PRIMARY CUTANEOUS T-cell lymphomas
|
|
|
- Tracy Hunt
- 5 years ago
- Views:
Transcription
1 Cutaneous T-Cell Lymphomas: A Review With Emphasis on New Treatment Approaches Christiane Querfeld, MD, Steven T. Rosen, MD, Timothy M. Kuzel, MD, and Joan Guitart, MD Primary cutaneous T-cell lymphomas represent a wide variety of non-hodgkin lymphomas that are characterized by a distinct clinical presentation. Advanced molecular and biological techniques have enhanced the recognition of cutaneous T- cell lymphomas. The most common subtypes of cutaneous T-cell lymphomas are the epidermotropic variants mycosis fungoides and Sézary syndrome. At present, a stage-adjusted therapy is the best concept available, since early aggressive treatment options did not improve the prognosis of patients with cutaneous T-cell lymphomas. Accurate diagnostic and clinical assessment as well as identification of prognostic factors provides a helpful basis for treatment strategies. Current medical literature on diagnosis, prognosis, and treatment is reviewed with emphasis on new biologic response-modifying treatment options Elsevier Inc. All rights reserved. PRIMARY CUTANEOUS T-cell lymphomas (CTCL) represent a heterogeneous group of lymphomas with a distinct clinical presentation, behaviour, and prognosis. Most classification systems were designed for non-hodgkin lymphomas and do not provide a helpful characterization of cutaneous lymphomas. In 1997, the European Organization for Research and Treatment of Cancer (EORTC) presented its own clinically oriented classification of primary cutaneous lymphomas taking into account the histological and molecular features. 1 Although for pathology reporting many pathologists prefer the currently developed scheme of From the Division of Hematology/Oncology, Departments of Dermatology and Medicine, Robert H. Lurie Comprehensive Cancer Center, Feinberg School of Medicine, Northwestern University, Chicago, IL. Address reprint requests to Christiane Querfeld, MD, Department of Dermatology, Research Fellow, Northwestern University, Feinberg School of Medicine, Galter Pavilion, Suite , 675 N St. Clair, Chicago, IL 60611; c-querfeld@northwestern.edu Elsevier Inc. All rights reserved /03/ $30.00/0 doi: /s (03) the World Health Organization (WHO), the EORTC classification still carries major clinical and therapeutical implications (Table 1). 2 Mycosis fungoides (MF) and Sézary syndrome (SS) are by far the most common types of CTCL in the general population comprising 50% of CTCL. Other, less common variants of CTCL include the CD30-positive lymphoproliferative disorders, CD30-negative large T-cell lymphoma, pleomorphic T-cell lymphoma, subcutaneous panniculitis-like T-cell lymphoma, and granulomatous slack skin. The origin of CTCL is poorly understood as viral and retroviral theories have not been conclusive to date, whereas the process of chronic antigenic stimulation remains possible. Studies of the cutaneous lymphocyte antigen (CLA), chemokines, and cell adhesion receptors have provided new insights into skin homing mechanisms, which play a role in cutaneous T-cell lymphomas. 3 It is believed that the process of T-lymphocytes homing to the skin is mediated by the CLA, which is a ligand for E-selectin. E-selectin exhibit selective lymphocyte-binding properties and is present on the cutaneous endothelial cells. 4 Other regulating skin homing receptors include intracellular adhesion molecule 1 (ICAM-1) with its ligand leukocyte function antigen (LFA-1) and the recently described chemokine receptor CCR4 and its ligand TARC (thymus and activation regulated chemokine). 5 While the underlying molecular pathogenesis remains unknown, but in its early stages MF is thought to develop from skin homing T-lymphocytes that accumulate because of defective apoptosis and in some cases progress into a true neoplasm. Recently published data of oncogene abnormalities in CTCL variants demonstrate decreased Fas expression on peripheral malignant CD4 T-lymphocytes indicating an impaired Fasmediated T-cell apoptosis. 6 Additional studies on 150 Seminars in Cutaneous Medicine and Surgery, Vol 22, No 3 (September), 2003: pp
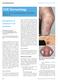
2 CUTANEOUS T-CELL LYMPHOMAS 151 Table 1. EORTC Classification for Primary Cutaneous T-cell Lymphomas and Corresponding Categories in the WHO Classification EORTC Cutaneous T-cell Lymphoma Indolent Mycosis fungoides Mycosis fungoides variants Follicular MF Pagetoid reticulosis CD30 large T-cell lymphoma Lymphomatoid Papulosis Aggressive Sézary syndrome CD30 large T-cell lymphoma Provisional entities CTCL, pleomorphic, small/ medium-sized Subcutaneous panniculitis-like T-cell lymphoma Granulomatous slack skin WHO Mycosis fungoides Mycosis fungoides variants Follicular MF Pagetoid reticulosis Primary cutaneous CD30 ALCL (CD30 lymphoproliferative diseases including lymphomatoid papulosis) Sézary syndrome Peripheral T-cell lymphoma, unspecified Peripheral T-cell lymphoma, unspecified Subcutaneous panniculitis-like T-cell lymphoma Granulomatous slack skin molecular pathogenesis identify a consistent upregulation of JUN-B in CTCL variants, suggesting this gene plays a critical role in pathogenesis of CTCL. 7 Following the EORTC classification scheme, we present a review of the distinct entities of primary CTCL with emphasis on new treatment options. blood) classification that is based by multivariate prognostic studies (Tables 2 and 3). Clinically, MF is typified by the development of patches, plaques, or tumors (Figs 2 and 3). In early stages, it might resemble eczematous dermatitis, psoriasis, or parapsoriasis. Varied subtypes have been described including granulomatous, hypopigmented, bullous, pustular, hyperkeratotic MF, and MF-associated follicular mucinosis, with or without alopecia. The d emblée presentation is defined by de novo appearance of tumors. Pagetoid reticulosis is a rare and controversial variant that presents with acral verrucous lesions with large epidermotropic lymphocytes and a benign prognosis. Microscopic assessment is required for diagnosis. Characteristic histologic features are a papillary dermal band-like infiltrate with small to medium-sized lymphocytes with hyperchromatic, hyperconvoluted nuclei, and variable findings of inflammatory cells. Epidermal exocytosis is classic (Fig 4). Pautrier s microabscesses are considered to be characteristic findings, but seen infrequently. Tumor lesions express more diffuse, superficial, and deep infiltrates with diminished epidermotropism. 10 MYCOSIS FUNGOIDES/SEZARY SYNDROME MF is the most common form of CTCL with a male predominance of approximately 2:1 and a predominance of patients of African descent about 1.6:1. It has a yearly incidence of 0.36 cases per 100,000 of the population that has remained constant over the last decade. 8 However, an increasing number of cases in children are reported. MF, was first described by Alibert in the 19th century, due to the mushroom-like appearance of tumors. It is classified as an indolent lymphoma by the EORTC. 9 Sézary syndrome is the leukemic and more aggressive variant of CTCL, which is characterized by circulating, atypical, malignant T-lymphocytes with cerebriform nuclei (Sézary cells), the presence of erythroderma, disabling pruritus, keratoderma, and lymphadenopathy (Fig 1). The recommended staging system is in according to the TNMB (tumor, node, metastasis, Fig 1. Sézary syndrome with generalized erythroderma.
3 152 QUERFELD ET AL Table 2. TNMB Classification for MF/SS T (skin) T1 T2 T3 T4 N (nodes) N0 N1 NP0 NP1 LNO LN1 LN2 LN3* LN4* M (viscera) M0 M1 B (blood) B0 B1 Limited patch/plaque ( 10% of BSA) Generalized patch/plaque( 10% of BSA) Tumors Generalized erythroderma No clinically abnormal peripheral lymphnodes Clinically abnormal peripheral lymphnodes Biopsy performed, not CTCL Biopsy performed, CTCL Uninvolved Reactive lymph node Dermatopathic node, small clusters of convoluted cells ( 6 cells per cluster) Dermatopathic node, small clusters of convoluted cells ( 6 cells per cluster) Lymph node effacement No visceral metastasis Visceral metastasis Atypical circulating cells not present ( 5%) Atypical circulating cells present ( 5%) Abbreviation: TNMB, tumor, node, metastasis, blood. *Pathologically involved lymph nodes. The malignant T-cell type variably expresses CD2, CD3, CD4, CD5, CD7, and CD45RO by immunohistochemistry. The majority of cases are of the helper/inducer T-cell subset with a CD4 phenotype. Rare cases of the cytotoxic/suppressor T-cell subset expressing the CD4 - /CD8 phenotype have been reported. In advanced stages, an aberrant phenotype with loss of T-cell markers is a common finding. Clonal rearrangement of the T-cell receptor (TCR) genes is demonstrated in most cases. Patients with SS and advanced MF show a helper T-cell type 1 (T h 1)/ (T h 2) imbalance with a predominant type 2 immune response followed by an impaired cell-mediated immunity. 11 Peripheral eosinophilia and hypergammaglobulinemia may occur. 12 Gene studies have shown allelic losses at 1p, 9p, 10q, and 17p with gains in chromosome 4q, 18, Fig 2. MF, patch stage. Multiple erythematous patches on the back and buttock area. and 17q, microsatellite instability, and rarely mutations of p53 in primary CTCL Acquired defects in apoptosis through inactivation of the p16 gene are also reported. 17 In addition, the antiapoptotic bcl-2 gene is overexpressed in MF and STAT 3 (signal transducer and transcription activator) is constitutively activated in SS cells. 18 In general, the T stage remains the best prognostic factor. However, several independent prognostic factors have been identified including the Table 3. Stage Classification for MF/SS Stage T N NP M IA IB IIA 1/ IIB 3 0/1 0 0 III 4 0/1 0 0 IVA 1-4 0/1 1 0 IVB 1-4 0/1 0/1 1 Fig 3. MF, tumor stage. Erythematous nodules on the forehead.
4 CUTANEOUS T-CELL LYMPHOMAS Fig 4. Histologic appearance of MF, with presence of a band-like mononuclear infiltrate and prominent epidermotropism. presence of visceral and/or lymph node involvement, follicular mucinosis, thickness of tumor infiltrate, and an increase in lactico-dehydrogenase (LDH). More recently, other predictive factors are reported The presence of cytotoxic CD8 T- lymphocytes in the dermal infiltrate, as well as the density of epidermal Langerhans cells greater than 90 cells/mm 2 is associated with a better prognosis. 24,25 In contrast, large cell transformation in MF is associated with an aggressive clinical course and shortened survival (Fig 5). 26 On histology, it is defined as the presence of large cells exceeding 25% of the dermal infiltrate or nodular aggregates. Morphometric studies revealed 2 types of Sézary cells, small and large type. Patients with large Sézary-cells were found to have a worse prognosis. A high Sézary cell count, loss of T-cell markers such as CD5 and CD7, existence of a T-cell clone in the blood and chromosomal abnormalities in T cells is also independently associated with a poor outcome Lymphomatoid Papulosis Lymphomatoid papulosis (LyP) represents a cutaneous CD30 lymphoproliferative disorder with histologic features resembling malignant lymphoma, in contrast to the benign clinical course. However, 10% to 20% of patients may develop a lymphoid malignancy. 28a LyP is most commonly associated with MF, CD30 LTCL, and Hodgkin s disease. The clinical features consist of recurrent eruptions of self-healing, frequently ulcerating, papulonodular lesions. 28b Three histologic types have been identified, characterized as type A, B, and C. Type A and C consist of large lymphocytes resembling Reed-Sternberg cells. Type A cells are embedded in a dense inflammatory background, whereas type C cells form large sheets imitating CD30 LTCL. Type B simulates classical MF features with epidermotropism and a dermal band-like infiltrate composed of small to medium-sized cells. 29 Clonality of TCR has been demonstrated. 30 Recently published immunohistochemical data suggest that fascin expression in LyP may become a predictive marker for tumor progression in LyP. 31 There is no curative treatment available. PUVA, methotrexate, interferon, topical or intralesional steroids, doxycyclin, and topical bexarotene are palliative, but probably do not alter the course of the disease. These agents should be used cautiously to avoid the harmful side effects in patients with an excellent prolonged survival. CD30 Positive Large T-Cell Lymphoma CD30 LTCL presents clinically as solitary or localized nodules or tumors that frequently ulcerate (Fig 6). Regional lymph node involvement is seen in 25% of patients at presentation. The neoplastic cells are of the CD4 helper T-cell phenotype with CD30 expression. This tumor has an excellent prognosis as confirmed in several studies, in contrast to the transformation of MF into a CTCL VARIANTS Fig 5. Histologic appearance of large cell transformation in MF, composed of large pleomorphic lymphocytes with presence of Pautrier s microabscesses.
