Clinical Connections April 16, 2014
|
|
|
- Denis Waters
- 6 years ago
- Views:
Transcription
1 Management of Burns Eric McCoy PA-C Kathy Johnston RN, BSN Trauma/Burn Service UPMC Mercy A Long Tradition of Caring Comprehensive burn care from initial treatment through rehabilitation Region s only Level I Regional Resource Trauma and Comprehensive Burn Center 24- hour in-house attending surgeon Adult ABA Verification Dedication to Our Pediatric Patients Enchanted Forest pediatric play area Newly appointed dedicated Child Life Specialist Learn Not to Burn Prevention Program 1
2 Vecta Mobile Sensory Unit Multisensory stimulation used to distract pediatric patients during treatment Optic cable lights, bubble column, projected imagery and aroma therapy Anatomy of the Skin Skin is the largest organ in the body. The skin consists of three layers: Epidermis Consists of five layers (stratum) Tough non-vascular protective barrier Dermis Consists of two layers Nerve endings, blood vessels, hair follicles, sebaceous and sweat glands & sensory fibers Subcutaneous Tissue Adipose tissue, major blood vessels and nerves Functions of the Skin Maintenance of Body Temperature Production of Vitamin D A Barrier Prevents evaporative water loss Protection for microorganisms Protection from environment Sensations of touch, pressure and pain Cosmetic Appearance 2
3 Incidence of Burn Injuries Overall a decreased incidence in the number of burn injuries as well as hospitalizations and deaths. Yet, annually in the United States: Approximately 1 million people require medical attention from burn injuries. 700,000 ER visits; of which 45,000 people are hospitalized Deaths from burn / smoke inhalation injuries account for 4,500 deaths. Most burn injuries occur in the home 75% are victims of their own actions Populations at highest risk: pediatric and elderly Special Populations Pediatric Clients Thinner skin; prone to more severe injury Greater body surface area / to weight ratio Greater evaporative fluid losses hypovolemia Rapid heat losses hypothermia Reduce metabolic reserves; prone to hypoglycemia Small airways more difficult to secure Immature immunological response sepsis Consider possibility of abuse / neglect Abuse & Burn Injuries Abuse & Burn Injuries Can occur in any age group; children highest incidence Burn injuries accounts for 10% of all child abuse cases Suspect Abuse When: Burn distribution inconsistent with reported incident Delay in seeking medical attention History of family instability Inability to cope with stress in time of crisis Laws Related to Suspicion of Abuse Must report suspected abuse cases!! 3
4 Causes of Burn Injuries Thermal Electrical Chemical Radiation Cold Injuries Inhalation Causes of Burn Injuries Thermal Injuries (most common) Contact Direct contact with hot object (i.e. pan or iron) Anything that sticks to skin (i.e. tar, grease or foods) Scalding Direct contact with hot liquid / vapors (moist heat) i.e. cooking, bathing or car radiator overheating Single most common injury in the pediatric client Flame Direct contact with flame (dry heat) i.e. structural fires / clothing catching on fire Causes of Burn Injuries Electrical Contact with an electrical current i.e. open wiring or being struck by lightening Pediatrics: chewing on electrical cord or placing object in outlet Require some different management Chemical Strong acids or alkaloids i.e. household cleaning products Management specific to chemical involved 4
5 Causes of Burn Injuries Radiation Prolonged exposure to ultraviolet rays of the sun Other sources: occupational or medical therapies Cold Injuries Frostbite Don t forget all burns not from heat!! Injury due to freezing & refreezing of intracellular fluid Ice crystals puncture the cells and destroy tissue Can result in amputation Causes of Burn Injuries Inhalation Injuries Suspect inhalation injury when: Burn occurred within a closed space Burns to face or neck Singed nasal hair or eyebrows Hoarseness, voice changes, wheezing or stridor Sooty sputum Brassy cough or drooling Labored breathing or tachypnea Erythema and blistering of oral or pharyngeal mucosa Often requires intubation & mechanical ventilation Causes of Burn Injuries Inhalation Injuries Cont., Carbon Monoxide Poisoning Most common inhalation injury May occur with or without cutaneous burns Hemoglobin s affinity for carbon monoxide is 200x greater than that for oxygen; result = hypoxia Diagnosis: Serum COHb levels & ABG s Pulse Ox: false readings!! Management: 100% O2 Face mask or mechanical ventilation 5
6 Classification of Burn Injuries Depth of Burn Injury Superficial-Thickness Partial Thickness Superficial Deep Full Thickness Deep-Full Thickness Size of Burn Injury Total body surface area (TBSA) burned Clinical Management of Burns Daily Hydrotherapy in the burn center by trained burn unit nurse in collaborating with techs, PA s and MD s. All burn dressings changed by burn nurse or technician. Goal of wound care is to promote healing and prevent infection. Teaching. 17 Principle of Wound Care Remove nonviable tissue Minimize risk of infection Promote epithelialization Decrease drying of wound bed 18 6
7 Superficial-Thickness Burns Involves the epidermis Wound Appearance: Red to pink Mild edema Dry and no blistering Pain / hypersensitivity to touch i.e. Classic sunburn Desquamation (peeling of dead skin) occurs 2-3 days post-burn Wound Healing: In 3 to 5 days (spontaneous) No scarring / other complications Partial-Thickness Burns Superficial, partial-thickness Involves upper 1/3 of dermis Wound Appearance: Red to pink Wet and weeping wounds Thin-walled, fluid-filled blisters Mild to moderate edema Extremely painful Wound Healing: In 2 weeks (spontaneous) Minimal scarring; minor pigment discoloration may occur Partial-Thickness Burns 7
8 Partial-Thickness Burns Care of Partial Thickness Burns Topical antimicrobials are used to control bacteria growth and decrease likelihood of wound infection. Signs of infection : Foul smell Green drainage Elevated temperature Erythema of skin and tissues surrounding wound Common Topical Agents Silvadene Sulfamylon cream Triple antibiotic ointment Santyl / Polysporin Mepilex Ag Medihoney 23 Deep Partial-Thickness Burns 8
9 Deep Partial-Thickness Burns Involves larger portion of dermis (not complete) Wound Appearance: Mottled: Red, pink, or white area Moist No blisters Moderate edema Painful; usually less severe Wound Healing: May heal spontaneously 2-6 weeks Hypertrophic scarring / formation of contractures Wound Management: Treatment of choice: surgical excision & skin grafting Deep Partial-Thickness Burns Deep Partial-Thickness Burns 9
10 Full-Thickness Burns Involves the entire epidermis and dermis Wound Appearance: Dry, leathery and rigid + Eschar (hard and in-elastic) Red, white, yellow, brown or black Severe edema Painless & insensitive to palpation Wound Healing: No spontaneous healing; weeks to months with graft Wound Management: Surgical excision & skin grafting Full-Thickness Burns Full-Thickness Burns 10
11 Complications Deep partial thickness to full thickness injury may cause increasing tissue pressure due to capillary leak, inelasticity and inflammatory response resulting in Compartment Syndrome. Signs and Symptoms are the 5 P s : Pain Pallor Pulselessness Paresthesia's Paralysis Surgical intervention such as escharotomy or fasciotomy are required to restore circulation to effected area. 31 Deep Full-Thickness Burns Extends beyond the skin to include muscle, tendons & possibly bone. Wound Appearance: Black (dry, dull and charred) Eschar tissue: hard, in-elastic No edema Painless & insensitive to palpation Wound Healing: No spontaneous healing; weeks to months with graft Wound Management: Surgical excision & skin grafting Frequently requires amputation if extremity involved Deep Full-Thickness Burns 11
12 Deep Full-Thickness Burns Classification of Burn Injuries Size of a Burn Injury Total Body Surface Area (TBSA) Burned Palmar Method A quick method to evaluate scattered or localized burns Client s palm = 1 % TBSA Rule of Nines A quick method to evaluate the extent of burns Major body surface areas divided into multiples of nine Modified version for children and infants Lund-Browder Method Most Accurate; based on age (growth) Can be used for the adult, children & infants Classification of Burn Injuries 12
13 Classification of Burn Injuries Severity of Burn Injuries Treatment of burns is directly related to the severity of injury! Severity is determined by: Depth of burn injury Total body surface (TBSA) burned Location of burn All burns of the face, hands, feet, face or perineum are considered severe!! Client s Age Presences of other preexisting medical conditions or trauma Critical Care Criteria Greater than 20% TBSA thermal burns Inhalation Injury Electrical Injury Fluid balance Temperature regulation Comorbid Conditions > extremes of age > pre-existing medical conditions > malnutrition > immunocompromised 39 13
14 Pain Management Critically ill patients requiring mechanical ventilation Fentanyl (narcotic opiate) continuous IV drip for pain control Propofol (hypnotic/amnestic) continuous IV drip for sedation Medications are ordered to be titrated for a riker sedation scale as ordered by the physician. 40 Pain Management, cont. Acute Interventional Pain Service Consult (AIPPS) Local blocks Ketamine infusions IV Selected Opiates Neurontin 41 Managing Pain for Dressings Pediatric Patients receive Conscious Sedation by pediatriccertified anesthesia personnel in the hydrotherapy and are recovered in their rooms by staff nurse. Adult patients receive pre-medication, usually PO opiates prior to dressing changes, with additional narcotic boluses during procedures as directed by physicians. Dedicated Physicians Assistant available at all times during dressing changes to evaluate wounds and pain control
15 Pain Conclusion Pain control is a huge issue for burn patients from initial injury through-out rehabilitation. Transition is made as healing occurs from AIPPS to the Chronic Pain Service as needed. 43 Prognosis Patient outcome dependent largely on depth and extent of injury. Also influenced by such indicators as. Age Location of wounds Mechanism of injury 44 Phases of Burn Care Resuscitation Acute Rehabilitation 15
