Arteriovenous malformations of the lateral ventricle. SHIRO WAGA, M.D., D.M.Sc., SHINICHI SHIMOSAKA, M.D., AND TADASHI KOJIMA, M.D., D.M.Sc.
|
|
|
- Alan Bond
- 5 years ago
- Views:
Transcription
1 J Neurosurg 63: , 1985 Arteriovenous malformations of the lateral ventricle SHIRO WAGA, M.D., D.M.Sc., SHINICHI SHIMOSAKA, M.D., AND TADASHI KOJIMA, M.D., D.M.Sc. Department of Neurosurgery, Mie University School of MAedicine and Hospital, Tsu, Mie, Japan o," Nine cases with arteriovenous malformations (AVM's) predominantly involving the lateral ventricle are presented. All the AVM's were small, but caused intraventricular hemorrhage in eight cases. Only two patients had an intracerebral hemorrhage large enough to warrant evacuation. Eight patients were under the age of 40 years at the onset of their disease. Computerized tomography demonstrated intraventricular hemorrhage in eight patients, and after intravenous administration of contrast medium a small area of enhancement with dilated subependymal draining veins was seen in seven. The lateral ventricles were of normal size in seven cases, and only two patients required a shunting procedure. Angiography demonstrated that the lesion was an AVM in eight patients, and did not visualize the lesion in the ninth. One patient suffered a recurrent inlraventricular hemorrhage when the AVM was demonstrated, although repeated angiography had failed to disclose a vascular lesion at his first intraventricular hemorrhage 14 months before. All nine lesions were resected by microsurgical techniques, and lhe results were excellent in eight patients. Of four caudate lesions, three were resected through a frontal transcortical approach and the other was operated on through an anterior transcallosal approach; the results were excellent in three of these patients. Only one (Case 4) was left with neurological deficits; he had confusion and disorientation following a right frontal transcortical approach. Even in the dominant hemisphere, lesions in the head of the caudate nucleus could be safely resected by an anterior transcallosal approach. Two choroidal lesions located in the temporal horn and trigone on the dominant side were resected through a middle temporal gyrus approach, and three thalamic lesions through a posterior transcallosal approach, all with excellent results. In all cases the brain opening required was about the width of the retractor (maximum 2.0 cm, average 1.5 cm). KEY WORDS " arteriovenous malformation 9 caudate nucleus 9 cerebral angiography 9 choroid plexus 9 intraventricular hemorrhage lateral ventricle A RTERIOVENOUS malformations (AVM's) located entirely or predominantly in the ventricular system are uncommon. Even in the large surgical experience of Drake 3 involving 166 patients with cerebral AVM's, only six (4%) lesions were predominantly intraventricular: three in the lateral ventricle, two in the third ventricle, and one in the fourth ventricle; another five AVM's (3%) involved the basal ganglia: four were located in the thalamus, and one was in the head of the caudate nucleus. From January, 1977, through June, 1984, 70 patients with intracranial vascular malformation underwent surgery at our institution. Nine lesions (13%) were entirely or predominantly located in the lateral ventricle, and form the subject of the present paper. We give particular attention to the clinical features and the operative approaches to these lesions. Case Reports Case 1 This I 1-year-old right-handed boy experienced the sudden onset of severe headache and vomiting followed by unconsciousness. He was admitted to another hospital where a spinal tap disclosed grossly bloody cerebrospinal fluid (CSF), and he was referred for further evaluation. Neurological examination 10 days postictus demonstrated a very mild right hemiparesis and a stiff neck. Computerized tomography (CT) demonstrated a high-density area in the head of the left caudate nucleus with slight ventricular dilatation (Fig. I left upper and lower). Angiography revealed a small AVM involving the head of the caudate nucleus, fed by the lenticulostriate arteries and drained chiefly via the anterior caudate vein (Fig. 1 upper right). J. Neurosurg. / Volume 63/August,
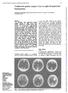
2 S. Waga, S. Shimosaka and T. Kojima FIG. 1. Case 1. Upper Left: Plain computerized tomography (CT) scans obtained 10 days after the ictus demonstrating hemorrhage in the head of the left caudate nucleus and slight ventricular dilatation. Lower Left: Contrast-enhanced CT scans disclosing the draining vein. Upper Right: Left carotid angiograms demonstrating an arteriovenous malformation (AVM) supplied by the lenticulostriate arteries and drained by an anterior caudate vein. Lower Right: Follow-up angiograms 1 year after the operation showing complete resection of the AVM. The AVM was located subependymally in the head of the caudate nucleus, and was approached through a left frontal transcortical incision. Using a bipolar coagulator, a plane of dissection was achieved with some difficulty, as most of the feeding arteries ascended from below through the head of the caudate nucleus. The AVM was resected, and immediately the patient suffered a slight expressive aphasia; the mild right hemiparesis was unchanged. Over the course of a month he regained the full strength in his fight arm and leg, and full recovery of speech. Postoperative angiography left some doubt about complete excision; however, followup angiography 1 year later demonstrated complete removal of the AVM (Fig. 1 lower right). Case 4 This 37-year-old right-handed man presented with sudden severe headache and vomiting. Neurological examination revealed marked neck stiffness, and CT scanning demonstrated a high-density area in the head of the caudate nucleus on the right as well as ventricular hemorrhage. On referral 2 weeks following the hemorrhage, there was no neurological abnormality. Computerized tomography scanning disclosed a small hemorrhage in the head of the caudate nucleus with moderate ventricular dilatation (Fig. 2 upper). Angiography revealed a small AVM in the head of the caudate nucleus (Fig. 2 lower). The AVM was subependymal in location and was totally resected through a fight frontal transcortical approach; complete removal of the AVM was con- firmed by angiography. Immediately after surgery, the patient was alert but apathetic. A week later he was uncooperative and markedly disoriented to place, time, and person. ACT scan disclosed only a small lowdensity area in the white matter and mild ventricular dilatation. Neither placement of a right ventriculoperitoneal shunt nor psychiatric consultation relieved his organic mental symptoms, although the lateral ventricle became smaller. At follow-up review 6 months, 1 year, and 2 years later, he remained markedly confused, disoriented, and disinterested. Case 5 This 35-year-old right-handed woman suddenly developed severe headache and a fight hemiparesis. Neurological examination 4 days following the ictus demonstrated slight papilledema, a slight fight hemiparesis with an extensor plantar response, and mild neck stiffness. A CT scan disclosed an intraventricular hemorrhage with a small high-density area in the head of the left caudate nucleus. Angiography demonstrated a small AVM in the head of the caudate nucleus, as seen in Cases 1 and 4. The AVM was located subependymally in the caudate nucleus, and was excised via an anterior transcallosal transventricular route. Postoperatively, the patient's neurological examination was normal except for the slight hemiparesis, which cleared completely in a month. Case 6 This 33-year-old right-handed man had the acute 186 J. Neurosurg. / Volume 63/August, 1985
3 Arteriovenous malformations of the lateral ventricle FIG. 2. Case 4. Upper Left Pair: Plain computerized tomography (CT) scans demonstrating a small hemorrhage in the head of the caudate nucleus on the right and moderate ventricular dilatation. Upper Right Pair: Contrast-enhanced CT scans disclosing an arteriovenous malformation (AVM) with its draining veins. Lower." Right carotid angiograms showing the AVM in the head of the caudate nucleus. onset of neck and shoulder pain followed by severe generalized headache. The following day the headache became more severe and he was evaluated at an outside hospital, where a spinal tap demonstrated grossly bloody CSF. Neurological examination at our institution 4 days following the ictus disclosed a right central facial paresis, a stiff neck, and moderate disorientation to place and time. ACT scan demonstrated intraventricular hemorrhage, and angiography disclosed an AVM in the temporal horn and trigone of the left lateral ventricle, supplied by the anterior and posterior choroidal arteries. Venous drainage was via an inferior ventricular wall vein (Fig. 3 left). The AVM was located in the choroid plexus, and was easily resected through a left temporal craniotomy and middle temporal gyrus approach. Following resection, the patient had a slight acalculia, finger agnosia, confusion of laterality, and a right homonymous hemianopsia, in addition to the preoperative findings. In the course of 2 weeks, the Gerstmann syndrome and the other signs had completely resolved, and the patient returned to his previous work. Angiography confirmed complete resection of the AVM (Fig. 3 right pair). Case 7 This 7-year-old right-handed boy presented with a sudden severe headache. He was evaluated at an outside hospital, where CT demonstrated intraventricular hemorrhage (Fig. 4 left) and angiography disclosed a small AVM in the dorsal aspect of the left thalamus, supplied by the posterior choroidal arteries and drained by the thalamostriate vein (Fig. 4 upper right). The AVM was located subependymally in the dorsal surface of the thalamus, but was not related to the choroid plexus. The lesion was resected through a left parieto-occipital craniotomy via the posterior transcauosal route. Some J. Neurosurg. / Volume 63/August,
