Temporary focal cerebral ischemia results in swollen astrocytic end-feet that compress microvessels and lead to focal cortical infarction
|
|
|
- Aldous Hart
- 5 years ago
- Views:
Transcription
1 & 211 ISCBFM All rights reserved X/11 Temporary focal cerebral ischemia results in swollen astrocytic end-feet that compress microvessels and lead to focal cortical infarction Umeo Ito 1, Yoji Hakamata 2, Emiko Kawakami 1 and Kiyomitsu Oyanagi 1,3 1 Department of Neuropathology, Tokyo Metropolitan Institute for Neuroscience, Tokyo, Japan; 2 Department of Basic Science, School of Veterinary Nursing and Technology, Faculty of Veterinary Science, Nippon Veterinary and Life Science University, Tokyo, Japan; 3 Division of Neuropathology, Department of Brain Disease Research, Shinshu University, School of Medicine, Tokyo, Japan We examined the mechanisms underlying the abrupt onset of the focal infarction in disseminated selective neuronal necrosis (DSNN) after temporary ischemia. Stroke-positive animals were selected according to their stroke-index score during the first 1 minutes after left carotid occlusion performed twice at a 5-hour interval. The animals were euthanized at various times after the second ischemia. Light- and electron-microscopical studies were performed chronologically on the coronalcut surface of the cerebral cortex at the chiasmatic level, where focal infarction evolved in the maturing DSNN. We counted the number of neurons, astrocytes, and astrocytic processes (APs); measured the areas of end-feet and astrocytes; and counted the numbers of obstructed microvessels and carbon-black-suspension-perfused microvessels (CBSPm). Between.5 and 5 hours after ischemia, DSNN matured, with the numbers of degenerated and dead neurons increasing, and those of APs cut-ends decreasing; whereas the area of the end-feet and the numbers of obstructed microvessels increased and those of CBSPm decreased. At 12 and 24 hours after ischemia, the infarction evolved, with the area of end-feet and astrocytic number decreased; whereas the numbers of obstructed microvessels decreased and the CBSPm number increased. The focal infarction evolved by temporary microvascular obstruction because of compression by swollen end-feet. ; doi:1.138/jcbfm.21.97; published online 3 June 21 Keywords: disseminated selective neuronal necrosis; evolution of focal infarction; maturation phenomenon; microvascular compression; swollen end-feet; temporary cerebral ischemia; tpa Abbreviations and Specific words: APs, astrocytic processes; CBSPm, carbon-black-suspension-perfused microvessels; cut-ends of APs, astrocytic processes appearing in cross-section on the EM photos; DSNN, disseminated selective neuronal necrosis or selective neuronal necrosis (selectively only neurons die not as a mass but in a disseminated manner among the surviving neurons); EM, electron microscopy; Face-A, coronal-cut surface at the chaismatic level of the gerbil brain; Face-B, coronal-cut surface at infundibular level of the gerbil brain; HE, hematoxylin-eosin; IF, interhemispheric fissure of the gerbil brain; LMS, light microscopy; PAS, periodic acid-fuchsin-schiff; rcbf, regional cerebral blood flow; RF, rhinal fissure of the gerbil brain; RPI, region peripheral to infarction of the gerbil brain; SDH, succinic dehydrogenase; TB, Toluidine blue. Introduction The maturation phenomenon of ischemic injury (Ito et al, 1975, 1979) or delayed neuronal death (Kirino, 1982) has been investigated with the main focus on neurons. However, astrocytes are known to support Correspondence: Dr U Ito, Department of Neuropathology, Tokyo Metropolitan Institute for Neuroscience, 2-6 Musashidai, Fuchu-shi, Tokyo , Japan. umeo-ito@nn.iij4u.or.jp This work was supported in part by grants from the Yumin Memorial Grant (to KO). Received 2 March 21; revised 2 June 21; accepted 8 June 21; published online 3 June 21 neuronal functions by regulating extracellular ionhomeostasis and neurotransmitters, as well as by providing energy substrates, for example, lactate to the neurons through their astrocytic processes (APs; Auer and Sutherland, 22; Bambrick et al, 24; Chen and Swanson, 23). An ischemic insult also injures astrocytes; however, no precise analysis of the APs had been reported before our earlier study (Ito et al, 29). In that study of the region peripheral to the cerebral cortical infarction (region peripheral to the infarction, RPI) or penumbra in Face-B (the coronal-cut surface of the gerbil brain at the level of the chiasma was termed as Face-A and that at the level of the infundibulum as Face-B), we found that
2 the heterogeneous degeneration of APs of the normal-appearing astrocytes was tightly associated with the appearance of disseminated selective neuronal necrosis (DSNN) and its maturation after temporary ischemia. Two types of morphological injury, DSNN and infarction, have been demonstrated in response to various temporary ischemic insults (Ito et al, 1975; Marcoux et al, 1982; DeGirolami et al, 1984). In temporary ischemia, brief moderate ischemia induces DSNN, whereas longer and severer ischemia produces an infarction (Ito et al, 1975; Marcoux et al, 1982; DeGirolami et al, 1984; Smith et al, 1984). Excitatory amino acids are thought to lead to DSNN; and tissue acidosis, to an infarction. However, the pathologic relationships between the two may not always be straightforward (Auer and Sutherland, 22). Infarction is defined as a pan-necrosis of both glial and neuronal elements and is different from DSNN in that astrocytes also die during the evolution of an infarction. Impairment of energy metabolism, as evidenced by reduced glucose utilization, progressive acidosis, and ATP depletion, has a pivotal function in the formation of an infarction. However, little is known about the mechanisms underlying the abrupt onset of astrocytic death and pan-necrosis in the DSNN (Auer and Sutherland, 22; Swanson et al, 1997). For thrombolytic therapy in acute stroke, prevention of the evolution of a focal infarction after restoration of blood flow is of paramount importance for a better recovery. Elucidation of the mechanisms and identification of targets for prevention of the abrupt onset of the focal infarction, and as well as the development of novel preventive measures, will have tremendous clinical implications for the treatment of acute stroke. Because of the difficulty involved in reproducibly producing either DSNN or an infarction in the cerebral cortex of experimental animals by imposing a single ischemic insult (Crowell and Olsson, 1972; Weinstein et al, 1984), we earlier devised a model that uses a modified, unilateral temporary carotid occlusion in Mongolian gerbils obtained by applying twice a 1-minute unilateral carotid occlusion with a 5-hour interval between them. This procedure afforded a threshold amount of ischemia needed to induce a unilateral cerebral cortical focal infarction in Face-A, around which DSNN slowly matured in a large RPI/or penumbra. The infarct size became uniform so that a focal infarction evolved in the DSNN of the coronal face sectioned at the chiasmatic level (Face-A; Figure 1A), and only DSNN matured in the coronal face sectioned at the infundibular level (Face-B; Figure 1A; Hanyu et al, 1997). In this model, by dividing the ischemic insult into two parts, the mortality rate of the animals caused by epileptic seizure is drastically decreased. In our earlier studies, we found that the threshold from DSNN to focal infarction after temporary ischemic insult was very narrow and that a small increase in the ischemic insult induced an infarction once a critical threshold of the intensity had been met (Hanyu et al, 1995, 1997). However, the temporal profile and mechanisms of transition from the maturing DSNN to evolution of the focal infarction still remained obscure. Our earlier study using the same gerbil model also revealed that, around 12 hours after ischemia, an abrupt drop in ATP content, SDH activity, and ph occurred in the cerebral cortex of gerbils at the chiasmatic level (Face-A) corresponding to the focal infarction, suggesting that some additional event had occurred in the cortical tissue (Kuroiwa et al, 2). Using this model, we presently investigated this transition, focusing on the ultrastructural temporal profiles of the astrocytic end-feet and patency of the microvessels during the appearance of a focal infarction in the maturing DSNN in Face-A, to elucidate the additional event that was required to induce the abrupt onset of the infarction. Materials and methods The animals used here were handled in accordance with the Guidelines for the Experimental Use of Animals of Tokyo Metropolitan Institute for Neuroscience. Animals were numbered and grouped by using a table of random numbers. Also using this table, an outsider numbered each specimen for light microscopy (LMS) and electron microscopic (EM) photographs in each of the settings, with measurements performed starting with the smallest number. Under anesthesia with 3% isoflurane, 7% nitrous oxide, and 3% oxygen, the left carotid artery of adult male Mongolian gerbils (6 to 8 g) was exposed by making a midline cervical incision. The carotid artery was occluded twice with a Heifetz aneurismal clip for 1 minutes each time, with a 5-hour interval between the two occlusions. Anesthesia was discontinued immediately after each cervical surgery, and the behavior of conscious animals was observed for 1 minutes during the carotid occlusion. Ischemia-positive animals were selected based on having a stroke-index score of over 13 points (Ohno et al, 1984). These animals were killed at (sham operated),.5, 3, 5, 12, 24, and 72 hours after the second ischemic insult, by transcardiac perfusion. The animals were perfused with diluted fixative (1% paraformaldehyde, 1.25% glutaraldehyde in.1 mol/l cacodylate buffer) for 5 minutes, followed by perfusion with concentrated fixative (4% paraformaldehyde, 5% glutaraldehyde in.1 mol/l cacodylate buffer) for 2 minutes for EM (three animals for each time group) or with 1% phosphate-buffered formaldehyde fixative for 3 minutes for LMS (four animals for each time group). For the EM study, we obtained cortical blocks including all cortical layers along a 2-mm-wide path from a point medial to one-half of the distance between the rhinal and interhemispheric fissures of the left cerebral cortex on Face-A. These blocks were divided into two adjacent column blocks of 1 mm width for each and embedded into Epon blocks. Ultrathin Epon sections including second through fifth cortical layers were double stained with 329
3 33 Figure 1 Light microscopic findings in the second to fifth cortical layers of Face-A. (A) Coronal section of Face-A and -B 72 hours after ischemia (periodic acid-fuchsin-schiff, PAS). The four cortical columns counted, each.25 mm in width, are indicated. 1/2 indicates the point medial between rhinal (RF) and interhemispheric (IF) fissures along the cortical surface. (B E) Hematoxylin-eosin (HE) staining; bars = 3.4 mm. (B) At.5 hour after ischemia, degenerated (arrows) and dead (arrowheads) neurons are seen. (C) At 5 hours after ischemia, degenerated (black arrows) and dead (arrowhead) neurons are seen along with obstructed microvessels showing stasis and surrounded by swollen end-feet (blue arrows). (D) By 12 hours after ischemia, flocks of foamy necrotic neuropils (black arrows) are noted among necrotic neurons. Blue arrows indicate patent microvessels. (E) At 24 hours after ischemia, dead neurons are scattered in diffusely spongy necrotic tissue. Almost all microvessels are patent (blue arrows). (F) At 3 hours after ischemia: carbon-black-suspension perfused (CBSP) and HE, bars = 3.4 mm. Carbon-black-suspension-perfused (blue arrows) and not-perfused (black arrows) microvessels are seen. (G) At 5 hours after ischemia, signs of stasis (arrows) and obstructed microvessels (arrowhead) are observed (Toluidine blue), bars = 12.2 mm. uranyl acetate and lead solution, and observed with an electron microscope (H9-Hitachi, Tokyo, Japan). A measure of 1-mm thick Epon sections of these column blocks were stained with Toluidine blue for LMS. Coronary paraffin sections of Face-A were separately stained with hematoxylin-eosin or periodic acid-fuchsin-schiff for LMS. We performed the following morphometric measurements. Number of Normal-Appearing, Degenerating, and Dead Neurons and of Astrocytes (Light Microscopy) Using an eye-piece micrometer (U-OCMSQ1/1) under 4-power magnification, we counted the number of normal-appearing, degenerated, and dead neurons in all six cortical layers in four adjacent columns, by vertically
