Respiratory Disorders in the Newborn: Identification and Diagnosis Hany Aly. DOI: /pir
|
|
|
- Randall Logan
- 5 years ago
- Views:
Transcription
1 Respiratory Disorders in the Newborn: Identification and Diagnosis Hany Aly Pediatr. Rev. 2004;25; DOI: /pir The online version of this article, along with updated information and services, is located on the World Wide Web at: Pediatrics in Review is the official journal of the American Academy of Pediatrics. A monthly publication, it has been published continuously since Pediatrics in Review is owned, published, and trademarked by the American Academy of Pediatrics, 141 Northwest Point Boulevard, Elk Grove Village, Illinois, Copyright 2004 by the American Academy of Pediatrics. All rights reserved. Print ISSN: Online ISSN:
2 Article neonatology Respiratory Disorders in the Newborn: Identification and Diagnosis Hany Aly, MD, FAAP* Objectives After reading this article, readers should be able to: 1. Describe the specific radiologic findings in neonatal syndrome. 2. Differentiate between the normal results of a newborn chest radiograph and the radiographic patterns that reflect meconium aspiration. 3. Differentiate between the normal results of a newborn chest radiograph and the radiographic patterns that reflect pneumonia. 4. Distinguish between pulmonary disease and cyanotic congenital heart disease as a cause of hypoxemia and acidosis in a neonate. Background Respiratory distress is encountered frequently in newborns and represents the most frequent indication for re-evaluation of the young infant. Because in the newborn may be a potentially life-threatening condition, physicians are expected to assess and manage affected infants promptly. The key to successful management of the infant who has is based on the ability to obtain a complete maternal and newborn history, perform a thorough physical examination, recognize the common respiratory disorders, differentiate among various diagnostic entities, and identify those that are life-threatening. Definition Respiratory distress in the newborn is characterized by one or more of the following: nasal flaring, chest retractions, tachypnea, and grunting. Nasal flaring is a relatively frequent finding in an infant attempting to decrease airway resistance. Suprasternal retraction indicates upper airway obstruction. Subcostal retraction, on the other hand, is a less specific sign that may be associated with either pulmonary or cardiac diseases. Normally, the neonate takes 30 to 60 breaths/min. The infant breathes at a faster rate to maintain ventilation in the face of decreased tidal volume. An infant in may try to maintain lung volume with adequate gas exchange by partially closing the glottis during expiration. This is the mechanism responsible for the audible grunting in these infants. An infant who has an advanced degree of may exhibit additional signs, such as cyanosis, gasping, choking, apnea, and stridor. The managing physician should consider these additional signs to be alarming. Initial Assessment The aim of the initial assessment of the infant in is to identify life-threatening conditions that require prompt support, such as inadequate or obstructed airway (gasping, choking, stridor), apnea or poor respiratory efforts, cyanosis, and circulatory collapse (bradycardia, hypotension, poor perfusion) (Table 1). The physician should manage these infants promptly with immediate oxygen support and possibly bag-and-mask ventilation or even intubation and mechanical ventilation. Therefore, resuscitation equipment and supplies always should be available for immediate use in the delivery room. Senior physicians and other health care team personnel should be prepared to perform resuscitation. Neonatal resuscitation guidelines should be followed in a stepwise manner. *Assistant Professor of Pediatrics and of Obstetrics & Gynecology; Director, Newborn Services, George Washington University, Washington, DC. Pediatrics in Review Vol.25 No.6 June
3 Table 1. Alarming Signs of Lifethreatening Conditions Obstructive Airway Gasping Choking Stridor Insufficient Breathing Apnea Poor respiratory effort Circulatory Collapse Bradycardia Hypotension Poor perfusion Poor Oxygenation Cyanosis History After the initial assessment and cardiorespiratory management, a history should be obtained. Maternal and obstetrical histories can provide invaluable information. Results of fetal assessment during pregnancy (triple screen, ultrasonography, biophysical profile) and fetal monitoring during labor and delivery (fetal heart rate, beat-to-beat variability, presence of decelerations) may provide useful information about a neonate in respiratory distress. Complications at delivery (eg, birth trauma, presence of meconium, perinatal depression) may be informative or play an important role in the development of. Figure 1 illustrates maternal and fetal conditions commonly associated with respiratory diseases. Details of the presenting respiratory symptoms may be helpful. A history of coughing and choking in relation to feeding should be clarified. If these symptoms occur during the feeding, both functional (eg, oropharyngeal aspiration occasionally seen in preterm infants) and structural (eg, tracheoesophageal fistula) should be considered. A maternal history of polyhydramnios is consistent with the latter diagnosis when esophageal atresia is also present. If these symptoms follow the feeding, gastroesophageal reflux with aspiration should be suspected. These infants may have a history of recurrent emesis. Gradually improving symptoms are consistent with transient tachypnea of the newborn (TTN); gradual deterioration may be consistent with pneumonia or sepsis. Many nonrespiratory conditions can present with respiratory symptoms, including hypoglycemia, metabolic acidosis, anemia, heart failure, and sepsis. Information that may help to ascertain these conditions should be obtained. Physical Examination Inspection is the first and most important tool in a physical examination. Infants who exhibit apnea, poor respiratory effort, marked retractions, cyanosis, or poor perfusion require urgent attention. Inspiratory stridor is consistent with upper airway obstruction. Stridor in an infant who has a previous history of endotracheal intubation may indicate airway injury, such as subglottic stenosis. Asymmetric chest movement combined with severe distress can be an alarming sign for tension pneumothorax. A scaphoid abdomen is the hallmark for congenital diaphragmatic hernia. Auscultation is helpful in determining the symmetry and adequacy of air exchange. Abnormal breath sounds also should be identified. The presence of a heart murmur deserves special attention, although a murmur alone is not diagnostic of congenital heart disease. Neonates frequently present with heart murmurs that are innocent, and some serious congenital heart diseases may present without any murmur. Transillumination of the chest is useful to detect a pneumothorax on an emergent basis. Differential Diagnosis of Respiratory Distress in the Newborn Respiratory distress of the newborn is a common presentation for a wide variety of other diseases (Fig. 2). Parenchymal lung diseases, such as pneumonia, surfactant deficiency, and meconium aspiration, are the most common causes of in the neonate. However, airway and chest wall deformities as well as abnormalities of the diaphragm and mediastinal structures also can cause. Additionally, neurologic, cardiac, and metabolic abnormalities must be considered. Neonates who have congenital heart diseases commonly present with. Seizures, asphyxia, and meningitis are examples of neurologic disorders associated with respiratory signs. Common metabolic causes of include hypoglycemia and acidosis. Respiratory distress can be a presentation of hypothermia, sepsis, acidosis, polycythemia, or anemia. Case Scenarios A few common scenarios of infants presenting with respiratory distress follow. 202 Pediatrics in Review Vol.25 No.6 June 2004
4 Figure 1. Maternal and obstetric conditions associated with in neonates. Case #1 A 3.5-kg newborn male has tachypnea and acrocyanosis. Delivery was via an elective cesarean section at 41 weeks of gestation. Apgar scores were 7 and 8 at 1 and 5 minutes, respectively. The infant s temperature is 96.4 F (35.8 C), heart rate is 153 beats/min, and respiratory rate is 82 breaths/min. He has slight subcostal retractions. The remainder of the examination is normal. The chest radiograph is shown in Figure 3. At 18 hours after birth, the infant s color is pink and respiratory rate is decreased to 48 breaths/min. Case #2 A 3.9-kg female infant appears blue and tachypneic immediately after vaginal delivery. Amniotic fluid was stained with thick meconium. Apgar scores were 4 and 6 at 1 and 5 minutes, respectively. The infant s temperature is 98.4 F (36.9 C), heart rate is 173 beats/min, respiratory rate is 110 breaths/min, and mean blood pressure is 61 mm Hg. She is barrel-chested and has retractions with poor-to-fair air entry. Coarse rales are audible bilaterally. The chest radiograph is shown in Figure 4. Case #3 A 1.2-kg male infant is born at 32 weeks gestation. Apgar scores are 7 and 8 at 1 and 5 minutes, respectively. The infant is acrocyanotic and has grunting and marked retractions with breathing. The infant s temperature is 96.8 F (36.0 C), heart rate is 170 beats/min, respiratory rate is 75 breaths/min, and mean blood pressure is 39 mm Hg. The chest radiograph is shown in Figure 5. Pediatrics in Review Vol.25 No.6 June
