NIH Public Access Author Manuscript Calcif Tissue Int. Author manuscript; available in PMC 2015 January 01.
|
|
|
- Wilfrid Brown
- 5 years ago
- Views:
Transcription
1 NIH Public Access Author Manuscript Published in final edited form as: Calcif Tissue Int January ; 94(1): doi: /s y. Osteocyte-Driven Bone Remodeling Teresita Bellido *,1,2,3 1 Department of Anatomy and Cell Biology, Division of Endocrinology, Indiana University School of Medicine 2 Department of Medicine, Division of Endocrinology, Indiana University School of Medicine 3 Roudebush Veterans Administration Medical Center, Indianapolis, Indiana Abstract Osteocytes, the most abundant cells in bone, have been long postulated to detect and respond to mechanical and hormonal stimuli and to coordinate the function of osteoblasts and osteoclasts. The discovery that the inhibitor of bone formation sclerostin is primarily expressed in osteocytes in bone and it is downregulated by anabolic stimuli provided a mechanism by which osteocytes influence the activity of osteoblasts. Advances of the last few years provided experimental evidence demonstrating that osteocytes also participate in the recruitment of osteoclasts and the initiation of bone remodeling. Apoptotic osteocytes trigger yet to be identified signals that attract osteoclast precursors to specific areas of bone, which in turn differentiate to mature, bone resorbing osteoclasts. Osteocytes are also the source of molecules that regulate generation and activity of osteoclasts, such as OPG and RANKL; and genetic manipulations of the mouse genome leading to loss or gain of function, or to altered expression of either molecule in osteocytes, markedly affect bone resorption. This review highlights these investigations and discusses how the novel concept of osteocyte-driven bone resorption and formation impacts our understanding of the mechanisms by which current therapies control bone remodeling. Keywords osteocyte; osteoclast; osteoblast; bone remodeling; RANKL; OPG; Sost 1. Osteocytes and their functions in bone homeostasis Osteocytes are former osteoblasts that become entombed during the process of bone deposition and remain regularly distributed throughout the mineralized bone matrix. Osteocytes comprise more than 90% of bone cells within the matrix or on the bone surfaces. It has been long hypothesized that osteocytes are the primary cells responsible for the adaptation of bone to mechanical force. Evidence accumulated in the last few years supports this notion and demonstrates that osteocytes are also involved in the response of bone to hormones. Few genes expressed in osteocytes have been identified as molecular mediators of the osteocyte-driven changes in bone remodeling. However, the molecular mechanisms by which osteocytes regulate the bone homeostasis are far from being understood. * Corresponding author and reprint requests: Teresita Bellido, Ph.D, Indiana University School of Medicine, 635 Barnhill Drive, MS5035, Indianapolis, IN 46202, tbellido@iupui.edu. The author has stated that there is no conflict of interest. Disclosures: None
2 Bellido Page 2 Osteocytogenesis and the relationship between osteocyte shape and function Between 5 to 20% of mature osteoblasts become entombed in the matrix that they generate and that subsequently mineralizes. The process of osteocyte formation was long thought to be stochastic. However, some osteoblasts might be prompted to extend cytoplasmic projections and to contact with already embedded cells, resulting in their differentiation into osteocytes. The mechanisms that regulate osteocytogenesis and osteocyte maturation have begun to be revealed. Expression of the membrane-associated proteins E11 and metalloproteinase MMP14 (also known as MT1-MMP) is required for the formation of osteocyte dendritic processes and canaliculi (1-3), suggesting that osteocytogenesis is an active process driven by changes in gene expression. Osteocyte formation is one of the three possible fates of mature osteoblasts, the other two being becoming lining cells or undergoing apoptosis (Figure 1). It is then expected that stimuli that alter one of the fates of osteoblasts would impact osteocyte formation. Consistent with this notion, inhibition of osteoblast apoptosis by intermittent administration of parathyroid hormone (PTH) leads to increased osteocyte density (4;5). However, it is still unknown whether this effect of the hormone is accompanied by changes in the expression of genes required for the osteoblast-osteocyte transition. Osteocytes express most of the genes expressed by osteoblasts, including osteoblast-specific transcription factors and proteins, although the levels of expression may differ (Figure 2) (6). Thus, alkaline phosphatase and type I collagen expression is lower whereas osteocalcin expression is higher in osteocytes. Keratocan, an extracellular matrix protein that belongs to the small leucine rich proteoglycan family, has emerged as an osteoblast marker because its expression is greatly reduced in osteocytes compared to osteoblasts (6;7). Another gene that appears to be expressed preferentially in osteoblasts is integrin binding sialoprotein (8;9). Osteocytes, on the other hand, are richer than osteoblasts in genes related to mineralization and phosphate metabolism, including phosphate-regulating neutral endopeptidase (Phex), dentin matrix protein 1 (DMP1), matrix extracellular phosphoglycoprotein (MEPE) and fibroblast growth factor 23 (FGF23) (6;10). Osteocytes also express molecules that affect bone formation, including Dkk1, which also can be found in osteoblasts, and Sost, which is primarily expressed in osteocytes, but not in osteoblasts (10;11). The product of the sost gene sclerostin potently antagonizes several members of the bone morphogenetic protein (BMP) family of proteins. In addition, both sclerostin and Dkk1 bind to LRP5 and LPR6 preventing activation of Wnt signaling. BMPs and Wnts are critical for osteoblast generation and function as they induce commitment of multipotential mesenchymal progenitors towards the osteoblast lineage, stimulate osteoblast differentiation, and regulate osteoblast activity (Figure 1A). Thus, through the expression of Wnt and BMP antagonists, osteocytes have the potential to regulate the formation and activity of osteoblasts. Osteocyte bodies are individually encased in lacunae and exhibit cytoplasmic dendritic processes that run along narrow canaliculi within the mineralized matrix (Figure 1) (10). Osteocyte morphology is dictated by the expression of genes involved in dendrite formation and branching, such as E11/gp38, CD44, and fimbrin (Figure 2), which are also expressed in neurons and give osteocytes their characteristic morphology in vivo as well as in culture. Numerous cytoplasmic projections (fifty in average in human bone) emerge from each osteocyte body. Projections from neighboring osteocytes touch each other within the canaliculi and establish intercellular communications through gap junctions. Osteocytic projections running inside canaliculi also reach the periosteal and endocortical surfaces of cortical bone as well as the surfaces adjacent to the bone marrow in cancellous bone. Thus, there is potential for direct cell-to-cell interactions between osteocytes and other bone cells (lining cells, osteoblasts and osteoclasts), and the marrow stroma. In turn, cells in the marrow establish contact with endothelial cells of the blood vessels. It appears that
3 Bellido Page 3 osteocytes also establish direct contact with blood vessels within the marrow and with capillaries derived from the Haversian canals in cortical bone (10). Nevertheless, it remains uncertain how proteins expressed by osteocytes reach their cellular targets. The fluid running in the lacunar-canalicular system could transport proteins secreted by osteocytes to their sites of action, provided that the osteocyte products are proteins up to 70kDa and 7 nm in diameter, as estimated by tracer experiments (9;12). However, it is less clear how and whether high molecular size proteins move through the osteocytic lacunar-canalicular system. Furthermore, in the case of membrane proteins which exert their effects through cell-to-cell interactions, direct contact between the osteocytic dendritic processes and the plasma membranes of the cellular targets must occur. The composition of the pericellular matrix surrounding osteocytes adds another layer of control over diffusion of molecules within the osteocyte network, as it will be discussed in section 2 latter in this review. 2. Modulation of bone formation and resorption by osteocyte-derived molecules Regulation of bone formation by osteocytes: role of sclerostin Mature osteocytes embedded in the matrix selectively secrete sclerostin, the product of the Sost gene, which antagonizes several members of the BMP family of proteins and also binds to LRP5/LRP6 preventing canonical Wnt signaling (11;13;14). Sclerostin is a potent inhibitor of bone formation (15). Genetic and pharmacologic evidence supports this mechanism. Loss of SOST expression in humans causes the high bone mass disorders Van Buchem's disease (16) and sclerosteosis (17). Mice with targeted deletion of the Sost gene display progressive high bone mass and increased bone strength (18;19); whereas, conversely, transgenic mice overexpressing human SOST exhibit low bone mass (15;20;21). These findings demonstrate conservation throughout the species of the inhibitory effect of sclerostin on bone formation. Pharmacologic inhibition of sclerostin with neutralizing antibodies leads to marked anabolic effects in several preclinical osteopenic animal models and it is currently in clinical trials for the treatment of postmenopausal osteoporosis, validating the high potential of targeting osteocytes for increasing bone mass and strength (22-25). Sclerostin is also regulated by stimuli with anabolic effects on the skeleton. In particular, elevation of parathyroid hormone (PTH), either in an intermittent or a continuous mode, downregulates sclerostin expression in osteocytes in mice and decreases the circulating levels of the protein in humans (11;26-29) (Figure 3). Furthermore, changes in sclerostin expression are responsible for the adaptive responses of the skeleton to mechanical stimulation. Thus, cortical bone areas exposed to high mechanical strain exhibit a reduction in sclerostin-positive osteocytes that is associated with higher bone formation on adjacent periosteal surfaces (30). Conversely, sost/sclerostin expression is high in unloaded bones (30). Taken together, these findings suggest that osteocytes coordinate the osteogenic response to mechanical force by downregulating sclerostin, thereby locally unleashing Wnt signaling. In fact, mice overexpressing a human SOST transgene in osteocytes, which cannot be downregulated by loading, failed to exhibit activation of the Wnt pathway and the anabolic response to mechanical stimulation (31). Therefore, Sost downregulation is an obligatory step for mechanotransduction. Regulation of bone resorption by osteocytes: RANKL and OPG The cues that signal bone resorption are not completely understood. One important event in the regulation of remodeling appears to be the apoptosis of osteocytes, which might prompt lining cells to form the bone remodeling compartment (BRC) (Figure 3 and Figure 4) and could also signal to neighboring cells (osteocytes or other osteoblast lineage cells) to change
