The surgical management of hyperparathyroidism and endocrine disease of the pancreas in the multiple endocrine neoplasia type 1 patient
|
|
|
- Rolf Walsh
- 5 years ago
- Views:
Transcription
1 lournal of Internal Medicine 1995: 238: The surgical management of hyperparathyroidism and endocrine disease of the pancreas in the multiple endocrine neoplasia type 1 patient N. W. THOMPSON Division of Endocrine Surgery. University of Michigan. Department of Surgery, Ann Arbor, Michigan. USA Abstract. Thompson NW (Division of Endocrine Surgery, University of Michigan, Department of Surgery, Ann Arbor, Michigan, USA). The surgical management of hyperparathyroidism and endocrine disease of the pancreas in the multiple endocrine neoplasia type 1 patient (Minisymposium: Multiple Endocrine Neoplasia 1). J Intern Med 1995; 238: The surgical management of multiple endocrine neoplasia type 1 (MEN1) parathyroid disease and involvement of the endocrine pancreas remains controversial. Hyperparathyroidism, usually the first clinical manifestation of the syndrome, requires surgical treatment in nearly all patients. We favour a subtotal parathyroidectomy and cervical thymectomy rather than a total parathyroidectomy and autotransplant because of good long-term results and the absence of permanent hypoparathyroidism. The results of treating 34 MENl patients during a 20-year period are reported. The most common functional pancreatic or duodenal tumours in MENl patients are gastrinomas and insulinomas. In addition to the management of functional syndromes, another major concern is the malignant potential of the neuroendocrine tumours that frequently develop. Our surgical management of gastrinomas and the ZES has evolved over a period of 15 years. We have found that distal pancreatectomy, enucleation of any neoplasms in the head, and duodenotomy and excision of any neuroendocrine tumours (gastrinomas) combined with a regional node dissection are effective in the majority of patients. The results of treating 21 MENl patients with ZES are reported. Keywords: MEN1, hyperparathyroidism ZJS, gastrinomas, neuroendocrine tumors. Introduction The surgical management of multiple endocrine neoplasia type 1 (MEN1) involvement in the parathyroid glands and pancreas remains controversial. Nearly all patients develop hyperparathyroidism (HPT), which is most frequently the first clinical manifestation of the syndrome [I+]. Overt pancreatic disease is less frequent and usually develops at a later age than the HPT [l, 51. It may initially be (D 1995 Blackwell Science Ltd detected after the development of specific symptoms caused by the hypersecretion of one or more of the gastrointestinal peptide hormones, mechanical effects of a nonfunctional tumour, or by screening imaging of the pancreas or liver. The most common functional pancreatic or duodenal tumours in MEN 1 patients are gastrinomas and their management is the subject of the greatest controversy El]. Their importance lies in the fact that up to 30% of MEN1 patients will develop gastrinomas and the Zollinger- 269
2 270 N. W. THOMPSON: SURGICAL MANAGEMENT OF MENl Ellison syndrome (ZES). The surgical management of MENl ZES has gradually evolved during a period of more than a decade in which important developments in pathology, localization techniques and drug therapy have played a significant role in determining the multifaceted operation we currently employ [ The optimal surgical management of insulinomas in MEN 1 patients is less controversial, but as yet, not standardized [ The purpose of this paper is to report our experience at the University of Michigan, Ann Arbor, MI, USA, in the management of the MENl patient with either or both HPT, and neuroendocrine disease of the pancreas or duodenum. Hyperparathyroidism Multiglandular disease is present in all MENl patients with HPT [l-3, 81. Furthermore, it is assumed that up to 20% of patients will have a supernumerary or fifth gland within the thymus that must be considered in operative strategy [l-3, 211. Frequently, one or more parathyroid glands may be normal in size and even in microscopic appearance from a limited biopsy. The asymmetrical parathyroid enlargement by a nodular type of hyperplasia is typical of MENl [l]. Only one or two parathyroid glands may be enlarged grossly, and a false impression that the disease is caused by an adenoma or 'double adenoma' may occur, especially in the patient without a known family history or other manifestation of the MENl syndrome. Two surgical procedures are widely employed in treating MENl HPT [l, 4, 22-29]. Both are based on the assumption that persistent or recurrent hypercalcemia can be anticipated if less than a subtotal parathyroidectomy is performed. One technique is to perform a total parathyroidectomy with excision of the cervically accessible thymus gland and autotransplantation of sufflcient parathyroid tissue into the forearm or other readily accessible location so that, should recurrence ever develop, re-operation using a local anaesthetic could be performed on an outpatient basis [27]. This procedure has the potential for permanent hypoparathyroidism if the transplanted tissue does not survive and the patients require replacement therapy with vitamin D and oral calcium until the graft functions adequately (4-8 weeks or longer). Its advantage is that, if recurrence develops, a second procedure in the neck can usually be avoided, providing all parathyroid tissue has been excised at the first operation. Graft size reduction can be accomplished readily under local anaesthesia. The second procedure is a subtotal parathyroidectomy with cervical thymectomy and is the one that we have used during the past 20 years and currently prefer [l, 261. Our surgical explorations in MENl patients have included a careful search for a minimum of four parathyroid glands and excision of the thymus. All parathyroid glands but one are excised. When all four glands are enlarged, a well vascularized gland is partially resected leaving a remnant weighing approximately mg. When a normalsized gland has been identified, regardless of its location, it is carefully preserved and marked with a metal clip for possible future identification. When all four glands are enlarged, the smallest inferior gland is mobilized and trimmed to the desired size after carefully placing a metal clip across the gland. The resected portion is cut on the clip after packing the surrounding area with gauze sponges to prevent possible implantation of hyperplastic parathyroid cells. The remnant with clip is then tacked with a stitch to the trachea for easy access should a subsequent recurrence caused by remnant hypertrophy develop. Results Thirty-four MENl patients with HPT treated at the University of Michigan Medical Center between 1972 and 1994 were available for follow-up studies ranging from 3 months to 20 years following parathyroidectomy. Twenty-four patients had their primary operations at the University of Michigan. One of these patients, in whom only three parathyroid glands were found at exploration, had persistent hypercalcemia (4.1%). At re-operation, the missing left inferior parathyroid gland was found within the lower pole of the thyroid gland. Three patients developed recurrent hyperparathyroidism diagnosed at intervals of 8, 16 and 17 years after a subtotal parathyroidectomy and thymectomy (12.5%). All three patients were reoperated and found to have remnant hypertrophy. Partial resection of the remnant has resulted in normocalcemia in each case. Twenty-three out of the 24 patients became transiently hypocalcemic after their initial operations and most required vitamin D preparations (Dihydrotachysterol) in addition to oral Q 1995 Blackwell Science Ltd journal 01 Internal Medirine 238:
3 MINISYMPOSIUM: MULTIPLE ENDOCRINE NEOPLASIA calcium carbonate supplements. Similarly, transient hypocalcemia developed in the four patients who were subsequently re-explored. No patient has developed permanent hypocalcemia, although one is taking daily oral calcium supplements. A subset of this group of 24 patients consists of seven patients who had synchronous primary HPT. and neuroendocrine pancreatic or duodenal neuroendocrine tumours. Each underwent a combined cervical and abdominal exploration, avoiding a second operative procedure. These patients, all explored between 1990 and are currently?ormocalcemic following subtotal parathyroidecomy and cervical thymectomy. Each of these patients tlso underwent a distal pancreatectomy. Five subjects with ZES also had duodenotomies and excision of submucosal gastrinomas. One patient with hypoglycemia had multiple neuroendocrine tumours in the neck, body and tail of the pancreas. One patient without symptoms was found to have a neuroendocrine tumour within the pancreatic head on routine CT screening. Based on the favourable results in this group, we recommend this combined approach for synchronous HPT and pancreatic disease, providing neither neck nor abdominal procedure is a re-operative exploration. None of these procedures exceeded 5 h in operative time. Eleven patients who were initially treated elsewhere underwent re-operative parathyroidectomies for persistent (n = 8) or recurrent disease (n = 3). A subtotal parathyroidectomy was accomplished in eight patients in which one or more enlarged hyperplastic glands was excised. Each patient also had a cervical thymectomy. The three patients with recurrences were found to have hypertrophy of remnants which were trimmed to an estimated mg. One out of the 11 patients has persistent hypercalcemia and another has serum calcium levels at the upper limit of normal. All but one patient was temporarily hypocalcemic, although none developed permanent hypoparathyroidism. Thirty-four out of the 35 MENl patients are normocalcemic. The one patient with persistent hypercalcemia is asymptomatic. However, it should be emphasized that 15 out of these 34 patients required two operations (44%). nine for persistent and six for recurrent disease. Remnant hypertrophy was the only cause of true recurrence in this group of patients and occurred at intervals ranging from 4 to 17 years after an initially successful operation. Re- operation for remnant recurrences was not difficult in those cases in which the surgeon had carefully documented the location of the remaining gland. Annual follow-up of these patients is indicated for life because late recurrences can be anticipated and occurred in 17.6% of all patients in this series. We favour subtotal parathyroidectomy and thymectomy because, if carefully performed. it completely avoids permanent hypoparathyroidism, and in our own primary cases, was associated with a long-term recurrence rate of only 12.5%. Furthermore, reoperation in this group was successful without any significant morbidity. Surgical disease of the pancreas and duodenum During the past 2 decades, several important developments have contributed to a more rational approach to the operative management of neuroendocrine disease in MENl patients. The first was the finding on immunohistochemical studies of MEN 1 pancreas and tumours that patients with functional hormonal syndromes had one or more discreet tumours as the cause of the syndrome, rather than islet-cell hyperplasia or microadenomastosis, even though the diffuse changes always accompanied the tumour(s) [7, 81. As a result, it became apparent that functional syndromes might be effectively treated if all gross tumour(s) could be excised without the need for total pancreatectomy. Another finding was that most patients with ZES had small gastrinomas arising within the duodenal wall which could be the only cause of hypergastrinemia. In many of these cases, gross tumours elsewhere in the pancreas were present, but based on immunohistochemical studies, were not found to be the cause of the ZES in the majority of patients [6, 8, 10, 18, Finally, it was discovered that duodenal gastrinomas, despite sizes as small as 1-2 mm, metastasized to the peripancreatic and periduodenal lymph nodes and were accompanied by liver metastases in about only 10% of cases, and usually, only after a long period without surgical intervention [9, , 16, , 32, Although MENl tumours were previously considered to be less malignant than those occurring sporadically, it became apparent that, eventually, both primary tumours and liver metastases were the cause of significant mortality. More recently, the development of antisecretory drugs Q 1995 Blackwell Science Ltd fournal of Internal Medicine 238:
