The role of PET with 18 F-FDG has largely been demonstrated in clinical oncology, especially lung cancer (1). In
|
|
|
- Randolf Harmon
- 5 years ago
- Views:
Transcription
1 Value of 4-Dimensional 18 F-FDG PET/CT in the Classification of Pulmonary Lesions Ana María García Vicente, Angel Soriano Castrejón, Antonio Alberto León Martín, Beatriz González García, John Patrick Pilkington Woll, and Azahara Palomar Muñoz Nuclear Medicine Department, General University Hospital, Ciudad Real, Spain Our aim was to evaluate the effect of 4-dimensional (4D) 18 F- FDG PET/CT in the detection of pulmonary lesions. Methods: Fifty-seven pulmonary lesions were prospectively assessed in 37 patients (26 men and 11 women) with a mean age of 66.3 y. Twenty-nine of these patients had a history of neoplasm. All patients underwent 3-dimensional (3D) total-body PET/CT and 4D thoracic PET/CT (synchronized with respiratory movement). Maximum standardized uptake value () was obtained for each lesion in both studies. For the 4D studies, we selected the in the respiratory period with the highest uptake ( best bin ) and the average value over all bins ( average gated ). percentage difference between 3D and 4D PET/CT and the relationship of this value to the diameter and location of the lesions were calculated. Statistical parameters were calculated for 3D and 4D PET/CT. Results: Fifty-four of 57 lesions showed an increase of in the 4D study with respect to the 3D study. The mean was 3.1 in the 3D study. 4D PET/CT studies showed a mean of 4.5 for the best-bin study and 3.9 for the average gated study. The percentage difference in mean between 3D and 4D studies (best bin and averaged gated) was 72.9% and 48.8%, respectively. The smaller the lesion, the greater was the percentage difference (P, 0.05). However, no statistical differences dependent on the location of the lesions were observed. Final diagnosis showed that 37 lesions were malignant. The sensitivity, specificity, positive predictive value, and negative predictive value were 37.8%, 95%, 93%, and 45%, respectively, for 3D studies and 70.3%, 70%, 81.2%, and 56%, respectively, for 4D best-bin studies. Conclusion: Characterization of malignant lung lesions was better with 4D PET/ CT than with standard PET/CT. Key Words: respiratory gating; PET/CT; 18 F-FDG; pulmonary lesions; diagnosis J Nucl Med Technol 2011; 39:91 99 DOI: /jnmt The role of PET with 18 F-FDG has largely been demonstrated in clinical oncology, especially lung cancer (1). In Received Aug. 27, 2010; revision accepted Mar. 8, For correspondence contact: Ana María García Vicente, Nuclear Medicine Department, General University Hospital, C/Obispo Rafael Torija s/n, 13005, Ciudad Real, Spain. angarvice@yahoo.es COPYRIGHT ª 2011 by the Society of Nuclear Medicine, Inc. addition to qualitative analysis, semiquantitative analysis using the standardized uptake value (SUV) may be helpful in distinguishing between benign and malignant lesions. However, several factors can influence this parameter, particularly organ motion due to respiratory movement. Although the global sensitivity and specificity of 18 F- FDG PET for diagnosis of solitary pulmonary nodes are 96.8% and 77.8%, respectively, sensitivity decreases for lesions smaller than 2 cm (70%) (2 4). Furthermore, the evaluation of small lesions in the base of the lungs presents challenges due to respiratory movement, in addition to the partial-volume effect (5,6). Movement results in image blurring, leading to imprecise quantification of the size and uptake of lesions (7). These inaccuracies may produce problems in diagnosis and in lesion volume definition for planning radiotherapy, especially if respiration-gated radiotherapy is used (8,9). In hybrid equipment, the use of CT as a transmission source offers several advantages over conventional 68 Ge or 137 Cs rod sources. CT data have a higher signal-to-noise ratio, and the acquisition time of a transmission scan is considerably reduced. However, the introduction of CT for attenuation correction is not free of disadvantages. During a helical CT scan of a patient with pulmonary nodules, the lesion may be captured at a phase of the respiratory cycle that is different from its respiration-averaged position in the PET emission data. This event has a significant frequency and may affect up to 85% of the cases, with mean coregistry differences of about 2 3 cm (10). Furthermore, these differences are more significant in the right hemithorax and inferobasal portions; therefore, some authors recommend that the emission study be viewed without attenuation correction (11,12). With the development of combined PET/CT devices, respiratory motion has greater impact. A PET image alone corresponds to an average of multiple respiratory cycles and is susceptible to motion-related distortion. However, CT data, which are used for attenuation correction, produce an image from a fraction in time that is on the order of seconds (13). These spatial misalignments between CT and PET images not only compromise the interpretation of PET images but also result in mislocalization of the lesion and inaccurate quantification of SUV. In fact, attenuation correction factors 4D PET/CT IN PULMONARY LESIONS García Vicente et al. 91
2 are calculated on the basis of the corresponding CT transmission images (14). Thereby, the effect of respiratory movement on the quantification of 18 F-FDG activity is particularly relevant for small lesions and those in the base of the lungs. Phantom studies suggest that SUV measurements are underestimated by 21% 45% because of respiratory blurring, depending on the lesion size (15). Semiquantitative evaluation of tumor metabolism with SUV is widely used to assess pulmonary nodules and to quantify tumor response to therapy. But this semiquantitative method has limitations. Different reports show that the threshold to differentiate benign from malignant lesions varies between 2.5 and 5.0, depending on the reconstruction method, filtering parameters, and postinjection scan time (16,17). In addition, it has been shown that the SUV is overestimated in large patients if 18 F-FDG uptake is normalized to the weight of the patient (18,19). SUV normalization can be done with the ideal body weight, lean body mass, or body surface area to reduce this effect (20). Other factors, such as the interval after injection, plasma glucose level, and size of the lesion, can also have significant effects on the image (21). Lesion motion within the lung is another determinant factor. Although this movement is highly variable (5,22), it is greater in the lung bases adjacent to the diaphragm (23)and in the craniocaudal direction (24), with a statistically significant correlation between lesion mobility and lesion localization. Therefore, respiratory movement may affect the diagnosis (11), and although an SUV of more than 2.5 has been reported to indicate a higher probability of malignancy (25), some authors believe that this cutoff should not be correlated with malignancy in lung lesions and that a new SUV cutoff must be investigated (7). Some previous studies have shown that respiratory gating, or 4D PET, may significantly improve the accuracy of tumor volume determination and 18 F-FDG quantitation in the thorax (7,26 30). However, 4D experience is still limited, and its clinical diagnostic impact has not been completely assessed (31). Our objective was to evaluate the impact of 4D imaging in the assessment of benign or malignant pulmonary lesions without a previous diagnosis. MATERIALS AND METHODS Patients To establish the added value of PET synchronized with respiratory movement, with respect to conventional PET, we studied 57 lung lesions in 37 patients (26 men and 11 women). The inclusion criteria were lesions without a definitive diagnosis and clinically suggestive of malignancy. Exclusion criteria included incapacity to perform 4D PET due to patient condition or 4D acquisitions with technical problems related to irregular breathing. The mean age of our patients was 66.3 y (range, y). Twentynine of the 37 patients had a history of neoplasm, colorectal carcinoma being the most common tumor in our sample (8), followed by lung primary tumors (6). The remaining patients had no known history of malignancy. Lesions The lung lesions had a maximum diameter of cm (mean 6 SD, cm). The size was determined on CT scans (lung window). These lesions were mainly in the upper right lobe (29.8%), upper left lobe (22.8%), and lower right lobe (26.3%). The distribution is shown in Table 1. Methodology All patients fasted for at least 4 h before undergoing PET/CT. Glucose levels were lower than 180 mg/dl in all but 4 patients. PET/CT was performed with a Discovery STE 16 scanner (GE Healthcare). Before PET acquisition, helical CT was performed from the head to the proximal thigh according to a standardized protocol (modulated CT: ma, 120 kv, slice thickness of 3 mm, rotation time of 0.5 s). No oral or intravenous contrast agents were used. Emission scans from the head to the proximal thigh were acquired 60 min after the injection of a mean dose of 370 MBq of 18 F-FDG. Images were acquired in 3-dimensional (3D) mode, at 3 min per table position. After completion of the standard 3D acquisition, the study was reconstructed using 2 iterations and 8 subsets and was evaluated on a dedicated workstation (Advantage; GE Healthcare). The suggestive lesions were evaluated (size and location), and thorax-gated 4D PET/CT was performed within 60 min after the standard PET/CT, with the following parameters: ma and 120 kv for CT; 12 min for PET. The gating tool was the Real-Time Position Management Respiratory Gating System (Varian Medical Systems), dividing the respiratory cycle into 6 periods, or bins. In each bin, a PET image and a CT image were acquired. The total scan duration was 12 min (2 min/bin). For the reconstruction, 4D PET was corrected with the helical CT. Analysis of Lesions Maximum SUV () was determined for each lesion in both studies. For the gated studies, was calculated for each bin. We selected the in the bin with the highest uptake ( best bin ) for lesion classification. The average over all bins ( average gated ) was also calculated. To compare techniques, we calculated the percentage difference between 3D and 4D studies (best bin and average gated) (% difference 5 4D 3D/ 3D 100). A threshold of 2.5 was selected; therefore, any lesion with an of 2.5 or higher was classified as malignant. Statistical Analysis Data are expressed as mean 6 SD and proportions. Sensitivity, specificity, and positive and negative predictive values were calculated for the diagnosis of malignancy on 3D and 4D images (best bin and average gated) for all groups of lesions. These values were also calculated for lesions greater than 1 cm and then for those greater than or equal 92 JOURNAL OF NUCLEAR MEDICINE TECHNOLOGY Vol. 39 No. 2 June 2011
3 TABLE 1 Patient Data, Lesion Data, Final Diagnosis, and Imaging Results Les no. Pt no. Sex Age (y) NB LC Hy NB Diam (cm) Location 3D (A) BB 4D (B) Bin %Dif (B 2 A) AG 4D (C) Classification Imaging result %Dif (C 2 A) 3D BB 4D AG 4D Hy 3D BB 4D AG 4D 1 1 M LUL B M M TN FP FP LUL B B B TN TN TN 3 2 F 71 Y Testicular 2.1 LUL M M M Mts melanoma TP TP TP 4 3 F LUL B M M Hamartoma TN FP FP 5 4 M 68 Y Prostate 2.0 RLL M M M NSCLC TP TP TP 6 5 M 78 Y Melanoma 2.5 LUL B M B FN TP FN 7 6 F LUL B B B TN TN TN 8 7 M LLL B B B Epidermal FN FN FN 9 8 M 70 Y Larynx 3.5 LUL M M M TP TP TP RUL M M M TP TP TP Lingula B B B FN FN FN 12 9 M RUL B B B TN TN TN Lingula B B B TN TN TN M 80 Y Y NSCLC 3.2 LUL M M M Adenoca TP TP TP LUL B M M Adenoca FN TP TP M 51 Y Y SCLC 4.0 RLL M M M SCLC TP TP TP RUL B B B SCLC FN FN FN M 52 Y Y NSCLC 2.1 RUL B M B Adenoca FN TP FN M 71 Y Colorectal 0.7 ML B B B TN TN TN RLL B B B TN TN TN M 73 Y HD 1.8 RUL B B B TN TN TN F 73 Y Colorectal 2.4 RLL M M M TP TP TP M 84 Y Y Epidermoid 1.6 RLL M M M Epidermoid TP TP TP F 50 Y Ovarian 0.6 RUL B B B TN TN TN M 58 Y Renal 0.8 RUL B B B Negative TN TN TN RUL B M M Negative TN FP FP RUL B M B Negative TN FP TN ML B B B Negative TN TN TN M 73 Y Colorectal 2.0 LUL M M M TP TP TP LUL B B B FN FN FN RUL B B B FN FN FN M RUL B B B TN TN TN F 61 Y Melanoma 1.3 Lingula B B B TN TN TN M 70 Y Colorectal 0.9 LLL M M M TP TP TP M 70 Y Colorectal 0.6 LLL B B B FN FN FN RLL B M B FN TP FN M 57 Y Epidermoid 1.6 RLL M M M TP TP TP Lingula B M B FN TP FN F 61 Y Endometrial 0.7 RUL B M B FN TP FN RUL B M M FN TP TP RLL B M M FN TP TP F 67 Y Y NSCLC 0.8 RUL B B B TN TN TN LLL B M M TN FP FP M 69 Y Colorectal 1.2 LLL B B B FN FN FN RLL B B B FN FN FN 4D PET/CT IN PULMONARY LESIONS García Vicente et al. 93
