Neurodegeneration with brain iron accumulation : clinical, radiographic and genetic heterogeneity and corresponding therapeutic options
|
|
|
- Dorothy Osborne
- 5 years ago
- Views:
Transcription
1 Acta neurol. belg., 2007, 107, Neurodegeneration with brain iron accumulation : clinical, radiographic and genetic heterogeneity and corresponding therapeutic options Frederik CLEMENT 1,3, David DEVOS 1, Caroline MOREAU 1, Philippe COUBES 2, Alain DESTEE 1 and Luc DEFEBVRE 1 1 Department of Neurology, Hôpital Roger Salengro, Lille, France ; 2 Department of Neurosurgery, Centre Gui de Chaulwiac, Montpellier, France ; 3 Department of Neuroradiology, H. Hart Ziekenhuis Roeselare-Menen, Belgium. Abstract Background : Neurodegeneration with brain iron accumulation (NBIA), formerly known as Hallervorden- Spatz syndrome, is a heterogeneous group of disorders with different treatment options. Case reports : In the first case, progressively generalizing dystonic symptoms appeared during childhood. A mutation in the gene encoding pantothenate kinase 2 (PANK2) was found. Brain MRI showed bilateral hypersignals within the globus pallidi on T2-weighted images. The patient was successfully treated by pallidal deep brain stimulation (DBS). In the second case an adult onset with parkinsonism was observed, for which no PANK2 mutation was found. T2-weighted brain MR images revealed multiple significant hyposignals (suggestive of iron deposits) localised in the cerebellar dentate nuclei and in the globi pallidi, the red nuclei and the substantia nigra. An antiparkinsonian treatment was proposed. Conclusion : The clinical, radiographic and genetic heterogeneity of NBIA has to be underlined. Key words : Neurodegeneration ; iron ; dystonia ; pantothenate kinase ; deep brain stimulation. Introduction Neurodegeneration with brain iron accumulation (NBIA) triggers cerebral neurodegeneration via iron deposition in the basal ganglia. It is a group of disorders with different onset times and heterogeneous clinical presentations (Carod-Artal et al., 2004). Patients with NBIA have a combination of motor symptoms - notably dystonia, parkinsonism, choreoathetosis, corticospinal tract involvement, optic atrophy, pigmentary retinopathy and cognitive impairment. Following the recent identification of mutations in the PANK2 gene on chromosome 20p12.3-p13 in some patients with the NBIA phenotype, the term pantothenate kinase-associated neurodegeneration has been proposed (Thomas et al., 2004). We compare the clinical, radiographic and genetic features of two patients and discuss different therapeutic approaches. In the first patient, the symptoms appeared during childhood period, whereas adult onset was observed in the second patient. Case reports PATIENT 1 A 14-year-old, right-handed boy consulted for the first time in our department because of dystonic right arm movements experienced over the previous three years. The condition had deteriorated progressively and had finally resulted in a significant functional deficit, making writing impossible. The patient s medical history included flat feet and distortion of the left ankle at the age of 18 months. Pregnancy, delivery and the subject s psychomotor development during the first decade had been completely normal. The patient s father had died at the age of 40 due to the complications of diabetes mellitus but the patient s mother and his two older sisters had never suffered from any major medical problems. There was no family history of neurological disorder. At the first clinical examination in 1997, we observed intermittent, dystonic movements with internal rotation of the right arm and wrist hyperextension, which worsened during writing. Indeed, writing was only possible when the arm was stretched out. Moderate hypokinesia was present : the patient had difficulty in performing fine movements with the fingers of either hand. Both knee tendon reflexes were brisk. Moderate dysarthria with dystonic characteristics was noticed. All the other neurological findings were normal. Neuropsychological investigations revealed modest intellectual capacities with an IQ score of 91 on the revised Wechsler Intelligence Scale for Children. Brain MRI showed bilateral hypersignals within the globi pallidi on T2-weighted images but no atrophy, no vascular lesions and no calcifications (Fig. 1). The differential diagnosis of this clinical presentation includes both the spectrum of inborn errors of metabolism and that of neurodegenerative
2 NEURODEGENERATION WITH BRAIN IRON ACCUMULATION 27 FIG. 1. Hypersignals bilaterally within the globi pallidi on T2-images. disorders with potential early onset. In both groups, various possibilities were ruled out on clinical, biochemical, genetic and radiographic grounds. In the absence of any evidence for other neurodegenerative or metabolic diseases we concluded that Hallervorden-Spatz disease was the most probable hypothesis. Then, in 2003, we found a mutation in the patient s PANK2 gene, thus definitively confirming the diagnosis of Hallervorden-Spatz disease or pantothenate kinase-associated neurodegeneration. The neurological symptoms remained stable for more than six months after the first consultation. During this period, patient was treated with a dopamine agonist (bromocriptine, 30 mg/day) and low doses of levodopa (300 mg/day). However, after one year, he presented oromandibular dystonia and spastic dysphonia of fluctuating intensity. Dystonic arm movements were also variable and now appeared to be more prominent in the left hand - exactly the opposite of the initial observations. An anticholinergic agent (trihexyfenidylhydrochloride, 15 mg/day) was combined with the ongoing drug treatment. Two years later, axial dystonia with scoliotic deformation was noticed. Oromandibular dystonia persisted, causing mastication difficulties. Gait problems were relatively mild, with discrete pes equinovarus on the right side. Oromandibular and left arm dystonia were treated with botulinum toxin injections. These injections temporarily improved mastication and swallowing but the effect on dysphonia was much less pronounced. Five years after the first visit, further worsening was marked by significant aggravation of right arm dystonia. Axial dystonia also increased (especially at the neck level), leading to an extended posture of the neck. MRI monitoring over this five-year period did not reveal any ongoing modifications. Nine years after the first neuropsychological evaluation, an IQ score of 82 was obtained on the revised Wechsler Adult Intelligence Survey scale. Anticholinergic treatment was increased (trihexyfenidylhydrochloride up to 60 mg/day) and dopamine agonist treatment (bromocriptine) was first decreased and then finally stopped. Due to the rise in dystonic symptoms despite conservative treatment, the patient underwent a neurosurgical operation for bilateral stimulation of the globus pallidum internum (Gpi). The operation was performed under standard, general anaesthesia. A pair of electrodes (each comprising four contacts numbered conventionally from 0 (distal) to 3 (proximal)) was implanted bilaterally. The surgical procedure was problem-free. Five months after the operation, a progressive improvement in the axial dystonia was noticed, leading to a more stable gait. Dystonic symptoms in the limbs decreased only slightly at first but a marked improvement of the right arm was noticed twelve months after the operation. The patient was then able to write again. Dystonia of the face was also less pronounced, although mastication difficulties and dysphonia remained. Eighteen months after the operation, evaluation of the dystonic syndrome revealed a Burke-Fahn-Marsden (BFM) score of 19/120 and a functional score of 8/30, compared to a BFM score of 55/120 and a functional score of 11/30 before the operation. Levodopa treatment was reduced. In June 2004, the stimulation frequency (130 Hertz), pulse width (450 ms) and amplitude (1,5 Volt) were equalized on both the right and left side. Levodopa treatment was stopped and the anticholinergic treatment was reduced. The social outcome also happened to be favourable : the patient obtained his driver s license and qualified as an accountant. In June 2005 we noticed no further aggravation of the symptoms and reduction of anticholinergic treatment was continued. The patient was professionally active in the financial department of the local authorities. PATIENT 2 A 47-year-old, professionally active woman (working as a secretary) consulted in our department because of involuntary buccolingual and facial movements. The patient s medical history included asthma, herniated disc, migraine and transitory tics (eye blinking) during childhood. She had never taken neuroleptic drugs. One of her two
3 28 F. CLEMENT FIG. 2. Hyposignals, evocative for iron deposits, localised in the dentate nuclei of the cerebellum on T2-images. FIG. 3. Hyposignals, evocative for iron deposits, localised in the globi pallidi on T2-images. sisters experienced involuntary movements of the cheek (starting at the age of 40) and she had also suffered from severe depression. The patient s father presented behavioural problems and motor agitation. The patient s paternal grandmother may have presented an episode of Sydenham s chorea but died due to phlebitis. The patient s history of movement disorders had started more than ten years before the first consultation, with the appearance of a left arm action tremor with mainly postural characteristics, relatively stable since then. In the six months before consultation, the patient had started experiencing difficulty in swallowing. Later on, dysarthria and mastication problems were noticed. This was linked to the presence of involuntary buccolingual, pharyngeal and facial movements. At the first clinical examination in December 2002, a gait pattern with extrapyramidal characteristics (marked by a discrete anteflexion of the trunk) was noted. Akinesia and rigidity predominated on the right side. Facial expression was less varied and hyperkinetic dysarthria was present. Dystonic buccolingual, pharyngeal and facial movements were noted : these appeared spontaneously but were also provoked by voluntary movement. Deep tendon reflexes were brisk, and both Hoffmann and Babinski signs were present. Finally, there was an action and postural tremor of both arms, with discrete dysmetria. All other neurological findings were normal. A cognitive evaluation appeared to be completely normal, since the following scores were obtained : a Mini Mental State Examination score of 29/30, a Mattis score of 144/144, a BREF score (frontal battery of psychological tests) of 17/18 and an IQ score of 87. The extrapyramidal syndrome appeared to be levodoparesponsive : following administration of 200 mg of levodopa, the motor UPDRS score decreased by 86%, passing from 17 to 4. Levodopa treatment (400 mg/day) was initiated and indeed induced a significant improvement not only in the dysarthria but also terms of the akinesia, rigidity and dystonia. No mutations in the DYT gene were found and there was no genetic evidence of Huntington s disease. T2-weighted brain MRI images showed significant hyposignals (suggestive of iron deposits) localised not only in the cerebellar dentate nuclei (Fig. 2) but also in the globi pallidi (Fig. 3), the red nuclei and the substantia nigra (Fig. 4). We ruled out neuroferritinopathy and aceruloplasminemia, both adult-onset, genetic, extrapyramidal disorders associated with increased iron accumulation in the brain. Finally, the possibility of neurodegeneration with brain iron accumulation was considered, even though no mutations in the PANK2 gene had been found. Further progression of the condition was marked by the appearance of dystonic right arm movements, especially when writing. An anticholinergic drug (trihexyfenidylhydrochloride) was
