Airway Inflammation and Bronchial Hyperresponsiveness after Mycoplasma pneumoniae Infection in a Murine Model
|
|
|
- Claude Carroll
- 5 years ago
- Views:
Transcription
1 Airway Inflammation and Bronchial Hyperresponsiveness after Mycoplasma pneumoniae Infection in a Murine Model Richard J. Martin, Hong Wei Chu, Joyce M. Honour, and Ronald J. Harbeck Department of Medicine, National Jewish Medical and Research Center, Denver, Colorado The interaction between chronic infection and chronic asthma is receiving increased investigation as a factor in the pathophysiology of asthma. To further understand this interaction, we used an animal model (BALB/c mice) with a Mycoplasma pneumoniae respiratory infection. Mice were studied 3, 7, 14, and 21 d after infection. Bronchial hyperresponsiveness (BHR) was assessed by methacholine challenge and was significantly heightened in the infected mice compared with saline controls at Days 3, 7, and 14. The associated inflammatory response was mainly neutrophils. The tissue inflammatory score significantly correlated to BHR (r 0.78, P ). Additionally, tissue interferon (IFN)- was significantly suppressed at Days 3 and 7 in the infected group compared with controls; and at Days 3, 7, and 14 compared with Day 21 in the infected group. There was a significant negative correlation between lung tissue messenger RNA levels of IFN- corrected for -actin and BHR (r 0.50, P 0.022). Thus, M. pneumoniae respiratory infection is associated with BHR in this murine model. It appears that acute mycoplasma infection suppresses IFN-, which may be a pivotal factor in the control of BHR. Increasingly, investigation into the relationship between chronic asthma and chronic infection has suggested that Mycoplasma pneumoniae and/or Chlamydia pneumoniae are present in a large proportion of asthmatic patients (1 5). This is an important finding because it suggests an infectious contribution to asthma pathophysiology and ultimately may lead to new therapeutic strategies. To better investigate the effects of these bacteria on airway function, animal models will need to be developed to study the pathophysiologic alterations that are induced by the bacterial infection. Respiratory infection with M. pulmonis in a murine model is commonly used because this is a natural pathogen for mice (6). However, it is not a human pathogen. Pietsch and colleagues demonstrated that mice infected with M. pneumoniae expressed proinflammatory cytokines similar to those found in human asthma (7). Recently, Wubbell and colleagues investigated the pathogenesis of acute M. pneumoniae respiratory infection in BALB/c mice (8). Thus, although not a natural mouse pathogen, M. pneumoniae respiratory murine infection can be used to investigate the pathophysiologic and inflammatory effects it produces. (Received in original form August 7, 2000 and in revised form December 14, 2000) Address correspondence to: Richard J. Martin, M.D., National Jewish Medical and Research Center, 1400 Jackson St., Denver, CO martinr@njc.org Abbreviations: bronchoalveolar lavage fluid, BALF; bronchial hyperresponsiveness, BHR; interferon, IFN; methacholine, Mch; messenger RNA, mrna; airway opening pressure, Pao; polymerase chain reaction, PCR; pulmonary resistance, R L ; reverse transcription, RT. Am. J. Respir. Cell Mol. Biol. Vol. 24, pp , 2001 Internet address: The present study was designed to determine the alterations in bronchial hyperresponsiveness (BHR) and the associated inflammatory responses over a 3-wk time interval in a mouse model of M. pneumoniae respiratory infection. Materials and Methods Organism M. pneumoniae (strain FH, ATCC 15531) was grown in SP-4 broth for 72 h at 37 C (9). Organisms were harvested, centrifuged at 10,000 g for 20 min, washed with sterile saline, and resuspended in saline to yield approximately organisms/50 l. Animals All experimental animals used in this study were covered by a protocol approved by the Institutional Animal Care and Use Committee. BALB/c mice were obtained from Jackson Laboratories (Bar Harbor, ME). They were quarantined for 4 wk before the experiment and bled to establish that they were virus-free, as indicated by negative antibody titers to six common murine pathogens. They were also negative for M. pulmonis. The mice were housed in autoclaved microisolation cages bedded with autoclaved pine chips (Sani Chips; J. P. Murphy Forest Products, Montville, NJ) using standard barrier techniques. The diet consisted of water and Purina 5015 Mouse Chow. After infection with M. pneumoniae, the infected mice and their saline controls were housed in a flexible film isolator (Model #M20; Isotec-Harlan Sprague Dawley, Indianapolis, IN) in the P3 facility of our vivarium. Inoculation for Groups Mice were inoculated with either M. pneumoniae or saline at Day 0. Before the inoculation, all the mice were intraperitoneally anesthetized with Avertin (ethanol) at 0.25 g/kg. Mice in the infected group were inoculated intranasally with 50 l of M. pneumoniae containing colony-forming units. A similar 50- l inoculation of saline was given to the mice in the control group. Measurement of Airway Resistance After a single inoculation of either M. pneumoniae or saline, BHR testing to increasing doses of methacholine (Mch) with resultant airway resistance measurements was performed in mice at Days 3, 7, 14, and 21. There were nine mice in each group at each time point. The BHR test was performed in anesthetized, tracheostomized mice mechanically ventilated in a body plethysmograph using a modification of methods described by Martin and colleagues (10). Mice were initially anesthetized with 90 mg/kg intraperitoneal pentobarbital sodium (Abbott Laboratories, North Chicago, IL), and the trachea was exposed. A metal 19-gauge endotracheal catheter was inserted and was sutured in the trachea. After surgery, the mice were placed in a plethysmograph and the tracheostomy tube was attached to a four-way connector (Y-Tc 13/ 4; Small Parts, Miami Lakes, FL), with one port connected to a catheter measuring airway opening pressure (Pao) and two ports connected to the inspiratory and expiratory ports of a volume cycled ventilator (Model #SN-480-7; Tokyo, Japan). The mice were ventilated at a rate of 160 breaths/min, with a tidal volume of 0.4
2 578 AMERICAN JOURNAL OF RESPIRATORY CELL AND MOLECULAR BIOLOGY VOL ml and 2 to 4 cm H 2 O positive end-expiratory pressure. Transpulmonary pressure was estimated as the Pao, referenced to pressure within the plethysmograph. Pao approximates transpulmonary pressure in the mouse, inasmuch as the chest wall contributes little to the overall compliance of the respiratory system. Changes in volume were determined by pressure changes in the plethysmographic chamber referenced to pressure in a reference box using a differential pressure transducer (Validyne CD19A Carrier Demo; Validyne Engineering, Northridge, CA), electronically phased with a timing delay circuit to 5 degrees at 10 Hz, and then converted from an analog to a digital signal using a 16-bit analog-to-digital board (model NB MIO-16x-18: National Instruments, Austin, TX) at 600 bits/s 1 /channel 1. The digitized signals were fed into a computer (Macintosh Quadra 8 model M1206; Apple Computer, Cupertino, CA) and were analyzed using a real-time computer program (LabVIEW 2.2.1; National Instruments). LabVIEW uses pressure, flow, volume, and average compliance to calculate pulmonary resistance (R L ) using a recursive least-squares method (11). The breath-by-breath results for R L were tabulated and the reported values are the average of at least 10 breaths at the peak response for each Mch dose. Results are expressed as means standard error of the mean for each dose. Acetyl- -methylcholine (Sigma Chemical Co., St. Louis, MO) was dissolved in normal saline and aerosolized with an ultrasonic nebulizer (Model #5500D DeVilbiss; Health Care, Inc., Somerset, PA). Twenty breaths, at a rate of 30 breaths a minute with tidal volume 0.5 ml of aerosolized mist, were delivered to the mouse with a volume-cycled ventilator (Model 680; Harvard Apparatus Rodent Ventilator, South Natick, MA). Airway resistance was measured during the baseline period before administration of Mch, then after a saline control dose and each subsequent doubling Mch dose from 1.6 to 50 mg ml. Bronchoalveolar Lavage After Mch challenge, a bronchoalveolar lavage (BAL) was performed using 1 ml of saline in all mice. The BAL fluid (BALF) was analyzed for cell count and differential, mycoplasma culture, and polymerase chain reaction (PCR) for M. pneumoniae. either the P1 adhesion gene or the 16S ribosomal RNA (rrna) gene of M. pneumoniae (1). The sizes of PCR products for P1 and 16S gene are 103 and 260 base pairs (bp), respectively. To further confirm the PCR specificity, 16S rrna gene PCR products (five positive and five negative) were tested by Southern blot analysis using a 32 P-labeled specific oligonucleotide probe. RT-PCR RT-PCR was performed to detect IFN- messenger RNA (mrna) expression in the lung tissue from both infected and saline control mice. Total cellular RNA was isolated from the lung using a microscale RNA isolation kit (5-3 Prime Inc., Boulder, CO). RT was performed on 2 g of total RNA as previously reported (13). After RT, the complementary DNA (cdna) for IFN- was amplified using the mouse IFN- primers (Clontech, Palo Alto, CA). The cdna for -actin was also amplified as a control using mouse -actin primers (Clontech). PCR was performed in a 50- l reaction mixture containing 0.4 M of each primer, 50 mm Tris-HCl (ph 8.3), 15 mm KCl, 0.2 mm of each deoxynucleotide triphosphate, 1.5 mm MgCl 2, and 0.04 U/ l Taq DNA polymerase (GIBCO Life Science, Gaithersburg, MD). The PCR reactions were carried out on a DNA Thermal Cycler GeneAmp PCR system 2400 (Perkin-Elmer, Norwalk, CT) for 35 cycles using the following step cycle: 94 C for 30 s, 60 C for 30 s, 72 C for 1 min. Aliquots (25 l) of the PCR products were electrophoresed in a 1.6% agarose gel, stained with ethidium bromide, and photographed. The specific PCR products for IFN- and -actin are 365 and 540 bp, respectively. IFN- and -actin bands were quantitated by densitometry (NIH Image Software; NIH, Bethesda, MD). IFN- / -actin ratio was used to represent IFN- mrna expression levels. Statistics The outcome variables were analyzed by using the Kruskal Wallis test for continuous responses. For correlative analyses the Spearman rho was used (14). Histologic Analysis After lavage, the lungs were excised. Part of the lung tissue was taken for mycoplasma culture and reverse transcription (RT) PCR for interferon (IFN)-. The rest of the lung was immersed in 4% paraformaldehyde and fixed in the same solution overnight at 4 C. Lung tissue specimens were then embedded in paraffin and cut at 4 m. Hematoxylin and eosin (H&E) stained lung sections were evaluated under the light microscope using a histopathologic inflammatory scoring system as described previously in a hamster M. pneumoniae infection model (12). A final score per mouse on a scale of 0 to 26 (least to most severe) was obtained on the assessment of quantity and quality of peribronchiolar and peribronchial inflammatory infiltrates, luminal exudates, perivascular infiltrates, and parenchymal pneumonia. Mycoplasma Culture Minced lung tissue (approximate total size mm) and 200 l BALF were collected from mice in both infected and saline control groups. The samples were cultured at 37 C in SP-4 broth for up to 4 wk. After a week of culture in SP-4 broth, an aliquot (about 50 l) of culture media was transferred, plated on PPLO agar plates, and incubated at 37 C for 3 more weeks. M. pneumoniae PCR After 6 wk of incubation, the culture solution was centrifuged and the resulting pellet was used for DNA extraction. The extracted DNA was analyzed by PCR using specific primer sets for Figure 1. The percent positivity of M. pneumoniae by culture and PCR in BALF (A) and lung tissue (B).