16 Current Status of Burn Resuscitation Initial management follows the guidelines established by ATLS course of the American College of Surgeons ABC s of critical burns have several complicating variables Airway Initial evaluation by history, symptoms and physical findings Intubation required Unconscious patients Obvious respiratory distress Hemodynamic instability Airway Hard signs and symptoms Dyspnea Chest tightness Tachypnea Stridor Use of accessory muscles Swelling of the tongue and oropharynx Immediate intubation!! 16
17 Inhalational Injuries Inhalational injuries complicate nearly one third of all major burns Doubles the mortality of cutaneous burns Three distinct components Carbon monoxide poisoning Upper airway thermal burns Lower airway chemical injuries Airway Suspect inhalational injury Fires in closed spaces Facial burns Singeing of facial hairs Oropharyngeal carbon deposits Carbonaceous sputum HOUSEFIRE SMOKE TOXIC ELEMENTS GAS SOURCE EFFECT Carbon Monoxide Organic Matter Tissue Hypoxia Carbon Dioxide Organic Matter Narcosis Hydrogen Chloride Plastics (PVC) Mucosal Irritation Hydrogen Cyanide Polyurethane Respiratory Failure Benzene Petroleum plastics Mucosal irritation Aldehydes Wood, cotton, paper Severe mucosal and lung damage 17
18 Carbon Monoxide Produced by the combustion of organic material Systemic poison Inhibits transport and mitochondrial use of oxygen Pulse oximeter gives spuriously high reading for O2 saturation COHgb assessment must be made by ABG Carbon Monoxide Poisoning 0% - 5% = Normal value 15% - 20% = Headache, confusion 20% - 40% = Visual changes, nausea 40% - 60% = Hallucinations, combativeness, coma > 60% = Mortality rate > 50% Carbon Monoxide Poisoning Treatment 1/2 life on room air = 240 minutes 1/2 life at 100% FIO2 = min (tight- fitting nonrebreather face mask or ET tube HBO (O2 at 3 atm.) will shorten 1/2 life even further Several randomized, controlled trials have failed to show significant benefit over 100% O2 (Tibbles, Perrota, Ann. Em. Med. 1994) 18
19 Upper Airway Thermal Injuries Occur due to hot air or chemical toxins Dx by direct laryngoscopy Swelling, sloughing, carbonaceous sputum below vocal cords Indication for prophylactic intubation Manifest within 48 hrs of injury Maximal swelling hrs Lower Airway Thermal Injuries Injury to tracheobronchial tree and lung parenchyma Due to combustion products in smoke and inhaled steam Atelectasis Decreased ciliary action Pooling of secretions Bronchorrhea Bronchospasm Lower Airway Thermal Injuries 19
20 Timeline of Inhalational Injuries 0-36 hours Carbon monoxide poisoining Upper airway obstruction Bronchospasm hours Pulmonary edema Atelectasis Tracheobronchiitis 3-10 days post injury Bronchopneumonia/ARDS Diagnosis of Inhalational Injuries High index of suspicion History/physical exam Chest x-ray and CT not helpful Fiberoptic bronchoscopy May use local anesthesia only Place appropriate sized endotracheal tube over scope Treatment of Inhalational Injuries Treatment begins at scene Secure airway 100% oxygen until COHgb <10% Carboxyhemoglobin and ABG obtained Consider checking cyanide level with hypoxia/acidosis Meticulous pulmonary hygiene Frequent airway suctioning Chest physiotherapy Early mobilization Percussive and vibratory techniques 20
21 Breathing Always recognize associated trauma!! Tension pneumothorax, pulmonary contusion, head/spinal injuries Circumferential third degree burns to the chest Restricts chest wall expansion Decreases lung compliance Increased airway pressures Escharotomy!! Circulation Two large bore IV s Access through unburned skin preferred Avoid in limbs distal to areas of circumferential burns Tourniquet effect Cutdowns associated with high infection rates Interosseous preferred 21
22 Circulation Goal is restoration of adequate tissue perfusion and cardiovascular function with the least amount of administered fluid Optimal survival Fewest adverse events Calculations based on weight and burn size Include only areas of partial and full thickness dermal injury Burn size initially based on rule of nines Rule of Nines 9% Head Each upper extremity 18% Each leg Anterior trunk Posterior trunk Underestimates head size in children Fluid Resuscitation Oral resuscitation Children with less than 10-15% TBSA Requires close monitoring Nausea and vomiting Gastric ileus 22
23 Adult Burn Resuscitation Formulas Crystalloid fluid resuscitation based on Parkland or modified Brooke formula LR most popular 4cc x kg x % TBSA Half of fluid requirements given over first eight hours, half over the next 16 hours Fluid Resuscitation in Pediatric Burn Patient Children require more fluid Greater ratio of surface area to volume Hypoglycemia Limited glycogen stores 5% dextrose maintenance fluid <2 years old Monitoring Resuscitation Gross tissue edema has no direct correlation to adequacy of intravascular volume Urinary output is prime indicator of adequate tissue perfusion Adults: 0.5 to 1 ml/kg/hr Children: 1 to 1.5 ml/kg/hr Infants: 1.5 ml/kg/hr 23
24 Fluid Resuscitation Factors associated with increased requirements Delayed resuscitation Scald burn injuries Inhalational injuries High-voltage electrical injuries Hyperglycemia Alcohol intoxication Patients on chronic diuretic therapy Associated trauma Fluid Resuscitation Rhabdomyolysis Suspect with deep burns, electrical burns, compartment syndromes Results in myoglobinuria and acute tubular necrosis Maintain urine output >100cc/hr Consider alkalinization and mannitol Fluid Resuscitation No single perfect formula Adverse consequences Poor tissue perfusion Abdominal compartment syndrome Extremity compartment syndrome Pulmonary edema Pleural effusion 24
25 Wound Management Wound Management Thermal injury disrupts protective barrier function of skin Dressings protect against environmental flora and evaporative heat loss Superficial wounds Promote re-epithelialization Partial-thickness, full-thickness Protect against microbial colonization Wound Management Topical antimicrobials Eschar devitalized and avascular systemic antibiotics do not reach Topicals delay wound colonization and infection Promote spontaneous wound healing Early excision and grafting still key 25
26 Topicals Burn Excision and Grafting Importance of excision not recognized until 1970 s Required for deep partial-thickness and full-thickness burns Necrotic tissue is nidus for development of infection and burn wound sepsis Improves survival, reduces infection rate, shortens hospital stay, decreases scarring Burn Excision and Grafting Excision may begin as early as post-burn day 3 Extensive burns - serial operations placed several days apart Temporarily cover with biologic dressing, xenograft, cadaveric allograft until autograft available 26
27 Grafting Selection of depth Full-thickness: entire thickness of dermis Partial-thickness: partial thickness of dermis (0.08 to 0.20 in.) Thicker grafts contract less Burn size may require re-cropping Grafting Applied as sheet (unmeshed) or meshed grafts Meshing minimizes hematoma/seroma formation Sheet more aesthetic Autograft: Sheet Autograft: Meshed 27
28 Donor Site: Wound Considerations The donor site is often the most painful aspect for the post-operative client. We have created a brand new wound!! Variety of products are used for donor sites. Most are left place for 24 hours and then left open to air. Donor sites usually heal in 7-10 days 28
29 Advances in Wound Closure: Biological Dressings Biological dressings Cadaver allograft Porcine xenograft Amniotic membranes Xenograft Allograft Advances in Wound Closure: Skin Substitutes Dermal replacement material Integra TM Bi-laminar composite with bovine collagen neodermis, silicone neoepidermis Alloderm TM Acellular allogenic dermal matrix Cultured epithelial autografts Stem cell culture technology Negative Pressure Wound Therapy Advances in Wound Closure Integra TM CEA 29
30 Rehabilitation Phase Begins day one and may last several years Nursing, OT and PT are major providers Meticulous asepsis continues to be important Major areas of focus: Support of adequate wound healing Prevention of hypertrophic scarring & contractures Psychosocial Support Client and family Promotion of maximal functional independence Hypertrophic Scar Formation Excessive scar formation, which rises above the level of the skin Management: Pressure Garments Elasticized garments that are custom fitted Maintains constant pressure on the wound Result: smoother skin & minimized scar appearance Client Considerations: Must be worn 23 hours a day Need to be worn for up to 1-2 years Are very hot and tight!! Contracture Formation Shrinkage and shortening of burned tissue Results in disfigurement Especially if burn injury involves joints Management is opposing force: Splints, proper positioning and ROM Must begin at day one!! Multidisciplinary approach is essential!! 30
31 Psychosocial Considerations Alterations in Body Image Loss of Self-Esteem Returning to community, work or school Sexuality Supports Services Psychologist, social work & vocational counselors Local or national burn injury support organizations Nursing Considerations Encourage client & family to express feelings Assist in developing positive coping strategies Psychosocial Considerations LISTEN AND PROVIDE REALISTIC SUPPORT!! Be honest about possible scarring Remember people come to terms with the change in their appearance at their own pace. Provide reassurance that skin grafts always look worse before they look better. Remember how a client looks at discharge is not how they will look in 2 years. The Skin Cell Gun Research collaborative with McGowan Institute of Regenerative Medicine Experimental study using human burn victims 31
32 32
33 Burn Center Criteria Partial thickness burns > 10% TBSA Face, hands, feet, genitalia, perineum, major joints Full thickness burns; any age or size Electrical burns Chemical burns Inhalation injury Pre-existing medical disorders Concomitant trauma, particularly if burn injury poses greatest risk Children Special social, emotional, or long-term rehabilitative intervention 33
BURNS MODULE. In the paediatric population consider non-accidental injury as a mechanism for burn injuries.
