Surgical Neurology International
|
|
|
- Norma Allen
- 5 years ago
- Views:
Transcription
1 Surgical Neurology International Review Article OPEN ACCESS For entire Editorial Board visit : Editor: James I. Ausman, MD, PhD University of California, Los Angeles, CA, USA Surgical resection of sporadic and hereditary hemangioblastoma: Our 10-year experience and a literature review Elisabeth Bründl, Petra Schödel, Odo-Winfried Ullrich, Alexander Brawanski, Karl-Michael Schebesch Department of Neurosurgery, University Medical Center Regensburg, Germany *Elisabeth Bründl - elisabeth.bruendl@ukr.de; Petra Schödel - petra.schoedel@ukr.de; Odo-Winfried Ullrich - winfried.ullrich@ukr.de; Alexander Brawanski - alexander.brawanski@ukr.de; Karl-Michael Schebesch - karl-michael.schebesch@ukr.de *Corresponding author Received: 20 May 14 Accepted: 30 July 14 Published: 22 September 14 This article may be cited as: Brundl E, Schodel P, Ullrich O, Brawanski A, Schebesch K. Surgical resection of sporadic and hereditary hemangioblastoma: Our 10-year experience and a literature review. Surg Neurol Int 2014;5:138. Available FREE in open access from: Copyright: 2014 Bründl E. This is an open access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited. Abstract Background: Hemangioblastomas (HBLs) are benign neoplasms that contribute to 1-2.5% of intracranial tumors and 7-12% of posterior fossa lesions in adult patients. HBLs either evolve hereditarily in association with von Hippel Lindau disease (vhl) or, more prevalently, as solitary sporadic tumors. Only few authors have reported on the clinical presentation and the neurological outcome of HBL. Methods: We retrospectively analyzed the clinical, radiological, surgical, and histopathologic records of 24 consecutive patients (11 men, 13 women; mean age 51.3 years) with HBL of the posterior cranial fossa, who had been treated at our center between 2001 and We reviewed the current literature, and discussed our findings in the context of previous publications on HBL. The study protocol was approved by the local ethics committee ( ). Results: Mean time to diagnosis was 14 weeks. The extent of resection (EOR) was total in 20 and near total in 4 patients. Four patients required revision within 24 h because of relevant postoperative bleeding. One patient died within 14 days. One patient required permanent shunting. At discharge, 75% of patients [n = 18, modified Rankin scale (mrs) 0-1] showed no or at least resolved symptoms. Mean follow-up was 21 months. Two recurrences were detected during follow-up. Conclusions:In comparison to other benign entities of the posterior fossa, time to diagnosis was significantly shorter for HBL. This finding indicates the rather aggressive biological behavior of these excessively vascularized tumors. In our series, however, the rate of complete resection was high, and morbidity and mortality rates were within the reported range. Access this article online Website: DOI: / Quick Response Code: Key Words: CNS hemangioblastoma, neurological outcome, posterior cranial fossa, von Hippel Lindau disease INTRODUCTION Hemangioblastomas (HBLs) represent benign capillary rich neoplasms of the central nervous system (CNS) that are derived from a blood vessel lineage. HBLs account for 1-2.5% of intracranial tumors and 7-12% of posterior fossa lesions in adult patients. [21,32,33] Morphologically, HBLs present heterogeneously, mainly as cystic, solid cystic,
2 or solid lesions that consist of a small, abundantly vascularized, mural nidus surrounded by a variably lipidized stromal cell component of unknown histogenesis. [2,4,7,13,30,38] HBLs predominantly evolve as solitary sporadic lesions, but may also grow hereditarily in association with von Hippel Lindau (vhl) disease. [4,8,21,24,30,42] vhl is a clinically heterogeneous syndrome of varying severity that is characterized by a predisposition to develop various benign and malignant tumors, for example, retinal angiomas, endolymphatic sac tumors, renal cell carcinomas (RCC), pancreatic tumors, and pheochromocytomas. However, solely cystic lesions may also develop, for example, of the epididymis or the mandible. [4,6,8,21,24,30,42] Hence, patients with vhl require interdisciplinary treatment by neurosurgeons or surgeons, geneticists, and internists. Approximately 25% of CNS HBLs arise in the setting of vhl. [11,22] HBLs are potentially curable, and the outcome is favorable provided that the solid component of the tumor can be resected. [8,44,46,49] Consulting our database, we wanted to retrospectively analyze the clinical presentation, neuroradiological findings, surgical aspects, and neurological outcome of patients with HBL of the posterior cranial fossa, both with and without vhl, who had undergone surgery at our center over the past 10 years. METHODS Between 2001 and 2012, 24 consecutive patients with HBL in the posterior cranial fossa underwent suboccipital craniotomy and consecutive microsurgical resection in our department. We retrospectively reviewed the patients clinical, neuroradiological, surgical, and histopathologic records. We excluded three patients with tumor recurrence because they had undergone initial surgery before All patients were treated according to our standardized postoperative treatment regimen: (1). all patients were transferred to the intensive care unit for postoperative monitoring for at least 24 h; (2). corticosteroids were routinely administered to avoid brain edema; and (3). post surgical computed tomography (CT) or magnetic resonance imaging (MRI) was obtained within 24 h. The nature and duration of symptoms, the manifestations of vhl, and associated positive family history were evaluated by analyzing the patients charts. vhl was diagnosed on a solely clinical basis according to previous updated criteria. [8,23,30] Fundoscopy and abdominal echography or CT scans were carried out to screen for vhl. Cerebral MRI and CT scans were analyzed with regard to tumor localization, tumor size (maximum diameter), and the number of lesions as well as their signal density in the T1 sequence after intravenous gadolinium injection. Further factors to be analyzed were surrounding tumor edema, hemorrhage, abnormally large vessels within or adjacent to the tumor, morphology (pure cyst, cyst with a mural nidus, mixed solid and cystic components, syrinx formation), and the presence or absence of hydrocephalus. Tumor location was defined by the predominant anatomical area of the solid part of the lesion. Preoperative hydrocephalus was diagnosed if external ventricular drainage (EVD) placement was required. Moreover, we assessed the surgical approach, the adhesive neurovascular structures, the duration of the surgical procedure, and the extent of resection (EOR; total or near total), as well as the complications and recurrence rates. The EOR was assessed by early control CT (n = 14) or MRI (n = 10) scans. During follow up, all patients underwent MRI to screen for residual or recurrent tumors, defined as residual or new areas of contrast enhancement along the borders of the resection cavity. Postoperative complications were treated within 24 h after surgery (early complications) and between 24 h and up to 10 days postoperatively (late complications). Patient outcome was assessed immediately after surgery, at discharge, and, if available, at follow up according to the modified Rankin scale (mrs) and the Glasgow Outcome Scale (GOS). Outcomes of mrs values of 0-1 or GOS values of 5-4 were considered good, mrs values of 2-3 or GOS value of 3 as fair, and mrs values of 4-5 or GOS values of 2-1 as poor. The overall follow up interval ranged from 2 to 99 months with a mean follow up time of 21 months. Two patients dropped out during follow up. We reviewed the current literature and discussed our findings in the context of previous publications on HBL. The study protocol was approved by the local ethics committee ( ). RESULTS Patient profiles During the study period, 27 patients had undergone 37 surgical procedures for CNS HBL. Three patients with tumor recurrence who had received initial surgery before 2001 were excluded. Of the 24 patients included in our study, 13 (54%) were women and 11 (46%) were men. The mean age was 51.3 years (ranging from 27 to 81 years) [see Figure 1]. Twenty two HBLs had been localized within the cerebellar hemispheres, and two were in the craniocervical junction area, of which one partially extended into the medulla oblongata. Clinical features The major presenting symptoms were headache, vertigo or ataxia, and nausea. The other symptoms were neck pain, emesis, dysarthria, and cranial nerve deficits [Table 1]. The mean time to diagnosis was 14 weeks (ranging from 1 day to 57 weeks) in the entire cohort, 7 weeks in the hereditary subgroup, and 15 weeks in the sporadic HBL subgroup [Figure 2].
3 Figure 1: Age distribution by decades of patients with hemangioblastoma in the posterior cranial fossa Table 1: Preoperative clinical features of hemangioblastoma in the posterior cranial fossa (n=24 patients) Clinical features and symptoms Age (years) >70 3 Sex Female 13 Male 11 Duration of symptoms (weeks) >32 5 Presenting symptoms Headache 22 Vertigo 15 Ataxia 15 Nausea 10 Emesis 7 Neck pain 7 Recurring syncopes 5 Dysarthria 3 Sensomotoric deficits or unilateral symptoms 3 Diplopia or anisocoria 3 Depressive mood 1 Dysgraphia 1 Neuroimaging On MRI scans (n = 12), eight lesions appeared to be cystic, showing a characteristic mural nodular component with strong homogenous enhancement after gadolinium injection. Two lesions were purely solid, two were both solid and cystic, and none of the lesions was purely cystic N Figure 2: Mean time to diagnosis in the entire cohort (n = 24, ranging from 1 day to 57 weeks) in the subgroup with sporadic hemangioblastoma (HBL) (n = 21) and in the subgroup with hereditary HBL [von Hippel Lindau disease (vhl), n = 3, ranging from 4 to 12 weeks]. Analyses showed a considerably shorter mean time from the onset of symptoms to diagnosis in patients with vhl disease-associated HBL [Figure 3]. The mean tumor size was 36.8 mm (ranging from 15.0 to 63.7 mm). Perifocal edema was found in 10 patients. All patients except one had only one solitary CNS HBL. There were no signs of any intratumoral hemorrhage. Among the five MRIs of the spinal cord available, no syrinx formation could be detected. Surgery Three patients required an EVD placement preoperatively because of occlusive hydrocephalus and one patient intraoperatively because of prolonged bleeding into the fourth ventricle. All operations were done via the retrosigmoid suboccipital approach, four operations included a laminectomy of the atlas, and one of those an additional laminectomy of the axis. The mean duration of the surgical procedure was 218 min (ranging from 75 to 900 min). Strong intraoperative bleeding due to abundant tumor vascularization was reported for five patients, and two of them required a blood transfusion. Cortical adherences were reported for three patients. The EOR was total in 20 patients and near total in 4 patients. Three of them were operated on again after the postoperative control MRI scan had shown a residual nodule. In one patient, complete removal could not be achieved because of a highly vascularized nidus. The histopathologic findings confirmed the diagnosis of HBL in all patients. Postoperative course and long term outcome Within 24 h postoperatively, 14 patients did not show any neurological deficits. Some patients had transient cranial nerve paresis (n = 3) (e.g. diplopia), hemiparesis (n = 1), ataxia (n = 1), or nausea and emesis (n = 1). Within the first 24 h after surgery, four patients underwent immediate surgical revision with hematoma evacuation because of relevant bleeding, and
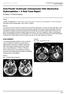
