Ultrasonographic-Surgical Correlation of Ankle Tendon Tears
|
|
|
- Cassandra Briggs
- 5 years ago
- Views:
Transcription
1 Ultrasonographic-Surgical Correlation of Ankle Tendon Tears Gayle M. Waitches, DO, Matthew Rockett, DPM, Michael Brage, MD, Gary Sudakoff, MD This study evaluates the accuracy of ultrasonography in detecting ankle tendon tears of the peroneal, posterior tibial, and flexor digitorum longus tendons based on operative findings and clinical follow-up. A prospective study was performed in 33 patients with clinically suspected tendon injury. Sixty-eight tendons were evaluated sonographically. The diagnosis of an intrasubstance tear was made when disruption of uniform tendon architecture by hypoechoic linear or globular clefts was observed. Criteria used to diagnose complete tendon rupture included discontinuity or gap within the tendon or complete nonvisualization of the tendon. Treatment decisions were based on a combination of clinical parameters and imaging studies. Twenty-six patients had the presence or absence of Ankle tendon tears can be both debilitating and difficult to diagnose. The most common pathologic tendon condition on the medial side of the ankle is rupture or dysfunction of ABBREVIATIONS PT, Posterior tibial; FDL, Flexor digitorum longus; FHL, Flexor hallucis longus; PB, Peroneus brevis; PL, Peroneus longus; MR, Magnetic resonance Received October 24, 1997, from the Department of Radiology, The University of Washington School of Medicine, Harborview Medical Center, Seattle, Washington (G.M.W.); Harris County Podiatric Surgical Residency, Houston, Texas (M.R.); Department of Orthopedics, The University of Chicago, Chicago, Illinois (M.B.); and Department of Radiology, The Hammond Clinic, Hammond, Indiana (G.S.). Revised manuscript accepted for publication January 11, Address correspondence and reprint requests to Gayle M. Waitches, DO, University of Washington School of Medicine, Department of Radiology, Harborview Hospital, 325 Ninth Ave., Seattle, WA tear confirmed at surgery. Five patients had a final diagnosis based on clinical findings, and two were lost to follow-up. Of the 68 tendons evaluated sonographically, 54 were directly inspected at surgery; 20 were found to be torn and 34 were intact. Ultrasonography was able to identify all tears correctly with an accuracy of 93%, a sensitivity of 100%, and a specificity of 88%. The positive and negative predictive values were 83% and 100%, respectively. The combined accuracy, sensitivity, and specificity of ultrasonography in detecting tendon tears in all patients evaluated both surgically and by clinical follow-up were 94%, 100%, and 90%, respectively. KEY WORDS: Ankle, tendons; Musculoskeletal system, ultrasonography; Posterior tibial tendon; Peroneal tendons. the PT tendon. Although medial ankle pain, unilateral flatfoot deformity, hindfoot valgus, and forefoot abduction are the typical clinical findings of PT tendon tear, 1,2 other, less frequent problems can cause similar symptoms. These include rupture of the flexor retinaculum, tarsal tunnel syndrome, and tears or tenosynovitis of the FDL and FHL tendons. 1 Lack of recognition of PT tendon tear can lead to progressive collapse of the medial longitudinal arch of the foot. 1 Peroneal tendon injuries often are more difficult to diagnose. 3,4 Patients typically have pain and weakness of these tendons on focused examination, together with ambulatory ankle instability. However, sinus tarsi syndrome, injury to the calcaneofibular ligament, and subtalar joint instability also can masquerade as peroneal tendon tear. 1 4 Accurate detection and confirmation of tendon tear is necessary to institute appropriate therapy. The imaging modality of choice in detecting ankle tendon tears has primarily been MR imaging by the American Institute of Ultrasound in Medicine J Ultrasound Med 17: , /98/$3.50
2 250 ANKLE TENDON TEARS J Ultrasound Med 17: , 1998 Although ultrasonography has been applied to the diagnosis of musculoskeletal abnormalities involving the shoulder, knee, and hand, aside from the Achilles tendon, ultrasonography has been a relatively underutilized modality for imaging ankle tendons The purpose of this prospective study was to determine if sonography is accurate in diagnosing ankle tendon tears, using operative findings and clinical follow-up as the gold standard. MATERIALS AND METHODS A prospective study of 33 patients was conducted between October 1995 and May Patients were referred for sonographic evaluation after examination by experienced orthopedic or podiatric physicians. The sonographic studies were performed prospectively and independently by two radiologists experienced in musculoskeletal imaging. The orthopedic and podiatric surgeons were not blinded to the results of the examinations, and each operative decision was based on a combination of clinical parameters and imaging results. Twenty-six patients underwent surgical tendon exploration, five patients were followed clinically, and two were lost to follow-up. The clinical, surgical, and sonographic findings were correlated in all cases. The duration of clinical follow-up ranged between 15 to 17 months (mean, 16.5 months). The range of time between the sonographic study and subsequent surgery was 1 day to 3 months (mean, 1.5 weeks). Two tendons were evaluated in all patients; the PT and FDL tendons were scanned in those with medial ankle pain, and both peroneal tendons (PB, PL) were scanned in patients with lateral ankle symptoms. One patient had both medial and lateral tendon pairs evaluated. The PT and FDL tendons were inspected directly at the time of medial ankle surgery, and both peroneal tendons were evaluated at the time of lateral ankle surgery. The FHL tendon was not visualized at surgery owing to its containment in a separate sheath, and was therefore not included in the sonographic data. Although the contralateral asymptomatic medial or lateral tendons also were scanned in all patients to provide a comparison of normal, these tendons were not confirmed to be normal at surgery, and therefore these tendons were not included in the data. Ultrasonographic examinations of the ankle were performed by a commercially available Siemens Elegra unit (Siemens, Issaquah, WA) or an ATL Ultra- Mark 9 HDI unit (Advanced Technology Laboratories, Bothell, WA) using either a 7.5 or a 10 MHz linear transducer. In most cases, imaging of the ankle tendons was done without the use of a commercially available acoustic stand-off pad. The medial aspect of the ankle was scanned after placing the patient in either the right or left lateral oblique position, with a small towel securing the ankle. Longitudinal and transverse images were obtained from approximately 8 cm superior to the tip of the malleolus to the navicular tuberosity for the PT tendon or deep to the navicular for the FDL tendon. Refractive artifact was avoided by placing the transducer perpendicular to the tendon throughout its course. To ensure that the correct tendon was evaluated, the foot was inverted and plantar flexed to visualize isolated PT tendon motion. Similar provocative kinetic maneuvers of the FDL tendon included flexion and extension of the lesser digits. Focused attention was always directed to the site of maximum patient complaint. The contralateral asymptomatic tendon also was evaluated in all cases, and hard copy images were obtained. Scanning of the lateral aspect of the ankle was accomplished in similar fashion; transverse and longitudinal images were obtained from approximately 8 cm superior to the tip of the lateral malleolus to either the point of insertion of the PB on the fifth metatarsal base or until the PL tendon coursed under the plantar tunnel. The foot and ankle were placed through active motion during scanning to ensure that the tendons were correctly identified. Eversion and inversion of the foot causes the PB to slide within its sheath while the PL tendon remains relatively motionless. Plantar flexion and dorsiflexion of the first metatarsal bone at the first metatarsal cuneiform joint prompts motion of the PL tendon while the PB remains static. Hard copy images were obtained. The sonographic criterion used to identify a tendon tear is disruption of the uniformly parallel echogenic fibrils by one or more hypoechoic clefts or gaps within a tendon (Figs. 1, 2). 23,26 28 These hypoechoic areas may or may not extend to the tendon s peripheral surface. The sonographic criteria compatible with a complete tendon rupture include nonvisualization of the tendon in the absence of surgery or tendon discontinuity, or both. 23,28 RESULTS Of the 68 tendons that were evaluated sonographically, 54 were inspected directly at the time of surgery (14 PT, 14 FDL, 13 PB, and 13 PL). Twenty of these tendons were found to be torn at surgery (13 PT, four PB, and three PL). Eighteen tendons were partially torn, and two were completely ruptured. Ultrasonography interpreted all surgically proven tendon tears correctly for a sensitivity of 100%, a specificity of 88%, and an accuracy of 93%. The positive and negative predictive values were 83% and 100%, respectively.
3 J Ultrasound Med 17: , 1998 WAITCHES ET AL 251 A Four tendons that were thought to be torn sonographically were found to be normal at surgery. Two cases occurred in a patient with suspected tears of both PL and PB tendons. Although tendon tears were not detected surgically, the abnormal sonographic findings in this patient were consistent with the final surgical diagnosis of stenosing tenosynovitis. Two other false positive examinations occurred early in the course of our study, when we were less experienced. Both errors were due in part to a failure to corroborate the abnormality in orthogonal planes. Of the 54 tendons inspected surgically, the 30 remaining tendons were considered normal sonographically. Four of these patients were taken to surgery on the basis of abnormal clinical parameters despite normal appearing tendons sonographically; all eight tendons were surgically intact. Two of these patients with intact tendons showed other sonographic peritendinous abnormalities, which were confirmed at surgery. One patient with a hypoechoic fluid collection inferior to the PB muscle at the level of the malleolus had a subtalar joint capsule rupture with a cyst that was closely associated with the peroneal tendon sheath. The second patient had a poorly defined hypoechoic area deep to the inframalleolar portion of the PT tendon, which was interpreted as a probable hematoma at the time of ultrasonography. This patient was found to have a ruptured retinaculum. Of the remaining two of the four patients with normal tendons who were taken to surgery, no detectable abnormalities were B C Figure 1 44 year old woman with history of left medial ankle pain, exacerbated with ambulation. A, Transverse image of the PT tendon just below the malleolus shows an enlarged and hypoechoic tendon, with a central focal area of hypoechogenicity within the substance of the tendon (straight arrow). The curved arrows point to the tibia just below the medial malleolus. B, Longitudinal imaging confirms the abnormality seen on transverse scanning. A linear hypoechoic area is observed coursing through the tendon in longitudinal fashion, consistent with an intrasubstance tear (straight arrow). C, Intraoperative photograph taken at the time of surgical repair demonstrates the partial longitudinal tear within the edematous tendon (small straight arrow).
