MatrixMIDFACE Preformed Orbital Plates. MatrixORBITAL. Surgical Technique
|
|
|
- Osborn Rose
- 5 years ago
- Views:
Transcription
1 MatrixMIDFACE Preformed Orbital Plates MatrixORBITAL Surgical Technique
2 Image intensifier control This description alone does not provide sufficient background for direct use of DePuy Synthes products. Instruction by a surgeon experienced in handling these products is highly recommended. Processing, Reprocessing, Care and Maintenance For general guidelines, function control and dismantling of multi-part instruments, as well as processing guidelines for implants, please contact your local sales representative or refer to: For general information about reprocessing, care and maintenance of Synthes reusable devices, instrument trays and cases, as well as processing of Synthes non-sterile implants, please consult the Important Information leaflet (SE_023827) or refer to:
3 Table of Contents Introduction MatrixORBITAL 2 Introduction 4 Intended Use, Indications, Contraindications, Warnings, Precautions, General Adverse Events and MRI Information 5 Clinical Case 8 Orbital Landmarks 9 Orbital Retractors 10 Surgical Technique 11 Product Information Plates 19 Screws 20 Instruments 21 Bibliography 22 MatrixORBITAL Surgical Technique DePuy Synthes 1
4 MatrixORBITAL MatrixMIDFACE Preformed Orbital Plates Features and benefits Designed from CT-scan data, the three-dimensional implants closely approximate the topographical anatomy of the human orbital floor and medial wall to provide accurate reconstruction even after significant two-wall fractures. 5,6 Preformed three-dimensional shape. For minimal bending and cutting which reduces the amount of time needed to contour plate. Contoured plate edges. For easier plate insertion through skin incision and less interference between the plate and surrounding soft tissue. Segmented design. To customize plate size to address orbital topography and to maintain contoured plate borders with minimal sharp edges. Rigid zone. Restores the shape of the posterior orbital floor to help maintain the correct position of the globe. Intersection bars for minimal cutting and contoured plate borders Medial wall Rigid zone ensures consistent form in the posterior orbit Orbital floor Fixation arms Screw hole pattern 2 DePuy Synthes MatrixORBITAL Surgical Technique
5 Intersection bars for minimal cutting and contoured plate borders S-shape to match the contour of the orbital floor Lateral edge MatrixORBITAL Surgical Technique DePuy Synthes 3
6 Introduction Orbital floor fractures are frequently associated with medial wall fractures. The complex geometry of the bony orbit makes anatomical reconstruction extremely challenging, particularly in two wall fractures and when the deep orbital cone is affected. The orbital floor has an initial shallow convex section behind the rim, then inclines upward behind the globe, and inclines upward to meet the medial wall, creating a distinct bulge behind the globe. These convex curves of the medial wall and floor create a postbulbar constriction of the orbital cavity, which must be reconstructed when the orbit is rebuilt following fractures. 2 Treatment is directed at precise anatomical reconstruction of orbital shape and volume in order to restore the correct position of the eye. 3,4 The MatrixMIDFACE Preformed Orbital Plates may be used for acute orbital fractures or in secondary reconstruction of enophthalmos and dystopia. 4 DePuy Synthes MatrixORBITAL Surgical Technique
7 Intended Use, Indications, Contraindications, Warnings, Precautions, General Adverse Events and MRI Information Intended Use MatrixMIDFACE Preformed Orbital Plates are intended for use as trauma repair and reconstruction of the cranio-maxillofacial skeleton. Indications MatrixMIDFACE Preformed Orbital Plates are indicated for use in: Orbital floor fractures Medial orbital wall fractures Combined orbital floor and medial wall fractures Contraindications No specific contraindications. Warnings: Using an internal fixation system on patients with active or latent infection may cause potential risks which may include construct failure and deterioration of infection. It is at the physician s discretion to evaluate the patient s medical conditions and select a fixation device most appropriate for the individual patient. It is also at the physician s discretion to consider all other necessary treatment methods to effectively manage the infection. Confirm the quality of bone at the selected plate position. Using an internal fixation system on patients with insufficient quantity or quality of bone may cause potential risks which may include device loosening and construct failure. It is at the physician s discretion to evaluate the patient s medical conditions and select a fixation device most appropriate for the individual patient. These devices can break during use (when subjected to excessive forces or outside the recommended surgical technique). While the surgeon must make the final decision on removal of the broken part based on associated risk in doing so, we recommend that whenever possible and practical for the individual patient, the broken part should be removed. Be aware that implants are not as strong as native bone. Implants subjected to substantial loads may fail. Instruments, screws and cut plates may have sharp edges or moving joints that may pinch or tear user s glove or skin. Take care to remove all fragments that are not fixated during the surgery. While the surgeon must make the final decision on implant removal, we recommend that whenever possible and practical for the individual patient, fixation devices should be removed once their service as an aid to healing is accomplished. Implant removal should be followed by adequate post-operative management to avoid refracture. Precautions: Confirm functionality of instruments and check for wear during reprocessing. Replace worn or damaged instruments prior to use. It is recommended to only use the instruments identified for use within the MatrixMIDFACE (DSEM/CMF/0216/0113) and MatrixORBITAL surgical techniques (DSEM/CMF/0216/0114) with the MatrixMIDFACE implants. Handle devices with care and dispose worn bone cutting instruments in an approved sharps container. Always irrigate and apply suction for removal of debris potentially generated during implantation or removal. General Adverse Events As with all major surgical procedures, risks, side effects and adverse events can occur. While many possible reactions may occur, some of the most common include: Problems resulting from anesthesia and patient positioning (e.g. nausea, vomiting, dental injuries, neurological impairments, etc.), thrombosis, embolism, infection, nerve and/or tooth root damage or injury of other critical structures including blood vessels, excessive bleeding, damage to soft tissues incl. swelling, abnormal scar formation, functional impairment of the musculoskeletal system, pain, discomfort or abnormal sensation due to the presence of the device, allergy or hypersensitivity reactions, side effects associated with hardware prominence, loosening, bending, or breakage of the device, mal-union, non-union or delayed union which may lead to breakage of the implant, reoperation. MatrixORBITAL Surgical Technique DePuy Synthes 5
