Differentiation of Papillary Renal Cell Carcinoma Subtypes on CT and MRI
|
|
|
- Rebecca Cain
- 6 years ago
- Views:
Transcription
1 Genitourinary Imaging Original Research Egbert et al. CT and MRI Differentiation of Papillary RCC Subtypes Genitourinary Imaging Original Research Nathan D. Egbert 1 Elaine M. Caoili 1 Richard H. Cohan 1 Matthew S. Davenport 1 Isaac R. Francis 1 L. Priya Kunju 2 James H. Ellis 1 Egbert ND, Caoili EM, Cohan RH, et al. Keywords: atypical papillary renal cell carcinoma, CT, MRI, papillary renal cell carcinoma, renal mass enhancement DOI: /JR Received June 20, 2012; accepted after revision November 15, Department of Radiology, University of Michigan Health System, 1500 E Medical Center Dr, nn rbor, MI ddress correspondence to N. D. Egbert (nathaneg@med.umich.edu). 2 Department of Pathology, University of Michigan Health System, nn rbor, MI. JR 2013; 201: X/13/ merican Roentgen Ray Society Differentiation of Papillary Renal Cell Carcinoma Subtypes on CT and MRI OJECTIVE. The objective of our study was to determine the frequency of atypical papillary renal cell carcinomas (RCCs) and identify imaging differences between type 1 and type 2 papillary RCCs once atypical papillary RCC tumors have been excluded. MTERILS ND METHODS. Eighty-two papillary RCC tumors were classified at pathology as type 1, type 2, or atypical. The CT and MRI examinations of these tumors were reviewed. Imaging features such as tumor size, margins, heterogeneity, and enhancement were assessed and the findings in type 1 and type 2 tumors were compared. RESULTS. There were 43 type 1 and 13 type 2 tumors. typical histologic features (i.e., tumors containing both type 1 and type 2 components, clear cells, or components with atypically high nuclear grade [in type 1 tumors] or low nuclear grade [in type 2 tumors]) were seen in 26 tumors. On CT, type 2 tumors more commonly had infiltrative margins (p = 0.05) and were more likely to have calcifications (p = 0.04) than type 1 tumors, although these features were seen in all tumor types. Type 2 tumors were also more heterogeneous than type 1 tumors (p = 0.04). On CT, 11 papillary RCCs showed enhancement of less than 20 HU, seven of which showed enhancement of less than 10 HU. On MRI, all tumors showed enhancement on subtraction images. CONCLUSION. Nearly one third of papillary RCCs in our patient population had atypical features at histology. On CT and MRI, there are some significant differences in imaging features between type 1 and type 2 tumors; however, substantial overlap precludes categorization on a per-patient basis. On CT, many papillary RCCs do not enhance, indicating that assessment of enhancement alone is insufficient for differentiating papillary RCCs from hyperdense cysts. P apillary renal cell carcinoma (RCC) is the second most common form of RCC, after clear cell RCC, accounting for 10 15% of cases [1]. In comparison with clear cell RCCs, papillary RCCs in general have less aggressive features, including being both smaller in size and lower in stage at presentation [2, 3]. Delahunt and Eble [4] divided papillary RCCs into two groups: type 1 and type 2 tumors. This classification of papillary RCC is important clinically because type 1 tumors, which are lowgrade neoplasms, have a much better prognosis than do type 2 tumors, which are high-grade neoplasms [2 4]. In several previous studies, investigators have reviewed the imaging features of type 1 and type 2 papillary RCCs to determine whether differences in appearance could predict subsequent tumor behavior [5, 6]. In the largest such study to date, consisting of 19 patients (including 12 type 1 tumors and eight type 2 tumors), Yamada et al. [6] found that, on CT, type 2 tumors were more likely to be heterogeneous and show indistinct margins. In that series, only one type 2 tumor was followed over time; it grew rapidly and was more aggressive than were the type 1 tumors. Some papillary RCCs cannot be neatly categorized into two types, suggesting that the description of the morphologic spectrum of papillary RCCs should be modified. For example, some papillary RCCs show separate regions with type 1 and type 2 features, whereas others contain both clear cell and papillary components [7, 8]. In addition, some type 1 papillary RCCs exhibit areas of high nuclear grade and some type 2 papillary RCCs exhibit areas of low nuclear grade [9]. The purpose of our study was to identify the frequency with which the various types of papillary RCC were encountered in our patient population. We also wished to determine whether different imaging features between type 1 and type 2 tumors would be revealed once atypical papillary RCCs had JR:201, ugust
2 Egbert et al. been removed from consideration. Finally, we sought to determine how many papillary RCCs fail to show detectable enhancement on CT and MRI, a characteristic that might make them indistinguishable from some complex hyperdense renal cysts. Materials and Methods Subjects This study complied with HIP. fter obtaining institutional review board approval with a waiver of patient informed consent due to the retrospective nature of this study, we searched a pathologic database for papillary RCCs diagnosed at our institution from January 1, 2004, through December 31, Only cases with available CT or MRI studies obtained before either biopsy or surgery were included. When multiple papillary renal cancers were present in the same patient, only the largest histologically proven papillary RCC was included in our analysis. Demographics Patient demographics are listed in Table 1. During the study period, 82 patients with histologically confirmed papillary RCCs underwent preoperative imaging with CT only (n = 53), MRI only (n = 18), or both CT and MRI (n = 11). There were 61 men and 21 women, with a mean age of 62.4 years (range, years). Forty-three (52%) papillary RCCs were classified as type 1 tumors, 13 (16%) as type 2 tumors, and 26 (32%) as atypical tumors; the 26 atypical tumors were further subcategorized into papillary RCC with clear cell features (n = 8), high-nuclear-grade type 1 (n = 8), mixed type 1 and type 2 (n = 7), and low-nuclear-grade type 2 (n = 3). Of the 64 patients evaluated by CT, 35 had type 1 papillary RCCs, nine had type 2 papillary RCCs, and 20 had atypical papillary RCCs. Of the 29 patients evaluated with MRI, 15 had type 1 papillary RCCs, six had type 2 papillary RCCs, and eight had atypical papillary RCCs. CT and MRI Technique ecause this study was retrospective, a variety of CT and MRI techniques were used on a variety of scanners; 14 CT studies and four MRI studies were performed at outside institutions. The CT examinations at our institution were performed on MDCT scanners (LightSpeed 16, LightSpeed 16 Pro, and LightSpeed VCT; GE Healthcare). The CT images were acquired at 120 kvp and between 150 and 400 ms and were reconstructed at 2.5- or 5-mm intervals. Contrast-enhanced CT images at our institution were obtained after the injection of 100 or 125 ml of a nonionic iodinated contrast material with a concentration of 300 mg/ml (iopromide [Ultravist 300, ayer HealthCare] or iopamidol [Isovue 300, racco Diagnostics]) at a rate of 2 or 3 ml/s. rterial, corticomedullary, nephrographic, and excretory phase images were obtained according to a variety of protocols using at least one of the following delays: 20, 70, 120, or 150 seconds. Forty-eight of the 64 CT studies performed in the papillary RCC patients were at least dual-phase studies, including unenhanced images and at least one of the following: arterial phase (n = 2 patients), corticomedullary phase (n = 21), nephrographic phase (n = 39), or excretory phase (n = 5) images. Forty-one of the 48 patients with at least dual-phase imaging (defined as having both unenhanced and at least one contrast-enhanced series) had images obtained before contrast material administration and during the nephrographic or excretory phase of enhancement (constituting an acceptable dedicated renal mass protocol CT technique [10, 11]). This group included 20 type 1, five type 2, and 16 atypical papillary RCCs. MRI was performed on a 1.5-T magnet (Signa HD, GE Healthcare) or a 3-T magnet (chieva, Philips Healthcare) with a body or torso phased-array coil using the following sequences: axial T1-weighted spin-echo breath-hold spoiled gradient-echo, axial T2- weighted fat-suppressed fast spin-echo (FSE), coronal non fat-suppressed breath-hold half-fourier singleshot FSE, and coronal T1-weighted dynamic breathhold gadolinium-enhanced spoiled gradient-recalled sequences. fter unenhanced acquisitions, gadolinium-enhanced imaging was performed in the corticomedullary, nephrographic, and delayed phases, with images obtained using delays of 30, 60, and 120 seconds, respectively. Enhancement after the administration of up to 20 ml of gadolinium-based contrast material (gadopentetate dimeglumine [Magnevist, ayer Pharmaceuticals] or gadoben ate dimeglumine [MultiHance, racco Diagnostics]) was determined by creating subtraction images derived from the nephrographic and unenhanced image acquisitions. total of 29 papillary RCCs were imaged with MRI, including 15 type 1 papillary RCCs, six type 2 papillary RCCs, and eight atypical papillary RCCs. Contrast-enhanced images were included in all but one of the MRI studies that were reviewed. ssessment of Imaging Features on oth CT and MRI The index CT and MRI examinations and the oldest available comparison study were assessed independently by two reviewers who were blinded to the histologic data, and discrepancies were resolved in consensus. For all masses, the following imaging features were recorded: maximal tumor diameter in the axial plane; location (upper pole, mid kidney, or lower pole); whether the tumor was exophytic, defined as having any margin extending beyond the edge of the renal parenchyma, or endophytic, defined as being located completely within the renal parenchyma; whether tumor margins were well defined or infiltrative; and whether the tumor was heterogeneous or homogeneous on all imaging sequences on CT or MRI. In addition, reviewers recorded whether any of the following features were present: inhomogeneity of perilesional fat, an identifiable capsule, renal vein invasion, regional lymph node enlargement, or distant metastatic disease. For masses imaged with CT, the presence or absence of calcification was also determined. Regions of interest were placed over the renal mass incorporating approximately three quarters of the mass on the axial image where the mass was at its largest dimension visually while excluding areas of calcification. Renal mass enhancement was calculated by subtracting the high-attenuation components of the mass on unenhanced images from the attenuation on each of the following phases: corticomedullary, nephrographic, and excretory, as available. The maximum degree of enhancement evident on contrast-enhanced images was recorded. n increase in attenuation of 20 HU or greater indicated definite enhancement, whereas TLE 1: Demographics of 82 Patients With Papillary Renal Cell Carcinoma (RCC) RCC No. of Patients ge (y) Total Male Female Mean Range Typical type Typical type typical Mixed type 1 and type Papillary RCC with clear cell features Type 1, high nuclear grade Type 2, low nuclear grade Total JR:201, ugust 2013
3 CT and MRI Differentiation of Papillary RCC Subtypes TLE 2: CT Imaging Features of 64 Papillary Renal Cell Carcinomas (RCCs) Characteristic an increase of HU was considered equivocal and an increase of less than 10 HU indicated lack of enhancement [3, 12, 13]. For masses imaged with MRI, the presence or absence of hemosiderin was determined, defined as the subjective identification of loss of signal intensity on longer-te in-phase images relative to opposed-phase T1-weighted dual-echo gradient-recalled echo images. Relative signal intensity in comparison with the normal renal parenchyma (i.e., hypointense, isointense, hyperintense) was also recorded on unenhanced T1-weighted, unenhanced T2-weighted, and contrast-enhanced T1-weighted images. In addition, the presence or absence of enhancement was determined subjectively on subtraction images. Papillary RCC Types Type 1 Type 2 typical Type 1, High Nuclear Grade Follow-Up ssessment To evaluate tumors for growth, we identified patients who had imaging studies obtained before the index study. For each patient, the most remote previous study available was used and compared with the index imaging study. The tumor growth rate was then calculated on the basis of the measured changes in the maximum axial diameter in centimeters per year. This calculation was performed only for patients who had at least two imaging studies obtained 6 months or more apart. Patient outcomes were assessed using the institutional electronic medical records. The following data were recorded: whether there was a surgical resection and findings at resection, the results of histologic sampling, whether the patient developed local recurrence, whether the patient developed regional or distant metastatic disease, and patient survival. The time interval between the index imaging study and each patient outcome was recorded. Review of Papillary Renal Cell Carcinoma Histopathology Histopathologic specimens of the tumors in this study were reviewed by an experienced genitourinary pathologist who classified each of the tumors into the following types: type 1, type 2, or atypical. Reclassification was performed for masses if typing had not been performed previously, which had occurred largely because some tumors in our series were encountered before the description of the papillary tumor types. Type 1 tumors were those that had low-fuhrman-grade nuclei and were composed of papillae lined by small cells in a single layer with scant typical Papillary RCC Subtypes Type 2, Low Nuclear Grade Mixed Types 1 and 2 Papillary RCC With Clear Cell Features No. of tumors Mean tumor size (cm) Homogeneous a 3 (9) 0 (0) 3 (15) Perilesional stranding a 4 (11) 3 (33) 3 (15) Central scar or necrosis a 1 (3) 1 (11) 2 (10) Calcifications a 4 (11) 4 (44) 4 (20) Margins b Well-defined 33 (94) 6 (67) 17 (85) Infiltrative 2 (6) 3 (33) 3 (15) No. of patients who underwent dual-phase imaging c Mean unenhanced attenuation (HU) Mean maximal enhancement (HU) No. of tumors with equivocal or no enhancement ( < 20 HU) No. of tumors with equivocal or no enhancement ( < 1 0 HU) Renal vein invasion d 0 (0) 1 (11) 0 (0) Enlarged regional lymph node(s) d 3 (9) 2 (22) 1 (5) Distant metastases d 0 (0) 0 (0) 0 (0) a No. (%) of tumors. No./total no. (%) of tumors. c Defined as unenhanced and at least one nephrographic or excretory phase contrast-enhanced imaging series. d No. (%) of patients. Fig year-old man with type 2 papillary renal cell carcinoma (RCC). xial CT image in nephrographic phase shows homogeneous, hypoenhancing mass with relatively indistinct borders with renal parenchyma. lthough there was overlap, type 2 papillary RCCs more commonly had indistinct margins than type 1 papillary RCCs (p = 0.05). pale to basophilic cytoplasm. Type 2 tumors were those that had high-fuhrman-grade nuclei, eosinophilic cytoplasm, and pseudostratification of nuclei JR:201, ugust
