Critical Evaluation of Chemical Neurolysis of the Sympathetic Axis for Cancer Pain
|
|
|
- Dorothy Burns
- 6 years ago
- Views:
Transcription
1 Neurolysis of the sympathetic nervous system can be effective in managing cancer-related visceral pain. Frank Wright. The Canoe Builders, Oil on canvas. Courtesy of Auckland Art Gallery Toi o Tamaki, presented by Mr. C. J. Parr, Critical Evaluation of Chemical Neurolysis of the Sympathetic Axis for Cancer Pain Oscar A. de Leon-Casasola, MD Background: Patients with pain caused by cancer frequently experience visceral pain. In addition to oral pharmacologic therapy to manage pain, neurolytic blocks of the sympathetic axis are also effective in controlling visceral cancer pain. Methods: Four types of neurolytic blocks (interpleural phenol, celiac plexus, superior hypogastric plexus, and ganglion impar) used in the treatment of visceral cancer pain are reviewed. Results: Several studies have documented the efficacy of neurolytic blocks in reducing pain intensity and opioid consumption. However, the narrow risk-benefit ratio associated with neurolysis techniques requires knowledge of the implications associated with the different neurolytic blocks to minimize undesirable effects. Conclusions: Neurolysis of the sympathetic axis has been shown to be an effective and safe approach to treat visceral pain in cancer patients and should be incorporated in the armamentarium of the pain specialist as a useful adjunct to oral pharmacologic therapy. Introduction Pain associated with cancer may be somatic, visceral, or neuropathic in origin. Approximately 50% of cancer patients experience a combination of pain types at the time of diagnosis. Stretching, compressing, From the Department of Anesthesiology, Roswell Park Cancer Institute, Buffalo, NY. Address reprint requests to Oscar A. de Leon-Casasola, MD, Department of Anesthesiology, SUNY-Buffalo, School of Medicine, Roswell Park Cancer Institute, Elm and Carlton Streets, Buffalo, NY No significant relationship exists between the author and the companies/organizations whose products or services may be referenced in this article. invading, or distending visceral structures can result in a poorly localized noxious pain. Patients experiencing visceral pain often describe the pain as vague, deep, squeezing, crampy, or colicky. Other signs and symptoms include referred pain (eg, shoulder pain that appears when the diaphragm is invaded with tumor) and nausea/vomiting due to vagal irritation. Visceral pain associated with cancer may be relieved with oral pharmacologic therapy that includes combinations of nonsteroidal anti-inflammatory drugs (NSAIDs), opioids, and coadjuvant therapy. In addition to pharmacologic therapy, neurolytic blocks of the sympathetic axis are also effective in controlling visceral cancer pain and should be considered as impor- 142 Cancer Control
2 tant adjuncts to pharmacologic therapy for the relief of severe pain experienced by cancer patients. These blocks rarely eliminate cancer pain because patients frequently experience coexisting somatic and neuropathic pain as well. Therefore,oral pharmacologic therapy must be continued, albeit at lower doses. The goals of performing a neurolytic block of the sympathetic axis are to maximize the analgesic effects of opioid or nonopioid analgesics and reduce the dosage of these agents to alleviate side effects. Since neurolysis techniques have a narrow risk-benefit ratio, undesirable effects due to neurolytic blocks can be minimized with sound clinical judgment and by assessing the probable effect of the technique on each patient. A detailed description of the techniques for these blocks is beyond the scope of this review but is available elsewhere. 1 This report describes several different approaches to achieve neurolysis, including the interpleural phenol block, celiac plexus block, superior hypogastric block, and ganglion impar block. Interpleural Phenol Block The role of interpleural analgesia in both acute and chronic pain management is still undergoing clinical scrutiny. Original work with this technique showed that interpleural analgesia could provide analgesia in patients with subcostal incisions and fractured ribs. 2,3 Inserting an interpleural catheter is a relatively easy technique, and an epidural tray can be utilized. Local anesthetics (0.5% bupivacaine or 2% lidocaine) traditionally have been used via intermittent bolus or a continuous infusion. Recently, interpleural phenol therapy has been described as an alternative for the treatment of visceral pain associated with esophageal cancer. 4 Unpublished data suggest that this may be an effective technique to treat visceral pain associated with cancer of the esophagus, liver, biliary tree, stomach and pancreas. A multicenter study is under way to determine the efficacy of this block in the treatment of pain associated with the above-mentioned malignancies (H. Silva, MD, and R. Plancarte, MD, personal communication, 1999). Drugs and Dosing For neurolytic blocks, increased concentrations of phenol are recommended. Since patients with cancer of the esophagus or the chest wall frequently have pleural effusions, several injections through a catheter are indicated. Initially, 10 ml of 6% phenol is recommended. A subsequent progressive increase in concentration of up to 10% is encouraged, depending on the results, because the pleural effusion acts as a diluting agent. However, further experience with patients with pleural effusions suggests that 5 to 10 ml of 6% phenol may render adequate results (H. Silva, MD, and R. Plancarte, MD, personal communication, 1999). Fig 1. Anteroposterior view of a patient with Chiba needles placed to perform a splanchnic nerve neurolysis. Note the contrast medium distribution. The black arrows demonstrate the needles, and the open arrows indicate the contrast medium. Fig 2. Lateral view of a patient with Chiba needles placed for a splanchnic nerve neurolysis. The black arrows demonstrate the needles, and the open arrows indicate the contrast medium. Cancer Control 143
3 For analgesia associated with cancer, a continuous infusion of 0.25% to 0.375% of bupivacaine (8 to 10 ml/hr) or intermittent bolus doses of 0.5% of bupivacaine (10 to 15 ml every 8 hours) also provide adequate analgesia. However, if the high concentration of bupivacaine is chosen, the risk of toxicity increases. Thus, a regimen of 0.375% to 0.5% of ropivacaine for a continuous infusion and 0.5% of ropivacaine (10 to 15 ml every 8 hours) is a better choice for patients who need higher doses of bupivacaine. Complications Complications from this procedure can be divided into two categories those produced by traumatic injuries caused by the needle or the catheter and those produced by the neurolytic agent injected in the interpleural space. Pneumothorax may occur in 2% of the patients, and lung injuries have been reported when a rigid catheter is used. 5 Phrenic nerve palsy resulting in respiratory failure may also occur following this block. Therefore, bilateral blocks should be avoided. Systemic effects from drug absorption may also occur since the pleural membranes are highly vascularized. Thus, at our center, doses of phenol are limited to 10 ml of a 10% solution. Efficacy No outcome information is available to determine the efficacy of this block for the treatment of visceral pain. Literature describing experience with this block is limited to a case report, 4 and the effects in a large population have not been reported. Celiac Plexus Block The celiac plexus is situated retroperitoneally in the upper abdomen. It is at the level of the T12 and L1 vertebrae, anterior to the crura of the diaphragm. The celiac plexus surrounds the abdominal aorta and the celiac and superior mesenteric arteries. The plexus is composed of a network of nerve fibers, from both the sympathetic and the parasympathetic systems. It contains two large ganglia that receive sympathetic fibers from the three splanchnic nerves (greater, lesser, and least). The plexus also receives parasympathetic fibers from the vagus nerve. Autonomic nerves supplying to the liver, pancreas, gallbladder, stomach, spleen, kidneys, intestines, and adrenal glands, as well as blood vessels, arise in the celiac plexus. Neurolytic blocks of the celiac plexus have been used for malignant and chronic nonmalignant pain. In patients with acute or chronic pancreatitis, the celiac plexus block has been used with significant success. 6 Likewise, patients with cancer in the upper abdomen who have a significant visceral pain component have responded well to this block. 7 Three approaches to block nociceptive impulses from the viscera of the upper abdomen include the retrocrural (or classic) approach, the anterocrural approach, and neurolysis of the splanchnic nerves. With all of these approaches, the needles are inserted at the level of the first lumbar vertebra,5 to 7 cm from the midline. Then, the tip of the needle is directed towards the body of L-1 for the retrocrural and anterocrural approaches and to the body of T-12 for neurolysis of the splanchnic nerves. Figs 1-2 illustrate the final position of the needles and the expected spread of contrast medium after successful placement. More recently, computed tomography and ultrasound techniques have allowed pain specialists to perform neurolysis of the celiac plexus via a transabdominal approach. This approach is frequently used when patients are unable to tolerate either the prone or lateral decubitus position or when their liver is so enlarged that a posterior approach is not feasible. Drugs and Dosing For neurolytic blocks, 50% to 100% alcohol, 20 ml per side, is used. Injected by itself, alcohol can produce severe pain. Thus, it is recommended to first inject 5 to 10 ml of 0.25% bupivacaine 5 minutes prior to the injection of alcohol or to dilute 100% alcohol by 50% with local anesthetic (0.25% bupivacaine). Phenol in a 10% final concentration may also be used; this has the advantage of being painless on injection. Both agents seem to have the same efficacy. Complications Complications associated with celiac plexus blocks appear to be related to the technique used: retrocrural, 8 transcrural, 9 or transaortic. 10 In a prospective, randomized study of 61 patients with cancer of the pancreas, Ischia et al 7 compared the efficacy and incidence of complications associated with these three approaches to celiac plexus neurolysis. Orthostatic hypotension occurred more often when the retrocrural (50%) or splanchnic (52%) technique was used than when the anterocrural approach (10%) was used. In contrast,transient diarrhea was more frequent with the anterocrural approach (65%) than with the splanchnic nerve block technique (5%) but not the retrocrural approach (25%). The incidence of dysesthesia, interscapular back pain, reactive pleurisy, hiccups, or hematuria was not statistically different among the three groups. 144 Cancer Control
