Burn wounds - Determining the size and type degree
|
|
|
- Kristina Gordon
- 5 years ago
- Views:
Transcription
1
2 1 Burn wounds - Determining the size and type degree Determining surface area of burn (Open hand only for small burns) 1
3 2 Burn depth Most burns are a combination of superficial and deeper burns and the best assessment is made 3 to 4 days after the injury when wound evolution is complete. 1. Superficial partial thickness: destruction of only superficial layers of the skin. These wounds will re-epithelialise spontaneously within 3 weeks; excision is contraindicated and the wounds rarely cause functional or cosmetic defects or hypertrophic scars. They characteristically have an erythematous, moist, homogeneous surface with blister formation, are painful and hypersensitive to touch, blanch readily on pressure and have a normal to firm texture on palpation. 2. Indeterminate depth (deep dermal burn): destruction of epidermis and varying amounts of dermis. These wounds are difficult to assess during the first 3 to 4 days after injury due to the ongoing evolution within the burn wound, which can be modulated by infection and dehydration. These wounds present with a reticulated red, white, dry surface and may blister. Capillary circulation may be sluggish or absent when pressure is applied to the wound. Wound pain is perceived as discomfort and the wound is often less sensitive to pinprick than the surrounding normal skin. The healing time for these wounds may be variable and may require several weeks leading to severe hypertrophic scarring. 3. Unequivocally full thickness: total irreversible destruction of all elements of the skin with or without extension into the deeper tissues and structures. These wounds will not heal spontaneously within 3 weeks and have unsatisfactory functional and cosmetic results. There is general consensus that the best treatment entails early eschar excision and immediate grafting. These wounds may mimic the appearance of an indeterminate burn and are usually mottled, white, red or charred and dry in appearance, insensitive to pain and leathery to palpation. Blisters are unusual and if present are thin walled and do not enlarge. Clotted superficial vessels may be visible. The appearance of the burn remains static with little change over the ensuing days. 2
4 3 PROTOCOL for Emergency Treatment of a Burn: 1. Assess airway/breathing (a) Careful airway assessment of both flame and scald burns to face and neck. Intubation is generally only necessary for unconscious patients, hypoxic patients with severe smoke inhalation, or patients with flame or flash burns involving face and neck. Indications include: pharyngeal burns, air hunger, stridor, carbonaceous sputum with hoarseness and any of the above. (b) All major burns must receive high flow oxygen for 24 hours (c) Carbon monoxide may present as restlessness, headache, nausea, poor coordination, memory impairment, disorientation, or coma. Administer 100% O 2 via non-rebreathing face mask. Useful lab: Blood gases with carboxyhaemoglobin level. (d) If breathing seems to be compromised by tight circumferential trunk burns an escharotomy must be performed urgently. 2. Circulation (a) Stop any external bleeding. (b) Identify potential sources of internal bleeding. (c) Establish large bore IV lines and provide resuscitation bolus fluid if required in all compromised patients. Perfusion of potentially viable burn wounds is critical. 3. Remove any sources of heat (a) Remove any clothing that may be burned, covered with chemicals or are constricting. (b) Cool any burns less than 3hours old with cold tap water for at least 30 min and then dry the patient. (c) Cover patient with clean dry sheet or blanket to prevent hypothermia. (d) Use of Burnshield is a very effective means for cooling and dressing for the first 24 hrs. (e) Rings and constricting garments must be removed. 4. Estimate percent total body surface area burned (%TBSA) (a) Initially, use Rule of Nines; for all pediatric patients and for a more accurate assessment, use attached Berkow diagram or patients outstretched open hand representing 1% Reminder: Accurate estimation of burn size is critical to ongoing fluid replacement and management 3
5 4 5. Ongoing losses (once the patient has been stabilised). Resuscitation must be commenced within two hours of injury (a) Burns <10% can be resuscitated orally, unless the patient has an electrical injury or associated trauma. This needs ongoing evaluation and still may require an IV line. (b) For 10 to 40% burns, secure a large bore IV line; add a second if the transport will be longer than 45 minutes. (c) Burns >40% require two large bore IV lines. (d) If the transfer will be less than 30 min. from the time of call, don t delay transfer for an IV line Reminder: IVs may be placed through a burnt area if necessary (suture to secure). Avoid saphenous vein if at all possible; avoid cut-downs through unburned skin if possible. Intraosseous is an excellent alternative in the hypovolaemic child. 4 (e) Initiate fluids for ongoing resuscitation and fluid losses: Parkland formula: 3-4ml Ringers lactate x kg body weight x % burn = mls in first 24 hours, with half of this total given in the first 8 hours post injury. Children must have their daily maintenance fluids added to the volume of fluids calculated by the Parkland formula (including dextrose). Glucose must be added to Ringer s lactate in children weighing less than 20kg. Example: Patient weighing 70kg with a 50% burn: (4 x 70 x 50) = 14,000ml needed in first 24 hours. 7000mls are needed in the first 8 hours (calculated from the time of burn injury) so IVs are initially started at 900mls/hour. Reminders: Do not give dextrose solutions (except for maintenance fluids in children) they may cause an osmotic diuresis and confuse adequacy of resuscitation assessment. Ideally use Ringers Lactate or Plasmalyte B for ongoing fluid losses and a 5% dextrose balanced salt solution for the child s maintenance This is only a guide and ongoing evaluation is essential, patients may need more fluids than calculated. 6. Assess urine output (this is the best guide to resuscitation) (a) Insert Foley catheter in patients with burns >15% TBSA. Adequate urine output is 0.5ml -1/kg/hr in adults and 1ml/kg/hr in children. Reminder: Lasix and other diuretics are never given to improve urine output; fluid rates are adjusted to increase urine output.
6 5 (b) Observe urine for burgundy colour (seen with massive injuries or electrical burns). There is a high incidence of renal failure associated with these injuries, requiring prompt and aggressive intervention. Reminder: If the urine is red or brown CONSULT BURN CENTRE. 7. Insert nasogastric tube (a) Insert nasogastric tube in any patient who is unresponsive, shocked or with burns >20% if preparing for air or long distance transport. 8. Decompression incisions (Escharotomy) Assess for circumferential full-thickness burns of extremities or trunk. Elevate burned extremities on pillows above level of the heart. If transfer will be delayed, discuss with a burn surgeon indications and methods for decompression incisions (escharotomies). If an escharotomy is required, do not delay the procedure. 9. Medications (a) Give tetanus immunization. (b) After fluid resuscitation has been started, pain medication may be titrated in small intravenous doses (not intramuscular). Blood pressure, pulse, respiratory rate and state of consciousness should be assessed after each increment of IV morphine. 10. Wound care during transport (a) Debridement and application of topical antimicrobials is usually unnecessary; transport patient wrapped in dry sheet, blanket or cling wrap and keep the patient warm. (b) Apply a thin layer of Silver Sulfadiazine to open areas if transport will be delayed longer than 12 hours. (c) Use of Burnshield is a very effective means for cooling and dressing for the first 24 hr. 11. General items (a) A history, including details of the accident and pre-existing diseases/allergies, should be recorded and sent with the patient. (b) Annotate the burn wound in TBSA and depth. (c) Copies of all medical records, including all fluids (calculations of fluids) and medications given, urine outputs and vital signs must accompany the patient. These specific details may be recorded on the back of the burn size assessment sheet. (d) The Burn Centre will arrange transport if appropriate. (e) In case of paediatric patients not accompanied by a parent get consent in consultation with your burn centre. 5