4 S. Waga, S. Shimosaka and T. Kojima FIG. 3. Case 6. Left Trio: Preoperative left carotid angiograms demonstrating an arteriovenous malformation (AVM) fed by the anterior and posterior choroidal arteries and drained by the inferior ventricular vein. Right Pair: Postoperative angiograms demonstrating complete resection of the AVM. feeding vessels, running superficially from posteriorly, were easily coagulated. A plane of dissection was achieved with some difficulty, because some of the feeding arteries ascended through the thalamus. Following resection of the AVM, the patient was confused and apathetic for 4 days, and diffident and reticent for another 4 days. His condition then improved. Followup neurological and neuropsychological examinations were normal. Angiography demonstrated complete resection of the AVM (Fig. 4 lower right), and CT demonstrated a small low-density area in the dorsal aspect of the thalamus. Case 8 This 23-year-old right-handed woman had the sudden onset of double vision, numbness in the left upper limb, weakness of the left lower limb, and gradual drowsiness 4 days prior to admission. She was first evaluated at an outside hospital, complaining of severe headache and frequent vomiting. A CT scan demonstrated a hemorrhagic lesion in the right thalamus, extending downward to the midbrain; dilatation of the lateral ventricles was also revealed (Fig. 5 upper). A cavum vergae was also seen. On referral the patient was drowsy, with bilateral FIG. 4. Case 7. Left: Plain computerized tomography scans demonstrating intraventricular hemorrhage without ventricular dilatation. Upper Right: Vertebral angiograms disclosing an arteriovenous malformation (AVM) in the dorsal aspect of the left thalamus, supplied by the posterior choroidal arteries and drained by the thalamostriate vein. Lower Right: Postoperative angiograms showing complete resection of the AVM. 188 J. Neurosurg. / Volume 63/August, 1985
5 Arteriovenous malformations of the lateral ventricle low-density area remaining in the left subthalamus (Fig. 5 lower). FIG. 5. Case 8. Upper." Plain computerized tomography (CT) scans demonstrating a hemorrhagic lesion in the right thalamus, extending downward to the upper midbrain. Lower: Postoperative CT scans demonstating complete removal of the lesion and a small low-density area in the left subthalamus. choked discs, a right oculomotor nerve palsy, bilateral medial longitudinal fascicle lesions, loss of corneal and ciliar reflexes, loss of oculocephalic and oculovestibular responses on the right, and a dense left hemiparesis with an extensor plantar response. Immediately after a left ventriculoperitoneal shunt was placed, the patient regained consciousness, corneal and ciliar reflexes returned, oculocephalic and oculovestibular responses became normal, and the papilledema disappeared. Angiography using a slow-injection technique demonstrated no vascular malformation. Through a right parieto-occipital craniotomy and a posterior transcallosal approach, the cavum vergae was exposed. A blue mass in the right thalamus was seen through the septum between the cavum vergae and the right lateral ventricle. The septum and ventricle were opened, and the mass, consisting of clot and moderately vascularized capsule-like tissues, was completely removed from the right thalamus and upper midbrain. The postoperative course was smooth and uneventful except for transient right hemiballismus. Histological examination demonstrated aggregation of many thinwalled abnormal vessels surrounded by hemorrhage, and a cryptic AVM was diagnosed. The right oculomotor palsy and the medial longitudinal fascicle lesions cleared in 4 weeks. The dense left hemiparesis, however, has not shown any improvement so far. The ventriculoperitoneal shunt was removed and CT scanning demonstrated complete removal of the mass, with a small Summary of Cases Table 1 provides clinical details of the nine patients in this series. The age at onset ranged from 7 to 51 years, and only one patient was over the age of 40 years. The presenting symptom was intraventricular hemorrhage in eight, with a small intracerebral hemorrhage in two. Only two patients (Cases 3 and 8) had an intracerebral hemorrhage large enough to be evacuated. Contrast-enhanced CT scans demonstrated a small area of enhancement, with a dilated subependymal draining vein in seven cases. The ventricles were of normal size in eight patients. Eight lesions were demonstrated by angiography; in only one (Case 8) was the AVM not visualized angiographically. In one patient (Case 9) repeated angiography had failed to demonstrate an earlier intraventricular hemorrhage, and 14 months later, when the hemorrhage recurred, the AVM was discovered in the dorsal surface of the thalamus. The AVM's were less than 2 cm in diameter in all patients. Four were located in the head of the caudate nucleus (in the anterior horn), two in the choroid plexus (in the temporal horn and trigone), and three in the dorsal surface of the thalamus (in the trigone); five were on the left side and four on the right. The AVM's were resected at a single-stage operation with microsurgical techniques, and total removal of the lesion was verified by angiography and CT scanning. The results were excellent in eight and persistent neuropsychological deficits occurred in only one patient (Case 4). In all patients, the size of brain opening and leukotomy required was approximately the width of the blade of a retractor, maximum 2 cm, average 1.5 cm. Discussion Arteriovenous malformations (AVM's) involving the lateral ventricle and basal ganglia comprise from 4% to 10% of all cerebral AVM's. 3"8"18'3~ They occurred in 8% of the 50 children reported by Harwood-Nash and Fitz. 9 In a series of 56 cases presented by Gerosa, et al., 7 these deep lesions were even more common in children; nine (16%) in the basal ganglia, seven (13%) in the trigone, and three (5%) in the thalamus. The small cryptic AVM's, angiographically invisible but detectable on CT scanning, are also present in the thalamus and caudate nucleus? ~ Luessenhop and GennarellP 6 have formulated an anatomical grading scheme to correspond to the number of tertiary arteries directly supplying AVM's and the degree of surgical difficulty involved in total excision; Grade I lesions can be operated on without morbidity and mortality regardless of clinical state and location, and Grade IV AVM's are probably not operable. The great majority of AVM's supplied by the lenticulostriate arteries are described as Grade IV, and operable periventricular AVM's are those supplied by J. Neurosurg. / Volume 63/August,
6 TABLE 1 Clinical features of nine cases of lateral ventricle A VM* S. Waga, S. Shimosaka and T. Kojima Case Age (yrs), Location of Presentation Preop Status Operative Follow-Up No. Sex AVM Approach Postop Status Results 1 1 l, M It head of IVH mild rt hemiparesis It frontal slight expressive aphasia, completely caudate nucl transcortical mild hemiparesis recovered unchanged 2 51, F It choroid plexus IVH normal It middle temporal gyrus normal healthy 3 18, M rt head of IVH, ICH lethargic, It hemiparesis rt frontal mild It upper extremity completely caudate nucl transcortical weakness recovered 4 37, M rt head of caudate nucl 1VH, ICH normal rt frontal transcortical confusion, disorientation no change, unemployed 5 35, F It head of caudate nucl IVH, ICH mild rt hemiparesis anterior transcallosal no change completely recovered 6 33, M It choroid plexus IVH normal It middle temporal gyrus slight Gerstmann syndrome completely recovered 7 7, M It thalamus IVH normal posterior transcallosal normal healthy 8 23, F rt thalamus ICH lethargic, rt 3rd nerve posterior dense It hemiparesis no change palsy, bilat MLF transcallosal lesions, loss of brainstem reflexes, dense It hemiparesis 9 39, M rt thalamus recurrent IVH normal posterior transcauosal normal healthy * Abbreviations: AVM = arteriovenous malformation; nucl = nucleus; IVH = intraventricular hemorrhage; ICH = intracerebral hemorrhage; MLF = medial longitudinal fascicle. one or two of these arteries. On the other hand, AVM's of the choroid plexus can be considered as Grade III. For Grade II! lesions, location and clinical state are probably more important than anatomical grading. One of the studies on the natural history of cerebral AVM's 8 has shown that average yearly risk for first hemorrhage is between 2% and 3%, the risk of rebleeding is 6% in the 1 st year, and thereafter the average rebleeding rate is 2% per year for up to 20 years. Luessenhop and Rosa, 17 taking into consideration this study and equating another grading scheme to the maximum measured diameter of AVM's in the lateral angiograms, have concluded that for Grade I (up to 2 cm) and Grade II (2 to 4 cm) cerebral AVM's, the risk involved in nonsurgical therapy exceeds that of surgical treatment, so excision is indicated; however, for Grade III (4 to 6 cm) and more extensive AVM's, the surgical risk probably exceeds the natural risk in most circumstances for patients after the fourth to fifth decade of life. The risk of initial bleeding appears to be greater with small lesions, 8A4"19-21'28 as seen in our limited series. Small AVM's predominantly involving the lateral ventricle can be resected without deficits on the nondominant hemisphere and without or with minimal and acceptable deficits on the dominant side. There are three main locations of AVM's in the lateral ventricle; anterior horn (the head of the caudate nucleus), trigone and temporal horn (the choroid plexus), and trigone (the dorsal surface of the thalamus). Surgical approaches are available that leave no neuropsychological sequelae, or at least reduce the possibility of sequelae. The AVM's located in the head of the caudate nucleus in the nondominant hemisphere can be resected via a frontal transcorticall'5 or an anterior transcallosa124 route without neuropsychological sequelae. For those located in the dominant hemisphere, an anterior transcallosal approach is preferable since frontal cortical incisions in the dominant hemisphere are not without complications. Although a frontal transcortical approach may give excellent results without sequelae, z3"3~ it can result in neuropsychological deficits. 2'22 In the patient reported by Carton and Hickey 2 transient mental confusion, poor memory, tendency to perseverate, and emotional lability were observed immediately postoperatively, and there was minimal reduction in perforrnance on psychological testing at 15-month followup review. Ralston and Papatheodorou 22 described postoperative neurological findings including limitation of upward gaze and slight difficulty in naming objects. As mentioned above, frontal cortical incisions are not without their complications, even in the nondominant hemisphere, as shown in our Case 4. We believe that lesions in the head of the caudate nucleus should be resected through an anterior transcallosal approach as recommended by Shucart and Stein. 24 The AVM's in the temporal horn and trigone on the nondominant side can be approached and resected 190 J. Neurosurg. / Volume 63/August, 1985
