Long survival in a child with a mutated K27M-H3.3 pilocytic astrocytoma
|
|
|
- Jemimah Blair
- 6 years ago
- Views:
Transcription
1 BRIEF COMMUNICATION Long survival in a child with a mutated K27M-H3.3 pilocytic astrocytoma Audrey Hochart 1, Fabienne Escande 2, Nathalie Rocourt 3, Jacques Grill 4, Valerie Koubi-Pick 5, Juliette Beaujot 6, Samuel Meignan 7, Matthieu Vinchon 8, Claude Alain Maurage 9 & Pierre Leblond 1,7 1 Pediatric Oncology Unit, Oscar Lambret Center, Lille, France 2 Biochemistry and Molecular Biology Department, Lille University Hospital, Lille, France 3 Department of Radiology, Oscar Lambret Center, Lille, France 4 Vectorology and New Anticancer Treatments UMR CNRS 8203 and Department of Pediatric Oncology, Gustave Roussy and University Paris sud, Villejuif, France 5 Department of Molecular Medicine and Translational Research Laboratory, Gustave Roussy, Villejuif, France 6 Neuropathology Department, Biology and Pathology Center, Lille University Hospital, Lille, France 7 Unite Tumorigenese et Resistance au Traitement, INSERM U908, Oscar Lambret Center, Lille, France 8 Department of Pediatric Neurosurgery, Lille University Hospital, Lille, France 9 Groupe d Etude en Neuropathologie Oncologique Pediatrique (GENOP) and Neuropathology Department, Biology and CHULille, F-59000, Lille, France Correspondence Audrey Hochart, Pediatric Oncology Unit, Centre Oscar Lambret, 3 Rue F. Combemale, Lille, France. Tel: ; Fax: ; Audrey. hochart@gmail.com Funding Information No funding information provided. Received: 6 January 2015; Accepted: 27 January 2015 Abstract We report the first case of a child with a H3F3A K27M mutated pilocytic astrocytoma, who presented with a 10 years survival, and underwent spontaneous malignant transformation. The complex tumoral chromosomal rearrangements were consistent for genomic instability and for the histopathological features of malignant transformation into glioblastoma. H3F3A K27M mutations are rarely observed in benign neoplasms and may be associated with an adverse outcome. This mutation might not be the major driver that led to the onset of tumorigenesis, and we could consider that the associated TP53 mutation, would be required for malignant transformation. Annals of Clinical and Translational Neurology 2015; 2(4): doi: /acn3.184 Introduction Pilocytic astrocytoma is the most common brain tumor in children. It is a well circumscribed tumor with a slow growth and is classified as a grade I tumor by the World Health Organization. 1 Malignant transformation (MT) of low-grade gliomas (LGG) is a very unusual event in the pediatric population. 2 H3.3 K27M and G34V/R histone mutations were recently identified as molecular drivers of a subgroup of pediatric high-grade gliomas (HGG), and the H3.3 K27M mutation is associated with worse overall survival. 3,4 Here, we describe the first case of spontaneous MT of a H3.3 K27M mutated cervical spinal cord WHO grade I juvenile pilocytic astrocytoma (JPA) to glioblastoma, after a symptom-free period of 10 years in a teenager. Interestingly, the H3.3-K27M mutation was already present at diagnosis and could explain the unusual evolution of the disease. Patient and Methods Case report A 7-year-old girl with no familial history of neurofibromatosis presented with torticollis and left hemiparesia in Sagittal T1 MRI revealed a well-defined heterogeneous tumor of the cervical spinal cord from level C2, down to C6, with solid and cystic tumor parts and marked contrast enhancement (Fig. 1). Complete surgical removal of the tumor was performed. Clinical, radiological, histological and immun ª 2015 The Authors. Annals of Clinical and Translational Neurology published by Wiley Periodicals, Inc on behalf of American Neurological Association. This is an open access article under the terms of the Creative Commons Attribution-NonCommercial-NoDerivs License, which permits use and distribution in any medium, provided the original work is properly cited, the use is non-commercial and no modifications or adaptations are made. 439
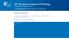
2 Long Survival in a Child With a K27M-H3.3 Glioma A. Hochart et al. ohistochemical data were consistent for WHO grade 1 pilocytic astrocytoma. The patient received no further treatment. Regular MRI after tumor removal showed no residual tumor. Ten years later, in 2012, the patient presented with rapidly evolving neck pain, worsening of her hemiparesis and balance disorders. Spinal MRI revealed a tumor relapse expanding from the cranio-cervical junction to level T1, with a hyperintense signal on T2 weight imaging and heterogeneous enhancement on postcontrast T1 weight imaging. There was also a hyperintense signal on T2 weight imaging down to level T4. Brainstem was normal and no metastatic dissemination was observed. Surgical resection was subtotal, and the tumor was diagnosed as a WHO grade IV glioblastoma. The patient underwent radiation therapy on the whole neuroaxis (40 Gy in 20 sessions with focal boost of Gy on tumor site) plus concomitant daily temozolomide, followed by maintenance temozolomide. Five months later, the patient received irinotecan and bevacizumab due to tumor progression. Finally, the patient died 12 months later. Histological and immunohistochemical examinations Figure 1. MRI from the first tumor in 2002 (left column) and the recurrence in 2012 (right column). (A) Initial MR Imaging at diagnosis in November 2002, sagittal postcontrast T1 spin echo weight imaging (TR: 400; TE: 16) showing a heterogeneous tumor of the cervical spinal cord from level C2, down to C6, with solid and cystic tumor parts and with marked contrast enhancement. (B) Three years postsurgery treatment, sagittal MRI postcontrast T1 weight imaging (TR: 463; TE: 10): no recurrence. (C) Ten years after surgery treatment, postcontrast sagittal T1 weight imaging (TR: 470; TE: 8.6) showing a relapse as a spinal expansion from the cranio-cervical junction to level T1, with heterogeneous enhancement. (D) Ten years after surgery treatment, sagittal T2 weight imaging (TR: 3405; TE: 122) showing relapse with a hyperintense signal down to level T4. In 2002, light microscopy examination revealed that the first tumor tissue fit with the criteria of a biphasic, WHO grade 1 pilocytic astrocytoma with only slight nuclear atypia. Rosenthal fibers and granular eosinophilic bodies were prominent in the most abundant piloid component, whereas oligodendroglioma-like fields were not so obvious. Mitoses were rare; there was a marked glomeruloid vascular proliferation. Necrosis was barely observed. Olig2 staining was positive, and CD34 immunochemistry was negative. The tumor was circumscribed, and synaptophysin labeling failed to show any neurites within the tumor tissue. Furthermore, 5% of the nuclei were immunoreactive for Ki67, and only rare nuclei exhibited a faint labeling of p53; EGFR (Epidermal Growth Factor Receptor) was negative. Microscopic features of a glioblastoma were present at examination of the tumor that was resected at recurrence in 2012 (Fig. 2). Tumor cells had a stellate or elongated morphology, with a brisk mitotic activity, necrosis and vascular festoons. They were labeled by anti-olig2 (70%) but not with anti-idh1 (R132H) antibodies, and the Ki67 index reached 30% of the tumor cell nuclei. In addition, p53 immunoreactivity was strong, and 20% of the cell tumors were EGFR-immunoreactive. CD34 labeling remained negative. Immunofluorescence staining revealed a reduction in H3K27 methylation. Molecular data After genomic DNA extraction, a mutation analysis of hotspot codons 27 and 34 of the H3F3A gene was investigated using pyrosequencing (Qiagen, Valencia, CA, USA). Exon 4 of the IDH1/2 genes, exon 15 of the BRAF gene and all of the exons of the activin A receptor type I (ACVR1) and TP53 genes were also analyzed using Sanger sequencing (Applied Biosystems, Foster City, CA, USA). Unexpectedly, these results showed the exclusive presence of a K27M (c.83a>t, p.lys27met) H3.3 mutation in the primary tumor from In the tumor recurrence from 2012, K27M mutation associated with a TP53 mutation (c.817c>t, p.arg273cys) were detected (Fig. 3). No IDH1/2, PTEN, BRAF, and ACVR1 mutations were found in both tumors. Array comparative genomic hybridization (acgh) was performed using a sureprint G3 Human CGH Microarray kit 60 K (Agilent Technologies, Santa Clara, CA, USA). 440 ª 2015 The Authors. Annals of Clinical and Translational Neurology published by Wiley Periodicals, Inc on behalf of American Neurological Association.
