Analysis of the Patellofemoral Region on MRI: Association of Abnormal Trochlear Morphology With Severe Cartilage Defects
|
|
|
- Naomi Simmons
- 6 years ago
- Views:
Transcription
1 Musculoskeletal Imaging Original Research li et al. MRI of the Patellofemoral Region Musculoskeletal Imaging Original Research Syed. li 1 Robert Helmer Michael R. Terk li S, Helmer R, Terk MR Keywords: articular cartilage defects, chondromalacia patella, femoral trochlea, knee instability, MRI, patella, patellofemoral region DOI: /JR Received May 4, 2009; accepted after revision ugust 17, ll authors: Department of Radiology, Emory University, 59 Executive Park South, 4th Fl., Ste. 4009, tlanta, G ddress correspondence to S.. li (saali4@emory.edu). JR 2010; 194: X/10/ merican Roentgen Ray Society nalysis of the Patellofemoral Region on MRI: ssociation of bnormal Trochlear Morphology With Severe Cartilage Defects OJECTIVE. The objective of our study was to assess patellofemoral measurements on MRI and to correlate the measurements with different grades of cartilage defect. MTERILS ND METHODS. xial and sagittal MR images of 100 patients with various pathologic knee conditions were analyzed. The patients were divided into two age groups: < 40 years and 40 years. Patellar measurements of facet asymmetry, the patellato-patellar tendon ratio, and the amount of patellotrochlear cartilage overlap were obtained in each subject. Similarly, trochlear measurements of the ventral trochlear prominence, trochlear depth, facet asymmetry, sulcus angle, and lateral inclination were obtained. xial and sagittal MR images were reviewed to grade the severity of focal cartilage defects in the patellofemoral region on the basis of the depth of the lesion. Measurements in knees without a chondral defect were compared with knees with mild and severe chondral defects. RESULTS. There was a statistically significant difference in the trochlear measurements of the ventral prominence (p = 0.012), trochlear depth (p = 0.001), sulcus angle (p = 0.208), and lateral inclination (p = 0.154) between normal knees and knees with severe cartilage defects in patients younger than 40 years. No significant difference was seen in the patellar measurements between normal knees and knees with severe cartilage defects. CONCLUSION. There is an association between abnormal trochlear morphology and severe patellofemoral cartilage defects in patients younger than 40 years. T he patellofemoral joint (PFJ) is a complex structure with high functional and biomechanical requirements. The normal function of this joint is dependent on the congruent relationship of the patella with the trochlear groove. Developmental or acquired alterations in the surface geometry of the PFJ are associated with multiple clinical problems such as patellar instability; chondromalacia patella; and, consequently, anterior knee pain [1 6]. Therefore, having knowledge about the exact anatomy and function of the joint is required to understand, diagnose, and treat these different abnormalities appropriately. Investigators have traditionally focused their attention on variations in patellar morphology when analyzing for disorders of the PFJ. In 1941, Wiberg [7] classified the patella into three types on the basis of the medial and lateral facet lengths. This classification has been studied extensively to determine a correlation between patellar morphology and chondromalacia patella using both radiogra phy [8 10] and MRI [11]. However, most authors have failed to establish a relationship between the two. Therefore, the region needs to be reevaluated with particular attention to the trochlear anatomy to understand the cartilage changes in the region. The femoral trochlea has been described in the literature using radiography [12, 13], CT [1], and MRI [14 16]. Dejour et al. [1] defined femoral trochlear dysplasia by one qualitative (the crossing sign) and two quantitative (trochlear bump and trochlear depth) features on true lateral radiographs. Pfirrmann et al. [14] used this classification to study the femoral trochlea on MRI. They found that trochlear dysplasia can be diagnosed reliably on sagittal and transverse images using measures of ventral prominence, trochlear depth, and facet asymmetry [14]. Later studies have added other quantitative measurements such as the sulcus angle and the lateral trochlear inclination [16, 17]. lthough these measurements have improved our understanding of the trochlear morphology, there remains a dearth of information JR:194, March
2 li et al. in the literature regarding the correlation of these measurements with PFJ abnormalities. Previous studies have investigated the correlation between chondral defects and different radiographic morphologic measurements such as the congruence angle, Q angle, and patellar height and shape [8, 18, 19]. However, to our knowledge, no study has used MRI to specifically analyze the relationship between the trochlear anatomy and patellofemoral cartilage defects. In this study, different trochlear and patellar morphologic parameters were measured using MRI and were correlated to different grades of cartilage defects. The purpose was to assess patellofemoral morphology on MRI and to determine its association with different grades of cartilage defects. Materials and Methods Patient Selection This retrospective study was performed in compliance with HIP regulations, with approval from our institutional review board and with a waiver of informed consent. MR images of 107 consecutive patients were retrospectively analyzed for the purpose of this study. Patients were imaged at our institution for various clinical conditions (Table 1). Subjects with a history of arthroscopic surgery were excluded from the study. ased on these criteria, seven patients with a history of arthroscopy for meniscus and anterior cruciate ligament injury repair were excluded from the study. Patients were divided into two age groups: 49 subjects (age range, years; 29 male, 20 female) were younger than 40 years and 51 subjects (range, years; 26 male, 25 female) were 40 years old or older. This was done to account for age-related osteoarthritic changes seen in TLE 1: Clinical Indications for MRI in 100 Patients Clinical Indication the older population. Only 30 subjects were found to have undergone arthroscopy after MRI. MRI MRI was performed with either a 1.5-T magnet (TR range/te range, 3,500 4,000/12 35; matrix size, ; field of view [FOV], or cm; 3-mm slice thickness) or a 3-T magnet (2,500 3,000/18 50; matrix size, ; FOV, cm; 3-mm slice thickness) (Signa, GE Healthcare) and an extremity coil. Sagittal proton density weighted fast spin-echo (FSE) sequences and axial proton density fat-saturated sequences were used to analyze the sagittal and axial images, respectively. The images were analyzed on a workstation and measured using software (efilm Workstation version 2.1, Merge Healthcare) and electronic calipers. Patellar Measurements ll measurements were made on the sagittal slice showing the greatest patella length. The patella was measured from the proximal margin to the distal anterior tip excluding osteophytes and No. of Patients Suspected medial meniscus injury 34 Suspected lateral meniscus injury 18 Suspected anterior cruciate ligament injury 13 Other (loose body, knee mass, swelling, posterior cruciate ligament) 10 Patella (patellar dislocation, tendon rupture) 9 Suspected medial collateral ligament injury 6 Suspected osteoarthritic changes 8 Suspected medial and lateral meniscus injuries 2 enthesophytes (Fig. 1). The following measurements were obtained: patellar length, the length of the patellar tendon, the length of the patellar articular cartilage, and the length of the trochlear articular cartilage overlapping with the patellar cartilage. These measurements were used to determine the patellotrochlear index, which is the ratio of the trochlear cartilage overlapping with the patellar cartilage in relation to the length of the patellar cartilage (Fig. 1), and to determine the Insall-Salvati index, which is the ratio of the length of the patellar tendon in relation to the diagonal length of the patella (Fig. 1C). xial slices were used to determine the patellar facet asymmetry, which is described as the ratio of the medial and lateral patellar facet lengths (Fig. 1). The slice for this measurement was the same as the one used for the axial trochlear measurements. The medial patellar so-called odd facet was not included in the medial facet measurements to prevent overestimation of the facet. Trochlear Measurements For each subject, the sagittal proton density weighted FSE sequence was initially analyzed to Fig. 1 Patellar measurements in 35-year-old woman who underwent knee MRI., Patellar facet asymmetry. Medial patellar facet (MF) and lateral patellar facet (LF) were measured., Patellotrochlear cartilage overlap. Patellar articular cartilage (PC) and trochlear articular cartilage (TC) were measured from caudal extent of patellar cartilage to cranial end of trochlear cartilage overlapping with patellar cartilage. C, Insall-Salvati index. Patellar length (PL) and length of patellar tendon (PT) were measured. C 722 JR:194, March 2010
