Mastocytosis and clonal mast cell activation syndrome
|
|
|
- Gregory Summers
- 5 years ago
- Views:
Transcription
1 Review paper Mastocytosis and clonal mast cell activation syndrome Aleksandra Górska 1, Marek Niedoszytko 1, Magdalena Lange 2 1 Department of Allergology, Medical University of Gdansk, Poland Head: Prof. Ewa Jassem MD, PhD 2 Department of Dermatology, Venerology and Allergology, Medical University of Gdansk, Poland Head: Prof. Jadwiga Roszkiewicz MD, PhD Post Dermatol Alergol 2011; XXVIII, 3: Abstract Mastocytosis is a group of disorders characterized by the abnormal proliferation and accumulation of atypical mast cells (MC) in one or more organs. In the majority of patients the bone marrow is affected. The clinical presentation of this disease is heterogeneous, ranging from asymptomatic to aggressive with fatal prognosis. Symptoms of mastocytosis result from MC-derived mediators and, less frequently, from destructive infiltration of MCs in tissues. The symptoms of mastocytosis include episodes of MC mediator release and anaphylactic reactions. The diagnosis of mast cell activation disorder (MCAD) has been proposed for subjects without skin lesions (such as urticaria pigmentosa) and unexplained anaphylactic reactions who only meet one or two minor criteria for systemic mastocytosis (SM) (so SM cannot be recognized). The presence of both KIT-mutated and aberrant CD25 expression on bone marrow MCs, defined as clonality, occurs in c-mcad. Those patients lacking both criteria are considered non-clonal (nc-mcad). Patients with c-mcad might correspond to indolent systemic mastocytosis (ISM) at the early phase of the disease. Further follow-up of patients fulfilling only one or two minor criteria for SM is required to determine whether they evolve to SM and to detect disease progression. The diagnosis of MCAD is crucial for the treatment of allergy and anaphylaxis, for example for Hymenoptera venom allergy therapy, which is similar to that applied in patients with SM. Key words: systemic mastocytosis, mast cell activation disorder, monoclonal mast cell activation syndrome, mast cell mediators, tryptase, anaphylaxis. Introduction Mastocytosis is a group of disorders characterized by the abnormal proliferation and accumulation of atypical mast cells (MC) in different organs including bone marrow, which is affected in the majority of patients, but also skin, liver, spleen, lymph nodes and the gastrointestinal tract [1]. The clinical presentation of the disease is heterogeneous, with the course ranging from asymptomatic to aggressive with fatal prognosis. Symptoms of mastocytosis result from MC-derived mediators and, less frequently, from destructive infiltration of MCs in tissues. The most favourable prognosis is assigned to cutaneous mastocytosis (CM), which is frequent in infancy and could resolve spontaneously during the second decade of life [2]. Depending on the age of onset, two main categories of the disease can be distinguished. In patients with typical childhood-onset mastocytosis, the disease is limited to the skin and the first symptoms develop in the first years of life. In these cases the prognosis is favourable [3]. Possible improvement of the skin lesions or remission of the disease usually occurs in adolescence. In contrast, patients with adult-onset mastocytosis present more often persistent systemic involvement, where not only skin but also other organs are affected first of all the bone marrow (systemic mastocytosis SM) [4]. A point mutation in codon D816V of C-KIT is usually present [5]. Diagnosis The disease cannot be diagnosed only on the basis of clinical symptoms. The most important step in the diagnostic process is the histological examination of the bone marrow biopsy, which is the reference test to diagnose SM in adult patients. Diagnostic work-up also includes examination of bone marrow aspirate: cytology, immunophenotype of mast cells with expression of CD2 Address for correspondence: Aleksandra Górska MD, Department of Allergology, Medical University of Gdansk, 7 Dębinki, Gdańsk, Poland, agorska@gumed.edu.pl Postępy Dermatologii i Alergologii XXVIII; 2011/3 217
2 Aleksandra Górska, Marek Niedoszytko, Magdalena Lange and CD25, activating point mutation of c-kit. Further, serum tryptase level must be determined [6]. The WHO classification of mastocytosis provides criteria of diagnosis of SM based on major and minor criteria. The major diagnostic criterion is the presence of compact multifocal dense infiltrates of MC in bone marrow or another extracutaneous organ (> 15 MC in aggregate). The minor diagnostic criteria are as follows: 1) the presence of > 25% spindle-shaped or atypical MCs in bone marrow aspirate, 2) activating point mutation in codon D816V of c-kit in any extracutaneous biopsy, 3) atypical immunophenotype of MC with CD2 and/or CD25 expression and 4) chronically elevated serum tryptase level more than 20 ng/ml. The diagnosis of SM can be established if the major and at least 1 minor or 3 minor criteria are present [2, 5, 7]. Initial diagnosis of SM based on gastrointestinal tract or spleen biopsy is exceptional. Furthermore, MC infiltrates may occur in chronic inflammatory diseases of the gastrointestinal tract with no connection with SM. The WHO classification defines 7 variants of mastocytosis: cutaneous mastocytosis (CM), indolent systemic mastocytosis (ISM), systemic mastocytosis with clonal haematological non- MC-lineage disease (SM-AHNMD), aggressive systemic mastocytosis (ASM), MC leukaemia (MCL), MC sarcoma (MCS), extracutaneous mastocytoma [1]. In order to differentiate the subtypes of SM it is necessary to assess the presence of clinical symptoms caused by tissue or organ infiltration of MC, especially so-called B-findings (borderline benign), referring to organomegaly, and C-findings, indicating organ failure and eligibility for cytoreductive therapy [1]. B-findings carry the message be careful, wait and watch if progression of this disease occurs and include the following: signs of multilineage involvement (hypercellular marrow, dysplasia), huge MC marrow infiltration (a massive MC burden), significantly elevated serum tryptase level (> 200 ng/ml) and organomegaly (hepatomegaly, splenomegaly, lymphadenopathy) [8, 9]. If at least 2 B-findings are documented, the diagnosis of smouldering systemic mastocytosis (SSM) should be established. Smouldering systemic mastocytosis is a type of SM associated with a higher risk of developing myelodysplastic, myeloproliferative or even leukaemic transformation syndrome [1]. C-findings mean consider cytoreduction with chemotherapy or with targeted drugs, and include: cytopenia, pathological fractures, hepatosplenomegaly with liver and/or spleen dysfunction, ascites, malabsorption syndrome, weight loss, lymphadenopathy and eosinophilia. These symptoms occur in ASM, MCL and MC lymphoma. Thus, C-findings result from clinically relevant impairment or loss of organ function due to MC infiltration and are eligible for intensive or targeted treatment [7]. The severity of skin lesions often shows an inverse correlation with bone marrow involvement. Absence of urticaria pigmentosa is often seen in ASM or MCL. The lack of skin lesions is also found in isolated bone marrow mastocytosis (BMM), a subtype of SM without skin involvement and low serum baseline tryptase (sbt) in contrast to SSM [6, 10]. Additionally, significantly increased serum sbt is considered as a potential indicator of ag - gressiveness of the disease in SM patients without skin lesions [10]. Mast cell activation syndrome Mast cell activation disorder (MCAD) is a mast cell disease characterized by abnormal MC activation leading to enhanced release of mediators without clear triggers. For subjects without skin lesions who experienced anaphylactic reactions but who only meet 1 or 2 minor criteria for SM (excluding raised sbt), the diagnosis of monoclonal mast cell activation syndrome (MMAS) has been proposed [11]. The presence of both KIT-mutated and aberrant CD25 expression in bone marrow MCs, defined as clonality, occurs in clonal mast cell activation disorder (c-mcad). Those patients lacking both criteria are considered to have non-clonal mast cell activation disorder (nc-mcad) [12]. Álvarez-Twose et al. [12] presented clinical, biological and molecular characteristics of adult patients with c-mcad and nc-mcad. Overall, the most common triggers for acute MC activation and mediator release were as follows: (1) Hymenoptera stings, horsefly and unidentified insects, (2) hypersensitivity to drugs: antibiotics, non-steroidal anti-inflammatory drugs (NSAIDs), codeine, mepivacaine, rocuronium, (3) food: fish, egg, sunflower oil, alcohol, and (4) intestinal manipulation during abdominal surgery. Insect venom allergy was the most common causative factor of anaphylaxis in patients with ISMs (indolent systemic mastocytosis without involvement of the skin), and drugs in patients with nc-mcad. Eigthy percent of patients had severe life-threatening respiratory and/or cardiovascular symptoms. Regarding the clinical presentation of the most severe anaphylaxis, significantly higher frequencies of skin and respiratory symptoms were found among nc-mcad, and cardiovascular symptoms among ISMs. Frequency and intensity of anaphylactic episodes were similar in both ISMs and ISMs+ groups. Interestingly, 14% of patients with ISMs+ with anaphylaxis in medical history had MC mediator release symptoms from 12 to 32 months before the occurrence of skin lesions and recognition of SM. These data suggest the need for long-term follow-up of patients with c-mcad to rule out the diagnosis of SM. Among patients with elevated sbt > 20 ng/ml, ISMs was diagnosed more frequently, while in patients with 218 Postępy Dermatologii i Alergologii XXVIII; 2011/3
3 Mastocytosis and clonal mast cell activation syndrome sbt < 20 ng/ml, nc-mcad was diagnosed more frequently. The average level of sbt in c-mcad patients was 14.3 μg/l. In this study the authors also found an increase in male predominance in ISMs patients, which is consistent with reports of male predominance among patients with ISM and IgE-mediated anaphylactic reactions versus patients without SM. Moreover, these data suggest a relationship between male gender and severity of reactions associated with the release of MC mediators in mastocytosis, especially in ISMs. The results show a high sensitivity and specificity of sbt > 25 μg/l or sbt < 15 μg/l for the diagnosis of MC clonality. Furthermore, there was no specific relationship between the sbt levels and the severity of clinical symptoms in ISMs, c-mcad and nc-mcad. The presence of KIT-mutated MC in bone marrow was detected mostly in ISMs patients. Based on clinical and laboratory findings, a screening model is proposed to predict MC clonality in patients presenting with anaphylaxis without skin lesions (Tab. 1) [12]. The authors of this study demonstrated that a significant proportion of patients with c-mcad correspond to an early stage of ISM [12]. Thus further follow-up of patients who meet only 1 or 2 criteria of SM is reasonable since there is a risk of progression to systemic disease. The presence of KIT mutations in MC should always prompt performance of diagnostics to find an early phase of progression [12]. Compared to patients with idiopathic anaphylaxis, patients with MCAD have more episodes of hypotension. The reason for this clinical distinction is unclear. Thus the exclusion of bone marrow involvement by the pathological process is important because it enables one to recognize MCAD as a cause of anaphylaxis [4]. The detection of activating point mutations in KIT tyrosine kinase of identifying mast cells is essential for the development of clinically symptomatic mast cell disease monoclonal mast cell activation syndrome (MMAS). Molderings et al. [13] showed that MMAS is a disease with clonal proliferation of mast cells which is usually