Lymph node hyalinisation in rheumatoid arthritis
|
|
|
- Morgan Underwood
- 6 years ago
- Views:
Transcription
1 Clin Pathol 1994;47: Department of Pathology, Royal Victoria Hospital, Belfast W G McCluggage Queen's University, Belfast H Bharucha Correspondence to: Dr W G McCluggage, Department of Pathology, Royal Victoria Hospital, Grosvenor Road, Belfast BT12 6BA, Northern Ireland Accepted for publication 7 September 1993 Lymph node hyalinisation in rheumatoid arthritis and systemic sclerosis W G McCluggage, H Bharucha Abstract Aims-To review the histological features of lymph nodes excised from seven patients with rheumatoid arthritis and one with systemic sclerosis. Methods-Lymph nodes excised from seven patients with rheumatoid arthritis and one patient with systemic sclerosis over a 10 year period were examined using the stains haematoxylin and eosin, periodic acid Schiff (PAS), Massontrichrome, and Congo red for amyloid. Results-Of the seven nodes examined from the cases of rheumatoid arthritis, three showed definite reactive follicular hyperplasia with a prominence of plasma cells in the interfollicular areas, two showed subtotal replacement of the node by numerous sarcoid like granulomata, and one contained a large central area of necrosis with a surrounding palisade of histiocytes. In all six cases, focal areas of PAS positive eosinophilic hyaline material were present, which did not stain with Congo red. In some cases this hyaline material was focally calcified. In the seventh patient with rheumatoid arthritis the excised lymph node was almost totally replaced by similar PAS positive hyaline material which showed extensive areas of calcification. The lymph node removed from the patient with systemic sclerosis similarly showed almost total replacement by PAS positive hyaline material. Conclusion-In all cases the nodes contained PAS positive extracellular hyaline material to a greater or lesser degree. The lymph nodes from two of the patients with rheumatoid arthritis contained numerous sarcoid like granulomata, further indicating a possible association between sarcoidosis and rheumatoid arthritis. Pathologists and clinicans should include rheumatoid arthritis and systemic sclerosis in their differential diagnosis of lymph node hyalinisation of unknown aetiology. (J Clin Pathol 1994;47: ) Local or generalised lymphadenopathy may occur in up to 75% of patients with rheumatoid arthritis.' Most commonly the axillary, supraclavicular, and cervical lymph nodes are enlarged, but other lymph node groups may be affected.'2 Lymphadenopathy in systemic sclerosis has not been so well documented. In both these conditions malignant lymphoma may supervene and lymph node biopsy may be undertaken to exclude this.35 Previous publications on node changes in rheumatoid arthritis have commented on the extreme reactive follicular hyperplasia and prominent plasma cell infiltration of the interfollicular areas.' 2 As far as we are aware, lymph node changes have only been reported in one previous necropsy case of systemic sclerosis and the histological findings were of obliteration of the nodal architecture by extensive hyaline fibrosis.6 Methods The clinical summaries stated on the request forms of all lymph nodes submitted to the Royal Victoria Hospital, Belfast, since 1984 were reviewed. Seven patients with rheumatoid arthritis and one with systemic sclerosis were identified. Sections from each node were routinely processed and stained with haematoxylin and eosin, periodic acid Schiff (PAS), Masson trichrome, and the Congo red stain for amyloid. The clinical notes of all eight patients were reviewed. Results CASE REPORTS Cases 1-3 Cases 1, 2, and 3 were a 50 year old man, a 59 year old woman, and a 71 year old woman, respectively. Each had had a five year, 10 year, and long history of seropositive rheumatoid arthritis, respectively. All had multiple joint disease. Case 1 developed bilateral axillary lymphadenopathy and an enlarged lymph node was removed from his right axilla. In case 2 an enlarged node was removed from the right groin, and in case 3 (a patient who developed bilateral axillary and inguinal lymphadenopathy) a node was removed from the right axilla. Histological examination of the excised nodes in all three cases showed essentially similar features. There was a noticeable degree of reactive follicular hyperplasia with lymphoid follicles and germinal centres situated throughout the cortex and medulla of the nodes. Many of these lymphoid follicles showed a "starry-sky" appearance of tingible body macrophages in their germinal centres. In the interfollicular areas there was a mixture of small lymphoid cells, among which were
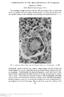
2 Lymph node hyalinisation in rheumatoid arthritis and systemic sclerosis Figure 1 Node showingfollicular hyperplasia with in interfollicular areas (haematoxylin and eosin). Figure 2 Node from case 4 showing extensive replacement by focally calcified eosinophilic hyaline material (haematoxylin and eosin). V '' l ~~~~~~~~~~~~~~~~~M6.t sil :j,~ ~ ~ ~ ~ ~ ~ ~ ~ ~ Figure 3 Node replaced by numerous sarcoid like granulomata with intervening (haematoxylin and eosin). 139 plasma cells in considerable numbers. The interfollicular areas contained focal deposits of which were calcified in case 2 (fig 1). This material gave a positive reaction with the PAS stain and stained green with the Masson trichrome stain. In all three cases the material did not stain with Congo red. Case 4 The patient was a 78 year old man with a long history of rheumatoid arthritis and Felty's syndrome. He had an enlarged lymph node in his right axilla. This was removed. Histological examination showed the node to be extensively replaced by eosinophilic hyaline material which was focally calcified (fig 2). A small amount of residual lymphoid tissue was identified, particularly around the periphery of the node. This was composed mainly of small lymphocytes with occasional scattered plasma cells. No follicular structures were identified. The staining reactions of the were identical with those of the above group (cases 1-3). Cases 5 and 6 These comprised a 50 year old man with a 10 year history of seropositive rheumatoid arthritis, and a 67 year old woman with a long history of seropositive rheumatoid arthritis. Both had multiple joint disease. The patient in case 6 also had autoimmune hypothyroidism, pernicious anaemia, and liver cirrhosis of presumed autoimmune aetiology. In case 5 an enlarged lymph node was removed from the right side of the neck, and in case 6 an enlarged node was removed from the left axilla. Histological examination of the excised nodes in cases 5 and 6 showed similar features. There was extensive replacement of the lymph nodes by numerous well formed sarcoid-like granulomata. These granulomata were composed of epithelioid histiocytes and Langhans' type giant cells. Small central areas of necrosis were present in a few of the granulomata. Plasma cells were identified admixed with small lymphocytes surrounding the granulomata. Between the granulomata, deposits of were present, similar to those described in the previous cases (fig 3). This hyaline material was also PAS positive, stained a green colour with the Masson-trichrome stain, and was Congo red negative. The Ziehl-Neelsen stain for acid fast bacilli was negative in both cases, and fungal organisms were not identified with the PAS stain. A chest x ray picture of case 5 showed bilateral hilar lymphadenopathy, and following the results of the lymph node pathology, the patient underwent a Kveim test which proved positive. After a node biopsy and before further investigation could be undertaken, case 6 died as a result of liver failure. A post mortem examination was not carried out.
3 140 Figure 4 Node from case 8 showing extensive replacement by eosinophilic hyaline material (haematoxylin and eosin). Summary ofclinicalfeatures and lymph node histology Case 7 This was a 62 year old woman with a four year history of seropositive rheumatoid arthritis, mainly affecting her hands. She developed an enlarged lymph node in her right axilla, and the lymph node was biopsied. She also had bilateral subcutaneous swellings on the extensor surfaces of both forearms, which clinically indicated rheumatoid nodules. Histological examination showed a large area of coagulative necrosis within the centre Case No AgelSex Clinicalfindings Lymph node histology 1 50 /M Five year history of rheumatoid Pronounced reactive follicular arthritis. Bilateral axillary hyperplasia. Plasma cells in lymphadenopathy interfollicular areas. Focal deposition of PAS positive 2 59/F 10 year history of rheumatoid Pronounced reactive follicular arthritis. Enlarged node right hyperplasia. Plasma cells in groin interfollicular areas. Focal deposition of calcified PAS positive eosinophilic hyaline material 3 71 /F Long history of rheumatoid Pronounced reactive follicular arthritis. Bilateral axillary and hyperplasia. Plasma cells in inguinal lymphadenopathy interfollicular areas. Focal deposition of PAS positive 4 78 / M Long history of rheumatoid Extensive replacement of node arthritis with Felty's syndrome. by focally calcified PAS Enlarged node right axilla positive eosinophilic hyaline material 5 50 /M 10 year history of rheumatoid Numerous well formed sarcoid artritis. Enlarged right like granulomata. PAS cervical node positive eosinophilic hyaline material between granulomata 6 67/F Long history of rheumatoid Numerous well formed sarcoid arthritis, autoimmune like granulomata. PAS hypothyroidism, pernicious positive eosinophilic hyaline anaemia, cirrhosis. Left axillary material between lymphadenopathy granulomata 7 62 /F Four year history of rheumatoid Large central area of necrosis arthritis. Enlarged nodes right with surrounding palisade of axilla histiocytes. PAS positive 8 39/ M Five year history of systemic Extensive replacement of node sclerosis by PAS positive eosinophilic hyaline material McCluggage, Bharucha of the lymph node, with a surrounding palisade of histiocytes. The remaining lymph node contained a few inactive lymphoid follicles, together with plasma cells and small lymphocytes. Deposits of eosinophillic hyaline material were also identified in interfollicular areas. This material was PAS positive, Congo red negative, and stained a green colour with the Masson-trichrome stain. The Ziehl-Neelsen stain was negative, as was the Warthin-Starry stain for cat scratch bacilli. Fungal organisms were not identified. Investigations performed following the biopsy included serology for toxoplasmosis, Q-fever and infectious mononucleosis. All tests yielded negative results. The lymphadenopathy disappeared and no infective cause was ever found. Case 8 A 39 year old man with a five year history of systemic sclerosis was found to have mediastinal lymphadenopathy on chest x ray. One of these nodes was removed for histological examination. Histological examination showed that the lymph node had been extensively replaced by similar to case 4 (fig 4). Occasional inactive lymphoid follicles were present in parts of the node which were not hyalinised. In contrast to case 4, calcification was not identified in the hyalinised areas. The staining reactions of the hyalinised material were similar to those in the previous cases. The clinical features and histological findings of the excised lymph nodes are summarised in the table. Discussion Localised or generalised lymphadenopathy may be found in up to 75% of patients with rheumatoid arthritis at some stage during the disease process.' In rheumatoid arthritis lymphadenopathy is most common when the symptoms in the joint are active. The most common nodes affected are the axillary, cervical, and supraclavicular groups,' 2 although other lymph nodes may also be enlarged. Lymphadenopathy may be particularly severe in Felty's syndrome (rheumatoid arthritis, splenomegaly, and autoimmune neutropenia) and in juvenile rheumatoid arthritis (Still's disease). As well as lymphadenopathy, patients with rheumatoid arthritis may have associated systemic features such as fever, weight loss, and anaemia. These clinical symptoms may raise the question of a malignant lymphoma, and lymph node biopsy may be undertaken to exclude this diagnosis. The clinical suspicion may be further heightened by the increased incidence of malignant lymphoma previously reported in patients with rheumatoid arthritis.'5 The histological findings reported in excised nodes comprise pronounced follicular hyperplasia with large active germinal centres.' 2 Increased numbers of plasma cells are generally found in interfollicular areas in the medullary cords.