4 Figure 3: Characteristics of available preoperative MRI of 12 out of 24 patients with hemangioblastoma. MN: Mural nodule three of them additionally required an EVD placement. Only one of these four patients underwent permanent ventriculoperitoneal shunting 1 month later. Within the first 10 postoperative days, we found cerebrospinal fluid (CSF) infections (n= 3, 13%), infratentorial ischemia (n = 2, 8%), pneumonia (n =2, 8%), psycho syndrome (n = 1, 4%), and a Mallory Weiss lesion (n = 1, 4%). Perioperative mortality was 4% (n = 1) as one patient died due to postoperative bleeding. At discharge, 75% (n = 18, mrs 0 1) of the patients showed no or at least resolved symptoms. The remaining patients (mrs 2 3 in n = 1 and mrs 4 5 in n = 4) had persistent ataxia (n = 3, 13%) and newly developed diplopia (n = 1, 4%) and hemiparesis (n = 1; 4%). According to the GOS grading, outcome at discharge was good in 18 patients (GOS 5 4), fair in 4 patients (GOS 3), and poor in 2 patients (GOS 2 1). The overall follow up period ranged from 2 to 99 months with a mean follow up time of 21 months. Differentiating between patients with vhl associated HBL and sporadic HBL, we found a mean follow up time of 75 months for vhl and 19 months for sporadic HBL. Two tumor recurrences were detected during follow up. One patient underwent re operation 32 months after initial surgery. The other patient (vhl subgroup) had regular MRI controls because of two small contrast enhanced nodules in the resection cavity that were stable and asymptomatic within the 57 months of follow up ( watch and wait ). At follow up, outcome was good in 14 (according to mrs) and 15 patients (according to GOS), fair in 2 (mrs) and 4 (GOS) patients, and poor in 5 (mrs) and 2 (GOS) patients. DISCUSSION HBLs are benign CNS lesions, classified as grade I according to the World Health Organization (WHO), with a highly vascularized solid tumor component. The posterior inferior cerebellar arteries and their drainage into the transverse, sigmoid, and rectus sinuses may occasionally require preoperative embolization. [31,48] Sometimes, preoperative embolization may significantly reduce the tumor blood supply and thus avoid profuse intraoperative bleeding. In this way, surgery in sensitive areas may be facilitated. [37,39,41] In our cohort, five patients underwent preoperative cerebral digital subtraction angiography. Embolization prior to surgery was not conducted in any of the patients. Besides, none of our patients received any adjuvant therapy after surgery. The effectiveness of both radiotherapy and chemotherapy in HBL has been questioned. [5,25,28] Both techniques are solely used for residual or recurrent tumors after microsurgery. Neurosurgical resection represents the treatment of choice, providing long term tumor control. [1,14,20,26,36] Commonly, HBLs develop within the cerebellar hemispheres, whereas HBLs in the cerebellopontine angle, brain stem, ventricles, or supratentorially are rather rare. [10,19,36,47] About 20% of CNS HBLs develop within the spinal cord, contributing to 2-4% of spinal tumors. [21,34,45] Accordingly, 92% of the infratentorial HBLs in our patients were localized in the cerebellum and none originated from the brain stem. In comparison to sporadic HBLs, vhl is more often associated with the brain stem, spinal cord, and the spinal nerve roots. [4,30] As depicted in Figure 1, our series comprised 13 (54%) women and 11 (46%) men, with a mean age of 51.3 years (ranging from 27 to 81 years) at the time of diagnosis. Consistent with our results [Table 1], recent trials [16,27] have identified headache, cerebellar signs, and nausea as the main presenting symptoms. Even in HBL, non specific clinical manifestations were reported that were localized in functionally important areas, such as the brain stem and the cerebellopontine angle. [31,48] Clinical diagnosis of vhl was solely based on the updated criteria described by Conway et al. [8] In the absence of any family history of CNS or retinal HBL, diagnosis of vhl requires the presence of multiple or of at least two HBLs or one HBL and one of the visceral manifestations described above. In the case of a positive family history of CNS or retinal HBL, diagnosis of vhl necessitates the presence of only one HBL or any other manifestation of vhl. [8,23,30] As previously stated in the literature, many patients with HBL do unfortunately not undergo appropriate screening for vhl. [6,27] A possibly underrated percentage of 10-40% of primary symptomatic HBL has been reported to be vhl associated. [6,8,21,27,35] Despite basically similar histological characteristics, the biological behavior of syndromic HBL may be more aggressive than that of sporadic HBL because of its rapid growth pattern or its multifocal evolvement. [29,32,42] Our results confirm the idea of the more aggressive nature of hereditary HBL because the mean time to diagnosis of 7 weeks of the three patients diagnosed with vhl was significantly shorter than that of the
5 patients with sporadic HBL who tended to present after 15 weeks [Figure 2]. Compared to a recent analysis of 10 patients with epidermoids of the posterior cranial fossa (unpublished data), we found a significantly longer mean duration from the onset of neurological symptoms to the time of diagnosis of 121 weeks (2.3 years). In contrast to other tumor entities of the posterior cranial fossa, such as histomorphologically inert and non vascularized epidermoids, HBLs, particularly of the syndromic subtype, seem to be considerably more aggressive. Such behavior may be due to a more rapid, space occupying expansion of the cyst, causing focal compression of the surrounding tissue. Lesion growth bears the risk of decompensation of the brain stem and bleeding. Despite being rare, bleeding significantly increases morbidity and mortality. [9,12] Because the majority of symptomatic HBL is associated with cysts, [42] solid and cystic lesions may differ regarding their clinical manifestation. When reviewing 17 patients with solid HBL, Rachinger and colleagues [31] emphasized that solid tumors are much more complex to handle than the microsurgical resection of a cystic compartment. This complexity is caused by the frequent localization of solid tumors in eloquent areas and their more complex vascular architecture and blood supply. Rachinger et al. yielded good functional results with en bloc removal and also discussed the histological features of HBL: The stromal cells, representing the neoplastic component of the tumor, express, among others, a high level of different growth factors and receptors, such as vascular endothelial growth factor (VEGF). Excessive expression of VEGF may result in peritumorous edema. We observed perifocal edema in two patients with solid HBL that account for approximately one third of HBLs. [17] In these tumors, peritumorous edema may mask radiological diagnosis by mimicking metastatic disease. [18] In our study population, the radiologically suspected diagnosis of HBL in preoperative MRI was histologically verified in all patients. Advances in MRI techniques, such as dynamic susceptibility contrast perfusion MRI, perfusion MRI, and susceptibility weighted imaging (SWI), facilitate differential diagnosis with other infratentorial lesions, for instance, pilocytic astrocytoma, [3,15] vestibular schwannoma, [50] or tumoral hemorrhage. Such technical advances also improve the potential identification of high velocity blood vessels. [40] In 8 out of 12 available preoperative MRI analyses [Figure 3], we observed the predominant radiological pattern of a cyst with an intense gadolinium enhanced mural nodule [Figure 4]. [38] We noted a mean maximum tumor size of 36.8 mm (ranging from 15.0 to 63.7 mm) that was within the previously reported range (5-57 mm [16] and mm [31] ) of HBL in the posterior cranial fossa. Patients with vhl tend to develop new lesions over time, thus requiring frequent surgery. [8,21] Frequent tumor recurrence and surgical a c Figure 4: (a) T1-weighted, axial and (b) T2-weighted, axial MRI of a cystic hemangioblastoma localized in the left cerebellar hemisphere, showing the characteristic mural nodule with strong gadolinium enhancement. (c) Postoperative MRI (T1-weighted, axial), confirming total tumor removal and resection of the cystic component after retrosigmoid suboccipital craniotomy. The spaceoccupying effect and the brain stem compression are alleviated resection represent the most common causes of morbidity and mortality in patients with vhl disease; in 30-50% of patients, RCC are the cause of death. Our surgical procedures were conventionally performed in Concorde position with the patient s upper body elevated approximately 15 above the horizontal level and head in neutral position, with the neck flexed. Craniotomy was done via a retrosigmoid suboccipital approach, based on the shape of the venous sinuses, the nidus, and the side and localization of the tumor. In four HBLs with either a space occupying cerebellar cyst or tumor localization in the craniocervical junction, a laminectomy of C1 (and C2) was required for sufficient exposure of the foramen magnum and the medulla oblongata. Prior to dural incision, an ultrasound guided localization of the tumor was usually conducted. The strategy of surgical tumor resection differed depending on the morphological characteristics of the HBL. In tumors with an expansive cystic component, the cyst was released before dissecting the mural nidus. In solid tumors, a circumferential dissection with devascularization and en bloc removal was favored whenever possible. We achieved complete resection in 83% of our patients (n = 20). In one patient with a strongly adhesive and highly vascularized solid HBL extending from the cerebellar vermis to the foramen magnum, complete removal of the tumor was not possible. Because of relevant bleeding on the first postoperative day, the patient underwent immediate surgical revision with hematoma evacuation but died 13 days later because of multi organ failure. Two patients underwent re craniotomy after a residual nodule was found in the postoperative b
6 MRI scan. Three tumor recurrences were detected within the follow up period (mean 21 months). Apart from the above mentioned difficulties in diagnosing vhl, another limitation in the current literature including the present study is the restricted duration of the follow up period. Similar follow up periods have been reported, ranging from 16 days to 132 months, [27] from 6 to 9 months, [31] and from 13 to 108 months. [16] Tumor control was achieved in all patients at the last follow up. In comparison to the reports by Conway et al. [8] and Padhi et al. [27] reporting a mortality rate of 5% and 8%, respectively, we observed a lower mortality rate of 4%. With regard to surgery associated morbidity, we noted relevant postoperative bleeding (n = 4, 17%), consecutive permanent shunting (n = 1, 4%), CSF infections (n = 3, 13%), infratentorial ischemia (n = 2, 8%), newly developed diplopia (n = 1, 4%), and newly developed hemiparesis (n = 1, 4%). However, 75% of patients (n = 18) were discharged without or at least with resolved symptoms. We found poor outcome at discharge in patients with preexisting encephalomyelitis disseminata (n = 1), postoperative cerebellopontine edema (n = 1), and postoperative hemorrhage (n = 2). In a series of 38 patients with sporadic intracranial HBL, Le Reste et al. [16] reported CSF leaks in 8%, transiently worsened cerebellar syndrome in 3%, peripheral facial palsy in 3%, postoperative external shunts for hydrocephalus in 11%, bulbar syndromes with tetraparesis in 8%, postoperative hematoma of the surgical bed in 3%, and both hemiparesia and lateral homonym hemianopsia in 3% of patients. Rachinger et al. [31] reported a favorable outcome in six patients with solid HBL of the cerebellar hemispheres. Despite improved clinical results because of progress in imaging and microsurgical techniques over the past decades, HBLs within the brain stem still have the most unfavorable prognosis. [43,48] Limitations This is a retrospective observational study with the commonly acknowledged methodological limitations given below. Preoperative MRI was only available for review for 12 patients of our study population, curtailing preoperative neuroradiological analysis. Furthermore, only in 10 out of 24 patients was an MRI scan assessed as early control imaging, whereas the remaining 14 patients had an early postoperative CT scan, limiting the analysis of residual tumor. However, all patients received MRI for follow up control. As previously reported by a number of authors, the exact