associated with the presence of different mutations in the tyrosine kinase kit. In mast cells of 13 out of 20 patients with MMAS multiple new point mutations or complex changes in the mrna sequences encoding the tyrosine kinase kit were detected. Interestingly, in all but one healthy subjects in the control group (in 19/20 persons) functionally irrelevant changes were not detected, which confirms earlier reports [14]. It is likely that the patient with multiple changes in c-kit transcripts suffered from the disease without clinical symptoms. In addition to the D816V point mutation in KIT, which occurs in more than 90% of patients with SM, there were evaluated functional consequences of mutations D419H and M541L [15]. However, more studies are needed in larger patient groups. Patients with mastocytosis often have symptoms resulting from the activation and release of mediators Tab. 1. Scoring model to predict MC clonality in patients presenting with anaphylaxis without skin lesions (before bone marrow study) [11] Variable Score Gender Male +1 Female 1 Clinical Absence of urticaria and angioedema +1 symptoms Urticaria and/or angioedema 2 Fainting and/or syncope +3 Tryptase sbt < 15 ng/ml 1 > 25 ng/ml +2 Score < 2 low probability of c-mcad, score > 2 high probability of c-mcad, sensitivity 0.92, specificity 0.81 from mast cells, such as generalized itching, redness, headache, abdominal cramps, diarrhoea, bone pain or arthritis, hypotension and shock [16]. Anaphylactic reactions occur in 30% of all patients with mastocytosis, and in 50% of patients with systemic mastocytosis [4, 17, 18]. The activation of mast cells might result from an immune response (e.g., allergy to food, insect venoms, drugs, latex), or non-allergic mechanisms of hypersensitivity after activation of non-specific stimuli such as heat, exercise, and also stress. Although the incidence of IgE-mediated allergic diseases is not higher than in the general population, it is believed that mast cells in mastocytosis patients may have an internal defect lowering the threshold for activation and/or increasing its sensitivity to activation [4]. A key factor in activating mast cells is insect stings. It is estimated that 30% of patients with mastocytosis have insect sting anaphylactic reactions [19], which are more severe than the general population of people with allergies to insect venom (1-3% of the general population) [20]. The treatment of choice in patients with insect venom allergy (IVA) is a specific venom immunotherapy (VIT) with the relevant insect venom. Meta-analysis of research on the effectiveness, safety and efficacy of treatment showed an overwhelming benefit of the treatment of patients and reduction of the risk of life-threatening anaphylaxis. Moreover, in contrast to patients without diagnosed mastocytosis, they have not diminished with time [21, 22]. The mechanism of increased risk of IVA in SM, as compared to the general population, is not completely understood. The introduction of the basophil activation test and histamine release assay from basophils to diagnostic procedures enables the detection of specific IgE in most cases of insect venom allergic patients with SM [23]. Non-IgE mediated IVA are rather rare [24], although specific IgE and skin tests are more often negative than in the general population with the IVA. The suggested explanation for this phenomenon is the adsorption of circulating IgE in numerous mast cells clustered in the tissues [23]. Postępy Dermatologii i Alergologii XXVIII; 2011/3 219
4 Aleksandra Górska, Marek Niedoszytko, Magdalena Lange The anaphylaxis may also result from the activation of mast cells by activation of a cascade of intracellular tyrosine kinases: Kit, Lyn, Syk and Fyn. The presence of KIT gene mutations, notably D816V, detectable in more than 90% of patients with SM and resulting in increased activation of mast cells, did not correlate with the severity or the prevalence of anaphylaxis [25]. However, the severity of anaphylaxis correlates with the levels of mast cell tryptase (sbt), which is the determinant of the number and activity of mast cells. The higher sbt serum level indicates an indirect link between SM and IVA. Insect venom allergy is present in 30% of SM patients, compared with a prevalence of 1% to 2.6% in the general population [16, 26]. Approximately 10% to 15% of patients with IVA have high sbt, and up to 5.5% suffer from mastocytosis [4, 16, 21]. Mueller [27] recommends measuring the sbt level in all patients with insect venom anaphylaxis in their history and diagnosing the possible SM in patients with elevated sbt above 20 ng/ml. Because of the reported fatalities of patients with mastocytosis after finishing VIT, in these patients it is recommended to continue VIT for life [27, 28]. The evaluation of sbt should be used routinely in all patients with VIT. The finding of elevated tryptase level significantly modifies the further treatment of the patient (prolonged period of treatment, the use of additional measures to prevent side effects). The diagnostic procedure to establish the diagnosis of SM is typically performed in patients with IVA accompanied by urticaria pigmentosa, although there are reports indicating the absence of skin lesions in 76% of cases with coexistent IVA and SM [29]. Patients with a history of insect sting anaphylaxis and negative results of skin tests and sige to insect venom may suffer from mastocytosis [30]. Thus there is an indication to establish a diagnosis of mastocytosis apart from the sbt level and dermatological examination for UP. Bonadonna et al. [16] reported that in all patients with non-ige-mediated venom anaphylaxis sbt was elevated and MCAD was finally diagnosed. The study confirms the association between mastocytosis and systemic reactions triggered by insect stings in patients, despite negative results of tests for insect venom allergy. The criterion for the diagnosis of SM was accepted only if a higher level of sbt (> 11.4 ng/ml) was detected. The study by Potier et al. compared the results of diagnostic tests to establish mastocytosis in patients with elevated sbt and IVA [31]. An elevated sbt level was found in 23/140 patients (16.4%) whose skin was less involved and more often with flushing during an anaphylactic reaction. Compared to those patients with normal sbt level the course of the systemic reaction was more severe. Mastocytosis was diagnosed in 7 patients. Among them 5 subjects had been suspected of SM in the past without a definitive diagnosis. These results show a specific clinical insect venom anaphylactic reaction in people with an elevated sbt level, characterized by greater severity, more frequent episodes of redness and rare skin lesions. In this study, the authors present the need to determine groups of patients with elevated sbt, who are at risk of mastocytosis. Carrying out sbt measurement is indicated in all patients with insect venom anaphylactic reaction in their history, and the diagnosis of mastocytosis should be made in patients with severe anaphylactic reaction, with redness, without urticaria pigmentosa. In systemic mastocytosis patients the course of Hymenoptera venom anaphylaxis is usually severe and includes the involvement of the cardiovascular system. Negative prognostic factors of the anaphylactic reaction include cardiovascular disease and β-blocker therapy. Mast cells are present in the heart and coronary arteries, and their number and/or density increases in coronary heart disease [32]. Some MC-derived mediators have cardiotoxic effects including vasoconstriction, negative inotropy and arrhythmia. In patients with anaphylaxis, co-existing cardiovascular disorders, mastocytosis and elevated sbt are risk factors for severe, even fatal anaphylactic reactions or consequences of myocardial infarction or stroke. Treatment with β-blockers or angiotensinconverting enzyme inhibitors (ACEI) may worsen the anaphylactic reaction and cause difficulties in the treatment of anaphylactic shock. However, because of their value in the treatment of cardiovascular diseases, which occur much more frequently than anaphylaxis, their withdrawal should be preceded by a thorough assessment of the relative risk of the consequences of each disease [27]. Idiopathic anaphylaxis is a difficult clinical problem. The triggering factor cannot be diagnosed even in two thirds of patients with a history of anaphylaxis, and preventive therapy is usually ineffective. Since idiopathic hypotension is typical for SM, Akin et al. [33] proposed evaluation of clonal proliferation of mast cells in patients with recurrent anaphylactic reactions and patients suspected of mastocytosis. Thus, in this group of patients the presence of clonal proliferation markers of mast cells was determined. The subgroup of patients who could benefit from c-kit targeted inhibitor therapy was indicated. Among patients enrolled in the study, the diagnosis of cutaneous or systemic mastocytosis was confirmed (36/72 persons), although these patients had no episodes of hypotension in the past. The evaluation of KIT gene point mutation D816 was made in two thirds of these patients, confirming its presence in 82% of individuals. There were 12 patients described with idiopathic anaphylaxis who did not have skin lesions typical for urticaria pigmentosa or multifocal infiltration of mast cells in bone marrow biopsy. In 5 of them at least one minor criterion for mastocytosis was confirmed. D816V KIT gene mutation was found in 3 patients with confirmed CD25+ immunophenotype in the bone marrow. These results confirm the presence of atypical mast cell populations and markers of clonality in the subgroup of patients with unexplained episodes of anaphylaxis. Such patients may benefit from C-KIT targeted inhibitor therapy [33]. 220 Postępy Dermatologii i Alergologii XXVIII; 2011/3
5 Mastocytosis and clonal mast cell activation syndrome Tab. 2. Classification of diseases associated with mast cell activation 1. Primary Hypotension with an associated clonal proliferative mast cell disorder (mastocytosis) MMAS 2. Secondary Allergic disorder Mast cell activation associated with chronic inflammatory or neoplastic disorder Physical urticaria Chronic autoimmune urticaria 3. Idiopathic Anaphylaxis Angioedema Urticaria MCAS Tab. 3. Criteria for the diagnosis of MCAS 1. Episodic symptoms consistent with MC mediator release affecting 2 organ systems as follows: skin: urticaria, angioedema, flushing gastrointestinal: nausea, vomiting, diarrhoea, abdominal cramps cardiovascular: hypotensive syncope, tachycardia respiratory: wheezing naso-ocular: conjunctival injection, pruritus, nasal congestion 2. Effectiveness of antihistamine therapy (H1 and H2 blockers), antileukotriene medications, mast cell stabilizers 3. Evidence of increased MC mediators while clinical symptoms occurred 4. Exclusion of primary, secondary and idiopathic causes of mast cell activation Although the incidence of anaphylactic reactions (IgE-dependent and IgE-independent) in patients with mastocytosis is significantly higher than in the general population, the frequency of atopy is similar in both populations [34]. De Olano et al. [35] showed that 23.9% of patients with CM or SM also suffer from allergic diseases (based on history, skin tests and specific IgE). In 36 patients there were signs of anaphylactic reactions in the medical history, including 9 patients with the IgE-dependent mechanism of anaphylaxis confirmed. In addition, the results of this study confirm the hypothesis that the total concentration of IgE in mastocytosis is generally reduced probably because of the binding to the surface of an increased number of mast cells [36]. The diagnosis is easier in the presence of urticaria pigmentosa or CM. Increasingly, mastocytosis is diagnosed in the case of recurrent anaphylactic reactions in patients without skin lesions with minimal changes in the bone marrow, but with