Anticoagulation policy after venous resection with a pancreatectomy: a systematic review
|
|
|
- Jonathan Oliver
- 5 years ago
- Views:
Transcription
1 DOI: /hpb HPB REVIEW ARTICLE Anticoagulation policy after venous resection with a pancreatectomy: a systematic review Manju D. Chandrasegaram 1,2, Guy D. Eslick 2, Wayne Lee 3, Mark E Brooke-Smith 1,4,5, Rob Padbury 1,5, Christopher S Worthley 4, John W Chen 1,4,5 & John A Windsor 6 1 HPB Department, Flinders Medical Centre, 3 School of Medicine, University of Adelaide, 4 HPB Unit, Royal Adelaide Hospital, 5 Flinders Clinical and Molecular Medicine, Flinders University, Adelaide, SA, 2 Department of Surgery, The University of Sydney, Sydney Medical School, Nepean, Penrith, NSW, Australia, and 6 HPB/Upper GI Unit, Auckland City Hospital, Auckland, New Zealand Abstract Background: Portal vein (PV) resection is used increasingly in pancreatic resections. There is no agreed policy regarding anticoagulation. Methods: A systematic review was performed to compare studies with an anticoagulation policy (AC+) to no anticoagulation policy (AC ) after venous resection. Results: There were eight AC+ studies (n = 266) and five AC studies (n = 95). The AC+ studies included aspirin, clopidogrel, heparin or warfarin. Only 50% of patients in the AC+ group received anticoagulation. There were more prosthetic grafts in the AC+ group (30 versus 2, Fisher's exact P < 0.001). The overall morbidity and mortality was similar in both groups. Early PV thrombosis (EPVT) was similar in the AC+ group and the AC group (7%, versus 3%, Fisher's exact P = 0.270) and was associated with a high mortality (8/20, 40%). When prosthetic grafts were excluded there was no difference in the incidence of EPVT between both groups (1% vs 2%, Fisher's exact test P = 0.621). Conclusion: There is significant heterogeneity in the use of anticoagulation after PV resection. Overall morbidity, mortality and EPVT in both groups were similar. EPVT has a high associated mortality. While we have been unable to demonstrate a benefit for anticoagulation, the incidence of EPVT is low in the absence of prosthetic grafts. Received 20 August 2013; accepted 30 October 2013 Correspondence Manju D. Chandrasegaram, Hepatobiliary Unit, Flinders Medical Centre, Flinders Drive, Bedfork Park, SA 5042, Australia. Tel: Fax: manjudashini@yahoo.com Introduction This paper was presented at the Annual Scientific Congress of the Royal Australasian College of Surgeons (RACS), in May 2013, in Auckland, New Zealand and the RACS Tri-state Western Australia, South Australia and Northern Territory Annual Scientific Meeting Portal vein involvement in pancreatic cancer historically represented unresectable disease. 1,2 Numerous contemporary reports have highlighted acceptable morbidity, mortality and respectable survival outcomes from venous resection provided an R0 resection is performed. 3 8 Pancreatic adenocarcinoma with portal vein involvement is no longer a contraindication to resection. 9 The clincher of unresectable disease now lies in superior mesenteric arterial (SMA) invasion and resectability has now shifted to clearance of the medial or SMA margin to facilitate an R0 resection when combined with a venous resection. 10 There are several techniques of performing mesentericoportal vein resection and reconstruction. These include tangential or lateral wedge venous resections with a non-occlusive side biting vascular clamp, and where a more extensive length of vein is resected this may be reconstructed primarily with an end-to-end anastomosis or with a venous or prosthetic graft. In the latter, portal vein clamping is required for the duration of the anastomosis, which may lead to bowel oedema that may complicate the subsequent pancreatico-enteric anastomosis. To prevent this some centres perform superior mesenteric arterial occlusion, and several Japanese centres have described the use of antithrombogenic bypass catheters to prevent portal congestion or hepatic ischaemia. 11 In view of the vast differences in technique,
2 692 HPB we can expect significant heterogeneity in the population of patients undergoing venous resection in the literature. To add to this, several major Eastern centres perform arterial resections in addition to venous resection, which make comparisons between Eastern and Western patients difficult. 12 Portal vein resection and clamping would intuitively be associated with an increased risk of portal vein thrombosis compared with patients not undergoing venous resection. The risk of venous thrombosis after a PV/SMV resection is estimated to be as high as 21 26% in some series There appears to be no published guidelines regarding anticoagulation after a venous resection with a pancreatic resection and no current systematic review addressing this question. The aim of this study was to review the different published anticoagulation policies and outcomes of patients with and without anticoagulation after a venous resection with a pancreatic resection, with special reference to early portal vein thrombosis. Methods Study protocol This systematic review followed the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) guidelines 16 (Fig. 1). Three databases (MEDLINE from 1946, PubMed from 1946, and EMBASE from 1949) were searched to June The search terms included pancreatectomy OR pancreaticoduodenectomy, portal vein OR mesenteric vein, and resection OR reconstruction. A search for unpublished literature was not performed. Study selection The studies that were included described patients that underwent a pancreatic resection (pancreaticoduodenectomy, distal pancreatectomy and total pancreatectomy) and a venous resection (portal and/or superior mesenteric vein). Studies were only included if they described a policy with respect to anticoagulation, of either administering this or not administering this. This resulted in two groups of publications, those with a policy of administering anticoagulation (AC+) and those with a policy of not administering anticoagulation (AC ). Studies that described an extended pancreatic resection, including an arterial resection involving the celiac axis or SMA in combination with venous resection were excluded. Studies that included an arterial resection alone without a portal vein resection were excluded from this review. Data extraction Data extraction was done using a standardized data extraction form. Information collected included the year of publication, country of origin, number of pancreatic resections, number of cases of venous resection, overall morbidity, mortality, incidence of bleeding, re-operations and portal vein thrombosis. Anticoagulation Anticoagulation (AC) was defined as the use of heparin, warfarin and included antiplatelet use such as aspirin and clopidogrel in the immediate post-operative period, irrespective of the duration. Although the purpose of this study was to assess anticoagulation beyond standard thromboprophylaxis, some patients in the anticoagulation group received only routine thromboprophylaxis. The dosing and duration of these anticoagulation is further elaborated in Table 1. Intra-operative techniques We have reported the practice of intra-operative heparinization in each of the studies and the practice of superior mesenteric artery occlusion at the time of venous anastomosis to prevent congestion and intestinal oedema in Tables 1 and 2. Venous resection and reconstruction Venous resection included tangential and segmental resections Tangential venous resections are lateral wedge resections of the portal vein (PV) or SMV or the SMV-PV confluence. Segmental venous resections involved resection of a cyclindrical portion of the portal vein, superior mesenteric vein or mesentericoportal confluence. Reconstruction after a tangential or segmental venous resection was with a primary repair or with the use of a graft (venous or prosthetic). 17 We have defined the type of venous resection used in these studies in Tables 1 and 2. Portal vein thrombosis The diagnosis of portal vein thrombosis was within 30 days, and is termed early portal vein thrombosis (EPVT). The basis for the diagnosis of EPVT varied between studies, but invariably used a combination of clinical, biochemical and imaging studies including Doppler ultrasound. Statistical analysis The data have been compared as descriptive statistics, with patient demographic and clinical characteristics reported as percentages for discrete characteristics. All P-values calculated were two-tailed; the alpha level of significance was set at Analysis was done on an intention-to-treat basis. Fisher s exact test was used for statistical analysis of categorical variables. Results Thirteen studies were included in this review. Eight studies (n = 266 patients) described a policy for anticoagulation after venous resection (AC+ group, Table 1). 14,15,18 23 There were five studies (n = 95 patients) that described a policy of no post-operative anticoagulation (AC group, Table 2) Pancreatic resection There was no significant difference between the two groups for the types of pancreatic resection. The AC+ group had similar proportions of pancreatoduodenectomies (242/266, 91% versus 86/95, 91%) and total pancreatectomies (14/266, 5% versus 9/95, 9%
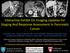
3 HPB 693 Identification Records identified through database searching (n = 1586) Additional records identified through other sources (n = 0) Records after duplicates removed (n = 897) Screening Records screened (n = 897) Records excluded (n = 859) Eligibility Included Full-text articles assessed for eligibility (n = 36) Studies included in qualitative synthesis (n = 13) Studies included in quantitative synthesis (n = 13) Full-text articles excluded (n = 23) Debate article n = 1 Technique paper n = 1 Extended pancreatectomy with celiac or SMA resection n = 3 Hepatic artery resection without PVR included in study n = 1 Review article n = 5 Survival study n = 2 No post-operative anticoagulation policy mentioned n = 7 Timing of post-op anticoagulation unclear n = 1 Correspondence n = 1 Not relevant n = 1 Figure 1 Flow chart showing the search strategy used to identify studies Fisher s exact P = 0.223). The only distal pancreatectomies were in the AC+ group (10/266, 4%) (Table 3). Venous resection and reconstruction There was a higher proportion of tangential resections in the AC+ group (147/266, 55%) compared with the AC group (7/95, 7% Fisher s exact P < 0.001). There was a correspondingly lower proportionof segmentalresectionsintheac+ group (119/266, 45%) compared with the AC group (88/95, 93% Fisher s exact P < 0.001) (Table 3). In regards to reconstruction there was a similar proportion of tangential resections with primary venous closure without use of a patch graft in the AC+ group (134/147, 91%) compared with the AC group (6/7, Fisher s exact P = 0.494). There were fewer segmental resections with primary end-to-end venous anastomosis without graft use in the AC+ group (71/119, 60%) compared with the AC group (66/88, 75% Fisher s exact P = 0.026). There was no difference between the two groups with respect to the proportion of patients who had some form of graft (venous or prosthetic) (AC+ group 61/265, 23% compared with the AC group 23/95, 24% Fisher s exact P = 0.888). There were