3 MRI of the Patellofemoral Region Fig. 2 Sagittal proton density weighted fast spinecho image shows measurement of ventral trochlear prominence (VTP) in 51-year-old man who underwent knee MRI. determine the slice with the greatest ventral trochlear prominence. The ventral trochlear prominence was described as the distance between the line paralleling the ventral cortical surface of the distal femur and the most ventral cortical point of the femoral trochlear floor (Fig. 2). The maximum ventral trochlear prominence was measured and was then used as a reference for determining the slice for the axial measurements. The slice corresponding to the horizontal line passing through the greatest ventral trochlear prominence was determined and used to calculate the axial measurement (Fig. 3). In PFJs with no trochlear prominence, the anterior physeal line was used as a reference for determining the axial slice (Fig. 3). Four different measurements were made on the axial proton density fat-saturated sequences: the trochlear depth, trochlear facet asymmetry, sulcus angle, and lateral trochlear inclination. For all trochlear measurements, the cartilage was excluded and only the osseous surfaces were used as a reference. The trochlear depth was defined as the maximum distance of the trochlear groove from the line connecting the medial and lateral trochlear facets (Fig. 4). The lengths of the medial and lateral trochlear facets were measured, and asymmetry was calculated as the ratio of the medial-tolateral facet length (Fig. 4). The angle formed between the medial and lateral trochlear facets was simultaneously measured and determined to be the sulcus angle (Fig. 4C). Similarly, the angle formed between the lateral trochlear facet and a line connecting the posterior-most cortical surfaces of the femoral condyles was measured and determined to be the lateral trochlear inclination (Fig. 4D). ll measurements were made by one observer using electronic calipers. Cartilage ssessment Only 30 patients in the study underwent arthroscopic surgery after MRI. Therefore, MRI was used to detect and grade the patellofemoral cartilage defects. Fig. 3 Proton density sagittal changes in 51-year-old man who underwent knee MRI show ventral trochlear prominence (VTP) and anterior physeal line., Sagittal MR image shows example of horizontal line passing through VTP that was to determine corresponding slice for axial measurements., Sagittal MR image shows example of anterior physeal line that was used as reference in knees with no VTP. For all 100 patients, the sagittal, axial, and coronal knee images, which were obtained using proton density weighted FSE and proton density fat-saturated sequences, were retrospectively reviewed by a fellowship-trained musculoskeletal Fig. 4 MR images show axial measurements in 16-year-old girl who underwent knee MRI., Trochlear facet asymmetry. MT = medial trochlea, LT = lateral trochlea., Trochlear depth (TD). C, Sulcus angle (S). D, Lateral trochlear inclination (LTI). C D JR:194, March
4 li et al. radiologist with 6 years of experience to assess for trochlear and patellar cartilage defects [20]. The reader was blinded to the patient s age and trochlear measurements. The severity of the chondral defect was determined according to the International Cartilage Repair Society Classification system using the depth of the lesion [21] (Table 2). In knees in which more than one cartilage defect was observed, the defect with the greatest severity was chosen. We correlated the MR findings with the reference standard arthroscopy in the 30 knees that underwent surgery. Statistical nalysis The knee measurements of the two age groups were analyzed separately. The distribution of each patellar and trochlear measurement was determined. Measurements (mean and SD) of patients with normal cartilage were compared with those with mild and those with severe cartilage defects. The p value was derived using a paired Student s t test calculated using statistics software (MedCalc version 9.6, MedCalc Software Company). statistical significance was defined by a p value of < The interobserver reliability (Cohen s kappa coefficient) was determined between the grading of patellofemoral chondral defects on arthroscopy and imaging in patients who underwent surgery. Results In patients younger than 40 years, 34 knees (69%) were assessed to have normal-appearing cartilage, eight (16%) to have mild cartilage defects, and seven (14%) to have severe cartilage defects. In patients 40 years old or older, 12 knees (24%) were assessed to have normal cartilage, whereas 17 (34%) had mild and 22 (44%) had severe cartilage defects. For the 30 subjects who underwent arthroscopy, substantial agreement (κ = 0.621) was found between the grade of the patellofemoral cartilage on arthroscopy and MRI [22]. Tables 3 and 4 compare the differences between various patellar and trochlear measurements in patients with no cartilage defects and those with mild or severe cartilage defects. No statistically significant difference was seen in the calculated patellar facet measurements (patients < 40 years, p = 0.37; patients 40 years, p = 0.21), patellar trochlear index (< 40 years, p = 0.64; 40 years, p = 0.34), and Insall-Salvati index (< 40 years, p = 0.14; 40 years, p = 0.12) between cases with normal and severe cartilage defects. These findings were similar in both age groups. nalysis of the sagittal trochlear measurements revealed a statistical difference in the TLE 2: MRI Indications for rthroscopy in 30 Patients Clinical Indication ventral trochlear prominence between patients with normal cartilage and patients with severe cartilage defects (< 40 years, p = 0.012; 40 years, p = 0.015) (Table 5). In knees with severe cartilage defects, the ventral trochlear prominence was always greater than 5 mm, with the maximum measurement being 10 mm. There were five knees with no trochlear prominence (0 mm) that had normal cartilage. No significant difference was seen in this measurement between patients with normal cartilage and those with mild cartilage defects in either age group. The comparison in axial trochlear measurements revealed a significant difference in No. of Patients Suspected medial meniscus injury 13 Suspected anterior cruciate ligament injury 6 Suspected anterior cruciate ligament and medial meniscus injury 5 Suspected lateral meniscus injury 3 Suspected medial and lateral meniscus injuries 2 Other (loose body) 1 TLE 3: International Cartilage Repair Society Classification System [21] Used to Classify Cartilage Defects None Grade 0 Mild defect Grade 1 Cartilage Defect Normal MR Finding Normal contour with abnormal increased signal Grade 2 Superficial erosion or ulceration of < 50% Severe defect Grade 3 Partial-thickness defect of > 50% but < 100% Grade 4 Fig. 5 MR images of knee in 16-year-old girl with no chondral surface defects (grade 0)., Sagittal proton density weighted fast spin-echo image shows lack of ventral trochlear prominence (0 mm)., xial proton density fat-saturated image shows deep trochlear groove (4 mm), sulcus angle of 133, lateral trochlear inclination of 27, and trochlear facet asymmetry of 66%. Full-thickness cartilage loss 724 JR:194, March 2010
5 MRI of the Patellofemoral Region Fig. 6 MR images of knee in 27-year-old man with arthroscopy-proven grades 3 and 4 lesions., Sagittal proton density weighted fast spin-echo image shows increased ventral trochlear prominence (arrows) of 10 mm., xial proton density fat-saturated image shows flattened trochlear groove (white arrows), trochlear depth of 0 mm, sulcus angle of 175, lateral trochlear inclination of 14, and trochlear facet asymmetry of 55%. Note presence of patellar subluxation (black arrow). the trochlear depth (p = 0.001), sulcus angle (p = 0.003), and lateral trochlear inclination (p = 0.007) between knees with normal-appearing cartilage and severe cartilage defects in patients younger than 40 years. Patients with severe cartilage defects had a trochlear groove that was seen to be less deep (mean = 0.29 mm; range, 3 to 4 mm) than that in patients with normal cartilage (mean, 3.68 mm; range, 3 to 7 mm). The negative value indicates a trochlea with a convex anterior surface. The sulcus angle was wider in patients with severe cartilage defects (mean = 173 ) than in patients with normal cartilage (mean = 151 ). decreased lateral trochlear inclination was seen in knees with severe cartilage defects (mean = 14.7 ), whereas this value was considerably greater in knees with normal cartilage (mean = 22.8 ). The trochlear facet asymmetry was calculated to be similar in knees with normal cartilage and knees with severe cartilage defects because there was no statistical difference between those measurements. dditionally, no significant difference was seen between any of the axial measurements of knees with normal cartilage and knees with mild cartilage defects. In patients 40 years old or older, all axial measurements of patients with normal cartilage, mild cartilage defects, and severe cartilage defects were found to be similar. Discussion In previous studies of the morphologic features of the patellofemoral region, investigators have focused their attention on the patellar aspect of the joint. We believe that the failures of these studies to conclusively show any correlation between patellofemoral morphology and chondromalacia patella are related in part to the neglect of the trochlear aspect of the joint. Our study shows that with the exception of trochlear facet asymmetry there is a significant correlation between trochlear measurements and severe cartilage defects. dditionally, we confirmed previous results indicating a lack of correlation between patellar morphology and cartilage defects in patients younger than 40 years. s early as 1964, Outerbridge [9] had proposed that the motion of the medial patellar facet on the rim of the medial femoral condyle may cause wear of the cartilage in the area. Over the years, many have investigated this theory using radiography [8, 23] and MRI [11] but without much success [24]. In our study, we found no statistical correlation between patellar facet measurements and different grades of cartilage defects. rticular cartilage congruence between the patella and femoral trochlea has been proposed as an alternate view in understanding the development of chondral changes in the region. Endo et al. [11] found no association between patellofemoral cartilage overlap and the presence of chondromalacia patella at surgery. We also did not find a significant correlation between patellofemoral articular congruency and different grades of patellofemoral cartilage defects on MRI. The lack of correlation in our study between patellar indices and cartilage defects provides evidence to conclude that patellar height and surface anatomy are not associated with patellofemoral chondral defects and to justify the importance of focusing our attention on the trochlear aspect of the joint. Pfirrmann et al. [14], Carrillon et al. [16], Tecklenburg et al. [25], and van Huyssteen et al. [26] have studied different trochlear measurements to describe trochlear dysplasia on MRI. The ventral trochlear prominence (> 8 mm), facet asymmetry (< 40%), trochlear depth (< 3 mm), lateral inclination (< 11 ), and sulcus angle (> 150 ) are some of the morphologic features used to classify the condition. In our study, the determined trochlear depth (mean, 0.29 mm) and sulcus angle (mean, 173 ) in knees with severe cartilage defects were found to correlate with the proposed cutoffs. TLE 4: Comparison of Patellar Measurements With Severity of Cartilage Defects in Subjects by Patient ge Patient Group Subjects < 40 y old No Cartilage Defect Mild Cartilage Severe Cartilage Defect p a Defect Patellar facet asymmetry (%) 73 ± ± ± Patellotrochlear index 0.49 ± ± ± Insall-Salvati index 1.08 ± ± ± Subjects 40 y old Patellar facet asymmetry (%) 75 ± ± ± Patellotrochlear index 0.51 ± ± ± Insall-Salvati index 0.98 ± ± ± Note Except p values, data are presented as mean ± SD. a The p value refers to the results of the Student s t test between measurements in knees with mild or severe cartilage defects and knees with normal cartilage. p a JR:194, March