3 Martin, Chu, Honour, et al.: Bronchial Hyperresponsiveness and Infection 579 Figure 2. Dose response curves to Mch on Days 3, 7, 14, and 21. *P 0.05 for control group (circles with solid lines) compared with the infected group (squares with dashed lines). Figure 4. The histology scores (see MATERIALS AND METHODS) for the saline group (filled bars) and infected group (open bars) are shown for Days 3, 7, 14, and 21 after infection. *P 0.05 between groups. Results Detection of M. pneumoniae Figure 1A shows the detection of M. pneumoniae by culture and PCR in the BALF from infected mice. There was 100% detection at Day 3 in culture and Days 3 and 7 by PCR. The other time points ranged from 40 to 70% detection. Detection of M. pneumoniae in the lung tissue had a positivity similar to that seen in the BALF (Figure 1B). All control group days were negative for M. pneumoniae. BHR Figure 2 shows that BHR on Day 3 was significantly increased at 12.5, 25, and 50 mg/ml and on Day 7 at 25 and 50 mg/ml compared with the control mice (P 0.05). On Day 14, the 25 mg/ml dose showed a significant difference (P 0.05) and a trend at 50 mg ml. No differences were found at Day 21. Figure 3. The total white-cell count in BALF (upper left panel) and differential are shown for Days 3, 7, 14, and 21 after infection. Eosinophils are not shown because they were 1% on all days. Saline control, filled bars; infected mice, open bars. *P 0.05 between groups. Inflammation Figure 3 shows the BALF total white cell count and the cell differential at the different time points. This was mainly a neutrophilic response with significantly elevated time points at Days 3 and 7 in the infected groups compared with controls (P 0.05). Correspondingly, the macrophages and lymphocytes were decreased on Day 3 (P 0.05) and elevated on Days 14 and 21, respectively (P 0.05). The histology score (Figure 4) demonstrated significant increases for the infected group on Days 3, 7, and 14 (P 0.05) compared with control. The lung tissue at Day 3 showed the most intense inflammatory response, characterized by peribronchiolar, bronchial, and perivascular infiltrates; parenchymal pneumoniae; and bronchial luminal exudate (Figure 5). There were large numbers of neutrophils and mononuclear cells in the inflammatory sites. After Day 3, the inflammatory response was seen mainly around the bronchioles and blood vessels, with decreasing numbers of both neutrophils and mononuclear cells. At all time points, tissue eosinophils were rarely seen. No inflammation was observed in saline control mice. There was a highly significant correlation between the tissue inflammation score and airway resistance to Mch (Figure 6), r 0.78, P IFN- mrna Expression The expression of IFN- mrna in the lung tissue was significantly depressed in the infected groups on Days 3 and 7 (P 0.03) compared with the control groups (Figure 7). In the infected group, the positivity of IFN- expression was significantly higher on Day 21 than on Days 3, 7, and 14 (P 0.002). There was a significant negative correlation (Figure 8) between IFN- / -actin and Mch airway resistance (r 0.50, P 0.022); whereas the suppression of IFN- appeared to allow BHR to increase, and its recovery to an elevated level (Figure 7) appeared to decrease BHR. Discussion A murine model of M. pneumoniae respiratory infection was developed to evaluate the alterations in BHR and air-
4 580 AMERICAN JOURNAL OF RESPIRATORY CELL AND MOLECULAR BIOLOGY VOL Figure 6. Correlation between the tissue inflammatory score and BHR at a Mch dose of 50 mg/ml on Days 3, 7, 14, and 21 after infection. way inflammation produced by this microorganism. The acute effect, at 3 d, demonstrated a neutrophil response associated with increased BHR. The increase in BHR was also seen at Days 7 and 14, which corresponded to the tissue inflammatory score being elevated through Day 14. At Day 21 the inflammatory response and BHR were similar to the control population. Indeed, the lung tissue inflammatory score had a high correlation with BHR (r 0.78, P 0.001), as shown in Figure 6. Of potential importance was the relationship between the tissue expression of IFN- mrna and BHR. It appeared that M. pneumoniae respiratory infection suppressed IFN- at Days 3 and 7 with a trend at Day 14, and as the infection waned at Day 21 there was a significant increase in IFN- (Figure 7). The IFN- mrna levels were significantly correlated in a reverse fashion to lung resistance (r 0.50, P 0.022). Our murine model of M. pneumoniae infection produced an acute lung tissue inflammatory response similar to that reported by Wubbel and coworkers (8). The fol- Figure 5. Histology of mouse lung tissue. Saline-treated mouse lung (A) at Day 3 shows no inflammatory response. M. pneumoniae infected mouse lung at Day 3 (B and C) shows intensive inflammatory responses. View in C amplifies part of B and details the inflammatory infiltrates around a bronchiole (yellow arrowhead) and a blood vessel (green arrowhead), in the airway lumen (green arrow) and lung parenchyma (black arrow). Neutrophils, mononuclear cells, and alveolar macrophages are the main components of the inflammatory infiltrates. (H&E staining; original magnification: A and B, 200; C, 400). Figure 7. IFN- mrna expression level in the infected group (open bars) is significantly depressed at Days 3 and 7 after infection compared with controls (filled bars). At Day 21, in the infected group, IFN- is significantly greater than at Days 3, 7, and 14. *P 0.03 control versus infected groups; **P for Day 21 in the infected group compared with other days.
5 Martin, Chu, Honour, et al.: Bronchial Hyperresponsiveness and Infection 581 sensitization in the absence of eosinophils and IgE increases. This finding has also been documented by others (17 19). In summary, we found that a murine model of acute respiratory mycoplasma infection can induce BHR. The involved mechanism needs further elucidation, but may be linked to IFN- suppression. As IFN- increased, BHR decreased. With regard to human asthma, chronic reoccurring mycoplasma or chlamydia infection may modulate IFN- and produce a state of chronic BHR. Additionally, the interaction between chronic infection and atopy may further modulate IFN- and BHR in the pathophysiology of asthma. This murine model of mycoplasma respiratory infection can serve to enlighten our knowledge of this potential interaction. Figure 8. The negative correlation between lung tissue mrna levels of IFN- corrected for -actin and BHR at 50 mg/ml of Mch on Days 3, 7, 14, and 21. Acknowledgments: The authors thank Peter Henson, Ph.D., for his guidance; and Ms. Mary Peterson for assistance in manuscript preparation. This work was supported by an Asthma Research Center Award from the American Lung Association. lowing areas are new in our current study. We measured the BHR to see whether acute M. pneumoniae infection would induce BHR. As stated earlier, a single infection significantly increased BHR for up to 14 d and the tissue inflammatory response appeared to have a pivotal role in inducing the BHR. As lung inflammation diminished, BHR decreased, especially at the lower concentrations of the bronchoconstrictor. IFN-, a cytokine involved in infection and the regulation of BHR, was demonstrated to be associated with the induction or suppression of BHR in this model, depending on the level of IFN- expression in the lung. This finding is supported by the work of Hofstra and colleagues (15), who demonstrated that ovalbumin-sensitized wild-type BALB/c mice upregulated immunoglobulin (Ig) E, airway hyperresponsiveness, and infiltration of eosinophils and mononuclear cells in BALF. However, in IFN- knockout mice, only a reduced eosinophilic infiltration was observed after challenge. Additionally, parenteral IFN- given to wild-type mice downregulated the IgE levels, airway hyperresponsiveness, and airway cellular infiltration. When given aerosolized IFN-, only suppression of hyperresponsiveness occurred. In our infection model, the initial suppression of IFN- was associated with marked BHR even in the absence of eosinophilia. As IFN- increased, BHR decreased. This may be a major controlling factor in BHR. It is interesting to note that a dramatic decrease of BALF total white-cell count at Day 7 was not accompanied by a similar decrease in lung tissue inflammation, as shown in Figure 4. In fact, at Days 7 and 14 there was still an increase in lung tissue inflammation as compared with the saline control groups. These data indicate that lung tissue inflammation lasts longer than BALF total white-cell count. As shown in Figure 6, this relatively long-lasting lung tissue inflammation may be responsible for BHR in infected mice. The lack of eosinophils but increased BHR has also been shown by Wilder and colleagues (16). In their model of BHR in BALBc mice, BHR was induced by ovalbumin References 1. Kraft, M., G. H. Cassell, J. E. Henson, H. Watson, J. Williamson, B. P. Marmion, C. A. Gaydos, and R. J. Martin Detection of Mycoplasma pneumoniae in the airways of adults with chronic asthma. Am. J. Respir. Crit. Care Med. 158: [Erratum Am. J. Respir. Crit. Care Med :1692] 2. Hahn, D. L., R. W. Dodge, and R. Golubjatnikov Association of Chlamydia pneumoniae (strain TWAR) infection with wheezing, asthmatic bronchitis, and adult-onset asthma. JAMA 266: Gil, J. C., R. L. Cedillo, B. G. Mayagoitia, and M. D. Puz Isolation of Mycoplasma pneumoniae from asthmatic patients. Ann. Allergy 70: Yuno, T., Y. Ichikawa, S. Kumatu, S. Arai, and K. Oizum Association of Mycoplasma pneumoniae antigen with initial onset of bronchial asthma. Am. J. Respir. Crit. Care Med. 149: Emre, U., P. M. Roblin, M. Gelling, W. Dumornay, M. Rao, M. R. Hammerschlag, and J. Schacter The association of Chlamydia pneumoniae infection and reactive airway disease in children. Arch. Pediatr. Adolesc. Med. 148: Bowden, J. J., T. R. Schoeb, J. R. Lindsey, and D. M. McDonald Dexamethasone and oxytetracycline reverse the potentiation of neurogenic inflammation in airways of rats with Mycoplasma pulmonis infection. Am. J. Respir. Crit. Care Med. 150: Pietsch, K., S. Ehlers, and E. Jacobs Cytokine gene expression in lungs of BALB c mice during primary and secondary intranasal infection with Mycoplasma pneumoniae. Microbiology 140: Wubbel, L., H. S. Jafri, K. Olsen, S. Shelton, B. Barton-Rogers, G. Gambill, P. Patel, E. Keysey, G. Cassell, and G. H. McCracken Mycoplasma pneumoniae pneumonia in a mouse model. J. Infect. Dis. 178: Tully, J. G Culture medium formulation for primary isolation and maintenance of mollicutes. In Molecular and Diagnostic Procedures in Mycoplasmology, Vol. I. S. Razin and J. G. Tully, editors. Academic Press, New York Martin, T. R., N. P. Gerard, S. J. Galli, and J. M. Drazen Pulmonary responses to bronchoconstrictor agonists in the mouse. J. Appl. Physiol. 64: Lauzon, A. M., and J. H. Bates Estimation of time-varying respiratory mechanical parameters by recursive least squares. J. Appl. Physiol. 71: Cimolai, N., G. P. Taylor, D. Mah, and B. J. Morrison Definition and application of a histopathological scoring scheme for an animal model of acute Mycoplasma pneumoniae pulmonary infection. Microbiol. Immunol. 36: Bosse, M., M. Audette, C. Ferland, G. Pelletier, H. W. Chu, A. Dakhama, S. Lavigne, L. P. Boulet, and M. Laviolette Gene expression of interleukin-2 in purified human peripheral blood eosinophils. Immunology 87: Snedecor, G. W., and W. G. Cochran Statistical Methods. Iowa State University Press, Ames, IA Hofstra, C. L., I. Van Ark, G. Hofman, F. P. Nijkamp, P. M. Jardieu, and A. J. M. Van Oosterhout Differential effects of endogenous and exogenous interferon- on immunoglobulin E, cellular infiltration, and airway responsiveness in a murine model of allergic asthma. Am. J. Respir. Cell Mol. Biol. 19: Wilder, J. A., D. S. Collic, B. S. Wilson, D. E. Bice, C. R. Lyons, and M. F.