4 Lymph node hyalinisation in rheumatoid arthitis and systemic sclerosis Lymph node changes have been described rarely in patients with systemic sclerosis. As far as we are aware, only one necropsy case has been reported, and the findings were of extensive nodal replacement by hyaline fibrosis.6 Malignant lymphomas have also been described arising in association with systemic sclerosis and so lymph node biopsy may be undertaken to exclude this.4 The histological findings in cases 1, 2, and 3 were of pronounced reactive follicular hyperplasia and prominent plasma cell infiltration of interfollicular areas. These findings were similar to those reported before.' 2 In all three cases there were focal deposits of PAS positive (focally calcified in case 2) in interfollicular areas. Hyaline material may be seen in burnt-out germinal centres in rheumatoid arthritis, and in other conditions where reactive follicular hyperplasia has been followed by involution of lymphoid follicles. As far as we are aware, however, the presence of such material within interfollicular areas in association with reactive follicular hyperplasia has not been commented on in other reviews of lymph node histology in patients with rheumatoid arthritis. In 1946 Poursines and Rochu7 mentioned lymphoid aplasia with pronounced sclerosis of the lymph nodes accompanying longstanding rheumatoid arthritis. They called this "lymph node cirrhosis". The changes they described are similar to those in case 4 in which the excised lymph node was almost totally replaced by focally calcified hyaline material. Similar hyaline material was also seen in cases 5, 6, and 7. In cases 5 and 6, numerous well formed sarcoid-like granulomata were present throughout the substance of the node. There is no doubt that in case 5 the patient also had active sarcoid disease as there was extensive bilateral hilar lymphadenopathy and the patient exhibited a positive Kveim reaction. In case 6 the patient died from hepatic failure soon after the lymph node biopsy and before it could be determined whether he had sarcoidosis. The histological findings of well formed granulomata, however, were certainly suggestive of this diagnosis. Sarcoidosis has many features in common with various autoimmune disease. Several studies have commented on a possible association between sarcoidosis and rheumatoid arthritis.89 The findings in cases 5 and 6 lend further support to the existence of such an association. In case 7, a large central area of necrosis was present in the node, with a surrounding palisade of histiocytes. The histological findings were suggestive of an infective process, but no infective cause was found despite detailed investigation following the lymph node biopsy. The findings also raised the question of a rheumatoid nodule arising in the lymph node, a phenomenon which has been described.'0 The pattern of coagulative necrosis found in this case, however, was not typical of that found in rheumatoid nodules were the necrosis generally has a more 141 basophilic appearance, typical of necrobiotic collagen. In the area of the node which was not affected by this necrotising process the same PAS positive seen in cases 1 to 6 was also present. In all seven cases of rheumatoid arthritis this was negative with Congo red stain for amyloid. Amyloid, of course, may complicate the course of rheumatoid arthritis and has been described in lymph nodes in patients with this condition." The nature of the hyaline material in our cases was unclear. It may represent immunoglobulin which does not have a /Bpleated structure when deposited in tissues, and therefore does not have the staining properties of amyloid. This material might have been produced by the plasma cells, commonly seen in nodes in rheumatoid arthritis and present to a greater or lesser degree in all of our cases examined. Interestingly, similar PAS positive amorphous eosinophilic material may also be seen in lymph nodes in angioimmunoblastic lymphadenopathy with dysproteinaemia (AILD)"2-'4 and in nodes affected by lymphoplasmacytoid lymphomas."5 Again this material may represent immunoglobulin products produced by plasma cells in AILD, and by the lymphoplasmacytoid cells in lymphoplasmacytoid lymphomas. Plasma cells may, of course, be present in large numbers in AILD. Amyloid has also been reported in lymph nodes in occasional cases of AILD.16 Some patients with AILD have a history of an autoimmune disease such as rheumatoid arthritis, although most cases arise de novo. We suggest that this characteristic hyaline material is produced in lymph nodes in cases of rheumatoid arthritis. Plasma cells, which are present in appreciable numbers in interfollicular areas in association with the pronounced reactive follicular hyperplasia seen in cases 1 to 3, were probably responsible. We have not seen such hyaline material in interfollicular areas of nodes showing reactive follicular hyperplasia in association with other conditions. More pronounced changes of extensive fibrosis and calcification (case 4) may occur in later stages of the disease process, in nodes where the reactive hyperplasia has subsided. These changes may lead to a confusing picture which the pathologist could find difficult to interpret. Hyaline material, similar to that which we have described, has been referred to as paraamyloid, and it is not uncommon in advanced stages of inflammatory or neoplastic conditions affecting nodes.'7 The hyaline material found in cases 5 and 6 may simply represent healed sarcoid granulomata, and in case 7 may represent the sequela of a healed infective process which has subsequently become reactivated. Alternatively, the material may have resulted from previous reactive changes and plasmacytosis secondary to the associated rheumatoid arthritis. Extensive lymph node fibrosis has been reported in one previous necropsy case of systemic sclerosis.6 Four visceral nodes
5 142 McCluggage, Bhamcha were examined histologically (one tracheobronchial, two bronchopulmonary, and one mesenteric) and all showed similar features. The findings described are similar to those seen in the mediastinal lymph node in case 8. The aetiology of this fibrosis is unknown, but fibrosis may be found in various other organs in systemic sclerosis. Extensive lymph node hyalinisation is particularly common in the inguinal and iliac group of nodes. These changes may result from longstanding non-specific low grade inflammation. Hyalinisation is also common following inflammatory conditions such as sarcoidosis and tuberculosis, and in association with certain neoplastic diseases such as nodular sclerosing Hodgkin's disease. Occasionally extensive lymph node hyalinisation may be found with no clue as to its possible aetiology. This hyaline material may calcify, in time. We suggest that rheumatoid arthritis and systemic sclerosis should be added to the list of causes of lymph node hyalinisation and calcification, and that pathologists and clinicians should consider these conditions in their differential diagnosis of nodal sclerosis. 1 Motulsky AG, Weinburg S, Saphir 0, Rosenberg E. Lymph nodes in rheumatoid arthritis. Arch Intern Med 1952;90: Nosanchuk JS, Schnitzer B. Follicular hyperplasia in lymph nodes from patients with rheumatoid arthritis: a clinicopathological study. Cancer 1969;24: Porter D, Madhok R, Capell H. Non-Hodgkin's lymphoma in rheumatoid arthritis. Ann Rheum Dis 1991;50: Sugai S. B cell malignant lymphoma in a patient with progressive systemic sclerosis and Sjogren's syndrome. Report of a case and review of the literature. Jpn Jf Med 1985;24: Symmons DPM, Ahern M, Bacon PA, et al. Lymphoproliferative malignancy in rheumatoid arthritis: a study of 20 cases. Ann Rheum Dis 1984;43: Symmers W St C. The Lymphoreticular system. In: System pathology. Vol 2. 2nd edn. Edinburgh: Churchill Livingstone, 1978: Poursines Y, Rochu P. Etude histopathologique des adenopathies dans les rhumatismes articulaires chroniques. Rev Rheum 1946;13: Kucera RF. A possible association of rheumatoid arthritis and sarcoidosis. Chest 1989;95: Fallahi S, Collins RD, Miller RK, Halla JT. Coexistence of rheumatoid arthritis and sarcoidosis: difficulties encountered in the differential diagnosis of common manifestations. J Rheum 1984;l1: Robb-Smith AHT, Taylor CR, eds. Follicular reactions. In: Lymph node biopsy: a diagnostic adas. London: Miller Heyden, 1981: Baggenstoss AH, Rosenberg EF. Visceral lesions associated with chronic infectious (rheumatoid) arthritis. Arch Pathol 1943;35: Neiman RS, Dervan P. Haudenschild C, Jaffe R. Angioimmunoblastic lymphadenopathy: an ultrastructural and immunologic study with review of the literature. Cancer 1978;41: Schnaidt H, Thiele J, Georgii A. Angioimmunoblastic lymphadenopathy. Fine structure of the lymph nodes by correlation of light and electron microscopical findings. Virchows Arch (PatholAnat) 1980;389: Matz LR, Papdimitriou JM, Carroll JR, et al. Angioimmunoblastic lymphadenopathy with dysproteinaemia. Cancer 1977;40: Symmers W St C, ed. Neoplastic Disorders of lymphoreticular tissue. In: Systemic pathology. Vol 7. 3rd edn. Edinburgh: Churchill Livingstone, 1992: Madri JA, Fromowitz F. Amyloid deposition in immunoblastic lymphadenopathy. Hum Pathol 1978;9: Stansfeld AG, d'ardenne AJ, eds. Primary and secondary immune disorders. In: Lymph node biopsy interpretation. 2nd edn. Edinburgh: Churchill Livingstone, 1992: J Clin Pathol: first published as /jcp on 1 February Downloaded from on 12 May 2018 by guest. Protected by copyright.
