IL-6: a regulator of the transition from neutrophil to monocyte recruitment during inflammation
|
|
|
- Theodora Stokes
- 6 years ago
- Views:
Transcription
1 Opinion TRENDS in Immunology Vol.24 No.1 January IL-6: a regulator of the transition from neutrophil to monocyte recruitment during inflammation Gilles Kaplanski 1, Valérie Marin 1,Félix Montero-Julian 2, Alberto Mantovani 3 and Catherine Farnarier 1 1 INSERM U387, Hôpital Sainte-Marguerite, 270, Boulevard de Sainte-Marguerite, Marseille, France 2 Immunotech, a Coulter-Beckman company, Marseille, France 3 Instituto di Ricerche Farmacologiche Mario Negri, Milano, Italy The transition from neutrophil to mononuclear-cell infiltrate is a hallmark of acute inflammation. The kinetics of leuko-endothelial adhesion molecule expression and chemokine secretion might participate in the initial recruitment of neutrophils. Neutrophils then die in situ by apoptosis, while mononuclear cells accumulate. We propose that interleukin-6 (IL-6) and its soluble receptor (sil-6ra) might regulate the leukocyte recruitment transition, through a shift of chemokine production. This new function of IL-6 might aid in the understanding of its complex role in inflammation: during acute inflammation, IL-6 might favor the resolution of the neutrophilic infiltrate and the initiation of the immune response; in chronic inflammation, IL-6 might increase the mononuclear-cell infiltrate and participate in disease pathogenesis. Inflammation is a complex defense mechanism characterized by leukocyte migration from the vasculature into damaged tissues to destroy the injurious agents. Acute inflammation is a limited beneficial response particularly during infectious challenges, whereas chronic inflammation is a persistent phenomenon, which can progress to inflammatory diseases. One hallmark of acute inflammation is that the leukocyte infiltrate is initially mostly neutrophilic but after 24 to 48 h, monocytic cells predominate [1 3]. By contrast, chronic inflammation is histologically associated with the presence of mononuclear cells, such as macrophages and lymphocytes [1,2]. Although several explanations have been suggested, the mechanisms controlling the transition from neutrophil to monocyte recruitment during acute inflammation are poorly known. Here, we review different possible mechanisms involved and propose that the IL-6 soluble IL-6Ra (sil-6ra) complex might have an important role in this transition. Why are polymorphonuclear (PMN) cells the first leukocytes recruited to the inflammatory site? In several different models of acute inflammation, Corresponding author: Gilles Kaplanski (gkaplanski@marseille.inserm.fr). neutrophils are the first cells to accumulate in tissues [1 3]. One explanation for the initial recruitment of PMN cells might be the high concentration of these cells in the blood compared to monocytes. Another explanation could be the kinetics of expression of leuko-endothelial adhesion molecules. Adhesion of leukocytes to endothelium is a multistep process characterized by an initial weak interaction mediated by selectins and their carbohydrated ligands, giving a rolling motion to leukocytes. Rolling enables leukocyte activation by chemotactic agents associated with the endothelial-cell membrane, inducing activation of b integrins on the white-cell surface. These molecules interact with endothelial members of the immunoglobulin superfamily for firm leuko-endothelial adhesion [4,5]. Leukocytes then begin to cross the endothelial layer through homologous interactions of PECAM-1 [platelet endothelial-cell adhesion molecule (CD31)] expressed on both leukocytes and the intercellular membranes of endothelial cells, and migrate following a chemoattractant gradient initiated in the injured tissue [6]. Neutrophil adhesion is mainly supported by the selectins CD62L on white cells and CD62P on endothelium, the leukocyte b2 integrins CD11a/b (CD18) and the two endothelial members of the immunoglobulin superfamily, intercellular adhesion molecule-1 (ICAM-1) and ICAM-2. Each of these molecules are either constitutively present on leukocytes and endothelium, such as CD62L, CD11a (CD18), ICAM-1 and ICAM-2 or are very rapidly translocated, activated and upregulated, for example, CD62P, CD11b (CD18) and ICAM-1. Moreover, neutrophil recruitment is facilitated by chemotactic agents, such as C5a, leucotriene B4 (LTB4) or the platelet activating factor which are synthesized in minutes. In addition, the chemokine IL-8 (CXCL8), which is important for neutrophil recruitment in vivo, exists as a preformed pool in endothelial cells [7]. By contrast, the endothelial selectin CD62E, the b1 integrin VLA-4 on leukocytes and the endothelial immunoglobulin superfamily member vascular-cell adhesion molecule-1 (VCAM-1), which are more important for monocyte adhesion, are absent from the surface of quiescent leukocytes or endothelium and require several /02/$ - see front matter q 2002 Elsevier Science Ltd. All rights reserved. PII: S (02)
2 26 Opinion TRENDS in Immunology Vol.24 No.1 January 2003 Table 1. Effects of IL-6 on various inflammatory cells a Type of cells Production of IL-6 a Expression of IL-6Ra Expression of gp130 Effects of IL-6 Neutrophil Yes Yes Yes Increases elastase, PAF, IL-1Ra secretion, phagocytosis (at high concentrations) and apoptosis Monocyte Macrophage Yes Yes Yes Favors differentiation into macrophages, increases oxydative burst, tissue factor expression, MCP-1, IL-1Ra production, decreases IL-1b, TNF-a, and IL-12 production Endothelial cell Yes No Yes Increases ICAM-1 expression (þ/2 VCAM-1, CD62E), MCP-1, IL-6 (þ/2 IL-8) production and protein S synthesis Fibroblast Yes No or weak Yes Increases or decreases proliferation, increases collagen, glycosaminoglycan and TIMP-1 synthesis, MCP-1 and IL-6 production Dendritic cell Yes (mature cells) No Yes Increases precursor cell proliferation, phagocytosis, naïve T-cell attraction, GM-CSF receptor expression, IL-12 secretion a Abbreviations: GM-CSF, granulocyte macrophage-colony stimulating factor; ICAM, intercellular adheson molecule; IL, interleukin; IL-1Ra, IL-1 receptor antagonist; MCP, monocyte chemotactic protein; PAF, platelet activating factor; TIMP, tissue inhibitor of metalloproteinase; TNF, tumor necrosis factor; VCAM, vascular-cell adhesion molecule. hours of de novo synthesis. Therefore, the mediators necessary for neutrophil adhesion are present early in the course of inflammation, whereas molecules leading to monocyte adhesion appear several hours later. Why are monocytes subsequently recruited? A role for IL-6 sil-6ra trans signaling in chemokine shift In addition to adhesion molecules, the recruitment of leukocytes is dependent on the specificity of chemokines produced in the inflammatory site. IL-8 and monocyte chemotactic protein-1 (MCP-1) are the most important chemokines for the recruitment of PMN cells and monocytes, respectively. The transition from neutrophil to monocyte accumulation might be linked to these two chemokine production kinetics and functional properties. When neutrophils or other cells are stimulated by inflammatory cytokines, IL-8 is usually produced early and for 24 h, recruiting and activating more neutrophils locally [8,9]. Prolonged production of IL-8 on the contrary, might induce high concentrations of this chemokine in vessels, which inhibits both neutrophil adhesion to endothelium and extravasation [10]. MCP-1 production is usually delayed but sustained for several days; its accumulation does not desensitize cells and leads to late monocyte recruitment [8,9]. The transition from neutrophil to monocyte accumulation might also be secondary to a shift of the type of chemokine produced by stromal cells, inflammatory macrophages or neutrophils. Indeed, neutrophils stimulated with inflammatory cytokines for several hours selectively produced MCP-1 and not IL-8 [9]. In addition, it has been shown that IL-6 has a rather unexpected role in leukocyte recruitment in vivo, asaresultofthefact that the IL-6 sil-6ra complex can activate endothelial cells to secrete IL-8 and MCP-1, as well as the expression of adhesion molecules [11]. Noticeably, IL-6 activation of endothelial cells occurs in vivo, although these cells, like other stromal cells, express the gp130 transducing protein of the IL-6 receptor complex but not the 80 kda ligand binding subunit, IL-6Ra, andin vitro, this activation could only be achieved when IL-6 was combined with soluble recombinant IL-6Ra. IL-6Ra expression is limited in humans to leukocyte and hepatocyte membranes [12] but can be shed from the neutrophil membrane into a soluble form, which is found at high concentrations in neutrophil-enriched inflammatory fluids [13]. The sil-6ra combines with IL-6 to bind gp130 on the membranes of stromal cells, and activates these cells in a mechanism called trans signaling, explaining the data obtained on endothelial cells [14]. Although the observation that IL-6-induced IL-8 secretion was reported by another group using supraphysiological sil-6ra concentrations [15], other investigators have reported that the IL-6 sil-6ra complex primarily induced MCP-1 and not IL-8 secretion by human mesangial cells, fibroblasts or blood mononuclear cells [16 18] (Table 1). Recently, two groups including ours, made the observation that the IL-6 sil-6ra complex favors the transition from neutrophil to monocyte in inflammation [19,20]. Weusedanin vitro model of thrombin-activated HUVECs (human umbilical vein endothelial cells), which have been shown to acquire an inflammatory phenotype characterized by IL-6, IL-8, MCP-1 secretion and adhesion molecule expression [21]. Addition of sil-6ra, at concentrations comparable to those measured in inflammatory synovial fluids, to thrombinactivated HUVECs induced MCP-1 but not IL-8 secretion, which was even slightly inhibited [20]. Moreover, we observed that activation of neutrophils by IL-8 and other chemoattractants induces IL-6Ra shedding, in a mechanism involving the TNF-a converting enzyme [22]. Interestingly, IL-6Ra is expressed on monocyte membranes but its shedding is not induced by chemokine activation of these cells [12] (V. Marin et al., unpublished). In accordance with early observations in a model of C5-induced acute inflammation, monocyte recruitment in lungs was dependent on prior neutrophil recruitment [3]. These data suggest an interesting cascade: thrombin (or another proinflammatory agent) might activate endothelium (or other stromal cells) to produce IL-8 and other chemoattractants favoring
