Glucosamine and Chondroitin for Osteoarthritis
|
|
|
- Berniece West
- 5 years ago
- Views:
Transcription
1 The Journal of International Medical Research 2008; 36(6) 6 Glucosamine and Chondroitin for Osteoarthritis EC USKISSON King Edward VII ospital, London, UK Osteoarthritis (OA) is a common, chronic disease that most frequently affects the knees and is a major cause of disability in the elderly. It is characterized by progressive cartilage loss, accompanied by secondary changes such as osteophyte formation and calcium deposition. Inflammatory processes are also involved, leading to stiffness and pain, for which patients seek treatment. Conventional treatment includes analgesics or non-steroidal antiinflammatory drugs, however life-style changes should also be recommended, such as weight reduction and specific exercises. Glucosamine and chondroitin, classed as over-the-counter supplements or nutraceuticals, are regularly selfadministered by patients with OA. Both agents are produced endogenously in the human body and are essential components of cartilage. This review discusses the evidence that supports the use of these agents either alone or in combination for pain relief and as disease-modifying agents in OA. KEY WORDS: GLUCOSAMINE; CONDROITIN; NUTRACEUTICALS; DIETARY SUPPLEMENTS; COMPLEMENTARY MEDICINE; OSTEOARTRITIS; ELDERLY PATIENTS; PAIN RELIEF Introduction Osteoarthritis (OA) is a huge global problem. It is a chronic disease and the most common of all the joint diseases, affecting about 15% of the world s population and three-times more common in women than in men. 1 It is characterized by joint pain and swelling. The knees are the joints most often involved; OA commonly affects the hips, lumbar and cervical spines and the small joints of the hands and feet, with the ankles and other upper limb joints less frequently affected. Involvement of the knees and hips limits mobility as well as causing pain and stiffness. Onset of symptoms is typically at about 50 years of age and OA is a major cause of disability in later life. Up to the age of 55 years, men are more prone to OA than women; after 55 years, this trend is reversed. 1 OA is economically important because of the need for joint replacements, the disability and the cost of treatment including drugs, operations and care. Osteoarthritis is a disease of cartilage and occurs through hereditary factors and trauma. 2 Most cases of OA present around 50 years of age for no obvious reason other than a family history of the disease. In a few cases, the disease appears at the site of an injury, such as a fracture, involving the joint surface or an open meniscectomy. In some cases, there may be a family history but trauma or some mechanical insult has led to the appearance of the disease at a particular 1
2 site or to more severe disease at that site. Although the nature of the initiating event in OA is unknown, a lot is known about the process. For example, disruption of the collagen matrix of cartilage is followed by an increase in water content and progressive loss of proteoglycan, the stuffing of cartilage and the material that provides its elasticity. 3 X-rays in patients with OA show progressive cartilage loss with secondary changes such as osteophyte formation and calcium deposition. OA is an active process, with cartilage apparently making vigorous efforts at repair, rather than just wearing out. 4 It is a process that is accompanied by inflammation, evident in the clinical manifestations of the disease such as stiffness, signs such as warmth, and the histopathology. Most patients consulting a primary care physician with the common problem of OA receive a prescription to help them deal with the symptoms, such as pain and stiffness, which limit their mobility. Most prescriptions for OA are for analgesics or antiinflammatory drugs such as non-steroidal anti-inflammatory drugs (NSAIDs). 2 In the author s opinion, too few consultations include advice about the nature of the disease and other measures to alleviate the pain and disability, like exercises for the knee, dietary measures (weight reduction especially in cases of OA of the weightbearing joints), acupuncture and supplements and, despite the remarkable achievements of pharmaceutical medicine in recent decades, patients yearn for the natural approach, alternative or complementary medicine. The combination of salts of glucosamine and chondroitin provide such an approach. Another reason for looking carefully at supplements like glucosamine and chondroitin is the side-effects of the antiinflammatory drugs that are widely used for OA. These drugs produce various adverse reactions, however the gastrointestinal tract is most frequently affected. Nausea and epigastric pain may limit the ability to take medication but the more serious problems are peptic ulceration and its complications, bleeding and perforation, which carry a significant mortality risk. 5 The elderly, who are particularly likely to be suffering from OA, are also at a higher risk of these problems. 6 They are also likely to be taking other drugs, including anticoagulants or diuretics with which NSAIDs may interact and are likely to have other medical problems, such as hypertension, which may be exacerbated by NSAID use. Glucosamine and chondroitin are essential components of the proteoglycan in normal cartilage, which was the main rationale for their use as supplements in the management of OA, although their mode of action may be complex. 7 Academics have rightly insisted that the same stringent criteria for efficacy and safety should be applied to supplements like glucosamine and chondroitin as to conventional drug treatments. This review is concerned with the available evidence about the properties of glucosamine and chondroitin and attempts to provide answers to some of the most basic questions about their use for the treatment of OA. Are they effective? Are they well tolerated? Are they safe? Are they safe for everyone including diabetics? When and how should they be given and for how long? What is glucosamine? Glucosamine is a monosaccharide (2-amino- 2-deoxy-D-glucose; C 6 14 NO 5 ) with a molecular weight of Da (Fig. 1). It is naturally produced in the human body and is an important precursor in the biosynthesis of glycosylated proteins and lipids. 2
3 O C O O FIGURE 1: Chemical structure of glucosamine Glucosamine is important because it is an essential component of proteoglycans, acting as one of the principal substrates in their synthesis. 7 Glucosamine is synthesized in vivo from glucose and is used to produce glycosaminoglycan chains from which proteoglycans are formed. Cartilage consists of a matrix of collagen fibres, stuffed with proteoglycans. The proteoglycans are high molecular weight complexes that attract water, creating a positive pressure within the cartilage and giving it the ability to withstand loading. In OA, breaks occur in the collagen network, the water content of O N O the cartilage increases and the proteoglycan stuffing of the cartilage is lost. 8 Glucosamine is used as an agent to help relieve the symptoms and delay the progression of OA. The rationale for its use is based on the hypothesis that OA is associated with a local deficiency in some key natural substances and that glucosamine might act as a substrate for cartilage repair, by stimulating proteoglycan synthesis by chondrocytes. 7,9 Glucosamine is considered to be a slow-acting substance because treatment is usually characterized by several weeks delay in the onset of improvement in symptoms of OA and by a carryover effect. 9,10 Glucosamine in the form of a dietary supplement typically derives from marine exoskeletons, such as shellfish or crab shells. Synthetic glucosamine is also available. What is chondroitin? Chondroitin is a high molecular weight ( Da) glycosaminoglycan, which is found in cartilage and connective tissue. It is a natural polymer of a disaccharide consisting of an alternating sequence of D-glucuronate and N-acetylgalactosamine-4-sulphate or -6-sulphate residues linked through alternating bonds (Fig. 2). 11 Chondroitin, like glucosamine, is COO C 2 O O O 2 SO O O O O O NCOC 3 FIGURE 2: Chemical structure of chondroitin 3
4 hydrophilic and soluble in water, producing a viscous fluid similar to sodium hyaluronate. Chondroitin sulphate is essential for the structural and functional integrity of the joints, since it constitutes the majority of glycosaminoglycans (GAGs) in articular cartilage. 12,13 It has been suggested that chondroitin helps maintain the viscosity in joints, stimulates cartilage repair and inhibits enzymes that degrade cartilage. 14 Clinically, these properties could result in pain relief and improved joint mobility in patients with OA as well as in decelerated joint destruction. Pharmacological and clinical data further suggest that concomitant use of glucosamine and chondroitin sulphate may work additively. 15 The use of glucosamine and chondroitin is believed to bridge the symptomatic and preventive approach since these compounds may have the ability to maintain and rebuild cartilage, with beneficial consequences on both chronic joint pain and progression of joint degeneration Chondroitin as a supplement is produced from animal sources, including bovine trachea and shark cartilage. Pharmacokinetics of glucosamine and chondroitin Glucosamine taken orally is 90% absorbed. 20 owever, there is extensive first-pass metabolism so that only 25% bioavailability is achieved by oral administration when compared with intravenous administration, which achieves bioactivity of 96%. 20,21 Glucosamine can be taken in the form of the sulphate or the hydrochloride. The salts of glucosamine are ionized in the stomach, making glucosamine available for absorption in the small bowel. 22 Glucosamine is extensively metabolized and the metabolites are excreted predominantly in urine. 23 Plasma levels of glucosamine after oral administration of a single dose of 1500 mg glucosamine sulphate peak at 1200 ng/ml after about 4 h, declining to baseline after about 48 h. 24 Plasma concentrations range from 600 to 4061 ng/ml and synovial fluid concentrations range from 577 to 3248 ng/ml. 24 Plasma and synovial fluid levels are highly correlated. 24 Studying the plasma and synovial fluid levels makes it clear that glucosamine is absorbed following oral administration, providing significant increases in levels of glucosamine both in plasma and synovial fluid. Chondroitin is larger and not as well absorbed as glucosamine. 14 The absorption of orally-administered sulphated GAGs, such as chondroitin sulphate, remains controversial due to the difficulty in accepting that charged, high molecular weight molecules can pass the gastric and/or intestinal mucosa. In dogs and rats, an oral dose of sodium 3-borohydride-labelled chondroitin resulted in 70% absorption, with a peak value at approximately 2 h. 25 The liver, intestine, kidneys, synovial fluid and cartilage had the highest radioactivity 24 h after administration. 25 Chondroitin sulphate given orally to human volunteers in one dose of 800 mg and in two daily doses of 400 mg led to a significant increase in plasma chondroitin concentration when compared with pre-dose values during a 24-h period. 26 A separate report determined oral absorption in 10 healthy human volunteers to be 30%, with a concentration peak at 240 min. 27 A fair proportion of orally administered chondroitin sulphate is absorbed as partially digested GAGs, both as high molecular weight forms and as oligosaccharides Chondroitin sulphate is absorbed in the 4
5 small intestine in low amounts (< 10%) in the intact form, while in the distal gastrointestinal tract, it acts as a prebiotic and is degraded by the enzymes in the intestinal flora to di- and monosaccharides. 7,31 Maximum plasma concentration occurs 1 5 h after oral administration. 26 uman studies have shown that, after oral administration, the mean plasma curve of exogenous chondroitin peaks after 2.4 h, h, h, 27 or 5.0 h. 25 Bioavailability has been estimated at 12 13%. 29,33 Mean plasma levels over a 30-day period of administration of 800 mg/day were between 1.7 and 1.89 µg/ml. 25 Radiolabelled chondroitin sulphate has been recovered in urine as both high and low molecular weight derivatives of chondroitin sulphate, 30,33 providing further support for its oral bioavailability. Is the combination of glucosamine and chondroitin effective? Glucosamine and chondroitin are often taken together and, therefore, it is appropriate to look first at the efficacy of the combination. The Glucosamine/Chondroitin Arthritis Intervention Trial (GAIT) compared glucosamine hydrochloride 1500 mg/day, chondroitin sulphate 1200 mg/day, both agents together, placebo and celecoxib 200 mg/day for 6 months on the relief of symptoms from OA of the knee in 1583 patients. 15 The study was initiated by the National Center for Complementary and Alternative Medicine, which is part of the US National Institutes of ealth, and was a multicentre, randomized, double-blind placebo- and celecoxib-controlled study. The treatment groups were stratified by pain according to baseline Western Ontario and McMaster Universities Osteoarthritis Index (WOMAC) scores. Mild pain was defined as on the WOMAC pain score and there were 1229 participants (78% of the study population) in this category. Moderate-to-severe pain was defined as on the WOMAC pain score with 354 participants (22%) included in this category. The primary outcome was at least a 20% reduction in the sum score of the WOMAC pain subscale at 24 weeks. Secondary outcomes were: the degree of stiffness and function subscales of the WOMAC index; patients global assessment of disease status; response to therapy using a visual analogue scale (VAS); investigators global assessment of disease status using a VAS; the presence or absence in the index knee of soft tissue swelling, effusion, or both; the quality of life improvement; the physical function, assessed using a health assessment questionnaire; and the use of paracetamol. In the 354 patients with moderate-to-severe pain, the response rate to the combination of glucosamine and chondroitin using the Outcome Measures in Rheumatology Clinical Trials and Osteoarthritis Research Society International (OMERACT-OARS) criteria was 79.2% compared with 54.3% with placebo (P = 0.002). There was, therefore, a significant reduction in pain in patients receiving the glucosamine chondroitin combination compared with placebo. This was the most effective of the treatments: glucosamine alone and celecoxib were less effective and chondroitin alone was only a little better than placebo. In the overall study population and in patients with mild pain, differences between glucosamine, chondroitin, the glucosamine chondroitin combination and placebo were not statistically significant. This might be expected because a 20% decrease in the pain score was unlikely to be achieved in patients 5