3 A. Hochart et al. Long Survival in a Child With a K27M-H3.3 Glioma (f) specific losses in large chromosomal regions in 5q, 8, 9q, 10, 12q, 13q, 14, 16q, 17, 18q, and 21 and a gain of 9p (Fig. 3). There was no loss of 16p. Focal high copy number amplification was observed in segments, including the PDGFR (Platelet-Derived Growth Factor Receptor), EGFR, and MDM2/CDK4 genes. To search for BRAF-KIAA1549 fusion transcript status (KIAA1549-Ex16_BRAF-Ex9, KIAA1549-Ex15_BRAF-Ex9, KIAA1549-Ex18_BRAF-Ex11, and KIAA1549-Ex16_BRAF- Ex11), total RNA was extracted and reverse transcriptase amplification chain reaction was performed. No KIAA- BRAF transcripts were detected. (e) Figure 2. Light microscopy data from the first tumor sample resected in 2002 (left column) and the recurrence sample (right column), showing routine hematoxylin erythrosin saffron staining (first line) and immunohistochemistry of Ki67, EGFR, Olig2 and p53 (lines 2 5). (A and F) the first tumor exhibited hallmarks of an pilocytic astrocytoma, that is, piloid cells, Rosenthal fibers, eosinophilic granular bodies, and glomeruloid vascular proliferation, whereas in the second tumor, the cells were poorly differentiated. There was severe nuclear atypia and numerous mitoses. (B and G) Olig2 immunoreactivity is present in both tumors but is stronger in the recurrence. (C and H) The Ki67 index was 5% in the first tumor, but reached an overall 30% on the recurrence with a foci of 70%. (D and I) p53 labeling was faint in the first tumor, but strong in the second tumor (70% of the stained nuclei). (E and J) EGFR labeling appeared in the second tumor, as a membrane signal on 20% of tumor cells, but is weak to intermediate in intensity. Profiles of acgh showed no chromosomal abnormalities in the tumor from 2002, whereas the specimen from 2012 demonstrated multiple chromosome rearrangements with (g) (h) (i) (j) Discussion To the best of our knowledge, we report here the first case of a long survival of a child with H3F3A K27M mutated JPA undergoing spontaneous MT into glioblastoma. 5 According to the WHO classification, 1 this patient initially had a pilocytic astrocytoma. Despite an unusually high Ki67 proliferation index, the long-term clinical course confirmed a benign slow-growing tumor. Expectedly, in our case, molecular analysis of the JPA did not disclose any alteration associated with circumscribed gliomas, that is, BRAF-KIAA 1549 fusion, V600E BRAF mutation and IDH1/IDH2 mutation. Indeed, BRAF-KIAA 1549 fusion mainly focuses on specific locations as infra-tentorial and optical pathway pilocytic astrocytomas. 6 The V600E BRAF activating mutation is commonly observed in supratentorial pediatric LGGs, mainly pleomorphic xanthoastrocytomas, gangliogliomas and extra-cerebellar pilocytic astrocytoma. 6,7 IDH1/IDH2 mutations are unusual in pediatric LGGs. 2 MT of LGG is rarer in children than in adults 2 (6.7% vs. 50%, respectively). The main risk factors suspected of malignant degeneration are ionizing radiation and tumorigenesis predisposition syndrome. In a previous pediatric study of 11 patients, this event was mainly related to an infiltrative astrocytoma grade II WHO that degenerated into a glioblastoma, with a median latency of 5.1 years, and was most likely related to treatment for most of the patients. 8 Only three cases of spontaneous malignant degeneration from JPA to full blown glioblastoma have been previously reported in children All of the tumors were located intracranially, two received prior radiotherapy and one patient had neurofibromatosis type I. This patient presented with a thalamic tumor degenerating in less than 2 years into anaplastic astrocytoma, which led to a discussion of the diagnosis The K27M H3F3A mutation was present not only in the high-grade recurrence tumor but also in the initial pilocytic astrocytoma, 10 years prior to the recurrence. ª 2015 The Authors. Annals of Clinical and Translational Neurology published by Wiley Periodicals, Inc on behalf of American Neurological Association. 441
4 Long Survival in a Child With a K27M-H3.3 Glioma A. Hochart et al. Figure 3. acgh and H3F3A K27 mutational status in the first tumor sample resected in 2002 (left column) and the recurrence sample (right column). (A and C) Array comparative genomic hybridization (acgh) genome plots indicating no aberration in the tumor of 2002 compared to the complex profile in 2012, which demonstrated multiple chromosome rearrangements with losses in large chromosomal regions in 5q, 8, 9q, 10, 12q, 13q, 14, 16q, 17, 18q, and 21 and gain of 9p. Focal high copy number amplification was observed in segments, including PDGFR, EGFR and MDM2/CDK4 genes. (B and D) Representative pyrograms showing the K27M (wt AAG? ATG) mutation in tumor recurrence and in the primary tumor leading to an amino acid exchange from lysine (Lys) 27 to methionine (Met). Histone H3.3 is a nuclear, replication-independent protein supporting DNA that is predominantly incorporated into transcription sites and associated with active and open chromatin. The K27M mutation is a gain-of-function mutation that impairs trimethylation at residue 27. H3.3 insertion is affected, and gene expression in the tumor cells is profoundly modified. 3,4,11 The H3F3A K27M mutation is characteristic of midline HGG in children. In a previous study, it was shown that K27M-H3.3 is associated with worse prognosis in children with diffuse intrinsic pontine glioma, and all of the longterm survivors were wild type for H3F3A. 4 Here, we described long survival despite the K27M-H3.3 mutation. Zhang et al. already reported two patients with LGG (diffuse glioma) and K27M H and Jones et al. describes a patient with JPA and K27M H3.3 in association to NF1 and FGFR1. 13 In four previous studies, 34, 3 12, 14 29, 12, and 15, 15 JPA were investigated for the H3F3A K27M mutation: no mutation was found. Thus, these data questioned the prognostic role of this mutation in pediatric Central Nervous System (CNS) glial tumors. The K27M H3.3 mutation may not be exclusively related to high-grade tumors, and studies of the histone mutation should be performed routinely in all pediatric glial tumors. This could result in the identification of genetic subgroups of distinct histologically indistinguishable entities, resulting in a better understanding the behavior of atypical tumors, as pilocytic astrocytoma with malignant features. No somatic mutations in the gene ACVR1 was found. These gain-of-function mutations occur in diffuse intrinsic pontine glioma in conjunction with the histone H3.1 p.lys27met substitution. 16 CGHa analysis performed in 2012 showed complex tumoral chromosomal rearrangements in comparison with 2002, which is consistent with the histopathological features of MT and genomic instability of glioblastoma. 17 In our case of MT, several hypotheses may be made. First, the occurrence of relapse suggests that the initial tumor resection was microscopically incomplete, leaving a residual tumor containing cells carrying the K27M H3.3 mutation. The existence of this significant delay between the initial surgical resection and the appearance of glioblastoma suggests that, in this case, the K27M H3.3 mutation was the first event, although it was potentially not sufficient to lead to transformation. Thus, this mutation might not be the major driver that led to the onset of glioblastoma, and it is possible that another event, such as the second associated mutation in TP53, was responsible for the MT as TP53 mutations are a crucial key in the cell cycle dysfunction. Another hypothesis could be that epigenetic events have suppressed the effect of the K27M H3.3 mutation. 442 ª 2015 The Authors. Annals of Clinical and Translational Neurology published by Wiley Periodicals, Inc on behalf of American Neurological Association.