4 694 HPB Table 1 Anticoagulation group (AC+ group, n = 8) First author Country Year Carrère N France n PVR Tangential PVR with primary repair Segmental PVR with primary repair Prosthetic grafts Vein patch or interposition Intra-operative heparinization Clamp time (min) NR Mean 19 ± 3 (range 7 58) SMA inflow occlusion Not used AC+ policy 1st 15 patients therapeutic systematic heparin, all others received subcutaneous prophylactic LMWH Smoot RL Not used Mean 14 Yes Aspirin n = 19, US Warfarin n = 11, Clopidogrel n = 4 Riedinger H Germany Smoot RL US Illuminati G Italy Ouaïssi M France Stauffer JA US Kendrick ML US NR NR NR Systemic therapeutic heparin aiming APTT for segmental resection (n = 17/53), all others received prophylactic low dose heparin Not used NR Yes One patient received clopidogrel, and the remainder daily aspirin if no clot on post-operative imaging. If clot noted on imaging systemic heparin used Systemic heparin 0.5 mg/kg 9 Not used LMWH for one month followed by aspirin 100 mg/daily NR <20 Not used Systemic therapeutic heparin 500 U/ kg/day for 10 days followed by warfarin for 3 months in n = 8/27; PTFE n = 2, t angential SMV/PV resection n = 6. All others, n = 19/27 received preventative LMWH Not used 18 NR Autologous PVR had standard perioperative thromboprophylaxis, PTFE grafts n = 10/28, had thromboprophylaxis plus low dose warfarin 1 2 mg for 3 months Systemic heparin intraoperative units 35 Not used Low dose aspirin 81 mg for 3 months. If cancer or previous thrombosis, warfarin given. AC+ EPVT Total (50%) 18 (7%) 22 (8%) PVR, portal vein resection; AR, arterial resection;; SMA, superior mesenteric artery; LMWH, low-molecular-weight heparin; NR, not reported. Bleeding
5 HPB 695 Table 2 No anticoagulation group (AC group, n = 5) First author Country Year Allema JH Netherlands Howard TJ US Zhang J China Kaneoka Y Japan Chakravarty DK Taiwan n PVR Tangential PVR with primary repair Segmental PVR with primary repair Prosthetic grafts Vein patch or interposition Intra-operative heparinization Clamp time (min) SMA inflow occlusion NR NR NR Systemic heparinization (100U/kg), for complete isolation not side bite clamp NR Not used NR Not used Within 15 min Not used Not used NR Yes Yes NR NR NR Total PVR, portal vein resection; AR, arterial resection; NR, not reported. EPVT Table 3 Type of pancreatic and venous resections in the AC+ and AC group AC+ (n = 266) AC (n = 95) P value Types of pancreatic resection Pancreaticoduodenectomy 242 (91%) 86 (91%) P = Total pancreatectomy 14 (5%) 9 (9%) Distal pancreatectomy 10 (4%) Type of venous resection Tangential 147 (55%) 7 (7%) P < Segmental 119 (45%) 88 (93%) Reconstruction by primary repair or anastomosis (no grafts used) Tangential 134/147 (91%) 6/7 P = Segmental 71/119 (60%) 66/88 (75%) P = Reconstruction by grafting Overall (venous and prosthetic) 61/266 (23%) 23/95 (24%) P = Venous grafts 31/61 21/23 P < Prosthetic grafts 30/61 2/23 P < correspondingly more prosthetic graft reconstructions in the AC+ group (30/61) compared with the AC group (2/23, Fisher s exact P < 0.001) (Table 3). Anticoagulation policies There was wide variation in the published anticoagulation policies. Table 1 outlines these policies that included the use of aspirin, clopidogrel, heparin and warfarin. In spite of the policy, only 50% of patients in the AC+ group actually received anticoagulation beyond described standard thromboprophylaxis. The anticoagulation policy was evaluated in relation to the type of venous resection and reconstruction in the AC+ group. Aspirin was used as an anticoagulant in four centres but only in a minority of patients (67/266, 26%) (Table 1), but this did not appear to be related to the type of venous resection or reconstruction. 19,21 23 There appeared to be a relationship between the type of graft used for reconstruction and whether anticoagulation was advocated. The AC+ group used a significantly higher proportion of prosthetic grafts (30/61) compared with the AC group (2/23, Fisher s exact P < 0.001) (Table 3). Clinical and surgical outcomes The overall mortality was similar in the AC+ group (12/266, 5%) compared with the AC group (6/95, 6% Fisher exact P = 0.583). TheoverallmorbiditywasalsosimilarintheAC+ group (125/266, 47%) compared with the AC group (38/95, 40% Fisher s exact
6 696 HPB Table 4 Overall morbidity, reoperations, bleeding and mortality in the AC+ and AC group AC+ (n = 266) AC (n = 95) P-value Mortality 12/266 (5%) 6/95 (6%) P = Overall morbidity 125/266 (47%) 38/95 (40%) P = Reoperations 23/225 (10%) *n = 6 studies reported outcome 6/75 (8%) *n = 3 studies reported outcome P = Bleeding 22/266 (8%) *n = 8 studies reported outcome 7/32 *n = 2 studies reported outcome P = P = 0.280). When studies using prosthetic grafts were excluded in subgroup analysis, no significant difference was found for mortality (AC+ 5/147, 3% versus AC 6/83, 7% Fisher s exact P = 0.211) or morbidity (AC+ 63/147, 43% versus AC 32/83, 39% Fisher s exact P = 0.578). The incidence of reoperations and bleeding was not reported by all the studies and were analysed in studies that reported these outcomes. The incidence of re-operations was similar in the reported studies in the AC+ group (n = 6, 23/225, 10%) compared with the AC group (n = 3, 6/75, 8% Fisher s exact test P = 0.658) The incidence of bleeding in the reported studies was lower in the AC+ group (n = 8, 22/266, 8%) compared with the AC group (n = 2, 7/32, Fisher s exact test P = 0.025) (Table 4). Early portal venous thrombosis There was a higher incidence of EPVT reported in the AC+ group (n = 9, 18/266, 7%) compared with the AC group (n = 3, 2/70, 3% Fisher s exact P = 0.270). The overall mortality associated with EPVT was 40% (8/20). The mortality associated with EPVT was similar in the AC+ group (7/18) compared with the AC group (1/2, Fisher s exact P = 1.000). The incidence of EPVT was also examined in relation to the type of resection and reconstruction. The type of vascular reconstruction was described for 19 of the 20 EPVT. In the AC + group there were comparable rates of EPVT in those who had a tangential resection (8/147, 5%) compared with a segmental resection (10/119, 8%, Fisher s exact test P = 0.462). There were also similar EPVT from a primary closure (13/205, 6%) compared with grafting (5/61, 8% Fisher s exact P = 0.571). There were more EPVT in prosthetic grafts (4/30) compared with vein grafts (1/31, Fisher s exact P = 0.195). When studies that used prosthetic grafts were excluded from analysis, there was no difference in the incidence of EPVT in the AC+ group (2/147) compared with the AC group (2/83, Fisher s exact test P = 0.621). 10,11,15,24 Discussion There is no agreed approach to anti-coagulation after a venous resection with a pancreatic resection in the published literature. This reflects the absence of high-level evidence and evidencebased guidelines. This review found that in centres with an anticoagulation policy only half of the patients received it, which made it difficult to derive firm conclusions about outcomes when comparing outcomes with centres that had no such policy. This difficulty was further compounded by differences in anticoagulation policy and also variations in the types of venous resection and reconstruction. There were higher proportions of patients having tangential (c.f. segmental) venous resections and prosthetic (c.f. venous) grafts in the group that had an anticoagulation policy. It was found that there was no difference between both anticoagulation groups, as implemented, in terms of overall morbidity and mortality. Early portal vein thrombosis was more common in the group with an anticoagulation policy (7% versus 3%), in those have prosthetic graft reconstruction (13% versus 3%) and this was associated with 40% mortality. Portal vein reconstruction is performed mostly in the setting of liver transplantation where anticoagulation is not routinely given, and EPVT is seen far less frequently than hepatic artery thrombosis (2% versus 9%). The incidence of vascular thrombosis in this group has been shown to be related to high fibrinogen levels, and low protein C levels suggesting future anticoagulation trials may be warranted in this high-risk group. 29 Anticoagulation has been shown to be safe and in paediatric liver transplantation has been shown to reduce early thrombotic events. 30,31 In contrast to pancreatic surgery, there is tendency to antoanticoagulation in liver transplantation particularly after liver reperfusion. 32 In contrast, there is tendency to procoagulation in patients with pancreatic cancer undergoing a pancreatectomy and venous resection. 33 Early portal vein thrombosis occurred more frequently in the AC+ group, and interestingly, there were a higher proportion of tangential resections and fewer segmental resections compared with the AC group. Tangential resections can be associated with a degree of luminal narrowing that can be avoided with a transverse repair or a patch graft, and historically this was advocated when the degree of luminal narrowing was more than one-third of the venous circumference. In this review, EPVT was not more likely with tangential or segmental resections in AC+ group. However, EPVT did occur more frequently with prosthetic grafts in our study (4/30, 13%) and this incidence is similar to a study by Chu et al. (3/33, 9%) in which PTFE grafts were used. Echoing the high mortality of 40% with EPVT in this review, the study by Chu et al. reported a mortality of 33%. 34 When prosthetic grafts were excluded, there was no difference in EPVT between the AC+ group and the AC group.