5 Figure 2. Differential diagnosis for infants in. 204 Pediatrics in Review Vol.25 No.6 June 2004
6 Figure 3. Chest radiograph of an infant who has transient tachypnea of the newborn. Arrows point at fluids in the interlobar fissures. Note the increased pulmonary interstitial markings in both lung fields. TTN TTN represents transient pulmonary edema resulting from delayed clearance of fetal lung liquid. It can occur in both term and preterm neonates. Lung liquid is produced actively in utero by a chloride pump that causes influx of chloride and water from the interstitium into the alveolar space. Approximately 2 to 3 days before delivery, lung liquid starts to clear due to an interesting Figure 4. Chest radiograph of an infant who has meconium aspiration syndrome, with course patches of atelectasis (arrows). Areas of hyperinflation also are present, best seen at both lung bases. Figure 5. Chest radiograph of a preterm infant who has hyaline membrane disease. Arrows on the right lung field point at the diffuse ground glass appearance. Arrows on the left demonstrate prominent air-filled bronchi, known as air bronchogram. transformation process in the pulmonary epithelium. The fetal pulmonary epithelium changes from a chloridesecreting membrane to a sodium-absorbing membrane, with reversal of the flow of lung liquid away from the airless alveolar spaces. Because this liquid contains very little protein, low oncotic pressure also favors the movement of water from the alveolar spaces into the interstitium. At this time, prostaglandin secretion by the fetoplacental unit increases to trigger labor. Prostaglandins are responsible for the lymphatic dilatation that accelerates clearance of liquid from the interstitium. After birth, when the lungs expand with air, water moves rapidly from air spaces to connective tissue, to be removed gradually from the lungs by the lymphatic system and pulmonary blood vessels. Infants who have TTN present clinically with tachypnea and occasionally grunting and nasal flaring immediately after birth (Case #1). The incidence of TTN may be increased in infants born via elective cesarean section, especially before the onset of labor. Typically, arterial blood gases reveal respiratory acidosis and mild-tomoderate hypoxemia. Chest radiography reveals increased interstitial markings and occasionally fluid in the interlobar fissures (Fig. 3). Occasionally, pleural effusion or signs of alveolar edema may be seen. TTN is generally a benign, self-limited disease that usually responds well Pediatrics in Review Vol.25 No.6 June
7 to oxygen therapy. Mechanical ventilation seldom is needed, although many infants require nasal continuous positive airway pressure support. The additional distending airway pressure may assist in maintaining alveolar surface area as well as absorbing the retained intraalveolar fluid. Infants whose disease is uncomplicated usually recover without long-term pulmonary sequelae. Full recovery is expected within 2 to 5 days. Meconium Aspiration Syndrome (MAS) Meconium staining of amniotic fluid occurs in approximately 10% to 26% of all deliveries and almost exclusively in term and postterm deliveries. Meconium consists of water, desquamated cells from the alimentary tract, skin, lanugo hair, vernix, bile pigments, lipid, and mucopolysaccharides. Passage of meconium in utero may represent fetal hypoxemia. Meconium can be aspirated before, during, or after delivery. Once aspirated, meconium can cause obstruction of the air passages, chemical pneumonitis with activation of several inflammatory mediators, and inactivation of lung surfactant. The infant who has MAS may present with varying degrees of and is likely to have a barrel chest with audible rales or rhonchi on auscultation (Case #2). The chest radiograph usually shows patchy areas of atelectasis alternating with areas of overinflation (Fig. 4). Pneumothorax is seen in 10% to 20% of infants who have MAS. It is recommended that obstetricians suction the infant s mouth, pharynx, and nose as soon as the head is delivered, before delivery of the body, to prevent MAS. Once the infant is delivered and placed under the radiant warmer, the hypopharynx should be suctioned to clear any residual meconium. If the newborn has absent or depressed respiration, a heart rate of less than 100 beats/min, or poor muscle tone, direct tracheal visualization and suctioning should be performed to remove meconium from the airway. Hyaline Membrane Disease (HMD) HMD is a common condition in preterm infants. The cause is insufficient pulmonary surfactant, a mixture of lipids and proteins produced by type II pneumocytes. It serves to create a thin alveolar-lining layer that reduces the surface tension inside the alveoli, preventing them from collapsing. The preterm infant who has HMD usually presents with beginning at or immediately after birth (Case #3). The blood gas typically reveals hypoxemia and respiratory acidosis. Radiographically, lungs demonstrate the typical ground glass appearance that represents diffuse atelectasis and air bronchograms that reflect the contrast of the relatively airless parenchyma against the air-filled bronchi (Fig. 5). Prevention of HMD relies on appropriate obstetric measures to continue gestation or treatment with antenatal steroids, which has been instrumental in reducing the incidence of HMD. Affected infants often are managed with mechanical ventilation and endotracheal surfactant replacement therapy. The use of continuous positive airway pressure is a less invasive alternative. Pneumonia Pneumonia, the most common infection in neonates, can be due to different antenatal, perinatal, or postnatal causes. Pneumonia can present with a diversity of signs in infancy, including any form of, lethargy, poor feeding, jaundice, or apnea. Temperature instability, if noted, is a good clue for considering pneumonia in the diagnosis. Findings on chest radiography depend on the cause of pneumonia. Bilateral consolidation ( whiteout ) is related primarily to in utero infections. Group B streptococcal pneumonia may be confused with HMD because it has a similar reticular appearance with air bronchogram. Other infections may cause a localized pneumonia that is confined to one or more lobes of the lung. It frequently is advisable to treat newborns in with antibiotics until the diagnosis of pneumonia or sepsis is absolutely ruled out. Congenital Heart Disease (CHD) Infants who have CHD may present with cyanosis or heart failure. Common CHDs in the early neonatal pe- Figure 6. Chest radiograph of an infant who has transposition of the great vessels. Note the prominent increased pulmonary vasculature (arrows). 206 Pediatrics in Review Vol.25 No.6 June 2004
8 Table 2. Differentiation of Cyanotic Heart Diseases From Pulmonary Diseases Among Infants in Respiratory Distress Criteria Cyanotic Heart Diseases Pulmonary Diseases History Physical Findings Chest Radiograph Previous sibling who has CHD Diagnosis of CHD by prenatal ultrasonography Cyanosis Gallop rhythm Single second heart sound Large liver Mild Increased heart size Decreased pulmonary vascularity (except in transposition of the great vessels and total anomalous pulmonary venous return) Maternal fever Meconium-stained amniotic fluid Preterm delivery Cyanosis Severe retraction Split second heart sound Fever Normal heart size Abnormal pulmonary parenchyma, such as a) total whiteout or patches of consolidation in pneumonia, b) fluid in the fissures in TTN, or c) ground glass appearance in HMD Increased PCO Arterial Blood Gases Normal or decreased PCO 2 Decreased PO 2 2 Decreased PO 2 Hyperoxygenation test PaO 2 <150 mm Hg PaO 2 >150 mm Hg (except in severe PPHN) Echocardiography Abnormal heart or vessels Normal heart and vessels CHD congenital heart diseases; HMD hyaline membrane disease; TTN transient tachypnea of the newborn: PPHN persistent pulmonary hypertension of the newborn riod are shown in Figure 2. Differentiation between CHD and pulmonary disease can be challenging, and the two can coexist. It is important to recognize that points of differentiation between heart and lung disease are cumulative rather than exclusive. A history of meconium staining of the amniotic fluid does not exclude the diagnosis of transposition of the great vessels. Alternatively, a heart murmur heard on physical