Airway Inflammation and Allergen Specific IgE Production May Persist Longer Than Airway Hyperresponsiveness in Mice
|
|
|
- Randolph Andrews
- 5 years ago
- Views:
Transcription
1 J Korean Med Sci 24; 19: ISSN Copyright The Korean Academy of Medical Sciences Airway Inflammation and Allergen Specific IgE Production May Persist Longer Than Airway Hyperrespoiveness in Mice During the preclinical study of new therapeutic modality, we evaluate whether the treatment can reverse the established asthma phenotypes in animal model. However, few have reported on the long term persistence of asthma phenotypes upon re-challenge with allergen (secondary challenge) in animal model. We evaluated the persistence of asthma phenotypes by secondary challenge at different times in previously challenged murine asthma model. BALB/c mice seitized by intraperitoneal injectio of 2 g of ovalbumin and 1 mg of alum on days 1 and 14 were challenged initially by the inhalation of 1% ovalbumin for 3 min on days 21, 22, and 23. Each group of mice was rechallenged at 5, 7, 9, or 12 weeks after the initial challenge. Airway hyperrespoiveness, BAL fluid, airway histology and serum ovalbumin-specific IgE level were evaluated. Airway eosinophilia, airway inflammation and serum ovalbumin-specific IgE production persisted upon secondary allergen challenges at least 12 weeks after the initial challenge. However, airway hyperrespoiveness persisted only until mice were rechallenged 7 weeks after the initial challenge. Airway inflammation and allergen specific IgE production may persist longer than airway hyperrespoiveness in a mouse asthma model of secondary allergen challenge. Key Words : Asthma; Disease Models, Animal; Mice; Allergen Challenge Yoon-Seok Chang*,,, Yoon-Keun Kim*,,, Tae-Bum Kim*,,, Hye-Ryun Kang*,,, Sun-Sin Kim*,,, Joon-Woo Bahn*,,, Kyung-Up Min*,,, You-Young Kim*,,, Sang-Heon Cho*,, *Department of Internal Medicine, Seoul National University College of Medicine, Ititute of Allergy and Clinical Immunology, Seoul National University Medical Research Center, and Clinical Research Ititute, Seoul National University Hospital, Seoul, Korea Received : 23 July 23 Accepted : 1 November 23 Address for correspondence Sang-Heon Cho, M.D. Department of Internal Medicine, Seoul National University College of Medicine, 28 Yongon-dong, Chongno-gu, Seoul , Korea Tel : , Fax : shcho@plaza.snu.ac.kr *This study was supported by the grant from the Ministry of Health & Welfare, Korea (HMP--CH-6-6). INTRODUCTION Allergic asthma is characterized by the intermediate phenotypes of chronic inflammation of airway with predominant eosinophilic infiltration, airway hyperrespoiveness, reversible airway obstruction, and allergen specific IgE production. The prevalence of asthma is increasing worldwide, also in Korea (1). Asthma reduces the quality of life and may result in mortality. It is regarded as one of most important public health problems. The morbidity and mortality associated with asthma are still increasing, especially during the last half 2th century, despite the currently available mediatio, which demands new therapeutic modalities (2). Animal models are essential in the study of the mechanisms of allergic diseases and for the development of new therapies. The mouse is one of the most popular species in the field of asthma study. It has several advantages; a well-known immune system, the availability of many tools to manipulate the immunological process, the availability of numerous genetically modified (tragenic or knockout) strai, and cost. The persistence of a disease phenotype is important in the evaluation of newly developed treatment modalities in animal models. During the preclinical study, we evaluate whether the treatment can reverse the established asthma phenotypes in animal model. Many reports have been issued on mouse models of asthma (3) but few have reported upon the long term persistence of asthma phenotypes upon secondary allergen challenge in previously seitized and challenged mice. For these reaso, we undertook to evaluate the persistence of asthma phenotypes in a mouse model after secondary allergen challenge at different times after seitization and initial challenge. Animals MATERIALS AND METHODS Seven weeks old BALB/c female mice were used in this study. The mice were purchased from Dae Han Biolink (Choongbuk, Korea) and kept in specific pathogen free conditio in the Preclinical Center of the Clinical Research Ititute of Seoul National University Hospital (Seoul, Korea). None of the mice was exposed to ovalbumin (OVA) before the experiment. The study was approved by the Committee on Animal Experimentation at our ititution and performed according to the guide for the care and use of laboratory animals issued 69
2 7 Y.-S. Chang, Y.-K. Kim, T.-B. Kim, et al. OVA 2 g+alum 1 mg IP (x2) 1% OVA inhalation by the Ititute of Laboratory Animal Resources Commission on Life Sciences, National Research Council, U.S.A. (4). Experimental protocol wk Initial Challenge, The protocol used for seitization and bronchial challenge was the same as previously described (5). There were five groups and each group coists of five mice; mice initially challenged, mice initially challenged and rechallenged at 5, 7, 9, or 12 weeks after the initally challenge (Fig. 1). Mice were seitized by intraperitoneal injectio of 2 g of ovalbumin (OVA, ICN, Costa Mesa, U.S.A.) with 1 mg of alum hydroxide (alum, Sigma, St. Louis, U.S.A.) on days 1 and 14. The initial inhalation challenge was done with 1% OVA for 3 min daily on days 21, 22 and 23 with an ultrasonic nebulizer (NE-U12, Omron, Japan). Each group of mice were rechallenged at different times (5, 7, 9, or 12 weeks after the initial challenge) with 1% OVA for 3 min daily and for 3 coecutive days. Mice seitized and challenged by PBS at each time were used as negative controls for possible environmental factors. Evaluation of asthma phenotypes Secondary Challenge, wk Fig. 1. Experimental protocols for seitization, initial challenge and secondary challenge. 7-week old female BALB/c mice were used for the experiment. Mice were seitized by intraperitoneal injection and initial provocative challenge was done on days 21, 22, 23 ( week). Secondary challenges were performed at 5, 7, 9, or 12 weeks after the initial challenge. PBS treated mice were used as controls. Five mice were used in each group. IP: intraperitoneal injection. Airway hyperrespoiveness: Twenty-four hours after the final OVA inhalation, airway hyperrespoiveness was assessed by methacholine-induced airflow limitation using single chamber whole body plethysmography (Allmedicus, Anyang, Korea) as previously described (5, 6). Increases in enhanced pause (Penh) were measured as an index of airway resistance {Penh= [(Te/RT-1) (PEF/ PIF)], where Penh=enhanced pause, Te= expiratory time (s), RT=relaxation time (s), PEF=peak expiratory flow (ml/s), PIF=peak ipiratory flow (ml/s)}. Increasing doses of methacholine (ranging from 2.5 to 5 mg/ml; Sigma, St. Louis, U.S.A.) were administered by nebulization for 3 min, and the values of Penh were calculated over the following 3 min. During the experiment, the activity of the mice and the barometric plethysmograph flow tracings were monitored. For the quantification of the dose-respoe to methacholine, the linear regression of Penh on log was calculated for individual mice. The log dose corresponding to an increase in Penh of 2%, respectively, was determined, and the average log doses of the different groups were compared. The results are presented as PC2, which is the concentration of methacholine required to increase the baseline Penh by 2%. Inflammatory cells in bronchoalveolar lavage (BAL) fluid: Forty-eight hours after the final OVA challenge, mice tracheae were cannulated and the lungs were lavaged five times with.4 ml aliquots of pyrogen-free saline. After Diff-quick R staining (Dade Behring AG, Dudingen, Switzerland) of lung lavage cells in a cytospin preparation, two investigators blindly counted more than 3 inflammatory cells under a light microscope and classified them as macrophages, lymphocytes, neutrophils, or eosinophils. Lung histology: Following BAL, the lungs were infused with 1% formalin and embedded in paraffin. Lung sectio were stained with hematoxylin and eosin. Slides were assessed by light microscopy and the degree of peribronchial and perivascular inflammation was evaluated on a subjective scale of - 3, as previously described (5, 7). The investigators who scored airway inflammation were blinded as to which preparation they were scoring. Briefly, a value of was assigned when no inflammation was detectable, a value of 1 for occasional cuffing with inflammatory cells, a value of 2 when most bronchi or vessels were surrounded by a thin layer (one to five cells) of inflammatory cells and a value of 3 when most bronchi or vessels were surrounded by a thick layer (more than five cells deep) of inflammatory cells. The total lung inflammation was defined as the average of the peribronchial and perivascular inflammation scores. Serum ovalbumin specific IgE: Forty-eight hours after the final OVA challenge, blood samples were obtained from the mice via the inferior vena cava. Anti-OVA specific antibodies were measured by ELISA, as previously described (5). Briefly, microtiter plates (Nunc, Roskilde, Denmark) were coated overnight with 2 g/ml of OVA in a 5 mm of carbonate buffer (ph 9.6) at 4 Nopecific binding was blocked with 2% bovine serum albumin for 1 hr at 2 After incubation of the test sera for 2 hr, the plates were incubated with horseradish peroxidase-labeled goat anti-mouse IgE (Pharmingen, San Diego, U.S.A.) for 1 hr at 2. The reaction was developed with a tetramethylbenzidine (Sigma, St. Louis, U.S.A.) and stopped by adding 2 N H2SO4. The optical deity was measured at 49 nm, and the antibody titers of the samples were related to pooled standards, which were generated in the laboratory; results are expressed in arbitrary units (AU) according to each O.D. value.