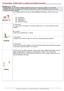
3 Opinion TRENDS in Immunology Vol.24 No.1 January IL-6Rα C5a LTB4 Neutrophil sil6-rα Monocyte PAF Endothelium activation IL-8 ICAM-1 IL-6 MCP-1 VCAM-1 Endothelial cells gp130 Polymorphonuclear-cell inflammation Mononuclear-cell inflammation TRENDS in Immunology Fig. 1. IL-6 sil-6ra autocrine loop of endothelial activation mediates a chemokine shift and the transition from neutrophil to monocyte recruitment. Endothelial (or stromal cells) activation by proinflammatory molecules leads to PAF, IL-8 and IL-6 secretion, as well as leuko-endothelial adhesion molecule expression (blue arrows). Chemoattractants, originating from the endothelium or other cell sources, recruit neutrophils and induce IL-6Ra shedding from their membranes (red arrows). The combination of sil- 6Ra with IL-6 enables ligation to gp130 on endothelial-cell membrane (black arrows) and increase both IL-6 and MCP-1 endothelial (or stromal) cell secretion (green arrows) but not IL-8, favoring a transition from neutrophil to monocyte recruitment. Abbreviations: ICAM, intercellular adhesion molecule; IL, interleukin; MCP, monocyte chemotactic protein; PAF, platelet activating factor; sil-6r, soluble IL-6 receptor; VCAM, vascular-cell adhesion molecule. early neutrophil recruitment in the inflammatory site. Activated PMN cells might release sil-6ra, which combines with locally produced IL-6, to activate endothelial cells to produce MCP-1 and not IL-8, decreasing neutrophil and favoring monocyte recruitment (Fig. 1). This could explain why in inflammatory animal models, the neutrophilic infiltrate is more dominant in IL-6 knockout mice than in wild-type animals [23]. Similar observations and conclusions have been made by Hurst et al. [19] using mesothelial cells and validated in IL-6 knockout mice. In wild-type animals, the local infiltrate of acute peritonitis was primarily made of neutrophils followed by monocytes, however, in the IL-6 knockout animals, neutrophils were the only cells present in the infiltrate. The injection of exogenous IL-6 sil-6ra complex restored the monocytic influx [19]. Role of apoptosis in neutrophil fate at the inflammatory site A transition from neutrophil to monocyte accumulation at the inflammatory site not only suggests a progression of events leading to monocyte recruitment but also the disappearance of neutrophils. Neutrophils are central cells in the defense of an organism against injury, notably infection, through their capacity to synthesise oxygen metabolites and to liberate various enzymes. However, these agents might also be toxic for normal surrounding tissues and potentially induce inflammatory diseases. Therefore, neutrophil functions must be rapidly negatively regulated. Numerous reports show that this is achieved through local death of aged PMN cells by apoptosis [24]. In addition, activation of PMN cells by phagocytosis of bacteria or more globally by phagocytosis mediated by Fc or complement receptors induces upregulation of programmed cell death genes and apoptosis [25]. Some cytokines and growth factors, such as granulocyte-colony-stimulating factor (G-CSF) prevent neutrophil death but interestingly, IL-6 has been shown to induce PMN-cell apoptosis [26]. More importantly, death by apoptosis induces loss of PMN-cell biological functions but prevents liberation of neutrophil intracellular toxic contents and further tissue injury [27]. Apoptosis induces the appearance of or changes of some molecules on leukocyte-cell membranes, notably negatively charged phosphatidylserine, sugars and ICAM-3. These molecules might be recognized by various receptors, such as the phosphatidylserine, the vitronectin, the scavenger receptors, or CD36 on macrophages leading to phagocytosis of dead cells [28]. In addition, CD44, the hyaluronan receptor, which is present on both neutrophil and macrophage surfaces also increases the phagocytosis of apoptotic neutrophils and has an important role in the resolution of
4 28 Opinion TRENDS in Immunology Vol.24 No.1 January 2003 IL-6 PMN SCV Rec IL-1β TNF-α IL-8 Sugars Apoptotic neutrophil PS PS Rec Macrophage TGF-β ICAM-3 TSP α53β CD36 MCP-1 Phagocytosis Mononuclear cells TRENDS in Immunology Fig. 2. Role of apoptotic neutrophil phagocytosis in the transition from neutrophil to monocyte recruitment. Apoptotic neutrophils expressing new membrane antigens (PS: phosphatidylserine, TSP: thrombospondin) are recognized by various receptors on macrophages (SCV Rec: scavenger receptors, PS Rec: phosphatidylserine receptor, a5b3: vitronectin receptor), leading to their phagocytosis. Phagocytosis of apoptotic PMN neutrophils by macrophages increases TGFb and MCP-1 secretion and decreases IL-8 production (red arrows), leading to a chemokine shift favoring monocyte recruitment (green arrows). Abbreviations: ICAM, intercellular adhesion molecule; MCP, monocyte chemotactic protein; TGF, transforming growth factor; TNF, tumor necrosis factor. inflammation [29,30]. For the phagocytosis process to be engaged, a previous persistent adhesive step mediated by homophilic CD31 interactions between apoptotic cells and phagocytes seems to be necessary, as recently reported [31]. A crucial aspect of this phenomenon is that in contrast to FCgR-mediated phagocytosis, phagocytosis of apoptotic cells decreases macrophage activation and cytokine production through secretion of transforming growth factor-b (TGF-b) [32,33]. Notably, IL-1b, TNF-a and IL-8 are decreased. TGF-b also decreases the production of G-CSF by macrophages, thus favoring PMN-cell death [33]. However, contrary to other main proinflammatory cytokines, phagocytosis of apoptotic neutrophils induces MCP-1 production by macrophages [33]. Thus, PMN-cell apoptosis not only participates in neutrophil elimination but could also favor a chemokine shift leading to monocyte recruitment (Fig. 2). Inflammatory macrophages emigrate to the draining lymph node Following these different steps, neutrophils are depleted from the inflammatory site; by contrast, blood monocytes accumulate and differentiate into inflammatory macrophages, which complete phagocytosis and destruction of the injurious agents [1 3]. Contrary to neutrophils, monocytes and macrophages do not die locally but emigrate after several days in the local lymph nodes [34]. During this migratory process, monocytes differentiate into dendritic cells, upregulating HLA class II antigen membrane expression, and acquiring costimulatory molecules, such as CD80 and CD86 [35]. These cells might then present antigenic peptides to lymphocytes, contributing to the generation of an immune response. Concluding remarks To be beneficial, the inflammatory reaction must be acute, destroying the injurious agent in a timeand space-limited fashion, and inducing an immune response. This is achieved through a complex series of events characterized by local leukocyte recruitment, death and emigration [36]. The transition from neutrophil to monocyte recruitment participates in the efficient destruction of the noxious agent by the combined destructive and phagocytic actions of neutrophils and inflammatory macrophages. However, it also participates in the resolution of inflammation through elimination of neutrophils and the initiation of an immune response. We discussed here the role of a shift of locally produced chemokines and the potential orchestrating functions of IL-6 in this phenomenon. It remains probable, however, that other signals exist that promote this shift in chemokine production and leukocyte recruitment. Moreover, this adds a new function for IL-6; its role in inflammation remains to be elucidated. In numerous models of chronic inflammatory diseases, such as collagen-induced arthritis, murine colitis or experimental autoimmune encephalomyelitis, IL-6 is pro-inflammatory [37,38], whereas in models of acute inflammation (except in a recently reported model [39] of viral ocular inflammation), IL-6 is rather protective [23]. A way to reconcile these different aspects and an attractive hypothesis might be that in acute inflammation, IL-6 could have a rather