5 154 QUERFELD ET AL Fig 6. CD30 large T-cell lymphoma. Clinical appearance with a solitary, ulcerated tumor. CD30 large cell variant. The characteristic histologic feature is a diffuse, nonepidermotropic infiltrate with cohesive sheets of large CD30 lymphocytes (Fig 7). In most cases, tumor cells show anaplastic features, less commonly a pleomorphic or immunoblastic appearance. However, there is no difference in the prognosis and survival rate. 32,33 T-cell clonality is demonstrated in most instances. In contrast to their nodal counterpart, chromosomal translocation t (2;5) leading to anaplastic lymphoma kinase (ALK) expression is rarely observed. CD30 LTCL may regress spontaneously. However, the mechanism of tumor regression remains unknown. CD30 ligand-mediated cytotoxicity may participate in the pathophysiology of clinical regression. 34,35 Risk factors predicting tumor progression or dissemination have not been identified. However, patients with multiple lesions exhibit extracutaneous manifestations in up to 17% of cases. 20 Coexpression of CD56 and CD30 may be associated with a more aggressive behavior. 36 In cases with progression, point mutations and deletions on TGF- receptor genes I and II have been found leading to the loss of its tumor suppressor properties. 37 Increased levels of fascin have also been correlated with disease progression. 31 Spot radiation or surgical excision is the preferred treatment with systemic chemotherapy reserved for cases with large tumor burden and extracutaneous involvement. More recently there has been reported a therapeutic efficacy of recombinant interferon. 38 CD30 Negative Large T-Cell Lymphoma These lymphomas are aggressive neoplasms with an abysmal 15% 5-year survival rate. Patients present with solitary, localized or generalized plaques, nodules, or tumors without spontaneous regression. Microscopically, a dense, nodular or diffuse, sometimes angiocentric, and epidermotropic infiltrate characterized by pleomorphic medium or large-sized cells and immunoblastic lymphocytes is present. 39 Large cells comprise over 30% and might resemble classical MF undergoing large cell transformation. In contrast to true MF, the neoplastic T cells do not display a T h 2 cytokine profile and do not express CD T-cell clonality is present. Multiagent systemic chemotherapy is recommended in most cases, with radiotherapy limited to localized disease. Pleomorphic T-Cell Lymphoma With Small/Medium-sized Cells These uncommon CTCL type appears clinically with single red-purple nodules or tumors. Histopathology shows a dermal dense, diffuse, or nodular infiltrate comprising small- and medium-sized pleomorphic cells with variable epidermotropism. Most cases express a classic T-helper cell phenotype and do not express CD30. T-cell rearrangement studies have shown clonality. The prognosis is favorable with a 5-year survival rate of 60% to 90%. 41,42 A predominance of small-sized pleomorphic cells is associated with a better prognosis whereas a CD4 / CD56 phenotype with loss of pan T-cell markers Fig 7. Histologic appearance of CD30 large T-cell lymphoma with presence of large CD30 lymphocytes.
6 CUTANEOUS T-CELL LYMPHOMAS appear to have a less favorable prognosis. 43 The optimal therapy of pleomorphic T-cell lymphoma has not been defined. Localized lesions have been treated with radiation or surgical excision. Patients with generalized skin disease or progression have been treated effective with systemic treatments including chemotherapy, retinoids, interferons, and monoclonal antibodies. Subcutaneous Panniculitis-like T-Cell Lymphoma Subcutaneous panniculitis-like T-cell lymphoma (SPTCL) is an extremely rare type of lymphoma. Approximately 100 cases are described to date. Patients, often young adults, present with subcutaneous nodules and plaques accompanied by constitutional symptoms including weight loss, fatigue, and low-grade fever. The primary subcutaneous involvement resembles panniculitis. On histology, there is a subcutaneous infiltrate including pleomorphic small- to medium-sized T cells, histiocytes, and variable component of fat necrosis, mixed inflammation, cytophagocytosis, and karyorrhexis. Two distinct patterns of TCR expression are known. The majority express / TCR with a CD8 phenotype, less commonly / TCR with variable CD8 phenotype which is frequently associated with systemic symptoms and hemophagocytic syndrome. 45,46 In general, the prognosis remains poor despite use of aggressive chemotherapy with an overall survival rate of less than 3 years Granulomatous Slack Skin This is a rare skin neoplasm characterized by large, erythematous, and indurated plaques slowly progressing into erythematous masses resembling cutis laxa-like appearance, often localized in intertriginous or flexural areas. The common histologic feature is a dense granulomatous infiltrate containing pleomorphic T cells with a varying number of histiocytes, multinucleated giant cells and elastophagocytosis. Elastic fiber destruction leads to the cutis laxa-like appearance. 48 The atypical cells usually express a CD4, and CD8 - phenotype. Clonality may occur. Although patients show an indolent clinical course, 30% of patients develop other lymphomatoid malignancies. MF and Hodgkin s disease are most common associated. Treatment options include radiation, PUVA, interferons, retinoids, steroids, and surgical excision. 49 However, the assessment of therapeutic alternatives is limited because of the modest number of patients reported to date. THERAPY Standard treatment options are typically palliative and can be divided into skin-targeted and systemic approaches. The skin-targeted modalities includes psoralens with ultraviolet light A (PUVA), narrowband-ultraviolet light B (NB- UVB), skin electron beam radiation, as well as topical preparations of steroids, retinoids, carmustine, and nitrogen mustard. In early CTCL, the cell-mediated immune response is usually normal. Therefore, the majority of these cases can be treated successfully with topical modalities, since early aggressive therapy did not improve the prognosis of patients with CTCL. Systemic therapies are reserved for more advanced stages. Established treatment options include single-agent or multiagent chemotherapy, extracorporeal photopheresis, interferon- or interferon-, monoclonal antibodies and recombinant toxins. In advanced CTCL, there is a shift from the helper T-cell type 1 (T h 1) to helper T-cell type 2 (T h 2) with up-regulation of T h 2 cytokines such as interleukin (IL)-4, IL-5, and IL-10 and downregulation of T h 1 cytokines such as IL-2 and interferon- leading to an impaired immune response. 50 Newer treatments such as biologic response modifiers target the reconstitution of immune function. Photochemotherapy PUVA is probably the preferred treatment option for early stage MF. 8-Methoxypsoralen (8- MOP) act at the nuclear level of cells, inhibiting DNA and RNA synthesis through formation of mono- or bifunctional thymine products, gene mutations, or sister chromatid exchanges. 51 In vitro studies have shown that peripheral blood mononuclear cells undergo apoptosis after exposure to PUVA MOP becomes only activated when exposed to UVA light and it is usually ingested 2 hours before UVA exposure. Initial exposure times of patients are limited to the phototype according to Fitzpatrick grading system, the ability to tan, and the patient s history of sunburns. The initial UVA dosage is approximately 0.5 J/cm 2 and will be increased per treatment as tolerated or up to the minimal erythema dose. Therapy is typically given 3 times a week
7 156 QUERFELD ET AL until complete remission is achieved. Additional maintenance therapy is necessary to achieve longer remission times. Several studies confirmed high remission rates in early stages of MF. Herrmann et al 53 reported complete remissions in 65% of patients. Similar results have been reported from the Scandinavian study group. 54 Reported side effects to PUVA can be divided into more acute short-term effects including nausea from ingestion of psoralen, erythema, pruritus, and photodermatitis and longterm effects such as chronic photodamage and secondary skin malignancies. 55 Narrowband-UVB phototherapy (NB-UVB) is considered to be less carcinogenic and may be an alternative treatment option in early stage MF. However, the remission time is short. 56 A few cases have been reported showing that UVA 1 phototherapy is also effective. 57 Radiotherapy CTCL s are radiosensitive and radiation therapy is effective in controlling localized tumors. Total electron beam treatment (TSEBT) should be reserved for more advanced and disseminated stages, because of its potential toxicity. 58 The standard total dose is 36 Gy applied over 8 to 10 weeks. Side effects consist of erythema, edema, scaling, ulcerating, and often, irreversible loss of skin adnexa. Recently published data of therapeutic efficacy of TSEBT from Hamilton, Ontario, and Yale University showed that 60% of patients with erythrodermic mycosis fungoides achieved complete remission with a 5-year progression free duration of 26% and with more intense TSEB 74% complete remission with a 10-year progression free duration of 26%. 59 TSEB should only be used in centers with extensive experience and often requires adjuvant therapy to maintain the time of remission. Systemic Chemotherapy Systemic chemotherapy is defined to patients with advanced stages or with relapsed and refractory stages. Established treatment options include single-agent or multiagent chemotherapy including steroids, methotrexate, chlorambucil, doxorubicin, and etoposide. 60 Newer purine analogs such as fludarabine and 2-chloro-deoxyadenosine showed initial response rates from 28% to 66%. However, most responses were short-lived and accompanied by harmful side effects related to prolonged immunosuppression. 61,62 Temozolomide, a new oral alkylating agent, is being evaluated in a phase II trial for patients with relapsed MF and SS. Patients with MF/SS have been shown to have low levels of DNA repair enzyme O 6 alkylguanine DNA alkyltransferase (AGT) and may be particularly sensitive to this alkylator. 63,64 Pegylated Doxorubicin, empirically tested for relapsing or recalcitrant CTCL, achieved an overall response rate of 83% with tolerable side effects. 65 BIOLOGICAL THERAPIES Retinoids Retinoids are vitamin A derivatives. The biological effects of retinoids are triggered through specific retinoid receptors, RAR and RXR. Wellknown retinoids such as 13-cis retinoic acid (isotretinoin), etretinate, acitretin, and trans-retinoic acid exert their effects by binding to the retinoic acid receptor resulting in controlling cell growth and differentiation. All of these retinoids have been used in CTCL and several studies have evaluated their effectiveness. However, the response rates remained to be shortly The most common side effects include mucous membrane dryness and headache. Bexarotene, a new synthetic retinoid identified, selectively binds to the retinoid X receptor. In vitro studies have shown that stimulation of RXR induces apoptosis, which is thought to be defect in CTCL. 69 Bexarotene (300 mg/m 2 administered daily) has been studied in several clinical trials for refractory early and advanced stage patients. The results are promising, with 54% of patients with refractory early stage and 45% of patients with refractory advanced stage, having an overall response. The median duration of response was 299 days. 70,71 Bexarotene, at recommended dosage, is associated with significant side effects, particularly hyperlipidemia and hypothyroidism. Therefore, patients should be monitored closely. It is commonly used in combination with PUVA to achieve optimal efficacy at lower dosage and increased response durability. A topical formulation as a 1% gel is also approved. It is indicated for early stage Ia and Ib of CTCL. A phase II trial demonstrated a 63% overall response rate. Side effects were restricted to the application side and were mostly mild to moderate irritation with erythema in 73% of cases. 72
8 CUTANEOUS T-CELL LYMPHOMAS Interferons Interferon- (INF ) is the most effective agent in the treatment of CTCL, as verified in several studies. Monotherapies achieved significant response rates in 50% to 80% of patients. 73 T h 1 cytokines support cytotoxic T-cell mediated immunity and therefore INF is used to boost the cell-mediated response to malignant T-lymphocytes. 74,75 It is administered sub-cutaneously, intramuscularly, or intralesionally. INF is initiated at low doses of between 1 and 3 million international units (IU) 3 times weekly with gradually increasing as treatment is tolerated by the patient. Most common side effects are flu-like symptoms such as chills, fever, headache, myalgia, and fatigue. With less frequency, depression, cytopenia, impaired liver function test, renal and cardiac dysfunction occur. 76 IFN is often used in combination with retinoids/rexinoids, PUVA, electron beam radiation, and extracorporeal photopheresis. The combination therapy IFN and PUVA resulted in high response rates in more than 90% of patients and shows superiority to other combinations. 77,78 Experience with INF is limited. It has been shown to inhibit T h 2 cytokine production by malignant T cells. In a single trial of 16 CTCL patients with refractory disease, five patients showed partial response rates with a median duration of 10 month. The side effects are similar to those of INF. 79 Extracorporeal Photochemotherapy Extracorporeal photochemotherapy or photopheresis (ECP) is a leukapheresis-based method in which 8-MOP treated blood mononuclear cells are exposed to UVA and returned to the patient. It is performed on 2 consecutive days every month. Although the mechanism of action is not completely understood, induction of apoptosis with subsequently release of tumor antigens leading to a systemic antitumor response against the malignant T-cell clone is suspected. 80,81 Few studies have reported response rates between 36% and 64% for patients with advanced disease. 82,83 Prolonged survival rates have also been reported. Ideal candidates for ECP are patients with Sézary syndrome with a short duration of disease, modest numbers of circulating atypical cells and near normal counts of circulating CD8 T- lymphocytes The results in patients with marked immunosuppression are disappointing. 85 IL-2 Fusion Protein (Denileukin Diftitox) Diphtherotoxin-interleukin-2 (DAB-IL-2) is a recombinant cytotoxic fusion protein that targets the IL-2 receptor on malignant and activated T- lymphocytes. It combines the receptor binding domain of IL-2 with diphtheria toxin. Once bound to the IL-2 receptor, it is internalized by endocytosis, the ADP-ribosyltransferase activity of diphtheria toxin compound is enzymatically cleaved with subsequently inhibition of protein synthesis. In phase I and II trials, 37% of patients showed an objective clinical response with a median duration of 10 month. A phase III study initiated for patients with refractory or advanced CTCL showed similar results with a 30% response rate. 86 However, predominant adverse effects including acute infusion-related hypersensitivity reaction such as fever, rash, chills, myalgias, and vascular leak syndrome have been witnessed in 74% of patients. In a subsequent study, premedication of steroids diminished the events. 87 Recombinant IL-12 In CTCL progression marked defects in cellmediated immunity are associated with the impaired production of T h 1 cytokines IL-2 and INF. In vitro studies have shown that IL-12 is a powerful inducer of INF production and cellmediated cytotoxicity. Based on these findings, a phase I dose escalation trial using ril-12 intralesionally or subcutaneously for CTCL patients was performed and showed an overall response in 56% of patients. 88 Subcutaneous application resulted in complete responses in 2 of 5 patients and partial responses in 2 of 5 patients with plaque disease and in one of 2 patients with Sézary syndrome. Recombinant IL-12 is a potent therapeutic agent. Repeated administration of ril-12, however, results in clinical refractoriness secondary to downregulation of the IL-12 receptor. A combination of ril-2 and ril-12 showed a synergistic enhancement of a cytotoxic T-cell response and upregulation of IL-12 receptors. 89 Further clinical trials are in progress to establish the effectiveness of the IL-2 plus IL-12 regimen in advanced CTCL.
