Respiratory Research. Open Access. Abstract. BioMed Central
|
|
|
- Albert Sims
- 5 years ago
- Views:
Transcription
1 Respiratory Research BioMed Central Research Exposure of neonates to Respiratory Syncytial Virus is critical in determining subsequent airway response in adults Dahui You, David Becnel, Kai Wang, Michael Ripple, Melissa Daly and Stephania A Cormier* Open Access Address: Louisiana State University, Department of Biological Sciences, Baton Rouge, USA Dahui You - dyou1@lsu.edu; David Becnel - dbecne1@lsu.edu; Kai Wang - kwang@lsu.edu; Michael Ripple - mrippl1@lsu.edu; Melissa Daly - mdaly2@lsu.edu; Stephania A Cormier* - scormier@lsu.edu * Corresponding author Published: 07 August 2006 doi: / This article is available from: Received: 27 March 2006 Accepted: 07 August You et al; licensee BioMed Central Ltd. This is an Open Access article distributed under the terms of the Creative Commons Attribution License ( which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited. Abstract Background: Respiratory syncytial virus (RSV) is the most common cause of acute bronchiolitis in infants and the elderly. Furthermore, epidemiological data suggest that RSV infection during infancy is a potent trigger of subsequent wheeze and asthma development. However, the mechanism by which RSV contributes to asthma is complex and remains largely unknown. A recent study indicates that the age of initial RSV infection is a key factor in determining airway response to RSV rechallenge. We hypothesized that severe RSV infection during neonatal development significantly alters lung structure and the pulmonary immune micro-environment; and thus, neonatal RSV infection is crucial in the development of or predisposition to allergic inflammatory diseases such as asthma. Methods: To investigate this hypothesis the present study was conducted in a neonatal mouse model of RSV-induced pulmonary inflammation and airway dysfunction. Seven-day-old mice were infected with RSV ( TCID 50 /g body weight) and allowed to mature to adulthood. To determine if neonatal RSV infection predisposed adult animals to enhanced pathophysiological responses to allergens, these mice were then sensitized and challenged with ovalbumin. Various endpoints including lung function, histopathology, cytokine production, and cellularity in bronchoalveolar lavage were examined. Results: RSV infection in neonates alone led to inflammatory airway disease characterized by airway hyperreactivity, peribronchial and perivascular inflammation, and subepithelial fibrosis in adults. If early RSV infection was followed by allergen exposure, this pulmonary phenotype was exacerbated. The initial response to neonatal RSV infection resulted in increased TNF-α levels in bronchoalveolar lavage. Interestingly, increased levels of IL-13 and mucus hyperproduction were observed almost three months after the initial infection with RSV. Conclusion: Neonatal RSV exposure results in long term pulmonary inflammation and exacerbates allergic airways disease. The early increase in TNF-α in the bronchoalveolar lavage implicates this inflammatory cytokine in orchestrating these events. Finally, the data presented emphasize IL-13 and TNF-α as potential therapeutic targets for treating RSV induced-asthma. Page 1 of 10
2 Background Respiratory syncytial virus (RSV) is the most common cause of upper and subsequent lower respiratory tract infection in children and the elderly and is most severe in children between the ages of 8 and 30 weeks [1]. Severe RSV infection occurs in 1 2% of the cases and may result in acute bronchiolitis that requires mechanical ventilation. [2]. Several studies have suggested that severe RSV lower respiratory tract infection in infancy may induce later development of asthma [3-8]. In 2000, Sigur and colleagues reported that RSV infection in infancy, severe enough to require hospitalization, was associated with asthma and allergy in children up to age 7 [9]. More recently, they reported that the relationship between severe RSV bronchiolitis in infancy and later development of asthma and allergy sensitization are still observed in children up to age 13. [10]. In murine models, numerous studies have been carried out and controversial results have been reported. While some studies propose that previous RSV infection enhances allergen sensitization and exacerbates asthma, others believe that RSV infection in infancy protects against later allergic sensitization [11]. This controversy is now thought to arise from the age of initial RSV infection and the different protocols used for RSV infection and allergen sensitization and challenge. In two independent experiments, researchers suggested that the timing of primary RSV infection is significant for predicting disease outcome. Culley and colleagues reported that if neonatal mice (1 d or 7 d of age) were infected with RSV and rechallenged at 12 wks of age, inflammatory cell recruitment was enhanced (including Th2 cells and eosinophils) [12]. Their data suggested that neonatal exposure to RSV exacerbated subsequent disease upon rechallenge in the adult. [12]. More recently, Dakhama and colleagues infected 1-wk old or 3-wk old mice with RSV, and they found that both primary infections led to increased lung resistance, mucus hyperproduction and inflammation along with increased lymphocytes in the lung. [13]. Furthermore, they demonstrated that the BAL fluid from mice infected with RSV at 1 wk of age had reduced levels of IFNγ and elevated levels of IL-13 compared to mice initially infected at 3 wks of age. This data indicated that a Th2 polarized response occurred in mice infected with RSV at 1 wk of age, while a Th1-biased response occurred in the mice infected with RSV at 3 wks of age. When rechallenged with RSV 5 weeks later (i.e., infection at 1 wk and reinfection at 6 wks of age), these mice displayed exacerbated disease as indicated by enhanced pulmonary resistance, mucus hyperproduction, eosinophilia, and elevated levels of Th2 cytokines. In contrast, initial infection of mice at 3 wks of age resulted in protection upon RSV rechallenge as indicated by the abolished lung resistance and enhanced viral clearance at rechallenge [13]. These experiments indicate that age at initial RSV infection influences the subsequent immune and physiologic response upon re-exposure to RSV. We hypothesized that neonatal exposure to RSV plays a critical role in the pathophysiological response to subsequent allergen exposure and the development of allergic asthma. To investigate whether neonatal exposure to RSV influences airway hyperreactivity (AHR), mice were infected with RSV at 1 wk of age. At 6 wks of age, these mice were then sensitized and challenged with ovalbumin (Ova). Pulmonary function, histopathology, and bronchoalveolar lavage fluid (BALF) cellularity and cytokine production were examined 24 hours after the last Ova challenge. The results were compared to sham infected and/or saline exposed mice and demonstrated that neonatal exposure to RSV resulted in elevated and prolonged AHR, chronic pulmonary inflammation, and subepithelial fibrosis in adult mice. These pathophysiological endpoints were most severe when neonatal RSV infection was followed by allergen sensitization and challenge. These studies demonstrate the ability of neonatal exposures to chronically alter lung function and the importance of preventing RSV exposure during infancy. Methods The study protocol is outlined in Figure 1. Mice were divided into four groups. RSS mice were infected with RSV and mock-sensitized and challenged. OVA mice were mock-infected then Ova sensitized and challenged. ROO mice were infected with RSV and then Ova-sensitized and challenged. As the control group, SAL mice were mock infected, mock-sensitized and challenged. Data were collected on protocol days 0, 4, 69 and 96. Mice BALB/c breeders were purchased from the Division of Laboratory Animal Medicine (School of Veterinary Medicine, Louisiana State University) and seven day old pups were obtained by time-mating. All mice were maintained in ventilated micro-isolator cages housed in a specific pathogen-free animal facility. Sentinel mice within this animal colony were negative for antibodies to viral and other known mouse pathogens. All animal protocols were prepared in accordance with the Guide for the Care and Use of Laboratory Animals (National Research Council, 1996) and approved by the Institutional Animal Care and Use Committee at Louisiana State University. Infection of mice with RSV and assessment of viral titers Seven day old mice (protocol day 0; Figure 1) were infected intranasally (i.n.) with TCID 50 RSV/g body weight (RSV A-2, Advanced Biotechnologies Incorporated, Columbia, MD) or culture media alone (OVA group). Four days post-infection, viral titer of whole lung Page 2 of 10
3 Schematic of study protocol and exposure groups Figure 1 Schematic of study protocol and exposure groups. Neonatal mice (7 days of age) were infected with RSV ( TCID50/g body weight; RSS, ROO groups). On protocol days 41 and 55, mice were injected i.p. with ovalbumin complexed to Imject Alum (OVA and ROO groups) or with isotonic saline (SAL and RSS groups). These mice were then exposed to aerosolized ovalbumin or saline for 20 minutes on protocol days 65, 66, and 67. n = 8/group. homogenates was determined using the TCID 50 method of Spearman-Kärber [14,15]. Ovalbumin sensitization and challenge Mice were sensitized and challenged with chicken ovalbumin (grade V; Sigma, St. Louis, MO) as previously described [16]. Mice were intraperitoneally (i.p.) injected with 20 µg Ova complexed with 2 mg Imject Alum (Al [OH]3/Mg [OH]2; Pierce, Rockford, IL) or Sal (RSS and SAL group) on protocol days 41 and 55 (Figure 1) and subsequently challenged with aerosolized 1% Ova (in isotonic Sal) or Sal (RSS and SAL group) using an ultrasonic nebulizer (PariNeb Pro Nebulizer) on protocol days (Figure 1). Assessment of pulmonary function A) Lung resistance in response to methacholine On protocol day 69, lung resistance to increasing doses of methacholine (MeCh, Sigma; 0, 6.25, 12.5, and 25 mg/ml in isotonic saline) was assessed using the forced oscillation technique as previously described [16]. Anesthetized animals were mechanically ventilated with a tidal volume of 10 ml/kg and a frequency of 2.5 Hz using a computercontrolled piston ventilator (FlexiVent, SCIREQ; Montreal, Canada). Resistance data were collected using single compartment model and plotted as the percent change from the 0 mg/ml MeCh dose. B) Airway hyperreactivity in response to methacholine Airway hyperresponsiveness to MeCh (Sigma; 0, 6.25, 12.5, 25 and 50 mg/ml in isotonic saline) was assessed by whole body plethysmography (Buxco Electronics, Troy, NY and EMKA Technologies, Falls Church, VA) as described previously [16]. Mice were exposed to aerosolized MeCh for 3 minutes at each dose and enhanced pause (Penh) was recorded for 3 minutes and averaged for each dose. Penh data were plotted as percent change from saline per dose. Determination of Bbronchoalveolar Lavage Fluid cellularity On protocol day 69, bronchoalveolar lavage fluid (BALF) was isolated in 1 ml of PBS containing 2% heat-inactivated FBS. Total BAL cellularity was determined with the use of a hemocytometer. Cytospin slides were fixed and stained using the Diff-Quick kit (IMEB, Chicago, IL), and differential cell counts by two unbiased observers were obtained using standard morphological criteria to classify individual leukocyte populations. Three mice from each group were used for these analyses, and cells were counted per cytospin preparation. Pulmonary histopathology On protocol day 69, lungs were inflated with 1 ml of 4% paraformaldehyde. The lungs were then excised and fixed in 4% paraformaldehyde for 24 hours at 4 C. These tissues were then embedded in paraffin, cut in 4 µm frontal sections and stained with hematoxylin and eosin (H&E), periodic acid-schiff (PAS) to show mucus production in airway goblet cells, or Masson's trichrome (MT) to indicate airway collagen deposition. Scores were assigned to these histological endpoints by two independent observers and were recorded on a scale of 0 3. Cytokine level in BAL fluid IL-2, IL-4, IL-5, IFN-γ, and TNF-α levels in the BALF were examined using the Mouse Th1/Th2 Cytokine Cytometric Bead Array Kit (BD Biosciences, San Diego, CA) as per the manufacturer's instructions. Data were acquired with a BD FACScan flow cytometer. Data analyses were performed using the BD Cytometric Bead Array Software to generate standard curves for each cytokine and to deter- Page 3 of 10
