Framework - Expectations for Physicians Who have Changed, or Plan to Change their Scope of Practice to Include Interventional Pain Management
|
|
|
- Crystal Watts
- 6 years ago
- Views:
Transcription
1 Framework - Expectations for Physicians Who have Changed, or Plan to Change their Scope of Practice to Include Interventional Pain Management Recommendations of the CPSO Interventional Pain Working Group on Change in Scope Working Group Objective: To develop a decision-making framework to assist the College of Physicians and Surgeons of Ontario (CPSO) in responding to requests from physicians who have changed or plan to change their scope of practice to include interventional pain management (IPM) in any setting including hospitals and out-of-hospital premises. CPSO s Changing Scope of Practice Policy: The CPSO Changing Scope of Practice Policy states that a physician s ability to perform competently in his or her scope of practice is determined by the physician s knowledge, skills and judgment, which are developed through training and experience in that scope of practice. The Policy also indicates a physician s scope of practice is determined by the: patients the physician cares for, procedures performed, treatments provided, and practice environment. In addition, the CPSO policy on Changing Scope of Practice (Policy number 1-08) states: All physicians who have undergone a significant change in scope of practice or who will be changing their scope of practice significantly and who do not have the training and/or experience to practise competently in the new area of practice, will have to participate in a process to ensure that they have the necessary competence to practise in that area. This process will be individualized for each physician but, in general, the core activities involved are training; supervision; and assessment. To learn more about the Scope policy, follow the link: Background: As with any area of medicine, in order to practise interventional pain medicine in Ontario, the College of Physicians and Surgeons (CPSO) expects physicians to practise according to any terms and limitations on their certificate of registration. All physicians in the province have limitations on their certificate that state that physicians are able to practise medicine in areas in which they are educated and experience. A physician s competence within a scope of practice is determined by their education and experience within that scope. Traditionally, physicians who commonly practise IPM are from the following specialties: Anaesthesia, Neurology, Physical Medicine, Psychiatry, General Surgery, Orthopaedic Surgery and Radiology. In addition, it is becoming increasingly common for general practitioners/family 1
2 physicians as well as emergency medicine physicians to practise IPM as well. Regardless of specialty background, a physician must ensure that s/he has the appropriate training and/or experience for the specific procedures that s/he plans to include in his or her practice. The CPSO relies primarily upon certification processes from the Royal College of Physicians and Surgeons of Canada (RCPSC) in order to determine which physicians can be designated as specialists in a given field of practice. At the present time, the RCPSC is working towards approving accredited residency programs in Pain Medicine, which will include the option to specialize or focus in a particular area, i.e. provide competency in some interventional pain management procedures. However, until such time, any physician who plans to practise IPM is expected to comply with both the Changing Scope of Practice policy and the expectations set out in this document. The purpose of this document is to clarify the CPSO s expectations for physicians choosing to change their scope of practice to include IPM. In this type of practice, as well as in others, physicians must ensure they are meeting the standard of practice, which includes conducting a risk/benefit analysis to assess the appropriateness of performing any given procedure. It must be emphasized that if a physician plans to practise IPM in an Out-of- Hospital Premises (OHP) they must meet the qualifications set out in the Out-of-Hospital Premises (OHP) Standards and also complete all CPSO requirements for Changing Scope of Practice. While the change in scope of practice process generally involves training, supervision and assessment, all of these components may not apply in every case. As with all requests for change in scope issues, in arriving at a decision, the CPSO will review each physician s individual circumstances. DEFINITION Interventional pain management is the diagnosis and treatment of pain involving the percutaneous introduction of medications into the body at sites involved in the production and/or modulation of pain. Interventions may be diagnostic, to determine which structures are involved in producing the pain or therapeutic, to treat the cause of pain or relieve symptoms. 1 The purpose of the definition is to provide guidance to physicians about how IPM is defined so that physicians understand when they need to contact the College to report a change in scope of practice. In addition, this document will deal with IPM procedures that fall into the following categories: (i) (ii) (iii) anaesthetic procedures for analgesia without sedation, divided into: a. those that are peripheral b. those that may include neuraxial or non-neurologic deep structures, and those that benefit from or require imaging. those that may require sedation For the purpose of this document, the procedures listed in Appendix 1 entitled List of Interventional Pain Procedures will be considered as interventional pain management procedures by the College. 1 Injections into tissues that are superficial and easily accessible (e.g. tendon, muscle, peripheral joints) are excluded. For example, trigger point and botox injections are excluded. 2
3 Although this document is directed at physicians who practise interventional pain management, the College also expects physicians who practise pain medicine without the use of interventional procedures (i.e. they usually refer patients to others for procedures when necessary) to fulfill general core competencies for IPM as set out in the section Expectations of General Knowledge, Skills and Judgment for Pain Medicine. Physicians who practise pain management using interventional procedures as well as other modalities of treatment are not only required to fulfill the core competencies set out in the Expectations of General Knowledge, Skills and Judgment for Pain Medicine, but also the Expectations of Procedural-Specific Knowledge, Skills and Judgment for IPM. Physicians who plan to include Interventional Pain Management as part of their scope of practice and who do not have the training and/or experience to practise competently in the new area of practice are required to comply with the College s Changing Scope of Practice policy: Training Requirements for Interventional Pain Management Physicians who have completed a RCPSC residency program, for example in anaesthesia, physical medicine, etc. may have recent relevant training in IPM. Regardless, the College needs to consider the physician s specialty background, prior training and/or experience, as well as his or her intended procedures when determining overall training needs. Moreover, physicians who have received formal training in IPM, but have not practised in this field in a number of years would likely need to go through a change of scope process despite their related training/specialty background. Each situation will be assessed on an individual basis and generally physicians who want to practise IPM will be required to fulfill the training requirements outlined in one of the pathways, as described further below. The goal of training is to ensure that the physician has achieved competence in the procedure, rather than simply relying on a minimum number of procedures and/or hours of training. The College expects a physician with NO prior training and/or experience in IPM procedures to complete the minimum number of overall hours of training (900 hours) as defined in Sections A and B of this document. If the physician has had prior training and/or experience in IPM procedures, then the College may exercise flexibility on the minimum number of hours. Each situation would be assessed individually. For each procedure a physician intends to add to his or her practice, the supervisor must ensure that the physician has completed an adequate number of procedures 2 so that s/he can attest to the fact that the physician has achieved competence in the given procedure(s). 2 An adequate number of procedures to achieve competence will vary from one physician to the next. For example, a physician may require 20 or more supervised trials to develop safety and competence in difficult high risk procedures. For other, less complex procedures the number could be less. Consideration would be given to the physician s prior training and/or experience, as well as whether the physician has transferrable skills that can be applied to the new procedure s/he is intending to add to his or her practice. Moreover, the infrequency of some rare interventional procedures, e.g. plexus blocks could make it difficult for the physician to achieve a high volume of those procedures. It is at the discretion of the supervisor to decide on the length and scope of training, and sign off on the physician s competence, especially in these circumstances. 3