9 158 QUERFELD ET AL Alemtuzumab (Campath-1H) Alemtuzumab, a humanized monoclonal IgG 1 antibody, targets the CD52 antigen that is expressed on most malignant B- and T-lymphocytes, but not on hematopoietic stem cells. The mechanism of this antibody is not completely understood, but is thought to regulate antibody-dependent cellular cytotoxicity, complement-mediated cell lysis, and apoptosis. Malignant T-lymphocytes express high numbers of CD52 cell-surface marker and correlate with the clinical benefits. Alemtuzumab is currently the focus of many clinical trials in hematologic malignancies and has been used in the treatment of lymphomas and lymphoid leukemias with promising results. 90 A phase II multicenter trial with advanced and pretreated low-grade non-hodgkin s lymphoma included 8 patients with MF/SS. Four of these patients responded and 2 achieved a complete remission. 91 A recently published study of alemtuzumab in 22 patients with advanced MF/SS recorded a clinical response in 55% of cases with 32% complete remission. The compound has an acceptable toxicity rate with mostly infusion-related events including fever, rigor, nausea, hypotension, rash, and fatigue. Cytopenias and prolonged immunosuppression require prophylactic antibiotics. The most impressive results for this agent are demonstrated in Sézary syndrome patients. 92 CONCLUSION At present, a stage-adapted therapy of cutaneous lymphoma is the best approach, since early aggressive therapies reveal no difference in longterm outcome. Many immunologic abnormalities in CTCL are associated with advanced disease and are caused by cytokine imbalances. The biologic response modifiers have the potential to reconstitute the immune function with a tolerable rate of adverse effects and improvement in quality of life. It is apparent that patients with advanced stages of disease are optimally treated with a combination of immune modifiers to prolong survival. Future studies will have to verify the role of this strategy. Other future directions are vaccinations that target specific TCRs or immunization via tumor-associated antigen loaded dendritic cells. 1. Willemze R, Kerl H, Sterry W, et al: EORTC classification for primary cutaneous lymphomas: A proposal from the Cutaneous Lymphoma Study Group of the European Organization for Research and Treatment of Cancer. Blood 90: , Fink-Puches R, Zenahlik P, Bäck B, et al: Primary cutaneous lymphomasapplicability of current classification schemes (European Organisation for Research and Treatment of Cancer, World Health Organization) based on clinicopathologic features observed in a large group of patients. Blood 99: , Drillenburg P, Pals T: Cell adhesion receptors in lymphoma dissemination. Blood 95: , Kansas GS: Selectins and their ligands: Current concepts and controversies. Blood 88: , Ferenci K, Fuhlbrigge RC, Pinkus JL, et al: Increased CCR4 expression in cutaneous T-cell lymphoma. J Invest Dermatol 119: , Zoi-Toli O, Vermeer MH, De Vries E, et al: Expression of Fas and Fas-ligand in primary cutaneous T-cell lymphoma (CTCL): Association between lack of FAS expression and aggressive types of CTCL. Brit J Dermatol 143: , Mao X, Orchard G, Lillington D, et al: Amplification and overexpression of JUNB is associated with primary cutaneous T-cell lymphomas. Blood 101: , Weinstock MA, Gardstein B: Twenty-year trends in the reported incidence of mycosis fungoides and associated mortality. Am J Public Health 89: , Alibert JLM: Tableau de plan fongoide: Description des REFERENCES maladies de la peau observeé à l hôpital St. Louis, et exposition des melleurs methods suivies pour leur trâitement. Paris, France, Barrois l Aine et Files, Fung MA, Murphy MJ, Hoss DM, et al: Practical evaluation and management of cutaneous lymphoma. J Am Acad Dermatol 46: , Rook AH, Lessin SR, Jaworsky C, et al: Immunopathogenesis of cutaneous T-cell lymphoma: Abnormal cytokine production by Sézary cells. Arch Dermatol 129: , Talpur R, Lifshitz O, Breuer-McHam J, et al: Increased serum immunoglobulin levels are common in mycosis fungoides and Sézary syndrome. J Am Acad Dermatol 47: , Scarisbrick JJ, Woolford AJ, Russel-Jones R, et al: Allelotyping in mycosis fungoides and Sézary syndrome: Common regions of allelic loss identified on 9p, 10q, and 17p. J Invest Dermatol 117: , Mao X, Lillington D, Scarisbrick JJ, et al: Molecular cytogenetic anlysis of cutaneous T-cell lymphomas: identification of common genetic alterations in Sézary syndrome and mycosis fungoides. Br J Dermatol 147: , Dereure O, Levi E, Vonderheid E, et al: Infrequent Fas mutations but no BAX or p53 mutations in early mycosis fungoides: A possible mechanism for the accumulation of malignant T lymphocytes in the skin. J Invest Dermatol 118: , Wu K, Lund M, Bang K, et al: Telomerase activity and telomere length in lymphocytes from patients with cutaneous T-cell lymphoma. Cancer 86: , 2000
10 CUTANEOUS T-CELL LYMPHOMAS Navas IC, Algara P, Mateo M, et al: p16 INK4a is selectively silenced in the tumoral progression of mycosis fungoides. Lab Invest 82: , Garatti SA, Roscetti E, Trecca D, et al: bcl-1, bcl-2, p53, c-myc, and lyt-fl10 analysis in cutaneous lymphomas. Recent Results Cancer Res 139: , Qin JZ, Kamarashev J, Zhang CL, et al: Constitutive and interleukin-7- and interleukin-15-stimulated DNA binding of STAT and novel factors in cutaneous T-cell lymphoma cells. J Invest Dermatol 117: , Grange F, Bagot M: Prognosis of primary cutaneous lymphomas. Ann Dermatol Venerol 129:30-40, Toro JR, Stoll HL, Stomper PC, et al: Prognostic factors and evaluation of mycosis fungoides and Sézary syndrome. J Am Acad Dermatol 37:58-67, Kim YH, Bishop K, Varghese A, et al: Prognostic factors in erythrodermic mycosis fungoides and Sézary syndrome. Arch Dermatol 131: , Diamandidou E, Colome M, Fayad L, et al: Prognostic factor analysis in mycosis fungoides/sézary syndrome. J Am Acad Dermatol 40: , Hoppe RT, Medeiros LJ, Warnke RA, et al: CD8-positive tumor-infiltrating lymphocytes influence the long-term survival in mycosis fungoides. J Am Acad Dermatol 32: , Meissner K, Michaelis K, Rehpenning W, et al: Epidermal Langerhans cell densities influence survival in mycosis fungoides and Sézary syndrome. Cancer 69: , Vergier B, de Muret A, Beylot-Barry M, et al: Transformation of mycosis fungoides: Clinicopathological and prognostic factors of 45 cases. Blood 95: , Vonderheid EC, Bernengo MG, Burg G, et al: Update on erythrodermic cutaneous T-cell lymphoma: Report of the International Society for Cutaneous Lymphomas. J Am Acad Dermatol 46:95-106, a. Wang HH, Myers T, Lach LJ, et al: Increased risk of lymphoid and non-lymphoid malignancies in patients with lymphomatoid papulosis. Cancer 86: , b. el-azhary RA, Gibson LE, Kurtin PJ, et al: Lymphomatoid papulosis: a clinical and histopathological review of 53 cases with leukocyte immunophenotyping, DNA flow cytometry, and T-cell receptor gene rearrangement studies. J Am Acad Dermatol 30: , LeBoit P: Lymphomatoid papulosis and cutaneous CD30 lymphoma. Am J Dermatopathol 18: , Steinhoff M, Hummel M, Anagnostopoulos I, et al: Single-cell analysis of CD30 cells in lymphomatoid papulosis demonstrates a common clonal T-cell origin. Blood 100: , Kempf W, Levi E, Kutzner H, et al: Fascin expression in CD30-positive cutaneous lymphoproliferative disorders. J Cutan Pathol 29: , Bekkenk MW, Greelen FA, van Voorst PC, et al: Primary and secondary cutaneous CD30 lymphoproliferative disorders with a report from the Dutch Cutaneous Lymphoma Group on the long-term follow-up of 219 patients and guidelines for diagnosis and treatment. Blood 95: , Stein H, Foss HD, Duerkop H, et al: CD30 anaplastic large cell lymphoma: A review of its histopathologic, genetic, and clinical features. Blood 96: , Mori M, Manuelli C, Pimpinelli N, et al: CD30-CD30 ligand interaction in primary cutaneous CD30 T-cell lymphomas: A clue to the pathophysiology of clinical regression. Blood 94: , Kadin ME, Levi E, Kempf W: Progression of lymphomatoid papulosis to systemic lymphoma is associated with escape from growth inhibition by transforming growth factor-b and CD30 ligand. Ann NY Acad Sci 941:59-68, Natkunam Y, Warnke RA, Haghighi B, et al: Co-expression of CD56 and CD30 in lymphomas with primary presentation in the skin: Clinicopathologic, immunohistochemical, and molecular analysis of seven cases. J Cutan Pathol 27: , Schiemann WP, Pfeifer WM, Levi E, et al: A deletion in the gene for transforming growth factor type I receptor abolishes growth regulation by transforming growth factor in a cutaneous T-cell lymphoma. Blood 94: , Yagi H, Furukawa F, Takigawa M, et al: T h 2 cytokine mrna expression in primary cutaneous CD30-positive lymphoproliferative disorders: successful treatment with recombinant interferon-gamma. J Invest Dermatol 107: , Beljaards RC, Meijer CJ, Van der Putte SC, et al: Primary cutaneous T-cell lymphoma: clinicopathological features and prognostic parameters of 35 cases other than mycosis fungoides and CD30-positive large cell lymphoma. J Pathol 172: 53-60, Vermeer MH, Tensen C, van der Stoop PM, et al: Absence of T h 2 cytokine messenger expression in CD30-negative primary cutaneous large T-cell lymphomas. Arch Dermatol 137: , Friedmann D, Wechsler J, Delfau MH, et al: Primary cutaneous pleomorphic small T-cell lymphoma. A review of 11 cases. The French Study Group on Cutaneous Lymphomas. Arch Dermatol 131: , von den Driesch P, Coors E: Localized cutaneous small to medium-sized pleomorphic T-cell lymphoma: a report of 3 cases stable for years. J Am Acad Dermatol 46: , Petrella T, Dalac S, Maynadie M, et al: CD4 /CD56 cutaneous neoplasms: A distinct hematological entity? Am Surg Pathol 23: , Papenfuss JS, Aoun P, Bierman PJ, et al: Subcutaneous panniculitis-like T-cell lymphoma: Presentation of 2 cases and observations. Clin Lymphoma 3: , Wang H, Medeiros JL, Jones D: Subcutaneous panniculitis-like T-cell lymphoma. Clin Lymphoma 3: , Kumar S, Krenacs L, Medeiros J, et al: Subcutaneous panniculitic T-cell lymphoma is a tumor of cytotoxic T lymphocytes. Hum Pathol 29: , McGinnis KS, Shapiro M, Junkins-Hopkins JM, et al: Denileukin Diftitox for the treatment of panniculitic lymphoma. Arch Dermatol 138: , LeBoit PE, Zackheim HS, White CR Jr: Granulomatous variants of cutaneous T-cell lymphoma: The histopathology of granulomatous mycosis fungoides and granulomatous slack skin. Am J Surg Pathol 12:83-95, van Haselen CW, Toonstra J, van der Putte SJ, et al: Granulomatous slack skin. Report of three patients with an updated review of the literature. Dermatology 196: , Rook AH, Lessin SR, Jaworsky C, et al: Immunopathogenesis of cutaneous T-cell lymphoma: abnormal cytokine