6 582 AMERICAN JOURNAL OF RESPIRATORY CELL AND MOLECULAR BIOLOGY VOL Lipscomb Dissociation of airway hyperresponsiveness from immunoglobulin E and airway eosinophilia in a murine model of allergic asthma. Am. J. Respir. Cell Mol. Biol. 20: Corry, D. B., H. G. Folkesson, M. L. Warnock, D. J. Erle, M. A. Matthay, J. P. Wiener-Kronish, and R. M. Locksley Interleukin-4, but not interleukin-5 or eosinophils, is required in a murine model of acute airway hyperreactivity. J. Exp. Med. 183: [Erratum J. Exp. Med :1715] 18. Kung, T. T., H. Jones, G. K. Adams, III, S. P. Umland, W. Kreutner, R. W. Egan, R. W. Chapman, and A. S. Watnick Characterization of a murine model of allergic pulmonary inflammation. Int. Arch. Allergy Immunol. 105: Zhang, Y., W. J. Lamm, R. K. Albert, E. Y. Chi, W. R. Henderson, Jr., and D. B. Lewis Influence of the route of allergen administration and genetic background on the murine allergic pulmonary response. Am. J. Respir. Crit. Care Med. 155:
Effects of Respiratory Mycoplasma pneumoniae Infection on Allergen-Induced Bronchial Hyperresponsiveness and Lung Inflammation in Mice
 INFECTION AND IMMUNITY, Mar. 2003, p. 1520 1526 Vol. 71, No. 3 0019-9567/03/$08.00 0 DOI: 10.1128/IAI.71.3.1520 1526.2003 Copyright 2003, American Society for Microbiology. All Rights Reserved. Effects
INFECTION AND IMMUNITY, Mar. 2003, p. 1520 1526 Vol. 71, No. 3 0019-9567/03/$08.00 0 DOI: 10.1128/IAI.71.3.1520 1526.2003 Copyright 2003, American Society for Microbiology. All Rights Reserved. Effects
Asthma, rhinitis, other respiratory diseases. A link between chronic asthma and chronic infection
 Asthma, rhinitis, other respiratory diseases A link between chronic asthma and chronic infection Richard J. Martin, MD, a Monica Kraft, MD, a Hong Wei Chu, MD, a Eric A. Berns, MS, b and Gail H. Cassell,
Asthma, rhinitis, other respiratory diseases A link between chronic asthma and chronic infection Richard J. Martin, MD, a Monica Kraft, MD, a Hong Wei Chu, MD, a Eric A. Berns, MS, b and Gail H. Cassell,
Soluble ADAM33 initiates airway remodeling to promote susceptibility for. Elizabeth R. Davies, Joanne F.C. Kelly, Peter H. Howarth, David I Wilson,
 Revised Suppl. Data: Soluble ADAM33 1 Soluble ADAM33 initiates airway remodeling to promote susceptibility for allergic asthma in early life Elizabeth R. Davies, Joanne F.C. Kelly, Peter H. Howarth, David
Revised Suppl. Data: Soluble ADAM33 1 Soluble ADAM33 initiates airway remodeling to promote susceptibility for allergic asthma in early life Elizabeth R. Davies, Joanne F.C. Kelly, Peter H. Howarth, David
Noninvasive Measurement of Airway Responsiveness in Allergic Mice Using Barometric Plethysmography
 Noninvasive Measurement of Airway Responsiveness in Allergic Mice Using Barometric Plethysmography E. HAMELMANN, J. SCHWARZE, K. TAKEDA, A. OSHIBA, G. L. LARSEN, C. G. IRVIN, and E. W. GELFAND Divisions
Noninvasive Measurement of Airway Responsiveness in Allergic Mice Using Barometric Plethysmography E. HAMELMANN, J. SCHWARZE, K. TAKEDA, A. OSHIBA, G. L. LARSEN, C. G. IRVIN, and E. W. GELFAND Divisions
Potent and Selective CRTh2 Antagonists are Efficacious in Models of Asthma, Allergic Rhinitis and Atopic Dermatitis
 Potent and Selective CRTh2 Antagonists are Efficacious in Models of Asthma, Allergic Rhinitis and Atopic Dermatitis Laura L. Carter, Yoshi Shiraishi, Yooseob Shin, Laurence Burgess, Christine Eberhardt,
Potent and Selective CRTh2 Antagonists are Efficacious in Models of Asthma, Allergic Rhinitis and Atopic Dermatitis Laura L. Carter, Yoshi Shiraishi, Yooseob Shin, Laurence Burgess, Christine Eberhardt,
Dissociation of Airway Hyperresponsiveness from Immunoglobulin E and Airway Eosinophilia in a Murine Model of Allergic Asthma
 Dissociation of Airway Hyperresponsiveness from Immunoglobulin E and Airway Eosinophilia in a Murine Model of Allergic Asthma Julie A. Wilder, D. David S. Collie,* Bridget S. Wilson, David E. Bice, C.
Dissociation of Airway Hyperresponsiveness from Immunoglobulin E and Airway Eosinophilia in a Murine Model of Allergic Asthma Julie A. Wilder, D. David S. Collie,* Bridget S. Wilson, David E. Bice, C.
/01/$ DOI: /IAI Copyright 2001, American Society for Microbiology. All Rights Reserved.
 INFECTION AND IMMUNITY, June 2001, p. 3869 3876 Vol. 69, No. 6 0019-9567/01/$04.00 0 DOI: 10.1128/IAI.69.6.3869 3876.2001 Copyright 2001, American Society for Microbiology. All Rights Reserved. Elevated
INFECTION AND IMMUNITY, June 2001, p. 3869 3876 Vol. 69, No. 6 0019-9567/01/$04.00 0 DOI: 10.1128/IAI.69.6.3869 3876.2001 Copyright 2001, American Society for Microbiology. All Rights Reserved. Elevated
(A) PCR primers (arrows) designed to distinguish wild type (P1+P2), targeted (P1+P2) and excised (P1+P3)14-
 1 Supplemental Figure Legends Figure S1. Mammary tumors of ErbB2 KI mice with 14-3-3σ ablation have elevated ErbB2 transcript levels and cell proliferation (A) PCR primers (arrows) designed to distinguish
1 Supplemental Figure Legends Figure S1. Mammary tumors of ErbB2 KI mice with 14-3-3σ ablation have elevated ErbB2 transcript levels and cell proliferation (A) PCR primers (arrows) designed to distinguish
Role of Tyk-2 in Th9 and Th17 cells in allergic asthma
 Supplementary File Role of Tyk-2 in Th9 and Th17 cells in allergic asthma Caroline Übel 1*, Anna Graser 1*, Sonja Koch 1, Ralf J. Rieker 2, Hans A. Lehr 3, Mathias Müller 4 and Susetta Finotto 1** 1 Laboratory
Supplementary File Role of Tyk-2 in Th9 and Th17 cells in allergic asthma Caroline Übel 1*, Anna Graser 1*, Sonja Koch 1, Ralf J. Rieker 2, Hans A. Lehr 3, Mathias Müller 4 and Susetta Finotto 1** 1 Laboratory
10.00 PBS OVA OVA+isotype antibody 8.00 OVA+anti-HMGB1. PBS Methatroline (mg/ml)
 RESEARCH ARTICLE Penh (100% of PBS) 1 PBS 8.00 +anti-hmgb1 6.00 4.00 p=0.054 Cellular & Molecular Immunology advance online publication, PBS 3.12 6.25 Methatroline (mg/ml) Neutrophil isolation and culture
RESEARCH ARTICLE Penh (100% of PBS) 1 PBS 8.00 +anti-hmgb1 6.00 4.00 p=0.054 Cellular & Molecular Immunology advance online publication, PBS 3.12 6.25 Methatroline (mg/ml) Neutrophil isolation and culture
Antimicrobial and Immunologic Activities of Clarithromycin in a Murine Model of Mycoplasma pneumoniae-induced Pneumonia
 ANTIMICROBIAL AGENTS AND CHEMOTHERAPY, May 2003, p. 1614 1620 Vol. 47, No. 5 0066-4804/03/$08.00 0 DOI: 10.1128/AAC.47.5.1614 1620.2003 Copyright 2003, American Society for Microbiology. All Rights Reserved.
