Lymphadenoma of the salivary gland: clinicopathological and immunohistochemical analysis of 33 tumors
|
|
|
- Lucinda Ray
- 5 years ago
- Views:
Transcription
1 26 & 2012 USCAP, Inc. All rights reserved /12 $32.00 Lymphadenoma of the salivary gland: clinicopathological and immunohistochemical analysis of 33 tumors Raja R Seethala 1, Lester DR Thompson 2, Douglas R Gnepp 3, E Leon Barnes 1, Alena Skalova 4, Kathleen Montone 5, Shubhada Kane 6, James S Lewis Jr 7, Lynn W Solomon 8, Roderick HW Simpson 9, Ashraf Khan 10 and Manju L Prasad 11 1 Departments of Pathology, Presbyterian University Hospital, Pittsburgh, PA, USA; 2 Woodland Hills Medical Center, Woodland Hills, CA, USA; 3 Rhode Island Hospital of Brown University, Providence, RI, USA; 4 Medical Faculty of Charles University, Prague, Czech Republic; 5 Hospital of the University of Pennsylvania, Philadelphia, PA, USA; 6 Tata Memorial Hospital, Mumbai, India; 7 Washington University School of Medicine, St Louis, MO, USA; 8 Tufts University School of Dental Medicine, Boston, MA, USA; 9 Royal Devon and Exeter Hospital, Exeter, UK; 10 UMass Memorial Medical Center, Worcester, MA, USA and 11 Yale School of Medicine, New Haven, CT, USA Lymphadenomas (LADs) are rare salivary gland tumors. Their clinicopathologic characteristics and etiopathogenesis are poorly understood. We examined 33 LADs in 31 patients (17 women and 14 men) aged years (median 65 years). There were 22 sebaceous LADs in 21 patients (9 women and 12 men) and 11 nonsebaceous LADs in 10 patients (8 women and 2 men). Two patients had synchronous double tumors. Twentysix tumors (79%) arose in parotid, three in the neck, and two each in submandibular gland and oral cavity. Extraparotid tumors were seen in 2 of 21 (10%) patients with sebaceous and 4 of 10 (40%) patients with nonsebaceous LADs. Seven of twenty-three (30%) patients had immunosuppressive therapy for unrelated diseases. The tumors were well circumscribed, encapsulated (n ¼ 28, 84%) painless masses, varying in size from 0.6 to 6 cm (median 2.2). The cut surfaces were gray-tan to yellow, homogeneous and multicystic (n ¼ 24, 72%). The epithelial cells were basaloid, squamous and glandular, forming solid nests, cords, tubules, and cysts. Sebaceous differentiation was restricted to sebaceous lymphadenoma. The epithelial cells expressed basal cell markers (p63, 34BE12, and/or CK5/6, 18/18, 100%) and the luminal glandular cells expressed CK7 (12/12, 100%). Myoepithelial cells were absent (n ¼ 10/16, 63%) or focal. The lymphoid stroma was reactive, with germinal centers in 28 (84%). There was no evidence of HPV (0/11), EBV (0/7), and HHV-8 (0/8). Malignant transformation to sebaceous and basal cell adenocarcinoma was seen in one patient each. None of the 11 patients with followup (1 8 years) recurred. In summary, sebaceous and non-sebaceous LADs are benign, encapsulated, solid and cystic tumors affecting older adults. Non-sebaceous LADs affect women and extraparotid sites more frequently than sebaceous LADs. Altered immune status may have a role in their etiopathogenesis. Multiple synchronous tumors, origin in buccal mucosa, and malignant transformation may rarely occur. ; doi: /modpathol ; published online 2 September 2011 Keywords: benign; lymphadenoma; neoplasm; salivary gland Correspondence: Associate Professor ML Prasad, MD, Department of Pathology, Yale University School of Medicine, PO Box , 310 Cedar Street, New Haven, CT 06520, USA. manju.prasad@yale.edu Received 17 February 2011; revised 8 June 2011; accepted 8 June 2011; published online 2 September 2011 Lymphadenomas (LADs) are rare benign tumors of the major salivary glands comprising biphasic tumor cell population that show groups of epithelial cells with or without sebaceous differentiation admixed with intense, reactive lymphoid proliferation. Since its first description in 1960 by McGavran et al, 1 o75 cases 2 5 have been published, the largest series comprising three cases only. 6 The clinicopathological
2 RR Seethala et al 27 features are poorly understood, and the etiology is unknown. LADs are typically tumors of the adults, and present as painless mass of long duration in the parotid gland. In most tumors, the epithelial component comprising benign basal and squamous cells with sebaceous differentiation. A much smaller number of tumors lack sebaceous differentiation. 7 Only 11 non-sebaceous LAD are reported in the literature. 5,6,8 16 We present a multicenter experience with 33 salivary LAD: 22 sebaceous and 11 non-sebaceous, in order to better define their clinicopathological characteristics, and explore their etiopathogenesis including association with malignancy, altered immune status, and viral infection. Materials and methods The study comprising 33 LAD diagnosed at 10 different institutions by head and neck pathologists with several years of experience in salivary gland pathology. Clinical information, pathologic findings, and results of immunohistochemistry (IHC) were analyzed (Table 1). In order to explore viral etiology, strong and diffuse (480%) cytoplasmic and nuclear expression of p16 was considered a surrogate marker of high risk type HPV infection, as described in tonsillar squamous cell carcinoma. In situ hybridization for HPV was performed in tumors strongly and diffusely positive for p16 17 using a wide spectrum HPV-DNA probe set (code Y1404, Dako, Carpinteria, CA), followed by subtyping, if positive. In situ hybridization for EBV-encoded RNA (EBER) was performed. One of the patients was included in a series of sclerosing polycystic adenosis, 18 and another was the subject of a case report on bilateral intraoral sebaceous LAD. 19 Results Twenty-two sebaceous and eleven non-sebaceous LADs were identified in thirty-one patients (Tables 2 4). The tumors were solitary in 29 patients (94%). A 54-year-old man developed bilateral sebaceous LAD as pedunculated masses in the right and left posterior buccal mucosa (patient SL18a,b in Table 3), and a 70-year-old man suffering from chronic lymphocytic leukemia developed two non-sebaceous LAD in right intraparotid lymph nodes (patient NSL8a,b in Table 4). Clinical Features Table 2 summarizes the age and sex distribution, and the tumor size, and Tables 3 and 4 show clinical features in the two subtypes of LAD. All but five patients were older than 50 years (84%), and only one was a child: an 11-year-old girl with nonsebaceous LAD (patient NSL7; Table 4). Twenty-six tumors (79%) arose in the parotid, two in the submandibular salivary gland, and two in the buccal mucosa. One tumor arose within the right cervical lymph node and in two tumors the location was reported as left neck. Nineteen of twenty-one (90%) patients had intraparotid sebaceous LAD, compared with 6 of 10 (60%) patients with nonsebaceous LAD. Thirty tumors presented as painless masses, some slowly enlarging (Figure 1a). The duration of symptoms, when known, ranged from a few months to several years. Medical history was available in 23 patients, and 11 of them (48%) had co-morbidities that included diabetes, hypertension, hyperlipidemia, coronary artery disease, depression, hypothyroidism, obesity, autoimmune and neoplastic diseases. Five patients had malignancies: basal cell carcinoma and squamous cell carcinoma of the skin in one patient each (patients SL7 and SL16, respectively; Table 3), breast carcinoma in one (patient SL20; Table 3), low-grade salivary duct carcinoma in one (patient NSL4; Table 4), and chronic lymphocytic leukemia in one patient (patient NSL8; Table 4). Two patients were on immunomodulatory drugs for rheumatoid arthritis Table 1 Immunohistochemistry panel Antibody Clone Dilution Antigen retrieval Vendor Calponin CALP 1:500 Dako TRS Dako, Carpinteria, CA CD3 Rabbit polyclonal 1:200 Dako TRS Dako CD5 4C7 1:100 Dako TRS Vector, Burlingame, CA CD20 L26 1:1000 Dako TRS Dako CD79a HM57 1:50 Dako TRS Dako CK5/6 D5/16 B4 1:50 EDTA ph8 Dako CK7 OV-TL 12/30 1:200 Dako TRS Dako CK20 K S :200 Dako TRS Dako EBV-LMP CS 1-4 1:50 Trypsin Dako HHV-8 13B10 1:25 Dako TRS Novocastra, UK HMWK 34bE12 1:50 Dako TRS Dako Ki-67 MIB-1 1:200 Dako TRS Dako p16 E6H4 Neat Dako TRS MTM Labs, Germany p63 4A4 1:20 Dako TRS Chemicon, Temecula, CA SMA 1A4 1:800 Dako TRS Dako SMMS SMMS-1 1:1600 Dako TRS Biogenex, San Ramon, CA S100 Rabbit polyclonal 1:1600 Dako TRS Dako
3 28 RR Seethala et al Table 2 Sebaceous and non-sebaceous lymphadenomas Lymphadenomas Age Median (range) Sex (ratio) Size Median (range) Sebaceous (n ¼ 22) 63.5 years (35 84) 9F:12M (1:1.3) 2.9 cm (1 6) Non-sebaceous (n ¼ 11) 65.5 years (11 78) 8F:2M (4:1) 1.5 cm (0.6 5) All lymphadenoma (n ¼ 33) 65 years (11 84) 17F:14M (1.2:1) 2.2 cm (0.6 6) Abbreviations: F, female; M, male. Table 3 Sebaceous lymphadenomas: clinical information Cases Age/sex Site Presentation Size (cm) SL1 42F L parotid Mass 2.2 SL2 48M R parotid Mass for 6 years 3.5 SL3 67F Parotid Unknown 2 SL4 84F L parotid Mass slowly enlarging 3.5 SL5 74F R parotid Mass a 1.5 SL6 74M L parotid Mass slowly enlarging 6 SL7 76M R parotid Mass b 5.5 SL8 53F L parotid Mass 2.9 SL9 59F R parotid Mass 1 SL10 74M R parotid Mass for 6 months 2.3 SL11 55M L neck Mass 2.1 SL12 53M R parotid Mass 5.1 SL13 74M L parotid Mass 3.2 SL14 60M L parotid Mass 1.8 SL15 43F R parotid Mass 2.3 SL16 76M R parotid Mass for 2 months 1.2 SL17 35M L parotid Mass long standing c 3.1 SL18a 54M R buccal Pedunculated mass Unknown SL18b Same patient as above L buccal Pedunculated mass Unknown SL19 64F R parotid Mass for 3 months 2.2 SL20 79M R parotid Mass for 2 months 3.5 SL21 77F R parotid Mass for many years 3.3 Abbreviations: F, female; L, left; M, male; R, right; SL, sebaceous lymphadenoma. Duration of presentation, side and location, when known is mentioned. a Malignant transformation to basal cell. b Malignant transformation to sebaceous adenocarcinoma. c Associated with Warthin tumor and sclerosing polycystic adenosis. Table 4 Non-sebaceous lymphadenomas: clinical information Cases Age/sex Site Presentation Size (cm) NSL1 62F L submandibular Mass 5 NSL2 52F Neck Mass 1.1 NSL3 76M R parotid Mass 1.5 NSL4 a 78F R cervical lymph node Mass 0.9 NSL5 66F L parotid Mass 2 NSL6 70F R parotid Mass 2.1 NSL7 11F L parotid Mass 3.5 NSL8a b 70M R Intraparotid lymph node Unknown 1.2 NSL8b b Same patient as above Same as above Unknown 0.6 NSL9 65F L parotid Mass for 4 months 1.5 NSL11 60F R submandibular Mass 2.9 Abbreviations: F, female; L, left; M, male; R, right; NSL, non-sebaceous lymphadenoma. Duration of presentation when known is mentioned. a History of low-grade salivary duct carcinoma. b Associated with chronic lymphocytic leukemia. for several years including one with breast carcinoma (patients SL16 and SL20; Table 3). Thus, in 7 of the 23 patients (30%) there was history of immunomodulatory drug therapy for autoimmune diseases, cancer chemotherapy or preexisting low-grade malignancies. The tumors were resected in 22 of 23 patients, the excisions designated as parotidectomy in 18 (superficial 5, deep 1, and not specified