4 Egbert et al. on papillary cores. typical papillary tumors were those exhibiting any of the following characteristics: tumors containing both type 1 and type 2 morphologic features, tumors containing clear cell and papillary components, tumors having type 1 cytoplasmic features but high nuclear grade (Fuhrman grade 3 or 4), and tumors having type 2 cytoplasmic features but low nuclear grade (Fuhrman grade 1 or 2). Statistical nalysis Descriptive statistics were used to summarize the data. Calculations were made using statistics software (SS, version 9.3, SS Institute). lthough three groups of papillary RCCs were evaluated in this study (type 1, type 2, and atypical), statistical comparisons were performed only between type 1 and type 2 tumors to assess any differences that might emerge once the atypical papillary RCC tumors had been excluded. comparison between atypical tumors and type 1 and type 2 tumors and a subgroup analysis of the atypical papillary RCC tumors were not performed because of the heterogeneity of the atypical group and insufficient numbers of the individual atypical variants. The Student t test was used to assess continuous variables, which are defined as variables that can take on any value unlike discrete variables that can assume only a few possible values (i.e., age, size, or attenuation measurements). The Fisher exact test was used to determine whether the presence of specific imaging features was associated with either papillary RCC type. For all analyses, p 0.05 was considered to indicate statistical significance. Results Combined CT and MR Data nalysis The mean maximum diameters of the papillary RCC types were 3.5 cm for type 1 tumors, Fig year-old man with type 2 papillary renal cell carcinoma. and, xial unenhanced () and nephrographic phase () CT images show complex mass in left kidney. Note that highest-attenuation component (arrow, ; arrowhead, ) of this mass does not show enhancement, measuring 60 HU on unenhanced image and 55 HU on contrast-enhanced nephrographic phase image. 6.0 cm for type 2 tumors, and 4.2 cm for atypical tumors. Type 2 tumors were significantly larger than type 1 tumors (p = 0.01). There were no significant differences (p > 0.05) between type 1 and type 2 tumors for the following additional characteristics assessed on CT and MRI studies: location (upper, mid, or lower pole), exophytic versus endophytic, perilesional inhomogeneity, venous invasion, presence of a capsule, enlarged regional lymph node or nodes, and distant metastatic disease. CT nalysis The results of the CT analysis are provided in Table 2. There was a significant difference in margin distinctness (p = 0.05) between type 1 and type 2 tumors, with indistinct margins more likely in type 2 tumors (Fig. 1); however, there was overlap. Three of nine (33%) type 2 lesions showed this imaging feature in comparison with only two of 35 (6%) type 1 lesions. The majority of papillary RCCs of all types were heterogeneous in appearance with only three type 1 (9%), zero type 2 (0%), and three atypical (15%) papillary RCCs appearing homogeneous. Calcifications were more frequent in type 2 papillary RCCs (4/9, 44%) than in type 1 papillary RCCs (4/35, 11%) (p = 0.04). Twenty papillary RCCs (17 [85%] type 1 and three [60%] type 2 papillary RCCs) showed enhancement on nephrographic or excretory phase images, defined as an increase in attenuation of 20 HU or more between unenhanced and any series of contrast-enhanced images. This difference was not significant. Three type 1 and two type 2 papillary RCCs showed an increase in attenuation between unenhanced and nephrographic or excretory enhanced images of less than 20 HU. Within this group, one type 1 papillary RCC and one type 2 papillary RCC showed a change in attenuation of less than 10 HU. Within the atypical papillary RCC group, six showed enhancement of less than 20 HU, with five of these atypical neoplasms changing less than 10 HU in attenuation. Overall, eight of the 11 papillary RCCs of all types that showed less than 20 HU of enhancement were heterogeneous (Fig. 2). The remaining three nonenhancing tumors (one type 1 papillary RCC and two atypical papillary RCCs showing type 1 morphology but high nuclear grade) were homogeneous (Fig. 3). Further histologic review of the 11 papillary RCCs of all types that showed less than 20 HU of enhancement revealed that six of the tu- Fig year-old man with type 1 papillary renal cell carcinoma. and, xial CT images in unenhanced () and delayed contrast-enhanced () phases show homogeneous mass in right kidney (27 HU on unenhanced image and 34 HU on delayed phase image). CT appearance of this mass is indistinguishable from that of hyperdense cyst. 350 JR:201, ugust 2013
5 CT and MRI Differentiation of Papillary RCC Subtypes TLE 3: MRI Features of 29 Papillary Renal Cell Carcinomas (RCCs) Characteristic mors (55%) were extensively necrotic and four (36%) were extensively cystic. The 11th tumor had undergone radiofrequency ablation before resection, which precluded assessment of the lesion for preablation cystic change or necrosis. Papillary RCC Types Type 1 Type 2 typical Type 1, High Nuclear Grade MRI nalysis Table 3 summarizes the MRI findings. We were not able to detect a significant difference between type 1 and type 2 papillary RCCs with respect to the presence of infiltrative margins, internal hemosiderin, or a surrounding capsule. lthough no significant difference was found, only eight (53%) type 1 papillary RCCs versus all six (100%) type 2 papillary RCCs showed heterogeneity on at least one imaging sequence. Type 1 papillary RCCs were most often hypointense on T2- weighted images (10/14, 71%), whereas type 2 papillary RCCs were more commonly hyperintense on T2-weighted images (3/5, 60%); however, there was overlap. On contrast-enhanced images, the majority of type 1 and type 2 papillary RCCs were hypointense to the typical Papillary RCC Subtypes Type 2, Low Nuclear Grade Mixed Types 1 and 2 Papillary RCC With Clear Cell Features No. of tumors Mean tumor size (cm) Capsule a 5 (33) 3 (50) 4 (50) Perilesional stranding a 4 (27) 2 (33) 3 (38) Central scar or necrosis a 1 (7) 1 (17) 1 (13) Hemosiderin b 2/13 (15) 2/6 (33) 1/8 (13) Margins a Well-defined 13 (87) 6 (100) 8 (100) Infiltrative 2 (13) 0 (0) 0 (0) Renal vein invasion c 0 (0) 0 (0) 0 (0) Enlarged regional lymph nodes c 2 (13) 2 (33) 0 (0) Distant metastases c 0 (0) 0 (0) 1 (13) T1 unenhanced signal Heterogeneous Homogeneous Hypointense to renal cortex Isointense to renal cortex Hyperintense to renal cortex T1 signal (nephrographic phase) Heterogeneous Homogeneous Hypointense to renal cortex Isointense to renal cortex Hyperintense to renal cortex T2 signal Heterogeneous Homogeneous Hypointense to renal cortex Isointense to renal cortex Hyperintense to renal cortex Enhancement, no. (%) 13/13 (100) 5/5 (100) 8/8 (100) a No. (%) of tumors. No./total no. (%) of tumors. No. (%) of patients. normal renal cortex (11/15 [73%] type 1, 5/6 [83%] type 2) (Fig. 4). Subtraction images revealed enhancement in all type 1 and type 2 tumors. Of the eight atypical papillary RCCs, seven (88%) showed hypointensity relative to the renal cortex on contrast-enhanced images and all eight also showed enhancement on subtraction images. Only two of the 11 papillary RCCs that showed equivocal or no enhancement on CT were imaged with MRI, and both of these lesions showed enhancement on subtraction MR images. JR:201, ugust
6 Egbert et al. Tumor Growth The results of the tumor growth assessment are listed in Table 4. Sequential examinations were available for only eight type 1 papillary RCCs, two type 2 papillary RCCs, and three atypical papillary RCCs, with a median time interval during which these were followed of 14.6 months (range, 6 36 months) (Fig. 5). We were not able to detect a significant difference between the growth rates for type 1 and type 2 tumors. Clinical Follow-Up Of the 82 patients with papillary RCCs, follow-up clinical information was available in the electronic medical records for 80 patients. The median length of clinical follow-up for all tumors was 29 months (range, 0 86 months). Of the 41 type 1 tumors in which clinical follow-up was available, one patient with an 8.1-cm papillary RCC developed local recurrence and distant metastatic Fig year-old man with type 1 papillary renal cell carcinoma in left kidney., Coronal T2-weighted image with fat saturation shows hypointense mass in lower pole., xial T1-weighted image also shows mass to be largely hypointense. C, xial contrastenhanced T1-weighted image in nephrographic phase with fat saturation shows hypoenhancing mass in comparison with normal renal parenchyma. This mass did show enhancement on subsequently created subtraction images (not shown). disease to the lungs and pelvis. Five of the 13 patients with type 2 papillary RCC developed recurrent or metastatic disease, a significantly higher frequency than was noted in the patients in the type 1 papillary RCC group (p = 0.002) (Fig. 6). The metastases in these patients occurred in the lungs (n = 3), bones (n = 3), adrenal glands (n = 2), and perihepatic space (n = 1). Of the 26 atypical papillary RCCs, only one patient with a papillary clear cell neoplasm developed distant C metastatic disease; in that case, metastatic disease to the bones was detected 15 months after initial presentation. Most of the patients who developed recurrent disease had large tumors at the time of diagnosis. The average and median sizes of the tumors in these patients were 7.2 and 5.6 cm (range, cm), respectively. In comparison, the average and median tumor sizes for patients who did not develop local or distant metastatic disease were 3.9 and 3.0 cm (range, cm), respectively. Only one patient (who had a type 2 papillary RCC) with a papillary RCC measuring less than 4.0 cm at the time of diagnosis subsequently developed metastatic disease. Discussion Histologically, papillary RCCs are characterized by variable proportions of papillae, each of which contains a fibrovascular core. dditional findings can include aggregates of foamy macrophages, calcifications, and frequent hemosiderin granules [2, 4]. Pathologists have recognized that all papillary cancers are not histologically similar and do not behave in a clinically identical fashion [2, 14]. This finding led to the classification of papillary RCCs into two major types [2, 4]. Type 1 papillary RCCs contain papillae covered by cells arranged in a single layer, have a small amount of clear to basophilic cytoplasm, are of low nuclear grade (Fuhrman grade 1 or 2), grow slowly, and have a better prognosis than do clear cell RCCs. In comparison, type 2 papillary RCCs contain abundant eosinophilic cytoplasm, have pseudostratified high-grade nuclei (Fuhrman grade 3 or 4) [2, 4], behave more aggressively, and have a prognosis that approximates that of clear cell RCCs. Once the classification of papillary cancers into two groups was recognized by the World Health Organization, several studies were undertaken to determine whether type 1 papillary RCCs have different cross-sectional imaging features than type 2 papillary RCCs. Yamada et al. [6] found that type 2 tu- TLE 4: Growth Rates of Papillary Renal Cell Carcinomas (RCCs) Papillary RCC Type No. of Patients With Comparison Studies Imaging Follow-Up (mo) Lesion Growth Rate (cm/y) Mean Range Mean Range Type 1 (n = 32) to 2.4 Type 2 (n = 8) typical (n = 19) to 1.8 Total (n = 59) to JR:201, ugust 2013
