CLINICAL PATHOLOGY. Diagnosis of Colitis: Making the Initial Diagnosis. Case History. Clinical Evaluation of New Onset Colitis
|
|
|
- Blake Hutchinson
- 6 years ago
- Views:
Transcription
1 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2007;5: CLINICAL PATHOLOGY Diagnosis of Colitis: Making the Initial Diagnosis MARIA T. ABREU* and NOAM HARPAZ*, *Division of Gastroenterology and the Inflammatory Bowel Disease Center, and Department of Pathology, Mount Sinai, New York, New York The evaluation of patients with colitis of recent onset is a relatively common clinical challenge. The main considerations are infectious colitides, idiopathic IBD, ie, ulcerative and Crohn s colitis, and colonic ischemia. An initial risk assessment on the basis of such factors as concurrent symptoms in contacts, travel history, medications, and human immunodeficiency virus risk factors should be followed by a thorough clinical history, physical examination, stool studies, blood tests, and, in selected cases, endoscopic examination and serologic tests. Biopsies can be decisive in distinguishing among the different types of acute colitis and might help identify specific etiologies. The diagnostic yield of biopsies is maximized by appropriate sampling of the colonic mucosa and by sharing the clinical and endoscopic findings with the pathologist, eg, via a copy of the endoscopy report. Case History A 30-year-old woman presented with non-bloody diarrhea, crampy lower abdominal pain, and headache of 10 days duration unrelieved by bismuth salicylate. Blood and mucus per rectum became apparent 5 days after symptom onset. The symptoms had begun on return from an overseas trip during which she had consumed unpasteurized honey. She had lost 5 pounds, but a physical examination was unremarkable. There were no significant medical conditions, human immunodeficiency virus risk factors, or family history of IBD. Stool studies were negative for pathogens and Clostridium difficile toxin. A flexible sigmoidoscopy 2 weeks after symptom onset revealed diffuse erythema, loss of vascular markings, friability, and inflammatory exudates extending beyond the limits of examination (Figure 1A). A biopsy showed acute colitis of infectious type (Figure 1B). Despite an initial response to ciprofloxacin 500 mg by mouth twice a day, her cramps and diarrhea recurred a week later. Stool samples remained culture negative but were now positive for C difficile toxin A. A repeat flexible sigmoidoscopy revealed scattered whitish pseudomembranes throughout the left colon (Figure 2A), and biopsies confirmed pseudomembranous colitis and no evidence of IBD (Figure 2B). Treatment with metronidazole 500 mg by mouth 3 times daily for 2 weeks resulted in gradual and complete resolution. Clinical Evaluation of New Onset Colitis Clinicians evaluating a patient with new onset colitis should first consider whether the colitis is due to a specific agent, eg, infectious, environmental, or a drug, or to idiopathic IBD. A thorough history should include a review of risk factors such as travel, antibiotic exposure, use of NSAIDs or other new drugs. Infectious colitis is responsible for the majority of cases of new onset diarrhea. Travelers are at particular risk of bacterial enterocolitis such as Campylobacter, including ciprofloxacin-resistant strains currently most common in Spain and Southeast Asia. C difficile colitis associated with hospitalization or antibiotic exposure is currently epidemic in North America. Nonetheless, a clear history of such exposure cannot always be elicited. The severity of the C difficile problem has been compounded by the emergence of a virulent strain characterized by deletion of the tcdt gene, which normally down-regulates the production of toxins A and B. 1,2 Currently, fluoroquinolones are the most common associated antibiotics. In patients with new onset colitis, C difficile should not be excluded until 3 sets of negative toxin assays have been reported, especially if the testing facility does not test for both toxins. Ischemic colitis must be considered in older patients with cardiovascular disease and in younger patients with specific risk factors such as use of various drugs (oral contraceptives, nasal decongestants, alosetron for treatment of irritable bowel syndrome, and cocaine, to name a few), heavy exercise, and coagulation disorders. Once suspected on clinical grounds, the diagnosis can usually be confirmed by endoscopy with biopsies. Once other causes of colitis have been ruled out, IBD such as Crohn s disease and ulcerative colitis should be considered. 1 A recent study has reported that patients with a history of bacterial gastroenteritis carry a 2.4-fold risk of developing IBD and a 4.1-fold risk during the first year. 2 Patients with colitis associated with IBD typically give a history of symptoms of several weeks duration. Even those with more recent onset will often relate rectal bleeding that had been attributed to hemorrhoids. Weight loss might be noted, as well as constitutional symptoms of fatigue, low-grade fevers, and night sweats; however, these are not specific for IBD unless protracted. The physical examination should evaluate the sclera for icterus and episcleritis and the buccal mucosa for volume status and aphthous stomatitis or other possible oral manifestations of inflammatory bowel. 3 Skin lesions such as erythema nodosum or pyoderma gangrenosum would support a diagnosis of idiopathic IBD. The abdominal examination might reveal a Abbreviations used in this paper: CMV, cytomegalovirus by the AGA Institute /07/$32.00 doi: /j.cgh
2 296 ABREU AND HARPAZ CLINICAL GASTROENTEROLOGY AND HEPATOLOGY Vol. 5, No. 3 right lower quadrant mass suggesting Crohn s disease, but patients with colitis will more often have a normal examination or left-sided tenderness. In thin patients, a thickened left colon might be palpable. Up to 20% of patients with Crohn s disease have perianal fistulas, 4 and 50% have other perianal complications, 5 and their prevalence is even higher among patients with isolated Crohn s colitis. Careful perianal examination might reveal large edematous tags or a sentinel tag associated with an anal fissure, and rectal examination might reveal an anal stricture. Heme-positive stool is not helpful in distinguishing IBD from infectious colitis. Routine laboratory tests focus on complications related to systemic inflammation and chronic blood loss. Elevated erythrocyte sedimentation rates and C-reactive protein levels occur in patients with infections and with idiopathic IBD. However, abnormalities in hemoglobin levels and mean corpuscular volume favor IBD, in which iron deficiency anemia and mixed anemia are common manifestations. The albumin level might be low in both infectious colitis and IBD, but more commonly in the latter. Early endoscopy is recommended in patients with colitis of new onset, especially when stool cultures are negative. Empirical treatment with antibiotics such as fluoroquinolones should be avoided when the risk of bacterial infection is low, and before culture results have returned. The potential adverse consequences include C difficile colitis, as described in the present case, and partial healing, either of which might confound the endoscopic and clinical picture. Figure 1. (A) Patient s endoscopic findings characterized by diffuse superficial ulcerations and exudates. (B) Biopsy revealing typical pattern of acute infectious colitis characterized by edema and infiltration by neutrophils. The crypts are separated from one another and from the muscularis mucosae by edema, but their architecture is preserved, and there is no significant increase in lymphocytes and plasma cells. Figure 2. (A) Pseudomembranous colitis is evident on repeat endoscopy. (B) Biopsy showing superficial necrosis, dilated crypts, and eruptive inflammatory exudates.
3 March 2007 INITIAL DIAGNOSIS OF COLITIS 297 While performing the initial endoscopic procedure, usually a flexible sigmoidoscopy, the gastroenterologist should observe and record the extent of inflammation and the nature of the inflammatory changes. 6 Is the rectum involved? Does the inflammation extend beyond the reach of the sigmoidoscope? Is it continuous? Are there punched out, stellate, or aphthous ulcers, or pinpoint granular mucosa? Are pseudomembranes present? All observations should be recorded in descriptive terms, because endoscopic findings are rarely if ever pathognomonic. To obtain adequate representative tissue, 4 biopsies should be sampled from each inflamed segment and an equal number from each uninflamed segment within reach. If ulcerations are extensive, some of the biopsies should sample areas that are not completely denuded to evaluate the residual crypt epithelial architecture. Fresh samples are desirable for C difficile toxin assays and for examination for ova and parasites. Our practice is to aspirate stool directly from the colon and forward it promptly to the clinical laboratory. Serologic markers have been developed as a means to help diagnose IBD and to distinguish ulcerative colitis from Crohn s disease. The combination of positive perinuclear antineutrophil cytoplasmic antibodies and negative antibodies to oligomannans in yeast, antibodies to the outer membrane porin of Escherichia coli, and antibodies to flagellin has a high positive predictive value for ulcerative colitis, whereas the converse results are associated with Crohn s disease. 7 9 However, some patients with Crohn s colitis are positive for perinuclear antineutrophil cytoplasmic antibodies, reducing the value of the test in this setting. 10 Importantly, these serologies are negative in patients with infectious colitis; the sole exception is antibody to flagellin, which is present in up to 8% of healthy controls (presumably a result of prior infection with flagellated pathogenics). 11 In patients with isolated colitis as in the present case, a positive serologic marker would be helpful because it would support a diagnosis of idiopathic IBD rather than infectious colitis. Additional tests will continue to improve the diagnostic capabilities of noninvasive methods to distinguish IBD from other entities. Finally, fecal markers such as lactoferrin and calprotectin are present in patients with idiopathic IBD. Although these have quite good sensitivity and specificity for distinguishing irritable bowel syndrome from IBD, they are not adequate for distinguishing IBD from infectious colitis. 