4 TABLE 1 (Continued ) Les no. Pt no. Sex Age (y) NB LC Hy NB Diam (cm) Location 3D (A) BB 4D (B) Bin %Dif (B 2 A) AG 4D (C) Classification Imaging result %Dif (C 2 A) 3D BB 4D AG 4D Hy 3D BB 4D AG 4D M 41 Y Testicular 1.5 RLL B B B Negative TN TN TN F 68 Y Colorectal 0.8 RUL B M B FN TP FN RLL B M B FN TP FN RLL B M M FN TP TP F 79 Y Renal 2.4 LLL B B B Mts FN FN FN M RLL M M M Epidermoid TP TP TP F 57 Y Cervix 1.2 RLL B B B FN FN FN M 81 Y Colorectal 1.0 LUL B M M FN TP TP M 65 Y Renal 1.6 LUL B B B FN FN FN M 61 Y SCLC 2.2 RLL M M M SCLC TP TP TP M 62 Y Larynx 4.7 RUL M M M Positive TP TP TP M RUL M M M FP FP FP Les 5 lesion; Pt 5 patient; NB 5 neoplastic background; LC 5 lung cancer; Hy 5 histopathology; Diam 5 diameter; BB 5 best bin; Dif 5 difference; AG 5 average gated; NSCLC 5 non small cell lung cancer; SCLC 5 small cell lung cancer; HD 5 Hodgkin disease; RUL: right upper lobe; LUL 5 left upper lobe; RLL 5 right lower lobe; LLL 5 left lower lobe; ML 5 middle lobe; B 5 benign; M 5 malignant; Mts 5 metastases; adenoca 5 adenocarcinoma; TN 5 true negative; FP 5 false positive; TP 5 true positive; FN 5 false negative. 94 JOURNAL OF NUCLEAR MEDICINE TECHNOLOGY Vol. 39 No. 2 June 2011
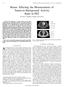
5 FIGURE 1. ROC curves of 3D and 4D (best bin and average gated) statistical parameters. Area under curve was for 3D, for 4D best bin, and for 4D average gated. 4D best bin showed best value, with no statistically significant differences from the other techniques. a.g. 5 average gated; b.b. 5 best bin. to 1.5 cm on 3D and best-bin 4D images. A P value of less than 0.05 was considered to be statistically significant. A receiver-operating-characteristic (ROC) analysis was performed to establish the best cutoff for the diagnostic test parameters. ROC curves were generated using nonparametric ROC analysis. To compare area under the curve for the 2 tests, a critical ratio z was calculated from the difference of the area under the curve, the SE of the ROC area, and the correlation between 3D and 4D images according to the method of McNeil and Hanley (32). Mann Whitney and Kruskal Wallis tests were used to compare quantitative variables. A P value of less than 0.05 was considered statistically significant. percentage difference and lesion diameter were compared by the Spearman test. We correlated the change in with lesion diameter and location. RESULTS The final diagnosis was confirmed by histologic assessment (19/57 lesions, or 33.3%) or clinical and radiologic follow-up for more than 12 mo (38/57 lesions, or 66.7%). In the final diagnosis, 37 lesions were found to be malignant and the others benign. Attending to semiquantitative data, 3D, best-bin 4D, and average gated 4D imaging classified 15, 32, and 24 lesions, respectively, as malignant. This assessment was correct for most lesions, although 4D imaging had a greater number of false-positives with respect to 3D (6 for best-bin 4D and 5 for average gated 4D vs. 1 for 3D). Therefore, 3D imaging diagnosed 14 (37.83%) malignant lesions, whereas best-bin and average gated 4D imaging diagnosed 26 (70.3%) and 19 (51.3%), respectively. The rate of false-negatives was greater for the 3D technique (23) than for the best-bin(11) and average gated 4D techniques (18) (Table 1). Sensitivity increased and specificity decreased significantly for 4D with respect to 3D imaging, although the diagnostic value did not show significant differences between any techniques (P ). In the ROC analysis, the area under the curve was for the 3D study, for the best-bin 4D study, and for the average gated 4D study (Fig. 1). Sensitivity, specificity, positive predictive value, negative predictive value, and accuracy for 3D and best-bin 4D imaging (all lesions, lesions. 1 cm, and lesions $ 1.5 cm) and for average gated 4D imaging (all lesions) are shown in Table 2. In the best-bin and average gated 4D images, 54 of 57 and 46 of 57 lesions, respectively, showed an increase in with respect to the 3D study. In 41 of the 54 lesions on best-bin 4D imaging, the greater increase in SUV was observed during the expiratory phase. One lesion was not detected on 3D imaging and showed metabolism in the best-bin 4D study (Fig. 2). Two lesions did not show any SUV variation, and another showed a decreased 18 F-FDG uptake on best-bin 4D imaging with respect to 3D imaging (23.3%). On average gated 4D imaging, 8 lesions did not show any increase in the semiquantitative parameters compared with 3D imaging, and 3 showed a decrease. Most of the smaller lesions were better defined in the 4D studies because of higher lesion contrast with respect to background lung activity (Fig. 3). The mean in the 3D and the best-bin and average gated 4D studies was , , and , TABLE 2 Statistical Parameters for the 3 Techniques 3D Best-bin 4D Index (%) Total.1 cm $1.5 cm AG 4D total Total.1 cm $1.5 cm Sensitivity Specificity Positive predictive value Negative predictive value Accuracy AG 5 average gated. 4D PET/CT IN PULMONARY LESIONS García Vicente et al. 95
6 FIGURE 2. Example of lesion that cannot be visualized on 3D axial image but is detectable on 4D best-bin axial image. Study is of patient 11, who had small cell lung cancer with 2 pulmonary lesions. CT image (center) shows one lesion in right lower lobe (maximum diameter, 4 cm) and another in right upper lobe (8 mm). Larger lesion has high avidity for 18 F-FDG ( in 3D and in best bin of 4D, 8.4 and 11.1, respectively), whereas smaller lesion (arrow) is detectable only in 4D study (, 1.1). respectively. The mean percentage difference between 3D and best-bin 4D studies was 72.9% %, and the range was 23.3% to 360%. Between the 3D and average gated 4D studies, the mean percentage difference was 48.8% %, and the range was 227.8% to 360%. After ROC analysis, an of 1.45 was shown to be the best diagnostic parameter of sensitivity and specificity for the 3D studies (63% and 69%, respectively). In the best-bin 4D studies, this value was 2.45 (68% sensitivity and 69% specificity), and in the average gated 4D studies, a cutoff of 1.45 showed a sensitivity of 71% but a low specificity (28%). Regarding the correlation between the percentage difference with other parameters, we observed a statistically significant (P, 0.05) higher increase in for smaller lesions with respect to larger ones. This correlation is represented in Figure 4. No statistically significant differences dependent on lesion location were observed, but the right lung showed higher SUV increases in 4D studies (best bin and average gated) with respect to the left lung. Detailed data are shown in Table 3. FIGURE 3. Example of higher lesion contrast with respect to background lung activity in 4D study than in 3D study in patient with 2 pulmonary lesions smaller than 1 cm. Study is of patient 26, who had history of treated non small cell lung cancer. CT images (center) show one lesion in right upper lobe (maximum diameter, 8 mm) and another in left lower lobe (8 mm). Both (arrows) show faint uptake on 3D axial images (, 0.8 and 1.4, respectively) that improves in best-bin 4D images (, 1.9 and 2.9, respectively). DISCUSSION Experience with 4D PET is still limited to few centers and small groups of patients. Nevertheless, results on the increase in SUV, the improvement in coregistration, and the reduction in lesion volume are encouraging (27). Some studies have used 4D acquisition exclusively in CT (cine CT) and have observed increases in SUV of up to 50% (26,28,29). Erdi et al. (26) examined PET/CT images of 5 patients with lung carcinoma and multiple lung lesions. CT images were acquired in cine mode and divided into 10 phases. Examination of all phases showed an SUV variation of up to 30%. Using 4D PET, the increase of SUVs is variable and ranges widely but is statistically significant. Our results show a mean increase of 73% for between 3D and best-bin 4D studies, with a range of 23.3% to 360%, similar to the results of Lupi et al. (30). Regarding how the respiratory phase influences quantitative parameters, we found that most lesions (76%) showed the highest during the expiratory phase. This condition, demonstrated also in other works (10,26), is explained by the low motion of lesions during this phase. Some authors have found that the effect of gating may depend on lesion size and intrapulmonary site, which corresponds to different motion amplitudes (7). Pevsner et al. (6) found that the range of SUV fluctuation for a given motion amplitude was inversely proportional to lesion size. We found a statistically significant correlation between percentage difference and lesion diameter (Fig. 4). A greater increase of was observed in smaller lesions, with respect to larger ones. These results are explained by the greater adverse effect of respiratory movement on lesions smaller than 1.5 cm than on larger ones. 96 JOURNAL OF NUCLEAR MEDICINE TECHNOLOGY Vol. 39 No. 2 June 2011
7 FIGURE 4. Correlation between lesion size and percentage difference between 3D and best-bin 4D studies (A) and between 3D and average gated 4D studies (B). Both graphs show statistically significant (P, 0.05) higher increase in in smaller lesions than in larger ones. Therefore, although motion amplitude was not assessed in our study, this correlation indirectly reflects the greater detriment of respiratory movement in smaller lesions. In relation to the semiquantitative assessment, other authors have remarked that a new SUV cutoff should be reconsidered for lung cancer when gating is used (7). We did not modify this threshold because we considered that the ideal cutoff of 2.5 was created under optimal conditions, without the disadvantages of partial-volume effect and respiratory movement, whereas lung lesions, especially the smaller ones, are studied under suboptimal conditions due to respiratory movement. Attending to our results, ROC analysis showed that a cutoff of 2.45 in best-bin 4D studies had the best sensitivity and specificity (68% and 69%, respectively). One main effect of respiratory motion is the decrease in concentration per pixel within the lesion a decrease sometimes exceeding 50% of maximum activity (12). Therefore, the problem of respiratory movement has such relevance that it may determine the therapeutic management of a patient. Any metabolic activity in a nodule of approximately 1 cm or less, even if the activity does not exceed the reference threshold, may indicate malignancy. Our ROC analysis showed that the best diagnostic for sensitivity and specificity in the 3D study (63% and 69%, respectively) was According to some authors, the likelihood of malignancy in any metabolically detectable lesion is 60%, which agrees with the prevalence (66.67%) that we found (4,33). Therefore, the absence of metabolic activity in a nodule, especially if it is smaller than 1 cm, cannot rule out malignancy, and radiologic follow-up should be recommended (27). Nehmeh et al. (27) reported in their conclusions that 4D PET/CT acquisition should improve the confidence of PET/ CT diagnosis, especially in lung cancer screening of small nodules. However, the clinical diagnostic impact of 4D studies has not been determined yet, particularly because all previous studies were performed on patients with known TABLE 3 Data with Reference to Lesion Location Lesion location Mean 6 SD percentage difference 6 SD Lesion distribution 3D BB 4D AG 4D 3D vs. BB 4D 3D vs. AG 4D RUL LUL RLL LLL Lingula ML RUL 5 right upper lobe; LUL 5 left upper lobe; RLL 5 right lower lobe; LLL 5 left lower lobe; ML 5 middle lobe; BB 5 best bin; AG 5 average gated. 4D PET/CT IN PULMONARY LESIONS García Vicente et al. 97