7 CT and MRI Differentiation of Papillary RCC Subtypes mors overall have less distinct margins, are less likely to be homogeneous, and are more likely to be advanced tumors at the time of diagnosis than type 1 tumors. s pathologists have gained more experience typing papillary cancers, it has become evident that many papillary RCCs cannot be classified easily as belonging to either of the two existing types. Specifically, some papillary RCCs can contain both type 1 and type 2 components in separate areas. Some RCCs have been identified that contain both papillary and clear cell components and recently classified as clear cell papillary RCC, with most being reported in patients with chronic kidney disease [7, 8]. In addition, some type 1 tumors may have high nuclear grade and some type 2 tumors may have low nuclear grade in contradiction to their otherwise overall behavior and prognosis [9, 15]. We undertook this study to determine whether there are imaging features that might allow differentiation of type 1 papillary RCCs from type 2 papillary RCCs that may have not been previously reported because they may have been masked by the presence of atypical papillary RCCs contaminating data analysis. We found that there are some significant differences in the imaging appearances of type 1 and type 2 papillary RCCs when the atypical papillary RCCs have been removed from consideration. The detected significant mean differences included each of the following: overall type 2 papillary RCCs were larger, more likely to have infiltrative margins on CT (which had been previously reported [6]), more likely to be Fig year-old man with type 1 papillary renal cell carcinoma., xial contrast-enhanced CT image in corticomedullary phase shows 1.6-cm hypoenhancing mass in left kidney., xial contrast-enhanced CT image in nephrographic phase obtained 3 years after shows growth to 3.2 cm (growth rate = 0.5 cm/y). Mass also now contains lobulated higher-attenuation components peripherally. heterogeneous, and more likely to contain calcifications than type 1 papillary RCCs. Unfortunately, there was overlap between both type 1 and type 2 papillary RCCs, and thus we believe that these features may not be able to distinguish between tumor types reliably in any given patient. This problem was even more substantial with respect to the MRI features: We were unable to find any significant differences in the MRI appearances of the type 1 and type 2 neoplasms. The presence of enhancing areas within a renal mass is a well-accepted indicator that a mass may be solid and potentially malignant. For CT, it is generally accepted that an increase in attenuation of greater than or equal to 20 HU on MDCT scanners indicates true enhancement, whereas measurements of less than 10 HU indicate an absence of enhancement. It is somewhat more controversial how to interpret differences measured to be between 10 and 20 HU, with some centers considering findings in this range to be equivocal [3, 10, 11]. For MRI, the presence of internal enhancement is often a qualitative assessment on subtraction images, with any remaining subjective nonartifactual internal signal intensity being indicative of true enhancement. Papillary RCC has classically been described as a poorly enhancing type of RCC [16, 17]. In fact, in our study, when a renal mass CT technique was used, a substantial minority of all papillary RCCs showed either no CT enhancement (7/41 [17%] tumors imaged using renal mass CT technique) or equivocal enhancement (4/41 [9.8%] tumors). Nonenhancing and equivocally enhancing tumors were found in all three papillary RCC groups. Our study confirms that a lack of CT enhancement in a renal lesion is not sufficient to indicate that a renal mass is benign (i.e., a hyperdense cyst). Instead, assessment of mass morphology (if it is homogeneous or heterogeneous) can be helpful in cases in which the attenuation measurements indicate a lack of enhancement. In our series, eight of the 11 (73%) nonenhancing or equivocally enhancing papillary tumors were heterogeneous on at least one series of contrastenhanced images. Only three nonenhancing or equivocally enhancing papillary RCCs were homogeneous on contrast-enhanced images, a feature that rendered these tumors indistinguishable from benign hyperdense cysts. In our study, MRI was more sensitive in detecting enhancement; areas of enhancement were detected on MRI in the two patients with equivocal or nonenhancing papillary RCCs on CT who also had MRI examinations. Investigators have observed that papillary RCCs account for approximately 25% of malignant cystic lesions [18], a feature that is thought to be a result of necrosis or cystic degeneration [19]. The results of our study further support those data because histologic reanalysis of the 10 equivocally enhancing or nonenhancing papillary RCCs in our study that could be assessed sufficiently at subsequent surgery were either extensively necrotic (6/10, 60%) or extensively cystic (4/10, 40%). Evaluation of an 11th papillary RCC in this group was limited because that tumor had been treated with radiofrequency ablation before resection. Overall, our MRI results for papillary RCCs support previously reported findings, with papillary RCCs usually being hypointense on T2- weighted images [5, 20, 21]. In our series, type 1 papillary RCCs were most often hypointense on T2-weighted images (10/14, 71%) (Fig. 4), whereas type 2 papillary RCCs were more commonly hyperintense on T2-weighted images (3/5, 60%). Regardless, relative signal intensity on T2-weighted imaging cannot be used for definitive prospective classification not only because some clear cell RCCs show signal patterns like those of papillary RCCs, but also because there is substantial overlap between the signal characteristics of type 1 and type 2 papillary RCCs. The majority of all papillary RCCs were also hypointense relative to normal renal parenchyma on contrast-enhanced images. However, enhancement was always identified on subtraction images even for two tumors that were equivocally enhancing or nonenhancing on JR:201, ugust
8 Egbert et al. Fig year-old man with type 2 papillary renal cell carcinoma., xial CT contrast-enhanced image shows large heterogeneous mass in left kidney and enlarged regional lymph nodes (arrow). and C, xial contrast-enhanced CT images through pelvis () and lower left ribs (C), show metastases to left ischium (arrowhead, ) and left ribs and chest wall. CT. Overall, there were no distinguishing features identified on MR images that allowed reliable differentiation of type 1 from type 2 papillary RCCs. s we have already noted, distinguishing between type 1 and type 2 papillary RCCs is clinically relevant because type 2 papillary RCCs have been associated with a worse prognosis. Our results confirm that type 2 papillary RCCs behave more aggressively than type 1 papillary RCCs. In our study, patients with type 2 papillary RCCs were more likely to develop locally recurrent or distant metastatic disease (5/13, 38.5%) than patients with either type 1 (1/41, 2.4%) or atypical (1/26, 3.8%) papillary RCCs, despite the fact that the average growth rates for the small number of followed type 1, type 2, and atypical papillary RCCs were not significantly different (0.5, 0.7, and 1.0 cm/y, respectively); however, we should note that only a small number of patients were followed. We also noticed that most of the patients who eventually developed metastatic disease overall had larger tumors at the time of diagnosis, with average and median sizes of 7.2 and 5.6 cm (range, cm), respectively. In fact, only one patient with a papillary RCC (type 2) less than 4 cm at the time of diagnosis developed metastatic disease. There are several limitations of our study. ecause our study was retrospective, a variety of imaging protocols were used, which may have contributed to the heterogeneity of our results. In addition, verification bias is a concern because it is possible that some additional patients with papillary RCC may have not been included in our study if these tumors were not properly identified. lso, although our study included 82 papillary RCCs, there were still a relatively small number of type 2 neoplasms and of the individual atypical types. This fact makes our comparisons limited. It is possible that more differences would emerge in a larger series. Nevertheless, we believe that the presence of overlapping features in even this small series suggests that papillary RCC classification will not be possible with CT or MRI alone in any given case. In summary, almost one third of papillary RCCs in our cohort were found on pathology to have atypical features that precluded strict type 1 or type 2 papillary RCC classification. lthough our results support prior work showing that type 2 papillary RCCs have a worse prognosis, we did not identify any reliable imaging characteristic that might allow noninvasive distinction between type 1 and type 2 papillary RCCs even when atypical tumors were considered separately. In addition, more than one quarter of all the papillary RCCs assessed with a renal mass CT technique that were reviewed in our study did not show definitive CT enhancement, although areas of enhancement could be identified on subtraction images of two papillary RCCs imaged with MRI that showed equivocal enhancement or no enhancement on CT. Reliance on the presence or absence of enhancement on CT to determine whether a mass is solid or cystic is inadequate. In such cases, the presence of tumor heterogeneity is a more reliable clue that the mass is solid. Contrast-enhanced MRI may be pref- C 354 JR:201, ugust 2013
9 CT and MRI Differentiation of Papillary RCC Subtypes erable for renal mass characterization because subtraction images show enhancement of papillary RCCs in some cases when CT does not. stage renal disease: an experience from 66 tumorbearing kidneys with emphasis on histologic patterns distinct from those in sporadic adult renal ma: a clinicopathologic and immunohistochemical study of 105 tumors. Mod Pathol 1997; 10: Park H, Ro JY, Park WS, et al. Oncocytic papil- References 1. Tse G, Chow DS, Hsu M, Margolis D, Raman SS. neoplasia. m J Surg Pathol 2006; 30: Gobbo S, Eble JN, Grignon DJ, et al. Clear cell papillary renal cell carcinoma: a distinct histo- lary renal cell carcinoma with inverted nuclear pattern: distinct subtype with an indolent clinical course. Pathol Int 2009; 59: Multidetector computed tomographic features of oncocytic papillary renal cell carcinoma, a new subtype. J Comput ssist Tomogr 2010; 34: Lopez-eltran, Scarpelli M, Montironi R, Kirkali Z WHO classification of the renal tumors of the adults. Eur Urol 2006; 49: Vikram R, Ng CS, Tamboli P, et al. Papillary renal cell carcinoma: radiologic-pathologic correlation and spectrum of disease. RadioGraphics 2009; 29: ; discussion, Delahunt, Eble JN. Papillary renal cell carcinoma. In: Eble JN, Sauter G, Epstein JI, Sesterhenn I, eds. World Health Organization classification of tumors. Lyon, France: IRC Press, 2004: Roy C, Sauer, Lindner V, Lang H, Saussine C, Jacqmin D. MR imaging of papillary renal neoplasms: potential application for characterization of small renal masses. Eur Radiol 2007; 17: Yamada T, Endo M, Tsuboi M, et al. Differentiation of pathologic subtypes of papillary renal cell carcinoma on CT. JR 2008; 191: Tickoo SK, de Peralta-Venturina MN, Harik LR, et al. Spectrum of epithelial neoplasms in end- pathologic and molecular genetic entity. m J Surg Pathol 2008; 32: Kunju LP, Wojno K, Wolf JS, Cheng L, Shah R. Papillary renal cell carcinoma with oncocytic cells and nonoverlapping low grade nuclei: expanding the morphologic spectrum with emphasis on clinicopathologic, immunohistochemical and molecular features. Hum Pathol 2008; 39: Yuh I, Cohan RH. Different phases of renal enhancement: role in detecting and characterizing renal masses during helical CT. JR 1999; 173: Yuh I, Cohan RH, Francis IR, Korobkin M, Ellis JH. Comparison of nephrographic with excretory phase helical CT for detection and characterization of renal masses. Can ssoc Radiol J 2000; 51: Chung EP, Herts R, Linnell G, et al. nalysis of changes in attenuation of proven renal cysts on different scanning phases of triphasic MDCT. JR 2004; 182: Silverman SG, Herts R, Israel GM, Richie JP. Management of the incidental renal mass. Radiology 2008; 249: Delahunt, Eble JN. Papillary renal cell carcino- 16. Ruppert-Kohlmayr J, Uggowitzer M, Meissnitzer T, Ruppert G. Differentiation of renal clear cell carcinoma and renal papillary carcinoma using quantitative CT enhancement parameters. JR 2004; 183: Zhang J, Lefkowitz R, Ishill NM, et al. Solid renal cortical tumors: differentiation with CT. Radiology 2007; 244: Smith D, Remer EM, Cox KL, et al. osniak category IIF and III cystic renal lesions: outcomes and associations. Radiology 2012; 262: rinker D, min M, de Peralta-Venturina M, Reuter V, Chan DY, Epstein JI. Extensively necrotic cystic renal cell carcinoma: a clinicopathologic study with comparison to other cystic and necrotic renal cancers. m J Surg Pathol 2000; 24: Sussman SK, Glickstein MF, Kryzmowski G. Hypointense renal cell carcinoma: MR imaging with pathologic correlation. Radiology 1990; 177: Yoshimitsu K, Kakihara D, Irie H, et al. Papillary renal carcinoma: diagnostic approach by chemical shift gradient-echo and echo-planar MR imaging. J Magn Reson Imaging 2006; 23: JR:201, ugust
MDCT Findings of Renal Cell Carcinoma Associated With Xp11.2 Translocation and TFE3 Gene Fusion and Papillary Renal Cell Carcinoma
 Genitourinary Imaging Original Research Woo et al. MDCT in Renal Cell Carcinoma Genitourinary Imaging Original Research Sungmin Woo 1 Sang Youn Kim 1 Myoung Seok Lee 1 Kyung Chul Moon 2 See Hyung Kim 3
Genitourinary Imaging Original Research Woo et al. MDCT in Renal Cell Carcinoma Genitourinary Imaging Original Research Sungmin Woo 1 Sang Youn Kim 1 Myoung Seok Lee 1 Kyung Chul Moon 2 See Hyung Kim 3
Chromophobe Renal Cell Carcinoma: Multiphase MDCT Enhancement Patterns and Morphologic Features
 Genitourinary Imaging Original Research Raman et al. Enhancement Patterns and Morphologic Features of Chromophobe Renal Cell Carcinoma Genitourinary Imaging Original Research Siva P. Raman 1 Pamela T.