manifestations are uncommon. Initial descriptions of the disease (Rosai and Dorfman, 1969) specifically
 Postgraduate Medical Journal (July 1980) 56, 521-525 Diffuse cutaneous involvement and sinus histiocytosis with massive lymphadenopathy A. A. WOODCOCK B.Sc., M.B., Ch.B., M.R.C.P. Summary Severe skin involvement
Postgraduate Medical Journal (July 1980) 56, 521-525 Diffuse cutaneous involvement and sinus histiocytosis with massive lymphadenopathy A. A. WOODCOCK B.Sc., M.B., Ch.B., M.R.C.P. Summary Severe skin involvement
A Retrospective Histological Evaluation of Non-neoplastic Superficial Lymphadenopathy
 ISPUB.COM The Internet Journal of Internal Medicine Volume 6 Number 1 A Retrospective Histological Evaluation of Non-neoplastic Superficial Lymphadenopathy S Chhabra, H Mohan, A Bal Citation S Chhabra,
ISPUB.COM The Internet Journal of Internal Medicine Volume 6 Number 1 A Retrospective Histological Evaluation of Non-neoplastic Superficial Lymphadenopathy S Chhabra, H Mohan, A Bal Citation S Chhabra,
A clinicopathological study of nodular sclerosing Hodgkin's disease
 A clinicopathological study of nodular sclerosing Hodgkin's disease R. M. CROSS J. clini. Path. (1968), 21, 0-10 From the Royal Air Force Institute ofpathology and Tropical Medicine, Halton, Buckinghamshire
A clinicopathological study of nodular sclerosing Hodgkin's disease R. M. CROSS J. clini. Path. (1968), 21, 0-10 From the Royal Air Force Institute ofpathology and Tropical Medicine, Halton, Buckinghamshire
FINE NEEDLE ASPIRATION (FNAC) AS A DIAGNOSTIC TOOL IN PAEDIATRIC LYMPHADENOPATHY.
 IJCRR Vol 06 issue 01 Section: Healthcare Category: Research Received on: 16/10/13 Revised on: 18/11/13 Accepted on: 20/12/13 FINE NEEDLE ASPIRATION (FNAC) AS A DIAGNOSTIC TOOL IN PAEDIATRIC Heming Agrawal,
IJCRR Vol 06 issue 01 Section: Healthcare Category: Research Received on: 16/10/13 Revised on: 18/11/13 Accepted on: 20/12/13 FINE NEEDLE ASPIRATION (FNAC) AS A DIAGNOSTIC TOOL IN PAEDIATRIC Heming Agrawal,
Necrotizing and suppurative lymphadenitis in Leishmania
 Tropical Medicine and International Health VOLUME I NO. 2 PP 243-250 APRIL 1996 Necrotizing and suppurative lymphadenitis in Leishmania major infections A. Gaafar r, A. Ismai13, A. Y. El Kadaro4, Elsir
Tropical Medicine and International Health VOLUME I NO. 2 PP 243-250 APRIL 1996 Necrotizing and suppurative lymphadenitis in Leishmania major infections A. Gaafar r, A. Ismai13, A. Y. El Kadaro4, Elsir
Cytopathological Study of Lymph Node Lesions - A 2 Years Retrospective Study
 Original Article Print ISSN: 2321-6379 Online ISSN: 2321-595X DOI: 10.17354/ijss/2018/24 Cytopathological Study of Lymph Node Lesions - A 2 Years Retrospective Study K Florence, K Suresh, K Lavanya Department
Original Article Print ISSN: 2321-6379 Online ISSN: 2321-595X DOI: 10.17354/ijss/2018/24 Cytopathological Study of Lymph Node Lesions - A 2 Years Retrospective Study K Florence, K Suresh, K Lavanya Department
Pathology of Hematopoietic and Lymphoid tissue
 Pathology of Hematopoietic and Lymphoid tissue Peerayut Sitthichaiyakul, M.D. Department of Pathology and Forensic Medicine Faculty of Medicine, Naresuan University CONTENTS White blood cells and lymph
Pathology of Hematopoietic and Lymphoid tissue Peerayut Sitthichaiyakul, M.D. Department of Pathology and Forensic Medicine Faculty of Medicine, Naresuan University CONTENTS White blood cells and lymph
Infections and nonmicrobial inflammatory stimuli can cause leukocytosis (as seen in Lab 1) as well as lymph node enlargement (lymphadenopathy).
 LAB 5: LYMPHOID TISSUE AND SKIN The focus of this week s lab will be pathology of the lymphoid tissue and skin. The lymphoid organs include the thymus, spleen, and lymph nodes. Abnormalities in the lymph
LAB 5: LYMPHOID TISSUE AND SKIN The focus of this week s lab will be pathology of the lymphoid tissue and skin. The lymphoid organs include the thymus, spleen, and lymph nodes. Abnormalities in the lymph
CHRONIC INFLAMMATION
 CHRONIC INFLAMMATION Chronic inflammation is an inflammatory response of prolonged duration often for months, years or even indefinitely. Its prolonged course is proved by persistence of the causative
CHRONIC INFLAMMATION Chronic inflammation is an inflammatory response of prolonged duration often for months, years or even indefinitely. Its prolonged course is proved by persistence of the causative
and plasmacytic type. of the proximal interphalangeal joints, morning on the left forearm, and positive rheumatoid factor.
 Annals of the Rheumatic Diseases, 1989; 48, 326-330 Case report Multicentric Castleman's disease associated with rheumatoid arthritis: a possible role of hepatitis B antigen ELDAD BEN-CHETRIT,1 DANIEL
Annals of the Rheumatic Diseases, 1989; 48, 326-330 Case report Multicentric Castleman's disease associated with rheumatoid arthritis: a possible role of hepatitis B antigen ELDAD BEN-CHETRIT,1 DANIEL
Lymphoma co existing with Tuberculosis granulomatous
 Available online at www.worldscientificnews.com WSN 90 (2017) 265-270 EISSN 2392-2192 SHORT COMMUNICATION Lymphoma co existing with Tuberculosis granulomatous Madeeha Subhan 1, *, Waleed Sadiq 2 1 Ayub
Available online at www.worldscientificnews.com WSN 90 (2017) 265-270 EISSN 2392-2192 SHORT COMMUNICATION Lymphoma co existing with Tuberculosis granulomatous Madeeha Subhan 1, *, Waleed Sadiq 2 1 Ayub
Contents. vii. Preface... Acknowledgments... v xiii
 Contents Preface... Acknowledgments... v xiii SECTION I 1. Introduction... 3 Knowledge-Based Diagnosis... 4 Systematic Examination of the Lymph Node... 7 Cell Type Identification... 9 Cell Size and Cellularity...
Contents Preface... Acknowledgments... v xiii SECTION I 1. Introduction... 3 Knowledge-Based Diagnosis... 4 Systematic Examination of the Lymph Node... 7 Cell Type Identification... 9 Cell Size and Cellularity...
Histopathology: granulomatous inflammation, including tuberculosis
 Histopathology: granulomatous inflammation, including tuberculosis These presentations are to help you identify basic histopathological features. They do not contain the additional factual information
Histopathology: granulomatous inflammation, including tuberculosis These presentations are to help you identify basic histopathological features. They do not contain the additional factual information
HISTOPATHOLOGY. Shannon Martinson
 HISTOPATHOLOGY Shannon Martinson March 2013 Case #1 History: 8 year old beagle Neck pain for the past couple of weeks Paresis, followed by paralysis developed over the past few days Gross Description courtesy
HISTOPATHOLOGY Shannon Martinson March 2013 Case #1 History: 8 year old beagle Neck pain for the past couple of weeks Paresis, followed by paralysis developed over the past few days Gross Description courtesy
MECHANISMS OF HUMAN DISEASE: LABORATORY SESSIONS LYMPHOMA. April 16, 2008
 MECHANISMS OF HUMAN DISEASE: LABORATORY SESSIONS LYMPHOMA April 16, 2008 FACULTY COPY GOAL: Learn the appearance of normal peripheral blood elements and lymph nodes. Recognize abnormal peripheral blood
MECHANISMS OF HUMAN DISEASE: LABORATORY SESSIONS LYMPHOMA April 16, 2008 FACULTY COPY GOAL: Learn the appearance of normal peripheral blood elements and lymph nodes. Recognize abnormal peripheral blood
LYMPHOBLASTOMA OF THE SPLEEN
 LYMPHOBLASTOMA OF THE SPLEEN By ELLIS KELLERT, M.D. (From the Ellis Hospital Laboratory, Schenectady, N. Y.) Several recently reported cases have stimulated interest in a newly described form of the ever
LYMPHOBLASTOMA OF THE SPLEEN By ELLIS KELLERT, M.D. (From the Ellis Hospital Laboratory, Schenectady, N. Y.) Several recently reported cases have stimulated interest in a newly described form of the ever
Case 3. Ann T. Moriarty,MD
 Case 3 Ann T. Moriarty,MD Case 3 59 year old male with asymptomatic cervical lymphadenopathy. These images are from a fine needle biopsy of a left cervical lymph node. Image 1 Papanicolaou Stained smear,100x.