6 li et al. TLE 5: Comparison of Trochlear Measurements With Severity of Cartilage Defects in Subjects by Patient ge Patient Group Subjects < 40 y old No Cartilage Defect However, the ventral trochlear prominence (mean, 6.9 mm), trochlear facet asymmetry (54%), and lateral trochlear inclination (mean, 14.7 mm) measurements were found to lie outside these cutoff values. The difference in our findings and those of the other studies [14, 16, 25, 26] can be attributed to multiple factors. Previous studies had used the mid sagittal and multiple axial slices to obtain measurements. We found that in knees with gross trochlear abnormalities, the most remarkable axial changes were seen in the slice corresponding to the greatest ventral trochlear prominence. Therefore, unlike the authors of previous studies, we used the maximum ventral trochlear prominence as a reference point to determine the axial slice for the measurements. Second, in our study we modified the measurements to exclude the cartilaginous surface and measured only to the most ventral cortical points. The purposes of doing so were to eliminate variability in cartilage encountered in knees with chondral defects and to counter differences in surface geometry of the articular cartilage and the corresponding subchondral osseous anatomy [10]. Last, we divided our population into two age groups to account for osteoarthritic changes in older knees [27 29]. ecause previous authors had made no such distinction, this difference in study design might also have led to the difference in measurements. However, with regard to variations in trochlear anatomy between knees with normal cartilage and those with severe chondral defects, our findings were in agreement with Mild Cartilage Severe Cartilage Defect p a Defect Ventral trochlear prominence (mm) 4.68 ± ± ± Trochlear depth (mm) 3.68 ± ± ± Sulcus angle ( ) 151 ± ± ± Trochlear facet asymmetry (%) 61 ± ± ± Lateral trochlear inclination ( ) 22.8 ± ± ± Subjects 40 y old Ventral trochlear prominence (mm) 3.08 ± ± ± Trochlear depth (mm) 4.33 ± ± ± Sulcus angle ( ) 148 ± ± ± Trochlear facet asymmetry (%) 62 ± ± ± Lateral trochlear inclination ( ) 21.5 ± ± ± Note Except p values, data are presented as mean ± SD. oldface indicates difference is statistically significant. a Student s t test. previously described differences between normal and dysplastic trochleae [14, 16, 17]. In knees with trochlear dysplasia, studies have shown that there is an increased ventral prominence, decreased trochlear depth, increased sulcus angle, and decreased lateral trochlear inclination [14, 16, 17]. We also found a larger prominence, shallower trochlear groove, wider sulcus angle, and more horizontal lateral facet to be associated with severe cartilage defects (Figs. 5 and 6). The correlation of our results with previously determined values strongly suggests the association of trochlear dysplasia in cases with severe cartilage defects. There may be various explanations for the correlation seen between the trochlear measurements and severe cartilage defects. One possible explanation could be the changes in articulation and contact patterns between the patella and trochlear groove during flexion extension of the knee. When the knee is fully extended, the patella sits above the trochlea and the contact area between the patella and femur is minimal. During knee flexion the patella moves inferiorly to be completely engaged with the trochlear groove and significant medial and lateral facet contact is evident [30]. In the presence of an increased trochlear prominence and decreased trochlear depth, the contact area between the patella and trochlea is reduced as it tracks along the femur. Moreover, in vivo findings suggest that a shallow trochlear groove and a trochlear facet with less angulation will allow the patella to be displaced laterally more easily [31, p a 32]. The resulting instability to the PFJ may cause an unequal distribution of forces and an unfavorable mechanical joint stress within the joint. With the shearing forces being constantly elevated, these knees remain susceptible to severe stresses that result in the pathologic changes in the surrounding cartilage. Furthermore, the correlation between the axial measurements and severe cartilage defects was evident only in the younger population. Physiologically, thinning of PFJ cartilage occurs with aging in the absence of cartilage disease [27, 28]. Experimental investigations have shown that cartilage may become less compliant to changes and stiffer with aging because of a decrease in interstitial water content [29]. lso, elderly individuals apply different motor strategies during physical exercise [33], potentially leading to lower joint loads during exercise. Therefore, in elderly subjects, deformation of cartilage is considerably less than in the young [27]. We believe that this might account for the lack of development of cartilage defects in cases with abnormal trochlear anatomy in the elderly. We recognize some limitations in our study. First, this study was retrospective and only knees of symptomatic patients were analyzed. ecause only 30 patients underwent arthroscopy, we had to rely on MRI to diagnose the articular cartilage defects. However, we found substantial agreement in the detection of the specific grade of defects between arthroscopy and MRI. Second, a relatively small population of patients was found to have severe cartilage defects on imaging in our study. lthough we saw a general trend in correlation between trochlear measurements and cartilage defects, future investigations should incorporate a larger sample of patients with severe chondral defects to determine this relationship. Last, we did not assess the correlation of trochlear measurements with cartilage defects in particular locations of the PFJ. Investigating defects in specific areas of the medial and lateral facets of the patella and trochlea may provide a better understanding regarding the mechanism of injury associated with specific trochlear morphology. In conclusion, our study has important diagnostic implications because it gives valuable information regarding the cause of patellofemoral degeneration. With regard to patellofemoral morphology, we established an association between abnormal femoral trochlear osseous anatomy and severe PFJ cartilage defects of the knee. Specifically, we found that knees with a large ventral trochlear prominence, 726 JR:194, March 2010
7 MRI of the Patellofemoral Region shallow trochlear groove, increased sulcus angle, and decreased lateral trochlear inclination in patients younger than 40 years are associated with severe PFJ chondral defects. Therefore, the evaluation of these trochlear measurements is important when evaluating MR images of patients with patellofemoral cartilage defects. References 1. Dejour H, Walch G, Nove-Josserand L, Guier C. Factors of patellar instability: an anatomic radiographic study. Knee Surg Sports Traumatol rthrosc 1994; 2: Sasaki T, Yagi T. Subluxation of the patella: investigation by computerized tomography. Int Orthop 1986; 10: MacNab I. Recurrent dislocation of the patella. J one Joint Surg m 1952; 34: glietti P, Insall JN, Cerulli G. Patellar pain and incongruence: measurements of incongruence. Clin Orthop Relat Res 1983; 176: Insall J, ullough PG, urstein H. Proximal tube realignment of the patella for chondromalacia patellae. Clin Orthop Relat Res 1979; 144: Christoforakis JJ, Strachan RK. Internal derangements of the knee associated with patellofemoral joint degeneration. Knee Surg Sports Traumatol rthrosc 2005; 13: Wiberg G. Roentgenographs and anatomic studies on the femoropatellar joint. cta Orthop 1941; 12: Insall J, Falvo K, Wise DW. Chondromalacia patellae: a prospective study. J one Joint Surg m 1976; 58: Outerbridge RE. Further studies on the etiology of chondromalacia patellae. J one Joint Surg r 1964; 46: Stäubli HU, Dürrenmatt U, Porcellini, Rauschning W. natomy and surface geometry of the patellofemoral joint in the axial plane. J one Joint Surg r 1999; 81: Endo Y, Schweitzer ME, ordalo-rodrigues M, Rokito S, abb JS. MRI quantitative morphologic analysis of patellofemoral region: lack of correlation with chondromalacia patellae at surgery. JR 2007; 189: Grelsamer RP, Tedder JL. The lateral trochlear sign: femoral trochlear dysplasia as seen on a lateral view roentgenograph. Clin Orthop Relat Res 1992; 281: Dejour H, Walch G, Neyret P, delein P. Dysplasia of the femoral trochlea [in French]. Rev Chir Orthop Reparatrice ppar Mot 1990; 76: Pfirrmann CW, Zanetti M, Romero J, Hodler J. Femoral trochlear dysplasia: MR findings. Radiology 2000; 216: Tavernier T, Dejour D. Knee imaging: what is the best modality [in French]? J Radiol 2001; 82: Carrillon Y, bidi H, Dejour D, Fantino O, Moyen, Tran-Minh V. Patellar instability: assessment on MR images by measuring the lateral trochlear inclination initial experience. Radiology 2000; 216: Davies P, Costa ML, Shepstone L, Glasgow MM, Donell S. The sulcus angle and malalignment of the extensor mechanism of the knee. J one Joint Surg r 2000; 82: Dowd GS, entley G. Radiographic assessment in patellar instability and chondromalacia patellae. J one Joint Surg r 1986; 68: glietti P, Cerulli G. Chondromalacia and recurrent subluxation of the patella: a study of malalignment, with some indications for radiography. Ital J Orthop Traumatol 1979; 5: Kijowski R, lankenbaker DG, Davis KW, Shinki K, Kaplan LD, De Smet. Comparison of 1.5- and 3.0-T MR imaging for evaluating the articular cartilage of the knee joint. Radiology 2009; 250: rittberg M, Winalski CS. Evaluation of cartilage injuries and repair. J one Joint Surg m 2003; 85[suppl 2]: Landis JR, Koch GG. The measurement of observer agreement for categorical data. iometrics 1977; 33: Goodfellow J, Hungerford DS, Zindel M. Patellofemoral joint mechanics and pathology: functional anatomy of the patello-femoral joint. J one Joint Surg r 1976; 58: Tria J Jr, licea J. Embryology and anatomy of the patella. In: Scuderi GR, ed. The patella. erlin, Germany: Springer-Verlag, 1995: Tecklenburg K, Dejour D, Hoser C, et al. ony and cartilaginous anatomy of the patellofemoral joint. Knee Surg Sports Traumatol rthrosc 2006; 14: van Huyssteen L, Hendrix MR, arnett J, Wakeley CJ, Eldridge JD. Cartilage bone mismatch in the dysplastic trochlea: an MRI study. J one Joint Surg r 2006; 88: Hudelmaier M, Glaser C, Hohe J, et al. ge-related changes in the morphology and deformational behavior of knee joint cartilage. rthritis Rheum 2001; 44: Karvonen RL, Negendank WG, Teitge R, Reed H, Miller PR, Fernandez-Madrid F. Factors affecting articular cartilage thickness in osteoarthritis and aging. J Rheumatol 1994; 21: Meachim G, entley G, aker R. Effect of age on thickness of adult patellar articular cartilage. nn Rheum Dis 1977; 36: Salsich G, Ward SR, Terk MR, Powers CM. In vivo assessment of patellofemoral joint contact area in individuals who are pain free. Clin Orthop Relat Res 2003; 417: rattström H. Shape of the intercondylar groove normally and in recurrent dislocation of the patella. cta Scand 1964; 68[suppl]: Jafaril, Farahmand F, Meghdari. The effects of trochlear groove geometry on patellofemoral joint stability: a computer model study. Proc Inst Mech Eng H 2008; 222: Papa E, Cappozzo. Sit-to-stand motor strategies in able-bodied young and elderly subjects. J iomech 2000; 33: JR:194, March