6 with mild pain, and there was also a very high placebo response rate of just over 60%, much higher than the 35% that had been predicted. There were 77 reports of serious adverse effects during the GAIT study. Of these, only three were attributed to study treatments. Most side-effects were mild, such as an upset stomach and they were spread evenly across the different treatment groups. No change in glucose tolerance was seen for glucosamine nor was an increased incidence of cardiovascular events seen with celecoxib. The conclusion of the GAIT study was that glucosamine hydrochloride and chondroitin sulphate alone or in combination showed only mild and infrequent side-effects and that the glucosamine chondroitin combination significantly reduced pain in patients with moderate-to-severe pain. Leffler et al. 18 conducted a double-blind, crossover trial comparing the combination of glucosamine hydrochloride 1500 mg/day, chondroitin sulphate 1200 mg/day and manganese ascorbate 228 mg/day for 16 weeks in 20 young (mean age 45 years), male patients with knee OA. There were significant differences in favour of the active treatment in pain (P = 0.05) and summary disease scores (P = 0.05). Das and ammad 16 used the combination of glucosamine hydrochloride 2000 mg/day, chondroitin sulphate 1600 mg/day and manganese ascorbate 304 mg/day in 93 patients aged years recruited from a single centre. They found the combination to be statistically superior to placebo in patients with mild-to-moderate OA of the knee (P = at 4 months). A total of 52% of patients responded to treatment compared with 28% to placebo. In contrast to the GAIT study in which moderate-to-severe OA was found to improve, 15 Das and ammad 16 found no significant improvement in patients with severe disease. Is glucosamine effective? An early trial compared 400 mg of glucosamine sulphate given twice weekly by intramuscular injection for 6 weeks with placebo in 155 patients with OA of the knee or spine. 34 Response was defined as a threepoint reduction in the Lequesne Index (a 10 question interview-style survey scored on a 0 24 scale comprising five questions related to pain, one related to walking distance and four about daily activities; lower score means less functional impairment) and this was achieved in 55% of patients on glucosamine sulphate compared with 33% on placebo (P = 0.012). The difference persisted for 2 weeks after stopping treatment and this sustained efficacy has been a feature of many studies. 35 Using a multicentre, randomized, placebo-controlled, double-blind, parallelgroup study design, Noack et al. 36 investigated the efficacy and safety of glucosamine sulphate in 252 out-patients with knee OA. The primary end point was a reduction in the Lequesne Index. Patients were treated with either placebo or oral glucosamine sulphate 500 mg three times daily for 4 weeks. The results were very similar to the intramuscular study 34 with response rates of 55% for glucosamine sulphate and 38% for placebo (P = 0.05). Both medications were well tolerated throughout the study with no difference between the groups. The authors concluded that glucosamine sulphate may be a safe and effective symptomatic slow-acting drug for OA. Rovati et al. 37 compared 1500 mg/day of glucosamine with placebo and piroxicam in 329 patients with medial femoro-tibial OA. Glucosamine demonstrated a marked effect compared with placebo and a more progressive and slower effect compared with 6
7 piroxicam. Glucosamine also showed fewer adverse events than piroxicam (14.8% versus 40.9%, respectively) and compared favourably with placebo (23.7%). oupt et al. 22 compared glucosamine hydrochloride and placebo in a randomized, double-blind study in 98 patients with OA of the knee over 8 weeks. They found a significant treatment effect on pain as measured by a daily questionnaire (P = 0.018), but not on the WOMAC index. The double-blind study was followed by an 8- week open-label trial, after the end of which 77% of patients continued to use glucosamine which they purchased themselves. The Glucosamine Unum In Die (GUIDE) study, carried out in Spain and Portugal, compared 1500 mg/day glucosamine sulphate with placebo and 3 g/day acetaminophen (paracetamol) in knee OA for 6 months. 38 At baseline, the study patients had moderately severe OA symptoms (mean Lequesne Index of approximately 11). The change in Lequesne Index was significant for glucosamine sulphate ( 3.1 points) versus placebo ( 1.9 points) (P = 0.032); acetaminophen was not significantly different from placebo. Similar results were observed for the WOMAC scale: there were more responders to glucosamine sulphate (39.6%) and acetaminophen (33.3%) than to placebo (21.2%) (P = and P = 0.047, respectively, versus placebo). Cohen et al. 39 compared a placebo cream and a spray containing glucosamine sulphate, chondroitin sulphate and shark cartilage in 63 patients with OA of the knee. They found a significant difference in favour of the active-treatment group in the reduction of pain measured by a VAS (mean difference 1.2 cm; P = 0.03) after 4 weeks. After 8 weeks, the mean difference was even greater (1.8 cm; P = 0.002). Braham et al. 40 carried out a 12-week randomized, placebo-controlled study comparing glucosamine supplementation and placebo in patients who had regular knee pain due to previous articular cartilage damage and OA. Patients received either glucosamine 2000 mg/day or placebo. Changes in knee pain and function were assessed by palpation, a 3-m duck walk, repeated walking stair climb, questionnaires and a pain scale. There was a significant improvement in the glucosamine-treated group for quality of life scores at weeks 8 and 12 (P < 0.05) and pain scores at week 8 (P < 0.05) compared with placebo. At the end of the study, 88% of the glucosamine-treated patients reported some improvement in knee pain compared with 17% in the placebo group. Not surprisingly, there have also been negative studies. For example, ughes and Carr 41 did not find significant pain relief in 80 patients with OA of the knee given either glucosamine sulphate 1500 mg/day or placebo for 6 months. They also reported negative results for VAS pain scores, although they did report an improvement in mobility. Rindone et al. 42 also failed to find significant pain relief in 98 patients given either 1500 mg/day glucosamine sulphate or placebo for 2 months. Comparison of glucosamine and NSAIDs Müller-Fassbender et al. 43 compared 1500 mg/day of glucosamine sulphate and 1200 mg/day of ibuprofen in 200 patients with OA of the knee. There was no significant difference in efficacy between the two treatments, with reported success rates of 48% for glucosamine sulphate and 52% for ibuprofen after 4 weeks. The success rates after the first week of treatment, however, were 48% for ibuprofen and 28% for 7
8 glucosamine sulphate, showing that ibuprofen works more quickly. Fewer patients had adverse effects in the glucosamine sulphate group (6%) compared with the ibuprofen group (35%) (P < 0.05) and there were fewer adverse event-related drop-outs with glucosamine sulphate (1%) compared with ibuprofen (7%). Qiu et al. 44 also compared the efficacy of glucosamine sulphate 1500 mg/day and ibuprofen 1200 mg/day in knee OA in a double-blind, randomized study in 178 Chinese patients. Knee pain at rest, under movement and under pressure, knee swelling, improvement, therapeutic facility, adverse events and drop-outs were measured. Both glucosamine and ibuprofen significantly reduced the symptoms of OA, with glucosamine showing a trend to greater efficacy (84% reduction with glucosamine versus 77% with ibuprofen), although the difference was not statistically significant. There were significantly fewer (P = 0.01) adverse events and fewer drop-outs because of adverse events in the glucosamine-treated patients. Two weeks after stopping the drugs, there was a remnant therapeutic effect in both groups, and there was a trend towards a greater remnant therapeutic effect in the glucosamine group. Thie et al. 45 compared glucosamine sulphate 1500 mg/day and ibuprofen 1200 mg/day given for 90 days in patients with temporomandibular OA. Both treatments were effective but glucosamine sulphate was significantly more effective and patients receiving it took less acetaminophen (paracetamol) after the end of therapy (days ). Pain reduction of at least 20% was achieved in 71% of the glucosamine group versus 61% of the ibuprofen group by the end of 90 days. Lopes Vaz 46 conducted a double-blind trial in 40 out-patients with unilateral knee OA, which was designed to compare the efficacy and tolerance of glucosamine sulphate 1500 mg/day and ibuprofen 1200 mg/day over an 8-week period. Pain scores decreased faster during the first 2 weeks in the ibuprofen group compared with the glucosamine group. Although the response to glucosamine was slower, the reduction in pain scores continued throughout the trial period and, at the end, there was a statistically significant difference in favour of glucosamine (P < 0.05). No significant differences were observed in swelling or any of the other parameters monitored. Tolerance was satisfactory with both treatments. There were only minor complaints recorded by two patients on glucosamine compared with five on ibuprofen. The efficacy and safety of glucosamine compared with NSAIDs is summarized in Table 1. Does glucosamine alter the course of the disease? Several studies have shown beneficial effects on the radiological features of OA in patients receiving glucosamine. One of the most important trials was conducted by Reginster et al. 47 The investigators assessed the effects of glucosamine sulphate on the long-term progression of OA and also on symptoms. They used a randomized, double-blind, placebo-controlled design in which 212 patients with knee OA were randomly assigned to receive either 1500 mg glucosamine sulphate or placebo once daily for 3 years. Changes in radiological signs and the WOMAC index were measured. Weight-bearing posterior anterior X-rays of the knees were used to measure joint space width in the medial compartment of the knee. Patients receiving placebo showed progressive narrowing of the joint space, 8
9 TABLE 1: Efficacy and safety of glucosamine compared with non-steroidal anti-inflammatory drugs (NSAIDs) in osteoarthritis (OA) Glucosamine versus NSAIDs Results 1500 mg/day glucosamine versus Lequesne Index improvement: 48% in the 1200 mg/day ibuprofen in OA of the knee 43 glucosamine group versus 52% in the ibuprofen group at the end of week 4. Lequesne s Index decrease: > 6 points in both groups. 35% of patients on ibuprofen reported adverse events versus 6% on glucosamine 1500 mg/day glucosamine versus Pain reduction: 71% in the glucosamine group 1200 mg/day ibuprofen in versus 61% in the ibuprofen group at the end of temporomandibular OA 45 month 3. Glucosamine treatment was associated with a significantly greater decrease in pain and acetaminophen (paracetamol) use between days 90 and 120 (carryover effect) 1500 mg/day glucosamine versus Pain reduction: 51% in the glucosamine group 1200 mg/day ibuprofen in OA of the knee 44 versus 57% in the ibuprofen group at the end of week 4. Knee swelling: 77% in the glucosamine group versus 78% in the ibuprofen group at the end of week 4. Symptom improvement: 84% in the glucosamine group versus 77% in the ibuprofen group at the end of week 4. Glucosamine was better tolerated than ibuprofen 1500 mg/day glucosamine versus Pain scores decreased faster during the first mg/day ibuprofen in OA of the knee 46 weeks in the ibuprofen than in the glucosamine treatment group. The reduction in pain scores was significantly in favour of glucosamine at week 8 (P < 0.05) whereas there was no significant joint space loss in the 106 patients receiving glucosamine sulphate. After 2 years, there was joint space loss of 0.31 mm in the placebo group but no significant loss in the glucosamine group. This difference was statistically significant (P < 0.05). There were also statistically significant improvements in both pain and physical function (P = 0.016) in the glucosamine-treated patients using WOMAC scores; symptoms worsened slightly in patients who received placebo. There were no significant differences in safety or reasons for early withdrawal between the treatment and placebo groups. Pavelká et al. 9 compared glucosamine sulphate 1500 mg/day and placebo over 3 years, using an identical protocol in 202 patients with knee OA. Measurements were made of the radiographic minimum joint space and width of the tibio-femoral joint, and OA symptoms were assessed by the Lequesne and WOMAC indices. The results showed a statistically significant difference 9
