management of this patient within the Enhanced Primary Care Pathway is appropriate, without need for specialist consultation at this time.
|
|
|
- Charles Melton
- 5 years ago
- Views:
Transcription
1 TRIAGE CATEGORY: Enhanced Primary Care Pathway CONSTIPATION Dear Colleague, The clinical and diagnostic information you have provided for the above-named patient is consistent with a diagnosis of chronic constipation. Based on full review of your referral, it has been determined that management of this patient within the Enhanced Primary Care Pathway is appropriate, without need for specialist consultation at this time. This clinical pathway has been developed by the Calgary Zone Primary Care Network in partnership with the Section of Gastroenterology and Alberta Health Services. These local guidelines are based on best available clinical evidence, and are practical in the primary care setting. This package includes: 1. Focused summary of constipation relevant to primary care 2. Checklist to guide your in-clinic patient review 3. Links to additional resources for this specific condition 4. Clinical flow diagram with expanded detail If you would like to discuss this referral with a Gastroenterologist, call SpecialistLINK, a dedicated GI phone consultation service, available 08:00-17:00 weekdays at or toll-free [LINK]. An Advice Request to Adult Gastroenterology can also be submitted through Alberta Netcare e- Referral ( ). If your patient completes the Enhanced Primary Care Pathway and remains symptomatic or if your patient s status or symptoms have changed, a new referral using the QURE guidelines (included in this package) indicating completed care pathway or new information should be faxed to for prioritized review. Thank you. Paul Belletrutti, MD FRCPC Medical Lead, Central Access and Triage Section of Gastroenterology
2 Enhanced Primary Care Pathway: CONSTIPATION 1. Focused summary of constipation relevant to primary care Definition. Chronic constipation is a functional bowel disorder defined as abnormal colonic transit (fewer than 3 bowel movements per week that are mostly hard or lumpy i.e. Bristol stool scale type 1-2) and/or defecatory dysfunction (difficult stool passage i.e. straining, sensation of incomplete evacuation/obstruction/blockage, digital evacuation/support of the perineum). Pain or bloating may be present in patients with constipation, but it is not a dominant symptom; patients with constipationpredominant irritable bowel syndrome (IBS-C) have abdominal discomfort or bloating as a major symptom, accompanied by constipation. There is significant overlap between chronic constipation and IBS-C in terms of clinical presentation and treatment. For additional advice about IBS-C, please refer to the Enhanced Primary Care Pathway for IBS Pathophysiology. Constipation may be due to a primary functional disorder of colonic motility (slow transit) and/or dyssynergic defecation (incoordination of rectal propulsion and anal sphincter relaxation). In the primary care setting, constipation is very often caused or compounded by secondary effects of medications or their underlying diseases. Mechanical or structural causes of constipation (e.g. mass or stricture) are relatively rare in practice and can usually be discerned by clinical red flags or physical findings on abdominal and anorectal exam. There is no increase in prevalence of colorectal cancer in patients with constipation and, therefore, constipation is generally not an indication for diagnostic colonoscopy; however, colorectal cancer screening should be undertaken in patients with constipation according to age and family history. Constipation in older adults is a special category, which can be particularly challenging to assess and treat. Secondary causes are most often at play in the elderly due to multiple medical conditions and medications that predispose to constipation, limited physical activity, less control or attention to diet and fluid intake, and failure to maintain a bowel regimen or recognize the call to stool. Evaluation. Routine laboratory testing is generally not recommended in patients with chronic constipation. Instead, a thorough and detailed history, medication review, and physical examination is of paramount importance and may then guide use of selected laboratory tests such as CBC, glucose, creatinine, calcium, and TSH to assess for anemia as a red flag or common contributory metabolic disturbances. There is no literature to support routine use of plain abdominal x-ray, radiopaque marker transit study, barium enema, or defecography for assessment of constipation in primary care. An abdominal radiograph may be useful in some elderly patients with episodic diarrhea and fecal incontinence to evaluate the possibility of severe constipation with overflow in order to avoid erroneous prescription of antidiarrheals. Anorectal manometry, barostat, and balloon expulsion studies are reserved for patients with suspected for anorectal dyssynergy under evaluation by a Gastroenterologist. Overview of management. A complete and thorough medical assessment, patient reassurance and education, dietary changes, and increased physical activity and fluid intake along with bulk-forming laxatives provide significant and prompt benefit in most patients. Polyethylene glycol and stimulant laxatives are used in those who fail to respond to initial conservative approaches. Addition of linaclotide or prucalopride should be considered for those with refractory constipation or for episodic use. Gastroenterology referral is appropriate if failed response to the above foundational treatments, presence of red flags, or strong suspicion of dyssynergic defecation at initial assessment. Enhanced Primary Care Pathway: CONSTIPATION Dec 2017
3 2. Checklist to guide your in-clinic review of this patient with constipation At least two symptoms of constipation: fewer than 3 bowel movements per week, stool form that is mostly hard or lumpy (Bristol 1-2), difficult stool passage leading to straining, incomplete evacuation, sensation of obstruction, or requirement for digital evacuation Absence of red flags: sudden or progressive change in bowel habit, blood in stool, iron deficiency anemia, unintended weight loss, family history of colorectal cancer in a first degree relative Full review of prescribed (Netcare) and over-the-counter medications that may cause constipation and timing with its onset or worsening; assess dietary fibre/fluid intake and physical activity Detailed abdominal and anorectal examination Assess for clinical and physical features of anorectal dyssynergy 3. References and links to additional resources for patients Canadian Digestive Health Foundation Understanding Constipation - zoom=100 UpToDate Beyond the Basics Patient Information about Constipation in Adults (freely accessible) UpToDate Beyond the Basics Patient Information about High Fibre Diet (freely accessible) Fibre pdf 4. Clinical flow diagram with expanded detail This AHS Calgary Zone pathway incorporates the most current evidence-based clinical guidelines for diagnosis and management of constipation from both Gastroenterology and Primary Care literature: Drossman DA and Hasler WL. Rome IV Functional GI disorders: Disorders of gut-brain interaction Gastroenterology 2016;150: Wald A. Constipation: Advances in diagnosis and treatment. JAMA 2016;315: Schuster BG, Kosar L, Kamrul R. Constipation in older adults: A stepwise approach to keeping things moving. Canadian Family Physician 2015;61: Full article CFPlus Additional Info Bharucha AE, Dorn SD, Lembo A, Pressman A. American Gastroenterological Association position statement on constipation. Gastroenterology. 2013;144: Jamshed N, Lee ZE, Olden KW. Diagnostic approach to chronic constipation in adults. American Family Physician 2011;84: The following is a best-practice clinical pathway for management of constipation in the primary care medical home, which includes a flow diagram and expanded explanation of treatment options: Enhanced Primary Care Pathway: CONSTIPATION Dec 2017
4 Enhanced Primary Care Pathway: CONSTIPATION Dec 2017
