The Heart. PowerPoint Lecture Presentations prepared by Jason LaPres. Lone Star College North Harris Pearson Education, Inc.
|
|
|
- Edwina Shelton
- 6 years ago
- Views:
Transcription
1 20 The Heart PowerPoint Lecture Presentations prepared by Jason LaPres Lone Star College North Harris
2 An Introduction to the Cardiovascular System Learning Outcomes Describe the superficial anatomy of the heart, and pericardium structure. Identify the major blood vessels, and chambers. Trace the flow of blood through the heart. Cellular architecture of the heart.
3 Figure 20-3c The Superficial Anatomy of the Heart Base of heart Ribs Apex of heart Heart position relative to the rib cage.
4 Figure 20-2a The Location of the Heart in the Thoracic Cavity Trachea Thyroid gland First rib (cut) Base of heart Right lung Diaphragm Left lung Apex of heart Parietal pericardium (cut) An anterior view of the chest, showing the position of the heart and major blood vessels relative to the ribs, lungs, and diaphragm.
5 20-1 Anatomy of the Heart Superficial Anatomy of the Heart Adult heart: 12 cm (5 in) in length, 8 cm (3.5 in) wide, and 6 cm (2.5 in) in thickness. Pumps 5 quarts of blood/ minute (4.7 litres) Atria Upper chambers/ thin-walled Expandable outer auricle (atrial appendage) Ventricles Lower chambers/ thick-walled Lack outer appendages
6 20-1 Anatomy of the Heart The Heart Includes Pointed tip is apex Surrounded by pericardial sac Sits between two pleural cavities in the mediastinum Great veins and arteries at the base
7 20-1 Anatomy of the Heart Superficial Anatomy of the Heart Sulci Coronary sulcus divides atria and ventricles Anterior interventricular sulcus and posterior interventricular sulcus Separate left and right ventricles Contain blood vessels of cardiac muscle
8 20-1 Anatomy of the Heart The Pericardium Double lining of the pericardial cavity Visceral pericardium Inner layer of pericardium Parietal pericardium Outer layer Forms inner layer of pericardial sac or cavity Filled with pericardial fluid
9 Figure 20-2c The Location of the Heart in the Thoracic Cavity Base of heart Cut edge of parietal pericardium Fibrous tissue of pericardial sac Wrist (corresponds to base of heart) Inner wall (corresponds to epicardium) Fibrous attachment to diaphragm Parietal pericardium Areolar tissue Mesothelium Cut edge of epicardium Apex of heart Air space (corresponds to pericardial cavity) Outer wall (corresponds to parietal pericardium) Balloon The relationship between the heart and the pericardial cavity; compare with the fist-and-balloon example.
10 20-1 Anatomy of the Heart Four Chambers of the Heart 1. Right atrium Collects blood from systemic circuit 2. Right ventricle Pumps blood to pulmonary circuit 3. Left atrium Collects blood from pulmonary circuit 4. Left ventricle Pumps blood to systemic circuit
11 Figure 20-3a The Superficial Anatomy of the Heart Left common carotid artery Brachiocephalic trunk Ascending aorta Superior vena cava Auricle of right atrium RIGHT ATRIUM Left subclavian artery Arch of aorta Ligamentum arteriosum Descending aorta Left pulmonary artery Pulmonary trunk Auricle of left atrium Fat and vessels in coronary sulcus RIGHT VENTRICLE Fat and vessels in anterior interventricular sulcus LEFT VENTRICLE Major anatomical features on the anterior surface.
12 Figure 20-3b The Superficial Anatomy of the Heart Left pulmonary artery Left pulmonary veins Fat and vessels in coronary sulcus Coronary sinus LEFT VENTRICLE LEFT ATRIUM RIGHT ATRIUM Arch of aorta Right pulmonary artery Superior vena cava Right pulmonary veins (superior and inferior) RIGHT VENTRICLE Inferior vena cava Fat and vessels in posterior interventricular sulcus Major landmarks on the posterior surface. Coronary arteries (which supply the heart itself) are shown in red; coronary veins are shown in blue.
13 20-1 Anatomy of the Heart Three Types of Blood Vessels 1. Arteries Carry blood away from heart 2. Veins Carry blood to heart 3. Capillaries Networks between arteries and veins Also called exchange vessels Exchange materials between blood and tissues Materials include dissolved gases, nutrients, waste products
14 20-1 Anatomy of the Heart The Pulmonary Circuit Carries blood to and from gas exchange surfaces of lungs The Systemic Circuit Carries blood to and from the body Blood alternates between pulmonary circuit and systemic circuit
15 Figure 20-1 An Overview of the Cardiovascular System PULMONARY CIRCUIT Pulmonary arteries Pulmonary veins SYSTEMIC CIRCUIT Systemic arteries Systemic veins Capillaries in lungs Right atrium Capillaries in head, neck, upper limbs Left atrium Right ventricle Left ventricle Capillaries in trunk and lower limbs
16 20-1 Anatomy of the Heart (External) Epicardium (Outer Layer) Visceral pericardium Covers the heart Myocardium (Middle Layer) Muscular wall of the heart Concentric layers of cardiac muscle tissue Atrial myocardium wraps around great vessels Two divisions of ventricular myocardium Endocardium (Inner Layer) Simple squamous epithelium
17 Figure 20-4a The Heart Wall Parietal pericardium Dense fibrous layer Areolar tissue Mesothelium Myocardium (cardiac muscle tissue) Cardiac muscle cells Connective tissues Pericardial cavity Epicardium (visceral pericardium) Mesothelium Areolar tissue Endocardium Areolar tissue Endothelium
18 Figure 20-4b The Heart Wall Atrial musculature Ventricular musculature Cardiac muscle tissue forms concentric layers that wrap around the atria or spiral within the walls of the ventricles.
19 20-1 Anatomy of the Heart Cardiac Muscle Tissue Intercalated discs Interconnect cardiac muscle cells Secured by desmosomes- notches and knots Linked by gap junctions- channels Convey force of contraction Propagate action potentials
20 20-1 Anatomy of the Heart Characteristics of Cardiac Muscle Cells 1. Small size 2. Single, central nucleus 3. Branching interconnections between cells 4. Intercalated discs
21 Figure 20-5a Cardiac Muscle Cells Cardiac muscle cell Mitochondria Intercalated disc (sectioned) Nucleus Cardiac muscle cell (sectioned) Bundles of myofibrils Intercalated discs Cardiac muscle cells
22 Figure 20-5b Cardiac Muscle Cells Intercalated disc Gap junction Opposing plasma membranes Desmosomes Structure of an intercalated disc
23 Figure 20-5c Cardiac Muscle Cells Intercalated discs Cardiac muscle tissue LM 575 Cardiac muscle tissue
24 Figure 20-4b The Heart Wall Atrial musculature Ventricular musculature Cardiac muscle tissue forms concentric layers that wrap around the atria or spiral within the walls of the ventricles.
25 Internal Anatomy of Heart
26 20-1 Anatomy of the Heart Internal Anatomy and Organization Interatrial septum separates atria Interventricular septum separates ventricles
27 20-1 Anatomy of the Heart Atrioventricular (AV) valves Connect right atrium to right ventricle and left atrium to left ventricle Are folds of fibrous tissue that extend into openings between atria and ventricles Permit blood flow in one direction From atria to ventricles
28 20-1 Anatomy of the Heart The Right Atrium Superior vena cava Receives blood from head, neck, upper limbs, and chest Inferior vena cava Receives blood from trunk, viscera, and lower limbs Coronary sinus Cardiac veins return blood to coronary sinus Coronary sinus opens into right atrium
29 20-1 Anatomy of the Heart The Right Atrium Foramen ovale Before birth, is an opening through interatrial septum Connects the two atria Seals off at birth, forming fossa ovalis
30 20-1 Anatomy of the Heart The Right Atrium Pectinate muscles Contain prominent muscular ridges On anterior atrial wall and inner surfaces of right auricle
31 Figure 20-6a The Sectional Anatomy of the Heart Superior vena cava Right pulmonary arteries Ascending aorta Fossa ovalis Opening of coronary sinus RIGHT ATRIUM Pectinate muscles Conus arteriosus Cusp of right AV (tricuspid) valve Chordae tendineae Papillary muscles RIGHT VENTRICLE Inferior vena cava Brachiocephalic trunk Aortic arch LEFT ATRIUM Left common carotid artery Left subclavian artery Ligamentum arteriosum Pulmonary trunk Pulmonary valve Left pulmonary arteries Left pulmonary veins Interatrial septum Aortic valve Cusp of left AV (mitral) valve LEFT VENTRICLE Interventricular septum Trabeculae carneae Moderator band Descending aorta
32 Figure 20-6c The Sectional Anatomy of the Heart Ascending aorta Cusp of aortic valve Inferior vena cava Fossa ovalis Pectinate muscles Coronary sinus RIGHT ATRIUM Cusps of right AV (tricuspid) valve Trabeculae carneae Left coronary artery branches (red) and great cardiac vein (blue) Cusp of left AV (bicuspid) valve Chordae tendineae Papillary muscles LEFT VENTRICLE Interventricular septum RIGHT VENTRICLE A frontal section, anterior view.
33 20-1 Anatomy of the Heart The Right Ventricle Free edges attach to chordae tendineae from papillary muscles of ventricle Prevent valve from opening backward Right atrioventricular (AV) valve Also called tricuspid valve Opening from right atrium to right ventricle Has three cusps Prevents backflow
34 20-1 Anatomy of the Heart The Right Ventricle Trabeculae carneae Muscular ridges on internal surface of right (and left) ventricle Includes moderator band Ridge contains part of conducting system Coordinates contractions of cardiac muscle cells
35 Figure 20-6b The Sectional Anatomy of the Heart Chordae tendineae Papillary muscles The papillary muscles and chordae tendinae supporting the right AV (tricuspid) valve. The photograph was taken from inside the right ventricle, looking toward a light shining from the right atrium.
