent Endovascular Treatment Trials
 Comparison of Five Major Recent Endovascular Treatment Trials Sample size 500 # sites 70 (100 planned) 316 (500 planned) 196 (833 estimated) 206 (690 planned) 16 10 22 39 4 Treatment contrasts Baseline
Comparison of Five Major Recent Endovascular Treatment Trials Sample size 500 # sites 70 (100 planned) 316 (500 planned) 196 (833 estimated) 206 (690 planned) 16 10 22 39 4 Treatment contrasts Baseline
NEURO IMAGING 2. Dr. Said Huwaijah Chairman of radiology Dep, Damascus Univercity
 NEURO IMAGING 2 Dr. Said Huwaijah Chairman of radiology Dep, Damascus Univercity I. EPIDURAL HEMATOMA (EDH) LOCATION Seventy to seventy-five percent occur in temporoparietal region. CAUSE Most likely caused
NEURO IMAGING 2 Dr. Said Huwaijah Chairman of radiology Dep, Damascus Univercity I. EPIDURAL HEMATOMA (EDH) LOCATION Seventy to seventy-five percent occur in temporoparietal region. CAUSE Most likely caused
Diagnosis of Subarachnoid Hemorrhage (SAH) and Non- Aneurysmal Causes
 Diagnosis of Subarachnoid Hemorrhage (SAH) and Non- Aneurysmal Causes By Sheila Smith, MD Swedish Medical Center 1 Disclosures I have no disclosures 2 Course Objectives Review significance and differential
Diagnosis of Subarachnoid Hemorrhage (SAH) and Non- Aneurysmal Causes By Sheila Smith, MD Swedish Medical Center 1 Disclosures I have no disclosures 2 Course Objectives Review significance and differential
Ischemic strokes are estimated to happen during sleep in
 Can Diffusion-Weighted Imaging Fluid-Attenuated Inversion Recovery Mismatch (Positive Diffusion-Weighted Imaging/ Negative Fluid-Attenuated Inversion Recovery) at 3 Tesla Identify Patients With Stroke
Can Diffusion-Weighted Imaging Fluid-Attenuated Inversion Recovery Mismatch (Positive Diffusion-Weighted Imaging/ Negative Fluid-Attenuated Inversion Recovery) at 3 Tesla Identify Patients With Stroke
OBSERVATION. Postpartum Angiopathy With Reversible Posterior Leukoencephalopathy
 Postpartum Angiopathy With Reversible Posterior Leukoencephalopathy Aneesh B. Singhal, MD OBSERVATION Background: Postpartum angiopathy (PPA) is a cerebral vasoconstriction syndrome of uncertain cause
Postpartum Angiopathy With Reversible Posterior Leukoencephalopathy Aneesh B. Singhal, MD OBSERVATION Background: Postpartum angiopathy (PPA) is a cerebral vasoconstriction syndrome of uncertain cause
Acute stroke. Ischaemic stroke. Characteristics. Temporal classification. Clinical features. Interpretation of Emergency Head CT
 Ischaemic stroke Characteristics Stroke is the third most common cause of death in the UK, and the leading cause of disability. 80% of strokes are ischaemic Large vessel occlusive atheromatous disease
Ischaemic stroke Characteristics Stroke is the third most common cause of death in the UK, and the leading cause of disability. 80% of strokes are ischaemic Large vessel occlusive atheromatous disease
with susceptibility-weighted imaging and computed tomography perfusion abnormalities in diagnosis of classic migraine
 Emerg Radiol (2012) 19:565 569 DOI 10.1007/s10140-012-1051-2 CASE REPORT Susceptibility-weighted imaging and computed tomography perfusion abnormalities in diagnosis of classic migraine Christopher Miller
Emerg Radiol (2012) 19:565 569 DOI 10.1007/s10140-012-1051-2 CASE REPORT Susceptibility-weighted imaging and computed tomography perfusion abnormalities in diagnosis of classic migraine Christopher Miller
Background. Recommendations for Imaging of Acute Ischemic Stroke: A Scientific Statement From the American Heart Association
 for Imaging of Acute Ischemic Stroke: A Scientific Statement From the American Heart Association An Scientific Statement from the Stroke Council, American Heart Association and American Stroke Association
for Imaging of Acute Ischemic Stroke: A Scientific Statement From the American Heart Association An Scientific Statement from the Stroke Council, American Heart Association and American Stroke Association
INSTITUTE OF NEUROSURGERY & DEPARTMENT OF PICU
 CEREBRAL BYPASS An Innovative Treatment for Arteritis INSTITUTE OF NEUROSURGERY & DEPARTMENT OF PICU CASE 1 q 1 year old girl -recurrent seizure, right side limb weakness, excessive cry and irritability.
CEREBRAL BYPASS An Innovative Treatment for Arteritis INSTITUTE OF NEUROSURGERY & DEPARTMENT OF PICU CASE 1 q 1 year old girl -recurrent seizure, right side limb weakness, excessive cry and irritability.