4 Bellido Page 4 the expression of pro- and anti-osteoclastogenic genes. Apoptotic osteocytes could regulate the recruitment of osteoclast precursors and their differentiation in two ways. Osteocyte apoptosis may indirectly stimulate osteoclastogenesis by inducing stromal/osteoblastic cells to secrete RANKL. In addition, osteocytes can directly produce and potentially secrete RANKL. Indeed, in vitro, purified osteocytes express higher levels of RANKL than osteoblasts and bone marrow stromal cells (32). The osteopetrotic phenotype observed in mice lacking RANKL in osteocytes supports the notion that osteocytes are a major source of RANKL in remodeling bone (32;33). As it will be discussed below, these conditional knockout mice are resistant to bone loss induced by tail suspension demonstrating that osteocytic RANKL contributes to disuse osteopenia (33). It remains unknown however whether osteocytic membrane-bound or soluble RANKL is involved in osteocyte-driven bone resorption. The decreased bone resorption exhibited by mice lacking RANKL in osteocytes was accompanied by lower expression of RANKL in bone but no decreased soluble RANKL in the circulation (33). Moreover, no changes in circulating soluble RANKL were found in tail suspended mice [(34) and Bellido et al, unpublished]. Furthermore, the contribution of soluble RANKL to osteoclastogenesis in a novel, 3D-coculture system between osteocytes and osteoclast precursors was found minimal. Instead, direct contact between membrane-bound RANKL expressed in the osteocytic dendrites and RANK expressed in osteoclast precursors appears to be required to initiate osteoclast development (35). Resorption induced by exclusive activation of the PTH receptor in osteocytes in transgenic mice is also associated to increased RANKL (36-38); and the bone loss induced during lactation, which is accompanied by increased PTHrP, is dependent on the expression of osteocytic PTH receptor (36;39) (Figure 3). In the latter case, it was shown that osteocytes can remove bone matrix by remodeling their perilacunar/canalicular matrix. Osteocytes from lactating animals exhibit elevated expression of genes known to be utilized by osteoclasts to remove bone, including tartrate-resistant acid phosphatase (TRAP) and cathepsin K, suggesting that osteocytes remove mineralized matrix through molecular mechanisms similar to those utilized by osteoclasts (39). Considering that the matrix surrounding osteocytes is a likely sieve regulating the diffusion of cellular products, control by osteocytes of their own pericellular matrix might have implications for the molecular transport within the lacunarcanalicular system. Thus, changes in matrix composition or mineral deposition surrounding osteocytes due to altered osteocyte function or decreased osteocyte viability might add an additional level of regulation to the movement of osteocytic products within the lacunaecanalicular system. Osteocytes also secrete OPG, which competes with RANKL for its receptor RANK on osteoclast precursors. In osteocytes, as in osteoblasts, OPG secretion is regulated by the Wnt/β-catenin pathway and mice lacking β-catenin in osteocytes are osteoporotic due to increased osteoclast numbers and bone resorption (9). In addition, emerging evidence also points to osteocytes as an additional source of secreted M-CSF in bone (40). Together, these novel findings suggest that osteocytes have the potential to control bone resorption through direct and indirect regulation of osteoclast differentiation and function under physiological and pathological conditions. 3. Osteocyte apoptosis: Regulation and consequences That osteocytes perceive changes in the level of both physical stimuli as well as circulating factors is evidenced by studies on the regulation of their life span (41-43). Osteocytes are long-lived cells. However, like osteoblasts and osteoclasts, they die by apoptosis. The early work of Noble and colleagues showed an association between osteocyte apoptosis and estrogen withdrawal (44). Subsequent studies by this and other research groups
5 Bellido Page 5 demonstrated the role of estrogen and SERMS preserving osteocyte viability (45-49). It is now recognized that decreased osteocyte viability accompanies not only the bone fragility syndrome that characterizes estrogen withdrawal, but also glucocorticoid excess, mechanical disuse, and aging (34;50;51). Conversely, preservation of osteocyte viability might result from physiological levels of mechanical stimulation (34;52) and is associated with the antifracture effects of treatment with sex steroids (48;49) or bisphosphonates (53). Inhibition of osteocyte apoptosis by mechanical stimulation and activation of Wnt signaling Mechanical stimulation of osteocytic cells or authentic osteocytes protects them from the pro-apoptotic action of death inducers including glucocorticoids (54;55). Mechanotransduction is accomplished by a signalsome assembled at caveolin-rich domains of the plasma membrane and composed of integrins, cytoskeletal proteins, the focal adhesion kinase FAK, and the Src kinase. Downstream activation of the ERK pathway results in preservation of osteocyte viability (54). Activation of Wnt signaling is an early response of osteocytes (and osteoblasts) to mechanical loading (5;56-58) that also promotes osteocyte survival by activating ERKs (59). Moreover, there is interaction between the caveolin-1/erk and Wnt/β-catenin signaling pathways in osteocytes (60). ERK nuclear translocation and anti-apoptosis induced by mechanical stretching or fluid flow is abolished by the Wnt antagonist DKK1 and the stimulator of β-catenin degradation Axin2. Conversely, glycogen synthase kinase 3β (GSK3β) phosphorylation and β-catenin accumulation induced by mechanical stimulation are abolished either by pharmacologic inhibition of ERKs or by silencing caveolin-1. The simultaneous requirement of β-catenin for ERK activation and of ERK activation for β-catenin accumulation suggests a bidirectional crosstalk between the caveolin-1/erks and the Wnt/β-catenin pathways in mechanotransduction leading to osteocyte survival (60). Remarkably, the inhibitor of transcription induced by canonical Wnt signaling dominant negative T cell factor (TCF) does not alter ERK nuclear translocation or survival induced by mechanical stimulation. Thus, β-catenin accumulation is an essential component of the mechanotransduction machinery in osteocytes, albeit β-catenin/tcf-mediated transcription is not required. Dying osteocytes: primary culprits for the bone loss induced by physical inactivity Mechanical forces also regulate osteocyte life span in vivo. Apoptotic osteocytes are found in unloaded bones (34) or in bones exposed to high levels of mechanical strain (41;61;62). In both cases, increased osteocyte apoptosis precedes osteoclastic resorption; and apoptotic osteocytes accumulate in areas subsequently removed by osteoclasts (34). These findings suggest that dying osteocytes become the beacons for osteoclast recruitment to the vicinity and the resulting increase in bone resorption (63) (Figure 4). Indeed, targeted ablation of osteocytes by genetic means is sufficient to induce osteoclast recruitment and resorption leading to bone loss (64). It is possible that osteocytes produce molecules that restrain osteoclast recruitment and/or formation; thereby when osteocytes die, there is a spontaneous increase in osteoclast genesis. A potential candidate mediating this phenomenon is OPG, the decoy receptor for RANKL, which is expressed in osteocytes at least at similar levels than in osteoblasts (9). Alternatively, in the process of undergoing apoptosis, osteocytes might produce molecular signals that attract osteoclast precursors and/or factors that stimulate osteoclast development. A potential molecular mediator in this case is the osteoclast chemotactic factor high mobility group box 1 (HMGB1) protein (65), which is released by osteocytes undergoing apoptosis and that upregulates the expression of RANKL, TNF and, IL6, and also decreases OPG expression. Apoptotic bodies released from dying osteocytes are another potential signal leading to changes in gene expression in surrounding cells (66). Apoptotic bodies produced by osteocytic cells, but not by osteoblastic cells, have been shown to stimulate osteoclast differentiation and to initiate localized bone resorption,
6 Bellido Page 6 although RANKL was apparently not involved (67). Furthermore, in overloaded rat bones, dead osteocytes are surrounded by still-living osteocytes in which the expression of VEGF and RANKL is elevated (68), suggesting that signals emanated from apoptotic cells alter the expression of molecules that influence angiogenesis and potentially osteoclast precursor recruitment, as well as osteoclast differentiation. In contrast to the increasing knowledge about the role of osteocyte apoptosis in remodeling bone, whether osteocyte apoptosis plays any role in bone modeling remains unknown. Future studies specifically designed to answer this question are still warranted. Mechanical loading is critical for the maintenance of bone mass; and skeletal unloading as with reduced physical activity with old age, immobilization of bed rest, and total or partial motor paralyses, causes bone loss leading to disuse osteoporosis (69). Furthermore, the bone loss that ensues under microgravity conditions represents the most significant hindrance for long-term space flying (70). The rapid decrease in osteocyte viability with unloading had suggested that osteocytes are the first responders to the change in mechanical forces (34). Consistent with this notion, mice depleted from osteocytes are protected from the bone loss induced by tail suspension indicating that in the absence of osteocytes the skeleton is unable to elicit the normal osteoclastogenic response (64). Mice with conditional deletion of RANKL in osteocytes are also protected from unloading-induced elevation in osteoclasts and bone loss (33), suggesting that osteocytes provide the required RANKL for osteoclast formation during skeletal disuse. These findings confirm that osteocytes are the primary culprit of the negative bone balance that ensues with weightlessness. Regulation of osteocyte survival by sex steroids and bisphosphonates Loss of sex steroids leads to increased prevalence of osteocyte apoptosis; and conversely, estrogens and androgens inhibit apoptosis of osteocytes as well as osteoblasts (5;48). This anti-apoptotic effect is due to rapid activation of the Src/Shc/ERK and PI3K signaling pathways through non-genotropic actions of the classical receptors for sex steroids (48;71). Bisphosphonates also preserve viability of osteocytes (and osteoblasts) in vitro and in vivo, by a mechanism that in this case involves opening of connexin (Cx) 43 hemichannels and ERK activation (42;53;72;73). The fact that apoptotic osteocytes trigger bone resorption, taken together with the evidence that osteocyte apoptosis is inhibited by estrogens and bisphosphonates, raises the possibility that preservation of osteocyte viability contributes to the anti-remodeling properties of these agents. Aging and osteocyte apoptosis One of the functions of the osteocyte network is to detect microdamage and trigger its repair (74;75). During aging, there is accumulation of microdamage and a decline in osteocyte density accompanied by decreased prevalence of osteocyte-occupied lacunae, an index of premature osteocyte death (76). Reduced osteocyte density might be a direct consequence of increased osteoblast apoptosis; whereas increase in the prevalence of apoptotic osteocytes might result from the decline in physical activity with old age leading to reduced skeletal loading, accumulation of reactive oxygen species (ROS) in bone (77) and/or increased levels of endogenous glucocorticoids with age (78). Age-related loss of osteocytes could be then at least partially responsible for the disparity between bone quantity and quality that occurs with aging. Connexin-43 and osteocyte survival Osteocytic expression of the gap junction channel/hemichannel protein C 43 is required in a cell autonomous fashion to preserve the viability of osteocytes, as well as to control in osteocytes the levels of proteins that regulate the generation and activity of osteoclast and