36 20-1 Anatomy of the Heart The Pulmonary Circuit Conus arteriosus (superior end of right ventricle) leads to pulmonary trunk Pulmonary trunk divides into left and right pulmonary arteries Blood flows from right ventricle to pulmonary trunk through pulmonary valve Pulmonary valve has three semilunar cusps
37 20-1 Anatomy of the Heart The Left Atrium Blood gathers into left and right pulmonary veins Pulmonary veins deliver to left atrium Blood from left atrium passes to left ventricle through left atrioventricular (AV) valve A two-cusped bicuspid valve or mitral valve
38 20-1 Anatomy of the Heart The Left Ventricle Holds same volume as right ventricle Is larger; muscle is thicker and more powerful Similar internally to right ventricle but does not have moderator band
39 20-1 Anatomy of the Heart The Left Ventricle Systemic circulation Blood leaves left ventricle through aortic valve into ascending aorta Ascending aorta turns (aortic arch) and becomes descending aorta
40 Figure 20-6c The Sectional Anatomy of the Heart Ascending aorta Cusp of aortic valve Inferior vena cava Fossa ovalis Pectinate muscles Coronary sinus RIGHT ATRIUM Cusps of right AV (tricuspid) valve Trabeculae carneae Left coronary artery branches (red) and great cardiac vein (blue) Cusp of left AV (bicuspid) valve Chordae tendineae Papillary muscles LEFT VENTRICLE Interventricular septum RIGHT VENTRICLE A frontal section, anterior view.
41 20-1 Anatomy of the Heart Structural Differences between the Left and Right Ventricles Right ventricle wall is thinner, develops less pressure than left ventricle Right ventricle is pouch-shaped, left ventricle is round ANIMATION The Heart: Heart Anatomy
42 Figure 20-7a Structural Differences between the Left and Right Ventricles Posterior interventricular sulcus Right ventricle Left ventricle Fat in anterior interventricular sulcus A diagrammatic sectional view through the heart, showing the relative thicknesses of the two ventricles. Notice the pouchlike shape of the right ventricle and the greater thickness of the left ventricle.
43 Figure 20-7b Structural Differences between the Left and Right Ventricles Right ventricle Left ventricle Dilated Contracted Diagrammatic views of the ventricles just before a contraction (dilated) and just after a contraction (contracted).
44 20-1 Anatomy of the Heart The Heart Valves Two pairs of one-way valves prevent backflow during contraction Atrioventricular (AV) valves Between atria and ventricles Blood pressure closes valve cusps during ventricular contraction Papillary muscles tense chordae tendineae to prevent valves from swinging into atria
45 20-1 Anatomy of the Heart The Heart Valves Semilunar valves Pulmonary and aortic tricuspid valves Prevent backflow from pulmonary trunk and aorta into ventricles Have no muscular support Three cusps support like tripod
46 20-1 Anatomy of the Heart Aortic Sinuses At base of ascending aorta Sacs that prevent valve cusps from sticking to aorta Origin of right and left coronary arteries
47 Figure 20-8a Valves of the Heart Transverse Sections, Superior View, Atria and Vessels Removed POSTERIOR Cardiac skeleton Left AV (bicuspid) valve (open) RIGHT VENTRICLE LEFT VENTRICLE Relaxed ventricles Right AV (tricuspid) valve (open) Aortic valve (closed) ANTERIOR Pulmonary valve (closed) Aortic valve closed When the ventricles are relaxed, the AV valves are open and the semilunar valves are closed. The chordae tendineae are loose, and the papillary muscles are relaxed.
48 Figure 20-8a Valves of the Heart Frontal Sections through Left Atrium and Ventricle Pulmonary veins Relaxed ventricles Aortic valve (closed) LEFT ATRIUM Left AV (bicuspid) valve (open) Chordae tendineae (loose) Papillary muscles (relaxed) LEFT VENTRICLE (relaxed and filling with blood)
49 Figure 20-8b Valves of the Heart Right AV (tricuspid) valve (closed) RIGHT VENTRICLE Cardiac skeleton Left AV (bicuspid) valve (closed) LEFT VENTRICLE Contracting ventricles Aortic valve (open) Pulmonary valve (open) Aortic valve open When the ventricles are contracting, the AV valves are closed and the semilunar valves are open. In the frontal section notice the attachment of the left AV valve to the chordae tendineae and papillary muscles.
50 Figure 20-8b Valves of the Heart Contracting ventricles Aorta Aortic sinus Aortic valve (open) LEFT ATRIUM Left AV (bicuspid) valve (closed) Chordae tendineae (tense) Papillary muscles (contracted) Left ventricle (contracted)
51 20-1 Anatomy of the Heart Connective Tissues and the Cardiac Skeleton Connective Tissue Fibers 1. Physically support cardiac muscle fibers 2. Distribute forces of contraction 3. Add strength and prevent overexpansion of heart 4. Provide elasticity that helps return heart to original size and shape after contraction
52 20-1 Anatomy of the Heart The Cardiac Skeleton Four bands around heart valves and bases of pulmonary trunk and aorta Stabilize valves Electrically insulate ventricular cells from atrial cells
53 20-1 Anatomy of the Heart The Blood Supply to the Heart = Coronary circulation Supplies blood to muscle tissue of heart Coronary arteries and cardiac veins
54 20-1 Anatomy of the Heart The Coronary Arteries Left and right Originate at aortic sinuses High blood pressure, elastic rebound forces blood through coronary arteries between contractions
55 20-1 Anatomy of the Heart Right Coronary Artery Supplies blood to: Right atrium Portions of both ventricles Cells of sinoatrial (SA) and atrioventricular nodes Marginal arteries (surface of right ventricle) Posterior interventricular artery
56 20-1 Anatomy of the Heart Left Coronary Artery Supplies blood to: Left ventricle Left atrium Interventricular septum
57 20-1 Anatomy of the Heart Two Main Branches of Left Coronary Artery 1. Circumflex artery 2. Anterior interventricular artery Arterial Anastomoses Interconnect anterior and posterior interventricular arteries Stabilize blood supply to cardiac muscle
58 20-1 Anatomy of the Heart The Cardiac Veins Great cardiac vein Drains blood from area of anterior interventricular artery into coronary sinus Anterior cardiac veins Empty into right atrium Posterior cardiac vein, middle cardiac vein, and small cardiac vein Empty into great cardiac vein or coronary sinus
59 Figure 20-9a Coronary Circulation Aortic arch Ascending aorta Right coronary artery Atrial arteries Anterior cardiac veins Small cardiac vein Marginal artery Left coronary artery Pulmonary trunk Circumflex artery Anterior interventricular artery Great cardiac vein Coronary vessels supplying and draining the anterior surface of the heart.
60 Figure 20-9b Coronary Circulation Circumflex artery Great cardiac vein Coronary sinus Marginal artery Posterior interventricular artery Posterior cardiac vein Left ventricle Small cardiac vein Right coronary artery Middle cardiac vein Marginal artery Coronary vessels supplying and draining the posterior surface of the heart.
61 Figure Heart Disease and Heart Attacks Normal Artery Narrowing of Artery Tunica externa Lipid deposit of plaque Tunica media Cross-section Cross-section
62 Figure Heart Disease and Heart Attacks Occluded Coronary Artery Damaged Heart Muscle
63 20-2 The Conducting System Heartbeat A single contraction of the heart The entire heart contracts in series First the atria Then the ventricles
64 20-2 The Conducting System Cardiac Physiology Two Types of Cardiac Muscle Cells 1. Conducting system Controls and coordinates heartbeat 2. Contractile cells Produce contractions that propel blood
65 20-2 The Conducting System The Cardiac Cycle Begins with action potential at SA node Transmitted through conducting system Produces action potentials in cardiac muscle cells (contractile cells) Electrocardiogram (ECG or EKG) Electrical events in the cardiac cycle can be recorded on an electrocardiogram
66 20-2 The Conducting System The Conducting System A system of specialized cardiac muscle cells Initiates and distributes electrical impulses that stimulate contraction Automaticity Cardiac muscle tissue contracts automatically
67 20-2 The Conducting System Structures of the Conducting System Sinoatrial (SA) node - wall of right atrium Atrioventricular (AV) node - junction between atria and ventricles Conducting cells - throughout myocardium
68 20-2 The Conducting System Conducting Cells Interconnect SA and AV nodes Distribute stimulus through myocardium In the atrium Internodal pathways In the ventricles AV bundle and the bundle branches
69 20-2 The Conducting System Prepotential Also called pacemaker potential Resting potential of conducting cells Gradually depolarizes toward threshold SA node depolarizes first, establishing heart rate ANIMATION The Heart: Conduction System
70 Figure 20-11a The Conducting System of the Heart Sinoatrial (SA) node Internodal pathways Atrioventricular (AV) node AV bundle Purkinje fibers Components of the conducting system Bundle branches
71 Figure 20-11b The Conducting System of the Heart Threshold Prepotential (spontaneous depolarization) Time (sec) Changes in the membrane potential of a pacemaker cell in the SA node that is establishing a heart rate of 72 beats per minute. Note the presence of a prepotential, a gradual spontaneous depolarization.
72 20-2 The Conducting System Heart Rate SA node generates action potentials per minute Parasympathetic stimulation slows heart rate AV node generates action potentials per minute
73 20-2 The Conducting System The Sinoatrial (SA) Node In posterior wall of right atrium Contains pacemaker cells Connected to AV node by internodal pathways Begins atrial activation (Step 1)
74 Figure Impulse Conduction through the Heart (Step 1) SA node activity and atrial activation begin. SA node Time = 0
75 20-2 The Conducting System The Atrioventricular (AV) Node In floor of right atrium Receives impulse from SA node (Step 2) Delays impulse (Step 3) Atrial contraction begins
76 Figure Impulse Conduction through the Heart (Step 2) Stimulus spreads across the atrial surfaces and reaches the AV node. AV node Elapsed time = 50 msec
77 Figure Impulse Conduction through the Heart (Step 3) There is a 100-msec delay at the AV node. Atrial contraction begins. AV bundle Elapsed time = 150 msec Bundle branches
78 20-2 The Conducting System The AV Bundle In the septum Carries impulse to left and right bundle branches Which conduct to Purkinje fibers (Step 4) And to the moderator band Which conducts to papillary muscles
79 Figure Impulse Conduction through the Heart (Step 4) The impulse travels along the interventricular septum within the AV bundle and the bundle branches to the Purkinje fibers and, via the moderator band, to the papillary muscles of the right ventricle. Moderator Elapsed time = 175 msec band
80 20-2 The Conducting System Purkinje Fibers Distribute impulse through ventricles (Step 5) Atrial contraction is completed Ventricular contraction begins
81 Figure Impulse Conduction through the Heart (Step 5) The impulse is distributed by Purkinje fibers and relayed throughout the ventricular myocardium. Atrial contraction is completed, and ventricular contraction begins. Elapsed time = 225 msec Purkinje fibers
82 20-2 The Conducting System Abnormal Pacemaker Function Bradycardia - abnormally slow heart rate Tachycardia - abnormally fast heart rate Ectopic pacemaker Abnormal cells Generate high rate of action potentials Bypass conducting system Disrupt ventricular contractions
83 20-2 The Conducting System The Electrocardiogram (ECG or EKG) A recording of electrical events in the heart Obtained by electrodes at specific body locations Abnormal patterns diagnose damage
84 20-2 The Conducting System Features of an ECG P wave Atria depolarize QRS complex Ventricles depolarize T wave Ventricles repolarize
85 20-2 The Conducting System Time Intervals between ECG Waves P R interval From start of atrial depolarization To start of QRS complex Q T interval From ventricular depolarization To ventricular repolarization