7 6 12. Special considerations with chemical burns Consult Burn Centre! (a) Remove ALL clothing. (b) Brush powdered chemicals off wound; then flush chemical burns for a minimum of 30 minutes or until all pain has disappeared,with copious volumes of running water. Be careful to protect yourself. Reminder: Never neutralize an acid with a base or vice versa. (c) Irrigate burned eyes with a gentle stream of saline. Follow with an ophthalmology consult if transport is not imminent. (d) Determine what chemical (and what concentration) caused the injury. 13. Special considerations with electrical injuries Consult Burn Centre! (a) Differentiate between low voltage(below 1000v) and high voltage (>1000v) (b) Attach cardiac monitor; treat life-threatening dysrythmias as needed. (c) Assess for associated trauma; assess central and peripheral neurologic function. (d) Administer Ringer s lactate; titrate fluids to maintain adequate urine output or to flush pigments through the urinary tract (see urine output above). Useful lab: ABG with acid/base balance. (e) Elevate burned extremities above the level of the heart on pillows. Monitor distal pulses. 14. Local Care The burn wound is carefully assessed for extent and depth and then treated topically with an antiseptic/antibacterial agent as a prophylactic or therapeutic measure against burn wound colonisation and burn wound infection. (a) (b) The burn wound is washed with water and soap or with chlorhexidine solution and then covered with the selected topical agent. Grease and road contamination can be removed by the application of petroleum jelly. A closed burn wound technique is used and the topical agents chosen according to burn unit protocol. Frequently used topical agents include silver sulphudiazine (changed daily), povidine iodine (changed daily), Mupirison with or without Chlorhexidine (changed daily) and a nanocrystalline dressing (Acticoat) changed every 3 days. 15. Wound Cleansing Hydrotherapy and Versajet The initial burn wounds can be washed with soap and water or Chlorhexidine or can be debrided under anaesthesia. 6
8 7 Transportation of the burned patient Ensure airway is safe. Transport as soon as possible to reach destination within 4 to 6 hours. Intravenous (IV) fluid therapy should be commenced. Ensure IV lines are reliable, especially if long journey. Secure lines with sutures if necessary. Transfer children only after fluid resuscitation has commenced, measures to maintain temperature have been instituted and the wound protected. Transfer with dry dressings or cling film, not wet towels. Arrange appropriate escort. Oxygen should be administered to all major burns or when carbon monoxide poisoning is suspected. Administer adequate analgesia. Infection prophylaxis: tetanus immunisation. Defer antibiotics if for burns only. Provide a full and complete record to the receiving service/clinician: o Medication given: dosage and route o Dressings o Fluids administered: type, volume and time of commencement o Urine output: catheterisation for accuracy o Procedures performed, if any o Contact details of relatives o Name and contact details of referring person Special Considerations: Circumferential Burns: assess distal circulation, remove jewellery. Evaluate for escharotomies as necessary. Contact the regional burn centre for further instructions. High Voltage Electrical Injuries: suspect myoglobinuria or haemoglobinuria. Keep urine output at 100ml/hr and urine alkaline. Place on cardiac monitor. Record ECG. Suspect compartmental syndrome, consider fasciotomies. Contact the regional burn centre for further instructions. 7
9 8 REFERRAL CRITERIA/GUIDELINES FOR TRANSFER TO BURNS CENTRE/HIGHER FACILITY Partial thickness (2 ) and full thickness burns (3 o ) > 10% total body surface area (TBSA) in patients under 10 and over 50 years of age Partial thickness (2 o ) and full thickness (3 o ) burns >20% TBSA in other age groups Full thickness (3 ) burns >5% (TBSA)in any age group Burns to the face, hands, feet, genitalia or major joints Electrical (including lightning), Chemical or Inhalation burns Patients with pre-existing medical disorders compromising outcome Patients with burns and concomitant trauma Patients requiring extensive social, emotional or long-term rehabilitation support Paediatric burns without qualified personnel or equipment Associated co-morbidity and injuries may complicate any burn and the patient needs to be carefully considered and the injuries be treated according to clinical needs. Before any transfer please consult with the receiving hospital unit. 1. Entry criteria for Level 3 burns centre: These are complex burns. a. Age under 2 and over 60 years. b. TBSA: c. Anatomical site: All partial thickness burns >15% TBSA in children. All partial thickness burns >25% TBSA in adults. All full thickness burns >15% TBSA. Face, Hands, Feet, Genitalia, Perineum, major joints, circumferential burns. These burns could also be dealt with at level 1 or 2 but discretion must be used. d. Inhalational injury requiring ventilation for more than 48 hours. e. Mechanism of injury Exposure to ionizing radiation injury 8
10 9 9 f. Existing Co-morbidity: High pressure steam injury High tension electrical injury (>1000 Volts) Hydrofluoric acid injury >1% TBSA Suspicion of non-accidental burn injury: paediatrics and adults Cardiac limitation and/or MI within 5 years Respiratory limitation of exercise Uncontrolled type 1 diabetes Pregnancy Medically or disease induced immune-suppression for any reason Existing psychiatric or suicidal tendencies Suspected drug/alcohol abuse g. Severe associated injuries e.g. polytrauma and crush syndrome Burns that may qualify for Level 2 care: a. Partial thickness burns of up to 25% TBSA in adults and up to 15% in b. Children older than 2 years c. Full thickness burns less than 10-15% TBSA in both adults and children excluding critical areas. d. Burns that require debridement, skin grafting and dressing changes. e. Inhalational burns requiring ventilation support for less than 48 hours. 16. Burns that may qualify for Level 1 care: These are non-complex injuries. a. A uncomplicated minor burn is: Partial thickness burn < 15% TBSA Full thickness burn <5% TBSA
11 10 b. Depending on the expertise of the available staff, additional criteria may include: Minor inhalational injury Electrical burns <400 Volts Minor burns in anatomically important sites Manageable and stabilised co-morbidities Surgery: debridement, skin grafting, dressing changes The quality of care at this level can be substantially improved by the development of clinical guidelines and educational programmes (e.g. EMSB Course). These programmes should also be made available to the Emergency and Ambulance Services to standardized burn care at pre-hospital and HPC levels. There is unfortunately no published information available on the outcome of burns treated at community level. Dosing schedule of simple analgesics Dosing schedule of Tilidine Dosing schedule of Clonidine 10
12 11 Dosing schedule of Ketamine Profile of Topical Antimicrobials Agent Application Eschar Penetration Action Sodium hypochlorite min Surface action Bacteriocidal Silver sulphadiazine 12 hourly Limited Bacteriocidal Povidone Iodine 6 hourly Limited Bacteriocidal Mupirocin Daily Excellent Bacteriocidal Chlorhexidine Daily Surface action Bacteriocidal Nano-silver 3-4 days Excellent Bacteriocidal Bactigras 48 hours Limited Bacteriocidal 11
BURNS MODULE. In the paediatric population consider non-accidental injury as a mechanism for burn injuries.
 BURNS MODULE INTRODUCTION Burns are a common cause of trauma. Most burn injuries are a result of flame burns, with scalds also occurring commonly. Electrical and chemical burns are less common. 1 Concurrent
BURNS MODULE INTRODUCTION Burns are a common cause of trauma. Most burn injuries are a result of flame burns, with scalds also occurring commonly. Electrical and chemical burns are less common. 1 Concurrent
Approved By: Airway and Breathing A. Initially give humidified high flow oxygen at 15 L (100%) using a nonrebreather
 Subject: BURN CARE CLINICAL GUIDELINE Originator: Approval Date: 2015 Approved By: Policy: All burn patients presenting to XXXXXX Hospital will have appropriate assessment, stabilization and evaluation
Subject: BURN CARE CLINICAL GUIDELINE Originator: Approval Date: 2015 Approved By: Policy: All burn patients presenting to XXXXXX Hospital will have appropriate assessment, stabilization and evaluation
IMMEDIATE EMERGENCY BURN CARE » THERMAL BURNS » ELECTRICAL BURNS » CHEMICAL BURNS FIRST AID FOR THE THREE MAJOR CATEGORIES
 IMMEDIATE EMERGENCY BURN CARE 1. Treat according to BLS or ACLS Protocol 2. Use airway and C-Spine precautions. 3. Stop the burning process. FIRST AID FOR THE THREE MAJOR CATEGORIES» THERMAL BURNS + Stop
IMMEDIATE EMERGENCY BURN CARE 1. Treat according to BLS or ACLS Protocol 2. Use airway and C-Spine precautions. 3. Stop the burning process. FIRST AID FOR THE THREE MAJOR CATEGORIES» THERMAL BURNS + Stop
EmergencyKT: Management of Thermal Injury in Adult Patients
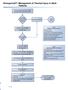 EmergencyKT: Management of Thermal Injury in Adult Patients Remove patient from source of injury, including burned clothing and jewelry Does patient appear to have minor burns? (See Box A) No Notify Burn
EmergencyKT: Management of Thermal Injury in Adult Patients Remove patient from source of injury, including burned clothing and jewelry Does patient appear to have minor burns? (See Box A) No Notify Burn
Burn Priorities of Care: Triage/Treatment/Transfer. Via Christi Regional Burn Center Sarah Fischer, MSN, RN
 Burn Priorities of Care: Triage/Treatment/Transfer Via Christi Regional Burn Center Sarah Fischer, MSN, RN Disclosure I have nothing to disclose Objectives Identify American Burn Association referral criteria
Burn Priorities of Care: Triage/Treatment/Transfer Via Christi Regional Burn Center Sarah Fischer, MSN, RN Disclosure I have nothing to disclose Objectives Identify American Burn Association referral criteria
Burns. A Comprehensive Review Assessment & Management
 Burns A Comprehensive Review Assessment & Management 1 Objectives Understand types of Burns Understand the pathophysiology of the Burns Understand Rule of Nine Understand Classification of Burns Identify
Burns A Comprehensive Review Assessment & Management 1 Objectives Understand types of Burns Understand the pathophysiology of the Burns Understand Rule of Nine Understand Classification of Burns Identify
The immediate management of burns patients should be similar to management of trauma.
