We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists. International authors and editors
|
|
|
- Jane Beasley
- 5 years ago
- Views:
Transcription
1 We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 3, , M Open access books available International authors and editors Downloads Our authors are among the 151 Countries delivered to TOP 1% most cited scientists 12.2% Contributors from top 500 universities Selection of our books indexed in the Book Citation Index in Web of Science Core Collection (BKCI) Interested in publishing with us? Contact book.department@intechopen.com Numbers displayed above are based on latest data collected. For more information visit
2 Chapter 8 Surgical Approaches to the Temporomandibular Joint Mohammad Esmaeelinejad and Maryam Sohrabi Additional information is available at the end of the chapter Abstract The temporomandibular joint (TMJ) acts as a sliding hinge between mandible and temporal bone. Disorders of temporomandibular joint are intolerable for the patients in severe cases. Furthermore, surgical treatment of temporomandibular joint problems is a challenge for surgeons in some cases. In that order, it is critical for the surgeon to choose the best surgical approach in treating the temporomandibular joint diseases. There are several surgical approaches in the management of temporomandibular joint problems including some pros and cons. So, in this chapter, we aim to present a comprehensive review of surgical approaches to the temporomandibular joint. Keywords: facial nerve, mandible, mandibular condyle, supericial musculoaponeurotic system, temporomandibular joint 1. Introduction Exact diagnosis and appropriate treatment plan are two important fundamentals of successful surgical results. Planning the treatment of temporomandibular joint (TMJ) problems is not an exception. TMJ is a hinge that connects the mandible to the temporal and serves the movement of lower jaw. TMJ problems such as disc derangement, pathologic lesions, and traumatic injuries would have a signiicant inluence on quality of life of the patients. Treatment of TMJ diseases is still one of the controversial issues in maxillofacial surgery ield. It is important to choose the best surgical technique to solve the problem and rehabilitate the TMJ function. There are several surgical approaches to the TMJ mentioned in the literature and a maxillofacial surgeon should know the technical aspects of these surgical procedures The Author(s). Licensee InTech. This chapter is distributed under the terms of the Creative Commons Attribution License ( which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
3 186 Temporomandibular Joint Pathology - Current Approaches and Understanding This chapter is based on recent investigations reported in the literature and briely presents the diferent aspects of available surgical approaches to TMJ including their indications, techniques, and beneits. 2. Applied anatomy TMJ is a synovial joint between the head of mandibular condyle and the temporal glenoid fossa. The space between the head of mandibular condyle and the glenoid fossa of temporal bone is divided into two separate cavities by the articular disc (Figure 1). The inferior compartment is involved in the hinge movement of the joint, while the superior joint space participates in the translation movement. The postglenoid process and articular eminence are the posterior and anterior limitations of the articular space, respectively. TMJ is surrounded by a ibrous capsule called articular capsule, and its extension is the articular disc (Figure 2). The movements of TMJ are restricted by three main ligaments. The temporomandibular ligament is the lateral portion of articular capsule. This fan-shaped ligament is responsible for synchronizing the condyle and articular disc. The other two ligaments are sphenomandibular and stylomandibular ligaments which are involved in controlling the mandibular movements (Figure 2) Regional nerves The most common anatomical structure facing during the approaches to the TMJ is the facial nerve. The main trunk of facial nerve exits the stylomastoid foramen and after passing about 2 cm distance divides into two main branches of temporofacial and cervicofacial divisions (Figure 3) [1]. The distance from the bony part of external auditory canal to the bifurcation is cm (mean is 2.3 cm) [2]. The assumed line connected from the tragus to the Figure 1. Anatomy of the TMJ.
4 Surgical Approaches to the Temporomandibular Joint Figure 2. Anatomy of the articular ligaments. Figure 3. Anatomy of the facial nerve. lateral palpebral commissure is considered the superior limit of temporal branch of the facial nerve. This branch of facial nerve is mostly located under this oblique line [3]. Temporal branch is the most susceptible branch of facial nerve that would be damaged during the approaches to the TMJ [4]. This nerve branch lies under the surface of temporoparietal fascia [5]. The average distance of bony part of external auditory canal to the location where temporal branch of facial nerve crosses the zygomatic arch is almost 2 cm (8 35 mm). In some surgical approaches to the subcondylar area, the most important anatomical structure that
5 188 Temporomandibular Joint Pathology - Current Approaches and Understanding should be preserved is the marginal mandibular branch of the facial nerve. This branch is superior to the mandibular inferior border in 74% of the cases [6]. The maximum distance to the mandibular inferior border is 1.2 cm; in other patients that marginal mandibular branch of facial nerve is located beneath the inferior border of the mandible. This branch is located superior to the facial artery and vein immediately deep to the supericial layer of the deep cervical fascia. The branches of trigeminal nerve are other critical structures adjacent to the TMJ. The auriculotemporal branch supplies sensation to the anterior external meatus and the temporal and preauricular region skin. This branch of trigeminal nerve passes behind the neck of mandibular condyle (Figure 4) Anatomy of regional vessels Maxillary artery and supericial temporal artery are two last branches of external carotid artery and important structures adjacent to the TMJ. The surgeons usually face the supericial temporal artery during the preauricular approaches. This terminal branch of external carotid artery runs posterolateral to the mandibular condyle within the temporoparietal fascia (Figure 5). Maxillary artery is important in condylectomy procedure. Middle meningeal artery is a branch of internal maxillary artery that passes medial to the mandibular condyle and could be damaged during the surgical procedures on TMJ. Figure 4. Relation of trigeminal nerve to the TMJ.
6 Surgical Approaches to the Temporomandibular Joint Figure 5. Vascular anatomy of the face encountered during surgical procedures of the TMJ. The important vein that the surgeon usually encounters in surgical treatment of the TMJ problems is retromandibular vein which is formed from the supericial temporal and the maxillary veins. 3. Surgical approaches 3.1. Preauricular surgical technique Preauricular incision is made along the natural crease anterior to the tragus (Figure 6). Dissection should be continued along the cartilage of external auditory canal in order to prevent damaging the auriculotemporal nerve and supericial temporal artery. Supericial layer of the temporalis fascia would be incised 2 cm above the zygomatic arch in an oblique line. Blunt dissection should be continued to reach the zygomatic arch. The periosteum of the zygomatic arch is incised at this time, and it should be relected laterally to achieve to the articular capsule (Figure 7). If the surgeon needs to expose the superior joint space, the incision should be made along the posterior slope of the articular eminence. Incising the disc along the superior joint space, lateral recess allows the surgeon to expose the inferior joint space. In some cases, to maximize the exposure to the TMJ, preauricular incision is modiied to a question mark patern presented by Al-Kayat and Bramley (Figure 8).
7 190 Temporomandibular Joint Pathology - Current Approaches and Understanding Figure 6. Surgical approaches to the TMJ. P1 and P2 preauricular approaches; PA postauricular approach; I inverted hockey stick approach; E endaural approach. R retromandibular approach. Figure 7. After exposing the articular capsule, it could be incised to reach to the joint spaces. Figure 8. Al-Kayat and Bramley incision to expose the TMJ for condylectomy.
8 Surgical Approaches to the Temporomandibular Joint Indications This approach is ideally used to manage the problems encountered in upper condylar process and TMJ compartments. Al-Kayat modiied preauricular incision is routinely used in TMJ ankylosis cases. Preauricular incision is also used in treatment of high condylar fractures Advantages Almost invisible scars are main advantages of a preauricular approach. This surgical technique provides access to the superior part of the TMJ and anteromedially displaced mandibular condyle Disadvantages There is no access to the lower portion of condylar process. Rigid ixation of mandibular condyle fracture is diicult in this approach [7]. The possibility of facial nerve damage is a major disadvantage of this surgical technique Endaural surgical technique This approach is provided to achieve the beneits of preauricular methods simultaneously with more cosmetic results. The incision is made behind the prominence of the tragus. The skin lap is relected over the cartilage of the tragus, and then, dissection is continued in the same manner of preauricular approach Indications This technique is indicated when there is the aim to provide the access to the TMJ and fractures of condylar head and neck Advantages The cosmetic result of scar is beter than preauricular incision [8] Disadvantages Tragus cartilage damage is the main disadvantage of this approach. When the problem happens, poor healing process is expected Postauricular surgical technique The incision is made 3 mm posterior to the posterior auricular fold and carried to the mastoid fascia (Figure 9). Dissection is continued above the mastoid fascia to the external auditory canal which is then transected to retract the pinna anteriorly. Dissection through the supericial layer of temporalis fascia is carried out to the zygomatic arch, and the periosteum is sharply incised to expose the joint. There is no need to suture the cartilage after the surgery, and closing the skin of the ear is enough.