4 252 ANKLE TENDON TEARS J Ultrasound Med 17: , 1998 Figure 2 Transverse images of the PB (short open black arrow) and PL (curved black arrow) tendons just below the level of the malleolus. The white arrow points to a longitudinal tear of the PL tendon, which was confirmed at the time of surgical repair. The solid straight black arrow points to the lateral malleolus. noted in one, and the other suffered from sinus tarsi syndrome. The 22 remaining tendons that were considered sonographically normal and were visualized surgically were all found to be normal (Fig. 3). Fourteen tendons in seven patients were examined sonographically without surgical confirmation. Two patients were lost to follow-up. Ten tendons were therefore followed in five patients (two PT, two FDL, three PB, three PL). The final diagnosis in these five patients was based on clinical parameters and longterm follow-up. Six tendons in three patients (three PB, three PL) had no evidence of a tear sonographically. Of these three patients, one had chronic symptoms compatible with diabetic neuropathy, another had pain relief after fusion of the calcaneocuboid joint, and the last had complete cessation of symptoms after a short-term period of conservative management. These three patients are considered true negative cases. Of the remaining two of the five patients followed clinically (four tendons; two PT, two FDL), both were diagnosed as having PT tendon tears sonographically. These patients refused surgery, and both continue to have clinical findings consistent with tear. These cases are considered true positives. In summary, 68 tendons were evaluated sonographically; 54 were inspected at surgery, and 14 were followed clinically. Of the 14 tendons followed clinically, four were not included because two patients were lost to follow-up. Of the remaining 10 tendons evaluated clinically, six were considered true negative and four were considered true positive. The combined accuracy, sensitivity, and specificity of ultrasonography in detecting tendons tears for all patients examined both surgically and by clinical follow-up are 94%, 100%, and 90%, respectively. The negative and positive predictive values are 100% and 86%, respectively (Tables 1, 2). DISCUSSION MR imaging has been the standard imaging modality in the evaluation of tendon abnormalities around the ankle Several authors have reported high accuracy in detecting ankle tendon tears involving the PT and peroneal tendons. 5 8 In 1988, Rosenberg and coworkers reported a sensitivity of 95% and specificity of 100% in the detection of PT tears using surgery as the gold standard. 6 More recently, Khoury and associates reported an MR imaging study of 12 patients with peroneal tendon tears in which MR imaging was Figure 3 A, Longitudinal image of a normal posterior tibial tendon (short arrows). Note the uniformity of the echogenic tendon fibril architecture. B, Transverse image of the normal PT and FDL tendons in the same asymptomatic patient. A B
5 J Ultrasound Med 17: , 1998 WAITCHES ET AL 253 Table 1: Surgical Sonographic Correlation of Tendon Tears Number Torn Tendons Torn Tendons Tendons (N) (Surgery) (Sonography) PT FDL PB PL Total Table 2: Combined Surgical, Clinical, and Sonographic Correlation of Tendon Tears Ultrasonography Combined Surgical Ultrasonography Correlation Clinical Correlation (N = 54) (N = 66) True positive tendon tears True negative tendon tears False positive tendon tears 4 4 False negative tendon tears 0 0 Sensitivity Specificity Accuracy Positive predictive value Negative predictive value equally accurate. 7 Ultrasonography, on the other hand, has been a relatively underutilized modality for imaging ankle tendons Aside from Achilles tendon imaging, little information on sonographicsurgical correlation has been published concerning additional ankle tendon tears. 6,26 A review of the literature shows a recent article by Miller and colleagues, who describe the use of ultrasonography in the evaluation of PT tendon pathologic conditions. 26 Coakley and coauthors reported on the use of ultrasonography in evaluating the PT tendon in patients with rheumatoid arthritis and found that tendon thinning and hindfoot deformity were common. 15 A case report by Stephenson and coworkers describes the detection of tenosynovitis of the PT tendon sonographically, concluding that ultrasonography may obviate additional diagnostic tests. 12 There have also been few articles comparing MR imaging with ultrasonography in evaluating ankle tendon injury. 10,26 Davies and coauthors in 1991 compared sonography, CT, and MR imaging in imaging patellar tendinitis and concluded that ultrasonography should be the initial imaging modality in these patients. 10 Our personal experience has been that MR imaging is less sensitive than ultrasonography in excluding ankle tendon tears. Ultrasonography has greater tendinous contrast resolution and can detect subtle tendon texture abnormalities that are not appreciable with MR imaging (Fig. 4). We therefore set out to investigate the overall accuracy of ultrasonography in detecting PT, FDL, and peroneal tendon tears using surgical and clinical correlation. The clinical utility of ultrasonography depends on how accurately it can distinguish tendon tear from other pathologic conditions such as tendinitis and tenosynovitis. Patients with tendon tears usually are treated surgically, whereas those with tendinitis or tenosynovitis are managed conservatively. 6 A complete tendon tear rarely presents a clinical or imaging dilemma. 23,27,28 Sonographic confirmation of an acute rupture often is not necessary, as this entity usually is appreciable clinically. Partial intrasubstance tears, on the other hand, are more common and more challenging clinically to diagnose. Ultrasonography can be most helpful to the clinician in this clinical setting to allow for distinction between tear and other disease processes. Our reported high accuracy and sensitivity in detecting tendon tears may be due in part to the specific imaging criteria used to diagnose tear. We defined partial tears as either globular or linear hypoechoic gaps within the substance of the tendon, which often extend to the tendon periphery. 23,26 28 While applying these specific imaging criteria results in a high sonographic accuracy, we did, however, visualize other sonographic findings in patients with tendon tears (Fig. 5). These include an enlarged and diffusely hypoechoic tendon, a large amount of peritendinous fluid, thinning of tendon contour, decreased mobility, and peritendinous material of mixed echogenicity (usually representing blood, fibrosis, synovial hypertrophy, or tendon debris). These additional findings are probably less specific for tendon tear, as they can also be found in tendinitis and tenosynovitis. We are pursuing further prospective trials to evaluate the accuracy of these findings in diagnosing tears. Tendon ultrasonography is able to assess the severity and extent of tendon injury. Often, the operative approach and type of surgical repair vary with the location and extent of the injury. Information regarding the size of the gap between the tendon ends or the condition of the torn tendon fibers in complete rupture can aid the surgeon in determining surgical approach. Persistent diastasis of tendon ends in plantar flexion often is treated operatively, whereas complete coaptation may be treated conservatively. 27 Ultrasonography also may be helpful in postoperative
6 254 ANKLE TENDON TEARS J Ultrasound Med 17: , 1998 patients with persistent pain, as approximately 2% of tendons treated surgically, and 10 to 35% of those treated medically, will rerupture. 17 All abnormal intratendinous areas must be corroborated in orthogonal planes to confirm the existence of a tear and avoid false positive diagnoses. We obtain the longitudinal view first because it provides a survey of overall tendon architecture. Any deviation or disruption of longitudinal tendon fibril uniformity should be reevaluated transversely. Two of our four false positive examinations occurred when we failed to confirm a suspected abnormality with transverse scanning. We now realize that there may be occasional slight variability in the normal longitudinal appearance of ankle tendons, which is not necessarily pathologic unless it can be confirmed in an orthogonal plane. This study is limited in that it was neither random nor blinded. The results of the sonographic examinations were made available to the surgeon preoperatively. This invariably produces a selection bias in that patients with abnormal ultrasonograms are more likely to have an operation, leading to a greater than normal prevalence of disease. Despite the fact that more patients with abnormal tendons were taken to surgery, every patient had at least two tendons scanned preoperatively: the questionable abnormal tendon and the adjacent tendon. The bias toward a higher number of positive tendon tears is offset by the simultaneous evaluation of true and false negative results in adjacent tendons. For example, the PB tendons are imaged simultaneously in a patient with suspected PB tear. Both tendons are inspected at surgery, confirming the normal appearance of the unaffected tendon. Moreover, four patients were taken to surgery despite a negative sonogram, and all eight tendons were confirmed to be normal at surgery. Finally, tendon ultrasonography is not meant to be a screening modality in which every patient with nonspecific ankle pain is referred for this examination. The inherent limitations of ultrasonography in evaluating osseous structures dictate that those referred for this modality should have a high pretest probability of tendon disease. We therefore believe that this study provides information regarding not only the positive but also the negative predictive value of ultrasonography in detecting tendon tears. Our study also was limited in that the final diagnosis in five patients was based only on clinical parameters. Some patients may have had tendon tears that which were not accurately detected by physical examination. The literature suggests, however, that the diagnosis of PT tears by an experienced clinician can be extremely accurate and may even be utilized as a standard. 30 Two of five patients examined clinically had medial ankle symptoms highly compatible with PT tear. Both refused surgery because of personal circumstances that do not allow them the anticipated postoperative convalescent period. Both patients continue to have clinical features compatible with tear. The three remaining patients followed clinically had lateral ankle symptoms with negative ultrasonograms and could conceivably have had tendon tears. Although the authors assume that patients with a negative examination who improve clinically do not have a torn tendon, it is possible that some of these patients may have had sonographically occult subtle tears that may have healed with conservative management. Another unavoidable limitation of this study is the possibility that subtle central intrasubstance tears that do not extend to the tendon periphery may not be visible during gross surgical inspection. These tears could go undetected at the time of surgical exploration, leading to a higher sonographic false positive rate. The clinical significance of missing subtle central Figure 4 Ultrasonogram and MR image of a partial longitudinal tear of PT tendon. A, The longitudinal ultrasonogram shows a linear area of hypoechogenicity within the central substance, suggestive of partial tear (white arrows). B, The T2-weighted sagittal MR image shows a normal appearing tendon (black arrows). A partial longitudinal tear was identified at the time of surgery. A B
