Life-threatening respiratory failure requiring extra-corporeal membrane oxygenation secondary to the anti-synthetase syndrome
|
|
|
- Valentine Wells
- 5 years ago
- Views:
Transcription
1 Case report Life-threatening respiratory failure requiring extra-corporeal membrane oxygenation secondary to the anti-synthetase syndrome Journal of the Intensive Care Society 0(0) 1 5! The Intensive Care Society 2019 Article reuse guidelines: sagepub.com/journals-permissions DOI: / journals.sagepub.com/home/jics Caroline Sampson 1, Jennifer Taylor 1, Luke Dyson 2 and Mostafa Hassanein 1 Abstract Veno-venous extra-corporeal membrane oxygenation (VV ECMO) provides support in severe acute respiratory failure (SARF) refractory to maximal conventional ventilatory support. ECMO does not treat the lungs per se, but allows time for the underlying condition to reverse or resolve. Common indications include acute respiratory distress syndrome (ARDS) and life-threatening asthma. On occasion, rarer conditions causing respiratory failure are diagnosed during ECMO support. The anti-synthetase syndrome (ASS) comprises of a group of conditions characterised by the presence of anti-aminoacyl-trna-synthetase antibodies with one or more of interstitial lung disease, inflammatory myositis and/or arthritis. Mainstay of management is immunosuppression. Here, we present two patients requiring ECMO support for SARF, whose respiratory function failed to respond to usual treatment for their assumed pneumonia. Both showed a rapid improvement in respiratory function and oxygenation once immunosuppressive therapy was instigated. Further testing revealed anti-synthetase antibodies, therefore both went on to receive further immunosuppression and an ultimately good outcome. Despite life-threatening respiratory failure, VV ECMO support allowed time for stabilisation, diagnosis and treatment. Outcomes in acute inflammatory interstitial pneumonitis are improved if immunosuppressive treatment is initiated as soon as possible. Our experience with these two cases have led to an institutional change in practice to send an urgent auto-antibody screen (including extractable nuclear antigen panel) on admission for all our SARF patients. Keywords Antisynthetase syndrome, extra-corporeal membrane oxygenation, severe acute respiratory failure Case report 1 Our first case is a 47-year-old previously fit and well male, who presented to his local hospital with a threeday history of shortness of breath, productive cough and fever. Clinical and radiological studies indicated multilobar community-acquired pneumonia of unknown organism and he was treated accordingly. He deteriorated into Type 2 respiratory failure, necessitating invasive ventilation. Despite maximal conventional treatment, hypoxia worsened and he was referred and accepted for extra-corporeal membrane oxygenation (ECMO) on day 5. He was commenced on Veno-venous (VV) ECMO support via a right internal jugular 31 F dual lumen Avalon Elite ß cannula, achieving flows of L/min prior to transfer to his local ECMO centre. Initial blood tests on transfer demonstrated raised inflammatory markers C- reactive protein 435 mg/l, white cell count (WCC) /L with a predominant neutrophilia. Percutaneous dilatational tracheostomy was performed on day 9. Despite an improvement in inflammatory markers with broad spectrum antimicrobial treatment, oxygenation and compliance issues persisted during the first two weeks of ECMO support. This necessitated 50 60% inspired oxygen concentration and the use of prone positioning alongside ECMO support to 1 Department of Anaesthesia and Critical Care, University Hospitals of Leicester NHS Trust, Leicester, UK 2 Department of Anaesthesia, Kettering General Hospital, Kettering, UK Corresponding author: Caroline Sampson, Department of Anaesthesia and Critical Care, Glenfield Hospital, University Hospitals of Leicester NHS Trust, Groby Road, Leicester, LE3 9QP, UK caroline.sampson@uhl-tr.nhs.uk
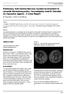
2 2 Journal of the Intensive Care Society 0(0) achieve an arterial partial pressure of oxygen greater than 6 kpa. Extensive microbiological investigations including sputum, blood, urine and broncho-alveolar lavage (BAL) culture for bacteria, mycobacteria and fungi, respiratory viral PCR from throat swab and BAL, legionella urinary antigen and atypical pneumonia screen (mycoplasma, Q fever and psittacosis) yielded no positive results. Initial chest X-rays demonstrated severe bilateral consolidation (Figure 1) and a computed tomography (CT) chest on day 10, five days post ECMO cannulation showed extensive consolidation with ground glass opacities affecting 70% of the pulmonary parenchyma, with pulmonary hypertension and right heart strain (Figure 2), which was confirmed by transoesophageal echocardiography. A trial of methylprednisolone (500 mg/day for three days followed by a 14- day tapering steroid regime) to treat acute respiratory distress syndrome (ARDS) with failure to progress as per our institution s policy was commenced on day 13. From day 16 onwards he demonstrated persistent improvement in oxygenation alongside slow radiological resolution allowing weaning from ECMO support after a successful 14-h trial off on day 28 with acceptable respiratory and gas exchange parameters (PaO kpa with ph on FiO %), spontaneously breathing with a pressure support of cmh 2 O over 10 cmh 2 O positive end expiratory pressure (PEEP) and respiratory rate 430. Unfortunately, 48 h post ECMO decannulation he deteriorated, requiring raised inspired oxygen to 80% and peak inspiration pressures of cmh 2 Oto achieve adequate gas exchange. Immunological testing yielded negative results for antineutrophil cytoplasmic antibodies (ANCA), antinuclear antibodies (ANA), anti-glomerular basement membrane (anti- GBM) and anti double-stranded DNA (antidsdna) with normal immunoglobulin and complement profiles, but on day 32, a standard extractable nuclear antigen (ENA) panel revealed the presence of anti-jo antibodies. Steroid therapy was recommenced at 60 mg prednisone daily, and, following discussion with rheumatology and respiratory consultant colleagues, rituximab 1 g was administered on day 33. There was a rapid and dramatic improvement in oxygenation and compliance in following days. Although critical care acquired weakness slowed his respiratory weaning, he was successfully tracheostomy decannulated on day 48 and transferred to the ward for ongoing rehabilitation on day 49. During follow-up at six months, imaging demonstrated bilateral peripheral and mainly lower zone interstitial shadowing consistent with a degree of pulmonary fibrosis (Figure 3), but he reported being back at work part-time with much improved exercise tolerance, and was cycling 2-3km several times a week. He remains on low-dose maintenance prednisone and six monthly rituximab infusions having experienced worsening of respiratory symptoms on both azathioprine Figure 1. Case 1: Chest X-ray on arrival to our ECMO centre. Figure 2. Case 1: CT thorax at day 10. and mycophenolate mofetil and is followed up 3 6 monthly by local rheumatology and respiratory teams. Case report 2 Our second case is a 39-year-old female with insulindependent diabetes, who presented to her local hospital with a seven-day history of productive cough and pyrexia. She was diagnosed with communityacquired pneumonia and treated accordingly. Three days after admission, her condition deteriorated, with increased oxygen requirements and she required intubation, invasive ventilation and renal replacement therapy for an acute kidney injury. As she was requiring a very high concentration of inspired oxygen to maintain an acceptable PaO 2, she was referred and accepted for ECMO support on day 4. VV ECMO was initiated at her local hospital via a 19 F multistage drainage cannula in her femoral vein and 17 F return cannula in her right internal jugular vein and
3 Sampson et al. 3 Figure 5. Case 2: CT thorax at day 18. Figure 3. Case 1: Chest X-ray at follow-up appointment (six months post ECMO de-cannulation). Figure 4. Case 2: Chest X-ray on arrival to our ECMO centre. she was transferred to our ECMO centre (Figure 4). Flows were maintained at L/min and she was weaned to rest ventilator settings (FiO , pressure controlled ventilation of 20/10 cm H20 with respiratory rate of 10 breaths per minute). Her admission blood tests were consistent with an infectious aetiology with a CRP of 245 mg/l and WCC of /L which was predominantly due to neutrophilia. She underwent percutaneous dilatational tracheostomy on day 9. She initially seemed to respond well to treatment and was successfully weaned off ECMO support by day 10. Unfortunately, oxygen requirements increased over subsequent days and despite numerous measures including prone positioning and inhaled nitric oxide, her respiratory function worsened and she was placed back on ECMO via a 27 F Avalon Elite ß dual lumen cannula in her right internal jugular vein on day 18 achieving similar ECMO and ventilator settings as before. CT scan post re-cannulation demonstrated frank bilateral lung consolidation with areas of necrosis (Figure 5). Microbiological testing revealed pneumococcus in the original sputum sample from the referring hospital, but all other microbiological tests were returned as negative, including blood, sputum, urine and BAL cultures, urinary antigen for legionella, PCR for respiratory viruses and atypical pneumonia screen. She failed to improve when treated with various antimicrobial regimens. Immunological tests yielded negative results for rheumatoid factor, ANCA, antidsdna, anti-ena and anti-gbm, with a normal immunoglobulin and complement profile, although a positive ANA was detected (1 in 400 with a positive homogeneous pattern). On closer questioning, her family reported that she had been suffering from muscle and joint pains, diagnosed as fibromyalgia, for a couple of years. Seven days post re-cannulation for ECMO, an extended myositis panel revealed the presence of anti-pl-12 antibodies. That same day she was started on three days of pulsed methyl-prednisolone 1 g once a day followed by maintenance steroids, and her immunosuppressive regime was consolidated with rituximab 1 g on day 24 with rapid and dramatic improvement in gas exchange and compliance. Twenty-four hours later, respiratory function had improved to the extent she could be successfully weaned off ECMO support with acceptable ventilatory and gas exchange parameters as in case 1. Within a week, her FiO 2 was down to 35%, and she was spontaneously breathing via a tracheostomy mask. Her critical care recovery was complicated by on-going need for renal replacement therapy, a prolonged ileus and critical care acquired weakness. She was transferred back to her local hospital on day 50 to continue rehabilitation. During follow-up at six months, her main symptom was myalgia with no reported breathlessness. Chest X-ray demonstrated no evidence of extensive volume loss or pulmonary fibrosis (Figure 6), and pulmonary function tests