4 mine sample cytokine levels. IL-13 levels in BALF were determined using the Mouse IL-13 ELISA Ready-SET-Go kit (ebioscience, San Diego, CA). The sensitivity for each cytokine is as follows: 5.0 pg/ml for IL-2, IL-4 and IL-5; 2.5 pg/ml for IFN-γ, 6.3 pg/ml for TNF-α and 30 pg/ml for IL- 13. Statistical analysis Data are presented as mean ± SEM and were obtained from experiments with n = 8 for whole body plethysmography analysis of AHR, n = 4 5 for invasive measurements of pulmonary mechanics, and n = 3 for BAL cellularity, cytokine assays, pulmonary viral titers and histology. For AHR, lung resistance and BAL cellularity, differences between groups were evaluated by means of two-way ANOVA using GraphPad Prism (GraphPad Software Inc, San Diago, CA). Bonferroni post-tests were performed to compare between pairs of groups. A one-way ANOVA was used to compare the mean cytokine levels among the various groups followed by the Tukey-Kramer multiple comparisons tests for significance between the groups. This was repeated for each individual cytokine. Differences between means were considered significant when p < Results Reduced pulmonary function was observed in mice infected with RSV as neonates To determine if neonatal exposure to RSV is sufficient to induce long-term pulmonary dysfunction, mice were infected with RSV ( TCID/g body weight) at seven days of age and then allowed to mature to adults (Figure 1). Four days post-infection, we assessed pulmonary viral titers for Sham and RSV infected mice. As expected, mice from the Sham infected groups displayed no evidence of viral replication. The mean viral titer in the lungs of neonatal mice exposed to RSV alone (RSS and ROO) was 2.67 ± TCID 50 /g lung tissue. After maturation, subsets of mice were then sensitized (protocol days 41 and 55) and challenged (protocol days 65, 66, and 67) with ovalbumin OVA and ROO groups. All other mice received saline RSS and SAL groups. AHR was assessed on protocol day 69 and 96 (2.5 and 3.5 months after infection). We observed no significant difference in baseline airway resistance between the RSV infected (mean ± SEM; 0.52 ± 0.01 cm H 2 O.s/mL) or sham infected mice (0.64 ± 0.06). For ease of comparison among all groups, lung resistance data was normalized by plotting the percentage difference from baseline (percent difference = 100 * ((value-baseline)/baseline). Lung resistance in response to increasing concentrations of inhaled MeCh was significantly greater in RSV infected neonates (RSS; ± 10.20) than control mice (SAL; ± 6.51) at 25 mg/ml MeCh (1.4 times, p < 0.01) (Figure 2A). Neonatal RSV infection followed by exposure to Ova (ROO) resulted in the highest lung resistance among the four groups ( ± 32.84). This increased airway resistance was greater than could be accounted for by Ova exposure alone (OVA; ± 23.01). Thus, neonatal exposure to RSV infection appears to predispose adults to the development of airway responsiveness to subsequent allergen exposure. To investigate the long-term influence of neonatal exposure to RSV, AHR was assessed by whole body plethysmography on protocol day 96 (103 days of age). Penh data was normalized and the percentage difference from baseline was plotted. Mice in the RSS group continued to demonstrate reduced airway function 3 months postinfection as evidenced by a significantly increased Penh compared to SAL mice at 25 and 50 mg/ml MeCh ( ± vs ± at 25 mg/ml; ± vs ± at 50 mg/ml; p < and p < 0.001, respectively) (Figure 2B). These data demonstrate that neonatal infection with RSV results in the development of chronic AHR, and furthermore, that airway function is further diminished due to an allergic phenotype. Neonatal RSV infection predisposes mice to chronic pulmonary inflammation indicated in BALF cellularity To evaluate the pulmonary immune response to RSV, BAL fluid was isolated, total cells recovered were counted, and the cellular composition of BALF was determined using morphological criteria. RSV and/or Ova exposed mice recruited significantly more leukocytes than control mice (SAL group, p < 0.001) (Figure 3). However, there was no significant difference in the total number of recovered cells among the RSS, OVA, and ROO groups. Interestingly, BALF cellularity was elevated in mice exposed to RSV as neonates (RSS) on protocol day 69. Upon allergen sensitization and challenge, total BALF cellularity was not significantly altered compared to RSS although the cell populations were changed. Neonatal RSV infection resulted in a predominantly monocyte/macrophage pulmonary infiltrate and these cells seemed to account for the elevation in the total number of recovered cells. In contrast, Ova exposure, in the absence (OVA) or presence of neonatal RSV (ROO) infection, resulted in a significant BALF eosinophilia (compared to control SAL group, p < 0.001). Concomitant with the observed increase in BALF eosinophil numbers in the OVA and ROO groups was a decrease in BALF macrophage numbers. Cytokine levels in BAL fluid is altered in mice exposed to RSV and/or Ova Cytokine levels in BAL fluid were examined to study the Th1/Th2 polarization in RSV and/or Ova exposed mice. As shown in Figure 4A, we assayed cytokine levels in BALF five hours post-infection, and observed greatly elevated Page 4 of 10
5 Airway hyperreactivity in RSV and/or Ova exposed mice Figure 2 Airway hyperreactivity in RSV and/or Ova exposed mice. Mice were infected with RSV as neonates (RSS) and exposed to Ova 5 wks later (ROO). Controls were sham infected and exposed to Saline (SAL) or Ova (OVA). A. Lung resistance of each group is plotted as a function of increasing doses of inhaled MeCh, using single compartment model. B. Penh is plotted as a function of increasing dose of inhaled MeCh (0 to 50 mg/ml). Data were collected on protocol days 69 (A) or 96 (B), normalized to saline airway responses as described in methods, and expressed as mean ± SEM. n = 4 5/group. ***p < 0.001; **p < TNF-α (21.4 times, p < 0.001) in RSV infected neonates. In addition, Th2 cytokines (IL-4 and IL-5) along with IL-2 were detected in BALF of neonatal infected mice whereas no IL-4, IL-5, or IL-2 was detected in control mice (SAL group). TNF-α levels declined by protocol day 69 in mice infected with RSV as neonates, but was elevated in RSV infected and Ova exposed mice (ROO group, Figure 4B). Intriguingly, IL-13 levels were elevated in RSS mice at protocol day 69 compared to SAL mice (p < 0.001). Mice exposed to RSV and Ova (ROO group) showed increased Th2 cytokines (IL-5 and IL-13) compared to SAL group. In addition, IL-13 levels in ROO mice were significantly elevated compared to the animals exposed to Ova alone (OVA group; p < 0.01). Neonatal infection with RSV also resulted in increased levels of TGF-β 1 protein in the lungs 4d post-infection (RSS: 29.8 ± 0.45 ng/g lung tissue) compared to mice exposed to Sal alone (22.1 ± 0.39 ng/g lung tissue). Enhanced pulmonary histopathology in mice exposed to RSV and/or Ova Airway inflammation, mucus hyperproduction, and collagen deposition in the subepithelial reticular layer of the airway were observed in mice exposed to RSV and/or Ova (Figure 5A: inflammation; Figure 5B: mucus production; Figure 5C: collagen deposition). Mice exposed to both RSV and Ova demonstrated the largest amount of inflammation, mucus production, and collagen deposition (Figure 5D), and this was consistent with the greatest lung resistance and airway hypersensitivity (Figure 2). In addition, tremendous perivascular inflammation was observed in both groups of mice exposed to Ova (i.e., OVA and ROO mice; Figure 5A). Mice infected with RSV as neonates displayed chronic (69d post infection) inflammation, mucus production and collagen deposition compared to control mice (SAL group), which also correlated to enhanced lung resistance and airway hyper- Page 5 of 10
6 BALF. In addition, TNF-α and IL-13 were significantly higher compared to mice exposed to Ova alone. The most severe lung histopathology was observed in mice exposed to both RSV and Ova, as indicated by severe peribronchial and perivascular inflammation, mucus production, and collagen deposition. Collectively, these data suggest that neonatal RSV infection influences adult immune response to allergen (Ova) and exacerbates allergic pathophysiology in mice long after viral titers are no longer detectable. BAL cellularity in RSV and/or Ova exposed mice Figure 3 BAL cellularity in RSV and/or Ova exposed mice. Bronchoalveolar lavage fluid was isolated on protocol day 69. RSV and/or Ova induced significant increase in total BAL cellularity. In mice exposed to RSV as neonates (RSS), this increase correlated with elevated levels of macrophages; whereas, in mice exposed to Ova (ROO and Ova), this increase correlated to elevation in eosinophil numbers. Data are expressed as means ± SEM, n = 3/group. ***p < sensitivity in the RSS group (Figure 2). Increased peribronchial and perivascular collagen deposition and peribronchial smooth muscle deposition indicated that airway remodeling occurred in mice exposed to RSV and/ or Ova (Figure 5B), and that neonatal RSV infection alone was sufficient to induce airway remodeling. Discussion In the present study, we have shown that neonatal exposure to RSV alone induced long-term airway hyperresponsiveness and pulmonary resistance in mice. This result was correlated with peribronchial inflammation, increased BALF cellularity, increased mucus production, and airway remodeling. Elevations in TNF-α and Th2 cytokines (IL-4 and IL-5) were observed in BALF immediately following neonatal RSV infection. Once these mice had matured (protocol day 69), only IL-13 remained elevated in the BALF. Neonatal RSV infection followed by adult exposure to allergen resulted in significantly higher lung resistance, along with increased total cellularity, eosinophilia, and increased TNF-α and Th2 cytokines (IL-5 and IL-13) in In contrast to previously published studies analyzing the effect of RSV infection on allergen exposure in adult mice. [17], the present study investigated the influence of neonatal RSV infection on adult allergen sensitization. Neonatal infection with RSV alone was sufficient to induce long-term pulmonary dysfunction and inflammation. Similarly, neonatal infection of brown Norway rats with parainfluenza type 1 (Sendai) virus also led to increases in pulmonary resistance and hyperresponsiveness to methacholine up to 65d after infection [18]. As in our model, persistent airway dysfunction following neonatal infection with Sendai virus correlated with increased peribronchial fibrosis and pulmonary inflammation. [19]. Furthermore, both models (i.e., neonatal RSV infection and neonatal Sendai virus infection) resulted in significantly increased mrna [19] and protein levels for TGF-β 1. Although numerous cytokines may contribute to airway remodeling, the elevation of TGF-β 1, a fibrogenic cytokine, in both neonatal viral infection models prior to the development of fibrosis suggests a role this cytokine in the regulation of viral-induced airway remodeling observed in neonates. More importantly, neonatal infection with RSV predisposed mice to the development of enhanced AHR and inflammation after allergen exposure. In contrast, adult RSV infection prior to allergen exposure seemed to assert a "protective" response as evidenced by significantly decreased allergen induced pulmonary resistance, tissue eosinophilia, and IL-13 levels [20]. Our data presented here and elsewhere [16] extend these findings and, more importantly, demonstrate that the age at initial RSV infection also determines whether RSV infection will exacerbate or prevent subsequent allergic inflammation. A more recent study using neonatal RSV infection followed by subsequent reinfection of adults with RSV demonstrated that early RSV infection also exacerbates RSV induced diseases in the adult [13]. Interestingly, if the primary RSV infection occurred at 3 wks of age, a protective effect upon secondary infection was observed similar to that reported by Peebles and colleagues [17]. Dakhama and colleagues further established that enhancement of AHR, pulmonary eosinophilia, and mucus hyperproduction during reinfection were dependent on IL-13 [13]. We Page 6 of 10