86 Figure 20-13a An Electrocardiogram Electrode placement for recording a standard ECG.
87 Figure 20-13b An Electrocardiogram 800 msec R R P wave (atria depolarize) T wave (ventricles repolarize) P R segment S T segment Millivolts P R interval Q S S T interval Q T interval QRS interval (ventricles depolarize)
88 Figure Cardiac Arrhythmias Premature Atrial Contractions (PACs) P P P Paroxysmal Atrial Tachycardia (PAT) P P P P P P Atrial Fibrillation (AF)
89 Figure Cardiac Arrhythmias Premature Ventricular Contractions (PVCs) P T P T P T Ventricular Tachycardia (VT) P Ventricular Fibrillation (VF)
90 20-2 The Conducting System Contractile Cells Purkinje fibers distribute the stimulus to the contractile cells, which make up most of the muscle cells in the heart Resting Potential Of a ventricular cell about 90 mv Of an atrial cell about 80 mv
91 Figure 20-15a The Action Potential in Skeletal and Cardiac Muscle Rapid Depolarization The Plateau Repolarization Cause: Na + entry Duration: 3 5 msec Ends with: Closure of voltage-gated fast sodium channels Cause: Ca 2+ entry Duration: ~175 msec Ends with: Closure of slow calcium channels Cause: K + loss Duration: 75 msec Ends with: Closure of slow potassium channels mv Absolute refractory period Relative refractory period Stimulus Time (msec) Events in an action potential in a ventricular muscle cell. KEY Absolute refractory period Relative refractory period
92 Figure 12-9 The Resting Potential is the Transmembrane Potential of an Undisturbed Cell EXTRACELLULAR FLUID Cl mv K + leak channel 3 Na + Na + leak channel Plasma membrane Sodium potassium exchange pump CYTOSOL Protein 2 K + Protein Protein
93 Figure 20-15b The Action Potential in Skeletal and Cardiac Muscle mv Action potential SKELETAL MUSCLE Tension Contraction Time (msec) CARDIAC MUSCLE mv Action potential KEY Absolute refractory period Relative refractory period Tension Contraction Time (msec) Action potentials and twitch contractions in a skeletal muscle (above) and cardiac muscle (below).
94 20-2 The Conducting System Refractory Period Absolute refractory period Long Cardiac muscle cells cannot respond Relative refractory period Short Response depends on degree of stimulus
95 20-2 The Conducting System The Role of Calcium Ions in Cardiac Contractions As slow calcium channels close Intracellular Ca 2+ is absorbed by the SR Or pumped out of cell Cardiac muscle tissue Very sensitive to extracellular Ca 2+ concentrations
96 20-2 The Conducting System The Energy for Cardiac Contractions Aerobic energy of heart From mitochondrial breakdown of fatty acids and glucose Oxygen from circulating hemoglobin Cardiac muscles store oxygen in myoglobin
97 20-3 The Cardiac Cycle The Cardiac Cycle Is the period between the start of one heartbeat and the beginning of the next Includes both contraction and relaxation
98 20-3 The Cardiac Cycle Two Phases of the Cardiac Cycle Within any one chamber 1. Systole (contraction) 2. Diastole (relaxation) Atrial systole Atrial diastole Ventricular systole Ventricular diastole
99 20-3 The Cardiac Cycle Atrial Systole 1. Atrial systole Atrial contraction begins Right and left AV valves are open 2. Atria eject blood into ventricles Filling ventricles 3. Atrial systole ends AV valves close Ventricles contain maximum blood volume Known as end-diastolic volume (EDV)
100 20-3 The Cardiac Cycle Ventricular Systole 4. Ventricles contract and build pressure AV valves close cause isovolumetric contraction 5. Ventricular ejection Ventricular pressure exceeds vessel pressure opening the semilunar valves and allowing blood to leave the ventricle Amount of blood ejected is called the stroke volume (SV)
101 20-3 The Cardiac Cycle Ventricular Systole 6. Ventricular pressure falls Semilunar valves close Ventricles contain end-systolic volume (ESV), about 40% of end-diastolic volume
102 Figure Phases of the Cardiac Cycle
103 20-3 The Cardiac Cycle Blood Pressure In any chamber Rises during systole Falls during diastole Blood flows from high to low pressure Controlled by timing of contractions Directed by one-way valves
104 20-3 The Cardiac Cycle Cardiac Cycle and Heart Rate At 75 beats per minute (bpm) Cardiac cycle lasts about 800 msec When heart rate increases All phases of cardiac cycle shorten, particularly diastole
105 Figure Pressure and Volume Relationships in the Cardiac Cycle ATRIAL DIASTOLE ATRIAL SYSTOLE VENTRICULAR DIASTOLE VENTRICULAR SYSTOLE ATRIAL DIASTOLE Aortic valve opens Aorta Atrial contraction begins. Pressure (mm Hg) Left ventricle Atria eject blood into ventricles. Atrial systole ends; AV valves close. Isovolumetric ventricular contraction. Ventricular ejection occurs. Left atrium Left AV valve closes Semilunar valves close. Isovolumetric relaxation occurs. AV valves open; passive ventricular filling occurs. End-diastolic volume Left ventricular volume (ml) Stroke volume Time (msec)
106 Figure Pressure and Volume Relationships in the Cardiac Cycle VENTRICULAR SYSTOLE ATRIAL DIASTOLE VENTRICULAR DIASTOLE ATRIAL SYSTOLE Aortic valve closes Pressure (mm Hg) Dicrotic notch Left AV valve opens Atrial contraction begins. Atria eject blood into ventricles. Atrial systole ends; AV valves close. Isovolumetric ventricular contraction. Ventricular ejection occurs. Semilunar valves close. Isovolumetric relaxation occurs. AV valves open; passive ventricular filling occurs. Left ventricular volume (ml) End-systolic volume Time (msec)
107 20-3 The Cardiac Cycle Heart Sounds S 1 Loud sounds Produced by AV valves S 2 Loud sounds Produced by semilunar valves
108 20-3 The Cardiac Cycle S 3, S 4 Soft sounds Blood flow into ventricles and atrial contraction Heart Murmur Sounds produced by regurgitation through valves
109 Figure 20-18a Heart Sounds Sounds heard Valve location Aortic valve Valve location Sounds heard Pulmonary valve Sounds heard Valve location Left AV valve Valve location Sounds heard Right AV valve Placements of a stethoscope for listening to the different sounds produced by individual valves
110 Figure 20-18b Heart Sounds Semilunar valves open Semilunar valves close Aorta Pressure (mm Hg) Left ventricle Left atrium AV valves close AV valves open Heart sounds S 1 S 4 S 4 S 2 S 3 Lubb Dubb The relationship between heart sounds and key events in the cardiac cycle
111 20-4 Cardiodynamics Cardiodynamics The movement and force generated by cardiac contractions End-diastolic volume (EDV) End-systolic volume (ESV) Stroke volume (SV) SV = EDV ESV Ejection fraction The percentage of EDV represented by SV SV= %EDV
112 20-4 Cardiodynamics Cardiac Output (CO) The volume pumped by left ventricle in 1 minute CO = HR SV CO = cardiac output (ml/min) HR = heart rate (beats/min) SV = stroke volume (ml/beat)
113 20-4 Cardiodynamics Factors Affecting Cardiac Output Cardiac output Adjusted by changes in heart rate or stroke volume Heart rate Adjusted by autonomic nervous system or hormones Stroke volume Adjusted by changing EDV or ESV
114 Figure Factors Affecting Cardiac Output Factors Affecting Heart Rate (HR) Factors Affecting Stroke Volume (SV) Autonomic innervation Hormones End-diastolic volume End-systolic volume HEART RATE (HR) STROKE VOLUME (SV) = EDV ESV CARDIAC OUTPUT (CO) = HR SV
115 20-4 Cardiodynamics Autonomic Innervation Cardiac plexuses innervate heart Vagus nerves (N X) carry parasympathetic preganglionic fibers to small ganglia in cardiac plexus Cardiac centers of medulla oblongata Cardioacceleratory center controls sympathetic neurons (increases heart rate) Cardioinhibitory center controls parasympathetic neurons (slows heart rate)
116 20-4 Cardiodynamics Cardiac reflexes Cardiac centers monitor: Blood pressure (baroreceptors) Arterial oxygen and carbon dioxide levels (chemoreceptors) Cardiac centers adjust cardiac activity Autonomic tone Dual innervation maintains resting tone by releasing ACh and NE Fine adjustments meet needs of other systems
117 Figure Autonomic Innervation of the Heart Cardioinhibitory center Vagal nucleus Cardioacceleratory center Medulla oblongata Vagus (N X) Spinal cord Sympathetic Sympathetic ganglia (cervical ganglia and superior thoracic ganglia [T 1 T 4 ]) Sympathetic preganglionic fiber Sympathetic postganglionic fiber Cardiac nerve Parasympathetic Parasympathetic preganglionic fiber Synapses in cardiac plexus Parasympathetic postganglionic fibers
118 20-4 Cardiodynamics Effects on the SA Node Membrane potential of pacemaker cells Lower than other cardiac cells Rate of spontaneous depolarization depends on: Resting membrane potential Rate of depolarization
119 Figure 20-22a Autonomic Regulation of Pacemaker Function Membrane potential (mv) Threshold Normal (resting) Prepotential (spontaneous depolarization) Heart rate: 75 bpm Pacemaker cells have membrane potentials closer to threshold than those of other cardiac muscle cells ( 60 mv versus 90 mv). Their plasma membranes undergo spontaneous depolarization to threshold, producing action potentials at a frequency determined by (1) the resting-membrane potential and (2) the rate of depolarization.