8 Intended Use, Indications, Contraindications, Warnings, Precautions, General Adverse Events and MRI Information Device-specific Adverse Events Device-specific adverse events include but are not limited to: Malunion / non-union that may be associated with: Implant inappropriately dimensioned for the intended use Hole deformation due to plate bending Construct failure due to inadequate strength design Construct strength too weak for post-operative loading forces Plate/mesh hole diameter too large or screw head too small Wrong implant material/design Misleading/incorrect label Information provided to the end-user (i.e. IFU, ST, care guide) is insufficient, incorrect or imprecise Insufficient screw holes left after plate has been cut Reverse and repeated bending applied Adverse Tissue Reaction that may be associated with: Instruments debris/particle created during cutting Instruments debris/particle created during implantation and/or removal Incorrect label i.e. wrong data provided on the LMD i.e. wrong text, missing symbols, wrong expiry date Damage to vital organs / surrounding structures that may be associated with: Premature plate/mesh failure Plate/mesh does not offer enough options for screw placement Plate/mesh too thick for anatomical area Fixation holes do not allow for appropriate fixation Insufficient mesh structure Screw placement into nerve, tooth buds/roots and or any other critical structures Screw core diameter is too small leading to screw breakage post-operatively Screw deforms or breaks during insertion with generation of fragments that the surgeon is unaware of or unable to retrieve, potentially resulting in fragment migration Screw recess strips due to blade cam-out Burrs/sharp edges on edge of plate Plate/mesh inadequately contoured resulting in inadequate reduction Screw breaks during insertion and fragments are not retrieved Screw breakage post-operatively Blade cams-out of screw recess Screw passes completely through plate Generation of particle debris during surgical procedure Screw strips bone post-operatively Screw not safely retained resulting in loss of screw intra-operatively Screw or plate migrates or deforms post-operatively Plate hole does not hold screw head Implant loses functionality post-operatively Improper use of implant resulting in treatment failure Wrong plate selection Incorrect plate/screw position resulting in irreversible damage Inappropriate use of screws or drill bits Overheating of drill bit causing thermal necrosis of bone Injury to user that may be associated with: Sharp edges caused during cutting of plates punctures surgical glove/hand Loosening that may be associated with: Insufficient implant fixation Screw breakage post-operatively Inappropriate screw used Peripheral Nerve that may be associated with: Screws inserted into nerve, tooth buds/roots and or any other critical structures Soft Tissue Damage that may be associated with: Premature plate/mesh failure Screw breakage post-operatively Burrs/sharp edges on edge of plate Implant loses its function post-operatively Systemic Infection that may be associated with: Incomplete/incorrect processing leading to implantation of a non-sterile product Sterile barrier compromised leading to implantation of a non-sterile product Implantation of non-sterile product Implantation of non-sterile unclean product due to incorrect label Reuse of single use implant 6 DePuy Synthes MatrixORBITAL Surgical Technique
9 MRI Information Torque, Displacement and Image Artifacts according to ASTM F , ASTM F and ASTM F Non-clinical testing of a worst case scenario in a 3 T MRI system did not reveal any relevant torque or displacement of the construct for an experimentally measured local spatial gradient of the magnetic field of 5.4 T/m. The largest image artifact extended approximately 20 mm from the construct when scanned using the Gradient Echo (GE). Testing was conducted on a Siemens Prisma 3 T MRI system. Radio-Frequency-(RF-)induced heating according to ASTM F a Non-clinical electromagnetic and thermal simulations of a worst case scenario lead to temperature rises of 9.3 C (1.5 T) and 6 C (3 T) under MRI Conditions using RF Coils (whole body averaged specific absorption rate [SAR] of 2 W/kg for 15 minutes). Precautions: The above mentioned test relies on nonclinical testing. The actual temperature rise in the patient will depend on a variety of factors beyond the SAR and time of RF application. Thus, it is recommended to pay particular attention to the following points: It is recommended to thoroughly monitor patients undergoing MR scanning for perceived temperature and/or pain sensations. Patients with impaired thermoregulation or temperature sensation should be excluded from MR scanning procedures. Generally, it is recommended to use an MRI system with low field strength in the presence of conductive implants. The employed specific absorption rate (SAR) should be reduced as far as possible. Using the ventilation system may further contribute to reduce temperature increase in the body. MatrixORBITAL Surgical Technique DePuy Synthes 7
10 Clinical Case* Preoperative CT 25-year old male sustaining blunt trauma to left orbit. Ophthalmological exam unremarkable except for severe soft tissue swelling and bruising. CT demonstrated severe displacement of medial wall and floor, including the transition zone, putting the patient at risk for late enophthalmos and dystopia as well as strabismus. Coronal preop Axial preop Postoperative CT Orbit approached through transconjunctival incision with lateral canthotomy. MatrixMIDFACE Preformed Orbital Plate, large, left placed without modification except slight bending and trimming of some of fixation holes. The implant was fixed to inferior orbital rim with two MatrixMIDFACE screws. Coronal postop Axial postop * Clinical Case and all images are courtesy of Dr. Bartlett, Children s Hospital of Philadelphia, University of Pennsylvania, USA. Results from case studies are not predictive of results in other cases. Results in other cases may vary. 8 DePuy Synthes MatrixORBITAL Surgical Technique
11 Orbital Landmarks Implant placement according to the orbital landmarks 1. Orbital rim 2. Inferior orbital fissure 3. Posterior orbital ledge 4. Transition zone* between the orbital floor and medial wall 5. Optic canal 6. Lacrimal fossa Preoperative planning** 3D Coronal Sagittal Axial * Transition zone is located at the infero-medial aspect of the orbital floor and refers to an inner buttress at the junction to the lower end of the medial orbital wall. ** Images courtesy of Prof. Dr. Dr. R. Schmelzeisen, Dr. Dr. M. C. Metzger, Department of Craniomaxillofacial Surgery, University of Freiburg, Germany. MatrixORBITAL Surgical Technique DePuy Synthes 9
12 Orbital Retractors Minimize orbital soft tissue prolapse Provide soft tissue protection Large and small retractor ends Right and left retractors Stainless steel, malleable Graduation on both sides Concave ends Design follows orbital anatomy 11 DePuy Synthes MatrixORBITAL Surgical Technique
13 Surgical Technique 1. Select implant Implants Preformed Orbital Plate, small, left Preformed Orbital Plate, large, left Preformed Orbital Plate, small, right Preformed Orbital Plate, large, right Select the preformed orbital plate that best suits the patient s orbital anatomy, the fracture type and extent, and which is based on the preoperative plan. Notes: In three-wall fractures involving the lateral wall, an additional orbital implant must be used (e. g. Synthes orbital mesh plate). For the surgical technique for MatrixMIDFACE, refer to the surgical technique DSEM/CMF/0216/0113. MatrixORBITAL Surgical Technique DePuy Synthes 11
14 Surgical Technique 2. Size implant (if required) Instruments Cutting Scissors for Mesh Plates, short Cutting Scissors for Mesh Plates, long Reduce the height of the medial wall and/or orbital floor length when not used for bridging the fracture. Always cut the implant along the cutting lines to ensure smooth edges, using scissors or mesh cutters. Precaution: Take care to protect soft tissue from trimmed plate edges. 11 DePuy Synthes MatrixORBITAL Surgical Technique
