Building bone to reverse osteoporosis and repair fractures
|
|
|
- Gary Skinner
- 5 years ago
- Views:
Transcription
1 Building bone to reverse osteoporosis and repair fractures Sundeep Khosla,, Jennifer J. Westendorf, Merry Jo Oursler J Clin Invest. 2008;118(2): Review Series An important, unfilled clinical need is the development of new approaches to improve fracture healing and to treat osteoporosis by increasing bone mass. Recombinant forms of bone morphogenetic protein 2 (BMP2) and BMP7 are FDA approved to promote spinal fusion and fracture healing, respectively, and the first FDA-approved anabolic drug for osteoporosis, parathyroid hormone, increases bone mass when administered intermittently but can only be given to patients in the US for two years. As we discuss here, the tremendous explosion over the last two decades in our fundamental understanding of the mechanisms of bone remodeling has led to the prospect of mechanism-based anabolic therapies for bone disorders. Find the latest version:
2 Building bone to reverse osteoporosis and repair fractures Sundeep Khosla, 1 Jennifer J. Westendorf, 2 and Merry Jo Oursler 1 Review series 1 Endocrine Research Unit and 2 Department of Orthopedic Surgery, College of Medicine, Mayo Clinic, Rochester, Minnesota, USA. An important, unfilled clinical need is the development of new approaches to improve fracture healing and to treat osteoporosis by increasing bone mass. Recombinant forms of bone morphogenetic protein 2 (BMP2) and BMP7 are FDA approved to promote spinal fusion and fracture healing, respectively, and the first FDA-approved anabolic drug for osteoporosis, parathyroid hormone, increases bone mass when administered intermittently but can only be given to patients in the US for two years. As we discuss here, the tremendous explosion over the last two decades in our fundamental understanding of the mechanisms of bone remodeling has led to the prospect of mechanismbased anabolic therapies for bone disorders. There are currently a number of FDA-approved drugs for the prevention and treatment of osteoporosis that work by inhibiting bone resorption (i.e., they are anticatabolic). However, these compounds, which include bisphosphonates, calcitonin, and selective estrogen receptor modulators, only prevent further loss of bone; they do not stimulate new bone formation. The only FDAapproved compound capable of stimulating new bone formation (and thus reversing bone loss) is parathyroid hormone (PTH). However, PTH is a protein that needs to be administered subcutaneously, and patients generally prefer taking an oral medication; there are potential side effects (e.g., hypercalcemia and hypercalciuria) associated with its use; and the duration of treatment with this drug is limited to 18 months in Europe and 24 months in the US, because rodents administered high doses of PTH were shown to develop osteosarcomas (1). Thus, there is a clear clinical need to develop new bone anabolic agents (particularly small molecules that can be used orally), and understanding the molecular details of the pathways that control bone formation is critical for the development of novel approaches to reverse osteoporosis. It might be possible to modulate these pathways not only for the treatment osteoporosis, but also to accelerate the healing of fractures and to treat the 5% 10% of fractures that fail to heal satisfactorily (2, 3). This Review focuses on current approaches, as well as those on the horizon, that have the potential to achieve these goals. Although the osteoblast, as the bone-forming cell, is the obvious target for agents that aim to mediate bone anabolism, other cells are now also being considered as therapeutic targets. For example, osteocytes, cells that have historically largely been ignored because they lie entombed in the bone matrix, and osteoclasts, the boneresorbing cells that have long been a target for agents that are anticatabolic, are now also potential targets for drugs that stimulate bone anabolism. The development of agents that target more than one of these cell types might be the most effective therapy, as there is some evidence to suggest that PTH utilizes all of the above cell types in achieving its anabolic effects on bone. Nonstandard abbreviations used: BMP, bone morphogenetic protein; BMU, basic multicellular unit; BRC, bone remodeling compartment; Dkk1, dickkopf homolog 1; EphB4, EPH receptor B4; Fz, Frizzled; GSK3β, glycogen synthase kinase 3β; LRP, LDL receptor related protein; OPG, osteoprotegerin; PTH, parathyroid hormone; Runx2, Runt-related transcription factor 2; SfrP, secreted frizzled-related protein. Conflict of interest: The authors have declared that no conflict of interest exists. Citation for this article: J. Clin. Invest. 118: (2008). doi: /jci Bone remodeling: evolving concepts Although macroscopically the skeleton seems to be a static organ, it is an extremely dynamic tissue at the microscopic level. Its ability to sustain the tremendous loads placed on it in everyday life depend on, among other factors, being able to remodel and repair the constant microcracks that develop both in cancellous bone the spongy bone present in the vertebrae, pelvis, and ends (metaphyses) of long bones and in cortical bone the compact bone present in the shafts (diaphyses) of the long bones and surrounding cancellous bone in the vertebrae and pelvis. Since remodeling sites in cancellous bone in the vertebrae and pelvis are close to red marrow, which is known to contain osteoprogenitor cells (4), whereas remodeling sites in cortical bone are distant from red marrow, it had been assumed that the mechanisms of bone remodeling were likely to be different in cancellous versus cortical bone. Specifically, the assumption was that the cells needed for bone remodeling traveled directly from the red marrow to bone surfaces in cancellous bone, whereas they accessed cortical bone via the vasculature (5). However, it now seems that the fundamental mechanisms of bone remodeling might be very similar in both bone compartments, occurring in what has been termed the basic multicellular unit (BMU), which comprises the osteoclasts, osteoblasts, and osteocytes within the bone-remodeling cavity (Figure 1). Although the existence of the BMU has been established for a long time, the intimate relationship between the BMU and the vasculature, particularly in cancellous bone, was less well appreciated. This intimate relationship was initially described by Burkhardt et al. (6) more than 20 years ago and analyzed in detail in subsequent studies by Hauge and colleagues (7). These investigators demonstrated that the cells in the BMU, even in cancellous bone, were not directly contiguous to the bone marrow, but rather they were covered by a canopy of cells (most probably bone-lining cells) that seem to be connected to bone-lining cells on the quiescent bone surface (7). In turn, these bone-lining cells on the quiescent bone surface are in communication with osteocytes embedded within the bone matrix (7). Penetrating the canopy of bone-lining cells, and presumably serving as a conduit for the cells needed in the BMU, are capillaries; thus, the work of Hauge et al. (7) placed the BMU (consisting of osteoclasts, osteoblasts, and osteocytes), both in cancellous (Figure 1A) and in cortical (Figure 1B) bone, within the bone remodeling compartment (BRC), which comprises the BMU, the canopy of bone-lining cells, and the associated capillaries (Figure 1C and depicted schematically in Figure 1D). The Journal of Clinical Investigation Volume 118 Number 2 February
3 Figure 1 Histology (A C; original magnification, 40) and composite schematic (D) of the BRC, which comprises the cells constituting the BMU specifically osteoclasts (OCs), osteoblasts (OBs), and osteocytes as well as the canopy of bone-lining cells and the associated capillary. (A) BRC in cancellous bone, demonstrating the location of the OBs along the bone-forming surface. The osteocytes are shown embedded in the bone matrix and the canopy of cells consists of bone-lining cells. (B) BRC in cortical bone (outer demarcation indicated by the broken line) that is filled with erythrocyte ghosts (EG) and OBs; a few OCs are also seen. CV denotes the central vessel of the Haversian system, which forms the basic structural unit in cortical bone. (C) BRC stained with an antibody specific for CD34, which demonstrates staining of endothelial cells in the marrow capillary adjacent to the BRC. (D) Composite schematic of the BRC, showing connections between the osteocyte network, surface bone-lining cells, and the BRC. All cells in this network are connected with gap junctions, which might provide a pathway (arrows) by which signals generated by osteocytes deep within the bone reach the surface and elicit remodeling events by OCs and OBs. Note also the potential direct physical contact between OCs and OBs, which would allow for signaling between these cells. A and C are reproduced from Hauge et al. (7), and B and D from Eriksen et al. (10), with permission from the American Society for Bone and Mineral Research. Given the structure of the BRC, it becomes easier to understand the key role that osteocytes have in controlling bone remodeling, despite being imprisoned in the bone matrix. It is now clear that osteocytes can sense microcracks and mechanical strain and be responsive to changes in the hormonal milieu of the bone (e.g., estrogen deficiency) to essentially trigger bone remodeling, perhaps by communicating with bone-lining cells (8, 9). The bone-lining cells, in turn, probably initiate the process of bone resorption (8), attract osteoclasts, and, together with adjoining bone-lining cells, begin to form the roof of the BRC. By analogy with remodeling in cortical bone, which is clearly associated with growth of a blood vessel into the remodeling site (5), the presumed ingrowth of a capillary into the BRC provides the vascular supply for the cells in the BMU of cancellous bone and might also provide the necessary osteoclasts and, subsequently, the osteoblasts that are needed for bone remodeling in both cancellous and cortical bone. Within the BMU, preosteoblastic cells, which express RANKL (10), probably control the differentiation of osteoclasts from hematopoietic progenitors; in turn, completion of the bone resorption phase is followed by a wave of bone formation, driven, in part, by factors produced by the osteoclast that stimulate osteoblast differentiation and activity, perhaps via direct cell-cell contact between the osteoclast and osteoblast within the confines of the BRC. In the context of this orchestrated activity in the BMU, there are thus a number of cells that can be targeted by agents that increase bone mass: the osteoblast, the osteocyte, the osteoclast, and perhaps even the endothelial cell in the vasculature. Indeed, a recent study by Wang et al. (11) showed that increased VEGF production by osteoblastic cells has a marked anabolic effect on bone, apparently due to increased angiogenesis and a subsequent influx of osteoblasts onto bone surfaces. However, although the interactions of endothelial cells with osteoblasts is an active area of investigation (reviewed in ref. 12), a detailed discussion of this is beyond the scope of the present Review. Targeting osteoblast differentiation to enhance bone formation Overview of osteoblast differentiation. Numerous secreted factors of paracrine, autocrine, and endocrine origin influence osteoblast development and maturation. These include some bone morphogenetic proteins (BMPs), PTH, FGF, IGF, endothelin-1, and prostaglandin agonists (13 16). Only a few are used clinically in the US to promote bone formation in response to injury or aging. Recombinant human BMP2 is used clinically to mediate spinal fusions, and BMP7 (also known as OP1) is used for the treatment of nonunion of long-bone fractures that occur secondary to trauma and for which an allograft is unsuitable. Neither is approved for osteoporosis therapy, because they both have a short half-life and cannot be administered systemically. As mentioned earlier, PTH is FDA approved to increase bone formation in patients with osteoporosis; however, it can only be prescribed for two years in the US. Thus, there is a clear need for more anabolic therapies to promote osteoblast activity. Targeting the Wnt pathway is one promising avenue. Available evidence indicates that Wnts and PTH stimulate bone formation via complementary pathways (17). BMP2 also synergizes with canonical Wnts to promote bone formation, and there seems to be considerable crosstalk between the Wnt and BMP signaling pathways (18, 19). Osteoblasts are mesenchymal cells derived from mesodermal and neural crest progenitors. As cells of the osteoblast lineage differentiate, they produce molecules essential for construction of the mineralized bone matrix and for support of hematopoiesis and angiogenesis. Sequential expression of several molecules facilitates the differentiation of the progenitor cell into a proliferating preosteoblast, then into a bone matrix producing osteoblast, and eventually into a mechanosensory osteocyte or a bone-lining cell (Figure 2). Runt-related transcription factor 2 (Runx2) is the earliest marker of an osteoblast lineage cell and is necessary, but not 422 The Journal of Clinical Investigation Volume 118 Number 2 February 2008