7 Cytokine levels in the BAL fluid of mice exposed to RSV and/or Ova Figure 4 Cytokine levels in the BAL fluid of mice exposed to RSV and/or Ova. Bronchoalveolar lavage fluid was isolated 5 hr post-infection with RSV (A) or on protocol day 69 (B). A. Elevated levels of TNF-α, IL-5, IL-4, and IL-2 were observed as early as 5 hrs post-infection, although significance over SAL controls was observed only for TNF-α. IL-2, IL-4 and IL-5 were below the limit of detection in the SAL mice. B. IL-13 was significantly elevated in RSS mice; while TNF-α, IL-5, and IL-13 were significantly enhanced in mice exposed to RSV and Ova (ROO). IL-13 was below the limit of detection in control animals (SAL). Data are expressed as means ± SEM, n = 3/group. ***p < 0.001, **p < 0.01, and *p < demonstrated that neonatal RSV infection alone leads to elevated levels of IL-13 in the lung and that exposure to allergen significantly increases IL-13 levels over RSV exposure alone. IL-13 has emerged as a major regulatory molecule involved in mucus hyperproduction and allergen induced AHR [21-23]. It is entirely possible that the longterm AHR, pulmonary inflammation, and mucus production observed in our neonatal RSV model is due to high levels of IL-13. In fact, elevated levels of IL-13 were observed in whole lung homogenates as early as 5 hours post-infection (data not shown) and were again observed in adult lungs on protocol day 69 suggesting that IL-13 is being chronically produced. Although the exact cellular source of IL-13 in this neonatal model of RSV infection is currently unknown, previous studies have demonstrated that epithelial cells and/or macrophages infected by RSV are a significant source of IL-13 and are capable of producing this cytokine for months after the initial infection. [24]. We are currently investigating this possibility. In our study, TNF-α was significantly elevated in the BALF shortly after infection with RSV. TNF-α is an important cytokine for innate immune responses and a central regulator of inflammatory processes, through binding to distinct membrane receptors, referred to as p55 or TNFR1 and p75 or TNFR2 [25]. TNF-α is likely a central mediator of airway inflammation and AHR in asthma, regulating inflammatory cell infiltration, locally enhancing vascular permeability, and inducing the release of the chemokines. Ultimately, this will lead to chronic inflammation and irreversible airway remodeling. Recently, depletion studies using monoclonal antibody therapy for TNF-α have shown promising effects in viral-specific lung immunopathology. [26], rheumatoid arthritis [27] and inflammatory Page 7 of 10
8 Figure Lung histopathology 5 of mice exposed to RSV and/or Ova Lung histopathology of mice exposed to RSV and/or Ova. Lung tissue sections were obtained from mice on protocol day 69. Tissue sections were stained with H&E (A), PAS (B), and MT (C). A. Lung inflammation, B. mucus (purple) hyperproduction, and C. collagen (blue) deposition were observed in mice exposed to RSV and/or Ova. D. Scores were assigned to these histological endpoints by two independent observers and were recorded on a scale of 0 4. Increased deposition of peribronchial and perivascular collagen was observed in the subepithelial reticular layer of the airways in RSS, OVA and ROO mice. In all cases, neonatal RSV infection (RSS) induced persistent lung pathologies including increased peribronchial inflammation, mucus production, and subepithelial fibrosis were exacerbated by subsequent exposure to allergen (ROO). n = 3/group. ***p < 0.001, *p < bowel disease [28]. Moreover, a soluble TNF receptor fusion protein, etanercept, has proven efficacious in treating juvenile rheumatoid arthritis in patients as young as 4 [27]. In viral models, TNF-α depletion reduced recruitment of inflammatory cells, reduced type 1 and type 2 cytokines in BALF, and decreased pulmonary pathology without inhibiting viral clearance [26,29]. Although the precise mechanism by which TNF-α leads to the pathol- ogy in lungs after RSV infection remains unknown, our data and these previous studies suggest a key role for TNFα in chronic inflammation in the lung and subsequent airway remodeling associated with asthma. Several studies along with our present data have established the correlation of severe RSV infection followed by allergen exposure and the development of allergic inflam- Page 8 of 10
9 matory disease (i.e., asthma) in mice. Although the mechanism by which the exposure causes asthma and the importance of such exposures in humans need to be further elucidated, our current and previously published data [16] demonstrate that the initial age of the RSV infection is capable of altering adult pulmonary function and exacerbating pulmonary immunopathology when followed by subsequent allergen exposure. Furthermore, enhanced AHR correlated with chronic pulmonary inflammation, upregulation of the Th2 cytokine, IL-13, and subepithelial fibrosis of the bronchial airways. Increases in TNF-α within 5 hours of RSV infection in our mouse model also suggest a role for this cytokine in the immunopathology of RSV-induced wheeze and asthma development in humans. Conclusion We have demonstrated that neonatal infection with RSV in mice leads to reduced lung function, which is associated with chronic inflammation, increased mucus production, and airway remodeling in the lung. In addition, RSV infection in neonates predisposes the adult to develop enhanced airway responses upon allergen exposure. The upregulation of TNF-α and IL-13 suggests that these cytokines may play a key role in mediating this process and highlights the importance of these cytokines as therapeutic targets for RSV induced asthma. Abbreviations RSV, respiratory syncytial virus; AHR, airway hyperreactivity; Ova, ovalbumin; Sal, saline; BAL, bronchoalveolar lavage; BALF, bronchoalveolar lavage fluid; MeCh, methacholine; Penh, enhanced pause, TNF-α: Tumor necrosis factor-α Competing interests The author(s) declare that they have no competing interests. Authors' contributions DY performed pulmonary function tests, cytokine assays, and assisted in the preparation of the manuscript. DB counted the BAL fluid differentials and assisted in the preparation of the manuscript. KW counted the BAL fluid differentials and assisted in the preparation of the manuscript and the micrographs. MR determined pulmonary viral titers. MD helped in preparation of reagents. SC conceived of the study, performed/assisted in all experiments, and prepared the manuscript. All authors read and approved the final manuscript. Acknowledgements Insightful comments and critical review of the manuscript was provided by Dr. Timothy Foster and Dr. Karin Peterson. The authors wish to thank those at the Louisiana State University School of Veterinary Medicine Core facilities (Histology: Cheryl Crowder; Flow analysis: Marilyn Dietrich). This publication was made possible by NIH grant number P20 RR from the LSU/Tulane COBRE-CEIDR Program of the National Center for Research Resources. Its contents are solely the responsibility of the authors and do not necessarily represent the official views of NIH. References 1. Openshaw PJ, Tregoning JS: Immune responses and disease enhancement during respiratory syncytial virus infection. Clin Microbiol Rev 2005, 18(3): Leader S, Kohlhase K: Respiratory syncytial virus-coded pediatric hospitalizations, 1997 to Pediatr Infect Dis J 2002, 21(7): McConnochie KM, Roghmann KJ: Bronchiolitis as a possible cause of wheezing in childhood: new evidence. Pediatrics 1984, 74(1): Pullan CR, Hey EN: Wheezing, asthma, and pulmonary dysfunction 10 years after infection with respiratory syncytial virus in infancy. Br Med J (Clin Res Ed) 1982, 284(6330): Sims DG, Downham MA, Gardner PS, Webb JK, Weightman D: Study of 8-year-old children with a history of respiratory syncytial virus bronchiolitis in infancy. Br Med J 1978, 1(6104): Mok JY, Simpson H: Outcome for acute bronchitis, bronchiolitis, and pneumonia in infancy. Arch Dis Child 1984, 59(4): Murray M, Webb MS, O'Callaghan C, Swarbrick AS, Milner AD: Respiratory status and allergy after bronchiolitis. Arch Dis Child 1992, 67(4): Noble V, Murray M, Webb MS, Alexander J, Swarbrick AS, Milner AD: Respiratory status and allergy nine to 10 years after acute bronchiolitis. Arch Dis Child 1997, 76(4): Sigurs N, Bjarnason R, Sigurbergsson F, Kjellman B: Respiratory syncytial virus bronchiolitis in infancy is an important risk factor for asthma and allergy at age 7. Am J Respir Crit Care Med 2000, 161(5): Sigurs N, Gustafsson PM, Bjarnason R, Lundberg F, Schmidt S, Sigurbergsson F, Kjellman B: Severe respiratory syncytial virus bronchiolitis in infancy and asthma and allergy at age 13. Am J Respir Crit Care Med 2005, 171(2): Kalina WV, Gershwin LJ: Progress in defining the role of RSV in allergy and asthma: from clinical observations to animal models. Clin Dev Immunol 2004, 11(2): Culley FJ, Pollott J, Openshaw PJ: Age at first viral infection determines the pattern of T cell-mediated disease during reinfection in adulthood. Journal of Experimental Medicine 2002, 196(10): Dakhama A, Park JW, Taube C, Joetham A, Balhorn A, Miyahara N, Takeda K, Gelfand EW: The Enhancement or Prevention of Airway Hyperresponsiveness during Reinfection with Respiratory Syncytial Virus Is Critically Dependent on the Age at First Infection and IL-13 Production. J Immunol 2005, 175(3): Spearman C: The Method of Right and Wrong Cases (constant stimuli) Without Gauss's Formulae. Brit J Psychol 1908, 2: Karber G: Beitrag zur kollektiven behandlung pharmakologischer reihenversuche. Arch exp Path Pharmak 1931, 162: Becnel D, You D, Erskin J, Dimina DM, Cormier SA: A role for airway remodeling during respiratory syncytial virus infection. Respir Res 2005, 6(1): Peebles RSJ, Hashimoto K, Collins RD, Jarzecka K, Furlong J, Mitchell DB, Sheller JR, Graham BS: Immune interaction between respiratory syncytial virus infection and allergen sensitization critically depends on timing of challenges. J Infect Dis 2001, 184(11): Sorkness R, Lemanske RFJ, Castleman WL: Persistent airway hyperresponsiveness after neonatal viral bronchiolitis in rats. J Appl Physiol 1991, 70(1): Uhl EW, Castleman WL, Sorkness RL, Busse WW, Lemanske RFJ, McAllister PK: Parainfluenza virus-induced persistence of airway inflammation, fibrosis, and dysfunction associated with TGF-beta 1 expression in brown Norway rats. Am J Respir Crit Care Med 1996, 154(6 Pt 1): Page 9 of 10