15 3. Contour implant (if required) Instrument Bending Pliers for MatrixMIDFACE Plates (two bending pliers required) The implant can be further contoured to match patient anatomy. Precautions: Avoid contouring of the implant in situ that may lead to implant malposition and/or posterior cantilever effect. The lateral anterior part of the plate (circled right) is intentionally prebent higher than the orbital rim anatomy to allow free plate movement during plate positioning. The lateral anterior part can be further contoured to match patient anatomy. If contouring is necessary, the surgeon should avoid bending the device at a screw hole. Avoid sharp bends, repetitive and reverse bending as it increases the risk of implant breakage. MatrixORBITAL Surgical Technique DePuy Synthes 11
16 Surgical Technique 4. Rectract soft tissue Instruments Orbital Retractor, left Orbital Retractor, right The malleable orbital retractors can be used to retract the soft tissue as well as size the defect. The spoon shaped shield of the malleable retractors is bent perpendicular to the handle. Fat prolapsing beside the retractor shield can be retracted by the additional insertion of a flexible foil. Note: Make an angled bend (red line) to allow the hand position to rest conveniently and away from the surgical view on the patient s forehead. Twisting of the bent end can further improve or facilitate the handling. 11 DePuy Synthes MatrixORBITAL Surgical Technique
17 5. Insert implant Position the lateral edge of the plate along the inferior orbital fissure. Since the implant is anatomic and preformed, it should be positioned in the same location for every patient. The orientation of the implant does not need to change based on the anatomy of the fracture. Place the plate on the stable bony contour. 1 Note: Confirm appropriate dissection. Insert the medial wall section of the plate first (1). While inserting the rest of the plate, turn the plate (2) until the implant is in the correct anatomical position (3). (Refer to page 9 for orbital landmarks.) 2 3 MatrixORBITAL Surgical Technique DePuy Synthes 11
18 Surgical Technique 6. Drill the hole (when using selftapping screws) Drill the hole with the appropriate diameter and length drill bit. Notes: Screws are available in self-drilling (silver), self-tapping (bronze), and emergency (blue) designs. If a pilot hole is desired, use the appropriate 1.1 mm diameter MatrixMIDFACE drill bit for drilling up to 8 mm length and the 1.25 mm diameter MatrixMIDFACE drill bit for screw lengths of 10 mm or more. Precautions: Confirm that plate positioning allows for adequate clearance of nerves and any other critical structures. Confirm that drill bit length and diameter correspond to selected screw length prior to drilling. Drill speed rate should never exceed 1,800 rpm, particularly in dense, hard bone. Higher drill speed rates can result in: thermal necrosis of the bone, soft tissue burns, an oversized hole, which can lead to reduced pull-out force, increased ease of the screws stripping in bone, suboptimal fixation, and/or the need for emergency screws. Always irrigate during drilling to avoid thermal damage to the bone and ensure drill bit is concentric to plate hole. Avoid drilling over nerve or tooth roots. Take care while drilling as to not damage, entrap, or tear a patient s soft tissue or damage critical structures. Be sure to keep drill clear of loose surgical materials. 11 DePuy Synthes MatrixORBITAL Surgical Technique
19 7. Secure implant Stabilize the implant with the appropriate number of MatrixMIDFACE screws inserted through selected screw holes in the plate. Fixation arms should be removed when not used for fixation. Note: Test for impingement A forced duction test must be completed to ensure unrestricted lateral and medial movement of the globe. Precautions: Confirm screw length prior to implantation. Tighten screws in a controlled manner. Applying too much torque to the screws may cause screw/ plate de formation or bone stripping. If bone becomes stripped, remove the screw from the bone and replace it with an emergency screw. In order to determine the appropriate amount of screws needed to achieve stable construct fixation, the surgeon should consider the fracture size and shape. MatrixORBITAL Surgical Technique DePuy Synthes 11
20 Surgical Technique 8. Confirm plate placement* Sagittal view of the correct plate placement is demonstrated in the image. Placement on the posterior ledge should be confirmed intraoperatively. * Image courtesy of Prof. Dr. Dr. M. Rasse, Department of Craniomaxillofacial Surgery, University of Innsbruck, Austria. 11 DePuy Synthes MatrixORBITAL Surgical Technique
21 Plates MatrixMIDFACE Preformed Orbital Plates, 0.4 mm thickness, malleable, pure titanium small left large left small right large right MatrixORBITAL Surgical Technique DePuy Synthes 11
22 Screws MatrixMIDFACE Screws, Titanium Alloy (TAN) Self-tapping screws B 1.5 mm length 4 mm length 5 mm length 6 mm length 8 mm Self-drilling screws B 1.5 mm length 4 mm length 5 mm length 6 mm length 8 mm Emergency screws B 1.8 mm, self-tapping length 4 mm length 5 mm length 6 mm length 8 mm Screw/plate overview Pack of 1 unit Pack of 4 units Pack of 1 unit, Pack of 4 units, Labelling clips sterile sterile Self-tapping screws xxx.01C xxx.04C xxx.01S xxx.04S xxxLC (in clips) Self-drilling screws xxx.01C xxx.04C xxx.01S xxx.04S xxxLC 1 (in clips) Emergency screws xxx.01C xxx.01S xxxLC (in clips) Plates xxx xxxS xxxLC 1 Labeling clips for self-drilling screws are marked with SD. 22 DePuy Synthes MatrixORBITAL Surgical Technique
23 Instruments Orbital Retractors Orbital Retractor, left Orbital Retractor, right Modules Module MatrixORBITAL Set MatrixMIDFACE Instrument Tray MatrixORBITAL MatrixORBITAL Surgical Technique DePuy Synthes 22
24 Bibliography 1. Müller ME, Allgöwer M, Schneider R, Willenegger H. Manual of Internal Fixation. 3 rd, expanded and completely revised edition. Berlin, Heidelberg, New York: Springer Prein J (ed.). Manual of Internal Fixation in the Cranio- Facial Skeleton. Berlin: Springer Hammer B. Orbital Fractures: Diagnosis, Operative Treatment, Secondary Corrections. Seattle, Toronto, Bern, Göttingen: Hogrefe & Huber Hammer B, Prein J. Correction of post-traumatic orbital deformities: operative techniques and review of 26 patients. J Craniomaxillofac Surg 1995; 23(2): Metzger MC, Schön R, Tetzlaf R, Weyer N, Rafii A, Gellrich NC, Schmelzeisen R. Topographical CT-data analysis of the human orbital floor. Int J Oral Maxillofac Surg 2007; 36(1): Metzger MC, Schön R, Weyer N, Rafii A, Gellrich NC, Schmelzeisen R, Strong BE. Anatomical 3-dimensional pre-bent titanium implant for orbital floor fractures. Ophthalmology 2006; 113(10): DePuy Synthes MatrixORBITAL Surgical Technique
25
26
27
28 Synthes GmbH Eimattstrasse Oberdorf Switzerland Tel: Fax: Not all products are currently available in all markets. This publication is not intended for distribution in the USA. All surgical techniques are available as PDF files at DePuy Synthes CMF, a division of Synthes GmbH All rights reserved DSEM/CMF/0216/0114(1) 03/18
MatrixMIDFACE Plate and Screw System. Surgical Technique
 MatrixMIDFACE Plate and Screw System Surgical Technique Image intensifier control This description alone does not provide sufficient background for direct use of DePuy Synthes products. Instruction by
MatrixMIDFACE Plate and Screw System Surgical Technique Image intensifier control This description alone does not provide sufficient background for direct use of DePuy Synthes products. Instruction by
Compact Midface. The systematic solution for craniomaxillofacial indications and displacement osteotomies.
