Assessment of the durability of robot-assisted laparoscopic sacrocolpopexy for treatment of vaginal vault prolapse
|
|
|
- Paul Houston
- 5 years ago
- Views:
Transcription
1 J Robotic Surg (2007) 1: DOI /s ORIGINAL ARTICLE Assessment of the durability of robot-assisted laparoscopic sacrocolpopexy for treatment of vaginal vault prolapse Daniel S. Elliott Sameer A. Siddiqui George K. Chow Received: 1 November 2006 / Accepted: 24 May 2007 / Published online: 19 June 2007 Springer London 2007 Abstract Transabdominal sacrocolpopexy has been shown, in multiple long-term studies of its success and durability, to be the dewnitive treatment option for posthysterectomy vaginal vault prolapse. It is, however, associated with greater morbidity than vaginal repair. We describe a minimally invasive technique for vaginal vault prolapse repair and present our experience with a minimum of one-year follow-up. The surgical technique involves Wve laparoscopic ports three for the da Vinci robot and two for the assistant. After appropriate dissection a polypropylene mesh is attached to the sacral promontory and to the vaginal apex by use of Gore-Tex sutures. The mesh material is then covered by the peritoneum. Patient analysis focused on complications, urinary continence, patient satisfaction, and morbidity, with a minimum of 12 months follow-up. Forty-two patients with post-hysterectomy vaginal vault prolapse underwent robot-assisted laparoscopic sacrocolpopexy at our institute and 35 have a minimum of 12 months follow-up, with a mean follow-up of 36 months (range 12 48) in the group. Mean age was 67 (47 83) years and mean operating time was 3.1 ( ) h for the entire cohort. All but one patient were discharged home on postoperative day one; one patient left on postoperative day two. One developed recurrent grade three rectocele, one had recurrent vault prolapse, and two suvered from vaginal extrusion of mesh. All patients were satiswed with their outcome. The robot-assisted laparoscopic sacrocolpopexy is a minimally invasive technique for vaginal vault prolapse repair, combining the advantages of open sacrocolpopexy D. S. Elliott (&) S. A. Siddiqui G. K. Chow Department of Urology, Section of Female Urology and Laparoscopy, Mayo Clinic, 200 First Street S.W., Rochester, MN 55905, USA Elliott.daniel@mayo.edu with the reduced morbidity of laparoscopy. We observed reduced hospital stay, low occurrence of complications, and high patient satisfaction, with a minimum of 1-year followup. Most importantly, the long-term results of the robotic repair are similar to those of open repair, but with signiwcantly less morbidity. Keywords Robotics Laparoscopy Sacrocolpopexy Vaginal vault prolapse Introduction More than one in nine women will undergo a hysterectomy and up to 10% of these will need surgical repair for treatment of a symptomatic vaginal prolapse [1, 2]. The search for the ideal repair with the best combination of eycacy, safety, and durability for treatment of vaginal vault prolapse is an ongoing process, as evidenced by the multiple surgical approaches to this problem. Clearly, no surgical approach is ideal for every patient. As known risk factors for prolapse, for example age, obesity, and hysterectomy, continue to increase in the United States, however, so does the search for better means to repair vaginal vault prolapse [2 4]. In multiple studies transabdominal sacrocolpopexy has been shown to have the highest long-term success for durable repair of severe vault prolapse (93 100%) [5 11]. In addition to high success and durable results, other advantages of the sacrocolpopexy approach with use of synthetic material to repair vault prolapse can be summarized as follows: 1. Support of the vaginal vault by the anterior surface of the sacrum preserves the normal axis of the vagina.
2 164 J Robotic Surg (2007) 1: Maximum vaginal depth is preserved, which is important to patients who desire continued sexual activity and to patients with an already foreshortened vagina from previous surgery. 3. Use of synthetic suspensory material can provide a source of strength in patients where the native tissue with prolapse is weak [5]. Young patients and those with an active life-style are usually ideal candidates for the open procedures. Other important indications are concurrent medical conditions such as chronic cough, COPD, and asthma, which place chronic and repeated increased intra-abdominal pressure on the repair. Unfortunately, because of the morbidity of the open transabdominal procedure, many patients are unable to tolerate the surgery and are, therefore, managed via a transvaginal approach or with more conservative therapies, for example expectant management, pessary, or even colpocleisis. Clearly, the objectives of any surgical repair of vaginal vault prolapse should include restoration of proper anatomy, maintenance of function (sexual, bowel, and urinary), and durability. Surgical approaches to correct the prolapse include either vaginal or abdominal approach or a combination. The main advantage of the vaginal approach has historically been reduced morbidity, including shorter hospitalization and convalescence [12, 13]. Unfortunately, the long-term success of transvaginal repairs is consistently lower than for abdominal sacrocolpopexy [14]. In an evort to balance the benewt of open sacrocolpopexy with the advantage of vaginal repair, many attempts have been made to treat vault prolapse by laparoscopic sacrocolpopexy [15 18]. Unfortunately, technical diyculties and the potentially signiwcant increase in operating time has greatly limited its widespread use. Recent advances in robotic surgery have helped to address the limitations of laparoscopy. Robotics provides technical features such as threedimensional vision, increased robotic instrument maneuverability, and Wltering of physiological tremor [19]. These factors provide an ergonomic environment for the surgeon and simplify complex laparoscopic tasks. We describe the technique of robot-assisted laparoscopic sacrocolpopexy using a polypropylene graft. Preliminary results of our approach have been reported elsewhere [20, 21]. Our objectives in this study were twofold: 1. To analyze the long-term durability of robot-assisted laparoscopic sacrocolpopexy on the basis of postoperative physical examination. 2. To determine the morbidity (postoperative pain, complications, and length of hospital stay) of the procedure compared to that associated with transabdominal procedures. Materials and methods After Institutional Review Board approval, 42 consecutive patients with post-hysterectomy vaginal vault prolapse were treated by robot-assisted laparoscopic sacrocolpopexy at the Mayo Clinic, Department of Urology, starting in September To meet selection criteria patient had to have a Grade 4/4 Baden Walker apical prolapse. Patients with multiple previous abdominal surgery or multiple other vaginal defects were excluded from the procedure. All patients were evaluated preoperatively with a history, physical examination, and post void residual check. Surgical options and informed consent were obtained in the standard fashion. The surgical procedure was conducted by a team comprising a fellowship-trained laparoscopic surgeon and a female urologist. Surgical technique The davinci robot is an integrated computer-based system consisting of two interactive robotic arms, a camera arm, and a remote control with three-dimensional vision capability. It uses instruments with 6 of freedom, providing the same Xexibility as the human wrist. The working robotic arms are attached to reusable 8-mm trocars and the camera is placed through a standard 12 mm laparoscopic port. For optimum collision-free robot function, the angle created by the camera port and each working robotic port should be obtuse and the distance between the ports at least one handbreadth. In robotic surgery the motions of the surgeon at the remote-control unit are replicated by the robotic arms placed within the patient. During robotic surgery an assistant surgeon is scrubbed at the operating table. The assistant performs a variety of important robot-related tasks including alignment and exchange of instruments on the robotic arms. The assistant also performs operative maneuvers with conventional instruments, including tissue countertraction, hemostasis, hemoclip application, suction, and assistance during suturing. For the procedure the patient is placed on the operating table in the dorsal lithotomy position. After general anesthesia is established a nasogastric tube is placed and both arms are tucked beside the torso. The patient is prepped from the nipples to proximal thigh including the vagina. After abdominal insuzation using a Veress needle, we place a periumbilical Visiport optical trocar (AutoSuture, Norwalk, CT, USA) under direct vision to avoid visceral or vascular injury. Two standard laparoscopic ports for retraction are next introduced under direct vision one 10-mm port right subcostal lateral to the rectus and one 5 mm port one hands-breadth inferior-laterally (Fig. 1). Next, two 8 mm robotic ports are placed lateral to the rectus two Wngerbreadths superior to the iliac crest.