4 Generally, on the recommendation of the supervisor(s), the College may require the physician to complete more, or in some cases less than the minimum number of hours of training where there is prior training and/or experience. Physicians applying for a change in scope of practice to include interventional pain management will have done so by satisfying the requirements listed in one of three different pathways: Pathway 1 - Academic Training Pathway a) Completed an accredited training program at a Canadian or an ACGME 3 recognized Medical School Department or Division that must be structured such that it includes: i. A designated program director ii. Standard, written training objectives iii. A formal, regular evaluation process iv. A mechanism to report the Program s assessment of the individual s competence at the end of the program. v. All components contained within this document entitled A) Expectations of General Knowledge, Skills and Judgment for Pain Medicine and B) Acquisition of Procedural-Specific Knowledge, Skills, and Judgment in IPM. vi. A mechanism to document all training experiences including the number and types of interventional pain procedures performed. 4 At a minimum, it is recommended that trainees complete 900 hours of overall training gaining skills as defined in Sections A and B of this document. 5 b) The program must be completed in less than 36 months. Pathway 2 Non-Academic Training Pathway a) Completed a personalized training program 6 in Interventional Pain that must be structured such that it includes: 3 Accreditation Council for Graduate Medical Education (ACGME) is responsible for the accreditation of post-md medical training programs within the United States. Accreditation is accomplished through a peer review process and is based upon established standards and guidelines. 4 Each situation would be assessed on an individual basis in order to assure competency has been achieved in procedure(s) that the physician intends to add to his or her practice. In addition, techniques involving the use of fluoroscopy or ultrasound imaging require specialized training that should be sponsored by an accredited organization. 5 The trainee should have a minimum of 450 documented hours of training under supervision completed during their training/residency program and any additional documented hours of training could be acquired through a period of supervised practice, i.e. post-residency (level of subsequent supervision will be determined by College). Total documented hours of training would need to total 900 hours. 6 A personalized training program relies on the physician finding a suitable Clinical Supervisor who will help develop a training/educational program, and supervise the physician for the duration of the training program. Both the proposed Clinical Supervisor and the content of the training program must be acceptable to the College. Refer to the Guidelines for College-Directed Supervision for more information about the responsibilities and characteristics necessary for a Clinical Supervisor: Supervision.pdf 4
5 i. All components contained within this document entitled A) Expectations of General Knowledge, Skills and Judgment for Pain Medicine and B) Expectations of Procedural-Specific Knowledge, Skills, and Judgment for IPM. ii. Supervision with supervisor(s) approved by the CPSO who agree to report on the content of the training no less than quarterly. iii. A formal, regular evaluation process iv. Written objectives of training v. A mechanism to report the supervisors assessment of the individual s competence at the end of the program. vi. A mechanism to document all training experiences including the number and types of interventional pain procedures performed. At a minimum, it is recommended that trainees complete 900 documented overall hours of training as defined in Sections A and B of this document. 7 b) The program must be completed in less than 36 months. Pathway 3 Significant Practice Experience in IPM This would essentially include physicians who are coming to Ontario from another jurisdiction 8 where they have demonstrated significant experience, and began practicing IPM after the Changing Scope of Practice Policy came into effect (2003). The need for training/supervision (length and level) is discretionary and it would depend on the physician s intended scope of procedures and previous training and experience. The assessment would be multi-modal in nature, e.g. chart review, interviewing colleagues, etc. The nature of the assessment will be determined by the physician s scope of procedures. 7 The trainee should have a minimum of 450 documented hours of training under high supervision with an additional 450 documented hours of training under moderate to low supervision. For a detailed description of each level of supervision, please refer to the Guidelines for College-Directed Supervision. 8 These physicians will have met the usual requirements for registration in Ontario. 5
6 Supervision and Assessment Requirements Training and supervision for IPM occur at the same time. Once the training/supervision phase is complete, the physician may be required to undergo a College-directed assessment prior to being granted a change in scope of practice. The table below summarizes the College s general expectations. However, each physician s situation would be assessed on an individual basis, and therefore, the levels and duration of supervision are discretionary. In addition, the supervisor s feedback in the form of supervision reports will be considered by the College when determining a change in level of supervision. PATHWAY SUPERVISION/ TRAINING PHASE REQUIRED? LEVEL OF SUPERVISION MINIMUM DURATION OF TRAINING/ SUPERVISION ASSESSMENT REQUIRED? Pathway 1: Academic Pathway YES DISCRETIONARY 900 HOURS 9 DISCRETIONARY 10 Pathway 2: Non- Academic, Pathway Pathway 3: Physicians with significant practice experience YES DISCRETIONARY (i.e. if CPSO deems applicable) HIGH, MODERATE, then LOW DISCRETIONARY 900 HOURS 10 (450 under HIGH supervision; 450 under MODERATE to LOW supervision) DISCRETIONARY YES The CPSO-directed assessment is required 11. YES The CPSO-directed assessment is required. 9 Total number of hours is discretionary, as it depends on the trainee s prior training and/or experience. 10 The need for an assessment will depend on the types of the procedures that the physician plans to add to his or her practice, as well as training completed. 11 In keeping with the usual quality assurance process, a re-assessment could be directed if the CPSO believes that the physician requires a period of additional training/supervision after the initial assessment is conducted. 6
7 (A) Expectations of General Knowledge, Skills, and Judgment for Pain Medicine Any physician planning to practise IPM should be competent in: accurate bedside and laboratory assessment and diagnosis of pain conditions, evidence-based medical, physical, and interventional treatment (to the degree that evidence-based literature exists), fluoroscopy and ultrasound techniques and imaging interpretation, if applicable, and conducting and documenting appropriate follow-up care. In order to acquire the necessary knowledge, skills and judgment required for IPM, physicians will acquire the core competencies through: 1. Practicing under supervision in an IPM practice where the physician will acquire competency in: Assessing and managing patients with regard to pain mechanism, co-morbidities, and functional impairment; Knowledge of the pathophysiology of chronic pain; Non-pharmacological rehabilitation strategies; Identifying and managing opioid misuse problems; The effective use of opioids in pain management; The effective use of non-opioid medications in pain management; Drug interactions and adverse effects; Epidemiology of pain and co-morbidity of psychological conditions, and; The use of measurement scales in pain practice. 2. Being familiar with basic cognitive behavioural techniques and aware of the interplay between psychiatric conditions and pain conditions. 3. Being familiar with the management of complications and preparation for handling emergency situations which may arise in the outpatient setting of an interventional pain practice. 4. Being familiar with : o Management of acute and chronic neck and back pain; o Management of headache; o Management of chronic soft tissue, myofascial, and fibromyalgia pain; o Management of chronic visceral pain; o Sleep disorders; o Neuropathic pain, and; o Pain in children, in elderly, in pregnancy and lactation (if applicable). 3. Completing specific courses 12 as recommended by his/her supervisor. 12 For example, Canadian Pain Society-sponsored interventional pain courses, or ISIS courses to provide basic knowledge and practice for fluoroscopy and ultrasound-guided interventions. 7
8 (B) Expectations of Procedural-Specific Knowledge, Skills and Judgment for IPM Physicians, having gained competencies and general knowledge, skills and judgment required for the diagnosis and management of pain are then required to have specific procedural competence for each procedure that they want to perform. For any given procedure, the physician must: 1) Demonstrate experience with all aspects of the clinical features of the procedure through working with an approved supervisor under HIGH supervision. Under HIGH supervision, the supervisor, at all times, remains the most responsible physician for all aspects of care. The supervising physician is expected to be on-site at all times for the immediate pre-procedure, the entire procedure and the immediately postprocedure periods. The supervisor(s), at their own discretion, can delegate increasing responsibility to the physician learning the new procedure much as would happen during a residency experience. The clinical features to be learned include: a) Assessing patients in consultation for suitability for the procedure, discussion of risks, benefits and alternatives, obtaining informed consent and routine preprocedure assessment; b) Assessing patients with regard to the risks/benefits of using sedation, with knowledge and experience in IV access and monitoring; c) Assessing patients in the immediate pre-procedure period, including patient positioning, identification of landmarks; d) Assisting and eventually performing the procedure, with knowledge and experience in managing complications; e) Management of the patient in the immediate post-procedure period, including any post-procedure complications, and; f) Management of the patient and complications at follow-up. 2) Demonstrate experience with all aspects of the clinical features of the procedure through working with an approved supervisor under LOWER levels of supervision. This stage of the change of scope can commence only after the supervisor(s) involved in high supervision feels that the physician is capable of practicing independently without risk to patient safety and the College approves it. Lower supervision (Moderate and Low) means that the physician is working independently but is visited by his/her supervisor on a regular basis in order to review records and observe procedures. The supervisor is also available to support the physician in his/her new field of practice. 3) Obtain Advanced Cardiac Life Support certification. Physicians who perform IPM procedures and manage recovery of paediatric patients (those patients age 18 and under) are also required to obtain Paediatric Advanced Life Support (PALS) certification. 4) Acquire competency in Imaging interpretation, if applicable. 5) Acquire competency in fluoroscopy and ultrasound techniques, if applicable; this would include basic knowledge of radiation safety. 8