 Compact Midface. The systematic solution for craniomaxillofacial indications and displacement osteotomies. Surgical Technique This publication is not intended for distribution in the USA. Instruments and
Compact Midface. The systematic solution for craniomaxillofacial indications and displacement osteotomies. Surgical Technique This publication is not intended for distribution in the USA. Instruments and
LOW PROFILE NEURO. This publication is not intended for distribution in the USA. SURGICAL TECHNIQUE
 LOW PROFILE NEURO This publication is not intended for distribution in the USA. SURGICAL TECHNIQUE TABLE OF CONTENTS INTRODUCTION Low Profile Neuro Plating System 2 Intended Use, Indications, Contraindications
LOW PROFILE NEURO This publication is not intended for distribution in the USA. SURGICAL TECHNIQUE TABLE OF CONTENTS INTRODUCTION Low Profile Neuro Plating System 2 Intended Use, Indications, Contraindications
MatrixNEURO. The next generation cranial plating system.
 MatrixNEURO. The next generation cranial plating system. Surgical Technique This publication is not intended for distribution in the USA. Instruments and implants approved by the AO Foundation. Image intensifier
MatrixNEURO. The next generation cranial plating system. Surgical Technique This publication is not intended for distribution in the USA. Instruments and implants approved by the AO Foundation. Image intensifier
The Calcaneal Plate. The Synthes non-locking solution for the Calcaneus.
 The Calcaneal Plate. The Synthes non-locking solution for the Calcaneus. Surgical Technique This publication is not intended for distribution in the USA. Instruments and implants approved by the AO Foundation.
The Calcaneal Plate. The Synthes non-locking solution for the Calcaneus. Surgical Technique This publication is not intended for distribution in the USA. Instruments and implants approved by the AO Foundation.
Orthodontic Bone Anchor (OBA) System
 Skeletal implants for the orthodontic movement of the teeth Orthodontic Bone Anchor (OBA) System Surgical Technique Image intensifier control This description alone does not provide sufficient background
Skeletal implants for the orthodontic movement of the teeth Orthodontic Bone Anchor (OBA) System Surgical Technique Image intensifier control This description alone does not provide sufficient background
Button Plate. Reinforcement for transosseous fixations.
 Button Plate. Reinforcement for transosseous fixations. Product Information This publication is not intended for distribution in the USA. Instruments and implants approved by the AO Foundation. Image intensifier
Button Plate. Reinforcement for transosseous fixations. Product Information This publication is not intended for distribution in the USA. Instruments and implants approved by the AO Foundation. Image intensifier
Low Profile Neuro Plating System. Surgical Technique
 Low Profile Neuro Plating System Surgical Technique TABLE OF CONTENTS INTRODUCTION Low Profile Neuro Plating System 2 SURGICAL TECHNIQUE Technique 5 PRODUCT INFORMATION Low Profile Neuro Plates 10 Low
Low Profile Neuro Plating System Surgical Technique TABLE OF CONTENTS INTRODUCTION Low Profile Neuro Plating System 2 SURGICAL TECHNIQUE Technique 5 PRODUCT INFORMATION Low Profile Neuro Plates 10 Low
Compact 2.0 LOCK Mandible. The locking system for the mandible.
 Compact 2.0 LOCK Mandible. The locking system for the mandible. Surgical Technique This publication is not intended for distribution in the USA. Instruments and implants approved by the AO Foundation.
Compact 2.0 LOCK Mandible. The locking system for the mandible. Surgical Technique This publication is not intended for distribution in the USA. Instruments and implants approved by the AO Foundation.
LCP Metaphyseal Plates. For extra-articular fractures.
 LCP Metaphyseal Plates. For extra-articular fractures. Surgical Technique This publication is not intended for distribution in the USA. Instruments and implants approved by the AO Foundation. Image intensifier
LCP Metaphyseal Plates. For extra-articular fractures. Surgical Technique This publication is not intended for distribution in the USA. Instruments and implants approved by the AO Foundation. Image intensifier
IMF Screw Set. For temporary, peri opera tive stabilisation of the occlusion in adults.
 IMF Screw Set. For temporary, peri opera tive stabilisation of the occlusion in adults. Surgical Technique This publication is not intended for distribution in the USA. Instruments and implants approved
IMF Screw Set. For temporary, peri opera tive stabilisation of the occlusion in adults. Surgical Technique This publication is not intended for distribution in the USA. Instruments and implants approved
Distal Radius Plate 2.4/2.7 dorsal and volar
 Distal Radius Plate 2.4/2.7 dorsal and volar Surgical Technique This publication is not intended for distribution in the USA. Instruments and implants approved by the AO Foundation. Distal Radius Plate
Distal Radius Plate 2.4/2.7 dorsal and volar Surgical Technique This publication is not intended for distribution in the USA. Instruments and implants approved by the AO Foundation. Distal Radius Plate
MatrixNEURO. The next generation cranial plating system.
 MatrixNEURO. The next generation cranial plating system. Technique Guide CMF Matrix This publication is not intended for distribution in the USA. Instruments and implants approved by the AO Foundation
MatrixNEURO. The next generation cranial plating system. Technique Guide CMF Matrix This publication is not intended for distribution in the USA. Instruments and implants approved by the AO Foundation
OBSOLETED. LCP Medial Distal Tibia Plate, without Tab. The Low Profile Anatomic Fixation System with Angular Stability and Optimal Screw Orientation.