12 Endoscopy and Biopsy Guidelines Patients whose symptoms have not improved within 1 week should undergo a flexible sigmoidoscopy. Use of a pediatric colonoscope might allow one to visualize mucosa normally outside of the reach of the sigmoidoscope if the patient can tolerate it. A Fleet enema before sigmoidoscopy improves visualization of the mucosa but might lower the yield from stool cultures sent directly from stool collected into a trap. If symptoms persist and the sigmoidoscopy reveals no abnormality, a colonoscopy should be performed. Biopsies can be decisive in achieving a specific diagnosis, but several guidelines and precautions should be observed to maximize their diagnostic yield. First, as is true for any other medical consultation, it is of the utmost importance for the pathologist to have access to the patient s clinical history and endoscopic findings. An excellent source is the endoscopy report, a copy of which should be attached to the pathology requisition. Copies of endoscopic images are helpful in selected cases, ie, when unusual endoscopic changes are encountered. Information regarding the type of bowel preparation and any prescription or over-the-counter drug use should be provided, because a host of agents can affect the histology and confound the evaluation. Among many examples are sodium phosphate purgatives, which can result in focal inflammation or aphthous lesions, NSAIDs, which can produce ischemic changes, and ranitidine, which can elicit intraepithelial lymphocytosis mimicking lymphocytic colitis. In patients whose diarrhea results in dehydration or arrhythmias, hypoperfusion of the colon might result in ischemic changes superimposed on the underlying pathology of the colitis. This will result in an erroneous interpretation if the clinician has withheld this information. Multiple biopsies should be sampled from each region examined; the main objective is to achieve a representative sampling of regional and local variations that naturally occur in various inflammatory disorders. Another objective is to compensate for the small dimensions of conventional forceps biopsies, for lost detail caused by crush and electrocautery artifacts, and for random variations in specimen orientation, all of which can reduce the likelihood of detecting diagnostic features. In most cases, 4 quadrant biopsies of affected and unaffected areas will suffice. Certain colitides such as pseudomembranous colitis, Crohn s disease, and resolving infectious colitis might be exquisitely patchy and are therefore apt to yield false-negative results if inadequately sampled. Random specimens from the same anatomic segment might be in a single specimen container, but any grossly distinctive areas should be sampled separately. The source of each container should always be identified by anatomic segment, because the morphology of normal mucosa varies with anatomic location. Sampling should include endoscopically normal mucosa, because significant and potentially important microscopic changes might be found even when unsuspected endoscopically. 13 Finally, supplemental ( special ) stains have a very limited role in evaluating acute colitides encountered in routine practice. Decisions regarding their use are best made after the pathologist has been apprised of any particular pathogens or disease entities that are suspected on clinical grounds and has evaluated the routine hematoxylin-eosin slides. Examples include immunoperoxidase staining for cytomegalovirus (CMV), especially when inclusion bodies are scarce or histologically atypical, the Congo red stain for amyloidosis, an acid-fast stain for mycobacterial infections, the Gram stain for enteroadherent coliform infections, and silver stains for opportunistic fungi. Normal Histology and Anatomic Variations Conventional forceps biopsies of the colon and rectum sample the entire lamina propria, all or part of the muscularis mucosae, and sometimes the superficial submucosa. Diagnostic yield is maximized by orienting the sample luminal side up on an adherent matrix such as an absorbable gelatin sponge to facilitate on-edge sectioning by the laboratory and then fixing the sample promptly in buffered formalin solution. 14
4 298 ABREU AND HARPAZ CLINICAL GASTROENTEROLOGY AND HEPATOLOGY Vol. 5, No. 3 Histologically, normal crypts present as uniform structures with tubular profiles if the mucosa is well-oriented but otherwise with elliptical or circular profiles. They are separated by a half crypt diameter or less and surrounded by a nearly transparent lamina propria. The upper half of the lamina propria contains a loose collection of mononuclear inflammatory cells, mainly plasma cells and lymphocytes, which dissipate toward the base of the mucosa. The resulting gradient is an important diagnostic feature but may be lost in poorly oriented biopsies. The epithelium lining the crypts and surface, at least at the light microscopic level, is dominated by columnar (absorptive) and goblet cells accompanied by small numbers of endocrine and Paneth s cells. The histology of the mucosa varies with anatomic location. Compared with the rest of the colon, the normal cecal mucosa is characterized by widely spaced crypts and a relative abundance of mononuclear inflammatory cells. Biopsies from this location might therefore be regarded as abnormal if their origin is unknown. Paneth s cells are normally limited to the ascending colon, but they might occur throughout the colon and rectum in ulcerative colitis and other chronic inflammatory states. Biopsies of the sigmoid might show nonspecific or IBDlike inflammation if sampled from the vicinity of diverticula. The rectal mucosa frequently contains mucin-laden macrophages that intervene between the crypt bases and the muscularis mucosae, simulating the crypt shortfall of chronic IBD (Figure 3A). Likewise, the mucosa approaching the anorectal junction is distorted and IBD-like. It follows that the common but unnecessary practices of submitting undesignated biopsy specimens ( colon biopsy ) and combining biopsies from different locations in a single container fall short of the best standards of care. Acute Infectious Colitis Conventional cases of acute or self-limited infectious colitis are characterized by an abrupt onset of diarrheal and associated symptoms and an overall duration of 10 days 3 weeks followed by permanent clinical resolution. They might be caused by a wide variety of bacterial pathogens including Campylobacter jejuni, E coli, Salmonella, and Shigella species and C difficile, as well as a host of viruses, but cultures and other laboratory techniques yield specific diagnoses in less than half of cases. Mucosal biopsies of the large intestine can afford a valuable adjunct to clinical and laboratory evaluation by excluding other disorders with similar clinical presentations, such as an initial attack of IBD or colonic ischemia, and by identifying or suggesting specific pathogens. 15 The conventional self-limited bacterial and viral colitides have similar histologic features. Their distinction as a group from other entities is best achieved when biopsies are taken during the first few days after symptom onset. 16 At this stage the mucosa is characterized by (1) edema; (2) neutrophil infiltration of the lamina propria, surface epithelium, and crypts, including distended crypt abscesses with flat epithelial lining; (3) reduced goblet cell mucin; (4) retention of the architectural features of parallel tubular crypts; and (5) little or no increase in the density or distribution of mononuclear inflammatory cells that are normally present in the upper regions of the colonic mucosa (Figure 1B). Clinical and histologic remission usually takes place in parallel toward the end of the first week and into the second. Histologically, one sees resolution of the edema, gradual dissipation of the neutrophil infiltrates, and signs of epithelial regeneration such as increased mitotic activity, enlarged nuclei, prominent nucleoli, and persistent mucin depletion. As the intensity of acute inflammation subsides, residual crypt inflammation might assume a patchy distribution, referred to as focal active colitis, in which scattered crypts continue to harbor cryptitis while others have normalized (Figure 3B). On complete clinical resolution, the mucosa is left with little or no microscopic residua. Initial Attack of Inflammatory Bowel Disease By contrast with infectious colitis, the mucosa during the early symptomatic stages of IBD evinces many of the same characteristics as long-standing disease, evidently reflecting the cumulative effects of preclinical inflammation of indeterminate duration. Biopsies taken even within a few days of a first bout of bloody diarrhea show expansion of the lamina propria and separation of the crypts by a dense, full-thickness inflammatory infiltrate dominated by plasma cells, lymphocytes, histiocytes, and eosinophils in varying proportions (Figure 3C). By comparison, neutrophils are relatively sparse within the lamina propria, concentrating instead within the crypts in the form of cryptitis and crypt abscesses, in the surface epithelium, and adjacent to capillaries. Although crypt abscesses are commonplace, the lining epithelial cells are more apt to be columnar or cuboidal than those of infectious colitis, and Paneth s cells might be found beyond their normal location in the ascending colon. However, crypt branching and disarray, considered hallmarks of chronic IBD, commonly develop gradually during the course of subsequent months Figure 3. (A) Normal rectal mucosa with muciphages separating the crypt bases from the muscularis mucosae. This should not be interpreted as postinflammatory crypt shortfall as seen in IBD. (B) Focal active colitis. This nonspecific pattern occurs in resolving infectious colitis, Crohn s disease, and after phosphosoda administration among other conditions. (C) Ulcerative colitis of recent onset characterized by full-thickness lymphoplasmacytic infiltrates, crypt shortfall, and selective neutrophil infiltration of the crypts. Focal branching of a crypt is noted in the lower right, but the degree of crypt disarray often seen in chronic IBD is not evident. (D) Chronic infectious colitis. In addition to mild edema and dense neutrophil infiltration, the lamina propria also contains mononuclear inflammatory cells surrounding the crypt bases. (E) Acute colonic ischemia. The crypts are devoid of goblet cells and taper toward the surface. The lamina propria is densely eosinophilic, and neutrophils are less abundant than in infections. (F) Colitis associated with E coli O157:H7. The edema, neutrophil infiltrates, and preserved crypt architecture resemble the findings in conventional acute infectious colitis. However, the diagnosis was suggested by the presence of an inflammatory pseudomembrane and evidence of ischemia in an adjoining biopsy. (G) CMV inclusion body in biopsy of a patient with ulcerative colitis on an immunosuppressive regimen. (Inset) High magnification.