4 NEURODEGENERATION WITH BRAIN IRON ACCUMULATION 29 FIG. 4. Hyposignals, evocative for iron deposits, localised in the substantia nigra and red nuclei on T2-images. initially combined with the ongoing drug treatment but was replaced by baclofen (15 mg/day) after the occurrence of side-effects. Levodopa treatment was progressively increased up to 800 mg/day. At a recent consultation (June 2005), dystonic and parkinsonian symptoms happened to be stabilized and thus treatment was not modified. Discussion Neurodegeneration with brain iron accumulation (NBIA, formerly known as Hallervorden-Spatz syndrome) is a heterogeneous group of disorders. A distinction must made between patients who bear mutations in the gene encoding pantothenate kinase 2 (PANK2) and those who do not. For disorders associated with PANK2 mutations, the term pantothenate kinase-associated neurodegeneration is now routinely used (Hayflick, 2003). Hallervorden-Spatz disease with early onset and rapid progression is the originally reported, classic form, as described in 1922 in a family of 12 siblings, with 5 individuals affected at the age between 7 and 9 years. This appears to be an autosomal, recessive neurodegenerative disorder, associated with iron accumulation in the globus pallidus, substantia nigra pars reticulata, with demyelination of the globus pallidus and widespread focal, axonal swellings in the pallidonigral system and the cerebral cortex (Hallervorden and Spatz, 1922). Although childhood-onset cases are the most common type of NBIA, adolescent- and adult-onset presentations have also been reported. Clinical symptoms vary greatly amongst patients and may notably include extrapyramidal signs (dystonia, bradykinesia, rigidity, tremor, choreoathetosis, dysarthria) as well as ataxia, seizures, dementia, visual impairment due to retinitis pigmentosa or indeed pyramidal signs like spasticity and hyperreflexia (Wigboldus and Bruyn 1968). In patients with the classic form of NBIA (age of onset ranging from 0.5 to 12 years), dystonia is almost always an early manifestation. Early dystonia often involves the cranial and limb musculature, whereas axial dystonia predominates in later symptoms as seen in our first patient. Other prominent features include dysarthria (also noticed here), rigidity and choreoathetosis. Cognitive decline (29%) and involvement of the corticospinal tract (25%) are also common (Hayflick et al., 2003). Our young patient showed normal intellectual development during childhood. An IQ score of 91 was noted at the first evaluation, and nine years later a score of 82 was achieved. Follow-up of this subject s cognitive state will be an important source of information. Apart from hyperreflexia of the legs, no pyramidal signs were observed. Hayflick found clinical or electroretinographic evidence of retinopathy present in 68% of patients with the classic disease variant (Hayflick et al., 2003). Our first patient had a normal electroretinogram. Adult-onset cases have a quite variable clinical presentation (Halliday 1995). Parkinsonism is a predominant feature (Jankovic et al., 1985 ; Grimes et al., 2000 ; Racette et al., 2001 ; Thomas et al., 2004), as noticed in our second case. Dementia is also often presented (Dooling et al., 1974 ; Jankovic et al., 1985 ; Wang et al., 1990), although to date our second patient has not shown any cognitive decline. MRI has been useful in the diagnosis of iron storage diseases. Iron, a paramagnetic substance, exerts a proton relaxation effect on neighbouring hydrogen nuclei, resulting in a decrease in T1 and T2 times. On T2-weighted images, the decrease in relaxation time results in a decreased signal. The low attenuation localized bilaterally in the globus pallidi suggests iron accumulation. The central, high signal within the hypodense zone may be due to intense gliosis or increased water content due to loss of cellular elements. This specific, hyperintensity pattern within the hypointense medial globus pallidus is known as the eye of the tiger sign (Sethi et al., 1998). In our first case, the first MRI revealed bilateral hypersignals within the globus pallidi on T2-weighted images. Monitoring brain MRI parameters over the next five years did not reveal any further modifications. An area of only high signal intensity on T2-weighted images (i.e. without any neighbouring hypodensity) may be
5 30 F. CLEMENT evident in the earlier stages and may become progressively smaller (Thomas et al., 2004). Gallucci and colleagues found that the MRI characteristics may change over the course of the disease. They give an example of a case with hyperintense pallidi which, over a period of 3 years, changed to a mixed-intensity, target-like appearance and then finally to the pattern known as the eye of the tiger (Gallucci et al., 1990). This pattern is not found in all patients with NBIA syndrome. MRI images of some patients show only T2-weighted hypointensity in the globus pallidus, without a central hypersignal : iron deposition in the red nucleus and dentate nucleus are common features in this group (Hayflick et al., 2003). This MRI feature with multiple significant hyposignals was noticed in our second patient. The first case corresponds to the classic NBIA syndrome, as we described earlier, and indeed a PANK2 mutation was found. Hayflick and colleagues have identified PANK2 mutations in a large subgroup of patients with NBIA syndrome. They found that all patients with the classic disease and one third of those with atypical disease had PANK2 mutations. The clinical features of the PANK2- mutation-positive patients with the classic disease were remarkably homogeneous, whilst those of patients with atypical NBIA syndrome and PANK2 mutations were heterogeneous (Hayflick et al., 2003). The presence of a mutation in the PANK2 gene is usually associated with younger age at onset and a higher frequency of dystonia, dysarthria, intellectual impairment and gait disturbance. The absence of a mutation in the PANK2 gene tends to be associated with onset of symptoms after the age of 20 and with parkinsonism, which was observed in the second PANK2-mutationnegative patient (Thomas et al., 2004). Once the PANK2 gene had been discovered on chromosome 20, it was found to code for pantothenate kinase an essential enzyme in the synthesis of coenzyme A from pantothenate. Coenzyme A plays a central role in fatty acid synthesis and energy metabolism. A deficiency can lead first to a high concentration of cysteine in the basal ganglia and then to iron accumulation in these same areas. The cysteineiron complex results in tissue damage by provoking oxidative stress (Gordon, 2002). Both iron accumulation and the loss of cellular elements explain the typical eye of the tiger pattern on T2-weighted brain MRI images. The study by Hayflick and colleagues found this pattern in all patients with pantothenate kinase-associated neurodegeneration, regardless of classic or atypical clinical presentation. No evidence of the eye-of-the-tiger pattern was found in PANK2 mutation-negative patients (Hayflick et al., 2003). The diversity of the lesions in this group of patients correlates with the clinical heterogeneity. MRI of our second patient showed multiple lesions without eye-of-the-tiger pattern. Our adult patient s extrapyramidal syndrome appeared to be levodopa-responsive. This has also been described in other adult-onset cases (Seibel et al., 1993 ; Carod-Artal et al., 2004). Anticholinergic therapy (even at high doses) did not influence our patients symptomatology. In our first subject, dopaminergic treatment had no effect on the clinical symptoms. The botulinum injections that were subsequently given to treat the patient s oromandibular dystonia temporarily improved mastication and swallowing. Other authors have mentioned the benefit of botulinum toxin for treatment of jaw-opening dystonia in Hallervorden- Spatz syndrome (Dressler et al., 2001). The general dystonic symptoms were finally treated by pallidal deep brain stimulation (DBS). Electrical stimulation of the globus pallidum internum (Gpi) has been proven to be an effective treatment for primary generalized dystonia (PGD), especially in DYT1 mutation carriers, and should be considered for conditions which are refractory to drug therapy (Vercueil et al., 2002). Coubes and colleagues found that the improvement of both clinical and functional Burke-Fahn-Marsden (BFM) scores at the 2-year follow-up examination was comparable for PGD patients with and without the DYT1 mutation (Coubes et al., 2004). The efficacy and safety of chronic, pallidal DBS in generalized non-dyt1 dystonia has been confirmed by other authors. Beneficial results have been achieved in patients with primary genetic segmental dystonia, myoclonic dystonia and complex cervical dystonia (Krauss, 2002 ; Krauss et al., 2003 ; Kupsch et al., 2003). Results of pallidal DBS in secondary dystonias (such as NBIA) are less conclusive (Volkmann and Benecke, 2002 ; Toda et al., 2004). The results are generally less helpful than those obtained in patients with primary dystonia (Eltahawy et al., 2004). After a 1-year follow-up, Coubes found a 71% improvement in the clinical BFM score in a group of 15 patients with DYT1 dystonia, compared to a 31% improvement in a group of 21 patients with secondary dystonia (varied etiologies as perinatal anoxia, foeto-maternal incompatibility in the Rhesus system, PKAN syndrome, mitochondrial cytopathies, type 1 tyrosinemia, postanoxic encephalopathies) (Cif et al., 2003) The BFM score of our first patient improved by 65% after 18 months. This is a favourable outcome when compared to most results in secondary dystonia. This was also confirmed in other cases of genetically confirmed PKAN. Bilateral internal globus pallidus stimulation was performed in six patients with genetically confirmed PKAN who obtained a major and longlasting improvement of their painful spasms, dystonia and functional autonomy (Castelnau et al., 2005). Follow-up of larger patient series will be needed to evaluate the impact of the bipallidal DBS technique on both PANK2-mutation-positive and -negative NBIA patients.