7 Arteriovenous malformations of the lateral ventricle without a field defect by a short transverse incision in the superior or middle temporal gyrus carried down in the trigone. 3'26 On the dominant side the lesions may be approached transcortically 1~176 or transcallosally through the splenium or just in front of it, TM with or without significant sequelae. Thalamic AVM's presenting on the ventricular surface may be resected via a prefrontal, temporal, or transcallosal approach. 3'12 When the lesions are small or medium-sized and receive blood supply from both the anterior and posterior choroidal arteries on the nondominant side, they can be resected via a temporal route if the cortical incision is made somewhat wider. We believe that it is better to approach lesions on the dominant side via a posterior transcallosal route or, as an alternative, via both the temporal and callosal routes. 26 The temporal route provides a better way to occlude the feeding vessels from the anterior choroidal artery, while the posterior transcallosal route facilitates occlusion of the feeding vessels from the posterior choroidal arteries. A large temporal incision may give good access to both the anterior and posterior choroidal arteries; however, this is not desirable on the dominant side. Wharen, et al,29 operated on a right-handed girl with a large AVM involving the left thalamus and glomus of the choroid plexus; they approached the lesion via a left parieto-occipital craniotomy by a leukotomy in the medial portion of the left parietal lobe, entering the atrium of the lateral ventricle. Immediately following surgery, the patient had an expressive aphasia, right homonymous hemianopsia, and a flaccid right hemiparesis. Three months later she could walk independently, but the right arm was still very weak; her speech is conversational, with some deficits in auditory processing and writing. Left trigonal 1~ and thalamic 3~ AVM's have been exposed and resected by a high parietal approach across the trigone of the lateral ventricle, with good results. Two patients reported by Wilson, et al,3~ were temporarily worse but then improved: one returned to the preoperative level of impairment and the condition of the other was ameliorated. With parapeduncular AVM's or those located medial to the trigone of the lateral ventricle, Stein 26 has recommended that the approach be transcortical via the posterior middle temporal gyms, and if the removal is difficult via this route, that the resection be done in two stages. The first stage of this procedure approaches via the posterior infratemporal route and the second stage via an interhemispheric parafalx exposure to remove the residual portion of the AVM's. In the series reported by Juh~isz, 12 one AVM located in the corpus striatum, the genu of the internal capsule, anterior part of the thalamus, and in centrum semiovale on the dominant side was supplied by the anterior and posterior choroidal and lenticulostriate arteries. It was removed via two cortical incisions, a parietal one for the feeding vessels from the posterior choroidal arteries when a portion of the AVM was removed, and a frontal one where the residual AVM was removed with considerable bleeding. Three years after the operation the patient had a slight motor aphasia. Another AVM located in the nondominant temporal horn was removed at that time without any neurological deficits after resection of the right laterobasal portion of the temporal lobe. Various approaches have been proposed for meningiomas of the lateral ventricle involving the trigone on the dominant side. 4"13"25 Approaches through the inferior parietal lobule or the temporal lobe very often cause transient or permanent speech, motor, or sensory deficits, in addition to the damage to the optic radiation. An approach via the posterior portion of the corpus callosum has been described as safe by Kempe and Blaylock, 13 although a disconnection syndrome with alexia without agraphia has been reported. 15 A paramedian parieto-occipital approach may carry the risk of damage to the higher function of the parietal lobule. 6;11'13 We believe that a posterior transcallosal approach, although it sacrifices a functionally significant portion of the corpus callosum, gives a better and less traumatic route for removal of AVM's and meningiomas located in the trigone. The neuropsychological sequelae are minimal and acceptable when the incision in the corpus callosum or splenium is small. 3'6'11,13 When the AVM's are large and there is need to split considerable amount of the corpus callosum, we do not know whether a temporal, high parietal, or posterior transcallosal approach is better or more desirable. Large AVM's involving the lateral ventricle in the dominant hemisphere may be unsuitable for a direct operative procedure, and it may be better to treat them with intravascular techniques. In the presence of sizable intracerebral hematoma, we find that it is wise to evacuate the hematoma to reduce intracranial pressure and save the life of the patient first. The AVM can then be resected with a microsurgical technique after the patient's condition has stabilized. 23'27 References 1. Bartal (Behmoaram) AD, Tirosh MS, Weinstein M: Angiographic control during total excision of a cerebral arteriovenous malformation. Technical note. J Neurnsurg 29: , Carton CA, Hickey WC: Arteriovenous malformation of the head of the caudate nucleus. Report of a case with total removal. J Neurosurg 12: , Drake CG: Cerebral arteriovenous malformations: considerations for and experience with surgical treatment in 166 cases. Clin Neurosurg 26: , Fornari M, Savoiardo M, Morello G, et al: Meningiomas of the lateral ventricles. Neuroradiological and surgical considerations in 18 cases. J Neurosurg 54:64-74, Garcia de Sola R, Cabezudo J, Areitio E, et al: Combined approach (stereotactic-microsurgical) to a paraventricular arteriovenous malformation. Case report. Acta Neurochir Suppl 30: , 1980 J. Neurosurg. / Volume 63/August,
8 S. Waga, S. Shimosaka and T. Kojima 6. Geffen G, Walsh A, Simpson D, et al: Comparison of the effects of transcortical and transcallosal removal of intraventricular tumours. Brain 103: , Gerosa MA, Cappellotto P, Licata C, et al: Cerebral arteriovenous malformations in children (56 cases). Childs Brain 8: , Graf C J, Perret GE, Torner JC: Bleeding from cerebral arteriovenous malformations as a part of their natural history. J Neurosurg 58: , Harwood-Nash DC, Fitz CR: Neuroradinlogy in Infants and Children. St Louis: CV Mosby, 1976, Vol 3, pp Hodge CJ Jr, King RB: Arteriovenous malformation of choroid plexus. Case report. J Nenrosurg 42: , Jeeves MA, Simpson DA, Geffen G: Functional consequences of the transcallosal removal of intraventricular tumours. J Neurol Neurosurg Psychiatry 42: , Juhfisz J: Surgical treatment of arteriovenous angiomas localised in the corpus callosum, basal ganglia and near the brain stem. Acta Neurochir 40:83-101, Kempe LG, Blaylock R: Lateral-trigonal intraventricular tumors. A new operative approach. Acta Neurochir 35: , Krayenbtihl H, Siebenmann R: Small vascular malformations as a cause of primary intracerebral hemorrhage. J Neurosurg 22:7-20, Levin HS, Rose JE: Alexia without agraphia in a musician after transcallosal removal of a left intraventricular meningioma. Neurosurgery 4: , Luessenhop AJ, Gennarelli TA: Anatomical grading of supratentorial arteriovenous malformations for determining operability. Neurosurgery 1:30-35, Luessenhop A J, Rosa L: Cerebral arteriovenous malformations. Indications for and results of surgery, and the role of intravascular techniques. J Neurosnrg 60:14-22, Moody RA, Poppen JL: Arteriovenous malformations. J Nenrosurg 32: , Parkinson D, Bathers G: Arteriovenous malformations. Summary of 100 consecutive supratentorial cases. J Neurosurg 53: , Paterson JH, McKissock W: A clinical survey ofintracranial angiomas with special reference to their mode of progression and surgical treatment: a report of 110 cases. Brain 79: , Pia HW: The surgical treatment of intracerebral and intraventricular haematomas. Acta Nenrachir 27: , Ralston BL, Papatheodorou CA: Vascular malformation of the left thalamus. Report of a case of successful treatment, with a note on occlusion of the left internal cerebral vein. J Nenrosnrg 17: , Rutka JT, Tucker WS: Successful removal of an arteriovenous malformation in the basal ganglia. Nenrosnrgery 14: , Shucart WA, Stein BM: Transcallosal approach to the anterior ventricular system. Neurosurgery 3: , Spencer DD, Collins WF: Surgical management of lateral intraventricular tumors, in Schmidek HH, Sweet WH (eds): Operative Neurosurgical Techniques. Indications, Methods, and Results. New York: Grune & Stratton, 1982, Vol 1, pp Stein BM: Arteriovenous malformations of the medial cerebral hemisphere and the limbic system. J Neurosurg 60:23-31, Stein BM: Comment on Rutka JT, Tucker WS: Successful removal of an arteriovenous malformation in the basal ganglia. Neurosurgery 14:474, Waltimo O: The relationship of size, density and localization of intracranial arteriovenous malformations to the type of initial symptom. J Neurol Sci 19:13-19, Wharen RE Jr, Anderson RE, Sundt TM Jr: The Nd:YAG laser in neurosurgery. Part 2. Clinical studies: an adjunctive measure for hemostasis in resection of arteriovenous malformations. J Neurosurg 60: , Wilson CB, U HS, Domingue J: Microsurgical treatment of intracranial vascular malformations. J Neurosurg 51: , 1979 Manuscript received September 20, Address reprint requests to: Shiro Waga, M.D., Department of Neurosurgery, Mie University School of Medicine, Edobashi, Tsu, Mie, 514 Japan. 192 J. Neurosurg. / Volume 63~August, 1985
Stroke School for Internists Part 1
 Stroke School for Internists Part 1 November 4, 2017 Dr. Albert Jin Dr. Gurpreet Jaswal Disclosures I receive a stipend for my role as Medical Director of the Stroke Network of SEO I have no commercial
Stroke School for Internists Part 1 November 4, 2017 Dr. Albert Jin Dr. Gurpreet Jaswal Disclosures I receive a stipend for my role as Medical Director of the Stroke Network of SEO I have no commercial
Brain AVM with Accompanying Venous Aneurysm with Intracerebral and Intraventricular Hemorrhage
 Cronicon OPEN ACCESS EC PAEDIATRICS Case Report Brain AVM with Accompanying Venous Aneurysm with Intracerebral and Intraventricular Hemorrhage Dimitrios Panagopoulos* Neurosurgical Department, University
Cronicon OPEN ACCESS EC PAEDIATRICS Case Report Brain AVM with Accompanying Venous Aneurysm with Intracerebral and Intraventricular Hemorrhage Dimitrios Panagopoulos* Neurosurgical Department, University
Marc Norman, Ph.D. - Do Not Use without Permission 1. Cerebrovascular Accidents. Marc Norman, Ph.D. Department of Psychiatry
 Cerebrovascular Accidents Marc Norman, Ph.D. Department of Psychiatry Neuropsychiatry and Behavioral Medicine Neuropsychology Clinical Training Seminar 1 5 http://www.nlm.nih.gov/medlineplus/ency/images/ency/fullsize/18009.jpg
Cerebrovascular Accidents Marc Norman, Ph.D. Department of Psychiatry Neuropsychiatry and Behavioral Medicine Neuropsychology Clinical Training Seminar 1 5 http://www.nlm.nih.gov/medlineplus/ency/images/ency/fullsize/18009.jpg
OBJECTIVES. At the end of the lecture, students should be able to: List the cerebral arteries.
 DR JAMILA EL MEDANY OBJECTIVES At the end of the lecture, students should be able to: List the cerebral arteries. Describe the cerebral arterial supply regarding the origin, distribution and branches.
DR JAMILA EL MEDANY OBJECTIVES At the end of the lecture, students should be able to: List the cerebral arteries. Describe the cerebral arterial supply regarding the origin, distribution and branches.