7 J Ultrasound Med 17: , 1998 WAITCHES ET AL 255 intrasubstance tears is uncertain when surgical findings are used as the gold standard, as these potential tears may or may not progress to more significant abnormalities. Of our four false positive examinations, two occurred in a patient with suspected tears of both PL and PB tendons. And although tendon tears were not detected surgically, the abnormal sonographic findings in this patient were consistent with the final diagnosis of stenosing tenosynovitis (Fig. 6). It is possible that in the remaining two false positive cases, an occult intrasubstance tear may have been present that was not seen at surgery. Further sonographic and clinical follow-up may be necessary in patients with inconsistent surgical-sonographic correlation and persistent symptoms. Ultrasonography as an imaging modality also has a few limitations. The examination is operator-dependent, with a variable learning curve. We found that the sonographic tendon anatomy and appearances became understandable after approximately 2 to 3 weeks. Another minor limitation is the amount of time required for the study. Including the contralateral ankle, the study can take from 30 to 45 min. However, the standard competitor for this modality is MR imaging, and a 45 min examination is not long in comparison to that. Finally, the major limitation of ultrasonography is its inability to image deeper tissues and bones around the ankle. If pathologic conditions other than ankle tendons are in question, MR imaging may be the more appropriate modality. A Figure 5 43 year old woman with history of progressively worsening right medial ankle pain over the last 2.5 years. The pain was recently exacerbated after tripping and twisting her ankle 4 months prior to presentation. A, Longitudinal scanning of the PT tendon shows mixed echogenicity material (short arrows) surrounding the tendon (long arrow), compatible with blood and fibrotic debris. The distended synovium is marked with calipers. B, Transverse image shows a vague hypoechoic mass-like structure adjacent to the insertion of the PT tendon (long arrows) on the navicular bone (NAV). This was found to represent torn and retracted tendon fibers and accompanying fibrosis. C, T1-weighted longitudinal MR image confirms the existence of multiple severe tendon tears (solid arrows) with surrounding intermediate signal intensity material, which was operatively shown to represent blood and fibrotic tissue. Note the corresponding MR imaging appearance of the retracted tendon fibers and accompanying fibrosis (open arrow) at the navicular tuberosity (arrowhead). C B
8 256 ANKLE TENDON TEARS J Ultrasound Med 17: , 1998 Figure 6 Example of a false positive case; this is a longitudinal image of the PL tendon, which was interpreted as a tear. The tendon appears thinned and irregular in contour and is surrounded by a large amount of fluid. The suggestion of a thin hypoechoic linear area within the substance of the tendon also is present (arrow). This patient was taken to surgery, and was found to have stenosing tenosynovitis without tear. CONCLUSION In conclusion, we have found that ultrasonography is an accurate and sensitive modality in detecting tears of the peroneal, PT, and FDL tendons. The ability to distinguish tendon tear from other pathologic conditions allows for more appropriate patient management and, it is hoped, more rapid patient recovery. REFERENCES l. Turek SL: Orthopaedics: Principles and Their Application. 4th Ed. Philadelphia, JB Lippincott, 1984, p Sarrafian SK: Anatomy of the Foot and Ankle. Philadelphia, JB Lippincott, 1983, pp 251, Sammarco GJ: Peroneus longus tendon tears: Acute and chronic. Foot Ankle Int 16:245, Bassett FH, Speer KP: Longitudinal rupture of the peroneal tendons. Am J Sports Med 21:354, Khoury NJ, El-Khoury GY, Saltzman CL, et al: MR imaging of posterior tibial tendon dysfunction. AJR 167:675, Rosenberg ZS, Cheung Y, Jahss MH, et al: Rupture of posterior tibial tendon: CT and MR imaging with surgical correlation. Radiology 169:229, Khoury NJ, El-Khoury GY, Saltzman CL, et al: Peroneus longus and brevis tendon tears: MR imaging evaluation. Radiology 200:833, Schweitzer ME, Caccese R, Karasick D, et al: Posterior tibial tendon tears: Utility of secondary signs for MR imaging diagnosis. Radiology 88:655, Schweitzer ME, van Leersum M, Ehrlich SS, et al: Fluid in normal and abnormal joints: Amount and distribution as seen on MR images. AJR 162:111, Davies SG, Baudouin CJ, King JB, et al: Ultrasound, computed tomography and magnetic resonance imaging in patellar tendinitis. Clin Radiol 43:52, Fornage BD: Achilles tendon: US examination. Radiology 159:759, Stephenson CA: Sonographic diagnosis of tenosynovitis of the posterior tibial tendon. J Clin Ultrasound 18: 114, Kaplan PA, Anderson JC, Norris MA, et al: Ultrasonography of post-traumatic soft-tissue lesions. Radiol Clin North Am 27:973, Bianchi S, Zwass A, Abdelwahab I, et al: Diagnosis of tears of the quadriceps tendon of the knee: Value of sonography. AJR 162:1137, Coakley FV, Samanta AK, Finlay DB: Ultrasonography of the tibialis posterior tendon in rheumatoid arthritis. Br J Rheumatol 33:273, Kainberger FM, Engel A, Barton P, et al: Injury of the Achilles tendon: Diagnosis with sonography. AJR 155:1031, Blei CL, Nirschl RP, Grant EG: Achilles tendon: US diagnosis of pathologic conditions. Radiology 159:765, Harcke HT, Grissom LE, Finkelstein MS: Evaluation of the musculoskeletal system with sonography. AJR 150:1253, Fornage BD, Rifkin MD: Ultrasound examination of tendons. Radiol Clin North Am 26: 87, Dillehay GL, Deschler T, Rogers LF, et al: The ultrasonographic characterization of tendons. Invest Radiol 19:338, Harcke HT, Grissom LE, Finklestein MS: Evaluation of the musculoskeletal system with sonography. AJR 150:1253, Crass JR, van de Vagte GL, Harkavy LA: Tendon echogenicity: Ex vivo study. Radiology 167:499, van Holsbeeck M, Powell A: Ankle and foot. In van Holsbeeck M, Introcaso JH: Musculoskeletal Ultrasound. St. Louis, Mosby Year Book, 1991, p Chhem RK, Beauregard G: Synovial diseases. In van Holsbeeck M, Introcaso JH: Musculoskeletal Ultrasound. St. Louis, Mosby Year Book, 1991, p Nazarian LN, Rawool NM, Martin CE, et al: Synovial fluid in the hindfoot and ankle: Detection of amount and distribution with US. Radiology 197:275, Miller SD, Van Holsbeeck M. Boruta PM, et al: Ultrasound in the diagnosis of posterior tibial pathology. Foot Ankle Int 17:555, Thermann H, Hoffman R, Zwipp H, et al: The use of ultrasound in the foot and ankle. Foot Ankle 13:386, Marcelis S, Daenen B, Ferrara MA: Peripheral Musculoskeletal Ultrasound Atlas. New York, Thieme Medical Publishers, 1996, pp 12, 30, Saltzman CL, Bonar SK: Tendon problems of the foot and ankle. In Lutter LD, Mizel MS, Pfeffer GB (Eds): Orthopedic Knowledge of Update of the Foot and Ankle. Chicago, American Academy of Orthopedic Surgeons, 1994, p Mann RA, Thompson FM: Rupture of the posterior tibial tendon causing flat foot. J Bone Joint Surg [Am] 67:556, 1985
Ultrasound of Mid and Hindfoot Pathology
 Ultrasound of Mid and Hindfoot Pathology Levon N. Nazarian, M.D. Professor of Radiology Thomas Jefferson University Hospital Disclosures None relevant to this presentation Educational Objective Following
Ultrasound of Mid and Hindfoot Pathology Levon N. Nazarian, M.D. Professor of Radiology Thomas Jefferson University Hospital Disclosures None relevant to this presentation Educational Objective Following
Longitudinal Split of the Peroneus Longus and Peroneus Brevis Tendons with Disruption of the Superior Peroneal Retinaculum
 Longitudinal Split of the Peroneus Longus and Peroneus Brevis Tendons with Disruption of the Superior Peroneal Retinaculum Gregory C. Diaz, MD, Marnix van Holsbeeck, MD, Jon A. Jacobson, MD Longitudinal
Longitudinal Split of the Peroneus Longus and Peroneus Brevis Tendons with Disruption of the Superior Peroneal Retinaculum Gregory C. Diaz, MD, Marnix van Holsbeeck, MD, Jon A. Jacobson, MD Longitudinal
Ultrasound Evaluation of Posteromedial Ankle Pathology. Andrew C Cordle, M.D., Ph.D. 9/21/2018
 Ultrasound Evaluation of Posteromedial Ankle Pathology Andrew C Cordle, M.D., Ph.D. 9/21/2018 Overview: Pathology of the Posteromedial Ankle Flexor Tendon Pathology Accessory Navicular Bone Pathology Tarsal
Ultrasound Evaluation of Posteromedial Ankle Pathology Andrew C Cordle, M.D., Ph.D. 9/21/2018 Overview: Pathology of the Posteromedial Ankle Flexor Tendon Pathology Accessory Navicular Bone Pathology Tarsal
Original Report. Sonography of Ankle Tendon Impingement with Surgical Correlation
 Downloaded from www.ajronline.org by 162.158.89.91 on 08/23/18 from IP address 162.158.89.91. Copyright RRS. For personal use only; all rights reserved Monisha Shetty 1 David P. Fessell 1 John E. Femino
Downloaded from www.ajronline.org by 162.158.89.91 on 08/23/18 from IP address 162.158.89.91. Copyright RRS. For personal use only; all rights reserved Monisha Shetty 1 David P. Fessell 1 John E. Femino
Musculoskeletal Ultrasound Technical Guidelines. VI. Ankle
 European Society of MusculoSkeletal Radiology Musculoskeletal Ultrasound Technical Guidelines VI. Ankle Ian Beggs, UK Stefano Bianchi, Switzerland Angel Bueno, Spain Michel Cohen, France Michel Court-Payen,
European Society of MusculoSkeletal Radiology Musculoskeletal Ultrasound Technical Guidelines VI. Ankle Ian Beggs, UK Stefano Bianchi, Switzerland Angel Bueno, Spain Michel Cohen, France Michel Court-Payen,
Shane A. Shapiro, M.D. Assistant Professor, Orthopedic Surgery Mayo Clinic 2012 MFMER slide MFMER slide-3
 Ultrasound Foot and Ankle Pathology Disclosures None relevant Shane A. Shapiro, M.D. Assistant Professor, Orthopedic Surgery Mayo Clinic Florida @ShaneShapiroMD 2012 MFMER slide-2 Foot and Ankle Fundamentals
Ultrasound Foot and Ankle Pathology Disclosures None relevant Shane A. Shapiro, M.D. Assistant Professor, Orthopedic Surgery Mayo Clinic Florida @ShaneShapiroMD 2012 MFMER slide-2 Foot and Ankle Fundamentals
11/2/17. Lateral Collateral Complex Medial Collateral Complex Distal Tibiofibular Syndesmosis Spring Ligament
 Andrew J Grainger Leeds, UK Lateral Collateral Complex ial Collateral Complex Distal Tibiofibular Syndesmosis Spring Ligament Brief anatomy review Scan tips and tricks Pathological appearances andrewgrainger@nhs.net
Andrew J Grainger Leeds, UK Lateral Collateral Complex ial Collateral Complex Distal Tibiofibular Syndesmosis Spring Ligament Brief anatomy review Scan tips and tricks Pathological appearances andrewgrainger@nhs.net
ANKLE PLANTAR FLEXION
 ANKLE PLANTAR FLEXION Evaluation and Measurements By Isabelle Devreux 1 Ankle Plantar Flexion: Gastrocnemius and Soleus ROM: 0 to 40-45 A. Soleus: Origin: Posterior of head of fibula and proximal1/3 of
ANKLE PLANTAR FLEXION Evaluation and Measurements By Isabelle Devreux 1 Ankle Plantar Flexion: Gastrocnemius and Soleus ROM: 0 to 40-45 A. Soleus: Origin: Posterior of head of fibula and proximal1/3 of
Ankle Tendons in Athletes. Laura W. Bancroft, M.D.