6 NEURODEGENERATION WITH BRAIN IRON ACCUMULATION 31 REFERENCES CAROD-ARTAL F. J., VARGAS A. P., MARINHO P. B., FERNANDES-SILVA T. V., PORTUGAL D. Tourettism, hemiballism and juvenile Parkinsonism : expanding the clinical spectrum of the neurodegeneration associated to panothenate kinase deficiency (Hallervorden Spatz syndrome). Rev. Neuro., 2004, 38 : THOMAS M., HAYFLICK S. J., JANKOVIC J. Clinical Heterogeneity of Neurodegeneration With Brain Iron Accumulation (Hallervorden-Spatz Syndrome) and Pantothenate Kinase-Associated Neurodegeneration. Mov. Disord., 2004, 19 : HAYFLICK S. J. Unraveling the Hallervorden-Spatz syndrome : pantothenate kinase-associated neurodegeneration is the name. Curr. Opin. Pediatr., 2003, 15 : HALLERVORDEN J., SPATZ H. Eigenartige Erkrankung im extrapyramidalen System mit besonderer Beteiligung des Globus pallidus und der Substantia nigra : Ein Beitrag zu den Beziehungen zwischen diesen beiden Zentren. Z Ges Neurol Psychiat, 1922, 79 : WIGBOLDUS J. M., BRUYN G. W. Hallervorden-Spatz disease. In : VINKEN P. J., BRUYN G. W. (eds.). Handbook of clinical neurology : diseases of the basal ganglia, 1968, 6 : HAYFLICK S. J., WESTAWAY S. K., LEVINSON B. Genetic, Clinical, and Radiographic Delineation of Hallervorden-Spatz Syndrome. N. Engl. J. Med., 2003, 348 : HALLIDAY W. The nosology of Hallervorden-Spatz disease. J. Neurol. Sci., 1995, 134 : GRIMES D. A., LANG A. E., BERGERON C. Late adult chorea with typical pathology of Hallervorden- Spatz syndrome. J Neurol. Neurosurg. Psychiatry, 2000, 69 : RACETTE B. A., PERRY A., D AVOSSA G., PERLMUTTER J. S. Late-onset neurodegeneration with brain iron accumulation type 1 : expanding the clinical spectrum. Mov. Disord., 2001, 16 : JANKOVIC J., KIRKPATRICK J. B., BLOMQUIST K. A., LANGLAIS P. J., BIRD E. D. Late-onset Hallervorden-Spatz disease presenting as familial parkinsonism. Neurology, 1985, 2 : DOOLING E. C., SCHOENE W. C., RICHARDSON E. P. Hallervorden-Spatz syndrome. Arch. Neurol., 1974, 30 : WANG L. N., HUANG K. W., LIU Z. Y. Sporadic late-onset type of Hallervorden-Spatz disease presenting as parkinsonism in a Chinese patient. Chin. Med. J., 1990, 103 : SETHI K. D., ADAMS R. J., LORING D. W., GAMMAL T. Hallervorden-Spatz Syndrome : Clinical and Magnetic Resonance Imaging Correlations. Ann. Neurol., 1998, 24 : GALLUCCI M., CARDONA F., ARACHI M., SPLENDIANI A., BOZZAO A. et al. Follow-up MR studies in Hallervorden-Spatz disease. J. Comput. Assist. Tomogr., 1990, 14 : GORDON N. Pantothenate kinase-associated neurodegeneration (Hallervorden-Spatz syndrome). Eur. J. Paediatr. Neurol., 2002, 6 : SEIBEL M. O., DATE E. S., ZEINER H., SCHWARTZ M. Rehabilitation of patients with Hallervorden- Spatz syndrome. Arch. Phys. Med. Rehabil., 1993, 74 : DRESSLER D., WITTSTOCK M., BENECKE R. Botulinum toxin for treatment of jaw opening dystonia in Hallervorden-Spatz syndrome. Eur. Neurol., 2001, 45 : VERCUEIL L., KRACK P., POLLAK P. Results of deep brain stimulation for dystonia : a critical reappraisal. Mov. Disord., 2002, 17 (suppl 3) : S COUBES P., CIF L., FERTIT H. Electrical stimulation of the globus pallidus internus in patients with primary generalized dystonia : long-term results. J. Neurosurg., 2004, 10 : KRAUSS J. K., LOHER T. J., WEIGEL R., CAPELLE H. H., WEBER S. Chronic stimulation of the globus pallidus internus for treatment of non-dyt 1 generalized dystonia and choreoathetosis : 2-year follow-up. J. Neurosurg., 2003, 98 : KUPSCH A., KUEHN A., KLAFFKE S. Deep brain stimulation in dystonia. J Neurol, 2003, 250 (suppl. 1) : KRAUSS J. K. Deep brain stimulation for dystonia in adults Overview and developments. Stereotact. Funct. Neurosurg., 2002, 78 : VOLKMANN J., BENECKE R. Deep brain stimulation for dystonia : patient selection and evaluation. Mov. Disord. Suppl., 2002, 3 : S TODA H., HAMANI C., LOZANO A. Deep brain stimulation in the treatment of dyskinesia and dystonia. Neurosurg. Focus, 2004, 17 : E2. ELTAHAWY H. A., SAINT-CYR J., GILADI N., LANG A. E., LOZANO A. M. Primary dystonia is more responsive than secondary dystonia to pallidal interventions : outcome after pallidotomy or pallidal deep brain stimulation. Neurosurgery, 2004, 54 : CIF L., EL FERTIT H., VAYSSIERE N., HEMM S., HARDOUIN E. et al. Treatment of dystonic syndromes by chronic electrical stimulation of the internal globus pallidusi. J. Neurosurg. Sci., 2003, 47 : CASTELNAU P., CIF L., VALENTE E. M., VAYSSIERE N., HEMM S. et al. Pallidal stimulation improves pantothenate kinase-associated neurodegeneration. Ann. Neurol, 2005, 57 : F. CLEMENT, Hôpital Roger Salengro, F Lille, France L. DEFEBVRE, Hôpital Roger Salengro, F Lille, France freclement@yahoo.com ldefebvre@chru-lille.fr.
Movement Disorders Will Garrett, M.D Assistant Professor of Neurology
 Movement Disorders Will Garrett, M.D Assistant Professor of Neurology I. The Basal Ganglia The basal ganglia are composed of several structures including the caudate and putamen (collectively called the
Movement Disorders Will Garrett, M.D Assistant Professor of Neurology I. The Basal Ganglia The basal ganglia are composed of several structures including the caudate and putamen (collectively called the
VL VA BASAL GANGLIA. FUNCTIONAl COMPONENTS. Function Component Deficits Start/initiation Basal Ganglia Spontan movements
 BASAL GANGLIA Chris Cohan, Ph.D. Dept. of Pathology/Anat Sci University at Buffalo I) Overview How do Basal Ganglia affect movement Basal ganglia enhance cortical motor activity and facilitate movement.
BASAL GANGLIA Chris Cohan, Ph.D. Dept. of Pathology/Anat Sci University at Buffalo I) Overview How do Basal Ganglia affect movement Basal ganglia enhance cortical motor activity and facilitate movement.
Overview of Neurodegeneration with Brain Iron Accumulation (NBIA) Disorders
 Overview of Neurodegeneration with Brain Iron Accumulation (NBIA) Disorders What is NBIA? Neurodegeneration with Brain Iron Accumulation is a group of inherited neurological disorders characterized by
Overview of Neurodegeneration with Brain Iron Accumulation (NBIA) Disorders What is NBIA? Neurodegeneration with Brain Iron Accumulation is a group of inherited neurological disorders characterized by
Deep brain stimulation of globus pallidus internus for DYT1 positive primary generalized dystonia
 Original Article Medical Journal of the Islamic Republic of Iran (MJIRI) Iran University of Medical Sciences Deep brain stimulation of globus pallidus internus for DYT1 positive primary generalized dystonia
Original Article Medical Journal of the Islamic Republic of Iran (MJIRI) Iran University of Medical Sciences Deep brain stimulation of globus pallidus internus for DYT1 positive primary generalized dystonia
DISORDERS OF THE MOTOR SYSTEM. Jeanette J. Norden, Ph.D. Professor Emerita Vanderbilt University School of Medicine
 DISORDERS OF THE MOTOR SYSTEM Jeanette J. Norden, Ph.D. Professor Emerita Vanderbilt University School of Medicine THE MOTOR SYSTEM To understand disorders of the motor system, we need to review how a
DISORDERS OF THE MOTOR SYSTEM Jeanette J. Norden, Ph.D. Professor Emerita Vanderbilt University School of Medicine THE MOTOR SYSTEM To understand disorders of the motor system, we need to review how a
Movement Disorders. Psychology 372 Physiological Psychology. Background. Myasthenia Gravis. Many Types
 Background Movement Disorders Psychology 372 Physiological Psychology Steven E. Meier, Ph.D. Listen to the audio lecture while viewing these slides Early Studies Found some patients with progressive weakness
Background Movement Disorders Psychology 372 Physiological Psychology Steven E. Meier, Ph.D. Listen to the audio lecture while viewing these slides Early Studies Found some patients with progressive weakness
An approach to movement disorders. Kailash Bhatia, DM, FRCP Professor of Clinical Neurology Institute of Neurology Queen Square, London
 An approach to movement disorders Kailash Bhatia, DM, FRCP Professor of Clinical Neurology Institute of Neurology Queen Square, London Neurology Diagnosis Two main questions: What parts of the nervous
An approach to movement disorders Kailash Bhatia, DM, FRCP Professor of Clinical Neurology Institute of Neurology Queen Square, London Neurology Diagnosis Two main questions: What parts of the nervous
Strick Lecture 4 March 29, 2006 Page 1
 Strick Lecture 4 March 29, 2006 Page 1 Basal Ganglia OUTLINE- I. Structures included in the basal ganglia II. III. IV. Skeleton diagram of Basal Ganglia Loops with cortex Similarity with Cerebellar Loops
Strick Lecture 4 March 29, 2006 Page 1 Basal Ganglia OUTLINE- I. Structures included in the basal ganglia II. III. IV. Skeleton diagram of Basal Ganglia Loops with cortex Similarity with Cerebellar Loops
Department of Neurology, Rigshospitalet, 9 Blegdamsvej, PAULSON, O.B. Involuntary Movements. Tohoku J. Exp. Med., 1990, 161,
 Tohoku J. Exp. Med., 1990, 161, Suppl., 21-27 Involuntary Movements OLAF B. PAULSON Department of Neurology, Rigshospitalet, 9 Blegdamsvej, DK-2100, Copenhagen, Denmark PAULSON, O.B. Involuntary Movements.