Patella Alta: Lack of Correlation Between Patellotrochlear Cartilage Congruence and Commonly Used Patellar Height Ratios
 Musculoskeletal Imaging Original Research Ali et al. Patella Alta Musculoskeletal Imaging Original Research Syed A. Ali 1 Robert Helmer Michael R. Terk Ali SA, Helmer R, Terk MR Keywords: Insall-Salvati
Musculoskeletal Imaging Original Research Ali et al. Patella Alta Musculoskeletal Imaging Original Research Syed A. Ali 1 Robert Helmer Michael R. Terk Ali SA, Helmer R, Terk MR Keywords: Insall-Salvati
Where to Draw the Line:
 Where to Draw the Line: Anatomical Measurements Used to Evaluate Patellofemoral Instability Murray Grissom, MD 1 Bao Do, MD 2 Kathryn Stevens, MD 2 1 Santa Clara Valley Medical Center, San Jose, CA 2 Stanford
Where to Draw the Line: Anatomical Measurements Used to Evaluate Patellofemoral Instability Murray Grissom, MD 1 Bao Do, MD 2 Kathryn Stevens, MD 2 1 Santa Clara Valley Medical Center, San Jose, CA 2 Stanford
CT Evaluation of Patellar Instability
 CT Evaluation of Patellar Instability Poster No.: C-2157 Congress: ECR 2014 Type: Educational Exhibit Authors: R. Ruef, C. Edgar, C. Lebedis, A. Guermazi, A. Kompel, A. Murakami; Boston, MA/US Keywords:
CT Evaluation of Patellar Instability Poster No.: C-2157 Congress: ECR 2014 Type: Educational Exhibit Authors: R. Ruef, C. Edgar, C. Lebedis, A. Guermazi, A. Kompel, A. Murakami; Boston, MA/US Keywords:
International Cartilage Repair Society
 OsteoArthritis and Cartilage (2005) 13, 1029e1036 ª 2005 OsteoArthritis Research Society International. Published by Elsevier Ltd. All rights reserved. doi:10.1016/j.joca.2005.07.004 Brief report Second-look
OsteoArthritis and Cartilage (2005) 13, 1029e1036 ª 2005 OsteoArthritis Research Society International. Published by Elsevier Ltd. All rights reserved. doi:10.1016/j.joca.2005.07.004 Brief report Second-look
Original Report. The Reverse Segond Fracture: Association with a Tear of the Posterior Cruciate Ligament and Medial Meniscus
 Eva M. Escobedo 1 William J. Mills 2 John. Hunter 1 Received July 10, 2001; accepted after revision October 1, 2001. 1 Department of Radiology, University of Washington Harborview Medical enter, 325 Ninth
Eva M. Escobedo 1 William J. Mills 2 John. Hunter 1 Received July 10, 2001; accepted after revision October 1, 2001. 1 Department of Radiology, University of Washington Harborview Medical enter, 325 Ninth
Clinical Evaluation and Imaging of the Patellofemoral Joint Common clinical syndromes
 Clinical Evaluation and Imaging of the Patellofemoral Joint Common clinical syndromes A. Panagopoulos Lecturer in Orthopaedics Medical School, Patras University Objectives Anatomy of patellofemoral joint
Clinical Evaluation and Imaging of the Patellofemoral Joint Common clinical syndromes A. Panagopoulos Lecturer in Orthopaedics Medical School, Patras University Objectives Anatomy of patellofemoral joint
Meniscal Tears: Role of Axial MRI Alone and in Combination with Other Imaging Planes
 Nefise Cagla Tarhan 1,2 Christine. Chung 1 urea Valeria Rosa Mohana-orges 1 Tudor Hughes 1 Donald Resnick 1 Received September 30, 2003; accepted after revision February 2, 2004. 1 Department of Radiology,
Nefise Cagla Tarhan 1,2 Christine. Chung 1 urea Valeria Rosa Mohana-orges 1 Tudor Hughes 1 Donald Resnick 1 Received September 30, 2003; accepted after revision February 2, 2004. 1 Department of Radiology,
Acute Trauma,c Disloca,on Am J Sports Med July 2000 vol. 28 no
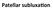 Patellar subluxa,on Acute Trauma,c Disloca,on Am J Sports Med July 2000 vol. 28 no. 4 472-479 History taking is important: a. Trivial or significant injury b. Requires Hospital or self reducion c. Bilateral,
Patellar subluxa,on Acute Trauma,c Disloca,on Am J Sports Med July 2000 vol. 28 no. 4 472-479 History taking is important: a. Trivial or significant injury b. Requires Hospital or self reducion c. Bilateral,
Patellofemoral Pathology
 Patellofemoral Pathology Matthew Murray, MD UT Health Science Center/UT Medicine Sports Medicine and Arthroscopic Surgery I have disclosed that I am a consultant for Biomet Orthopaedics. Anterior Knee
Patellofemoral Pathology Matthew Murray, MD UT Health Science Center/UT Medicine Sports Medicine and Arthroscopic Surgery I have disclosed that I am a consultant for Biomet Orthopaedics. Anterior Knee
Superolateral Hoffa s Fat Pad Edema: Association With Patellofemoral Maltracking and Impingement
 Musculoskeletal Imaging Original Research Subhawong et al. Imaging of Superolateral Hoffa s Fat Pad Edema Musculoskeletal Imaging Original Research Ty K. Subhawong 1 John Eng John. Carrino vneesh Chhabra
Musculoskeletal Imaging Original Research Subhawong et al. Imaging of Superolateral Hoffa s Fat Pad Edema Musculoskeletal Imaging Original Research Ty K. Subhawong 1 John Eng John. Carrino vneesh Chhabra
Patellar malalignment: a new method on knee MRI
 DOI 10.1186/s40064-016-3195-0 RESEARCH Open Access Patellar malalignment: a new method on knee MRI Hülya Kurtul Yildiz * and Elif Evrim Ekin Abstract Purpose: The medial patellofemoral ligament (MPFLL)/lateral
DOI 10.1186/s40064-016-3195-0 RESEARCH Open Access Patellar malalignment: a new method on knee MRI Hülya Kurtul Yildiz * and Elif Evrim Ekin Abstract Purpose: The medial patellofemoral ligament (MPFLL)/lateral
Chronic patellar dislocation in adults
 CASE STUDY 11 Chronic patellar dislocation in adults What are the reasons for chronic dislocation? Which is the best imaging modality for documentation? How can we treat it? Table CS11 Patellofemoral joint
CASE STUDY 11 Chronic patellar dislocation in adults What are the reasons for chronic dislocation? Which is the best imaging modality for documentation? How can we treat it? Table CS11 Patellofemoral joint
Sensitivity and Specificity in Detection of Labral Tears with 3.0-T MRI of the Shoulder
 Magee and Williams MRI for Detection of Labral Tears Musculoskeletal Imaging Clinical Observations C M E D E N T U R I C L I M G I N G JR 2006; 187:1448 1452 0361 803X/06/1876 1448 merican Roentgen Ray
Magee and Williams MRI for Detection of Labral Tears Musculoskeletal Imaging Clinical Observations C M E D E N T U R I C L I M G I N G JR 2006; 187:1448 1452 0361 803X/06/1876 1448 merican Roentgen Ray
Trochleaplasty for recurrent patellar dislocation in association with trochlear dysplasia
 Trochleaplasty for recurrent patellar dislocation in association with trochlear dysplasia A 4- TO 14-YEAR FOLLOW-UP STUDY F. von Knoch, T. Böhm, M. L. Bürgi, M. von Knoch, H. Bereiter From the Kantonsspital
Trochleaplasty for recurrent patellar dislocation in association with trochlear dysplasia A 4- TO 14-YEAR FOLLOW-UP STUDY F. von Knoch, T. Böhm, M. L. Bürgi, M. von Knoch, H. Bereiter From the Kantonsspital
Mr. S. Tanweer Ashraf MS, MRCS (Ed), FRCS (Eng). FRCS (Tr&Orth) MSc Ortho Engineering (Cardiff),
 Mr. S. Tanweer Ashraf MS, MRCS (Ed), FRCS (Eng). FRCS (Tr&Orth) MSc Ortho Engineering (Cardiff), Consultant Knee Surgeon NHS: The Royal Orthopaedic Hospital & Queen Elizabeth Hospital, Birmingham MRI Knee:
Mr. S. Tanweer Ashraf MS, MRCS (Ed), FRCS (Eng). FRCS (Tr&Orth) MSc Ortho Engineering (Cardiff), Consultant Knee Surgeon NHS: The Royal Orthopaedic Hospital & Queen Elizabeth Hospital, Birmingham MRI Knee:
PRE & POST OPERATIVE RADIOLOGICAL ASSESSMENT IN TOTAL KNEE REPLACEMENT. Dr. Divya Rani K 2 nd Year Resident Dept. of Radiology
 PRE & POST OPERATIVE RADIOLOGICAL ASSESSMENT IN TOTAL KNEE REPLACEMENT Dr. Divya Rani K 2 nd Year Resident Dept. of Radiology PRE OPERATIVE ASSESSMENT RADIOGRAPHS Radiographs are used for assessment and
PRE & POST OPERATIVE RADIOLOGICAL ASSESSMENT IN TOTAL KNEE REPLACEMENT Dr. Divya Rani K 2 nd Year Resident Dept. of Radiology PRE OPERATIVE ASSESSMENT RADIOGRAPHS Radiographs are used for assessment and
MRI of Osteochondral Defects of the Lateral Femoral Condyle: Incidence and Pattern of Injury After Transient Lateral Dislocation of the Patella
 Sanders et al. MRI of Osteochond ral Defects of the Lateral Femoral Condyle Musculoskeletal Imaging Clinical Observations A C M E D E N T U R I C A L I M A G I N G AJR 2006; 187:1332 1337 0361 803X/06/1875
Sanders et al. MRI of Osteochond ral Defects of the Lateral Femoral Condyle Musculoskeletal Imaging Clinical Observations A C M E D E N T U R I C A L I M A G I N G AJR 2006; 187:1332 1337 0361 803X/06/1875
Surgical Technique. Poly UHMWPE. Bio Hyaluronic Acid. Advancing Materials. Advancing Outcomes.
 Surgical Technique Bio Hyaluronic Acid Poly UHMWPE Advancing Materials. Advancing Outcomes. Pre-Operative Planning Prior to implantation of the BioPoly RS-Trochlea Implant, pre-operative planning will
Surgical Technique Bio Hyaluronic Acid Poly UHMWPE Advancing Materials. Advancing Outcomes. Pre-Operative Planning Prior to implantation of the BioPoly RS-Trochlea Implant, pre-operative planning will
MRI KNEE WHAT TO SEE. Dr. SHEKHAR SRIVASTAV. Sr.Consultant KNEE & SHOULDER ARTHROSCOPY
 MRI KNEE WHAT TO SEE Dr. SHEKHAR SRIVASTAV Sr.Consultant KNEE & SHOULDER ARTHROSCOPY MRI KNEE - WHAT TO SEE MRI is the most accurate and frequently used diagnostic tool for evaluation of internal derangement
MRI KNEE WHAT TO SEE Dr. SHEKHAR SRIVASTAV Sr.Consultant KNEE & SHOULDER ARTHROSCOPY MRI KNEE - WHAT TO SEE MRI is the most accurate and frequently used diagnostic tool for evaluation of internal derangement
Is a malady commonly seen in the orthopaedic office. MPFL to be the major medial so: ;ssue stabilizer, providing 53% of the total restraining force.