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists. International authors and editors
 We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 3,800 116,000 120M Open access books available International authors and editors Downloads Our
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 3,800 116,000 120M Open access books available International authors and editors Downloads Our
Blood Supply of the CNS
 Blood Supply of the CNS Lecture Objectives Describe the four arteries supplying the CNS. Follow up each artery to its destination. Describe the circle of Willis and its branches. Discuss the principle
Blood Supply of the CNS Lecture Objectives Describe the four arteries supplying the CNS. Follow up each artery to its destination. Describe the circle of Willis and its branches. Discuss the principle
Arteriovenous malformations in the basal ganglia and thalamus: management and results in 101 cases
 J Neurosurg 88:285 292, 1998 Arteriovenous malformations in the basal ganglia and thalamus: management and results in 101 cases TOMIO SASAKI, M.D., PH.D., HIROKI KURITA, M.D., ISAMU SAITO, M.D., PH.D.,
J Neurosurg 88:285 292, 1998 Arteriovenous malformations in the basal ganglia and thalamus: management and results in 101 cases TOMIO SASAKI, M.D., PH.D., HIROKI KURITA, M.D., ISAMU SAITO, M.D., PH.D.,
External carotid blood supply to acoustic neurinomas
 External carotid blood supply to acoustic neurinomas Report of two cases HARVEY L. LEVINE, M.D., ERNEST J. FERmS, M.D., AND EDWARD L. SPATZ, M.D. Departments of Radiology, Neurology, and Neurosurgery,
External carotid blood supply to acoustic neurinomas Report of two cases HARVEY L. LEVINE, M.D., ERNEST J. FERmS, M.D., AND EDWARD L. SPATZ, M.D. Departments of Radiology, Neurology, and Neurosurgery,
The dura is sensitive to stretching, which produces the sensation of headache.
 Dural Nerve Supply Branches of the trigeminal, vagus, and first three cervical nerves and branches from the sympathetic system pass to the dura. Numerous sensory endings are in the dura. The dura is sensitive
Dural Nerve Supply Branches of the trigeminal, vagus, and first three cervical nerves and branches from the sympathetic system pass to the dura. Numerous sensory endings are in the dura. The dura is sensitive
Medical Neuroscience Tutorial Notes
 Medical Neuroscience Tutorial Notes Blood Supply to the Brain MAP TO NEUROSCIENCE CORE CONCEPTS 1 NCC1. The brain is the body's most complex organ. LEARNING OBJECTIVES After study of the assigned learning
Medical Neuroscience Tutorial Notes Blood Supply to the Brain MAP TO NEUROSCIENCE CORE CONCEPTS 1 NCC1. The brain is the body's most complex organ. LEARNING OBJECTIVES After study of the assigned learning
Introduction to the Central Nervous System: Internal Structure
 Introduction to the Central Nervous System: Internal Structure Objective To understand, in general terms, the internal organization of the brain and spinal cord. To understand the 3-dimensional organization
Introduction to the Central Nervous System: Internal Structure Objective To understand, in general terms, the internal organization of the brain and spinal cord. To understand the 3-dimensional organization
SURGICAL MANAGEMENT OF BRAIN TUMORS
 SURGICAL MANAGEMENT OF BRAIN TUMORS LIGIA TATARANU, MD, Ph D NEUROSURGICAL CLINIC, BAGDASAR ARSENI CLINICAL HOSPITAL BUCHAREST, ROMANIA SURGICAL INDICATIONS CONFIRMING HISTOLOGIC DIAGNOSIS REDUCING TUMOR
SURGICAL MANAGEMENT OF BRAIN TUMORS LIGIA TATARANU, MD, Ph D NEUROSURGICAL CLINIC, BAGDASAR ARSENI CLINICAL HOSPITAL BUCHAREST, ROMANIA SURGICAL INDICATIONS CONFIRMING HISTOLOGIC DIAGNOSIS REDUCING TUMOR
Brain Arteriovenous Malformations Endovascular Therapy and Associated Therapeutic Protocols Jorge Guedes Cabral de Campos
 Endovascular Therapy and Associated Therapeutic Protocols Jorge Guedes Cabral de Campos Neuroradiology Department Hospital de Santa Maria University of Lisbon CEREBRAL AVM CLINICAL / EPIDEMIOLOGY Brain
Endovascular Therapy and Associated Therapeutic Protocols Jorge Guedes Cabral de Campos Neuroradiology Department Hospital de Santa Maria University of Lisbon CEREBRAL AVM CLINICAL / EPIDEMIOLOGY Brain
What Is an Arteriovenous malformation (AVM)?
 American Society of Neuroradiology What Is an Arteriovenous malformation (AVM)? From the Cerebrovascular Imaging and Intervention Committee of the American Heart Association Cardiovascular Council Randall
American Society of Neuroradiology What Is an Arteriovenous malformation (AVM)? From the Cerebrovascular Imaging and Intervention Committee of the American Heart Association Cardiovascular Council Randall
Blood Supply. Allen Chung, class of 2013
 Blood Supply Allen Chung, class of 2013 Objectives Understand the importance of the cerebral circulation. Understand stroke and the types of vascular problems that cause it. Understand ischemic penumbra
Blood Supply Allen Chung, class of 2013 Objectives Understand the importance of the cerebral circulation. Understand stroke and the types of vascular problems that cause it. Understand ischemic penumbra
Telencephalon (Cerebral Hemisphere)
 Telencephalon (Cerebral Hemisphere) OUTLINE The Cortex - Lobes, Sulci & Gyri - Functional Subdivisions - Limbic Lobe & Limbic System The Subcortex - Basal Ganglia - White Matter (Internal Capsule) - Relations
Telencephalon (Cerebral Hemisphere) OUTLINE The Cortex - Lobes, Sulci & Gyri - Functional Subdivisions - Limbic Lobe & Limbic System The Subcortex - Basal Ganglia - White Matter (Internal Capsule) - Relations
Pathologies of postchiasmatic visual pathways and visual cortex
 Pathologies of postchiasmatic visual pathways and visual cortex Optic radiation: anatomy Pathologies of the postchiamsatic visual pathways and visual cortex Characterized by homonymous hemianopsia. This
Pathologies of postchiasmatic visual pathways and visual cortex Optic radiation: anatomy Pathologies of the postchiamsatic visual pathways and visual cortex Characterized by homonymous hemianopsia. This
Supratentorial cerebral arteriovenous malformations : a clinical analysis
 Original article: Supratentorial cerebral arteriovenous malformations : a clinical analysis Dr. Rajneesh Gour 1, Dr. S. N. Ghosh 2, Dr. Sumit Deb 3 1Dept.Of Surgery,Chirayu Medical College & Research Centre,
Original article: Supratentorial cerebral arteriovenous malformations : a clinical analysis Dr. Rajneesh Gour 1, Dr. S. N. Ghosh 2, Dr. Sumit Deb 3 1Dept.Of Surgery,Chirayu Medical College & Research Centre,
Principles Arteries & Veins of the CNS LO14
 Principles Arteries & Veins of the CNS LO14 14. Identify (on cadaver specimens, models and diagrams) and name the principal arteries and veins of the CNS: Why is it important to understand blood supply
Principles Arteries & Veins of the CNS LO14 14. Identify (on cadaver specimens, models and diagrams) and name the principal arteries and veins of the CNS: Why is it important to understand blood supply
Effect of clot removal on cerebral vasospasm TETSUJI INAGAWA, M.D., MITSUO YAMAMOTO, M.D., AND KAZUKO KAMIYA, M.D.
 J Neurosurg 72:224-230, 1990 Effect of clot removal on cerebral vasospasm TETSUJI INAGAWA, M.D., MITSUO YAMAMOTO, M.D., AND KAZUKO KAMIYA, M.D. Department of Neurosurgery, Shimane Prefectural Central Hospital,
J Neurosurg 72:224-230, 1990 Effect of clot removal on cerebral vasospasm TETSUJI INAGAWA, M.D., MITSUO YAMAMOTO, M.D., AND KAZUKO KAMIYA, M.D. Department of Neurosurgery, Shimane Prefectural Central Hospital,
Anatomy Lab (1) Theoretical Part. Page (2 A) Page (2B)
 Anatomy Lab (1) This sheet only includes the extra notes for the lab handout regarding the theoretical part, as for the practical part it includes everything the doctor mentioned. Theoretical Part Page
Anatomy Lab (1) This sheet only includes the extra notes for the lab handout regarding the theoretical part, as for the practical part it includes everything the doctor mentioned. Theoretical Part Page
Assessing the Stroke Patient. Arlene Boudreaux, MSN, RN, CCRN, CNRN
 Assessing the Stroke Patient Arlene Boudreaux, MSN, RN, CCRN, CNRN Cincinnati Pre-Hospital Stroke Scale May be done by EMS o One of many o F facial droop on one side o A arm drift (hold a pizza box, close
Assessing the Stroke Patient Arlene Boudreaux, MSN, RN, CCRN, CNRN Cincinnati Pre-Hospital Stroke Scale May be done by EMS o One of many o F facial droop on one side o A arm drift (hold a pizza box, close
Cerebro-vascular stroke
 Cerebro-vascular stroke CT Terminology Hypodense lesion = lesion of lower density than the normal brain tissue Hyperdense lesion = lesion of higher density than normal brain tissue Isodense lesion = lesion
Cerebro-vascular stroke CT Terminology Hypodense lesion = lesion of lower density than the normal brain tissue Hyperdense lesion = lesion of higher density than normal brain tissue Isodense lesion = lesion
[(PHY-3a) Initials of MD reviewing films] [(PHY-3b) Initials of 2 nd opinion MD]
![[(PHY-3a) Initials of MD reviewing films] [(PHY-3b) Initials of 2 nd opinion MD] [(PHY-3a) Initials of MD reviewing films] [(PHY-3b) Initials of 2 nd opinion MD]](/thumbs/89/98619893.jpg) 2015 PHYSICIAN SIGN-OFF (1) STUDY NO (PHY-1) CASE, PER PHYSICIAN REVIEW 1=yes 2=no [strictly meets case definition] (PHY-1a) CASE, IN PHYSICIAN S OPINION 1=yes 2=no (PHY-2) (PHY-3) [based on all available
2015 PHYSICIAN SIGN-OFF (1) STUDY NO (PHY-1) CASE, PER PHYSICIAN REVIEW 1=yes 2=no [strictly meets case definition] (PHY-1a) CASE, IN PHYSICIAN S OPINION 1=yes 2=no (PHY-2) (PHY-3) [based on all available
CLEAR III TRIAL : UPDATE ON SURGICAL MATTERS THAT MATTER
 CLEAR III TRIAL : UPDATE ON SURGICAL MATTERS THAT MATTER CLEAR Surgical Center Team July 2011 Trial Enrollment Status Updates Insert latest enrollment update chart from most recent CLEAR newsletter Imaging
CLEAR III TRIAL : UPDATE ON SURGICAL MATTERS THAT MATTER CLEAR Surgical Center Team July 2011 Trial Enrollment Status Updates Insert latest enrollment update chart from most recent CLEAR newsletter Imaging
Principles of Anatomy and Physiology
 Principles of Anatomy and Physiology 14 th Edition CHAPTER 14 The Brain and Cranial Nerves Introduction The purpose of the chapter is to: 1. Understand how the brain is organized, protected, and supplied
Principles of Anatomy and Physiology 14 th Edition CHAPTER 14 The Brain and Cranial Nerves Introduction The purpose of the chapter is to: 1. Understand how the brain is organized, protected, and supplied
TRANSVERSE SECTION PLANE Scalp 2. Cranium. 13. Superior sagittal sinus
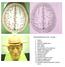 TRANSVERSE SECTION PLANE 1 1. Scalp 2. Cranium 3. Superior sagittal sinus 4. Dura mater 5. Falx cerebri 6. Frontal lobes of the cerebrum 7. Middle meningeal artery 8. Cortex, grey matter 9. Cerebral vessels
TRANSVERSE SECTION PLANE 1 1. Scalp 2. Cranium 3. Superior sagittal sinus 4. Dura mater 5. Falx cerebri 6. Frontal lobes of the cerebrum 7. Middle meningeal artery 8. Cortex, grey matter 9. Cerebral vessels
DIRECT SURGERY FOR INTRA-AXIAL
 Kitakanto Med. J. (S1) : 23 `28, 1998 23 DIRECT SURGERY FOR INTRA-AXIAL BRAINSTEM LESIONS Kazuhiko Kyoshima, Susumu Oikawa, Shigeaki Kobayashi Department of Neurosurgery, Shinshu University School of Medicine,
Kitakanto Med. J. (S1) : 23 `28, 1998 23 DIRECT SURGERY FOR INTRA-AXIAL BRAINSTEM LESIONS Kazuhiko Kyoshima, Susumu Oikawa, Shigeaki Kobayashi Department of Neurosurgery, Shinshu University School of Medicine,
GEORGE E. PERRET, M.D., AND CARL J. GRAF, M.D.