7 HPB 697 The need for interposition grafts is debated as several centres report successful direct end-to-end venous anastomosis even when the length of the resected vein is up to 5 cm. Several previous studies have shown that an adequate length of SMV/PV can be achieved with adequate mobilization of the root of mesentery and dividing the ligaments of the liver as well to enable a primary end-to-end anastomosis and obviating the need for an interposition graft. 35 Early portal vein thrombosis can also be caused by technical factors. In the Carrere study, two cases of EPVT were thought to be the result of technical factors. In one the venous anastomosis was twisted, and flow was successfully re-established by re-operation, and in the other the narrow diameter anastomosis led to mesenteric infarction. Stauffer et al. hypothesised that their four cases of EPVT after a segmental resection may have been due to the lack of expansion of the anastomosis or increased anastomotic tension upon return of the bowel and closure of the abdomen. Surgical technique during venous anastomosis requires provision of a growth factor to enable adequate venous expansion upon re-establishing blood flow. Before anticoagulation is dismissed on the basis that this review has been unable to demonstrate a benefit for it, there are several factors that need to be considered. First, only 50% of patients in the AC+ group received anticoagulation beyond standard peri-operative thromboprophylaxis. Second, the use of standard thromboprophylaxis in these studies was not controlled for and the effect due to this could not be accounted for in this review. Thirdly, there was a higher frequency of vein and prosthetic grafts in the AC+ group. These factors mean that a firm conclusion about anticoagulation in this setting cannot be drawn from the available data. This highlights the need for better designed studies on which to determine an evidence-based policy for the use of anticoagulation in this setting. This is now more important with the increased use of venous resection with pancreatectomy. In conclusion this review demonstrates highly variable practice with the use of anticoagulation after venous resection with a pancreatectomy. The data heterogeneity makes it impossible to perform a formal meta-analysis. As we do not know what policy should be instituted in this setting, there is equipoise regarding anticoagulation and this should provide a strong impetus for a well-designed, multi-centre randomized controlled trial. Such a study should include standardized definitions to describe the types of vascular resection (e.g. Type 1 Tangentialresection and Type 2 Segmental resection) and reconstruction techniques (e.g. a. Primary venous anastomosis, b. venous graft, c. prosthetic graft use). The data from this review indicate that early portal vein thrombosis still occurs, is four times more likely after prosthetic graft reconstruction and is associated with a 40% mortality. Conflicts of interest There are no sources of funding to disclose. References 1. Warshaw AL, Gu Z, Wittenberg J, Waltmann AC. (1990) Preoperative staging and assessment of resectability of pancreatic cancer. Arch Surg 125: Warshaw AL, Castillo CF. (1992) Pancreatic carcinoma. N Engl J Med 362: Siriwardana HPP, Siriwardena AK. (2006) Systematic review of outcome of synchronous portal-superior mesenteric vein resection during pancreatectomy for cancer. Br J Surg 93: Chua TC, Saxena A. (2010) Extended Pancreaticoduodenectomy with vascular resection for pancreatic cancer: a systematic review. J Gastrointest Surg 14: Tseng JF, Raut CP, Lee JE, Pisters PWT, Vauthey J, Abdalla EK et al. (2004) Pancreaticoduodenectomy with vascular resection: margin status and survival duration. J Gastrointest Surg 8: Christians KK, Lal A, Pappas S, Quebbeman E, Evans DB. (2010) Portal vein resection. Surg Clin N Am 90: Banz VM, Croagh D, Coldham C, Tanière P, Buckels J, Isaac J et al. (2012) Factors influencing outcome in patients undergoing portal vein resection for adenocarcinoma of the pancreas. Eur J Surg Oncol 38: Zhou Y, Zhang Z, Liu Y, Li B, Xu D. (2012) Pancreatectomy combined with superior mesenteric vein-portal vein resection for pancreatic cancer: a meta-analysis. World J Surg 36: Callery MP, Chang KJ, Fishman EK, Talamonti MS, William Traverso L, Linehan DC. (2009) Pretreatment assessment of resectable and borderline resectable pancreatic cancer: expert consensus statement. Ann Surg Oncol 16: Sanjay P, Takaori K, Govil S, Shrikhande SV, Windsor JA. (2012) Arteryfirst approaches to pancreatoduodenectomy. Br J Surg 99: Nakao A, Takeda S, Inoue S, Nomoto S, Kanazumi N, Sugimoto H et al. (2006) Indications and technique of extended resection for pancreatic cancer. World J Surg 30: Li B, Chen FZ, Ge XH, Cai MZ, Jiang JS, Li JP et al. (2004) Pancreatoduodenectomy with vascular reconstruction in treating carcinoma of the pancreatic head. Hepatobiliary Pancreat Dis Int 3: Leach SD, Lee JE, Charnsangavej C, Cleary KR, Lowy AM, Fenoglio CJ et al. (1998) Survival following pancreaticoduodenectomy with resection of the superior mesenteric-portal vein confluence for adenocarcinoma of the pancreatic head. Br J Surg 85: Stauffer JA, Dougherty MK, Kim GP, Nguyen JH. (2009) Interposition graft with polytetrafluoroethylene for mesenteric and portal vein reconstruction after pancreaticoduodenectomy. Br J Surg 96: Ouaïssi M, Sielezneff I, Pirro N, Bon Mardion R, Chaix JB, Merad A et al. (2008) Therapeutic anticoagulant does not modify thromboses rate vein after venous reconstruction following pancreaticoduodenectomy. Gastroenterol Res Pract 2008: Moher D, Liberati A, Tetzlaff J, Altman DG. (2009) Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. J Clin Epidemiol 62: Lai ECS. (2012) Vascular resection and reconstruction at pancreaticoduodenectomy: technical issues. Hepatobiliary Pancreat Dis Int 11: Carrère N, Sauvanet A, Goere D, Kianmanesh R, Vullierme MP, Couvelard A et al. (2006) Pancreaticoduodenectomy with mesentericoportal vein resection for adenocarcinoma of the pancreatic head. World J Surg 30: Smoot RL, Christein JD, Farnell MB. (2006) Durability of portal venous reconstruction following resection during pancreaticoduodenectomy. J Gastrointest Surg 10:
8 698 HPB 20. Riediger H, Makowiec F, Fischer E, Adam U, Hopt UT. (2006) Postoperative morbidity and long-term survival after pancreaticoduodenectomy with superior mesenterico-portal vein resection. J Gastrointest Surg 10: Smoot RL, Christein JD, Farnell MB. (2007) An innovative option for venous reconstruction after ancreaticoduodenectomy: the left renal vein. J Gastrointest Surg 11: Illuminati G, Carboni F, Lorusso R, D'Urso A, Ceccanei G, Papaspyropoulos C et al. (2008) Results of a pancreatectomy with a limited venous resection for pancreatic cancer. Surg Today 38: Kendrick ML, Sciabas GM. (2011) Major venous resection during total laparoscopic pancreaticodeuodenectomy. HPB 13: Allema JH, Reinders ME, van Gulick TM, van Leeuwen DJ, de Wit LT, Verbeek PC et al. (1994) Portal vein resection in patients undergoing pancreatoduodenectomy for carcinoma of the pancreatic head. Br J Surg 81: Howard TJ, Villanustre N, Moore SA, DeWitt J, LeBlanc J, Maglinte D et al. (2003) Efficacy of venous reconstruction in patients with adenocarcinoma of the pancreatic head. J Gastrointest Surg 7: Zhang J, Qian HG, Leng JH, Cui M, Qiu H, Zhou GQ et al. (2009) Long mesentericoportal vein resection and end-to-end anastomosis without graft in pancreaticoduodenectomy. J Gastrointest Surg 13: Kaneoka Y, Yamaguchi A, Isogai M. (2009) Portal or superior mesenteric vein resection for pancreatic head adenocarcinoma: prognostic value of the length of venous resection. Surgery 145: Chakravarty KD, Hsu JT, Liu KH, Yeh CN, Yeh TS, Hwang TL et al. (2010) Prognosis and feasibility of en-bloc vascular resection in stage II pancreatic adenocarcinoma. World J Gastroenterol 16: Ayala R, Martínez-López J, Cedena T, Bustelos R, Jimenez C, Moreno E et al. (2011) Recipient and donor thrombophilia and the risk of portal venous thrombosis and hepatic artery thrombosis in liver receipients. BMC Gastroenterol 11: Widén A, Rolando N, Manousou P, Rolles K, Davidson B, Sharma D et al. (2009) Anticoagulation after liver transplantation: a retrospective audit and case-control study. Blood Coagul Fibrinolysis 20: McLin VA, Rimensberger P, Belli DC, Wildhaber BE. (2011) Anticoagulation following pediatric liver transplantation reduces early thrombotic events. Pediatr Transplant 15: Senzolo M, Burra P, Cholongitas E, Burroughs AK. (2006) New insights into the coagulopathy of liver disease and liver transplantation. World J Gastroenterol 28: Khorana AA, Fine RL. (2004) Pancreatic cancer and thromboembolic disease. Lancet Oncol 5: Chu CK, Farnell MB, Nguyen JH, Stauffer JA, Kooby DA, Sclabas GM et al. (2010) Prosthetic graft reconstruction after portal vein resection in pancreaticoduodenectomy: a multicenter analysis. J Am Coll Surg 211: Wang F, Arianayagam R, Gill A, Puttaswamy V, Neale M, Gananadha S et al. (2012) Grafts for mesenterico-portal vein resections can be avoided during pancreaticoduodenectomy. J Am Coll Surg 215:
PANCREATECTOMY WITH MESENTERIC AND PORTAL VEIN RESECTION FOR BORDERLINE RESECTABLE PANCREATIC CANCER: MULTICENTER STUDY
 PROPOSAL: PANCREATECTOMY WITH MESENTERIC AND PORTAL VEIN RESECTION FOR BORDERLINE RESECTABLE PANCREATIC CANCER: MULTICENTER STUDY Pancreatic carcinoma represents the fourth-leading cause of cancer-related
PROPOSAL: PANCREATECTOMY WITH MESENTERIC AND PORTAL VEIN RESECTION FOR BORDERLINE RESECTABLE PANCREATIC CANCER: MULTICENTER STUDY Pancreatic carcinoma represents the fourth-leading cause of cancer-related
An Innovative Option for Venous Reconstruction After Pancreaticoduodenectomy: the Left Renal Vein
 J Gastrointest Surg (2007) 11:425 431 DOI 10.1007/s11605-007-0131-1 An Innovative Option for Venous Reconstruction After Pancreaticoduodenectomy: the Left Renal Vein Rory L. Smoot & John D. Christein &
J Gastrointest Surg (2007) 11:425 431 DOI 10.1007/s11605-007-0131-1 An Innovative Option for Venous Reconstruction After Pancreaticoduodenectomy: the Left Renal Vein Rory L. Smoot & John D. Christein &
What to expect with major vascular reconstruction during Whipple procedures: a single institution experience and literature review
 Original Article What to expect with major vascular reconstruction during Whipple procedures: a single institution experience and literature review Matthew S. Jorgensen 1, Tariq Almerey 2, Houssam Farres