4 Figure 2 The central role of canonical Wnt signaling in regulating osteoblast lineage specification, expansion, and terminal differentiation. Osteoblasts are derived from multipotent mesodermal or neural crest progenitors. Activation of the canonical (ca) Wnt signaling pathway, manifest through β-catenin stabilization, prevents the formation of cartilage (chondrogenesis). Wnt10b prevents adipogenesis (40). The canonical Wnt signaling pathway promotes survival of all cells of the osteoblast lineage and induces the proliferation of preosteoblasts. +, canonical Wnt signaling promotes the process;, canonical Wnt signaling inhibits the process; AP, alkaline phosphatase; Cola1, collagen a1; DMP1, dentin matrix protein 1; OCN, osteocalcin; Osx, osterix; PTHR, receptor for PTH. sufficient, for a progenitor cell to differentiate along the osteoblast lineage (20, 21). Runx2 regulates cellular proliferation, integrates numerous signaling pathways, and controls the expression of many genes (e.g., those encoding osteocalcin, VEGF, RANKL, sclerostin, and dentin matrix protein 1 [DMP1]) throughout osteoblast maturation (22, 23). Osterix is another transcription factor essential for the formation of preosteoblasts from multipotent progenitors (24). It acts downstream of Runx2, but its expression is downregulated in bone marrow stromal cells by endothelial cells (25); osterix, in turn, impairs osteoblast differentiation (24). Osterix is also a suppressor of VEGF expression following endothelin-1 exposure (26); therefore, it might be a crucial mediator of osteoblast function within the context of the BRC. During the matrix-forming and maturation phases of osteoblast differentiation, the simultaneous coexpression of alkaline phosphatase and type I collagen sets the stage for mineralization (27). Mature osteoblasts also produce osteocalcin, RANKL, and the receptor for PTH (PTHR1), which, among other actions, regulate bone formation and resorption. As osteoblasts become embedded in the mineralized matrix, they transform into osteocytes and begin expressing several molecules, including DMP1 and sclerostin, that control bone formation and phosphate metabolism (28). Wnts and osteoblast differentiation. Wnts are secreted glycoproteins crucial for the development and homeostatic renewal of many tissues, including bone. Figure 2 depicts the central role played by the canonical Wnt signaling pathway in regulating osteoblast development. Wnts stimulate several signaling pathways by binding a receptor complex consisting of LDL receptor related protein 5 (LRP5) or LRP6 and one of ten Frizzled (Fz) molecules (18). The canonical Wnt signaling pathway has been the most extensively studied Wnt signaling pathway in osteoblasts. It involves the stabilization of β-catenin and regulation of multiple transcription factors, namely lymphoid enhancer factor 1 (Lef1) and the T cell factors Tcf7 (often referred to as Tcf1), Tcf7L1 (often referred to as Tcf3), and Tcf7L2 (often referred to as Tcf4) (Figure 3). This pathway is active in all cells of the osteoblast lineage, including preosteoblasts, bone-lining cells, and osteocytes (29). Notably, Wnt/β-catenin signaling is a normal physiological response to mechanical loading (30) and participates in the fracture healing process (31). Wnt signaling has three major functions in osteoblast lineage cells: dictating osteoblast specification from osteo-/chondroprogenitors; stimulating osteoblast proliferation; and enhancing osteoblast and osteocyte survival. Within the BMU, Wnts influence osteoclast maturation by regulating RANKL levels in osteoblasts (32). The crucial role of the canonical Wnt signaling pathway in bone cells was revealed earlier this decade in seminal studies showing that loss-of-function mutations in the gene encoding LRP5 decrease bone mass, whereas gain-of-function mutations increase bone mass in both humans and mice (33 36). The mouse models also revealed that Lrp5 is mechanistically essential for regulating osteoblast number, through both increasing the proliferation of progenitors and enhancing the survival of committed osteoblasts and osteocytes (35, 36). In accordance with these findings, adding Wnts or deleting secreted Wnt inhibitors enhances osteoblast and osteocyte survival (37 39). Since the LRP5 discoveries, many other components of the Wnt signaling pathway (e.g., Wnt10b, β-catenin, Tcf1, adenomatosis polyposis coli [APC], Axin-2, secreted frizzled-related protein 1 [Sfrp1], Sfrp4, and dickkopf homolog 1 [Dkk1]) have been deleted or overexpressed in mice. The general conclusion derived from all these studies is that activation of the canonical Wnt signaling pathway facilitates osteoblast specification from mesenchymal progenitors at the expense of adipogenesis and enhances bone mass and strength, whereas suppression causes bone loss (38, 40 50). Several of these studies also revealed that the canonical Wnt signaling pathway cooperates with the essential transcription factors Runx2 and osterix to maintain and promote osteoblast maturation (41 43, 45, 50). Although the final conclusion (that stimulation of the canonical Wnt signaling pathway increases bone mass) was similar in the above-mentioned studies (38, 40 50), the underlying mechanisms The Journal of Clinical Investigation Volume 118 Number 2 February
5 Figure 3 A partial view of the canonical Wnt signaling pathway. Wnts bind a receptor complex consisting of LRP5 or LRP6 and one of ten Fz proteins. This prevents phosphorylation of β-catenin by GSK3β and other kinases and its subsequent degradation. Of note, mutating the residues that can be phosphorylated to alanine creates stable, gainof-function β-catenin proteins. Stabilized β-catenin accumulates and translocates to the nucleus, where it interacts with Tcf7 and related transcription factors (Lef1, Tcf7L1, Tcf7L2) to regulate gene expression. Outside the cell, molecules that sequester either LRP5 (e.g., Dkk1 and sclerostin) or the Wnt ligand (e.g., Sfrp) negatively control the canonical Wnt signaling pathway. Lithium chloride inhibits GSK3β inside the cell. APC, adenomatosis polyposis coli. sometimes differed. For example, constitutively active β-catenin increases bone mass by inducing the expression of the gene encoding osteoprotegerin (OPG) and thereby inhibits osteoclast maturation (41, 50). In contrast, Lrp5 gain-of-function mutations or administration of Wnt3a enhance the proliferation of preosteoblasts and prevent apoptosis of osteoblasts and osteocytes without affecting osteoclasts (35, 37, 51, 52). Thus, activation of Wnt signaling pathways through Wnt proteins binding to their receptors triggers different signaling pathways than if β-catenin is the starting point (37). β-catenin participates in other signaling pathways, including ones induced by activated receptor tyrosine kinases and nuclear hormone receptors, and physically links E-cadherin to the actin cytoskeleton (53). Additional studies are needed to unravel the complex roles that individual Wnts have within the BMU and to determine the extent to which stabilized β-catenin can be used as a reliable surrogate for measuring Wnt activity. Much remains to be learned about the molecular mechanisms of Wnt signaling, but it is clear that Wnts are potential targets for therapeutics designed to increase bone mass. One possible therapeutic approach would be to deliver Wnt agonists. The limitation of this approach, however, is that Wnts are historically very difficult and expensive to purify; thus, using Wnts as an anabolic agonist is impractical at this time. Efforts to therapeutically target the Wnt signaling pathway have instead focused on two alternative approaches (Figure 3): the first is to inhibit Wnt antagonists (e.g. Dkk1, sclerostin, and Sfrp1) with neutralizing antibodies (discussed below), and the second is to inhibit glycogen synthase kinase 3β (GSK3β), which is a kinase that phosphorylates β-catenin and promotes its degradation. The latter approach has been accomplished in mice, whereby administration of lithium chloride and other small-molecule inhibitors of GSK3β reversed bone loss caused by aging, estrogen deficiency, and Lrp5 mutations (54); increased the sensitivity of osteoblasts and osteocytes to mechanical loading (30); and improved fracture healing (31). Lithium chloride is a commonly prescribed mood-stabilizing drug. Two studies examining fracture risk in humans found that lithium chloride use decreased fracture incidence in a dose-dependent manner (55); however, one study found that fracture incidence did not remain lower and actually increased after lithium chloride use was discontinued (56). Thus, the long-term effects of GSK3β inhibitors and other Wnt pathway agonists on bone formation and quality require careful evaluation before they can be used clinically as bone anabolic agents. The other therapeutic approach being actively pursued to stimulate Wnt signaling to increase bone mass is the use of humanized monoclonal antibodies to neutralize antagonists of the Wnt signaling pathway. The canonical Wnt signaling pathway can be inhibited extracellularly by sequestering either the ligand or the receptor (Figure 3). Dkk1 and sclerostin inhibit Wnt signaling by dissociating LRP5 from Fz and Wnts. Sfrps, in contrast, bind Wnts and prevent them from associating with the LRP5/Fz complex. Serum Dkk1 levels are inversely proportional to bone mass in mice (48, 49, 57) and are a prognostic biomarker of the osteolysis that is associated with multiple myeloma in humans (58). Similarly, Sfrp1 levels are inversely related to bone formation, but in mouse gene deletion studies, the results were more compelling in female mice than in male mice, indicating that Sfrp1 effects might be tied to hormonal influences (38). Sfrp1-specific neutralizing antibodies and antagonists have not yet been described. In contrast, Dkk1- specific neutralizing antibodies have been tested in several studies (59, 60). Diarra and colleagues reversed bone destruction in a mouse model of rheumatoid arthritis by administering Dkk1-specific antibodies (59). This was accompanied by increased numbers of osteoblasts, rates of bone formation, and expression of OPG and by decreased numbers of osteoclasts. Interestingly, osteophytes (bone spurs) developed in the animals treated with Dkk1-specific antibodies, which effectively converted the phenotype to an osteoarthritic model. In a different study using a mouse model of multiple myeloma, a Dkk1-specific antibody promoted bone formation in tumor-bearing and non tumor-bearing femurs (60). The Dkk1- specific antibody reduced the number of osteoclasts expressing tartrate-resistant acid phosphatase (TRAP) and increased the number of osteoblasts producing osteocalcin. Testing of Dkk1-specific neutralizing antibodies is ongoing in preclinical animal models and these agents are likely to enter phase I clinical trials. Although early results indicate that Dkk1-specific antibodies can promote bone formation, there are some concerns about their safety and potency. The development of osteophytes following administration of Dkk1-specific antibodies in the mouse model of rheumatoid arthritis suggests a role for Dkk1 in preventing osteoarthritis and bone spurs. However, optimization of dosage and delivery methods might control this outcome, and more studies are needed to define the appropriate doses and routes of delivery. Tumor formation is also a general concern, because the Wnt signaling pathway is activated by mutations in many cancers. However, it is well established that tumor formation requires multiple events; therefore, even though overstimulation of Wnt signaling 424 The Journal of Clinical Investigation Volume 118 Number 2 February 2008
6 pathways might contribute to tumorigenesis, it would be highly unlikely to be the sole initiating event. In anecdotal support of this, neither aged Dkk1 haploinsufficient mice nor humans using lithium chloride or with high bone mass due to gain-of-function mutations in LRP5 have increased cancer incidence (61). Targeting osteocyte function as a potential approach to enhancing bone anabolism Sclerostin is another promising target of biologic therapies to increase bone mass. Sclerostin is secreted exclusively by osteocytes, apparently as a mechanism to reduce bone formation (62, 63). Accordingly, sclerostin expression levels are repressed in response to mechanical loading and intermittent PTH treatment (64 66). Sclerostin is the product of the SOST gene, which is mutated and downregulated in patients with sclerosteosis and van Buchem disease (67, 68), diseases characterized by high bone density. Sclerostin inhibits osteoblast activity and bone formation by sequestering LRP5 and LRP6, thereby slowing the Wnt signaling pathway (Figure 3) (69). Interestingly, an LRP5 mutant that is associated with high bone mass prevents sclerostin from binding LRP5 (70), in both mice and humans. Sclerostin also binds BMPs, but with low affinity, nondiscriminately, and without directly affecting BMP2 target genes in osteoblasts (62, 63). Sclerostin thus seems to indirectly block BMP-induced bone formation by inhibiting Wnt signaling pathways. Preliminary studies with a humanized sclerostin-specific monoclonal antibody were promising and have shown bone anabolic activities in animal models and postmenopausal women (71, 72). Thus, inhibition of sclerostin activity seems to be a bone anabolic approach that is likely to progress rapidly toward clinical testing and ultimate clinical use. Targeting osteoblast-osteoclast cross-talk as a potential approach to enhancing bone anabolism Under most conditions, resorbed bone is nearly precisely replaced in location and amount by new bone. Thus, it has long been recognized that bone loss through osteoclast-mediated bone resorption and bone replacement through osteoblast-mediated bone formation are tightly coupled. There is now clear evidence that osteoblasts direct osteoclast differentiation by membrane presentation of RANKL and M-CSF (73, 74). The promotion of osteoclast differentiation by RANKL can be dampened through regulation of expression of the RANKL decoy receptor, OPG (74). In many instances, suppression of OPG, usually combined with increased expression of M-CSF and RANKL, enhances bone resorption (74). However, questions remain as to how osteoblasts are recruited to the site following the resorption phase and how the amount of bone laid down is controlled. This has led to consideration of how osteoclasts and/or their activity could promote bone formation. Stored within the bone matrix are considerable quantities of several growth factors that could promote bone formation, such as TGF-β, IGF-I, and IGF-II (75, 76). Because osteoclast-mediated bone resorption releases IGFs and TGF-β from bone, it has been posited that these play a part in coupling bone resorption to subsequent bone formation, although there is no direct evidence of this (77, 78). Examination of both mouse models and humans in whom osteoclastogenesis is perturbed has provided important insights into the role of bone resorption in promoting bone formation (79, 80). In mouse models where osteoclasts are present but not able to resorb bone (mice lacking either c-src or chloride-7 channel), there is no defect in bone formation (81 83). Likewise, in humans who have one of their genes encoding the chloride-7 channel inactivated, osteoclasts are present, but there is inhibition of bone resorption with no reduction in bone formation (84 86). These data are in sharp contrast to mouse models that result in defective osteoclastogenesis, such as mice lacking c-fos or M-CSF, which have no osteoclasts and also exhibit defective bone formation (87 89). Thus, it seems that the presence of osteoclasts, whether or not they are resorbing bone, is needed for normal bone formation