4 RR Seethala et al 29 Figure 1 Sebaceous lymphadenoma. (a, b) Sixty-four-year-old woman (SL19): contrast enhanced computerized tomography shows a well-defined mass (arrow) in the right preauricular area (a). The tumor was firm and well circumscribed, measured 2.2 cm in size and had a tan, homogeneous cut surface (b). (c, d) Seventy-nine-year-old man with a 3.5-cm encapsulated mass in the right parotid (SL20). The cut surface is tan yellow and multicystic (c) with cysts measuring up to 5 mm (d). 12). No recurrences were noted in 11 patients with follow-up ranging from 1 to 8 years (median 2.5 years). Pathology All tumors were well circumscribed with a median size of 2.2 cm, and 28 of 33 (84%) tumors were encapsulated (Figures 1b d). Twenty-four of thirtythree (72%) tumors were homogenous, multicystic, gray-tan to yellow. The cyst contents in four grossly cystic tumors were gelatinous, yellow sebum like, and chalky white in one case each, and not specified in the fourth tumor. Microscopically, in sebaceous LAD the epithelial component comprising solid nests, trabeculae, cords, glands, and tubules of basal, glandular,
5 30 RR Seethala et al squamous, and sebaceous cells (Figures 2a c). Most cell clusters had a basal cell layer at the periphery, and solid or cystic centers. Tubuloglandular structures showed two cell layers with an outer basal cell layer and an inner luminal glandular cell layer comprising cuboidal or low columnar cells. Keratinization was frequent in squamous cells. Clusters of sebaceous cells, tubules, and cysts with sebaceous cells in lining epithelium were frequent. Cyst contents were keratinous material, eosinophilic proteinaceous fluid, or sebaceous secretions. In non-sebaceous LAD, the epithelial component comprising predominantly solid cords and trabeculae of basal cells admixed with low columnar cells around tubuloglandular spaces without any sebaceous differentiation (Figures 3a and b). Squamous differentiation with keratinization was seen less frequently (2/11, 18%). The lymphocytic infiltrate comprising mixed populations of B and T lymphocytes was prominent in all LAD, with germinal centers in 28 of 33 (84%) tumors (Figure 2d). Stromal foreign body type giant cell granulomatous reaction (Figure 2d) was frequently noted in association with ruptured cyst in sebaceous LAD (n ¼ 11/22, 50%), and less frequently in non-sebaceous LAD (n ¼ 2/11, 18%). Intraepithelial B and T lymphocytes were noted in 13 of 13 tumors, but were remarkable in only 1 case (Figure 3b). Five tumors appeared to be intranodal with intact lymph node capsule. Two of these (40%) also had adjacent normal salivary tissue elements within the lymph node. Oncocytic change was seen in a combined sebaceous LAD and Warthin tumor that was associated with an adjacent sclerosing polycystic adenosis tumor within the same parotid gland (patient SL17; Table 3). The epithelial cells were typically negative for mucin by mucicarmine stain (8/8 tumors). Intraluminal mucin was occasionally detected (2/8 tumors). Periodic Schiff s stain (with and without diastase) highlighted the basement membrane and stained the intraluminal secretions (5/5) cases. Figure 2 Sebaceous lymphadenoma (a, b from SL19, same case as in Figures 1a and b). The tumor is biphasic with epithelial and lymphoid components, and is separated from the adjacent uninvolved parotid gland by a thin fibrous capsule (a, 10). Solid and microcystic clusters with squamous and sebaceous differentiation on the inside and basal cells on the outside. Focal keratinization (arrow) is seen (b, 40). Sebaceous lymphadenoma (SL17) showing a cyst lined by columnar cells, large foamy sebaceous cells, a small area of squamous cells (arrow) and basal cells at the periphery (c, 40). Foreign body type giant cell reaction to ruptured cyst contents is seen adjacent to a lymphoid follicle with germinal center (d, 20).
6 RR Seethala et al 31 Figure 3 Non-sebaceous lymphadenoma in an 11-year-old girl (NSL7) showing solid clusters of basaloid cells with keratinizing (arrows) squamous cells (a, 20) and low columnar cells lining tubules with intraepithelial lymphocytes (b, 40). Table 5 Ancillary studies in lymphadenomas Study Sebaceous lymphadenoma Non-sebaceous lymphadenoma All tumors Immunohistochemistry Basal cell markers p63 11/11 7/7 18/18 (100%) HMWK 3/3 2/2 5/5 (100%) CK5/6 8/8 1/1 9/9 (100%) Epithelial markers CK7 8/8 4/4 12/12 (100%) CK20 1/7 0/4 1/11 (0.9%) Myoepithelial markers (calponin, 3/8 3/8 6/16 (37.5%) SMA, SMMS, S100) Proliferation index (Ki-67) a 0/3 0/2 0/5 Lymphoid component Reactive mixed B and T cells 4/4 2/4 b 6/8 b (75%) Viral markers HPV 0/9 0/2 0/11 (0%) P16 7/8 0/2 0/10 c HPV-ISH 0/5 0/2 0/7 EBV 0/7 0/6 0/13 (0%) EBER 0/7 0/4 0/11 EBV-LMP 0/3 0/3 HHV-8 (KSHV) 0/6 0/2 0/8 (0%) a Proliferation index was evaluated in epithelial cells and considered negative when o5%. b The lymphoid component was immunophenotypically consistent with CLL in one patient with preexisting diagnosis of CLL. c Strong, diffuse nuclear and cytoplasmic expression of p16 has been correlated with HPV infection and was not seen in any tumor. IHC results are summarized in Table 5. The basal cells were positive for at least one of the basal cell markers (p63, CK5/6, and/or high molecular weight keratin) in all cases that were tested. In tubuloglandular structures, the luminal cells expressed CK7 while the abluminal basal cells, sebaceous and squamous cells were negative. All tumors were negative for CK20 except for focal expression in a sebaceous LAD. Myoepithelial markers (calponin, smooth muscle actin, smooth muscle myosin, and/ or S100 protein) were negative in 10 of 16 cases (63%), and focally expressed in a few abluminal basaloid cells in 5 tumors. Proliferation marker (Ki-67) showed appropriately intense expression in the germinal centers but absent or occasional expression (o5%) in epithelial cells. The lymphoid population was reactive and mixed B- and T-cell types. The germinal centers were populated by B cells (CD20 and/or CD79a positive) and the interfollicular areas by T cells (CD3 and/or CD5) as seen in reactive follicular hyperplasia. Intraepithelial lymphocytes were T-cell type in one, and mixed B-and T-cell types in another tumor where their immunophenotype was examined. In one patient
7 32 RR Seethala et al with two non-sebaceous LAD in the right parotid, the lymphoid infiltrate was malignant, positive for CD20, CD5, CD23, and negative for cyclin D1, consistent with his preexisting chronic lymphocytic leukemia (patient NSL8a,b in Table 4; Figures 4a c). Viral Studies Focal weak-to-moderate p16 expression was noted in epithelial cells in 8 of 10 cases, but none showed strong, diffuse nuclear and cytoplasmic expression of p16 as is typical of HPV-associated squamous cell carcinomas. None of the tumors tested were positive for HPV, EBV, and HHV-8 (Table 5). Malignant Transformation and Associated Salivary Gland Pathology Two sebaceous LADs showed malignant transformation: a 74-year-old woman developed basal cell adenocarcinoma (patient SL5; Table 3; Figures 5a and b) and a 76-year-old man developed sebaceous carcinoma (patient SL7; Table 3; Figures 5c and d). Both tumors showed benign component and areas of transition from benign to malignant (Figures 5b and c). The diagnosis of malignancy was based on mitoses and increased cellularity in basal cell adenocarcinoma where the tumor cells remained monomorphic (Figure 5a). In the sebaceous carcinoma, there was significant cytologic atypia, nuclei were large and vesicular with prominent nucleoli, and the cytoplasm was foamy (Figures 5c and d). A 70-year-old man with preexisting chronic lymphocytic leukemia developed two non-sebaceous LAD in two intraparotid lymph nodes in the right parotid (patient NSL8; Table 4; Figure 4). A 78-year-old woman with intranodal nonsebaceous LAD in the right neck had prior history of low-grade intraductal carcinoma in the right parotid gland (patient NSL4; Table 4). The LAD was morphologically not consistent with metastatic adenocarcinoma. No follow-up was available in these patients after resection of their LAD. A 35-year-old man (patient SL17; Table 3) had combined sebaceous LAD and Warthin tumor associated with an adjacent but separate sclerosing polycystic adenosis tumor. Figure 4 (a c) Non-sebaceous lymphadenoma in a 70-year-old man with chronic lymphocytic leukemia (NSL8). The basaloid epithelial cells are arranged in solid clusters and cords with intraepithelial and stromal malignant small B lymphocytes (a, 40) that are positive for CD20 (b, 40) and CD5 (c, 40).