4 272 N. W. THOMPSON: SURGICAL MANAGEMENT OF MENl such as omeprazole has allowed for effective medical management of MENl ZES patients without the need for total gastrectomy in patients with either acute complications of peptic ulcer disease or unremitting symptoms. Because of an almost universal failure in previous surgical efforts to render MENl ZES patients, eugastrinemic, total gastrectomy had previously been the standard operative procedure performed in these patients. After omeprazole became available, many groups elected to treat MEN1 ZES patients with drug therapy only, avoiding an exploration unless a pancreatic tumour was imaged by CT or any other localization study [4245]. The obvious disadvantages of medical therapy in MENl ZES include life-long dependency on therapy with H2 blockers or omeprazole, the possible progression of localized malignancy to Iymph nodes and liver, and the possible development of multiple gastric ECL (enterochromaffin-like tumours [ Our surgical approach, developed during the past 15 years, is based on the premise that MENl patients with neuroendocrine disease of the pancreas or duodenum can be 'cured' of their syndrome or nonfunctional tumours, providing that the tumour has not metastasized to the liver and that the operation is extensive enough to excise all sites of disease [31-33, 381. An aggressive surgical approach is indicated because the incidence of malignancy is similar to that in patients with sporadic islet-cell tumours, although liver metastases are less common at the time of diagnosis, perhaps because of the younger age of patients at the time of diagnosis and the frequency of duodenal primary tumours in MENl ZES patients [18. 40, 431. MENl non-functional turnours Both benign and malignant neuroendocrine tumours develop in the pancreas in patients with MEN1. In our experience. the majority of patients with functional tumours have had other neuroendocrine tumours that were non-functional or secreting hormones that produce no identifiable syndrome. Additionally, some patients, estimated to represent 5-10% of MEN1 patients, have developed neuroendocrine tumours producing symptoms entirely related to their size, local invasion or hepatic metastases. Three recent patients illustrate the management of these tumours. A 41-year-old male patient with no family history of MENl developed Flg. 1 CT scan of a 41-year-old MENl male showing a 12-cm tumour &sing from the neck and the body of the pancreas with obstruction of the splenic and superior mesentedc veins with portal hypertension. There was no evidence of llver metastases. FIg. 2 Venous phase In same patlent as Fig. 1 : selectlve visceral angiogram showing complete occlusion of the splenic and distal superior mesentedc and proximal portal veins. Note reconstruction of portal veins from large venous collaterals (white arrows) coursing through the pancreatic head. Black arrows point to proximal SMV and distal portal vein. hyperparathyroidism at 3 7 years of age. Parathyroid explorations were performed elsewhere in and 1990 for what was eventually determined to be asymmetrical parathyroid hyperplasia. During the autumn of 199 1, he developed crampy abdominal pain, a 9 kg weight loss and a palpable abdominal mass. A CT scan showed a 12-cm mass in the pancreas in the region of its neck and body [Fig. 17. An angiogram showed a large hypervascular mass completely occluding the superior mesenteric, splenic and proximal portal veins [Fig. 21. Imaging showed 1995 Blackwell Science Ltd Iournal 01 Internal Medfrfne 238:
5 MINISYMPOSIUM: MULTIPLE ENDOCRINE NEOPLASIA Flg. 3 The operatlve specimen showing a 12-cm invasive neuroendocrine tumour involving the mid-portion of the pancreas and contlguous veins. The superior mesenteric and proximal portal veins were resected and replaced with a ribbed dacron graft. Flg. 5 The operatlve specimen of resected distal pancreas, tumour and spleen. A 2-mm gastrinoma was exclsed from the second portion of the duodenum. No hlstoologlcal evidence of malignancy was found in lymph nodes. and liver was negative for metastases. Flg. 4 CT scan In a 22-year-old female MEN1 patlent who developed left upper quadrant paln 3 years arer a subtotal parathyroldectomy and thymectomy. When 19 years of age. screening studies for endocrine dlsease of the pitultary, pancreas and adrenal glands had been negative. GI hormone levels were normal at the time of this CT except for a sllghtly elevated serum gastrin and a positive secretin test. CT demonstrates a 13-cm tumour Involving the body and tall. The arrow points to non-invaded plane between the tumour and the left kldney. no liver metastases. Because of progressive pain and weight loss, an exploration was performed in January After a difficult dissection, it was possible to isolate the proximal superior mesenteric and distal portal veins for interposition of a ribbed dacron vascular graft after a distal pancreatectomy which included the enlarged tumour and invaded portal and superior mesenteric veins [Fig. 31. Despite a complicated post-operative recovery, this patient did well for the next 3 years and is working full-time, although recently, a CT scan has shown possible local tumour recurrence and liver metastases. A 22-year-old female with a known family history of MEN1 was found to be hypercalcemic at 19 years of age after developing a renal stone. A subtotal parathyroidectomy and cervical thymectomy were performed, and she remained asymptomatic until 3 years later, when she suffered left upper quadrant pain for several weeks following a minor fall on ice. A CT scan then demonstrated a 13-cm mass in the distal pancreas and a normal spleen and liver [Fig. 41. The only abnormality in her hormonal screen was a slightly elevated serum gastrin (1 60 mg ml-'). A secretin test was positive for gastrinoma. At exploration in March of 1993, a large tumour involving the entire body and tail was resected with the spleen [Fig. 51. There was no evidence of local invasion, or lymph node or liver metastases. A duodenotomy was also performed and a 2-mm neuroendocrine tumour was rocally excised from the distal second portion of the duodenum. Peripancreatic lymph nodes were negative for metastases. The duodenal microadenoma stained positive for gastrin, whereas the large neuroendocrine tumour, which was histologically benign, stained only for neuron specific enolase (NSE) and chromogranin. She has remained asymptomatic since the operation and has no displayed evidence of recurrence. The third patient, a 54-year-old female, presented with recurrent hyperparathyroidism 10 years after a Blackwell Sclence Ltd journal of Internal Medicine 238:
6 274 N. W. THOMPSON: SURGICAL MANAGEMENT OF MENl subtotal parathyroidectomy for multiple gland disease. At that time, there was no family history of MEN1. but subsequently, a daughter developed a prolactinoma and HPT. As a result, she had hormonal screening and a CT scan which demonstrated a 3-cm tumour within the pancreatic head. During a combined operation consisting of parathyroid reexploration and abdominal exploration, the neuroendocrine tumour in the head was enucleated, and a distal pancreatectomy was performed for multiple small palpable tumours in the body and tail. She has been asymptomatic and normocalcemic for the last 2 years. None of these tumours were histologically malignant. The results from this group of patients suggest that periodic screening of the pancreas in all proven MENl patients is indicated. In most patients without liver metastases, determining whether a tumour is benign or malignant cannot be made until resection, histopathological study, and in some cases, longterm follow-up. Functional islet-cell tumour syndromes A spectrum of islet-cell tumours syndromes have been reported in MENl patients, including VIP oma, glucagonoma, ectopic ACTH and somatostatinoma. Only the two most common, resulting from insulinomas and gastrinomas, will be considered in further detail. Insulinoma It is estimated that lo-15% of MENl patients will develop insulinomas as the only functional component in their pancreatic neuroendocrine disease. Approximately 5% of all insolinomas occur in MENl patients. As a general rule, sporadic insulinomas are solitary tumours, whereas insulinomas in MENl patients are likely to be multiple. Nevertheless, multiple tumours in MENl patients are not always insulinomas, and their designation as such must be proven by immunohistochemical staining [8, 18-20, 31,41,44-45]. Whenever a presumed sporadic insulinoma patient is found to have multiple islet-cell tumours, a complete evaluation for MENl should be undertaken. Most of these patients will eventually be proven to have the syndrome. Five patients with symptomatic insulinomas occurring in association with the MENl syndrome Fig. 6 Operative specimen from a 27-year old MENl male with a 7cm pedunculated malignant insulinoma. a 2-cm benign insulinoma (black arrows) and three non-functional neuroendocrine tumours (white arrows). were treated at the University of Michigan over the past 20 years. One additional patient, operated upon elsewhere, underwent an enucleation of an insulinoma located in the tail of the pancreas at the age of 9 years. At that time, there was no known family history of MEN1, and apparently, this was a solitary tumour. She did well until 3 5 years of age, at which time both hyperparathyroidism and ZES were diagnosed. When re-explored, six macroneuroendocrine tumours were excised from the pancreas and seven microgastrinomas from the duodenum. At least two or more insulinomas were excised in each of the other five patients. One patient, a 2 7-year-old male with a large (7-cm) predunculated insulinoma arising from the neck of the pancreas was also found to have an additional insulinoma, as well as three other nonfunctioning neuroendocrine tumours [Fig. 61. The largest insulinoma was histologically malignant and one contiguous lymph node contained a metastatic neuroendocrine tumour which stained positively for insulin. Two patients developed insulinomas within 2 and 3 years, respectively, after the surgical treatment of ZES, successfully treated by excision of duodenal gastrinomas. Neither patient had undergone a distal pancreatectomy at the time of their first operation. Multiple insulinomas were found in the body and tail in each patient at reoperation. All six patients are euglycemic at the present time with follow-ups ranging from 2 to 16 years. Although we relied upon percutaneous transhepatic selective venous sampling of insulin for Q 1995 Blackwell Science Ltd Iournal ojintemal Medirlne 238:
7 MINISYMPOSIUM: MULTIPLE ENDOCRINE NEOPLASIA YEN-1 Im~linOM Confirmed dhgnosb of Inaullnm(e) m serum gastrin I Measure serum gastrin 1 1 Fig. 7 Algorithm of a management plan currently employed in MENl patlents with hyperinsullnism. Endoscoplc ultrasound Is the only localization study used primarily to evaluate the head and uncinate process of the pancreas. Expkn 1 MzUmlpancrentectomy 2 Enucbate any tumwr(s) In head or uncinate 1 L localization of insulinomas for more than a decade, we no longer consider that study necessary [19]. The only localization we recommend in MEN 1 patients is endoscoplc ultrasonography of the head and uncinate process of the pancreas. Our current management algorithm is shown in Fig. 7. In addition to a confirmed biochemical diagnosis of organic hyperinsulinism, a serum gastrin level is obtained to rule out concomitant preclinical gastrinoma. The operative procedure we perform is a distal pancreatectomy to the level of the superior mesenteric vein, and enucleation of any neuroendocrine tumours in the head or uncinate process. A duodenotomy is not performed unless the pre-operative serum gastrin levels are elevated and a secretin test is positive. Extrapancreatic insulinomas are extremely rare and have not been reported in MENl patients. In our experience, neuroendocrine duodenal tumours in both MEN1 and sporadic patients have rarely shown any cells staining positive for insulin. A lymphatic dissection is performed only in those patients with concomitant duodenal gastrinomas or in the rare MENl patient with a malignant insulinoma. Gastrinomas The surgical treatment of ZES in MEN1 patients is predicated on the facts that all gastrinomas, whether in the duodenum or the pancreas, have malignant Q 1995 Blackwell Science Ltd joirrnal of Intprnal Medicine 238:
