Laparoscopic sacrocolpopexy for the correction of vaginal vault prolapse
|
|
|
- Roy Anthony
- 5 years ago
- Views:
Transcription
1 Washington University School of Medicine Digital Open Access Publications 2004 Laparoscopic sacrocolpopexy for the correction of vaginal vault prolapse Chandru P. Sundaram Indiana University - Purdue University Indianapolis Ramakrishna Venkatesh Washington University School of Medicine in St. Louis Jaime Landman Washington University School of Medicine in St. Louis Carl G. Klutke Washington University School of Medicine in St. Louis Follow this and additional works at: Recommended Citation Sundaram, Chandru P.; Venkatesh, Ramakrishna; Landman, Jaime; and Klutke, Carl G.,,"Laparoscopic sacrocolpopexy for the correction of vaginal vault prolapse." Journal of Endourology.18, (2004). This Open Access Publication is brought to you for free and open access by Digital Commons@Becker. It has been accepted for inclusion in Open Access Publications by an authorized administrator of Digital Commons@Becker. For more information, please contact engeszer@wustl.edu.
2 JOURNAL OF ENDOUROLOGY Volume 18, Number 7, September 2004 Mary Ann Liebert, Inc. Techniques in Endourology Laparoscopic Sacrocolpopexy for the Correction of Vaginal Vault Prolapse* CHANDRU P. SUNDARAM, M.D., 1 RAMAKRISHNA VENKATESH, M.D., 2 JAIME LANDMAN, M.D., 2 and CARL G. KLUTKE, M.D. 2 ABSTRACT Background and Purpose: Laparoscopic sacrocolpopexy offers a minimally invasive approach to correcting vaginal vault prolapse. We describe our operative technique and review our experience. Patients and Methods: A retrospective study of 10 patients who underwent laparoscopic sacrocolpopexy between February 2000 and June 2002 for posthysterectomy vaginal vault prolapse was performed. Data collected included operative time, complications, hospital stay, and postoperative morbidity. Results: One patient underwent primary laparoscopic repair of an intraoperative bladder injury. Conversion from a laparoscopic to an open procedure was required in one patient because of dense bowel adhesions in the pelvis. The mean analgesic (morphine sulfate equivalent) requirement was 7.3 mg (range 5 21 mg). With a mean follow-up of 16 months (range 5 32 months), prolapse recurred in one patient. Conclusion: In the short term, laparoscopic sacrocolpopexy appears to be an effective approach for the treatment of vaginal vault prolapse with minimal postoperative pain and morbidity. INTRODUCTION VAGINAL VAULT PROLAPSE is descent of the apex of the vagina below the introitus, turning the vagina inside out. Vaginal vault prolapse is uncommon in the United States, occurring in only 900 to 1200 women annually, and is estimated to develop in 0.2% to 1% of women who have undergone hysterectomy. 1 The goals of correcting vault prolapse are relief of symptoms, restoration of normal vaginal anatomic relations, and preservation of coital function. Abdominal sacrocolpopexy, by suspending a mesh hammock between the prolapsed vaginal vault and sacrum, provides durable support to the vagina that has prolapsed after hysterectomy. 2 4 The laparoscopic approach to sacrocolpopexy for vaginal vault prolapse is a relatively new procedure, carried out in very few specialized centers across the country. We demonstrate our technique for this procedure and review the outcome. TECHNIQUE The laparoscopic sacrocolpopexy was performed with the intent of applying the principles of open sacrocolpopexy. Laparoscopic techniques and instruments were adapted to duplicate open surgery. Our procedures were performed by an experienced laparoscopic surgeon (CPS) assisted by an experienced open surgeon (CGK). The equipment used is listed in Table 1. Patient preparation The patient is placed in the dorsal lithotomy position, and the vagina and the abdomen are prepared and draped in a sterile fashion. The vagina, including the apex, is thoroughly prepared with povidone-iodine solution. The bladder is drained with a Foley catheter. Preoperatively, intravenous cefazolin and gentamicin are administered. 1 1Department of Urology, Indiana University School of Medicine, Indianapolis, Indiana. 2 Department of Surgery, Division of Urologic Surgery, Washington University School of Medicine, St. Louis, Missouri. *The technique described here is illustrated on the enclosed CD-ROM. Videoclips available online at 620
3 LAPAROSCOPIC SACROCOLPOPEXY FOR THE CORRECTION OF VAGINAL VAULT PROLAPSE 621 TABLE 1. INSTRUMENTS FOR LAPAROSCOPIC SACROCOLPOPEXY Trocars, two 12 mm, three 5 mm 30 laparoscope Harmonic Scalpel (Ethicon Endosurgery, Cincinnati, OH) 5-mm grasping forceps Suction irrigator Bowel retractor (fan shaped) Ethicon drivers (non-self-righting), two Gore-Tex mesh (W.L. Gore and Associates, Flagstaff, AZ) 2-0 Ethibond suture on CT-1 needle (Ethicon, Inc., Somerville, NJ) Endostitch device with 2-0 polyglactin suture (US Surgical, Norwalk, CT) Protack helical tacker (US Surgical) with clips Endoscissors Sponge-holding forceps Approach FIG. 2. Pelvic anatomy with patient in Trendelenberg position and sigmoid colon retracted to left. After the pneumoperitoneum is established with a Veress needle, the trocars are introduced in a fan-shaped or inverted- U configuration (Fig. 1). We use five trocars: two 12-mm trocars and three 5-mm trocars. A 30 laparoscope is introduced through the umbilical 12-mm trocar. The trocars on the left are used by the surgeon, who stands on the left of the patient, facing the patient s right leg, while the assistant utilizes the trocars on the right. The patient is placed in a steep Trendelenburg position to help move the bowel out of the pelvis. The sigmoid colon is retracted superiorly and to the left with a fan retractor to facilitate exposure of the anterior sacral surface (Fig. 2). A sponge stick in the vagina is used by an assistant to push the vaginal vault to facilitate vaginal dissection. Presacral dissection The peritoneum over the sacral promontory is incised in the midline to the right of the sigmoid mesocolon using ultrasonic shears (Fig. 3). The prominent sacral promontory is identified, and the presacral fascia is exposed for fixation of the Gore-Tex patch (W.L. Gore and Associates, Flagstaff, AZ). Care is taken not to shear the presacral veins by excessive blunt dissection. During the surgeon s early experience, prior placement of external ureteral catheters can facilitate identification of the FIG. 1. Trocar positions. Large dot: 10/12 mm; small dot: 5 mm. FIG. 3. Incision of peritoneum overlying sacrum exposes presacral fascia.
4 622 SUNDARAM ET AL. ureters. Rolled gauze is placed in the presacral region to keep this area dry until fixation of the Gore-Tex patch is performed (Fig. 4). Vaginal vault dissection The apex of the vagina is identified and elevated using a lubricated intravaginal sponge stick, and the overlying peritoneum is incised transversely. The peritoneal surface is dissected off the vaginal apex while simultaneously mobilizing the bladder anteriorly and the rectum posteriorly. The vault apex is exposed about 3 cm anteriorly and posteriorly. An appropriate length of Gore-Tex patch is taken, usually 2 8 cm, one end of which is fixed to the vault of the vagina with interrupted 2-O Ethibond suture on a CT1 needle (Ethicon, Somerville, NJ). We now use polypropylene mesh. Culdoplasty Culdoplasty is performed by closing the cul-de-sac linearly (Halban s method) with 2-0 Vicryl sutures by opposing the remnants of the uterosacral ligaments using an Endostitch device (US Surgical, Norwalk, CT). Alternatively. the closure of the cul-de-sac can be achieved with a 2-0 polyglactin pursestring suture using the Moschcowitz technique. Care is taken not to injure the ureters during this procedure. Constriction of the colon must also be avoided. Patch fixation to sacrum The Gore-Tex patch is affixed to the presacral fascia and periosteum using a laparoscopic 5-mm Protack helical tacker (US Surgical), making sure there is no tension on the patch (Fig. 5). The excess patch is excised. The patch is retroperitonealized by bringing the peritoneal edges back together over the sacrum using 2-0 polyglactin sutures on an Endostitch device (Fig. 6). Postoperative care Postoperatively, the patient is given three doses of antibiotics intravenously, and an oral antibiotic is prescribed for 1 week. FIG. 5. Gore-Tex patch is sutured to vaginal vault and fixed to sacrum with helical tacker. The Foley catheter is removed on the first postoperative day, after which most patients are discharged from the hospital. The patient is advised to refrain from strenuous activity and heavy lifting for 6 weeks. RESULTS In our series, the mean patient age was 61 years (range years), and the average body mass index was 29 (range 22 34). The mean operative time was 196 minutes (range minutes), and the average blood loss was 65 ml (range ml). One patient underwent primary laparoscopic repair of an intraoperative bladder injury. One of the six patients with associated preoperative urinary symptoms got worse after surgery, requiring a TVT sling procedure for stress urinary incontinence. The average hospital stay was 2 days (range days), and the mean postoperative analgesic requirement (mor- FIG. 4. Rolled gauze overlying presacral fascia. Sponge stick inserted through vagina helps identify vaginal vault. FIG. 6. Gore-Tex patch has been peritonealized with continuous 2-0 polyglactin suture using Endostitch device. Lapra-Ty clip is visible at one end of suture line.