examination does not exclude the possibility of pneumonia. Signs that generally are consistent with CHD include: visibly hyperactive precordial impulse, gallop rhythm, poor capillary refill, weak pulses, decreased or delayed pulses in lower extremities, hepatomegaly, and abnormal vascularity or cardiomegaly on chest radiography (Fig. 6). A single second heart sound without split also may be indicative of CHD. Recognition of this finding in infants requires considerable experience, and appreciating this can be challenging, especially in the presence of tachycardia. Infants who have isolated CHD usually do not have hypercapnia. The Paco 2 may be decreased unless CHD is associated with lung disease. Metabolic acidosis is slightly more common in patients who have low cardiac output as a consequence of CHD, but it can occur in newborns who have infections or inborn errors of metabolism. Finally, it should be emphasized that complete echocardiography can detect most congenital heart defects. Infants who have cyanotic heart diseases typically do not present with severe chest retraction. However, tachypnea is common. Oxygen saturation usually is decreased. Increasing the concentration of inspired oxygen to 100% for 20 minutes ( hyperoxygenation test ) will not produce a significant increase in Pao 2 in most infants who have cyanotic CHD. Table 2 describes steps to help differentiate cyanotic heart diseases from pulmonary diseases. Suggested Reading Fletcher MA. Physical Diagnosis in Neonatology. Philadelphia, Pa: Lippincott-Raven Publishers; 1998: International guidelines for neonatal resuscitation: an excerpt from the guidelines 2000 for cardiopulmonary resuscitation and emergency cardiovascular care: international consensus on science. Pediatrics. 2000;106:e29. Available at: aappubliations.org/cgi/content/full/106/3/e29 Moses D, Holm BA, Spitale P, Liu MY, Enhorning G. Inhibition of pulmonary surfactant function by meconium. Am J Obstet Gynecol. 1991;164:477 Nathan L, Leveno KJ, Carnody TJ III, Kelly MA, Sherman ML. Meconium: a 1990s perspective on an old obstetrics hazard. Obstet Gynecol. 1994;83:329 Peterson HG, Pendleton ME. Contrasting roentgenographic pulmonary patterns of the hyaline membrane and fetal-aspiration syndromes. AJR. 1989;73:800 Singer JI, Losek JD. Grunting respiration: chest or abdominal pathology? Pediatr Emerg Care. 1992;8: Stokes DC. Respiratory failure. Pediatr Rev. 1997;18: Pediatrics in Review Vol.25 No.6 June
9 PIR Quiz Quiz also available online at A radiograph that reveals increased interstitial markings with fluid in the interlobar fissures in an infant who has is most likely to represent: A. Hyaline membrane disease. B. Lobar pneumonia. C. Meconium aspiration syndrome. D. Transient tachypnea of the newborn. E. Transposition of the great vessels. 11. The most likely diagnosis associated with the radiographic findings of a diffuse ground glass appearance to the parenchyma in an infant who has is: A. Hyaline membrane disease. B. Lobar pneumonia. C. Meconium aspiration syndrome. D. Transient tachypnea of the newborn. E. Transposition of the great vessels. 12. The radiographic finding of patchy atelectasis with areas of hyperinflation in an infant who has syndrome is most indicative of: A. Hyaline membrane disease. B. Lobar pneumonia. C. Meconium aspiration syndrome. D. Transient tachypnea of the newborn. E. Transposition of the great vessels. 13. For an infant who has syndrome, increased pulmonary vascularity on a radiograph most likely represents: A. Hyaline membrane disease. B. Lobar pneumonia. C. Meconium aspiration syndrome. D. Transient tachypnea of the newborn. E. Transposition of the great vessels. 14. Among the following, the information that is most helpful in distinguishing cyanotic heart disease from pulmonary parenchymal disease in a newborn who has is: A. Decreased Po 2 in blood gas analysis. B. Gestational age less than 32 weeks. C. Maternal infection during the third trimester. D. Respiratory rate of 70 breaths/min. E. Results of a hyperoxygenation test. 208 Pediatrics in Review Vol.25 No.6 June 2004
10 Respiratory Disorders in the Newborn: Identification and Diagnosis Hany Aly Pediatr. Rev. 2004;25; DOI: /pir Updated Information & Services Supplementary Material Subspecialty Collections Permissions & Licensing Reprints including high-resolution figures, can be found at: Supplementary material can be found at: /DC1 This article, along with others on similar topics, appears in the following collection(s): Fetus and Newborn Infant born_infant Information about reproducing this article in parts (figures, tables) or in its entirety can be found online at: Information about ordering reprints can be found online:
1st Annual Clinical Simulation Conference
 1st Annual Clinical Simulation Conference Newborns with Acute Respiratory Distress: Diagnosis and Management Ma Teresa C. Ambat, MD Assistant Professor Division of Neonatology, Department of Pediatrics
1st Annual Clinical Simulation Conference Newborns with Acute Respiratory Distress: Diagnosis and Management Ma Teresa C. Ambat, MD Assistant Professor Division of Neonatology, Department of Pediatrics
Review of Neonatal Respiratory Problems
 Review of Neonatal Respiratory Problems Respiratory Distress Occurs in about 7% of infants Clinical presentation includes: Apnea Cyanosis Grunting Inspiratory stridor Nasal flaring Poor feeding Tachypnea
Review of Neonatal Respiratory Problems Respiratory Distress Occurs in about 7% of infants Clinical presentation includes: Apnea Cyanosis Grunting Inspiratory stridor Nasal flaring Poor feeding Tachypnea
Hyaline membrane disease. By : Dr. Ch Sarishma Peadiatric Pg
 Hyaline membrane disease By : Dr. Ch Sarishma Peadiatric Pg Also called Respiratory distress syndrome. It occurs primarily in premature infants; its incidence is inversely related to gestational age and
Hyaline membrane disease By : Dr. Ch Sarishma Peadiatric Pg Also called Respiratory distress syndrome. It occurs primarily in premature infants; its incidence is inversely related to gestational age and
Karen Corlett, RN, MSN, CPNP-AC/PC Pediatric Nurse Practitioner Congenital Heart Surgery Unit Pediatric Cardiac Intensivists of North Texas Medical
 Karen Corlett, RN, MSN, CPNP-AC/PC Pediatric Nurse Practitioner Congenital Heart Surgery Unit Pediatric Cardiac Intensivists of North Texas Medical City Children s Hospital, Dallas Hypoxia Shortage of
Karen Corlett, RN, MSN, CPNP-AC/PC Pediatric Nurse Practitioner Congenital Heart Surgery Unit Pediatric Cardiac Intensivists of North Texas Medical City Children s Hospital, Dallas Hypoxia Shortage of
Presented By : Kamlah Olaimat
 Presented By : Kamlah Olaimat 18\7\2010 Transient Tachpnea of the Definition:- newborn (TTN) TTN is a benign disease of near term or term infant who display respiratory distress shortly after delivery.
Presented By : Kamlah Olaimat 18\7\2010 Transient Tachpnea of the Definition:- newborn (TTN) TTN is a benign disease of near term or term infant who display respiratory distress shortly after delivery.
The Blue Baby. Network Stabilisation of the Term Infant Study Day 15 th March 2017 Joanna Behrsin
 The Blue Baby Network Stabilisation of the Term Infant Study Day 15 th March 2017 Joanna Behrsin Session Structure Definitions and assessment of cyanosis Causes of blue baby Structured approach to assessing
The Blue Baby Network Stabilisation of the Term Infant Study Day 15 th March 2017 Joanna Behrsin Session Structure Definitions and assessment of cyanosis Causes of blue baby Structured approach to assessing
 NEONATAL LIFE SUPPORT PROVIDER (NLSP) CERTIFICATION EXAMINATION 1. To determine if an infant requires resuscitation, you must rapidly assess gestation period, presence of meconium in amniotic fluid, breaths
NEONATAL LIFE SUPPORT PROVIDER (NLSP) CERTIFICATION EXAMINATION 1. To determine if an infant requires resuscitation, you must rapidly assess gestation period, presence of meconium in amniotic fluid, breaths
MODULE VII. Delivery and Immediate Neonatal Care
 MODULE VII Delivery and Immediate Neonatal Care NEONATAL ASPHYXIA About one million deaths per year In Latin America 12% of newborns suffer some degree of asphyxia Main cause of perinatal and neonatal
MODULE VII Delivery and Immediate Neonatal Care NEONATAL ASPHYXIA About one million deaths per year In Latin America 12% of newborns suffer some degree of asphyxia Main cause of perinatal and neonatal
Pediatrics. Blue Baby Syndrome (Cyanotic Newborn) and Hyperoxia Test. Definition. See online here
 Pediatrics Blue Baby Syndrome (Cyanotic Newborn) and Hyperoxia Test See online here Blue babies lack sufficient hemoglobin, resulting in the bluish discoloration of tissues, a term referred to as cyanosis.
Pediatrics Blue Baby Syndrome (Cyanotic Newborn) and Hyperoxia Test See online here Blue babies lack sufficient hemoglobin, resulting in the bluish discoloration of tissues, a term referred to as cyanosis.