9 192 Temporomandibular Joint Pathology - Current Approaches and Understanding Figure 9. The incision patern of postauricular approach (Courtesy of Dr. F. Pourdanesh) Indications Exposing the entire joint is the main indication of this technique. This approach is also indicated in the patients with the tendency to form keloids who should undergo TMJ surgery Advantages The resulting scar is not very noticeable, and an excellent exposure to the TMJ is provided by this method Disadvantages Auricular stenosis is the main disadvantage of this procedure. External otitis and infection of the TMJ are the contraindications of this approach Submandibular surgical technique To provide the safety zone of marginal mandibular nerve, the incision is made 2 cm below the inferior border of the mandible (Figure 10). The sharp incision is made through the skin and subcutaneous tissue. Then, the platysma is sharply incised to expose the supericial layer of deep cervical fascia. The fascia is incised at the level of the skin incision. The facial artery and vein are retracted or ligated. According to the Hayes-Martin maneuver, ligation and upward retraction of facial vessels protect the marginal mandibular nerve from injury [9]. The dissection is carried to the pterygomasseteric sling. The sling is sharply incised by the blade, and the inferior border of the mandible is exposed (Figure 11) Indications This approach is usually used for mandibular angle and body fractures and sometimes for low subcondylar factures.
10 Surgical Approaches to the Temporomandibular Joint Figure 10. Outline of lateral ramus and submandibular incision. The distance from the inferior border of mandible to the incision should be about 2 cm. Figure 11. Exposure of mandibular angle, body, and lateral ramus area by submandibular approach Advantages The advantage of this technique is the ability to retract the mandibular angle when the surgeon atempts to reduct the condylar fracture. Also, this method provides good accessibility for anchor screw ixation technique of mandibular subcondyle fractures Disadvantages There is limited access to the high condylar portion and joint spaces Retromandibular surgical technique The incision is made along the posterior border of mandible 5 mm below the earlobe inferiorly for a distance of about 3 cm. Incision is continued through the skin, subcutaneous tissue, platysma, and supericial musculoaponeuretic system (SMAS). The SMAS layer is undermined,
11 194 Temporomandibular Joint Pathology - Current Approaches and Understanding and blunt dissection is continued to the substance of the parotid. The dissection is carried to the periosteum of the posterior border of the mandible. The periosteum is sharply incised, and the access to the lower portion of condylar process is provided Indications This technique is used for internal rigid ixation of low condylar fracture. This approach is also used for ixation of costochondral graft in TMJ region Advantages Good accessibility to the lower portion of condylar fracture and subcondylar area is the main advantage of retromandibular approach. A less noticeable scar in comparison with the submandibular technique is the other advantage of this approach Disadvantages A more visible scar than preauricular incision is the disadvantage of this technique. The access to the joint spaces and anteromedially displaced condyle is limited in this surgical method Rhytidectomy surgical technique The incision is made in preauricular area and in the neck hairline (Figure 12). The skin and subcutaneous tissue are incised, and dissection is carried above the level of SMAS (Figure 13). Figure 12. Outline of incision for rhytidectomy approach is combined of preauricular incision and an incision in neck hairline.
12 Surgical Approaches to the Temporomandibular Joint Figure 13. After incising the skin and subcutaneous tissue for rhytidectomy approach, dissection is continued over the SMAS. A vertical incision is made through the SMAS onto the parotid gland, extending from just below the ear lobe toward the gonial angle. Blunt dissection through the substance of parotid is continued to the posterior border of the mandible. The periosteum is sharply incised, and the entire mandibular ramus is exposed (Figure 14) Indications This approach is indicated when the accessibility to the lower portion of TMJ is needed similar to the retromandibular technique although its cosmetic results are much beter than the later technique Advantages Good cosmetic results of the scar and enough access to the condylar process are the most important advantages. Figure 14. Exposure of condylar neck fracture by rhytidectomy approach. The fracture was reduced and ixed by two miniplates.
13 196 Temporomandibular Joint Pathology - Current Approaches and Understanding Disadvantages Damage to the branches of facial nerve is the most important disaster that could happen in this method Intraoral approach surgical technique Incision is made in an external oblique ridge area. Subperiosteal dissection is carried out over the mandibular ramus (Figure 15) Indications Reduction and ixation of subcondyle fracture are two usual indications of intraoral approach. This method is also used sometimes for condylectomy [10] Advantages Invisible scar and preventing from facial nerve damage are the beneits of current approach Disadvantages Limited access to the TMJ is the main problem during this surgical method Endoscopic approach surgical technique Subperiosteal dissection is performed following the incision of posterior mandibular buccal sulcus. A percutaneous incision is then made perpendicular to the mandibular condyle just to pass the endoscope. Further dissection is then carried under direct vision provided by the endoscope Indications Mandibular condyle fractures are the main indications of this approach. Figure 15. Intraoral approach to manage mandibular subcondyle fracture in a 9-year-old boy.
14 Surgical Approaches to the Temporomandibular Joint Advantages This method is minimally invasive with invisible scars. The possibility of nerve damage during this technique is very low [11] Disadvantages Increasing the operation time is a disadvantage of endoscopic technique [12]. 4. Conclusion Deciding on choosing a unique surgical technique for the treatment of all pathologies and diseases of the TMJ is impossible. It is important to understand the pros and cons of all available procedures and choose the best approach with most beneits which provides the best access to the TMJ. Acknowledgements We would like to thank Hossein Esmaeelinejad for providing the illustrations of the chapter. Conlict of interest The authors declare that they have no conlict of interest. Author details Mohammad Esmaeelinejad 1 * and Maryam Sohrabi 2 *Address all correspondence to: esmaeelnejad@gmail.com 1 Department of Oral and Maxillofacial Surgery, School of Dentistry, Semnan University of Medical Sciences, Semnan, Iran 2 Department of Oral and Maxillofacial Surgery, School of Dentistry, Azad University of Medical Sciences, Tehran, Iran References [1] Yang HM, Won SY, Kim HJ, Hu KS. Neurovascular structures of the mandibular angle and condyle: a comprehensive anatomical review. Surgical and Radiologic Anatomy: SRA. 2015;37:
15 198 Temporomandibular Joint Pathology - Current Approaches and Understanding [2] Al-Kayat A, Bramley P. A modiied pre-auricular approach to the temporomandibular joint and malar arch. The British Journal of Oral Surgery. 1979;17: [3] Saylam C, Ucerler H, Orhan M, Ozek C. Anatomic guides to precisely localize the zygomatic branches of the facial nerve. The Journal of Craniofacial Surgery. 2006;17:50-53 [4] de Bonnecaze G, Chaput B, Filleron T, Al Hawat A, Vergez S, Chaynes P. The frontal branch of the facial nerve: can we deine a safety zone? Surgical and radiologic anatomy: SRA. 2015;37: [5] Pourdanesh F, Esmaeelinejad M, Jafari SM, Nematollahi Z. Facelift: Current Concepts, Techniques, and Principles. In: A Textbook of Advanced Oral and Maxillofacial Surgery Volume 3. InTech; 2016 [6] Saylam C, Ucerler H, Orhan M, Uckan A, Ozek C. Localization of the marginal mandibular branch of the facial nerve. Journal of Craniofacial Surgery. 2007;18: [7] Jayavelu P, Riaz R, Tariq Salam AR, Saravanan B, Karthick R. Diiculties encountered in preauricular approach over retromandibular approach in condylar fracture. Journal of Pharmacy & Bioallied Sciences. 2016;8:S175-S1s8 [8] Santos GS, Nogueira LM, Sonoda CK, de Melo WM. Using endaural approach for temporomandibular joint access. The Journal of Craniofacial Surgery. 2014;25: [9] Richards AT. Chapter 14 - Surgical Exposures for the Nerves of the Neck A2 - Tubbs, R. Shane. In: Rizk E, Shoja MM, Loukas M, Barbaro N, Spinner RJ, editors. Nerves and Nerve Injuries. San Diego: Academic Press; p [10] Li B, Sun H, Zhang L, Wang X. Simple way of facilitating intraoral condylectomy and securing the excised condyle: technical note. The British journal of oral & maxillofacial surgery. 2013;51:e305-e306 [11] You HJ, Moon KC, Yoon ES, Lee BI, Park SH. Clinical and radiological outcomes of transoral endoscope-assisted treatment of mandibular condylar fractures. International Journal of Oral and Maxillofacial Surgery. 2016;45: [12] Schmelzeisen R, Cienfuegos-Monroy R, Schon R, Chen CT, Cunningham L Jr, Goldhahn S. Patient beneit from endoscopically assisted ixation of condylar neck fractures--a randomized controlled trial. Journal of oral and maxillofacial surgery : Oicial Journal of the American Association of Oral and Maxillofacial Surgeons. 2009;67:
Parotid Gland, Temporomandibular Joint and Infratemporal Fossa
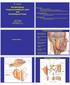 M1 - Anatomy Parotid Gland, Temporomandibular Joint and Infratemporal Fossa Jeff Dupree Sanger 9-057 jldupree@vcu.edu Parotid gland: wraps around the mandible positioned between the mandible and the sphenoid
M1 - Anatomy Parotid Gland, Temporomandibular Joint and Infratemporal Fossa Jeff Dupree Sanger 9-057 jldupree@vcu.edu Parotid gland: wraps around the mandible positioned between the mandible and the sphenoid
Parotid Gland. Parotid Gland. Largest of 3 paired salivary glands (submandibular; sublingual) Ramus of Mandible. Medial pterygoid.