5 LAPAROSCOPIC SACROCOLPOPEXY FOR THE CORRECTION OF VAGINAL VAULT PROLAPSE 623 phine sulfate equivalent) was 7.3 mg (range 5 21 mg). The average time of return to normal activity was 1.5 weeks (range weeks). With a mean follow-up of 16 months (range 5 32 months), there was recurrence of prolapse in one patient that was repaired laparoscopically. ROLE IN UROLOGIC PRACTICE Laparoscopic sacrocolpopexy offers a new approach to vaginal vault prolapse, providing a good view of the anterior and posterior pelvic compartments to correct the problem with minimal morbidity. The open procedure requires a midline abdominal incision, abdominal packing, and bowel manipulation and has the potential for morbidity such as infection, wound separation or dehiscence, and ileus or bowel obstruction. 5 On the other hand, reported failures necessitating repeat operation with a long-term follow-up are few. 6,7 Addison and coworkers 6 observed 3 recurrences in 250 patients treated with abdominal sacrocolpopexy over a 20-year period, and Livengood and associates 7 reported only 1 failure following 143 procedures. Nezhat and colleagues 2 and Dorsey and Cundiff 8 reported the first cases of laparoscopic sacrocolpopexy in A synthetic material such as Gore-Tex was used for fixation of the vaginal vault to the sacral promontory. Y-shaped mesh for anterior and posterior fixation to the vaginal apex has been used. Cosson et al from France 9 reported on their experience with 77 patients who underwent laparoscopic sacral colpopexy. Subtotal laparoscopic hysterectomy and laparoscopic Burch colposuspension was performed in 60 and 74 patients, respectively. There were one rectal and two bladder injuries. Only five of these patients had prior hysterectomy. Open conversion was performed in six patients. Their mean follow-up was nearly 1 year, with three patients requiring reoperation: one for a thirddegree cystocele and two for recurrent stress incontinence. Fedele and coauthors 10 reported on their experience with 12 operations by the laparoscopic approach for posthysterectomy vaginal vault prolapse and reported no complications and no recurrence with a follow-up ranging from 9 to 28 months. CONCLUSION Laparoscopic sacrocolpopexy can be performed with minimal complications and morbidity. At least in the short term, the procedure appears to be an effective approach for the treatment of vaginal vault prolapse with minimal postoperative pain and morbidity. REFERENCES 1. Dunton JD, Mikuta J. Posthysterectomy vaginal vault prolapse. Postgrad Obstet Gynecol 1988;8: Nezhat CH, Nezhat C, Nezhat F. Laparoscopic sacral colpopexy for vaginal vault prolapse. Obstet Gynecol 1994;84: Timmons MC, Addison WA, Cavenar MG. Abdominal sacral colpopexy in 163 women with posthysterectomy vaginal vault prolapse and enterocele. J Reprod Med 1992;37: Arthur HG, Savage D. Uterine prolapse and prolapse of vaginal vault treated by sacral hysteropexy. J Obstet Gynaecol Br Emp 1957;64: Symmonds RE, Williams TJ, Lee RA, Webb MJ. Post-hysterectomy entereocele and vaginal vault prolapse. Am J Obstet Gynecol 1981;140: Addison WA, Livengood CH, Parker RT. Posthysterectomy vaginal vault prolapse with emphasis on management by transabdominal sacral colpopexy. Postgrad Obstet Gynecol 1988;8: Livengood CH, Addison WA. Failed abdominal sacral colpopexy: Observations and recommendations. Obstet Gynecol 1989;74: Dorsey JH and Cundiff G. Laparoscopic procedures for incontinence and prolapse. Curr Opin Obstet Gynecol 1994;6: Cosson M, Bogaert E, Narducci F, Querleu D, Crepin G. Laparoscopic sacral colpopexy: Short-term results and complications in 83 patients. J Gynecol Obstet Biol Reprod (Paris) 2000;8: Fedele L, Garsia S, Bianchi S, Albiero A, Dorta M. A new laparoscopic procedure for the correction of vaginal vault prolapse. J Urol 1998;159: Address reprint requests to: Chandru P. Sundaram, M.D., FRCS Dept. of Urology University of Indiana School of Medicine Indianapolis, IN EDITORIAL COMMENT sundaram@iupui.edu Pelvic vault prolapse can be an extremely distressing problem for the small percentage of women who suffer this condition after hysterectomy. While there is a paucity of reports in the literature with regard to the laparoscopic approach to sacrocolpopexy, the open counterpart has certainly demonstrated excellent long-term success rates. I concur with the authors that the laparoscopic approach affords excellent access to the pelvis and magnification of the surgical site, which facilitates this minimally invasive approach to the surgical repair. Abdominal and pelvic adhesions secondary to the prior gynecologic surgery may be a limiting factor in the laparoscopic access for these patients. However, often, the pneumoperitoneum, in conjunction with articulating laparoscopic scissors or the Harmonic Shears, can facilitate adhesiolysis and access to the pelvis. A variety of materials has been used to perform the sacrocolpopexy, and we have found Marlex mesh to be as successful as the Gore-Tex patch the authors describe. The key component of this surgical procedure is secure attachment of the chosen piece of material to the apex of the vaginal vault and then securing the cephalad aspect of the material to the presacral ligaments without any tension. This facilitates return of the vagina to its normal anatomic position. One aspect of the surgical procedure that has limited the enthusiasm for the laparoscopic approach has been the challenge of intracorporeal suturing and knot tying. However, as the authors have demonstrated in the description of their technique, the use of the helical tacking device reduces the difficulty of securing the mesh to the sacral ligaments. We have also incorporated several time-saving tricks in our technique of performing the laparoscopic sacrocolpopexy. These allow laparoscopic
6 624 suturing of both the vaginal and the sacral ends of the mesh and include use of a pre-formed loop at the end of the suture and the incorporation of the Lapra-Ty suture clips to complete the securing of the continuous suturing of both ends of the mesh. The recent introduction of the robot-assisted laparoscopic approach has further enhanced our ability to perform sacrocolpopexy with a 50% reduction of our operative time. It is essential that these patients be adequately assessed preoperatively for concomitant stress incontinence. Such incontinence can be addressed effectively at the same operative procedure. We have been incorporating the TVT procedure at the commencement of the operation to manage the stress incontinence and follow this with the laparoscopic sacrocolpopexy. It is important to perform the TVT procedure first, as the degree of elevation of the anterior vaginal vault as a result of the sacrocolpopexy may make access to the anterior vaginal wall difficult. Performing the TVT procedure initially facilitates this portion of the surgery and does not adversely affect the ability to complete the sacrocolpopexy. A formal posterior closure of the cul-de-sac can be performed in those patients with a significant SUNDARAM ET AL. rectocele. Even in patients without evidence of an enterocele or posterior prolapse, we routinely use a purse-string suture to close the posterior cul-de-sac with a Moschcowitz technique. This maneuver alone will isolate the mesh material from the abdominal contents. As the authors have demonstrated, laparoscopic sacrocolpopexy affords the patient with vaginal vault prolapse effective surgical management with minimal postoperative morbidity. While a randomized study comparing the open and laparoscopic approaches for sacrocolpopexy is unlikely to happen, I commend the authors on their report as an addition to the literature on this topic. I encourage them to continue accruing patients to their study population and to provide further long-term (5-year) follow-up with regard to this technique in the future. Elspeth M. McDougall, M.D. University of California Irvine Medical Center Orange, California
REPAIR OF LARGE CYSTOCELE
 REPAIR OF LARGE CYSTOCELE WITH RAZ SUSPENSION 17 VAGINAL INCISION AND DISSECTION Premarin cream application to the anterior vagina daily for 1 month before cystocele repair enriches the vasculature and
REPAIR OF LARGE CYSTOCELE WITH RAZ SUSPENSION 17 VAGINAL INCISION AND DISSECTION Premarin cream application to the anterior vagina daily for 1 month before cystocele repair enriches the vasculature and
Gynecology Dr. Sallama Lecture 3 Genital Prolapse
 Gynecology Dr. Sallama Lecture 3 Genital Prolapse Genital(utero-vaginal )prolapse is extremely common, with an estimated 11% of women undergoing at least one operation for this condition. Definition: A
Gynecology Dr. Sallama Lecture 3 Genital Prolapse Genital(utero-vaginal )prolapse is extremely common, with an estimated 11% of women undergoing at least one operation for this condition. Definition: A
Interventional procedures guidance Published: 28 June 2017 nice.org.uk/guidance/ipg583
 Sacrocolpopexy using mesh to repair vaginal vault prolapse Interventional procedures guidance Published: 28 June 2017 nice.org.uk/guidance/ipg583 Your responsibility This guidance represents the view of
Sacrocolpopexy using mesh to repair vaginal vault prolapse Interventional procedures guidance Published: 28 June 2017 nice.org.uk/guidance/ipg583 Your responsibility This guidance represents the view of
Robot Assisted Rectopexy
 1. Abdominal cavity approach 1A Trocars Introduce Introduce five trocars to gain access to the abdominal cavity (in da Vinci Si type; In Xi type the trocar placement may differ slightly). First the camera
1. Abdominal cavity approach 1A Trocars Introduce Introduce five trocars to gain access to the abdominal cavity (in da Vinci Si type; In Xi type the trocar placement may differ slightly). First the camera
RECTAL INJURY IN UROLOGIC SURGERY. Inadvertent rectal injury from a urologic procedure is often subtle but has serious postoperative consequences.