Methods. Yahya Paksoy, Bülent Oğuz Genç, and Emine Genç. AJNR Am J Neuroradiol 24: , August 2003
 AJNR Am J Neuroradiol 24:1364 1368, August 2003 Retrograde Flow in the Left Inferior Petrosal Sinus and Blood Steal of the Cavernous Sinus Associated with Central Vein Stenosis: MR Angiographic Findings
AJNR Am J Neuroradiol 24:1364 1368, August 2003 Retrograde Flow in the Left Inferior Petrosal Sinus and Blood Steal of the Cavernous Sinus Associated with Central Vein Stenosis: MR Angiographic Findings
Nicolas Bianchi M.D. May 15th, 2012
 Nicolas Bianchi M.D. May 15th, 2012 New concepts in TIA Differential Diagnosis Stroke Syndromes To learn the new definitions and concepts on TIA as a condition of high risk for stroke. To recognize the
Nicolas Bianchi M.D. May 15th, 2012 New concepts in TIA Differential Diagnosis Stroke Syndromes To learn the new definitions and concepts on TIA as a condition of high risk for stroke. To recognize the
ISCHEMIC STROKE IMAGING
 ISCHEMIC STROKE IMAGING ผศ.พญ พญ.จ ร ร ตน ธรรมโรจน ภาคว ชาร งส ว ทยา คณะแพทยศาสตร มหาว ทยาล ยขอนแก น A case of acute hemiplegia Which side is the abnormality, right or left? Early Right MCA infarction
ISCHEMIC STROKE IMAGING ผศ.พญ พญ.จ ร ร ตน ธรรมโรจน ภาคว ชาร งส ว ทยา คณะแพทยศาสตร มหาว ทยาล ยขอนแก น A case of acute hemiplegia Which side is the abnormality, right or left? Early Right MCA infarction
Imaging of Moya Moya Disease
 Abstract Imaging of Moya Moya Disease Pages with reference to book, From 181 To 185 Rashid Ahmed, Hurnera Ahsan ( Liaquat National Hospital, Karachi. ) Moya Moya disease is a rare disease causing occlusion
Abstract Imaging of Moya Moya Disease Pages with reference to book, From 181 To 185 Rashid Ahmed, Hurnera Ahsan ( Liaquat National Hospital, Karachi. ) Moya Moya disease is a rare disease causing occlusion
A report of nontraumatic cortical subarachnoid hemorrhage and subsequent management
 For reprint orders, please contact: reprints@futuremedicine.com A report of nontraumatic cortical subarachnoid hemorrhage and subsequent management David Qiyuan Mao*,1, Daniel Addess 1 & Helen Valsamis
For reprint orders, please contact: reprints@futuremedicine.com A report of nontraumatic cortical subarachnoid hemorrhage and subsequent management David Qiyuan Mao*,1, Daniel Addess 1 & Helen Valsamis
Pearls and Pitfalls in Neuroradiology of Cerebrovascular Disease The Essentials with MR and CT
 Pearls and Pitfalls in Neuroradiology of Cerebrovascular Disease The Essentials with MR and CT Val M. Runge, MD Wendy R. K. Smoker, MD Anton Valavanis, MD Control # 823 Purpose The focus of this educational
Pearls and Pitfalls in Neuroradiology of Cerebrovascular Disease The Essentials with MR and CT Val M. Runge, MD Wendy R. K. Smoker, MD Anton Valavanis, MD Control # 823 Purpose The focus of this educational
NEURORADIOLOGY DIL part 4
 NEURORADIOLOGY DIL part 4 Strokes and infarcts K. Agyem MD, G. Hall MD, D. Palathinkal MD, Alexandre Menard March/April 2015 OVERVIEW Introduction to Neuroimaging - DIL part 1 Basic Brain Anatomy - DIL
NEURORADIOLOGY DIL part 4 Strokes and infarcts K. Agyem MD, G. Hall MD, D. Palathinkal MD, Alexandre Menard March/April 2015 OVERVIEW Introduction to Neuroimaging - DIL part 1 Basic Brain Anatomy - DIL
Surface Appearance of the Vertebrobasilar Artery Revealed on Basiparallel Anatomic Scanning (BPAS) MR Imaging: Its Role for Brain MR Examination
 AJNR Am J Neuroradiol 26:2508 2513, November/December 2005 Surface Appearance of the Vertebrobasilar Artery Revealed on Basiparallel Anatomic Scanning (BPAS) MR Imaging: Its Role for Brain MR Examination
AJNR Am J Neuroradiol 26:2508 2513, November/December 2005 Surface Appearance of the Vertebrobasilar Artery Revealed on Basiparallel Anatomic Scanning (BPAS) MR Imaging: Its Role for Brain MR Examination
CT INTERPRETATION COURSE
 CT INTERPRETATION COURSE Refresher Course ASTRACAT October 2012 Stroke is a Clinical Diagnosis A clinical syndrome characterised by rapidly developing clinical symptoms and/or signs of focal loss of cerebral
CT INTERPRETATION COURSE Refresher Course ASTRACAT October 2012 Stroke is a Clinical Diagnosis A clinical syndrome characterised by rapidly developing clinical symptoms and/or signs of focal loss of cerebral
Spontaneous Recanalization after Complete Occlusion of the Common Carotid Artery with Subsequent Embolic Ischemic Stroke
 Original Contribution Spontaneous Recanalization after Complete Occlusion of the Common Carotid Artery with Subsequent Embolic Ischemic Stroke Abstract Introduction: Acute carotid artery occlusion carries
Original Contribution Spontaneous Recanalization after Complete Occlusion of the Common Carotid Artery with Subsequent Embolic Ischemic Stroke Abstract Introduction: Acute carotid artery occlusion carries
Longitudinal anterior-to-posterior shift of collateral channels in patients with moyamoya disease: an implication for its hemorrhagic onset
 CLINICAL ARTICLE Longitudinal anterior-to-posterior shift of collateral channels in patients with moyamoya disease: an implication for its hemorrhagic onset Shusuke Yamamoto, MD, Satoshi Hori, MD, PhD,
CLINICAL ARTICLE Longitudinal anterior-to-posterior shift of collateral channels in patients with moyamoya disease: an implication for its hemorrhagic onset Shusuke Yamamoto, MD, Satoshi Hori, MD, PhD,
The central nervous system
 Sectc.qxd 29/06/99 09:42 Page 81 Section C The central nervous system CNS haemorrhage Subarachnoid haemorrhage Cerebral infarction Brain atrophy Ring enhancing lesions MRI of the pituitary Multiple sclerosis
Sectc.qxd 29/06/99 09:42 Page 81 Section C The central nervous system CNS haemorrhage Subarachnoid haemorrhage Cerebral infarction Brain atrophy Ring enhancing lesions MRI of the pituitary Multiple sclerosis