 CATS Clinical Guideline Burns The National Burn Care Review recommends that children with burns should be treated in a Burn Centre. Chelsea and Westminster may take non-ventilated children, Broomfield
CATS Clinical Guideline Burns The National Burn Care Review recommends that children with burns should be treated in a Burn Centre. Chelsea and Westminster may take non-ventilated children, Broomfield
At the conclusion of this course the learner will be able to
 Objectives At the conclusion of this course the learner will be able to 1. Discuss basic anatomy and pathophysiology of burns 2. Describe burn injuries in terms of size, depth, coloration and characteristics
Objectives At the conclusion of this course the learner will be able to 1. Discuss basic anatomy and pathophysiology of burns 2. Describe burn injuries in terms of size, depth, coloration and characteristics
1/3/2008. Karen Burke Priscilla LeMone Elaine Mohn-Brown. Medical-Surgical Nursing Care, 2e Karen Burke, Priscilla LeMone, and Elaine Mohn-Brown
 Medical-Surgical Nursing Care Second Edition Karen Burke Priscilla LeMone Elaine Mohn-Brown Chapter 46 Caring for Clients with Burns Types of Burns Thermal Dry heat flame Moist heat steam or hot liquid
Medical-Surgical Nursing Care Second Edition Karen Burke Priscilla LeMone Elaine Mohn-Brown Chapter 46 Caring for Clients with Burns Types of Burns Thermal Dry heat flame Moist heat steam or hot liquid
Pediatric Burn Management Justin D. Klein, MD Associate Burn Director Lisa C. Vitale, RN Burn Program Coordinator
 Pediatric Burn Management Justin D. Klein, MD Associate Burn Director Lisa C. Vitale, RN Burn Program Coordinator Lecture Overview Burn statistics and etiologies Pre-hospital evaluation Anatomy of a burn
Pediatric Burn Management Justin D. Klein, MD Associate Burn Director Lisa C. Vitale, RN Burn Program Coordinator Lecture Overview Burn statistics and etiologies Pre-hospital evaluation Anatomy of a burn
Responsibility This guideline applies to teams of health professions caring for burn patients.
 Page 1 of 9 Guideline: Initial Assessment & Management of Burn Injuries Purpose This document provides a guideline for the initial assessment and management of burn patients. It is not intended as a full
Page 1 of 9 Guideline: Initial Assessment & Management of Burn Injuries Purpose This document provides a guideline for the initial assessment and management of burn patients. It is not intended as a full
PEDIATRIC TRAUMA I: ABDOMINAL TRAUMA BURNS. December 19, 2012
 PEDIATRIC TRAUMA I: ABDOMINAL TRAUMA BURNS Niel F. Miele,, M.D. December 19, 2012 EPIDEMIOLOGY Major Trauma responsible for
PEDIATRIC TRAUMA I: ABDOMINAL TRAUMA BURNS Niel F. Miele,, M.D. December 19, 2012 EPIDEMIOLOGY Major Trauma responsible for
Dóra Ujvárosy MD. Medical University of Debrecen Oxyology and Emergency Department
 Dóra Ujvárosy MD. Medical University of Debrecen Oxyology and Emergency Department Functions Definition A burn is a type of injury to the skin caused by heat, electricity, chemicals, light, radiation or
Dóra Ujvárosy MD. Medical University of Debrecen Oxyology and Emergency Department Functions Definition A burn is a type of injury to the skin caused by heat, electricity, chemicals, light, radiation or
Children's National Medical Center The Division of Trauma and Burn Burn Education Module Post-test
 Children's National Medical Center The Division of Trauma and Burn Burn Education Module Post-test Purpose: To provide nurses with on overview of burn injuries in pediatric patients. Learning Objectives:
Children's National Medical Center The Division of Trauma and Burn Burn Education Module Post-test Purpose: To provide nurses with on overview of burn injuries in pediatric patients. Learning Objectives:
Objectives. Initial Burn Care and Fluid Resuscitation 6/5/2015 INITIAL MANAGEMENT
 Initial Burn Care and Fluid Resuscitation Sarah Taylor MSN, RN, ACNS-BC Clinical Nurse Specialist Trauma Burn Center University of Michigan Health System Ann Arbor, MI Objectives Discuss the initial assessment
Initial Burn Care and Fluid Resuscitation Sarah Taylor MSN, RN, ACNS-BC Clinical Nurse Specialist Trauma Burn Center University of Michigan Health System Ann Arbor, MI Objectives Discuss the initial assessment
Management of Acute Burn Injuries: The First 24 Hours
 Speaker Disclosure I, Debbie Harrell, MSN, RN, NE BC, have no financial relationships to disclose. I will not discuss off label uses of any pharmaceutical products or medical devices. Management of Acute
Speaker Disclosure I, Debbie Harrell, MSN, RN, NE BC, have no financial relationships to disclose. I will not discuss off label uses of any pharmaceutical products or medical devices. Management of Acute
Speaker Disclosure Emergent Burn Care I, Debbie Harrell, MSN, RN, NE BC, have no financial relationships to disclose.