three minor criteria for mastocytosis fulfilled [37]. In some patients the disease is not diagnosed for a long time because its symptoms are similar to those occurring in allergic diseases, pseudoallergic reactions, gastrointestinal disorders, vasculitis, endocrine diseases and idiopathic anaphylaxis [38]. In all patients suspected of mastocytosis the serum concentrations of sbt should be determined [39]. Recent studies showed that the upper limit of normal sbt is 11.4 ng/ml, and sbt higher than 20 ng/ml is a minor criterion of SM [40]. An elevated level of sbt can also be detected in myeloproliferative disorders, in chronic eosinophilic leukaemia associated with the occurrence of mutations FIP1L1/PDGFRA, as well as in end-stage renal failure, amniotic fluid congestion, and orthostatic tachycardia [40]. Moreover, an increased number of atypical mast cells in tissues is also found in reactive hyperplasia present in many inflammatory and neoplastic diseases [38]. Akin et al. [41] have proposed criteria for diagnosis of mast cell activation syndrome (MCAS) including other diseases in which mast cells are involved. The authors proposed a classification of diseases associated with proliferation and/or activation of mast cells (Tab. 2) [41]. The presence of separate MCAS, with the exclusion of MMAS, has not met with general acceptance. Despite the lack of guidelines MCAS is recognized among patients with unexplained clinical symptoms. The diagnosis of MCAS can be considered after the exclusion of primary, secondary, and idiopathic diseases associated with activation of mast cells and when at least three additional criteria from the following were fulfilled (Tab. 3) [41]. Applying these criteria, MCAS should be considered if the patient has recurrent symptoms from at least two organ systems resulting from the activation of mast cells and these episodes do not meet the clinical criteria for idiopathic anaphylaxis or other well-defined diseases mentioned above. These criteria could be a starting point to classify and diagnose MCAS [41]. Conclusions Mastocytosis is a proliferative disease, with clonal proliferation of mast cells and their progenitor cells. The symptoms of mastocytosis include episodes of MC mediator release and anaphylactic reactions. In the absence of skin lesions of urticaria pigmentosa type, the clinical presentation may suggest allergic disease. However, patients with severe anaphylaxis, particularly when the cardiovascular and/or respiratory system is involved, should be Postępy Dermatologii i Alergologii XXVIII; 2011/3 221
6 Aleksandra Górska, Marek Niedoszytko, Magdalena Lange diagnosed with SM (regardless of the causative factor). It is believed that during the routine diagnosis of anaphylaxis the evaluation of the sbt level and of the KIT gene mutation D816V should be applied. Patients with an elevated level of sbt and with the presence of Kit mutations should be further referred to specialist centres [3]. Perhaps the development of knowledge concerning the mechanisms of mast cell proliferation will result, in the near future, in new tests to diagnose mastocytosis, even in patients without typical urticaria pigmentosa. References 1. Valent P, Akin C, Escribano L, et al. Standards and standardization in mastocytosis: Consensus Statements on Diagnostics, Treatment Recommendations and Response Criteria. Eur J Clin Invest 2007; 37: Florian S, Krauth MT, Simonitsch-Klupp, et al. Indolent systemic mastocytosis with elevated serum tryptase, absence of skin lesions, and recurrent severe anaphylactoid episodes. Int Arch Allergy Immunol 2005; 136: Lesiak A, Olejniczak I, Narbutt J. Cutaneous forms of mastocytosis in children report of three cases. Diagnosis and treatment. Post Dermatol Alergol 2010; 27: Akin C. Anaphylaxis and mast cell disease: what is the risk? Curr Allergy Asthma Rep 2010; 10: Valent P, Akin C, Sperr WR, et al. Mastocytosis: pathology, genetics, and current options for therapy. Leuk Lymphoma 2005; 46: Valent P, Horny HP, Escribano L, et al. Diagnostic criteria and classification of mastocytosis: a consensus proposal. Leuk Res 2001; 25: Horny HP. An unusual clonal disorder of bone marrow-derrived hematopoetic progenitor cells. Am J Clin Pathol 2009; 132: Escribano L. Mastocytosis: current concepts in diagnosis and treatment. Ann Hematol 2002; 81: Vrdima J. The World Health Organization (WHO) classification of the myeloid neoplasms. Blood 2002; 100: Valent P, Horny HP, Li CY, et al. World Health Organization (WHO) Classification of Tumours. Pathology and Genetics. Tumours of Haematopoietic and Lymphoid Tissues. Oxford University Press 2001; 1: Sonneck K, Florian S, Müllauer L, et al. Diagnostic and subdiagnostic accumulation of mast cells in the bone marrow of patients with anaphylaxis: monoclonal mast cell activation syndrome. Int Arch Allergy Immunol 2007; 142: Álvarez-Twose I, de Olano DG, Sánchez-Mun ~ oz L, et al. Clinical, biological, and molecular characteristics of clonal mast cell disorders presenting with systemic mast cell activation symptoms. J Allergy Clin Immunol 2010; 6: Molderings GJ, Meis K, Kolck UW, et al. Comperative analysis of mutation of tyrosine kinase kit in mast cells from patients with systemic mast cell activation syndrome and healthy subject. Immunogenetics 2010; 62: Fontanabla A, Real PJ, Fernandez-Luna JL, et al. Identification of c-kit gene mutations in patients with polycythemia vera. Leuk Res 2006; 30: Yang Y, Letard S, Borge L. Pediatric mastocytosis associated KIT extracellular domain mutations exhibit different functional and signaling properties compared with KIT-phosphotransferase domain mutations. Blood 2010; 116: Bonadonna P, Perbellini O, Passalacqua G, et al. Clonal mast cell disorders in patients with systemic reactions to Hymenoptera stings and increased serum tryptase levels. J Allergy Clin Immunol 2009; 3: Ruëff F, Wenderoth A, Przybilla B. Patients still reacting to a sting challenge while receiving conventional Hymenoptera venom immunotherapy are protected by increased venom doses. J Allergy Clin Immunol 2001; 108: Brockow K, Jofer C, Behrendt H, Ring J. Anaphylaxis in patients with mastocytosis: a study on history, clinical features and risk factors in 120 patients. Allergy 2008; 63: Brockow K, Jofer C, Behrendt H, Ring J. Anaphylaxis in patients with mastocytosis: a study on history, clinical features and risk factors in 120 patients. Allergy 2008; 63: Ludolph-Hauser D, Ruëff F, Fries C, et al. Constitutively raised serum concentrations of mast-cell tryptase and severe anaphylactic reactions to Hymenoptera stings. Lancet 2001; 357: Niedoszytko M, de Monchy J, van Doormaal J, et al. Mastocytosis and insect venom allergy: diagnosis, safety and efficacy of venom immunotherapy. Allergy 2009; 64: Górska A, Niedoszytko M, Chełmińska M, et al. Prevalence of insect venom allergy in mastocytosis patients and safety of VIT in Polish patients with mastocytosis [abstract]. EAACI th Congress of the European Academy of Allergy and Clinical Immunology. 23. Műller UR, Horat W, Wűthrich B, et al. Anaphylaxis after hymenoptera stings in three patients with urticaria pigmentosa. J Allergy Clin Immunol 1983; 72: Haeberli G, Brönnimann M, Hunziker T, Műller U. Elevated basal serum tryptase and hymenoptera venom allergy: relation to severity of sting reactions and to safety and efficacy of venom immunotherapy. Clin Exp Allergy 2003; 33: Peavy R, Metcalfe D. Understanding the mechanisms of anaphylaxis. Curr Opin Allergy Clin Immunol 2008; 8: Ruëff F, Placzek M, Przybilla B. Mastocytosis and hymenoptera venom allergy. Curr Opin Allergy Clin Immunol 2006; 6: Mueller UR. Cardiovascular disease and anaphylaxis. Curr Opin Allergy Clin Immunol 2007; 7: Oude Elberink JN, de Monchy JG, Kors JW, et al. Fatal anaphylaxis after a yellow jacket sting, despite immunotherapy, in two patients with mastocytosis. J Allergy Clin Immunol 1997; 99: de Olano DG, de la Hoz Caballer B, Nűn ~ ez López R, et al. Prevalence of allergy and anaphylactic symptoms in 210 adult and pediatric patients with mastocytosis in Spain: a study of the Spanish network on mastocytosis (REMA). Clin Exp Allergy 2007; 37: Kränke B, Sturm G, Aberer W. Negative venom skin test results and mastocytosis. J Allergy Clin Immunol 2004; 113: Potier A, Lavigne CD, Chappardz J, et al. Cutaneous manifestations in Hymenoptera and Diptera anaphylaxis: relationship with basal serum tryptase. Clin Exp Allergy 2009; 39: Marone G, Betoraki A, Onorati AM, et al. The human heart as a shock organ in anaphylaxis. Novartis Found Symp 2004; 257: Akin C, Scott LM, Kocabas CN, et al. Demonstration of an aberrant mast-cell population with clonal markers in a subset of patients with idiopathic anaphylaxis. Blood 2007; 110: Postępy Dermatologii i Alergologii XXVIII; 2011/3
7 Mastocytosis and clonal mast cell activation syndrome 34. Brockow K, Jofer C, Ring J. Anaphylaxis in patients with mastocytosis: a prospective study on prevalence, severity and trigger factors in 121 patients [abstract]. J Allergy Clin Immunol 2006; 117: S de Olano GD, de la Hoz Caballer MB, Nunez-Lopez R, et al. Prevalence of allergy and anaphylaxis in 210 patients with mastocytosis: a study from the Spanish network on mastocytosis (REMA) [abstract]. J Allergy Clin Immunol 2007; 119: S Muller U, Helbling A, Hunziker T, et al. Mastocytosis and atopy: a study of 33 patients with urticaria pigmentosa. Allergy 1990; 45: Sonneck K, Florian S, Mullauer L, et al. Diagnostic and subdiagnostic accumulation of mast cells in the bone marrow of patients with anaphylaxis: monoclonal mast cell activation syndrome. Int Arch Allergy Immunol 2007; 142: Greenhawt M, Akin C. Mastocytosis and allergy. Curr Opin Allergy Clin Immunol 2007; 7: Akin C, Schwartz LB, Kitoh T, et al. Soluble stem cell factor receptor (CD117) and IL-2 receptor alpha chain (CD25) levels in the plasma of patients with mastocytosis: relationships to disease severity and bone marrow pathology. Blood 2000; 96: Schwartz LB. Diagnostic value of tryptase in anaphylaxis and mastocytosis. Immunol Allergy Clin North Am 2006; 26: Akin C, Valent P, Metcalfe D. Mast cell activation syndrome: proposed diagnostic criteria. J Allergy Clin Immunol 2010; 126: Postępy Dermatologii i Alergologii XXVIII; 2011/3 223
Mastocytosis and insect venom allergy Patrizia Bonadonna a,c, Roberta Zanotti b,c and Ulrich Müller d
 Mastocytosis and insect venom allergy Patrizia Bonadonna a,c, Roberta Zanotti b,c and Ulrich Müller d a Allergy Unit, b Department of Clinical and Experimental Medicine, Division of Hematology, c Multidisciplinary
Mastocytosis and insect venom allergy Patrizia Bonadonna a,c, Roberta Zanotti b,c and Ulrich Müller d a Allergy Unit, b Department of Clinical and Experimental Medicine, Division of Hematology, c Multidisciplinary
Evaluation of Mast Cell Activation Syndromes: Impact of Pathology and Immunohistology
 Review DOI: 10.1159/000336374 Published online: April 27, 2012 Evaluation of Mast Cell Activation Syndromes: Impact of Pathology and Immunohistology H.-P. Horny a K. Sotlar a P. Valent b a Institute of
Review DOI: 10.1159/000336374 Published online: April 27, 2012 Evaluation of Mast Cell Activation Syndromes: Impact of Pathology and Immunohistology H.-P. Horny a K. Sotlar a P. Valent b a Institute of
Fortgeschrittene systemische Mastozytose Hintergrundinformationen zu einer seltenen Erkrankung und zur ersten zugelassenen Therapie
 Fortgeschrittene systemische Mastozytose Hintergrundinformationen zu einer seltenen Erkrankung und zur ersten zugelassenen Therapie Georgia Metzgeroth Hämatologie und Onkologie III. Medizinische Klinik
Fortgeschrittene systemische Mastozytose Hintergrundinformationen zu einer seltenen Erkrankung und zur ersten zugelassenen Therapie Georgia Metzgeroth Hämatologie und Onkologie III. Medizinische Klinik
CME/SAM. Olga Pozdnyakova, MD, PhD, 1 Svetlana Kondtratiev, MD, 1,2 Betty Li, MS, 1 Karry Charest, 1 and David M. Dorfman, MD, PhD 1.