5 A. Hochart et al. Long Survival in a Child With a K27M-H3.3 Glioma Concerning the management of a similar tumor in 2014, we probably performed a more aggressive therapeutic approach with adjuvant chemotherapy or radiotherapy. This approach should have been suboptimal but unfortunately pharmacologic inhibition of histone demethylation is not currently available. 18 Acknowledgments None. Author Contributions A. Hochart, F. Escande, N. Rocourt, C.-A. Maurage, and P. Leblond wrote the body of the manuscript. C.-A. Maurage and J. Beaujot provided tissue samples and performed histopathological analyses and performed validation experiments. S. Meignan produced figures. J. Grill, F. Escande, and V. Koubi-Pick performed mutation analysis and produced molecular data. All authors contributed to the final manuscript. Conflict of Interest The ICMJE requirements for the authors have been met and the authors have nothing to report. References 1. Louis DN, Ohgaki H, Wiestler OD, et al. The 2007 WHO classification of tumours of the central nervous system. Acta Neuropathol 2007;114: Jones C, Perryman L, Hargrave D. Paediatric and adult malignant glioma: close relatives or distant cousins? Nat Rev Clin Oncol 2012;9: Schwartzentruber J, Korshunov A, Liu X-Y, et al. Driver mutations in histone H3.3 and chromatin remodelling genes in paediatric glioblastoma. Nature 2012;482: Khuong-Quang D-A, Buczkowicz P, Rakopoulos P, et al. K27M mutation in histone H3.3 defines clinically and biologically distinct subgroups of pediatric diffuse intrinsic pontine gliomas. Acta Neuropathol 2012;124: Parsa CF, Givrad S. Juvenile pilocytic astrocytomas do not undergo spontaneous malignant transformation: grounds for designation as hamartomas. Br J Ophthalmol 2008;92: Figarella-Branger D, Chappe C, Padovani L, et al. Glial and glioneuronal tumors in adults and children: main genetic alterations and towards a histomolecular classification. Bull Cancer 2013;100: Horbinski C. To BRAF or not to BRAF: is that even a question anymore? J Neuropathol Exp Neurol 2013;72: Broniscer A, Baker SJ, West AN, et al. Clinical and molecular characteristics of malignant transformation of low-grade glioma in children. J Clin Oncol 2007;25: Privett BJ, Liubinas SV, Tsui A, et al. Pilocytic astrocytoma with neoplastic gemistocytes undergoing spontaneous transformation to glioblastoma multiforme without prior radiotherapy. J Clin Neurosci 2011;18: Amene CS, Yeh-Nayre LA, Crawford JR. Secondary glioblastoma multiforme in a child with disseminated juvenile pilocytic astrocytoma. Case Rep Oncol Med 2012;2012: Chan K-M, Fang D, Gan H, et al. The histone H3.3K27M mutation in pediatric glioma reprograms H3K27 methylation and gene expression. Genes Dev 2013;27: Zhang J, Wu G, Miller CP, et al. Whole-genome sequencing identifies genetic alterations in pediatric lowgrade gliomas. Nat Genet 2013;45: Jones D, Hutter B, J ager NCP, et al. Recurrent somatic alterations of FGFR1 and NKTRK2 in pilocytic astrocytoma. Nat Genet 2013;45: Wu G, Broniscer A, McEachron TA, et al. Somatic histone H3 alterations in pediatric diffuse intrinsic pontine gliomas and non-brainstem glioblastomas. Nat Genet 2012;44: Gielen GH, Gessi M, Hammes J, et al. H3F3A K27M mutation in pediatric CNS tumors: a marker for diffuse high-grade astrocytomas. Am J Clin Pathol 2013;139: Fontebasso AM, Papillon-Cavanagh S, Schwartzentruber J, et al. Recurrent somatic mutations in ACVR1 in pediatric midline high-grade astrocytoma. Nat Genet 2014;46: Paugh BS, Qu C, Jones C, et al. Integrated molecular genetic profiling of pediatric high-grade gliomas reveals key differences with the adult disease. J Clin Oncol 2010;28: Hashizume R, Andor N, Ihara Y, et al. Pharmacologic inhibition of histone demethylation as a therapy for pediatric brainstem glioma. Nat Med 2014;20: ª 2015 The Authors. Annals of Clinical and Translational Neurology published by Wiley Periodicals, Inc on behalf of American Neurological Association. 443
Enterprise Interest None
 Enterprise Interest None Heterogeneous chromosomal profiles in a unique series of DIPG in children and young adults European Congress of Pathology Amsterdam, 6 th September 2017 Charlotte Dufour, Romain
Enterprise Interest None Heterogeneous chromosomal profiles in a unique series of DIPG in children and young adults European Congress of Pathology Amsterdam, 6 th September 2017 Charlotte Dufour, Romain
Neuropathology Evening Session: Case 3
 Neuropathology Evening Session: Case 3 Christine E. Fuller, MD Cincinnati Children s Hospital Medical Center Disclosure of Relevant Financial Relationships USCAP requires that all faculty in a position
Neuropathology Evening Session: Case 3 Christine E. Fuller, MD Cincinnati Children s Hospital Medical Center Disclosure of Relevant Financial Relationships USCAP requires that all faculty in a position
H3F3A K27M Mutation in Pediatric CNS Tumors. A Marker for Diffuse High-Grade Astrocytomas
 Anatomic Pathology / H3.3 Mutations in Pediatric Diffuse High-Grade Astrocytomas H3F3A K27M Mutation in Pediatric CNS Tumors A Marker for Diffuse High-Grade Astrocytomas Gerrit H. Gielen, MD, 1 Marco Gessi,
Anatomic Pathology / H3.3 Mutations in Pediatric Diffuse High-Grade Astrocytomas H3F3A K27M Mutation in Pediatric CNS Tumors A Marker for Diffuse High-Grade Astrocytomas Gerrit H. Gielen, MD, 1 Marco Gessi,
CNS pathology Third year medical students. Dr Heyam Awad 2018 Lecture 12: CNS tumours 2/3
 CNS pathology Third year medical students Dr Heyam Awad 2018 Lecture 12: CNS tumours 2/3 Pilocytic astrocytoma Relatively benign ( WHO grade 1) Occurs in children and young adults Mostly: in the cerebellum
CNS pathology Third year medical students Dr Heyam Awad 2018 Lecture 12: CNS tumours 2/3 Pilocytic astrocytoma Relatively benign ( WHO grade 1) Occurs in children and young adults Mostly: in the cerebellum
Genomic analysis of childhood High grade glial (HGG) brain tumors
 Genomic analysis of childhood High grade glial (HGG) brain tumors Linda D Cooley Children s Mercy, Kansas City The Children s Mercy Hospital, 2017 Genomic analysis of childhood High grade glial (HGG) brain
Genomic analysis of childhood High grade glial (HGG) brain tumors Linda D Cooley Children s Mercy, Kansas City The Children s Mercy Hospital, 2017 Genomic analysis of childhood High grade glial (HGG) brain
Anaplastic Pilocytic Astrocytoma: The fusion of good and bad
 Anaplastic Pilocytic Astrocytoma: The fusion of good and bad Alexandrina Nikova 1, Charalampos-Chrysovalantis Chytoudis-Peroudis 2, Penelope Korkolopoulou 3 and Dimitrios Kanakis 4 Abstract 5 Pilocytic
Anaplastic Pilocytic Astrocytoma: The fusion of good and bad Alexandrina Nikova 1, Charalampos-Chrysovalantis Chytoudis-Peroudis 2, Penelope Korkolopoulou 3 and Dimitrios Kanakis 4 Abstract 5 Pilocytic
Morphological features and genetic alterations
 Morphological features and genetic alterations Tutor : Audrey Rousseau Caget Lise: Université d Angers Iorio Vittoria: Seconda Università degli studi di Napoli Manaila Roxana: Iuliu Hatieganu University
Morphological features and genetic alterations Tutor : Audrey Rousseau Caget Lise: Université d Angers Iorio Vittoria: Seconda Università degli studi di Napoli Manaila Roxana: Iuliu Hatieganu University
General: Brain tumors are lesions that have mass effect distorting the normal tissue and often result in increased intracranial pressure.
 1 Lecture Objectives Know the histologic features of the most common tumors of the CNS. Know the differences in behavior of the different tumor types. Be aware of the treatment modalities in the various
1 Lecture Objectives Know the histologic features of the most common tumors of the CNS. Know the differences in behavior of the different tumor types. Be aware of the treatment modalities in the various
2017 Diagnostic Slide Session Case 3
 2017 Diagnostic Slide Session Case 3 Andrew Gao, MD Lili-Naz Hazrati, MD, PhD Cynthia Hawkins, MD, PhD Hospital for Sick Children and University of Toronto, Toronto, Canada Disclosures: none Clinical History
2017 Diagnostic Slide Session Case 3 Andrew Gao, MD Lili-Naz Hazrati, MD, PhD Cynthia Hawkins, MD, PhD Hospital for Sick Children and University of Toronto, Toronto, Canada Disclosures: none Clinical History
Tumors of the Nervous System
 Tumors of the Nervous System Peter Canoll MD. PhD. What I want to cover What are the most common types of brain tumors? Who gets them? How do they present? What do they look like? How do they behave? 1
Tumors of the Nervous System Peter Canoll MD. PhD. What I want to cover What are the most common types of brain tumors? Who gets them? How do they present? What do they look like? How do they behave? 1
Clinical significance of genetic analysis in glioblastoma treatment
 Clinical significance of genetic analysis in glioblastoma treatment Department of Neurosurgery, Graduate School of Medical Sciences, Kyushu University, Fukuoka, Japan Koji Yoshimoto Can we get prognostic
Clinical significance of genetic analysis in glioblastoma treatment Department of Neurosurgery, Graduate School of Medical Sciences, Kyushu University, Fukuoka, Japan Koji Yoshimoto Can we get prognostic
CNS TUMORS. D r. Ali Eltayb ( U. of Omdurman. I ). M. Path (U. of Alexandria)
 CNS TUMORS D r. Ali Eltayb ( U. of Omdurman. I ). M. Path (U. of Alexandria) CNS TUMORS The annual incidence of intracranial tumors of the CNS ISmore than intraspinal tumors May be Primary or Secondary
CNS TUMORS D r. Ali Eltayb ( U. of Omdurman. I ). M. Path (U. of Alexandria) CNS TUMORS The annual incidence of intracranial tumors of the CNS ISmore than intraspinal tumors May be Primary or Secondary
Classification of Diffuse Gliomas: Progress, Pearls and Pitfalls. Rob Macaulay Neuropathologist, MCC October 21, 2017
 Classification of Diffuse Gliomas: Progress, Pearls and Pitfalls Rob Macaulay Neuropathologist, MCC October 21, 2017 Objectives Explain why the designation high grade glioma is preferable to GBM for intraoperative
Classification of Diffuse Gliomas: Progress, Pearls and Pitfalls Rob Macaulay Neuropathologist, MCC October 21, 2017 Objectives Explain why the designation high grade glioma is preferable to GBM for intraoperative
I have no conflicts of interest in relation to this presentation. Vogel FS & Burger PC 3/28/2016
 IF THIS IS NOT GLIOBLASTOMA, THEN WHAT IS IT? Murat Gokden, MD Department of Pathology/Neuropathology University of Arkansas for Medical Sciences Little Rock, AR mgokden@uams.edu I have no conflicts of
IF THIS IS NOT GLIOBLASTOMA, THEN WHAT IS IT? Murat Gokden, MD Department of Pathology/Neuropathology University of Arkansas for Medical Sciences Little Rock, AR mgokden@uams.edu I have no conflicts of
Understanding general brain tumor pathology, Part I: The basics. Craig Horbinski, M.D., Ph.D. Department of Pathology University of Kentucky
 Understanding general brain tumor pathology, Part I: The basics Craig Horbinski, M.D., Ph.D. Department of Pathology University of Kentucky plan of attack what IS a pathologist, anyway? what s so special
Understanding general brain tumor pathology, Part I: The basics Craig Horbinski, M.D., Ph.D. Department of Pathology University of Kentucky plan of attack what IS a pathologist, anyway? what s so special
Tumors of the Central Nervous System
 Tumors of the Central Nervous System 1 Financial Disclosures I have NO SIGNIFICANT FINANCIAL, GENERAL, OR OBLIGATION INTERESTS TO REPORT Introduction General: Brain tumors are lesions that have mass effect
Tumors of the Central Nervous System 1 Financial Disclosures I have NO SIGNIFICANT FINANCIAL, GENERAL, OR OBLIGATION INTERESTS TO REPORT Introduction General: Brain tumors are lesions that have mass effect
Case Report Atypical Presentation of Atypical Teratoid Rhabdoid Tumor in a Child
 Case Reports in Oncological Medicine Volume 2013, Article ID 815923, 4 pages http://dx.doi.org/10.1155/2013/815923 Case Report Atypical Presentation of Atypical Teratoid Rhabdoid Tumor in a Child Y. T.