 BURNS MODULE INTRODUCTION Burns are a common cause of trauma. Most burn injuries are a result of flame burns, with scalds also occurring commonly. Electrical and chemical burns are less common. 1 Concurrent
BURNS MODULE INTRODUCTION Burns are a common cause of trauma. Most burn injuries are a result of flame burns, with scalds also occurring commonly. Electrical and chemical burns are less common. 1 Concurrent
At the conclusion of this course the learner will be able to
 Objectives At the conclusion of this course the learner will be able to 1. Discuss basic anatomy and pathophysiology of burns 2. Describe burn injuries in terms of size, depth, coloration and characteristics
Objectives At the conclusion of this course the learner will be able to 1. Discuss basic anatomy and pathophysiology of burns 2. Describe burn injuries in terms of size, depth, coloration and characteristics
1/3/2008. Karen Burke Priscilla LeMone Elaine Mohn-Brown. Medical-Surgical Nursing Care, 2e Karen Burke, Priscilla LeMone, and Elaine Mohn-Brown
 Medical-Surgical Nursing Care Second Edition Karen Burke Priscilla LeMone Elaine Mohn-Brown Chapter 46 Caring for Clients with Burns Types of Burns Thermal Dry heat flame Moist heat steam or hot liquid
Medical-Surgical Nursing Care Second Edition Karen Burke Priscilla LeMone Elaine Mohn-Brown Chapter 46 Caring for Clients with Burns Types of Burns Thermal Dry heat flame Moist heat steam or hot liquid
Pediatric Burn Management Justin D. Klein, MD Associate Burn Director Lisa C. Vitale, RN Burn Program Coordinator
 Pediatric Burn Management Justin D. Klein, MD Associate Burn Director Lisa C. Vitale, RN Burn Program Coordinator Lecture Overview Burn statistics and etiologies Pre-hospital evaluation Anatomy of a burn
Pediatric Burn Management Justin D. Klein, MD Associate Burn Director Lisa C. Vitale, RN Burn Program Coordinator Lecture Overview Burn statistics and etiologies Pre-hospital evaluation Anatomy of a burn
Approved By: Airway and Breathing A. Initially give humidified high flow oxygen at 15 L (100%) using a nonrebreather
 Subject: BURN CARE CLINICAL GUIDELINE Originator: Approval Date: 2015 Approved By: Policy: All burn patients presenting to XXXXXX Hospital will have appropriate assessment, stabilization and evaluation
Subject: BURN CARE CLINICAL GUIDELINE Originator: Approval Date: 2015 Approved By: Policy: All burn patients presenting to XXXXXX Hospital will have appropriate assessment, stabilization and evaluation
Children's National Medical Center The Division of Trauma and Burn Burn Education Module Post-test
 Children's National Medical Center The Division of Trauma and Burn Burn Education Module Post-test Purpose: To provide nurses with on overview of burn injuries in pediatric patients. Learning Objectives:
Children's National Medical Center The Division of Trauma and Burn Burn Education Module Post-test Purpose: To provide nurses with on overview of burn injuries in pediatric patients. Learning Objectives:
Burn Priorities of Care: Triage/Treatment/Transfer. Via Christi Regional Burn Center Sarah Fischer, MSN, RN
 Burn Priorities of Care: Triage/Treatment/Transfer Via Christi Regional Burn Center Sarah Fischer, MSN, RN Disclosure I have nothing to disclose Objectives Identify American Burn Association referral criteria
Burn Priorities of Care: Triage/Treatment/Transfer Via Christi Regional Burn Center Sarah Fischer, MSN, RN Disclosure I have nothing to disclose Objectives Identify American Burn Association referral criteria
IMMEDIATE EMERGENCY BURN CARE » THERMAL BURNS » ELECTRICAL BURNS » CHEMICAL BURNS FIRST AID FOR THE THREE MAJOR CATEGORIES
 IMMEDIATE EMERGENCY BURN CARE 1. Treat according to BLS or ACLS Protocol 2. Use airway and C-Spine precautions. 3. Stop the burning process. FIRST AID FOR THE THREE MAJOR CATEGORIES» THERMAL BURNS + Stop
IMMEDIATE EMERGENCY BURN CARE 1. Treat according to BLS or ACLS Protocol 2. Use airway and C-Spine precautions. 3. Stop the burning process. FIRST AID FOR THE THREE MAJOR CATEGORIES» THERMAL BURNS + Stop
Objectives. Initial Burn Care and Fluid Resuscitation 6/5/2015 INITIAL MANAGEMENT
 Initial Burn Care and Fluid Resuscitation Sarah Taylor MSN, RN, ACNS-BC Clinical Nurse Specialist Trauma Burn Center University of Michigan Health System Ann Arbor, MI Objectives Discuss the initial assessment
Initial Burn Care and Fluid Resuscitation Sarah Taylor MSN, RN, ACNS-BC Clinical Nurse Specialist Trauma Burn Center University of Michigan Health System Ann Arbor, MI Objectives Discuss the initial assessment
Burn Injuries & Its Management M JARI.MD
 Burn Injuries & Its Management M JARI.MD 1 BURNS Wounds caused by exposure to: 1. excessive heat 2. Chemicals 3. fire/steam 4. radiation 5. electricity 2 BURNS Results in 10-20 thousand deaths annually
Burn Injuries & Its Management M JARI.MD 1 BURNS Wounds caused by exposure to: 1. excessive heat 2. Chemicals 3. fire/steam 4. radiation 5. electricity 2 BURNS Results in 10-20 thousand deaths annually
Dóra Ujvárosy MD. Medical University of Debrecen Oxyology and Emergency Department
 Dóra Ujvárosy MD. Medical University of Debrecen Oxyology and Emergency Department Functions Definition A burn is a type of injury to the skin caused by heat, electricity, chemicals, light, radiation or
Dóra Ujvárosy MD. Medical University of Debrecen Oxyology and Emergency Department Functions Definition A burn is a type of injury to the skin caused by heat, electricity, chemicals, light, radiation or
Burns. A Comprehensive Review Assessment & Management
 Burns A Comprehensive Review Assessment & Management 1 Objectives Understand types of Burns Understand the pathophysiology of the Burns Understand Rule of Nine Understand Classification of Burns Identify
Burns A Comprehensive Review Assessment & Management 1 Objectives Understand types of Burns Understand the pathophysiology of the Burns Understand Rule of Nine Understand Classification of Burns Identify
EmergencyKT: Management of Thermal Injury in Adult Patients
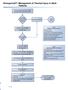 EmergencyKT: Management of Thermal Injury in Adult Patients Remove patient from source of injury, including burned clothing and jewelry Does patient appear to have minor burns? (See Box A) No Notify Burn
EmergencyKT: Management of Thermal Injury in Adult Patients Remove patient from source of injury, including burned clothing and jewelry Does patient appear to have minor burns? (See Box A) No Notify Burn
PEDIATRIC TRAUMA I: ABDOMINAL TRAUMA BURNS. December 19, 2012
 PEDIATRIC TRAUMA I: ABDOMINAL TRAUMA BURNS Niel F. Miele,, M.D. December 19, 2012 EPIDEMIOLOGY Major Trauma responsible for