Case 3 Ann T. Moriarty,MD Case 3 59 year old male with asymptomatic cervical lymphadenopathy. These images are from a fine needle biopsy of a left cervical lymph node. Image 1 Papanicolaou Stained smear,100x.
A Descriptive Study of Histopathological Patterns of Lymph Node Biopsies In A Tertiary Care Hospital
 Original Article DOI: 10.21276/APALM.1089 A Descriptive Study of Histopathological Patterns of Lymph Node Biopsies In A Tertiary Care Hospital Rajshri P. Damle*, Kishor H. Suryawanshi, N.V.Dravid, D.V.Newadkar
Original Article DOI: 10.21276/APALM.1089 A Descriptive Study of Histopathological Patterns of Lymph Node Biopsies In A Tertiary Care Hospital Rajshri P. Damle*, Kishor H. Suryawanshi, N.V.Dravid, D.V.Newadkar
Pathology of Hematopoietic and Lymphoid tissue
 CONTENTS Pathology of Hematopoietic and Lymphoid tissue White blood cells and lymph nodes Quantitative disorder of white blood cells Reactive lymphadenopathies Infectious lymphadenitis Tumor metastasis
CONTENTS Pathology of Hematopoietic and Lymphoid tissue White blood cells and lymph nodes Quantitative disorder of white blood cells Reactive lymphadenopathies Infectious lymphadenitis Tumor metastasis
Pathology of the Lymphoid System
 Pathology of the Lymphoid System Learning Objectives: Define lymphadenitis and enumerate its types. Briefly describe the morphological appearance of reactive lymph node. Describe the microscopic picture
Pathology of the Lymphoid System Learning Objectives: Define lymphadenitis and enumerate its types. Briefly describe the morphological appearance of reactive lymph node. Describe the microscopic picture
FOLLICULARITY in LYMPHOMA
 FOLLICULARITY in LYMPHOMA Reactive Follicular Hyperplasia Follicular Hyperplasia irregular follicles Follicular Hyperplasia dark and light zones Light Zone Dark Zone Follicular hyperplasia MIB1 Follicular
FOLLICULARITY in LYMPHOMA Reactive Follicular Hyperplasia Follicular Hyperplasia irregular follicles Follicular Hyperplasia dark and light zones Light Zone Dark Zone Follicular hyperplasia MIB1 Follicular
Lymphoma Read with the experts
 Lymphoma Read with the experts Marc Seltzer, MD Associate Professor of Radiology Geisel School of Medicine at Dartmouth Director, PET-CT Course American College of Radiology Learning Objectives Recognize
Lymphoma Read with the experts Marc Seltzer, MD Associate Professor of Radiology Geisel School of Medicine at Dartmouth Director, PET-CT Course American College of Radiology Learning Objectives Recognize
HENATOLYMPHOID SYSTEM THIRD YEAR MEDICAL STUDENTS- UNIVERSITY OF JORDAN AHMAD T. MANSOUR, MD. Part 1
 HENATOLYMPHOID SYSTEM THIRD YEAR MEDICAL STUDENTS- UNIVERSITY OF JORDAN AHMAD T. MANSOUR, MD Part 1 NONNEOPLASTIC DISEASES OF THE WHITE BLOOD CELLS There are five major types of WBCs in the blood: neutrophils,
HENATOLYMPHOID SYSTEM THIRD YEAR MEDICAL STUDENTS- UNIVERSITY OF JORDAN AHMAD T. MANSOUR, MD Part 1 NONNEOPLASTIC DISEASES OF THE WHITE BLOOD CELLS There are five major types of WBCs in the blood: neutrophils,
11/8/2018 DISCLOSURES. I have NO Conflicts of Interest to Disclose. UTILTY OF DETECTING PATTERNS
 Bharat N. Nathwani, M.D. City of Hope Medical Center Professor, Director of Pathology Consultation Services, 1500 East Duarte Road, Duarte, California, 91010 DISCLOSURES -------------------------------------------------------
Bharat N. Nathwani, M.D. City of Hope Medical Center Professor, Director of Pathology Consultation Services, 1500 East Duarte Road, Duarte, California, 91010 DISCLOSURES -------------------------------------------------------
Normal thyroid tissue
 Thyroid Pathology Overview Normal thyroid tissue Normal thyroid tissue with follicles filled with colloid. Thyroid cells form follicles, spheres of epithelial cells (always single layered in health, usually
Thyroid Pathology Overview Normal thyroid tissue Normal thyroid tissue with follicles filled with colloid. Thyroid cells form follicles, spheres of epithelial cells (always single layered in health, usually
PROBABLE HODGKIN'S DISEASE IN A DOG: REPORT OF A CASE 1
 PROBABLE HODGKIN'S DISEASE IN A DOG: REPORT OF A CASE 1 LEONARD K. STALKER, M.D. Fellow in Surgery, The Mayo Foundation CARL F. SCHLOTTHAUER, D.V.M. AND WILLIAM H. FELDMAN, D.V.M., M.S. Division of Experimental
PROBABLE HODGKIN'S DISEASE IN A DOG: REPORT OF A CASE 1 LEONARD K. STALKER, M.D. Fellow in Surgery, The Mayo Foundation CARL F. SCHLOTTHAUER, D.V.M. AND WILLIAM H. FELDMAN, D.V.M., M.S. Division of Experimental
Perifollicular granulomatous inflammation in reactive lymph nodes: a possible morphologic marker for IgG4 plasmacytosis
 J Hematopathol (2011) 4:207 214 DOI 10.1007/s12308-011-0117-5 ORIGINAL ARTICLE Perifollicular granulomatous inflammation in reactive lymph nodes: a possible morphologic marker for IgG4 plasmacytosis Imran
J Hematopathol (2011) 4:207 214 DOI 10.1007/s12308-011-0117-5 ORIGINAL ARTICLE Perifollicular granulomatous inflammation in reactive lymph nodes: a possible morphologic marker for IgG4 plasmacytosis Imran
, , 2011 HODGKIN LYMPHOMA
 European Federation of Cytology Societies 4tu Annual Tutorial in Cytopathology Trieste, June 6-10, 2011 HODGKIN LYMPHOMA Classification The World Health Organization Classification of Lymphomas (2001)
European Federation of Cytology Societies 4tu Annual Tutorial in Cytopathology Trieste, June 6-10, 2011 HODGKIN LYMPHOMA Classification The World Health Organization Classification of Lymphomas (2001)
Radiology- Pathology Conference 4/29/2012. Lymph Nodes. John McGrath
 Radiology- Pathology Conference 4/29/2012 Lymph Nodes John McGrath 1 Presentation material is for education purposes only. All rights reserved. 2012 URMC Radiology Page 1 of 24 Case 1: 51 year-old male
Radiology- Pathology Conference 4/29/2012 Lymph Nodes John McGrath 1 Presentation material is for education purposes only. All rights reserved. 2012 URMC Radiology Page 1 of 24 Case 1: 51 year-old male
Pathology lab 4 DONE BY : MORAD ABU QAMAR
 Pathology lab 4 DONE BY : MORAD ABU QAMAR Chronic interstitial inflammation, lung Certain etiologic agents such as viruses are more likely to lead to chronic inflammation, as seen here in the lung of a
Pathology lab 4 DONE BY : MORAD ABU QAMAR Chronic interstitial inflammation, lung Certain etiologic agents such as viruses are more likely to lead to chronic inflammation, as seen here in the lung of a
Abstracting Hematopoietic Neoplasms
 CASE 1: LYMPHOMA PHYSICAL EXAMINATION 43yo male with a history of lower gastrointestinal bleeding and melena undergoing colonoscopy and biopsy to rule out neoplasm versus inflammation. Patient had no other
CASE 1: LYMPHOMA PHYSICAL EXAMINATION 43yo male with a history of lower gastrointestinal bleeding and melena undergoing colonoscopy and biopsy to rule out neoplasm versus inflammation. Patient had no other
ACHIEVING EXCELLENCE IN ABSTRACTING: LYMPHOMA
 ACHIEVING EXCELLENCE IN ABSTRACTING: LYMPHOMA ACHIEVING EXCELLENCE IN ABSTRACTING LYMPHOMA Recoding Audit Performed in 2009 260 cases audited 17 data items audited per case 4420 possible discrepancies
ACHIEVING EXCELLENCE IN ABSTRACTING: LYMPHOMA ACHIEVING EXCELLENCE IN ABSTRACTING LYMPHOMA Recoding Audit Performed in 2009 260 cases audited 17 data items audited per case 4420 possible discrepancies
Osteosclerotic Myeloma (POEMS Syndrome)
 Osteosclerotic Myeloma (POEMS Syndrome) Osteosclerotic Myeloma (POEMS Syndrome) Synonyms Crow-Fukase syndrome Multicentric Castleman disease Takatsuki syndrome Acronym coined by Bardwick POEMS Scheinker,
Osteosclerotic Myeloma (POEMS Syndrome) Osteosclerotic Myeloma (POEMS Syndrome) Synonyms Crow-Fukase syndrome Multicentric Castleman disease Takatsuki syndrome Acronym coined by Bardwick POEMS Scheinker,
In our paper, we suggest that tuberculosis and sarcoidosis are two ends of the same spectrum. Given the pathophysiological and clinical link between
 In our paper, we suggest that tuberculosis and sarcoidosis are two ends of the same spectrum. Given the pathophysiological and clinical link between the two, we also propose a classification system for
In our paper, we suggest that tuberculosis and sarcoidosis are two ends of the same spectrum. Given the pathophysiological and clinical link between the two, we also propose a classification system for
Diagnosis and patient pathway in lymphomas
 The Royal Marsden Diagnosis and patient pathway in lymphomas Dr Ian Chau Consultant Medical Oncologist The Royal Marsden Hospital London & Surrey Change Presentation title and date in Footer dd.mm.yyyy
The Royal Marsden Diagnosis and patient pathway in lymphomas Dr Ian Chau Consultant Medical Oncologist The Royal Marsden Hospital London & Surrey Change Presentation title and date in Footer dd.mm.yyyy
Hepatic vein lesions in alcoholic liver disease:
 Hepatic vein lesions in alcoholic liver disease: retrospective biopsy and necropsy study AD BURT, RNM MacSWEEN University Department of Pathology Western Infirmary, Glasgow J Clin Pathol 1986;39:63-67
Hepatic vein lesions in alcoholic liver disease: retrospective biopsy and necropsy study AD BURT, RNM MacSWEEN University Department of Pathology Western Infirmary, Glasgow J Clin Pathol 1986;39:63-67
Dr Rodney Itaki Lecturer Anatomical Pathology Discipline
 Lymphoid Neoplasia & Hodgkin s Disease Dr Rodney Itaki Lecturer Anatomical Pathology Discipline Lymphomas Are neoplasms of lymphoid cells. Classified as: Hodgkin Disease (30%) Non-Hodgkin lymphoma (70%).