Case Reports in Oncological Medicine Volume 2013, Article ID 815923, 4 pages http://dx.doi.org/10.1155/2013/815923 Case Report Atypical Presentation of Atypical Teratoid Rhabdoid Tumor in a Child Y. T.
Supplemental Information. Molecular, Pathological, Radiological, and Immune. Profiling of Non-brainstem Pediatric High-Grade
 Cancer Cell, Volume 33 Supplemental Information Molecular, Pathological, Radiological, and Immune Profiling of Non-brainstem Pediatric High-Grade Glioma from the HERBY Phase II Randomized Trial Alan Mackay,
Cancer Cell, Volume 33 Supplemental Information Molecular, Pathological, Radiological, and Immune Profiling of Non-brainstem Pediatric High-Grade Glioma from the HERBY Phase II Randomized Trial Alan Mackay,
Peter Canoll MD. PhD.
 Tumors of the Nervous System Peter Canoll MD. PhD. What I want to cover What are the most common types of brain tumors? Who gets them? How do they ypresent? What do they look like? How do they behave?
Tumors of the Nervous System Peter Canoll MD. PhD. What I want to cover What are the most common types of brain tumors? Who gets them? How do they ypresent? What do they look like? How do they behave?
The New WHO Classification and the Role of Integrated Molecular Profiling in the Diagnosis of Malignant Gliomas
 The New WHO Classification and the Role of Integrated Molecular Profiling in the Diagnosis of Malignant Gliomas Stefan Prokop, MD Neuropathology Fellow Hospital of the University of Pennsylvania Background
The New WHO Classification and the Role of Integrated Molecular Profiling in the Diagnosis of Malignant Gliomas Stefan Prokop, MD Neuropathology Fellow Hospital of the University of Pennsylvania Background
Diffuse mid-line glioma with H3K27M mutation
 Diffuse mid-line glioma with H3K27M mutation Sonikpreet PGY5 Hematology/Oncology fellow Mayo Clinic, Florida 2017 MFMER slide-1 Learning objectives Case discussion Diffuse mid-line glioma with H3K27M mutation.
Diffuse mid-line glioma with H3K27M mutation Sonikpreet PGY5 Hematology/Oncology fellow Mayo Clinic, Florida 2017 MFMER slide-1 Learning objectives Case discussion Diffuse mid-line glioma with H3K27M mutation.
Precision medicine: How to exploit the growing knowledge on the evolving genomes of cells to improve cancer prevention and therapy.
 Precision medicine: How to exploit the growing knowledge on the evolving genomes of cells to improve cancer prevention and therapy Joe Costello, PhD Department of Neurological Surgery A more accurate and
Precision medicine: How to exploit the growing knowledge on the evolving genomes of cells to improve cancer prevention and therapy Joe Costello, PhD Department of Neurological Surgery A more accurate and
Pediatric Brain Tumors: Updates in Treatment and Care
 Pediatric Brain Tumors: Updates in Treatment and Care Writer Classroom Rishi R. Lulla, MD MS Objectives Introduce the common pediatric brain tumors Discuss current treatment strategies for pediatric brain
Pediatric Brain Tumors: Updates in Treatment and Care Writer Classroom Rishi R. Lulla, MD MS Objectives Introduce the common pediatric brain tumors Discuss current treatment strategies for pediatric brain
Cynthia Hawkins. Division of Pathology, Labatt Brain Tumour Research Centre, The Hospital for Sick Children, University of Toronto, Canada
 Cynthia Hawkins Division of Pathology, Labatt Brain Tumour Research Centre, The Hospital for Sick Children, University of Toronto, Canada To apply a practical diagnostic approach to pediatric high grade
Cynthia Hawkins Division of Pathology, Labatt Brain Tumour Research Centre, The Hospital for Sick Children, University of Toronto, Canada To apply a practical diagnostic approach to pediatric high grade
Applications of molecular neuro-oncology - a review of diffuse glioma integrated diagnosis and emerging molecular entities
 Wood et al. Diagnostic Pathology (2019) 14:29 https://doi.org/10.1186/s13000-019-0802-8 REVIEW Applications of molecular neuro-oncology - a review of diffuse glioma integrated diagnosis and emerging molecular
Wood et al. Diagnostic Pathology (2019) 14:29 https://doi.org/10.1186/s13000-019-0802-8 REVIEW Applications of molecular neuro-oncology - a review of diffuse glioma integrated diagnosis and emerging molecular
Five Most Common Problems in Surgical Neuropathology
 Five Most Common Problems in Surgical Neuropathology If the brain were so simple that we could understand it, we would be so simple that we couldn t Emerson Pugh What is your greatest difficulty in neuropathology?
Five Most Common Problems in Surgical Neuropathology If the brain were so simple that we could understand it, we would be so simple that we couldn t Emerson Pugh What is your greatest difficulty in neuropathology?
Case year old female presented with asymmetric enlargement of the left lobe of the thyroid
 Case 4 22 year old female presented with asymmetric enlargement of the left lobe of the thyroid gland. No information available relative to a prior fine needle aspiration biopsy. A left lobectomy was performed.
Case 4 22 year old female presented with asymmetric enlargement of the left lobe of the thyroid gland. No information available relative to a prior fine needle aspiration biopsy. A left lobectomy was performed.
Case 4 Diagnosis 2/21/2011 TGB
 Case 4 22 year old female presented with asymmetric enlargement of the left lobe of the thyroid gland. No information available relative to a prior fine needle aspiration biopsy. A left lobectomy was performed.
Case 4 22 year old female presented with asymmetric enlargement of the left lobe of the thyroid gland. No information available relative to a prior fine needle aspiration biopsy. A left lobectomy was performed.
Title. CitationBrain Tumor Pathology, 34(4): Issue Date Doc URL. Rights. Type. Additional There Information.
 Title Diencephalic pediatric low-grade glioma harboring th sequential biopsy specimens Ishi, Yukitomo; Hatanaka, Kanako C.; Yamaguchi, Shig Author(s) Terasaka, Shunsuke; Houkin, Kiyohiro CitationBrain
Title Diencephalic pediatric low-grade glioma harboring th sequential biopsy specimens Ishi, Yukitomo; Hatanaka, Kanako C.; Yamaguchi, Shig Author(s) Terasaka, Shunsuke; Houkin, Kiyohiro CitationBrain
Advances In Orbital Neuropathology
 Advances In Orbital Neuropathology Charles G. Eberhart, MD PhD Associate Professor of Pathology, Ophthalmology and Oncology Johns Hopkins University School of Medicine Overview Non-neoplastic lesions Microphthalmos/pseudoglioma
Advances In Orbital Neuropathology Charles G. Eberhart, MD PhD Associate Professor of Pathology, Ophthalmology and Oncology Johns Hopkins University School of Medicine Overview Non-neoplastic lesions Microphthalmos/pseudoglioma
CHINESE MEDICAL ASSOCIATION
 Zhu et al. Chinese Neurosurgical Journal (2017) 3:22 DOI 10.1186/s41016-017-0087-2 CHINESE NEUROSURGICAL SOCIETY CASE REPORT CHINESE MEDICAL ASSOCIATION Anaplastic pleomorphic xanthoastrocytoma with disseminated
Zhu et al. Chinese Neurosurgical Journal (2017) 3:22 DOI 10.1186/s41016-017-0087-2 CHINESE NEUROSURGICAL SOCIETY CASE REPORT CHINESE MEDICAL ASSOCIATION Anaplastic pleomorphic xanthoastrocytoma with disseminated
2018 Diagnostic Slide Session Case #8
 2018 Diagnostic Slide Session Case #8 Angela N. Viaene, MacLean P. Nasrallah, and Zissimos Mourelatos Hospital of the University of Pennsylvania AANP June 9, 2018 Disclosures: none Clinical History Healthy,
2018 Diagnostic Slide Session Case #8 Angela N. Viaene, MacLean P. Nasrallah, and Zissimos Mourelatos Hospital of the University of Pennsylvania AANP June 9, 2018 Disclosures: none Clinical History Healthy,
Astroblastoma: Radiologic-Pathologic Correlation and Distinction from Ependymoma
 AJNR Am J Neuroradiol 23:243 247, February 2002 Case Report Astroblastoma: Radiologic-Pathologic Correlation and Distinction from Ependymoma John D. Port, Daniel J. Brat, Peter C. Burger, and Martin G.