9 6) Demonstrate knowledge of how to identify and manage emergency situations in IPM related to: a. Vasovagal Reaction b. Hypotension c. Hypertension d. Local anaesthetic toxicity e. High Spinal f. Pneumothorax g. Anaphylaxis h. Spinal cord ischemia/paralysis (e.g. related to transforaminal epidural steroid injections, or celiac plexus blocks/splanchnic blocks i. Seizures 7) Demonstrate competence in the above areas through a College-directed assessment of his/her practice in the relevant area. The College assessment may include, but is not limited to: a) A review of all educational outcomes and supervision reports from the entire educational process; b) A review patient charts in private office, or hospital, or Out-of-Hospital Premises c) Observation of physician performing procedures requested in the change of scope of practice application; d) Multi-source feedback including, but not limited to, interviews with significant stakeholders including all supervisors, staff including nursing, and medical staff and physicians who refer to the physician and patients, and; e) Review of CPSO physician profile. Revised: May12,
10 Appendix 1 List of Interventional Pain Procedures Below is a listing of interventional procedures appropriately performed in interventional clinics. Some of these benefit from imaging guidance. Treatment may include injection of medications and/or use of radio frequency lesioning or pulsed treatment. Interventional Pain Management Procedures RISK LEVEL TYPE OF NERVE BLOCK DEFINITION CRANIAL NERVE BLOCKS/DEEP NERVES OF THE HEAD AND NECK HIGH RISK Trigeminal/Ganglion Block A block of the trigeminal ganglion (semilunar ganglion, gasserian ganglion) situated in Meckel s cavity. The block is used in the treatment of trigeminal neuralgia, cluster headaches, pain in the eye region and other head and facial pain. Sphenopalatine Ganglion Block A block of the nasoplatine nerve(s) used for treating facial and head pain located in pterygopalatine fossa. Glossopharyngeal Nerve Block A block of the glossopharyngeal nerve in the extracranial course for treatment of facial and head pain. Hypoglossal Nerve Block Maxillary Nerve Block A block of the XII cranial nerve involving the tongue. The nerve emerges from the skull through the round foramen. The nerve can be accessed intra-orally (medial to the posterior edge of the second maxillary molar through the greater palatine foramen) or extra orally above or beneath (mandibular fossa) the zygomatic arch for nerve blocks. LOW RISK Spinal Accessory Nerve Block A block of the spinal accessory nerve (cranial nerve XI). Superficial branches of CN V A block of the 3 divisions of the Cranial V nerve or trigeminal nerve. This includes V1, V2 and V3 distribution or ophthalmic, maxillary and mandibular nerves respectively. Mandibular Nerve Block A block of the mandibular nerve for treatment of facial pain in the V3 distribution. Auriculotemporal Nerve Block Infraorbital Nerve Block Mental Nerve Block Supraorbital Block Zygomatic Temporal Nerve Block Occipital Block of the nerve at the origin of the zygoma between the otic canal and temporomandibular Joint. Block of the nerve at the infra-orbital foramen. The mental nerve is the sensory end branch of the mandibular nerve as it emerges from the mental foramen. Nerve blocks can be carried out intra or extra orally. The supraorbital nerve passes through the supraorbital notch. The nerve block is carried out after palpation of the supraorbital foramen. Block of the nerve between the orbit and the ear superior to the zygomatic arch. Occipital nerve blocks including greater or lesser occipital nerves. 10
11 RISK LEVEL NEURAXIAL BLOCKS HIGH RISK Interventional Pain Management Procedures TYPE OF NERVE BLOCK DEFINITION Central neuraxial blocks including: Intrathecal blocks Neuraxial anesthesia pertains to local anesthetics placed around the nerves of the central nervous system, such as spinal anesthesia (also called subarachnoid anesthesia), and epidural anesthesia. Intrathecal Block is administration of drugs into the subarachnoid space. Spinal cord stimulation A spinal cord stimulator is a device used to exert pulsed electrical signals to the spinal cord to control chronic pain. Spinal cord stimulation (SCS), in the simplest form, consists of stimulating electrodes, implanted in the epidural space, an electrical pulse generator, implanted in the lower abdominal area or gluteal region, conducting wires connecting the electrodes to the generator, and the generator remote control. SCS has notable analgesic properties and, at the present, is used mostly in the treatment of failed back surgery syndrome, complex regional pain syndrome and refractory pain due to ischemia. Epidural blocks Interlaminar Transforaminal Caudal Epidural Adhesiolysis Nerve root blocks Epidural steroid injection - There are three types of epidural steroid injection: interlaminar, caudal, and transforaminal epidural steroid injection Epidural lysis of adhesions is performed by placement of a catheter/guide wire into the epidural space using X-ray guidance for proper placement. Once the catheter is in the proper location where the scar tissue is affecting the nerve root, medications are injected into the space in order to dissolve the scar tissue and reduce the inflammation and irritation on the nerve. Selective lumbar nerve root block in the vicinity of, but distal to the foramen. Blocks involving the facet joints: Medial branch block The target is the medial branch of the cervical, thoracic or lumbar dorsal rami where the nerves course around the articular pillar (cervical) or between superior articular process (SAP) and transverse process Peri-articular facet blocks Intra articular facet block. Injection inside or around the facet joint. 11
12 RISK LEVEL Interventional Pain Management Procedures TYPE OF NERVE BLOCK DEFINITION NEURAXIAL BLOCKS (continued) HIGH RISK Paravertebral nerve blocks A paravertebral block is a block of the spinal nerve where local anesthetic is injected in the paravertebral space. Thoracic: The boundaries of thoracic paravertebral space are defined anterior-laterally by the parietal pleura; posteriorly by the superior costotransverse ligament (thoracic levels); medially by the vertebrae, vertebral disk, and intervertebral foramina; and superiorly and inferiorly by the heads of the ribs. When the needle is inserted posteriorly, it has to pass through the transverse process to get into the space. Lumbar: The boundaries are the psoas muscle anterolaterally, vertebral body/disc intervertebral foramen, and pedicle medially, and transverse process posteriorly. Cervical: The cervical paravertebral space is not a discrete space as in thoracic and lumbar paravertebral space. The nerve block is a block of the cervical spinal nerve. Provocative discography Kyphoplasty Injection of contrast to the nucleus pulposus of the intervertebral disc. A form of Vertebral augmentation used to stabilize a fractured vertebra with the goal of reducing the patient's pain caused by a compression fracture. Kyphoplasty involves a small incision, and fluoroscopically guided balloon reduction of the fractured vertabrae, followed by injection of vertebral cement into the affected vertebral level for stabilization of the fractured vertebral fragments. Biacuplasty A disc denervation procedure which involves fluoroscopic electrode placement onto intervertebral discs with the purpose of application of a radiofrequency current through the disc. The goal is to achieve of ablation of the neurons that generate pain sensations. The indication is for the reduction of chronic back pain caused by the intervertebral disc. 12
13 RISK TYPE OF NERVE BLOCK LEVEL PERIPHERAL NERVE BLOCKS Interventional Pain Management Procedures DEFINITION HIGH RISK Femoral Peri-nerual injection of the femoral nerve and the target is usually in the infrainguinal region. Sciatic Perineural injection of the sciatic nerve. Popliteal Perineural injection of the sciatic nerve at the popliteal fossa. Intercostal Pudendal Perineural injection of the intercostal nerve, principally the lateral cutaneous branch. Perineural injection of the pudendal nerve (S2-4) at the ischial spine level or Alcock canal. It can be achieved by transgluteal, transvaginal or transperineal approach. LOW RISK Proximal Radial/Median/Ulnar Nerve block of the Proximal Radial/Median/Ulnar nerve. Suprascapular/transcapular Ilioinguinal/iliohypogastric Genitofemoral Suprascapular nerve blocks at the notch or the suprascapular fossa. A block of the Ilioinguinal nerve and/or illiohypogastric nerve in the abdominal wall A block of the Genitofemoral nerve. PLEXUS BLOCKS HIGH RISK Deep Cervical A deep cervical plexus block is of the C2-C4 spinal nerves as they emerge from the foramina of their respective vertebrae. Upper extremity/brachial Coeliac Lower Extremity/Lumbar Hypogastric plexus Ganglion of impar A brachial plexus block is a block of the brachial plexus. A coeliac plexus block is an injection of medication into or around the coeliac plexus that surround the aorta. A modification of the target is splanchnic nerves. A lumbar plexus block is a nerve block of this plexus. A block of the Hypogastric plexus in the anterior aspect of lumbosacral junction. A block of the ganglion anterior to the sacrococcygeal junction. LOW RISK Superficial Cervical Nerve plexus deep to the SCM muscle. SYMPATHETIC NERVE BLOCKS HIGH RISK Stellate ganglion A block of the sympathetic ganglion formed by the fusion of inferior cervical and first thoracic ganglion. It is commonly approached at the cervical sympathetic chain. Lumbar sympathetic A block of the sympathetic chain to the lower limb in the anteriolateral aspect of L2-L4. 13
14 RISK LEVEL TYPE OF NERVE BLOCK INTRAVENOUS BLOCKS HIGH RISK Local Anaesthetic Bretylium Interventional Pain Management Procedures DEFINITION Injection of medication intravenously requiring pneumatic tourniquet and monitoring; limb exsanguinated and tourniquet inflation for minutes INTRAVENOUS INFUSIONS HIGH RISK Lidocaine Ketamine JOINTS Continuous IV infusion of ketamine and/or lidocaine for pain relief. LOW RISK Sacroiliac joints An injection of medication either intra or peri-articular of the joint. NEUROABLATIVE BLOCKS HIGH RISK Radiofrequency Ablation Is a percutaneous therapeutic image-guided procedure in which a radiofrequency electrode is used to coagulate one or more nerves 14
Cover page DRAFT PROCEDURAL PAIN MANAGEMENT
 Cover page DRAFT PROCEDURAL PAIN MANAGEMENT 3 April 2018 Please find attached the DRAFT privileges for PROCEDURAL (INTERVENTIONAL) PAIN MANAGEMENT. THE PANEL: This draft was developed by a provincial panel