Original Article What to expect with major vascular reconstruction during Whipple procedures: a single institution experience and literature review Matthew S. Jorgensen 1, Tariq Almerey 2, Houssam Farres
Douglas B. Evans, MD 1, Ben George, MD 2, and Susan Tsai, MD, MHS 1
 Ann Surg Oncol (2015) 22:3409 3413 DOI 10.1245/s10434-015-4649-2 EDITORIAL PANCREATIC TUMORS Non-metastatic Pancreatic Cancer: Resectable, Borderline Resectable, and Locally Advanced-Definitions of Increasing
Ann Surg Oncol (2015) 22:3409 3413 DOI 10.1245/s10434-015-4649-2 EDITORIAL PANCREATIC TUMORS Non-metastatic Pancreatic Cancer: Resectable, Borderline Resectable, and Locally Advanced-Definitions of Increasing
Pancreaticoduodenectomy the anatomy and the surgical approaches
 Pancreaticoduodenectomy the anatomy and the surgical approaches Paul BS LAI Division of Hepato biliary and Pancreatic Surgery Department of Surgery The Chinese Univesity of Hong Kong Whipple s operation
Pancreaticoduodenectomy the anatomy and the surgical approaches Paul BS LAI Division of Hepato biliary and Pancreatic Surgery Department of Surgery The Chinese Univesity of Hong Kong Whipple s operation
The Whipple Operation Illustrations
 The Whipple Operation Illustrations Fig. 1. Illustration of the sixstep pancreaticoduodenectomy (Whipple operation) as described in a number of recent text books by Dr. Evans. The operation is divided
The Whipple Operation Illustrations Fig. 1. Illustration of the sixstep pancreaticoduodenectomy (Whipple operation) as described in a number of recent text books by Dr. Evans. The operation is divided
Neoadjuvant chemoradiotherapy for locally advanced pancreas cancer rarely leads to radiological evidence of tumour regression
 DOI:10.1111/hpb.12015 HPB ORIGINAL ARTICLE Neoadjuvant chemoradiotherapy for locally advanced pancreas cancer rarely leads to radiological evidence of tumour regression Vikas Dudeja 1, Edward W. Greeno
DOI:10.1111/hpb.12015 HPB ORIGINAL ARTICLE Neoadjuvant chemoradiotherapy for locally advanced pancreas cancer rarely leads to radiological evidence of tumour regression Vikas Dudeja 1, Edward W. Greeno
Cattell-Braasch maneuver combined with superior mesenteric artery first approach for resection of borderline resectable pancreatic cancer
 Masters of Surgery Page 1 of 5 Cattell-Braasch maneuver combined with superior mesenteric artery first approach for resection of borderline resectable pancreatic cancer Tingsong Yang 1, Fairweather Mark
Masters of Surgery Page 1 of 5 Cattell-Braasch maneuver combined with superior mesenteric artery first approach for resection of borderline resectable pancreatic cancer Tingsong Yang 1, Fairweather Mark
Correspondence to: Dr R. Ravikumar, Department of Hepatopancreatobiliary and Liver Transplant
 Impact of portal vein infiltration and type of venous reconstruction in surgery for borderline resectable pancreatic cancer R. Ravikumar 1, C. Sabin 2, M. Abu Hilal 4, A. Al-Hilli 4, S. Aroori 5, G. Bond-Smith
Impact of portal vein infiltration and type of venous reconstruction in surgery for borderline resectable pancreatic cancer R. Ravikumar 1, C. Sabin 2, M. Abu Hilal 4, A. Al-Hilli 4, S. Aroori 5, G. Bond-Smith
Neoadjuvant radiotherapy for pancreatic cancer: rationale and outcomes
 Review Article Neoadjuvant radiotherapy for pancreatic cancer: rationale and outcomes Rohan Deraniyagala, Emily D. Tanzler The University of Florida College of Medicine Department of Radiation Oncology,
Review Article Neoadjuvant radiotherapy for pancreatic cancer: rationale and outcomes Rohan Deraniyagala, Emily D. Tanzler The University of Florida College of Medicine Department of Radiation Oncology,
Surgical management of HCC. Evangelos Prassas Hepatobiliary and Pancreatic Surgery / Liver Transplantation Kings College Hospital / London
 Surgical management of HCC Evangelos Prassas Hepatobiliary and Pancreatic Surgery / Liver Transplantation Kings College Hospital / London Global distribution of HCC and staging systems WEST 1. Italy (Milan,
Surgical management of HCC Evangelos Prassas Hepatobiliary and Pancreatic Surgery / Liver Transplantation Kings College Hospital / London Global distribution of HCC and staging systems WEST 1. Italy (Milan,
Surgical Management of Pancreatic Cancer
 I Congresso de Oncologia D Or July 5-6, 2013 Surgical Management of Pancreatic Cancer Michael A. Choti, MD, MBA, FACS Department of Surgery Johns Hopkins University School of Medicine, Baltimore, MD Estimated
I Congresso de Oncologia D Or July 5-6, 2013 Surgical Management of Pancreatic Cancer Michael A. Choti, MD, MBA, FACS Department of Surgery Johns Hopkins University School of Medicine, Baltimore, MD Estimated
Outcomes associated with robotic approach to pancreatic resections
 Short Communication (Management of Foregut Malignancies and Hepatobiliary Tract and Pancreas Malignancies) Outcomes associated with robotic approach to pancreatic resections Caitlin Takahashi 1, Ravi Shridhar
Short Communication (Management of Foregut Malignancies and Hepatobiliary Tract and Pancreas Malignancies) Outcomes associated with robotic approach to pancreatic resections Caitlin Takahashi 1, Ravi Shridhar
Pancreatic cancer is a common malignant tumor of
 PDVR Original in treatment Article / of Pancreas pancreatic cancer Pancreaticoduodenectomy with portal vein/superior mesenteric vein resection for patients with pancreatic cancer with venous invasion Wei-Lin
PDVR Original in treatment Article / of Pancreas pancreatic cancer Pancreaticoduodenectomy with portal vein/superior mesenteric vein resection for patients with pancreatic cancer with venous invasion Wei-Lin
Visceral aneurysm. Diagnosis and Interventions M.NEDEVSKA
 Visceral aneurysm Diagnosis and Interventions M.NEDEVSKA History 1953 De Bakeyand Cooley Visceral aneurysm VAAs rare, reported incidence of 0.01 to 0.2% on routine autopsies. Clinically important Potentially
Visceral aneurysm Diagnosis and Interventions M.NEDEVSKA History 1953 De Bakeyand Cooley Visceral aneurysm VAAs rare, reported incidence of 0.01 to 0.2% on routine autopsies. Clinically important Potentially
Objectives. Intraoperative Consultation of the Whipple Resection Specimen. Pancreas Anatomy. Pancreatic ductal carcinoma 11/10/2014
 Intraoperative Consultation of the Whipple Resection Specimen Pathology Update Faculty of Medicine, University of Toronto November 15, 2014 John W. Wong, MD, FRCPC Department of Anatomical Pathology Sunnybrook
Intraoperative Consultation of the Whipple Resection Specimen Pathology Update Faculty of Medicine, University of Toronto November 15, 2014 John W. Wong, MD, FRCPC Department of Anatomical Pathology Sunnybrook
Case Presentation. PMH: HTN, BPH, strabismus PSH: appendectomy Medications: norvasc, tamsulosin NKDA SH/FH: negative
 Case Presentation 68yM referred for incidental finding of pancreatic head mass on CT scan for elevated PSA. No symptoms. Denied pruritus, jaundice, change in color of urine/stool, anorexia, or weight loss.
Case Presentation 68yM referred for incidental finding of pancreatic head mass on CT scan for elevated PSA. No symptoms. Denied pruritus, jaundice, change in color of urine/stool, anorexia, or weight loss.
ORIGINAL ARTICLE. Helical Computed Tomography in the Diagnosis of Portal Vein Invasion by Pancreatic Head Carcinoma
 ORIGINAL ARTICLE Helical Computed Tomography in the Diagnosis of Portal Vein Invasion by Pancreatic Head Carcinoma Usefulness for Selecting Surgical Procedures and Predicting the Outcome Hiroyoshi Furukawa,
ORIGINAL ARTICLE Helical Computed Tomography in the Diagnosis of Portal Vein Invasion by Pancreatic Head Carcinoma Usefulness for Selecting Surgical Procedures and Predicting the Outcome Hiroyoshi Furukawa,
ARROCase: Borderline Resectable Pancreatic Cancer
 ARROCase: Borderline Resectable Pancreatic Cancer Resident: Jordan Kharofa, MD Staff: Beth Erickson, MD 8/2012 Medical College of Wisconsin Department of Radiation Oncology Case Presentation: 60 year old
ARROCase: Borderline Resectable Pancreatic Cancer Resident: Jordan Kharofa, MD Staff: Beth Erickson, MD 8/2012 Medical College of Wisconsin Department of Radiation Oncology Case Presentation: 60 year old
WARFARIN: PERI OPERATIVE MANAGEMENT
 WARFARIN: PERI OPERATIVE MANAGEMENT OBJECTIVE: To provide an approach to the perioperative management of warfarin treated patients who require an elective or urgent surgery/procedure. To provide an approach
WARFARIN: PERI OPERATIVE MANAGEMENT OBJECTIVE: To provide an approach to the perioperative management of warfarin treated patients who require an elective or urgent surgery/procedure. To provide an approach
WARFARIN: PERI-OPERATIVE MANAGEMENT
 WARFARIN: PERI-OPERATIVE MANAGEMENT OBJECTIVE: To provide an approach to the perioperative management of warfarin-treated patients who require an elective or urgent surgery/procedure. To provide an approach
WARFARIN: PERI-OPERATIVE MANAGEMENT OBJECTIVE: To provide an approach to the perioperative management of warfarin-treated patients who require an elective or urgent surgery/procedure. To provide an approach
Interactive Exhibit On Imaging Updates For Staging And Response Assessment In Pancreatic Cancer
 Interactive Exhibit On Imaging Updates For Staging And Response Assessment In Pancreatic Cancer 1 Vinit Baliyan, MD; 1 Hamed Kordbacheh, MD; 2 Eric P Tamm, MD; 3 Theodore S Hong, MD; 4 Carlos Fernandez-Del
Interactive Exhibit On Imaging Updates For Staging And Response Assessment In Pancreatic Cancer 1 Vinit Baliyan, MD; 1 Hamed Kordbacheh, MD; 2 Eric P Tamm, MD; 3 Theodore S Hong, MD; 4 Carlos Fernandez-Del
Surgery for hilar cholangiocirconoma
 Department of Surgery University Hospital RWTH Aachen Surgery for hilar cholangiocirconoma Ulf Peter Neumann Agenda Operating on the most complex tumor in HBP Surgery Preoperative management Does the patient
Department of Surgery University Hospital RWTH Aachen Surgery for hilar cholangiocirconoma Ulf Peter Neumann Agenda Operating on the most complex tumor in HBP Surgery Preoperative management Does the patient
Leiomyosarcoma involving the inferior vena cava in an. elderly patient with reference to its operative modalities: a case report
 Leiomyosarcoma involving the inferior vena cava in an elderly patient with reference to its operative modalities: a case report Hiroshi Ushida 1, Ryosuke Murai 1, Mitsuhiro Narita 1, Fumiyoshi Kojima 2
Leiomyosarcoma involving the inferior vena cava in an elderly patient with reference to its operative modalities: a case report Hiroshi Ushida 1, Ryosuke Murai 1, Mitsuhiro Narita 1, Fumiyoshi Kojima 2
Index. Note: Page numbers of article titles are in boldface type.