10 20. Peebles RSJ, Sheller JR, Collins RD, Jarzecka K, Mitchell DB, Graham BS: Respiratory syncytial virus (RSV)-induced airway hyperresponsiveness in allergically sensitized mice is inhibited by live RSV and exacerbated by formalin-inactivated RSV. J Infect Dis 2000, 182(3): Taube C, Duez C, Cui ZH, Takeda K, Rha YH, Park JW, Balhorn A, Donaldson DD, Dakhama A, Gelfand EW: The Role of IL-13 in Established Allergic Airway Disease. J Immunol 2002, 169(11): Wills-Karp M, Chiaramonte M: Interleukin-13 in asthma. Current Opinion in Pulmonary Medicine 2003, 9(1): Kuperman DA, Huang XZ, Koth LL, Chang GH, Dolganov GM, Zhu Z, Elias JA, Sheppard D, Erle DJ: Direct effects of interleukin-13 on epithelial cells cause airway hyperreactivity and mucus overproduction in asthma. Nature Medicine 2002, 8(8): Schwarze J, O'Donnell DR, Rohwedder A, Openshaw PJ: Latency and persistence of respiratory syncytial virus despite T cell immunity. Am J Respir Crit Care Med 2004, 169(7): Peschon JJ, Torrance DS, Stocking KL, Glaccum MB, Otten C, Willis CR, Charrier K, Morrissey PJ, Ware CB, Mohler KM: TNF receptor-deficient mice reveal divergent roles for p55 and p75 in several models of inflammation. J Immunol 1998, 160(2): Hussell T, Pennycook A, Openshaw PJM: Inhibition of tumor necrosis factor reduces the severity of virus-specific lung immunopathology. European Journal of Immunology 2001, 31(9): Lovell DJ, Giannini EH, Reiff A, Cawkwell GD, Silverman ED, Nocton JJ, Stein LD, Gedalia A, Ilowite NT, Wallace CA, Whitmore J, Finck BK: Etanercept in children with polyarticular juvenile rheumatoid arthritis. New England Journal of Medicine 2000, 342(11): Bell S, Kamm MA: Antibodies to tumour necrosis factor alpha as treatment for Crohn's disease. Lancet 2000, 355(9207): Rutigliano JA, Graham BS: Prolonged Production of TNF-{alpha} Exacerbates Illness during Respiratory Syncytial Virus Infection. J Immunol 2004, 173(5): Publish with BioMed Central and every scientist can read your work free of charge "BioMed Central will be the most significant development for disseminating the results of biomedical research in our lifetime." Sir Paul Nurse, Cancer Research UK Your research papers will be: available free of charge to the entire biomedical community peer reviewed and published immediately upon acceptance cited in PubMed and archived on PubMed Central yours you keep the copyright BioMedcentral Submit your manuscript here: Page 10 of 10
Defining Asthma: Clinical Criteria. Defining Asthma: Bronchial Hyperresponsiveness
 Defining Asthma: Clinical Criteria Atopy 34% Recent wheeze 20% Asthma 11% AHR 19% n = 807 From: Woolcock, AJ. Asthma in Textbook of Respiratory Medicine, 2nd ed. Murray, Nadel, eds.(saunders:philadelphia)
Defining Asthma: Clinical Criteria Atopy 34% Recent wheeze 20% Asthma 11% AHR 19% n = 807 From: Woolcock, AJ. Asthma in Textbook of Respiratory Medicine, 2nd ed. Murray, Nadel, eds.(saunders:philadelphia)
Role of Tyk-2 in Th9 and Th17 cells in allergic asthma
 Supplementary File Role of Tyk-2 in Th9 and Th17 cells in allergic asthma Caroline Übel 1*, Anna Graser 1*, Sonja Koch 1, Ralf J. Rieker 2, Hans A. Lehr 3, Mathias Müller 4 and Susetta Finotto 1** 1 Laboratory
Supplementary File Role of Tyk-2 in Th9 and Th17 cells in allergic asthma Caroline Übel 1*, Anna Graser 1*, Sonja Koch 1, Ralf J. Rieker 2, Hans A. Lehr 3, Mathias Müller 4 and Susetta Finotto 1** 1 Laboratory
Defining Asthma: Clinical Criteria. Defining Asthma: Bronchial Hyperresponsiveness
 Defining Asthma: Clinical Criteria Atopy 34% Recent wheeze 20% Asthma 11% AHR 19% n = 807 From: Woolcock, AJ. Asthma in Textbook of Respiratory Medicine, 2nd ed. Murray, Nadel, eds.(saunders:philadelphia)
Defining Asthma: Clinical Criteria Atopy 34% Recent wheeze 20% Asthma 11% AHR 19% n = 807 From: Woolcock, AJ. Asthma in Textbook of Respiratory Medicine, 2nd ed. Murray, Nadel, eds.(saunders:philadelphia)
Defining Asthma: Bronchial Hyperresponsiveness. Defining Asthma: Clinical Criteria. Impaired Ventilation in Asthma. Dynamic Imaging of Asthma
 Defining Asthma: Clinical Criteria Defining Asthma: Bronchial Hyperresponsiveness Atopy 34% Recent wheeze 20% Asthma 11% AHR 19% n = 807 From: Woolcock, AJ. Asthma in Textbook of Respiratory Medicine,
Defining Asthma: Clinical Criteria Defining Asthma: Bronchial Hyperresponsiveness Atopy 34% Recent wheeze 20% Asthma 11% AHR 19% n = 807 From: Woolcock, AJ. Asthma in Textbook of Respiratory Medicine,
The Effect of BTP on the Development of Allergic Asthma in Mice
 93 The Effect of BTP on the Development of Allergic Asthma in Mice Alana Curry, McNair Scholar, Virginia State University Faculty Advisor: Avery August, Ph.D Associate Professor of Immunology Department
93 The Effect of BTP on the Development of Allergic Asthma in Mice Alana Curry, McNair Scholar, Virginia State University Faculty Advisor: Avery August, Ph.D Associate Professor of Immunology Department
Abstract. IgE. IgE Th2. x x IL-4 IL-5 IgE CD4 +
 D. o ƒf 6,''!" # + % %$ '& ' '' & " k n k x k k k k k x k IgE k x IgE Ò1Ó k Ò2Ó v k x IgE Th2 x } x x IL-4 IL-5 IgE IgE j IFN-γ IgG j j CD4 + { k d «d j B7 w k k x IgE k 1 k Abstract Parental immunization
D. o ƒf 6,''!" # + % %$ '& ' '' & " k n k x k k k k k x k IgE k x IgE Ò1Ó k Ò2Ó v k x IgE Th2 x } x x IL-4 IL-5 IgE IgE j IFN-γ IgG j j CD4 + { k d «d j B7 w k k x IgE k 1 k Abstract Parental immunization
The Link Between Viruses and Asthma
 The Link Between Viruses and Asthma CATHERINE KIER, MD Professor of Clinical Pediatrics Division Chief, Pediatric Pulmonary, and Cystic Fibrosis Center Director, Pediatric Sleep Disorders Center SUNY Stony
The Link Between Viruses and Asthma CATHERINE KIER, MD Professor of Clinical Pediatrics Division Chief, Pediatric Pulmonary, and Cystic Fibrosis Center Director, Pediatric Sleep Disorders Center SUNY Stony
Identifying Biologic Targets to Attenuate or Eliminate Asthma Exacerbations
 Identifying Biologic Targets to Attenuate or Eliminate Exacerbations exacerbations are a major cause of disease morbidity and costs. For both children and adults, viral respiratory infections are the major
Identifying Biologic Targets to Attenuate or Eliminate Exacerbations exacerbations are a major cause of disease morbidity and costs. For both children and adults, viral respiratory infections are the major
Immunology of Asthma. Kenneth J. Goodrum,Ph. Ph.D. Ohio University College of Osteopathic Medicine
 Immunology of Asthma Kenneth J. Goodrum,Ph Ph.D. Ohio University College of Osteopathic Medicine Outline Consensus characteristics/incidence data Immune/inflammatory basis Etiology/Genetic basis Hygiene
Immunology of Asthma Kenneth J. Goodrum,Ph Ph.D. Ohio University College of Osteopathic Medicine Outline Consensus characteristics/incidence data Immune/inflammatory basis Etiology/Genetic basis Hygiene
Supplementary Figure S1. Flow cytometric analysis of the expression of Thy1 in NH cells. Flow cytometric analysis of the expression of T1/ST2 and
 Supplementary Figure S1. Flow cytometric analysis of the expression of Thy1 in NH cells. Flow cytometric analysis of the expression of T1/ST2 and Thy1 in NH cells derived from the lungs of naïve mice.
Supplementary Figure S1. Flow cytometric analysis of the expression of Thy1 in NH cells. Flow cytometric analysis of the expression of T1/ST2 and Thy1 in NH cells derived from the lungs of naïve mice.
Immunology of Asthma. Kenneth J. Goodrum,Ph. Ph.D. Ohio University College of Osteopathic Medicine
 Immunology of Asthma Kenneth J. Goodrum,Ph Ph.D. Ohio University College of Osteopathic Medicine Outline! Consensus characteristics! Allergens:role in asthma! Immune/inflammatory basis! Genetic basis!
Immunology of Asthma Kenneth J. Goodrum,Ph Ph.D. Ohio University College of Osteopathic Medicine Outline! Consensus characteristics! Allergens:role in asthma! Immune/inflammatory basis! Genetic basis!
Building a better neonatal mouse model to understand infant respiratory syncytial virus disease
 You et al. Respiratory Research (2015) 16:91 DOI 10.1186/s12931-015-0244-0 RESEARCH Building a better neonatal mouse model to understand infant respiratory syncytial virus disease Dahui You 1,2, David
You et al. Respiratory Research (2015) 16:91 DOI 10.1186/s12931-015-0244-0 RESEARCH Building a better neonatal mouse model to understand infant respiratory syncytial virus disease Dahui You 1,2, David
The Role of T Cells in the Enhancement of Respiratory Syncytial Virus Infection Severity during Adult Reinfection of Neonatally Sensitized Mice
 JOURNAL OF VIROLOGY, Apr. 2008, p. 4115 4124 Vol. 82, No. 8 0022-538X/08/$08.00 0 doi:10.1128/jvi.02313-07 Copyright 2008, American Society for Microbiology. All Rights Reserved. The Role of T Cells in
JOURNAL OF VIROLOGY, Apr. 2008, p. 4115 4124 Vol. 82, No. 8 0022-538X/08/$08.00 0 doi:10.1128/jvi.02313-07 Copyright 2008, American Society for Microbiology. All Rights Reserved. The Role of T Cells in
Respiratory Syncytial Virus Infection Results in Airway Hyperresponsiveness and Enhanced Airway Sensitization to Allergen
 Respiratory Syncytial Virus Infection Results in Airway Hyperresponsiveness and Enhanced Airway Sensitization to Allergen Jürgen Schwarze, Eckard Hamelmann, Katherine L. Bradley, Katsuyuki Takeda, and
Respiratory Syncytial Virus Infection Results in Airway Hyperresponsiveness and Enhanced Airway Sensitization to Allergen Jürgen Schwarze, Eckard Hamelmann, Katherine L. Bradley, Katsuyuki Takeda, and
Inhibition of airway remodeling in IL-5 deficient mice
 Inhibition of airway remodeling in IL-5 deficient mice See the related Commentary beginning on page 507. Jae Youn Cho, Marina Miller, Kwang Je Baek, Ji Won Han, Jyothi Nayar, Sook Young Lee, Kirsti McElwain,
Inhibition of airway remodeling in IL-5 deficient mice See the related Commentary beginning on page 507. Jae Youn Cho, Marina Miller, Kwang Je Baek, Ji Won Han, Jyothi Nayar, Sook Young Lee, Kirsti McElwain,
Searching for Targets to Control Asthma
 Searching for Targets to Control Asthma Timothy Craig Distinguished Educator Professor Medicine and Pediatrics Penn State University Hershey, PA, USA Inflammation and Remodeling in Asthma The most important
Searching for Targets to Control Asthma Timothy Craig Distinguished Educator Professor Medicine and Pediatrics Penn State University Hershey, PA, USA Inflammation and Remodeling in Asthma The most important
Impact of Asthma in the U.S. per Year. Asthma Epidemiology and Pathophysiology. Risk Factors for Asthma. Childhood Asthma Costs of Asthma
 American Association for Respiratory Care Asthma Educator Certification Prep Course Asthma Epidemiology and Pathophysiology Robert C. Cohn, MD, FAARC MetroHealth Medical Center Cleveland, OH Impact of
American Association for Respiratory Care Asthma Educator Certification Prep Course Asthma Epidemiology and Pathophysiology Robert C. Cohn, MD, FAARC MetroHealth Medical Center Cleveland, OH Impact of
Kun Jiang 1, He-Bin Chen 1, Ying Wang 1, Jia-Hui Lin 2, Yan Hu 1, Yu-Rong Fang 1
 Original Article Changes in interleukin-17 and transforming growth factor beta 1 levels in serum and bronchoalveolar lavage fluid and their clinical significance among children with asthma Kun Jiang 1,
Original Article Changes in interleukin-17 and transforming growth factor beta 1 levels in serum and bronchoalveolar lavage fluid and their clinical significance among children with asthma Kun Jiang 1,
Phenotypes of asthma; implications for treatment. Medical Grand Rounds Feb 2018 Jim Martin MD DSc
 Phenotypes of asthma; implications for treatment Medical Grand Rounds Feb 2018 Jim Martin MD DSc No conflicts to declare Objectives To understand the varied clinical forms of asthma To understand the pathobiologic
Phenotypes of asthma; implications for treatment Medical Grand Rounds Feb 2018 Jim Martin MD DSc No conflicts to declare Objectives To understand the varied clinical forms of asthma To understand the pathobiologic
Airway Inflammation in Asthma Chih-Yung Chiu 1,2, Kin-Sun Wong 2 1 Department of Pediatrics, Chang Gung Memorial Hospital, Keelung, Taiwan.