4 The incidence of complications from neurolytic celiac plexus blocks was recently determined by Davis 11 in 2,730 patients having blocks performed from 1986 to The overall incidence of major complications (eg, paraplegia, bladder, and bowel dysfunction) was 1 in 683 procedures. However, the report does not describe which approach or approaches were used to perform the blocks. Following are several aspects in the diagnosis and management of specific complications. Malposition of the needle is avoided with radiologic imaging prior to the injection of a neurolytic agent, as the tip of the needle may be intravascular, in the peritoneal cavity, or in a viscus. Imaging techniques currently used include biplanar fluoroscopy, computed tomography, or ultrasound guidance. However, no study has evaluated the superiority of one technique over the others. Wong and Brown 12 suggest that the use of radiologic imaging does not alter the quality of the block or the incidence of complications based on a retrospective study of 136 patients with pancreatic cancer pain treated with a celiac plexus block with or without radiologic control of the position of the needle s tip. However, it is not clear how many of those patients had radiologic imaging. Assuming that half of the patients did not,the upper 95% confidence limit for complications is 5%. 13 Orthostatic hypotension may occur up to 5 days after the block in 1% to 3% of patients. Treatment includes resting in bed, avoiding sudden changes in position, and replacing fluids. Once compensatory vascular reflexes are fully activated, this side effect disappears. Wrapping the lower extremities from the toes to the upper thighs with elastic bandages has been successful in patients who developed orthostatic hypotension and thus needed to walk during the first week after the block. Backache may result from local trauma during the needle placement resulting in a retroperitoneal hematoma,from alcohol irritation of the retroperitoneal structures, or from injury to the lumbar plexus. Patients with a backache should have at least two hematocrit measurements at a 1-hour interval. If there is a decrease in the hematocrit, radiologic imaging is indicated to rule out a retroperitoneal hematoma. A urine analysis positive for red blood cells suggests renal injury. Retroperitoneal hemorrhage is rare; however, in patients who present with orthostatic hypotension, the possibility of hemorrhage must be ruled out before assuming that it is a physiologic response to the block. Patients who present with backache and orthostatic hypotension after a celiac plexus block should be admitted to the hospital for serial hematocrit monitoring. If the hematocrit level is low or decreasing, patients should undergo radiologic evaluation to rule out injury to the kidneys, the aorta, or other vascular structures. A surgical consult should be obtained as soon as feasible. Diarrhea may occur due to the sympathetic block of the bowel. Treatment includes hydration and antidiarrheal agents. Oral loperamide is a good choice, although any anticholinergic agent may be used. Matson and colleagues 14 reported near-fatal dehydration from diarrhea following this block. In debilitated patients, diarrhea must be treated aggressively. Abdominal aortic dissection has also been reported. 15,16 The mechanism of aortic injury is direct damage with the needle during the performance of the block. As expected, the anterocrural approach is more frequently associated with this complication. Thus, this approach should be avoided if atherosclerotic disease of the abdominal aorta is present. Paraplegia and transient motor paralysis have occurred after celiac plexus block These neurologic complications may occur due to a spasm of the lumbar segmental arteries that perfuse the spinal cord. 23 In fact, canine lumbar arteries undergo contraction when exposed to low concentrations of alcohol. 24 Thus, empirical data suggest that alcohol should not be used if there is evidence of significant atherosclerotic disease of the aorta, suggesting that the circulation to the spinal cord may also be impaired. However,there is also a report of paraplegia after phenol use, 17 thus suggesting that other factors (eg,direct vascular or neurologic injury or retrograde spread to the spinal cord) may come into play. These complications further support the use of radiologic imaging during the performance of the block. Efficacy To date, only two randomized, controlled trials 7,25 and one prospective study 26 have evaluated the efficacy of celiac plexus neurolysis in pain due to cancer of the upper abdomen. In a prospective, randomized study, Ischia et al 7 evaluated the efficacy of three different approaches to celiac plexus neurolysis in pancreatic cancer. Of 61 patients with pancreatic cancer pain, 29 (48%) experienced complete pain relief after the neurolytic block. The remaining 32 patients (52%) required further therapy for residual visceral pain due to technical failure in 15 patients and neuropathic/somatic pains in 17 patients. The second trial, 25 which compared the procedure with oral pharmaco- Cancer Control 145
5 logic therapy in 20 patients, concluded that celiac plexus neurolysis resulted in an equal reduction in visual analog pain score (VAPS) as therapy with a combination of NSAIDs and opioids. However, opioid consumption was significantly lower in the group of patients who underwent neurolysis when compared to the group receiving oral pharmacologic therapy during the 7 weeks of the study. Moreover, the incidence of side effects was greater in patients who received oral pharmacologic therapy when compared to those who underwent neurolysis block. The prospective, nonrandomized study 26 compared 41 patients treated according to the World Health Organization (WHO) guidelines for cancer pain relief with 21 patients treated with a neurolytic celiac plexus block. The authors concluded that this technique can play an important role in managing pancreatic cancer pain. Since one of the two studies that used a randomized, controlled design compared different approaches to the celiac plexus and had no control group 7 and the other study compared the procedure with an analgesic drug, 25 it is not possible to estimate the success rate of this technique. In contrast, the results of a meta-analysis that evaluated the results of 21 retrospective studies in 1,145 patients concluded that adequate to excellent pain relief can be achieved in 89% of the patients during the first two weeks following the block. 27 Partial to complete pain relief continued in approximately 90% of the patients who were alive at the 3-month interval and in 70% to 90% of the patients during the 3-month interval before death. Moreover, the efficacy was similar in patients with pancreatic cancer than in those with other intra-abdominal malignancies of the upper abdomen. However, these results are based on retrospective evaluations that may not yield reliable information or may be subject to publication bias. In addition, statistical techniques used for the analysis must account for the heterogeneity produced by the patients selection criteria, technical differences in the performance of the blocks, choice of neurolytic agents and doses, diversity in the tools for the evaluation of pain, goals of therapy, etc. Thus, the meta-analysis must be interpreted with caution as the reports may be overly enthusiastic. As previously discussed, oral pharmacologic therapy with opioids, NSAIDs, and coadjuvants is frequently used for the treatment of cancer pain. However, evidence suggests that chronic use of high doses of opioids may have a negative effect on immunity. 28 Thus, analgesic techniques that lower opioid consumption may have a positive effect on patient outcomes. Lillemoe and colleagues 29 showed in a prospective, randomized trial that patients with nonresectable cancer of the pancreas who received a splanchnic neurolysis lived longer than patients who did not. These findings may be the result of lower opioid use in the neurolysis patients who not only had better-preserved immune functions, but also experienced fewer side effects (eg, nausea and vomiting), thus allowing them to eat better. This hypothesis is currently being tested in a prospective, randomized trial. Superior Hypogastric Plexus Block Cancer patients with tumor extension into the pelvis may experience severe pain that is unresponsive to oral or parenteral opioids. Also, excessive sedation or other side effects may limit the acceptability and usefulness of oral opioid therapy. Therefore, a more invasive approach is needed to control pain and improve the quality of life of these patients. Pelvic pain associated with cancer and chronic nonmalignant conditions may be alleviated by blocking the superior hypogastric plexus Analgesia to the organs in the pelvis is possible because the afferent fibers innervating these structures travel in the sympathetic nerves, trunks, ganglia, and rami. Thus, a sympathectomy for visceral pain is analogous to a peripheral neurectomy or dorsal rhizotomy for somat- New Perspectives Fig 3. Anteroposterior view showing adequate needle placement (black arrows) and contrast medium spread (open arrow) for neurolysis of the superior hypogastric plexus. 146 Cancer Control