4 4 Journal of the Intensive Care Society 0(0) Figure 6. Chest X-ray at follow-up appointment (six months post ECMO de-cannulation). were within normal limits. She had regained independent renal function. Discussion Anti-synthetase syndrome (ASS) is a term used to describe a group of rare chronic autoimmune inflammatory myopathies comprising a subset of polymyositis and dermatomyositis of unknown cause. 1 Clinical features include fever, rash, myositis and myopathy, polyarthritis, Raynaud s phenomenon, mechanic s hands, Gottron s papules and interstitial lung disease (ILD). It is 2 3 times more prevalent in women and presents throughout adulthood with a peak age of onset in the fifth and sixth decades of life. 2 The hallmark of the syndrome is the presence of serum autoantibodies against aminoacyl-trna synthetases. At least 10 different antibodies have been described including anti-jo-1 (anti-histadyl trna synthetase), anti-pl-7 and PL-12, anti-oj, anti-zo, anti-ej, anti-ks, anti-yrs, anti-srp and anti-wa with anti-jo-1 being by far the most commonly described. 1 The diagnosis is confirmed by the presence of one or more of these antibodies alongside evidence of at least one of: (i) ILD (ii) inflammatory myopathy (iii) inflammatory polyarthritis affecting small joints. 3 Acute respiratory failure as the first presentation in ASS is rare, but reports within the literature are increasing. 3,4 The use of ECMO in these patients is rarer still but there are published case series from Germany 5 and England 6 describing the use of ECMO in ILD with at least one patient from each series having a confirmed diagnosis of the ASS. 5,6 Once the diagnosis has been confirmed, the mainstay of treatment is immunosuppression. Corticosteroids are typically used first-line, with other immunosuppressants, including cyclophosphamide, azathioprine, cyclosporine and tacrolimus, used in those who fail to respond to steroids. 7 It is policy at our institution to consider a trial of IV methylprednisolone in all patients with unresolving ARDS who are still reliant on ECMO support by day 10 (to be commenced before day 14), particularly in those with any suspicion of underlying autoimmune pathology and those with signs of fibrotic change on CT imaging. Whilst the evidence base behind steroid treatment in ARDS is controversial, we have observed that some patients demonstrate dramatic clinical improvement within a few days of starting treatment, whilst others are non-responders. We give a pulse of 500 mg IV methylprednisolone for three days in younger patients with single organ failure, followed by a tapering regime in responders and use a more conservative dose of 2 mg/kg infusion over 24 h in older patients or those with on-going need for multiorgan support with a slower taper. The initial improvement in case 1 was most likely secondary to the dose of intravenous methylprednisolone with subsequent deterioration related to weaning and discontinuation of steroids. It is perfectly possible that many or all of the steroid responders we encounter have a previously undiagnosed underlying steroid-responsive condition causing or perpetuating their ARDS. Rituximab is a chimeric monoclonal antibody which targets a cluster of 20 different antigens (CD20) found on the surface of B-cells. It is licensed for primary treatment of certain lymphomas, granulomatosis with polyangitis and microscopic polyangitis and in severe active rheumatoid arthritis resistant to other disease-modifying antirheumatic drugs, but is increasingly used off label for a wide range of autoimmune and inflammatory diseases. 8,9 There are published case series describing the use of rituximab to good effect in patients with treatment refractory ASS However, its use as second line following steroids in the absence of other immunosuppressants or in combination with cyclophosphamide is limited to case reports 13 Rituximab has been associated with a number of adverse events in the critically ill, most relating to developing new infections, but also isolated cases of cytokine release syndrome, a potentially lifethreatening systemic inflammatory reaction. Pulmonary toxicity (organising, desuamative, interstitial or granulomatous pneumonitis) has also been reported. 14 As in the cases described above, patients receiving rituximab should always be pre-medicated with steroids, antihistamine and antipyretic agents to minimise the risk of infusion reactions. In both of these cases, rituximab was advised by rheumatology and respiratory colleagues due to previous experience with the use of rituximab in ASS for both induction and maintenance of remission, the lifethreatening nature of their respiratory failure and to minimise consequences on future fertility.
5 Sampson et al. 5 Prognosis in ASS is most affected by the degree of ILD and any irreversible fibrosis that may have developed underlining the vital importance of early diagnosis and treatment. 1 Both of our patients required immunosuppression to reverse their respiratory failure. Results from ENA testing, particularly the extended panels, may take some time, and the tests are not available universally. Immunosuppression in the face of potential infection, without serological confirmation of appropriate autoantibodies, risks causing significant deterioration. Within our institution we have changed practice to send an ENA panel on admission in all our severe acute respiratory failure (SARF) patients, with an extended myositis panel sent after discussion with rheumatology and respiratory colleagues in those with a suggestive history of ASS. Case 2 also highlights the vital importance of taking a thorough history from family members, as her joint pains, previously labelled as fibromyalgia, may have expedited discussion with rheumatology colleagues and led to an earlier diagnosis and treatment had their importance been appreciated on admission. Conclusions Both these patients presented with life-threatening respiratory failure requiring ECMO support for presumed community-acquired pneumonia but failed to improve with standard treatment. When this occurs, it is imperative not to get fixated on the initial diagnosis and to consider a wide differential of alternative diagnoses. In both of these patients, positive antibody results led us to diagnose ASS and treat with immunosuppressive agents, with dramatic improvements noted shortly thereafter. Outcomes are improved if immunosuppressive treatment in acute inflammatory pneumonitis is commenced rapidly, but this must be balanced with substantial risks of immunosuppression in a patient with a severe infective pneumonia. It is therefore vital to diagnose these patients promptly. As a direct result of these cases, we have changed our clinical practice to request an urgent auto-antibody screen including ENA panel in all of our SARF patients on admission. ASS should be remembered as a rare form of acute ILD presenting with all the clinical and radiological hallmark features of a severe community-acquired pneumonia, and the inflammatory ILDs must be considered in the differential diagnosis of all presumed infective pneumoniae that fail to respond to appropriate antimicrobial treatment. Declaration of conflicting interests The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article. Funding The author(s) received no financial support for the research, authorship, and/or publication of this article. References 1. Cojocaru M, Cojocaru IM, and Chicos B. New insights into antisynthetase syndrome. Mædica 2016; 11: Imbert-Masseau A, Hamidou M, Agard C, et al. Antisynthetase syndrome. Joint Bone Spine 2003; 70: Toujani S, Ben Mansour A, Mjid M, et al. Acute respiratory failure as the first manifestation of antisynthetase syndrome. Tanaffos 2017; 16: Piroddi IM, Ferraioli G, Barlascini C, et al. Severe respiratory failure as a presenting feature of an interstitial lung disease associated with anti-synthetase syndrome. Respir Investig 2016; 54: Trudzinski FC, Kaestner F, Schafers HJ, et al. Outcome of patients with interstitial lung disease treated with extracorporeal membrane oxygenation for acute respiratory failure. Am J Resp Crit Care Med 2016; 193: Starsmore L, Lams B, Agarwal S, et al. Acute Inflammatory presentation associates with survival in interstitial lung disease and extracorporeal membrane oxygenation-requiring severe respiratory failure: a single centre case series. Thorax 2014; 69: A1 A Marie I, Dominique S, Janvresse A, et al. Rituximab therapy for refractory interstitial lung disease related to antisynthetase syndrome. Respir Med 2012; 106: Harb D, Moukadem H, Nayfe R, et al. The off-label use of rituximab for the management of inflammatory disorders. American University of Beirut Medical Centre experience. Arch Rheumatol 2014; 29: Sem M, Molberg O, Lund MB, et al. Rituximab treatment of the anti-synthetase syndrome: a retrospective case series. Rheumatology 2009; 48: Marie I, Dominique S, Jamyresse A, et al. Rituximab therapy for refractory interstitial lung disease related to antisynthetase syndrome. Resp Med 2012; 106: Keir G, Maher T, Ming D, et al. Rituximab in severe, treatment-refractory interstitial lung disease. Respirology 2014; 19: Dasa O, Ruzieh M, and Oraibi O. Successful treatment of life-threatening interstitial lung disease secondary to antisynthetase syndrome using rituximab: a case report and review of the literature. Am J Ther 2016; 23: e639 e Kulkarni H, and Aggarwal R. Successful treatment of acute respiratory failure using rituximab and cyclophosphamide as a combination immunosuppressive regimen in a ventilator-dependent patient having antisynthetase syndrome. Am J Resp CCM 2011; 183: A Kroschinsky F, Sto lzel F, Bonin S, et al. New drugs, new toxicities: severe side effects of modern targeted and immunotherapy of cancer and their management. Crit Care 2017; 21: 89.