8 RR Seethala et al 33 Figure 5 Malignant transformation in lymphadenoma. (a b) Seventy-four-year-old man with 1.5 cm sebaceous lymphadenoma in the right parotid gland. Tumor shows an area of basal cell adenocarcinoma comprising sheets of monomorphic basaloid cells with frequent mitoses (arrows, a, 40). The capsule is intact and benign areas consistent with lymphadenoma are present within the tumor (b, 40). (c, d) Sebaceous carcinoma arising in a sebaceous lymphadenoma with area of transition between benign (upper left) and malignant (lower right) epithelial cells (c, 40). Tumor cells show significant cytologic atypia with abundant foamy cytoplasm, large pleomorphic vesicular nuclei, and prominent nucleoli (d, 40). Discussion We present clinicopathological and immunophenotypic profile of 33 salivary LAD, the largest series to date. Our observations confirm that LADs are typically benign tumors affecting adults over the age of 50 years (84%), and two thirds of them show some sebaceous differentiation. Interestingly, 48% of patients in the current series suffered from additional co-morbidities, including a subset (30%) that received immunomodulatory drug therapy for autoimmune diseases and/or chemotherapy for cancers, or had associated low-grade malignancies, raising the question of altered immune status as a predisposing factor. Multiple co-morbidities may be coincidental given the advanced age of most patients, although chronic diseases may further alter immune status. We questioned a possible viral etiology but found no evidence of EBV, HPV, and HHV-8 viruses. Negative results with in situ hybridization for EBER have been reported previously in three non-sebaceous LAD. 6,16 We add another 13 tumors that were negative for EBV. To the best of our knowledge, this is the first study exploring the role of HPV or HHV-8 viruses in LAD. Sebaceous LAD showed a slight male preponderance (1.3 1). This is similar to other sebaceous salivary gland tumors. 2 This may be due to the generally higher concentration of sebaceous glands in men than in women, associated with the higher density of facial hair in the former. Additionally, the site distribution of sebaceous LAD mirrors the distribution of sebaceous rests seen in salivary glands and the oral cavity. Sebaceous cells have been found in 30 40% of normal adult parotid glands 3 and 6% of submandibular glands. 2 Fordyce granules in the buccal mucosa comprising sebaceous glands and may be seen in as many as 80% of normal adults. 3 Despite this, salivary tumors with
9 34 RR Seethala et al sebaceous differentiation are rare. Intraoral sebaceous LAD was first reported by Gnepp and Brannon, 2 included in a series of 21 sebaceous tumors of the salivary gland. Origin in the Fordyce granuloma has been proposed. 19 To date, 11 non-sebaceous LAD have been reported in the literature, the largest series comprising three cases only. 6,16 We add another 11 cases. Unlike their sebaceous counterparts, the non-sebaceous tumors were more common in women than in men, similar to most salivary gland tumors. Additionally, 40% of the patients had extraparotid nonsebaceous LAD in contrast to sebaceous LAD that was intraparotid in nearly 90% of patients. No other demographic, clinical, or pathologic differences were found in these two subtypes. Some investigators argue that non-sebaceous LAD may not be a distinct entity but rather a basal cell adenoma or cystadenoma with extensive lymphoid infiltrate. 4,6,9,11 The non-sebaceous LAD tend to have more focal keratinization, less peripheral palisading, generally lack the production of basement membrane material and have a small or non-existent myoepithelial component as compared with basal cell adenomas. 6,12 14,16 The prominent reactive mixed B- and T-cell proliferation with germinal centers is identical to follicular hyperplasia of reactive lymph nodes, and is a defining feature of LAD. We frequently noted a granulomatous reaction in sebaceous LAD, likely secondary to ruptured cyst contents. The possibility that LAD are intranodal tumors arising in intranodal sebaceous or salivary inclusions akin to Warthin tumor has been proposed. 1 3 In a recent report, Dardick and Thomas 13 used a definition of nonsebaceous LAD that excluded cases with any evidence of lymph node architecture. Our diagnostic criteria are admittedly more liberal in that one sebaceous and four non-sebaceous LADs in the current series were intranodal, three in cervical lymph nodes, and two in intraparotid lymph nodes. Intraparotid and cervical nodes in the vicinity of the parotid may have salivary inclusions, and as such may develop primary intranodal salivary gland neoplasms, both benign and malignant. Thus, we felt that it was justifiable to retain these cases for this study. In fact, two of the intranodal tumors also had normal salivary tissue elements within the lymph node. LADs are exceedingly rare in children with only four reported cases (Table 6). 6,16,20,21 To our knowledge, the 11-year-old girl in the present series is the youngest patient with LAD. Table 6 shows a trend to non-sebaceous LAD in the children. This may be because sebaceous differentiation in salivary glands develops later in life and is not present in infants and children. 3 Mayorga et al 22 reported a sebaceous LAD arising in association with acinic cell carcinoma in the parotid gland in a 78-year-old woman. The current series includes seven patients with synchronous or Table 6 Review of lymphadenomas in children Reports Age/ sex Lymphadenoma Location Size (cm) Ma et al 6 13M Non-sebaceous Preauricular 3 Rawlinson et al 20 13F Sebaceous Left parotid 2.4 Chang et al 16 15F Non-sebaceous Right parotid 4.5 Sun et al 21 16M Sebaceous Left parotid 2.4 Current series 11F Non-sebaceous Left parotid 3.5 metachronous salivary or non-salivary malignant tumors. Two sebaceous LAD in the current series showed transformation into basal cell adenocarcinoma and sebaceous carcinoma, respectively. Carcinomatous change is rare in LAD, and should be suspected when the epithelial component in an otherwise typical LAD begins to show frequent mitoses and significant cytologic atypia with areas of transition from benign to malignant, even in the absence of infiltration of the tumor capsule. Among the five reported cases of sebaceous lymphadenocarcinoma including one in the current series and four in the literature, there were four men and one woman. 2,23,24 Rarely, LAD may be associated with other benign salivary tumors as in one of our cases where a 35-year-old man had a combined sebaceous LAD and Warthin tumor, adjacent to a separate sclerosing polycystic adenosis tumor. 18 Both sebaceous and non-sebaceous LAD raise several differential diagnostic considerations, 13 most important being metastatic low-grade adenocarcinoma and adenosquamous carcinoma involving intraparotid lymph node. Nodal metastasis is not the primary presentation in low-grade adenocarcinomas. Mitoses in LAD are restricted to the germinal centers in the lymphoid component, and were absent or rare in the epithelial cells. Epithelial cells in LAD do not show cellular atypia or other overt features of malignancy. The lack of sinusoidal pattern of epithelial growth may be helpful in ruling out nodal metastasis. Primary or metastatic lymphoepithelial carcinoma may mimic non-sebaceous LAD; however, severe atypia, brisk mitosis, infiltrating growth, and frequent association with EBV distinguish them from benign tumors. Tumor cell nests in lymphoepithelial carcinoma tend to be more syncytial in nature, comprising cells with indistinct membranes and characteristic large vesicular nuclei with prominent nucleoli. Mucoepidermoid carcinoma may occasionally show prominent lymphoid stroma and focal sebaceous differentiation. Identification of the three basic cell types, epidermoid, intermediate and, especially, mucous cells, and the absence of keratinization are useful features in recognizing mucoepidermoid carcinoma. Additionally, when present, infiltration may help distinguish mucoepidermoid carcinoma from LAD. Occasionally, the lymphoid component may lead to the consideration of lymphoma. Demonstration of
10 RR Seethala et al 35 mixed B and T cells and lack of light chain restriction should help rule it out. Among benign conditions lymphoepithelial cysts, lymphoepithelial sialadenitis and other salivary gland tumors with sebaceous differentiation may need to be distinguished from LAD. Lymphoepithelial cysts tend to be multifocal and bilateral, and do not have the distinct circumscription and encapsulation seen in LAD. Lymphoepithelial sialadenitis tends to involve the gland diffusely. Of note, none of our LAD arose in the setting of lymphoepithelial sialadenitis. In fine needle aspirations, LAD may be mistaken for Warthin tumor due to their lymphoid contents, 15,21 but the absence of oncocytic cells should help rule out the latter. In summary, LADs are encapsulated, benign solid and/or cystic tumors of major salivary glands affecting patient in their sixth to eighth decade. A remarkable female preponderance was noted for non-sebaceous LAD, similar to other salivary gland tumors, and in contrast to sebaceous LAD, that showed a slight male predilection. The former is also more frequently extraparotid compared with the latter. The prominent reactive lymphoid proliferation is a defining feature. Basal cells appear to be the most predominant epithelial component with frequent sebaceous and squamous differentiation, and show little proliferative activity. Myoepithelial cell participation appears to be insignificant in this neoplastic process. Synchronous or metachronous salivary or non-salivary tumors may be associated with some LAD. Malignant transformation may rarely occur in the epithelial component. Although the etiology remains unknown, altered immune status may be a risk factor in a subset of patients. Disclosure/conflict of interest The authors declare no conflict of interest. References 1 McGavran MH, Bauer WC, Ackerman LV. Sebaceous lymphadenoma of the parotid salivary gland. Cancer 1960;13: Gnepp DR, Brannon R. Sebaceous neoplasms of salivary gland origin. Report of 21 cases. Cancer 1984;53: Batsakis JG, el-naggar AK. Sebaceous lesions of salivary glands and oral cavity. Ann Otol Rhinol Laryngol 1990;99: Auclair PL. Tumor-associated lymphoid proliferation in the parotid gland. A potential diagnostic pitfall. Oral Surg Oral Med Oral Pathol 1994;77: Bos I, Meyer S, Merz H. Lymphadenoma of the parotid gland without sebaceous differentiation. Immunohistochemical investigations. Pathologe 2004;25: Ma J, Chan JK, Chow CW, et al. Lymphadenoma: a report of three cases of an uncommon salivary gland neoplasm. Histopathology 2002;41: Gnepp DR, Henley JD, Simpson RHW, et al. Salivary and Lacrimal glands. In: Gnepp DR (ed). Diagnostic Surgical Pathology of the Head and Neck. 2nd edn. Elsevier: Philadelphia, 2009, pp Kwon GY, Kim EJ, Go JH. Lymphadenoma arising in the parotid gland: a case report. Yonsei Med J 2002;43: Chang JY, Hsiao CH. Lymphadenoma lacking sebaceous differentiation in the parotid gland. J Formos Med Assoc 2004;103: Musthyala NB, Low SE, Seneviratne RH. Lymphadenoma of the salivary gland: a rare tumour. J Clin Pathol 2004;57: Cheuk W, Chan JK. Advances in salivary gland pathology. Histopathology 2007;51: Yang S, Chen X, Wang L, et al. Non-sebaceous lymphadenoma of the salivary gland: case report with immunohistochemical investigation. Virchows Arch 2007;450: Dardick I, Thomas MJ. Lymphadenoma of parotid gland: Two additional cases and a literature review. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 2008;105: Gallego L, Junquera L, Fresno MF. Non-sebaceous lymphadenoma of the parotid gland: immunohistochemical study and DNA ploidy analysis. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 2009;107: Castelino-Prabhu S, Li QK, Ali SZ. Nonsebaceous lymphadenoma of the parotid gland: cytopathologic findings and differential diagnosis. Diagn Cytopathol 2010;38: Chang KT, Chadha NK, Leung R, et al. Lymphadenoma: case report of a rare salivary gland tumor in childhood. Pediatr Dev Pathol 2010;13: Begum S, Gillison ML, Ansari-Lari MA, et al. Detection of human papillomavirus in cervical lymph nodes: a highly effective strategy for localizing site of tumor origin. Clin Cancer Res 2003;9: Gnepp DR, Wang LJ, Brandwein-Gensler M, et al. Sclerosing polycystic adenosis of the salivary gland: a report of 16 cases. Am J Surg Pathol 2006;30: Abdool RA, Solomon LW, Papageorge MB. A clinicopathologic correlation. Sebaceous lymphadenoma. J Mass Dent Soc 2008;57: Rawlinson NJ, Almarzooqi S, Nicol K. Sebaceous lymphadenoma of the parotid gland in a 13-year-old girl: a case report. Head Neck Pathol 2010;4: Sun G, Hu Q, Huang X, et al. Sebaceous lymphadenoma of parotid gland in a child. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 2009;107: Mayorga M, Fernandez N, Val-Bernal JF. Synchronous ipsilateral sebaceous lymphadenoma and acinic cell adenocarcinoma of the parotid gland. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 1999;88: Linhartova A. Sebaceous glands in salivary gland tissue. Arch Pathol 1974;98: Croitoru CM, Mooney JE, Luna MA. Sebaceous lymphadenocarcinoma of salivary glands. Ann Diagn Pathol 2003;7:
Lymphadenoma of the salivary gland: Report of 10 cases
 ONCOLOGY LETTERS 7: 1097-1101, 2014 Lymphadenoma of the salivary gland: Report of 10 cases GUANGLONG LIU 1,2, JIE HE 1, CHUNYE ZHANG 3, SHUITING FU 1,2 and YUE HE 1 1 Department of Oral and Maxillofacial
ONCOLOGY LETTERS 7: 1097-1101, 2014 Lymphadenoma of the salivary gland: Report of 10 cases GUANGLONG LIU 1,2, JIE HE 1, CHUNYE ZHANG 3, SHUITING FU 1,2 and YUE HE 1 1 Department of Oral and Maxillofacial
My Journey into the World of Salivary Gland Sebaceous Neoplasms
 My Journey into the World of Salivary Gland Sebaceous Neoplasms Douglas R. Gnepp Warren Alpert Medical School at Brown University Rhode Island Hospital Pathology Department Providence RI Asked to present
My Journey into the World of Salivary Gland Sebaceous Neoplasms Douglas R. Gnepp Warren Alpert Medical School at Brown University Rhode Island Hospital Pathology Department Providence RI Asked to present
Oncocytic-Appearing Salivary Gland Tumors. Oncocytic, Cystic, Mucinous, and High Grade Salivary Gland Tumors SALIVARY GLAND FNA: PART II
 William C. Faquin, MD, PhD Professor of Pathology Harvard Medical School Director of Head and Neck Pathology Massachusetts Eye and Ear Massachusetts General Hospital SALIVARY GLAND FNA: PART II Oncocytic,
William C. Faquin, MD, PhD Professor of Pathology Harvard Medical School Director of Head and Neck Pathology Massachusetts Eye and Ear Massachusetts General Hospital SALIVARY GLAND FNA: PART II Oncocytic,
Salivary Glands 3/7/2017
 Salivary Glands 3/7/2017 Goals and objectives Focus on the entities unique to H&N Common board type facts Information for your future practice Salivary Glands Salivary Glands Major gland. Paratid. Submandibular.