120 20-4 Cardiodynamics Effects on the SA Node Sympathetic and parasympathetic stimulation Greatest at SA node (heart rate) ACh (parasympathetic stimulation) Slows the heart NE (sympathetic stimulation) Speeds the heart
121 Figure 20-22b Autonomic Regulation of Pacemaker Function Membrane potential (mv) Parasympathetic stimulation Threshold Hyperpolarization Heart rate: 40 bpm Slower depolarization Parasympathetic stimulation releases ACh, which extends repolarization and decreases the rate of spontaneous depolarization. The heart rate slows.
122 Figure 20-22c Autonomic Regulation of Pacemaker Function Membrane potential (mv) Sympathetic stimulation Threshold Reduced repolarization Heart rate: 120 bpm More rapid depolarization Time (sec) Sympathetic stimulation releases NE, which shortens repolarization and accelerates the rate of spontaneous depolarization. As a result, the heart rate increases.
123 20-4 Cardiodynamics Atrial Reflex Also called Bainbridge reflex Adjusts heart rate in response to venous return Stretch receptors in right atrium Trigger increase in heart rate Through increased sympathetic activity
124 20-4 Cardiodynamics Hormonal Effects on Heart Rate Increase heart rate (by sympathetic stimulation of SA node) Epinephrine (E) Norepinephrine (NE) Thyroid hormone
125 20-4 Cardiodynamics Factors Affecting the Stroke Volume The EDV amount of blood a ventricle contains at the end of diastole Filling time Duration of ventricular diastole Venous return Rate of blood flow during ventricular diastole
126 20-4 Cardiodynamics Preload The degree of ventricular stretching during ventricular diastole Directly proportional to EDV Affects ability of muscle cells to produce tension
127 20-4 Cardiodynamics The EDV and Stroke Volume At rest EDV is low Myocardium stretches less Stroke volume is low With exercise EDV increases Myocardium stretches more Stroke volume increases
128 20-4 Cardiodynamics The Frank Starling Principle As EDV increases, stroke volume increases Physical Limits Ventricular expansion is limited by: Myocardial connective tissue The cardiac (fibrous) skeleton The pericardial sac
129 20-4 Cardiodynamics End-Systolic Volume (ESV) Is the amount of blood that remains in the ventricle at the end of ventricular systole
130 20-4 Cardiodynamics Three Factors That Affect ESV 1. Preload Ventricular stretching during diastole 2. Contractility Force produced during contraction, at a given preload 3. Afterload Tension the ventricle produces to open the semilunar valve and eject blood
131 20-4 Cardiodynamics Contractility Is affected by: Autonomic activity Hormones
132 20-4 Cardiodynamics Effects of Autonomic Activity on Contractility Sympathetic stimulation NE released by postganglionic fibers of cardiac nerves Epinephrine and NE released by adrenal medullae Causes ventricles to contract with more force Increases ejection fraction and decreases ESV
133 20-4 Cardiodynamics Effects of Autonomic Activity on Contractility Parasympathetic activity Acetylcholine released by vagus nerves Reduces force of cardiac contractions
134 20-4 Cardiodynamics Hormones Many hormones affect heart contraction Pharmaceutical drugs mimic hormone actions Stimulate or block beta receptors Affect calcium ions (e.g., calcium channel blockers)
135 20-4 Cardiodynamics Afterload Is increased by any factor that restricts arterial blood flow As afterload increases, stroke volume decreases
136 Figure Factors Affecting Stroke Volume Factors Affecting Stroke Volume (SV) Venous return (VR) Filling time (FT) VR = EDV FT = EDV VR = EDV FT = EDV Increased by sympathetic stimulation Decreased by parasympathetic stimulation Increased by E, NE, glucagon, thyroid hormones Preload Contractility (Cont) of muscle cells Cont = ESV Increased by Cont = ESV vasoconstriction Decreased by vasodilation End-diastolic volume (EDV) End-systolic volume (ESV) Afterload (AL) AL = ESV AL = ESV EDV = EDV = STROKE VOLUME (SV) SV SV ESV = ESV = SV SV
137 20-4 Cardiodynamics Summary: The Control of Cardiac Output Heart Rate Control Factors Autonomic nervous system Sympathetic and parasympathetic Circulating hormones Venous return and stretch receptors
138 20-4 Cardiodynamics Summary: The Control of Cardiac Output Stroke Volume Control Factors EDV Filling time, and rate of venous return ESV Preload, contractility, afterload
139 20-4 Cardiodynamics Cardiac Reserve The difference between resting and maximal cardiac output
140 20-4 Cardiodynamics The Heart and Cardiovascular System Cardiovascular regulation Ensures adequate circulation to body tissues Cardiovascular centers Control heart and peripheral blood vessels Cardiovascular system responds to: Changing activity patterns Circulatory emergencies
141 Figure A Summary of the Factors Affecting Cardiac Output Factors affecting heart fate (HR) Factors affecting stroke volume (SV) Skeletal muscle activity Blood volume Changes in peripheral circulation Atrial reflex Venous return Filling time Autonomic innervation Hormones Preload Contractility Vasodilation or vasoconstriction Autonomic innervation Hormones End-diastolic volume End-systolic volume Afterload HEART RATE (HR) STROKE VOLUME (SV) = EDV ESV CARDIAC OUTPUT (CO) = HR SV
The Heart. C h a p t e r. PowerPoint Lecture Slides prepared by Jason LaPres Lone Star College - North Harris
 C h a p t e r 20 The Heart PowerPoint Lecture Slides prepared by Jason LaPres Lone Star College - North Harris Copyright 2009 Pearson Education, Inc., publishing as Pearson Benjamin Cummings Introduction
C h a p t e r 20 The Heart PowerPoint Lecture Slides prepared by Jason LaPres Lone Star College - North Harris Copyright 2009 Pearson Education, Inc., publishing as Pearson Benjamin Cummings Introduction
The Cardiovascular System: The Heart
 PowerPoint Lecture Slides prepared by Meg Flemming Austin Community College C H A P T E R 12 The Cardiovascular System: The Heart Chapter 12 Learning Outcomes 12-1 12-2 Describe the anatomy of the heart,
PowerPoint Lecture Slides prepared by Meg Flemming Austin Community College C H A P T E R 12 The Cardiovascular System: The Heart Chapter 12 Learning Outcomes 12-1 12-2 Describe the anatomy of the heart,
Cardiovascular System
 Cardiovascular System The Heart Cardiovascular System The Heart Overview What does the heart do? By timed muscular contractions creates pressure gradients blood moves then from high pressure to low pressure
Cardiovascular System The Heart Cardiovascular System The Heart Overview What does the heart do? By timed muscular contractions creates pressure gradients blood moves then from high pressure to low pressure
Chapter 18 - Heart. I. Heart Anatomy: size of your fist; located in mediastinum (medial cavity)
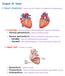 Chapter 18 - Heart I. Heart Anatomy: size of your fist; located in mediastinum (medial cavity) A. Coverings: heart enclosed in double walled sac called the pericardium 1. Fibrous pericardium: dense connective
Chapter 18 - Heart I. Heart Anatomy: size of your fist; located in mediastinum (medial cavity) A. Coverings: heart enclosed in double walled sac called the pericardium 1. Fibrous pericardium: dense connective
Chapter 20: Cardiovascular System: The Heart
 Chapter 20: Cardiovascular System: The Heart I. Functions of the Heart A. List and describe the four functions of the heart: 1. 2. 3. 4. II. Size, Shape, and Location of the Heart A. Size and Shape 1.
Chapter 20: Cardiovascular System: The Heart I. Functions of the Heart A. List and describe the four functions of the heart: 1. 2. 3. 4. II. Size, Shape, and Location of the Heart A. Size and Shape 1.
The Heart. The Heart A muscular double pump. The Pulmonary and Systemic Circuits
 C H A P T E R 19 The Heart The Heart A muscular double pump circuit takes blood to and from the lungs Systemic circuit vessels transport blood to and from body tissues Atria receive blood from the pulmonary
C H A P T E R 19 The Heart The Heart A muscular double pump circuit takes blood to and from the lungs Systemic circuit vessels transport blood to and from body tissues Atria receive blood from the pulmonary
Approximately the size of your fist Location. Pericardial physiology
 Heart Anatomy Approximately the size of your fist Location Superior surface of diaphragm Left of the midline Anterior to the vertebral column, posterior to the sternum Wednesday, March 28, 2012 Muscle
Heart Anatomy Approximately the size of your fist Location Superior surface of diaphragm Left of the midline Anterior to the vertebral column, posterior to the sternum Wednesday, March 28, 2012 Muscle
11/10/2014. Muscular pump Two atria Two ventricles. In mediastinum of thoracic cavity 2/3 of heart's mass lies left of midline of sternum
 It beats over 100,000 times a day to pump over 1,800 gallons of blood per day through over 60,000 miles of blood vessels. During the average lifetime, the heart pumps nearly 3 billion times, delivering
It beats over 100,000 times a day to pump over 1,800 gallons of blood per day through over 60,000 miles of blood vessels. During the average lifetime, the heart pumps nearly 3 billion times, delivering
THE CARDIOVASCULAR SYSTEM. Heart 2
 THE CARDIOVASCULAR SYSTEM Heart 2 PROPERTIES OF CARDIAC MUSCLE Cardiac muscle Striated Short Wide Branched Interconnected Skeletal muscle Striated Long Narrow Cylindrical PROPERTIES OF CARDIAC MUSCLE Intercalated
THE CARDIOVASCULAR SYSTEM Heart 2 PROPERTIES OF CARDIAC MUSCLE Cardiac muscle Striated Short Wide Branched Interconnected Skeletal muscle Striated Long Narrow Cylindrical PROPERTIES OF CARDIAC MUSCLE Intercalated
The Heart. Size, Form, and Location of the Heart. 1. Blunt, rounded point; most inferior part of the heart.