Radiological evaluation of neonatal lesions in 118 neonates
 Original Research Article ISSN: 394-006 (P) Radiological evaluation of neonatal thoracic lesions in 8 neonates Konark Sarvaiya *, Himanshu Singla, Nirav Patel, Jai Inder Dhillon, Babubhai Patel 3 nd year
Original Research Article ISSN: 394-006 (P) Radiological evaluation of neonatal thoracic lesions in 8 neonates Konark Sarvaiya *, Himanshu Singla, Nirav Patel, Jai Inder Dhillon, Babubhai Patel 3 nd year
MODULE VII. Delivery and Immediate Neonatal Care
 MODULE VII Delivery and Immediate Neonatal Care NEONATAL ASPHYXIA About one million deaths per year In Latin America 12% of newborns suffer some degree of asphyxia A major cause of perinatal and neonatal
MODULE VII Delivery and Immediate Neonatal Care NEONATAL ASPHYXIA About one million deaths per year In Latin America 12% of newborns suffer some degree of asphyxia A major cause of perinatal and neonatal
SUMPh N. Testemitanu Radiology and Medical imaging department PEDIATRIC IMAGING. M. Crivceanschii, assistant professor
 SUMPh N. Testemitanu Radiology and Medical imaging department PEDIATRIC IMAGING M. Crivceanschii, assistant professor GOALS AND OBJECTIVES to be aware of the role of modern diagnostic imaging modalities
SUMPh N. Testemitanu Radiology and Medical imaging department PEDIATRIC IMAGING M. Crivceanschii, assistant professor GOALS AND OBJECTIVES to be aware of the role of modern diagnostic imaging modalities
Infection. Risk factor for infection ACoRN alerting sign with * Clinical deterioration. Problem List. Respiratory. Cardiovascular
 The ACoRN Process Baby at risk Unwell Risk factors Post-resuscitation requiring stabilization Resuscitation Ineffective breathing Heart rate < 100 bpm Central cyanosis Support Infection Risk factor for
The ACoRN Process Baby at risk Unwell Risk factors Post-resuscitation requiring stabilization Resuscitation Ineffective breathing Heart rate < 100 bpm Central cyanosis Support Infection Risk factor for
Simulation 08: Cyanotic Preterm Infant in Respiratory Distress
 Flow Chart Simulation 08: Cyanotic Preterm Infant in Respiratory Distress Opening Scenario Section 1 Type: DM As staff therapist assigned to a Level 2 NICU in a 250 bed rural medical center you are called
Flow Chart Simulation 08: Cyanotic Preterm Infant in Respiratory Distress Opening Scenario Section 1 Type: DM As staff therapist assigned to a Level 2 NICU in a 250 bed rural medical center you are called
Screening for Critical Congenital Heart Disease
 Screening for Critical Congenital Heart Disease Caroline K. Lee, MD Pediatric Cardiology Disclosures I have no relevant financial relationships or conflicts of interest 1 Most Common Birth Defect Most
Screening for Critical Congenital Heart Disease Caroline K. Lee, MD Pediatric Cardiology Disclosures I have no relevant financial relationships or conflicts of interest 1 Most Common Birth Defect Most
A radiological perspective of assessing neonatal respiratory distress syndrome
 Original Research Article A radiological perspective of assessing neonatal respiratory distress syndrome Jayesh Shah 1, Nikhil Parvatkar 2*, C. Raychaudhuri 3 1 Associate Professor, 2 1 st Year Resident,
Original Research Article A radiological perspective of assessing neonatal respiratory distress syndrome Jayesh Shah 1, Nikhil Parvatkar 2*, C. Raychaudhuri 3 1 Associate Professor, 2 1 st Year Resident,
Neonatal Life Support Provider (NLSP) Certification Preparatory Materials
 Neonatal Life Support Provider (NLSP) Certification Preparatory Materials NEONATAL LIFE SUPPORT PROVIDER (NRP) CERTIFICATION TABLE OF CONTENTS NEONATAL FLOW ALGORITHM.2 INTRODUCTION 3 ANTICIPATION OF RESUSCITATION
Neonatal Life Support Provider (NLSP) Certification Preparatory Materials NEONATAL LIFE SUPPORT PROVIDER (NRP) CERTIFICATION TABLE OF CONTENTS NEONATAL FLOW ALGORITHM.2 INTRODUCTION 3 ANTICIPATION OF RESUSCITATION
Simulation 3: Post-term Baby in Labor and Delivery
 Simulation 3: Post-term Baby in Labor and Delivery Opening Scenario (Links to Section 1) You are an evening-shift respiratory therapist in a large hospital with a level III neonatal unit. You are paged
Simulation 3: Post-term Baby in Labor and Delivery Opening Scenario (Links to Section 1) You are an evening-shift respiratory therapist in a large hospital with a level III neonatal unit. You are paged
Semiology of respiratory system in children Simple choice 1. Mark the intrauterine age of lung development onset from the gut: a) 1 week b) 24 days
 Semiology of respiratory system in children Simple choice 1. Mark the intrauterine age of lung development onset from the gut: a) 1 week b) 24 days c) 6 weeks d) 12 weeks e) 35 weeks 2. Stridor is not
Semiology of respiratory system in children Simple choice 1. Mark the intrauterine age of lung development onset from the gut: a) 1 week b) 24 days c) 6 weeks d) 12 weeks e) 35 weeks 2. Stridor is not
Chest X rays and Case Studies. No disclosures. Outline 5/31/2018. Carlo Manalo, M.D. Department of Radiology Loma Linda University Children s Hospital
 Chest X rays and Case Studies Carlo Manalo, M.D. Department of Radiology Loma Linda University Children s Hospital No disclosures. Outline Importance of history Densities delineated on radiography An approach
Chest X rays and Case Studies Carlo Manalo, M.D. Department of Radiology Loma Linda University Children s Hospital No disclosures. Outline Importance of history Densities delineated on radiography An approach
Pulmonary Problems of the Neonate. Jon Palmer, VMD, DACVIM Chief, Neonatal Intensive Care Service New Bolton Center, University of Pennsylvania, USA
 Pulmonary Problems of the Neonate Jon Palmer, VMD, DACVIM Chief, Neonatal Intensive Care Service New Bolton Center, University of Pennsylvania, USA Lower Respiratory Diseases Ventilation/Perfusion Abnormalities
Pulmonary Problems of the Neonate Jon Palmer, VMD, DACVIM Chief, Neonatal Intensive Care Service New Bolton Center, University of Pennsylvania, USA Lower Respiratory Diseases Ventilation/Perfusion Abnormalities
An Overview of Bronchopulmonary Dysplasia and Chronic Lung Disease in Infancy
 An Overview of Bronchopulmonary Dysplasia and Chronic Lung Disease in Infancy Housekeeping: I have no financial disclosures Learning objectives: Develop an understanding of bronchopulmonary dysplasia (BPD)
An Overview of Bronchopulmonary Dysplasia and Chronic Lung Disease in Infancy Housekeeping: I have no financial disclosures Learning objectives: Develop an understanding of bronchopulmonary dysplasia (BPD)
When is Risky to Apply Oxygen for Congenital Heart Disease 부천세종병원 소아청소년과최은영
 When is Risky to Apply Oxygen for Congenital Heart Disease 부천세종병원 소아청소년과최은영 The Korean Society of Cardiology COI Disclosure Eun-Young Choi The author have no financial conflicts of interest to disclose
When is Risky to Apply Oxygen for Congenital Heart Disease 부천세종병원 소아청소년과최은영 The Korean Society of Cardiology COI Disclosure Eun-Young Choi The author have no financial conflicts of interest to disclose
Competency Title: Continuous Positive Airway Pressure
 Competency Title: Continuous Positive Airway Pressure Trainee Name: ------------------------------------------------------------- Title: ---------------------------------------------------------------
Competency Title: Continuous Positive Airway Pressure Trainee Name: ------------------------------------------------------------- Title: ---------------------------------------------------------------
CONTINUOUS POSITIVE AIRWAY PRESSURE (CPAP) DEFINITION
 CONTINUOUS POSITIVE AIRWAY PRESSURE (CPAP) DEFINITION Method of maintaining low pressure distension of lungs during inspiration and expiration when infant breathing spontaneously Benefits Improves oxygenation
CONTINUOUS POSITIVE AIRWAY PRESSURE (CPAP) DEFINITION Method of maintaining low pressure distension of lungs during inspiration and expiration when infant breathing spontaneously Benefits Improves oxygenation
Pediatric Shock. Hypovolemia. Sepsis. Most common cause of pediatric shock Small blood volumes (80cc/kg)
 Critical Concepts: Shock Inadequate peripheral perfusion where oxygen delivery does not meet metabolic demand Adult vs Pediatric Shock - Same causes/different frequencies Pediatric Shock Hypovolemia Most
Critical Concepts: Shock Inadequate peripheral perfusion where oxygen delivery does not meet metabolic demand Adult vs Pediatric Shock - Same causes/different frequencies Pediatric Shock Hypovolemia Most
1 Chapter 13 Respiratory Emergencies 2 Respiratory Distress Patients often complain about. Shortness of breath Symptom of many different Cause can be
 1 Chapter 13 Respiratory Emergencies 2 Respiratory Distress Patients often complain about. Shortness of breath Symptom of many different Cause can be difficult to determine. Even for physician in hospital
1 Chapter 13 Respiratory Emergencies 2 Respiratory Distress Patients often complain about. Shortness of breath Symptom of many different Cause can be difficult to determine. Even for physician in hospital
TRAINING NEONATOLOGY SILVANA PARIS