6 ic pain. A recent study 31 suggests that visceral pain is an important component of the cancer pain syndrome experienced by patients with cancer of the pelvis, even in advanced stages. Thus, percutaneous neurolytic blocks of the superior hypogastric plexus should be considered more often for patients with advanced stages of pelvic cancer. The superior hypogastric plexus is situated in the retroperitoneum, bilaterally extending from the lower third of the fifth lumbar vertebral body to the upper third of the first sacral vertebral body. The technique for the blockade has been described elsewhere Fig 3 shows adequate needle placement and contrast medium spread prior to neurolysis of the superior hypogastric plexus. Complications The combined experience of more than 200 cases from the Mexican Institute of Cancer,Roswell Park Cancer Institute, and M.D. Anderson Cancer Center indicates that neurologic complications do not occur as a result of this block. 32 Efficacy The effectiveness of the block was originally demonstrated by documenting a significant decrease in pain via VAPS scores. In this study, Plancarte et al 30 showed that this block was effective in reducing VAPS scores in 70% of the patients with pelvic pain associated with cancer. The majority of the enrolled patients had cervical cancer. In a subsequent study, 69% of the patients experienced a decrease in VAPS scores. Moreover, a mean daily opioid morphine reduction of 67% was seen in the success group (736 ± 633 reduced to 251 ± 191 mg/day), and 45% in the failure group (1,443 ± 703 reduced to 800 ± 345 mg/day). 31 In a more recent multicentric study, 159 patients with pelvic pain associated with cancer were evaluated. Overall, 115 patients (72%) had satisfactory pain relief after one or two neurolytic procedures. Mean opioid use decreased by 40% from 58 ± 43 reduced to 35 ± 18 equianalgesic mg/day of morphine 3 weeks after treatment in all the studied patients. This decrease in opioid consumption was significant for both the success group (56 ± 32 reduced to 32 ± 16 mg/day) and the failure group (65 ± 28 reduced to 48 ± 21 mg/day). 32 Success was defined in these two studies as the ability to reduce opioid consumption by at least 50% in the 3 weeks following the block and a decrease in the pain scores below 4/10 in the VAPS scores. 32,33 In a recent case report, Rosenberg and colleagues 33 reported on the efficacy of this block in a patient with severe chronic nonmalignant penile pain after transurethral resection of the prostate. Although the patient did not receive a neurolytic agent, a diagnostic block performed with 0.25% bupivacaine and 20 mg of methylprednisolone acetate was effective in relieving the pain for more than 6 months. The usefulness of this block in chronic benign pain conditions has not been adequately documented. Fig 4. Anteroposterior view of the pelvis showing contrast medium distribution (arrow) prior to ganglion impar neurolysis. Fig 5. Lateral view of the same patient in Fig 4. Cancer Control 147
7 Ganglion Impar Block The ganglion impar is a solitary retroperitoneal structure located at the level of the sacrococcygeal junction. This unpaired ganglion marks the end of the two sympathetic chains. Visceral pain in the perineal area associated with malignancies may be effectively treated with neurolysis of the ganglion impar (Walther s). 34 Patients who will benefit from this block frequently present with a vague, poorly localized pain that is frequently accompanied by sensations of burning and urgency. However, the clinical value of this block is not clear as the published experienced is limited. This block may be performed with the patient in the left lateral decubitus position with the knees flexed, in the lithotomy position, or in the prone position. The easiest approach is with the patient in the prone position,where a 20-g 1.5-inch needle is inserted through the sacrococcygeal ligament in the midline. The needle is then advanced until the tip is placed posterior to the rectum. Figs 4-5 illustrate adequate needle placement and contrast medium spread. No complications have been reported with this block. Conclusions Neurolysis of the sympathetic axis appears to be a safe, cost-effective approach to treating visceral pain associated with cancer. The benefits include improved analgesia, reduced opioid consumption, favorable economic implications, and superior clinical effects due to the deleterious properties of high-dose chronic opioid therapy. Current knowledge and techniques to perform these blocks allow these procedures to be performed safely and expeditiously. Pain practitioners should consider the role of these blocks in adjuvant therapy for the optimal treatment of cancer pain. References 1. Regional anesthetic techniques for the management of cancer pain. In: Urmey W, ed. Techniques in Regional Anesthesia and Pain Management. Vol 1, No 1. Philadelphia, Pa: WB Saunders; Reiestad FL, Stromskag KE. Interpleural catheter in the management of postoperative pain: a preliminary report. Reg Anesth. 1986;11: Rocco A, Reiestad F, Gudman J, et al. Intrapleural administration of local anesthetics for pain relief in patients with multiple rib fractures: preliminary report. Reg Anesth. 1987;12: Lema MJ, Myers DP, de Leon-Casasola O, et al. Pleural phenol therapy for the treatment of chronic esophageal cancer pain. Reg Anesth. 1992;17: Stromskag KE, Reiestad F, Holmqvist EL, et al. Intrapleural administration of 0.25%, 0.375%, and 0.5% bupivacaine with epinephrine after cholecystectomy. Anesth Analg. 1988;67: Rykowski JJ, Hilgier M. Continuous celiac plexus block in acute pancreatitis. Reg Anesth. 1995;20: Ischia S, Ischia A, Polati E, et al. Three posterior percutaneous celiac plexus block techniques: a prospective randomized study in 61 patients with pancreatic cancer pain. Anesthesiology. 1992;76: Singler RC. An improved technique for alcohol neurolysis of the celiac plexus block. Anesthesiology. 1982;56: Hilgier M, Rykowski JJ. One needle transcrural celiac plexus block: single shot, or continuous technique, or both. Reg Anesth. 1994;19: Ischia S, Luzzani A, Ischia A, et al. A new approach to the neurolytic block of the coeliac plexus: the transaortic technique. Pain. 1983;16: Davis DD. Incidence of major complications of neurolytic coeliac plexus block. J Royal Soc Med. 1993;86: Wong GY,Brown DL. Celiac plexus block for cancer pain. In: Urmey W, ed. Techniques in Regional Anesthesia and Pain Management. Vol 1, No 1. Philadelphia, Pa: WB Saunders; Hanley JA, Lippman-Hand A. If nothing goes wrong, is everything all right? Interpreting zero numerators. JAMA. 1983;249: Matson JA, Ghia JN, Levy JH. A case report of a potentially fatal complications associated with Ischia s transaortic method of celiac plexus block. Reg Anesth. 1985;10: Sett SS,Taylor DC. Aortic pseudoaneurysm secondary to celiac plexus block. Ann Vasc Surg. 1991;5: Kaplan R, Schiff-Keren B,Alt E. Aortic dissection as a complication of celiac plexus block. Anesthesiology. 1995;83: Galizia EJ, Lahiri SK. Paraplegia following coeliac plexus block with phenol. Case report. Br J Anaesth. 1974;46: Lo JN,Buckley JJ. Spinal cord ischemia a complication of celiac plexus block. Reg Anesth. 1982;7: Cherry DA, Lamberty J. Paraplegia following coeliac plexus block. Anaesth Intensive Care. 1984;12: Woodham MJ, Hanna MH. Paraplegia after coeliac plexus block. Anaesthesia. 1989;44: van Dongen RT, Crul BJ. Paraplegia following coeliac plexus block. Anaesthesia. 1991;46: Jabbal SS, Hunton J. Reversible paraplegia following coeliac plexus block. Anaesthesia. 1992;47: Wong GY, Brown DL. Transient paraplegia following alcohol celiac plexus block. Reg Anesth. 1995;20: Brown DL, Rorie DK. Altered reactivity of isolated segmental lumbar arteries of dogs following exposure to ethano and phenol. Pain. 1994;56: Mercadante S. Celiac plexus block versus analgesics in pancreatic cancer pain. Pain. 1993;52: Ventafridda GV, Caraceni AT, Sbanotto AM, et al. Pain treatment in cancer of the pancreas. Eur J Surg Oncol. 1990;16: Eisenberg E, Carr DB, Chalmers TC. Neurolytic celiac plexus block for treatment of cancer pain: a meta-analysis. Anesth Analg. 1995;80: Yeager MP. Morphine inhibits spontaneous and cytokineenhanced natural killer cell cytotoxicity in volunteers. Anesthesiology. 1995;83: Lillemoe KD, Cameron JL, Kaufman HS, et al. Chemical splanchnicectomy in patients with unresectable pancreatic cancer: a prospective randomized trial. Ann Surg. 1993;217: Plancarte R, Amescua C, Patt RB, et al. Superior hypogastric plexus block for pelvic cancer pain. Anesthesiology. 1990;73: de Leon-Casasola OA, Kent E, Lema MJ. Neurolytic superior hypogastric plexus block for chronic pelvic pain associated with cancer. Pain. 1993;54: Plancarte R, de Leon-Casasola OA, El-Helaly M, et al. Neurolytic superior hypogastric plexus block for chronic pelvic pain associated with cancer. Reg Anesth. 1997;22: Rosenberg SK,Tewari R, Boswell MV, et al. Superior hypogastric plexus block successfully treats severe penile pain after transurethral resection of the prostate. Reg Anesth Pain Med. 1998;23: Plancarte R, Amescua C, Patt RB. Presacral blockade of the ganglion of Walther (ganglion impar). Anesthesiology. 1990;73:A Cancer Control
Celiac plexus block. Dr.Kasturi Bhagawati Asst.professor Dept. of Emergency Medicine & Critical care.
 Celiac plexus block Dr.Kasturi Bhagawati Asst.professor Dept. of Emergency Medicine & Critical care. Introduction A celiac plexus block is an injection of local anesthetic into or around the celiac plexus
Celiac plexus block Dr.Kasturi Bhagawati Asst.professor Dept. of Emergency Medicine & Critical care. Introduction A celiac plexus block is an injection of local anesthetic into or around the celiac plexus