3 J Robotic Surg (2007) 1: Fig. 1 Standard laparoscopic port placement for the robot-assisted laparoscopic sacrocolpopexy. The laparoscopic ports are the 10 mm right subcostal port and the 5 mm port inferior laterally. The robotic ports are the paraumbilical camera port and the two 8-mm working ports lateral to the rectus muscle superior to the iliac crest Using standard laparoscopy, a retracting suture is placed through the sigmoid tenia to help in exposing the sacral promontory. The bladder is then dissected from the anterior vaginal wall using forceps and cautery scissors. A customized hand-held vaginal retractor manufactured at the Mayo Clinic (Fig. 2) is used to facilitate the dissection, which should be a relatively bloodless plane. Posteriorly, the peritoneal rexection is then incised to mobilize the vagina. Rectovaginal dissection is greatly facilitated by the vaginal retractor. Both of these dissections should be performed as distal (toward the introitus) as possible to maximize the support given by the Y-graft. After vaginal mobilization the sacral dissection is accomplished with avoidance of the sacral venous complexes. When the periosteum is exposed, the polypropylene Y-graft (IntePro American Medical Systems, Minnetonka, MN,USA) (Fig. 3) is brought into the Weld through the 10 mm port. In our experience the aforementioned steps are usually accomplished within min. The robot is then docked with the base positioned at the foot of the bed. The robot is used to facilitate and greatly reduce the operating time needed for suturing of the graft to the vagina and the sacrum. The Y-graft is robotically sutured using 1.0 Gore-Tex. The 30 lens and vaginal retractor maximize exposure for placement of the sutures. We have found placing the more diycult posterior sutures Wrst followed by suturing the anterior portion of the Y-graft reduces the diyculty of the process. The tail of the graft is then sutured to the sacral promontory in an interrupted fashion with careful attention to avoiding tension on the vagina. Usually, three to Wve 1.0 Gore-Tex sutures are used to adequately Wx the mesh to the sacrum. It is our preference to perform a standard Halban s culdoplasty with plication of the uterosacral ligaments at this time. The posterior peritoneum is then closed to completely retroperitonealize the graft [20, 21]. Postoperatively, pain is managed with scheduled Toradol mg every 6 h. Antibiotics are continued for two days postoperatively. Diet is advanced immediately and the patient is encouraged to ambulate on the evening of the procedure. All patients were discharged home on three months of vaginal estrogen postoperative, irrespective of preoperative estrogen status. The patients were followed with routine clinic visits and physical examination every three months for year. Fig. 2 The hand-held vaginal retractor (patent pending) used to facilitate dissection between the bladder and vagina Fig. 3 The polypropylene Y-graft is used to tack the vaginal vault to the sacral promontory
4 166 J Robotic Surg (2007) 1: Results At our institute we have performed robot-assisted laparoscopic sacrocolpopexy on 42 patients for treatment of grade 4/4 Baden Walker, symptomatic vaginal vault prolapse. Mean age is 67 (47 83) years. Thirty-Wve of these patients have met the minimum requirement of at least one-year follow-up (mean follow-up 24 months, range months). Mean total operating time was 3.1 ( ) hours. Figure 4 summarizes the operating time. Initially, the skinto-skin time was 4.75 h. With experience, however, and use of several diverent time-saving steps we are now routinely completing the procedure in less than 2.5 h. Of the 42 patients 19 had procedures less than 3 h and 5 had procedures less than 2.5 h. Twenty-six (61%) of the patients underwent a concurrent anti-incontinence procedure at the time of prolapse repair. These procedures included one cadaveric pubovaginal sling, twenty-two synthetic pubovaginal slings, and four transobturator slings. The anti-incontinence procedure was performed concurrently with the sacrocolpopexy and did not, therefore, lengthen the operating time. Two patients were converted to an open procedure secondary to unfavorable anatomy. In both of these patients the bladder was densely adherent to the vagina from a previous anterior colporrhaphy and laparoscopic dissection was not possible. The open procedures were completed without diyculty. All but one patient treated with the robotic sacrocolpopexy were discharged from the hospital after an overnight stay; one patient left on postoperative day two. All patients were dismissed on oral pain medication. Ten patients reported they only required non-steroidal Hours Procedure Time Case Number Fig. 4 Comparative operating time of robot-assisted laparoscopic sacrocolpopexy anti-inxammatory medication for control of their pain. One patient had persistent vaginal bleeding for 2 days post-operation, a complication related to the anti-incontinence portion of the procedure, because all bleeding was from the vaginal incision site. Although her hemoglobin remained stable with no further sequelae, this did require her to stay an extra night in the hospital. All patients treated with the robotic sacrocolpopexy reported being satiswed with the outcome of their surgery and 41/42 would recommend it to a friend. The one patient who did not recommend the procedure was the one converted to an open procedure. Complications Immediate postoperative complication Complications were limited to mild port site infections in two patients, which resolved with oral antibiotic therapy. Long-term complications With a mean follow up of 36 months (range 12 48), 34/35 (97%) have had a successful repair of their apical prolapse, on the basis of visual speculum examination one year postoperation. Examinations were performed by one of the authors (DSE). One patient, seven months after surgery, developed a recurrent vault prolapse. We elected to treat her recurrence with a transabdominal sacrocolpopexy. At the time of re-operation it was found the mesh was Wrmly attached to the sacrum but had completely separated from the vagina. Sutures were still attached to the mesh indicating the sutures had pulled through the vaginal mucosa. This was the Wfth patient in our series leading us to adjust our suturing technique by adding two to four more sutures attaching the mesh to the vagina. Since this adjustment we have had no further recurrences, including those with less than one-year follow-up. Another patient developed a recurrent grade 3/4 Baden Walker rectocele, without evidence of anterior or apical prolapse. This was the second patient in our series. The rectocele developed nine months after the sacrocolpopexy and was treated with an outpatient posterior colporrhaphy. It is now 36 months since the patient s posterior colporrhaphy and 47 months since sacrocolpopexy and she has not experienced any further recurrence of prolapse. As a result of this case we modiwed our robotic repair by placing the posterior leaf of the Y- graft to cover the entire vaginal length. Great evort is taken to place the mesh on the posterior aspect of the vagina as close to the level of the introitus as possible. Since this modiwcation no patient in our series has experienced prolapse recurrence.
5 J Robotic Surg (2007) 1: Two patients developed a small (1 cm 1 cm) vaginal extrusion of the mesh at the level of the vaginal cuv. Each extrusion developed at 6 months after the procedure. The extrusion was managed as an outpatient with transvaginal excision of the mesh and primary closure. None experienced recurrence of their prolapse. These two patients were among our initial eight patients treated. We surmise that because all patients were treated with postoperative vaginal estrogen, overly aggressive dissection of the bladder ov the vagina most probably contributed to this complication. Since modifying our dissection technique by avoiding excessive tension with our vaginal retractor and avoiding dissecting the vagina too thinly, no further patient has experienced this complication. SigniWcant postoperative incontinence (>1 pad/day) was experienced by two patients. Discussion The transabdominal sacrocolpopexy is a durable and evective treatment of post-hysterectomy vaginal vault prolapse. Not every patient is a candidate for this procedure, however, because of age, concurrent medical conditions, or concerns about postoperative recovery time. We feel the robot-assisted laparoscopic sacrocolpopexy accomplishes a repair identical with that of the open transabdominal technique. The morbidity associated with the open procedure is greatly reduced and the hospital stay has been reduced from 2 to 5 days with the open procedure to 1 day with the laparoscopic repair [22]. Also, on the basis of a minimum of one-year follow-up (mean 36 months), our results are as durable as the long-term results of the open procedure. Potentially, many more women will be overed the strongest repair for prolapse while still minimizing morbidity. Relative contraindications would be the same for most laparoscopic procedures including patients with prior abdominal surgeries and those with morbid obesity. Clearly, longer follow-up is needed; the robot-assisted laparoscopic sacrocolpopexy described in this report may, however, be an ideal approach to surgical repair of vaginal vault prolapse. Last, it must be stressed that we take great measures to perform the robot-assisted laparoscopic sacrocolpopexy to mimic the classic repair of the open transabdominal sacrocolpopexy including the Halban s culdoplasty. Recent reports have described laparoscopic sacrocolpopexy but on close review it becomes evident that even though highly skilled laparoscopic techniques were utilized, unfortunately, the basic principles of prolapse repair were not followed. Caution must be taken, because vaginal vault prolapse repair is not just a procedure of laparoscopic skills. We do recognize some limitations of this study. It is a single surgical team, single institute experience and therefore the exact results may not be translatable to other institutes. Because this is a newly developed technique, time will be required to determine other institutes success rates. This study was also of a relatively small cohort of patients. Despite these limitations, the study provides supporting evidence for durable long-term success and minimum complications of this minimally invasive procedure for treatment of pelvic organ prolapse. Conclusion We report the largest single institute series of robot-assisted laparoscopic sacrocolpopexy for treatment of high-grade vaginal vault prolapse. This minimally invasive technique provides the durable repair benewts of the open procedure with the minimal morbidity associated with laparoscopic surgery. Our series was characterized by a short inpatient hospital stay, minimal recurrence and conversion rates, minimal complications, and high overall patient satisfaction. The initial benewts associated with this novel procedure are promising and we expect more widespread use of robot-assisted laparoscopic sacrocolpopexy in the future. Acknowledgments Authorship and contribution to this manuscript is limited to the three authors indicated. There was neither outside funding nor technical assistance with the production of this manuscript. References 1. Marchionni M, Bracco GL, Checcucci V, Carabaneanu A, Coccia EM, Mecacci F et al (1999) True incidence of vaginal vault prolapse. Thirteen years of experience. J Reprod Med 44: Olsen A, Smith V, Bergstrom J, Colling J, Clark A (1997) Epidemiology of surgically managed pelvic organ prolapse and urinary incontinence. Obstet Gynecol 89: Dwyer PL, Lee ETC, Hay DM (1988) Obesity and urinary incontinence in women. Br J Obstet Gynaecol 95:91 4. Virtanen HS, Makinen JI (1993) Retrospective analysis of 711 patients operated on for pelvic relaxation in Int J Gynecol Obstet 42: Addison WA, Timmons MC (1993) Abdominal approach to vaginal eversion. Clin Obstet Gynecol 36: Timmons MC, Addison WA, Addison SB, Cavenar MG (1992) Abdominal sacral colpopexy in 163 women with posthysterectomy vaginal vault prolapse and enterocele. J Repro Med 37: CundiV GW, Harris RL, Coates K, Low VHS, Bump RC, Addison WA (1997) Abdominal sacral colpoperineopexy: a new approach for correction of posterior compartment defects and perineal descent associated with vaginal vault prolapse. Am J Obstet Gynecol 177: Snyder TE, Krantz KE (1991) Abdominal-retroperitoneal sacral colpopexy for the correction of vaginal prolapse. Obstet Gynecol 77:944
6 168 J Robotic Surg (2007) 1: Menefee SA, Miller KF, Wall LL (1999) Results of abdominal sacral colpopexy using polyester mesh in the treatment of posthysterectomy vaginal vault prolapse and enterocele. Obstet Gynecol 54: Reddy K, Malik TG. (2002) Short-term and long-term follow-up of abdominal sacrocolpopexy for vaginal vault prolapse: initial experience in a district general hospital. J Obstet Gynaecol. 22: Webb MJ, Aronson MP, Ferguson LK, Lee RA (1998) Posthysterectomy vaginal vault prolapse: primary repair in 693 patients. Obstet Gynecol 92: Podratz LK, Ferguson VR, Lee RA, Symmonds RE (1995) Abdominal sacral colpopexy for posthysterectomy vaginal vault descensus. Obstet Gynecol 50: Karram M, Goldwasser S, Kleeman S, Steele A, Vassallo B, Walsh P (2001) High uterosacral vaginal vault suspension with fascial reconstruction for vaginal repair of enterocele and vaginal vault prolapse. Am J Obstet Gynecol 185: Benson JT, Lucente V, McClellan E (1996) Vaginal versus abdominal reconstructive surgery for the treatment of pelvic support defects: a prospective randomized study with long-term outcome evaluation. Am J Obstet Gynecol 175: Ostrzenski A (1996) Laparoscopic colposuspension for total vaginal prolapse. Int J Gynaecol Obstet 55: Cosson M, Rajabally R, Bogaert E, Querleu D, Crepin G (2002) Laparoscopic sacrocolpopexy, hysterectomy, and burch colposuspension: feasibility and short-term complications of 77 procedures. J Soc Laparoendosc Surg 6: Paraiso MF, Walters MD, Rackley RR, Melek S, Hugney C (2005) Laparoscopic and abdominal sacral colpopexies: a comparative cohort study. Am J Obstet Gynecol 192: Higgs PJ, Chua HL, Smith AR (2005) Long term review of laparoscopic sacrocolpopexy. BJOG 112: Hubens G, Coveliers H, Balliu L, Ruppert M, Vaneerdweg W (2003) A performance study comparing manual and robotically assisted laparoscopic surgery using the da Vinci system. Surg Endosc 17: DiMarco DS, Chow GC, Gettman MT, Elliott DS (2004) Roboticassisted laparoscopic sacrocolpopexy for treatment of vaginal vault prolapse. Urology 63: Elliott DS, Krambeck AE, Chow GK (2006) Long-term results of robotic assisted laparoscopic sacrocolpopexy for the treatment of high grade vaginal vault prolapse. J Urol 176: Cosson M, Bogaert E, Narducci F, Querleu D, Crepin G (2000) Laparoscopic sacral colpopexy: short-term results and complications in 83 patients. J Gynecol Obstet Biol Reprod (Paris) 29:746
Considering Surgery for Vaginal or Uterine Prolapse? Learn why da Vinci Surgery may be your best treatment option.