Salivary Glands 3/7/2017 Goals and objectives Focus on the entities unique to H&N Common board type facts Information for your future practice Salivary Glands Salivary Glands Major gland. Paratid. Submandibular.
Objectives. Salivary Gland FNA: The Milan System. Role of Salivary Gland FNA 04/26/2018
 Salivary Gland FNA: The Milan System Dr. Jennifer Brainard Section Head Cytopathology Cleveland Clinic Objectives Introduce the Milan System for reporting salivary gland cytopathology Define cytologic
Salivary Gland FNA: The Milan System Dr. Jennifer Brainard Section Head Cytopathology Cleveland Clinic Objectives Introduce the Milan System for reporting salivary gland cytopathology Define cytologic
Lesions Mimicking Adenoid Cystic Carcinoma. Diagnostic Problems in Salivary Gland Pathology An Update 5/29/2009
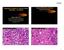 Diagnostic Problems in Salivary Gland Pathology An Update Lesions Mimicking Adenoid Cystic Carcinoma Stacey E. Mills, M.D. W.S. Royster Professor of Pathology Director of Surgical and Cytopathology University
Diagnostic Problems in Salivary Gland Pathology An Update Lesions Mimicking Adenoid Cystic Carcinoma Stacey E. Mills, M.D. W.S. Royster Professor of Pathology Director of Surgical and Cytopathology University
Update in Salivary Gland Pathology. Benjamin L. Witt University of Utah/ARUP Laboratories February 9, 2016
 Update in Salivary Gland Pathology Benjamin L. Witt University of Utah/ARUP Laboratories February 9, 2016 Objectives Review the different appearances of a selection of salivary gland tumor types Establish
Update in Salivary Gland Pathology Benjamin L. Witt University of Utah/ARUP Laboratories February 9, 2016 Objectives Review the different appearances of a selection of salivary gland tumor types Establish
Los Angeles Society Of Pathologists Dr. Shobha Castelino Prabhu
 Los Angeles Society Of Pathologists Dr. Shobha Castelino Prabhu Loma Linda University Medical Center June 12, 2007 CASE 1 76 year-old gentleman Status post right parotidectomy 1 year ago for a rare tumor
Los Angeles Society Of Pathologists Dr. Shobha Castelino Prabhu Loma Linda University Medical Center June 12, 2007 CASE 1 76 year-old gentleman Status post right parotidectomy 1 year ago for a rare tumor
Salivary Gland Cytology
 Salivary Gland Cytology Diagnostic challenges and potential pitfalls Tarik M. Elsheikh, MD Professor and Medical Director Anatomic Pathology Cleveland Clinic FNA Salivary Gland Lesions Indications Distinguish
Salivary Gland Cytology Diagnostic challenges and potential pitfalls Tarik M. Elsheikh, MD Professor and Medical Director Anatomic Pathology Cleveland Clinic FNA Salivary Gland Lesions Indications Distinguish
Salivary gland tumor cytologic and histologic correlation: Algorithmic and risk stratification based approaches
 Salivary gland tumor cytologic and histologic correlation: Algorithmic and risk stratification based approaches Christopher C. Griffith, MD, PhD Raja R. Seethala, MD 1. Salivary gland tumor cytology: A
Salivary gland tumor cytologic and histologic correlation: Algorithmic and risk stratification based approaches Christopher C. Griffith, MD, PhD Raja R. Seethala, MD 1. Salivary gland tumor cytology: A
ARIZONA SOCIETY OF PATHOLOGISTS 13 TH APRIL 2013 HEAD AND NECK CYTOPATHOLOGY. F ZAHRA ALY, MD, PhD
 ARIZONA SOCIETY OF PATHOLOGISTS 13 TH APRIL 2013 HEAD AND NECK CYTOPATHOLOGY F ZAHRA ALY, MD, PhD The main areas sites amenable for cytopathology include lymph nodes, thyroid, major salivary glands especially
ARIZONA SOCIETY OF PATHOLOGISTS 13 TH APRIL 2013 HEAD AND NECK CYTOPATHOLOGY F ZAHRA ALY, MD, PhD The main areas sites amenable for cytopathology include lymph nodes, thyroid, major salivary glands especially
Papillary Lesions of the breast
 Papillary Lesions of the breast Emad Rakha Professor of Breast Pathology The University of Nottingham Papillary lesions of the breast are a heterogeneous group of disease, which are characterised by neoplastic
Papillary Lesions of the breast Emad Rakha Professor of Breast Pathology The University of Nottingham Papillary lesions of the breast are a heterogeneous group of disease, which are characterised by neoplastic
3/28/2017. Head and Neck/Endocrine Pathology Specialty Conference Case 4 Raja R. Seethala, M.D. University of Pittsburgh Medical Center
 Head and Neck/Endocrine Pathology Specialty Conference Case 4 Raja R. Seethala, M.D. University of Pittsburgh Medical Center Disclosure of Relevant Financial Relationships Disclosure of Relevant Financial
Head and Neck/Endocrine Pathology Specialty Conference Case 4 Raja R. Seethala, M.D. University of Pittsburgh Medical Center Disclosure of Relevant Financial Relationships Disclosure of Relevant Financial
FNA OF SALIVARY GLANDS: A PRACTICAL APPROACH
 FNA OF SALIVARY GLANDS: A PRACTICAL APPROACH FNA of Salivary Glands: Challenges Wide range of neoplastic and non-neoplastic lesions Cytological overlap between the different benign and malignant tumors
FNA OF SALIVARY GLANDS: A PRACTICAL APPROACH FNA of Salivary Glands: Challenges Wide range of neoplastic and non-neoplastic lesions Cytological overlap between the different benign and malignant tumors
04/09/2018. Salivary Gland Pathology in the Molecular Era Old Friends, Old Foes, & New Acquaintances
 Salivary Gland Pathology in the Molecular Era Old Friends, Old Foes, & New Acquaintances Jennifer L. Hunt, MD, MEd Aubrey J. Hough Jr, MD, Endowed Professor of Pathology Chair of Pathology and Laboratory
Salivary Gland Pathology in the Molecular Era Old Friends, Old Foes, & New Acquaintances Jennifer L. Hunt, MD, MEd Aubrey J. Hough Jr, MD, Endowed Professor of Pathology Chair of Pathology and Laboratory
Fine-needle aspiration (FNA) has been used increasingly
 Worrisome Histologic Alterations Following Fine-Needle Aspiration of Benign Parotid Lesions Shiyong Li, MD, PhD; Zubair W. Baloch, MD, PhD; John E. Tomaszewski, MD; Virginia A. LiVolsi, MD Objective. To
Worrisome Histologic Alterations Following Fine-Needle Aspiration of Benign Parotid Lesions Shiyong Li, MD, PhD; Zubair W. Baloch, MD, PhD; John E. Tomaszewski, MD; Virginia A. LiVolsi, MD Objective. To
Papillary Lesions of the Breast A Practical Approach to Diagnosis. (Arch Pathol Lab Med. 2016;140: ; doi: /arpa.
 Papillary Lesions of the Breast A Practical Approach to Diagnosis (Arch Pathol Lab Med. 2016;140:1052 1059; doi: 10.5858/arpa.2016-0219-RA) Papillary lesions of the breast Span the spectrum of benign,
Papillary Lesions of the Breast A Practical Approach to Diagnosis (Arch Pathol Lab Med. 2016;140:1052 1059; doi: 10.5858/arpa.2016-0219-RA) Papillary lesions of the breast Span the spectrum of benign,
Diseases of the breast (1 of 2)
 Diseases of the breast (1 of 2) Introduction A histology introduction Normal ducts and lobules of the breast are lined by two layers of cells a layer of luminal cells overlying a second layer of myoepithelial
Diseases of the breast (1 of 2) Introduction A histology introduction Normal ducts and lobules of the breast are lined by two layers of cells a layer of luminal cells overlying a second layer of myoepithelial
USCAP 2012: Companion Meeting of the AAOOP. Update on lacrimal gland neoplasms: Molecular pathology of interest
 USCAP 2012: Companion Meeting of the AAOOP Vancouver BC, Canada, March 17, 2012 Update on lacrimal gland neoplasms: Molecular pathology of interest Valerie A. White MD, MHSc, FRCPC Department of Pathology
USCAP 2012: Companion Meeting of the AAOOP Vancouver BC, Canada, March 17, 2012 Update on lacrimal gland neoplasms: Molecular pathology of interest Valerie A. White MD, MHSc, FRCPC Department of Pathology
Educational Cases EQA November T.J. Palmer Raigmore Hospital Inverness
 Educational Cases EQA November 2013 T.J. Palmer Raigmore Hospital Inverness Case 2 Clinical Details Dob 11 February 1951 PMH: 1964 Extraction of 45 aet 13 yr 1966 Cyst between 44 and 46 enucleated 1973
Educational Cases EQA November 2013 T.J. Palmer Raigmore Hospital Inverness Case 2 Clinical Details Dob 11 February 1951 PMH: 1964 Extraction of 45 aet 13 yr 1966 Cyst between 44 and 46 enucleated 1973
Review and Updates of Immunohistochemistry in Selected Salivary Gland and Head and Neck Tumors
 Review and Updates of Immunohistochemistry in Selected Salivary Gland and Head and Neck Tumors. Monophasic tumors : myoepithelioma, acinic cell carcinoma, and salivary duct carcinoma. Biphasic tumors includes
Review and Updates of Immunohistochemistry in Selected Salivary Gland and Head and Neck Tumors. Monophasic tumors : myoepithelioma, acinic cell carcinoma, and salivary duct carcinoma. Biphasic tumors includes
Slide Seminar of the Head and Neck Session of the European Congress of Pathology Bilbao, Spain, 2018.