nerve blocks in the diagnosis and therapy of visceral disease
 Visceral Pain nerve blocks in the diagnosis and therapy of visceral disease Guy Hans, MD, PhD Dept. of Anesthesiology, Multidisciplinary Pain Center Visceral Pain? Type of nociceptive pain (although often
Visceral Pain nerve blocks in the diagnosis and therapy of visceral disease Guy Hans, MD, PhD Dept. of Anesthesiology, Multidisciplinary Pain Center Visceral Pain? Type of nociceptive pain (although often
SYMPATHETIC BLOCKS AND THEIR ROLE IN MANAGEMENT AND DIAGNOSIS OF CHRONIC PAIN SYNDROMES
 SYMPATHETIC BLOCKS AND THEIR ROLE IN MANAGEMENT AND DIAGNOSIS OF CHRONIC PAIN SYNDROMES Overview Eugene Mitchell, MD Activity of the sympathetic efferents and their role in the pathology of chronic pain
SYMPATHETIC BLOCKS AND THEIR ROLE IN MANAGEMENT AND DIAGNOSIS OF CHRONIC PAIN SYNDROMES Overview Eugene Mitchell, MD Activity of the sympathetic efferents and their role in the pathology of chronic pain
[ANATOMY #12] April 28, 2013
![[ANATOMY #12] April 28, 2013 [ANATOMY #12] April 28, 2013](/thumbs/86/93473883.jpg) Sympathetic chain : Sympathetic chain is each of the pair of ganglionated longitudinal cords of the sympathetic nervous system; extend from level of atlas (base of skull) till coccyx. It is paravertebral
Sympathetic chain : Sympathetic chain is each of the pair of ganglionated longitudinal cords of the sympathetic nervous system; extend from level of atlas (base of skull) till coccyx. It is paravertebral
Increasing the Efficacy of a Celiac Plexus Block in Patients with Severe Pancreatic Cancer Pain
 966 Journal of Pain and Symptom Management Vol. 22 No. 5 November 2001 Original Article Increasing the Efficacy of a Celiac Plexus Block in Patients with Severe Pancreatic Cancer Pain Jan H. Vranken, MD,
966 Journal of Pain and Symptom Management Vol. 22 No. 5 November 2001 Original Article Increasing the Efficacy of a Celiac Plexus Block in Patients with Severe Pancreatic Cancer Pain Jan H. Vranken, MD,
Fig Glossopharyngeal nerve transmits signals to medulla oblongata. Integrating center. Receptor. Baroreceptors sense increased blood pressure
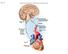 Fig. 5. Integrating center Glossopharyngeal nerve transmits signals to medulla oblongata Receptor 3 Vagus nerve transmits inhibitory signals to cardiac pacemaker Baroreceptors sense increased blood pressure
Fig. 5. Integrating center Glossopharyngeal nerve transmits signals to medulla oblongata Receptor 3 Vagus nerve transmits inhibitory signals to cardiac pacemaker Baroreceptors sense increased blood pressure
Computed Tomography (CT) Simulated Fluoroscopy-Guided Transdiscal Approach in Transcrural Celiac Plexus Block
 Brief Report Korean J Pain 2013 October; Vol. 26, No. 4: 396-400 pissn 2005-9159 eissn 2093-0569 http://dx.doi.org/10.3344/kjp.2013.26.4.396 Computed Tomography (CT) Simulated Fluoroscopy-Guided Transdiscal
Brief Report Korean J Pain 2013 October; Vol. 26, No. 4: 396-400 pissn 2005-9159 eissn 2093-0569 http://dx.doi.org/10.3344/kjp.2013.26.4.396 Computed Tomography (CT) Simulated Fluoroscopy-Guided Transdiscal
The Neurolytic Celiac Plexus Block Efficacy in Patients with Severe, Chronic Upper-abdominal Cancer Pain
 Original Article Cent Asian J Med Sci. 2016 May;2(1):76-82. The Neurolytic Celiac Plexus Block Efficacy in Patients with Severe, Chronic Upper-abdominal Cancer Pain Byambasuren Yondonjamts 1, Odontuya
Original Article Cent Asian J Med Sci. 2016 May;2(1):76-82. The Neurolytic Celiac Plexus Block Efficacy in Patients with Severe, Chronic Upper-abdominal Cancer Pain Byambasuren Yondonjamts 1, Odontuya
A New Technique for Superior Hypogastric Plexus Block: The Posteromedian Transdiscal Approach
 Tohoku J. Exp. Med., 2005, A New 206, Transdiscal 277-281Approach for Hypogastric Plexus Block 277 A New Technique for Superior Hypogastric Plexus Block: The Posteromedian Transdiscal Approach Case Report
Tohoku J. Exp. Med., 2005, A New 206, Transdiscal 277-281Approach for Hypogastric Plexus Block 277 A New Technique for Superior Hypogastric Plexus Block: The Posteromedian Transdiscal Approach Case Report
Types of blocks. Clinical considerations 8/11/2009. Let s Discuss Sympathetic Blocks. Stellate Celiac plexis Lumbar sympathetic Hypogastric
 Let s Discuss Sympathetic Blocks Janette Elliott, RN-BC, MSN, AOCN ASPMN 19 th Annual Conference September 2009 Types of blocks Stellate Celiac plexis Lumbar sympathetic Hypogastric Clinical considerations
Let s Discuss Sympathetic Blocks Janette Elliott, RN-BC, MSN, AOCN ASPMN 19 th Annual Conference September 2009 Types of blocks Stellate Celiac plexis Lumbar sympathetic Hypogastric Clinical considerations
CELIAC PLEXUS NEUROLYSIS WITH REPEATED AMMONIUM SULPHATE INJECTION FOR THE TREATMENT OF CHRONIC NON- CANCER ABDOMINAL PAIN UNDER CT SCAN GUIDANCE
 CELIAC PLEXUS NEUROLYSIS WITH REPEATED AMMONIUM SULPHATE INJECTION FOR THE TREATMENT OF CHRONIC NON- CANCER ABDOMINAL PAIN UNDER CT SCAN GUIDANCE By Eshaq AlShaqaq Clinical fellow Introduction Celiac Plexus
CELIAC PLEXUS NEUROLYSIS WITH REPEATED AMMONIUM SULPHATE INJECTION FOR THE TREATMENT OF CHRONIC NON- CANCER ABDOMINAL PAIN UNDER CT SCAN GUIDANCE By Eshaq AlShaqaq Clinical fellow Introduction Celiac Plexus
Organisation of the nervous system
 Chapter1 Organisation of the nervous system 1. Subdivisions of the nervous system The nervous system is divided: i) Structurally The central nervous system (CNS) composed of the brain and spinal cord.
Chapter1 Organisation of the nervous system 1. Subdivisions of the nervous system The nervous system is divided: i) Structurally The central nervous system (CNS) composed of the brain and spinal cord.
Nerves on the Posterior Abdominal Wall
 Nerves on the Posterior Abdominal Wall Lumbar Plexus The lumbar plexus, which is one of the main nervous pathways supplying the lower limb, is formed in the psoasmuscle from the anterior ramiof the upper
Nerves on the Posterior Abdominal Wall Lumbar Plexus The lumbar plexus, which is one of the main nervous pathways supplying the lower limb, is formed in the psoasmuscle from the anterior ramiof the upper
The Nervous System: Autonomic Nervous System
 17 The Nervous System: Autonomic Nervous System PowerPoint Lecture Presentations prepared by Steven Bassett Southeast Community College Lincoln, Nebraska Introduction The autonomic nervous system functions
17 The Nervous System: Autonomic Nervous System PowerPoint Lecture Presentations prepared by Steven Bassett Southeast Community College Lincoln, Nebraska Introduction The autonomic nervous system functions
Chapter 15: The Autonomic Nervous System. Copyright 2009, John Wiley & Sons, Inc.
 Chapter 15: The Autonomic Nervous System Comparison of Somatic and Autonomic Nervous Systems Comparison of Somatic and Autonomic Nervous Systems Anatomy of Autonomic Motor Pathways Preganglionic neuron
Chapter 15: The Autonomic Nervous System Comparison of Somatic and Autonomic Nervous Systems Comparison of Somatic and Autonomic Nervous Systems Anatomy of Autonomic Motor Pathways Preganglionic neuron
Sympathetic Nervous System
 Sympathetic Nervous System Lecture Objectives Review the subdivisions of the nervous system. Review the general arrangement and compare the sympathetic and parasympathetic parts. Describe the following
Sympathetic Nervous System Lecture Objectives Review the subdivisions of the nervous system. Review the general arrangement and compare the sympathetic and parasympathetic parts. Describe the following
Chapter 16. APR Enhanced Lecture Slides
 Chapter 16 APR Enhanced Lecture Slides See separate PowerPoint slides for all figures and tables pre-inserted into PowerPoint without notes and animations. Copyright The McGraw-Hill Companies, Inc. Permission
Chapter 16 APR Enhanced Lecture Slides See separate PowerPoint slides for all figures and tables pre-inserted into PowerPoint without notes and animations. Copyright The McGraw-Hill Companies, Inc. Permission
Interventional Techniques for Cancer Pain Management
 Interventional Techniques for Cancer Pain Management Musa M. Aner, MD Director, Cancer Pain Service Arnold Pain Management Center Beth Israel Deaconess Medical Center Disclosure No financial or industry
Interventional Techniques for Cancer Pain Management Musa M. Aner, MD Director, Cancer Pain Service Arnold Pain Management Center Beth Israel Deaconess Medical Center Disclosure No financial or industry
The Nervous System: Autonomic Nervous System Pearson Education, Inc.
 17 The Nervous System: Autonomic Nervous System Introduction The autonomic nervous system: Functions outside of our conscious awareness Makes routine adjustments in our body s systems The autonomic nervous
17 The Nervous System: Autonomic Nervous System Introduction The autonomic nervous system: Functions outside of our conscious awareness Makes routine adjustments in our body s systems The autonomic nervous
Ultrasound-Guided Superior Hypogastric Plexus Block: A Cadaveric Feasibility Study with Fluoroscopic Confirmation
 ORIGINAL ARTICLE Ultrasound-Guided Superior Hypogastric Plexus Block: A Cadaveric Feasibility Study with Fluoroscopic Confirmation Michael Gofeld, MD; Chuan-Whei Lee, MBChB Department of Anesthesia, St
ORIGINAL ARTICLE Ultrasound-Guided Superior Hypogastric Plexus Block: A Cadaveric Feasibility Study with Fluoroscopic Confirmation Michael Gofeld, MD; Chuan-Whei Lee, MBChB Department of Anesthesia, St
Group of students. - Rawan almujabili د. محمد المحتسب - 1 P a g e
 - 14 - Group of students - Rawan almujabili د. محمد المحتسب - 1 P a g e Nerves of the posterior abdominal wall The spinal cord gives off spinal nerves between the vertebrae. In the abdomen, through the
- 14 - Group of students - Rawan almujabili د. محمد المحتسب - 1 P a g e Nerves of the posterior abdominal wall The spinal cord gives off spinal nerves between the vertebrae. In the abdomen, through the
ANATOMY & PHYSIOLOGY - CLUTCH CH THE AUTONOMIC NERVOUS SYSTEM.