 Note: Page numbers of article titles are in boldface type. A Adenocarcinoma, pancreatic ductal, laparoscopic distal pancreatectomy for, 61 Adrenal cortical carcinoma, laparoscopic adrenalectomy for, 114
Note: Page numbers of article titles are in boldface type. A Adenocarcinoma, pancreatic ductal, laparoscopic distal pancreatectomy for, 61 Adrenal cortical carcinoma, laparoscopic adrenalectomy for, 114
Portal vein stent placement for the treatment of postoperative portal vein stenosis: long-term success and factor associated with stent failure
 Kato et al. BMC Surgery (2017) 17:11 DOI 10.1186/s12893-017-0209-y RESEARCH ARTICLE Portal vein stent placement for the treatment of postoperative portal vein stenosis: long-term success and factor associated
Kato et al. BMC Surgery (2017) 17:11 DOI 10.1186/s12893-017-0209-y RESEARCH ARTICLE Portal vein stent placement for the treatment of postoperative portal vein stenosis: long-term success and factor associated
Bridging anticoagulant therapy early after mechanical heart. valve surgery: systematic review with meta-analysis.
 Bridging anticoagulant therapy early after mechanical heart valve surgery: systematic review with meta-analysis. Luiz Guilherme Passaglia, MD; Guilherme M. Barros, MD; Marcos R. de Sousa, MD, MSc, PhD.
Bridging anticoagulant therapy early after mechanical heart valve surgery: systematic review with meta-analysis. Luiz Guilherme Passaglia, MD; Guilherme M. Barros, MD; Marcos R. de Sousa, MD, MSc, PhD.
How to deal with synchronous primary and liver metastases
 How to deal with synchronous primary and liver metastases Luis Sabater Ortí MD, PhD Associate Professor University of Valencia European Board Surgical Qualification HBP (EBSQ-HPB) Department of Surgery.
How to deal with synchronous primary and liver metastases Luis Sabater Ortí MD, PhD Associate Professor University of Valencia European Board Surgical Qualification HBP (EBSQ-HPB) Department of Surgery.
Minimally Invasive Esophagectomy- Valuable. Jayer Chung, MD University of Colorado Health Sciences Center December 11, 2006
 Minimally Invasive Esophagectomy- Valuable Jayer Chung, MD University of Colorado Health Sciences Center December 11, 2006 Overview Esophageal carcinoma What is minimally invasive esophagectomy (MIE)?
Minimally Invasive Esophagectomy- Valuable Jayer Chung, MD University of Colorado Health Sciences Center December 11, 2006 Overview Esophageal carcinoma What is minimally invasive esophagectomy (MIE)?
Feasibility of portal or superior mesenteric vein resection and reconstruction by allogeneic vein for pancreatic head cancer a case-control study
 Zhang et al. BMC Gastroenterology (2018) 18:49 https://doi.org/10.1186/s12876-018-0778-y RESEARCH ARTICLE Open Access Feasibility of portal or superior mesenteric vein resection and reconstruction by allogeneic
Zhang et al. BMC Gastroenterology (2018) 18:49 https://doi.org/10.1186/s12876-018-0778-y RESEARCH ARTICLE Open Access Feasibility of portal or superior mesenteric vein resection and reconstruction by allogeneic
Patient Selection for Surgery in RCC with Thrombus. E. Jason Abel, M.D.
 Patient Selection for Surgery in RCC with Thrombus E. Jason Abel, M.D. RCC with venous invasion Venous invasion occurs in ~10% of RCC Surgery more complex Increased risk for morbidity Thrombus may be confined
Patient Selection for Surgery in RCC with Thrombus E. Jason Abel, M.D. RCC with venous invasion Venous invasion occurs in ~10% of RCC Surgery more complex Increased risk for morbidity Thrombus may be confined
Total laparoscopic pancreaticoduodenectomy: a retrospective study of 27 cases treated in a single institution
 Original Article Total laparoscopic pancreaticoduodenectomy: a retrospective study of 27 cases treated in a single institution Hong Li 1, Jie Zhu 2, Bin Zhang 1, Gencong Li 1, Xinhua Zhou 3, Dansong Yu
Original Article Total laparoscopic pancreaticoduodenectomy: a retrospective study of 27 cases treated in a single institution Hong Li 1, Jie Zhu 2, Bin Zhang 1, Gencong Li 1, Xinhua Zhou 3, Dansong Yu
Successful Application of Supraceliac Aortohepatic Conduit Using Saphenous Venous Graft in Right Lobe Living Donor Liver Transplantation
 LETTERS FROM THE FRONTLINE Successful Application of Supraceliac Aortohepatic Conduit Using Saphenous Venous Graft in Right Lobe Living Donor Liver Transplantation TO THE EDITOR: Hepatic artery (HA) reconstruction
LETTERS FROM THE FRONTLINE Successful Application of Supraceliac Aortohepatic Conduit Using Saphenous Venous Graft in Right Lobe Living Donor Liver Transplantation TO THE EDITOR: Hepatic artery (HA) reconstruction
Neoadjuvant therapy prior to surgical resection for previously explored pancreatic cancer patients is associated with improved survival
 Original Article Neoadjuvant therapy prior to surgical resection for previously explored pancreatic cancer patients is associated with improved survival Fengchun Lu 1,2, Kevin C. Soares 1, Jin He 1, Ammar
Original Article Neoadjuvant therapy prior to surgical resection for previously explored pancreatic cancer patients is associated with improved survival Fengchun Lu 1,2, Kevin C. Soares 1, Jin He 1, Ammar
Pylorus Preserving Pancreaticoduodenectomy
 REVIEW Pylorus Preserving Pancreaticoduodenectomy Jacqueline M. Garonzik-Wang, M. B. Majella Doyle Pancreaticoduodenectomy (PD) has become the standard of care for resectable pancreatic cancer and premalignant
REVIEW Pylorus Preserving Pancreaticoduodenectomy Jacqueline M. Garonzik-Wang, M. B. Majella Doyle Pancreaticoduodenectomy (PD) has become the standard of care for resectable pancreatic cancer and premalignant
MANAGEMENT OF OVERANTICOAGULATION AND PREOPERATIVE MANAGEMENT OF WARFARIN DOSE 1. GUIDELINES FOR THE MANAGEMENT OF AN ELEVATED INR
 MANAGEMENT OF OVERANTICOAGULATION AND PREOPERATIVE MANAGEMENT OF WARFARIN DOSE 1. GUIDELINES FOR THE MANAGEMENT OF AN ELEVATED INR 1.1 Time to lower INR Prothrombinex-VF - 15 minutes Fresh Frozen Plasma
MANAGEMENT OF OVERANTICOAGULATION AND PREOPERATIVE MANAGEMENT OF WARFARIN DOSE 1. GUIDELINES FOR THE MANAGEMENT OF AN ELEVATED INR 1.1 Time to lower INR Prothrombinex-VF - 15 minutes Fresh Frozen Plasma
Recommendations for Follow-up After Vascular Surgery Arterial Procedures SVS Practice Guidelines
 Recommendations for Follow-up After Vascular Surgery Arterial Procedures 2018 SVS Practice Guidelines vsweb.org/svsguidelines About the guidelines Published in the July 2018 issue of Journal of Vascular
Recommendations for Follow-up After Vascular Surgery Arterial Procedures 2018 SVS Practice Guidelines vsweb.org/svsguidelines About the guidelines Published in the July 2018 issue of Journal of Vascular
Financial and Other Disclosures
 Financial and Other Disclosures Off-label use of drugs, devices, or other agents: None Data from IRB-approved human research is not presented I have the following financial interests or relationships to
Financial and Other Disclosures Off-label use of drugs, devices, or other agents: None Data from IRB-approved human research is not presented I have the following financial interests or relationships to
Donor Hypernatremia Influences Outcomes Following Pediatric Liver Transplantation
 8 Original Article Donor Hypernatremia Influences Outcomes Following Pediatric Liver Transplantation Neema Kaseje 1 Samuel Lüthold 2 Gilles Mentha 3 Christian Toso 3 Dominique Belli 2 Valérie McLin 2 Barbara
8 Original Article Donor Hypernatremia Influences Outcomes Following Pediatric Liver Transplantation Neema Kaseje 1 Samuel Lüthold 2 Gilles Mentha 3 Christian Toso 3 Dominique Belli 2 Valérie McLin 2 Barbara
Management of Extensive Portal Vein Thrombosis
 Management of Extensive Portal Vein Thrombosis Deok-Bog Moon, Sung-Gyu Lee, Chul-Soo Ahn, Shin Hwang, Ki-Hun Kim, Gi-Won Song, Dong-Hwan Jung, Gil-Chun Park, Kyu-Bo Sung 1, Gi- Young Ko 1, Dong-Il Kweon
Management of Extensive Portal Vein Thrombosis Deok-Bog Moon, Sung-Gyu Lee, Chul-Soo Ahn, Shin Hwang, Ki-Hun Kim, Gi-Won Song, Dong-Hwan Jung, Gil-Chun Park, Kyu-Bo Sung 1, Gi- Young Ko 1, Dong-Il Kweon
Prevention Of Pancreaticojejunal Fistula After Whipple Procedure
 ISPUB.COM The Internet Journal of Surgery Volume 4 Number 2 Prevention Of Pancreaticojejunal Fistula After Whipple Procedure N Barbetakis, K Setsiz Citation N Barbetakis, K Setsiz. Prevention Of Pancreaticojejunal
ISPUB.COM The Internet Journal of Surgery Volume 4 Number 2 Prevention Of Pancreaticojejunal Fistula After Whipple Procedure N Barbetakis, K Setsiz Citation N Barbetakis, K Setsiz. Prevention Of Pancreaticojejunal
DATA REPORT. August 2014
 AUDIT DATA REPORT August 2014 Prepared for the Australian and New Zealand Gastric and Oesophageal Surgical Association by the Royal Australasian College of Surgeons 199 Ward St, North Adelaide, SA 5006
AUDIT DATA REPORT August 2014 Prepared for the Australian and New Zealand Gastric and Oesophageal Surgical Association by the Royal Australasian College of Surgeons 199 Ward St, North Adelaide, SA 5006
Multiple Primary Quiz
 Multiple Primary Quiz Case 1 A 72 year old man was found to have a 12 mm solid lesion in the pancreatic tail by computed tomography carried out during a routine follow up study of this patient with adult
Multiple Primary Quiz Case 1 A 72 year old man was found to have a 12 mm solid lesion in the pancreatic tail by computed tomography carried out during a routine follow up study of this patient with adult
PROGNOSIS AND SURVIVAL
 CANCER ASSOCIATED THROMBOSIS PROGNOSIS AND SURVIVAL Since French internist Armand Trousseau reported the occurrence of mysterious thrombotic disorders in cancer patients in the mid-19th century, the link
CANCER ASSOCIATED THROMBOSIS PROGNOSIS AND SURVIVAL Since French internist Armand Trousseau reported the occurrence of mysterious thrombotic disorders in cancer patients in the mid-19th century, the link
Vascular Imaging in the Pediatric Abdomen. Jonathan Swanson, MD
 Vascular Imaging in the Pediatric Abdomen Jonathan Swanson, MD Goals and Objectives To understand the imaging approach, appearance, and clinical manifestations of the common pediatric abdominal vascular
Vascular Imaging in the Pediatric Abdomen Jonathan Swanson, MD Goals and Objectives To understand the imaging approach, appearance, and clinical manifestations of the common pediatric abdominal vascular
ECMO vs. CPB for Intraoperative Support: How do you Choose?