8 276 N. W. THOMPSON: SURGICAL MANAGEMENT OF MENl MEN-1 ZES Conflnned dlagnwls of gnslrlnoma 1. r c 1 u a) Omeprazole b) Chemotherapy c) Embolbatbn d) Surgicalresectlon e) Uver lranplantatbn hepatk VBnOIg Mmpllng (Immura bat) I Expkmtkn 1 Dietalpancrwtectomy 2 Enucktkm d p.ncrwlc head tumwr(8) 3 Duodenolmyexclsbn d any tumwr(8) 4 Regkmal node dbaectbn optknlal Flg. 8 Algorithm of a management plan in MEN1 ZES patients. Elther (T or MRI Is used to evaluate the liver for metastases and the adrenal glands for posslble cortical tumours. Endoscopie ultrasound Is used to evaluate the head and uncinate process. Duodenal microadenomas present in the majority of these patients are usually too small to be detected by any localization technique. potential or are already malignant, and that surgical treatment can be successful in patients without liver metastases, providing the operative procedure performed is appropriate. All patients without liver metastases should be explored with the intent to 'cure' the disease, short of a Whipple procedure or total pancreatectomy. The following principles are guidelines in all explorations for ZE!3 in MENl patients: (1) A duodenotomy is performed and the wall is circumferentially palpated from the pylorus through the third portion. Any small (less than 0.5 cm) gastrinomas are locally excised. Larger gastrinomas are excised with a full thickness margin of duodenal wall. (2) All peripancreatic lymph nodes are excised, including those along the common bile duct and within the porta hepatis medially to the celiac axis. (3) After full mobilization of the head and uncinate, any palpable or ultrasonically identified tumour is enucleated. (4) A distal pancreatectomy, including the neck, body and tail, preserving the spleen when feasible, is routinely performed. The majority of MENl patients have palpable neuroendocrine tumours within the body or tail. The only pre-operative localization studies we now utilize are a CT or MRI scan to rule out liver metastases and to evaluate the adrenal glands. Endoscopic ultrasonography is used to evaluate the head and uncinate process for possible neuro Blackwell Science Ltd ]ournu/ oj1ntcmal Medicine 238:
9 MINISYMPOSIUM: MULTIPLE ENDOCRINE NEOPLASIA Table 1 Locatlon of ImmunohlstochemIcally proven gastdnomas In 17 patients with MENl ZES Location No. (%) Gastdnoma(s) In duodenum 13 (76%) Gashinomas(s) In duodenum and pancreas 6 (35%) Multlple gashinomas In duodenum 8 (47%) Gastrlnoma(s) In pancreas 10 (59%) Castdnomas(s) only In pancreas 4 (24%) endocrine tumours too small to be palpated during exploration. An algorithm of our current management scheme is shown in Fig. 8. During the 15-year period from to 199 3,17 MENl patients without liver metastases underwent pancreatic exploration with intent to 'cure ' their biochemically proven ZES. Eleven patients were female and six were male. Their mean age was 36.7 years at the time of exploration. Twelve patients had previously undergone a parathyroidectomy, whereas five with a synchronous diagnosis of HPT and ZES were treated with a combined operation. Gastrinoma(s) were found in the duodenum of 76% and in both pancreas and duodenum of 35% (Table 1). A minimum of 46% with duodenal gastrinomas were proven to be malignant, as determined by lymph node metastases. Gaastrinoma(s) were only found in the pancreas in 24%, although 59% had pancreatic gastrinomas in the entire group. None of the pancreatic gastrinomas have proven to be malignant, as determined by local invasion, lymph node or liver metastases. Other neuroendocrine tumours were found in the body or tail of the pancreas at the initial exploration in 82%. Additional neuroendocrine tumours developed which were proven at a subsequent exploration in the remaining three patients after periods ranging from 2 to 8 years. Thus, 100% of these patients had or developed neuroendocrine tumours of the body or tail. Thirteen out of 17 patients (76%) had a distal pancreatectomy as a component of their initial operation. Of the four with a remaining body and tail. one with three duodenal and two pancreatic head gastrinomas had lower but persistent hypergastrinemia. At a second exploration, 2 months later. a 1.5-cm gastrinoma was found and excised from the distal pancreatic tail. Another patient had normal basal gastrin levels but a positive secretin study for 8 years. At re-exploration, a 1.5-cm gastrinoma was found and excised from the pan- creatic neck. Both patients have had normal gastrin levels and negative secretin tests for periods of 4 and 5 years. The other two patients both became eugastrinemic after excision of gastrinomas from the duodenum, but developed organic hyperinsulinism after 2 and 3 year intervals, respectively. At re-exploration, multiple insulinomas were found in the distal pancreas in both patients. These patients were successfully treated by distal pancreatectomy. After follow-up periods ranging from one to 16 years, 11 out of 17 (65%) patients have normal basal gastrin levels, are asymptomatic, and require no drug therapy for diarrhoea or peptic ulcer symptoms. Five of these patients have had one or more negative secretin-stimulated studies (29%). The six patients (3 5%) currently with increased basal gastrin levels have all had a decrease in gastrin levels, a decrease in symptoms and a decrease in drug requirements for variable periods after operation, although none became eugastrinemic. Because none of these patients have liver metastases, they are considered potential candidates for a re-exploration. One of these patients has recently undergone endoscopic ultrasonography and two 0.5-cm neuroendocrine tumours were identified in the remaining pancreatic head. Discussion Neuroendocrine tumours of the pancreas develop in 50% of patients with MENl and may cause significantmorbidityormortality[ , 45, 461. Their treatment is surgical when detected by imaging, biochemical screening or biochemical confirmation of a hormonal syndrome. The objective in all patients is to detect and excise the tumour(s) before their malignant potential has been conhed by hepatic metastases. In patients with functional syndromes caused by hypersecretion of a specific hormone, surgical treatment may be life saving (glucagonoma. VIPoma or insulinoma), or eliminate the need for expensive daily drug therapy (gastrinoma). These objects need to be re-emphasized in MENl patients with ZES because many groups have excluded these patients for operation based on historical failures caused by previous inadequate knowledge of tumour pathophysiology. Our current operation has evolved during a 15- year period, and is based on an improved under- Q 1995 Blackwell Science Ltd lournu1 of Internal Medirine 238:
10 ~ ~ 278 N. W. THOMPSON: SURGICAL MANAGEMENT OF MENl standing of the extent and locations of gastrinomas in MENl [7, , 381. The fact that some patients become eugastrinemic yet have positive secretin stimulation tests suggests that either a very small duodenal or pancreatic head gastrinoma, or micrometastases in a lymph node was overlooked at exploration. Initially, it was assumed that all of these patients would develop symptomatic recurrences, but surprisingly, that has not been the case [33]. One patient in this category has been symptom free without drug therapy for 16 years, and two others had similar courses for 8 and 9 years, respectively, before developing recurrent hyperparathyroidism and then elevated basal serum gastrin levels. In both cases, successful parathyroid re-operations resulted in eugastrinemia, which has been maintained for 4 and 6 years, respectively [47]. Whether MENl patients with hypergastrinemia have a greater propensity to have concomitant neuroendocrine tumours in the pancreas is not known. The fact that 100% of our patients had or developed neuroendocrine tumours in the body or tail of the pancreas is the basis for our recommendation to include a distal pancreatectomy as a routine step in the MENl ZES operation. An alternative approach, which has been advocated by several authors, is to perform a pancreaticoduodectomy resection which would eliminate any neuroendocrine tumours in the duodenum, head, uncinate and peripancreatic lymph nodes [ 16, Any tumour in the remaining pancreatic body and tail could be enucleated. It is not unreasonable to assume that an even higher cure rate of the ZES could be achieved with this procedure. Whether the potential added morbidity and possible mortality associated with this operation is justifiable remains to be answered. In those patients who are not cured after the procedure, we perform a ' second look' procedure, which can be performed after a year or so with the reasonable assumption that a previously occult tumour may have grown to detectable size. We are currently considering re-exploration in several patients who have had a rising gastrin level after a previous operation failed to return the serum gastrin level to the normal range. In one of these patients, two small neuroendocrine tumours have been identified in the remaining pancreatic head by endoscopic ultrasound. Another approach would be to excise all duodenal tumours and to enculeate any pancreatic tumours rather than resect the distal pancreas. Failures after this procedure would still be Table 2 The Occurrence of malignancy In MENl ZES patients Occurrence No. (%I Malignant duodenal gastrinoma(s) 6 (46%) Malignant pancreatic gastrinoma(s) 0 (0%) Malignant E pancreatic tumour 1(6%) Liver metastases including follow-up 0 (0%) (range years) amenable to a pancreaticoduodenectomy without resorting to a total pancreatectomy. In patients without liver metastases, a total pancreatectomy. including any involved lymph nodes, would cure the MENl patient of pancreatic and duodenal neuroendocrine disease. Considering the potential longterm side effects of this procedure and the relative indolence of most neuroendocrine malignancies of MEN1, the benefits gained would be likely to overcome by the subsequent morbidity in all but the rare MENl families with proven highly aggressive pancreatic malignancies [48]. Although our series is small, several observations can be emphasized. The fist is that the majority of the MENl ZES patients can be rendered eugastrinemic if diagnosed and explored before liver metastases have developed (Table 2). The second is that excision of tumours and lymph node metastases when present may prevent the subsequent progression to liver metastases. Although our longest follow-up in this series is only 16 years, no patient has developed liver metastases. These initial results encourage us to recommend pancreatic duodenal exploration in all MENl ZES patients without liver metastases. There is increasing evidence that, after a procedure appropriate for the neuroendocrine disease present, most patients will obtain significant longterm benefits. To do nothing but observe and treat with drug therapy until a tumour is obvious may eliminate the potential opportunity to cure many of these patients. References 1 A110 M. Thompson NW. Hyperparathyroidlsm as a part of the MEN I Syndrome. In: Kaplan EL. ed. Surgery ofthe Thyroid and Parathyroid Glands. Cllnlcal Surgery International. Churchill Livlngston. 1983: Block MA. Famlllal hyperparathyroidism and hyperparathyroldlsm associated with multiple endocrine neoplasia syndrome. In: Cady B. Ross1 RL. eds. Surgery ofthe Thyroid and Parathyroid GIunds. 3rd edn. Philadelphia. PA: W. B. Saunders & Co Q 1995 Blackwell Sclence Ltd journal of Internal Medicine 238:
11 MINISYMPOSIUM: MULTIPLE ENDOCRINE NEOPLASIA Lamers CB. Frwling PG. Clinlcal Significance of hyperparathyroidlsm in familial multiple endocrine adenomatosis type I (MEA 1). Am / Md 1979: 66: Malmaeus J. Benson L. Johansson H. Ljunghall S. Rastad 1, Akerstrom G. et al. Parathyroid surgery in the multlple endocrine neoplasia type I syndrome: Choice of surgical procedure. World 1 Surg 1986: 10: Shepherd JJ. The natural history of multiple endocrine neoplasia type I. Arrh Surg 1991 : 126: Donow C. Pipeleers-Marichal M. Schroder S. Surgical pathology of gastrinoma : site. sk. multicentricity. association with multiple neoplasia Type I and malignancy. Cunrer 1991 : 68: Thompson NW. Lloyd RB. Nishiyama RH. Vinik AI. Strode1 WE. Allo MD. et al. MEN4 pancreas: A histological and immunohlstological study. World I Surg 1984; 8: Kloppel G. Willemer S. Stamm B. Hacki WH. Heitz PU. Pancreatic lesions and hormonal profile of pancreatic tumors in multiple endocrine neoplasia type I: An lmmunocytochemical study of nine patients. Canrer 1986: 57: MacGilllvay DC. Rushin JM. Zeiger MA. Shakir KMM. The significance of gastrinomas found in peripancreatic lymph nodes. Surgery 1991: 109: Pipeleers-Marlchal M. Somers G. Wlllems G. Foulis A, Imrie C. Bishop AE. el al. Gastrinomas in the duodenums of patients with multiple endocrine neoplasia type I and the Zolllnger- Elllson syndrome. N Engl] Med 1990; 322: Vinik AI. Moattarl AR. Cho K. Thompson NW. Transhepatic portal vein catheterization for localization of sporadic and MEN gastrinomas: A ten-year experience. Surgery 1990: 107: Imamura M. Takahashi K. Adachl H. Mlnematsu S. Shimada Y. Naito M. Suzuki T. et al. Usefullness of selective arterial secretin Injection test for localization of gastrinoma in the Zollinger-Ellison Syndrome. Ann Surg 1987: 205: 23&6. 13 Delcore R. Jr, Cheung LY. Friesen SR. Characteristics of duodenal wall gastrinomas. Am 1 Surg 1990: 160: Thom AK. Norton JA. Axiotis CA. Jensen RT. Location. incidence and malignant potential of duodenal gastrinomas. Surg 1991; 110: Bornman PC. Marks IN. Mee AS. Price S. Favorable response to conservatlve surgery for extra-pancreatic gasmnoma wlth lymph nodes metastases. Brit 1 Surg 1987: 74: Imamura M. Kanda M. Takahashi K. Shimada Y. Miyahara T. Wagata T. ef al. Clinlcopathologlcal characteristics ofduodenal microgastrinomas. World 1 Surg 1992; 16: Sugg SL. Norton JA. Fraker DL. Metz DC. Pisegna JR. Fishbeyne V. et ul. A prospective study of intraoperative methods to diagnose and resect duodenal gastrinomas. Ann Surg 1993: 218: Shepherd JJ. Challis DR. Davies PF. McArdle JP, Teh BT. Wilkinson S. et al. Multiple endocrine neoplasia. type I: gastrinomas. pancreatic neoplasms, microcarcinoids. the Zolllnger-Ellison Syndrome. lymph nodes and hepatic metastases. Arrh Surgery 1993: 128: Pasieka JL. Mcleod MK. Thompson NW. Burney RE. Surglcal approach to lnsullnomas: Assessing the need for preoperative localization. Arch Surg 1992: 127: Service FJ. McMahon MM. O'Brlen PC. Ballard DJ. Functioning Insullnoma-incldence recurrence and long-term survival of patients: A 60-year study. Mayo Clin Proc 1991 : 66: Akerstmm G. Malmaes J. Bergstrom R. Surgical anatomy of human parathyroid glands. Surgery 1984 : 95 : Block MA. Frame B. Jackson CF. The efficacy of subtotal parathyroidectomy for primary hyperparathyroidlsm due to multiple gland involvement. Surg Gynecol Obstet 1978: 147: Light GS. Hensley MI. Management of familial hyperparathyroidism. Prog Surg 1986: 18: Prim RA. Gamvros 01, Sellu D. Lynn JA. Subtotal parathyroldectomy for primary chief cell hyperplasia of the multiple endocrine neoplasla type I syndrome. Ann Surg 1981: 193: Rhll R. Green J Marx SJ. Primary hyperparathyroidlsm In familial multiple endocrine neoplasia type 1. Long-term follow-up of serum calclum levels after parathyroidectomy. Am] Med 1985: 78: Thompson NW. The techniques of initial parathyroid explorative and reoperative parathyroidectomy. In : Thompson NW, Vlnik AI. eds. Endocrine Surgery Update. New York. NY: Grune 81 Stratton. 1983: Wells SA. Jr, Farndon JR, Dale JK, Leight GS. Dilley WG. Longterm evaluation of patients wlth primary parathyroid hyperplasla managed by total parathyroldectomy and heterotopic autotransplantation. Ann Surg 1980: 192: van Heerden JA, Kent RB. 111, Shemore GW. Grant CS. ReMlne WH. Kent RB. Primary hyperparathyroidlsm In patients with multiple endocrine neoplasla syndrome. Surgical experience. Arch Surg 1983: 118: Thompson NW. Eckhauser FE. Harness JK. Anatomy of primary hyperparathyroidlsm. Surgery 1982 : 92: Thompson NW, Vlnlk AI. Eckhauser FE. MlcrogastrInomas of the duodenum. A cause of failed operatlons for the Zolllnger- Elllson syndrome. Ann Surg 1989: 209: Thompson NW. The surgical treatment of the Zolllnger-Elllson Syndrome in sporadic and MEN I Syndrome. Actn Chir Austrlaca 1992: 24: Thompson NW. The surgical treatment of the endocrine pancreas and Zollinger-Elllson syndrome in the MEN-I Syndrome. Henry Ford Hospital Med Journul 1992: 40: Thompson NW. Bondeson AG. Bondeson L. Vinik AI. The surgical treatment of gastrlnoma in MEN-I syndrome patients. Surgery 1989; 106: Delcore R. Herumreck AS. Friesen SR. Selectlve surglcal management of correctable hypergastrinemia. Surgery 1989 : 106: Delcore R. Friesen SR. Zollinger-EllIson Syndrome. A new look at regresslon of gastrinomas. Arch Surg 1991: 126: Friesen SR. Are ' aberrant nodal gasmnomas' pathogenetlcally sidlar to 'lateral aberrant thyroid' nodules? Surgery 1990; 107: Delcore R. Friesen SR. The role of pancreatoduodenectomy of primary duodenal wall gastrlnomas in patients with the ZollInger-Elllson Syndrome. Surgery 1992; 112: Thompson NW, Pasieka J, Fukuuchi A. Duodenal gastrinomas, duodenotomy and duodenal exploration in the surgical management of Zollinger-Elllson Syndrome. World 1 Surg 1993; 17: Pipeleers-Marlchal M. Donow C. Heik PU. Kloppel G. Pathologic aspects of gastrinomas In patients with Zolllnger-Elllson Syndrome wlth and without multiple endocrine neoplasia Type I. World I Surgery 1993; 17: Cheruer JA, Sawyers JL. Benefit of resectlon of metastatlc Blackwell Science Ltd lournal of Internal Medirlne 238:
12 280 N. W. THOMPSON: SURGICAL MANAGEMENT OF MEN1 gastrinoma in Multiple Endocrine Neoplasia Type I. Cmtroenkrology 1992: 102: Akerstrom G. Johansson H. Grama D. Surgical treatment of endocrine pancreatic leslons in MEN I. ACTA Onrologica 1991 : 30: van Heerden JA. Smith SL. Miller L. Management of the Zolllnger-Ellison Syndrome In patients with multiple endocrine neoplasia type I. Surgery 1986: 100: Norton JA. Doppman JL. Jensen RT. Curative resection in Zolllnger-Ellison Syndrome: Results of a 10 year prospective study. Ann Surg 1992: 215: Mignon M. Ruszniewski P. Podevin P. et al. Current approach to the management of gastrinoma and lnsulinoma in adults with multlple endocrine neoplasia I. World Surgery 1993: 17: Sheppard BC. Norton JA. Doppman JL. et al. Management of islet-cell tumors In patients with multlple endocrine neoplasla : a prospectlve study. Surgery 1989; 106: Solcia E. Capella C. Fiocca R. Rlndi G. Rosa1 J. Gastric argyrophil carcinoldosls in patients wlth Zolllnger-Ellison Syndrome due to Type I multiple Endocrine Neoplasia. Am I Surg Pathol 1990: 14: Norton JA. Cornelius MJ. Doppman JL. Maton PN. Gardner JD. Jensen RT. Effect of parathyroldectomy in patients with hyperparathyroldisrn. Zollinger-Elllson syndrome and multlple endocrine neoplasia type I: A prospective study. Surgerg 1987: 102: Tisell LE. Ahlman H. Jansson S. Grimelius L. Total pancreatectomy in the MEN-I syndrome. Br 1 Surg 1988: 75: Recelved 18 October 1994: accepted 15 May Correspondence: Norman W. Thompson MD. University of Mlchlgan. Department of Surgery E Medical Center Drive. Ann Arbor, MI 48109, USA. Q 1995 Blackwell Science Ltd Iournal ojhternal Medirine 238:
MINISYMPOSIUM MEN & VHL. N. W. THOMPSON From the Division of Endocrine Surgery, University of Michigan, Ann Arbor, MI, USA
 Journal of Internal Medicine 1998; 243: 495 500 MINISYMPOSIUM MEN & VHL Current concepts in the surgical management of multiple endocrine neoplasia type 1 pancreatic-duodenal disease. Results in the treatment
Journal of Internal Medicine 1998; 243: 495 500 MINISYMPOSIUM MEN & VHL Current concepts in the surgical management of multiple endocrine neoplasia type 1 pancreatic-duodenal disease. Results in the treatment
Surgical treatment and prognosis of gastrinoma
 Best Practice & Research Clinical Gastroenterology Vol. 19, No. 5, pp. 799 805, 2005 doi:10.1016/j.bpg.2005.05.003 available online at http://www.sciencedirect.com 10 Surgical treatment and prognosis of
Best Practice & Research Clinical Gastroenterology Vol. 19, No. 5, pp. 799 805, 2005 doi:10.1016/j.bpg.2005.05.003 available online at http://www.sciencedirect.com 10 Surgical treatment and prognosis of
Diagnosis abnormal morphology and /or abnormal biochemistry
 Diagnosis abnormal morphology and /or abnormal biochemistry MEN 1 GEP Tumours Pancreatico-Nodal (-Duodenal) Affects 35-80% of MEN1 patients Functioning or non functioning Hyperplasia microadenoma macrotumours
Diagnosis abnormal morphology and /or abnormal biochemistry MEN 1 GEP Tumours Pancreatico-Nodal (-Duodenal) Affects 35-80% of MEN1 patients Functioning or non functioning Hyperplasia microadenoma macrotumours
AN ARGUMENT FOR SURGERY FOR GASTRINOMA. Lauren Wilson R1 General Surgery
 AN ARGUMENT FOR SURGERY FOR GASTRINOMA Lauren Wilson R1 General Surgery WHAT IS A GASTRINOMA? Gastrin secreting cells derived from multipotential stem cells of endodermal origin or enteroendocrine cells
AN ARGUMENT FOR SURGERY FOR GASTRINOMA Lauren Wilson R1 General Surgery WHAT IS A GASTRINOMA? Gastrin secreting cells derived from multipotential stem cells of endodermal origin or enteroendocrine cells
Management of Pancreatic Islet Cell Tumors
 Management of Pancreatic Islet Cell Tumors Ravi Dhanisetty, MD November 5, 2009 Morbidity and Mortality Conference Case Presentation 42 yr female with chronic abdominal pain. PMHx: Uterine fibroids Medications:
Management of Pancreatic Islet Cell Tumors Ravi Dhanisetty, MD November 5, 2009 Morbidity and Mortality Conference Case Presentation 42 yr female with chronic abdominal pain. PMHx: Uterine fibroids Medications:
Gastrinoma: Medical Management. Haley Gallup
 Gastrinoma: Medical Management Haley Gallup Also known as When to put your knife down Gastrinoma Definition and History Diagnosis Historic Management Sporadic vs MEN-1 Defining surgical candidates Nonsurgical
Gastrinoma: Medical Management Haley Gallup Also known as When to put your knife down Gastrinoma Definition and History Diagnosis Historic Management Sporadic vs MEN-1 Defining surgical candidates Nonsurgical
Pancreas Quizzes c. Both A and B a. Directly into the blood stream (not using ducts)
 Pancreas Quizzes Quiz 1 1. The pancreas produces hormones. Which type of hormone producing organ is the pancreas? a. Endocrine b. Exocrine c. Both A and B d. Neither A or B 2. Endocrine indicates hormones
Pancreas Quizzes Quiz 1 1. The pancreas produces hormones. Which type of hormone producing organ is the pancreas? a. Endocrine b. Exocrine c. Both A and B d. Neither A or B 2. Endocrine indicates hormones
NEUROENDOCRINE CARCINOID TUMORS PANCREATIC NEUROENDOCRINE TUMORS
 University of Miami Jackson Memorial Hospital Role of the Surgeon in the Approach to Neuroendocrine tumors Dido Franceschi, MD Professor of Surgery University of Miami Karzinoide Siegfried Oberndorfer,
University of Miami Jackson Memorial Hospital Role of the Surgeon in the Approach to Neuroendocrine tumors Dido Franceschi, MD Professor of Surgery University of Miami Karzinoide Siegfried Oberndorfer,
Biopsy needle, thyroid gland, 74 technique, Bone hunger syndrome, 23