 !! www.clutchprep.com ANATOMY & PHYSIOLOGY - CLUTCH CONCEPT: THE AUTONOMIC NERVOUS SYSTEM: DIVISIONS AND STRUCTURE The Autonomic Nervous System and its Divisions: Autonomic Nervous System (ANS) controls
!! www.clutchprep.com ANATOMY & PHYSIOLOGY - CLUTCH CONCEPT: THE AUTONOMIC NERVOUS SYSTEM: DIVISIONS AND STRUCTURE The Autonomic Nervous System and its Divisions: Autonomic Nervous System (ANS) controls
14RC1-PERRUCHOUD Interventional management of cancer pain
 14RC1-PERRUCHOUD Interventional management of cancer pain Christophe Perruchoud Department of Anaesthesiology and Pain Management, University Hospital Centre and University of Lausanne, Lausanne Background
14RC1-PERRUCHOUD Interventional management of cancer pain Christophe Perruchoud Department of Anaesthesiology and Pain Management, University Hospital Centre and University of Lausanne, Lausanne Background
cardiac plexus is continuous with the coronary and no named branches pain from the heart and lungs
 Nerves of the Thoracic Region Nerve Source Branches Motor Sensory Notes cardiac plexus cardiac brs. of the vagus n. and cervical ; thoracic l nn. the heart and lungs cardiac, cervical cardiac, vagal vagus
Nerves of the Thoracic Region Nerve Source Branches Motor Sensory Notes cardiac plexus cardiac brs. of the vagus n. and cervical ; thoracic l nn. the heart and lungs cardiac, cervical cardiac, vagal vagus
Pain Management Clinic ISIC
 Pain Management Clinic ISIC Let us rebuild a pain free life Pain is one of the commonest symptoms in patients attending OPDs of various hospitals and clinics. Chronic pain is any pain that has persisted
Pain Management Clinic ISIC Let us rebuild a pain free life Pain is one of the commonest symptoms in patients attending OPDs of various hospitals and clinics. Chronic pain is any pain that has persisted
Human Anatomy. Autonomic Nervous System
 Human Anatomy Autonomic Nervous System 1 Autonomic Nervous System ANS complex system of nerves controls involuntary actions. Works with the somatic nervous system (SNS) regulates body organs maintains
Human Anatomy Autonomic Nervous System 1 Autonomic Nervous System ANS complex system of nerves controls involuntary actions. Works with the somatic nervous system (SNS) regulates body organs maintains
ParasymPathetic Nervous system. Done by : Zaid Al-Ghnaneem
 ParasymPathetic Nervous system Done by : Zaid Al-Ghnaneem In this lecture we are going to discuss Parasympathetic, in the last lecture we took sympathetic and one of the objectives of last lecture was
ParasymPathetic Nervous system Done by : Zaid Al-Ghnaneem In this lecture we are going to discuss Parasympathetic, in the last lecture we took sympathetic and one of the objectives of last lecture was
HBA 531 THE BODY. Trunk Examination September 30, What is the effect of the parasympathetic nervous system on: (2.5)
 HBA 531 THE BODY Trunk Examination September 30, 2013 Name: 1. What is the effect of the parasympathetic nervous system on: (2.5) a) Heart rate b) Male reproductive function c) Pylorus d) Internal anal
HBA 531 THE BODY Trunk Examination September 30, 2013 Name: 1. What is the effect of the parasympathetic nervous system on: (2.5) a) Heart rate b) Male reproductive function c) Pylorus d) Internal anal
Autonomic Nervous System DR JAMILA EL MEDANY
 Autonomic Nervous System DR JAMILA EL MEDANY OBJECTIVES At the end of the lecture, students should be able to: Define the autonomic nervous system. Describe the structure of autonomic nervous system Trace
Autonomic Nervous System DR JAMILA EL MEDANY OBJECTIVES At the end of the lecture, students should be able to: Define the autonomic nervous system. Describe the structure of autonomic nervous system Trace
Computed tomography versus fluoroscopy guidance in celiac plexus neurolysis for treatment of upper abdominal malignant pain
 Computed tomography versus fluoroscopy guidance in celiac plexus neurolysis for treatment of upper abdominal malignant pain Thesis Submitted for the partial fulfillment of MD Degree in anesthesiology and
Computed tomography versus fluoroscopy guidance in celiac plexus neurolysis for treatment of upper abdominal malignant pain Thesis Submitted for the partial fulfillment of MD Degree in anesthesiology and
Celiac Plexus Block for Pancreatic Cancer Pain: Factors Influencing Pain, Symptoms and Quality of Life
 1140 Journal of Pain and Symptom Management Vol. 26 No. 6 December 2003 Original Article Celiac Plexus Block for Pancreatic Cancer Pain: Factors Influencing Pain, Symptoms and Quality of Life Sebastiano
1140 Journal of Pain and Symptom Management Vol. 26 No. 6 December 2003 Original Article Celiac Plexus Block for Pancreatic Cancer Pain: Factors Influencing Pain, Symptoms and Quality of Life Sebastiano
Perioperative Pain Management
 Perioperative Pain Management Overview and Update As defined by the Anesthesiologist's Task Force on Acute Pain Management are from the practice guidelines from the American Society of Anesthesiologists
Perioperative Pain Management Overview and Update As defined by the Anesthesiologist's Task Force on Acute Pain Management are from the practice guidelines from the American Society of Anesthesiologists
Transsacrococcygeal Approach to Ganglion Impar Block for Management Of Chronic Perineal Pain: A Prospective Observational Study
 Pain Physician 2007; 10:661-666 ISSN 1533-3159 Prospective Evaluation Transsacrococcygeal Approach to Ganglion Impar Block for Management Of Chronic Perineal Pain: A Prospective Observational Study Gokul
Pain Physician 2007; 10:661-666 ISSN 1533-3159 Prospective Evaluation Transsacrococcygeal Approach to Ganglion Impar Block for Management Of Chronic Perineal Pain: A Prospective Observational Study Gokul
ISPUB.COM. Lumbar Sympathectomy by Laser Technique. S Kantha, B Kantha METHODS AND MATERIALS
 ISPUB.COM The Internet Journal of Minimally Invasive Spinal Technology Volume 1 Number 2 Lumbar Sympathectomy by Laser Technique S Kantha, B Kantha Citation S Kantha, B Kantha. Lumbar Sympathectomy by
ISPUB.COM The Internet Journal of Minimally Invasive Spinal Technology Volume 1 Number 2 Lumbar Sympathectomy by Laser Technique S Kantha, B Kantha Citation S Kantha, B Kantha. Lumbar Sympathectomy by
Long-Term Results of Celiac Ganglia Block: Correlation of Grade of Tumoral Invasion and Pain Relief
 Long-Term Results of Celiac Ganglia Block: Correlation of Grade of Tumoral Invasion and Pain Relief Okan Akhan 1 Mustafa N. Ozmen Nuri Basgun Devrim Akinci Oguzhan Oguz Mert Koroglu Musturay Karcaaltincaba
Long-Term Results of Celiac Ganglia Block: Correlation of Grade of Tumoral Invasion and Pain Relief Okan Akhan 1 Mustafa N. Ozmen Nuri Basgun Devrim Akinci Oguzhan Oguz Mert Koroglu Musturay Karcaaltincaba
ALTERNATIVAS A LA ADMINISTRACION: OPIOIDES IT
 ALTERNATIVAS A LA ADMINISTRACION: OPIOIDES IT Oscar A. de Leon-Casasola, MD Professor of Anesthesiology and Medicine Senior Vice-Chair Dept. of Anesthesiology, The Jacobs School of Medicine Chief, Pain
ALTERNATIVAS A LA ADMINISTRACION: OPIOIDES IT Oscar A. de Leon-Casasola, MD Professor of Anesthesiology and Medicine Senior Vice-Chair Dept. of Anesthesiology, The Jacobs School of Medicine Chief, Pain
Paraspinal Blocks a new paradigm in truncal analgesia
 Paraspinal Blocks a new paradigm in truncal analgesia Ki Jinn Chin, MBBS (Hons), MMed, FRCPC Associate Professor Toronto Western Hospital University of Toronto Online Resources https://youtu.be/lockhd
Paraspinal Blocks a new paradigm in truncal analgesia Ki Jinn Chin, MBBS (Hons), MMed, FRCPC Associate Professor Toronto Western Hospital University of Toronto Online Resources https://youtu.be/lockhd
Autonomic Nervous System. Ms. DS Pillay Room 2P24
 Autonomic Nervous System Ms. DS Pillay Room 2P24 OVERVIEW OF THE NERVOUS SYSTEM NERVOUS SYSTEM CNS PNS BRAIN SPINAL CORD SOMATIC ANS SYMPATHEIC PARASYMPATHEIC LOCATION OF GANGLIA IN THE ANS Short post-ganglionic
Autonomic Nervous System Ms. DS Pillay Room 2P24 OVERVIEW OF THE NERVOUS SYSTEM NERVOUS SYSTEM CNS PNS BRAIN SPINAL CORD SOMATIC ANS SYMPATHEIC PARASYMPATHEIC LOCATION OF GANGLIA IN THE ANS Short post-ganglionic
The abdominal Esophagus, Stomach and the Duodenum. Prof. Oluwadiya KS
 The abdominal Esophagus, Stomach and the Duodenum Prof. Oluwadiya KS www.oluwadiya.com Viscera of the abdomen Abdominal esophagus: Terminal part of the esophagus The stomach Intestines: Small and Large
The abdominal Esophagus, Stomach and the Duodenum Prof. Oluwadiya KS www.oluwadiya.com Viscera of the abdomen Abdominal esophagus: Terminal part of the esophagus The stomach Intestines: Small and Large
Part 1. Copyright 2011 Pearson Education, Inc. Copyright 2011 Pearson Education, Inc. Stimulatory
 PowerPoint Lecture Slides prepared by Leslie Hendon University of Alabama, Birmingham C H A P T E R 15 Part 1 The Autonomic Nervous System and Visceral Sensory Neurons The ANS and Visceral Sensory Neurons
PowerPoint Lecture Slides prepared by Leslie Hendon University of Alabama, Birmingham C H A P T E R 15 Part 1 The Autonomic Nervous System and Visceral Sensory Neurons The ANS and Visceral Sensory Neurons
Epidural Analgesia in Labor - Whats s New
 Epidural Analgesia in Labor - Whats s New Wichelewski Josef 821 Selective neural blockade has many clinical applications in medicine but nowhere has its use been so well accepted than in the field of Obstetrics.
Epidural Analgesia in Labor - Whats s New Wichelewski Josef 821 Selective neural blockade has many clinical applications in medicine but nowhere has its use been so well accepted than in the field of Obstetrics.