5 March 2007 INITIAL DIAGNOSIS OF COLITIS 299
6 300 ABREU AND HARPAZ CLINICAL GASTROENTEROLOGY AND HEPATOLOGY Vol. 5, No. 3 Prolonged Infectious Colitis Versus Inflammatory Bowel Disease Infections that persist beyond 2 3 weeks might gradually evolve histologic features that overlap with those of early IBD, resulting in diagnostic ambiguity just when persistent symptoms begin to elicit clinical concerns for IBD. One common pattern in chronic infections is focal active colitis, which occurs in persistent infections and Crohn s colitis as well as in other unrelated disorders. Another pattern is basal lymphoplasmacytosis resulting from increased density and downward expansion of the mononuclear inflammatory cell population, mimicking the basal lymphoplasmacytosis of IBD (Figure 3D). This expansion is typically less dense, uniform, and diffuse than in ulcerative colitis, but it is well within the range of findings in Crohn s disease. Distortion of the crypt architecture and Paneth s cell metaplasia are uncommon even in prolonged infectious colitis, and the appearance of either favors IBD. In addition, the dichotomous patterns of neutrophil infiltration that characterize acute infectious colitis and IBD, ie, nonselective (lamina propria and epithelium) in infectious colitis versus epitheliotropic in IBD, remain useful discriminating criteria in the subacute and chronic settings as well. Acute Colonic Ischemia Acute colonic ischemia is usually microscopically distinctive, but its distribution might be patchy at both the gross and microscopic levels. Diagnostic yield is therefore optimized by submitting multiple biopsy samples from affected areas. Histologically, mild degrees of ischemia preferentially affect the superficial mucosa, whereas severe ischemia leads to progressively deeper changes. The earliest findings reflect injury to the capillary endothelial cells, ie, superficial capillary microthrombi or extravasation of red cells and plasma protein into the lamina propria, and are accompanied by near disappearance of goblet cells. The crypts assume shrunken, microcystic profiles with diameters tapering from the base to the surface, and the lamina propria takes on a characteristic dense hyaline eosinophilia, a feature that is often mistaken for fibrosis (Figure 3E). Inflammatory cells are usually sparse at this stage. Ultimately the mucosa undergoes coagulative necrosis of increasing depth accompanied by erosions and acute inflammatory pseudomembranes, which might simulate pseudomembranous colitis. 18 Although biopsies are informative in distinguishing ischemia from other disorders, they are of limited value in assessing the severity of ischemia or ruling out colonic infarction. Patient management therefore will depend primarily on the clinical assessment. C difficile Colitis Pseudomembranous colitis associated with C difficile colitis presents relatively distinctive histologic findings consisting of patchy necrosis of the superficial lamina propria, massive crypt dilatation, and volcano-like exudates of mucus, fibrin, and streaming neutrophils arranged in single file (Figure 2B). Endoscopic sampling of the pseudomembranes is important, because biopsies of the intervening mucosa will appear normal or resemble conventional acute infection. A relatively common problem is detachment of pseudomembranes from the mucosa during processing of biopsies, which can result in their being overlooked by the pathologist. This error can be avoided if the pathologist is suitably apprised of the endoscopic findings. Persistent C difficile colitis might result in severe and extensive mucosal injury, the cumulative manifestations of which might include significant architectural disarray closely mimicking chronic IBD. E coli O157:H7 Colitis Enterohemorrhagic colitis caused by E coli O157:H7 presents endoscopically with erythema, friability, longitudinal ulcers, and pseudomembranes, but these are usually more prominent in the right colon than in the left. The histologic features combine the motifs of acute infectious colitis, pseudomembranous colitis, and ischemia (Figure 3F), manifesting the combined effects of toxin-mediated injury to both the epithelial and endothelial cells. 19 Diagnostic yield is enhanced by taking multiple biopsies, especially from the right colon if possible, and conveying the endoscopic picture and any suspicion of a diarrheal outbreak to the pathologist. Cytomegalovirus Colitis Although usually encountered in immunocompromised individuals, including IBD patients on immunosuppressive therapies, CMV colitis can occur in otherwise healthy persons and in untreated IBD patients. It manifests grossly as discrete ulcerations of the cecum and ascending colon or, less commonly, as a segmental colitis, pancolitis, or flare-up of underlying IBD. Biopsies of ulcerated or intact mucosa reveal cytomegalic epithelial, endothelial, or mesenchymal cells of various types containing basophilic nuclear and eosinophilic cytoplasmic inclusion bodies (Figure 3G). The inclusions might be histologically atypical or extremely sparse, requiring a high index of suspicion and use of immunohistochemical staining for confirmation. Conclusions Evaluation of the patient with new onset colitis entails a thorough clinical evaluation and stool testing. When the latter results are negative or symptoms fail to resolve, endoscopic examination and biopsies are indicated. Biopsies will frequently permit distinction among acute infectious colitis, IBD, and colonic ischemia and might identify specific infectious etiologies. However, the endoscopist can do much to maximize their yield, principally by sharing clinical and endoscopic data with the pathologist and by following certain practical guidelines to achieve an adequate representation of the pathology. References 1. Carter MJ, Lobo AJ, Travis SP. Guidelines for the management of inflammatory bowel disease in adults. Gut 2004;53(Suppl 5):V1 V Garcia Rodriguez LA, Ruigomez A, Panes J. Acute gastroenteritis is followed by an increased risk of inflammatory bowel disease. Gastroenterology 2006;130: Harty S, Fleming P, Rowland M, et al. A prospective study of the oral manifestations of Crohn s disease. Clin Gastroenterol Hepatol 2005;3: Schwartz DA, Loftus EV Jr, Tremaine WJ, et al. The natural history of fistulizing Crohn s disease in Olmsted County, Minnesota. Gastroenterology 2002;122:
7 March 2007 INITIAL DIAGNOSIS OF COLITIS Harper PH, Fazio VW, Lavery IC, et al. The long-term outcome in Crohn s disease. Dis Colon Rectum 1987;30: Leighton JA, Shen B, Baron TH, et al. ASGE guideline: endoscopy in the diagnosis and treatment of inflammatory bowel disease. Gastrointest Endosc 2006;63: Landers CJ, Cohavy O, Misra R, et al. Selected loss of tolerance evidenced by Crohn s disease-associated immune responses to auto- and microbial antigens. Gastroenterology 2002;123: Targan SR, Landers CJ, Yang H, et al. Antibodies to CBir1 flagellin define a unique response that is associated independently with complicated Crohn s disease. Gastroenterology 2005;128: Lodes MJ, Cong Y, Elson CO, et al. Bacterial flagellin is a dominant antigen in Crohn disease. J Clin Invest 2004;113: Vasiliauskas EA, Plevy SE, Landers CJ, et al. Perinuclear antineutrophil cytoplasmic antibodies in patients with Crohn s disease define a clinical subgroup. Gastroenterology 1996;110: Targan SR, Landers CJ, Yang H, et al. Antibodies to CBir1 flagellin define a unique response that is associated independently with complicated Crohn s disease. Gastroenterology 2005;128: Kane SV, Sandborn WJ, Rufo PA, et al. Fecal lactoferrin is a sensitive and specific marker in identifying intestinal inflammation. Am J Gastroenterol 2003;98: Mathy C, Schneider K, Chen YY, et al. Gross versus microscopic pancolitis and the occurrence of neoplasia in ulcerative colitis. Inflamm Bowel Dis 2003;9: Weinstein WM. Mucosal biopsy techniques and interaction with the pathologist. Gastrointest Endosc Clin N Am 2000;10: Jenkins D, Balsitis M, Gallivan S, et al. Guidelines for the initial biopsy diagnosis of suspected chronic idiopathic inflammatory bowel disease: the British Society of Gastroenterology Initiative. J Clin Pathol 1997;50: Kumar NB, Nostrant TT, Appelman HD. The histopathologic spectrum of acute self-limited colitis (acute infectious-type colitis). Am J Surg Pathol 1982;6: Schumacher G, Kollberg B, Sandstedt B. A prospective study of first attacks of inflammatory bowel disease and infectious colitis: histologic course during the 1st year after presentation. Scand J Gastroenterol 1994;29: Dignan CR, Greenson JK. Can ischemic colitis be differentiated from C difficile colitis in biopsy specimens? Am J Surg Pathol 1997;21: Griffin PM, Olmstead LC, Petras RE. Escherichia coli O157:H7- associated colitis: a clinical and histological study of 11 cases. Gastroenterology 1990;99: Address requests for reprints to: Maria T. Abreu, MD, Mount Sinai IBD Center, Gastroenterology, 1425 Madison Ave, Rm 11-23, New York, New York maria.abreu@mssm.edu; fax: (212)
하부위장관비종양성질환의 감별진단 주미인제의대일산백병원
 하부위장관비종양성질환의 감별진단 주미인제의대일산백병원 Solutions for diagnostic problems in Colitis : Please ask yourself five questions Normal or Inflamed? Acute or Chronic? IBD or Other chronic colitis? Ulcerative colitis or
하부위장관비종양성질환의 감별진단 주미인제의대일산백병원 Solutions for diagnostic problems in Colitis : Please ask yourself five questions Normal or Inflamed? Acute or Chronic? IBD or Other chronic colitis? Ulcerative colitis or
11/1/2017. Tetyana Mettler, MD Department of Laboratory Medicine and Pathology University of Minnesota. Cerilli & Greenson
 Tetyana Mettler, MD Department of Laboratory Medicine and Pathology University of Minnesota Acute infectious (self-limited) colitis Focal active colitis Pseudomembranous colitis Ischemic colitis Collagenous
Tetyana Mettler, MD Department of Laboratory Medicine and Pathology University of Minnesota Acute infectious (self-limited) colitis Focal active colitis Pseudomembranous colitis Ischemic colitis Collagenous
GUIDELINES FOR THE INITIAL BIOPSY DIAGNOSIS OF CHRONIC IDIOPATHIC INFLAMMATORY BOWEL DISEASE A STRUCTURED APPROACH TO COLORECTAL BIOPSY ASSESSMENT
 Guidelines for the Initial Biopsy Diagnosis of Chronic Idiopathic Inflammatory Bowel Disease 1 GUIDELINES FOR THE INITIAL BIOPSY DIAGNOSIS OF CHRONIC IDIOPATHIC INFLAMMATORY BOWEL DISEASE A STRUCTURED
Guidelines for the Initial Biopsy Diagnosis of Chronic Idiopathic Inflammatory Bowel Disease 1 GUIDELINES FOR THE INITIAL BIOPSY DIAGNOSIS OF CHRONIC IDIOPATHIC INFLAMMATORY BOWEL DISEASE A STRUCTURED
The Spectrum of IBD. Inflammatory Bowel Disease. Symptoms. Epidemiology. Tests for IBD. CD or UC? Inflamatory Bowel Disease. Fernando Vega, M.D.
 The Spectrum of IBD Inflammatory Bowel Disease Fernando Vega, M.D. Epidemiology CD and UC together 1:400 UC Prevalence 1:500 UC Incidence 6-12K/annum CD Prevalence 1:1000 CD Incidence 3-6K/annum Symptoms
The Spectrum of IBD Inflammatory Bowel Disease Fernando Vega, M.D. Epidemiology CD and UC together 1:400 UC Prevalence 1:500 UC Incidence 6-12K/annum CD Prevalence 1:1000 CD Incidence 3-6K/annum Symptoms
BIOPSY DIAGNOSIS OF COLITIS Common and Unusual Forms of Inflammatory Bowel disease
 BIOPSY DIAGNOSIS OF COLITIS Common and Unusual Forms of Inflammatory Bowel disease David A Owen University of British Columbia CAUSES OF DIARRHEA DIARRHEA COLITIS PRESENT COLITIS ABSENT INFECTIOUS NON-INFECTIOUS
BIOPSY DIAGNOSIS OF COLITIS Common and Unusual Forms of Inflammatory Bowel disease David A Owen University of British Columbia CAUSES OF DIARRHEA DIARRHEA COLITIS PRESENT COLITIS ABSENT INFECTIOUS NON-INFECTIOUS
Inflammatory Bowel Disease When is diarrhea not just diarrhea?