11 160 QUERFELD ET AL production by Sézary T-cells. Arch Dermatol 129: , Loveday KS, Donahue BA: Induction of sister chromatid exchanges and gene mutations in Chinese hamster ovary cells by psoralens. NCI Monograph 66: , Yoo EK, Rook AH, Elenitsas R, et al: Apoptosis induction by ultraviolet light A and photochemotherapy in cutaneous T-cell lymphoma: Relevance to mechanism of therapeutic action. J Invest Dermatol 107: , Herrmann JJ, Roenigk HH, Hurria A, et al: Treatment of mycosis fungoides with photochemotherapy (PUVA): Long term follow-up. J Am Acad Dermatol 33: , Molin L, Thomsen K, Volden G, et al: Photochemotherapy (PUVA) in the pretumor stage of mycosis fungoides: A report from the Scandinavian Mycosis Fungoides Study Group. Act Dermatol Venereol 61:47-51, Stern RS, Bolshakov S, Nataraj AJ, et al: p53 mutation in nonmelanoma skin cancers occurring in psoralen ultraviolet A-treated patients: Evidence for heterogeneity and field cancerization. J Invest Dermatol 119: , Cochran Gathers R, Scherschun L, Malick F, et al: Narrowband UVB phototherapy for early-stage mycosis fungoides. J Am Acad Dermatol 47: , Plettenberg H, Stege H, Megahed M, et al: Ultraviolet A1 ( nm) phototherapy for cutaneous T-cell lymphoma. J Am Acad Dermatol 47: , Jones GW, Kacinski BM, Wilson LD, et al: Total skin radiation in the management of mycosis fungoides: Consensus of the European Organization for Research and Treatment of Cancer (EORTC) Cutaneous Lymphoma Project Group. J Am Acad Dermatol 47: , Jones GW, Rosenthal D, Wilson LD: Total skin electron radiation for patients with erythrodermic cutaneous T-cell lymphoma (mycosis fungoides and Sézary syndrome). Cancer 85: , Rosen ST, Foss FM: Chemotherapy for Mycosis fungoides and the Sézary syndrome. Hematol Oncol Clin North Am 9: , von Hoff D, Dahlberg S, Hartstock R, et al: Activity of fludarabine monophosphate in patients with advanced mycosis fungoides/sézary syndrome. J Natl Cancer Inst 82: , Kuzel TM, Huria A, Samuelson E, et al: Phase II trial of 2-chloro-desoxyadenosine for the treatment of cutaneous T- cell lymphoma. Blood 87:906, Dolan ME, McRae BL, Ferries-Rowe E, et al: O 6 -Alkylguanine-DNA alkyltransferase in cutaneous T-cell lymphoma: Implications for treatment with alkylating agents. Clin Cancer Res 5: , Kyrtopoulos SA: O 6 -Alkylguanine-DNA alkyltransferase: influence on susceptibility to the genetic effects of alkylating agents. Toxicol Lett 102:53-57, Wollina U, Graefe T, Karte K: Treatment of relapsing or recalcitrant cutaneous T-cell lymphoma with pegylated liposomal doxorubicin. J Am Acad Dermatol 42:40-46, Kessler JF, Jones SE, Levine N, et al: Isotretinoin and cutaneous helper T-cell lymphoma (mycosis fungoides). Arch Dermatol 123: , Molin L, Thomson K, Volden G, et al: 13-cis-retinoic Acid in Mycosis Fungoides. Retinoids. New Trends in Research and Therapy. Basel, Switzerland, Karger, 1985, pp Siegel RS, Martone B, Guitart J, et al: Phase II trial of all-trans retinoic acid in the treatment of relapsed/refractory mycosis fungoides/sezary syndrome: Proc of American Society of Hematology. Blood 94:97a, 1999 (suppl, abstr) 69. Zhang C, Hazarika P, Ni X, et al: Induction of apoptosis by bexarotene in cutaneous T-cell lymphoma cells: Relevance to mechanism of therapeutic action. Clin Cancer Res 8: , Duvic M, Hymes K, Heald P, et al: Bexarotene is effective and safe for treatment of refractory advanced-stage cutaneous T-cell lymphoma: Multinational phase II-III trial results. J Clin Oncol 19: , Talpur R, War S, Apisarnthanarax N, et al: Optimizing bexarotene therapy for cutaneous T cell lymphoma. J Am Acad Dermatol 47: , Breneman D, Duvic M, Kuzel T, et al: Phase I and II trial of bexarotene gel for skin-directed treatment of patients with cutaneous T-cell lymphoma. Arch Dermatol 138: , Jumbou O, N Guyen MJ, Tessier MH, et al: Long-term follow-up in 51 patients with mycosis fungoides and Sézary syndrome treated by interferon-alfa. 140: , Platsoucas CD, Fox FE, Oleszak E, et al: Regulation of natural killer cytotoxicity by recombinant alpha interferons: Augmentation by INF-alpha 7, an interferon similar to IFNalpha. J Anticancer Res 9: , Suchin KR, Cassin M, Gottleib SL, et al: Increased interleukin 5 production in eosinophilic Sézary syndrome: Regulation by interferon alfa and interleukin 12. J Am Acad Dermatol 44:28-32, Olsen EA, Rosen ST, Vollmer RT, et al: Interferon alfa-2a in the therapy of cutaneous T-cell lymphoma. J Am Acad Dermatol 20: , Rupoli S, Barulli S, Guiducci B, et al: Low dose interferon- 2b combined with PUVA is an effective treatment of early stage mycosis fungoides: Results of a multicenter study. 84: , Chiarion-Sileni V, Bononi A, Fornasa Veller C, et al: Phase II trial of interferon- -2a plus Psoralen with ultraviolet light A in patients with cutaneous T-cell lymphoma. Cancer 95: , Kaplan FH, Rosen ST, Norris DB, et al: Phase II study of recombinant human interferon gamma for treatment of cutaneous T-cell lymphoma. J Natl Cancer Inst 82: , Yoo EK, Rook AH, Elenitsas R, et al: Apoptosis induction by ultraviolet light A and photochemotherapy in cutaneous T-cell lymphoma: Relevance to mechanism of therapeutic action. J Invest Dermatol 107: , Rook AH, Suchin KR, Kao DMF, et al: Photopheresis: Clinical applications and mechanisms of action. J Invest Dermatol Symp Proc 4:85-89, Gottleib SL, Wolfe JT, Fox FE, et al: Treatment of cutaneous T-cell lymphoma with extracorporeal photophoresis monotherapy and in combination with recombinant interferon alpha: A 10-year experience at a single institution. J Am Acad Dermatol 35: , Edelson R, Berger C, Gasparro F, et al: Treatment of cutaneous T-cell lymphoma by extracorporeal photochemotherapy: Preliminary results. N Engl J Med 316: , 1987
12 CUTANEOUS T-CELL LYMPHOMAS Suchin KR, Cucchiara AJ, Gottleib SL, et al: Treatment of cutaneous T-cell lymphoma with combined immunomodulatory therapy. Arch Dermatol 138: , Fraser-Andrews E, Seed P, Whittaker S, et al: Extracorporeal photophoresis in Sézary syndrome: No significant effect in the survival of 44 patients with a peripheral blood T-cell clone. Arch Dermatol 134: , Foss FM: DAB 389 IL-2 (ONTAK): A novel fusion toxin therapy for lymphoma. Clin Lymph 1: , Foss FM, Bacha P, Osann KE, et al: Biological correlates of acute hypersensitivity events with DAB 389 IL-2 (Denileukin Diftitox, ONTAK ) in cutaneous T-cell lymphoma: Decreased frequency and severity with steroid premedication. Clin Lymph 1: , Rook A, Wood GS, Yoo EK: Interleukin-12 therapy of cutaneous T-cell lymphoma induces lesion regression and cytotoxic T-cell responses. Blood 94: , Zaki MH, Wysocka M, Everetts SE, et al: Synergistic enhancement of cell-mediated immunity by interleukin-12 plus interleukin-2: Basis for therapy of cutaneous T cell lymphoma. J Invest Dermatol 118: , Pawson R, Dyer MJ, Barge R, et al: Treatment of T-cell prolymphocytic leukemia with human CD52 antibody. J Clin Oncol 15: , Lundin J, Osterborg A, Brittinger G, et al: Campath-1H monoclonal antibody in therapy for previously treated lowgrade non-hodgkin s lymphomas: A phase II multicenter study. European Study Group of CAMPATH-1H Treatment in Low-Grade Non-Hodgkin s Lymphoma. J Clin Oncol 16: , Lundin J, Hagberg H, Repp R, et al: Phase II study of alemtuzumab (anti-cd52 monoclonal antibody, Campath- 1H) in patients with advanced mycosis fungoides/sézary syndrome. Blood 101: , 2003
Therapeutic Management of Early Cutaneous Mycosis Fungoides
 Therapeutic Management of Early Cutaneous Mycosis Fungoides L Frank Glass, MD Cutaneous Lymphoma Programs H Lee Moffitt Cancer Center and Research Institute George Washington University Dermatology and
Therapeutic Management of Early Cutaneous Mycosis Fungoides L Frank Glass, MD Cutaneous Lymphoma Programs H Lee Moffitt Cancer Center and Research Institute George Washington University Dermatology and
Primary Cutaneous CD30-Positive T-cell Lymphoproliferative Disorders
 Primary Cutaneous CD30-Positive T-cell Lymphoproliferative Disorders Definition A spectrum of related conditions originating from transformed or activated CD30-positive T-lymphocytes May coexist in individual
Primary Cutaneous CD30-Positive T-cell Lymphoproliferative Disorders Definition A spectrum of related conditions originating from transformed or activated CD30-positive T-lymphocytes May coexist in individual
Disclosures. Advisory Board. Consultant. Investigator. MiRagen, Actelion, Celgene, Therakos. Mindera
 Cutaneous Lymphomas Christiane Querfeld, MD, PhD Director, Cutaneous Lymphoma Program City of Hope ~ How the Experts Treat Hematologic Malignancies Symposium March 10 13, 2017 Disclosures Advisory Board
Cutaneous Lymphomas Christiane Querfeld, MD, PhD Director, Cutaneous Lymphoma Program City of Hope ~ How the Experts Treat Hematologic Malignancies Symposium March 10 13, 2017 Disclosures Advisory Board
Overview of Cutaneous Lymphomas: Diagnosis and Staging. Lauren C. Pinter-Brown MD, FACP Health Sciences Professor of Medicine and Dermatology
 Overview of Cutaneous Lymphomas: Diagnosis and Staging Lauren C. Pinter-Brown MD, FACP Health Sciences Professor of Medicine and Dermatology Definition of Lymphoma A cancer or malignancy that comes from
Overview of Cutaneous Lymphomas: Diagnosis and Staging Lauren C. Pinter-Brown MD, FACP Health Sciences Professor of Medicine and Dermatology Definition of Lymphoma A cancer or malignancy that comes from
Cover Page. The handle holds various files of this Leiden University dissertation.