Dermatomyositis with Rapidly Progressive Interstitial Lung Disease Treated with Rituximab: A Report of 3 Cases in Japan
 CASE REPORT Dermatomyositis with Rapidly Progressive Interstitial Lung Disease Treated with Rituximab: A Report of 3 Cases in Japan Kenichiro Tokunaga 1 and Noboru Hagino 2 Abstract We performed a retrospective
CASE REPORT Dermatomyositis with Rapidly Progressive Interstitial Lung Disease Treated with Rituximab: A Report of 3 Cases in Japan Kenichiro Tokunaga 1 and Noboru Hagino 2 Abstract We performed a retrospective
Myositis and Your Lungs
 Myositis and Your Lungs 2013 TMA Annual Patient Meeting Louisville, Kentucky Chester V. Oddis, MD University of Pittsburgh Director, Myositis Center Myositis Heterogeneous group of autoimmune syndromes
Myositis and Your Lungs 2013 TMA Annual Patient Meeting Louisville, Kentucky Chester V. Oddis, MD University of Pittsburgh Director, Myositis Center Myositis Heterogeneous group of autoimmune syndromes
New respiratory symptoms and lung imaging findings in a woman with polymyositis
 Maria Bolaki 1, Konstantinos Karagiannis 1, George Bertsias 2, Ioanna Mitrouska 1, Nikolaos Tzanakis 1, Katerina M. Antoniou 1 kantoniou@uoc.gr 1 Dept of Thoracic Medicine, Heraklion University Hospital,
Maria Bolaki 1, Konstantinos Karagiannis 1, George Bertsias 2, Ioanna Mitrouska 1, Nikolaos Tzanakis 1, Katerina M. Antoniou 1 kantoniou@uoc.gr 1 Dept of Thoracic Medicine, Heraklion University Hospital,
Autoantibodies in the Idiopathic Inflammatory Myopathies
 Autoantibodies in the Idiopathic Inflammatory Myopathies Steven R. Ytterberg, M.D. Division of Rheumatology Mayo Clinic Rochester, MN The Myositis Association Annual Conference St. Louis, MO Sept. 25,
Autoantibodies in the Idiopathic Inflammatory Myopathies Steven R. Ytterberg, M.D. Division of Rheumatology Mayo Clinic Rochester, MN The Myositis Association Annual Conference St. Louis, MO Sept. 25,
DRAFT FOR POC BOARD Clinical Commissioning Policy Proposition: Rituximab in Connective Tissue Disease associated Interstitial Lung Disease (adults)
 Clinical Commissioning Policy Proposition: Rituximab in Connective Tissue Disease associated Interstitial Lung Disease (adults) Reference: NHS England A/14/X01 CHECK Information Reader Box (IRB) to be
Clinical Commissioning Policy Proposition: Rituximab in Connective Tissue Disease associated Interstitial Lung Disease (adults) Reference: NHS England A/14/X01 CHECK Information Reader Box (IRB) to be
SCLERODERMA LUNG DISEASE: WHAT THE PATIENT SHOULD KNOW
 SCLERODERMA LUNG DISEASE: WHAT THE PATIENT SHOULD KNOW Lung disease can be a serious complication of scleroderma. The two most common types of lung disease in patients with scleroderma are interstitial
SCLERODERMA LUNG DISEASE: WHAT THE PATIENT SHOULD KNOW Lung disease can be a serious complication of scleroderma. The two most common types of lung disease in patients with scleroderma are interstitial
Anestesia Pediatrica e Neonatale, Vol. 10, N. 1, May-July 2012
 Goodpasture s Syndrome in a 17 years girl. Fast track ICU support as bridge to full recovery after pulmonary failure. Daniela Codazzi 1, Antonio di Coste 2, Maria A. Scalera 1, Maria T. Ficarella 1 1 Division
Goodpasture s Syndrome in a 17 years girl. Fast track ICU support as bridge to full recovery after pulmonary failure. Daniela Codazzi 1, Antonio di Coste 2, Maria A. Scalera 1, Maria T. Ficarella 1 1 Division
ECMO for Severe Hypoxemic Respiratory Failure: Pro-Con Debate. Carolyn Calfee, MD MAS Mark Eisner, MD MPH
 ECMO for Severe Hypoxemic Respiratory Failure: Pro-Con Debate Carolyn Calfee, MD MAS Mark Eisner, MD MPH June 3, 2010 Case Presentation Setting: Community hospital, November 2009 29 year old woman with
ECMO for Severe Hypoxemic Respiratory Failure: Pro-Con Debate Carolyn Calfee, MD MAS Mark Eisner, MD MPH June 3, 2010 Case Presentation Setting: Community hospital, November 2009 29 year old woman with
DAILY SCREENING FORM
 DAILY SCREENING FORM Patient s initials: Date of admission: Time of admission: Gender: M F Year of Birth: Type of admission: Medical/Surgical/Postoperative (elective) Days Date Mechanical ventilation Lung
DAILY SCREENING FORM Patient s initials: Date of admission: Time of admission: Gender: M F Year of Birth: Type of admission: Medical/Surgical/Postoperative (elective) Days Date Mechanical ventilation Lung
Treatment of Coccidioidomycosis-associated Eosinophilic Pneumonia with Corticosteroids
 Treatment of Coccidioidomycosis-associated Eosinophilic Pneumonia with Corticosteroids Joshua Malo, MD Yuval Raz, MD Linda Snyder, MD Kenneth Knox, MD University of Arizona Medical Center Department of
Treatment of Coccidioidomycosis-associated Eosinophilic Pneumonia with Corticosteroids Joshua Malo, MD Yuval Raz, MD Linda Snyder, MD Kenneth Knox, MD University of Arizona Medical Center Department of
CASE PRESENTATION VV ECMO
 CASE PRESENTATION VV ECMO Joshua Huelster, MD Fellow in Critical Care Medicine Department of Pulmonary and Critical Care Medicine Hennepin County Medical Center Disclosure There are no conflicts of interest
CASE PRESENTATION VV ECMO Joshua Huelster, MD Fellow in Critical Care Medicine Department of Pulmonary and Critical Care Medicine Hennepin County Medical Center Disclosure There are no conflicts of interest
ACUTE RESPIRATORY DISTRESS SYNDROME
 ACUTE RESPIRATORY DISTRESS SYNDROME Angel Coz MD, FCCP, DCE Assistant Professor of Medicine UCSF Fresno November 4, 2017 No disclosures OBJECTIVES Identify current trends and risk factors of ARDS Describe
ACUTE RESPIRATORY DISTRESS SYNDROME Angel Coz MD, FCCP, DCE Assistant Professor of Medicine UCSF Fresno November 4, 2017 No disclosures OBJECTIVES Identify current trends and risk factors of ARDS Describe
The use of proning in the management of Acute Respiratory Distress Syndrome
 Case 3 The use of proning in the management of Acute Respiratory Distress Syndrome Clinical Problem This expanded case summary has been chosen to explore the rationale and evidence behind the use of proning
Case 3 The use of proning in the management of Acute Respiratory Distress Syndrome Clinical Problem This expanded case summary has been chosen to explore the rationale and evidence behind the use of proning
Emerging Therapies for Lung Fibrosis. Helen Garthwaite Respiratory Registrar/ Clinical Research Fellow
 Emerging Therapies for Lung Fibrosis Helen Garthwaite Respiratory Registrar/ Clinical Research Fellow Lung Fibrosis/Interstitial Lung Disease Disease that affects the tissue that supports the lungs alveoli
Emerging Therapies for Lung Fibrosis Helen Garthwaite Respiratory Registrar/ Clinical Research Fellow Lung Fibrosis/Interstitial Lung Disease Disease that affects the tissue that supports the lungs alveoli
Clinical Laboratory. [None
 Clinical Laboratory Procedure Result Units Ref Interval Accession Collected Received Double-Stranded DNA (dsdna) Ab IgG ELISA Detected * [None 18-289-900151 Detected] Double-Stranded DNA (dsdna) Ab IgG
Clinical Laboratory Procedure Result Units Ref Interval Accession Collected Received Double-Stranded DNA (dsdna) Ab IgG ELISA Detected * [None 18-289-900151 Detected] Double-Stranded DNA (dsdna) Ab IgG
Clinical Commissioning Policy Proposition:
 Clinical Commissioning Policy Proposition: Rituximab for the treatment of dermatomyositis and polymyositis (Adults) Reference: NHS England A13X05/01 Information Reader Box (IRB) to be inserted on inside
Clinical Commissioning Policy Proposition: Rituximab for the treatment of dermatomyositis and polymyositis (Adults) Reference: NHS England A13X05/01 Information Reader Box (IRB) to be inserted on inside
What your autoantibodies tell us about your disease. Mark Gourley, MD
 What your autoantibodies tell us about your disease Mark Gourley, MD The Importance of the Immune System Defends us against foreign invaders Self (cancer) and Nonself (virus, bacteria, etc.) But, if the
What your autoantibodies tell us about your disease Mark Gourley, MD The Importance of the Immune System Defends us against foreign invaders Self (cancer) and Nonself (virus, bacteria, etc.) But, if the
Steroids for ARDS. Clinical Problem. Management
 Steroids for ARDS James Beck Clinical Problem A 60 year old lady re-presented to ICU with respiratory failure. She had previously been admitted for fluid management and electrolyte correction having presented
Steroids for ARDS James Beck Clinical Problem A 60 year old lady re-presented to ICU with respiratory failure. She had previously been admitted for fluid management and electrolyte correction having presented
New Evidence reports on presentations given at EULAR Rituximab for the Treatment of Rheumatoid Arthritis and Vasculitis
 New Evidence reports on presentations given at EULAR 2011 Rituximab for the Treatment of Rheumatoid Arthritis and Vasculitis Report on EULAR 2011 presentations Anti-TNF failure and response to rituximab
New Evidence reports on presentations given at EULAR 2011 Rituximab for the Treatment of Rheumatoid Arthritis and Vasculitis Report on EULAR 2011 presentations Anti-TNF failure and response to rituximab
Does proning patients with refractory hypoxaemia improve mortality?