 Inflammatory Bowel Disease When is diarrhea not just diarrhea? Jackie Kazik, MA, PA C CME Resources CAPA Annual Conference, 2011 Inflammatory Bowel Disease Objectives Discuss what is known about the pathophysiology
Inflammatory Bowel Disease When is diarrhea not just diarrhea? Jackie Kazik, MA, PA C CME Resources CAPA Annual Conference, 2011 Inflammatory Bowel Disease Objectives Discuss what is known about the pathophysiology
Patterns of Colonic Involvement at Initial Presentation in Ulcerative Colitis A Retrospective Study of 46 Newly Diagnosed Cases
 Anatomic Pathology / PATTERNS OF INVOLVEMENT IN ULCERATIVE COLITIS Patterns of Colonic Involvement at Initial Presentation in Ulcerative Colitis A Retrospective Study of 46 Newly Diagnosed Cases Marie
Anatomic Pathology / PATTERNS OF INVOLVEMENT IN ULCERATIVE COLITIS Patterns of Colonic Involvement at Initial Presentation in Ulcerative Colitis A Retrospective Study of 46 Newly Diagnosed Cases Marie
HDF Case CRYPTOSPORIDIOSE
 HDF Case 986949 CRYPTOSPORIDIOSE 45 yo male with severe diarrhea. Known HIV positive. Endoscopic biopsy of duodenum, the colon and ileum. EXUDATIVE CHANGES GRANULAR BASOPHILIC BODIES Colonic biopsy shows
HDF Case 986949 CRYPTOSPORIDIOSE 45 yo male with severe diarrhea. Known HIV positive. Endoscopic biopsy of duodenum, the colon and ileum. EXUDATIVE CHANGES GRANULAR BASOPHILIC BODIES Colonic biopsy shows
Original Article. Atypical histological features of ulcerative colitis. Siddharth N Shah, 1 Anjali D Amarapurkar, 1 N Shrinivas, 2 Rathi PM 2 ABSTRACT
 Tropical Gastroenterology 2011;32(2):107 111 Original Article Atypical histological features of ulcerative colitis Siddharth N Shah, 1 Anjali D Amarapurkar, 1 N Shrinivas, 2 Rathi PM 2 ABSTRACT Department
Tropical Gastroenterology 2011;32(2):107 111 Original Article Atypical histological features of ulcerative colitis Siddharth N Shah, 1 Anjali D Amarapurkar, 1 N Shrinivas, 2 Rathi PM 2 ABSTRACT Department
... Inflammatory disorder of the colon that occurs as a complication of antibiotic treatment.
 Definition Inflammatory disorder of the colon that occurs as a complication of antibiotic treatment. " Epidemiology Humans represent the main reservoir of Clostridium difficile, which is not part of the
Definition Inflammatory disorder of the colon that occurs as a complication of antibiotic treatment. " Epidemiology Humans represent the main reservoir of Clostridium difficile, which is not part of the
IBD. Crohn s. Outline. Ulcerative colitis versus Crohn s disease: is biopsy useful? UC vs. Crohn s? Is it easy? Biopsy settings 21/07/2017 IBD
 Outline Ulcerative colitis versus Crohn s disease: is biopsy useful? Roger Feakins Colorectal biopsies Ileal and upper GI biopsies Special situations New techniques Summary Inflammatory bowel disease (IBD)
Outline Ulcerative colitis versus Crohn s disease: is biopsy useful? Roger Feakins Colorectal biopsies Ileal and upper GI biopsies Special situations New techniques Summary Inflammatory bowel disease (IBD)
What do we need for diagnosis of IBD
 What do we need for diagnosis of IBD Kaichun Wu Dept. of Gastroenterology, Xijing Hospital Fourth Military Medical University Xi an an,, China In China UC 11.6/10 5,CD 1.4/10 5 Major cause of chronic diarrhea
What do we need for diagnosis of IBD Kaichun Wu Dept. of Gastroenterology, Xijing Hospital Fourth Military Medical University Xi an an,, China In China UC 11.6/10 5,CD 1.4/10 5 Major cause of chronic diarrhea
Case History B Female patient 1970 Clinical History : crampy abdominal pain and episodes of bloody diarrhea Surgical treatment
 Case History B-1325945 Female patient 1970 Clinical History : crampy abdominal pain and episodes of bloody diarrhea Surgical treatment Case History B-1325945 Pathology Submucosa & Muscularis Endometriosis
Case History B-1325945 Female patient 1970 Clinical History : crampy abdominal pain and episodes of bloody diarrhea Surgical treatment Case History B-1325945 Pathology Submucosa & Muscularis Endometriosis
IBD 101. Ronen Stein, MD Assistant Professor of Clinical Pediatrics Division of Gastroenterology, Hepatology, and Nutrition
 IBD 101 Ronen Stein, MD Assistant Professor of Clinical Pediatrics Division of Gastroenterology, Hepatology, and Nutrition Objectives Identify factors involved in the development of inflammatory bowel
IBD 101 Ronen Stein, MD Assistant Professor of Clinical Pediatrics Division of Gastroenterology, Hepatology, and Nutrition Objectives Identify factors involved in the development of inflammatory bowel
IBD 101. Ronen Stein, MD Assistant Professor of Clinical Pediatrics Division of Gastroenterology, Hepatology, and Nutrition
 IBD 101 Ronen Stein, MD Assistant Professor of Clinical Pediatrics Division of Gastroenterology, Hepatology, and Nutrition Objectives Identify factors involved in the development of inflammatory bowel
IBD 101 Ronen Stein, MD Assistant Professor of Clinical Pediatrics Division of Gastroenterology, Hepatology, and Nutrition Objectives Identify factors involved in the development of inflammatory bowel
A Case of Crohn s Disease with Mesalazine Allergy that was Difficult to Differentiate from Comorbid Ulcerative Colitis
 doi: 10.2169/internalmedicine.1607-18 http://internmed.jp CASE REPORT A Case of Crohn s Disease with Mesalazine Allergy that was Difficult to Differentiate from Comorbid Ulcerative Colitis Rumiko Tsuboi,
doi: 10.2169/internalmedicine.1607-18 http://internmed.jp CASE REPORT A Case of Crohn s Disease with Mesalazine Allergy that was Difficult to Differentiate from Comorbid Ulcerative Colitis Rumiko Tsuboi,
Biopsy Evaluation of Non- Neoplastic Diseases of the Large Bowel: an algorithmic approach
 Biopsy Evaluation of Non- Neoplastic Diseases of the Large Bowel: an algorithmic approach Laura W. Lamps, M.D. Godfrey D. Stobbe Professor and Director of GI Pathology University of Michigan Health System
Biopsy Evaluation of Non- Neoplastic Diseases of the Large Bowel: an algorithmic approach Laura W. Lamps, M.D. Godfrey D. Stobbe Professor and Director of GI Pathology University of Michigan Health System
What is your diagnosis? a. Lymphocytic colitis. b. Collagenous colitis. c. Common variable immunodeficiency (CVID) associated colitis
 Case History A 24 year old male presented with fatigue, fever, watery diarrhea, and a cough with sputum production for the past three weeks. His past medical history was significant for recurrent bouts
Case History A 24 year old male presented with fatigue, fever, watery diarrhea, and a cough with sputum production for the past three weeks. His past medical history was significant for recurrent bouts
Treatment of Inflammatory Bowel Disease. Michael Weiss MD, FACG
 Treatment of Inflammatory Bowel Disease Michael Weiss MD, FACG What is IBD? IBD is an immune-mediated chronic intestinal disorder, characterized by chronic or relapsing inflammation within the GI tract.
Treatment of Inflammatory Bowel Disease Michael Weiss MD, FACG What is IBD? IBD is an immune-mediated chronic intestinal disorder, characterized by chronic or relapsing inflammation within the GI tract.
-2002: Rectal blood loss, UC? (no definite diagnosis) rectal mesalazine. -June 2008: Recurrence of rectal blood loss and urgency
 SD, male 40 yrs. old. (680718M467.) -2002: Rectal blood loss, UC? (no definite diagnosis) rectal mesalazine -June 2008: Recurrence of rectal blood loss and urgency Total colonoscopy: ulcerative rectitis,
SD, male 40 yrs. old. (680718M467.) -2002: Rectal blood loss, UC? (no definite diagnosis) rectal mesalazine -June 2008: Recurrence of rectal blood loss and urgency Total colonoscopy: ulcerative rectitis,
Chapter 8 Ischemic Colitis
 Chapter 8 Ischemic Colitis Peter Van Eyken, Daniela Fanni, and Clara Gerosa Abstract The large bowel accounts for roughly half of all episodes of gastrointestinal ischemia. Three major manifestations of
Chapter 8 Ischemic Colitis Peter Van Eyken, Daniela Fanni, and Clara Gerosa Abstract The large bowel accounts for roughly half of all episodes of gastrointestinal ischemia. Three major manifestations of
SAMs Guidelines DEVELOPING SELF-ASSESSMENT MODULES TEST QUESTIONS. Ver. #
 SAMs Guidelines DEVELOPING SELF-ASSESSMENT MODULES TEST Ver. #5-02.12.17 GUIDELINES FOR DEVELOPING SELF-ASSESSMENT MODULES TEST The USCAP is accredited by the American Board of Pathology (ABP) to offer
SAMs Guidelines DEVELOPING SELF-ASSESSMENT MODULES TEST Ver. #5-02.12.17 GUIDELINES FOR DEVELOPING SELF-ASSESSMENT MODULES TEST The USCAP is accredited by the American Board of Pathology (ABP) to offer
Cytomegalovirus Colitis in an Immunocompetent Patient: A Case Report
 ISPUB.COM The Internet Journal of Surgery Volume 17 Number 2 Cytomegalovirus Colitis in an Immunocompetent Patient: A Case Report M Ud Citation M Ud. Cytomegalovirus Colitis in an Immunocompetent Patient:
ISPUB.COM The Internet Journal of Surgery Volume 17 Number 2 Cytomegalovirus Colitis in an Immunocompetent Patient: A Case Report M Ud Citation M Ud. Cytomegalovirus Colitis in an Immunocompetent Patient:
Gastrooesophageal reflux disease. Jera Jeruc Institute of pathology, Faculty of Medicine, Ljubljana, Slovenia
 Gastrooesophageal reflux disease Jera Jeruc Institute of pathology, Faculty of Medicine, Ljubljana, Slovenia Reflux esophagitis (RE) GERD: a spectrum of clinical conditions and histologic alterations resulting
Gastrooesophageal reflux disease Jera Jeruc Institute of pathology, Faculty of Medicine, Ljubljana, Slovenia Reflux esophagitis (RE) GERD: a spectrum of clinical conditions and histologic alterations resulting
Pitfalls in the Diagnosis of Inflammatory Bowel Disease