 REVIEW ARTICLE Chih-Yung Chiu 1,2, Kin-Sun Wong 2 1 Department of Pediatrics, Chang Gung Memorial Hospital, Keelung, Taiwan. 2 Division of Pediatric Pulmonology, Department of Pediatrics, Chang Gung Memorial
REVIEW ARTICLE Chih-Yung Chiu 1,2, Kin-Sun Wong 2 1 Department of Pediatrics, Chang Gung Memorial Hospital, Keelung, Taiwan. 2 Division of Pediatric Pulmonology, Department of Pediatrics, Chang Gung Memorial
Identification of an IFN-γ/mast cell axis in a mouse model of chronic asthma
 Research article Identification of an IFN-γ/mast cell axis in a mouse model of chronic asthma Mang Yu, 1 Michael R. Eckart, 2 Alexander A. Morgan, 3 Kaori Mukai, 1 Atul J. Butte, 3 Mindy Tsai, 1 and Stephen
Research article Identification of an IFN-γ/mast cell axis in a mouse model of chronic asthma Mang Yu, 1 Michael R. Eckart, 2 Alexander A. Morgan, 3 Kaori Mukai, 1 Atul J. Butte, 3 Mindy Tsai, 1 and Stephen
Supplementary Figures
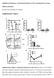 Inhibition of Pulmonary Anti Bacterial Defense by IFN γ During Recovery from Influenza Infection By Keer Sun and Dennis W. Metzger Supplementary Figures d a Ly6G Percentage survival f 1 75 5 1 25 1 5 1
Inhibition of Pulmonary Anti Bacterial Defense by IFN γ During Recovery from Influenza Infection By Keer Sun and Dennis W. Metzger Supplementary Figures d a Ly6G Percentage survival f 1 75 5 1 25 1 5 1
Role of C5 in the development of airway inflammation, airway hyperresponsiveness, and ongoing airway response
 Research article Role of C5 in the development of airway inflammation, airway hyperresponsiveness, and ongoing airway response Tao Peng, 1 Liming Hao, 2 Joseph A. Madri, 2 Xiao Su, 1 Jack A. Elias, 3 Gregory
Research article Role of C5 in the development of airway inflammation, airway hyperresponsiveness, and ongoing airway response Tao Peng, 1 Liming Hao, 2 Joseph A. Madri, 2 Xiao Su, 1 Jack A. Elias, 3 Gregory
Chemical Chaperones Mitigate Experimental Asthma By Attenuating Endoplasmic
 Chemical Chaperones Mitigate Experimental Asthma By Attenuating Endoplasmic Reticulum Stress Lokesh Makhija, BE, Veda Krishnan, MSc, Rakhshinda Rehman, MTech, Samarpana Chakraborty, MSc, Shuvadeep Maity,
Chemical Chaperones Mitigate Experimental Asthma By Attenuating Endoplasmic Reticulum Stress Lokesh Makhija, BE, Veda Krishnan, MSc, Rakhshinda Rehman, MTech, Samarpana Chakraborty, MSc, Shuvadeep Maity,
Maintenance of Airway Hyperresponsiveness in Chronic Asthma May Be Mediated by Th2-Independent Mechanisms
 12 The Open Allergy Journal, 2008, 1, 12-18 Open Access Maintenance of Airway Hyperresponsiveness in Chronic Asthma May Be Mediated by Th2-Independent Mechanisms Nora J. Lin 1, Jane M. Schuh 2 and Cory
12 The Open Allergy Journal, 2008, 1, 12-18 Open Access Maintenance of Airway Hyperresponsiveness in Chronic Asthma May Be Mediated by Th2-Independent Mechanisms Nora J. Lin 1, Jane M. Schuh 2 and Cory
Potent and Selective CRTh2 Antagonists are Efficacious in Models of Asthma, Allergic Rhinitis and Atopic Dermatitis
 Potent and Selective CRTh2 Antagonists are Efficacious in Models of Asthma, Allergic Rhinitis and Atopic Dermatitis Laura L. Carter, Yoshi Shiraishi, Yooseob Shin, Laurence Burgess, Christine Eberhardt,
Potent and Selective CRTh2 Antagonists are Efficacious in Models of Asthma, Allergic Rhinitis and Atopic Dermatitis Laura L. Carter, Yoshi Shiraishi, Yooseob Shin, Laurence Burgess, Christine Eberhardt,
B220 CD4 CD8. Figure 1. Confocal Image of Sensitized HLN. Representative image of a sensitized HLN
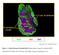 B220 CD4 CD8 Natarajan et al., unpublished data Figure 1. Confocal Image of Sensitized HLN. Representative image of a sensitized HLN showing B cell follicles and T cell areas. 20 µm thick. Image of magnification
B220 CD4 CD8 Natarajan et al., unpublished data Figure 1. Confocal Image of Sensitized HLN. Representative image of a sensitized HLN showing B cell follicles and T cell areas. 20 µm thick. Image of magnification
감초 (Glycyrrhiza uralensis Fisch, GLU) 가천식모델생쥐의 BALF 내면역세포및 Cytokine 에미치는효과
 감초 (Glycyrrhiza uralensis Fisch, GLU) 가천식모델생쥐의 BALF 내면역세포및 Cytokine 에미치는효과 Effects of Glycyrrhiza uralensis Fisch on Immunocyte and Cytokine Production in Asthma Model Mouse Young-Joo Han, Yang-Chun Park
감초 (Glycyrrhiza uralensis Fisch, GLU) 가천식모델생쥐의 BALF 내면역세포및 Cytokine 에미치는효과 Effects of Glycyrrhiza uralensis Fisch on Immunocyte and Cytokine Production in Asthma Model Mouse Young-Joo Han, Yang-Chun Park
Pulmonary Perspective
 Pulmonary Perspective Bronchiolitis to Asthma A Review and Call for Studies of Gene Virus Interactions in Asthma Causation Anne Marie Singh, Paul E. Moore, James E. Gern, Robert F. Lemanske, Jr., and Tina
Pulmonary Perspective Bronchiolitis to Asthma A Review and Call for Studies of Gene Virus Interactions in Asthma Causation Anne Marie Singh, Paul E. Moore, James E. Gern, Robert F. Lemanske, Jr., and Tina
Supplementary Information
 Supplementary Information TABLE S1. SUBJECT CHARACTERISTICS* Normal Control Subjects Subjects with Asthma p Value Number 23 48 Age (years) 35±10 35±10 0.75 Sex, M:F (% F) 9:12 (57) 17:26 (60) 0.76 FEV1
Supplementary Information TABLE S1. SUBJECT CHARACTERISTICS* Normal Control Subjects Subjects with Asthma p Value Number 23 48 Age (years) 35±10 35±10 0.75 Sex, M:F (% F) 9:12 (57) 17:26 (60) 0.76 FEV1
Soluble ADAM33 initiates airway remodeling to promote susceptibility for. Elizabeth R. Davies, Joanne F.C. Kelly, Peter H. Howarth, David I Wilson,
 Revised Suppl. Data: Soluble ADAM33 1 Soluble ADAM33 initiates airway remodeling to promote susceptibility for allergic asthma in early life Elizabeth R. Davies, Joanne F.C. Kelly, Peter H. Howarth, David
Revised Suppl. Data: Soluble ADAM33 1 Soluble ADAM33 initiates airway remodeling to promote susceptibility for allergic asthma in early life Elizabeth R. Davies, Joanne F.C. Kelly, Peter H. Howarth, David
Modulation of hyperresponsiveness by glutathione in a murine in vivo model of allergic asthma
 6 Modulation of hyperresponsiveness by glutathione in a murine in vivo model of allergic asthma J. Kloek, I. Van Ark, G. Folkerts, F. De Clerck,, N. Bloksma,, F.P. Nijkamp. Department of Pharmacology and
6 Modulation of hyperresponsiveness by glutathione in a murine in vivo model of allergic asthma J. Kloek, I. Van Ark, G. Folkerts, F. De Clerck,, N. Bloksma,, F.P. Nijkamp. Department of Pharmacology and
10.00 PBS OVA OVA+isotype antibody 8.00 OVA+anti-HMGB1. PBS Methatroline (mg/ml)
 RESEARCH ARTICLE Penh (100% of PBS) 1 PBS 8.00 +anti-hmgb1 6.00 4.00 p=0.054 Cellular & Molecular Immunology advance online publication, PBS 3.12 6.25 Methatroline (mg/ml) Neutrophil isolation and culture
RESEARCH ARTICLE Penh (100% of PBS) 1 PBS 8.00 +anti-hmgb1 6.00 4.00 p=0.054 Cellular & Molecular Immunology advance online publication, PBS 3.12 6.25 Methatroline (mg/ml) Neutrophil isolation and culture
Interleukin-17 enhances the removal of respiratory syncytial virus in mice by promoting neutrophil migration and reducing interferon-gamma expression
 Interleukin-17 enhances the removal of respiratory syncytial virus in mice by promoting neutrophil migration and reducing interferon-gamma expression G. Zhang 1, K.F. Zhou 2 and Z.H. Lu 1 1 Department
Interleukin-17 enhances the removal of respiratory syncytial virus in mice by promoting neutrophil migration and reducing interferon-gamma expression G. Zhang 1, K.F. Zhou 2 and Z.H. Lu 1 1 Department
Concurrent dual allergen exposure and its effects on airway hyperresponsiveness, inflammation and remodeling in mice
 Disease Models & Mechanisms, 75-8 (9) doi:1.14/dmm.1859 RESEARCH ARTICLE Concurrent dual allergen exposure and its effects on airway hyperresponsiveness, inflammation and remodeling in mice Franco A. DiGiovanni
Disease Models & Mechanisms, 75-8 (9) doi:1.14/dmm.1859 RESEARCH ARTICLE Concurrent dual allergen exposure and its effects on airway hyperresponsiveness, inflammation and remodeling in mice Franco A. DiGiovanni
Health professionals. 8Asthma. and Wheezing in the First Years of Life. A guide for health professionals
 Health professionals 8Asthma and Wheezing in the First Years of Life A guide for health professionals Asthma and Wheezing in the First Years of Life An information paper for health professionals The aim
Health professionals 8Asthma and Wheezing in the First Years of Life A guide for health professionals Asthma and Wheezing in the First Years of Life An information paper for health professionals The aim
Asthma. - A chronic inflammatory disorder which causes recurrent episodes of wheezing, breathlessness, cough and chest tightness.
 Obstructive diseases Asthma - A chronic inflammatory disorder which causes recurrent episodes of wheezing, breathlessness, cough and chest tightness. - Characterized by Intermittent and reversible (the
Obstructive diseases Asthma - A chronic inflammatory disorder which causes recurrent episodes of wheezing, breathlessness, cough and chest tightness. - Characterized by Intermittent and reversible (the
IL-4R on CD4 T cells plays a pathogenic role in respiratory syncytial virus reinfection in mice infected initially as neonates
 Article IL-4R on CD4 T cells plays a pathogenic role in respiratory syncytial virus reinfection in mice infected initially as neonates Dahui You,* Nico Marr, Jordy Saravia,* Bishwas Shrestha,* Greg I.