AJNR Am J Neuroradiol 23:243 247, February 2002 Case Report Astroblastoma: Radiologic-Pathologic Correlation and Distinction from Ependymoma John D. Port, Daniel J. Brat, Peter C. Burger, and Martin G.
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES
 PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES CENTRAL NERVOUS SYSTEM MEDULLOBLASTOMA AND PNET CNS Site Group Medulloblastoma and PNET Author: Dr. Norm Laperriere 1. INTRODUCTION 3 2. PREVENTION
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES CENTRAL NERVOUS SYSTEM MEDULLOBLASTOMA AND PNET CNS Site Group Medulloblastoma and PNET Author: Dr. Norm Laperriere 1. INTRODUCTION 3 2. PREVENTION
MOLECULAR DIAGNOSTICS OF GLIOMAS
 MOLECULAR DIAGNOSTICS OF GLIOMAS Arie Perry, M.D. Director, Neuropathology Division DIFFUSE GLIOMAS Cell types Astrocytomas (A) Oligodendrogliomas (O) Mixed oligoastrocytoma (MOA) Three WHO grades: II,
MOLECULAR DIAGNOSTICS OF GLIOMAS Arie Perry, M.D. Director, Neuropathology Division DIFFUSE GLIOMAS Cell types Astrocytomas (A) Oligodendrogliomas (O) Mixed oligoastrocytoma (MOA) Three WHO grades: II,
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES
 PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES CENTRAL NERVOUS SYSTEM LOW GRADE GLIOMAS CNS Site Group Low Grade Gliomas Author: Dr. Norm Laperriere 1. INTRODUCTION 3 2. PREVENTION 3 3. SCREENING
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES CENTRAL NERVOUS SYSTEM LOW GRADE GLIOMAS CNS Site Group Low Grade Gliomas Author: Dr. Norm Laperriere 1. INTRODUCTION 3 2. PREVENTION 3 3. SCREENING
Histopathological Study and Categorisation of Brain Tumors
 Histopathological Study and Categorisation of Brain Tumors Ruchira Wadhwa 1*, Purvi Patel 2, Hansa Goswami 3 1 Third Year Resident, 2 Assistant Professor, 3 Professor and Head, Department of Pathology,
Histopathological Study and Categorisation of Brain Tumors Ruchira Wadhwa 1*, Purvi Patel 2, Hansa Goswami 3 1 Third Year Resident, 2 Assistant Professor, 3 Professor and Head, Department of Pathology,
SYSTEMIC MANAGEMENT OF PEDIATRIC PRIMARY BRAIN TUMORS
 SYSTEMIC MANAGEMENT OF PEDIATRIC PRIMARY BRAIN TUMORS María E. Echevarría, MD Assistant Professor University of Puerto Rico Medical Sciences Campus DISCLOSURES No disclosures INTRODUCTION Pediatric CNS
SYSTEMIC MANAGEMENT OF PEDIATRIC PRIMARY BRAIN TUMORS María E. Echevarría, MD Assistant Professor University of Puerto Rico Medical Sciences Campus DISCLOSURES No disclosures INTRODUCTION Pediatric CNS
Pleomorphic Xanthoastrocytoma
 Pleomorphic Xanthoastrocytoma Christine E. Fuller Keywords Pleomorphic xanthoastrocytoma; Pleomorphic xanthoastrocytoma with anaplastic features 2.1 OVERVIEW Pleomorphic xanthoastrocytoma (PXA) is an uncommon
Pleomorphic Xanthoastrocytoma Christine E. Fuller Keywords Pleomorphic xanthoastrocytoma; Pleomorphic xanthoastrocytoma with anaplastic features 2.1 OVERVIEW Pleomorphic xanthoastrocytoma (PXA) is an uncommon
MALIGNANT GLIOMAS: TREATMENT AND CHALLENGES
 MALIGNANT GLIOMAS: TREATMENT AND CHALLENGES DISCLOSURE No conflicts of interest to disclose Patricia Bruns APRN, CNS Givens Brain Tumor Center Abbott Northwestern Hospital October 12, 2018 OBJECTIVES THEN
MALIGNANT GLIOMAS: TREATMENT AND CHALLENGES DISCLOSURE No conflicts of interest to disclose Patricia Bruns APRN, CNS Givens Brain Tumor Center Abbott Northwestern Hospital October 12, 2018 OBJECTIVES THEN
Gliomas in the 2016 WHO Classification of CNS Tumors
 Gliomas in the 2016 WHO Classification of CNS Tumors Hindi N Al-Hindi, MD, FCAP Consultant Neuropathologist and Head Section of Anatomic Pathology Department of Pathology and Laboratory Medicine King Faisal
Gliomas in the 2016 WHO Classification of CNS Tumors Hindi N Al-Hindi, MD, FCAP Consultant Neuropathologist and Head Section of Anatomic Pathology Department of Pathology and Laboratory Medicine King Faisal
Radioterapia no Tratamento dos Gliomas de Baixo Grau
 Radioterapia no Tratamento dos Gliomas de Baixo Grau Dr. Luis Souhami University Montreal - Canada Low Grade Gliomas Relatively rare Heterogeneous, slow growing tumors WHO Classification Grade I Pilocytic
Radioterapia no Tratamento dos Gliomas de Baixo Grau Dr. Luis Souhami University Montreal - Canada Low Grade Gliomas Relatively rare Heterogeneous, slow growing tumors WHO Classification Grade I Pilocytic
21/03/2017. Disclosure. Practice Changing Articles in Neuro Oncology for 2016/17. Gliomas. Objectives. Gliomas. No conflicts to declare
 Practice Changing Articles in Neuro Oncology for 2016/17 Disclosure No conflicts to declare Frances Cusano, BScPharm, ACPR April 21, 2017 Objectives Gliomas To describe the patient selection, methodology
Practice Changing Articles in Neuro Oncology for 2016/17 Disclosure No conflicts to declare Frances Cusano, BScPharm, ACPR April 21, 2017 Objectives Gliomas To describe the patient selection, methodology
AMERICAN ASSOCIATION OF NEUROPATHOLOGISTS COMPANION SOCIETY MEETING at the 106 th ANNUAL MEETING OF THE USCAP San Antonio, March 4, 2017
 AMERICAN ASSOCIATION OF NEUROPATHOLOGISTS COMPANION SOCIETY MEETING at the 106 th ANNUAL MEETING OF THE USCAP San Antonio, March 4, 2017 SYLLABUS Papillary Tumor of the Pineal Region and the Differential
AMERICAN ASSOCIATION OF NEUROPATHOLOGISTS COMPANION SOCIETY MEETING at the 106 th ANNUAL MEETING OF THE USCAP San Antonio, March 4, 2017 SYLLABUS Papillary Tumor of the Pineal Region and the Differential
Chapter 1 Introduction
 Chapter 1 Introduction Men think epilepsy divine, merely because they do not understand it. But if they called everything divine which they do not understand, why, there would be no end to divine things.
Chapter 1 Introduction Men think epilepsy divine, merely because they do not understand it. But if they called everything divine which they do not understand, why, there would be no end to divine things.