ANATOMY OF PELVICAYCEAL SYSTEM -DR. RAHUL BEVARA
 1 ANATOMY OF PELVICAYCEAL SYSTEM -DR. RAHUL BEVARA 2 KIDNEY:ANATOMY OVERVIEW Kidneys are retroperitoneal, in posterior abdominal region, extending from T12 L3 Bean-shaped Right kidney is lower than left
1 ANATOMY OF PELVICAYCEAL SYSTEM -DR. RAHUL BEVARA 2 KIDNEY:ANATOMY OVERVIEW Kidneys are retroperitoneal, in posterior abdominal region, extending from T12 L3 Bean-shaped Right kidney is lower than left
Neural Blocks in Pain Medicine D R M A R G A R E T E B O N E M B C H B F R C A F F P M R C A C O N S U LTA N T I N PA I N M E D I C I N E
 Neural Blocks in Pain Medicine D R M A R G A R E T E B O N E M B C H B F R C A F F P M R C A C O N S U LTA N T I N PA I N M E D I C I N E Stellate Ganglion Block Lumbar Sympathetic Block Requirements Diagnosis
Neural Blocks in Pain Medicine D R M A R G A R E T E B O N E M B C H B F R C A F F P M R C A C O N S U LTA N T I N PA I N M E D I C I N E Stellate Ganglion Block Lumbar Sympathetic Block Requirements Diagnosis
A New Technique for Inferior Hypogastric Plexus Block: A Coccygeal Transverse Approach
 Case Report Korean J Pain 2012 January; Vol. 25, No. 1: 38-42 pissn 2005-9159 eissn 2093-0569 http://dx.doi.org/10.3344/kjp.2012.25.1.38 A New Technique for Inferior Hypogastric Plexus Block: A Coccygeal
Case Report Korean J Pain 2012 January; Vol. 25, No. 1: 38-42 pissn 2005-9159 eissn 2093-0569 http://dx.doi.org/10.3344/kjp.2012.25.1.38 A New Technique for Inferior Hypogastric Plexus Block: A Coccygeal
The posterior abdominal wall. Prof. Oluwadiya KS
 The posterior abdominal wall Prof. Oluwadiya KS www.oluwadiya.sitesled.com Posterior Abdominal Wall Lumbar vertebrae and discs. Muscles opsoas, quadratus lumborum, iliacus, transverse, abdominal wall
The posterior abdominal wall Prof. Oluwadiya KS www.oluwadiya.sitesled.com Posterior Abdominal Wall Lumbar vertebrae and discs. Muscles opsoas, quadratus lumborum, iliacus, transverse, abdominal wall
The TAP Block: Rapidly Evolving From Managing Acute Post-Op Pain to Treating Chronic Abdominal Pain
 Interventional APRIL 9, 2018 The TAP Block: Rapidly Evolving From Managing Acute Post-Op Pain to Treating Chronic Abdominal Pain By Anil P. Pisharoty, MD Purpose This review article describes the increasing
Interventional APRIL 9, 2018 The TAP Block: Rapidly Evolving From Managing Acute Post-Op Pain to Treating Chronic Abdominal Pain By Anil P. Pisharoty, MD Purpose This review article describes the increasing
Interventional Techniques for Cancer Pain Management
 Interventional Techniques for Cancer Pain Management Musa M. Aner, MD Director, Cancer Pain Service Arnold - Warfield Pain Center Beth Israel Deaconess Medical Center Boston, MA Disclosure No financial
Interventional Techniques for Cancer Pain Management Musa M. Aner, MD Director, Cancer Pain Service Arnold - Warfield Pain Center Beth Israel Deaconess Medical Center Boston, MA Disclosure No financial
Labor Epidural: Local Anesthetics and Beyond
 Goals: Labor Epidural: Local Anesthetics and Beyond Pedram Aleshi MD The Changing Practice of Anesthesia September 2012 Review Concept of MLAC Local anesthetic efficacy Local anesthetic sparing effects:
Goals: Labor Epidural: Local Anesthetics and Beyond Pedram Aleshi MD The Changing Practice of Anesthesia September 2012 Review Concept of MLAC Local anesthetic efficacy Local anesthetic sparing effects:
Non-Pharmacological Management of Pain. Anesthetic interventions Neurosurgical interventions Cognitive behavioral therapy Physical Therapies
 Non-Pharmacological Management of Pain Anesthetic interventions Neurosurgical interventions Cognitive behavioral therapy Physical Therapies Practice Pharmacotherapy treats majority of pain(90%). Occasionally
Non-Pharmacological Management of Pain Anesthetic interventions Neurosurgical interventions Cognitive behavioral therapy Physical Therapies Practice Pharmacotherapy treats majority of pain(90%). Occasionally
Lecture 56 Kidney and Urinary System
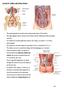 Lecture 56 Kidney and Urinary System The adrenal glands are located on the superomedial aspect of the kidney The right diagram shows a picture of the kidney with the abdominal walls and organs removed
Lecture 56 Kidney and Urinary System The adrenal glands are located on the superomedial aspect of the kidney The right diagram shows a picture of the kidney with the abdominal walls and organs removed
Tymaa Al-zaben & Amin Al-ajalouni
 Done by: Tymaa Al-zaben & Amin Al-ajalouni ** Hello SERTONIN! SLIDE 3 note:: the slide included within the sheet but make sure back to slide for pictures The Autonomic Nervous System Function : Regulate
Done by: Tymaa Al-zaben & Amin Al-ajalouni ** Hello SERTONIN! SLIDE 3 note:: the slide included within the sheet but make sure back to slide for pictures The Autonomic Nervous System Function : Regulate
THE GOOFY ANATOMIST QUIZZES
 THE GOOFY ANATOMIST QUIZZES 5. NERVES Q1. Which of the following classifications of the nervous systems is correct? A. The autonomic nervous system is composed of the brain, cranial nerves and spinal nerves.
THE GOOFY ANATOMIST QUIZZES 5. NERVES Q1. Which of the following classifications of the nervous systems is correct? A. The autonomic nervous system is composed of the brain, cranial nerves and spinal nerves.
Principles of Anatomy and Physiology
 Principles of Anatomy and Physiology 14 th Edition CHAPTER 15 The Autonomic Nervous System Comparison of Somatic and Autonomic Nervous Systems The somatic nervous system includes both sensory and motor
Principles of Anatomy and Physiology 14 th Edition CHAPTER 15 The Autonomic Nervous System Comparison of Somatic and Autonomic Nervous Systems The somatic nervous system includes both sensory and motor
I. Autonomic Nervous System (ANS) A. Dual Innervation B. Autonomic Motor Pathway 1. Preganglionic Neuron a. Preganglionic Fibers (Axons) (1)
 I. Autonomic Nervous System (ANS) A. Dual Innervation B. Autonomic Motor Pathway 1. Preganglionic Neuron a. Preganglionic Fibers (Axons) (1) Acetylcholine - ACh 2. Ganglion (Ganglia) 3. Ganglionic Neuron
I. Autonomic Nervous System (ANS) A. Dual Innervation B. Autonomic Motor Pathway 1. Preganglionic Neuron a. Preganglionic Fibers (Axons) (1) Acetylcholine - ACh 2. Ganglion (Ganglia) 3. Ganglionic Neuron
HBA THE BODY Trunk Examination - October 1, 2012
 HBA 531 - THE BODY Trunk Examination - October 1, 2012 1. On the right is a lettered list of different functional types of neurons. On the left is a list of structures. In the blank following each named
HBA 531 - THE BODY Trunk Examination - October 1, 2012 1. On the right is a lettered list of different functional types of neurons. On the left is a list of structures. In the blank following each named
01/07/2018 MANAGEMENT OF RECTAL TENESMUS PRESENTATION OUTLINE
 MANAGEMENT OF RECTAL TENESMUS Dr. Áine Ní Laoire The Oxford Advanced Pain & Symptom Management Course Nottingham 27 th June 2018 PRESENTATION OUTLINE Definition A Clinical Case Epidemiology Pathophysiology
MANAGEMENT OF RECTAL TENESMUS Dr. Áine Ní Laoire The Oxford Advanced Pain & Symptom Management Course Nottingham 27 th June 2018 PRESENTATION OUTLINE Definition A Clinical Case Epidemiology Pathophysiology
Dana Alrafaiah. - Amani Nofal. - Ahmad Alsalman. 1 P a g e
 - 2 - Dana Alrafaiah - Amani Nofal - Ahmad Alsalman 1 P a g e This lecture will discuss five topics as follows: 1- Arrangement of pelvic viscera. 2- Muscles of Pelvis. 3- Blood Supply of pelvis. 4- Nerve
- 2 - Dana Alrafaiah - Amani Nofal - Ahmad Alsalman 1 P a g e This lecture will discuss five topics as follows: 1- Arrangement of pelvic viscera. 2- Muscles of Pelvis. 3- Blood Supply of pelvis. 4- Nerve
Chp. 16: AUTONOMIC N.S. (In Review: Peripheral N. S.)
 Chp. 16: AUTONOMIC N.S. (In Review: Peripheral N. S.) Peripheral nerves contain both motor and sensory neurons Among the motor neurons, some of these are somatic and innervate skeletal muscles while some
Chp. 16: AUTONOMIC N.S. (In Review: Peripheral N. S.) Peripheral nerves contain both motor and sensory neurons Among the motor neurons, some of these are somatic and innervate skeletal muscles while some
Gross Anatomy of Lower Spinal Cord
 Chapter 13 Spinal Cord, Spinal Nerves and Somatic Reflexes Spinal cord Spinal nerves Somatic reflexes Gross Anatomy of Lower Spinal Cord Meninges of Vertebra & Spinal Cord Spina Bifida Congenital defect
Chapter 13 Spinal Cord, Spinal Nerves and Somatic Reflexes Spinal cord Spinal nerves Somatic reflexes Gross Anatomy of Lower Spinal Cord Meninges of Vertebra & Spinal Cord Spina Bifida Congenital defect
The Thoracic wall including the diaphragm. Prof Oluwadiya KS
 The Thoracic wall including the diaphragm Prof Oluwadiya KS www.oluwadiya.com Components of the thoracic wall Skin Superficial fascia Chest wall muscles (see upper limb slides) Skeletal framework Intercostal
The Thoracic wall including the diaphragm Prof Oluwadiya KS www.oluwadiya.com Components of the thoracic wall Skin Superficial fascia Chest wall muscles (see upper limb slides) Skeletal framework Intercostal
Physiologic Anatomy and Nervous Connections of the Bladder
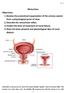 Micturition Objectives: 1. Review the anatomical organization of the urinary system from a physiological point of view. 2. Describe the micturition reflex. 3. Predict the lines of treatment of renal failure.