7 Bellido Page 7 osteoblasts (79;80). C 43 deficiency causes an intrinsic reduction in OPG expression and loss of viable osteocytes, with the consequent decrease in local levels of the bone formation inhibitor sclerostin. Anatomical mapping of apoptotic osteocytes, osteocytic protein expression, and resorption and formation suggests that C 43 controls osteoclast and osteoblast activity by regulating OPG and sclerostin levels, respectively, in osteocytes located in specific areas of cortical bone. Whereas empty lacunae and living osteocytes lacking OPG are distributed throughout cortical bone of mice lacking osteocytic C 43, apoptotic osteocytes preferentially locate in areas containing osteoclasts, suggesting that osteoclast recruitment requires active signaling from dying osteocytes. Furthermore, cultured osteocytic cells lacking C 43 exhibit increased rate of apoptosis, decreased OPG and increased RANKL expression (79;81). Similar molecular changes are observed in bones of mice lacking C 43 in osteocytes. Moreover, these conditional knockout mice display increased endocortical resorption and exaggerated periosteal bone apposition resulting in altered cortical bone geometry. As a consequence, long bones from mice deficient in C 43 in osteocytes exhibit enlarged bone marrow cavities and increased cross sectional diameter (79;81;82). Accumulation of apoptotic osteocytes and empty lacunae, increased endocortical resorption and periosteal expansion of the long bones resemble bones from aging rodents and humans (51;83). C 43 is a Wnt target gene (84) and Wnt signaling as well as C 43 expression decrease with age in bone [(51) and Plotkin et al, unpublished]. Therefore, reduced C 43 expression might mediate at least some of the changes induced by aging in the skeleton. 4. Therapeutic implications of osteocyte-driven bone remodeling and closing remarks Acknowledgments References In closing, research from the last decade greatly increased our understanding of the biology of osteocytes and revealed previously unrecognized mechanisms by which bone acting stimuli regulate the skeleton through effects on these cells. We now know that some of the most profound effects that hormones, such as PTH or glucocorticoids, exert on bone are mediated by actions on osteocytes. The fact that osteocyte apoptosis underlies osteocytedriven bone resorption raises the possibility that bisphosphonates and estrogens, which prevent osteocyte apoptosis, exert part of their anti-remodeling effects acting on osteocytes. Moreover, the discovery that osteocytes are the major source of RANKL in remodeling bone strongly suggest that the potent antiresorptive effects of the anti-rankl antibody are exerted by inhibiting osteolytic RANKL. Our current knowledge of the molecular events by which osteocytes influence the function of osteoblasts and osteoclasts has opened new opportunities for developing therapeutic strategies to regulate bone remodeling targeting osteocytes. The neutralizing antibody against sclerostin is the best example of an approach that positively impacts the skeleton by controlling an osteocytic product. It is expected that future investigations will identify new genes expressed in osteocytes, thereby increasing the number of potential targets of pharmacological intervention towards an improved management of bone diseases. This research was supported by the National Institutes of Health (R01-AR053643, KO2-AR02127, R03 TW006919, R01-DK076007, and P01-AG13918). 1. Zhang K, Barragan-Adjemian C, Ye L, Kotha S, Dallas M, Lu Y, Zhao S, et al. E11/gp38 selective expression in osteocytes: regulation by mechanical strain and role in dendrite elongation. Mol Cell Biol. 2006; 26: [PubMed: ]
8 Bellido Page 8 2. Holmbeck K, Bianco P, Caterina J, Yamada S, Kromer M, Kuznetsov SA, Mankani M, et al. MT1- MMP-deficient mice develop dwarfism, osteopenia, arthritis, and connective tissue disease due to inadequate collagen turnover. Cell. 1999; 99: [PubMed: ] 3. Holmbeck K, Bianco P, Pidoux I, Inoue S, Billinghurst RC, Wu W, Chrysovergis K, et al. The metalloproteinase MT1-MMP is required for normal development and maintenance of osteocyte processes in bone. J Cell Sci. 2005; 118: [PubMed: ] 4. Jilka RL, Weinstein RS, Bellido T, Roberson P, Parfitt AM, Manolagas SC. Increased bone formation by prevention of osteoblast apoptosis with parathyroid hormone. J Clin Invest. 1999; 104: [PubMed: ] 5. Boyce, BF.; Xing, L.; Jilka, RL.; Bellido, T.; Weinstein, RS.; Parfitt, AM.; Manolagas, SC. Apoptosis in bone cells. In: Bilezikian, JP.; Raisz, LG.; Rodan, GA., editors. Principles of Bone Biology. Academic Press; San Diego, San Francisco, New York, London, Sydney, Tokyo: p Paic F, Igwe JC, Nori R, Kronenberg MS, Franceschetti T, Harrington P, Kuo L, et al. Identification of differentially expressed genes between osteoblasts and osteocytes. Bone. 2009; 45: [PubMed: ] 7. Igwe JC, Gao Q, Kizivat T, Kao WW, Kalajzic I. Keratocan is Expressed by Osteoblasts and Can Modulate Osteogenic Differentiation. Connect Tissue Res. 2011; 52: [PubMed: ] 8. Benson MD, Aubin JE, Xiao G, Thomas PE, Franceschi RT. Cloning of a 2.5 kb murine bone sialoprotein promoter fragment and functional analysis of putative Osf2 binding sites. J Bone Miner Res. 1999; 14: [PubMed: ] 9. Kramer I, Halleux C, Keller H, Pegurri M, Gooi JH, Weber PB, Feng JQ, et al. Osteocyte Wnt/betacatenin signaling is required for normal bone homeostasis. Mol Cell Biol. 2010; 30: [PubMed: ] 10. Bonewald LF. The Amazing Osteocyte. J Bone Miner Res. 2011; 26: [PubMed: ] 11. Bellido T, Ali AA, Gubrij I, Plotkin LI, Fu Q, O'Brien CA, Manolagas SC, et al. Chronic elevation of PTH in mice reduces expression of sclerostin by osteocytes: a novel mechanism for hormonal control of osteoblastogenesis. Endocrinology. 2005; 146: [PubMed: ] 12. Wang L, Ciani C, Doty SB, Fritton SP. Delineating bone's interstitial fluid pathway in vivo. Bone. 2004; 34: [PubMed: ] 13. Poole KE, Van Bezooijen RL, Loveridge N, Hamersma H, Papapoulos SE, Lowik CW, Reeve J. Sclerostin is a delayed secreted product of osteocytes that inhibits bone formation. FASEB J. 2005; 19: [PubMed: ] 14. Van Bezooijen RL, Roelen BA, Visser A, Wee-Pals L, de Wilt E, Karperien M, Hamersma H, et al. Sclerostin is an osteocyte-expressed negative regulator of bone formation, but not a classical BMP antagonist. J Exp Med. 2004; 199: [PubMed: ] 15. Winkler DG, Sutherland MK, Geoghegan JC, Yu C, Hayes T, Skonier JE, Shpektor D, et al. Osteocyte control of bone formation via sclerostin, a novel BMP antagonist. EMBO J. 2003; 22: [PubMed: ] 16. Balemans W, Ebeling M, Patel N, Van Hul E, Olson P, Dioszegi M, Lacza C, et al. Increased bone density in sclerosteosis is due to the deficiency of a novel secreted protein (SOST). Hum Mol Genet. 2001; 10: [PubMed: ] 17. Brunkow ME, Gardner JC, Van Ness J, Paeper BW, Kovacevich BR, Proll S, Skonier JE, et al. Bone dysplasia sclerosteosis results from loss of the SOST gene product, a novel cystine knotcontaining protein. Am J Hum Genet. 2001; 68: [PubMed: ] 18. Li X, Ominsky MS, Niu QT, Sun N, Daugherty B, D'Agostin D, Kurahara C, et al. Targeted deletion of the sclerostin gene in mice results in increased bone formation and bone strength. J Bone Miner Res. 2008; 23: [PubMed: ] 19. Lin C, Jiang X, Dai Z, Guo X, Weng T, Wang J, Li Y, et al. Sclerostin mediates bone response to mechanical unloading through antagonizing Wnt/beta-catenin signaling. J Bone Miner Res. 2009; 24: [PubMed: ]
9 Bellido Page Loots GG, Kneissel M, Keller H, Baptist M, Chang J, Collette NM, Ovcharenko D, et al. Genomic deletion of a long-range bone enhancer misregulates sclerostin in Van Buchem disease. Genome Res. 2005; 15: [PubMed: ] 21. Rhee Y, Allen MR, Condon K, Lezcano V, Ronda AC, Galli C, Olivos N, et al. PTH receptor signaling in osteocytes governs periosteal bone formation and intra-cortical remodeling. J Bone Miner Res. 2011; 26: [PubMed: ] 22. Warmington K, Morony S, Sarosi I, Gong G, Stepphens P, Winkler DG, Sutherland MK, et al. Sclerostin antagonism in adult rodents, via monoclonal antibody mediated blockade, increases bone mineral density and implicates sclerostin as a key regulator of bone mass during adulthood. J Bone Min Res. 2004; 19:S Warmington K, Ominsky M, Bolon B, Cattley R, Stephens P, Lawson A, Lightwood D, et al. Sclerostin monoclonal antibody treatment of osteoporotic rats completely reverses one year of ovariectomy-induced systemic bone loss. J Bone Min Res. 2005; 20:S Paszty C, Turner CH, Robinson MK. Sclerostin: a gem from the genome leads to bone-building antibodies. J Bone Miner Res. 2010; 25: [PubMed: ] 25. Jilka RL. Inhibiting the inhibitor: a new route to bone anabolism. J Bone Miner Res. 2009; 24: [PubMed: ] 26. Keller H, Kneissel M. SOST is a target gene for PTH in bone. Bone. 2005; 37: [PubMed: ] 27. van Lierop AH, Witteveen J, Hamdy N, Papapoulos S. Patients with primary hyperparathyroidism have lower circulating sclerostin levels than euparathyroid controls. Eur J Endocrinol. 2010; 163: [PubMed: ] 28. Drake MT, Srinivasan B, Modder UI, Peterson JM, McCready LK, Riggs BL, Dwyer D, et al. Effects of parathyroid hormone treatment on circulating sclerostin levels in postmenopausal women. J Clin Endocrinol Metab. 2010; 95: [PubMed: ] 29. Mirza FS, Padhi ID, Raisz LG, Lorenzo JA. Serum sclerostin levels negatively correlate with parathyroid hormone levels and free estrogen index in postmenopausal women. J Clin Endocrinol Metab. 2010; 95: [PubMed: ] 30. Robling AG, Niziolek PJ, Baldridge LA, Condon KW, Allen MJ, Alam I, Mantila SM, et al. Mechanical stimulation of bone in vivo reduces osteocyte expression of Sost/sclerostin. J Biol Chem. 2008; 283: [PubMed: ] 31. Tu X, Rhee Y, Condon KW, Bivi N, Allen MR, Dwyer D, Stolina M, et al. Sost downregulation and local Wnt signaling are required for the osteogenic response to mechanical loading. Bone. 2012; 50: [PubMed: ] 32. Nakashima T, Hayashi M, Fukunaga T, Kurata K, Oh-hora M, Feng JQ, Bonewald LF, et al. Evidence for osteocyte regulation of bone homeostasis through RANKL expression. Nat Med. 2011; 17: [PubMed: ] 33. Xiong J, Onal M, Jilka RL, Weinstein RS, Manolagas SC, O'Brien CA. Matrix-embedded cells control osteoclast formation. Nat Med. 2011; 17: [PubMed: ] 34. Aguirre JI, Plotkin LI, Stewart SA, Weinstein RS, Parfitt AM, Manolagas SC, Bellido T. Osteocyte apoptosis is induced by weightlessness in mice and precedes osteoclast recruitment and bone loss. J Bone Min Res. 2006; 21: Honma M, Ikebuchi Y, Kariya Y, Hayashi M, Hayashi N, Aoki S, Suzuki H. RANKL subcellular trafficking and regulatory mechanisms in osteocytes. J Bone Miner Res Bellido T, Saini V, Divieti Pajevic P Effects of PTH on osteocyte function. Bone Sep 24. pii: S (12) Epub ahead of print /j.bone Rhee Y, Allen MR, Condon K, Plotkin LI, Lezcano V, Vyas K, O'Brien CA, et al. PTH receptor signaling in osteocytes governs periosteal bone formation and intra-cortical remodeling: divergent role of Sost and the Wnt pathway. J Bone Min Res. 2009; 24:S O'Brien CA, Plotkin LI, Galli C, Goellner J, Gortazar AR, Allen MR, Robling AG, et al. Control of bone mass and remodeling by PTH receptor signaling in osteocytes. PLoS ONE. 2008; 3:e2942. [PubMed: ]