5 Opinion TRENDS in Immunology Vol.24 No.1 January protective role decreasing neutrophil and favoring monocyte recruitment leading to the resolution of inflammation and the initiation of an immune response. Alternatively, in chronic inflammation, as supported by experimental models of rheumatoid arthritis and Crohn s disease, IL-6 could have a rather detrimental role favoring mononuclear-cell accumulation at the site of injury, through continuous MCP-1 secretion, angioproliferation and anti-apoptotic functions on T cells [40]. Better knowledge of these mechanisms could help our understanding of how and why mediators of acute inflammation lead, in some circumstances, to chronic inflammation. References 1 Ryan, G.B. and Majno, G. (1977) Acute inflammation. Am. J. Pathol. 86, Melnicoff, M.J. et al. (1989) Kinetics of changes in peritoneal-cell populations following acute inflammation. Cell. Immunol. 118, Doherty, D.E. et al. (1988) Monocyte retention and migration in pulmonary inflammation. Requirement for neutrophils. Lab. Invest. 59, Springer, T.A. (1994) Traffic signals for lymphocyte recirculation and leukocyte emigration: the multistep paradigm. Cell 76, Bevilacqua, M.P. and Nelson, R.M. (1993) Selectins. J. Clin. Invest. 91, Newman, P.J. (1997) The biology of PECAM-1. J. Clin. Invest. 100, S25 S29 7 Utgaard, J.O. et al. (1998) Rapid secretion of prestored interleukin-8 from Weibel-Palade bodies of microvascular endothelial cells. J. Exp. Med. 188, Sallusto, F. et al. (1999) Distinct patterns and kinectics of chemokine production regulate dendritic-cell function. Eur. J. Immunol. 29, Yamashiro, S. et al. (1999) MCP-1 is selectively expressed in the late phase by cytokine-stimulated human neutrophils: TNF-a plays a role in maximal MCP-1 mrna expression. J. Leukoc. Biol. 65, Gimbrone, M.A. et al. (1989) Interleukin-8: a novel inhibitor of leukocyte-endothelial interactions. Science 246, Romano, M. et al. (1997) Role of IL-6 and its soluble receptor in induction of chemokines and leukocyte recruitment. Immunity 6, Müllberg, J. et al. (1993) The soluble interleukin-6 receptor is generated by shedding. Eur. J. Immunol. 23, Desgeorges, A. et al. (1997) Concentrations and origins of soluble interleukin-6 receptor-a in serum and synovial fluid. J. Rheumatol. 24, Taga, T. et al. (1989) Interleukin-6 triggers the association of its receptor with a possible signal transducer, gp130. Cell 58, Modur, V. et al. (1997) Retrograde inflammatory signaling from neutrophils to endothelial cells by soluble interleukin-6 receptor a. J. Clin. Invest. 100, Coletta, I. et al. (2000) Selective induction of MCP-1 in human mesangial cells by the IL-6/sIL-6R complex. Exp. Nephrol. 8, Sporri, B. et al. (1999) Soluble IL-6 receptor induces calcium flux and selectively modulates chemokine expression in human dermal fibroblasts. Int. Immunol. 11, Biswas, P. et al. (1998) Interleukin-6 induces monocyte chemotactic protein-1 in peripheral blood mononuclear cells and in the U937 cell line. Blood 91, Hurst, S.M. et al. (2001) IL-6 and its soluble receptor orchestrate a temporal switch in the pattern of leukocyte recruitment seen during acute inflammation. Immunity 14, Marin, V. et al. (2001) The IL-6/soluble IL-6Ra autocrine loop of endothelial activation as an intermediate between acute and chronic inflammation: an experimental model involving thrombin. J. Immunol. 167, Kaplanski, G. et al. (1997) Thrombin induces endothelial type II activation in vitro: IL-1andTNF-a-independent IL-8 secretion and E-selectin expression. J. Immunol. 158, Marin, V. et al. (2002) Chemotactic agents induces IL-6Ra shedding from polymorphonuclear cells through involvement of a metalloproteinase of the TNF-a converting enzyme (TACE)-type. Eur. J. Immunol. 32, Xing, Z.et al. (1998) IL-6 is an anti-inflammatory cytokine required for controlling local or systemic acute inflammatory responses. J. Clin. Invest. 101, Savill, J.S. et al. (1989) Macrophage phagocytosis of aging neutrophils in inflammation. Programmed cell death in the neutrophil leads to its recognition by macrophages. J. Clin. Invest. 83, Kobayashi, S.D. et al. (2002) Global changes in gene expression by human polymorphonuclear leukocytes during receptor-mediated phagocytosis: cell fate is regulated at the level of gene expression. Proc. Natl Acad. Sci. USA 99, Afford, S.C. et al. (1992) The induction by human interleukin-6 of apoptosis in the promonocytic cell line U937 and human neutrophils. J. Biol. Chem. 267, Whyte, M.K.B. et al. (1993) Impairment of function in aging neutrophils is associated with apoptosis. J. Immunol. 150, Savill, J.S. (1998) Phagocytic docking without shocking. Nature 392, Hart, S.P. et al. (1997) CD44 regulates phagocytosis of apoptotic neutrophil granulocytes, but not apoptotic lymphocytes, by human macrophages. J. Immunol. 159, Teder,P. et al. (2002) Resolution of lung inflammation by CD44. Science 296, Brown, S. et al. (2002) Apoptosis disables CD31-mediated cell detachment from phagocytes promoting binding and engulfment. Nature 418, Fadok, V.A. et al. (1998) Macrophages that have ingested apoptotic cells in vitro inhibit proinflammatory cytokine production through autocrine/paracrine mechanisms involving TGF-b, PGE2, and PAF. J. Clin. Invest. 101, McDonald, P.P. et al. (1999) Transcriptional and translational regulation of inflammatory mediator production by endogenous TGF-b in macrophages that have ingested apoptotic cells. J. Immunol. 163, Bellingan, G.J. et al. (1996) In vivo fate of the inflammatory macrophage during the resolution of inflammation. Inflammatory macrophages do not die locally but emigrate to the draining lymph nodes. J. Immunol. 157, Randolph, G.J. et al. (1998) Differentiation of monocytes into dendritic cells in a model of transendothelial trafficking. Science 282, Buckley, C.D. et al. (2001) Fibroblasts regulate the switch from acute resolving to chronic persistent inflammation. Trends Immunol. 22, Alonzi, T. et al. (1998) Interleukin-6 is required for the development of collagen-induced arthritis. J. Exp. Med. 187, Yamamoto, M. et al. (2000) IL-6 is required for the development of Th-1 cell-mediated murine colitis. J. Immunol. 164, Fenton, R.R. et al. (2002) Linkage of IL-6 with neutrophil chemoattractant expression in virus-induced ocular inflammation. Invest. Ophthalmol. Vis. Sci. 43, Atreya, R. et al. (2000) Blockade of interleukin-6 trans signaling suppresses T-cell resistance against apoptosis in chronic intestinal inflammation: evidence in Crohn disease and experimental colitis in vivo. Nat. Med. 6,
Chapter 3, Part A (Pages 37-45): Leukocyte Migration into Tissues
 Allergy and Immunology Review Corner: Chapter 3, Part A (pages 37-45) of Cellular and Molecular Immunology (Seventh Edition), by Abul K. Abbas, Andrew H. Lichtman and Shiv Pillai. Chapter 3, Part A (Pages
Allergy and Immunology Review Corner: Chapter 3, Part A (pages 37-45) of Cellular and Molecular Immunology (Seventh Edition), by Abul K. Abbas, Andrew H. Lichtman and Shiv Pillai. Chapter 3, Part A (Pages
Cytokines, adhesion molecules and apoptosis markers. A comprehensive product line for human and veterinary ELISAs
 Cytokines, adhesion molecules and apoptosis markers A comprehensive product line for human and veterinary ELISAs IBL International s cytokine product line... is extremely comprehensive. The assays are
Cytokines, adhesion molecules and apoptosis markers A comprehensive product line for human and veterinary ELISAs IBL International s cytokine product line... is extremely comprehensive. The assays are
ACTIVATION OF T LYMPHOCYTES AND CELL MEDIATED IMMUNITY
 ACTIVATION OF T LYMPHOCYTES AND CELL MEDIATED IMMUNITY The recognition of specific antigen by naïve T cell induces its own activation and effector phases. T helper cells recognize peptide antigens through
ACTIVATION OF T LYMPHOCYTES AND CELL MEDIATED IMMUNITY The recognition of specific antigen by naïve T cell induces its own activation and effector phases. T helper cells recognize peptide antigens through
The recruitment of leukocytes and plasma proteins from the blood to sites of infection and tissue injury is called inflammation
 The migration of a particular type of leukocyte into a restricted type of tissue, or a tissue with an ongoing infection or injury, is often called leukocyte homing, and the general process of leukocyte
The migration of a particular type of leukocyte into a restricted type of tissue, or a tissue with an ongoing infection or injury, is often called leukocyte homing, and the general process of leukocyte
Subject Index. Bcl-2, apoptosis regulation Bone marrow, polymorphonuclear neutrophil release 24, 26
 Subject Index A1, apoptosis regulation 217, 218 Adaptive immunity, polymorphonuclear neutrophil role 31 33 Angiogenesis cancer 178 endometrium remodeling 172 HIV Tat induction mechanism 176 inflammatory
Subject Index A1, apoptosis regulation 217, 218 Adaptive immunity, polymorphonuclear neutrophil role 31 33 Angiogenesis cancer 178 endometrium remodeling 172 HIV Tat induction mechanism 176 inflammatory
Cytokines modulate the functional activities of individual cells and tissues both under normal and pathologic conditions Interleukins,
 Cytokines http://highered.mcgraw-hill.com/sites/0072507470/student_view0/chapter22/animation the_immune_response.html Cytokines modulate the functional activities of individual cells and tissues both under
Cytokines http://highered.mcgraw-hill.com/sites/0072507470/student_view0/chapter22/animation the_immune_response.html Cytokines modulate the functional activities of individual cells and tissues both under
The T cell receptor for MHC-associated peptide antigens
 1 The T cell receptor for MHC-associated peptide antigens T lymphocytes have a dual specificity: they recognize polymporphic residues of self MHC molecules, and they also recognize residues of peptide
1 The T cell receptor for MHC-associated peptide antigens T lymphocytes have a dual specificity: they recognize polymporphic residues of self MHC molecules, and they also recognize residues of peptide
ACTIVATION AND EFFECTOR FUNCTIONS OF CELL-MEDIATED IMMUNITY AND NK CELLS. Choompone Sakonwasun, MD (Hons), FRCPT
 ACTIVATION AND EFFECTOR FUNCTIONS OF CELL-MEDIATED IMMUNITY AND NK CELLS Choompone Sakonwasun, MD (Hons), FRCPT Types of Adaptive Immunity Types of T Cell-mediated Immune Reactions CTLs = cytotoxic T lymphocytes
ACTIVATION AND EFFECTOR FUNCTIONS OF CELL-MEDIATED IMMUNITY AND NK CELLS Choompone Sakonwasun, MD (Hons), FRCPT Types of Adaptive Immunity Types of T Cell-mediated Immune Reactions CTLs = cytotoxic T lymphocytes
Generation of post-germinal centre myeloma plasma B cell.