Lymphoid Neoplasia & Hodgkin s Disease Dr Rodney Itaki Lecturer Anatomical Pathology Discipline Lymphomas Are neoplasms of lymphoid cells. Classified as: Hodgkin Disease (30%) Non-Hodgkin lymphoma (70%).
HISTOPATHOLOGIC FINDINGS OF LYMPH NODE BIOPSY CASES IN COMPARISON WITH CLINICAL FEATURES
 Original Article HISTOPATHOLOGIC FINDINGS OF LYMPH NODE BIOPSY CASES IN COMPARISON WITH CLINICAL FEATURES Shokouh Taghipour Zahir 1, Alireza Azimi 2 ABSTRACT Objective: To determine useful and important
Original Article HISTOPATHOLOGIC FINDINGS OF LYMPH NODE BIOPSY CASES IN COMPARISON WITH CLINICAL FEATURES Shokouh Taghipour Zahir 1, Alireza Azimi 2 ABSTRACT Objective: To determine useful and important
NON-SPECIFIC REACTIVE HYPERPIASIA OF CERVICAL LYMPH NODES: A FOLLOW-UP
 NON-SPECIFIC REACTIVE HYPERPIASIA OF CERVICAL LYMPH NODES: A FOLLOW-UP ABSTRACT Pages with reference to book, From 237 To 238 Ijaz Ahmad ( Department of Surgery, K.E. Medical College, Lahore. ) Non-specific
NON-SPECIFIC REACTIVE HYPERPIASIA OF CERVICAL LYMPH NODES: A FOLLOW-UP ABSTRACT Pages with reference to book, From 237 To 238 Ijaz Ahmad ( Department of Surgery, K.E. Medical College, Lahore. ) Non-specific
Diagnostic Value of EBUS-TBNA in Various Lung Diseases (Lymphoma, Tuberculosis, Sarcoidosis)
 Diagnostic Value of EBUS-TBNA in Various Lung Diseases (Lymphoma, Tuberculosis, Sarcoidosis) Sevda Sener Cömert, MD, FCCP. SBU, Kartal Dr.Lütfi Kırdar Training and Research Hospital Department of Pulmonary
Diagnostic Value of EBUS-TBNA in Various Lung Diseases (Lymphoma, Tuberculosis, Sarcoidosis) Sevda Sener Cömert, MD, FCCP. SBU, Kartal Dr.Lütfi Kırdar Training and Research Hospital Department of Pulmonary
Mimics of Lymphoma in Routine Biopsies. Mixed follicular and paracortical hyperplasia. Types of Lymphoid Hyperplasia
 Mimics of Lymphoma in Routine Biopsies Patrick Treseler, MD, PhD Professor of Pathology University of California San Francisco Types of Lymphoid Hyperplasia Follicular hyperplasia (B-cells) Paracortical
Mimics of Lymphoma in Routine Biopsies Patrick Treseler, MD, PhD Professor of Pathology University of California San Francisco Types of Lymphoid Hyperplasia Follicular hyperplasia (B-cells) Paracortical
Glistening, Skin-Colored Nodule
 To Print: Click your browser's PRINT button. NOTE: To view the article with Web enhancements, go to: http://www.medscape.com/viewarticle/436334 Medscape Dermatology Clinic Glistening, Skin-Colored Nodule
To Print: Click your browser's PRINT button. NOTE: To view the article with Web enhancements, go to: http://www.medscape.com/viewarticle/436334 Medscape Dermatology Clinic Glistening, Skin-Colored Nodule
Mimics of Lymphoma in Routine Biopsies. I have nothing to disclose regarding the information to be reported in this talk.
 Mimics of Lymphoma in Routine Biopsies Patrick Treseler, MD, PhD Professor of Pathology University of California San Francisco I have nothing to disclose regarding the information to be reported in this
Mimics of Lymphoma in Routine Biopsies Patrick Treseler, MD, PhD Professor of Pathology University of California San Francisco I have nothing to disclose regarding the information to be reported in this
( Rosai Dorfman disease)
 Sinus histiocytosis with massive lymphadenopathy ( Rosai Dorfman disease) BIBI SHAIN SHAMSIAN Rosai Dorfman disease Rosai-Dorfman Disease (RDD) or Sinus Histiocytosis with massive lymhadenopathy (SHML):
Sinus histiocytosis with massive lymphadenopathy ( Rosai Dorfman disease) BIBI SHAIN SHAMSIAN Rosai Dorfman disease Rosai-Dorfman Disease (RDD) or Sinus Histiocytosis with massive lymhadenopathy (SHML):
number Done by Corrected by Doctor Mousa Al-Abbadi
 number 11 Done by Husam Abu-Awad Corrected by Muhammad Tarabieh Doctor Mousa Al-Abbadi The possible outcomes of an acute inflammation are the following: 1- A complete resolution in which the tissue returns
number 11 Done by Husam Abu-Awad Corrected by Muhammad Tarabieh Doctor Mousa Al-Abbadi The possible outcomes of an acute inflammation are the following: 1- A complete resolution in which the tissue returns
Among the benign intraepithelial melanocytic proliferations, Inflamed Conjunctival Nevi. Histopathological Criteria. Resident Short Reviews
 Resident Short Reviews Inflamed conjunctival nevi (ICN) may suggest malignancy because of their rapid growth and atypical histology. The objective of this study was to characterize the diagnostic features
Resident Short Reviews Inflamed conjunctival nevi (ICN) may suggest malignancy because of their rapid growth and atypical histology. The objective of this study was to characterize the diagnostic features
A Rare case of Tubercular Gingivitis Case Report
 Case Report A Rare case of Tubercular Gingivitis Case Report *Dr. Ansh Chugh 1, Dr. Firoz A Hakkim 2, Dr. Rajesh. V 3, Dr. Raghava Sharma 4 1: JUNIOR RESIDENT IN GENERAL MEDICINE 2: SENIOR RESIDENT IN
Case Report A Rare case of Tubercular Gingivitis Case Report *Dr. Ansh Chugh 1, Dr. Firoz A Hakkim 2, Dr. Rajesh. V 3, Dr. Raghava Sharma 4 1: JUNIOR RESIDENT IN GENERAL MEDICINE 2: SENIOR RESIDENT IN
Dr Vidya Devarajan DNB(Gen Med),FNB(ID), Fellowship ID,SCE (UK) Consultant ID Apollo Cancer Hospital
 Dr Vidya Devarajan DNB(Gen Med),FNB(ID), Fellowship ID,SCE (UK) Consultant ID Apollo Cancer Hospital Knowledge of nodal distribution and anatomic drainage Provide an approach to the patient with peripheral
Dr Vidya Devarajan DNB(Gen Med),FNB(ID), Fellowship ID,SCE (UK) Consultant ID Apollo Cancer Hospital Knowledge of nodal distribution and anatomic drainage Provide an approach to the patient with peripheral
J of Evolution of Med and Dent Sci/ eissn , pissn / Vol. 3/ Issue 37/Aug 21, 2014 Page 9580
 THE SPECTRUM OF CERVICAL LYMPHADENOPATHY IN CHILDREN: A STUDY IN RURAL NORTH INDIA Pawan Tiwari 1, Satya Kiran Kapoor 2, Madhu Tiwari 3, Yogesh Yadav 4 HOW TO CITE THIS ARTICLE: Pawan Tiwari, Satya Kiran
THE SPECTRUM OF CERVICAL LYMPHADENOPATHY IN CHILDREN: A STUDY IN RURAL NORTH INDIA Pawan Tiwari 1, Satya Kiran Kapoor 2, Madhu Tiwari 3, Yogesh Yadav 4 HOW TO CITE THIS ARTICLE: Pawan Tiwari, Satya Kiran
Pattern of lymph node pathology in a private pathology laboratory
 Malaysian J Parhol1999; 21(2): 87-93 Pattern of lymph node pathology in a private pathology laboratory LH KIM, BSc (Biomedical), SC PEH, MBBS, FRCPath, *K S CHAN, MBBS, MPath and SP CHAI, BSc (Biomedical)
Malaysian J Parhol1999; 21(2): 87-93 Pattern of lymph node pathology in a private pathology laboratory LH KIM, BSc (Biomedical), SC PEH, MBBS, FRCPath, *K S CHAN, MBBS, MPath and SP CHAI, BSc (Biomedical)
Hematopathology Lab. Third year medical students
 Hematopathology Lab Third year medical students Objectives Identify the lesion Know the specific name of the lesion Know associated disease Know relevant pathologic background Spherocytes: appear small,
Hematopathology Lab Third year medical students Objectives Identify the lesion Know the specific name of the lesion Know associated disease Know relevant pathologic background Spherocytes: appear small,
Clinicopathologic Self- Assessment S003 AAD 2017
 Clinicopathologic Self- Assessment S003 AAD 2017 Clay J. Cockerell, M.D. Director, Cockerell Dermatopathology Director, Division of Dermatopathology UT Southwestern Medical Center July 2017 No relevant
Clinicopathologic Self- Assessment S003 AAD 2017 Clay J. Cockerell, M.D. Director, Cockerell Dermatopathology Director, Division of Dermatopathology UT Southwestern Medical Center July 2017 No relevant
CONTRIBUTION TO THE HISTOPATHOLOGY OF FILARIASIS