 Slide Seminar of the Head and Neck Session of the European Congress of Pathology Bilbao, Spain, 2018. Prof Sulen Sarioglu, MD Dokuz Eylul University Faculty of Medicine Department of Pathology Graduate
Slide Seminar of the Head and Neck Session of the European Congress of Pathology Bilbao, Spain, 2018. Prof Sulen Sarioglu, MD Dokuz Eylul University Faculty of Medicine Department of Pathology Graduate
CASE REPORT Malignant transformation of breast ductal adenoma: a diagnostic pitfall
 Malaysian J Pathol 2015; 37(3) : 281 285 CASE REPORT Malignant transformation of breast ductal adenoma: a diagnostic pitfall Hiroko HAYASHI, Hiroshi OHTANI,* Junzo YAMAGUCHI,** and Isao SHIMOKAWA Department
Malaysian J Pathol 2015; 37(3) : 281 285 CASE REPORT Malignant transformation of breast ductal adenoma: a diagnostic pitfall Hiroko HAYASHI, Hiroshi OHTANI,* Junzo YAMAGUCHI,** and Isao SHIMOKAWA Department
Mammary analogue secretory carcinoma of salivary gland A case report of new entity
 Case Report Mammary analogue secretory carcinoma of salivary gland A case report of new entity Vaibhav Bhika Bari 1*, Sandhya Unmesh Bholay 2 1 Assistant Professor, 2 Associate Professor Rajiv Gandhi Medical
Case Report Mammary analogue secretory carcinoma of salivary gland A case report of new entity Vaibhav Bhika Bari 1*, Sandhya Unmesh Bholay 2 1 Assistant Professor, 2 Associate Professor Rajiv Gandhi Medical
DISORDERS OF THE SALIVARY GLANDS Neoplasms Dr.M.Baskaran Selvapathy S IV
 DISORDERS OF THE SALIVARY GLANDS Neoplasms Dr.M.Baskaran Selvapathy S IV NEOPLASMS A) Epithelial I. Benign Pleomorphic adenoma( Mixed tumour) Adenolymphoma (Warthin s tumour) Oxyphil adenoma (Oncocytoma)
DISORDERS OF THE SALIVARY GLANDS Neoplasms Dr.M.Baskaran Selvapathy S IV NEOPLASMS A) Epithelial I. Benign Pleomorphic adenoma( Mixed tumour) Adenolymphoma (Warthin s tumour) Oxyphil adenoma (Oncocytoma)
Enterprise Interest None
 Enterprise Interest None What are triple negative breast cancers? A synopsis of their histological patterns Ian Ellis Molecular Medical Sciences, University of Nottingham Department of Histopathology,
Enterprise Interest None What are triple negative breast cancers? A synopsis of their histological patterns Ian Ellis Molecular Medical Sciences, University of Nottingham Department of Histopathology,
doi: /j.anl
 doi: 10.1016/j.anl.2006.07.001 Synchronous unilateral parotid gland neoplasms of three different histological types Shuho Tanaka 1, Keiji Tabuchi 1, Keiko Oikawa 1, Rika Kohanawa 1, Hideki Okubo 1, Dai
doi: 10.1016/j.anl.2006.07.001 Synchronous unilateral parotid gland neoplasms of three different histological types Shuho Tanaka 1, Keiji Tabuchi 1, Keiko Oikawa 1, Rika Kohanawa 1, Hideki Okubo 1, Dai
Low-grade cribriform cystadenocarcinoma arising from a minor salivary gland: a case report
 145 Journal of Oral Science, Vol. 58, No. 1, 145-149, 2016 Case Report Low-grade cribriform cystadenocarcinoma arising from a minor salivary gland: a case report Masashi Kimura 1), Shinji Mii 2), Shinichi
145 Journal of Oral Science, Vol. 58, No. 1, 145-149, 2016 Case Report Low-grade cribriform cystadenocarcinoma arising from a minor salivary gland: a case report Masashi Kimura 1), Shinji Mii 2), Shinichi
3/27/2017. Pulmonary Pathology Specialty Conference. Disclosure of Relevant Financial Relationships. Clinical History:
 Pulmonary Pathology Specialty Conference Saul Suster, M.D. Medical College of Wisconsin Disclosure of Relevant Financial Relationships USCAP requires that all planners (Education Committee) in a position
Pulmonary Pathology Specialty Conference Saul Suster, M.D. Medical College of Wisconsin Disclosure of Relevant Financial Relationships USCAP requires that all planners (Education Committee) in a position
PRELIMINARY CYTOLOGIC DIAGNOSIS: Suspicious for Acinic Cell Carcinoma. Cell Block: Immunohistochemical Studies CYTOLOGIC DIAGNOSIS:
 1 PRELIMINARY CYTOLOGIC DIAGNOSIS: Suspicious for Acinic Cell Carcinoma. Cell Block: Immunohistochemical Studies GCDFP-15 S-100 CYTOLOGIC DIAGNOSIS: Consistent with mammary analogue secretory carcinoma.
1 PRELIMINARY CYTOLOGIC DIAGNOSIS: Suspicious for Acinic Cell Carcinoma. Cell Block: Immunohistochemical Studies GCDFP-15 S-100 CYTOLOGIC DIAGNOSIS: Consistent with mammary analogue secretory carcinoma.
Oncocytic carcinoma: A rare malignancy of the parotid gland
 ISPUB.COM The Internet Journal of Pathology Volume 8 Number 2 Oncocytic carcinoma: A rare malignancy of the parotid gland K Mardi, J Sharma Citation K Mardi, J Sharma.. The Internet Journal of Pathology.
ISPUB.COM The Internet Journal of Pathology Volume 8 Number 2 Oncocytic carcinoma: A rare malignancy of the parotid gland K Mardi, J Sharma Citation K Mardi, J Sharma.. The Internet Journal of Pathology.
THYMIC CARCINOMAS AN UPDATE
 THYMIC CARCINOMAS AN UPDATE Mark R. Wick, M.D. University of Virginia Medical Center Charlottesville, VA CARCINOMA OF THE THYMUS General Clinical Features No apparent gender predilection Age range of 35-75
THYMIC CARCINOMAS AN UPDATE Mark R. Wick, M.D. University of Virginia Medical Center Charlottesville, VA CARCINOMA OF THE THYMUS General Clinical Features No apparent gender predilection Age range of 35-75
Synonyms. Nephrogenic metaplasia Mesonephric adenoma
 Nephrogenic Adenoma Synonyms Nephrogenic metaplasia Mesonephric adenoma Definition Benign epithelial lesion of urinary tract with tubular, glandular, papillary growth pattern Most frequently in the urinary
Nephrogenic Adenoma Synonyms Nephrogenic metaplasia Mesonephric adenoma Definition Benign epithelial lesion of urinary tract with tubular, glandular, papillary growth pattern Most frequently in the urinary
University Journal of Pre and Para Clinical Sciences
 ISSN 2455 2879 Volume 2 Issue 1 2016 Metaplastic carcinoma breast a rare case report Abstract : Metaplastic carcinoma of the breast is a rare malignancy with two distinct cell lines described as a breast
ISSN 2455 2879 Volume 2 Issue 1 2016 Metaplastic carcinoma breast a rare case report Abstract : Metaplastic carcinoma of the breast is a rare malignancy with two distinct cell lines described as a breast
Human Papillomavirus Testing in Head and Neck Carcinomas
 Human Papillomavirus Testing in Head and Neck Carcinomas Guideline from the College of American Pathologists Early Online Release Publication: Archives of Pathology & Laboratory Medicine 12/18/2017 Overview
Human Papillomavirus Testing in Head and Neck Carcinomas Guideline from the College of American Pathologists Early Online Release Publication: Archives of Pathology & Laboratory Medicine 12/18/2017 Overview
Evening Specialty Conference: Cytopathology
 : Cytopathology N. Paul Ohori, M.D. University of Pittsburgh Medical Center Disclosure of Relevant Financial Relationships Disclosure of Relevant Financial Relationships USCAP requires that all planners
: Cytopathology N. Paul Ohori, M.D. University of Pittsburgh Medical Center Disclosure of Relevant Financial Relationships Disclosure of Relevant Financial Relationships USCAP requires that all planners
Small Cell Carcinoma ex-pleomorphic Adenoma of the Parotid Gland
 Head and Neck Pathol (2012) 6:502 506 DOI 10.1007/s12105-012-0376-1 CASE REPORT Small Cell Carcinoma ex-pleomorphic Adenoma of the Parotid Gland Ashley Cimino-Mathews Brian M. Lin Steven S. Chang Kofi
Head and Neck Pathol (2012) 6:502 506 DOI 10.1007/s12105-012-0376-1 CASE REPORT Small Cell Carcinoma ex-pleomorphic Adenoma of the Parotid Gland Ashley Cimino-Mathews Brian M. Lin Steven S. Chang Kofi
DISCUSSION: PLGA accounts for about 2% of all salivary gland tumours and occurs almost exclusively in the minor salivary glands.