prevalence of vhl disease may also be misleading in our series because not every patient with HBL was subjected to vhl screening as an in patient. A precise differentiation between sporadic HBL and vhl patients is of utmost importance because the complexity of vhl associated lesions requires interdisciplinary management and prolonged endeavor. Family members of affected patients also have to be counseled and subjected to the full screening protocol, ideally to identify HBL or any other vhl manifestation before the disease could become symptomatic. These issues should be addressed in clinical practice and further prospective research projects. CONCLUSIONS In the present study, we correlated our 10 year results with the various findings of previous clinical trials on HBLs. In contrast to other benign tumor entities of the posterior cranial fossa, the biological behavior of excessively vascularized HBLs seems to be rather aggressive as reflected by the short time to diagnosis. We achieved a high rate of complete resection, and morbidity and mortality rates were within the reported range. vhl disease requires early diagnosis, adequate surgical management, a multimodal therapeutic approach, a lifelong follow up, and the counseling of patients and their relatives at risk. These issues are all the more important because of the rather high estimated number of unreported cases due to patients not undergoing the appropriate screening for vhl. REFERENCES 1. Ahyai A, Woerner U, Markakis E. Surgical treatment of intramedullary tumors (spinal cord and medulla oblongata). Analysis of 16 cases. Neurosurg Rev 1990;13: Baker KB, Moran CJ, Wippold FJ, 2nd, Smirniotopoulos JG, Rodriguez FJ, Meyers SP, et al. MR imaging of spinal hemangioblastoma. AJR Am J Roentgenol 2000;174: Bing F, Kremer S, Lamalle L, Chabardes S, Ashraf A, Pasquier B, et al. Value of perfusion MRI in the study of pilocytic astrocytoma and hemangioblastoma: Preliminary findings. J Neuroradiol 2009;36: Burger PC, Scheithauer BW. Hemangioblastoma. Tumors of the central nervous system, AFIP atlas of tumor pathology. ; 4 th series, Fascicle 7: Washington DC: ARC Press; Capitanio JF, Mazza E, Motta M, Mortini P, Reni M. Mechanisms, indications and results of salvage systemic therapy for sporadic and von Hippel-Lindau related hemangioblastomas of the central nervous system. Crit Rev Oncol Hematol 2013;86: Catapano D, Muscarella LA, Guarnieri V, Zelante L, D'Angelo VA, D'Agruma L. Hemangioblastomas of central nervous system: Molecular genetic analysis and clinical management. Neurosurgery 2005;56: Choyke PL, Glenn GM, Walther MM, Patronas NJ, Linehan WM, Zbar B. von Hippel-Lindau disease: Genetic, clinical, and imaging features. Radiology 1995;194: Conway JE, Chou D, Clatterbuck RE, Brem H, Long DM, Rigamonti D. Hemangioblastomas of the central nervous system in von Hippel-Lindau syndrome and sporadic disease. Neurosurgery 2001;48: de San Pedro JR, Rodriguez FA, Niguez BF, Sanchez JF, Lopez-Guerrero AL, Murcia MF, et al. Massive hemorrhage in hemangioblastomas Literature review. Neurosurg Rev 2010;33: Dow GR, Sim DW, O'Sullivan MG. Excision of large solid haemangioblastomas of the cerebellopontine angle by a skull base approach. Br J Neurosurg 2002;16:
7 11. Filling-Katz MR, Choyke PL, Oldfield E, Charnas L, Patronas NJ, Glenn GM, et al. Central nervous system involvement in von Hippel-Lindau disease. Neurology 1991;41: Glasker S, Van Velthoven V. Risk of hemorrhage in hemangioblastomas of the central nervous system. Neurosurgery 2005;57: Ho VB, Smirniotopoulos JG, Murphy FM, Rushing EJ. Radiologic-pathologic correlation: Hemangioblastoma. AJNR Am J Neuroradiol 1992;13: Kohno K, Matsui S, Nishizaki A, Takeda S, Sadamoto K, Sakaki S. Successful total removal of intramedullary hemangioblastoma from the medulla oblongata. Surg Neurol 1993;39: Kumar VA, Knopp EA, Zagzag D. Magnetic resonance dynamic susceptibilityweighted contrast-enhanced perfusion imaging in the diagnosis of posterior fossa hemangioblastomas and pilocytic astrocytomas: Initial results. J Comput Assist Tomogr 2010;34: Le Reste PJ, Henaux PL, Morandi X, Carsin-Nicol B, Brassier G, Riffaud L. Sporadic intracranial haemangioblastomas: Surgical outcome in a single institution series. Acta Neurochir 2013;155: Lee SR, Sanches J, Mark AS, Dillon WP, Norman D, Newton TH. Posterior fossa hemangioblastomas: MR imaging. Radiology 1989;171: Machein MR, Plate KH. VEGF in brain tumors. J Neurooncol 2000;50: Naik RT, Purohit AK, Dinakar I, Ratnakar KS. Hemangioblastoma of the IV ventricle. Childs Nerv Syst 1995;11: Nakamura N, Sekino H, Taguchi Y, Fuse T. Successful total extirpation of hemangioblastoma originating in the medulla oblongata. Surg Neurol 1985;24: Neumann HP, Eggert HR, Weigel K, Friedburg H, Wiestler OD, Schollmeyer P. Hemangioblastomas of the central nervous system. A 10-year study with special reference to von Hippel-Lindau syndrome. J Neurosurg 1989;70: Neumann HP, Wiestler OD. Von Hippel-Lindau disease: A syndrome providing insights into growth control and tumorigenesis. Nephrol Dial Transplant 1994;9: Neumann HP. Basic criteria for clinical diagnosis and genetic counseling in von Hippel-Lindau syndrome. Vasa 1987;16: Niemela M, Lemeta S, Summanen P, Bohling T, Sainio M, Kere J, et al. Long-term prognosis of haemangioblastoma of the CNS: Impact of von Hippel-Lindau disease. Acta Neurochir 1999;141: Niemela M, Lim YJ, Soderman M, Jaaskelainen J, Lindquist C. Gamma knife radiosurgery in 11 hemangioblastomas. J Neurosurg 1996;85: Nishimoto A, Kawakami Y. Surgical removal of hemangioblastoma in the fourth ventricle. Surg Neurol 1980;13: Padhi S, Sarangi R, Challa S, Bussary P, Panigrahi MK, Purohit AK. A 10-year retrospective study of hemangioblastomas of the central nervous system with reference to von Hippel-Lindau (VHL) disease. J Clin Neurosci 2011;18: Pan L, Wang EM, Wang BJ, Zhou LF, Zhang N, Cai PW, et al. Gamma knife radiosurgery for hemangioblastomas. Stereotact Funct Neurosurg 1998;70 Suppl 1: Peyre M, David P, Van Effenterre R, Francois P, Thys M, Emery E, et al. Natural history of supratentorial hemangioblastomas in von Hippel-Lindau disease. Neurosurgery 2010;67: Plate KH, Vortmeyer AO, Zagzag D, Neumann HPH. Von Hippel-Lindau disease and hemangioblastoma. In: Louis DN, Ohgaki H, Weistler OC, editors World Health Organization classification of tumors of the central nervous system. 4 th ed. Lyon: IARC Press; p Rachinger J, Buslei R, Prell J, Strauss C. Solid haemangioblastomas of the CNS: A review of 17 consecutive cases. Neurosurg Rev 2009;32: Resche F, Moisan JP, Mantoura J, de Kersaint-Gilly A, Andre MJ, Perrin-Resche I, et al. Haemangioblastoma, haemangioblastomatosis, and von Hippel-Lindau disease. Adv Tech Stand Neurosurg 1993;20: Russel DS, Rubinstein LJ. Pathology of tumors of the nervous system. 5 th ed. London: Arnold Publishers; Singounas EG. Haemangioblastomas of the central nervous system. Acta Neurochir 1978;44: Sora S, Ueki K, Saito N, Kawahara N, Shitara N, Kirino T. Incidence of von Hippel-Lindau disease in hemangioblastoma patients: The University of Tokyo Hospital experience from Acta Neurochir 2001;143: Spetzger U, Bertalanffy H, Huffmann B, Mayfrank L, Reul J, Gilsbach JM. Hemangioblastomas of the spinal cord and the brainstem: Diagnostic and therapeutic features. Neurosurg Rev 1996;19: Standard SC, Ahuja A, Livingston K, Guterman LR, Hopkins LN. Endovascular embolization and surgical excision for the treatment of cerebellar and brain stem hemangioblastomas. Surg Neurol 1994;41: Sundaram C, Rammurti S, Reddy JJ, Prasad SS, Purohit AK. Hemangioblastoma: A study of radiopathologic correlation. Neurol India 2003;51: Takeuchi S, Tanaka R, Fujii Y, Abe H, Ito Y. Surgical treatment of hemangioblastomas with presurgical endovascular embolization. Neurol Med Chir 2001;41: Thomas B, Somasundaram S, Thamburaj K, Kesavadas C, Gupta AK, Bodhey NK, et al Clinical applications of susceptibility weighted MR imaging of the brain - a pictorial review. Neuroradiology 2008;50: Tognetti F, Galassi E, Servadei F, Gaist G. Haemangioblastomas of the brain stem. Neurochirurgia 1986;29: Wanebo JE, Lonser RR, Glenn GM, Oldfield EH. The natural history of hemangioblastomas of the central nervous system in patients with von Hippel-Lindau disease. J Neurosurg 2003;98: Wang C, Zhang J, Liu A, Sun B. Surgical management of medullary hemangioblastoma. Report of 47 cases. Surg Neurol 2001;56: Weil RJ, Lonser RR, DeVroom HL, Wanebo JE, Oldfield EH. Surgical management of brainstem hemangioblastomas in patients with von Hippel- Lindau disease. J Neurosurg 2003;98: Yasargil MG, Antic J, Laciga R, de Preux J, Fideler RW, Boone SC. The microsurgical removal of intramedullary spinal hemangioblastomas. Report of twelve cases and a review of the literature. Surg Neurol 1976: Young S, Richardson AE. Solid haemangioblastomas of the posterior fossa: Radiological features and results of surgery. J Neurol Neurosurg Psychiatry 1987;50: Zhou LF. Intracranial epidermoid tumours: Thirty-seven years of diagnosis and treatment. Br J Neurosurg 1990;4: Zhou LF, Du G, Mao Y, Zhang R. Diagnosis and surgical treatment of brainstem hemangioblastomas. Surg Neurol 2005;63: Zimmermann M, Seifert V, Schreyer F, Stolke D, Dietz H. Hemangioblastoma: Description of a disease picture and report of 41 cases. Zentralbl Neurochir 1997;58: Zimny A, Sasiadek M. Contribution of perfusion-weighted magnetic resonance imaging in the differentiation of meningiomas and other extra-axial tumors: Case reports and literature review. J Neurooncol 2011;103:
The Natural History of Cerebellar Hemangioblastomas in von Hippel-Lindau Disease
 AJNR Am J Neuroradiol 24:1570 1574, September 2003 The Natural History of Cerebellar Hemangioblastomas in von Hippel-Lindau Disease Andrew Slater, Niall R. Moore, and Susan M. Huson BACKGROUND AND PURPOSE:
AJNR Am J Neuroradiol 24:1570 1574, September 2003 The Natural History of Cerebellar Hemangioblastomas in von Hippel-Lindau Disease Andrew Slater, Niall R. Moore, and Susan M. Huson BACKGROUND AND PURPOSE:
Clinical Factors Predicting Outcomes After Surgical Resection for Sporadic Cerebellar Hemangioblastomas
 Clinical Factors Predicting Outcomes After Surgical Resection for Sporadic Cerebellar Hemangioblastomas Masafumi Fukuda, Tetsuro Takao, Tetsuya Hiraishi, Junichi Yoshimura, Naoki Yajima, Akihiko Saito,
Clinical Factors Predicting Outcomes After Surgical Resection for Sporadic Cerebellar Hemangioblastomas Masafumi Fukuda, Tetsuro Takao, Tetsuya Hiraishi, Junichi Yoshimura, Naoki Yajima, Akihiko Saito,
Haemangioblastomas of the central nervous system in von Hippel Lindau Syndrome involving cerebellum and spinal cord
 Romanian Neurosurgery Volume XXXII Number 1 2018 January-March Article Haemangioblastomas of the central nervous system in von Hippel Lindau Syndrome involving cerebellum and spinal cord V.A. Kiran Kumar,
Romanian Neurosurgery Volume XXXII Number 1 2018 January-March Article Haemangioblastomas of the central nervous system in von Hippel Lindau Syndrome involving cerebellum and spinal cord V.A. Kiran Kumar,
Disclosures. Neurological Manifestations of Von Hippel Lindau Syndrome. Objectives. Overview. None No conflicts of interest
 Neurological Manifestations of Von Hippel Lindau Syndrome ARNOLD B. ETAME MD, PhD NEURO-ONCOLOGY/NEUROSURGERY Moffitt Cancer Center Disclosures None No conflicts of interest VHL Alliance Annual Family
Neurological Manifestations of Von Hippel Lindau Syndrome ARNOLD B. ETAME MD, PhD NEURO-ONCOLOGY/NEUROSURGERY Moffitt Cancer Center Disclosures None No conflicts of interest VHL Alliance Annual Family
Disseminated Hemangioblastoma of the Central Nervous System without Von Hippel-Lindau Disease
 CASE REPORT Brain Tumor Res Treat 2014;2(2):96-101 / pissn 2288-2405 / eissn 2288-2413 http://dx.doi.org/10.14791/btrt.2014.2.2.96 Disseminated Hemangioblastoma of the Central Nervous System without Von
CASE REPORT Brain Tumor Res Treat 2014;2(2):96-101 / pissn 2288-2405 / eissn 2288-2413 http://dx.doi.org/10.14791/btrt.2014.2.2.96 Disseminated Hemangioblastoma of the Central Nervous System without Von
G. Aksu, C. Ulutin, M. Fayda, M. Saynak Gulhane Military Faculty of Medicine, Department of Radiation Oncology, Ankara, Turkey CLINICAL CASE.