 LCP Medial Distal Tibia Plate, without Tab. The Low Profile Anatomic Fixation System with Angular Stability and Optimal Screw Orientation. Surgical Technique LCP Small Fragment System This publication
LCP Medial Distal Tibia Plate, without Tab. The Low Profile Anatomic Fixation System with Angular Stability and Optimal Screw Orientation. Surgical Technique LCP Small Fragment System This publication
LCP Proximal Radius Plates 2.4. Plates for radial head rim and for radial head neck address individual fracture patterns of the proximal radius.
 LCP Proximal Radius Plates 2.4. Plates for radial head rim and for radial head neck address individual fracture patterns of the proximal radius. Surgical Technique This publication is not intended for
LCP Proximal Radius Plates 2.4. Plates for radial head rim and for radial head neck address individual fracture patterns of the proximal radius. Surgical Technique This publication is not intended for
Mandible External Fixator II
 Provides treatment for fractures of the mandible Mandible External Fixator II Surgical Technique Image intensifier control This description alone does not provide sufficient background for direct use of
Provides treatment for fractures of the mandible Mandible External Fixator II Surgical Technique Image intensifier control This description alone does not provide sufficient background for direct use of
low ProfIle neuro PlaTIng system
 low ProfIle neuro PlaTIng system surgical TeChnIque Table of Contents Introduction Low Profile Neuro Cranial Plating System 2 Surgical Technique Technique 5 Product Information Low Profile Neuro Plates
low ProfIle neuro PlaTIng system surgical TeChnIque Table of Contents Introduction Low Profile Neuro Cranial Plating System 2 Surgical Technique Technique 5 Product Information Low Profile Neuro Plates
LCP Proximal Radius Plates 2.4. Plates for radial head rim and for radial head neck address individual fracture patterns of the proximal radius.
 LCP Proximal Radius Plates 2.4. Plates for radial head rim and for radial head neck address individual fracture patterns of the proximal radius. Surgical Technique This publication is not intended for
LCP Proximal Radius Plates 2.4. Plates for radial head rim and for radial head neck address individual fracture patterns of the proximal radius. Surgical Technique This publication is not intended for
2.4 mm Variable Angle LCP Volar Extra-Articular Distal Radius System. For fragment-specific fracture fixation with variable angle locking technology.
 2.4 mm Variable Angle LCP Volar Extra-Articular Distal Radius System. For fragment-specific fracture fixation with variable angle locking technology. Surgical Technique This publication is not intended
2.4 mm Variable Angle LCP Volar Extra-Articular Distal Radius System. For fragment-specific fracture fixation with variable angle locking technology. Surgical Technique This publication is not intended
Internal Midface Distractor.
 Internal Midface Distractor. Surgical Technique This publication is not intended for distribution in the USA. Instruments and implants approved by the AO Foundation. Image intensifier control This description
Internal Midface Distractor. Surgical Technique This publication is not intended for distribution in the USA. Instruments and implants approved by the AO Foundation. Image intensifier control This description
orthodontic Bone anchor (oba) SYStem
 orthodontic Bone anchor (oba) SYStem Skeletal implants for the orthodontic movement of teeth SurgIcal technique Table of Contents Introduction Orthodontic Bone Anchor (OBA) System 2 Indications and Contraindications
orthodontic Bone anchor (oba) SYStem Skeletal implants for the orthodontic movement of teeth SurgIcal technique Table of Contents Introduction Orthodontic Bone Anchor (OBA) System 2 Indications and Contraindications
LCP DISTAL TIBIA PLATE
 LCP DISTAL TIBIA PLATE Instruments and implants approved by the AO Foundation. This publication is not intended for distribution in the USA. SURGICAL TECHNIQUE Image intensifier control This description
LCP DISTAL TIBIA PLATE Instruments and implants approved by the AO Foundation. This publication is not intended for distribution in the USA. SURGICAL TECHNIQUE Image intensifier control This description
Wrist Fusion Instrument and Implant Set.
 Wrist Fusion Instrument and Implant Set. Surgical Technique Discontinued December 2016 DSEM/TRM/0815/0479(2) This publication is not intended for distribution in the USA. Instruments and implants approved
Wrist Fusion Instrument and Implant Set. Surgical Technique Discontinued December 2016 DSEM/TRM/0815/0479(2) This publication is not intended for distribution in the USA. Instruments and implants approved
Technique Guide. Compact 2.0 LOCK Mandible. The locking system for the mandible.
 Technique Guide Compact 2.0 LOCK Mandible. The locking system for the mandible. Table of Contents Introduction Compact 2.0 LOCK Mandible 2 AO Principles 4 Indications and Contraindications 5 Surgical
Technique Guide Compact 2.0 LOCK Mandible. The locking system for the mandible. Table of Contents Introduction Compact 2.0 LOCK Mandible 2 AO Principles 4 Indications and Contraindications 5 Surgical
Titanium Wire with Barb and Needle. Surgical Technique Guide for Canthal Tendon Procedures.
 Titanium Wire with Barb and Needle. Surgical Technique Guide for Canthal Tendon Procedures. Technique Guide This publication is not intended for distribution in the USA. Instruments and implants approved
Titanium Wire with Barb and Needle. Surgical Technique Guide for Canthal Tendon Procedures. Technique Guide This publication is not intended for distribution in the USA. Instruments and implants approved
Condylar Head Add-on System. Adjustable system for condylar head reconstruction.
 Condylar Head Add-on System. Adjustable system for condylar head reconstruction. Surgical Technique This publication is not intended for distribution in the USA. Instruments and implants approved by the
Condylar Head Add-on System. Adjustable system for condylar head reconstruction. Surgical Technique This publication is not intended for distribution in the USA. Instruments and implants approved by the
2.0 mm Mandible Locking Plate System
 Advanced Plating System for Trauma, Microvascular Reconstruction, and Orthognathic Surgery 2.0 mm Mandible Locking Plate System Surgical Technique TABLE OF CONTENTS INTRODUCTION 2.0 mm Mandible Locking
Advanced Plating System for Trauma, Microvascular Reconstruction, and Orthognathic Surgery 2.0 mm Mandible Locking Plate System Surgical Technique TABLE OF CONTENTS INTRODUCTION 2.0 mm Mandible Locking
Titanium Wire With Barb and Needle
 For Canthal Tendon Procedures Titanium Wire With Barb and Needle Surgical Technique Table of Contents Introduction Titanium Wire With Barb and Needle 2 Indications 2 Surgical Technique Preoperative Planning
For Canthal Tendon Procedures Titanium Wire With Barb and Needle Surgical Technique Table of Contents Introduction Titanium Wire With Barb and Needle 2 Indications 2 Surgical Technique Preoperative Planning
Mandible External Fixator II. Provides treatment for fractures of the maxillofacial area.