 The following figures were reproduced by permission, courtesy of the Mayo Clinic: Figures 2-7, 2-l4a, 2-l5a, 2-l5c, 2-l6a, 2-l8a, 3-l5a, 3-21a The following figure was slightly modified and reproduced
The following figures were reproduced by permission, courtesy of the Mayo Clinic: Figures 2-7, 2-l4a, 2-l5a, 2-l5c, 2-l6a, 2-l8a, 3-l5a, 3-21a The following figure was slightly modified and reproduced
Multiple endocrine neoplasia type 1: duodenopancreatic tumours
 Journal of Internal Medicine 2003; 253: 590 598 MINISYMPOSIUM Multiple endocrine neoplasia type 1: duodenopancreatic tumours G. M. DOHERTY & N. W. THOMPSON Division of Endocrine Surgery, Department of
Journal of Internal Medicine 2003; 253: 590 598 MINISYMPOSIUM Multiple endocrine neoplasia type 1: duodenopancreatic tumours G. M. DOHERTY & N. W. THOMPSON Division of Endocrine Surgery, Department of
Imaging and Management of Pancreatic Endocrine Tumors in MEN 1
 October 20, 2008 Imaging and Management of Pancreatic Endocrine Tumors in MEN 1 Marie Elaine Stevens Georgetown University School of Medicine, Year IV Dr. Agenda Discuss Our Patient s Presentation Review
October 20, 2008 Imaging and Management of Pancreatic Endocrine Tumors in MEN 1 Marie Elaine Stevens Georgetown University School of Medicine, Year IV Dr. Agenda Discuss Our Patient s Presentation Review
Unusual Pancreatic Neoplasms RTC 2/11/2011
 Unusual Pancreatic Neoplasms RTC 2/11/2011 Objectives Intraductal Papillary Mucinous Neoplasm (IPMN) Mucinous Cystic Neoplasm (MCN) Islet Cell Tumors Insulinoma Glucagonoma VIPoma Somatostatinoma Gastrinoma
Unusual Pancreatic Neoplasms RTC 2/11/2011 Objectives Intraductal Papillary Mucinous Neoplasm (IPMN) Mucinous Cystic Neoplasm (MCN) Islet Cell Tumors Insulinoma Glucagonoma VIPoma Somatostatinoma Gastrinoma
An Unexpected Cause of Hypoglycemia
 An Unexpected Cause of Hypoglycemia Stacey A. Milan, MD FACS Surgical Oncology Nothing to disclose Disclosures Objectives Identify indications for workup of hypoglycemia Define work up for hypoglycemic
An Unexpected Cause of Hypoglycemia Stacey A. Milan, MD FACS Surgical Oncology Nothing to disclose Disclosures Objectives Identify indications for workup of hypoglycemia Define work up for hypoglycemic
Multiple Endocrine Neoplasia Type 1
 Journal of Surgical Oncology 2005;89:143 150 Multiple Endocrine Neoplasia Type 1 GERARD M. DOHERTY, MD* NW Thompson Professor of Surgery, University of Michigan, Ann Arbor, Michigan Multiple endocrine
Journal of Surgical Oncology 2005;89:143 150 Multiple Endocrine Neoplasia Type 1 GERARD M. DOHERTY, MD* NW Thompson Professor of Surgery, University of Michigan, Ann Arbor, Michigan Multiple endocrine
Greater Manchester and Cheshire HPB Unit Guidelines for the Assessment & Management of Hepatobiliary and Pancreatic Disease Chapter 14
 Greater Manchester and Cheshire HPB Unit Guidelines for the Assessment & Management of Hepatobiliary and Pancreatic Disease Chapter 14 Contents 14. Neuroendocrine Tumours 161 14.1. Diagnostic algorithm
Greater Manchester and Cheshire HPB Unit Guidelines for the Assessment & Management of Hepatobiliary and Pancreatic Disease Chapter 14 Contents 14. Neuroendocrine Tumours 161 14.1. Diagnostic algorithm
Surgical Therapy of GEP-NET: An Overview
 Surgical Therapy of GEP-NET: An Overview Pierce K.H Chow MBBS, MMed, FRCSE, FAMS, PhD Professor, Duke-NUS Graduate School of Medicine Senior Consultant Surgeon, Singapore General Hospital Visiting Senior
Surgical Therapy of GEP-NET: An Overview Pierce K.H Chow MBBS, MMed, FRCSE, FAMS, PhD Professor, Duke-NUS Graduate School of Medicine Senior Consultant Surgeon, Singapore General Hospital Visiting Senior
General Surgery Curriculum Royal Australasian College of Surgeons, General Surgeons Australia & New Zealand Association of General Surgeons
 General Surgery Curriculum Royal Australasian College of Surgeons, General Surgeons Australia & New Zealand Association of General Surgeons MODULE TITLE: ENDOCRINE 5-May-2013 DEVELOPED BY: Jonathan Serpell
General Surgery Curriculum Royal Australasian College of Surgeons, General Surgeons Australia & New Zealand Association of General Surgeons MODULE TITLE: ENDOCRINE 5-May-2013 DEVELOPED BY: Jonathan Serpell
Surgical Management of Zollinger-Ellison Syndrome; State of the Art
 Surgical Management of Zollinger-Ellison Syndrome; State of the Art Ellen H. Morrow, MD, JeffreyA. Norton, MD* KEYWORDS Gastrinoma Surgery Diagnosis Localization Outcome MEN-1 Zollinger-Ellison Syndrome
Surgical Management of Zollinger-Ellison Syndrome; State of the Art Ellen H. Morrow, MD, JeffreyA. Norton, MD* KEYWORDS Gastrinoma Surgery Diagnosis Localization Outcome MEN-1 Zollinger-Ellison Syndrome
Endoscopic Ultrasound Is Highly Accurate and Directs Management in Patients With Neuroendocrine Tumors of the Pancreas
 THE AMERICAN JOURNAL OF GASTROENTEROLOGY Vol. 95, No. 9, 2000 2000 by Am. Coll. of Gastroenterology ISSN 0002-9270/00/$20.00 Published by Elsevier Science Inc. PII S0002-9270(00)01272-7 Endoscopic Ultrasound
THE AMERICAN JOURNAL OF GASTROENTEROLOGY Vol. 95, No. 9, 2000 2000 by Am. Coll. of Gastroenterology ISSN 0002-9270/00/$20.00 Published by Elsevier Science Inc. PII S0002-9270(00)01272-7 Endoscopic Ultrasound
SURGERY TO CURE THE ZOLLINGER ELLISON SYNDROME SURGERY TO CURE THE ZOLLINGER ELLISON SYNDROME
 SURGERY TO CURE THE ZOLLINGER ELLISON SYNDROME SURGERY TO CURE THE ZOLLINGER ELLISON SYNDROME JEFFREY A. NORTON, M.D., DOUGLAS L. FRAKER, M.D., H. RICHARD ALEXANDER, M.D., DAVID J. VENZON, PH.D., JOHN
SURGERY TO CURE THE ZOLLINGER ELLISON SYNDROME SURGERY TO CURE THE ZOLLINGER ELLISON SYNDROME JEFFREY A. NORTON, M.D., DOUGLAS L. FRAKER, M.D., H. RICHARD ALEXANDER, M.D., DAVID J. VENZON, PH.D., JOHN
Case Scenario 1. Discharge Summary
 Case Scenario 1 Discharge Summary A 69-year-old woman was on vacation and noted that she was becoming jaundiced. Two months prior to leaving on that trip, she had had a workup that included an abdominal
Case Scenario 1 Discharge Summary A 69-year-old woman was on vacation and noted that she was becoming jaundiced. Two months prior to leaving on that trip, she had had a workup that included an abdominal
Multiple Primary Quiz
 Multiple Primary Quiz Case 1 A 72 year old man was found to have a 12 mm solid lesion in the pancreatic tail by computed tomography carried out during a routine follow up study of this patient with adult
Multiple Primary Quiz Case 1 A 72 year old man was found to have a 12 mm solid lesion in the pancreatic tail by computed tomography carried out during a routine follow up study of this patient with adult
Type 2 gastric neuroendocrine tumor: report of one case
 Case Report Type 2 gastric neuroendocrine tumor: report of one case Yuanliang Li, Xin Su, Huangying Tan Department of Integrative Oncology, China-Japan Friendship Hospital, Beijing 100029, China Correspondence
Case Report Type 2 gastric neuroendocrine tumor: report of one case Yuanliang Li, Xin Su, Huangying Tan Department of Integrative Oncology, China-Japan Friendship Hospital, Beijing 100029, China Correspondence
An Unusual Case of Concurrent Insulinoma and Nesidioblastosis
 CASE REPORT An Unusual Case of Concurrent Insulinoma and Nesidioblastosis Elizabeth Bright 1, Giuseppe Garcea 1, Seok L Ong 1, Webster Madira 2, David P Berry 1, Ashley R Dennison 1 Departments of 1 Hepatobiliary
CASE REPORT An Unusual Case of Concurrent Insulinoma and Nesidioblastosis Elizabeth Bright 1, Giuseppe Garcea 1, Seok L Ong 1, Webster Madira 2, David P Berry 1, Ashley R Dennison 1 Departments of 1 Hepatobiliary
INDEX. Note: Page numbers of issue and article titles are in boldface type. cell carcinoma. ENDOCRINE SURGERY
 ENDOCRINE SURGERY INDEX Note: Page numbers of issue and article titles are in boldface type. Adenylate cyclase, in signal transduction 425-426 Adrenal incidentalomas, 499-509 imaging of, 502-504 in patients
ENDOCRINE SURGERY INDEX Note: Page numbers of issue and article titles are in boldface type. Adenylate cyclase, in signal transduction 425-426 Adrenal incidentalomas, 499-509 imaging of, 502-504 in patients
Color Codes Pathology and Genetics Medicine and Clinical Pathology Surgery Imaging
 Saturday, November 5, 2005 8:30-10:30 a. m. Poorly Differentiated Endocrine Carcinomas Chairman: E. Van Cutsem, Leuven, Belgium 9:00-9:30 a. m. Working Group Sessions Pathology and Genetics Group leaders:
Saturday, November 5, 2005 8:30-10:30 a. m. Poorly Differentiated Endocrine Carcinomas Chairman: E. Van Cutsem, Leuven, Belgium 9:00-9:30 a. m. Working Group Sessions Pathology and Genetics Group leaders:
NEOPLASMS OF THE THYROID PATHOLOGY OF PARATHYROID GLANDS. BY: Shifaa Qa qa
 NEOPLASMS OF THE THYROID PATHOLOGY OF PARATHYROID GLANDS BY: Shifaa Qa qa Neoplasmas of the thyroid thyroid nodules Neoplastic ---- benign, malignant Non neoplastic Solitary nodules ----- neoplastic Nodules
NEOPLASMS OF THE THYROID PATHOLOGY OF PARATHYROID GLANDS BY: Shifaa Qa qa Neoplasmas of the thyroid thyroid nodules Neoplastic ---- benign, malignant Non neoplastic Solitary nodules ----- neoplastic Nodules
The role of routine surgical exploration for gastrinoma
 ORIGINAL ARTICLES Surgery Increases Survival in Patients With Gastrinoma Jeffrey A. Norton, MD, Douglas L. Fraker, MD, H. R. Alexander, MD, Fathia Gibril, MD, David J. Liewehr, MS, David J. Venzon, PhD,
ORIGINAL ARTICLES Surgery Increases Survival in Patients With Gastrinoma Jeffrey A. Norton, MD, Douglas L. Fraker, MD, H. R. Alexander, MD, Fathia Gibril, MD, David J. Liewehr, MS, David J. Venzon, PhD,
B. Environmental Factors. a. The major risk factor to papillary thyroid cancer is exposure to ionizing radiation, during the first 2 decades of life.
 B. Environmental Factors. a. The major risk factor to papillary thyroid cancer is exposure to ionizing radiation, during the first 2 decades of life. b. Deficiency of dietary iodine: - Is linked with a
B. Environmental Factors. a. The major risk factor to papillary thyroid cancer is exposure to ionizing radiation, during the first 2 decades of life. b. Deficiency of dietary iodine: - Is linked with a
Imaging Pancreatic Neuroendocrine Tumors (PNETs): CT, MRI, EUS, Nuclear
 Imaging Pancreatic Neuroendocrine Tumors (PNETs): CT, MRI, EUS, Nuclear Eric Tamm, M.D. Department of Diagnostic Radiology Division of Diagnostic Imaging MD Anderson Cancer Center Houston, TX Disclosure
Imaging Pancreatic Neuroendocrine Tumors (PNETs): CT, MRI, EUS, Nuclear Eric Tamm, M.D. Department of Diagnostic Radiology Division of Diagnostic Imaging MD Anderson Cancer Center Houston, TX Disclosure
Surgical Experiences of Functioning Neuroendocrine Neoplasm of the Pancreas
 Yonsei Medical Journal Vol. 47, No. 6, pp. 833-839, 2006 Surgical Experiences of Functioning Neuroendocrine Neoplasm of the Pancreas Chang Moo Kang, Se Ho Park, Kyung Sik Kim, Jin Sub Choi, Woo Jung Lee,
Yonsei Medical Journal Vol. 47, No. 6, pp. 833-839, 2006 Surgical Experiences of Functioning Neuroendocrine Neoplasm of the Pancreas Chang Moo Kang, Se Ho Park, Kyung Sik Kim, Jin Sub Choi, Woo Jung Lee,
Index. Note: Page numbers of article titles are in boldface type.
 Note: Page numbers of article titles are in boldface type. A Adenocarcinoma, pancreatic ductal, laparoscopic distal pancreatectomy for, 61 Adrenal cortical carcinoma, laparoscopic adrenalectomy for, 114
Note: Page numbers of article titles are in boldface type. A Adenocarcinoma, pancreatic ductal, laparoscopic distal pancreatectomy for, 61 Adrenal cortical carcinoma, laparoscopic adrenalectomy for, 114
Surgical treatment of neuroendocrine metastases
 Best Practice & Research Clinical Gastroenterology Vol. 19, No. 4, pp. 577 583, 2005 doi:10.1016/j.bpg.2005.04.003 available online at http://www.sciencedirect.com 6 Surgical treatment of neuroendocrine
Best Practice & Research Clinical Gastroenterology Vol. 19, No. 4, pp. 577 583, 2005 doi:10.1016/j.bpg.2005.04.003 available online at http://www.sciencedirect.com 6 Surgical treatment of neuroendocrine
Neuroendocrine Tumors
 Neuroendocrine Tumors Neuroendocrine tumors arise from cells that release a hormone in response to a signal from the nervous system. Neuro refers to the nervous system. Endocrine refers to the hormones.