PEDIATRIC TRAUMA I: ABDOMINAL TRAUMA BURNS Niel F. Miele,, M.D. December 19, 2012 EPIDEMIOLOGY Major Trauma responsible for
Advanced Paediatric Nursing. Burn Trauma. 26 April Wong Tze Wing NC (Burns), Burns Centre, Surgery, PWH
 Advanced Paediatric Nursing Burn Trauma 26 April 2016 Wong Tze Wing NC (Burns), Burns Centre, Surgery, PWH Objective: Understand burn trauma in children Understand Important nursing interventions in burn
Advanced Paediatric Nursing Burn Trauma 26 April 2016 Wong Tze Wing NC (Burns), Burns Centre, Surgery, PWH Objective: Understand burn trauma in children Understand Important nursing interventions in burn
Wisecracks 1. What are the indications for an escharotomy 2. What are the primary considerations in mechanical ventilation of burn patients
 Chapter 63 Thermal Burns Episode Overview Questions 1. List zones of burns 2. List 6 indications for intubation in the burn patient 3. List and describe 2 formulas for fluid resuscitation 4. Describe depth
Chapter 63 Thermal Burns Episode Overview Questions 1. List zones of burns 2. List 6 indications for intubation in the burn patient 3. List and describe 2 formulas for fluid resuscitation 4. Describe depth
Management of Acute Burn Injuries: The First 24 Hours
 Speaker Disclosure I, Debbie Harrell, MSN, RN, NE BC, have no financial relationships to disclose. I will not discuss off label uses of any pharmaceutical products or medical devices. Management of Acute
Speaker Disclosure I, Debbie Harrell, MSN, RN, NE BC, have no financial relationships to disclose. I will not discuss off label uses of any pharmaceutical products or medical devices. Management of Acute
BLS, ILS, ALS OTEP BURNS BURN INTRODUCTION TYPES OF BURNS
 BURNS BLS, ILS, ALS OTEP While we do understand this presentation is an instructional tool for all levels of certification, taking this into consideration everyone taking this class must remember that
BURNS BLS, ILS, ALS OTEP While we do understand this presentation is an instructional tool for all levels of certification, taking this into consideration everyone taking this class must remember that
Burns and electrical injuries. Shelley Westwood, RN, BSN
 Burns and electrical injuries Shelley Westwood, RN, BSN Burns A burn is an injury caused by fire, heat, chemicals, radiation, or electricity. Burns are traumatic in that they can cause extreme pain, permanent
Burns and electrical injuries Shelley Westwood, RN, BSN Burns A burn is an injury caused by fire, heat, chemicals, radiation, or electricity. Burns are traumatic in that they can cause extreme pain, permanent
INITIAL CARE AND TREATMENT OF BURN INJURIES. November 10,
 INITIAL CARE AND TREATMENT OF BURN INJURIES 2 11/10/2012 November 10, 2012 2 Oregon Burn Center Only burn center in Oregon and SW Washington New unit 16 beds, 20,000 square feet Opened in February 2002
INITIAL CARE AND TREATMENT OF BURN INJURIES 2 11/10/2012 November 10, 2012 2 Oregon Burn Center Only burn center in Oregon and SW Washington New unit 16 beds, 20,000 square feet Opened in February 2002
Epidemiology. Burn Rehabilitation. Epidemiology. Epidemiology. United States. United States Cause of injury. Incidence has declined
 Burn Rehabilitation Peter Esselman, MD Professor and Chair Department of Rehabilitation Medicine University of Washington Epidemiology United States 450,000 burn injuries/year in USA that receive medical
Burn Rehabilitation Peter Esselman, MD Professor and Chair Department of Rehabilitation Medicine University of Washington Epidemiology United States 450,000 burn injuries/year in USA that receive medical
Lecture Notes. Chapter 9: Smoke Inhalation Injury and Burns
 Lecture Notes Chapter 9: Smoke Inhalation Injury and Burns Objectives List the factors that influence mortality rate Describe the nature of smoke inhalation and the fire environment Recognize the pulmonary
Lecture Notes Chapter 9: Smoke Inhalation Injury and Burns Objectives List the factors that influence mortality rate Describe the nature of smoke inhalation and the fire environment Recognize the pulmonary
Current Trends in Burn Care
 Objectives Current Trends in Burn Care Jordan Murphy, BSN, CFRN Clinical Educator-KY/FL PHI Air Medical Describes normal skin anatomy. Differentiates pathophysiology related to etiology of injury. Identify
Objectives Current Trends in Burn Care Jordan Murphy, BSN, CFRN Clinical Educator-KY/FL PHI Air Medical Describes normal skin anatomy. Differentiates pathophysiology related to etiology of injury. Identify
Speaker Disclosure Emergent Burn Care I, Debbie Harrell, MSN, RN, NE BC, have no financial relationships to disclose.
 Speaker Disclosure Emergent Burn Care I, Debbie Harrell, MSN, RN, NE BC, have no financial relationships to disclose. Debbie Harrell RN, MSN, Shriners Hospitals for Children Cincinnati Cincinnati, Ohio
Speaker Disclosure Emergent Burn Care I, Debbie Harrell, MSN, RN, NE BC, have no financial relationships to disclose. Debbie Harrell RN, MSN, Shriners Hospitals for Children Cincinnati Cincinnati, Ohio
Pediatrics Grand Rounds 1 June University of Texas Health Science Center at San Antonio. Management of Burn Wounds. Management of Burn Wounds
 Management of Burn Wounds Management of Burn Wounds History of Burn Care Pathophysiology of Burn Lillian F. Liao, MD, MPH Division of Trauma and Emergency Surgery Department of Surgery UTHSCSA Acute burn
Management of Burn Wounds Management of Burn Wounds History of Burn Care Pathophysiology of Burn Lillian F. Liao, MD, MPH Division of Trauma and Emergency Surgery Department of Surgery UTHSCSA Acute burn
Erin P. Frazier, OTR/L Occupational Therapist Jessica Maher, PT, MSPT Physical Therapist
 Management of Burns for The Pediatric Patient Erin P. Frazier, OTR/L Occupational Therapist efrazier@mwph.org Jessica Maher, PT, MSPT Physical Therapist jmaher@mwph.org Mt. Washington Pediatric Hospital
Management of Burns for The Pediatric Patient Erin P. Frazier, OTR/L Occupational Therapist efrazier@mwph.org Jessica Maher, PT, MSPT Physical Therapist jmaher@mwph.org Mt. Washington Pediatric Hospital
Chapter 23 Caring for Clients with Burns
 Chapter 23 Caring for Clients with Burns Burn Injuries 4500 people die from burns each year High risk group ~ children and the elderly The most common cause of burns Smoking material Scalding Lighting
Chapter 23 Caring for Clients with Burns Burn Injuries 4500 people die from burns each year High risk group ~ children and the elderly The most common cause of burns Smoking material Scalding Lighting
The immediate management of burns patients should be similar to management of trauma.