10 in favour of glucosamine (P = 0.001). The mean joint space narrowing after 3 years was 0.19 mm in the placebo group and 0.04 mm in the glucosamine group. In the placebo group, 14% of patients showed joint space narrowing > 0.5 mm compared with 5% of the glucosamine group (P = 0.05). Symptoms of OA improved by as much as 20 25% with glucosamine sulphate, but there was only modest improvement with placebo. Differences in the Lequesne and WOMAC indices for pain function and stiffness were statistically significant in favour of glucosamine sulphate (P < 0.05). Safety was good with no significant differences between the groups. Bruyere et al. 48 carried out a pre-planned study consisting of two 3-year independent studies and a post-hoc analysis of the results obtained in 319 post-menopausal women with knee OA given either glucosamine sulphate 1500 mg/day or placebo. There was joint space loss of 0.33 mm with placebo and a small gain of mm in patients receiving glucosamine sulphate (P < ). A 14.1% improvement in the WOMAC Index with glucosamine sulphate and a deterioration of 5.4% with placebo (P = 0.003) were also found. Altman et al. 49 looked at the need for arthritis-related surgery in two groups of patients followed-up 5 years after the original glucosamine sulphate and placebo comparison. Surgery was required in 14.7% of 177 patients studied. Twice as many patients originally treated with placebo required surgery compared with patients treated with glucosamine, a difference that almost reached significance. Time-to-event analysis confirmed a decreased cumulative reduction in risk in patients who had been treated with glucosamine (P = 0.05). Finally, Christgau et al., 50 in a study of 212 knee OA patients participating in a trial of glucosamine sulphate, showed that collagen II degradation, a measure of cartilage turnover, decreased over 12 months on glucosamine and the changes correlated with changes in joint space (P < 0.05). This indicated that the best response to glucosamine was achieved in patients with the highest cartilage turnover or the most active disease. These studies indicate that long-term treatment with glucosamine may help to delay the progression of knee OA, suggesting that glucosamine can be considered as a disease-modifying agent for OA. Is chondroitin effective? Many studies have confirmed the efficacy of chondroitin. Bourgeois et al. 51 compared 1200 mg/day of chondroitin and placebo over 3 months in 127 patients with knee OA. The Lequesne Index was reduced by 40 45% in the chondroitin-treated patients and 10% in the placebo-treated patients (P < from day 42 throughout the remaining treatment period). Chondroitin was given either in a single daily dose or in three divided doses but this did not influence the efficacy. The benefits of chondroitin were evident after 2 weeks of treatment and patients on chondroitin needed less paracetamol. The overall judgement of patients and physicians correlated well; both showed a statistically significant difference between chondroitin and placebo at day 42 (P < 0.05) and at day 91 (P < 0.01). Bucsi and Poór 52 compared chondroitin 800 mg/day and placebo in 85 patients with OA, finding a significant difference in favour of chondroitin. Pain was reduced by 36% after 3 months and 43% after 6 months of chondroitin therapy. The difference between chondroitin and placebo was statistically significant from 3 months onwards (P < 0.001). 10
11 Uebelhart et al. 53 compared chondroitin sulphate 800 mg/day and placebo in 46 patients with knee OA, finding a significant difference in favour of chondroitin. The VAS pain scores in the chondroitin-treated group were reduced from 5.76 to 3.6 after 3 months and to 2.1 after 12 months compared with values of 6.4, 5.2 and 4.8 in the placebo group, respectively. The differences were statistically significant at 3 months (P < 0.05) and 12 months (P < 0.01). Overall mobility capacity increased by 69% after 12 months in the chondroitin-treated patients compared with 19% in the placebo group (P < 0.001). Biochemical markers of cartilage metabolism increased in the placebo group and showed little change in the chondroitin group. Mazières et al. 54 compared chondroitin sulphate 1000 mg/day and placebo given for 3 months to 130 patients with knee OA. The results at the end of 3 months favoured chondroitin, but were not statistically significant since the Lequesne Index fell by 2.4 in the chondroitin group and 1.6 in the placebo group. Taking only patients who completed the 3 months of treatment, the difference was significant in favour of chondroitin (P = 0.02). owever, 1 month after the end of the treatment period, there were significantly greater persistent effects in the patients treated with chondroitin sulphate compared with the placebo group for the Lequesne Index (P < 0.01) as well as pain at rest (P = 0.03), pain with activity (P = 0.001), effect on daily living (P = 0.001), and patient and physician assessments (P = 0.02 and P = 0.05, respectively). Uebelhart et al. 55 compared chondroitin sulphate 800 mg/day and placebo in 120 patients with knee OA. Treatment was given for two 3-month periods in 1 year. There was a statistically significant difference in favour of chondroitin at the end of the year. The Lequesne Index improved by 36% in the chondroitin group and 22% in the placebo group (P < 0.01). There were also significant improvements in VAS pain scores and walking time (P < 0.05). Improvement occurred during both treatment periods and results were stable in the 3 months without treatment, suggesting that chondroitin could be given for alternate 3-month periods. Mazières et al. 56 compared 1 g/day chondroitin sulphate and placebo in 307 patients with knee OA over a period of 24 weeks. There was no significant difference in pain and the Lequesne Index but there was a significant difference in response rate that showed improvement in 68% of patients receiving chondroitin and 56% receiving placebo (P = 0.03). The primary efficacy measures showed trends in favour of chondroitin; VAS pain scores fell by 26.2 mm and 19.9 mm and improved function was 22.4 mm and 21.7 mm in the chondroitin and placebo groups, respectively (P = and P = 0.109, respectively). Morreale et al. 57 carried out a doubleblind, double-dummy study in which 146 patients with knee OA were randomized to either chondroitin sulphate or diclofenac sodium over a period of 6 months. Both groups showed similar improvements in pain, but the onset of events was more rapid in the diclofenac group. owever, the effect of diclofenac ceased upon discontinuation whereas that of chondroitin continued for 3 months after the end of treatment. The physicians global assessment at the end of the study was in favour of chondroitin compared with diclofenac (P < 0.01). Does chondroitin alter the course of the disease? Verbruggen et al. 58 compared chondroitin sulphate 1200 mg/day and placebo in 165 patients with hand OA over a 3-year period. Treatment with chondroitin did not prevent 11
12 the development of OA in normal joints. owever, substantially fewer patients treated with chondroitin developed erosive OA; 8.8% in the chondroitin group and 29.4% in the placebo group. Uebelhart et al. 53 compared chondroitin sulphate 800 mg/day and placebo over 12 months. In this trial, the medial compartment joint space narrowing was studied in a small number of patients (14 treated with chondroitin and 12 with placebo). The joint space decreased in the placebo group, but not in the chondroitin group. Despite the small number of participants, this study was able to show a significant difference between chondroitin and placebo (P = 0.001). Biochemical markers of cartilage metabolism were unchanged in the chondroitin group and rose in the placebo group. Uebelhart et al. 55 reported that, in a multicentre study of 110 patients given either chondroitin sulphate 800 mg/day (n = 54) or placebo (n = 56), the medial compartment joint space narrowing was unchanged in the chondroitin group, but there was a significant loss of joint space in the placebo group (P 0.01 between group comparisons). The Lequesne Index improved by 36% in the chondroitin group compared with 23% in the placebo group (P < 0.01) and there were also significant improvements in VAS pain scores and walking time in the chondroitin group compared with placebo (P < 0.05 for each). Physicians (P < 0.01) and patients (P < 0.01) overall assessments were also statistically significant in favour of chondroitin. Michel et al. 59 compared chondroitin sulphate 800 mg/day and placebo in 300 patients with knee OA treated for 2 years. Compared with baseline, there was no change in joint space in chondroitin-treated patients after 2 years, but a significant reduction in those receiving placebo (P = for mean and P = 0.05 for minimum joint space width). Between-group comparison showed a statistically significant difference in both mean (P = 0.04) and minimum joint space width (P = 0.05), favouring chondroitin. Meta-analysis of glucosamine studies With plenty of large studies available, it is doubtful whether a meta-analysis is going to provide additional information. Not surprisingly, Poolsup et al., 60 in combining the results of the studies by Reginster et al. 47 and Pavelká et al., 9 showed symptomatic relief and delayed progression of knee OA. The risk of disease progression was reduced by 54%. Glucosamine sulphate caused no more side-effects than placebo. Richy et al. 10 similarly confirmed the chondroprotective action of both glucosamine and chondroitin in knee OA, as well as a pronounced effect on symptoms and no more adverse effects than placebo. Confounding factors in clinical trials It is not surprising to see some variation in the results of different studies and this is evident in trials of anti-inflammatory drugs and other types of medication. There are various reasons why the effects of glucosamine and chondroitin may vary between trials. For example, it is clear that different preparations of glucosamine provide different amounts of elemental glucosamine and many studies have failed to document the bioavailability of the compound used. 61 The placebo effect has been large in many studies, over 60% of patients responding in the GAIT study 15 for example. The OA patient population is diverse and it is clear from some studies that 12
13 different effects are seen in patients with different disease severity. It is the author s view that concomitant use of antiinflammatory and analgesic medications might also alter responses. Some preparations of glucosamine and chondroitin contain other potentially active ingredients, such as manganese. Mode of action The original rationale for taking glucosamine and chondroitin was to provide substrate or building blocks for the biosynthesis of proteoglycan. It is probably naïve to think that this is the mode of action of these compounds since there is no evidence of a shortage of proteoglycan in patients with OA. It seems more likely that glucosamine and chondroitin promote proteoglycan synthesis by chondrocytes and inhibit the degradative enzymes that lead to the premature breakdown of cartilage in OA. The possible modes of action of glucosamine and chondroitin are summarized in Table 2. Side-effects and safety No serious adverse events have been reported with glucosamine or chondroitin and treatment-related deaths do not appear in the literature. For both these agents, the incidence of adverse events is comparable with that of placebo and caution should be exercised in patients who are highly allergic; for glucosamine, particularly in those who are allergic to shellfish since it is usually made from crustacea shells. A photosensitivity reaction has been reported 62 as well as one case of angioedema, 63 while exacerbation of asthma has also been recorded. 64 The common side-effects reported in studies of glucosamine are gastrointestinal, including abdominal pain, diarrhoea, heartburn, nausea, epigastric pain and flatulence. These occurred in 3.5% of 1208 patients reported by Tapadinhas et al. 65 treated with glucosamine sulphate 1500 mg/day. Amongst the non-gastrointestinal adverse events are drowsiness and skin reactions of doubtful significance. 21 Chondroitin is also well tolerated with gastrointestinal events being the most common recorded adverse reactions in trials and with an incidence comparable to placebo. 51,55 Contraindications and interactions There is no evidence of any clinically significant interactions with glucosamine or chondroitin. There has been some concern TABLE 2: Possible modes of action of glucosamine and chondroitin in osteoarthritis Glucosamine Provides substrate Increases proteoglycan synthesis Inhibits cytokines (IL-1β) Inhibits proteases (matrix metalloproteinase and collagenase) Reduces PGE 2 production Interferes with binding of NFκB in chondrocytes IL-1β, interleukin-1β; PGE 2, prostaglandin E 2 ; NFκB, nuclear factor κb. Chondroitin Provides substrate Increases proteoglycan synthesis by chondrocytes Inhibits cytokines Inhibits proteases (collagenase) Increases viscosity of synovial fluid Increases bone mineralization and repair 13