 RECTAL INJURY IN 27 UROLOGIC SURGERY Inadvertent rectal injury from a urologic procedure is often subtle but has serious postoperative consequences. With good mechanical bowel preparation plus antibiotic
RECTAL INJURY IN 27 UROLOGIC SURGERY Inadvertent rectal injury from a urologic procedure is often subtle but has serious postoperative consequences. With good mechanical bowel preparation plus antibiotic
By:Dr:ISHRAQ MOHAMMED
 By:Dr:ISHRAQ MOHAMMED Protrusion of an organ or structure beyond its normal confines. Prolapses are classified according to their location and the organs contained within them. 1-Anterior vaginal wall
By:Dr:ISHRAQ MOHAMMED Protrusion of an organ or structure beyond its normal confines. Prolapses are classified according to their location and the organs contained within them. 1-Anterior vaginal wall
CHAU KHAC TU M.D., Ph.D.
 CHAU KHAC TU M.D., Ph.D. Hue Central Hospital Vietnam LAPAROSCOPIC PROMONTOFIXATION FOR THE GENITAL PROLAPSE TREATMENT Chau Khac Tu MD.PhD. Hue central hospital CONTENT 3 1 INTRODUCTION 2 OBJECTIVE AND
CHAU KHAC TU M.D., Ph.D. Hue Central Hospital Vietnam LAPAROSCOPIC PROMONTOFIXATION FOR THE GENITAL PROLAPSE TREATMENT Chau Khac Tu MD.PhD. Hue central hospital CONTENT 3 1 INTRODUCTION 2 OBJECTIVE AND
Laparoscopic sacrocolpopexy: an observational study of functional and anatomical outcomes
 DOI 10.1007/s00192-010-1241-y ORIGINAL ARTICLE Laparoscopic sacrocolpopexy: an observational study of functional and anatomical outcomes Natalia Price & Alex Slack & Simon R. Jackson Received: 26 April
DOI 10.1007/s00192-010-1241-y ORIGINAL ARTICLE Laparoscopic sacrocolpopexy: an observational study of functional and anatomical outcomes Natalia Price & Alex Slack & Simon R. Jackson Received: 26 April
Traditional Anterior, Posterior, and Apical Compartment Repairs A Technique Based Review
 Traditional Anterior, Posterior, and Apical Compartment Repairs A Technique Based Review Sandip Vasavada, MD Center for Female Urology and Pelvic Reconstructive Surgery The Glickman Urological and Kidney
Traditional Anterior, Posterior, and Apical Compartment Repairs A Technique Based Review Sandip Vasavada, MD Center for Female Urology and Pelvic Reconstructive Surgery The Glickman Urological and Kidney
Stop Coping. Start Living. Talk to your doctor about pelvic organ prolapse and sacrocolpopexy
 Stop Coping. Start Living Talk to your doctor about pelvic organ prolapse and sacrocolpopexy Did you know? One in three women will suffer from a pelvic health condition in her lifetime. Four of the most
Stop Coping. Start Living Talk to your doctor about pelvic organ prolapse and sacrocolpopexy Did you know? One in three women will suffer from a pelvic health condition in her lifetime. Four of the most
A Laparoscopic-Assisted Extraperitoneal Bladder Neck Suspension: An Initial Experience
 Journal Of Laparoendoscopic Surgery Volume 4, Number 5, 1994 Mary Ann Liebert, Inc., Publishers A Laparoscopic-Assisted Extraperitoneal Bladder Neck Suspension: An Initial Experience E.D. RIZA, M.D.(1)
Journal Of Laparoendoscopic Surgery Volume 4, Number 5, 1994 Mary Ann Liebert, Inc., Publishers A Laparoscopic-Assisted Extraperitoneal Bladder Neck Suspension: An Initial Experience E.D. RIZA, M.D.(1)
PL Narducci Department of Obstetrics and Gynecology General Hospital San Giovanni Battista Foligno, ITALY
 NESA DAYS 2018 New European Surgical Academy Perugia, April 19-21, 2018 EXCELLENCE IN FEMALE SURGERY PROLAPSE RECONSTRUCTIVE SURGERY IN SEXUALLY ACTIVE WOMEN LAPAROSCOPIC ANTERIOR ABDOMINAL WALL COLPOPEXY
NESA DAYS 2018 New European Surgical Academy Perugia, April 19-21, 2018 EXCELLENCE IN FEMALE SURGERY PROLAPSE RECONSTRUCTIVE SURGERY IN SEXUALLY ACTIVE WOMEN LAPAROSCOPIC ANTERIOR ABDOMINAL WALL COLPOPEXY
W23: Approaches to pelvic organ prolapse surgery Workshop Chair: Philippe Zimmern, United States 21 October :00-12:00
 W23: Approaches to pelvic organ prolapse surgery Workshop Chair: Philippe Zimmern, United States 21 October 2014 09:00-12:00 Start End Topic Speakers 09:00 09:30 Goals of repair and anatomical principles
W23: Approaches to pelvic organ prolapse surgery Workshop Chair: Philippe Zimmern, United States 21 October 2014 09:00-12:00 Start End Topic Speakers 09:00 09:30 Goals of repair and anatomical principles
Vaginal McCall culdoplasty versus laparoscopic uterosacral plication to prophylactically address vaginal vault prolapse
 Vaginal McCall culdoplasty versus laparoscopic uterosacral to prophylactically address vaginal vault prolapse Niblock, K., Bailie, E., McCracken, G., & Johnston, K. (2017). Vaginal McCall culdoplasty versus
Vaginal McCall culdoplasty versus laparoscopic uterosacral to prophylactically address vaginal vault prolapse Niblock, K., Bailie, E., McCracken, G., & Johnston, K. (2017). Vaginal McCall culdoplasty versus
Robotic-Assisted Surgery in Urogynecology: Beyond Sacrocolpopexy
 Robotic-Assisted Surgery in Urogynecology: Beyond Sacrocolpopexy Marie Fidela R. Paraiso, M.D. Professor of Surgery Section Head, Urogynecology and Reconstructive Pelvic Surgery Cleveland, OH Disclosures
Robotic-Assisted Surgery in Urogynecology: Beyond Sacrocolpopexy Marie Fidela R. Paraiso, M.D. Professor of Surgery Section Head, Urogynecology and Reconstructive Pelvic Surgery Cleveland, OH Disclosures
SURGICAL. How to manage the cuff at vaginal hysterectomy. For personal use only. Copyright Dowden Health Media TECHNIQUES
 For mass reproduction, content licensing and permissions contact Dowden Health Media. How to manage the cuff at vaginal hysterectomy The high McCall culdoplasty and its modifications can prevent apical
For mass reproduction, content licensing and permissions contact Dowden Health Media. How to manage the cuff at vaginal hysterectomy The high McCall culdoplasty and its modifications can prevent apical
Laparoscopic Sacrocolpopexy with & without the Robot: Tips and Tricks for success and avoidance / management of complications
 Laparoscopic Sacrocolpopexy with & without the Robot: Tips and Tricks for success and avoidance / management of complications Course Faculty: Patrick Culligan, MD Peter Rosenblatt, MD What is a Sacrocolpopexy?
Laparoscopic Sacrocolpopexy with & without the Robot: Tips and Tricks for success and avoidance / management of complications Course Faculty: Patrick Culligan, MD Peter Rosenblatt, MD What is a Sacrocolpopexy?