 Hematopathology / New Mastocytosis Flow Cytometry Approach High-Sensitivity Flow Cytometric Analysis for the Evaluation of Systemic Mastocytosis Including the Identification of a New Flow Cytometric Criterion
Hematopathology / New Mastocytosis Flow Cytometry Approach High-Sensitivity Flow Cytometric Analysis for the Evaluation of Systemic Mastocytosis Including the Identification of a New Flow Cytometric Criterion
Mast Cell Disease. Daniel A. Arber, MD Stanford University, Stanford CA
 Mast Cell Disease Daniel A. Arber, MD Stanford University, Stanford CA Mast cell disease, or mastocytosis, includes a variety of disorders that are characterized by the presence of mast cell aggregates
Mast Cell Disease Daniel A. Arber, MD Stanford University, Stanford CA Mast cell disease, or mastocytosis, includes a variety of disorders that are characterized by the presence of mast cell aggregates
Mastocytosis and Hymenoptera venom allergy Franziska Ruëff, Marianne Placzek and Bernhard Przybilla
 Mastocytosis and Hymenoptera venom allergy Franziska Ruëff, Marianne Placzek and Bernhard Przybilla Purpose of review Mastocytosis is a rare disease characterized by increased mast cells in skin and/or
Mastocytosis and Hymenoptera venom allergy Franziska Ruëff, Marianne Placzek and Bernhard Przybilla Purpose of review Mastocytosis is a rare disease characterized by increased mast cells in skin and/or
Mastocytosis. Dr Sarah Sasson SydPath Registrar 24 th November 2014
 Mastocytosis Dr Sarah Sasson SydPath Registrar 24 th November 2014 Introduction to Mastocytosis A rare myeloid malignancy resulting from a clonal, neoplastic proliferation of morphologically and immunotypically
Mastocytosis Dr Sarah Sasson SydPath Registrar 24 th November 2014 Introduction to Mastocytosis A rare myeloid malignancy resulting from a clonal, neoplastic proliferation of morphologically and immunotypically
Systemic mastocytosis: overview and new insights in prognosis and therapy
 3 Systemic mastocytosis: overview and new insights in prognosis and therapy G. Deslypere, MD 1, T. Devos, MD, PhD 2, M. Delforge, MD, PhD 2, G. Verhoef, MD, PhD 2 Systemic mastocytosis is an orphan myeloproliferative
3 Systemic mastocytosis: overview and new insights in prognosis and therapy G. Deslypere, MD 1, T. Devos, MD, PhD 2, M. Delforge, MD, PhD 2, G. Verhoef, MD, PhD 2 Systemic mastocytosis is an orphan myeloproliferative
Case Report. Introduction. Mastocytosis associated with CML Hematopathology - March K. David Li 1,*, Xinjie Xu 1, and Anna P.
 Mastocytosis associated with CML Hematopathology - March 2016 Case Report Systemic mastocytosis with associated clonal hematologic non-mast cell lineage disease (SM-AHNMD) involving chronic myelogenous
Mastocytosis associated with CML Hematopathology - March 2016 Case Report Systemic mastocytosis with associated clonal hematologic non-mast cell lineage disease (SM-AHNMD) involving chronic myelogenous
Expanding Spectrum of Mast Cell Activation Disorders: Monoclonal and Idiopathic Mast Cell Activation Syndromes
 Review Article Clinical Therapeutics/Volume 35, Number 5, 2013 Atopic Clinical Entities Update Expanding Spectrum of Mast Cell Activation Disorders: Monoclonal and Idiopathic Mast Cell Activation Syndromes
Review Article Clinical Therapeutics/Volume 35, Number 5, 2013 Atopic Clinical Entities Update Expanding Spectrum of Mast Cell Activation Disorders: Monoclonal and Idiopathic Mast Cell Activation Syndromes
ImmunoCAP Tryptase Product information
 ImmunoCAP Tryptase Product information 1 Clinical utility of ImmunoCAP Tryptase Risk marker for severe reactions elevated baseline levels indicate increased risk for severe reactions (1-3) in insect and
ImmunoCAP Tryptase Product information 1 Clinical utility of ImmunoCAP Tryptase Risk marker for severe reactions elevated baseline levels indicate increased risk for severe reactions (1-3) in insect and
Systemic Mastocytosis: Seldomly Seen, Multiple Manifestations
 Systemic Mastocytosis: Seldomly Seen, Multiple Manifestations Ryan Cassaday, MD HematologyFellows Conference June 3, 2011 Outline Why this topic, and case discussion Brief background Classification i of
Systemic Mastocytosis: Seldomly Seen, Multiple Manifestations Ryan Cassaday, MD HematologyFellows Conference June 3, 2011 Outline Why this topic, and case discussion Brief background Classification i of
9/25/2017. Disclosure. I have nothing to disclose. Young S. Kim MD Dept. of Pathology
 Disclosure MAST CELLNEOPLASM I have nothing to disclose. Young S. Kim MD Dept. of Pathology 1 Objectives What is mast cell lineage? Changes in updated WHO 2016 mastocytosis Issues of Mastocytosis CD30
Disclosure MAST CELLNEOPLASM I have nothing to disclose. Young S. Kim MD Dept. of Pathology 1 Objectives What is mast cell lineage? Changes in updated WHO 2016 mastocytosis Issues of Mastocytosis CD30
Idiopathic Anaphylaxis. Paul A. Greenberger, MD, FAAAAI 2/28/2014 Course # 1605
 Idiopathic Anaphylaxis Paul A. Greenberger, MD, FAAAAI 2/28/2014 Course # 1605 Objectives Review definition and classification of idiopathic anaphylaxis Consider the differential diagnosis Critique lab
Idiopathic Anaphylaxis Paul A. Greenberger, MD, FAAAAI 2/28/2014 Course # 1605 Objectives Review definition and classification of idiopathic anaphylaxis Consider the differential diagnosis Critique lab
2007 Workshop of Society for Hematopathology & European Association for Hematopathology Indianapolis, IN, USA Case # 228
 2007 Workshop of Society for Hematopathology & European Association for Hematopathology Indianapolis, IN, USA Case # 228 Vishnu V. B Reddy, MD University of Alabama at Birmingham Birmingham, AL USA 11/03/07
2007 Workshop of Society for Hematopathology & European Association for Hematopathology Indianapolis, IN, USA Case # 228 Vishnu V. B Reddy, MD University of Alabama at Birmingham Birmingham, AL USA 11/03/07
Immunophenotyping of mast cells: a sensitive and specific diagnostic tool for systemic mastocytosis
 O R I G I N A L A R T I C L E Immunophenotyping of mast cells: a sensitive and specific diagnostic tool for systemic mastocytosis P.L.A. van Daele 1,2*, B.S. Beukenkamp 2, W.M.C. Geertsma-Kleinekoort 3,
O R I G I N A L A R T I C L E Immunophenotyping of mast cells: a sensitive and specific diagnostic tool for systemic mastocytosis P.L.A. van Daele 1,2*, B.S. Beukenkamp 2, W.M.C. Geertsma-Kleinekoort 3,
Clonal mast cell disorders in patients with systemic reactions to Hymenoptera stings and increased serum tryptase levels
 Food, drug, insect sting allergy, and anaphylaxis Clonal mast cell disorders in patients with systemic reactions to Hymenoptera stings and increased serum tryptase levels Patrizia Bonadonna, MD, a,i Omar
Food, drug, insect sting allergy, and anaphylaxis Clonal mast cell disorders in patients with systemic reactions to Hymenoptera stings and increased serum tryptase levels Patrizia Bonadonna, MD, a,i Omar
The Role of TRAF4 and B3GAT1 Gene Expression in the Food Hypersensitivity and Insect Venom Allergy in Mastocytosis
 DOI 10.1007/s00005-016-0397-7 ORIGINAL ARTICLE The Role of TRAF4 and B3GAT1 Gene Expression in the Food Hypersensitivity and Insect Venom Allergy in Mastocytosis Aleksandra Górska 1 Marta Gruchała-Niedoszytko
DOI 10.1007/s00005-016-0397-7 ORIGINAL ARTICLE The Role of TRAF4 and B3GAT1 Gene Expression in the Food Hypersensitivity and Insect Venom Allergy in Mastocytosis Aleksandra Górska 1 Marta Gruchała-Niedoszytko
Update on Diagnosis and Treatment of Mastocytosis
 Curr Allergy Asthma Rep (2011) 11:292 299 DOI 10.1007/s11882-011-0199-2 Update on Diagnosis and Treatment of Mastocytosis Knut Brockow & Johannes Ring Published online: 27 April 2011 # Springer Science+Business
Curr Allergy Asthma Rep (2011) 11:292 299 DOI 10.1007/s11882-011-0199-2 Update on Diagnosis and Treatment of Mastocytosis Knut Brockow & Johannes Ring Published online: 27 April 2011 # Springer Science+Business
Diagnostic Approach for Eosinophilia and Mastocytosis. Curtis A. Hanson, M.D.