and that the release of bone-bound factors might not be required to couple osteoclasts to the bone formation phase of bone turnover. What are possible osteoclast-osteoblast coupling factors? One intriguing recent discovery is the bidirectional signaling mediated by the transmembrane proteins ephrinb2 and EPH receptor B4 (EphB4), which are expressed on osteoclasts and osteoblasts, respectively (90). The engagement of these molecules stimulates osteoblast differentiation and represses osteoclast differentiation. A potential scenario is that osteoclast ephrinb2 stimulates osteoblast differentiation by binding EphB4 on osteoprogenitor cells, promoting bone formation. Conversely, EphB4 on osteoblastic cells binding ephrinb2 on osteoclast precursors represses further osteoclast differentiation. These interactions require close physical contact of osteoblast lineage cells with preosteoclasts and mature osteoclasts and are likely to occur in the BRC, as depicted in Figure 1D. Indeed, the close proximity of osteoblast lineage cells to preosteoclasts and mature osteoclasts has already been demonstrated by the finding that membrane-bound RANKL and M-CSF on osteoblast lineage cells promote osteoclast differentiation (91, 92). There is evidence that osteoclasts might also recruit osteoblast lineage cells. Ryu et al. (93) have shown that sphingosine 1-phosphate (S1P), which is produced by osteoclasts, stimulates osteoblast migration, as well as promoting osteoblast survival. Thus, osteoclasts might recruit osteoprogenitors to sites of bone resorption by secretion of S1P and stimulate osteoblast differentiation by stimulating EphB4 signaling. In turn, osteoblast-stimulated reverse signaling through EphB4 binding to ephrinb2 on osteoclast precursors would repress osteoclast differentiation. This sequence of events would shut down bone resorption and set the stage for the next phase of bone remodeling, when osteoblasts are recruited to the site to replace the resorbed bone. Interest is growing in whether this stage of the bone remodeling cycle could provide novel anabolic targets. PTH uses multiple pathways to promote bone formation Although an excess of PTH, as in severe hyperparathyroidism, is often catabolic for bone, Fuller Albright observed almost 80 years ago that PTH can also have anabolic effects on bone (94). This led ultimately to a clinical trial clearly demonstrating that intermittent exposure of bone to PTH can increase bone formation and bone mass in humans (95). This is in marked contrast to continuous PTH exposure, which often leads to bone loss (96). Even though PTH is now approved by the FDA as a bone anabolic agent for patients with osteoporosis, determining the precise mechanism(s) by which it exerts its anabolic effects on bone still remains an area of intensive investigation. Emerging evidence indicates that part of the difficulty in unequivocally defining the mechanism(s) for the anabolic effects of PTH is that these effects probably involve multiple cell types and pathways. Thus, as summarized in Figure 4 and discussed below, PTH probably impacts osteoblasts, bone-lining cells, osteocytes, and osteoclasts and activates multiple pathways that collectively result in stimulation of bone formation. This The Journal of Clinical Investigation Volume 118 Number 2 February
7 Figure 4 Potential cellular targets for the anabolic effects of PTH. PTH targets multiple cell types to mediate its bone anabolic effects. Specifically, PTH decreases apoptosis and proliferation of osteoblasts (OBs), as well as increasing their differentiation. It can activate bone-lining cells into functioning osteoblasts and decrease sclerostin production by osteocytes, which would be expected to increase Wnt signaling to osteoblasts. Finally, PTH is postulated to stimulate factors produced by osteoclasts (OCs) that stimulate osteoblasts. complexity has recently been demonstrated in microarray analyses of bones harvested from rats treated with PTH, where a large number of genes ( 1,000) were modulated by PTH (97). These included genes involved in Wnt signaling (Wnt4 and Sfrp4), transcription factors (camp responsive element modulator [CREM]), growth factors (amphiregulin [AREG]), and chemokines (CCL2, also known as MCP-1]), and understanding how theses genes and gene regulatory networks ultimately result in an anabolic effect on bone is clearly an ongoing challenge. As recently summarized by Jilka (98), the osteoblast is clearly a target for PTH action. Studies in mice have demonstrated that intermittent PTH treatment inhibits osteoblast apoptosis, at least in cancellous bone, leading to the suggestion that this might account, in large part, for the increase in osteoblast numbers and subsequent increase in bone formation seen following PTH therapy (99, 100). However, inhibition of osteoblast apoptosis by PTH is yet to be confirmed in humans (101); this might, in part, be due to the much lower basal prevalence of osteoblast apoptosis in mice versus humans (98). In terms of the specific mechanisms by which apoptosis is inhibited, studies in cultured osteoblastic cells have shown that PTH rapidly activates antiapoptotic signaling pathways that involve camp-mediated activation of PKA and its subsequent phosphorylation and inactivation of the proapoptotic protein BCL2-antagonist of cell death (Bad), as well as increased expression of survival genes such as B cell leukemia/lymphoma 2 (Bcl-2) (100). PTH also seems to decrease osteoblast proliferation, leading to a reciprocal increase in osteoblast differentiation (102); these effects might be due to decreased expression of cyclin D1, which is required for cell cycle progression, as well as increased expression of cyclin-dependent kinase inhibitors (102, 103). Concomitantly, PTH transiently increases the level and activity of Runx2 (100), and there are data supporting a role for LRP5-mediated Wnt signaling in mediating at least part of the anabolic effect of PTH (104). Some of the effects of PTH on osteoblastic cells might also be due to increased production and subsequent autocrine/paracrine effects of IGF-I and FGF-2 (105, 106). In addition, there is also evidence that PTH can activate previously quiescent bone-lining cells on bone surfaces (107), which might explain the very early increase in bone formation seen following PTH therapy. In contrast to these effects on differentiated osteoblastic cells, PTH does not seem to influence the proliferation or differentiation of uncommitted osteoprogenitor cells (99), in part because the PTH receptor is not expressed until these cells have progressed down the osteoblast lineage (108). As noted earlier, until recently, the osteocyte was regarded as a relatively inert, quiescent cell entrapped in the bone matrix, but there is increasing evidence of a key role for the osteocyte in the regulation of bone remodeling (9). Consistent with this role, PTH has been shown to cause a transient reduction in the level of mrna encoding sclerostin in osteocytes (65). This would, in turn, lead to increased Wnt signaling in the local microenvironment, and this might be an important mechanism by which PTH regulates osteoblast development via actions on the osteocyte. Prior to the approval of PTH as a therapy for osteoporosis, there were a number of FDA-approved drugs, such as alendronate, that inhibited bone resorption. Since PTH stimulates bone formation, a logical hypothesis was that the simultaneous administration of PTH with an anticatabolic drug would lead to even larger increases in bone mass than administration of either agent alone. Surprisingly, however, this has proven not to be the case: studies in both women (109) and men (110) show that alendronate in fact blunts the anabolic action of PTH, at least in cancellous bone. This clinical observation combined with animal work showing that absence of c-fos, which leads to a block in osteoclast differentiation, also results in loss of the anabolic response to PTH (111) has led to the plausible hypothesis that at least part of the anabolic actions of PTH on bone are mediated by its activation of the osteoclast (79). Indeed, as discussed earlier, there is intense interest in identifying the factor(s) produced by osteoclasts that stimulate bone formation by osteoblasts. The future of bone anabolic therapies It is clear that within the closed compartment constituting the BRC, there is an intimate cross-talk among osteoblasts, osteo- 426 The Journal of Clinical Investigation Volume 118 Number 2 February 2008
8 clasts, and bone-lining cells forming the canopy of the BRC. Moreover, the connections between the bone-lining canopy cells and bone-lining cells on the bone surface, which communicate with osteocytes, also allow the osteocytes embedded deep within the bone matrix to influence the numbers and activity of the osteoblasts. Understanding better these complex cellular interactions and the molecules that mediate them, such as those discussed in this Review, will ultimately lead to the development of new compounds, such as the sclerostin-specific antibody discussed above, with potent bone anabolic effects. This would, in turn, fulfill an important clinical need, since, although there are numerous compounds available that inhibit bone resorption, treatment options for reversing bone loss with bone formation stimulating agents are currently limited to PTH. Interestingly, it is somewhat ironic that despite the tremendous advances in basic bone biology that might lead to targeted anabolic therapies, PTH, which was discovered empirically to have anabolic effects on bone, continues to remain somewhat of a mystery in terms of its specific mechanisms of action. Acknowledgments This work was supported by NIH grants AG004875, AG028936, AR048147, AR050074, DE14680, and AR Address correspondence to: Sundeep Khosla, Guggenheim 7, College of Medicine, Mayo Clinic, 200 First Street SW, Rochester, Minnesota 55905, USA. Phone: (507) ; Fax: (507) ; khosla.sundeep@mayo.edu. 1. Vahle, J.L., et al Skeletal changes in rats given daily subcutaneous injections of recombinant human parathyroid human (1-34) for 2 years and relevance to human safety. Toxicol. Pathol. 30: Rodriguez-Merchan, E.C., and Forriol, F Nonunion: general principles and experimental data. Clin. Orthop. Rel. Res. 419: Marsh, D Concepts of fracture union, delayed union, and nonunion. Clin. Orthop. Rel. Res. 355(Suppl.):S22 S Owen, M The origin of bone cells in the postnatal organism. Arthritis Rheum. 23: Parfitt, A.M The mechanism of coupling: role for the vasculature. Bone. 26: Burkhardt, R., et al The structural relationship of bone forming and endothelial cells of the bone marrow. In Bone Circulation. J. Arlet, R.P. Ficat, and D.S. Hungerford, editors. Williams & Wilkins. Baltimore, Maryland, USA Hauge, E.M., Qvesel, D., Eriksen, E.F., Mosekilde, L., and Melsen, F Cancellous bone remodeling occurs in specialized compartments lined by cells expressing osteoblastic markers. J. Bone Miner. Res. 16: Everts, V., et al The bone lining cell: its role in cleaning Howship s lacunae and initiating bone formation. J. Bone Miner. Res. 17: Bonewald, L.F Osteocyte messages from a bony tomb. Cell Metab. 5: Eriksen, E.F., Eghbali-Fatourechi, G.Z., and Khosla, S Remodeling and vascular spaces in bone. J. Bone Miner. Res. 22: Wang, Y., et al The hypoxia-inducible factor alpha pathway couples angiogenesis to osteogenesis during skeletal development. J. Clin. Invest. 117: Brandi, M.L., and Collin-Osdoby, P Perspective: Vascular biology and the skeleton. J. Bone Miner. Res. 21: Iwaniec, U.T., et al A comparative study of the bone-restorative efficacy of anabolic agents in aged ovariectomized rates. Osteoporos. Int. 18: Li, M., et al A novel, non-prostanoid EP2 receptor-selective prostaglandin E2 agonist stimulates local bone formation and enhances fracture healing. J. Bone Miner. Res. 18: Qin, L., et al Gene expression profiles and transcription factors involved in parathyroid hormone signaling in osteoblasts revealed by microarray and bioinformatics. J. Biol. Chem. 278: Onyia, J.E., et al Molecular profile of catabolic versus anabolic treatment regimens of parathyroid hormone (PTH) in rat bone: an analysis by DNA microarray. J. Cell. Biochem. 95: Bodine, P.V.N., Seestaller-Wehr, L., Kharode, Y.P., Bex, F.J., and Komm, B.S Bone anabolic effects of parathyroid hormone are blunted by deletion of the Wnt antagonist secreted frizzledrelated protein-1. J. Cell Physiol. 210: Westendorf, J.J., Kahler, R.A., and Schroeder, T.M Wnt signaling in osteoblasts and bone diseases. Gene. 341: Mbalaviele, G., et al Beta-catenin and BMP-2 synergize to promote osteoblast differentiation and new bone formation. J. Cell. Biochem. 94: Komori, T., et al Targeted disruption of Cbfa1 results in a complete lack of bone formation owing to maturational arrest of osteoblasts. Cell. 89: Otto, F., et al Cbfa1, a candidate gene for cleidocranial dysplasia syndrome, is essential for osteoblast differentiation and bone development. Cell. 89: Otto, F., Lubbert, M., and Stock, M Upstream and downstream targets of RUNX proteins. J. Cell. Biochem. 89: Lian, J.B., et al Networks and hubs for the transcriptional control of osteoblastogenesis. Rev. Endocr. Metab. Disord. 7: Nakashima, K., et al The novel zinc fingercontaining transcription factor osterix is required for osteoblast differentiation and bone formation. Cell. 108: Qu, G., and von Schroeder, H.P Role of osterix in endothelin-1-induces downregulation of vascular endothelial growth factor in osteoblastic cells. Bone. 38: Meury, T., Verrier, S., and Alini, M Human endothelial cells inhibit BMSC differentiation into mature osteoblasts in vitro by interfering with osterix expression. J. Cell. Biochem. 98: Murshed, M., Harmey, D., Millan, J.L., McKee, M.D., and Karsenty, G Unique coexpression in osteoblasts of broadly expressed genes accounts for the spatial restriction of ECM mineralization to bone. Genes Dev. 19: Bonewald, L Osteocytes as multifunctional cells. J. Musculoskelet. Neuronal Interact. 6: Hens, J.R., et al TOPGAL mice show that the canonical Wnt signaling pathway is active during bone development and growth and is activated by mechanical loading in vitro. J. Bone Miner. Res. 20: Robinson, J.A., et al Wnt/beta-catenin signaling is a normal physiological response to mechanical leading in bone. J. Biol. Chem. 281: Chen, Y., et al Beta-catenin signaling plays a disparate role in different phases of fracture repair: implications for therapy to improve bone healing. PLoS Med. 4: Spencer, G.J., Utting, J.C., Etheridge, S.L., Arnett, T.R., and Genever, P.G Wnt signalling in osteoblasts regulates expression of the receptor activator of NFkappaB ligand and inhibits osteoclastogenesis in vitro. J. Cell Sci. 119: Gong, Y., et al LDL receptor-related protein 5 (LRP5) affects bone accrual and eye development. Cell. 107: Little, R.D., et al A mutation in the LDL receptor-related protein 5 gene results in the autosomal dominant high-bone-mass trait. Am. J. Hum. Genet. 