5 Flow Diagram: CONSTIPATION Diagnosis and Management - Expanded Detail 1. A presumptive diagnosis of functional constipation can be made based on Rome IV criteria (2016). In order to apply these criteria, it is essential to collect a detailed history of stool frequency and form (see Bristol Stool Scale on page 6) and features of defecatory dysfunction. It is well recognized that patients who meet these criteria for diagnosis of functional constipation commonly will also meet criteria for IBS-C and therefore additional approaches should be considered if significant abdominal bloating or discomfort co-exist with constipation (see Enhanced Primary Care Pathway for IBS-C Important additional history includes: (1) duration and progression of symptoms (problem since childhood or more recent onset and worsening), (2) precipitating events (changes in diet, fluid intake, physical activity, medications introduced around symptom onset), (3) laxatives tried already (most products are accessible over-the-counter, noting type, duration, and combination of agents helps discern undertreated from treatment resistant cases), (4) alarm features. 2. Focused physical examination provides information about mass or structural lesions and clues about dysfunctional defecation, which would require specialist consultation. Abdomen: noting distention, focal discomfort, palpable mass, inguinal lymphadenopathy. Inspection of perineum: noting skin conditions, anal wink reflex and sensory deficits, strain maneuvers to assess degree of perineal descent and elicit hemorrhoidal or rectal prolapse, seepage; apply traction to examine the anal canal for presence and location of fissure which usually evokes sharp localized pain. Digital anorectal examination: noting stricture, high resting anal sphincter tone and voluntary squeeze pressure, mass or irregularity of anal canal and distal rectum on circumferential finger sweep, and presence and form of stool or blood. A rectocoele is prolapse of the anterior rectal wall into the vagina and is associated with obstructive defecation. When the patient bears down during DRE, the anal sphincter and puborectalis sling (felt posteriorly) should relax and the perineum should descend. During DRE, high resting anal sphincter tone or, on bear down manoeuver, paradoxical contraction of the puborectalis and failure of the perineum to descend are clues to anorectal dyssynergy. 3. Consider secondary causes of constipation. For Primary Care physicians, it is important to do a thorough review of medications. Netcare is a valuable tool to identify medications that could contribute to constipation. Choosing Medication Profile > All > Summary Report in Netcare will generate a chronological list which provides focus on medications associated with time of onset of constipation. There are many medical conditions and their drug treatments that are associated with constipation and recognition of this may allow disease-specific intervention (e.g. hypothyroidism, diabetes). See page 6 for further details. 4. General approach to treating functional constipation. There is a wide range of what is considered normal bowel function in adults. Education, reassurance, management of expectations: some patients believe they must have a bowel movement every day in order to be healthy. Reminding patients that a bowel movement every 2-3 days is considered within normal limits and some variability of stool form is expected and normal. It is often helpful to show patients the Bristol Stool Scale to better quantify stool form and, in many patients, reveals normal or ideal stool form much of the time. Patients gain reassurance and hope in knowing that bowel function usually improves with very simple interventions, that the medical literature consistently shows that most patients with constipation do not require extensive initial investigation, and that colonoscopy almost never reveals relevant abnormalities. Fibre, fluid, physical activity: There is a dose-response relationship between fibre and fluid intake and stool output, and it is important to quantify at initial visit, as patients with constipation whose fibre and fluid intakes are inadequate are most likely to benefit from this intervention. Most Canadians consume only 10-20g of fibre per day, which is far less than the recommended 30g/d target. It is challenging for most patients to achieve this amount of daily fibre intake due to palatability, adverse effects (intestinal gas and cramps), and lack of knowledge about what 30g/d of fibre looks like in practical terms. Although there is very little evidence of clinical effect, increased exercise may have favorable effects on intestinal fluid handling and motility and seems sensible in terms of overall patient well-being. Patient adherence to these principles of therapy for constipation tends to be poor and needs frequent monitoring, reinforcement, and enablement by Primary Care physicians. Laxatives: Bulk-forming agents are natural or synthetic polysaccharides that bind fluid in the gut to increase stool volume and mass. Osmotic agents are poorly absorbed sugars that draw water into the bowel to loosen stool. Stimulant laxatives increase secretory and propulsive activity in the intestine. Surfactants soften stool by breaking surface tension on formed stool allowing water to penetrate. 5. Specific additional approaches. Failure to improve after the above general approaches are exhausted is diagnostically useful, suggesting specific additional or dominant mechanisms underlying constipation in a particular patient. This may bolster clinical impression of IBS-C or defecatory dysfunction, or may indicate a subtype of constipation known as slow transit which guides next steps in helping these patients.
6 The Bristol Stool Scale: An index of colonic transit time Lewis SJ, Heaton KW. Stool form scale as a useful guide to intestinal transit time. Scand J Gastroenterol. 1997;32: Figure adapted from Canadian Digestive Health Foundation Important secondary causes of constipation to consider Medications Medical Conditions Common Common Iron and calcium supplements Cerebrovascular disease Antihypertensives Cognitive impairment Antidepressants Renal dysfunction Antacids Diabetes mellitus NSAIDs Hypothyroidism Opioids Depression Less common Less common Antiparkinsonian agents Hypomagnesemia and hypokalemia Bile acid sequestrants Hypercalcemia and hypocalcemia Bisphosphonates Hyperparathyroidism Anticonvulsants Anorexia nervosa Antispasmodics Autonomic neuropathy Antihistamine Muscular dystrophies Antipsychotics Parkinson disease Antiemetics Multiple sclerosis Enhanced Primary Care Pathway: CONSTIPATION Dec 2017
7 General Principles Dietary Fibre Fluid Intake Physical Activity Self-Management Counsel patients to target of 30g/d of fibre per day from various food sources. Fibre is categorized by solubility in water and fermentability by intestinal bacteria. There is limited evidence to guide choice of best dietary fibre for management of constipation. Insoluble fibre mechanically stimulates the GI mucosa thus promoting secretion and peristalsis. Soluble fibre increases stool bulk by osmotic and gel-forming effects and by selectively increasing bacterial biomass, which probably has additional beneficial effects on gut function. However, some forms of soluble fibre also contain highly fermentable substrates that lead to gas production, pain, and bloating. Nonetheless, it is worthwhile making a general recommendation to patients simultaneously increase dietary fibre and fluid intake in a graded manner, building in some expectation that some foods may cause bloating, pain, or flatulence. Prunes contain insoluble fibre as well as sorbitol and fructans and have been shown to be effective in management of constipation through both bulk-forming and osmotic effects at a dose of 12 medium-sized prunes per day. Provide patient handout: Fibre 101 Consumption of L of fluid per day significantly enhances the effectiveness of fibre. Moderate to vigorous exercise for minutes 3-5x per week, as per general health guidelines. Although exercise speeds up intestinal transit, there is no evidence to inform specific recommendations of frequency, duration, or intensity of exercise in management of constipation. It is reasonable to talk to patients about possible beneficial effects of exercise on GI function and the well-established benefits to overall physical health and well-being. Alberta Healthy Living Program (ahs.ca/info/cdmcalgaryzone.asp) Bulk-Forming Agents Psyllium Methylcellulose Calcium Polycarbophil Inulin Metamucil 1 tablespoon OD-TID ($5-10/mo.) Intermediate soluble and fermentable fibre which has good laxative effect but some risk of bloating and flatus. Start with low dose and titrate to effect. Citrucel 2 caplets OD-QID ($10-40/mo.) Good laxative effect, onset of action 12-72h. Insoluble, non-fermentable fibre producing less bloating and flatulence. Prodiem 2 caplets OD-QID ($5-20/mo.) Good laxative effect, onset of action 12-72h. Less risk of flatulence and bloating compared with other bulk-forming agents. Benefibre 1-2 teaspoon OD-TID ($10-20/mo.) Mild laxative effect, onset of action 24-48h. Non-absorbed fermentable sugar may cause bloating, pain, or flatulence. Osmotic Laxatives Polyethylene glycol Lactulose PEG3350 (Lax-A-Day RestoraLAX PEGalax Relaxa ) 17-34g/d ($25-50/mo.) Start with 17g at night dissolved in 250mL of water, juice, or soda; titrate up to effect or maximum of 34g/d. Onset of action 48-96h. Studies suggest superior to lactulose. Lactulose 15-30mL OD to TID ($10-20/mo.) Onset of action 24-48h. Non-absorbed fermentable sugar, which may cause bloating, pain, or flatulence. Stimulant Laxatives Bisacodyl Sennosides Bisacodyl (Dulcolax ) 5-10mg PO QHS ($ /dose) Bisacodyl (Dulcolax The Magic Bullet ) 10mg suppository PRN max. 30mg/d ($1.00/dose) Sennosides 8.6mg tab (Senokot ) 2-4 tab OD-BID max. 4 tab BID ($ /dose) Prokinetics Linaclotide Prucalopride Constella 145µg/d, 30 minutes before breakfast ($100/mo.) Resotran 2mg/d, 4 week trial ($120/mo.) Enhanced Primary Care Pathway: CONSTIPATION Dec 2017