Cover page DRAFT PROCEDURAL PAIN MANAGEMENT 3 April 2018 Please find attached the DRAFT privileges for PROCEDURAL (INTERVENTIONAL) PAIN MANAGEMENT. THE PANEL: This draft was developed by a provincial panel
2017 FINAL - Physician Payment Rates rates compared to 2016 rates
 Injection, therapeutic (eg, local anesthetic; corticosteroid), carpal tunnel 20526 $79.18 $59.47 $79.06 $59.74 $78.96 $59.58-0.3% 0.2% tendon sheath, ligament injection 20550 $60.19 $42.99 $54.02 $40.78
Injection, therapeutic (eg, local anesthetic; corticosteroid), carpal tunnel 20526 $79.18 $59.47 $79.06 $59.74 $78.96 $59.58-0.3% 0.2% tendon sheath, ligament injection 20550 $60.19 $42.99 $54.02 $40.78
UBC Pain Medicine Residency Program: CanMEDS Goals and Objectives of the 4 week UBC Interventional Pain Management Elective: Goals & Objectives
 UBC Pain Medicine Residency Program: CanMEDS Goals and Objectives of the 4 week UBC Interventional Pain Management Elective: Goals & Objectives Overview Further Interventional Pain training over 4 weeks
UBC Pain Medicine Residency Program: CanMEDS Goals and Objectives of the 4 week UBC Interventional Pain Management Elective: Goals & Objectives Overview Further Interventional Pain training over 4 weeks
2019 PROPOSED - Physician Payment Rates rates compared to 2018 rates
 Injection, therapeutic (eg, local anesthetic; corticosteroid), carpal tunnel 20526 $78.96 $59.58 $79.56 $59.76 $79.30 $59.84-0.3% 0.1% tendon sheath, ligament injection 20550 $53.83 $40.55 $54.36 $40.68
Injection, therapeutic (eg, local anesthetic; corticosteroid), carpal tunnel 20526 $78.96 $59.58 $79.56 $59.76 $79.30 $59.84-0.3% 0.1% tendon sheath, ligament injection 20550 $53.83 $40.55 $54.36 $40.68
2013 FINAL - Physician Payment Rates
 ASC/Hospital) Injection, therapeutic (eg, local anesthetic; corticosteroid), 20526 carpal tunnel $74.88 $56.50 $76.55 $56.48 2.2% 0.0% tendon sheath, ligament injection 20550 $57.18 $40.85 $58.52 $41.17
ASC/Hospital) Injection, therapeutic (eg, local anesthetic; corticosteroid), 20526 carpal tunnel $74.88 $56.50 $76.55 $56.48 2.2% 0.0% tendon sheath, ligament injection 20550 $57.18 $40.85 $58.52 $41.17
Basic Standards for. Fellowship Training in. Acute and Chronic Pain Management. in Anesthesiology
 Basic Standards for Fellowship Training in Acute and Chronic Pain Management in Anesthesiology American Osteopathic Association and American Osteopathic College of Anesthesiologists BOT, 7/1995 BOT, 11/2002
Basic Standards for Fellowship Training in Acute and Chronic Pain Management in Anesthesiology American Osteopathic Association and American Osteopathic College of Anesthesiologists BOT, 7/1995 BOT, 11/2002
Regions Hospital Delineation of Privileges Pain Medicine
 Regions Hospital Delineation of s Pain Medicine Applicant s Name: Last First M. Instructions: Place a check-mark where indicated for each core group you are requesting. Review education and basic formal
Regions Hospital Delineation of s Pain Medicine Applicant s Name: Last First M. Instructions: Place a check-mark where indicated for each core group you are requesting. Review education and basic formal
BAYLOR SCOTT & WHITE TEXAS SPINE & JOINT HOSPITAL
 BAYLOR SCOTT & WHITE TEXAS SPINE & JOINT HOSPITAL NAME: Initial Appointment / Reappointment / Update (Circle One) REQUESTED PRIVILEGE PAIN BLOCKS Blood Patch Hardware Block Epidurogram Fluoroscopy Intradural/Intrathecal
BAYLOR SCOTT & WHITE TEXAS SPINE & JOINT HOSPITAL NAME: Initial Appointment / Reappointment / Update (Circle One) REQUESTED PRIVILEGE PAIN BLOCKS Blood Patch Hardware Block Epidurogram Fluoroscopy Intradural/Intrathecal
2018 ASC FINAL Payment Rates
 20526 20550 20551 20552 20553 20600 20605 20610 22510 22511 22513 22514 62263 62264 62268 62269 62270 62272 62273 Injection, therapeutic tendon sheath, ligament injection Tendon origin/insertion injection
20526 20550 20551 20552 20553 20600 20605 20610 22510 22511 22513 22514 62263 62264 62268 62269 62270 62272 62273 Injection, therapeutic tendon sheath, ligament injection Tendon origin/insertion injection
Beth Israel Deaconess Medical Center Department of Anesthesia, Critical Care, and Pain Medicine Rotation: Interventional Pain
 Beth Israel Deaconess Medical Center Department of Anesthesia, Critical Care, and Pain Medicine Rotation: Interventional Pain Goals GOALS AND OBJECTIVES The ACGME recognizes that interventional pain medicine
Beth Israel Deaconess Medical Center Department of Anesthesia, Critical Care, and Pain Medicine Rotation: Interventional Pain Goals GOALS AND OBJECTIVES The ACGME recognizes that interventional pain medicine
2019 ASC FINAL Payment Rates
 20526 20550 20551 20552 20553 20600 20605 20610 22510 22511 22513 22514 22869 27279 62263 62264 62268 62269 62270 Injection, therapeutic tendon sheath, ligament injection Tendon origin/insertion injection
20526 20550 20551 20552 20553 20600 20605 20610 22510 22511 22513 22514 22869 27279 62263 62264 62268 62269 62270 Injection, therapeutic tendon sheath, ligament injection Tendon origin/insertion injection
2019 ASC Proposed Payment Rates
 20526 20550 20551 20552 20553 20600 20605 20610 22510 22511 22513 22514 22869 27279 62263 62264 62268 62269 62270 Injection, therapeutic tendon sheath, ligament injection Tendon origin/insertion injection
20526 20550 20551 20552 20553 20600 20605 20610 22510 22511 22513 22514 22869 27279 62263 62264 62268 62269 62270 Injection, therapeutic tendon sheath, ligament injection Tendon origin/insertion injection
INDIANA HEALTH COVERAGE PROGRAMS
 INDIANA HEALTH COVERAGE PROGRAMS PROVIDER CODE TABLES Note: Due to possible changes in Indiana Health Coverage Programs (IHCP) policy or national coding updates, inclusion of a code on the code tables
INDIANA HEALTH COVERAGE PROGRAMS PROVIDER CODE TABLES Note: Due to possible changes in Indiana Health Coverage Programs (IHCP) policy or national coding updates, inclusion of a code on the code tables
PAIN MANAGEMENT CODES PRIOR AUTHORIZATION REQUIRED THROUGH EVICORE HEALTHCARE
 PAIN MANAGEMENT CODES PRIOR AUTHORIZATION REQUIRED THROUGH EVICORE HEALTHCARE The following CPT/HCPCS codes for pain management require prior authorization through evicore healthcare. In order to request
PAIN MANAGEMENT CODES PRIOR AUTHORIZATION REQUIRED THROUGH EVICORE HEALTHCARE The following CPT/HCPCS codes for pain management require prior authorization through evicore healthcare. In order to request
Pain Management Clinic ISIC
 Pain Management Clinic ISIC Let us rebuild a pain free life Pain is one of the commonest symptoms in patients attending OPDs of various hospitals and clinics. Chronic pain is any pain that has persisted
Pain Management Clinic ISIC Let us rebuild a pain free life Pain is one of the commonest symptoms in patients attending OPDs of various hospitals and clinics. Chronic pain is any pain that has persisted
Epidural Steroid Injection
 Epidural Steroid Injection Epidural steroid injections (ESI) are performed to place anti-inflammatory medication (steroid) and local anesthetic in the epidural space to target irritated nerves and relieve
Epidural Steroid Injection Epidural steroid injections (ESI) are performed to place anti-inflammatory medication (steroid) and local anesthetic in the epidural space to target irritated nerves and relieve
Management of Neuropathic pain
 Management of Neuropathic pain Ravi Parekodi Consultant in Anaesthetics and Pain Management 08/04/2014 Ref: BJA July2013, Map of Medicine2013, Pain Physician 2007, IASP 2012, Nice guideline 2013 Aims Highlight
Management of Neuropathic pain Ravi Parekodi Consultant in Anaesthetics and Pain Management 08/04/2014 Ref: BJA July2013, Map of Medicine2013, Pain Physician 2007, IASP 2012, Nice guideline 2013 Aims Highlight
Synapse Homework. Back page last question not counted. 4 pts total, each question worth 0.18pts. 26/34 students answered correctly!
 Synapse Homework Back page last question not counted 26/34 students answered correctly! 4 pts total, each question worth 0.18pts Business TASS hours extended! MWF 1-2pm, Willamette 204 T and Th 9:30-10:30am,
Synapse Homework Back page last question not counted 26/34 students answered correctly! 4 pts total, each question worth 0.18pts Business TASS hours extended! MWF 1-2pm, Willamette 204 T and Th 9:30-10:30am,
Policy Specific Section:
 Payment Policy Anesthesia Services Type: Payment Policy Policy Specific Section: Payment Original Policy Date: Effective Date: October 1, 2010 06-16-2014 Description Anesthesia services consist of the
Payment Policy Anesthesia Services Type: Payment Policy Policy Specific Section: Payment Original Policy Date: Effective Date: October 1, 2010 06-16-2014 Description Anesthesia services consist of the
Placename CCG. Policies for the Commissioning of Healthcare. Policy for Managing Back Pain- Spinal Injections
 Placename CCG Policies for the Commissioning of Healthcare Policy for Managing Back Pain- Spinal Injections 1 Introduction 1.1 This document is part of a suite of policies that the CCG uses to drive its
Placename CCG Policies for the Commissioning of Healthcare Policy for Managing Back Pain- Spinal Injections 1 Introduction 1.1 This document is part of a suite of policies that the CCG uses to drive its
Infratemporal fossa: Tikrit University college of Dentistry Dr.Ban I.S. head & neck Anatomy 2 nd y.
 Infratemporal fossa: This is a space lying beneath the base of the skull between the lateral wall of the pharynx and the ramus of the mandible. It is also referred to as the parapharyngeal or lateral pharyngeal
Infratemporal fossa: This is a space lying beneath the base of the skull between the lateral wall of the pharynx and the ramus of the mandible. It is also referred to as the parapharyngeal or lateral pharyngeal
Human Anatomy and Physiology - Problem Drill 07: The Skeletal System Axial Skeleton
 Human Anatomy and Physiology - Problem Drill 07: The Skeletal System Axial Skeleton Question No. 1 of 10 Which of the following statements about the axial skeleton is correct? Question #01 A. The axial
Human Anatomy and Physiology - Problem Drill 07: The Skeletal System Axial Skeleton Question No. 1 of 10 Which of the following statements about the axial skeleton is correct? Question #01 A. The axial
Organisation of the nervous system
 Chapter1 Organisation of the nervous system 1. Subdivisions of the nervous system The nervous system is divided: i) Structurally The central nervous system (CNS) composed of the brain and spinal cord.
Chapter1 Organisation of the nervous system 1. Subdivisions of the nervous system The nervous system is divided: i) Structurally The central nervous system (CNS) composed of the brain and spinal cord.