4 and medially moving the specimen along a.25-mm-wide 4 path of the cortex. We started medially from a point one-half of the distance between the rhinal and interhemispheric fissures on hematoxylin-eosin-stained Face-A (Figure 1A) in each of the four animals (Supplementary Table A). We calculated the average number of normalappearing, degenerated, and dead neurons in each column. The average number of all neurons counted was 8,641.±256.6 per time point. In the same way, we determined the average number of astrocytes on the periodic acid-fuchsin-schiff-stained sections. The average number of all astrocytes counted was 663.2±115.7 per time point. The following criteria were used to classify the neurons. For normal-appearing neurons, a clear cytoplasm containing a large round nucleus with homogenous chromatin and a centrally located large nucleolus was required. For degenerating neurons, an eosinophilic dark or foamy cytoplasm surrounded by a clear halo (swollen APs) along with nuclear chromatin condensation or aggregation was requisite. For dead neurons, either (1) an asterisk-shaped condensed eosinophilic cytoplasm surrounded by a clear halo and a nucleus showing karyorrhexsis or pyknosis or (2) ghost cells with homogeneously, faintly stained eosinophilic cytoplasm occasionally having a faintly stained basophilic nucleus with an obscure nuclear margin met the requirement. The following criteria were used to identify astrocytes: those cells with a round or elliptical or occasionally polygonal nucleus surrounded by a conspicuous nuclear membrane and having a clear, homogenous chromatin and an eccentrically located single small nucleolus, along with an irregular foamy cytoplasm filled with periodic acidfuchsin-schiff-positive glycogen particles. Area and Number of Mitochondria in the Astrocytic Cytoplasm and End-Feet (Electron Microscopy) Using a computer-assisted digitizer (Measure-5, System Supply, Nagano Japan), we measured the area (mm 2 ) and the number of mitochondria in the astrocytic cytoplasm in each of three animals at,.5, 3, 5, 12, and 24 hours after ischemia. These values were expressed as the average with respect to time point, obtained from 26.3±1.7 evenly distributed EM photographs of astrocytes taken at 4,5 to 1,8-fold magnification (Supplementary Table B). Similarly, we used the same animals to measure the area (mm 2 ) of the end-feet and number of mitochondria in them. These data were expressed as the average per time point, obtained from 32.7±2.9 evenly distributed EM pictures of end-feet at the same magnification as used for the astrocytes. Percent Volume of Astrocytic Processes and Numbers of Cut-Ends of Astrocytic Processes and Mitochondria in them in Neuropils (Electron Microscopy) Placing a.5.5 cm 2 quadratic lattice on each of 22.4±.8 evenly distributed EM photographs (magnified 1,8) of neuropil for three animals in each time group, we determined the percent volume of the APs in the neuropil by using the point-counting method (Weibel, 1963; Supplementary Table C). By this method, we counted the number of intersecting points of the lattice touched by the cut-ends of the APs among an average of 38,595.6±1,421.9 evenly distributed points in the neuropil of the EM pictures in each time group, and converted the counted number to the number per 1 intersecting points of the lattice for each EM picture (percent volume) and expressed them as the average per time point. According to the equation for the relative error for different volumetric proportions, all values had < 5% error (Weibel, 1963). We also measured the numbers of cut-ends of APs and their mitochondria in an average of 36,916.4±1,313.8 evenly distributed areas of.25 cm 2 in size in the neuropil of the EM pictures in each time group. The counted number was converted to the number per a 25-cm 2 area of each EM picture (21.53 mm 2, after correcting for magnification by real size) and expressed them as the average per time point. Ultrastructural appearance of APs: Electron microscopically, APs pervade the neuropil and are recognized by their irregular contours. Some of them form perivascular end-feet that make a complete layer of varying width that is imposed between the nerve fibers and the endothelial cells. In the APs, glial fibrils occur in bundles; and the mitochondria are oriented parallel to the long axis of the APs. Glycogen granules are observed, more frequently in end-feet and APs near the neuronal perikaryon than in other areas. In the smaller processes, the only structures found are ribosomes, glycogen granules, and bundle of fibrils. Ultrastructural criteria for cut-ends of APs: Structures that contained astrocytic microorganelles (e.g., endoplasmic reticulum, rough-surfaced endoplasmic reticulum, ribosomes, glial fibrils, mitochondria, and glycogen granules) but were negative for components of neurites (e.g., microtubules, neurofilaments, synapses, synaptic vesicles, and spine or thorn with spine apparatus). The APs showed various degrees of swelling. Number of Obstructed Microvessels (Light Microscopy) We prepared Toluidine blue-stained 1-mm thick cortical Epon sections along a 2-mm-wide path divided into two adjacent columns of 1 mm width from each of three animals killed at,.5, 3, 5, 12, and 24 hours after ischemia and trimmed them to contain all cortical layers in each column of 1-mm width. Using an eye-piece micrometer (U-OCMSQ1/1) under 1-power magnification (oil immersion), we determined the percentage of all obstructed microvessels ( < 1 mm in diameter) showing microcirculatory obstruction and stasis (Little et al, 1981) among all counted microvessels in each section (Supplementary Table D). The average number of all counted microvessels was 2,532.4±262.8 per time point. Number of Patent Carbon-Black-Suspension-Perfused Microvessels (Light Microscopy) Under anesthesia, gerbils were perfused for 3 seconds with 1. ml of carbon-black-suspension (Platina-Ink, Tokyo, Japan) through a femoral vein by using a microinfusion 331
5 332 pump (KDS1, KD Scientific, MA, USA). Thereafter, each animal was guillotined immediately; and its brain was then removed and fixed in 1% phosphate-buffered formaldehyde for 3 days. Using an eye-piece micrometer (U-OCMSQ1/1) under 4-power magnification, we counted the number of carbon-black-suspension-perfused microvessels (CBSPm) in all six cerebral cortical layers in four columns of Face-A and of -B. This was performed by vertically and medially moving the specimen along a.25-mm-wide 4 path of the cortex starting medially from a point one-half of the distance between the rhinal and interhemispheric fissures on hematoxylin-eosin-stained Face-A (,.5, 3, 5, 8, 12, and 24 hours) and Face-B (3, 5, and 12 hours) for each of the three animals (Figure 1A). We also counted the number of CBSPm in each of the four columns located at the corresponding position of the opposite nonischemic right cerebral hemisphere, and expressed the number of CBSPm in each column of the ischemic left hemisphere as a percentage of the number for the nonischemic right hemisphere per each time point (Supplementary Table E). The average numbers of all CBSPm per each time point of the right hemisphere of Face-A and Face-B were 2,111.3±46.3 and 1,359.±7.8, respectively. Statistical Analysis We analyzed the statistical difference between each time group by using analysis of variance, followed by the Bonferroni Dunn test. All data in the text and in Figures 2 and 5 were presented as the average±s.e.m., and a statistically significant difference was accepted at P <.5. Results Maturation of Disseminated Selective Neuronal Necrosis (from.5 to 5 hours After Last Ischemic Insult) By LMS observations, DSNN was found to have matured in the cerebral cortex of Face-A (Figure 1A), where degenerating neurons with a halo of swollen APs and dead neurons appeared and increased in number in disseminated manner (DSNN) among the normal-appearing neurons at.5 (Figure 1B) and 5 hours after ischemia (Figure 1C). These changes were more intense in laminar manner in the third, fifth, and sixth cortical layers. On morphometry by LMS, normal-appearing neurons decreased, whereas degenerated and dead neurons increased, in number (Figure 2A). Astrocytes slightly decreased in number from 55.3±.92 at hours to 43.9±1.76 per column at 5 hours (Figure 2B), but there were no statistical differences among -,.5-, and 3-hour values. At 3 hours after ischemia, we compared APs in EM pictures taken around the normal-appearing, degenerated, and dead neurons. No necrotic hallmarks were observed in the slightly darkened degenerated neurons with slight condensations of nuclear chromatin. Some of these neurons may have later recovered during the maturation period (Figure 3B). Dead neurons appeared as variously condensed dark cell bodies with necrotic hallmarks such as flocculent densities in mitochondria, disruption of the nuclear and/or cellular membrane, and advanced nuclear chromatin condensates or karyorrhexis (Figure 3C). In these areas, where DSNN was maturing in the cerebral cortex of Face-A, swelling and degeneration of the APs in the neuropil were more advanced in that order around the normal-appearing (Figure 3A), degenerated (Figure 3B), and dead neurons (Figure 3C) at an even earlier stage, that is at 3 hours after ischemia, than at 12 hours in the cerebral cortical RPI or penumbra in Face-B (Ito et al, 29). In EM photos, the astrocytic cytoplasm was swollen at.5 (Figure 4A) and 5 hours (Figure 4D) and the area of the astrocytes increased (Figure 2C). However, there were no statistically significant differences in the number of their mitochondria among all time courses examined (Figure 2D). The cut-ends of APs in the neuropil at.5 hour (Figure 4C) and 5 hours (Figure 4F) decreased in number from 9.79±.48 at hour to 5.16±.19/21.53 mm 2 at 5 hours. However, there were no statistical differences among.5-, 3-, and 5-hour values (Figure 2E). However, the APs increased in percent volume from 5.62%±.45% at hour to 24.15%±1.2% at 5 hours (Figure 2F), and the density of their glycogen granules also increased (Figure 4F). In contrast, their mitochondrial number decreased (Figure 2G), associated with a decrease in the number of their cutends (Figure 2E). In EM pictures, the end-feet also showed increased swelling at.5 hour (Figure 4B) and at 3 hours (Figure 4E); and the area of the end-feet increased markedly from 6.1±.64 at hour to 67.83± 8.11 mm 2 at 5 hours (Figure 5A). The number of mitochondria in the end-feet decreased at 24 hours; however, there were no statistical differences among the values at the other time periods (Figure 5B). Obstructed microvessels with stasis were observed at 5 hours in LMS (Figures 1C and 1G). They increased in percentage from % at hour to 57.3%± 16.1% at 5 hours (Figure 5C), whereas the CBSPm in Face-A (Figure 1F) decreased in number from 97.5%±4.16% at hour to 31.9%±1.85% at 5 hours; and further decreased to 23.8%±.69% at 8 hours after ischemia (Figure 5D). The EM revealed obstructed microvessels of various shapes that had been compressed by swollen end-feet and had developed microvascular stasis (Figure 6). In Face-B where only DSNN matured without evolution of an infarction, no significant reduction in the number of CBSPm was observed during 3 to 12 hours after the final insult (Figure 5D). Evolution of Focal Infarction (at 12 and 24 hours After Ischemia) At 12 hours after ischemia, flocks of foamy necrotic foci were scattered in the cerebral cortex; and
6 A no. of neurons per column hr.5-hr B # 5 4 # hr 5-hr 12-hr 24-hr -hr.5-hr 3-hr 5-hr 12-hr 24-hr -hr.5-hr 3-hr 5-hr 12-hr 24-hr no. of astrocytes per column C area (sq.μm) of astrocytes 333 D E F no. of mitochondria in astrocytes hr.5-hr 3-hr 5-hr 12-hr 24-hr no. of cut-ends of APs in neuropil area hr.5-hr 3-hr 5-hr 12-hr 24-hr % volume of APs in neuropil hr.5-hr 3-hr 5-hr 12-hr 24-hr G no. of mitochondria of PAs in neuropil area hr.5-hr 3-hr 5-hr 12-hr 24-hr Figure 2 (A) Number of normal-appearing, degenerated, and dead neurons per cortical column of.25 mm width. *P <.5 versus, 3, and 12 hours; w P <.5 versus, 3, 5, and 24 hours; # P <.5 versus,.5, 12, and 24 hours. (B) Number of astrocytes per cortical column of.25 mm in width. *P <.5 versus 5, 12, and 24 hours; w P <.5 versus 5, and 24 hours. (C) Astrocytic area (mm 2 ). *P <.5 versus.5, 3, 5, and 12 hours; w P <.5 versus 12, and 24 hours. (D) Number of mitochondria in astrocytic cytoplasm. No statistically significant differences were found. (E) Number of cut-ends of astrocytic processes (APs) in a neuropil area of mm 2. *P <.5 versus and 12 hours. (F) Percent volume of cut-ends of APs in the neuropil area. *P <.5 versus.5, 3, and 5 hours; w P <.5 versus 12 hours. (G) Number of mitochondria of APs in the neuropil area of mm 2. *P <.5 versus.5, 3, 5, and 12 hours. Figure 3 Electron microscopic findings on three kinds of neurons in the second to fifth cortical layers of Face-A (bars = 2.4 mm), at 3 hours after ischemia. (A) Normal-appearing neuron with slightly swollen astrocytic processes (APs) (arrows). (B) Degenerated neuron with advanced swelling of APs, especially around the neuron (arrows). (C) Dead neuron surrounded by remarkably swollen degenerated APs (arrows).