8 Enhanced Primary Care Pathway: CONSTIPATION Dec 2017
9 Enhanced Primary Care Pathway: CONSTIPATION Dec 2017
10 IMPORTANT INFORMATION REGARDING YOUR RECENT REFERRAL To ensure that your referral is triaged appropriately, please review this quality referral checklist as you create the referral. Free pocket sized copies of this checklist are available through Quality Referral Evolution (QuRE) at PATIENT INFORMATION Name, DOB, PHN, Address, Phone, Alternate contact, Translator required PRIMARY CARE PROVIDER INFORMATION Name, Phone, Fax, cc/indicate if different from family physician REFERRING PHYSICIAN INFORMATION Name, Phone, Fax TIPS REASON FOR REFERRAL Diagnosis, management and/or treatment Procedure issue / care transfer PATIENT S CURRENT STATUS Stable, worsening or urgent/emergent Understanding of situation Key symptoms and findings Symptom onset / duration Red flags FINDINGS AND/OR INVESTIGATIONS (RELEVANT RESULTS ATTACHED) What has been done & is available What has been ordered & is pending CURRENT & PAST MANAGEMENT (LIST WITH OUTCOMES) None Unsuccessful / successful treatment(s) Previous or concurrent consultations for this issue Assist with patient communication by indicating patient s preferred method of contact and if they will be unavailable (holiday, etc) Don t forget that the referring physician isn t always the family physician. Keep everyone in the loop with a cc. Make sure to express clear expectations for the consult and, when possible, outline a specific question. Current status is must-know clinical information that has direct impact on triage of the referral. Ensure you have listed all ordered tests so the receiving consultant does not unknowingly order the same tests again. COMORBIDITIESNone Medical history Pertinent concurrent medical problems Current & recent medications (name, dosage, PRN basis) Allergies Warnings & challenges Provide information on what has been tried previously and why a consult is required. A complete medical history can help the consultant determine the complexity and urgency of the referral. Enhanced Primary Care Pathway: CONSTIPATION Dec 2017
Constipation an Old Friend. Presented by Dr. Keith Harris
 Constipation an Old Friend Presented by Dr. Keith Harris Irregularity and the Tricks of the Trade." CONSTIPATION What is constipation? INFREQUENT BOWEL MOVEMENTS DIFFICULTY DURING DEFECATION SENSATION
Constipation an Old Friend Presented by Dr. Keith Harris Irregularity and the Tricks of the Trade." CONSTIPATION What is constipation? INFREQUENT BOWEL MOVEMENTS DIFFICULTY DURING DEFECATION SENSATION
Elderly Man With Chronic Constipation
 Elderly Man With Chronic Constipation Linda Nguyen, MD Director, Neurogastroenterology and Motility Clinical Assistant Professor Stanford University Overview Normal bowel function Defining Constipation:
Elderly Man With Chronic Constipation Linda Nguyen, MD Director, Neurogastroenterology and Motility Clinical Assistant Professor Stanford University Overview Normal bowel function Defining Constipation:
Constipation An Overview. Definition Physiology of GI tract Etiology Assessment Treatment
 CONSTIPATION Constipation An Overview Definition Physiology of GI tract Etiology Assessment Treatment Definition Constipation = the infrequent passage of hard feces Definition of Infrequent The meaning
CONSTIPATION Constipation An Overview Definition Physiology of GI tract Etiology Assessment Treatment Definition Constipation = the infrequent passage of hard feces Definition of Infrequent The meaning
IBS CLOSED REFERRAL STATUS: Dear Dr.,
 Name: PHN/ULI: DOB: RHRN: RefMD: Dr. RefMD Fax: RefDate: Date Today: CONFIRMATION: TRIAGE CATEGORY: REFERRAL STATUS: Dear Dr., Referral Received Enhanced Primary Care Pathway CLOSED IBS The clinical and
Name: PHN/ULI: DOB: RHRN: RefMD: Dr. RefMD Fax: RefDate: Date Today: CONFIRMATION: TRIAGE CATEGORY: REFERRAL STATUS: Dear Dr., Referral Received Enhanced Primary Care Pathway CLOSED IBS The clinical and
Chronic constipation in the elderly
 Chronic constipation in the elderly 1 Dec,2011 R 2 Natta Asanaleykha Epidemiology Definition Scope The impact of chronic constipation in the elderly Pathophysiology Evaluation the elderly patient with
Chronic constipation in the elderly 1 Dec,2011 R 2 Natta Asanaleykha Epidemiology Definition Scope The impact of chronic constipation in the elderly Pathophysiology Evaluation the elderly patient with
Understanding & Alleviating Constipation. Living (Well!) with Gastroparesis Program Warm-Up Class
 Understanding & Alleviating Constipation Living (Well!) with Gastroparesis Program Warm-Up Class Please Remember The information presented is for educational purposes only and is in no way intended as
Understanding & Alleviating Constipation Living (Well!) with Gastroparesis Program Warm-Up Class Please Remember The information presented is for educational purposes only and is in no way intended as
Constipation. What is constipation? What is the criteria for having constipation? What are the different types of constipation?
 What is constipation? is defined as having a bowel movement less than 3 times per week. It is usually associated with hard stools or difficulty passing stools. You may have pain while passing stools or
What is constipation? is defined as having a bowel movement less than 3 times per week. It is usually associated with hard stools or difficulty passing stools. You may have pain while passing stools or
What Is Constipation?
 CONSTIPATION What Is Constipation? Constipation is when you have infrequent or hard-to-pass bowel movements (meaning they are painful or you have to strain), have hard stools or feel like your bowel movements
CONSTIPATION What Is Constipation? Constipation is when you have infrequent or hard-to-pass bowel movements (meaning they are painful or you have to strain), have hard stools or feel like your bowel movements
Common Gastrointestinal Problems in the Elderly
 Common Gastrointestinal Problems in the Elderly Brian Viviano, D.O. Objectives Understand the pathophysiology, clinical manifestations, diagnosis and management of GI diseases of the elderly. Differentiate
Common Gastrointestinal Problems in the Elderly Brian Viviano, D.O. Objectives Understand the pathophysiology, clinical manifestations, diagnosis and management of GI diseases of the elderly. Differentiate
Constipation. (Medical Aspects)
 Constipation (Medical Aspects) By Dr. Ehab Abdel Khalik MD. Anatomy of the anorectum The rectum is 12-15 15 cm. long. It connects with the sigmoid colon by the rectosigmoid junction which is believed to
Constipation (Medical Aspects) By Dr. Ehab Abdel Khalik MD. Anatomy of the anorectum The rectum is 12-15 15 cm. long. It connects with the sigmoid colon by the rectosigmoid junction which is believed to
ACG Clinical Guideline: Management of Benign Anorectal Disorders
 ACG Clinical Guideline: Management of Benign Anorectal Disorders Arnold Wald, MD, MACG 1, Adil E. Bharucha, MBBS, MD 2, Bard C. Cosman, MD, MPH, FASCRS 3 and William E. Whitehead, PhD, MACG 4 1 Division
ACG Clinical Guideline: Management of Benign Anorectal Disorders Arnold Wald, MD, MACG 1, Adil E. Bharucha, MBBS, MD 2, Bard C. Cosman, MD, MPH, FASCRS 3 and William E. Whitehead, PhD, MACG 4 1 Division
UNDERSTANDING IBS AND CC Implications for diagnosis and management
 UNDERSTANDING IBS AND CC Implications for diagnosis and management J. TACK, M.D., Ph.D. Department of Gastroenterology University Hospitals, K.U. Leuven Leuven, Belgium TYPES OF GASTROINTESTINAL DISORDERS
UNDERSTANDING IBS AND CC Implications for diagnosis and management J. TACK, M.D., Ph.D. Department of Gastroenterology University Hospitals, K.U. Leuven Leuven, Belgium TYPES OF GASTROINTESTINAL DISORDERS
10/10/16. Disclosures. Educational Objectives
 Nimish Vakil, MD, FACP, FACG, AGAF, FASGE Clinical Adjunct Professor University of Wisconsin Madison, Wisconsin Disclosures All faculty, course directors, planning committee, content reviewers and others
Nimish Vakil, MD, FACP, FACG, AGAF, FASGE Clinical Adjunct Professor University of Wisconsin Madison, Wisconsin Disclosures All faculty, course directors, planning committee, content reviewers and others
Scoop on the poop: Constipation in the Elderly
 Scoop on the poop: Constipation in the Elderly Laurie Archbald-Pannone, MD, MPH Assistant Professor Division of General Medicine, Geriatrics, & Palliative Care Division of Infectious Diseases and International
Scoop on the poop: Constipation in the Elderly Laurie Archbald-Pannone, MD, MPH Assistant Professor Division of General Medicine, Geriatrics, & Palliative Care Division of Infectious Diseases and International
Aging Persons with Intellectual Developmental Disorders (IDD): Constipation KEYPOINTS OVERVIEW
 Aging Persons with Intellectual Developmental Disorders (IDD): Constipation KEYPOINTS A major medical conditions that commonly is seen among persons with IDD and may lead to serious complications is constipation.
Aging Persons with Intellectual Developmental Disorders (IDD): Constipation KEYPOINTS A major medical conditions that commonly is seen among persons with IDD and may lead to serious complications is constipation.