8 lung malignancies. In a preliminary assessment of 18 lesions, 4D studies reduced the false-negative rate by 50% when compared with the 3D technique but at the expense of an increase in the false-positive rate to 11% (31). Above all, this study introduced an important factor with respect to the previous studies. Although most of our patients had a history of neoplasm, the objective of 4D PET was the diagnostic assessment of suggestive lesions. Among all lesions, best-bin 4D studies increased the sensitivity significantly (from 38% to 70%) although specificity decreased (from 95% to 70%), and accuracy was higher for best-bin 4D studies with respect to 3D (70% vs. 58%). In contrast, the global parameters assessed by ROC curves did not show statistically significant differences. In our opinion, more important than the decrease in specificity is the increase in sensitivity, because it enables a recommendation that lesions suggestive on 4D PET be followed up closely or biopsied to establish an earlier diagnosis of malignancy, but these results should be verified in a larger sample of lesions. Our study had some limitations. The delay of acquisition of the 4D study could contribute to the SUV parameters obtained. But we do not believe this delay was the main cause of the observed SUV increase, taking into account the short acquisition time in each bin (2 min) of the 4D acquisitions with respect to the 3D acquisition (3 min/bed position). On the other hand, the effect of double-phase or dual-time-point PET/CT has not been fully assessed. Therefore, determining the diagnostic impact of both techniques on the same group of patients would clear these doubts and enable comparison of the 2 available techniques to improve lesion detection. Another controversial aspect is lesion classification using a semiquantitative approach. Despite the assumption that the best bin is defined by its lowest motion, statistical noise is also a factor, particularly when is used. In theory, delayed gated acquisition should lead to improved contrast between lesion and background, but the delay additionally causes a reduced rate of true coincidences due to radioactive decay. Furthermore, the shorter acquisition time of 4D studies (2 min) increases the statistical noise in each bin. To reduce this effect, an average was obtained, but the derived diagnostic parameters of this procedure did not show significant differences from standard 3D acquisition (Fig. 1). With respect to attenuation correction, we were aware that helical CT could limit the accuracy of the corrected images and, therefore, influence the results. The combined synchronization technique offers more accurate quantification than separate synchronization because of the greater coincidence in each respiratory phase. Therefore, tumor images and intralesional SUVs are more correct, as has been demonstrated by Nehmeh et al. (27) and Hamill et al. (12). Furthermore, the number of lesions histologically studied was limited, but many lesions were smaller than 1.5 cm. The fact that some patients had multiple lesions and that most patients had a history of neoplasm makes us consider clinical follow-up to be the most ethical option and, in the opinion of oncologists, enough to assess the probable diagnosis. The limited sensitivity of PET in small lesions has been previously documented (70% for lesions, 2 cm)(3,4) and was observed by us using a cutoff of 2.5. When lesions 1 cm or smaller were excluded (42% of our sample), sensitivity increased from 37.8% to 52.2%, and when we assessed only lesions 1.5 cm or larger (25/57 lesions), sensitivity increased even more, reaching a value (68.4%) similar to that reported in the literature. However, this sensitivity is not quite sufficient for diagnostic purposes: there is an inherent limitation in the detection of small lesions, and in our study more than half the lesions were smaller than 1.5 cm. This fact and our different criteria for selecting patients could be the reasons for the reduced sensitivity with respect to other works. A possible solution would be the normalization or correction of SUVs according to tumor size (34), although this procedure has not previously been shown to significantly improve diagnosis (6,39). Other works have calculated the recovery coefficient in phantoms with spheres of different sizes (6,36). Although the calculation depends on the resolution and reconstruction parameters, among other factors, Soret et al. (36) found that for a system with a spatial resolution of 6 mm (similar to our PET system), the recovery coefficient was 3.7 for 1-cm-diameter lesions and greater than 2.5 for 1.5-cm lesions. The application of this approach in our 11 falsenegative lesions in best-bin 4D PET correctly classified all as malignant although erroneously classifying all but one benign lesion as malignant, increasing the number of falsepositives from 6 to 19. Therefore, methods of correcting partial-volume effect are not a perfect solution, because other factors such as tumor density, 18 F-FDG avidity, and background activity play a role in semiquantitative parameters. Therefore, the main limitation of standard PET/CT continues to be the study of small lung nodules, with an error rate possibly exceeding 50% in the diagnosis of subcentimeter lesions, and at the expense of false-negative results (37). In the present work, 4D studies showed a lower rate of false-negatives than standard acquisition (11 vs. 23). Therefore, 4D studies offer more efficient identification, as Lupi et al. (30) concluded in their publication, and may be recommended to improve the detection of these lesions. On the other hand, 4D studies detected more false-positive lesions, a factor that must be considered although we believed the best parameter to be the increased sensitivity, which improved the correct classification of malignant lesions. CONCLUSION The acquisition of 18 F-FDG PET/CT scans in 4 dimensions increases the sensitivity of lesion detection from a metabolic point of view. To our knowledge, this work is the first reported assessment of the diagnostic impact of this technique, showing it to have higher diagnostic accuracy than standard acquisition. If this finding is confirmed in 98 JOURNAL OF NUCLEAR MEDICINE TECHNOLOGY Vol. 39 No. 2 June 2011
9 future studies, 4D PET/CT acquisitions should be recommended for the screening of small lung lesions to improve diagnostic confidence. REFERENCES 1. Hellwig D, Baum RP, Kirsch C. FDG-PET, PET/CT and conventional nuclear medicine procedures in the evaluation of lung cancer: a systematic review. Nuklearmedizin. 2009;48: Gould MK, Maclean CC, Kuschner WG, et al. Accuracy of positron emission tomography for diagnosis of pulmonary nodules and mass lesions: a meta-analysis. JAMA. 2001;285: Degirmenci B, Wilson D, Laymon CM, et al. Standarized uptake value-based evaluations of solitary pulmonary nodules using F-18 fluorodeoxyglucose-pet/ computed tomography. Nucl Med Commun. 2008;29: Kim SC, Machac J, Krynyckyi BR, et al. FDG PET for evaluation of indeterminate lung nodules: assigning a probability of malignancy may be preferable to binary readings. Ann Nucl Med. 2008;22: Goerres GW, Kamel E, Seifert B, et al. Accuracy of image coregistration of pulmonary lesions in patients with non-small cell lung cancer using an integrated PET/CT system. J Nucl Med. 2002;43: Pevsner A, Hehmeh SA, Humm JL, et al. Effect of motion on tracer activity determination in CT attenuation corrected PET images: a lung phantom study. Med Phys. 2005;32: Nehmeh SA, Erdi Y, Ling CC, et al. Effect of respiratory gating on quantifying PET images of lung cancer. J Nucl Med. 2002;43: Dawson LA, Brock KK, Kayanjian S, et al. The reproducibility of organ position using active breathing control during lever radiotherapy. Int J Radiat Oncol Biol Phys. 2001;51: Underberg RW, Lagerwaard FJ, Slotman BJ, et al. Benefit of respiration-gated stereotactic radiotherapy for stage I lung cancer: an analysis of 4DCT datasets. Int J Radiat Oncol Biol Phys. 2005;62: Larson SM, Nehmeh SA, Erdi Y, et al. PET-CT in non-small-cell lung cancer: value of respiratory-gated PET. Chang Gung Med J. 2005;28: Beyer T, Antoch G, Blodgett T, et al. Dual-modality PET/CT imaging: the effect of respiratory motion on combined image quality in clinical oncology. Eur J Nucl Med Mol Imaging. 2003;30: Hamill JJ, Bosmans G, Dekker A. Respiratory-gated CT as a tool for the simulation of breathing artifacts in PET and PET-CT. Med Phys. 2008;35: Cohade C, Osman M, Marschall LN, et al. PET-CT: accuracy of PET and CT spatial registration of lung lesions. Eur J Nucl Med Mol Imaging. 2003;30: Kinahan P, Hasegawa B, Beyer T. X-ray based attenuation correction for PET-CT scanners. Semin Nucl Med. 2003;33: Boucher L, Rodrigue S, Lecomte R, et al. Respiratory gating for 3-dimensional PET of the thorax: feasibility and initial results. J Nucl Med. 2004;45: Hickeson M, Yun M, Matthies A, et al. Use of corrected standardized uptake value based on the lesion size on CT permits accurate characterization of lung nodules on FDG-PET. Eur J Nucl Med Mol Imaging. 2002;29: Inoue T, Kim EE, Komaki R, et al. Detecting recurrent or residual lung cancer with FDG PET. J Nucl Med. 1995;36: Kim CK, Gupta NC. Dependency of SUV of F18 FDG on body size: comparison of body surface area correction and lean body mass correction. Nucl Med Commun. 1996;17: Schomburg A, Bender H, Reichel C, et al. SUV value of F18 FDG: the value of different normalization procedures. Eur J Nucl Med. 1996;23: Sugawara Y, Zasadny KR, Neuhoff AW, et al. Reevaluation of the SUV for FDG: variations with body weight and methods for correction. Radiology. 1999;213: Keyes JW. SUV: standard uptake or silly useless value? J Nucl Med. 1995;36: Seppenwoolde Y, Shirato H, Kitamura K, et al. Precise and real-time measurement of 3D tumor motion in lung due to breathing and heartbeat, measured during radiotherapy. Int J Radiat Oncol Biol Phys. 2002;53: Plathow C, Ley S, Fink C, et al. Analysis of intrathoracic tumor mobility during whole breathing cycle by dynamic MRI. Int J Radiat Oncol Biol Phys. 2004;59: Bundschuh RA, Martinez-Moeller A, Essler M, et al. Postacquisition detection of tumor motion in the lung and upper abdomen using list-mode PET data: feasibility study. J Nucl Med. 2007;48: Lowe VJ, Fletcher JW, Gobar L, et al. Prospective investigation of positron emission tomography in lung nodules. J Clin Oncol. 1998;16: Erdi YE, Nehmeh SA, Pan T, et al. The CT motion quantitation of lung lesions and its impact on PET-measured SUVs. J Nucl Med. 2004;45: Nehmeh SA, Erdi YE, Ling CC, et al. Four dimensional (4D) PET/CT imaging in the thorax. Med Phys. 2004;31: Cheng NM, Yu CT, Ho KC, et al. Respiration-averaged CT for attenuation correction in non-small-cell lung cancer. Eur J Nucl Med Mol Imaging. 2009; 36: Pan T, Mawlawi O, Nehmeh SA, et al. Attenuation correction of PET images with respiration-averaged CT images in PET/CT. J Nucl Med. 2005;46: Lupi A, Zaroccolo M, Salgarello M, Malfatti V, Zanco P. The effect of 18 F-FDG- PET/CT respiratory gating on detected metabolic activity in lung lesions. Ann Nucl Med. 2009;23: García Vicente AM, Soriano Castrejón A, Talavera Rubio MP, et al. 18 F-FDG PET/CT and respiratory synchronization: effect in the detection and classification of pulmonary lesions. Rev Esp Med Nucl. 2009;28: McNeil BJ, Hanley JA. Statistical approaches to the analysis of receiver operating characteristic (ROC) curves. Med Decis Making. 1984;4: Hashimoto Y, Tsujikawa T, Kondo C, et al. Accuracy of PET for diagnosis of solid pulmonary lesions with 18 F-FDG uptake below the standardized uptake value of 2.5. J Nucl Med. 2006;47: Rousset OG, Rahmim A, Alavi A, Zaidi H. Partial volume correction strategies in PET. PET Clin. 2007;2: Menda Y, Bushnell DL, Madsen MT, et al. Evaluation of various corrections to the standardized uptake value for diagnosis of pulmonary malignancy. Nucl Med Commun. 2001;22: Soret M, Bacharach SL, Buvat I. Partial-volume effect in PET tumor imaging. J Nucl Med. 2007;48: Bryant AS, Cerfolio RJ. The maximum standardized uptake value on integrated FDG-PET/CT is useful in differentiating benign from malignant pulmonary nodules. Ann Thorac Surg. 2006;82: D PET/CT IN PULMONARY LESIONS García Vicente et al. 99
10 Value of 4-Dimensional 18 F-FDG PET/CT in the Classification of Pulmonary Lesions Ana María García Vicente, Angel Soriano Castrejón, Antonio Alberto León Martín, Beatriz González García, John Patrick Pilkington Woll and Azahara Palomar Muñoz J. Nucl. Med. Technol. 2011;39: Published online: May 12, Doi: /jnmt This article and updated information are available at: Information about reproducing figures, tables, or other portions of this article can be found online at: Information about subscriptions to JNMT can be found at: Journal of Nuclear Medicine Technology is published quarterly. SNMMI Society of Nuclear Medicine and Molecular Imaging 1850 Samuel Morse Drive, Reston, VA (Print ISSN: , Online ISSN: ) Copyright 2011 SNMMI; all rights reserved.