10 Bellido Page Qing H, Ardeshirpour L, Pajevic PD, Dusevich V, Jahn K, Kato S, Wysolmerski J, et al. Demonstration of osteocytic perilacunar/canalicular remodeling in mice during lactation. J Bone Miner Res. 2012; 27: [PubMed: ] 40. Harris SE, MacDougall M, Horn D, Woodruff K, Zimmer SN, Rebel VI, Fajardo R, et al. Meox2Cre-mediated disruption of CSF-1 leads to osteopetrosis and osteocyte defects. Bone. 2012; 50: [PubMed: ] 41. Noble BS, Peet N, Stevens HY, Brabbs A, Mosley JR, Reilly GC, Reeve J, et al. Mechanical loading: biphasic osteocyte survival and the targeting of osteoclasts for bone destruction in rat cortical bone. Am J Physiol Cell Physiol. 2003; 284:C934 C943. [PubMed: ] 42. Bellido T, Plotkin LI. Novel actions of bisphosphonates in bone: Preservation of osteoblast and osteocyte viability. Bone. 2011; 49: [PubMed: ] 43. Jilka, RL.; Bellido, T.; Almeida, M.; Plotkin, LI.; O'Brien, CA.; Weinstein, RS.; Manolagas, SC. Apoptosis in bone cells. In: Bilezikian, JP.; Raisz, LG.; Martin, TJ., editors. Principles of Bone Biology. Academic Press; San Diego, San Francisco, New York, London, Sydney, Tokyo: p Tomkinson A, Reeve J, Shaw RW, Noble BS. The death of osteocytes via apoptosis accompanies estrogen withdrawal in human bone. J Clin Endocrinol Metab. 1997; 82: [PubMed: ] 45. Tomkinson A, Gevers EF, Wit JM, Reeve J, Noble BS. The role of estrogen in the control of rat osteocyte apoptosis. J Bone Min Res. 1998; 13: Huber C, Collishaw S, Mosley JR, Reeve J, Noble BS. Selective estrogen receptor modulator inhibits osteocyte apoptosis during abrupt estrogen withdrawal: implications for bone quality maintenance. Calcif Tissue Int. 2007; 81: [PubMed: ] 47. Mann V, Huber C, Kogianni G, Collins F, Noble B. The antioxidant effect of estrogen and Selective Estrogen Receptor Modulators in the inhibition of osteocyte apoptosis in vitro. Bone. 2007; 40: [PubMed: ] 48. Kousteni S, Bellido T, Plotkin LI, O'Brien CA, Bodenner DL, Han L, Han K, et al. Nongenotropic, sex-nonspecific signaling through the estrogen or androgen receptors: dissociation from transcriptional activity. Cell. 2001; 104: [PubMed: ] 49. Kousteni S, Chen JR, Bellido T, Han L, Ali AA, O'Brien CA, Plotkin LI, et al. Reversal of bone loss in mice by nongenotropic signaling of sex steroids. Science. 2002; 298: [PubMed: ] 50. Weinstein RS, Jilka RL, Parfitt AM, Manolagas SC. Inhibition of osteoblastogenesis and promotion of apoptosis of osteoblasts and osteocytes by glucocorticoids: potential mechanisms of their deleterious effects on bone. J Clin Invest. 1998; 102: [PubMed: ] 51. Almeida M, Han L, Martin-Millan M, Plotkin LI, Stewart SA, Roberson PK, Kousteni S, et al. Skeletal involution by age-associated oxidative stress and its acceleration by loss of sex steroids. J Biol Chem. 2007; 282: [PubMed: ] 52. Bellido T. Antagonistic interplay between mechanical forces and glucocorticoids in bone: a tale of kinases. J Cell Biochem. 2010; 111:1 6. [PubMed: ] 53. Plotkin LI, Weinstein RS, Parfitt AM, Roberson PK, Manolagas SC, Bellido T. Prevention of osteocyte and osteoblast apoptosis by bisphosphonates and calcitonin. J Clin Invest. 1999; 104: [PubMed: ] 54. Plotkin LI, Mathov I, Aguirre JI, Parfitt AM, Manolagas SC, Bellido T. Mechanical stimulation prevents osteocyte apoptosis: requirement of integrins, Src kinases and ERKs. Am J Physiol Cell Physiol. 2005; 289:C633 C643. [PubMed: ] 55. Bakker A, Klein-Nulend J, Burger E. Shear stress inhibits while disuse promotes osteocyte apoptosis. Biochem Biophys Res Commun. 2004; 320: [PubMed: ] 56. Bonewald LF, Johnson ML. Osteocytes, mechanosensing and Wnt signaling. Bone. 2008; 42: [PubMed: ] 57. Armstrong VJ, Muzylak M, Sunters A, Zaman G, Saxon LK, Price JS, Lanyon LE. Wnt/β-catenin signaling Is a component of osteoblastic bone cell early responses to load-bearing and requires estrogen receptor α. J Biol Chem. 2007; 282: [PubMed: ]
11 Bellido Page Sunters A, Armstrong VJ, Zaman G, Kypta RM, Kawano Y, Lanyon LE, Price JS. Mechanotransduction in osteoblastic cells involves strain-regulated, Estrogen Receptor {alpha&rcub - mediated, control of IGF-IR sensitivity to ambient IGF, leading to PI3-K/ AKT dependent, Wnt/ LRP5 receptor-independent activation of { beta} -catenin signaling. J Biol Chem. 2010; 285: [PubMed: ] 59. Almeida M, Han L, Bellido T, Manolagas SC, Kousteni S. Wnt proteins prevent apoptosis of both uncommitted osteoblast progenitors and differentiated osteoblasts by beta-catenin-dependent and - independent signaling cascades involving Src/ERK and phosphatidylinositol 3-kinase/AKT. J Biol Chem. 2005; 280: [PubMed: ] 60. Gortazar AR, Martin-Millan M, Bravo B, Plotkin LI, Bellido T. Crosstalk between caveolin-1/ ERKs and ß-catenin survival pathways in osteocyte mechanotransduction. J Biol Chem /jbc.M Verborgt O, Gibson G, Schaffler MB. Loss of osteocyte integrity in association with microdamage and bone remodeling after fatigue in vivo. J Bone Min Res. 2000; 15: Verborgt O, Tatton NA, Majeska RJ, Schaffler MB. Spatial distribution of Bax and Bcl-2 in osteocytes after bone fatigue: complementary roles in bone remodeling regulation? J Bone Miner Res. 2002; 17: [PubMed: ] 63. Bellido T. Osteocyte apoptosis induces bone resorption and impairs the skeletal response to weightlessness. BoneKEy-osteovision. 2007; 4: Tatsumi S, Ishii K, Amizuka N, Li M, Kobayashi T, Kohno K, Ito M, et al. Targeted ablation of osteocytes induces osteoporosis with defective mechanotransduction. Cell Metab. 2007; 5: [PubMed: ] 65. Yang J, Shah R, Robling AG, Templeton E, Yang H, Tracey KJ, Bidwell JP. HMGB1 is a boneactive cytokine. J Cell Physiol. 2008; 214: [PubMed: ] 66. Jilka RL, Noble B, Weinstein RS. Osteocyte apoptosis. Bone Kogianni G, Mann V, Noble BS. Apoptotic bodies convey activity capable of initiating osteoclastogenesis and localised bone destruction. J Bone Miner Res. 2008; 23: [PubMed: ] 68. Kennedy OD, Herman BC, Laudier DM, Majeska RJ, Sun HB, Schaffler MB. Activation of resorption in fatigue-loaded bone involves both apoptosis and active pro-osteoclastogenic signaling by distinct osteocyte populations. Bone. 2012; 50: [PubMed: ] 69. Marcus, R. Mechanisms of exercise effects on bone. In: Bilezikian, JP.; Raisz, LG.; Rodan, GA., editors. Principles of Bone Biology. Academic Press; San Diego: p Bikle DD, Halloran BP, Morey-Holton E. Spaceflight and the skeleton: lessons for the earthbound. Gravit Space Biol Bull. 1997; 10: [PubMed: ] 71. Kousteni S, Han L, Chen JR, Almeida M, Plotkin LI, Bellido T, Manolagas SC. Kinase-mediated regulation of common transcription factors accounts for the bone-protective effects of sex steroids. J Clin Invest. 2003; 111: [PubMed: ] 72. Plotkin LI, Manolagas SC, Bellido T. Transduction of cell survival signals by connexin-43 hemichannels. J Biol Chem. 2002; 277: [PubMed: ] 73. Plotkin LI, Bellido T. Bisphosphonate-induced, hemichannel-mediated, anti-apoptosis through the Src/ERK pathway: a gap junction-independent action of connexin43. Cell Adhes Commun. 2001; 8: Parfitt AM. Life history of osteocytes: relationship to bone age, bone remodeling, and bone fragility. J Musculoskelet Neuronal Interact. 2002; 2: [PubMed: ] 75. Parfitt AM. Targeted and nontargeted bone remodeling: relationship to basic multicellular unit origination and progression. Bone. 2002; 30:5 7. [PubMed: ] 76. Manolagas SC, Parfitt AM. What old means to bone. Trends Endocrinol Metab. 2010; 21: [PubMed: ] 77. Manolagas SC. From Estrogen-Centric to Aging and Oxidative Stress: A Revised Perspective of the Pathogenesis of Osteoporosis. Endocr Rev. 2010; 31: [PubMed: ] 78. Weinstein RS, Wan C, Liu Q, Wang Y, Almeida M, O'Brien CA, Thostenson J, et al. Endogenous glucocorticoids decrease skeletal angiogenesis, vascularity, hydration, and strength in 21-monthold mice. Aging Cell. 2009; 9: [PubMed: ]
12 Bellido Page Bivi N, Condon KW, Allen MR, Farlow N, Passeri G, Brun L, Rhee Y, et al. Cell autonomous requirement of connexin 43 for osteocyte survival: consequences for endocortical resorption and periosteal bone formation. J Bone Min Res. 2012; 27: Plotkin LI, Bellido T. Beyond gap junctions: Connexin43 and bone cell signaling. Bone. 2013; 52: [PubMed: ] 81. Zhang Y, Paul EM, Sathyendra V, Davidson A, Bronson S, Srinivasan S, Gross TS, et al. Enhanced osteoclastic resorption and responsiveness to mechanical load in gap junction deficient bone. PLoS ONE. 2011; 6:e [PubMed: ] 82. Grimston SK, Brodt MD, Silva MJ, Civitelli R. Attenuated response to in vivo mechanical loading in mice with conditional osteoblast ablation of the Connexin43 gene ( Gja1. J Bone Miner Res. 2008; 23: [PubMed: ] 83. Qiu S, Rao DS, Palnitkar S, Parfitt AM. Age and distance from the surface but not menopause reduce osteocyte density in human cancellous bone. Bone. 2002; 31: [PubMed: ] 84. Robinson JA, Chatterjee-Kishore M, Yaworsky PJ, Cullen DM, Zhao W, Li C, Kharode Y, et al. WNT/beta-catenin signaling is a normal physiological response to mechanical loading in bone. J Biol Chem. 2006; 281: [PubMed: ]
13 Bellido Page 13 Figure 1. Osteocytogenesis and osteocyte maturation (A) Stages of osteocytogenesis and main transcription factors involved in differentiation of osteoblast precursors towards mature osteocytes. (B) Row of osteoblasts (bottom red arrows); an osteocyte recently embedded (top red arrow); two osteocytes completely embedded in osteoid (bottom white arrows); an osteocyte fully embedded in mineralized bone matrix (top white arrow). Picture was contributed by Keith Condon, Indiana University School of Medicine, IN, USA. (C) Morphology of an early osteocyte being embedded in bone; with part of the cell surface partially embedded (left) and the other part totally embedded (right) in mineralized matrix, 10,000, rat bone. Picture was contributed by Stephen B. Doty, Hospital for Special Surgery, New York, NY, USA. (Reprinted with kind permission of Elsevier, Basic and Applied Bone Biology, Chapter 2 Bone Cells, Bellido, Plotkin and Bruzzaniti).
14 Bellido Page 14 Figure 2. Gene expression at different stages of osteocyte development and maturation The osteocyte phenotype is characterized by the expression of groups of genes closely related to their morphology and function. Expression of some of these genes changes at different stages of osteocyte development and maturation. Boxes group four main categories: 1) Genes related to dendritic morphology and canaliculi formation; 2) genes related to phosphate metabolism and matrix mineralization; 3) genes that regulate bone formation; and 4) genes that regulate bone resorption. Please, note that several of these genes are also expressed in other cell types, besides cells of the osteoblastic lineage. (Reprinted with kind permission of Elsevier, Basic and Applied Bone Biology, Chapter 2 Bone Cells, Bellido, Plotkin and Bruzzaniti).
15 Bellido Page 15 Figure 3. Regulation of osteoblast and osteoclast production and function by osteocytes Osteocytes regulate bone formation through sost/sclerostin. Thus, bone formation induced by systemic elevation of PTH or local mechanical loading is associated with decreased expression of sclerostin. Osteocytes regulate bone resorption through pro- and antiosteoclastogenic cytokines. Resorption under basal conditions, induced by PTH elevation or by PTHrP increased during lactation is regulated by RANKL through the PTH receptor (PTHR) expressed in osteocytes. Activation of Wnt signaling in osteocytes increases OPG expression leading to inhibition of resorption. Osteocyte apoptosis induced by immobilization, fatigue loading, sex steroid deficiency, or genetically induced by activating diphtheria toxin receptor signaling, is sufficient to recruit osteoclasts to specific bone areas and increase resorption; likely through a mechanism that increases RANKL expression in still-living osteocytes surrounding dead osteocytes. (Reprinted with kind permission of Elsevier, Basic and Applied Bone Biology, Chapter 2 Bone Cells, Bellido, Plotkin and Bruzzaniti).
16 Bellido Page 16 Figure 4. Osteocytes and the bone remodeling compartment (BRC) Apoptotic osteocytes might initiate bone remodeling by sending signals to lining cells, which retract from the bone surface to form a structure named the bone remodeling compartment (BRC). Osteoclast precursors are transported to the BRC by marrow capillaries, differentiate to mature osteoclasts under the influence of pro- and antiosteoclastogenic cytokines (RANKL, M-CSF and OPG) derived from osteocytes, and initiate bone remodeling. Osteoblast precursors from the bone marrow or the circulation differentiate into mature, bone synthesizing cells in response to factors released from the bone matrix by resorption. Differentiation and function of osteoblasts is controlled by molecules derived from osteocytes, including sclerostin and Dkk1. (Reprinted with kind permission of Elsevier, Basic and Applied Bone Biology, Chapter 2 Bone Cells, Bellido, Plotkin and Bruzzaniti).