 Journal of BUON 10: 405-409, 2005 2005 Zerbinis Medical Publications. Printed in Greece CLINICAL CASE Cerebellar and multiple spinal hemangioblastomas and intraventricular meningioma managed with subtotal
Journal of BUON 10: 405-409, 2005 2005 Zerbinis Medical Publications. Printed in Greece CLINICAL CASE Cerebellar and multiple spinal hemangioblastomas and intraventricular meningioma managed with subtotal
ASJ. Microsurgical Treatment of Sporadic and von Hippel-Lindau Disease Associated Spinal Hemangioblastomas: A Single-Institution Experience
 Asian Spine Journal 548 Joe M. Das Clinical et al. Study Asian Spine J 217;11(4):548-555 https://doi.org/1.4184/asj.217.11.4.548 Asian Spine J 217;11(4):548-555 Microsurgical Treatment of Sporadic and
Asian Spine Journal 548 Joe M. Das Clinical et al. Study Asian Spine J 217;11(4):548-555 https://doi.org/1.4184/asj.217.11.4.548 Asian Spine J 217;11(4):548-555 Microsurgical Treatment of Sporadic and
Hemangioblastoma located in the posterior incisural space mimicking a tentorial meningioma: a case report
 Rabadán et al. Journal of Medical Case Reports (2016) 10:183 DOI 10.1186/s13256-016-0962-z CASE REPORT Open Access Hemangioblastoma located in the posterior incisural space mimicking a tentorial meningioma:
Rabadán et al. Journal of Medical Case Reports (2016) 10:183 DOI 10.1186/s13256-016-0962-z CASE REPORT Open Access Hemangioblastoma located in the posterior incisural space mimicking a tentorial meningioma:
Case Report Intracranial Capillary Hemangioma in the Posterior Fossa of an Adult Male
 Case Reports in Radiology Volume 2016, Article ID 6434623, 4 pages http://dx.doi.org/10.1155/2016/6434623 Case Report Intracranial Capillary Hemangioma in the Posterior Fossa of an Adult Male Jordan Nepute,
Case Reports in Radiology Volume 2016, Article ID 6434623, 4 pages http://dx.doi.org/10.1155/2016/6434623 Case Report Intracranial Capillary Hemangioma in the Posterior Fossa of an Adult Male Jordan Nepute,
Anaplastic Pilocytic Astrocytoma: The fusion of good and bad
 Anaplastic Pilocytic Astrocytoma: The fusion of good and bad Alexandrina Nikova 1, Charalampos-Chrysovalantis Chytoudis-Peroudis 2, Penelope Korkolopoulou 3 and Dimitrios Kanakis 4 Abstract 5 Pilocytic
Anaplastic Pilocytic Astrocytoma: The fusion of good and bad Alexandrina Nikova 1, Charalampos-Chrysovalantis Chytoudis-Peroudis 2, Penelope Korkolopoulou 3 and Dimitrios Kanakis 4 Abstract 5 Pilocytic
Multifocal central nervous system hemangioblastoma: a case report and review of the literature
 Multifocal central nervous system hemangioblastoma: a case report and review of the literature L.Z. Chu 1,3, Z.Z. Guan 1,2, J. Liu 3, H. Yang 3, X.L. Qi 2, M.G. Dong 3, Y.M. Chen 3, Y.N. Xiang 1 and Y.
Multifocal central nervous system hemangioblastoma: a case report and review of the literature L.Z. Chu 1,3, Z.Z. Guan 1,2, J. Liu 3, H. Yang 3, X.L. Qi 2, M.G. Dong 3, Y.M. Chen 3, Y.N. Xiang 1 and Y.
WHOLE SPECTRUM OF NATURAL PROGRESSION OF HAEMANGIOBLASTOMA SEEN WITHIN A SINGLE PATIENT: A VERY RARE CASE REPORT AND LITERATURE REVIEW
 WHOLE SPECTRUM OF NATURAL PROGRESSION OF HAEMANGIOBLASTOMA SEEN WITHIN A SINGLE PATIENT: A VERY RARE CASE REPORT AND LITERATURE REVIEW *Sunil Munakomi, Binod Bhattarai Department of Neurosurgery, College
WHOLE SPECTRUM OF NATURAL PROGRESSION OF HAEMANGIOBLASTOMA SEEN WITHIN A SINGLE PATIENT: A VERY RARE CASE REPORT AND LITERATURE REVIEW *Sunil Munakomi, Binod Bhattarai Department of Neurosurgery, College
Microsurgery for ruptured cerebellar arteriovenous malformations
 European Review for Medical and Pharmacological Sciences Microsurgery for ruptured cerebellar arteriovenous malformations S.-F. GONG 1,2, X.-B. WANG 1,3, Y.-Q. LIAO 1,2, T.-P. JIANG 1,2, J.-B. HE 1,2,
European Review for Medical and Pharmacological Sciences Microsurgery for ruptured cerebellar arteriovenous malformations S.-F. GONG 1,2, X.-B. WANG 1,3, Y.-Q. LIAO 1,2, T.-P. JIANG 1,2, J.-B. HE 1,2,
Integra Foundation Award: Long-term Natural History of Hemangioblastomas in von Hippel-Lindau Disease: Implications for Treatment
 CHAPTER 38 Integra Foundation Award: Long-term Natural History of Hemangioblastomas in von Hippel-Lindau Disease: Implications for Treatment Joshua M. Ammerman, M.D., Russell R. Lonser, M.D., James Dambrosia,
CHAPTER 38 Integra Foundation Award: Long-term Natural History of Hemangioblastomas in von Hippel-Lindau Disease: Implications for Treatment Joshua M. Ammerman, M.D., Russell R. Lonser, M.D., James Dambrosia,
Year 2003 Paper two: Questions supplied by Tricia
 question 43 A 42-year-old man presents with a two-year history of increasing right facial numbness. He has a history of intermittent unsteadiness, mild hearing loss and vertigo but has otherwise been well.
question 43 A 42-year-old man presents with a two-year history of increasing right facial numbness. He has a history of intermittent unsteadiness, mild hearing loss and vertigo but has otherwise been well.
CNS TUMORS. D r. Ali Eltayb ( U. of Omdurman. I ). M. Path (U. of Alexandria)
 CNS TUMORS D r. Ali Eltayb ( U. of Omdurman. I ). M. Path (U. of Alexandria) CNS TUMORS The annual incidence of intracranial tumors of the CNS ISmore than intraspinal tumors May be Primary or Secondary
CNS TUMORS D r. Ali Eltayb ( U. of Omdurman. I ). M. Path (U. of Alexandria) CNS TUMORS The annual incidence of intracranial tumors of the CNS ISmore than intraspinal tumors May be Primary or Secondary
Haemangioblastoma of the posterior cranial fossa: clinico-neuropathological study
 ORIGINAL ARTICLE Folia Neuropathol. Vol. 41, No. 4, pp. 245 249 Copyright 2003 Via Medica ISSN 1641 4640 Haemangioblastoma of the posterior cranial fossa: clinico-neuropathological study Teresa Wierzba-Bobrowicz
ORIGINAL ARTICLE Folia Neuropathol. Vol. 41, No. 4, pp. 245 249 Copyright 2003 Via Medica ISSN 1641 4640 Haemangioblastoma of the posterior cranial fossa: clinico-neuropathological study Teresa Wierzba-Bobrowicz
Hemorrhagic vestibular schwannoma: an unusual clinical entity Case report
 Neurosurg Focus 5 (3):Article 9, 1998 Hemorrhagic vestibular schwannoma: an unusual clinical entity Case report Dean Chou, M.D., Prakash Sampath, M.D., and Henry Brem, M.D. Departments of Neurological
Neurosurg Focus 5 (3):Article 9, 1998 Hemorrhagic vestibular schwannoma: an unusual clinical entity Case report Dean Chou, M.D., Prakash Sampath, M.D., and Henry Brem, M.D. Departments of Neurological
Intra-Fourth Ventricular Schwannoma With Obstructive Hydrocephalus A Rare Case Report
 ISPUB.COM The Internet Journal of Neurosurgery Volume 7 Number 1 Intra-Fourth Ventricular Schwannoma With Obstructive Hydrocephalus A Rare Case Report A Babbu, R Katheerayson Citation A Babbu, R Katheerayson..
ISPUB.COM The Internet Journal of Neurosurgery Volume 7 Number 1 Intra-Fourth Ventricular Schwannoma With Obstructive Hydrocephalus A Rare Case Report A Babbu, R Katheerayson Citation A Babbu, R Katheerayson..