 Speaker Disclosure Emergent Burn Care I, Debbie Harrell, MSN, RN, NE BC, have no financial relationships to disclose. Debbie Harrell RN, MSN, Shriners Hospitals for Children Cincinnati Cincinnati, Ohio
Speaker Disclosure Emergent Burn Care I, Debbie Harrell, MSN, RN, NE BC, have no financial relationships to disclose. Debbie Harrell RN, MSN, Shriners Hospitals for Children Cincinnati Cincinnati, Ohio
Burns Management in the Emergency Department
 Management in the Emergency Department (Referral Proforma) Time/Date of injury (24hr) Patient demographic data sticker Airway Please remember to protect C-spine until clinically cleared as stable Administer
Management in the Emergency Department (Referral Proforma) Time/Date of injury (24hr) Patient demographic data sticker Airway Please remember to protect C-spine until clinically cleared as stable Administer
INITIAL CARE AND TREATMENT OF BURN INJURIES. November 10,
 INITIAL CARE AND TREATMENT OF BURN INJURIES 2 11/10/2012 November 10, 2012 2 Oregon Burn Center Only burn center in Oregon and SW Washington New unit 16 beds, 20,000 square feet Opened in February 2002
INITIAL CARE AND TREATMENT OF BURN INJURIES 2 11/10/2012 November 10, 2012 2 Oregon Burn Center Only burn center in Oregon and SW Washington New unit 16 beds, 20,000 square feet Opened in February 2002
BLS, ILS, ALS OTEP BURNS BURN INTRODUCTION TYPES OF BURNS
 BURNS BLS, ILS, ALS OTEP While we do understand this presentation is an instructional tool for all levels of certification, taking this into consideration everyone taking this class must remember that
BURNS BLS, ILS, ALS OTEP While we do understand this presentation is an instructional tool for all levels of certification, taking this into consideration everyone taking this class must remember that
Burn Injuries & Its Management M JARI.MD
 Burn Injuries & Its Management M JARI.MD 1 BURNS Wounds caused by exposure to: 1. excessive heat 2. Chemicals 3. fire/steam 4. radiation 5. electricity 2 BURNS Results in 10-20 thousand deaths annually
Burn Injuries & Its Management M JARI.MD 1 BURNS Wounds caused by exposure to: 1. excessive heat 2. Chemicals 3. fire/steam 4. radiation 5. electricity 2 BURNS Results in 10-20 thousand deaths annually
Chapter 29. Objectives. Objectives 01/09/2013. Burns
 Chapter 29 Burns Prehospital Emergency Care, Ninth Edition Joseph J. Mistovich Keith J. Karren Copyright 2010 by Pearson Education, Inc. All rights reserved. Objectives 1. Define key terms introduced in
Chapter 29 Burns Prehospital Emergency Care, Ninth Edition Joseph J. Mistovich Keith J. Karren Copyright 2010 by Pearson Education, Inc. All rights reserved. Objectives 1. Define key terms introduced in
Wisecracks 1. What are the indications for an escharotomy 2. What are the primary considerations in mechanical ventilation of burn patients
 Chapter 63 Thermal Burns Episode Overview Questions 1. List zones of burns 2. List 6 indications for intubation in the burn patient 3. List and describe 2 formulas for fluid resuscitation 4. Describe depth
Chapter 63 Thermal Burns Episode Overview Questions 1. List zones of burns 2. List 6 indications for intubation in the burn patient 3. List and describe 2 formulas for fluid resuscitation 4. Describe depth
EMERGENCYROOM BURN MANAGEMENT
 EMERGENCYROOM INITIAL ASSESSMENT PRIMARY SURVEY A = Airway and C-spine immobilization B = Breathing and Ventilation C = Circulation D = Disability, Neurologic Deficit E = Expose (remove all clothing and
EMERGENCYROOM INITIAL ASSESSMENT PRIMARY SURVEY A = Airway and C-spine immobilization B = Breathing and Ventilation C = Circulation D = Disability, Neurologic Deficit E = Expose (remove all clothing and
LRI Emergency Department. Burn injuries management in adults
 LRI Emergency Department Clinical guideline for: Burn injuries management in adults Authors: Approved by: Martin Wiese Reena Agarwal Claire Porter EF guidelines committee Approval date: 21 Sep 16 Approval
LRI Emergency Department Clinical guideline for: Burn injuries management in adults Authors: Approved by: Martin Wiese Reena Agarwal Claire Porter EF guidelines committee Approval date: 21 Sep 16 Approval
Printed copies of this document may not be up to date, obtain the most recent version from Author Position
 Children s Acute Transport Service Clinical Guidelines Burns Management Document Control Information Author E Borrows E Randle Author Position PICU/BURNS Consultant CATS Consultant Document Owner E. Polke
Children s Acute Transport Service Clinical Guidelines Burns Management Document Control Information Author E Borrows E Randle Author Position PICU/BURNS Consultant CATS Consultant Document Owner E. Polke
Advanced Paediatric Nursing. Burn Trauma. 26 April Wong Tze Wing NC (Burns), Burns Centre, Surgery, PWH
 Advanced Paediatric Nursing Burn Trauma 26 April 2016 Wong Tze Wing NC (Burns), Burns Centre, Surgery, PWH Objective: Understand burn trauma in children Understand Important nursing interventions in burn
Advanced Paediatric Nursing Burn Trauma 26 April 2016 Wong Tze Wing NC (Burns), Burns Centre, Surgery, PWH Objective: Understand burn trauma in children Understand Important nursing interventions in burn
Modern management of paediatric burns
 Modern management of paediatric burns Burn injuries pose a major threat to children in South Africa and remain a devastating injury, because of the resulting severe emotional and physical scarring and
Modern management of paediatric burns Burn injuries pose a major threat to children in South Africa and remain a devastating injury, because of the resulting severe emotional and physical scarring and
Mr Zachary Moaveni Plastic Surgeon, Middlemore Hospital. Mr Adam Bialostocki Plastic Surgeon, Tauranga
 Mr Zachary Moaveni Plastic Surgeon, Middlemore Hospital Mr Adam Bialostocki Plastic Surgeon, Tauranga Mr. Adam Bialostocki Plastic Surgeon Minor Burns First Aid Remove the burning agent / wet clothes
Mr Zachary Moaveni Plastic Surgeon, Middlemore Hospital Mr Adam Bialostocki Plastic Surgeon, Tauranga Mr. Adam Bialostocki Plastic Surgeon Minor Burns First Aid Remove the burning agent / wet clothes
Printed copies of this document may not be up to date, obtain the most recent version from Author Position
 Children s Acute Transport Service Clinical Guidelines Burns Management Document Control Information Author E Borrows E Randle, L Chigaru Author Position PICU/BURNS Consultant CATS Consultants Document
Children s Acute Transport Service Clinical Guidelines Burns Management Document Control Information Author E Borrows E Randle, L Chigaru Author Position PICU/BURNS Consultant CATS Consultants Document
Guidelines for the management of paediatric burns
 Guidelines for the management of paediatric burns Are there signs of airway injury? If yes contact anaesthetist! Is burn TBSA >10% If appropriate COOL THE BURN! Heat room. Insert IVC. Obtain FBC, U&,E
Guidelines for the management of paediatric burns Are there signs of airway injury? If yes contact anaesthetist! Is burn TBSA >10% If appropriate COOL THE BURN! Heat room. Insert IVC. Obtain FBC, U&,E
Cellular and Tissue Effects. Pathophysiology of the Burn Wound. Special Topics: Thermal Burns & Smoke Inhalation
 Special Topics: Thermal Burns & Smoke Inhalation MEDICAL RESPONDER AND RECEIVER SEMINAR; EXPLOSION AND BLAST INJURIES Pathophysiology of the Burn Wound The burn wound is the source of virtually all ill
Special Topics: Thermal Burns & Smoke Inhalation MEDICAL RESPONDER AND RECEIVER SEMINAR; EXPLOSION AND BLAST INJURIES Pathophysiology of the Burn Wound The burn wound is the source of virtually all ill
Burn injury. A : patent airway with smoking inhalation, stridor. D: E4V5M6,pupil 2mm RTLBE
 Burn injury Pinyong Uthaitas Emergency Department Faculty of Medicine, Ramathibodi Hospital A Thai man 52 year old came to the hospital due to flam burn ½ hr ago at his house. He gain conscious but hoarseness
Burn injury Pinyong Uthaitas Emergency Department Faculty of Medicine, Ramathibodi Hospital A Thai man 52 year old came to the hospital due to flam burn ½ hr ago at his house. He gain conscious but hoarseness
Burns. Chapter 9. Burns
 Burns Chapter 9 Burns Introduction Natural childhood curiosity and lack of supervision frequently combine to make thermal injuries a major cause of morbidity and mortality in the pediatric patient. Whether
Burns Chapter 9 Burns Introduction Natural childhood curiosity and lack of supervision frequently combine to make thermal injuries a major cause of morbidity and mortality in the pediatric patient. Whether
Current Trends in Burn Care
 Objectives Current Trends in Burn Care Jordan Murphy, BSN, CFRN Clinical Educator-KY/FL PHI Air Medical Describes normal skin anatomy. Differentiates pathophysiology related to etiology of injury. Identify
Objectives Current Trends in Burn Care Jordan Murphy, BSN, CFRN Clinical Educator-KY/FL PHI Air Medical Describes normal skin anatomy. Differentiates pathophysiology related to etiology of injury. Identify
Dr. Muhammad Shamim. FCPS (Pak), FACS (USA), FICS (USA), MHPE (Nl & Eg)
 Dr. Muhammad Shamim FCPS (Pak), FACS (USA), FICS (USA), MHPE (Nl & Eg) Assistant Professor, Dept. of Surgery College of Medicine, Salman bin Abdulaziz University Email: surgeon.shamim@gmail.com Web: surgeonshamim.com
Dr. Muhammad Shamim FCPS (Pak), FACS (USA), FICS (USA), MHPE (Nl & Eg) Assistant Professor, Dept. of Surgery College of Medicine, Salman bin Abdulaziz University Email: surgeon.shamim@gmail.com Web: surgeonshamim.com
Review. A. abrasion B. contusion C. hematoma D. avulsion
 Chapter 24 Review Review 1. A young male was struck in the forearm with a baseball and complains of pain to the area. Slight swelling and ecchymosis are present, but no external bleeding. What type of
Chapter 24 Review Review 1. A young male was struck in the forearm with a baseball and complains of pain to the area. Slight swelling and ecchymosis are present, but no external bleeding. What type of
Burns and electrical injuries. Shelley Westwood, RN, BSN
 Burns and electrical injuries Shelley Westwood, RN, BSN Burns A burn is an injury caused by fire, heat, chemicals, radiation, or electricity. Burns are traumatic in that they can cause extreme pain, permanent
Burns and electrical injuries Shelley Westwood, RN, BSN Burns A burn is an injury caused by fire, heat, chemicals, radiation, or electricity. Burns are traumatic in that they can cause extreme pain, permanent
Chapter 23 Caring for Clients with Burns
 Chapter 23 Caring for Clients with Burns Burn Injuries 4500 people die from burns each year High risk group ~ children and the elderly The most common cause of burns Smoking material Scalding Lighting
Chapter 23 Caring for Clients with Burns Burn Injuries 4500 people die from burns each year High risk group ~ children and the elderly The most common cause of burns Smoking material Scalding Lighting
Purpose To outline the pre-hospital and inter-hospital assessment and management of patients with major burns.