 Considering Surgery for Vaginal or Uterine Prolapse? Learn why da Vinci Surgery may be your best treatment option. The Condition(s): Vaginal Prolapse, Uterine Prolapse Vaginal prolapse occurs when the
Considering Surgery for Vaginal or Uterine Prolapse? Learn why da Vinci Surgery may be your best treatment option. The Condition(s): Vaginal Prolapse, Uterine Prolapse Vaginal prolapse occurs when the
Laparoscopic sacrocolpopexy for the correction of vaginal vault prolapse
 Washington University School of Medicine Digital Commons@Becker Open Access Publications 2004 Laparoscopic sacrocolpopexy for the correction of vaginal vault prolapse Chandru P. Sundaram Indiana University
Washington University School of Medicine Digital Commons@Becker Open Access Publications 2004 Laparoscopic sacrocolpopexy for the correction of vaginal vault prolapse Chandru P. Sundaram Indiana University
International Federation of Gynecology and Obstetrics
 International Federation of Gynecology and Obstetrics COMMITTEE FOR UROGYNAECOLOGY AND PELVIC FLOOR MEMBER: TSUNG-HSIEN (CHARLES) SU, CHAIR (TAIWAN) DAVID RICHMOND, CO-CHAIR (UK) CHITTARANJAN PURANDARE,
International Federation of Gynecology and Obstetrics COMMITTEE FOR UROGYNAECOLOGY AND PELVIC FLOOR MEMBER: TSUNG-HSIEN (CHARLES) SU, CHAIR (TAIWAN) DAVID RICHMOND, CO-CHAIR (UK) CHITTARANJAN PURANDARE,
Traditional Anterior, Posterior, and Apical Compartment Repairs A Technique Based Review
 Traditional Anterior, Posterior, and Apical Compartment Repairs A Technique Based Review Sandip Vasavada, MD Center for Female Urology and Pelvic Reconstructive Surgery The Glickman Urological and Kidney
Traditional Anterior, Posterior, and Apical Compartment Repairs A Technique Based Review Sandip Vasavada, MD Center for Female Urology and Pelvic Reconstructive Surgery The Glickman Urological and Kidney
ROBOTIC MESH SACROCOLPOPEXY
 ROBOTIC MESH SACROCOLPOPEXY Philippe E. Zimmern, MD, FACS Professor of Urology Mesh sacrocolpopexy Background First described in 1962 by Lane Until then, treatment options were: Pessary Colpocleisis Vaginal
ROBOTIC MESH SACROCOLPOPEXY Philippe E. Zimmern, MD, FACS Professor of Urology Mesh sacrocolpopexy Background First described in 1962 by Lane Until then, treatment options were: Pessary Colpocleisis Vaginal
Laparoscopic sacrocolpopexy: an observational study of functional and anatomical outcomes
 DOI 10.1007/s00192-010-1241-y ORIGINAL ARTICLE Laparoscopic sacrocolpopexy: an observational study of functional and anatomical outcomes Natalia Price & Alex Slack & Simon R. Jackson Received: 26 April
DOI 10.1007/s00192-010-1241-y ORIGINAL ARTICLE Laparoscopic sacrocolpopexy: an observational study of functional and anatomical outcomes Natalia Price & Alex Slack & Simon R. Jackson Received: 26 April
PL Narducci Department of Obstetrics and Gynecology General Hospital San Giovanni Battista Foligno, ITALY
 NESA DAYS 2018 New European Surgical Academy Perugia, April 19-21, 2018 EXCELLENCE IN FEMALE SURGERY PROLAPSE RECONSTRUCTIVE SURGERY IN SEXUALLY ACTIVE WOMEN LAPAROSCOPIC ANTERIOR ABDOMINAL WALL COLPOPEXY
NESA DAYS 2018 New European Surgical Academy Perugia, April 19-21, 2018 EXCELLENCE IN FEMALE SURGERY PROLAPSE RECONSTRUCTIVE SURGERY IN SEXUALLY ACTIVE WOMEN LAPAROSCOPIC ANTERIOR ABDOMINAL WALL COLPOPEXY
Gynecology Dr. Sallama Lecture 3 Genital Prolapse
 Gynecology Dr. Sallama Lecture 3 Genital Prolapse Genital(utero-vaginal )prolapse is extremely common, with an estimated 11% of women undergoing at least one operation for this condition. Definition: A
Gynecology Dr. Sallama Lecture 3 Genital Prolapse Genital(utero-vaginal )prolapse is extremely common, with an estimated 11% of women undergoing at least one operation for this condition. Definition: A
Karanvir Virk M.D. Minimally Invasive & Pelvic Reconstructive Surgery 01/28/2015
 Karanvir Virk M.D. Minimally Invasive & Pelvic Reconstructive Surgery 01/28/2015 Disclosures I have none Objectives Identify the basic Anatomy and causes of Pelvic Organ Prolapse Examine office diagnosis
Karanvir Virk M.D. Minimally Invasive & Pelvic Reconstructive Surgery 01/28/2015 Disclosures I have none Objectives Identify the basic Anatomy and causes of Pelvic Organ Prolapse Examine office diagnosis
SURGICAL. How to manage the cuff at vaginal hysterectomy. For personal use only. Copyright Dowden Health Media TECHNIQUES
 For mass reproduction, content licensing and permissions contact Dowden Health Media. How to manage the cuff at vaginal hysterectomy The high McCall culdoplasty and its modifications can prevent apical
For mass reproduction, content licensing and permissions contact Dowden Health Media. How to manage the cuff at vaginal hysterectomy The high McCall culdoplasty and its modifications can prevent apical
Supracervical Robotic-Assisted Laparoscopic Sacrocolpopexy for Pelvic Organ Prolapse
 SCIENTIFIC PAPER Supracervical Robotic-Assisted Laparoscopic Sacrocolpopexy for Pelvic Organ Prolapse Aaron D. Benson, MD, Brandan A. Kramer, MD, Robert O. Wayment, MD, Bradley F. Schwartz, DO ABSTRACT
SCIENTIFIC PAPER Supracervical Robotic-Assisted Laparoscopic Sacrocolpopexy for Pelvic Organ Prolapse Aaron D. Benson, MD, Brandan A. Kramer, MD, Robert O. Wayment, MD, Bradley F. Schwartz, DO ABSTRACT
Robotic-Assisted Surgery in Urogynecology: Beyond Sacrocolpopexy
 Robotic-Assisted Surgery in Urogynecology: Beyond Sacrocolpopexy Marie Fidela R. Paraiso, M.D. Professor of Surgery Section Head, Urogynecology and Reconstructive Pelvic Surgery Cleveland, OH Disclosures
Robotic-Assisted Surgery in Urogynecology: Beyond Sacrocolpopexy Marie Fidela R. Paraiso, M.D. Professor of Surgery Section Head, Urogynecology and Reconstructive Pelvic Surgery Cleveland, OH Disclosures
Interventional procedures guidance Published: 28 June 2017 nice.org.uk/guidance/ipg583
 Sacrocolpopexy using mesh to repair vaginal vault prolapse Interventional procedures guidance Published: 28 June 2017 nice.org.uk/guidance/ipg583 Your responsibility This guidance represents the view of
Sacrocolpopexy using mesh to repair vaginal vault prolapse Interventional procedures guidance Published: 28 June 2017 nice.org.uk/guidance/ipg583 Your responsibility This guidance represents the view of
Colorectal procedure guide
 Colorectal procedure guide Illustrations by Lisa Clark Biodesign ADVANCED TISSUE REPAIR cookmedical.com 2 INDEX Anal fistula repair Using the Biodesign plug with no button.... 4 Anal fistula repair Using
Colorectal procedure guide Illustrations by Lisa Clark Biodesign ADVANCED TISSUE REPAIR cookmedical.com 2 INDEX Anal fistula repair Using the Biodesign plug with no button.... 4 Anal fistula repair Using
Understanding Pelvic Organ Prolapse. Stephanie Pickett, MD, MS Female Pelvic Medicine and Reconstructive Surgery
 Understanding Pelvic Organ Prolapse Stephanie Pickett, MD, MS Female Pelvic Medicine and Reconstructive Surgery Disclosures None I am the daughter of a physician assistant. Objectives List types of pelvic
Understanding Pelvic Organ Prolapse Stephanie Pickett, MD, MS Female Pelvic Medicine and Reconstructive Surgery Disclosures None I am the daughter of a physician assistant. Objectives List types of pelvic
Long-Term Effectiveness of Uterosacral Colpopexy and Minimally Invasive Sacral Colpopexy for Treatment of Pelvic Organ Prolapse