Reimbursement Guidelines for Pain Management Procedures 1
 GE Healthcare Reimbursement Guidelines for Pain Management Procedures 1 April 2015 www.gehealthcare.com/reimbursement This overview addresses coding, coverage, and payment for pain management procedures
GE Healthcare Reimbursement Guidelines for Pain Management Procedures 1 April 2015 www.gehealthcare.com/reimbursement This overview addresses coding, coverage, and payment for pain management procedures
Nonsurgical Interventional Treatments for Spinal Pain Management
 Nonsurgical Interventional Treatments for Spinal Pain Management I. Policy University Health Alliance (UHA) will reimburse for nonsurgical interventional treatment for subacute and chronic spinal pain
Nonsurgical Interventional Treatments for Spinal Pain Management I. Policy University Health Alliance (UHA) will reimburse for nonsurgical interventional treatment for subacute and chronic spinal pain
Surgery Under Regional Anesthesia
 Surgery Under Regional Anesthesia Jean Daniel Eloy, MD Assistant Professor Residency Program Director Rutgers-New Jersey Medical School Rutgers The State University of New Jersey Peripheral Nerve Block
Surgery Under Regional Anesthesia Jean Daniel Eloy, MD Assistant Professor Residency Program Director Rutgers-New Jersey Medical School Rutgers The State University of New Jersey Peripheral Nerve Block
Interventional Pain. Judith Dunipace MD Board certified in Anesthesiology, Pain Management and Hospice and Palliative Care
 Interventional Pain Judith Dunipace MD Board certified in Anesthesiology, Pain Management and Hospice and Palliative Care IASP Definition of Pain Pain is an unpleasant sensory or emotional experience associated
Interventional Pain Judith Dunipace MD Board certified in Anesthesiology, Pain Management and Hospice and Palliative Care IASP Definition of Pain Pain is an unpleasant sensory or emotional experience associated
Corporate Medical Policy
 Corporate Medical Policy Epidural Steroid Injections for Back Pain File Name: Origination: Last CAP Review: Next CAP Review: Last Review: epidural_steroid_injections_for_back_pain 2/2016 4/2017 4/2018
Corporate Medical Policy Epidural Steroid Injections for Back Pain File Name: Origination: Last CAP Review: Next CAP Review: Last Review: epidural_steroid_injections_for_back_pain 2/2016 4/2017 4/2018
Spinal and Trigger Point Injections
 Spinal and Trigger Point Injections I. Policy University Health Alliance (UHA) will reimburse for nonsurgical interventional treatment for subacute and chronic spinal pain when determined to be medically
Spinal and Trigger Point Injections I. Policy University Health Alliance (UHA) will reimburse for nonsurgical interventional treatment for subacute and chronic spinal pain when determined to be medically
22110 vertebral segment; cervical vertebral segment; thoracic vertebral segment; lumbar
 The following codes are authorized by Palladian Health for applicable product lines. Visit palladianhealth.com to request authorization and to access guidelines. Palladian Musculoskeletal Program Codes
The following codes are authorized by Palladian Health for applicable product lines. Visit palladianhealth.com to request authorization and to access guidelines. Palladian Musculoskeletal Program Codes
Human Anatomy Biology 351
 nnnnn 1 Human Anatomy Biology 351 Exam #2 Please place your name on the back of the last page of this exam. You must answer all questions on this exam. Because statistics demonstrate that, on average,
nnnnn 1 Human Anatomy Biology 351 Exam #2 Please place your name on the back of the last page of this exam. You must answer all questions on this exam. Because statistics demonstrate that, on average,
nerve blocks in the diagnosis and therapy of visceral disease
 Visceral Pain nerve blocks in the diagnosis and therapy of visceral disease Guy Hans, MD, PhD Dept. of Anesthesiology, Multidisciplinary Pain Center Visceral Pain? Type of nociceptive pain (although often
Visceral Pain nerve blocks in the diagnosis and therapy of visceral disease Guy Hans, MD, PhD Dept. of Anesthesiology, Multidisciplinary Pain Center Visceral Pain? Type of nociceptive pain (although often
PERIPHERAL NERVOUS SYSTEM
 CHAPTER 13 PERIPHERAL NERVOUS SYSTEM Functional division of nervous system = afferent info to the CNS ascending spinal cord = efferent info from CNS descending spinal cord somatic skin, muscles visceral
CHAPTER 13 PERIPHERAL NERVOUS SYSTEM Functional division of nervous system = afferent info to the CNS ascending spinal cord = efferent info from CNS descending spinal cord somatic skin, muscles visceral
Human Anatomy. Spinal Cord and Spinal Nerves
 Human Anatomy Spinal Cord and Spinal Nerves 1 The Spinal Cord Link between the brain and the body. Exhibits some functional independence from the brain. The spinal cord and spinal nerves serve two functions:
Human Anatomy Spinal Cord and Spinal Nerves 1 The Spinal Cord Link between the brain and the body. Exhibits some functional independence from the brain. The spinal cord and spinal nerves serve two functions:
Spinal nerves and cervical plexus Prof. Abdulameer Al Nuaimi. E mail: a.al E. mail:
 Spinal nerves and cervical plexus Prof. Abdulameer Al Nuaimi E mail: a.al nuaimi@sheffield.ac.uk E. mail: abdulameerh@yahoo.com Branches of ophthalmic artery Muscles of face A spinal nerve Spinal
Spinal nerves and cervical plexus Prof. Abdulameer Al Nuaimi E mail: a.al nuaimi@sheffield.ac.uk E. mail: abdulameerh@yahoo.com Branches of ophthalmic artery Muscles of face A spinal nerve Spinal
2012 CPT Changes Affecting Radiology REVISIONS
 2012 CPT Changes Affecting Radiology REVISIONS 22520 Percutaneous vertebroplasty (bone biopsy included when performed), 1 vertebral body, unilateral or bilateral injection; thoracic 22521 lumbar 22522
2012 CPT Changes Affecting Radiology REVISIONS 22520 Percutaneous vertebroplasty (bone biopsy included when performed), 1 vertebral body, unilateral or bilateral injection; thoracic 22521 lumbar 22522
Blackburn with Darwen Clinical Commissioning Group and East Lancashire Clinical Commissioning Group. Policies for the Commissioning of Healthcare
 Blackburn with Darwen Clinical Commissioning Group and East Lancashire Clinical Commissioning Group Policies for the Commissioning of Healthcare Policy for Managing Back Pain Spinal /Facet Joint and Epidural
Blackburn with Darwen Clinical Commissioning Group and East Lancashire Clinical Commissioning Group Policies for the Commissioning of Healthcare Policy for Managing Back Pain Spinal /Facet Joint and Epidural
Discussion Points 10/17/16. Spine Pain is Ubiquitous. Interventional Pain Management
 Interventional Pain Management Blake Christensen, D.O. Fellowship Trained Interventional Pain Management Board Eligible in Anesthesiology and Interventional Pain Management Oklahoma Interventional Pain
Interventional Pain Management Blake Christensen, D.O. Fellowship Trained Interventional Pain Management Board Eligible in Anesthesiology and Interventional Pain Management Oklahoma Interventional Pain
The Thoracic wall including the diaphragm. Prof Oluwadiya KS
 The Thoracic wall including the diaphragm Prof Oluwadiya KS www.oluwadiya.com Components of the thoracic wall Skin Superficial fascia Chest wall muscles (see upper limb slides) Skeletal framework Intercostal
The Thoracic wall including the diaphragm Prof Oluwadiya KS www.oluwadiya.com Components of the thoracic wall Skin Superficial fascia Chest wall muscles (see upper limb slides) Skeletal framework Intercostal
Autonomic Nervous System. Ms. DS Pillay Room 2P24
 Autonomic Nervous System Ms. DS Pillay Room 2P24 OVERVIEW OF THE NERVOUS SYSTEM NERVOUS SYSTEM CNS PNS BRAIN SPINAL CORD SOMATIC ANS SYMPATHEIC PARASYMPATHEIC LOCATION OF GANGLIA IN THE ANS Short post-ganglionic
Autonomic Nervous System Ms. DS Pillay Room 2P24 OVERVIEW OF THE NERVOUS SYSTEM NERVOUS SYSTEM CNS PNS BRAIN SPINAL CORD SOMATIC ANS SYMPATHEIC PARASYMPATHEIC LOCATION OF GANGLIA IN THE ANS Short post-ganglionic
Clarification of Terms
 Clarification of Terms The Spine, Spinal Column, and Vertebral Column are synonymous terms referring to the bony components housing the spinal cord Spinal Cord = made of nervous tissue Facet = a small,
Clarification of Terms The Spine, Spinal Column, and Vertebral Column are synonymous terms referring to the bony components housing the spinal cord Spinal Cord = made of nervous tissue Facet = a small,
Clarification of Terms
 Clarification of Terms The Spine, Spinal Column, and Vertebral Column are synonymous terms referring to the bony components housing the spinal cord Spinal Cord = made of nervous tissue Facet = a small,
Clarification of Terms The Spine, Spinal Column, and Vertebral Column are synonymous terms referring to the bony components housing the spinal cord Spinal Cord = made of nervous tissue Facet = a small,
Medical Affairs Policy
 Medical Affairs Policy Service: Back Pain Procedures-Epidural Injection (Caudal Epidural, Selective Nerve Root Block, Interlaminar, Transforaminal, Translaminar Epidural Injection) PUM 250-0015-1706 Medical
Medical Affairs Policy Service: Back Pain Procedures-Epidural Injection (Caudal Epidural, Selective Nerve Root Block, Interlaminar, Transforaminal, Translaminar Epidural Injection) PUM 250-0015-1706 Medical
PERCUTANEOUS FACET JOINT DENERVATION
 Status Active Medical and Behavioral Health Policy Section: Surgery Policy Number: IV-95 Effective Date: 10/22/2014 Blue Cross and Blue Shield of Minnesota medical policies do not imply that members should
Status Active Medical and Behavioral Health Policy Section: Surgery Policy Number: IV-95 Effective Date: 10/22/2014 Blue Cross and Blue Shield of Minnesota medical policies do not imply that members should
Pain Management. Medicine. without limits
 Pain Management Medicine without limits Minimally invasive therapies for chronic pain relief Thanks to advances in medicine, you don t have to live with the debilitating effects of chronic pain. The physicians
Pain Management Medicine without limits Minimally invasive therapies for chronic pain relief Thanks to advances in medicine, you don t have to live with the debilitating effects of chronic pain. The physicians
Parotid Gland, Temporomandibular Joint and Infratemporal Fossa
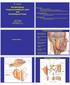 M1 - Anatomy Parotid Gland, Temporomandibular Joint and Infratemporal Fossa Jeff Dupree Sanger 9-057 jldupree@vcu.edu Parotid gland: wraps around the mandible positioned between the mandible and the sphenoid
M1 - Anatomy Parotid Gland, Temporomandibular Joint and Infratemporal Fossa Jeff Dupree Sanger 9-057 jldupree@vcu.edu Parotid gland: wraps around the mandible positioned between the mandible and the sphenoid
The posterior abdominal wall. Prof. Oluwadiya KS
 The posterior abdominal wall Prof. Oluwadiya KS www.oluwadiya.sitesled.com Posterior Abdominal Wall Lumbar vertebrae and discs. Muscles opsoas, quadratus lumborum, iliacus, transverse, abdominal wall
The posterior abdominal wall Prof. Oluwadiya KS www.oluwadiya.sitesled.com Posterior Abdominal Wall Lumbar vertebrae and discs. Muscles opsoas, quadratus lumborum, iliacus, transverse, abdominal wall
THE THORACIC WALL. Boundaries Posteriorly by the thoracic part of the vertebral column. Anteriorly by the sternum and costal cartilages
 THE THORACIC WALL Boundaries Posteriorly by the thoracic part of the vertebral column Anteriorly by the sternum and costal cartilages Laterally by the ribs and intercostal spaces Superiorly by the suprapleural
THE THORACIC WALL Boundaries Posteriorly by the thoracic part of the vertebral column Anteriorly by the sternum and costal cartilages Laterally by the ribs and intercostal spaces Superiorly by the suprapleural
Parotid Gland. Parotid Gland. Largest of 3 paired salivary glands (submandibular; sublingual) Ramus of Mandible. Medial pterygoid.