Case Report Multiple Intracranial Meningiomas: A Review of the Literature and a Case Report
 Case Reports in Surgery Volume 2013, Article ID 131962, 4 pages http://dx.doi.org/10.1155/2013/131962 Case Report Multiple Intracranial Meningiomas: A Review of the Literature and a Case Report F. Koech,
Case Reports in Surgery Volume 2013, Article ID 131962, 4 pages http://dx.doi.org/10.1155/2013/131962 Case Report Multiple Intracranial Meningiomas: A Review of the Literature and a Case Report F. Koech,
SURGICAL MANAGEMENT OF BRAIN TUMORS
 SURGICAL MANAGEMENT OF BRAIN TUMORS LIGIA TATARANU, MD, Ph D NEUROSURGICAL CLINIC, BAGDASAR ARSENI CLINICAL HOSPITAL BUCHAREST, ROMANIA SURGICAL INDICATIONS CONFIRMING HISTOLOGIC DIAGNOSIS REDUCING TUMOR
SURGICAL MANAGEMENT OF BRAIN TUMORS LIGIA TATARANU, MD, Ph D NEUROSURGICAL CLINIC, BAGDASAR ARSENI CLINICAL HOSPITAL BUCHAREST, ROMANIA SURGICAL INDICATIONS CONFIRMING HISTOLOGIC DIAGNOSIS REDUCING TUMOR
Br a i n s t e m hemangioblastomas account for approximately
 J Neurosurg 114:1312 1318, 2011 Long-term outcome after resection of brainstem hemangioblastomas in von Hippel-Lindau disease Clinical article Jo s h u a J. Wi n d, M.D., 1,2 Ka m r a n D. Ba k h t i a
J Neurosurg 114:1312 1318, 2011 Long-term outcome after resection of brainstem hemangioblastomas in von Hippel-Lindau disease Clinical article Jo s h u a J. Wi n d, M.D., 1,2 Ka m r a n D. Ba k h t i a
Update on Pediatric Brain Tumors
 Update on Pediatric Brain Tumors David I. Sandberg, M.D. Director of Pediatric Neurosurgery & Associate Professor Dr. Marnie Rose Professorship in Pediatric Neurosurgery Pre-talk Questions for Audience
Update on Pediatric Brain Tumors David I. Sandberg, M.D. Director of Pediatric Neurosurgery & Associate Professor Dr. Marnie Rose Professorship in Pediatric Neurosurgery Pre-talk Questions for Audience
Otolaryngologist s Perspective of Stereotactic Radiosurgery
 Otolaryngologist s Perspective of Stereotactic Radiosurgery Douglas E. Mattox, M.D. 25 th Alexandria International Combined ORL Conference April 18-20, 2007 Acoustic Neuroma Benign tumor of the schwann
Otolaryngologist s Perspective of Stereotactic Radiosurgery Douglas E. Mattox, M.D. 25 th Alexandria International Combined ORL Conference April 18-20, 2007 Acoustic Neuroma Benign tumor of the schwann
Tumors of the Nervous System
 Tumors of the Nervous System Peter Canoll MD. PhD. What I want to cover What are the most common types of brain tumors? Who gets them? How do they present? What do they look like? How do they behave? 1
Tumors of the Nervous System Peter Canoll MD. PhD. What I want to cover What are the most common types of brain tumors? Who gets them? How do they present? What do they look like? How do they behave? 1
Original Article Surgical Management of Tentorial Meningiomas: Analysis of 14 Cases Experience
 Egyptian Journal of Neurosurgery Volume 29 / No. 1 / January - March 2014 39-44 Original Article Surgical Management of Tentorial Meningiomas: Analysis of 14 Cases Experience Ahmed M Zaater*, Mohamed I
Egyptian Journal of Neurosurgery Volume 29 / No. 1 / January - March 2014 39-44 Original Article Surgical Management of Tentorial Meningiomas: Analysis of 14 Cases Experience Ahmed M Zaater*, Mohamed I
THE EFFECTIVE OF BRAIN CANCER AND XAY BETWEEN THEORY AND IMPLEMENTATION. Mustafa Rashid Issa
 THE EFFECTIVE OF BRAIN CANCER AND XAY BETWEEN THEORY AND IMPLEMENTATION Mustafa Rashid Issa ABSTRACT: Illustrate malignant tumors that form either in the brain or in the nerves originating in the brain.
THE EFFECTIVE OF BRAIN CANCER AND XAY BETWEEN THEORY AND IMPLEMENTATION Mustafa Rashid Issa ABSTRACT: Illustrate malignant tumors that form either in the brain or in the nerves originating in the brain.
Original Article Remote cerebellar hemorrhage after microsurgical clipping of intracranial aneurysms: diagnosis and treatment a review of 13 cases
 Int J Clin Exp Med 2016;9(2):3681-3686 www.ijcem.com /ISSN:1940-5901/IJCEM0012155 Original Article Remote cerebellar hemorrhage after microsurgical clipping of intracranial aneurysms: diagnosis and treatment
Int J Clin Exp Med 2016;9(2):3681-3686 www.ijcem.com /ISSN:1940-5901/IJCEM0012155 Original Article Remote cerebellar hemorrhage after microsurgical clipping of intracranial aneurysms: diagnosis and treatment
The Use of Early Postoperative MR in Detecting Residual Juvenile Cerebellar Pilocytic Astrocytoma
 AJNR Am J Neuroradiol 19:151 156, January 1998 The Use of Early Postoperative MR in Detecting Residual Juvenile Cerebellar Pilocytic Astrocytoma Nancy K. Rollins, Perry Nisen, and Kenneth N. Shapiro PURPOSE:
AJNR Am J Neuroradiol 19:151 156, January 1998 The Use of Early Postoperative MR in Detecting Residual Juvenile Cerebellar Pilocytic Astrocytoma Nancy K. Rollins, Perry Nisen, and Kenneth N. Shapiro PURPOSE:
Brain AVM with Accompanying Venous Aneurysm with Intracerebral and Intraventricular Hemorrhage
 Cronicon OPEN ACCESS EC PAEDIATRICS Case Report Brain AVM with Accompanying Venous Aneurysm with Intracerebral and Intraventricular Hemorrhage Dimitrios Panagopoulos* Neurosurgical Department, University
Cronicon OPEN ACCESS EC PAEDIATRICS Case Report Brain AVM with Accompanying Venous Aneurysm with Intracerebral and Intraventricular Hemorrhage Dimitrios Panagopoulos* Neurosurgical Department, University
Rapid recurrence of a malignant meningioma: case report
 Romanian Neurosurgery Volume XXXI Number 2 2017 April-June Article Rapid recurrence of a malignant meningioma: case report Oguz Baran, Sima Sayyahmeli, Taner Tanriverdi, Pamir Erdincler TURKEY DOI: 10.1515/romneu-2017-0027
Romanian Neurosurgery Volume XXXI Number 2 2017 April-June Article Rapid recurrence of a malignant meningioma: case report Oguz Baran, Sima Sayyahmeli, Taner Tanriverdi, Pamir Erdincler TURKEY DOI: 10.1515/romneu-2017-0027
DIRECT SURGERY FOR INTRA-AXIAL
 Kitakanto Med. J. (S1) : 23 `28, 1998 23 DIRECT SURGERY FOR INTRA-AXIAL BRAINSTEM LESIONS Kazuhiko Kyoshima, Susumu Oikawa, Shigeaki Kobayashi Department of Neurosurgery, Shinshu University School of Medicine,
Kitakanto Med. J. (S1) : 23 `28, 1998 23 DIRECT SURGERY FOR INTRA-AXIAL BRAINSTEM LESIONS Kazuhiko Kyoshima, Susumu Oikawa, Shigeaki Kobayashi Department of Neurosurgery, Shinshu University School of Medicine,
Radiographic and statistical analysis of Brain Arteriovenous Malformations.
 Radiographic and statistical analysis of Brain Arteriovenous Malformations. Poster No.: C-0996 Congress: ECR 2017 Type: Educational Exhibit Authors: C. E. Rodriguez 1, A. Lopez Moreno 1, D. Sánchez Paré
Radiographic and statistical analysis of Brain Arteriovenous Malformations. Poster No.: C-0996 Congress: ECR 2017 Type: Educational Exhibit Authors: C. E. Rodriguez 1, A. Lopez Moreno 1, D. Sánchez Paré
Results of Surgery of Cerebellopontine angle Tumors
 Original Article Iranian Journal of Otorhinolaryngology, Vol. 27(1), Serial No.78, Jan 2015 Abstract Results of Surgery of Cerebellopontine angle Tumors Faramarz Memari 1, * Fatemeh Hassannia 1, Seyed
Original Article Iranian Journal of Otorhinolaryngology, Vol. 27(1), Serial No.78, Jan 2015 Abstract Results of Surgery of Cerebellopontine angle Tumors Faramarz Memari 1, * Fatemeh Hassannia 1, Seyed
Von Hippel Lindau Disease, Involvement of Multiple Members of the Same Families
 ORIGINAL ARTICLE Von Hippel Lindau Disease, Involvement of Multiple Members of the Same Families AMIR AZIZ, YASER-UD-DIN HOTI, KHURRAM ISHAQ Tariq Salah-ud-Din Department of Neurosurgery Unit II, Lahore
ORIGINAL ARTICLE Von Hippel Lindau Disease, Involvement of Multiple Members of the Same Families AMIR AZIZ, YASER-UD-DIN HOTI, KHURRAM ISHAQ Tariq Salah-ud-Din Department of Neurosurgery Unit II, Lahore
Essentials of Clinical MR, 2 nd edition. 51. Primary Neoplasms
 51. Primary Neoplasms As with spinal central canal neoplasms in other regions, those of the lumbar spine may be classified as extradural, intradural extramedullary, and medullary. If an extradural lesion
51. Primary Neoplasms As with spinal central canal neoplasms in other regions, those of the lumbar spine may be classified as extradural, intradural extramedullary, and medullary. If an extradural lesion
Surgical management of brainstem hemangioblastomas in patients with von Hippel Lindau disease
 J Neurosurg 98:95 105, 2003 Surgical management of brainstem hemangioblastomas in patients with von Hippel Lindau disease ROBERT J. WEIL, M.D., RUSSELL R. LONSER, M.D., HETTY L. DEVROOM, R.N., JOHN E.
J Neurosurg 98:95 105, 2003 Surgical management of brainstem hemangioblastomas in patients with von Hippel Lindau disease ROBERT J. WEIL, M.D., RUSSELL R. LONSER, M.D., HETTY L. DEVROOM, R.N., JOHN E.