7 334 Figure 4 Electron microscopic findings on the second to fifth cortical layers of Face-A (bars = 2.4 mm). (A C) Obtained at.5 hours after ischemia. (A) Swollen astrocytic cytoplasm. (B) Slightly swollen end-feet. (C) Decreased number of astrocytic processes (APs) and their mitochondria in the neuropil (arrows). (D) At 5 hours after ischemia, swollen astrocytic cytoplasm is noted. (E) At 3 hours after ischemia, remarkably swollen end-feet are present. (F) At 5 hours after ischemia, swollen APs are evident in the neuropil (arrows). (G) At 24 hours after ischemia, swollen degenerative astrocytic cytoplasm with condensed nuclear chromatin is noted. (H) At 24 hours after ischemia, necrotic end-feet (arrows) are evident. (Inset) Magnified necrotic end-foot (arrow; bar = 1.5 mm). (I) At 12 hours after ischemia, a remarkably decreased number of swollen APs (arrows) are found in the neuropil. many microvessels became patent (Figure 1D). The cut-ends of APs had degenerated (Figure 4I) and become decreased in number to 1.29±.31 (Figure 2E). The numbers of degenerated and normal-looking neurons decreased, whereas those of dead neurons increased drastically (Figure 2A). The numbers of astrocytes also markedly decreased to 25.25±1.88 (Figure 2B). By 24 hours, the numbers of normal-appearing and degenerated neurons were greatly reduced (Figure 2A); and dead neurons were observed throughout the diffusely spongy necrotic tissue, and almost all microvessels had become patent (Figure 1E; see temporal profiles of results in Supplementary Table F). The number of astrocytes further decreased to 15.25±1.65 (Figure 2B), and almost all of the astrocytes had disintegrated. The remaining ones were swollen remarkably with degenerated cytoplasm (Figure 4G), and the cut-ends of APs had disappeared from the necrotic tissue (Figure 2E). In accordance with this drastic disintegration of astrocytes, their remaining end-feet had thinned out to 8.92±1.67 mm 2,
8 A % of obstructed micro-vessels area (sq. μm) of end-feet C hr.5-hr 3-hr 5-hr 12-hr 24-hr -hr.5-hr 3-hr 5-hr 12-hr 24-hr # B no. of mitochondria in end-feet D % of carbon-black perfused micro-vessels hr.5-hr 3-hr 5-hr 12-hr 24-hr Face A Face B -hr.5-hr 3-hr # 5-hr 8-hr 12-hr 24-hr Figure 5 (A) Area of end-feet (mm 2 ). *P <.5 versus.5, 3, 5, and 12 hours; w P <.5 versus 5, and 24 hours; # P <.5 versus 12, and 24 hours. (B) Number of mitochondria in end-feet. *P <.5 versus.5, 3, 5, and 12 hours. (C) Percentage of obstructed microvessels among all counted microvessels. *P <.5 versus 3, 5, and 12 hours; w P <.5 versus.5, 12, and 24 hours. (D) Percentage ratio of carbon-black-suspension-perfused microvessels (CBSPm) in the left ischemic hemisphere to all CBSPm in the corresponding position of the opposite (right) nonischemic hemisphere. *P <.5 versus 3, 5, 8, and 12 hours; w P <.5 versus,.5, 3, 5, 12, and 24 hours. # P <.5 versus, 12, and 24 hours. 335 Figure 6 Electron microscopic findings of narrowed and obstructed microvessels resulting from compression by swollen end-feet, at 5 hours after ischemia. (A) Obstructed microvessel with evidence of stasis is seen. (bar = 7.5 mm). (B) This microvascular lumen is remarkably deformed (bar = 2.4 mm). (C) A narrowed microvascular lumen showing stasis (arrow) is seen. (bar = 1.8 mm). (D) This microvascular lumen is remarkably narrowed (bar = 3. mm). (E) A completely obstructed microvascular lumen is shown (bar = 2.1 mm). (Figure 5A) and/or had become necrotic (Figure 4H); and then the vascular compression disappeared (Figure 1E). Therefore, obstructed microvessels decreased to 3.6%±1.3% (Figure 5C); and that of CBSPm increased to 76.2%±7.11% (Figure 5D). However, pannecrosis was already complete. At 72 hours after ischemia, a sharply demarcated focal infarction became more prominent and was surrounded by the RPI or penumbra, where DSNN matured in both Face-A and -B (Figure 1A) (see Supplementary Table F: temporal profiles of evolution of infarction in maturing DSNN).
9 336 Discussion In this study in Face-A, during.5 and 5 hours after ischemia, degenerated and dead neurons increased in number in a disseminated manner (DSNN) associated with heterogeneously impaired interaction between neurons and degenerating APs, as in the case of the maturing DSNN in the earlier study on Face-B (Ito et al, 29). As no necrotic hallmarks were observed in the slightly darkened degenerated neurons with slight nuclear chromatin condensations, some of these neurons may have later recovered during the maturation period in the DSNN. But, by 12 and 24 hours after ischemia, the numbers of normal-appearing and degenerated neurons decreased; and the dead neurons increased in number drastically. The remaining astrocytes degenerated, and their APs completely disappeared around 24 hours, associated with tissue necrosis, that is, focal infarction. Different from the earlier study in the Face-B where the astrocytic density was constant during DSNN maturation, the ischemic insult in the Face-A induced injury of astrocytic function, resulting in a slight decrease in the number of astrocytes and marked swelling of the astrocytic end-feet from.5 to 5 hours in the maturing DSNN. That swelling induced compression of microvessels and decreased microvascular perfusion, which induced sharply circumscribed tissue necrosis surrounded by RPI where only DSNN progressed (Figure 1A; Face-A). In our earlier study on energy metabolism using the same experimental model, we found an abrupt drop in ATP content, reduced SDH activity, and a drop in ph around 12 hours after ischemia in the cerebral cortex corresponding to the sharply circumscribed focal infarction in the Face-A. However, the cause of these drops has remained unknown. On the other hand, in the cerebral cortex of RPI where only maturation of DSNN occurred in the Face-B, energy metabolism showed only slight changes over the periods during which circulation was restored (Kuroiwa et al, 2). In an earlier study, we performed unilateral carotid occlusion, and 3 minutes later investigated the noreflow phenomenon immediately after recirculation by perfusion of the animals with a carbon-blacksuspension and by performing C 14 -antipyrine radioautography. In this ischemic model where the cerebral blood flow (CBF) did not cease completely, but was reduced during ischemia, we found that the no-reflow phenomenon was transient; it continued for <.5 minutes after recanalization, and the regional CBF (rcbf) returned to normal (Ito et al, 198). In this study, we found that a focal cerebral cortical infarction evolved in the maturing DSNN. It was being induced by delayed occurrence of temporary microvascular obstruction because of compression of microvessels by swollen end-feet at 3 to 8 hours after the insult, and it later resulted in tissue pan-necrosis at 12 to 24 hours after ischemia (Figures 1A and 7; Supplementary Table F). In primates, the rate of rcbf in control animals is 5 ml per 1 g per minute; and when it is < 18 ml per 1 g per minute, an infarction evolves, occurring with a delay of < 3 to 4 hours along a rising sigmoid Temporary micro-vascular obstruction resulting from compression by swollen end-feet A.5-hr B 3~8-hr C 12-hr D 24-hr thinned end-feet basal lamina swollen end-feet endothelium necrotic end-feet Figure 7 Illustration of temporary microvascular obstruction resulting from compression by swollen end-feet. (A) At.5 hour after ischemia, no microvascular obstruction is observed. (B) By 3 to 8 hours after ischemia, swollen end-feet compressed the microvessels and induced microvascular obstruction as evidenced by stasis. (C) By 12 hours after ischemia, there is a decrease in the number and thickness of end-feet, resulting in restoration of blood flow in the microvessels. (D) At 24 hours after ischemia, astrocytes and end-feet have become necrotic; and microvascular compression has disappeared. Upper: longitudinal scheme along microvessels. Lower: transverse section of microvessels. Long arrows: bloodstream.
10 function between rcbf and the duration before the appearance of an infarction (Jones et al, 1981). Although the rcbf in the cerebral cortex of conscious gerbils is 11 ml per 1 g per minute (Ohno et al, 1984), the ratio of the normal blood flow to the blood flow at the threshold necessary to induce infarction remains roughly constant across species at 3:1 (Auer and Sutherland, 22). In this study, the percentage of microvessels perfused by the carbonblack-suspension was reduced to 32% and 24% of the total perfused microvessels at 5 and 8 hours after ischemia, respectively. Thus, the rcbf in primates can be calculated simply as reduced to 16 and 12 ml per 1 g per minute, respectively. On the basis of the rising sigmoid function observed in primates, infarction evolved, occurring with a delay of about 3 to 4 hours after the microvascular obstruction. As vascular compression by swollen end-feet became less severe because of the rapid reduction in the number of astrocytes and swelling of their end-feet caused by their necrosis, the patency of the obstructed microvessels eventually recovered at B12 to 24 hours after ischemia. However, pan-necrosis had already completed (Figure 7; Supplementary Table F). The following reports were found in the past literature: during permanent MCA occlusion, microvascular obstruction and stasis induce further development of pan-necrosis during MCA occlusion (Crowell and Olsson, 1972; Little et al, 1981; Garcia et al, 1994). After temporary MCA occlusion, secondary occlusion of microvessels by polymorphonuclear leukocytes demonstrates a role of these cells in early microvascular injuries and the no-reflow phenomenon (del Zoppo et al, 1991). In this study, an occasional mixture of polymorphs and platelets was observed among the erythrocytes in the microvessels where stasis had occurred. However, neither microthrombi nor microvascular obstruction by polymorphs was observed. Swelling of end-feet and temporary compressive obstruction of microvessels may occur in the early phase after reopening of an obstructed major vessel (e.g., after tissue plasminogen activator (tpa) administration). Therefore, before evolution of an infarction, strategies to prevent swelling of end-feet should commence soon after stroke onset, before or immediately after the reopening of the obstructed major vessels but before infarction evolution. Osmotherapy using low-molecular-weight dextran (Crowell and Olsson, 1972), mannitol (Little, 1978), or glycerol (Meyer et al, 1972), as well as high colloid-oncotic pressure therapy (Hakamata et al, 1995), might be effective. Aquaporin 4, a member of the family of membrane water channels, is present as orthogonal arrays in the cell surface of the end-feet in contact with microvessels (Berry et al, 22), and pharmacological manipulations of AQP-4 and -9 expression may offer a therapeutic strategy (Lo et al, 25; Badaut et al, 27). In conclusion, during DSNN maturation in the cerebral cortex, focal infarction did not develop continuously from DSNN. Instead, it evolved by secondary microvascular obstruction and stasis resulting from compression by the swollen astrocytic end-feet. Disclosure/conflict of interest The authors declare no conflict of interest. References Auer R, Sutherland G (22) Hypoxia and related conditions. In: Greenfield s neuropathology (Graham D, Lantos P, eds), 