Neuroendocrine Tumors Neuroendocrine tumors arise from cells that release a hormone in response to a signal from the nervous system. Neuro refers to the nervous system. Endocrine refers to the hormones.
hypercalcemia of malignancy hyperparathyroidism PHPT the most common cause of hypercalcemia in the outpatient setting the second most common cause
 hyperparathyroidism A 68-year-old woman with documented osteoporosis has blood tests showing elevated serum calcium and parathyroid hormone (PTH) levels: 11.2 mg/dl (8.8 10.1 mg/dl) and 88 pg/ml (10-60),
hyperparathyroidism A 68-year-old woman with documented osteoporosis has blood tests showing elevated serum calcium and parathyroid hormone (PTH) levels: 11.2 mg/dl (8.8 10.1 mg/dl) and 88 pg/ml (10-60),
Pancreas Case Scenario #1
 Pancreas Case Scenario #1 An 85 year old white female presented to her primary care physician with increasing abdominal pain. On 8/19 she had a CT scan of the abdomen and pelvis. This showed a 4.6 cm mass
Pancreas Case Scenario #1 An 85 year old white female presented to her primary care physician with increasing abdominal pain. On 8/19 she had a CT scan of the abdomen and pelvis. This showed a 4.6 cm mass
Pancreaticoduodenectomy the anatomy and the surgical approaches
 Pancreaticoduodenectomy the anatomy and the surgical approaches Paul BS LAI Division of Hepato biliary and Pancreatic Surgery Department of Surgery The Chinese Univesity of Hong Kong Whipple s operation
Pancreaticoduodenectomy the anatomy and the surgical approaches Paul BS LAI Division of Hepato biliary and Pancreatic Surgery Department of Surgery The Chinese Univesity of Hong Kong Whipple s operation
HYPERPARATHYROIDIS M FAISAL GHANI SIDDIQUI MBBS; FCPS; PGDIP-BIOMEDICAL ETHICS; MCPS-HPE
 HYPERPARATHYROIDIS M FAISAL GHANI SIDDIQUI MBBS; FCPS; PGDIP-BIOMEDICAL ETHICS; MCPS-HPE PROFESSOR OF SURGERY J I N N A H S I N D H M E D I C A L U N I V E R S I T Y PREAMBLE Anatomy & physiology of the
HYPERPARATHYROIDIS M FAISAL GHANI SIDDIQUI MBBS; FCPS; PGDIP-BIOMEDICAL ETHICS; MCPS-HPE PROFESSOR OF SURGERY J I N N A H S I N D H M E D I C A L U N I V E R S I T Y PREAMBLE Anatomy & physiology of the
Multiple endocrine neoplasia type 1 (MEN1) is an autosomal
 ORIGINAL ARTICLES Outcome of Duodenopancreatic Resections in Patients With Multiple Endocrine Neoplasia Type 1 Detlef K. Bartsch, MD,* Volker Fendrich, MD,* Peter Langer, MD,* Ilhan Celik, MD, Peter H.
ORIGINAL ARTICLES Outcome of Duodenopancreatic Resections in Patients With Multiple Endocrine Neoplasia Type 1 Detlef K. Bartsch, MD,* Volker Fendrich, MD,* Peter Langer, MD,* Ilhan Celik, MD, Peter H.
Coexistence of parathyroid adenoma and papillary thyroid carcinoma. Yong Sang Lee, Kee-Hyun Nam, Woong Youn Chung, Hang-Seok Chang, Cheong Soo Park
 J Korean Surg Soc 2011;81:316-320 http://dx.doi.org/10.4174/jkss.2011.81.5.316 ORIGINAL ARTICLE JKSS Journal of the Korean Surgical Society pissn 2233-7903 ㆍ eissn 2093-0488 Coexistence of parathyroid
J Korean Surg Soc 2011;81:316-320 http://dx.doi.org/10.4174/jkss.2011.81.5.316 ORIGINAL ARTICLE JKSS Journal of the Korean Surgical Society pissn 2233-7903 ㆍ eissn 2093-0488 Coexistence of parathyroid
Index. Surg Oncol Clin N Am 15 (2006) Note: Page numbers of article titles are in boldface type.
 Surg Oncol Clin N Am 15 (2006) 681 685 Index Note: Page numbers of article titles are in boldface type. A Ablative therapy, for liver metastases in patients with neuroendocrine tumors, 517 with radioiodine
Surg Oncol Clin N Am 15 (2006) 681 685 Index Note: Page numbers of article titles are in boldface type. A Ablative therapy, for liver metastases in patients with neuroendocrine tumors, 517 with radioiodine
Original Report. Carcinoid Tumors of the Stomach: A Clinical and Radiographic Study
 Aaron J. Binstock 1 C. Daniel Johnson 1 David H. Stephens 1 Ricardo V. Lloyd 2 Joel G. Fletcher 1 Received July 25, 2000; accepted after revision September 29, 2000. 1 Department of Radiology, Mayo Clinic,
Aaron J. Binstock 1 C. Daniel Johnson 1 David H. Stephens 1 Ricardo V. Lloyd 2 Joel G. Fletcher 1 Received July 25, 2000; accepted after revision September 29, 2000. 1 Department of Radiology, Mayo Clinic,
Update on Surgical Management of NETs
 Update on Surgical Management of Neuroendocrine Tumors James R. Howe, M.D. Director, Surgical Oncology and Endocrine Surgery University of Iowa College of Medicine Distribution of NETs 2000-2004 27% ---
Update on Surgical Management of Neuroendocrine Tumors James R. Howe, M.D. Director, Surgical Oncology and Endocrine Surgery University of Iowa College of Medicine Distribution of NETs 2000-2004 27% ---
Avi Khafif, MD, Rami Ben-Yosef, MD, Avrum Abergel, MD, Ada Kesler, MD, Roee Landsberg, MD, Dan M. Fliss, MD
 ORIGINAL ARTICLE ELECTIVE PARATRACHEAL NECK DISSECTION FOR LATERAL METASTASES FROM PAPILLARY CARCINOMA OF THE THYROID: IS IT INDICATED? Avi Khafif, MD, Rami Ben-Yosef, MD, Avrum Abergel, MD, Ada Kesler,
ORIGINAL ARTICLE ELECTIVE PARATRACHEAL NECK DISSECTION FOR LATERAL METASTASES FROM PAPILLARY CARCINOMA OF THE THYROID: IS IT INDICATED? Avi Khafif, MD, Rami Ben-Yosef, MD, Avrum Abergel, MD, Ada Kesler,
Objectives. Intraoperative Consultation of the Whipple Resection Specimen. Pancreas Anatomy. Pancreatic ductal carcinoma 11/10/2014
 Intraoperative Consultation of the Whipple Resection Specimen Pathology Update Faculty of Medicine, University of Toronto November 15, 2014 John W. Wong, MD, FRCPC Department of Anatomical Pathology Sunnybrook
Intraoperative Consultation of the Whipple Resection Specimen Pathology Update Faculty of Medicine, University of Toronto November 15, 2014 John W. Wong, MD, FRCPC Department of Anatomical Pathology Sunnybrook
Endoscopic Ultrasonography Assessment for Ampullary and Bile Duct Malignancy
 Diagnostic and Therapeutic Endoscopy, Vol. 3, pp. 35-40 Reprints available directly from the publisher Photocopying permitted by license only (C) 1996 OPA (Overseas Publishers Association) Amsterdam B.V.
Diagnostic and Therapeutic Endoscopy, Vol. 3, pp. 35-40 Reprints available directly from the publisher Photocopying permitted by license only (C) 1996 OPA (Overseas Publishers Association) Amsterdam B.V.
Imaging in gastric cancer
 Imaging in gastric cancer Gastric cancer remains a deadly disease because of late diagnosis. Adenocarcinoma represents 90% of malignant tumors. Diagnosis is based on endoscopic examination with biopsies.
Imaging in gastric cancer Gastric cancer remains a deadly disease because of late diagnosis. Adenocarcinoma represents 90% of malignant tumors. Diagnosis is based on endoscopic examination with biopsies.
Surgery for NET Challenges and specific aspects
 Surgery for NET Challenges and specific aspects Raymond Aerts, MD Department of Abdominal Surgery and Liver Transplantation University Clinics Leuven ESMO Preceptorship on GI neuroendocrine tumours (NETs)
Surgery for NET Challenges and specific aspects Raymond Aerts, MD Department of Abdominal Surgery and Liver Transplantation University Clinics Leuven ESMO Preceptorship on GI neuroendocrine tumours (NETs)
Evaluation of Suspected Pancreatic Cancer
 Evaluation of Suspected Pancreatic Cancer October 15, 2015 If you experience technical difficulty during the presentation: Contact WebEx Technical Support directly at: US Toll Free: 1-866-779-3239 Toll
Evaluation of Suspected Pancreatic Cancer October 15, 2015 If you experience technical difficulty during the presentation: Contact WebEx Technical Support directly at: US Toll Free: 1-866-779-3239 Toll
Imaging Pancreatic Neuroendocrine Tumors (PNETs): CT, MRI, EUS, Nuclear
 Imaging Pancreatic Neuroendocrine Tumors (PNETs): CT, MRI, EUS, Nuclear Eric Tamm, M.D. Department of Diagnostic Radiology Division of Diagnostic Imaging MD Anderson Cancer Center Houston, TX Disclosure
Imaging Pancreatic Neuroendocrine Tumors (PNETs): CT, MRI, EUS, Nuclear Eric Tamm, M.D. Department of Diagnostic Radiology Division of Diagnostic Imaging MD Anderson Cancer Center Houston, TX Disclosure
The Whipple Operation Illustrations
 The Whipple Operation Illustrations Fig. 1. Illustration of the sixstep pancreaticoduodenectomy (Whipple operation) as described in a number of recent text books by Dr. Evans. The operation is divided
The Whipple Operation Illustrations Fig. 1. Illustration of the sixstep pancreaticoduodenectomy (Whipple operation) as described in a number of recent text books by Dr. Evans. The operation is divided
Primary hyperparathyroidism (HPT) has an incidence of
 Dual-Phase Tc-Sestamibi Imaging: Its Utility in Parathyroid Hyperplasia and Use of Immediate/ Delayed Image Ratios to Improve Diagnosis of Hyperparathyroidism Leonie Gordon, MD; William Burkhalter, MD;
Dual-Phase Tc-Sestamibi Imaging: Its Utility in Parathyroid Hyperplasia and Use of Immediate/ Delayed Image Ratios to Improve Diagnosis of Hyperparathyroidism Leonie Gordon, MD; William Burkhalter, MD;
Surgical management of pancreatico-duodenal tumors in multiple endocrine neoplasia syndrome type 1
 CLINICS 2012;67(S1):173-178 DOI:10.6061/clinics/2012(Sup01)29 REVIEW Surgical management of pancreatico-duodenal tumors in multiple endocrine neoplasia syndrome type 1 Göran Åkerström, Peter Stålberg,
CLINICS 2012;67(S1):173-178 DOI:10.6061/clinics/2012(Sup01)29 REVIEW Surgical management of pancreatico-duodenal tumors in multiple endocrine neoplasia syndrome type 1 Göran Åkerström, Peter Stålberg,
Zollinger-Ellison Syndrome
 Zollinger-Ellison Syndrome National Digestive Diseases Information Clearinghouse U.S. Department of Health and Human Services NATIONAL INSTITUTES OF HEALTH What is Zollinger-Ellison syndrome (ZES)? ZES
Zollinger-Ellison Syndrome National Digestive Diseases Information Clearinghouse U.S. Department of Health and Human Services NATIONAL INSTITUTES OF HEALTH What is Zollinger-Ellison syndrome (ZES)? ZES
Prospective Study of the Ability of Computed Axial Tomography to Localize Gastrinomas in Patients With Zollinger-Ellison Syndrome
 GASTROENTEROLOGY 1987;92;905-12 Prospective Study of the Ability of Computed Axial Tomography to Localize Gastrinomas in Patients With Zollinger-Ellison Syndrome S. A. WANK, J. L. DOPPMAN, D. L. MILLER,
GASTROENTEROLOGY 1987;92;905-12 Prospective Study of the Ability of Computed Axial Tomography to Localize Gastrinomas in Patients With Zollinger-Ellison Syndrome S. A. WANK, J. L. DOPPMAN, D. L. MILLER,
Index. radiologic.theclinics.com. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A ACC. See Adrenal cortical carcinoma. Acromegaly and the pituitary gland, 551 Acute suppurative thyroiditis, 405, 406 Addison, Thomas and
Index Note: Page numbers of article titles are in boldface type. A ACC. See Adrenal cortical carcinoma. Acromegaly and the pituitary gland, 551 Acute suppurative thyroiditis, 405, 406 Addison, Thomas and
Q&A Session NAACCR Webinar Series Collecting Cancer Data: Pancreas January 05, 2012
 Q&A Session NAACCR Webinar Series Collecting Cancer Data: Pancreas January 05, 2012 Q: Will sticky notes be transferrable from the previous electronic version of CS to the updated version? A: It is our
Q&A Session NAACCR Webinar Series Collecting Cancer Data: Pancreas January 05, 2012 Q: Will sticky notes be transferrable from the previous electronic version of CS to the updated version? A: It is our
Diagnosing and monitoring NET
 Diagnosing and monitoring NET Inaccurate or delayed diagnosis of neuroendocrine tumors (NET) is common, because many NET are small and asymptomatic. 1 When symptoms are present, they are usually nonspecific