 Does proning patients with refractory hypoxaemia improve mortality? Clinical problem and domain I selected this case because although this was the second patient we had proned in our unit within a week,
Does proning patients with refractory hypoxaemia improve mortality? Clinical problem and domain I selected this case because although this was the second patient we had proned in our unit within a week,
The many faces of myositis. Marianne de Visser Academic Medical Centre Dept of Neurology Amsterdam The Netherlands
 The many faces of myositis Marianne de Visser Academic Medical Centre Dept of Neurology Amsterdam The Netherlands Outline of the presentation Classification Diagnosis Therapy Prognosis Diagnostic criteria
The many faces of myositis Marianne de Visser Academic Medical Centre Dept of Neurology Amsterdam The Netherlands Outline of the presentation Classification Diagnosis Therapy Prognosis Diagnostic criteria
A 72-year-old male with worsening interstitial infiltrates and respiratory failure
 A 72-year-old male with worsening interstitial infiltrates and respiratory failure Case report On November 24, 2004, a 72-year-old male was admitted to the medical intensive care unit (ICU) with a history
A 72-year-old male with worsening interstitial infiltrates and respiratory failure Case report On November 24, 2004, a 72-year-old male was admitted to the medical intensive care unit (ICU) with a history
Extracorporeal support in acute respiratory failure. Dr Anthony Bastin Consultant in critical care Royal Brompton Hospital, London
 Extracorporeal support in acute respiratory failure Dr Anthony Bastin Consultant in critical care Royal Brompton Hospital, London Objectives By the end of this session, you will be able to: Describe different
Extracorporeal support in acute respiratory failure Dr Anthony Bastin Consultant in critical care Royal Brompton Hospital, London Objectives By the end of this session, you will be able to: Describe different
Clinical Laboratory. 14:41:00 Complement Component 3 50 mg/dl Oct-18
 Clinical Laboratory Procedure Result Units Ref Interval Accession Collected Received Thyroid Peroxidase (TPO) Antibody 5.0 IU/mL [0.0-9.0] 18-289-900139 16-Oct-18 Complement Component 3 50 mg/dl 18-289-900139
Clinical Laboratory Procedure Result Units Ref Interval Accession Collected Received Thyroid Peroxidase (TPO) Antibody 5.0 IU/mL [0.0-9.0] 18-289-900139 16-Oct-18 Complement Component 3 50 mg/dl 18-289-900139
Test Name Results Units Bio. Ref. Interval
 LL - LL-ROHINI (NATIONAL REFERENCE 135091593 Age 25 Years Gender Male 30/8/2017 91600AM 30/8/2017 93946AM 31/8/2017 84826AM Ref By Final COLLAGEN DISEASES ANTIBODY ANEL ANTI NUCLEAR ANTIBODY / FACTOR (ANA/ANF),
LL - LL-ROHINI (NATIONAL REFERENCE 135091593 Age 25 Years Gender Male 30/8/2017 91600AM 30/8/2017 93946AM 31/8/2017 84826AM Ref By Final COLLAGEN DISEASES ANTIBODY ANEL ANTI NUCLEAR ANTIBODY / FACTOR (ANA/ANF),
Ventilator ECMO Interactions
 Ventilator ECMO Interactions Lorenzo Del Sorbo, MD CCCF Toronto, October 2 nd 2017 Disclosure Relevant relationships with commercial entities: none Potential for conflicts within this presentation: none
Ventilator ECMO Interactions Lorenzo Del Sorbo, MD CCCF Toronto, October 2 nd 2017 Disclosure Relevant relationships with commercial entities: none Potential for conflicts within this presentation: none
Immune-mediated lung disease. Ian Sabroe
 Immune-mediated lung disease Ian Sabroe It s all immune? Diseases that doesn t have immune involvement? The processes of response to injury and tissue repair are key homeostatic pathways involved in all
Immune-mediated lung disease Ian Sabroe It s all immune? Diseases that doesn t have immune involvement? The processes of response to injury and tissue repair are key homeostatic pathways involved in all
Managing Checkpoint Inhibitor Toxicities. Megan L. Menon, Pharm.D., BCOP Roswell Park Cancer Institute
 Managing Checkpoint Inhibitor Toxicities Megan L. Menon, Pharm.D., BCOP Roswell Park Cancer Institute Approved Indications Ipilimumab Nivolumab Pembrolizumab* Atezolizumab Avelumab Durvalumab Ipi + Nivol
Managing Checkpoint Inhibitor Toxicities Megan L. Menon, Pharm.D., BCOP Roswell Park Cancer Institute Approved Indications Ipilimumab Nivolumab Pembrolizumab* Atezolizumab Avelumab Durvalumab Ipi + Nivol
UIP OR NOT UIP PATTERN: THAT IS NOT THE ONLY QUESTION!
 UIP OR NOT UIP PATTERN: THAT IS NOT THE ONLY QUESTION! STÉPHANE JOUNEAU 11 JULY 2014 Respiratory Medicine Department, Pontchaillou Hospital, Rennes, France CASE OVERVIEW This case highlights how a usual
UIP OR NOT UIP PATTERN: THAT IS NOT THE ONLY QUESTION! STÉPHANE JOUNEAU 11 JULY 2014 Respiratory Medicine Department, Pontchaillou Hospital, Rennes, France CASE OVERVIEW This case highlights how a usual
INTERSTITIAL LUNG DISEASE. Radhika Reddy MD Pulmonary/Critical Care Long Beach VA Medical Center January 5, 2018
 INTERSTITIAL LUNG DISEASE Radhika Reddy MD Pulmonary/Critical Care Long Beach VA Medical Center January 5, 2018 Interstitial Lung Disease Interstitial Lung Disease Prevalence by Diagnosis: Idiopathic Interstitial
INTERSTITIAL LUNG DISEASE Radhika Reddy MD Pulmonary/Critical Care Long Beach VA Medical Center January 5, 2018 Interstitial Lung Disease Interstitial Lung Disease Prevalence by Diagnosis: Idiopathic Interstitial
Evidence Review: Title. Month/ Year. Evidence Review:
 Evidence Review: Title Month/ Year Evidence Review: Rituximab for connective tissue disease associated interstitial lung disease October 2014 Standard Operating Procedure: NHS England Evidence Review:
Evidence Review: Title Month/ Year Evidence Review: Rituximab for connective tissue disease associated interstitial lung disease October 2014 Standard Operating Procedure: NHS England Evidence Review:
Clinical Laboratory. 14:42:00 SSA-52 (Ro52) (ENA) Antibody, IgG 1 AU/mL [0-40] Oct-18
![Clinical Laboratory. 14:42:00 SSA-52 (Ro52) (ENA) Antibody, IgG 1 AU/mL [0-40] Oct-18 Clinical Laboratory. 14:42:00 SSA-52 (Ro52) (ENA) Antibody, IgG 1 AU/mL [0-40] Oct-18](/thumbs/95/125595183.jpg) Clinical Laboratory Procedure Result Units Ref Interval Accession Collected Received Rheumatoid Factor
Clinical Laboratory Procedure Result Units Ref Interval Accession Collected Received Rheumatoid Factor
ECLS as Bridge to Transplant
 ECLS as Bridge to Transplant Marcelo Cypel MD, MSc Assistant Professor of Surgery Division of Thoracic Surgery Toronto General Hospital University of Toronto Application of ECLS Bridge to lung recovery
ECLS as Bridge to Transplant Marcelo Cypel MD, MSc Assistant Professor of Surgery Division of Thoracic Surgery Toronto General Hospital University of Toronto Application of ECLS Bridge to lung recovery
Jones slide di 23
 1 di 23 The patient with ANCA- associated vasculitis and pulmonary haemorrhage Rachel B Jones, Cambridge, UK Chairs:Hans-Joachim Anders, Munich, Germany Vladimir Tesar, Prague, Czech Republic Prof. Rachel
1 di 23 The patient with ANCA- associated vasculitis and pulmonary haemorrhage Rachel B Jones, Cambridge, UK Chairs:Hans-Joachim Anders, Munich, Germany Vladimir Tesar, Prague, Czech Republic Prof. Rachel
Case discussion Acute severe asthma during pregnancy. J.G. van der Hoeven