14 about the use of parenteral glucosamine in patients with diabetes but, despite the fact that studies in animals have shown that glucosamine may have a negative impact on insulin levels, 66 studies in humans have demonstrated that supplementation with the normal recommended dosages of glucosamine does not cause any concern. For example, Tannis et al. 67 showed no changes in glucose levels or serum insulin concentrations in healthy individuals, while a study in patients with type II diabetes over a 90-day period, during which they received either placebo or glucosamine hydrochloride 1500 mg/day and chondroitin sulphate 1200 mg/day, showed no significant changes in haemoglobin A 1C. 68 Glucosamine sulphate or glucosamine hydrochloride? Two different salts of glucosamine (glucosamine hydrochloride and glucosamine sulphate) are commonly used for the treatment of OA. Following absorption, the salt is broken down in the acid environment of the stomach, making glucosamine available 14 so that it is unlikely that the nature of the salt would affect the efficacy of the product. Furthermore, the bioavailability of the two salts is the same. 22 The hydrochloride salt, however, provides more elemental glucosamine than the sulphate so that, in theory, 2608 mg of glucosamine sulphate would be required to provide the same amount of glucosamine as 1500 mg of the hydrochloride. 4 This is because glucosamine hydrochloride has a higher compound purity than glucosamine sulphate, which requires sodium and potassium for stability. Qiu et al. 69 compared glucosamine sulphate 1500 mg/day and glucosamine hydrochloride 1440 mg/day for 4 weeks in 142 patients with knee OA. Treatments were randomized, but the study was not double-blind. Both groups showed considerable improvement in symptoms of OA: The Lequesne Index decreased from a baseline of 9.4 ± 1.8 to 3.4 ± 1.9 (P < 0.05) in the glucosamine hydrochloride group and from a baseline of 9.5 ± 1.4 to 3.4 ± 1.8 (P < 0.05) in the glucosamine sulphate group. There was no significant difference between the two different glucosamine salts. Response rates were 91.4% and 90.0% in the hydrochloride and sulphate groups, respectively, and responses persisted for 2 weeks after stopping treatment. Side-effects occurred in 4.2% and 7.0% of the hydrochloride and sulphate groups, respectively, and they were mainly mild stomach discomfort and constipation. It has been argued that the effect of glucosamine sulphate is not mediated by glucosamine, but by sulphate since sulphate is required for GAG production. 70,71 offer et al. 70 suggested that sulphate might be the important part of glucosamine sulphate based on the finding that, in seven healthy volunteers, sulphate levels increased after ingestion of glucosamine sulphate but glucosamine levels did not. In addition, there was a close correlation between serum and synovial fluid sulphate levels, and coadministration of glucosamine and acetaminophen (paracetamol) resulted in decreased serum sulphate levels. The authors argued that the lack of increase in serum glucosamine levels would make it impossible for glucosamine to stimulate GAG synthesis in the joint space. This is in striking contrast to other studies reviewed above, which clearly showed increased levels of glucosamine in plasma and synovial fluid after administration of both salts. Furthermore, the sulphate hypothesis is clearly contradicted by studies with 14 C-labelled glucosamine in 14
15 which radioactivity was recovered in femoral cartilage after both intravenous and oral administration. 20,72 In addition, a recently published study in which glucosamine levels were determined in plasma and synovial fluid by liquid chromatography tandem mass spectrometry after oral administration of glucosamine sulphate 1500 mg/day for 14 days, clearly demonstrated that glucosamine is bioavailable in the plasma and synovial fluid. 24 It has recently been noted that some proprietary glucosamine sulphate preparations are stabilized with potassium chloride and that at recommended doses the potassium intake may be as much as 6.6 mmol/day. The Swedish Medical Products Agency recently issued a warning that the risk of hyperkalaemia should be considered in patients with impaired renal function who receive concomitant treatment with other drugs that have a risk of hyperkalaemia or in patients prescribed a low potassium diet. 73 Potassium salts are not present in glucosamine hydrochloride preparations. Conclusion Glucosamine, chondroitin and the combination of these two agents have stood the test of time. What patients say and do, continuing to pay for and take this particular treatment, and what physicians say on the basis of experience, support the view that these are effective treatments for OA. Patients will not, as a rule, continue to take medicines that do not work. The views of physicians are set out in the European League Against Rheumatism (EULAR) recommendations for the management of knee OA, which includes glucosamine and chondroitin as symptomatic slow acting drugs for OA which may modify the structure of cartilage. 74 While the knee is the most common site of OA and, thus, has received the most attention in studies, trials involving the hand, 58 spine 18 and temporomandibular joints 45 suggest that the efficacy of supplementation is similar, and it would be surprising if it were not so. The evidence reviewed above confirms the efficacy of glucosamine, chondroitin and the combination of both agents in the treatment of OA. These treatments are widely and easily available in comparison with antiinflammatory drugs, better tolerated and safer. Occasional adverse reactions have occurred, mainly involving the stomach, but their incidence is comparable with placebo. It is wise to avoid the use of glucosamine in highly allergic individuals and those with shellfish allergy but, apart from this, it appears to be suitable for the great majority of patients. The evidence suggests that glucosamine hydrochloride is as effective as glucosamine sulphate, as one would expect from theoretical considerations. The evidence also suggests that the combination of glucosamine and chondroitin is probably slightly more effective than either drug alone but larger studies in suitable patients would be desirable to confirm this. The combination of glucosamine and chondroitin is effective, but further, welldesigned trials are necessary to confirm their short- and long-term efficacy in OA. Clinical experience as well as the continued taking of glucosamine and chondroitin by patients and the recommending of them by doctors supports the view that they are useful for many patients and clinical trials have confirmed this. Glucosamine and chondroitin are better tolerated and much safer than NSAIDs particularly for elderly and high-risk patients. The X-ray evidence of a disease-modifying effect makes a strong case for the use of these agents, particularly in early disease when good symptomatic 15
16 benefit can be achieved. In conclusion, glucosamine and chondroitin deserve a prominent place amongst the very important non-drug measures to be considered in a patient presenting with painful osteoarthritic joints, measures designed not only to relieve symptoms but also to limit the long-term impact of the disease. Glucosamine and chondroitin work slowly, taking a few weeks to become effective and should be given for at least 4 weeks before an assessment is made. Supplementation should be continued because of their potential chondroprotective effect, particularly in knee OA. The most striking experimental evidence is related to knee surgery. To avoid an operation is every patient s wish and it has been shown that glucosamine and chondroitin may increase the likelihood of this. 49 Conflicts of interest The author had no conflicts of interest to declare in relation to this article. Received for publication 1 July 2008 Accepted subject to revision 3 July 2008 Revised accepted 22 September 2008 Copyright 2008 Field ouse Publishing LLP References 1 Spector TD, MacGregor AJ: Epidermiology of rheumatic diseases. In: ABC of Rheumatology, 2nd edn (Snaith ML, ed). London: BMJ Books, 1999; pp American College of Rheumatology Subcommittee on Osteoarthritis Guidelines: ACR recommendations for the medical management of osteoarthritis of the hip and knee: 2000 update. Arthritis Rheum 2000; 43: Dieppe PA, Lohmander LS: Pathogenesis and management of pain in osteoarthritis. Lancet 2005; 365: Owens S, Wagner P, Vangsness CT: Recent advances in glucosamine and chondroitin supplementation. J Knee Surg 2004; 17: Lichtenstein DR, Syngal S, Wolfe MM: Nonsteroidal antiinflammatory drugs and the gastrointestinal tract. The double-edged sword. Arthritis Rheum 1995; 38: Lozada CJ, Altman RD: Management of limb joint osteoarthritis. Section 11: Osteoarthritis and related disorders. In: Practical Rheumatology, 3rd edn (ochberg MC, Silman AJ, Smolen JS, et al, eds). Philadelphia: Elsevier (Mosby), 2004; pp Simanek V, Kren V, Ulrichova J, et al: The efficacy of glucosamine and chondroitin sulfate in the treatment of osteoarthritis: are these saccharides drugs or nutraceuticals? Biomed Pap Med Fac Univ Palacky Olomouc Czech Repub 2005; 149: Brion P, Kalunian KC: Osteoarthritis. Section In: Oxford Textbook of Medicine, 4th edn (Warrell DA, Cox TM, Firth JD, eds). London: Oxford University Press, 2004; pp Pavelká K, Gatterová J, Olejarová M, et al: Glucosamine sulfate use and delay of progression of knee osteoarthritis: a 3-year, randomized, placebo-controlled, double-blind study. Arch Intern Med 2002; 162: Richy F, Bruyere O, Ethgen O, et al: Structural and symptomatic efficacy of glucosamine and chondroitin in knee osteoarthritis: a comprehensive meta-analysis. Arch Intern Med 2003; 163: Steinmeyer J, Konttinen YT: Oral treatment options for degenerative joint disease presence and future. Adv Drug Deliv Rev 2006; 58: Kelly GS: The role of glucosamine sulfate and chondroitin sulfates in the treatment of degenerative joint disease. Altern Med Rev 1998; 3: Lippiello L, Woodward J, Karpman R, et al: In vivo chondroprotection and metabolic synergy of glucosamine and chondroitin sulfate. Clin Orthop Rel Res 2000; 381: Deal CL, Moskowitz RW: Nutraceuticals as therapeutic agents in osteoarthritis. The role of glucosamine, chondroitin sulfate, and collagen hydrolysate. Rheum Dis Clin North Am 1999; 25: Clegg DO, Reda DJ, arris CL, et al: Glucosamine, chondroitin sulfate, and the two in combination for painful knee osteoarthritis. N Engl J Med 2006; 354: Das A, ammad TA: Efficacy of a combination of FCG49 glucosamine hydrochloride, TR122 low molecular weight sodium chondroitin sulfate and manganese ascorbate in the management of knee osteoarthritis. Osteoarthritis Cartilage 2000; 8: Denham AC, Newton WP: Are glucosamine and chondroitin effective in treating osteoarthritis? J Fam Pract 2000; 49:
REVIEW I-Flex and Management of Inflammation in Osteoarthritis
 1 REVIEW I-Flex and Management of Inflammation in Osteoarthritis Tammy Wolhuter, RD (SA) & Anne Till, RD(SA) From: Anne Till & Associates, Registered Dietitians 1. Introduction Osteoarthritis (OA) is a
1 REVIEW I-Flex and Management of Inflammation in Osteoarthritis Tammy Wolhuter, RD (SA) & Anne Till, RD(SA) From: Anne Till & Associates, Registered Dietitians 1. Introduction Osteoarthritis (OA) is a
TRANSPARENCY COMMITTEE OPINION. 26 November 2008
 The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION 26 November 2008 CHONDROSULF 400 mg, capsule Box containing 84 capsules (CIP: 335 917-3) CHONDROSULF 400 mg, granules
The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION 26 November 2008 CHONDROSULF 400 mg, capsule Box containing 84 capsules (CIP: 335 917-3) CHONDROSULF 400 mg, granules
4 2 Osteoarthritis 1
 Osteoarthritis 1 Osteoarthritis ( OA) Osteoarthritis is a chronic disease and the most common of all rheumatological disorders. It particularly affects individuals over the age of 65 years. The prevalence
Osteoarthritis 1 Osteoarthritis ( OA) Osteoarthritis is a chronic disease and the most common of all rheumatological disorders. It particularly affects individuals over the age of 65 years. The prevalence
New Medicines Profile
 New Medicines Profile May 2008 Issue No. 08/05 (Alateris ) Concise evaluated information to support the managed entry of new medicines in the NHS Brand Name, (Manufacturer): Alateris (William Ransom &
New Medicines Profile May 2008 Issue No. 08/05 (Alateris ) Concise evaluated information to support the managed entry of new medicines in the NHS Brand Name, (Manufacturer): Alateris (William Ransom &
The legally binding text is the original French version
 The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION 22 July 2009 ENDOSTA 625 mg, tablet Box of 60 (CIP: 380 534-2) Box of 180 (CIP: 380 535-9) Applicant: EXPANSCIENCE
The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION 22 July 2009 ENDOSTA 625 mg, tablet Box of 60 (CIP: 380 534-2) Box of 180 (CIP: 380 535-9) Applicant: EXPANSCIENCE
NOTOPAIN CAPLETS. Diclofenac Sodium + Paracetamol. Composition. Each tablet contains: Diclofenac Sodium BP 50mg Paracetamol BP 500mg.