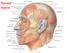 Parotid region Parotid Gland Largest of 3 paired salivary glands (submandibular; sublingual) Ramus of Mandible Medial pterygoid Cross section of mandible Masseter D S SCM Parotid Gland Mastoid Process
Parotid region Parotid Gland Largest of 3 paired salivary glands (submandibular; sublingual) Ramus of Mandible Medial pterygoid Cross section of mandible Masseter D S SCM Parotid Gland Mastoid Process
ISPUB.COM. Lumbar Sympathectomy by Laser Technique. S Kantha, B Kantha METHODS AND MATERIALS
 ISPUB.COM The Internet Journal of Minimally Invasive Spinal Technology Volume 1 Number 2 Lumbar Sympathectomy by Laser Technique S Kantha, B Kantha Citation S Kantha, B Kantha. Lumbar Sympathectomy by
ISPUB.COM The Internet Journal of Minimally Invasive Spinal Technology Volume 1 Number 2 Lumbar Sympathectomy by Laser Technique S Kantha, B Kantha Citation S Kantha, B Kantha. Lumbar Sympathectomy by
INDEX. Cancerpain alcohol neurolysis for, 5, 20, 53-54
 INDEX Alcohol advantages of, 54 celiac plexus block with, 19-20, 165 chemical hypophysectomy with, 20 complications and side effects of, 18, 19, 45-46, 54-55 contraindications for, 54 doses with, 52 drug
INDEX Alcohol advantages of, 54 celiac plexus block with, 19-20, 165 chemical hypophysectomy with, 20 complications and side effects of, 18, 19, 45-46, 54-55 contraindications for, 54 doses with, 52 drug
Clarification of Terms
 Clarification of Terms The Spine, Spinal Column, and Vertebral Column are synonymous terms referring to the bony components housing the spinal cord Spinal Cord = made of nervous tissue Facet = a small,
Clarification of Terms The Spine, Spinal Column, and Vertebral Column are synonymous terms referring to the bony components housing the spinal cord Spinal Cord = made of nervous tissue Facet = a small,
cardiac plexus is continuous with the coronary and no named branches pain from the heart and lungs
 Nerves of the Thoracic Region Nerve Source Branches Motor Sensory Notes cardiac plexus cardiac brs. of the vagus n. and cervical ; thoracic l nn. the heart and lungs cardiac, cervical cardiac, vagal vagus
Nerves of the Thoracic Region Nerve Source Branches Motor Sensory Notes cardiac plexus cardiac brs. of the vagus n. and cervical ; thoracic l nn. the heart and lungs cardiac, cervical cardiac, vagal vagus
PTERYGOPALATINE FOSSA
 PTERYGOPALATINE FOSSA Outline Anatomical Structure and Boundaries Foramina and Communications with other spaces and cavities Contents Pterygopalatine Ganglion Especial emphasis on certain arteries and
PTERYGOPALATINE FOSSA Outline Anatomical Structure and Boundaries Foramina and Communications with other spaces and cavities Contents Pterygopalatine Ganglion Especial emphasis on certain arteries and
Table of Contents: Part 1 General principles. Section 1: Introduction. 1. Past, present and future of interventional physiatry 2.
 Table of Contents: Part 1 General principles Section 1: Introduction 1. Past, present and future of interventional physiatry 2. Epidemiology Section 2: Spinal pain 3. Inflammatory basis of spinal pain
Table of Contents: Part 1 General principles Section 1: Introduction 1. Past, present and future of interventional physiatry 2. Epidemiology Section 2: Spinal pain 3. Inflammatory basis of spinal pain
2. The vertebral arch is composed of pedicles (projecting from the body) and laminae (uniting arch posteriorly).
 VERTEBRAL COLUMN 2018zillmusom I. VERTEBRAL COLUMN - functions to support weight of body and protect spinal cord while permitting movements of trunk and providing for muscle attachments. A. Typical vertebra
VERTEBRAL COLUMN 2018zillmusom I. VERTEBRAL COLUMN - functions to support weight of body and protect spinal cord while permitting movements of trunk and providing for muscle attachments. A. Typical vertebra
OBJECTIVE: To obtain a fundamental knowledge of the root of the neck with respect to structure and function
 The root of the neck Jeff Dupree, Ph.D. e mail: jldupree@vcu.edu OBJECTIVE: To obtain a fundamental knowledge of the root of the neck with respect to structure and function READING ASSIGNMENT: Moore and
The root of the neck Jeff Dupree, Ph.D. e mail: jldupree@vcu.edu OBJECTIVE: To obtain a fundamental knowledge of the root of the neck with respect to structure and function READING ASSIGNMENT: Moore and
Thoracic Cooled-RF Training Presentation
 Thoracic Cooled-RF Training Presentation Patient Selection Anatomy Overview Neuroanatomy Lesion targets Technique Diagnostic Block Cooled-RF Precautions Summary Appendix AGENDA Patient Selection Thoracic
Thoracic Cooled-RF Training Presentation Patient Selection Anatomy Overview Neuroanatomy Lesion targets Technique Diagnostic Block Cooled-RF Precautions Summary Appendix AGENDA Patient Selection Thoracic
Group of students. - Rawan almujabili د. محمد المحتسب - 1 P a g e
 - 14 - Group of students - Rawan almujabili د. محمد المحتسب - 1 P a g e Nerves of the posterior abdominal wall The spinal cord gives off spinal nerves between the vertebrae. In the abdomen, through the
- 14 - Group of students - Rawan almujabili د. محمد المحتسب - 1 P a g e Nerves of the posterior abdominal wall The spinal cord gives off spinal nerves between the vertebrae. In the abdomen, through the
Putting You at the Forefront of Applied Interventional Pain Medicine
 Cadaver Workshop, Palm Springs Putting You at the Forefront of Applied Interventional Pain Medicine a non-cme Educational offering February 23, 2012 Palm springs, CA Purpose and Audience AAPM s non-cme
Cadaver Workshop, Palm Springs Putting You at the Forefront of Applied Interventional Pain Medicine a non-cme Educational offering February 23, 2012 Palm springs, CA Purpose and Audience AAPM s non-cme
Temporal region. temporal & infratemporal fossae. Zhou Hong Ying Dept. of Anatomy
 Temporal region temporal & infratemporal fossae Zhou Hong Ying Dept. of Anatomy Temporal region is divided by zygomatic arch into temporal & infratemporal fossae. Temporal Fossa Infratemporal fossa Temporal
Temporal region temporal & infratemporal fossae Zhou Hong Ying Dept. of Anatomy Temporal region is divided by zygomatic arch into temporal & infratemporal fossae. Temporal Fossa Infratemporal fossa Temporal
Effective Date: 1/1/2019 Section: MED Policy No: 391 Medical Policy Committee Approved Date: 6/17; 12/18
 Effective Date: 1/1/2019 Section: MED Policy No: 391 Medical Policy Committee Approved Date: 6/17; 12/18 1/1/2019 Medical Officer Date APPLIES TO: Medicare Only See Policy CPT/HCPCS CODE section below
Effective Date: 1/1/2019 Section: MED Policy No: 391 Medical Policy Committee Approved Date: 6/17; 12/18 1/1/2019 Medical Officer Date APPLIES TO: Medicare Only See Policy CPT/HCPCS CODE section below
[ANATOMY #12] April 28, 2013
![[ANATOMY #12] April 28, 2013 [ANATOMY #12] April 28, 2013](/thumbs/86/93473883.jpg) Sympathetic chain : Sympathetic chain is each of the pair of ganglionated longitudinal cords of the sympathetic nervous system; extend from level of atlas (base of skull) till coccyx. It is paravertebral
Sympathetic chain : Sympathetic chain is each of the pair of ganglionated longitudinal cords of the sympathetic nervous system; extend from level of atlas (base of skull) till coccyx. It is paravertebral
Introduction to Pain. What Is Pain Management Or Pain Medicine? What is Interventional pain management? What is a pain clinic?