 12 The Heart FOCUS: The heart is composed of cardiac muscle cells, which are elongated, branching cells that appear striated. Cardiac muscle cells behave as a single electrical unit, and the highly coordinated
12 The Heart FOCUS: The heart is composed of cardiac muscle cells, which are elongated, branching cells that appear striated. Cardiac muscle cells behave as a single electrical unit, and the highly coordinated
Ch 19: Cardiovascular System - The Heart -
 Ch 19: Cardiovascular System - The Heart - Give a detailed description of the superficial and internal anatomy of the heart, including the pericardium, the myocardium, and the cardiac muscle. Trace the
Ch 19: Cardiovascular System - The Heart - Give a detailed description of the superficial and internal anatomy of the heart, including the pericardium, the myocardium, and the cardiac muscle. Trace the
Human Anatomy, First Edition
 Human Anatomy, First Edition McKinley & O'Loughlin Chapter 22 : Heart 1 Functions of the Heart Center of the cardiovascular system, the heart. Connects to blood vessels that transport blood between the
Human Anatomy, First Edition McKinley & O'Loughlin Chapter 22 : Heart 1 Functions of the Heart Center of the cardiovascular system, the heart. Connects to blood vessels that transport blood between the
2. right heart = pulmonary pump takes blood to lungs to pick up oxygen and get rid of carbon dioxide
 A. location in thorax, in inferior mediastinum posterior to sternum medial to lungs superior to diaphragm anterior to vertebrae orientation - oblique apex points down and to the left 2/3 of mass on left
A. location in thorax, in inferior mediastinum posterior to sternum medial to lungs superior to diaphragm anterior to vertebrae orientation - oblique apex points down and to the left 2/3 of mass on left
10/23/2017. Muscular pump Two atria Two ventricles. In mediastinum of thoracic cavity 2/3 of heart's mass lies left of midline of sternum
 It beats over 100,000 times a day to pump over 1,800 gallons of blood per day through over 60,000 miles of blood vessels. During the average lifetime, the heart pumps nearly 3 billion times, delivering
It beats over 100,000 times a day to pump over 1,800 gallons of blood per day through over 60,000 miles of blood vessels. During the average lifetime, the heart pumps nearly 3 billion times, delivering
the Cardiovascular System I
 the Cardiovascular System I By: Dr. Nabil A Khouri MD, MsC, Ph.D MEDIASTINUM 1. Superior Mediastinum 2. inferior Mediastinum Anterior mediastinum. Middle mediastinum. Posterior mediastinum Anatomy of
the Cardiovascular System I By: Dr. Nabil A Khouri MD, MsC, Ph.D MEDIASTINUM 1. Superior Mediastinum 2. inferior Mediastinum Anterior mediastinum. Middle mediastinum. Posterior mediastinum Anatomy of
- what other structures, besides the heart, does the mediastinum contain?
 Basic A & P II Dr. L. Bacha Chapter Outline (Martini & Nath 2010) An Introduction to the Cardiovascular System - read the paragraphs under this heading on page 580 The Heart is a Four Chambered Organ describe
Basic A & P II Dr. L. Bacha Chapter Outline (Martini & Nath 2010) An Introduction to the Cardiovascular System - read the paragraphs under this heading on page 580 The Heart is a Four Chambered Organ describe
Chapter 20 (1) The Heart
 Chapter 20 (1) The Heart Learning Objectives Describe the location and structure of the heart Describe the path of a drop of blood from the superior vena cava or inferior vena cava through the heart out
Chapter 20 (1) The Heart Learning Objectives Describe the location and structure of the heart Describe the path of a drop of blood from the superior vena cava or inferior vena cava through the heart out
THE HEART. A. The Pericardium - a double sac of serous membrane surrounding the heart
 THE HEART I. Size and Location: A. Fist-size weighing less than a pound (250 to 350 grams). B. Located in the mediastinum between the 2 nd rib and the 5 th intercostal space. 1. Tipped to the left, resting
THE HEART I. Size and Location: A. Fist-size weighing less than a pound (250 to 350 grams). B. Located in the mediastinum between the 2 nd rib and the 5 th intercostal space. 1. Tipped to the left, resting
THE CARDIOVASCULAR SYSTEM. Part 1
 THE CARDIOVASCULAR SYSTEM Part 1 CARDIOVASCULAR SYSTEM Blood Heart Blood vessels What is the function of this system? What other systems does it affect? CARDIOVASCULAR SYSTEM Functions Transport gases,
THE CARDIOVASCULAR SYSTEM Part 1 CARDIOVASCULAR SYSTEM Blood Heart Blood vessels What is the function of this system? What other systems does it affect? CARDIOVASCULAR SYSTEM Functions Transport gases,
10. Thick deposits of lipids on the walls of blood vessels, called, can lead to serious circulatory issues. A. aneurysm B. atherosclerosis C.
 Heart Student: 1. carry blood away from the heart. A. Arteries B. Veins C. Capillaries 2. What is the leading cause of heart attack and stroke in North America? A. alcohol B. smoking C. arteriosclerosis
Heart Student: 1. carry blood away from the heart. A. Arteries B. Veins C. Capillaries 2. What is the leading cause of heart attack and stroke in North America? A. alcohol B. smoking C. arteriosclerosis
Collin County Community College. ! BIOL Anatomy & Physiology! WEEK 5. The Heart
 Collin County Community College! BIOL. 2402 Anatomy & Physiology! WEEK 5 The Heart 1 (1578-1657) A groundbreaking work in the history of medicine, English physician William Harvey s Anatomical Essay on
Collin County Community College! BIOL. 2402 Anatomy & Physiology! WEEK 5 The Heart 1 (1578-1657) A groundbreaking work in the history of medicine, English physician William Harvey s Anatomical Essay on
Chapter 14. The Cardiovascular System
 Chapter 14 The Cardiovascular System Introduction Cardiovascular system - heart, blood and blood vessels Cardiac muscle makes up bulk of heart provides force to pump blood Function - transports blood 2
Chapter 14 The Cardiovascular System Introduction Cardiovascular system - heart, blood and blood vessels Cardiac muscle makes up bulk of heart provides force to pump blood Function - transports blood 2
The Cardiovascular System: The Heart: Part A
 PowerPoint Lecture Slides prepared by Janice Meeking, Mount Royal College CHAPTER 18 The Cardiovascular System: The Heart: Part A Heart Anatomy Approximately the size of a fist Location In the mediastinum
PowerPoint Lecture Slides prepared by Janice Meeking, Mount Royal College CHAPTER 18 The Cardiovascular System: The Heart: Part A Heart Anatomy Approximately the size of a fist Location In the mediastinum
Chapter 13 The Cardiovascular System: Cardiac Function
 Chapter 13 The Cardiovascular System: Cardiac Function Overview of the Cardiovascular System The Path of Blood Flow through the Heart and Vasculature Anatomy of the Heart Electrical Activity of the Heart
Chapter 13 The Cardiovascular System: Cardiac Function Overview of the Cardiovascular System The Path of Blood Flow through the Heart and Vasculature Anatomy of the Heart Electrical Activity of the Heart
*Generating blood pressure *Routing blood: separates. *Ensuring one-way blood. *Regulating blood supply *Changes in contraction
 *Generating blood pressure *Routing blood: separates pulmonary and systemic circulations *Ensuring one-way blood flow: valves *Regulating blood supply *Changes in contraction rate and force match blood
*Generating blood pressure *Routing blood: separates pulmonary and systemic circulations *Ensuring one-way blood flow: valves *Regulating blood supply *Changes in contraction rate and force match blood
Anatomy of the Heart. Figure 20 2c
 Anatomy of the Heart Figure 20 2c Pericardium & Myocardium Remember, the heart sits in it s own cavity, known as the mediastinum. The heart is surrounded by the Pericardium, a double lining of the pericardial
Anatomy of the Heart Figure 20 2c Pericardium & Myocardium Remember, the heart sits in it s own cavity, known as the mediastinum. The heart is surrounded by the Pericardium, a double lining of the pericardial
The Heart. PowerPoint Lecture Presentations prepared by Jason LaPres
 20 The Heart PowerPoint Lecture Presentations prepared by Jason LaPres Lone Star College North Harris NOTE: Presentations extensively modi6ied for use in MCB 244 & 246 at the University of Illinois by
20 The Heart PowerPoint Lecture Presentations prepared by Jason LaPres Lone Star College North Harris NOTE: Presentations extensively modi6ied for use in MCB 244 & 246 at the University of Illinois by
Functions of the Heart
 Cardiovascular System The Heart What is the Cardiovascular System? Blood circulated in Arteries, veins, and capillaries by the Pumping action of the heart Functions of the Heart Generating blood pressure
Cardiovascular System The Heart What is the Cardiovascular System? Blood circulated in Arteries, veins, and capillaries by the Pumping action of the heart Functions of the Heart Generating blood pressure
Chapter 20! The Heart!
 Chapter 20! The Heart! SECTION 20-1! The heart is a four-chambered organ, supplied by the coronary circulation, that pumps oxygen-poor blood to the lungs and oxygen-rich blood to the rest of the body!
Chapter 20! The Heart! SECTION 20-1! The heart is a four-chambered organ, supplied by the coronary circulation, that pumps oxygen-poor blood to the lungs and oxygen-rich blood to the rest of the body!
The Heart. Happy Friday! #takeoutyournotes #testnotgradedyet
 The Heart Happy Friday! #takeoutyournotes #testnotgradedyet Introduction Cardiovascular system distributes blood Pump (heart) Distribution areas (capillaries) Heart has 4 compartments 2 receive blood (atria)
The Heart Happy Friday! #takeoutyournotes #testnotgradedyet Introduction Cardiovascular system distributes blood Pump (heart) Distribution areas (capillaries) Heart has 4 compartments 2 receive blood (atria)
Lab Activity 23. Cardiac Anatomy. Portland Community College BI 232
 Lab Activity 23 Cardiac Anatomy Portland Community College BI 232 Cardiac Muscle Histology Branching cells Intercalated disc: contains many gap junctions connecting the adjacent cell cytoplasm, creates
Lab Activity 23 Cardiac Anatomy Portland Community College BI 232 Cardiac Muscle Histology Branching cells Intercalated disc: contains many gap junctions connecting the adjacent cell cytoplasm, creates
CARDIOVASCULAR SYSTEM
 CARDIOVASCULAR SYSTEM Overview Heart and Vessels 2 Major Divisions Pulmonary Circuit Systemic Circuit Closed and Continuous Loop Location Aorta Superior vena cava Right lung Pulmonary trunk Base of heart
CARDIOVASCULAR SYSTEM Overview Heart and Vessels 2 Major Divisions Pulmonary Circuit Systemic Circuit Closed and Continuous Loop Location Aorta Superior vena cava Right lung Pulmonary trunk Base of heart
Chapter 20 (2) The Heart
 Chapter 20 (2) The Heart ----------------------------------------------------------------------------------------------------------------------------------------- Describe the component and function of
Chapter 20 (2) The Heart ----------------------------------------------------------------------------------------------------------------------------------------- Describe the component and function of
The Cardiovascular System
 The Cardiovascular System The Cardiovascular System A closed system of the heart and blood vessels The heart pumps blood Blood vessels allow blood to circulate to all parts of the body The function of
The Cardiovascular System The Cardiovascular System A closed system of the heart and blood vessels The heart pumps blood Blood vessels allow blood to circulate to all parts of the body The function of
The Circulatory System. The Heart, Blood Vessels, Blood Types
 The Circulatory System The Heart, Blood Vessels, Blood Types The Closed Circulatory System Humans have a closed circulatory system, typical of all vertebrates, in which blood is confined to vessels and
The Circulatory System The Heart, Blood Vessels, Blood Types The Closed Circulatory System Humans have a closed circulatory system, typical of all vertebrates, in which blood is confined to vessels and
CV Anatomy Quiz. Dr Ella Kim Dr Pip Green
 CV Anatomy Quiz Dr Ella Kim Dr Pip Green Q1 The location of the heart is correctly described as A) lateral to the lungs. B) medial to the sternum. C) superior to the diaphragm. D) posterior to the spinal
CV Anatomy Quiz Dr Ella Kim Dr Pip Green Q1 The location of the heart is correctly described as A) lateral to the lungs. B) medial to the sternum. C) superior to the diaphragm. D) posterior to the spinal
This lab activity is aligned with Visible Body s A&P app. Learn more at visiblebody.com/professors
 1 This lab activity is aligned with Visible Body s A&P app. Learn more at visiblebody.com/professors 2 PRE-LAB EXERCISES: A. Watch the video 29.1 Heart Overview and make the following observations: 1.