 NOTOPAIN CAPLETS Diclofenac Sodium + Paracetamol Composition Each tablet contains: Diclofenac Sodium BP 50mg Paracetamol BP 500mg Pharmacology Phamacodynamics Diclofenac relieves pain and inflammation
NOTOPAIN CAPLETS Diclofenac Sodium + Paracetamol Composition Each tablet contains: Diclofenac Sodium BP 50mg Paracetamol BP 500mg Pharmacology Phamacodynamics Diclofenac relieves pain and inflammation
Osteoarthritis What is new? Dr Peter Cheung, Rheumatologist, NUHS
 Osteoarthritis What is new? Dr Peter Cheung, Rheumatologist, NUHS Objective Outline some clinical features that are not well appreciated in OA patients Recent advances in knowledge and management of OA
Osteoarthritis What is new? Dr Peter Cheung, Rheumatologist, NUHS Objective Outline some clinical features that are not well appreciated in OA patients Recent advances in knowledge and management of OA
SUMMARY OF PRODUCT CHARACTERISTICS
 SUMMARY OF PRODUCT CHARACTERISTICS 1. NAME OF THE MEDICINAL PRODUCT Comfora 595 mg film-coated tablets 2. QUALITATIVE AND QUANTITATIVE COMPOSITION One film-coated tablet contains: glucosamine sulphate
SUMMARY OF PRODUCT CHARACTERISTICS 1. NAME OF THE MEDICINAL PRODUCT Comfora 595 mg film-coated tablets 2. QUALITATIVE AND QUANTITATIVE COMPOSITION One film-coated tablet contains: glucosamine sulphate
Glucosamine hydrochloride for the treatment of osteoarthritis symptoms
 REVIEW Glucosamine hydrochloride for the treatment of osteoarthritis symptoms Beth Anne Fox Mary M Stephens East Tennessee State University, Family Physicians of Kingsport, Kingsport, TN, USA Abstract:
REVIEW Glucosamine hydrochloride for the treatment of osteoarthritis symptoms Beth Anne Fox Mary M Stephens East Tennessee State University, Family Physicians of Kingsport, Kingsport, TN, USA Abstract:
Arthritis of the Knee
 Arthritis of the Knee There are three basic types of arthritis that may affect the knee joint. Osteoarthritis Osteoarthritis (OA) is the most common form of knee arthritis. OA is usually a slowly progressive
Arthritis of the Knee There are three basic types of arthritis that may affect the knee joint. Osteoarthritis Osteoarthritis (OA) is the most common form of knee arthritis. OA is usually a slowly progressive
Osteoarthritis. Dr Anthony Feher. With special thanks to Dr. Tim Williams and Dr. Bhatia for allowing me to use some of their slides
 Osteoarthritis Dr Anthony Feher With special thanks to Dr. Tim Williams and Dr. Bhatia for allowing me to use some of their slides No Financial Disclosures Number one chronic disability in the United States
Osteoarthritis Dr Anthony Feher With special thanks to Dr. Tim Williams and Dr. Bhatia for allowing me to use some of their slides No Financial Disclosures Number one chronic disability in the United States
Safety and efficacy of flavocoxid compared with naproxen in subjects with osteoarthritis of the knee: a pilot study
 Osteoarthritis and Cartilage. 15(suppl B):B91 Safety and efficacy of flavocoxid compared with naproxen in subjects with osteoarthritis of the knee: a pilot study Levy R*, Saikovsky R, Shmidt E, Khokhlov
Osteoarthritis and Cartilage. 15(suppl B):B91 Safety and efficacy of flavocoxid compared with naproxen in subjects with osteoarthritis of the knee: a pilot study Levy R*, Saikovsky R, Shmidt E, Khokhlov
Is Ginger Effective in Reducing Knee Pain in Adults With Osteoarthritis?
 Philadelphia College of Osteopathic Medicine DigitalCommons@PCOM PCOM Physician Assistant Studies Student Scholarship Student Dissertations, Theses and Papers 2015 Is Ginger Effective in Reducing Knee
Philadelphia College of Osteopathic Medicine DigitalCommons@PCOM PCOM Physician Assistant Studies Student Scholarship Student Dissertations, Theses and Papers 2015 Is Ginger Effective in Reducing Knee
Suffolk PCT Drug & Therapeutics Committee New Medicine Report (Adopted by the CCG until review and further notice)
 Suffolk PCT Drug & Therapeutics Committee New Medicine Report (Adopted by the CCG until review and further notice) This drug has been reviewed because it is a product that may be prescribed in primary
Suffolk PCT Drug & Therapeutics Committee New Medicine Report (Adopted by the CCG until review and further notice) This drug has been reviewed because it is a product that may be prescribed in primary
The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION. 9 January 2013
 The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION 9 January 2013 The opinion adopted by the Transparency Committee on 4 July 2012 was given a hearing on 5 December
The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION 9 January 2013 The opinion adopted by the Transparency Committee on 4 July 2012 was given a hearing on 5 December
RISK MANAGEMENT PLAN (RMP) PUBLIC SUMMARY ETORICOXIB ORION (ETORICOXIB) 30 MG, 60 MG, 90 MG & 120 MG FILM-COATED TABLET DATE: , VERSION 1.
 RISK MANAGEMENT PLAN (RMP) PUBLIC SUMMARY ETORICOXIB ORION (ETORICOXIB) 30 MG, 60 MG, 90 MG & 120 MG FILM-COATED TABLET DATE: 07-10-2016, VERSION 1.2 VI.2 Elements for a Public Summary Etoricoxib Orion
RISK MANAGEMENT PLAN (RMP) PUBLIC SUMMARY ETORICOXIB ORION (ETORICOXIB) 30 MG, 60 MG, 90 MG & 120 MG FILM-COATED TABLET DATE: 07-10-2016, VERSION 1.2 VI.2 Elements for a Public Summary Etoricoxib Orion
Risk Management Plan Etoricoxib film-coated tablets
 VI.2 Elements for a Public Summary VI.2.1 Overview of disease epidemiology Osteoarthritis (OA): OA is a condition in which the cartilage of the joints is broken down. This causes stiffness, pain and leads
VI.2 Elements for a Public Summary VI.2.1 Overview of disease epidemiology Osteoarthritis (OA): OA is a condition in which the cartilage of the joints is broken down. This causes stiffness, pain and leads
Prevention Diagnosis Assessment Prescription and /or application of wide range of interventions and PRM program management
 OA PATHOLOGY Characterized by progressive deterioration and ultimate loss of articular cartilage Reactive changes of joint margins and joint thickening of the capsule When OA symptomatic leads to: Pain
OA PATHOLOGY Characterized by progressive deterioration and ultimate loss of articular cartilage Reactive changes of joint margins and joint thickening of the capsule When OA symptomatic leads to: Pain
GLUCOSAMINE SP TABLETS
 Executive Executive Summary Summary GLUCOSAMINE SP TABLETS WHAT IS GLUCOSAMINE? Glucosamine is widely used in Europe and is popular as a health food ingredient in Japan. Glucosamine is originally produced
Executive Executive Summary Summary GLUCOSAMINE SP TABLETS WHAT IS GLUCOSAMINE? Glucosamine is widely used in Europe and is popular as a health food ingredient in Japan. Glucosamine is originally produced
Glucosamine May Reduce Pain in Individuals with Knee Osteoarthritis
 1 Glucosamine May Reduce Pain in Individuals with Knee Osteoarthritis Prepared by: Jacqueline Pierce, MSc (PT) candidate, Queen's University Date: April 2005 (planned review date April 2007) Clinical Scenario:
1 Glucosamine May Reduce Pain in Individuals with Knee Osteoarthritis Prepared by: Jacqueline Pierce, MSc (PT) candidate, Queen's University Date: April 2005 (planned review date April 2007) Clinical Scenario:
Iroko Pharmaceuticals Receives FDA Approval for VIVLODEX - First Low Dose SoluMatrix Meloxicam for Osteoarthritis Pain
 Iroko Pharmaceuticals Receives FDA Approval for VIVLODEX - First Low Dose SoluMatrix Meloxicam for Osteoarthritis Pain VIVLODEX Developed to Align with FDA NSAID Recommendations Proven Efficacy at Low
Iroko Pharmaceuticals Receives FDA Approval for VIVLODEX - First Low Dose SoluMatrix Meloxicam for Osteoarthritis Pain VIVLODEX Developed to Align with FDA NSAID Recommendations Proven Efficacy at Low
Webinar 2. Natures Aid: Joint Health
 Webinar 2 Natures Aid: Joint Health The Scale of The Problem Joint problems such as osteoarthritis affect many millions of people throughout the world, leading to agonising pain and disability. Arthritis
Webinar 2 Natures Aid: Joint Health The Scale of The Problem Joint problems such as osteoarthritis affect many millions of people throughout the world, leading to agonising pain and disability. Arthritis
Glucosamine Natural Standard Monograph (www.naturalstandard.com) Copyright 2008.
 Glucosamine Natural Standard Monograph (www.naturalstandard.com) Copyright 2008. Synonyms/Common Names/Related Substances: 2-acetamido-2-deoxyglucose, acetylglucosamine, Arth-X Plus, chitosamine, D- glucosamine,
Glucosamine Natural Standard Monograph (www.naturalstandard.com) Copyright 2008. Synonyms/Common Names/Related Substances: 2-acetamido-2-deoxyglucose, acetylglucosamine, Arth-X Plus, chitosamine, D- glucosamine,
OSTEOARTHRITIS An introduction to aging science brought to you by the American Federation for Aging Research
 infoaging guides DISEASES OF AGING OSTEOARTHRITIS An introduction to aging science brought to you by the American Federation for Aging Research WHAT IS OSTEOARTHRITIS? Osteoarthritis (OA) is the most common
infoaging guides DISEASES OF AGING OSTEOARTHRITIS An introduction to aging science brought to you by the American Federation for Aging Research WHAT IS OSTEOARTHRITIS? Osteoarthritis (OA) is the most common
PRIMARY CARE BRIEFING GLUSARTEL (GLUCOSAMINE SULPHATE)
 Summary This Primary Care Briefing informs healthcare professionals of a new preparation of glucosamine sulphate, Glusartel, licensed for the relief of symptoms in mild to moderate osteoarthritis of the
Summary This Primary Care Briefing informs healthcare professionals of a new preparation of glucosamine sulphate, Glusartel, licensed for the relief of symptoms in mild to moderate osteoarthritis of the
THE RESEARCH STATUS OF GLUCOSAMINE SULFATE JAMES MESCHINO DC, MS, ND. Introduction
 THE RESEARCH STATUS OF GLUCOSAMINE SULFATE JAMES MESCHINO DC, MS, ND Introduction Osteoarthritis has been reported to affect 40 million Americans, involving more than 13% of the population. Eighty percent
THE RESEARCH STATUS OF GLUCOSAMINE SULFATE JAMES MESCHINO DC, MS, ND Introduction Osteoarthritis has been reported to affect 40 million Americans, involving more than 13% of the population. Eighty percent
UPDATES ON MANAGEMENT OF OSTEOARTHRITIS
 UPDATES ON MANAGEMENT OF OSTEOARTHRITIS August 10, 2014 Dr. Suneil Kapur Assistant Professor of Medicine, University of Ottawa Associate Staff Rheumatologist, The Ottawa Hospital Learning Objectives Upon
UPDATES ON MANAGEMENT OF OSTEOARTHRITIS August 10, 2014 Dr. Suneil Kapur Assistant Professor of Medicine, University of Ottawa Associate Staff Rheumatologist, The Ottawa Hospital Learning Objectives Upon
ART 50 Capsules. Symptomatic treatment of functional symptoms and signs of osteoarthritis.
 Doctor leaflet Art50-DL-March2012-01 ART 50 Capsules 1. NAME OF THE MEDICINAL PRODUCT Art 50 mg, capsule. 2. QUALITATIVE AND QUANTITATIVE COMPOSITION Each capsule of ART 50 contains Diacerein 50 mg. For
Doctor leaflet Art50-DL-March2012-01 ART 50 Capsules 1. NAME OF THE MEDICINAL PRODUCT Art 50 mg, capsule. 2. QUALITATIVE AND QUANTITATIVE COMPOSITION Each capsule of ART 50 contains Diacerein 50 mg. For
DISEASES AND DISORDERS
 DISEASES AND DISORDERS 9. 53 10. Rheumatoid arthritis 59 11. Spondyloarthropathies 69 12. Connective tissue diseases 77 13. Osteoporosis and metabolic bone disease 95 14. Crystal arthropathies 103 15.
DISEASES AND DISORDERS 9. 53 10. Rheumatoid arthritis 59 11. Spondyloarthropathies 69 12. Connective tissue diseases 77 13. Osteoporosis and metabolic bone disease 95 14. Crystal arthropathies 103 15.