 Diagnostic Approach for Eosinophilia and Mastocytosis Curtis A. Hanson, M.D. 2014 MFMER slide-1 DISCLOSURES: Relevant Financial Relationship(s) None Off Label Usage None 2014 MFMER slide-2 Molecular Classification
Diagnostic Approach for Eosinophilia and Mastocytosis Curtis A. Hanson, M.D. 2014 MFMER slide-1 DISCLOSURES: Relevant Financial Relationship(s) None Off Label Usage None 2014 MFMER slide-2 Molecular Classification
Evaluation of the WHO criteria for the classification of patients with mastocytosis
 2011 USCAP, Inc. All rights reserved 0893-3952/11 $32.00 1 Evaluation of the WHO criteria for the classification of patients with Laura Sánchez-Muñoz 1, Ivan Alvarez-Twose 1, Andrés C García-Montero 2,
2011 USCAP, Inc. All rights reserved 0893-3952/11 $32.00 1 Evaluation of the WHO criteria for the classification of patients with Laura Sánchez-Muñoz 1, Ivan Alvarez-Twose 1, Andrés C García-Montero 2,
EPIPEN INSERVICE Emergency Administration of Epinephrine for the Basic EMT. Michael J. Calice MD, FACEP St. Mary Mercy Hospital
 EPIPEN INSERVICE Emergency Administration of Epinephrine for the Basic EMT Michael J. Calice MD, FACEP St. Mary Mercy Hospital Case #1 NR is an 8 yo male c/o hot mouth and stomach ache after eating jelly
EPIPEN INSERVICE Emergency Administration of Epinephrine for the Basic EMT Michael J. Calice MD, FACEP St. Mary Mercy Hospital Case #1 NR is an 8 yo male c/o hot mouth and stomach ache after eating jelly
Serum tryptase and SCORMA (SCORing MAstocytosis) Index as disease severity parameters in childhood and adult cutaneous mastocytosis
 Clinical dermatology Original article Clinical and Experimental Dermatology Serum tryptase and (SCORing MAstocytosis) Index as disease severity parameters in childhood and adult cutaneous mastocytosis
Clinical dermatology Original article Clinical and Experimental Dermatology Serum tryptase and (SCORing MAstocytosis) Index as disease severity parameters in childhood and adult cutaneous mastocytosis
How I Handle Mast Cells in GI Biopsies
 How I Handle Mast Cells in GI Biopsies Dora Lam-Himlin, MD Rodger C. Haggitt Gastrointestinal Pathology Society Forum United States and Canadian Academy of Pathologists Seattle, Washington, March 12, 2016
How I Handle Mast Cells in GI Biopsies Dora Lam-Himlin, MD Rodger C. Haggitt Gastrointestinal Pathology Society Forum United States and Canadian Academy of Pathologists Seattle, Washington, March 12, 2016
Recognition & Management of Anaphylaxis in the Community. S. Shahzad Mustafa, MD, FAAAAI
 Recognition & Management of Anaphylaxis in the Community S. Shahzad Mustafa, MD, FAAAAI Disclosures None Outline Define anaphylaxis Pathophysiology Common causes Recognition and Management Definition Acute,
Recognition & Management of Anaphylaxis in the Community S. Shahzad Mustafa, MD, FAAAAI Disclosures None Outline Define anaphylaxis Pathophysiology Common causes Recognition and Management Definition Acute,
Synonyms. Mast cell disease Mast cell proliferative disease
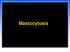 Mastocytosis Definition Mastocytosis is a proliferation of mast cells and their subsequent accumulation in one or more organ systems. Mast cells are derived from hematopoietic progenitors, thus mastocytosis
Mastocytosis Definition Mastocytosis is a proliferation of mast cells and their subsequent accumulation in one or more organ systems. Mast cells are derived from hematopoietic progenitors, thus mastocytosis
ICCS e-newsletter CSI Case Laura Sánchez-Muñoz, Jose Mario T. Morgado, Cristina Teodosio
 ICCS e-newsletter CSI Case Laura Sánchez-Muñoz, Jose Mario T. Morgado, Cristina Teodosio Instituto de Estudios de Mastocitosis and Centro de Investigación del Cáncer Spanish Network on Mastocytosis Spain
ICCS e-newsletter CSI Case Laura Sánchez-Muñoz, Jose Mario T. Morgado, Cristina Teodosio Instituto de Estudios de Mastocitosis and Centro de Investigación del Cáncer Spanish Network on Mastocytosis Spain
Mast cell activation syndrome: Proposed diagnostic criteria
 Mast cell activation syndrome: Proposed diagnostic criteria Cem Akin, MD, PhD, a * Peter Valent, MD, b and Dean D. Metcalfe, MD c Ann Arbor, Mich, Vienna, Austria, and Bethesda, Md The term mast cell activation
Mast cell activation syndrome: Proposed diagnostic criteria Cem Akin, MD, PhD, a * Peter Valent, MD, b and Dean D. Metcalfe, MD c Ann Arbor, Mich, Vienna, Austria, and Bethesda, Md The term mast cell activation
Mastocytosis An Unusual Clonal Disorder of Bone Marrow Derived Hematopoietic Progenitor Cells
 Mastocytosis An Unusual Clonal Disorder of Bone Marrow Derived Hematopoietic Progenitor Cells Hans-Peter Horny, MD Key Words: Mastocytosis; Mast cell; Bone marrow; KITD816V; Systemic mastocytosis with
Mastocytosis An Unusual Clonal Disorder of Bone Marrow Derived Hematopoietic Progenitor Cells Hans-Peter Horny, MD Key Words: Mastocytosis; Mast cell; Bone marrow; KITD816V; Systemic mastocytosis with
Urticaria Moderate Allergic Reaction Mild signs/symptoms with any of following: Dyspnea, possibly with wheezes Angioneurotic edema Systemic, not local
 Allergic Reactions & Anaphylaxis Incidence In USA - 400 to 800 deaths/year Parenterally administered penicillin accounts for 100 to 500 deaths per year Hymenoptera stings account for 40 to 100 deaths per
Allergic Reactions & Anaphylaxis Incidence In USA - 400 to 800 deaths/year Parenterally administered penicillin accounts for 100 to 500 deaths per year Hymenoptera stings account for 40 to 100 deaths per
How I Handle Mast Cells in GI Biopsies
 How I Handle Mast Cells in GI Biopsies Dora Lam-Himlin, MD Mayo Clinic Scottsdale, AZ Rodger C. Haggitt Gastrointestinal Pathology Society Forum United States and Canadian Academy of Pathologists Seattle,
How I Handle Mast Cells in GI Biopsies Dora Lam-Himlin, MD Mayo Clinic Scottsdale, AZ Rodger C. Haggitt Gastrointestinal Pathology Society Forum United States and Canadian Academy of Pathologists Seattle,
Mast Cell Disease Case 054 Session 7
 Mast Cell Disease Case 054 Session 7 Rodney R. Miles, M.D., Ph.D. Lauren B. Smith, M.D. Cem Akin, M.D. Diane Roulston,, Ph.D. Charles W. Ross, M.D. Departments of Pathology and Internal Medicine University
Mast Cell Disease Case 054 Session 7 Rodney R. Miles, M.D., Ph.D. Lauren B. Smith, M.D. Cem Akin, M.D. Diane Roulston,, Ph.D. Charles W. Ross, M.D. Departments of Pathology and Internal Medicine University
FLOCK Cluster Analysis of Mast Cell Event Clustering by High-Sensitivity Flow Cytometry Predicts Systemic Mastocytosis
 FLOCK Cluster Analysis of Mast Cell Event Clustering by High-Sensitivity Flow Cytometry Predicts Systemic Mastocytosis David M. Dorfman, MD, PhD, Charlotte D. LaPlante, Olga Pozdnyakova, MD, PhD, and Betty
FLOCK Cluster Analysis of Mast Cell Event Clustering by High-Sensitivity Flow Cytometry Predicts Systemic Mastocytosis David M. Dorfman, MD, PhD, Charlotte D. LaPlante, Olga Pozdnyakova, MD, PhD, and Betty
Mast Cell Disorders. Andrew M. Smith, MD, MS
 Mast Cell Disorders Andrew M. Smith, MD, MS Division of Immunology, Allergy, and Rheumatology University of Cincinnati and Cincinnati VA Medical Centers August 10 and 11, 2012 Disclosures None The contents
Mast Cell Disorders Andrew M. Smith, MD, MS Division of Immunology, Allergy, and Rheumatology University of Cincinnati and Cincinnati VA Medical Centers August 10 and 11, 2012 Disclosures None The contents
Myelodysplastic syndrome (MDS) & Myeloproliferative neoplasms
 Myelodysplastic syndrome (MDS) & Myeloproliferative neoplasms Myelodysplastic syndrome (MDS) A multipotent stem cell that can differentiate into any of the myeloid lineage cells (RBCs, granulocytes, megakaryocytes)
Myelodysplastic syndrome (MDS) & Myeloproliferative neoplasms Myelodysplastic syndrome (MDS) A multipotent stem cell that can differentiate into any of the myeloid lineage cells (RBCs, granulocytes, megakaryocytes)
7/25/2016. Use of Epinephrine in the Community. Knowledge Amongst Paramedics. Knowledge Amongst Paramedics survey of 3479 paramedics
 Recognition & Management of Anaphylaxis in the Community S. Shahzad Mustafa, MD, FAAAAI Disclosures Speaker s bureau Genentech, Teva Consultant Genentech, Teva Outline Knowledge gap Definition Pathophysiology
Recognition & Management of Anaphylaxis in the Community S. Shahzad Mustafa, MD, FAAAAI Disclosures Speaker s bureau Genentech, Teva Consultant Genentech, Teva Outline Knowledge gap Definition Pathophysiology
Natural history of insect ir, g allergy: Relationship of severity of sym oms of initial sting anaphylaxis to re-sting rea ions
 Natural history of insect ir, g allergy: Relationship of severity of sym oms of initial sting anaphylaxis to re-sting rea ions Robert E. Reisman, MD Buffalo, N.Y. To examine the postulate that the nature
Natural history of insect ir, g allergy: Relationship of severity of sym oms of initial sting anaphylaxis to re-sting rea ions Robert E. Reisman, MD Buffalo, N.Y. To examine the postulate that the nature
University of Groningen. Hymenoptera venom allergy Vos, Byrthe
 University of Groningen Hymenoptera venom allergy Vos, Byrthe IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check the document
University of Groningen Hymenoptera venom allergy Vos, Byrthe IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check the document
Integrated Diagnostic Approach to the Classification of Myeloid Neoplasms. Daniel A. Arber, MD Stanford University
 Integrated Diagnostic Approach to the Classification of Myeloid Neoplasms Daniel A. Arber, MD Stanford University What is an integrated approach? What is an integrated approach? Incorporating all diagnostic
Integrated Diagnostic Approach to the Classification of Myeloid Neoplasms Daniel A. Arber, MD Stanford University What is an integrated approach? What is an integrated approach? Incorporating all diagnostic
Anaphylaxis: The Atypical Varieties
 Anaphylaxis: The Atypical Varieties John Johnson, D.O., PGY-4 Allergy/Immunology Fellow University Hospitals of Cleveland Case Western Reserve University School of Medicine Disclosures: None What is Anaphylaxis?