Tohoku J. Exp. Med., 1990, 161, Suppl., 21-27 Involuntary Movements OLAF B. PAULSON Department of Neurology, Rigshospitalet, 9 Blegdamsvej, DK-2100, Copenhagen, Denmark PAULSON, O.B. Involuntary Movements.
Basal ganglia Sujata Sofat, class of 2009
 Basal ganglia Sujata Sofat, class of 2009 Basal ganglia Objectives Describe the function of the Basal Ganglia in movement Define the BG components and their locations Describe the motor loop of the BG
Basal ganglia Sujata Sofat, class of 2009 Basal ganglia Objectives Describe the function of the Basal Ganglia in movement Define the BG components and their locations Describe the motor loop of the BG
Functional Distinctions
 Functional Distinctions FUNCTION COMPONENT DEFICITS Start Basal Ganglia Spontaneous Movements Move UMN/LMN Cerebral Cortex Brainstem, Spinal cord Roots/peripheral nerves Plan Cerebellum Ataxia Adjust Cerebellum
Functional Distinctions FUNCTION COMPONENT DEFICITS Start Basal Ganglia Spontaneous Movements Move UMN/LMN Cerebral Cortex Brainstem, Spinal cord Roots/peripheral nerves Plan Cerebellum Ataxia Adjust Cerebellum
CN V! touch! pain! Touch! P/T!
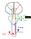 CN V! touch! pain! Touch! P/T! Visual Pathways! L! R! B! A! C! D! LT! E! F! RT! G! hypothalamospinal! and! ALS! Vestibular Pathways! 1. Posture/Balance!!falling! 2. Head Position! 3. Eye-Head Movements
CN V! touch! pain! Touch! P/T! Visual Pathways! L! R! B! A! C! D! LT! E! F! RT! G! hypothalamospinal! and! ALS! Vestibular Pathways! 1. Posture/Balance!!falling! 2. Head Position! 3. Eye-Head Movements
The motor regulator. 1) Basal ganglia/nucleus
 The motor regulator 1) Basal ganglia/nucleus Neural structures involved in the control of movement Basal Ganglia - Components of the basal ganglia - Function of the basal ganglia - Connection and circuits
The motor regulator 1) Basal ganglia/nucleus Neural structures involved in the control of movement Basal Ganglia - Components of the basal ganglia - Function of the basal ganglia - Connection and circuits
Professor Tim Anderson
 Professor Tim Anderson Neurologist University of Otago Christchurch 11:00-11:55 WS #91: Shakes Jerks and Spasms - Recognition and Differential Diagnosis 12:05-13:00 WS #102: Shakes Jerks and Spasms - Recognition
Professor Tim Anderson Neurologist University of Otago Christchurch 11:00-11:55 WS #91: Shakes Jerks and Spasms - Recognition and Differential Diagnosis 12:05-13:00 WS #102: Shakes Jerks and Spasms - Recognition
Professor Tim Anderson
 Professor Tim Anderson Neurologist University of Otago Christchurch 11:00-11:55 WS #91: Shakes Jerks and Spasms - Recognition and Differential Diagnosis 12:05-13:00 WS #102: Shakes Jerks and Spasms - Recognition
Professor Tim Anderson Neurologist University of Otago Christchurch 11:00-11:55 WS #91: Shakes Jerks and Spasms - Recognition and Differential Diagnosis 12:05-13:00 WS #102: Shakes Jerks and Spasms - Recognition
Subthalamic Nucleus Deep Brain Stimulation (STN-DBS)
 Subthalamic Nucleus Deep Brain Stimulation (STN-DBS) A Neurosurgical Treatment for Parkinson s Disease Parkinson s Disease Parkinson s disease is a common neurodegenerative disorder that affects about
Subthalamic Nucleus Deep Brain Stimulation (STN-DBS) A Neurosurgical Treatment for Parkinson s Disease Parkinson s Disease Parkinson s disease is a common neurodegenerative disorder that affects about
10/13/2017. Disclosures. Deep Brain Stimulation in the Treatment of Movement Disorders. Deep Brain Stimulation: Objectives.
 Deep Brain Stimulation in the Treatment of Movement Disorders Disclosures None Eleanor K Orehek, M.D. Movement Disorders Specialist Noran Neurological Clinic 1 2 Objectives To provide an overview of deep
Deep Brain Stimulation in the Treatment of Movement Disorders Disclosures None Eleanor K Orehek, M.D. Movement Disorders Specialist Noran Neurological Clinic 1 2 Objectives To provide an overview of deep
Lecture XIII. Brain Diseases I - Parkinsonism! Brain Diseases I!
 Lecture XIII. Brain Diseases I - Parkinsonism! Bio 3411! Wednesday!! Lecture XIII. Brain Diseases - I.! 1! Brain Diseases I! NEUROSCIENCE 5 th ed! Page!!Figure!!Feature! 408 18.9 A!!Substantia Nigra in
Lecture XIII. Brain Diseases I - Parkinsonism! Bio 3411! Wednesday!! Lecture XIII. Brain Diseases - I.! 1! Brain Diseases I! NEUROSCIENCE 5 th ed! Page!!Figure!!Feature! 408 18.9 A!!Substantia Nigra in
Deep Brain Stimulation: Patient selection
 Deep Brain Stimulation: Patient selection Halim Fadil, MD Movement Disorders Neurologist Kane Hall Barry Neurology Bedford/Keller, TX 1991: Thalamic (Vim) DBS for tremor Benabid AL, et al. Lancet. 1991;337(8738):403-406.
Deep Brain Stimulation: Patient selection Halim Fadil, MD Movement Disorders Neurologist Kane Hall Barry Neurology Bedford/Keller, TX 1991: Thalamic (Vim) DBS for tremor Benabid AL, et al. Lancet. 1991;337(8738):403-406.
Review Article Dystonia and the Role of Deep Brain Stimulation
 International Scholarly Research Network ISRN Surgery Volume 2011, Article ID 193718, 5 pages doi:10.5402/2011/193718 Review Article Dystonia and the Role of Deep Brain Stimulation Thomas L. Ellis Wake
International Scholarly Research Network ISRN Surgery Volume 2011, Article ID 193718, 5 pages doi:10.5402/2011/193718 Review Article Dystonia and the Role of Deep Brain Stimulation Thomas L. Ellis Wake
III./3.1. Movement disorders with akinetic rigid symptoms
 III./3.1. Movement disorders with akinetic rigid symptoms III./3.1.1. Parkinson s disease Parkinson s disease (PD) is the second most common neurodegenerative disorder worldwide after Alzheimer s disease.
III./3.1. Movement disorders with akinetic rigid symptoms III./3.1.1. Parkinson s disease Parkinson s disease (PD) is the second most common neurodegenerative disorder worldwide after Alzheimer s disease.