 ORIGINAL ARTICLE Long-Term Effectiveness of Uterosacral Colpopexy and Minimally Invasive Sacral Colpopexy for Treatment of Pelvic Organ Prolapse Cecile A. Unger, MD, MPH, Matthew D. Barber, MD, MHS, Mark
ORIGINAL ARTICLE Long-Term Effectiveness of Uterosacral Colpopexy and Minimally Invasive Sacral Colpopexy for Treatment of Pelvic Organ Prolapse Cecile A. Unger, MD, MPH, Matthew D. Barber, MD, MHS, Mark
PRACTICE BULLETIN Female Pelvic Medicine & Reconstructive Surgery Volume 23, Number 4, July/August 2017
 PRACTICE BULLETIN Number 176, April 2017 (Replaces Committee Opinion Number 513, December 2011) Pelvic Organ Prolapse Pelvic organ prolapse (POP) is a common, benign condition in women. For many women
PRACTICE BULLETIN Number 176, April 2017 (Replaces Committee Opinion Number 513, December 2011) Pelvic Organ Prolapse Pelvic organ prolapse (POP) is a common, benign condition in women. For many women
LAPAROSCOPIC REPAIR OF PELVIC FLOOR
 LAPAROSCOPIC REPAIR OF PELVIC FLOOR Dr. R. K. Mishra Elements comprising the Pelvis Bones Ilium, ischium and pubis fusion Ligaments Muscles Obturator internis muscle Arcus tendineus levator ani or white
LAPAROSCOPIC REPAIR OF PELVIC FLOOR Dr. R. K. Mishra Elements comprising the Pelvis Bones Ilium, ischium and pubis fusion Ligaments Muscles Obturator internis muscle Arcus tendineus levator ani or white
Current status in pelvic organ prolapse surgery: an evidence based review
 Current status in pelvic organ prolapse surgery: an evidence based review Christian Falconer, MD, PhD Department of Obstetrics and Gynecology Danderyd University Hospital Stockholm, Sweden Finnish Society
Current status in pelvic organ prolapse surgery: an evidence based review Christian Falconer, MD, PhD Department of Obstetrics and Gynecology Danderyd University Hospital Stockholm, Sweden Finnish Society
By:Dr:ISHRAQ MOHAMMED
 By:Dr:ISHRAQ MOHAMMED Protrusion of an organ or structure beyond its normal confines. Prolapses are classified according to their location and the organs contained within them. 1-Anterior vaginal wall
By:Dr:ISHRAQ MOHAMMED Protrusion of an organ or structure beyond its normal confines. Prolapses are classified according to their location and the organs contained within them. 1-Anterior vaginal wall
A Laparoscopic-Assisted Extraperitoneal Bladder Neck Suspension: An Initial Experience
 Journal Of Laparoendoscopic Surgery Volume 4, Number 5, 1994 Mary Ann Liebert, Inc., Publishers A Laparoscopic-Assisted Extraperitoneal Bladder Neck Suspension: An Initial Experience E.D. RIZA, M.D.(1)
Journal Of Laparoendoscopic Surgery Volume 4, Number 5, 1994 Mary Ann Liebert, Inc., Publishers A Laparoscopic-Assisted Extraperitoneal Bladder Neck Suspension: An Initial Experience E.D. RIZA, M.D.(1)
Stop Coping. Start Living. Talk to your doctor about pelvic organ prolapse and sacrocolpopexy
 Stop Coping. Start Living Talk to your doctor about pelvic organ prolapse and sacrocolpopexy Did you know? One in three women will suffer from a pelvic health condition in her lifetime. Four of the most
Stop Coping. Start Living Talk to your doctor about pelvic organ prolapse and sacrocolpopexy Did you know? One in three women will suffer from a pelvic health condition in her lifetime. Four of the most
INGUINAL HERNIA REPAIR PROCEDURE GUIDE
 ROOM CONFIGURATION The following figure shows an overhead view of the recommended OR configuration for a da Vinci Inguinal Hernia Repair (Figure 1). NOTE: Configuration of the operating room suite is dependent
ROOM CONFIGURATION The following figure shows an overhead view of the recommended OR configuration for a da Vinci Inguinal Hernia Repair (Figure 1). NOTE: Configuration of the operating room suite is dependent
SACROSPINOUS LIGAMENT FIXATION, A SAFE AND EFFECTIVE WAY TO MANAGE VAGINAL VAULT PROLAPSE.A 10-YEAR OBSERVATIONAL STUDY OF CLINICAL PRACTICE
 Original Article, A SAFE AND EFFECTIVE WAY TO MANAGE VAGINAL VAULT PROLAPSE.A 10-YEAR OBSERVATIONAL STUDY OF CLINICAL PRACTICE * ** Fauzia Rasool Memon, Mohamed Matar * Consultant Obstetrician and Gynecologist
Original Article, A SAFE AND EFFECTIVE WAY TO MANAGE VAGINAL VAULT PROLAPSE.A 10-YEAR OBSERVATIONAL STUDY OF CLINICAL PRACTICE * ** Fauzia Rasool Memon, Mohamed Matar * Consultant Obstetrician and Gynecologist
Posterior intravaginal slingplasty for vault and uterovaginal prolapse: an initial experience
 Gynecol Surg (2006) 3: 88 92 DOI 10.1007/s10397-005-0168-7 ORIGINAL ARTICLE R. Oliver. C. Dasgupta. A. Coker Posterior intravaginal slingplasty for vault and uterovaginal prolapse: an initial experience
Gynecol Surg (2006) 3: 88 92 DOI 10.1007/s10397-005-0168-7 ORIGINAL ARTICLE R. Oliver. C. Dasgupta. A. Coker Posterior intravaginal slingplasty for vault and uterovaginal prolapse: an initial experience
Robot Assisted Rectopexy
 1. Abdominal cavity approach 1A Trocars Introduce Introduce five trocars to gain access to the abdominal cavity (in da Vinci Si type; In Xi type the trocar placement may differ slightly). First the camera
1. Abdominal cavity approach 1A Trocars Introduce Introduce five trocars to gain access to the abdominal cavity (in da Vinci Si type; In Xi type the trocar placement may differ slightly). First the camera
Surgical repair of vaginal wall prolapse using mesh
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Surgical repair of vaginal wall prolapse using mesh Vaginal wall prolapse happens when the normal support
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Surgical repair of vaginal wall prolapse using mesh Vaginal wall prolapse happens when the normal support
Considering Surgery for Pelvic Prolapse? Learn about minimally invasive da Vinci Surgery
 Considering Surgery for Pelvic Prolapse? Learn about minimally invasive da Vinci Surgery The Surgery: Pelvic Prolapse Surgery If you have pelvic prolapse symptoms, your doctor may suggest medicine or lifestyle
Considering Surgery for Pelvic Prolapse? Learn about minimally invasive da Vinci Surgery The Surgery: Pelvic Prolapse Surgery If you have pelvic prolapse symptoms, your doctor may suggest medicine or lifestyle
Index. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Abdominal mesh background of, 84 85 Age as factor in PFDs, 8 Anal plugs in FI management in women, 107 Anterior compartment native tissue
Index Note: Page numbers of article titles are in boldface type. A Abdominal mesh background of, 84 85 Age as factor in PFDs, 8 Anal plugs in FI management in women, 107 Anterior compartment native tissue
With our aging population, the rate of pelvic
 Original Research Short-Term Outcomes of Robotic Sacrocolpopexy Compared With Abdominal Sacrocolpopexy Elizabeth J. Geller, MD, Nazema Y. Siddiqui, MD, Jennifer M. Wu, MD, MPH, and Anthony G. Visco, MD
Original Research Short-Term Outcomes of Robotic Sacrocolpopexy Compared With Abdominal Sacrocolpopexy Elizabeth J. Geller, MD, Nazema Y. Siddiqui, MD, Jennifer M. Wu, MD, MPH, and Anthony G. Visco, MD
Laparoscopic Sacrocolpopexy with & without the Robot: Tips and Tricks for success and avoidance / management of complications
 Laparoscopic Sacrocolpopexy with & without the Robot: Tips and Tricks for success and avoidance / management of complications Course Faculty: Patrick Culligan, MD Peter Rosenblatt, MD What is a Sacrocolpopexy?