 Is a malady commonly seen in the orthopaedic office. MPFL to be the major medial so: ;ssue stabilizer, providing 53% of the total restraining force. Symptoms are occasionally preceded by a trauma;c event
Is a malady commonly seen in the orthopaedic office. MPFL to be the major medial so: ;ssue stabilizer, providing 53% of the total restraining force. Symptoms are occasionally preceded by a trauma;c event
ORIGINAL ARTICLE. ROLE OF MRI IN EVALUATION OF TRAUMATIC KNEE INJURIES Saurabh Chaudhuri, Priscilla Joshi, Mohit Goel
 ROLE OF MRI IN EVALUATION OF TRAUMATIC KNEE INJURIES Saurabh Chaudhuri, Priscilla Joshi, Mohit Goel 1. Associate Professor, Department of Radiodiagnosis & imaging, Bharati Vidyapeeth Medical College and
ROLE OF MRI IN EVALUATION OF TRAUMATIC KNEE INJURIES Saurabh Chaudhuri, Priscilla Joshi, Mohit Goel 1. Associate Professor, Department of Radiodiagnosis & imaging, Bharati Vidyapeeth Medical College and
Usefulness of Unenhanced MRI and MR Arthrography of the Shoulder in Detection of Unstable Labral Tears
 Musculoskeletal Imaging Original Research Unenhanced MRI and MR rthrography for Unstable Labral Tears Musculoskeletal Imaging Original Research Thomas 1,2 T Keywords: labral tear, MRI, shoulder DOI:10.2214/JR.14.14262
Musculoskeletal Imaging Original Research Unenhanced MRI and MR rthrography for Unstable Labral Tears Musculoskeletal Imaging Original Research Thomas 1,2 T Keywords: labral tear, MRI, shoulder DOI:10.2214/JR.14.14262
Where are we now? A little bit of History.. Is menu à la carte relevant in 2019? Medial PatelloFemoral Ligament the Queen of the PF Joint
 Surgical Algorithm for PF Stablization Can we get there? Elizabeth A. Arendt, M.D. Professor & Vice Chair University of Minnesota, USA Department of Orthopedic Surgery A little bit of History.. TRIA 4
Surgical Algorithm for PF Stablization Can we get there? Elizabeth A. Arendt, M.D. Professor & Vice Chair University of Minnesota, USA Department of Orthopedic Surgery A little bit of History.. TRIA 4
Acute Injury of the Articular Cartilage and Subchondral Bone: A Common but Unrecognized Lesion in the Immature Knee
 Rachel S. Oeppen 1,2 Susan. Connolly 3 Jenny T. encardino 4 Diego Jaramillo 1 Received May 19, 2003; accepted after revision July 28, 2003. 1 Department of Pediatric Radiology, Massachusetts General Hospital,
Rachel S. Oeppen 1,2 Susan. Connolly 3 Jenny T. encardino 4 Diego Jaramillo 1 Received May 19, 2003; accepted after revision July 28, 2003. 1 Department of Pediatric Radiology, Massachusetts General Hospital,
Patellofemoral Instability in Children: Correlation Between Risk Factors, Injury Patterns, and Severity of Cartilage Damage
 Pediatric Imaging Original Research Kim et al. Patellofemoral Instability in Children Pediatric Imaging Original Research Hee Kyung Kim 1 Sahar Shiraj 1 Chang Ho Kang 2 Christopher Anton 1 Dong Hoon Kim
Pediatric Imaging Original Research Kim et al. Patellofemoral Instability in Children Pediatric Imaging Original Research Hee Kyung Kim 1 Sahar Shiraj 1 Chang Ho Kang 2 Christopher Anton 1 Dong Hoon Kim
Correlating Femoral Shape with Patellar Kinematics in Patients with Patellofemoral Pain
 Correlating Femoral Shape with Patellar Kinematics in Patients with Patellofemoral Pain Calista M. Harbaugh, 1 Nicole A. Wilson, 2 Frances T. Sheehan 2 1 University of Michigan, College of Engineering,
Correlating Femoral Shape with Patellar Kinematics in Patients with Patellofemoral Pain Calista M. Harbaugh, 1 Nicole A. Wilson, 2 Frances T. Sheehan 2 1 University of Michigan, College of Engineering,
Patellofemoral Instability Jacqueline Munch, MD April 23, 2016
 Patellofemoral Instability Jacqueline Munch, MD April 23, 2016 With many thanks to Beth Shubin Stein, MD What is the Problem??? THIS IS THE PROBLEM Patella Stability Factors contributing to stability Articular
Patellofemoral Instability Jacqueline Munch, MD April 23, 2016 With many thanks to Beth Shubin Stein, MD What is the Problem??? THIS IS THE PROBLEM Patella Stability Factors contributing to stability Articular
Imaging in patellofemoral instability is essential to the accurate
 REVIEW ARTICLE Imaging in Patellofemoral Instability: An Abnormality-based Approach Paulo Renato Fernandes Saggin, MD,* Jose Idıĺio Saggin, MD,* and David Dejour, MDw Abstract: Imaging in patellofemoral
REVIEW ARTICLE Imaging in Patellofemoral Instability: An Abnormality-based Approach Paulo Renato Fernandes Saggin, MD,* Jose Idıĺio Saggin, MD,* and David Dejour, MDw Abstract: Imaging in patellofemoral
Axial Scan Orientation and the Tibial Tubercle Trochlear Groove Distance: Error Analysis and Correction
 Musculoskeletal Imaging Original Research Yao et al. MRI Measurements of the TT-TG Distance Musculoskeletal Imaging Original Research Lawrence Yao 1 Neville Gai 1 Robert D. Boutin 2 Yao L, Gai N, Boutin
Musculoskeletal Imaging Original Research Yao et al. MRI Measurements of the TT-TG Distance Musculoskeletal Imaging Original Research Lawrence Yao 1 Neville Gai 1 Robert D. Boutin 2 Yao L, Gai N, Boutin
Patella position in the trochlea groove: comparison between supine and standing radiographs
 Patella position in the trochlea groove: comparison between supine and standing radiographs Award: Winner Poster No.: P-0098 Congress: ESSR 2014 Type: Authors: Keywords: DOI: Scientific Poster N. Skou,
Patella position in the trochlea groove: comparison between supine and standing radiographs Award: Winner Poster No.: P-0098 Congress: ESSR 2014 Type: Authors: Keywords: DOI: Scientific Poster N. Skou,
Prevalence of Meniscal Radial Tears of the Knee Revealed by MRI After Surgery
 Downloaded from www.ajronline.org by 46.3.207.114 on 12/22/17 from IP address 46.3.207.114. Copyright RRS. For personal use only; all rights reserved Thomas Magee 1 Marc Shapiro David Williams Received
Downloaded from www.ajronline.org by 46.3.207.114 on 12/22/17 from IP address 46.3.207.114. Copyright RRS. For personal use only; all rights reserved Thomas Magee 1 Marc Shapiro David Williams Received
Variability in Patellofemoral Alignment Measurements on MRI: Influence of Knee Position
 Musculoskeletal Imaging Original Research Marquez-Lara et al. Variability in Patellofemoral lignment Measurements on MRI Musculoskeletal Imaging Original Research lejandro Marquez-Lara 1 Jason ndersen
Musculoskeletal Imaging Original Research Marquez-Lara et al. Variability in Patellofemoral lignment Measurements on MRI Musculoskeletal Imaging Original Research lejandro Marquez-Lara 1 Jason ndersen
FAI syndrome with or without labral tear.
 Case This 16-year-old female, soccer athlete was treated for pain in the right groin previously. Now has acute onset of pain in the left hip. The pain was in the groin that was worse with activities. Diagnosis
Case This 16-year-old female, soccer athlete was treated for pain in the right groin previously. Now has acute onset of pain in the left hip. The pain was in the groin that was worse with activities. Diagnosis
Radiological evaluation of the causes of patellar instability.
 Radiological evaluation of the causes of patellar instability. Poster No.: C-0054 Congress: ECR 2014 Type: Authors: Keywords: DOI: Educational Exhibit J. M. Spaccesi Pau, D. Pomato, N. CEDOLA; La Plata/AR
Radiological evaluation of the causes of patellar instability. Poster No.: C-0054 Congress: ECR 2014 Type: Authors: Keywords: DOI: Educational Exhibit J. M. Spaccesi Pau, D. Pomato, N. CEDOLA; La Plata/AR
Stability of Post Traumatic Osteochondritis Dissecans of the Knee: MR Imaging Findings
 Chin J Radiol 2005; 30: 199-204 199 Stability of Post Traumatic Osteochondritis Dissecans of the Knee: MR Imaging Findings YU-CHUNG HUNG 1 JON-KWAY HUANG 1,2 Department of Radiology 1, Mackay Memorial
Chin J Radiol 2005; 30: 199-204 199 Stability of Post Traumatic Osteochondritis Dissecans of the Knee: MR Imaging Findings YU-CHUNG HUNG 1 JON-KWAY HUANG 1,2 Department of Radiology 1, Mackay Memorial
Diagnostic Utility of MRI and MR Arthrography for Detection of Ligamentum Teres Tears: A Retrospective Analysis of 187 Patients With Hip Pain
 Musculoskeletal Imaging Original Research Datir et al. MRI and MR for Ligamentum Teres Tears Musculoskeletal Imaging Original Research bhijit Datir 1 Minzhi Xing 1 Jian Kang 2 Paul Harkey 1 parna Kakarala
Musculoskeletal Imaging Original Research Datir et al. MRI and MR for Ligamentum Teres Tears Musculoskeletal Imaging Original Research bhijit Datir 1 Minzhi Xing 1 Jian Kang 2 Paul Harkey 1 parna Kakarala
Department of Orthopedic Surgery, Ewha Womans University Mokdong Hospital, Seoul, Korea
 Case Report https://doi.org/10.14517/aosm16016 pissn 2289-005X eissn 2289-0068 Revision surgery for recurrent lateral patellar dislocation despite proximal realignment: a report of three cases You Keun
Case Report https://doi.org/10.14517/aosm16016 pissn 2289-005X eissn 2289-0068 Revision surgery for recurrent lateral patellar dislocation despite proximal realignment: a report of three cases You Keun
This presentation is the intellectual property of the author. Contact them for permission to reprint and/or distribute.
 MRI of the Knee Jennifer Swart, M.D. Musculoskeletal Radiology South Texas Radiology Group Outline Coils, Patient Positioning Acquisition Parameters, Planes and Pulse Sequences Knee Arthrography Normal
MRI of the Knee Jennifer Swart, M.D. Musculoskeletal Radiology South Texas Radiology Group Outline Coils, Patient Positioning Acquisition Parameters, Planes and Pulse Sequences Knee Arthrography Normal
Peggers Super Summaries: PFJ
 Patellofemoral Joint: ANATOMY: Largest sesamoid ossifying at 3-5 years of age Multiple foci having a sec ossification centre SUPEROLATERAL Helps increase moment arm PATELLOFEMORAL OA Incidence 10% of knee
Patellofemoral Joint: ANATOMY: Largest sesamoid ossifying at 3-5 years of age Multiple foci having a sec ossification centre SUPEROLATERAL Helps increase moment arm PATELLOFEMORAL OA Incidence 10% of knee
This presentation is the intellectual property of the author. Contact them at for permission to reprint and/or distribute.
 MRI of the Knee Jennifer Swart, M.D. Musculoskeletal Radiology South Texas Radiology Group Financial Disclosure Dr. Jennifer Swart has no relevant financial relationships with commercial interests to disclose.
MRI of the Knee Jennifer Swart, M.D. Musculoskeletal Radiology South Texas Radiology Group Financial Disclosure Dr. Jennifer Swart has no relevant financial relationships with commercial interests to disclose.