Article IL-4R on CD4 T cells plays a pathogenic role in respiratory syncytial virus reinfection in mice infected initially as neonates Dahui You,* Nico Marr, Jordy Saravia,* Bishwas Shrestha,* Greg I.
Potential therapeutic implications of new insights into respiratory syncytial virus disease Peter JM Openshaw
 Available online http://respiratory-research.com/content/3/s1/s15 Potential therapeutic implications of new insights into respiratory syncytial virus disease Peter JM Openshaw Department of Respiratory
Available online http://respiratory-research.com/content/3/s1/s15 Potential therapeutic implications of new insights into respiratory syncytial virus disease Peter JM Openshaw Department of Respiratory
Airway Inflammation and Allergen Specific IgE Production May Persist Longer Than Airway Hyperresponsiveness in Mice
 J Korean Med Sci 24; 19: 69-73 ISSN 111-8934 Copyright The Korean Academy of Medical Sciences Airway Inflammation and Allergen Specific IgE Production May Persist Longer Than Airway Hyperrespoiveness in
J Korean Med Sci 24; 19: 69-73 ISSN 111-8934 Copyright The Korean Academy of Medical Sciences Airway Inflammation and Allergen Specific IgE Production May Persist Longer Than Airway Hyperrespoiveness in
COPD lungs show an attached stratified mucus layer that separate. bacteria from the epithelial cells resembling the protective colonic
 COPD lungs show an attached stratified mucus layer that separate bacteria from the epithelial cells resembling the protective colonic mucus SUPPLEMENTARY TABLES AND FIGURES Tables S1 S8, page 1 and separate
COPD lungs show an attached stratified mucus layer that separate bacteria from the epithelial cells resembling the protective colonic mucus SUPPLEMENTARY TABLES AND FIGURES Tables S1 S8, page 1 and separate
Dr Rodney Itaki Lecturer Division of Pathology Anatomical Pathology Discipline
 Pathology of Asthma Dr Rodney Itaki Lecturer Division of Pathology Anatomical Pathology Discipline Bronchial Asthma Definition: chronic, relapsing inflammatory lung disorder characterised by reversible
Pathology of Asthma Dr Rodney Itaki Lecturer Division of Pathology Anatomical Pathology Discipline Bronchial Asthma Definition: chronic, relapsing inflammatory lung disorder characterised by reversible
Online Data Supplement
 Modulatory role for retinoid-related orphan receptor α (RORα) in allergen-induced lung inflammation Maisa Jaradat, Cliona Stapleton, Stephen L. Tilley, Darlene Dixon, Christopher J. Erikson, Joshua G.
Modulatory role for retinoid-related orphan receptor α (RORα) in allergen-induced lung inflammation Maisa Jaradat, Cliona Stapleton, Stephen L. Tilley, Darlene Dixon, Christopher J. Erikson, Joshua G.
Interleukin-4 and interleukin-13 induce fibronectin production by human lung fibroblasts
 Allergology International (2001) 50: 197 202 Original Article Interleukin-4 and interleukin-13 induce fibronectin production by human lung fibroblasts Tatsuya Machino, Shu Hashimoto, Yasuhiro Gon, Kosei
Allergology International (2001) 50: 197 202 Original Article Interleukin-4 and interleukin-13 induce fibronectin production by human lung fibroblasts Tatsuya Machino, Shu Hashimoto, Yasuhiro Gon, Kosei
Neonatal Exposure to Microbial Phosphorylcholine Modulates the Development of House Dust Mite Allergy During Adult Life
 Neonatal Exposure to Microbial Phosphorylcholine Modulates the Development of House Dust Mite Allergy During Adult Life J. Sides SEM Preeyam Patel Mentor: Dr John Kearney 015 CAMBAC Research Day 9/18/15
Neonatal Exposure to Microbial Phosphorylcholine Modulates the Development of House Dust Mite Allergy During Adult Life J. Sides SEM Preeyam Patel Mentor: Dr John Kearney 015 CAMBAC Research Day 9/18/15
Th17 Pathway Research By Bio-Plex
 Th17 Pathway Research By Bio-Plex Zhiyang Shen, Senior Product Manager Bio-Rad Laboratories, Inc 2011 年 6 月 28 日星期二 T helper cell research Timeline: advances on T helper research. Figure depicts some of
Th17 Pathway Research By Bio-Plex Zhiyang Shen, Senior Product Manager Bio-Rad Laboratories, Inc 2011 年 6 月 28 日星期二 T helper cell research Timeline: advances on T helper research. Figure depicts some of
Diagnosis and Management of Fungal Allergy Monday, 9-139
 Diagnosis and Management of Fungal Allergy Monday, 9-139 13-2010 Alan P. Knutsen,, MD Director, Pediatric Allergy & Immunology Director, Jeffrey Modell Diagnostic Center for Primary Immunodeficiencies
Diagnosis and Management of Fungal Allergy Monday, 9-139 13-2010 Alan P. Knutsen,, MD Director, Pediatric Allergy & Immunology Director, Jeffrey Modell Diagnostic Center for Primary Immunodeficiencies
Original Article. ÎË T cell is essential for allergen-induced late asthmatic response in a murine model of asthma
 J Med Dent Sci 2008; 55: 113 120 Original Article ÎË T cell is essential for allergen-induced late asthmatic response in a murine model of asthma Kanna Tamura-Yamashita 1,2, Junji Endo 1,3, Susumu Isogai
J Med Dent Sci 2008; 55: 113 120 Original Article ÎË T cell is essential for allergen-induced late asthmatic response in a murine model of asthma Kanna Tamura-Yamashita 1,2, Junji Endo 1,3, Susumu Isogai
Noninvasive Measurement of Airway Responsiveness in Allergic Mice Using Barometric Plethysmography
 Noninvasive Measurement of Airway Responsiveness in Allergic Mice Using Barometric Plethysmography E. HAMELMANN, J. SCHWARZE, K. TAKEDA, A. OSHIBA, G. L. LARSEN, C. G. IRVIN, and E. W. GELFAND Divisions
Noninvasive Measurement of Airway Responsiveness in Allergic Mice Using Barometric Plethysmography E. HAMELMANN, J. SCHWARZE, K. TAKEDA, A. OSHIBA, G. L. LARSEN, C. G. IRVIN, and E. W. GELFAND Divisions
Biomerker onderzoek voor isocyanaatgeïnduceerd
 CGC en NVAB meeting, 6 Juni 2013, s-hertogenbosch Biomerker onderzoek voor isocyanaatgeïnduceerd astma Jeroen Vanoirbeek Asthma 1. Chronic airway disease: prevalence: 5-10%, 300.000 people affected world-wide
CGC en NVAB meeting, 6 Juni 2013, s-hertogenbosch Biomerker onderzoek voor isocyanaatgeïnduceerd astma Jeroen Vanoirbeek Asthma 1. Chronic airway disease: prevalence: 5-10%, 300.000 people affected world-wide
Effects of Respiratory Mycoplasma pneumoniae Infection on Allergen-Induced Bronchial Hyperresponsiveness and Lung Inflammation in Mice
 INFECTION AND IMMUNITY, Mar. 2003, p. 1520 1526 Vol. 71, No. 3 0019-9567/03/$08.00 0 DOI: 10.1128/IAI.71.3.1520 1526.2003 Copyright 2003, American Society for Microbiology. All Rights Reserved. Effects
INFECTION AND IMMUNITY, Mar. 2003, p. 1520 1526 Vol. 71, No. 3 0019-9567/03/$08.00 0 DOI: 10.1128/IAI.71.3.1520 1526.2003 Copyright 2003, American Society for Microbiology. All Rights Reserved. Effects
Interferon γ regulates idiopathic pneumonia syndrome, a. Th17 + CD4 + T-cell-mediated GvH disease
 Interferon γ regulates idiopathic pneumonia syndrome, a Th17 + CD4 + T-cell-mediated GvH disease Nora Mauermann, Julia Burian, Christophe von Garnier, Stefan Dirnhofer, Davide Germano, Christine Schuett,
Interferon γ regulates idiopathic pneumonia syndrome, a Th17 + CD4 + T-cell-mediated GvH disease Nora Mauermann, Julia Burian, Christophe von Garnier, Stefan Dirnhofer, Davide Germano, Christine Schuett,
Re: SCN-Lifequest: Bird flu study in mice, H1 N1/MAE-01
 ST&T DEPARTMENTS: PRODUCT DEVELOPMENT & CLINICAL RESEARCH MS. SIMONE DERAYEH PHARMACOLOGY/TOXICOLOGY DR. ALDRICH DR. SNODGRASS GENERAL MEDICINE, MEDICAL CONSULTATION DR. ALDRICH DR. SNODGRASS INTERNATIONAL
ST&T DEPARTMENTS: PRODUCT DEVELOPMENT & CLINICAL RESEARCH MS. SIMONE DERAYEH PHARMACOLOGY/TOXICOLOGY DR. ALDRICH DR. SNODGRASS GENERAL MEDICINE, MEDICAL CONSULTATION DR. ALDRICH DR. SNODGRASS INTERNATIONAL
DNA vaccine, peripheral T-cell tolerance modulation 185
 Subject Index Airway hyperresponsiveness (AHR) animal models 41 43 asthma inhibition 45 overview 41 mast cell modulation of T-cells 62 64 respiratory tolerance 40, 41 Tregs inhibition role 44 respiratory
Subject Index Airway hyperresponsiveness (AHR) animal models 41 43 asthma inhibition 45 overview 41 mast cell modulation of T-cells 62 64 respiratory tolerance 40, 41 Tregs inhibition role 44 respiratory
Property of Presenter
 Have We Missed A Role For Neutrophils In Asthma? In Steroid-Refractory Asthma? Erwin W. Gelfand, MD Chairman, Department of Pediatrics National Jewish Health Professor of Pediatrics and Immunology University
Have We Missed A Role For Neutrophils In Asthma? In Steroid-Refractory Asthma? Erwin W. Gelfand, MD Chairman, Department of Pediatrics National Jewish Health Professor of Pediatrics and Immunology University
Supplemental Figures: Supplemental Figure 1
 Supplemental Figures: Supplemental Figure 1 Suppl. Figure 1. BM-DC infection with H. pylori does not induce cytotoxicity and treatment of BM-DCs with H. pylori sonicate, but not heat-inactivated bacteria,
Supplemental Figures: Supplemental Figure 1 Suppl. Figure 1. BM-DC infection with H. pylori does not induce cytotoxicity and treatment of BM-DCs with H. pylori sonicate, but not heat-inactivated bacteria,
Grup de fisiologia digestiva i adaptacions nutricionals Institut de Nutrició i Seguretat Alimentaria
 Grup de fisiologia digestiva i adaptacions nutricionals Institut de Nutrició i Seguretat Alimentaria 1 Outline Weaning and the consequences of stress Animal blood plasma Spray-drying SDP SDP in a model
Grup de fisiologia digestiva i adaptacions nutricionals Institut de Nutrició i Seguretat Alimentaria 1 Outline Weaning and the consequences of stress Animal blood plasma Spray-drying SDP SDP in a model
METHODS Penh. Measurements and ribonuclease protection assay. Intracellular cytokine staining. ELISAs RT-PCR. Lung morphometry.