 J Neurosurg 47:590-595, 1977 Subgaleal shunt for temporary ventricle decompression and subdural drainage GEORGE E. PERRET, M.D., AND CARL J. GRAF, M.D. Division of Neurological Surgery, University of Iowa
J Neurosurg 47:590-595, 1977 Subgaleal shunt for temporary ventricle decompression and subdural drainage GEORGE E. PERRET, M.D., AND CARL J. GRAF, M.D. Division of Neurological Surgery, University of Iowa
PARIETAL LOBE. Vasilios A. Zerris MD, MPH, MSc, FAANS
 PARIETAL LOBE Vasilios A. Zerris MD, MPH, MSc, FAANS Diplomate of the American Board of Neurological Surgery Fellow of the American Association of Neurological Surgeons Professor of Neurosurgery, European
PARIETAL LOBE Vasilios A. Zerris MD, MPH, MSc, FAANS Diplomate of the American Board of Neurological Surgery Fellow of the American Association of Neurological Surgeons Professor of Neurosurgery, European
The outcome of treatment for arteriovenous malformations of the brain: A five-year retrospective series from the Philippines
 Neurology Asia 2006; 11 : 91 96 ORIGINAL ARTICLES The outcome of treatment for arteriovenous malformations of the brain: A five-year retrospective series from the Philippines Roland Mark M GIGATARAS MD,
Neurology Asia 2006; 11 : 91 96 ORIGINAL ARTICLES The outcome of treatment for arteriovenous malformations of the brain: A five-year retrospective series from the Philippines Roland Mark M GIGATARAS MD,
Fig.1: A, Sagittal 110x110 mm subimage close to the midline, passing through the cingulum. Note that the fibers of the corpus callosum run at a
 Fig.1 E Fig.1:, Sagittal 110x110 mm subimage close to the midline, passing through the cingulum. Note that the fibers of the corpus callosum run at a slight angle are through the plane (blue dots with
Fig.1 E Fig.1:, Sagittal 110x110 mm subimage close to the midline, passing through the cingulum. Note that the fibers of the corpus callosum run at a slight angle are through the plane (blue dots with
Cerebrovascular Disorders. Blood, Brain, and Energy. Blood Supply to the Brain 2/14/11
 Cerebrovascular Disorders Blood, Brain, and Energy 20% of body s oxygen usage No oxygen/glucose reserves Hypoxia - reduced oxygen Anoxia - Absence of oxygen supply Cell death can occur in as little as
Cerebrovascular Disorders Blood, Brain, and Energy 20% of body s oxygen usage No oxygen/glucose reserves Hypoxia - reduced oxygen Anoxia - Absence of oxygen supply Cell death can occur in as little as
Brain Meninges, Ventricles and CSF
 Brain Meninges, Ventricles and CSF Lecture Objectives Describe the arrangement of the meninges and their relationship to brain and spinal cord. Explain the occurrence of epidural, subdural and subarachnoid
Brain Meninges, Ventricles and CSF Lecture Objectives Describe the arrangement of the meninges and their relationship to brain and spinal cord. Explain the occurrence of epidural, subdural and subarachnoid
Announcement. Danny to schedule a time if you are interested.
 Announcement If you need more experiments to participate in, contact Danny Sanchez (dsanchez@ucsd.edu) make sure to tell him that you are from LIGN171, so he will let me know about your credit (1 point).
Announcement If you need more experiments to participate in, contact Danny Sanchez (dsanchez@ucsd.edu) make sure to tell him that you are from LIGN171, so he will let me know about your credit (1 point).
Ruptured Cerebral Aneurysm of the Anterior Circulation
 Original Articles * Division of Neurosurgery Department of Surgery Ruptured Cerebral Aneurysm of the Anterior Circulation Management and Microsurgical Treatment Ossama Al-Mefty, MD* ABSTRACT Based on the
Original Articles * Division of Neurosurgery Department of Surgery Ruptured Cerebral Aneurysm of the Anterior Circulation Management and Microsurgical Treatment Ossama Al-Mefty, MD* ABSTRACT Based on the
Inside Your Patient s Brain Michelle Peterson, APRN, CNP Centracare Stroke and Vascular Neurology
 Inside Your Patient s Brain Michelle Peterson, APRN, CNP Centracare Stroke and Vascular Neurology Activity Everyone stand up, raise your right hand, tell your neighbors your name 1 What part of the brain
Inside Your Patient s Brain Michelle Peterson, APRN, CNP Centracare Stroke and Vascular Neurology Activity Everyone stand up, raise your right hand, tell your neighbors your name 1 What part of the brain
Chapter 3. Structure and Function of the Nervous System. Copyright (c) Allyn and Bacon 2004
 Chapter 3 Structure and Function of the Nervous System 1 Basic Features of the Nervous System Neuraxis: An imaginary line drawn through the center of the length of the central nervous system, from the
Chapter 3 Structure and Function of the Nervous System 1 Basic Features of the Nervous System Neuraxis: An imaginary line drawn through the center of the length of the central nervous system, from the
Regional and Lobe Parcellation Rhesus Monkey Brain Atlas. Manual Tracing for Parcellation Template
 Regional and Lobe Parcellation Rhesus Monkey Brain Atlas Manual Tracing for Parcellation Template Overview of Tracing Guidelines A) Traces are performed in a systematic order they, allowing the more easily
Regional and Lobe Parcellation Rhesus Monkey Brain Atlas Manual Tracing for Parcellation Template Overview of Tracing Guidelines A) Traces are performed in a systematic order they, allowing the more easily
CEREBRUM Dr. Jamila Elmedany Dr. Essam Eldin Salama
 CEREBRUM Dr. Jamila Elmedany Dr. Essam Eldin Salama Objectives At the end of the lecture, the student should be able to: List the parts of the cerebral hemisphere (cortex, medulla, basal nuclei, lateral
CEREBRUM Dr. Jamila Elmedany Dr. Essam Eldin Salama Objectives At the end of the lecture, the student should be able to: List the parts of the cerebral hemisphere (cortex, medulla, basal nuclei, lateral
Slide 1. Slide 2. Slide 3. Tomography vs Topography. Computed Tomography (CT): A simplified Topographical review of the Brain. Learning Objective
 Slide 1 Computed Tomography (CT): A simplified Topographical review of the Brain Jon Wheiler, ACNP-BC Slide 2 Tomography vs Topography Tomography: A technique for displaying a representation of a cross
Slide 1 Computed Tomography (CT): A simplified Topographical review of the Brain Jon Wheiler, ACNP-BC Slide 2 Tomography vs Topography Tomography: A technique for displaying a representation of a cross
CEREBRUM & CEREBRAL CORTEX
 CEREBRUM & CEREBRAL CORTEX Seonghan Kim Dept. of Anatomy Inje University, College of Medicine THE BRAIN ANATOMICAL REGIONS A. Cerebrum B. Diencephalon Thalamus Hypothalamus C. Brain Stem Midbrain Pons
CEREBRUM & CEREBRAL CORTEX Seonghan Kim Dept. of Anatomy Inje University, College of Medicine THE BRAIN ANATOMICAL REGIONS A. Cerebrum B. Diencephalon Thalamus Hypothalamus C. Brain Stem Midbrain Pons
HEAD AND NECK IMAGING. James Chen (MS IV)
 HEAD AND NECK IMAGING James Chen (MS IV) Anatomy Course Johns Hopkins School of Medicine Sept. 27, 2011 OBJECTIVES Introduce cross sectional imaging of head and neck Computed tomography (CT) Review head
HEAD AND NECK IMAGING James Chen (MS IV) Anatomy Course Johns Hopkins School of Medicine Sept. 27, 2011 OBJECTIVES Introduce cross sectional imaging of head and neck Computed tomography (CT) Review head
Epilepsy after two different neurosurgical approaches
 Journal ofneurology, Neurosurgery, and Psychiatry, 1976, 39, 1052-1056 Epilepsy after two different neurosurgical approaches to the treatment of ruptured intracranial aneurysm R. J. CABRAL, T. T. KING,
Journal ofneurology, Neurosurgery, and Psychiatry, 1976, 39, 1052-1056 Epilepsy after two different neurosurgical approaches to the treatment of ruptured intracranial aneurysm R. J. CABRAL, T. T. KING,
Intraventricular neoplasms are uncommon, Intraventricular Tumor: An. Analysis of 18 Cases Dhaka, Bangladesh
 Original Article Nepal Journal of Neuroscience 13:23-29, 2016 Shamsul Alam, MS Intraventricular Tumor: An Analysis of 18 Cases Abu N W Uddin, MS Mashiur R Majumder, MS Comilla Medical College Comilla,
Original Article Nepal Journal of Neuroscience 13:23-29, 2016 Shamsul Alam, MS Intraventricular Tumor: An Analysis of 18 Cases Abu N W Uddin, MS Mashiur R Majumder, MS Comilla Medical College Comilla,
P. Hitchcock, Ph.D. Department of Cell and Developmental Biology Kellogg Eye Center. Wednesday, 16 March 2009, 1:00p.m. 2:00p.m.