 Major Burns HELI.CLI.08 Purpose To outline the pre-hospital and inter-hospital assessment and management of patients with major burns. Procedure Management of Severe Burns For Review Aug 2015 1. Introduction
Major Burns HELI.CLI.08 Purpose To outline the pre-hospital and inter-hospital assessment and management of patients with major burns. Procedure Management of Severe Burns For Review Aug 2015 1. Introduction
Pediatrics Grand Rounds 1 June University of Texas Health Science Center at San Antonio. Management of Burn Wounds. Management of Burn Wounds
 Management of Burn Wounds Management of Burn Wounds History of Burn Care Pathophysiology of Burn Lillian F. Liao, MD, MPH Division of Trauma and Emergency Surgery Department of Surgery UTHSCSA Acute burn
Management of Burn Wounds Management of Burn Wounds History of Burn Care Pathophysiology of Burn Lillian F. Liao, MD, MPH Division of Trauma and Emergency Surgery Department of Surgery UTHSCSA Acute burn
INTRODUCTION OBJECTIVES. When the student has finished this module, he/she will be able to:
 Burn Care and Management WWW.RN.ORG Reviewed September 2017, Expires September 2019 Provider Information and Specifics available on our Website Unauthorized Distribution Prohibited 2017 RN.ORG, S.A., RN.ORG,
Burn Care and Management WWW.RN.ORG Reviewed September 2017, Expires September 2019 Provider Information and Specifics available on our Website Unauthorized Distribution Prohibited 2017 RN.ORG, S.A., RN.ORG,
TBSA Burn Estimation Chart Adult Major Burn Clinical Practice Guideline
 TBSA Burn Estimation Chart Adult Major Burn Clinical Practice Guideline Patient Label Anatomical Subunit Percent Total Percent One Side Anterior Posterior Injury Subtotal 3.5% 2nd and 3rd degree burns
TBSA Burn Estimation Chart Adult Major Burn Clinical Practice Guideline Patient Label Anatomical Subunit Percent Total Percent One Side Anterior Posterior Injury Subtotal 3.5% 2nd and 3rd degree burns
Modern management of paediatric burns
 Modern management of paediatric burns Burn injuries pose a major threat to children in South Africa and remain a devastating injury, because of the resulting severe emotional and physical scarring and
Modern management of paediatric burns Burn injuries pose a major threat to children in South Africa and remain a devastating injury, because of the resulting severe emotional and physical scarring and
Fire Deaths. Dr Julie McAdam Consultant Forensic Pathologist Glasgow University
 Fire Deaths Dr Julie McAdam Consultant Forensic Pathologist Glasgow University Forensic investigation multidisciplinary fire officers, police officers, scientists, photographers, pathologist, procurator
Fire Deaths Dr Julie McAdam Consultant Forensic Pathologist Glasgow University Forensic investigation multidisciplinary fire officers, police officers, scientists, photographers, pathologist, procurator
Applicable to. Team Members Performing MD House Staff APRN/PA RN LPN
 Protocol: Adult Burn Fluid Resuscitation Category Clinical Practice Protocol Number Approval Date vember 1, 2016 Due for review vember 1, 2018 Applicable to VUH Children s DOT VMG Off-site locations VMG
Protocol: Adult Burn Fluid Resuscitation Category Clinical Practice Protocol Number Approval Date vember 1, 2016 Due for review vember 1, 2018 Applicable to VUH Children s DOT VMG Off-site locations VMG
INSTRUCTOR GUIDE FOR TACTICAL FIELD CARE 3B BURNS AND FRACTURES
 INSTRUCTOR GUIDE FOR TACTICAL FIELD CARE 3B BURNS AND FRACTURES 180801 1 Tactical Combat Casualty Care for Medical Personnel 1. August 2017 (Based on TCCC-MP Guidelines 180801 In this presentation, we
INSTRUCTOR GUIDE FOR TACTICAL FIELD CARE 3B BURNS AND FRACTURES 180801 1 Tactical Combat Casualty Care for Medical Personnel 1. August 2017 (Based on TCCC-MP Guidelines 180801 In this presentation, we
WOUNDS. Emergency Procedures in PT
 WOUNDS Emergency Procedures in PT Types of Wounds Abrasions uppermost layer scraped away, minor capillary bleeding occurs, nerve endings exposed Lacerations skin tear with edges jagged and uneven Incisions
WOUNDS Emergency Procedures in PT Types of Wounds Abrasions uppermost layer scraped away, minor capillary bleeding occurs, nerve endings exposed Lacerations skin tear with edges jagged and uneven Incisions
Northern Burn Care Operational Delivery Network Referral Information Pack
 Northern Burn Care Operational Delivery Network Referral Information Pack Northern Burn Care ODN Burns Referral Pack Pack includes: 1. NBCODN Burns services Contact information 2. Burns Referral Flow chart.
Northern Burn Care Operational Delivery Network Referral Information Pack Northern Burn Care ODN Burns Referral Pack Pack includes: 1. NBCODN Burns services Contact information 2. Burns Referral Flow chart.
Initial assessment. ATLS/ABLS protocol and assess for other injuries/fractures based on mechanism. Inhalational injury. Vascular compromise:
 Complex Hand Burns Brent Egeland, MD Assistant Professor Dell Medical School Department of Surgery and Perioperative Care Institute of Reconstructive Plastic Surgery Plastic, Hand, and Reconstructive Microsurgery
Complex Hand Burns Brent Egeland, MD Assistant Professor Dell Medical School Department of Surgery and Perioperative Care Institute of Reconstructive Plastic Surgery Plastic, Hand, and Reconstructive Microsurgery
Chapter 24 Soft Tissue Injuries Presentation Notes
 Names: Chapter 24 Soft Tissue Injuries Presentation Notes Anatomy of the Skin - Function of the Skin control Soft-Tissue Injuries injuries Soft-tissue damage the skin injuries Break in the of the skin
Names: Chapter 24 Soft Tissue Injuries Presentation Notes Anatomy of the Skin - Function of the Skin control Soft-Tissue Injuries injuries Soft-tissue damage the skin injuries Break in the of the skin
Wound Care in the Community. Lisa Sutherland MSc Tissue Viability Senior Lead Ipswich Hospital & Community NHS Trusts
 Wound Care in the Community Lisa Sutherland MSc Tissue Viability Senior Lead Ipswich Hospital & Community NHS Trusts What are the key elements? What is the patient s goal or aim for the wound? What are
Wound Care in the Community Lisa Sutherland MSc Tissue Viability Senior Lead Ipswich Hospital & Community NHS Trusts What are the key elements? What is the patient s goal or aim for the wound? What are
Sidney Miller, MD, FACS Professor of Surgery Director of Research and Development Ohio State University Burn Center
 Management of the Burn Patient Sidney Miller, MD, FACS Professor of Surgery Director of Research and Development Ohio State University Burn Center American Burn Association Transfer Criteria Burn > 10%
Management of the Burn Patient Sidney Miller, MD, FACS Professor of Surgery Director of Research and Development Ohio State University Burn Center American Burn Association Transfer Criteria Burn > 10%
Management of Burns under Prolonged Field Care
 This Role 1, prolonged field care (PFC) guideline is intended to be used after TCCC Guidelines when evacuation to higher level of care is not immediately possible. A provider of PFC must first and foremost
This Role 1, prolonged field care (PFC) guideline is intended to be used after TCCC Guidelines when evacuation to higher level of care is not immediately possible. A provider of PFC must first and foremost
STANDARD OPERATING PROCEDURE #203 LARGE ANIMAL SURGERY
 STANDARD OPERATING PROCEDURE #203 LARGE ANIMAL SURGERY 1. PURPOSE This Standard Operating Procedure (SOP) describes procedures for general surgery of large animal species such as swine, dogs, rabbits,
STANDARD OPERATING PROCEDURE #203 LARGE ANIMAL SURGERY 1. PURPOSE This Standard Operating Procedure (SOP) describes procedures for general surgery of large animal species such as swine, dogs, rabbits,
Patient Details Hospital number NHS number. Surname First name DOB. Permanent address. Post code. Mobile No. Temporary. Mother DOB. Father.