Pr D.Figarella-Branger Service d Anatomie Pathologique et de Neuropathologie, La Timone, Marseille UMR 911 Inserm, Université d Aix-Marseille
 Novelties in the WHO 2016 classification of brain tumours Pr D.Figarella-Branger Service d Anatomie Pathologique et de Neuropathologie, La Timone, Marseille UMR 911 Inserm, Université d Aix-Marseille The
Novelties in the WHO 2016 classification of brain tumours Pr D.Figarella-Branger Service d Anatomie Pathologique et de Neuropathologie, La Timone, Marseille UMR 911 Inserm, Université d Aix-Marseille The
R1601 Essential Immunohistochemical and Molecular Markers for General CNS Glial Tumors
 October 22, 2018 12:00-1:00 PM Background The World Health Organization Classification of tumors of the Central Nervous System has recently been revised. There is now greater emphasis on molecular phenotype
October 22, 2018 12:00-1:00 PM Background The World Health Organization Classification of tumors of the Central Nervous System has recently been revised. There is now greater emphasis on molecular phenotype
Nature Genetics: doi: /ng.2995
 Supplementary Figure 1 Kaplan-Meier survival curves of patients with brainstem tumors. (a) Comparison of patients with PPM1D mutation versus wild-type PPM1D. (b) Comparison of patients with PPM1D mutation
Supplementary Figure 1 Kaplan-Meier survival curves of patients with brainstem tumors. (a) Comparison of patients with PPM1D mutation versus wild-type PPM1D. (b) Comparison of patients with PPM1D mutation
Disclaimers. Molecular pathology of brain tumors. Some aspects only. Some details are inevitably personal opinions
 Molecular pathology of brain tumors Disclaimers Some aspects only H.K. Ng The Chinese University of Hong Kong Some details are inevitably personal opinions Free ppt : http://www.acp.cuhk.edu.hk/hkng Why
Molecular pathology of brain tumors Disclaimers Some aspects only H.K. Ng The Chinese University of Hong Kong Some details are inevitably personal opinions Free ppt : http://www.acp.cuhk.edu.hk/hkng Why
Karl Kashofer, Phd Institut für Pathologie Medizinische Universität Graz
 Expanding on WHO guideline compliant molecular testing of central nervous system tumors by low density whole genome sequencing. Karl Kashofer, Phd Institut für Pathologie Medizinische Universität Graz
Expanding on WHO guideline compliant molecular testing of central nervous system tumors by low density whole genome sequencing. Karl Kashofer, Phd Institut für Pathologie Medizinische Universität Graz
Integrating molecular markers into the World Health Organization classification of CNS tumors: a survey of the neuro-oncology community
 Integrating molecular markers into the World Health Organization classification of CNS tumors: a survey of the neuro-oncology community The Harvard community has made this article openly available. Please
Integrating molecular markers into the World Health Organization classification of CNS tumors: a survey of the neuro-oncology community The Harvard community has made this article openly available. Please
성균관대학교삼성창원병원신경외과학교실신경종양학 김영준. KNS-MT-03 (April 15, 2015)
 성균관대학교삼성창원병원신경외과학교실신경종양학 김영준 INTRODUCTIONS Low grade gliomas (LGG) - heterogeneous group of tumors with astrocytic, oligodendroglial, ependymal, or mixed cellular histology - In adults diffuse, infiltrating
성균관대학교삼성창원병원신경외과학교실신경종양학 김영준 INTRODUCTIONS Low grade gliomas (LGG) - heterogeneous group of tumors with astrocytic, oligodendroglial, ependymal, or mixed cellular histology - In adults diffuse, infiltrating
Case Report A Rare Cutaneous Adnexal Tumor: Malignant Proliferating Trichilemmal Tumor
 Case Reports in Medicine Volume 2015, Article ID 742920, 4 pages http://dx.doi.org/10.1155/2015/742920 Case Report A Rare Cutaneous Adnexal Tumor: Malignant Proliferating Trichilemmal Tumor Omer Alici,
Case Reports in Medicine Volume 2015, Article ID 742920, 4 pages http://dx.doi.org/10.1155/2015/742920 Case Report A Rare Cutaneous Adnexal Tumor: Malignant Proliferating Trichilemmal Tumor Omer Alici,
SUPPLEMENTARY INFORMATION
 VOLUME: 1 ARTICLE NUMBER: 0027 In the format provided by the authors and unedited. Rapid intraoperative histology of unprocessed surgical specimens via fibre-laser-based stimulated Raman scattering microscopy
VOLUME: 1 ARTICLE NUMBER: 0027 In the format provided by the authors and unedited. Rapid intraoperative histology of unprocessed surgical specimens via fibre-laser-based stimulated Raman scattering microscopy
Novel BRAF alteration in a sporadic pilocytic astrocytoma
 Washington University School of Medicine Digital Commons@Becker Open Access Publications 2012 Novel BRAF alteration in a sporadic pilocytic astrocytoma Sonika Dahiya Jinsheng Yu Aparna Kaul Jeffrey R.
Washington University School of Medicine Digital Commons@Becker Open Access Publications 2012 Novel BRAF alteration in a sporadic pilocytic astrocytoma Sonika Dahiya Jinsheng Yu Aparna Kaul Jeffrey R.
Pediatr Blood Cancer 2014
 Low grade Glioma! 40% of pediatric brain tumors Pathologically, anatomically, clinically and biologically heterogeneous Leptomeningeal metastases in 5% Frequently protracted clinical course Long-Term Outcome
Low grade Glioma! 40% of pediatric brain tumors Pathologically, anatomically, clinically and biologically heterogeneous Leptomeningeal metastases in 5% Frequently protracted clinical course Long-Term Outcome
A clinical perspective on neuropathology and molecular genetics in brain tumors
 A clinical perspective on neuropathology and molecular genetics in brain tumors M.J. van den Bent Erasmus MC Cancer Institute Rotterdam, the Netherlands Disclosures Member speakersbureau: MSD Consultancy:
A clinical perspective on neuropathology and molecular genetics in brain tumors M.J. van den Bent Erasmus MC Cancer Institute Rotterdam, the Netherlands Disclosures Member speakersbureau: MSD Consultancy:
Case Report Complex Form Variant of Dysembryoplastic Neuroepithelial Tumor of the Cerebellum
 Case Reports in Pathology Volume 2012, Article ID 718651, 4 pages doi:10.1155/2012/718651 Case Report Complex Form Variant of Dysembryoplastic Neuroepithelial Tumor of the Cerebellum Jesús Vaquero, 1,
Case Reports in Pathology Volume 2012, Article ID 718651, 4 pages doi:10.1155/2012/718651 Case Report Complex Form Variant of Dysembryoplastic Neuroepithelial Tumor of the Cerebellum Jesús Vaquero, 1,
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES
 PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES CENTRAL NERVOUS SYSTEM ANAPLASTIC GLIOMAS CNS Site Group Anaplastic Gliomas Author: Dr. Norm Laperriere Date: February 20, 2018 1. INTRODUCTION
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES CENTRAL NERVOUS SYSTEM ANAPLASTIC GLIOMAS CNS Site Group Anaplastic Gliomas Author: Dr. Norm Laperriere Date: February 20, 2018 1. INTRODUCTION
Imaging for suspected glioma
 Imaging for suspected glioma 1.1.1 Offer standard structural MRI (defined as T2 weighted, FLAIR, DWI series and T1 pre- and post-contrast volume) as the initial diagnostic test for suspected glioma, unless
Imaging for suspected glioma 1.1.1 Offer standard structural MRI (defined as T2 weighted, FLAIR, DWI series and T1 pre- and post-contrast volume) as the initial diagnostic test for suspected glioma, unless
Protocol Abstract and Schema
 Protocol Abstract and Schema A Phase I Trial of p28 (NSC745104), a Non-HDM2 mediated peptide inhibitor of p53 ubiquitination in pediatric patients with recurrent or progressive CNS tumors Description and
Protocol Abstract and Schema A Phase I Trial of p28 (NSC745104), a Non-HDM2 mediated peptide inhibitor of p53 ubiquitination in pediatric patients with recurrent or progressive CNS tumors Description and
No financial or other disclosures
 Case 2014-5 Esther N. Bit-Ivan, DO Northwestern University Jason Wang, MD Jason Park, MD Korgun Koral, MD Children s Medical Center Charles Timmons, MD Veena Rajaram, MD No financial or other disclosures
Case 2014-5 Esther N. Bit-Ivan, DO Northwestern University Jason Wang, MD Jason Park, MD Korgun Koral, MD Children s Medical Center Charles Timmons, MD Veena Rajaram, MD No financial or other disclosures
Brain tumors are, as a group, the most common
 See the corresponding editorial in this issue, pp 133 134. J Neurosurg Pediatrics 8:000 000, 8:135 148, 2011 Multidisciplinary management of childhood brain tumors: a review of outcomes, recent advances,
See the corresponding editorial in this issue, pp 133 134. J Neurosurg Pediatrics 8:000 000, 8:135 148, 2011 Multidisciplinary management of childhood brain tumors: a review of outcomes, recent advances,
What yield in the last decade about Molecular Diagnostics in Neuro
 What yield in the last decade about Molecular Diagnostics in Neuro Oncology? Raphael Salles S.Medeiros Neuropathologist at HC FMUSP Clinical Research Project Manager at Oncology department at Hospital
What yield in the last decade about Molecular Diagnostics in Neuro Oncology? Raphael Salles S.Medeiros Neuropathologist at HC FMUSP Clinical Research Project Manager at Oncology department at Hospital
HHS Public Access Author manuscript Nat Genet. Author manuscript; available in PMC 2012 September 01.
 Somatic Histone H3 Alterations in Paediatric Diffuse Intrinsic Pontine Gliomas and Non-Brainstem Glioblastomas Gang Wu 1,*, Alberto Broniscer 2,*, Troy A McEachron 3,*, Charles Lu 4, Barbara S Paugh 3,
Somatic Histone H3 Alterations in Paediatric Diffuse Intrinsic Pontine Gliomas and Non-Brainstem Glioblastomas Gang Wu 1,*, Alberto Broniscer 2,*, Troy A McEachron 3,*, Charles Lu 4, Barbara S Paugh 3,
Neurosurgical Management of Brain Tumours. Nicholas Little Neurosurgeon RNSH
 Neurosurgical Management of Brain Tumours Nicholas Little Neurosurgeon RNSH General Most common tumours are metastatic 10x more common than primary Incidence of primary neoplasms is 20 per 100000 per year
Neurosurgical Management of Brain Tumours Nicholas Little Neurosurgeon RNSH General Most common tumours are metastatic 10x more common than primary Incidence of primary neoplasms is 20 per 100000 per year
Examining large groups of cancer patients to identify ways of predicting which therapies cancers might respond to.