70: Kato, M., et al Cbfa1-independent decrease in osteoblast proliferation, osteopenia, and persistent embryonic eye vascularization in mice deficient in Lrp5, a Wnt coreceptor. J. Cell Biol. 157: Babij, P., et al High bone mass in mice expressing a mutant LRP5 gene. J. Bone Miner. Res. 18: Almeida, M., Han, L., Bellido, T., Manolagas, S.C., and Kousteni, S Wnt proteins prevent apoptosis of both uncommitted osteoblast progenitors and differentiated osteoblasts by beta-catenindependent and -independent signaling cascades involving Src/ERK and phosphatidylinositol 3-kinase/AKT. J. Biol. Chem. 280: Bodine, P.V.N., et al The Wnt antagonist secreted frizzled-related protein-1 is a negative regulator of trabecular bone formation in adult mice. Mol. Endocrinol. 18: Bodine, P.V.N., et al The Wnt antagonist secreted frizzled-related protein-1 controls osteoblast and osteocyte apoptosis. J. Cell. Biochem. 96: Bennett, C.N., et al Regulation of osteoblastogenesis and bone mass by Wnt10b. Proc. Natl. Acad. Sci. U. S. A. 102: Glass, D.A., II, et al Canonical Wnt signaling in differentiated osteoblasts controls osteoclast differentiation. Dev. Cell. 8: Hill, T.P., Spater, D., Taket, M.M., Birchmeier, W., and Hartmann, C Canonical Wnt/betacatenin signaling prevents osteoblasts from differentiating into chondrocytes. Dev. Cell. 8: Hu, H., et al Sequential roles of hedgehog and Wnt signaling in osteoblast development. Development. 132: Tamamura, Y., et al Developmental regulation of Wnt/beta-catenin signals is required for growth plate assembly, cartilage integrity, and endochondral ossification. J. Biol. Chem. 280: Day, T.F., Guo, X., Garrett-Beal, L., and Yang, Y Wnt/beta-catenin signaling in mesenchymal progenitors controls osteoblast and chondrocyte differentiation during vertebrate skeletogenesis. Dev. Cell. 8: Liu, H., et al Augmented Wnt signaling in a mammalian model of accelerated aging. Science. 317: Nakanishi, R., et al Secreted frizzled-related protein 4 is a negative regulator of peak BMD in SAMP6 mice. J. Bone Miner. Res. 21: Li, J., et al Dkk1-mediated inhibition of Wnt signaling in bone results in osteopenia. Bone. 39: The Journal of Clinical Investigation Volume 118 Number 2 February
9 49. Morvan, F., et al Deletion of a single allele of the Dkk1 gene leads to an increase in bone formation and bone mass. J. Bone Miner. Res. 21: Rodda, S.J., and McMahon, A.P Distinct roles for hedgehog and canonical Wnt in specification, differentiation and maintenance of osteoblast progenitors. Development. 133: Kang, S., et al Wnt signaling stimulates osteoblastogenesis of mesenchymal precursors by suppressing CCAAT/enhancer-binding protein alpha and peroxisome proliferator-activated receptor gamma. J. Biol. Chem. 282: Boland, G.M., Perkins, G., Hall, D.J., and Tuan, R.S Wnt 3a promotes proliferation and suppresses osteogenic differentiation of adult human mesenchymal stem cells. J. Cell. Biochem. 93: McCrea, P.D., Turck, C.W., and Gumbiner, B A homolog of the armadillo protein in drosophila (plakoglobin)associated with E-cadherin. Science. 254: Clement-Lacroix, P., et al Lrp5-independent activation of Wnt signaling by lithium chloride increases bone formation and bone mass in mice. Proc. Natl. Acad. Sci. U. S. A. 102: Vestergaard, P., Rejnmark, L., and Mosekilde, L Reduced relative risk of fractures among users of lithium. Calcif. Tissue Int. 77: Wilting, I., et al Lithium use and the risk of fractures. Bone. 40: Macdonald, B.T., et al Bone mass is inversely proportional to Dkk1 levels in mice. Bone. 41: Tian, E., et al The role of the Wnt-signaling antagonist DKK1 in the development of osteolytic lesions in multiple myeloma. N. Engl. J. Med. 349: Diarra, D., et al Dickkopf-1 is a master regulator of joint remodeling. Nat. Med. 13: Yaccoby, S., et al Antibody-based inhibition of DKK1 suppresses tumor-induced bone resorption and multiple myelome growth in vivo. Blood. 109: Baron, R., and Rawadi, G Targeting the Wnt/ beta-catenin pathway to regulate bone formation in the adult skeleton. Endocrinology. 148: van Bezooijen, R.L., et al Wnt but not BMP signaling is involved in the inhibitory action of sclerostin on BMP-stimulated bone formation. J. Bone Miner. Res. 22: Winkler, D.G., et al Osteocyte control of bone formation via sclerostin, a novel BMP antagonist. EMBO J. 22: Keller, H., and Kneissel, M SOST is a target gene for PTH in bone. Bone. 37: Bellido, T., et al Chronic elevation of parathyroid hormone in mice reduces expression of sclerostin by osteocytes: a novel mechanism for hormonal control of osteoblastogenesis. Endocrinology. 146: Robling, A.G., Bellido, T., and Turner, C.H Mechanical stimulation in vivo reduces osteocyte expression of sclerostin. J. Musculoskelet. Neuronal. Interact. 6: Balemans, W., et al Increase bone density in sclerosteosis is due to the deficiency of a novel secreted protein (SOST). Hum. Mol. Genet. 10: Brunkow, M.E., et al Bone dysplasia sclerosteosis results from loss of the SOST gene product, a novel cystine knot-containing protein. Am. J. Hum. Genet. 68: Li, X., et al Dkk2 has a role in terminal osteoblast differentiation and mineralized matrix formation. Nat. Genet. 37: Ellies, D.L., et al Bone density ligand, sclerostin, directly interacts with LRP5 but not LRP- 5G171V to modulate Wnt activity. J. Bone Miner. Res. 21: Ominsky, M.S., et al Sclerostin monoclonal antibody treatment increases bone strength in osteopenic ovariectomized rats. J. Bone Miner. Res. 21:S Padhi, D., et al Anti-sclerostin antibody increases markers of bone formation in healthy postmenopausal women [abstract]. J. Bone Miner. Res. 22(Suppl. 1):S Suda, T., Kobayashi, K., Jimi, E., Udagawa, N., and Takahashi, N The molecular basis of osteoclast differentiation and activation. Novartis Found. Symp. 232: ; discussion Khosla, S Minireview: the OPG/RANKL/ RANK system. Endocrinology. 142: Dallas, S.L., Rosser, J.L., Mundy, G.R., and Bonewald, L.F Proteolysis of latent transforming growth factor-beta (TGF-beta)-binding protein-1 by osteoclasts. A cellular mechanism for release of TGF-beta from bone matrix. J. Biol. Chem. 277: Linkhart, T.A., and MacCharles, D.C Interleukin-1 stimulates release of insulin-like growth factor-i from neonatal mouse calvaria by a prostaglandin synthesis-dependent mechanism. Endocrinology. 131: Mohan, S., and Baylink, D.J Insulin-like growth factor system components and the coupling of bone formation to resorption. Horm. Res. 45(Suppl.): Bonewald, L.F., and Mundy, G.R Role of transforming growth factor-beta in bone remodeling. Clin. Orthop. Relat. Res. 250: Martin, T.J., and Sims, N.A Osteoclastderived activity in the coupling of bone formation to resorption. Trends Mol. Med. 11: Karsdal, M.A., Martin, T.J., Bollerslev, J., Christiansen, C., and Henriksen, K Are nonresorbing osteoclasts sources of bone anabolic activity? J. Bone Miner. Res. 22: Marzia, M., et al Decreased c-src expression enhances osteoblast differentiation and bone formation. J. Cell Biol. 151: Kornak, U., et al Loss of the CiC-7 chloride channel leads to osteopetrosis in mice and man. Cell. 104: Soriano, P., Montgomery, C., Geske, R., and Bradley, A Targeted disruption of the c-src proto-oncogene leads to osteopetrosis in mice. Cell. 64: Bollerslev, J., Steiniche, T., Melsen, F., and Mosekilde, L Structural and histomorphometric studies of iliac crest trabecular and cortical bone in autosomal dominant osteopetrosis: a study of two radiological types. Bone. 10: Atlatalo, S.L., et al Osteoclast-derived serum tartrate-resistant acid phosphatase 5b in Albers- Schonberg disease (type II autosomal dominant osteopetrosis). Clin. Chem. 50: Del Fattore, A., et al Clinical, genetic, and cellular analysis of 49 osteopetrotic patients: implications for diagnosis and treatment. J. Med. Genet. 43: Dai, X.M., Zong, X.H., Akhter, M.P., and Stanley, E.R Osteoclast deficiency results in disorganized matrix, reduced mineralization, and abnormal osteoblast behavior in developing bone. J. Bone Miner. Res. 19: Sakagami, N., et al Reduced osteoblastic population and defective mineralization in osteopetrotic (op/op) mice. Micron. 36: Tuukkanen, J., et al Mineral density and bone strength are dissociated in long bones of rat osteopetrotic mutations. J. Bone Miner. Res. 15: Zhao, C., et al Bidirectional ephrinb2-ephb4 signaling controls bone homeostasis. Cell Metab. 4: Yasuda, H., et al Osteoclast differentiation factor is a ligand for osteoprotegerin osteoclastogenesis-inhibitory factor and is identical to TRANCE/ RANKL. Proc. Natl. Acad. Sci. U. S. A. 95: Lacey, D.L., et al Osteoprotegerin ligand is a cytokine that regulates osteoclast differentiation and activation. Cell. 93: Ryu, J., et al Sphingosine 1-phosphate as a regulator of osteoclast differentiation and osteoclast-osteoblast coupling. EMBO J. 25: Bauer, W., Aub, J.C., and Albright, F Studies of calcium and phosphorus metabolism. J. Exp. Med. 49: Neer, R.M., et al Effect of parathyroid hormone (1-34) on fractures and bone mineral density in postmenopausal women with osteoporosis. N. Engl. J. Med. 344: Tam, C.S., Heersche, J.N.M., Murray, T.M., and Parsons, J.A Parathyroid hormone stimulates the bone apposition rate independently of its resorptive action: differential effects of intermittent and continuous administration. Endocrinology. 110: Li, X., et al Determination of dual effects of parathyroid hormone on skeletal gene expression in vivo by microarray and network analysis. J. Biol. Chem. 282: Jilka, R.L Molecular and cellular mechanisms of the anabolic effect of intermittent PTH. Bone. 40: Jilka, R.L., et al Increased bone formation by prevention of osteoblast apoptosis with parathyroid hormone. J. Clin. Invest. 104: Bellido, T., et al Proteasomal degradation of Runx2 shortens parathyroid hormone-induced anti-apoptotic signaling in osteoblasts. J. Biol. Chem. 278: Lindsay, R., et al Effects if a one-month treatment with PTH(1-34) on bone formation on cancellous, endocortical, and periosteal surfaces of the human ilium. J. Bone Miner. Res. 22: Qin, L., Li, X., Ko, J.K., and Partridge, N.C Parathyroid hormone uses multiple mechanisms to arrest the cell cycle progression of osteoblastic cells from G1 to S phase. J. Biol. Chem. 280: Datta, N.S., Chen, C., Berry, J.E., and McCauley, L.K PTHrP signaling targets cyclin D1 and induces osteoblastic cell growth arrest. J. Bone Miner. Res. 20: Kharode, Y.P., et al Selective involvement of WNT signaling pathway in bone anabolic action of parathyroid hormone. J. Bone Miner. Res. 21:S Bikle, D.D., et al Insulin-like growth factor I is required for the anabolic actions of parathyroid hormone on mouse bone. J. Bone Miner. Res. 17: Hurley, M.M., et al Parathyroid hormone regulates the expression of fibroblast growth factor-2 mrna in osteoblastic cells. J. Bone Miner. Res. 14: Dobnig, H., and Turner, R.T Evidence that intermittent treatment with parathyroid hormone increases bone formation in adult rats by activation of bone lining cells. Endocrinology. 136: Gronthos, S., et al Differential cell surface expression of the STRO-1 and alkaline phosphatase antigens on discrete developmental stages in primary cultures of human bone cells. J. Bone Miner. Res. 14: Black, D.M., et al The effects of parathyroid hormone and alendronate alone or in combination in postmenopausal osteoporosis. N. Engl. J. Med. 349: Finkelstein, J.S., et al The effects of parathyroid hormone, alendronate, or both in men with osteoporosis. N. Engl. J. Med. 349: Koh, A.J., et al Cells of the osteoclast lineage as mediators of the anabolic actions of parathyroid hormone in bone. Endocrinology. 146: The Journal of Clinical Investigation Volume 118 Number 2 February 2008
Pathophysiology of Postmenopausal & Glucocorticoid Induced Osteoporosis. March 15, 2016 Bone ECHO Kate T Queen, MD
 Pathophysiology of Postmenopausal & Glucocorticoid Induced Osteoporosis March 15, 2016 Bone ECHO Kate T Queen, MD Review: normal bone formation Bone Modeling Remodeling Peak Bone Mass Maximum bone mass
Pathophysiology of Postmenopausal & Glucocorticoid Induced Osteoporosis March 15, 2016 Bone ECHO Kate T Queen, MD Review: normal bone formation Bone Modeling Remodeling Peak Bone Mass Maximum bone mass
Bone. Development. Tim Arnett. University College London. Department of Anatomy and Developmental Biology
 Bone Development Tim Arnett Department of Anatomy and Developmental Biology University College London Bone development Outline Bone composition matrix + mineral Bone formation - intramembranous & endochondral
Bone Development Tim Arnett Department of Anatomy and Developmental Biology University College London Bone development Outline Bone composition matrix + mineral Bone formation - intramembranous & endochondral
Anabolic Therapy With Teriparatide Indications Beyond Osteoporosis
 Anabolic Therapy With Teriparatide Indications Beyond Osteoporosis Andreas Panagopoulos MD, PhD Upper Limb & Sports Medicine Orthopaedic Surgeon Assistant Professor, University of Patras Outline Teriparatide
Anabolic Therapy With Teriparatide Indications Beyond Osteoporosis Andreas Panagopoulos MD, PhD Upper Limb & Sports Medicine Orthopaedic Surgeon Assistant Professor, University of Patras Outline Teriparatide
THE GROWING GAP IN OSTEOPOROSIS TREATMENT
 THE GROWING GAP IN OSTEOPOROSIS TREATMENT Sundeep Khosla, M.D. Mayo Clinic, Rochester, MN DISCLOSURES SUNDEEP KHOSLA, M.D. NONE 1 OVERALL CONCLUSIONS There has been remarkable progress in our understanding
THE GROWING GAP IN OSTEOPOROSIS TREATMENT Sundeep Khosla, M.D. Mayo Clinic, Rochester, MN DISCLOSURES SUNDEEP KHOSLA, M.D. NONE 1 OVERALL CONCLUSIONS There has been remarkable progress in our understanding
DISCLOSURES TOPICS" PATHOPHYSIOLOGY of OSTEOPOROSIS: Pathways That Control Bone Remodeling! Why Do Bones Remodel?" Nothing to disclose
 PATHOPHYSIOLOGY of OSTEOPOROSIS: Pathways That Control Bone Remodeling Dolores Shoback, MD Professor of Medicine, UCSF Staff Physician SF/VAMC May 19, 2017 DISCLOSURES Nothing to disclose No conflicts
PATHOPHYSIOLOGY of OSTEOPOROSIS: Pathways That Control Bone Remodeling Dolores Shoback, MD Professor of Medicine, UCSF Staff Physician SF/VAMC May 19, 2017 DISCLOSURES Nothing to disclose No conflicts
Središnja medicinska knjižnica.