 Introduction to Pain Pain is actually a wide spectrum of disorders including acute pain, chronic pain and cancer pain and sometimes a combination of these. Pain can arise from many different reasons such
Introduction to Pain Pain is actually a wide spectrum of disorders including acute pain, chronic pain and cancer pain and sometimes a combination of these. Pain can arise from many different reasons such
NERVOUS SYSTEM ANATOMY
 INTRODUCTION to NERVOUS SYSTEM ANATOMY M1 - Gross and Developmental Anatomy Dr. Milton M. Sholley Professor of Anatomy and Neurobiology and Dr. Michael H. Peters Professor of Chemical and Life Science
INTRODUCTION to NERVOUS SYSTEM ANATOMY M1 - Gross and Developmental Anatomy Dr. Milton M. Sholley Professor of Anatomy and Neurobiology and Dr. Michael H. Peters Professor of Chemical and Life Science
Temporal fossa Infratemporal fossa Pterygopalatine fossa Terminal branches of external carotid artery Pterygoid venous plexus
 Outline of content Temporal fossa Infratemporal fossa Pterygopalatine fossa Terminal branches of external carotid artery Pterygoid venous plexus Boundary Content Communication Mandibular division of trigeminal
Outline of content Temporal fossa Infratemporal fossa Pterygopalatine fossa Terminal branches of external carotid artery Pterygoid venous plexus Boundary Content Communication Mandibular division of trigeminal
For the following questions, indicate the letter that corresponds to the SINGLE MOST APPROPRIATE ANSWER
 GROSS ANATOMY EXAMINATION May 15, 2000 For the following questions, indicate the letter that corresponds to the SINGLE MOST APPROPRIATE ANSWER 1. Pain associated with an infection limited to the middle
GROSS ANATOMY EXAMINATION May 15, 2000 For the following questions, indicate the letter that corresponds to the SINGLE MOST APPROPRIATE ANSWER 1. Pain associated with an infection limited to the middle
Axial Skeleton: Vertebrae and Thorax
 Axial Skeleton: Vertebrae and Thorax Function of the vertebral column (spine or backbone): 1) 2) 3) Composition of Vertebral column The vertebral column is formed by 33 individual vertebrae (some of which
Axial Skeleton: Vertebrae and Thorax Function of the vertebral column (spine or backbone): 1) 2) 3) Composition of Vertebral column The vertebral column is formed by 33 individual vertebrae (some of which
Mohammad Hisham Al-Mohtaseb. Lina Mansour. Reyad Jabiri. 0 P a g e
 2 Mohammad Hisham Al-Mohtaseb Lina Mansour Reyad Jabiri 0 P a g e This is only correction for the last year sheet according to our record. If you already studied this sheet just read the yellow notes which
2 Mohammad Hisham Al-Mohtaseb Lina Mansour Reyad Jabiri 0 P a g e This is only correction for the last year sheet according to our record. If you already studied this sheet just read the yellow notes which
Brain and spinal nerve. By: shirin Kashfi
 Brain and spinal nerve By: shirin Kashfi Nervous system: central nervous system (CNS) peripheral nervous system (PNS) Brain (cranial) nerves Spinal nerves Ganglions (dorsal root ganglions, sympathetic
Brain and spinal nerve By: shirin Kashfi Nervous system: central nervous system (CNS) peripheral nervous system (PNS) Brain (cranial) nerves Spinal nerves Ganglions (dorsal root ganglions, sympathetic
issps2014 Day 1 - Session 1: Plenary Lecture Series I. Moderator: Dr. M.K. Karmakar
 International Symposium on Spine and Paravertebral Sonography for Anaesthesia and Pain Medicine 2014 Dates: 31 st October 2 nd November 2014 Organized by: The Department of Anaesthesia and Intensive Care,
International Symposium on Spine and Paravertebral Sonography for Anaesthesia and Pain Medicine 2014 Dates: 31 st October 2 nd November 2014 Organized by: The Department of Anaesthesia and Intensive Care,
EPIDURAL STEROID AND FACET INJECTIONS FOR SPINAL PAIN
 EPIDURAL STEROID AND FACET INJECTIONS FOR SPINAL PAIN UnitedHealthcare Oxford Clinical Policy Policy Number: PAIN 019.21 T2 Effective Date: October 1, 2017 Table of Contents Page INSTRUCTIONS FOR USE...
EPIDURAL STEROID AND FACET INJECTIONS FOR SPINAL PAIN UnitedHealthcare Oxford Clinical Policy Policy Number: PAIN 019.21 T2 Effective Date: October 1, 2017 Table of Contents Page INSTRUCTIONS FOR USE...
Anesthesia Processing Guidelines
 Anesthesia Processing Guidelines Policy Number: 10.01.511 Last Review: 5/2014 Origination: 10/1988 Next Review: 5/2015 Policy The following guidelines are utilized in processing anesthesia claims: 1) Anesthesia
Anesthesia Processing Guidelines Policy Number: 10.01.511 Last Review: 5/2014 Origination: 10/1988 Next Review: 5/2015 Policy The following guidelines are utilized in processing anesthesia claims: 1) Anesthesia
Nerves on the Posterior Abdominal Wall
 Nerves on the Posterior Abdominal Wall Lumbar Plexus The lumbar plexus, which is one of the main nervous pathways supplying the lower limb, is formed in the psoasmuscle from the anterior ramiof the upper
Nerves on the Posterior Abdominal Wall Lumbar Plexus The lumbar plexus, which is one of the main nervous pathways supplying the lower limb, is formed in the psoasmuscle from the anterior ramiof the upper
INJECTION-BASED PAIN PROCEDURES
 Introduction INJECTION-BASED PAIN PROCEDURES The most commonly performed pain procedures include facet joint procedures, neurotomies ( rhizotomies ), epidurals and nerve blocks. More advanced procedures
Introduction INJECTION-BASED PAIN PROCEDURES The most commonly performed pain procedures include facet joint procedures, neurotomies ( rhizotomies ), epidurals and nerve blocks. More advanced procedures
MEDICAL HISTORY CHIRO PHYSICAL
 Overview of Spinal Injection Procedures Blake A. Johnson, MD, FACR 1 PATIENT MANAGEMENT EVALUATION TREATMENT P.T. MEDICAL CHIRO S SURGICAL Effective treatment requires a precise diagnosis! HISTORY PHYSICAL
Overview of Spinal Injection Procedures Blake A. Johnson, MD, FACR 1 PATIENT MANAGEMENT EVALUATION TREATMENT P.T. MEDICAL CHIRO S SURGICAL Effective treatment requires a precise diagnosis! HISTORY PHYSICAL
Regional Anaesthesia of the Thoracic Limb
 Regional Anaesthesia of the Thoracic Limb Trauma and inflammation cause sensitization of the peripheral nervous system and the subsequent barrage of nociceptive input (usually by surgery) produces sensitization
Regional Anaesthesia of the Thoracic Limb Trauma and inflammation cause sensitization of the peripheral nervous system and the subsequent barrage of nociceptive input (usually by surgery) produces sensitization
Nervous System. Student Learning Objectives:
 Nervous System Student Learning Objectives: Identify the primary parts of the neuron Identify the major structures of the central nervous system Identify the major structures of the peripheral nervous
Nervous System Student Learning Objectives: Identify the primary parts of the neuron Identify the major structures of the central nervous system Identify the major structures of the peripheral nervous
Skull-2. Norma Basalis Interna Norma Basalis Externa. Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology
 Skull-2 Norma Basalis Interna Norma Basalis Externa Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology Norma basalis interna Base of the skull- superior view The interior of the base of the
Skull-2 Norma Basalis Interna Norma Basalis Externa Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology Norma basalis interna Base of the skull- superior view The interior of the base of the
Cranium Facial bones. Sternum Rib
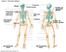 Figure 7.1 The human skeleton. Skull Thoracic cage (ribs and sternum) Cranium Facial bones Sternum Rib Bones of pectoral girdle Vertebral column Sacrum Vertebra Bones of pelvic girdle (a) Anterior view
Figure 7.1 The human skeleton. Skull Thoracic cage (ribs and sternum) Cranium Facial bones Sternum Rib Bones of pectoral girdle Vertebral column Sacrum Vertebra Bones of pelvic girdle (a) Anterior view
THE AORTA AND IT S MAJOR BRANCHES
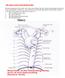 1 THE AORTA AND IT S MAJOR BRANCHES The aorta commences at the aortic valve, above the vestible of the left ventricle and terminates at the level of the fourth lumbar vertebra (L4), where it bifurcates
1 THE AORTA AND IT S MAJOR BRANCHES The aorta commences at the aortic valve, above the vestible of the left ventricle and terminates at the level of the fourth lumbar vertebra (L4), where it bifurcates
Orthopedic Coding Changes for 2012
 Orthopedic Coding Changes for Lynn M. Anderanin, CPC,CPC-I, COSC Vertebroplasty 22520- Percutaneous vertebroplasty, 1 vertebral body, unilateral or bilateral injection; thoracic 22520- Percutaneous vertebroplasty,
Orthopedic Coding Changes for Lynn M. Anderanin, CPC,CPC-I, COSC Vertebroplasty 22520- Percutaneous vertebroplasty, 1 vertebral body, unilateral or bilateral injection; thoracic 22520- Percutaneous vertebroplasty,
Classification of the nervous system. Prof. Dr. Nikolai Lazarov 2
 1 1. Formation and general organization 2. Spinal ganglia 3. Zonal and segmental innervation 4. Dorsal rami of the spinal nerves 5. Ventral rami of the spinal nerves 6. Cervical plexus Classification of
1 1. Formation and general organization 2. Spinal ganglia 3. Zonal and segmental innervation 4. Dorsal rami of the spinal nerves 5. Ventral rami of the spinal nerves 6. Cervical plexus Classification of
UNMH Physical Medicine and Rehabilitation Clinical Privileges. Name: Effective Dates: From To
 All new applicants must meet the following requirements as approved by the UNMH Board of Trustees, effective July 29, 2016: Initial Privileges (initial appointment) Renewal of Privileges (reappointment)
All new applicants must meet the following requirements as approved by the UNMH Board of Trustees, effective July 29, 2016: Initial Privileges (initial appointment) Renewal of Privileges (reappointment)
General Anatomy p. 1 Organization of the Human Body p. 1 Skeleton of the Human Body p. 4 Ossification of the Bones p. 6 Bone Structure p. 8 Joints p.