1 This lab activity is aligned with Visible Body s A&P app. Learn more at visiblebody.com/professors 2 PRE-LAB EXERCISES: A. Watch the video 29.1 Heart Overview and make the following observations: 1.
Principles of Anatomy and Physiology
 Principles of Anatomy and Physiology 14 th Edition CHAPTER 20 The Cardiovascular System: The Heart Introduction The purpose of the chapter is to: 1. Learn about the components of the cardiovascular system
Principles of Anatomy and Physiology 14 th Edition CHAPTER 20 The Cardiovascular System: The Heart Introduction The purpose of the chapter is to: 1. Learn about the components of the cardiovascular system
Figure ) The specific chamber of the heart that is indicated by letter A is called the. Diff: 1 Page Ref: 364
 Essentials of Anatomy and Physiology, 9e (Marieb) Chapter 11 The Cardiovascular System Short Answer Figure 11.1 Using Figure 11.1, identify the following: 1) The Purkinje fibers are indicated by label.
Essentials of Anatomy and Physiology, 9e (Marieb) Chapter 11 The Cardiovascular System Short Answer Figure 11.1 Using Figure 11.1, identify the following: 1) The Purkinje fibers are indicated by label.
Cardiovascular system
 BIO 301 Human Physiology Cardiovascular system The Cardiovascular System: consists of the heart plus all the blood vessels transports blood to all parts of the body in two 'circulations': pulmonary (lungs)
BIO 301 Human Physiology Cardiovascular system The Cardiovascular System: consists of the heart plus all the blood vessels transports blood to all parts of the body in two 'circulations': pulmonary (lungs)
4. The two inferior chambers of the heart are known as the atria. the superior and inferior vena cava, which empty into the left atrium.
 Answer each statement true or false. If the statement is false, change the underlined word to make it true. 1. The heart is located approximately between the second and fifth ribs and posterior to the
Answer each statement true or false. If the statement is false, change the underlined word to make it true. 1. The heart is located approximately between the second and fifth ribs and posterior to the
The Cardiovascular System. Chapter 15. Cardiovascular System FYI. Cardiology Closed systemof the heart & blood vessels. Functions
 Chapter 15 Cardiovascular System FYI The heart pumps 7,000 liters (4000 gallons) of blood through the body each day The heart contracts 2.5 billion times in an avg. lifetime The heart & all blood vessels
Chapter 15 Cardiovascular System FYI The heart pumps 7,000 liters (4000 gallons) of blood through the body each day The heart contracts 2.5 billion times in an avg. lifetime The heart & all blood vessels
Heart Anatomy. 7/5/02 Stephen G Davenport 1
 Heart Anatomy Copyright 1999, Stephen G. Davenport, No part of this publication may be reproduced, stored in a retrieval system, or transmitted, in any form without prior written permission. 7/5/02 Stephen
Heart Anatomy Copyright 1999, Stephen G. Davenport, No part of this publication may be reproduced, stored in a retrieval system, or transmitted, in any form without prior written permission. 7/5/02 Stephen
BIOL 4350 Cardiovascular Physiology Dr. Hamilton. Using the figure above, match the following: 1. Purkinje fibers. 2. SA node. 3. AV node.
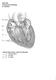 BIOL 4350 Cardiovascular Physiology Dr. Hamilton Using the figure above, match the following: 1. Purkinje fibers. 2. SA node. 3. AV node. 1 Using the figure above, match the following: 4. Atrial depolarization.
BIOL 4350 Cardiovascular Physiology Dr. Hamilton Using the figure above, match the following: 1. Purkinje fibers. 2. SA node. 3. AV node. 1 Using the figure above, match the following: 4. Atrial depolarization.
Heart. Structure Physiology of blood pressure and heartbeat
 Heart Structure Physiology of blood pressure and heartbeat Location and Anatomy Location and Anatomy Pericardial cavity: surrounds, isolates, and anchors heart Parietal pericardium lined with serous membrane
Heart Structure Physiology of blood pressure and heartbeat Location and Anatomy Location and Anatomy Pericardial cavity: surrounds, isolates, and anchors heart Parietal pericardium lined with serous membrane
The HEART. What is it???? Pericardium. Heart Facts. This muscle never stops working It works when you are asleep
 This muscle never stops working It works when you are asleep The HEART It works when you eat It really works when you exercise. What is it???? Located between the lungs in the mid thoracic region Apex
This muscle never stops working It works when you are asleep The HEART It works when you eat It really works when you exercise. What is it???? Located between the lungs in the mid thoracic region Apex
Cardiovascular System
 Cardiovascular System I. Structure of the Heart A. Average adult heart is 14 cm long and 9 cm wide. B. Lies in the mediastinum. C. Enclosed in the pericardium. 1. Fibrous pericardium- Outer, tough connective
Cardiovascular System I. Structure of the Heart A. Average adult heart is 14 cm long and 9 cm wide. B. Lies in the mediastinum. C. Enclosed in the pericardium. 1. Fibrous pericardium- Outer, tough connective
Heart. Heart 2-Tunica media: middle layer (media ='middle') muscle fibers (smooth or cardiac).
 t. innermost lumenal General Circulatory system heart and blood vessels walls have 3 layers (inside to outside) 1-Tunica interna: aka tunica intima layer--lumenal layer epithelium--endothelium simple squamous
t. innermost lumenal General Circulatory system heart and blood vessels walls have 3 layers (inside to outside) 1-Tunica interna: aka tunica intima layer--lumenal layer epithelium--endothelium simple squamous
Heart Overview. Chapter 18. Heart. Heart. Two Circuits. Organization of the Cardiovascular System. The Heart. Located directly behind sternum
 Heart Overview Chapter 18 The Heart Heart anatomy Cardiac muscle cells Heart chambers, valves and vessels Conducting system EKG Cardiac cycle Contractile and pacemaker cells Cardiodynamics Cardiac disorders
Heart Overview Chapter 18 The Heart Heart anatomy Cardiac muscle cells Heart chambers, valves and vessels Conducting system EKG Cardiac cycle Contractile and pacemaker cells Cardiodynamics Cardiac disorders
Electrical Conduction
 Sinoatrial (SA) node Electrical Conduction Sets the pace of the heartbeat at 70 bpm AV node (50 bpm) and Purkinje fibers (25 40 bpm) can act as pacemakers under some conditions Internodal pathway from
Sinoatrial (SA) node Electrical Conduction Sets the pace of the heartbeat at 70 bpm AV node (50 bpm) and Purkinje fibers (25 40 bpm) can act as pacemakers under some conditions Internodal pathway from
Principles of Biomedical Systems & Devices. Lecture 8: Cardiovascular Dynamics Dr. Maria Tahamont
 Principles of Biomedical Systems & Devices Lecture 8: Cardiovascular Dynamics Dr. Maria Tahamont Review of Cardiac Anatomy Four chambers Two atria-receive blood from the vena cave and pulmonary veins Two
Principles of Biomedical Systems & Devices Lecture 8: Cardiovascular Dynamics Dr. Maria Tahamont Review of Cardiac Anatomy Four chambers Two atria-receive blood from the vena cave and pulmonary veins Two
BIO 136 Human Anatomy & Physiology For Non-Majors 11:39 am, Mar 08, 2006
 Jim Swan 1 These slides are from class presentations, reformatted for static viewing. The content contained in these pages is also in the Class Notes pages in a narrative format. Best screen resolution
Jim Swan 1 These slides are from class presentations, reformatted for static viewing. The content contained in these pages is also in the Class Notes pages in a narrative format. Best screen resolution
Major Function of the Cardiovascular System. Transportation. Structures of the Cardiovascular System. Heart - muscular pump
 Structures of the Cardiovascular System Heart - muscular pump Blood vessels - network of tubes Blood - liquid transport vehicle brachiocephalic trunk superior vena cava right pulmonary arteries right pulmonary
Structures of the Cardiovascular System Heart - muscular pump Blood vessels - network of tubes Blood - liquid transport vehicle brachiocephalic trunk superior vena cava right pulmonary arteries right pulmonary
BIOLOGY 2060 LECTURE NOTES ANATOMY & PHYSIOLOGY II (A. IMHOLTZ) HEART P1 OF 5
 BIOLOGY 2060 LECTURE NOTES ANATOMY & PHYSIOLOGY II (A. IMHOLTZ) HEART P1 OF 5 1. Heart Functions a. Generates pressure that propels blood thru blood vessels. (Tissue perfusion.) b. Separates oxygenated
BIOLOGY 2060 LECTURE NOTES ANATOMY & PHYSIOLOGY II (A. IMHOLTZ) HEART P1 OF 5 1. Heart Functions a. Generates pressure that propels blood thru blood vessels. (Tissue perfusion.) b. Separates oxygenated
Cardiovascular System
 Cardiovascular System Purpose Transport oxygen and nutrients Take waste products away from tissues & organs Things we learned Blood pressure: the force of blood pushing against the walls of blood vessels
Cardiovascular System Purpose Transport oxygen and nutrients Take waste products away from tissues & organs Things we learned Blood pressure: the force of blood pushing against the walls of blood vessels
THE HEART Dr. Ali Ebneshahidi
 THE HEART Dr. Ali Ebneshahidi Functions is of the heart & blood vessels 1. The heart is an essential pumping organ in the cardiovascular system where the right heart pumps deoxygenated blood (returned
THE HEART Dr. Ali Ebneshahidi Functions is of the heart & blood vessels 1. The heart is an essential pumping organ in the cardiovascular system where the right heart pumps deoxygenated blood (returned
Cardiovascular System: The Heart
 Cardiovascular System: The Heart I. Anatomy of the Heart (See lab handout for terms list) A. Describe the size, shape and location of the heart B. Describe the structure and function of the pericardium
Cardiovascular System: The Heart I. Anatomy of the Heart (See lab handout for terms list) A. Describe the size, shape and location of the heart B. Describe the structure and function of the pericardium
Cardiovascular System Notes: Physiology of the Heart
 Cardiovascular System Notes: Physiology of the Heart Interesting Heart Fact Capillaries are so small it takes ten of them to equal the thickness of a human hair. Review What are the 3 parts of the cardiovascular
Cardiovascular System Notes: Physiology of the Heart Interesting Heart Fact Capillaries are so small it takes ten of them to equal the thickness of a human hair. Review What are the 3 parts of the cardiovascular
The Cardiovascular System
 Essentials of Human Anatomy & Physiology Elaine N. Marieb Slides 11.1 11.19 Seventh Edition Chapter 11 The Cardiovascular System Functions of the Cardiovascular system Function of the heart: to pump blood
Essentials of Human Anatomy & Physiology Elaine N. Marieb Slides 11.1 11.19 Seventh Edition Chapter 11 The Cardiovascular System Functions of the Cardiovascular system Function of the heart: to pump blood
The cardiovascular system is composed of the heart and blood vessels that carry blood to and from the body s organs. There are 2 major circuits:
 1 The cardiovascular system is composed of the heart and blood vessels that carry blood to and from the body s organs. There are 2 major circuits: pulmonary and systemic. The pulmonary goes out to the
1 The cardiovascular system is composed of the heart and blood vessels that carry blood to and from the body s organs. There are 2 major circuits: pulmonary and systemic. The pulmonary goes out to the
BIOLOGY 2060 LECTURE NOTES ANATOMY & PHYSIOLOGY II (A. IMHOLTZ) HEART P1 OF 7
 BIOLOGY 2060 LECTURE NOTES ANATOMY & PHYSIOLOGY II (A. IMHOLTZ) HEART P1 OF 7 1. Heart a. Generates the pressure that propels blood thru blood vessels. b. Separates oxygenated and deoxygenated blood separate.