 ECMO vs. CPB for Intraoperative Support: How do you Choose? Shaf Keshavjee MD MSc FRCSC FACS Director, Toronto Lung Transplant Program Surgeon-in-Chief, University Health Network James Wallace McCutcheon
ECMO vs. CPB for Intraoperative Support: How do you Choose? Shaf Keshavjee MD MSc FRCSC FACS Director, Toronto Lung Transplant Program Surgeon-in-Chief, University Health Network James Wallace McCutcheon
Intended for use by Clinicians and Health Care Providers involved in the Management or Referral of adult patients with pancreatic
 Intended for use by Clinicians and Health Care Providers involved in the Management or Referral of adult patients with pancreatic cancer Section AA Cancer Centre Referrals In the absence of metastatic
Intended for use by Clinicians and Health Care Providers involved in the Management or Referral of adult patients with pancreatic cancer Section AA Cancer Centre Referrals In the absence of metastatic
PANCREATIC CANCER GUIDELINES
 PANCREATIC CANCER GUIDELINES North-East London Cancer Network & Barts and the London HPB Centre PROTOCOL FOR MANAGEMENT OF PANCREATIC CANCER (SEPTEMBER 2010) I. PRE-REFERRAL GUIDELINES Screening 1. Offer
PANCREATIC CANCER GUIDELINES North-East London Cancer Network & Barts and the London HPB Centre PROTOCOL FOR MANAGEMENT OF PANCREATIC CANCER (SEPTEMBER 2010) I. PRE-REFERRAL GUIDELINES Screening 1. Offer
The role of adjuvant chemotherapy following resection of early stage thymoma
 Perspective The role of adjuvant chemotherapy following resection of early stage thymoma Masatsugu Hamaji Department of Thoracic Surgery, Kyoto University Hospital, 54 Kawaharacho, Shogoin, Sakyo-ku, Kyoto,
Perspective The role of adjuvant chemotherapy following resection of early stage thymoma Masatsugu Hamaji Department of Thoracic Surgery, Kyoto University Hospital, 54 Kawaharacho, Shogoin, Sakyo-ku, Kyoto,
The Choice of Palliative Treatment for Biliary and Duodenal Obstruction in Patients With Unresectable Pancreatic Cancer: Is Surgery Bypass Better?
 Int Surg 2016;101:58 63 DOI: 10.9738/INTSURG-D-14-00247.1 The Choice of Palliative Treatment for Biliary and Duodenal Obstruction in Patients With Unresectable Pancreatic Cancer: Is Surgery Bypass Better?
Int Surg 2016;101:58 63 DOI: 10.9738/INTSURG-D-14-00247.1 The Choice of Palliative Treatment for Biliary and Duodenal Obstruction in Patients With Unresectable Pancreatic Cancer: Is Surgery Bypass Better?
Laparoscopy-assisted D2 radical distal subtotal gastrectomy
 Masters of Gastrointestinal Surgery Laparoscopy-assisted D2 radical distal subtotal gastrectomy Xiaogeng Chen, Weihua Li, Jinsi Wang, Changshun Yang Department of Tumor Surgery, Fujian Provincial Hospital,
Masters of Gastrointestinal Surgery Laparoscopy-assisted D2 radical distal subtotal gastrectomy Xiaogeng Chen, Weihua Li, Jinsi Wang, Changshun Yang Department of Tumor Surgery, Fujian Provincial Hospital,
Distal pancreatectomy with en bloc celiac axis resection for pancreatic body-tail cancer: Is it justified?
 e-issn 1643-3750 DOI: 10.12659/MSM.889847 Received: 2013.10.01 Accepted: 2013.10.21 Published: 2014.01.02 Distal pancreatectomy with en bloc celiac axis resection for pancreatic body-tail cancer: Is it
e-issn 1643-3750 DOI: 10.12659/MSM.889847 Received: 2013.10.01 Accepted: 2013.10.21 Published: 2014.01.02 Distal pancreatectomy with en bloc celiac axis resection for pancreatic body-tail cancer: Is it
Laparoscopic vs Robotic Rectal Cancer Surgery: Making it better!
 Laparoscopic vs Robotic Rectal Cancer Surgery: Making it better! Francis Seow- Choen Medical Director Seow-Choen Colorectal Centre Singapore In all situations: We have to use the right tool for the job
Laparoscopic vs Robotic Rectal Cancer Surgery: Making it better! Francis Seow- Choen Medical Director Seow-Choen Colorectal Centre Singapore In all situations: We have to use the right tool for the job
pitfall Table 1 4 disorientation pitfall pitfall Table 1 Tel:
 11 687 692 2002 pitfall 1078 29 17 9 1 2 3 dislocation outflow block 11 1 2 3 9 1 2 3 4 disorientation pitfall 11 687 692 2002 Tel: 075-751-3606 606-8507 54 2001 8 27 2002 10 31 29 4 pitfall 16 1078 Table
11 687 692 2002 pitfall 1078 29 17 9 1 2 3 dislocation outflow block 11 1 2 3 9 1 2 3 4 disorientation pitfall 11 687 692 2002 Tel: 075-751-3606 606-8507 54 2001 8 27 2002 10 31 29 4 pitfall 16 1078 Table
Slide 1: Perioperative Management of Anticoagulation
 Perioperative Management of Anticoagulation by Steven L. Cohn, MD, FACP Director, Medical Consultation Service, Kings County Hospital Center, Clinical Professor of Medicine, SUNY Downstate, Brooklyn, NY
Perioperative Management of Anticoagulation by Steven L. Cohn, MD, FACP Director, Medical Consultation Service, Kings County Hospital Center, Clinical Professor of Medicine, SUNY Downstate, Brooklyn, NY
Zhengtao Liu 1,2,3*, Shuping Que 4*, Lin Zhou 1,2,3 Author affiliation:
 Dose-response Relationship of Serum Uric Acid with Metabolic Syndrome and Non-alcoholic Fatty Liver Disease Incidence: AMeta-analysis of Prospective Studies Zhengtao Liu 1,2,3*, Shuping Que 4*, Lin Zhou
Dose-response Relationship of Serum Uric Acid with Metabolic Syndrome and Non-alcoholic Fatty Liver Disease Incidence: AMeta-analysis of Prospective Studies Zhengtao Liu 1,2,3*, Shuping Que 4*, Lin Zhou
Hemostasis and thrombosis in patients with liver disease. Ton Lisman, Dept Surgery, UMC Groningen, The Netherlands
 Hemostasis and thrombosis in patients with liver disease Ton Lisman, Dept Surgery, UMC Groningen, The Netherlands Importance of the liver in hemostasis Synthesis of Coagulation factors Fibrinolytic proteins
Hemostasis and thrombosis in patients with liver disease Ton Lisman, Dept Surgery, UMC Groningen, The Netherlands Importance of the liver in hemostasis Synthesis of Coagulation factors Fibrinolytic proteins
Symptomatic venous thromboembolism after femoral vein harvest
 From the Western Vascular Society Symptomatic venous thromboembolism after femoral vein harvest Ravi V. Dhanisetty, MD, a Timothy K. Liem, MD, a Gregory J. Landry, MD, a Brett C. Sheppard, MD, b Erica
From the Western Vascular Society Symptomatic venous thromboembolism after femoral vein harvest Ravi V. Dhanisetty, MD, a Timothy K. Liem, MD, a Gregory J. Landry, MD, a Brett C. Sheppard, MD, b Erica
Thirty-Day Outcomes of Laparoscopic vs. Open Total Proctocolectomy with Ileoanal Anastomosis in Children
 Thirty-Day Outcomes of Laparoscopic vs. Open Total Proctocolectomy with Ileoanal Anastomosis in Children Jeremy D. Kauffman MD, Paul D. Danielson MD, Nicole M. Chandler MD Johns Hopkins All Children s
Thirty-Day Outcomes of Laparoscopic vs. Open Total Proctocolectomy with Ileoanal Anastomosis in Children Jeremy D. Kauffman MD, Paul D. Danielson MD, Nicole M. Chandler MD Johns Hopkins All Children s
Management of Colorectal Liver Metastases
 Management of Colorectal Liver Metastases MM Bernon, JEJ Krige HPB Surgical Unit, Groote Schuur Hospital Department of Surgery, University of Cape Town 50% of patients with colorectal cancer develop liver
Management of Colorectal Liver Metastases MM Bernon, JEJ Krige HPB Surgical Unit, Groote Schuur Hospital Department of Surgery, University of Cape Town 50% of patients with colorectal cancer develop liver
Vasile Goldiş Western University of Arad Faculty of Medicine, Pharmacy and Dental Medicine, Arad, Romania
 ENDOVASCULAR TREATMENT FOR VASCULAR GRAFT RESTENOSIS Bogdan Totolici 1, Francisca Blanca Călinescu 1*, Ionel Droc 2, Carmen Neamţu 1 1 Vasile Goldiş Western University of Arad Faculty of Medicine, Pharmacy
ENDOVASCULAR TREATMENT FOR VASCULAR GRAFT RESTENOSIS Bogdan Totolici 1, Francisca Blanca Călinescu 1*, Ionel Droc 2, Carmen Neamţu 1 1 Vasile Goldiş Western University of Arad Faculty of Medicine, Pharmacy
Acute abdominal venous thromboses- the hyperdense noncontrast CT sign
 Acute abdominal venous thromboses- the hyperdense noncontrast CT sign Poster No.: C-1095 Congress: ECR 2011 Type: Educational Exhibit Authors: M. Goldstein, K. Jhaveri; Toronto, ON/CA Keywords: Abdomen,
Acute abdominal venous thromboses- the hyperdense noncontrast CT sign Poster No.: C-1095 Congress: ECR 2011 Type: Educational Exhibit Authors: M. Goldstein, K. Jhaveri; Toronto, ON/CA Keywords: Abdomen,
Deep vein thrombosis and its prevention in critically ill adults Attia J, Ray J G, Cook D J, Douketis J, Ginsberg J S, Geerts W H
 Deep vein thrombosis and its prevention in critically ill adults Attia J, Ray J G, Cook D J, Douketis J, Ginsberg J S, Geerts W H Authors' objectives To systematically review the incidence of deep vein
Deep vein thrombosis and its prevention in critically ill adults Attia J, Ray J G, Cook D J, Douketis J, Ginsberg J S, Geerts W H Authors' objectives To systematically review the incidence of deep vein
Thrombin injection vs Conventional Surgical Repair in Treatment of Iatrogenic Post-cath Femoral Artery Pseudoaneurysm (IFAP)
 Kasr El Aini Journal of Surgery VOL., 11, NO 3 September 2010 31 Thrombin injection vs Conventional Surgical Repair in Treatment of Iatrogenic Post-cath Femoral Artery Pseudoaneurysm (IFAP) Farghaly A,
Kasr El Aini Journal of Surgery VOL., 11, NO 3 September 2010 31 Thrombin injection vs Conventional Surgical Repair in Treatment of Iatrogenic Post-cath Femoral Artery Pseudoaneurysm (IFAP) Farghaly A,
Celsion Symposium New Paradigms in HCC Staging: HKLC vs. BCLC Staging
 Celsion Symposium New Paradigms in HCC Staging: HKLC vs. BCLC Staging Ronnie T.P. Poon, MBBS, MS, PhD Chair Professor of Hepatobiliary and Pancreatic Surgery Chief of Hepatobiliary and Pancreatic Surgery
Celsion Symposium New Paradigms in HCC Staging: HKLC vs. BCLC Staging Ronnie T.P. Poon, MBBS, MS, PhD Chair Professor of Hepatobiliary and Pancreatic Surgery Chief of Hepatobiliary and Pancreatic Surgery
General Surgery Curriculum Royal Australasian College of Surgeons, General Surgeons Australia & New Zealand Association of General Surgeons
 General Surgery Curriculum Royal Australasian College of Surgeons, General Surgeons Australia & New Zealand Association of General Surgeons MODULE TITLE: TRANSPLANTATION 7-Nov-2016 DEVELOPED BY: Daryl
General Surgery Curriculum Royal Australasian College of Surgeons, General Surgeons Australia & New Zealand Association of General Surgeons MODULE TITLE: TRANSPLANTATION 7-Nov-2016 DEVELOPED BY: Daryl
Acute Diverticulitis. Andrew B. Peitzman, MD Mark M. Ravitch Professor of Surgery University of Pittsburgh
 Acute Diverticulitis Andrew B. Peitzman, MD Mark M. Ravitch Professor of Surgery University of Pittsburgh Focus today: when to operate n Recurrent, uncomplicated diverticulitis; after how many episodes?