 Case discussion Acute severe asthma during pregnancy J.G. van der Hoeven Case (1) 32-year-old female - gravida 3 - para 2 Previous medical history - asthma Pregnant (33 w) Acute onset fever with wheezing
Case discussion Acute severe asthma during pregnancy J.G. van der Hoeven Case (1) 32-year-old female - gravida 3 - para 2 Previous medical history - asthma Pregnant (33 w) Acute onset fever with wheezing
ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) Rv
 ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) Rv.8.18.18 ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) SUDDEN PROGRESSIVE FORM OF ACUTE RESPIRATORY FAILURE ALVEOLAR CAPILLARY MEMBRANE BECOMES DAMAGED AND MORE
ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) Rv.8.18.18 ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) SUDDEN PROGRESSIVE FORM OF ACUTE RESPIRATORY FAILURE ALVEOLAR CAPILLARY MEMBRANE BECOMES DAMAGED AND MORE
Acute Emergencies in Rheumatology
 Acute Emergencies in Rheumatology Clare Higgens Northwick Park hospital and St George s Hospital London Acute Rheumatological Emergencies The Acute Hot joint Inflammatory back pain.. Systemic lupus erythematosus(sle)
Acute Emergencies in Rheumatology Clare Higgens Northwick Park hospital and St George s Hospital London Acute Rheumatological Emergencies The Acute Hot joint Inflammatory back pain.. Systemic lupus erythematosus(sle)
Landmark articles on ventilation
 Landmark articles on ventilation Dr Shrikanth Srinivasan MD,DNB,FNB,EDIC Consultant, Critical Care Medicine Medanta, The Medicity ARDS AECC DEFINITION-1994 ALI Acute onset Bilateral chest infiltrates PCWP
Landmark articles on ventilation Dr Shrikanth Srinivasan MD,DNB,FNB,EDIC Consultant, Critical Care Medicine Medanta, The Medicity ARDS AECC DEFINITION-1994 ALI Acute onset Bilateral chest infiltrates PCWP
ECMO: a breakthrough in care for respiratory failure. PD Dr. Thomas Müller Regensburg no conflict of interest
 ECMO: a breakthrough in care for respiratory failure? PD Dr. Thomas Müller Regensburg no conflict of interest 1 Overview Mortality of severe ARDS Indication for ECMO PaO 2 /FiO 2 Efficiency of ECMO: gas
ECMO: a breakthrough in care for respiratory failure? PD Dr. Thomas Müller Regensburg no conflict of interest 1 Overview Mortality of severe ARDS Indication for ECMO PaO 2 /FiO 2 Efficiency of ECMO: gas
Differential diagnosis
 Differential diagnosis Idiopathic pulmonary fibrosis (IPF) is part of a large family of idiopathic interstitial pneumonias (IIP), one of four subgroups of interstitial lung disease (ILD). Differential
Differential diagnosis Idiopathic pulmonary fibrosis (IPF) is part of a large family of idiopathic interstitial pneumonias (IIP), one of four subgroups of interstitial lung disease (ILD). Differential
Protocol Version 2.0 Synopsis
 Protocol Version 2.0 Synopsis Title Short Title Plasma exchange and glucocorticoid dosing in anti-neutrophil cytoplasm antibody associated vasculitis: a randomized controlled trial. PEXIVAS PEXIVAS Clinical
Protocol Version 2.0 Synopsis Title Short Title Plasma exchange and glucocorticoid dosing in anti-neutrophil cytoplasm antibody associated vasculitis: a randomized controlled trial. PEXIVAS PEXIVAS Clinical
Management of Acute Vasculitis. CMT teaching 3 rd June 2015 Caroline Wroe
 Management of Acute Vasculitis CMT teaching 3 rd June 2015 Caroline Wroe Vasculitis pub quiz Match the date with the event Dr Peter McBride, Scottish Otolaryngologist describes a disease of rapid destruction
Management of Acute Vasculitis CMT teaching 3 rd June 2015 Caroline Wroe Vasculitis pub quiz Match the date with the event Dr Peter McBride, Scottish Otolaryngologist describes a disease of rapid destruction
Eosinophils and effusion: a clinical conundrum
 Ruth Sobala, Kevin Conroy, Hilary Tedd, Salem Elarbi kevin.peter.conroy@gmail.com Respiratory Dept, Queen Elizabeth Hospital, Gateshead, UK. Eosinophils and effusion: a clinical conundrum Case report A
Ruth Sobala, Kevin Conroy, Hilary Tedd, Salem Elarbi kevin.peter.conroy@gmail.com Respiratory Dept, Queen Elizabeth Hospital, Gateshead, UK. Eosinophils and effusion: a clinical conundrum Case report A
AKI Case study -Vasculitis. Sarah Mackie Renal Practice Development Nurse King s College Hospital - London
 AKI Case study -Vasculitis Sarah Mackie Renal Practice Development Nurse King s College Hospital - London What is vasculitis Vasculitis refers to inflammation of the blood vessels, including arteries,
AKI Case study -Vasculitis Sarah Mackie Renal Practice Development Nurse King s College Hospital - London What is vasculitis Vasculitis refers to inflammation of the blood vessels, including arteries,
Test Name Results Units Bio. Ref. Interval
 135091660 Age 44 Years Gender Male 29/8/2017 120000AM 29/8/2017 100219AM 29/8/2017 105510AM Ref By Final EXTRACTABLENUCLEAR ANTIGENS (ENA), QUANTITATIVE ROFILE CENTROMERE ANTIBODY, SERUM 20-30 Weak ositive
135091660 Age 44 Years Gender Male 29/8/2017 120000AM 29/8/2017 100219AM 29/8/2017 105510AM Ref By Final EXTRACTABLENUCLEAR ANTIGENS (ENA), QUANTITATIVE ROFILE CENTROMERE ANTIBODY, SERUM 20-30 Weak ositive
The Egyptian Journal of Hospital Medicine (July 2017) Vol.68 (2), Page
 The Egyptian Journal of Hospital Medicine (July 2017) Vol.68 (2), Page 1135-1140 Role of High Resolution Computed Tomography in Diagnosis of Interstitial Lung Diseases in Patients with Collagen Diseases
The Egyptian Journal of Hospital Medicine (July 2017) Vol.68 (2), Page 1135-1140 Role of High Resolution Computed Tomography in Diagnosis of Interstitial Lung Diseases in Patients with Collagen Diseases
Understanding Myositis Medications
 Understanding Myositis Medications 2015 TMA Annual Patient Conference Orlando, Florida Chester V. Oddis, MD University of Pittsburgh Director, Myositis Center Disclosures Mallinckrodt: Research Grant Genentech:
Understanding Myositis Medications 2015 TMA Annual Patient Conference Orlando, Florida Chester V. Oddis, MD University of Pittsburgh Director, Myositis Center Disclosures Mallinckrodt: Research Grant Genentech:
EXTRACORPOREAL MEMBRANE OXYGENATION (ECMO) REFERRAL FORM
 Patient Label This form is accessible on www.royalpapworth.nhs.uk Intensive Care Unit EXTRACORPOREAL MEMBRANE OXYGENATION (ECMO) REFERRAL FORM Please always phone Papworth ECMO Coordinator on 01480 830541,
Patient Label This form is accessible on www.royalpapworth.nhs.uk Intensive Care Unit EXTRACORPOREAL MEMBRANE OXYGENATION (ECMO) REFERRAL FORM Please always phone Papworth ECMO Coordinator on 01480 830541,
Steroids in ARDS: if, when, how much? John Fowler, MD, FACEP Dept. of Emergency Medicine Kent Hospital, İzmir, Türkiye
 Steroids in ARDS: if, when, how much? John Fowler, MD, FACEP Dept. of Emergency Medicine Kent Hospital, İzmir, Türkiye Steroids in ARDS: conclusion Give low-dose steroids if indicated for another problem
Steroids in ARDS: if, when, how much? John Fowler, MD, FACEP Dept. of Emergency Medicine Kent Hospital, İzmir, Türkiye Steroids in ARDS: conclusion Give low-dose steroids if indicated for another problem
PL-7 and Anti-Jo-1 Antibodies. publication is available at link.sp
 NAOSITE: Nagasaki University's Ac Title Author(s) Comparison of Pulmonary Involvement PL-7 and Anti-Jo-1 Antibodies Tomonaga, Masaomi; Sakamoto, Noriho Tomoyuki; Harada, Tatsuhiko; Nakash Shintaro; Horai,