 TRAINING ON NEONATOLOGY SILVANA PARIS RESUSCITATION IN DELIVERY ROOM INTRODUCTION THE GLOBAL RESUSCITATION BURDEN IN NEWBORN 136 MILL NEWBORN BABIES EACH YEAR (WHO WORLD REPORT) 5-8 MILL NEWBORN INFANTS
TRAINING ON NEONATOLOGY SILVANA PARIS RESUSCITATION IN DELIVERY ROOM INTRODUCTION THE GLOBAL RESUSCITATION BURDEN IN NEWBORN 136 MILL NEWBORN BABIES EACH YEAR (WHO WORLD REPORT) 5-8 MILL NEWBORN INFANTS
ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) Rv
 ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) Rv.8.18.18 ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) SUDDEN PROGRESSIVE FORM OF ACUTE RESPIRATORY FAILURE ALVEOLAR CAPILLARY MEMBRANE BECOMES DAMAGED AND MORE
ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) Rv.8.18.18 ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) SUDDEN PROGRESSIVE FORM OF ACUTE RESPIRATORY FAILURE ALVEOLAR CAPILLARY MEMBRANE BECOMES DAMAGED AND MORE
Practical Application of CPAP
 CHAPTER 3 Practical Application of CPAP Dr. Srinivas Murki Neonatologist Fernadez Hospital, Hyderabad. A.P. Practical Application of CPAP Continuous positive airway pressure (CPAP) applied to premature
CHAPTER 3 Practical Application of CPAP Dr. Srinivas Murki Neonatologist Fernadez Hospital, Hyderabad. A.P. Practical Application of CPAP Continuous positive airway pressure (CPAP) applied to premature
Duct Dependant Congenital Heart Disease
 Children s Acute Transport Service Clinical Guidelines Duct Dependant Congenital Heart Disease Document Control Information Author CATS/NTS Author Position CC Transport Services Document Owner E. Polke
Children s Acute Transport Service Clinical Guidelines Duct Dependant Congenital Heart Disease Document Control Information Author CATS/NTS Author Position CC Transport Services Document Owner E. Polke
Duct Dependant Congenital Heart Disease
 Children s Acute Transport Service Clinical Guidelines Duct Dependant Congenital Heart Disease This guideline has been agreed by both NTS & CATS Document Control Information Author CATS/NTS Author Position
Children s Acute Transport Service Clinical Guidelines Duct Dependant Congenital Heart Disease This guideline has been agreed by both NTS & CATS Document Control Information Author CATS/NTS Author Position
INTRODUCTION The effect of CPAP works on lung mechanics to improve oxygenation (PaO 2
 2 Effects of CPAP INTRODUCTION The effect of CPAP works on lung mechanics to improve oxygenation (PaO 2 ). The effect on CO 2 is only secondary to the primary process of improvement in lung volume and
2 Effects of CPAP INTRODUCTION The effect of CPAP works on lung mechanics to improve oxygenation (PaO 2 ). The effect on CO 2 is only secondary to the primary process of improvement in lung volume and
PHYSIOLOGICAL CONSIDERATION OF
 PHYSIOLOGICAL CONSIDERATION OF RESPIRATORY DISEASE A Symposium JULIUS H. COMROE, M.D., Chair,nan Graduate School of Medicine, University of Pennsylvania, Philadelphia RESPIRATORY AND PULMONARY PHYSIOLOGY
PHYSIOLOGICAL CONSIDERATION OF RESPIRATORY DISEASE A Symposium JULIUS H. COMROE, M.D., Chair,nan Graduate School of Medicine, University of Pennsylvania, Philadelphia RESPIRATORY AND PULMONARY PHYSIOLOGY
How to Recognize a Suspected Cardiac Defect in the Neonate
 Neonatal Nursing Education Brief: How to Recognize a Suspected Cardiac Defect in the Neonate https://www.seattlechildrens.org/healthcareprofessionals/education/continuing-medical-nursing-education/neonatalnursing-education-briefs/
Neonatal Nursing Education Brief: How to Recognize a Suspected Cardiac Defect in the Neonate https://www.seattlechildrens.org/healthcareprofessionals/education/continuing-medical-nursing-education/neonatalnursing-education-briefs/
Guslihan Dasa Tjipta Division of Perinatology Department of Child Health Medical School University of Sumatera Utara
 Guslihan Dasa Tjipta Division of Perinatology Department of Child Health Medical School University of Sumatera Utara 1 Definition Perinatal asphyxia is a fetus/newborn, due to: is an insult to the Lack
Guslihan Dasa Tjipta Division of Perinatology Department of Child Health Medical School University of Sumatera Utara 1 Definition Perinatal asphyxia is a fetus/newborn, due to: is an insult to the Lack
Chapter 11: Respiratory Emergencies
 29698_CH11_ANS_p001_005 4/12/05 2:02 PM Page 1 Answer Key Chapter 11 1 Chapter 11: Respiratory Emergencies Matching 1. B (page 373) 8. E (page 370) 2. D (page 369) 9. M(page 389) 3. H (page 370) 10. A
29698_CH11_ANS_p001_005 4/12/05 2:02 PM Page 1 Answer Key Chapter 11 1 Chapter 11: Respiratory Emergencies Matching 1. B (page 373) 8. E (page 370) 2. D (page 369) 9. M(page 389) 3. H (page 370) 10. A
1
 1 2 3 RIFAI 5 6 Dublin cohort, retrospective review. Milrinone was commenced at an initial dose of 0.50 μg/kg/minute up to 0.75 μg/kg/minute and was continued depending on clinical response. No loading
1 2 3 RIFAI 5 6 Dublin cohort, retrospective review. Milrinone was commenced at an initial dose of 0.50 μg/kg/minute up to 0.75 μg/kg/minute and was continued depending on clinical response. No loading
Epiglottitis. Bronchitis. Bronchiolitis. Pneumonia. Croup syndrome. Miss. kamlah 2
 Miss. kamlah 1 Epiglottitis. Bronchitis. Bronchiolitis. Pneumonia. Croup syndrome. Miss. kamlah 2 Acute Epiglottitis Is an infection of the epiglottis, the long narrow structure that closes off the glottis
Miss. kamlah 1 Epiglottitis. Bronchitis. Bronchiolitis. Pneumonia. Croup syndrome. Miss. kamlah 2 Acute Epiglottitis Is an infection of the epiglottis, the long narrow structure that closes off the glottis
NON INVASIVE LIFE SAVERS. Non Invasive Ventilation (NIV)
 Table 1. NIV: Mechanisms Of Action Decreases work of breathing Increases functional residual capacity Recruits collapsed alveoli Improves respiratory gas exchange Reverses hypoventilation Maintains upper
Table 1. NIV: Mechanisms Of Action Decreases work of breathing Increases functional residual capacity Recruits collapsed alveoli Improves respiratory gas exchange Reverses hypoventilation Maintains upper
Addendum to the NRP Provider Textbook 6 th Edition Recommendations for specific modifications in the Canadian context
 Addendum to the NRP Provider Textbook 6 th Edition Recommendations for specific modifications in the Canadian context A subcommittee of the Canadian Neonatal Resuscitation Program (NRP) Steering Committee
Addendum to the NRP Provider Textbook 6 th Edition Recommendations for specific modifications in the Canadian context A subcommittee of the Canadian Neonatal Resuscitation Program (NRP) Steering Committee
Surfactant Administration
 Approved by: Surfactant Administration Gail Cameron Senior Director Operations, Maternal, Neonatal & Child Health Programs Dr. Paul Byrne Medical Director, Neonatology Neonatal Policy & Procedures Manual
Approved by: Surfactant Administration Gail Cameron Senior Director Operations, Maternal, Neonatal & Child Health Programs Dr. Paul Byrne Medical Director, Neonatology Neonatal Policy & Procedures Manual
Respiratory Failure. Causes of Acute Respiratory Failure (ARF): a- Intrapulmonary:
 Respiratory failure exists whenever the exchange of O 2 for CO 2 in the lungs cannot keep up with the rate of O 2 consumption & CO 2 production in the cells of the body. This results in a fall in arterial
Respiratory failure exists whenever the exchange of O 2 for CO 2 in the lungs cannot keep up with the rate of O 2 consumption & CO 2 production in the cells of the body. This results in a fall in arterial
Neonatal/Pediatric Cardiopulmonary Care
 Neonatal/Pediatric Cardiopulmonary Care Resuscitation 2 When To Resuscitate Need usually related Combination of Can occur in 3 Causes of Fetal Asphyxia 1 4 Apnea Hypoxia Stimulates chemoreceptors & baroreceptors
Neonatal/Pediatric Cardiopulmonary Care Resuscitation 2 When To Resuscitate Need usually related Combination of Can occur in 3 Causes of Fetal Asphyxia 1 4 Apnea Hypoxia Stimulates chemoreceptors & baroreceptors
Neonatal/Pediatric Cardiopulmonary Care. Persistent Pulmonary Hypertension of the Neonate (PPHN) PPHN. Other. Other Diseases
 Neonatal/Pediatric Cardiopulmonary Care Other Diseases Persistent Pulmonary Hypertension of the Neonate (PPHN) PPHN 3 Also known as Persistent Fetal Circulation (PFC) Seen most frequently in term, post-term
Neonatal/Pediatric Cardiopulmonary Care Other Diseases Persistent Pulmonary Hypertension of the Neonate (PPHN) PPHN 3 Also known as Persistent Fetal Circulation (PFC) Seen most frequently in term, post-term
5 Million neonatal deaths each year worldwide. 20% caused by neonatal asphyxia. Improvement of the outcome of 1 million newborns every year
 1 5 Million neonatal deaths each year worldwide 20% caused by neonatal asphyxia Improvement of the outcome of 1 million newborns every year International Liaison Committee on Resuscitation (ILCOR) American
1 5 Million neonatal deaths each year worldwide 20% caused by neonatal asphyxia Improvement of the outcome of 1 million newborns every year International Liaison Committee on Resuscitation (ILCOR) American
BRUE and Apnea at Term, how do they relate?