Constipation Information Leaflet THE DIGESTIVE SYSTEM. gutscharity.org.uk
 THE DIGESTIVE SYSTEM http://healthfavo.com/digestive-system-for-kids.html This factsheet is about Constipation Constipation is a symptom that can mean different things to different people but the usual
THE DIGESTIVE SYSTEM http://healthfavo.com/digestive-system-for-kids.html This factsheet is about Constipation Constipation is a symptom that can mean different things to different people but the usual
FOOT OFF THE BRAKES. Kerri Novak MD MSc FRCPC. Chronic Constipation: Taking the Foot off the Brakes Dr. Kerri Novak
 CHRONIC CONSTIPATION: TAKING THE FOOT OFF THE BRAKES Kerri Novak MD MSc FRCPC www.seacourses.com 1 OUTLINE Epidemiology i Quality of life Approach Therapies www.seacourses.com 2 DEFINING CHRONIC CONSTIPATION
CHRONIC CONSTIPATION: TAKING THE FOOT OFF THE BRAKES Kerri Novak MD MSc FRCPC www.seacourses.com 1 OUTLINE Epidemiology i Quality of life Approach Therapies www.seacourses.com 2 DEFINING CHRONIC CONSTIPATION
3D Dynamic Ultrasound In Obstructed Defecation
 3D Dynamic Ultrasound In Obstructed Defecation By Ramy Salahudin Abdelkader Assist. Lecturer of General Surgery Cairo University Introduction Pelvic floor is complex system, with passive and active components
3D Dynamic Ultrasound In Obstructed Defecation By Ramy Salahudin Abdelkader Assist. Lecturer of General Surgery Cairo University Introduction Pelvic floor is complex system, with passive and active components
Drugs Affecting the Gastrointestinal System. Antidiarrheal and Laxatives
 Drugs Affecting the Gastrointestinal System Antidiarrheal and Laxatives Diarrhea Abnormal frequent passage of loose stools or Abnormal passage of stools with increased frequency, fluidity, and weight,
Drugs Affecting the Gastrointestinal System Antidiarrheal and Laxatives Diarrhea Abnormal frequent passage of loose stools or Abnormal passage of stools with increased frequency, fluidity, and weight,
CENTENE PHARMACY AND THERAPEUTICS DRUG REVIEW 2Q17 April May
 BRAND NAME Trulance GENERIC NAME Plecanatide MANUFACTURER Synergy Pharmaceuticals, Inc. DATE OF APPROVAL January 19, 2017 PRODUCT LAUNCH DATE Anticipated in 1Q2017 REVIEW TYPE Review type 1 (RT1): New
BRAND NAME Trulance GENERIC NAME Plecanatide MANUFACTURER Synergy Pharmaceuticals, Inc. DATE OF APPROVAL January 19, 2017 PRODUCT LAUNCH DATE Anticipated in 1Q2017 REVIEW TYPE Review type 1 (RT1): New
Identify electrolytes that should be monitored whenever prolonged or severe diarrhea is present
 Chapter 35 Drugs Used to Treat Constipation and Diarrhea Learning Objectives State the underlying causes of constipation Explain the meaning of normal bowel habits Cite nine causes of diarrhea Describe
Chapter 35 Drugs Used to Treat Constipation and Diarrhea Learning Objectives State the underlying causes of constipation Explain the meaning of normal bowel habits Cite nine causes of diarrhea Describe
OCTOBER 7-10 PHILADELPHIA, PENNSYLVANIA
 OMED 17 OCTOBER 7-10 PHILADELPHIA, PENNSYLVANIA 29.5 Category 1-A CME credits anticipated ACOFP / AOA s 122 nd Annual Osteopathic Medical Conference & Exposition Joint Session with ACOFP and Cleveland
OMED 17 OCTOBER 7-10 PHILADELPHIA, PENNSYLVANIA 29.5 Category 1-A CME credits anticipated ACOFP / AOA s 122 nd Annual Osteopathic Medical Conference & Exposition Joint Session with ACOFP and Cleveland
Irritable Bowel Syndrome Now. George M. Logan, MD Friday, May 5, :35 4:05 PM
 Irritable Bowel Syndrome Now George M. Logan, MD Friday, May 5, 2017 3:35 4:05 PM Dr. Logan indicated no potential conflict of interest to this presentation. He does not intend to discuss any unapproved/investigative
Irritable Bowel Syndrome Now George M. Logan, MD Friday, May 5, 2017 3:35 4:05 PM Dr. Logan indicated no potential conflict of interest to this presentation. He does not intend to discuss any unapproved/investigative
Efficacy and Safety of Lubiprostone. Laura Wozniak February 23, 2010 K30 Monthly Journal Club
 Efficacy and Safety of Lubiprostone Laura Wozniak February 23, 2010 K30 Monthly Journal Club Objectives Brief overview of constipation Review of article Discussion Constipation in Children 3-5% of all
Efficacy and Safety of Lubiprostone Laura Wozniak February 23, 2010 K30 Monthly Journal Club Objectives Brief overview of constipation Review of article Discussion Constipation in Children 3-5% of all
A 27-Year-Old Woman With Constipation: Diagnosis and Treatment
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2010;8:838 842 EDUCATION PRACTICE A 27-Year-Old Woman With Constipation: Diagnosis and Treatment ARNOLD WALD Section of Gastroenterology and Hepatology, University
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2010;8:838 842 EDUCATION PRACTICE A 27-Year-Old Woman With Constipation: Diagnosis and Treatment ARNOLD WALD Section of Gastroenterology and Hepatology, University
Fecal Incontinence. What is fecal incontinence?
 Scan for mobile link. Fecal Incontinence Fecal incontinence is the inability to control the passage of waste material from the body. It may be associated with constipation or diarrhea and typically occurs
Scan for mobile link. Fecal Incontinence Fecal incontinence is the inability to control the passage of waste material from the body. It may be associated with constipation or diarrhea and typically occurs
Constipation in Children. Amani Al Hajeri, MD, CABFM, IBFM, MSc MG*
 1 Bahrain Medical Bulletin, Vol. 33, No. 4, December 2011 Education-Family Physician Corner Constipation in Children Amani Al Hajeri, MD, CABFM, IBFM, MSc MG* Constipation in pediatrics age group is frequently
1 Bahrain Medical Bulletin, Vol. 33, No. 4, December 2011 Education-Family Physician Corner Constipation in Children Amani Al Hajeri, MD, CABFM, IBFM, MSc MG* Constipation in pediatrics age group is frequently
Primary Management of Irritable Bowel Syndrome
 Primary Management of Irritable Bowel Syndrome Jasmine Zia, MD Acting Instructor, Division of Gastroenterology Current Concepts in Drug Therapy CME Course April 23, 2015 Irritable Bowel Syndrome (IBS)
Primary Management of Irritable Bowel Syndrome Jasmine Zia, MD Acting Instructor, Division of Gastroenterology Current Concepts in Drug Therapy CME Course April 23, 2015 Irritable Bowel Syndrome (IBS)
A Nursing Assessment Tool for Adults With Fecal Incontinence
 Journal of Wound, Ostomy and Continence Nursing 2000, 279- A Nursing Assessment Tool for Adults With Fecal Incontinence Christine Norton, MA, RN, and Sonya Chelvanayagam, MSc, RN Abstract Fecal incontinence
Journal of Wound, Ostomy and Continence Nursing 2000, 279- A Nursing Assessment Tool for Adults With Fecal Incontinence Christine Norton, MA, RN, and Sonya Chelvanayagam, MSc, RN Abstract Fecal incontinence
Chapter 31 Bowel Elimination
 Chapter 31 Bowel Elimination Defecation Defecation: the act of expelling feces from the body Peristalsis: rhythmic contractions of intestinal smooth muscle to facilitate defecation Gastrocolic reflex:
Chapter 31 Bowel Elimination Defecation Defecation: the act of expelling feces from the body Peristalsis: rhythmic contractions of intestinal smooth muscle to facilitate defecation Gastrocolic reflex:
I ve had it with you and your emotional constipation.
 I ve had it with you and your emotional constipation. Washington Irving If Mother had to be told not to put the entire brick of ivory up Junior s hindquarters, constipation is the least of his problems.
I ve had it with you and your emotional constipation. Washington Irving If Mother had to be told not to put the entire brick of ivory up Junior s hindquarters, constipation is the least of his problems.