Original Article CT grouping and microsurgical treatment strategies of hypertensive cerebellar hemorrhage
 Int J Clin Exp Med 2016;9(8):15921-15927 www.ijcem.com /ISSN:1940-5901/IJCEM0022273 Original Article CT grouping and microsurgical treatment strategies of hypertensive cerebellar hemorrhage Xielin Tang
Int J Clin Exp Med 2016;9(8):15921-15927 www.ijcem.com /ISSN:1940-5901/IJCEM0022273 Original Article CT grouping and microsurgical treatment strategies of hypertensive cerebellar hemorrhage Xielin Tang
Surgical treatment of cerebellar hemangioblastomas
 SNI: Neurovascular OPEN ACCESS For entire Editorial Board visit : http://www.surgicalneurologyint.com Editor: Kazuhiro Hongo, M.D., Shinsui University, Matsomoto, Japan Original Article Surgical treatment
SNI: Neurovascular OPEN ACCESS For entire Editorial Board visit : http://www.surgicalneurologyint.com Editor: Kazuhiro Hongo, M.D., Shinsui University, Matsomoto, Japan Original Article Surgical treatment
BRAIN & SPINAL LESIONS: NOT JUST A SCIENCE. Rimas V. Lukas, MD Associate Professor Director of Medical Neuro-Oncology University of Chicago
 BRAIN & SPINAL LESIONS: NOT JUST A SCIENCE Rimas V. Lukas, MD Associate Professor Director of Medical Neuro-Oncology University of Chicago OVERVIEW Background Clinical Presentation Clinical Management
BRAIN & SPINAL LESIONS: NOT JUST A SCIENCE Rimas V. Lukas, MD Associate Professor Director of Medical Neuro-Oncology University of Chicago OVERVIEW Background Clinical Presentation Clinical Management
MINERVA MEDICA COPYRIGHT
 ORIGINAL ARTICLES J NEUROSURG SCI 2008;52:29-36 Neurosurgical treatment of von Hippel-Lindau-associated hemangioblastomas: benefits, risks and outcome G. PAVESI 1, A. FELETTI 2, S. BERLUCCHI 1, G. OPOCHER
ORIGINAL ARTICLES J NEUROSURG SCI 2008;52:29-36 Neurosurgical treatment of von Hippel-Lindau-associated hemangioblastomas: benefits, risks and outcome G. PAVESI 1, A. FELETTI 2, S. BERLUCCHI 1, G. OPOCHER
Original Research Article
 Original Research Article Study Determining Correlation between Histopathological Diagnosis and MRI Findings of Posterior Fossa Tumors Srinivasarao S. Gummadidala 1, B. Jyothi 2 1 Assistant Professor,
Original Research Article Study Determining Correlation between Histopathological Diagnosis and MRI Findings of Posterior Fossa Tumors Srinivasarao S. Gummadidala 1, B. Jyothi 2 1 Assistant Professor,
NEURORADIOLOGY-NEUROPATHOLOGY CONFERENCE
 THE UNIVERSITY OF NORTH CAROLINA at CHAPEL HILL SEPTEMBER 2013 NEURORADIOLOGY-NEUROPATHOLOGY CONFERENCE Claudia da Costa Leite, MD, PhD Thomas Bouldin, MD CASE 1 6 y-o female with headaches and vomiting
THE UNIVERSITY OF NORTH CAROLINA at CHAPEL HILL SEPTEMBER 2013 NEURORADIOLOGY-NEUROPATHOLOGY CONFERENCE Claudia da Costa Leite, MD, PhD Thomas Bouldin, MD CASE 1 6 y-o female with headaches and vomiting
FOR PUBLIC CONSULTATION ONLY STEREOTACTIC RADIOSURGERY/ STEROTACTIC RADIOTHERAPY FOR HAEMANGIOBLASTOMA
 1 EVIDENCE SUMMARY REPORT FOR PUBLIC CONSULTATION ONLY STEREOTACTIC RADIOSURGERY/ STEROTACTIC RADIOTHERAPY FOR HAEMANGIOBLASTOMA QUESTIONS TO BE ADDRESSED: 1. What is the evidence for the clinical effectiveness
1 EVIDENCE SUMMARY REPORT FOR PUBLIC CONSULTATION ONLY STEREOTACTIC RADIOSURGERY/ STEROTACTIC RADIOTHERAPY FOR HAEMANGIOBLASTOMA QUESTIONS TO BE ADDRESSED: 1. What is the evidence for the clinical effectiveness
Selected radiosurgery cases from the Rotating Gamma Institute Debrecen, Hungary
 Selected radiosurgery cases from the Rotating Gamma Institute Debrecen, Hungary László Bognár M.D., Ph.D., József G. Dobai M.D., Gábor Csiky and Imre Fedorcsák M.D., Ph.D. Department of Neurosurgery, Medical
Selected radiosurgery cases from the Rotating Gamma Institute Debrecen, Hungary László Bognár M.D., Ph.D., József G. Dobai M.D., Gábor Csiky and Imre Fedorcsák M.D., Ph.D. Department of Neurosurgery, Medical
10/11/2018. Disclosures TOC. von Hippel-Lindau disease. CNS correlations
 Disclosures CLINICAL DEBATE: Optimal Treatment of Hemangioblastomas Ashok R. Asthagiri, MD Ian McCutcheon, MD TOC Background ELST Asymptomatic growth Peritumoral edema Pregnancy Radiosurgery Difficult
Disclosures CLINICAL DEBATE: Optimal Treatment of Hemangioblastomas Ashok R. Asthagiri, MD Ian McCutcheon, MD TOC Background ELST Asymptomatic growth Peritumoral edema Pregnancy Radiosurgery Difficult
Astroblastoma: Radiologic-Pathologic Correlation and Distinction from Ependymoma
 AJNR Am J Neuroradiol 23:243 247, February 2002 Case Report Astroblastoma: Radiologic-Pathologic Correlation and Distinction from Ependymoma John D. Port, Daniel J. Brat, Peter C. Burger, and Martin G.
AJNR Am J Neuroradiol 23:243 247, February 2002 Case Report Astroblastoma: Radiologic-Pathologic Correlation and Distinction from Ependymoma John D. Port, Daniel J. Brat, Peter C. Burger, and Martin G.
Neurosurgery Review. Mudit Sharma, MD May 16 th, 2008
 Neurosurgery Review Mudit Sharma, MD May 16 th, 2008 Dr. Mudit Sharma, Neurosurgeon Manassas, Fredericksburg, Virginia http://www.virginiaspinespecialists.com Phone: 1-855-SPINE FIX (774-6334) Fundamentals
Neurosurgery Review Mudit Sharma, MD May 16 th, 2008 Dr. Mudit Sharma, Neurosurgeon Manassas, Fredericksburg, Virginia http://www.virginiaspinespecialists.com Phone: 1-855-SPINE FIX (774-6334) Fundamentals
Diagnostic and Therapeutic Consequences of Repeat Brain Imaging and Follow-up Vascular Imaging in Stroke Patients
 AJNR Am J Neuroradiol 0:7, January 999 Diagnostic and Therapeutic Consequences of Repeat Brain Imaging and Follow-up Vascular Imaging in Stroke Patients Birgit Ertl-Wagner, Tobias Brandt, Christina Seifart,
AJNR Am J Neuroradiol 0:7, January 999 Diagnostic and Therapeutic Consequences of Repeat Brain Imaging and Follow-up Vascular Imaging in Stroke Patients Birgit Ertl-Wagner, Tobias Brandt, Christina Seifart,
HEAD AND NECK IMAGING. James Chen (MS IV)
 HEAD AND NECK IMAGING James Chen (MS IV) Anatomy Course Johns Hopkins School of Medicine Sept. 27, 2011 OBJECTIVES Introduce cross sectional imaging of head and neck Computed tomography (CT) Review head
HEAD AND NECK IMAGING James Chen (MS IV) Anatomy Course Johns Hopkins School of Medicine Sept. 27, 2011 OBJECTIVES Introduce cross sectional imaging of head and neck Computed tomography (CT) Review head
General: Brain tumors are lesions that have mass effect distorting the normal tissue and often result in increased intracranial pressure.
 1 Lecture Objectives Know the histologic features of the most common tumors of the CNS. Know the differences in behavior of the different tumor types. Be aware of the treatment modalities in the various
1 Lecture Objectives Know the histologic features of the most common tumors of the CNS. Know the differences in behavior of the different tumor types. Be aware of the treatment modalities in the various
Infratentorial and Intraparenchymal Subependymoma in the Cerebellum: Case Report
 Case Report Neuroimaging and Head and Neck http://dx.doi.org/10.3348/kjr.2014.15.1.151 pissn 1229-6929 eissn 2005-8330 Korean J Radiol 2014;15(1):151-155 Infratentorial and Intraparenchymal Subependymoma
Case Report Neuroimaging and Head and Neck http://dx.doi.org/10.3348/kjr.2014.15.1.151 pissn 1229-6929 eissn 2005-8330 Korean J Radiol 2014;15(1):151-155 Infratentorial and Intraparenchymal Subependymoma
Brain tumors: tumor types
 Brain tumors: tumor types Tumor types There are more than 120 types of brain tumors. Today, most medical institutions use the World Health Organization (WHO) classification system to identify brain tumors.
Brain tumors: tumor types Tumor types There are more than 120 types of brain tumors. Today, most medical institutions use the World Health Organization (WHO) classification system to identify brain tumors.
INTRACRANIAL ARACHNOID CYSTS: CLASSIFICATION AND MANAGEMENT. G. Tamburrini, Rome
 INTRACRANIAL ARACHNOID CYSTS: CLASSIFICATION AND MANAGEMENT G. Tamburrini, Rome Incidence 2% of occasional neuroradiological findings From clinical studies (1960 s): 0.4-1% of intracranial space occupying
INTRACRANIAL ARACHNOID CYSTS: CLASSIFICATION AND MANAGEMENT G. Tamburrini, Rome Incidence 2% of occasional neuroradiological findings From clinical studies (1960 s): 0.4-1% of intracranial space occupying
Spinal Cord Hemangioblastomas in von Hippel-Lindau Disease: Management of Asymptomatic and Symptomatic Tumors
 Original Article http://dx.doi.org/10.3349/ymj.2012.53.6.1073 pissn: 0513-5796, eissn: 1976-2437 Yonsei Med J 53(6):1073-1080, 2012 Spinal Cord Hemangioblastomas in von Hippel-Lindau Disease: Management
Original Article http://dx.doi.org/10.3349/ymj.2012.53.6.1073 pissn: 0513-5796, eissn: 1976-2437 Yonsei Med J 53(6):1073-1080, 2012 Spinal Cord Hemangioblastomas in von Hippel-Lindau Disease: Management
NON MALIGNANT BRAIN TUMOURS Facilitator. Ros Taylor Advanced Neurosurgical Nurse Practitioner Southmead Hospital Bristol
 NON MALIGNANT BRAIN TUMOURS Facilitator Ros Taylor Advanced Neurosurgical Nurse Practitioner Southmead Hospital Bristol Neurosurgery What will be covered? Meningioma Vestibular schwannoma (acoustic neuroma)
NON MALIGNANT BRAIN TUMOURS Facilitator Ros Taylor Advanced Neurosurgical Nurse Practitioner Southmead Hospital Bristol Neurosurgery What will be covered? Meningioma Vestibular schwannoma (acoustic neuroma)
Update on IGKRF Activities
 Stereotactic radiosurgery research, education and publishing for the purpose of improving public health Fall 2016 In this issue: Update on IGKRF Activities The IGKRF Recently Published Articles Topics
Stereotactic radiosurgery research, education and publishing for the purpose of improving public health Fall 2016 In this issue: Update on IGKRF Activities The IGKRF Recently Published Articles Topics
Case Report Complex Form Variant of Dysembryoplastic Neuroepithelial Tumor of the Cerebellum
 Case Reports in Pathology Volume 2012, Article ID 718651, 4 pages doi:10.1155/2012/718651 Case Report Complex Form Variant of Dysembryoplastic Neuroepithelial Tumor of the Cerebellum Jesús Vaquero, 1,
Case Reports in Pathology Volume 2012, Article ID 718651, 4 pages doi:10.1155/2012/718651 Case Report Complex Form Variant of Dysembryoplastic Neuroepithelial Tumor of the Cerebellum Jesús Vaquero, 1,
Primary intracranial malignant melanoma: A case with review of literature
 ISSN (print form): 25931431 Primary intracranial malignant melanoma: A case with review of literature K.SAHRAOUI 1, M.A KAIM 2, K.BOUYOUCEF 3 ABSTRACT Introduction: Primary intracranial melanoma is an
ISSN (print form): 25931431 Primary intracranial malignant melanoma: A case with review of literature K.SAHRAOUI 1, M.A KAIM 2, K.BOUYOUCEF 3 ABSTRACT Introduction: Primary intracranial melanoma is an
CT & MRI Evaluation of Brain Tumour & Tumour like Conditions
 CT & MRI Evaluation of Brain Tumour & Tumour like Conditions Dr. Anjana Trivedi 1, Dr. Jay Thakkar 2, Dr. Maulik Jethva 3, Dr. Ishita Virda 4 1 M.D. Radiology, Professor and Head, P.D.U. Medical College
CT & MRI Evaluation of Brain Tumour & Tumour like Conditions Dr. Anjana Trivedi 1, Dr. Jay Thakkar 2, Dr. Maulik Jethva 3, Dr. Ishita Virda 4 1 M.D. Radiology, Professor and Head, P.D.U. Medical College
Nature and Science 2017;15(7) Surgical Options for Treatment of Posterior Fossa Tumors with Hydrocephalus
 Surgical Options for Treatment of Posterior Fossa Tumors with Hydrocephalus Mohamed Mahmoud Abohashima; Ahmed Mohamed Hasan Salem; Magdy Asaad El-Hawary Neurosurgery department, Faculty of Medicine, Al-azhar
Surgical Options for Treatment of Posterior Fossa Tumors with Hydrocephalus Mohamed Mahmoud Abohashima; Ahmed Mohamed Hasan Salem; Magdy Asaad El-Hawary Neurosurgery department, Faculty of Medicine, Al-azhar
Peter Canoll MD. PhD.