 Cover Page The handle http://hdl.handle.net/1887/2010 holds various files of this Leiden University dissertation. Author: Benner, Marchina Frederika Title: Cutaneous CD30-positive lymphoproliferations
Cover Page The handle http://hdl.handle.net/1887/2010 holds various files of this Leiden University dissertation. Author: Benner, Marchina Frederika Title: Cutaneous CD30-positive lymphoproliferations
Michi Shinohara MD Associate Professor University of Washington/Seattle Cancer Care Alliance Dermatology, Dermatopathology
 Michi Shinohara MD Associate Professor University of Washington/Seattle Cancer Care Alliance Dermatology, Dermatopathology Agenda Overview of cutaneous T and B- cell lymphomas Diagnosis, Staging, Prognosis
Michi Shinohara MD Associate Professor University of Washington/Seattle Cancer Care Alliance Dermatology, Dermatopathology Agenda Overview of cutaneous T and B- cell lymphomas Diagnosis, Staging, Prognosis
Classification of Cutaneous T cell Lymphomas (CTCLs) Hernani Cualing, MD
 Classification of Cutaneous T cell Lymphomas (CTCLs) Hernani Cualing, MD Pathology and Cell Biology, USF IFLOW, Inc. CTCL, MF, and Sézary syndrome In 1806, mycosis fungoides (MF) was first described 1
Classification of Cutaneous T cell Lymphomas (CTCLs) Hernani Cualing, MD Pathology and Cell Biology, USF IFLOW, Inc. CTCL, MF, and Sézary syndrome In 1806, mycosis fungoides (MF) was first described 1
clinical recommendations
 19 (Supplement 2): ii72 ii76, 2008 doi:10.1093/annonc/mdn095 Primary cutaneous lymphoma: ESMO Clinical Recommendations for diagnosis, treatment and follow-up R. Dummer 1 & M. Dreyling 2 On behalf of the
19 (Supplement 2): ii72 ii76, 2008 doi:10.1093/annonc/mdn095 Primary cutaneous lymphoma: ESMO Clinical Recommendations for diagnosis, treatment and follow-up R. Dummer 1 & M. Dreyling 2 On behalf of the
Case Report A Severe Case of Lymphomatoid Papulosis Type E Successfully Treated with Interferon-Alfa 2a
 Hindawi Case Reports in Dermatological Medicine Volume 2017, Article ID 3194738, 5 pages https://doi.org/10.1155/2017/3194738 Case Report A Severe Case of Lymphomatoid Papulosis Type E Successfully Treated
Hindawi Case Reports in Dermatological Medicine Volume 2017, Article ID 3194738, 5 pages https://doi.org/10.1155/2017/3194738 Case Report A Severe Case of Lymphomatoid Papulosis Type E Successfully Treated
Sezary Syndrome(SS) and other malignancies. Hernani Cualing MD Hematopathologist IHCFLOW Lab
 Sezary Syndrome(SS) and other malignancies Hernani Cualing MD Hematopathologist IHCFLOW Lab Disclosures IHCFLOW Laboratory:consultant and director NEOGENOMICS: contract consultant USF: contract reviewer
Sezary Syndrome(SS) and other malignancies Hernani Cualing MD Hematopathologist IHCFLOW Lab Disclosures IHCFLOW Laboratory:consultant and director NEOGENOMICS: contract consultant USF: contract reviewer
CUTANEOUS T-CELL LYMPHOMA PROFORMA
 STATE OF KUWAIT MINISTRY OF HEALTH AS AD ALHAMAD DERMATOLOGY CENTER ALSABAH HOSPITAL دولة الكویت وزارة الصحة مرآز أسعد الحمد للا مراض الجلدیة مستشفى الصباح بسم االله الرحمن الرحيم CUTANEOUS TCELL LYMPHOMA
STATE OF KUWAIT MINISTRY OF HEALTH AS AD ALHAMAD DERMATOLOGY CENTER ALSABAH HOSPITAL دولة الكویت وزارة الصحة مرآز أسعد الحمد للا مراض الجلدیة مستشفى الصباح بسم االله الرحمن الرحيم CUTANEOUS TCELL LYMPHOMA
OBSERVATION. Psoralen Plus Long-Wave UV-A (PUVA) and Bexarotene Therapy
 OBSERVATION Psoralen Plus Long-Wave UV-A (PUVA) and Bexarotene Therapy An Effective and Synergistic Combined Adjunct to Therapy for Patients With Advanced Cutaneous T-Cell Lymphoma Karen S. McGinnis, MD;
OBSERVATION Psoralen Plus Long-Wave UV-A (PUVA) and Bexarotene Therapy An Effective and Synergistic Combined Adjunct to Therapy for Patients With Advanced Cutaneous T-Cell Lymphoma Karen S. McGinnis, MD;
Index. derm.theclinics.com. Note: Page numbers of article titles are in boldface type.
 Note: Page numbers of article titles are in boldface type. A Acitretin and cutaneous T-cell lymphomas, 716 719, 722, 725 ADCC. See Antibody-dependent cell-mediated cytotoxicity. Adjunctive therapies and
Note: Page numbers of article titles are in boldface type. A Acitretin and cutaneous T-cell lymphomas, 716 719, 722, 725 ADCC. See Antibody-dependent cell-mediated cytotoxicity. Adjunctive therapies and
ISPUB.COM. Primary Cutaneous Anaplastic Large Cell Lymphoma Long-term Management with Low Dose Methotrexate. S Parker INTRODUCTION
 ISPUB.COM The Internet Journal of Dermatology Volume 7 Number 3 Primary Cutaneous Anaplastic Large Cell Lymphoma Long-term Management with Low Dose S Parker Citation S Parker.. The Internet Journal of
ISPUB.COM The Internet Journal of Dermatology Volume 7 Number 3 Primary Cutaneous Anaplastic Large Cell Lymphoma Long-term Management with Low Dose S Parker Citation S Parker.. The Internet Journal of
Clinical Policy: Vorinostat (Zolinza) Reference Number: CP.PHAR.83 Effective Date: 10/11
 Clinical Policy: (Zolinza) Reference Number: CP.PHAR.83 Effective Date: 10/11 Last Review Date: 12/16 Revision Log See Important Reminder at the end of this policy for important regulatory and legal information.
Clinical Policy: (Zolinza) Reference Number: CP.PHAR.83 Effective Date: 10/11 Last Review Date: 12/16 Revision Log See Important Reminder at the end of this policy for important regulatory and legal information.
Narrow band UVB (311 nm), psoralen UVB (311 nm) and PUVA therapy in the treatment of early-stage mycosis fungoides: a right left comparative study
 Photodermatol Photoimmunol Photomed 2005; 21: 281 286 Blackwell Munksgaard Copyright r Blackwell Munksgaard 2005 Narrow band UVB (311 nm), psoralen UVB (311 nm) and therapy in the treatment of early-stage
Photodermatol Photoimmunol Photomed 2005; 21: 281 286 Blackwell Munksgaard Copyright r Blackwell Munksgaard 2005 Narrow band UVB (311 nm), psoralen UVB (311 nm) and therapy in the treatment of early-stage
Lymphoma and Pseudolymphoma
 Lymphoma and Pseudolymphoma Laura B. Pincus, MD Co-Director, Cutaneous Lymphoma Clinic Associate Professor Dermatology and Pathology University of California, San Francisco I HAVE NO RELEVANT RELATIONSHIPS
Lymphoma and Pseudolymphoma Laura B. Pincus, MD Co-Director, Cutaneous Lymphoma Clinic Associate Professor Dermatology and Pathology University of California, San Francisco I HAVE NO RELEVANT RELATIONSHIPS
CASE 15 Patient: A 41-year-old Thai female Chief Compliant: Generalized papulovesicular rash for 1 month Present Illness: She presented with a 1-week
 CASE 15 Patient: A 41-year-old Thai female Chief Compliant: Generalized papulovesicular rash for 1 month Present Illness: She presented with a 1-week history of the generalized asymptomatic erythematous
CASE 15 Patient: A 41-year-old Thai female Chief Compliant: Generalized papulovesicular rash for 1 month Present Illness: She presented with a 1-week history of the generalized asymptomatic erythematous
Non-Hodgkin lymphomas (NHLs) Hodgkin lymphoma )HL)
 Non-Hodgkin lymphomas (NHLs) Hodgkin lymphoma )HL) Lymphoid Neoplasms: 1- non-hodgkin lymphomas (NHLs) 2- Hodgkin lymphoma 3- plasma cell neoplasms Non-Hodgkin lymphomas (NHLs) Acute Lymphoblastic Leukemia/Lymphoma
Non-Hodgkin lymphomas (NHLs) Hodgkin lymphoma )HL) Lymphoid Neoplasms: 1- non-hodgkin lymphomas (NHLs) 2- Hodgkin lymphoma 3- plasma cell neoplasms Non-Hodgkin lymphomas (NHLs) Acute Lymphoblastic Leukemia/Lymphoma
Sézary syndrome presenting with leonine facies ajd_560
 285..288 Australasian Journal of Dermatology (2009) 50, 285 288 doi: 10.1111/j.1440-0960.2009.00560.x CASE REPORT Sézary syndrome presenting with leonine facies ajd_560 Shano Nassem, 1 Rajesh Kashyap,
285..288 Australasian Journal of Dermatology (2009) 50, 285 288 doi: 10.1111/j.1440-0960.2009.00560.x CASE REPORT Sézary syndrome presenting with leonine facies ajd_560 Shano Nassem, 1 Rajesh Kashyap,
Microscopic study of the normal skin in cases of mycosis fungoides
 Microscopic study of the normal skin in cases of mycosis fungoides M. El Darouti, S. Marzook, M. Bosseila, O. Abu Zeid, O. El- Safouri, A. Zayed, A. El-Ramly Egyptian Dermatology Online Journal 2 (1):
Microscopic study of the normal skin in cases of mycosis fungoides M. El Darouti, S. Marzook, M. Bosseila, O. Abu Zeid, O. El- Safouri, A. Zayed, A. El-Ramly Egyptian Dermatology Online Journal 2 (1):
A middle-aged man with self-healing papulonecrotic lesions over the trunk and proximal limbs
 Hong Kong J. Dermatol. Venereol. (2011) 19, 30-34 Case Report A middle-aged man with self-healing papulonecrotic lesions over the trunk and proximal limbs JC Chan, N Trendell-Smith, CK Yeung Lymphomatoid
Hong Kong J. Dermatol. Venereol. (2011) 19, 30-34 Case Report A middle-aged man with self-healing papulonecrotic lesions over the trunk and proximal limbs JC Chan, N Trendell-Smith, CK Yeung Lymphomatoid
Allogeneic Stem Cell Transplantation for Cutaneous T-cell Lymphoma: Updated results from a single center
 Allogeneic Stem Cell Transplantation for Cutaneous T-cell Lymphoma: Updated results from a single center Madeleine Duvic, MD Professor and Deputy Chairman Blanche Bender Professor in Cancer Research Departments
Allogeneic Stem Cell Transplantation for Cutaneous T-cell Lymphoma: Updated results from a single center Madeleine Duvic, MD Professor and Deputy Chairman Blanche Bender Professor in Cancer Research Departments
Fig. 3.1 Fig Past history: She was previously healthy and not taking any medication.
 Case 3 A 41-year-old Thai female from Bangkok Chief compliant: Erythematous patch at left thigh for 2 months Present illness: The patient presented with a 10- year history of erythematous patch on her
Case 3 A 41-year-old Thai female from Bangkok Chief compliant: Erythematous patch at left thigh for 2 months Present illness: The patient presented with a 10- year history of erythematous patch on her
CD30+ Lymphoproliferative Disorders Associated with Longstanding Mycosis Fungoides
 Case Report DOI: 10.6003/jtad.16102c5 CD30+ Lymphoproliferative Disorders Associated with Longstanding Mycosis Fungoides Esra Adışen, 1 MD, Özlem Erdem, 2 MD, Mehmet Ali Gürer, 1 MD Address: 1 Gazi University
Case Report DOI: 10.6003/jtad.16102c5 CD30+ Lymphoproliferative Disorders Associated with Longstanding Mycosis Fungoides Esra Adışen, 1 MD, Özlem Erdem, 2 MD, Mehmet Ali Gürer, 1 MD Address: 1 Gazi University
Dermatologica Sinica
 DERMATOLOGICA SINICA 31 (2013) 3e Contents lists available at SciVerse ScienceDirect Dermatologica Sinica journal homepage: http://www.derm-sinica.com CASE REPORT Early stage mycosis fungoides with focal
DERMATOLOGICA SINICA 31 (2013) 3e Contents lists available at SciVerse ScienceDirect Dermatologica Sinica journal homepage: http://www.derm-sinica.com CASE REPORT Early stage mycosis fungoides with focal
Forum 115 Management Issues in Cutaneous Lymphomas. Management of Transformed Mycosis Fungoides
 Forum 115 Management Issues in Cutaneous Lymphomas Management of Transformed Mycosis Fungoides Madeleine Duvic, MD Deputy Chairman -Department of Dermatology Blanche Bender Professor of Cancer Research
Forum 115 Management Issues in Cutaneous Lymphomas Management of Transformed Mycosis Fungoides Madeleine Duvic, MD Deputy Chairman -Department of Dermatology Blanche Bender Professor of Cancer Research
ISPUB.COM. Management of Co-existing Mycosis Fungoides and Lymphomatoid Papulosis. E Kim PHYSICAL FINDINGS INTRODUCTION INITIAL PRESENTATION
 ISPUB.COM The Internet Journal of Dermatology Volume 7 Number 3 Management of Co-existing Mycosis Fungoides and Lymphomatoid Papulosis E Kim Citation E Kim. Management of Co-existing Mycosis Fungoides
ISPUB.COM The Internet Journal of Dermatology Volume 7 Number 3 Management of Co-existing Mycosis Fungoides and Lymphomatoid Papulosis E Kim Citation E Kim. Management of Co-existing Mycosis Fungoides
Cutaneous Lymphoid Proliferations: A Comprehensive Textbook of Lymphocytic Infiltrates of the Skin
 Cutaneous Lymphoid Proliferations: A Comprehensive Textbook of Lymphocytic Infiltrates of the Skin Magro, Cynthia M., MD ISBN-13: 9780471695981 Table of Contents Chapter One: Introduction to the Classification
Cutaneous Lymphoid Proliferations: A Comprehensive Textbook of Lymphocytic Infiltrates of the Skin Magro, Cynthia M., MD ISBN-13: 9780471695981 Table of Contents Chapter One: Introduction to the Classification
Primary cutaneous lymphomas: ESMO Clinical Practice Guidelines for diagnosis, treatment and follow-up
 Annals of Oncology 24 (Supplement 6): vi149 vi154, 2013 doi:10.1093/annonc/mdt242 Published online 17 July 2013 Primary cutaneous lymphomas: ESMO Clinical Practice Guidelines for diagnosis, treatment and
Annals of Oncology 24 (Supplement 6): vi149 vi154, 2013 doi:10.1093/annonc/mdt242 Published online 17 July 2013 Primary cutaneous lymphomas: ESMO Clinical Practice Guidelines for diagnosis, treatment and
Sézary syndrome. Diagnosis and staging
 CME DERMATOLOGY Clinical Medicine 2012, Vol 12, No 2: 160 4 Edited by Clive B Archer, consultant dermatologist and lead for Medical Education, St John s Institute of Dermatology, Guy s and St Thomas NHS
CME DERMATOLOGY Clinical Medicine 2012, Vol 12, No 2: 160 4 Edited by Clive B Archer, consultant dermatologist and lead for Medical Education, St John s Institute of Dermatology, Guy s and St Thomas NHS
CUTANEOUS T-CELL LYMPHOMA: SYSTEMIC THERAPY. Anne W. Beaven, MD Associate Professor Director, Lymphoma Program University of North Carolina
 CUTANEOUS T-CELL LYMPHOMA: SYSTEMIC THERAPY Anne W. Beaven, MD Associate Professor Director, Lymphoma Program University of North Carolina CTCL Extranodal Nodal Leukemia Mycosis fungoides Sezary Syndrome
CUTANEOUS T-CELL LYMPHOMA: SYSTEMIC THERAPY Anne W. Beaven, MD Associate Professor Director, Lymphoma Program University of North Carolina CTCL Extranodal Nodal Leukemia Mycosis fungoides Sezary Syndrome
Mycosis Fungoides, then and now Have we travelled?