 Ankle Tendons in Athletes Laura W. Bancroft, M.D. Outline Protocols Normal Anatomy Tendinopathy, partial and complete tears Posterior tibial, Flexor Hallucis Longus, Achilles, Peroneal and Anterior Tibial
Ankle Tendons in Athletes Laura W. Bancroft, M.D. Outline Protocols Normal Anatomy Tendinopathy, partial and complete tears Posterior tibial, Flexor Hallucis Longus, Achilles, Peroneal and Anterior Tibial
Clarification of Terms
 Clarification of Terms The plantar aspect of the foot refers to the role or its bottom The dorsal aspect refers to the top or its superior portion The ankle and foot perform three main functions: 1. shock
Clarification of Terms The plantar aspect of the foot refers to the role or its bottom The dorsal aspect refers to the top or its superior portion The ankle and foot perform three main functions: 1. shock
Therapeutic Foot Care Certificate Program Part I: Online Home Study Program
 Therapeutic Foot Care Certificate Program Part I: Online Home Study Program 1 Anatomy And Terminology Of The Lower Extremity Joan E. Edelstein, MA, PT, FISPO Associate Professor of Clinical Physical Therapy
Therapeutic Foot Care Certificate Program Part I: Online Home Study Program 1 Anatomy And Terminology Of The Lower Extremity Joan E. Edelstein, MA, PT, FISPO Associate Professor of Clinical Physical Therapy
The Lower Limb VII: The Ankle & Foot. Anatomy RHS 241 Lecture 7 Dr. Einas Al-Eisa
 The Lower Limb VII: The Ankle & Foot Anatomy RHS 241 Lecture 7 Dr. Einas Al-Eisa Ankle joint Synovial, hinge joint Allow movement of the foot in the sagittal plane only (1 degree of freedom): dorsiflexion:
The Lower Limb VII: The Ankle & Foot Anatomy RHS 241 Lecture 7 Dr. Einas Al-Eisa Ankle joint Synovial, hinge joint Allow movement of the foot in the sagittal plane only (1 degree of freedom): dorsiflexion:
17/10/2017. Foot and Ankle
 17/10/2017 Alicia M. Yochum RN, DC, DACBR, RMSK Foot and Ankle Plantar Fasciitis Hallux Valgus Deformity Achilles Tendinosis Posterior Tibialis Tendon tendinopathy Stress Fracture Ligamentous tearing Turf
17/10/2017 Alicia M. Yochum RN, DC, DACBR, RMSK Foot and Ankle Plantar Fasciitis Hallux Valgus Deformity Achilles Tendinosis Posterior Tibialis Tendon tendinopathy Stress Fracture Ligamentous tearing Turf
musculoskeletal system anatomy muscles of foot sheet done by: dina sawadha & mohammad abukabeer
 musculoskeletal system anatomy muscles of foot sheet done by: dina sawadha & mohammad abukabeer Extensor retinaculum : A- superior extensor retinaculum (SER) : originates from the distal ends of the tibia
musculoskeletal system anatomy muscles of foot sheet done by: dina sawadha & mohammad abukabeer Extensor retinaculum : A- superior extensor retinaculum (SER) : originates from the distal ends of the tibia
«Foot & Ankle Surgery» 04. Sept THE PAINFUL FLATFOOT. Norman Espinosa, MD
 THE PAINFUL FLATFOOT Norman Espinosa, MD Department of Orthopaedics University of Zurich Balgrist Switzerland www.balgrist.ch WHAT TO DO? INTRINSIC > EXTRINSIC ETIOLOGIES Repetitive microtrauma combined
THE PAINFUL FLATFOOT Norman Espinosa, MD Department of Orthopaedics University of Zurich Balgrist Switzerland www.balgrist.ch WHAT TO DO? INTRINSIC > EXTRINSIC ETIOLOGIES Repetitive microtrauma combined
BLUE SKY SCHOOL OF PROFESSIONAL MASSAGE AND THERAPEUTIC BODYWORK Musculoskeletal Anatomy & Kinesiology KNEE & ANKLE MUSCLES
 BLUE SKY SCHOOL OF PROFESSIONAL MASSAGE AND THERAPEUTIC BODYWORK Musculoskeletal Anatomy & Kinesiology KNEE & ANKLE MUSCLES MSAK201-I Session 3 1) REVIEW a) THIGH, LEG, ANKLE & FOOT i) Tibia Medial Malleolus
BLUE SKY SCHOOL OF PROFESSIONAL MASSAGE AND THERAPEUTIC BODYWORK Musculoskeletal Anatomy & Kinesiology KNEE & ANKLE MUSCLES MSAK201-I Session 3 1) REVIEW a) THIGH, LEG, ANKLE & FOOT i) Tibia Medial Malleolus
Posterior Tibialis Tendon Dysfunction & Repair
 1 Posterior Tibialis Tendon Dysfunction & Repair Surgical Indications and Considerations Anatomical Considerations: The posterior tibialis muscle arises from the interosseous membrane and the adjacent
1 Posterior Tibialis Tendon Dysfunction & Repair Surgical Indications and Considerations Anatomical Considerations: The posterior tibialis muscle arises from the interosseous membrane and the adjacent
Clin Podiatr Med Surg 19 (2002) Index
 Clin Podiatr Med Surg 19 (2002) 335 344 Index Note: Page numbers of article titles are in bold face type. A Accessory soleus muscle, magnetic resonance imaging of, 300 Achilles tendon injury of, magnetic
Clin Podiatr Med Surg 19 (2002) 335 344 Index Note: Page numbers of article titles are in bold face type. A Accessory soleus muscle, magnetic resonance imaging of, 300 Achilles tendon injury of, magnetic
Knee, Ankle, and Foot: Normal and Abnormal Features with MRI and Ultrasound Correlation. Disclosures. Outline. Joint Effusion. Suprapatellar recess
 Knee, Ankle, and Foot: Normal and Abnormal Features with MRI and Ultrasound Correlation Jon A. Jacobson, M.D. Professor of Radiology Director, Division of Musculoskeletal Radiology University of Michigan
Knee, Ankle, and Foot: Normal and Abnormal Features with MRI and Ultrasound Correlation Jon A. Jacobson, M.D. Professor of Radiology Director, Division of Musculoskeletal Radiology University of Michigan
Copyright 2004, Yoshiyuki Shiratori. All right reserved.
 Ankle and Leg Evaluation 1. History Chief Complaint: A. What happened? B. Is it a sharp or dull pain? C. How long have you had the pain? D. Can you pinpoint the pain? E. Do you have any numbness or tingling?
Ankle and Leg Evaluation 1. History Chief Complaint: A. What happened? B. Is it a sharp or dull pain? C. How long have you had the pain? D. Can you pinpoint the pain? E. Do you have any numbness or tingling?
The Leg. Prof. Oluwadiya KS
 The Leg Prof. Oluwadiya KS www.oluwadiya.sitesled.com Compartments of the leg 4 Four Compartments: 1. Anterior compartment Deep fibular nerve Dorsiflexes the foot and toes 2. Lateral Compartment Superficial
The Leg Prof. Oluwadiya KS www.oluwadiya.sitesled.com Compartments of the leg 4 Four Compartments: 1. Anterior compartment Deep fibular nerve Dorsiflexes the foot and toes 2. Lateral Compartment Superficial
Extraarticular Lateral Ankle Impingement
 Extraarticular Lateral Ankle Impingement Poster No.: C-1282 Congress: ECR 2016 Type: Educational Exhibit Authors: C. Cevikol; Keywords: Trauma, Diagnostic procedure, MR, CT, Musculoskeletal system, Musculoskeletal
Extraarticular Lateral Ankle Impingement Poster No.: C-1282 Congress: ECR 2016 Type: Educational Exhibit Authors: C. Cevikol; Keywords: Trauma, Diagnostic procedure, MR, CT, Musculoskeletal system, Musculoskeletal
Urgent Cases and Foreign Bodies
 Urgent Cases and Foreign Bodies Catherine J. Brandon, MD, MS University of Michigan Ann Arbor, MI, USA Introduction: Patients added on to the schedule from the emergency department or as urgent add-on
Urgent Cases and Foreign Bodies Catherine J. Brandon, MD, MS University of Michigan Ann Arbor, MI, USA Introduction: Patients added on to the schedule from the emergency department or as urgent add-on
European Journal of Radiology
 European Journal of Radiology 84 (2015) 1777 1781 Contents lists available at ScienceDirect European Journal of Radiology journal homepage: www.elsevier.com/locate/ejrad Imaging of posterior tibial tendon
European Journal of Radiology 84 (2015) 1777 1781 Contents lists available at ScienceDirect European Journal of Radiology journal homepage: www.elsevier.com/locate/ejrad Imaging of posterior tibial tendon
SUBTALAR ARTHROEREISIS IN THE OLDER PATIENT
 C H A P T E R 1 7 SUBTALAR ARTHROEREISIS IN THE OLDER PATIENT William D. Fishco, DPM, MS INTRODUCTION Arthroereisis is a surgical procedure designed to limit the motion of a joint. Subtalar joint arthroereisis
C H A P T E R 1 7 SUBTALAR ARTHROEREISIS IN THE OLDER PATIENT William D. Fishco, DPM, MS INTRODUCTION Arthroereisis is a surgical procedure designed to limit the motion of a joint. Subtalar joint arthroereisis
Anatomy of Foot and Ankle
 Anatomy of Foot and Ankle Surface anatomy of the ankle & foot Surface anatomy of the ankle & foot Medial orientation point medial malleous sustentaculum tali tuberosity of navicular TA muscle TP muscle
Anatomy of Foot and Ankle Surface anatomy of the ankle & foot Surface anatomy of the ankle & foot Medial orientation point medial malleous sustentaculum tali tuberosity of navicular TA muscle TP muscle
Section Three: The Leg, Ankle, and Foot Lecture: Review of Clinical Anatomy, Patterns of Dysfunction and Injury, and
 Section Three: The Leg, Ankle, and Foot Lecture: Review of Clinical Anatomy, Patterns of Dysfunction and Injury, and Treatment Implications for the Leg, Ankle, and Foot Levels I and II Demonstration and
Section Three: The Leg, Ankle, and Foot Lecture: Review of Clinical Anatomy, Patterns of Dysfunction and Injury, and Treatment Implications for the Leg, Ankle, and Foot Levels I and II Demonstration and
Sonographic Evaluation of Tears of the Gastrocnemius Medial Head ( Tennis Leg )
 Sonographic Evaluation of Tears of the Gastrocnemius Medial Head ( Tennis Leg ) Stefano Bianchi, MD, Carlo Martinoli, MD, Ibrahim Fikry Abdelwahab, MD, Lorenzo E. Derchi, MD, Sandro Damiani, MD Rupture
Sonographic Evaluation of Tears of the Gastrocnemius Medial Head ( Tennis Leg ) Stefano Bianchi, MD, Carlo Martinoli, MD, Ibrahim Fikry Abdelwahab, MD, Lorenzo E. Derchi, MD, Sandro Damiani, MD Rupture
Ultrasound and MRI Findings of Tennis Leg with Differential Diagnosis.