Anaphylaxis: The Atypical Varieties John Johnson, D.O., PGY-4 Allergy/Immunology Fellow University Hospitals of Cleveland Case Western Reserve University School of Medicine Disclosures: None What is Anaphylaxis?
CONCLUSIONS: For the primary end point in the total population, there were no significant differences between treatments. There were small, but statis
 V. Clinical Sciences A. Allergic Diseases and Related Disorders 1. Upper airway disease a. Clinical skills and interpretive strategies for diagnosis of upper airway diseases: skin testing (epicutaneous
V. Clinical Sciences A. Allergic Diseases and Related Disorders 1. Upper airway disease a. Clinical skills and interpretive strategies for diagnosis of upper airway diseases: skin testing (epicutaneous
VACCINE-RELATED ALLERGIC REACTIONS
 VACCINE-RELATED ALLERGIC REACTIONS Management of Anaphylaxis Public Health Immunization Program June 2018 VACCINE-RELATED ADVERSE EVENTS Local reactions pain, edema, erythema Systemic reactions fever,
VACCINE-RELATED ALLERGIC REACTIONS Management of Anaphylaxis Public Health Immunization Program June 2018 VACCINE-RELATED ADVERSE EVENTS Local reactions pain, edema, erythema Systemic reactions fever,
Supervisor: Prof. Dr. P Vandenberghe Dr. C Brusselmans
 Contribution of molecular diagnosis in eosinophilia/hypereosinophilia Eosinophilia Hypereosinophilia Hypereosinophilic syndrome Immune mediated hypereosinophilia Chronic eosinophilic leukemia (NOS)/ Idiopathic
Contribution of molecular diagnosis in eosinophilia/hypereosinophilia Eosinophilia Hypereosinophilia Hypereosinophilic syndrome Immune mediated hypereosinophilia Chronic eosinophilic leukemia (NOS)/ Idiopathic
Acute myeloid leukaemia with t(8;21) associated with occult mastocytosis. Report of an unusual case and review of the literature
 324 CASE REPORT Acute myeloid leukaemia with t(8;21) associated with occult mastocytosis. Report of an unusual case and review of the literature H-W Bernd, K Sotlar, J Lorenzen, R Osieka, U Fabry, P Valent,
324 CASE REPORT Acute myeloid leukaemia with t(8;21) associated with occult mastocytosis. Report of an unusual case and review of the literature H-W Bernd, K Sotlar, J Lorenzen, R Osieka, U Fabry, P Valent,
Mast cell leukemia with prolonged survival on PKC412/midostaurin
 Washington University School of Medicine Digital Commons@Becker Open Access Publications 2014 Mast cell leukemia with prolonged survival on PKC412/midostaurin Xiangdong Xu Friederike H. Kreisel John L.
Washington University School of Medicine Digital Commons@Becker Open Access Publications 2014 Mast cell leukemia with prolonged survival on PKC412/midostaurin Xiangdong Xu Friederike H. Kreisel John L.
Chapter 16 Anaphylaxis in Mastocytosis*
 Chapter 16 Anaphylaxis in Mastocytosis* Luis Escribano and Alberto Orfao Abstract An increase in anaphylaxis has been reported in mastocytosis, with a predominance of males. Recurrent idiopathic anaphylaxis
Chapter 16 Anaphylaxis in Mastocytosis* Luis Escribano and Alberto Orfao Abstract An increase in anaphylaxis has been reported in mastocytosis, with a predominance of males. Recurrent idiopathic anaphylaxis
Survey on practice of venom immunotherapy in France
 Public health Survey on practice of venom immunotherapy in France Charles Dzviga 1, Catherine Matevi 2, Philippe Bonniaud 3, François Lavaud 4, Bruno Girodet 5, Joelle Birnbaum 6, Claude Lambert 7, the
Public health Survey on practice of venom immunotherapy in France Charles Dzviga 1, Catherine Matevi 2, Philippe Bonniaud 3, François Lavaud 4, Bruno Girodet 5, Joelle Birnbaum 6, Claude Lambert 7, the
Transient hypogammaglobulinaemia of infants in children with mastocytosis strengthened indications for vaccinations
 Clinical immunology DOI: 10.5114/ceji.2016.63128 Transient hypogammaglobulinaemia of infants in children with mastocytosis strengthened indications for vaccinations Joanna Renke 1,2, Magdalena Lange 3,
Clinical immunology DOI: 10.5114/ceji.2016.63128 Transient hypogammaglobulinaemia of infants in children with mastocytosis strengthened indications for vaccinations Joanna Renke 1,2, Magdalena Lange 3,
Terms What is Anaphylaxis? Causes Signs & Symptoms Management Education Pictures Citations. Anaphylaxis; LBodak
 Leslie Bodak, EMT-P Terms What is Anaphylaxis? Causes Signs & Symptoms Management Education Pictures Citations Allergic Reaction: an abnormal immune response the body develops when a person has been previously
Leslie Bodak, EMT-P Terms What is Anaphylaxis? Causes Signs & Symptoms Management Education Pictures Citations Allergic Reaction: an abnormal immune response the body develops when a person has been previously
Lymphoma: What You Need to Know. Richard van der Jagt MD, FRCPC
 Lymphoma: What You Need to Know Richard van der Jagt MD, FRCPC Overview Concepts, classification, biology Epidemiology Clinical presentation Diagnosis Staging Three important types of lymphoma Conceptualizing
Lymphoma: What You Need to Know Richard van der Jagt MD, FRCPC Overview Concepts, classification, biology Epidemiology Clinical presentation Diagnosis Staging Three important types of lymphoma Conceptualizing
Multidisciplinary Management of Mastocytosis: Nordic Expert Group Consensus
 Acta Derm Venereol 2016; 96: 602 612 SPECIAL REPORT Multidisciplinary Management of Mastocytosis: Nordic Expert Group Consensus Sigurd BROESBY-OLSEN 1, Ingunn DYBEDAL 2, Theo GÜLEN 3, Thomas K. KRISTENSEN
Acta Derm Venereol 2016; 96: 602 612 SPECIAL REPORT Multidisciplinary Management of Mastocytosis: Nordic Expert Group Consensus Sigurd BROESBY-OLSEN 1, Ingunn DYBEDAL 2, Theo GÜLEN 3, Thomas K. KRISTENSEN
Diagnosis and Treatment of Anaphylaxis in Patients with Mastocytosis
 Current Treatment Options in Allergy (2014) 1:247 261 DOI 10.1007/s40521-014-0021-1 Anaphylaxis (P Lieberman, Section Editor) Diagnosis and Treatment of Anaphylaxis in Patients with Mastocytosis Peter
Current Treatment Options in Allergy (2014) 1:247 261 DOI 10.1007/s40521-014-0021-1 Anaphylaxis (P Lieberman, Section Editor) Diagnosis and Treatment of Anaphylaxis in Patients with Mastocytosis Peter
ANAPHYLAXIS EMET 2015
 ANAPHYLAXIS EMET 2015 ANA = AGAINST PHYLAX = PROTECTION No standardised definition (they re working on it) All include the similar concept of: A serious, generalised or systemic, allergic or hypersensitivity
ANAPHYLAXIS EMET 2015 ANA = AGAINST PHYLAX = PROTECTION No standardised definition (they re working on it) All include the similar concept of: A serious, generalised or systemic, allergic or hypersensitivity
REFERRAL GUIDELINES - SUMMARY
 Clinical Immunology & Allergy Unit LEEDS TEACHING HOSPITALS NHS TRUST REFERRAL GUIDELINES - SUMMARY THESE GUIDELINES ARE DESIGNED TO ENSURE THAT PATIENTS REQUIRING SECONDARY CARE ARE SEEN EFFICIENTLY AND
Clinical Immunology & Allergy Unit LEEDS TEACHING HOSPITALS NHS TRUST REFERRAL GUIDELINES - SUMMARY THESE GUIDELINES ARE DESIGNED TO ENSURE THAT PATIENTS REQUIRING SECONDARY CARE ARE SEEN EFFICIENTLY AND
Mast Cell Tumors in Dogs
 Mast Cell Tumors in Dogs 803-808-7387 www.gracepets.com These notes are provided to help you understand the diagnosis or possible diagnosis of cancer in your pet. For general information on cancer in pets
Mast Cell Tumors in Dogs 803-808-7387 www.gracepets.com These notes are provided to help you understand the diagnosis or possible diagnosis of cancer in your pet. For general information on cancer in pets
VACCINE-RELATED ALLERGIC REACTIONS
 VACCINE-RELATED ALLERGIC REACTIONS Management of Anaphylaxis IERHA Immunization Program September 2016 VACCINE-RELATED ADVERSE EVENTS Local reactions pain, edema, erythema Systemic reactions fever, lymphadenopathy
VACCINE-RELATED ALLERGIC REACTIONS Management of Anaphylaxis IERHA Immunization Program September 2016 VACCINE-RELATED ADVERSE EVENTS Local reactions pain, edema, erythema Systemic reactions fever, lymphadenopathy
Path2220 INTRODUCTION TO HUMAN DISEASE ALLERGY. Dr. Erika Bosio
 Path2220 INTRODUCTION TO HUMAN DISEASE ALLERGY Dr. Erika Bosio Research Fellow Centre for Clinical Research in Emergency Medicine, Harry Perkins Institute of Medical Research University of Western Australia
Path2220 INTRODUCTION TO HUMAN DISEASE ALLERGY Dr. Erika Bosio Research Fellow Centre for Clinical Research in Emergency Medicine, Harry Perkins Institute of Medical Research University of Western Australia
Eosinophilia: A Diagnostic Approach and Test Utilization Strategies for Bone Marrow Evaluation