Constipation. H. David Vargas, MD. Overview
 Constipation H. David Vargas, MD Overview Constipation is a very common complaint affecting upwards of 15% of all Americans. Fortunately, constipation usually is simple to avoid and easy to treat when
Constipation H. David Vargas, MD Overview Constipation is a very common complaint affecting upwards of 15% of all Americans. Fortunately, constipation usually is simple to avoid and easy to treat when
Constipation a symptom NOT a disease! Bowels/Constipation Documentation The A-B-C-D. Documentation: Bowels/Constipation
 Documentation The A-B-C-D Terry Broda, RN(EC), BScN, NPHC,CDDN Elizabeth Kacew, RN(EC), MScN, NP-PHC October 30, 2014 Constipation a symptom NOT a disease! 1 How serious a problem? 50-85% of older people
Documentation The A-B-C-D Terry Broda, RN(EC), BScN, NPHC,CDDN Elizabeth Kacew, RN(EC), MScN, NP-PHC October 30, 2014 Constipation a symptom NOT a disease! 1 How serious a problem? 50-85% of older people
Antidiarrheals Antidiarrheal
 Antidiarrheals Major factors in diarrhea Increased motility of the GI tract. Decreased absorption of fluid. Antidiarrheal drugs include: Antimotility agents. Adsorbents. Drugs that modify fluid and electrolyte
Antidiarrheals Major factors in diarrhea Increased motility of the GI tract. Decreased absorption of fluid. Antidiarrheal drugs include: Antimotility agents. Adsorbents. Drugs that modify fluid and electrolyte
Understanding the Prevalence and Impact of Constipation in Canada. A Special Report from the Canadian Digestive Health Foundation
 Understanding the Prevalence and Impact of Constipation in Canada A Special Report from the Canadian Digestive Health Foundation February 2014 Understanding the Prevalence and Impact of Constipation in
Understanding the Prevalence and Impact of Constipation in Canada A Special Report from the Canadian Digestive Health Foundation February 2014 Understanding the Prevalence and Impact of Constipation in
Constipation. Disease Review
 bowel. 1 Constipation is a symptom, not a disease. Almost everyone experiences Disease Review Constipation Introduction: Constipation is exceedingly common and is rarely associated with mortality in developed
bowel. 1 Constipation is a symptom, not a disease. Almost everyone experiences Disease Review Constipation Introduction: Constipation is exceedingly common and is rarely associated with mortality in developed
Biofeedback for Pelvic Floor Disorders and Incontinence
 The UNC Center for Functional GI & Motility Disorders www.med.unc.edu/ibs Biofeedback for Pelvic Floor Disorders and Incontinence Olafur S. Palsson, Psy.D. Associate Professor of Medicine UNC Center for
The UNC Center for Functional GI & Motility Disorders www.med.unc.edu/ibs Biofeedback for Pelvic Floor Disorders and Incontinence Olafur S. Palsson, Psy.D. Associate Professor of Medicine UNC Center for
Diagnosis and Management of Irritable Bowel Syndrome (IBS) For the Primary Care Provider
 Diagnosis and Management of Irritable Bowel Syndrome (IBS) For the Primary Care Provider Elizabeth Coss, MD General Gastroenterologist Audie Murphy Veterans Hospital UT Health This presentation does not
Diagnosis and Management of Irritable Bowel Syndrome (IBS) For the Primary Care Provider Elizabeth Coss, MD General Gastroenterologist Audie Murphy Veterans Hospital UT Health This presentation does not
Angie Jefferson Registered Dietitian & Consultant Nutritionist
 Angie Jefferson Registered Dietitian & Consultant Nutritionist Constipation & Haemorrhoids are two of the most common problems experienced by pregnant women Incidence increases dramatically 40% women reportedto
Angie Jefferson Registered Dietitian & Consultant Nutritionist Constipation & Haemorrhoids are two of the most common problems experienced by pregnant women Incidence increases dramatically 40% women reportedto
Irritable Bowel Syndrome. Mustafa Giaffer March 2017
 Irritable Bowel Syndrome Mustafa Giaffer March 2017 Introduction First described in 1771. 50% of patients present
Irritable Bowel Syndrome Mustafa Giaffer March 2017 Introduction First described in 1771. 50% of patients present
Irritable Bowel Disease. Dr. Alexandra Ilnyckyj MD
 Irritable Bowel Disease Dr. Alexandra Ilnyckyj MD Exactly what is IBS? Common condition affecting mostly women Symptoms are variable but they reflect altered gut movement (motility) and sensation Commonly
Irritable Bowel Disease Dr. Alexandra Ilnyckyj MD Exactly what is IBS? Common condition affecting mostly women Symptoms are variable but they reflect altered gut movement (motility) and sensation Commonly
Human Anatomy rectum
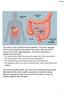 rectum The colon is also called the large intestine. The ileum (last part of the small intestine) connects to the cecum (first part of the colon) in the lower right abdomen. The rest of the colon is divided
rectum The colon is also called the large intestine. The ileum (last part of the small intestine) connects to the cecum (first part of the colon) in the lower right abdomen. The rest of the colon is divided
CHRONIC DIARRHEA DR. PHILIP K. BLUSTEIN M.D. F.R.C.P.(C) DEFINITION: *LOOSE, WATERY STOOLS *MORE THAN 3 TIMES A DAY *FOR MORE THAN 4 WEEKS
 DR. PHILIP K. BLUSTEIN M.D. F.R.C.P.(C) 415 14 TH ST. NW. CALGARY AB T2N2A1 PHONE (403) 270-9555 FAX (403) 270-7479 CHRONIC DIARRHEA DEFINITION: *LOOSE, WATERY STOOLS *MORE THAN 3 TIMES A DAY *FOR MORE
DR. PHILIP K. BLUSTEIN M.D. F.R.C.P.(C) 415 14 TH ST. NW. CALGARY AB T2N2A1 PHONE (403) 270-9555 FAX (403) 270-7479 CHRONIC DIARRHEA DEFINITION: *LOOSE, WATERY STOOLS *MORE THAN 3 TIMES A DAY *FOR MORE
Management of Neurogenic Bowel Dysfunction. Fiona Paul, DNP, RN, CPNP Center for Motility and Functional Gastrointestinal Disorders
 Management of Neurogenic Bowel Dysfunction Fiona Paul, DNP, RN, CPNP Center for Motility and Functional Gastrointestinal Disorders DEFECATION Delivery of colon contents to the rectum Rectal compliance
Management of Neurogenic Bowel Dysfunction Fiona Paul, DNP, RN, CPNP Center for Motility and Functional Gastrointestinal Disorders DEFECATION Delivery of colon contents to the rectum Rectal compliance
Don t let. Irritable irregularity 2.0
 Don t let constipation Over 2 million Americans visit their health care providers each year for constipationrelated problems, yet constipation is often overlooked until it becomes serious. We ll help you
Don t let constipation Over 2 million Americans visit their health care providers each year for constipationrelated problems, yet constipation is often overlooked until it becomes serious. We ll help you
Presenter. Irritable Bowel Syndrome. Objectives. Introduction. Rome Criteria. Irritable Bowel Syndrome 2/28/2018
 Presenter Irritable Bowel Syndrome Current evidence for diagnosis & management Julie Daniels DNP, CNM Assistant Professor Course Coordinator of Primary Care of Women Faculty at Frontier Nursing University
Presenter Irritable Bowel Syndrome Current evidence for diagnosis & management Julie Daniels DNP, CNM Assistant Professor Course Coordinator of Primary Care of Women Faculty at Frontier Nursing University
Protectives and Adsorbents. Inorganic chemistry Course 1 Third year Assist. Lecturer Ahlam A. Shafeeq MSc. Pharmaceutical chemistry
 Protectives and Adsorbents Inorganic chemistry Course 1 Third year 2016-2017 Assist. Lecturer Ahlam A. Shafeeq MSc. Pharmaceutical chemistry Protectives and Adsorbents This group of gastrointestinal agents
Protectives and Adsorbents Inorganic chemistry Course 1 Third year 2016-2017 Assist. Lecturer Ahlam A. Shafeeq MSc. Pharmaceutical chemistry Protectives and Adsorbents This group of gastrointestinal agents
Primary Care Constipation Guidelines. Version 1 November 2016
 Primary Care Constipation Guidelines Version 1 November 2016 VERSION CONTROL Version Date Amendments made Version 1 November 2016 New guideline Contents 1. Management of constipation in adults: acute and
Primary Care Constipation Guidelines Version 1 November 2016 VERSION CONTROL Version Date Amendments made Version 1 November 2016 New guideline Contents 1. Management of constipation in adults: acute and
CONSTIPATION. Atan Baas Sinuhaji
 CONSTIPATION Atan Baas Sinuhaji Sub Division of Pediatrics Gastroentero-Hepatolgy Department of ChildHealth,School of Medicine University of Sumatera Utara MEDAN DEFECATION REGULAR PATTERN CONSTIPATION
CONSTIPATION Atan Baas Sinuhaji Sub Division of Pediatrics Gastroentero-Hepatolgy Department of ChildHealth,School of Medicine University of Sumatera Utara MEDAN DEFECATION REGULAR PATTERN CONSTIPATION
IRRITABLE BOWEL SYNDROME
 DR. PHILIP K. BLUSTEIN M.D. F.R.C.P.(C) 415 14 TH ST. NW. CALGARY AB T2N2A1 PHONE (403) 270-9555 FAX (403) 270-7479 IRRITABLE BOWEL SYNDROME DEFINITION: *FUNCTIONAL GASTROINTESTINAL DISORDER CHARACTERIZED
DR. PHILIP K. BLUSTEIN M.D. F.R.C.P.(C) 415 14 TH ST. NW. CALGARY AB T2N2A1 PHONE (403) 270-9555 FAX (403) 270-7479 IRRITABLE BOWEL SYNDROME DEFINITION: *FUNCTIONAL GASTROINTESTINAL DISORDER CHARACTERIZED
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE SCOPE
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE 1 Guideline title SCOPE Constipation: management of idiopathic constipation in children in primary and secondary care 1.1 Short title Constipation
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE 1 Guideline title SCOPE Constipation: management of idiopathic constipation in children in primary and secondary care 1.1 Short title Constipation
CONSTIPATION OR STYPSIS. Prof. G. Zuliani
 CONSTIPATION OR STYPSIS Prof. G. Zuliani How Do We Define Constipation? The American College of Gastroenterology (ACG) definition of constipation: Unsatisfactory defecation characterized by infrequent
CONSTIPATION OR STYPSIS Prof. G. Zuliani How Do We Define Constipation? The American College of Gastroenterology (ACG) definition of constipation: Unsatisfactory defecation characterized by infrequent
SYMPROIC (naldemedine tosylate) oral capsule
 SYMPROIC (naldemedine tosylate) oral capsule Coverage for services, procedures, medical devices and drugs are dependent upon benefit eligibility as outlined in the member's specific benefit plan. This
SYMPROIC (naldemedine tosylate) oral capsule Coverage for services, procedures, medical devices and drugs are dependent upon benefit eligibility as outlined in the member's specific benefit plan. This
Are you aware there are many different reasons for having irregular bowels? This chart is to help you get back into balance during and post detox.