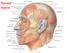 Parotid region Parotid Gland Largest of 3 paired salivary glands (submandibular; sublingual) Ramus of Mandible Medial pterygoid Cross section of mandible Masseter D S SCM Parotid Gland Mastoid Process
Parotid region Parotid Gland Largest of 3 paired salivary glands (submandibular; sublingual) Ramus of Mandible Medial pterygoid Cross section of mandible Masseter D S SCM Parotid Gland Mastoid Process
The Skull and Temporomandibular joint II Prof. Abdulameer Al-Nuaimi. E. mail:
 The Skull and Temporomandibular joint II Prof. Abdulameer Al-Nuaimi E-mail: a.al-nuaimi@sheffield.ac.uk E. mail: abdulameerh@yahoo.com Temporal fossa The temporal fossa is a depression on the temporal
The Skull and Temporomandibular joint II Prof. Abdulameer Al-Nuaimi E-mail: a.al-nuaimi@sheffield.ac.uk E. mail: abdulameerh@yahoo.com Temporal fossa The temporal fossa is a depression on the temporal
Temporal region. temporal & infratemporal fossae. Zhou Hong Ying Dept. of Anatomy
 Temporal region temporal & infratemporal fossae Zhou Hong Ying Dept. of Anatomy Temporal region is divided by zygomatic arch into temporal & infratemporal fossae. Temporal Fossa Infratemporal fossa Temporal
Temporal region temporal & infratemporal fossae Zhou Hong Ying Dept. of Anatomy Temporal region is divided by zygomatic arch into temporal & infratemporal fossae. Temporal Fossa Infratemporal fossa Temporal
Temporomandibular Joint. Dr Noman ullah wazir
 Temporomandibular Joint Dr Noman ullah wazir Type of Joint TMJ is a Synovial joint between : The condylar head of the mandible. The mandibular fossa of squamous part of temporal bone. The joint cavity
Temporomandibular Joint Dr Noman ullah wazir Type of Joint TMJ is a Synovial joint between : The condylar head of the mandible. The mandibular fossa of squamous part of temporal bone. The joint cavity
be very thin and variable. Facial nerve branches that exit the parotid gland are deep to the SMAS.
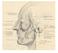 The Superficial musculoaponeurotic system (SMAS) fascia is a fanlike fascia that envelops the face and provides a suspensory sheet which distributes forces of facial expression.. The SMAS is continuous
The Superficial musculoaponeurotic system (SMAS) fascia is a fanlike fascia that envelops the face and provides a suspensory sheet which distributes forces of facial expression.. The SMAS is continuous
Muscles of mastication [part 1]
![Muscles of mastication [part 1] Muscles of mastication [part 1]](/thumbs/76/73586850.jpg) Muscles of mastication [part 1] In this lecture well have the muscles of mastication, neuromuscular function, and its relationship to the occlusion morphology. The fourth determinant of occlusion is the
Muscles of mastication [part 1] In this lecture well have the muscles of mastication, neuromuscular function, and its relationship to the occlusion morphology. The fourth determinant of occlusion is the
Clinical Study Open Reduction of Subcondylar Fractures Using a New Retractor
 Plastic Surgery International Volume 2011, Article ID 421245, 5 pages doi:10.1155/2011/421245 Clinical Study Open Reduction of Subcondylar Fractures Using a New Retractor Akira Sugamata, 1 Naoki Yoshizawa,
Plastic Surgery International Volume 2011, Article ID 421245, 5 pages doi:10.1155/2011/421245 Clinical Study Open Reduction of Subcondylar Fractures Using a New Retractor Akira Sugamata, 1 Naoki Yoshizawa,
Use of Modified Retro-mandibular subparotid approach for treatment of Condylar fracture: a Technical note
 Original article: Use of Modified Retro-mandibular subparotid approach for treatment of Condylar fracture: a Technical note 1 DR.Sonal Anchlia, 2 DR.BIPIN.S.SADHWANI, 3 DR.ROHIT KUMAR, 4 Dr.Vipul 1Assistant
Original article: Use of Modified Retro-mandibular subparotid approach for treatment of Condylar fracture: a Technical note 1 DR.Sonal Anchlia, 2 DR.BIPIN.S.SADHWANI, 3 DR.ROHIT KUMAR, 4 Dr.Vipul 1Assistant
Tikrit University collage of dentistry Dr.Ban I.S. head & neck anatomy 2 nd y. Lec [5] / Temporal fossa :
![Tikrit University collage of dentistry Dr.Ban I.S. head & neck anatomy 2 nd y. Lec [5] / Temporal fossa : Tikrit University collage of dentistry Dr.Ban I.S. head & neck anatomy 2 nd y. Lec [5] / Temporal fossa :](/thumbs/88/115294566.jpg) Lec [5] / Temporal fossa : Borders of the Temporal Fossa: Superior: Superior temporal line. Inferior: gap between zygomatic arch and infratemporal crest of sphenoid bone. Anterior: Frontal process of the
Lec [5] / Temporal fossa : Borders of the Temporal Fossa: Superior: Superior temporal line. Inferior: gap between zygomatic arch and infratemporal crest of sphenoid bone. Anterior: Frontal process of the
Infratemporal fossa: Tikrit University college of Dentistry Dr.Ban I.S. head & neck Anatomy 2 nd y.
 Infratemporal fossa: This is a space lying beneath the base of the skull between the lateral wall of the pharynx and the ramus of the mandible. It is also referred to as the parapharyngeal or lateral pharyngeal
Infratemporal fossa: This is a space lying beneath the base of the skull between the lateral wall of the pharynx and the ramus of the mandible. It is also referred to as the parapharyngeal or lateral pharyngeal
Tikrit University College of Dentistry Dr.Ban I.S. head & neck anatomy 2 nd y.