Genitourinary Imaging Original Research Raman et al. Enhancement Patterns and Morphologic Features of Chromophobe Renal Cell Carcinoma Genitourinary Imaging Original Research Siva P. Raman 1 Pamela T.
ESUR 2018, Sept. 13 th.-16 th., 2018 Barcelona, Spain
 ESUR 2018, Sept. 13 th.-16 th., 2018 Barcelona, Spain OUR APPROACH Incidental adrenal nodule/mass Isaac R Francis, M.B;B.S University of Michigan, Ann Arbor, Michigan Disclosures None (in memory) M Korobkin,
ESUR 2018, Sept. 13 th.-16 th., 2018 Barcelona, Spain OUR APPROACH Incidental adrenal nodule/mass Isaac R Francis, M.B;B.S University of Michigan, Ann Arbor, Michigan Disclosures None (in memory) M Korobkin,
Diagnostic accuracy of percutaneous renal tumor biopsy May 10 th 2018
 Diagnostic accuracy of percutaneous renal tumor biopsy May 10 th 2018 Dr. Tzahi Neuman Dep.Of Pathology Hadassah Medical Center Jerusalem, Israel, (tneuman@hadassah.org.il) Disclosure: 1 no conflicts of
Diagnostic accuracy of percutaneous renal tumor biopsy May 10 th 2018 Dr. Tzahi Neuman Dep.Of Pathology Hadassah Medical Center Jerusalem, Israel, (tneuman@hadassah.org.il) Disclosure: 1 no conflicts of
Imaging characterization of renal clear cell carcinoma
 Imaging characterization of renal clear cell carcinoma Poster No.: C-0327 Congress: ECR 2011 Type: Educational Exhibit Authors: S. Ballester 1, A. Gaser 2, M. Dotta 1, M. F. CAPPA 1, F. Hammar 1 ; 1 2
Imaging characterization of renal clear cell carcinoma Poster No.: C-0327 Congress: ECR 2011 Type: Educational Exhibit Authors: S. Ballester 1, A. Gaser 2, M. Dotta 1, M. F. CAPPA 1, F. Hammar 1 ; 1 2
Qualitative and Quantitative MDCT Features for Differentiating Clear Cell Renal Cell Carcinoma From Other Solid Renal Cortical Masses
 Genitourinary Imaging Original Research Lee-Felker et al. MDCT Differentiation of Clear Cell RCC Genitourinary Imaging Original Research Stephanie A. Lee-Felker 1 Ely R. Felker 1 Nelly Tan 1 Daniel J.
Genitourinary Imaging Original Research Lee-Felker et al. MDCT Differentiation of Clear Cell RCC Genitourinary Imaging Original Research Stephanie A. Lee-Felker 1 Ely R. Felker 1 Nelly Tan 1 Daniel J.
Sarcomatoid renal cell carcinoma: A case report and literature review
 Sarcomatoid renal cell carcinoma: A case report and literature review Michael Reiter 1*, Ryan Schwope 1, Arthur Clarkson 2 1. Department of Radiology, Brooke Army Medical Center, San Antonio USA 2. Department
Sarcomatoid renal cell carcinoma: A case report and literature review Michael Reiter 1*, Ryan Schwope 1, Arthur Clarkson 2 1. Department of Radiology, Brooke Army Medical Center, San Antonio USA 2. Department
MRI IN THE CHARACTERIZATION OF SEMINOMATOUS AND NONSEMINOMATOUS GERM CELL TUMORS OF THE TESTIS
 MRI IN THE CHARACTERIZATION OF SEMINOMATOUS AND NONSEMINOMATOUS GERM CELL TUMORS OF THE TESTIS Ambesh Deshar *, Gyanendra KC and Zhang Lopsang *Department of Medical Imaging and Nuclear Medicine, First
MRI IN THE CHARACTERIZATION OF SEMINOMATOUS AND NONSEMINOMATOUS GERM CELL TUMORS OF THE TESTIS Ambesh Deshar *, Gyanendra KC and Zhang Lopsang *Department of Medical Imaging and Nuclear Medicine, First
Role of imaging in RCC. Ultrasonography. Solid lesion. Cystic RCC. Solid RCC 31/08/60. From Diagnosis to Treatment: the Radiologist Perspective
 Role of imaging in RCC From Diagnosis to Treatment: the Radiologist Perspective Diagnosis Staging Follow up Imaging modalities Limitations and pitfalls Duangkamon Prapruttam, MD Department of Therapeutic
Role of imaging in RCC From Diagnosis to Treatment: the Radiologist Perspective Diagnosis Staging Follow up Imaging modalities Limitations and pitfalls Duangkamon Prapruttam, MD Department of Therapeutic
Imaging findings of papillary renal cell carcinoma
 Imaging findings of papillary renal cell carcinoma Poster No.: C-0286 Congress: ECR 2015 Type: Educational Exhibit Authors: J. Praia, R. Dias, C. Macedo, J. Albuquerque, M. Certo ; 1 1 2 2 1 2 2 Barreiro/PT,
Imaging findings of papillary renal cell carcinoma Poster No.: C-0286 Congress: ECR 2015 Type: Educational Exhibit Authors: J. Praia, R. Dias, C. Macedo, J. Albuquerque, M. Certo ; 1 1 2 2 1 2 2 Barreiro/PT,
Anatomical and Functional MRI of the Pancreas
 Anatomical and Functional MRI of the Pancreas MA Bali, MD, T Metens, PhD Erasme Hospital Free University of Brussels Belgium mbali@ulb.ac.be Introduction The use of MRI to investigate the pancreas has
Anatomical and Functional MRI of the Pancreas MA Bali, MD, T Metens, PhD Erasme Hospital Free University of Brussels Belgium mbali@ulb.ac.be Introduction The use of MRI to investigate the pancreas has
Kidney Case 1 SURGICAL PATHOLOGY REPORT
 Kidney Case 1 Surgical Pathology Report February 9, 2007 Clinical History: This 45 year old woman was found to have a left renal mass. CT urography with reconstruction revealed a 2 cm medial mass which
Kidney Case 1 Surgical Pathology Report February 9, 2007 Clinical History: This 45 year old woman was found to have a left renal mass. CT urography with reconstruction revealed a 2 cm medial mass which
CME Article Clinics in diagnostic imaging (135)
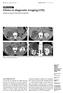 Medical Education Singapore Med J 2011; 52(5) : 384 CME Article Clinics in diagnostic imaging (135) Pojchamarnwiputh S, Muttarak M, Sriplakich S H 1a 1b 1c 1d Fig. 1 (a) Axial unenhanced; (b & c) delayed
Medical Education Singapore Med J 2011; 52(5) : 384 CME Article Clinics in diagnostic imaging (135) Pojchamarnwiputh S, Muttarak M, Sriplakich S H 1a 1b 1c 1d Fig. 1 (a) Axial unenhanced; (b & c) delayed
Recommendations for cross-sectional imaging in cancer management, Second edition
 www.rcr.ac.uk Recommendations for cross-sectional imaging in cancer management, Second edition Renal and adrenal tumours Faculty of Clinical Radiology www.rcr.ac.uk Contents Renal cell carcinoma 3 Clinical
www.rcr.ac.uk Recommendations for cross-sectional imaging in cancer management, Second edition Renal and adrenal tumours Faculty of Clinical Radiology www.rcr.ac.uk Contents Renal cell carcinoma 3 Clinical
Cystic Renal Cell Carcinomas: Do They Grow, Metastasize, or Recur?