ANTIMICROBIAL AGENTS AND CHEMOTHERAPY, May 2003, p. 1614 1620 Vol. 47, No. 5 0066-4804/03/$08.00 0 DOI: 10.1128/AAC.47.5.1614 1620.2003 Copyright 2003, American Society for Microbiology. All Rights Reserved.
Chemical Chaperones Mitigate Experimental Asthma By Attenuating Endoplasmic
 Chemical Chaperones Mitigate Experimental Asthma By Attenuating Endoplasmic Reticulum Stress Lokesh Makhija, BE, Veda Krishnan, MSc, Rakhshinda Rehman, MTech, Samarpana Chakraborty, MSc, Shuvadeep Maity,
Chemical Chaperones Mitigate Experimental Asthma By Attenuating Endoplasmic Reticulum Stress Lokesh Makhija, BE, Veda Krishnan, MSc, Rakhshinda Rehman, MTech, Samarpana Chakraborty, MSc, Shuvadeep Maity,
ORIGINAL ARTICLE. Chiung-Zuei Chen, 1 Bei-Chang Yang, 2 Tsun-Mei Lin, 3 Cheng-Hung Lee, 1 Tzuen-Ren Hsiue 1 *
 ORIGINAL ARTICLE Chronic and Repeated Chlamydophila pneumoniae Lung Infection can Result in Increasing IL-4 Gene Expression and Thickness of Airway Subepithelial Basement Membrane in Mice Chiung-Zuei Chen,
ORIGINAL ARTICLE Chronic and Repeated Chlamydophila pneumoniae Lung Infection can Result in Increasing IL-4 Gene Expression and Thickness of Airway Subepithelial Basement Membrane in Mice Chiung-Zuei Chen,
Effect of Azithromycin plus Rifampin versus That of Azithromycin Alone on the Eradication of Chlamydia pneumoniae
 Antimicrobial Agents and Chemotherapy, June 1999, p. 1491-1493, Vol. 43, No. 6 0066-4804/99/$04.00+0 Copyright 1999, American Society for Microbiology. All rights reserved. Effect of Azithromycin plus
Antimicrobial Agents and Chemotherapy, June 1999, p. 1491-1493, Vol. 43, No. 6 0066-4804/99/$04.00+0 Copyright 1999, American Society for Microbiology. All rights reserved. Effect of Azithromycin plus
Effects of Mycoplasma pneumoniae infection on airway neurokinin-1 receptor expression in BALB/c mice
 Effects of Mycoplasma pneumoniae infection on airway neurokinin-1 receptor expression in BALB/c mice H. Zhang 1, B. Wei 2, Y.X. Shang 1, X.Y. Jiao 1, L. Wang 1, M.B. He 3, X.H. Han 1 and G.Z. Wang 3 1
Effects of Mycoplasma pneumoniae infection on airway neurokinin-1 receptor expression in BALB/c mice H. Zhang 1, B. Wei 2, Y.X. Shang 1, X.Y. Jiao 1, L. Wang 1, M.B. He 3, X.H. Han 1 and G.Z. Wang 3 1
Supplementary Figure S1. Flow cytometric analysis of the expression of Thy1 in NH cells. Flow cytometric analysis of the expression of T1/ST2 and
 Supplementary Figure S1. Flow cytometric analysis of the expression of Thy1 in NH cells. Flow cytometric analysis of the expression of T1/ST2 and Thy1 in NH cells derived from the lungs of naïve mice.
Supplementary Figure S1. Flow cytometric analysis of the expression of Thy1 in NH cells. Flow cytometric analysis of the expression of T1/ST2 and Thy1 in NH cells derived from the lungs of naïve mice.
Supplementary Information
 Supplementary Information TABLE S1. SUBJECT CHARACTERISTICS* Normal Control Subjects Subjects with Asthma p Value Number 23 48 Age (years) 35±10 35±10 0.75 Sex, M:F (% F) 9:12 (57) 17:26 (60) 0.76 FEV1
Supplementary Information TABLE S1. SUBJECT CHARACTERISTICS* Normal Control Subjects Subjects with Asthma p Value Number 23 48 Age (years) 35±10 35±10 0.75 Sex, M:F (% F) 9:12 (57) 17:26 (60) 0.76 FEV1
IgE-mediated allergy in elderly patients with asthma
 Allergology international (1997) 46: 237-241 Original Article IgE-mediated allergy in elderly patients with asthma Fumihiro Mitsunobu, Takashi Mifune, Yasuhiro Hosaki, Kouzou Ashida, Hirofumi Tsugeno,
Allergology international (1997) 46: 237-241 Original Article IgE-mediated allergy in elderly patients with asthma Fumihiro Mitsunobu, Takashi Mifune, Yasuhiro Hosaki, Kouzou Ashida, Hirofumi Tsugeno,
SUPPLEMENTAL MATERIAL. Supplementary Methods
 SUPPLEMENTAL MATERIAL Supplementary Methods Culture of cardiomyocytes, fibroblasts and cardiac microvascular endothelial cells The isolation and culturing of neonatal rat ventricular cardiomyocytes was
SUPPLEMENTAL MATERIAL Supplementary Methods Culture of cardiomyocytes, fibroblasts and cardiac microvascular endothelial cells The isolation and culturing of neonatal rat ventricular cardiomyocytes was
Therapeutic efficacy of an anti IL-5 monoclonal antibody delivered into the respiratory tract in a murine model of
 Therapeutic efficacy of an anti IL-5 monoclonal antibody delivered into the respiratory tract in a murine model of asthma Felix R. Shardonofsky, MD, Joe Venzor III, MD, Roberto Barrios, MD, Khai-Pang Leong,
Therapeutic efficacy of an anti IL-5 monoclonal antibody delivered into the respiratory tract in a murine model of asthma Felix R. Shardonofsky, MD, Joe Venzor III, MD, Roberto Barrios, MD, Khai-Pang Leong,
The Effect of BTP on the Development of Allergic Asthma in Mice
 93 The Effect of BTP on the Development of Allergic Asthma in Mice Alana Curry, McNair Scholar, Virginia State University Faculty Advisor: Avery August, Ph.D Associate Professor of Immunology Department
93 The Effect of BTP on the Development of Allergic Asthma in Mice Alana Curry, McNair Scholar, Virginia State University Faculty Advisor: Avery August, Ph.D Associate Professor of Immunology Department
감초 (Glycyrrhiza uralensis Fisch, GLU) 가천식모델생쥐의 BALF 내면역세포및 Cytokine 에미치는효과
 감초 (Glycyrrhiza uralensis Fisch, GLU) 가천식모델생쥐의 BALF 내면역세포및 Cytokine 에미치는효과 Effects of Glycyrrhiza uralensis Fisch on Immunocyte and Cytokine Production in Asthma Model Mouse Young-Joo Han, Yang-Chun Park
감초 (Glycyrrhiza uralensis Fisch, GLU) 가천식모델생쥐의 BALF 내면역세포및 Cytokine 에미치는효과 Effects of Glycyrrhiza uralensis Fisch on Immunocyte and Cytokine Production in Asthma Model Mouse Young-Joo Han, Yang-Chun Park
Abstract. IgE. IgE Th2. x x IL-4 IL-5 IgE CD4 +
 D. o ƒf 6,''!" # + % %$ '& ' '' & " k n k x k k k k k x k IgE k x IgE Ò1Ó k Ò2Ó v k x IgE Th2 x } x x IL-4 IL-5 IgE IgE j IFN-γ IgG j j CD4 + { k d «d j B7 w k k x IgE k 1 k Abstract Parental immunization
D. o ƒf 6,''!" # + % %$ '& ' '' & " k n k x k k k k k x k IgE k x IgE Ò1Ó k Ò2Ó v k x IgE Th2 x } x x IL-4 IL-5 IgE IgE j IFN-γ IgG j j CD4 + { k d «d j B7 w k k x IgE k 1 k Abstract Parental immunization
Modulation of hyperresponsiveness by glutathione in a murine in vivo model of allergic asthma
 6 Modulation of hyperresponsiveness by glutathione in a murine in vivo model of allergic asthma J. Kloek, I. Van Ark, G. Folkerts, F. De Clerck,, N. Bloksma,, F.P. Nijkamp. Department of Pharmacology and
6 Modulation of hyperresponsiveness by glutathione in a murine in vivo model of allergic asthma J. Kloek, I. Van Ark, G. Folkerts, F. De Clerck,, N. Bloksma,, F.P. Nijkamp. Department of Pharmacology and
Pair-fed % inkt cells 0.5. EtOH 0.0
 MATERIALS AND METHODS Histopathological analysis Liver tissue was collected 9 h post-gavage, and the tissue samples were fixed in 1% formalin and paraffin-embedded following a standard procedure. The embedded
MATERIALS AND METHODS Histopathological analysis Liver tissue was collected 9 h post-gavage, and the tissue samples were fixed in 1% formalin and paraffin-embedded following a standard procedure. The embedded
The Link Between Viruses and Asthma
 The Link Between Viruses and Asthma CATHERINE KIER, MD Professor of Clinical Pediatrics Division Chief, Pediatric Pulmonary, and Cystic Fibrosis Center Director, Pediatric Sleep Disorders Center SUNY Stony
The Link Between Viruses and Asthma CATHERINE KIER, MD Professor of Clinical Pediatrics Division Chief, Pediatric Pulmonary, and Cystic Fibrosis Center Director, Pediatric Sleep Disorders Center SUNY Stony
Supplementary Figures
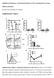 Inhibition of Pulmonary Anti Bacterial Defense by IFN γ During Recovery from Influenza Infection By Keer Sun and Dennis W. Metzger Supplementary Figures d a Ly6G Percentage survival f 1 75 5 1 25 1 5 1
Inhibition of Pulmonary Anti Bacterial Defense by IFN γ During Recovery from Influenza Infection By Keer Sun and Dennis W. Metzger Supplementary Figures d a Ly6G Percentage survival f 1 75 5 1 25 1 5 1
Role of C5 in the development of airway inflammation, airway hyperresponsiveness, and ongoing airway response
 Research article Role of C5 in the development of airway inflammation, airway hyperresponsiveness, and ongoing airway response Tao Peng, 1 Liming Hao, 2 Joseph A. Madri, 2 Xiao Su, 1 Jack A. Elias, 3 Gregory
Research article Role of C5 in the development of airway inflammation, airway hyperresponsiveness, and ongoing airway response Tao Peng, 1 Liming Hao, 2 Joseph A. Madri, 2 Xiao Su, 1 Jack A. Elias, 3 Gregory
Online Data Supplement
 Modulatory role for retinoid-related orphan receptor α (RORα) in allergen-induced lung inflammation Maisa Jaradat, Cliona Stapleton, Stephen L. Tilley, Darlene Dixon, Christopher J. Erikson, Joshua G.