ORIGINAL CONTRIBUTION. Acute Deep-Brain Stimulation of the Internal and External Globus Pallidus in Primary Dystonia
 ORIGINAL CONTRIBUTION Acute Deep-Brain Stimulation of the Internal and External Globus Pallidus in Primary Dystonia Functional Mapping of the Pallidum Jean-Luc Houeto, MD, PhD; Jérôme Yelnik, MD, PhD;
ORIGINAL CONTRIBUTION Acute Deep-Brain Stimulation of the Internal and External Globus Pallidus in Primary Dystonia Functional Mapping of the Pallidum Jean-Luc Houeto, MD, PhD; Jérôme Yelnik, MD, PhD;
Movement disorders in childhood: assessment and diagnosis. Lucinda Carr
 Movement disorders in childhood: assessment and diagnosis Lucinda Carr Movement disorders in childhood: Assessment Classification Causes Diagnosis Presentation of movement disorders in childhood: Concerns
Movement disorders in childhood: assessment and diagnosis Lucinda Carr Movement disorders in childhood: Assessment Classification Causes Diagnosis Presentation of movement disorders in childhood: Concerns
Deep Brain Stimulation: Indications and Ethical Applications
 Deep Brain Stimulation Overview Kara D. Beasley, DO, MBe, FACOS Boulder Neurosurgical and Spine Associates (303) 562-1372 Deep Brain Stimulation: Indications and Ethical Applications Instrument of Change
Deep Brain Stimulation Overview Kara D. Beasley, DO, MBe, FACOS Boulder Neurosurgical and Spine Associates (303) 562-1372 Deep Brain Stimulation: Indications and Ethical Applications Instrument of Change
GENETICS AND TREATMENT OF DYSTONIA
 GENETICS AND TREATMENT OF DYSTONIA Oksana Suchowersky, M.D., FRCPC, FCCMG Professor of Medicine, Medical Genetics, and Psychiatry Toupin Research Chair in Neurology DYSTONIA Definition: abnormal sustained
GENETICS AND TREATMENT OF DYSTONIA Oksana Suchowersky, M.D., FRCPC, FCCMG Professor of Medicine, Medical Genetics, and Psychiatry Toupin Research Chair in Neurology DYSTONIA Definition: abnormal sustained
Parkinson's Disease Center and Movement Disorders Clinic
 Parkinson's Disease Center and Movement Disorders Clinic 7200 Cambridge Street, 9th Floor, Suite 9A Houston, Texas 77030 713-798-2273 phone www.jankovic.org Dystonia Diagnosis Dystonia is a neurologic
Parkinson's Disease Center and Movement Disorders Clinic 7200 Cambridge Street, 9th Floor, Suite 9A Houston, Texas 77030 713-798-2273 phone www.jankovic.org Dystonia Diagnosis Dystonia is a neurologic
Disorders of Movement M A R T I N H A R L E Y N E U R O L O G Y
 Disorders of Movement M A R T I N H A R L E Y N E U R O L O G Y Educational Objectives Improved history taking in patients with movement disorders. Develop a systematic approach to observing and describing
Disorders of Movement M A R T I N H A R L E Y N E U R O L O G Y Educational Objectives Improved history taking in patients with movement disorders. Develop a systematic approach to observing and describing
Palladotomy and Pallidal Deep Brain Stimulation
 Palladotomy and Pallidal Deep Brain Stimulation Parkinson s disease Parkinson s Disease is a common neurodegenerative disorder that affects about 1:100 individuals over the age of 60. In a small percentage
Palladotomy and Pallidal Deep Brain Stimulation Parkinson s disease Parkinson s Disease is a common neurodegenerative disorder that affects about 1:100 individuals over the age of 60. In a small percentage
Outcome predictors of pallidal stimulation in patients with primary dystonia: the role of disease duration
 doi:10.1093/brain/awn120 Brain (2008), 131,1895^1902 Outcome predictors of pallidal stimulation in patients with primary dystonia: the role of disease duration Ioannis U. Isaias, 1 Ron L. Alterman 2 and
doi:10.1093/brain/awn120 Brain (2008), 131,1895^1902 Outcome predictors of pallidal stimulation in patients with primary dystonia: the role of disease duration Ioannis U. Isaias, 1 Ron L. Alterman 2 and
Dystonia: Title. A real pain in the neck. in All the Wrong Places
 Focus on CME at the University of Western Ontario Dystonia: Title in All the Wrong Places A real pain in the neck By Mandar Jog, MD, FRCPC and; Mary Jenkins, MD, FRCPC What is dystonia? Dystonia is a neurologic
Focus on CME at the University of Western Ontario Dystonia: Title in All the Wrong Places A real pain in the neck By Mandar Jog, MD, FRCPC and; Mary Jenkins, MD, FRCPC What is dystonia? Dystonia is a neurologic
Diagnosis and treatment of dystonia
 Diagnosis and treatment of dystonia Professor Tom Warner, Reta Lila Weston Institute of Neurological Studies UCL Institute of Neurology National Hospital for Neurology and Neurosurgery Queen Square What
Diagnosis and treatment of dystonia Professor Tom Warner, Reta Lila Weston Institute of Neurological Studies UCL Institute of Neurology National Hospital for Neurology and Neurosurgery Queen Square What
Dr Barry Snow. Neurologist Auckland District Health Board
 Dr Barry Snow Neurologist Auckland District Health Board Dystonia and Parkinson s disease Barry Snow Gowers 1888: Tetanoid chorea Dystonia a movement disorder characterized by sustained or intermittent
Dr Barry Snow Neurologist Auckland District Health Board Dystonia and Parkinson s disease Barry Snow Gowers 1888: Tetanoid chorea Dystonia a movement disorder characterized by sustained or intermittent
COGNITIVE SCIENCE 107A. Motor Systems: Basal Ganglia. Jaime A. Pineda, Ph.D.
 COGNITIVE SCIENCE 107A Motor Systems: Basal Ganglia Jaime A. Pineda, Ph.D. Two major descending s Pyramidal vs. extrapyramidal Motor cortex Pyramidal system Pathway for voluntary movement Most fibers originate
COGNITIVE SCIENCE 107A Motor Systems: Basal Ganglia Jaime A. Pineda, Ph.D. Two major descending s Pyramidal vs. extrapyramidal Motor cortex Pyramidal system Pathway for voluntary movement Most fibers originate
Diagnosis and treatment of dystonia
 Diagnosis and treatment of dystonia Professor Tom Warner, Reta Lila Weston Institute of Neurological Studies UCL Institute of Neurology National Hospital for Neurology and Neurosurgery Queen Square What
Diagnosis and treatment of dystonia Professor Tom Warner, Reta Lila Weston Institute of Neurological Studies UCL Institute of Neurology National Hospital for Neurology and Neurosurgery Queen Square What
Dr. Farah Nabil Abbas. MBChB, MSc, PhD
 Dr. Farah Nabil Abbas MBChB, MSc, PhD The Basal Ganglia *Functions in association with motor cortex and corticospinal pathways. *Regarded as accessory motor system besides cerebellum. *Receive most of
Dr. Farah Nabil Abbas MBChB, MSc, PhD The Basal Ganglia *Functions in association with motor cortex and corticospinal pathways. *Regarded as accessory motor system besides cerebellum. *Receive most of
Review Article MRI Findings in Neuroferritinopathy
 Neurology Research International Volume 2012, Article ID 197438, 7 pages doi:10.1155/2012/197438 Review Article MRI Findings in Neuroferritinopathy Emiko Ohta and Yoshihisa Takiyama Department of Neurology,
Neurology Research International Volume 2012, Article ID 197438, 7 pages doi:10.1155/2012/197438 Review Article MRI Findings in Neuroferritinopathy Emiko Ohta and Yoshihisa Takiyama Department of Neurology,
A. General features of the basal ganglia, one of our 3 major motor control centers:
 Reading: Waxman pp. 141-146 are not very helpful! Computer Resources: HyperBrain, Chapter 12 Dental Neuroanatomy Suzanne S. Stensaas, Ph.D. March 1, 2012 THE BASAL GANGLIA Objectives: 1. What are the main
Reading: Waxman pp. 141-146 are not very helpful! Computer Resources: HyperBrain, Chapter 12 Dental Neuroanatomy Suzanne S. Stensaas, Ph.D. March 1, 2012 THE BASAL GANGLIA Objectives: 1. What are the main
A. General features of the basal ganglia, one of our 3 major motor control centers:
 Reading: Waxman pp. 141-146 are not very helpful! Computer Resources: HyperBrain, Chapter 12 Dental Neuroanatomy Suzanne S. Stensaas, Ph.D. April 22, 2010 THE BASAL GANGLIA Objectives: 1. What are the
Reading: Waxman pp. 141-146 are not very helpful! Computer Resources: HyperBrain, Chapter 12 Dental Neuroanatomy Suzanne S. Stensaas, Ph.D. April 22, 2010 THE BASAL GANGLIA Objectives: 1. What are the
Basal Ganglia. Steven McLoon Department of Neuroscience University of Minnesota
 Basal Ganglia Steven McLoon Department of Neuroscience University of Minnesota 1 Course News Graduate School Discussion Wednesday, Nov 1, 11:00am MoosT 2-690 with Paul Mermelstein (invite your friends)
Basal Ganglia Steven McLoon Department of Neuroscience University of Minnesota 1 Course News Graduate School Discussion Wednesday, Nov 1, 11:00am MoosT 2-690 with Paul Mermelstein (invite your friends)
No Financial Disclosures
 Deep Brain Stimulation: A Physician and Patient Perspective Jessica McClure Warren Marks, MD Cook Children s Medical Center Cook Children s Health Foundation Endowed Chair in Neurosciences Department of
Deep Brain Stimulation: A Physician and Patient Perspective Jessica McClure Warren Marks, MD Cook Children s Medical Center Cook Children s Health Foundation Endowed Chair in Neurosciences Department of
Parkinson s Disease. Sirilak yimcharoen
 Parkinson s Disease Sirilak yimcharoen EPIDEMIOLOGY ~1% of people over 55 years Age range 35 85 years peak age of onset is in the early 60s ~5% of cases characterized by an earlier age of onset (typically
Parkinson s Disease Sirilak yimcharoen EPIDEMIOLOGY ~1% of people over 55 years Age range 35 85 years peak age of onset is in the early 60s ~5% of cases characterized by an earlier age of onset (typically
Patient selection for surgery: Hyperkinetic movement disorders
 Patient selection for surgery: Hyperkinetic movement disorders Alfons Schnitzler, MD, PhD Dept. of Neurology, Movement Disorder and Neuromodulation, Heinrich-Heine-University Düsseldorf, Germany Hyperkinetic
Patient selection for surgery: Hyperkinetic movement disorders Alfons Schnitzler, MD, PhD Dept. of Neurology, Movement Disorder and Neuromodulation, Heinrich-Heine-University Düsseldorf, Germany Hyperkinetic
EMERGING TREATMENTS FOR PARKINSON S DISEASE
 EMERGING TREATMENTS FOR PARKINSON S DISEASE Katerina Markopoulou, MD, PhD Director Neurodegenerative Diseases Program Department of Neurology NorthShore University HealthSystem Clinical Assistant Professor
EMERGING TREATMENTS FOR PARKINSON S DISEASE Katerina Markopoulou, MD, PhD Director Neurodegenerative Diseases Program Department of Neurology NorthShore University HealthSystem Clinical Assistant Professor
An Approach to Patients with Movement Disorders
 An Approach to Patients with Movement Disorders Joaquim Ferreira, MD, PhD Laboratory of Clinical Pharmacology and Therapeutics Faculty of Medicine University of Lisbon EDUCATIONAL TOOLS MDS video library
An Approach to Patients with Movement Disorders Joaquim Ferreira, MD, PhD Laboratory of Clinical Pharmacology and Therapeutics Faculty of Medicine University of Lisbon EDUCATIONAL TOOLS MDS video library
Critical Review: What effects do neurosurgical treatments for generalized dystonia have on speech?