Respiratory gated PET/CT in a European multicentre retrospective study: added diagnostic value in detection and characterization of lung lesions
 Eur J Nucl Med Mol Imaging (2012) 39:1381 1390 DOI 10.1007/s00259-012-2148-2 ORIGINAL ARTICLE Respiratory gated PET/CT in a European multicentre retrospective study: added diagnostic value in detection
Eur J Nucl Med Mol Imaging (2012) 39:1381 1390 DOI 10.1007/s00259-012-2148-2 ORIGINAL ARTICLE Respiratory gated PET/CT in a European multicentre retrospective study: added diagnostic value in detection
4D PET: promises and limitations
 4D PET: promises and limitations Tinsu Pan, Ph.D. M.D. Anderson Cancer Center The University of Texas Background Outlines Gating techniques: Deep inspiration breath hold 4D PET/CT Non-gating techniques
4D PET: promises and limitations Tinsu Pan, Ph.D. M.D. Anderson Cancer Center The University of Texas Background Outlines Gating techniques: Deep inspiration breath hold 4D PET/CT Non-gating techniques
Respiratory-gated 18 F-FDG PET imaging in lung cancer: effects on sensitivity and specificity
 Original article Respiratory-gated 18 F-FDG PET imaging in lung cancer: effects on sensitivity and specificity Joël Daouk 1,2, Marie Leloir 2, Loïc Fin 3, Pascal Bailly 1, Julie Morvan 1,2, Isabelle EI
Original article Respiratory-gated 18 F-FDG PET imaging in lung cancer: effects on sensitivity and specificity Joël Daouk 1,2, Marie Leloir 2, Loïc Fin 3, Pascal Bailly 1, Julie Morvan 1,2, Isabelle EI
Biases affecting tumor uptake measurements in FDG-PET
 Biases affecting tumor uptake measurements in FDG-PET M. Soret, C. Riddell, S. Hapdey, and I. Buvat Abstract-- The influence of tumor diameter, tumor-tobackground activity ratio, attenuation, spatial resolution,
Biases affecting tumor uptake measurements in FDG-PET M. Soret, C. Riddell, S. Hapdey, and I. Buvat Abstract-- The influence of tumor diameter, tumor-tobackground activity ratio, attenuation, spatial resolution,
PET-CT for radiotherapy planning in lung cancer: current recommendations and future directions
 PET-CT for radiotherapy planning in lung cancer: current recommendations and future directions Gerry Hanna Centre for Cancer Research and Cell Biology Queen s University of Belfast @gerryhanna Talk Outline
PET-CT for radiotherapy planning in lung cancer: current recommendations and future directions Gerry Hanna Centre for Cancer Research and Cell Biology Queen s University of Belfast @gerryhanna Talk Outline
Imaging Decisions Start Here SM
 Owing to its high resolution and wide anatomic coverage, dynamic first-pass perfusion 320-detector-row CT outperforms PET/CT for distinguishing benign from malignant lung nodules, researchers from Japan
Owing to its high resolution and wide anatomic coverage, dynamic first-pass perfusion 320-detector-row CT outperforms PET/CT for distinguishing benign from malignant lung nodules, researchers from Japan
Utility of 18 F-FDG PET/CT in metabolic response assessment after CyberKnife radiosurgery for early stage non-small cell lung cancer
 Utility of F-FDG PET/CT in metabolic response assessment after CyberKnife radiosurgery for early stage non-small cell lung cancer Ngoc Ha Le 1*, Hong Son Mai 1, Van Nguyen Le 2, Quang Bieu Bui 2 1 Department
Utility of F-FDG PET/CT in metabolic response assessment after CyberKnife radiosurgery for early stage non-small cell lung cancer Ngoc Ha Le 1*, Hong Son Mai 1, Van Nguyen Le 2, Quang Bieu Bui 2 1 Department
Effectiveness of FDG-PET Scans in the Evaluation of Patients with Single Pulmonary Nodules in Taiwan
 Effectiveness of FDG-PET Scans in the Evaluation of Patients with Single Pulmonary Nodules in Taiwan Wan-Yu Lin 1, Gee-Chen Chang 2, Shyh-Jen Wang 1 1 Department of Nuclear Medicine, Taichung Veterans
Effectiveness of FDG-PET Scans in the Evaluation of Patients with Single Pulmonary Nodules in Taiwan Wan-Yu Lin 1, Gee-Chen Chang 2, Shyh-Jen Wang 1 1 Department of Nuclear Medicine, Taichung Veterans
Positron Emission Tomography in Lung Cancer
 May 19, 2003 Positron Emission Tomography in Lung Cancer Andrew Wang, HMS III Patient DD 53 y/o gentleman presented with worsening dyspnea on exertion for the past two months 30 pack-year smoking Hx and
May 19, 2003 Positron Emission Tomography in Lung Cancer Andrew Wang, HMS III Patient DD 53 y/o gentleman presented with worsening dyspnea on exertion for the past two months 30 pack-year smoking Hx and
Research Article The Advantage of PET and CT Integration in Examination of Lung Tumors
 Hindawi Publishing Corporation International Journal of Biomedical Imaging Volume 2007, Article ID 17131, 5 pages doi:10.1155/2007/17131 Research Article The Advantage of PET and CT Integration in Examination
Hindawi Publishing Corporation International Journal of Biomedical Imaging Volume 2007, Article ID 17131, 5 pages doi:10.1155/2007/17131 Research Article The Advantage of PET and CT Integration in Examination
IAEA RTC. PET/CT and Planning of Radiation Therapy 20/08/2014. Sarajevo (Bosnia & Hercegovina) Tuesday, June :40-12:20 a.
 IAEA RTC PET/CT and Planning of Radiation Therapy Sarajevo (Bosnia & Hercegovina) Tuesday, June 17 2014 11:40-12:20 a.m María José García Velloso Servicio de Medicina Nuclear Clínica Universidad de Navarra
IAEA RTC PET/CT and Planning of Radiation Therapy Sarajevo (Bosnia & Hercegovina) Tuesday, June 17 2014 11:40-12:20 a.m María José García Velloso Servicio de Medicina Nuclear Clínica Universidad de Navarra
Los Angeles Radiological Society 62 nd Annual Midwinter Radiology Conference January 31, 2010
 Los Angeles Radiological Society 62 nd Annual Midwinter Radiology Conference January 31, 2010 Self Assessment Module on Nuclear Medicine and PET/CT Case Review FDG PET/CT IN LYMPHOMA AND MELANOMA Submitted
Los Angeles Radiological Society 62 nd Annual Midwinter Radiology Conference January 31, 2010 Self Assessment Module on Nuclear Medicine and PET/CT Case Review FDG PET/CT IN LYMPHOMA AND MELANOMA Submitted
Pitfalls and Remedies in PET/CT imaging for RT planning
 Pitfalls and Remedies in PET/CT imaging for RT planning Tinsu Pan, Ph.D. M.D. Anderson Cancer Center The University of Texas Outlines Background Average CT (< 1 msv) to reduce mis-alignment of PET and
Pitfalls and Remedies in PET/CT imaging for RT planning Tinsu Pan, Ph.D. M.D. Anderson Cancer Center The University of Texas Outlines Background Average CT (< 1 msv) to reduce mis-alignment of PET and
Molecular Imaging and Cancer
 Molecular Imaging and Cancer Cancer causes one in every four deaths in the United States, second only to heart disease. According to the U.S. Department of Health and Human Services, more than 512,000
Molecular Imaging and Cancer Cancer causes one in every four deaths in the United States, second only to heart disease. According to the U.S. Department of Health and Human Services, more than 512,000
Clinical PET/CT imaging. PET/CT - Optimization of torso imaging. CT-based attenuation correction. PET/CT torso imaging
 / - Optimization of torso imaging Clinical / imaging Torso FDG, 1976 Torso FDG-/, 2007 Thomas Beyer thomas.beyer@cmi-experts.com CE 30, SNM Annual Meeting, Toronto, June 2009 Software Hardware Neck Thorax
/ - Optimization of torso imaging Clinical / imaging Torso FDG, 1976 Torso FDG-/, 2007 Thomas Beyer thomas.beyer@cmi-experts.com CE 30, SNM Annual Meeting, Toronto, June 2009 Software Hardware Neck Thorax
PET/CT Frequently Asked Questions
 PET/CT Frequently Asked Questions General Q: Is FDG PET specific for cancer? A: No, it is a marker of metabolism. In general, any disease that causes increased metabolism can result in increased FDG uptake
PET/CT Frequently Asked Questions General Q: Is FDG PET specific for cancer? A: No, it is a marker of metabolism. In general, any disease that causes increased metabolism can result in increased FDG uptake
Biases Affecting the Measurements of Tumor-to-Background Activity Ratio in PET
 2112 IEEE TRANSACTIONS ON NUCLEAR SCIENCE, VOL. 49, NO. 5, OCTOBER 2002 Biases Affecting the Measurements of Tumor-to-Background Activity Ratio in PET M. Soret, C. Riddell, S. Hapdey, and I. Buvat Abstract
2112 IEEE TRANSACTIONS ON NUCLEAR SCIENCE, VOL. 49, NO. 5, OCTOBER 2002 Biases Affecting the Measurements of Tumor-to-Background Activity Ratio in PET M. Soret, C. Riddell, S. Hapdey, and I. Buvat Abstract
Photon Attenuation Correction in Misregistered Cardiac PET/CT
 Photon Attenuation Correction in Misregistered Cardiac PET/CT A. Martinez-Möller 1,2, N. Navab 2, M. Schwaiger 1, S. G. Nekolla 1 1 Nuklearmedizinische Klinik der TU München 2 Computer Assisted Medical
Photon Attenuation Correction in Misregistered Cardiac PET/CT A. Martinez-Möller 1,2, N. Navab 2, M. Schwaiger 1, S. G. Nekolla 1 1 Nuklearmedizinische Klinik der TU München 2 Computer Assisted Medical
Endobronchial Ultrasound in the Diagnosis & Staging of Lung Cancer
 Endobronchial Ultrasound in the Diagnosis & Staging of Lung Cancer Dr Richard Booton PhD FRCP Lead Lung Cancer Clinician, Consultant Respiratory Physician & Speciality Director Manchester University NHS
Endobronchial Ultrasound in the Diagnosis & Staging of Lung Cancer Dr Richard Booton PhD FRCP Lead Lung Cancer Clinician, Consultant Respiratory Physician & Speciality Director Manchester University NHS
Title: TC simulation versus TC/PET simulation for radiotherapy in lung cancer: volumes comparison in two cases.