 Tumors of the Nervous System Peter Canoll MD. PhD. What I want to cover What are the most common types of brain tumors? Who gets them? How do they ypresent? What do they look like? How do they behave?
Tumors of the Nervous System Peter Canoll MD. PhD. What I want to cover What are the most common types of brain tumors? Who gets them? How do they ypresent? What do they look like? How do they behave?
Supratentorial cerebral arteriovenous malformations : a clinical analysis
 Original article: Supratentorial cerebral arteriovenous malformations : a clinical analysis Dr. Rajneesh Gour 1, Dr. S. N. Ghosh 2, Dr. Sumit Deb 3 1Dept.Of Surgery,Chirayu Medical College & Research Centre,
Original article: Supratentorial cerebral arteriovenous malformations : a clinical analysis Dr. Rajneesh Gour 1, Dr. S. N. Ghosh 2, Dr. Sumit Deb 3 1Dept.Of Surgery,Chirayu Medical College & Research Centre,
Impact of Gamma Knife Radiosurgery on the neurosurgical management of skull-base lesions: The Combined Approach
 Radiosurgery as part of the neurosurgical armamentarium: Educational Symposium November 24 th 2011 Impact of Gamma Knife Radiosurgery on the neurosurgical management of skull-base lesions: The Combined
Radiosurgery as part of the neurosurgical armamentarium: Educational Symposium November 24 th 2011 Impact of Gamma Knife Radiosurgery on the neurosurgical management of skull-base lesions: The Combined
Case 7391 Intraventricular Lesion
 Case 7391 Intraventricular Lesion Bastos Lima P1, Marques C1, Cabrita F2, Barbosa M2, Rebelo O3, Rio F1. 1Neuroradiology, 2Neurosurgery, 3Neuropathology, Coimbra University Hospitals, Portugal. University
Case 7391 Intraventricular Lesion Bastos Lima P1, Marques C1, Cabrita F2, Barbosa M2, Rebelo O3, Rio F1. 1Neuroradiology, 2Neurosurgery, 3Neuropathology, Coimbra University Hospitals, Portugal. University
Brainstem diffuse gliomas: radiologic findings.
 Brainstem diffuse gliomas: radiologic findings. Poster No.: C-2220 Congress: ECR 2013 Type: Educational Exhibit Authors: E. GARCIA MARTINEZ 1, D. H. Jiménez 1, L. Navarro Vilar 2, C. P. Fernandez Ruiz
Brainstem diffuse gliomas: radiologic findings. Poster No.: C-2220 Congress: ECR 2013 Type: Educational Exhibit Authors: E. GARCIA MARTINEZ 1, D. H. Jiménez 1, L. Navarro Vilar 2, C. P. Fernandez Ruiz
Pathologic Analysis of CNS Surgical Specimens
 2015 Kenneth M. Earle Memorial Neuropathology Review Pathologic Analysis of CNS Surgical Specimens Peter C. Burger, MD Interdisciplinary Quality Control Familiarity with entities Use of diagnostic algorithm
2015 Kenneth M. Earle Memorial Neuropathology Review Pathologic Analysis of CNS Surgical Specimens Peter C. Burger, MD Interdisciplinary Quality Control Familiarity with entities Use of diagnostic algorithm
Meningioma tumor. Meningiomas are named according to their location (Fig. 1) and cause various symptoms: > 1
 Meningioma tumor Overview A meningioma is a type of tumor that grows from the protective membranes, called meninges, which surround the brain and spinal cord. Most meningiomas are benign (not cancer) and
Meningioma tumor Overview A meningioma is a type of tumor that grows from the protective membranes, called meninges, which surround the brain and spinal cord. Most meningiomas are benign (not cancer) and
Pancreatic Involvement in Von Hippel-Lindau Disease: The Role of Integrated Imaging
 MULTIMEDIA ARTICLE - Clinical Imaging Pancreatic Involvement in Von Hippel-Lindau Disease: The Role of Integrated Imaging Lucia Calculli 1, Marta Fiscaletti 1, Riccardo Casadei 2, Raffaele Pezzilli 3,
MULTIMEDIA ARTICLE - Clinical Imaging Pancreatic Involvement in Von Hippel-Lindau Disease: The Role of Integrated Imaging Lucia Calculli 1, Marta Fiscaletti 1, Riccardo Casadei 2, Raffaele Pezzilli 3,
Nicolas Bianchi M.D. May 15th, 2012
 Nicolas Bianchi M.D. May 15th, 2012 New concepts in TIA Differential Diagnosis Stroke Syndromes To learn the new definitions and concepts on TIA as a condition of high risk for stroke. To recognize the
Nicolas Bianchi M.D. May 15th, 2012 New concepts in TIA Differential Diagnosis Stroke Syndromes To learn the new definitions and concepts on TIA as a condition of high risk for stroke. To recognize the
Introduction to Neurosurgical Subspecialties:
 Introduction to Neurosurgical Subspecialties: Tumor and Skull Base Neurosurgery Brian L. Hoh, MD 1 and Gregory J. Zipfel, MD 2 1 University of Florida, 2 Washington University Tumor / Skull Base Neurosurgery
Introduction to Neurosurgical Subspecialties: Tumor and Skull Base Neurosurgery Brian L. Hoh, MD 1 and Gregory J. Zipfel, MD 2 1 University of Florida, 2 Washington University Tumor / Skull Base Neurosurgery
Case Report Optic Nerve Hemangioblastoma: A Case Report
 Case Reports in Pathology Volume 2012, Article ID 915408, 4 pages doi:10.1155/2012/915408 Case Report Optic Nerve Hemangioblastoma: A Case Report Holly Zywicke, 1 Cheryl Ann Palmer, 2 Michael S. Vaphiades,
Case Reports in Pathology Volume 2012, Article ID 915408, 4 pages doi:10.1155/2012/915408 Case Report Optic Nerve Hemangioblastoma: A Case Report Holly Zywicke, 1 Cheryl Ann Palmer, 2 Michael S. Vaphiades,
Posterior fossa tumors: clues to differential diagnosis with case-based review
 Posterior fossa tumors: clues to differential diagnosis with case-based review Poster No.: C-0323 Congress: ECR 2017 Type: Educational Exhibit Authors: H. A. Aboughalia, M. Abdelhady; Doha/QA Keywords:
Posterior fossa tumors: clues to differential diagnosis with case-based review Poster No.: C-0323 Congress: ECR 2017 Type: Educational Exhibit Authors: H. A. Aboughalia, M. Abdelhady; Doha/QA Keywords:
Dr. T. Venkat Kishan Asst. Prof Department of Radiodiagnosis
 Dr. T. Venkat Kishan Asst. Prof Department of Radiodiagnosis Schwannomas (also called neurinomas or neurilemmomas) constitute the most common primary cranial nerve tumors. They are benign slow-growing
Dr. T. Venkat Kishan Asst. Prof Department of Radiodiagnosis Schwannomas (also called neurinomas or neurilemmomas) constitute the most common primary cranial nerve tumors. They are benign slow-growing
What Every Spine Surgeon Should Know About Neurosurgical Issues
 What Every Spine Surgeon Should Know About Neurosurgical Issues Amer Samdani, MD Chief of Surgery Shriners Hospitals for Children Philadelphia, PA Objectives Main intraspinal lesions Chiari malformation
What Every Spine Surgeon Should Know About Neurosurgical Issues Amer Samdani, MD Chief of Surgery Shriners Hospitals for Children Philadelphia, PA Objectives Main intraspinal lesions Chiari malformation
Cystic Meningioma in the Inter-Hemisferic Space Location
 Case Cystic Meningioma in the Inter-Hemisferic Space Location Muhammad Zafrullah Arifin, Firman Priguna Tjahjono, Agung Budi Sutiono, Ahmad Faried Department of Neurosurgery, Faculty of Medicine, Universitas
Case Cystic Meningioma in the Inter-Hemisferic Space Location Muhammad Zafrullah Arifin, Firman Priguna Tjahjono, Agung Budi Sutiono, Ahmad Faried Department of Neurosurgery, Faculty of Medicine, Universitas
SUCCESSFUL TREATMENT OF METASTATIC BRAIN TUMOR BY CYBERKNIFE: A CASE REPORT
 SUCCESSFUL TREATMENT OF METASTATIC BRAIN TUMOR BY CYBERKNIFE: A CASE REPORT Cheng-Ta Hsieh, 1 Cheng-Fu Chang, 1 Ming-Ying Liu, 1 Li-Ping Chang, 2 Dueng-Yuan Hueng, 3 Steven D. Chang, 4 and Da-Tong Ju 1
SUCCESSFUL TREATMENT OF METASTATIC BRAIN TUMOR BY CYBERKNIFE: A CASE REPORT Cheng-Ta Hsieh, 1 Cheng-Fu Chang, 1 Ming-Ying Liu, 1 Li-Ping Chang, 2 Dueng-Yuan Hueng, 3 Steven D. Chang, 4 and Da-Tong Ju 1
Case Report Suprasellar hemangioblastoma without von Hippel-Lindau disease: a case report and literature review
 Int J Clin Exp Pathol 2015;8(6):7553-7558 www.ijcep.com /ISSN:1936-2625/IJCEP0008755 Case Report Suprasellar hemangioblastoma without von Hippel-Lindau disease: a case report and literature review Zhen
Int J Clin Exp Pathol 2015;8(6):7553-7558 www.ijcep.com /ISSN:1936-2625/IJCEP0008755 Case Report Suprasellar hemangioblastoma without von Hippel-Lindau disease: a case report and literature review Zhen
Intra-cranial malignant peripheral nerve sheath tumor of olfactory nerve: a case report and review of literature
 DOI: 10.2478/romneu-2018-0059 Article Intra-cranial malignant peripheral nerve sheath tumor of olfactory nerve: a case report and review of literature Varun Aggarwal, Amit Narang, Chandni Maheshwari, Divya
DOI: 10.2478/romneu-2018-0059 Article Intra-cranial malignant peripheral nerve sheath tumor of olfactory nerve: a case report and review of literature Varun Aggarwal, Amit Narang, Chandni Maheshwari, Divya
Radiologic Evaluation of Petrous Apex Masses. Pavan Kavali, MS-IV Morehouse School of Medicine November 16, 2009
 Radiologic Evaluation of Petrous Apex Masses Pavan Kavali, MS-IV Morehouse School of Medicine November 16, 2009 Roadmap Petrous Apex Anatomy Patient D.S.: Clinical Presentation Differential diagnosis of
Radiologic Evaluation of Petrous Apex Masses Pavan Kavali, MS-IV Morehouse School of Medicine November 16, 2009 Roadmap Petrous Apex Anatomy Patient D.S.: Clinical Presentation Differential diagnosis of
Chiari Malformations. Google. Objectives Seventh Annual NKY TBI Conference 3/22/13. Kerry R. Crone, M.D.