 Ultrasound and MRI Findings of Tennis Leg with Differential Diagnosis. Poster No.: R-0057 Congress: 2015 ASM Type: Educational Exhibit Authors: M. George, A. Thomas, R. Dutta, K. Gummalla; Singapore/SG
Ultrasound and MRI Findings of Tennis Leg with Differential Diagnosis. Poster No.: R-0057 Congress: 2015 ASM Type: Educational Exhibit Authors: M. George, A. Thomas, R. Dutta, K. Gummalla; Singapore/SG
بسم هللا الرحمن الرحيم
 بسم هللا الرحمن الرحيم Laboratory RHS 221 Manual Muscle Testing Theory 1 hour practical 2 hours Dr. Ali Aldali, MS, PT Department of Physical Therapy King Saud University Talocrural and Subtalar Joint
بسم هللا الرحمن الرحيم Laboratory RHS 221 Manual Muscle Testing Theory 1 hour practical 2 hours Dr. Ali Aldali, MS, PT Department of Physical Therapy King Saud University Talocrural and Subtalar Joint
~, /' ~::'~ EXTENSOR HALLUCIS LONGUS. Leg-anterolateral :.:~ / ~\,
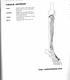 TIBIALIS ANTERIOR Lateral condyle of tibia, upper half of lateral surface of tibia, interosseous membrane Medial side and plantar surface of medial cuneiform bone, and base of first metatarsal bone Dorsiflexes
TIBIALIS ANTERIOR Lateral condyle of tibia, upper half of lateral surface of tibia, interosseous membrane Medial side and plantar surface of medial cuneiform bone, and base of first metatarsal bone Dorsiflexes
First & second layers of muscles of the sole
 The FOOT First & second layers of muscles of the sole introduction The muscles acting on the foot can be divided into two distinct groups; extrinsic and intrinsic muscles. The extrinsic muscles arise from
The FOOT First & second layers of muscles of the sole introduction The muscles acting on the foot can be divided into two distinct groups; extrinsic and intrinsic muscles. The extrinsic muscles arise from
Detection and Measurement of Rotator Cuff Tears with Sonography: Analysis of Diagnostic Errors
 Musculoskeletal Imaging Teefey et al. Detection of Rotator Cuff Tears with Sonography Sharlene A. Teefey 1 William D. Middleton 1 William T. Payne 2 Ken Yamaguchi 3 Teefey SA, Middleton WD, Payne WT, Yamaguchi
Musculoskeletal Imaging Teefey et al. Detection of Rotator Cuff Tears with Sonography Sharlene A. Teefey 1 William D. Middleton 1 William T. Payne 2 Ken Yamaguchi 3 Teefey SA, Middleton WD, Payne WT, Yamaguchi
Sonographic Findings of Adductor Insertion Avulsion Syndrome With Magnetic Resonance Imaging Correlation
 Case Report Sonographic Findings of Adductor Insertion Avulsion Syndrome With Magnetic Resonance Imaging Correlation Jennifer S. Weaver, MD, Jon A. Jacobson, MD, David A. Jamadar, MBBS, Curtis W. Hayes,
Case Report Sonographic Findings of Adductor Insertion Avulsion Syndrome With Magnetic Resonance Imaging Correlation Jennifer S. Weaver, MD, Jon A. Jacobson, MD, David A. Jamadar, MBBS, Curtis W. Hayes,
Introduction to Anatomy. Dr. Maher Hadidi. Laith Al-Hawajreh. Mar/25 th /2013
 Introduction to Anatomy Dr. Maher Hadidi Laith Al-Hawajreh 22 Mar/25 th /2013 Lower limb - The leg The skeleton of the leg is formed by two bones: 1) Medial: Tibia 2) Lateral: Fibula The two bones are
Introduction to Anatomy Dr. Maher Hadidi Laith Al-Hawajreh 22 Mar/25 th /2013 Lower limb - The leg The skeleton of the leg is formed by two bones: 1) Medial: Tibia 2) Lateral: Fibula The two bones are
Leg. Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology
 Leg Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology Skin of the Leg Cutaneous Nerves Medially: The saphenous nerve, a branch of the femoral nerve supplies the skin on the medial surface
Leg Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology Skin of the Leg Cutaneous Nerves Medially: The saphenous nerve, a branch of the femoral nerve supplies the skin on the medial surface
Physical Examination of the Foot & Ankle
 Inspection Standing, feet straight forward facing toward examiner Swelling Deformity Flatfoot (pes planus and hindfoot valgus) High arch (pes cavus and hindfoot varus) Peek-a-boo heel Varus Too many toes
Inspection Standing, feet straight forward facing toward examiner Swelling Deformity Flatfoot (pes planus and hindfoot valgus) High arch (pes cavus and hindfoot varus) Peek-a-boo heel Varus Too many toes
Main Menu. Ankle and Foot Joints click here. The Power is in Your Hands
 1 The Ankle and Foot Joints click here Main Menu Copyright HandsOn Therapy Schools 2009 K.8 http://www.handsonlineeducation.com/classes/k8/k8entry.htm[3/27/18, 1:40:03 PM] Ankle and Foot Joint 26 bones
1 The Ankle and Foot Joints click here Main Menu Copyright HandsOn Therapy Schools 2009 K.8 http://www.handsonlineeducation.com/classes/k8/k8entry.htm[3/27/18, 1:40:03 PM] Ankle and Foot Joint 26 bones
The Egyptian Journal of Hospital Medicine (October 2017) Vol.69 (3), Page
 The Egyptian Journal of Hospital Medicine (October 2017) Vol.69 (3), Page 2016-2024 Role of MRI in Evaluation of Traumatic Ankle Injuries Mervat Mohamed Ibrahim Ali Elgohary*, Susan Adel Ali Abdul Rahim*,
The Egyptian Journal of Hospital Medicine (October 2017) Vol.69 (3), Page 2016-2024 Role of MRI in Evaluation of Traumatic Ankle Injuries Mervat Mohamed Ibrahim Ali Elgohary*, Susan Adel Ali Abdul Rahim*,
Understanding Leg Anatomy and Function THE UPPER LEG
 Understanding Leg Anatomy and Function THE UPPER LEG The long thigh bone is the femur. It connects to the pelvis to form the hip joint and then extends down to meet the tibia (shin bone) at the knee joint.
Understanding Leg Anatomy and Function THE UPPER LEG The long thigh bone is the femur. It connects to the pelvis to form the hip joint and then extends down to meet the tibia (shin bone) at the knee joint.
Sonographic Differences in the Appearance of Acute and Chronic Full-Thickness Rotator Cuff Tears
 Sonographic Differences in the Appearance of Acute and Chronic Full-Thickness Rotator Cuff Tears Sharlene A. Teefey, MD, William D. Middleton, MD, Gregory S. Bauer, MD, Charles F. Hildebolt, DDS, PhD,
Sonographic Differences in the Appearance of Acute and Chronic Full-Thickness Rotator Cuff Tears Sharlene A. Teefey, MD, William D. Middleton, MD, Gregory S. Bauer, MD, Charles F. Hildebolt, DDS, PhD,
What Happens to the Paediatric Flat Foot? Peter J Briggs Freeman Hospital Newcastle upon Tyne
 What Happens to the Paediatric Flat Foot? Peter J Briggs Freeman Hospital Newcastle upon Tyne We don t know!! Population Studies 2300 children aged 4-13 years Shoe wearers Flat foot 8.6% Non-shoe wearers
What Happens to the Paediatric Flat Foot? Peter J Briggs Freeman Hospital Newcastle upon Tyne We don t know!! Population Studies 2300 children aged 4-13 years Shoe wearers Flat foot 8.6% Non-shoe wearers
Pragmatic ultrasound in the diagnosis of soft tissue rheumatic pain. Plamen Todorov
 Pragmatic ultrasound in the diagnosis of soft tissue rheumatic pain Plamen Todorov INTRODUCTION Soft tissue rheumatism: nonsystemic, focal pathological syndromes involving the periarticular structures.
Pragmatic ultrasound in the diagnosis of soft tissue rheumatic pain Plamen Todorov INTRODUCTION Soft tissue rheumatism: nonsystemic, focal pathological syndromes involving the periarticular structures.