NEURORADIOLOGY Part I
 NEURORADIOLOGY Part I Vörös Erika University of Szeged Department of Radiology SZEGED BRAIN IMAGING METHODS Plain film radiography Ultrasonography (US) Computer tomography (CT) Magnetic resonance imaging
NEURORADIOLOGY Part I Vörös Erika University of Szeged Department of Radiology SZEGED BRAIN IMAGING METHODS Plain film radiography Ultrasonography (US) Computer tomography (CT) Magnetic resonance imaging
/ / / / / / Hospital Abstraction: Stroke/TIA. Participant ID: Hospital Code: Multi-Ethnic Study of Atherosclerosis
 Multi-Ethnic Study of Atherosclerosis Participant ID: Hospital Code: Hospital Abstraction: Stroke/TIA History and Hospital Record 1. Was the participant hospitalized as an immediate consequence of this
Multi-Ethnic Study of Atherosclerosis Participant ID: Hospital Code: Hospital Abstraction: Stroke/TIA History and Hospital Record 1. Was the participant hospitalized as an immediate consequence of this
Moyamoya Disease A Vasculopathy and an Uncommon Cause of Recurrent Cerebrovascular Accidents
 Moyamoya Disease A Vasculopathy and an Uncommon Cause of Recurrent Cerebrovascular Accidents Yasmin S. Hamirani, Md 1 *, Mohammad Valikhani, Md 2, Allison Sweney, Ms Iii 2, Hafsa Khan, Md 2, Mohammad Pathan,
Moyamoya Disease A Vasculopathy and an Uncommon Cause of Recurrent Cerebrovascular Accidents Yasmin S. Hamirani, Md 1 *, Mohammad Valikhani, Md 2, Allison Sweney, Ms Iii 2, Hafsa Khan, Md 2, Mohammad Pathan,
Cerebro-vascular stroke
 Cerebro-vascular stroke CT Terminology Hypodense lesion = lesion of lower density than the normal brain tissue Hyperdense lesion = lesion of higher density than normal brain tissue Isodense lesion = lesion
Cerebro-vascular stroke CT Terminology Hypodense lesion = lesion of lower density than the normal brain tissue Hyperdense lesion = lesion of higher density than normal brain tissue Isodense lesion = lesion
Detection of Leptomeningeal CNS Metastases in Children
 Detection of Leptomeningeal CNS Metastases in Children Noah D. Sabin, M.D. Julie H. Harreld M.D. Kathleen J. Helton M.D. Zoltan Patay M.D., Ph.D. St. Jude Children s Research Hospital Memphis, TN Leptomeningeal
Detection of Leptomeningeal CNS Metastases in Children Noah D. Sabin, M.D. Julie H. Harreld M.D. Kathleen J. Helton M.D. Zoltan Patay M.D., Ph.D. St. Jude Children s Research Hospital Memphis, TN Leptomeningeal
IMAGING IN ACUTE ISCHEMIC STROKE
 IMAGING IN ACUTE ISCHEMIC STROKE Timo Krings MD, PhD, FRCP (C) Professor of Radiology & Surgery Braley Chair of Neuroradiology, Chief and Program Director of Diagnostic and Interventional Neuroradiology;
IMAGING IN ACUTE ISCHEMIC STROKE Timo Krings MD, PhD, FRCP (C) Professor of Radiology & Surgery Braley Chair of Neuroradiology, Chief and Program Director of Diagnostic and Interventional Neuroradiology;
Vascular Disorders. Nervous System Disorders (Part B-1) Module 8 -Chapter 14. Cerebrovascular disease S/S 1/9/2013
 Nervous System Disorders (Part B-1) Module 8 -Chapter 14 Overview ACUTE NEUROLOGIC DISORDERS Vascular Disorders Infections/Inflammation/Toxins Metabolic, Endocrinologic, Nutritional, Toxic Neoplastic Traumatic
Nervous System Disorders (Part B-1) Module 8 -Chapter 14 Overview ACUTE NEUROLOGIC DISORDERS Vascular Disorders Infections/Inflammation/Toxins Metabolic, Endocrinologic, Nutritional, Toxic Neoplastic Traumatic
Moyamoya Syndrome with contra lateral DACA aneurysm: First Case report with review of literature
 Romanian Neurosurgery Volume XXXI Number 3 2017 July-September Article Moyamoya Syndrome with contra lateral DACA aneurysm: First Case report with review of literature Ashish Kumar Dwivedi, Pradeep Kumar,
Romanian Neurosurgery Volume XXXI Number 3 2017 July-September Article Moyamoya Syndrome with contra lateral DACA aneurysm: First Case report with review of literature Ashish Kumar Dwivedi, Pradeep Kumar,
Intraventricular CSF Pulsation Artifact on Fast Fluid-Attenuated Inversion-Recovery MR Images: Analysis of 100 Consecutive Normal Studies
 AJNR Am J Neuroradiol 21:503 508, March 2000 Intraventricular CSF Pulsation Artifact on Fast Fluid-Attenuated Inversion-Recovery MR Images: Analysis of 100 Consecutive Normal Studies Rohit Bakshi, Shelton
AJNR Am J Neuroradiol 21:503 508, March 2000 Intraventricular CSF Pulsation Artifact on Fast Fluid-Attenuated Inversion-Recovery MR Images: Analysis of 100 Consecutive Normal Studies Rohit Bakshi, Shelton
I schaemic stroke is currently the third leading cause
 1426 PAPER The probability of middle cerebral artery MRA flow signal abnormality with quantified CT ischaemic change: targets for future therapeutic studies P A Barber, A M Demchuk, M D Hill, J H Warwick
1426 PAPER The probability of middle cerebral artery MRA flow signal abnormality with quantified CT ischaemic change: targets for future therapeutic studies P A Barber, A M Demchuk, M D Hill, J H Warwick
High Signal Intensity of the Infundibular Stalk on Fluid-Attenuated Inversion Recovery MR
 High Signal Intensity of the Infundibular Stalk on Fluid-Attenuated Inversion Recovery MR Yutaka Araki, Ryuichirou Ashikaga, Satoru Takahashi, Jun Ueda, and Osamu Ishida PURPOSE: To determine the MR imaging
High Signal Intensity of the Infundibular Stalk on Fluid-Attenuated Inversion Recovery MR Yutaka Araki, Ryuichirou Ashikaga, Satoru Takahashi, Jun Ueda, and Osamu Ishida PURPOSE: To determine the MR imaging
Internal Carotid Artery Dissection
 May 2011 Internal Carotid Artery Dissection Carolyn April, HMS IV Agenda Presentation of a clinical case Discussion of the clinical features of ICA dissection Discussion of the imaging modalities used