 BRISTOL POOP CHART The Bristol Poop Chart was created in the United Kingdom by a group of gastroenterologists at the University of Bristol. This chart is designed to help you determine the health of your
BRISTOL POOP CHART The Bristol Poop Chart was created in the United Kingdom by a group of gastroenterologists at the University of Bristol. This chart is designed to help you determine the health of your
IBS - Definition. Chronic functional disorder of GI generally characterized by:
 IBS - Definition Chronic functional disorder of GI generally characterized by: 3500 3000 No. of Publications 2500 2000 1500 1000 Irritable Bowel syndrome Irritable Bowel Syndrome 500 0 1968-1977 1978-1987
IBS - Definition Chronic functional disorder of GI generally characterized by: 3500 3000 No. of Publications 2500 2000 1500 1000 Irritable Bowel syndrome Irritable Bowel Syndrome 500 0 1968-1977 1978-1987
ABC s of Bowel Management
 ABC s of Bowel Management Spina Bifida Education Day Conference SBA of Northeastern New York Albany, New York April 14, 2018 Eric Levey, M.D. Pediatrics & Neurodevelopmental Disabilities Chief Medical
ABC s of Bowel Management Spina Bifida Education Day Conference SBA of Northeastern New York Albany, New York April 14, 2018 Eric Levey, M.D. Pediatrics & Neurodevelopmental Disabilities Chief Medical
Managing constipation in residential care
 Managing constipation in residential care Amanda Lee Lecturer, Hull University ; PhD Candidate, Gastroesophageal cancers Key Points Constipation is a major problem in residential care Early detection and
Managing constipation in residential care Amanda Lee Lecturer, Hull University ; PhD Candidate, Gastroesophageal cancers Key Points Constipation is a major problem in residential care Early detection and
11/04/2011 OVERVIEW. Neurogenic Bowel Management. in adults with Spinal Cord Injury (S.C.I.) Sequence of events in normal Defecation
 Neurogenic Bowel Management in adults with Spinal Cord Injury (S.C.I.) Dimitrios D. Ergeletzis MD Physiatrist Director of Physical Medicine & Rehabilitation Dept.- GIROKOMEION ATHENS, Greece OVERVIEW Anatomy
Neurogenic Bowel Management in adults with Spinal Cord Injury (S.C.I.) Dimitrios D. Ergeletzis MD Physiatrist Director of Physical Medicine & Rehabilitation Dept.- GIROKOMEION ATHENS, Greece OVERVIEW Anatomy
Why does my stomach hurt? Exploring irritable bowel syndrome
 Why does my stomach hurt? Exploring irritable bowel syndrome By Flavio M. Habal, MD, PhD, FRCPC Case In this article: 1. What is IBS? A 45-year-old female is referred to your office with recurrent 2. How
Why does my stomach hurt? Exploring irritable bowel syndrome By Flavio M. Habal, MD, PhD, FRCPC Case In this article: 1. What is IBS? A 45-year-old female is referred to your office with recurrent 2. How
Episode 3.2 Show Notes Constipation
 Episode 3.2 Show Notes Constipation Presented by: Dr Jo Preston, Dr Iain Wilkinson & Mairéad O Malley Faculty: Clare Watson, Wendy Grosvenor Guest faculty: Dr Gaggandeep Singh Alg Broadcast Date: 28th
Episode 3.2 Show Notes Constipation Presented by: Dr Jo Preston, Dr Iain Wilkinson & Mairéad O Malley Faculty: Clare Watson, Wendy Grosvenor Guest faculty: Dr Gaggandeep Singh Alg Broadcast Date: 28th
Class Review: Drugs for Constipation
 Copyright 2012 Oregon State University. All Rights Reserved Drug Use Research & Management Program Oregon State University, 500 Summer Street NE, E35 Salem, Oregon 97301-1079 Phone 503-947-5220 Fax 503-947-1119
Copyright 2012 Oregon State University. All Rights Reserved Drug Use Research & Management Program Oregon State University, 500 Summer Street NE, E35 Salem, Oregon 97301-1079 Phone 503-947-5220 Fax 503-947-1119
CHAPTER 11 Functional Gastrointestinal Disorders (FGID) Mr. Ashok Kumar Dept of Pharmacy Practice SRM College of Pharmacy SRM University
 CHAPTER 11 Functional Gastrointestinal Disorders (FGID) Mr. Ashok Kumar Dept of Pharmacy Practice SRM College of Pharmacy SRM University 1 Definition of FGID Chronic and recurrent symptoms of the gastrointestinal
CHAPTER 11 Functional Gastrointestinal Disorders (FGID) Mr. Ashok Kumar Dept of Pharmacy Practice SRM College of Pharmacy SRM University 1 Definition of FGID Chronic and recurrent symptoms of the gastrointestinal
Diagnosis of Impaired Defecatory Function with Special Reference to Physiological Tests
 Defecatory Dysfunction Diagnosis of Impaired Defecatory Function with Special Reference to Physiological Tests JMAJ 46(9): 373 377, 2003 Masatoshi OYA, Masashi UENO, and Tetsuichiro MUTO Department of
Defecatory Dysfunction Diagnosis of Impaired Defecatory Function with Special Reference to Physiological Tests JMAJ 46(9): 373 377, 2003 Masatoshi OYA, Masashi UENO, and Tetsuichiro MUTO Department of
Treatment of Constipation in Adults
 This Clinical Resource gives subscribers additional insight related to the Recommendations published in April 2017 ~ Resource #330407 Treatment of Constipation in Adults Use this document as a stepwise
This Clinical Resource gives subscribers additional insight related to the Recommendations published in April 2017 ~ Resource #330407 Treatment of Constipation in Adults Use this document as a stepwise
GI Physiology - Investigating and treating patients with pelvic floor dysfunction. Lynne Smith Department of GI Physiology NGH Sheffield
 GI Physiology - Investigating and treating patients with pelvic floor dysfunction Lynne Smith Department of GI Physiology NGH Sheffield Aims o o o To give an overview of lower GI investigations To demonstrate
GI Physiology - Investigating and treating patients with pelvic floor dysfunction Lynne Smith Department of GI Physiology NGH Sheffield Aims o o o To give an overview of lower GI investigations To demonstrate
Tana's Habitat - Vim and Vigor - They Don t Call Them High Bars For Nothin
 http://www.tanashabitat.com/vim/0404151of6.asp Do you have a tummy ache that ver seems to go away? Do you wish your gu would just calm down and let you live your life? If so, you re not alo. You may suffer
http://www.tanashabitat.com/vim/0404151of6.asp Do you have a tummy ache that ver seems to go away? Do you wish your gu would just calm down and let you live your life? If so, you re not alo. You may suffer
Constipation. Information for adults. GI Motility Clinic (UMCCC University Medical Clinics of Campbelltown and Camden) Page 1
 Constipation Information for adults GI Motility Clinic (UMCCC University Medical Clinics of Campbelltown and Camden) Page 1 Contents Role of the large intestine..3 Mass movements in the large intestine..4
Constipation Information for adults GI Motility Clinic (UMCCC University Medical Clinics of Campbelltown and Camden) Page 1 Contents Role of the large intestine..3 Mass movements in the large intestine..4
Irritable bowel syndrome (IBS) is a ... PRESENTATION... Defining and Diagnosing Irritable Bowel Syndrome
 ... PRESENTATION... Defining and Diagnosing Irritable Bowel Syndrome Based on a presentation by Marvin M. Schuster, MD Presentation Summary Approximately 20% of the general population has irritable bowel
... PRESENTATION... Defining and Diagnosing Irritable Bowel Syndrome Based on a presentation by Marvin M. Schuster, MD Presentation Summary Approximately 20% of the general population has irritable bowel
Constipation David A Smith MD, FAAFP, CMD
 A Program of Morningside Ministries Constipation David A Smith MD, FAAFP, CMD President, Geriatric Consultants of Central Texas, PA Webcast This webcast is possible through the generous support of donors
A Program of Morningside Ministries Constipation David A Smith MD, FAAFP, CMD President, Geriatric Consultants of Central Texas, PA Webcast This webcast is possible through the generous support of donors
Revisionary Capsulorrhaphy Surgery Aftercare Guidelines Following Day Date:
 Surgery Sleep in a reclined positon Medications- take as directed Soft Diet and liquids Stool softener/high Fiber foods Leave on all dressing Surgical Stockings First Night Revisionary Capsulorrhaphy Surgery
Surgery Sleep in a reclined positon Medications- take as directed Soft Diet and liquids Stool softener/high Fiber foods Leave on all dressing Surgical Stockings First Night Revisionary Capsulorrhaphy Surgery
Constipation. What is constipation? What causes constipation? How common is constipation?