 Genitourinary Imaging Original Research Jhaveri et al. Growth Patterns of Cystic Renal Cell Carcinomas Genitourinary Imaging Original Research Kartik Jhaveri 1 Priya Gupta 1 Azadeh Elmi 2 Lior Flor 1 Hadas
Genitourinary Imaging Original Research Jhaveri et al. Growth Patterns of Cystic Renal Cell Carcinomas Genitourinary Imaging Original Research Kartik Jhaveri 1 Priya Gupta 1 Azadeh Elmi 2 Lior Flor 1 Hadas
Renal masses - the role of diagnostic imaging
 Renal masses - the role of diagnostic imaging Poster No.: C-2471 Congress: ECR 2015 Type: Educational Exhibit Authors: V. Rai#; Bjelovar/HR Keywords: Cysts, Cancer, Structured reporting, Ultrasound, MR,
Renal masses - the role of diagnostic imaging Poster No.: C-2471 Congress: ECR 2015 Type: Educational Exhibit Authors: V. Rai#; Bjelovar/HR Keywords: Cysts, Cancer, Structured reporting, Ultrasound, MR,
Multidetector Computed Tomography Evaluation of Subtypes of Renal Cell Carcinoma
 Original Article Print ISSN: 2321-6379 Online ISSN: 2321-595X DOI: 10.17354/ijss/2017/390 Multidetector Computed Tomography Evaluation of Subtypes of Renal Cell Carcinoma A Rohini 1, Vidya Bhargavi 2,
Original Article Print ISSN: 2321-6379 Online ISSN: 2321-595X DOI: 10.17354/ijss/2017/390 Multidetector Computed Tomography Evaluation of Subtypes of Renal Cell Carcinoma A Rohini 1, Vidya Bhargavi 2,
Original Report. Imaging Features of Fat Necrosis. Lai Peng Chan 1 R. Gee 2 Ciaran Keogh 2 Peter L. Munk 2
 Lai Peng Chan 1 R. Gee 2 Ciaran Keogh 2 Peter L. Munk 2 Received September 16, 2002; accepted after revision pril 29, 2003. 1 Department of Diagnostic Radiology, Singapore General Hospital, Outram Rd.,
Lai Peng Chan 1 R. Gee 2 Ciaran Keogh 2 Peter L. Munk 2 Received September 16, 2002; accepted after revision pril 29, 2003. 1 Department of Diagnostic Radiology, Singapore General Hospital, Outram Rd.,
Analysis of Changes in Attenuation of Proven Renal Cysts on Different Scanning Phases of Triphasic MDCT
 Eugene P. Chung 1 Brian R. Herts 1,2 Grant Linnell 1 Andrew C. Novick 2 Nancy Obuchowski 1,3 Deirdre M. Coll 1,4 Mark E. Baker 1 Received June 24, 2003; accepted after revision August 28, 2003. Presented
Eugene P. Chung 1 Brian R. Herts 1,2 Grant Linnell 1 Andrew C. Novick 2 Nancy Obuchowski 1,3 Deirdre M. Coll 1,4 Mark E. Baker 1 Received June 24, 2003; accepted after revision August 28, 2003. Presented
Renal Mass Biopsy: Needed Now More than Ever
 Renal Mass Biopsy: Needed Now More than Ever Stuart G. Silverman, MD, FACR Professor of Radiology Harvard Medical School Director, Abdominal Imaging and Intervention Brigham and Women s Hospital Boston,
Renal Mass Biopsy: Needed Now More than Ever Stuart G. Silverman, MD, FACR Professor of Radiology Harvard Medical School Director, Abdominal Imaging and Intervention Brigham and Women s Hospital Boston,
REVIEW. Distinguishing benign from malignant adrenal masses
 Cancer Imaging (2003) 3, 102 110 DOI: 10.1102/1470-7330.2003.0006 CI REVIEW Distinguishing benign from malignant adrenal masses Isaac R Francis Professor of Radiology, Department of Radiology, University
Cancer Imaging (2003) 3, 102 110 DOI: 10.1102/1470-7330.2003.0006 CI REVIEW Distinguishing benign from malignant adrenal masses Isaac R Francis Professor of Radiology, Department of Radiology, University
4,3,2,1...How Many Phases are Needed? Balancing Diagnostic Efficacy and Radiation Modulation for MDCT Imaging of Renal Cell Carcinoma
 4,3,2,1...How Many Phases are Needed? Balancing Diagnostic Efficacy and Radiation Modulation for MDCT Imaging of Renal Cell Carcinoma Jeremy Hackworth, MD, MS Steven P Rowe, MD, PhD Satomi Kawamoto, MD
4,3,2,1...How Many Phases are Needed? Balancing Diagnostic Efficacy and Radiation Modulation for MDCT Imaging of Renal Cell Carcinoma Jeremy Hackworth, MD, MS Steven P Rowe, MD, PhD Satomi Kawamoto, MD
MR Imaging Features of Small Solid Pseudopapillary Tumors: Retrospective Differentiation From Other Small Solid Pancreatic Tumors
 Gastrointestinal Imaging Original Research Gastrointestinal Imaging Original Research Mi Hye Yu 1 Jae Young Lee 1 Min Kim 2 Se Hyung Kim 1 Jeong Min Lee 1 Joon Koo Han 1 yung-ihn Choi 1 Yu MH, Lee JY,
Gastrointestinal Imaging Original Research Gastrointestinal Imaging Original Research Mi Hye Yu 1 Jae Young Lee 1 Min Kim 2 Se Hyung Kim 1 Jeong Min Lee 1 Joon Koo Han 1 yung-ihn Choi 1 Yu MH, Lee JY,
Segmental Enhancement Inversion of Small Renal Oncocytoma: Differences in Prevalence According to Tumor Size
 Genitourinary Imaging Original Research Woo et al. Renal Oncocytoma Genitourinary Imaging Original Research Sungmin Woo 1 Jeong Yeon Cho 1,2 Seung Hyup Kim 1,2 Sang Youn Kim 1 Hak Jong Lee 3 Sung Il Hwang
Genitourinary Imaging Original Research Woo et al. Renal Oncocytoma Genitourinary Imaging Original Research Sungmin Woo 1 Jeong Yeon Cho 1,2 Seung Hyup Kim 1,2 Sang Youn Kim 1 Hak Jong Lee 3 Sung Il Hwang
Hyperechoic renal masses
 Hyperechoic renal masses Jean-Yves Meuwly, MD Department of Diagnostic and Interventional Radiology, University Hospital Lausanne, Switzerland Department of Diagnostic and Interventional Radiology Renal
Hyperechoic renal masses Jean-Yves Meuwly, MD Department of Diagnostic and Interventional Radiology, University Hospital Lausanne, Switzerland Department of Diagnostic and Interventional Radiology Renal
NIFTP: Histopathology of a Cytological Monkey Wrench. B. Wehrli
 NIFTP: Histopathology of a Cytological Monkey Wrench B. Wehrli Non-Invasive Encapsulated Follicular Variant of Papillary Thyroid Carcinoma Before 2016 Non-Invasive Follicular Thyroid Neoplasm with Papillary-Like
NIFTP: Histopathology of a Cytological Monkey Wrench B. Wehrli Non-Invasive Encapsulated Follicular Variant of Papillary Thyroid Carcinoma Before 2016 Non-Invasive Follicular Thyroid Neoplasm with Papillary-Like
MRI Features of Renal Oncocytoma and Chromophobe Renal Cell Carcinoma
 Genitourinary Imaging Original Research Rosenkrantz et al. MRI of Renal Tumors Genitourinary Imaging Original Research ndrew. Rosenkrantz 1 Nicole Hindman 1 Erin F. Fitzgerald 1 enjamin E. Niver 1 Jonathan
Genitourinary Imaging Original Research Rosenkrantz et al. MRI of Renal Tumors Genitourinary Imaging Original Research ndrew. Rosenkrantz 1 Nicole Hindman 1 Erin F. Fitzgerald 1 enjamin E. Niver 1 Jonathan
Sensitivity and Specificity in Detection of Labral Tears with 3.0-T MRI of the Shoulder
 Magee and Williams MRI for Detection of Labral Tears Musculoskeletal Imaging Clinical Observations C M E D E N T U R I C L I M G I N G JR 2006; 187:1448 1452 0361 803X/06/1876 1448 merican Roentgen Ray
Magee and Williams MRI for Detection of Labral Tears Musculoskeletal Imaging Clinical Observations C M E D E N T U R I C L I M G I N G JR 2006; 187:1448 1452 0361 803X/06/1876 1448 merican Roentgen Ray
Small renal mass: differential diagnosis on image
 Small renal mass: differential diagnosis on image Poster No.: R-0166 Congress: RANZCR-AOCR 2012 Type: Educational Exhibit Authors: H. Lee, K. S. Lee, M. J. Kim; Anyang/KR Keywords: Cysts, Cancer, Staging,
Small renal mass: differential diagnosis on image Poster No.: R-0166 Congress: RANZCR-AOCR 2012 Type: Educational Exhibit Authors: H. Lee, K. S. Lee, M. J. Kim; Anyang/KR Keywords: Cysts, Cancer, Staging,
Pseudoenhancement of Renal Cysts: Influence of Lesion Size, Lesion Location, Slice Thickness, and Number of MDCT Detectors
 Genitourinary Imaging Original Research Tappouni et al. MDCT of Renal Cysts Genitourinary Imaging Original Research Rafel Tappouni 1 Jennifer Kissane 2 Nabeel Sarwani 1 Erik B. Lehman 1 Tappouni R, Kissane
Genitourinary Imaging Original Research Tappouni et al. MDCT of Renal Cysts Genitourinary Imaging Original Research Rafel Tappouni 1 Jennifer Kissane 2 Nabeel Sarwani 1 Erik B. Lehman 1 Tappouni R, Kissane
DIAGNOSTIC SLIDE SEMINAR: PART 1 RENAL TUMOUR BIOPSY CASES
 DIAGNOSTIC SLIDE SEMINAR: PART 1 RENAL TUMOUR BIOPSY CASES Dr. Andrew J. Evans MD, PhD, FACP, FRCPC Consultant in Genitourinary Pathology University Health Network, Toronto, ON Case 1 43 year-old female,
DIAGNOSTIC SLIDE SEMINAR: PART 1 RENAL TUMOUR BIOPSY CASES Dr. Andrew J. Evans MD, PhD, FACP, FRCPC Consultant in Genitourinary Pathology University Health Network, Toronto, ON Case 1 43 year-old female,
Imaging Features of Sclerosed Hemangioma
 Sclerosed Hemangioma Abdominal Imaging Clinical Observations Deirdre J. Doyle 1 Korosh Khalili 1 Maha Guindi 2 Mostafa Atri 3 Doyle DJ, Khalili K, Guindi M, Atri M Keywords: abdominal imaging, CT, liver,
Sclerosed Hemangioma Abdominal Imaging Clinical Observations Deirdre J. Doyle 1 Korosh Khalili 1 Maha Guindi 2 Mostafa Atri 3 Doyle DJ, Khalili K, Guindi M, Atri M Keywords: abdominal imaging, CT, liver,
Renal Cell Carcinoma: Attenuation Values on Unenhanced CT
 Genitourinary Imaging Original Research Pooler et al. Attenuation Values of Unenhanced CT of Renal Cell Carcinoma Genitourinary Imaging Original Research B. Dustin Pooler 1 Perry J. Pickhardt 1 Stacy D.
Genitourinary Imaging Original Research Pooler et al. Attenuation Values of Unenhanced CT of Renal Cell Carcinoma Genitourinary Imaging Original Research B. Dustin Pooler 1 Perry J. Pickhardt 1 Stacy D.
The Incidental Renal lesion
 The Incidental Renal lesion BACKGROUND Increase in abdominal CT/US in last 15 years Resulted in detection of many (small) renal lesions 50% > 50yrs has at least 1 lesion majority simple cysts Renal lesions
The Incidental Renal lesion BACKGROUND Increase in abdominal CT/US in last 15 years Resulted in detection of many (small) renal lesions 50% > 50yrs has at least 1 lesion majority simple cysts Renal lesions
Yield of Urinary Tract Cancer Diagnosis With Repeat CT Urography in Patients With Hematuria
 Genitourinary Imaging Original Research Mullen et al. CT Urography in Urinary Tract Cancer Genitourinary Imaging Original Research Katherine M. Mullen 1 V. nik Sahni Cheryl. Sadow Stuart G. Silverman Mullen
Genitourinary Imaging Original Research Mullen et al. CT Urography in Urinary Tract Cancer Genitourinary Imaging Original Research Katherine M. Mullen 1 V. nik Sahni Cheryl. Sadow Stuart G. Silverman Mullen
CT and MR Imaging Manifestation of Adrenal Hemangioma: a case report
 Chin J Radiol 2004; 29: 371-375 371 CT and MR Imaging Manifestation of Adrenal Hemangioma: a case report MING-TSUNG WANG 1 WEN-SHENG TZENG 2 CHEE-WAI MAK 2 JYH-CHING CHEN 1 JINN-MING CHANG 2 DAVID LU 3
Chin J Radiol 2004; 29: 371-375 371 CT and MR Imaging Manifestation of Adrenal Hemangioma: a case report MING-TSUNG WANG 1 WEN-SHENG TZENG 2 CHEE-WAI MAK 2 JYH-CHING CHEN 1 JINN-MING CHANG 2 DAVID LU 3
Pulmonary Nodule Volumetric Measurement Variability as a Function of CT Slice Thickness and Nodule Morphology
 CT of Pulmonary Nodules Chest Imaging Original Research Myria Petrou 1 Leslie E. Quint 1 in Nan 2 Laurence H. aker 3 Petrou M, Quint LE, Nan, aker LH Keywords: chest, lung disease, MDCT, oncologic imaging,
CT of Pulmonary Nodules Chest Imaging Original Research Myria Petrou 1 Leslie E. Quint 1 in Nan 2 Laurence H. aker 3 Petrou M, Quint LE, Nan, aker LH Keywords: chest, lung disease, MDCT, oncologic imaging,
ADRENAL MR: PEARLS AND PITFALLS
 ADRENAL MR: PEARLS AND PITFALLS Frank Miller, M.D. Lee F. Rogers MD Professor of Medical Education Chief, Body Imaging Section and Fellowship Medical Director, MR Imaging Professor of Radiology Northwestern
ADRENAL MR: PEARLS AND PITFALLS Frank Miller, M.D. Lee F. Rogers MD Professor of Medical Education Chief, Body Imaging Section and Fellowship Medical Director, MR Imaging Professor of Radiology Northwestern
Essentials of Clinical MR, 2 nd edition. 73. Urinary Bladder and Male Pelvis
 73. Urinary Bladder and Male Pelvis Urinary bladder carcinoma is best locally staged with MRI. It is important however to note that a thickened wall (> 5 mm) is a non-specific finding seen in an underfilled
73. Urinary Bladder and Male Pelvis Urinary bladder carcinoma is best locally staged with MRI. It is important however to note that a thickened wall (> 5 mm) is a non-specific finding seen in an underfilled
Invasive Ductal Carcinoma with Fibrotic Focus: Mammographic and Sonographic Findings with Histopathologic Correlation
 Mammograp hy and Sonography of Invasive Ductal arcinoma reast Imaging linical Observations Shara Millman Oken 1 ecilia L. Mercado 2 Lorenzo Memeo 3 Hanina Hibshoosh 3 Oken SM, Mercado L, Memeo L, Hibshoosh
Mammograp hy and Sonography of Invasive Ductal arcinoma reast Imaging linical Observations Shara Millman Oken 1 ecilia L. Mercado 2 Lorenzo Memeo 3 Hanina Hibshoosh 3 Oken SM, Mercado L, Memeo L, Hibshoosh
Papillary Lesions of the Breast: WHO Update
 Papillary Lesions of the Breast: WHO Update Stuart J. Schnitt, M.D. Department of Pathology Beth Israel Deaconess Medical Center and Harvard Medical School Boston, MA, USA Papillary Lesions of the Breast
Papillary Lesions of the Breast: WHO Update Stuart J. Schnitt, M.D. Department of Pathology Beth Israel Deaconess Medical Center and Harvard Medical School Boston, MA, USA Papillary Lesions of the Breast
Oncocytic Neoplasms of the Adrenal Gland
 Genitourinary Imaging linical Perspective Tirkes et al. drenal Oncocytic Neoplasms Genitourinary Imaging linical Perspective Downloaded from www.ajronline.org by 37.44.205.11 on 12/20/17 from IP address
Genitourinary Imaging linical Perspective Tirkes et al. drenal Oncocytic Neoplasms Genitourinary Imaging linical Perspective Downloaded from www.ajronline.org by 37.44.205.11 on 12/20/17 from IP address
(2/3 PRCC!) (2/3 PRCC!)