Laparoscopic Sacrocolpopexy with & without the Robot: Tips and Tricks for success and avoidance / management of complications Course Faculty: Patrick Culligan, MD Peter Rosenblatt, MD What is a Sacrocolpopexy?
Innovations in mesh kit technology for vaginal wall prolapse
 Available at www.obgmanagement.com s u p p l e m e n t t o This supplement is supported by American Medical Systems, Inc., and has been peer reviewed by the editors of OBG Management. J a n u a r y 2 0
Available at www.obgmanagement.com s u p p l e m e n t t o This supplement is supported by American Medical Systems, Inc., and has been peer reviewed by the editors of OBG Management. J a n u a r y 2 0
Factors associated with intraoperative conversion during robotic sacrocolpopexy
 ORIGINAL ARTICLE Vol. 41 (2): 319-324, March - April, 2015 doi: 10.1590/S1677-5538.IBJU.2015.02.19 Factors associated with intraoperative conversion during robotic sacrocolpopexy Brian J. Linder 1, George
ORIGINAL ARTICLE Vol. 41 (2): 319-324, March - April, 2015 doi: 10.1590/S1677-5538.IBJU.2015.02.19 Factors associated with intraoperative conversion during robotic sacrocolpopexy Brian J. Linder 1, George
Vaginal McCall culdoplasty versus laparoscopic uterosacral plication to prophylactically address vaginal vault prolapse
 Vaginal McCall culdoplasty versus laparoscopic uterosacral to prophylactically address vaginal vault prolapse Niblock, K., Bailie, E., McCracken, G., & Johnston, K. (2017). Vaginal McCall culdoplasty versus
Vaginal McCall culdoplasty versus laparoscopic uterosacral to prophylactically address vaginal vault prolapse Niblock, K., Bailie, E., McCracken, G., & Johnston, K. (2017). Vaginal McCall culdoplasty versus
Medium-term follow-up on use of freeze-dried, irradiated donor fascia for sacrocolpopexy and sling procedures
 Int Urogynecol J (2004) 15: 238 242 DOI 10.1007/s00192-004-1146-8 ORIGINAL ARTICLE Mary Pat FitzGerald Æ S. Renee Edwards Æ Dee Fenner Medium-term follow-up on use of freeze-dried, irradiated donor fascia
Int Urogynecol J (2004) 15: 238 242 DOI 10.1007/s00192-004-1146-8 ORIGINAL ARTICLE Mary Pat FitzGerald Æ S. Renee Edwards Æ Dee Fenner Medium-term follow-up on use of freeze-dried, irradiated donor fascia
REPAIR OF LARGE CYSTOCELE
 REPAIR OF LARGE CYSTOCELE WITH RAZ SUSPENSION 17 VAGINAL INCISION AND DISSECTION Premarin cream application to the anterior vagina daily for 1 month before cystocele repair enriches the vasculature and
REPAIR OF LARGE CYSTOCELE WITH RAZ SUSPENSION 17 VAGINAL INCISION AND DISSECTION Premarin cream application to the anterior vagina daily for 1 month before cystocele repair enriches the vasculature and
INJ. Transvaginal Cystocele Repair by Purse-String Technique Reinforced with Three Simple Sutures: Surgical Technique and Results.
 Original Article Int Neurourol J 2012;16:144-148 pissn 2093-4777 eissn 2093-6931 International Neurourology Journal Transvaginal Cystocele Repair by Purse-String Technique Reinforced with Three Simple
Original Article Int Neurourol J 2012;16:144-148 pissn 2093-4777 eissn 2093-6931 International Neurourology Journal Transvaginal Cystocele Repair by Purse-String Technique Reinforced with Three Simple
Paravaginal Repair: A Laparoscopic Approach
 44 Paravaginal Repair: A Laparoscopic Approach John R. Miklos and Robert Moore Atlanta Urogynecology Associates, Atlanta, Georgia, U.S.A. Neeraj Kohli Harvard University, Boston, Massachusetts, U.S.A.
44 Paravaginal Repair: A Laparoscopic Approach John R. Miklos and Robert Moore Atlanta Urogynecology Associates, Atlanta, Georgia, U.S.A. Neeraj Kohli Harvard University, Boston, Massachusetts, U.S.A.
A Long-Term Treatment Outcome of Abdominal Sacrocolpopexy
 Original Article DOI 10.3349/ymj.2009.50.6.807 pissn: 0513-5796, eissn: 1976-2437 Yonsei Med J 50(6): 807-813, 2009 A Long-Term Treatment Outcome of Abdominal Sacrocolpopexy Myung Jae Jeon, 1 Yeo Jung
Original Article DOI 10.3349/ymj.2009.50.6.807 pissn: 0513-5796, eissn: 1976-2437 Yonsei Med J 50(6): 807-813, 2009 A Long-Term Treatment Outcome of Abdominal Sacrocolpopexy Myung Jae Jeon, 1 Yeo Jung
What are we talking about? Symptoms. Prolapse Risk Factors. Vaginal bulge 1 Splinting. ?? Pelvic pressure Back pain 1 Urinary complaints 2
 Options for Vaginal Prolapse What are we talking about? Michelle Y. Morrill, M.D. Director of Urogynecology The Permanente Medical Group Kaiser, San Francisco Assistant Professor, Volunteer Faculty Department
Options for Vaginal Prolapse What are we talking about? Michelle Y. Morrill, M.D. Director of Urogynecology The Permanente Medical Group Kaiser, San Francisco Assistant Professor, Volunteer Faculty Department
CHAU KHAC TU M.D., Ph.D.
 CHAU KHAC TU M.D., Ph.D. Hue Central Hospital Vietnam LAPAROSCOPIC PROMONTOFIXATION FOR THE GENITAL PROLAPSE TREATMENT Chau Khac Tu MD.PhD. Hue central hospital CONTENT 3 1 INTRODUCTION 2 OBJECTIVE AND
CHAU KHAC TU M.D., Ph.D. Hue Central Hospital Vietnam LAPAROSCOPIC PROMONTOFIXATION FOR THE GENITAL PROLAPSE TREATMENT Chau Khac Tu MD.PhD. Hue central hospital CONTENT 3 1 INTRODUCTION 2 OBJECTIVE AND
We welcome comments and corrections which will be used to improve the system annually.
 ACGME Case Log Instructions: Female Pelvic Medicine and Reconstructive Surgery (FPMRS) Review Committees for Obstetrics and Gynecology, and Urology Updated July 2013 BACKGROUND The ACGME Case Log System
ACGME Case Log Instructions: Female Pelvic Medicine and Reconstructive Surgery (FPMRS) Review Committees for Obstetrics and Gynecology, and Urology Updated July 2013 BACKGROUND The ACGME Case Log System
University College Hospital
 University College Hospital Surgery for prolapse Helping you to make the right choice Urogynaecology and Pelvic Floor Unit, Women s Health Contents Page 1. What type of surgery should I choose? 2 2. What
University College Hospital Surgery for prolapse Helping you to make the right choice Urogynaecology and Pelvic Floor Unit, Women s Health Contents Page 1. What type of surgery should I choose? 2 2. What
Introduction. Regarding the Section of the UPDATE Entitled Purpose
 Time to Rethink: an Evidence-Based Response from Pelvic Surgeons to the FDA Safety Communication: UPDATE on Serious Complications Associated with Transvaginal Placement of Surgical Mesh for Pelvic Organ
Time to Rethink: an Evidence-Based Response from Pelvic Surgeons to the FDA Safety Communication: UPDATE on Serious Complications Associated with Transvaginal Placement of Surgical Mesh for Pelvic Organ
Clinical Curriculum: Urogynecology
 Updated July 201 Clinical Curriculum: Urogynecology GOAL: The primary goal of the Urogynecology rotation at the University of Alabama at Birmingham (UAB) is to train physicians to have a broad knowledge
Updated July 201 Clinical Curriculum: Urogynecology GOAL: The primary goal of the Urogynecology rotation at the University of Alabama at Birmingham (UAB) is to train physicians to have a broad knowledge
9/24/2015. Pelvic Floor Disorders. Agenda. What is the Pelvic Floor? Pelvic Floor Problems
 Management of Pelvic Floor Disorders Doctor, I don t want THAT mesh! Agenda What are pelvic floor disorders (PFDs)? What are the treatment options? Expectant. Conservative. Surgical. How and when are grafts
Management of Pelvic Floor Disorders Doctor, I don t want THAT mesh! Agenda What are pelvic floor disorders (PFDs)? What are the treatment options? Expectant. Conservative. Surgical. How and when are grafts
Step by step High uterosacral vaginal vault suspension to repair enterocele and apical prolapse
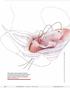 When performing high uterosacral suspension, it is possible to pass sutures through the coccygeus muscle-sacrospinous ligament complex (arrow) because a segment of the uterosacral ligament inserts into
When performing high uterosacral suspension, it is possible to pass sutures through the coccygeus muscle-sacrospinous ligament complex (arrow) because a segment of the uterosacral ligament inserts into
Research Article The Impact of Training Residents on the Outcome of Robotic-Assisted Sacrocolpopexy
 Minimally Invasive Surgery Volume 2012, Article ID 289342, 6 pages doi:10.1155/2012/289342 Research Article The Impact of Training Residents on the Outcome of Robotic-Assisted Sacrocolpopexy Mohamed A.
Minimally Invasive Surgery Volume 2012, Article ID 289342, 6 pages doi:10.1155/2012/289342 Research Article The Impact of Training Residents on the Outcome of Robotic-Assisted Sacrocolpopexy Mohamed A.