Pain therapeutics. Acetaminophen/NSAIDs Acute pain Osteoarthritis Migraine Acute Gout Neuropathic pain
 Pain therapeutics Acetaminophen/NSAIDs Acute pain Osteoarthritis Migraine Acute Gout Neuropathic pain James McCormack, Pharm.D. Professor Faculty of Pharmaceutical Sciences, UBC Common types of pain killers
Pain therapeutics Acetaminophen/NSAIDs Acute pain Osteoarthritis Migraine Acute Gout Neuropathic pain James McCormack, Pharm.D. Professor Faculty of Pharmaceutical Sciences, UBC Common types of pain killers
GLUCOSAMINE COMPLEX WORLDWIDE HEALTH CENTER. CONTAINS: No gluten Wheat Lactose 100 CAPSULES. www
 WORLDWIDE HEALTH CENTER www Natural Health Products & Remedies Important note: This product fact sheet is for professional use and contains guideline information only. A direct copy of the information
WORLDWIDE HEALTH CENTER www Natural Health Products & Remedies Important note: This product fact sheet is for professional use and contains guideline information only. A direct copy of the information
Q&A for Algaea-X 1. What is Algaea-X? 2. What are the ingredients of Algaea-X? 3. How does Algaea-X work?
 Q&A for Algaea-X 1. What is Algaea-X? Algaea-X is a topical cream developed to help relieve pain and inflammation caused by arthritis and helps the regeneration of damaged cartilage. Developed by utilizing
Q&A for Algaea-X 1. What is Algaea-X? Algaea-X is a topical cream developed to help relieve pain and inflammation caused by arthritis and helps the regeneration of damaged cartilage. Developed by utilizing
Etoricoxib STADA 30 mg, 60 mg, 90 mg and 120 mg film-coated tablets , Version V1.2 PUBLIC SUMMARY OF THE RISK MANAGEMENT PLAN
 Etoricoxib STADA 30 mg, 60 mg, 90 mg and 120 mg film-coated tablets 23.5.2016, Version V1.2 PUBLIC SUMMARY OF THE RISK MANAGEMENT PLAN VI.2 Elements for a Public Summary Etoricoxib STADA 30 mg film-coated
Etoricoxib STADA 30 mg, 60 mg, 90 mg and 120 mg film-coated tablets 23.5.2016, Version V1.2 PUBLIC SUMMARY OF THE RISK MANAGEMENT PLAN VI.2 Elements for a Public Summary Etoricoxib STADA 30 mg film-coated
Osteoarthritis (OA), Safety & Efficacy of Glucosamine & Chondroitin in Osteoarthritis. Clinical studies. show these. agents are very.
 FEATURE Safety & Efficacy of Glucosamine & Chondroitin in Osteoarthritis by DARRELL T. HULISZ, Pharm.D., R.Ph. Assistant Professor of Family Medicine Case Western Reserve University School of Medicine;
FEATURE Safety & Efficacy of Glucosamine & Chondroitin in Osteoarthritis by DARRELL T. HULISZ, Pharm.D., R.Ph. Assistant Professor of Family Medicine Case Western Reserve University School of Medicine;
Children Enteric coated tablet : 1-3 mg/kg per day in divided doses.
 Ultrafen Tablet/SR Tablet/Suppository/Gel Description Ultrafen is a preparation of Diclofenac is a non-steroidal antiinflammatory agent with marked analgesic, anti-inflammatory and antipyretic properties.
Ultrafen Tablet/SR Tablet/Suppository/Gel Description Ultrafen is a preparation of Diclofenac is a non-steroidal antiinflammatory agent with marked analgesic, anti-inflammatory and antipyretic properties.
10 April 2014 Osteoarthritis SSalman 2
 10 April 2014 Osteoarthritis SSalman 2 Updates on therapies of knee Osteoarthritis Prof Sami Salman, FRCP, MRCP, DMR, CES, MB ChB College of Medicine University of Baghdad Introduction Investigational
10 April 2014 Osteoarthritis SSalman 2 Updates on therapies of knee Osteoarthritis Prof Sami Salman, FRCP, MRCP, DMR, CES, MB ChB College of Medicine University of Baghdad Introduction Investigational
Public Assessment Report Scientific discussion SE/H/639/01/MR
 Public Assessment Report Scientific discussion Comfora (Glucosamine sulphate potassium chloride (2:1:2)) SE/H/639/01/MR This module reflects the scientific discussion for the approval of Comfora. The procedure
Public Assessment Report Scientific discussion Comfora (Glucosamine sulphate potassium chloride (2:1:2)) SE/H/639/01/MR This module reflects the scientific discussion for the approval of Comfora. The procedure
Some illustrations are from the internet and intended for educational purpose only
 Some illustrations are from the internet and intended for educational purpose only นพ. ส หธ ช งามอ โฆษ ภาคว ชา ออร โธป ด กส คณะแพทย ศาสตร จ ฬาลงกรณ มหาว ทยาล ย Knee anatomy Femur Pathophysiology Symptoms
Some illustrations are from the internet and intended for educational purpose only นพ. ส หธ ช งามอ โฆษ ภาคว ชา ออร โธป ด กส คณะแพทย ศาสตร จ ฬาลงกรณ มหาว ทยาล ย Knee anatomy Femur Pathophysiology Symptoms
The New Science of Osteoarthritis
 The New Science of Osteoarthritis What it means in managing our patients Terence W. Starz MD Clinical Professor of Medicine University of Pittsburgh School of Medicine Osteoarthritis: Key Points Perspective:
The New Science of Osteoarthritis What it means in managing our patients Terence W. Starz MD Clinical Professor of Medicine University of Pittsburgh School of Medicine Osteoarthritis: Key Points Perspective:
TRANSPARENCY COMMITTEE OPINION. 26 November 2008
 The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION 26 November 2008 ZONDAR 50 mg, capsules Pack of 30 capsules (CIP: 335 530-01) Applicant : PHARMA 2000 Diacerein ATC
The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION 26 November 2008 ZONDAR 50 mg, capsules Pack of 30 capsules (CIP: 335 530-01) Applicant : PHARMA 2000 Diacerein ATC
Month/Year of Review: January 2012 Date of Last Review: February 2007
 Drug Use Research & Management Program Oregon State University, 500 Summer Street NE, E35, Salem, Oregon 97301-1079 Phone 503-945-5220 Fax 503-947-1119 Month/Year of Review: January 2012 Date of Last Review:
Drug Use Research & Management Program Oregon State University, 500 Summer Street NE, E35, Salem, Oregon 97301-1079 Phone 503-945-5220 Fax 503-947-1119 Month/Year of Review: January 2012 Date of Last Review:
TBC Providing the Missing Piece
 Put simplistically, Spring is a twisted collagen hydrolysate molecule. Spring stimulates the body to repair and maintain its own connective tissue. It is not possible to overdose on Spring as the body
Put simplistically, Spring is a twisted collagen hydrolysate molecule. Spring stimulates the body to repair and maintain its own connective tissue. It is not possible to overdose on Spring as the body
Effectiveness of True Acupuncture as an Adjunct to Standard Care or Electro-Physiotherapy in Osteoarthritis of the Knee
 Cronicon OPEN ACCESS ORTHOPAEDICS Research article Effectiveness of True Acupuncture as an Adjunct to Standard Care or Electro-Physiotherapy in Osteoarthritis of Dimitar Tonev 1 *, Stoyka Radeva 2 and
Cronicon OPEN ACCESS ORTHOPAEDICS Research article Effectiveness of True Acupuncture as an Adjunct to Standard Care or Electro-Physiotherapy in Osteoarthritis of Dimitar Tonev 1 *, Stoyka Radeva 2 and
For more information about how to cite these materials visit
 Author(s): Seetha Monrad, M.D., 2009 License: Unless otherwise noted, this material is made available under the terms of the Creative Commons Attribution Noncommercial Share Alike 3.0 License: http://creativecommons.org/licenses/by-nc-sa/3.0/
Author(s): Seetha Monrad, M.D., 2009 License: Unless otherwise noted, this material is made available under the terms of the Creative Commons Attribution Noncommercial Share Alike 3.0 License: http://creativecommons.org/licenses/by-nc-sa/3.0/
Pain in Osteoarthritis
 Pain in Osteoarthritis By Edward L. Treadwell, MD Professor of Medicine- Rheumatology/Immunology Brody School of Medicine at East Carolina University School of Medicine Greenville, NC 27834 E-mail: treadwelle@ecu.edu
Pain in Osteoarthritis By Edward L. Treadwell, MD Professor of Medicine- Rheumatology/Immunology Brody School of Medicine at East Carolina University School of Medicine Greenville, NC 27834 E-mail: treadwelle@ecu.edu
Live On Screen: Knee Injections ABCs of Musculoskeletal Care. Knee aspiration. Objectives. I have no disclosures.
 I have no disclosures. Live On Screen: Knee Injections ABCs of Musculoskeletal Care Carlin Senter, MD Primary Care Sports Medicine Departments of Medicine and Orthopaedics December 11, 2015 Objectives
I have no disclosures. Live On Screen: Knee Injections ABCs of Musculoskeletal Care Carlin Senter, MD Primary Care Sports Medicine Departments of Medicine and Orthopaedics December 11, 2015 Objectives
160 Belmore Rd, Randwick
 www.orthosports.com.au 160 Belmore Rd, Randwick The Non Operative Management of Knee Joint Osteoarthritis (KJOA) KJOA Prevalence and burden Chronic disease joint pain, swelling, altered qol OA sufferers
www.orthosports.com.au 160 Belmore Rd, Randwick The Non Operative Management of Knee Joint Osteoarthritis (KJOA) KJOA Prevalence and burden Chronic disease joint pain, swelling, altered qol OA sufferers
Elements for a Public Summary
 VI.2 Elements for a Public Summary VI.2.1 Overview of disease epidemiology Osteoarthritis Osteoarthritis is the most common type of joint disease. It represents a group of conditions that result in changes
VI.2 Elements for a Public Summary VI.2.1 Overview of disease epidemiology Osteoarthritis Osteoarthritis is the most common type of joint disease. It represents a group of conditions that result in changes
Elements for a Public Summary Overview of disease epidemiology
 VI.2 VI.2.1 Elements for a Public Summary Overview of disease epidemiology Acute pain usually responds to medication and should settle in less than three months. Inadequate pain relief may lead to other
VI.2 VI.2.1 Elements for a Public Summary Overview of disease epidemiology Acute pain usually responds to medication and should settle in less than three months. Inadequate pain relief may lead to other
A rthritis is a major cause of limitation in daily functional
 45 ORIGINAL ARTICLE The effect of glucosamine supplementation on people experiencing regular knee pain R Braham, B Dawson, C Goodman... See end of article for authors affiliations... Correspondence to:
45 ORIGINAL ARTICLE The effect of glucosamine supplementation on people experiencing regular knee pain R Braham, B Dawson, C Goodman... See end of article for authors affiliations... Correspondence to:
Strontium ranolate effect on knee osteoarthritis
 Available online www.jocpr.com Journal of Chemical and harmaceutical Research, 2014, 6(4):623-627 Research Article ISSN : 0975-7384 CODEN(USA) : JCRC5 Strontium ranolate effect on knee osteoarthritis Alireza
Available online www.jocpr.com Journal of Chemical and harmaceutical Research, 2014, 6(4):623-627 Research Article ISSN : 0975-7384 CODEN(USA) : JCRC5 Strontium ranolate effect on knee osteoarthritis Alireza
Your Joint Pain and Treatment Options
 Your Joint Pain and Treatment Options Pinnacle Orthopedics Pinnacle Medical Network About Pinnacle Orthopedics and Pinnacle Medical Network South Louisiana s Premier System for the Delivery of Musculoskeletal
Your Joint Pain and Treatment Options Pinnacle Orthopedics Pinnacle Medical Network About Pinnacle Orthopedics and Pinnacle Medical Network South Louisiana s Premier System for the Delivery of Musculoskeletal
Non-Steroidal Anti- Inflammatory Drugs. ATPE 410 Chapter 6
 Non-Steroidal Anti- Inflammatory Drugs ATPE 410 Chapter 6 Inflammatory Process A normal, beneficial process that begins immediately after injury to facilitate repair and return the tissue to normal function
Non-Steroidal Anti- Inflammatory Drugs ATPE 410 Chapter 6 Inflammatory Process A normal, beneficial process that begins immediately after injury to facilitate repair and return the tissue to normal function
Introduction. Absorption and Metabolism of Oral Glucosamine Sulfate
 GLUCOSAMINE SULFATE AND ARTHRITIS: THE SCIENTIFIC EVIDENCE Written by Dr. James Meschino, D.C., M.S., -- Research and Clinical Director, RenaiSanté Institute of Integrative Medicine Introduction Osteoarthritis
GLUCOSAMINE SULFATE AND ARTHRITIS: THE SCIENTIFIC EVIDENCE Written by Dr. James Meschino, D.C., M.S., -- Research and Clinical Director, RenaiSanté Institute of Integrative Medicine Introduction Osteoarthritis
NON-SURGICAL TREATMENTS FOR OSTEOARTHRITIS of the KNEE
 Dr C S Waller MB BS FRCS(Ed) FRACS FA(Orth)A Specialist Hip and Knee Surgeon NON-SURGICAL TREATMENTS FOR OSTEOARTHRITIS of the KNEE The knee is the largest joint in the body, and is also the joint most
Dr C S Waller MB BS FRCS(Ed) FRACS FA(Orth)A Specialist Hip and Knee Surgeon NON-SURGICAL TREATMENTS FOR OSTEOARTHRITIS of the KNEE The knee is the largest joint in the body, and is also the joint most
Arthritis of the Knee
 Copyright 2007 American Academy of Orthopaedic Surgeons Arthritis of the Knee There are three basic types of arthritis that may affect the knee joint. Osteoarthritis Osteoarthritis (OA) is the most common
Copyright 2007 American Academy of Orthopaedic Surgeons Arthritis of the Knee There are three basic types of arthritis that may affect the knee joint. Osteoarthritis Osteoarthritis (OA) is the most common
Evidence supporting the use of glucosamine and chondroitin is scant, anecdotal
 Supplements for OA: An Unconvincing Story Evidence supporting the use of glucosamine and chondroitin is scant, anecdotal Terry Stanton The glory days for glucosamine began in 1996 with the publication
Supplements for OA: An Unconvincing Story Evidence supporting the use of glucosamine and chondroitin is scant, anecdotal Terry Stanton The glory days for glucosamine began in 1996 with the publication
Is Viscosupplementation Effective in Reducing Osteoarthritis Knee Pain?