 Constipation What is constipation? Constipation is the word we use to describe any difficulty having a bowel movement. This does not just mean infrequent bowel movements, (two or fewer bowel movements
Constipation What is constipation? Constipation is the word we use to describe any difficulty having a bowel movement. This does not just mean infrequent bowel movements, (two or fewer bowel movements
 Page 1 of 7 Official reprint from UpToDate www.uptodate.com 2017 UpToDate The content on the UpToDate website is not intended nor recommended as a substitute for medical advice, diagnosis, or treatment.
Page 1 of 7 Official reprint from UpToDate www.uptodate.com 2017 UpToDate The content on the UpToDate website is not intended nor recommended as a substitute for medical advice, diagnosis, or treatment.
Objectives. Identify age-related changes in the gastrointestinal tract
 The Primary Care Physician s Approach to Gastrointestinal Complaints in the Elderly Brian Viviano, D.O. Medical Associates of Erie Objectives Identify age-related changes in the gastrointestinal tract
The Primary Care Physician s Approach to Gastrointestinal Complaints in the Elderly Brian Viviano, D.O. Medical Associates of Erie Objectives Identify age-related changes in the gastrointestinal tract
The Digestive System or tract extends from the mouth to the anus.
 The Digestive System or tract extends from the mouth to the anus. FUNCTION The Digestive System breaks down and absorbs food materials e.g. amino acids, glucose DEFINITIONS: Ingestion: Ingestion is the
The Digestive System or tract extends from the mouth to the anus. FUNCTION The Digestive System breaks down and absorbs food materials e.g. amino acids, glucose DEFINITIONS: Ingestion: Ingestion is the
Constipation. Self-study course
 Constipation Self-study course 2 Course objectives: At the end of this course you will be able to: 1. Define the term constipation 2. Explain three reasons why older adults are at greater risk for constipation
Constipation Self-study course 2 Course objectives: At the end of this course you will be able to: 1. Define the term constipation 2. Explain three reasons why older adults are at greater risk for constipation
Constipation. National Digestive Diseases Information Clearinghouse
 Constipation National Digestive Diseases Information Clearinghouse National Institute of Diabetes and Digestive and Kidney Diseases NATIONAL INSTITUTES OF HEALTH Constipation is defined as having a bowel
Constipation National Digestive Diseases Information Clearinghouse National Institute of Diabetes and Digestive and Kidney Diseases NATIONAL INSTITUTES OF HEALTH Constipation is defined as having a bowel
Anorectal Diagnostic Overview
 Anorectal Diagnostic Overview 11-25-09 3.11.2010 2009 2010 Anorectal Manometry Overview Measurement of pressures and the annotation of rectal sensation throughout the rectum and anal canal to determine:
Anorectal Diagnostic Overview 11-25-09 3.11.2010 2009 2010 Anorectal Manometry Overview Measurement of pressures and the annotation of rectal sensation throughout the rectum and anal canal to determine:
Slide #43. Functional Disorders - An Update 11/8/ MA ACP Annual Scientific Meeting. Functional Disorders: An Update
 Functional Disorders: An Update Anthony Lembo, M.D. Associate Professor of Medicine Beth Israel Deaconess Medical Center Harvard Medical School Boston, MA Disclosure of Financial Relationships Anthony
Functional Disorders: An Update Anthony Lembo, M.D. Associate Professor of Medicine Beth Israel Deaconess Medical Center Harvard Medical School Boston, MA Disclosure of Financial Relationships Anthony
MANAGING CONSTIPATION
 MANAGING CONSTIPATION INFORMATION FOR OLDER ADULTS, FAMILIES, AND CAREGIVERS READ THIS PAMPHLET TO LEARN: What Constipation is. The Symptoms of Constipation. How to Help Manage Constipation. WHAT IS CONSTIPATION?
MANAGING CONSTIPATION INFORMATION FOR OLDER ADULTS, FAMILIES, AND CAREGIVERS READ THIS PAMPHLET TO LEARN: What Constipation is. The Symptoms of Constipation. How to Help Manage Constipation. WHAT IS CONSTIPATION?
Chronic Constipation. written by Harvard Medical School.
 Chronic Constipation written by Harvard Medical School www.patientedu.org What is Constipation? Although estimates vary widely, up to 28% of adult Americans may suffer from constipation. The problem is
Chronic Constipation written by Harvard Medical School www.patientedu.org What is Constipation? Although estimates vary widely, up to 28% of adult Americans may suffer from constipation. The problem is
Irritable bowel syndrome in adults
 Irritable bowel syndrome in adults NICE provided the content for this booklet which is independent of any company or product advertised Welcome In February 2008, NICE published a clinical guideline on
Irritable bowel syndrome in adults NICE provided the content for this booklet which is independent of any company or product advertised Welcome In February 2008, NICE published a clinical guideline on
OPIOID-INDUCED CONSTIPATION DR ANDREW DAVIES
 OPIOID-INDUCED CONSTIPATION DR ANDREW DAVIES Introduction Introduction Mean faecal weight 128 g / cap / day Mean range 51-796 g Absolute range 15-1505 g Main factors affecting mass are caloric intake,
OPIOID-INDUCED CONSTIPATION DR ANDREW DAVIES Introduction Introduction Mean faecal weight 128 g / cap / day Mean range 51-796 g Absolute range 15-1505 g Main factors affecting mass are caloric intake,
Morning Report S a p n a P a t e l K u e h l M D F A C P S t. A g n e s H o s p i t a l, B a l t i m o r e M D
 Morning Report Sapna Patel Kuehl MD FACP St. Agnes Hospital, Baltimore MD Chief complaint Found confused in bathtub History of present illness 74 yo woman with PMHx of COPD, on home oxygen 2L presented
Morning Report Sapna Patel Kuehl MD FACP St. Agnes Hospital, Baltimore MD Chief complaint Found confused in bathtub History of present illness 74 yo woman with PMHx of COPD, on home oxygen 2L presented
Is one of the most common chronic disorders. causing patients to seek medical treatment.