 BRUE and Apnea at Term, how do they relate? Mary Elaine Patrinos, M.D. Attending Neonatologist Rainbow Babies and Children s Hospital Director, Infant Apnea Program Apnea at Term Can it happen? How does
BRUE and Apnea at Term, how do they relate? Mary Elaine Patrinos, M.D. Attending Neonatologist Rainbow Babies and Children s Hospital Director, Infant Apnea Program Apnea at Term Can it happen? How does
Cyanosis and Pulmonary Disease in Infancy
 CLINICAL CONFERENCE Cyanosis and Pulmonary Disease in Infancy By Robert A. Miller, M.D. Division of Cardiology, Children s Memorial Hospital, and the Department of Pediatrics, Northwestern University Medical
CLINICAL CONFERENCE Cyanosis and Pulmonary Disease in Infancy By Robert A. Miller, M.D. Division of Cardiology, Children s Memorial Hospital, and the Department of Pediatrics, Northwestern University Medical
Dr. (Kate) Katherine Miller GUELPH ON 121 RESPIRATORY DISTRESS IN THE NEWBORN
 Society of Rural Physicians of Canada 26TH ANNUAL RURAL AND REMOTE MEDICINE COURSE ST. JOHN'S NEWFOUNDLAND AND LABRADOR APRIL 12-14, 2018 Dr. (Kate) Katherine Miller GUELPH ON 121 RESPIRATORY DISTRESS
Society of Rural Physicians of Canada 26TH ANNUAL RURAL AND REMOTE MEDICINE COURSE ST. JOHN'S NEWFOUNDLAND AND LABRADOR APRIL 12-14, 2018 Dr. (Kate) Katherine Miller GUELPH ON 121 RESPIRATORY DISTRESS
disease, bronchopulmonary dysplasia, pulmonary hypoplasia and congenital diaphragmatic hernia.
 Neonatal Chest Imaging - What the Nurse Should Know Expires Monday, April 30, 2018 Nursing Michael J. Diament, M.D. Objectives 1. Describe a good technique for positioning a neonate for the purpose of
Neonatal Chest Imaging - What the Nurse Should Know Expires Monday, April 30, 2018 Nursing Michael J. Diament, M.D. Objectives 1. Describe a good technique for positioning a neonate for the purpose of
Lecture Notes. Chapter 2: Introduction to Respiratory Failure
 Lecture Notes Chapter 2: Introduction to Respiratory Failure Objectives Define respiratory failure, ventilatory failure, and oxygenation failure List the causes of respiratory failure Describe the effects
Lecture Notes Chapter 2: Introduction to Respiratory Failure Objectives Define respiratory failure, ventilatory failure, and oxygenation failure List the causes of respiratory failure Describe the effects
Pediatric Advanced Life Support
 Pediatric Advanced Life Support Pediatric Chain of Survival Berg M D et al. Circulation 2010;122:S862-S875 Prevention Early cardiopulmonary resuscitation (CPR) Prompt access to the emergency response system
Pediatric Advanced Life Support Pediatric Chain of Survival Berg M D et al. Circulation 2010;122:S862-S875 Prevention Early cardiopulmonary resuscitation (CPR) Prompt access to the emergency response system
Neonatal Resuscitation. Dustin Coyle, M.D. Anesthesiology
 Neonatal Resuscitation Dustin Coyle, M.D. Anesthesiology Recognize complications Maternal-fetal factors Maternal DM PIH Chronic HTN Previous stillbirth Rh sensitization Infection Substance abuse/certain
Neonatal Resuscitation Dustin Coyle, M.D. Anesthesiology Recognize complications Maternal-fetal factors Maternal DM PIH Chronic HTN Previous stillbirth Rh sensitization Infection Substance abuse/certain
Equipment: NRP algorithm, MRSOPA table, medication chart, SpO 2 table Warm
 NRP Skills Stations Performance Skills Station OR Integrated Skills Station STATION: Assisting with and insertion of endotracheal tube (ETT) Equipment: NRP algorithm, MRSOPA table, medication chart, SpO
NRP Skills Stations Performance Skills Station OR Integrated Skills Station STATION: Assisting with and insertion of endotracheal tube (ETT) Equipment: NRP algorithm, MRSOPA table, medication chart, SpO
Respiratory Emergencies. Chapter 11
 Respiratory Emergencies Chapter 11 Respiratory System Anatomy and Function of the Lung Characteristics of Adequate Breathing Normal rate and depth Regular breathing pattern Good breath sounds on both sides
Respiratory Emergencies Chapter 11 Respiratory System Anatomy and Function of the Lung Characteristics of Adequate Breathing Normal rate and depth Regular breathing pattern Good breath sounds on both sides
-Tamara Wahbeh. -Razan Abu Rumman. Dr. Mohammed Al-Muhtaseb
 -2 -Tamara Wahbeh -Razan Abu Rumman Dr. Mohammed Al-Muhtaseb I tried to include everything the doctor mentioned in both the lecture and his slides in the simplest way possible, so hopefully there would
-2 -Tamara Wahbeh -Razan Abu Rumman Dr. Mohammed Al-Muhtaseb I tried to include everything the doctor mentioned in both the lecture and his slides in the simplest way possible, so hopefully there would
Arabian Gulf University Kingdom of Bahrain Year 5 Pediatrics 3 rd Week Discussion with Dr. Muna Al-Jufairi (Part 2)
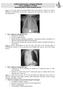 Arabian Gulf University Kingdom of Bahrain Year 5 Pediatrics 3 rd Week Discussion with Dr. Muna Al-Jufairi (Part 2) - Case 1: a 32 weeks preterm developed RDS 4 hours after delivery. Chest X-ray shows:
Arabian Gulf University Kingdom of Bahrain Year 5 Pediatrics 3 rd Week Discussion with Dr. Muna Al-Jufairi (Part 2) - Case 1: a 32 weeks preterm developed RDS 4 hours after delivery. Chest X-ray shows:
Daniel A. Beals MD, FACS, FAAP Pediatric Surgery and Urology Community Medical Center Associate Professor of Surgery and Pediatrics University of
 Daniel A. Beals MD, FACS, FAAP Pediatric Surgery and Urology Community Medical Center Associate Professor of Surgery and Pediatrics University of Washington Seattle Children s Hospital Objectives Define
Daniel A. Beals MD, FACS, FAAP Pediatric Surgery and Urology Community Medical Center Associate Professor of Surgery and Pediatrics University of Washington Seattle Children s Hospital Objectives Define
NEONATOLOGY Healthy newborn. Neonatal sequelaes
 NEONATOLOGY Healthy newborn. Neonatal sequelaes Ágnes Harmath M.D. Ph.D. senior lecturer 11. November 2016. Tasks of the neonatologist Prenatal diagnosed condition Inform parents, preparation of necessary
NEONATOLOGY Healthy newborn. Neonatal sequelaes Ágnes Harmath M.D. Ph.D. senior lecturer 11. November 2016. Tasks of the neonatologist Prenatal diagnosed condition Inform parents, preparation of necessary
GUIDELINE PHYSIOLOGY OF BIRTH ASPHYXIA
 GUIDELINE PHYSIOLOGY OF BIRTH ASPHYXIA The newborn is not an adult, nor a child. In people of all ages, death can occur from a failure of breathing and / or circulation. The interventions required to aid
GUIDELINE PHYSIOLOGY OF BIRTH ASPHYXIA The newborn is not an adult, nor a child. In people of all ages, death can occur from a failure of breathing and / or circulation. The interventions required to aid
Handling Common Problems & Pitfalls During. Oxygen desaturation in patients receiving mechanical ventilation ACUTE SEVERE RESPIRATORY FAILURE
 Handling Common Problems & Pitfalls During ACUTE SEVERE RESPIRATORY FAILURE Pravit Jetanachai, MD QSNICH Oxygen desaturation in patients receiving mechanical ventilation Causes of oxygen desaturation 1.
Handling Common Problems & Pitfalls During ACUTE SEVERE RESPIRATORY FAILURE Pravit Jetanachai, MD QSNICH Oxygen desaturation in patients receiving mechanical ventilation Causes of oxygen desaturation 1.