BIOLOGY 2060 LECTURE NOTES ANATOMY & PHYSIOLOGY II (A. IMHOLTZ) HEART P1 OF 7 1. Heart a. Generates the pressure that propels blood thru blood vessels. b. Separates oxygenated and deoxygenated blood separate.
Blood must move! 4/15/2014. Heart Basics
 What is the CARDIOVASCULAR system? The cardiovascular system carries blood and dissolved substances to and from different places in the body. The Heart has the job of pumping these things around the body.
What is the CARDIOVASCULAR system? The cardiovascular system carries blood and dissolved substances to and from different places in the body. The Heart has the job of pumping these things around the body.
INTRODUCTORY REMARKS:
 INTRODUCTORY REMARKS: The circulatory system provides a way for the blood to be transported throughout the body. This provides nutrients to the cells and allows wastes to be removed. Open vs. Closed Circulatory
INTRODUCTORY REMARKS: The circulatory system provides a way for the blood to be transported throughout the body. This provides nutrients to the cells and allows wastes to be removed. Open vs. Closed Circulatory
Circulation. Circulation = is a process used for the transport of oxygen, carbon! dioxide, nutrients and wastes through-out the body
 Circulation Circulation = is a process used for the transport of oxygen, carbon! dioxide, nutrients and wastes through-out the body Heart = muscular organ about the size of your fist which pumps blood.
Circulation Circulation = is a process used for the transport of oxygen, carbon! dioxide, nutrients and wastes through-out the body Heart = muscular organ about the size of your fist which pumps blood.
Chapter 20 THE CARDIOVASCULAR SYSTEM: THE HEART
 Chapter 20 THE CARDIOVASCULAR SYSTEM: THE HEART INTRODUCTION A. The cardiovascular system consists of the blood, heart, and blood vessels. B. The heart is the pump that circulates the blood through an
Chapter 20 THE CARDIOVASCULAR SYSTEM: THE HEART INTRODUCTION A. The cardiovascular system consists of the blood, heart, and blood vessels. B. The heart is the pump that circulates the blood through an
The Cardiovascular System
 Essentials of Human Anatomy & Physiology Elaine N. Marieb Seventh Edition Chapter 11 The Cardiovascular System Slides 11.1 11.19 Lecture Slides in PowerPoint by Jerry L. Cook The Cardiovascular System
Essentials of Human Anatomy & Physiology Elaine N. Marieb Seventh Edition Chapter 11 The Cardiovascular System Slides 11.1 11.19 Lecture Slides in PowerPoint by Jerry L. Cook The Cardiovascular System
The Cardiovascular System
 The Cardiovascular System The Manila Times College of Subic Prepared by: Stevens B. Badar, RN, MANc THE HEART Anatomy of the Heart Location and Size approx. the size of a person s fist, hollow and cone-shaped,
The Cardiovascular System The Manila Times College of Subic Prepared by: Stevens B. Badar, RN, MANc THE HEART Anatomy of the Heart Location and Size approx. the size of a person s fist, hollow and cone-shaped,
The Cardiovascular System
 Chapter 18 Part A The Cardiovascular System 1/19/16 1 Annie Leibovitz/Contact Press Images Similarities of Cardiac and Skeletal Muscle RMP Ion concentration Deploarization Action Potential Repolarization
Chapter 18 Part A The Cardiovascular System 1/19/16 1 Annie Leibovitz/Contact Press Images Similarities of Cardiac and Skeletal Muscle RMP Ion concentration Deploarization Action Potential Repolarization
37 1 The Circulatory System
 H T H E E A R T 37 1 The Circulatory System The circulatory system and respiratory system work together to supply cells with the nutrients and oxygen they need to stay alive. a) The respiratory system:
H T H E E A R T 37 1 The Circulatory System The circulatory system and respiratory system work together to supply cells with the nutrients and oxygen they need to stay alive. a) The respiratory system:
Part 1. Copyright 2011 Pearson Education, Inc. Figure Copyright 2011 Pearson Education, Inc.
 PowerPoint Lecture Slides prepared by Leslie Hendon University of Alabama, Birmingham C H A P T E R The Heart 19 Part 1 The Heart A muscular double pump circuit vessels transport blood to and from the
PowerPoint Lecture Slides prepared by Leslie Hendon University of Alabama, Birmingham C H A P T E R The Heart 19 Part 1 The Heart A muscular double pump circuit vessels transport blood to and from the
Anatomy of the Heart
 Biology 212: Anatomy and Physiology II Anatomy of the Heart References: Saladin, KS: Anatomy and Physiology, The Unity of Form and Function 8 th (2018). Required reading before beginning this lab: Chapter
Biology 212: Anatomy and Physiology II Anatomy of the Heart References: Saladin, KS: Anatomy and Physiology, The Unity of Form and Function 8 th (2018). Required reading before beginning this lab: Chapter
IB TOPIC 6.2 THE BLOOD SYSTEM
 IB TOPIC 6.2 THE BLOOD SYSTEM THE BLOOD SYSTEM TERMS TO KNOW circulation ventricle artery vein 6.2.U1 - Arteries convey blood at high pressure from the ventricles to the tissues of the body Circulation
IB TOPIC 6.2 THE BLOOD SYSTEM THE BLOOD SYSTEM TERMS TO KNOW circulation ventricle artery vein 6.2.U1 - Arteries convey blood at high pressure from the ventricles to the tissues of the body Circulation
THE HEART OBJECTIVES: LOCATION OF THE HEART IN THE THORACIC CAVITY CARDIOVASCULAR SYSTEM
 BIOLOGY II CARDIOVASCULAR SYSTEM ACTIVITY #3 NAME DATE HOUR THE HEART OBJECTIVES: Describe the anatomy of the heart and identify and give the functions of all parts. (pp. 356 363) Trace the flow of blood
BIOLOGY II CARDIOVASCULAR SYSTEM ACTIVITY #3 NAME DATE HOUR THE HEART OBJECTIVES: Describe the anatomy of the heart and identify and give the functions of all parts. (pp. 356 363) Trace the flow of blood
human anatomy 2016 lecture thirteen Dr meethak ali ahmed neurosurgeon
 Heart The heart is a hollow muscular organ that is somewhat pyramid shaped and lies within the pericardium in the mediastinum. It is connected at its base to the great blood vessels but otherwise lies
Heart The heart is a hollow muscular organ that is somewhat pyramid shaped and lies within the pericardium in the mediastinum. It is connected at its base to the great blood vessels but otherwise lies
The Cardiovascular System
 11 PART A The Cardiovascular System PowerPoint Lecture Slide Presentation by Jerry L. Cook, Sam Houston University ESSENTIALS OF HUMAN ANATOMY & PHYSIOLOGY EIGHTH EDITION ELAINE N. MARIEB The Cardiovascular
11 PART A The Cardiovascular System PowerPoint Lecture Slide Presentation by Jerry L. Cook, Sam Houston University ESSENTIALS OF HUMAN ANATOMY & PHYSIOLOGY EIGHTH EDITION ELAINE N. MARIEB The Cardiovascular
The Heart and Cardiovascular System
 The Heart and Cardiovascular System What you will learn The location of the heart 3 layers and covering of the heart Explain the function of the heart as 2 separate pumps Identify the 4 chambers of the
The Heart and Cardiovascular System What you will learn The location of the heart 3 layers and covering of the heart Explain the function of the heart as 2 separate pumps Identify the 4 chambers of the
Pearson's Comprehensive Medical Assisting Administrative and Clinical Competencies
 Pearson's Comprehensive Medical Assisting Administrative and Clinical Competencies THIRD EDITION CHAPTER 27 The Cardiovascular System Lesson 1: Overview of the Cardiovascular System Lesson Objectives Upon
Pearson's Comprehensive Medical Assisting Administrative and Clinical Competencies THIRD EDITION CHAPTER 27 The Cardiovascular System Lesson 1: Overview of the Cardiovascular System Lesson Objectives Upon
The Cardiovascular System. anatom.ua 1
 The Cardiovascular System anatom.ua 1 The Closed Circulatory System Humans have a closed circulatory system, typical of all vertebrates, in which blood is confined to vessels and is distinct from the interstitial
The Cardiovascular System anatom.ua 1 The Closed Circulatory System Humans have a closed circulatory system, typical of all vertebrates, in which blood is confined to vessels and is distinct from the interstitial
Large Arteries of Heart
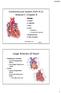 Cardiovascular System (Part A-2) Module 5 -Chapter 8 Overview Arteries Capillaries Veins Heart Anatomy Conduction System Blood pressure Fetal circulation Susie Turner, M.D. 1/5/13 Large Arteries of Heart
Cardiovascular System (Part A-2) Module 5 -Chapter 8 Overview Arteries Capillaries Veins Heart Anatomy Conduction System Blood pressure Fetal circulation Susie Turner, M.D. 1/5/13 Large Arteries of Heart
IP: Regulation of Cardiac Output
 ANP 1105D Winter 2013 Assignment 9: The Heart, part 2: Chap... Assignment 9: The Heart, part 2: Chapter 18 Signed in as Alex Sokolowski Help Close Resources Due: 11:59pm on Monday, March 25, 2013 Note:
ANP 1105D Winter 2013 Assignment 9: The Heart, part 2: Chap... Assignment 9: The Heart, part 2: Chapter 18 Signed in as Alex Sokolowski Help Close Resources Due: 11:59pm on Monday, March 25, 2013 Note:
Chapter 12 Lecture Outline
 Chapter 12 Lecture Outline See separate PowerPoint slides for all figures and tables preinserted into PowerPoint without notes. Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction
Chapter 12 Lecture Outline See separate PowerPoint slides for all figures and tables preinserted into PowerPoint without notes. Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction
Function: Transportation of. Oxygen Nutrients Waste Hormones gases
 Function: Transportation of Oxygen Nutrients Waste Hormones gases Pericardium: double sac of serous membrane filled with fluid (pericardial fluid to be exact) that surrounds the heart. Parietal pericardium:
Function: Transportation of Oxygen Nutrients Waste Hormones gases Pericardium: double sac of serous membrane filled with fluid (pericardial fluid to be exact) that surrounds the heart. Parietal pericardium:
The Cardiovascular System (Heart)
 The Cardiovascular System The Cardiovascular System (Heart) A closed system of the heart and blood vessels The heart pumps blood Blood vessels allow blood to circulate to all parts of the body The function
The Cardiovascular System The Cardiovascular System (Heart) A closed system of the heart and blood vessels The heart pumps blood Blood vessels allow blood to circulate to all parts of the body The function
Anatomy & Physiology of Cardiovascular System. Chapter 18 & 19
 Anatomy & Physiology of Cardiovascular System Chapter 18 & 19 Objectives..cont 1. Discuss the physiological stages of cardiac muscle contraction. 2. Trace a typical ECG and label each wave or complex 3.