7th ed. Vol. 1. London, New York, New Delhi: Arnold, Badaut J, Ashwal S, Tone B, Regli L, Tian HR, Obenaus A (27) Temporal and regional evolution of aquaporin-4 expression and magnetic resonance imaging in a rat pup model of neonatal stroke. Pediatr Res 62: Bambrick L, Kristian T, Fiskum G (24) Astrocyte mitochondrial mechanisms of ischemic brain injury and neuroprotection. Neurochem Res 29:61 8 Berry M, Butt A, Wilkins G, Perry V (22) Structure and function of glia in the central nervous system. In: Greenfield s neuropathology (Graham D, Lantos P, eds), 7th ed. Vol. 1. London, New York, New Delhi: Arnold, Chen Y, Swanson RA (23) Astrocytes and brain injury. J Cereb Blood Flow Metab 23: Crowell RM, Olsson Y (1972) Impaired microvascular filling after focal cerebral ischemia in the monkey. Modification by treatment. Neurology 22:5 4 DeGirolami U, Crowell RM, Marcoux FW (1984) Selective necrosis and total necrosis in focal cerebral ischemia. Neuropathologic observations on experimental middle cerebral artery occlusion in the macaque monkey. J Neuropathol Exp Neurol 43:57 71 del Zoppo GJ, Schmid-Schonbein GW, Mori E, Copeland BR, Chang CM (1991) Polymorphonuclear leukocytes occlude capillaries following middle cerebral artery occlusion and reperfusion in baboons. Stroke 22: Garcia JH, Liu KF, Yoshida Y, Chen S, Lian J (1994) Brain microvessels: factors altering their patency after the occlusion of a middle cerebral artery (Wistar rat). Am J Pathol 145:728 4 Hakamata Y, Ito U, Hanyu S, Yoshida M (1995) Long-term high-colloid oncotic therapy for ischemic brain edema in gerbils. Stroke 26: Hanyu S, Ito U, Hakamata Y, Nakano I (1997) Topographical analysis of cortical neuronal loss associated with disseminated selective neuronal necrosis and infarction after repeated ischemia. Brain Res 29:154 7 Hanyu S, Ito U, Hakamata Y, Yoshida M (1995) Transition from ischemic neuronal necrosis to infarction in repeated ischemia. Brain Res 686:44 8 Ito U, Hakamata Y, Kawakami E, Oyanagi K (29) Degeneration of astrocytic processes and their mitochondria in cerebral cortical regions peripheral to the cortical infarction: heterogeneity of their disintegration is closely associated with disseminated selective neuronal necrosis and maturation of injury. Stroke 4: Ito U, Ohno K, Nakamura R, Suganuma F, Inaba Y (1979) Brain edema during ischemia and after restoration of blood flow. Measurement of water, sodium, potassium 337
11 338 content and plasma protein permeability. Stroke 1:542 7 Ito U, Ohno K, Yamaguchi T, Tomita H, Inaba Y, Kashima M (198) Transitional appearance of no-reflow phenomenon in Mongolian gerbils. Stroke 11: Ito U, Spatz M, Walker Jr J, Klatzo I (1975) Experimental cerebral ischemia in mongolian gerbils. I. Light microscopic observations. Acta Neuropathol Berl 32:29 23 Jones TH, Morawetz RB, Crowell RM, Marcoux FW, FitzGibbon SJ, DeGirolami U, Ojemann RG (1981) Thresholds of focal cerebral ischemia in awake monkeys. J Neurosurg 54: Kirino T (1982) Delayed neuronal death in the gerbil hippocampus following ischemia. Brain Res 239:57 69 Kuroiwa T, Mies G, Hermann D, Hakamata Y, Hanyu S, Ito U (2) Regional differences in the rate of energy impairment after threshold level ischemia for induction of cerebral infarction in gerbils. Acta Nueropathol 1: Little JR (1978) Modification of acute focal ischemia by treatment with mannitol. Stroke 9:4 9 Little JR, Cook A, Cook SA, MacIntyre WJ (1981) Microcirculatory obstruction in focal cerebral ischemia: albumin and erythrocyte transit. Stroke 12: Lo AC, Chen AY, Hung VK, Yaw LP, Fung MK, Ho MC, Tsang MC, Chung SS, Chung SK (25) Endothelin-1 overexpression leads to further water accumulation and brain edema after middle cerebral artery occlusion via aquaporin 4 expression in astrocytic end-feet. J Cereb Blood Flow Metab 25: Marcoux FW, Morawetz RB, Crowell RM, DeGirolami U, Halsey Jr JH (1982) Differential regional vulnerability in transient focal cerebral ischemia. Stroke 13: Meyer JS, Fukuuchi Y, Shimazu K, Ouchi T, Ericsson AD (1972) Effect of intravenous infusion of glycerol on hemispheric blood flow and metabolism in patients with acute cerebral infarction. Stroke 3:168 8 Ohno K, Ito U, Inaba Y (1984) Regional cerebral blood flow and stroke index after left carotid artery ligation in the conscious gerbil. Brain Res 297:151 7 Smith ML, Auer RN, Siesjo BK (1984) The density and distribution of ischemic brain injury in the rat following 2-1 min of forebrain ischemia. Acta Neuropathol 64: Swanson RA, Farrell K, Stein BA (1997) Astrocyte energetics, function, and death under conditions of incomplete ischemia: a mechanism of glial death in the penumbra. Glia 21: Weibel E (1963) Morphometry of the human lung. Berlin, Gowttingen, Heidelberg: Springer-Verlag Weinstein PR, Anderson GG, Telles DA (1984) Neurological deficit and cerebral infarction after temporary middle cerebral artery occlusion in unanesthetized cats. Stroke 17: This work is licensed under the Creative Commons Attribution-NonCommercial-Share Alike 3. Unported License. To view a copy of this license, visit Supplementary Information accompanies the paper on the Journal of Cerebral Blood Flow & Metabolism website (
Part II Ischemia and the Blood-Brain Barrier Disorders
 Part II Ischemia and the Blood-Brain Barrier Disorders Experimental Cerebral Ischemia: The Contribution of the Bethesda Group Toshihiko Kuroiwa Abstract Igor Klatzo started his research on cerebral ischemia
Part II Ischemia and the Blood-Brain Barrier Disorders Experimental Cerebral Ischemia: The Contribution of the Bethesda Group Toshihiko Kuroiwa Abstract Igor Klatzo started his research on cerebral ischemia
Imaging ischemic strokes: Correlating radiological findings with the pathophysiological evolution of an infarct
 Imaging ischemic strokes: Correlating radiological findings with the pathophysiological evolution of an infarct Jay Chyung,, PhD, HMS III Patient A: history 91 y.o. woman Acute onset R sided weakness and
Imaging ischemic strokes: Correlating radiological findings with the pathophysiological evolution of an infarct Jay Chyung,, PhD, HMS III Patient A: history 91 y.o. woman Acute onset R sided weakness and
Fine Structure of the Normal Trigeminal Ganglion in the Cat and Monkey*
 Fine Structure of the Normal Trigeminal Ganglion in the Cat and Monkey* DAVID S. MAXWELL, PH.D. Principal Contributor and Leader of Discussion HE inclusion of animal material m a y be justified as a means
Fine Structure of the Normal Trigeminal Ganglion in the Cat and Monkey* DAVID S. MAXWELL, PH.D. Principal Contributor and Leader of Discussion HE inclusion of animal material m a y be justified as a means
Mechanisms of Cell Injury
 Causes of Cell Injury 1- oxygen deprivation (anoxia) 2- physical agents 3- chemical agents 4- infections agents 5- immunologic reactions 6- genetic defects 7- nutritional imbalances Mechanisms of Cell
Causes of Cell Injury 1- oxygen deprivation (anoxia) 2- physical agents 3- chemical agents 4- infections agents 5- immunologic reactions 6- genetic defects 7- nutritional imbalances Mechanisms of Cell
Chapter 7 Nerve tissue 1 Liu Jiamei
 Chapter 7 Nerve tissue 1 Liu Jiamei General description: nerve tissue nerve cells (neurons): show numerous long processes receive the stimulation make contact with each other, conduct the nerve impulse
Chapter 7 Nerve tissue 1 Liu Jiamei General description: nerve tissue nerve cells (neurons): show numerous long processes receive the stimulation make contact with each other, conduct the nerve impulse
Microcirculatory Obstruction in Focal Cerebral Ischemia: An Electron Microscopic Investigation in Monkeys
 MICROCIRCULATORY OBSTRUCTION IN FOCAL CEREBRAL ISCHEMIA/Z.;»/e et al. 25 References 1. Brock M, Furuse M, Weber R, et al: Brain tissue pressure gradients. In Lundberg N, Ponten U, Brock M (eds): Intracranial
MICROCIRCULATORY OBSTRUCTION IN FOCAL CEREBRAL ISCHEMIA/Z.;»/e et al. 25 References 1. Brock M, Furuse M, Weber R, et al: Brain tissue pressure gradients. In Lundberg N, Ponten U, Brock M (eds): Intracranial
number Done by Corrected by Doctor Heyam Awad
 number 4 Done by Waseem Abu Obeida Corrected by Saad Al-Hayek Doctor Heyam Awad Cell injury -in the previous lectures we talked about the causes (etiology) and the mechanism (pathogenesis) of cell injury.
number 4 Done by Waseem Abu Obeida Corrected by Saad Al-Hayek Doctor Heyam Awad Cell injury -in the previous lectures we talked about the causes (etiology) and the mechanism (pathogenesis) of cell injury.
Morphological Responses of Cerebral Tissues to Temporary Ischemia
 Morphological Responses of Cerebral Tissues to Temporary Ischemia RONALD F. DODSON, YUKIO TAGASHIRA, YASUO KAWAMURA AND LENA WAI-FONG CHU SUMMARY: The ultrastructural responses of cerebral tissue following
Morphological Responses of Cerebral Tissues to Temporary Ischemia RONALD F. DODSON, YUKIO TAGASHIRA, YASUO KAWAMURA AND LENA WAI-FONG CHU SUMMARY: The ultrastructural responses of cerebral tissue following
NACC Vascular Consortium. NACC Vascular Consortium. NACC Vascular Consortium
 NACC Vascular Consortium NACC Vascular Consortium Participating centers: Oregon Health and Science University ADC Rush University ADC Mount Sinai School of Medicine ADC Boston University ADC In consultation
NACC Vascular Consortium NACC Vascular Consortium Participating centers: Oregon Health and Science University ADC Rush University ADC Mount Sinai School of Medicine ADC Boston University ADC In consultation
What Cell Make Up the Brain and Spinal Cord
 What Cell Make Up the Brain and Spinal Cord Jennifer LaVail, Ph.D. (http://anatomy.ucsf.edu/pages/lavaillab/index.html) What kinds of cells are these?" Neuron?" Epithelial cell?" Glial cell?" What makes
What Cell Make Up the Brain and Spinal Cord Jennifer LaVail, Ph.D. (http://anatomy.ucsf.edu/pages/lavaillab/index.html) What kinds of cells are these?" Neuron?" Epithelial cell?" Glial cell?" What makes
Synoptic Alterations in Developing. Investigation in Monkeys
 Synoptic Alterations in Developing Cortical Infarction: An Experimental Investigation in Monkeys BY JOHN R. LITTLE, M.D., FREDERICK W. L. KERR, M.D., AND THORALF M. SUNDT, JR., M.D. Abstract: Synaptic
Synoptic Alterations in Developing Cortical Infarction: An Experimental Investigation in Monkeys BY JOHN R. LITTLE, M.D., FREDERICK W. L. KERR, M.D., AND THORALF M. SUNDT, JR., M.D. Abstract: Synaptic
Immunohistochemical investigation of cerebral ischemia after middle cerebral artery occlusion in gerbils
 J Neurosurg 67:414-42, 1987 Immunohistochemical investigation of cerebral ischemia after middle cerebral artery occlusion in gerbils KAZUMI YAMAMOTO, M.D., FUMIHARU AKAI, M.D., TOSHIKI YOSHIMINE, M.D.,
J Neurosurg 67:414-42, 1987 Immunohistochemical investigation of cerebral ischemia after middle cerebral artery occlusion in gerbils KAZUMI YAMAMOTO, M.D., FUMIHARU AKAI, M.D., TOSHIKI YOSHIMINE, M.D.,
ENHANCEMENT OF THE GRANULATION OF ADRFNERGIC STORAGE VESICLES IN DRUG-FREE SOLUTION
 ENHANCEMENT OF THE GRANULATION OF ADRFNERGIC STORAGE VESICLES IN DRUG-FREE SOLUTION TAKASHI IWAYAMA and J. B. FURNESS. From the Department of Zoology, University of Melbourne, Victoria, Australia. Dr.
ENHANCEMENT OF THE GRANULATION OF ADRFNERGIC STORAGE VESICLES IN DRUG-FREE SOLUTION TAKASHI IWAYAMA and J. B. FURNESS. From the Department of Zoology, University of Melbourne, Victoria, Australia. Dr.