 METHODS Penh In addition to measurement of APTI, airway hyperresponsiveness to methacholine was also evaluated within 24 hours of the last allergen challenge by means of measurement of Penh (Buxco Electronics,
METHODS Penh In addition to measurement of APTI, airway hyperresponsiveness to methacholine was also evaluated within 24 hours of the last allergen challenge by means of measurement of Penh (Buxco Electronics,
IKKα Causes Chromatin Modification on Pro-Inflammatory Genes by Cigarette Smoke in Mouse Lung
 IKKα Causes Chromatin Modification on Pro-Inflammatory Genes by Cigarette Smoke in Mouse Lung Se-Ran Yang, Samantha Valvo, Hongwei Yao, Aruna Kode, Saravanan Rajendrasozhan, Indika Edirisinghe, Samuel
IKKα Causes Chromatin Modification on Pro-Inflammatory Genes by Cigarette Smoke in Mouse Lung Se-Ran Yang, Samantha Valvo, Hongwei Yao, Aruna Kode, Saravanan Rajendrasozhan, Indika Edirisinghe, Samuel
Mouse Anti-OVA IgM Antibody Assay Kit
 Mouse Anti-OVA IgM Antibody Assay Kit Catalog # 3017 For Research Use Only - Not Human or Therapeutic Use INTRODUCTION Ovalbumin (OVA) is a widely used antigen for inducing allergic reactions in experimental
Mouse Anti-OVA IgM Antibody Assay Kit Catalog # 3017 For Research Use Only - Not Human or Therapeutic Use INTRODUCTION Ovalbumin (OVA) is a widely used antigen for inducing allergic reactions in experimental
Nishino, Tomoya; Fukushima, Chizu; Asthma and Immunology, 113, 2, (201
 NAOSITE: Nagasaki University's Ac Title Author(s) Citation Clearance of Aspergillus fumigatus inflammation Fukahori, Susumu; Matsuse, Hiroto; Nishino, Tomoya; Fukushima, Chizu; Annals of Allergy, Asthma
NAOSITE: Nagasaki University's Ac Title Author(s) Citation Clearance of Aspergillus fumigatus inflammation Fukahori, Susumu; Matsuse, Hiroto; Nishino, Tomoya; Fukushima, Chizu; Annals of Allergy, Asthma
Asthma is a major chronic respiratory. Streptococcus pneumoniae infection suppresses allergic airways disease by inducing regulatory T-cells
 Eur Respir J 11; 7: DOI: 1.11/919.91 CopyrightßERS 11 Streptococcus pneumoniae infection suppresses allergic airways disease by inducing regulatory T-cells J.A. Preston*,, A.N. Thorburn*,, M.R. Starkey*,
Eur Respir J 11; 7: DOI: 1.11/919.91 CopyrightßERS 11 Streptococcus pneumoniae infection suppresses allergic airways disease by inducing regulatory T-cells J.A. Preston*,, A.N. Thorburn*,, M.R. Starkey*,
The natural history of asthma and early intervention
 The natural history of asthma and early intervention Stanley J. Szefler, MD Denver, Colo The understanding of the natural history of asthma has changed significantly during the last 4 decades, with the
The natural history of asthma and early intervention Stanley J. Szefler, MD Denver, Colo The understanding of the natural history of asthma has changed significantly during the last 4 decades, with the
Christopher M. Carosino and Kent E. Pinkerton Center for Health and the Environment University of California, Davis
 Christopher M. Carosino and Kent E. Pinkerton Center for Health and the Environment University of California, Davis Particulate Pollution in the San Joaquin Valley: Translating Science into Policy June
Christopher M. Carosino and Kent E. Pinkerton Center for Health and the Environment University of California, Davis Particulate Pollution in the San Joaquin Valley: Translating Science into Policy June
Small Airways Disease. Respiratory Function In Small Airways And Asthma. Pathophysiologic Changes in the Small Airways of Asthma Patients
 Small Airways Disease Respiratory Function In Small Airways And Relevant Questions On Small Airway Involvement In How can small airway disease be defined? What is the link between small airway abnormalities
Small Airways Disease Respiratory Function In Small Airways And Relevant Questions On Small Airway Involvement In How can small airway disease be defined? What is the link between small airway abnormalities
HHS Public Access Author manuscript Mucosal Immunol. Author manuscript; available in PMC 2015 March 01.
 The Complex Relationship Between Inflammation And Lung Function In Severe Asthma Michelle L. Manni 1, John B. Trudeau 2, Erich V. Scheller 1, Sivanarayana Mandalapu 1, M. Merle Elloso 3, Jay K. Kolls 4,
The Complex Relationship Between Inflammation And Lung Function In Severe Asthma Michelle L. Manni 1, John B. Trudeau 2, Erich V. Scheller 1, Sivanarayana Mandalapu 1, M. Merle Elloso 3, Jay K. Kolls 4,
RSV bronchiolitis and risk of wheeze and allergic sensitisation in the first year of life
 Eur Respir J 2002; 20: 1277 1283 DOI: 10.1183/09031936.02.00019902 Printed in UK all rights reserved Copyright #ERS Journals Ltd 2002 European Respiratory Journal ISSN 0903-1936 RSV bronchiolitis and risk
Eur Respir J 2002; 20: 1277 1283 DOI: 10.1183/09031936.02.00019902 Printed in UK all rights reserved Copyright #ERS Journals Ltd 2002 European Respiratory Journal ISSN 0903-1936 RSV bronchiolitis and risk
CD4 + and CD8 + T cells play a central role in a HDM driven model of allergic asthma
 Raemdonck et al. Respiratory Research (2016)17:45 DOI 10.1186/s12931-016-0359-y RESEARCH CD4 + and CD8 + T cells play a central role in a HDM driven model of allergic asthma Open Access Kristof Raemdonck
Raemdonck et al. Respiratory Research (2016)17:45 DOI 10.1186/s12931-016-0359-y RESEARCH CD4 + and CD8 + T cells play a central role in a HDM driven model of allergic asthma Open Access Kristof Raemdonck
Mouse Total IgA Antibody Detection Kit
 Mouse Total IgA Antibody Detection Kit Catalog # 3019 For Research Use Only - Not Human or Therapeutic Use INTRODUCTION The total IgA levels in specimens are often determined in mouse disease models involving
Mouse Total IgA Antibody Detection Kit Catalog # 3019 For Research Use Only - Not Human or Therapeutic Use INTRODUCTION The total IgA levels in specimens are often determined in mouse disease models involving
Cysteinyl leukotriene receptor antagonist regulates allergic airway inflammation in an organ- and cytokine-specific manner
 e-issn 1643-375 Med Sci Monit, 214; 2: 297-32 DOI: 1.12659/MSM.889865 Received: 213.1.6 Accepted: 213.12.2 Published: 214.2.22 Cysteinyl leukotriene receptor antagonist regulates allergic airway inflammation
e-issn 1643-375 Med Sci Monit, 214; 2: 297-32 DOI: 1.12659/MSM.889865 Received: 213.1.6 Accepted: 213.12.2 Published: 214.2.22 Cysteinyl leukotriene receptor antagonist regulates allergic airway inflammation
Respiratory syncytial virus (RSV) is the
 [haematologica reports] 2006;2(10):50-55 IMMUNE RESPONSE TO RSV INFECTION Respiratory Syncytial Virus (RSV): Characteristics of Infection and the Role of Immune Response in the Evolution of Disease PEARAY
[haematologica reports] 2006;2(10):50-55 IMMUNE RESPONSE TO RSV INFECTION Respiratory Syncytial Virus (RSV): Characteristics of Infection and the Role of Immune Response in the Evolution of Disease PEARAY
Bitter Taste Receptor Agonists Mitigate Features of Allergic Asthma in Mice.
 Thomas Jefferson University Jefferson Digital Commons Department of Medicine Faculty Papers Department of Medicine 4-11-2017 Bitter Taste Receptor Agonists Mitigate Features of Allergic Asthma in Mice.
Thomas Jefferson University Jefferson Digital Commons Department of Medicine Faculty Papers Department of Medicine 4-11-2017 Bitter Taste Receptor Agonists Mitigate Features of Allergic Asthma in Mice.
Novel biomarkers of chemical-induced asthma: a murine model. Jeroen Vanoirbeek
 Novel biomarkers of chemical-induced asthma: a murine model Jeroen Vanoirbeek Asthma 1. Chronic airway disease: prevalence: 5-10%, 300.000 people affected world-wide 2. Reversible airflow limitation, airway
Novel biomarkers of chemical-induced asthma: a murine model Jeroen Vanoirbeek Asthma 1. Chronic airway disease: prevalence: 5-10%, 300.000 people affected world-wide 2. Reversible airflow limitation, airway
Distinction and Overlap. Allergy Dpt, 2 nd Pediatric Clinic, University of Athens
 Asthma Phenotypes: Distinction and Overlap Nikos Papadopoulos Allergy Dpt, 2 nd Pediatric Clinic, University of Athens Asthma as a syndrome From the Iliad to ADAM 33 and back again Bronchoconstriction,
Asthma Phenotypes: Distinction and Overlap Nikos Papadopoulos Allergy Dpt, 2 nd Pediatric Clinic, University of Athens Asthma as a syndrome From the Iliad to ADAM 33 and back again Bronchoconstriction,
Diesel exhaust particles exert acute effects on airway inflammation and function in murine allergen provocation models
 Diesel exhaust particles exert acute effects on airway inflammation and function in murine allergen provocation models Minqi Hao, MD, PhD, a Stephania Comier, PhD, b Meiying Wang, MD, a James J. Lee, PhD,
Diesel exhaust particles exert acute effects on airway inflammation and function in murine allergen provocation models Minqi Hao, MD, PhD, a Stephania Comier, PhD, b Meiying Wang, MD, a James J. Lee, PhD,
Effect of Influenza Virus Infection in a Murine Model of Asthma
 ORIGINAL ARTICLE Iran J Allergy Asthma Immunol August 2015; 14(4):392-401. Effect of Influenza Virus Infection in a Murine Model of Asthma Hwan Soo Kim, Huisu Lee, Hyun Sook Kim, Sulmui Won, Eu Kyoung
ORIGINAL ARTICLE Iran J Allergy Asthma Immunol August 2015; 14(4):392-401. Effect of Influenza Virus Infection in a Murine Model of Asthma Hwan Soo Kim, Huisu Lee, Hyun Sook Kim, Sulmui Won, Eu Kyoung
RESPIRATORY BLOCK. Bronchial Asthma. Dr. Maha Arafah Department of Pathology KSU
 RESPIRATORY BLOCK Bronchial Asthma Dr. Maha Arafah Department of Pathology KSU marafah@ksu.edu.sa Jan 2018 Objectives Define asthma (BA) Know the two types of asthma 1. Extrinsic or atopic allergic 2.
RESPIRATORY BLOCK Bronchial Asthma Dr. Maha Arafah Department of Pathology KSU marafah@ksu.edu.sa Jan 2018 Objectives Define asthma (BA) Know the two types of asthma 1. Extrinsic or atopic allergic 2.