 Lec [3]/The scalp The scalp extends from the supraorbital margins anteriorly to the nuchal lines at the back of the skull and down to the temporal lines at the sides. The forehead, from eyebrows to hairline,
Lec [3]/The scalp The scalp extends from the supraorbital margins anteriorly to the nuchal lines at the back of the skull and down to the temporal lines at the sides. The forehead, from eyebrows to hairline,
Head and Face Anatomy
 Head and Face Anatomy Epicranial region The Scalp The soft tissue that covers the vault of skull. Extends from supraorbital margin to superior nuchal line. Layers of the scalp S C A L P = skin = connective
Head and Face Anatomy Epicranial region The Scalp The soft tissue that covers the vault of skull. Extends from supraorbital margin to superior nuchal line. Layers of the scalp S C A L P = skin = connective
STEP 1 INCISION AND ELEVATION OF SKIN FLAP STEP 3 SEPARATE PAROTID GLAND FROM SCM STEP 2 IDENTIFICATON OF GREAT AURICULAR NERVE
 STEP 1 INCISION AND ELEVATION OF SKIN FLAP Create a modified Blair Figure 1 or facelift incision. Figure 2 Raise a superficial cervico-fascial flap between the Superficial Musculo Aponeurotic System (SMAS)
STEP 1 INCISION AND ELEVATION OF SKIN FLAP Create a modified Blair Figure 1 or facelift incision. Figure 2 Raise a superficial cervico-fascial flap between the Superficial Musculo Aponeurotic System (SMAS)
Temporal fossa Infratemporal fossa Pterygopalatine fossa Terminal branches of external carotid artery Pterygoid venous plexus
 Outline of content Temporal fossa Infratemporal fossa Pterygopalatine fossa Terminal branches of external carotid artery Pterygoid venous plexus Boundary Content Communication Mandibular division of trigeminal
Outline of content Temporal fossa Infratemporal fossa Pterygopalatine fossa Terminal branches of external carotid artery Pterygoid venous plexus Boundary Content Communication Mandibular division of trigeminal
Oral & Maxillofacial Surgery
 Chapter 2 Oral & Maxillofacial Surgery Ruchi Singhal 1 ; Virendra Singh 2 ; Amrish Bhagol* 1 Jaipur Dental College, Jaipur, India 2 Senior Professor, PGIDS, Rohtak, India Amrish Bhagol Condylar Fractures
Chapter 2 Oral & Maxillofacial Surgery Ruchi Singhal 1 ; Virendra Singh 2 ; Amrish Bhagol* 1 Jaipur Dental College, Jaipur, India 2 Senior Professor, PGIDS, Rohtak, India Amrish Bhagol Condylar Fractures
Anatomy and Physiology. Bones, Sutures, Teeth, Processes and Foramina of the Human Skull
 Anatomy and Physiology Chapter 6 DRO Bones, Sutures, Teeth, Processes and Foramina of the Human Skull Name: Period: Bones of the Human Skull Bones of the Cranium: Frontal bone: forms the forehead and the
Anatomy and Physiology Chapter 6 DRO Bones, Sutures, Teeth, Processes and Foramina of the Human Skull Name: Period: Bones of the Human Skull Bones of the Cranium: Frontal bone: forms the forehead and the
For the following questions, indicate the letter that corresponds to the SINGLE MOST APPROPRIATE ANSWER
 GROSS ANATOMY EXAMINATION May 15, 2000 For the following questions, indicate the letter that corresponds to the SINGLE MOST APPROPRIATE ANSWER 1. Pain associated with an infection limited to the middle
GROSS ANATOMY EXAMINATION May 15, 2000 For the following questions, indicate the letter that corresponds to the SINGLE MOST APPROPRIATE ANSWER 1. Pain associated with an infection limited to the middle
Skull-2. Norma Basalis Interna Norma Basalis Externa. Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology
 Skull-2 Norma Basalis Interna Norma Basalis Externa Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology Norma basalis interna Base of the skull- superior view The interior of the base of the
Skull-2 Norma Basalis Interna Norma Basalis Externa Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology Norma basalis interna Base of the skull- superior view The interior of the base of the
Dr. Sami Zaqout Faculty of Medicine IUG
 Auricle External Ear External auditory meatus The Ear Middle Ear (Tympanic Cavity) Auditory ossicles Internal Ear (Labyrinth) Bony labyrinth Membranous labyrinth External Ear Auricle External auditory
Auricle External Ear External auditory meatus The Ear Middle Ear (Tympanic Cavity) Auditory ossicles Internal Ear (Labyrinth) Bony labyrinth Membranous labyrinth External Ear Auricle External auditory
The Melbourne Temporomandibular Total Joint Replacement System
 The Melbourne Temporomandibular Total Joint Replacement System Device Description: The Melbourne TMJ Total Joint Replacement System is used to reconstruct a damaged or diseased temporomandibular joint
The Melbourne Temporomandibular Total Joint Replacement System Device Description: The Melbourne TMJ Total Joint Replacement System is used to reconstruct a damaged or diseased temporomandibular joint
Omran Saeed. Luma Taweel. Mohammad Almohtaseb. 1 P a g e
 2 Omran Saeed Luma Taweel Mohammad Almohtaseb 1 P a g e I didn t include all the photos in this sheet in order to keep it as small as possible so if you need more clarification please refer to slides In
2 Omran Saeed Luma Taweel Mohammad Almohtaseb 1 P a g e I didn t include all the photos in this sheet in order to keep it as small as possible so if you need more clarification please refer to slides In
Lec [8]: Mandibular nerve:
![Lec [8]: Mandibular nerve: Lec [8]: Mandibular nerve:](/thumbs/94/121295776.jpg) Lec [8]: Mandibular nerve: The mandibular branch from the trigeminal ganglion lies in the middle cranial fossa lateral to the cavernous sinus. With the motor root of the trigeminal nerve [motor roots lies
Lec [8]: Mandibular nerve: The mandibular branch from the trigeminal ganglion lies in the middle cranial fossa lateral to the cavernous sinus. With the motor root of the trigeminal nerve [motor roots lies
Dr.Ban I.S. head & neck anatomy 2 nd y. جامعة تكريت كلية طب االسنان املرحلة الثانية أ.م.د. بان امساعيل صديق 6102/6102
 جامعة تكريت كلية طب االسنان التشريح مادة املرحلة الثانية أ.م.د. بان امساعيل صديق 6102/6102 Parotid region The part of the face in front of the ear and below the zygomatic arch is the parotid region. The
جامعة تكريت كلية طب االسنان التشريح مادة املرحلة الثانية أ.م.د. بان امساعيل صديق 6102/6102 Parotid region The part of the face in front of the ear and below the zygomatic arch is the parotid region. The
PTERYGOPALATINE FOSSA
 PTERYGOPALATINE FOSSA Outline Anatomical Structure and Boundaries Foramina and Communications with other spaces and cavities Contents Pterygopalatine Ganglion Especial emphasis on certain arteries and
PTERYGOPALATINE FOSSA Outline Anatomical Structure and Boundaries Foramina and Communications with other spaces and cavities Contents Pterygopalatine Ganglion Especial emphasis on certain arteries and
Face. Definition: The area between the two ears and from the chin to the eye brows. The muscles of the face
 Face Definition: The area between the two ears and from the chin to the eye brows. The muscles of the face The muscle of facial expression (include the muscle of the face and the scalp). All are derived
Face Definition: The area between the two ears and from the chin to the eye brows. The muscles of the face The muscle of facial expression (include the muscle of the face and the scalp). All are derived
Anatomy and physiology of Temporomandibular Joint
 Anatomy and physiology of Temporomandibular Joint Temporomandibular joint (TMJ): It is the articulation of the condyle of the mandible, and the inter-articular disc; with the mandibular fossa (glenoid
Anatomy and physiology of Temporomandibular Joint Temporomandibular joint (TMJ): It is the articulation of the condyle of the mandible, and the inter-articular disc; with the mandibular fossa (glenoid
Bones Ethmoid bone Inferior nasal concha Lacrimal bone Maxilla Nasal bone Palatine bone Vomer Zygomatic bone Mandible
 splanchnocranium - Consists of part of skull that is derived from branchial arches - The facial bones are the bones of the anterior and lower human skull Bones Ethmoid bone Inferior nasal concha Lacrimal
splanchnocranium - Consists of part of skull that is derived from branchial arches - The facial bones are the bones of the anterior and lower human skull Bones Ethmoid bone Inferior nasal concha Lacrimal
3. The Jaw and Related Structures