Mouse Models for the Evaluation of Osteocyte Functions
 J Bone Metab 2014;21:55-60 http://dx.doi.org/10.11005/jbm.2014.21.1.55 pissn 2287-6375 eissn 2287-7029 Review Article Mouse Models for the Evaluation of Osteocyte Functions Toshihisa Komori Department
J Bone Metab 2014;21:55-60 http://dx.doi.org/10.11005/jbm.2014.21.1.55 pissn 2287-6375 eissn 2287-7029 Review Article Mouse Models for the Evaluation of Osteocyte Functions Toshihisa Komori Department
The Osteocyte Network as a Source and Reservoir of Signaling Factors
 Endocrinol Metab 25(3):161-165, September 2010 REVIEW ARTICLE The Osteocyte Network as a Source and Reservoir of Signaling Factors Lynda F. Bonewald Department of Oral Biology, University of Missouri at
Endocrinol Metab 25(3):161-165, September 2010 REVIEW ARTICLE The Osteocyte Network as a Source and Reservoir of Signaling Factors Lynda F. Bonewald Department of Oral Biology, University of Missouri at
Parathyroid Hormone Receptor Signaling Induces Bone Resorption in the Adult Skeleton by Directly Regulating the RANKL Gene in Osteocytes
 CALCIUM-REGULATING HORMONES Parathyroid Hormone Receptor Signaling Induces Bone Resorption in the Adult Skeleton by Directly Regulating the RANKL Gene in Osteocytes Abdullah N. Ben-awadh, Jesus Delgado-Calle,
CALCIUM-REGULATING HORMONES Parathyroid Hormone Receptor Signaling Induces Bone Resorption in the Adult Skeleton by Directly Regulating the RANKL Gene in Osteocytes Abdullah N. Ben-awadh, Jesus Delgado-Calle,
silent epidemic,. (WHO),
 Tel: 02-740-8686; E-mail: hhbkim@snu.ac.kr silent epidemic,. (WHO),. 5 3, 1. 50 70. 50%, 25%, 20% (12~35%). 2.8% 0.7% 4. ( ). bone remodeling (osteoblast), (osteoclast),.. 3~4.. 70% (osteocyte) (bone lining
Tel: 02-740-8686; E-mail: hhbkim@snu.ac.kr silent epidemic,. (WHO),. 5 3, 1. 50 70. 50%, 25%, 20% (12~35%). 2.8% 0.7% 4. ( ). bone remodeling (osteoblast), (osteoclast),.. 3~4.. 70% (osteocyte) (bone lining
Pathophysiology of Postmenopausal & Glucocorticoid Induced Osteoporosis. March 15, 2016 Bone ECHO Kate T Queen, MD
 Pathophysiology of Postmenopausal & Glucocorticoid Induced Osteoporosis March 15, 2016 Bone ECHO Kate T Queen, MD Review: normal bone formation Bone Modeling Remodeling Peak Bone Mass Maximum bone mass
Pathophysiology of Postmenopausal & Glucocorticoid Induced Osteoporosis March 15, 2016 Bone ECHO Kate T Queen, MD Review: normal bone formation Bone Modeling Remodeling Peak Bone Mass Maximum bone mass
Functions of the osteocyte network in the regulation of bone mass
 Cell Tissue Res (2013) 352:191 198 DOI 10.1007/s00441-012-1546-x REVIEW Functions of the osteocyte network in the regulation of bone mass Toshihisa Komori Received: 3 September 2012 / Accepted: 5 December
Cell Tissue Res (2013) 352:191 198 DOI 10.1007/s00441-012-1546-x REVIEW Functions of the osteocyte network in the regulation of bone mass Toshihisa Komori Received: 3 September 2012 / Accepted: 5 December
Integrity of the osteocyte bone cell network in osteoporotic fracture: Implications for mechanical load adaptation
 IOP Conference Series: Materials Science and Engineering Integrity of the osteocyte bone cell network in osteoporotic fracture: Implications for mechanical load adaptation To cite this article: J S Kuliwaba
IOP Conference Series: Materials Science and Engineering Integrity of the osteocyte bone cell network in osteoporotic fracture: Implications for mechanical load adaptation To cite this article: J S Kuliwaba
Osteocytes in Health and Disease
 Osteocytes in Health and Disease Nigel Loveridge Bone Research Group Cambridge With the very grateful help of: Andy Pitsillides, Ken Poole, Brendon Noble, Jonathan Reeve, Mitch Schaffler Osteocytes Entombed
Osteocytes in Health and Disease Nigel Loveridge Bone Research Group Cambridge With the very grateful help of: Andy Pitsillides, Ken Poole, Brendon Noble, Jonathan Reeve, Mitch Schaffler Osteocytes Entombed
The Osteocyte: An Endocrine Cell... and More. Sarah L. Dallas, Matthew Prideaux, and Lynda F. Bonewald
 REVIEW The Osteocyte: An Endocrine Cell... and More Sarah L. Dallas, Matthew Prideaux, and Lynda F. Bonewald Department of Oral and Craniofacial Sciences, School of Dentistry, University of Missouri-Kansas
REVIEW The Osteocyte: An Endocrine Cell... and More Sarah L. Dallas, Matthew Prideaux, and Lynda F. Bonewald Department of Oral and Craniofacial Sciences, School of Dentistry, University of Missouri-Kansas
Osteocytes-The Known and Unknown Osteositler-Bilinenler ve Bilinmeyenler
 Review Derleme 23 Osteocytes-The Known and Unknown Osteositler-Bilinenler ve Bilinmeyenler Celal Bayar University, Medical Faculty, Department of Internal Medicine, Division of Endocrinology and Metabolism,
Review Derleme 23 Osteocytes-The Known and Unknown Osteositler-Bilinenler ve Bilinmeyenler Celal Bayar University, Medical Faculty, Department of Internal Medicine, Division of Endocrinology and Metabolism,
Cover Page. The handle holds various files of this Leiden University dissertation.
 Cover Page The handle http://hdl.handle.net/1887/20541 holds various files of this Leiden University dissertation. Author: Lierop, Antoon van Title: Sclerostin : a key regulator of bone metabolism Issue
Cover Page The handle http://hdl.handle.net/1887/20541 holds various files of this Leiden University dissertation. Author: Lierop, Antoon van Title: Sclerostin : a key regulator of bone metabolism Issue
BONE REMODELLING. Tim Arnett. University College London. Department of Anatomy and Developmental Biology
 BONE REMODELLING Tim Arnett Department of Anatomy and Developmental Biology University College London The skeleton, out of sight and often out of mind, is a formidable mass of tissue occupying about 9%
BONE REMODELLING Tim Arnett Department of Anatomy and Developmental Biology University College London The skeleton, out of sight and often out of mind, is a formidable mass of tissue occupying about 9%
PTH and PTHR1 in osteocytes. New insights into old partners
 HORMONES 2017, 16(2):150-160 Mini Review PTH and PTHR1 in osteocytes. New insights into old partners Maria P. Yavropoulou, Alexandros Michopoulos, John G. Yovos Laboratory of Clinical and Molecular Endocrinology,
HORMONES 2017, 16(2):150-160 Mini Review PTH and PTHR1 in osteocytes. New insights into old partners Maria P. Yavropoulou, Alexandros Michopoulos, John G. Yovos Laboratory of Clinical and Molecular Endocrinology,
BIOLOGY and BIOMECHANICS OF NORMAL & OSTEOPOROTIC BONE
 BIOLOGY and BIOMECHANICS OF NORMAL & OSTEOPOROTIC BONE Andreas Panagopoulos, MD, PhD Assistant Professor in Orthopaedics University Hospital of Patras, Orthopaedic Clinic Objectives Bone structure and
BIOLOGY and BIOMECHANICS OF NORMAL & OSTEOPOROTIC BONE Andreas Panagopoulos, MD, PhD Assistant Professor in Orthopaedics University Hospital of Patras, Orthopaedic Clinic Objectives Bone structure and
Osteocytes The galaxy within
 Osteocytes The galaxy within Buenzli PR, Sims NA. Quantifying the osteocyte network in the human skeleton. Bone 2015;75:144-50. Buenzli and Sims present a fascinating insight into the intergalactic vastness
Osteocytes The galaxy within Buenzli PR, Sims NA. Quantifying the osteocyte network in the human skeleton. Bone 2015;75:144-50. Buenzli and Sims present a fascinating insight into the intergalactic vastness
Biology. Dr. Khalida Ibrahim
 Biology Dr. Khalida Ibrahim BONE TISSUE Bone tissue is a specialized form of connective tissue and is the main element of the skeletal tissues. It is composed of cells and an extracellular matrix in which
Biology Dr. Khalida Ibrahim BONE TISSUE Bone tissue is a specialized form of connective tissue and is the main element of the skeletal tissues. It is composed of cells and an extracellular matrix in which
SKELETAL SYSTEM I NOTE: LAB ASSIGNMENTS for this topic will run over 3 Weeks. A SEPARATE WORKSHEET WILL BE PROVIDED.
 BIO 211; Anatomy and Physiology I REFERENCE: CHAPTER 07 1 Dr. Lawrence Altman Naugatuck Valley Community College LECTURE TOPICS OUTLINE SKELETAL SYSTEM I NOTE: LAB ASSIGNMENTS for this topic will run over
BIO 211; Anatomy and Physiology I REFERENCE: CHAPTER 07 1 Dr. Lawrence Altman Naugatuck Valley Community College LECTURE TOPICS OUTLINE SKELETAL SYSTEM I NOTE: LAB ASSIGNMENTS for this topic will run over
Bone Cell Biology. David W. Dempster, PhD. Professor of Clinical Pathology Columbia University. Bone Remodeling
 Bone Cell Biology David W. Dempster, PhD Professor of Clinical Pathology Columbia University Bone Remodeling The skeleton, out of site and often out of mind, is a formidable mass of tissue occupying about
Bone Cell Biology David W. Dempster, PhD Professor of Clinical Pathology Columbia University Bone Remodeling The skeleton, out of site and often out of mind, is a formidable mass of tissue occupying about
Bone Cell Biology. The Remodeling Cycle. Bone Remodeling. Remodeling Maintains Mechanical Strength. David W. Dempster, PhD
 Bone Remodeling Bone Cell Biology David W. Dempster, PhD Professor of Clinical Pathology Columbia University The skeleton, out of site and often out of mind, is a formidable mass of tissue occupying about
Bone Remodeling Bone Cell Biology David W. Dempster, PhD Professor of Clinical Pathology Columbia University The skeleton, out of site and often out of mind, is a formidable mass of tissue occupying about
Osteocyte RANKL: New Insights Into the Control of Bone Remodeling
 PERSPECTIVE JBMR Osteocyte RANKL: New Insights Into the Control of Bone Remodeling Jinhu Xiong and Charles A O Brien Center for Osteoporosis and Metabolic Bone Diseases, University of Arkansas for Medical
PERSPECTIVE JBMR Osteocyte RANKL: New Insights Into the Control of Bone Remodeling Jinhu Xiong and Charles A O Brien Center for Osteoporosis and Metabolic Bone Diseases, University of Arkansas for Medical
What are the parts of the skeletal system? Chapter 6- Part I Bones and Skeletal Tissues. Growth of Cartilage. Bones come in many shapes
 Chapter 6- Part I Bones and Skeletal Tissues Components of the skeletal system Classification of Bone (bone shapes) Functions of bone Bone structure Microscopic structure of bone and bone cells What are
Chapter 6- Part I Bones and Skeletal Tissues Components of the skeletal system Classification of Bone (bone shapes) Functions of bone Bone structure Microscopic structure of bone and bone cells What are
Functions of the Skeletal System. Chapter 6: Osseous Tissue and Bone Structure. Classification of Bones. Bone Shapes
 Chapter 6: Osseous Tissue and Bone Structure Functions of the Skeletal System 1. Support 2. Storage of minerals (calcium) 3. Storage of lipids (yellow marrow) 4. Blood cell production (red marrow) 5. Protection
Chapter 6: Osseous Tissue and Bone Structure Functions of the Skeletal System 1. Support 2. Storage of minerals (calcium) 3. Storage of lipids (yellow marrow) 4. Blood cell production (red marrow) 5. Protection
Regulation of the skeletal mass through the life span
 Regulation of the skeletal mass through the life span Functions of the skeletal system Mechanical protection skull Movement leverage for muscles Mineral metabolism calcium store Erythropoiesis red blood
Regulation of the skeletal mass through the life span Functions of the skeletal system Mechanical protection skull Movement leverage for muscles Mineral metabolism calcium store Erythropoiesis red blood
Glucocorticoid excess increases bone loss and fragility
 JCEM ONLINE Brief Report Endocrine Research Circulating Sclerostin Levels Are Decreased in Patients with Endogenous Hypercortisolism and Increase after Treatment A. H. van Lierop, A. W. van der Eerden,
JCEM ONLINE Brief Report Endocrine Research Circulating Sclerostin Levels Are Decreased in Patients with Endogenous Hypercortisolism and Increase after Treatment A. H. van Lierop, A. W. van der Eerden,
THE GROWING GAP IN OSTEOPOROSIS TREATMENT
 THE GROWING GAP IN OSTEOPOROSIS TREATMENT Sundeep Khosla, M.D. Mayo Clinic, Rochester, MN DISCLOSURES SUNDEEP KHOSLA, M.D. NONE 1 OVERALL CONCLUSIONS There has been remarkable progress in our understanding
THE GROWING GAP IN OSTEOPOROSIS TREATMENT Sundeep Khosla, M.D. Mayo Clinic, Rochester, MN DISCLOSURES SUNDEEP KHOSLA, M.D. NONE 1 OVERALL CONCLUSIONS There has been remarkable progress in our understanding
BONE TISSUE. Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology
 BONE TISSUE Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology BONE FUNCTION Support Protection (protect internal organs) Movement (provide leverage system for skeletal muscles, tendons, ligaments
BONE TISSUE Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology BONE FUNCTION Support Protection (protect internal organs) Movement (provide leverage system for skeletal muscles, tendons, ligaments
Tanya Zappitelli. Copyright by Tanya Zappitelli 2015
 Characterization of the Gja1 Jrt /+ Skeletal Phenotype and the Cellular and Molecular Effects of the G60S Connexin 43 Mutation in the Long Bone Microenvironment by Tanya Zappitelli A thesis submitted in
Characterization of the Gja1 Jrt /+ Skeletal Phenotype and the Cellular and Molecular Effects of the G60S Connexin 43 Mutation in the Long Bone Microenvironment by Tanya Zappitelli A thesis submitted in
Deposition of Bone by the Osteoblasts. Bone is continually being deposited by osteoblasts, and it is continually being resorbed where osteoclasts are
 Bone remodeling Deposition of Bone by the Osteoblasts. Bone is continually being deposited by osteoblasts, and it is continually being resorbed where osteoclasts are active. This mechanism is always is
Bone remodeling Deposition of Bone by the Osteoblasts. Bone is continually being deposited by osteoblasts, and it is continually being resorbed where osteoclasts are active. This mechanism is always is
Signaling Vascular Morphogenesis and Maintenance
 Signaling Vascular Morphogenesis and Maintenance Douglas Hanahan Science 277: 48-50, in Perspectives (1997) Blood vessels are constructed by two processes: vasculogenesis, whereby a primitive vascular
Signaling Vascular Morphogenesis and Maintenance Douglas Hanahan Science 277: 48-50, in Perspectives (1997) Blood vessels are constructed by two processes: vasculogenesis, whereby a primitive vascular
A KL/R / AN A K/O / P O G G
 Outline and New Treatments on the Horizon Steven R. Cummings, MD CPMC and UCSF San Francisco Coordinating Center Support from Lilly and Amgen New treatments, new mechanisms of action Cathepsin K inhibition
Outline and New Treatments on the Horizon Steven R. Cummings, MD CPMC and UCSF San Francisco Coordinating Center Support from Lilly and Amgen New treatments, new mechanisms of action Cathepsin K inhibition
Silent Killer: Osteoporosis
 Special Dedication to the Old Females Silent Killer: Osteoporosis David Goltzman, Discoveries, Drugs and Skeletal Disorders Nature, Volume 1, October 2002, pp784-796 BII Journal Club Wang Zhengyuan 5:00-5:30pm
Special Dedication to the Old Females Silent Killer: Osteoporosis David Goltzman, Discoveries, Drugs and Skeletal Disorders Nature, Volume 1, October 2002, pp784-796 BII Journal Club Wang Zhengyuan 5:00-5:30pm
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists. International authors and editors
 We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 3,350 108,000 1.7 M Open access books available International authors and editors Downloads Our
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 3,350 108,000 1.7 M Open access books available International authors and editors Downloads Our
Osteoporosis: current treatment and future prospects. Juliet Compston Professor Emeritus of Bone Medicine Cambridge Biomedical Campus
 Osteoporosis: current treatment and future prospects Juliet Compston Professor Emeritus of Bone Medicine Cambridge Biomedical Campus Disclosures Consultancy and speaking fees for Gilead, related to development
Osteoporosis: current treatment and future prospects Juliet Compston Professor Emeritus of Bone Medicine Cambridge Biomedical Campus Disclosures Consultancy and speaking fees for Gilead, related to development
Outline. Estrogens and SERMS The forgotten few! How Does Estrogen Work in Bone? Its Complex!!! 6/14/2013
 Outline Estrogens and SERMS The forgotten few! Clifford J Rosen MD rosenc@mmc.org Physiology of Estrogen and estrogen receptors Actions of estrogen on bone BMD, fracture, other off target effects Cohort
Outline Estrogens and SERMS The forgotten few! Clifford J Rosen MD rosenc@mmc.org Physiology of Estrogen and estrogen receptors Actions of estrogen on bone BMD, fracture, other off target effects Cohort
Chapter 6: SKELETAL SYSTEM
 Chapter 6: SKELETAL SYSTEM I. FUNCTIONS A. Support B. Protection C. Movement D. Mineral storage E. Lipid storage (Fig. 6.8b) F. Blood cell production (Fig. 6.4) II. COMPONENTS A. Cartilage 1. Hyaline 2.