 Normal CNS, Special Senses, Head and Neck TOPIC: CEREBRAL HEMISPHERES FACULTY: LECTURE: READING: P. Hitchcock, Ph.D. Department of Cell and Developmental Biology Kellogg Eye Center Wednesday, 16 March
Normal CNS, Special Senses, Head and Neck TOPIC: CEREBRAL HEMISPHERES FACULTY: LECTURE: READING: P. Hitchcock, Ph.D. Department of Cell and Developmental Biology Kellogg Eye Center Wednesday, 16 March
Stroke - Intracranial hemorrhage. Dr. Amitesh Aggarwal Associate Professor Department of Medicine
 Stroke - Intracranial hemorrhage Dr. Amitesh Aggarwal Associate Professor Department of Medicine Etiology and pathogenesis ICH accounts for ~10% of all strokes 30 day mortality - 35 45% Incidence rates
Stroke - Intracranial hemorrhage Dr. Amitesh Aggarwal Associate Professor Department of Medicine Etiology and pathogenesis ICH accounts for ~10% of all strokes 30 day mortality - 35 45% Incidence rates
Essentials of Clinical MR, 2 nd edition. 14. Ischemia and Infarction II
 14. Ischemia and Infarction II Lacunar infarcts are small deep parenchymal lesions involving the basal ganglia, internal capsule, thalamus, and brainstem. The vascular supply of these areas includes the
14. Ischemia and Infarction II Lacunar infarcts are small deep parenchymal lesions involving the basal ganglia, internal capsule, thalamus, and brainstem. The vascular supply of these areas includes the
Anatomy and Physiology (Bio 220) The Brain Chapter 14 and select portions of Chapter 16
 Anatomy and Physiology (Bio 220) The Brain Chapter 14 and select portions of Chapter 16 I. Introduction A. Appearance 1. physical 2. weight 3. relative weight B. Major parts of the brain 1. cerebrum 2.
Anatomy and Physiology (Bio 220) The Brain Chapter 14 and select portions of Chapter 16 I. Introduction A. Appearance 1. physical 2. weight 3. relative weight B. Major parts of the brain 1. cerebrum 2.
CEREBRAL ANEURYSMS PRESENTING WITH VISUAL FIELD DEFECTS*
 Brit. J. Ophthal. (1966) 50, 251 CEREBRAL ANEURYSMS PRESENTING WITH VISUAL FIELD DEFECTS* BY University Department of Ophthalmology and Royal Infirmary, Edinburgh ANEURYSMS occur more frequently within
Brit. J. Ophthal. (1966) 50, 251 CEREBRAL ANEURYSMS PRESENTING WITH VISUAL FIELD DEFECTS* BY University Department of Ophthalmology and Royal Infirmary, Edinburgh ANEURYSMS occur more frequently within
Clinical Symptoms in the Lateral Type of Hypertensive Intracerebral Hemorrhage
 676 Correlation Between the Location of Hematoma and its Clinical Symptoms in the Lateral Type of Hypertensive Intracerebral Hemorrhage Observations on Pantopaque Radiography of the Hematoma Cavity in
676 Correlation Between the Location of Hematoma and its Clinical Symptoms in the Lateral Type of Hypertensive Intracerebral Hemorrhage Observations on Pantopaque Radiography of the Hematoma Cavity in
If I Only Had a Brain
 If I Only Had a Brain A Heart. (The Nerve!) Regions of the Brain Cerebral hemisphere Diencephalon Cerebellum (b) Adult brain Brain stem Regions of the Brain: Cerebrum Precentral gyrus Frontal lobe Central
If I Only Had a Brain A Heart. (The Nerve!) Regions of the Brain Cerebral hemisphere Diencephalon Cerebellum (b) Adult brain Brain stem Regions of the Brain: Cerebrum Precentral gyrus Frontal lobe Central
Longitudinal anterior-to-posterior shift of collateral channels in patients with moyamoya disease: an implication for its hemorrhagic onset
 CLINICAL ARTICLE Longitudinal anterior-to-posterior shift of collateral channels in patients with moyamoya disease: an implication for its hemorrhagic onset Shusuke Yamamoto, MD, Satoshi Hori, MD, PhD,
CLINICAL ARTICLE Longitudinal anterior-to-posterior shift of collateral channels in patients with moyamoya disease: an implication for its hemorrhagic onset Shusuke Yamamoto, MD, Satoshi Hori, MD, PhD,
Spasm of the extracranial internal carotid artery resulting from blunt trauma demonstrated by angiography
 Spasm of the extracranial internal carotid artery resulting from blunt trauma demonstrated by angiography Case report ELISHA S. GURDJIAN, M.D., BLAISE AUDET, M.D., RENATO W. SIBAYAN, M.D., AND LLYWELLYN
Spasm of the extracranial internal carotid artery resulting from blunt trauma demonstrated by angiography Case report ELISHA S. GURDJIAN, M.D., BLAISE AUDET, M.D., RENATO W. SIBAYAN, M.D., AND LLYWELLYN
Cerebral Cortex Structure, Function, Dysfunction Reading Ch 10 Waxman Dental Neuroanatomy Lecture. Suzanne Stensaas, Ph.D.
 Cerebral Cortex Structure, Function, Dysfunction Reading Ch 10 Waxman Dental Neuroanatomy Lecture Suzanne Stensaas, Ph.D. March 7, 2012 Anatomy Review Lobes and layers Brodmann s areas Vascular Supply
Cerebral Cortex Structure, Function, Dysfunction Reading Ch 10 Waxman Dental Neuroanatomy Lecture Suzanne Stensaas, Ph.D. March 7, 2012 Anatomy Review Lobes and layers Brodmann s areas Vascular Supply
Transient obstructive hydrocephalus due to intraventricular hemorrhage: A case report and review of literature
 Digital Commons@Becker Open Access Publications 2013 Transient obstructive hydrocephalus due to intraventricular hemorrhage: A case report and review of literature Eriks A. Lusis Ananth K. Vellimana Wilson
Digital Commons@Becker Open Access Publications 2013 Transient obstructive hydrocephalus due to intraventricular hemorrhage: A case report and review of literature Eriks A. Lusis Ananth K. Vellimana Wilson
INTRACRANIAL ARACHNOID CYSTS: CLASSIFICATION AND MANAGEMENT. G. Tamburrini, Rome
 INTRACRANIAL ARACHNOID CYSTS: CLASSIFICATION AND MANAGEMENT G. Tamburrini, Rome Incidence 2% of occasional neuroradiological findings From clinical studies (1960 s): 0.4-1% of intracranial space occupying
INTRACRANIAL ARACHNOID CYSTS: CLASSIFICATION AND MANAGEMENT G. Tamburrini, Rome Incidence 2% of occasional neuroradiological findings From clinical studies (1960 s): 0.4-1% of intracranial space occupying
INTRACEREBRAL HEMORRHAGE FOLLOWING ENUCLEATION: A RESULT OF SURGERY OR ANESTHESIA?
 INTRACEREBRAL HEMORRHAGE FOLLOWING ENUCLEATION: A RESULT OF SURGERY OR ANESTHESIA? - A Case Report - DIDEM DAL *, AYDIN ERDEN *, FATMA SARICAOĞLU * AND ULKU AYPAR * Summary Choroidal melanoma is the most
INTRACEREBRAL HEMORRHAGE FOLLOWING ENUCLEATION: A RESULT OF SURGERY OR ANESTHESIA? - A Case Report - DIDEM DAL *, AYDIN ERDEN *, FATMA SARICAOĞLU * AND ULKU AYPAR * Summary Choroidal melanoma is the most
b. The groove between the two crests is called 2. The neural folds move toward each other & the fuse to create a
 Chapter 13: Brain and Cranial Nerves I. Development of the CNS A. The CNS begins as a flat plate called the B. The process proceeds as: 1. The lateral sides of the become elevated as waves called a. The
Chapter 13: Brain and Cranial Nerves I. Development of the CNS A. The CNS begins as a flat plate called the B. The process proceeds as: 1. The lateral sides of the become elevated as waves called a. The
MENTAL HOSPITAL PHONE MENU
 If you have low self-esteem, please hang up. Our operators are too busy to talk with you. MENTAL HOSPITAL PHONE MENU Hello and thank you for calling The State Mental Hospital. Please select from the following
If you have low self-esteem, please hang up. Our operators are too busy to talk with you. MENTAL HOSPITAL PHONE MENU Hello and thank you for calling The State Mental Hospital. Please select from the following
Stroke in the ED. Dr. William Whiteley. Scottish Senior Clinical Fellow University of Edinburgh Consultant Neurologist NHS Lothian
 Stroke in the ED Dr. William Whiteley Scottish Senior Clinical Fellow University of Edinburgh Consultant Neurologist NHS Lothian 2016 RCP Guideline for Stroke RCP guidelines for acute ischaemic stroke
Stroke in the ED Dr. William Whiteley Scottish Senior Clinical Fellow University of Edinburgh Consultant Neurologist NHS Lothian 2016 RCP Guideline for Stroke RCP guidelines for acute ischaemic stroke
CEREBRUM. Dr. Jamila EL Medany
 CEREBRUM Dr. Jamila EL Medany Objectives At the end of the lecture, the student should be able to: List the parts of the cerebral hemisphere (cortex, medulla, basal nuclei, lateral ventricle). Describe
CEREBRUM Dr. Jamila EL Medany Objectives At the end of the lecture, the student should be able to: List the parts of the cerebral hemisphere (cortex, medulla, basal nuclei, lateral ventricle). Describe
meninges Outermost layer of the meninge dura mater arachnoid mater pia mater membranes located between bone and soft tissue of the nervous system
 membranes located between bone and soft tissue of the nervous system meninges Outermost layer of the meninge dura mater middle layer of the meninges, contains no blood vessels arachnoid mater Innermost
membranes located between bone and soft tissue of the nervous system meninges Outermost layer of the meninge dura mater middle layer of the meninges, contains no blood vessels arachnoid mater Innermost
NEURORADIOLOGY DIL part 4
 NEURORADIOLOGY DIL part 4 Strokes and infarcts K. Agyem MD, G. Hall MD, D. Palathinkal MD, Alexandre Menard March/April 2015 OVERVIEW Introduction to Neuroimaging - DIL part 1 Basic Brain Anatomy - DIL
NEURORADIOLOGY DIL part 4 Strokes and infarcts K. Agyem MD, G. Hall MD, D. Palathinkal MD, Alexandre Menard March/April 2015 OVERVIEW Introduction to Neuroimaging - DIL part 1 Basic Brain Anatomy - DIL
Neurosonography: State of the art
 Neurosonography: State of the art Lisa H Lowe, MD, FAAP Professor and Academic Chair, University MO-Kansas City Pediatric Radiologist, Children s Mercy Hospitals and Clinics Learning objectives After this
Neurosonography: State of the art Lisa H Lowe, MD, FAAP Professor and Academic Chair, University MO-Kansas City Pediatric Radiologist, Children s Mercy Hospitals and Clinics Learning objectives After this
INSTITUTE OF NEUROSURGERY & DEPARTMENT OF PICU
 CEREBRAL BYPASS An Innovative Treatment for Arteritis INSTITUTE OF NEUROSURGERY & DEPARTMENT OF PICU CASE 1 q 1 year old girl -recurrent seizure, right side limb weakness, excessive cry and irritability.