 Burns Unit Page 12 Paediatric Burn Injuries - Assessment & Admission Burns Unit Page 1 Discharge Patient Details Hospital number NHS number Admission date Injury date Hospital Use time time Time: Discharge
Burns Unit Page 12 Paediatric Burn Injuries - Assessment & Admission Burns Unit Page 1 Discharge Patient Details Hospital number NHS number Admission date Injury date Hospital Use time time Time: Discharge
Epidemiology. Burn Rehabilitation. Epidemiology. Epidemiology. United States. United States Cause of injury. Incidence has declined
 Burn Rehabilitation Peter Esselman, MD Professor and Chair Department of Rehabilitation Medicine University of Washington Epidemiology United States 450,000 burn injuries/year in USA that receive medical
Burn Rehabilitation Peter Esselman, MD Professor and Chair Department of Rehabilitation Medicine University of Washington Epidemiology United States 450,000 burn injuries/year in USA that receive medical
Thermal Burns PFN: SOMEML07. Terminal Learning Objective. References. Hours: 3.0 Instructor: Action: Communicate knowledge of thermal burns
 Thermal Burns PFN: SOMEML07 Hours: 3.0 Instructor: Slide 1 Terminal Learning Objective Action: Communicate knowledge of thermal burns Condition: Given a lecture in a classroom environment Standard: Received
Thermal Burns PFN: SOMEML07 Hours: 3.0 Instructor: Slide 1 Terminal Learning Objective Action: Communicate knowledge of thermal burns Condition: Given a lecture in a classroom environment Standard: Received
Outpatient Burn Care for Primary Care: Who needs a referral?
 Outpatient Burn Care for Primary Care: Who needs a referral? J. Kevin Bailey, MD Associate Professor Department of Surgery Division of Trauma, Critical Care and Burn The Ohio State University Wexner Medical
Outpatient Burn Care for Primary Care: Who needs a referral? J. Kevin Bailey, MD Associate Professor Department of Surgery Division of Trauma, Critical Care and Burn The Ohio State University Wexner Medical
Burns and Scalds. Treatment and Management. Accident and Emergency Department. Royal Surrey County Hospital. Patient information leaflet
 Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Burns and Scalds Treatment and Management Accident and Emergency Department A Burn is an injury caused to the skin by thermal
Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Burns and Scalds Treatment and Management Accident and Emergency Department A Burn is an injury caused to the skin by thermal
Printed copies of this document may not be up to date, obtain the most recent version from
 Children s Acute Transport Service Clinical Guidelines Septic Shock Document Control Information Author Claire Fraser P.Ramnarayan Author Position tanp CATS Consultant Document Owner E. Polke Document
Children s Acute Transport Service Clinical Guidelines Septic Shock Document Control Information Author Claire Fraser P.Ramnarayan Author Position tanp CATS Consultant Document Owner E. Polke Document
Sussex Trauma Network Guidelines for: The Management of Compartment Syndrome
 Sussex Trauma Network Guidelines for: The Management of Compartment Syndrome Management of Compartment Syndrome Control Page Version: 1 Category number: Approved by: Date approved: Name of author: and
Sussex Trauma Network Guidelines for: The Management of Compartment Syndrome Management of Compartment Syndrome Control Page Version: 1 Category number: Approved by: Date approved: Name of author: and
STS Care of Thermal Burns 20% Total Body Surface Area
 Temp Regulation Transfer Pain Fluids Airway Initial Assessment STS Care of Thermal Burns 20% Total Body Surface Area Remove burned clothing, rings, watches, and jewelry Cervical spine precautions (if history
Temp Regulation Transfer Pain Fluids Airway Initial Assessment STS Care of Thermal Burns 20% Total Body Surface Area Remove burned clothing, rings, watches, and jewelry Cervical spine precautions (if history
Case Report: Burns Reid Sadoway PGY1 Emergency Medicine, Dalhousie
 Case Report: Burns Reid Sadoway PGY1 Emergency Medicine, Dalhousie History 3 yo boy, presents to pediatric ED with mother Child can be heard crying inside waiting/patient room, has both hands bandaged
Case Report: Burns Reid Sadoway PGY1 Emergency Medicine, Dalhousie History 3 yo boy, presents to pediatric ED with mother Child can be heard crying inside waiting/patient room, has both hands bandaged
January Adult Burn Injured patients
 Guideline Full Title of Guideline: Author (include email and role): Division & Speciality: Scope (Target audience, state if Trust wide): Review date (when this version goes out of date): Explicit definition
Guideline Full Title of Guideline: Author (include email and role): Division & Speciality: Scope (Target audience, state if Trust wide): Review date (when this version goes out of date): Explicit definition
Essex and Herts Air Ambulance Trust (EHAAT) Essex and Herts Air Ambulance: a focused case series for pre-hospital practice
 Essex and Herts Air Ambulance: a focused case series for pre-hospital practice Case 1: management of a paediatric burn Erica Ley, critical care paramedic, Essex and Herts Air Ambulance; Adam Chesters,
Essex and Herts Air Ambulance: a focused case series for pre-hospital practice Case 1: management of a paediatric burn Erica Ley, critical care paramedic, Essex and Herts Air Ambulance; Adam Chesters,
TRAUMATIC EMERGENCIES
 TRAUMATIC EMERGENCIES I. General. A. Follow General Principles/Routine Care protocol unless otherwise indicated. B. Limit scene time for trauma patients, with goal of 15 minutes. C. See Appendix B for
TRAUMATIC EMERGENCIES I. General. A. Follow General Principles/Routine Care protocol unless otherwise indicated. B. Limit scene time for trauma patients, with goal of 15 minutes. C. See Appendix B for
Emergency management of the patient with severe burns in the emergency unit
 Emergency management of the patient with severe burns in the emergency unit Grobler RC, DipNurs, DipCliNursSc Netcare Union Hospital, Level 1 Trauma Centre Abstract Burns are one of the common causes of
Emergency management of the patient with severe burns in the emergency unit Grobler RC, DipNurs, DipCliNursSc Netcare Union Hospital, Level 1 Trauma Centre Abstract Burns are one of the common causes of
Surgical Care at the District Hospital. EMERGENCY & ESSENTIAL SURGICAL CARE
 Surgical Care at the District Hospital 1 13 Resuscitation and Preparation for Anesthesia & Surgery Key Points 2 13.1 Management of Emergencies and Cardiopulmonary Resuscitation The emergency measures that
Surgical Care at the District Hospital 1 13 Resuscitation and Preparation for Anesthesia & Surgery Key Points 2 13.1 Management of Emergencies and Cardiopulmonary Resuscitation The emergency measures that
Thermal Injuries. Manika Bhandari, Malika Bhola, Rucha Desai, Dhruvika Joshi, Abir Shamim Life Science 4M03
 Thermal Injuries Manika Bhandari, Malika Bhola, Rucha Desai, Dhruvika Joshi, Abir Shamim Life Science 4M03 INTRODUCTION Anatomy of the skin The skin has three anatomical layers Epidermis Dermis Subcutaneous
Thermal Injuries Manika Bhandari, Malika Bhola, Rucha Desai, Dhruvika Joshi, Abir Shamim Life Science 4M03 INTRODUCTION Anatomy of the skin The skin has three anatomical layers Epidermis Dermis Subcutaneous
ITLS Pediatric Provider Course Advanced Pre-Test