 Title: TC simulation versus TC/PET simulation for radiotherapy in lung cancer: volumes comparison in two cases. Authors: Franzone, P.; 1* Muni, A; 2 Cazzulo, E.; 3 Berretta, L.; 1 Pozzi, G. 1 ; Todisco,
Title: TC simulation versus TC/PET simulation for radiotherapy in lung cancer: volumes comparison in two cases. Authors: Franzone, P.; 1* Muni, A; 2 Cazzulo, E.; 3 Berretta, L.; 1 Pozzi, G. 1 ; Todisco,
The development of combined PET/CT scanners has
 Decreased Perfusion in the Lateral Wall of the Left Ventricle in PET/CT Studies with 13 N-Ammonia: Evaluation in Healthy Adults William C. Klingensmith III 1, Carolyn Noonan 2, Jack H. Goldberg 2, Dedra
Decreased Perfusion in the Lateral Wall of the Left Ventricle in PET/CT Studies with 13 N-Ammonia: Evaluation in Healthy Adults William C. Klingensmith III 1, Carolyn Noonan 2, Jack H. Goldberg 2, Dedra
GE Healthcare. Rad Rx. White Paper
 GE Healthcare Rad Rx White Paper Introduction This publication is part of a series of white papers aimed at communicating the importance of each component in the image chain of a PET/CT study. From data
GE Healthcare Rad Rx White Paper Introduction This publication is part of a series of white papers aimed at communicating the importance of each component in the image chain of a PET/CT study. From data
MEASUREMENT OF EFFECT SOLID TUMOR EXAMPLES
 MEASUREMENT OF EFFECT SOLID TUMOR EXAMPLES Although response is not the primary endpoint of this trial, subjects with measurable disease will be assessed by standard criteria. For the purposes of this
MEASUREMENT OF EFFECT SOLID TUMOR EXAMPLES Although response is not the primary endpoint of this trial, subjects with measurable disease will be assessed by standard criteria. For the purposes of this
WHAT DOES PET IMAGING ADD TO CONVENTIONAL STAGING OF HEAD AND NECK CANCER PATIENTS?
 doi:10.1016/j.ijrobp.2006.12.044 Int. J. Radiation Oncology Biol. Phys., Vol. 68, No. 2, pp. 383 387, 2007 Copyright 2007 Elsevier Inc. Printed in the USA. All rights reserved 0360-3016/07/$ see front
doi:10.1016/j.ijrobp.2006.12.044 Int. J. Radiation Oncology Biol. Phys., Vol. 68, No. 2, pp. 383 387, 2007 Copyright 2007 Elsevier Inc. Printed in the USA. All rights reserved 0360-3016/07/$ see front
Early detection of prostate cancer (PCa) may feasibly lead
 ORIGINAL ARTICLE C-11 Choline PET/CT Imaging for Differentiating Malignant From Benign Prostate Lesions Xin Li, MD,* Qi Liu, MD, PhD,* Muwen Wang, MD, PhD,* Xunbo Jin, MD,* Qingwei Liu, MD, PhD,* Shuzhan
ORIGINAL ARTICLE C-11 Choline PET/CT Imaging for Differentiating Malignant From Benign Prostate Lesions Xin Li, MD,* Qi Liu, MD, PhD,* Muwen Wang, MD, PhD,* Xunbo Jin, MD,* Qingwei Liu, MD, PhD,* Shuzhan
Reproducibility of Uptake Estimates in FDG PET: a Monte Carlo study
 Reproducibility of Uptake Estimates in FDG PET: a Monte Carlo study Juliette Feuardent, Marine Soret, Irène Buvat 1 Abstract Tumor glucose metabolism measurements from Fluoro-deoxyglucose (FDG) Positron
Reproducibility of Uptake Estimates in FDG PET: a Monte Carlo study Juliette Feuardent, Marine Soret, Irène Buvat 1 Abstract Tumor glucose metabolism measurements from Fluoro-deoxyglucose (FDG) Positron
Reevaluation of the Standardized Uptake Value for FDG: Variations with Body Weight and Methods for Correction 1
 Nuclear Medicine Yoshifumi Sugawara, MD Kenneth R. Zasadny, PhD Alex W. Neuhoff, BS Richard L. Wahl, MD Index terms: Breast neoplasms, PET, 00.12163, 00.32 Breast neoplasms, radionuclide studies, 00.12163,
Nuclear Medicine Yoshifumi Sugawara, MD Kenneth R. Zasadny, PhD Alex W. Neuhoff, BS Richard L. Wahl, MD Index terms: Breast neoplasms, PET, 00.12163, 00.32 Breast neoplasms, radionuclide studies, 00.12163,
PET/CT for Therapy Assessment in Oncology
 PET/CT for Therapy Assessment in Oncology Rodolfo Núñez Miller, M.D. Nuclear Medicine Section Division of Human Health International Atomic Energy Agency Vienna, Austria Clinical Applications of PET/CT
PET/CT for Therapy Assessment in Oncology Rodolfo Núñez Miller, M.D. Nuclear Medicine Section Division of Human Health International Atomic Energy Agency Vienna, Austria Clinical Applications of PET/CT
Noninvasive Differential Diagnosis of Pulmonary Nodules Using the Standardized Uptake Value Index
 doi: 10.5761/atcs.oa.14-00241 Original Article Noninvasive Differential Diagnosis of Pulmonary Nodules Using the Standardized Uptake Value Index Satoshi Shiono, MD, 1 Naoki Yanagawa, MD, 2 Masami Abiko,
doi: 10.5761/atcs.oa.14-00241 Original Article Noninvasive Differential Diagnosis of Pulmonary Nodules Using the Standardized Uptake Value Index Satoshi Shiono, MD, 1 Naoki Yanagawa, MD, 2 Masami Abiko,
Imaging for Lung Adenocarcinoma 1 to 3 cm in Size With Ground-Glass Opacity Images on Computed Tomography
 GENERAL THORACIC 11 C-Acetate Positron Emission Tomography Imaging for Lung Adenocarcinoma 1 to 3 cm in Size With Ground-Glass Opacity Images on Computed Tomography Hiroaki Nomori, MD, PhD, Noboru Kosaka,
GENERAL THORACIC 11 C-Acetate Positron Emission Tomography Imaging for Lung Adenocarcinoma 1 to 3 cm in Size With Ground-Glass Opacity Images on Computed Tomography Hiroaki Nomori, MD, PhD, Noboru Kosaka,
Utility of PET-CT for detection of N2 or N3 nodal mestastases in the mediastinum in patients with non-small cell lung cancer (NSCLC)
 Utility of PET-CT for detection of N2 or N3 nodal mestastases in the mediastinum in patients with non-small cell lung cancer (NSCLC) Poster No.: C-1360 Congress: ECR 2015 Type: Scientific Exhibit Authors:
Utility of PET-CT for detection of N2 or N3 nodal mestastases in the mediastinum in patients with non-small cell lung cancer (NSCLC) Poster No.: C-1360 Congress: ECR 2015 Type: Scientific Exhibit Authors:
First Clinical Experience with
 First Clinical Experience with Discovery MI Digital PET/CT Martin Huellner Department of Nuclear Medicine University Hospital Zurich / University of Zurich Switzerland Agenda BelNuc GE Symposium 1. Digital
First Clinical Experience with Discovery MI Digital PET/CT Martin Huellner Department of Nuclear Medicine University Hospital Zurich / University of Zurich Switzerland Agenda BelNuc GE Symposium 1. Digital
Dr Sneha Shah Tata Memorial Hospital, Mumbai.
 Dr Sneha Shah Tata Memorial Hospital, Mumbai. Topics covered Lymphomas including Burkitts Pediatric solid tumors (non CNS) Musculoskeletal Ewings & osteosarcoma. Neuroblastomas Nasopharyngeal carcinomas
Dr Sneha Shah Tata Memorial Hospital, Mumbai. Topics covered Lymphomas including Burkitts Pediatric solid tumors (non CNS) Musculoskeletal Ewings & osteosarcoma. Neuroblastomas Nasopharyngeal carcinomas
Typical PET Image. Elevated uptake of FDG (related to metabolism) Lung cancer example: But where exactly is it located?
 Typical PET Image Elevated uptake of FDG (related to metabolism) Lung cancer example: But where exactly is it located? PET/CT Oncology Imaging Anatometabolic fusion images are useful in the management
Typical PET Image Elevated uptake of FDG (related to metabolism) Lung cancer example: But where exactly is it located? PET/CT Oncology Imaging Anatometabolic fusion images are useful in the management
The Proper Use of PET/CT in Tumoring Imaging
 The Proper Use of PET/CT in Tumoring Imaging Mijin Yun, M.D. Jong Doo Lee, M.D. Department of Radiology / Division of Nuclear Medicine Yonsei University College of Medicine, Severance Hospital E mail :
The Proper Use of PET/CT in Tumoring Imaging Mijin Yun, M.D. Jong Doo Lee, M.D. Department of Radiology / Division of Nuclear Medicine Yonsei University College of Medicine, Severance Hospital E mail :
FDG PET/CT STAGING OF LUNG CANCER. Dr Shakher Ramdave
 FDG PET/CT STAGING OF LUNG CANCER Dr Shakher Ramdave FDG PET/CT STAGING OF LUNG CANCER FDG PET/CT is used in all patients with lung cancer who are considered for curative treatment to exclude occult disease.
FDG PET/CT STAGING OF LUNG CANCER Dr Shakher Ramdave FDG PET/CT STAGING OF LUNG CANCER FDG PET/CT is used in all patients with lung cancer who are considered for curative treatment to exclude occult disease.