 Stratified Medicine Examining large groups of cancer patients to identify ways of predicting which therapies cancers might respond to. Looking in detail at cancer cells and their genetic make up. Permit
Stratified Medicine Examining large groups of cancer patients to identify ways of predicting which therapies cancers might respond to. Looking in detail at cancer cells and their genetic make up. Permit
patients in the era of
 Communicating with cancer patients in the era of personalized medicine September 9 th, 2017 Gerald Prager, M.D. Comprehensive Cancer Center Vienna Medical University of Vienna, Austria Gerald Prager, M.D.
Communicating with cancer patients in the era of personalized medicine September 9 th, 2017 Gerald Prager, M.D. Comprehensive Cancer Center Vienna Medical University of Vienna, Austria Gerald Prager, M.D.
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES
 PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES CENTRAL NERVOUS SYSTEM MENINGIOMA CNS Site Group Meningioma Author: Dr. Norm Laperriere Date: February 20, 2018 1. INTRODUCTION 3 2. PREVENTION
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES CENTRAL NERVOUS SYSTEM MENINGIOMA CNS Site Group Meningioma Author: Dr. Norm Laperriere Date: February 20, 2018 1. INTRODUCTION 3 2. PREVENTION
USCAP Pediatrics Evening Subspecialty Conference 2015
 USCAP Pediatrics Evening Subspecialty Conference 2015 Sunday 22 March 2015 Alexander Lazar MD/PhD Department of Pathology S Section of Bone Soft TIssue Pathology Sarcoma Research Center The Case Patient
USCAP Pediatrics Evening Subspecialty Conference 2015 Sunday 22 March 2015 Alexander Lazar MD/PhD Department of Pathology S Section of Bone Soft TIssue Pathology Sarcoma Research Center The Case Patient
Rapid recurrence of a malignant meningioma: case report
 Romanian Neurosurgery Volume XXXI Number 2 2017 April-June Article Rapid recurrence of a malignant meningioma: case report Oguz Baran, Sima Sayyahmeli, Taner Tanriverdi, Pamir Erdincler TURKEY DOI: 10.1515/romneu-2017-0027
Romanian Neurosurgery Volume XXXI Number 2 2017 April-June Article Rapid recurrence of a malignant meningioma: case report Oguz Baran, Sima Sayyahmeli, Taner Tanriverdi, Pamir Erdincler TURKEY DOI: 10.1515/romneu-2017-0027
AGGRESSIVE VARIANTS OF PAPILLARY THYROID CARCINOMA DIAGNOSIS AND PROGNOSIS
 AGGRESSIVE VARIANTS OF PAPILLARY THYROID CARCINOMA DIAGNOSIS AND PROGNOSIS PAPILLARY THYROID CARCINOMA Clinical Any age Microscopic to large Female: Male= 2-4:1 Radiation history Lymph nodes Prognosis
AGGRESSIVE VARIANTS OF PAPILLARY THYROID CARCINOMA DIAGNOSIS AND PROGNOSIS PAPILLARY THYROID CARCINOMA Clinical Any age Microscopic to large Female: Male= 2-4:1 Radiation history Lymph nodes Prognosis
Osamu Tetsu, MD, PhD Associate Professor Department of Otolaryngology-Head and Neck Surgery School of Medicine, University of California, San
 Osamu Tetsu, MD, PhD Associate Professor Department of Otolaryngology-Head and Neck Surgery School of Medicine, University of California, San Francisco Lung Cancer Classification Pathological Classification
Osamu Tetsu, MD, PhD Associate Professor Department of Otolaryngology-Head and Neck Surgery School of Medicine, University of California, San Francisco Lung Cancer Classification Pathological Classification
The Radiologic Evaluation of Glioblastoma (GBM) and Differentiation from Pseudoprogression
 The Radiologic Evaluation of Glioblastoma (GBM) and Differentiation from Pseudoprogression Alexis Roy, Harvard Medical School, Year III Our Patient AB: Clinical Presentation 53 year old female with a past
The Radiologic Evaluation of Glioblastoma (GBM) and Differentiation from Pseudoprogression Alexis Roy, Harvard Medical School, Year III Our Patient AB: Clinical Presentation 53 year old female with a past
LOW GRADE ASTROCYTOMAS
 LOW GRADE ASTROCYTOMAS This article was provided to us by David Schiff, MD, Associate Professor of Neurology, Neurosurgery, and Medicine at University of Virginia, Charlottesville. We appreciate his generous
LOW GRADE ASTROCYTOMAS This article was provided to us by David Schiff, MD, Associate Professor of Neurology, Neurosurgery, and Medicine at University of Virginia, Charlottesville. We appreciate his generous
Corporate Medical Policy
 Corporate Medical Policy Analysis of MGMT Promoter Methylation in Malignant Gliomas File Name: Origination: Last CAP Review: Next CAP Review: Last Review: analysis_of_mgmt_promoter_methylation_in_malignant_gliomas
Corporate Medical Policy Analysis of MGMT Promoter Methylation in Malignant Gliomas File Name: Origination: Last CAP Review: Next CAP Review: Last Review: analysis_of_mgmt_promoter_methylation_in_malignant_gliomas
Pharmacologic inhibition of histone demethylation as a therapy for pediatric brainstem glioma
 Supplementary information for: Pharmacologic inhibition of histone demethylation as a therapy for pediatric brainstem glioma Rintaro Hashizume 1, Noemi Andor 2, Yuichiro Ihara 2, Robin Lerner 2, Haiyun
Supplementary information for: Pharmacologic inhibition of histone demethylation as a therapy for pediatric brainstem glioma Rintaro Hashizume 1, Noemi Andor 2, Yuichiro Ihara 2, Robin Lerner 2, Haiyun
Diplomate of the American Board of Pathology in Anatomic and Clinical Pathology
 A 33-year-old male with a left lower leg mass. Contributed by Shaoxiong Chen, MD, PhD Assistant Professor Indiana University School of Medicine/ IU Health Partners Department of Pathology and Laboratory
A 33-year-old male with a left lower leg mass. Contributed by Shaoxiong Chen, MD, PhD Assistant Professor Indiana University School of Medicine/ IU Health Partners Department of Pathology and Laboratory
The Pathology of Neoplasia Part II
 The Pathology of Neoplasia Part II February 2018 PAUL BOGNER, MD A S S O C I A T E P R O F E S S O R O F O N C O L O G Y P A T H O L O G Y A N D D E R M A T O L O G Y Clinical goals of cancer pathology
The Pathology of Neoplasia Part II February 2018 PAUL BOGNER, MD A S S O C I A T E P R O F E S S O R O F O N C O L O G Y P A T H O L O G Y A N D D E R M A T O L O G Y Clinical goals of cancer pathology
IDH1 R132H/ATRX Immunohistochemical validation
 IDH1 R132H/ATRX Immunohistochemical validation CIQC/DSM 2016 12 June 2016 0835-0905 Stephen Yip, M.D., Ph.D., FRCPC University of British Columbia Disclosure Statement I have nothing to disclose I will
IDH1 R132H/ATRX Immunohistochemical validation CIQC/DSM 2016 12 June 2016 0835-0905 Stephen Yip, M.D., Ph.D., FRCPC University of British Columbia Disclosure Statement I have nothing to disclose I will
Whole Genome and Transcriptome Analysis of Anaplastic Meningioma. Patrick Tarpey Cancer Genome Project Wellcome Trust Sanger Institute
 Whole Genome and Transcriptome Analysis of Anaplastic Meningioma Patrick Tarpey Cancer Genome Project Wellcome Trust Sanger Institute Outline Anaplastic meningioma compared to other cancers Whole genomes
Whole Genome and Transcriptome Analysis of Anaplastic Meningioma Patrick Tarpey Cancer Genome Project Wellcome Trust Sanger Institute Outline Anaplastic meningioma compared to other cancers Whole genomes
Precision medicine for gliomas
 Precision medicine for YAZMIN ODIA, MD MS LEAD PHYSICIAN OF MEDICAL NEURO-ONCOLOGY DISCLOSURES Novocure: Advisory Board for Optune in No other financial conflicts of interest Glioma OVERVIEW INFILTRATIVE,
Precision medicine for YAZMIN ODIA, MD MS LEAD PHYSICIAN OF MEDICAL NEURO-ONCOLOGY DISCLOSURES Novocure: Advisory Board for Optune in No other financial conflicts of interest Glioma OVERVIEW INFILTRATIVE,
Development of Carcinoma Pathways
 The Construction of Genetic Pathway to Colorectal Cancer Moriah Wright, MD Clinical Fellow in Colorectal Surgery Creighton University School of Medicine Management of Colon and Diseases February 23, 2019
The Construction of Genetic Pathway to Colorectal Cancer Moriah Wright, MD Clinical Fellow in Colorectal Surgery Creighton University School of Medicine Management of Colon and Diseases February 23, 2019
Contemporary Management of Glioblastoma
 Contemporary Management of Glioblastoma Incidence Rates of Primary Brain Tumors Central Brain Tumor Registry of the United States, 1992-1997 100 Number of Cases per 100,000 Population 10 1 0.1 x I x I