3 Airway Inflammation, IgE and Airway Hyperrespoives 71 Statistical Analysis Statistical analysis was performed using the Kruskal-Wallis and the Mann-Whitney U tests. Statistical significance was accepted at p<.5. Analysis was performed using SPSS 9.. Data are expressed as the mea±standard error with the exception of the inflammatory scores, which are expressed as the mea±standard deviation. RESULTS Airway hyperrespoiveness PC2 (mg/ml) p< week Fig. 2. Airway hyperrespoiveness upon a secondary OVA challenge is persistent when mice were rechallenged 5 or 7 weeks after the initial inhalation challenge. However, airway hyperrespoiveness disappeared when mice were rechallenged 9 or 12 weeks after the initial challenge. The results are presented as PC2 values, where PC2 is the concentration of methacholine required to increase the baseline Penh by 2%. BALF eosinophil (%) OVA PBS Airway hyperrespoiveness upon a secondary OVA challenge was persistent when mice were rechallenged 5 or 7 weeks after the initial inhalation challenge. The values of PC2 observed in the rechallenged animals at 5, or 7 weeks after the initial challenge were similar to that of initially challenged group (5.3±.3, 1.6±3.5 vs. 7.37±3.63 mg/ml, p>.5), but the values of PC2 at 9 and 12 weeks after the initial challenge were higher than that of initially challenged group (3.2±11.6, 19.5±15.2 vs. 7.37±3.63 mg/ml, p<.5). Mice seentized and challenged with PBS showed cotantly high values of PC2 from the initial challenge (41.3 ±8.67, 39.3±1.7, 33.48±1.2, 41.49±8.5, 45.2± 4.8 mg/ml, p>.5), which mea that there was no environmal factor that may alter the physiological air flow during the experiment (Fig. 2). Bronchoalveolar lavage fluid (BALF) The percentages of BALF eosinophils in the secondarily challenged mice were higher even in mice that were rechallenged 12 weeks after initial challenge. The proportio of BALF eosinophils observed in the rechallenged animals at 5, 7, 9, or 12 weeks after the initial challenge were similar to that of initially challenged group (37.8±9.7, 34.7±4.6, 29.4±9.1, 23.3±6. vs. 39.6±9.3 %, p>.5). PBS treated mice showed no eosinophil in BAL fluid at initial challenge and even at the end of the study (.±. %). (Fig. 3A) Histopathology of the lung The degree of inflammation was evaluated in 1 random high power fields ( 4). Peribronchial, perivascular and total inflammation scores in the rechallenged animals at 5, 7, 9, or 12 weeks were similar to that of initially challenged group (p>.5). The inflammatory scores of PBS treated mice were lower than those of OVA treated mice (p<.5) (Fig. 3B). Epithelial shedding was not found and the thickness of subepithelial fibrosis was similar in all groups. Inflammatory score * Peribronch perivascular total * * wk PBS A wk PBS B Fig. 3. (A) The proportion of eosinophils in bronchoalveolar lavage fluid. Eosinophils are increased even when mice were rechallenged 12 weeks after the initial challenge. (*p<.5, compared to the PBS treated mice, BALF: bronchoalveolar lavage fluid). (B) The degrees of airway inflammation observed in the initially and rechallenged animals at 5, 7, 9, or 12 weeks after the initial challenge are similar each other and higher than that of the PBS treated mice. Total lung inflammation was defined as the average value of the peribronchial and perivascular inflammation scores. (*p<.5, compared to initially challenged mice).
4 72 Y.-S. Chang, Y.-K. Kim, T.-B. Kim, et al. Serum OVA-specific IgE (A.U.) * wk PBS Fig. 4. The serum ovalbumin specific IgE level is still increased when mice were rechallenged 12 weeks after the initial challenge. The level of the specific IgE in the initially challenged or rechallenged mice are similar (p>.5, by Kruskal-Willis test) and higher than that of PBS treated group (*p<.5, compared to all allergen challenged groups). Sera of four to five mice were evaluated in each group. BALF: bronchoalveolar lavage fluid. Serum OVA specific IgE The serum anti-ova specific IgE level was still increased when mice were rechallenged 12 weeks after the initial challenge. The levels of serum anti-ova specific IgE observed in the rechallenged animals at 5, 7, 9, or 12 weeks were not different to that of initially changed group (72.8±24.7, 18. ±5.6, 65.2±45.8, 21.5±5. vs. 5.2±12.1 A.U., p>.5). We could not detect serum OVA-specific IgE production in PBS treated mice (.±. A.U.) (Fig. 4). DISCUSSION In this study, we found that eosinophilic airway inflammation and the increased serum allergen-specific IgE production persisted upon a secondary challenge at least 12 weeks after the initial challenge in a murine model of asthma. Airway hyperrespoiveness, another characteristic of asthma, persisted when asthmatic mice were reexposed to allergen only 5 to 7 weeks after the initial challenge. It is important to determine the duration of a persistent disease phenotype in an experimental protocol. The majority of previous investigatio have examined the effects of therapeutic intervention at the time of seitization or before the initiation of allergic respoes in mouse models (5, 8-1). However, we see patients who have established asthma in a clinical situation. Therefore, we should be aware as to whether the therapeutic intervention can reverse the established asthma phenotypes. In this study, we evaluated the persistence of asthma phenotypes upon a secondary challenge in previously challenged murine asthma model. The persistence of asthma phenotypes might vary according to the experimental protocols used, especially in terms of the types and dosages of allerge, adjuvants, and the strai of mice. We chose ovalbumin, alum, and BALB/c mice because they are one of the most popular systems used in asthma study (3). It has been reported that asthma phenotypes, including airway hyperrespoiveness persist for at least 7 weeks in a mouse model of asthma using ragweed allergen. However, the study used a different allergen and three ragweed challenges were performed during the experiment (11). Another study revealed that eosinophilic inflammation of airways persisted for 8 weeks in a mouse model of asthma using ovalbumin (1). Recently, Kanehiro et al. (12) rechallenged previously challenged animals 6 weeks after the initial challenge using ovalbumin, and measured airway resistance and dynamic compliance in anesthetized, mechanically ventilated mice. They found that airway hyperrespoiveness and eosinophilic inflammation of airway persisted. We evaluated the persistence of asthma phenotypes over a longer period with different model system. Though our results concur with those of the previous reports in similar period (1-12), we found that airway hyperrespoiveness upon a secondary challenge disappeared when mice were reexposed to allergen 9 or 12 weeks after initial challenge. However, airway eosinophilia (IL-5 dependent) and serum allergen specific IgE production (IL-4 dependent) were found to be elevated when mice were rechallenged even 12 weeks after the initial challenge. This finding suggests that the airway inflammation, allergen-specific IgE production and airway hyperrespoiveness may be regulated by different mechanisms. Airway hyperrespoiveness is a characteristic feature of asthma and is used as an index of the asthma phenotype in a mouse model (3). Airway inflammation, airway wall thickening, airway epithelial damage, edema of the airways, alteration of presynaptic control of acetylcholine release, activation of local axonal reflexes, altered airway smooth muscle function, or a combination of several of these events have been suggested as possible mechanisms of airway hyperrespoiveness (13). As for the cytokines, there was initial confusion about the relative importance of IL-4 and IL-5 in the pathogenesis of airway hyperrespoiveness (3). Anti-IL-4 antibody treatment reduced airway hyperrespoiveness in seitized BALB/c mice without affecting airway eosinophilia while anti-il-5 antibody did not reduce the airway hyperrespoiveness in one study (14), but deleting the IL-5 gene in C57BL/6 mice was found to abolish their ability to generate airway hyperrespoiveness and tissue eosinophilia in another (15). Now, three distinct pathways leading to airway hyperrespoiveness after T cell activation have been suggested (3). First, the IL-4 dependent pathway, which involves that IgE-stimulated activation of mast cells discharge mediators, such as histamine and leukotrienes that induce airway hyperrespoiveness upon exposure to the allergen (16). Second, the IL-5 dependent pathway, which involves allergen-activated T cell release of IL-5 that promotes eosinophil mediated epithelial cell damage and airway hyperrespoiveness (16). Finally, the IL-4 and IL-5 independent pathway, which involves a novel CD4+ T cell pathway for modulating airway hyperrespon-
5 Airway Inflammation, IgE and Airway Hyperrespoives 73 siveness, was suggested to function in IL-4- and IL-5- deficient BALB/c mice (17). IL-13 shares a common alpha chain with IL-4 and enhances IgE production, mucus production, and eotaxin expression (3, 18). It has been reported that IL- 13 can induce airway hyperrespoiveness independent of serum allergen-specific IgE, airway eosinophilia, IL-4, and IL-5; blockade of IL-13 before the allergen provocation resulted in decreased airway hyperseitivity without affecting airway eosinophilic inflammation or serum ovalbumin specific IgE level (18). IL-13 is important during antigen challenge, whereas IL-4 is useful during seitization (18). This finding is concordant with our results. In the present study, no difference was found in the extents of the mainly IL-5 dependent processes (i.e., the proportion of eosinophils in BAL fluid, the degree of airway inflammation, or epithelial damage) or in the extent of the mainly IL-4 dependent process (i.e., serum allergen-specific IgE level) in mice that were rechallenged at different times. However, airway hyperrespoiveness persisted for only 7 weeks after the initial challenge. Therefore, an IL- 4- and IL-5- independent regulatory mechanism, such as the regulation of IL-13 or novel CD4+ T cell pathway, might be involved in the modulation of airway hyperrespoiveness upon secondary allergen challenge. However, the actual mechanism of this phenomenon remai to be elucidated. We should admit that the number of mice in each group might be small as this study was done as a preliminary experiment before the evaluation of a new therapeutic modality. There were some variation in the level of serum specific IgE and the average value might seem to be somewhat decreased in the last part of study. However, the levels of serum specific IgE in the challenged or rechallenged mice were not statistically different by Kruskall-Willis test (p>.5) and definitely higher than that of PBS treated mice (p<.5). In summary, we report that airway