This information is intended as an overview only
 This information is intended as an overview only Please refer to the INSTRUCTIONS FOR USE included with this device for indications, contraindications, warnings, precautions and other important information
This information is intended as an overview only Please refer to the INSTRUCTIONS FOR USE included with this device for indications, contraindications, warnings, precautions and other important information
Assessment of the durability of robot-assisted laparoscopic sacrocolpopexy for treatment of vaginal vault prolapse
 J Robotic Surg (2007) 1:163 168 DOI 10.1007/s11701-007-0028-8 ORIGINAL ARTICLE Assessment of the durability of robot-assisted laparoscopic sacrocolpopexy for treatment of vaginal vault prolapse Daniel
J Robotic Surg (2007) 1:163 168 DOI 10.1007/s11701-007-0028-8 ORIGINAL ARTICLE Assessment of the durability of robot-assisted laparoscopic sacrocolpopexy for treatment of vaginal vault prolapse Daniel
Step by step High uterosacral vaginal vault suspension to repair enterocele and apical prolapse
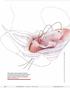 When performing high uterosacral suspension, it is possible to pass sutures through the coccygeus muscle-sacrospinous ligament complex (arrow) because a segment of the uterosacral ligament inserts into
When performing high uterosacral suspension, it is possible to pass sutures through the coccygeus muscle-sacrospinous ligament complex (arrow) because a segment of the uterosacral ligament inserts into
INGUINAL HERNIA REPAIR PROCEDURE GUIDE
 ROOM CONFIGURATION The following figure shows an overhead view of the recommended OR configuration for a da Vinci Inguinal Hernia Repair (Figure 1). NOTE: Configuration of the operating room suite is dependent
ROOM CONFIGURATION The following figure shows an overhead view of the recommended OR configuration for a da Vinci Inguinal Hernia Repair (Figure 1). NOTE: Configuration of the operating room suite is dependent
Pelvic Prolapse. A Patient Guide to Pelvic Floor Reconstruction
 Pelvic Prolapse A Patient Guide to Pelvic Floor Reconstruction Pelvic Prolapse When an organ becomes displaced, or slips down in the body, it is referred to as a prolapse. Your physician has diagnosed
Pelvic Prolapse A Patient Guide to Pelvic Floor Reconstruction Pelvic Prolapse When an organ becomes displaced, or slips down in the body, it is referred to as a prolapse. Your physician has diagnosed
Supracervical Robotic-Assisted Laparoscopic Sacrocolpopexy for Pelvic Organ Prolapse
 SCIENTIFIC PAPER Supracervical Robotic-Assisted Laparoscopic Sacrocolpopexy for Pelvic Organ Prolapse Aaron D. Benson, MD, Brandan A. Kramer, MD, Robert O. Wayment, MD, Bradley F. Schwartz, DO ABSTRACT
SCIENTIFIC PAPER Supracervical Robotic-Assisted Laparoscopic Sacrocolpopexy for Pelvic Organ Prolapse Aaron D. Benson, MD, Brandan A. Kramer, MD, Robert O. Wayment, MD, Bradley F. Schwartz, DO ABSTRACT
Colorectal procedure guide
 Colorectal procedure guide Illustrations by Lisa Clark Biodesign ADVANCED TISSUE REPAIR cookmedical.com 2 INDEX Anal fistula repair Using the Biodesign plug with no button.... 4 Anal fistula repair Using
Colorectal procedure guide Illustrations by Lisa Clark Biodesign ADVANCED TISSUE REPAIR cookmedical.com 2 INDEX Anal fistula repair Using the Biodesign plug with no button.... 4 Anal fistula repair Using
Determination of cell viability after laparoscopic tissue stapling in a porcine model
 Washington University School of Medicine Digital Commons@Becker Open Access Publications 2005 Determination of cell viability after laparoscopic tissue stapling in a porcine model Ramakrishna Venkatesh
Washington University School of Medicine Digital Commons@Becker Open Access Publications 2005 Determination of cell viability after laparoscopic tissue stapling in a porcine model Ramakrishna Venkatesh
Posterior intravaginal slingplasty for vault and uterovaginal prolapse: an initial experience
 Gynecol Surg (2006) 3: 88 92 DOI 10.1007/s10397-005-0168-7 ORIGINAL ARTICLE R. Oliver. C. Dasgupta. A. Coker Posterior intravaginal slingplasty for vault and uterovaginal prolapse: an initial experience
Gynecol Surg (2006) 3: 88 92 DOI 10.1007/s10397-005-0168-7 ORIGINAL ARTICLE R. Oliver. C. Dasgupta. A. Coker Posterior intravaginal slingplasty for vault and uterovaginal prolapse: an initial experience
Karanvir Virk M.D. Minimally Invasive & Pelvic Reconstructive Surgery 01/28/2015
 Karanvir Virk M.D. Minimally Invasive & Pelvic Reconstructive Surgery 01/28/2015 Disclosures I have none Objectives Identify the basic Anatomy and causes of Pelvic Organ Prolapse Examine office diagnosis
Karanvir Virk M.D. Minimally Invasive & Pelvic Reconstructive Surgery 01/28/2015 Disclosures I have none Objectives Identify the basic Anatomy and causes of Pelvic Organ Prolapse Examine office diagnosis
Blue Ridge Urogynecology
 Surgery for Stress Urinary Incontinence Surgery has proved to be a very effective treatment for stress incontinence. The best surgical procedures improve or cure the incontinence in 85 to 90 percent of
Surgery for Stress Urinary Incontinence Surgery has proved to be a very effective treatment for stress incontinence. The best surgical procedures improve or cure the incontinence in 85 to 90 percent of
Index. B Bladder, injury of, Bowel, injury of, , Brachytherapy, for cervical cancer, 357 Burns, electrosurgical,
 Perioperative Nursing Clinics 1 (2006) 375 379 Index Note: Page numbers of article titles are in boldface type. A Abdominal hysterectomy Acidosis, from insufflation, 323 Active electrode monitoring, in
Perioperative Nursing Clinics 1 (2006) 375 379 Index Note: Page numbers of article titles are in boldface type. A Abdominal hysterectomy Acidosis, from insufflation, 323 Active electrode monitoring, in
A New Technique for Performing a Laparoscopic Hysterectomy Using Microlaparoscopy: Microlaparoscopic Assisted Vaginal Hysterectomy (mlavh)
 A New Technique for Performing a Laparoscopic Hysterectomy Using Microlaparoscopy: Microlaparoscopic Assisted Vaginal Hysterectomy (mlavh) ABSTRACT In an effort to further decrease patient postoperative
A New Technique for Performing a Laparoscopic Hysterectomy Using Microlaparoscopy: Microlaparoscopic Assisted Vaginal Hysterectomy (mlavh) ABSTRACT In an effort to further decrease patient postoperative
Dr John Short. Obstetrician and Gynaecologist Christchurch Women s Hospital, Oxford Women's Health, Christchurch
 Dr John Short Obstetrician and Gynaecologist Christchurch Women s Hospital, Oxford Women's Health, Christchurch 8:30-9:25 WS #142: Peeling Back the Layers - The Pelvic Floor Uncovered 9:35-10:30 WS #152:
Dr John Short Obstetrician and Gynaecologist Christchurch Women s Hospital, Oxford Women's Health, Christchurch 8:30-9:25 WS #142: Peeling Back the Layers - The Pelvic Floor Uncovered 9:35-10:30 WS #152:
Female Urology. The Results of Grade IV Cystocele Repair Using Mesh. Introduction ZARGAR MA, EMAMI M*, ZARGAR K, JAMSHIDI M
 Urology Journal UNRC/IUA Vol. 1, No. 4, 263-267 Autumn 2004 Printed in IRAN Female Urology The Results of Grade IV Cystocele Repair Using Mesh ZARGAR MA, EMAMI M*, ZARGAR K, JAMSHIDI M Department of Urology,
Urology Journal UNRC/IUA Vol. 1, No. 4, 263-267 Autumn 2004 Printed in IRAN Female Urology The Results of Grade IV Cystocele Repair Using Mesh ZARGAR MA, EMAMI M*, ZARGAR K, JAMSHIDI M Department of Urology,
Prevention of Surgical Injuries in Gynecology
 in Gynecology John K. Chan, M.D. Division of Gynecologic Oncology Overview Review anatomy, etiology, intraoperative, postoperative management, prevention of injuries to: 1. Urinary tract 2. Gastrointestinal
in Gynecology John K. Chan, M.D. Division of Gynecologic Oncology Overview Review anatomy, etiology, intraoperative, postoperative management, prevention of injuries to: 1. Urinary tract 2. Gastrointestinal
International Federation of Gynecology and Obstetrics
 International Federation of Gynecology and Obstetrics COMMITTEE FOR UROGYNAECOLOGY AND PELVIC FLOOR MEMBER: TSUNG-HSIEN (CHARLES) SU, CHAIR (TAIWAN) DAVID RICHMOND, CO-CHAIR (UK) CHITTARANJAN PURANDARE,
International Federation of Gynecology and Obstetrics COMMITTEE FOR UROGYNAECOLOGY AND PELVIC FLOOR MEMBER: TSUNG-HSIEN (CHARLES) SU, CHAIR (TAIWAN) DAVID RICHMOND, CO-CHAIR (UK) CHITTARANJAN PURANDARE,
ROBOTIC MESH SACROCOLPOPEXY
 ROBOTIC MESH SACROCOLPOPEXY Philippe E. Zimmern, MD, FACS Professor of Urology Mesh sacrocolpopexy Background First described in 1962 by Lane Until then, treatment options were: Pessary Colpocleisis Vaginal
ROBOTIC MESH SACROCOLPOPEXY Philippe E. Zimmern, MD, FACS Professor of Urology Mesh sacrocolpopexy Background First described in 1962 by Lane Until then, treatment options were: Pessary Colpocleisis Vaginal
Surgical repair of vaginal wall prolapse using mesh
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Surgical repair of vaginal wall prolapse using mesh Vaginal wall prolapse happens when the normal support
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Surgical repair of vaginal wall prolapse using mesh Vaginal wall prolapse happens when the normal support
Desara TV and Desara Blue TV
 Desara TV and Desara Blue TV Sling for Female Stress Urinary Incontinence Instructions For Use D I Prescription Use only Do not reuse Sterilized using ethylene oxide Available Electronically M Manufactured
Desara TV and Desara Blue TV Sling for Female Stress Urinary Incontinence Instructions For Use D I Prescription Use only Do not reuse Sterilized using ethylene oxide Available Electronically M Manufactured
Desara and Desara Blue
 Desara and Desara Blue Sling for Female Stress Urinary Incontinence Instructions For Use D I Prescription Use only Do not reuse Sterilized using ethylene oxide M Manufactured by: Caldera Medical, Inc.