 USCAP 103 rd Annual Meeting 2014 American Society of Dermatopathology Companion Meeting Mycosis Fungoides, then and now Have we travelled? Vijaya B. Reddy, MD, MBA Professor of Pathology Rush University
USCAP 103 rd Annual Meeting 2014 American Society of Dermatopathology Companion Meeting Mycosis Fungoides, then and now Have we travelled? Vijaya B. Reddy, MD, MBA Professor of Pathology Rush University
Immunopathogenesis and therapy of cutaneous T cell lymphoma
 Science in medicine Immunopathogenesis and therapy of cutaneous T cell lymphoma Ellen J. Kim, Stephen Hess, Stephen K. Richardson, Sara Newton, Louise C. Showe, Bernice M. Benoit, Ravi Ubriani, Carmela
Science in medicine Immunopathogenesis and therapy of cutaneous T cell lymphoma Ellen J. Kim, Stephen Hess, Stephen K. Richardson, Sara Newton, Louise C. Showe, Bernice M. Benoit, Ravi Ubriani, Carmela
Synthetic hypericin (SGX301; VIMRxyn) for cutaneous T cell lymphoma, unspecified
 NIHR Innovation Observatory Evidence Briefing: May 2017 Synthetic hypericin (SGX301; VIMRxyn) for cutaneous T cell lymphoma, unspecified NIHRIO (HSRIC) ID: 10761 NICE ID: 8375 LAY SUMMARY Cutaneous T cell
NIHR Innovation Observatory Evidence Briefing: May 2017 Synthetic hypericin (SGX301; VIMRxyn) for cutaneous T cell lymphoma, unspecified NIHRIO (HSRIC) ID: 10761 NICE ID: 8375 LAY SUMMARY Cutaneous T cell
Supportive Care in the Management of T-cell Lymphomas
 Supportive Care in the Management of T-cell Lymphomas Erin Kopp, ACNP-BC City of Hope Comprehensive Cancer Center NCCN.org For Clinicians NCCN.org/patients For Patients Objectives Discuss the role of supportive
Supportive Care in the Management of T-cell Lymphomas Erin Kopp, ACNP-BC City of Hope Comprehensive Cancer Center NCCN.org For Clinicians NCCN.org/patients For Patients Objectives Discuss the role of supportive
ISPUB.COM. Advanced Stage CTCL, PTCL with Cutaneous Involvement. J Messenger, P Porcu INTRODUCTION INITIAL PRESENTATION
 ISPUB.COM The Internet Journal of Dermatology Volume 7 Number 3 Advanced Stage CTCL, PTCL with Cutaneous Involvement J Messenger, P Porcu Citation J Messenger, P Porcu. Advanced Stage CTCL, PTCL with Cutaneous
ISPUB.COM The Internet Journal of Dermatology Volume 7 Number 3 Advanced Stage CTCL, PTCL with Cutaneous Involvement J Messenger, P Porcu Citation J Messenger, P Porcu. Advanced Stage CTCL, PTCL with Cutaneous
ISPUB.COM. M Duvic, E Olsen PURPOSE OF REVISION
 ISPUB.COM The Internet Journal of Dermatology Volume 7 Number 3 International Society of Cutaneous Lymphoma (ISCL) and the European Organization of Research and Treatment of Cancer (EORTC) revisions to
ISPUB.COM The Internet Journal of Dermatology Volume 7 Number 3 International Society of Cutaneous Lymphoma (ISCL) and the European Organization of Research and Treatment of Cancer (EORTC) revisions to
Plenary paper. Introduction
 Plenary paper Primary and secondary cutaneous CD30 lymphoproliferative disorders: a report from the Dutch Cutaneous Lymphoma Group on the long-term follow-up data of 219 patients and guidelines for diagnosis
Plenary paper Primary and secondary cutaneous CD30 lymphoproliferative disorders: a report from the Dutch Cutaneous Lymphoma Group on the long-term follow-up data of 219 patients and guidelines for diagnosis
Review Article. Cutaneous lymphoproliferative disorders. NJ Trendell-Smith
 Hong Kong J. Dermatol. Venereol. (2010) 18, 190-201 Review Article Cutaneous lymphoproliferative disorders NJ Trendell-Smith Cutaneous lymphoproliferative disorders (CLD) include reactive lymphoid hyperplasias,
Hong Kong J. Dermatol. Venereol. (2010) 18, 190-201 Review Article Cutaneous lymphoproliferative disorders NJ Trendell-Smith Cutaneous lymphoproliferative disorders (CLD) include reactive lymphoid hyperplasias,
TARGRETIN (bexarotene) oral capsule & external gel
 TARGRETIN (bexarotene) oral capsule & external gel Coverage for services, procedures, medical devices and drugs are dependent upon benefit eligibility as outlined in the member's specific benefit plan.
TARGRETIN (bexarotene) oral capsule & external gel Coverage for services, procedures, medical devices and drugs are dependent upon benefit eligibility as outlined in the member's specific benefit plan.
Granulomatous Slack Skin with an unusually aggressive course due to the subsequent development of a CD30-positive Large Cell Lymphoma
 Granulomatous Slack Skin with an unusually aggressive course due to the subsequent development of a CD30-positive Large Cell Lymphoma Alexandra Papoudou-Bai 1, Eleni Kapsali 2, Ioannis Kostas-Agnantis
Granulomatous Slack Skin with an unusually aggressive course due to the subsequent development of a CD30-positive Large Cell Lymphoma Alexandra Papoudou-Bai 1, Eleni Kapsali 2, Ioannis Kostas-Agnantis
See Important Reminder at the end of this policy for important regulatory and legal information.
 Clinical Policy: Vorinostat (Zolinza) Reference Number: CP.PHAR.83 Effective Date: 10.01.18 Last Review Date: 07.13.18 Line of Business: Oregon Health Plan Revision Log See Important Reminder at the end
Clinical Policy: Vorinostat (Zolinza) Reference Number: CP.PHAR.83 Effective Date: 10.01.18 Last Review Date: 07.13.18 Line of Business: Oregon Health Plan Revision Log See Important Reminder at the end
Cluster of differentiation (CD) markers in erythrodermic patients: A case series study
 Original Article Cluster of differentiation (CD) markers in erythrodermic patients: A case series study Fariba Ghalamkarpour, MD Faranak Niknafs, MD Shima Younespour, PhD Skin Research Center, Shahid Beheshti
Original Article Cluster of differentiation (CD) markers in erythrodermic patients: A case series study Fariba Ghalamkarpour, MD Faranak Niknafs, MD Shima Younespour, PhD Skin Research Center, Shahid Beheshti
Denileukin diftitox for the treatment of cutaneous T-cell lymphoma
 REVIEW Denileukin diftitox for the treatment of cutaneous T-cell lymphoma David Kaminetzky 1 Kenneth B Hymes 2 1 Division of Hematology/Oncology, New York University School of Medicine, New York, USA;
REVIEW Denileukin diftitox for the treatment of cutaneous T-cell lymphoma David Kaminetzky 1 Kenneth B Hymes 2 1 Division of Hematology/Oncology, New York University School of Medicine, New York, USA;
Skin SSG (Anglia East & Anglia West)
 Guidelines for the Management of Primary Cutaneous T-Cell Lymphomas Skin SSG (Anglia East & Anglia West) Author: S J Whittaker, J R Marsden, M Spittle and R Russell Jones Approved by: Anglia Cancer Network
Guidelines for the Management of Primary Cutaneous T-Cell Lymphomas Skin SSG (Anglia East & Anglia West) Author: S J Whittaker, J R Marsden, M Spittle and R Russell Jones Approved by: Anglia Cancer Network
Large cell immunoblastic Diffuse histiocytic (DHL) Lymphoblastic lymphoma Diffuse lymphoblastic Small non cleaved cell Burkitt s Non- Burkitt s
 Non Hodgkin s Lymphoma Introduction 6th most common cause of cancer death in United States. Increasing in incidence and mortality. Since 1970, the incidence of has almost doubled. Overview The types of
Non Hodgkin s Lymphoma Introduction 6th most common cause of cancer death in United States. Increasing in incidence and mortality. Since 1970, the incidence of has almost doubled. Overview The types of
UKCLG Guidelines for Primary Cutaneous Lymphomas
 UKCLG Guidelines for Primary Cutaneous Lymphomas Sean Whi:aker Di Gilson Fiona Child Julia Scarisbrick Tim Illidge Eileen Parry Katy Rezvani Claire Dearden and Stephen Morris Diagnosis, staging, prognosis
UKCLG Guidelines for Primary Cutaneous Lymphomas Sean Whi:aker Di Gilson Fiona Child Julia Scarisbrick Tim Illidge Eileen Parry Katy Rezvani Claire Dearden and Stephen Morris Diagnosis, staging, prognosis
88-year-old Female with Lymphadenopathy. Faizi Ali, MD
 88-year-old Female with Lymphadenopathy Faizi Ali, MD Clinical History A 88-year-old caucasian female presented to our hospital with the complaints of nausea, vomiting,diarrhea, shortness of breath and
88-year-old Female with Lymphadenopathy Faizi Ali, MD Clinical History A 88-year-old caucasian female presented to our hospital with the complaints of nausea, vomiting,diarrhea, shortness of breath and
Management of Mycosis Fungoides: Part 2. Treatment
 Review Article [1] October 01, 2003 By Benjamin D. Smith, MD [2] and Lynn D. Wilson, MD, MPH [3] Mycosis fungoides is a low-grade lymphoproliferative disorder of skin-homing CD4+ lymphocytes that may produce
Review Article [1] October 01, 2003 By Benjamin D. Smith, MD [2] and Lynn D. Wilson, MD, MPH [3] Mycosis fungoides is a low-grade lymphoproliferative disorder of skin-homing CD4+ lymphocytes that may produce
2. Sézary syndrome (SS)
 Go Back to the Top To Order, Visit the Purchasing Page for Details Clinical images are available in hardcopy only. Clinical images are available in Clinical images are available in d e f g h i j Fig..36-2
Go Back to the Top To Order, Visit the Purchasing Page for Details Clinical images are available in hardcopy only. Clinical images are available in Clinical images are available in d e f g h i j Fig..36-2
1/19/2018. Early CTCL: treatment considerations
 Treatment of early stage CTCL Joan Guitart, MD Chicago, IL USA Disclosures: Actelion (grants, consultant), Tetralogic/Medivir (grant, consultant), Solygenix (grant) Therakos (grant) Early CTCL: treatment
Treatment of early stage CTCL Joan Guitart, MD Chicago, IL USA Disclosures: Actelion (grants, consultant), Tetralogic/Medivir (grant, consultant), Solygenix (grant) Therakos (grant) Early CTCL: treatment
Important Decisions in Dermatopathology: The Clinico- Pathologic Correlation. Dermatopathology Specialists Needed. Changing Trends
 Important Decisions in Dermatopathology: The Clinico- Pathologic Correlation Uma Sundram, MD, PhD Departments of Pathology and Dermatology Stanford University May 29, 2008 Dermatopathology Specialists
Important Decisions in Dermatopathology: The Clinico- Pathologic Correlation Uma Sundram, MD, PhD Departments of Pathology and Dermatology Stanford University May 29, 2008 Dermatopathology Specialists
Plasma cell myeloma (multiple myeloma)
 Plasma cell myeloma (multiple myeloma) Common lymphoid neoplasm, present at old age (70 years average) Remember: plasma cells are terminally differentiated B-lymphocytes that produces antibodies. B-cells
Plasma cell myeloma (multiple myeloma) Common lymphoid neoplasm, present at old age (70 years average) Remember: plasma cells are terminally differentiated B-lymphocytes that produces antibodies. B-cells
Renaissance of Low-Dose Radiotherapy Concepts for Cutaneous Lymphomas
 Review Article DOI: 10.1159/000470845 Received: February 06, 2017 Accepted: March 13, 2017 Published online: April 6, 2017 Renaissance of Low-Dose Radiotherapy Concepts for Cutaneous Lymphomas Bouthaina