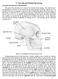 Overview and objectives of this dissection 3. The Jaw and Related Structures The goal of this dissection is to observe the muscles of jaw raising. You will also have the opportunity to observe several
Overview and objectives of this dissection 3. The Jaw and Related Structures The goal of this dissection is to observe the muscles of jaw raising. You will also have the opportunity to observe several
Alexander C Vlantis. Selective Neck Dissection 33
 05 Modified Radical Neck Dissection Type II Alexander C Vlantis Selective Neck Dissection 33 Modified Radical Neck Dissection Type II INCISION Various incisions can be used for a neck dissection. The incision
05 Modified Radical Neck Dissection Type II Alexander C Vlantis Selective Neck Dissection 33 Modified Radical Neck Dissection Type II INCISION Various incisions can be used for a neck dissection. The incision
Trigeminal Nerve Worksheets, Distributions Page 1
 Trigeminal Nerve Worksheet #1 Distribution by Nerve Dr. Darren Hoffmann Dental Gross Anatomy, Spring 2013 We have drawn out each of the branches of CN V in lecture and you have an idea now for their basic
Trigeminal Nerve Worksheet #1 Distribution by Nerve Dr. Darren Hoffmann Dental Gross Anatomy, Spring 2013 We have drawn out each of the branches of CN V in lecture and you have an idea now for their basic
Veins of the Face and the Neck
 Veins of the Face and the Neck Facial Vein The facial vein is formed at the medial angle of the eye by the union of the supraorbital and supratrochlear veins. connected through the ophthalmic veins with
Veins of the Face and the Neck Facial Vein The facial vein is formed at the medial angle of the eye by the union of the supraorbital and supratrochlear veins. connected through the ophthalmic veins with
THIEME. Scalp and Superficial Temporal Region
 CHAPTER 2 Scalp and Superficial Temporal Region Scalp Learning Objectives At the end of the dissection of the scalp, you should be able to identify, understand and correlate the clinical aspects: Layers
CHAPTER 2 Scalp and Superficial Temporal Region Scalp Learning Objectives At the end of the dissection of the scalp, you should be able to identify, understand and correlate the clinical aspects: Layers
3-Deep fascia: is absent (except over the parotid gland & buccopharngeal fascia covering the buccinator muscle)
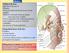 The Face 1-Skin of the Face The skin of the face is: Elastic Vascular (bleed profusely however heal rapidly) Rich in sweat and sebaceous glands (can cause acne in adults) It is connected to the underlying
The Face 1-Skin of the Face The skin of the face is: Elastic Vascular (bleed profusely however heal rapidly) Rich in sweat and sebaceous glands (can cause acne in adults) It is connected to the underlying
ANTERIOR CERVICAL TRIANGLE (Fig. 2.1 )
 2 Neck Anatomy ANTERIOR CERVICAL TRIANGLE (Fig. 2.1 ) The boundaries are: Lateral: sternocleidomastoid muscle Superior: inferior border of the mandible Medial: anterior midline of the neck This large triangle
2 Neck Anatomy ANTERIOR CERVICAL TRIANGLE (Fig. 2.1 ) The boundaries are: Lateral: sternocleidomastoid muscle Superior: inferior border of the mandible Medial: anterior midline of the neck This large triangle
SCHOOL OF ANATOMICAL SCIENCES Mock Run Questions. 4 May 2012
 SCHOOL OF ANATOMICAL SCIENCES Mock Run Questions 4 May 2012 1. With regard to the muscles of the neck: a. the platysma muscle is supplied by the accessory nerve. b. the stylohyoid muscle is supplied by
SCHOOL OF ANATOMICAL SCIENCES Mock Run Questions 4 May 2012 1. With regard to the muscles of the neck: a. the platysma muscle is supplied by the accessory nerve. b. the stylohyoid muscle is supplied by
REVIEW/PREVIEW OF HEAD AND NECK ANATOMY FOR ENT EXAM
 REVIEW/PREVIEW OF HEAD AND NECK ANATOMY FOR ENT EXAM - 2017 PALPATE CAROTID ARTERY: AT LEVEL OF CAROTID BIFURCATION VERTEBRAL LEVEL C4 Sternocleidomastoid Muscle INTERNAL CAROTID EXTERNAL CAROTID COMMON
REVIEW/PREVIEW OF HEAD AND NECK ANATOMY FOR ENT EXAM - 2017 PALPATE CAROTID ARTERY: AT LEVEL OF CAROTID BIFURCATION VERTEBRAL LEVEL C4 Sternocleidomastoid Muscle INTERNAL CAROTID EXTERNAL CAROTID COMMON
Bones of the skull & face
 Bones of the skull & face Cranium= brain case or helmet Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display. The cranium is composed of eight bones : frontal Occipital
Bones of the skull & face Cranium= brain case or helmet Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display. The cranium is composed of eight bones : frontal Occipital
The Visible Ear Simulator Dissection Manual.
 The Visible Ear Simulator Dissection Manual. Stereoscopic Tutorialized Version 3.1, August 2017 Peter Trier Mikkelsen, the Alexandra Institute A/S, Aarhus, Denmark Mads Sølvsten Sørensen & Steven Andersen,
The Visible Ear Simulator Dissection Manual. Stereoscopic Tutorialized Version 3.1, August 2017 Peter Trier Mikkelsen, the Alexandra Institute A/S, Aarhus, Denmark Mads Sølvsten Sørensen & Steven Andersen,
Dr.Noor Hashem Mohammad Lecture (5)
 Dr.Noor Hashem Mohammad Lecture (5) 2016-2017 If the mandible is discarded, the anterior part of this aspect of the skull is seen to be formed by the hard palate. The palatal processes of the maxillae
Dr.Noor Hashem Mohammad Lecture (5) 2016-2017 If the mandible is discarded, the anterior part of this aspect of the skull is seen to be formed by the hard palate. The palatal processes of the maxillae
THE ANGULAR TRACT: AN ANATOMICAL
 British Journal of Oral Surgery (1981) 19, 116-120 0 The British Association of Oral Surgeons 0007-117X/81/00170116$02.00 THE ANGULAR TRACT: AN ANATOMICAL OF SURGICAL SIGNIFICANCE STRUCTURE HAITHEM A.
British Journal of Oral Surgery (1981) 19, 116-120 0 The British Association of Oral Surgeons 0007-117X/81/00170116$02.00 THE ANGULAR TRACT: AN ANATOMICAL OF SURGICAL SIGNIFICANCE STRUCTURE HAITHEM A.
Mohammad Hisham Al-Mohtaseb. Lina Mansour. Reyad Jabiri. 0 P a g e
 2 Mohammad Hisham Al-Mohtaseb Lina Mansour Reyad Jabiri 0 P a g e This is only correction for the last year sheet according to our record. If you already studied this sheet just read the yellow notes which
2 Mohammad Hisham Al-Mohtaseb Lina Mansour Reyad Jabiri 0 P a g e This is only correction for the last year sheet according to our record. If you already studied this sheet just read the yellow notes which
Upper arch. 1Prosthodontics. Dr.Bassam Ali Al-Turaihi. Basic anatomy & & landmark of denture & mouth
 1Prosthodontics Lecture 2 Dr.Bassam Ali Al-Turaihi Basic anatomy & & landmark of denture & mouth Upper arch Palatine process of maxilla: it form the anterior three quarter of the hard palate. Horizontal
1Prosthodontics Lecture 2 Dr.Bassam Ali Al-Turaihi Basic anatomy & & landmark of denture & mouth Upper arch Palatine process of maxilla: it form the anterior three quarter of the hard palate. Horizontal
Introduction to Occlusion and Mechanics of Mandibular Movement
 Introduction to Occlusion and Mechanics of Mandibular Movement Dr. Pauline Hayes Garrett Department of Endodontics, Prosthodontics, and Operative Dentistry University of Maryland, Baltimore Assigned reading
Introduction to Occlusion and Mechanics of Mandibular Movement Dr. Pauline Hayes Garrett Department of Endodontics, Prosthodontics, and Operative Dentistry University of Maryland, Baltimore Assigned reading
Structure Location Function
 Frontal Bone Cranium forms the forehead and roof of the orbits Occipital Bone Cranium forms posterior and inferior portions of the cranium Temporal Bone Cranium inferior to the parietal bone forms the
Frontal Bone Cranium forms the forehead and roof of the orbits Occipital Bone Cranium forms posterior and inferior portions of the cranium Temporal Bone Cranium inferior to the parietal bone forms the
Conventional radiograph verses CT for evaluation of sagittal fracture of mandibular condyle
 Case Report: Conventional radiograph verses CT for evaluation of sagittal fracture of mandibular condyle Dr Anjali Wadhwa, Dr Gaurav Shah, Dr Shweta Sharma, Dr Anand Bhatnagar, Dr Pallavi Malaviya NIMS
Case Report: Conventional radiograph verses CT for evaluation of sagittal fracture of mandibular condyle Dr Anjali Wadhwa, Dr Gaurav Shah, Dr Shweta Sharma, Dr Anand Bhatnagar, Dr Pallavi Malaviya NIMS
Skeletal System: Skull.