 Mandible External Fixator II. Provides treatment for fractures of the maxillofacial area. Technique Guide This publication is not intended for distribution in the USA. Instruments and implants approved
Mandible External Fixator II. Provides treatment for fractures of the maxillofacial area. Technique Guide This publication is not intended for distribution in the USA. Instruments and implants approved
Technique Guide. Orthodontic Bone Anchor (OBA) System. Skeletal implants for the orthodontic movement of the teeth.
 Technique Guide Orthodontic Bone Anchor (OBA) System. Skeletal implants for the orthodontic movement of the teeth. Table of Contents Introduction Orthodontic Bone Anchor (OBA) System 2 Indications and
Technique Guide Orthodontic Bone Anchor (OBA) System. Skeletal implants for the orthodontic movement of the teeth. Table of Contents Introduction Orthodontic Bone Anchor (OBA) System 2 Indications and
MatrixNEURO Cranial Plating System
 The Next Generation Cranial Plating System MatrixNEURO Cranial Plating System Surgical Technique TABLE OF CONTENTS INTRODUCTION MatrixNEURO Cranial Plating System 2 MatrixNEURO Reconstruction Mesh 6 MatrixNEURO
The Next Generation Cranial Plating System MatrixNEURO Cranial Plating System Surgical Technique TABLE OF CONTENTS INTRODUCTION MatrixNEURO Cranial Plating System 2 MatrixNEURO Reconstruction Mesh 6 MatrixNEURO
MatrixORTHOGNATHIC TM Plating System
 Specialized Implants and Instruments for Orthognathic Surgery MatrixORTHOGNATHIC TM Plating System Surgical Technique TABLE OF CONTENTS INTRODUCTION MatrixORTHOGNATHIC Plating System 2 Features and Benefits
Specialized Implants and Instruments for Orthognathic Surgery MatrixORTHOGNATHIC TM Plating System Surgical Technique TABLE OF CONTENTS INTRODUCTION MatrixORTHOGNATHIC Plating System 2 Features and Benefits
LCP Medial Proximal Tibial Plate 3.5. Part of the Synthes small fragment Locking Compression Plate (LCP) system.
 LCP Medial Proximal Tibial Plate 3.5. Part of the Synthes small fragment Locking Compression Plate (LCP) system. Surgical Technique This publication is not intended for distribution in the USA. Instruments
LCP Medial Proximal Tibial Plate 3.5. Part of the Synthes small fragment Locking Compression Plate (LCP) system. Surgical Technique This publication is not intended for distribution in the USA. Instruments
Specialized Implants and Instruments for Orthognathic Surgery. MatrixORTHOGNATHIC. Surgical Technique
 Specialized Implants and Instruments for Orthognathic Surgery MatrixORTHOGNATHIC Surgical Technique Image intensifier control This description alone does not provide sufficient background for direct use
Specialized Implants and Instruments for Orthognathic Surgery MatrixORTHOGNATHIC Surgical Technique Image intensifier control This description alone does not provide sufficient background for direct use
LCP Low Bend Medial Distal Tibia Plates 3.5 mm. Anatomic plates with low profile head for intra- and extraarticular fractures.
 LCP Low Bend Medial Distal Tibia Plates 3.5 mm. Anatomic plates with low profile head for intra- and extraarticular fractures. Surgical Technique This publication is not intended for distribution in the
LCP Low Bend Medial Distal Tibia Plates 3.5 mm. Anatomic plates with low profile head for intra- and extraarticular fractures. Surgical Technique This publication is not intended for distribution in the
Femoral Neck System. Surgical Technique
 Femoral Neck System Surgical Technique Image intensifier control This description alone does not provide sufficient background for direct use of DePuy Synthes products. Instruction by a surgeon experienced
Femoral Neck System Surgical Technique Image intensifier control This description alone does not provide sufficient background for direct use of DePuy Synthes products. Instruction by a surgeon experienced
LCP Condylar Plate 4.5/5.0. Part of the LCP Periarticular Plating System.
 LCP Condylar Plate 4.5/5.0. Part of the LCP Periarticular Plating System. Surgical Technique This publication is not intended for distribution in the USA. Instruments and implants approved by the AO Foundation.
LCP Condylar Plate 4.5/5.0. Part of the LCP Periarticular Plating System. Surgical Technique This publication is not intended for distribution in the USA. Instruments and implants approved by the AO Foundation.
VA-Locking Intercarpal Fusion System. Variable angle locking technology for mediocarpal partial arthrodesis.
 VA-Locking Intercarpal Fusion System. Variable angle locking technology for mediocarpal partial arthrodesis. Surgical Technique This publication is not intended for distribution in the USA. Image intensifier
VA-Locking Intercarpal Fusion System. Variable angle locking technology for mediocarpal partial arthrodesis. Surgical Technique This publication is not intended for distribution in the USA. Image intensifier
External Distal Radius Fixator. Supplement to the 8 mm rod fixator system
 External Distal Radius Fixator. Supplement to the 8 mm rod fixator system Surgical technique This publication is not intended for distribution in the USA. Instruments and implants approved by the AO Foundation
External Distal Radius Fixator. Supplement to the 8 mm rod fixator system Surgical technique This publication is not intended for distribution in the USA. Instruments and implants approved by the AO Foundation
ARCH Laminoplasty System. Dedicated System for Open-door Laminoplasty.
 ARCH Laminoplasty System. Dedicated System for Open-door Laminoplasty. Surgical Technique This publication is not intended for distribution in the USA. Instruments and implants approved by the AO Foundation.
ARCH Laminoplasty System. Dedicated System for Open-door Laminoplasty. Surgical Technique This publication is not intended for distribution in the USA. Instruments and implants approved by the AO Foundation.
VECTRA-T SURGICAL TECHNIQUE. The Translational Anterior Cervical Palate System. This publication is not intended for distribution in the USA.
 VECTRA-T The Translational Anterior Cervical Palate System This publication is not intended for distribution in the USA. SURGICAL TECHNIQUE Image intensifier control This description alone does not provide
VECTRA-T The Translational Anterior Cervical Palate System This publication is not intended for distribution in the USA. SURGICAL TECHNIQUE Image intensifier control This description alone does not provide
Lag Screw Device Intended for symphyseal fracture fixation of the mandible
 Lag Screw Device Intended for symphyseal fracture fixation of the mandible SUrgicaL TecHNiqUe Lag Screw Device Intended for symphyseal fracture fixation of the mandible Simplifies the lag screw fixation
Lag Screw Device Intended for symphyseal fracture fixation of the mandible SUrgicaL TecHNiqUe Lag Screw Device Intended for symphyseal fracture fixation of the mandible Simplifies the lag screw fixation
LCP Condylar Plate 4.5/5.0. Part of the LCP Periarticular Plating System.