Review Article DOI: 10.1159/000470845 Received: February 06, 2017 Accepted: March 13, 2017 Published online: April 6, 2017 Renaissance of Low-Dose Radiotherapy Concepts for Cutaneous Lymphomas Bouthaina
Cutaneous T-Cell Lymphoma
 PROVIDING THE LATEST INFORMATION FOR PATIENTS & CAREGIVERS Cutaneous T-Cell Lymphoma Revised 2019 Support for this publication provided by A six-word narrative about living with blood cancer from patients
PROVIDING THE LATEST INFORMATION FOR PATIENTS & CAREGIVERS Cutaneous T-Cell Lymphoma Revised 2019 Support for this publication provided by A six-word narrative about living with blood cancer from patients
Burkitt lymphoma. Sporadic Endemic in Africa associated with EBV Translocations involving MYC gene on chromosome 8
 Heme 8 Burkitt lymphoma Sporadic Endemic in Africa associated with EBV Translocations involving MYC gene on chromosome 8 Most common is t(8;14) Believed to be the fastest growing tumor in humans!!!! Morphology
Heme 8 Burkitt lymphoma Sporadic Endemic in Africa associated with EBV Translocations involving MYC gene on chromosome 8 Most common is t(8;14) Believed to be the fastest growing tumor in humans!!!! Morphology
SH/EAHP Workshop 2011 Los Angeles, California, USA
 SH/EAHP Workshop 2011 Los Angeles, California, USA October 27-29, 2011 Session 3 Non-Mycosis Fungoides CTCL Patty Jansen & Rein Willemze Introduction Submitted: 101 cases + 7 cases group 1: 108 Deactivated
SH/EAHP Workshop 2011 Los Angeles, California, USA October 27-29, 2011 Session 3 Non-Mycosis Fungoides CTCL Patty Jansen & Rein Willemze Introduction Submitted: 101 cases + 7 cases group 1: 108 Deactivated
Mycosis Fungoides and Variants
 Mycosis Fungoides and Variants Jennifer Madison McNiff, M.D. Associate Professor, Dermatology and Pathology Yale University School of Medicine Classic mycosis fungoides The most common cutaneous lymphoma
Mycosis Fungoides and Variants Jennifer Madison McNiff, M.D. Associate Professor, Dermatology and Pathology Yale University School of Medicine Classic mycosis fungoides The most common cutaneous lymphoma
Lymphoma: What You Need to Know. Richard van der Jagt MD, FRCPC
 Lymphoma: What You Need to Know Richard van der Jagt MD, FRCPC Overview Concepts, classification, biology Epidemiology Clinical presentation Diagnosis Staging Three important types of lymphoma Conceptualizing
Lymphoma: What You Need to Know Richard van der Jagt MD, FRCPC Overview Concepts, classification, biology Epidemiology Clinical presentation Diagnosis Staging Three important types of lymphoma Conceptualizing
Primary cutaneous large cell lymphoma CD30+: a case-based review
 Case-based review Primary cutaneous large cell lymphoma CD30+: a case-based review Anna Campanati 1 Katia Giuliodori 1 Emanuela Martina 1 Luca Conocchiari 1 Giulia Ganzetti 1 Gaia Goteri 2 Annamaria Offidani
Case-based review Primary cutaneous large cell lymphoma CD30+: a case-based review Anna Campanati 1 Katia Giuliodori 1 Emanuela Martina 1 Luca Conocchiari 1 Giulia Ganzetti 1 Gaia Goteri 2 Annamaria Offidani
Malignant Lymphomas Decision Making and Problem Solving
 Malignant Lymphomas Decision Making and Problem Solving Cutaneous T-cell lymphomas (including rare subtypes). Current concepts. II. [haematologica] 2004;89:1372-1388 MARCO PAULLI EMILIO BERTI A B S T R
Malignant Lymphomas Decision Making and Problem Solving Cutaneous T-cell lymphomas (including rare subtypes). Current concepts. II. [haematologica] 2004;89:1372-1388 MARCO PAULLI EMILIO BERTI A B S T R
Mycosis Fungoides: A Retrospective Study of 44 Swedish Cases
 Acta Derm Venereol 2016; 96: 669 673 CLINICAL REPORT Mycosis Fungoides: A Retrospective Study of 44 Swedish Cases Yvonne EKLUND 1, Annika ARONSSON 1, Artur SCHMIDTCHEN 1 and Thomas RELANDER 2 1 Section
Acta Derm Venereol 2016; 96: 669 673 CLINICAL REPORT Mycosis Fungoides: A Retrospective Study of 44 Swedish Cases Yvonne EKLUND 1, Annika ARONSSON 1, Artur SCHMIDTCHEN 1 and Thomas RELANDER 2 1 Section
Research Article Characteristics of Primary Cutaneous T-Cell Lymphoma in Iran: A 10-Year Retrospective Study
 International Scholarly Research Notices, Article ID 820921, 5 pages http://dx.doi.org/10.1155/2014/820921 Research Article Characteristics of Primary Cutaneous T-Cell Lymphoma in Iran: A 10-Year Retrospective
International Scholarly Research Notices, Article ID 820921, 5 pages http://dx.doi.org/10.1155/2014/820921 Research Article Characteristics of Primary Cutaneous T-Cell Lymphoma in Iran: A 10-Year Retrospective
Corporate Medical Policy
 Corporate Medical Policy Extracorporeal Photopheresis File Name: Origination: Last CAP Review: Next CAP Review: Last Review: extracorporeal_photopheresis 9/2010 8/2017 8/2018 8/2017 Description of Procedure
Corporate Medical Policy Extracorporeal Photopheresis File Name: Origination: Last CAP Review: Next CAP Review: Last Review: extracorporeal_photopheresis 9/2010 8/2017 8/2018 8/2017 Description of Procedure
Clinical Trial Outcomes
 l Recent clinical evidence for topical mechlorethamine in mycosis fungoides Mycosis fungoides (MF) is a rare, potentially life-threatening cutaneous T-cell lymphoma characterized by cutaneous homing of
l Recent clinical evidence for topical mechlorethamine in mycosis fungoides Mycosis fungoides (MF) is a rare, potentially life-threatening cutaneous T-cell lymphoma characterized by cutaneous homing of
Bone Marrow Histopathologic and Molecular Staging in Epidermotropic T-Cell Lymphomas
 Hematopathology / BONE MARROW STAGING IN CUTANEOUS T-CELL LYMPHOMA Bone Marrow Histopathologic and Molecular Staging in Epidermotropic T-Cell Lymphomas Vincent Sibaud, MD, 1,2 Marie Beylot-Barry, MD, PhD,
Hematopathology / BONE MARROW STAGING IN CUTANEOUS T-CELL LYMPHOMA Bone Marrow Histopathologic and Molecular Staging in Epidermotropic T-Cell Lymphomas Vincent Sibaud, MD, 1,2 Marie Beylot-Barry, MD, PhD,
Case 1 A 61 year-old Thai woman from Bangkok Chief complaint: Multiple nodules and ulcerative masses on both arms, forearms and legs for 2 weeks
 Case 1 A 61 year-old Thai woman from Bangkok Chief complaint: Multiple nodules and ulcerative masses on both arms, forearms and legs for 2 weeks Fig. 1.1 Present illness: Five years ago, the patient presented
Case 1 A 61 year-old Thai woman from Bangkok Chief complaint: Multiple nodules and ulcerative masses on both arms, forearms and legs for 2 weeks Fig. 1.1 Present illness: Five years ago, the patient presented
Mycosis fungoides (MF) is the most common type of cutaneous
 Mycosis fungoides variants clinicopathologic features, differential diagnosis, and treatment Rein Willemze, MD, PhD Abstract Mycosis fungoides (MF) is the most common type of cutaneous T-cell lymphoma,
Mycosis fungoides variants clinicopathologic features, differential diagnosis, and treatment Rein Willemze, MD, PhD Abstract Mycosis fungoides (MF) is the most common type of cutaneous T-cell lymphoma,
Clusterin Expression Correlates With Stage and Presence of Large Cells in Mycosis Fungoides
 Anatomic Pathology / Clusterin Expression in Mycosis Fungoides Clusterin Expression Correlates With Stage and Presence of Large Cells in Mycosis Fungoides Pranil Chandra, DO, 1 Jose A. Plaza, MD, 2,4 Zhuang
Anatomic Pathology / Clusterin Expression in Mycosis Fungoides Clusterin Expression Correlates With Stage and Presence of Large Cells in Mycosis Fungoides Pranil Chandra, DO, 1 Jose A. Plaza, MD, 2,4 Zhuang
Clinical Study The Influence of the Coexpression of CD4 and CD8 in Cutaneous Lesions on Prognosis of Mycosis Fungoides: A Preliminary Study
 Skin Cancer, Article ID 624143, 4 pages http://dx.doi.org/10.1155/2014/624143 Clinical Study The Influence of the Coexpression of CD4 and CD8 in Cutaneous Lesions on Prognosis of Mycosis Fungoides: A Preliminary
Skin Cancer, Article ID 624143, 4 pages http://dx.doi.org/10.1155/2014/624143 Clinical Study The Influence of the Coexpression of CD4 and CD8 in Cutaneous Lesions on Prognosis of Mycosis Fungoides: A Preliminary
Cutaneous T cell lymphoma: update on treatment
 Review Cutaneous T cell lymphoma: update on treatment Uwe Wollina, MD Department of Dermatology, Dresden- Friedrichstadt Hospital, Dresden, Germany Correspondence Uwe Wollina, MD Department of Dermatology
Review Cutaneous T cell lymphoma: update on treatment Uwe Wollina, MD Department of Dermatology, Dresden- Friedrichstadt Hospital, Dresden, Germany Correspondence Uwe Wollina, MD Department of Dermatology
Classification of Hematologic Malignancies. Patricia Aoun MD MPH
 Classification of Hematologic Malignancies Patricia Aoun MD MPH Objectives Know the basic principles of the current classification system for hematopoietic and lymphoid malignancies Understand the differences
Classification of Hematologic Malignancies Patricia Aoun MD MPH Objectives Know the basic principles of the current classification system for hematopoietic and lymphoid malignancies Understand the differences
Commentary on the 2008 WHO classification of mature T- and NK-cell neoplasms
 J Hematopathol (2009) 2:65 73 DOI 10.1007/s12308-009-0034-z COMMENT Commentary on the 2008 WHO classification of mature T- and NK-cell neoplasms Megan S. Lim & Laurence de Leval & Leticia Quintanilla-Martinez
J Hematopathol (2009) 2:65 73 DOI 10.1007/s12308-009-0034-z COMMENT Commentary on the 2008 WHO classification of mature T- and NK-cell neoplasms Megan S. Lim & Laurence de Leval & Leticia Quintanilla-Martinez
Mycosis Fungoides Presentation in Emergency
 The Open Emergency Medicine Journal, 2011, 4, 17-21 17 Mycosis Fungoides Presentation in Emergency Asaad Shujaa*,1 and M. Owais Suriya 2 Open Access Department of Emergency Medicine College of Medicine,
The Open Emergency Medicine Journal, 2011, 4, 17-21 17 Mycosis Fungoides Presentation in Emergency Asaad Shujaa*,1 and M. Owais Suriya 2 Open Access Department of Emergency Medicine College of Medicine,
NCCN Guidelines Version Mycosis Fungoides/Sezary Syndrome
 DIAGNOSIS ESSENTIAL: Biopsy of suspicious skin sites Dermatopathology review of slides USEFUL UNDER CERTAIN CIRCUMSTANCES: Immunohistochemical studies of skin biopsy a,b (CD2, CD3, CD4, CD5, CD7, CD8,
DIAGNOSIS ESSENTIAL: Biopsy of suspicious skin sites Dermatopathology review of slides USEFUL UNDER CERTAIN CIRCUMSTANCES: Immunohistochemical studies of skin biopsy a,b (CD2, CD3, CD4, CD5, CD7, CD8,
Lymphomatoid Papulosis. اللمفواني الحطاطي الداء = lymphomatoide Papulose Thursday, 21 October :16 - Last Updated Friday, 03 December :54
 Lymphomatoid Papulosis 1 / 12 Lymphomatoid papulosis (LyP) is a chronic papulonecrotic or papulonodular skin disease with histologic features suggestive of a malignant lymphoma. The disease is characterized