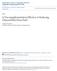 Philadelphia College of Osteopathic Medicine DigitalCommons@PCOM PCOM Physician Assistant Studies Student Scholarship Student Dissertations, Theses and Papers 2016 Is Viscosupplementation Effective in
Philadelphia College of Osteopathic Medicine DigitalCommons@PCOM PCOM Physician Assistant Studies Student Scholarship Student Dissertations, Theses and Papers 2016 Is Viscosupplementation Effective in
Iroko Pharmaceuticals Announces Acceptance for Filing of ZORVOLEX snda for the Treatment of Osteoarthritis Pain in Adults
 Iroko Pharmaceuticals Announces Acceptance for Filing of ZORVOLEX snda for the Treatment of Osteoarthritis Pain in Adults First Lower Dose NSAID Using SoluMatrix Fine Particle Technology to be Reviewed
Iroko Pharmaceuticals Announces Acceptance for Filing of ZORVOLEX snda for the Treatment of Osteoarthritis Pain in Adults First Lower Dose NSAID Using SoluMatrix Fine Particle Technology to be Reviewed
Bone/Joint Health. Bone and Joint Nourishment. Products. Bone/Joint Health Regimen nutrametrix Custom Health Solutions
 Bone/Joint Health Bone/Joint Health Regimen nutrametrix Custom Health Solutions Bone and Joint Nourishment Active people as well as the elderly often need joint support. The Bone/Joint Health Regimen includes
Bone/Joint Health Bone/Joint Health Regimen nutrametrix Custom Health Solutions Bone and Joint Nourishment Active people as well as the elderly often need joint support. The Bone/Joint Health Regimen includes
Joint Health Optimum Flex Plus, Hi- Victory, Yucca, Herbal Respond
 Joint Health Optimum Flex Plus, Hi- Victory, Yucca, Herbal Respond May Educational Webinar 2018 Dr Tania Cubitt Performance Horse Nutrition COMPARATIVE ANATOMY 2 JOINT A joint is defined as a structure
Joint Health Optimum Flex Plus, Hi- Victory, Yucca, Herbal Respond May Educational Webinar 2018 Dr Tania Cubitt Performance Horse Nutrition COMPARATIVE ANATOMY 2 JOINT A joint is defined as a structure
Salicylates: Interactions 10/14/2009. Salicylates DRUGS USED IN THE MANAGEMENT OF MUSCULOSKELETAL DISORDERS. Chapters 17, 18, 34 & Pages 577 &
 DRUGS USED IN THE MANAGEMENT OF MUSCULOSKELETAL DISORDERS Chapters 17, 18, 34 & Pages 577 & 579-586 Salicylates aspirin Have analgesic, antipyretic, and anti-inflammatory effects. Inhibits the production
DRUGS USED IN THE MANAGEMENT OF MUSCULOSKELETAL DISORDERS Chapters 17, 18, 34 & Pages 577 & 579-586 Salicylates aspirin Have analgesic, antipyretic, and anti-inflammatory effects. Inhibits the production
Is Tanezumab More Effective than a Placebo in Reducing Pain in Patients with Osteoarthritis?
 Philadelphia College of Osteopathic Medicine DigitalCommons@PCOM PCOM Physician Assistant Studies Student Scholarship Student Dissertations, Theses and Papers 2018 Is Tanezumab More Effective than a Placebo
Philadelphia College of Osteopathic Medicine DigitalCommons@PCOM PCOM Physician Assistant Studies Student Scholarship Student Dissertations, Theses and Papers 2018 Is Tanezumab More Effective than a Placebo
STRIDE PLUS STRIDE PLUS. Nutritional Maintenance of Healthy Cartilage and Joints in Dogs. 100%
 STRIDE STRIDE Nutritional Maintenance of Healthy Cartilage and Joints in Dogs. WITH HYALURONIC ACID NATURAL YEAST FLAVOURING CERTIFIED VEGAN 100% The Joint The joint is where two or more bones meet. Each
STRIDE STRIDE Nutritional Maintenance of Healthy Cartilage and Joints in Dogs. WITH HYALURONIC ACID NATURAL YEAST FLAVOURING CERTIFIED VEGAN 100% The Joint The joint is where two or more bones meet. Each
ARTHRITIS. What happens when Arthritis goes untreated? Often people take arthritis to be a natural part of aging and do not seek medical advice.
 ARTHRITIS Move again with Life ARTHRITIS needn't control your life anymore Now you can control it. Joint pain, restricted joint mobility, joint swelling and inflammation can steal happiness from your life.
ARTHRITIS Move again with Life ARTHRITIS needn't control your life anymore Now you can control it. Joint pain, restricted joint mobility, joint swelling and inflammation can steal happiness from your life.
Efficacy and tolerability of celecoxib in osteoarthritis patients who previously failed naproxen and ibuprofen: results from two trials
 International Journal of Clinical Rheumatology A - Efficacy and tolerability of celecoxib in osteoarthritis patients who previously failed naproxen and ibuprofen: results from two trials Aims: To evaluate
International Journal of Clinical Rheumatology A - Efficacy and tolerability of celecoxib in osteoarthritis patients who previously failed naproxen and ibuprofen: results from two trials Aims: To evaluate
High Impact Rheumatology
 High Impact Rheumatology Evaluation and Management of Osteoarthritis Osteoarthritis: Case 1 A 65-year-old man comes to your office complaining of knee pain that began insidiously about a year ago. He has
High Impact Rheumatology Evaluation and Management of Osteoarthritis Osteoarthritis: Case 1 A 65-year-old man comes to your office complaining of knee pain that began insidiously about a year ago. He has
Is Phlogenzym Effective in Reducing Moderate to Severe Osteoarthritis Pain in Adults?
 Philadelphia College of Osteopathic Medicine DigitalCommons@PCOM PCOM Physician Assistant Studies Student Scholarship Student Dissertations, Theses and Papers 2013 Is Phlogenzym Effective in Reducing Moderate
Philadelphia College of Osteopathic Medicine DigitalCommons@PCOM PCOM Physician Assistant Studies Student Scholarship Student Dissertations, Theses and Papers 2013 Is Phlogenzym Effective in Reducing Moderate
Maria Lourdes R. Bernardo and Alfredo C. Azarcon, Jr. Department of Rehabi/itation Medicine, Veterans Memorial Medica! Center
 A Randomized Controlled Trial on the Effects of Oral Collagen Treatment on the Media) Knee Joint Space aod Functional Outcome among Veterans Memorial Medical Center Patients Diagnosed with Osteoarthritis
A Randomized Controlled Trial on the Effects of Oral Collagen Treatment on the Media) Knee Joint Space aod Functional Outcome among Veterans Memorial Medical Center Patients Diagnosed with Osteoarthritis
Action Rufenal contains a non - steroidal compound with pronounced antirheumatic, anti-inflammatory, analgesic and antipyretic properties.
 RUFENAL Composition Rufenal Injection Each ampoule of 3 ml contains Diclofenac sodium 75 mg. Ampoule, Tablets & Suppositories Rufenal 12.5 Suppositories Each suppository contains Diclofenac sodium 12.5
RUFENAL Composition Rufenal Injection Each ampoule of 3 ml contains Diclofenac sodium 75 mg. Ampoule, Tablets & Suppositories Rufenal 12.5 Suppositories Each suppository contains Diclofenac sodium 12.5
COMPOUNDING PHARMACY SOLUTIONS PRESCRIPTION COMPOUNDING FOR PAIN MANAGEMENT
 JANUARY 2012 COMPOUNDING PHARMACY SOLUTIONS PRESCRIPTION COMPOUNDING WWW.CPSRXS. COM We customize individual prescriptions for the specific needs of our patients. INSIDE THIS ISSUE: Osteoarthritis Pain
JANUARY 2012 COMPOUNDING PHARMACY SOLUTIONS PRESCRIPTION COMPOUNDING WWW.CPSRXS. COM We customize individual prescriptions for the specific needs of our patients. INSIDE THIS ISSUE: Osteoarthritis Pain
Osteoarthritis. RA Hughes
 Osteoarthritis RA Hughes Osteoarthritis (OA) OA is the most common form of arthritis and the most common joint disease Most of the people who have OA are older than age 45, and women are more commonly
Osteoarthritis RA Hughes Osteoarthritis (OA) OA is the most common form of arthritis and the most common joint disease Most of the people who have OA are older than age 45, and women are more commonly
Osteoarthritis (OA) is a major cause of pain
 Menopause: The Journal of The North American Menopause Society Vol. 11, No. 2, pp. 138 143 DOI: 10.1097/01.GME.0000087983.28957.5D 2004 The North American Menopause Society Text printed on acid-free paper.
Menopause: The Journal of The North American Menopause Society Vol. 11, No. 2, pp. 138 143 DOI: 10.1097/01.GME.0000087983.28957.5D 2004 The North American Menopause Society Text printed on acid-free paper.