 Skeletal System: Skull www.fisiokinesiterapia.biz Bones of the Skull SPLANCHNOCRANIUM Nasal (2) Maxilla (2) Lacrimal (2) Zygomatic (2) Palatine (2) Inferior concha (2) Vomer Mandible NEUROCRANIUM Frontal
Skeletal System: Skull www.fisiokinesiterapia.biz Bones of the Skull SPLANCHNOCRANIUM Nasal (2) Maxilla (2) Lacrimal (2) Zygomatic (2) Palatine (2) Inferior concha (2) Vomer Mandible NEUROCRANIUM Frontal
Functional components
 Facial Nerve VII cranial nerve Emerges from Pons Two roots Functional components: 1. GSA (general somatic afferent) 2. SA (Somatic afferent) 3. GVE (general visceral efferent) 4. BE (Special visceral/branchial
Facial Nerve VII cranial nerve Emerges from Pons Two roots Functional components: 1. GSA (general somatic afferent) 2. SA (Somatic afferent) 3. GVE (general visceral efferent) 4. BE (Special visceral/branchial
Temporomandibular Joint
 6 Temporomandibular Joint Most human bones are joined with one another. These connections of bones to each other are termed articulations or joints. Some joints are immovable as in the articulations of
6 Temporomandibular Joint Most human bones are joined with one another. These connections of bones to each other are termed articulations or joints. Some joints are immovable as in the articulations of
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists. International authors and editors
 We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 4,000 116,000 120M Open access books available International authors and editors Downloads Our
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 4,000 116,000 120M Open access books available International authors and editors Downloads Our
The Neck the lower margin of the mandible above the suprasternal notch and the upper border of the clavicle
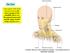 The Neck is the region of the body that lies between the lower margin of the mandible above and the suprasternal notch and the upper border of the clavicle below Nerves of the neck Cervical Plexus Is formed
The Neck is the region of the body that lies between the lower margin of the mandible above and the suprasternal notch and the upper border of the clavicle below Nerves of the neck Cervical Plexus Is formed
Anatomical Landmarks to Avoid Injury to the Great Auricular Nerve During Rhytidectomy
 Facial Surgery Anatomical Landmarks to Avoid Injury to the Great Auricular Nerve During Rhytidectomy Todd Lefkowitz, MD; Ron Hazani, MD; Saeed Chowdhry, MD; Josh Elston, BS; Michael J. Yaremchuk, MD; and
Facial Surgery Anatomical Landmarks to Avoid Injury to the Great Auricular Nerve During Rhytidectomy Todd Lefkowitz, MD; Ron Hazani, MD; Saeed Chowdhry, MD; Josh Elston, BS; Michael J. Yaremchuk, MD; and
Gross Anatomy of the. TEMPORAL BONE, EXTERNAL EAR, and MIDDLE EAR. Assignment: Head to Toe Temporomandibular Joint (TMJ)
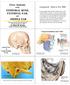 Gross Anatomy the TEMPORAL BONE, EXTERNAL EAR, and MIDDLE EAR M1 Gross and Developmental Anatomy 9:00 AM, December 11, 2008 Dr. Milton M. Sholley Pressor Anatomy and Neurobiology Assignment: Head to Toe
Gross Anatomy the TEMPORAL BONE, EXTERNAL EAR, and MIDDLE EAR M1 Gross and Developmental Anatomy 9:00 AM, December 11, 2008 Dr. Milton M. Sholley Pressor Anatomy and Neurobiology Assignment: Head to Toe
Report of Ankylosis of the Temporomandibular Joint: Treatment with a Temporalis Muscle Flap and Augmentation Genioplasty
 Report of Ankylosis of the Temporomandibular Joint: Treatment with a Temporalis Muscle Flap and Augmentation Genioplasty Abstract A case of true bilateral ankylosis of the temporomandibular joint (TMJ)
Report of Ankylosis of the Temporomandibular Joint: Treatment with a Temporalis Muscle Flap and Augmentation Genioplasty Abstract A case of true bilateral ankylosis of the temporomandibular joint (TMJ)
Chapter 7 Part A The Skeleton
 Chapter 7 Part A The Skeleton Why This Matters Understanding the anatomy of the skeleton enables you to anticipate problems such as pelvic dimensions that may affect labor and delivery The Skeleton The
Chapter 7 Part A The Skeleton Why This Matters Understanding the anatomy of the skeleton enables you to anticipate problems such as pelvic dimensions that may affect labor and delivery The Skeleton The
Gross Anatomy of the. TEMPORAL BONE, EXTERNAL EAR, and MIDDLE EAR
 Gross Anatomy of the TEMPORAL BONE, EXTERNAL EAR, and MIDDLE EAR M1 Gross and Developmental Anatomy 9:00 AM, December 11, 2008 Dr. Milton M. Sholley Professor of Anatomy and Neurobiology Assignment: Head
Gross Anatomy of the TEMPORAL BONE, EXTERNAL EAR, and MIDDLE EAR M1 Gross and Developmental Anatomy 9:00 AM, December 11, 2008 Dr. Milton M. Sholley Professor of Anatomy and Neurobiology Assignment: Head
Small access postaural parotidectomy: an analysis of techniques, feasibility and safety
 Eur Arch Otorhinolaryngol (2016) 273:1879 1883 DOI 10.1007/s00405-015-3691-9 HEAD AND NECK Small access postaural parotidectomy: an analysis of techniques, feasibility and safety Anthony Po-Wing Yuen 1
Eur Arch Otorhinolaryngol (2016) 273:1879 1883 DOI 10.1007/s00405-015-3691-9 HEAD AND NECK Small access postaural parotidectomy: an analysis of techniques, feasibility and safety Anthony Po-Wing Yuen 1
Maxilla, ORBIT and infratemporal fossa. Neophytos C Demetriades MD, DDS, MSc Associate professor European University of Cyprus School of Medicine
 Maxilla, ORBIT and infratemporal fossa Neophytos C Demetriades MD, DDS, MSc Associate professor European University of Cyprus School of Medicine MAXILLA Superior, middle, and inferior meatus Frontal sinus
Maxilla, ORBIT and infratemporal fossa Neophytos C Demetriades MD, DDS, MSc Associate professor European University of Cyprus School of Medicine MAXILLA Superior, middle, and inferior meatus Frontal sinus
Dr. Sami Zaqout, IUG Medical School
 The skull The skull is composed of several separate bones united at immobile joints called sutures. Exceptions? Frontal bone Occipital bone Vault Cranium Sphenoid bone Zygomatic bones Base Ethmoid bone
The skull The skull is composed of several separate bones united at immobile joints called sutures. Exceptions? Frontal bone Occipital bone Vault Cranium Sphenoid bone Zygomatic bones Base Ethmoid bone
Skull-2. Norma Basalis Interna. Dr. Heba Kalbouneh Assistant Professor of Anatomy and Histology
 Skull-2 Norma Basalis Interna Dr. Heba Kalbouneh Assistant Professor of Anatomy and Histology Norma basalis interna Base of the skull- superior view The interior of the base of the skull is divided into
Skull-2 Norma Basalis Interna Dr. Heba Kalbouneh Assistant Professor of Anatomy and Histology Norma basalis interna Base of the skull- superior view The interior of the base of the skull is divided into
AXIAL SKELETON SKULL
 AXIAL SKELETON SKULL CRANIAL BONES (8 total flat bones w/ 2 paired) 1. Frontal forms forehead & upper portion of eyesocket (orbital) 2. Parietal paired bones; form superior & lateral walls of cranium 3.
AXIAL SKELETON SKULL CRANIAL BONES (8 total flat bones w/ 2 paired) 1. Frontal forms forehead & upper portion of eyesocket (orbital) 2. Parietal paired bones; form superior & lateral walls of cranium 3.