 Critical Review: What effects do neurosurgical treatments for generalized dystonia have on speech? Jana Zalmanowitz M.Cl.Sc (SLP) Candidate University of Western Ontario: School of Communication Sciences
Critical Review: What effects do neurosurgical treatments for generalized dystonia have on speech? Jana Zalmanowitz M.Cl.Sc (SLP) Candidate University of Western Ontario: School of Communication Sciences
Surgical Treatment: Patient Edition
 Parkinson s Disease Clinic and Research Center University of California, San Francisco 505 Parnassus Ave., Rm. 795-M, Box 0114 San Francisco, CA 94143-0114 (415) 476-9276 http://pdcenter.neurology.ucsf.edu
Parkinson s Disease Clinic and Research Center University of California, San Francisco 505 Parnassus Ave., Rm. 795-M, Box 0114 San Francisco, CA 94143-0114 (415) 476-9276 http://pdcenter.neurology.ucsf.edu
Movement disorders. Dr Rick Leventer Royal Children s Hospital
 Movement disorders Dr Rick Leventer Royal Children s Hospital richard.leventer@rch.org.au Movement disorders! conditions that affect the speed, fluency, quality, and ease of movement! usually affect TONE
Movement disorders Dr Rick Leventer Royal Children s Hospital richard.leventer@rch.org.au Movement disorders! conditions that affect the speed, fluency, quality, and ease of movement! usually affect TONE
Moving fast or moving slow: an overview of Movement Disorders
 Moving fast or moving slow: an overview of Movement Disorders Mini Medical School October 25, 2018 Heather Rigby, MD, FRCPC 2014 MFMER slide-1 2014 MFMER slide-2 Basal Ganglia Dysfunction - Movement Disorders
Moving fast or moving slow: an overview of Movement Disorders Mini Medical School October 25, 2018 Heather Rigby, MD, FRCPC 2014 MFMER slide-1 2014 MFMER slide-2 Basal Ganglia Dysfunction - Movement Disorders
Connections of basal ganglia
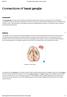 Connections of basal ganglia Introduction The basal ganglia, or basal nuclei, are areas of subcortical grey matter that play a prominent role in modulating movement, as well as cognitive and emotional
Connections of basal ganglia Introduction The basal ganglia, or basal nuclei, are areas of subcortical grey matter that play a prominent role in modulating movement, as well as cognitive and emotional
C. Moreau, MD L. Defebvre, MD, PhD A. Destée, MD, PhD S. Bleuse, PhD F. Clement, MD J.L. Blatt, MD, PhD P. Krystkowiak, MD, PhD D.
 ARTICLES STN-DBS frequency effects on freezing of gait in advanced Parkinson disease C. Moreau, MD L. Defebvre, MD, PhD A. Destée, MD, PhD S. Bleuse, PhD F. Clement, MD J.L. Blatt, MD, PhD P. Krystkowiak,
ARTICLES STN-DBS frequency effects on freezing of gait in advanced Parkinson disease C. Moreau, MD L. Defebvre, MD, PhD A. Destée, MD, PhD S. Bleuse, PhD F. Clement, MD J.L. Blatt, MD, PhD P. Krystkowiak,
Neurodegenerative Disease. April 12, Cunningham. Department of Neurosciences
 Neurodegenerative Disease April 12, 2017 Cunningham Department of Neurosciences NEURODEGENERATIVE DISEASE Any of a group of hereditary and sporadic conditions characterized by progressive dysfunction,
Neurodegenerative Disease April 12, 2017 Cunningham Department of Neurosciences NEURODEGENERATIVE DISEASE Any of a group of hereditary and sporadic conditions characterized by progressive dysfunction,
P rimary generalised dystonia (PGD) is a movement disorder
 1314 PAPER Effect of electrode contact location on clinical efficacy of pallidal deep brain stimulation in primary generalised dystonia S Tisch, L Zrinzo, P Limousin, K P Bhatia, N Quinn, K Ashkan, M Hariz...
1314 PAPER Effect of electrode contact location on clinical efficacy of pallidal deep brain stimulation in primary generalised dystonia S Tisch, L Zrinzo, P Limousin, K P Bhatia, N Quinn, K Ashkan, M Hariz...
Diffusion-Weighted and Conventional MR Imaging Findings of Neuroaxonal Dystrophy
 AJNR Am J Neuroradiol 25:1269 1273, August 2004 Diffusion-Weighted and Conventional MR Imaging Findings of Neuroaxonal Dystrophy R. Nuri Sener BACKGROUND AND PURPOSE: Neuroaxonal dystrophy is a rare progressive
AJNR Am J Neuroradiol 25:1269 1273, August 2004 Diffusion-Weighted and Conventional MR Imaging Findings of Neuroaxonal Dystrophy R. Nuri Sener BACKGROUND AND PURPOSE: Neuroaxonal dystrophy is a rare progressive
Making Things Happen 2: Motor Disorders
 Making Things Happen 2: Motor Disorders How Your Brain Works Prof. Jan Schnupp wschnupp@cityu.edu.hk HowYourBrainWorks.net On the Menu in This Lecture In the previous lecture we saw how motor cortex and
Making Things Happen 2: Motor Disorders How Your Brain Works Prof. Jan Schnupp wschnupp@cityu.edu.hk HowYourBrainWorks.net On the Menu in This Lecture In the previous lecture we saw how motor cortex and
Differential Diagnosis of Hypokinetic Movement Disorders
 Differential Diagnosis of Hypokinetic Movement Disorders Dr Donald Grosset Consultant Neurologist - Honorary Professor Institute of Neurological Sciences - Glasgow University Hypokinetic Parkinson's Disease
Differential Diagnosis of Hypokinetic Movement Disorders Dr Donald Grosset Consultant Neurologist - Honorary Professor Institute of Neurological Sciences - Glasgow University Hypokinetic Parkinson's Disease
Dystonia. The condition can vary from very mild to severe. Dystonia may get worse over time or it may stay the same or get better.
 Dystonia What are movement disorders? Movement disorders are conditions that cause involuntary body movements. With all movement disorders, abnormal signals from the brain cause patients to have trouble
Dystonia What are movement disorders? Movement disorders are conditions that cause involuntary body movements. With all movement disorders, abnormal signals from the brain cause patients to have trouble
Deep Brain Stimulation for Parkinson s Disease & Essential Tremor
 Deep Brain Stimulation for Parkinson s Disease & Essential Tremor Albert Fenoy, MD Assistant Professor University of Texas at Houston, Health Science Center Current US Approvals Essential Tremor and Parkinsonian
Deep Brain Stimulation for Parkinson s Disease & Essential Tremor Albert Fenoy, MD Assistant Professor University of Texas at Houston, Health Science Center Current US Approvals Essential Tremor and Parkinsonian
symptoms of Parkinson s disease EXCEPT.