 Eosinophilia: A Diagnostic Approach and Test Utilization Strategies for Bone Marrow Evaluation American Society for Clinical Pathology 2014 Annual Meeting Presented by: Matthew T. Howard, MD Assistant
Eosinophilia: A Diagnostic Approach and Test Utilization Strategies for Bone Marrow Evaluation American Society for Clinical Pathology 2014 Annual Meeting Presented by: Matthew T. Howard, MD Assistant
De novo mast cell leukemia without CD25 expression and KIT mutations: a rare case report in a 13-year-old child
 Zheng et al. Diagnostic Pathology (2018) 13:14 https://doi.org/10.1186/s13000-018-0691-2 CASE REPORT Open Access De novo mast cell leukemia without CD25 expression and KIT mutations: a rare case report
Zheng et al. Diagnostic Pathology (2018) 13:14 https://doi.org/10.1186/s13000-018-0691-2 CASE REPORT Open Access De novo mast cell leukemia without CD25 expression and KIT mutations: a rare case report
contact activation in formation diseases 67 endothelial cells and kinin formation 73 processing and degradation 68 70
 Subject Index Adenosine, mast cell activation modulation 60 Age, risk factor 17, 18 Allergen elicitors 9, 10 insects, see Insect venom-induced microarrays for 136 overview of characteristics 23 recognition
Subject Index Adenosine, mast cell activation modulation 60 Age, risk factor 17, 18 Allergen elicitors 9, 10 insects, see Insect venom-induced microarrays for 136 overview of characteristics 23 recognition
Mast Cells and Basophil Biology and Disorders. Sarbjit S. Saini, M.D. Associate Professor of Medicine Johns Hopkins University
 Mast Cells and Basophil Biology and Disorders Sarbjit S. Saini, M.D. Associate Professor of Medicine Johns Hopkins University Disclosure Research Interests-NIH, AstraZeneca, Genentech, Novartis Consultant:
Mast Cells and Basophil Biology and Disorders Sarbjit S. Saini, M.D. Associate Professor of Medicine Johns Hopkins University Disclosure Research Interests-NIH, AstraZeneca, Genentech, Novartis Consultant:
Osteosclerotic Myeloma (POEMS Syndrome)
 Osteosclerotic Myeloma (POEMS Syndrome) Osteosclerotic Myeloma (POEMS Syndrome) Synonyms Crow-Fukase syndrome Multicentric Castleman disease Takatsuki syndrome Acronym coined by Bardwick POEMS Scheinker,
Osteosclerotic Myeloma (POEMS Syndrome) Osteosclerotic Myeloma (POEMS Syndrome) Synonyms Crow-Fukase syndrome Multicentric Castleman disease Takatsuki syndrome Acronym coined by Bardwick POEMS Scheinker,
Myth: Prior Episodes Predict Future Reactions REALITY: No predictable pattern Severity depends on: Sensitivity of the individual Dose of the allergen
 Myth: Prior Episodes Predict Future Reactions REALITY: No predictable pattern Severity depends on: Sensitivity of the individual Dose of the allergen Anaphylaxis Fatalities Estimated 500 1000 deaths annually
Myth: Prior Episodes Predict Future Reactions REALITY: No predictable pattern Severity depends on: Sensitivity of the individual Dose of the allergen Anaphylaxis Fatalities Estimated 500 1000 deaths annually
Welcome to Master Class for Oncologists. Session 3: 9:15 AM - 10:00 AM
 Welcome to Master Class for Oncologists Session 3: 9:15 AM - 10:00 AM Miami, FL December 18, 2009 Myeloproliferative Neoplasms: Bringing Order to Complexity and Achieving Optimal Outcomes Speaker: Andrew
Welcome to Master Class for Oncologists Session 3: 9:15 AM - 10:00 AM Miami, FL December 18, 2009 Myeloproliferative Neoplasms: Bringing Order to Complexity and Achieving Optimal Outcomes Speaker: Andrew
Policy for the Treatment of Anaphylaxis in Adults and Children
 Policy for the Treatment of Anaphylaxis in Adults and Children June 2008 Policy Title: Policy for the Treatment of Anaphylaxis in Adults or Children Policy Reference Number: PrimCare08/17 Implementation
Policy for the Treatment of Anaphylaxis in Adults and Children June 2008 Policy Title: Policy for the Treatment of Anaphylaxis in Adults or Children Policy Reference Number: PrimCare08/17 Implementation
Pathology. #11 Acute Leukemias. Farah Banyhany. Dr. Sohaib Al- Khatib 23/2/16
 35 Pathology #11 Acute Leukemias Farah Banyhany Dr. Sohaib Al- Khatib 23/2/16 1 Salam First of all, this tafreegh is NOT as long as you may think. If you just focus while studying this, everything will
35 Pathology #11 Acute Leukemias Farah Banyhany Dr. Sohaib Al- Khatib 23/2/16 1 Salam First of all, this tafreegh is NOT as long as you may think. If you just focus while studying this, everything will
T he World Health Organisation (WHO) classification of
 604 ORIGINAL ARTICLE Systemic mastocytosis with associated clonal haematological non-mast cell lineage diseases: a histopathological challenge H-P Horny, K Sotlar, W R Sperr, P Valent... See end of article
604 ORIGINAL ARTICLE Systemic mastocytosis with associated clonal haematological non-mast cell lineage diseases: a histopathological challenge H-P Horny, K Sotlar, W R Sperr, P Valent... See end of article
Pathology of Hematopoietic and Lymphoid tissue
 CONTENTS Pathology of Hematopoietic and Lymphoid tissue White blood cells and lymph nodes Quantitative disorder of white blood cells Reactive lymphadenopathies Infectious lymphadenitis Tumor metastasis
CONTENTS Pathology of Hematopoietic and Lymphoid tissue White blood cells and lymph nodes Quantitative disorder of white blood cells Reactive lymphadenopathies Infectious lymphadenitis Tumor metastasis
Five things to know about anaphylaxis
 Five things to know about anaphylaxis Magdalena Berger, MD FRCPC Allergist and Clinical Immunologist New Brunswick Internal Medicine Update April 22, 2016 Disclosures None relevant to this presentation
Five things to know about anaphylaxis Magdalena Berger, MD FRCPC Allergist and Clinical Immunologist New Brunswick Internal Medicine Update April 22, 2016 Disclosures None relevant to this presentation
Urticaria and Angioedema. Allergy and Immunology Awareness Program
 Urticaria and Angioedema Allergy and Immunology Awareness Program 1 Urticaria and Angioedema Allergy and Immunology Awareness Program Urticaria Commonly known as hives, urticarial is an itchy rash with
Urticaria and Angioedema Allergy and Immunology Awareness Program 1 Urticaria and Angioedema Allergy and Immunology Awareness Program Urticaria Commonly known as hives, urticarial is an itchy rash with
Basal Serum Tryptase Level Correlates With Severity of Hymenoptera Sting and Age
 ORIGINAL ARTICLE Basal Serum Tryptase Level Correlates With Severity of Hymenoptera Sting and Age I Kucharewicz, 1 A Bodzenta-Lukaszyk, 1 W Szymanski, 1 B Mroczko, 2 M Szmitkowski 2 1 Department of Allergology
ORIGINAL ARTICLE Basal Serum Tryptase Level Correlates With Severity of Hymenoptera Sting and Age I Kucharewicz, 1 A Bodzenta-Lukaszyk, 1 W Szymanski, 1 B Mroczko, 2 M Szmitkowski 2 1 Department of Allergology
The Diagnosis and Management of Anaphylaxis
 Transcript Details This is a transcript of an educational program accessible on the ReachMD network. Details about the program and additional media formats for the program are accessible by visiting: https://reachmd.com/programs/focus-on-allergy/the-diagnosis-and-management-of-anaphylaxis/3919/
Transcript Details This is a transcript of an educational program accessible on the ReachMD network. Details about the program and additional media formats for the program are accessible by visiting: https://reachmd.com/programs/focus-on-allergy/the-diagnosis-and-management-of-anaphylaxis/3919/
Allergy School on Investigating allergic effects of environmental exposures. Brindisi, Italy, 2-5 July Venom Allergy. M.
 Allergy School on Investigating allergic effects of environmental exposures Brindisi, Italy, 2-5 July 2014 Venom Allergy M.Beatrice Bilò Department of Internal Medicine Allergy Unit University Hospital,
Allergy School on Investigating allergic effects of environmental exposures Brindisi, Italy, 2-5 July 2014 Venom Allergy M.Beatrice Bilò Department of Internal Medicine Allergy Unit University Hospital,
Case #16: Diagnosis. T-Lymphoblastic lymphoma. But wait, there s more... A few weeks later the cytogenetics came back...
 Case #16: Diagnosis T-Lymphoblastic lymphoma But wait, there s more... A few weeks later the cytogenetics came back... 46,XY t(8;13)(p12;q12)[12] Image courtesy of Dr. Xinyan Lu Further Studies RT-PCR
Case #16: Diagnosis T-Lymphoblastic lymphoma But wait, there s more... A few weeks later the cytogenetics came back... 46,XY t(8;13)(p12;q12)[12] Image courtesy of Dr. Xinyan Lu Further Studies RT-PCR
MYELOPROLIFARATIVE NEOPLASMS. Dr. Hasan Fahmawi, MRCP(UK), FRCP(Edin).