 CONTRIBUTION TO THE HISTOPATHOLOGY OF FILARIASIS PHILIP H. HARTZ Public Health Service, Curacao, N.W.I. The histologic changes caused by filariasis (Wucheria Bancrofti) are considered to be non-specific
CONTRIBUTION TO THE HISTOPATHOLOGY OF FILARIASIS PHILIP H. HARTZ Public Health Service, Curacao, N.W.I. The histologic changes caused by filariasis (Wucheria Bancrofti) are considered to be non-specific
Non-Hodgkin lymphomas (NHLs) Hodgkin lymphoma )HL)
 Non-Hodgkin lymphomas (NHLs) Hodgkin lymphoma )HL) Lymphoid Neoplasms: 1- non-hodgkin lymphomas (NHLs) 2- Hodgkin lymphoma 3- plasma cell neoplasms Non-Hodgkin lymphomas (NHLs) Acute Lymphoblastic Leukemia/Lymphoma
Non-Hodgkin lymphomas (NHLs) Hodgkin lymphoma )HL) Lymphoid Neoplasms: 1- non-hodgkin lymphomas (NHLs) 2- Hodgkin lymphoma 3- plasma cell neoplasms Non-Hodgkin lymphomas (NHLs) Acute Lymphoblastic Leukemia/Lymphoma
Differential Diagnosis in Conventional Radiology
 Differential Diagnosis in Conventional Radiology Bearbeitet von Francis A. Burgener, Martti Kormano, Tomi Pudas Neuausgabe 2007. Buch. 872 S. Hardcover ISBN 978 3 13 656103 4 Format (B x L): 21 x 29,7
Differential Diagnosis in Conventional Radiology Bearbeitet von Francis A. Burgener, Martti Kormano, Tomi Pudas Neuausgabe 2007. Buch. 872 S. Hardcover ISBN 978 3 13 656103 4 Format (B x L): 21 x 29,7
Differential cell counts in the histiocytic variant of lymphocytic predominance subtype of Hodgkin's
 Journal of Clinical Pathology, 1978, 31, 1234-1238 Differential cell counts in the histiocytic variant of lymphocytic predominance subtype of Hodgkin's disease FIONA I. SUTHERLAND, J. B. MAcGILLIVRAY,
Journal of Clinical Pathology, 1978, 31, 1234-1238 Differential cell counts in the histiocytic variant of lymphocytic predominance subtype of Hodgkin's disease FIONA I. SUTHERLAND, J. B. MAcGILLIVRAY,
Atypical Palisaded Myofibroblastoma of Lymph Node: Report of a rare case.
 ISPUB.COM The Internet Journal of Pathology Volume 10 Number 1 Atypical Palisaded Myofibroblastoma of Lymph Node: Report of a rare case. V Kinnera, R Nandyala, M Yootla, K Mandyam Citation V Kinnera, R
ISPUB.COM The Internet Journal of Pathology Volume 10 Number 1 Atypical Palisaded Myofibroblastoma of Lymph Node: Report of a rare case. V Kinnera, R Nandyala, M Yootla, K Mandyam Citation V Kinnera, R
Arthritis and Rosai-Dorfman Disease of the Skin: A Diagnostic Dilemma
 Arthritis and Rosai-Dorfman Disease of the Skin: A Diagnostic Dilemma Introduction Pages with reference to book, From 280 To 282 Irshad Nabi Soomro ( Department of Pathology, The Aga Khan University Hospital,
Arthritis and Rosai-Dorfman Disease of the Skin: A Diagnostic Dilemma Introduction Pages with reference to book, From 280 To 282 Irshad Nabi Soomro ( Department of Pathology, The Aga Khan University Hospital,
Pulmonary Sarcoidosis - Radiological Evaluation
 Original Research Article Pulmonary Sarcoidosis - Radiological Evaluation Jayesh Shah 1, Darshan Shah 2*, C. Raychaudhuri 3 1 Associate Professor, 2 1 st Year Resident, 3 Professor and HOD Radiology Department,
Original Research Article Pulmonary Sarcoidosis - Radiological Evaluation Jayesh Shah 1, Darshan Shah 2*, C. Raychaudhuri 3 1 Associate Professor, 2 1 st Year Resident, 3 Professor and HOD Radiology Department,
Diagnosis of lymphadenopathies by FNAC: a prospective study
 Original article: Diagnosis of lymphadenopathies by FNAC: a prospective study Dr. Kandukuri Mahesh Kumar, Dr. Chinthakindi Sravan, Dr. Swarupa Ravuri, Dr. Divyagna Department of Pathology, Malla Reddy
Original article: Diagnosis of lymphadenopathies by FNAC: a prospective study Dr. Kandukuri Mahesh Kumar, Dr. Chinthakindi Sravan, Dr. Swarupa Ravuri, Dr. Divyagna Department of Pathology, Malla Reddy
An Introduction to Radiology for TB Nurses
 An Introduction to Radiology for TB Nurses Garold O. Minns, MD September 14, 2017 TB Nurse Case Management September 12 14, 2017 EXCELLENCE EXPERTISE INNOVATION Garold O. Minns, MD has the following disclosures
An Introduction to Radiology for TB Nurses Garold O. Minns, MD September 14, 2017 TB Nurse Case Management September 12 14, 2017 EXCELLENCE EXPERTISE INNOVATION Garold O. Minns, MD has the following disclosures
Pathology of the Lymphoid System
 Pathology of the Lymphoid System Learning Objectives: Define lymphadenitis and enumerate its types. Briefly describe the morphological appearance of reactive lymph node. Describe the microscopic picture
Pathology of the Lymphoid System Learning Objectives: Define lymphadenitis and enumerate its types. Briefly describe the morphological appearance of reactive lymph node. Describe the microscopic picture
Case Report Pulmonary Sarcoidosis following Etanercept Treatment
 Case Reports in Rheumatology Volume 2012, Article ID 724013, 4 pages doi:10.1155/2012/724013 Case Report Pulmonary Sarcoidosis following Etanercept Treatment Kuljeet Bhamra and Richard Stevens Department
Case Reports in Rheumatology Volume 2012, Article ID 724013, 4 pages doi:10.1155/2012/724013 Case Report Pulmonary Sarcoidosis following Etanercept Treatment Kuljeet Bhamra and Richard Stevens Department
New lung lesion in a 55 year-old male treated with chemoradiation for non-small cell lung carcinoma
 July 2016 New lung lesion in a 55 year-old male treated with chemoradiation for non-small cell lung carcinoma Contributed by: Laurel Rose, MD, Resident Physician, Indiana University School of Medicine,
July 2016 New lung lesion in a 55 year-old male treated with chemoradiation for non-small cell lung carcinoma Contributed by: Laurel Rose, MD, Resident Physician, Indiana University School of Medicine,
LYMPHOMA Joginder Singh, MD Medical Oncologist, Mercy Cancer Center
 LYMPHOMA Joginder Singh, MD Medical Oncologist, Mercy Cancer Center Lymphoma is cancer of the lymphatic system. The lymphatic system is made up of organs all over the body that make up and store cells
LYMPHOMA Joginder Singh, MD Medical Oncologist, Mercy Cancer Center Lymphoma is cancer of the lymphatic system. The lymphatic system is made up of organs all over the body that make up and store cells
Lymphatic System Disorders
 Lymphatic System Disorders Lymphomas Malignant neoplasms involving lymphocyte proliferation in lymph nodes Specific causes not identified // Higher risk in adults who received radiation during childhood
Lymphatic System Disorders Lymphomas Malignant neoplasms involving lymphocyte proliferation in lymph nodes Specific causes not identified // Higher risk in adults who received radiation during childhood
Incidence. Bimodal age incidence 15-40, >55 years Childhood form (0-14) more common in developing countries M:F=1.5:1; in all subtypes except NS
 Hodgkin Lymphoma Hodgkin Lymphoma 30% of all lymphomas Absolute incidence unchanged Arise in lymph node, cervical region Neoplastic tissues usually contain a small number of tumor cells Incidence Bimodal
Hodgkin Lymphoma Hodgkin Lymphoma 30% of all lymphomas Absolute incidence unchanged Arise in lymph node, cervical region Neoplastic tissues usually contain a small number of tumor cells Incidence Bimodal
ISPUB.COM. A Kochhar, G Duggal, K Singh, S Kochhar INTRODUCTION MATERIAL AND METHOD
 ISPUB.COM The Internet Journal of Pathology Volume 13 Number 2 Spectrum Of Cytological Findings In Patients With Lymphadenopathy In Rural Population Of Southern A Kochhar, G Duggal, K Singh, S Kochhar
ISPUB.COM The Internet Journal of Pathology Volume 13 Number 2 Spectrum Of Cytological Findings In Patients With Lymphadenopathy In Rural Population Of Southern A Kochhar, G Duggal, K Singh, S Kochhar
Figure 2: Lymph node Cortical follicular (F) and paracortical (PC) atrophy, with narrowing of the cortex relative to the medulla (M).