RECENT ADVANCES IN CLINICAL MR OF ARTICULAR CARTILAGE
 In Practice RECENT ADVANCES IN CLINICAL MR OF ARTICULAR CARTILAGE By Atsuya Watanabe, MD, PhD, Director, Advanced Diagnostic Imaging Center and Associate Professor, Department of Orthopedic Surgery, Teikyo
In Practice RECENT ADVANCES IN CLINICAL MR OF ARTICULAR CARTILAGE By Atsuya Watanabe, MD, PhD, Director, Advanced Diagnostic Imaging Center and Associate Professor, Department of Orthopedic Surgery, Teikyo
Patellofemoral Joint. Question? ANATOMY
 Doug Elenz is a paid Consultant/Advisor for the Biomet Manufacturing Corporation. Doug Elenz, MD Team Orthopaedic Surgeon The University of Texas Men s Athletic Department Question? Patellofemoral Joint
Doug Elenz is a paid Consultant/Advisor for the Biomet Manufacturing Corporation. Doug Elenz, MD Team Orthopaedic Surgeon The University of Texas Men s Athletic Department Question? Patellofemoral Joint
The Problem of Patellofemoral Pain. The Low Back Pain of the Lower Extremity. Objectives. Christopher M. Powers, PhD, PT, FACSM, FAPTA
 Mechanisms Underlying Patellofemoral Joint Pain: What have we learned over the last 20 years? Professor Co Director, Musculoskeletal Biomechanics Research Laboratory Objectives 1. Highlight recent research
Mechanisms Underlying Patellofemoral Joint Pain: What have we learned over the last 20 years? Professor Co Director, Musculoskeletal Biomechanics Research Laboratory Objectives 1. Highlight recent research
CHRONIC PATELLOFEMORAL INSTABILITY
 INSTRUCTIONAL COURSE LECTURE DAVID J. DANDY From Addenbrooke s Hospital, Cambridge, England This article aims to discuss the many causes of patellofemoral instability so that an appropriate stabilisation
INSTRUCTIONAL COURSE LECTURE DAVID J. DANDY From Addenbrooke s Hospital, Cambridge, England This article aims to discuss the many causes of patellofemoral instability so that an appropriate stabilisation
Patella Instability 1 st Time Dislocation
 Patella Instability 1 st Time Dislocation American Medical Society for Sports Medicine April 6, 2014 Beth E. Shubin Stein, MD Sports Medicine & Shoulder Surgery Hospital for Special Surgery Beth E. Shubin
Patella Instability 1 st Time Dislocation American Medical Society for Sports Medicine April 6, 2014 Beth E. Shubin Stein, MD Sports Medicine & Shoulder Surgery Hospital for Special Surgery Beth E. Shubin
Computational Evaluation of Predisposing Factors to Patellar Dislocation
 Computational Evaluation of Predisposing Factors to Patellar Dislocation Clare K. Fitzpatrick 1, Robert Steensen, MD 2, Jared Bentley, MD 2, Thai Trinh 2, Paul Rullkoetter 1. 1 University of Denver, Denver,
Computational Evaluation of Predisposing Factors to Patellar Dislocation Clare K. Fitzpatrick 1, Robert Steensen, MD 2, Jared Bentley, MD 2, Thai Trinh 2, Paul Rullkoetter 1. 1 University of Denver, Denver,
What is the most effective MRI specific findings for lateral meniscus posterior root tear in ACL injuries
 What is the most effective MRI specific findings for lateral meniscus posterior root tear in ACL injuries Kazuki Asai 1), Junsuke Nakase 1), Kengo Shimozaki 1), Kazu Toyooka 1), Hiroyuki Tsuchiya 1) 1)
What is the most effective MRI specific findings for lateral meniscus posterior root tear in ACL injuries Kazuki Asai 1), Junsuke Nakase 1), Kengo Shimozaki 1), Kazu Toyooka 1), Hiroyuki Tsuchiya 1) 1)
GENDER DIFFERENCE IN THE MODIFIED INSALL-SALVATI RATIO IN A BLACK KENYAN POPULATION
 ORIGINAL ARTICLE Anatomy Journal of Africa. 2016. Vol 5 (1): 686-692 GENDER DIFFERENCE IN THE MODIFIED INSALL-SALVATI RATIO IN A BLACK KENYAN POPULATION * Wambua Brian, Awori Kirsteen, Ongeti Kevin, Kigera
ORIGINAL ARTICLE Anatomy Journal of Africa. 2016. Vol 5 (1): 686-692 GENDER DIFFERENCE IN THE MODIFIED INSALL-SALVATI RATIO IN A BLACK KENYAN POPULATION * Wambua Brian, Awori Kirsteen, Ongeti Kevin, Kigera
PART III Case Studies
 PART III Case Studies Patellofemoral Disorders: Diagnosis and Treatment. Edited by Roland M. Biedert 2004 John Wiley & Sons, Ltd ISBN: 0-470-85011-6 CASE STUDY 1 Unspecific patellofemoral pain What do
PART III Case Studies Patellofemoral Disorders: Diagnosis and Treatment. Edited by Roland M. Biedert 2004 John Wiley & Sons, Ltd ISBN: 0-470-85011-6 CASE STUDY 1 Unspecific patellofemoral pain What do
Recurrent Traumatic Patellar Dislocation: Case Example and Tying it all Together?? Christopher M. Larson MD
 Recurrent Traumatic Patellar Dislocation: Case Example and Tying it all Together?? Christopher M. Larson MD Disclosures Consultant: Smith & Nephew A3 surgical Stockholder: A3 surgical Case Presentation:
Recurrent Traumatic Patellar Dislocation: Case Example and Tying it all Together?? Christopher M. Larson MD Disclosures Consultant: Smith & Nephew A3 surgical Stockholder: A3 surgical Case Presentation:
Patellofemoral instability: evaluation by magnetic resonance imaging
 Rev Bras Ortop. 2013;48(2):159-164 www.rbo.org.br/ Original Article Patellofemoral instability: evaluation by magnetic resonance imaging Patrícia Martins e Souza, 1,* Marcelo Sadock de Sá Gabetto, 2 Marcelo
Rev Bras Ortop. 2013;48(2):159-164 www.rbo.org.br/ Original Article Patellofemoral instability: evaluation by magnetic resonance imaging Patrícia Martins e Souza, 1,* Marcelo Sadock de Sá Gabetto, 2 Marcelo
Knee Joint Anatomy 101
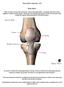 Knee Joint Anatomy 101 Bone Basics There are three bones at the knee joint femur, tibia and patella commonly referred to as the thighbone, shinbone and kneecap. The fibula is not typically associated with
Knee Joint Anatomy 101 Bone Basics There are three bones at the knee joint femur, tibia and patella commonly referred to as the thighbone, shinbone and kneecap. The fibula is not typically associated with
MR imaging of the knee in marathon runners before and after competition
 Skeletal Radiol (2001) 30:72 76 International Skeletal Society 2001 ARTICLE W. Krampla R. Mayrhofer J. Malcher K.H. Kristen M. Urban W. Hruby MR imaging of the knee in marathon runners before and after
Skeletal Radiol (2001) 30:72 76 International Skeletal Society 2001 ARTICLE W. Krampla R. Mayrhofer J. Malcher K.H. Kristen M. Urban W. Hruby MR imaging of the knee in marathon runners before and after
Excessive lateral tracking
 Patellofemoral Kinematics During Weight-earing and Non Weight-earing Knee Extension in Persons With Lateral Subluxation of the Patella: Preliminary Study Christopher M. Powers, PT, PhD 1 Samuel R. Ward,
Patellofemoral Kinematics During Weight-earing and Non Weight-earing Knee Extension in Persons With Lateral Subluxation of the Patella: Preliminary Study Christopher M. Powers, PT, PhD 1 Samuel R. Ward,
HOW DO WE DIAGNOSE LAMENESS IN YOUR HORSE?
 HOW DO WE DIAGNOSE LAMENESS IN YOUR HORSE? To help horse owners better understand the tools we routinely use at VetweRx to evaluate their horse s soundness, the following section of this website reviews
HOW DO WE DIAGNOSE LAMENESS IN YOUR HORSE? To help horse owners better understand the tools we routinely use at VetweRx to evaluate their horse s soundness, the following section of this website reviews
of the lumbar facet joints there
 Skeletal Radiol (1999) 28:215±219 International Skeletal Society 1999 A R T I C L E Dominik Weishaupt Marco Zanetti Norbert Boos Juerg Hodler MR imaging and CT in osteoarthritis of the lumbar facet joints
Skeletal Radiol (1999) 28:215±219 International Skeletal Society 1999 A R T I C L E Dominik Weishaupt Marco Zanetti Norbert Boos Juerg Hodler MR imaging and CT in osteoarthritis of the lumbar facet joints
8/9/2017. Case Based: Beyond Medial Patellofemoral Ligament. Editorial Board AJSM Social Media. Consultant. Not talking about PF pain/chondrosis Rehab
 Case Based: Beyond Medial Patellofemoral Ligament Dr Alan Getgood MD FRCS(Tr&Orth) DipSEM Assistant Professor Orthopaedic Sport Medicine Fellowship Director The Fowler Kennedy Sport Medicine Clinic University
Case Based: Beyond Medial Patellofemoral Ligament Dr Alan Getgood MD FRCS(Tr&Orth) DipSEM Assistant Professor Orthopaedic Sport Medicine Fellowship Director The Fowler Kennedy Sport Medicine Clinic University
Personal use only. MRI of the extensor mechanism of the knee. 5 th Musculoskeletal MRI meeting. Falkowski, MD, MHBA
 MRI of the extensor mechanism of the knee 5 th Musculoskeletal MRI meeting Falkowski, MD, MHBA Outline extensor mechanism - anatomy - pathology - controversies anterior knee pain biomechanics 05.05.2018
MRI of the extensor mechanism of the knee 5 th Musculoskeletal MRI meeting Falkowski, MD, MHBA Outline extensor mechanism - anatomy - pathology - controversies anterior knee pain biomechanics 05.05.2018
MRI of the Knee: Part 4 - normal variants that may simulate disease. Mark Anderson, M.D. University of Virginia
 MRI of the Knee: Part 4 - normal variants that may simulate disease Mark Anderson, M.D. University of Virginia discuss the most common normal variants in the pediatric knee that may simulate pathology
MRI of the Knee: Part 4 - normal variants that may simulate disease Mark Anderson, M.D. University of Virginia discuss the most common normal variants in the pediatric knee that may simulate pathology
The Meniscal Roots: Gross Anatomic Correlation with 3-T MRI Findings
 rody et al. Meniscal Root MRI Musculoskeletal Imaging Pictorial Essay Jeffrey M. rody 1 Michael J. Hulstyn 2 raden. Fleming 3 Glenn. Tung 1 rody JM, Hulstyn MJ, Fleming, Tung G Keywords: anatomy, knee,
rody et al. Meniscal Root MRI Musculoskeletal Imaging Pictorial Essay Jeffrey M. rody 1 Michael J. Hulstyn 2 raden. Fleming 3 Glenn. Tung 1 rody JM, Hulstyn MJ, Fleming, Tung G Keywords: anatomy, knee,
First-Time Patellofemoral Dislocation: Risk Factors for Recurrent Instability
 Special Focus Section 303 First-Time Patellofemoral Dislocation: Risk Factors for Recurrent Instability Laura Lewallen, MD 1 Amy McIntosh, MD 1 Diane Dahm, MD 1 1 Department of Orthopedic Surgery, Mayo
Special Focus Section 303 First-Time Patellofemoral Dislocation: Risk Factors for Recurrent Instability Laura Lewallen, MD 1 Amy McIntosh, MD 1 Diane Dahm, MD 1 1 Department of Orthopedic Surgery, Mayo
Imaging the Athlete s Knee. Peter Lowry, MD Musculoskeletal Radiology University of Colorado