Desara and Desara Blue Sling for Female Stress Urinary Incontinence Instructions For Use D I Prescription Use only Do not reuse Sterilized using ethylene oxide M Manufactured by: Caldera Medical, Inc.
Paravaginal Repair: A Laparoscopic Approach
 44 Paravaginal Repair: A Laparoscopic Approach John R. Miklos and Robert Moore Atlanta Urogynecology Associates, Atlanta, Georgia, U.S.A. Neeraj Kohli Harvard University, Boston, Massachusetts, U.S.A.
44 Paravaginal Repair: A Laparoscopic Approach John R. Miklos and Robert Moore Atlanta Urogynecology Associates, Atlanta, Georgia, U.S.A. Neeraj Kohli Harvard University, Boston, Massachusetts, U.S.A.
LAPAROSCOPIC REPAIR OF PELVIC FLOOR
 LAPAROSCOPIC REPAIR OF PELVIC FLOOR Dr. R. K. Mishra Elements comprising the Pelvis Bones Ilium, ischium and pubis fusion Ligaments Muscles Obturator internis muscle Arcus tendineus levator ani or white
LAPAROSCOPIC REPAIR OF PELVIC FLOOR Dr. R. K. Mishra Elements comprising the Pelvis Bones Ilium, ischium and pubis fusion Ligaments Muscles Obturator internis muscle Arcus tendineus levator ani or white
Anatomical and functional results of McCall culdoplasty in the prevention of enteroceles and vaginal vault prolapse after vaginal hysterectomy
 Int Urogynecol J (2008) 19:1007 1011 DOI 10.1007/s00192-007-0549-8 ORIGINAL ARTICLE Anatomical and functional results of McCall culdoplasty in the prevention of enteroceles and vaginal vault prolapse after
Int Urogynecol J (2008) 19:1007 1011 DOI 10.1007/s00192-007-0549-8 ORIGINAL ARTICLE Anatomical and functional results of McCall culdoplasty in the prevention of enteroceles and vaginal vault prolapse after
Posterior Deep Endometriosis. What is the best approach? Posterior Deep Endometriosis. Should we perform a routine excision of the vagina??
 Posterior Deep Endometriosis What is the best approach? Dept Gyn Obst Polyclinique Hotel Dieu CHU Clermont Ferrand France Posterior Deep Endometriosis Organs involved - Peritoneum - Uterine cervix -Rectum
Posterior Deep Endometriosis What is the best approach? Dept Gyn Obst Polyclinique Hotel Dieu CHU Clermont Ferrand France Posterior Deep Endometriosis Organs involved - Peritoneum - Uterine cervix -Rectum
DISMEMBERED LAPAROSCOPIC PYELOPLASTY WITH ANTEGRADE PLACEMENT OF URETERAL STENT: SIMPLIFICATION OF THE TECHNIQUE
 Surgical Technique International Braz J Urol Official Journal of the Brazilian Society of Urology Vol. 28 (5): 439-445, September - October, 2002 DISMEMBERED LAPAROSCOPIC PYELOPLASTY WITH ANTEGRADE PLACEMENT
Surgical Technique International Braz J Urol Official Journal of the Brazilian Society of Urology Vol. 28 (5): 439-445, September - October, 2002 DISMEMBERED LAPAROSCOPIC PYELOPLASTY WITH ANTEGRADE PLACEMENT
PRACTICE BULLETIN Female Pelvic Medicine & Reconstructive Surgery Volume 23, Number 4, July/August 2017
 PRACTICE BULLETIN Number 176, April 2017 (Replaces Committee Opinion Number 513, December 2011) Pelvic Organ Prolapse Pelvic organ prolapse (POP) is a common, benign condition in women. For many women
PRACTICE BULLETIN Number 176, April 2017 (Replaces Committee Opinion Number 513, December 2011) Pelvic Organ Prolapse Pelvic organ prolapse (POP) is a common, benign condition in women. For many women
Stephen T Jeffery. University of Cape Town, South Africa
 Stephen T Jeffery University of Cape Town, South Africa I still think there s a role for mesh in Prolapse surgery Examples of my most recent mesh cases Case 1 62 yr old Sacrocolpopexy for vault prolapse
Stephen T Jeffery University of Cape Town, South Africa I still think there s a role for mesh in Prolapse surgery Examples of my most recent mesh cases Case 1 62 yr old Sacrocolpopexy for vault prolapse
Current status in pelvic organ prolapse surgery: an evidence based review
 Current status in pelvic organ prolapse surgery: an evidence based review Christian Falconer, MD, PhD Department of Obstetrics and Gynecology Danderyd University Hospital Stockholm, Sweden Finnish Society
Current status in pelvic organ prolapse surgery: an evidence based review Christian Falconer, MD, PhD Department of Obstetrics and Gynecology Danderyd University Hospital Stockholm, Sweden Finnish Society
Surgical treatment of urinary stress incontinence with tension free vaginal tape
 Surgical treatment of urinary stress incontinence with tension free vaginal tape Gynaecology department 01935 384 385 yeovilhospital.nhs.uk Many surgical operations are available for the treatment of
Surgical treatment of urinary stress incontinence with tension free vaginal tape Gynaecology department 01935 384 385 yeovilhospital.nhs.uk Many surgical operations are available for the treatment of
Laparoscopic Sacral ColpopexyApproach for Genito-Urinary Prolapse: Experience with 363 Cases
 European Urology European Urology 47 (2005) 230 236 Laparoscopic Sacral ColpopexyApproach for Genito-Urinary Prolapse: Experience with 363 Cases Francois Rozet a, *, Eric Mandron b, Carlos Arroyo a,1,
European Urology European Urology 47 (2005) 230 236 Laparoscopic Sacral ColpopexyApproach for Genito-Urinary Prolapse: Experience with 363 Cases Francois Rozet a, *, Eric Mandron b, Carlos Arroyo a,1,
Posterior Deep Endometriosis. What is the best approach? Dept Gyn Obst CHU Clermont Ferrand France
 Posterior Deep Endometriosis What is the best approach? Dept Gyn Obst CHU Clermont Ferrand France Posterior Deep Endometriosis Organs involved - Peritoneum - Uterine cervix - Rectum - Vagina Should we
Posterior Deep Endometriosis What is the best approach? Dept Gyn Obst CHU Clermont Ferrand France Posterior Deep Endometriosis Organs involved - Peritoneum - Uterine cervix - Rectum - Vagina Should we
Surgery for vaginal vault prolapse. Patient decision aid
 Surgery for vaginal vault prolapse Patient decision aid? i What is vaginal vault prolapse? Vaginal vault prolapse happens when the top of the vagina (the vault) slips from its normal position and sags
Surgery for vaginal vault prolapse Patient decision aid? i What is vaginal vault prolapse? Vaginal vault prolapse happens when the top of the vagina (the vault) slips from its normal position and sags
Robotic Ventral Rectopexy
 Robotic Ventral Rectopexy What is a robotic ventral rectopexy? The term rectopexy refers to an operation in which the rectum (the part of the bowel nearest the anus) is put back into its normal position
Robotic Ventral Rectopexy What is a robotic ventral rectopexy? The term rectopexy refers to an operation in which the rectum (the part of the bowel nearest the anus) is put back into its normal position
Laparoscopic Hysteropexy
 Page 1 of 10 Laparoscopic Hysteropexy Introduction This leaflet will provide information on uterine prolapse and laparoscopic hysteropexy. This procedure is performed for women who wish to have uterine
Page 1 of 10 Laparoscopic Hysteropexy Introduction This leaflet will provide information on uterine prolapse and laparoscopic hysteropexy. This procedure is performed for women who wish to have uterine
EndoFast Reliant System vs. Tension- free Mesh in a Sheep Model; three arm Comparative Study Assessing the Mechanical Pullout Force of Mesh Over Time
 EndoFast Reliant System vs. Tension- free Mesh in a Sheep Model; three arm Comparative Study Assessing the Mechanical Pullout Force of Mesh Over Time Menachem Alcalay,M.D, Urogynecology unit, Sheba Medical
EndoFast Reliant System vs. Tension- free Mesh in a Sheep Model; three arm Comparative Study Assessing the Mechanical Pullout Force of Mesh Over Time Menachem Alcalay,M.D, Urogynecology unit, Sheba Medical
Urethrolysis; When, Why & How. M Karram Professor of Ob/Gyn & Urology University of Cincinnati
 Urethrolysis; When, Why & How M Karram Professor of Ob/Gyn & Urology University of Cincinnati Anatomy Urethra may be fixed to the pubic bone with dense scar tissue Goal of urethrolysis is to completely
Urethrolysis; When, Why & How M Karram Professor of Ob/Gyn & Urology University of Cincinnati Anatomy Urethra may be fixed to the pubic bone with dense scar tissue Goal of urethrolysis is to completely
Considering Surgery for Vaginal or Uterine Prolapse? Learn why da Vinci Surgery may be your best treatment option.