 Approach to the Incidental Solid Renal Mass Stuart G. Silverman, MD, FACR Professor of Radiology Harvard ard Medical School Director, Abdominal Imaging and Intervention Brigham and Women s Hospital Boston,
Approach to the Incidental Solid Renal Mass Stuart G. Silverman, MD, FACR Professor of Radiology Harvard ard Medical School Director, Abdominal Imaging and Intervention Brigham and Women s Hospital Boston,
Characteristic Enhancement Patterns of Renal Epithelioid Angiomyolipoma: a case report and literature review
 J Radiol Sci 2015; 40: 51-56 Characteristic Enhancement Patterns of Renal Epithelioid Angiomyolipoma: a case report and literature review I-Chang LIn 1 nan-han Lu 1 KaI-Jen LIn 2 VICtor C. LIn 3 Department
J Radiol Sci 2015; 40: 51-56 Characteristic Enhancement Patterns of Renal Epithelioid Angiomyolipoma: a case report and literature review I-Chang LIn 1 nan-han Lu 1 KaI-Jen LIn 2 VICtor C. LIn 3 Department
INTERDISCIPLINARY DISCUSSIONS IN LOCALISED RCC DIAGNOSIS AND SURGICAL STRATEGIES FOR ATYPICAL RENAL CYSTIC LESIONS. Maria Cova
 INTERDISCIPLINARY DISCUSSIONS IN LOCALISED RCC DIAGNOSIS AND SURGICAL STRATEGIES FOR ATYPICAL RENAL CYSTIC LESIONS Maria Cova Radiology Department University of Trieste (IT) Eleventh European International
INTERDISCIPLINARY DISCUSSIONS IN LOCALISED RCC DIAGNOSIS AND SURGICAL STRATEGIES FOR ATYPICAL RENAL CYSTIC LESIONS Maria Cova Radiology Department University of Trieste (IT) Eleventh European International
Primary Synovial Sarcoma of the Kidney: a case report
 Chin J Radiol 2004; 29: 359-363 359 Primary Synovial Sarcoma of the Kidney: a case report YU-KUN TSUI 1 CHUNG-JUNG LIN 1 JIA-HWIA WANG 1,4 SHU-HUEI SHEN 1,4 CHIN-CHEN PAN 2,4 YEN-HWA CHANG 3,4 CHENG-YEN
Chin J Radiol 2004; 29: 359-363 359 Primary Synovial Sarcoma of the Kidney: a case report YU-KUN TSUI 1 CHUNG-JUNG LIN 1 JIA-HWIA WANG 1,4 SHU-HUEI SHEN 1,4 CHIN-CHEN PAN 2,4 YEN-HWA CHANG 3,4 CHENG-YEN
CT-imaging features of renal epithelioid angiomyolipoma
 Liu et al. World Journal of Surgical Oncology (2015) 13:280 DOI 10.1186/s12957-015-0700-9 WORLD JOURNAL OF SURGICAL ONCOLOGY RESEARCH Open Access CT-imaging features of renal epithelioid angiomyolipoma
Liu et al. World Journal of Surgical Oncology (2015) 13:280 DOI 10.1186/s12957-015-0700-9 WORLD JOURNAL OF SURGICAL ONCOLOGY RESEARCH Open Access CT-imaging features of renal epithelioid angiomyolipoma
Update on RECIST and Staging of Common Pediatric Tumors Ethan A. Smith, MD
 Update on RECIST and Staging of Common Pediatric Tumors Ethan A. Smith, MD Section of Pediatric Radiology C.S. Mott Children s Hospital University of Michigan ethans@med.umich.edu Disclosures No relevant
Update on RECIST and Staging of Common Pediatric Tumors Ethan A. Smith, MD Section of Pediatric Radiology C.S. Mott Children s Hospital University of Michigan ethans@med.umich.edu Disclosures No relevant
Pediatric Retroperitoneal Masses Radiologic-Pathologic Correlation
 Acta Radiológica Portuguesa, Vol.XVIII, nº 70, pág. 61-70, Abr.-Jun., 2006 Pediatric Retroperitoneal Masses Radiologic-Pathologic Correlation Marilyn J. Siegel Mallinckrodt Institute of Radiology, Washington
Acta Radiológica Portuguesa, Vol.XVIII, nº 70, pág. 61-70, Abr.-Jun., 2006 Pediatric Retroperitoneal Masses Radiologic-Pathologic Correlation Marilyn J. Siegel Mallinckrodt Institute of Radiology, Washington
Disclosure. Relevant Financial Relationship(s) None. Off Label Usage None MFMER slide-1
 Disclosure Relevant Financial Relationship(s) None Off Label Usage None 2013 MFMER slide-1 Case Presentation A 43 year old male, with partial nephrectomy for a right kidney mass 2013 MFMER slide-2 2013
Disclosure Relevant Financial Relationship(s) None Off Label Usage None 2013 MFMER slide-1 Case Presentation A 43 year old male, with partial nephrectomy for a right kidney mass 2013 MFMER slide-2 2013
International Journal of Pharma and Bio Sciences CHROMOPHOBE VARIANT OF RENAL CELL CARCINOMA MASQUARDING AS RENAL ONCOCYTOMA ON CYTOLOGY.
 Case Report Pathology International Journal of Pharma and Bio Sciences ISSN 0975-6299 CHROMOPHOBE VARIANT OF RENAL CELL CARCINOMA MASQUARDING AS RENAL ONCOCYTOMA ON CYTOLOGY. DR.MAMATHA K*, DR. ARAKERI
Case Report Pathology International Journal of Pharma and Bio Sciences ISSN 0975-6299 CHROMOPHOBE VARIANT OF RENAL CELL CARCINOMA MASQUARDING AS RENAL ONCOCYTOMA ON CYTOLOGY. DR.MAMATHA K*, DR. ARAKERI
Brief History. Identification : Past History : HTN without regular treatment.
 Brief History Identification : Name : 陳 x - Admission : 94/10/06 Gender : male Age : 75 y/o Chief Complaint : Urinary difficulty for months. Past History : HTN without regular treatment. Brief History
Brief History Identification : Name : 陳 x - Admission : 94/10/06 Gender : male Age : 75 y/o Chief Complaint : Urinary difficulty for months. Past History : HTN without regular treatment. Brief History
Steven Herwick 1 Frank H. Miller Ana L. Keppke
 Herwick et al. MRI of Islet ell Tumors of the Pancreas bdominal Imaging Pictorial Essay Downloaded from www.ajronline.org by 37.44.203.29 on 02/19/18 from IP address 37.44.203.29. opyright RRS. For personal
Herwick et al. MRI of Islet ell Tumors of the Pancreas bdominal Imaging Pictorial Essay Downloaded from www.ajronline.org by 37.44.203.29 on 02/19/18 from IP address 37.44.203.29. opyright RRS. For personal
Multilocular Cystic Renal Cell Carcinoma: Comparison of Imaging and Pathologic Findings
 Genitourinary Imaging Original Research Hindman et al. Multilocular ystic Renal ell arcinoma Genitourinary Imaging Original Research Nicole M. Hindman 1 Morton. osniak 1 ndrew. Rosenkrantz 1 Stephanie
Genitourinary Imaging Original Research Hindman et al. Multilocular ystic Renal ell arcinoma Genitourinary Imaging Original Research Nicole M. Hindman 1 Morton. osniak 1 ndrew. Rosenkrantz 1 Stephanie
Common and unusual CT and MRI manifestations of pancreatic adenocarcinoma: a pictorial review
 Review Article Common and unusual CT and MRI manifestations of pancreatic adenocarcinoma: a pictorial review Min-Jie Yang, Su Li, Yong-Guang Liu, Na Jiao, Jing-Shan Gong Department of Radiology, Shenzhen
Review Article Common and unusual CT and MRI manifestations of pancreatic adenocarcinoma: a pictorial review Min-Jie Yang, Su Li, Yong-Guang Liu, Na Jiao, Jing-Shan Gong Department of Radiology, Shenzhen
Differentiation of Subtypes of Renal Cell Carcinoma on Helical CT Scans
 Jeong Kon Kim 1 Tae Kyoung Kim 1 Han Jong hn 2 hung Soo Kim 2 Kyu-Rae Kim 3 Kyoung-Sik ho 1 Received September 21, 2001; accepted after revision December 28, 2001. 1 Department of Radiology, san Medical
Jeong Kon Kim 1 Tae Kyoung Kim 1 Han Jong hn 2 hung Soo Kim 2 Kyu-Rae Kim 3 Kyoung-Sik ho 1 Received September 21, 2001; accepted after revision December 28, 2001. 1 Department of Radiology, san Medical
Essentials of Clinical MR, 2 nd edition. 65. Benign Hepatic Masses
 65. Benign Hepatic Masses Pulse sequences acquired for abdominal MRI typically consist of fast acquisition schemes such as single-shot turbo spin echo (i.e. HASTE) and gradient echo schemes such as FLASH
65. Benign Hepatic Masses Pulse sequences acquired for abdominal MRI typically consist of fast acquisition schemes such as single-shot turbo spin echo (i.e. HASTE) and gradient echo schemes such as FLASH
CYSTIC TUMORS OF THE KIDNEY JOHN N. EBLE, M.D. CYSTIC NEPHROMA
 Page 1 CYSTIC TUMORS OF THE KIDNEY JOHN N. EBLE, M.D. Department of Pathology & Laboratory Medicine Phone (317) 274-4806 Medical Science A-128 FAX: (317) 278-2018 635 Barnhill Drive jeble @iupui.edu Indianapolis,
Page 1 CYSTIC TUMORS OF THE KIDNEY JOHN N. EBLE, M.D. Department of Pathology & Laboratory Medicine Phone (317) 274-4806 Medical Science A-128 FAX: (317) 278-2018 635 Barnhill Drive jeble @iupui.edu Indianapolis,
MR of Intraparotid Masses
 MR of Intraparotid Masses Bruce N. Schlakman and David M. Yousem PURPOSE: To determine which MR techniques are best for identifying intraparotid masses and to assess the utility of MR for predicting specific
MR of Intraparotid Masses Bruce N. Schlakman and David M. Yousem PURPOSE: To determine which MR techniques are best for identifying intraparotid masses and to assess the utility of MR for predicting specific
ARTHUR PURDY STOUT SOCIETY COMPANION MEETING: DIFFICULT NEW DIFFERENTIAL DIAGNOSES IN PROSTATE PATHOLOGY. Jonathan I. Epstein.