 Imaging the Athlete s Knee Peter Lowry, MD Musculoskeletal Radiology University of Colorado None Disclosures Knee Imaging: Radiographs Can be performed weight-bearing or non-weight-bearing View options
Imaging the Athlete s Knee Peter Lowry, MD Musculoskeletal Radiology University of Colorado None Disclosures Knee Imaging: Radiographs Can be performed weight-bearing or non-weight-bearing View options
Why does it matter? Patellar Instability 7/23/2018. What is the current operation de jour? Common. Poorly taught. Poorly treated
 Patellar Instability It s Really Not That Difficult! David Shneider MD East Lansing, MI www.patellamdcom Detroit Sports Medicine Foundation July 2018 Why does it matter? Common Poorly taught Poorly treated
Patellar Instability It s Really Not That Difficult! David Shneider MD East Lansing, MI www.patellamdcom Detroit Sports Medicine Foundation July 2018 Why does it matter? Common Poorly taught Poorly treated
Distribution of MR-detected cartilage defects of the patellofemoral joint in chronic knee pain
 OsteoArthritis and Cartilage (2003) 11, 494 498 Crown Copyright 2003 Published by Elsevier Science Ltd on behalf of OsteoArthritis Research Society International. All rights reserved. doi:10.1016/s1063-4584(03)00084-0
OsteoArthritis and Cartilage (2003) 11, 494 498 Crown Copyright 2003 Published by Elsevier Science Ltd on behalf of OsteoArthritis Research Society International. All rights reserved. doi:10.1016/s1063-4584(03)00084-0
Musculoskeletal Imaging Clinical Perspective
 Musculoskeletal Imaging linical Perspective McMonagle et al. MRI of the PL Musculoskeletal Imaging linical Perspective J. Scott McMonagle 1 lyde. Helms 1 William E. Garrett, Jr. 2 Emily N. Vinson 1 McMonagle
Musculoskeletal Imaging linical Perspective McMonagle et al. MRI of the PL Musculoskeletal Imaging linical Perspective J. Scott McMonagle 1 lyde. Helms 1 William E. Garrett, Jr. 2 Emily N. Vinson 1 McMonagle
Traumatic Patellar Dislocation and Cartilage Injury A Follow- Up Study of Long-Term Cartilage Deterioration
 Traumatic Patellar Dislocation and Cartilage Injury A Follow- Up Study of Long-Term Cartilage Deterioration Salonen EE 1 M.D., Magga T 2 M.D., Sillanpää PJ 3 M.D. Ph.D., Kiekara T 2 M.D., Ph.D., Mäenpää
Traumatic Patellar Dislocation and Cartilage Injury A Follow- Up Study of Long-Term Cartilage Deterioration Salonen EE 1 M.D., Magga T 2 M.D., Sillanpää PJ 3 M.D. Ph.D., Kiekara T 2 M.D., Ph.D., Mäenpää
Comparative study of imaging at 3.0 T versus 1.5 T of the knee
 Skeletal Radiol (2009) 38:761 769 DOI 10.1007/s00256-009-0683-0 SCIENTIFIC ARTICLE Comparative study of imaging at 3.0 T versus 1.5 T of the knee Scott Wong & Lynne Steinbach & Jian Zhao & Christoph Stehling
Skeletal Radiol (2009) 38:761 769 DOI 10.1007/s00256-009-0683-0 SCIENTIFIC ARTICLE Comparative study of imaging at 3.0 T versus 1.5 T of the knee Scott Wong & Lynne Steinbach & Jian Zhao & Christoph Stehling
A Review of Radiographic Measurements to assess the Patellofemoral Joint
 DOJ Review Article A Review of Radiographic Measurements 10.5005/jp-journals-10017-1085 to assess the Patellofemoral Joint A Review of Radiographic Measurements to assess the Patellofemoral Joint 1 Christopher
DOJ Review Article A Review of Radiographic Measurements 10.5005/jp-journals-10017-1085 to assess the Patellofemoral Joint A Review of Radiographic Measurements to assess the Patellofemoral Joint 1 Christopher
Validation of MRI Classification System for Tibial Stress Injuries
 Musculoskeletal Imaging Original Research Kijowski et al. MRI lassification for Tibial Stress Injuries Musculoskeletal Imaging Original Research Richard Kijowski 1 James hoi 2 Kazuhiko Shinki 3 lejandro
Musculoskeletal Imaging Original Research Kijowski et al. MRI lassification for Tibial Stress Injuries Musculoskeletal Imaging Original Research Richard Kijowski 1 James hoi 2 Kazuhiko Shinki 3 lejandro
Elbow Effusions in Trauma in Adults and Children: Is There an Occult Fracture?
 Downloaded from www.ajronline.org by 46.3.193.109 on 01/20/18 from IP address 46.3.193.109. Copyright RRS. For personal use only; all rights reserved Nancy M. Major 1 Steven T. Crawford 1,2 Received July
Downloaded from www.ajronline.org by 46.3.193.109 on 01/20/18 from IP address 46.3.193.109. Copyright RRS. For personal use only; all rights reserved Nancy M. Major 1 Steven T. Crawford 1,2 Received July
JMSCR Vol 05 Issue 01 Page January
 www.jmscr.igmpublication.org Impact Factor 5.244 Index Copernicus Value: 83.27 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v5i1.28 Diagnostic Accuracy of Magnetic Resonance
www.jmscr.igmpublication.org Impact Factor 5.244 Index Copernicus Value: 83.27 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v5i1.28 Diagnostic Accuracy of Magnetic Resonance
Downloaded from by on 12/22/17 from IP address Copyright ARRS. For personal use only; all rights reserved
 Downloaded from www.ajronline.org by 46.3.205.8 on 12/22/17 from IP address 46.3.205.8. opyright RRS. For personal use only; all rights reserved Pictorial Essay MR Imaging of the natomy of and Injuries
Downloaded from www.ajronline.org by 46.3.205.8 on 12/22/17 from IP address 46.3.205.8. opyright RRS. For personal use only; all rights reserved Pictorial Essay MR Imaging of the natomy of and Injuries
Proximal tibial bony and meniscal slopes are higher in ACL injured subjects than controls: a comparative MRI study
 Proximal tibial bony and meniscal slopes are higher in ACL injured subjects than controls: a comparative MRI study Ashraf Elmansori, Timothy Lording, Raphaël Dumas, Khalifa Elmajri, Philippe Neyret, Sebastien
Proximal tibial bony and meniscal slopes are higher in ACL injured subjects than controls: a comparative MRI study Ashraf Elmansori, Timothy Lording, Raphaël Dumas, Khalifa Elmajri, Philippe Neyret, Sebastien
THE KNEE SOCIETY VIRTUAL FELLOWSHIP
 THE KNEE SOCIETY VIRTUAL FELLOWSHIP CHAPTER 2: RADIOGRAPHIC EVALUATION OF THE KNEE Radiographic Evaluation of the Knee Presented by: R. Michael Meneghini, MD COPYRIGHT 2016 THE KNEE SOCIETY Disclosures
THE KNEE SOCIETY VIRTUAL FELLOWSHIP CHAPTER 2: RADIOGRAPHIC EVALUATION OF THE KNEE Radiographic Evaluation of the Knee Presented by: R. Michael Meneghini, MD COPYRIGHT 2016 THE KNEE SOCIETY Disclosures
Distal Femoral Osteotomy to Treat Patellar Instability with Valgus Lower Extremity Alignment in Adolescents
 Distal Femoral Osteotomy to Treat Patellar Instability with Valgus Lower Extremity Alignment in Adolescents Sheena R. Black, MD, Henry B. Ellis, MD, Philip L. Wilson, MD, David A. Podeszwa, MD LLRS Annual
Distal Femoral Osteotomy to Treat Patellar Instability with Valgus Lower Extremity Alignment in Adolescents Sheena R. Black, MD, Henry B. Ellis, MD, Philip L. Wilson, MD, David A. Podeszwa, MD LLRS Annual
Meniscus T2 Relaxation Time at Various Stages of Knee Joint Degeneration
 Meniscus T2 Relaxation Time at Various Stages of Knee Joint Degeneration Richard Kijowski, Michael Fazio, Benjamin Beduhn, and Fang Liu Department of Radiology University of Wisconsin School of Medicine
Meniscus T2 Relaxation Time at Various Stages of Knee Joint Degeneration Richard Kijowski, Michael Fazio, Benjamin Beduhn, and Fang Liu Department of Radiology University of Wisconsin School of Medicine
Evaluation of the Glenoid Labrum With 3-T MRI: Is Intraarticular Contrast Necessary?
 Musculoskeletal Imaging Original Research Major et al. 3-T MRI of the Glenoid Labrum Musculoskeletal Imaging Original Research Evaluation of the Glenoid Labrum With 3-T MRI: Is Intraarticular Contrast
Musculoskeletal Imaging Original Research Major et al. 3-T MRI of the Glenoid Labrum Musculoskeletal Imaging Original Research Evaluation of the Glenoid Labrum With 3-T MRI: Is Intraarticular Contrast
MRI Characteristics of Healed and Unhealed Peripheral Vertical Meniscal Tears
 Musculoskeletal Imaging Original Research Kijowski et al. MRI of Peripheral Meniscal Tears Musculoskeletal Imaging Original Research Richard Kijowski 1 Humberto G. Rosas 1 Kenneth S. Lee 1 rnold Cheung
Musculoskeletal Imaging Original Research Kijowski et al. MRI of Peripheral Meniscal Tears Musculoskeletal Imaging Original Research Richard Kijowski 1 Humberto G. Rosas 1 Kenneth S. Lee 1 rnold Cheung
7/20/14. Patella Instability. Alignment. PF contact areas. Tissue Restraints. Pain. Acute Blunt force trauma Disorders of the Patellafemoral Joint
 Patella Instability Acute Blunt force trauma Disorders of the Patellafemoral Joint Evan G. Meeks, M.D. Orthopaedic Surgery Sports Medicine The University of Texas - Houston Pivoting action Large effusion
Patella Instability Acute Blunt force trauma Disorders of the Patellafemoral Joint Evan G. Meeks, M.D. Orthopaedic Surgery Sports Medicine The University of Texas - Houston Pivoting action Large effusion
Sonographic Detection of Baker s Cysts: Comparison with MR Imaging
 Eric E. Ward 1 Jon. Jacobson 2 David P. Fessell 2 Curtis W. Hayes 2 Marnix van Holsbeeck 1 Received June 20, 2000; accepted after revision ugust 14, 2000. Presented at the annual meeting of the merican
Eric E. Ward 1 Jon. Jacobson 2 David P. Fessell 2 Curtis W. Hayes 2 Marnix van Holsbeeck 1 Received June 20, 2000; accepted after revision ugust 14, 2000. Presented at the annual meeting of the merican
MRI findings associated with distal. Tibiofibular Syndesmosis Injury
 Kevin W. Brown 1 William B. Morrison 1 Mark E. Schweitzer 1,2 J. ntoni Parellada 1 Henry Nothnagel 1 Received January 6, 2003; accepted after revision July 30, 2003. 1 Department of Radiology, Thomas Jefferson
Kevin W. Brown 1 William B. Morrison 1 Mark E. Schweitzer 1,2 J. ntoni Parellada 1 Henry Nothnagel 1 Received January 6, 2003; accepted after revision July 30, 2003. 1 Department of Radiology, Thomas Jefferson
Variations of the grand-piano sign during total knee replacement
 Knee Variations of the grand-piano sign during total knee replacement A COMPUTER-SIMULATION STUDY W.-Q. Cui, Y.-Y. Won, M.-H. Baek, K.-K. Kim, J.-H. Cho From Ajou University School of Medicine, Suwon City,
Knee Variations of the grand-piano sign during total knee replacement A COMPUTER-SIMULATION STUDY W.-Q. Cui, Y.-Y. Won, M.-H. Baek, K.-K. Kim, J.-H. Cho From Ajou University School of Medicine, Suwon City,
Shaw-Ruey Lyu, M.D., Ph.D., and Chia-Chen Hsu, M.D.