Cell Overview. Hanan Jafar BDS.MSc.PhD
 Cell Overview Hanan Jafar BDS.MSc.PhD THE CELL is made of: 1- Nucleus 2- Cell Membrane 3- Cytoplasm THE CELL Formed of: 1. Nuclear envelope 2. Chromatin 3. Nucleolus 4. Nucleoplasm (nuclear matrix) NUCLEUS
Cell Overview Hanan Jafar BDS.MSc.PhD THE CELL is made of: 1- Nucleus 2- Cell Membrane 3- Cytoplasm THE CELL Formed of: 1. Nuclear envelope 2. Chromatin 3. Nucleolus 4. Nucleoplasm (nuclear matrix) NUCLEUS
Implication of aquaporins in ischemic stroke. New target?
 Implication of aquaporins in ischemic stroke. New target? Balseanu Tudor-Adrian, MD, PhD EXPERIMENTAL RESEARCH CENTER OF NORMAL AND PATHOLOGICAL AGING University of Medicine and Pharmacy of Craiova, Romania
Implication of aquaporins in ischemic stroke. New target? Balseanu Tudor-Adrian, MD, PhD EXPERIMENTAL RESEARCH CENTER OF NORMAL AND PATHOLOGICAL AGING University of Medicine and Pharmacy of Craiova, Romania
Cells and Tissues. Lesson 2.1: Molecules of Life Lesson 2.2: Cells Lesson 2.3: Tissues
 2 Cells and Tissues Lesson 2.1: Molecules of Life Lesson 2.2: Cells Lesson 2.3: Tissues Chapter 2: Cells and Tissues Lesson 2.1 Molecules of Life Molecules of Life carbohydrates proteins lipids nucleic
2 Cells and Tissues Lesson 2.1: Molecules of Life Lesson 2.2: Cells Lesson 2.3: Tissues Chapter 2: Cells and Tissues Lesson 2.1 Molecules of Life Molecules of Life carbohydrates proteins lipids nucleic
mm Distance (mm)
 b a Magnet Illumination Coverslips MPs Objective 2575 µm 1875 µm 1575 µm 1075 µm 875 µm 545 µm 20µm 2 3 0.5 0.3mm 1 1000 100 10 1 0.1 1000 100 10 1 0.1 Field Induction (Gauss) 1.5 0 5 10 15 20 Distance
b a Magnet Illumination Coverslips MPs Objective 2575 µm 1875 µm 1575 µm 1075 µm 875 µm 545 µm 20µm 2 3 0.5 0.3mm 1 1000 100 10 1 0.1 1000 100 10 1 0.1 Field Induction (Gauss) 1.5 0 5 10 15 20 Distance
Endothelial cell damage by temporary arterial occlusion with surgical clips
 Endothelial cell damage by temporary arterial occlusion with surgical clips Study of the clip site by scanning and transmission electron microscopy S. DAVID GERTZ, PH.D., MARSHALL L. RENNELS, PH.D., MICHAEL
Endothelial cell damage by temporary arterial occlusion with surgical clips Study of the clip site by scanning and transmission electron microscopy S. DAVID GERTZ, PH.D., MARSHALL L. RENNELS, PH.D., MICHAEL
Elastic Skeleton of Intracranial Cerebral Aneurysms in Rats
 1722 Elastic Skeleton of Intracranial Cerebral Aneurysms in Rats Naohiro Yamazoe, MD, Nobuo Hashimoto, MD, Haruhiko Kikuchi, MD, and Fumitada Hazama, MD In an attempt to clarify the developmental mechanism
1722 Elastic Skeleton of Intracranial Cerebral Aneurysms in Rats Naohiro Yamazoe, MD, Nobuo Hashimoto, MD, Haruhiko Kikuchi, MD, and Fumitada Hazama, MD In an attempt to clarify the developmental mechanism
African Trypanosomes
 African Trypanosomes Giemsa-stained blood smear of African trypanosomes viewed under the 100X objective lens. The block arrows denote trypomastigote forms of the African trypanosomes found within the blood
African Trypanosomes Giemsa-stained blood smear of African trypanosomes viewed under the 100X objective lens. The block arrows denote trypomastigote forms of the African trypanosomes found within the blood
Supplementary Figure 1
 Supplementary Figure 1 The average sigmoid parametric curves of capillary dilation time courses and average time to 50% peak capillary diameter dilation computed from individual capillary responses averaged
Supplementary Figure 1 The average sigmoid parametric curves of capillary dilation time courses and average time to 50% peak capillary diameter dilation computed from individual capillary responses averaged
Basophilic. Basophilic structures are stained by basic dyes: Mnemonic: Basophilic = Blue
 Cell Overview Basophilic Basophilic structures are stained by basic dyes: Basic dyes are positive Basophilic structures are negative (ex. DNA, RNA, ribosomes, RER) Mnemonic: Basophilic = Blue Acidophilic
Cell Overview Basophilic Basophilic structures are stained by basic dyes: Basic dyes are positive Basophilic structures are negative (ex. DNA, RNA, ribosomes, RER) Mnemonic: Basophilic = Blue Acidophilic
Introduction. BY W. R. HUDGINS, M.D.,* AND JULIO H. GARCIA, M.D.t. Abstract: ADDITIONAL KEY WORDS focal cerebral ischemia
 Transorbital Approach to the Middle Cerebral Artery of the Squirrel Monkey: A Technique for Experimental Cerebral Infarction Applicable to Ultrastructural Studies BY W. R. HUDGINS, M.D.,* AND JULIO H.
Transorbital Approach to the Middle Cerebral Artery of the Squirrel Monkey: A Technique for Experimental Cerebral Infarction Applicable to Ultrastructural Studies BY W. R. HUDGINS, M.D.,* AND JULIO H.
TOXIC AND NUTRITIONAL DISORDER MODULE
 TOXIC AND NUTRITIONAL DISORDER MODULE Objectives: For each of the following entities the student should be able to: 1. Describe the etiology/pathogenesis and/or pathophysiology, gross and microscopic morphology
TOXIC AND NUTRITIONAL DISORDER MODULE Objectives: For each of the following entities the student should be able to: 1. Describe the etiology/pathogenesis and/or pathophysiology, gross and microscopic morphology
Muscle and Neuromuscular Junction. Peter Takizawa Department of Cell Biology
 Muscle and Neuromuscular Junction Peter Takizawa Department of Cell Biology Types and structure of muscle cells Structural basis of contraction Triggering muscle contraction Skeletal muscle consists of
Muscle and Neuromuscular Junction Peter Takizawa Department of Cell Biology Types and structure of muscle cells Structural basis of contraction Triggering muscle contraction Skeletal muscle consists of
Complete Recovery of Perfusion Abnormalities in a Cardiac Arrest Patient Treated with Hypothermia: Results of Cerebral Perfusion MR Imaging
 pissn 2384-1095 eissn 2384-1109 imri 2018;22:56-60 https://doi.org/10.13104/imri.2018.22.1.56 Complete Recovery of Perfusion Abnormalities in a Cardiac Arrest Patient Treated with Hypothermia: Results
pissn 2384-1095 eissn 2384-1109 imri 2018;22:56-60 https://doi.org/10.13104/imri.2018.22.1.56 Complete Recovery of Perfusion Abnormalities in a Cardiac Arrest Patient Treated with Hypothermia: Results
Early Angiographic and CT Findings in Patients with Hemorrhagic Infarction in the Distribution of the Middle Cerebral Artery
 1115 Early Angiographic and CT Findings in Patients with Hemorrhagic Infarction in the Distribution of the Middle Cerebral Artery L. Bozzao 1 U. Angeloni S. Bastianello L. M. Fantozzi A. Pierallini C.
1115 Early Angiographic and CT Findings in Patients with Hemorrhagic Infarction in the Distribution of the Middle Cerebral Artery L. Bozzao 1 U. Angeloni S. Bastianello L. M. Fantozzi A. Pierallini C.
occlusions. Cerebral perfusion is driven fundamentally by regional cerebral
 Appendix Figures Figure A1. Hemodynamic changes that may occur in major anterior circulation occlusions. Cerebral perfusion is driven fundamentally by regional cerebral perfusion pressure (CPP). In response
Appendix Figures Figure A1. Hemodynamic changes that may occur in major anterior circulation occlusions. Cerebral perfusion is driven fundamentally by regional cerebral perfusion pressure (CPP). In response
Blood Cells. Dr. Sami Zaqout. Dr. Sami Zaqout Faculty of Medicine IUG
 Blood Cells Dr. Sami Zaqout Blood Blood Blood cells (45%) Erythrocytes Platelets Leukocytes Plasma (55%) Hematocrit tubes with blood Composition of Plasma Plasma Aqueous solution (90%) Substances (10%)
Blood Cells Dr. Sami Zaqout Blood Blood Blood cells (45%) Erythrocytes Platelets Leukocytes Plasma (55%) Hematocrit tubes with blood Composition of Plasma Plasma Aqueous solution (90%) Substances (10%)
Blood: Functions. Liquid connective tissue 3 general functions 1. Transportation. 2. Regulation. 3. Protection
 Blood Elements Lecture Objectives List blood components. Classify formed elements of blood. Discuss the scientific basis of the above classification. Describe the basic structure of erythrocytes and criteria
Blood Elements Lecture Objectives List blood components. Classify formed elements of blood. Discuss the scientific basis of the above classification. Describe the basic structure of erythrocytes and criteria
Cellular Injury. Intracellular degeneration. By Dr. Hemn Hassan Othman PhD, Pathology Fall /20/2018 1
 Cellular Injury Intracellular degeneration By Dr. Hemn Hassan Othman PhD, Pathology Fall 2018 10/20/2018 1 Types of cell injury Cell injury is divided into: 1. Reversible cell injury 2. Irreversible cell
Cellular Injury Intracellular degeneration By Dr. Hemn Hassan Othman PhD, Pathology Fall 2018 10/20/2018 1 Types of cell injury Cell injury is divided into: 1. Reversible cell injury 2. Irreversible cell
STUDIES OF THE HUMAN UNFERTILIZED TUBAL OVUM*t
 FERTILITY AND STERILITY Copyright @ 1973 by The Williams & Wilkins Co. Vol. 24, No.8, August 1973 Printed in U.S.A. STUDIES OF THE HUMAN UNFERTILIZED TUBAL OVUM*t C. NORIEGA, M.D., AND C. OBERTI, M.D.
FERTILITY AND STERILITY Copyright @ 1973 by The Williams & Wilkins Co. Vol. 24, No.8, August 1973 Printed in U.S.A. STUDIES OF THE HUMAN UNFERTILIZED TUBAL OVUM*t C. NORIEGA, M.D., AND C. OBERTI, M.D.