May 2011 Internal Carotid Artery Dissection Carolyn April, HMS IV Agenda Presentation of a clinical case Discussion of the clinical features of ICA dissection Discussion of the imaging modalities used
Postoperative Assessment of Extracranial Intracranial Bypass by Time- Resolved 3D Contrast-Enhanced MR Angiography Using Parallel Imaging
 AJNR Am J Neuroradiol 26:2243 2247, October 2005 Postoperative Assessment of Extracranial Intracranial Bypass by Time- Resolved 3D Contrast-Enhanced MR Angiography Using Parallel Imaging Kazuhiro Tsuchiya,
AJNR Am J Neuroradiol 26:2243 2247, October 2005 Postoperative Assessment of Extracranial Intracranial Bypass by Time- Resolved 3D Contrast-Enhanced MR Angiography Using Parallel Imaging Kazuhiro Tsuchiya,
Diagnosis of Middle Cerebral Artery Occlusion with Transcranial Color-Coded Real-Time Sonography
 Diagnosis of Middle Cerebral Artery Occlusion with Transcranial Color-Coded Real-Time Sonography Kazumi Kimura, Yoichiro Hashimoto, Teruyuki Hirano, Makoto Uchino, and Masayuki Ando PURPOSE: To determine
Diagnosis of Middle Cerebral Artery Occlusion with Transcranial Color-Coded Real-Time Sonography Kazumi Kimura, Yoichiro Hashimoto, Teruyuki Hirano, Makoto Uchino, and Masayuki Ando PURPOSE: To determine
Dynamic 3D MR Angiography of Intra- and Extracranial Vascular Malformations at 3T: A Technical Note
 AJNR Am J Neuroradiol 26:630 634, March 2005 Technical Note Dynamic 3D MR Angiography of Intra- and Extracranial Vascular Malformations at 3T: A Technical Note S. Ziyeh, R. Strecker, A. Berlis, J. Weber,
AJNR Am J Neuroradiol 26:630 634, March 2005 Technical Note Dynamic 3D MR Angiography of Intra- and Extracranial Vascular Malformations at 3T: A Technical Note S. Ziyeh, R. Strecker, A. Berlis, J. Weber,
Outline. Neuroradiology. Diffusion Imaging in. Clinical Applications of. Basics of Diffusion Imaging. Basics of Diffusion Imaging
 Clinical Applications of Diffusion Imaging in Neuroradiology No disclosures Stephen F. Kralik Assistant Professor of Radiology Indiana University School of Medicine Department of Radiology and Imaging
Clinical Applications of Diffusion Imaging in Neuroradiology No disclosures Stephen F. Kralik Assistant Professor of Radiology Indiana University School of Medicine Department of Radiology and Imaging
Intra-arterial nimodipine for the treatment of vasospasm due to aneurysmal subarachnoid hemorrhage
 Romanian Neurosurgery (2016) XXX 4: 461 466 461 DOI: 10.1515/romneu-2016-0074 Intra-arterial nimodipine for the treatment of vasospasm due to aneurysmal subarachnoid hemorrhage A. Chiriac, Georgiana Ion*,
Romanian Neurosurgery (2016) XXX 4: 461 466 461 DOI: 10.1515/romneu-2016-0074 Intra-arterial nimodipine for the treatment of vasospasm due to aneurysmal subarachnoid hemorrhage A. Chiriac, Georgiana Ion*,
Analysis of Characteristics in Patients with Non-Hemorrhagic Reversible Cerebral Vasoconstriction syndrome NH-RCVS
 Analysis of Characteristics in Patients with Non-Hemorrhagic Reversible Cerebral Vasoconstriction syndrome NH-RCVS Owais Mufti, MBBS Aaron McMurtray, MD, PhD and Bijal K. Mehta, MD, MPH, MA Department
Analysis of Characteristics in Patients with Non-Hemorrhagic Reversible Cerebral Vasoconstriction syndrome NH-RCVS Owais Mufti, MBBS Aaron McMurtray, MD, PhD and Bijal K. Mehta, MD, MPH, MA Department
1Pulse sequences for non CE MRA
 MRI: Principles and Applications, Friday, 8.30 9.20 am Pulse sequences for non CE MRA S. I. Gonçalves, PhD Radiology Department University Hospital Coimbra Autumn Semester, 2011 1 Magnetic resonance angiography
MRI: Principles and Applications, Friday, 8.30 9.20 am Pulse sequences for non CE MRA S. I. Gonçalves, PhD Radiology Department University Hospital Coimbra Autumn Semester, 2011 1 Magnetic resonance angiography
Long-term Observation of Lateral Medullary Infarction due to Vertebral Artery Dissection Assessed with Multimodal Neuroimaging
 Case Reports Long-term Observation of Lateral Medullary Infarction due to Vertebral Artery Dissection Assessed with Multimodal Neuroimaging Koichi Nomura 1, Masahiro Mishina 1,SeijiOkubo 1, Satoshi Suda
Case Reports Long-term Observation of Lateral Medullary Infarction due to Vertebral Artery Dissection Assessed with Multimodal Neuroimaging Koichi Nomura 1, Masahiro Mishina 1,SeijiOkubo 1, Satoshi Suda
Clinical Study Circle of Willis Variants: Fetal PCA
 Stroke Research and Treatment Volume 2013, Article ID 105937, 6 pages http://dx.doi.org/10.1155/2013/105937 Clinical Study Circle of Willis Variants: Fetal PCA Amir Shaban, 1 Karen C. Albright, 2,3,4,5
Stroke Research and Treatment Volume 2013, Article ID 105937, 6 pages http://dx.doi.org/10.1155/2013/105937 Clinical Study Circle of Willis Variants: Fetal PCA Amir Shaban, 1 Karen C. Albright, 2,3,4,5
Vasculitides in Surgical Neuropathology Practice
 Vasculitides in Surgical Neuropathology Practice USCAP requires that all faculty in a position to influence or control the content of CME disclose any relevant financial relationship WITH COMMERCIAL INTERESTS
Vasculitides in Surgical Neuropathology Practice USCAP requires that all faculty in a position to influence or control the content of CME disclose any relevant financial relationship WITH COMMERCIAL INTERESTS
Occlusion of All Four Extracranial Vessels With Minimal Clinical Symptomatology. Case Report
 Occlusion of All Four Extracranial Vessels With Minimal Clinical Symptomatology. Case Report BY JIRI J. VITEK, M.D., JAMES H. HALSEY, JR., M.D., AND HOLT A. McDOWELL, M.D. Abstract: Occlusion of All Four