inflammation and allergen specific IgE production may persist longer than airway hyperrespoiveness in a mouse asthma model of secondary allergen challenge. It is important to know the persistence of a disease phenotype in an animal model, especially in the evaluation of newly developed treatment modalities. This study also supports the hypothesis that airway inflammation, allergen-specific IgE production and airway hyperrespoiveness may be regulated by different mechanisms. REFERENCES 1. Kim YY, Cho SH, Kim WK, Park JK, Song SH, Kim YK, Jee YK, Ha MN, Ahn YO, Lee SI, Min KU. Prevalence of childhood asthma based on questionnaires and methacholine bronchial provocation test in Korea. Clin Exp Allergy 1997; 27: Beasly R. The burden of asthma with specific reference to the United States. J Allergy Clin Immunol 22; 19 (Suppl 5): S Leong KP, Huston DP. Understanding the pathogenesis of allergic asthma using mouse models. Ann Allergy Asthma Immunol 21; 87: Ititute of laboratory animal resources, commission on life sciences, National research council, USA Guide for the care and use of laboratory animals. National academy press. Washington D.C Park YJ, Chang YS, Lee SW, Cho SY, Kim YK, Min KU, Kim YY, Cho SH, Sung YC. The enhanced effect of a hexameric deoxyriboguanosine run conjugation to CpG oligodeoxynucleotides on the protection agait allergic asthma. J Allergy Clin Immunol 21; 18: Hamelmann E, Schwarze J, Takeda SK, Oshiba A, Larsen GL, Irvin CG, Gelfand E. Noninvasive measurement of airway respoiveness in allergic mice using barometric plethysmography. Am J Respir Crit Care Med 1997; 156: Tournoy KG, Kips JC, Schou C, Pauwels RA. Airway eosinophilia is not a requirement for allergen-induced airway hyperrespoiveness. Clin Exp Allergy 2; 3: Kline JN, Waldschmidt TJ, Businga TR, Lemish JE Weitock JV, Thorne PS, Krieg AM. Modulation of airway inflammation by CpG oligodeoxynucleotides in a murine model of asthma. J Immunol 1998; 16: Broide D, Schwarze J, Tighe H, Gifford T, Nguyen MD, Malek S, Van Uden J, Martin-Orozco E, Gelfand EW, Raz E. Immunostimulatory DNA sequences inhibit IL-5, eosinophilic inflammation, and airway hyperrespoiveness in mice. J Immunol 1998; 161: Shirota H, Sano K, Kikuchi T, Tamura G, Shirato K. Regulation of murine airway eosinophilia and Th2 cells by antigen-conjugated CpG oligodeoxynucleotides as a novel antigen-specific immunomodulator. J Immunol 2; 164: Sur S, Wild JS, Choudhury BK, Sur N, Alam R, Klinman DM. Long term prevention of allergic lung inflammation in a mouse model of asthma by CpG oligodeoxynucleotides. J Immunol 1999; 162: Kanehiro A, Ikemura T, Makela MJ, Lahn M, Joetham A, Dakhama A, Gelfand EW. Inhibition of phosphodiesterase 4 attenuates airway hyperrespoiveness and airway inflammation in a model of secondary allergen challenge. Am J Respir Crit Care Med 21; 163: O Byrne PM. Airway hyperrespoiveness. In: Middletone E. Jr., et al., editors. Allergy principles & practice. 5th ed., St. Louis: Mosby, 1998: Corry DB, Folkesson HG, Warnock ML, Erle DJ, Matthay MA, Wiener-Kronish JP, Locksley RM. Interleukin 4, but not Interleukin 5 or eosinophils, is required in a murine model of acute airway hyperreactivity. J Exp Med 1996; 183: Foster PS, Hogan SP, Ramsay AJ, Matthaei KI, Young IG. Interleukin 5 deficiency abolishes eosinophilia, airway hyperreactivity, and lung damage in a mouse asthma model. J Exp Med 1996; 183: Drazen JM, Arm JP, Austen KF. Sorting out the cytokines of asthma. J Exp Med 1996; 183: Hogan SP, Matthaei KI, Young JM, Koskinen A, Young IG, Foster PS. A novel T cell-regulated mechanism modulating allergen-induced airways hyperreactivity in BALB/c mice independently of IL-4 and IL-5. J Immunol 1998; 161: Wills-Karp M, Luyimbazi J, Xu X, Schofield B, Neben TY, Karp CL, Donaldson DD. Interleukin-13: Central mediator of allergic asthma. Science 1998; 282:
Influence of the Adjuvants and Genetic Background on the Asthma Model Using Recombinant Der f 2 in Mice
 http://dx.doi.org/10.4110/in.2013.13.6.295 pissn 1598-2629 eissn 2092-6685 BRIEF COMMUNICATION Influence of the Adjuvants and Genetic Background on the Asthma Model Using Recombinant Der f 2 in Mice Yoon-Seok
http://dx.doi.org/10.4110/in.2013.13.6.295 pissn 1598-2629 eissn 2092-6685 BRIEF COMMUNICATION Influence of the Adjuvants and Genetic Background on the Asthma Model Using Recombinant Der f 2 in Mice Yoon-Seok
Role of Tyk-2 in Th9 and Th17 cells in allergic asthma
 Supplementary File Role of Tyk-2 in Th9 and Th17 cells in allergic asthma Caroline Übel 1*, Anna Graser 1*, Sonja Koch 1, Ralf J. Rieker 2, Hans A. Lehr 3, Mathias Müller 4 and Susetta Finotto 1** 1 Laboratory
Supplementary File Role of Tyk-2 in Th9 and Th17 cells in allergic asthma Caroline Übel 1*, Anna Graser 1*, Sonja Koch 1, Ralf J. Rieker 2, Hans A. Lehr 3, Mathias Müller 4 and Susetta Finotto 1** 1 Laboratory
감초 (Glycyrrhiza uralensis Fisch, GLU) 가천식모델생쥐의 BALF 내면역세포및 Cytokine 에미치는효과
 감초 (Glycyrrhiza uralensis Fisch, GLU) 가천식모델생쥐의 BALF 내면역세포및 Cytokine 에미치는효과 Effects of Glycyrrhiza uralensis Fisch on Immunocyte and Cytokine Production in Asthma Model Mouse Young-Joo Han, Yang-Chun Park
감초 (Glycyrrhiza uralensis Fisch, GLU) 가천식모델생쥐의 BALF 내면역세포및 Cytokine 에미치는효과 Effects of Glycyrrhiza uralensis Fisch on Immunocyte and Cytokine Production in Asthma Model Mouse Young-Joo Han, Yang-Chun Park
Modulation of hyperresponsiveness by glutathione in a murine in vivo model of allergic asthma
 6 Modulation of hyperresponsiveness by glutathione in a murine in vivo model of allergic asthma J. Kloek, I. Van Ark, G. Folkerts, F. De Clerck,, N. Bloksma,, F.P. Nijkamp. Department of Pharmacology and
6 Modulation of hyperresponsiveness by glutathione in a murine in vivo model of allergic asthma J. Kloek, I. Van Ark, G. Folkerts, F. De Clerck,, N. Bloksma,, F.P. Nijkamp. Department of Pharmacology and
The Effect of BTP on the Development of Allergic Asthma in Mice
 93 The Effect of BTP on the Development of Allergic Asthma in Mice Alana Curry, McNair Scholar, Virginia State University Faculty Advisor: Avery August, Ph.D Associate Professor of Immunology Department
93 The Effect of BTP on the Development of Allergic Asthma in Mice Alana Curry, McNair Scholar, Virginia State University Faculty Advisor: Avery August, Ph.D Associate Professor of Immunology Department
Potent and Selective CRTh2 Antagonists are Efficacious in Models of Asthma, Allergic Rhinitis and Atopic Dermatitis
 Potent and Selective CRTh2 Antagonists are Efficacious in Models of Asthma, Allergic Rhinitis and Atopic Dermatitis Laura L. Carter, Yoshi Shiraishi, Yooseob Shin, Laurence Burgess, Christine Eberhardt,
Potent and Selective CRTh2 Antagonists are Efficacious in Models of Asthma, Allergic Rhinitis and Atopic Dermatitis Laura L. Carter, Yoshi Shiraishi, Yooseob Shin, Laurence Burgess, Christine Eberhardt,
Abstract. IgE. IgE Th2. x x IL-4 IL-5 IgE CD4 +
 D. o ƒf 6,''!" # + % %$ '& ' '' & " k n k x k k k k k x k IgE k x IgE Ò1Ó k Ò2Ó v k x IgE Th2 x } x x IL-4 IL-5 IgE IgE j IFN-γ IgG j j CD4 + { k d «d j B7 w k k x IgE k 1 k Abstract Parental immunization
D. o ƒf 6,''!" # + % %$ '& ' '' & " k n k x k k k k k x k IgE k x IgE Ò1Ó k Ò2Ó v k x IgE Th2 x } x x IL-4 IL-5 IgE IgE j IFN-γ IgG j j CD4 + { k d «d j B7 w k k x IgE k 1 k Abstract Parental immunization
Noninvasive Measurement of Airway Responsiveness in Allergic Mice Using Barometric Plethysmography
 Noninvasive Measurement of Airway Responsiveness in Allergic Mice Using Barometric Plethysmography E. HAMELMANN, J. SCHWARZE, K. TAKEDA, A. OSHIBA, G. L. LARSEN, C. G. IRVIN, and E. W. GELFAND Divisions
Noninvasive Measurement of Airway Responsiveness in Allergic Mice Using Barometric Plethysmography E. HAMELMANN, J. SCHWARZE, K. TAKEDA, A. OSHIBA, G. L. LARSEN, C. G. IRVIN, and E. W. GELFAND Divisions
Mouse Anti-OVA IgM Antibody Assay Kit
 Mouse Anti-OVA IgM Antibody Assay Kit Catalog # 3017 For Research Use Only - Not Human or Therapeutic Use INTRODUCTION Ovalbumin (OVA) is a widely used antigen for inducing allergic reactions in experimental
Mouse Anti-OVA IgM Antibody Assay Kit Catalog # 3017 For Research Use Only - Not Human or Therapeutic Use INTRODUCTION Ovalbumin (OVA) is a widely used antigen for inducing allergic reactions in experimental
Maintenance of Airway Hyperresponsiveness in Chronic Asthma May Be Mediated by Th2-Independent Mechanisms
 12 The Open Allergy Journal, 2008, 1, 12-18 Open Access Maintenance of Airway Hyperresponsiveness in Chronic Asthma May Be Mediated by Th2-Independent Mechanisms Nora J. Lin 1, Jane M. Schuh 2 and Cory
12 The Open Allergy Journal, 2008, 1, 12-18 Open Access Maintenance of Airway Hyperresponsiveness in Chronic Asthma May Be Mediated by Th2-Independent Mechanisms Nora J. Lin 1, Jane M. Schuh 2 and Cory
Effects of CpG oligodeoxynucleotide on transcription factors GATA-3 and T-bet mrna expression in asthmatic mice
 Acta Pharmacologica Sinica 2005 Sep; 26 (9): 1117 1122 Full-length article Effects of CpG oligodeoxynucleotide on transcription factors GATA-3 and T-bet mrna expression in asthmatic mice Zu-qun WU 1,2,
Acta Pharmacologica Sinica 2005 Sep; 26 (9): 1117 1122 Full-length article Effects of CpG oligodeoxynucleotide on transcription factors GATA-3 and T-bet mrna expression in asthmatic mice Zu-qun WU 1,2,
CD4 + and CD8 + T cells play a central role in a HDM driven model of allergic asthma
 Raemdonck et al. Respiratory Research (2016)17:45 DOI 10.1186/s12931-016-0359-y RESEARCH CD4 + and CD8 + T cells play a central role in a HDM driven model of allergic asthma Open Access Kristof Raemdonck
Raemdonck et al. Respiratory Research (2016)17:45 DOI 10.1186/s12931-016-0359-y RESEARCH CD4 + and CD8 + T cells play a central role in a HDM driven model of allergic asthma Open Access Kristof Raemdonck
Searching for Targets to Control Asthma
 Searching for Targets to Control Asthma Timothy Craig Distinguished Educator Professor Medicine and Pediatrics Penn State University Hershey, PA, USA Inflammation and Remodeling in Asthma The most important
Searching for Targets to Control Asthma Timothy Craig Distinguished Educator Professor Medicine and Pediatrics Penn State University Hershey, PA, USA Inflammation and Remodeling in Asthma The most important
Key words: Asthma, remodeling, MMP-9, TIMP-1, ISS. 1 The potential role of MMP-9 in matrix remodeling
 Remodeling associated expression of matrix metalloproteinase 9 but not tissue inhibitor of metalloproteinase 1 in airway epithelium: Modulation by immunostimulatory DNA Jae Youn Cho, MD, PhD, a Marina
Remodeling associated expression of matrix metalloproteinase 9 but not tissue inhibitor of metalloproteinase 1 in airway epithelium: Modulation by immunostimulatory DNA Jae Youn Cho, MD, PhD, a Marina
METHODS Penh. Measurements and ribonuclease protection assay. Intracellular cytokine staining. ELISAs RT-PCR. Lung morphometry.