 Središnja medicinska knjižnica Pećina, M., Vukičević, S. (2007) Biological aspects of bone, cartilage and tendon regeneration. International Orthopaedics, 31 (6). pp. 719-720. The original publication
Središnja medicinska knjižnica Pećina, M., Vukičević, S. (2007) Biological aspects of bone, cartilage and tendon regeneration. International Orthopaedics, 31 (6). pp. 719-720. The original publication
Clinical Biochemistry
 Clinical Biochemistry 45 (2012) 863 873 Contents lists available at SciVerse ScienceDirect Clinical Biochemistry journal homepage: www.elsevier.com/locate/clinbiochem Review An overview of the regulation
Clinical Biochemistry 45 (2012) 863 873 Contents lists available at SciVerse ScienceDirect Clinical Biochemistry journal homepage: www.elsevier.com/locate/clinbiochem Review An overview of the regulation
Generation of post-germinal centre myeloma plasma B cell.
 Generation of post-germinal centre myeloma. DNA DAMAGE CXCR4 Homing to Lytic lesion activation CD38 CD138 CD56 Phenotypic markers Naive Secondary lymphoid organ Multiple myeloma is a malignancy of s caused
Generation of post-germinal centre myeloma. DNA DAMAGE CXCR4 Homing to Lytic lesion activation CD38 CD138 CD56 Phenotypic markers Naive Secondary lymphoid organ Multiple myeloma is a malignancy of s caused
silent epidemic,. (WHO),
 Tel: 02-740-8686; E-mail: hhbkim@snu.ac.kr silent epidemic,. (WHO),. 5 3, 1. 50 70. 50%, 25%, 20% (12~35%). 2.8% 0.7% 4. ( ). bone remodeling (osteoblast), (osteoclast),.. 3~4.. 70% (osteocyte) (bone lining
Tel: 02-740-8686; E-mail: hhbkim@snu.ac.kr silent epidemic,. (WHO),. 5 3, 1. 50 70. 50%, 25%, 20% (12~35%). 2.8% 0.7% 4. ( ). bone remodeling (osteoblast), (osteoclast),.. 3~4.. 70% (osteocyte) (bone lining
Comment les cellules osseuses communiquent entre elles. Gérard Friedlander Journées UPA 2011
 Comment les cellules osseuses communiquent entre elles Gérard Friedlander Journées UPA 2011 Structure de l os Osteocyte Ostéoclaste Remodelage osseux RANKL RANK NF-kB pathway Stem cell progenitor precursor
Comment les cellules osseuses communiquent entre elles Gérard Friedlander Journées UPA 2011 Structure de l os Osteocyte Ostéoclaste Remodelage osseux RANKL RANK NF-kB pathway Stem cell progenitor precursor
BIOLOGY and BIOMECHANICS OF NORMAL & OSTEOPOROTIC BONE
 BIOLOGY and BIOMECHANICS OF NORMAL & OSTEOPOROTIC BONE Andreas Panagopoulos, MD, PhD Assistant Professor in Orthopaedics University Hospital of Patras, Orthopaedic Clinic Objectives Bone structure and
BIOLOGY and BIOMECHANICS OF NORMAL & OSTEOPOROTIC BONE Andreas Panagopoulos, MD, PhD Assistant Professor in Orthopaedics University Hospital of Patras, Orthopaedic Clinic Objectives Bone structure and
BONE REMODELLING. Tim Arnett. University College London. Department of Anatomy and Developmental Biology
 BONE REMODELLING Tim Arnett Department of Anatomy and Developmental Biology University College London The skeleton, out of sight and often out of mind, is a formidable mass of tissue occupying about 9%
BONE REMODELLING Tim Arnett Department of Anatomy and Developmental Biology University College London The skeleton, out of sight and often out of mind, is a formidable mass of tissue occupying about 9%
Bone Cell Precursors and the Pathophysiology of Bone Loss
 Bone Cell Precursors and the Pathophysiology of Bone Loss HARRY C. BLAIR, a AND JILL L. CARRINGTON b a Departments of Pathology and Cell Biology, University of Pittsburgh, and Pittsburgh VA Medical Center,
Bone Cell Precursors and the Pathophysiology of Bone Loss HARRY C. BLAIR, a AND JILL L. CARRINGTON b a Departments of Pathology and Cell Biology, University of Pittsburgh, and Pittsburgh VA Medical Center,
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists. International authors and editors
 We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 3,350 108,000 1.7 M Open access books available International authors and editors Downloads Our
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 3,350 108,000 1.7 M Open access books available International authors and editors Downloads Our
Download slides:
 Download slides: https://www.tinyurl.com/m67zcnn https://tinyurl.com/kazchbn OSTEOPOROSIS REVIEW AND UPDATE Boca Raton Regional Hospital Internal Medicine Conference 2017 Benjamin Wang, M.D., FRCPC Division
Download slides: https://www.tinyurl.com/m67zcnn https://tinyurl.com/kazchbn OSTEOPOROSIS REVIEW AND UPDATE Boca Raton Regional Hospital Internal Medicine Conference 2017 Benjamin Wang, M.D., FRCPC Division
SKELETAL SYSTEM I NOTE: LAB ASSIGNMENTS for this topic will run over 3 Weeks. A SEPARATE WORKSHEET WILL BE PROVIDED.
 BIO 211; Anatomy and Physiology I REFERENCE: CHAPTER 07 1 Dr. Lawrence Altman Naugatuck Valley Community College LECTURE TOPICS OUTLINE SKELETAL SYSTEM I NOTE: LAB ASSIGNMENTS for this topic will run over
BIO 211; Anatomy and Physiology I REFERENCE: CHAPTER 07 1 Dr. Lawrence Altman Naugatuck Valley Community College LECTURE TOPICS OUTLINE SKELETAL SYSTEM I NOTE: LAB ASSIGNMENTS for this topic will run over
The Skeletal System:Bone Tissue
 The Skeletal System:Bone Tissue Dynamic and ever-changing throughout life Skeleton composed of many different tissues cartilage, bone tissue, epithelium, nerve, blood forming tissue, adipose, and dense
The Skeletal System:Bone Tissue Dynamic and ever-changing throughout life Skeleton composed of many different tissues cartilage, bone tissue, epithelium, nerve, blood forming tissue, adipose, and dense
BONE TISSUE. Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology
 BONE TISSUE Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology BONE FUNCTION Support Protection (protect internal organs) Movement (provide leverage system for skeletal muscles, tendons, ligaments
BONE TISSUE Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology BONE FUNCTION Support Protection (protect internal organs) Movement (provide leverage system for skeletal muscles, tendons, ligaments
Skeletal Tissues. Skeletal tissues. Frame; muscles, organs and CT attach. Brain, spinal cord, thoracic organs; heart and lungs.
 Skeletal Tissues Functions 1) support 2) protection 3) movement Skeletal tissues Frame; muscles, organs and CT attach. Brain, spinal cord, thoracic organs; heart and lungs. Aids muscle contraction; generate
Skeletal Tissues Functions 1) support 2) protection 3) movement Skeletal tissues Frame; muscles, organs and CT attach. Brain, spinal cord, thoracic organs; heart and lungs. Aids muscle contraction; generate
Functions of the Skeletal System. Chapter 6: Osseous Tissue and Bone Structure. Classification of Bones. Bone Shapes
 Chapter 6: Osseous Tissue and Bone Structure Functions of the Skeletal System 1. Support 2. Storage of minerals (calcium) 3. Storage of lipids (yellow marrow) 4. Blood cell production (red marrow) 5. Protection
Chapter 6: Osseous Tissue and Bone Structure Functions of the Skeletal System 1. Support 2. Storage of minerals (calcium) 3. Storage of lipids (yellow marrow) 4. Blood cell production (red marrow) 5. Protection
Lecture 3: Skeletogenesis and diseases
 Jilin University School of Stomatology Skeletogenesis Lecture 3: Skeletogenesis and diseases Aug. 21, 2015 Yuji Mishina, Ph.D. mishina@umich.edu Bone Development Mouse embryo, E14.5 Mouse embryo, E18.0
Jilin University School of Stomatology Skeletogenesis Lecture 3: Skeletogenesis and diseases Aug. 21, 2015 Yuji Mishina, Ph.D. mishina@umich.edu Bone Development Mouse embryo, E14.5 Mouse embryo, E18.0
For more information about how to cite these materials visit
 Author(s): University of Michigan Medical School, Department of Cell and Developmental Biology License: Unless otherwise noted, the content of this course material is licensed under a Creative Commons
Author(s): University of Michigan Medical School, Department of Cell and Developmental Biology License: Unless otherwise noted, the content of this course material is licensed under a Creative Commons
Regulation of bone mass by Wnt signaling
 Review series Regulation of bone mass by Wnt signaling Venkatesh Krishnan, 1 Henry U. Bryant, 1 and Ormond A. MacDougald 2 1 Musculoskeletal Research, Lilly Research Laboratories, Indianapolis, Indiana,
Review series Regulation of bone mass by Wnt signaling Venkatesh Krishnan, 1 Henry U. Bryant, 1 and Ormond A. MacDougald 2 1 Musculoskeletal Research, Lilly Research Laboratories, Indianapolis, Indiana,
Canonical Wnt Signaling in Osteoblasts Is Required for Osteoclast Differentiation
 Canonical Wnt Signaling in Osteoblasts Is Required for Osteoclast Differentiation DONALD A. GLASS, II AND GERARD KARSENTY Department of Molecular and Human Genetics, Bone Disease Program of Texas, Baylor
Canonical Wnt Signaling in Osteoblasts Is Required for Osteoclast Differentiation DONALD A. GLASS, II AND GERARD KARSENTY Department of Molecular and Human Genetics, Bone Disease Program of Texas, Baylor
ANATOMY C027A: MINERALIZED TISSUE BIOLOGY: SKELETAL TISSUES. Please answer THREE Questions. All questions carry equal marks.