Modulatory role for retinoid-related orphan receptor α (RORα) in allergen-induced lung inflammation Maisa Jaradat, Cliona Stapleton, Stephen L. Tilley, Darlene Dixon, Christopher J. Erikson, Joshua G.
METHODS Penh. Measurements and ribonuclease protection assay. Intracellular cytokine staining. ELISAs RT-PCR. Lung morphometry.
 METHODS Penh In addition to measurement of APTI, airway hyperresponsiveness to methacholine was also evaluated within 24 hours of the last allergen challenge by means of measurement of Penh (Buxco Electronics,
METHODS Penh In addition to measurement of APTI, airway hyperresponsiveness to methacholine was also evaluated within 24 hours of the last allergen challenge by means of measurement of Penh (Buxco Electronics,
Antigen-Induced Airway Hyperresponsiveness, Pulmonary Eosinophilia, and Chemokine Expression in B Cell Deficient Mice
 Antigen-Induced Airway Hyperresponsiveness, Pulmonary Eosinophilia, and Chemokine Expression in B Cell Deficient Mice James A. MacLean, Alain Sauty, Andrew D. Luster, Jeffrey M. Drazen, and George T. De
Antigen-Induced Airway Hyperresponsiveness, Pulmonary Eosinophilia, and Chemokine Expression in B Cell Deficient Mice James A. MacLean, Alain Sauty, Andrew D. Luster, Jeffrey M. Drazen, and George T. De
Mouse Anti-OVA IgM Antibody Assay Kit
 Mouse Anti-OVA IgM Antibody Assay Kit Catalog # 3017 For Research Use Only - Not Human or Therapeutic Use INTRODUCTION Ovalbumin (OVA) is a widely used antigen for inducing allergic reactions in experimental
Mouse Anti-OVA IgM Antibody Assay Kit Catalog # 3017 For Research Use Only - Not Human or Therapeutic Use INTRODUCTION Ovalbumin (OVA) is a widely used antigen for inducing allergic reactions in experimental
Impact of Asthma in the U.S. per Year. Asthma Epidemiology and Pathophysiology. Risk Factors for Asthma. Childhood Asthma Costs of Asthma
 American Association for Respiratory Care Asthma Educator Certification Prep Course Asthma Epidemiology and Pathophysiology Robert C. Cohn, MD, FAARC MetroHealth Medical Center Cleveland, OH Impact of
American Association for Respiratory Care Asthma Educator Certification Prep Course Asthma Epidemiology and Pathophysiology Robert C. Cohn, MD, FAARC MetroHealth Medical Center Cleveland, OH Impact of
Immunology of Asthma. Kenneth J. Goodrum,Ph. Ph.D. Ohio University College of Osteopathic Medicine
 Immunology of Asthma Kenneth J. Goodrum,Ph Ph.D. Ohio University College of Osteopathic Medicine Outline! Consensus characteristics! Allergens:role in asthma! Immune/inflammatory basis! Genetic basis!
Immunology of Asthma Kenneth J. Goodrum,Ph Ph.D. Ohio University College of Osteopathic Medicine Outline! Consensus characteristics! Allergens:role in asthma! Immune/inflammatory basis! Genetic basis!
Basic mechanisms disturbing lung function and gas exchange
 Basic mechanisms disturbing lung function and gas exchange Blagoi Marinov, MD, PhD Pathophysiology Department, Medical University of Plovdiv Respiratory system 1 Control of breathing Structure of the lungs
Basic mechanisms disturbing lung function and gas exchange Blagoi Marinov, MD, PhD Pathophysiology Department, Medical University of Plovdiv Respiratory system 1 Control of breathing Structure of the lungs
Zheng, BJ; Du, LY; Zhao, GY; Lin, YP; Sui, HY; Chan, C; Ma, S; Guan, Y; Yuen, KY. Citation Hong Kong Medical Journal, 2008, v. 14 suppl. 4, p.
 Title Studies of SARS virus vaccines Author(s) Zheng, BJ; Du, LY; Zhao, GY; Lin, YP; Sui, HY; Chan, C; Ma, S; Guan, Y; Yuen, KY Citation Hong Kong Medical Journal, 2008, v. 14 suppl. 4, p. 39-43 Issued
Title Studies of SARS virus vaccines Author(s) Zheng, BJ; Du, LY; Zhao, GY; Lin, YP; Sui, HY; Chan, C; Ma, S; Guan, Y; Yuen, KY Citation Hong Kong Medical Journal, 2008, v. 14 suppl. 4, p. 39-43 Issued
Identifying Biologic Targets to Attenuate or Eliminate Asthma Exacerbations
 Identifying Biologic Targets to Attenuate or Eliminate Exacerbations exacerbations are a major cause of disease morbidity and costs. For both children and adults, viral respiratory infections are the major
Identifying Biologic Targets to Attenuate or Eliminate Exacerbations exacerbations are a major cause of disease morbidity and costs. For both children and adults, viral respiratory infections are the major
Lecture Notes. Chapter 3: Asthma
 Lecture Notes Chapter 3: Asthma Objectives Define asthma and status asthmaticus List the potential causes of asthma attacks Describe the effect of asthma attacks on lung function List the clinical features
Lecture Notes Chapter 3: Asthma Objectives Define asthma and status asthmaticus List the potential causes of asthma attacks Describe the effect of asthma attacks on lung function List the clinical features
Respiratory Syncytial Virus Infection Results in Airway Hyperresponsiveness and Enhanced Airway Sensitization to Allergen
 Respiratory Syncytial Virus Infection Results in Airway Hyperresponsiveness and Enhanced Airway Sensitization to Allergen Jürgen Schwarze, Eckard Hamelmann, Katherine L. Bradley, Katsuyuki Takeda, and
Respiratory Syncytial Virus Infection Results in Airway Hyperresponsiveness and Enhanced Airway Sensitization to Allergen Jürgen Schwarze, Eckard Hamelmann, Katherine L. Bradley, Katsuyuki Takeda, and
Hepatitis B Virus Genemer
 Product Manual Hepatitis B Virus Genemer Primer Pair for amplification of HBV Viral Specific Fragment Catalog No.: 60-2007-10 Store at 20 o C For research use only. Not for use in diagnostic procedures
Product Manual Hepatitis B Virus Genemer Primer Pair for amplification of HBV Viral Specific Fragment Catalog No.: 60-2007-10 Store at 20 o C For research use only. Not for use in diagnostic procedures
Maintenance of Airway Hyperresponsiveness in Chronic Asthma May Be Mediated by Th2-Independent Mechanisms
 12 The Open Allergy Journal, 2008, 1, 12-18 Open Access Maintenance of Airway Hyperresponsiveness in Chronic Asthma May Be Mediated by Th2-Independent Mechanisms Nora J. Lin 1, Jane M. Schuh 2 and Cory
12 The Open Allergy Journal, 2008, 1, 12-18 Open Access Maintenance of Airway Hyperresponsiveness in Chronic Asthma May Be Mediated by Th2-Independent Mechanisms Nora J. Lin 1, Jane M. Schuh 2 and Cory
Bronchial hyperresponsiveness in type Ia (simple bronchoconstriction) asthma Relationship to patient age and the proportions of bronchoalveolar cells
 28 Bronchial hyperresponsiveness in type I Bronchial hyperresponsiveness in type Ia (simple bronchoconstriction) Relationship to patient age and the proportions of bronchoalveolar cells Kouzou Ashida,
28 Bronchial hyperresponsiveness in type I Bronchial hyperresponsiveness in type Ia (simple bronchoconstriction) Relationship to patient age and the proportions of bronchoalveolar cells Kouzou Ashida,
Defining Asthma: Clinical Criteria. Defining Asthma: Bronchial Hyperresponsiveness
 Defining Asthma: Clinical Criteria Atopy 34% Recent wheeze 20% Asthma 11% AHR 19% n = 807 From: Woolcock, AJ. Asthma in Textbook of Respiratory Medicine, 2nd ed. Murray, Nadel, eds.(saunders:philadelphia)
Defining Asthma: Clinical Criteria Atopy 34% Recent wheeze 20% Asthma 11% AHR 19% n = 807 From: Woolcock, AJ. Asthma in Textbook of Respiratory Medicine, 2nd ed. Murray, Nadel, eds.(saunders:philadelphia)
Defining Asthma: Bronchial Hyperresponsiveness. Defining Asthma: Clinical Criteria. Impaired Ventilation in Asthma. Dynamic Imaging of Asthma