 SWELLING ON THE HARD PALATE PRESENTING AS POLYMORPHOUS LOW GRADE ADENOCARCINOMA: A AND REVIEW OF LITERATURE Swapnil D. Chandekar 1, Sunita S. Dantkale 2, Rahul R. Narkhede 3, Snehal V. Chavhan 4, Khushboo
SWELLING ON THE HARD PALATE PRESENTING AS POLYMORPHOUS LOW GRADE ADENOCARCINOMA: A AND REVIEW OF LITERATURE Swapnil D. Chandekar 1, Sunita S. Dantkale 2, Rahul R. Narkhede 3, Snehal V. Chavhan 4, Khushboo
Among the benign intraepithelial melanocytic proliferations, Inflamed Conjunctival Nevi. Histopathological Criteria. Resident Short Reviews
 Resident Short Reviews Inflamed conjunctival nevi (ICN) may suggest malignancy because of their rapid growth and atypical histology. The objective of this study was to characterize the diagnostic features
Resident Short Reviews Inflamed conjunctival nevi (ICN) may suggest malignancy because of their rapid growth and atypical histology. The objective of this study was to characterize the diagnostic features
(CYLINDROMA) ATLAS OF HEAD AND NECK PATHOLOGY ADENOID CYSTIC CARCINOMA
 (CYLINDROMA) This malignant tumor is poorly encapsulated and while seemingly well defined within the affected gland, there is usually infiltration of surrounding tissue on closer examination. The cut surface
(CYLINDROMA) This malignant tumor is poorly encapsulated and while seemingly well defined within the affected gland, there is usually infiltration of surrounding tissue on closer examination. The cut surface
1 NORMAL HISTOLOGY AND METAPLASIAS
 1 NORMAL HISTOLOGY AND METAPLASIAS, MD Anatomy and Histology 1 Metaplasias 2 ANATOMY AND HISTOLOGY The female breast is composed of a branching duct system, which begins at the nipple with the major lactiferous
1 NORMAL HISTOLOGY AND METAPLASIAS, MD Anatomy and Histology 1 Metaplasias 2 ANATOMY AND HISTOLOGY The female breast is composed of a branching duct system, which begins at the nipple with the major lactiferous
Pleomorphic adenoma of breast - a case report and distinction with metaplastic carcinoma D Gupta, S Agrawal, N Trivedi, A Tewari
 of breast - a case report and distinction with metaplastic carcinoma D Gupta, S Agrawal, N Trivedi, A Tewari Introduction, also known as mixed tumour, is a benign tumour which typically presents as a painless,
of breast - a case report and distinction with metaplastic carcinoma D Gupta, S Agrawal, N Trivedi, A Tewari Introduction, also known as mixed tumour, is a benign tumour which typically presents as a painless,
PLEOMORPHIC ADENOMA ( BENIGN MIXED TUMOR )
 ( BENIGN MIXED TUMOR ) Grossly, the tumor is freely movable, solid, sometimes lobulated and occasionally cystic. If recurrent, multinodular masses are common. Histologically, within a fibrous capsule,
( BENIGN MIXED TUMOR ) Grossly, the tumor is freely movable, solid, sometimes lobulated and occasionally cystic. If recurrent, multinodular masses are common. Histologically, within a fibrous capsule,
Ben Witt, MD University of Utah/ARUP Laboratories Assistant Professor of Anatomic Pathology
 Ben Witt, MD University of Utah/ARUP Laboratories Assistant Professor of Anatomic Pathology Review some of the more common cytodiagnoses of the Head and Neck Establish an approach to some of the diagnostic
Ben Witt, MD University of Utah/ARUP Laboratories Assistant Professor of Anatomic Pathology Review some of the more common cytodiagnoses of the Head and Neck Establish an approach to some of the diagnostic
Fine-Needle Aspiration Cytology of Low-Grade Cribriform Cystadenocarcinoma with Many Psammoma Bodies of the Salivary Gland
 The Korean Journal of Pathology 2013; 47: 481-485 CASE STUDY Fine-Needle Aspiration Cytology of Low-Grade Cribriform Cystadenocarcinoma with Many Psammoma Bodies of the Salivary Gland Ji Yun Jeong Dongbin
The Korean Journal of Pathology 2013; 47: 481-485 CASE STUDY Fine-Needle Aspiration Cytology of Low-Grade Cribriform Cystadenocarcinoma with Many Psammoma Bodies of the Salivary Gland Ji Yun Jeong Dongbin
Note: The cause of testicular neoplasms remains unknown
 - In the 15- to 34-year-old age group, they are the most common tumors of men. - Tumors of the testis are a heterogeneous group of neoplasms that include: I. Germ cell tumors : 95%; all are malignant.
- In the 15- to 34-year-old age group, they are the most common tumors of men. - Tumors of the testis are a heterogeneous group of neoplasms that include: I. Germ cell tumors : 95%; all are malignant.
Proliferative Epithelial lesions of the Breast. Sami Shousha, MD, FRCPath Charing Cross Hospital & Imperial College, London
 Proliferative Epithelial lesions of the Breast Sami Shousha, MD, FRCPath Charing Cross Hospital & Imperial College, London Amman, November2013 Proliferative Epithelial Lesions of the Breast Usual type
Proliferative Epithelial lesions of the Breast Sami Shousha, MD, FRCPath Charing Cross Hospital & Imperial College, London Amman, November2013 Proliferative Epithelial Lesions of the Breast Usual type
04/10/2018. Intraductal Papillary Neoplasms Of Breast INTRADUCTAL PAPILLOMA
 Intraductal Papillary Neoplasms Of Breast Savitri Krishnamurthy MD Professor of Pathology Deputy Division Head The University of Texas MD Anderson Cancer Center 25 th Annual Seminar in Pathology Pittsburgh,
Intraductal Papillary Neoplasms Of Breast Savitri Krishnamurthy MD Professor of Pathology Deputy Division Head The University of Texas MD Anderson Cancer Center 25 th Annual Seminar in Pathology Pittsburgh,
Select problems in cystic pancreatic lesions
 Disclosure Select problems in cystic pancreatic lesions Five Prime Therapeutics shareholder Adicet Bio shareholder Bristol-Meyer Squibb advisory board grace.kim@ucsf.edu Pancreatic cystic lesions Intraductal
Disclosure Select problems in cystic pancreatic lesions Five Prime Therapeutics shareholder Adicet Bio shareholder Bristol-Meyer Squibb advisory board grace.kim@ucsf.edu Pancreatic cystic lesions Intraductal
Mody. AIS vs. Invasive Adenocarcinoma of the Cervix
 Common Problems in Gynecologic Pathology Michael T. Deavers, M.D. Houston Methodist Hospital, Houston, Texas Common Problems in Gynecologic Pathology Adenocarcinoma in-situ (AIS) of the Cervix vs. Invasive
Common Problems in Gynecologic Pathology Michael T. Deavers, M.D. Houston Methodist Hospital, Houston, Texas Common Problems in Gynecologic Pathology Adenocarcinoma in-situ (AIS) of the Cervix vs. Invasive
Glycogen-rich adenocarcinoma in the lower lip: report of a case with particular emphasis on differential diagnosis
 Open Journal of Stomatology, 2011, 1, 109-113 doi:10.4236/ojst.2011.13017 Published Online September 2011 (http://www.scirp.org/journal//). Glycogen-rich adenocarcinoma in the lower lip: report of a case
Open Journal of Stomatology, 2011, 1, 109-113 doi:10.4236/ojst.2011.13017 Published Online September 2011 (http://www.scirp.org/journal//). Glycogen-rich adenocarcinoma in the lower lip: report of a case
Gross appearance of nodular hyperplasia in material obtained from suprapubic prostatectomy. Note the multinodular appearance and the admixture of
 Tiền liệt tuyến Tiền liệt tuyến Gross appearance of nodular hyperplasia in material obtained from suprapubic prostatectomy. Note the multinodular appearance and the admixture of solid and microcystic areas.
Tiền liệt tuyến Tiền liệt tuyến Gross appearance of nodular hyperplasia in material obtained from suprapubic prostatectomy. Note the multinodular appearance and the admixture of solid and microcystic areas.
Spinal Cord Compression caused by Metastatic Epithelial Myoepithelial Carcinoma of the Parotid Gland
 Spinal Cord Compression caused by Metastatic Epithelial Myoepithelial Carcinoma of the Parotid Gland Pages with reference to book, From 249 To 250 Irshad N. Soomro,Akber S. Hussainy,Rashida Ahmed,Sheema
Spinal Cord Compression caused by Metastatic Epithelial Myoepithelial Carcinoma of the Parotid Gland Pages with reference to book, From 249 To 250 Irshad N. Soomro,Akber S. Hussainy,Rashida Ahmed,Sheema
Objectives. Atypical Glandular Cells. Atypical Endocervical Cells. Reactive Endocervical Cells
 2013 California Society of Pathologists 66 th Annual Meeting San Francisco, CA Atypical Glandular Cells to Early Invasive Adenocarcinoma: Cervical Cytology and Histology Christina S. Kong, MD Associate
2013 California Society of Pathologists 66 th Annual Meeting San Francisco, CA Atypical Glandular Cells to Early Invasive Adenocarcinoma: Cervical Cytology and Histology Christina S. Kong, MD Associate
Salivary gland Workshop Trondheim 31th may 2012
 Salivary gland Workshop Trondheim 31th may 2012 Peter Jebsen cytopathologist Oslo University Hospital Rikshospitalet Anna Bofin ass. Professor St. Olavs Hospital, Trondheim Drying artifacts Lymfocytes
Salivary gland Workshop Trondheim 31th may 2012 Peter Jebsen cytopathologist Oslo University Hospital Rikshospitalet Anna Bofin ass. Professor St. Olavs Hospital, Trondheim Drying artifacts Lymfocytes
Pitfalls in thyroid tumor pathology. Prof.Valdi Pešutić-Pisac MD, PhD
 Pitfalls in thyroid tumor pathology Prof.Valdi Pešutić-Pisac MD, PhD Too many or... Tumour herniation through a torn capsule simulating capsular invasion fibrous capsule with a sharp discontinuity, suggestive
Pitfalls in thyroid tumor pathology Prof.Valdi Pešutić-Pisac MD, PhD Too many or... Tumour herniation through a torn capsule simulating capsular invasion fibrous capsule with a sharp discontinuity, suggestive
Salivary gland cytology. Salivary gland cytology. Triage helps the clinician. Salivary gland tumors. Diagnostic difficulties
 Salivary gland cytology Salivary Gland Cytology Pınar Fırat, MD Professor of Pathology İ.U. İstanbul Faculty of Medicine Çapa, İstanbul It is a reliable diagnostic test However, definitive subclassification
Salivary gland cytology Salivary Gland Cytology Pınar Fırat, MD Professor of Pathology İ.U. İstanbul Faculty of Medicine Çapa, İstanbul It is a reliable diagnostic test However, definitive subclassification
Biliary tract tumors
 Short Course 2010 Annual Fall Meeting of the Korean Society for Pathologists Biliary tract tumors Joon Hyuk Choi, M.D., Ph.D. Professor, Department of Pathology, Yeungnam Univ. College of Medicine, Daegu,
Short Course 2010 Annual Fall Meeting of the Korean Society for Pathologists Biliary tract tumors Joon Hyuk Choi, M.D., Ph.D. Professor, Department of Pathology, Yeungnam Univ. College of Medicine, Daegu,
Disclosure of Relevant Financial Relationships
 Squamous entities of the thyroid: Reactive to Neoplastic Michelle D. Williams Associate Professor Dept of Pathology, Head & Neck Section University of Texas MD Anderson Cancer Center Disclosure of Relevant
Squamous entities of the thyroid: Reactive to Neoplastic Michelle D. Williams Associate Professor Dept of Pathology, Head & Neck Section University of Texas MD Anderson Cancer Center Disclosure of Relevant
A 60-year old Man with Left Jaw Mass. Simon Chiosea, MD University of Pittsburgh medical Center 3/15/2016
 ACCME/Disclosures The USCAP requires that anyone in a position to influence or control the content of CME disclose any relevant financial relationship WITH COMMERCIAL INTERESTS which they or their spouse/partner
ACCME/Disclosures The USCAP requires that anyone in a position to influence or control the content of CME disclose any relevant financial relationship WITH COMMERCIAL INTERESTS which they or their spouse/partner
BSD 2015 Case 19. Female 21. Nodule on forehead. The best diagnosis is:
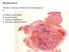 BSD 2015 Case 19 Female 21. Nodule on forehead. The best diagnosis is: A. mixed tumour of skin B. porocarcinoma C. nodular hidradenoma D. metastatic adenocarcinoma BSD 2015 Case 19 Female 21 Nodule on
BSD 2015 Case 19 Female 21. Nodule on forehead. The best diagnosis is: A. mixed tumour of skin B. porocarcinoma C. nodular hidradenoma D. metastatic adenocarcinoma BSD 2015 Case 19 Female 21 Nodule on
Case Presentation. Maha Akkawi, MD, Fatima Obeidat, MD, Tariq Aladily, MD. Department of Pathology Jordan University Hospital Amman, Jordan
 Case Presentation Maha Akkawi, MD, Fatima Obeidat, MD, Tariq Aladily, MD Department of Pathology Jordan University Hospital Amman, Jordan The 25th Annual Congress of the ADIAP The 8/11/2013 1 5th International
Case Presentation Maha Akkawi, MD, Fatima Obeidat, MD, Tariq Aladily, MD Department of Pathology Jordan University Hospital Amman, Jordan The 25th Annual Congress of the ADIAP The 8/11/2013 1 5th International
Journal of International Academy of Forensic Science & Pathology (JIAFP)
 Journal of International Academy of Forensic Science & Pathology (JIAFP) ISSN 2395-0722 MICROCYSTIC ADNEXAL CARCINOMA-A CASE REPORT WITH REVIEW OF LITERATURE Case Report Sulakshana M S 1,Natarajan M 2
Journal of International Academy of Forensic Science & Pathology (JIAFP) ISSN 2395-0722 MICROCYSTIC ADNEXAL CARCINOMA-A CASE REPORT WITH REVIEW OF LITERATURE Case Report Sulakshana M S 1,Natarajan M 2
Case Scenario 1: Thyroid
 Case Scenario 1: Thyroid History and Physical Patient is an otherwise healthy 80 year old female with the complaint of a neck mass first noticed two weeks ago. The mass has increased in size and is palpable.