 M. Angele Theard, M.D Asst. Professor, Washington University, St. Louis, MO Quiz team; Shobana Rajan, M.D; Suneeta Gollapudy, MD; Verghese Cherian, M.D, M. Angele Theard, MD This quiz is being published
M. Angele Theard, M.D Asst. Professor, Washington University, St. Louis, MO Quiz team; Shobana Rajan, M.D; Suneeta Gollapudy, MD; Verghese Cherian, M.D, M. Angele Theard, MD This quiz is being published
Identification number: TÁMOP /1/A
 Manifestation of Novel Social Challenges of the European Union in the Teaching Material of Medical Biotechnology Master s Programmes at the University of Pécs and at the University of Debrecen Identification
Manifestation of Novel Social Challenges of the European Union in the Teaching Material of Medical Biotechnology Master s Programmes at the University of Pécs and at the University of Debrecen Identification
162 Cangül H, et al The Turkish Journal of Pediatrics March - April 2009
 The Turkish Journal of ediatrics 2009; 51: 161-165 Case Report antothenate kinase-associated neurodegeneration (KN): molecular confirmation of a Turkish patient with a rare frameshift mutation in the coding
The Turkish Journal of ediatrics 2009; 51: 161-165 Case Report antothenate kinase-associated neurodegeneration (KN): molecular confirmation of a Turkish patient with a rare frameshift mutation in the coding
Understanding Dystonia
 Understanding Dystonia Sand Sharks Anthony Richardsen, Lindsey Rathbun, Evan Harrington, Chris Erzen The Essentials What, Why, How What is Dystonia? Dystonias are movement disorders often characterized
Understanding Dystonia Sand Sharks Anthony Richardsen, Lindsey Rathbun, Evan Harrington, Chris Erzen The Essentials What, Why, How What is Dystonia? Dystonias are movement disorders often characterized
SELECTIVE VULNERABILITY (HYPOXIA AND HYPOGLYCEMIA)
 DEFICIENCY OF METABOLITE -HYPOXIA AND HYPOGLYCEMIA -HYPOVITAMINOSIS SELECTIVE VULNERABILITY (HYPOXIA AND HYPOGLYCEMIA) -SPECIFIC CELL TYPE NEURONS>OLIGODENDROCYTES>ASTROCYTES -SPECIFIC BRAIN REGION PYRAMIDAL
DEFICIENCY OF METABOLITE -HYPOXIA AND HYPOGLYCEMIA -HYPOVITAMINOSIS SELECTIVE VULNERABILITY (HYPOXIA AND HYPOGLYCEMIA) -SPECIFIC CELL TYPE NEURONS>OLIGODENDROCYTES>ASTROCYTES -SPECIFIC BRAIN REGION PYRAMIDAL
The symptoms of the Parkinson s disease may vary from person to person. The symptoms might include the following:
 1 PARKINSON S DISEASE Parkinson's disease is a long term disease related to the central nervous system that mainly affects the motor system, resulting in the loss of dopamine, which helps in producing
1 PARKINSON S DISEASE Parkinson's disease is a long term disease related to the central nervous system that mainly affects the motor system, resulting in the loss of dopamine, which helps in producing
levodopa-induced dyskinesia
 Journal of Neurology, Neurosurgery, and Psychiatry, 1978, 41, 702-706 Sodium valproate in the treatment of levodopa-induced dyskinesia P. A. PRICE, J. D. PARKES, AND C. D. MARSDEN From the University Department
Journal of Neurology, Neurosurgery, and Psychiatry, 1978, 41, 702-706 Sodium valproate in the treatment of levodopa-induced dyskinesia P. A. PRICE, J. D. PARKES, AND C. D. MARSDEN From the University Department
Punit Agrawal, DO Clinical Assistant Professor of Neurology Division of Movement Disorders OSU Department of Neurology
 Deep Brain Stimulation for Movement Disorders Punit Agrawal, DO Clinical Assistant Professor of Neurology Division of Movement Disorders OSU Department of Neurology History of DBS 1 History of DBS 1987
Deep Brain Stimulation for Movement Disorders Punit Agrawal, DO Clinical Assistant Professor of Neurology Division of Movement Disorders OSU Department of Neurology History of DBS 1 History of DBS 1987
Extrapyramidal Motor System. Basal Ganglia or Striatum. Basal Ganglia or Striatum 3/3/2010
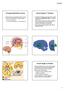 Extrapyramidal Motor System Basal Ganglia or Striatum Descending extrapyramidal paths receive input from other parts of motor system: From the cerebellum From the basal ganglia or corpus striatum Caudate
Extrapyramidal Motor System Basal Ganglia or Striatum Descending extrapyramidal paths receive input from other parts of motor system: From the cerebellum From the basal ganglia or corpus striatum Caudate
Role of Magnetic Resonance Imaging in the Diagnosis of Adult Onset Movement Disorders
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 17, Issue 3 Ver.11 March. (2018), PP 73-84 www.iosrjournals.org Role of Magnetic Resonance Imaging in
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 17, Issue 3 Ver.11 March. (2018), PP 73-84 www.iosrjournals.org Role of Magnetic Resonance Imaging in
Natural History of JNCL and other NCLs
 Natural History of JNCL and other NCLs Jonathan W. Mink, MD PhD Departments of Neurology, Neurobiology & Anatomy, Brain & Cognitive Sciences, and Pediatrics University of Rochester Neuronal Ceroid Lipofuscinosis
Natural History of JNCL and other NCLs Jonathan W. Mink, MD PhD Departments of Neurology, Neurobiology & Anatomy, Brain & Cognitive Sciences, and Pediatrics University of Rochester Neuronal Ceroid Lipofuscinosis
Source: *Dystonia facts medically edited by: Charles Patrick Davis, MD, PhD
 Source: http://www.medicinenet.com/script/main/art.asp?articlekey=349 Dystonia facts* *Dystonia facts medically edited by: Charles Patrick Davis, MD, PhD Dystonia is a disorder of muscle control; it can
Source: http://www.medicinenet.com/script/main/art.asp?articlekey=349 Dystonia facts* *Dystonia facts medically edited by: Charles Patrick Davis, MD, PhD Dystonia is a disorder of muscle control; it can
Deep brain stimulation in the treatment of dyskinesia and dystonia
 Neurosurg Focus 17 (1):E2, 2004, Click here to return to Table of Contents Deep brain stimulation in the treatment of dyskinesia and dystonia HIROKI TODA, M.D., PH.D., CLEMENT HAMANI, M.D., PH.D., AND
Neurosurg Focus 17 (1):E2, 2004, Click here to return to Table of Contents Deep brain stimulation in the treatment of dyskinesia and dystonia HIROKI TODA, M.D., PH.D., CLEMENT HAMANI, M.D., PH.D., AND
Deep Brain Stimulation and Movement Disorders
 Deep Brain Stimulation and Movement Disorders Farrokh Farrokhi, MD Neurosurgery Maria Marsans, PA-C Neurosurgery Virginia Mason June 27, 2017 OBJECTIVES Understand the role of Deep Brain Stimulation (DBS)
Deep Brain Stimulation and Movement Disorders Farrokh Farrokhi, MD Neurosurgery Maria Marsans, PA-C Neurosurgery Virginia Mason June 27, 2017 OBJECTIVES Understand the role of Deep Brain Stimulation (DBS)
Pallidal Deep Brain Stimulation
 Pallidal Deep Brain Stimulation Treatment for Dystonia Dystonia Dystonia is a neurological disorder characterized by involuntary muscle contractions resulting in abnormal postures. These movements may
Pallidal Deep Brain Stimulation Treatment for Dystonia Dystonia Dystonia is a neurological disorder characterized by involuntary muscle contractions resulting in abnormal postures. These movements may
1.1. Parkinson disease
 1.TREMOR 1.1. Parkinson disease Parkinson Disease Progressive disorder: tremor, rigidity, and slowness of movements Neuronal loss of the substantia nigra Non motor features (dementia and dysautonomia),
1.TREMOR 1.1. Parkinson disease Parkinson Disease Progressive disorder: tremor, rigidity, and slowness of movements Neuronal loss of the substantia nigra Non motor features (dementia and dysautonomia),
Clinical aspects of pterin disorders
 Clinical aspects of pterin disorders Thomas Opladen, MD University Children s Hospital Department of Inborn Errors of Metabolism Heidelberg Germany Introductory words Brain function depends on the capacity
Clinical aspects of pterin disorders Thomas Opladen, MD University Children s Hospital Department of Inborn Errors of Metabolism Heidelberg Germany Introductory words Brain function depends on the capacity
ORIGINAL CONTRIBUTION. Subthalamic Stimulation in Parkinson Disease
 Subthalamic Stimulation in Parkinson Disease A Multidisciplinary Approach ORIGINAL CONTRIBUTION J. L. Houeto, MD; P. Damier, MD, PhD; P. B. Bejjani, MD; C. Staedler, MD; A. M. Bonnet, MD; I. Arnulf, MD;
Subthalamic Stimulation in Parkinson Disease A Multidisciplinary Approach ORIGINAL CONTRIBUTION J. L. Houeto, MD; P. Damier, MD, PhD; P. B. Bejjani, MD; C. Staedler, MD; A. M. Bonnet, MD; I. Arnulf, MD;
static encephalopathy of childhood with neurodegeneration in adulthood
 De novo mutations in the autophagy gene encoding WDR45 cause static encephalopathy of childhood with neurodegeneration in adulthood Hirotomo Saitsu, Taki Nishimura, Kazuhiro Muramatsu, Hirofumi Kodera,
De novo mutations in the autophagy gene encoding WDR45 cause static encephalopathy of childhood with neurodegeneration in adulthood Hirotomo Saitsu, Taki Nishimura, Kazuhiro Muramatsu, Hirofumi Kodera,
Clinical, imaging, and molecular findings in a sample of Mexican families with pantothenate kinase-associated neurodegeneration
 Clin Genet 2015: 87: 259 265 Printed in Singapore. All rights reserved Short Report 2014 John Wiley & Sons A/S. Published by John Wiley & Sons Ltd CLINICAL GENETICS doi: 10.1111/cge.12400 Clinical, imaging,
Clin Genet 2015: 87: 259 265 Printed in Singapore. All rights reserved Short Report 2014 John Wiley & Sons A/S. Published by John Wiley & Sons Ltd CLINICAL GENETICS doi: 10.1111/cge.12400 Clinical, imaging,
Case Report Neuropsychiatric Outcome of an Adolescent Who Received Deep Brain Stimulation for Tourette s Syndrome
 Case Reports in Neurological Medicine Volume 2011, Article ID 209467, 4 pages doi:10.1155/2011/209467 Case Report Neuropsychiatric Outcome of an Adolescent Who Received Deep Brain Stimulation for Tourette
Case Reports in Neurological Medicine Volume 2011, Article ID 209467, 4 pages doi:10.1155/2011/209467 Case Report Neuropsychiatric Outcome of an Adolescent Who Received Deep Brain Stimulation for Tourette
Dystonia and Brain Iron Accumulation
 Dystonia and Brain Iron Accumulation Introduction An Overview of the Current Understanding, Diagnosis and Treatment of Neurodegeneration with Brain Iron Accumulation The term dystonia describes the disordered
Dystonia and Brain Iron Accumulation Introduction An Overview of the Current Understanding, Diagnosis and Treatment of Neurodegeneration with Brain Iron Accumulation The term dystonia describes the disordered
Basal Ganglia. Today s lecture is about Basal Ganglia and it covers:
 Basal Ganglia Motor system is complex interaction between Lower motor neurons (spinal cord and brainstem circuits) and Upper motor neurons (pyramidal and extrapyramidal tracts) plus two main regulators
Basal Ganglia Motor system is complex interaction between Lower motor neurons (spinal cord and brainstem circuits) and Upper motor neurons (pyramidal and extrapyramidal tracts) plus two main regulators
Basal Ganglia George R. Leichnetz, Ph.D.