 Figure 1: Lymph node Follicular hyperplasia, with expansion of the follicular germinal centres (F) by large blast cells. Paracortical hyperplasia, with expansion of the paracortex (PC) by small lymphocytes.
Figure 1: Lymph node Follicular hyperplasia, with expansion of the follicular germinal centres (F) by large blast cells. Paracortical hyperplasia, with expansion of the paracortex (PC) by small lymphocytes.
Histopathological findings in 29 lymph node biopsies with increased IgG4 plasma cells
 480 & 2012 USCAP, Inc. All rights reserved 0893-3952/12 $32.00 Histopathological findings in 29 lymph node biopsies with increased IgG4 plasma cells Kate E Grimm 1, Todd S Barry 1, Vladislav Chizhevsky
480 & 2012 USCAP, Inc. All rights reserved 0893-3952/12 $32.00 Histopathological findings in 29 lymph node biopsies with increased IgG4 plasma cells Kate E Grimm 1, Todd S Barry 1, Vladislav Chizhevsky
Lymphoma: What You Need to Know. Richard van der Jagt MD, FRCPC
 Lymphoma: What You Need to Know Richard van der Jagt MD, FRCPC Overview Concepts, classification, biology Epidemiology Clinical presentation Diagnosis Staging Three important types of lymphoma Conceptualizing
Lymphoma: What You Need to Know Richard van der Jagt MD, FRCPC Overview Concepts, classification, biology Epidemiology Clinical presentation Diagnosis Staging Three important types of lymphoma Conceptualizing
Histological features of the nephrotic syndrome
 J. clin. Path. (1967), 2, 117 Histological features of the nephrotic syndrome associated with quartan malaria J. W. KIBUKAMUSOKE AND M. S. R. HUTT From the Makerere University College Medical School and
J. clin. Path. (1967), 2, 117 Histological features of the nephrotic syndrome associated with quartan malaria J. W. KIBUKAMUSOKE AND M. S. R. HUTT From the Makerere University College Medical School and
Peripheral mycobacterial lymphadenitis (TB, NTM and BCG)
 Peripheral mycobacterial lymphadenitis (TB, NTM and BCG) H Simon Schaaf Desmond Tutu TB Centre, Department of Paediatrics and Child Health, Stellenbosch University, Cape Town, South Africa Questions Peripheral
Peripheral mycobacterial lymphadenitis (TB, NTM and BCG) H Simon Schaaf Desmond Tutu TB Centre, Department of Paediatrics and Child Health, Stellenbosch University, Cape Town, South Africa Questions Peripheral
88-year-old Female with Lymphadenopathy. Faizi Ali, MD
 88-year-old Female with Lymphadenopathy Faizi Ali, MD Clinical History A 88-year-old caucasian female presented to our hospital with the complaints of nausea, vomiting,diarrhea, shortness of breath and
88-year-old Female with Lymphadenopathy Faizi Ali, MD Clinical History A 88-year-old caucasian female presented to our hospital with the complaints of nausea, vomiting,diarrhea, shortness of breath and
Bone Marrow Involvement in Malignant Lymphomas (Non-Hodgkin ' s) Eman Sadiq Jalal MSc
 MSc Abstract: Background: Bone marrow biopsies are taken routinely in the initial investigation of patients with non-hodgkin, s lymphomas to estimate the progression of disease at time of presentation
MSc Abstract: Background: Bone marrow biopsies are taken routinely in the initial investigation of patients with non-hodgkin, s lymphomas to estimate the progression of disease at time of presentation
Lipid content of malignant lymphomas
 J. clin. Path. (1968), 1, 6-69 Lipid content of malignant lymphomas D. H. WRIGHT1 From Makerere University College Medical School, Kampala, Uganda SYNOPSIS Lipid staining, using oil red 0 and Sudan black
J. clin. Path. (1968), 1, 6-69 Lipid content of malignant lymphomas D. H. WRIGHT1 From Makerere University College Medical School, Kampala, Uganda SYNOPSIS Lipid staining, using oil red 0 and Sudan black
Distribution of malignant lymphoid cells
 J. clin. Path., 32, Suppl. (Roy. Coll. Path.), 13, 70-75 Distribution of malignant lymphoid cells R. I. VANHEGAN From the University of Oxford, Pathology Department, Radcliffe Infirmary, Oxford About two-thirds
J. clin. Path., 32, Suppl. (Roy. Coll. Path.), 13, 70-75 Distribution of malignant lymphoid cells R. I. VANHEGAN From the University of Oxford, Pathology Department, Radcliffe Infirmary, Oxford About two-thirds
Case Report CT Findings of Axillary Tuberculosis Lymphadenitis: A Case Detected by Breast Cancer Screening Examination
 Hindawi Publishing Corporation Case Reports in Radiology Volume 2016, Article ID 9016517, 5 pages http://dx.doi.org/10.1155/2016/9016517 Case Report CT Findings of Axillary Tuberculosis Lymphadenitis:
Hindawi Publishing Corporation Case Reports in Radiology Volume 2016, Article ID 9016517, 5 pages http://dx.doi.org/10.1155/2016/9016517 Case Report CT Findings of Axillary Tuberculosis Lymphadenitis:
encapsulated thyroid nodule with a follicular architecture and some form of atypia. The problem is when to diagnose
 Histological Spectrum of Papillary Carcinoma of Thyroid A Two Years Study Gomathi Srinivasan 1, M. Vennila 2 1 Associate Professor Pathology, Government Medical College, Omandurar Estate, Chennai 600 002
Histological Spectrum of Papillary Carcinoma of Thyroid A Two Years Study Gomathi Srinivasan 1, M. Vennila 2 1 Associate Professor Pathology, Government Medical College, Omandurar Estate, Chennai 600 002
Benign, Reactive and Inflammatory Lesions of the Breast
 Benign, Reactive and Inflammatory Lesions of the Breast Marilin Rosa, MD Associate Member Section Head of Breast Pathology Department of Anatomic Pathology Program Director, Breast Pathology Fellowship
Benign, Reactive and Inflammatory Lesions of the Breast Marilin Rosa, MD Associate Member Section Head of Breast Pathology Department of Anatomic Pathology Program Director, Breast Pathology Fellowship
HISTOLOGIC PATTERN OF LYMPH NODE BIOPSIES IN A TERTIARY HOSPITAL IN SOUTH EASTERN NIGERIA.
 HISTOLOGIC PATTERN OF LYMPH NODE BIOPSIES IN A TERTIARY HOSPITAL IN SOUTH EASTERN NIGERIA. MBATA G. C. 1,3, NWEKE IG 2, EGEJURU RO 2, OMEJUA EG 1, NWAKO OF 1, CHIMA E I 3. INTRODUCTION Lymphadenopathy
HISTOLOGIC PATTERN OF LYMPH NODE BIOPSIES IN A TERTIARY HOSPITAL IN SOUTH EASTERN NIGERIA. MBATA G. C. 1,3, NWEKE IG 2, EGEJURU RO 2, OMEJUA EG 1, NWAKO OF 1, CHIMA E I 3. INTRODUCTION Lymphadenopathy
22 year old QH mare with regionally extensive alopecia and scaling on one front limb and ventral chest (Figure 1 and 2).