 Generation of post-germinal centre myeloma. DNA DAMAGE CXCR4 Homing to Lytic lesion activation CD38 CD138 CD56 Phenotypic markers Naive Secondary lymphoid organ Multiple myeloma is a malignancy of s caused
Generation of post-germinal centre myeloma. DNA DAMAGE CXCR4 Homing to Lytic lesion activation CD38 CD138 CD56 Phenotypic markers Naive Secondary lymphoid organ Multiple myeloma is a malignancy of s caused
Immunology for the Rheumatologist
 Immunology for the Rheumatologist Rheumatologists frequently deal with the immune system gone awry, rarely studying normal immunology. This program is an overview and discussion of the function of the
Immunology for the Rheumatologist Rheumatologists frequently deal with the immune system gone awry, rarely studying normal immunology. This program is an overview and discussion of the function of the
CYTOKINE RECEPTORS AND SIGNAL TRANSDUCTION
 CYTOKINE RECEPTORS AND SIGNAL TRANSDUCTION What is Cytokine? Secreted popypeptide (protein) involved in cell-to-cell signaling. Acts in paracrine or autocrine fashion through specific cellular receptors.
CYTOKINE RECEPTORS AND SIGNAL TRANSDUCTION What is Cytokine? Secreted popypeptide (protein) involved in cell-to-cell signaling. Acts in paracrine or autocrine fashion through specific cellular receptors.
Cytokines (II) Dr. Aws Alshamsan Department of Pharmaceu5cs Office: AA87 Tel:
 Cytokines (II) Dr. Aws Alshamsan Department of Pharmaceu5cs Office: AA87 Tel: 4677363 aalshamsan@ksu.edu.sa Learning Objectives By the end of this lecture you will be able to: 1 Understand the physiological
Cytokines (II) Dr. Aws Alshamsan Department of Pharmaceu5cs Office: AA87 Tel: 4677363 aalshamsan@ksu.edu.sa Learning Objectives By the end of this lecture you will be able to: 1 Understand the physiological
Chapter 2 (pages 22 33): Cells and Tissues of the Immune System. Prepared by Kristen Dazy, MD, Scripps Clinic Medical Group
 Allergy and Immunology Review Corner: Cellular and Molecular Immunology, 8th Edition By Abul K. Abbas, MBBS; Andrew H. H. Lichtman, MD, PhD; and Shiv Pillai, MBBS, PhD. Chapter 2 (pages 22 33): Cells and
Allergy and Immunology Review Corner: Cellular and Molecular Immunology, 8th Edition By Abul K. Abbas, MBBS; Andrew H. H. Lichtman, MD, PhD; and Shiv Pillai, MBBS, PhD. Chapter 2 (pages 22 33): Cells and
The Immune Response in Time and Space
 The Immune Response in Time and Space Chapters 14 & 4 Sharon S. Evans, Ph.D. Department of Immunology 845-3421 sharon.evans@roswellpark.org September 18 & 23, 2014 Inflammation Inflammation Complex response
The Immune Response in Time and Space Chapters 14 & 4 Sharon S. Evans, Ph.D. Department of Immunology 845-3421 sharon.evans@roswellpark.org September 18 & 23, 2014 Inflammation Inflammation Complex response
MACROPHAGE "MONOCYTES" SURFACE RECEPTORS
 LECTURE: 13 Title: MACROPHAGE "MONOCYTES" SURFACE RECEPTORS LEARNING OBJECTIVES: The student should be able to: Describe the blood monocytes (size, and shape of nucleus). Enumerate some of the monocytes
LECTURE: 13 Title: MACROPHAGE "MONOCYTES" SURFACE RECEPTORS LEARNING OBJECTIVES: The student should be able to: Describe the blood monocytes (size, and shape of nucleus). Enumerate some of the monocytes
Basis of Immunology and
 Basis of Immunology and Immunophysiopathology of Infectious Diseases Jointly organized by Institut Pasteur in Ho Chi Minh City and Institut Pasteur with kind support from ANRS & Université Pierre et Marie
Basis of Immunology and Immunophysiopathology of Infectious Diseases Jointly organized by Institut Pasteur in Ho Chi Minh City and Institut Pasteur with kind support from ANRS & Université Pierre et Marie
Test Bank for Basic Immunology Functions and Disorders of the Immune System 4th Edition by Abbas
 Test Bank for Basic Immunology Functions and Disorders of the Immune System 4th Edition by Abbas Chapter 04: Antigen Recognition in the Adaptive Immune System Test Bank MULTIPLE CHOICE 1. Most T lymphocytes
Test Bank for Basic Immunology Functions and Disorders of the Immune System 4th Edition by Abbas Chapter 04: Antigen Recognition in the Adaptive Immune System Test Bank MULTIPLE CHOICE 1. Most T lymphocytes
MAF Shalaby Prof. Rheumatology Al Azhar University, Cairo, Egypt.
 MAF Shalaby Prof. Rheumatology Al Azhar University, Cairo, Egypt. AUTOIMMUNE DISEASE RA SLE VASCULITIS RELAPSING POLYCHONDRITIS SS DM/PM SJOGREN S SYNDROME RHEUMATOID ARTHRITIS Classically immune mediated
MAF Shalaby Prof. Rheumatology Al Azhar University, Cairo, Egypt. AUTOIMMUNE DISEASE RA SLE VASCULITIS RELAPSING POLYCHONDRITIS SS DM/PM SJOGREN S SYNDROME RHEUMATOID ARTHRITIS Classically immune mediated
Newly Recognized Components of the Innate Immune System
 Newly Recognized Components of the Innate Immune System NOD Proteins: Intracellular Peptidoglycan Sensors NOD-1 NOD-2 Nod Protein LRR; Ligand Recognition CARD RICK I-κB p50 p65 NF-κB Polymorphisms in Nod-2
Newly Recognized Components of the Innate Immune System NOD Proteins: Intracellular Peptidoglycan Sensors NOD-1 NOD-2 Nod Protein LRR; Ligand Recognition CARD RICK I-κB p50 p65 NF-κB Polymorphisms in Nod-2
Effector mechanisms of cell-mediated immunity: Properties of effector, memory and regulatory T cells
 ICI Basic Immunology course Effector mechanisms of cell-mediated immunity: Properties of effector, memory and regulatory T cells Abul K. Abbas, MD UCSF Stages in the development of T cell responses: induction
ICI Basic Immunology course Effector mechanisms of cell-mediated immunity: Properties of effector, memory and regulatory T cells Abul K. Abbas, MD UCSF Stages in the development of T cell responses: induction
INFLAMMATION: Cellular Functions
 INFLAMMATION: Cellular Functions Sequence of Vascular Events 1. Vasodilation (increased blood flow) CALOR & RUBOR 2. Increased microvascular permeability: fluids into tissues TUMOR 3. Blood flow slows
INFLAMMATION: Cellular Functions Sequence of Vascular Events 1. Vasodilation (increased blood flow) CALOR & RUBOR 2. Increased microvascular permeability: fluids into tissues TUMOR 3. Blood flow slows
HIV AND INFLAMMATION: A NEW THREAT
 HIV AND INFLAMMATION: A NEW THREAT KAP ANNUAL SCIENTIFIC CONFERENC MAY 2013 DR JOSEPH ALUOCH FRCP,EBS Basic Components of the Immune System Immunology: cells and tissues involved in recognizing and attacking
HIV AND INFLAMMATION: A NEW THREAT KAP ANNUAL SCIENTIFIC CONFERENC MAY 2013 DR JOSEPH ALUOCH FRCP,EBS Basic Components of the Immune System Immunology: cells and tissues involved in recognizing and attacking
Cell Mediated Immunity CELL MEDIATED IMMUNITY. Basic Elements of Cell Mediated Immunity (CMI) Antibody-dependent cell-mediated cytotoxicity (ADCC)
 Chapter 16 CELL MEDIATED IMMUNITY Cell Mediated Immunity Also known as Cellular Immunity or CMI The effector phase T cells Specificity for immune recognition reactions TH provide cytokines CTLs do the
Chapter 16 CELL MEDIATED IMMUNITY Cell Mediated Immunity Also known as Cellular Immunity or CMI The effector phase T cells Specificity for immune recognition reactions TH provide cytokines CTLs do the
Immune response to infection
 Immune response to infection Dr. Sandra Nitsche (Sandra.Nitsche@rub.de ) 20.06.2018 1 Course of acute infection Typical acute infection that is cleared by an adaptive immune reaction 1. invasion of pathogen
Immune response to infection Dr. Sandra Nitsche (Sandra.Nitsche@rub.de ) 20.06.2018 1 Course of acute infection Typical acute infection that is cleared by an adaptive immune reaction 1. invasion of pathogen
ANATOMY OF THE IMMUNE SYSTEM
 Immunity Learning objectives Explain what triggers an immune response and where in the body the immune response occurs. Understand how the immune system handles exogenous and endogenous antigen differently.
Immunity Learning objectives Explain what triggers an immune response and where in the body the immune response occurs. Understand how the immune system handles exogenous and endogenous antigen differently.