 CATS Clinical Guideline Burns The National Burn Care Review recommends that children with burns should be treated in a Burn Centre. Chelsea and Westminster may take non-ventilated children, Broomfield
CATS Clinical Guideline Burns The National Burn Care Review recommends that children with burns should be treated in a Burn Centre. Chelsea and Westminster may take non-ventilated children, Broomfield
INTRODUCTION OBJECTIVES. When the student has finished this module, he/she will be able to:
 Burn Care and Management WWW.RN.ORG Reviewed September 2017, Expires September 2019 Provider Information and Specifics available on our Website Unauthorized Distribution Prohibited 2017 RN.ORG, S.A., RN.ORG,
Burn Care and Management WWW.RN.ORG Reviewed September 2017, Expires September 2019 Provider Information and Specifics available on our Website Unauthorized Distribution Prohibited 2017 RN.ORG, S.A., RN.ORG,
Burns Management in the Emergency Department
 Management in the Emergency Department (Referral Proforma) Time/Date of injury (24hr) Patient demographic data sticker Airway Please remember to protect C-spine until clinically cleared as stable Administer
Management in the Emergency Department (Referral Proforma) Time/Date of injury (24hr) Patient demographic data sticker Airway Please remember to protect C-spine until clinically cleared as stable Administer
Mr Zachary Moaveni Plastic Surgeon, Middlemore Hospital. Mr Adam Bialostocki Plastic Surgeon, Tauranga
 Mr Zachary Moaveni Plastic Surgeon, Middlemore Hospital Mr Adam Bialostocki Plastic Surgeon, Tauranga Mr. Adam Bialostocki Plastic Surgeon Minor Burns First Aid Remove the burning agent / wet clothes
Mr Zachary Moaveni Plastic Surgeon, Middlemore Hospital Mr Adam Bialostocki Plastic Surgeon, Tauranga Mr. Adam Bialostocki Plastic Surgeon Minor Burns First Aid Remove the burning agent / wet clothes
Burn & Soft Tissue Service Orientation Slides
 Burn & Soft Tissue Service Orientation Slides Damien Wilson Carter, MD Director, Burn/Soft Tissue Service Sue Reeder, BSN, CWOCN Burn Resource Nurse Specialist Scope ALL Burn injuries (> Age 12) Cold injury/
Burn & Soft Tissue Service Orientation Slides Damien Wilson Carter, MD Director, Burn/Soft Tissue Service Sue Reeder, BSN, CWOCN Burn Resource Nurse Specialist Scope ALL Burn injuries (> Age 12) Cold injury/
Initial assessment. ATLS/ABLS protocol and assess for other injuries/fractures based on mechanism. Inhalational injury. Vascular compromise:
 Complex Hand Burns Brent Egeland, MD Assistant Professor Dell Medical School Department of Surgery and Perioperative Care Institute of Reconstructive Plastic Surgery Plastic, Hand, and Reconstructive Microsurgery
Complex Hand Burns Brent Egeland, MD Assistant Professor Dell Medical School Department of Surgery and Perioperative Care Institute of Reconstructive Plastic Surgery Plastic, Hand, and Reconstructive Microsurgery
CARE OF PATIENTS WITH BURNS. NUR 240 Donna Ricketts, MSN, RN, OCN
 CARE OF PATIENTS WITH BURNS NUR 240 Donna Ricketts, MSN, RN, OCN INCIDENCE/PREVALENCE OF BURN INJURY 5 th most common unintentional injury deaths 3 rd leading cause of fatal home injuries 4,000 burn deaths
CARE OF PATIENTS WITH BURNS NUR 240 Donna Ricketts, MSN, RN, OCN INCIDENCE/PREVALENCE OF BURN INJURY 5 th most common unintentional injury deaths 3 rd leading cause of fatal home injuries 4,000 burn deaths
Burns and Scalds. Treatment and Management. Accident and Emergency Department. Royal Surrey County Hospital. Patient information leaflet
 Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Burns and Scalds Treatment and Management Accident and Emergency Department A Burn is an injury caused to the skin by thermal
Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Burns and Scalds Treatment and Management Accident and Emergency Department A Burn is an injury caused to the skin by thermal
Thermal Burns PFN: SOMEML07. Terminal Learning Objective. References. Hours: 3.0 Instructor: Action: Communicate knowledge of thermal burns
 Thermal Burns PFN: SOMEML07 Hours: 3.0 Instructor: Slide 1 Terminal Learning Objective Action: Communicate knowledge of thermal burns Condition: Given a lecture in a classroom environment Standard: Received
Thermal Burns PFN: SOMEML07 Hours: 3.0 Instructor: Slide 1 Terminal Learning Objective Action: Communicate knowledge of thermal burns Condition: Given a lecture in a classroom environment Standard: Received
Applicable to. Team Members Performing
 Protocol: Pediatric Burn Inhalation Injury Category Clinical Practice Protocol Number Approval Date November 1, 2016 Due for review November 1, 2018 Applicable to VUH Children s DOT VMG Off-site locations
Protocol: Pediatric Burn Inhalation Injury Category Clinical Practice Protocol Number Approval Date November 1, 2016 Due for review November 1, 2018 Applicable to VUH Children s DOT VMG Off-site locations
EMERGENCYROOM BURN MANAGEMENT
 EMERGENCYROOM INITIAL ASSESSMENT PRIMARY SURVEY A = Airway and C-spine immobilization B = Breathing and Ventilation C = Circulation D = Disability, Neurologic Deficit E = Expose (remove all clothing and
EMERGENCYROOM INITIAL ASSESSMENT PRIMARY SURVEY A = Airway and C-spine immobilization B = Breathing and Ventilation C = Circulation D = Disability, Neurologic Deficit E = Expose (remove all clothing and
Burns. Chapter 9. Burns
 Burns Chapter 9 Burns Introduction Natural childhood curiosity and lack of supervision frequently combine to make thermal injuries a major cause of morbidity and mortality in the pediatric patient. Whether
Burns Chapter 9 Burns Introduction Natural childhood curiosity and lack of supervision frequently combine to make thermal injuries a major cause of morbidity and mortality in the pediatric patient. Whether
BASICS OF BURN MANAGEMENT
 BASICS OF BURN MANAGEMENT Dr S M Keswani Cosmetic Surgeon National Burns Centre, Airoli,Navi-Mumbai Breach Candy Hospital Wockhardt Hospital National Burns Centre, Airoli, Navi-Mumbai. CLASSIFICATION 1.
BASICS OF BURN MANAGEMENT Dr S M Keswani Cosmetic Surgeon National Burns Centre, Airoli,Navi-Mumbai Breach Candy Hospital Wockhardt Hospital National Burns Centre, Airoli, Navi-Mumbai. CLASSIFICATION 1.
Burn wounds - Determining the size and type degree
 1 Burn wounds - Determining the size and type degree Determining surface area of burn (Open hand only for small burns) 1 2 Burn depth Most burns are a combination of superficial and deeper burns and the
1 Burn wounds - Determining the size and type degree Determining surface area of burn (Open hand only for small burns) 1 2 Burn depth Most burns are a combination of superficial and deeper burns and the
Outpatient Burn Care for Primary Care: Who needs a referral?
 Outpatient Burn Care for Primary Care: Who needs a referral? J. Kevin Bailey, MD Associate Professor Department of Surgery Division of Trauma, Critical Care and Burn The Ohio State University Wexner Medical
Outpatient Burn Care for Primary Care: Who needs a referral? J. Kevin Bailey, MD Associate Professor Department of Surgery Division of Trauma, Critical Care and Burn The Ohio State University Wexner Medical
Due next week in lab - Scientific America Article Select one article to read and complete article summary
 Due in Lab 1. Skeletal System 33-34 2. Skeletal System 26 3. PreLab 6 Due next week in lab - Scientific America Article Select one article to read and complete article summary Cell Defenses and the Sunshine
Due in Lab 1. Skeletal System 33-34 2. Skeletal System 26 3. PreLab 6 Due next week in lab - Scientific America Article Select one article to read and complete article summary Cell Defenses and the Sunshine
Trauma Life Support Pre-Hospital (TLS-P) Preparatory Materials
 Trauma Life Support Pre-Hospital (TLS-P) Preparatory Materials 1 1. A high-risk bodily fluid for spreading infection is blood. 2. Items that can reduce the spread of infection include masks, gloves, and
Trauma Life Support Pre-Hospital (TLS-P) Preparatory Materials 1 1. A high-risk bodily fluid for spreading infection is blood. 2. Items that can reduce the spread of infection include masks, gloves, and
Printed copies of this document may not be up to date, obtain the most recent version from Author Position
 Children s Acute Transport Service Clinical Guidelines Burns Management Document Control Information Author E Borrows E Randle Author Position PICU/BURNS Consultant CATS Consultant Document Owner E. Polke
Children s Acute Transport Service Clinical Guidelines Burns Management Document Control Information Author E Borrows E Randle Author Position PICU/BURNS Consultant CATS Consultant Document Owner E. Polke
Applicable to. Team Members Performing MD House Staff APRN/PA RN LPN
 Protocol: Adult Burn Fluid Resuscitation Category Clinical Practice Protocol Number Approval Date vember 1, 2016 Due for review vember 1, 2018 Applicable to VUH Children s DOT VMG Off-site locations VMG
Protocol: Adult Burn Fluid Resuscitation Category Clinical Practice Protocol Number Approval Date vember 1, 2016 Due for review vember 1, 2018 Applicable to VUH Children s DOT VMG Off-site locations VMG
Current Concepts in Burn Rehabilitation
 Current Concepts in Burn Rehabilitation 7 th Congress of the Baltic Association of Rehabilitation Tallinn, Estonia September 2010 R. Scott Ward, PT, PhD Professor and Chair Department of Physical Therapy
Current Concepts in Burn Rehabilitation 7 th Congress of the Baltic Association of Rehabilitation Tallinn, Estonia September 2010 R. Scott Ward, PT, PhD Professor and Chair Department of Physical Therapy
Responsibility This guideline applies to teams of health professions caring for burn patients.