 Considering Surgery for Vaginal or Uterine Prolapse? Learn why da Vinci Surgery may be your best treatment option. The Condition(s): Vaginal Prolapse, Uterine Prolapse Vaginal prolapse occurs when the
Considering Surgery for Vaginal or Uterine Prolapse? Learn why da Vinci Surgery may be your best treatment option. The Condition(s): Vaginal Prolapse, Uterine Prolapse Vaginal prolapse occurs when the
T h e C o m p l e t e Tr e a t m e n t o f P e l v i c F l o o r P r o l a p s e by Laparoscopy Technique, Tips and Tricks
 T h e C o m p l e t e Tr e a t m e n t o f P e l v i c F l o o r P r o l a p s e by Laparoscopy Technique, Tips and Tricks R Botchorishvili, A Wattiez, G Mage, M Canis, B Rabischong, K Jardon, C Rivoire,
T h e C o m p l e t e Tr e a t m e n t o f P e l v i c F l o o r P r o l a p s e by Laparoscopy Technique, Tips and Tricks R Botchorishvili, A Wattiez, G Mage, M Canis, B Rabischong, K Jardon, C Rivoire,
Prediction and prevention of stress urinary incontinence after prolapse surgery van der Ploeg, J.M.
 UvA-DARE (Digital Academic Repository) Prediction and prevention of stress urinary incontinence after prolapse surgery van der Ploeg, J.M. Link to publication Citation for published version (APA): van
UvA-DARE (Digital Academic Repository) Prediction and prevention of stress urinary incontinence after prolapse surgery van der Ploeg, J.M. Link to publication Citation for published version (APA): van
A Long-Term Treatment Outcome of Abdominal Sacrocolpopexy
 Original Article DOI 10.3349/ymj.2009.50.6.807 pissn: 0513-5796, eissn: 1976-2437 Yonsei Med J 50(6): 807-813, 2009 A Long-Term Treatment Outcome of Abdominal Sacrocolpopexy Myung Jae Jeon, 1 Yeo Jung
Original Article DOI 10.3349/ymj.2009.50.6.807 pissn: 0513-5796, eissn: 1976-2437 Yonsei Med J 50(6): 807-813, 2009 A Long-Term Treatment Outcome of Abdominal Sacrocolpopexy Myung Jae Jeon, 1 Yeo Jung
The accomplished gynecologic surgeon
 For mass reproduction, content licensing and permissions contact Dowden Health Media. SURGICAL TECHNIQUES THE RETROPERITONEAL SPACE Keeping vital structures out of harm s way Knowledge of the retroperitoneal
For mass reproduction, content licensing and permissions contact Dowden Health Media. SURGICAL TECHNIQUES THE RETROPERITONEAL SPACE Keeping vital structures out of harm s way Knowledge of the retroperitoneal
INJ. Transvaginal Cystocele Repair by Purse-String Technique Reinforced with Three Simple Sutures: Surgical Technique and Results.
 Original Article Int Neurourol J 2012;16:144-148 pissn 2093-4777 eissn 2093-6931 International Neurourology Journal Transvaginal Cystocele Repair by Purse-String Technique Reinforced with Three Simple
Original Article Int Neurourol J 2012;16:144-148 pissn 2093-4777 eissn 2093-6931 International Neurourology Journal Transvaginal Cystocele Repair by Purse-String Technique Reinforced with Three Simple
Pelvic Support Problems
 AP012, April 2010 ACOG publications are protected by copyright and all rights are reserved. ACOG publications may not be reproduced in any form or by any means without written permission from the copyright
AP012, April 2010 ACOG publications are protected by copyright and all rights are reserved. ACOG publications may not be reproduced in any form or by any means without written permission from the copyright
Technique Guide. Bard MK Hernia Repair. Featuring Modified Onflex Mesh SOFT TISSUE REPAIR. Anterior Approach to a Preperitoneal Inguinal Hernia Repair
 Bard MK Hernia Repair Featuring Modified Onflex Mesh Technique Guide Anterior Approach to a Preperitoneal Inguinal Hernia Repair SOFT TISSUE REPAIR Right Procedure. Right Product. Right Outcome. The opinions
Bard MK Hernia Repair Featuring Modified Onflex Mesh Technique Guide Anterior Approach to a Preperitoneal Inguinal Hernia Repair SOFT TISSUE REPAIR Right Procedure. Right Product. Right Outcome. The opinions
Procedure related complications and how to prevent them
 Procedure related complications and how to prevent them Rama Jayanthi, M.D. Section of Urology Nationwide Children s Hospital The Ohio State University Retroperitoneoscopic surgery Inadvertent peritoneal
Procedure related complications and how to prevent them Rama Jayanthi, M.D. Section of Urology Nationwide Children s Hospital The Ohio State University Retroperitoneoscopic surgery Inadvertent peritoneal
Research Article The Impact of Training Residents on the Outcome of Robotic-Assisted Sacrocolpopexy
 Minimally Invasive Surgery Volume 2012, Article ID 289342, 6 pages doi:10.1155/2012/289342 Research Article The Impact of Training Residents on the Outcome of Robotic-Assisted Sacrocolpopexy Mohamed A.
Minimally Invasive Surgery Volume 2012, Article ID 289342, 6 pages doi:10.1155/2012/289342 Research Article The Impact of Training Residents on the Outcome of Robotic-Assisted Sacrocolpopexy Mohamed A.
Understanding Pelvic Organ Prolapse. Stephanie Pickett, MD, MS Female Pelvic Medicine and Reconstructive Surgery
 Understanding Pelvic Organ Prolapse Stephanie Pickett, MD, MS Female Pelvic Medicine and Reconstructive Surgery Disclosures None I am the daughter of a physician assistant. Objectives List types of pelvic
Understanding Pelvic Organ Prolapse Stephanie Pickett, MD, MS Female Pelvic Medicine and Reconstructive Surgery Disclosures None I am the daughter of a physician assistant. Objectives List types of pelvic
Early View Article: Online published version of an accepted article before publication in the final form.
 : Online published version of an accepted article before publication in the final form. Journal Name: Journal of Case Reports and Images in Surgery doi: To be assigned Early view version published: November
: Online published version of an accepted article before publication in the final form. Journal Name: Journal of Case Reports and Images in Surgery doi: To be assigned Early view version published: November
Laparoscopic surgery for pelvic support defects
 ~ Laparoscopic surgery for pelvic support defects John R. Miklosa, Robert D. Mooreb and Neeraj Kohlia Reconstructive pelvic surgery for the treatment of vaginal prolapse continues to evolve as surgeons
~ Laparoscopic surgery for pelvic support defects John R. Miklosa, Robert D. Mooreb and Neeraj Kohlia Reconstructive pelvic surgery for the treatment of vaginal prolapse continues to evolve as surgeons
Robotic distal ureterectomy with psoas hitch and ureteroneocystostomy: Surgical technique and outcomes
 Asian Journal of Urology (2015) 2, 123e127 HOSTED BY Available online at www.sciencedirect.com ScienceDirect journal homepage: www.elsevier.com/locate/ajur CASE REPORT Robotic distal with psoas hitch and
Asian Journal of Urology (2015) 2, 123e127 HOSTED BY Available online at www.sciencedirect.com ScienceDirect journal homepage: www.elsevier.com/locate/ajur CASE REPORT Robotic distal with psoas hitch and
Sacrocolpopexy. Department of Gynaecology. Patient Information
 Sacrocolpopexy Department of Gynaecology 2 Patient Information What What is is a a sacrocolpopexy? This is an operation carried out to correct prolapse of the vaginal vault in patients who had a hysterectomy.