Immunology lecture: 14. Cytokines: Main source: Fibroblast, but actually it can be produced by other types of cells
 Immunology lecture: 14 Cytokines: 1)Interferons"IFN" : 2 types Type 1 : IFN-Alpha : Main source: Macrophages IFN-Beta: Main source: Fibroblast, but actually it can be produced by other types of cells **There
Immunology lecture: 14 Cytokines: 1)Interferons"IFN" : 2 types Type 1 : IFN-Alpha : Main source: Macrophages IFN-Beta: Main source: Fibroblast, but actually it can be produced by other types of cells **There
INFLAMMATION & REPAIR
 INFLAMMATION & REPAIR Lecture 7 Chemical Mediators of Inflammation Winter 2013 Chelsea Martin Special thanks to Drs. Hanna and Forzan Course Outline i. Inflammation: Introduction and generalities (lecture
INFLAMMATION & REPAIR Lecture 7 Chemical Mediators of Inflammation Winter 2013 Chelsea Martin Special thanks to Drs. Hanna and Forzan Course Outline i. Inflammation: Introduction and generalities (lecture
Immunological Aspect of Ozone in Rheumatic Diseases
 Immunological Aspect of Ozone in Rheumatic Diseases Prof. Dr. med. Z. Fahmy Chief Consulting Rheumatologist Augusta Clinic for Rheumatic Diseases And Rehabilitation Bad Kreuznach Germany Rheumatoid arthritis
Immunological Aspect of Ozone in Rheumatic Diseases Prof. Dr. med. Z. Fahmy Chief Consulting Rheumatologist Augusta Clinic for Rheumatic Diseases And Rehabilitation Bad Kreuznach Germany Rheumatoid arthritis
T-cell activation T cells migrate to secondary lymphoid tissues where they interact with antigen, antigen-presenting cells, and other lymphocytes:
 Interactions between innate immunity & adaptive immunity What happens to T cells after they leave the thymus? Naïve T cells exit the thymus and enter the bloodstream. If they remain in the bloodstream,
Interactions between innate immunity & adaptive immunity What happens to T cells after they leave the thymus? Naïve T cells exit the thymus and enter the bloodstream. If they remain in the bloodstream,
T-cell activation T cells migrate to secondary lymphoid tissues where they interact with antigen, antigen-presenting cells, and other lymphocytes:
 Interactions between innate immunity & adaptive immunity What happens to T cells after they leave the thymus? Naïve T cells exit the thymus and enter the bloodstream. If they remain in the bloodstream,
Interactions between innate immunity & adaptive immunity What happens to T cells after they leave the thymus? Naïve T cells exit the thymus and enter the bloodstream. If they remain in the bloodstream,
Effector T Cells and
 1 Effector T Cells and Cytokines Andrew Lichtman, MD PhD Brigham and Women's Hospital Harvard Medical School 2 Lecture outline Cytokines Subsets of CD4+ T cells: definitions, functions, development New
1 Effector T Cells and Cytokines Andrew Lichtman, MD PhD Brigham and Women's Hospital Harvard Medical School 2 Lecture outline Cytokines Subsets of CD4+ T cells: definitions, functions, development New
Medical Virology Immunology. Dr. Sameer Naji, MB, BCh, PhD (UK) Head of Basic Medical Sciences Dept. Faculty of Medicine The Hashemite University
 Medical Virology Immunology Dr. Sameer Naji, MB, BCh, PhD (UK) Head of Basic Medical Sciences Dept. Faculty of Medicine The Hashemite University Human blood cells Phases of immune responses Microbe Naïve
Medical Virology Immunology Dr. Sameer Naji, MB, BCh, PhD (UK) Head of Basic Medical Sciences Dept. Faculty of Medicine The Hashemite University Human blood cells Phases of immune responses Microbe Naïve
Lymphoid System: cells of the immune system. Answer Sheet
 Lymphoid System: cells of the immune system Answer Sheet Q1 Which areas of the lymph node have most CD3 staining? A1 Most CD3 staining is present in the paracortex (T cell areas). This is towards the outside
Lymphoid System: cells of the immune system Answer Sheet Q1 Which areas of the lymph node have most CD3 staining? A1 Most CD3 staining is present in the paracortex (T cell areas). This is towards the outside
Lymphoid architecture & Leukocyte recirculation. Thursday Jan 26th, 2017
 Lymphoid architecture & Leukocyte recirculation Thursday Jan 26th, 2017 Topics The life of immune cells Where are they born? Where are they educated? Where do they function? How do they get there? The
Lymphoid architecture & Leukocyte recirculation Thursday Jan 26th, 2017 Topics The life of immune cells Where are they born? Where are they educated? Where do they function? How do they get there? The
Neuronal guidance protein semaphorin 7A influences neutrophil arrest and aggravates inflammatory lung injury. Dr. Tiago Granja
 Neuronal guidance protein semaphorin 7A influences neutrophil arrest and aggravates inflammatory lung injury Dr. Tiago Granja Neuronal guidance proteins (NGPs) force cells to move NPGs give axons and dendrites
Neuronal guidance protein semaphorin 7A influences neutrophil arrest and aggravates inflammatory lung injury Dr. Tiago Granja Neuronal guidance proteins (NGPs) force cells to move NPGs give axons and dendrites
1) Mononuclear phagocytes : 2) Regarding acute inflammation : 3) The epithelioid cells of follicular granulomas are :
 Pathology Second 1) Mononuclear phagocytes : - Are the predominant cells in three day old wounds - Are common in liver, spleen and pancreasd - Produce fibroblast growth factor - Secrete interferon-g -
Pathology Second 1) Mononuclear phagocytes : - Are the predominant cells in three day old wounds - Are common in liver, spleen and pancreasd - Produce fibroblast growth factor - Secrete interferon-g -
M.Sc. III Semester Biotechnology End Semester Examination, 2013 Model Answer LBTM: 302 Advanced Immunology
 Code : AS-2246 M.Sc. III Semester Biotechnology End Semester Examination, 2013 Model Answer LBTM: 302 Advanced Immunology A. Select one correct option for each of the following questions:- 2X10=10 1. (b)
Code : AS-2246 M.Sc. III Semester Biotechnology End Semester Examination, 2013 Model Answer LBTM: 302 Advanced Immunology A. Select one correct option for each of the following questions:- 2X10=10 1. (b)
The Adaptive Immune Responses
 The Adaptive Immune Responses The two arms of the immune responses are; 1) the cell mediated, and 2) the humoral responses. In this chapter we will discuss the two responses in detail and we will start
The Adaptive Immune Responses The two arms of the immune responses are; 1) the cell mediated, and 2) the humoral responses. In this chapter we will discuss the two responses in detail and we will start
Title: NATURAL KILLER CELL FUNCTIONS AND SURFACE RECEPTORS
 LECTURE: 14 Title: NATURAL KILLER CELL FUNCTIONS AND SURFACE RECEPTORS LEARNING OBJECTIVES: The student should be able to: Describe the general morphology of the NK-cells. Enumerate the different functions
LECTURE: 14 Title: NATURAL KILLER CELL FUNCTIONS AND SURFACE RECEPTORS LEARNING OBJECTIVES: The student should be able to: Describe the general morphology of the NK-cells. Enumerate the different functions
Antigen Presentation and T Lymphocyte Activation. Abul K. Abbas UCSF. FOCiS
 1 Antigen Presentation and T Lymphocyte Activation Abul K. Abbas UCSF FOCiS 2 Lecture outline Dendritic cells and antigen presentation The role of the MHC T cell activation Costimulation, the B7:CD28 family
1 Antigen Presentation and T Lymphocyte Activation Abul K. Abbas UCSF FOCiS 2 Lecture outline Dendritic cells and antigen presentation The role of the MHC T cell activation Costimulation, the B7:CD28 family
T Lymphocyte Activation and Costimulation. FOCiS. Lecture outline
 1 T Lymphocyte Activation and Costimulation Abul K. Abbas, MD UCSF FOCiS 2 Lecture outline T cell activation Costimulation, the B7:CD28 family Inhibitory receptors of T cells Targeting costimulators for
1 T Lymphocyte Activation and Costimulation Abul K. Abbas, MD UCSF FOCiS 2 Lecture outline T cell activation Costimulation, the B7:CD28 family Inhibitory receptors of T cells Targeting costimulators for
TCR, MHC and coreceptors
 Cooperation In Immune Responses Antigen processing how peptides get into MHC Antigen processing involves the intracellular proteolytic generation of MHC binding proteins Protein antigens may be processed
Cooperation In Immune Responses Antigen processing how peptides get into MHC Antigen processing involves the intracellular proteolytic generation of MHC binding proteins Protein antigens may be processed
Immune response. This overview figure summarizes simply how our body responds to foreign molecules that enter to it.