Case Scenario 1: Thyroid History and Physical Patient is an otherwise healthy 80 year old female with the complaint of a neck mass first noticed two weeks ago. The mass has increased in size and is palpable.
Salivary Gland FNA ATYPICAL : Criteria and Controversies
 Salivary Gland FNA ATYPICAL : Criteria and Controversies W.C. Faquin, M.D., Ph.D. Director, Head and Neck Pathology Massachusetts General Hospital Massachusetts Eye and Ear Infirmary Harvard Medical School
Salivary Gland FNA ATYPICAL : Criteria and Controversies W.C. Faquin, M.D., Ph.D. Director, Head and Neck Pathology Massachusetts General Hospital Massachusetts Eye and Ear Infirmary Harvard Medical School
Spartan Medical Research Journal
 Spartan Medical Research Journal Research at Michigan State University College of Osteopathic Medicine Volume 1 Number 1 Fall 2016 Pages: 66-72 Title: Submandibular Gland Epithelial-Myoepithelial Carcinoma
Spartan Medical Research Journal Research at Michigan State University College of Osteopathic Medicine Volume 1 Number 1 Fall 2016 Pages: 66-72 Title: Submandibular Gland Epithelial-Myoepithelial Carcinoma
SESSION 1: GENERAL (BASIC) PATHOLOGY CONCEPTS Thursday, October 16, :30am - 11:30am FACULTY COPY
 SESSION 1: GENERAL (BASIC) PATHOLOGY CONCEPTS Thursday, October 16, 2008 9:30am - 11:30am FACULTY COPY GOAL: Describe the basic morphologic (structural) changes which occur in various pathologic conditions.
SESSION 1: GENERAL (BASIC) PATHOLOGY CONCEPTS Thursday, October 16, 2008 9:30am - 11:30am FACULTY COPY GOAL: Describe the basic morphologic (structural) changes which occur in various pathologic conditions.
Salivary Gland Pathology
 IN THE NAME OF GOD Salivary Gland Pathology CHAPTER 11 Dr.kheirandish Oral and maxillofacial pathology Sialadenosis Adenomatoid Hyperplasia of the Minor Salivary Glands Necrotizing Sialometaplasia Pleomorphic
IN THE NAME OF GOD Salivary Gland Pathology CHAPTER 11 Dr.kheirandish Oral and maxillofacial pathology Sialadenosis Adenomatoid Hyperplasia of the Minor Salivary Glands Necrotizing Sialometaplasia Pleomorphic
Cystic lymphoid hyperplasia of the parotid gland as the initial manifestation of HIV infection
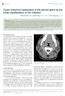 Singapore Med J 2014; 55(1): e12-e16 doi: 10.11622/smedj.2014010 Cystic lymphoid hyperplasia of the parotid gland as the initial manifestation of HIV infection Bingcheng Wu 1, MBBS, Raymond Ngo 2, MBBCh
Singapore Med J 2014; 55(1): e12-e16 doi: 10.11622/smedj.2014010 Cystic lymphoid hyperplasia of the parotid gland as the initial manifestation of HIV infection Bingcheng Wu 1, MBBS, Raymond Ngo 2, MBBCh
Neoplasia 2018 Lecture 2. Dr Heyam Awad MD, FRCPath
 Neoplasia 2018 Lecture 2 Dr Heyam Awad MD, FRCPath ILOS 1. List the differences between benign and malignant tumors. 2. Recognize the histological features of malignancy. 3. Define dysplasia and understand
Neoplasia 2018 Lecture 2 Dr Heyam Awad MD, FRCPath ILOS 1. List the differences between benign and malignant tumors. 2. Recognize the histological features of malignancy. 3. Define dysplasia and understand
4/17/2015. Case 1. A 37 year old man with a 2.2 cm solitary left thyroid mass.
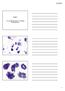 Case 1 A 37 year old man with a 2.2 cm solitary left thyroid mass. Case 1 Case 1 1 Case 1: Diagnosis? A. Benign B. Atypia of undetermined significance/follicular lesion of undetermined significance C.
Case 1 A 37 year old man with a 2.2 cm solitary left thyroid mass. Case 1 Case 1 1 Case 1: Diagnosis? A. Benign B. Atypia of undetermined significance/follicular lesion of undetermined significance C.
Pathology of Selected Head and Neck Lesions. Adel Assaad MD Department of Pathology
 Pathology of Selected Head and Neck Lesions Adel Assaad MD Department of Pathology 1 NOSE Infections 2 Zygomycosis (Mucormycosis) Opportunistic infection caused by "bread mold fungi," including Rhizopus,
Pathology of Selected Head and Neck Lesions Adel Assaad MD Department of Pathology 1 NOSE Infections 2 Zygomycosis (Mucormycosis) Opportunistic infection caused by "bread mold fungi," including Rhizopus,
Myoepithelial carcinoma (malignant myoepithelioma) of the parotid gland arising in a pleomorphic adenoma
 552 Royal Group of Hospitals Trust, Belfast, UK Department of Pathology W G McCluggage P G Toner Department of Otorhinolaryngology W J Primrose Correspondence to: Dr W G McCluggage, Department of Pathology,
552 Royal Group of Hospitals Trust, Belfast, UK Department of Pathology W G McCluggage P G Toner Department of Otorhinolaryngology W J Primrose Correspondence to: Dr W G McCluggage, Department of Pathology,
Benign Mimics of Malignancy in Breast Pathology
 Arthur Purdy Stout Society of Surgical Pathologists Companion Meeting Benign Mimics of Malignancy in Breast Pathology Stuart J. Schnitt, M.D. Beth Israel Deaconess Medical Center and Harvard Medical School,
Arthur Purdy Stout Society of Surgical Pathologists Companion Meeting Benign Mimics of Malignancy in Breast Pathology Stuart J. Schnitt, M.D. Beth Israel Deaconess Medical Center and Harvard Medical School,
Case Report A Case of Primary Submandibular Gland Oncocytic Carcinoma
 Case Reports in Otolaryngology Volume 2013, Article ID 384238, 4 pages http://dx.doi.org/10.1155/2013/384238 Case Report A Case of Primary Submandibular Gland Oncocytic Carcinoma Kunihiko Tokashiki, Kiyoaki
Case Reports in Otolaryngology Volume 2013, Article ID 384238, 4 pages http://dx.doi.org/10.1155/2013/384238 Case Report A Case of Primary Submandibular Gland Oncocytic Carcinoma Kunihiko Tokashiki, Kiyoaki
Diagnostically Challenging Cases in Gynecologic Pathology
 Diagnostically Challenging Cases in Gynecologic Pathology Eric C. Huang, M.D., Ph.D. Department of Pathology and Laboratory Medicine University of California, Davis Medical Center Case 1 Presentation 38
Diagnostically Challenging Cases in Gynecologic Pathology Eric C. Huang, M.D., Ph.D. Department of Pathology and Laboratory Medicine University of California, Davis Medical Center Case 1 Presentation 38
Histopathology: Cervical HPV and neoplasia
 Histopathology: Cervical HPV and neoplasia These presentations are to help you identify basic histopathological features. They do not contain the additional factual information that you need to learn about
Histopathology: Cervical HPV and neoplasia These presentations are to help you identify basic histopathological features. They do not contain the additional factual information that you need to learn about
ARTHUR PURDY STOUT SOCIETY COMPANION MEETING: DIFFICULT NEW DIFFERENTIAL DIAGNOSES IN PROSTATE PATHOLOGY. Jonathan I. Epstein.