 METHODS Penh In addition to measurement of APTI, airway hyperresponsiveness to methacholine was also evaluated within 24 hours of the last allergen challenge by means of measurement of Penh (Buxco Electronics,
METHODS Penh In addition to measurement of APTI, airway hyperresponsiveness to methacholine was also evaluated within 24 hours of the last allergen challenge by means of measurement of Penh (Buxco Electronics,
Mouse Total IgA Antibody Detection Kit
 Mouse Total IgA Antibody Detection Kit Catalog # 3019 For Research Use Only - Not Human or Therapeutic Use INTRODUCTION The total IgA levels in specimens are often determined in mouse disease models involving
Mouse Total IgA Antibody Detection Kit Catalog # 3019 For Research Use Only - Not Human or Therapeutic Use INTRODUCTION The total IgA levels in specimens are often determined in mouse disease models involving
Role of immunoglobulin E and mast cells in murine models of asthma
 Brazilian Murine models Journal of of asthma Medical and Biological Research (2003) 36: 821-827 ISSN 0100-879X Review 821 Role of immunoglobulin E and mast cells in murine models of asthma S.I. Mayr 1,
Brazilian Murine models Journal of of asthma Medical and Biological Research (2003) 36: 821-827 ISSN 0100-879X Review 821 Role of immunoglobulin E and mast cells in murine models of asthma S.I. Mayr 1,
Role of C5 in the development of airway inflammation, airway hyperresponsiveness, and ongoing airway response
 Research article Role of C5 in the development of airway inflammation, airway hyperresponsiveness, and ongoing airway response Tao Peng, 1 Liming Hao, 2 Joseph A. Madri, 2 Xiao Su, 1 Jack A. Elias, 3 Gregory
Research article Role of C5 in the development of airway inflammation, airway hyperresponsiveness, and ongoing airway response Tao Peng, 1 Liming Hao, 2 Joseph A. Madri, 2 Xiao Su, 1 Jack A. Elias, 3 Gregory
Defining Asthma: Clinical Criteria. Defining Asthma: Bronchial Hyperresponsiveness
 Defining Asthma: Clinical Criteria Atopy 34% Recent wheeze 20% Asthma 11% AHR 19% n = 807 From: Woolcock, AJ. Asthma in Textbook of Respiratory Medicine, 2nd ed. Murray, Nadel, eds.(saunders:philadelphia)
Defining Asthma: Clinical Criteria Atopy 34% Recent wheeze 20% Asthma 11% AHR 19% n = 807 From: Woolcock, AJ. Asthma in Textbook of Respiratory Medicine, 2nd ed. Murray, Nadel, eds.(saunders:philadelphia)
Time Sequence of Airway Remodeling in a Mouse Model of Chronic Asthma: the Relation with Airway Hyperresponsiveness
 J Korean Med Sci 7; : 183-91 ISSN 111-893 Copyright The Korean Academy of Medical Sciences Time Sequence of Airway Remodeling in a Mouse Model of Chronic Asthma: the Relation with Airway Hyperresponsiveness
J Korean Med Sci 7; : 183-91 ISSN 111-893 Copyright The Korean Academy of Medical Sciences Time Sequence of Airway Remodeling in a Mouse Model of Chronic Asthma: the Relation with Airway Hyperresponsiveness
Supplementary Information
 Supplementary Information TABLE S1. SUBJECT CHARACTERISTICS* Normal Control Subjects Subjects with Asthma p Value Number 23 48 Age (years) 35±10 35±10 0.75 Sex, M:F (% F) 9:12 (57) 17:26 (60) 0.76 FEV1
Supplementary Information TABLE S1. SUBJECT CHARACTERISTICS* Normal Control Subjects Subjects with Asthma p Value Number 23 48 Age (years) 35±10 35±10 0.75 Sex, M:F (% F) 9:12 (57) 17:26 (60) 0.76 FEV1
Respiratory Syncytial Virus Infection Results in Airway Hyperresponsiveness and Enhanced Airway Sensitization to Allergen
 Respiratory Syncytial Virus Infection Results in Airway Hyperresponsiveness and Enhanced Airway Sensitization to Allergen Jürgen Schwarze, Eckard Hamelmann, Katherine L. Bradley, Katsuyuki Takeda, and
Respiratory Syncytial Virus Infection Results in Airway Hyperresponsiveness and Enhanced Airway Sensitization to Allergen Jürgen Schwarze, Eckard Hamelmann, Katherine L. Bradley, Katsuyuki Takeda, and
Inhibition of airway remodeling in IL-5 deficient mice
 Inhibition of airway remodeling in IL-5 deficient mice See the related Commentary beginning on page 507. Jae Youn Cho, Marina Miller, Kwang Je Baek, Ji Won Han, Jyothi Nayar, Sook Young Lee, Kirsti McElwain,
Inhibition of airway remodeling in IL-5 deficient mice See the related Commentary beginning on page 507. Jae Youn Cho, Marina Miller, Kwang Je Baek, Ji Won Han, Jyothi Nayar, Sook Young Lee, Kirsti McElwain,
Impact of Asthma in the U.S. per Year. Asthma Epidemiology and Pathophysiology. Risk Factors for Asthma. Childhood Asthma Costs of Asthma
 American Association for Respiratory Care Asthma Educator Certification Prep Course Asthma Epidemiology and Pathophysiology Robert C. Cohn, MD, FAARC MetroHealth Medical Center Cleveland, OH Impact of
American Association for Respiratory Care Asthma Educator Certification Prep Course Asthma Epidemiology and Pathophysiology Robert C. Cohn, MD, FAARC MetroHealth Medical Center Cleveland, OH Impact of
Inhibition of Phosphodiesterase 4 Attenuates Airway Hyperresponsiveness and Airway Inflammation in a Model of Secondary Allergen Challenge
 Inhibition of Phosphodiesterase 4 Attenuates Airway Hyperresponsiveness and Airway Inflammation in a Model of Secondary Allergen Challenge ARIHIKO KANEHIRO, TOSHIHIDE IKEMURA, MIKA J. MÄKELÄ, MICHAEL LAHN,
Inhibition of Phosphodiesterase 4 Attenuates Airway Hyperresponsiveness and Airway Inflammation in a Model of Secondary Allergen Challenge ARIHIKO KANEHIRO, TOSHIHIDE IKEMURA, MIKA J. MÄKELÄ, MICHAEL LAHN,
10.00 PBS OVA OVA+isotype antibody 8.00 OVA+anti-HMGB1. PBS Methatroline (mg/ml)
 RESEARCH ARTICLE Penh (100% of PBS) 1 PBS 8.00 +anti-hmgb1 6.00 4.00 p=0.054 Cellular & Molecular Immunology advance online publication, PBS 3.12 6.25 Methatroline (mg/ml) Neutrophil isolation and culture
RESEARCH ARTICLE Penh (100% of PBS) 1 PBS 8.00 +anti-hmgb1 6.00 4.00 p=0.054 Cellular & Molecular Immunology advance online publication, PBS 3.12 6.25 Methatroline (mg/ml) Neutrophil isolation and culture
Defining Asthma: Clinical Criteria. Defining Asthma: Bronchial Hyperresponsiveness
 Defining Asthma: Clinical Criteria Atopy 34% Recent wheeze 20% Asthma 11% AHR 19% n = 807 From: Woolcock, AJ. Asthma in Textbook of Respiratory Medicine, 2nd ed. Murray, Nadel, eds.(saunders:philadelphia)
Defining Asthma: Clinical Criteria Atopy 34% Recent wheeze 20% Asthma 11% AHR 19% n = 807 From: Woolcock, AJ. Asthma in Textbook of Respiratory Medicine, 2nd ed. Murray, Nadel, eds.(saunders:philadelphia)
Defining Asthma: Bronchial Hyperresponsiveness. Defining Asthma: Clinical Criteria. Impaired Ventilation in Asthma. Dynamic Imaging of Asthma
 Defining Asthma: Clinical Criteria Defining Asthma: Bronchial Hyperresponsiveness Atopy 34% Recent wheeze 20% Asthma 11% AHR 19% n = 807 From: Woolcock, AJ. Asthma in Textbook of Respiratory Medicine,
Defining Asthma: Clinical Criteria Defining Asthma: Bronchial Hyperresponsiveness Atopy 34% Recent wheeze 20% Asthma 11% AHR 19% n = 807 From: Woolcock, AJ. Asthma in Textbook of Respiratory Medicine,
Effect of Influenza Virus Infection in a Murine Model of Asthma
 ORIGINAL ARTICLE Iran J Allergy Asthma Immunol August 2015; 14(4):392-401. Effect of Influenza Virus Infection in a Murine Model of Asthma Hwan Soo Kim, Huisu Lee, Hyun Sook Kim, Sulmui Won, Eu Kyoung
ORIGINAL ARTICLE Iran J Allergy Asthma Immunol August 2015; 14(4):392-401. Effect of Influenza Virus Infection in a Murine Model of Asthma Hwan Soo Kim, Huisu Lee, Hyun Sook Kim, Sulmui Won, Eu Kyoung
RESPIRATORY BLOCK. Bronchial Asthma. Dr. Maha Arafah Department of Pathology KSU
 RESPIRATORY BLOCK Bronchial Asthma Dr. Maha Arafah Department of Pathology KSU marafah@ksu.edu.sa Jan 2018 Objectives Define asthma (BA) Know the two types of asthma 1. Extrinsic or atopic allergic 2.