 Page 1 of 9 Guideline: Initial Assessment & Management of Burn Injuries Purpose This document provides a guideline for the initial assessment and management of burn patients. It is not intended as a full
Page 1 of 9 Guideline: Initial Assessment & Management of Burn Injuries Purpose This document provides a guideline for the initial assessment and management of burn patients. It is not intended as a full
Printed copies of this document may not be up to date, obtain the most recent version from Author Position
 Children s Acute Transport Service Clinical Guidelines Burns Management Document Control Information Author E Borrows E Randle, L Chigaru Author Position PICU/BURNS Consultant CATS Consultants Document
Children s Acute Transport Service Clinical Guidelines Burns Management Document Control Information Author E Borrows E Randle, L Chigaru Author Position PICU/BURNS Consultant CATS Consultants Document
Update on Burn Care and Resuscitation
 Niknam Eshraghi, M.D., F.A.C.S General and Burn Surgery; The Oregon Clinic Director; Oregon Burn Center, Legacy Emanuel Medical Center Affiliate Professor of Surgery, Oregon Health Sciences University
Niknam Eshraghi, M.D., F.A.C.S General and Burn Surgery; The Oregon Clinic Director; Oregon Burn Center, Legacy Emanuel Medical Center Affiliate Professor of Surgery, Oregon Health Sciences University
Chapter 24 Soft Tissue Injuries Presentation Notes
 Names: Chapter 24 Soft Tissue Injuries Presentation Notes Anatomy of the Skin - Function of the Skin control Soft-Tissue Injuries injuries Soft-tissue damage the skin injuries Break in the of the skin
Names: Chapter 24 Soft Tissue Injuries Presentation Notes Anatomy of the Skin - Function of the Skin control Soft-Tissue Injuries injuries Soft-tissue damage the skin injuries Break in the of the skin
Fire Deaths. Dr Julie McAdam Consultant Forensic Pathologist Glasgow University
 Fire Deaths Dr Julie McAdam Consultant Forensic Pathologist Glasgow University Forensic investigation multidisciplinary fire officers, police officers, scientists, photographers, pathologist, procurator
Fire Deaths Dr Julie McAdam Consultant Forensic Pathologist Glasgow University Forensic investigation multidisciplinary fire officers, police officers, scientists, photographers, pathologist, procurator
HEAVY METALS : Review
 HEAVY METALS : Review INHALED TOXINS Dr. Tawfiq Almezeiny MBBS FRCPC (CCM) Introduction Airborne toxins typically produce local noxious effects on the airways and lungs. Examples of Inhalational exposure:
HEAVY METALS : Review INHALED TOXINS Dr. Tawfiq Almezeiny MBBS FRCPC (CCM) Introduction Airborne toxins typically produce local noxious effects on the airways and lungs. Examples of Inhalational exposure:
Wound Care in the Community. Lisa Sutherland MSc Tissue Viability Senior Lead Ipswich Hospital & Community NHS Trusts
 Wound Care in the Community Lisa Sutherland MSc Tissue Viability Senior Lead Ipswich Hospital & Community NHS Trusts What are the key elements? What is the patient s goal or aim for the wound? What are
Wound Care in the Community Lisa Sutherland MSc Tissue Viability Senior Lead Ipswich Hospital & Community NHS Trusts What are the key elements? What is the patient s goal or aim for the wound? What are
MY STRATEGY FOR TREATING BURN INJURIES. Warren Garner MD FACS Keck School of Medicine at USC Los Angeles, CA
 MY STRATEGY FOR TREATING BURN INJURIES Warren Garner MD FACS Keck School of Medicine at USC Los Angeles, CA ASSUMPTIONS: Burns which heal to normal have best outcome. Medical risk, functional recovery,
MY STRATEGY FOR TREATING BURN INJURIES Warren Garner MD FACS Keck School of Medicine at USC Los Angeles, CA ASSUMPTIONS: Burns which heal to normal have best outcome. Medical risk, functional recovery,
Purpose To outline the pre-hospital and inter-hospital assessment and management of patients with major burns.
 Major Burns HELI.CLI.08 Purpose To outline the pre-hospital and inter-hospital assessment and management of patients with major burns. Procedure Management of Severe Burns For Review Aug 2015 1. Introduction
Major Burns HELI.CLI.08 Purpose To outline the pre-hospital and inter-hospital assessment and management of patients with major burns. Procedure Management of Severe Burns For Review Aug 2015 1. Introduction
Integumentary System
 Chapter 5 Integumentary System 5-1 Skin: composed of dermis and epidermis Dermis. Gives structural strength. C.T. with many fibers, fibroblasts, macrophages. Some adipocytes and blood vessels. Contains
Chapter 5 Integumentary System 5-1 Skin: composed of dermis and epidermis Dermis. Gives structural strength. C.T. with many fibers, fibroblasts, macrophages. Some adipocytes and blood vessels. Contains
Case Report: Burns Reid Sadoway PGY1 Emergency Medicine, Dalhousie
 Case Report: Burns Reid Sadoway PGY1 Emergency Medicine, Dalhousie History 3 yo boy, presents to pediatric ED with mother Child can be heard crying inside waiting/patient room, has both hands bandaged
Case Report: Burns Reid Sadoway PGY1 Emergency Medicine, Dalhousie History 3 yo boy, presents to pediatric ED with mother Child can be heard crying inside waiting/patient room, has both hands bandaged
Not All That Blisters Is a Burn! Jamie Hoffman-Rosenfeld, MD CHAMP Webinar December 6, 2012
 Not All That Blisters Is a Burn! Jamie Hoffman-Rosenfeld, MD CHAMP Webinar December 6, 2012 Objectives To review the epidemiology of burns in children including burns caused by abuse To review the steps
Not All That Blisters Is a Burn! Jamie Hoffman-Rosenfeld, MD CHAMP Webinar December 6, 2012 Objectives To review the epidemiology of burns in children including burns caused by abuse To review the steps
Skin Anatomy and Physiology
 Skin Anatomy and Physiology Body s largest organ Three layers: Epidermis Dermis Subcutaneous tissue 1 2 Skin Anatomy and Physiology Complex system, variety of functions Sensation Control of water loss
Skin Anatomy and Physiology Body s largest organ Three layers: Epidermis Dermis Subcutaneous tissue 1 2 Skin Anatomy and Physiology Complex system, variety of functions Sensation Control of water loss
Human Anatomy & Physiology
 PowerPoint Lecture Slides prepared by Barbara Heard, Atlantic Cape Community College Ninth Edition Human Anatomy & Physiology C H A P T E R 5 Annie Leibovitz/Contact Press Images 2013 Pearson Education,
PowerPoint Lecture Slides prepared by Barbara Heard, Atlantic Cape Community College Ninth Edition Human Anatomy & Physiology C H A P T E R 5 Annie Leibovitz/Contact Press Images 2013 Pearson Education,
Burns. There is also technically a fourth-degree burn. In this type, the damage of third-degree burns extends beyond the skin into tendons and bones.