Occlusion of All Four Extracranial Vessels With Minimal Clinical Symptomatology. Case Report BY JIRI J. VITEK, M.D., JAMES H. HALSEY, JR., M.D., AND HOLT A. McDOWELL, M.D. Abstract: Occlusion of All Four
Fluid-attenuated inversion recovery (FLAIR) imaging has been reported to be a sensitive and specific method in the diagnosis of disease of the sub-
 AJNR Am J Neuroradiol 22:1698 1703, October 2001 Imaging of Acute Subarachnoid Hemorrhage with a Fluid-Attenuated Inversion Recovery Sequence in an Animal Model: Comparison with Non Contrast-Enhanced CT
AJNR Am J Neuroradiol 22:1698 1703, October 2001 Imaging of Acute Subarachnoid Hemorrhage with a Fluid-Attenuated Inversion Recovery Sequence in an Animal Model: Comparison with Non Contrast-Enhanced CT
Subtraction CT Angiography with Controlled- Orbit Helical Scanning for Detection of Intracranial Aneurysms
 AJNR Am J Neuroradiol 19:291 295, February 1998 Subtraction CT Angiography with Controlled- Orbit Helical Scanning for Detection of Intracranial Aneurysms Satoshi Imakita, Yoshitaka Onishi, Tokihiro Hashimoto,
AJNR Am J Neuroradiol 19:291 295, February 1998 Subtraction CT Angiography with Controlled- Orbit Helical Scanning for Detection of Intracranial Aneurysms Satoshi Imakita, Yoshitaka Onishi, Tokihiro Hashimoto,
Tutorials. By Dr Sharon Truter
 Tutorials By Dr Sharon Truter To the Tutorials By Dr Sharon Truter What to expect from the Tutorials What to expect from these tutorials Outlines, structure, guided reading, explanations, mnemonics Begin
Tutorials By Dr Sharon Truter To the Tutorials By Dr Sharon Truter What to expect from the Tutorials What to expect from these tutorials Outlines, structure, guided reading, explanations, mnemonics Begin
Case 37 Clinical Presentation
 Case 37 73 Clinical Presentation The patient is a 62-year-old woman with gastrointestinal (GI) bleeding. 74 RadCases Interventional Radiology Imaging Findings () Image from a selective digital subtraction
Case 37 73 Clinical Presentation The patient is a 62-year-old woman with gastrointestinal (GI) bleeding. 74 RadCases Interventional Radiology Imaging Findings () Image from a selective digital subtraction
Assessment Of Collateral Pathways In Acute Ischemic Cerebrovascular Stroke Using A Mansour Grading Scale; A New Scale, A Pilot Study
 ISPUB.COM The Internet Journal of Interventional Medicine Volume 3 Number 1 Assessment Of Collateral Pathways In Acute Ischemic Cerebrovascular Stroke Using A Mansour Grading Scale; A New Scale, A Pilot
ISPUB.COM The Internet Journal of Interventional Medicine Volume 3 Number 1 Assessment Of Collateral Pathways In Acute Ischemic Cerebrovascular Stroke Using A Mansour Grading Scale; A New Scale, A Pilot
Hemodynamic patterns of status epilepticus detected by susceptibility weighted imaging (SWI)
 Hemodynamic patterns of status epilepticus detected by susceptibility weighted imaging (SWI) Poster No.: C-1086 Congress: ECR 014 Type: Scientific Exhibit Authors: J. AELLEN, E. Abela, R. Kottke, E. Springer,
Hemodynamic patterns of status epilepticus detected by susceptibility weighted imaging (SWI) Poster No.: C-1086 Congress: ECR 014 Type: Scientific Exhibit Authors: J. AELLEN, E. Abela, R. Kottke, E. Springer,
PTA 106 Unit 1 Lecture 3
 PTA 106 Unit 1 Lecture 3 The Basics Arteries: Carry blood away from the heart toward tissues. They typically have thicker vessels walls to handle increased pressure. Contain internal and external elastic
PTA 106 Unit 1 Lecture 3 The Basics Arteries: Carry blood away from the heart toward tissues. They typically have thicker vessels walls to handle increased pressure. Contain internal and external elastic
Acute stroke imaging
 Acute stroke imaging Aims Imaging modalities and differences Why image acute stroke Clinical correlation to imaging appearance What is stroke Classic definition: acute focal injury to the central nervous
Acute stroke imaging Aims Imaging modalities and differences Why image acute stroke Clinical correlation to imaging appearance What is stroke Classic definition: acute focal injury to the central nervous
Blunt Carotid Injury- CT Angiography is Adequate For Screening. Kelly Knudson, M.D. UCHSC April 3, 2006
 Blunt Carotid Injury- CT Angiography is Adequate For Screening Kelly Knudson, M.D. UCHSC April 3, 2006 CT Angiography vs Digital Subtraction Angiography Blunt carotid injury screening is one of the very
Blunt Carotid Injury- CT Angiography is Adequate For Screening Kelly Knudson, M.D. UCHSC April 3, 2006 CT Angiography vs Digital Subtraction Angiography Blunt carotid injury screening is one of the very
ACUTE STROKE IMAGING
 ACUTE STROKE IMAGING Mahesh V. Jayaraman M.D. Director, Inter ventional Neuroradiology Associate Professor Depar tments of Diagnostic Imaging and Neurosurger y Alper t Medical School at Brown University
ACUTE STROKE IMAGING Mahesh V. Jayaraman M.D. Director, Inter ventional Neuroradiology Associate Professor Depar tments of Diagnostic Imaging and Neurosurger y Alper t Medical School at Brown University
Magnetic Resonance Angiography
 Magnetic Resonance Angiography 1 Magnetic Resonance Angiography exploits flow enhancement of GR sequences saturation of venous flow allows arterial visualization saturation of arterial flow allows venous
Magnetic Resonance Angiography 1 Magnetic Resonance Angiography exploits flow enhancement of GR sequences saturation of venous flow allows arterial visualization saturation of arterial flow allows venous
Remission of diffusion lesions in acute stroke magnetic resonance imaging
 ORIGINAL RESEARCH Remission of diffusion lesions in acute stroke magnetic resonance imaging F. A. Fellner 1, M. R. Vosko 2, C. M. Fellner 1, D. Flöry 1 1. AKH Linz, Institute of Radiology, Austria. 2.