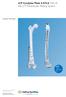 LCP Condylar Plate 4.5/5.0. Part of the LCP Periarticular Plating System. Surgical Technique This publication is not intended for distribution in the USA. Instruments and implants approved by the AO Foundation.
LCP Condylar Plate 4.5/5.0. Part of the LCP Periarticular Plating System. Surgical Technique This publication is not intended for distribution in the USA. Instruments and implants approved by the AO Foundation.
MEFiSTO. Monolateral External Fixation System for Trauma and Orthopaedics.
 MEFiSTO. Monolateral External Fixation System for Trauma and Orthopaedics. Surgical Technique This publication is not intended for distribution in the USA. Instruments and implants approved by the AO Foundation.
MEFiSTO. Monolateral External Fixation System for Trauma and Orthopaedics. Surgical Technique This publication is not intended for distribution in the USA. Instruments and implants approved by the AO Foundation.
3.0/3.5/4.0/4.5/6.5/7.0/7.3. Cannulated Screws. Surgical Technique
 3.0/3.5/4.0/4.5/6.5/7.0/7.3 Cannulated Screws Surgical Technique Image intensifier control This description alone does not provide sufficient background for direct use of DePuy Synthes products. Instruction
3.0/3.5/4.0/4.5/6.5/7.0/7.3 Cannulated Screws Surgical Technique Image intensifier control This description alone does not provide sufficient background for direct use of DePuy Synthes products. Instruction
ARCH Laminoplasty System
 Dedicated System for Open-door Laminoplasty ARCH Laminoplasty System Surgical Technique Image intensifier control This description alone does not provide sufficient background for direct use of DePuy Synthes
Dedicated System for Open-door Laminoplasty ARCH Laminoplasty System Surgical Technique Image intensifier control This description alone does not provide sufficient background for direct use of DePuy Synthes
LCP Superior Anterior Clavicle Plate. The anatomically precontoured fixation system with angular stability for clavicle shaft and lateral clavicle.
 LCP Superior Anterior Clavicle Plate. The anatomically precontoured fixation system with angular stability for clavicle shaft and lateral clavicle. Surgical Technique This publication is not intended for
LCP Superior Anterior Clavicle Plate. The anatomically precontoured fixation system with angular stability for clavicle shaft and lateral clavicle. Surgical Technique This publication is not intended for
Surgical Technique. This publication is not intended for distribution in the USA. Instruments and implants approved by the AO Foundation.
 LCP Extra-articular Distal Humerus Plate. The anatomically shaped and angular stable fixation system for extraarticular fractures of the distal humerus. Surgical Technique This publication is not intended
LCP Extra-articular Distal Humerus Plate. The anatomically shaped and angular stable fixation system for extraarticular fractures of the distal humerus. Surgical Technique This publication is not intended
LCP Distal Fibula Plates. Part of the Synthes locking compression plate (LCP) system.
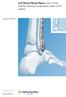 LCP Distal Fibula Plates. Part of the Synthes locking compression plate (LCP) system. Surgical Technique This publication is not intended for distribution in the USA. Instruments and implants approved
LCP Distal Fibula Plates. Part of the Synthes locking compression plate (LCP) system. Surgical Technique This publication is not intended for distribution in the USA. Instruments and implants approved
SynPOR HD Facial Shape System. For the augmentation or reconstruction of the craniomaxillofacial skeleton.
 SynPOR HD Facial Shape System. For the augmentation or reconstruction of the craniomaxillofacial skeleton. Technique Guide This publication is not intended for distribution in the USA. Instruments and
SynPOR HD Facial Shape System. For the augmentation or reconstruction of the craniomaxillofacial skeleton. Technique Guide This publication is not intended for distribution in the USA. Instruments and
CSLP-Cervical Spine Locking Plate
 For anterior, cervical fixation CSLP-Cervical Spine Locking Plate Surgical Technique Image intensifier control This description alone does not provide sufficient background for direct use of DePuy Synthes
For anterior, cervical fixation CSLP-Cervical Spine Locking Plate Surgical Technique Image intensifier control This description alone does not provide sufficient background for direct use of DePuy Synthes
VA-LCP Anterior Clavicle Plate. The anatomically precontoured fixation system with angular stability for clavicle shaft and lateral clavicle.
 VA-LCP Anterior Clavicle Plate. The anatomically precontoured fixation system with angular stability for clavicle shaft and lateral clavicle. Surgical Technique This publication is not intended for distribution
VA-LCP Anterior Clavicle Plate. The anatomically precontoured fixation system with angular stability for clavicle shaft and lateral clavicle. Surgical Technique This publication is not intended for distribution
TSLP Thoracolumbar Spine Locking Plate
 Anterior thoracolumbar spine locking plate TSLP Thoracolumbar Spine Locking Plate Surgical Technique Image intensifier control This description alone does not provide sufficient background for direct use
Anterior thoracolumbar spine locking plate TSLP Thoracolumbar Spine Locking Plate Surgical Technique Image intensifier control This description alone does not provide sufficient background for direct use
VA LOCKING CALCANEAL PLATES 2.7
 VA LOCKING CALCANEAL PLATES 2.7 Instruments and Implants approved by the AO Foundation. This publication is not intended for distribution in the USA. SURGICAL TECHNIQUE Image intensifier control Warning
VA LOCKING CALCANEAL PLATES 2.7 Instruments and Implants approved by the AO Foundation. This publication is not intended for distribution in the USA. SURGICAL TECHNIQUE Image intensifier control Warning
LCP Medial Proximal Tibial Plate 3.5. Part of the Synthes small fragment Locking Compression Plate (LCP) system.
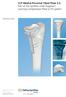 LCP Medial Proximal Tibial Plate 3.5. Part of the Synthes small fragment Locking Compression Plate (LCP) system. Technique Guide This publication is not intended for distribution in the USA. Instruments
LCP Medial Proximal Tibial Plate 3.5. Part of the Synthes small fragment Locking Compression Plate (LCP) system. Technique Guide This publication is not intended for distribution in the USA. Instruments
MATRIX PLATFORM FEATURES DESIGNED TO COMPLEMENT AO FIXATION PRINCIPLES
 MATRIX PLATFORM FEATURES DESIGNED TO COMPLEMENT AO FIXATION PRINCIPLES The aim of surgical fracture treatment is to reconstruct the bony anatomy and restore its function. Internal fixation is distinguished
MATRIX PLATFORM FEATURES DESIGNED TO COMPLEMENT AO FIXATION PRINCIPLES The aim of surgical fracture treatment is to reconstruct the bony anatomy and restore its function. Internal fixation is distinguished
LCP Distal Fibula Plates. Part of the Synthes locking compression plate (LCP) system.