RESPIRATORY BLOCK Bronchial Asthma Dr. Maha Arafah Department of Pathology KSU marafah@ksu.edu.sa Jan 2018 Objectives Define asthma (BA) Know the two types of asthma 1. Extrinsic or atopic allergic 2.
Allergy and Immunology Review Corner: Chapter 75 of Middleton s Allergy Principles and Practice, 7 th Edition, edited by N. Franklin Adkinson, et al.
 Allergy and Immunology Review Corner: Chapter 75 of Middleton s Allergy Principles and Practice, 7 th Edition, edited by N. Franklin Adkinson, et al. Chapter 75: Approach to Infants and Children with Asthma
Allergy and Immunology Review Corner: Chapter 75 of Middleton s Allergy Principles and Practice, 7 th Edition, edited by N. Franklin Adkinson, et al. Chapter 75: Approach to Infants and Children with Asthma
Antigen-Induced Airway Hyperresponsiveness, Pulmonary Eosinophilia, and Chemokine Expression in B Cell Deficient Mice
 Antigen-Induced Airway Hyperresponsiveness, Pulmonary Eosinophilia, and Chemokine Expression in B Cell Deficient Mice James A. MacLean, Alain Sauty, Andrew D. Luster, Jeffrey M. Drazen, and George T. De
Antigen-Induced Airway Hyperresponsiveness, Pulmonary Eosinophilia, and Chemokine Expression in B Cell Deficient Mice James A. MacLean, Alain Sauty, Andrew D. Luster, Jeffrey M. Drazen, and George T. De
The Role of Plasmacytoid and Myeloid Dendritic Cells in Induction of Asthma in a Mouse Model and the Effect of a TLR9 Agonist on Dendritic Cells
 Original Article Allergy Asthma Immunol Res. 211 July;3(3):199-24. doi: 1.4168/aair.211.3.3.199 pissn 292-7355 eissn 292-7363 The Role of Plasmacytoid and Myeloid Dendritic Cells in Induction of Asthma
Original Article Allergy Asthma Immunol Res. 211 July;3(3):199-24. doi: 1.4168/aair.211.3.3.199 pissn 292-7355 eissn 292-7363 The Role of Plasmacytoid and Myeloid Dendritic Cells in Induction of Asthma
E-1 Role of IgE and IgE receptors in allergic airway inflammation and remodeling
 E-1 Role of IgE and IgE receptors in allergic airway inflammation and remodeling Ruby Pawankar, MD, Ph.D. FRCP, FAAAAI Prof. Div of Allergy, Dept of Pediatrics Nippon Medical School Tokyo, Japan pawankar.ruby@gmail.com
E-1 Role of IgE and IgE receptors in allergic airway inflammation and remodeling Ruby Pawankar, MD, Ph.D. FRCP, FAAAAI Prof. Div of Allergy, Dept of Pediatrics Nippon Medical School Tokyo, Japan pawankar.ruby@gmail.com
Original Article. ÎË T cell is essential for allergen-induced late asthmatic response in a murine model of asthma
 J Med Dent Sci 2008; 55: 113 120 Original Article ÎË T cell is essential for allergen-induced late asthmatic response in a murine model of asthma Kanna Tamura-Yamashita 1,2, Junji Endo 1,3, Susumu Isogai
J Med Dent Sci 2008; 55: 113 120 Original Article ÎË T cell is essential for allergen-induced late asthmatic response in a murine model of asthma Kanna Tamura-Yamashita 1,2, Junji Endo 1,3, Susumu Isogai
Airway Inflammation in Asthma Chih-Yung Chiu 1,2, Kin-Sun Wong 2 1 Department of Pediatrics, Chang Gung Memorial Hospital, Keelung, Taiwan.
 REVIEW ARTICLE Chih-Yung Chiu 1,2, Kin-Sun Wong 2 1 Department of Pediatrics, Chang Gung Memorial Hospital, Keelung, Taiwan. 2 Division of Pediatric Pulmonology, Department of Pediatrics, Chang Gung Memorial
REVIEW ARTICLE Chih-Yung Chiu 1,2, Kin-Sun Wong 2 1 Department of Pediatrics, Chang Gung Memorial Hospital, Keelung, Taiwan. 2 Division of Pediatric Pulmonology, Department of Pediatrics, Chang Gung Memorial
Soluble ADAM33 initiates airway remodeling to promote susceptibility for. Elizabeth R. Davies, Joanne F.C. Kelly, Peter H. Howarth, David I Wilson,
 Revised Suppl. Data: Soluble ADAM33 1 Soluble ADAM33 initiates airway remodeling to promote susceptibility for allergic asthma in early life Elizabeth R. Davies, Joanne F.C. Kelly, Peter H. Howarth, David
Revised Suppl. Data: Soluble ADAM33 1 Soluble ADAM33 initiates airway remodeling to promote susceptibility for allergic asthma in early life Elizabeth R. Davies, Joanne F.C. Kelly, Peter H. Howarth, David
Heat-killed Lactobacillus casei
 Heat-killed Lactobacillus casei confers broad protection against influenza A virus primary infection and develops heterosubtypic immunity against future secondary infection Yu-Jin Jung, Young-Tae Lee,
Heat-killed Lactobacillus casei confers broad protection against influenza A virus primary infection and develops heterosubtypic immunity against future secondary infection Yu-Jin Jung, Young-Tae Lee,
Therapeutic efficacy of an anti IL-5 monoclonal antibody delivered into the respiratory tract in a murine model of
 Therapeutic efficacy of an anti IL-5 monoclonal antibody delivered into the respiratory tract in a murine model of asthma Felix R. Shardonofsky, MD, Joe Venzor III, MD, Roberto Barrios, MD, Khai-Pang Leong,
Therapeutic efficacy of an anti IL-5 monoclonal antibody delivered into the respiratory tract in a murine model of asthma Felix R. Shardonofsky, MD, Joe Venzor III, MD, Roberto Barrios, MD, Khai-Pang Leong,
Induced sputum to assess airway inflammation: a study of reproducibility
 Clinical and Experimental Allergy. 1997. Volume 27. pages 1138-1144 Induced sputum to assess airway inflammation: a study of reproducibility A. SPANEVELLO, G. B. MIGLIORI. A. SHARARA*, L. BALLARDlNIt,
Clinical and Experimental Allergy. 1997. Volume 27. pages 1138-1144 Induced sputum to assess airway inflammation: a study of reproducibility A. SPANEVELLO, G. B. MIGLIORI. A. SHARARA*, L. BALLARDlNIt,
Diesel exhaust particles exert acute effects on airway inflammation and function in murine allergen provocation models
 Diesel exhaust particles exert acute effects on airway inflammation and function in murine allergen provocation models Minqi Hao, MD, PhD, a Stephania Comier, PhD, b Meiying Wang, MD, a James J. Lee, PhD,
Diesel exhaust particles exert acute effects on airway inflammation and function in murine allergen provocation models Minqi Hao, MD, PhD, a Stephania Comier, PhD, b Meiying Wang, MD, a James J. Lee, PhD,
Chemical Chaperones Mitigate Experimental Asthma By Attenuating Endoplasmic
 Chemical Chaperones Mitigate Experimental Asthma By Attenuating Endoplasmic Reticulum Stress Lokesh Makhija, BE, Veda Krishnan, MSc, Rakhshinda Rehman, MTech, Samarpana Chakraborty, MSc, Shuvadeep Maity,
Chemical Chaperones Mitigate Experimental Asthma By Attenuating Endoplasmic Reticulum Stress Lokesh Makhija, BE, Veda Krishnan, MSc, Rakhshinda Rehman, MTech, Samarpana Chakraborty, MSc, Shuvadeep Maity,
IL-12-STAT4-IFN-γ axis is a key downstream pathway in the development of IL-13-mediated asthma phenotypes in a Th2 type asthma model
 EXPERIMENTAL and MOLECULAR MEDICINE, Vol. 42, No. 8, 533-546, August 2010 IL-12-STAT4-IFN-γ axis is a key downstream pathway in the development of IL-13-mediated asthma phenotypes in a Th2 type asthma
EXPERIMENTAL and MOLECULAR MEDICINE, Vol. 42, No. 8, 533-546, August 2010 IL-12-STAT4-IFN-γ axis is a key downstream pathway in the development of IL-13-mediated asthma phenotypes in a Th2 type asthma
IKKα Causes Chromatin Modification on Pro-Inflammatory Genes by Cigarette Smoke in Mouse Lung
 IKKα Causes Chromatin Modification on Pro-Inflammatory Genes by Cigarette Smoke in Mouse Lung Se-Ran Yang, Samantha Valvo, Hongwei Yao, Aruna Kode, Saravanan Rajendrasozhan, Indika Edirisinghe, Samuel
IKKα Causes Chromatin Modification on Pro-Inflammatory Genes by Cigarette Smoke in Mouse Lung Se-Ran Yang, Samantha Valvo, Hongwei Yao, Aruna Kode, Saravanan Rajendrasozhan, Indika Edirisinghe, Samuel
Chronic cough is defined as a cough persisting for. Airway Inflammation as an Assessment of Chronic Nonproductive Cough*
 Airway Inflammation as an Assessment of Chronic Nonproductive Cough* Sang Yeub Lee, MD ; Jae Youn Cho, MD; Jae Jeong Shim, MD; Han Kyeom Kim, MD; Kyung Ho Kang, MD, FCCP; Se Hwa Yoo, MD; and Kwang Ho In,
Airway Inflammation as an Assessment of Chronic Nonproductive Cough* Sang Yeub Lee, MD ; Jae Youn Cho, MD; Jae Jeong Shim, MD; Han Kyeom Kim, MD; Kyung Ho Kang, MD, FCCP; Se Hwa Yoo, MD; and Kwang Ho In,
Dissociation of Airway Hyperresponsiveness from Immunoglobulin E and Airway Eosinophilia in a Murine Model of Allergic Asthma
 Dissociation of Airway Hyperresponsiveness from Immunoglobulin E and Airway Eosinophilia in a Murine Model of Allergic Asthma Julie A. Wilder, D. David S. Collie,* Bridget S. Wilson, David E. Bice, C.