Respiratory Management in Pediatrics
 Respiratory Management in Pediatrics Children s Hospital Omaha Critical Care Transport Sue Holmer RN, C-NPT Objectives Examine the differences between the pediatric and adults airways. Recognize respiratory
Respiratory Management in Pediatrics Children s Hospital Omaha Critical Care Transport Sue Holmer RN, C-NPT Objectives Examine the differences between the pediatric and adults airways. Recognize respiratory
The Goal of the Respiratory Assessment. Two Parts of the Respiratory Assessment
 The Respiratory System Respiratory Assessment of the Adult Patient Mary Douglas, MSN, RN Nurse Educator Minneapolis VA Health Care System Respiratory system: moves oxygen into the body and carbon dioxide
The Respiratory System Respiratory Assessment of the Adult Patient Mary Douglas, MSN, RN Nurse Educator Minneapolis VA Health Care System Respiratory system: moves oxygen into the body and carbon dioxide
Airway and Breathing
 Airway and Breathing ETAT Module 2 Adapted from Emergency Triage Assessment and Treatment (ETAT): Manual for Participants, World Health Organization, 2005 Learning Objectives Accurately determine whether
Airway and Breathing ETAT Module 2 Adapted from Emergency Triage Assessment and Treatment (ETAT): Manual for Participants, World Health Organization, 2005 Learning Objectives Accurately determine whether
Lecture Notes. Chapter 9: Smoke Inhalation Injury and Burns
 Lecture Notes Chapter 9: Smoke Inhalation Injury and Burns Objectives List the factors that influence mortality rate Describe the nature of smoke inhalation and the fire environment Recognize the pulmonary
Lecture Notes Chapter 9: Smoke Inhalation Injury and Burns Objectives List the factors that influence mortality rate Describe the nature of smoke inhalation and the fire environment Recognize the pulmonary
PUMANI bcpap GUIDELINES FOR CLINICIANS. An Overview of the Pumani bcpap, Indications for bcpap, and Instructions for Use
 An Overview of the Pumani bcpap, Indications for bcpap, and Instructions for Use What is bcpap? bcpap stands for bubble Continuous Positive Airway Pressure. Sometimes called Continuous Distending Pressure,
An Overview of the Pumani bcpap, Indications for bcpap, and Instructions for Use What is bcpap? bcpap stands for bubble Continuous Positive Airway Pressure. Sometimes called Continuous Distending Pressure,
Respiratory Distress Syndrome
 Respiratory Distress Syndrome -Introduction: Generally speaking, there s an overlap between the presentations of cardiac and respiratory illnesses in neonates. Also there s a considerable overlap between
Respiratory Distress Syndrome -Introduction: Generally speaking, there s an overlap between the presentations of cardiac and respiratory illnesses in neonates. Also there s a considerable overlap between
INDEPENDENT LUNG VENTILATION
 INDEPENDENT LUNG VENTILATION Giuseppe A. Marraro, MD Director Anaesthesia and Intensive Care Department Paediatric Intensive Care Unit Fatebenefratelli and Ophthalmiatric Hospital Milan, Italy gmarraro@picu.it
INDEPENDENT LUNG VENTILATION Giuseppe A. Marraro, MD Director Anaesthesia and Intensive Care Department Paediatric Intensive Care Unit Fatebenefratelli and Ophthalmiatric Hospital Milan, Italy gmarraro@picu.it
Stabilization of the Newborn for Transport. Relevant Disclosure. Learning Objectives
 Stabilization of the Newborn for Transport Arlen Foulks, DO FAAP FACOP Medical Director, CCMH Level II NICU Medical Director, NeoFlight Assistant Professor of Pediatrics Neonatal Perinatal Medicine Section,
Stabilization of the Newborn for Transport Arlen Foulks, DO FAAP FACOP Medical Director, CCMH Level II NICU Medical Director, NeoFlight Assistant Professor of Pediatrics Neonatal Perinatal Medicine Section,
Protocol for performing chest clearance techniques by nursing staff
 Protocol for performing chest clearance techniques by nursing staff Rationale The main indications for performing chest clearance techniques (CCT) are to assist in the removal of thick, tenacious secretions
Protocol for performing chest clearance techniques by nursing staff Rationale The main indications for performing chest clearance techniques (CCT) are to assist in the removal of thick, tenacious secretions
Congenital Lung Malformations: Radiologic-Pathologic Correlation
 Acta Radiológica Portuguesa, Vol.XVIII, nº 70, pág. 51-60, Abr.-Jun., 2006 Congenital Lung Malformations: Radiologic-Pathologic Correlation Marilyn J. Siegel Mallinckrodt Institute of Radiology, Washington
Acta Radiológica Portuguesa, Vol.XVIII, nº 70, pág. 51-60, Abr.-Jun., 2006 Congenital Lung Malformations: Radiologic-Pathologic Correlation Marilyn J. Siegel Mallinckrodt Institute of Radiology, Washington
ACoRN Workbook 2012 Update
 ACoRN Neonatal Society Société néonatale ACoRN www.acornprogram.net A Canadian non-profit Society Vancouver, British Columbia ACoRN Workbook 2012 Update Name: The ACoRN Process The Resuscitation Sequence
ACoRN Neonatal Society Société néonatale ACoRN www.acornprogram.net A Canadian non-profit Society Vancouver, British Columbia ACoRN Workbook 2012 Update Name: The ACoRN Process The Resuscitation Sequence
Shedding Light on Neonatal X-rays. Objectives. Indications for X-Rays 5/14/2018
 Shedding Light on Neonatal X-rays Barbara C. Mordue, MSN, NNP-BC Neonatal Nurse Practitioner LLUH Children s Hospital, NICU Objectives Utilize a systematic approach to neonatal x-ray interpretation Identify
Shedding Light on Neonatal X-rays Barbara C. Mordue, MSN, NNP-BC Neonatal Nurse Practitioner LLUH Children s Hospital, NICU Objectives Utilize a systematic approach to neonatal x-ray interpretation Identify
Lecture Notes. Chapter 3: Asthma
 Lecture Notes Chapter 3: Asthma Objectives Define asthma and status asthmaticus List the potential causes of asthma attacks Describe the effect of asthma attacks on lung function List the clinical features
Lecture Notes Chapter 3: Asthma Objectives Define asthma and status asthmaticus List the potential causes of asthma attacks Describe the effect of asthma attacks on lung function List the clinical features
Cardiovascular Pathophysiology: Right to Left Shunts aka Cyanotic Lesions
 Cardiovascular Pathophysiology: Right to Left Shunts aka Cyanotic Lesions Ismee A. Williams, MD, MS iib6@columbia.edu Pediatric Cardiology Learning Objectives To discuss the hemodynamic significance of
Cardiovascular Pathophysiology: Right to Left Shunts aka Cyanotic Lesions Ismee A. Williams, MD, MS iib6@columbia.edu Pediatric Cardiology Learning Objectives To discuss the hemodynamic significance of
Cardiovascular Pathophysiology: Right to Left Shunts aka Cyanotic Lesions Ismee A. Williams, MD, MS Pediatric Cardiology
 Cardiovascular Pathophysiology: Right to Left Shunts aka Cyanotic Lesions Ismee A. Williams, MD, MS iib6@columbia.edu Pediatric Cardiology Learning Objectives To discuss the hemodynamic significance of
Cardiovascular Pathophysiology: Right to Left Shunts aka Cyanotic Lesions Ismee A. Williams, MD, MS iib6@columbia.edu Pediatric Cardiology Learning Objectives To discuss the hemodynamic significance of
A retrospective review of tracheal suction at birth in neonates with meconium aspiration syndrome
 A retrospective review of tracheal suction at birth in neonates with meconium aspiration syndrome D. Manickam MBBS, DCH, MRCP, MIAC, Paediatric Department, Penang General Hospital, 10450 Pulau Pinang Summary
A retrospective review of tracheal suction at birth in neonates with meconium aspiration syndrome D. Manickam MBBS, DCH, MRCP, MIAC, Paediatric Department, Penang General Hospital, 10450 Pulau Pinang Summary
Neonatal Resuscitation in What is new? How did we get here? Steven Ringer MD PhD Harvard Medical School May 25, 2011
 Neonatal Resuscitation in 2011- What is new? How did we get here? Steven Ringer MD PhD Harvard Medical School May 25, 2011 Conflicts I have no actual or potential conflict of interest in relation to this
Neonatal Resuscitation in 2011- What is new? How did we get here? Steven Ringer MD PhD Harvard Medical School May 25, 2011 Conflicts I have no actual or potential conflict of interest in relation to this
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists. International authors and editors
 We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 3,800 116,000 120M Open access books available International authors and editors Downloads Our
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 3,800 116,000 120M Open access books available International authors and editors Downloads Our
Usefulness of DuoPAP in the treatment of very low birth weight preterm infants with neonatal respiratory distress syndrome
 European Review for Medical and Pharmacological Sciences 2015; 19: 573-577 Usefulness of DuoPAP in the treatment of very low birth weight preterm infants with neonatal respiratory distress syndrome B.
European Review for Medical and Pharmacological Sciences 2015; 19: 573-577 Usefulness of DuoPAP in the treatment of very low birth weight preterm infants with neonatal respiratory distress syndrome B.