 1 ARTHUR PURDY STOUT SOCIETY COMPANION MEETING: DIFFICULT NEW DIFFERENTIAL DIAGNOSES IN PROSTATE PATHOLOGY Jonathan I. Epstein Professor Pathology, Urology, Oncology The Reinhard Professor of Urological
1 ARTHUR PURDY STOUT SOCIETY COMPANION MEETING: DIFFICULT NEW DIFFERENTIAL DIAGNOSES IN PROSTATE PATHOLOGY Jonathan I. Epstein Professor Pathology, Urology, Oncology The Reinhard Professor of Urological
Imaging of Kidney Cancer
 119 Imaging of Kidney Cancer RADIOLOGIC CLINICS OF NORTH AMERICA Radiol Clin N Am 45 (2007) 119 147 Jingbo Zhang, MD*, Robert A. Lefkowitz, MD, Ariadne Bach, MD - Detection and diagnosis - CT scan Solid
119 Imaging of Kidney Cancer RADIOLOGIC CLINICS OF NORTH AMERICA Radiol Clin N Am 45 (2007) 119 147 Jingbo Zhang, MD*, Robert A. Lefkowitz, MD, Ariadne Bach, MD - Detection and diagnosis - CT scan Solid
CT & MRI of Benign Liver Neoplasms Srinivasa R Prasad
 CT & MRI of Benign Liver Neoplasms Srinivasa R Prasad No financial disclosures Acknowledgements Many thanks to Drs. Heiken, Narra & Menias (MIR) Dr. Sahani (MGH) for sharing images Benign Liver Tumors:
CT & MRI of Benign Liver Neoplasms Srinivasa R Prasad No financial disclosures Acknowledgements Many thanks to Drs. Heiken, Narra & Menias (MIR) Dr. Sahani (MGH) for sharing images Benign Liver Tumors:
Using Superparamagnetic Iron Oxide Enhanced MRI to Differentiate Metastatic Hepatic Tumors and Nonsolid Benign Lesions
 Downloaded from www.ajronline.org by 46.3.202.96 on 11/27/17 from IP address 46.3.202.96. Copyright RRS. For personal use only; all rights reserved Seishi Kumano 1 Takamichi Murakami Tonsok Kim Masatoshi
Downloaded from www.ajronline.org by 46.3.202.96 on 11/27/17 from IP address 46.3.202.96. Copyright RRS. For personal use only; all rights reserved Seishi Kumano 1 Takamichi Murakami Tonsok Kim Masatoshi
Radiologic Pathologic Correlation of Intraosseous Lipomas. Tim Propeck 1, Mary Anne Bullard 1, John Lin 1, Kei Doi 2, William Martel 1
 Downloaded from www.ajronline.org by 148.251.232.83 on 04/10/18 from IP address 148.251.232.83. opyright RRS. For personal use only; all rights reserved Radiologic Pathologic orrelation of Intraosseous
Downloaded from www.ajronline.org by 148.251.232.83 on 04/10/18 from IP address 148.251.232.83. opyright RRS. For personal use only; all rights reserved Radiologic Pathologic orrelation of Intraosseous
I mportant prognostic factors in renal cell carcinoma (RCC)
 39 ORIGINAL ARTICLE Prognostic relevance of extensive necrosis in renal cell carcinoma V Foria, T Surendra, D N Poller... See end of article for authors affiliations... Correspondence to: Dr D N Poller,
39 ORIGINAL ARTICLE Prognostic relevance of extensive necrosis in renal cell carcinoma V Foria, T Surendra, D N Poller... See end of article for authors affiliations... Correspondence to: Dr D N Poller,
1/25/13 Right partial nephrectomy followed by completion right radical nephrectomy.
 History and Physical Case Scenario 1 45 year old white male presents with complaints of nausea, weight loss, and back pain. A CT of the chest, abdomen and pelvis was done on 12/8/12 that revealed a 12
History and Physical Case Scenario 1 45 year old white male presents with complaints of nausea, weight loss, and back pain. A CT of the chest, abdomen and pelvis was done on 12/8/12 that revealed a 12
Traumatic and Non Traumatic Adrenal Emergencies
 Traumatic and Non Traumatic Adrenal Emergencies Michael N. Patlas, MD, FRCPC (1), Christine O. Menias, MD (2), Douglas S. Katz, MD, FACR (3), Ania Z. Kielar, MD, FRCPC (4), Alla M. Rozenblit, MD (5), Jorge
Traumatic and Non Traumatic Adrenal Emergencies Michael N. Patlas, MD, FRCPC (1), Christine O. Menias, MD (2), Douglas S. Katz, MD, FACR (3), Ania Z. Kielar, MD, FRCPC (4), Alla M. Rozenblit, MD (5), Jorge
Prostate cancer ~ diagnosis and impact of pathology on prognosis ESMO 2017
 Prostate cancer ~ diagnosis and impact of pathology on prognosis ESMO 2017 Dr Puay Hoon Tan Division of Pathology Singapore General Hospital Prostate cancer (acinar adenocarcinoma) Invasive carcinoma composed
Prostate cancer ~ diagnosis and impact of pathology on prognosis ESMO 2017 Dr Puay Hoon Tan Division of Pathology Singapore General Hospital Prostate cancer (acinar adenocarcinoma) Invasive carcinoma composed
Case Scenario 1: Thyroid
 Case Scenario 1: Thyroid History and Physical Patient is an otherwise healthy 80 year old female with the complaint of a neck mass first noticed two weeks ago. The mass has increased in size and is palpable.
Case Scenario 1: Thyroid History and Physical Patient is an otherwise healthy 80 year old female with the complaint of a neck mass first noticed two weeks ago. The mass has increased in size and is palpable.
Renal Masses in Patients with Known Extrarenal Primary Primary Cancer Primary Primary n Met Mets s RCC Beni L mphoma Lung Breast Others
 The Importance of Stuart G. Silverman, MD, FACR Professor of Radiology Harvard ard Medical School Director, Abdominal Imaging and Intervention Brigham and Women s Hospital Boston, MA The Importance of
The Importance of Stuart G. Silverman, MD, FACR Professor of Radiology Harvard ard Medical School Director, Abdominal Imaging and Intervention Brigham and Women s Hospital Boston, MA The Importance of
CT evaluation of small bowel carcinoid tumors
 CT evaluation of small bowel carcinoid tumors Poster No.: C-0060 Congress: ECR 2015 Type: Educational Exhibit Authors: N. V. V. P. Costa, L. Nascimento, T. Bilhim ; Estoril/PT, PT, 1 2 3 1 2 3 Lisbon/PT
CT evaluation of small bowel carcinoid tumors Poster No.: C-0060 Congress: ECR 2015 Type: Educational Exhibit Authors: N. V. V. P. Costa, L. Nascimento, T. Bilhim ; Estoril/PT, PT, 1 2 3 1 2 3 Lisbon/PT
MULTILOCULAR CYSTIC RENAL CELL CARCINOMA
 MULTILOCULAR CYSTIC RENAL CELL CARCINOMA Khalaf M. Al-Jader, MD* ABSTRACT Objective: Multilocular cystic renal cell carcinoma appears to be uncommon subtype of renal cell carcinoma with characteristic
MULTILOCULAR CYSTIC RENAL CELL CARCINOMA Khalaf M. Al-Jader, MD* ABSTRACT Objective: Multilocular cystic renal cell carcinoma appears to be uncommon subtype of renal cell carcinoma with characteristic
Cystic Lesions of the Pancreas
 Residents Section Pattern of the Month w668 04.29.11 Khan et al. Residents Section Pattern of the Month Residents inradiology tif Khan 1 Faisal Khosa Ronald L. Eisenberg Khan, Khosa F, Eisenberg RL Keywords:
Residents Section Pattern of the Month w668 04.29.11 Khan et al. Residents Section Pattern of the Month Residents inradiology tif Khan 1 Faisal Khosa Ronald L. Eisenberg Khan, Khosa F, Eisenberg RL Keywords:
The role of Bosniak classification in malignant tumor diagnosis: A single institution experience
 Original Article - Urological Oncology http://dx.doi.org/10.4111/icu.2016.57.2.100 pissn 2466-0493 eissn 2466-054X The role of Bosniak classification in malignant tumor diagnosis: A single institution
Original Article - Urological Oncology http://dx.doi.org/10.4111/icu.2016.57.2.100 pissn 2466-0493 eissn 2466-054X The role of Bosniak classification in malignant tumor diagnosis: A single institution
Value of the Diffusion-Weighted MRI in the Differential Diagnostics of Malignant and Benign Kidney Neoplasms Our Clinical Experience
 Signature: Pol J Radiol, 2014; 79: 290-295 DOI: 10.12659/PJR.890604 ORIGINAL ARTICLE Received: 2014.02.27 Accepted: 2014.03.24 Published: 2014.09.01 Authors Contribution: A Study Design B Data Collection
Signature: Pol J Radiol, 2014; 79: 290-295 DOI: 10.12659/PJR.890604 ORIGINAL ARTICLE Received: 2014.02.27 Accepted: 2014.03.24 Published: 2014.09.01 Authors Contribution: A Study Design B Data Collection
Five Views of Transitional Cell Carcinoma: One Man s Journey
 September 2006 Five Views of Transitional Cell Carcinoma: One Man s Journey Amsalu Dabela, Harvard Medical School III Outline Overview: Renal Anatomy Our Patient s Story Diagnostic Imaging Studies Appearance
September 2006 Five Views of Transitional Cell Carcinoma: One Man s Journey Amsalu Dabela, Harvard Medical School III Outline Overview: Renal Anatomy Our Patient s Story Diagnostic Imaging Studies Appearance
STANDARDIZED MANAGEMENT RECOMMENDATIONS FOR ADRENAL NODULES: EVIDENCE-BASED CONSENSUS POWERSCRIBE MACROS FROM AN ACADEMIC/PRIVATE PRACTICE
 STANDARDIZED MANAGEMENT RECOMMENDATIONS FOR ADRENAL NODULES: EVIDENCE-BASED CONSENSUS POWERSCRIBE MACROS FROM AN ACADEMIC/PRIVATE PRACTICE COLLABORATIVE Pamela Johnson 1, Darcy Wolfman 2, Upma Rawal 3,
STANDARDIZED MANAGEMENT RECOMMENDATIONS FOR ADRENAL NODULES: EVIDENCE-BASED CONSENSUS POWERSCRIBE MACROS FROM AN ACADEMIC/PRIVATE PRACTICE COLLABORATIVE Pamela Johnson 1, Darcy Wolfman 2, Upma Rawal 3,
CTA/MRA of Pediatric Hepatic Masses Radiology-Pathology Correlation
 Acta Radiológica Portuguesa, Vol.XVIII, nº70, pág. 41-50, Abr.-Jun., 2006 CTA/MRA of Pediatric Hepatic Masses Radiology-Pathology Correlation Marilyn J. Siegel Mallinckrodt Institute of Radiology, Washington
Acta Radiológica Portuguesa, Vol.XVIII, nº70, pág. 41-50, Abr.-Jun., 2006 CTA/MRA of Pediatric Hepatic Masses Radiology-Pathology Correlation Marilyn J. Siegel Mallinckrodt Institute of Radiology, Washington
MRI of Small Hepatocellular Carcinoma: Typical Features Are Less Frequent Below a Size Cutoff of 1.5 cm
 Gastrointestinal Imaging Original Research Choi et al. MRI of Small HCC Gastrointestinal Imaging Original Research Moon Hyung Choi 1 Joon-Il Choi 1 Young Joon Lee 1 Michael Yong Park 1 Sung Eun Rha 1 Chandana
Gastrointestinal Imaging Original Research Choi et al. MRI of Small HCC Gastrointestinal Imaging Original Research Moon Hyung Choi 1 Joon-Il Choi 1 Young Joon Lee 1 Michael Yong Park 1 Sung Eun Rha 1 Chandana
Papillary Lesions of the Breast A Practical Approach to Diagnosis. (Arch Pathol Lab Med. 2016;140: ; doi: /arpa.