 ITLS Pediatric Provider Course Advanced Pre-Test 1. You arrive at the scene of a motor vehicle crash and are directed to evaluate a child who was in one of the vehicles. The patient appears to be a child
ITLS Pediatric Provider Course Advanced Pre-Test 1. You arrive at the scene of a motor vehicle crash and are directed to evaluate a child who was in one of the vehicles. The patient appears to be a child
The Affects of Music Therapy on Management of Pain and Anxiety During Burn Dressing Changes
 Philadelphia College of Osteopathic Medicine DigitalCommons@PCOM PCOM Physician Assistant Studies Student Scholarship Student Dissertations, Theses and Papers 2014 The Affects of Music Therapy on Management
Philadelphia College of Osteopathic Medicine DigitalCommons@PCOM PCOM Physician Assistant Studies Student Scholarship Student Dissertations, Theses and Papers 2014 The Affects of Music Therapy on Management
CARE OF PATIENTS WITH BURNS. NUR 240 Donna Ricketts, MSN, RN, OCN
 CARE OF PATIENTS WITH BURNS NUR 240 Donna Ricketts, MSN, RN, OCN INCIDENCE/PREVALENCE OF BURN INJURY 5 th most common unintentional injury deaths 3 rd leading cause of fatal home injuries 4,000 burn deaths
CARE OF PATIENTS WITH BURNS NUR 240 Donna Ricketts, MSN, RN, OCN INCIDENCE/PREVALENCE OF BURN INJURY 5 th most common unintentional injury deaths 3 rd leading cause of fatal home injuries 4,000 burn deaths
PRE-HOSPITAL PATIENT CARE PROTOCOLS BASIC LIFE SUPPORT/ADVANCED LIFE SUPPORT
 PRE-HOSPITAL PATIENT CARE PROTOCOLS BASIC LIFE SUPPORT/ADVANCED LIFE SUPPORT Board Approved June 2007 Revised December 2009 Revised July 2011 Revised June 2015 435 Hunter Street Fredericksburg, VA 22401
PRE-HOSPITAL PATIENT CARE PROTOCOLS BASIC LIFE SUPPORT/ADVANCED LIFE SUPPORT Board Approved June 2007 Revised December 2009 Revised July 2011 Revised June 2015 435 Hunter Street Fredericksburg, VA 22401
Burn & Soft Tissue Service Orientation Slides
 Burn & Soft Tissue Service Orientation Slides Damien Wilson Carter, MD Director, Burn/Soft Tissue Service Sue Reeder, BSN, CWOCN Burn Resource Nurse Specialist Scope ALL Burn injuries (> Age 12) Cold injury/
Burn & Soft Tissue Service Orientation Slides Damien Wilson Carter, MD Director, Burn/Soft Tissue Service Sue Reeder, BSN, CWOCN Burn Resource Nurse Specialist Scope ALL Burn injuries (> Age 12) Cold injury/
Skin Anatomy and Physiology
 Skin Anatomy and Physiology Body s largest organ Three layers: Epidermis Dermis Subcutaneous tissue 1 2 Skin Anatomy and Physiology Complex system, variety of functions Sensation Control of water loss
Skin Anatomy and Physiology Body s largest organ Three layers: Epidermis Dermis Subcutaneous tissue 1 2 Skin Anatomy and Physiology Complex system, variety of functions Sensation Control of water loss
European Resuscitation Council
 European Resuscitation Council Incidence of Trauma in Childhood Leading cause of death and disability in children older than one year all over the world Structured approach Primary survey and resuscitation
European Resuscitation Council Incidence of Trauma in Childhood Leading cause of death and disability in children older than one year all over the world Structured approach Primary survey and resuscitation
Research Article The Introduction of a Protocol for the Use of Biobrane for Facial Burns in Children
 Hindawi Publishing Corporation Plastic Surgery International Volume 2011, Article ID 858093, 5 pages doi:10.1155/2011/858093 Research Article The Introduction of a Protocol for the Use of Biobrane for
Hindawi Publishing Corporation Plastic Surgery International Volume 2011, Article ID 858093, 5 pages doi:10.1155/2011/858093 Research Article The Introduction of a Protocol for the Use of Biobrane for
Urgent Care Burn Management. Neil Uspal Division of Emergency Medicine Seattle Children s Hospital October 6 th, 2017
 Urgent Care Burn Management Neil Uspal Division of Emergency Medicine Seattle Children s Hospital October 6 th, 2017 Objectives Epidemiology of Burn Injuries Classification of Burns Initial Burn Management
Urgent Care Burn Management Neil Uspal Division of Emergency Medicine Seattle Children s Hospital October 6 th, 2017 Objectives Epidemiology of Burn Injuries Classification of Burns Initial Burn Management
ELECTRICAL INJURY 9/21/2015 I HAVE NO DISCLOSURES WE HAVE OBTAINED APPROVAL FOR USE OF IDENTIFIABLE PATIENT PHOTOS
 ELECTRICAL INJURY SAMUEL P. MANDELL, MD, MPH ASSISTANT PROFESSOR OF SURGERY UNIVERSITY OF WASHINGTON SEPTEMBER 28, 2015 I HAVE NO DISCLOSURES WE HAVE OBTAINED APPROVAL FOR USE OF IDENTIFIABLE PATIENT PHOTOS
ELECTRICAL INJURY SAMUEL P. MANDELL, MD, MPH ASSISTANT PROFESSOR OF SURGERY UNIVERSITY OF WASHINGTON SEPTEMBER 28, 2015 I HAVE NO DISCLOSURES WE HAVE OBTAINED APPROVAL FOR USE OF IDENTIFIABLE PATIENT PHOTOS
PROOF. Many people will 2REMEMBER ANALGESIA 1PROMPT FIRST AID IS ESSENTIAL 3EFFECTIVE CLEANSING. Ten Top Tips... The management of burn wounds
 ... The management of burn wounds Author: John McRobert Author: Krissie Stiles Many people will experience a burn injury in their lifetime. Burn injuries range from the most severe requiring high levels
... The management of burn wounds Author: John McRobert Author: Krissie Stiles Many people will experience a burn injury in their lifetime. Burn injuries range from the most severe requiring high levels
Burns & its Homoeopathic Management - Pawan Satyanarayan Chandak
 Page 1 of 7 Burns & its Homoeopathic Management Pawan Satyanarayan Chandak A burn is a tissue injury from thermal heat or cold application or from the absorption of physical energy or chemical contact.
Page 1 of 7 Burns & its Homoeopathic Management Pawan Satyanarayan Chandak A burn is a tissue injury from thermal heat or cold application or from the absorption of physical energy or chemical contact.
Continuous Nitrous Oxide Sedation in Paediatrics
 Guideline: Page 1 of 6 Continuous Nitrous Oxide Sedation in Paediatrics Purpose This guideline applies to all nitrous oxide sedation of all children under 15 years of age The aim of this guideline is to
Guideline: Page 1 of 6 Continuous Nitrous Oxide Sedation in Paediatrics Purpose This guideline applies to all nitrous oxide sedation of all children under 15 years of age The aim of this guideline is to
Trauma Life Support Pre-Hospital (TLS-P) Preparatory Materials
 Trauma Life Support Pre-Hospital (TLS-P) Preparatory Materials 1 1. A high-risk bodily fluid for spreading infection is blood. 2. Items that can reduce the spread of infection include masks, gloves, and
Trauma Life Support Pre-Hospital (TLS-P) Preparatory Materials 1 1. A high-risk bodily fluid for spreading infection is blood. 2. Items that can reduce the spread of infection include masks, gloves, and
Arizona Emergency Medical Systems, Inc. RED BOOK CHAPTER 5. Triage: PEDIATRIC Pediatric Emergencies Triage Guidelines
 5-1 Arizona Emergency Medical Systems, Inc. RED BOOK CHAPTER 5 Triage: PEDIATRIC Pediatric Emergencies Triage Guidelines DISCLAIMER The AEMS Red Book is designed to be a resource document for use by Medical
5-1 Arizona Emergency Medical Systems, Inc. RED BOOK CHAPTER 5 Triage: PEDIATRIC Pediatric Emergencies Triage Guidelines DISCLAIMER The AEMS Red Book is designed to be a resource document for use by Medical
Presentation Menu. Walk-in Slide. Full Presentation. Access. Site. Needle. Flush. Comfort. Monitor. Removing the EZ-IO catheter.