Micturition Objectives: 1. Review the anatomical organization of the urinary system from a physiological point of view. 2. Describe the micturition reflex. 3. Predict the lines of treatment of renal failure.
Biology 218 Human Anatomy
 Chapter 20 Adapted form Tortora 10 th ed. LECTURE OUTLINE A. Introduction (p. 632) 1. The autonomic nervous system (ANS) regulates the activity of smooth muscle, cardiac muscle, and certain glands. 2.
Chapter 20 Adapted form Tortora 10 th ed. LECTURE OUTLINE A. Introduction (p. 632) 1. The autonomic nervous system (ANS) regulates the activity of smooth muscle, cardiac muscle, and certain glands. 2.
OBJECTIVE: To obtain a fundamental knowledge of the root of the neck with respect to structure and function
 The root of the neck Jeff Dupree, Ph.D. e mail: jldupree@vcu.edu OBJECTIVE: To obtain a fundamental knowledge of the root of the neck with respect to structure and function READING ASSIGNMENT: Moore and
The root of the neck Jeff Dupree, Ph.D. e mail: jldupree@vcu.edu OBJECTIVE: To obtain a fundamental knowledge of the root of the neck with respect to structure and function READING ASSIGNMENT: Moore and
Human Anatomy & Physiology
 PowerPoint Lecture Slides prepared by Barbara Heard, Atlantic Cape Community College Ninth Edition Human Anatomy & Physiology C H A P T E R 14 Annie Leibovitz/Contact Press Images 2013 Pearson Education,
PowerPoint Lecture Slides prepared by Barbara Heard, Atlantic Cape Community College Ninth Edition Human Anatomy & Physiology C H A P T E R 14 Annie Leibovitz/Contact Press Images 2013 Pearson Education,
2012 CPT Changes Affecting Radiology REVISIONS
 2012 CPT Changes Affecting Radiology REVISIONS 22520 Percutaneous vertebroplasty (bone biopsy included when performed), 1 vertebral body, unilateral or bilateral injection; thoracic 22521 lumbar 22522
2012 CPT Changes Affecting Radiology REVISIONS 22520 Percutaneous vertebroplasty (bone biopsy included when performed), 1 vertebral body, unilateral or bilateral injection; thoracic 22521 lumbar 22522
Paraplegia after celiac plexus neurolysis in a patient with pancreatic cancer - A case report and literature review -
 Anesth Pain Med 2019;14:85-90 https://doi.org/10.17085/apm.2019.14.1.85 pissn 1975-5171 ㆍ eissn 2383-7977 Case Report Received March 13, 2018 Revised 1st, May 8, 2018 2nd, July 18, 2018 Accepted August
Anesth Pain Med 2019;14:85-90 https://doi.org/10.17085/apm.2019.14.1.85 pissn 1975-5171 ㆍ eissn 2383-7977 Case Report Received March 13, 2018 Revised 1st, May 8, 2018 2nd, July 18, 2018 Accepted August
Comparison of Bolus Bupivacaine, Fentanyl, and Mixture of Bupivacaine with Fentanyl in Thoracic Epidural Analgesia for Upper Abdominal Surgery
 Original Article DOI: 10.17354/ijss/2016/156 Comparison of Bolus Bupivacaine, Fentanyl, and Mixture of Bupivacaine with Fentanyl in Thoracic Epidural Analgesia for Upper Abdominal Surgery Sachin Gajbhiye
Original Article DOI: 10.17354/ijss/2016/156 Comparison of Bolus Bupivacaine, Fentanyl, and Mixture of Bupivacaine with Fentanyl in Thoracic Epidural Analgesia for Upper Abdominal Surgery Sachin Gajbhiye
Human Anatomy and Physiology - Problem Drill 15: The Autonomic Nervous System
 Human Anatomy and Physiology - Problem Drill 15: The Autonomic Nervous System Question No. 1 of 10 Which of the following statements is correct about the component of the autonomic nervous system identified
Human Anatomy and Physiology - Problem Drill 15: The Autonomic Nervous System Question No. 1 of 10 Which of the following statements is correct about the component of the autonomic nervous system identified
THORACIC AND ABDOMINAL BLOCKS. Giovanni Cucchiaro MD MPP The Children s Hospital Los Angeles
 THORACIC AND ABDOMINAL BLOCKS Giovanni Cucchiaro MD MPP The Children s Hospital Los Angeles 1 CONFLICTS OF INTEREST??? NONE ZERO 2 John Fiadjoe 3 DIFFERENT ANSWERS TO MY DILEMMA 4 WHICH? WHAT? WHY? 5 RAGIONAL
THORACIC AND ABDOMINAL BLOCKS Giovanni Cucchiaro MD MPP The Children s Hospital Los Angeles 1 CONFLICTS OF INTEREST??? NONE ZERO 2 John Fiadjoe 3 DIFFERENT ANSWERS TO MY DILEMMA 4 WHICH? WHAT? WHY? 5 RAGIONAL
Department of Anaesthesiology, Shanghai Tenth People s Hospital, Tongji University, Shanghai , China. *
 Int J Clin Exp Med 2015;8(11):20092-20096 www.ijcem.com /ISSN:1940-5901/IJCEM0014323 Original Article Clinical research of percutaneous bilateral splanchnic nerve lesion for pain relief in patients with
Int J Clin Exp Med 2015;8(11):20092-20096 www.ijcem.com /ISSN:1940-5901/IJCEM0014323 Original Article Clinical research of percutaneous bilateral splanchnic nerve lesion for pain relief in patients with
CLINICAL PRESENTATION AND RADIOLOGY QUIZ QUESTION
 Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 6/23/2012 Radiology Quiz of the Week # 78 Page 1 CLINICAL PRESENTATION AND RADIOLOGY
Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 6/23/2012 Radiology Quiz of the Week # 78 Page 1 CLINICAL PRESENTATION AND RADIOLOGY
GUIDELINES ON PAIN MANAGEMENT IN UROLOGY
 GUIDELINES ON PAIN MANAGEMENT IN UROLOGY F. Francesca (chairman), P. Bader, D. Echtle, F. Giunta, J. Williams Eur Urol 2003; 44(4):383-389 Introduction Pain is defined as an unpleasant sensory and emotional
GUIDELINES ON PAIN MANAGEMENT IN UROLOGY F. Francesca (chairman), P. Bader, D. Echtle, F. Giunta, J. Williams Eur Urol 2003; 44(4):383-389 Introduction Pain is defined as an unpleasant sensory and emotional
Management of Neuropathic pain
 Management of Neuropathic pain Ravi Parekodi Consultant in Anaesthetics and Pain Management 08/04/2014 Ref: BJA July2013, Map of Medicine2013, Pain Physician 2007, IASP 2012, Nice guideline 2013 Aims Highlight
Management of Neuropathic pain Ravi Parekodi Consultant in Anaesthetics and Pain Management 08/04/2014 Ref: BJA July2013, Map of Medicine2013, Pain Physician 2007, IASP 2012, Nice guideline 2013 Aims Highlight
Y A L E S C H O O L O F M E D I C I N E. This is a CME accredited activity. The presenters and there are no conflicts of interest.
 This is a CME accredited activity. The presenters and there are no conflicts of interest. Pain in Pancreatic Cancer More than 50% of patients with pancreatic cancer suffer from abdominal and back pain
This is a CME accredited activity. The presenters and there are no conflicts of interest. Pain in Pancreatic Cancer More than 50% of patients with pancreatic cancer suffer from abdominal and back pain
2014 Deleted CPT Codes
 2014 Deleted CPT Codes Surgery 13150 - Repair, complex, eyelids, nose, ears and/or lips; 1.0 cm or less 19102 - Biopsy of breast; percutaneous, needle core, using imaging guidance 19103 - Biopsy of breast;
2014 Deleted CPT Codes Surgery 13150 - Repair, complex, eyelids, nose, ears and/or lips; 1.0 cm or less 19102 - Biopsy of breast; percutaneous, needle core, using imaging guidance 19103 - Biopsy of breast;
Fig. A.1. Frontal. plane. Transverse. plane. Sagittal plane. Copyright McGraw-Hill Education. Permission required for reproduction or display.