 Pitfalls in the Diagnosis of Inflammatory Bowel Disease Robert H Riddell MD Mt Sinai Hospital Toronto Prof of Lab. Medicine and Pathobiology University of Toronto Atypical gross / endoscopic distribution
Pitfalls in the Diagnosis of Inflammatory Bowel Disease Robert H Riddell MD Mt Sinai Hospital Toronto Prof of Lab. Medicine and Pathobiology University of Toronto Atypical gross / endoscopic distribution
Patho Basic Chronic Inflammatory Bowel Diseases. Jürg Vosbeck Pathology
 Patho Basic Chronic Inflammatory Bowel Diseases Jürg Vosbeck Pathology General Group of chronic relapsing diseases with chronic bloody or watery diarrhea Usually ulcerative colitis (UC) or Crohn s disease
Patho Basic Chronic Inflammatory Bowel Diseases Jürg Vosbeck Pathology General Group of chronic relapsing diseases with chronic bloody or watery diarrhea Usually ulcerative colitis (UC) or Crohn s disease
For the past 40 years, it has been standard practice to obtain
 ORIGINAL ARTICLE: GASTROENTEROLOGY Good Agreement Between Endoscopic Findings and Biopsy Reports Supports Limited Tissue Sampling During Pediatric Colonoscopy Michael A. Manfredi, Hongyu Jiang, Lawrence
ORIGINAL ARTICLE: GASTROENTEROLOGY Good Agreement Between Endoscopic Findings and Biopsy Reports Supports Limited Tissue Sampling During Pediatric Colonoscopy Michael A. Manfredi, Hongyu Jiang, Lawrence
Inflammatory Bowel Disease Ischemic bowel disease
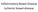 Inflammatory Bowel Disease Ischemic bowel disease Inflammatory Bowel Disease The two disorders that comprise IBD are: ulcerative colitis Crohn disease The distinction between ulcerative colitis and Crohn
Inflammatory Bowel Disease Ischemic bowel disease Inflammatory Bowel Disease The two disorders that comprise IBD are: ulcerative colitis Crohn disease The distinction between ulcerative colitis and Crohn
NEW CONCEPTS IN CROHN S DISEASE GLENDON BURRESS, MD PEDIATRIC GASTROENTEROLOGY ROCKFORD, IL
 NEW CONCEPTS IN CROHN S DISEASE GLENDON BURRESS, MD PEDIATRIC GASTROENTEROLOGY ROCKFORD, IL CROHN S DISEASE Chronic disease of uncertain etiology Etiology- genetic, environmental, and infectious Transmural
NEW CONCEPTS IN CROHN S DISEASE GLENDON BURRESS, MD PEDIATRIC GASTROENTEROLOGY ROCKFORD, IL CROHN S DISEASE Chronic disease of uncertain etiology Etiology- genetic, environmental, and infectious Transmural
A Practical Approach to Small Bowel Biopsies: All that flattens is not sprue
 A Practical Approach to Small Bowel Biopsies: All that flattens is not sprue UCSF Liver and Gastrointestinal Pathology Update Sept. 4, 2009 How to Go Wrong When Evaluating Small Bowel Biopsies, Based on
A Practical Approach to Small Bowel Biopsies: All that flattens is not sprue UCSF Liver and Gastrointestinal Pathology Update Sept. 4, 2009 How to Go Wrong When Evaluating Small Bowel Biopsies, Based on
Surgical Management of IBD. Val Jefford Grand Rounds October 14, 2003
 Surgical Management of IBD Val Jefford Grand Rounds October 14, 2003 Introduction Important Features Clinical Presentation Evaluation Medical Treatment Surgical Treatment Cases Overview Introduction Two
Surgical Management of IBD Val Jefford Grand Rounds October 14, 2003 Introduction Important Features Clinical Presentation Evaluation Medical Treatment Surgical Treatment Cases Overview Introduction Two
INTERNATIONAL COURSE ON THE PATHOLOGY OF THE DIGESTIVE SYSTEM VICTOR BABES NATIONAL INSTITUTE OF PATHOLOGY BUCHAREST 7-8 BUCHAREST 2014
 INTERNATIONAL COURSE ON THE PATHOLOGY OF THE DIGESTIVE SYSTEM VICTOR BABES NATIONAL INSTITUTE OF PATHOLOGY BUCHAREST 7-8 BUCHAREST 2014 Endoscopic biopsy samples of naïve colitides patients: Role of basal
INTERNATIONAL COURSE ON THE PATHOLOGY OF THE DIGESTIVE SYSTEM VICTOR BABES NATIONAL INSTITUTE OF PATHOLOGY BUCHAREST 7-8 BUCHAREST 2014 Endoscopic biopsy samples of naïve colitides patients: Role of basal
SURGICAL MANAGEMENT OF ULCERATIVE COLITIS
 SURGICAL MANAGEMENT OF ULCERATIVE COLITIS Cary B. Aarons, MD Associate Professor of Surgery Division of Colon & Rectal Surgery University of Pennsylvania AGENDA Background Diagnosis/Work-up Medical Management
SURGICAL MANAGEMENT OF ULCERATIVE COLITIS Cary B. Aarons, MD Associate Professor of Surgery Division of Colon & Rectal Surgery University of Pennsylvania AGENDA Background Diagnosis/Work-up Medical Management
What Every Pathologist Wants the GI Nurse to Know (and how you can help us help you)
 What Every Pathologist Wants the GI Nurse to Know (and how you can help us help you) Jonathan N. Glickman MD PhD Director, GI Pathology, Caris Diagnostics, Newton, MA Associate Professor of Pathology,
What Every Pathologist Wants the GI Nurse to Know (and how you can help us help you) Jonathan N. Glickman MD PhD Director, GI Pathology, Caris Diagnostics, Newton, MA Associate Professor of Pathology,
INFLAMMATORY BOWEL DISEASE. Jean-Paul Achkar, MD Center for Inflammatory Bowel Disease Cleveland Clinic
 INFLAMMATORY BOWEL DISEASE Jean-Paul Achkar, MD Center for Inflammatory Bowel Disease Cleveland Clinic WHAT IS INFLAMMATORY BOWEL DISEASE (IBD)? Chronic inflammation of the intestinal tract Two related
INFLAMMATORY BOWEL DISEASE Jean-Paul Achkar, MD Center for Inflammatory Bowel Disease Cleveland Clinic WHAT IS INFLAMMATORY BOWEL DISEASE (IBD)? Chronic inflammation of the intestinal tract Two related
Diagnostic and Therapeutic Approaches to Dysplasia in Inflammatory Bowel Diseases
 Diagnostic and Therapeutic Approaches to Dysplasia in Inflammatory Bowel Diseases Parakkal Deepak, M.B.B.S., M.S. Assistant Professor of Medicine Division of Gastroenterology John T. Milliken Department
Diagnostic and Therapeutic Approaches to Dysplasia in Inflammatory Bowel Diseases Parakkal Deepak, M.B.B.S., M.S. Assistant Professor of Medicine Division of Gastroenterology John T. Milliken Department
Implementation of disease and safety predictors during disease management in UC
 Implementation of disease and safety predictors during disease management in UC DR ARIELLA SHITRIT DIGESTIVE DISEASES INSTITUTE SHAARE ZEDEK MEDICAL CENTER JERUSALEM Case presentation A 52 year old male
Implementation of disease and safety predictors during disease management in UC DR ARIELLA SHITRIT DIGESTIVE DISEASES INSTITUTE SHAARE ZEDEK MEDICAL CENTER JERUSALEM Case presentation A 52 year old male
HDF Case Whipple s disease
 HDF Case 952556 Whipple s disease 63 yo female complaining of a diarrhea for 2 months, weigth loss (12 Kg in 3 months), and joint pains. Duodenal biopsy performed. Scanning view, enlarged intestinal villi,
HDF Case 952556 Whipple s disease 63 yo female complaining of a diarrhea for 2 months, weigth loss (12 Kg in 3 months), and joint pains. Duodenal biopsy performed. Scanning view, enlarged intestinal villi,
Histological and immunological characteristics of colitis associated with anti-ctla 4 antibody therapy
 Histological and immunological characteristics of colitis associated with anti-ctla 4 antibody therapy M. Perdiki 2, G. Bamias 1, D. Pouloudi 2, H. Gogas 3, I. Delladetsima 2 1 Academic Dpt. of Gastroenterology,
Histological and immunological characteristics of colitis associated with anti-ctla 4 antibody therapy M. Perdiki 2, G. Bamias 1, D. Pouloudi 2, H. Gogas 3, I. Delladetsima 2 1 Academic Dpt. of Gastroenterology,
Fibrin thrombi, a cause of clindamycin-associated
 Gut, 1976, 17, 483487 Fibrin thrombi, a cause of clindamycin-associated colitis? W. V. BOGOMOLETZ From the Department of Pathology, Queen Mary's Hospital, London summary Rectal biopsies from five patients
Gut, 1976, 17, 483487 Fibrin thrombi, a cause of clindamycin-associated colitis? W. V. BOGOMOLETZ From the Department of Pathology, Queen Mary's Hospital, London summary Rectal biopsies from five patients
Beyond Anti TNFs: positioning of other biologics for Crohn s disease. Christina Ha, MD Cedars Sinai Inflammatory Bowel Disease Center
 Beyond Anti TNFs: positioning of other biologics for Crohn s disease Christina Ha, MD Cedars Sinai Inflammatory Bowel Disease Center Objectives: To define high and low risk patient and disease features
Beyond Anti TNFs: positioning of other biologics for Crohn s disease Christina Ha, MD Cedars Sinai Inflammatory Bowel Disease Center Objectives: To define high and low risk patient and disease features
Pouchitis and Cuffitis A bloody mess. Sze-Lin Peng Colorectal Surgeon Counties Manukau District Health Board
 Pouchitis and Cuffitis A bloody mess Sze-Lin Peng Colorectal Surgeon Counties Manukau District Health Board Ileal-pouch anal anastomosis https://www.pennmedicine.org/for-health-care-professionals/for-physicians/physician-education-and-resources/clinicalbriefings/2018/february/total-proctocolectomy-with-jpouch-reconstruction-for-ulcerative-colitis
Pouchitis and Cuffitis A bloody mess Sze-Lin Peng Colorectal Surgeon Counties Manukau District Health Board Ileal-pouch anal anastomosis https://www.pennmedicine.org/for-health-care-professionals/for-physicians/physician-education-and-resources/clinicalbriefings/2018/february/total-proctocolectomy-with-jpouch-reconstruction-for-ulcerative-colitis
Simple objective criteria for diagnosis of causes of
 5808 JClin Pathol 1997;50:580-585 Simple objective criteria for diagnosis of causes of acute diarrhoea on rectal biopsy Division of Pathology, Queen's Medical Centre, Nottingham, UK D Jenkins Department
5808 JClin Pathol 1997;50:580-585 Simple objective criteria for diagnosis of causes of acute diarrhoea on rectal biopsy Division of Pathology, Queen's Medical Centre, Nottingham, UK D Jenkins Department
How to differentiate Segmental Colitis Associated with Diverticulosis and Inflammatory Bowel Diseases?