Acute Diverticulitis Andrew B. Peitzman, MD Mark M. Ravitch Professor of Surgery University of Pittsburgh Focus today: when to operate n Recurrent, uncomplicated diverticulitis; after how many episodes?
Is it Time to Stop Checking Frozen Section Neck Margins During Pancreaticoduodenectomy?
 Ann Surg Oncol (2013) 20:3626 3633 DOI 10.1245/s10434-013-3080-9 ORIGINAL ARTICLE PANCREATIC TUMORS Is it Time to Stop Checking Frozen Section Neck Margins During Pancreaticoduodenectomy? Neha L. Lad,
Ann Surg Oncol (2013) 20:3626 3633 DOI 10.1245/s10434-013-3080-9 ORIGINAL ARTICLE PANCREATIC TUMORS Is it Time to Stop Checking Frozen Section Neck Margins During Pancreaticoduodenectomy? Neha L. Lad,
1. Epidemiology of Esophageal Cancer 2. Operative Strategies 3. Minimally Invasive Esophagectomy 4. Video
 Minimally Invasive Esophagectomy Guilherme M Campos, MD, FACS Assistant Professor of Surgery Director G.I. Motility Center Director Bariatric Surgery Program University of California San Francisco ESOPHAGEAL
Minimally Invasive Esophagectomy Guilherme M Campos, MD, FACS Assistant Professor of Surgery Director G.I. Motility Center Director Bariatric Surgery Program University of California San Francisco ESOPHAGEAL
TITLE: Acetylsalicylic Acid for Venous Thromboembolism Prophylaxis: A Review of Clinical Evidence, Benefits and Harms
 TITLE: Acetylsalicylic Acid for Venous Thromboembolism Prophylaxis: A Review of Clinical Evidence, Benefits and Harms DATE: 23 August 2011 CONTEXT AND POLICY ISSUES: Thromboembolism occurs when a blood
TITLE: Acetylsalicylic Acid for Venous Thromboembolism Prophylaxis: A Review of Clinical Evidence, Benefits and Harms DATE: 23 August 2011 CONTEXT AND POLICY ISSUES: Thromboembolism occurs when a blood
OPEN ACCESS TEXTBOOK OF GENERAL SURGERY
 OPEN ACCESS TEXTBOOK OF GENERAL SURGERY MESENTERIC ISCHAEMIA P Zwanepoel INTRODUCTION Mesenteric ischaemia results from hypoperfusion of the gut, most commonly due to occlusion, thrombosis or vasospasm.
OPEN ACCESS TEXTBOOK OF GENERAL SURGERY MESENTERIC ISCHAEMIA P Zwanepoel INTRODUCTION Mesenteric ischaemia results from hypoperfusion of the gut, most commonly due to occlusion, thrombosis or vasospasm.
Superior vena cava replacement combined with venovenous shunt for lung cancer and thymoma: a case series
 Original Article Superior vena cava replacement combined with venovenous shunt for lung cancer and thymoma: a case series Wei Dai 1 *, Jifu Dong 2 *, Hongwei Zhang 2, Xiaojun Yang 1, Qiang Li 1 1 Department
Original Article Superior vena cava replacement combined with venovenous shunt for lung cancer and thymoma: a case series Wei Dai 1 *, Jifu Dong 2 *, Hongwei Zhang 2, Xiaojun Yang 1, Qiang Li 1 1 Department
NOACS/DOACS*: PERI-OPERATIVE MANAGEMENT
 NOACS/DOACS*: PERI-OPERATIVE MANAGEMENT OBJECTIVE: To provide guidance for the peri-operative management of patients who are receiving a newer direct oral anticoagulant (DOAC) and require an elective surgery/procedure.
NOACS/DOACS*: PERI-OPERATIVE MANAGEMENT OBJECTIVE: To provide guidance for the peri-operative management of patients who are receiving a newer direct oral anticoagulant (DOAC) and require an elective surgery/procedure.
Treatment of Colorectal Liver Metastases State of the Art
 Treatment of Colorectal Liver Metastases State of the Art Eddie K. Abdalla, MD, FACS Professor and Chairman of Surgery Chief of Hepatobiliary Surgery Hilton Metropolitan Palace Hotel Beirut 16 November,
Treatment of Colorectal Liver Metastases State of the Art Eddie K. Abdalla, MD, FACS Professor and Chairman of Surgery Chief of Hepatobiliary Surgery Hilton Metropolitan Palace Hotel Beirut 16 November,
Review Article Controversies in the Management of Borderline Resectable Proximal Pancreatic Adenocarcinoma with Vascular Involvement
 HPB Surgery Volume 2008, Article ID 839503, 8 pages doi:10.1155/2008/839503 Review Article Controversies in the Management of Borderline Resectable Proximal Pancreatic Adenocarcinoma with Vascular Involvement
HPB Surgery Volume 2008, Article ID 839503, 8 pages doi:10.1155/2008/839503 Review Article Controversies in the Management of Borderline Resectable Proximal Pancreatic Adenocarcinoma with Vascular Involvement
Review of radiological classifications of pancreatic cancer with peripancreatic vessel invasion: are new grading criteria required?
 Shen et al. Cancer Imaging (2017) 17:14 DOI 10.1186/s40644-017-0115-7 REVIEW Review of radiological classifications of pancreatic cancer with peripancreatic vessel invasion: are new grading criteria required?
Shen et al. Cancer Imaging (2017) 17:14 DOI 10.1186/s40644-017-0115-7 REVIEW Review of radiological classifications of pancreatic cancer with peripancreatic vessel invasion: are new grading criteria required?