Chapter 6: SKELETAL SYSTEM I. FUNCTIONS A. Support B. Protection C. Movement D. Mineral storage E. Lipid storage (Fig. 6.8b) F. Blood cell production (Fig. 6.4) II. COMPONENTS A. Cartilage 1. Hyaline 2.
Rama Nada. - Mousa Al-Abbadi. 1 P a g e
 - 1 - Rama Nada - - Mousa Al-Abbadi 1 P a g e Bones, Joints and Soft tissue tumors Before we start: the first 8 minutes was recalling to Dr.Mousa s duties, go over them in the slides. Wherever you see
- 1 - Rama Nada - - Mousa Al-Abbadi 1 P a g e Bones, Joints and Soft tissue tumors Before we start: the first 8 minutes was recalling to Dr.Mousa s duties, go over them in the slides. Wherever you see
The Skeletal System:Bone Tissue
 The Skeletal System:Bone Tissue Dynamic and ever-changing throughout life Skeleton composed of many different tissues cartilage, bone tissue, epithelium, nerve, blood forming tissue, adipose, and dense
The Skeletal System:Bone Tissue Dynamic and ever-changing throughout life Skeleton composed of many different tissues cartilage, bone tissue, epithelium, nerve, blood forming tissue, adipose, and dense
Bone and Cancer. Peter Croucher
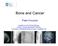 Bone and Cancer Peter Croucher Academic Unit of Bone Biology, Section of Musculoskeletal Science, University of Sheffield Medical School, Sheffield, UK Learning Objectives To Develop Understanding of:
Bone and Cancer Peter Croucher Academic Unit of Bone Biology, Section of Musculoskeletal Science, University of Sheffield Medical School, Sheffield, UK Learning Objectives To Develop Understanding of:
A Novel Murine Model Of Adynamic Bone Disease (ABD)
 A Novel Murine Model Of Adynamic Bone Disease (ABD) Adeline H. Ng 1,2, Thomas L. Willett, PhD 2,1, Benjamin A. Alman 3,1, Marc D. Grynpas 1,2. 1 University of Toronto, Toronto, ON, Canada, 2 Samuel Lunenfeld
A Novel Murine Model Of Adynamic Bone Disease (ABD) Adeline H. Ng 1,2, Thomas L. Willett, PhD 2,1, Benjamin A. Alman 3,1, Marc D. Grynpas 1,2. 1 University of Toronto, Toronto, ON, Canada, 2 Samuel Lunenfeld
Bone Cell Precursors and the Pathophysiology of Bone Loss
 Bone Cell Precursors and the Pathophysiology of Bone Loss HARRY C. BLAIR, a AND JILL L. CARRINGTON b a Departments of Pathology and Cell Biology, University of Pittsburgh, and Pittsburgh VA Medical Center,
Bone Cell Precursors and the Pathophysiology of Bone Loss HARRY C. BLAIR, a AND JILL L. CARRINGTON b a Departments of Pathology and Cell Biology, University of Pittsburgh, and Pittsburgh VA Medical Center,
Osteoporosis - Pathophysiology and diagnosis. Bente L Langdahl Department of Endocrinology Aarhus University Hospital Aarhus, Denmark
 Osteoporosis - Pathophysiology and diagnosis Bente L Langdahl Department of Endocrinology Aarhus University Hospital Aarhus, Denmark Objective General knowledge about osteoporosis Optimise your protocols
Osteoporosis - Pathophysiology and diagnosis Bente L Langdahl Department of Endocrinology Aarhus University Hospital Aarhus, Denmark Objective General knowledge about osteoporosis Optimise your protocols
Osteoporosis and its Association with Rheumatoid Arthritis and Prednisolone Therapy
 Osteoporosis and its Association with Rheumatoid Arthritis and Prednisolone Therapy Master s Thesis Ane Eriksen Medicine with Industrial Specialization Aalborg University Osteoporosis and its Association
Osteoporosis and its Association with Rheumatoid Arthritis and Prednisolone Therapy Master s Thesis Ane Eriksen Medicine with Industrial Specialization Aalborg University Osteoporosis and its Association
Bone mechanics bone strength and beyond
 Bone mechanics bone strength and beyond Tim Arnett Bone Curriculum Symposium 2018 Department of Cell & Developmental Biology University College London Factors affecting bone strength Mass Architectural
Bone mechanics bone strength and beyond Tim Arnett Bone Curriculum Symposium 2018 Department of Cell & Developmental Biology University College London Factors affecting bone strength Mass Architectural
Chapter 6: Skeletal System: Bones and Bone Tissue
 Chapter 6: Skeletal System: Bones and Bone Tissue I. Functions A. List and describe the five major functions of the skeletal system: 1. 2. 3.. 4. 5.. II. Cartilage A. What do chondroblasts do? B. When
Chapter 6: Skeletal System: Bones and Bone Tissue I. Functions A. List and describe the five major functions of the skeletal system: 1. 2. 3.. 4. 5.. II. Cartilage A. What do chondroblasts do? B. When
Review. Role of osteocytes in the adaptation of bone to mechanical loading. Future Rheumatology
 Role of osteocytes in the adaptation of bone to mechanical loading Astrid D Bakker & Jenneke Klein-Nulend Author for correspondence: ACTA-Vrije Universiteit, Department of Oral Cell Biology, Van der Boechorststraat
Role of osteocytes in the adaptation of bone to mechanical loading Astrid D Bakker & Jenneke Klein-Nulend Author for correspondence: ACTA-Vrije Universiteit, Department of Oral Cell Biology, Van der Boechorststraat
Clinical Biochemistry
 Clinical Biochemistry 45 (2012) 863 873 Contents lists available at SciVerse ScienceDirect Clinical Biochemistry journal homepage: www.elsevier.com/locate/clinbiochem Review An overview of the regulation
Clinical Biochemistry 45 (2012) 863 873 Contents lists available at SciVerse ScienceDirect Clinical Biochemistry journal homepage: www.elsevier.com/locate/clinbiochem Review An overview of the regulation
Chapter 6: Osseous Tissue and Bone Structure
 Chapter 6: Osseous Tissue and Bone Structure I. An Introduction to the Skeletal System, p. 180 Objective: Describe the functions of the skeletal system The skeletal system includes: - bones of the skeleton
Chapter 6: Osseous Tissue and Bone Structure I. An Introduction to the Skeletal System, p. 180 Objective: Describe the functions of the skeletal system The skeletal system includes: - bones of the skeleton
Fructose Upregulates FGF23 Expression In MC3T3 Pre-osteoblasts
 Fructose Upregulates FGF23 Expression In MC3T3 Pre-osteoblasts Edek A. Williams, B.S.E., Veronique Douard, Ph.D., Joseph M. Lomuti, B.S., Ronaldo Ferraris, Ph.D., J. C. Fritton, Ph.D.. Rutgers University,
Fructose Upregulates FGF23 Expression In MC3T3 Pre-osteoblasts Edek A. Williams, B.S.E., Veronique Douard, Ph.D., Joseph M. Lomuti, B.S., Ronaldo Ferraris, Ph.D., J. C. Fritton, Ph.D.. Rutgers University,
Download slides:
 Download slides: https://www.tinyurl.com/m67zcnn https://tinyurl.com/kazchbn OSTEOPOROSIS REVIEW AND UPDATE Boca Raton Regional Hospital Internal Medicine Conference 2017 Benjamin Wang, M.D., FRCPC Division
Download slides: https://www.tinyurl.com/m67zcnn https://tinyurl.com/kazchbn OSTEOPOROSIS REVIEW AND UPDATE Boca Raton Regional Hospital Internal Medicine Conference 2017 Benjamin Wang, M.D., FRCPC Division
Drugs Affecting Bone. Rosa McCarty PhD. Department of Pharmacology & Therapeutics
 Drugs Affecting Bone Rosa McCarty PhD Department of Pharmacology & Therapeutics rmccarty@unimelb.edu.au Objectives At the end of this lecture you should have gained: An understanding of bone metabolism
Drugs Affecting Bone Rosa McCarty PhD Department of Pharmacology & Therapeutics rmccarty@unimelb.edu.au Objectives At the end of this lecture you should have gained: An understanding of bone metabolism
The Microenvironment Matters: Estrogen Deficiency Fuels Cancer Bone Metastases
 CCR Translations CCR-14-0576 Commentary on Ottewell et al. The Microenvironment Matters: Estrogen Deficiency Fuels Cancer Bone Metastases Laura E. Wright 1 and Theresa A. Guise 1,2 Authors Affiliations:
CCR Translations CCR-14-0576 Commentary on Ottewell et al. The Microenvironment Matters: Estrogen Deficiency Fuels Cancer Bone Metastases Laura E. Wright 1 and Theresa A. Guise 1,2 Authors Affiliations:
DISCLOSURES TOPICS" PATHOPHYSIOLOGY of OSTEOPOROSIS: Pathways That Control Bone Remodeling! Why Do Bones Remodel?" Nothing to disclose
 PATHOPHYSIOLOGY of OSTEOPOROSIS: Pathways That Control Bone Remodeling Dolores Shoback, MD Professor of Medicine, UCSF Staff Physician SF/VAMC May 19, 2017 DISCLOSURES Nothing to disclose No conflicts
PATHOPHYSIOLOGY of OSTEOPOROSIS: Pathways That Control Bone Remodeling Dolores Shoback, MD Professor of Medicine, UCSF Staff Physician SF/VAMC May 19, 2017 DISCLOSURES Nothing to disclose No conflicts
Assessment and Treatment of Osteoporosis Professor T.Masud
 Assessment and Treatment of Osteoporosis Professor T.Masud Nottingham University Hospitals NHS Trust University of Nottingham University of Derby University of Southern Denmark What is Osteoporosis? Osteoporosis
Assessment and Treatment of Osteoporosis Professor T.Masud Nottingham University Hospitals NHS Trust University of Nottingham University of Derby University of Southern Denmark What is Osteoporosis? Osteoporosis
Generation of post-germinal centre myeloma plasma B cell.