Dissociation of Airway Hyperresponsiveness from Immunoglobulin E and Airway Eosinophilia in a Murine Model of Allergic Asthma Julie A. Wilder, D. David S. Collie,* Bridget S. Wilson, David E. Bice, C.
Physicians Preferences for Asthma Guidelines Implementation
 Original Article Allergy Asthma Immunol Res. 2010 October;2(4):247-253. doi: 10.4168/aair.2010.2.4.247 pissn 2092-7355 eissn 2092-7363 Physicians Preferences for Asthma Guidelines Implementation Min-Koo
Original Article Allergy Asthma Immunol Res. 2010 October;2(4):247-253. doi: 10.4168/aair.2010.2.4.247 pissn 2092-7355 eissn 2092-7363 Physicians Preferences for Asthma Guidelines Implementation Min-Koo
Interleukin (IL)-5 but Not Immunoglobulin E Reconstitutes Airway Inflammation and Airway Hyperresponsiveness in IL-4 Deficient Mice
 Interleukin (IL)-5 but Not Immunoglobulin E Reconstitutes Airway Inflammation and Airway Hyperresponsiveness in IL-4 Deficient Mice Eckard Hamelmann, Katsuyuki Takeda, Angela Haczku, Grzegorz Cieslewicz,
Interleukin (IL)-5 but Not Immunoglobulin E Reconstitutes Airway Inflammation and Airway Hyperresponsiveness in IL-4 Deficient Mice Eckard Hamelmann, Katsuyuki Takeda, Angela Haczku, Grzegorz Cieslewicz,
IgE-mediated allergy in elderly patients with asthma
 Allergology international (1997) 46: 237-241 Original Article IgE-mediated allergy in elderly patients with asthma Fumihiro Mitsunobu, Takashi Mifune, Yasuhiro Hosaki, Kouzou Ashida, Hirofumi Tsugeno,
Allergology international (1997) 46: 237-241 Original Article IgE-mediated allergy in elderly patients with asthma Fumihiro Mitsunobu, Takashi Mifune, Yasuhiro Hosaki, Kouzou Ashida, Hirofumi Tsugeno,
Airway Smooth Muscle Sensitivity to Methacholine in Precision-Cut Lung Slices (PCLS) from Ovalbumin-induced Asthmatic Mice
 Korean J Physiol Pharmacol Vol 19: 65-71, January, 2015 http://dx.doi.org/10.4196/kjpp.2015.19.1.65 Airway Smooth Muscle Sensitivity to Methacholine in Precision-Cut Lung Slices (PCLS) from Ovalbumin-induced
Korean J Physiol Pharmacol Vol 19: 65-71, January, 2015 http://dx.doi.org/10.4196/kjpp.2015.19.1.65 Airway Smooth Muscle Sensitivity to Methacholine in Precision-Cut Lung Slices (PCLS) from Ovalbumin-induced
Identification of an IFN-γ/mast cell axis in a mouse model of chronic asthma
 Research article Identification of an IFN-γ/mast cell axis in a mouse model of chronic asthma Mang Yu, 1 Michael R. Eckart, 2 Alexander A. Morgan, 3 Kaori Mukai, 1 Atul J. Butte, 3 Mindy Tsai, 1 and Stephen
Research article Identification of an IFN-γ/mast cell axis in a mouse model of chronic asthma Mang Yu, 1 Michael R. Eckart, 2 Alexander A. Morgan, 3 Kaori Mukai, 1 Atul J. Butte, 3 Mindy Tsai, 1 and Stephen
Supplementary Figure S1. Flow cytometric analysis of the expression of Thy1 in NH cells. Flow cytometric analysis of the expression of T1/ST2 and
 Supplementary Figure S1. Flow cytometric analysis of the expression of Thy1 in NH cells. Flow cytometric analysis of the expression of T1/ST2 and Thy1 in NH cells derived from the lungs of naïve mice.
Supplementary Figure S1. Flow cytometric analysis of the expression of Thy1 in NH cells. Flow cytometric analysis of the expression of T1/ST2 and Thy1 in NH cells derived from the lungs of naïve mice.
Comparative Study of Nasal Smear and Biopsy in Patients of Allergic Rhinitis
 Indian J Allergy Asthma Immunol 2002; 16(1) : 27-31 Comparative Study of Nasal Smear and Biopsy in Patients of Allergic Rhinitis Rakesh Chanda, Ajay Kumar Aggarwal, G.S. Kohli, T.S. Jaswal*, and K.B. Gupta**
Indian J Allergy Asthma Immunol 2002; 16(1) : 27-31 Comparative Study of Nasal Smear and Biopsy in Patients of Allergic Rhinitis Rakesh Chanda, Ajay Kumar Aggarwal, G.S. Kohli, T.S. Jaswal*, and K.B. Gupta**
SERIES 'OCCUPATIONAL ASTHMA' Edited by C. Mapp
 Eur Respir J, 1994, 7, 555 568 DOI: 10.1183/09031936.94.07030555 Printed in UK - all rights reserved Copyright ERS Journals Ltd 1994 European Respiratory Journal ISSN 0903-1936 SERIES 'OCCUPATIONAL ASTHMA'
Eur Respir J, 1994, 7, 555 568 DOI: 10.1183/09031936.94.07030555 Printed in UK - all rights reserved Copyright ERS Journals Ltd 1994 European Respiratory Journal ISSN 0903-1936 SERIES 'OCCUPATIONAL ASTHMA'
Immunology of Asthma. Kenneth J. Goodrum,Ph. Ph.D. Ohio University College of Osteopathic Medicine
 Immunology of Asthma Kenneth J. Goodrum,Ph Ph.D. Ohio University College of Osteopathic Medicine Outline! Consensus characteristics! Allergens:role in asthma! Immune/inflammatory basis! Genetic basis!
Immunology of Asthma Kenneth J. Goodrum,Ph Ph.D. Ohio University College of Osteopathic Medicine Outline! Consensus characteristics! Allergens:role in asthma! Immune/inflammatory basis! Genetic basis!
Immunostimulatory oligonucleotides block allergic airway inflammation by inhibiting Th2 cell activation and IgE-mediated cytokine induction
 Immunostimulatory oligonucleotides block allergic airway inflammation by inhibiting Th2 cell activation and IgE-mediated cytokine induction Edith M. Hessel, 1 Mabel Chu, 1 Jennifer O. Lizcano, 1 Bonnie
Immunostimulatory oligonucleotides block allergic airway inflammation by inhibiting Th2 cell activation and IgE-mediated cytokine induction Edith M. Hessel, 1 Mabel Chu, 1 Jennifer O. Lizcano, 1 Bonnie
Immunology of Asthma. Kenneth J. Goodrum,Ph. Ph.D. Ohio University College of Osteopathic Medicine
 Immunology of Asthma Kenneth J. Goodrum,Ph Ph.D. Ohio University College of Osteopathic Medicine Outline Consensus characteristics/incidence data Immune/inflammatory basis Etiology/Genetic basis Hygiene
Immunology of Asthma Kenneth J. Goodrum,Ph Ph.D. Ohio University College of Osteopathic Medicine Outline Consensus characteristics/incidence data Immune/inflammatory basis Etiology/Genetic basis Hygiene
PIERIS PHARMACEUTICALS, INC. (Exact Name of Registrant as Specified in its Charter)
 UNITED STATES SECURITIES AND EXCHANGE COMMISSION Washington, D.C. 20549 FORM 8-K CURRENT REPORT Pursuant to Section 13 or 15(d) of the Securities Exchange Act of 1934 Date of Report (Date of earliest event
UNITED STATES SECURITIES AND EXCHANGE COMMISSION Washington, D.C. 20549 FORM 8-K CURRENT REPORT Pursuant to Section 13 or 15(d) of the Securities Exchange Act of 1934 Date of Report (Date of earliest event
INTERNATIONAL JOURNAL OF MOLECULAR MEDICINE 20: ,
 INTERNATIONAL JOURNAL OF MOLECULAR MEDICINE 20: 631-635, 2007 631 Effective microorganism fermentation extract (EM-X) attenuates airway hyperreactivity and inflammation through selective inhibition of
INTERNATIONAL JOURNAL OF MOLECULAR MEDICINE 20: 631-635, 2007 631 Effective microorganism fermentation extract (EM-X) attenuates airway hyperreactivity and inflammation through selective inhibition of
Supporting Information
 Supporting Information Valkenburg et al. 10.1073/pnas.1403684111 SI Materials and Methods ELISA and Microneutralization. Sera were treated with Receptor Destroying Enzyme II (RDE II, Accurate) before ELISA
Supporting Information Valkenburg et al. 10.1073/pnas.1403684111 SI Materials and Methods ELISA and Microneutralization. Sera were treated with Receptor Destroying Enzyme II (RDE II, Accurate) before ELISA
Respiratory Research. Open Access. Abstract. BioMed Central
 Respiratory Research BioMed Central Research Exposure of neonates to Respiratory Syncytial Virus is critical in determining subsequent airway response in adults Dahui You, David Becnel, Kai Wang, Michael
Respiratory Research BioMed Central Research Exposure of neonates to Respiratory Syncytial Virus is critical in determining subsequent airway response in adults Dahui You, David Becnel, Kai Wang, Michael
Asthma is induced by intranasal coadministration of allergen and natural killer T-cell ligand in a mouse model
 Asthma is induced by intranasal coadministration of allergen and natural killer T-cell ligand in a mouse model Jae-Ouk Kim, PhD, a Dong-Hyeon Kim, MS, a Woo-Sung Chang, BS, a Changwan Hong, MS, b Se-Ho
Asthma is induced by intranasal coadministration of allergen and natural killer T-cell ligand in a mouse model Jae-Ouk Kim, PhD, a Dong-Hyeon Kim, MS, a Woo-Sung Chang, BS, a Changwan Hong, MS, b Se-Ho
Airway Inflammation and Bronchial Hyperresponsiveness after Mycoplasma pneumoniae Infection in a Murine Model
 Airway Inflammation and Bronchial Hyperresponsiveness after Mycoplasma pneumoniae Infection in a Murine Model Richard J. Martin, Hong Wei Chu, Joyce M. Honour, and Ronald J. Harbeck Department of Medicine,
Airway Inflammation and Bronchial Hyperresponsiveness after Mycoplasma pneumoniae Infection in a Murine Model Richard J. Martin, Hong Wei Chu, Joyce M. Honour, and Ronald J. Harbeck Department of Medicine,
Concurrent dual allergen exposure and its effects on airway hyperresponsiveness, inflammation and remodeling in mice
 Disease Models & Mechanisms, 75-8 (9) doi:1.14/dmm.1859 RESEARCH ARTICLE Concurrent dual allergen exposure and its effects on airway hyperresponsiveness, inflammation and remodeling in mice Franco A. DiGiovanni
Disease Models & Mechanisms, 75-8 (9) doi:1.14/dmm.1859 RESEARCH ARTICLE Concurrent dual allergen exposure and its effects on airway hyperresponsiveness, inflammation and remodeling in mice Franco A. DiGiovanni
Dr Rodney Itaki Lecturer Division of Pathology Anatomical Pathology Discipline
 Pathology of Asthma Dr Rodney Itaki Lecturer Division of Pathology Anatomical Pathology Discipline Bronchial Asthma Definition: chronic, relapsing inflammatory lung disorder characterised by reversible
Pathology of Asthma Dr Rodney Itaki Lecturer Division of Pathology Anatomical Pathology Discipline Bronchial Asthma Definition: chronic, relapsing inflammatory lung disorder characterised by reversible
Inhibition of Protein Kinase C Delta Attenuates Allergic Airway Inflammation through Suppression of PI3K/Akt/ mtor/hif-1 Alpha/VEGF Pathway
 Inhibition of Protein Kinase C Delta Attenuates Allergic Airway Inflammation through Suppression of PI3K/Akt/ mtor/hif-1 Alpha/VEGF Pathway Yun Ho Choi 1., Guang Yu Jin 2., Liang chang Li 3, Guang Hai
Inhibition of Protein Kinase C Delta Attenuates Allergic Airway Inflammation through Suppression of PI3K/Akt/ mtor/hif-1 Alpha/VEGF Pathway Yun Ho Choi 1., Guang Yu Jin 2., Liang chang Li 3, Guang Hai
Review What have transgenic and knockout animals taught us about respiratory disease? Yanira Riffo Vasquez and Domenico Spina
 Review What have transgenic and knockout animals taught us about respiratory disease? Yanira Riffo Vasquez and Domenico Spina The Sackler Institute of Pulmonary Pharmacology, King s College London, London,
Review What have transgenic and knockout animals taught us about respiratory disease? Yanira Riffo Vasquez and Domenico Spina The Sackler Institute of Pulmonary Pharmacology, King s College London, London,
Asthma Pathophysiology and Treatment. John R. Holcomb, M.D.