 Module Code: C27A UNIVERSITY OF LONDON (University College London) BSc DEGREE 2001 ANATOMY C027A: MINERALIZED TISSUE BIOLOGY: SKELETAL TISSUES 16 May 2001, 10.00am 1) Discuss the roles of ph, po2, phosphate
Module Code: C27A UNIVERSITY OF LONDON (University College London) BSc DEGREE 2001 ANATOMY C027A: MINERALIZED TISSUE BIOLOGY: SKELETAL TISSUES 16 May 2001, 10.00am 1) Discuss the roles of ph, po2, phosphate
Peggers Super Summaries Basic Sciences Bone
 Bone Overview & Turnover BONES Function o Support o Protection o Assisting movement o Storage of minerals o Production of red blood cells from marrow Types o Cancellous o Compact with Haversian systems
Bone Overview & Turnover BONES Function o Support o Protection o Assisting movement o Storage of minerals o Production of red blood cells from marrow Types o Cancellous o Compact with Haversian systems
Skeletal System. The skeletal System... Components
 Skeletal System The skeletal System... What are the general components of the skeletal system? What does the skeletal system do for you & how does it achieve these functions? Components The skeletal system
Skeletal System The skeletal System... What are the general components of the skeletal system? What does the skeletal system do for you & how does it achieve these functions? Components The skeletal system
Reviewers' comments: Reviewer #1 (Expert in GPCRs; Remarks to the Author): General and major comments
 Editorial Note: this manuscript has been previously reviewed at another journal that is not operating a transparent peer review scheme. This document only contains reviewer comments and rebuttal letters
Editorial Note: this manuscript has been previously reviewed at another journal that is not operating a transparent peer review scheme. This document only contains reviewer comments and rebuttal letters
Bone and Cancer. Peter Croucher
 Bone and Cancer Peter Croucher Academic Unit of Bone Biology, Section of Musculoskeletal Science, University of Sheffield Medical School, Sheffield, UK Learning Objectives To Develop Understanding of:
Bone and Cancer Peter Croucher Academic Unit of Bone Biology, Section of Musculoskeletal Science, University of Sheffield Medical School, Sheffield, UK Learning Objectives To Develop Understanding of:
Rama Nada. - Mousa Al-Abbadi. 1 P a g e
 - 1 - Rama Nada - - Mousa Al-Abbadi 1 P a g e Bones, Joints and Soft tissue tumors Before we start: the first 8 minutes was recalling to Dr.Mousa s duties, go over them in the slides. Wherever you see
- 1 - Rama Nada - - Mousa Al-Abbadi 1 P a g e Bones, Joints and Soft tissue tumors Before we start: the first 8 minutes was recalling to Dr.Mousa s duties, go over them in the slides. Wherever you see
Pathogenesis of osteoporosis: concepts, conflicts, and prospects
 Science in medicine Pathogenesis of osteoporosis: concepts, conflicts, and prospects Lawrence G. Raisz University of Connecticut Health Center, Musculoskeletal Institute, Farmington, Connecticut, USA.
Science in medicine Pathogenesis of osteoporosis: concepts, conflicts, and prospects Lawrence G. Raisz University of Connecticut Health Center, Musculoskeletal Institute, Farmington, Connecticut, USA.
SKELETAL SYSTEM CHAPTER 07. Bone Function BIO 211: ANATOMY & PHYSIOLOGY I. Body Movement interacts with muscles bones act as rigid bar of a lever
 Page 1 BIO 211: ANATOMY & PHYSIOLOGY I 1 CHAPTER 07 SKELETAL SYSTEM Dr. Lawrence G. G. Altman www.lawrencegaltman.com Some illustrations are courtesy of McGraw-Hill. Some illustrations are courtesy of
Page 1 BIO 211: ANATOMY & PHYSIOLOGY I 1 CHAPTER 07 SKELETAL SYSTEM Dr. Lawrence G. G. Altman www.lawrencegaltman.com Some illustrations are courtesy of McGraw-Hill. Some illustrations are courtesy of
SKELETAL SYSTEM CHAPTER 07 BIO 211: ANATOMY & PHYSIOLOGY I
 BIO 211: ANATOMY & PHYSIOLOGY I 1 CHAPTER 07 SKELETAL SYSTEM Dr. Lawrence G. G. Altman www.lawrencegaltman.com Some illustrations are courtesy of McGraw-Hill. Some illustrations are courtesy of McGraw-Hill.
BIO 211: ANATOMY & PHYSIOLOGY I 1 CHAPTER 07 SKELETAL SYSTEM Dr. Lawrence G. G. Altman www.lawrencegaltman.com Some illustrations are courtesy of McGraw-Hill. Some illustrations are courtesy of McGraw-Hill.
Regulation of the skeletal mass through the life span
 Regulation of the skeletal mass through the life span Functions of the skeletal system Mechanical protection skull Movement leverage for muscles Mineral metabolism calcium store Erythropoiesis red blood
Regulation of the skeletal mass through the life span Functions of the skeletal system Mechanical protection skull Movement leverage for muscles Mineral metabolism calcium store Erythropoiesis red blood
Osteoporosis: current treatment and future prospects. Juliet Compston Professor Emeritus of Bone Medicine Cambridge Biomedical Campus
 Osteoporosis: current treatment and future prospects Juliet Compston Professor Emeritus of Bone Medicine Cambridge Biomedical Campus Disclosures Consultancy and speaking fees for Gilead, related to development
Osteoporosis: current treatment and future prospects Juliet Compston Professor Emeritus of Bone Medicine Cambridge Biomedical Campus Disclosures Consultancy and speaking fees for Gilead, related to development
Signaling Vascular Morphogenesis and Maintenance
 Signaling Vascular Morphogenesis and Maintenance Douglas Hanahan Science 277: 48-50, in Perspectives (1997) Blood vessels are constructed by two processes: vasculogenesis, whereby a primitive vascular
Signaling Vascular Morphogenesis and Maintenance Douglas Hanahan Science 277: 48-50, in Perspectives (1997) Blood vessels are constructed by two processes: vasculogenesis, whereby a primitive vascular
Meeting Report. From December 8 to 11, 2012 at Atlanta, GA, U.S.A
 Meeting Report Affiliation Department of Transfusion Medicine and Cell Therapy Name Hisayuki Yao Name of the meeting Period and venue Type of your presentation Title of your presentation The 54 th Annual
Meeting Report Affiliation Department of Transfusion Medicine and Cell Therapy Name Hisayuki Yao Name of the meeting Period and venue Type of your presentation Title of your presentation The 54 th Annual
Mutation in Osteoactivin Enhances RANKL-Mediated Signaling, Promoting Osteoclast Differentiation, Survival and Inhibiting Bone Resorption
 Mutation in Osteoactivin Enhances RANKL-Mediated Signaling, Promoting Osteoclast Differentiation, Survival and Inhibiting Bone Resorption Samir Abdelmagid, MD, PhD, Fouad Moussa, BS, Sondag Gregory, MS,
Mutation in Osteoactivin Enhances RANKL-Mediated Signaling, Promoting Osteoclast Differentiation, Survival and Inhibiting Bone Resorption Samir Abdelmagid, MD, PhD, Fouad Moussa, BS, Sondag Gregory, MS,
Deposition of Bone by the Osteoblasts. Bone is continually being deposited by osteoblasts, and it is continually being resorbed where osteoclasts are
 Bone remodeling Deposition of Bone by the Osteoblasts. Bone is continually being deposited by osteoblasts, and it is continually being resorbed where osteoclasts are active. This mechanism is always is
Bone remodeling Deposition of Bone by the Osteoblasts. Bone is continually being deposited by osteoblasts, and it is continually being resorbed where osteoclasts are active. This mechanism is always is
Tanya Zappitelli. Copyright by Tanya Zappitelli 2015
 Characterization of the Gja1 Jrt /+ Skeletal Phenotype and the Cellular and Molecular Effects of the G60S Connexin 43 Mutation in the Long Bone Microenvironment by Tanya Zappitelli A thesis submitted in
Characterization of the Gja1 Jrt /+ Skeletal Phenotype and the Cellular and Molecular Effects of the G60S Connexin 43 Mutation in the Long Bone Microenvironment by Tanya Zappitelli A thesis submitted in
Elecsys bone marker panel. Optimal patient management starts in the laboratory
 bone marker panel Optimal patient management starts in the laboratory Complete solution for osteoporosis The most complete bone metabolism panel on a single platform bone marker assays are important diagnostic
bone marker panel Optimal patient management starts in the laboratory Complete solution for osteoporosis The most complete bone metabolism panel on a single platform bone marker assays are important diagnostic
Fig Articular cartilage. Epiphysis. Red bone marrow Epiphyseal line. Marrow cavity. Yellow bone marrow. Periosteum. Nutrient foramen Diaphysis
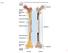 Fig. 7.1 Articular cartilage Epiphysis Red bone marrow Epiphyseal line Marrow cavity Yellow bone marrow Nutrient foramen Diaphysis Site of endosteum Compact bone Spongy bone Epiphyseal line Epiphysis Articular
Fig. 7.1 Articular cartilage Epiphysis Red bone marrow Epiphyseal line Marrow cavity Yellow bone marrow Nutrient foramen Diaphysis Site of endosteum Compact bone Spongy bone Epiphyseal line Epiphysis Articular
CHAPTER 6 LECTURE OUTLINE
 CHAPTER 6 LECTURE OUTLINE I. INTRODUCTION A. Bone is made up of several different tissues working together: bone, cartilage, dense connective tissue, epithelium, various blood forming tissues, adipose
CHAPTER 6 LECTURE OUTLINE I. INTRODUCTION A. Bone is made up of several different tissues working together: bone, cartilage, dense connective tissue, epithelium, various blood forming tissues, adipose
The bone remodelling cycle
 DOI: 0./000 The bone remodelling cycle Journal: Manuscript ID ACB-- Manuscript Type: Review Article Date Submitted by the Author: 0-Nov- Complete List of Authors: Kenkre, Julia; Imperial College London,
DOI: 0./000 The bone remodelling cycle Journal: Manuscript ID ACB-- Manuscript Type: Review Article Date Submitted by the Author: 0-Nov- Complete List of Authors: Kenkre, Julia; Imperial College London,
Cell Communication and Cell Signaling
 Cell Communication and Cell Signaling Why is cell signaling important? Why is cell signaling important? Allows cells to communicate and coordinate functions/activities of the organism Usually involves
Cell Communication and Cell Signaling Why is cell signaling important? Why is cell signaling important? Allows cells to communicate and coordinate functions/activities of the organism Usually involves
Module 2:! Functional Musculoskeletal Anatomy A! Semester 1! !!! !!!! Hard Tissues, Distal Upper Limb & Neurovascular Supply of Upper Limb!