 Generation of post-germinal centre myeloma. DNA DAMAGE CXCR4 Homing to Lytic lesion activation CD38 CD138 CD56 Phenotypic markers Naive Secondary lymphoid organ Multiple myeloma is a malignancy of s caused
Generation of post-germinal centre myeloma. DNA DAMAGE CXCR4 Homing to Lytic lesion activation CD38 CD138 CD56 Phenotypic markers Naive Secondary lymphoid organ Multiple myeloma is a malignancy of s caused
Peggers Super Summaries Basic Sciences Bone
 Bone Overview & Turnover BONES Function o Support o Protection o Assisting movement o Storage of minerals o Production of red blood cells from marrow Types o Cancellous o Compact with Haversian systems
Bone Overview & Turnover BONES Function o Support o Protection o Assisting movement o Storage of minerals o Production of red blood cells from marrow Types o Cancellous o Compact with Haversian systems
Sclerostin is essential for alveolar bone loss in occlusal hypofunction
 1812 Sclerostin is essential for alveolar bone loss in occlusal hypofunction YANG XU 1*, LUFEI WANG 1*, YAO SUN 2, XIANGLONG HAN 2, TIAN GAO 3, XIN XU 1, TIAN CHEN 1, XUEFENG ZHAO 1, HUAN ZENG 1, YANMIN
1812 Sclerostin is essential for alveolar bone loss in occlusal hypofunction YANG XU 1*, LUFEI WANG 1*, YAO SUN 2, XIANGLONG HAN 2, TIAN GAO 3, XIN XU 1, TIAN CHEN 1, XUEFENG ZHAO 1, HUAN ZENG 1, YANMIN
Phospho-AKT Sampler Kit
 Phospho-AKT Sampler Kit E 0 5 1 0 0 3 Kits Includes Cat. Quantity Application Reactivity Source Akt (Ab-473) Antibody E021054-1 50μg/50μl IHC, WB Human, Mouse, Rat Rabbit Akt (Phospho-Ser473) Antibody
Phospho-AKT Sampler Kit E 0 5 1 0 0 3 Kits Includes Cat. Quantity Application Reactivity Source Akt (Ab-473) Antibody E021054-1 50μg/50μl IHC, WB Human, Mouse, Rat Rabbit Akt (Phospho-Ser473) Antibody
Space radiation and osteoclastogenesis:the effects of radiation and microgravity on bone resorption:
 Space radiation and osteoclastogenesis:the effects of radiation and microgravity on bone resorption: Alamelu Sundaresan1, Sukesh Aghara2, Terrell Gibson1and Indi Siripirasan2 1: Texas Southern University-3100
Space radiation and osteoclastogenesis:the effects of radiation and microgravity on bone resorption: Alamelu Sundaresan1, Sukesh Aghara2, Terrell Gibson1and Indi Siripirasan2 1: Texas Southern University-3100
CHAPTER 6 LECTURE OUTLINE
 CHAPTER 6 LECTURE OUTLINE I. INTRODUCTION A. Bone is made up of several different tissues working together: bone, cartilage, dense connective tissue, epithelium, various blood forming tissues, adipose
CHAPTER 6 LECTURE OUTLINE I. INTRODUCTION A. Bone is made up of several different tissues working together: bone, cartilage, dense connective tissue, epithelium, various blood forming tissues, adipose
Effects of Anti RANK ligand Denosumab on Beta Thalassemia induced osteoporosis
 Effects of Anti RANK ligand Denosumab on Beta Thalassemia induced osteoporosis Mohamed Yassin 1 Ashraf T. Soliman2, Mohamed O. Abdelrahman3, Vincenzo De Sanctis 4 Departments of, 1 Hematology 2Pediatric
Effects of Anti RANK ligand Denosumab on Beta Thalassemia induced osteoporosis Mohamed Yassin 1 Ashraf T. Soliman2, Mohamed O. Abdelrahman3, Vincenzo De Sanctis 4 Departments of, 1 Hematology 2Pediatric
Endocrine secretion cells secrete substances into the extracellular fluid
 Animal Hormones Concept 30.1 Hormones Are Chemical Messengers Endocrine secretion cells secrete substances into the extracellular fluid Exocrine secretion cells secrete substances into a duct or a body
Animal Hormones Concept 30.1 Hormones Are Chemical Messengers Endocrine secretion cells secrete substances into the extracellular fluid Exocrine secretion cells secrete substances into a duct or a body
An Introduction to the Skeletal System Skeletal system includes Bones of the skeleton Cartilages, ligaments, and connective tissues
 An Introduction to the Skeletal System Skeletal system includes Bones of the skeleton Cartilages, ligaments, and connective tissues Functions of the Skeletal System Support Storage of minerals (calcium)
An Introduction to the Skeletal System Skeletal system includes Bones of the skeleton Cartilages, ligaments, and connective tissues Functions of the Skeletal System Support Storage of minerals (calcium)
For more information about how to cite these materials visit
 Author(s): University of Michigan Medical School, Department of Cell and Developmental Biology License: Unless otherwise noted, the content of this course material is licensed under a Creative Commons
Author(s): University of Michigan Medical School, Department of Cell and Developmental Biology License: Unless otherwise noted, the content of this course material is licensed under a Creative Commons
The Skeletal System:Bone Tissue
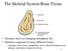 The Skeletal System:Bone Tissue Dynamic and ever-changing throughout life Skeleton composed of many different tissues cartilage, bone tissue, epithelium, nerve, blood forming tissue, adipose, and dense
The Skeletal System:Bone Tissue Dynamic and ever-changing throughout life Skeleton composed of many different tissues cartilage, bone tissue, epithelium, nerve, blood forming tissue, adipose, and dense
Pathogenesis of osteoporosis: concepts, conflicts, and prospects
 Science in medicine Pathogenesis of osteoporosis: concepts, conflicts, and prospects Lawrence G. Raisz University of Connecticut Health Center, Musculoskeletal Institute, Farmington, Connecticut, USA.
Science in medicine Pathogenesis of osteoporosis: concepts, conflicts, and prospects Lawrence G. Raisz University of Connecticut Health Center, Musculoskeletal Institute, Farmington, Connecticut, USA.
Introduction: 年 Fas signal-mediated apoptosis. PI3K/Akt
 Fas-ligand (CD95-L; Fas-L) Fas (CD95) Fas (apoptosis) 年 了 不 度 Fas Fas-L 力 不 Fas/Fas-L T IL-10Fas/Fas-L 不 年 Fas signal-mediated apoptosis 度降 不 不 力 U-118, HeLa, A549, Huh-7 MCF-7, HepG2. PI3K/Akt FasPI3K/Akt
Fas-ligand (CD95-L; Fas-L) Fas (CD95) Fas (apoptosis) 年 了 不 度 Fas Fas-L 力 不 Fas/Fas-L T IL-10Fas/Fas-L 不 年 Fas signal-mediated apoptosis 度降 不 不 力 U-118, HeLa, A549, Huh-7 MCF-7, HepG2. PI3K/Akt FasPI3K/Akt
Module 2:! Functional Musculoskeletal Anatomy A! Semester 1! !!! !!!! Hard Tissues, Distal Upper Limb & Neurovascular Supply of Upper Limb!
 Functional Musculoskeletal Anatomy A Module 2: Hard Tissues, Distal Upper Limb & Neurovascular Supply of Upper Limb Semester 1 1 18. Bone Tissue & Growth of Bones 18.1 Describe the structure of bone tissue
Functional Musculoskeletal Anatomy A Module 2: Hard Tissues, Distal Upper Limb & Neurovascular Supply of Upper Limb Semester 1 1 18. Bone Tissue & Growth of Bones 18.1 Describe the structure of bone tissue
Principles of Genetics and Molecular Biology
 Cell signaling Dr. Diala Abu-Hassan, DDS, PhD School of Medicine Dr.abuhassand@gmail.com Principles of Genetics and Molecular Biology www.cs.montana.edu Modes of cell signaling Direct interaction of a
Cell signaling Dr. Diala Abu-Hassan, DDS, PhD School of Medicine Dr.abuhassand@gmail.com Principles of Genetics and Molecular Biology www.cs.montana.edu Modes of cell signaling Direct interaction of a
Crosstalk between Adiponectin and IGF-IR in breast cancer. Prof. Young Jin Suh Department of Surgery The Catholic University of Korea
 Crosstalk between Adiponectin and IGF-IR in breast cancer Prof. Young Jin Suh Department of Surgery The Catholic University of Korea Obesity Chronic, multifactorial disorder Hypertrophy and hyperplasia
Crosstalk between Adiponectin and IGF-IR in breast cancer Prof. Young Jin Suh Department of Surgery The Catholic University of Korea Obesity Chronic, multifactorial disorder Hypertrophy and hyperplasia
Bone Health in the Cancer Patient. Stavroula Otis, M.D. Primary Care and Oncology: Practical Lessons Conference Brea Community Center May 10, 2018
 Bone Health in the Cancer Patient Stavroula Otis, M.D. Primary Care and Oncology: Practical Lessons Conference Brea Community Center May 10, 2018 Overview Healthy bone is in a constant state of remodelling
Bone Health in the Cancer Patient Stavroula Otis, M.D. Primary Care and Oncology: Practical Lessons Conference Brea Community Center May 10, 2018 Overview Healthy bone is in a constant state of remodelling
AACE Southern States Chapter Lecture. Basics
 AACE Southern States Chapter Lecture Unusual Bone Cases Basics Osteoporosis Osteomalacia Renal Osteodystrophy Multiple Myeloma 1 Osteoporosis Definition Modeling, Bone Remodeling Bone Resorption > Bone
AACE Southern States Chapter Lecture Unusual Bone Cases Basics Osteoporosis Osteomalacia Renal Osteodystrophy Multiple Myeloma 1 Osteoporosis Definition Modeling, Bone Remodeling Bone Resorption > Bone
From Fragile to Firm. Monika Starosta MD. Advocate Medical Group
 From Fragile to Firm Monika Starosta MD Advocate Medical Group Bone Remodeling 10% remodeled each year Calcium homoeostasis Maintain Mechanical strength Replace Osteocytes Release Growth Factors Bone remodeling
From Fragile to Firm Monika Starosta MD Advocate Medical Group Bone Remodeling 10% remodeled each year Calcium homoeostasis Maintain Mechanical strength Replace Osteocytes Release Growth Factors Bone remodeling
Quiz 6. Cartilage and Bone
 Quiz 6 Cartilage and Bone MCQs X type (true or false): 1. Cartilage tissue: a. Has a rich blood supply. b. Develops from mesenchyme. c. Has ability for a quick regeneration. d. Has chondrocytes as precursor
Quiz 6 Cartilage and Bone MCQs X type (true or false): 1. Cartilage tissue: a. Has a rich blood supply. b. Develops from mesenchyme. c. Has ability for a quick regeneration. d. Has chondrocytes as precursor
7/5/2016. We need drugs that. Disclosures. New Osteoporosis Treatments. What we have today. Maintain or promote bone formation
 New Osteoporosis Treatments Disclosures Mary L. Bouxsein, PhD Department of Orthopedic Surgery Harvard Medical School, Boston, MA Advisory Board: Research funding: Merck, Eli Lilly, Radius Merck, Amgen
New Osteoporosis Treatments Disclosures Mary L. Bouxsein, PhD Department of Orthopedic Surgery Harvard Medical School, Boston, MA Advisory Board: Research funding: Merck, Eli Lilly, Radius Merck, Amgen
SKELETAL TISSUES CHAPTER 7 INTRODUCTION TO THE SKELETAL SYSTEM TYPES OF BONES
 SKELETAL TISSUES CHAPTER 7 By John McGill Supplement Outlines: Beth Wyatt Original PowerPoint: Jack Bagwell INTRODUCTION TO THE SKELETAL SYSTEM STRUCTURE Organs: Bones Related Tissues: Cartilage and Ligaments
SKELETAL TISSUES CHAPTER 7 By John McGill Supplement Outlines: Beth Wyatt Original PowerPoint: Jack Bagwell INTRODUCTION TO THE SKELETAL SYSTEM STRUCTURE Organs: Bones Related Tissues: Cartilage and Ligaments
OSSEOUS TISSUE & BONE STRUCTURE PART I: OVERVIEW & COMPONENTS
 OSSEOUS TISSUE & BONE STRUCTURE PART I: OVERVIEW & COMPONENTS The Skeletal System Skeletal system includes: bones of the skeleton, cartilages, ligaments, and connective tissues What are the functions of
OSSEOUS TISSUE & BONE STRUCTURE PART I: OVERVIEW & COMPONENTS The Skeletal System Skeletal system includes: bones of the skeleton, cartilages, ligaments, and connective tissues What are the functions of
Comment les cellules osseuses communiquent entre elles. Gérard Friedlander Journées UPA 2011