Diagnosing and monitoring NET Inaccurate or delayed diagnosis of neuroendocrine tumors (NET) is common, because many NET are small and asymptomatic. 1 When symptoms are present, they are usually nonspecific
The parathyroid glands participate in the regulation
 41 HERNAN I. VARGAS STANLEY R. KLEIN The parathyroid glands participate in the regulation of calcium metabolism. Disorders of the parathyroid gland are most commonly a result of hyperfunction and rarely
41 HERNAN I. VARGAS STANLEY R. KLEIN The parathyroid glands participate in the regulation of calcium metabolism. Disorders of the parathyroid gland are most commonly a result of hyperfunction and rarely
5/17/2013. Pancreatic Cancer. Postgraduate Course in General Surgery CASE 1: CASE 1: Overview. Case presentation. Differential diagnosis
 Overview Case presentation Postgraduate Course in General Surgery Differential diagnosis Diagnosis and therapy Eric K. Nakakura Koloa, HI March 26, 2013 Outcomes CASE 1: CASE 1: A 78-year-old man developed
Overview Case presentation Postgraduate Course in General Surgery Differential diagnosis Diagnosis and therapy Eric K. Nakakura Koloa, HI March 26, 2013 Outcomes CASE 1: CASE 1: A 78-year-old man developed
HEPATIC METASTASES. We can state 3 types of metastases depending on their treatment options:
 HEPATIC METASTASES 1. Definition Metastasis means the spread of cancer. Cancerous cells can separate from the primary tumor and enter the bloodstream or the lymphatic system (the one that produces, stores,
HEPATIC METASTASES 1. Definition Metastasis means the spread of cancer. Cancerous cells can separate from the primary tumor and enter the bloodstream or the lymphatic system (the one that produces, stores,
Reoperative central neck surgery
 Reoperative central neck surgery R. Pandev, I. Tersiev, M. Belitova, A. Kouizi, D. Damyanov University Clinic of Surgery, Section Endocrine Surgery University Hospital Queen Johanna ISUL Medical University
Reoperative central neck surgery R. Pandev, I. Tersiev, M. Belitova, A. Kouizi, D. Damyanov University Clinic of Surgery, Section Endocrine Surgery University Hospital Queen Johanna ISUL Medical University
Pancreas & Biliary System. Dr. Vohra & Dr. Jamila
 Pancreas & Biliary System Dr. Vohra & Dr. Jamila 1 Objectives At the end of the lecture, the student should be able to describe the: Location, surface anatomy, parts, relations & peritoneal reflection
Pancreas & Biliary System Dr. Vohra & Dr. Jamila 1 Objectives At the end of the lecture, the student should be able to describe the: Location, surface anatomy, parts, relations & peritoneal reflection
PANCREATIC CANCER GUIDELINES
 PANCREATIC CANCER GUIDELINES North-East London Cancer Network & Barts and the London HPB Centre PROTOCOL FOR MANAGEMENT OF PANCREATIC CANCER (SEPTEMBER 2010) I. PRE-REFERRAL GUIDELINES Screening 1. Offer
PANCREATIC CANCER GUIDELINES North-East London Cancer Network & Barts and the London HPB Centre PROTOCOL FOR MANAGEMENT OF PANCREATIC CANCER (SEPTEMBER 2010) I. PRE-REFERRAL GUIDELINES Screening 1. Offer
DIABETES MELLITUS: COMPLICATION. Benyamin Makes Dept. of Anatomic Pathology FMUI - Jakarta
 DIABETES MELLITUS: COMPLICATION Benyamin Makes Dept. of Anatomic Pathology FMUI - Jakarta COMPLICATION OF DIABETES Susceptibility to infections including tuberculosis, pneumonia, pyelonephritis, and mucocutaneous
DIABETES MELLITUS: COMPLICATION Benyamin Makes Dept. of Anatomic Pathology FMUI - Jakarta COMPLICATION OF DIABETES Susceptibility to infections including tuberculosis, pneumonia, pyelonephritis, and mucocutaneous
Endocrine Tumors of the Gastrointestinal System. F. V. Nowak Ohio University March 22, 2005
 Endocrine Tumors of the Gastrointestinal System F. V. Nowak Ohio University March 22, 2005 Gastroenteropancreatic Endocrine System Clear cells of endodermal origin found in the pancreas, stomach, small
Endocrine Tumors of the Gastrointestinal System F. V. Nowak Ohio University March 22, 2005 Gastroenteropancreatic Endocrine System Clear cells of endodermal origin found in the pancreas, stomach, small
Radiology Pathology Conference
 Radiology Pathology Conference Nadia F. Yusaf, M.D. PGY-3 1/29/2010 Presentation material is for education purposes only. All rights reserved. 2010 URMC Radiology Page 1 of 90 Case 1 60 year- old man presents
Radiology Pathology Conference Nadia F. Yusaf, M.D. PGY-3 1/29/2010 Presentation material is for education purposes only. All rights reserved. 2010 URMC Radiology Page 1 of 90 Case 1 60 year- old man presents
EUS FNA NEUROENDOCRINE TUMORS. A. Ginès Endocopy Unit Hospital Cínic. Barcelona (Spain)
 EUS FNA NEUROENDOCRINE TUMORS A. Ginès Endocopy Unit Hospital Cínic. Barcelona (Spain) GI NEUROENDOCRINE TUMORS GENERAL CONCEPTS Rare neoplasms arising from the neuroendocrine cells of the GI tract Include:
EUS FNA NEUROENDOCRINE TUMORS A. Ginès Endocopy Unit Hospital Cínic. Barcelona (Spain) GI NEUROENDOCRINE TUMORS GENERAL CONCEPTS Rare neoplasms arising from the neuroendocrine cells of the GI tract Include:
Parathyroid Imaging: Current Concepts. Maria Gule-Monroe, M.D. Nancy Perrier, M.D.
 Parathyroid Imaging: Current Concepts Maria Gule-Monroe, M.D. Nancy Perrier, M.D. Disclosures None Objectives Ultrasound characteristics of parathyroid adenomas vs. lymph nodes 4D-CT evaluation of hyperparathyroidism
Parathyroid Imaging: Current Concepts Maria Gule-Monroe, M.D. Nancy Perrier, M.D. Disclosures None Objectives Ultrasound characteristics of parathyroid adenomas vs. lymph nodes 4D-CT evaluation of hyperparathyroidism
Intended for use by Clinicians and Health Care Providers involved in the Management or Referral of adult patients with pancreatic
 Intended for use by Clinicians and Health Care Providers involved in the Management or Referral of adult patients with pancreatic cancer Section AA Cancer Centre Referrals In the absence of metastatic
Intended for use by Clinicians and Health Care Providers involved in the Management or Referral of adult patients with pancreatic cancer Section AA Cancer Centre Referrals In the absence of metastatic
Gangliocytic Paraganglioma: Report of A Case
 2014 25 122-126 Gangliocytic Paraganglioma: Report of A Case Hsiu-Mei Su, Chi-Hung Chen, Jen-Chieh Huang, and Jeng-Shiann Shin Department of Gastroenterology, Chen-Chin General Hospital, Taichung, Taiwan
2014 25 122-126 Gangliocytic Paraganglioma: Report of A Case Hsiu-Mei Su, Chi-Hung Chen, Jen-Chieh Huang, and Jeng-Shiann Shin Department of Gastroenterology, Chen-Chin General Hospital, Taichung, Taiwan
Cross-sectional Imaging of Neuroendocrine Tumors of the Gastrointestinal Tract
 Cross-sectional Imaging of Neuroendocrine Tumors of the Gastrointestinal Tract Eric J. May 1, Shannon P. Sheedy 1, Joel G. Fletcher 1, Mark J. Truty 2, Thomas C. Smyrk 3, Jeff L. Fidler 1 1. Radiology,
Cross-sectional Imaging of Neuroendocrine Tumors of the Gastrointestinal Tract Eric J. May 1, Shannon P. Sheedy 1, Joel G. Fletcher 1, Mark J. Truty 2, Thomas C. Smyrk 3, Jeff L. Fidler 1 1. Radiology,
Lu Hao Feng et al., IJSIT, 2016, 5(6),
 AN UNUSUAL PRESENTATION OF PANCREATIC VASOACTIVE INTESTINAL PEPTIDE TUMOUR (VIP OMAS) WITH GASTROINTESTINAL STROMAL TUMOUR (GIST) WITHOUT HYPOKALEMIA AND HPERCALCEMIA: A CASE REPORT WITH REVIEW ARTICLES
AN UNUSUAL PRESENTATION OF PANCREATIC VASOACTIVE INTESTINAL PEPTIDE TUMOUR (VIP OMAS) WITH GASTROINTESTINAL STROMAL TUMOUR (GIST) WITHOUT HYPOKALEMIA AND HPERCALCEMIA: A CASE REPORT WITH REVIEW ARTICLES
Stomach. R.B. Kolachalam, MD
 Stomach R.B. Kolachalam, MD Relevent Anatomy 1.four regions: Cardia, Fundus, Body, and the Pylorus 2. fixed in two locations- at the GEJ and the duodenum Gastric Anatomy body of the stomach: site of mechanical
Stomach R.B. Kolachalam, MD Relevent Anatomy 1.four regions: Cardia, Fundus, Body, and the Pylorus 2. fixed in two locations- at the GEJ and the duodenum Gastric Anatomy body of the stomach: site of mechanical
Liver Tumors. Prof. Dr. Ahmed El - Samongy
 Liver Tumors Prof. Dr. Ahmed El - Samongy Objective 1. Identify the most important features of common benign liver tumors 2. Know the risk factors, diagnosis, and management of hepatocellular carcinoma
Liver Tumors Prof. Dr. Ahmed El - Samongy Objective 1. Identify the most important features of common benign liver tumors 2. Know the risk factors, diagnosis, and management of hepatocellular carcinoma
The Pancreas. Basic Anatomy. Endocrine pancreas. Exocrine pancreas. Pancreas vasculature. Islets of Langerhans. Acinar cells Ductal System
 SGNA: Back to Basics Rogelio G. Silva, MD Assistant Clinical Professor of Medicine University of Illinois at Chicago Department of Medicine Division of Gastroenterology Advocate Christ Medical Center GI
SGNA: Back to Basics Rogelio G. Silva, MD Assistant Clinical Professor of Medicine University of Illinois at Chicago Department of Medicine Division of Gastroenterology Advocate Christ Medical Center GI
PANCREAS DUCTAL ADENOCARCINOMA PDAC
 CONTENTS PANCREAS DUCTAL ADENOCARCINOMA PDAC I. What is the pancreas? II. III. IV. What is pancreas cancer? What is the epidemiology of Pancreatic Ductal Adenocarcinoma (PDAC)? What are the risk factors
CONTENTS PANCREAS DUCTAL ADENOCARCINOMA PDAC I. What is the pancreas? II. III. IV. What is pancreas cancer? What is the epidemiology of Pancreatic Ductal Adenocarcinoma (PDAC)? What are the risk factors
Health Sciences Centre, Team A, Dr. L. Bohacek (Endocrine Surgery) Medical Expert
 Health Sciences Centre, Team A, Dr. L. Bohacek (Endocrine Surgery) Introduction Medical Expert This is a three month PGY 1-5 rotation in which residents gain exposure in the care and management of patients
Health Sciences Centre, Team A, Dr. L. Bohacek (Endocrine Surgery) Introduction Medical Expert This is a three month PGY 1-5 rotation in which residents gain exposure in the care and management of patients
Ultrasound for Pre-operative Evaluation of Well Differentiated Thyroid Cancer
 Ultrasound for Pre-operative Evaluation of Well Differentiated Thyroid Cancer Its Not Just About the Nodes AACE Advances in Medical and Surgical Management of Thyroid Cancer - 2017 Robert A. Levine, MD,
Ultrasound for Pre-operative Evaluation of Well Differentiated Thyroid Cancer Its Not Just About the Nodes AACE Advances in Medical and Surgical Management of Thyroid Cancer - 2017 Robert A. Levine, MD,
GEP NEN. Personalised approach. Curative and Palliative Surgery. ESMO Preceptorship Programme Neuroendocrine Neoplasms Lugano April 2018
 GEP NEN Personalised approach Curative and Palliative Surgery ESMO Preceptorship Programme Neuroendocrine Neoplasms Lugano 13 14 April 2018 Professor Andrea Frilling Department of Surgery and Cancer Imperial
GEP NEN Personalised approach Curative and Palliative Surgery ESMO Preceptorship Programme Neuroendocrine Neoplasms Lugano 13 14 April 2018 Professor Andrea Frilling Department of Surgery and Cancer Imperial
Kidney Case 1 SURGICAL PATHOLOGY REPORT
 Kidney Case 1 Surgical Pathology Report February 9, 2007 Clinical History: This 45 year old woman was found to have a left renal mass. CT urography with reconstruction revealed a 2 cm medial mass which
Kidney Case 1 Surgical Pathology Report February 9, 2007 Clinical History: This 45 year old woman was found to have a left renal mass. CT urography with reconstruction revealed a 2 cm medial mass which
Minimally Invasive Endocrine Surgery. How far have we come?