NAOSITE: Nagasaki University's Ac Title Author(s) Comparison of Pulmonary Involvement PL-7 and Anti-Jo-1 Antibodies Tomonaga, Masaomi; Sakamoto, Noriho Tomoyuki; Harada, Tatsuhiko; Nakash Shintaro; Horai,
ARDS: an update 6 th March A. Hakeem Al Hashim, MD, FRCP SQUH
 ARDS: an update 6 th March 2017 A. Hakeem Al Hashim, MD, FRCP SQUH 30M, previously healthy Hx: 1 week dry cough Gradually worsening SOB No travel Hx Case BP 130/70, HR 100/min ph 7.29 pco2 35 po2 50 HCO3
ARDS: an update 6 th March 2017 A. Hakeem Al Hashim, MD, FRCP SQUH 30M, previously healthy Hx: 1 week dry cough Gradually worsening SOB No travel Hx Case BP 130/70, HR 100/min ph 7.29 pco2 35 po2 50 HCO3
Sub-category: Intensive Care for Respiratory Distress
 Course n : Course 3 Title: RESPIRATORY PHYSIOLOGY, PHYSICS AND PATHOLOGY IN RELATION TO ANAESTHESIA AND INTENSIVE CARE Sub-category: Intensive Care for Respiratory Distress Topic: Acute Respiratory Distress
Course n : Course 3 Title: RESPIRATORY PHYSIOLOGY, PHYSICS AND PATHOLOGY IN RELATION TO ANAESTHESIA AND INTENSIVE CARE Sub-category: Intensive Care for Respiratory Distress Topic: Acute Respiratory Distress
CASE REPORT. Introduction. Case Report
 doi: 10.2169/internalmedicine.9553-17 http://internmed.jp CASE REPORT Successful Treatment of Rapidly Progressive Unclassifiable Idiopathic Interstitial Pneumonia with Anti-melanoma Differentiation-associated
doi: 10.2169/internalmedicine.9553-17 http://internmed.jp CASE REPORT Successful Treatment of Rapidly Progressive Unclassifiable Idiopathic Interstitial Pneumonia with Anti-melanoma Differentiation-associated
Hospital-acquired Pneumonia
 Hospital-acquired Pneumonia Hospital-acquired pneumonia (HAP) Pneumonia that occurs at least 2 days after hospital admission. The second most common and the leading cause of death due to hospital-acquired
Hospital-acquired Pneumonia Hospital-acquired pneumonia (HAP) Pneumonia that occurs at least 2 days after hospital admission. The second most common and the leading cause of death due to hospital-acquired
The Onset of Eosinophilic Pneumonia Preceding Anti-synthetase Syndrome
 doi: 10.2169/internalmedicine.8955-17 http://internmed.jp CASE REPORT The Onset of Eosinophilic Pneumonia Preceding Anti-synthetase Syndrome Yoshimasa Hachisu 1, Yasuhiko Koga 1, Noriaki Sunaga 1,2, Chiharu
doi: 10.2169/internalmedicine.8955-17 http://internmed.jp CASE REPORT The Onset of Eosinophilic Pneumonia Preceding Anti-synthetase Syndrome Yoshimasa Hachisu 1, Yasuhiko Koga 1, Noriaki Sunaga 1,2, Chiharu
Connective Tissue Disorder- Associated Interstitial Lung Disease (CTD-ILD) and Updates
 Connective Tissue Disorder- Associated Interstitial Lung Disease (CTD-ILD) and Updates Maria Elena Vega, M.D Assistant Professor of Medicine Lewis Katz School of Medicine at Temple University Nothing to
Connective Tissue Disorder- Associated Interstitial Lung Disease (CTD-ILD) and Updates Maria Elena Vega, M.D Assistant Professor of Medicine Lewis Katz School of Medicine at Temple University Nothing to
Patient Management Code Blue in the CT Suite
 Patient Management Code Blue in the CT Suite David Stultz, MD November 28, 2001 Case Presentation A 53-year-old woman experienced acute respiratory distress during an IV contrast enhanced CT scan of the
Patient Management Code Blue in the CT Suite David Stultz, MD November 28, 2001 Case Presentation A 53-year-old woman experienced acute respiratory distress during an IV contrast enhanced CT scan of the
Interstitial Lung Disease
 Interstitial Lung Disease Interstitial lung disease (ILD) is a broad category of lung diseases that includes more than 130 disorders which are characterized by scarring (i.e. fibrosis ) and/or inflammation
Interstitial Lung Disease Interstitial lung disease (ILD) is a broad category of lung diseases that includes more than 130 disorders which are characterized by scarring (i.e. fibrosis ) and/or inflammation
Acute Respiratory Distress Syndrome (ARDS) An Update
 Acute Respiratory Distress Syndrome (ARDS) An Update Prof. A.S.M. Areef Ahsan FCPS(Medicine) MD(Critical Care Medicine) MD ( Chest) Head, Dept. of Critical Care Medicine BIRDEM General Hospital INTRODUCTION
Acute Respiratory Distress Syndrome (ARDS) An Update Prof. A.S.M. Areef Ahsan FCPS(Medicine) MD(Critical Care Medicine) MD ( Chest) Head, Dept. of Critical Care Medicine BIRDEM General Hospital INTRODUCTION
GRANULOMATOSIS WITH POLYANGIITIS
 What is granulomatosis with polyangiitis (GPA)? Granulomatosis with polyangiitis (GPA) is a form of vasculitis a family of rare disorders characterized by inflammation of the blood vessels, which can restrict
What is granulomatosis with polyangiitis (GPA)? Granulomatosis with polyangiitis (GPA) is a form of vasculitis a family of rare disorders characterized by inflammation of the blood vessels, which can restrict
Acute Onset Anti-Synthetase Syndrome With Pericardial Effusion and Non-Specific Interstitial Pneumonia
 Elmer ress Case Report J Clin Med Res. 2016;8(9):683-687 Acute Onset Anti-Synthetase Syndrome With Pericardial Effusion and Non-Specific Interstitial Pneumonia Aditya Shah a, b, Samir R. Patel a Abstract
Elmer ress Case Report J Clin Med Res. 2016;8(9):683-687 Acute Onset Anti-Synthetase Syndrome With Pericardial Effusion and Non-Specific Interstitial Pneumonia Aditya Shah a, b, Samir R. Patel a Abstract
CTD-related Lung Disease
 13 th Cambridge Chest Meeting King s College, Cambridge April 2015 Imaging of CTD-related Lung Disease Dr Sujal R Desai King s College Hospital, London Disclosure Statement No Disclosures / Conflicts of
13 th Cambridge Chest Meeting King s College, Cambridge April 2015 Imaging of CTD-related Lung Disease Dr Sujal R Desai King s College Hospital, London Disclosure Statement No Disclosures / Conflicts of
Clinical syndromes: experience from the bedside. Professor Rob Miller University College Hospital, London
 Clinical syndromes: experience from the bedside Professor Rob Miller University College Hospital, London Presented at ECCMID Berlin April 30 th 2013 Pneumocystis jirovecii pneumonia http://commons.wikimedia.org/wiki/file
Clinical syndromes: experience from the bedside Professor Rob Miller University College Hospital, London Presented at ECCMID Berlin April 30 th 2013 Pneumocystis jirovecii pneumonia http://commons.wikimedia.org/wiki/file
Acute Respiratory Distress Syndrome as the Initial Clinical Manifestation of an Antisynthetase Syndrome
 CASE REPORT http://dx.doi.org/10.4046/trd.2016.79.3.188 ISSN: 1738-3536(Print)/2005-6184(Online) Tuberc Respir Dis 2016;79:188-192 Acute Respiratory Distress Syndrome as the Initial Clinical Manifestation
CASE REPORT http://dx.doi.org/10.4046/trd.2016.79.3.188 ISSN: 1738-3536(Print)/2005-6184(Online) Tuberc Respir Dis 2016;79:188-192 Acute Respiratory Distress Syndrome as the Initial Clinical Manifestation
ד"ר דוד ירדני המכון לגסטרואנטרולוגיה ומחלות כבד מרכז רפואי סורוקה
 ד"ר דוד ירדני המכון לגסטרואנטרולוגיה ומחלות כבד מרכז רפואי סורוקה Presentation: S.A is 25 years old. Referred to a gastroentrologist because of abdominal pain and bloody diarrhea in the last few weeks.
ד"ר דוד ירדני המכון לגסטרואנטרולוגיה ומחלות כבד מרכז רפואי סורוקה Presentation: S.A is 25 years old. Referred to a gastroentrologist because of abdominal pain and bloody diarrhea in the last few weeks.
This resource was first published in 2014 and revised in 2017.