The Fine Structure and Function of the Mechanically Injured Renal Lymphatic Capillary M. Ohkuma
 Lymphology 7 (1974) 1-6 Georg Thieme Verlag Stuttgart The Fine Structure and Function of the Mechanically Injured Renal Lymphatic Capillary M. Ohkuma Electron Microscopic Laboratory, Department of Dermatology,
Lymphology 7 (1974) 1-6 Georg Thieme Verlag Stuttgart The Fine Structure and Function of the Mechanically Injured Renal Lymphatic Capillary M. Ohkuma Electron Microscopic Laboratory, Department of Dermatology,
Mansoura university Faculty of medicine Histology and cell Biology Department Curriculum Content And Logbook
 Mansoura university Faculty of medicine Histology and cell Biology Department Curriculum Content And Logbook For the 1 st year Medical Student s In Histology and cell Biology Mansoura university Faculty
Mansoura university Faculty of medicine Histology and cell Biology Department Curriculum Content And Logbook For the 1 st year Medical Student s In Histology and cell Biology Mansoura university Faculty
ON THE PRESENCE OF A CILIATED COLUMNAR EPITHELIAL CELL TYPE WITHIN THE BOVINE CERVICAL MUCOSA 1
 ON THE PRESENCE OF A CILIATED COLUMNAR EPITHELIAL CELL TYPE WITHIN THE BOVINE CERVICAL MUCOSA 1 R. I. Wordinger, 2 J. B. Ramsey, I. F. Dickey and I. R. Hill, Jr. Clemson University, Clemson, South Carolina
ON THE PRESENCE OF A CILIATED COLUMNAR EPITHELIAL CELL TYPE WITHIN THE BOVINE CERVICAL MUCOSA 1 R. I. Wordinger, 2 J. B. Ramsey, I. F. Dickey and I. R. Hill, Jr. Clemson University, Clemson, South Carolina
IV. Brain Edema in Stroke
 REPORT OF JOINT COMMITTEE FOR STROKE RESOURCES IV. Brain Edema in Stroke STUDY GROUP ON BRAIN EDEMA IN STROKE ROBERT KATZMAN, M.D., CHAIRMAN, RAYMOND CLASEN, M.D., IGOR KLATZO, M.D., JOHN STIRLING MEYER,
REPORT OF JOINT COMMITTEE FOR STROKE RESOURCES IV. Brain Edema in Stroke STUDY GROUP ON BRAIN EDEMA IN STROKE ROBERT KATZMAN, M.D., CHAIRMAN, RAYMOND CLASEN, M.D., IGOR KLATZO, M.D., JOHN STIRLING MEYER,
******************************************************************************************************* MUSCLE CYTOLOGY AND HISTOLOGY
 BIOLOGY 211: HUMAN ANATOMY & PHYSIOLOGY ******************************************************************************************************* MUSCLE CYTOLOGY AND HISTOLOGY *******************************************************************************************************
BIOLOGY 211: HUMAN ANATOMY & PHYSIOLOGY ******************************************************************************************************* MUSCLE CYTOLOGY AND HISTOLOGY *******************************************************************************************************
Glycogen Aggregates in Cardiac Muscle Cell: A Cytopathological Study on Endomyocardial Biopsies
 Arch. histol. jap., Vol. 45, No. 4 (1982) p. 347-354 Glycogen Aggregates in Cardiac Muscle Cell: A Cytopathological Study on Endomyocardial Biopsies Kazumasa MIURA, Tohru IZUMI, Junichi FUKUDA, Masaru
Arch. histol. jap., Vol. 45, No. 4 (1982) p. 347-354 Glycogen Aggregates in Cardiac Muscle Cell: A Cytopathological Study on Endomyocardial Biopsies Kazumasa MIURA, Tohru IZUMI, Junichi FUKUDA, Masaru
The Neuron. Consists Of: - cell body. - Dendrites - axon - axon terminal - myelin. dendrites Axon terminal. Cell body. nucleus. axon.
 The Neuron Consists Of: - cell body - Dendrites - axon - axon terminal - myelin dendrites Axon terminal Cell body nucleus myelin axon THE SYNAPSE Definition: It is a point of contact between the axon of
The Neuron Consists Of: - cell body - Dendrites - axon - axon terminal - myelin dendrites Axon terminal Cell body nucleus myelin axon THE SYNAPSE Definition: It is a point of contact between the axon of
Biology Dr. Khalida Ibrahim Nervous system The nervous system is responsible for communication between different regions of the body, it is divided
 Biology Dr. Khalida Ibrahim Nervous system The nervous system is responsible for communication between different regions of the body, it is divided into: CNS (central nervous system) = brain + spinal cord
Biology Dr. Khalida Ibrahim Nervous system The nervous system is responsible for communication between different regions of the body, it is divided into: CNS (central nervous system) = brain + spinal cord
Experimental Assessment of Infarct Lesion Growth in Mice using Time-Resolved T2* MR Image Sequences
 Experimental Assessment of Infarct Lesion Growth in Mice using Time-Resolved T2* MR Image Sequences Nils Daniel Forkert 1, Dennis Säring 1, Andrea Eisenbeis 2, Frank Leypoldt 3, Jens Fiehler 2, Heinz Handels
Experimental Assessment of Infarct Lesion Growth in Mice using Time-Resolved T2* MR Image Sequences Nils Daniel Forkert 1, Dennis Säring 1, Andrea Eisenbeis 2, Frank Leypoldt 3, Jens Fiehler 2, Heinz Handels
ELECTRON MICROSCOPIC STUDIES ON EQUINE ENCEPHALOSIS VIRUS
 Onderstepoort]. vet. Res. 40 (2), 53-58 (1973) ELECTRON MICROSCOPIC STUDIES ON EQUINE ENCEPHALOSIS VIRUS G. LECATSAS, B. J. ERASMUS and H. J. ELS, Veterinary Research Institute, Onderstepoort ABSTRACT
Onderstepoort]. vet. Res. 40 (2), 53-58 (1973) ELECTRON MICROSCOPIC STUDIES ON EQUINE ENCEPHALOSIS VIRUS G. LECATSAS, B. J. ERASMUS and H. J. ELS, Veterinary Research Institute, Onderstepoort ABSTRACT
Major Structures of the Nervous System. Brain, cranial nerves, spinal cord, spinal nerves, ganglia, enteric plexuses and sensory receptors
 Major Structures of the Nervous System Brain, cranial nerves, spinal cord, spinal nerves, ganglia, enteric plexuses and sensory receptors Nervous System Divisions Central Nervous System (CNS) consists
Major Structures of the Nervous System Brain, cranial nerves, spinal cord, spinal nerves, ganglia, enteric plexuses and sensory receptors Nervous System Divisions Central Nervous System (CNS) consists
Characteristic features of CNS pathology. By: Shifaa AlQa qa
 Characteristic features of CNS pathology By: Shifaa AlQa qa Normal brain: - The neocortex (gray matter): six layers: outer plexiform, outer granular, outer pyramidal, inner granular, inner pyramidal, polymorphous
Characteristic features of CNS pathology By: Shifaa AlQa qa Normal brain: - The neocortex (gray matter): six layers: outer plexiform, outer granular, outer pyramidal, inner granular, inner pyramidal, polymorphous
In the space provided, write the letter of the term or phrase that best completes each statement or best answers each question.
 CHAPTER 3 TEST Cell Structure Circle T if the statement is true or F if it is false. T F 1. Small cells can transport materials and information more quickly than larger cells can. T F 2. Newly made proteins
CHAPTER 3 TEST Cell Structure Circle T if the statement is true or F if it is false. T F 1. Small cells can transport materials and information more quickly than larger cells can. T F 2. Newly made proteins
WHITE PAPER: A GUIDE TO UNDERSTANDING SUBARACHNOID HEMORRHAGE
 WHITE PAPER: A GUIDE TO UNDERSTANDING SUBARACHNOID HEMORRHAGE Subarachnoid Hemorrhage is a serious, life-threatening type of hemorrhagic stroke caused by bleeding into the space surrounding the brain,
WHITE PAPER: A GUIDE TO UNDERSTANDING SUBARACHNOID HEMORRHAGE Subarachnoid Hemorrhage is a serious, life-threatening type of hemorrhagic stroke caused by bleeding into the space surrounding the brain,
Yara shwabkeh. Osama Alkhader. Heba Kalbouneh
 2 Yara shwabkeh Osama Alkhader Heba Kalbouneh CELL OVERVIEW -Note ; the important thing is to know how the organelles appear under the microscope - the stains we usually use in Histology are composed of
2 Yara shwabkeh Osama Alkhader Heba Kalbouneh CELL OVERVIEW -Note ; the important thing is to know how the organelles appear under the microscope - the stains we usually use in Histology are composed of
Nervous system is the most complex system in our body. It is formed by a network of more than 100 million nerve cells (neurons) assisted by many more
 Nervous system Nervous system is the most complex system in our body. It is formed by a network of more than 100 million nerve cells (neurons) assisted by many more glial cells. Devoid from connective
Nervous system Nervous system is the most complex system in our body. It is formed by a network of more than 100 million nerve cells (neurons) assisted by many more glial cells. Devoid from connective
A. Subdivisions of the Nervous System: 1. The two major subdivisions of the nervous system:
 BIO 211: ANATOMY & PHYSIOLOGY I 1 Ch 10 A Ch 10 B CHAPTER 10 NERVOUS SYSTEM 1 BASIC STRUCTURE and FUNCTION Dr. Lawrence G. Altman www.lawrencegaltman.com Some illustrations are courtesy of McGraw-Hill.
BIO 211: ANATOMY & PHYSIOLOGY I 1 Ch 10 A Ch 10 B CHAPTER 10 NERVOUS SYSTEM 1 BASIC STRUCTURE and FUNCTION Dr. Lawrence G. Altman www.lawrencegaltman.com Some illustrations are courtesy of McGraw-Hill.
Reperfusion Injury: How Can We Reduce It?
 MI/CAD: Practical Question in Management of AMI Patients Reperfusion Injury: How Can We Reduce It? Hyun-Jai Cho, M.D., Ph.D Cardiovascular Center & Department of Internal Medicine Seoul National University
MI/CAD: Practical Question in Management of AMI Patients Reperfusion Injury: How Can We Reduce It? Hyun-Jai Cho, M.D., Ph.D Cardiovascular Center & Department of Internal Medicine Seoul National University
The Cell. BIOLOGY OF HUMANS Concepts, Applications, and Issues. Judith Goodenough Betty McGuire
 BIOLOGY OF HUMANS Concepts, Applications, and Issues Fifth Edition Judith Goodenough Betty McGuire 3 The Cell Lecture Presentation Anne Gasc Hawaii Pacific University and University of Hawaii Honolulu
BIOLOGY OF HUMANS Concepts, Applications, and Issues Fifth Edition Judith Goodenough Betty McGuire 3 The Cell Lecture Presentation Anne Gasc Hawaii Pacific University and University of Hawaii Honolulu
Pathophysiology and treatment of focal cerebral ischemia
 J Neurosurg 77: 169-184, 1992 Review Article Pathophysiology and treatment of focal cerebral ischemia Part I: Pathophysiology Bo K. SIESJO, M.D. Laborutory for Experimental Bruin Reseurch, Experrmc~ntul
J Neurosurg 77: 169-184, 1992 Review Article Pathophysiology and treatment of focal cerebral ischemia Part I: Pathophysiology Bo K. SIESJO, M.D. Laborutory for Experimental Bruin Reseurch, Experrmc~ntul
MOLECULAR AND CELLULAR NEUROSCIENCE
 MOLECULAR AND CELLULAR NEUROSCIENCE BMP-218 November 4, 2014 DIVISIONS OF THE NERVOUS SYSTEM The nervous system is composed of two primary divisions: 1. CNS - Central Nervous System (Brain + Spinal Cord)
MOLECULAR AND CELLULAR NEUROSCIENCE BMP-218 November 4, 2014 DIVISIONS OF THE NERVOUS SYSTEM The nervous system is composed of two primary divisions: 1. CNS - Central Nervous System (Brain + Spinal Cord)
Organization of the nervous system. [See Fig. 48.1]
![Organization of the nervous system. [See Fig. 48.1] Organization of the nervous system. [See Fig. 48.1]](/thumbs/90/103926552.jpg) Nervous System [Note: This is the text version of this lecture file. To make the lecture notes downloadable over a slow connection (e.g. modem) the figures have been replaced with figure numbers as found
Nervous System [Note: This is the text version of this lecture file. To make the lecture notes downloadable over a slow connection (e.g. modem) the figures have been replaced with figure numbers as found
The Brain & Homeostasis. The Brain & Technology. CAT, PET, and MRI Scans
 The Brain & Homeostasis Today, scientists have a lot of information about what happens in the different parts of the brain; however they are still trying to understand how the brain functions. We know