CEREBRAL BYPASS An Innovative Treatment for Arteritis INSTITUTE OF NEUROSURGERY & DEPARTMENT OF PICU CASE 1 q 1 year old girl -recurrent seizure, right side limb weakness, excessive cry and irritability.
14 - Central Nervous System. The Brain Taft College Human Physiology
 14 - Central Nervous System The Brain Taft College Human Physiology Development of the Brain The brain begins as a simple tube, a neural tube. The tube or chamber (ventricle) is filled with cerebrospinal
14 - Central Nervous System The Brain Taft College Human Physiology Development of the Brain The brain begins as a simple tube, a neural tube. The tube or chamber (ventricle) is filled with cerebrospinal
Microsurgery for ruptured cerebellar arteriovenous malformations
 European Review for Medical and Pharmacological Sciences Microsurgery for ruptured cerebellar arteriovenous malformations S.-F. GONG 1,2, X.-B. WANG 1,3, Y.-Q. LIAO 1,2, T.-P. JIANG 1,2, J.-B. HE 1,2,
European Review for Medical and Pharmacological Sciences Microsurgery for ruptured cerebellar arteriovenous malformations S.-F. GONG 1,2, X.-B. WANG 1,3, Y.-Q. LIAO 1,2, T.-P. JIANG 1,2, J.-B. HE 1,2,
CVA. Alison Atwater PA-C
 CVA Alison Atwater PA-C Types of CVAs Ischemic strokes 80% of strokes 2/3 are thrombotic 1/3 are embolic emboli from the heart or arteries feeding the brain such as carotids, vertebral and basilar etc
CVA Alison Atwater PA-C Types of CVAs Ischemic strokes 80% of strokes 2/3 are thrombotic 1/3 are embolic emboli from the heart or arteries feeding the brain such as carotids, vertebral and basilar etc
Distal anterior cerebral artery (DACA) aneurysms are. Case Report
 248 Formos J Surg 2010;43:248-252 Distal Anterior Cerebral Artery Aneurysm: an Infrequent Cause of Transient Ischemic Attack Followed by Diffuse Subarachnoid Hemorrhage: Report of a Case Che-Chuan Wang
248 Formos J Surg 2010;43:248-252 Distal Anterior Cerebral Artery Aneurysm: an Infrequent Cause of Transient Ischemic Attack Followed by Diffuse Subarachnoid Hemorrhage: Report of a Case Che-Chuan Wang
Vascular Malformations of the Brain: A Review of Imaging Features and Risks
 Vascular Malformations of the Brain: A Review of Imaging Features and Risks Comprehensive Neuroradiology: Best Practices October 27-30, 2016 Sudhakar R. Satti, MD Associate Director Neurointerventional
Vascular Malformations of the Brain: A Review of Imaging Features and Risks Comprehensive Neuroradiology: Best Practices October 27-30, 2016 Sudhakar R. Satti, MD Associate Director Neurointerventional
THE VISUAL PATHWAY FOR DENTAL STUDENTS
 Neuroanatomy Suzanne S. Stensaas, Ph.D. February 16, 2012 Objectives: THE VISUAL PATHWAY FOR DENTAL STUDENTS A. Draw the expected visual fields seen in classic lesions of the nerve, chiasm, thalamus, optic
Neuroanatomy Suzanne S. Stensaas, Ph.D. February 16, 2012 Objectives: THE VISUAL PATHWAY FOR DENTAL STUDENTS A. Draw the expected visual fields seen in classic lesions of the nerve, chiasm, thalamus, optic
Unilateral spatial neglect due to right frontal lobe haematoma
 J7ournal ofneurology, Neurosurgery, and Psychiatry 1994;57:89-93 Unilateral spatial neglect due to right frontal lobe haematoma Shinichiro Maeshima, Kazuyoshi Funahashi, Mitsuhiro Ogura, Toru Itakura,
J7ournal ofneurology, Neurosurgery, and Psychiatry 1994;57:89-93 Unilateral spatial neglect due to right frontal lobe haematoma Shinichiro Maeshima, Kazuyoshi Funahashi, Mitsuhiro Ogura, Toru Itakura,
Cortical Organization. Functionally, cortex is classically divided into 3 general types: 1. Primary cortex:. - receptive field:.
 Cortical Organization Functionally, cortex is classically divided into 3 general types: 1. Primary cortex:. - receptive field:. 2. Secondary cortex: located immediately adjacent to primary cortical areas,
Cortical Organization Functionally, cortex is classically divided into 3 general types: 1. Primary cortex:. - receptive field:. 2. Secondary cortex: located immediately adjacent to primary cortical areas,
Neuroanatomy Dr. Maha ELBeltagy Assistant Professor of Anatomy Faculty of Medicine The University of Jordan 2018
 Neuroanatomy Dr. Maha ELBeltagy Assistant Professor of Anatomy Faculty of Medicine The University of Jordan 2018 Blood Supply of Brain and Spinal Cord Arterial Supply of Brain The brain receives blood
Neuroanatomy Dr. Maha ELBeltagy Assistant Professor of Anatomy Faculty of Medicine The University of Jordan 2018 Blood Supply of Brain and Spinal Cord Arterial Supply of Brain The brain receives blood
Anatomy & Physiology Central Nervous System Worksheet
 1. What are the two parts of the CNS? 2. What are the four functions of the CNS Anatomy & Physiology Central Nervous System Worksheet 3. What are the four functions of the meninges? (p430) 4. Starting
1. What are the two parts of the CNS? 2. What are the four functions of the CNS Anatomy & Physiology Central Nervous System Worksheet 3. What are the four functions of the meninges? (p430) 4. Starting
/ / / / / / Hospital Abstraction: Stroke/TIA. Participant ID: Hospital Code: Multi-Ethnic Study of Atherosclerosis
 Multi-Ethnic Study of Atherosclerosis Participant ID: Hospital Code: Hospital Abstraction: Stroke/TIA History and Hospital Record 1. Was the participant hospitalized as an immediate consequence of this
Multi-Ethnic Study of Atherosclerosis Participant ID: Hospital Code: Hospital Abstraction: Stroke/TIA History and Hospital Record 1. Was the participant hospitalized as an immediate consequence of this
CNS Imaging. Dr Amir Monir, MD. Lecturer of radiodiagnosis.
 CNS Imaging Dr Amir Monir, MD Lecturer of radiodiagnosis www.dramir.net Types of radiological examinations you know Plain X ray X ray with contrast GIT : barium (swallow, meal, follow through, enema) ERCP
CNS Imaging Dr Amir Monir, MD Lecturer of radiodiagnosis www.dramir.net Types of radiological examinations you know Plain X ray X ray with contrast GIT : barium (swallow, meal, follow through, enema) ERCP
NEURO IMAGING 2. Dr. Said Huwaijah Chairman of radiology Dep, Damascus Univercity
 NEURO IMAGING 2 Dr. Said Huwaijah Chairman of radiology Dep, Damascus Univercity I. EPIDURAL HEMATOMA (EDH) LOCATION Seventy to seventy-five percent occur in temporoparietal region. CAUSE Most likely caused
NEURO IMAGING 2 Dr. Said Huwaijah Chairman of radiology Dep, Damascus Univercity I. EPIDURAL HEMATOMA (EDH) LOCATION Seventy to seventy-five percent occur in temporoparietal region. CAUSE Most likely caused
Vascular Disorders. Nervous System Disorders (Part B-1) Module 8 -Chapter 14. Cerebrovascular disease S/S 1/9/2013
 Nervous System Disorders (Part B-1) Module 8 -Chapter 14 Overview ACUTE NEUROLOGIC DISORDERS Vascular Disorders Infections/Inflammation/Toxins Metabolic, Endocrinologic, Nutritional, Toxic Neoplastic Traumatic
Nervous System Disorders (Part B-1) Module 8 -Chapter 14 Overview ACUTE NEUROLOGIC DISORDERS Vascular Disorders Infections/Inflammation/Toxins Metabolic, Endocrinologic, Nutritional, Toxic Neoplastic Traumatic
ANALYSIS OF TREATMENT OUTCOMES WITH LINAC BASED STEREOTACTIC RADIOSURGERY IN INTRACRANIAL ARTERIOVENOUS MALFORMATIONS
 ANALYSIS OF TREATMENT OUTCOMES WITH LINAC BASED STEREOTACTIC RADIOSURGERY IN INTRACRANIAL ARTERIOVENOUS MALFORMATIONS Dr. Maitri P Gandhi 1, Dr. Chandni P Shah 2 1 Junior resident, Gujarat Cancer & Research
ANALYSIS OF TREATMENT OUTCOMES WITH LINAC BASED STEREOTACTIC RADIOSURGERY IN INTRACRANIAL ARTERIOVENOUS MALFORMATIONS Dr. Maitri P Gandhi 1, Dr. Chandni P Shah 2 1 Junior resident, Gujarat Cancer & Research
Student Lab #: Date. Lab: Gross Anatomy of Brain Sheep Brain Dissection Organ System: Nervous Subdivision: CNS (Central Nervous System)
 Lab: Gross Anatomy of Brain Sheep Brain Dissection Organ System: Nervous Subdivision: CNS (Central Nervous System) Student Lab #: Date 1 Objectives: 1. Learn the main components making up a motor neuron.