 This resource was first published in 2014 and revised in 2017. 0 There is good evidence to suggest that patients eventually diagnosed with HIV infection have had contact with medical services, with symptoms
This resource was first published in 2014 and revised in 2017. 0 There is good evidence to suggest that patients eventually diagnosed with HIV infection have had contact with medical services, with symptoms
Extracorporeal Membrane Oxygenation in Nivolumab Associated Pneumonitis
 The Journal of Critical Care Medicine 2017;3(2):84-88 CASE REPORT Extracorporeal Membrane Oxygenation in Nivolumab Associated Pneumonitis Thomas-Michael Schneider 1*, Friederike Klenner 2, Franz Brettner
The Journal of Critical Care Medicine 2017;3(2):84-88 CASE REPORT Extracorporeal Membrane Oxygenation in Nivolumab Associated Pneumonitis Thomas-Michael Schneider 1*, Friederike Klenner 2, Franz Brettner
ICU management and referral guidelines for severe hypoxic respiratory failure
 Aim: ICU management and referral guidelines for severe hypoxic respiratory failure 1) To provide a concise management plan Non ventilatory Ventilatory 2) Timeline for referring patient with refractory
Aim: ICU management and referral guidelines for severe hypoxic respiratory failure 1) To provide a concise management plan Non ventilatory Ventilatory 2) Timeline for referring patient with refractory
INTERSTITIAL LUNG DISEASE Dr. Zulqarnain Ashraf
 Indep Rev Jul-Dec 2018;20(7-12) Dr. Zulqarnain Ashraf IR-653 Abstract: ILD is a group of diseases affect interstitium of the lung. Repeated insult to the lung cause the interstitium to be damaged. Similarly
Indep Rev Jul-Dec 2018;20(7-12) Dr. Zulqarnain Ashraf IR-653 Abstract: ILD is a group of diseases affect interstitium of the lung. Repeated insult to the lung cause the interstitium to be damaged. Similarly
Pulmonary And Central Nervous System Involvement In Juvenile Dermatomyositis: Vasculopathy And/Or Steroids As Causative Agents - A Case Report
 ISPUB.COM The Internet Journal of Radiology Volume 4 Number 1 Pulmonary And Central Nervous System Involvement In Juvenile Dermatomyositis: Vasculopathy And/Or Steroids As Causative Agents - A Case Report
ISPUB.COM The Internet Journal of Radiology Volume 4 Number 1 Pulmonary And Central Nervous System Involvement In Juvenile Dermatomyositis: Vasculopathy And/Or Steroids As Causative Agents - A Case Report
Common things are common, but not always the answer
 Kevin Conroy, Joe Mackenzie, Stephen Cowie kevin.conroy@nhs.net Respiratory Dept, Darlington Memorial Hospital, Darlington, UK. Common things are common, but not always the answer Case report Cite as:
Kevin Conroy, Joe Mackenzie, Stephen Cowie kevin.conroy@nhs.net Respiratory Dept, Darlington Memorial Hospital, Darlington, UK. Common things are common, but not always the answer Case report Cite as:
Arthritis & Rheumatology Clinics of Kansas PATIENT EDUCATION SYSTEMIC LUPUS ERYTHEMATOSUS
 Arthritis & Rheumatology Clinics of Kansas PATIENT EDUCATION SYSTEMIC LUPUS ERYTHEMATOSUS Introduction: There is perhaps no rheumatic disease that evokes so much fear and confusion among both patients
Arthritis & Rheumatology Clinics of Kansas PATIENT EDUCATION SYSTEMIC LUPUS ERYTHEMATOSUS Introduction: There is perhaps no rheumatic disease that evokes so much fear and confusion among both patients
Annual Rheumatology & Therapeutics Review for Organizations & Societies
 Annual Rheumatology & Therapeutics Review for Organizations & Societies A Rheumatologist s Approach to Interstitial Lung Disease Outline ILD classification and patterns in CTD The clinical landscape and
Annual Rheumatology & Therapeutics Review for Organizations & Societies A Rheumatologist s Approach to Interstitial Lung Disease Outline ILD classification and patterns in CTD The clinical landscape and
ERJ Express. Published on August 9, 2012 as doi: /
 ERJ Express. Published on August 9, 2012 as doi: 10.1183/09031936.00076912 Extracorporeal membrane oxygenation in a non intubated patient with acute respiratory distress syndrome (ARDS) Olaf Wiesner, *
ERJ Express. Published on August 9, 2012 as doi: 10.1183/09031936.00076912 Extracorporeal membrane oxygenation in a non intubated patient with acute respiratory distress syndrome (ARDS) Olaf Wiesner, *
ECMO Experience from ECMO-ICU, Karolinska
 ECMO Experience from ECMO-ICU, Karolinska X Curso de Ventilacion Mecanica en Anestesia, Cuidados Criticos y Transplantes Madrid 2012 International numbers Totally since 1989; 46500 patients as of July
ECMO Experience from ECMO-ICU, Karolinska X Curso de Ventilacion Mecanica en Anestesia, Cuidados Criticos y Transplantes Madrid 2012 International numbers Totally since 1989; 46500 patients as of July
Surviving Sepsis Campaign. Guidelines for Management of Severe Sepsis/Septic Shock. An Overview
 Surviving Sepsis Campaign Guidelines for Management of Severe Sepsis/Septic Shock An Overview Mechanical Ventilation of Sepsis-Induced ALI/ARDS ARDSnet Mechanical Ventilation Protocol Results: Mortality
Surviving Sepsis Campaign Guidelines for Management of Severe Sepsis/Septic Shock An Overview Mechanical Ventilation of Sepsis-Induced ALI/ARDS ARDSnet Mechanical Ventilation Protocol Results: Mortality
UPDATE IN HOSPITAL MEDICINE
 UPDATE IN HOSPITAL MEDICINE FLORIDA CHAPTER ACP MEETING 2016 Himangi Kaushal, M.D., F.A.C.P. Program Director Memorial Healthcare System Internal Medicine Residency DISCLOSURES None OBJECTIVES Review some
UPDATE IN HOSPITAL MEDICINE FLORIDA CHAPTER ACP MEETING 2016 Himangi Kaushal, M.D., F.A.C.P. Program Director Memorial Healthcare System Internal Medicine Residency DISCLOSURES None OBJECTIVES Review some
COBIS Management of airway burns and inhalation injury PAEDIATRIC
 COBIS Management of airway burns and inhalation injury PAEDIATRIC 1 A multidisciplinary team should provide the management of the child with inhalation injury. Childhood inhalation injury mandates transfer
COBIS Management of airway burns and inhalation injury PAEDIATRIC 1 A multidisciplinary team should provide the management of the child with inhalation injury. Childhood inhalation injury mandates transfer
Early View Article: Online published version of an accepted article before publication in the final form.
 : Online published version of an accepted article before publication in the final form. Journal Name: International Journal of Case Reports and Images (IJCRI) Type of Article: Clinical Images Title: Successful
: Online published version of an accepted article before publication in the final form. Journal Name: International Journal of Case Reports and Images (IJCRI) Type of Article: Clinical Images Title: Successful
Case Report Repository Corticotropin Injection for Treatment of Idiopathic Inflammatory Myopathies
 Case Reports in Rheumatology Volume 2016, Article ID 9068061, 4 pages http://dx.doi.org/10.1155/2016/9068061 Case Report Repository Corticotropin Injection for Treatment of Idiopathic Inflammatory Myopathies
Case Reports in Rheumatology Volume 2016, Article ID 9068061, 4 pages http://dx.doi.org/10.1155/2016/9068061 Case Report Repository Corticotropin Injection for Treatment of Idiopathic Inflammatory Myopathies
Guideline for the Management of Acute Chest Syndrome in Children with Sickle Cell Disease
 Guideline for the Management of Acute Chest Syndrome in Children with Sickle Cell Disease Definition Acute chest syndrome (ACS) is defined as an acute illness characterized by fever and/or respiratory
Guideline for the Management of Acute Chest Syndrome in Children with Sickle Cell Disease Definition Acute chest syndrome (ACS) is defined as an acute illness characterized by fever and/or respiratory
Back to the Future: Updated Guidelines for Evaluation and Management of Adrenal Insufficiency in the Critically Ill
 Back to the Future: Updated Guidelines for Evaluation and Management of Adrenal Insufficiency in the Critically Ill Joe Palumbo PGY-2 Critical Care Pharmacy Resident Buffalo General Medical Center Disclosures
Back to the Future: Updated Guidelines for Evaluation and Management of Adrenal Insufficiency in the Critically Ill Joe Palumbo PGY-2 Critical Care Pharmacy Resident Buffalo General Medical Center Disclosures
Is it Autoimmune or NOT! Presented to AONP! October 2015!