The Brain & Homeostasis Today, scientists have a lot of information about what happens in the different parts of the brain; however they are still trying to understand how the brain functions. We know
Blood Supply. Allen Chung, class of 2013
 Blood Supply Allen Chung, class of 2013 Objectives Understand the importance of the cerebral circulation. Understand stroke and the types of vascular problems that cause it. Understand ischemic penumbra
Blood Supply Allen Chung, class of 2013 Objectives Understand the importance of the cerebral circulation. Understand stroke and the types of vascular problems that cause it. Understand ischemic penumbra
Neurological Deficit and Cerebral Infarction after Temporary Middle Cerebral Artery Occlusion in Unanesthetized Cats
 8 Neurological Deficit and Cerebral Infarction after Temporary Middle Cerebral Artery Occlusion in Unanesthetized Cats PHILIP R. WEINSTEIN, M.D., GARY G. ANDERSON, B.S., AND DAVID A. TELLES, B.S. SUMMARY
8 Neurological Deficit and Cerebral Infarction after Temporary Middle Cerebral Artery Occlusion in Unanesthetized Cats PHILIP R. WEINSTEIN, M.D., GARY G. ANDERSON, B.S., AND DAVID A. TELLES, B.S. SUMMARY
Unit 2 Warm Ups. Equilibrium
 Unit 2 Warm Ups Equilibrium 1. Cell wall 2. Mitochondria 3. Chloroplast 4. Vesicle 5. Vacuole 6. Rough Endoplasmic Reticulum 7. Smooth Endoplasmic Reticulum 8. Cytoskeleton 9. Lysosomes 10.Cell Membrane
Unit 2 Warm Ups Equilibrium 1. Cell wall 2. Mitochondria 3. Chloroplast 4. Vesicle 5. Vacuole 6. Rough Endoplasmic Reticulum 7. Smooth Endoplasmic Reticulum 8. Cytoskeleton 9. Lysosomes 10.Cell Membrane
Essentials of Clinical MR, 2 nd edition. 14. Ischemia and Infarction II
 14. Ischemia and Infarction II Lacunar infarcts are small deep parenchymal lesions involving the basal ganglia, internal capsule, thalamus, and brainstem. The vascular supply of these areas includes the
14. Ischemia and Infarction II Lacunar infarcts are small deep parenchymal lesions involving the basal ganglia, internal capsule, thalamus, and brainstem. The vascular supply of these areas includes the
CEREBROVASCULAR DISEASES. By: Shifaa AlQa qa
 CEREBROVASCULAR DISEASES By: Shifaa AlQa qa Cerebrovascular diseases Brain disorders caused by pathologic processes involving blood vessels 3 pathogenic mechanisms (1) thrombotic occlusion, (2) embolic
CEREBROVASCULAR DISEASES By: Shifaa AlQa qa Cerebrovascular diseases Brain disorders caused by pathologic processes involving blood vessels 3 pathogenic mechanisms (1) thrombotic occlusion, (2) embolic
HYPERTENSIVE ENCEPHALOPATHY
 HYPERTENSIVE ENCEPHALOPATHY Reversible posterior leukoencephalopathy syndrome Cause Renal disease Pheochromocytoma Disseminated vasculitis Eclampsia Acute toxemia Medications & illicit drugs (cocaine)
HYPERTENSIVE ENCEPHALOPATHY Reversible posterior leukoencephalopathy syndrome Cause Renal disease Pheochromocytoma Disseminated vasculitis Eclampsia Acute toxemia Medications & illicit drugs (cocaine)
Early Diffusion MR Imaging Findings and Short-Term Outcome in Comatose Patients with Hypoglycemia
 ORIGINAL RESEARCH K. Johkura Y. Nakae Y. Kudo T.N. Yoshida Y. Kuroiwa Early Diffusion MR Imaging Findings and Short-Term Outcome in Comatose Patients with Hypoglycemia BACKGROUND AND PURPOSE: The relationship
ORIGINAL RESEARCH K. Johkura Y. Nakae Y. Kudo T.N. Yoshida Y. Kuroiwa Early Diffusion MR Imaging Findings and Short-Term Outcome in Comatose Patients with Hypoglycemia BACKGROUND AND PURPOSE: The relationship
Fine structural appearances of glomerular capillaries in a case of malignant hypertension
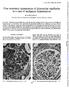 J. clin. Path. (1969), 22, 579-583 Fine structural appearances of glomerular capillaries in a case of malignant hypertension R. F. MACADAM From the University Department of Pathology, Western Infirmary,
J. clin. Path. (1969), 22, 579-583 Fine structural appearances of glomerular capillaries in a case of malignant hypertension R. F. MACADAM From the University Department of Pathology, Western Infirmary,
The Fine Structure of the Epithelial Cells of the Mouse Prostate* II. Ventral Lobe Epithelium
 Published Online: 1 June, 1960 Supp Info: http://doi.org/10.1083/jcb.7.3.511 Downloaded from jcb.rupress.org on September 28, 2018 The Fine Structure of the Epithelial Cells of the Mouse Prostate* II.
Published Online: 1 June, 1960 Supp Info: http://doi.org/10.1083/jcb.7.3.511 Downloaded from jcb.rupress.org on September 28, 2018 The Fine Structure of the Epithelial Cells of the Mouse Prostate* II.
Ischemic heart disease
 Ischemic heart disease Introduction In > 90% of cases: the cause is: reduced coronary blood flow secondary to: obstructive atherosclerotic vascular disease so most of the time it is called: coronary artery
Ischemic heart disease Introduction In > 90% of cases: the cause is: reduced coronary blood flow secondary to: obstructive atherosclerotic vascular disease so most of the time it is called: coronary artery
ALTERATIONS IN BEHAVIOR, BRAIN ELECTRICAL ACTIVITY, CBF, ICP/Marshall et al. 21
 ALTERATIONS IN BEHAVIOR, BRAIN ELECTRICAL ACTIVITY, CBF, ICP/Marshall et al. 21 occur. If a bruit is heard over the common carotid artery low in the neck, compression is deferred until angiography establishes
ALTERATIONS IN BEHAVIOR, BRAIN ELECTRICAL ACTIVITY, CBF, ICP/Marshall et al. 21 occur. If a bruit is heard over the common carotid artery low in the neck, compression is deferred until angiography establishes
THE NERVOUS SYSTEM AS A TARGET ORGAN
 THE NERVOUS SYSTEM AS A TARGET ORGAN Summary A target organ is an organ or organs of the body which adversely responds to systemic exposure of a chemical. The function of the nervous system is to communicate
THE NERVOUS SYSTEM AS A TARGET ORGAN Summary A target organ is an organ or organs of the body which adversely responds to systemic exposure of a chemical. The function of the nervous system is to communicate
WHITE PAPER: A GUIDE TO UNDERSTANDING LARGE HEMISPHERIC INFARCTION
 WHITE PAPER: A GUIDE TO UNDERSTANDING LARGE HEMISPHERIC INFARCTION Large Hemispheric Infarction (LHI) represents a minority of strokes, yet is responsible for a disproportionately large share of stroke-related
WHITE PAPER: A GUIDE TO UNDERSTANDING LARGE HEMISPHERIC INFARCTION Large Hemispheric Infarction (LHI) represents a minority of strokes, yet is responsible for a disproportionately large share of stroke-related
Graefe's Archive. Ophthalmology Springer-Verlag Artificial anterior chamber for the growing of membranes on lens implants*
 Graefe's Arch Clin Exp Ophthalmol (1983) 221:55-60 Graefe's Archive for Clinical and Experimental Ophthalmology Springer-Verlag 1983 Artificial anterior chamber for the growing of membranes on lens implants*
Graefe's Arch Clin Exp Ophthalmol (1983) 221:55-60 Graefe's Archive for Clinical and Experimental Ophthalmology Springer-Verlag 1983 Artificial anterior chamber for the growing of membranes on lens implants*
Cell Structure and Function. Biology 12 Unit 1 Cell Structure and Function Inquiry into Life pages and 68-69
 Cell Structure and Function Biology 12 Unit 1 Cell Structure and Function Inquiry into Life pages 45 59 and 68-69 Assignments for this Unit Pick up the notes/worksheet for this unit and the project There
Cell Structure and Function Biology 12 Unit 1 Cell Structure and Function Inquiry into Life pages 45 59 and 68-69 Assignments for this Unit Pick up the notes/worksheet for this unit and the project There
The 7 th lecture. Anatomy and Physiology For the. 1 st Class. By Dr. Ala a Hassan Mirza
 The 7 th lecture In Anatomy and Physiology For the 1 st Class By Dr. Ala a Hassan Mirza Nervous System (part I) The Nerve Tissue and the Nervous System The Tissues of the Body There are 4 types of tissues
The 7 th lecture In Anatomy and Physiology For the 1 st Class By Dr. Ala a Hassan Mirza Nervous System (part I) The Nerve Tissue and the Nervous System The Tissues of the Body There are 4 types of tissues
Lecture name: blood 2 & The Circulatory System Edited by: Buthainah Al masaeed & Yousef Qandeel
 Lecture name: blood 2 & The Circulatory System Edited by: Buthainah Al masaeed & Yousef Qandeel Now we will take about A granulocytes : Lymphocyte Monocytes 1- Lymphocyte - The second major type of presence
Lecture name: blood 2 & The Circulatory System Edited by: Buthainah Al masaeed & Yousef Qandeel Now we will take about A granulocytes : Lymphocyte Monocytes 1- Lymphocyte - The second major type of presence
Lesson 14. The Nervous System. Introduction to Life Processes - SCI 102 1
 Lesson 14 The Nervous System Introduction to Life Processes - SCI 102 1 Structures and Functions of Nerve Cells The nervous system has two principal cell types: Neurons (nerve cells) Glia The functions
Lesson 14 The Nervous System Introduction to Life Processes - SCI 102 1 Structures and Functions of Nerve Cells The nervous system has two principal cell types: Neurons (nerve cells) Glia The functions
Sheet: microscopic structures of the ns Done by: Rasha Rakan and Nisreen Obiedat
 Sheet: microscopic structures of the ns Done by: Rasha Rakan and Nisreen Obiedat Lecture Objectives Classify the types of neurons. Describe the structure of the different parts of neurons. Describe the
Sheet: microscopic structures of the ns Done by: Rasha Rakan and Nisreen Obiedat Lecture Objectives Classify the types of neurons. Describe the structure of the different parts of neurons. Describe the
Plants, Animals, Fungi and Protists have Eukaryotic Cell(s)
 Cell Structure Plants, Animals, Fungi and Protists have Eukaryotic Cell(s) Plant Cell Animal Cell straight edges curved edges Cell Organization cytoplasm cell membrane Eukaryotic cells have 3 major parts:
Cell Structure Plants, Animals, Fungi and Protists have Eukaryotic Cell(s) Plant Cell Animal Cell straight edges curved edges Cell Organization cytoplasm cell membrane Eukaryotic cells have 3 major parts:
The pinealocytes of the human pineal gland: a light and electron microscopic study
 O R I G I N A L A R T I C L E Folia Morphol. Vol. 65, No. 3, pp. 181 187 Copyright 2006 Via Medica ISSN 0015 5659 www.fm.viamedica.pl The pinealocytes of the human pineal gland: a light and electron microscopic
O R I G I N A L A R T I C L E Folia Morphol. Vol. 65, No. 3, pp. 181 187 Copyright 2006 Via Medica ISSN 0015 5659 www.fm.viamedica.pl The pinealocytes of the human pineal gland: a light and electron microscopic
Some Observations on the Fine Structure of the Goblet Cells. Special Reference to the Well-Developed Agranular Endoplasmic Reticulum
 Okajimas Folia Anat. Jpn., 58(4-6) : 583-594, March 1982 Some Observations on the Fine Structure of the Goblet Cells in the Nasal Respiratory Epithelium of the Rat, with Special Reference to the Well-Developed
Okajimas Folia Anat. Jpn., 58(4-6) : 583-594, March 1982 Some Observations on the Fine Structure of the Goblet Cells in the Nasal Respiratory Epithelium of the Rat, with Special Reference to the Well-Developed
Announcement. Danny to schedule a time if you are interested.
 Announcement If you need more experiments to participate in, contact Danny Sanchez (dsanchez@ucsd.edu) make sure to tell him that you are from LIGN171, so he will let me know about your credit (1 point).
Announcement If you need more experiments to participate in, contact Danny Sanchez (dsanchez@ucsd.edu) make sure to tell him that you are from LIGN171, so he will let me know about your credit (1 point).