 Functional Musculoskeletal Anatomy A Module 2: Hard Tissues, Distal Upper Limb & Neurovascular Supply of Upper Limb Semester 1 1 18. Bone Tissue & Growth of Bones 18.1 Describe the structure of bone tissue
Functional Musculoskeletal Anatomy A Module 2: Hard Tissues, Distal Upper Limb & Neurovascular Supply of Upper Limb Semester 1 1 18. Bone Tissue & Growth of Bones 18.1 Describe the structure of bone tissue
Upcoming Agents for Osteoporosis
 Upcoming Agents for Osteoporosis May 5, 2017 Michael R. McClung, MD, FACP Director, Oregon Osteoporosis Center Portland, Oregon, USA Professorial Fellow, Institute of Health and Ageing Australian Catholic
Upcoming Agents for Osteoporosis May 5, 2017 Michael R. McClung, MD, FACP Director, Oregon Osteoporosis Center Portland, Oregon, USA Professorial Fellow, Institute of Health and Ageing Australian Catholic
Osteocytes The galaxy within
 Osteocytes The galaxy within Buenzli PR, Sims NA. Quantifying the osteocyte network in the human skeleton. Bone 2015;75:144-50. Buenzli and Sims present a fascinating insight into the intergalactic vastness
Osteocytes The galaxy within Buenzli PR, Sims NA. Quantifying the osteocyte network in the human skeleton. Bone 2015;75:144-50. Buenzli and Sims present a fascinating insight into the intergalactic vastness
What are the parts of the skeletal system? Chapter 6- Part I Bones and Skeletal Tissues. Growth of Cartilage. Bones come in many shapes
 Chapter 6- Part I Bones and Skeletal Tissues Components of the skeletal system Classification of Bone (bone shapes) Functions of bone Bone structure Microscopic structure of bone and bone cells What are
Chapter 6- Part I Bones and Skeletal Tissues Components of the skeletal system Classification of Bone (bone shapes) Functions of bone Bone structure Microscopic structure of bone and bone cells What are
CHAPTER 6 SUMMARIZING DISCUSSION
 CHAPTER 6 SUMMARIZING DISCUSSION More than 20 years ago the founding member of the Wnt gene family, Wnt-1/Int1, was discovered as a proto-oncogene activated in mammary gland tumors by the mouse mammary
CHAPTER 6 SUMMARIZING DISCUSSION More than 20 years ago the founding member of the Wnt gene family, Wnt-1/Int1, was discovered as a proto-oncogene activated in mammary gland tumors by the mouse mammary
Derived copy of Bone *
 OpenStax-CNX module: m57739 1 Derived copy of Bone * Shannon McDermott Based on Bone by OpenStax This work is produced by OpenStax-CNX and licensed under the Creative Commons Attribution License 4.0 By
OpenStax-CNX module: m57739 1 Derived copy of Bone * Shannon McDermott Based on Bone by OpenStax This work is produced by OpenStax-CNX and licensed under the Creative Commons Attribution License 4.0 By
BIOH111. o Cell Module o Tissue Module o Integumentary system o Skeletal system o Muscle system o Nervous system o Endocrine system
 BIOH111 o Cell Module o Tissue Module o Integumentary system o Skeletal system o Muscle system o Nervous system o Endocrine system Endeavour College of Natural Health endeavour.edu.au 1 TEXTBOOK AND REQUIRED/RECOMMENDED
BIOH111 o Cell Module o Tissue Module o Integumentary system o Skeletal system o Muscle system o Nervous system o Endocrine system Endeavour College of Natural Health endeavour.edu.au 1 TEXTBOOK AND REQUIRED/RECOMMENDED
2015 AP Biology Unit #4 Quiz 1 Cell Communication, Cancer and The Cell Cycle Week of November
 Name: Class: Date: 2015 AP Biology Unit #4 Quiz 1 Cell Communication, Cancer and The Cell Cycle Week of 16-20 November Multiple Choice Identify the choice that best completes the statement or answers the
Name: Class: Date: 2015 AP Biology Unit #4 Quiz 1 Cell Communication, Cancer and The Cell Cycle Week of 16-20 November Multiple Choice Identify the choice that best completes the statement or answers the
Biology. Dr. Khalida Ibrahim
 Biology Dr. Khalida Ibrahim BONE TISSUE Bone tissue is a specialized form of connective tissue and is the main element of the skeletal tissues. It is composed of cells and an extracellular matrix in which
Biology Dr. Khalida Ibrahim BONE TISSUE Bone tissue is a specialized form of connective tissue and is the main element of the skeletal tissues. It is composed of cells and an extracellular matrix in which
Osteoporosis and its Association with Rheumatoid Arthritis and Prednisolone Therapy
 Osteoporosis and its Association with Rheumatoid Arthritis and Prednisolone Therapy Master s Thesis Ane Eriksen Medicine with Industrial Specialization Aalborg University Osteoporosis and its Association
Osteoporosis and its Association with Rheumatoid Arthritis and Prednisolone Therapy Master s Thesis Ane Eriksen Medicine with Industrial Specialization Aalborg University Osteoporosis and its Association
Chapter 6: Skeletal System: Bones and Bone Tissue
 Chapter 6: Skeletal System: Bones and Bone Tissue I. Functions A. List and describe the five major functions of the skeletal system: 1. 2. 3.. 4. 5.. II. Cartilage A. What do chondroblasts do? B. When
Chapter 6: Skeletal System: Bones and Bone Tissue I. Functions A. List and describe the five major functions of the skeletal system: 1. 2. 3.. 4. 5.. II. Cartilage A. What do chondroblasts do? B. When
The Skeletal System:Bone Tissue
 The Skeletal System:Bone Tissue Dynamic and ever-changing throughout life Skeleton composed of many different tissues cartilage, bone tissue, epithelium, nerve, blood forming tissue, adipose, and dense
The Skeletal System:Bone Tissue Dynamic and ever-changing throughout life Skeleton composed of many different tissues cartilage, bone tissue, epithelium, nerve, blood forming tissue, adipose, and dense
Bone Health in Patients with Multiple Myeloma
 Bone Health in Patients with Multiple Myeloma Amrita Y. Krishnan, MD Director Judy and Bernard Briskin Myeloma Center City of Hope Comprehensive Cancer Center Bone Health Bisphosphonates in Space Bone
Bone Health in Patients with Multiple Myeloma Amrita Y. Krishnan, MD Director Judy and Bernard Briskin Myeloma Center City of Hope Comprehensive Cancer Center Bone Health Bisphosphonates in Space Bone
Osteoporosis - Pathophysiology and diagnosis. Bente L Langdahl Department of Endocrinology Aarhus University Hospital Aarhus, Denmark
 Osteoporosis - Pathophysiology and diagnosis Bente L Langdahl Department of Endocrinology Aarhus University Hospital Aarhus, Denmark Objective General knowledge about osteoporosis Optimise your protocols
Osteoporosis - Pathophysiology and diagnosis Bente L Langdahl Department of Endocrinology Aarhus University Hospital Aarhus, Denmark Objective General knowledge about osteoporosis Optimise your protocols
CHAPTER 2. Literature Review. Bone Homeostasis. 2.1 Introduction. 2.2 Composition of bone
 CHAPTER 2 Literature Review I Bone Homeostasis 2.1 Introduction The mature skeleton is a metabolically active organ that undergoes continuous remodeling by a process that replaces old bone with new bone.
CHAPTER 2 Literature Review I Bone Homeostasis 2.1 Introduction The mature skeleton is a metabolically active organ that undergoes continuous remodeling by a process that replaces old bone with new bone.
Space radiation and osteoclastogenesis:the effects of radiation and microgravity on bone resorption:
 Space radiation and osteoclastogenesis:the effects of radiation and microgravity on bone resorption: Alamelu Sundaresan1, Sukesh Aghara2, Terrell Gibson1and Indi Siripirasan2 1: Texas Southern University-3100
Space radiation and osteoclastogenesis:the effects of radiation and microgravity on bone resorption: Alamelu Sundaresan1, Sukesh Aghara2, Terrell Gibson1and Indi Siripirasan2 1: Texas Southern University-3100
Interplay between Cartilage and Subchondral Bone Contributing to Pathogenesis of Osteoarthritis
 Int. J. Mol. Sci. 2013, 14, 19805-19830; doi:10.3390/ijms141019805 Review OPEN ACCESS International Journal of Molecular Sciences ISSN 1422-0067 www.mdpi.com/journal/ijms Interplay between Cartilage and
Int. J. Mol. Sci. 2013, 14, 19805-19830; doi:10.3390/ijms141019805 Review OPEN ACCESS International Journal of Molecular Sciences ISSN 1422-0067 www.mdpi.com/journal/ijms Interplay between Cartilage and
SKELETAL TISSUES CHAPTER 7 INTRODUCTION TO THE SKELETAL SYSTEM TYPES OF BONES
 SKELETAL TISSUES CHAPTER 7 By John McGill Supplement Outlines: Beth Wyatt Original PowerPoint: Jack Bagwell INTRODUCTION TO THE SKELETAL SYSTEM STRUCTURE Organs: Bones Related Tissues: Cartilage and Ligaments
SKELETAL TISSUES CHAPTER 7 By John McGill Supplement Outlines: Beth Wyatt Original PowerPoint: Jack Bagwell INTRODUCTION TO THE SKELETAL SYSTEM STRUCTURE Organs: Bones Related Tissues: Cartilage and Ligaments
A KL/R / AN A K/O / P O G G
 Outline and New Treatments on the Horizon Steven R. Cummings, MD CPMC and UCSF San Francisco Coordinating Center Support from Lilly and Amgen New treatments, new mechanisms of action Cathepsin K inhibition
Outline and New Treatments on the Horizon Steven R. Cummings, MD CPMC and UCSF San Francisco Coordinating Center Support from Lilly and Amgen New treatments, new mechanisms of action Cathepsin K inhibition
Cell Cell Communication
 IBS 8102 Cell, Molecular, and Developmental Biology Cell Cell Communication January 29, 2008 Communicate What? Why do cells communicate? To govern or modify each other for the benefit of the organism differentiate
IBS 8102 Cell, Molecular, and Developmental Biology Cell Cell Communication January 29, 2008 Communicate What? Why do cells communicate? To govern or modify each other for the benefit of the organism differentiate
Supplemental Data. Wnt/β-Catenin Signaling in Mesenchymal Progenitors. Controls Osteoblast and Chondrocyte
 Supplemental Data Wnt/β-Catenin Signaling in Mesenchymal Progenitors Controls Osteoblast and Chondrocyte Differentiation during Vertebrate Skeletogenesis Timothy F. Day, Xizhi Guo, Lisa Garrett-Beal, and
Supplemental Data Wnt/β-Catenin Signaling in Mesenchymal Progenitors Controls Osteoblast and Chondrocyte Differentiation during Vertebrate Skeletogenesis Timothy F. Day, Xizhi Guo, Lisa Garrett-Beal, and
Cancer. The fundamental defect is. unregulated cell division. Properties of Cancerous Cells. Causes of Cancer. Altered growth and proliferation
 Cancer The fundamental defect is unregulated cell division. Properties of Cancerous Cells Altered growth and proliferation Loss of growth factor dependence Loss of contact inhibition Immortalization Alterated
Cancer The fundamental defect is unregulated cell division. Properties of Cancerous Cells Altered growth and proliferation Loss of growth factor dependence Loss of contact inhibition Immortalization Alterated
New treatment targets in osteoporosis
 National University of Athens Greece New treatment targets in osteoporosis Gourzi Vassiliki PhD Candidate Dept. of Pathophysiology School of Medicine Bone remodeling Physiological process < bone tissue
National University of Athens Greece New treatment targets in osteoporosis Gourzi Vassiliki PhD Candidate Dept. of Pathophysiology School of Medicine Bone remodeling Physiological process < bone tissue
Chapter 6: SKELETAL SYSTEM
 Chapter 6: SKELETAL SYSTEM I. FUNCTIONS A. Support B. Protection C. Movement D. Mineral storage E. Lipid storage (Fig. 6.8b) F. Blood cell production (Fig. 6.4) II. COMPONENTS A. Cartilage 1. Hyaline 2.
Chapter 6: SKELETAL SYSTEM I. FUNCTIONS A. Support B. Protection C. Movement D. Mineral storage E. Lipid storage (Fig. 6.8b) F. Blood cell production (Fig. 6.4) II. COMPONENTS A. Cartilage 1. Hyaline 2.