 How to differentiate Segmental Colitis Associated with Diverticulosis and Inflammatory Bowel Diseases? Alessandro Armuzzi Lead IBD Unit Complesso Integrato Columbus Fondazione Policlinico Gemelli Università
How to differentiate Segmental Colitis Associated with Diverticulosis and Inflammatory Bowel Diseases? Alessandro Armuzzi Lead IBD Unit Complesso Integrato Columbus Fondazione Policlinico Gemelli Università
Terumitsu; Nagayasu, Takeshi
 NAOSITE: Nagasaki University's Ac Title Author(s) Citation A rare case of segmental ulcerative Tominaga, Tetsuro; Nonaka, Takashi; Shuichi; Kunizaki, Masaki; Sumida, Terumitsu; Nagayasu, Takeshi Acta medica
NAOSITE: Nagasaki University's Ac Title Author(s) Citation A rare case of segmental ulcerative Tominaga, Tetsuro; Nonaka, Takashi; Shuichi; Kunizaki, Masaki; Sumida, Terumitsu; Nagayasu, Takeshi Acta medica
Small intestine. Small intestine
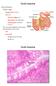 General features Tubular organ longest part; 5-6 m most of chemical digestion absorption of nutrients reabsorption of H2O occurs. Two structural features; maximize the lumenal surface area villi microvilli
General features Tubular organ longest part; 5-6 m most of chemical digestion absorption of nutrients reabsorption of H2O occurs. Two structural features; maximize the lumenal surface area villi microvilli
Endoscopy in Inflammatory Bowel Disease DR. REENA KHANNA
 Endoscopy in Inflammatory Bowel Disease DR. REENA KHANNA ASSISTANT PROFESSOR, UNIVERSITY OF WESTERN ONTARIO Background Clinical trials in ulcerative colitis and Crohn s disease require validated instruments
Endoscopy in Inflammatory Bowel Disease DR. REENA KHANNA ASSISTANT PROFESSOR, UNIVERSITY OF WESTERN ONTARIO Background Clinical trials in ulcerative colitis and Crohn s disease require validated instruments
Chromoendoscopy and Endomicroscopy for detecting colonic dysplasia
 Chromoendoscopy and Endomicroscopy for detecting colonic dysplasia Ralf Kiesslich I. Medical Department Johannes Gutenberg University Mainz, Germany Cumulative cancer risk in ulcerative colitis 0.5-1.0%
Chromoendoscopy and Endomicroscopy for detecting colonic dysplasia Ralf Kiesslich I. Medical Department Johannes Gutenberg University Mainz, Germany Cumulative cancer risk in ulcerative colitis 0.5-1.0%
TRICHURIASIS : LOCALIZED INFLAMMATORY RESPONSES IN THE COLON
 TRICHURIASIS : LOCALIZED INFLAMMATORY RESPONSES IN THE COLON Gurjeet Kaur 1, S Mahendra Raj 2 and Nyi Nyi Naing 3 Departments of 1 Pathology and 2 Medicine and the 3 Epidemiology and Medical Statistics
TRICHURIASIS : LOCALIZED INFLAMMATORY RESPONSES IN THE COLON Gurjeet Kaur 1, S Mahendra Raj 2 and Nyi Nyi Naing 3 Departments of 1 Pathology and 2 Medicine and the 3 Epidemiology and Medical Statistics
Endoscopy in IBD. F.Hartmann K.Kasper-Kliniken (St.Marienkrankenhaus) Frankfurt/M.
 F.Hartmann K.Kasper-Kliniken (St.Marienkrankenhaus) Frankfurt/M. F.Hartmann@em.uni-frankfurt.de Indications for endoscopy Diagnosis Management Surveillance Diagnosis Single most valuable tool: ileocolonoscopy
F.Hartmann K.Kasper-Kliniken (St.Marienkrankenhaus) Frankfurt/M. F.Hartmann@em.uni-frankfurt.de Indications for endoscopy Diagnosis Management Surveillance Diagnosis Single most valuable tool: ileocolonoscopy
Cytomegalovirus Colitis
 GASTROENTEROLOGY 1985;88:171-5 CASE REPORTS Cytomegalovirus Colitis Report of the Clinical, Endoscopic, and Pathologic Findings in Two Patients With the Acquired Immune Deficiency Syndrome MICK SCOTT MEISELMAN,
GASTROENTEROLOGY 1985;88:171-5 CASE REPORTS Cytomegalovirus Colitis Report of the Clinical, Endoscopic, and Pathologic Findings in Two Patients With the Acquired Immune Deficiency Syndrome MICK SCOTT MEISELMAN,
WSC , Conference 9, Case 1. Tissue from a nyala.
 WSC 2009-2010, Conference 9, Case 1. Tissue from a nyala. MICROSCOPIC DESCRIPTION: Heart, atrium (1 pt.): Approximately 40% of the atrial myocardium is replaced by areas of fibrous connective tissue (1
WSC 2009-2010, Conference 9, Case 1. Tissue from a nyala. MICROSCOPIC DESCRIPTION: Heart, atrium (1 pt.): Approximately 40% of the atrial myocardium is replaced by areas of fibrous connective tissue (1
(b) Stomach s function 1. Dilution of food materials 2. Acidification of food (absorption of dietary Fe in small intestine) 3. Partial chemical digest
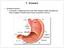 (1) General features a) Stomach is widened portion of gut-tube: between tubular and spherical; Note arranged of smooth muscle tissue in muscularis externa. 1 (b) Stomach s function 1. Dilution of food
(1) General features a) Stomach is widened portion of gut-tube: between tubular and spherical; Note arranged of smooth muscle tissue in muscularis externa. 1 (b) Stomach s function 1. Dilution of food
Frequency and Distribution of Microscopic Findings in Patients with Chronic Non-Bloody Diarrhea and Normal Colonoscopy
 IJMS Vol 33, No 2, June 2008 Original Article Frequency and Distribution of Microscopic Findings in Patients with Chronic Non-Bloody Diarrhea and Normal Colonoscopy H. Tabrizchie, M.J. Zahedie 1, M. Hayatbakhsh
IJMS Vol 33, No 2, June 2008 Original Article Frequency and Distribution of Microscopic Findings in Patients with Chronic Non-Bloody Diarrhea and Normal Colonoscopy H. Tabrizchie, M.J. Zahedie 1, M. Hayatbakhsh
Crohn s Disease: Should We Treat Based on Symptoms or Based on Objective Markers of Inflammation?
 Crohn s Disease: Should We Treat Based on Symptoms or Based on Objective Markers of Inflammation? Edward V. Loftus, Jr., M.D. Professor of Medicine Division of Gastroenterology and Hepatology Mayo Clinic
Crohn s Disease: Should We Treat Based on Symptoms or Based on Objective Markers of Inflammation? Edward V. Loftus, Jr., M.D. Professor of Medicine Division of Gastroenterology and Hepatology Mayo Clinic
CHRONIC DIARRHEA DR. PHILIP K. BLUSTEIN M.D. F.R.C.P.(C) DEFINITION: *LOOSE, WATERY STOOLS *MORE THAN 3 TIMES A DAY *FOR MORE THAN 4 WEEKS
 DR. PHILIP K. BLUSTEIN M.D. F.R.C.P.(C) 415 14 TH ST. NW. CALGARY AB T2N2A1 PHONE (403) 270-9555 FAX (403) 270-7479 CHRONIC DIARRHEA DEFINITION: *LOOSE, WATERY STOOLS *MORE THAN 3 TIMES A DAY *FOR MORE
DR. PHILIP K. BLUSTEIN M.D. F.R.C.P.(C) 415 14 TH ST. NW. CALGARY AB T2N2A1 PHONE (403) 270-9555 FAX (403) 270-7479 CHRONIC DIARRHEA DEFINITION: *LOOSE, WATERY STOOLS *MORE THAN 3 TIMES A DAY *FOR MORE
How do I choose amongst medicines for inflammatory bowel disease. Maria T. Abreu, MD
 How do I choose amongst medicines for inflammatory bowel disease Maria T. Abreu, MD Overview of IBD Pathogenesis Bacterial Products Moderately Acutely Inflamed Chronic Inflammation = IBD Normal Gut Mildly
How do I choose amongst medicines for inflammatory bowel disease Maria T. Abreu, MD Overview of IBD Pathogenesis Bacterial Products Moderately Acutely Inflamed Chronic Inflammation = IBD Normal Gut Mildly
Case Report Successful Long-Term Use of Infliximab in Refractory Pouchitis in an Adolescent
 Gastroenterology Research and Practice Volume 2010, Article ID 860394, 4 pages doi:10.1155/2010/860394 Case Report Successful Long-Term Use of Infliximab in Refractory Pouchitis in an Adolescent Jessica
Gastroenterology Research and Practice Volume 2010, Article ID 860394, 4 pages doi:10.1155/2010/860394 Case Report Successful Long-Term Use of Infliximab in Refractory Pouchitis in an Adolescent Jessica
Gastritis (and gastropathy) Dr Ian Brown Envoi Pathology Brisbane, Australia
 Gastritis (and gastropathy) Dr Ian Brown Envoi Pathology Brisbane, Australia ianbrown@envoi.com.au Topics for discussion Classification of gastritis Minimal diagnostic criteria for gastritis H.pylori negative
Gastritis (and gastropathy) Dr Ian Brown Envoi Pathology Brisbane, Australia ianbrown@envoi.com.au Topics for discussion Classification of gastritis Minimal diagnostic criteria for gastritis H.pylori negative
PERSISTENT DIARRHOEA. IAP UG Teaching slides
 PERSISTENT DIARRHOEA 1 DEFINITION Prolongation of acute diarrhoea / dysentery for more than 14 days Generally associated with weight loss. 2 PROTRACTED DIARRHOEA Prolongation of acute diarrhoea or dysentery
PERSISTENT DIARRHOEA 1 DEFINITION Prolongation of acute diarrhoea / dysentery for more than 14 days Generally associated with weight loss. 2 PROTRACTED DIARRHOEA Prolongation of acute diarrhoea or dysentery
Standard of care Inflammatory Bowel Disease (IBD)
 Standard of care Inflammatory Bowel Disease (IBD) Inflammatory bowel disease (IBD) Tens of thousands of Australians live with the debilitating symptoms of Crohn s disease or ulcerative colitis the two
Standard of care Inflammatory Bowel Disease (IBD) Inflammatory bowel disease (IBD) Tens of thousands of Australians live with the debilitating symptoms of Crohn s disease or ulcerative colitis the two
PARASITOLOGY CASE HISTORY 15 (HISTOLOGY) (Lynne S. Garcia)
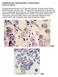 PARASITOLOGY CASE HISTORY 15 (HISTOLOGY) (Lynne S. Garcia) A biopsy was performed on a 27-year-old man with no known travel history, presenting with a perianal ulcer. The specimen was preserved in formalin
PARASITOLOGY CASE HISTORY 15 (HISTOLOGY) (Lynne S. Garcia) A biopsy was performed on a 27-year-old man with no known travel history, presenting with a perianal ulcer. The specimen was preserved in formalin
MANAGEMENT OF IMMUNOTHERAPY RELATED GI AND HEPATIC ADVERSE EVENTS
 MANAGEMENT OF IMMUNOTHERAPY RELATED GI AND HEPATIC ADVERSE EVENTS Wai K. Leung Li Shu Fan Medical Foundation Professor in Gastroenterology Associate Dean (Human Capital), LKS Faculty of Medicine, University
MANAGEMENT OF IMMUNOTHERAPY RELATED GI AND HEPATIC ADVERSE EVENTS Wai K. Leung Li Shu Fan Medical Foundation Professor in Gastroenterology Associate Dean (Human Capital), LKS Faculty of Medicine, University
Crohn's Disease. What causes Crohn s disease? What are the symptoms?