PET CT for Staging Lung Cancer
 PET CT for Staging Lung Cancer Rohit Kochhar Consultant Radiologist Disclosures Neither I nor my immediate family members have financial relationships with commercial organizations that may have a direct
PET CT for Staging Lung Cancer Rohit Kochhar Consultant Radiologist Disclosures Neither I nor my immediate family members have financial relationships with commercial organizations that may have a direct
Nuclear Medicine and PET. D. J. McMahon rev cewood
 Nuclear Medicine and PET D. J. McMahon 150504 rev cewood 2018-02-15 Key Points Nuclear Medicine and PET: Imaging: Understand how Nuc Med & PET differ from Radiography & CT by the source of radiation. Be
Nuclear Medicine and PET D. J. McMahon 150504 rev cewood 2018-02-15 Key Points Nuclear Medicine and PET: Imaging: Understand how Nuc Med & PET differ from Radiography & CT by the source of radiation. Be
The Role of PET / CT in Lung Cancer Staging
 July 2004 The Role of PET / CT in Lung Cancer Staging Vlad Vinarsky, Harvard Medical School Year IV Patient AM HPI: 81 yo F p/w hemoptysis x 1 month LLL lesion on CXR, not responsive to Abx 35 pack-year
July 2004 The Role of PET / CT in Lung Cancer Staging Vlad Vinarsky, Harvard Medical School Year IV Patient AM HPI: 81 yo F p/w hemoptysis x 1 month LLL lesion on CXR, not responsive to Abx 35 pack-year
Deformation Effect on SUV max Changes in Thoracic Tumors Using 4-D PET/CT Scan
 Deformation Effect on SUV max Changes in Thoracic Tumors Using 4-D PET/CT Scan Tzung-Chi Huang 1 *, Yao-Ching Wang 2 1 Department of Biomedical Imaging and Radiological Science, China Medical University,
Deformation Effect on SUV max Changes in Thoracic Tumors Using 4-D PET/CT Scan Tzung-Chi Huang 1 *, Yao-Ching Wang 2 1 Department of Biomedical Imaging and Radiological Science, China Medical University,
Average CT in PET studies of colorectal cancer patients with metastasis in the liver and esophageal cancer patients
 JOURNAL OF APPLIED CLINICAL MEDICAL PHYSICS, VOLUME 11, NUMBER 1, WINTER 2010 Average CT in PET studies of colorectal cancer patients with metastasis in the liver and esophageal cancer patients Elena Tonkopi,
JOURNAL OF APPLIED CLINICAL MEDICAL PHYSICS, VOLUME 11, NUMBER 1, WINTER 2010 Average CT in PET studies of colorectal cancer patients with metastasis in the liver and esophageal cancer patients Elena Tonkopi,
Regular PET Scanning Without CT. Christian Cohade and Richard L. Wahl
 Applications of Positron Emission Tomography/Computed Tomography Image Fusion in Clinical Positron Emission Tomography Clinical Use, Interpretation Methods, Diagnostic Improvements Christian Cohade and
Applications of Positron Emission Tomography/Computed Tomography Image Fusion in Clinical Positron Emission Tomography Clinical Use, Interpretation Methods, Diagnostic Improvements Christian Cohade and
Evaluation of Lung Cancer Response: Current Practice and Advances
 Evaluation of Lung Cancer Response: Current Practice and Advances Jeremy J. Erasmus I have no financial relationships, arrangements or affiliations and this presentation will not include discussion of
Evaluation of Lung Cancer Response: Current Practice and Advances Jeremy J. Erasmus I have no financial relationships, arrangements or affiliations and this presentation will not include discussion of
PET/CT in lung cancer
 PET/CT in lung cancer Andrei Šamarin North Estonia Medical Centre 3 rd Baltic Congress of Radiology 08.10.2010 Imaging in lung cancer Why do we need PET/CT? CT is routine imaging modality for staging of
PET/CT in lung cancer Andrei Šamarin North Estonia Medical Centre 3 rd Baltic Congress of Radiology 08.10.2010 Imaging in lung cancer Why do we need PET/CT? CT is routine imaging modality for staging of
Bone PET/MRI : Diagnostic yield in bone metastases and malignant primitive bone tumors
 Bone PET/MRI : Diagnostic yield in bone metastases and malignant primitive bone tumors Lars Stegger, Benjamin Noto Department of Nuclear Medicine University Hospital Münster, Germany Content From PET to
Bone PET/MRI : Diagnostic yield in bone metastases and malignant primitive bone tumors Lars Stegger, Benjamin Noto Department of Nuclear Medicine University Hospital Münster, Germany Content From PET to
PET in Radiation Therapy. Outline. Tumor Segmentation in PET and in Multimodality Images for Radiation Therapy. 1. Tumor segmentation in PET
 Tumor Segmentation in PET and in Multimodality Images for Radiation Therapy Wei Lu, Ph.D. Department of Radiation Oncology Mallinckrodt Institute of Radiology Washington University in St. Louis Outline
Tumor Segmentation in PET and in Multimodality Images for Radiation Therapy Wei Lu, Ph.D. Department of Radiation Oncology Mallinckrodt Institute of Radiology Washington University in St. Louis Outline
A Snapshot on Nuclear Cardiac Imaging
 Editorial A Snapshot on Nuclear Cardiac Imaging Khalil, M. Department of Physics, Faculty of Science, Helwan University. There is no doubt that nuclear medicine scanning devices are essential tool in the
Editorial A Snapshot on Nuclear Cardiac Imaging Khalil, M. Department of Physics, Faculty of Science, Helwan University. There is no doubt that nuclear medicine scanning devices are essential tool in the
Relation of external surface to internal tumor motion studied with cine CT
 Relation of external surface to internal tumor motion studied with cine CT Pai-Chun Melinda Chi, a Peter Balter, Dershan Luo, Radhe Mohan, and Tinsu Pan Departments of Imaging Physics and Radiation Physics,
Relation of external surface to internal tumor motion studied with cine CT Pai-Chun Melinda Chi, a Peter Balter, Dershan Luo, Radhe Mohan, and Tinsu Pan Departments of Imaging Physics and Radiation Physics,
8/10/2016. PET/CT Radiomics for Tumor. Anatomic Tumor Response Assessment in CT or MRI. Metabolic Tumor Response Assessment in FDG-PET
 PET/CT Radiomics for Tumor Response Evaluation August 1, 2016 Wei Lu, PhD Department of Medical Physics www.mskcc.org Department of Radiation Oncology www.umaryland.edu Anatomic Tumor Response Assessment
PET/CT Radiomics for Tumor Response Evaluation August 1, 2016 Wei Lu, PhD Department of Medical Physics www.mskcc.org Department of Radiation Oncology www.umaryland.edu Anatomic Tumor Response Assessment
New Visions in PET: Surgical Decision Making and PET/CT
 New Visions in PET: Surgical Decision Making and PET/CT Stanley J. Goldsmith, MD Director, Nuclear Medicine Professor, Radiology & Medicine New York Presbyterian Hospital- Weill Cornell Medical Center
New Visions in PET: Surgical Decision Making and PET/CT Stanley J. Goldsmith, MD Director, Nuclear Medicine Professor, Radiology & Medicine New York Presbyterian Hospital- Weill Cornell Medical Center
FDG-18 PET/CT - radiation dose and dose-reduction strategy
 FDG-18 PET/CT - radiation dose and dose-reduction strategy Poster No.: C-1856 Congress: ECR 2014 Type: Authors: Keywords: DOI: Scientific Exhibit P. Nicholson, S. McSweeney, K. O'Regan; Cork/IE Radiation
FDG-18 PET/CT - radiation dose and dose-reduction strategy Poster No.: C-1856 Congress: ECR 2014 Type: Authors: Keywords: DOI: Scientific Exhibit P. Nicholson, S. McSweeney, K. O'Regan; Cork/IE Radiation
An audit of radiation dose of 4D CT in a radiotherapy department
 An audit of radiation dose of 4D CT in a radiotherapy department Poster No.: R-0097 Congress: Type: Authors: Keywords: DOI: 2014 CSM Scientific Exhibit T. Hubbard, J. Callahan, J. Cramb, R. Budd, T. Kron;
An audit of radiation dose of 4D CT in a radiotherapy department Poster No.: R-0097 Congress: Type: Authors: Keywords: DOI: 2014 CSM Scientific Exhibit T. Hubbard, J. Callahan, J. Cramb, R. Budd, T. Kron;
Recent advances in positron emission tomography (PET)
 Evaluation of Semiquantitative Assessments of Fluorodeoxyglucose Uptake on Positron Emission Tomography Scans for the Diagnosis of Pulmonary Malignancies 1 to 3 cm in Size Yasuomi Ohba, MD, Hiroaki Nomori,
Evaluation of Semiquantitative Assessments of Fluorodeoxyglucose Uptake on Positron Emission Tomography Scans for the Diagnosis of Pulmonary Malignancies 1 to 3 cm in Size Yasuomi Ohba, MD, Hiroaki Nomori,
Introduction Pediatric malignancies Changing trends & Radiation burden Radiation exposure from PET/CT Image gently PET & CT modification - PET/CT
 Introduction Pediatric malignancies Changing trends & Radiation burden Radiation exposure from PET/CT Image gently PET & CT modification - PET/CT protocols Tips Leukaemia / lymphoma: ~ 35% acute lymphoblastic
Introduction Pediatric malignancies Changing trends & Radiation burden Radiation exposure from PET/CT Image gently PET & CT modification - PET/CT protocols Tips Leukaemia / lymphoma: ~ 35% acute lymphoblastic
Breast Cancer PET/CT Imaging Protocol
 Breast Cancer PET/CT Imaging Protocol Scanning Protocol: Patients are scanned from the top of the neck through the pelvis. Arms-up position is used to avoid beam-hardening artifact in the chest and abdomen.
Breast Cancer PET/CT Imaging Protocol Scanning Protocol: Patients are scanned from the top of the neck through the pelvis. Arms-up position is used to avoid beam-hardening artifact in the chest and abdomen.
Learning Objectives. 1. Identify which patients meet criteria for annual lung cancer screening
 Disclosure I, Taylor Rowlett, DO NOT have a financial interest /arrangement or affiliation with one or more organizations that could be perceived as a real or apparent conflict of interest in the context
Disclosure I, Taylor Rowlett, DO NOT have a financial interest /arrangement or affiliation with one or more organizations that could be perceived as a real or apparent conflict of interest in the context
Patterns and Prevalence of Misregistration in 18 F-FDG PET/CT
 Egyptian J. Nucl. Med., Vol 2, No. 2, Dec. 2009 55 ONCOLOGY, Original Article Patterns and Prevalence of Misregistration in 18 F-FDG PET/CT Farghaly HR,* Muzaffar R,** Bohle RJ,** Nguyen NC,** Osman MM,**
Egyptian J. Nucl. Med., Vol 2, No. 2, Dec. 2009 55 ONCOLOGY, Original Article Patterns and Prevalence of Misregistration in 18 F-FDG PET/CT Farghaly HR,* Muzaffar R,** Bohle RJ,** Nguyen NC,** Osman MM,**
An Introduction to PET Imaging in Oncology
 January 2002 An Introduction to PET Imaging in Oncology Janet McLaren, Harvard Medical School Year III Basics of PET Principle of Physiologic Imaging: Allows in vivo visualization of structures by their
January 2002 An Introduction to PET Imaging in Oncology Janet McLaren, Harvard Medical School Year III Basics of PET Principle of Physiologic Imaging: Allows in vivo visualization of structures by their
PET-MRI in malignant bone tumours. Lars Stegger Department of Nuclear Medicine University Hospital Münster, Germany
 PET-MRI in malignant bone tumours Lars Stegger Department of Nuclear Medicine University Hospital Münster, Germany Content From PET to PET/MRI General considerations Bone metastases Primary bone tumours
PET-MRI in malignant bone tumours Lars Stegger Department of Nuclear Medicine University Hospital Münster, Germany Content From PET to PET/MRI General considerations Bone metastases Primary bone tumours
Shozo Yamashita Kunihiko Yokoyama Masahisa Onoguchi Haruki Yamamoto Shigeaki Hiko Akihiro Horita Kenichi Nakajima
 Ann Nucl Med (2014) 28:1 10 DOI 10.1007/s12149-013-0774-9 ORIGINAL ARTICLE Feasibility of deep-inspiration breath-hold PET/CT with short-time acquisition: detectability for pulmonary lesions compared with
Ann Nucl Med (2014) 28:1 10 DOI 10.1007/s12149-013-0774-9 ORIGINAL ARTICLE Feasibility of deep-inspiration breath-hold PET/CT with short-time acquisition: detectability for pulmonary lesions compared with
Mathieu Hatt, Dimitris Visvikis. To cite this version: HAL Id: inserm
 Defining radiotherapy target volumes using 18F-fluoro-deoxy-glucose positron emission tomography/computed tomography: still a Pandora s box?: in regard to Devic et al. (Int J Radiat Oncol Biol Phys 2010).