Sacrocolpopexy Department of Gynaecology 2 Patient Information What What is is a a sacrocolpopexy? This is an operation carried out to correct prolapse of the vaginal vault in patients who had a hysterectomy.
Gökmen Sukgen, 1 Esra SaygJlJ YJlmaz, 2 and Eralp BaGer Introduction. 2. Case Presentation
 Case Reports in Obstetrics and Gynecology Volume 2016, Article ID 2906596, 4 pages http://dx.doi.org/10.1155/2016/2906596 Case Report Vaginal Hysterectomy with Anterior Four-Arm Mesh Implant Technique
Case Reports in Obstetrics and Gynecology Volume 2016, Article ID 2906596, 4 pages http://dx.doi.org/10.1155/2016/2906596 Case Report Vaginal Hysterectomy with Anterior Four-Arm Mesh Implant Technique
Anus,Rectum and Colon
 JOURNAL OF THE Anus,Rectum and Colon http://journal-arc.jp CLINICAL RESEARCH Laparoscopic ventral rectopexy with sacrocolpopexy for coexisting pelvic organ prolapse and external rectal prolapse Yoshiyuki
JOURNAL OF THE Anus,Rectum and Colon http://journal-arc.jp CLINICAL RESEARCH Laparoscopic ventral rectopexy with sacrocolpopexy for coexisting pelvic organ prolapse and external rectal prolapse Yoshiyuki
Surgical treatments for vaginal apical prolapse
 Review Article Obstet Gynecol Sci 2016;59(4):253-260 http://dx.doi.org/10.5468/ogs.2016.59.4.253 pissn 2287-8572 eissn 2287-8580 Surgical treatments for vaginal apical prolapse Mi Kyung Kong, Sang Wook
Review Article Obstet Gynecol Sci 2016;59(4):253-260 http://dx.doi.org/10.5468/ogs.2016.59.4.253 pissn 2287-8572 eissn 2287-8580 Surgical treatments for vaginal apical prolapse Mi Kyung Kong, Sang Wook
Laparoscopic pectopexy: initial experience of single center with a new technique for apical prolapse surgery
 ORIGINAL ARTICLE Vol. 43 (5): 903-909, September - October, 2017 doi: 10.1590/S1677-5538.IBJU.2017.0070 Laparoscopic pectopexy: initial experience of single center with a new technique for apical surgery
ORIGINAL ARTICLE Vol. 43 (5): 903-909, September - October, 2017 doi: 10.1590/S1677-5538.IBJU.2017.0070 Laparoscopic pectopexy: initial experience of single center with a new technique for apical surgery
Laparoscopic hysteropexy
 Page 1 of 10 Laparoscopic hysteropexy Introduction This leaflet will provide information on uterine prolapse and laparoscopic hysteropexy. This procedure is performed for women who wish to have uterine
Page 1 of 10 Laparoscopic hysteropexy Introduction This leaflet will provide information on uterine prolapse and laparoscopic hysteropexy. This procedure is performed for women who wish to have uterine
STOMA SITING & PARASTOMAL HERNIA MANAGEMENT
 STOMA SITING & PARASTOMAL HERNIA MANAGEMENT Professor Hany S. Tawfik Head of the Department of Surgery & Chairman of Colorectal Surgery Unit Benha University Disclosure No financial affiliation to disclose
STOMA SITING & PARASTOMAL HERNIA MANAGEMENT Professor Hany S. Tawfik Head of the Department of Surgery & Chairman of Colorectal Surgery Unit Benha University Disclosure No financial affiliation to disclose
Management of Vaginal Prolapse
 Information for Patients Saint Mary s Hospital/Trafford General Hospital Uro-gynaecology Service Management of Vaginal Prolapse Before reading this leaflet you should read What is vaginal prolapse? If
Information for Patients Saint Mary s Hospital/Trafford General Hospital Uro-gynaecology Service Management of Vaginal Prolapse Before reading this leaflet you should read What is vaginal prolapse? If
Index. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Ablation in uterine leiomyoma management, 719 723 Adnexal masses diagnosis of, 664 667 imaging in, 664 665 laboratory studies in, 665
Index Note: Page numbers of article titles are in boldface type. A Ablation in uterine leiomyoma management, 719 723 Adnexal masses diagnosis of, 664 667 imaging in, 664 665 laboratory studies in, 665
Site-specific fascial defects in the diagnosis and surgical management of enterocele
 Site-specific fascial defects in the diagnosis and surgical management of enterocele John R. Miklos, MD,a Neeraj Kohli, MD,b Vincent Lucente, MD,c and William B. Safe, MDd Atlanta and Marietta, GeO1gia,
Site-specific fascial defects in the diagnosis and surgical management of enterocele John R. Miklos, MD,a Neeraj Kohli, MD,b Vincent Lucente, MD,c and William B. Safe, MDd Atlanta and Marietta, GeO1gia,
Clinical Study Initial Experience with Robotic Retropubic Urethropexy Compared to Open Retropubic Urethropexy
 Obstetrics and Gynecology International Volume 2013, Article ID 315680, 5 pages http://dx.doi.org/10.1155/2013/315680 Clinical Study Initial Experience with Retropubic Urethropexy Compared to Open Retropubic
Obstetrics and Gynecology International Volume 2013, Article ID 315680, 5 pages http://dx.doi.org/10.1155/2013/315680 Clinical Study Initial Experience with Retropubic Urethropexy Compared to Open Retropubic
Considering Surgery for Pelvic Prolapse? Learn about minimally invasive da Vinci Surgery
 Considering Surgery for Pelvic Prolapse? Learn about minimally invasive da Vinci Surgery The Surgery: Pelvic Prolapse Surgery If you have pelvic prolapse symptoms, your doctor may suggest medicine or lifestyle
Considering Surgery for Pelvic Prolapse? Learn about minimally invasive da Vinci Surgery The Surgery: Pelvic Prolapse Surgery If you have pelvic prolapse symptoms, your doctor may suggest medicine or lifestyle
With our aging population, the rate of pelvic
 Original Research Short-Term Outcomes of Robotic Sacrocolpopexy Compared With Abdominal Sacrocolpopexy Elizabeth J. Geller, MD, Nazema Y. Siddiqui, MD, Jennifer M. Wu, MD, MPH, and Anthony G. Visco, MD
Original Research Short-Term Outcomes of Robotic Sacrocolpopexy Compared With Abdominal Sacrocolpopexy Elizabeth J. Geller, MD, Nazema Y. Siddiqui, MD, Jennifer M. Wu, MD, MPH, and Anthony G. Visco, MD
ARTIFICIAL MESH REPAIR FOR TREATMENT OF PELVIC ORGAN PROLAPSE
 Pelvic Floor Unit / Department of Gynaecology Ward 17, Singleton Hospital, Sketty, Swansea, SA2 8QA 01792 205666 Secretary Direct Line: 01792 285688. Fax: 01792 285874 ARTIFICIAL MESH REPAIR FOR TREATMENT
Pelvic Floor Unit / Department of Gynaecology Ward 17, Singleton Hospital, Sketty, Swansea, SA2 8QA 01792 205666 Secretary Direct Line: 01792 285688. Fax: 01792 285874 ARTIFICIAL MESH REPAIR FOR TREATMENT
Sacrohysteropexy with synthetic mesh for the management of uterovaginal prolapse
 British Journal of Obstetrics and Gynaecology June 2001, Vol. 108, pp. 629±633 Sacrohysteropexy with synthetic mesh for the management of uterovaginal prolapse Elad Leron a, Stuart L. Stanton b, * Objective
British Journal of Obstetrics and Gynaecology June 2001, Vol. 108, pp. 629±633 Sacrohysteropexy with synthetic mesh for the management of uterovaginal prolapse Elad Leron a, Stuart L. Stanton b, * Objective
Prospective study of an ultra-lightweight polypropylene Y mesh for robotic sacrocolpopexy
 Int Urogynecol J (2013) 24:1371 1375 DOI 10.1007/s00192-012-2021-7 ORIGINAL ARTICLE Prospective study of an ultra-lightweight polypropylene Y mesh for robotic sacrocolpopexy Charbel G. Salamon & Christa
Int Urogynecol J (2013) 24:1371 1375 DOI 10.1007/s00192-012-2021-7 ORIGINAL ARTICLE Prospective study of an ultra-lightweight polypropylene Y mesh for robotic sacrocolpopexy Charbel G. Salamon & Christa
Long-Term Effectiveness of Uterosacral Colpopexy and Minimally Invasive Sacral Colpopexy for Treatment of Pelvic Organ Prolapse
 ORIGINAL ARTICLE Long-Term Effectiveness of Uterosacral Colpopexy and Minimally Invasive Sacral Colpopexy for Treatment of Pelvic Organ Prolapse Cecile A. Unger, MD, MPH, Matthew D. Barber, MD, MHS, Mark