ORIGINAL RESEARCH Remission of diffusion lesions in acute stroke magnetic resonance imaging F. A. Fellner 1, M. R. Vosko 2, C. M. Fellner 1, D. Flöry 1 1. AKH Linz, Institute of Radiology, Austria. 2.
How to interpret an unenhanced CT brain scan. Part 2: Clinical cases
 How to interpret an unenhanced CT brain scan. Part 2: Clinical cases Thomas Osborne a, Christine Tang a, Kivraj Sabarwal b and Vineet Prakash c a Radiology Registrar; b Radiology Foundation Year 1 Doctor;
How to interpret an unenhanced CT brain scan. Part 2: Clinical cases Thomas Osborne a, Christine Tang a, Kivraj Sabarwal b and Vineet Prakash c a Radiology Registrar; b Radiology Foundation Year 1 Doctor;
IMAGING IN ACUTE ISCHEMIC STROKE
 IMAGING IN ACUTE ISCHEMIC STROKE Timo Krings MD, PhD, FRCP (C) Professor of Radiology & Surgery Braley Chair of Neuroradiology, Chief and Program Director of Diagnostic and Interventional Neuroradiology;
IMAGING IN ACUTE ISCHEMIC STROKE Timo Krings MD, PhD, FRCP (C) Professor of Radiology & Surgery Braley Chair of Neuroradiology, Chief and Program Director of Diagnostic and Interventional Neuroradiology;
Advances in MR imaging have recently allowed better characterization
 ORIGINAL RESEARCH BRAIN Do FLAIR Vascular Hyperintensities beyond the DWI Lesion Represent the Ischemic Penumbra? L. Legrand, M. Tisserand, G. Turc, O. Naggara, M. Edjlali, C. Mellerio, J.-L. Mas, J.-F.
ORIGINAL RESEARCH BRAIN Do FLAIR Vascular Hyperintensities beyond the DWI Lesion Represent the Ischemic Penumbra? L. Legrand, M. Tisserand, G. Turc, O. Naggara, M. Edjlali, C. Mellerio, J.-L. Mas, J.-F.
Alan Barber. Professor of Clinical Neurology University of Auckland
 Alan Barber Professor of Clinical Neurology University of Auckland Presented with L numbness & slurred speech 2 episodes; 10 mins & 2 hrs Hypertension Type II DM Examination P 80/min reg, BP 160/95, normal
Alan Barber Professor of Clinical Neurology University of Auckland Presented with L numbness & slurred speech 2 episodes; 10 mins & 2 hrs Hypertension Type II DM Examination P 80/min reg, BP 160/95, normal
Index. aneurysm, 92 carotid occlusion, 94 ICA stenosis, 95 intracranial, 92 MCA, 94
 A ADC. See Apparent diffusion coefficient (ADC) Aneurysm cerebral artery aneurysm, 93 CT scan, 93 gadolinium, 93 Angiography, 13 Anoxic brain injury, 25 Apparent diffusion coefficient (ADC), 7 Arachnoid
A ADC. See Apparent diffusion coefficient (ADC) Aneurysm cerebral artery aneurysm, 93 CT scan, 93 gadolinium, 93 Angiography, 13 Anoxic brain injury, 25 Apparent diffusion coefficient (ADC), 7 Arachnoid
Diagnostic improvement from average image in acute ischemic stroke
 Diagnostic improvement from average image in acute ischemic stroke N. Magne (1), E.Tollard (1), O. Ozkul- Wermester (2), V. Macaigne (1), J.-N. Dacher (1), E. Gerardin (1) (1) Department of Radiology,
Diagnostic improvement from average image in acute ischemic stroke N. Magne (1), E.Tollard (1), O. Ozkul- Wermester (2), V. Macaigne (1), J.-N. Dacher (1), E. Gerardin (1) (1) Department of Radiology,
Recurring Extracranial Internal Carotid Artery Vasospasm Detected by Intravascular Ultrasound
 CSE EPOT ecurring Extracranial Internal Carotid rtery Vasospasm Detected by Intravascular Ultrasound Tomohisa Dembo 1,2 and Norio Tanahashi 2 bstract 24-year-old woman presented with headache and left-sided
CSE EPOT ecurring Extracranial Internal Carotid rtery Vasospasm Detected by Intravascular Ultrasound Tomohisa Dembo 1,2 and Norio Tanahashi 2 bstract 24-year-old woman presented with headache and left-sided
Carotid artery stenting for long CTO and pseudo occlusion of carotid artery -2 case reports-
 Carotid artery stenting for long CTO and pseudo occlusion of carotid artery -2 case reports- Katsutoshi Takayama, MD, Ph.D Department of Radiology and Interventional Neuroradiology Ishinkai Yao General
Carotid artery stenting for long CTO and pseudo occlusion of carotid artery -2 case reports- Katsutoshi Takayama, MD, Ph.D Department of Radiology and Interventional Neuroradiology Ishinkai Yao General
MR Imaging of Leptomeningeal Metastases: Comparison of Three Sequences
 AJNR Am J Neuroradiol 23:817 821, May 2002 MR Imaging of Leptomeningeal Metastases: Comparison of Three Sequences Sanjay K. Singh, Norman E. Leeds, and Lawrence E. Ginsberg BACKGROUND AND PURPOSE: Recent
AJNR Am J Neuroradiol 23:817 821, May 2002 MR Imaging of Leptomeningeal Metastases: Comparison of Three Sequences Sanjay K. Singh, Norman E. Leeds, and Lawrence E. Ginsberg BACKGROUND AND PURPOSE: Recent
S pontaneous dissection of the internal
 Pictorial Essay Dissections of the Internal Carotid Artery: Th ree- Dimensional Time-of-Flight M R Angiography and MR Imaging Features S pontaneous dissection of the internal carotid artery is now recognized
Pictorial Essay Dissections of the Internal Carotid Artery: Th ree- Dimensional Time-of-Flight M R Angiography and MR Imaging Features S pontaneous dissection of the internal carotid artery is now recognized
EMBOLIZATION OF ARTERIOVENOUS FISTULA AFTER RADIOSURGERY FOR MULTIPLE CEREBRAL ARTERIOVENOUS MALFORMATIONS