 Asthma Pathophysiology and Treatment John R. Holcomb, M.D. Objectives Definition of Asthma Epidemiology and risk factors of Asthma Pathophysiology of Asthma Diagnostics test of Asthma Management of Asthma
Asthma Pathophysiology and Treatment John R. Holcomb, M.D. Objectives Definition of Asthma Epidemiology and risk factors of Asthma Pathophysiology of Asthma Diagnostics test of Asthma Management of Asthma
B220 CD4 CD8. Figure 1. Confocal Image of Sensitized HLN. Representative image of a sensitized HLN
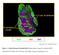 B220 CD4 CD8 Natarajan et al., unpublished data Figure 1. Confocal Image of Sensitized HLN. Representative image of a sensitized HLN showing B cell follicles and T cell areas. 20 µm thick. Image of magnification
B220 CD4 CD8 Natarajan et al., unpublished data Figure 1. Confocal Image of Sensitized HLN. Representative image of a sensitized HLN showing B cell follicles and T cell areas. 20 µm thick. Image of magnification
Boswellic acid attenuates asthma phenotype by downregulation of GATA3 via nhibition of PSTAT6
 Boswellic acid attenuates asthma phenotype by downregulation of GATA3 via nhibition of PSTAT6 X. Zhou 1 *, J.G. Cai 2 *, W.W. Zhu 1, H.Y. Zhao 1, K. Wang 2 and X.F. Zhang 2 1 Department of Pediatrics,
Boswellic acid attenuates asthma phenotype by downregulation of GATA3 via nhibition of PSTAT6 X. Zhou 1 *, J.G. Cai 2 *, W.W. Zhu 1, H.Y. Zhao 1, K. Wang 2 and X.F. Zhang 2 1 Department of Pediatrics,
Influenza A virus infection increases IgE production and airway responsiveness in aerosolized antigen-exposed mice
 Influenza A virus infection increases IgE production and airway responsiveness in aerosolized antigen-exposed mice Shunsuke Suzuki, MD, Yuzo Suzuki, MD, PhD, Naomi Yamamoto, MD, Yutaka Matsumoto, MD, PhD,
Influenza A virus infection increases IgE production and airway responsiveness in aerosolized antigen-exposed mice Shunsuke Suzuki, MD, Yuzo Suzuki, MD, PhD, Naomi Yamamoto, MD, Yutaka Matsumoto, MD, PhD,
Implications on therapy. Prof. of Medicine and Allergy Faculty of Medicine, Cairo University
 Implications on therapy Dr. Hisham Tarraf MD,FRCP(Edinb.) Prof. of Medicine and Allergy Faculty of Medicine, Cairo University Need for better understanding Global health problem Impact on quality of life
Implications on therapy Dr. Hisham Tarraf MD,FRCP(Edinb.) Prof. of Medicine and Allergy Faculty of Medicine, Cairo University Need for better understanding Global health problem Impact on quality of life
The role of exogen proteases in Th 2 cell differentiation and in the pathogenesis of asthma
 Ph.D Thesis The role of exogen proteases in Th 2 cell differentiation and in the pathogenesis of asthma By Attila Kiss M.D. Semmelweis University Doctoral School Semmelweis University Faculty of Pulmonology
Ph.D Thesis The role of exogen proteases in Th 2 cell differentiation and in the pathogenesis of asthma By Attila Kiss M.D. Semmelweis University Doctoral School Semmelweis University Faculty of Pulmonology
Effect of early vitamin D supplementation on asthma and the possible mechanisms
 Effect of early vitamin D supplementation on asthma and the possible mechanisms X. Chen 1, S.Q. Rao 2, B.H. Gao 3 and Z.Q. Jiang 1 1 Department of Nutrition, College of Public Health, Sun Yat-Sen University,
Effect of early vitamin D supplementation on asthma and the possible mechanisms X. Chen 1, S.Q. Rao 2, B.H. Gao 3 and Z.Q. Jiang 1 1 Department of Nutrition, College of Public Health, Sun Yat-Sen University,
CONTENTS. STUDY DESIGN METHODS ELISA protocol for quantitation of mite (Dermatophagoides spp.) Der p 1 or Der f 1
 CONTENTS STUDY DESIGN METHODS ELISA protocol for quantitation of mite (Dermatophagoides spp.) Der p 1 or Der f 1 ELISA protocol for mite (Dermatophagoides spp.) Group 2 ALLERGENS RESULTS (SUMMARY) TABLE
CONTENTS STUDY DESIGN METHODS ELISA protocol for quantitation of mite (Dermatophagoides spp.) Der p 1 or Der f 1 ELISA protocol for mite (Dermatophagoides spp.) Group 2 ALLERGENS RESULTS (SUMMARY) TABLE
Full Paper. Hiroyasu Hirose, Jian Jiang, and Masaru Nishikibe*
 J Pharmacol Sci 92, 209 217 (2003) Journal of Pharmacological Sciences 2003 The Japanese Pharmacological Society Full Paper Effects of Muscarinic Receptor Antagonists With or Without M 2 Antagonist Activity
J Pharmacol Sci 92, 209 217 (2003) Journal of Pharmacological Sciences 2003 The Japanese Pharmacological Society Full Paper Effects of Muscarinic Receptor Antagonists With or Without M 2 Antagonist Activity
Alveolar macrophages modulate allergic inflammation in a murine model of asthma
 EXPERIMENTAL and MOLECULAR MEDICINE, Vol. 43, No. 5, 275-280, May 2011 Alveolar macrophages modulate allergic inflammation in a murine model of asthma Bo-Ram Bang 1,2, Eunyoung Chun 1,2, Eun-Jin Shim 1,2,
EXPERIMENTAL and MOLECULAR MEDICINE, Vol. 43, No. 5, 275-280, May 2011 Alveolar macrophages modulate allergic inflammation in a murine model of asthma Bo-Ram Bang 1,2, Eunyoung Chun 1,2, Eun-Jin Shim 1,2,
Depletion of Alveolar Macrophages by Treatment with 2-Chloroadenosine Aerosol
 CLINICAL AND DIAGNOSTIC LABORATORY IMMUNOLOGY, July 1999, p. 452 456 Vol. 6, No. 4 1071-412X/99/$04.00 0 Copyright 1999, American Society for Microbiology. All Rights Reserved. Depletion of Alveolar Macrophages
CLINICAL AND DIAGNOSTIC LABORATORY IMMUNOLOGY, July 1999, p. 452 456 Vol. 6, No. 4 1071-412X/99/$04.00 0 Copyright 1999, American Society for Microbiology. All Rights Reserved. Depletion of Alveolar Macrophages
Asthma. - A chronic inflammatory disorder which causes recurrent episodes of wheezing, breathlessness, cough and chest tightness.