Contemporary Management of Glioblastoma Incidence Rates of Primary Brain Tumors Central Brain Tumor Registry of the United States, 1992-1997 100 Number of Cases per 100,000 Population 10 1 0.1 x I x I
SPECIAL SLIDE SEMINAR CASE 3
 SPECIAL SLIDE SEMINAR CASE 3 Tihana Džombeta, MD Leo Pažanin, MD, PhD Department of Pathology, School of Medicine, University of Zagreb Department of Pathology, Clinical Hospital Centre Sestre milosrdnice
SPECIAL SLIDE SEMINAR CASE 3 Tihana Džombeta, MD Leo Pažanin, MD, PhD Department of Pathology, School of Medicine, University of Zagreb Department of Pathology, Clinical Hospital Centre Sestre milosrdnice
Avastin (bevacizumab) DRUG.00028, CG-DRUG-68
 Avastin (bevacizumab) DRUG.00028, CG-DRUG-68 Override(s) Prior Authorization Approval Duration 1 year Medications Avastin (bevacizumab) APPROVAL CRITERIA Requests for Avastin (bevacizumab) may be approved
Avastin (bevacizumab) DRUG.00028, CG-DRUG-68 Override(s) Prior Authorization Approval Duration 1 year Medications Avastin (bevacizumab) APPROVAL CRITERIA Requests for Avastin (bevacizumab) may be approved
Childhood Brain and Spinal Cord Tumors Treatment Overview (PDQ )
 1 di 8 04/03/2017 07.31 NCBI Bookshelf. A service of the National Library of Medicine, National Institutes of Health. PDQ Cancer Information Summaries [Internet]. Bethesda (MD): National Cancer Institute
1 di 8 04/03/2017 07.31 NCBI Bookshelf. A service of the National Library of Medicine, National Institutes of Health. PDQ Cancer Information Summaries [Internet]. Bethesda (MD): National Cancer Institute
Systemic Treatment. Third International Neuro-Oncology Course. 23 May 2014
 Low-Grade Astrocytoma of the CNS: Systemic Treatment Third International Neuro-Oncology Course São Paulo, Brazil 23 May 2014 John de Groot, MD Associate Professor, Neuro-Oncology UT MD Anderson Cancer
Low-Grade Astrocytoma of the CNS: Systemic Treatment Third International Neuro-Oncology Course São Paulo, Brazil 23 May 2014 John de Groot, MD Associate Professor, Neuro-Oncology UT MD Anderson Cancer
USCAP 2012: Companion Meeting of the AAOOP. Update on lacrimal gland neoplasms: Molecular pathology of interest
 USCAP 2012: Companion Meeting of the AAOOP Vancouver BC, Canada, March 17, 2012 Update on lacrimal gland neoplasms: Molecular pathology of interest Valerie A. White MD, MHSc, FRCPC Department of Pathology
USCAP 2012: Companion Meeting of the AAOOP Vancouver BC, Canada, March 17, 2012 Update on lacrimal gland neoplasms: Molecular pathology of interest Valerie A. White MD, MHSc, FRCPC Department of Pathology
BRAF mutation and CDKN2A deletion define a clinically distinct subgroup of childhood secondary high-grade glioma
 BRAF mutation and CDKN2A deletion define a clinically distinct subgroup of childhood secondary high-grade glioma by Matthew R. Mistry A thesis submitted in conformity with the requirements for the degree
BRAF mutation and CDKN2A deletion define a clinically distinct subgroup of childhood secondary high-grade glioma by Matthew R. Mistry A thesis submitted in conformity with the requirements for the degree
Adult intramedullary astrocytomas of the spinal cord
 J Neurosurg 77:355-359, 1992 Adult intramedullary astrocytomas of the spinal cord FRED J. EPSTEIN, M.D., JEAN-PIERRE FARMER, M.D., F.R.C.S., AND DIANA FREED Division of Pediatric Neurosurgery, Department
J Neurosurg 77:355-359, 1992 Adult intramedullary astrocytomas of the spinal cord FRED J. EPSTEIN, M.D., JEAN-PIERRE FARMER, M.D., F.R.C.S., AND DIANA FREED Division of Pediatric Neurosurgery, Department
Supra- and infratentorial brain tumors from childhood to maternity
 Supra- and infratentorial brain tumors from childhood to maternity What to expect? I am going to show you the characteristic imaging findings of following tumors: Thierry A.G.M. Huisman, MD, FICIS, EQNR
Supra- and infratentorial brain tumors from childhood to maternity What to expect? I am going to show you the characteristic imaging findings of following tumors: Thierry A.G.M. Huisman, MD, FICIS, EQNR
Oligodendroglioma: imaging findings, radio-pathological correlation and evolution
 Oligodendroglioma: imaging findings, radio-pathological correlation and evolution Poster No.: C-2104 Congress: ECR 2013 Type: Authors: Keywords: DOI: Scientific Exhibit A. Hernandez Castro, M. D. Monedero
Oligodendroglioma: imaging findings, radio-pathological correlation and evolution Poster No.: C-2104 Congress: ECR 2013 Type: Authors: Keywords: DOI: Scientific Exhibit A. Hernandez Castro, M. D. Monedero
Biomarkers in Neuro-Ophthalmic Tumors
 Biomarkers in Neuro-Ophthalmic Tumors Fausto J. Rodríguez MD Department of Pathology Johns Hopkins University School of Medicine Disclosure of Relevant Financial Relationships Disclosure of Relevant Financial
Biomarkers in Neuro-Ophthalmic Tumors Fausto J. Rodríguez MD Department of Pathology Johns Hopkins University School of Medicine Disclosure of Relevant Financial Relationships Disclosure of Relevant Financial
Pediatric CNS Tumors. Disclosures. Acknowledgements. Introduction. Introduction. Posterior Fossa Tumors. Whitney Finke, MD
 Pediatric CNS Tumors Disclosures Whitney Finke, MD Neuroradiology Fellow PGY-6 University of Utah Health Sciences Center Salt Lake City, Utah None Acknowledgements Introduction Nicholas A. Koontz, MD Luke
Pediatric CNS Tumors Disclosures Whitney Finke, MD Neuroradiology Fellow PGY-6 University of Utah Health Sciences Center Salt Lake City, Utah None Acknowledgements Introduction Nicholas A. Koontz, MD Luke
5-hydroxymethylcytosine loss is associated with poor prognosis for
 5-hydroxymethylcytosine loss is associated with poor prognosis for patients with WHO grade II diffuse astrocytomas Feng Zhang 1,*, Yifan Liu 2, Zhiwen Zhang 1, Jie Li 1, Yi Wan 3, Liying Zhang 1, Yangmei
5-hydroxymethylcytosine loss is associated with poor prognosis for patients with WHO grade II diffuse astrocytomas Feng Zhang 1,*, Yifan Liu 2, Zhiwen Zhang 1, Jie Li 1, Yi Wan 3, Liying Zhang 1, Yangmei
Case Presentation. Maha Akkawi, MD, Fatima Obeidat, MD, Tariq Aladily, MD. Department of Pathology Jordan University Hospital Amman, Jordan
 Case Presentation Maha Akkawi, MD, Fatima Obeidat, MD, Tariq Aladily, MD Department of Pathology Jordan University Hospital Amman, Jordan The 25th Annual Congress of the ADIAP The 8/11/2013 1 5th International
Case Presentation Maha Akkawi, MD, Fatima Obeidat, MD, Tariq Aladily, MD Department of Pathology Jordan University Hospital Amman, Jordan The 25th Annual Congress of the ADIAP The 8/11/2013 1 5th International
Disclosures. The Thin Red Line Between Neuropathology and Head & Neck Pathology. Introduction CASE 1. Current Issues Tihan
 Disclosures I have nothing to disclose The Thin Red Line Between Neuropathology and Head & Neck Pathology Tarik Tihan, MD, PhD UCSF, Department of Pathology Neuropathology Division Introduction Three cases
Disclosures I have nothing to disclose The Thin Red Line Between Neuropathology and Head & Neck Pathology Tarik Tihan, MD, PhD UCSF, Department of Pathology Neuropathology Division Introduction Three cases
Key Words: Brain tumor, BRAF, Glioneuronal, MAPK, Pilocytic astrocytoma.
 J Neuropathol Exp Neurol Copyright Ó 2012 by the American Association of Neuropathologists, Inc. Vol. 71, No. 1 January 2012 pp. 66Y72 ORIGINAL ARTICLE BRAF Alterations in Primary Glial and Glioneuronal
J Neuropathol Exp Neurol Copyright Ó 2012 by the American Association of Neuropathologists, Inc. Vol. 71, No. 1 January 2012 pp. 66Y72 ORIGINAL ARTICLE BRAF Alterations in Primary Glial and Glioneuronal
3/27/2017. Pulmonary Pathology Specialty Conference. Disclosure of Relevant Financial Relationships. Clinical History:
 Pulmonary Pathology Specialty Conference Saul Suster, M.D. Medical College of Wisconsin Disclosure of Relevant Financial Relationships USCAP requires that all planners (Education Committee) in a position
Pulmonary Pathology Specialty Conference Saul Suster, M.D. Medical College of Wisconsin Disclosure of Relevant Financial Relationships USCAP requires that all planners (Education Committee) in a position