Anatomic Relations Summary. Done by: Sohayyla Yasin Dababseh
 Anatomic Relations Summary Done by: Sohayyla Yasin Dababseh Anatomic Relations Lecture 1 Part-1 - The medial wall of the nose is the septum. - The vestibule lies directly inside the nostrils (Nares). -
Anatomic Relations Summary Done by: Sohayyla Yasin Dababseh Anatomic Relations Lecture 1 Part-1 - The medial wall of the nose is the septum. - The vestibule lies directly inside the nostrils (Nares). -
By : Prof Saeed Abuel Makarem & Dr.Sanaa Alshaarawi
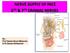 By : Prof Saeed Abuel Makarem & Dr.Sanaa Alshaarawi OBJECTIVES By the end of the lecture, students shouldbe able to: List the nuclei of the deep origin of the trigeminal and facial nerves in the brain
By : Prof Saeed Abuel Makarem & Dr.Sanaa Alshaarawi OBJECTIVES By the end of the lecture, students shouldbe able to: List the nuclei of the deep origin of the trigeminal and facial nerves in the brain
Original Article Analysis of neurologic complications after modified temporomandibular joint disc anchorage surgery
 Int J Clin Exp Med 2017;10(3):5440-5444 www.ijcem.com /ISSN:1940-5901/IJCEM0041511 Original Article Analysis of neurologic complications after modified temporomandibular joint disc anchorage surgery Jin-Ze
Int J Clin Exp Med 2017;10(3):5440-5444 www.ijcem.com /ISSN:1940-5901/IJCEM0041511 Original Article Analysis of neurologic complications after modified temporomandibular joint disc anchorage surgery Jin-Ze
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists. International authors and editors
 We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 4,000 116,000 120M Open access books available International authors and editors Downloads Our
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 4,000 116,000 120M Open access books available International authors and editors Downloads Our
Assessment of Relapse Following Intraoral Vertical Ramus Osteotomy Mandibular Setback and Short-term Immobilization
 Assessment of Relapse Following Intraoral Vertical Ramus Osteotomy Mandibular Setback and Short-term Immobilization Koroush Taheri Talesh, DDS, a Mohammad Hosein Kalantar Motamedi, DDS, b Mahdi Sazavar,
Assessment of Relapse Following Intraoral Vertical Ramus Osteotomy Mandibular Setback and Short-term Immobilization Koroush Taheri Talesh, DDS, a Mohammad Hosein Kalantar Motamedi, DDS, b Mahdi Sazavar,
Bony orbit Roof The orbital plate of the frontal bone Lateral wall: the zygomatic bone and the greater wing of the sphenoid
 Bony orbit Roof: Formed by: The orbital plate of the frontal bone, which separates the orbital cavity from the anterior cranial fossa and the frontal lobe of the cerebral hemisphere Lateral wall: Formed
Bony orbit Roof: Formed by: The orbital plate of the frontal bone, which separates the orbital cavity from the anterior cranial fossa and the frontal lobe of the cerebral hemisphere Lateral wall: Formed
Biology 218 Human Anatomy. Adapted from Martini Human Anatomy 7th ed. Chapter 6 The Skeletal System: Axial Division
 Adapted from Martini Human Anatomy 7th ed. Chapter 6 The Skeletal System: Axial Division Introduction The axial skeleton: Composed of bones along the central axis of the body Divided into three regions:
Adapted from Martini Human Anatomy 7th ed. Chapter 6 The Skeletal System: Axial Division Introduction The axial skeleton: Composed of bones along the central axis of the body Divided into three regions:
PCM1 Physical Exam Skills Session: Head and Neck FACILITATOR & STUDENT COPY
 PATIENT CENTERED MEDICINE - 1 GOALS & OUTCOMES: PCM1 Physical Exam Skills Session: Head and Neck FACILITATOR & STUDENT COPY 1. To introduce the applied anatomy relevant for the examination of the head
PATIENT CENTERED MEDICINE - 1 GOALS & OUTCOMES: PCM1 Physical Exam Skills Session: Head and Neck FACILITATOR & STUDENT COPY 1. To introduce the applied anatomy relevant for the examination of the head
The Ear The ear consists of : 1-THE EXTERNAL EAR 2-THE MIDDLE EAR, OR TYMPANIC CAVITY 3-THE INTERNAL EAR, OR LABYRINTH 1-THE EXTERNAL EAR.
 The Ear The ear consists of : 1-THE EXTERNAL EAR 2-THE MIDDLE EAR, OR TYMPANIC CAVITY 3-THE INTERNAL EAR, OR LABYRINTH 1-THE EXTERNAL EAR Made of A-AURICLE B-EXTERNAL AUDITORY MEATUS A-AURICLE It consists
The Ear The ear consists of : 1-THE EXTERNAL EAR 2-THE MIDDLE EAR, OR TYMPANIC CAVITY 3-THE INTERNAL EAR, OR LABYRINTH 1-THE EXTERNAL EAR Made of A-AURICLE B-EXTERNAL AUDITORY MEATUS A-AURICLE It consists
Skeletal System -Axial System. Chapter 7 Part A
 Skeletal System -Axial System Chapter 7 Part A Skeleton Learn: Names of the s. Identify specific landmarks that allow: Bones to fit into each other, Organs to fit into the cavities, Muscles to attach,
Skeletal System -Axial System Chapter 7 Part A Skeleton Learn: Names of the s. Identify specific landmarks that allow: Bones to fit into each other, Organs to fit into the cavities, Muscles to attach,
NIDCD NATIONAL TEMPORAL BONE, HEARING AND BALANCE PATHOLOGY RESOURCE REGISTRY
 NIDCD NATIONAL TEMPORAL BONE, HEARING AND BALANCE PATHOLOGY RESOURCE REGISTRY Guidelines for Removal of Temporal Bones for Pathological Study The temporal bones should be removed as soon as possible. If
NIDCD NATIONAL TEMPORAL BONE, HEARING AND BALANCE PATHOLOGY RESOURCE REGISTRY Guidelines for Removal of Temporal Bones for Pathological Study The temporal bones should be removed as soon as possible. If
Anatomy and Physiology II. Review Spine and Neck
 Anatomy and Physiology II Review Spine and Neck Spine regions How many cervical vertibrae are there? 7 The curvature is the cervical region posterior? Concave posterior How many thoracic? And curvature?
Anatomy and Physiology II Review Spine and Neck Spine regions How many cervical vertibrae are there? 7 The curvature is the cervical region posterior? Concave posterior How many thoracic? And curvature?
OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY
 OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY BUCCINATOR MYOMUCOSAL FLAP The Buccinator Myomucosal Flap is an axial flap, based on the facial and/or buccal arteries. It is a flexible
OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY BUCCINATOR MYOMUCOSAL FLAP The Buccinator Myomucosal Flap is an axial flap, based on the facial and/or buccal arteries. It is a flexible
The Temporomandibular joint: Anatomy, Mechanics, Pathology. Aditya Bahel, DO
 The Temporomandibular joint: Anatomy, Mechanics, Pathology Aditya Bahel, DO Outline Anatomy Mechanics and function Indications for TMJ imaging MR Protocols and pitfalls Pathology Treatment options Anatomy
The Temporomandibular joint: Anatomy, Mechanics, Pathology Aditya Bahel, DO Outline Anatomy Mechanics and function Indications for TMJ imaging MR Protocols and pitfalls Pathology Treatment options Anatomy
ACTIVITY 3: AXIAL SKELETON AND LONG BONE DISSECTION COW BONE DISSECTION
 ACTIVITY 3: AXIAL SKELETON AND LONG BONE DISSECTION Objectives: 1) How to get ready: Read Chapter 7, McKinley et al., Human Anatomy, 4e. All text references are for this textbook. Learning the meanings
ACTIVITY 3: AXIAL SKELETON AND LONG BONE DISSECTION Objectives: 1) How to get ready: Read Chapter 7, McKinley et al., Human Anatomy, 4e. All text references are for this textbook. Learning the meanings
Scholars Journal of Medical Case Reports
 DOI: 10.21276/sjmcr.2016.4.11.17 Scholars Journal of Medical Case Reports Sch J Med Case Rep 2016; 4(11):863-868 Scholars Academic and Scientific Publishers (SAS Publishers) (An International Publisher
DOI: 10.21276/sjmcr.2016.4.11.17 Scholars Journal of Medical Case Reports Sch J Med Case Rep 2016; 4(11):863-868 Scholars Academic and Scientific Publishers (SAS Publishers) (An International Publisher
Anatomy of the Trigeminal Nerve
 19 Anatomy of the Trigeminal Nerve.1 Introduction 0. The Central Part of the Trigeminal Nerve 1..1 Origin 1.. Trigeminal Nuclei.3 The Peripheral Part of the Trigeminal Nerve 4.3.1 Ophthalmic Nerve 4.3.
19 Anatomy of the Trigeminal Nerve.1 Introduction 0. The Central Part of the Trigeminal Nerve 1..1 Origin 1.. Trigeminal Nuclei.3 The Peripheral Part of the Trigeminal Nerve 4.3.1 Ophthalmic Nerve 4.3.
TRANSVERSE SECTION PLANE Scalp 2. Cranium. 13. Superior sagittal sinus
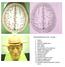 TRANSVERSE SECTION PLANE 1 1. Scalp 2. Cranium 3. Superior sagittal sinus 4. Dura mater 5. Falx cerebri 6. Frontal lobes of the cerebrum 7. Middle meningeal artery 8. Cortex, grey matter 9. Cerebral vessels
TRANSVERSE SECTION PLANE 1 1. Scalp 2. Cranium 3. Superior sagittal sinus 4. Dura mater 5. Falx cerebri 6. Frontal lobes of the cerebrum 7. Middle meningeal artery 8. Cortex, grey matter 9. Cerebral vessels
Prevertebral Region, Pharynx and Soft Palate
 Unit 20: Prevertebral Region, Pharynx and Soft Palate Dissection Instructions: Step1 Step 2 Step 1: Insert your fingers posterior to the sternocleidomastoid muscle, vagus nerve, internal jugular vein,
Unit 20: Prevertebral Region, Pharynx and Soft Palate Dissection Instructions: Step1 Step 2 Step 1: Insert your fingers posterior to the sternocleidomastoid muscle, vagus nerve, internal jugular vein,
Techniques of local anesthesia in the mandible
 Techniques of local anesthesia in the mandible The technique of choice for anesthesia of the mandible is the block injection and this is attributed to the absence of the advantages which are present in
Techniques of local anesthesia in the mandible The technique of choice for anesthesia of the mandible is the block injection and this is attributed to the absence of the advantages which are present in
YOU MUST BRING YOUR OWN GLOVES FOR THIS ACTIVITY.