 Fig. A.1 Frontal plane Transverse plane Sagittal plane McGraw-Hill Education/Joe DeGrandis Fig. A.2 (a) Sagittal section (b) Frontal section (c) Transverse section Table A.1 Fig. A.3 Cephalic r. (head)
Fig. A.1 Frontal plane Transverse plane Sagittal plane McGraw-Hill Education/Joe DeGrandis Fig. A.2 (a) Sagittal section (b) Frontal section (c) Transverse section Table A.1 Fig. A.3 Cephalic r. (head)
Role and safety of epidural analgesia
 Anaesthesia for Liver Resection Surgery The Association of Anaesthetists Seminars 21 Portland Place, London Thursday 15 th December 2005 Role and safety of epidural analgesia Lennart Christiansson MD,
Anaesthesia for Liver Resection Surgery The Association of Anaesthetists Seminars 21 Portland Place, London Thursday 15 th December 2005 Role and safety of epidural analgesia Lennart Christiansson MD,
Regional Anaesthesia of the Thoracic Limb
 Regional Anaesthesia of the Thoracic Limb Trauma and inflammation cause sensitization of the peripheral nervous system and the subsequent barrage of nociceptive input (usually by surgery) produces sensitization
Regional Anaesthesia of the Thoracic Limb Trauma and inflammation cause sensitization of the peripheral nervous system and the subsequent barrage of nociceptive input (usually by surgery) produces sensitization
Surgery Under Regional Anesthesia
 Surgery Under Regional Anesthesia Jean Daniel Eloy, MD Assistant Professor Residency Program Director Rutgers-New Jersey Medical School Rutgers The State University of New Jersey Peripheral Nerve Block
Surgery Under Regional Anesthesia Jean Daniel Eloy, MD Assistant Professor Residency Program Director Rutgers-New Jersey Medical School Rutgers The State University of New Jersey Peripheral Nerve Block
Intraspinal (Neuraxial) Analgesia Community Nurses Competency Test
 Intraspinal (Neuraxial) Analgesia Community Nurses Competency Test 1 Intraspinal (Neuraxial) Analgesia for Community Nurses Competency Test 1) Name the two major classifications of pain. i. ii. 2) Neuropathic
Intraspinal (Neuraxial) Analgesia Community Nurses Competency Test 1 Intraspinal (Neuraxial) Analgesia for Community Nurses Competency Test 1) Name the two major classifications of pain. i. ii. 2) Neuropathic
INDIANA HEALTH COVERAGE PROGRAMS
 INDIANA HEALTH COVERAGE PROGRAMS PROVIDER CODE TABLES Note: Due to possible changes in Indiana Health Coverage Programs (IHCP) policy or national coding updates, inclusion of a code on the code tables
INDIANA HEALTH COVERAGE PROGRAMS PROVIDER CODE TABLES Note: Due to possible changes in Indiana Health Coverage Programs (IHCP) policy or national coding updates, inclusion of a code on the code tables
Introduction to The Human Body
 1 Introduction to The Human Body FOCUS: The human organism is often examined at seven structural levels: chemical, organelle, cell, tissue, organ, organ system, and the organism. Anatomy examines the structure
1 Introduction to The Human Body FOCUS: The human organism is often examined at seven structural levels: chemical, organelle, cell, tissue, organ, organ system, and the organism. Anatomy examines the structure
Biology Human Anatomy Abdominal and Pelvic Cavities
 Biology 351 - Human Anatomy Abdominal and Pelvic Cavities You must answer all questions on this exam. Because statistics demonstrate that, on average, between 2-5 questions on every 100-point exam are
Biology 351 - Human Anatomy Abdominal and Pelvic Cavities You must answer all questions on this exam. Because statistics demonstrate that, on average, between 2-5 questions on every 100-point exam are
Intercostal nerve blockade for cancer pain: effectiveness and selection of patients
 O R I G I N A L A R T I C L E Frank CS Wong TW Lee KK Yuen SH Lo WK Sze Stewart Y Tung Intercostal nerve blockade for cancer pain: effectiveness and selection of patients Objectives To review treatment
O R I G I N A L A R T I C L E Frank CS Wong TW Lee KK Yuen SH Lo WK Sze Stewart Y Tung Intercostal nerve blockade for cancer pain: effectiveness and selection of patients Objectives To review treatment
The Kidneys. (L., ren; Gk, nephros; hence the adjectives renal and nephric) & Suprarenal (Adrenal) Glands. Dr Maan Al-Abbasi PhD, MBChB
 The Kidneys (L., ren; Gk, nephros; hence the adjectives renal and nephric) & Suprarenal (Adrenal) Glands Dr Maan Al-Abbasi PhD, MBChB Functions of Urinary System Regulate electrolytes (K+, Na+, etc) Regulate
The Kidneys (L., ren; Gk, nephros; hence the adjectives renal and nephric) & Suprarenal (Adrenal) Glands Dr Maan Al-Abbasi PhD, MBChB Functions of Urinary System Regulate electrolytes (K+, Na+, etc) Regulate
Objectives 9/7/2012. Optimizing Analgesia to Enhance the Recovery After Surgery CME FACULTY DISCLOSURE
 Optimizing Analgesia to Enhance the Recovery After Surgery Francesco Carli, M.D.. McGill University, Montreal, QC, Canada. ASPMN, Baltimore, 2012 CME FACULTY DISCLOSURE Francesco Carli has no affiliation
Optimizing Analgesia to Enhance the Recovery After Surgery Francesco Carli, M.D.. McGill University, Montreal, QC, Canada. ASPMN, Baltimore, 2012 CME FACULTY DISCLOSURE Francesco Carli has no affiliation
Stimulation of the Sacral Anterior Root Combined with Posterior Sacral Rhizotomy in Patients with Spinal Cord Injury. Original Policy Date
 MP 7.01.58 Stimulation of the Sacral Anterior Root Combined with Posterior Sacral Rhizotomy in Patients with Spinal Cord Injury Medical Policy Section Issue 12:2013 Original Policy Date 12:2013 Last Review
MP 7.01.58 Stimulation of the Sacral Anterior Root Combined with Posterior Sacral Rhizotomy in Patients with Spinal Cord Injury Medical Policy Section Issue 12:2013 Original Policy Date 12:2013 Last Review
3 Circulatory Pathways
 40 Chapter 3 Circulatory Pathways Systemic Arteries -Arteries carry blood away from the heart to the various organs of the body. -The aorta is the longest artery in the body; it branches to give rise to
40 Chapter 3 Circulatory Pathways Systemic Arteries -Arteries carry blood away from the heart to the various organs of the body. -The aorta is the longest artery in the body; it branches to give rise to
AUTONOMIC NERVOUS SYSTEM PART I: SPINAL CORD
 AUTONOMIC NERVOUS SYSTEM PART I: SPINAL CORD How is the organization of the autonomic nervous system different from that of the somatic nervous system? Peripheral Nervous System Divisions Somatic Nervous
AUTONOMIC NERVOUS SYSTEM PART I: SPINAL CORD How is the organization of the autonomic nervous system different from that of the somatic nervous system? Peripheral Nervous System Divisions Somatic Nervous
Human Anatomy. Spinal Cord and Spinal Nerves
 Human Anatomy Spinal Cord and Spinal Nerves 1 The Spinal Cord Link between the brain and the body. Exhibits some functional independence from the brain. The spinal cord and spinal nerves serve two functions:
Human Anatomy Spinal Cord and Spinal Nerves 1 The Spinal Cord Link between the brain and the body. Exhibits some functional independence from the brain. The spinal cord and spinal nerves serve two functions:
The Human Body: An Overview of Anatomy. Anatomy. Physiology. Anatomy - Study of internal and external body structures
 C H A P T E R 1 The Human Body: An Orientation An Overview of Anatomy Anatomy The study of the structure of the human body Physiology The study of body function Anatomy - Study of internal and external
C H A P T E R 1 The Human Body: An Orientation An Overview of Anatomy Anatomy The study of the structure of the human body Physiology The study of body function Anatomy - Study of internal and external
NERVOUS SYSTEM ANATOMY
 INTRODUCTION to NERVOUS SYSTEM ANATOMY M1 - Gross and Developmental Anatomy Dr. Milton M. Sholley Professor of Anatomy and Neurobiology and Dr. Michael H. Peters Professor of Chemical and Life Science
INTRODUCTION to NERVOUS SYSTEM ANATOMY M1 - Gross and Developmental Anatomy Dr. Milton M. Sholley Professor of Anatomy and Neurobiology and Dr. Michael H. Peters Professor of Chemical and Life Science
How and why to do an epidural in dogs and cats? Which Indications and which drugs?
 AMVAC/RoSAVA 2014 How and why to do an epidural in dogs and cats? Which Indications and which drugs? Prof. Yves Moens Dipl ECVAA Why do epidurals? A part of a balanced anesthesia A means to provide analgesia
AMVAC/RoSAVA 2014 How and why to do an epidural in dogs and cats? Which Indications and which drugs? Prof. Yves Moens Dipl ECVAA Why do epidurals? A part of a balanced anesthesia A means to provide analgesia
Autonomic Nervous System Dr. Ali Ebneshahidi
 Autonomic Nervous System Dr. Ali Ebneshahidi Nervous System Divisions of the nervous system The human nervous system consists of the central nervous System (CNS) and the Peripheral Nervous System (PNS).
Autonomic Nervous System Dr. Ali Ebneshahidi Nervous System Divisions of the nervous system The human nervous system consists of the central nervous System (CNS) and the Peripheral Nervous System (PNS).
Vatsal Patel 1, Kamla Mehta 2, Kirti Patel 3, Hiren Parmar 4* Original Research Article. Abstract
 Original Research Article Comparison of USG guided modified rectus sheath block with intraperitoneal instillation with Inj. Bupivacaine for postoperative pain relief in diagnostic laparoscopy Vatsal Patel
Original Research Article Comparison of USG guided modified rectus sheath block with intraperitoneal instillation with Inj. Bupivacaine for postoperative pain relief in diagnostic laparoscopy Vatsal Patel
Interventional Pain. Judith Dunipace MD Board certified in Anesthesiology, Pain Management and Hospice and Palliative Care
 Interventional Pain Judith Dunipace MD Board certified in Anesthesiology, Pain Management and Hospice and Palliative Care IASP Definition of Pain Pain is an unpleasant sensory or emotional experience associated
Interventional Pain Judith Dunipace MD Board certified in Anesthesiology, Pain Management and Hospice and Palliative Care IASP Definition of Pain Pain is an unpleasant sensory or emotional experience associated
Chapter 1: Introduction to the Human Body Test Bank
 Chapter 1: Introduction to the Human Body Test Bank MULTIPLE CHOICE 1. What is the branch of science that studies how the body functions? a. Anatomy b. Histology c. Pathology d. Physiology 2. Which word
Chapter 1: Introduction to the Human Body Test Bank MULTIPLE CHOICE 1. What is the branch of science that studies how the body functions? a. Anatomy b. Histology c. Pathology d. Physiology 2. Which word
Divisions of ANS. Divisions of ANS 2 Divisions dualing innervate most organs. Autonomic Nervous System (Chapter 9)
 Autonomic Nervous System (Chapter 9) Autonomic Nervous System (ANS) general properties anatomy Autonomic Effects on Target Organs Subs of Nervous System Central nervous system Brain Spinal cord Peripheral
Autonomic Nervous System (Chapter 9) Autonomic Nervous System (ANS) general properties anatomy Autonomic Effects on Target Organs Subs of Nervous System Central nervous system Brain Spinal cord Peripheral