 Arteriovenous fistula after radiosurgery for multiple CAVM EMBOLIZATION OF ARTERIOVENOUS FISTULA AFTER RADIOSURGERY FOR MULTIPLE CEREBRAL ARTERIOVENOUS MALFORMATIONS Chao-Bao Luo, Wan-Yuo Guo, Michael
Arteriovenous fistula after radiosurgery for multiple CAVM EMBOLIZATION OF ARTERIOVENOUS FISTULA AFTER RADIOSURGERY FOR MULTIPLE CEREBRAL ARTERIOVENOUS MALFORMATIONS Chao-Bao Luo, Wan-Yuo Guo, Michael
Extracranial CAD accounts for nearly 20% of cases of stroke
 ORIGINAL RESEARCH O. Naggara F. Soares E. Touze D. Roy X. Leclerc J.-P. Pruvo J.-L. Mas J.-F. Meder C. Oppenheim Is It Possible to Recognize Cervical Artery Dissection on Stroke Brain MR Imaging? A Matched
ORIGINAL RESEARCH O. Naggara F. Soares E. Touze D. Roy X. Leclerc J.-P. Pruvo J.-L. Mas J.-F. Meder C. Oppenheim Is It Possible to Recognize Cervical Artery Dissection on Stroke Brain MR Imaging? A Matched
Heejin Shim, Hyun Seok Choi, So-Lyung Jung, Kook-Jin Ahn, Bum-soo Kim
 Susceptibility Weighted MR Imaging at 3T in Patients with Occlusion of Middle Cerebral Artery : Comparison with Diffusion Weighted Imaging Score (ASPECTS) Heejin Shim, Hyun Seok Choi, So-Lyung Jung, Kook-Jin
Susceptibility Weighted MR Imaging at 3T in Patients with Occlusion of Middle Cerebral Artery : Comparison with Diffusion Weighted Imaging Score (ASPECTS) Heejin Shim, Hyun Seok Choi, So-Lyung Jung, Kook-Jin
The Role of Neuroimaging in Acute Stroke. Bradley Molyneaux, HMS IV
 The Role of Neuroimaging in Acute Stroke Bradley Molyneaux, HMS IV Patient CR 62 yo F w/ 2 wk h/o altered mental status Presents to ED w/ confusion following a fall 1 day prior New onset left facial droop
The Role of Neuroimaging in Acute Stroke Bradley Molyneaux, HMS IV Patient CR 62 yo F w/ 2 wk h/o altered mental status Presents to ED w/ confusion following a fall 1 day prior New onset left facial droop
FLAIR is a valuable MR imaging technique for the detection
 ORIGINAL RESEARCH N. Lummel V. Schoepf M. Burke H. Brueckmann J. Linn 3D Fluid-Attenuated Inversion Recovery Imaging: Reduced CSF Artifacts and Enhanced Sensitivity and Specificity for Subarachnoid Hemorrhage
ORIGINAL RESEARCH N. Lummel V. Schoepf M. Burke H. Brueckmann J. Linn 3D Fluid-Attenuated Inversion Recovery Imaging: Reduced CSF Artifacts and Enhanced Sensitivity and Specificity for Subarachnoid Hemorrhage
Vascular Malformations of the Brain. William A. Cox, M.D. Forensic Pathologist/Neuropathologist. September 8, 2014
 Vascular Malformations of the Brain William A. Cox, M.D. Forensic Pathologist/Neuropathologist September 8, 2014 Vascular malformations of the brain are classified into four principal groups: arteriovenous
Vascular Malformations of the Brain William A. Cox, M.D. Forensic Pathologist/Neuropathologist September 8, 2014 Vascular malformations of the brain are classified into four principal groups: arteriovenous
Complete Recovery of Perfusion Abnormalities in a Cardiac Arrest Patient Treated with Hypothermia: Results of Cerebral Perfusion MR Imaging
 pissn 2384-1095 eissn 2384-1109 imri 2018;22:56-60 https://doi.org/10.13104/imri.2018.22.1.56 Complete Recovery of Perfusion Abnormalities in a Cardiac Arrest Patient Treated with Hypothermia: Results
pissn 2384-1095 eissn 2384-1109 imri 2018;22:56-60 https://doi.org/10.13104/imri.2018.22.1.56 Complete Recovery of Perfusion Abnormalities in a Cardiac Arrest Patient Treated with Hypothermia: Results
Place for Interventional Radiology in Acute Stroke
 Place for Interventional Radiology in Acute Stroke Dr Lakmalie Paranahewa MBBS, MD(Radiology), FRCR Consultant Interventional Radiologist Asiri Group of Hospitals Objectives Imaging in Stroke Neurovascular
Place for Interventional Radiology in Acute Stroke Dr Lakmalie Paranahewa MBBS, MD(Radiology), FRCR Consultant Interventional Radiologist Asiri Group of Hospitals Objectives Imaging in Stroke Neurovascular
Applicable Neuroradiology
 For the Clinical Neurology Clerkship LSU Medical School New Orleans Amy W Voigt, MD Clerkship Director Introduction The field of Radiology first developed following the discovery of X-Rays by Wilhelm Roentgen
For the Clinical Neurology Clerkship LSU Medical School New Orleans Amy W Voigt, MD Clerkship Director Introduction The field of Radiology first developed following the discovery of X-Rays by Wilhelm Roentgen
Imaging Acute Stroke and Cerebral Ischemia
 Department of Radiology University of California San Diego Imaging Acute Stroke and Cerebral Ischemia John R. Hesselink, M.D. Causes of Stroke Arterial stenosis Thrombosis Embolism Dissection Hypotension
Department of Radiology University of California San Diego Imaging Acute Stroke and Cerebral Ischemia John R. Hesselink, M.D. Causes of Stroke Arterial stenosis Thrombosis Embolism Dissection Hypotension
11/1/2018. Disclosure. Imaging in Acute Ischemic Stroke 2018 Neuro Symposium. Is NCCT good enough? Keystone Heart Consultant, Stock Options