 ILOs After this lecture you should be able to : Define IBS Identify causes and risk factors of IBS Determine the appropriate therapeutic options for IBS Is one of the most common chronic disorders causing
ILOs After this lecture you should be able to : Define IBS Identify causes and risk factors of IBS Determine the appropriate therapeutic options for IBS Is one of the most common chronic disorders causing
A guide to Anoplasty (anal surgery)
 Saint Mary s Hospital Newborn Intensive Care Unit Information for Parents A guide to Anoplasty (anal surgery) Introduction This information leaflet is designed to help parents and families to care for
Saint Mary s Hospital Newborn Intensive Care Unit Information for Parents A guide to Anoplasty (anal surgery) Introduction This information leaflet is designed to help parents and families to care for
Advancing gastroenterology, improving patient care
 American College of Gastroenterology Advancing gastroenterology, improving patient care Note to Visitors: A fully updated ACG Systematic Review on the Management of Chronic Idiopathic Constipation and
American College of Gastroenterology Advancing gastroenterology, improving patient care Note to Visitors: A fully updated ACG Systematic Review on the Management of Chronic Idiopathic Constipation and
What is Irritable Bowel Syndrome (IBS)?
 What is Irritable Bowel Syndrome (IBS)? Irritable bowel syndrome (IBS) is a health issue found in your intestines (gut). IBS can cause symptoms such as: Belly pain. Cramping. Gas. Bloating (or swelling)
What is Irritable Bowel Syndrome (IBS)? Irritable bowel syndrome (IBS) is a health issue found in your intestines (gut). IBS can cause symptoms such as: Belly pain. Cramping. Gas. Bloating (or swelling)
A Case of Fecal Incontinence: Medical and Interventional Treatment Options
 A Case of Fecal Incontinence: Medical and Interventional Treatment Options HPI JP is a 69 year-old F with a 12-month history of FI. Her symptoms began after a colonoscopy She has been experiencing passive
A Case of Fecal Incontinence: Medical and Interventional Treatment Options HPI JP is a 69 year-old F with a 12-month history of FI. Her symptoms began after a colonoscopy She has been experiencing passive
PELVIC PAIN : Gastroenterological Conditions
 PELVIC PAIN : Gastroenterological Conditions Departman Tarih Prof. A. Melih OZEL, MD Department of Gastroenterology Anadolu Medical Center Hospital Gebze Kocaeli - TURKEY Presentation plan 15 min. Introduction
PELVIC PAIN : Gastroenterological Conditions Departman Tarih Prof. A. Melih OZEL, MD Department of Gastroenterology Anadolu Medical Center Hospital Gebze Kocaeli - TURKEY Presentation plan 15 min. Introduction
Active ingredients per ml: Docusate sodium 1 mg/sorbitol solution (70%) (crystallising) 357 mg Structural formula: Docusate.
 NAME OF THE MEDICINE KLYX Enema Active ingredients per ml: Docusate sodium 1 mg/sorbitol solution (70%) (crystallising) 357 mg Structural formula: Docusate Sorbitol C20H37NaO7S MW: 444.56 CAS no: 577-11-7
NAME OF THE MEDICINE KLYX Enema Active ingredients per ml: Docusate sodium 1 mg/sorbitol solution (70%) (crystallising) 357 mg Structural formula: Docusate Sorbitol C20H37NaO7S MW: 444.56 CAS no: 577-11-7
CENTENE PHARMACY AND THERAPEUTICS DRUG REVIEW 3Q17 July August
 BRAND NAME Symproic GENERIC NAME Naldemedine MANUFACTURER Shionogi Inc. DATE OF APPROVAL March 23, 2017 PRODUCT LAUNCH DATE Anticipated to launch mid-summer 2017 REVIEW TYPE Review type 1 (RT1): New Drug
BRAND NAME Symproic GENERIC NAME Naldemedine MANUFACTURER Shionogi Inc. DATE OF APPROVAL March 23, 2017 PRODUCT LAUNCH DATE Anticipated to launch mid-summer 2017 REVIEW TYPE Review type 1 (RT1): New Drug
Constipation and bowel obstruction
 Constipation and bowel obstruction Constipation Infrequent or difficult defecation with reduced number of bowel movements, which may or may not be abnormally hard with increased difficulty or discomfort
Constipation and bowel obstruction Constipation Infrequent or difficult defecation with reduced number of bowel movements, which may or may not be abnormally hard with increased difficulty or discomfort
Evidence-based Treatment Strategies for
 Evidence-based Treatment Strategies for Chronic Constipation William D. Chey, MD Professor of Medicine University of Michigan Rome III criteria*: Chronic constipation Must include 2 of the following (>25%
Evidence-based Treatment Strategies for Chronic Constipation William D. Chey, MD Professor of Medicine University of Michigan Rome III criteria*: Chronic constipation Must include 2 of the following (>25%
Biofeedback Program. GI Motility Clinic (UMCCC University Medical Clinics of Campbelltown and Camden) Page 1
 Biofeedback Program GI Motility Clinic (UMCCC University Medical Clinics of Campbelltown and Camden) Page 1 Biofeedback Checklist Bristol Stool Form Scale Digestive process 4F s Fibre, Fluid, Fitness,
Biofeedback Program GI Motility Clinic (UMCCC University Medical Clinics of Campbelltown and Camden) Page 1 Biofeedback Checklist Bristol Stool Form Scale Digestive process 4F s Fibre, Fluid, Fitness,
Chapter 34. Nursing Care of Patients with Lower Gastrointestinal Disorders
 Chapter 34 Nursing Care of Patients with Lower Gastrointestinal Disorders Lower Gastrointestinal System Small Intestines Large Intestines Rectum Anus Constipation Fecal Mass Held In Rectum Feces Become
Chapter 34 Nursing Care of Patients with Lower Gastrointestinal Disorders Lower Gastrointestinal System Small Intestines Large Intestines Rectum Anus Constipation Fecal Mass Held In Rectum Feces Become
Breast Augmentation Saline Overfilled Surgery Aftercare Guidelines
 Surgery Breast Augmentation Saline Overfilled Surgery Aftercare Guidelines First Night Following Day 3-5 Days 1 st Post op Visit 7-10 Days 2 nd Post op Visit 2 Weeks Post op 4-6 Weeks Post op 8-12Weeks
Surgery Breast Augmentation Saline Overfilled Surgery Aftercare Guidelines First Night Following Day 3-5 Days 1 st Post op Visit 7-10 Days 2 nd Post op Visit 2 Weeks Post op 4-6 Weeks Post op 8-12Weeks
Current Pharmacological Treatment Options in Chronic Constipation and IBS with Constipation
 Current Pharmacological Treatment Options in Chronic Constipation and IBS with Constipation Anthony Lembo, M.D. Associate Professor of Medicine Harvard Medical School Director, GI Motility Center Beth
Current Pharmacological Treatment Options in Chronic Constipation and IBS with Constipation Anthony Lembo, M.D. Associate Professor of Medicine Harvard Medical School Director, GI Motility Center Beth
Anal Fissure. The basis of conservative treatment for an anal fissure is simple. If you have
 Anal Fissure An anal fissure is a cut in the anal canal resulting from trauma. Most people suffering from an anal fissure experience pain during or after defecation (the act of moving one s bowels, a number
Anal Fissure An anal fissure is a cut in the anal canal resulting from trauma. Most people suffering from an anal fissure experience pain during or after defecation (the act of moving one s bowels, a number
Bowel and Bladder Dysfunction (BBD) Naida Kalloo, MD Pediatric Urology Children s National
 Bowel and Bladder Dysfunction (BBD) Naida Kalloo, MD Pediatric Urology Children s National What is Bowel and Bladder Dysfunction? Lower urinary tract symptoms (LUTS) and bowel movement disorders Majority
Bowel and Bladder Dysfunction (BBD) Naida Kalloo, MD Pediatric Urology Children s National What is Bowel and Bladder Dysfunction? Lower urinary tract symptoms (LUTS) and bowel movement disorders Majority
Long-Term Bowel Symptoms Following Corrective Surgery
 HIRSCHSPRUNG'S DISEASE Samuel Nurko MD MPH Center for Motility and Functional Gastrointestinal Disorders Children s Hospital Medical Center, Boston Ma Long-Term Bowel Symptoms Following Corrective Surgery
HIRSCHSPRUNG'S DISEASE Samuel Nurko MD MPH Center for Motility and Functional Gastrointestinal Disorders Children s Hospital Medical Center, Boston Ma Long-Term Bowel Symptoms Following Corrective Surgery