Results of Calcaneal Osteotomy & Flexor Digitorum Longus transfer in Stage II Acquired Flatfoot Deformity
 Results of Calcaneal Osteotomy & Flexor Digitorum Longus transfer in Stage II Acquired Flatfoot Deformity Mr Amit Chauhan Mr Prasad Karpe Ms Maire-claire Killen Mr Rajiv Limaye University Hospital of North
Results of Calcaneal Osteotomy & Flexor Digitorum Longus transfer in Stage II Acquired Flatfoot Deformity Mr Amit Chauhan Mr Prasad Karpe Ms Maire-claire Killen Mr Rajiv Limaye University Hospital of North
Ultrasound Evaluation of Masses
 Ultrasound Evaluation of Masses Jon A. Jacobson, M.D. Professor of Radiology Director, Division of Musculoskeletal Radiology University of Michigan Disclosures: Consultant: Bioclinica Advisory Panel: GE,
Ultrasound Evaluation of Masses Jon A. Jacobson, M.D. Professor of Radiology Director, Division of Musculoskeletal Radiology University of Michigan Disclosures: Consultant: Bioclinica Advisory Panel: GE,
The University Of Jordan Faculty Of Medicine FOOT. Dr.Ahmed Salman Assistant Prof. of Anatomy. The University Of Jordan
 The University Of Jordan Faculty Of Medicine FOOT Dr.Ahmed Salman Assistant Prof. of Anatomy. The University Of Jordan Tarsal Tunnel Syndrome Due to compression of Tibial nerve as it travels through the
The University Of Jordan Faculty Of Medicine FOOT Dr.Ahmed Salman Assistant Prof. of Anatomy. The University Of Jordan Tarsal Tunnel Syndrome Due to compression of Tibial nerve as it travels through the
Case Report Painful Os Peroneum Syndrome: Underdiagnosed Condition in the Lateral Midfoot Pain
 Case Reports in Radiology Volume 2016, Article ID 8739362, 4 pages http://dx.doi.org/10.1155/2016/8739362 Case Report Painful Os Peroneum Syndrome: Underdiagnosed Condition in the Lateral Midfoot Pain
Case Reports in Radiology Volume 2016, Article ID 8739362, 4 pages http://dx.doi.org/10.1155/2016/8739362 Case Report Painful Os Peroneum Syndrome: Underdiagnosed Condition in the Lateral Midfoot Pain
A Patient s Guide to Adult-Acquired Flatfoot Deformity
 A Patient s Guide to Adult-Acquired Flatfoot Deformity Glendale Adventist Medical Center 1509 Wilson Terrace Glendale, CA 91206 Phone: (818) 409-8000 DISCLAIMER: The information in this booklet is compiled
A Patient s Guide to Adult-Acquired Flatfoot Deformity Glendale Adventist Medical Center 1509 Wilson Terrace Glendale, CA 91206 Phone: (818) 409-8000 DISCLAIMER: The information in this booklet is compiled
TENDON TRANSFER IN CAVUS FOOT
 TENDON TRANSFER IN CAVUS FOOT Cavovarus deformity is defined by fixed equinus of the forefoot on the hindfoot, resulting in a pathologic elevation of the longitudinal arch, with either a fixed or flexible
TENDON TRANSFER IN CAVUS FOOT Cavovarus deformity is defined by fixed equinus of the forefoot on the hindfoot, resulting in a pathologic elevation of the longitudinal arch, with either a fixed or flexible
Tears of the knee menisci frequently occur not. Is There a Role for Sonography in the Diagnosis of Tears of the Knee Menisci?
 Is There a Role for Sonography in the Diagnosis of Tears of the Knee Menisci? Roberto Azzoni, MD, Paolo Cabitza, MD Orthopedic and Trauma Surgery Department, Policlinico San Donato Institute, University
Is There a Role for Sonography in the Diagnosis of Tears of the Knee Menisci? Roberto Azzoni, MD, Paolo Cabitza, MD Orthopedic and Trauma Surgery Department, Policlinico San Donato Institute, University
The Foot. Dr. Wegdan Moh.Mustafa Medicine Faculty Assistant Professor Mob:
 The Foot Dr. Wegdan Moh.Mustafa Medicine Faculty Assistant Professor Mob: 0127155717 The skeleton of the foot Cutaneous innervations Sole of foot layers of muscles First layer -Abductor hallucis -Flexor
The Foot Dr. Wegdan Moh.Mustafa Medicine Faculty Assistant Professor Mob: 0127155717 The skeleton of the foot Cutaneous innervations Sole of foot layers of muscles First layer -Abductor hallucis -Flexor
5.1 Identify, describe the attachments of and deduce the actions of the muscles of the thigh:
 5.1 Identify, describe the attachments of and deduce the actions of the muscles of the thigh: Anterior group Proximal attachment Distal attachment Sartorius ASIS» Upper part of shaft tibia (middle surface)»
5.1 Identify, describe the attachments of and deduce the actions of the muscles of the thigh: Anterior group Proximal attachment Distal attachment Sartorius ASIS» Upper part of shaft tibia (middle surface)»
Introduction to Ultrasound Examination of the Hand and upper
 Introduction to Ultrasound Examination of the Hand and upper Emil Dionysian, M.D. Ultrasound of upper ext. Upside Convenient Opens another exam dimension Can be like a stethoscope Helps 3-D D visualization
Introduction to Ultrasound Examination of the Hand and upper Emil Dionysian, M.D. Ultrasound of upper ext. Upside Convenient Opens another exam dimension Can be like a stethoscope Helps 3-D D visualization
Your diagnosis? The case: n radiologic case study. For answer see page 807
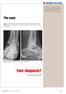 Enhance your diagnostic skills with this test yourself monthly column, which features a radiograph and challenges you to make a diagnosis. The case: 45-year-old man presented with acute lateral hindfoot
Enhance your diagnostic skills with this test yourself monthly column, which features a radiograph and challenges you to make a diagnosis. The case: 45-year-old man presented with acute lateral hindfoot
Original Report. Sonography of Tears of the Distal Biceps Tendon. Theodore T. Miller 1,2 Ronald S. Adler 3
 Theodore T. Miller 1,2 Ronald S. dler 3 Received October 15, 1999; accepted after revision March 21, 2000. Presented at the annual meeting of the merican Roentgen Ray Society, Washington, DC, May 2000.
Theodore T. Miller 1,2 Ronald S. dler 3 Received October 15, 1999; accepted after revision March 21, 2000. Presented at the annual meeting of the merican Roentgen Ray Society, Washington, DC, May 2000.
Ultrasound of the Knee
 Ultrasound of the Knee Jon A. Jacobson, M.D. Professor of Radiology Director, Division of Musculoskeletal Radiology University of Michigan Disclosures: Consultant: Bioclinica Book Royalties: Elsevier Advisory
Ultrasound of the Knee Jon A. Jacobson, M.D. Professor of Radiology Director, Division of Musculoskeletal Radiology University of Michigan Disclosures: Consultant: Bioclinica Book Royalties: Elsevier Advisory
Case Report Ultrasound Guidance in Performing a Tendoscopic Surgery to Treat Posterior Tibial Tendinitis: A Useful Tool?
 Case Reports in Orthopedics Volume 2016, Article ID 7262413, 5 pages http://dx.doi.org/10.1155/2016/7262413 Case Report Ultrasound Guidance in Performing a Tendoscopic Surgery to Treat Posterior Tibial
Case Reports in Orthopedics Volume 2016, Article ID 7262413, 5 pages http://dx.doi.org/10.1155/2016/7262413 Case Report Ultrasound Guidance in Performing a Tendoscopic Surgery to Treat Posterior Tibial
SUPERIOR PERONEAL RETINACULAR INJURIES IN CALCANEAL FRACTURES
 SUPERIOR PERONEAL RETINACULAR INJURIES IN CALCANEAL FRACTURES Justin J. Fleming, DPM Kwasi Y. Kwaadu, DPM Derek J. Florek, DPM INTRODUCTION Calcaneal fractures are devastating injuries with historically
SUPERIOR PERONEAL RETINACULAR INJURIES IN CALCANEAL FRACTURES Justin J. Fleming, DPM Kwasi Y. Kwaadu, DPM Derek J. Florek, DPM INTRODUCTION Calcaneal fractures are devastating injuries with historically
fig fig For the following diagrams
 fig. 1271 For the following diagrams Please draw small circles at the following points (pts in bold are main syllabus pts): Liver-1 Liver-2 Liver-3 Liver-4 Spleen-4 Spleen-5 Stomach-41 Stomach-42 Stomach-43
fig. 1271 For the following diagrams Please draw small circles at the following points (pts in bold are main syllabus pts): Liver-1 Liver-2 Liver-3 Liver-4 Spleen-4 Spleen-5 Stomach-41 Stomach-42 Stomach-43
OVERUSE AND SPORTS-RELATED INJURIES. Overuse and sports-related injuries of the ankle and hindfoot: MR imaging findings
 OVERUSE ND SPORTS-RELTED INJURIES CHPTER 10 Overuse and sports-related injuries of the ankle and hindfoot: MR imaging findings Elizabeth S. Sijbrandij 1, d P.G. van Gils 1, Eduard E. de Lange 2 From the
OVERUSE ND SPORTS-RELTED INJURIES CHPTER 10 Overuse and sports-related injuries of the ankle and hindfoot: MR imaging findings Elizabeth S. Sijbrandij 1, d P.G. van Gils 1, Eduard E. de Lange 2 From the
Managing Tibialis Posterior Tendon Injuries
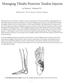 Managing Tibialis Posterior Tendon Injuries by Thomas C. Michaud, DC Published April 1, 2015 by Dynamic Chiropractic Magazine Tibialis posterior is the deepest, strongest, and most central muscle of the
Managing Tibialis Posterior Tendon Injuries by Thomas C. Michaud, DC Published April 1, 2015 by Dynamic Chiropractic Magazine Tibialis posterior is the deepest, strongest, and most central muscle of the
Lower limb summary. Anterior compartment of the thigh. Done By: Laith Qashou. Doctor_2016
 Lower limb summary Done By: Laith Qashou Doctor_2016 Anterior compartment of the thigh Sartorius Anterior superior iliac spine Upper medial surface of shaft of tibia 1. Flexes, abducts, laterally rotates
Lower limb summary Done By: Laith Qashou Doctor_2016 Anterior compartment of the thigh Sartorius Anterior superior iliac spine Upper medial surface of shaft of tibia 1. Flexes, abducts, laterally rotates
Original Report. The Reverse Segond Fracture: Association with a Tear of the Posterior Cruciate Ligament and Medial Meniscus
 Eva M. Escobedo 1 William J. Mills 2 John. Hunter 1 Received July 10, 2001; accepted after revision October 1, 2001. 1 Department of Radiology, University of Washington Harborview Medical enter, 325 Ninth
Eva M. Escobedo 1 William J. Mills 2 John. Hunter 1 Received July 10, 2001; accepted after revision October 1, 2001. 1 Department of Radiology, University of Washington Harborview Medical enter, 325 Ninth
Your diagnosis? The case: radiologic case study. For answer see page 872
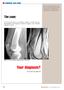 Enhance your diagnostic skills with this test yourself monthly column, which features a radiograph and challenges you to make a diagnosis. The case: A 56-year-old man was suddenly unable to extend his
Enhance your diagnostic skills with this test yourself monthly column, which features a radiograph and challenges you to make a diagnosis. The case: A 56-year-old man was suddenly unable to extend his
Pelvic cavity. Gross anatomy of the lower limb. Walking. Sándor Katz M.D.,Ph.D.