Supporting Information
 Supporting Information Desnues et al. 10.1073/pnas.1314121111 SI Materials and Methods Mice. Toll-like receptor (TLR)8 / and TLR9 / mice were generated as described previously (1, 2). TLR9 / mice were
Supporting Information Desnues et al. 10.1073/pnas.1314121111 SI Materials and Methods Mice. Toll-like receptor (TLR)8 / and TLR9 / mice were generated as described previously (1, 2). TLR9 / mice were
HYPERSENSITIVITY REACTIONS D R S H O AI B R AZ A
 HYPERSENSITIVITY REACTIONS D R S H O AI B R AZ A HYPERSENSITIVITY REACTIONS Are exaggerated immune response upon antigenic stimulation Individuals who have been previously exposed to an antigen are said
HYPERSENSITIVITY REACTIONS D R S H O AI B R AZ A HYPERSENSITIVITY REACTIONS Are exaggerated immune response upon antigenic stimulation Individuals who have been previously exposed to an antigen are said
Therapeutic Dosing with Anti-Interleukin-13 Monoclonal Antibody Inhibits Asthma Progression in Mice
 0022-3565/05/3131-8 15$20.00 THE JOURNAL OF PHARMACOLOGY AND EXPERIMENTAL THERAPEUTICS Vol. 313, No. 1 Copyright 2005 by The American Society for Pharmacology and Experimental Therapeutics 76133/134368
0022-3565/05/3131-8 15$20.00 THE JOURNAL OF PHARMACOLOGY AND EXPERIMENTAL THERAPEUTICS Vol. 313, No. 1 Copyright 2005 by The American Society for Pharmacology and Experimental Therapeutics 76133/134368
IL-13Rα2 and IL-10 coordinately suppress airway inflammation, airwayhyperreactivity,
 Research article IL-13Rα2 and IL-10 coordinately suppress airway inflammation, airwayhyperreactivity, and fibrosis in mice Mark S. Wilson, 1 Eldad Elnekave, 1 Margaret M. Mentink-Kane, 1 Marcus G. Hodges,
Research article IL-13Rα2 and IL-10 coordinately suppress airway inflammation, airwayhyperreactivity, and fibrosis in mice Mark S. Wilson, 1 Eldad Elnekave, 1 Margaret M. Mentink-Kane, 1 Marcus G. Hodges,
Optimal Assessment of Asthma Control in Clinical Practice: Is there a role for biomarkers?
 Disclosures: Optimal Assessment of Asthma Control in Clinical Practice: Is there a role for biomarkers? Stanley Fineman, MD Past-President, American College of Allergy, Asthma & Immunology Adjunct Associate
Disclosures: Optimal Assessment of Asthma Control in Clinical Practice: Is there a role for biomarkers? Stanley Fineman, MD Past-President, American College of Allergy, Asthma & Immunology Adjunct Associate
Systems Pharmacology Respiratory Pharmacology. Lecture series : General outline
 Systems Pharmacology 3320 2017 Respiratory Pharmacology Associate Professor Peter Henry (Rm 1.34) Peter.Henry@uwa.edu.au Division of Pharmacology, School of Biomedical Sciences Lecture series : General
Systems Pharmacology 3320 2017 Respiratory Pharmacology Associate Professor Peter Henry (Rm 1.34) Peter.Henry@uwa.edu.au Division of Pharmacology, School of Biomedical Sciences Lecture series : General
E-1 Role of IgE and IgE receptors in allergic airway inflammation and remodeling
 E-1 Role of IgE and IgE receptors in allergic airway inflammation and remodeling Ruby Pawankar, MD, Ph.D. FRCP, FAAAAI Prof. Div of Allergy, Dept of Pediatrics Nippon Medical School Tokyo, Japan pawankar.ruby@gmail.com
E-1 Role of IgE and IgE receptors in allergic airway inflammation and remodeling Ruby Pawankar, MD, Ph.D. FRCP, FAAAAI Prof. Div of Allergy, Dept of Pediatrics Nippon Medical School Tokyo, Japan pawankar.ruby@gmail.com
Severe Asthma(s): Can THEY be prevented or reversed?
 Severe Asthma(s): Can THEY be prevented or reversed? Sally Wenzel, MD Professor of Medicine UPMC Chair in Translational Airway Biology Disclosures Sally Wenzel, M.D. Grant/Research Support: Boehringer-Ingelheim,
Severe Asthma(s): Can THEY be prevented or reversed? Sally Wenzel, MD Professor of Medicine UPMC Chair in Translational Airway Biology Disclosures Sally Wenzel, M.D. Grant/Research Support: Boehringer-Ingelheim,
IgE-mediated allergy in elderly patients with asthma
 Allergology international (1997) 46: 237-241 Original Article IgE-mediated allergy in elderly patients with asthma Fumihiro Mitsunobu, Takashi Mifune, Yasuhiro Hosaki, Kouzou Ashida, Hirofumi Tsugeno,
Allergology international (1997) 46: 237-241 Original Article IgE-mediated allergy in elderly patients with asthma Fumihiro Mitsunobu, Takashi Mifune, Yasuhiro Hosaki, Kouzou Ashida, Hirofumi Tsugeno,
/06/ PEDIATRIC RESEARCH Vol. 59, No. 2, 2006 Copyright 2006 International Pediatric Research Foundation, Inc.
 0031-3998/06/5902-0210 PEDIATRIC RESEARCH Vol. 59, No. 2, 2006 Copyright 2006 International Pediatric Research Foundation, Inc. Printed in U.S.A. Respiratory Syncytial Virus Infection Reversed Anti-Asthma
0031-3998/06/5902-0210 PEDIATRIC RESEARCH Vol. 59, No. 2, 2006 Copyright 2006 International Pediatric Research Foundation, Inc. Printed in U.S.A. Respiratory Syncytial Virus Infection Reversed Anti-Asthma
Viral infections in airway remodeling
 Viral infections in airway remodeling Nikos Papadopoulos As. Proffesor,Head, Allergy Dpt, 2 nd Pediatric Clinic, University of Athens Overview Acute events may have long term consequences Remodeling appears
Viral infections in airway remodeling Nikos Papadopoulos As. Proffesor,Head, Allergy Dpt, 2 nd Pediatric Clinic, University of Athens Overview Acute events may have long term consequences Remodeling appears
Effects of Respiratory Syncytial Virus Infection on Dendritic Cells and Cysteinyl Leukotrienes in Lung Tissues of a Murine Model of Asthma
 Allergology International. 27;56:165-169 DOI: 1.2332allergolint.O-6-476 Awarded Article, Annual Meeting of JSA ORIGINAL ARTICLE Effects of Respiratory Syncytial Virus Infection on Dendritic Cells and Cysteinyl
Allergology International. 27;56:165-169 DOI: 1.2332allergolint.O-6-476 Awarded Article, Annual Meeting of JSA ORIGINAL ARTICLE Effects of Respiratory Syncytial Virus Infection on Dendritic Cells and Cysteinyl
COPYRIGHTED MATERIAL. Definition and Pathology CHAPTER 1. John Rees
 CHAPTER 1 Definition and Pathology John Rees Sherman Education Centre, Guy s Hospital, London, UK OVERVIEW Asthma is an overall descriptive term but there are a number of more or less distinct phenotypes
CHAPTER 1 Definition and Pathology John Rees Sherman Education Centre, Guy s Hospital, London, UK OVERVIEW Asthma is an overall descriptive term but there are a number of more or less distinct phenotypes
Clinical & Experimental Allergy
 doi: 10.1111/j.1365-2222.2010.03459.x Clinical & Experimental Allergy, 40, 933 941 ORIGINAL ARTICLE Experimental Models of Allergic Disease c 2010 Blackwell Publishing Ltd Attenuated Bordetella pertussis
doi: 10.1111/j.1365-2222.2010.03459.x Clinical & Experimental Allergy, 40, 933 941 ORIGINAL ARTICLE Experimental Models of Allergic Disease c 2010 Blackwell Publishing Ltd Attenuated Bordetella pertussis
The FDA Critical Path Initiative
 The FDA Critical Path Initiative Clinical Considerations for Demonstration of Dose-response for Inhaled Corticosteroids - Exhaled Nitric Oxide Model Badrul A. Chowdhury, MD, PhD Director Division of Pulmonary
The FDA Critical Path Initiative Clinical Considerations for Demonstration of Dose-response for Inhaled Corticosteroids - Exhaled Nitric Oxide Model Badrul A. Chowdhury, MD, PhD Director Division of Pulmonary
NIH Public Access Author Manuscript J Invest Dermatol. Author manuscript; available in PMC 2015 February 01.
 NIH Public Access Author Manuscript Published in final edited form as: J Invest Dermatol. 2014 August ; 134(8): 2071 2074. doi:10.1038/jid.2014.141. A possible role for IL-17A in establishing Th2 inflammation
NIH Public Access Author Manuscript Published in final edited form as: J Invest Dermatol. 2014 August ; 134(8): 2071 2074. doi:10.1038/jid.2014.141. A possible role for IL-17A in establishing Th2 inflammation
R espiratory syncytial virus (RSV) bronchiolitis is one of the
 922 ORIGINAL ARTICLE Bronchoalveolar lavage cellularity in infants with severe respiratory syncytial virus bronchiolitis P S McNamara, P Ritson, A Selby, C A Hart, R L Smyth... See end of article for authors
922 ORIGINAL ARTICLE Bronchoalveolar lavage cellularity in infants with severe respiratory syncytial virus bronchiolitis P S McNamara, P Ritson, A Selby, C A Hart, R L Smyth... See end of article for authors
Medicine Dr. Kawa Lecture 1 Asthma Obstructive & Restrictive Pulmonary Diseases Obstructive Pulmonary Disease Indicate obstruction to flow of air
 Medicine Dr. Kawa Lecture 1 Asthma Obstructive & Restrictive Pulmonary Diseases Obstructive Pulmonary Disease Indicate obstruction to flow of air through the airways. As asthma, COPD ( chronic bronchitis
Medicine Dr. Kawa Lecture 1 Asthma Obstructive & Restrictive Pulmonary Diseases Obstructive Pulmonary Disease Indicate obstruction to flow of air through the airways. As asthma, COPD ( chronic bronchitis
PIERIS PHARMACEUTICALS, INC. (Exact Name of Registrant as Specified in its Charter)
 UNITED STATES SECURITIES AND EXCHANGE COMMISSION Washington, D.C. 20549 FORM 8-K CURRENT REPORT Pursuant to Section 13 or 15(d) of the Securities Exchange Act of 1934 Date of Report (Date of earliest event
UNITED STATES SECURITIES AND EXCHANGE COMMISSION Washington, D.C. 20549 FORM 8-K CURRENT REPORT Pursuant to Section 13 or 15(d) of the Securities Exchange Act of 1934 Date of Report (Date of earliest event
Immune Responses and Disease Enhancement during Respiratory Syncytial Virus Infection
 CLINICAL MICROBIOLOGY REVIEWS, July 2005, p. 541 555 Vol. 18, No. 3 0893-8512/05/$08.00 0 doi:10.1128/cmr.18.3.541 555.2005 Copyright 2005, American Society for Microbiology. All Rights Reserved. Immune
CLINICAL MICROBIOLOGY REVIEWS, July 2005, p. 541 555 Vol. 18, No. 3 0893-8512/05/$08.00 0 doi:10.1128/cmr.18.3.541 555.2005 Copyright 2005, American Society for Microbiology. All Rights Reserved. Immune
Autoimmune Diseases. Betsy Kirchner CNP The Cleveland Clinic
 Autoimmune Diseases Betsy Kirchner CNP The Cleveland Clinic Disclosures (financial) No relevant disclosures Learning Objectives Explain the pathophysiology of autoimmune disease Discuss safe administration
Autoimmune Diseases Betsy Kirchner CNP The Cleveland Clinic Disclosures (financial) No relevant disclosures Learning Objectives Explain the pathophysiology of autoimmune disease Discuss safe administration
COPD and Asthma: Similarities and differences Prof. Peter Barnes
 and Asthma: Similarities and Differences and Asthma: 1 Imperial College Peter Barnes FRS, FMedSci, National Heart & Lung Institute Imperial College, London, UK p.j.barnes@imperial.ac.uk Royal Brompton
and Asthma: Similarities and Differences and Asthma: 1 Imperial College Peter Barnes FRS, FMedSci, National Heart & Lung Institute Imperial College, London, UK p.j.barnes@imperial.ac.uk Royal Brompton