 MYELOPROLIFARATIVE NEOPLASMS Dr. Hasan Fahmawi, MRCP(UK), FRCP(Edin). These are a group of chronic conditions characterised by clonal proliferation of marrow precursor cells. PRV, essential thrombocyathaemia,
MYELOPROLIFARATIVE NEOPLASMS Dr. Hasan Fahmawi, MRCP(UK), FRCP(Edin). These are a group of chronic conditions characterised by clonal proliferation of marrow precursor cells. PRV, essential thrombocyathaemia,
Definitions, Criteria and Global Classification of Mast Cell Disorders with Special Reference to Mast Cell Activation Syndromes: A Consensus Proposal
 Position Paper DOI: 10.1159/000328760 Received: January 24, 2011 Accepted after revision: April 18, 2011 Published online: October 27, 2011 Definitions, Criteria and Global Classification of Mast Cell
Position Paper DOI: 10.1159/000328760 Received: January 24, 2011 Accepted after revision: April 18, 2011 Published online: October 27, 2011 Definitions, Criteria and Global Classification of Mast Cell
by accumulation of pathological mast cells in potentially any or all organs and tissues and/or
 1 Supplementary Material to Seidel et al. Bleeding diathesis in patients with mast cell activation disease (Thromb Haemost 2011; 106.5) Definition of mast cell activation disease The term mast cell activation
1 Supplementary Material to Seidel et al. Bleeding diathesis in patients with mast cell activation disease (Thromb Haemost 2011; 106.5) Definition of mast cell activation disease The term mast cell activation
FOLLICULARITY in LYMPHOMA
 FOLLICULARITY in LYMPHOMA Reactive Follicular Hyperplasia Follicular Hyperplasia irregular follicles Follicular Hyperplasia dark and light zones Light Zone Dark Zone Follicular hyperplasia MIB1 Follicular
FOLLICULARITY in LYMPHOMA Reactive Follicular Hyperplasia Follicular Hyperplasia irregular follicles Follicular Hyperplasia dark and light zones Light Zone Dark Zone Follicular hyperplasia MIB1 Follicular
Allergy Management Policy
 Allergy Management Policy Food Allergy People with allergies have over-reactive immune systems that target otherwise harmless elements of our diet and environment. During an allergic reaction to food,
Allergy Management Policy Food Allergy People with allergies have over-reactive immune systems that target otherwise harmless elements of our diet and environment. During an allergic reaction to food,
Transfusion and Allergy: What is it, and what is it not? Prof. Olivier GARRAUD INTS, Paris Université de Lyon/Saint-Etienne France
 Transfusion and Allergy: What is it, and what is it not? Prof. Olivier GARRAUD INTS, Paris Université de Lyon/Saint-Etienne France The commonest picture of Allergy Allergy is commonly sensed as an Antibody
Transfusion and Allergy: What is it, and what is it not? Prof. Olivier GARRAUD INTS, Paris Université de Lyon/Saint-Etienne France The commonest picture of Allergy Allergy is commonly sensed as an Antibody
The Tryptase Test Clinical Use in Dermatology and Allergy
 The Tryptase Test Clinical Use in Dermatology and Allergy Knut Brockow 1, Lawrence B Schwartz 2 1 Department of Dermatology and Allergy Biederstein, Technical University Munich, Munich, Germany 2 Department
The Tryptase Test Clinical Use in Dermatology and Allergy Knut Brockow 1, Lawrence B Schwartz 2 1 Department of Dermatology and Allergy Biederstein, Technical University Munich, Munich, Germany 2 Department
Anaphylaxis School First results of a national multicenter study
 Anaphylaxis School First results of a national multicenter study J. Kupfer, S. Schallmayer, I. Fell, U. Gieler for the German study group Anaphylaxis is an acute, potentially life-threatening hypersensitivity
Anaphylaxis School First results of a national multicenter study J. Kupfer, S. Schallmayer, I. Fell, U. Gieler for the German study group Anaphylaxis is an acute, potentially life-threatening hypersensitivity
Chapter 65 Allergy and Immunology for the Internist. ingestion provoke an IgE antibody response and clinical symptoms in sensitive individuals.
 Chapter 65 Allergy and Immunology for the Internist 1 I. Basic Information A. Definition of Allergens: Proteins of appropriate size that after inhalation, injection (e.g. drug, venom) or ingestion provoke
Chapter 65 Allergy and Immunology for the Internist 1 I. Basic Information A. Definition of Allergens: Proteins of appropriate size that after inhalation, injection (e.g. drug, venom) or ingestion provoke
Single venom-based immunotherapy effectively protects patients with double positive tests to honey bee and Vespula venom
 Stoevesandt et al. Allergy, Asthma & Clinical Immunology 2013, 9:33 ALLERGY, ASTHMA & CLINICAL IMMUNOLOGY RESEARCH Open Access Single venom-based immunotherapy effectively protects patients with double
Stoevesandt et al. Allergy, Asthma & Clinical Immunology 2013, 9:33 ALLERGY, ASTHMA & CLINICAL IMMUNOLOGY RESEARCH Open Access Single venom-based immunotherapy effectively protects patients with double
Pathology of Hematopoietic and Lymphoid tissue
 Pathology of Hematopoietic and Lymphoid tissue Peerayut Sitthichaiyakul, M.D. Department of Pathology and Forensic Medicine Faculty of Medicine, Naresuan University CONTENTS White blood cells and lymph
Pathology of Hematopoietic and Lymphoid tissue Peerayut Sitthichaiyakul, M.D. Department of Pathology and Forensic Medicine Faculty of Medicine, Naresuan University CONTENTS White blood cells and lymph
Course Objectives: Upon completion of this presentation, the attendee will be able to:
 Course Objectives: Upon completion of this presentation, the attendee will be able to: Kevin Letz DNP, MBA, MSN, RN, CNE, CEN, FNP-C, PNP-BC, ANP-BC, FAPPex, FAANP 1. Identify the newest diagnostic criteria
Course Objectives: Upon completion of this presentation, the attendee will be able to: Kevin Letz DNP, MBA, MSN, RN, CNE, CEN, FNP-C, PNP-BC, ANP-BC, FAPPex, FAANP 1. Identify the newest diagnostic criteria
Immunocompetence The immune system responds appropriately to a foreign stimulus
 Functions of the immune system Protect the body s internal environment against invading organisms Maintain homeostasis by removing damaged cells from the circulation Serve as a surveillance network for
Functions of the immune system Protect the body s internal environment against invading organisms Maintain homeostasis by removing damaged cells from the circulation Serve as a surveillance network for
Anaphylaxis: Treatment in the Community
 : Treatment in the Community is likely if a patient who, within minutes of exposure to a trigger (allergen), develops a sudden illness with rapidly progressing skin changes and life-threatening airway
: Treatment in the Community is likely if a patient who, within minutes of exposure to a trigger (allergen), develops a sudden illness with rapidly progressing skin changes and life-threatening airway
Allergy & Anaphylaxis
 Allergy & Anaphylaxis (why, where, and what to do) Robert H. Brown, M.D., M.P.H. Professor Departments of Anesthesiology, Environmental Health Sciences, Medicine, and Radiology The Johns Hopkins Medical
Allergy & Anaphylaxis (why, where, and what to do) Robert H. Brown, M.D., M.P.H. Professor Departments of Anesthesiology, Environmental Health Sciences, Medicine, and Radiology The Johns Hopkins Medical
Heme 9 Myeloid neoplasms
 Heme 9 Myeloid neoplasms The minimum number of blasts to diagnose acute myeloid leukemia is 5% 10% 20% 50% 80% AML with the best prognosis is AML with recurrent cytogenetic abnormality AML with myelodysplasia
Heme 9 Myeloid neoplasms The minimum number of blasts to diagnose acute myeloid leukemia is 5% 10% 20% 50% 80% AML with the best prognosis is AML with recurrent cytogenetic abnormality AML with myelodysplasia
Myeloid neoplasms. Early arrest in the blast cell or immature cell "we call it acute leukemia" Myoid neoplasm divided in to 3 major categories:
 Myeloid neoplasms Note: Early arrest in the blast cell or immature cell "we call it acute leukemia" Myoid neoplasm divided in to 3 major categories: 1. AML : Acute myeloid leukemia(stem cell with myeloid
Myeloid neoplasms Note: Early arrest in the blast cell or immature cell "we call it acute leukemia" Myoid neoplasm divided in to 3 major categories: 1. AML : Acute myeloid leukemia(stem cell with myeloid
Who Should Be Premediciated for Contrast-Enhanced Exams?
 Who Should Be Premediciated for Contrast-Enhanced Exams? Jeffrey C. Weinreb, MD,FACR Yale University School of Medicine jeffrey.weinreb@yale.edu Types of Intravenous Contrast Media Iodinated Contrast Agents
Who Should Be Premediciated for Contrast-Enhanced Exams? Jeffrey C. Weinreb, MD,FACR Yale University School of Medicine jeffrey.weinreb@yale.edu Types of Intravenous Contrast Media Iodinated Contrast Agents
59 Manifestações cutâneas em indivíduos infectados ou com doenças 59
 59 Manifestações cutâneas em indivíduos infectados ou com doenças 59 INVESTIGATION s Adult mastocytosis: a review of the Santo António Hospital 's experience and an evaluation of World Health Organization
59 Manifestações cutâneas em indivíduos infectados ou com doenças 59 INVESTIGATION s Adult mastocytosis: a review of the Santo António Hospital 's experience and an evaluation of World Health Organization
Are Gastrointestinal Mucosal Mast Cells Increased in Patients With Systemic Mastocytosis?
 Anatomic Pathology / GASTRODUODENAL MAST CELLS IN MASTOCYTOSIS Are Gastrointestinal Mucosal Mast Cells Increased in Patients With Systemic Mastocytosis? Sabine I. Siegert, MD, 1 Joachim Diebold, MD, PhD,
Anatomic Pathology / GASTRODUODENAL MAST CELLS IN MASTOCYTOSIS Are Gastrointestinal Mucosal Mast Cells Increased in Patients With Systemic Mastocytosis? Sabine I. Siegert, MD, 1 Joachim Diebold, MD, PhD,
Systemic mastocytosis:
 Systemic mastocytosis: Flow cytometry and Molecular Biology Katrien Vermeulen 21 oktober 2016 Cuteanous mastocytosis Major criterion Typical skin lesions of mastocytosis associated with Darier s sign Minor
Systemic mastocytosis: Flow cytometry and Molecular Biology Katrien Vermeulen 21 oktober 2016 Cuteanous mastocytosis Major criterion Typical skin lesions of mastocytosis associated with Darier s sign Minor
University of Groningen. Hymenoptera venom allergy Vos, Byrthe
 University of Groningen Hymenoptera venom allergy Vos, Byrthe IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check the document
University of Groningen Hymenoptera venom allergy Vos, Byrthe IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check the document
Preliminary Communication Cichocka-Jarosz, Dorynska, Pietrzyk & Spiewak
 For reprint orders, please contact: reprints@futuremedicine.com Laboratory markers of mast cell and basophil activation in monitoring rush immunotherapy in bee venom-allergic children Aim: To evaluate
For reprint orders, please contact: reprints@futuremedicine.com Laboratory markers of mast cell and basophil activation in monitoring rush immunotherapy in bee venom-allergic children Aim: To evaluate
OBJECTIVES DEFINITION TYPE I HYPERSENSITIVITY TYPES OF HYPERSENSITIVITY ACUTE ALLERGIC REACTION 11/5/2016
 OBJECTIVES ACUTE ALLERGIC REACTION Wei Zhao, MD, PhD Ambulatory Medical Director Children s Hospital of Richmond at VCU Associate Professor, Chief Chief, Division of Allergy and Immunology Virginia Commonwealth
OBJECTIVES ACUTE ALLERGIC REACTION Wei Zhao, MD, PhD Ambulatory Medical Director Children s Hospital of Richmond at VCU Associate Professor, Chief Chief, Division of Allergy and Immunology Virginia Commonwealth