 Burns can be caused by a variety of household items, including electrical equipment and chemicals. Very light burns can be treated at home and only cause superficial damage, while more severe burns need
Burns can be caused by a variety of household items, including electrical equipment and chemicals. Very light burns can be treated at home and only cause superficial damage, while more severe burns need
Dr. Muhammad Shamim. FCPS (Pak), FACS (USA), FICS (USA), MHPE (Nl & Eg)
 Dr. Muhammad Shamim FCPS (Pak), FACS (USA), FICS (USA), MHPE (Nl & Eg) Assistant Professor, Dept. of Surgery College of Medicine, Salman bin Abdulaziz University Email: surgeon.shamim@gmail.com Web: surgeonshamim.com
Dr. Muhammad Shamim FCPS (Pak), FACS (USA), FICS (USA), MHPE (Nl & Eg) Assistant Professor, Dept. of Surgery College of Medicine, Salman bin Abdulaziz University Email: surgeon.shamim@gmail.com Web: surgeonshamim.com
Appendix. Sedatives and Pain Medications. Gabapentin ( mg po q8h) or Pregabalin ( mg po q8h)
 Appendix Sedatives and Pain Medications Non-intubated patients Non-opioid analgesics Acetaminophen (500 1,000 mg po q6h) NSAID (Ibuprofen, Naprosyn, Celebrex) Gabapentin (100 300 mg po q8h) or Pregabalin
Appendix Sedatives and Pain Medications Non-intubated patients Non-opioid analgesics Acetaminophen (500 1,000 mg po q6h) NSAID (Ibuprofen, Naprosyn, Celebrex) Gabapentin (100 300 mg po q8h) or Pregabalin
1 Inhalational Injury: pathophysiology, diagnosis, treatment. O.M. Oluwatosin Department of Surgery
 1 Inhalational Injury: pathophysiology, diagnosis, treatment O.M. Oluwatosin Department of Surgery 2 At the end of this lecture you should be able to: Describe the physiology of the respiration of the
1 Inhalational Injury: pathophysiology, diagnosis, treatment O.M. Oluwatosin Department of Surgery 2 At the end of this lecture you should be able to: Describe the physiology of the respiration of the
Proceedings of the 36th World Small Animal Veterinary Congress WSAVA
 www.ivis.org Proceedings of the 36th World Small Animal Veterinary Congress WSAVA Oct. 14-17, 2011 Jeju, Korea Next Congress: Reprinted in IVIS with the permission of WSAVA http://www.ivis.org 14(Fri)
www.ivis.org Proceedings of the 36th World Small Animal Veterinary Congress WSAVA Oct. 14-17, 2011 Jeju, Korea Next Congress: Reprinted in IVIS with the permission of WSAVA http://www.ivis.org 14(Fri)
Principles of Anatomy and Physiology
 Principles of Anatomy and Physiology 14 th Edition CHAPTER 5 The Integumentary System Introduction The organs of the integumentary system include the skin and its accessory structures including hair, nails,
Principles of Anatomy and Physiology 14 th Edition CHAPTER 5 The Integumentary System Introduction The organs of the integumentary system include the skin and its accessory structures including hair, nails,
COBIS Management of airway burns and inhalation injury PAEDIATRIC
 COBIS Management of airway burns and inhalation injury PAEDIATRIC 1 A multidisciplinary team should provide the management of the child with inhalation injury. Childhood inhalation injury mandates transfer
COBIS Management of airway burns and inhalation injury PAEDIATRIC 1 A multidisciplinary team should provide the management of the child with inhalation injury. Childhood inhalation injury mandates transfer
Burn injury. A : patent airway with smoking inhalation, stridor. D: E4V5M6,pupil 2mm RTLBE
 Burn injury Pinyong Uthaitas Emergency Department Faculty of Medicine, Ramathibodi Hospital A Thai man 52 year old came to the hospital due to flam burn ½ hr ago at his house. He gain conscious but hoarseness
Burn injury Pinyong Uthaitas Emergency Department Faculty of Medicine, Ramathibodi Hospital A Thai man 52 year old came to the hospital due to flam burn ½ hr ago at his house. He gain conscious but hoarseness
Smoke inhalation damages the body by simple asphyxiation (lack of oxygen), chemical irritation, chemical asphyxiation, or a combination of these.
 Print Close 2011 WebMD, LLC. All rights reserved. Smoke Inhalation Recommend 13 Medical Author: Christopher P Holstege, MD Medical Editor: Melissa Conrad Stöppler, MD Smoke Inhalation Overview Smoke Inhalation
Print Close 2011 WebMD, LLC. All rights reserved. Smoke Inhalation Recommend 13 Medical Author: Christopher P Holstege, MD Medical Editor: Melissa Conrad Stöppler, MD Smoke Inhalation Overview Smoke Inhalation
11/9/2015. Lehigh Valley Health Network Allentown, PA Lisa LePage, OTR/L
 Lehigh Valley Health Network Allentown, PA Lisa LePage, OTR/L Regional Burn Center 18 Bed Unit located in Kasych Building Critical and non-critical beds on the unit 3 Burn Surgeons, 6 Physician Assistants
Lehigh Valley Health Network Allentown, PA Lisa LePage, OTR/L Regional Burn Center 18 Bed Unit located in Kasych Building Critical and non-critical beds on the unit 3 Burn Surgeons, 6 Physician Assistants
Spinal Cord Injury Info Sheet An information series produced by the Spinal Cord Program at GF Strong Rehab Centre.
 Spinal Cord Injury Info Sheet An information series produced by the Spinal Cord Program at GF Strong Rehab Centre. What does skin do? 1. It protects you. 2. It provides sensory information. 3. It helps
Spinal Cord Injury Info Sheet An information series produced by the Spinal Cord Program at GF Strong Rehab Centre. What does skin do? 1. It protects you. 2. It provides sensory information. 3. It helps
Cellular and Tissue Effects. Pathophysiology of the Burn Wound. Special Topics: Thermal Burns & Smoke Inhalation
 Special Topics: Thermal Burns & Smoke Inhalation MEDICAL RESPONDER AND RECEIVER SEMINAR; EXPLOSION AND BLAST INJURIES Pathophysiology of the Burn Wound The burn wound is the source of virtually all ill
Special Topics: Thermal Burns & Smoke Inhalation MEDICAL RESPONDER AND RECEIVER SEMINAR; EXPLOSION AND BLAST INJURIES Pathophysiology of the Burn Wound The burn wound is the source of virtually all ill
WOUNDS. Emergency Procedures in PT
 WOUNDS Emergency Procedures in PT Types of Wounds Abrasions uppermost layer scraped away, minor capillary bleeding occurs, nerve endings exposed Lacerations skin tear with edges jagged and uneven Incisions
WOUNDS Emergency Procedures in PT Types of Wounds Abrasions uppermost layer scraped away, minor capillary bleeding occurs, nerve endings exposed Lacerations skin tear with edges jagged and uneven Incisions
Skin is the largest, most important organ % of total body weight Functions: - -Sensation - Regulation AKA: System
 1 Chapter 20 Soft-Tissue Injury 2 Introduction to Soft-Tissue Injury Skin is the largest, most important organ % of total body weight Functions: - -Sensation - Regulation AKA: System 3 Epidemiology Most
1 Chapter 20 Soft-Tissue Injury 2 Introduction to Soft-Tissue Injury Skin is the largest, most important organ % of total body weight Functions: - -Sensation - Regulation AKA: System 3 Epidemiology Most
Integumentary System and Body Membranes
 Integumentary System and Body Membranes The Skin and its appendages hair, nails, and skin glands Anatomy/Physiology NHS http://www.lab.anhb.uwa.edu.au/mb140/corepages/integumentary/integum.htm I. System
Integumentary System and Body Membranes The Skin and its appendages hair, nails, and skin glands Anatomy/Physiology NHS http://www.lab.anhb.uwa.edu.au/mb140/corepages/integumentary/integum.htm I. System
C H A P T E R 8 T H E R M A L I N J U R I E S
 CHAPTER 8 THERMAL INJURIES Thermal destruction of the skin results in severe local and systemic alterations. This destruction can occur from thermal energy, chemical reactions, electricity, or the response
CHAPTER 8 THERMAL INJURIES Thermal destruction of the skin results in severe local and systemic alterations. This destruction can occur from thermal energy, chemical reactions, electricity, or the response
LRI Emergency Department. Burn injuries management in adults
 LRI Emergency Department Clinical guideline for: Burn injuries management in adults Authors: Approved by: Martin Wiese Reena Agarwal Claire Porter EF guidelines committee Approval date: 21 Sep 16 Approval
LRI Emergency Department Clinical guideline for: Burn injuries management in adults Authors: Approved by: Martin Wiese Reena Agarwal Claire Porter EF guidelines committee Approval date: 21 Sep 16 Approval
Hole s Human Anatomy and Physiology Eleventh Edition. Mrs. Hummer. Chapter 6
 Hole s Human Anatomy and Physiology Eleventh Edition Mrs. Hummer Chapter 6 1 Chapter 6 Skin and the Integumentary System Composed of several tissues Maintains homeostasis Protective covering Retards water
Hole s Human Anatomy and Physiology Eleventh Edition Mrs. Hummer Chapter 6 1 Chapter 6 Skin and the Integumentary System Composed of several tissues Maintains homeostasis Protective covering Retards water
Warm Up. You have 10 minutes to complete your poster and prepare what you would like to share with the class.
 Warm Up You have 10 minutes to complete your poster and prepare what you would like to share with the class. Reflection 1. What were 2 similarities between your classification scheme and others in the
Warm Up You have 10 minutes to complete your poster and prepare what you would like to share with the class. Reflection 1. What were 2 similarities between your classification scheme and others in the
Describe the functions of the vertebrate integumentary system. Discuss the structure of the skin and how it relates to function.