 Defining Asthma: Clinical Criteria Defining Asthma: Bronchial Hyperresponsiveness Atopy 34% Recent wheeze 20% Asthma 11% AHR 19% n = 807 From: Woolcock, AJ. Asthma in Textbook of Respiratory Medicine,
Defining Asthma: Clinical Criteria Defining Asthma: Bronchial Hyperresponsiveness Atopy 34% Recent wheeze 20% Asthma 11% AHR 19% n = 807 From: Woolcock, AJ. Asthma in Textbook of Respiratory Medicine,
Mouse Total IgA Antibody Detection Kit
 Mouse Total IgA Antibody Detection Kit Catalog # 3019 For Research Use Only - Not Human or Therapeutic Use INTRODUCTION The total IgA levels in specimens are often determined in mouse disease models involving
Mouse Total IgA Antibody Detection Kit Catalog # 3019 For Research Use Only - Not Human or Therapeutic Use INTRODUCTION The total IgA levels in specimens are often determined in mouse disease models involving
E-1 Role of IgE and IgE receptors in allergic airway inflammation and remodeling
 E-1 Role of IgE and IgE receptors in allergic airway inflammation and remodeling Ruby Pawankar, MD, Ph.D. FRCP, FAAAAI Prof. Div of Allergy, Dept of Pediatrics Nippon Medical School Tokyo, Japan pawankar.ruby@gmail.com
E-1 Role of IgE and IgE receptors in allergic airway inflammation and remodeling Ruby Pawankar, MD, Ph.D. FRCP, FAAAAI Prof. Div of Allergy, Dept of Pediatrics Nippon Medical School Tokyo, Japan pawankar.ruby@gmail.com
The lungs as the site of delayed-type hypersensitivity reactions in guinea pigs
 BRIEF COMMUNICATION The lungs as the site of delayed-type hypersensitivity reactions in guinea pigs Terumasa Miyamoto, M.D., and Junzaburo Kobe, M.D. Tokyo, Japan Guinea pigs immunized hy a single intramuscular
BRIEF COMMUNICATION The lungs as the site of delayed-type hypersensitivity reactions in guinea pigs Terumasa Miyamoto, M.D., and Junzaburo Kobe, M.D. Tokyo, Japan Guinea pigs immunized hy a single intramuscular
Neonatal Pneumonia-2 assay
 Neonatal Pneumonia-2 assay For the detection of Ureaplasma species (Ureaplasma parvum and Ureaplasma urealyticum), Chlamydia trachomatis and Mycoplasma hominis using the BD MAX TM system. Instructions
Neonatal Pneumonia-2 assay For the detection of Ureaplasma species (Ureaplasma parvum and Ureaplasma urealyticum), Chlamydia trachomatis and Mycoplasma hominis using the BD MAX TM system. Instructions
What is the immune system? Types of Immunity. Pasteur and rabies vaccine. Historical Role of smallpox. Recognition Response
 Recognition Response Effector memory What is the immune system? Types of Immunity Innate Adaptive Anergy: : no response Harmful response: Autoimmunity Historical Role of smallpox Pasteur and rabies vaccine
Recognition Response Effector memory What is the immune system? Types of Immunity Innate Adaptive Anergy: : no response Harmful response: Autoimmunity Historical Role of smallpox Pasteur and rabies vaccine
SUPPLEMENTAL INFORMATIONS
 1 SUPPLEMENTAL INFORMATIONS Figure S1 Cumulative ZIKV production by testis explants over a 9 day-culture period. Viral titer values presented in Figure 1B (viral release over a 3 day-culture period measured
1 SUPPLEMENTAL INFORMATIONS Figure S1 Cumulative ZIKV production by testis explants over a 9 day-culture period. Viral titer values presented in Figure 1B (viral release over a 3 day-culture period measured
Novel biomarkers of chemical-induced asthma: a murine model. Jeroen Vanoirbeek
 Novel biomarkers of chemical-induced asthma: a murine model Jeroen Vanoirbeek Asthma 1. Chronic airway disease: prevalence: 5-10%, 300.000 people affected world-wide 2. Reversible airflow limitation, airway
Novel biomarkers of chemical-induced asthma: a murine model Jeroen Vanoirbeek Asthma 1. Chronic airway disease: prevalence: 5-10%, 300.000 people affected world-wide 2. Reversible airflow limitation, airway
Gastric Carcinoma with Lymphoid Stroma: Association with Epstein Virus Genome demonstrated by PCR
 Gastric Carcinoma with Lymphoid Stroma: Association with Epstein Virus Genome demonstrated by PCR Pages with reference to book, From 305 To 307 Irshad N. Soomro,Samina Noorali,Syed Abdul Aziz,Suhail Muzaffar,Shahid
Gastric Carcinoma with Lymphoid Stroma: Association with Epstein Virus Genome demonstrated by PCR Pages with reference to book, From 305 To 307 Irshad N. Soomro,Samina Noorali,Syed Abdul Aziz,Suhail Muzaffar,Shahid
Simultaneous and Rapid Detection of Causative Pathogens in Community-acquired Pneumonia by Real-time PCR (1167)
 From the Japanese Association of Medical Sciences The Japanese Association for Infectious Diseases Simultaneous and Rapid Detection of Causative Pathogens in Community-acquired Pneumonia by Real-time PCR
From the Japanese Association of Medical Sciences The Japanese Association for Infectious Diseases Simultaneous and Rapid Detection of Causative Pathogens in Community-acquired Pneumonia by Real-time PCR
Islet viability assay and Glucose Stimulated Insulin Secretion assay RT-PCR and Western Blot
 Islet viability assay and Glucose Stimulated Insulin Secretion assay Islet cell viability was determined by colorimetric (3-(4,5-dimethylthiazol-2-yl)-2,5- diphenyltetrazolium bromide assay using CellTiter
Islet viability assay and Glucose Stimulated Insulin Secretion assay Islet cell viability was determined by colorimetric (3-(4,5-dimethylthiazol-2-yl)-2,5- diphenyltetrazolium bromide assay using CellTiter
Pathology of Asthma Epidemiology
 Asthma A Presentation on Asthma Management and Prevention What Is Asthma? A chronic disease of the airways that may cause Wheezing Breathlessness Chest tightness Nighttime or early morning coughing Pathology
Asthma A Presentation on Asthma Management and Prevention What Is Asthma? A chronic disease of the airways that may cause Wheezing Breathlessness Chest tightness Nighttime or early morning coughing Pathology
CD4 + and CD8 + T cells play a central role in a HDM driven model of allergic asthma
 Raemdonck et al. Respiratory Research (2016)17:45 DOI 10.1186/s12931-016-0359-y RESEARCH CD4 + and CD8 + T cells play a central role in a HDM driven model of allergic asthma Open Access Kristof Raemdonck
Raemdonck et al. Respiratory Research (2016)17:45 DOI 10.1186/s12931-016-0359-y RESEARCH CD4 + and CD8 + T cells play a central role in a HDM driven model of allergic asthma Open Access Kristof Raemdonck
Influenza A virus infection increases IgE production and airway responsiveness in aerosolized antigen-exposed mice
 Influenza A virus infection increases IgE production and airway responsiveness in aerosolized antigen-exposed mice Shunsuke Suzuki, MD, Yuzo Suzuki, MD, PhD, Naomi Yamamoto, MD, Yutaka Matsumoto, MD, PhD,
Influenza A virus infection increases IgE production and airway responsiveness in aerosolized antigen-exposed mice Shunsuke Suzuki, MD, Yuzo Suzuki, MD, PhD, Naomi Yamamoto, MD, Yutaka Matsumoto, MD, PhD,
Nishino, Tomoya; Fukushima, Chizu; Asthma and Immunology, 113, 2, (201
 NAOSITE: Nagasaki University's Ac Title Author(s) Citation Clearance of Aspergillus fumigatus inflammation Fukahori, Susumu; Matsuse, Hiroto; Nishino, Tomoya; Fukushima, Chizu; Annals of Allergy, Asthma
NAOSITE: Nagasaki University's Ac Title Author(s) Citation Clearance of Aspergillus fumigatus inflammation Fukahori, Susumu; Matsuse, Hiroto; Nishino, Tomoya; Fukushima, Chizu; Annals of Allergy, Asthma
Outline FEF Reduced FEF25-75 in asthma. What does it mean and what are the clinical implications?