 Basal Ganglia George R. Leichnetz, Ph.D. OBJECTIVES 1. To understand the brain structures which constitute the basal ganglia, and their interconnections 2. To understand the consequences (clinical manifestations)
Basal Ganglia George R. Leichnetz, Ph.D. OBJECTIVES 1. To understand the brain structures which constitute the basal ganglia, and their interconnections 2. To understand the consequences (clinical manifestations)
Pathogenesis of Degenerative Diseases and Dementias. D r. Ali Eltayb ( U. of Omdurman. I ). M. Path (U. of Alexandria)
 Pathogenesis of Degenerative Diseases and Dementias D r. Ali Eltayb ( U. of Omdurman. I ). M. Path (U. of Alexandria) Dementias Defined: as the development of memory impairment and other cognitive deficits
Pathogenesis of Degenerative Diseases and Dementias D r. Ali Eltayb ( U. of Omdurman. I ). M. Path (U. of Alexandria) Dementias Defined: as the development of memory impairment and other cognitive deficits
ORIGINAL CONTRIBUTION
 ORIGINAL CONTRIBUTION Common Misdiagnosis of a Common Neurological Disorder How Are We Misdiagnosing Essential Tremor? Samay Jain, MD; Steven E. Lo, MD; Elan D. Louis, MD, MS Background: As a common neurological
ORIGINAL CONTRIBUTION Common Misdiagnosis of a Common Neurological Disorder How Are We Misdiagnosing Essential Tremor? Samay Jain, MD; Steven E. Lo, MD; Elan D. Louis, MD, MS Background: As a common neurological
Surgical Treatment for Movement Disorders
 Surgical Treatment for Movement Disorders Seth F Oliveria, MD PhD The Oregon Clinic Neurosurgery Director of Functional Neurosurgery: Providence Brain and Spine Institute Portland, OR Providence St Vincent
Surgical Treatment for Movement Disorders Seth F Oliveria, MD PhD The Oregon Clinic Neurosurgery Director of Functional Neurosurgery: Providence Brain and Spine Institute Portland, OR Providence St Vincent
Involuntary Movements in Children and Adolescents: Is it Seizure, Tic or Something Else?
 Involuntary Movements in Children and Adolescents: Is it Seizure, Tic or Something Else? California Association of Nurse Practitioners Monterey, March 22, 2013 Julie Sprague-McRae, MS, RN, PPCNP-BC Ruth
Involuntary Movements in Children and Adolescents: Is it Seizure, Tic or Something Else? California Association of Nurse Practitioners Monterey, March 22, 2013 Julie Sprague-McRae, MS, RN, PPCNP-BC Ruth
Parkinson Disease. Lorraine Kalia, MD, PhD, FRCPC. Presented by: Ontario s Geriatric Steering Committee
 Parkinson Disease Lorraine Kalia, MD, PhD, FRCPC Key Learnings Parkinson Disease (L. Kalia) Key Learnings Parkinson disease is the most common but not the only cause of parkinsonism Parkinson disease is
Parkinson Disease Lorraine Kalia, MD, PhD, FRCPC Key Learnings Parkinson Disease (L. Kalia) Key Learnings Parkinson disease is the most common but not the only cause of parkinsonism Parkinson disease is
Tremor. Mario Zappia. Università degli Studi di Catania
 Tremor Mario Zappia Università degli Studi di Catania Tremor: Definition Rhythmical, Involuntary, Oscillatory movement of a body part Classification of Dyskinesias Based on Rhythmicity Rhythmical Dyskinesias:
Tremor Mario Zappia Università degli Studi di Catania Tremor: Definition Rhythmical, Involuntary, Oscillatory movement of a body part Classification of Dyskinesias Based on Rhythmicity Rhythmical Dyskinesias:
Citation for published version (APA): Contarino, M. F. (2013). Improving surgical treatment for movement disorders
 UvA-DARE (Digital Academic Repository) Improving surgical treatment for movement disorders Contarino, M.F. Link to publication Citation for published version (APA): Contarino, M. F. (2013). Improving surgical
UvA-DARE (Digital Academic Repository) Improving surgical treatment for movement disorders Contarino, M.F. Link to publication Citation for published version (APA): Contarino, M. F. (2013). Improving surgical
DEEP BRAIN STIMULATION
 DEEP BRAIN STIMULATION Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices and drugs
DEEP BRAIN STIMULATION Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices and drugs
Transcranial sonography in movement disorders
 Transcranial sonography in movement disorders Uwe Walter 1st Residential Training of the European Society of Neurosonology and Cerebral Hemodynamics September 7-12, 2008 Bertinoro, Italy Department of
Transcranial sonography in movement disorders Uwe Walter 1st Residential Training of the European Society of Neurosonology and Cerebral Hemodynamics September 7-12, 2008 Bertinoro, Italy Department of
MODULE 6: CEREBELLUM AND BASAL GANGLIA
 MODULE 6: CEREBELLUM AND BASAL GANGLIA This module will summarize the important neuroanatomical and key clinical concepts from Chapters 15 and 16 of the textbook for the course. The first part of this
MODULE 6: CEREBELLUM AND BASAL GANGLIA This module will summarize the important neuroanatomical and key clinical concepts from Chapters 15 and 16 of the textbook for the course. The first part of this
Voluntary Movement. Ch. 14: Supplemental Images
 Voluntary Movement Ch. 14: Supplemental Images Skeletal Motor Unit: The basics Upper motor neuron: Neurons that supply input to lower motor neurons. Lower motor neuron: neuron that innervates muscles,
Voluntary Movement Ch. 14: Supplemental Images Skeletal Motor Unit: The basics Upper motor neuron: Neurons that supply input to lower motor neurons. Lower motor neuron: neuron that innervates muscles,
Parkinson disease: Parkinson Disease
 Surgical Surgical treatment treatment for for Parkinson disease: Parkinson Disease the Present and the Future the Present and the Future Olga Klepitskaya, MD Associate Professor of Neurology Co-Director,
Surgical Surgical treatment treatment for for Parkinson disease: Parkinson Disease the Present and the Future the Present and the Future Olga Klepitskaya, MD Associate Professor of Neurology Co-Director,
Deep Brain Stimulation: Surgical Process
 Deep Brain Stimulation: Surgical Process Kia Shahlaie, MD, PhD Assistant Professor Bronte Endowed Chair in Epilepsy Research Director of Functional Neurosurgery Minimally Invasive Neurosurgery Department
Deep Brain Stimulation: Surgical Process Kia Shahlaie, MD, PhD Assistant Professor Bronte Endowed Chair in Epilepsy Research Director of Functional Neurosurgery Minimally Invasive Neurosurgery Department
Deep brain stimulation: What can patients expect from it?
 MEDICAL GRAND ROUNDS ANDRE MACHADO, MD, PhD* Director, Center for Neurological Restoration, Neurological Institute, Cleveland Clinic HUBERT H. FERNANDEZ, MD Section Head, Movement Disorders, Center for
MEDICAL GRAND ROUNDS ANDRE MACHADO, MD, PhD* Director, Center for Neurological Restoration, Neurological Institute, Cleveland Clinic HUBERT H. FERNANDEZ, MD Section Head, Movement Disorders, Center for
Basal nuclei, cerebellum and movement
 Basal nuclei, cerebellum and movement MSTN121 - Neurophysiology Session 9 Department of Myotherapy Basal Nuclei (Ganglia) Basal Nuclei (Ganglia) Role: Predict the effects of various actions, then make
Basal nuclei, cerebellum and movement MSTN121 - Neurophysiology Session 9 Department of Myotherapy Basal Nuclei (Ganglia) Basal Nuclei (Ganglia) Role: Predict the effects of various actions, then make
THE CLINICAL USE OF BOTULINUM TOXIN IN THE TREATMENT OF MOVEMENT DISORDERS, SPASTICITY, AND SOFT TISSUE PAIN
 THE CLINICAL USE OF BOTULINUM TOXIN IN THE TREATMENT OF MOVEMENT DISORDERS, SPASTICITY, AND SOFT TISSUE PAIN Spasmodic torticollis (cervical dystonia), blepharospasm, and writer s cramp are specific types
THE CLINICAL USE OF BOTULINUM TOXIN IN THE TREATMENT OF MOVEMENT DISORDERS, SPASTICITY, AND SOFT TISSUE PAIN Spasmodic torticollis (cervical dystonia), blepharospasm, and writer s cramp are specific types
Indications. DBS for Tremor. What is the PSA? 6/08/2014. Tremor. 1. Tremor. 2. Gait freezing/postural instability. 3. Motor fluctuations
 Indications Deep brain stimulation for Parkinson s disease A Tailored Approach 1. Tremor 2. Gait freezing/postural instability Wesley Thevathasan FRACP DPhil.Oxf 3. Motor fluctuations Consultant Neurologist,
Indications Deep brain stimulation for Parkinson s disease A Tailored Approach 1. Tremor 2. Gait freezing/postural instability Wesley Thevathasan FRACP DPhil.Oxf 3. Motor fluctuations Consultant Neurologist,
Deep brain stimulation in movement disorders: stereotactic coregistration of two-dimensional electrical field modeling and magnetic resonance imaging
 J Neurosurg 103:949 955, 2005 Deep brain stimulation in movement disorders: stereotactic coregistration of two-dimensional electrical field modeling and magnetic resonance imaging SIMONE HEMM, PH.D, GÉRARD
J Neurosurg 103:949 955, 2005 Deep brain stimulation in movement disorders: stereotactic coregistration of two-dimensional electrical field modeling and magnetic resonance imaging SIMONE HEMM, PH.D, GÉRARD