 Obstructive diseases Asthma - A chronic inflammatory disorder which causes recurrent episodes of wheezing, breathlessness, cough and chest tightness. - Characterized by Intermittent and reversible (the
Obstructive diseases Asthma - A chronic inflammatory disorder which causes recurrent episodes of wheezing, breathlessness, cough and chest tightness. - Characterized by Intermittent and reversible (the
Safety, PK and PD of ARRY-502, a CRTh2 Antagonist, in Healthy Subjects with a History of Seasonal Allergies
 Safety, PK and PD of ARRY502, a CRTh2 Antagonist, in Healthy Subjects with a History of Seasonal Allergies L. Burgess*, L. Anderson, C. Nugent, N. Klopfenstein, C. Eberhardt, L. Carter, C. Kass, S. RojasCaro,
Safety, PK and PD of ARRY502, a CRTh2 Antagonist, in Healthy Subjects with a History of Seasonal Allergies L. Burgess*, L. Anderson, C. Nugent, N. Klopfenstein, C. Eberhardt, L. Carter, C. Kass, S. RojasCaro,
special communication
 Am J Physiol Lung Cell Mol Physiol 280: L565 L573, 2001. special communication Tidal midexpiratory flow as a measure of airway hyperresponsiveness in allergic mice THOMAS GLAAB, 1 ANGELIKA DASER, 2 ARMIN
Am J Physiol Lung Cell Mol Physiol 280: L565 L573, 2001. special communication Tidal midexpiratory flow as a measure of airway hyperresponsiveness in allergic mice THOMAS GLAAB, 1 ANGELIKA DASER, 2 ARMIN
Allergic diseases and treatment. Feng Qian ( 钱峰 )
 Allergic diseases and treatment Feng Qian ( 钱峰 ) fengqian@sjtu.edu.cn Hypersensitivity Antigen Host Adaptive responses protective to the host harmful to the host The deleterious consequences of the adaptive
Allergic diseases and treatment Feng Qian ( 钱峰 ) fengqian@sjtu.edu.cn Hypersensitivity Antigen Host Adaptive responses protective to the host harmful to the host The deleterious consequences of the adaptive
Protocols for the Induction and Evaluation of Systemic Anaphylaxis in Mice
 Chapter 10 Protocols for the Induction and Evaluation of Systemic Anaphylaxis in Mice Elizabeth Doyle, Julia Trosien, and Martin Metz Abstract Mouse models of systemic anaphylaxis are important tools for
Chapter 10 Protocols for the Induction and Evaluation of Systemic Anaphylaxis in Mice Elizabeth Doyle, Julia Trosien, and Martin Metz Abstract Mouse models of systemic anaphylaxis are important tools for
Interleukin-13 Mediates Airways Hyperreactivity through the IL-4 Receptor-Alpha Chain and STAT-6 Independently of IL-5 and Eotaxin
 Interleukin-13 Mediates Airways Hyperreactivity through the IL-4 Receptor-Alpha Chain and STAT-6 Independently of IL-5 and Eotaxin Ming Yang, Simon P. Hogan, Peter J. Henry, Klaus I. Matthaei, Andrew N.
Interleukin-13 Mediates Airways Hyperreactivity through the IL-4 Receptor-Alpha Chain and STAT-6 Independently of IL-5 and Eotaxin Ming Yang, Simon P. Hogan, Peter J. Henry, Klaus I. Matthaei, Andrew N.
Immunotoxicology in Food and Ingredient Safety Assessment: Approaches and Case Studies
 Immunotoxicology in Food and Ingredient Safety Assessment: Approaches and Case Studies April 14, 2015 Toxicology and Food Allergy: Case Study of tbhq Cheryl Rockwell Assistant Professor Department of Pharmacology
Immunotoxicology in Food and Ingredient Safety Assessment: Approaches and Case Studies April 14, 2015 Toxicology and Food Allergy: Case Study of tbhq Cheryl Rockwell Assistant Professor Department of Pharmacology
Small Airways Disease. Respiratory Function In Small Airways And Asthma. Pathophysiologic Changes in the Small Airways of Asthma Patients
 Small Airways Disease Respiratory Function In Small Airways And Relevant Questions On Small Airway Involvement In How can small airway disease be defined? What is the link between small airway abnormalities
Small Airways Disease Respiratory Function In Small Airways And Relevant Questions On Small Airway Involvement In How can small airway disease be defined? What is the link between small airway abnormalities
Eosinophils are not required to induce airway hyperresponsiveness after nematode infection
 2640 A.J.Coyleetal. Eur.J.Immunol.1998.28: 2640 2647 Eosinophils are not required to induce airway hyperresponsiveness after nematode infection Anthony J. Coyle 1, Gabriele Köhler 2, Shogo Tsuyuki 3, Frank
2640 A.J.Coyleetal. Eur.J.Immunol.1998.28: 2640 2647 Eosinophils are not required to induce airway hyperresponsiveness after nematode infection Anthony J. Coyle 1, Gabriele Köhler 2, Shogo Tsuyuki 3, Frank
ASTHMA. Epidemiology. Pathophysiology. Diagnosis. IAP UG Teaching slides
 BRONCHIAL ASTHMA ASTHMA Epidemiology Pathophysiology Diagnosis 2 CHILDHOOD ASTHMA Childhood bronchial asthma is characterized by Airway obstruction which is reversible Airway inflammation Airway hyper
BRONCHIAL ASTHMA ASTHMA Epidemiology Pathophysiology Diagnosis 2 CHILDHOOD ASTHMA Childhood bronchial asthma is characterized by Airway obstruction which is reversible Airway inflammation Airway hyper
IL-13 Augments Compressive Stress-induced Tissue Factor Expression in Human Airway Epithelial Cells
 IL-13 Augments Compressive Stress-induced Tissue Factor Expression in Human Airway Epithelial Cells Jennifer A. Mitchel, Silvio Antoniak, Joo-Hyeon Lee, Sae-Hoon Kim, Maureen McGill, David I. Kasahara,
IL-13 Augments Compressive Stress-induced Tissue Factor Expression in Human Airway Epithelial Cells Jennifer A. Mitchel, Silvio Antoniak, Joo-Hyeon Lee, Sae-Hoon Kim, Maureen McGill, David I. Kasahara,
Therapeutic target validation of protein kinase C (PKC)- for asthma using a mouse model
 INTERNATIONAL JOURNAL OF MOLECULAR MEDICINE 23: 561-566, 2009 561 Therapeutic target validation of protein kinase C (PKC)- for asthma using a mouse model JEONG-SU DO 1*, KANG-SEO PARK 2, HYO-JUNG SEO 1,
INTERNATIONAL JOURNAL OF MOLECULAR MEDICINE 23: 561-566, 2009 561 Therapeutic target validation of protein kinase C (PKC)- for asthma using a mouse model JEONG-SU DO 1*, KANG-SEO PARK 2, HYO-JUNG SEO 1,
Treatment of Allergic Airway Inflammation and Hyperresponsiveness by Antisense-induced Local Blockade of GATA-3 Expression
 Published Online: 29 May, 2001 Supp Info: http://doi.org/10.1084/jem.193.11.1247 Downloaded from jem.rupress.org on July 3, 2018 Treatment of Allergic Airway Inflammation and Hyperresponsiveness by Antisense-induced
Published Online: 29 May, 2001 Supp Info: http://doi.org/10.1084/jem.193.11.1247 Downloaded from jem.rupress.org on July 3, 2018 Treatment of Allergic Airway Inflammation and Hyperresponsiveness by Antisense-induced
Clinical & Experimental Allergy
 doi: 10.1111/j.1365-2222.2010.03459.x Clinical & Experimental Allergy, 40, 933 941 ORIGINAL ARTICLE Experimental Models of Allergic Disease c 2010 Blackwell Publishing Ltd Attenuated Bordetella pertussis
doi: 10.1111/j.1365-2222.2010.03459.x Clinical & Experimental Allergy, 40, 933 941 ORIGINAL ARTICLE Experimental Models of Allergic Disease c 2010 Blackwell Publishing Ltd Attenuated Bordetella pertussis
December 7, 2010 Future Use of Biologics in Allergy and Asthma
 December 7, 2010 Future Use of Biologics in Allergy and Asthma Lanny J. Rosenwasser, M.D. Dee Lyons/Missouri Endowed Chair in Immunology Research Professor of Pediatrics Allergy-Immunology Division Childrens
December 7, 2010 Future Use of Biologics in Allergy and Asthma Lanny J. Rosenwasser, M.D. Dee Lyons/Missouri Endowed Chair in Immunology Research Professor of Pediatrics Allergy-Immunology Division Childrens
Exhaled Nitric Oxide: An Adjunctive Tool in the Diagnosis and Management of Asthma
 Exhaled Nitric Oxide: An Adjunctive Tool in the Diagnosis and Management of Asthma Jason Debley, MD, MPH Assistant Professor, Pediatrics Division of Pulmonary Medicine University of Washington School of
Exhaled Nitric Oxide: An Adjunctive Tool in the Diagnosis and Management of Asthma Jason Debley, MD, MPH Assistant Professor, Pediatrics Division of Pulmonary Medicine University of Washington School of
Combined Rho-kinase inhibition and immunogenic cell death triggers and propagates immunity against cancer
 Supplementary Information Combined Rho-kinase inhibition and immunogenic cell death triggers and propagates immunity against cancer Gi-Hoon Nam, Eun-Jung Lee, Yoon Kyoung Kim, Yeonsun Hong, Yoonjeong Choi,
Supplementary Information Combined Rho-kinase inhibition and immunogenic cell death triggers and propagates immunity against cancer Gi-Hoon Nam, Eun-Jung Lee, Yoon Kyoung Kim, Yeonsun Hong, Yoonjeong Choi,
Using Patient Characteristics to Individualize and Improve Asthma Care
 Using Patient Characteristics to Individualize and Improve Asthma Care Leonard B. Bacharier, M.D. Associate Professor of Pediatrics Clinical Director, Division of Allergy, Immunology, & Pulmonary Medicine
Using Patient Characteristics to Individualize and Improve Asthma Care Leonard B. Bacharier, M.D. Associate Professor of Pediatrics Clinical Director, Division of Allergy, Immunology, & Pulmonary Medicine
Kun Jiang 1, He-Bin Chen 1, Ying Wang 1, Jia-Hui Lin 2, Yan Hu 1, Yu-Rong Fang 1
 Original Article Changes in interleukin-17 and transforming growth factor beta 1 levels in serum and bronchoalveolar lavage fluid and their clinical significance among children with asthma Kun Jiang 1,
Original Article Changes in interleukin-17 and transforming growth factor beta 1 levels in serum and bronchoalveolar lavage fluid and their clinical significance among children with asthma Kun Jiang 1,
Mouse Anti-HDM IgG Antibody Assay Kit
 Mouse Anti-HDM IgG Antibody Assay Kit Catalog # 3030 For Research Use Only - Not Human or Therapeutic Use INTRODUCTION Asthma is a common chronic inflammatory disease that affects 300 million people of
Mouse Anti-HDM IgG Antibody Assay Kit Catalog # 3030 For Research Use Only - Not Human or Therapeutic Use INTRODUCTION Asthma is a common chronic inflammatory disease that affects 300 million people of
Bronchial hyperresponsiveness in type Ia (simple bronchoconstriction) asthma Relationship to patient age and the proportions of bronchoalveolar cells
 28 Bronchial hyperresponsiveness in type I Bronchial hyperresponsiveness in type Ia (simple bronchoconstriction) Relationship to patient age and the proportions of bronchoalveolar cells Kouzou Ashida,
28 Bronchial hyperresponsiveness in type I Bronchial hyperresponsiveness in type Ia (simple bronchoconstriction) Relationship to patient age and the proportions of bronchoalveolar cells Kouzou Ashida,