Incidence rate and risk factors for vaginal vault prolapse repair after hysterectomy
 Int Urogynecol J (2008) 19:1623 1629 DOI 10.1007/s00192-008-0718-4 ORIGINAL ARTICLE Incidence rate and risk factors for vaginal vault prolapse repair after hysterectomy Patrick Dällenbach & Isabelle Kaelin-Gambirasio
Int Urogynecol J (2008) 19:1623 1629 DOI 10.1007/s00192-008-0718-4 ORIGINAL ARTICLE Incidence rate and risk factors for vaginal vault prolapse repair after hysterectomy Patrick Dällenbach & Isabelle Kaelin-Gambirasio
EndoFast Reliant System vs. Tension- free Mesh in a Sheep Model; three arm Comparative Study Assessing the Mechanical Pullout Force of Mesh Over Time
 EndoFast Reliant System vs. Tension- free Mesh in a Sheep Model; three arm Comparative Study Assessing the Mechanical Pullout Force of Mesh Over Time Menachem Alcalay,M.D, Urogynecology unit, Sheba Medical
EndoFast Reliant System vs. Tension- free Mesh in a Sheep Model; three arm Comparative Study Assessing the Mechanical Pullout Force of Mesh Over Time Menachem Alcalay,M.D, Urogynecology unit, Sheba Medical
Laparoscopic sacrocolpopexy
 ORIGINAL ARTICLE Laparoscopic sacrocolpopexy Marquina-Sánchez M, 1 Esquivel-Pedraza P. 2 Abstract Resumen Sacrocolpopexy (SCP) performed as open surgery is the best definitive treatment option for vaginal
ORIGINAL ARTICLE Laparoscopic sacrocolpopexy Marquina-Sánchez M, 1 Esquivel-Pedraza P. 2 Abstract Resumen Sacrocolpopexy (SCP) performed as open surgery is the best definitive treatment option for vaginal
W23: Approaches to pelvic organ prolapse surgery Workshop Chair: Philippe Zimmern, United States 21 October :00-12:00
 W23: Approaches to pelvic organ prolapse surgery Workshop Chair: Philippe Zimmern, United States 21 October 2014 09:00-12:00 Start End Topic Speakers 09:00 09:30 Goals of repair and anatomical principles
W23: Approaches to pelvic organ prolapse surgery Workshop Chair: Philippe Zimmern, United States 21 October 2014 09:00-12:00 Start End Topic Speakers 09:00 09:30 Goals of repair and anatomical principles
This information is intended as an overview only
 This information is intended as an overview only Please refer to the INSTRUCTIONS FOR USE included with this device for indications, contraindications, warnings, precautions and other important information
This information is intended as an overview only Please refer to the INSTRUCTIONS FOR USE included with this device for indications, contraindications, warnings, precautions and other important information
Prospective study of an ultra-lightweight polypropylene Y mesh for robotic sacrocolpopexy
 Int Urogynecol J (2013) 24:1371 1375 DOI 10.1007/s00192-012-2021-7 ORIGINAL ARTICLE Prospective study of an ultra-lightweight polypropylene Y mesh for robotic sacrocolpopexy Charbel G. Salamon & Christa
Int Urogynecol J (2013) 24:1371 1375 DOI 10.1007/s00192-012-2021-7 ORIGINAL ARTICLE Prospective study of an ultra-lightweight polypropylene Y mesh for robotic sacrocolpopexy Charbel G. Salamon & Christa
Content. Terminology Anatomy Aetiology Presentation Classification Management
 Prolapse Content Terminology Anatomy Aetiology Presentation Classification Management Terminology Prolapse Descent of pelvic organs into the vagina Cystocele ant. vaginal wall involving bladder Uterine
Prolapse Content Terminology Anatomy Aetiology Presentation Classification Management Terminology Prolapse Descent of pelvic organs into the vagina Cystocele ant. vaginal wall involving bladder Uterine
Robot-Assisted Gynecologic Surgery. Gynecologic Surgery
 Robot-Assisted Gynecologic Surgery Alison F. Jacoby, MD Department of Obstetrics, Gynecology and Reproductive Sciences University of California, San Francisco Robot-Assisted Gynecologic Surgery Clinical
Robot-Assisted Gynecologic Surgery Alison F. Jacoby, MD Department of Obstetrics, Gynecology and Reproductive Sciences University of California, San Francisco Robot-Assisted Gynecologic Surgery Clinical
Protective effect of suburethral slings on postoperative cystocele recurrence after reconstructive pelvic operation
 Protective effect of suburethral slings on postoperative cystocele recurrence after reconstructive pelvic operation Roger P. Goldberg, MD, MPH, Sumana Koduri, MD, Robert W. Lobel, MD, Patrick J. Culligan,
Protective effect of suburethral slings on postoperative cystocele recurrence after reconstructive pelvic operation Roger P. Goldberg, MD, MPH, Sumana Koduri, MD, Robert W. Lobel, MD, Patrick J. Culligan,
Prolapse & Stress Incontinence
 Advanced Pelvic Floor Course Prolapse & Stress Incontinence OVERVIEW Day One and morning of Day Two- Pelvic Organ Prolapse The Prolapse component covers the detailed anatomy of POP including the DeLancey
Advanced Pelvic Floor Course Prolapse & Stress Incontinence OVERVIEW Day One and morning of Day Two- Pelvic Organ Prolapse The Prolapse component covers the detailed anatomy of POP including the DeLancey
Laparoscopic Compared With Robotic Sacrocolpopexy for Vaginal Prolapse A Randomized Controlled Trial
 Compared With for Vaginal Prolapse A Randomized Controlled Trial Marie Fidela R. Paraiso, MD, J. Eric Jelovsek, MD, Anna Frick, MD, MPH, Chi Chung Grace Chen, MD, and Matthew D. Barber, MD, MHS OBJECTIVE:
Compared With for Vaginal Prolapse A Randomized Controlled Trial Marie Fidela R. Paraiso, MD, J. Eric Jelovsek, MD, Anna Frick, MD, MPH, Chi Chung Grace Chen, MD, and Matthew D. Barber, MD, MHS OBJECTIVE:
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of laparoscopic mesh pectopexy for apical prolapse of the uterus or vagina Apical
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of laparoscopic mesh pectopexy for apical prolapse of the uterus or vagina Apical
Avoiding Mesh Disasters: Tips and Tricks for Success and Handling Complications
 Avoiding Mesh Disasters: Tips and Tricks for Success and Handling Complications Karyn S. Eilber, M.D. Cedars-Sinai FPMRS Associate Professor, Cedars-Sinai Dept of Surgery Associate Director, Urology Residency
Avoiding Mesh Disasters: Tips and Tricks for Success and Handling Complications Karyn S. Eilber, M.D. Cedars-Sinai FPMRS Associate Professor, Cedars-Sinai Dept of Surgery Associate Director, Urology Residency
Pelvic Organ Prolapse. Natural Solutions
 Pelvic Organ Prolapse Natural Solutions Bringing your body back to its natural state There is a very common problem affecting millions of women. Many women are too embarrassed to talk to their physicians
Pelvic Organ Prolapse Natural Solutions Bringing your body back to its natural state There is a very common problem affecting millions of women. Many women are too embarrassed to talk to their physicians
Pelvic Prolapse. A Patient Guide to Pelvic Floor Reconstruction
 Pelvic Prolapse A Patient Guide to Pelvic Floor Reconstruction Pelvic Prolapse When an organ becomes displaced, or slips down in the body, it is referred to as a prolapse. Your physician has diagnosed
Pelvic Prolapse A Patient Guide to Pelvic Floor Reconstruction Pelvic Prolapse When an organ becomes displaced, or slips down in the body, it is referred to as a prolapse. Your physician has diagnosed
da Vinci Hysterectomy Overview Hysterectomy Facts
 da Vinci Hysterectomy for Benign Gynecologic Conditions K. Toursarkissian,MD Beaver Medical Group Dept of OB/GYN Banning, California Overview Welcome & Introductions Hysterectomy in the US da Vinci Surgery
da Vinci Hysterectomy for Benign Gynecologic Conditions K. Toursarkissian,MD Beaver Medical Group Dept of OB/GYN Banning, California Overview Welcome & Introductions Hysterectomy in the US da Vinci Surgery
Does trocar-guided tension-free vaginal mesh (Prolift ) repair provoke prolapse of the unaffected compartments?
 Int Urogynecol J (2010) 21:271 278 DOI 10.1007/s00192-009-1028-1 ORIGINAL ARTICLE Does trocar-guided tension-free vaginal mesh (Prolift ) repair provoke prolapse of the unaffected compartments? Mariëlla
Int Urogynecol J (2010) 21:271 278 DOI 10.1007/s00192-009-1028-1 ORIGINAL ARTICLE Does trocar-guided tension-free vaginal mesh (Prolift ) repair provoke prolapse of the unaffected compartments? Mariëlla
Female Urology. The Results of Grade IV Cystocele Repair Using Mesh. Introduction ZARGAR MA, EMAMI M*, ZARGAR K, JAMSHIDI M
 Urology Journal UNRC/IUA Vol. 1, No. 4, 263-267 Autumn 2004 Printed in IRAN Female Urology The Results of Grade IV Cystocele Repair Using Mesh ZARGAR MA, EMAMI M*, ZARGAR K, JAMSHIDI M Department of Urology,
Urology Journal UNRC/IUA Vol. 1, No. 4, 263-267 Autumn 2004 Printed in IRAN Female Urology The Results of Grade IV Cystocele Repair Using Mesh ZARGAR MA, EMAMI M*, ZARGAR K, JAMSHIDI M Department of Urology,
Assia A. Stepanian, MD*, John R. Miklos, MD, Robert D. Moore, DO, and T. Fleming Mattox, MD
 Risk of Mesh Extrusion and Other Mesh-Related Complications After Laparoscopic Sacral Colpopexy with or without Concurrent Laparoscopic-Assisted Vaginal Hysterectomy: Experience of 402 Patients Assia A.