Revised Annual Program Volumes for ASTS Accreditation Approved May 2013 Revised June 2016
 Overview This document outlines new requirements and processes for ASTS accreditation of transplant surgery fellowships including volume requirements for ASTS accreditation, as well as the individual training
Overview This document outlines new requirements and processes for ASTS accreditation of transplant surgery fellowships including volume requirements for ASTS accreditation, as well as the individual training
Laparoscopic Bladder-Preserving Surgery for Enterovesical Fistula Complicated with Benign Gastrointestinal Disease
 This is an Open Access article licensed under the terms of the Creative Commons Attribution-NonCommercial-NoDerivs 3.0 License (www.karger.com/oa-license), applicable to the online version of the article
This is an Open Access article licensed under the terms of the Creative Commons Attribution-NonCommercial-NoDerivs 3.0 License (www.karger.com/oa-license), applicable to the online version of the article
In the Clinic: Annals Sweta Kakaraparthi 1/23/15
 In the Clinic: Annals Sweta Kakaraparthi 1/23/15 Case Scenerio 56 year old female with breast cancer presents to the clinic for her 3 month followup! She is concerned about blood clots and asks you about
In the Clinic: Annals Sweta Kakaraparthi 1/23/15 Case Scenerio 56 year old female with breast cancer presents to the clinic for her 3 month followup! She is concerned about blood clots and asks you about
Role and safety of epidural analgesia
 Anaesthesia for Liver Resection Surgery The Association of Anaesthetists Seminars 21 Portland Place, London Thursday 15 th December 2005 Role and safety of epidural analgesia Lennart Christiansson MD,
Anaesthesia for Liver Resection Surgery The Association of Anaesthetists Seminars 21 Portland Place, London Thursday 15 th December 2005 Role and safety of epidural analgesia Lennart Christiansson MD,
2006 NKF-DOQI Guidelines Preferred Vascular Access Order 1. Radiocephalic (wrist) fistula 2. Brachiocephalic (elbow) fistula 3. Basilic vein transposi
 Stage 5 Chronic Kidney Disease Assessing the Results of AV Access: Realistic Outcomes in 2009 Sean P. Roddy, MD Albany, NY Defined as a GFR
Stage 5 Chronic Kidney Disease Assessing the Results of AV Access: Realistic Outcomes in 2009 Sean P. Roddy, MD Albany, NY Defined as a GFR
Lung cancer or primary malignant tumors of the mediastinum
 Technique of Superior Vena Cava Resection for Lung Carcinomas David R. Jones, MD Division of Thoracic and Cardiovascular Surgery, Department of Surgery, University of Virginia School of Medicine, Charlottesville,
Technique of Superior Vena Cava Resection for Lung Carcinomas David R. Jones, MD Division of Thoracic and Cardiovascular Surgery, Department of Surgery, University of Virginia School of Medicine, Charlottesville,
Pancreatic Adenocarcinoma: Everything You Need to Know From Cross-Sectional Imaging to Treatment
 Pancreatic Adenocarcinoma: Everything You Need to Know From Cross-Sectional Imaging to Treatment Andrew W. Bowman, MD PhD Assistant Professor of Radiology Mayo Clinic Florida SCBT-MR Annual Meeting Nashville,
Pancreatic Adenocarcinoma: Everything You Need to Know From Cross-Sectional Imaging to Treatment Andrew W. Bowman, MD PhD Assistant Professor of Radiology Mayo Clinic Florida SCBT-MR Annual Meeting Nashville,
Satisfactory surgical outcome of T2 gastric cancer after modified D2 lymphadenectomy
 Original Article Satisfactory surgical outcome of T2 gastric cancer after modified D2 lymphadenectomy Shupeng Zhang 1, Liangliang Wu 2, Xiaona Wang 2, Xuewei Ding 2, Han Liang 2 1 Department of General
Original Article Satisfactory surgical outcome of T2 gastric cancer after modified D2 lymphadenectomy Shupeng Zhang 1, Liangliang Wu 2, Xiaona Wang 2, Xuewei Ding 2, Han Liang 2 1 Department of General
Dental Management Considerations for Patients on Antithrombotic Therapy
 Dental Management Considerations for Patients on Antithrombotic Therapy Warfarin and Antiplatelet Joel J. Napeñas DDS FDSRCS(Ed) Program Director General Practice Residency Program Department of Oral Medicine
Dental Management Considerations for Patients on Antithrombotic Therapy Warfarin and Antiplatelet Joel J. Napeñas DDS FDSRCS(Ed) Program Director General Practice Residency Program Department of Oral Medicine
Diagnosis and Treatment of Deep Venous Thrombosis and Pulmonary Embolism
 Agency for Healthcare Research and Quality Evidence Report/Technology Assessment Diagnosis and Treatment of Deep Venous Thrombosis and Pulmonary Embolism Summary Number 68 Overview Venous thromboembolism
Agency for Healthcare Research and Quality Evidence Report/Technology Assessment Diagnosis and Treatment of Deep Venous Thrombosis and Pulmonary Embolism Summary Number 68 Overview Venous thromboembolism
Alliance A Alliance SWOG ECOG/ACRIN - NRG
 Preoperative chemotherapy and chemotherapy plus hypofractionated radiation therapy for borderline resectable adenocarcinoma of the head of the pancreas Alliance A021501 Alliance SWOG ECOG/ACRIN - NRG Clinical
Preoperative chemotherapy and chemotherapy plus hypofractionated radiation therapy for borderline resectable adenocarcinoma of the head of the pancreas Alliance A021501 Alliance SWOG ECOG/ACRIN - NRG Clinical
Correction of Extrahepatic Portal Vein Thrombosis by the Mesenteric to Left Portal Vein Bypass
 ORIGINAL ARTICLES Correction of Extrahepatic Portal Vein Thrombosis by the Mesenteric to Left Portal Vein Bypass Riccardo Superina, MD,* Daniel A. Bambini, MD,* Joan Lokar, RN, Cynthia Rigsby, MD, and
ORIGINAL ARTICLES Correction of Extrahepatic Portal Vein Thrombosis by the Mesenteric to Left Portal Vein Bypass Riccardo Superina, MD,* Daniel A. Bambini, MD,* Joan Lokar, RN, Cynthia Rigsby, MD, and
Radical nerve dissection for the carcinoma of head of pancreas: report of 30 cases
 Original Article Radical nerve dissection for the carcinoma of head of pancreas: report of 30 cases Qing Lin, Langping Tan, Yu Zhou, Quanbo Zhou, Rufu Chen Department of Biliary and Pancreatic Surgery,
Original Article Radical nerve dissection for the carcinoma of head of pancreas: report of 30 cases Qing Lin, Langping Tan, Yu Zhou, Quanbo Zhou, Rufu Chen Department of Biliary and Pancreatic Surgery,
THE CRITICAL COMPLCATIONS AND MANAGEMENTS AFTER PANCREATIC SURGERY 2013/12/21
 THE CRITICAL COMPLCATIONS AND MANAGEMENTS AFTER PANCREATIC SURGERY Tsann-Long Hwang, MD, FACS Department of Surgery Chang Gung Memorial Hospital Chang Gung University Taipei, TAIWAN 2013/12/21 THE DIFFICULTY
THE CRITICAL COMPLCATIONS AND MANAGEMENTS AFTER PANCREATIC SURGERY Tsann-Long Hwang, MD, FACS Department of Surgery Chang Gung Memorial Hospital Chang Gung University Taipei, TAIWAN 2013/12/21 THE DIFFICULTY
Open and minimally invasive pancreatic surgery a review of the literature
 Systematic Review Open and minimally invasive pancreatic surgery a review of the literature Brandon C. Chapman 1, Kristen DeSanto 2, Bulent Salman 3, Barish H. Edil 1 1 Department of Surgery, 2 Health
Systematic Review Open and minimally invasive pancreatic surgery a review of the literature Brandon C. Chapman 1, Kristen DeSanto 2, Bulent Salman 3, Barish H. Edil 1 1 Department of Surgery, 2 Health
Superficialización de la vena basílica. Pierre BOURQUELOT, Paris
 Superficialización de la vena basílica. Pierre BOURQUELOT, Paris 1 Basilic Vein Superficialization. Pierre BOURQUELOT, Paris 2 (Upper arm) Basilic Vein 3 Technique 2-stage Basilic Vein Tunnel-Superficialization
Superficialización de la vena basílica. Pierre BOURQUELOT, Paris 1 Basilic Vein Superficialization. Pierre BOURQUELOT, Paris 2 (Upper arm) Basilic Vein 3 Technique 2-stage Basilic Vein Tunnel-Superficialization
Anticoagulation for prevention of venous thromboembolism
 Anticoagulation for prevention of venous thromboembolism Original article by: Michael Tam Note: updated in June 2009 with the eighth edition (from the seventh) evidence-based clinical practice guidelines
Anticoagulation for prevention of venous thromboembolism Original article by: Michael Tam Note: updated in June 2009 with the eighth edition (from the seventh) evidence-based clinical practice guidelines
Pancreatic Cancer and Radiation Therapy
 Pancreatic Cancer and Radiation Therapy Why? Is there a role for local therapy with radiation in a disease with such a high rate of distant metastases? When? Resectable Disease Is there a role for post-op
Pancreatic Cancer and Radiation Therapy Why? Is there a role for local therapy with radiation in a disease with such a high rate of distant metastases? When? Resectable Disease Is there a role for post-op
Chronic Pancreatitis
 Gastro Foundation Fellows Weekend 2017 Chronic Pancreatitis Jose Ramos University of the Witwatersrand Donald Gordon Medical Centre Aetiology in SA Alcohol (up to 80%) Idiopathic Tropical Obstruction Autoimmune
Gastro Foundation Fellows Weekend 2017 Chronic Pancreatitis Jose Ramos University of the Witwatersrand Donald Gordon Medical Centre Aetiology in SA Alcohol (up to 80%) Idiopathic Tropical Obstruction Autoimmune
Surgical approach for DVT. Division of Vascular Surgery Department of Surgery Seoul National University College of Medicine
 Surgical approach for DVT Seung-Kee Min Division of Vascular Surgery Department of Surgery Seoul National University College of Medicine Treatment Options for Venous Thrombosis Unfractionated heparin &
Surgical approach for DVT Seung-Kee Min Division of Vascular Surgery Department of Surgery Seoul National University College of Medicine Treatment Options for Venous Thrombosis Unfractionated heparin &
EAST MULTICENTER STUDY DATA DICTIONARY. Temporary Intravascular Shunt Study Data Dictionary
 EAST MULTICENTER STUDY DATA DICTIONARY Temporary Intravascular Shunt Study Data Dictionary Data Entry Points and appropriate definitions / clarifications: Entry space Definition / Instructions 1. Specific
EAST MULTICENTER STUDY DATA DICTIONARY Temporary Intravascular Shunt Study Data Dictionary Data Entry Points and appropriate definitions / clarifications: Entry space Definition / Instructions 1. Specific
Trattamento chirurgico delle lesioni epatiche secondarie difficili. Adelmo Antonucci Chirurgia Oncologica e Epato-bilio-pancreatica
 Trattamento chirurgico delle lesioni epatiche secondarie difficili Adelmo Antonucci Chirurgia Oncologica e Epato-bilio-pancreatica What does it mean difficult lesions? Diagnosis Treatment Small size Unfit
Trattamento chirurgico delle lesioni epatiche secondarie difficili Adelmo Antonucci Chirurgia Oncologica e Epato-bilio-pancreatica What does it mean difficult lesions? Diagnosis Treatment Small size Unfit
Patients on anticoagulant or antiplatelet therapy undergoing elective endoscopic procedures
 This is an official Northern Trust policy and should not be edited in any way Patients on anticoagulant or antiplatelet therapy undergoing elective endoscopic procedures Reference Number: NHSCT/11/454
This is an official Northern Trust policy and should not be edited in any way Patients on anticoagulant or antiplatelet therapy undergoing elective endoscopic procedures Reference Number: NHSCT/11/454
Management of new onset atrial fibrillation McNamara R L, Bass E B, Miller M R, Segal J B, Goodman S N, Kim N L, Robinson K A, Powe N R
 Management of new onset atrial fibrillation McNamara R L, Bass E B, Miller M R, Segal J B, Goodman S N, Kim N L, Robinson K A, Powe N R Authors' objectives To synthesise the evidence that exists to guide
Management of new onset atrial fibrillation McNamara R L, Bass E B, Miller M R, Segal J B, Goodman S N, Kim N L, Robinson K A, Powe N R Authors' objectives To synthesise the evidence that exists to guide