An Introduction to the Skeletal System Skeletal system includes Bones of the skeleton Cartilages, ligaments, and connective tissues
 An Introduction to the Skeletal System Skeletal system includes Bones of the skeleton Cartilages, ligaments, and connective tissues Functions of the Skeletal System Support Storage of minerals (calcium)
An Introduction to the Skeletal System Skeletal system includes Bones of the skeleton Cartilages, ligaments, and connective tissues Functions of the Skeletal System Support Storage of minerals (calcium)
Drugs Affecting Bone. Rosa McCarty PhD. Department of Pharmacology & Therapeutics
 Drugs Affecting Bone Rosa McCarty PhD Department of Pharmacology & Therapeutics rmccarty@unimelb.edu.au Objectives At the end of this lecture you should have gained: An understanding of bone metabolism
Drugs Affecting Bone Rosa McCarty PhD Department of Pharmacology & Therapeutics rmccarty@unimelb.edu.au Objectives At the end of this lecture you should have gained: An understanding of bone metabolism
Lecture 2: Skeletogenesis
 Jilin University School of Stomatology Skeletogenesis Lecture 2: Skeletogenesis Aug. 18, 2015 Yuji Mishina, Ph.D. mishina@umich.edu Student will describe Development of Bone - the general anatomy of bone
Jilin University School of Stomatology Skeletogenesis Lecture 2: Skeletogenesis Aug. 18, 2015 Yuji Mishina, Ph.D. mishina@umich.edu Student will describe Development of Bone - the general anatomy of bone
Assessment and Treatment of Osteoporosis Professor T.Masud
 Assessment and Treatment of Osteoporosis Professor T.Masud Nottingham University Hospitals NHS Trust University of Nottingham University of Derby University of Southern Denmark What is Osteoporosis? Osteoporosis
Assessment and Treatment of Osteoporosis Professor T.Masud Nottingham University Hospitals NHS Trust University of Nottingham University of Derby University of Southern Denmark What is Osteoporosis? Osteoporosis
Cancer. The fundamental defect is. unregulated cell division. Properties of Cancerous Cells. Causes of Cancer. Altered growth and proliferation
 Cancer The fundamental defect is unregulated cell division. Properties of Cancerous Cells Altered growth and proliferation Loss of growth factor dependence Loss of contact inhibition Immortalization Alterated
Cancer The fundamental defect is unregulated cell division. Properties of Cancerous Cells Altered growth and proliferation Loss of growth factor dependence Loss of contact inhibition Immortalization Alterated
FORMATION OF BONE. Intramembranous Ossification. Bone-Lec-10-Prof.Dr.Adnan Albideri
 FORMATION OF BONE All bones are of mesodermal origin. The process of bone formation is called ossification. We have seen that formation of most bones is preceded by the formation of a cartilaginous model,
FORMATION OF BONE All bones are of mesodermal origin. The process of bone formation is called ossification. We have seen that formation of most bones is preceded by the formation of a cartilaginous model,
The Contribution Of Tie2-Lineage Cells To rhbmp-2 Induced Bone Formation
 The Contribution Of Tie2-Lineage Cells To rhbmp-2 Induced Bone Formation Mille P. Kolind, Ph.D 1, Alastair Aiken 1, Kathy Mikulec 1, Lauren Peacock 1, David Little 1,2, Aaron Schindeler, PhD 1,2. 1 Orthopaedic
The Contribution Of Tie2-Lineage Cells To rhbmp-2 Induced Bone Formation Mille P. Kolind, Ph.D 1, Alastair Aiken 1, Kathy Mikulec 1, Lauren Peacock 1, David Little 1,2, Aaron Schindeler, PhD 1,2. 1 Orthopaedic
Cell Biology Lecture 9 Notes Basic Principles of cell signaling and GPCR system
 Cell Biology Lecture 9 Notes Basic Principles of cell signaling and GPCR system Basic Elements of cell signaling: Signal or signaling molecule (ligand, first messenger) o Small molecules (epinephrine,
Cell Biology Lecture 9 Notes Basic Principles of cell signaling and GPCR system Basic Elements of cell signaling: Signal or signaling molecule (ligand, first messenger) o Small molecules (epinephrine,
Fructose Upregulates FGF23 Expression In MC3T3 Pre-osteoblasts
 Fructose Upregulates FGF23 Expression In MC3T3 Pre-osteoblasts Edek A. Williams, B.S.E., Veronique Douard, Ph.D., Joseph M. Lomuti, B.S., Ronaldo Ferraris, Ph.D., J. C. Fritton, Ph.D.. Rutgers University,
Fructose Upregulates FGF23 Expression In MC3T3 Pre-osteoblasts Edek A. Williams, B.S.E., Veronique Douard, Ph.D., Joseph M. Lomuti, B.S., Ronaldo Ferraris, Ph.D., J. C. Fritton, Ph.D.. Rutgers University,
Early cell death (FGF) B No RunX transcription factor produced Yes No differentiation
 Solution Key - Practice Questions Question 1 a) A recent publication has shown that the fat stem cells (FSC) can act as bone stem cells to repair cavities in the skull, when transplanted into immuno-compromised
Solution Key - Practice Questions Question 1 a) A recent publication has shown that the fat stem cells (FSC) can act as bone stem cells to repair cavities in the skull, when transplanted into immuno-compromised
KEY CONCEPTS Unit 6 THE SKELETAL SYSTEM
 ANATOMY & PHYSIOLOGY 1 (101-805 - AB) PAUL ANDERSON 2011 KEY CONCEPTS Unit 6 THE SKELETAL SYSTEM A Overview of The Skeletal System 1. Definition: Anatomically the SKELETAL SYSTEM consists of bones, cartilages,
ANATOMY & PHYSIOLOGY 1 (101-805 - AB) PAUL ANDERSON 2011 KEY CONCEPTS Unit 6 THE SKELETAL SYSTEM A Overview of The Skeletal System 1. Definition: Anatomically the SKELETAL SYSTEM consists of bones, cartilages,
Species differences in histomorphometry
 Species differences in histomorphometry Reinhold G. Erben Department of Biomedical Sciences Institute of Physiology and Pathophysiology University of Veterinary Medicine Vienna Purpose of histomorphometry
Species differences in histomorphometry Reinhold G. Erben Department of Biomedical Sciences Institute of Physiology and Pathophysiology University of Veterinary Medicine Vienna Purpose of histomorphometry
Silent Killer: Osteoporosis
 Special Dedication to the Old Females Silent Killer: Osteoporosis David Goltzman, Discoveries, Drugs and Skeletal Disorders Nature, Volume 1, October 2002, pp784-796 BII Journal Club Wang Zhengyuan 5:00-5:30pm
Special Dedication to the Old Females Silent Killer: Osteoporosis David Goltzman, Discoveries, Drugs and Skeletal Disorders Nature, Volume 1, October 2002, pp784-796 BII Journal Club Wang Zhengyuan 5:00-5:30pm
Cell Cell Communication
 IBS 8102 Cell, Molecular, and Developmental Biology Cell Cell Communication January 29, 2008 Communicate What? Why do cells communicate? To govern or modify each other for the benefit of the organism differentiate
IBS 8102 Cell, Molecular, and Developmental Biology Cell Cell Communication January 29, 2008 Communicate What? Why do cells communicate? To govern or modify each other for the benefit of the organism differentiate
Skeletal System worksheet
 Skeletal System worksheet Name Section A: Intro to Skeletal System The skeletal system performs vital functions that enable us to move through our daily lives. Support - The skeleton provides support and
Skeletal System worksheet Name Section A: Intro to Skeletal System The skeletal system performs vital functions that enable us to move through our daily lives. Support - The skeleton provides support and
Chapter 6: Osseous Tissue and Bone Structure
 Chapter 6: Osseous Tissue and Bone Structure I. An Introduction to the Skeletal System, p. 180 Objective: Describe the functions of the skeletal system The skeletal system includes: - bones of the skeleton
Chapter 6: Osseous Tissue and Bone Structure I. An Introduction to the Skeletal System, p. 180 Objective: Describe the functions of the skeletal system The skeletal system includes: - bones of the skeleton
Anabolic Therapies. Nancy E. Lane & Stuart L. Silverman
 Curr Osteoporos Rep (2010) 8:23 27 DOI 10.1007/s11914-010-0005-4 Anabolic Therapies Nancy E. Lane & Stuart L. Silverman Published online: 19 February 2010 # The Author(s) 2010. This article is published
Curr Osteoporos Rep (2010) 8:23 27 DOI 10.1007/s11914-010-0005-4 Anabolic Therapies Nancy E. Lane & Stuart L. Silverman Published online: 19 February 2010 # The Author(s) 2010. This article is published
Novel therapies for Myeloma bone disease. Dr. Naif AlJohani ABIM,FRCPC Adult Hematology/BMT King Faisal specialist hospital & Research center Jeddah
 Novel therapies for Myeloma bone disease Dr. Naif AlJohani ABIM,FRCPC Adult Hematology/BMT King Faisal specialist hospital & Research center Jeddah 1 Introduction Multiple myeloma (MM) is a plasma cell
Novel therapies for Myeloma bone disease Dr. Naif AlJohani ABIM,FRCPC Adult Hematology/BMT King Faisal specialist hospital & Research center Jeddah 1 Introduction Multiple myeloma (MM) is a plasma cell
TEAM SCIENCE AT A PROGRAMMATIC LEVEL. Sundeep Khosla, M.D. Mayo Clinic College of Medicine
 TEAM SCIENCE AT A PROGRAMMATIC LEVEL Sundeep Khosla, M.D. Mayo Clinic College of Medicine APPROACH TO TRANSLATIONAL RESEARCH IN OSTEOPOROSIS Epidemiological Studies Clinical Investigation Mouse and Cellular
TEAM SCIENCE AT A PROGRAMMATIC LEVEL Sundeep Khosla, M.D. Mayo Clinic College of Medicine APPROACH TO TRANSLATIONAL RESEARCH IN OSTEOPOROSIS Epidemiological Studies Clinical Investigation Mouse and Cellular
Regulation of the IGF axis by TGF-b during periosteal chondrogenesis: implications for articular cartilage repair
 Regulation of the IGF axis by TGF-b during periosteal chondrogenesis: implications for articular cartilage repair Chapter 04 Boek 1_Gie.indb 55 21-05-2007 12:27:33 Chapter 04 Abstract Goal: TGF-b and IGF-I
Regulation of the IGF axis by TGF-b during periosteal chondrogenesis: implications for articular cartilage repair Chapter 04 Boek 1_Gie.indb 55 21-05-2007 12:27:33 Chapter 04 Abstract Goal: TGF-b and IGF-I
Molecular biology :- Cancer genetics lecture 11
 Molecular biology :- Cancer genetics lecture 11 -We have talked about 2 group of genes that is involved in cellular transformation : proto-oncogenes and tumour suppressor genes, and it isn t enough to
Molecular biology :- Cancer genetics lecture 11 -We have talked about 2 group of genes that is involved in cellular transformation : proto-oncogenes and tumour suppressor genes, and it isn t enough to
The Role of the Laboratory in Metabolic Bone Disease
 The Role of the Laboratory in Metabolic Bone Disease Howard Morris PhD, FAACB, FFSc(RCPA) President, IFCC Professor of Medical Sciences, University of South Australia, Clinical Scientist, SA Pathology
The Role of the Laboratory in Metabolic Bone Disease Howard Morris PhD, FAACB, FFSc(RCPA) President, IFCC Professor of Medical Sciences, University of South Australia, Clinical Scientist, SA Pathology
Awaisheh. Mousa Al-Abbadi. Abdullah Alaraj. 1 Page
 f #3 Awaisheh Abdullah Alaraj Mousa Al-Abbadi 1 Page *This sheet was written from Section 1 s lecture, in the first 10 mins the Dr. repeated all the previous material relating to osteoporosis from the
f #3 Awaisheh Abdullah Alaraj Mousa Al-Abbadi 1 Page *This sheet was written from Section 1 s lecture, in the first 10 mins the Dr. repeated all the previous material relating to osteoporosis from the
TITLE: Effect of COX-2 (PGE2) and IL-6 on Prostate Cancer Bone Mets
 AD Award Number: W81XWH-05-1-0166 TITLE: Effect of COX-2 (PGE2) and IL-6 on Prostate Cancer Bone Mets PRINCIPAL INVESTIGATOR: Alice C. Levine, M.D. CONTRACTING ORGANIZATION: Mount Sinai School of Medicine
AD Award Number: W81XWH-05-1-0166 TITLE: Effect of COX-2 (PGE2) and IL-6 on Prostate Cancer Bone Mets PRINCIPAL INVESTIGATOR: Alice C. Levine, M.D. CONTRACTING ORGANIZATION: Mount Sinai School of Medicine
Effects of Anti RANK ligand Denosumab on Beta Thalassemia induced osteoporosis
 Effects of Anti RANK ligand Denosumab on Beta Thalassemia induced osteoporosis Mohamed Yassin 1 Ashraf T. Soliman2, Mohamed O. Abdelrahman3, Vincenzo De Sanctis 4 Departments of, 1 Hematology 2Pediatric
Effects of Anti RANK ligand Denosumab on Beta Thalassemia induced osteoporosis Mohamed Yassin 1 Ashraf T. Soliman2, Mohamed O. Abdelrahman3, Vincenzo De Sanctis 4 Departments of, 1 Hematology 2Pediatric
AACE Southern States Chapter Lecture. Basics
 AACE Southern States Chapter Lecture Unusual Bone Cases Basics Osteoporosis Osteomalacia Renal Osteodystrophy Multiple Myeloma 1 Osteoporosis Definition Modeling, Bone Remodeling Bone Resorption > Bone
AACE Southern States Chapter Lecture Unusual Bone Cases Basics Osteoporosis Osteomalacia Renal Osteodystrophy Multiple Myeloma 1 Osteoporosis Definition Modeling, Bone Remodeling Bone Resorption > Bone
Osseous Tissue and Bone Structure
 C h a p t e r 6 Osseous Tissue and Bone Structure PowerPoint Lecture Slides prepared by Jason LaPres Lone Star College - North Harris Copyright 2009 Pearson Education, Inc., publishing as Pearson Benjamin
C h a p t e r 6 Osseous Tissue and Bone Structure PowerPoint Lecture Slides prepared by Jason LaPres Lone Star College - North Harris Copyright 2009 Pearson Education, Inc., publishing as Pearson Benjamin
The Osteocyte: An Endocrine Cell... and More. Sarah L. Dallas, Matthew Prideaux, and Lynda F. Bonewald
 REVIEW The Osteocyte: An Endocrine Cell... and More Sarah L. Dallas, Matthew Prideaux, and Lynda F. Bonewald Department of Oral and Craniofacial Sciences, School of Dentistry, University of Missouri-Kansas
REVIEW The Osteocyte: An Endocrine Cell... and More Sarah L. Dallas, Matthew Prideaux, and Lynda F. Bonewald Department of Oral and Craniofacial Sciences, School of Dentistry, University of Missouri-Kansas
Bones. The division of bones anatomically is : long, short, irregular, flat and sesamoid.
 Bones Osteocytes : Are responsible for maintenance of bones Present in lacunae, and send processes. Unable to divide. The division of bones anatomically is : long, short, irregular, flat and sesamoid.
Bones Osteocytes : Are responsible for maintenance of bones Present in lacunae, and send processes. Unable to divide. The division of bones anatomically is : long, short, irregular, flat and sesamoid.
New Agents for Myeloma Bone Disease
 New Agents for Myeloma Bone Disease G. David Roodman MD PhD University of Pittsburgh Bone Remodeling is Uncoupled in Myeloma Normal Myeloma Hattner R et al. Nature. 1965;206:489. 1 Myeloma Bone Disease
New Agents for Myeloma Bone Disease G. David Roodman MD PhD University of Pittsburgh Bone Remodeling is Uncoupled in Myeloma Normal Myeloma Hattner R et al. Nature. 1965;206:489. 1 Myeloma Bone Disease