 22 year old QH mare with regionally extensive alopecia and scaling on one front limb and ventral chest (Figure 1 and 2). Which of the following is the most likely disease? a. Sterile granuloma complex
22 year old QH mare with regionally extensive alopecia and scaling on one front limb and ventral chest (Figure 1 and 2). Which of the following is the most likely disease? a. Sterile granuloma complex
SYNDROME) BY. these instances they are considered as possibly " rheumatoid " in origin. The inflammation was
 Thorax (1955), 10, 9. PATHOLOGICAL STUDIES OF MODIFIED PNEUMOCONIOSIS IN COAL-MINERS WITH RHEUMATOID ARTHRITIS (CAPLAN'S SYNDROME) BY J. GOUGH, D. RIVERS, AND R. M. E. SEAL From the Department of Pathology
Thorax (1955), 10, 9. PATHOLOGICAL STUDIES OF MODIFIED PNEUMOCONIOSIS IN COAL-MINERS WITH RHEUMATOID ARTHRITIS (CAPLAN'S SYNDROME) BY J. GOUGH, D. RIVERS, AND R. M. E. SEAL From the Department of Pathology
Tuberculosis. By: Shefaa Q aqa
 Tuberculosis By: Shefaa Q aqa Tuberculosis is a communicable chronic granulomatous disease caused by Mycobacterium tuberculosis. It usually involves the lungs but may affect any organ or tissue in the
Tuberculosis By: Shefaa Q aqa Tuberculosis is a communicable chronic granulomatous disease caused by Mycobacterium tuberculosis. It usually involves the lungs but may affect any organ or tissue in the
PROFILE OF PAEDIATRIC PATIENTS WITH CERVICAL LYMPHADENOPATHY: A STUDY FROM CENTRAL INDIA Jharna Mishra 1, M. Maheshwari 2, Roshan Chanchlani 3
 PROFILE OF PAEDIATRIC PATIENTS WITH CERVICAL LYMPHADENOPATHY: A STUDY FROM CENTRAL INDIA Jharna Mishra 1, M. Maheshwari 2, Roshan Chanchlani 3 HOW TO CITE THIS ARTICLE: Jharna Mishra, M. Maheshwari, Roshan
PROFILE OF PAEDIATRIC PATIENTS WITH CERVICAL LYMPHADENOPATHY: A STUDY FROM CENTRAL INDIA Jharna Mishra 1, M. Maheshwari 2, Roshan Chanchlani 3 HOW TO CITE THIS ARTICLE: Jharna Mishra, M. Maheshwari, Roshan
Amyloid-like Pulmonary Nodules, Including Localized Light-Chain Deposition Clinicopathologic Analysis of Three Cases
 Anatomic Pathology / AMYLOID-LIKE PULMONARY NODULES Amyloid-like Pulmonary Nodules, Including Localized Light-Chain Deposition Clinicopathologic Analysis of Three Cases Andras Khoor, MD, 1 Jeffrey L. Myers,
Anatomic Pathology / AMYLOID-LIKE PULMONARY NODULES Amyloid-like Pulmonary Nodules, Including Localized Light-Chain Deposition Clinicopathologic Analysis of Three Cases Andras Khoor, MD, 1 Jeffrey L. Myers,
RETICULUM-CELLED MEDULLARY RETICULOSIS IN A YOUNG ADULT
 J. clin. Path. (1955), 8, 99. RETICULUM-CELLED MEDULLARY RETICULOSIS IN A YOUNG ADULT BY F. G. J. HAYHOE From the Department of Medicine, University of Cambridge (RECEIVED FOR PUBLICATION AUGUST 3, 1954)
J. clin. Path. (1955), 8, 99. RETICULUM-CELLED MEDULLARY RETICULOSIS IN A YOUNG ADULT BY F. G. J. HAYHOE From the Department of Medicine, University of Cambridge (RECEIVED FOR PUBLICATION AUGUST 3, 1954)
CELL AND TISSUE INJURY COURSE-II PATHOLOGY LABORATORY
 CELL AND TISSUE INJURY COURSE-II PATHOLOGY LABORATORY PATHOLOGY of INFECTIOUS DISEASES MICROSCOPY Rengin Ahıskalı Macroscopy samples are shown in the macroscopy presentations of the first two courses.
CELL AND TISSUE INJURY COURSE-II PATHOLOGY LABORATORY PATHOLOGY of INFECTIOUS DISEASES MICROSCOPY Rengin Ahıskalı Macroscopy samples are shown in the macroscopy presentations of the first two courses.
Autoimmune Liver Diseases
 2nd Pannonia Congress of pathology Hepato-biliary pathology Autoimmune Liver Diseases Vera Ferlan Marolt Institute of pathology, Medical faculty, University of Ljubljana Slovenia Siofok, Hungary, May 2012
2nd Pannonia Congress of pathology Hepato-biliary pathology Autoimmune Liver Diseases Vera Ferlan Marolt Institute of pathology, Medical faculty, University of Ljubljana Slovenia Siofok, Hungary, May 2012
Histodemography of Lymphadenopathy
 Abstract Histodemography of Nadira Majid 1, MA Samad Talukder 2, Syed Mukarram Ali 3 Background: Lymph node enlargement presents a clinical problem whose significance can range from trivial to critical,
Abstract Histodemography of Nadira Majid 1, MA Samad Talukder 2, Syed Mukarram Ali 3 Background: Lymph node enlargement presents a clinical problem whose significance can range from trivial to critical,
A Practical Guide To Diagnose B-Cell Lymphomas on FNAs. Nancy P. Caraway, M.D.
 A Practical Guide To Diagnose B-Cell Lymphomas on FNAs Nancy P. Caraway, M.D. Major Factors Impacting Dx Lymphomas on Small Bxs Classification systems Immunophenotyping by multiprobe flow cytometry and
A Practical Guide To Diagnose B-Cell Lymphomas on FNAs Nancy P. Caraway, M.D. Major Factors Impacting Dx Lymphomas on Small Bxs Classification systems Immunophenotyping by multiprobe flow cytometry and
Basic patterns of liver damage what information can a liver biopsy provide and what clinical information does the pathologist need?
 Basic patterns of liver damage what information can a liver biopsy provide and what clinical information does the pathologist need? Rob Goldin r.goldin@imperial.ac.uk Fatty liver disease Is there fatty
Basic patterns of liver damage what information can a liver biopsy provide and what clinical information does the pathologist need? Rob Goldin r.goldin@imperial.ac.uk Fatty liver disease Is there fatty
DETERMINATION OF A LYMPHOID PROCESS
 Chapter 2 Applications of Touch Preparation Cytology to Intraoperative Consultations: Lymph Nodes and Extranodal Tissues for Evaluation of Hematolymphoid Disorders INTRODUCTION As discussed in Chap. 1,
Chapter 2 Applications of Touch Preparation Cytology to Intraoperative Consultations: Lymph Nodes and Extranodal Tissues for Evaluation of Hematolymphoid Disorders INTRODUCTION As discussed in Chap. 1,
Case Report A case of EBV positive diffuse large B-cell lymphoma of the adolescent
 Int J Clin Exp Med 2014;7(1):307-311 www.ijcem.com /ISSN:1940-5901/IJCEM1311029 Case Report A case of EBV positive diffuse large B-cell lymphoma of the adolescent Qilin Ao 2, Ying Wang 1, Sanpeng Xu 2,
Int J Clin Exp Med 2014;7(1):307-311 www.ijcem.com /ISSN:1940-5901/IJCEM1311029 Case Report A case of EBV positive diffuse large B-cell lymphoma of the adolescent Qilin Ao 2, Ying Wang 1, Sanpeng Xu 2,
Lách
 Lách Lách Lách Lách Splenogonadal fusion. Splenic tissue is attached to testicular tissue. Pseudocyst (false or secondary cyst). A, Outer aspect. Pseudocyst (false or secondary cyst). B, Inner surface.
Lách Lách Lách Lách Splenogonadal fusion. Splenic tissue is attached to testicular tissue. Pseudocyst (false or secondary cyst). A, Outer aspect. Pseudocyst (false or secondary cyst). B, Inner surface.
Correlation of fine needle aspiration cytology lymph node with histopathological diagnosis
 International Journal of Research in Medical Sciences Gupta ML et al. Int J Res Med Sci. 2016 Nov;4(11):4719-4723 www.msjonline.org pissn 2320-6071 eissn 2320-6012 Original Research Article DOI: http://dx.doi.org/10.18203/2320-6012.ijrms20163644
International Journal of Research in Medical Sciences Gupta ML et al. Int J Res Med Sci. 2016 Nov;4(11):4719-4723 www.msjonline.org pissn 2320-6071 eissn 2320-6012 Original Research Article DOI: http://dx.doi.org/10.18203/2320-6012.ijrms20163644
Lymphoma and Pseudolymphoma
 Lymphoma and Pseudolymphoma Laura B. Pincus, MD Co-Director, Cutaneous Lymphoma Clinic Associate Professor Dermatology and Pathology University of California, San Francisco I HAVE NO RELEVANT RELATIONSHIPS
Lymphoma and Pseudolymphoma Laura B. Pincus, MD Co-Director, Cutaneous Lymphoma Clinic Associate Professor Dermatology and Pathology University of California, San Francisco I HAVE NO RELEVANT RELATIONSHIPS
Lymphoma/CLL 101: Know your Subtype. Dr. David Macdonald Hematologist, The Ottawa Hospital
 Lymphoma/CLL 101: Know your Subtype Dr. David Macdonald Hematologist, The Ottawa Hospital Function of the Lymph System Lymph Node Lymphocytes B-cells develop in the bone marrow and influence the immune
Lymphoma/CLL 101: Know your Subtype Dr. David Macdonald Hematologist, The Ottawa Hospital Function of the Lymph System Lymph Node Lymphocytes B-cells develop in the bone marrow and influence the immune