 Chiari Malformations Kerry R. Crone, M.D. Professor of Neurosurgery and Pediatrics University of Cincinnati College of Medicine University of Cincinnati Medical Center Cincinnati Children s Hospital Medical
Chiari Malformations Kerry R. Crone, M.D. Professor of Neurosurgery and Pediatrics University of Cincinnati College of Medicine University of Cincinnati Medical Center Cincinnati Children s Hospital Medical
Neuro-oncology Update Andrew Kokkino, MD Medical Director, The Neurosciences Institute at Sacred Heart at Riverbend May 20, 2013
 Neuro-oncology Update 2013 Andrew Kokkino, MD Medical Director, The Neurosciences Institute at Sacred Heart at Riverbend May 20, 2013 Case 1 58 year old man with recent facial droop and HA s Thin, cachectic
Neuro-oncology Update 2013 Andrew Kokkino, MD Medical Director, The Neurosciences Institute at Sacred Heart at Riverbend May 20, 2013 Case 1 58 year old man with recent facial droop and HA s Thin, cachectic
HAEMANGIOBLASTOMA CASE REPORT
 HAEMANGIOBLASTOMA Pages with reference to book, From 113 To 115 Saleem Sadiq, K.C. Kyriacou ( Department of Pathology, College of Medicine, King Saud University, Riyadh, Saudi Arabia. ) Z.B. Jamjoom (
HAEMANGIOBLASTOMA Pages with reference to book, From 113 To 115 Saleem Sadiq, K.C. Kyriacou ( Department of Pathology, College of Medicine, King Saud University, Riyadh, Saudi Arabia. ) Z.B. Jamjoom (
Case Report Malignant Transformation Six Months after Removal of Intracranial Epidermoid Cyst: A Case Report
 Case Reports in Neurological Medicine Volume 2011, Article ID 525289, 4 pages doi:10.1155/2011/525289 Case Report Malignant Transformation Six Months after Removal of Intracranial Epidermoid Cyst: A Case
Case Reports in Neurological Medicine Volume 2011, Article ID 525289, 4 pages doi:10.1155/2011/525289 Case Report Malignant Transformation Six Months after Removal of Intracranial Epidermoid Cyst: A Case
Brain and Spine Tumors
 Brain and Spine Tumors Andrew J. Fabiano, MD FAANS Associate Professor of Neurosurgery Roswell Park Cancer Institute SUNY at Buffalo School of Medicine Brain Tumors Brain Tumor Basics Types of Tumors Cases
Brain and Spine Tumors Andrew J. Fabiano, MD FAANS Associate Professor of Neurosurgery Roswell Park Cancer Institute SUNY at Buffalo School of Medicine Brain Tumors Brain Tumor Basics Types of Tumors Cases
Magnetic Resonance Imaging. Basics of MRI in practice. Generation of MR signal. Generation of MR signal. Spin echo imaging. Generation of MR signal
 Magnetic Resonance Imaging Protons aligned with B0 magnetic filed Longitudinal magnetization - T1 relaxation Transverse magnetization - T2 relaxation Signal measured in the transverse plane Basics of MRI
Magnetic Resonance Imaging Protons aligned with B0 magnetic filed Longitudinal magnetization - T1 relaxation Transverse magnetization - T2 relaxation Signal measured in the transverse plane Basics of MRI
Management of pediatric brain tumors, strategies and long term outcome
 Management of pediatric brain tumors, strategies and long term outcome SAN The Sudanese association of neurosurgeons By Dr. Abubakr Darrag Salim Ahmed Dr. Mohammed Awad Elzain Khartoum Sudan Pediatric
Management of pediatric brain tumors, strategies and long term outcome SAN The Sudanese association of neurosurgeons By Dr. Abubakr Darrag Salim Ahmed Dr. Mohammed Awad Elzain Khartoum Sudan Pediatric
10/11/2018. Clinical and Surgical Management of VHL-Related Cysts and Cystic RCC. Outline. VHL Renal Manifestations. VHL Renal Manifestations
 Outline Clinical and Surgical Management of VHL-Related Cysts and Cystic RCC Mark W. Ball, MD Assistant Research Physician Attending Surgeon Urologic Oncology Branch, National Cancer Institute Prevalence
Outline Clinical and Surgical Management of VHL-Related Cysts and Cystic RCC Mark W. Ball, MD Assistant Research Physician Attending Surgeon Urologic Oncology Branch, National Cancer Institute Prevalence
Temporal Lobe Cystic Collection and Associated Oedema: A Rare Complication of Translabyrinthine Resection of Vestibular Schwannoma
 Open Access Case Report DOI: 10.7759/cureus.2217 Temporal Lobe Cystic Collection and Associated Oedema: A Rare Complication of Translabyrinthine Resection of Vestibular Schwannoma Abdurrahman Raeiq 1 1.
Open Access Case Report DOI: 10.7759/cureus.2217 Temporal Lobe Cystic Collection and Associated Oedema: A Rare Complication of Translabyrinthine Resection of Vestibular Schwannoma Abdurrahman Raeiq 1 1.
Renal Cell Carcinoma: Genetics & Imaging Srinivasa R Prasad University of Texas San Antonio
 Renal Cell Carcinoma: Genetics & Imaging Srinivasa R Prasad University of Texas HSC @ San Antonio No financial disclosures Acknowledgements Dr. Peter Choyke, NIH My Gurus @ MIR, MGH 2004 WHO Taxonomy of
Renal Cell Carcinoma: Genetics & Imaging Srinivasa R Prasad University of Texas HSC @ San Antonio No financial disclosures Acknowledgements Dr. Peter Choyke, NIH My Gurus @ MIR, MGH 2004 WHO Taxonomy of
STUDY OFPAEDIATRIC CNS TUMORS IN TERTIARY CARE CENTER
 IJCRR Section: Healthcare Sci. Journal Impact Factor 4.016 Original Article STUDY OFPAEDIATRIC CNS TUMORS IN TERTIARY CARE CENTER Grishma P. Jobanputra Tutor, Department of Pathology, B.J. Medical College,
IJCRR Section: Healthcare Sci. Journal Impact Factor 4.016 Original Article STUDY OFPAEDIATRIC CNS TUMORS IN TERTIARY CARE CENTER Grishma P. Jobanputra Tutor, Department of Pathology, B.J. Medical College,
Oligodendroglioma: imaging findings, radio-pathological correlation and evolution
 Oligodendroglioma: imaging findings, radio-pathological correlation and evolution Poster No.: C-2104 Congress: ECR 2013 Type: Authors: Keywords: DOI: Scientific Exhibit A. Hernandez Castro, M. D. Monedero
Oligodendroglioma: imaging findings, radio-pathological correlation and evolution Poster No.: C-2104 Congress: ECR 2013 Type: Authors: Keywords: DOI: Scientific Exhibit A. Hernandez Castro, M. D. Monedero
Untangling Cerebral Dural Arteriovenous Fistulas
 Untangling Cerebral Dural Arteriovenous Fistulas Bradley A. Gross, MD Assistant Professor, Dept of Neurosurgery, University of Pittsburgh September 2017 davfs Definition Clinical Presentation Natural History
Untangling Cerebral Dural Arteriovenous Fistulas Bradley A. Gross, MD Assistant Professor, Dept of Neurosurgery, University of Pittsburgh September 2017 davfs Definition Clinical Presentation Natural History
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES
 PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES CENTRAL NERVOUS SYSTEM MEDULLOBLASTOMA AND PNET CNS Site Group Medulloblastoma and PNET Author: Dr. Norm Laperriere 1. INTRODUCTION 3 2. PREVENTION
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES CENTRAL NERVOUS SYSTEM MEDULLOBLASTOMA AND PNET CNS Site Group Medulloblastoma and PNET Author: Dr. Norm Laperriere 1. INTRODUCTION 3 2. PREVENTION
CHAPTER 11 Tumors Originating in the Brain Medulloblastomas, PNETs and Ependymomas
 Tumors Originating in the Brain Medulloblastomas, PNETs and Ependymomas Foolishly, I waited 7 months before I joined this (or any) group. By that time, my son had radiation, chemo, and a recurrence of
Tumors Originating in the Brain Medulloblastomas, PNETs and Ependymomas Foolishly, I waited 7 months before I joined this (or any) group. By that time, my son had radiation, chemo, and a recurrence of
Case Report Atypical Presentation of Atypical Teratoid Rhabdoid Tumor in a Child
 Case Reports in Oncological Medicine Volume 2013, Article ID 815923, 4 pages http://dx.doi.org/10.1155/2013/815923 Case Report Atypical Presentation of Atypical Teratoid Rhabdoid Tumor in a Child Y. T.
Case Reports in Oncological Medicine Volume 2013, Article ID 815923, 4 pages http://dx.doi.org/10.1155/2013/815923 Case Report Atypical Presentation of Atypical Teratoid Rhabdoid Tumor in a Child Y. T.
Diffusion-weighted imaging and ADC mapping in the differentiation of intraventricular brain tumors
 Diffusion-weighted imaging and ADC mapping in the differentiation of intraventricular brain tumors Poster No.: C-2652 Congress: ECR 2010 Type: Educational Exhibit Topic: Neuro Authors: M. Gavrilov, T.
Diffusion-weighted imaging and ADC mapping in the differentiation of intraventricular brain tumors Poster No.: C-2652 Congress: ECR 2010 Type: Educational Exhibit Topic: Neuro Authors: M. Gavrilov, T.
Complex Hydrocephalus
 2012 Hydrocephalus Association Conference Washington, DC - June 27-July1, 2012 Complex Hydrocephalus Marion L. Walker, MD Professor of Neurosurgery & Pediatrics Primary Children s Medical Center University
2012 Hydrocephalus Association Conference Washington, DC - June 27-July1, 2012 Complex Hydrocephalus Marion L. Walker, MD Professor of Neurosurgery & Pediatrics Primary Children s Medical Center University
PA SYLLABUS. Syllabus for students of the FACULTY OF MEDICINE No.2
 Approved At the meeting of the Faculty Council Medicine No. of Approved At the meeting of the chair of Neurosurgery No. of Dean of the Faculty Medicine No.2 PhD, associate professor M. Betiu Head of the
Approved At the meeting of the Faculty Council Medicine No. of Approved At the meeting of the chair of Neurosurgery No. of Dean of the Faculty Medicine No.2 PhD, associate professor M. Betiu Head of the
CS Tumor Size CS Extension CS Tumor Size/Ext Eval CS Lymph Nodes CS Lymph Nodes Eval Reg LN Pos Reg LN Exam CS Mets at DX CS Mets Eval
 C70.0, C71.0-C71.9 C70.0 Cerebral meninges C71.0 Cerebrum C71.1 Frontal lobe C71.2 Temporal lobe C71.3 Parietal lobe C71.4 Occipital lobe C71.5 Ventricle, NOS C71.6 Cerebellum, NOS C71.7 Brain stem C71.8
C70.0, C71.0-C71.9 C70.0 Cerebral meninges C71.0 Cerebrum C71.1 Frontal lobe C71.2 Temporal lobe C71.3 Parietal lobe C71.4 Occipital lobe C71.5 Ventricle, NOS C71.6 Cerebellum, NOS C71.7 Brain stem C71.8