 ACTIVITY 3: AXIAL SKELETON AND LONG BONE DISSECTION Objectives: 1) How to get ready: Read Chapter 7, McKinley et al., Human Anatomy, 5e. All text references are for this textbook. Learning the meanings
ACTIVITY 3: AXIAL SKELETON AND LONG BONE DISSECTION Objectives: 1) How to get ready: Read Chapter 7, McKinley et al., Human Anatomy, 5e. All text references are for this textbook. Learning the meanings
Posterior Triangle of the Neck By Prof. Dr. Muhammad Imran Qureshi
 Posterior Triangle of the Neck By Prof. Dr. Muhammad Imran Qureshi For the purpose of anatomical description the neck is sub divided into two major triangles, the Anterior and the Posterior by muscle bellies
Posterior Triangle of the Neck By Prof. Dr. Muhammad Imran Qureshi For the purpose of anatomical description the neck is sub divided into two major triangles, the Anterior and the Posterior by muscle bellies
The sebaceous glands (glands of Zeis) open directly into the eyelash follicles, ciliary glands (glands of Moll) are modified sweat glands that open
 The Orbital Region The orbits are a pair of bony cavities that contain the eyeballs; their associated muscles, nerves, vessels, and fat; and most of the lacrimal apparatus upper eyelid is larger and more
The Orbital Region The orbits are a pair of bony cavities that contain the eyeballs; their associated muscles, nerves, vessels, and fat; and most of the lacrimal apparatus upper eyelid is larger and more
Anatomy images for MSS practical exam- 2019
 Anatomy images for MSS practical exam- 2019 Ilium Ischium Pubis Acetabulaum Iliac crest Iliac tubercle ASIS (muscle and ligament attached) AIIS (muscle attached) PSIS PIIS Ischial spine Ischial tuberosity
Anatomy images for MSS practical exam- 2019 Ilium Ischium Pubis Acetabulaum Iliac crest Iliac tubercle ASIS (muscle and ligament attached) AIIS (muscle attached) PSIS PIIS Ischial spine Ischial tuberosity
Lecture 07. Lymphatic's of Head & Neck. By: Dr Farooq Amanullah Khan PMC
 Lecture 07 Lymphatic's of Head & Neck By: Dr Farooq Amanullah Khan PMC Dated: 28.11.2017 Lymphatic Vessels Of the 800 lymph nodes in the human body, 300 are in the Head & neck region. The lymphatic vessels
Lecture 07 Lymphatic's of Head & Neck By: Dr Farooq Amanullah Khan PMC Dated: 28.11.2017 Lymphatic Vessels Of the 800 lymph nodes in the human body, 300 are in the Head & neck region. The lymphatic vessels
Dr.Ban I.S. head & neck anatomy 2 nd y. جامعة تكريت كلية طب االسنان مادة التشريح املرحلة الثانية أ.م.د. بان امساعيل صديق 6102/6102
 جامعة تكريت كلية طب االسنان مادة التشريح املرحلة الثانية أ.م.د. بان امساعيل صديق 6102/6102 The scalp The scalp extends from the supraorbital margins anteriorly to the nuchal lines at the back of the skull
جامعة تكريت كلية طب االسنان مادة التشريح املرحلة الثانية أ.م.د. بان امساعيل صديق 6102/6102 The scalp The scalp extends from the supraorbital margins anteriorly to the nuchal lines at the back of the skull
Tympanic Bulla Temporal Bone. Digastric Muscle. Masseter Muscle
 Superior view Hyoid Bone The hyoid bone does not articulate with any other bones. It is held in place by ligaments to the styloid process of the temporal bone and the thyroid cartilage of the larynx. It
Superior view Hyoid Bone The hyoid bone does not articulate with any other bones. It is held in place by ligaments to the styloid process of the temporal bone and the thyroid cartilage of the larynx. It
THE SURGICAL ANATOMY OF THE CERVICAL DISTRIBUTION OF THE FACIAL NERVE. Biology and Anatomy, University of Shefield
 British Journal of Oral Surgery (1981), 19, 171-179 @ The British Association of Oral Surgeons 0007-117X/81/00260171$02.00 THE SURGICAL ANATOMY OF THE CERVICAL DISTRIBUTION OF THE FACIAL NERVE HAITHEM
British Journal of Oral Surgery (1981), 19, 171-179 @ The British Association of Oral Surgeons 0007-117X/81/00260171$02.00 THE SURGICAL ANATOMY OF THE CERVICAL DISTRIBUTION OF THE FACIAL NERVE HAITHEM
The Subzygomatic Triangle: Rapid, minimally invasive identification of the masseteric nerve for facial ACCEPTED
 Plastic and Reconstructive Surgery Advance Online Article DOI: 10.1097/PRS.0b013e318290f6dc The Subzygomatic Triangle: Rapid, minimally invasive identification of the masseteric nerve for facial reanimation
Plastic and Reconstructive Surgery Advance Online Article DOI: 10.1097/PRS.0b013e318290f6dc The Subzygomatic Triangle: Rapid, minimally invasive identification of the masseteric nerve for facial reanimation
1 Eyelids. Lacrimal Apparatus. Orbital Region. 3 The Orbit. The Eye
 1 1 Eyelids Orbital Region 2 Lacrimal Apparatus 3 The Orbit 4 The Eye 2 Eyelids The eyelids protect the eye from injury and excessive light by their closure. The upper eyelid is larger and more mobile
1 1 Eyelids Orbital Region 2 Lacrimal Apparatus 3 The Orbit 4 The Eye 2 Eyelids The eyelids protect the eye from injury and excessive light by their closure. The upper eyelid is larger and more mobile
Introduction to Local Anesthesia and Review of Anatomy
 5-Sep Introduction and Anatomy Review 12-Sep Neurophysiology and Pain 19-Sep Physiology and Pharmacology part 1 26-Sep Physiology and Pharmacology part 2 Introduction to Local Anesthesia and Review of
5-Sep Introduction and Anatomy Review 12-Sep Neurophysiology and Pain 19-Sep Physiology and Pharmacology part 1 26-Sep Physiology and Pharmacology part 2 Introduction to Local Anesthesia and Review of
Human Anatomy and Physiology - Problem Drill 07: The Skeletal System Axial Skeleton
 Human Anatomy and Physiology - Problem Drill 07: The Skeletal System Axial Skeleton Question No. 1 of 10 Which of the following statements about the axial skeleton is correct? Question #01 A. The axial
Human Anatomy and Physiology - Problem Drill 07: The Skeletal System Axial Skeleton Question No. 1 of 10 Which of the following statements about the axial skeleton is correct? Question #01 A. The axial
8 External Ear Canal Surgery
 30 Chapter 8 8 External Ear Canal Surgery Henning Hildmann, Holger Sudhoff Surgery in the external auditory canal without surgery in the middle ear may be necessary: 1. After surgery 2. After trauma 3.
30 Chapter 8 8 External Ear Canal Surgery Henning Hildmann, Holger Sudhoff Surgery in the external auditory canal without surgery in the middle ear may be necessary: 1. After surgery 2. After trauma 3.
Cranial Nerve VII - Facial Nerve. The facial nerve has 3 main components with distinct functions
 Cranial Nerve VII - Facial Nerve The facial nerve has 3 main components with distinct functions Somatic motor efferent Supplies the muscles of facial expression; posterior belly of digastric muscle; stylohyoid,
Cranial Nerve VII - Facial Nerve The facial nerve has 3 main components with distinct functions Somatic motor efferent Supplies the muscles of facial expression; posterior belly of digastric muscle; stylohyoid,
Oral cavity landmarks
 By: Dr. Ahmed Rabah Oral cavity landmarks The knowledge of oral anatomy and physiology will help the operator and provides enough landmarks to act as positive guide during denture construction. This subject
By: Dr. Ahmed Rabah Oral cavity landmarks The knowledge of oral anatomy and physiology will help the operator and provides enough landmarks to act as positive guide during denture construction. This subject
Chapter 7. Skeletal System
 Chapter 7 Skeletal System 1 Skull A. The skull is made up of 22 bones: 8 cranial bones, 13 facial bones, and the mandible. B. The Cranium encloses and protects the brain, provides attachments for muscles,
Chapter 7 Skeletal System 1 Skull A. The skull is made up of 22 bones: 8 cranial bones, 13 facial bones, and the mandible. B. The Cranium encloses and protects the brain, provides attachments for muscles,