Defining radiotherapy target volumes using 18F-fluoro-deoxy-glucose positron emission tomography/computed tomography: still a Pandora s box?: in regard to Devic et al. (Int J Radiat Oncol Biol Phys 2010).
Identifying Image Artifacts, Their Causes and How to Fix Them: PET. Brad J Kemp, PhD Mayo Clinic, Rochester, MN
 Identifying Image Artifacts, Their Causes and How to Fix Them: PET Brad J Kemp, PhD Mayo Clinic, Rochester, MN Case 1 Can we scan with a defective block detector? Daily Quality Assurance Results Singles
Identifying Image Artifacts, Their Causes and How to Fix Them: PET Brad J Kemp, PhD Mayo Clinic, Rochester, MN Case 1 Can we scan with a defective block detector? Daily Quality Assurance Results Singles
PET/CT in Gynaecological Cancers. Stroobants Sigrid, MD, PhD Departement of Nuclear Medicine University Hospital,Antwerp
 PET/CT in Gynaecological Cancers Stroobants Sigrid, MD, PhD Departement of Nuclear Medicine University Hospital,Antwerp Cervix cancer Outline of this talk Initial staging Treatment monitoring/guidance
PET/CT in Gynaecological Cancers Stroobants Sigrid, MD, PhD Departement of Nuclear Medicine University Hospital,Antwerp Cervix cancer Outline of this talk Initial staging Treatment monitoring/guidance
Ryan Niederkohr, M.D. Slides are not to be reproduced without permission of author
 Ryan Niederkohr, M.D. CMS: PET/CT CPT CODES 78814 Limited Area (e.g., head/neck only; chest only) 78815 78816 Regional (skull base to mid-thighs) True Whole Body (skull vertex to feet) SELECTING FIELD
Ryan Niederkohr, M.D. CMS: PET/CT CPT CODES 78814 Limited Area (e.g., head/neck only; chest only) 78815 78816 Regional (skull base to mid-thighs) True Whole Body (skull vertex to feet) SELECTING FIELD
Direct Comparison of 18 F-FDG PET and PET/CT in Patients with Colorectal Carcinoma
 Direct Comparison of F-FDG PET and PET/CT in Patients with Colorectal Carcinoma Christian Cohade, MD; Medhat Osman, MD, PhD; Jeffrey Leal, BA; and Richard L. Wahl, MD Division of Nuclear Medicine, Russell
Direct Comparison of F-FDG PET and PET/CT in Patients with Colorectal Carcinoma Christian Cohade, MD; Medhat Osman, MD, PhD; Jeffrey Leal, BA; and Richard L. Wahl, MD Division of Nuclear Medicine, Russell
Q.SUV. Quantitative SUV you and your patients can trust. GE Healthcare Q.SUV 6.4 Q.SUV 9.6. Conventional SUV 3.1 (49% Convergence)
 GE Healthcare Q. 9.6 Q. 6.4 Conventional 3.1 (49% Convergence) Conventional 7.0 (73% Convergence) Q. TM Quantitative you and your patients can trust What if s were accurate and consistent? 2 Introduction
GE Healthcare Q. 9.6 Q. 6.4 Conventional 3.1 (49% Convergence) Conventional 7.0 (73% Convergence) Q. TM Quantitative you and your patients can trust What if s were accurate and consistent? 2 Introduction
Molecular Imaging in the Development of Cancer Therapeutics. Johannes Czernin
 Molecular Imaging in the Development of Cancer Therapeutics Johannes Czernin Ahmanson Biological Imaging Division University of California Los Angeles Cancer Statistics Cancer Type 5-year Survival Rate
Molecular Imaging in the Development of Cancer Therapeutics Johannes Czernin Ahmanson Biological Imaging Division University of California Los Angeles Cancer Statistics Cancer Type 5-year Survival Rate
Nuclear medicine in oncology. 1. Diagnosis 2. Therapy
 Nuclear medicine in oncology 1. Diagnosis 2. Therapy Diagnosis - Conventional methods - Nonspecific radiopharmaceuticals cumulating in tumours - Specific radiopharmaceuticals (receptor- and immunoscintigraphy)
Nuclear medicine in oncology 1. Diagnosis 2. Therapy Diagnosis - Conventional methods - Nonspecific radiopharmaceuticals cumulating in tumours - Specific radiopharmaceuticals (receptor- and immunoscintigraphy)
Disclosure. Acknowledgement. What is the Best Workup for Rectal Cancer Staging: US/MRI/PET? Rectal cancer imaging. None
 What is the Best Workup for Rectal Cancer Staging: US/MRI/PET? Zhen Jane Wang, MD Assistant Professor in Residence UC SF Department of Radiology Disclosure None Acknowledgement Hueylan Chern, MD, Department
What is the Best Workup for Rectal Cancer Staging: US/MRI/PET? Zhen Jane Wang, MD Assistant Professor in Residence UC SF Department of Radiology Disclosure None Acknowledgement Hueylan Chern, MD, Department
Uptake of 18 F-FDG in malignant tumors is subject to
 Time Course of Tumor SUV in 18 F-FDG PET of Breast Cancer: Presentation of a Simple Model Using a Single Reference Point for Time Corrections of Tumor SUVs Alexander R. Stahl 1, Till A. Heusner 2, Verena
Time Course of Tumor SUV in 18 F-FDG PET of Breast Cancer: Presentation of a Simple Model Using a Single Reference Point for Time Corrections of Tumor SUVs Alexander R. Stahl 1, Till A. Heusner 2, Verena
Radiological staging of lung cancer. Shukri Loutfi,MD,FRCR Consultant Thoracic Radiologist KAMC-Riyadh
 Radiological staging of lung cancer Shukri Loutfi,MD,FRCR Consultant Thoracic Radiologist KAMC-Riyadh Bronchogenic Carcinoma Accounts for 14% of new cancer diagnoses in 2012. Estimated to kill ~150,000
Radiological staging of lung cancer Shukri Loutfi,MD,FRCR Consultant Thoracic Radiologist KAMC-Riyadh Bronchogenic Carcinoma Accounts for 14% of new cancer diagnoses in 2012. Estimated to kill ~150,000
Image Guided Stereotactic Radiotherapy of the Lung
 Image Guided Stereotactic Radiotherapy of the Lung Jamie Marie Harris, MS DABR Avera McKennan Radiation Oncology September 25, 2015 Stereotactic Body Radiotherapy - Clinical Dose/Fractionation - Normal
Image Guided Stereotactic Radiotherapy of the Lung Jamie Marie Harris, MS DABR Avera McKennan Radiation Oncology September 25, 2015 Stereotactic Body Radiotherapy - Clinical Dose/Fractionation - Normal
Research Article Invalidity of SUV Measurements of Lesions in Close Proximity to Hot Sources due to Shine-Through Effect on FDG PET-CT Interpretation
 Radiology Research and Practice Volume 2012, rticle ID 867218, 4 pages doi:10.1155/2012/867218 Research rticle Invalidity of SUV Measurements of Lesions in Close Proximity to Hot Sources due to Shine-Through
Radiology Research and Practice Volume 2012, rticle ID 867218, 4 pages doi:10.1155/2012/867218 Research rticle Invalidity of SUV Measurements of Lesions in Close Proximity to Hot Sources due to Shine-Through
Principles of nuclear metabolic imaging. Prof. Dr. Alex Maes AZ Groeninge Kortrijk and KULeuven Belgium
 Principles of nuclear metabolic imaging Prof. Dr. Alex Maes AZ Groeninge Kortrijk and KULeuven Belgium I. Molecular imaging probes A. Introduction - Chemical disturbances will precede anatomical abnormalities
Principles of nuclear metabolic imaging Prof. Dr. Alex Maes AZ Groeninge Kortrijk and KULeuven Belgium I. Molecular imaging probes A. Introduction - Chemical disturbances will precede anatomical abnormalities
8/10/2016. PET/CT for Tumor Response. Staging and restaging Early treatment response evaluation Guiding biopsy
 PET/CT for Tumor Response Evaluation August 4, 2016 Wei Lu, PhD Department of Medical Physics www.mskcc.org Department of Radiation Oncology www.umaryland.edu FDG PET/CT for Cancer Imaging Staging and
PET/CT for Tumor Response Evaluation August 4, 2016 Wei Lu, PhD Department of Medical Physics www.mskcc.org Department of Radiation Oncology www.umaryland.edu FDG PET/CT for Cancer Imaging Staging and
4D-MRI for Radiotherapy of moving Tumours: Latest developments, comparison to 4D-CT. J. Biederer Vancouver, August 2, 2011
 4D-MRI for Radiotherapy of moving Tumours: Latest developments, comparison to 4D-CT Vancouver, August 2, 2011 Indications for Radiotherapy of Lung Cancer primary radiotherapy in NCSLC - stage III Oertel
4D-MRI for Radiotherapy of moving Tumours: Latest developments, comparison to 4D-CT Vancouver, August 2, 2011 Indications for Radiotherapy of Lung Cancer primary radiotherapy in NCSLC - stage III Oertel
Case Report PET/CT Imaging in Oncology: Exceptions That Prove the Rule
 Case Reports in Oncological Medicine Volume 2013, Article ID 865032, 4 pages http://dx.doi.org/10.1155/2013/865032 Case Report PET/CT Imaging in Oncology: Exceptions That Prove the Rule M. Casali, 1 A.
Case Reports in Oncological Medicine Volume 2013, Article ID 865032, 4 pages http://dx.doi.org/10.1155/2013/865032 Case Report PET/CT Imaging in Oncology: Exceptions That Prove the Rule M. Casali, 1 A.