Risk of Mesh Extrusion and Other Mesh-Related Complications After Laparoscopic Sacral Colpopexy with or without Concurrent Laparoscopic-Assisted Vaginal Hysterectomy: Experience of 402 Patients Assia A.
Index. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Ablation in uterine leiomyoma management, 719 723 Adnexal masses diagnosis of, 664 667 imaging in, 664 665 laboratory studies in, 665
Index Note: Page numbers of article titles are in boldface type. A Ablation in uterine leiomyoma management, 719 723 Adnexal masses diagnosis of, 664 667 imaging in, 664 665 laboratory studies in, 665
Site-specific fascial defects in the diagnosis and surgical management of enterocele
 Site-specific fascial defects in the diagnosis and surgical management of enterocele John R. Miklos, MD,a Neeraj Kohli, MD,b Vincent Lucente, MD,c and William B. Safe, MDd Atlanta and Marietta, GeO1gia,
Site-specific fascial defects in the diagnosis and surgical management of enterocele John R. Miklos, MD,a Neeraj Kohli, MD,b Vincent Lucente, MD,c and William B. Safe, MDd Atlanta and Marietta, GeO1gia,
Total vs Subtotal Hysterectomy
 Total vs Subtotal Hysterectomy AN UNSOLVED PROBLEM? G Centini, E Zupi, A Wattiez 153 patient with 15 years of follow-up The Timeline The first successful hysterectomy (Subtotal)! First Laparoscopic Hysterectomy!
Total vs Subtotal Hysterectomy AN UNSOLVED PROBLEM? G Centini, E Zupi, A Wattiez 153 patient with 15 years of follow-up The Timeline The first successful hysterectomy (Subtotal)! First Laparoscopic Hysterectomy!
Dr John Short. Obstetrician and Gynaecologist Christchurch Women s Hospital, Oxford Women's Health, Christchurch
 Dr John Short Obstetrician and Gynaecologist Christchurch Women s Hospital, Oxford Women's Health, Christchurch 8:30-9:25 WS #142: Peeling Back the Layers - The Pelvic Floor Uncovered 9:35-10:30 WS #152:
Dr John Short Obstetrician and Gynaecologist Christchurch Women s Hospital, Oxford Women's Health, Christchurch 8:30-9:25 WS #142: Peeling Back the Layers - The Pelvic Floor Uncovered 9:35-10:30 WS #152:
Index. B Bladder, injury of, Bowel, injury of, , Brachytherapy, for cervical cancer, 357 Burns, electrosurgical,
 Perioperative Nursing Clinics 1 (2006) 375 379 Index Note: Page numbers of article titles are in boldface type. A Abdominal hysterectomy Acidosis, from insufflation, 323 Active electrode monitoring, in
Perioperative Nursing Clinics 1 (2006) 375 379 Index Note: Page numbers of article titles are in boldface type. A Abdominal hysterectomy Acidosis, from insufflation, 323 Active electrode monitoring, in
Stephen T Jeffery. University of Cape Town, South Africa
 Stephen T Jeffery University of Cape Town, South Africa I still think there s a role for mesh in Prolapse surgery Examples of my most recent mesh cases Case 1 62 yr old Sacrocolpopexy for vault prolapse
Stephen T Jeffery University of Cape Town, South Africa I still think there s a role for mesh in Prolapse surgery Examples of my most recent mesh cases Case 1 62 yr old Sacrocolpopexy for vault prolapse
Original article J Bas Res Med Sci 2015; 2(2): The incidence of recurrent pelvic organ prolapse: A cross sectional study
 The incidence of recurrent pelvic organ prolapse: A cross sectional study Ashraf Direkvand-Moghadam 1, Ali Delpisheh 2, Azadeh Direkvand-Moghadam 3* 1. Psychosocial Injuries Research Center, Faculty of
The incidence of recurrent pelvic organ prolapse: A cross sectional study Ashraf Direkvand-Moghadam 1, Ali Delpisheh 2, Azadeh Direkvand-Moghadam 3* 1. Psychosocial Injuries Research Center, Faculty of
da Vinci Prostatectomy
 da Vinci Prostatectomy Justin T. Lee MD Director of Robotic Surgery Urology Associates of North Texas (UANT) USMD Prostate Cancer Center (www.usmdpcc.com) Prostate Cancer Facts Prostate cancer Leading
da Vinci Prostatectomy Justin T. Lee MD Director of Robotic Surgery Urology Associates of North Texas (UANT) USMD Prostate Cancer Center (www.usmdpcc.com) Prostate Cancer Facts Prostate cancer Leading
Suture complications in a teaching institution among patients undergoing uterosacral ligament suspension with permanent braided suture
 Int Urogynecol J (2010) 21:813 818 DOI 10.1007/s00192-010-1109-1 ORIGINAL ARTICLE Suture complications in a teaching institution among patients undergoing uterosacral ligament suspension with permanent
Int Urogynecol J (2010) 21:813 818 DOI 10.1007/s00192-010-1109-1 ORIGINAL ARTICLE Suture complications in a teaching institution among patients undergoing uterosacral ligament suspension with permanent
MIDLAND MEMORIAL HOSPITAL Delineation of Privileges FEMALE PELVIC MEDICINE AND RECONSTRUCTIVE SURGERY (UROGYNECOLOGY)
 MIDLAND MEMORIAL HOSPITAL Delineation of Privileges FEMALE PELVIC MEDICINE AND RECONSTRUCTIVE SURGERY (UROGYNECOLOGY) Physician Name: Your home for healthcare Female Pelvic Medicine and Reconstructive
MIDLAND MEMORIAL HOSPITAL Delineation of Privileges FEMALE PELVIC MEDICINE AND RECONSTRUCTIVE SURGERY (UROGYNECOLOGY) Physician Name: Your home for healthcare Female Pelvic Medicine and Reconstructive
Le fort s operation for prolapse uterus: A forgotten procedure
 2017; 1(2): 52-56 ISSN (P): 2522-6614 ISSN (E): 2522-6622 Gynaecology Journal www.gynaecologyjournal.com 2017; 1(2): 52-56 Received: 12-09-2017 Accepted: 13-10-2017 Dr. Jasmine Lall 3 rd Year Resident,
2017; 1(2): 52-56 ISSN (P): 2522-6614 ISSN (E): 2522-6622 Gynaecology Journal www.gynaecologyjournal.com 2017; 1(2): 52-56 Received: 12-09-2017 Accepted: 13-10-2017 Dr. Jasmine Lall 3 rd Year Resident,
Subjective and objective results 1 year after robotic sacrocolpopexy using a lightweight Y-mesh
 DOI 10.1007/s00192-013-2265-x ORIGINAL ARTICLE Subjective and objective results 1 year after robotic sacrocolpopexy using a lightweight Y-mesh Patrick J. Culligan & Emil Gurshumov & Christa Lewis & Jennifer
DOI 10.1007/s00192-013-2265-x ORIGINAL ARTICLE Subjective and objective results 1 year after robotic sacrocolpopexy using a lightweight Y-mesh Patrick J. Culligan & Emil Gurshumov & Christa Lewis & Jennifer
Vaginally-Assisted Laparoscopic Hysterosacropexy for Advanced Utero-Vaginal Prolapse: A Series of 32 Cases
 ARS Medica Tomitana - 2014; 2(77): 63-70 10.2478/arsm-2014-0012 Brătilă V. Elvira 1, Brătilă P.C. 2, Negroiu Andra-Teodora 3 Vaginally-Assisted Laparoscopic Hysterosacropexy for Advanced Utero-Vaginal
ARS Medica Tomitana - 2014; 2(77): 63-70 10.2478/arsm-2014-0012 Brătilă V. Elvira 1, Brătilă P.C. 2, Negroiu Andra-Teodora 3 Vaginally-Assisted Laparoscopic Hysterosacropexy for Advanced Utero-Vaginal
Urethrolysis; When, Why & How. M Karram Professor of Ob/Gyn & Urology University of Cincinnati
 Urethrolysis; When, Why & How M Karram Professor of Ob/Gyn & Urology University of Cincinnati Anatomy Urethra may be fixed to the pubic bone with dense scar tissue Goal of urethrolysis is to completely
Urethrolysis; When, Why & How M Karram Professor of Ob/Gyn & Urology University of Cincinnati Anatomy Urethra may be fixed to the pubic bone with dense scar tissue Goal of urethrolysis is to completely
Female Pelvic Prolapse: Considerations on Mesh Surgery and our Experience with Prolift Mesh in 84 Women with Complicated Pelvic Prolapses
 Journal of Applied Medical Sciences, vol.5, no. 2, 2016, 19-30 ISSN: 2241-2328 (print version), 2241-2336 (online) Scienpress Ltd, 2016 Female Pelvic Prolapse: Considerations on Mesh Surgery and our Experience
Journal of Applied Medical Sciences, vol.5, no. 2, 2016, 19-30 ISSN: 2241-2328 (print version), 2241-2336 (online) Scienpress Ltd, 2016 Female Pelvic Prolapse: Considerations on Mesh Surgery and our Experience
RECTAL INJURY IN UROLOGIC SURGERY. Inadvertent rectal injury from a urologic procedure is often subtle but has serious postoperative consequences.
 RECTAL INJURY IN 27 UROLOGIC SURGERY Inadvertent rectal injury from a urologic procedure is often subtle but has serious postoperative consequences. With good mechanical bowel preparation plus antibiotic
RECTAL INJURY IN 27 UROLOGIC SURGERY Inadvertent rectal injury from a urologic procedure is often subtle but has serious postoperative consequences. With good mechanical bowel preparation plus antibiotic
Laparoscopic sacrocolpopexy: how low does the mesh go?