 Papillary Lesions of the Breast A Practical Approach to Diagnosis (Arch Pathol Lab Med. 2016;140:1052 1059; doi: 10.5858/arpa.2016-0219-RA) Papillary lesions of the breast Span the spectrum of benign,
Papillary Lesions of the Breast A Practical Approach to Diagnosis (Arch Pathol Lab Med. 2016;140:1052 1059; doi: 10.5858/arpa.2016-0219-RA) Papillary lesions of the breast Span the spectrum of benign,
Characterization of adrenal lesions on CT and MRI: all that a radiologist must know
 Characterization of adrenal lesions on CT and MRI: all that a radiologist must know Poster No.: C-2476 Congress: ECR 2013 Type: Educational Exhibit Authors: N. Benzina, S. MAJDOUB, C. H. ZARRAD, H. Zaghouani,
Characterization of adrenal lesions on CT and MRI: all that a radiologist must know Poster No.: C-2476 Congress: ECR 2013 Type: Educational Exhibit Authors: N. Benzina, S. MAJDOUB, C. H. ZARRAD, H. Zaghouani,
Sex: 女 Age: 51 Occupation: 無 Admission date:92/07/22
 Sex: 女 Age: 51 Occupation: 無 Admission date:92/07/22 Chief complaint Unknown fever for one month Hand tremor and left huge renal tumor was noted Present illness Suffered from fever for one month, hand
Sex: 女 Age: 51 Occupation: 無 Admission date:92/07/22 Chief complaint Unknown fever for one month Hand tremor and left huge renal tumor was noted Present illness Suffered from fever for one month, hand
MRI of Adenocarcinoma of the Pancreas
 MRI of the Pancreas bdominal Imaging Pictorial Essay Downloaded from www.ajronline.org by 37.44.192.155 on 12/14/17 from IP address 37.44.192.155. opyright RRS. For personal use only; all rights reserved
MRI of the Pancreas bdominal Imaging Pictorial Essay Downloaded from www.ajronline.org by 37.44.192.155 on 12/14/17 from IP address 37.44.192.155. opyright RRS. For personal use only; all rights reserved
Imaging of Gastrointestinal Stromal Tumors (GIST) Amir Reza Radmard, MD Assistant Professor Shariati hospital Tehran University of Medical Sciences
 Imaging of Gastrointestinal Stromal Tumors (GIST) Amir Reza Radmard, MD Assistant Professor Shariati hospital Tehran University of Medical Sciences Describe the typical imaging findings of GIST at initial
Imaging of Gastrointestinal Stromal Tumors (GIST) Amir Reza Radmard, MD Assistant Professor Shariati hospital Tehran University of Medical Sciences Describe the typical imaging findings of GIST at initial
Radiation-induced Brachial Plexopathy: MR Imaging
 Radiation-induced Brachial Plexopathy 85 Chapter 5 Radiation-induced Brachial Plexopathy: MR Imaging Neurological symptoms and signs of brachial plexopathy may develop in patients who have had radiation
Radiation-induced Brachial Plexopathy 85 Chapter 5 Radiation-induced Brachial Plexopathy: MR Imaging Neurological symptoms and signs of brachial plexopathy may develop in patients who have had radiation
Update on Thyroid FNA The Bethesda System. Shikha Bose M.D. Associate Professor Cedars Sinai Medical Center
 Update on Thyroid FNA The Bethesda System Shikha Bose M.D. Associate Professor Cedars Sinai Medical Center Thyroid Nodules Frequent occurrence Palpable: 4-7% of adults Ultrasound: 10-31% Majority benign
Update on Thyroid FNA The Bethesda System Shikha Bose M.D. Associate Professor Cedars Sinai Medical Center Thyroid Nodules Frequent occurrence Palpable: 4-7% of adults Ultrasound: 10-31% Majority benign
Mucinous Adenocarcinoma of the Prostate: MRI and MR Spectroscopy Features
 Genitourinary Imaging Clinical Observations Westphalen et al. MRI of Mucinous Adenocarcinoma of the Prostate Genitourinary Imaging Clinical Observations Antonio C. Westphalen 1 Fergus V. Coakley 1 John
Genitourinary Imaging Clinical Observations Westphalen et al. MRI of Mucinous Adenocarcinoma of the Prostate Genitourinary Imaging Clinical Observations Antonio C. Westphalen 1 Fergus V. Coakley 1 John
Atypical kidney tumors and pseudotumors: Imaging features in 44 patients.
 Atypical kidney tumors and pseudotumors: Imaging features in 44 patients. Poster No.: C-1472 Congress: ECR 2011 Type: Scientific Exhibit Authors: M. Kasbi, Y. kallel, M. basly, Z. fitouri, K. Nouira, Y.
Atypical kidney tumors and pseudotumors: Imaging features in 44 patients. Poster No.: C-1472 Congress: ECR 2011 Type: Scientific Exhibit Authors: M. Kasbi, Y. kallel, M. basly, Z. fitouri, K. Nouira, Y.
Nonfunctioning Islet Cell Tumors of the Pancreas: Computed Tomography Findings
 Chin J Radiol 2002; 27: 239-243 239 Nonfunctioning Islet Cell Tumors of the Pancreas: Computed Tomography Findings CHAO-HSUAN YEN 1 JEN-HWEY CHIANG 1 JEN-I HUANG 3 CHENG-SHI SU 2 YI-YOU CHIOU 1 CHENG-YEN
Chin J Radiol 2002; 27: 239-243 239 Nonfunctioning Islet Cell Tumors of the Pancreas: Computed Tomography Findings CHAO-HSUAN YEN 1 JEN-HWEY CHIANG 1 JEN-I HUANG 3 CHENG-SHI SU 2 YI-YOU CHIOU 1 CHENG-YEN
This article appeared in a journal published by Elsevier. The attached copy is furnished to the author for internal non-commercial research and
 This article appeared in a journal published by Elsevier. The attached copy is furnished to the author for internal non-commercial research and education use, including for instruction at the authors institution
This article appeared in a journal published by Elsevier. The attached copy is furnished to the author for internal non-commercial research and education use, including for instruction at the authors institution
Enhancement Characteristics of Papillary Renal Neoplasms Revealed on Triphasic Helical CT of the Kidneys
 Brian R. Herts 1 Deirdre M. Coll 1,2 Andrew C. Novick 3 Nancy Obuchowski 1,4 Grant Linnell 1 Susan L. Wirth 1 Mark E. Baker 1 Received June 29, 2001; accepted after revision August 23, 2001. 1 Department
Brian R. Herts 1 Deirdre M. Coll 1,2 Andrew C. Novick 3 Nancy Obuchowski 1,4 Grant Linnell 1 Susan L. Wirth 1 Mark E. Baker 1 Received June 29, 2001; accepted after revision August 23, 2001. 1 Department
Management of the Incidental Renal Mass on CT: A White Paper of the ACR Incidental Findings Committee
 ORIGINAL ARTICLE Management of the Incidental Renal Mass on CT: A White Paper of the ACR Incidental Findings Committee Brian R. Herts, MD a, Stuart G. Silverman, MD b, Nicole M. Hindman, MD c, Robert G.
ORIGINAL ARTICLE Management of the Incidental Renal Mass on CT: A White Paper of the ACR Incidental Findings Committee Brian R. Herts, MD a, Stuart G. Silverman, MD b, Nicole M. Hindman, MD c, Robert G.
W J R. World Journal of Radiology. Advances of multidetector computed tomography in the characterization and staging of renal cell carcinoma.
 W J R World Journal of Radiology Submit a Manuscript: http://www.wjgnet.com/esps/ Help Desk: http://www.wjgnet.com/esps/helpdesk.aspx DOI: 10.4329/wjr.v7.i6.110 World J Radiol 2015 June 28; 7(6): 110-127
W J R World Journal of Radiology Submit a Manuscript: http://www.wjgnet.com/esps/ Help Desk: http://www.wjgnet.com/esps/helpdesk.aspx DOI: 10.4329/wjr.v7.i6.110 World J Radiol 2015 June 28; 7(6): 110-127
Diseases of the breast (1 of 2)
 Diseases of the breast (1 of 2) Introduction A histology introduction Normal ducts and lobules of the breast are lined by two layers of cells a layer of luminal cells overlying a second layer of myoepithelial
Diseases of the breast (1 of 2) Introduction A histology introduction Normal ducts and lobules of the breast are lined by two layers of cells a layer of luminal cells overlying a second layer of myoepithelial
performed to help sway the clinician in what the appropriate diagnosis is, which can substantially alter the treatment of management.
 Hello, I am Maura Polansky at the University of Texas MD Anderson Cancer Center. I am a Physician Assistant in the Department of Gastrointestinal Medical Oncology and the Program Director for Physician
Hello, I am Maura Polansky at the University of Texas MD Anderson Cancer Center. I am a Physician Assistant in the Department of Gastrointestinal Medical Oncology and the Program Director for Physician
Histogram Analysis of Small Solid Renal Masses: Differentiating Minimal Fat Angiomyolipoma From Renal Cell Carcinoma
 Genitourinary Imaging Original Research Chaudhry et al. Histogram Analysis of Small Solid Renal Masses Genitourinary Imaging Original Research Humaira S. Chaudhry 1,2 Matthew S. Davenport 1,3 Christopher
Genitourinary Imaging Original Research Chaudhry et al. Histogram Analysis of Small Solid Renal Masses Genitourinary Imaging Original Research Humaira S. Chaudhry 1,2 Matthew S. Davenport 1,3 Christopher
REVIEW. Rossella Graziani 1, Simona Mautone 2, Mario Vigo 1, Riccardo Manfredi 2, Giuseppe Opocher 4, Massimo Falconi 3
 REVIEW Spectrum of Magnetic Resonance Imaging Findings in Pancreatic and Other Abdominal Manifestations of Von Hippel-Lindau Disease in a Series of 23 patients: A Pictorial Review Rossella Graziani 1,
REVIEW Spectrum of Magnetic Resonance Imaging Findings in Pancreatic and Other Abdominal Manifestations of Von Hippel-Lindau Disease in a Series of 23 patients: A Pictorial Review Rossella Graziani 1,
Pitfalls and Limitations of Breast MRI. Susan Orel Roth, MD Professor of Radiology University of Pennsylvania
 Pitfalls and Limitations of Breast MRI Susan Orel Roth, MD Professor of Radiology University of Pennsylvania Objectives Review the etiologies of false negative breast MRI examinations Discuss the limitations
Pitfalls and Limitations of Breast MRI Susan Orel Roth, MD Professor of Radiology University of Pennsylvania Objectives Review the etiologies of false negative breast MRI examinations Discuss the limitations
Delayed Imaging in Routine CT Examinations of the Abdomen and Pelvis: Is It Worth the Additional Cost of Radiation and Time?
 Genitourinary Imaging Original Research Chan et al. CT of the bdomen and Pelvis Genitourinary Imaging Original Research Downloaded from www.ajronline.org by 46.3.194.249 on 01/02/18 from IP address 46.3.194.249.
Genitourinary Imaging Original Research Chan et al. CT of the bdomen and Pelvis Genitourinary Imaging Original Research Downloaded from www.ajronline.org by 46.3.194.249 on 01/02/18 from IP address 46.3.194.249.