 Chapter 5 Describe the functions of the vertebrate integumentary system. Discuss the structure of the skin and how it relates to function. Explain the basis for different skin colors. Describe the structure
Chapter 5 Describe the functions of the vertebrate integumentary system. Discuss the structure of the skin and how it relates to function. Explain the basis for different skin colors. Describe the structure
ITLS Pediatric Provider Course Advanced Pre-Test
 ITLS Pediatric Provider Course Advanced Pre-Test 1. You arrive at the scene of a motor vehicle crash and are directed to evaluate a child who was in one of the vehicles. The patient appears to be a child
ITLS Pediatric Provider Course Advanced Pre-Test 1. You arrive at the scene of a motor vehicle crash and are directed to evaluate a child who was in one of the vehicles. The patient appears to be a child
Anatomy Ch 6: Integumentary System
 Anatomy Ch 6: Integumentary System Introduction: A. Organs are body structures composed of two or more different tissues. B. The skin and its accessory organs make up the integumentary system. Types of
Anatomy Ch 6: Integumentary System Introduction: A. Organs are body structures composed of two or more different tissues. B. The skin and its accessory organs make up the integumentary system. Types of
Review. A. abrasion B. contusion C. hematoma D. avulsion
 Chapter 24 Review Review 1. A young male was struck in the forearm with a baseball and complains of pain to the area. Slight swelling and ecchymosis are present, but no external bleeding. What type of
Chapter 24 Review Review 1. A young male was struck in the forearm with a baseball and complains of pain to the area. Slight swelling and ecchymosis are present, but no external bleeding. What type of
1 Chapter 13 Respiratory Emergencies 2 Respiratory Distress Patients often complain about. Shortness of breath Symptom of many different Cause can be
 1 Chapter 13 Respiratory Emergencies 2 Respiratory Distress Patients often complain about. Shortness of breath Symptom of many different Cause can be difficult to determine. Even for physician in hospital
1 Chapter 13 Respiratory Emergencies 2 Respiratory Distress Patients often complain about. Shortness of breath Symptom of many different Cause can be difficult to determine. Even for physician in hospital
Thermal Injuries. Manika Bhandari, Malika Bhola, Rucha Desai, Dhruvika Joshi, Abir Shamim Life Science 4M03
 Thermal Injuries Manika Bhandari, Malika Bhola, Rucha Desai, Dhruvika Joshi, Abir Shamim Life Science 4M03 INTRODUCTION Anatomy of the skin The skin has three anatomical layers Epidermis Dermis Subcutaneous
Thermal Injuries Manika Bhandari, Malika Bhola, Rucha Desai, Dhruvika Joshi, Abir Shamim Life Science 4M03 INTRODUCTION Anatomy of the skin The skin has three anatomical layers Epidermis Dermis Subcutaneous
Epicel (cultured epidermal autografts) HDE# BH Patient Information
 Epicel (cultured epidermal autografts) HDE# BH990200 Patient Information This leaflet is designed to help you understand Epicel (cultured epidermal autografts) and its use for the treatment of burn wound.
Epicel (cultured epidermal autografts) HDE# BH990200 Patient Information This leaflet is designed to help you understand Epicel (cultured epidermal autografts) and its use for the treatment of burn wound.
Chapter 29. Objectives. Objectives 01/09/2013. Burns
 Chapter 29 Burns Prehospital Emergency Care, Ninth Edition Joseph J. Mistovich Keith J. Karren Copyright 2010 by Pearson Education, Inc. All rights reserved. Objectives 1. Define key terms introduced in
Chapter 29 Burns Prehospital Emergency Care, Ninth Edition Joseph J. Mistovich Keith J. Karren Copyright 2010 by Pearson Education, Inc. All rights reserved. Objectives 1. Define key terms introduced in
Structure and Movement
 Structure and Movement The Skin Key Concepts What does the skin do? How do the three layers of skin differ? How does the skin interact with other body systems? What do you think? Read the two statements
Structure and Movement The Skin Key Concepts What does the skin do? How do the three layers of skin differ? How does the skin interact with other body systems? What do you think? Read the two statements
The Affects of Music Therapy on Management of Pain and Anxiety During Burn Dressing Changes
 Philadelphia College of Osteopathic Medicine DigitalCommons@PCOM PCOM Physician Assistant Studies Student Scholarship Student Dissertations, Theses and Papers 2014 The Affects of Music Therapy on Management
Philadelphia College of Osteopathic Medicine DigitalCommons@PCOM PCOM Physician Assistant Studies Student Scholarship Student Dissertations, Theses and Papers 2014 The Affects of Music Therapy on Management
Skin Integrity and Wound Care
 Skin Integrity and Wound Care By Dr. Amer Hasanien & Dr. Ali Saleh Skin Integrity and Wound Care Skin integrity: the presence of normal Skin & Uninterrupted skin layers by wounds. Factors affecting appearance
Skin Integrity and Wound Care By Dr. Amer Hasanien & Dr. Ali Saleh Skin Integrity and Wound Care Skin integrity: the presence of normal Skin & Uninterrupted skin layers by wounds. Factors affecting appearance
INSTRUCTOR GUIDE FOR TACTICAL FIELD CARE 3B BURNS AND FRACTURES
 INSTRUCTOR GUIDE FOR TACTICAL FIELD CARE 3B BURNS AND FRACTURES 180801 1 Tactical Combat Casualty Care for Medical Personnel 1. August 2017 (Based on TCCC-MP Guidelines 180801 In this presentation, we
INSTRUCTOR GUIDE FOR TACTICAL FIELD CARE 3B BURNS AND FRACTURES 180801 1 Tactical Combat Casualty Care for Medical Personnel 1. August 2017 (Based on TCCC-MP Guidelines 180801 In this presentation, we
II. Skin and Its Tissues. I. Introduction. Unit Two. Integument URLs.
 6 Integument URLs http://www.nurseminerva.co.uk/integ.html http://www.aap.org/policy/s010116.html Chapter 6 Karen Webb Smith Unit Two I. Introduction A. Organs are body structures composed of two or more
6 Integument URLs http://www.nurseminerva.co.uk/integ.html http://www.aap.org/policy/s010116.html Chapter 6 Karen Webb Smith Unit Two I. Introduction A. Organs are body structures composed of two or more
INTEGUMENTARY SYSTEM PART I: FUNCTIONS & EPIDERMIS
 INTEGUMENTARY SYSTEM PART I: FUNCTIONS & EPIDERMIS Integumentary System Cutaneous membrane Epidermis (5-layers) made up of epithelial tissue only Dermis (2-layers) contains connective tissue, vessels,
INTEGUMENTARY SYSTEM PART I: FUNCTIONS & EPIDERMIS Integumentary System Cutaneous membrane Epidermis (5-layers) made up of epithelial tissue only Dermis (2-layers) contains connective tissue, vessels,
Pediatric Shock. Hypovolemia. Sepsis. Most common cause of pediatric shock Small blood volumes (80cc/kg)
 Critical Concepts: Shock Inadequate peripheral perfusion where oxygen delivery does not meet metabolic demand Adult vs Pediatric Shock - Same causes/different frequencies Pediatric Shock Hypovolemia Most
Critical Concepts: Shock Inadequate peripheral perfusion where oxygen delivery does not meet metabolic demand Adult vs Pediatric Shock - Same causes/different frequencies Pediatric Shock Hypovolemia Most
STS Care of Thermal Burns 20% Total Body Surface Area
 Temp Regulation Transfer Pain Fluids Airway Initial Assessment STS Care of Thermal Burns 20% Total Body Surface Area Remove burned clothing, rings, watches, and jewelry Cervical spine precautions (if history
Temp Regulation Transfer Pain Fluids Airway Initial Assessment STS Care of Thermal Burns 20% Total Body Surface Area Remove burned clothing, rings, watches, and jewelry Cervical spine precautions (if history
Applicable to. Team Members Performing
 Protocol: Category Clinical Practice Approval Date March 13, 2019 Due for review March 13, 2021 Applicable to VUH Children s DOT VMG Off-site locations VMG VPH Other All faculty & staff Other: Faculty
Protocol: Category Clinical Practice Approval Date March 13, 2019 Due for review March 13, 2021 Applicable to VUH Children s DOT VMG Off-site locations VMG VPH Other All faculty & staff Other: Faculty
Pressure Injury Definition and Stages
 Program Objective Pressure Injury Definition and Stages Identify the changes to the 2016 NPUAP staging system Changes to the Staging System in 2016 2 Anatomy of the Skin Anatomy of the Skin Largest organ
Program Objective Pressure Injury Definition and Stages Identify the changes to the 2016 NPUAP staging system Changes to the Staging System in 2016 2 Anatomy of the Skin Anatomy of the Skin Largest organ
Oxygenation. Chapter 45. Re'eda Almashagba 1
 Oxygenation Chapter 45 Re'eda Almashagba 1 Respiratory Physiology Structure and function Breathing: inspiration, expiration Lung volumes and capacities Pulmonary circulation Respiratory gas exchange: oxygen,
Oxygenation Chapter 45 Re'eda Almashagba 1 Respiratory Physiology Structure and function Breathing: inspiration, expiration Lung volumes and capacities Pulmonary circulation Respiratory gas exchange: oxygen,
MANAGING THE BURN WOUND
 MANAGING THE BURN WOUND Robert H. Demling, M.D. Leslie DeSanti R.N., Brigham and Women s Hospital Burn Center Harvard Medical School Boston, MA TABLE OF CONTENTS Section I: Section II: Section III: Section
MANAGING THE BURN WOUND Robert H. Demling, M.D. Leslie DeSanti R.N., Brigham and Women s Hospital Burn Center Harvard Medical School Boston, MA TABLE OF CONTENTS Section I: Section II: Section III: Section