SWISS SOCIETY OF NEONATOLOGY. Supercarbia in an infant with meconium aspiration syndrome
 SWISS SOCIETY OF NEONATOLOGY Supercarbia in an infant with meconium aspiration syndrome January 2006 2 Wilhelm C, Frey B, Department of Intensive Care and Neonatology, University Children s Hospital Zurich,
SWISS SOCIETY OF NEONATOLOGY Supercarbia in an infant with meconium aspiration syndrome January 2006 2 Wilhelm C, Frey B, Department of Intensive Care and Neonatology, University Children s Hospital Zurich,
ROLE OF EARLY POSTNATAL DEXAMETHASONE IN RESPIRATORY DISTRESS SYNDROME
 INDIAN PEDIATRICS VOLUME 35-FEBRUAKY 1998 ROLE OF EARLY POSTNATAL DEXAMETHASONE IN RESPIRATORY DISTRESS SYNDROME Kanya Mukhopadhyay, Praveen Kumar and Anil Narang From the Division of Neonatology, Department
INDIAN PEDIATRICS VOLUME 35-FEBRUAKY 1998 ROLE OF EARLY POSTNATAL DEXAMETHASONE IN RESPIRATORY DISTRESS SYNDROME Kanya Mukhopadhyay, Praveen Kumar and Anil Narang From the Division of Neonatology, Department
October Paediatric Respiratory Workbook APCP RESPIRATORY COMMITTEE
 October 2017 Paediatric Respiratory Workbook APCP RESPIRATORY COMMITTEE This workbook is designed to introduce to you the difference between paediatric and adult anatomy and physiology. It will also give
October 2017 Paediatric Respiratory Workbook APCP RESPIRATORY COMMITTEE This workbook is designed to introduce to you the difference between paediatric and adult anatomy and physiology. It will also give
Chapter 10 The Respiratory System
 Chapter 10 The Respiratory System Biology 2201 Why do we breathe? Cells carry out the reactions of cellular respiration in order to produce ATP. ATP is used by the cells for energy. All organisms need
Chapter 10 The Respiratory System Biology 2201 Why do we breathe? Cells carry out the reactions of cellular respiration in order to produce ATP. ATP is used by the cells for energy. All organisms need
From Buds to Branches to Tubes!
 : Respiratory and Ingestive Consequences of Premature Birth 2007 ASHA KAYPentax Lecture Session 1260 JL Miller, Ph.D. National Institutes of Health jmiller@cc.nih.gov From buds to branches to tubes, the
: Respiratory and Ingestive Consequences of Premature Birth 2007 ASHA KAYPentax Lecture Session 1260 JL Miller, Ph.D. National Institutes of Health jmiller@cc.nih.gov From buds to branches to tubes, the
** SURFACTANT THERAPY**
 ** SURFACTANT THERAPY** Full Title of Guideline: Surfactant Therapy Author (include email and role): Stephen Wardle (V4) Reviewed by Dushyant Batra Consultant Neonatologist Division & Speciality: Division:
** SURFACTANT THERAPY** Full Title of Guideline: Surfactant Therapy Author (include email and role): Stephen Wardle (V4) Reviewed by Dushyant Batra Consultant Neonatologist Division & Speciality: Division:
Patient Management Code Blue in the CT Suite
 Patient Management Code Blue in the CT Suite David Stultz, MD November 28, 2001 Case Presentation A 53-year-old woman experienced acute respiratory distress during an IV contrast enhanced CT scan of the
Patient Management Code Blue in the CT Suite David Stultz, MD November 28, 2001 Case Presentation A 53-year-old woman experienced acute respiratory distress during an IV contrast enhanced CT scan of the
Objectives. Health care significance of ARF 9/10/15 TREATMENT OF ACUTE RESPIRATORY FAILURE OF VARIABLE CAUSES: INVASIVE VS. NON- INVASIVE VENTILATION
 TREATMENT OF ACUTE RESPIRATORY FAILURE OF VARIABLE CAUSES: INVASIVE VS. NON- INVASIVE VENTILATION Louisa Chika Ikpeama, DNP, CCRN, ACNP-BC Objectives Identify health care significance of acute respiratory
TREATMENT OF ACUTE RESPIRATORY FAILURE OF VARIABLE CAUSES: INVASIVE VS. NON- INVASIVE VENTILATION Louisa Chika Ikpeama, DNP, CCRN, ACNP-BC Objectives Identify health care significance of acute respiratory
Respiratory Physiology
 Respiratory Physiology Dr. Aida Korish Associate Prof. Physiology KSU The main goal of respiration is to 1-Provide oxygen to tissues 2- Remove CO2 from the body. Respiratory system consists of: Passages
Respiratory Physiology Dr. Aida Korish Associate Prof. Physiology KSU The main goal of respiration is to 1-Provide oxygen to tissues 2- Remove CO2 from the body. Respiratory system consists of: Passages
Table 1: The major changes in AHA / AAP neonatal resuscitation guidelines2010 compared to previous recommendations in 2005
 Table 1: The major changes in AHA / AAP neonatal guidelines2010 compared to previous recommendations in 2005 Resuscitation step Recommendations (2005) Recommendations (2010) Comments/LOE 1) Assessment
Table 1: The major changes in AHA / AAP neonatal guidelines2010 compared to previous recommendations in 2005 Resuscitation step Recommendations (2005) Recommendations (2010) Comments/LOE 1) Assessment
Appendix 1. Causes of Neonatal Deaths. Interval between. Gestation at birth. birth and death. Allocation. (weeks +days ) Cause of death.
 Appendix 1. Causes of Neonatal Deaths Interval between Gestation at birth birth and death Allocation (weeks +days ) (days) Cause of death Amnioinfusion 25 +1/7 20 Respiratory and circulatory insufficiency
Appendix 1. Causes of Neonatal Deaths Interval between Gestation at birth birth and death Allocation (weeks +days ) (days) Cause of death Amnioinfusion 25 +1/7 20 Respiratory and circulatory insufficiency
Pediatric Advanced Life Support Overview Judy Haluka BS, RCIS, EMT-P
 Pediatric Advanced Life Support Overview 2006 Judy Haluka BS, RCIS, EMT-P General Our Database is lacking in pediatrics Pediatrics are DIFFERENT than Adults not just smaller The same procedure may require
Pediatric Advanced Life Support Overview 2006 Judy Haluka BS, RCIS, EMT-P General Our Database is lacking in pediatrics Pediatrics are DIFFERENT than Adults not just smaller The same procedure may require
Difficulty Breathing and Respiratory Distress Basics
 Difficulty Breathing and Respiratory Distress Basics OVERVIEW Difficulty breathing (known as dyspnea ) a subjective term that in human medicine means an uncomfortable sensation in breathing or a sensation
Difficulty Breathing and Respiratory Distress Basics OVERVIEW Difficulty breathing (known as dyspnea ) a subjective term that in human medicine means an uncomfortable sensation in breathing or a sensation
Provide guidelines for the management of mechanical ventilation in infants <34 weeks gestation.
 Page 1 of 5 PURPOSE: Provide guidelines for the management of mechanical ventilation in infants
Page 1 of 5 PURPOSE: Provide guidelines for the management of mechanical ventilation in infants
DAYTON CHILDREN S HOSPITAL CLINICAL PRACTICE GUIDELINES
 DAYTON CHILDREN S HOSPITAL CLINICAL PRACTICE GUIDELINES DISCLAIMER: This Clinical Practice Guideline (CPG) generally describes a recommended course of treatment for patients with the identified health
DAYTON CHILDREN S HOSPITAL CLINICAL PRACTICE GUIDELINES DISCLAIMER: This Clinical Practice Guideline (CPG) generally describes a recommended course of treatment for patients with the identified health
Volume Guarantee Initiation and ongoing clinical management of an infant supported by Volume Guarantee A Case Study
 D-32084-2011 Volume Guarantee Initiation and ongoing clinical management of an infant supported by Volume Guarantee A Case Study Robert DiBlasi RRT-NPS, FAARC Respiratory Care Manager of Research & Quality
D-32084-2011 Volume Guarantee Initiation and ongoing clinical management of an infant supported by Volume Guarantee A Case Study Robert DiBlasi RRT-NPS, FAARC Respiratory Care Manager of Research & Quality
Recent Advances in Respiratory Medicine
 Recent Advances in Respiratory Medicine Dr. R KUMAR Pulmonologist Non Invasive Ventilation (NIV) NIV Noninvasive ventilation (NIV) refers to the administration of ventilatory support without using an invasive
Recent Advances in Respiratory Medicine Dr. R KUMAR Pulmonologist Non Invasive Ventilation (NIV) NIV Noninvasive ventilation (NIV) refers to the administration of ventilatory support without using an invasive
Life Science Journal 2015;12(4)
 Efficacy of elected Chest Physical Therapy on Neonates with Respiratory Distress yndrome Amira M. El-Tohamy 1, Ola. Darwish 2 and El-ayed. alem 3. 1 Professor of Physical Therapy for Growth and Development
Efficacy of elected Chest Physical Therapy on Neonates with Respiratory Distress yndrome Amira M. El-Tohamy 1, Ola. Darwish 2 and El-ayed. alem 3. 1 Professor of Physical Therapy for Growth and Development