 Crohn's Disease Crohn s disease is an ongoing disorder that causes inflammation of the digestive tract, also referred to as the gastrointestinal (GI) tract. Crohn s disease can affect any area of the GI
Crohn's Disease Crohn s disease is an ongoing disorder that causes inflammation of the digestive tract, also referred to as the gastrointestinal (GI) tract. Crohn s disease can affect any area of the GI
Hompes Method. Practitioner Training Level II. Lesson Seven Part A DRG Pathogen Plus Interpretation
 Hompes Method Practitioner Training Level II Lesson Seven Part A DRG Pathogen Plus Interpretation Health for the People Ltd not for reuse without expressed permission Hompes Method is a trading name of
Hompes Method Practitioner Training Level II Lesson Seven Part A DRG Pathogen Plus Interpretation Health for the People Ltd not for reuse without expressed permission Hompes Method is a trading name of
Ulcerative Colitis after Multidisciplinary Treatment for Colorectal Cancer with Multiple Liver Metastases : A Case Report
 Showa Univ J Med Sci 29 3, 315 319, September 2017 Case Report Ulcerative Colitis after Multidisciplinary Treatment for Colorectal Cancer with Multiple Liver Metastases : A Case Report Kodai TOMIOKA 1
Showa Univ J Med Sci 29 3, 315 319, September 2017 Case Report Ulcerative Colitis after Multidisciplinary Treatment for Colorectal Cancer with Multiple Liver Metastases : A Case Report Kodai TOMIOKA 1
NON INVASIVE MONITORING OF MUCOSAL HEALING IN IBD. THE ROLE OF BOWEL ULTRASOUND. Fabrizio Parente
 NON INVASIVE MONITORING OF MUCOSAL HEALING IN IBD. THE ROLE OF BOWEL ULTRASOUND Fabrizio Parente Gastrointestinal Unit, A.Manzoni Hospital, Lecco & L.Sacco School of Medicine,University of Milan - Italy
NON INVASIVE MONITORING OF MUCOSAL HEALING IN IBD. THE ROLE OF BOWEL ULTRASOUND Fabrizio Parente Gastrointestinal Unit, A.Manzoni Hospital, Lecco & L.Sacco School of Medicine,University of Milan - Italy
Ulcerative Colitis. ulcerative colitis usually only affects the colon.
 Ulcerative Colitis Introduction Ulcerative colitis is an inflammatory bowel disease. It is one of the 2 most common inflammatory bowel diseases. The other one is Crohn s disease. Ulcerative colitis and
Ulcerative Colitis Introduction Ulcerative colitis is an inflammatory bowel disease. It is one of the 2 most common inflammatory bowel diseases. The other one is Crohn s disease. Ulcerative colitis and
Corporate Medical Policy
 Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: fecal_calprotectin_test 8/2009 11/2017 11/2018 11/2017 Description of Procedure or Service Fecal calprotectin
Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: fecal_calprotectin_test 8/2009 11/2017 11/2018 11/2017 Description of Procedure or Service Fecal calprotectin
The Morphologic Profile of Inflammatory Bowel Disease and the Diagnostic Problem of Crohn s Disease versus TB Colitis A Case Series
 OPEN ACCESS CASE REPORT The Morphologic Profile of Inflammatory Bowel Disease and the Diagnostic Problem of Crohn s Disease versus TB Colitis A Case Series Maria Lourdes Tilbe, Francia Victoria De Los
OPEN ACCESS CASE REPORT The Morphologic Profile of Inflammatory Bowel Disease and the Diagnostic Problem of Crohn s Disease versus TB Colitis A Case Series Maria Lourdes Tilbe, Francia Victoria De Los
SAM PROVIDER TOOLKIT
 THE AMERICAN BOARD OF PATHOLOGY Maintenance of Certification (MOC) Program SAM PROVIDER TOOLKIT Developing Self-Assessment Modules (SAMs) www.abpath.org The American Board of Pathology (ABP) approves educational
THE AMERICAN BOARD OF PATHOLOGY Maintenance of Certification (MOC) Program SAM PROVIDER TOOLKIT Developing Self-Assessment Modules (SAMs) www.abpath.org The American Board of Pathology (ABP) approves educational
Glutaraldehyde Colitis Following Endoscopy: Clinical and Pathological Features and Investigation of an Outbreak
 GASTROENTEROLOGY 1995;108:1250-1255 Glutaraldehyde Colitis Following Endoscopy: Clinical and Pathological Features and Investigation of an Outbreak A. BRIAN WEST,* SHIH-FAN KUAN,* MICHAEL BENNICK, t and
GASTROENTEROLOGY 1995;108:1250-1255 Glutaraldehyde Colitis Following Endoscopy: Clinical and Pathological Features and Investigation of an Outbreak A. BRIAN WEST,* SHIH-FAN KUAN,* MICHAEL BENNICK, t and
Certain genes passed on from parent to child increase the risk of developing Crohn's disease, if the right trigger occurs.
 Topic Page: Crohn's disease Definition: Crohn's disease from Benders' Dictionary of Nutrition and Food Technology Chronic inflammatory disease of the bowel, commonly the terminal ileum, of unknown aetiology,
Topic Page: Crohn's disease Definition: Crohn's disease from Benders' Dictionary of Nutrition and Food Technology Chronic inflammatory disease of the bowel, commonly the terminal ileum, of unknown aetiology,
Interpretation of inflammatory colorectal biopsies has
 The of Colitis in Endoscopic Biopsy Specimens A Review Article Lisa A. Cerilli, MD; Joel K. Greenson, MD Context. A variety of inflammatory disorders may affect the colon, with widely differing clinical
The of Colitis in Endoscopic Biopsy Specimens A Review Article Lisa A. Cerilli, MD; Joel K. Greenson, MD Context. A variety of inflammatory disorders may affect the colon, with widely differing clinical
INFLAMMATORY BOWEL DISEASE
 National University Faculty of Medicine INFLAMMATORY BOWEL DISEASE Gehan M. Osman, MD. MBBS Pediatrician Jaffar Ibn Auf Specialized Hospital EDUCATIONAL OBJECTIVES Definitions and spectrum of (IBD) Epidemiology
National University Faculty of Medicine INFLAMMATORY BOWEL DISEASE Gehan M. Osman, MD. MBBS Pediatrician Jaffar Ibn Auf Specialized Hospital EDUCATIONAL OBJECTIVES Definitions and spectrum of (IBD) Epidemiology
General Structure of Digestive Tract
 Dr. Nabil Khouri General Structure of Digestive Tract Common Characteristics: Hollow tube composed of a lumen whose diameter varies. Surrounded by a wall made up of 4 principal layers: Mucosa Epithelial
Dr. Nabil Khouri General Structure of Digestive Tract Common Characteristics: Hollow tube composed of a lumen whose diameter varies. Surrounded by a wall made up of 4 principal layers: Mucosa Epithelial
Crohn s Disease. Resident Lecture 1/17/19
 Crohn s Disease Resident Lecture 1/17/19 Objectives Features/Classification of Crohn s Disease Medical Treatment Surgical Indications Surgical Considerations 2 Case 25 yo F presents to your office with
Crohn s Disease Resident Lecture 1/17/19 Objectives Features/Classification of Crohn s Disease Medical Treatment Surgical Indications Surgical Considerations 2 Case 25 yo F presents to your office with
Rectal biopsy in patients presenting to an infectious disease unit with diarrhoeal disease
 Gut, 1979, 20, 141-148 Rectal biopsy in patients presenting to an infectious disease unit with diarrhoeal disease R. J. DICKINSON, H. M. GILMOUR, AND D. B. L. McCLELLAND' From the Department of Infectious
Gut, 1979, 20, 141-148 Rectal biopsy in patients presenting to an infectious disease unit with diarrhoeal disease R. J. DICKINSON, H. M. GILMOUR, AND D. B. L. McCLELLAND' From the Department of Infectious
The pathology of IBD and its modification by liver disease. Roger Feakins ESP/H-ECCO
 The pathology of IBD and its modification by liver disease Roger Feakins ESP/H-ECCO Enterprise Interest None IBD UC [IBDU] Crohn s IBD: distribution of disease Ulcerative colitis continuous Crohn s colitis
The pathology of IBD and its modification by liver disease Roger Feakins ESP/H-ECCO Enterprise Interest None IBD UC [IBDU] Crohn s IBD: distribution of disease Ulcerative colitis continuous Crohn s colitis
Oncologist-induced Disease of the GI tract: New Developments
 Oncologist-induced Disease of the GI tract: New Developments Jeffrey D Goldsmith, MD Children s Hospital Boston, Beth Israel Deaconess Medical Center, Harvard Medical School Boston, MA Everyone s on drugs
Oncologist-induced Disease of the GI tract: New Developments Jeffrey D Goldsmith, MD Children s Hospital Boston, Beth Israel Deaconess Medical Center, Harvard Medical School Boston, MA Everyone s on drugs
children Crohn s disease in MR enterography for GI Complications Microscopy Characterization Primary sclerosing cholangitis Anorectal fistulae
 MR enterography for Crohn s disease in children BOAZ KARMAZYN, MD PEDIATRIC RADIOLOGY ASSOCIATE PROFESSOR Characterization Crohn disease Idiopathic chronic transmural IBD Increasing incidence Age 7/100,000
MR enterography for Crohn s disease in children BOAZ KARMAZYN, MD PEDIATRIC RADIOLOGY ASSOCIATE PROFESSOR Characterization Crohn disease Idiopathic chronic transmural IBD Increasing incidence Age 7/100,000
Clinical Trials in IBD. Bruce Yacyshyn MD Professor of Medicine Division of Digestive Diseases
 Clinical Trials in IBD Bruce Yacyshyn MD Professor of Medicine Division of Digestive Diseases Objectives Today s discussion will address the following topics: Similarities and differences between Crohn
Clinical Trials in IBD Bruce Yacyshyn MD Professor of Medicine Division of Digestive Diseases Objectives Today s discussion will address the following topics: Similarities and differences between Crohn
Diarrhoea for the Acute Physician
 Diarrhoea for the Acute Physician STEPHEN INNS GASTROENTEROLOGIST AND PHYSICIAN HUTT VALLEY DHB August 2013 Outline Case History 1 Initial assessment of acute diarrhoea Management of fulminant UC Management
Diarrhoea for the Acute Physician STEPHEN INNS GASTROENTEROLOGIST AND PHYSICIAN HUTT VALLEY DHB August 2013 Outline Case History 1 Initial assessment of acute diarrhoea Management of fulminant UC Management
Diarrhoea on the AMU. Dr Chris Roseveare
 Diarrhoea on the AMU Dr Chris Roseveare The Society for Acute Medicine, Spring Meeting, Radisson Blu Hotel, Dublin 3-4 May 2012 Acute diarrhoea in developed countries adult populations Mainly a primary
Diarrhoea on the AMU Dr Chris Roseveare The Society for Acute Medicine, Spring Meeting, Radisson Blu Hotel, Dublin 3-4 May 2012 Acute diarrhoea in developed countries adult populations Mainly a primary
CT Evaluation of Bowel Wall Thickening. Dr: Adel El Badrawy; M.D. Lecturer of Radio Diagnosis Faculty of Medicine Mansoura University.