 Ultrasound Obstet Gynecol 2017; 49: 404 408 Published online 7 February 2017 in Wiley Online Library (wileyonlinelibrary.com). DOI: 10.1002/uog.15882 Laparoscopic sacrocolpopexy: how low does the mesh
Ultrasound Obstet Gynecol 2017; 49: 404 408 Published online 7 February 2017 in Wiley Online Library (wileyonlinelibrary.com). DOI: 10.1002/uog.15882 Laparoscopic sacrocolpopexy: how low does the mesh
Anatomical and Functional Results of Pelvic Organ Prolapse Mesh Repair: A Prospective Study of 105 Cases
 International Journal of Clinical Urology 2018; 2(1): 20-24 http://www.sciencepublishinggroup.com/j/ijcu doi: 10.11648/j.ijcu.20180201.14 Anatomical and Functional Results of Pelvic Organ Prolapse Mesh
International Journal of Clinical Urology 2018; 2(1): 20-24 http://www.sciencepublishinggroup.com/j/ijcu doi: 10.11648/j.ijcu.20180201.14 Anatomical and Functional Results of Pelvic Organ Prolapse Mesh
Pelvic Floor Reconstruction
 3.9 Curriculum in Urology Trauma and Reconstruction Pelvic Floor Reconstruction W. Artibani a, Stuart L. Stanton b, D. Kumar c, R. Villet d a University of Verona, Italy; b Saint George Hospital Medical
3.9 Curriculum in Urology Trauma and Reconstruction Pelvic Floor Reconstruction W. Artibani a, Stuart L. Stanton b, D. Kumar c, R. Villet d a University of Verona, Italy; b Saint George Hospital Medical
Anorectal malformations include a wide spectrum of
 JOURNAL OF LAPAROENDOSCOPIC & ADVANCED SURGICAL TECHNIQUES Volume 20, Number 1, 2010 ª Mary Ann Liebert, Inc. DOI: 10.1089=lap.2008.0343 Laparoscopic-Assisted Pull-Through for Congenital Rectal Stenosis
JOURNAL OF LAPAROENDOSCOPIC & ADVANCED SURGICAL TECHNIQUES Volume 20, Number 1, 2010 ª Mary Ann Liebert, Inc. DOI: 10.1089=lap.2008.0343 Laparoscopic-Assisted Pull-Through for Congenital Rectal Stenosis
Surgical treatments for vaginal apical prolapse
 Review Article Obstet Gynecol Sci 2016;59(4):253-260 http://dx.doi.org/10.5468/ogs.2016.59.4.253 pissn 2287-8572 eissn 2287-8580 Surgical treatments for vaginal apical prolapse Mi Kyung Kong, Sang Wook
Review Article Obstet Gynecol Sci 2016;59(4):253-260 http://dx.doi.org/10.5468/ogs.2016.59.4.253 pissn 2287-8572 eissn 2287-8580 Surgical treatments for vaginal apical prolapse Mi Kyung Kong, Sang Wook
FRANZCOG Training Program Logbook Procedure List and Classification
 FRANZCOG Training Program Logbook Procedure List and Classification This logbook procedure list provides sites and trainees with the major/minor classification of procedures in the online logbook. As detailed
FRANZCOG Training Program Logbook Procedure List and Classification This logbook procedure list provides sites and trainees with the major/minor classification of procedures in the online logbook. As detailed
Prolaps: Anteriore Rektopexie nach D Hoore. Prof. Dr. med. F. Hetzer
 Prolaps: Anteriore Rektopexie nach D Hoore Prof. Dr. med. F. Hetzer franc.hetzer@spital-linth.ch Rectal prolapse pathophysiology 24 22 20 18 congenital female pathology (90%) 16 14 straining weakened pelvic
Prolaps: Anteriore Rektopexie nach D Hoore Prof. Dr. med. F. Hetzer franc.hetzer@spital-linth.ch Rectal prolapse pathophysiology 24 22 20 18 congenital female pathology (90%) 16 14 straining weakened pelvic
Laparoscopic surgery for pelvic support defects
 ~ Laparoscopic surgery for pelvic support defects John R. Miklosa, Robert D. Mooreb and Neeraj Kohlia Reconstructive pelvic surgery for the treatment of vaginal prolapse continues to evolve as surgeons
~ Laparoscopic surgery for pelvic support defects John R. Miklosa, Robert D. Mooreb and Neeraj Kohlia Reconstructive pelvic surgery for the treatment of vaginal prolapse continues to evolve as surgeons
Prediction and prevention of stress urinary incontinence after prolapse surgery van der Ploeg, J.M.
 UvA-DARE (Digital Academic Repository) Prediction and prevention of stress urinary incontinence after prolapse surgery van der Ploeg, J.M. Link to publication Citation for published version (APA): van
UvA-DARE (Digital Academic Repository) Prediction and prevention of stress urinary incontinence after prolapse surgery van der Ploeg, J.M. Link to publication Citation for published version (APA): van
PUBOVAGINAL SLING IN THE TREATMENT OF STRESS URINARY INCONTINENCE FOR URETHRAL HYPERMOBILITY AND INTRINSIC SPHINCTERIC DEFICIENCY
 Urological Neurology International Braz J Urol Official Journal of the Brazilian Society of Urology PUBOVAGINAL SLING IN SUI Vol. 29 (6): 540-544, November - December, 2003 PUBOVAGINAL SLING IN THE TREATMENT
Urological Neurology International Braz J Urol Official Journal of the Brazilian Society of Urology PUBOVAGINAL SLING IN SUI Vol. 29 (6): 540-544, November - December, 2003 PUBOVAGINAL SLING IN THE TREATMENT
Laparoscopic Sacral ColpopexyApproach for Genito-Urinary Prolapse: Experience with 363 Cases
 European Urology European Urology 47 (2005) 230 236 Laparoscopic Sacral ColpopexyApproach for Genito-Urinary Prolapse: Experience with 363 Cases Francois Rozet a, *, Eric Mandron b, Carlos Arroyo a,1,
European Urology European Urology 47 (2005) 230 236 Laparoscopic Sacral ColpopexyApproach for Genito-Urinary Prolapse: Experience with 363 Cases Francois Rozet a, *, Eric Mandron b, Carlos Arroyo a,1,
Laparoscopic Uterine Conservation in Uterovaginal Prolapse
 SMGr up Laparoscopic Uterine Conservation in Uterovaginal Prolapse Hasan Cilgin Medicine Faculty of Kafkas University, Kars, Turkey *Corresponding author: Hasan Cilgin, Medicine Faculty of Kafkas University,
SMGr up Laparoscopic Uterine Conservation in Uterovaginal Prolapse Hasan Cilgin Medicine Faculty of Kafkas University, Kars, Turkey *Corresponding author: Hasan Cilgin, Medicine Faculty of Kafkas University,
HYSTERECTOMY FOR BENIGN CONDITIONS
 UnitedHealthcare Commercial Medical Policy HYSTERECTOMY FOR BENIGN CONDITIONS Policy Number: 2018T0572G Effective Date: September 1, 2018 Table of Contents Page INSTRUCTIONS FOR USE... 1 BENEFIT CONSIDERATIONS...
UnitedHealthcare Commercial Medical Policy HYSTERECTOMY FOR BENIGN CONDITIONS Policy Number: 2018T0572G Effective Date: September 1, 2018 Table of Contents Page INSTRUCTIONS FOR USE... 1 BENEFIT CONSIDERATIONS...
Surgery for women with apical vaginal prolapse(review)
 Cochrane Database of Systematic Reviews (Review) Maher C, Feiner B, Baessler K, Christmann-Schmid C, Haya N, Brown J Maher C, Feiner B, Baessler K, Christmann-Schmid C, Haya N, Brown J.. Cochrane Database
Cochrane Database of Systematic Reviews (Review) Maher C, Feiner B, Baessler K, Christmann-Schmid C, Haya N, Brown J Maher C, Feiner B, Baessler K, Christmann-Schmid C, Haya N, Brown J.. Cochrane Database
John Laughlin 4 th year Cardiff University Medical Student
 John Laughlin 4 th year Cardiff University Medical Student Prolapse/incontinence You need to know: Pelvic floor anatomy in relation to uterovaginal support and continence The classification of uterovaginal
John Laughlin 4 th year Cardiff University Medical Student Prolapse/incontinence You need to know: Pelvic floor anatomy in relation to uterovaginal support and continence The classification of uterovaginal
Postoperative Care for Pelvic Fistulae. Peter Jeppson, MD October 3, 2017
 Postoperative Care for Pelvic Fistulae Peter Jeppson, MD October 3, 2017 No Disclosures Rational for Postoperative Care Intraoperative injury may be managed by: Identification Closure Continuous post-operative
Postoperative Care for Pelvic Fistulae Peter Jeppson, MD October 3, 2017 No Disclosures Rational for Postoperative Care Intraoperative injury may be managed by: Identification Closure Continuous post-operative
Anatomical and functional results of McCall culdoplasty in the prevention of enteroceles and vaginal vault prolapse after vaginal hysterectomy
 Int Urogynecol J (2008) 19:1007 1011 DOI 10.1007/s00192-007-0549-8 ORIGINAL ARTICLE Anatomical and functional results of McCall culdoplasty in the prevention of enteroceles and vaginal vault prolapse after
Int Urogynecol J (2008) 19:1007 1011 DOI 10.1007/s00192-007-0549-8 ORIGINAL ARTICLE Anatomical and functional results of McCall culdoplasty in the prevention of enteroceles and vaginal vault prolapse after