45 Hr PET Registry Review Course
 45 HR PET/CT REGISTRY REVIEW COURSE Course Control Document Timothy K. Marshel, MBA, R.T. (R), (N)(CT)(MR)(NCT)(PET)(CNMT) The PET/CT Training Institute, Inc. SNMMI-TS 028600-028632 45hr CEH s Voice Credits
45 HR PET/CT REGISTRY REVIEW COURSE Course Control Document Timothy K. Marshel, MBA, R.T. (R), (N)(CT)(MR)(NCT)(PET)(CNMT) The PET/CT Training Institute, Inc. SNMMI-TS 028600-028632 45hr CEH s Voice Credits
Molecular Imaging and Breast Cancer
 Molecular Imaging and Breast Cancer Breast cancer forms in tissues of the breast usually in the ducts, tubes that carry milk to the nipple, and lobules, the glands that make milk. It occurs in both men
Molecular Imaging and Breast Cancer Breast cancer forms in tissues of the breast usually in the ducts, tubes that carry milk to the nipple, and lobules, the glands that make milk. It occurs in both men
Bilateral hilar 18 F-FDG avid foci are often noted on
 Bilateral Hilar Foci on F-FDG PET Scan in Patients Without Lung Cancer: Variables Associated with Benign and Malignant Etiology Maroun Karam 1, Shayna Roberts-Klein 1, Narendra Shet 2, Johanna Chang 2,
Bilateral Hilar Foci on F-FDG PET Scan in Patients Without Lung Cancer: Variables Associated with Benign and Malignant Etiology Maroun Karam 1, Shayna Roberts-Klein 1, Narendra Shet 2, Johanna Chang 2,
The Use of PET Scanning in Urologic Oncology
 The Use of PET Scanning in Urologic Oncology Dr Nicholas C. Buchan Uro-oncology Fellow 1 2 Aims To understand the basic concepts underlying PET scanning. Understand the emerging role of PET Scanning for
The Use of PET Scanning in Urologic Oncology Dr Nicholas C. Buchan Uro-oncology Fellow 1 2 Aims To understand the basic concepts underlying PET scanning. Understand the emerging role of PET Scanning for
Index. Surg Oncol Clin N Am 16 (2007) Note: Page numbers of article titles are in boldface type.
 Surg Oncol Clin N Am 16 (2007) 465 469 Index Note: Page numbers of article titles are in boldface type. A Adjuvant therapy, preoperative for gastric cancer, staging and, 339 B Breast cancer, metabolic
Surg Oncol Clin N Am 16 (2007) 465 469 Index Note: Page numbers of article titles are in boldface type. A Adjuvant therapy, preoperative for gastric cancer, staging and, 339 B Breast cancer, metabolic
Comparison of three mathematical prediction models in patients with a solitary pulmonary nodule
 Original Article Comparison of three mathematical prediction models in patients with a solitary pulmonary nodule Xuan Zhang*, Hong-Hong Yan, Jun-Tao Lin, Ze-Hua Wu, Jia Liu, Xu-Wei Cao, Xue-Ning Yang From
Original Article Comparison of three mathematical prediction models in patients with a solitary pulmonary nodule Xuan Zhang*, Hong-Hong Yan, Jun-Tao Lin, Ze-Hua Wu, Jia Liu, Xu-Wei Cao, Xue-Ning Yang From
S taging non-small lung cancer (NSCLC) is an important
 696 LUNG CANCER Integrated FDG-PET/CT does not make invasive staging of the intrathoracic lymph nodes in non-small cell lung cancer redundant: a prospective study K G Tournoy, S Maddens, R Gosselin, G
696 LUNG CANCER Integrated FDG-PET/CT does not make invasive staging of the intrathoracic lymph nodes in non-small cell lung cancer redundant: a prospective study K G Tournoy, S Maddens, R Gosselin, G
Small Pulmonary Nodules: Our Preliminary Experience in Volumetric Analysis of Doubling Times
 Small Pulmonary Nodules: Our Preliminary Experience in Volumetric Analysis of Doubling Times Andrea Borghesi, MD Davide Farina, MD Roberto Maroldi, MD Department of Radiology University of Brescia Brescia,
Small Pulmonary Nodules: Our Preliminary Experience in Volumetric Analysis of Doubling Times Andrea Borghesi, MD Davide Farina, MD Roberto Maroldi, MD Department of Radiology University of Brescia Brescia,
Cardiac Imaging Tests
 Cardiac Imaging Tests http://www.medpagetoday.com/upload/2010/11/15/23347.jpg Standard imaging tests include echocardiography, chest x-ray, CT, MRI, and various radionuclide techniques. Standard CT and
Cardiac Imaging Tests http://www.medpagetoday.com/upload/2010/11/15/23347.jpg Standard imaging tests include echocardiography, chest x-ray, CT, MRI, and various radionuclide techniques. Standard CT and
Ultralow Dose Chest CT with MBIR
 Ultralow Dose Chest CT with MBIR Ella A. Kazerooni, M.D. Professor & Director Cardiothoracic Radiology Associate Chair for Clinical Affairs University of Michigan Disclosures Consultant: GE Healthcare
Ultralow Dose Chest CT with MBIR Ella A. Kazerooni, M.D. Professor & Director Cardiothoracic Radiology Associate Chair for Clinical Affairs University of Michigan Disclosures Consultant: GE Healthcare
CARDIAC PET PERFUSION IMAGING with RUBIDIUM-82
 CARDIAC PET PERFUSION IMAGING with RUBIDIUM-82 Pr Denis AGOSTINI Président du Groupe de Cardiologie Nucléaire et IRM CHU Caen Bordeaux 2006 Cardiac Perfusion-Metabolism Mismatch with PET Cumulative Survival
CARDIAC PET PERFUSION IMAGING with RUBIDIUM-82 Pr Denis AGOSTINI Président du Groupe de Cardiologie Nucléaire et IRM CHU Caen Bordeaux 2006 Cardiac Perfusion-Metabolism Mismatch with PET Cumulative Survival
Disclosures. Diffusion and Perfusion Imaging in the Head and Neck. Learning objectives ???
 Disclosures No relevant financial disclosures Diffusion and Perfusion Imaging in the Head and Neck Ashok Srinivasan, MD Associate Professor Director of Neuroradiology University of Michigan Health System
Disclosures No relevant financial disclosures Diffusion and Perfusion Imaging in the Head and Neck Ashok Srinivasan, MD Associate Professor Director of Neuroradiology University of Michigan Health System
Clinical evaluation of respiration-induced attenuation uncertainties in pulmonary 3D PET/CT
 Kruis et al. EJNMMI Physics (2015) 2:4 DOI 10.1186/s40658-014-0107-7 ORIGINAL RESEARCH Open Access Clinical evaluation of respiration-induced attenuation uncertainties in pulmonary 3D PET/CT Matthijs F
Kruis et al. EJNMMI Physics (2015) 2:4 DOI 10.1186/s40658-014-0107-7 ORIGINAL RESEARCH Open Access Clinical evaluation of respiration-induced attenuation uncertainties in pulmonary 3D PET/CT Matthijs F
FDG-PET/CT in Gynaecologic Cancers
 Friday, August 31, 2012 Session 6, 9:00-9:30 FDG-PET/CT in Gynaecologic Cancers (Uterine) cervical cancer Endometrial cancer & Uterine sarcomas Ovarian cancer Little mermaid (Edvard Eriksen 1913) honoring
Friday, August 31, 2012 Session 6, 9:00-9:30 FDG-PET/CT in Gynaecologic Cancers (Uterine) cervical cancer Endometrial cancer & Uterine sarcomas Ovarian cancer Little mermaid (Edvard Eriksen 1913) honoring
REVIEW. Distinguishing benign from malignant adrenal masses
 Cancer Imaging (2003) 3, 102 110 DOI: 10.1102/1470-7330.2003.0006 CI REVIEW Distinguishing benign from malignant adrenal masses Isaac R Francis Professor of Radiology, Department of Radiology, University
Cancer Imaging (2003) 3, 102 110 DOI: 10.1102/1470-7330.2003.0006 CI REVIEW Distinguishing benign from malignant adrenal masses Isaac R Francis Professor of Radiology, Department of Radiology, University
1 Introduction. 2 Materials and methods. LI Na 1 LI Yaming 1,* YANG Chunming 2 LI Xuena 1 YIN Yafu 1 ZHOU Jiumao 1
 Nuclear Science and Techniques 20 (2009) 354 358 18 F-FDG PET/CT in diagnosis of skeletal metastases LI Na 1 LI Yaming 1,* YANG Chunming 2 LI Xuena 1 YIN Yafu 1 ZHOU Jiumao 1 1 Department of Nuclear Medicine,
Nuclear Science and Techniques 20 (2009) 354 358 18 F-FDG PET/CT in diagnosis of skeletal metastases LI Na 1 LI Yaming 1,* YANG Chunming 2 LI Xuena 1 YIN Yafu 1 ZHOU Jiumao 1 1 Department of Nuclear Medicine,
8/3/2016. Outline. Site Specific IGRT Considerations for Clinical Imaging Protocols. Krishni Wijesooriya, PhD University of Virginia
 Site Specific IGRT Considerations for Clinical Imaging Protocols Krishni Wijesooriya, PhD University of Virginia Outline Image registration accuracies for different modalities What imaging modality best
Site Specific IGRT Considerations for Clinical Imaging Protocols Krishni Wijesooriya, PhD University of Virginia Outline Image registration accuracies for different modalities What imaging modality best
Precision of pre-sirt predictive dosimetry
 International Course on THERANOSTICS AND MOLECULAR RADIOTHERAPY Precision of pre-sirt predictive dosimetry Hugo Levillain Department of Nuclear Medicine Medical Physics Jules Bordet Institute, Université
International Course on THERANOSTICS AND MOLECULAR RADIOTHERAPY Precision of pre-sirt predictive dosimetry Hugo Levillain Department of Nuclear Medicine Medical Physics Jules Bordet Institute, Université
Deppen S, et al. Annals of Thoracic Surgery 2011;92:
 Deppen S, et al. Annals of Thoracic Surgery 2011;92:428-33. http://www.nationmaster.com/graph/ mor_his-mortality-histoplasmosis http://www.humirarems.com/brochure.aspx Baddley, John W., et al. Emerging
Deppen S, et al. Annals of Thoracic Surgery 2011;92:428-33. http://www.nationmaster.com/graph/ mor_his-mortality-histoplasmosis http://www.humirarems.com/brochure.aspx Baddley, John W., et al. Emerging
patients with urinary tract infection and distended bladder
 J of Nuclear Medicine Technology, first published online December 23, 2014 as doi:10.2967/jnmt.114.148031 Interesting layering of excreted 18 F-FDG in the urinary bladder in patients with urinary tract
J of Nuclear Medicine Technology, first published online December 23, 2014 as doi:10.2967/jnmt.114.148031 Interesting layering of excreted 18 F-FDG in the urinary bladder in patients with urinary tract
Measurement of Respiratory and Cardiac Motion Using a Multi Antenna Continuous Wave Radar Operating in the Near Field
 Measurement of Respiratory and Cardiac Motion Using a Multi Antenna Continuous Wave Radar Operating in the Near Field Florian Pfanner 1,2, Thomas Allmendinger 2, Thomas Flohr 2, and Marc Kachelrieß 1,3
Measurement of Respiratory and Cardiac Motion Using a Multi Antenna Continuous Wave Radar Operating in the Near Field Florian Pfanner 1,2, Thomas Allmendinger 2, Thomas Flohr 2, and Marc Kachelrieß 1,3
Optimized PET/CT protocols: how much CT is needed? Increasing use of PET-CT. Imaging in Lymphoma
 BVS/ABR Workshop 2011 on dose related to multimodality imaging Optimized PET/CT protocols: how much CT is needed? 2008 Mean medical radiation exposure/head Belgium= 2.42 msv The Netherlands= 0.8 msv Belgium
BVS/ABR Workshop 2011 on dose related to multimodality imaging Optimized PET/CT protocols: how much CT is needed? 2008 Mean medical radiation exposure/head Belgium= 2.42 msv The Netherlands= 0.8 msv Belgium