 Disclosure Imaging in Acute Ischemic Stroke 2018 Neuro Symposium Keystone Heart Consultant, Stock Options Kevin Abrams, M.D. Chief of Radiology Medical Director of Neuroradiology Baptist Hospital, Miami,
Disclosure Imaging in Acute Ischemic Stroke 2018 Neuro Symposium Keystone Heart Consultant, Stock Options Kevin Abrams, M.D. Chief of Radiology Medical Director of Neuroradiology Baptist Hospital, Miami,
Subclavian artery Stenting
 Subclavian artery Stenting Etiology Atherosclerosis Takayasu s arteritis Fibromuscular dysplasia Giant Cell Arteritis Radiation-induced Vascular Injury Thoracic Outlet Syndrome Neurofibromatosis Incidence
Subclavian artery Stenting Etiology Atherosclerosis Takayasu s arteritis Fibromuscular dysplasia Giant Cell Arteritis Radiation-induced Vascular Injury Thoracic Outlet Syndrome Neurofibromatosis Incidence
Original Research Article
 MAGNETIC RESONANCE IMAGING IN MIDDLE CEREBRAL ARTERY INFARCT AND ITS CORRELATION WITH FUNCTIONAL RECOVERY Neethu Tressa Jose 1, Rajan Padinharoot 2, Vadakooth Raman Rajendran 3, Geetha Panarkandy 4 1Junior
MAGNETIC RESONANCE IMAGING IN MIDDLE CEREBRAL ARTERY INFARCT AND ITS CORRELATION WITH FUNCTIONAL RECOVERY Neethu Tressa Jose 1, Rajan Padinharoot 2, Vadakooth Raman Rajendran 3, Geetha Panarkandy 4 1Junior
Evaluation of Intracranial Vasculatures in Healthy Subjects with Arterial-Spin-Labeling-Based 4D-MR Angiography at 3T
 Magn Reson Med Sci, Vol. 15, No. 3, pp. 335 339, 2016 doi:10.2463/mrms.tn.2015-0081 TECHNICAL NOTE Evaluation of Intracranial Vasculatures in Healthy Subjects with Arterial-Spin-Labeling-Based 4D-MR Angiography
Magn Reson Med Sci, Vol. 15, No. 3, pp. 335 339, 2016 doi:10.2463/mrms.tn.2015-0081 TECHNICAL NOTE Evaluation of Intracranial Vasculatures in Healthy Subjects with Arterial-Spin-Labeling-Based 4D-MR Angiography
Three-Dimensional Time-of-Flight MR Angiography in the Evaluation of Intracranial Aneurysms Treated by Endovascular Balloon Occlusion
 Three-Dimensional Time-of-Flight MR Angiography in the Evaluation of Intracranial Aneurysms Treated by Endovascular Balloon Occlusion JayS. Tsuruda, Robert J. Sevick, 1 and Van V. Halbach Summary: The
Three-Dimensional Time-of-Flight MR Angiography in the Evaluation of Intracranial Aneurysms Treated by Endovascular Balloon Occlusion JayS. Tsuruda, Robert J. Sevick, 1 and Van V. Halbach Summary: The
AMSER Case of the Month: March 2019
 AMSER Case of the Month: March 2019 62 year-old male with left-sided weakness Ashley Graziano OMS IV, Lake Erie College of Osteopathic Medicine Erik Yannone MD, Charles Q. Li MD, Warren Chang MD, Matthew
AMSER Case of the Month: March 2019 62 year-old male with left-sided weakness Ashley Graziano OMS IV, Lake Erie College of Osteopathic Medicine Erik Yannone MD, Charles Q. Li MD, Warren Chang MD, Matthew
NEURORADIOLOGY DIL part 3
 NEURORADIOLOGY DIL part 3 Bleeds and hemorrhages K. Agyem MD, G. Hall MD, D. Palathinkal MD, Alexandre Menard March/April 2015 OVERVIEW Introduction to Neuroimaging - DIL part 1 Basic Brain Anatomy - DIL
NEURORADIOLOGY DIL part 3 Bleeds and hemorrhages K. Agyem MD, G. Hall MD, D. Palathinkal MD, Alexandre Menard March/April 2015 OVERVIEW Introduction to Neuroimaging - DIL part 1 Basic Brain Anatomy - DIL
Non-Traumatic Neuro Emergencies
 Department of Radiology University of California San Diego Non-Traumatic Neuro Emergencies John R. Hesselink, M.D. Nontraumatic Neuroemergencies 1. Acute focal neurological deficit 2. Worst headache of
Department of Radiology University of California San Diego Non-Traumatic Neuro Emergencies John R. Hesselink, M.D. Nontraumatic Neuroemergencies 1. Acute focal neurological deficit 2. Worst headache of
Time-resolved Magnetic Resonance Angiography for assessment of recanalization after coil embolization of visceral artery aneurysms
 Signature: Pol J Radiol, 2013; 78(1): 64-68 DOI: 10.12659/PJR.883769 CASE REPORT Received: 2012.09.29 Accepted: 2013.01.15 Time-resolved Magnetic Resonance Angiography for assessment of recanalization
Signature: Pol J Radiol, 2013; 78(1): 64-68 DOI: 10.12659/PJR.883769 CASE REPORT Received: 2012.09.29 Accepted: 2013.01.15 Time-resolved Magnetic Resonance Angiography for assessment of recanalization
Department of Radiology, Huashan Hospital, Fudan University, Shanghai, China
 Neurology Asia 2017; 22(3) : 193 202 ORIGINAL ARTICLES Fluid-attenuated inversion recovery vascular hyperintensity: Correlation with other radiologic findings in acute ischemic stroke with middle cerebral
Neurology Asia 2017; 22(3) : 193 202 ORIGINAL ARTICLES Fluid-attenuated inversion recovery vascular hyperintensity: Correlation with other radiologic findings in acute ischemic stroke with middle cerebral
An Introduc+on to Stroke
 An Introduc+on to Stroke Elizabeth Huntoon MS, MD Assistant Professor Department of Physical Medicine and Rehabilita>on Vanderbilt University School of Medicine Defini+on Sudden focal neurologic deficit
An Introduc+on to Stroke Elizabeth Huntoon MS, MD Assistant Professor Department of Physical Medicine and Rehabilita>on Vanderbilt University School of Medicine Defini+on Sudden focal neurologic deficit