 Presentation Menu Walk-in Slide Full Presentation Access Site Needle Flush Comfort Monitor Removing the EZ-IO catheter Clinical Support Explore. Discover. Examine. Vidacare Workshop Programmes www.vidacare.com
Presentation Menu Walk-in Slide Full Presentation Access Site Needle Flush Comfort Monitor Removing the EZ-IO catheter Clinical Support Explore. Discover. Examine. Vidacare Workshop Programmes www.vidacare.com
Homework Assignment Complete and Place in Binder
 Homework Assignment Complete and Place in Binder Chapter # 34/35: Pediatric & Geriatric Emergencies 1. The first month of life after birth is referred to as the: A) neonatal period. B) toddler period.
Homework Assignment Complete and Place in Binder Chapter # 34/35: Pediatric & Geriatric Emergencies 1. The first month of life after birth is referred to as the: A) neonatal period. B) toddler period.
MANAGEMENT OF DENGUE INFECTION IN ADULTS (Revised 2 nd Edition) QUICK REFERENCE FOR HEALTHCARE PROVIDERS
 1 KEY MESSAGES Dengue is a dynamic disease and presented in three phases - febrile phase, critical phase and recovery phase. Clinical deterioration often occurs in the critical phase and is marked by plasma
1 KEY MESSAGES Dengue is a dynamic disease and presented in three phases - febrile phase, critical phase and recovery phase. Clinical deterioration often occurs in the critical phase and is marked by plasma
Directions for the Creation and Use of GHS Labels
 Directions for the Creation and Use of GHS Labels Globally Harmonized System (GHS) labels must have the following elements: 1. Product Name or Identifier 2. Pictograms (See Final Page) 3. Signal Word (Danger
Directions for the Creation and Use of GHS Labels Globally Harmonized System (GHS) labels must have the following elements: 1. Product Name or Identifier 2. Pictograms (See Final Page) 3. Signal Word (Danger
Pediatric Trauma Care
 2013 Standard Trauma Care Procedures (Pediatric) Traumatic injuries require prompt care and transportation. Always suspect cervical injury. Note the mechanism of injury and any other condition that may
2013 Standard Trauma Care Procedures (Pediatric) Traumatic injuries require prompt care and transportation. Always suspect cervical injury. Note the mechanism of injury and any other condition that may
BASICS OF BURN MANAGEMENT
 BASICS OF BURN MANAGEMENT Dr S M Keswani Cosmetic Surgeon National Burns Centre, Airoli,Navi-Mumbai Breach Candy Hospital Wockhardt Hospital National Burns Centre, Airoli, Navi-Mumbai. CLASSIFICATION 1.
BASICS OF BURN MANAGEMENT Dr S M Keswani Cosmetic Surgeon National Burns Centre, Airoli,Navi-Mumbai Breach Candy Hospital Wockhardt Hospital National Burns Centre, Airoli, Navi-Mumbai. CLASSIFICATION 1.
Prehospital Resuscitation for the 21 st Century Simulation Case. VF/Asystole
 Prehospital Resuscitation for the 21 st Century Simulation Case VF/Asystole Case History 1 (hypovolemic cardiac arrest secondary to massive upper GI bleed) 56 year-old male patient who fainted in the presence
Prehospital Resuscitation for the 21 st Century Simulation Case VF/Asystole Case History 1 (hypovolemic cardiac arrest secondary to massive upper GI bleed) 56 year-old male patient who fainted in the presence
RCH Trauma Guideline. Management of Traumatic Pneumothorax & Haemothorax. Trauma Service, Division of Surgery
 RCH Trauma Guideline Management of Traumatic Pneumothorax & Haemothorax Trauma Service, Division of Surgery Aim To describe safe and competent management of traumatic pneumothorax and haemothorax at RCH.
RCH Trauma Guideline Management of Traumatic Pneumothorax & Haemothorax Trauma Service, Division of Surgery Aim To describe safe and competent management of traumatic pneumothorax and haemothorax at RCH.
Clinical Connections April 16, 2014
 Management of Burns Eric McCoy PA-C Kathy Johnston RN, BSN Trauma/Burn Service UPMC Mercy A Long Tradition of Caring Comprehensive burn care from initial treatment through rehabilitation Region s only
Management of Burns Eric McCoy PA-C Kathy Johnston RN, BSN Trauma/Burn Service UPMC Mercy A Long Tradition of Caring Comprehensive burn care from initial treatment through rehabilitation Region s only
Update on Burn Care and Resuscitation
 Niknam Eshraghi, M.D., F.A.C.S General and Burn Surgery; The Oregon Clinic Director; Oregon Burn Center, Legacy Emanuel Medical Center Affiliate Professor of Surgery, Oregon Health Sciences University
Niknam Eshraghi, M.D., F.A.C.S General and Burn Surgery; The Oregon Clinic Director; Oregon Burn Center, Legacy Emanuel Medical Center Affiliate Professor of Surgery, Oregon Health Sciences University
Burn Wound Assessment and Infections
 Burn Wound Assessment and Infections Title of Guideline (must include the word Guideline (not protocol, policy, procedure etc) Contact Name and Job Title (author) Directorate & Speciality Family Health:
Burn Wound Assessment and Infections Title of Guideline (must include the word Guideline (not protocol, policy, procedure etc) Contact Name and Job Title (author) Directorate & Speciality Family Health:
PEMSS PROTOCOLS INVASIVE PROCEDURES
 PEMSS PROTOCOLS INVASIVE PROCEDURES Panhandle Emergency Medical Services System SURGICAL AND NEEDLE CRICOTHYROTOMY Inability to intubate is the primary indication for creating an artificial airway. Care
PEMSS PROTOCOLS INVASIVE PROCEDURES Panhandle Emergency Medical Services System SURGICAL AND NEEDLE CRICOTHYROTOMY Inability to intubate is the primary indication for creating an artificial airway. Care
Wound Management for Nurses/Technicians What do we need to know?
 Wound Management for Nurses/Technicians What do we need to know? Laura Owen European Specialist in Small Animal Surgery Lecturer in Small Animal Surgery, University of Cambridge The Acute Open Wound PPE
Wound Management for Nurses/Technicians What do we need to know? Laura Owen European Specialist in Small Animal Surgery Lecturer in Small Animal Surgery, University of Cambridge The Acute Open Wound PPE
MANAGING THE BURN WOUND
 MANAGING THE BURN WOUND Robert H. Demling, M.D. Leslie DeSanti R.N., Brigham and Women s Hospital Burn Center Harvard Medical School Boston, MA TABLE OF CONTENTS Section I: Section II: Section III: Section
MANAGING THE BURN WOUND Robert H. Demling, M.D. Leslie DeSanti R.N., Brigham and Women s Hospital Burn Center Harvard Medical School Boston, MA TABLE OF CONTENTS Section I: Section II: Section III: Section
Lecture Notes. Chapter 9: Smoke Inhalation Injury and Burns
 Lecture Notes Chapter 9: Smoke Inhalation Injury and Burns Objectives List the factors that influence mortality rate Describe the nature of smoke inhalation and the fire environment Recognize the pulmonary
Lecture Notes Chapter 9: Smoke Inhalation Injury and Burns Objectives List the factors that influence mortality rate Describe the nature of smoke inhalation and the fire environment Recognize the pulmonary