Pathophysiology and treatment of focal cerebral ischemia
 J Neurosurg 77:337-354, 1992 Review Article Pathophysiology and treatment of focal cerebral ischemia Part 11: Mechanisms of damage and treatment Bo K. SIESJO, M.D. Laboratory for Experimental Brain Research,
J Neurosurg 77:337-354, 1992 Review Article Pathophysiology and treatment of focal cerebral ischemia Part 11: Mechanisms of damage and treatment Bo K. SIESJO, M.D. Laboratory for Experimental Brain Research,
R. Pluta, M. Ułamek, and S. Januszewski. relatively high [3] and an e ect of this incidence is irreversible. Summary
![R. Pluta, M. Ułamek, and S. Januszewski. relatively high [3] and an e ect of this incidence is irreversible. Summary R. Pluta, M. Ułamek, and S. Januszewski. relatively high [3] and an e ect of this incidence is irreversible. Summary](/thumbs/88/117553410.jpg) Acta Neurochir (2006) [Suppl] 96: 267 271 6 Springer-Verlag 2006 Printed in Austria Micro-blood-brain barrier openings and cytotoxic fragments of amyloid precursor protein accumulation in white matter
Acta Neurochir (2006) [Suppl] 96: 267 271 6 Springer-Verlag 2006 Printed in Austria Micro-blood-brain barrier openings and cytotoxic fragments of amyloid precursor protein accumulation in white matter
UPSTATE Comprehensive Stroke Center. Neurosurgical Interventions Satish Krishnamurthy MD, MCh
 UPSTATE Comprehensive Stroke Center Neurosurgical Interventions Satish Krishnamurthy MD, MCh Regional cerebral blood flow is important Some essential facts Neurons are obligatory glucose users Under anerobic
UPSTATE Comprehensive Stroke Center Neurosurgical Interventions Satish Krishnamurthy MD, MCh Regional cerebral blood flow is important Some essential facts Neurons are obligatory glucose users Under anerobic
FIXATION BY MEANS OF GLUTARALDEHYDE-HYDROGEN PEROXIDE REACTION PRODUCTS
 FIXATION BY MEANS OF GLUTARALDEHYDE-HYDROGEN PEROXIDE REACTION PRODUCTS CAMILLO PERACCHIA and BRANT S. MITTLER. From the Department of Anatomy, Duke University Medical Center, Durham, North Carolina 27706,
FIXATION BY MEANS OF GLUTARALDEHYDE-HYDROGEN PEROXIDE REACTION PRODUCTS CAMILLO PERACCHIA and BRANT S. MITTLER. From the Department of Anatomy, Duke University Medical Center, Durham, North Carolina 27706,
Acute stroke. Ischaemic stroke. Characteristics. Temporal classification. Clinical features. Interpretation of Emergency Head CT
 Ischaemic stroke Characteristics Stroke is the third most common cause of death in the UK, and the leading cause of disability. 80% of strokes are ischaemic Large vessel occlusive atheromatous disease
Ischaemic stroke Characteristics Stroke is the third most common cause of death in the UK, and the leading cause of disability. 80% of strokes are ischaemic Large vessel occlusive atheromatous disease
(From The Rockefeller Institute) Materials and Methods. Observations with the Electron Microscope
 ELECTRON MICROSCOPE STUDY OF THE DEVELOPMENT OF THE PAPILLOMA VIRUS IN THE SKIN OF THE RABBIT* BY ROBERT S. STONE,~ M.D., RICHARD E. SHOPE, M.D., DAN H. MOORE, P,~.D. (From The Rockefeller Institute) PLATES
ELECTRON MICROSCOPE STUDY OF THE DEVELOPMENT OF THE PAPILLOMA VIRUS IN THE SKIN OF THE RABBIT* BY ROBERT S. STONE,~ M.D., RICHARD E. SHOPE, M.D., DAN H. MOORE, P,~.D. (From The Rockefeller Institute) PLATES
Neurovascular Coupling
 Cerebral Blood Flow and Brain Activation UCLA NITP July 2012 Neurovascular Coupling Richard B. Buxton University of California, San Diego rbuxton@ucsd.edu... The subject to be observed lay on a delicately
Cerebral Blood Flow and Brain Activation UCLA NITP July 2012 Neurovascular Coupling Richard B. Buxton University of California, San Diego rbuxton@ucsd.edu... The subject to be observed lay on a delicately
Human height. Length of some nerve and muscle cells. Chicken egg. Frog egg. Most plant and animal cells Nucleus Most bacteria Mitochondrion
 10 m 1 m 0.1 m 1 cm Human height Length of some nerve and muscle cells Chicken egg Unaided eye 1 mm Frog egg 100 µm 10 µm 1 µm 100 nm 10 nm Most plant and animal cells Nucleus Most bacteria Mitochondrion
10 m 1 m 0.1 m 1 cm Human height Length of some nerve and muscle cells Chicken egg Unaided eye 1 mm Frog egg 100 µm 10 µm 1 µm 100 nm 10 nm Most plant and animal cells Nucleus Most bacteria Mitochondrion
Cell Structure and Function
 Cell Structure and Function Agre and cells in the news Cells Smallest living unit Most are microscopic Discovery of Cells Robert Hooke (mid-1600s) Observed sliver of cork Saw row of empty boxes Coined
Cell Structure and Function Agre and cells in the news Cells Smallest living unit Most are microscopic Discovery of Cells Robert Hooke (mid-1600s) Observed sliver of cork Saw row of empty boxes Coined
1. General characteristics of muscle tissues: 2. A. Skeletal muscle tissue ("striated muscle tissue")
 1. General characteristics of muscle tissues: Muscle fibers, AKA, muscle cells Vascularized. Other tissues dense and loose C.T. nerves and nerve fibers Muscle fibers (muscle cells) close together. From
1. General characteristics of muscle tissues: Muscle fibers, AKA, muscle cells Vascularized. Other tissues dense and loose C.T. nerves and nerve fibers Muscle fibers (muscle cells) close together. From
1. (a) (i) Ability to distinguish points (close together); 1 (ii) Electrons have a shorter wavelength; 1
 1. (a) (i) Ability to distinguish points (close together); 1 Electrons have a shorter wavelength; 1 (b) (i) Golgi / nucleus / mitochondrion / endoplasmic reticulum / chromosome / larger ribosomes; R Membrane
1. (a) (i) Ability to distinguish points (close together); 1 Electrons have a shorter wavelength; 1 (b) (i) Golgi / nucleus / mitochondrion / endoplasmic reticulum / chromosome / larger ribosomes; R Membrane
Hypertension and Acute Focal Cerebral Ischemia
 Hypertension and Acute Focal Cerebral Ischemia 6 Infarction and Edema after Occlusion of a Middle Cerebral Artery in Cats TORU HAYAKAWA, M.D., ARTHUR G. WALTZ, M.D., RONALD L. JACOBSON, PH.D. SUMMARY Hypertension
Hypertension and Acute Focal Cerebral Ischemia 6 Infarction and Edema after Occlusion of a Middle Cerebral Artery in Cats TORU HAYAKAWA, M.D., ARTHUR G. WALTZ, M.D., RONALD L. JACOBSON, PH.D. SUMMARY Hypertension
1. This is the location where N-linked oligosaccharide is initially synthesized and attached to glycoproteins.
 Biology 4410 Name Spring 2006 Exam 2 A. Multiple Choice, 2 pt each Pick the best choice from the list of choices, and write it in the space provided. Some choices may be used more than once, and other
Biology 4410 Name Spring 2006 Exam 2 A. Multiple Choice, 2 pt each Pick the best choice from the list of choices, and write it in the space provided. Some choices may be used more than once, and other
ANNEX II: Atlas of histopathological lesions of Isolated Chicken Eyes
 ANNEX II: Atlas of histopathological lesions of Isolated Chicken Eyes (from Triskelion, Zeist, The Netherlands) 1. Introduction... 1 2. Semi-quantitative microscopic evaluation of the cornea... 1 3. Histopathology
ANNEX II: Atlas of histopathological lesions of Isolated Chicken Eyes (from Triskelion, Zeist, The Netherlands) 1. Introduction... 1 2. Semi-quantitative microscopic evaluation of the cornea... 1 3. Histopathology
Cell Adaptation, Cell Injury and Cell Death
 Cell Adaptation, Cell Injury and Cell Death Pathology:- is the study of structural and functional abnormalities that are expressed as diseases of organs and systems. Modern pathology, proposed that injury
Cell Adaptation, Cell Injury and Cell Death Pathology:- is the study of structural and functional abnormalities that are expressed as diseases of organs and systems. Modern pathology, proposed that injury
1. endoplasmic reticulum This is the location where N-linked oligosaccharide is initially synthesized and attached to glycoproteins.
 Biology 4410 Name Spring 2006 Exam 2 A. Multiple Choice, 2 pt each Pick the best choice from the list of choices, and write it in the space provided. Some choices may be used more than once, and other
Biology 4410 Name Spring 2006 Exam 2 A. Multiple Choice, 2 pt each Pick the best choice from the list of choices, and write it in the space provided. Some choices may be used more than once, and other
ETIOLOGY AND PATHOGENESIS OF HYPOXIC-ISCHEMIC ENCEPHALOPATHY
 ETIOLOGY AND PATHOGENESIS OF HYPOXIC-ISCHEMIC ENCEPHALOPATHY HYPOXIC-ISCHEMIC ENCEPHALOPATHY Hypoxic-İschemic Encephalopathy Encephalopathy due to hypoxic-ischemic injury [Hypoxic-ischemic encephalopathy
ETIOLOGY AND PATHOGENESIS OF HYPOXIC-ISCHEMIC ENCEPHALOPATHY HYPOXIC-ISCHEMIC ENCEPHALOPATHY Hypoxic-İschemic Encephalopathy Encephalopathy due to hypoxic-ischemic injury [Hypoxic-ischemic encephalopathy
FLASH CARDS. Kalat s Book Chapter 2 Alphabetical
 FLASH CARDS www.biologicalpsych.com Kalat s Book Chapter 2 Alphabetical absolute refractory period absolute refractory period Time when neuron will not re-fire no matter how much stimulus it gets. action
FLASH CARDS www.biologicalpsych.com Kalat s Book Chapter 2 Alphabetical absolute refractory period absolute refractory period Time when neuron will not re-fire no matter how much stimulus it gets. action
8.2. Types of Neurons
 Chapter 8 Nervous Tissue The neuron is the functional and the structural unit of the nervous system. It displays two highly developed physiological traits: 1. Irritability - the capacity to generate a
Chapter 8 Nervous Tissue The neuron is the functional and the structural unit of the nervous system. It displays two highly developed physiological traits: 1. Irritability - the capacity to generate a
Coagulative Necrosis of Myocardium. Dr Rodney Itaki Division of Pathology
 Coagulative Necrosis of Myocardium Dr Rodney Itaki Division of Pathology Coagulative Necrosis Gross pathology: 3 day old infarct: Yellow necrosis surrounded by hyperemic borders. Arrow points to a transmural
Coagulative Necrosis of Myocardium Dr Rodney Itaki Division of Pathology Coagulative Necrosis Gross pathology: 3 day old infarct: Yellow necrosis surrounded by hyperemic borders. Arrow points to a transmural
Srikara V Peelukhana Shilpi Goenka Dr. Jay Kim Dr. Rupak K. Banerjee
 Srikara V Peelukhana Shilpi Goenka Dr. Jay Kim Dr. Rupak K. Banerjee Introduction Exposure to excessive vibration: Musculoskeletal disorder (MSD) Estimated cost : $13 - $54 billion annually ( NORA Musculoskeletal
Srikara V Peelukhana Shilpi Goenka Dr. Jay Kim Dr. Rupak K. Banerjee Introduction Exposure to excessive vibration: Musculoskeletal disorder (MSD) Estimated cost : $13 - $54 billion annually ( NORA Musculoskeletal
STRUCTURAL ELEMENTS OF THE NERVOUS SYSTEM
 STRUCTURAL ELEMENTS OF THE NERVOUS SYSTEM STRUCTURE AND MAINTENANCE OF NEURONS (a) (b) Dendrites Cell body Initial segment collateral terminals (a) Diagrammatic representation of a neuron. The break in
STRUCTURAL ELEMENTS OF THE NERVOUS SYSTEM STRUCTURE AND MAINTENANCE OF NEURONS (a) (b) Dendrites Cell body Initial segment collateral terminals (a) Diagrammatic representation of a neuron. The break in