 Immune response This overview figure summarizes simply how our body responds to foreign molecules that enter to it. It s highly recommended to watch Dr Najeeb s lecture that s titled T Helper cells and
Immune response This overview figure summarizes simply how our body responds to foreign molecules that enter to it. It s highly recommended to watch Dr Najeeb s lecture that s titled T Helper cells and
Innate Immunity II. Integration. Lindsay Nicholson Advanced Immunology L2
 Innate Immunity II Integration Lindsay Nicholson Advanced Immunology L2 l.nicholson@bristol.ac.uk Lecture 1 Defining Innate Immunity Recognition and effector mechanisms (I) Lecture 2 Recognition and effector
Innate Immunity II Integration Lindsay Nicholson Advanced Immunology L2 l.nicholson@bristol.ac.uk Lecture 1 Defining Innate Immunity Recognition and effector mechanisms (I) Lecture 2 Recognition and effector
Inflammation I. Dr. Nabila Hamdi MD, PhD
 Inflammation I Dr. Nabila Hamdi MD, PhD http://library.med.utah.edu/webpath/exam/m ULTGEN/examidx.htm 2 ILOs Distinguish between acute and chronic inflammation with respect to causes, nature of the inflammatory
Inflammation I Dr. Nabila Hamdi MD, PhD http://library.med.utah.edu/webpath/exam/m ULTGEN/examidx.htm 2 ILOs Distinguish between acute and chronic inflammation with respect to causes, nature of the inflammatory
Basic immunology. Lecture 9. Innate immunity: inflammation, leukocyte migration. Péter Engelmann
 Basic immunology Lecture 9. Innate immunity: inflammation, leukocyte migration Péter Engelmann Different levels of the immune response Recognition molecules of innate immunity Initiation of local and systemic
Basic immunology Lecture 9. Innate immunity: inflammation, leukocyte migration Péter Engelmann Different levels of the immune response Recognition molecules of innate immunity Initiation of local and systemic
Time course of immune response
 Time course of immune response Route of entry Route of entry (cont.) Steps in infection Barriers to infection Mf receptors Facilitate engulfment Glucan, mannose Scavenger CD11b/CD18 Allows immediate response
Time course of immune response Route of entry Route of entry (cont.) Steps in infection Barriers to infection Mf receptors Facilitate engulfment Glucan, mannose Scavenger CD11b/CD18 Allows immediate response
T Cell Effector Mechanisms I: B cell Help & DTH
 T Cell Effector Mechanisms I: B cell Help & DTH Ned Braunstein, MD The Major T Cell Subsets p56 lck + T cells γ δ ε ζ ζ p56 lck CD8+ T cells γ δ ε ζ ζ Cα Cβ Vα Vβ CD3 CD8 Cα Cβ Vα Vβ CD3 MHC II peptide
T Cell Effector Mechanisms I: B cell Help & DTH Ned Braunstein, MD The Major T Cell Subsets p56 lck + T cells γ δ ε ζ ζ p56 lck CD8+ T cells γ δ ε ζ ζ Cα Cβ Vα Vβ CD3 CD8 Cα Cβ Vα Vβ CD3 MHC II peptide
CYTOKINES. Based on: Cellular and Molecular Immunology, 4 th ed.,abbas A.K., Lichtman A.H. and Pober J.S. Sounders company; Philadelphia, 2010.
 CYTOKINES Based on: Cellular and Molecular Immunology, 4 th ed.,abbas A.K., Lichtman A.H. and Pober J.S. Sounders company; Philadelphia, 2010. 1 What are cytokines? Glycoproteins (15 25 kda): Interleukins
CYTOKINES Based on: Cellular and Molecular Immunology, 4 th ed.,abbas A.K., Lichtman A.H. and Pober J.S. Sounders company; Philadelphia, 2010. 1 What are cytokines? Glycoproteins (15 25 kda): Interleukins
Overview of the Lymphoid System
 Overview of the Lymphoid System The Lymphoid System Protects us against disease Lymphoid system cells respond to Environmental pathogens Toxins Abnormal body cells, such as cancers Overview of the Lymphoid
Overview of the Lymphoid System The Lymphoid System Protects us against disease Lymphoid system cells respond to Environmental pathogens Toxins Abnormal body cells, such as cancers Overview of the Lymphoid
10. Which of the following immune cell is unable to phagocytose (a) neutrophils (b) eosinophils (c) macrophages (d) T-cells (e) monocytes
 Chapter 2. Acute and chronic inflammation(6): 1. In acute inflammation, which events occur in the correct chronological order? (Remembered from 2000, 2004 exam.) p50 (a) transient vasoconstriction, stasis
Chapter 2. Acute and chronic inflammation(6): 1. In acute inflammation, which events occur in the correct chronological order? (Remembered from 2000, 2004 exam.) p50 (a) transient vasoconstriction, stasis
Question 1. Kupffer cells, microglial cells and osteoclasts are all examples of what type of immune system cell?
 Abbas Chapter 2: Sarah Spriet February 8, 2015 Question 1. Kupffer cells, microglial cells and osteoclasts are all examples of what type of immune system cell? a. Dendritic cells b. Macrophages c. Monocytes
Abbas Chapter 2: Sarah Spriet February 8, 2015 Question 1. Kupffer cells, microglial cells and osteoclasts are all examples of what type of immune system cell? a. Dendritic cells b. Macrophages c. Monocytes
Monocytes must also leave the circulation in response to inflammatory signals, and neutrophils and other granulocytes must be able to do so as well.
 Immunology Dr. John J. Haddad Chapter 15 Leukocyte Migration and inflammation Lymphocytes must recirculate in the body in search of antigens. Since antigens are brought to lymph nodes and the spleen, the
Immunology Dr. John J. Haddad Chapter 15 Leukocyte Migration and inflammation Lymphocytes must recirculate in the body in search of antigens. Since antigens are brought to lymph nodes and the spleen, the
Autoimmune Diseases. Betsy Kirchner CNP The Cleveland Clinic
 Autoimmune Diseases Betsy Kirchner CNP The Cleveland Clinic Disclosures (financial) No relevant disclosures Learning Objectives Explain the pathophysiology of autoimmune disease Discuss safe administration
Autoimmune Diseases Betsy Kirchner CNP The Cleveland Clinic Disclosures (financial) No relevant disclosures Learning Objectives Explain the pathophysiology of autoimmune disease Discuss safe administration
Immunology. T-Lymphocytes. 16. Oktober 2014, Ruhr-Universität Bochum Karin Peters,
 Immunology T-Lymphocytes 16. Oktober 2014, Ruhr-Universität Bochum Karin Peters, karin.peters@rub.de The role of T-effector cells in the immune response against microbes cellular immunity humoral immunity
Immunology T-Lymphocytes 16. Oktober 2014, Ruhr-Universität Bochum Karin Peters, karin.peters@rub.de The role of T-effector cells in the immune response against microbes cellular immunity humoral immunity
HYPERSENSITIVITY REACTIONS D R S H O AI B R AZ A
 HYPERSENSITIVITY REACTIONS D R S H O AI B R AZ A HYPERSENSITIVITY REACTIONS Are exaggerated immune response upon antigenic stimulation Individuals who have been previously exposed to an antigen are said
HYPERSENSITIVITY REACTIONS D R S H O AI B R AZ A HYPERSENSITIVITY REACTIONS Are exaggerated immune response upon antigenic stimulation Individuals who have been previously exposed to an antigen are said
Cellular Immune response. Jianzhong Chen, Ph.D Institute of immunology, ZJU
 Cellular Immune response Jianzhong Chen, Ph.D Institute of immunology, ZJU Concept of adaptive immune response T cell-mediated adaptive immune response I. Concept of immune response A collective and coordinated
Cellular Immune response Jianzhong Chen, Ph.D Institute of immunology, ZJU Concept of adaptive immune response T cell-mediated adaptive immune response I. Concept of immune response A collective and coordinated
Advances in Cancer Immunotherapy
 Advances in Cancer Immunotherapy Immunology 101 for the Non-Immunologist Arnold H. Zea, PhD azea@lsuhsc.edu Disclosures No relevant financial relationships to disclose This presentation does not contain
Advances in Cancer Immunotherapy Immunology 101 for the Non-Immunologist Arnold H. Zea, PhD azea@lsuhsc.edu Disclosures No relevant financial relationships to disclose This presentation does not contain
Adaptive immune responses: T cell-mediated immunity
 MICR2209 Adaptive immune responses: T cell-mediated immunity Dr Allison Imrie allison.imrie@uwa.edu.au 1 Synopsis: In this lecture we will discuss the T-cell mediated immune response, how it is activated,
MICR2209 Adaptive immune responses: T cell-mediated immunity Dr Allison Imrie allison.imrie@uwa.edu.au 1 Synopsis: In this lecture we will discuss the T-cell mediated immune response, how it is activated,
Innate vs Adaptive Response
 General Immunology Innate vs Adaptive Response Innate- non-specific (4 types of barriers) anatomic- ato mechanical ca (skin), ph, mucous, normal flora Physiologic- temperature, ph, chemicals (lysozyme,
General Immunology Innate vs Adaptive Response Innate- non-specific (4 types of barriers) anatomic- ato mechanical ca (skin), ph, mucous, normal flora Physiologic- temperature, ph, chemicals (lysozyme,
Independent Study Guide The Innate Immune Response (Chapter 15)
 Independent Study Guide The Innate Immune Response (Chapter 15) I. General types of immunity (Chapter 15 introduction) a. Innate i. inborn ii. pattern recognition b. Adaptive i. "learned" through exposure
Independent Study Guide The Innate Immune Response (Chapter 15) I. General types of immunity (Chapter 15 introduction) a. Innate i. inborn ii. pattern recognition b. Adaptive i. "learned" through exposure
Adaptive Immunity. Jeffrey K. Actor, Ph.D. MSB 2.214,
 Adaptive Immunity Jeffrey K. Actor, Ph.D. MSB 2.214, 500-5344 Lecture Objectives: Understand role of various molecules including cytokines, chemokines, costimulatory and adhesion molecules in the development
Adaptive Immunity Jeffrey K. Actor, Ph.D. MSB 2.214, 500-5344 Lecture Objectives: Understand role of various molecules including cytokines, chemokines, costimulatory and adhesion molecules in the development
1. The scavenger receptor, CD36, functions as a coreceptor for which TLR? a. TLR ½ b. TLR 3 c. TLR 4 d. TLR 2/6
 Allergy and Immunology Review Corner: Cellular and Molecular Immunology, 8th Edition By Abul K. Abbas, MBBS, Andrew H. H. Lichtman, MD, PhD and Shiv Pillai, MBBS, PhD. Chapter 4 (pages 62-74): Innate Immunity
Allergy and Immunology Review Corner: Cellular and Molecular Immunology, 8th Edition By Abul K. Abbas, MBBS, Andrew H. H. Lichtman, MD, PhD and Shiv Pillai, MBBS, PhD. Chapter 4 (pages 62-74): Innate Immunity
Requirements in the Development of an Autoimmune Disease Amino Acids in the Shared Epitope
 + T cell MHC/self-peptide MHC/Vβ Induction of + T H 1 mediated autoimmunity: A paradigm for the pathogenesis of rheumatoid arthritis, multiple sclerosis and type I diabetes APC Activated autoreactive +
+ T cell MHC/self-peptide MHC/Vβ Induction of + T H 1 mediated autoimmunity: A paradigm for the pathogenesis of rheumatoid arthritis, multiple sclerosis and type I diabetes APC Activated autoreactive +
Chapter 13: Cytokines
 Chapter 13: Cytokines Definition: secreted, low-molecular-weight proteins that regulate the nature, intensity and duration of the immune response by exerting a variety of effects on lymphocytes and/or
Chapter 13: Cytokines Definition: secreted, low-molecular-weight proteins that regulate the nature, intensity and duration of the immune response by exerting a variety of effects on lymphocytes and/or
Cutaneous Immunology: Innate Immune Responses. Skin Biology Lecture Series
 Cutaneous Immunology: Innate Immune Responses Skin Biology Lecture Series The Immune Response: Innate and Adaptive Components Source: Wolff, Goldsmith, Katz, Gilchrest, Paller, Leffell. Fitzpatrick s Dermatology
Cutaneous Immunology: Innate Immune Responses Skin Biology Lecture Series The Immune Response: Innate and Adaptive Components Source: Wolff, Goldsmith, Katz, Gilchrest, Paller, Leffell. Fitzpatrick s Dermatology
T Cell Activation, Costimulation and Regulation
 1 T Cell Activation, Costimulation and Regulation Abul K. Abbas, MD University of California San Francisco 2 Lecture outline T cell antigen recognition and activation Costimulation, the B7:CD28 family
1 T Cell Activation, Costimulation and Regulation Abul K. Abbas, MD University of California San Francisco 2 Lecture outline T cell antigen recognition and activation Costimulation, the B7:CD28 family
Basic Immunology. Cytokines, cytokine receptors. Lecture 8th. Timea Berki MD, PhD
 Basic Immunology Lecture 8th Cytokines, cytokine receptors Timea Berki MD, PhD 1. By direct cell-cell interactions: through adhesion molecules 2. By low MW regulatory proteins, called cytokines: messengers
Basic Immunology Lecture 8th Cytokines, cytokine receptors Timea Berki MD, PhD 1. By direct cell-cell interactions: through adhesion molecules 2. By low MW regulatory proteins, called cytokines: messengers
Corso di Laurea Specialistica in Biotecnologie Molecolari aa 2006/2007 Presentazione di Immunologia Molecolare INTERFERON GAMMA.