 General Anatomy p. 1 Organization of the Human Body p. 1 Skeleton of the Human Body p. 4 Ossification of the Bones p. 6 Bone Structure p. 8 Joints p. 10 Principal Joints (Immovable) p. 12 Synovial Joints
General Anatomy p. 1 Organization of the Human Body p. 1 Skeleton of the Human Body p. 4 Ossification of the Bones p. 6 Bone Structure p. 8 Joints p. 10 Principal Joints (Immovable) p. 12 Synovial Joints
Lecture 14: The Spinal Cord
 Lecture 14: The Spinal Cord M/O Chapters 16 69. Describe the relationship(s) between the following structures: root, nerve, ramus, plexus, tract, nucleus, and ganglion. 70. Trace the path of information
Lecture 14: The Spinal Cord M/O Chapters 16 69. Describe the relationship(s) between the following structures: root, nerve, ramus, plexus, tract, nucleus, and ganglion. 70. Trace the path of information
Cervical Cooled RF Training Presentation
 Cervical Cooled RF Training Presentation Agenda Patient Selection Considerations Diagnostic Block General Considerations COOLIEF* Cooled RF Technique Posterior Lateral Precautions Summary Appendix 2 Disclaimer
Cervical Cooled RF Training Presentation Agenda Patient Selection Considerations Diagnostic Block General Considerations COOLIEF* Cooled RF Technique Posterior Lateral Precautions Summary Appendix 2 Disclaimer
Trigeminal Nerve Worksheets, Distributions Page 1
 Trigeminal Nerve Worksheet #1 Distribution by Nerve Dr. Darren Hoffmann Dental Gross Anatomy, Spring 2013 We have drawn out each of the branches of CN V in lecture and you have an idea now for their basic
Trigeminal Nerve Worksheet #1 Distribution by Nerve Dr. Darren Hoffmann Dental Gross Anatomy, Spring 2013 We have drawn out each of the branches of CN V in lecture and you have an idea now for their basic
UCSD DEPARTMENT OF ANESTHESIOLOGY
 UCSD DEPARTMENT OF ANESTHESIOLOGY LEARNING OBJECTIVES FOR ADVANCED PAIN MEDICINE ROTATION, UCSD MEDICAL CENTER Competencies Objective Learning Environment Instructional Method Assessment Tool Patient Care:
UCSD DEPARTMENT OF ANESTHESIOLOGY LEARNING OBJECTIVES FOR ADVANCED PAIN MEDICINE ROTATION, UCSD MEDICAL CENTER Competencies Objective Learning Environment Instructional Method Assessment Tool Patient Care:
Phillip Weidner, DO, DABA, BCPM May 20th, 2014
 Phillip Weidner, DO, DABA, BCPM May 20th, 2014 Introduction Comprehensive Pain Management Center Interventional therapies Epidural steroid injections Sacroiliac interventions Facet joint disease Who to
Phillip Weidner, DO, DABA, BCPM May 20th, 2014 Introduction Comprehensive Pain Management Center Interventional therapies Epidural steroid injections Sacroiliac interventions Facet joint disease Who to
Comprehensive Centers for Pain Management. Common Injection and Implant Procedures for the Treatment of Acute and Chronic Back Pain
 Comprehensive Centers for Pain Management Common Injection and Implant Procedures for the Treatment of Acute and Chronic Back Pain There are many different treatments for back pain. Taking lots of drugs
Comprehensive Centers for Pain Management Common Injection and Implant Procedures for the Treatment of Acute and Chronic Back Pain There are many different treatments for back pain. Taking lots of drugs
UNMH Neurosurgery Clinical Privileges
 All new applicants must meet the following requirements as approved by the UNMH Board of Trustees effective: 02/20/2015 INSTRUCTIONS Applicant: Check off the "Requested" box for each privilege requested.
All new applicants must meet the following requirements as approved by the UNMH Board of Trustees effective: 02/20/2015 INSTRUCTIONS Applicant: Check off the "Requested" box for each privilege requested.
APPENDICULAR SKELETON 126 AXIAL SKELETON SKELETAL SYSTEM. Cranium. Skull. Face. Skull and associated bones. Auditory ossicles. Associated bones.
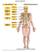 SKELETAL SYSTEM 206 AXIAL SKELETON 80 APPENDICULAR SKELETON 26 Skull Skull and associated s 29 Cranium Face Auditory ossicles 8 4 6 Associated s Hyoid Thoracic cage 25 Sternum Ribs 24 Vertebrae 24 column
SKELETAL SYSTEM 206 AXIAL SKELETON 80 APPENDICULAR SKELETON 26 Skull Skull and associated s 29 Cranium Face Auditory ossicles 8 4 6 Associated s Hyoid Thoracic cage 25 Sternum Ribs 24 Vertebrae 24 column
NASS Diagnosis and Treatment of Low-Back Pain Guideline Draft Clinical Question Protocol
 NASS Diagnosis and Treatment of Low-Back Pain Draft Clinical Questions Public Comment period: June 16-July 14, 2015 Comments should be sent to guidelines@spine.org Background The North American Spine Society
NASS Diagnosis and Treatment of Low-Back Pain Draft Clinical Questions Public Comment period: June 16-July 14, 2015 Comments should be sent to guidelines@spine.org Background The North American Spine Society
Lab 16: PNS: Nerves and Autonomic NS Hamilton Answers to Pre- Lab Assignments
 Lab 16: PNS: Nerves and Autonomic NS Hamilton Answers to Pre- Lab Assignments Pre-Lab Activity 1: 1. a. olfactory nerve b. optic nerve c. oculomotor nerve d. abducens nerve e. trochlear nerve f. trigeminal
Lab 16: PNS: Nerves and Autonomic NS Hamilton Answers to Pre- Lab Assignments Pre-Lab Activity 1: 1. a. olfactory nerve b. optic nerve c. oculomotor nerve d. abducens nerve e. trochlear nerve f. trigeminal
Peripheral Nervous System Dr. Gary Mumaugh
 Peripheral Nervous System Dr. Gary Mumaugh Spinal Nerves Overview Thirty-one pairs of spinal nerves are connected to the spinal cord No special names; numbered by level of vertebral column at which they
Peripheral Nervous System Dr. Gary Mumaugh Spinal Nerves Overview Thirty-one pairs of spinal nerves are connected to the spinal cord No special names; numbered by level of vertebral column at which they
Facility Payments for Interventional Pain Management Procedures: Impact of Proposed Rules
 Pain Physician 2016; 19:E957-E984 ISSN 2150-1149 Health Policy Review Payments for Interventional Pain Management Procedures: Impact of Proposed Rules Laxmaiah Manchikanti, MD 1, Vijay Singh, MD 2, and
Pain Physician 2016; 19:E957-E984 ISSN 2150-1149 Health Policy Review Payments for Interventional Pain Management Procedures: Impact of Proposed Rules Laxmaiah Manchikanti, MD 1, Vijay Singh, MD 2, and
Chapter 4 Section 20.1
 Surgery Chapter 4 Section 20.1 Issue Date: August 29, 1985 Authority: 32 CFR 199.4(c)(2) and (c)(3) 1.0 CPT 1 PROCEDURE CODES 61000-61626, 61680-62264, 62268-62284, 62290-63048, 63055-64484, 64505-64595,
Surgery Chapter 4 Section 20.1 Issue Date: August 29, 1985 Authority: 32 CFR 199.4(c)(2) and (c)(3) 1.0 CPT 1 PROCEDURE CODES 61000-61626, 61680-62264, 62268-62284, 62290-63048, 63055-64484, 64505-64595,
Chapter 4 Section 20.1
 Surgery Chapter 4 Section 20.1 Issue Date: August 29, 1985 Authority: 32 CFR 199.4(c)(2) and (c)(3) Copyright: CPT only 2006 American Medical Association (or such other date of publication of CPT). All
Surgery Chapter 4 Section 20.1 Issue Date: August 29, 1985 Authority: 32 CFR 199.4(c)(2) and (c)(3) Copyright: CPT only 2006 American Medical Association (or such other date of publication of CPT). All
Structure Location Function
 Frontal Bone Cranium forms the forehead and roof of the orbits Occipital Bone Cranium forms posterior and inferior portions of the cranium Temporal Bone Cranium inferior to the parietal bone forms the
Frontal Bone Cranium forms the forehead and roof of the orbits Occipital Bone Cranium forms posterior and inferior portions of the cranium Temporal Bone Cranium inferior to the parietal bone forms the