Anatomy & Physiology of Cardiovascular System Chapter 18 & 19 Objectives..cont 1. Discuss the physiological stages of cardiac muscle contraction. 2. Trace a typical ECG and label each wave or complex 3.
1. What kind of blood is found in the rt. atrium? (oxygenated or deoxygenated)
 Carl Christennsen, PhD Chap. 19, 20, & 21 - Circulatory System Bio. 2304 Human Anatomy HEART 1. What kind of blood is found in the rt. atrium? (oxygenated or deoxygenated) Where does this blood come from?
Carl Christennsen, PhD Chap. 19, 20, & 21 - Circulatory System Bio. 2304 Human Anatomy HEART 1. What kind of blood is found in the rt. atrium? (oxygenated or deoxygenated) Where does this blood come from?
QUIZ/TEST REVIEW NOTES SECTION 1 CARDIAC MYOCYTE PHYSIOLOGY [CARDIOLOGY]
![QUIZ/TEST REVIEW NOTES SECTION 1 CARDIAC MYOCYTE PHYSIOLOGY [CARDIOLOGY] QUIZ/TEST REVIEW NOTES SECTION 1 CARDIAC MYOCYTE PHYSIOLOGY [CARDIOLOGY]](/thumbs/96/126998162.jpg) QUIZ/TEST REVIEW NOTES SECTION 1 CARDIAC MYOCYTE PHYSIOLOGY [CARDIOLOGY] Learning Objectives: Describe the ionic basis of action potentials in cardiac contractile and autorhythmic cells Explain the relationship
QUIZ/TEST REVIEW NOTES SECTION 1 CARDIAC MYOCYTE PHYSIOLOGY [CARDIOLOGY] Learning Objectives: Describe the ionic basis of action potentials in cardiac contractile and autorhythmic cells Explain the relationship
LECTURE 5. Anatomy of the heart
 LECTURE 5. Anatomy of the heart Main components of the CVS: Heart Blood circulatory system arterial compartment haemomicrocirculatory (=microvascular) compartment venous compartment Lymphatic circulatory
LECTURE 5. Anatomy of the heart Main components of the CVS: Heart Blood circulatory system arterial compartment haemomicrocirculatory (=microvascular) compartment venous compartment Lymphatic circulatory
d) Cardiovascular System Higher Human Biology
 d) Cardiovascular System Higher Human Biology What can your remember about the heart and blood vessels? What is the Cardiovascular System? The cardiovascular system, also known as the circulatory system,
d) Cardiovascular System Higher Human Biology What can your remember about the heart and blood vessels? What is the Cardiovascular System? The cardiovascular system, also known as the circulatory system,
Chapter 13. Cardiovascular System
 Chapter 13 Cardiovascular System 1 Introduction A. The cardiovascular system consists of the heart and vessels (arteries, capillaries and veins.) B. A functional cardiovascular system is vital for supplying
Chapter 13 Cardiovascular System 1 Introduction A. The cardiovascular system consists of the heart and vessels (arteries, capillaries and veins.) B. A functional cardiovascular system is vital for supplying
8:49 am, Jan 28, 2008
 Jim Swan 1 These slides are from class presentations, reformatted for static viewing. The content contained in these pages is also in the Class Notes pages in a narrative format. Best screen resolution
Jim Swan 1 These slides are from class presentations, reformatted for static viewing. The content contained in these pages is also in the Class Notes pages in a narrative format. Best screen resolution
Practice Exercises for the Cardiovascular System
 Practice Exercises for the Cardiovascular System On the diagram below, color the oxygen-rich blood red and the oxygen-poor blood blue. Label the parts: Continued on the next page... Label the parts on
Practice Exercises for the Cardiovascular System On the diagram below, color the oxygen-rich blood red and the oxygen-poor blood blue. Label the parts: Continued on the next page... Label the parts on
CIRCULATORY SYSTEM BLOOD VESSELS
 Name: Block: CIRCULATORY SYSTEM Multicellular organisms (above the level of roundworms) rely on a circulatory system to bring nutrients to, and take wastes away from, cells. In higher organisms such as
Name: Block: CIRCULATORY SYSTEM Multicellular organisms (above the level of roundworms) rely on a circulatory system to bring nutrients to, and take wastes away from, cells. In higher organisms such as
LAB 12-1 HEART DISSECTION GROSS ANATOMY OF THE HEART
 LAB 12-1 HEART DISSECTION GROSS ANATOMY OF THE HEART Because mammals are warm-blooded and generally very active animals, they require high metabolic rates. One major requirement of a high metabolism is
LAB 12-1 HEART DISSECTION GROSS ANATOMY OF THE HEART Because mammals are warm-blooded and generally very active animals, they require high metabolic rates. One major requirement of a high metabolism is
Chapter 14. Circulatory System Images. VT-122 Anatomy & Physiology II
 Chapter 14 Circulatory System Images VT-122 Anatomy & Physiology II The mediastinum Dog heart Dog heart Cat heart Dog heart ultrasound Can see pericardium as distinct bright line Pericardial effusion Fluid
Chapter 14 Circulatory System Images VT-122 Anatomy & Physiology II The mediastinum Dog heart Dog heart Cat heart Dog heart ultrasound Can see pericardium as distinct bright line Pericardial effusion Fluid
Cardiac physiology. b. myocardium -- cardiac muscle and fibrous skeleton of heart
 I. Heart anatomy -- general gross. A. Size/orientation - base/apex B. Coverings D. Chambers 1. parietal pericardium 2. visceral pericardium 3. Layers of heart wall a. epicardium Cardiac physiology b. myocardium
I. Heart anatomy -- general gross. A. Size/orientation - base/apex B. Coverings D. Chambers 1. parietal pericardium 2. visceral pericardium 3. Layers of heart wall a. epicardium Cardiac physiology b. myocardium
Anatomy Review: The Heart Graphics are used with permission of A.D.A.M. Software, Inc. and Benjamin/Cummings Publishing Co.
 Anatomy Review: The Heart Graphics are used with permission of A.D.A.M. Software, Inc. and Benjamin/Cummings Publishing Co. Anatomy Views Label the diagrams of the heart below: Interactive Physiology Study
Anatomy Review: The Heart Graphics are used with permission of A.D.A.M. Software, Inc. and Benjamin/Cummings Publishing Co. Anatomy Views Label the diagrams of the heart below: Interactive Physiology Study
HUMAN HEART. Learn the following structures on the heart models.
 HUMAN HEART Learn the following structures on the heart models. The human heart has four chambers that consist of the right atrium, left atrium, right ventricle, and left ventricle. The atria are smaller
HUMAN HEART Learn the following structures on the heart models. The human heart has four chambers that consist of the right atrium, left atrium, right ventricle, and left ventricle. The atria are smaller
The Cardiovascular System
 PowerPoint Lecture Slide Presentation by Patty Bostwick-Taylor, Florence-Darlington Technical College The Cardiovascular System 11 PART A The Cardiovascular System A closed system of the heart and blood
PowerPoint Lecture Slide Presentation by Patty Bostwick-Taylor, Florence-Darlington Technical College The Cardiovascular System 11 PART A The Cardiovascular System A closed system of the heart and blood
IB TOPIC 6.2 THE BLOOD SYSTEM
 IB TOPIC 6.2 THE BLOOD SYSTEM TERMS TO KNOW circulation ventricle artery vein THE BLOOD SYSTEM 6.2.U1 - Arteries convey blood at high pressure from the ventricles to the tissues of the body Circulation
IB TOPIC 6.2 THE BLOOD SYSTEM TERMS TO KNOW circulation ventricle artery vein THE BLOOD SYSTEM 6.2.U1 - Arteries convey blood at high pressure from the ventricles to the tissues of the body Circulation