 Minimally Invasive Endocrine Surgery How far have we come? Introduction Minimally invasive surgery describes a field of surgery that crosses all traditional disciplines. It is not a discipline into itself
Minimally Invasive Endocrine Surgery How far have we come? Introduction Minimally invasive surgery describes a field of surgery that crosses all traditional disciplines. It is not a discipline into itself
3/28/2012. Periampullary Tumors. Postgraduate Course in General Surgery CASE 1: CASE 1: Overview. Eric K. Nakakura Ko Olina, HI
 Overview Postgraduate Course in General Surgery Case presentation Differential diagnosis Diagnosis and therapy Outcomes Principles of palliative care Eric K. Nakakura Ko Olina, HI March 27, 2012 CASE 1:
Overview Postgraduate Course in General Surgery Case presentation Differential diagnosis Diagnosis and therapy Outcomes Principles of palliative care Eric K. Nakakura Ko Olina, HI March 27, 2012 CASE 1:
Hepatobiliary and Pancreatic Malignancies
 Hepatobiliary and Pancreatic Malignancies Gareth Eeson MD MSc FRCSC Surgical Oncologist and General Surgeon Kelowna General Hospital Interior Health Consultant, Surgical Oncology BC Cancer Agency Centre
Hepatobiliary and Pancreatic Malignancies Gareth Eeson MD MSc FRCSC Surgical Oncologist and General Surgeon Kelowna General Hospital Interior Health Consultant, Surgical Oncology BC Cancer Agency Centre
PARATHYROID IMAGING. James Lee, MD Chief, Endocrine Surgery Co-Director NY Thyroid-Parathyroid Center Columbia University Medical Center
 PARATHYROID IMAGING James Lee, MD Chief, Endocrine Surgery Co-Director NY Thyroid-Parathyroid Center Columbia University Medical Center NO DISCLOSURES Overview The hallmarks of the ideal test Benefits
PARATHYROID IMAGING James Lee, MD Chief, Endocrine Surgery Co-Director NY Thyroid-Parathyroid Center Columbia University Medical Center NO DISCLOSURES Overview The hallmarks of the ideal test Benefits
10/24/2008. Surgery for Well-differentiated Thyroid Carcinoma- The Primary
 Surgery for Well-differentiated Thyroid Carcinoma- The Primary Head and Neck Endocrine Surgery Department of Otolaryngology-Head and Neck Surgery, UCSF October 24-25, 2008 Robert A. Sofferman, MD Professor
Surgery for Well-differentiated Thyroid Carcinoma- The Primary Head and Neck Endocrine Surgery Department of Otolaryngology-Head and Neck Surgery, UCSF October 24-25, 2008 Robert A. Sofferman, MD Professor
Fig. 59 Malignant phaeochromocytoma, hepatic metastasis.
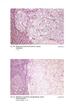 Fig. 59 Malignant phaeochromocytoma, hepatic metastasis. X 120 Hyperte nsion Fig. 60 Malignant sympathetic paraganglioma, lymph node metastasis Primary in bladder. x 1 20 Hypertension Fig. 61 Malignant
Fig. 59 Malignant phaeochromocytoma, hepatic metastasis. X 120 Hyperte nsion Fig. 60 Malignant sympathetic paraganglioma, lymph node metastasis Primary in bladder. x 1 20 Hypertension Fig. 61 Malignant
Neuro-endocrine and pancreatic non-adenocarcinomas. Marc Engelbrecht, AMC, Amsterdam
 Neuro-endocrine and pancreatic non-adenocarcinomas Marc Engelbrecht, AMC, Amsterdam Pancreatic Tumors q Epithelial Exocrine q Mesenchymal Ductal Adenocarcinoma (85-95%) Metastasis Lymfoma Acinar Cell Carcinoma
Neuro-endocrine and pancreatic non-adenocarcinomas Marc Engelbrecht, AMC, Amsterdam Pancreatic Tumors q Epithelial Exocrine q Mesenchymal Ductal Adenocarcinoma (85-95%) Metastasis Lymfoma Acinar Cell Carcinoma
Sporadic versus hereditary gastrinomas of the duodenum and pancreas: Distinct clinico-pathological and epidemiological features
 PO Box 2345, Beijing 100023, China World J Gastroenterol 2006 September 14; 12(34): 5440-5446 World Journal of Gastroenterology ISSN 1007-9327 wjg@wjgnet.com 2006 The WJG Press. All rights reserved. EDITORIAL
PO Box 2345, Beijing 100023, China World J Gastroenterol 2006 September 14; 12(34): 5440-5446 World Journal of Gastroenterology ISSN 1007-9327 wjg@wjgnet.com 2006 The WJG Press. All rights reserved. EDITORIAL
Peptic ulcer disease. Nomin-Erdene. D SOM-531
 Peptic ulcer disease Nomin-Erdene. D SOM-531 Learning objectives Stomach gross anatomy PUD Epidemiology Pathogenesis Clinical manifestation Diagnosing Treatment Complicated ulcer disease Surgical procedures
Peptic ulcer disease Nomin-Erdene. D SOM-531 Learning objectives Stomach gross anatomy PUD Epidemiology Pathogenesis Clinical manifestation Diagnosing Treatment Complicated ulcer disease Surgical procedures
Secondary and Familial Hyperparathyroidism
 Secondary and Familial Jeffrey F. Moley, M.D. Chief, Endocrine and Oncologic Surgery Section, Professor of Surgery Associate Director, The Alvin J. Siteman Cancer Center Occurs in setting of CRF Chronic
Secondary and Familial Jeffrey F. Moley, M.D. Chief, Endocrine and Oncologic Surgery Section, Professor of Surgery Associate Director, The Alvin J. Siteman Cancer Center Occurs in setting of CRF Chronic
PANCREATITIS: MEDICAL AND TRANSPLANT CONSIDERATIONS, DHIRAJ YADAV, MD 1
 DHIRAJ YADAV, MD 1 Good afternoon. This is actually an interesting time of the day to do pancreas topic since you just had lunch and this is the time when the pancreas is the most active with a lot of
DHIRAJ YADAV, MD 1 Good afternoon. This is actually an interesting time of the day to do pancreas topic since you just had lunch and this is the time when the pancreas is the most active with a lot of
CT 101 :Pancreas and Spleen
 CT 101 :Pancreas and Spleen Shikha Khullar,, MD, MPH Division of Radiology University of South Alabama The Pancreas Normal Pancreas 3 Phase Pancreatic CT Non contrast Arterial phase : 30-35 35 second
CT 101 :Pancreas and Spleen Shikha Khullar,, MD, MPH Division of Radiology University of South Alabama The Pancreas Normal Pancreas 3 Phase Pancreatic CT Non contrast Arterial phase : 30-35 35 second
Nonfunctioning Islet Cell Tumors of the Pancreas: Computed Tomography Findings
 Chin J Radiol 2002; 27: 239-243 239 Nonfunctioning Islet Cell Tumors of the Pancreas: Computed Tomography Findings CHAO-HSUAN YEN 1 JEN-HWEY CHIANG 1 JEN-I HUANG 3 CHENG-SHI SU 2 YI-YOU CHIOU 1 CHENG-YEN
Chin J Radiol 2002; 27: 239-243 239 Nonfunctioning Islet Cell Tumors of the Pancreas: Computed Tomography Findings CHAO-HSUAN YEN 1 JEN-HWEY CHIANG 1 JEN-I HUANG 3 CHENG-SHI SU 2 YI-YOU CHIOU 1 CHENG-YEN
THE RESULTS OF SURGICAL TREATMENT IN NODULAR GOITRE
 POSTGRAD. MED. J. (1966) 42, 490 THE RESULTS OF SURGICAL TREATMENT IN NODULAR GOITRE P. H. DICKINSON, M.B., B.S. (Durh.), M.S. (I11.), F.R.C.S. I. F. MCNEILL, M.S., F.R.C.S. Department of Surgery, Royal
POSTGRAD. MED. J. (1966) 42, 490 THE RESULTS OF SURGICAL TREATMENT IN NODULAR GOITRE P. H. DICKINSON, M.B., B.S. (Durh.), M.S. (I11.), F.R.C.S. I. F. MCNEILL, M.S., F.R.C.S. Department of Surgery, Royal
patients.1-7 Other associated endocrinopathies patients Furthermore, the other MENI test.13-'5 17 Indeed, in a series of patients with
 Gut 1996; 39: 273-278 Service de Gastroent6rologie, H6pital Bichat-Claude Bernard, Paris, France G Cadiot A Allouch M Mignon Departement de Physiologie, Universite Pierre et Marie Curie, H6pital Broussais,
Gut 1996; 39: 273-278 Service de Gastroent6rologie, H6pital Bichat-Claude Bernard, Paris, France G Cadiot A Allouch M Mignon Departement de Physiologie, Universite Pierre et Marie Curie, H6pital Broussais,
Afternoon Session Cases
 Afternoon Session Cases Case 1 19 year old woman Presented with abdominal pain to community hospital Mild incr WBC a14, 000, Hg normal, lipase 100 (normal to 75) US 5.2 x 3.7 x 4 cm mass in porta hepatis
Afternoon Session Cases Case 1 19 year old woman Presented with abdominal pain to community hospital Mild incr WBC a14, 000, Hg normal, lipase 100 (normal to 75) US 5.2 x 3.7 x 4 cm mass in porta hepatis
A retrospective analysis of neuroendocrine tumour of pancreas: a single institute study
 International Journal of Research in Medical Sciences Chheda YP et al. Int J Res Med Sci. 2015 Nov;3(11):3041-3045 www.msjonline.org pissn 2320-6071 eissn 2320-6012 Research Article DOI: http://dx.doi.org/10.18203/2320-6012.ijrms20150928
International Journal of Research in Medical Sciences Chheda YP et al. Int J Res Med Sci. 2015 Nov;3(11):3041-3045 www.msjonline.org pissn 2320-6071 eissn 2320-6012 Research Article DOI: http://dx.doi.org/10.18203/2320-6012.ijrms20150928
Parathyroid Imaging. A Guide to Parathyroid Surgery
 Parathyroid Imaging A Guide to Parathyroid Surgery Primary Hyperparathyroidism (PHPT) 3 rd most common endocrine disorder after diabetes and hyperthyroidism Prevalence in women 2% Often discovered in asymptomatic
Parathyroid Imaging A Guide to Parathyroid Surgery Primary Hyperparathyroidism (PHPT) 3 rd most common endocrine disorder after diabetes and hyperthyroidism Prevalence in women 2% Often discovered in asymptomatic
Calcitonin. 1
 Calcitonin Medullary thyroid carcinoma (MTC) is characterized by a high concentration of serum calcitonin. Routine measurement of serum calcitonin concentration has been advocated for detection of MTC
Calcitonin Medullary thyroid carcinoma (MTC) is characterized by a high concentration of serum calcitonin. Routine measurement of serum calcitonin concentration has been advocated for detection of MTC