 Pelvic cavity. Gross anatomy of the lower limb. Walking. Sándor Katz M.D.,Ph.D. Lower limb Pelvic girdle Free lower extremity Hip bone Definitive fusion of the Y- shaped growth plate occurs 16th -18th
Pelvic cavity. Gross anatomy of the lower limb. Walking. Sándor Katz M.D.,Ph.D. Lower limb Pelvic girdle Free lower extremity Hip bone Definitive fusion of the Y- shaped growth plate occurs 16th -18th
Review relevant anatomy of the foot and ankle. Learn the approach to examining the foot and ankle
 Objectives Review relevant anatomy of the foot and ankle Learn the approach to examining the foot and ankle Learn the basics of diagnosis and treatment of ankle sprains Overview of other common causes
Objectives Review relevant anatomy of the foot and ankle Learn the approach to examining the foot and ankle Learn the basics of diagnosis and treatment of ankle sprains Overview of other common causes
The Relationship between Medial Longitudinal Arch and Peroneal Tubercle
 The Relationship between Medial Longitudinal Arch and Peroneal Tubercle -Anatomical Study- Department of Orthopaedic Surgery Kangwon National University Hospital Chuncheon, Republic of Korea Chang Hyun
The Relationship between Medial Longitudinal Arch and Peroneal Tubercle -Anatomical Study- Department of Orthopaedic Surgery Kangwon National University Hospital Chuncheon, Republic of Korea Chang Hyun
Peripheral Nerve Ultrasound
 Peripheral Nerve Ultrasound Jon A. Jacobson, M.D. Professor of Radiology Director, Division of Musculoskeletal Radiology University of Michigan Normal Peripheral Nerve Ultrasound appearance: Hypoechoic
Peripheral Nerve Ultrasound Jon A. Jacobson, M.D. Professor of Radiology Director, Division of Musculoskeletal Radiology University of Michigan Normal Peripheral Nerve Ultrasound appearance: Hypoechoic
Proceedings of the 55th Annual Convention of the American Association of Equine Practitioners
 Close this window to return to IVIS www.ivis.org Proceedings of the 55th Annual Convention of the American Association of Equine Practitioners December 5 9, 2009, Las Vegas, Nevada Program Chair : Nathaniel
Close this window to return to IVIS www.ivis.org Proceedings of the 55th Annual Convention of the American Association of Equine Practitioners December 5 9, 2009, Las Vegas, Nevada Program Chair : Nathaniel
Knee: Cruciate Ligaments
 72 Knee: Cruciate Ligaments R. Kent Sanders Sagittal oblique 2.5-mm sequences along the plane of the anterior cruciate ligament (ACL) typically yield three to four images of the ACL, with the first medial
72 Knee: Cruciate Ligaments R. Kent Sanders Sagittal oblique 2.5-mm sequences along the plane of the anterior cruciate ligament (ACL) typically yield three to four images of the ACL, with the first medial
The plantar aponeurosis
 Anatomy of the foot The plantar aponeurosis Is a triangular thickening of the deep fascia Its apex is attached to the medial and lateral tubercles of the calcaneum. The base of the aponeurosis divides
Anatomy of the foot The plantar aponeurosis Is a triangular thickening of the deep fascia Its apex is attached to the medial and lateral tubercles of the calcaneum. The base of the aponeurosis divides
Podiatry Ultrasound Report Templates
 Podiatry Ultrasound Report Templates 1 st Edition Compiled exclusively for the clients of Fisher Biomedical Inc. Podiatric Ultrasound Report Templates Welcome to our first edition of sample podiatric ultrasound
Podiatry Ultrasound Report Templates 1 st Edition Compiled exclusively for the clients of Fisher Biomedical Inc. Podiatric Ultrasound Report Templates Welcome to our first edition of sample podiatric ultrasound
ELENI ANDIPA General Hospital of Athens G. Gennimatas
 ELENI ANDIPA General Hospital of Athens G. Gennimatas Technological advances over the last years have caused a dramatic improvement in ultrasound quality and resolution An established imaging modality
ELENI ANDIPA General Hospital of Athens G. Gennimatas Technological advances over the last years have caused a dramatic improvement in ultrasound quality and resolution An established imaging modality
MIDFOOT INJURIES-ARE WE UNDERTREATING IT? Mr Rajiv Limaye Mr Prasad Karpe University Hospital of North Tees 3 rd Foot and Ankle Symposium
 MIDFOOT INJURIES-ARE WE UNDERTREATING IT? Mr Rajiv Limaye Mr Prasad Karpe University Hospital of North Tees 3 rd Foot and Ankle Symposium Introduction Increasing sports injuries RTA and traumatic injuries
MIDFOOT INJURIES-ARE WE UNDERTREATING IT? Mr Rajiv Limaye Mr Prasad Karpe University Hospital of North Tees 3 rd Foot and Ankle Symposium Introduction Increasing sports injuries RTA and traumatic injuries
Impingement Syndromes of the Ankle. Noaman W Siddiqi MD 5/4/2006
 Impingement Syndromes of the Ankle Noaman W Siddiqi MD 5/4/2006 Ankle Impingement Overview Clinical DX Increasingly recognized cause of chronic ankle pain Etiology can be soft tissue or osseous Professional
Impingement Syndromes of the Ankle Noaman W Siddiqi MD 5/4/2006 Ankle Impingement Overview Clinical DX Increasingly recognized cause of chronic ankle pain Etiology can be soft tissue or osseous Professional
.org. Posterior Tibial Tendon Dysfunction. Anatomy. Cause. Symptoms
 Posterior Tibial Tendon Dysfunction Page ( 1 ) Posterior tibial tendon dysfunction is one of the most common problems of the foot and ankle. It occurs when the posterior tibial tendon becomes inflamed
Posterior Tibial Tendon Dysfunction Page ( 1 ) Posterior tibial tendon dysfunction is one of the most common problems of the foot and ankle. It occurs when the posterior tibial tendon becomes inflamed
Ultrasonography of the Rotator Cuff
 Ultrasonography of the Rotator Cuff A COMPARISON OF ULTRASONOGRAPHIC AND ARTHROSCOPIC FINDINGS IN ONE HUNDRED CONSECUTIVE CASES* BY SHARLENE A. TEEFEY, M.D., S. ASHFAQ HASAN, M.D., WILLIAM D. MIDDLETON,
Ultrasonography of the Rotator Cuff A COMPARISON OF ULTRASONOGRAPHIC AND ARTHROSCOPIC FINDINGS IN ONE HUNDRED CONSECUTIVE CASES* BY SHARLENE A. TEEFEY, M.D., S. ASHFAQ HASAN, M.D., WILLIAM D. MIDDLETON,
Scar Engorged veins. Size of the foot [In clubfoot, small foot]
![Scar Engorged veins. Size of the foot [In clubfoot, small foot] Scar Engorged veins. Size of the foot [In clubfoot, small foot]](/thumbs/78/77722241.jpg) 6. FOOT HISTORY Pain: Walking, Running Foot wear problem Swelling; tingly feeling Deformity Stiffness Disability: At work; recreation; night; walk; ADL, Sports Previous Rx Comorbidities Smoke, Sugar, Steroid
6. FOOT HISTORY Pain: Walking, Running Foot wear problem Swelling; tingly feeling Deformity Stiffness Disability: At work; recreation; night; walk; ADL, Sports Previous Rx Comorbidities Smoke, Sugar, Steroid
MRI KNEE WHAT TO SEE. Dr. SHEKHAR SRIVASTAV. Sr.Consultant KNEE & SHOULDER ARTHROSCOPY
 MRI KNEE WHAT TO SEE Dr. SHEKHAR SRIVASTAV Sr.Consultant KNEE & SHOULDER ARTHROSCOPY MRI KNEE - WHAT TO SEE MRI is the most accurate and frequently used diagnostic tool for evaluation of internal derangement
MRI KNEE WHAT TO SEE Dr. SHEKHAR SRIVASTAV Sr.Consultant KNEE & SHOULDER ARTHROSCOPY MRI KNEE - WHAT TO SEE MRI is the most accurate and frequently used diagnostic tool for evaluation of internal derangement
Lateral epicondylitis, or ``tennis elbow,'' is
 Comparison of Sonography and MRI for Diagnosing Epicondylitis Theodore T. Miller, MD, 1,2 Micheal A. Shapiro, MD, 1,2 Elizabeth Schultz, MD, 1,2 Paul E. Kalish, MD 3 1 Department of Radiology, North Shore
Comparison of Sonography and MRI for Diagnosing Epicondylitis Theodore T. Miller, MD, 1,2 Micheal A. Shapiro, MD, 1,2 Elizabeth Schultz, MD, 1,2 Paul E. Kalish, MD 3 1 Department of Radiology, North Shore
EDL EHL. Extensor Hallucis Longus L5 Extensor Digitorum longus L5,1 Peroneus Tertius L5 1 Extensor Digitorum Brevis S1,2 [like intrinsic muscle]
![EDL EHL. Extensor Hallucis Longus L5 Extensor Digitorum longus L5,1 Peroneus Tertius L5 1 Extensor Digitorum Brevis S1,2 [like intrinsic muscle] EDL EHL. Extensor Hallucis Longus L5 Extensor Digitorum longus L5,1 Peroneus Tertius L5 1 Extensor Digitorum Brevis S1,2 [like intrinsic muscle]](/thumbs/78/77875930.jpg) ANATOMY OF ANKLE AND FOOT Lateral aspect: [Dorsal medial to lateral= dorsal under extensor retinaculum] Tibialis Anterior EHL Artery [Dorsal pedal A] and Anterior tibial N EDL Peroneus Tertius Behind the
ANATOMY OF ANKLE AND FOOT Lateral aspect: [Dorsal medial to lateral= dorsal under extensor retinaculum] Tibialis Anterior EHL Artery [Dorsal pedal A] and Anterior tibial N EDL Peroneus Tertius Behind the
THE LOWER EXTREMITY EXAM FOR THE FAMILY PRACTITIONER
 THE LOWER EXTREMITY EXAM FOR THE FAMILY PRACTITIONER Melinda A. Scott, D.O. Orthopedic Associates of Dayton Board Certified in Primary Care Sports Medicine GOALS Identify landmarks necessary for exam of
THE LOWER EXTREMITY EXAM FOR THE FAMILY PRACTITIONER Melinda A. Scott, D.O. Orthopedic Associates of Dayton Board Certified in Primary Care Sports Medicine GOALS Identify landmarks necessary for exam of
Joints and muscles of the foot. Architecture of the foot. Sándor Katz M.D.,Ph.D.