Lymphomatoid Papulosis 1 / 12 Lymphomatoid papulosis (LyP) is a chronic papulonecrotic or papulonodular skin disease with histologic features suggestive of a malignant lymphoma. The disease is characterized
Granulomatous mycosis fungoides (GMF) is
 CASE REPORT Granulomatous mycosis fungoides, a rare subtype of cutaneous T-cell lymphoma Marta Kogut, MD, a Eva Hadaschik, MD, a Stephan Grabbe, MD, b Mindaugas Andrulis, MD, c Alexander Enk, MD, a and
CASE REPORT Granulomatous mycosis fungoides, a rare subtype of cutaneous T-cell lymphoma Marta Kogut, MD, a Eva Hadaschik, MD, a Stephan Grabbe, MD, b Mindaugas Andrulis, MD, c Alexander Enk, MD, a and
A rare clinical presentation of non Hodgkin Lymphoma as multiple neurofibromas with review of literature
 Original article A rare clinical presentation of non Hodgkin Lymphoma as multiple neurofibromas with review of literature Dr.C.R.Sirajunnisa Begum, Professor 1, Dr. Ira Bharadhwaj, Professor 1, Dr. Lavanya,
Original article A rare clinical presentation of non Hodgkin Lymphoma as multiple neurofibromas with review of literature Dr.C.R.Sirajunnisa Begum, Professor 1, Dr. Ira Bharadhwaj, Professor 1, Dr. Lavanya,
Lymphoma/CLL 101: Know your Subtype. Dr. David Macdonald Hematologist, The Ottawa Hospital
 Lymphoma/CLL 101: Know your Subtype Dr. David Macdonald Hematologist, The Ottawa Hospital Function of the Lymph System Lymph Node Lymphocytes B-cells develop in the bone marrow and influence the immune
Lymphoma/CLL 101: Know your Subtype Dr. David Macdonald Hematologist, The Ottawa Hospital Function of the Lymph System Lymph Node Lymphocytes B-cells develop in the bone marrow and influence the immune
Cutaneous T-Cell Lymphoma: Mycosis Fungoides/Sézary Syndrome: Part 1
 FEATURE ARTICLE Cutaneous T-Cell Lymphoma: Mycosis Fungoides/Sézary Syndrome: Part 1 Susan Booher, MS, RN, Sue Ann McCann, MSN, RN, DNC, Marianne C. Tawa, RN, MSN, ANP INTRODUCTION Cutaneous T-cell lymphoma
FEATURE ARTICLE Cutaneous T-Cell Lymphoma: Mycosis Fungoides/Sézary Syndrome: Part 1 Susan Booher, MS, RN, Sue Ann McCann, MSN, RN, DNC, Marianne C. Tawa, RN, MSN, ANP INTRODUCTION Cutaneous T-cell lymphoma
Lymphocytoma Cutis. Cynthia M. Magro MD. Director of Dermatopathology Weill Medical College of Cornell University New York, New York
 Lymphocytoma Cutis Cynthia M. Magro MD Professor of Pathology Director of Dermatopathology Weill Medical College of Cornell University New York, New York Lymphocytoma Cutis Falls under other designations
Lymphocytoma Cutis Cynthia M. Magro MD Professor of Pathology Director of Dermatopathology Weill Medical College of Cornell University New York, New York Lymphocytoma Cutis Falls under other designations
Primary cutaneous lymphomas: ESMO Clinical Practice Guidelines for diagnosis, treatment and follow-up
 Annals of Oncology 29 (Supplement 4): iv30 iv40, 2018 doi:10.1093/annonc/mdy133 CLINICAL PRACTICE GUIDELINES Primary cutaneous lymphomas: ESMO Clinical Practice Guidelines for diagnosis, treatment and
Annals of Oncology 29 (Supplement 4): iv30 iv40, 2018 doi:10.1093/annonc/mdy133 CLINICAL PRACTICE GUIDELINES Primary cutaneous lymphomas: ESMO Clinical Practice Guidelines for diagnosis, treatment and
Primary Cutaneous Acral CD8 þ T-Cell Lymphoma
 Primary Cutaneous Acral CD8 þ T-Cell Lymphoma Vivian M. Hathuc, DO; Alexandra C. Hristov, MD; Lauren B. Smith, MD Primary cutaneous acral CD8 þ T-cell lymphoma is a new provisional entity in the 2016 revision
Primary Cutaneous Acral CD8 þ T-Cell Lymphoma Vivian M. Hathuc, DO; Alexandra C. Hristov, MD; Lauren B. Smith, MD Primary cutaneous acral CD8 þ T-cell lymphoma is a new provisional entity in the 2016 revision
Subject Index. Dry desquamation, see Skin reactions, radiotherapy
 Subject Index Actinic keratosis disseminated disease 42 surgical excision 42 AIDS, see Kaposi s sarcoma Amifostine, skin reaction prophylaxis 111 Basal cell carcinoma, superficial X-ray therapy Bowen s
Subject Index Actinic keratosis disseminated disease 42 surgical excision 42 AIDS, see Kaposi s sarcoma Amifostine, skin reaction prophylaxis 111 Basal cell carcinoma, superficial X-ray therapy Bowen s
Cutaneous T cell lymphoma
 Cutaneous T cell lymphoma Belgian Hematology Society (BHS) course on indolent lymphomas 05-02-2015 Pascal Wolter, Department of General Medical Oncology, pascal.wolter@uzleuven.be Overview: I. Cutaneous
Cutaneous T cell lymphoma Belgian Hematology Society (BHS) course on indolent lymphomas 05-02-2015 Pascal Wolter, Department of General Medical Oncology, pascal.wolter@uzleuven.be Overview: I. Cutaneous
Summary. lymphoma/myeloma, regulatory T cells (T reg) Introduction. Clinical and Experimental Immunology ORIGINAL ARTICLE doi: /cei.
 bs_bs_banner Clinical and Experimental Immunology ORIGINAL ARTICLE doi:1.1111/cei.1273 Increased frequency of skin-infiltrating FoxP3 + regulatory T cells as a diagnostic indicator of severe atopic dermatitis
bs_bs_banner Clinical and Experimental Immunology ORIGINAL ARTICLE doi:1.1111/cei.1273 Increased frequency of skin-infiltrating FoxP3 + regulatory T cells as a diagnostic indicator of severe atopic dermatitis
NCCN Guidelines Version Primary Cutaneous CD30+ T-Cell Lymphoproliferative Disorders
 Primary Cutaneous CD30+ T-Cell Lymphoproliferative Disders OVERVIEW & DEFINITION Primary cutaneous CD30+ T-cell lymphoproliferative disders (LPDs) represent a spectrum that includes primary cutaneous anaplastic
Primary Cutaneous CD30+ T-Cell Lymphoproliferative Disders OVERVIEW & DEFINITION Primary cutaneous CD30+ T-cell lymphoproliferative disders (LPDs) represent a spectrum that includes primary cutaneous anaplastic
Dermatopathology: The tumor is composed of keratinocytes which show atypia, increase mitoses and abnormal mitoses.
 Squamous cell carcinoma (SCC): A common malignant tumor of keratinocytes arising in the epidermis, usually from a precancerous condition: 1- UV induced actinic keratosis, usually of low grade malignancy.
Squamous cell carcinoma (SCC): A common malignant tumor of keratinocytes arising in the epidermis, usually from a precancerous condition: 1- UV induced actinic keratosis, usually of low grade malignancy.
U006 Primary Cutaneous Lymphomas: Diagnosis, Staging and When to Refer M. Yadira Hurley, MD
 U006 Primary Cutaneous Lymphomas: Diagnosis, Staging and When to Refer M. Yadira Hurley, MD hurleyy@slu.edu DISCLOSURE OF RELATIONSHIPS WITH INDUSTRY Actelion: Speaker Honoraria, Investigator Grants, Consultant
U006 Primary Cutaneous Lymphomas: Diagnosis, Staging and When to Refer M. Yadira Hurley, MD hurleyy@slu.edu DISCLOSURE OF RELATIONSHIPS WITH INDUSTRY Actelion: Speaker Honoraria, Investigator Grants, Consultant
Defined lymphoma entities in the current WHO classification
 Defined lymphoma entities in the current WHO classification Luca Mazzucchelli Istituto cantonale di patologia, Locarno Bellinzona, January 29-31, 2016 Evolution of lymphoma classification Rappaport Lukes
Defined lymphoma entities in the current WHO classification Luca Mazzucchelli Istituto cantonale di patologia, Locarno Bellinzona, January 29-31, 2016 Evolution of lymphoma classification Rappaport Lukes
BJD British Journal of Dermatology. 1.0 Purpose and scope. 2.0 Methodology GUIDELINES. Linked Editorial: Wang and Bagot. Br J Dermatol 2019; 180:
 GUIDELINES BJD British Journal of Dermatology British Association of Dermatologists and U.K. Cutaneous Lymphoma Group guidelines for the management of primary cutaneous lymphomas 2018 D. Gilson, 1 S.J.
GUIDELINES BJD British Journal of Dermatology British Association of Dermatologists and U.K. Cutaneous Lymphoma Group guidelines for the management of primary cutaneous lymphomas 2018 D. Gilson, 1 S.J.
Interhospital Dermatology Conference 2013
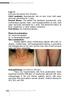 Case 21 A 50-year-old woman from Chonburi. Chief complaint: Asymptomatic rash on neck, trunk, both upper and lower extremities for 2 years. Present illness: The patient has developed asymptomatic scaly
Case 21 A 50-year-old woman from Chonburi. Chief complaint: Asymptomatic rash on neck, trunk, both upper and lower extremities for 2 years. Present illness: The patient has developed asymptomatic scaly
A Retrospective Study on the Risk of Non-Melanoma Skin Cancer in PUVA and Narrowband UVB Treated Patients
 Volume 1, Issue 3 Research Article A Retrospective Study on the Risk of Non-Melanoma Skin Cancer in PUVA and Narrowband UVB Treated Patients Darukarnphut P, Rattanakaemakorn P *, Rajatanavin N Division
Volume 1, Issue 3 Research Article A Retrospective Study on the Risk of Non-Melanoma Skin Cancer in PUVA and Narrowband UVB Treated Patients Darukarnphut P, Rattanakaemakorn P *, Rajatanavin N Division
Clinical manifestations and pathogenesis of cutaneous lymphomas: current status and future directions
 review Clinical manifestations and pathogenesis of cutaneous lymphomas: current status and future directions Belen Rubio-Gonzalez, 1 Jasmine Zain, 2 Steven T. Rosen 2 and Christiane Querfeld 1,2,3 1 Department
review Clinical manifestations and pathogenesis of cutaneous lymphomas: current status and future directions Belen Rubio-Gonzalez, 1 Jasmine Zain, 2 Steven T. Rosen 2 and Christiane Querfeld 1,2,3 1 Department
Phase 1 Trial Evaluating MRG-106, a Synthetic Inhibitor of microrna- 155, in Patients with CTCL
 EORTC CLTF 2017 meeting on Cutaneous Lymphomas: Insights & Therapeutic Progress Phase 1 Trial Evaluating MRG-106, a Synthetic Inhibitor of microrna- 155, in Patients with CTCL Christiane Querfeld, Francine
EORTC CLTF 2017 meeting on Cutaneous Lymphomas: Insights & Therapeutic Progress Phase 1 Trial Evaluating MRG-106, a Synthetic Inhibitor of microrna- 155, in Patients with CTCL Christiane Querfeld, Francine
Guidelines for the management of cutaneous lymphomas (2011): A consensus statement by the Japanese Skin Cancer Society Lymphoma Study Group
 doi: 10.1111/j.1346-8138.2012.01639.x Journal of Dermatology 2013; 40: 2 14 GUIDELINE Guidelines for the management of cutaneous lymphomas (2011): A consensus statement by the Japanese Skin Cancer Society
doi: 10.1111/j.1346-8138.2012.01639.x Journal of Dermatology 2013; 40: 2 14 GUIDELINE Guidelines for the management of cutaneous lymphomas (2011): A consensus statement by the Japanese Skin Cancer Society
The complex nature of the immunology of the skin
 Menus for Managing Patients With Cutaneous T-Cell Lymphoma Brian Poligone, MD, PhD,* and Peter Heald, MD In the management of patients with cutaneous T-cell lymphoma (CTCL), there are numerous distinct
Menus for Managing Patients With Cutaneous T-Cell Lymphoma Brian Poligone, MD, PhD,* and Peter Heald, MD In the management of patients with cutaneous T-cell lymphoma (CTCL), there are numerous distinct