 Medial Plicae and Degeneration of the Medial Femoral Condyle Shaw-Ruey Lyu, M.D., Ph.D., and Chia-Chen Hsu, M.D. Purpose: The purpose of this study was to evaluate and analyze the chronological changes
Medial Plicae and Degeneration of the Medial Femoral Condyle Shaw-Ruey Lyu, M.D., Ph.D., and Chia-Chen Hsu, M.D. Purpose: The purpose of this study was to evaluate and analyze the chronological changes
Medical Practice for Sports Injuries and Disorders of the Knee
 Sports-Related Injuries and Disorders Medical Practice for Sports Injuries and Disorders of the Knee JMAJ 48(1): 20 24, 2005 Hirotsugu MURATSU*, Masahiro KUROSAKA**, Tetsuji YAMAMOTO***, and Shinichi YOSHIDA****
Sports-Related Injuries and Disorders Medical Practice for Sports Injuries and Disorders of the Knee JMAJ 48(1): 20 24, 2005 Hirotsugu MURATSU*, Masahiro KUROSAKA**, Tetsuji YAMAMOTO***, and Shinichi YOSHIDA****
MRI Appearance of Posterior Cruciate Ligament Tears
 Musculoskeletal Imaging Clinical Observations Musculoskeletal Imaging Clinical Observations William Rodriguez, Jr. 1 Emily N. Vinson 1 Clyde. Helms 1 lison P. Toth 2 Rodriguez W Jr, Vinson EN, Helms C,
Musculoskeletal Imaging Clinical Observations Musculoskeletal Imaging Clinical Observations William Rodriguez, Jr. 1 Emily N. Vinson 1 Clyde. Helms 1 lison P. Toth 2 Rodriguez W Jr, Vinson EN, Helms C,
Dimensions of the intercondylar notch and the distal femur throughout life
 Dimensions of the intercondylar notch and the distal femur throughout life Poster No.: P-0089 Congress: ESSR 2013 Type: Scientific Exhibit Authors: L. Hirtler, S. Röhrich, F. Kainberger; Vienna/AT Keywords:
Dimensions of the intercondylar notch and the distal femur throughout life Poster No.: P-0089 Congress: ESSR 2013 Type: Scientific Exhibit Authors: L. Hirtler, S. Röhrich, F. Kainberger; Vienna/AT Keywords:
Viviane Khoury, MD. Assistant Professor Department of Radiology University of Pennsylvania
 U Penn Diagnostic Imaging: On the Cape Chatham, MA July 11-15, 2016 Viviane Khoury, MD Assistant Professor Department of Radiology University of Pennsylvania Hip imaging has changed in recent years: new
U Penn Diagnostic Imaging: On the Cape Chatham, MA July 11-15, 2016 Viviane Khoury, MD Assistant Professor Department of Radiology University of Pennsylvania Hip imaging has changed in recent years: new
And...WHAT DO WE KNOW ABOUT THE EXCESSIVE LATERAL PRESSURE SYNDROME?
 And...WHAT DO WE KNOW ABOUT THE EXCESSIVE LATERAL PRESSURE SYNDROME? Poster No.: C-1107 Congress: ECR 2011 Type: Scientific Exhibit Authors: E. Yllera Contreras, C. Jimenez Zapater, J. Arnaiz, A. Salvador
And...WHAT DO WE KNOW ABOUT THE EXCESSIVE LATERAL PRESSURE SYNDROME? Poster No.: C-1107 Congress: ECR 2011 Type: Scientific Exhibit Authors: E. Yllera Contreras, C. Jimenez Zapater, J. Arnaiz, A. Salvador
Why Talk About Technique? MRI of the Knee:
 Why Talk About Technique? MRI of the Knee: Part 1 - Imaging Techniques Mark Anderson, M.D. University of Virginia Health Sciences Center Charlottesville, Virginia Always had an interest teach our fellows
Why Talk About Technique? MRI of the Knee: Part 1 - Imaging Techniques Mark Anderson, M.D. University of Virginia Health Sciences Center Charlottesville, Virginia Always had an interest teach our fellows
Does the patellofemoral joint need articular cartilage? clinical relevance
 Review Article Page 1 of 6 Does the patellofemoral joint need articular cartilage? clinical relevance Lars Blønd 1,2 1 Department of Orthopaedic Surgery, Aleris-Hamlet Parken, Copenhagen, Denmark; 2 Department
Review Article Page 1 of 6 Does the patellofemoral joint need articular cartilage? clinical relevance Lars Blønd 1,2 1 Department of Orthopaedic Surgery, Aleris-Hamlet Parken, Copenhagen, Denmark; 2 Department
And...WHAT DO WE KNOW ABOUT THE EXCESSIVE LATERAL PRESSURE SYNDROME?
 And...WHAT DO WE KNOW ABOUT THE EXCESSIVE LATERAL PRESSURE SYNDROME? Poster No.: C-1107 Congress: ECR 2011 Type: Scientific Exhibit Authors: E. Yllera Contreras, C. Jimenez Zapater, J. Arnaiz García, 1
And...WHAT DO WE KNOW ABOUT THE EXCESSIVE LATERAL PRESSURE SYNDROME? Poster No.: C-1107 Congress: ECR 2011 Type: Scientific Exhibit Authors: E. Yllera Contreras, C. Jimenez Zapater, J. Arnaiz García, 1
ANATOMIC. Navigated Surgical Technique 4 in 1 TO.G.GB.016/1.0
 ANATOMIC Navigated Surgical Technique 4 in 1 TO.G.GB.016/1.0 SCREEN LAYOUT Take screenshot Surgical step Dynamic navigation zone Information area and buttons 2 SCREEN LAYOUT Indicates action when yellow
ANATOMIC Navigated Surgical Technique 4 in 1 TO.G.GB.016/1.0 SCREEN LAYOUT Take screenshot Surgical step Dynamic navigation zone Information area and buttons 2 SCREEN LAYOUT Indicates action when yellow
BASELINE QUESTIONNAIRE (SURGEON)
 SECTION A: STUDY INFORMATION Subject ID: - - Study Visit: Baseline Site Number: Date: / / Surgeon ID: SECTION B: INITIAL SURGEON HISTORY B1. Previous Knee Surgery: Yes No Not recorded B2. Number of Previous
SECTION A: STUDY INFORMATION Subject ID: - - Study Visit: Baseline Site Number: Date: / / Surgeon ID: SECTION B: INITIAL SURGEON HISTORY B1. Previous Knee Surgery: Yes No Not recorded B2. Number of Previous
Patellofemoral Instability
 Disclaimer This movie is an educational resource only and should not be used to manage Patellofemoral Instability. All decisions about the management of Patellofemoral Instability must be made in conjunction
Disclaimer This movie is an educational resource only and should not be used to manage Patellofemoral Instability. All decisions about the management of Patellofemoral Instability must be made in conjunction
Anterior Tibial Translation Sign: Factors Affecting Interpretation of Anterior Cruciate Ligament Tear
 Anterior Tibial Translation Sign: Factors Affecting Interpretation of Anterior Cruciate Ligament Tear J Med Assoc Thai 2015; 98 (Suppl. 1): S57-S62 Full text. e-journal: http://www.jmatonline.com Numphung
Anterior Tibial Translation Sign: Factors Affecting Interpretation of Anterior Cruciate Ligament Tear J Med Assoc Thai 2015; 98 (Suppl. 1): S57-S62 Full text. e-journal: http://www.jmatonline.com Numphung
CLINICAL PRESENTATION AND RADIOLOGY QUIZ QUESTION
 Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 12/01/2012 Radiology Quiz of the Week # 101 Page 1 CLINICAL PRESENTATION AND RADIOLOGY
Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 12/01/2012 Radiology Quiz of the Week # 101 Page 1 CLINICAL PRESENTATION AND RADIOLOGY
MRI of Acute Meniscal Injury Associated with Tibial Plateau Fractures: Prevalence, Type, and Location
 Musculoskeletal Imaging Original Research Mustonen et al. MRI of Meniscal Injury Musculoskeletal Imaging Original Research ntti O. T. Mustonen 1 Mika P. Koivikko 1 Jan Lindahl 2 Seppo K. Koskinen 1 Mustonen
Musculoskeletal Imaging Original Research Mustonen et al. MRI of Meniscal Injury Musculoskeletal Imaging Original Research ntti O. T. Mustonen 1 Mika P. Koivikko 1 Jan Lindahl 2 Seppo K. Koskinen 1 Mustonen
Musculoskeletal Applications for CT. Tal Laor, MD Cincinnati Children s Hospital University of Cincinnati College of Medicine
 Musculoskeletal Applications for CT Tal Laor, MD Cincinnati Children s Hospital University of Cincinnati College of Medicine I have no commercial disclosures. Why CT? Complimentary to other modalities
Musculoskeletal Applications for CT Tal Laor, MD Cincinnati Children s Hospital University of Cincinnati College of Medicine I have no commercial disclosures. Why CT? Complimentary to other modalities
TOTAL KNEE ARTHROPLASTY (TKA)
 TOTAL KNEE ARTHROPLASTY (TKA) 1 Anatomy, Biomechanics, and Design 2 Femur Medial and lateral condyles Convex, asymmetric Medial larger than lateral 3 Tibia Tibial plateau Medial tibial condyle: concave
TOTAL KNEE ARTHROPLASTY (TKA) 1 Anatomy, Biomechanics, and Design 2 Femur Medial and lateral condyles Convex, asymmetric Medial larger than lateral 3 Tibia Tibial plateau Medial tibial condyle: concave
Rehabilitation Guidelines for Medial Patellofemoral Ligament Repair and Reconstruction
 UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Medial Patellofemoral Ligament Repair and Reconstruction The knee consists of four bones that form three joints. The femur is the large bone
UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Medial Patellofemoral Ligament Repair and Reconstruction The knee consists of four bones that form three joints. The femur is the large bone