 Comment les cellules osseuses communiquent entre elles Gérard Friedlander Journées UPA 2011 Structure de l os Osteocyte Ostéoclaste Remodelage osseux RANKL RANK NF-kB pathway Stem cell progenitor precursor
Comment les cellules osseuses communiquent entre elles Gérard Friedlander Journées UPA 2011 Structure de l os Osteocyte Ostéoclaste Remodelage osseux RANKL RANK NF-kB pathway Stem cell progenitor precursor
Mutation in Osteoactivin Enhances RANKL-Mediated Signaling, Promoting Osteoclast Differentiation, Survival and Inhibiting Bone Resorption
 Mutation in Osteoactivin Enhances RANKL-Mediated Signaling, Promoting Osteoclast Differentiation, Survival and Inhibiting Bone Resorption Samir Abdelmagid, MD, PhD, Fouad Moussa, BS, Sondag Gregory, MS,
Mutation in Osteoactivin Enhances RANKL-Mediated Signaling, Promoting Osteoclast Differentiation, Survival and Inhibiting Bone Resorption Samir Abdelmagid, MD, PhD, Fouad Moussa, BS, Sondag Gregory, MS,
FORMATION OF BONE. Intramembranous Ossification. Bone-Lec-10-Prof.Dr.Adnan Albideri
 FORMATION OF BONE All bones are of mesodermal origin. The process of bone formation is called ossification. We have seen that formation of most bones is preceded by the formation of a cartilaginous model,
FORMATION OF BONE All bones are of mesodermal origin. The process of bone formation is called ossification. We have seen that formation of most bones is preceded by the formation of a cartilaginous model,
Recent Progress in Osteocyte Research
 Recent Progress in Osteocyte Research The Harvard community has made this article openly available. Please share how this access benefits you. Your story matters. Citation Published Version Accessed Citable
Recent Progress in Osteocyte Research The Harvard community has made this article openly available. Please share how this access benefits you. Your story matters. Citation Published Version Accessed Citable
Building bone to reverse osteoporosis and repair fractures
 Building bone to reverse osteoporosis and repair fractures Sundeep Khosla,, Jennifer J. Westendorf, Merry Jo Oursler J Clin Invest. 2008;118(2):421-428. https://doi.org/10.1172/jci33612. Review Series
Building bone to reverse osteoporosis and repair fractures Sundeep Khosla,, Jennifer J. Westendorf, Merry Jo Oursler J Clin Invest. 2008;118(2):421-428. https://doi.org/10.1172/jci33612. Review Series
KEY CONCEPTS Unit 6 THE SKELETAL SYSTEM
 ANATOMY & PHYSIOLOGY 1 (101-805 - AB) PAUL ANDERSON 2011 KEY CONCEPTS Unit 6 THE SKELETAL SYSTEM A Overview of The Skeletal System 1. Definition: Anatomically the SKELETAL SYSTEM consists of bones, cartilages,
ANATOMY & PHYSIOLOGY 1 (101-805 - AB) PAUL ANDERSON 2011 KEY CONCEPTS Unit 6 THE SKELETAL SYSTEM A Overview of The Skeletal System 1. Definition: Anatomically the SKELETAL SYSTEM consists of bones, cartilages,
SKELETAL SYSTEM CHAPTER 07. Bone Function BIO 211: ANATOMY & PHYSIOLOGY I. Body Movement interacts with muscles bones act as rigid bar of a lever
 Page 1 BIO 211: ANATOMY & PHYSIOLOGY I 1 CHAPTER 07 SKELETAL SYSTEM Dr. Lawrence G. G. Altman www.lawrencegaltman.com Some illustrations are courtesy of McGraw-Hill. Some illustrations are courtesy of
Page 1 BIO 211: ANATOMY & PHYSIOLOGY I 1 CHAPTER 07 SKELETAL SYSTEM Dr. Lawrence G. G. Altman www.lawrencegaltman.com Some illustrations are courtesy of McGraw-Hill. Some illustrations are courtesy of
Upcoming Agents for Osteoporosis
 Upcoming Agents for Osteoporosis May 5, 2017 Michael R. McClung, MD, FACP Director, Oregon Osteoporosis Center Portland, Oregon, USA Professorial Fellow, Institute of Health and Ageing Australian Catholic
Upcoming Agents for Osteoporosis May 5, 2017 Michael R. McClung, MD, FACP Director, Oregon Osteoporosis Center Portland, Oregon, USA Professorial Fellow, Institute of Health and Ageing Australian Catholic
SKELETAL SYSTEM CHAPTER 07 BIO 211: ANATOMY & PHYSIOLOGY I
 BIO 211: ANATOMY & PHYSIOLOGY I 1 CHAPTER 07 SKELETAL SYSTEM Dr. Lawrence G. G. Altman www.lawrencegaltman.com Some illustrations are courtesy of McGraw-Hill. Some illustrations are courtesy of McGraw-Hill.
BIO 211: ANATOMY & PHYSIOLOGY I 1 CHAPTER 07 SKELETAL SYSTEM Dr. Lawrence G. G. Altman www.lawrencegaltman.com Some illustrations are courtesy of McGraw-Hill. Some illustrations are courtesy of McGraw-Hill.
SIBLINGs, cancer's multifunctional weapons
 SIBLINGs, cancer's multifunctional weapons 6/18/08 Akeila Bellahcène and Vincent Castronovo of the Metastasis Research laboratory of the University of Liège are among the first researchers to have discovered
SIBLINGs, cancer's multifunctional weapons 6/18/08 Akeila Bellahcène and Vincent Castronovo of the Metastasis Research laboratory of the University of Liège are among the first researchers to have discovered
ANATOMY AND ULTRASTRUCTURE OF BONE HISTOGENESIS, GROWTH AND REMODELING
 ANATOMY AND ULTRASTRUCTURE OF BONE HISTOGENESIS, GROWTH AND REMODELING Updated: May 13, 2008 Authors: Roland Baron, DDS, PhD. Summary 1. Bones have three major functions: to serve as mechanical support,
ANATOMY AND ULTRASTRUCTURE OF BONE HISTOGENESIS, GROWTH AND REMODELING Updated: May 13, 2008 Authors: Roland Baron, DDS, PhD. Summary 1. Bones have three major functions: to serve as mechanical support,
CHAPTER 2. Literature Review. Bone Homeostasis. 2.1 Introduction. 2.2 Composition of bone
 CHAPTER 2 Literature Review I Bone Homeostasis 2.1 Introduction The mature skeleton is a metabolically active organ that undergoes continuous remodeling by a process that replaces old bone with new bone.
CHAPTER 2 Literature Review I Bone Homeostasis 2.1 Introduction The mature skeleton is a metabolically active organ that undergoes continuous remodeling by a process that replaces old bone with new bone.
HOMEWORK RUBRICS MECHANOTRANSDUCTION UNIT: HOMEWORK #1 (20 pts towards your grade)
 HOMEWORK RUBRICS MECHANOTRANSDUCTION UNIT: HOMEWORK #1 (20 pts towards your grade) 1. Mesenchymal stem cells (MSC) cultured on extracellular matrices with different stiffness exhibit diverse lineage commitment
HOMEWORK RUBRICS MECHANOTRANSDUCTION UNIT: HOMEWORK #1 (20 pts towards your grade) 1. Mesenchymal stem cells (MSC) cultured on extracellular matrices with different stiffness exhibit diverse lineage commitment
Anabolic Therapies. Nancy E. Lane & Stuart L. Silverman
 Curr Osteoporos Rep (2010) 8:23 27 DOI 10.1007/s11914-010-0005-4 Anabolic Therapies Nancy E. Lane & Stuart L. Silverman Published online: 19 February 2010 # The Author(s) 2010. This article is published
Curr Osteoporos Rep (2010) 8:23 27 DOI 10.1007/s11914-010-0005-4 Anabolic Therapies Nancy E. Lane & Stuart L. Silverman Published online: 19 February 2010 # The Author(s) 2010. This article is published
Osseous Tissue and Bone Structure
 C h a p t e r 6 Osseous Tissue and Bone Structure PowerPoint Lecture Slides prepared by Jason LaPres Lone Star College - North Harris Copyright 2009 Pearson Education, Inc., publishing as Pearson Benjamin
C h a p t e r 6 Osseous Tissue and Bone Structure PowerPoint Lecture Slides prepared by Jason LaPres Lone Star College - North Harris Copyright 2009 Pearson Education, Inc., publishing as Pearson Benjamin
Research Article The Effect of Renal Dysfunction on Circulating Sclerostin Level in Patients with Type 2 Diabetes
 International Endocrinology, Article ID 715908, 5 pages http://dx.doi.org/10.1155/2014/715908 Research Article The Effect of Renal Dysfunction on Circulating Sclerostin Level in Patients with Type 2 Diabetes
International Endocrinology, Article ID 715908, 5 pages http://dx.doi.org/10.1155/2014/715908 Research Article The Effect of Renal Dysfunction on Circulating Sclerostin Level in Patients with Type 2 Diabetes
Osteocytes as Dynamic Multifunctional Cells
 Osteocytes as Dynamic Multifunctional Cells LYNDA F. BONEWALD University of Missouri, School of Dentistry, Kansas City, Missouri, USA ABSTRACT: The target of bone systemic factors and therapeutics has
Osteocytes as Dynamic Multifunctional Cells LYNDA F. BONEWALD University of Missouri, School of Dentistry, Kansas City, Missouri, USA ABSTRACT: The target of bone systemic factors and therapeutics has
New treatment targets in osteoporosis
 National University of Athens Greece New treatment targets in osteoporosis Gourzi Vassiliki PhD Candidate Dept. of Pathophysiology School of Medicine Bone remodeling Physiological process < bone tissue
National University of Athens Greece New treatment targets in osteoporosis Gourzi Vassiliki PhD Candidate Dept. of Pathophysiology School of Medicine Bone remodeling Physiological process < bone tissue
Novel therapies for Myeloma bone disease. Dr. Naif AlJohani ABIM,FRCPC Adult Hematology/BMT King Faisal specialist hospital & Research center Jeddah
 Novel therapies for Myeloma bone disease Dr. Naif AlJohani ABIM,FRCPC Adult Hematology/BMT King Faisal specialist hospital & Research center Jeddah 1 Introduction Multiple myeloma (MM) is a plasma cell
Novel therapies for Myeloma bone disease Dr. Naif AlJohani ABIM,FRCPC Adult Hematology/BMT King Faisal specialist hospital & Research center Jeddah 1 Introduction Multiple myeloma (MM) is a plasma cell
Skeletal Tissues. Skeletal tissues. Frame; muscles, organs and CT attach. Brain, spinal cord, thoracic organs; heart and lungs.
 Skeletal Tissues Functions 1) support 2) protection 3) movement Skeletal tissues Frame; muscles, organs and CT attach. Brain, spinal cord, thoracic organs; heart and lungs. Aids muscle contraction; generate
Skeletal Tissues Functions 1) support 2) protection 3) movement Skeletal tissues Frame; muscles, organs and CT attach. Brain, spinal cord, thoracic organs; heart and lungs. Aids muscle contraction; generate
b. Adult bones produce 2.5 million RBCs each second.
 Ch 6 Skeletal System I. Functions of the Skeletal System A. The skeletal system consists of: 1. bones, cartilage, tendons and ligaments B. Living bone is not Gr. dried up 1. It is dynamic and adaptable
Ch 6 Skeletal System I. Functions of the Skeletal System A. The skeletal system consists of: 1. bones, cartilage, tendons and ligaments B. Living bone is not Gr. dried up 1. It is dynamic and adaptable
Enzyme-coupled Receptors. Cell-surface receptors 1. Ion-channel-coupled receptors 2. G-protein-coupled receptors 3. Enzyme-coupled receptors
 Enzyme-coupled Receptors Cell-surface receptors 1. Ion-channel-coupled receptors 2. G-protein-coupled receptors 3. Enzyme-coupled receptors Cell-surface receptors allow a flow of ions across the plasma
Enzyme-coupled Receptors Cell-surface receptors 1. Ion-channel-coupled receptors 2. G-protein-coupled receptors 3. Enzyme-coupled receptors Cell-surface receptors allow a flow of ions across the plasma
OSTEONECROSI DEI MASCELLARI (ONJ): PREVENZIONE, DIAGNOSI, TRATTAMENTO UPDATE 2010
 OSTEONECROSI DEI MASCELLARI (ONJ): PREVENZIONE, DIAGNOSI, TRATTAMENTO UPDATE 2010 Alessandria, 5 giugno 2010 Novità nel trattamento dell osteoporosi Stefania Boldini Francesco Bertoldo Dipartimento di
OSTEONECROSI DEI MASCELLARI (ONJ): PREVENZIONE, DIAGNOSI, TRATTAMENTO UPDATE 2010 Alessandria, 5 giugno 2010 Novità nel trattamento dell osteoporosi Stefania Boldini Francesco Bertoldo Dipartimento di