 Reduced FEF25-75 in asthma. What does it mean and what are the clinical implications? Fernando Holguin MD MPH Director, Asthma Clinical & Research Program Center for lungs and Breathing University of Colorado
Reduced FEF25-75 in asthma. What does it mean and what are the clinical implications? Fernando Holguin MD MPH Director, Asthma Clinical & Research Program Center for lungs and Breathing University of Colorado
Depletion of Alveolar Macrophages by Treatment with 2-Chloroadenosine Aerosol
 CLINICAL AND DIAGNOSTIC LABORATORY IMMUNOLOGY, July 1999, p. 452 456 Vol. 6, No. 4 1071-412X/99/$04.00 0 Copyright 1999, American Society for Microbiology. All Rights Reserved. Depletion of Alveolar Macrophages
CLINICAL AND DIAGNOSTIC LABORATORY IMMUNOLOGY, July 1999, p. 452 456 Vol. 6, No. 4 1071-412X/99/$04.00 0 Copyright 1999, American Society for Microbiology. All Rights Reserved. Depletion of Alveolar Macrophages
Bronchoalveolar lavage (BAL) with surfactant in pediatric ARDS
 Bronchoalveolar lavage (BAL) with surfactant in pediatric ARDS M. Luchetti, E. M. Galassini, A. Galbiati, C. Pagani,, F. Silla and G. A. Marraro gmarraro@picu.it www.picu.it Anesthesia and Intensive Care
Bronchoalveolar lavage (BAL) with surfactant in pediatric ARDS M. Luchetti, E. M. Galassini, A. Galbiati, C. Pagani,, F. Silla and G. A. Marraro gmarraro@picu.it www.picu.it Anesthesia and Intensive Care
IL-13 Augments Compressive Stress-induced Tissue Factor Expression in Human Airway Epithelial Cells
 IL-13 Augments Compressive Stress-induced Tissue Factor Expression in Human Airway Epithelial Cells Jennifer A. Mitchel, Silvio Antoniak, Joo-Hyeon Lee, Sae-Hoon Kim, Maureen McGill, David I. Kasahara,
IL-13 Augments Compressive Stress-induced Tissue Factor Expression in Human Airway Epithelial Cells Jennifer A. Mitchel, Silvio Antoniak, Joo-Hyeon Lee, Sae-Hoon Kim, Maureen McGill, David I. Kasahara,
SERIES 'OCCUPATIONAL ASTHMA' Edited by C. Mapp
 Eur Respir J, 1994, 7, 555 568 DOI: 10.1183/09031936.94.07030555 Printed in UK - all rights reserved Copyright ERS Journals Ltd 1994 European Respiratory Journal ISSN 0903-1936 SERIES 'OCCUPATIONAL ASTHMA'
Eur Respir J, 1994, 7, 555 568 DOI: 10.1183/09031936.94.07030555 Printed in UK - all rights reserved Copyright ERS Journals Ltd 1994 European Respiratory Journal ISSN 0903-1936 SERIES 'OCCUPATIONAL ASTHMA'
SUPPLEMENTARY METHODS
 SUPPLEMENTARY METHODS Histological analysis. Colonic tissues were collected from 5 parts of the middle colon on day 7 after the start of DSS treatment, and then were cut into segments, fixed with 4% paraformaldehyde,
SUPPLEMENTARY METHODS Histological analysis. Colonic tissues were collected from 5 parts of the middle colon on day 7 after the start of DSS treatment, and then were cut into segments, fixed with 4% paraformaldehyde,
Small Airways Disease. Respiratory Function In Small Airways And Asthma. Pathophysiologic Changes in the Small Airways of Asthma Patients
 Small Airways Disease Respiratory Function In Small Airways And Relevant Questions On Small Airway Involvement In How can small airway disease be defined? What is the link between small airway abnormalities
Small Airways Disease Respiratory Function In Small Airways And Relevant Questions On Small Airway Involvement In How can small airway disease be defined? What is the link between small airway abnormalities
B220 CD4 CD8. Figure 1. Confocal Image of Sensitized HLN. Representative image of a sensitized HLN
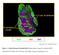 B220 CD4 CD8 Natarajan et al., unpublished data Figure 1. Confocal Image of Sensitized HLN. Representative image of a sensitized HLN showing B cell follicles and T cell areas. 20 µm thick. Image of magnification
B220 CD4 CD8 Natarajan et al., unpublished data Figure 1. Confocal Image of Sensitized HLN. Representative image of a sensitized HLN showing B cell follicles and T cell areas. 20 µm thick. Image of magnification
Isolation and identification of Mycoplasma gallisepticum in chickensbn from industrial farms in Kerman province
 Available online at http://www.ijabbr.com International journal of Advanced Biological and Biomedical Research Volume 2, Issue 1, 2014: 100-104 Isolation and identification of Mycoplasma gallisepticum
Available online at http://www.ijabbr.com International journal of Advanced Biological and Biomedical Research Volume 2, Issue 1, 2014: 100-104 Isolation and identification of Mycoplasma gallisepticum
Cytokine expression in normal, atopic, and. sputum induction and the polymerase chain reaction. asthmatic subjects using the combination of
 Thorax 1995;5:133-137 133 Original articles Department of Thoracic Medicine, Royal Brompton Hospital, National Heart and Lung Institute, Dovehouse Street, London SW3 6LY, UK C M Gelder P S Thomas D H Yates
Thorax 1995;5:133-137 133 Original articles Department of Thoracic Medicine, Royal Brompton Hospital, National Heart and Lung Institute, Dovehouse Street, London SW3 6LY, UK C M Gelder P S Thomas D H Yates
Supplementary methods:
 Supplementary methods: Primers sequences used in real-time PCR analyses: β-actin F: GACCTCTATGCCAACACAGT β-actin [11] R: AGTACTTGCGCTCAGGAGGA MMP13 F: TTCTGGTCTTCTGGCACACGCTTT MMP13 R: CCAAGCTCATGGGCAGCAACAATA
Supplementary methods: Primers sequences used in real-time PCR analyses: β-actin F: GACCTCTATGCCAACACAGT β-actin [11] R: AGTACTTGCGCTCAGGAGGA MMP13 F: TTCTGGTCTTCTGGCACACGCTTT MMP13 R: CCAAGCTCATGGGCAGCAACAATA
Exercise Alters Stress and Inflammatory Response in Lungs of Mice
 Exercise Alters Stress and Inflammatory Response in Lungs of Mice Joseph Sevcik1, Shibani Naik2, Marian L Kohut1,2 1Department of Kinesiology, Iowa State University, Ames, IA 2Immunobiology Department,
Exercise Alters Stress and Inflammatory Response in Lungs of Mice Joseph Sevcik1, Shibani Naik2, Marian L Kohut1,2 1Department of Kinesiology, Iowa State University, Ames, IA 2Immunobiology Department,
Asthma and obesity, implications for airway inflammation and Bronchial Hyperresponsiveness
 Asthma and obesity, implications for airway inflammation and Bronchial Hyperresponsiveness Fernando Holguin MD MPH Asthma Institute University of Pittsburgh Obesity Trends* Among U.S. Adults BRFSS, 1990,
Asthma and obesity, implications for airway inflammation and Bronchial Hyperresponsiveness Fernando Holguin MD MPH Asthma Institute University of Pittsburgh Obesity Trends* Among U.S. Adults BRFSS, 1990,
Immune-mediated inflammation directly impairs pulmonary function, contributing to the pathogenesis of Pneumocystis carinii pneumonia
 Immune-mediated inflammation directly impairs pulmonary function, contributing to the pathogenesis of Pneumocystis carinii pneumonia Terry W. Wright, 1 Francis Gigliotti, 1,2 Jacob N. Finkelstein, 1 John
Immune-mediated inflammation directly impairs pulmonary function, contributing to the pathogenesis of Pneumocystis carinii pneumonia Terry W. Wright, 1 Francis Gigliotti, 1,2 Jacob N. Finkelstein, 1 John
In vitro bactericidal assay Fig. S8 Gentamicin protection assay Phagocytosis assay
 In vitro bactericidal assay Mouse bone marrow was isolated from the femur and the tibia. Cells were suspended in phosphate buffered saline containing.5% BSA and 2 mm EDTA and filtered through a cell strainer.
In vitro bactericidal assay Mouse bone marrow was isolated from the femur and the tibia. Cells were suspended in phosphate buffered saline containing.5% BSA and 2 mm EDTA and filtered through a cell strainer.
DYNAMICS IN EXPRESSION OF THE IL-12 RELATED CYTOKINE TRANSCRIPTS OF IL-12A, IL-12B AND IL-23 AFTER STIMULATION OF HUMAN PBMC
 Trakia Journal of Sciences, Vol. 6, No. 1, pp 7-11, 2008 Copyright 2008 Trakia University Available online at: http://www.uni-sz.bg ISSN 1312-1723 (print) ISSN 1313-3551 (online) Original Contribution
Trakia Journal of Sciences, Vol. 6, No. 1, pp 7-11, 2008 Copyright 2008 Trakia University Available online at: http://www.uni-sz.bg ISSN 1312-1723 (print) ISSN 1313-3551 (online) Original Contribution
Current Asthma Therapy: Little Need to Phenotype. Phenotypes of Severe Asthma. Cellular Phenotypes 12/7/2012
 Subbasement Membrane Thickness(µm) 12/7/212 Current Asthma Therapy: Little Need to Phenotype Phenotypes of Severe Asthma Most mild and to some degree moderate asthmatics respond well to currently available
Subbasement Membrane Thickness(µm) 12/7/212 Current Asthma Therapy: Little Need to Phenotype Phenotypes of Severe Asthma Most mild and to some degree moderate asthmatics respond well to currently available
DNA vaccine, peripheral T-cell tolerance modulation 185
 Subject Index Airway hyperresponsiveness (AHR) animal models 41 43 asthma inhibition 45 overview 41 mast cell modulation of T-cells 62 64 respiratory tolerance 40, 41 Tregs inhibition role 44 respiratory
Subject Index Airway hyperresponsiveness (AHR) animal models 41 43 asthma inhibition 45 overview 41 mast cell modulation of T-cells 62 64 respiratory tolerance 40, 41 Tregs inhibition role 44 respiratory
IKKα Causes Chromatin Modification on Pro-Inflammatory Genes by Cigarette Smoke in Mouse Lung
 IKKα Causes Chromatin Modification on Pro-Inflammatory Genes by Cigarette Smoke in Mouse Lung Se-Ran Yang, Samantha Valvo, Hongwei Yao, Aruna Kode, Saravanan Rajendrasozhan, Indika Edirisinghe, Samuel
IKKα Causes Chromatin Modification on Pro-Inflammatory Genes by Cigarette Smoke in Mouse Lung Se-Ran Yang, Samantha Valvo, Hongwei Yao, Aruna Kode, Saravanan Rajendrasozhan, Indika Edirisinghe, Samuel
Interleukin-17 enhances the removal of respiratory syncytial virus in mice by promoting neutrophil migration and reducing interferon-gamma expression
 Interleukin-17 enhances the removal of respiratory syncytial virus in mice by promoting neutrophil migration and reducing interferon-gamma expression G. Zhang 1, K.F. Zhou 2 and Z.H. Lu 1 1 Department
Interleukin-17 enhances the removal of respiratory syncytial virus in mice by promoting neutrophil migration and reducing interferon-gamma expression G. Zhang 1, K.F. Zhou 2 and Z.H. Lu 1 1 Department
1/30/2016 RESPIRATORY INFECTIONS AND ASTHMA NO DISCLOSURES NO FINANCIAL INTEREST INFORMATION OBTAINED JACI AJRCCM
 RESPIRATORY INFECTIONS AND ASTHMA NO DISCLOSURES NO FINANCIAL INTEREST INFORMATION OBTAINED JACI AJRCCM 1 2 year old male HISTORY -Daycare since 9 months of age -Recurrent symptoms since 10 months of age:
RESPIRATORY INFECTIONS AND ASTHMA NO DISCLOSURES NO FINANCIAL INTEREST INFORMATION OBTAINED JACI AJRCCM 1 2 year old male HISTORY -Daycare since 9 months of age -Recurrent symptoms since 10 months of age:
Epithelial interleukin-25 is a key mediator in Th2-high, corticosteroid-responsive
 Online Data Supplement: Epithelial interleukin-25 is a key mediator in Th2-high, corticosteroid-responsive asthma Dan Cheng, Zheng Xue, Lingling Yi, Huimin Shi, Kan Zhang, Xiaorong Huo, Luke R. Bonser,
Online Data Supplement: Epithelial interleukin-25 is a key mediator in Th2-high, corticosteroid-responsive asthma Dan Cheng, Zheng Xue, Lingling Yi, Huimin Shi, Kan Zhang, Xiaorong Huo, Luke R. Bonser,
Airway Inflammation and Allergen Specific IgE Production May Persist Longer Than Airway Hyperresponsiveness in Mice
 J Korean Med Sci 24; 19: 69-73 ISSN 111-8934 Copyright The Korean Academy of Medical Sciences Airway Inflammation and Allergen Specific IgE Production May Persist Longer Than Airway Hyperrespoiveness in
J Korean Med Sci 24; 19: 69-73 ISSN 111-8934 Copyright The Korean Academy of Medical Sciences Airway Inflammation and Allergen Specific IgE Production May Persist Longer Than Airway Hyperrespoiveness in
3) What part of a feedback loop processes information and determines an appropriate response? A) receptor B) effector C) set point D) integrator
 AnS SI 214 Practice Exam 1 Introduction, Respiratory Immune Sunday, 1/31, 7pm Select the best answer choice in the questions below. 1) Which of the following is a characteristic of a secondary immune response?