Lab: Gross Anatomy of Brain Sheep Brain Dissection Organ System: Nervous Subdivision: CNS (Central Nervous System) Student Lab #: Date 1 Objectives: 1. Learn the main components making up a motor neuron.
Meninges and Ventricles
 Meninges and Ventricles Irene Yu, class of 2019 LEARNING OBJECTIVES Describe the meningeal layers, the dural infolds, and the spaces they create. Name the contents of the subarachnoid space. Describe the
Meninges and Ventricles Irene Yu, class of 2019 LEARNING OBJECTIVES Describe the meningeal layers, the dural infolds, and the spaces they create. Name the contents of the subarachnoid space. Describe the
2/20/2019 BRAIN DISSECTION CODING AND DOCUMENTATION OBJECTIVES INTRODUCTION
 BRAIN DISSECTION CODING AND DOCUMENTATION Diana R. Phelps, CPC, CPC-I, CEMC OBJECTIVES Identify general structure of the human brain Describe how the different parts work Recognized the two hemispheres
BRAIN DISSECTION CODING AND DOCUMENTATION Diana R. Phelps, CPC, CPC-I, CEMC OBJECTIVES Identify general structure of the human brain Describe how the different parts work Recognized the two hemispheres
Classical CNS Disease Patterns
 Classical CNS Disease Patterns Inflammatory Traumatic In response to the trauma of having his head bashed in GM would have experienced some of these features. NOT TWO LITTLE PEENY WEENY I CM LACERATIONS.
Classical CNS Disease Patterns Inflammatory Traumatic In response to the trauma of having his head bashed in GM would have experienced some of these features. NOT TWO LITTLE PEENY WEENY I CM LACERATIONS.
Intracerebral haematoma complicating ruptured cerebral berry aneurysm
 J. Neurol. Neurosurg. Psychiat., 196, 5, 378 Intracerebral haematoma complicating ruptured cerebral berry aneurysm M. R. CROMPTON From the Neurosurgical Department of St. George's Hospital at Atkinson
J. Neurol. Neurosurg. Psychiat., 196, 5, 378 Intracerebral haematoma complicating ruptured cerebral berry aneurysm M. R. CROMPTON From the Neurosurgical Department of St. George's Hospital at Atkinson
Nicolas Bianchi M.D. May 15th, 2012
 Nicolas Bianchi M.D. May 15th, 2012 New concepts in TIA Differential Diagnosis Stroke Syndromes To learn the new definitions and concepts on TIA as a condition of high risk for stroke. To recognize the
Nicolas Bianchi M.D. May 15th, 2012 New concepts in TIA Differential Diagnosis Stroke Syndromes To learn the new definitions and concepts on TIA as a condition of high risk for stroke. To recognize the
Methods. Treatment options for intracranial arteriovenous malformations
 AJNR Am J Neuroradiol 25:1139 1143, August 2004 Complete Obliteration of Intracranial Arteriovenous Malformation with Endovascular Cyanoacrylate Embolization: Initial Success and Rate of Permanent Cure
AJNR Am J Neuroradiol 25:1139 1143, August 2004 Complete Obliteration of Intracranial Arteriovenous Malformation with Endovascular Cyanoacrylate Embolization: Initial Success and Rate of Permanent Cure
Moyamoya Syndrome with contra lateral DACA aneurysm: First Case report with review of literature
 Romanian Neurosurgery Volume XXXI Number 3 2017 July-September Article Moyamoya Syndrome with contra lateral DACA aneurysm: First Case report with review of literature Ashish Kumar Dwivedi, Pradeep Kumar,
Romanian Neurosurgery Volume XXXI Number 3 2017 July-September Article Moyamoya Syndrome with contra lateral DACA aneurysm: First Case report with review of literature Ashish Kumar Dwivedi, Pradeep Kumar,
N EOPLASMS of the optic nerves occur
 Tumors of the optic nerve and optic chiasm COLLINS. MAcCARTY~ M.D., ALLEN S. BOYD, JR., M.D., AND DONALD S. CHILDS, JR,, M.D. Departments of Neurologic Surgery and Therapeutic Radiology, Mayo Clinic and
Tumors of the optic nerve and optic chiasm COLLINS. MAcCARTY~ M.D., ALLEN S. BOYD, JR., M.D., AND DONALD S. CHILDS, JR,, M.D. Departments of Neurologic Surgery and Therapeutic Radiology, Mayo Clinic and
Biological Bases of Behavior. 3: Structure of the Nervous System
 Biological Bases of Behavior 3: Structure of the Nervous System Neuroanatomy Terms The neuraxis is an imaginary line drawn through the spinal cord up to the front of the brain Anatomical directions are
Biological Bases of Behavior 3: Structure of the Nervous System Neuroanatomy Terms The neuraxis is an imaginary line drawn through the spinal cord up to the front of the brain Anatomical directions are
Lab 2. we will look into several angled horizontal sections ( orbitomeatal plane ) i.e passing from the orbit into the ear
 we will look into several angled horizontal sections ( orbitomeatal plane ) i.e passing from the orbit into the ear Figure I page 76 : looking at the key on the left side this section passed through the
we will look into several angled horizontal sections ( orbitomeatal plane ) i.e passing from the orbit into the ear Figure I page 76 : looking at the key on the left side this section passed through the
Fistula between three main cerebral arteries and a large occipital vein
 J. Neurol. Neurosurg. Psychiat., 1969, 32, 308-312 Fistula between three main cerebral arteries and a large occipital vein J. BRET AND Z. KUNC From the Neurosurgical Clinic of the Charles University, Prague,
J. Neurol. Neurosurg. Psychiat., 1969, 32, 308-312 Fistula between three main cerebral arteries and a large occipital vein J. BRET AND Z. KUNC From the Neurosurgical Clinic of the Charles University, Prague,
Endovascular Treatment of Cerebral Arteriovenous Malformations. Bs. Nguyễn Ngọc Pi Doanh- Bs Đặng Ngọc Dũng Khoa Ngoại Thần Kinh
 Endovascular Treatment of Cerebral Arteriovenous Malformations Bs. Nguyễn Ngọc Pi Doanh- Bs Đặng Ngọc Dũng Khoa Ngoại Thần Kinh Stroke Vascular Malformations of the Brain Epidemiology: - Incidence: 0.1%,
Endovascular Treatment of Cerebral Arteriovenous Malformations Bs. Nguyễn Ngọc Pi Doanh- Bs Đặng Ngọc Dũng Khoa Ngoại Thần Kinh Stroke Vascular Malformations of the Brain Epidemiology: - Incidence: 0.1%,
ANASTAMOSIS FOR BRAIN STEM ISCHEMIA/Khodadad et al.
 ANASTAMOSIS FOR BRAIN STEM ISCHEMIA/Khodadad et al. visualization of the posterior inferior cerebellar artery. The patient, now 11 months post-operative, has shown further neurological improvement since
ANASTAMOSIS FOR BRAIN STEM ISCHEMIA/Khodadad et al. visualization of the posterior inferior cerebellar artery. The patient, now 11 months post-operative, has shown further neurological improvement since
TIA AND STROKE. Topics/Order of the day 1. Topics/Order of the day 2 01/08/2012
 Charles Ashton Medical Director TIA AND STROKE Topics/Order of the day 1 What Works? Clinical features of TIA inc the difference between Carotid and Vertebral territories When is a TIA not a TIA TIA management
Charles Ashton Medical Director TIA AND STROKE Topics/Order of the day 1 What Works? Clinical features of TIA inc the difference between Carotid and Vertebral territories When is a TIA not a TIA TIA management
T HIS paper is based upon experience
 DIAGNOSIS OF TUBERCULOMAS OF THE BRAIN CLINICAL AND RADIOLOGICAL CORRELATION* B. RAMAMURTHI, M.D., AND M. G. VARADARAJAN, M.D. Department of Neurosurgery, Madras Medical College, Madras, India (Received
DIAGNOSIS OF TUBERCULOMAS OF THE BRAIN CLINICAL AND RADIOLOGICAL CORRELATION* B. RAMAMURTHI, M.D., AND M. G. VARADARAJAN, M.D. Department of Neurosurgery, Madras Medical College, Madras, India (Received
Pulmonary Arteriovenous Malformations Complicated with Paradoxical Embolic Stroke
 Archives of Clinical and Medical Case Reports doi: 10.26502/acmcr.96550032 Volume 2, Issue 4 Case Report Pulmonary Arteriovenous Malformations Complicated with Paradoxical Embolic Stroke Cheah Wai Hun
Archives of Clinical and Medical Case Reports doi: 10.26502/acmcr.96550032 Volume 2, Issue 4 Case Report Pulmonary Arteriovenous Malformations Complicated with Paradoxical Embolic Stroke Cheah Wai Hun
Neurosurgical Management of Stroke
 Overview Hemorrhagic Stroke Ischemic Stroke Aneurysmal Subarachnoid hemorrhage Neurosurgical Management of Stroke Jesse Liu, MD Instructor, Neurological Surgery Initial management In hospital management
Overview Hemorrhagic Stroke Ischemic Stroke Aneurysmal Subarachnoid hemorrhage Neurosurgical Management of Stroke Jesse Liu, MD Instructor, Neurological Surgery Initial management In hospital management