 Joints and muscles of the foot. Architecture of the foot. Sándor Katz M.D.,Ph.D. Ankle (talocrural) joint type: hinge Talocrural joint - medial collateral ligament Medial collateral = deltoid ligament
Joints and muscles of the foot. Architecture of the foot. Sándor Katz M.D.,Ph.D. Ankle (talocrural) joint type: hinge Talocrural joint - medial collateral ligament Medial collateral = deltoid ligament
Sonographically Guided Flexor Hallucis Longus Tendon Sheath Injection
 Technical dvance Sonographically Guided Flexor Hallucis Longus Tendon Sheath Injection mir Mehdizade, MD, Ronald S. dler, PhD, MD Objective. The purpose of this study was to describe a sonographically
Technical dvance Sonographically Guided Flexor Hallucis Longus Tendon Sheath Injection mir Mehdizade, MD, Ronald S. dler, PhD, MD Objective. The purpose of this study was to describe a sonographically
Ankle Sprains and Their Imitators
 Ankle Sprains and Their Imitators Mark Halstead, MD Dr. Mark Halstead is the Associate Professor of the Departments of Orthopedics and Pediatrics at Washington University School of Medicine; Director of
Ankle Sprains and Their Imitators Mark Halstead, MD Dr. Mark Halstead is the Associate Professor of the Departments of Orthopedics and Pediatrics at Washington University School of Medicine; Director of
Title. Issue Date Right.
 NOSITE: Nagasaki University's c Title uthor(s) Dynamic supination and hindfoot var tendons of both peroneus longus and Matsubayashi, Shohei; Tsujimoto, i Citation cta medica Nagasakiensia, 61(2), p Issue
NOSITE: Nagasaki University's c Title uthor(s) Dynamic supination and hindfoot var tendons of both peroneus longus and Matsubayashi, Shohei; Tsujimoto, i Citation cta medica Nagasakiensia, 61(2), p Issue
1. A worker falls from a height and lands on his feet. Radiographs reveal a fracture of the sustentaculum tali. The muscle passing immediately
 1. A worker falls from a height and lands on his feet. Radiographs reveal a fracture of the sustentaculum tali. The muscle passing immediately beneath it that would be adversely affected is the: fibularis
1. A worker falls from a height and lands on his feet. Radiographs reveal a fracture of the sustentaculum tali. The muscle passing immediately beneath it that would be adversely affected is the: fibularis
Hallux Valgus Deformity: Preoperative Radiologic Assessment
 119 Pictorial Essay H............ - Hallux Valgus Deformity: Preoperative Radiologic Assessment David Karasick1 and Keith L. Wapner An estimated 40% of the American adult population experiences foot problems,
119 Pictorial Essay H............ - Hallux Valgus Deformity: Preoperative Radiologic Assessment David Karasick1 and Keith L. Wapner An estimated 40% of the American adult population experiences foot problems,
Peritalar Dislocation After Tibio-Talar Arthrodesis: Fact or Fiction?
 AOFAS Annual Meeting, July 17-20th 2013 Hollywood, Florida Peritalar Dislocation After Tibio-Talar Arthrodesis: Fact or Fiction? Fabrice Colin, MD; Lukas Zwicky, MSc; Alexej Barg, MD; Beat Hintermann,
AOFAS Annual Meeting, July 17-20th 2013 Hollywood, Florida Peritalar Dislocation After Tibio-Talar Arthrodesis: Fact or Fiction? Fabrice Colin, MD; Lukas Zwicky, MSc; Alexej Barg, MD; Beat Hintermann,
Dr Nabil khouri MD. MSc. Ph.D
 Dr Nabil khouri MD. MSc. Ph.D Foot Anatomy The foot consists of 26 bones: 14 phalangeal, 5 metatarsal, and 7 tarsal. Toes are used to balance the body. Metatarsal Bones gives elasticity to the foot in
Dr Nabil khouri MD. MSc. Ph.D Foot Anatomy The foot consists of 26 bones: 14 phalangeal, 5 metatarsal, and 7 tarsal. Toes are used to balance the body. Metatarsal Bones gives elasticity to the foot in
Equine Diagnostic Radiography & Ultrasonography
 Equine Diagnostic adiography & Ultrasonography Dr. ussell Tucker DACV Prof Emeritus, WSU 90 ~30 DLPMO ~ projects medial forward lateral backward ~30 PL to DM projection 1 EQUINE DISTAL LIMB TENDONS & LIGAMENTS
Equine Diagnostic adiography & Ultrasonography Dr. ussell Tucker DACV Prof Emeritus, WSU 90 ~30 DLPMO ~ projects medial forward lateral backward ~30 PL to DM projection 1 EQUINE DISTAL LIMB TENDONS & LIGAMENTS
Claw toes after tibial fracture in children
 J Child Orthop (2009) 3:339 343 DOI 10.1007/s11832-009-0200-y ORIGINAL CLINICAL ARTICLE Claw toes after tibial fracture in children Frank Fitoussi Æ Brice Ilharreborde Æ Florent Guerin Æ Philippe Souchet
J Child Orthop (2009) 3:339 343 DOI 10.1007/s11832-009-0200-y ORIGINAL CLINICAL ARTICLE Claw toes after tibial fracture in children Frank Fitoussi Æ Brice Ilharreborde Æ Florent Guerin Æ Philippe Souchet
EASILY MISSED FOOT AND ANKLE FRACTURES NORDIC TRAUMA COURSE 2016, AARHUS
 EASILY MISSED FOOT AND ANKLE FRACTURES NORDIC TRAUMA COURSE 2016, AARHUS Ken F. Linnau, MD, MS Emergency Radiology Harborview Medical Center University of Washington Seattle, WA Thanks to Claire K Sandstrom
EASILY MISSED FOOT AND ANKLE FRACTURES NORDIC TRAUMA COURSE 2016, AARHUS Ken F. Linnau, MD, MS Emergency Radiology Harborview Medical Center University of Washington Seattle, WA Thanks to Claire K Sandstrom
Recognizing common injuries to the lower extremity
 Recognizing common injuries to the lower extremity Bones Femur Patella Tibia Tibial Tuberosity Medial Malleolus Fibula Lateral Malleolus Bones Tarsals Talus Calcaneus Metatarsals Phalanges Joints - Knee
Recognizing common injuries to the lower extremity Bones Femur Patella Tibia Tibial Tuberosity Medial Malleolus Fibula Lateral Malleolus Bones Tarsals Talus Calcaneus Metatarsals Phalanges Joints - Knee
MR Imaging of Disorders of the Posterior Tibialis Tendon
 MR Imaging of Disorders of the Posterior Tibialis Tendon Fig. 1. Drawing shows relationship of posterior tibialis tendon to remainder of tarsal tunnel. Note relative sites and distal extent of tendon sheaths
MR Imaging of Disorders of the Posterior Tibialis Tendon Fig. 1. Drawing shows relationship of posterior tibialis tendon to remainder of tarsal tunnel. Note relative sites and distal extent of tendon sheaths
BIOMECHANICAL EXAMINATION OF THE PEDIATRIC LOWER EXTREMITY
 BIOMECHANICAL EXAMINATION OF THE PEDIATRIC LOWER EXTREMITY B.Resseque, D.P.M. ARCH HEIGHT OFF WEIGHTBEARING Evaluate arch height by placing a ruler from the heel to the first metatarsal head Compare arch
BIOMECHANICAL EXAMINATION OF THE PEDIATRIC LOWER EXTREMITY B.Resseque, D.P.M. ARCH HEIGHT OFF WEIGHTBEARING Evaluate arch height by placing a ruler from the heel to the first metatarsal head Compare arch
Imaging of posterior ankle pain : Main etiologies and differential diagnosis
 Imaging of posterior ankle pain : Main etiologies and differential diagnosis Poster No.: C-2399 Congress: ECR 2017 Type: Educational Exhibit Authors: W. Frikha, M. MECHRI, S. boukriba, H. RIAHI, M. CHELLI
Imaging of posterior ankle pain : Main etiologies and differential diagnosis Poster No.: C-2399 Congress: ECR 2017 Type: Educational Exhibit Authors: W. Frikha, M. MECHRI, S. boukriba, H. RIAHI, M. CHELLI
New Radiographic Parameter Assessing Hindfoot Alignment in Stage II Adult Acquired Flatfoot Deformity
 New Radiographic Parameter Assessing Hindfoot Alignment in Stage II Adult Acquired Flatfoot Deformity Emilie Williamson, BS; Jeremy Chan, MD; Jayme C Burket, PhD; Jonathan T Deland, MD; Scott Ellis, MD
New Radiographic Parameter Assessing Hindfoot Alignment in Stage II Adult Acquired Flatfoot Deformity Emilie Williamson, BS; Jeremy Chan, MD; Jayme C Burket, PhD; Jonathan T Deland, MD; Scott Ellis, MD