OsteoDenx<<<TM. Bio-replenishment Technology. Bone Health Management. Where better bones begins. for
 OsteoDenx
OsteoDenx
Evaluation and Treatment of Knee Arthritis Classification of Knee Arthritis Osteoarthritis Osteoarthritis Osteoarthritis of Knee
 1 2 Evaluation and Treatment of Knee Arthritis John Zebrack, MD Reno Orthopaedic Clinic Classification of Knee Arthritis Non-inflammatory Osteoarthritis Primary Secondary Post-traumatic, dysplasia, neuropathic,
1 2 Evaluation and Treatment of Knee Arthritis John Zebrack, MD Reno Orthopaedic Clinic Classification of Knee Arthritis Non-inflammatory Osteoarthritis Primary Secondary Post-traumatic, dysplasia, neuropathic,
Important facts about ORTHOVISC mini
 ORTHOVISC mini A targeted treatment for small joint pain. An increasing number of patients suffer from osteoarthritis (OA), the multisymptomatic joint disease characterized by cartilage degeneration and
ORTHOVISC mini A targeted treatment for small joint pain. An increasing number of patients suffer from osteoarthritis (OA), the multisymptomatic joint disease characterized by cartilage degeneration and
Treatment of Knee OA With Glucosamine and Hyaluronan - Asian Perspective
 Treatment of Knee OA With Glucosamine and Hyaluronan - Asian Perspective Dr. NICOLAAS C. BUDHIPARAMA Jr., SpOT., F.I.C.S. Head of Department Orthopaedic Surgery - Medistra Hospital President and Founder
Treatment of Knee OA With Glucosamine and Hyaluronan - Asian Perspective Dr. NICOLAAS C. BUDHIPARAMA Jr., SpOT., F.I.C.S. Head of Department Orthopaedic Surgery - Medistra Hospital President and Founder
FORTIGEL for sustainable mobility
 FORTIGEL for sustainable mobility Scientifically studied to regenerate joint cartilage Stimulates the body s own mechanisms for maintaining healthy joints and optimum mobility Promotes joint health naturally
FORTIGEL for sustainable mobility Scientifically studied to regenerate joint cartilage Stimulates the body s own mechanisms for maintaining healthy joints and optimum mobility Promotes joint health naturally
Analgesic Subcommittee of PTAC Meeting held 1 March 2016
 Analgesic Subcommittee of PTAC Meeting held 1 March 2016 (minutes for web publishing) The Analgesic Subcommittee minutes are published in accordance with the Terms of Reference for the Pharmacology and
Analgesic Subcommittee of PTAC Meeting held 1 March 2016 (minutes for web publishing) The Analgesic Subcommittee minutes are published in accordance with the Terms of Reference for the Pharmacology and
Is Curcumin Effective in Reducing Pain in Arthritis Patients?
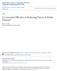 Philadelphia College of Osteopathic Medicine DigitalCommons@PCOM PCOM Physician Assistant Studies Student Scholarship Student Dissertations, Theses and Papers 2018 Is Curcumin Effective in Reducing Pain
Philadelphia College of Osteopathic Medicine DigitalCommons@PCOM PCOM Physician Assistant Studies Student Scholarship Student Dissertations, Theses and Papers 2018 Is Curcumin Effective in Reducing Pain
Osteoarthritis Research Society /98/ $12.00/0
 Osteoarthritis and Cartilage (1998) 6, (Supplement A), 31 36 9 1998 Osteoarthritis Research Society 1063-4584/98/030031 + 06 $12.00/0 OSTEOARTHRITIS and CARTILAGE Efficacy and tolerability of oral chondroitin
Osteoarthritis and Cartilage (1998) 6, (Supplement A), 31 36 9 1998 Osteoarthritis Research Society 1063-4584/98/030031 + 06 $12.00/0 OSTEOARTHRITIS and CARTILAGE Efficacy and tolerability of oral chondroitin
Diagnosis & Nonoperative Treatment of the Osteoarthritic Knee. Randall R Wroble MD Orthopedic One Columbus OH
 Diagnosis & Nonoperative Treatment of the Osteoarthritic Knee Randall R Wroble MD Orthopedic One Columbus OH There are 2 things a good doctor does First Step: Finds out what's wrong Second step Makes the
Diagnosis & Nonoperative Treatment of the Osteoarthritic Knee Randall R Wroble MD Orthopedic One Columbus OH There are 2 things a good doctor does First Step: Finds out what's wrong Second step Makes the
Collagen peptides improve knee osteoarthritis in elderly women - a 6-month randomized, double-blind, placebo-controlled study
 See discussions, stats, and author profiles for this publication at: https://www.researchgate.net/publication/282653960 Collagen peptides improve knee osteoarthritis in elderly women - a 6-month randomized,
See discussions, stats, and author profiles for this publication at: https://www.researchgate.net/publication/282653960 Collagen peptides improve knee osteoarthritis in elderly women - a 6-month randomized,
TRANSPARENCY COMMITTEE
 The legally binding text is the original French version TRANSPARENCY COMMITTEE Opinion 20 November 2013 FLEXEA 625 mg, tablet Box of 60 tablets (CIP: 34009 380 534 2 5) Box of 180 tablets (CIP: 34009 380
The legally binding text is the original French version TRANSPARENCY COMMITTEE Opinion 20 November 2013 FLEXEA 625 mg, tablet Box of 60 tablets (CIP: 34009 380 534 2 5) Box of 180 tablets (CIP: 34009 380
Targeted Health Regimen Every Targeted Health Regimen builds upon the Foundation of Optimal Health Regimen. Bone/Joint Health Regimen
 Targeted Health Regimen Every Targeted Health Regimen builds upon the Foundation of Optimal Health Regimen. Bone/Joint Health Regimen Active people as well as the elderly often need joint support. The
Targeted Health Regimen Every Targeted Health Regimen builds upon the Foundation of Optimal Health Regimen. Bone/Joint Health Regimen Active people as well as the elderly often need joint support. The
Guide to Understanding and Managing Arthritis
 Guide to Understanding and Managing Arthritis The content in this guide is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician
Guide to Understanding and Managing Arthritis The content in this guide is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician
SELECTED ABSTRACTS. Figure. Risk Stratification Matrix A CLINICIAN S GUIDE TO THE SELECTION OF NSAID THERAPY
 SELECTED ABSTRACTS A CLINICIAN S GUIDE TO THE SELECTION OF NSAID THERAPY The authors of this article present a 4-quadrant matrix based on 2 key clinical parameters: risk for adverse gastrointestinal (GI)
SELECTED ABSTRACTS A CLINICIAN S GUIDE TO THE SELECTION OF NSAID THERAPY The authors of this article present a 4-quadrant matrix based on 2 key clinical parameters: risk for adverse gastrointestinal (GI)
Intestinal absorption of Mobilee
 Pre-Clinical Data Intestinal absorption of To determine the intestinal absorption of using an everted gut sac model. Male OFA-strain rats weighing approximately g were used. Three different parts of the
Pre-Clinical Data Intestinal absorption of To determine the intestinal absorption of using an everted gut sac model. Male OFA-strain rats weighing approximately g were used. Three different parts of the
Non-Surgical vs. Surgical Treatment of Meniscus Tears of the Knee
 Non-Surgical vs. Surgical Treatment of Meniscus Tears of the Knee Greg I. Nakamoto, MD FACP Section of Orthopedics and Sports Medicine Virginia Mason Medical Center CASE 1 45 y/o construction worker sent
Non-Surgical vs. Surgical Treatment of Meniscus Tears of the Knee Greg I. Nakamoto, MD FACP Section of Orthopedics and Sports Medicine Virginia Mason Medical Center CASE 1 45 y/o construction worker sent
Zahra Jahangard Clinical pharmacy Resident
 Zahra Jahangard Clinical pharmacy Resident OA, or degenerative joint disease, is the most common form of arthritis A clinical syndrome of joint pain accompanied by varying degrees of functional limitation
Zahra Jahangard Clinical pharmacy Resident OA, or degenerative joint disease, is the most common form of arthritis A clinical syndrome of joint pain accompanied by varying degrees of functional limitation
THAT S PROVEN FOR THE LONG RUN
 A GUIDE FOR PATIENTS KNEE PAIN RELIEF THAT S PROVEN FOR THE LONG RUN TREATMENT OPTIONS FOR OA KNEE PAIN There are several things you can do to help reduce knee pain due to OA. Lifestyle changes Losing
A GUIDE FOR PATIENTS KNEE PAIN RELIEF THAT S PROVEN FOR THE LONG RUN TREATMENT OPTIONS FOR OA KNEE PAIN There are several things you can do to help reduce knee pain due to OA. Lifestyle changes Losing
A GUIDE FOR PATIENTS KNEE PAIN RELIEF THAT JUST CAN T WAIT
 A GUIDE FOR PATIENTS KNEE PAIN RELIEF THAT JUST CAN T WAIT TREATMENT OPTIONS FOR OA KNEE PAIN There are several things you can do to help reduce knee pain due to OA. Lifestyle changes Losing weight, if
A GUIDE FOR PATIENTS KNEE PAIN RELIEF THAT JUST CAN T WAIT TREATMENT OPTIONS FOR OA KNEE PAIN There are several things you can do to help reduce knee pain due to OA. Lifestyle changes Losing weight, if
Matthew Husa, MD Assistant Professor of Medicine
 Evidence-based Review of Non-surgical Management of Osteoarthritis Matthew Husa, MD Assistant Professor of Medicine Division i i of Rheumatlogy and Immunology The Ohio State University Wexner Medical Center
Evidence-based Review of Non-surgical Management of Osteoarthritis Matthew Husa, MD Assistant Professor of Medicine Division i i of Rheumatlogy and Immunology The Ohio State University Wexner Medical Center
Pain: A Public Health Challenge. NSAIDS for Managing Pain. Iroko: Innovators in Analgesia
 Pain: A Public Health Challenge Despite advances in understanding and treatment, pain remains a major public health challenge 1 that exacts a significant personal and economic toll on Americans. 1 Pain
Pain: A Public Health Challenge Despite advances in understanding and treatment, pain remains a major public health challenge 1 that exacts a significant personal and economic toll on Americans. 1 Pain
PDF of Trial CTRI Website URL -
 Clinical Trial Details (PDF Generation Date :- Tue, 01 Jan 2019 02:42:38 GMT) CTRI Number CTRI/2008/091/000063 [Registered on: 08/07/2008] - Last Modified On Post Graduate Thesis Type of Trial Type of
Clinical Trial Details (PDF Generation Date :- Tue, 01 Jan 2019 02:42:38 GMT) CTRI Number CTRI/2008/091/000063 [Registered on: 08/07/2008] - Last Modified On Post Graduate Thesis Type of Trial Type of
Types of osteoarthritis
 ARTHRITIS Osteoarthritis is a degenerative joint disease is the most common joint disorder. It is a frequent part of aging and is an important cause of physical disability in persons older than 65 years
ARTHRITIS Osteoarthritis is a degenerative joint disease is the most common joint disorder. It is a frequent part of aging and is an important cause of physical disability in persons older than 65 years
TIVORBEX Now Available in U.S. Pharmacies for the Treatment of Acute Pain
 TIVORBEX Now Available in U.S. Pharmacies for the Treatment of Acute Pain Second Low-Dose SoluMatrix NSAID from Iroko Now Available by Prescription PHILADELPHIA, June 29, 2015 Iroko Pharmaceuticals, LLC,
TIVORBEX Now Available in U.S. Pharmacies for the Treatment of Acute Pain Second Low-Dose SoluMatrix NSAID from Iroko Now Available by Prescription PHILADELPHIA, June 29, 2015 Iroko Pharmaceuticals, LLC,
Pain: A Public Health Challenge. NSAIDS for Managing Pain. Iroko: Innovators in Analgesia
 Pain: A Public Health Challenge Despite advances in understanding and treatment, pain remains a major public health challenge 1 that exacts a significant personal and economic toll on Americans 2. Pain
Pain: A Public Health Challenge Despite advances in understanding and treatment, pain remains a major public health challenge 1 that exacts a significant personal and economic toll on Americans 2. Pain
1. Understand the basic epidemiology of OA 2. Understand challenges facing OA therapy development
 Evidence-based Review of Non-surgical Management of Osteoarthritis Matthew Husa, MD Assistant Professor of Medicine Division of Rheumatlogy and Immunology The Ohio State University Wexner Medical Center
Evidence-based Review of Non-surgical Management of Osteoarthritis Matthew Husa, MD Assistant Professor of Medicine Division of Rheumatlogy and Immunology The Ohio State University Wexner Medical Center
MSM NPN What is MSM?
 MSM NPN 80044805 What is MSM? MSM is a natural sulfur compound and nutritional component contained in various foods. It is part of the staple diet of humans and almost all other vertebrates. As the main
MSM NPN 80044805 What is MSM? MSM is a natural sulfur compound and nutritional component contained in various foods. It is part of the staple diet of humans and almost all other vertebrates. As the main