 1 ARTHUR PURDY STOUT SOCIETY COMPANION MEETING: DIFFICULT NEW DIFFERENTIAL DIAGNOSES IN PROSTATE PATHOLOGY Jonathan I. Epstein Professor Pathology, Urology, Oncology The Reinhard Professor of Urological
1 ARTHUR PURDY STOUT SOCIETY COMPANION MEETING: DIFFICULT NEW DIFFERENTIAL DIAGNOSES IN PROSTATE PATHOLOGY Jonathan I. Epstein Professor Pathology, Urology, Oncology The Reinhard Professor of Urological
ISPUB.COM. Salivary duct carcinoma of parotid gland. V Kinnera, R Nandyala, M Yootla, K Mandyam INTRODUCTION CASE REPORT
 ISPUB.COM The Internet Journal of Pathology Volume 10 Number 1 V Kinnera, R Nandyala, M Yootla, K Mandyam Citation V Kinnera, R Nandyala, M Yootla, K Mandyam.. The Internet Journal of Pathology. 2008 Volume
ISPUB.COM The Internet Journal of Pathology Volume 10 Number 1 V Kinnera, R Nandyala, M Yootla, K Mandyam Citation V Kinnera, R Nandyala, M Yootla, K Mandyam.. The Internet Journal of Pathology. 2008 Volume
Pancreatitis: A Potential Pitfall in Endoscopic Ultrasound Guided Pancreatic FNA
 Pancreatitis: A Potential Pitfall in Endoscopic Ultrasound Guided Pancreatic FNA Jack Yang, MD Department of Pathology, Medical University of South Carolina Objectives Understand the indication of EUS
Pancreatitis: A Potential Pitfall in Endoscopic Ultrasound Guided Pancreatic FNA Jack Yang, MD Department of Pathology, Medical University of South Carolina Objectives Understand the indication of EUS
Differential Diagnosis of Oral Masses. Palatal Lesions
 Differential Diagnosis of Oral Masses Palatal Lesions Palatal Masses Periapical Abscess Torus Palatinus Mucocele Lymphoid Hyperplasia Adenomatous Hyperplasia Benign Salivary Neoplasms Malignant Salivary
Differential Diagnosis of Oral Masses Palatal Lesions Palatal Masses Periapical Abscess Torus Palatinus Mucocele Lymphoid Hyperplasia Adenomatous Hyperplasia Benign Salivary Neoplasms Malignant Salivary
They Do Look Alike : Mimics of Prostate Cancer in Biopsy Samples
 They Do Look Alike : in Biopsy Samples Gladell P. Paner, MD Departments of Pathology and Surgery (Urology) University of Chicago, IL USA Gladell.paner@uchospitals.edu Benign in Needle Biopsy 1. Benign
They Do Look Alike : in Biopsy Samples Gladell P. Paner, MD Departments of Pathology and Surgery (Urology) University of Chicago, IL USA Gladell.paner@uchospitals.edu Benign in Needle Biopsy 1. Benign
ORIGINAL ARTICLE. Fine-Needle Aspiration Biopsy of Salivary Gland Lesions in a Selected Patient Population
 ORIGINAL ARTICLE Fine-Needle Aspiration Biopsy of Salivary Gland Lesions in a Selected Patient Population Erik G. Cohen, MD; Snehal G. Patel, MD; Oscar Lin, MD; Jay O. Boyle, MD; Dennis H. Kraus, MD; Bhuvanesh
ORIGINAL ARTICLE Fine-Needle Aspiration Biopsy of Salivary Gland Lesions in a Selected Patient Population Erik G. Cohen, MD; Snehal G. Patel, MD; Oscar Lin, MD; Jay O. Boyle, MD; Dennis H. Kraus, MD; Bhuvanesh
Epithelial Columnar Breast Lesions: Histopathology and Molecular Markers
 29th Annual International Conference Advances in the Application of Monoclonal Antibodies in Clinical Oncology and Symposium on Cancer Stem Cells 25 th -27t h June, 2012, Mykonos, Greece Epithelial Columnar
29th Annual International Conference Advances in the Application of Monoclonal Antibodies in Clinical Oncology and Symposium on Cancer Stem Cells 25 th -27t h June, 2012, Mykonos, Greece Epithelial Columnar
Case year old female presented with asymmetric enlargement of the left lobe of the thyroid
 Case 4 22 year old female presented with asymmetric enlargement of the left lobe of the thyroid gland. No information available relative to a prior fine needle aspiration biopsy. A left lobectomy was performed.
Case 4 22 year old female presented with asymmetric enlargement of the left lobe of the thyroid gland. No information available relative to a prior fine needle aspiration biopsy. A left lobectomy was performed.
Presentation material is for education purposes only. All rights reserved URMC Radiology Page 1 of 98
 Presentation material is for education purposes only. All rights reserved. 2011 URMC Radiology Page 1 of 98 Radiology / Pathology Conference February 2011 Brooke Koltz, Cytopathology Resident Presentation
Presentation material is for education purposes only. All rights reserved. 2011 URMC Radiology Page 1 of 98 Radiology / Pathology Conference February 2011 Brooke Koltz, Cytopathology Resident Presentation
CENTRE. Stanley Medical College Chennai India
 ISSN: 2250-0359 Volume 5 Issue 4 2015 ROLE OF FINE NEEDLE ASPIRATION CYTOLOGY IN SALIVARY GLAND PATHOLOGY AND ITS HISTOPATHOLOGICAL CORRELATION: A FIVE YEAR DESCRIPTIVE STUDY IN A TERTIARY CAR CENTRE Yogambal
ISSN: 2250-0359 Volume 5 Issue 4 2015 ROLE OF FINE NEEDLE ASPIRATION CYTOLOGY IN SALIVARY GLAND PATHOLOGY AND ITS HISTOPATHOLOGICAL CORRELATION: A FIVE YEAR DESCRIPTIVE STUDY IN A TERTIARY CAR CENTRE Yogambal
EQA Circulation 43 Educational Cases
 EQA Circulation 43 Educational Cases E1-E2 Monica Agarwal Monklands Hospital E1 38 yrs male Submandibular gland tumour E1 Formal excision following diagnosis of poorly differentiated carcinoma on core
EQA Circulation 43 Educational Cases E1-E2 Monica Agarwal Monklands Hospital E1 38 yrs male Submandibular gland tumour E1 Formal excision following diagnosis of poorly differentiated carcinoma on core
Case 4 Diagnosis 2/21/2011 TGB
 Case 4 22 year old female presented with asymmetric enlargement of the left lobe of the thyroid gland. No information available relative to a prior fine needle aspiration biopsy. A left lobectomy was performed.
Case 4 22 year old female presented with asymmetric enlargement of the left lobe of the thyroid gland. No information available relative to a prior fine needle aspiration biopsy. A left lobectomy was performed.
Pleomorphic Adenoma of Parotid in a Young Patient. Key words: Pleomophic, Adenoma, Salivary Glands, Parotid Neoplasms, Neoplasm Recurrence.
 JOURNAL OF CASE REPORTS 2013;3(1):142-147 Pleomorphic Adenoma of Parotid in a Young Patient Sangeeta R. Patankar, Megha A. Meshram, Vasant Shewale 1, Gokul S. From the Department of Oral Pathology & Microbiology
JOURNAL OF CASE REPORTS 2013;3(1):142-147 Pleomorphic Adenoma of Parotid in a Young Patient Sangeeta R. Patankar, Megha A. Meshram, Vasant Shewale 1, Gokul S. From the Department of Oral Pathology & Microbiology
Af elt her dentures no longer fit. On performing an oral. Polymorphous Low-Grade Adenocarcinoma. Lester D. R. Thompson, MD
 Polymorphous Low-Grade Adenocarcinoma Lester D. R. Thompson, MD Abstract: Polymorphous low-grade adenocarcinomas are minor salivary gland neoplasms with a predilection for intraoral sites. Women are affected
Polymorphous Low-Grade Adenocarcinoma Lester D. R. Thompson, MD Abstract: Polymorphous low-grade adenocarcinomas are minor salivary gland neoplasms with a predilection for intraoral sites. Women are affected
Disclosure. Relevant Financial Relationship(s) None. Off Label Usage None MFMER slide-1
 Disclosure Relevant Financial Relationship(s) None Off Label Usage None 2013 MFMER slide-1 Case Presentation A 43 year old male, with partial nephrectomy for a right kidney mass 2013 MFMER slide-2 2013
Disclosure Relevant Financial Relationship(s) None Off Label Usage None 2013 MFMER slide-1 Case Presentation A 43 year old male, with partial nephrectomy for a right kidney mass 2013 MFMER slide-2 2013
Human Papillomavirus and Head and Neck Cancer. Ed Stelow, MD
 Human Papillomavirus and Head and Neck Cancer Ed Stelow, MD No conflict of interest Declaration Cancer 1974 Lancet Oncol 2016; 17: e477-8 JAMA 1984; 252: 1857 JAMA 1988;259(13):1943-1944 Clin Cancer Res
Human Papillomavirus and Head and Neck Cancer Ed Stelow, MD No conflict of interest Declaration Cancer 1974 Lancet Oncol 2016; 17: e477-8 JAMA 1984; 252: 1857 JAMA 1988;259(13):1943-1944 Clin Cancer Res
Immunohistochemical Evaluation of Necrotic Malignant Melanomas
 Anatomic Pathology / EVALUATION OF NECROTIC MALIGNANT MELANOMAS Immunohistochemical Evaluation of Necrotic Malignant Melanomas Daisuke Nonaka, MD, Jordan Laser, MD, Rachel Tucker, HTL(ASCP), and Jonathan
Anatomic Pathology / EVALUATION OF NECROTIC MALIGNANT MELANOMAS Immunohistochemical Evaluation of Necrotic Malignant Melanomas Daisuke Nonaka, MD, Jordan Laser, MD, Rachel Tucker, HTL(ASCP), and Jonathan
Acantholytic Anaplastic Extramammary Paget s Disease: A Case Report and Review of the Literature
 Ann Dermatol Vol. 23, Suppl. 2, 2011 http://dx.doi.org/10.5021/ad.2011.23.s2.s226 CASE REPORT Acantholytic Anaplastic Extramammary Paget s Disease: A Case Report and Review of the Literature Yu-Jin Oh,
Ann Dermatol Vol. 23, Suppl. 2, 2011 http://dx.doi.org/10.5021/ad.2011.23.s2.s226 CASE REPORT Acantholytic Anaplastic Extramammary Paget s Disease: A Case Report and Review of the Literature Yu-Jin Oh,
Diagnostic Cytology of Cancer Cases
 Diagnostic Cytology of Cancer Cases Somporn Techangamsuwan Companion Animal Cancer Research Unit (CAC-RU) Department of Pathology, Faculty of Veterinary Science, Chulalongkorn University 1 Tumor or Non-tumor
Diagnostic Cytology of Cancer Cases Somporn Techangamsuwan Companion Animal Cancer Research Unit (CAC-RU) Department of Pathology, Faculty of Veterinary Science, Chulalongkorn University 1 Tumor or Non-tumor
Carcinoma ex Pleomorphic Adenoma (CXPA)-A rare parotid malignancy
 Indian Journal of Mednodent and Allied Sciences, pp- 54-58 Indian journals.com Case Report Carcinoma ex Pleomorphic Adenoma (CXPA)-A rare parotid malignancy Vani Padmaja GJ 1 *, Sireesha A 2, Sunderi Devi
Indian Journal of Mednodent and Allied Sciences, pp- 54-58 Indian journals.com Case Report Carcinoma ex Pleomorphic Adenoma (CXPA)-A rare parotid malignancy Vani Padmaja GJ 1 *, Sireesha A 2, Sunderi Devi
Intraductal carcinoma of the prostate on needle biopsy: histologic features and clinical significance
 & 2006 USCAP, Inc All rights reserved 0893-3952/06 $30.00 www.modernpathology.org Intraductal carcinoma of the prostate on needle biopsy: histologic features and clinical significance Charles C Guo 1 and
& 2006 USCAP, Inc All rights reserved 0893-3952/06 $30.00 www.modernpathology.org Intraductal carcinoma of the prostate on needle biopsy: histologic features and clinical significance Charles C Guo 1 and
Molecular Diagnostics of Head and Neck Tumors Justin A. Bishop, M.D. Associate Professor of Pathology The Johns Hopkins University Baltimore, Maryland
 Molecular Diagnostics of Head and Neck Tumors Justin A. Bishop, M.D. Associate Professor of Pathology The Johns Hopkins University Baltimore, Maryland Two Main Topics Molecular insights in salivary gland
Molecular Diagnostics of Head and Neck Tumors Justin A. Bishop, M.D. Associate Professor of Pathology The Johns Hopkins University Baltimore, Maryland Two Main Topics Molecular insights in salivary gland
GOBLET CELL CARCINOID. Hanlin L. Wang, MD, PhD University of California Los Angeles
 GOBLET CELL CARCINOID Hanlin L. Wang, MD, PhD University of California Los Angeles Disclosure of Relevant Financial Relationships USCAP requires that all planners (Education Committee) in a position to
GOBLET CELL CARCINOID Hanlin L. Wang, MD, PhD University of California Los Angeles Disclosure of Relevant Financial Relationships USCAP requires that all planners (Education Committee) in a position to