 CT Evaluation of Bowel Wall Thickening By Dr: Adel El Badrawy; M.D. Lecturer of Radio Diagnosis Faculty of Medicine Mansoura University. The CT findings of bowel wall thickening includes 1 Degree of thickening.
CT Evaluation of Bowel Wall Thickening By Dr: Adel El Badrawy; M.D. Lecturer of Radio Diagnosis Faculty of Medicine Mansoura University. The CT findings of bowel wall thickening includes 1 Degree of thickening.
Dr David Epstein Vincent Pallotti Hospital and University of Cape Town
 Inflammatory Bowel Disease Management in South Africa in 2016 Pharmaceutical Care Management Association Dr David Epstein Vincent Pallotti Hospital and University of Cape Town Inflammatory Bowel Disease
Inflammatory Bowel Disease Management in South Africa in 2016 Pharmaceutical Care Management Association Dr David Epstein Vincent Pallotti Hospital and University of Cape Town Inflammatory Bowel Disease
This is the second learning component (Learning Component 2) in our first learning module (Learning Module 1). In this component we review a very
 This is the second learning component (Learning Component 2) in our first learning module (Learning Module 1). In this component we review a very basic response to injury inflammation. We ll look at examples
This is the second learning component (Learning Component 2) in our first learning module (Learning Module 1). In this component we review a very basic response to injury inflammation. We ll look at examples
DIGESTIVE TRACT ESOPHAGUS
 DIGESTIVE TRACT From the lower esophagus to the lower rectum four fundamental layers comprise the wall of the digestive tube: mucosa, submucosa, muscularis propria (externa), and adventitia or serosa (see
DIGESTIVE TRACT From the lower esophagus to the lower rectum four fundamental layers comprise the wall of the digestive tube: mucosa, submucosa, muscularis propria (externa), and adventitia or serosa (see
Colon ischemia. Bible class 12 September Stefan Christen. ACG Clinical Guideline: Am J Gastroenterol 2015
 Colon ischemia Bible class 12 September 2018 Stefan Christen ACG Clinical Guideline: Am J Gastroenterol 2015 Definition Definition Imbalance between blood supply and metabolic demands of the colonocytes
Colon ischemia Bible class 12 September 2018 Stefan Christen ACG Clinical Guideline: Am J Gastroenterol 2015 Definition Definition Imbalance between blood supply and metabolic demands of the colonocytes
Allergic Colitis Clinical and Endoscopic Aspects of Infants. with Rectal Bleeding
 Allergic Colitis Clinical and Endoscopic Aspects of Infants. with Rectal Bleeding Allergic Colitis is an inflammatory disorder of the colon which occurs mainly in preschool children. It is caused by an
Allergic Colitis Clinical and Endoscopic Aspects of Infants. with Rectal Bleeding Allergic Colitis is an inflammatory disorder of the colon which occurs mainly in preschool children. It is caused by an
Diagnostic difficulty arising from rectal recovery
 J Clin Pathol 1996;49:319-323 319 Cellular Pathology, Northwick Park and St Mark's NHS Trust, Harrow T S Levine A B Price Gastroenterology S Mitchell Histopathology, Heraklion University General Hospital,
J Clin Pathol 1996;49:319-323 319 Cellular Pathology, Northwick Park and St Mark's NHS Trust, Harrow T S Levine A B Price Gastroenterology S Mitchell Histopathology, Heraklion University General Hospital,
Supplemental Digital Content 1. Endoscopic and histolological findings in INR and FR study subjects
 Supplemental Digital Content 1. Endoscopic and histolological findings in INR and FR study subjects Patient Group Macroscopic examination Ileum Histology Colon/rectum Histology 1 INR Normal Acute and chronic
Supplemental Digital Content 1. Endoscopic and histolological findings in INR and FR study subjects Patient Group Macroscopic examination Ileum Histology Colon/rectum Histology 1 INR Normal Acute and chronic
Keep microscopic colitis in mind!
 Keep microscopic in mind! Information for gastroenterologists and pathologists D. Aust (Dresden), S. Miehlke (Hamburg) An initiative of the EUROPEAN MICROSCOPIC COLITIS GROUP Microscopic is a chronic inflammatory
Keep microscopic in mind! Information for gastroenterologists and pathologists D. Aust (Dresden), S. Miehlke (Hamburg) An initiative of the EUROPEAN MICROSCOPIC COLITIS GROUP Microscopic is a chronic inflammatory
UNDERSTANDING X-RAYS: ABDOMINAL IMAGING THE ABDOMEN
 UNDERSTANDING X-RAYS: ABDOMINAL IMAGING THE ABDOMEN Radiology Enterprises radiologyenterprises@gmail.com www.radiologyenterprises.com STOMACH AND SMALL BOWEL STOMACH AND SMALL BOWEL Swallowed air is a
UNDERSTANDING X-RAYS: ABDOMINAL IMAGING THE ABDOMEN Radiology Enterprises radiologyenterprises@gmail.com www.radiologyenterprises.com STOMACH AND SMALL BOWEL STOMACH AND SMALL BOWEL Swallowed air is a
What is Crohn's disease?
 What is Crohn's disease? Crohn's disease is a chronic inflammatory disorder that causes inflammation of the digestive tract. It can affect any area of the GI tract, from the mouth to the anus, but it most
What is Crohn's disease? Crohn's disease is a chronic inflammatory disorder that causes inflammation of the digestive tract. It can affect any area of the GI tract, from the mouth to the anus, but it most
Clinico-pathological study of colonoscopic biopsies in patients with chronic diarrhea
 International Journal of Research in Medical Sciences Bhagyalakshmi A et al. Int J Res Med Sci. 2016 Jul;4(7):2738-2744 www.msjonline.org pissn 2320-6071 eissn 2320-6012 Research Article DOI: http://dx.doi.org/10.18203/2320-6012.ijrms20161942
International Journal of Research in Medical Sciences Bhagyalakshmi A et al. Int J Res Med Sci. 2016 Jul;4(7):2738-2744 www.msjonline.org pissn 2320-6071 eissn 2320-6012 Research Article DOI: http://dx.doi.org/10.18203/2320-6012.ijrms20161942
Histopathology: Glomerulonephritis and other renal pathology
 Histopathology: Glomerulonephritis and other renal pathology These presentations are to help you identify basic histopathological features. They do not contain the additional factual information that you
Histopathology: Glomerulonephritis and other renal pathology These presentations are to help you identify basic histopathological features. They do not contain the additional factual information that you
Inflammatory disorders of the intestines can be
 Seymour Katz, M.D., Series Editor Practical Approach to Microscopic Colitis and Inflammatory Bowel Disease by Noel R. Fajardo and Darrell S. Pardi INTRODUCTION Inflammatory disorders of the intestines
Seymour Katz, M.D., Series Editor Practical Approach to Microscopic Colitis and Inflammatory Bowel Disease by Noel R. Fajardo and Darrell S. Pardi INTRODUCTION Inflammatory disorders of the intestines
Review Histological evaluation in ulcerative colitis
 Gastroenterology Report 2 (2014) 178 192, doi:10.1093/gastro/gou031 Advance access publication 18 June 2014 Review Histological evaluation in ulcerative colitis Tom C. DeRoche 1, Shu-Yuan Xiao 2 and Xiuli
Gastroenterology Report 2 (2014) 178 192, doi:10.1093/gastro/gou031 Advance access publication 18 June 2014 Review Histological evaluation in ulcerative colitis Tom C. DeRoche 1, Shu-Yuan Xiao 2 and Xiuli
Kids Like to Break the Rules: Gastrointestinal Pathology in Children
 Kids Like to Break the Rules: Gastrointestinal Pathology in Children Jeffrey Goldsmith MD Director of Surgical Pathology, Beth Israel Deaconess Medical Center; Consultant in Gastrointestinal Pathology,
Kids Like to Break the Rules: Gastrointestinal Pathology in Children Jeffrey Goldsmith MD Director of Surgical Pathology, Beth Israel Deaconess Medical Center; Consultant in Gastrointestinal Pathology,