 Is it Autoimmune or NOT! Presented to AONP! October 2015! Four main jobs of immune system Detects Contains and eliminates Self regulates Protects Innate Immune System! Epithelial cells, phagocytic cells
Is it Autoimmune or NOT! Presented to AONP! October 2015! Four main jobs of immune system Detects Contains and eliminates Self regulates Protects Innate Immune System! Epithelial cells, phagocytic cells
EXTRA CORPOREAL MEMBRANE OXYGENATION
 EXTRA CORPOREAL MEMBRANE OXYGENATION Basic Overview and Case Study Bob Hayes, Chief Perfusionist Enloe Medical Center Jenny Humphries, RN, BSN, MBA, CFRN Chief Flight Nurse, Enloe FlightCare Normal Cardiopulmonary
EXTRA CORPOREAL MEMBRANE OXYGENATION Basic Overview and Case Study Bob Hayes, Chief Perfusionist Enloe Medical Center Jenny Humphries, RN, BSN, MBA, CFRN Chief Flight Nurse, Enloe FlightCare Normal Cardiopulmonary
ENFERMEDADES AUTOINMUNES SISTÉMICAS. Dr. J. María Pego Reigosa
 ENFERMEDADES AUTOINMUNES SISTÉMICAS Dr. J. María Pego Reigosa ABSTRACT NUMBER: 888 PHASE 3 TRIAL RESULTS WITH BLISIBIMOD, A SELECTIVE INHIBITOR OF B-CELL ACTIVATING FACTOR, IN SUBJECTS WITH MODERATE-TO-SEVERE
ENFERMEDADES AUTOINMUNES SISTÉMICAS Dr. J. María Pego Reigosa ABSTRACT NUMBER: 888 PHASE 3 TRIAL RESULTS WITH BLISIBIMOD, A SELECTIVE INHIBITOR OF B-CELL ACTIVATING FACTOR, IN SUBJECTS WITH MODERATE-TO-SEVERE
4/17/2010 C ini n ca c l a Ev E a v l a ua u t a ion o n of o ILD U dat a e t e i n I LDs
 Update in ILDs Diagnosis 101: Clinical Evaluation April 17, 2010 Jay H. Ryu, MD Mayo Clinic, Rochester MN Clinical Evaluation of ILD Outline General aspects of ILDs Classification of ILDs Clinical evaluation
Update in ILDs Diagnosis 101: Clinical Evaluation April 17, 2010 Jay H. Ryu, MD Mayo Clinic, Rochester MN Clinical Evaluation of ILD Outline General aspects of ILDs Classification of ILDs Clinical evaluation
HYPERSENSITIVITY PNEUMONITIS
 HYPERSENSITIVITY PNEUMONITIS A preventable fibrosis MOSAVIR ANSARIE MB., FCCP INTERSTITIAL LUNG DISEASES A heterogeneous group of non infectious, non malignant diffuse parenchymal disorders of the lower
HYPERSENSITIVITY PNEUMONITIS A preventable fibrosis MOSAVIR ANSARIE MB., FCCP INTERSTITIAL LUNG DISEASES A heterogeneous group of non infectious, non malignant diffuse parenchymal disorders of the lower
All I Need Is The Air That I Breathe: A Case Study of Immunotherapy and Severe Pneumonitis
 All I Need Is The Air That I Breathe: A Case Study of Immunotherapy and Severe Pneumonitis Presenter Disclosure Faculty/Speaker: Dr. Brett Finney BSc MD CCFP Relationships with financial sponsors: Grants/Research
All I Need Is The Air That I Breathe: A Case Study of Immunotherapy and Severe Pneumonitis Presenter Disclosure Faculty/Speaker: Dr. Brett Finney BSc MD CCFP Relationships with financial sponsors: Grants/Research
Systemic lupus erythematosus (SLE): Pleuropulmonary Manifestations
 08/30/10 09/26/10 Systemic lupus erythematosus (SLE): Pleuropulmonary Manifestations Camila Downey S. Universidad de Chile, School of Medicine, Year VII Harvard University, School of Medicine Sept 17,
08/30/10 09/26/10 Systemic lupus erythematosus (SLE): Pleuropulmonary Manifestations Camila Downey S. Universidad de Chile, School of Medicine, Year VII Harvard University, School of Medicine Sept 17,
Rituximab treatment for ANCA-associated vasculitis in childhood
 Rituximab treatment for ANCA-associated vasculitis in childhood DISCLOSURE I have no relevant financial relationships to disclose Katharine Moore MD Nov 14, 2012 University of Colorado School of Medicine
Rituximab treatment for ANCA-associated vasculitis in childhood DISCLOSURE I have no relevant financial relationships to disclose Katharine Moore MD Nov 14, 2012 University of Colorado School of Medicine
CLINICAL GUIDELINES. Summary of Literature and Recommendations Concerning Immunization and Steroid Injections Thomas J. Gilbert M.D., M.P.P.
 CLINICAL GUIDELINES Summary of Literature and Recommendations Concerning Immunization and Steroid Injections Thomas J. Gilbert M.D., M.P.P. 11/2/15 Several practices routinely delay steroid injections
CLINICAL GUIDELINES Summary of Literature and Recommendations Concerning Immunization and Steroid Injections Thomas J. Gilbert M.D., M.P.P. 11/2/15 Several practices routinely delay steroid injections
Prone ventilation revisited in H1N1 patients
 International Journal of Advanced Multidisciplinary Research ISSN: 2393-8870 www.ijarm.com DOI: 10.22192/ijamr Volume 5, Issue 10-2018 Case Report DOI: http://dx.doi.org/10.22192/ijamr.2018.05.10.005 Prone
International Journal of Advanced Multidisciplinary Research ISSN: 2393-8870 www.ijarm.com DOI: 10.22192/ijamr Volume 5, Issue 10-2018 Case Report DOI: http://dx.doi.org/10.22192/ijamr.2018.05.10.005 Prone
EULAR/ERA-EDTA recommendations for the management of ANCAassociated
 EULAR/ERA-EDTA recommendations for the management of ANCAassociated vasculitis Dr. Meharunnisha Syed III year DNB Resident (General Medicine) Narayana Health-MSH Fifteen recommendations were developed,
EULAR/ERA-EDTA recommendations for the management of ANCAassociated vasculitis Dr. Meharunnisha Syed III year DNB Resident (General Medicine) Narayana Health-MSH Fifteen recommendations were developed,
CENTENE PHARMACY AND THERAPEUTICS DRUG REVIEW 1Q18 January February
 BRAND NAME Soliris GENERIC NAME Eculizumab MANUFACTURER Alexion Pharmaceuticals, Inc. DATE OF APPROVAL October 23, 2017 PRODUCT LAUNCH DATE Currently commercially available REVIEW TYPE Review type 1 (RT1):
BRAND NAME Soliris GENERIC NAME Eculizumab MANUFACTURER Alexion Pharmaceuticals, Inc. DATE OF APPROVAL October 23, 2017 PRODUCT LAUNCH DATE Currently commercially available REVIEW TYPE Review type 1 (RT1):
Recent advances in diagnosis and management of ABPA. Arindam SR(Pulmonary Medicine)
 Recent advances in diagnosis and management of ABPA Arindam SR(Pulmonary Medicine) Conventional diagnostic criteria for ABPA Primary Episodic bronchial obstruction (asthma) Peripheral blood eosinophilia
Recent advances in diagnosis and management of ABPA Arindam SR(Pulmonary Medicine) Conventional diagnostic criteria for ABPA Primary Episodic bronchial obstruction (asthma) Peripheral blood eosinophilia
Extracorporeal Life Support (ECLS) as a Bridge to Decision in Lung Transplantation
 Extracorporeal Life Support (ECLS) as a Bridge to Decision in Lung Transplantation Gabriel Loor, MD Baylor St. Lukes Medical Center Surgical Director Lung Transplantation Co-chief Section of Adult Cardiac
Extracorporeal Life Support (ECLS) as a Bridge to Decision in Lung Transplantation Gabriel Loor, MD Baylor St. Lukes Medical Center Surgical Director Lung Transplantation Co-chief Section of Adult Cardiac
ARDS - a must know. Page 1 of 14
 ARDS - a must know Poster No.: C-1683 Congress: ECR 2016 Type: Authors: Keywords: DOI: Educational Exhibit M. Cristian; Turda/RO Education and training, Edema, Acute, Localisation, Education, Digital radiography,
ARDS - a must know Poster No.: C-1683 Congress: ECR 2016 Type: Authors: Keywords: DOI: Educational Exhibit M. Cristian; Turda/RO Education and training, Edema, Acute, Localisation, Education, Digital radiography,
The Management of Acute Chest Syndrome in Children with Sickle Cell Disease
 The Management of Acute Chest Syndrome in Children with Sickle Cell Disease Document Information Version: 4 Date: Dec 2013 Authors (incl. job title): Professor David Rees and Dr Sue Height, consultant
The Management of Acute Chest Syndrome in Children with Sickle Cell Disease Document Information Version: 4 Date: Dec 2013 Authors (incl. job title): Professor David Rees and Dr Sue Height, consultant
Case Report Pulmonary Sarcoidosis following Etanercept Treatment
 Case Reports in Rheumatology Volume 2012, Article ID 724013, 4 pages doi:10.1155/2012/724013 Case Report Pulmonary Sarcoidosis following Etanercept Treatment Kuljeet Bhamra and Richard Stevens Department
Case Reports in Rheumatology Volume 2012, Article ID 724013, 4 pages doi:10.1155/2012/724013 Case Report Pulmonary Sarcoidosis following Etanercept Treatment Kuljeet Bhamra and Richard Stevens Department
Management of refractory ARDS. Saurabh maji
 Management of refractory ARDS Saurabh maji Refractory hypoxemia as PaO2/FIO2 is less than 100 mm Hg, inability to keep plateau pressure below 30 cm H2O despite a VT of 4 ml/kg development of barotrauma
Management of refractory ARDS Saurabh maji Refractory hypoxemia as PaO2/FIO2 is less than 100 mm Hg, inability to keep plateau pressure below 30 cm H2O despite a VT of 4 ml/kg development of barotrauma