ORIGINAL ARTICLE Long-Term Effectiveness of Uterosacral Colpopexy and Minimally Invasive Sacral Colpopexy for Treatment of Pelvic Organ Prolapse Cecile A. Unger, MD, MPH, Matthew D. Barber, MD, MHS, Mark
PROCEDURE EDUCATION LITERATURE AND CONSENT FORM SURGERY FOR UTEROVAGINAL PROLAPSE
 Premier Women s Health a division of MaternOhio Clinical Associates 3600 Olentangy River Rd, Ste 490, Columbus, OH 43215 Tel: 614-459-1000 Fax 614-459-1382 http://www.moca-obgyns.com/practice-premier/
Premier Women s Health a division of MaternOhio Clinical Associates 3600 Olentangy River Rd, Ste 490, Columbus, OH 43215 Tel: 614-459-1000 Fax 614-459-1382 http://www.moca-obgyns.com/practice-premier/
yechniques,!nd Instrumentation
 yechniques,!nd Instrumentation l FERTILITY AND STERILITY Copyright 1996 American Society for Reproductive Medicine Vol. 6, No.1, January 1996 Printed on acid-free paper in U. S. A Laparoscopically assisted
yechniques,!nd Instrumentation l FERTILITY AND STERILITY Copyright 1996 American Society for Reproductive Medicine Vol. 6, No.1, January 1996 Printed on acid-free paper in U. S. A Laparoscopically assisted
FIG The inferior and posterior peritoneal reflection is easily
 PSOAS HITCH, BOARI FLAP, AND COMBINATION OF PSOAS 7 HITCH AND BOARI FLAP The psoas hitch procedure, Boari flap, and transureteroureterostomy are useful operative procedures for reestablishing continuity
PSOAS HITCH, BOARI FLAP, AND COMBINATION OF PSOAS 7 HITCH AND BOARI FLAP The psoas hitch procedure, Boari flap, and transureteroureterostomy are useful operative procedures for reestablishing continuity
Innovations in mesh kit technology for vaginal wall prolapse
 Available at www.obgmanagement.com s u p p l e m e n t t o This supplement is supported by American Medical Systems, Inc., and has been peer reviewed by the editors of OBG Management. J a n u a r y 2 0
Available at www.obgmanagement.com s u p p l e m e n t t o This supplement is supported by American Medical Systems, Inc., and has been peer reviewed by the editors of OBG Management. J a n u a r y 2 0
Pelvic Organ Prolapse. Natural Solutions
 Pelvic Organ Prolapse Natural Solutions Bringing your body back to its natural state There is a very common problem affecting millions of women. Many women are too embarrassed to talk to their physicians
Pelvic Organ Prolapse Natural Solutions Bringing your body back to its natural state There is a very common problem affecting millions of women. Many women are too embarrassed to talk to their physicians
Avoiding Mesh Disasters: Tips and Tricks for Success and Handling Complications
 Avoiding Mesh Disasters: Tips and Tricks for Success and Handling Complications Karyn S. Eilber, M.D. Cedars-Sinai FPMRS Associate Professor, Cedars-Sinai Dept of Surgery Associate Director, Urology Residency
Avoiding Mesh Disasters: Tips and Tricks for Success and Handling Complications Karyn S. Eilber, M.D. Cedars-Sinai FPMRS Associate Professor, Cedars-Sinai Dept of Surgery Associate Director, Urology Residency
9/24/2015. Pelvic Floor Disorders. Agenda. What is the Pelvic Floor? Pelvic Floor Problems
 Management of Pelvic Floor Disorders Doctor, I don t want THAT mesh! Agenda What are pelvic floor disorders (PFDs)? What are the treatment options? Expectant. Conservative. Surgical. How and when are grafts
Management of Pelvic Floor Disorders Doctor, I don t want THAT mesh! Agenda What are pelvic floor disorders (PFDs)? What are the treatment options? Expectant. Conservative. Surgical. How and when are grafts
1) What conditions is vaginal mesh used to commonly treat? Vaginal mesh is used to treat two different health issues in women:
 Vaginal Mesh Frequently Asked Questions 1) What conditions is vaginal mesh used to commonly treat? Vaginal mesh is used to treat two different health issues in women: a) stress urinary incontinence (SUI)
Vaginal Mesh Frequently Asked Questions 1) What conditions is vaginal mesh used to commonly treat? Vaginal mesh is used to treat two different health issues in women: a) stress urinary incontinence (SUI)
Desara Blue OV D I. Sling for Female Stress Urinary Incontinence. Instructions For Use
 Desara Blue OV Sling for Female Stress Urinary Incontinence Instructions For Use D I Prescription Use only Do not reuse Sterilized using ethylene oxide M Manufactured by: Caldera Medical, Inc. 5171 Clareton
Desara Blue OV Sling for Female Stress Urinary Incontinence Instructions For Use D I Prescription Use only Do not reuse Sterilized using ethylene oxide M Manufactured by: Caldera Medical, Inc. 5171 Clareton
Protective effect of suburethral slings on postoperative cystocele recurrence after reconstructive pelvic operation
 Protective effect of suburethral slings on postoperative cystocele recurrence after reconstructive pelvic operation Roger P. Goldberg, MD, MPH, Sumana Koduri, MD, Robert W. Lobel, MD, Patrick J. Culligan,
Protective effect of suburethral slings on postoperative cystocele recurrence after reconstructive pelvic operation Roger P. Goldberg, MD, MPH, Sumana Koduri, MD, Robert W. Lobel, MD, Patrick J. Culligan,
12/1/13. What are Pelvic Floor Disorders? What is the Pelvic Floor? Facts. Prevalence of Urinary InconOnence. What s New in Pelvic Floor Disorders?
 What are Pelvic Floor Disorders? Urinary Control Problems - InconOnence or leakage of urine Prolapse of pelvic organs - Vagina, bladder, rectum What s New in Pelvic Floor Disorders? Kimberly Kenton MD,
What are Pelvic Floor Disorders? Urinary Control Problems - InconOnence or leakage of urine Prolapse of pelvic organs - Vagina, bladder, rectum What s New in Pelvic Floor Disorders? Kimberly Kenton MD,
Laparoscopic total mesorectal excision (TME) with electric hook for rectal cancer
 Technical Note Page 1 of 8 Laparoscopic total mesorectal excision (TME) with electric hook for rectal cancer Gong Chen, Rong-Xin Zhang, Zhi-Tao Xiao Department of Colorectal Surgery, Sun Yat-sen University
Technical Note Page 1 of 8 Laparoscopic total mesorectal excision (TME) with electric hook for rectal cancer Gong Chen, Rong-Xin Zhang, Zhi-Tao Xiao Department of Colorectal Surgery, Sun Yat-sen University
Las Vegas Urogynecology
 Las Vegas Urogynecology 7500 Smoke Ranch Road - #200 Las Vegas, NV 89128 Telephone: (702) 233-0727 Fax: (702) 233-4799 Physician's Surgical Procedure Disclosure and Patient s Consent TO THE PATIENT: You
Las Vegas Urogynecology 7500 Smoke Ranch Road - #200 Las Vegas, NV 89128 Telephone: (702) 233-0727 Fax: (702) 233-4799 Physician's Surgical Procedure Disclosure and Patient s Consent TO THE PATIENT: You
Subjective and objective results 1 year after robotic sacrocolpopexy using a lightweight Y-mesh
 DOI 10.1007/s00192-013-2265-x ORIGINAL ARTICLE Subjective and objective results 1 year after robotic sacrocolpopexy using a lightweight Y-mesh Patrick J. Culligan & Emil Gurshumov & Christa Lewis & Jennifer
DOI 10.1007/s00192-013-2265-x ORIGINAL ARTICLE Subjective and objective results 1 year after robotic sacrocolpopexy using a lightweight Y-mesh Patrick J. Culligan & Emil Gurshumov & Christa Lewis & Jennifer
Hysterectomy. What is a hysterectomy? Why is hysterectomy done? Are there alternatives to hysterectomy?
 301.681.3400 OBGYNCWC.COM What is a hysterectomy? Hysterectomy Hysterectomy is surgery to remove the uterus. It is a very common type of surgery for women in the United States. Removing your uterus means
301.681.3400 OBGYNCWC.COM What is a hysterectomy? Hysterectomy Hysterectomy is surgery to remove the uterus. It is a very common type of surgery for women in the United States. Removing your uterus means