AnS SI 214 Practice Exam 1 Introduction, Respiratory Immune Sunday, 1/31, 7pm Select the best answer choice in the questions below. 1) Which of the following is a characteristic of a secondary immune response?
Defining Asthma: Clinical Criteria. Defining Asthma: Bronchial Hyperresponsiveness
 Defining Asthma: Clinical Criteria Atopy 34% Recent wheeze 20% Asthma 11% AHR 19% n = 807 From: Woolcock, AJ. Asthma in Textbook of Respiratory Medicine, 2nd ed. Murray, Nadel, eds.(saunders:philadelphia)
Defining Asthma: Clinical Criteria Atopy 34% Recent wheeze 20% Asthma 11% AHR 19% n = 807 From: Woolcock, AJ. Asthma in Textbook of Respiratory Medicine, 2nd ed. Murray, Nadel, eds.(saunders:philadelphia)
MAJOR ARTICLE. along with the high density of pigeons in urban areas, it has been suggested that pulmonary infection
 MAJOR ARTICLE Enhanced Allergic Inflammation and Airway Responsiveness in Rats with Chronic Cryptococcus neoformans Infection: Potential Role for Fungal Pulmonary Infection in the Pathogenesis of Asthma
MAJOR ARTICLE Enhanced Allergic Inflammation and Airway Responsiveness in Rats with Chronic Cryptococcus neoformans Infection: Potential Role for Fungal Pulmonary Infection in the Pathogenesis of Asthma
SUPPLEMENTARY INFORMATION
 SUPPLEMENTARY INFORMATION FOR Liver X Receptor α mediates hepatic triglyceride accumulation through upregulation of G0/G1 Switch Gene 2 (G0S2) expression I: SUPPLEMENTARY METHODS II: SUPPLEMENTARY FIGURES
SUPPLEMENTARY INFORMATION FOR Liver X Receptor α mediates hepatic triglyceride accumulation through upregulation of G0/G1 Switch Gene 2 (G0S2) expression I: SUPPLEMENTARY METHODS II: SUPPLEMENTARY FIGURES
Neonatal Exposure to Microbial Phosphorylcholine Modulates the Development of House Dust Mite Allergy During Adult Life
 Neonatal Exposure to Microbial Phosphorylcholine Modulates the Development of House Dust Mite Allergy During Adult Life J. Sides SEM Preeyam Patel Mentor: Dr John Kearney 015 CAMBAC Research Day 9/18/15
Neonatal Exposure to Microbial Phosphorylcholine Modulates the Development of House Dust Mite Allergy During Adult Life J. Sides SEM Preeyam Patel Mentor: Dr John Kearney 015 CAMBAC Research Day 9/18/15
Asthma Pathophysiology and Treatment. John R. Holcomb, M.D.
 Asthma Pathophysiology and Treatment John R. Holcomb, M.D. Objectives Definition of Asthma Epidemiology and risk factors of Asthma Pathophysiology of Asthma Diagnostics test of Asthma Management of Asthma
Asthma Pathophysiology and Treatment John R. Holcomb, M.D. Objectives Definition of Asthma Epidemiology and risk factors of Asthma Pathophysiology of Asthma Diagnostics test of Asthma Management of Asthma
Aspirin antagonism in isonizaid treatment of tuberculosis in mice ACCEPTED. Department of Molecular Microbiology & Immunology, Bloomberg School of
 AAC Accepts, published online ahead of print on 4 December 2006 Antimicrob. Agents Chemother. doi:10.1128/aac.01145-06 Copyright 2006, American Society for Microbiology and/or the Listed Authors/Institutions.
AAC Accepts, published online ahead of print on 4 December 2006 Antimicrob. Agents Chemother. doi:10.1128/aac.01145-06 Copyright 2006, American Society for Microbiology and/or the Listed Authors/Institutions.
Clinical significance of airway inflammation in bronchcial asthma. Comparison with chronic obstructive bronchiolitis.
 24 Airway inflammation in asthma Clinical significance of airway inflammation in bronchcial asthma. Comparison with chronic obstructive bronchiolitis. Yoshiro Tanizaki, Hikaru Kitani, Takashi Mifune, Fumihiro
24 Airway inflammation in asthma Clinical significance of airway inflammation in bronchcial asthma. Comparison with chronic obstructive bronchiolitis. Yoshiro Tanizaki, Hikaru Kitani, Takashi Mifune, Fumihiro
Airway resistance due to alveolar gas compression measured by barometric plethysmography in mice
 J Appl Physiol 98: 2204 2218, 2005. First published January 27, 2005; doi:10.1152/japplphysiol.00869.2004. Airway resistance due to alveolar gas compression measured by barometric plethysmography in mice
J Appl Physiol 98: 2204 2218, 2005. First published January 27, 2005; doi:10.1152/japplphysiol.00869.2004. Airway resistance due to alveolar gas compression measured by barometric plethysmography in mice
General Laboratory methods Plasma analysis: Gene Expression Analysis: Immunoblot analysis: Immunohistochemistry:
 General Laboratory methods Plasma analysis: Plasma insulin (Mercodia, Sweden), leptin (duoset, R&D Systems Europe, Abingdon, United Kingdom), IL-6, TNFα and adiponectin levels (Quantikine kits, R&D Systems
General Laboratory methods Plasma analysis: Plasma insulin (Mercodia, Sweden), leptin (duoset, R&D Systems Europe, Abingdon, United Kingdom), IL-6, TNFα and adiponectin levels (Quantikine kits, R&D Systems
Analysis of Pulmonary Inflammation and Function in the Mouse and Baboon after Exposure to Mycoplasma pneumoniae CARDS Toxin
 Analysis of Pulmonary Inflammation and Function in the Mouse and Baboon after Exposure to Mycoplasma pneumoniae CARDS Toxin R. Doug Hardy 4,6, Jacqueline J. Coalson 3,5, Jay Peters 2,5, Adriana Chaparro
Analysis of Pulmonary Inflammation and Function in the Mouse and Baboon after Exposure to Mycoplasma pneumoniae CARDS Toxin R. Doug Hardy 4,6, Jacqueline J. Coalson 3,5, Jay Peters 2,5, Adriana Chaparro
Title: Oral administration of PPC enhances antigen-specific CD8+ T cell responses while reducing IgE levels in sensitized mice.
 Author's response to reviews Title: Oral administration of PPC enhances antigen-specific CD8+ T cell responses while reducing IgE levels in sensitized mice. Authors: Mike Burrows (mburrows@tampabayresearch.org)
Author's response to reviews Title: Oral administration of PPC enhances antigen-specific CD8+ T cell responses while reducing IgE levels in sensitized mice. Authors: Mike Burrows (mburrows@tampabayresearch.org)
Cell counting (EtBr) Before cell-lysis. Cell-lysis by 3% SDS beads beating. After cell-lysis
 Key words Sample Cell counting (EtBr) DNA extraction Cell-lysis by 3% SDS beads beating Before cell-lysis After cell-lysis Cell-lysis efficiency (Maintained70%) PCR PCR amplification of partial fragments
Key words Sample Cell counting (EtBr) DNA extraction Cell-lysis by 3% SDS beads beating Before cell-lysis After cell-lysis Cell-lysis efficiency (Maintained70%) PCR PCR amplification of partial fragments
Asthma Management for the Athlete
 Asthma Management for the Athlete Khanh Lai, MD Assistant Professor Division of Pediatric Pulmonary and Sleep Medicine University of Utah School of Medicine 2 nd Annual Sports Medicine Symposium: The Pediatric
Asthma Management for the Athlete Khanh Lai, MD Assistant Professor Division of Pediatric Pulmonary and Sleep Medicine University of Utah School of Medicine 2 nd Annual Sports Medicine Symposium: The Pediatric
Expression of acid base transporters in the kidney collecting duct in Slc2a7 -/-
 Supplemental Material Results. Expression of acid base transporters in the kidney collecting duct in Slc2a7 -/- and Slc2a7 -/- mice. The expression of AE1 in the kidney was examined in Slc26a7 KO mice.
Supplemental Material Results. Expression of acid base transporters in the kidney collecting duct in Slc2a7 -/- and Slc2a7 -/- mice. The expression of AE1 in the kidney was examined in Slc26a7 KO mice.
The FDA Critical Path Initiative
 The FDA Critical Path Initiative Clinical Considerations for Demonstration of Dose-response for Inhaled Corticosteroids - Exhaled Nitric Oxide Model Badrul A. Chowdhury, MD, PhD Director Division of Pulmonary
The FDA Critical Path Initiative Clinical Considerations for Demonstration of Dose-response for Inhaled Corticosteroids - Exhaled Nitric Oxide Model Badrul A. Chowdhury, MD, PhD Director Division of Pulmonary
Asthma is a major chronic respiratory. Streptococcus pneumoniae infection suppresses allergic airways disease by inducing regulatory T-cells
 Eur Respir J 11; 7: DOI: 1.11/919.91 CopyrightßERS 11 Streptococcus pneumoniae infection suppresses allergic airways disease by inducing regulatory T-cells J.A. Preston*,, A.N. Thorburn*,, M.R. Starkey*,
Eur Respir J 11; 7: DOI: 1.11/919.91 CopyrightßERS 11 Streptococcus pneumoniae infection suppresses allergic airways disease by inducing regulatory T-cells J.A. Preston*,, A.N. Thorburn*,, M.R. Starkey*,