 Corso di Laurea Specialistica in Biotecnologie Molecolari aa 2006/2007 Presentazione di Immunologia Molecolare INTERFERON GAMMA Valentina Grosso The Inteferons 1957: Isaacs and Lindenmann discovered a
Corso di Laurea Specialistica in Biotecnologie Molecolari aa 2006/2007 Presentazione di Immunologia Molecolare INTERFERON GAMMA Valentina Grosso The Inteferons 1957: Isaacs and Lindenmann discovered a
The Adaptive Immune Response. B-cells
 The Adaptive Immune Response B-cells The innate immune system provides immediate protection. The adaptive response takes time to develop and is antigen specific. Activation of B and T lymphocytes Naive
The Adaptive Immune Response B-cells The innate immune system provides immediate protection. The adaptive response takes time to develop and is antigen specific. Activation of B and T lymphocytes Naive
MOLECULAR IMMUNOLOGY Manipulation of immune response Autoimmune diseases & the pathogenic mechanism
 MOLECULAR IMMUNOLOGY Manipulation of immune response Autoimmune diseases & the pathogenic mechanism SCHMAIEL SHIRDEL CONTENT 2 Introduction Autoimmune diseases Classification Involved components Autoimmune
MOLECULAR IMMUNOLOGY Manipulation of immune response Autoimmune diseases & the pathogenic mechanism SCHMAIEL SHIRDEL CONTENT 2 Introduction Autoimmune diseases Classification Involved components Autoimmune
Allergic rhinitis (Hay fever) Asthma Anaphylaxis Urticaria Atopic dermatitis
 Hypersensitivity Disorders Hypersensitivity Disorders Immune Response IgE Disease Example Ragweed hay fever IgG Cytotoxic Immune complex T Cell Hemolytic anemia Serum sickness Poison ivy IgE-mediated Diseases
Hypersensitivity Disorders Hypersensitivity Disorders Immune Response IgE Disease Example Ragweed hay fever IgG Cytotoxic Immune complex T Cell Hemolytic anemia Serum sickness Poison ivy IgE-mediated Diseases
Cell-Derived Inflammatory Mediators
 Cell-Derived Inflammatory Mediators Introduction about chemical mediators in inflammation Mediators may be Cellular mediators cell-produced or cell-secreted derived from circulating inactive precursors,
Cell-Derived Inflammatory Mediators Introduction about chemical mediators in inflammation Mediators may be Cellular mediators cell-produced or cell-secreted derived from circulating inactive precursors,
Introduction to Immunology Lectures 1-3 by Bellur S. Prabhakar. March 13-14, 2007
 Introduction to Immunology Lectures 1-3 by Bellur S. Prabhakar. March 13-14, 2007 TheComponents Of The Immune System and Innate Immunity: Ref: Immunobiology-5 th edition. Janeway et al. Chapters-1 & 2.
Introduction to Immunology Lectures 1-3 by Bellur S. Prabhakar. March 13-14, 2007 TheComponents Of The Immune System and Innate Immunity: Ref: Immunobiology-5 th edition. Janeway et al. Chapters-1 & 2.
There are 2 major lines of defense: Non-specific (Innate Immunity) and. Specific. (Adaptive Immunity) Photo of macrophage cell
 There are 2 major lines of defense: Non-specific (Innate Immunity) and Specific (Adaptive Immunity) Photo of macrophage cell Development of the Immune System ery pl neu mφ nk CD8 + CTL CD4 + thy TH1 mye
There are 2 major lines of defense: Non-specific (Innate Immunity) and Specific (Adaptive Immunity) Photo of macrophage cell Development of the Immune System ery pl neu mφ nk CD8 + CTL CD4 + thy TH1 mye
Date of preparation: 06/ IBD/
 Mechanisms Mechanisms of of Disease Disease: The The Science of of IBD IBD 64002 Date of preparation: 06/11 2013 IBD/2013-11-01 Table of Contents IBD Background and Disease Management Etiology and Pathophysiology
Mechanisms Mechanisms of of Disease Disease: The The Science of of IBD IBD 64002 Date of preparation: 06/11 2013 IBD/2013-11-01 Table of Contents IBD Background and Disease Management Etiology and Pathophysiology
Physiology of Inflammation and Innate Immunity. สรช ย ศร ส มะ พ.บ., Ph.D. ภาคว ชาสร รว ทยา คณะแพทยศาสตร ศ ร ราชพยาบาล มหาว ทยาล ยมห ดล
 Physiology of Inflammation and Innate Immunity สรช ย ศร ส มะ พ.บ., Ph.D. ภาคว ชาสร รว ทยา คณะแพทยศาสตร ศ ร ราชพยาบาล มหาว ทยาล ยมห ดล Overview Pathogens infectious agents capable of causing pathology,
Physiology of Inflammation and Innate Immunity สรช ย ศร ส มะ พ.บ., Ph.D. ภาคว ชาสร รว ทยา คณะแพทยศาสตร ศ ร ราชพยาบาล มหาว ทยาล ยมห ดล Overview Pathogens infectious agents capable of causing pathology,
The Innate Immune Response
 The Innate Immune Response FUNCTIONS OF THE IMMUNE SYSTEM: Recognize, destroy and clear a diversity of pathogens. Initiate tissue and wound healing processes. Recognize and clear damaged self components.
The Innate Immune Response FUNCTIONS OF THE IMMUNE SYSTEM: Recognize, destroy and clear a diversity of pathogens. Initiate tissue and wound healing processes. Recognize and clear damaged self components.
Structure and Function of Antigen Recognition Molecules
 MICR2209 Structure and Function of Antigen Recognition Molecules Dr Allison Imrie allison.imrie@uwa.edu.au 1 Synopsis: In this lecture we will examine the major receptors used by cells of the innate and
MICR2209 Structure and Function of Antigen Recognition Molecules Dr Allison Imrie allison.imrie@uwa.edu.au 1 Synopsis: In this lecture we will examine the major receptors used by cells of the innate and
Role of Inflammatory and Progenitor Cells in Pulmonary Vascular Remodeling: Potential Role for Targeted Therapies. Traditional Hypothesis Stress
 3/1/212 Role of Inflammatory and Progenitor Cells in Pulmonary Vascular Remodeling: Potential Role for Targeted Therapies K.R. Stenmark University of Colorado Denver, CO 845 Prominent Fibroproliferative
3/1/212 Role of Inflammatory and Progenitor Cells in Pulmonary Vascular Remodeling: Potential Role for Targeted Therapies K.R. Stenmark University of Colorado Denver, CO 845 Prominent Fibroproliferative
Review Questions: Janeway s Immunobiology 8th Edition by Kenneth Murphy
 Review Questions: Janeway s Immunobiology 8th Edition by Kenneth Murphy Chapter 11 (pages 429-460): Dynamics of Adaptive Immunity prepared by Kelly von Elten, Walter Reed National Military Medical Center,
Review Questions: Janeway s Immunobiology 8th Edition by Kenneth Murphy Chapter 11 (pages 429-460): Dynamics of Adaptive Immunity prepared by Kelly von Elten, Walter Reed National Military Medical Center,
Principles of Adaptive Immunity
 Principles of Adaptive Immunity Chapter 3 Parham Hans de Haard 17 th of May 2010 Agenda Recognition molecules of adaptive immune system Features adaptive immune system Immunoglobulins and T-cell receptors
Principles of Adaptive Immunity Chapter 3 Parham Hans de Haard 17 th of May 2010 Agenda Recognition molecules of adaptive immune system Features adaptive immune system Immunoglobulins and T-cell receptors
Part III Innate and Adaptive Immune Cells: General Introduction
 Innate and Adaptive Immune Cells: General Introduction Iván López-Expósito As an organ specialized in food digestion and nutrient absorption, the intestinal mucosa presents a huge surface area (almost
Innate and Adaptive Immune Cells: General Introduction Iván López-Expósito As an organ specialized in food digestion and nutrient absorption, the intestinal mucosa presents a huge surface area (almost
windows of my lab Prof. Allan Wiik, emeritus director Department of Autoimmunology Statens Serum Institute, Copenhagen
 The normal immune system windows of my lab, Prof. Allan Wiik, emeritus director Department of Autoimmunology Statens Serum Institute, Copenhagen The immune defence Theinnateimmune system Cells: Eater cells
The normal immune system windows of my lab, Prof. Allan Wiik, emeritus director Department of Autoimmunology Statens Serum Institute, Copenhagen The immune defence Theinnateimmune system Cells: Eater cells
IMMUNE CELL SURFACE RECEPTORS AND THEIR FUNCTIONS
 LECTURE: 07 Title: IMMUNE CELL SURFACE RECEPTORS AND THEIR FUNCTIONS LEARNING OBJECTIVES: The student should be able to: The chemical nature of the cellular surface receptors. Define the location of the
LECTURE: 07 Title: IMMUNE CELL SURFACE RECEPTORS AND THEIR FUNCTIONS LEARNING OBJECTIVES: The student should be able to: The chemical nature of the cellular surface receptors. Define the location of the
IL-17 in health and disease. March 2014 PSO13-C051n
 IL-17 in health and disease March 2014 PSO13-C051n Originally Researchers Suggested That IL-12 and IL-4 drove Th Cell Differentiation Naïve CD4 + T cell Question: Which of these cell types is responsible
IL-17 in health and disease March 2014 PSO13-C051n Originally Researchers Suggested That IL-12 and IL-4 drove Th Cell Differentiation Naïve CD4 + T cell Question: Which of these cell types is responsible
Chapter 22: The Lymphatic System and Immunity
 Bio40C schedule Lecture Immune system Lab Quiz 2 this week; bring a scantron! Study guide on my website (see lab assignments) Extra credit Critical thinking questions at end of chapters 5 pts/chapter Due
Bio40C schedule Lecture Immune system Lab Quiz 2 this week; bring a scantron! Study guide on my website (see lab assignments) Extra credit Critical thinking questions at end of chapters 5 pts/chapter Due
Hematopoiesis. Hematopoiesis. Hematopoiesis
 Chapter. Cells and Organs of the Immune System Hematopoiesis Hematopoiesis- formation and development of WBC and RBC bone marrow. Hematopoietic stem cell- give rise to any blood cells (constant number,
Chapter. Cells and Organs of the Immune System Hematopoiesis Hematopoiesis- formation and development of WBC and RBC bone marrow. Hematopoietic stem cell- give rise to any blood cells (constant number,
NEUTROPHIL, BASOPHIL, EOSINOPHIL, AND PLATELETS SURFACE RECEPTORS
 LECTURE: 15 Title NEUTROPHIL, BASOPHIL, EOSINOPHIL, AND PLATELETS SURFACE RECEPTORS LEARNING OBJECTIVES: The student should be able to: Determine the relative percentages in blood for the various types
LECTURE: 15 Title NEUTROPHIL, BASOPHIL, EOSINOPHIL, AND PLATELETS SURFACE RECEPTORS LEARNING OBJECTIVES: The student should be able to: Determine the relative percentages in blood for the various types
Follicular Lymphoma. ced3 APOPTOSIS. *In the nematode Caenorhabditis elegans 131 of the organism's 1031 cells die during development.
 Harvard-MIT Division of Health Sciences and Technology HST.176: Cellular and Molecular Immunology Course Director: Dr. Shiv Pillai Follicular Lymphoma 1. Characterized by t(14:18) translocation 2. Ig heavy
Harvard-MIT Division of Health Sciences and Technology HST.176: Cellular and Molecular Immunology Course Director: Dr. Shiv Pillai Follicular Lymphoma 1. Characterized by t(14:18) translocation 2. Ig heavy
DEPARTMENT OF PHYSIOLOGY
 UNIVERSITY OF MEDICAL SCIENCES, ONDO DEPARTMENT OF PHYSIOLOGY BLOOD AND BODY FLUID PHYSIOLOGY LECTURER: MR A.O. AKINOLA OBJECTIVES Leukopoiesis Thrombopoiesis Leukopoiesis and Lymphopoiesis White blood
UNIVERSITY OF MEDICAL SCIENCES, ONDO DEPARTMENT OF PHYSIOLOGY BLOOD AND BODY FLUID PHYSIOLOGY LECTURER: MR A.O. AKINOLA OBJECTIVES Leukopoiesis Thrombopoiesis Leukopoiesis and Lymphopoiesis White blood
Darwinian selection and Newtonian physics wrapped up in systems biology
 Darwinian selection and Newtonian physics wrapped up in systems biology Concept published in 1957* by Macfarland Burnet (1960 Nobel Laureate for the theory of induced immune tolerance, leading to solid
Darwinian selection and Newtonian physics wrapped up in systems biology Concept published in 1957* by Macfarland Burnet (1960 Nobel Laureate for the theory of induced immune tolerance, leading to solid
MCB 4211 Basic Immunology 2nd Exam; 10/26/17 Peoplesoft #:
 For this first section, circle the letter that precedes the best answer for each of the following multiple-choice questions. LOOK AT ALL ALTERNATIVES BEFORE CHOOSING YOUR ANSWER. 1. The TcR (T cell receptor)
For this first section, circle the letter that precedes the best answer for each of the following multiple-choice questions. LOOK AT ALL ALTERNATIVES BEFORE CHOOSING YOUR ANSWER. 1. The TcR (T cell receptor)
Fc receptors, phagocytosis role 128
 Subject Index Adaptive immunity dependence on innate immunity 9, 10 evolution 10 Aging anti-inflammatory agents in counteraction 202 beneficial polymorphisms 199 201 definition 18, 189 innate immunity
Subject Index Adaptive immunity dependence on innate immunity 9, 10 evolution 10 Aging anti-inflammatory agents in counteraction 202 beneficial polymorphisms 199 201 definition 18, 189 innate immunity
Chapter 24 The Immune System
 Chapter 24 The Immune System The Immune System Layered defense system The skin and chemical barriers The innate and adaptive immune systems Immunity The body s ability to recognize and destroy specific
Chapter 24 The Immune System The Immune System Layered defense system The skin and chemical barriers The innate and adaptive immune systems Immunity The body s ability to recognize and destroy specific
Topics. Humoral Immune Response Part II Accessory cells Fc Receptors Opsonization and killing mechanisms of phagocytes NK, mast, eosynophils
 Topics Humoral Immune Response Part II Accessory cells Fc Receptors Opsonization and killing mechanisms of phagocytes NK, mast, eosynophils Immune regulation Idiotypic network 2/15/2005 MICR 415 / 515
Topics Humoral Immune Response Part II Accessory cells Fc Receptors Opsonization and killing mechanisms of phagocytes NK, mast, eosynophils Immune regulation Idiotypic network 2/15/2005 MICR 415 / 515
Immunology Basics Relevant to Cancer Immunotherapy: T Cell Activation, Costimulation, and Effector T Cells
 Immunology Basics Relevant to Cancer Immunotherapy: T Cell Activation, Costimulation, and Effector T Cells Andrew H. Lichtman, M.D. Ph.D. Department of Pathology Brigham and Women s Hospital and Harvard
Immunology Basics Relevant to Cancer Immunotherapy: T Cell Activation, Costimulation, and Effector T Cells Andrew H. Lichtman, M.D. Ph.D. Department of Pathology Brigham and Women s Hospital and Harvard
Innate immune cells---- one time migration preprogrammed homing properties
 Innate immune cells---- one time migration preprogrammed homing properties neutrophils---acute inflammation monocytes---subacute/chronic inflammation eosinophils---parasitic or allergic inflammation natural
Innate immune cells---- one time migration preprogrammed homing properties neutrophils---acute inflammation monocytes---subacute/chronic inflammation eosinophils---parasitic or allergic inflammation natural
A. Incorrect! It s not correct. Synergism of cytokines refers to two or more cytokines acting together.
 Immunology - Problem Drill 11: Cytokine and Cytokine Receptors Question No. 1 of 10 1. A single cytokine can act on several different cell types, which is known as. Question #1 (A) Synergism (B) Pleiotropism
Immunology - Problem Drill 11: Cytokine and Cytokine Receptors Question No. 1 of 10 1. A single cytokine can act on several different cell types, which is known as. Question #1 (A) Synergism (B) Pleiotropism
Introduction to Immune System
 Introduction to Immune System Learning outcome You will be able to understand, at a fundamental level, the STRUCTURES and FUNCTIONS of cell surface and soluble molecules involved in recognition of foreign
Introduction to Immune System Learning outcome You will be able to understand, at a fundamental level, the STRUCTURES and FUNCTIONS of cell surface and soluble molecules involved in recognition of foreign