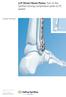 LCP Distal Fibula Plates. Part of the Synthes locking compression plate (LCP) system. Surgical Technique This publication is not intended for distribution in the USA. Instruments and implants approved
LCP Distal Fibula Plates. Part of the Synthes locking compression plate (LCP) system. Surgical Technique This publication is not intended for distribution in the USA. Instruments and implants approved
VA-LCP Olecranon Plates 2.7/3.5. The fracture-specific low-profile fixation system with variable angle locking technology.
 VA-LCP Olecranon Plates 2.7/3.5. The fracture-specific low-profile fixation system with variable angle locking technology. Surgical Technique This publication is not intended for distribution in the USA.
VA-LCP Olecranon Plates 2.7/3.5. The fracture-specific low-profile fixation system with variable angle locking technology. Surgical Technique This publication is not intended for distribution in the USA.
ANGLED BLADE PLATES FOR ADULTS
 ANGLED BLADE PLATES FOR ADULTS Instruments and implants approved by the AO Foundation. This publication is not intended for distribution in the USA. SURGICAL TECHNIQUE Image intensifier control This description
ANGLED BLADE PLATES FOR ADULTS Instruments and implants approved by the AO Foundation. This publication is not intended for distribution in the USA. SURGICAL TECHNIQUE Image intensifier control This description
The Versatile Polyaxial Solution for the Universal Spine Systems. USS II Polyaxial. Surgical Technique
 The Versatile Polyaxial Solution for the Universal Spine Systems USS II Polyaxial Surgical Technique Image intensifier control This description alone does not provide sufficient background for direct use
The Versatile Polyaxial Solution for the Universal Spine Systems USS II Polyaxial Surgical Technique Image intensifier control This description alone does not provide sufficient background for direct use
PHILOS and PHILOS Long. The anatomic fixation system for the proximal humerus.
 PHILOS and PHILOS Long. The anatomic fixation system for the proximal humerus. Surgical Technique This publication is not intended for distribution in the USA. Instruments and implants approved by the
PHILOS and PHILOS Long. The anatomic fixation system for the proximal humerus. Surgical Technique This publication is not intended for distribution in the USA. Instruments and implants approved by the
Orbital Plating System OPS 1.5
 PRODUCT INFORMATION Orbital Plating System OPS 1.5 MODUS Midface 2 Orbital Plating System OPS 1.5 At a glance Orbital Plating System OPS 1.5 INTRODUCTION Fractures of the orbit occur in about 50% of all
PRODUCT INFORMATION Orbital Plating System OPS 1.5 MODUS Midface 2 Orbital Plating System OPS 1.5 At a glance Orbital Plating System OPS 1.5 INTRODUCTION Fractures of the orbit occur in about 50% of all
ECD EXPANDABLE CORPECTOMY DEVICE Continuously Expandable Vertebral Body Replacement for Tumour Cases
 ECD EXPANDABLE CORPECTOMY DEVICE Continuously Expandable Vertebral Body Replacement for Tumour Cases Instruments and implants approved by the AO Foundation. This publication is not intended for distribution
ECD EXPANDABLE CORPECTOMY DEVICE Continuously Expandable Vertebral Body Replacement for Tumour Cases Instruments and implants approved by the AO Foundation. This publication is not intended for distribution
LCP Ulna Osteotomy System 2.7. Low profile angular stable fixation for ulna shortening osteotomies.
 LCP Ulna Osteotomy System 2.7. Low profile angular stable fixation for ulna shortening osteotomies. Surgical Technique This publication is not intended for distribution in the USA. Instruments and implants
LCP Ulna Osteotomy System 2.7. Low profile angular stable fixation for ulna shortening osteotomies. Surgical Technique This publication is not intended for distribution in the USA. Instruments and implants
Technique Guide. Midface Distractor System. For the temporary stabilization and gradual lengthening of the cranial or midfacial bones.
 Technique Guide Midface Distractor System. For the temporary stabilization and gradual lengthening of the cranial or midfacial bones. Table of Contents Introduction Midface Distractor System 2 Indications
Technique Guide Midface Distractor System. For the temporary stabilization and gradual lengthening of the cranial or midfacial bones. Table of Contents Introduction Midface Distractor System 2 Indications
Low Bend Distal Tibia Plates
 Part of the DePuy Synthes Locking Compression Plate (LCP ) System 3.5 mm LCP Low Bend Medial Distal Tibia Plates Surgical Technique Table of Contents Introduction 3.5 mm LCP Low Bend Medial Distal Tibia
Part of the DePuy Synthes Locking Compression Plate (LCP ) System 3.5 mm LCP Low Bend Medial Distal Tibia Plates Surgical Technique Table of Contents Introduction 3.5 mm LCP Low Bend Medial Distal Tibia
Mini External Fixator.
 Mini External Fixator. Assembly and Surgical Technique This publication is not intended for distribution in the USA. Instruments and implants approved by the AO Foundation. Image intensifier control Warning
Mini External Fixator. Assembly and Surgical Technique This publication is not intended for distribution in the USA. Instruments and implants approved by the AO Foundation. Image intensifier control Warning
Mandible External Fixator II
 Provides Treatment for Fractures of the Mandible Mandible External Fixator II Surgical Technique Table of Contents Introduction Mandible External Fixator II 2 AO Principles 4 Indications 5 MRI Information
Provides Treatment for Fractures of the Mandible Mandible External Fixator II Surgical Technique Table of Contents Introduction Mandible External Fixator II 2 AO Principles 4 Indications 5 MRI Information
Technique Guide. 3.5 mm LCP Low Bend Medial Distal Tibia Plates. Part of the Synthes locking compression plate (LCP) system.
 Technique Guide 3.5 mm LCP Low Bend Medial Distal Tibia Plates. Part of the Synthes locking compression plate (LCP) system. Table of Contents Introduction 3.5 mm LCP Low Bend Medial Distal Tibia Plates
Technique Guide 3.5 mm LCP Low Bend Medial Distal Tibia Plates. Part of the Synthes locking compression plate (LCP) system. Table of Contents Introduction 3.5 mm LCP Low Bend Medial Distal Tibia Plates
Cannulated Angled Blade Plate 3.5 and 4.5, 90.
 Cannulated Angled Blade Plate 3.5 and 4.5, 90. Technique Guide This publication is not intended for distribution in the USA. Instruments and implants approved by the AO Foundation. Table of Contents Introduction
Cannulated Angled Blade Plate 3.5 and 4.5, 90. Technique Guide This publication is not intended for distribution in the USA. Instruments and implants approved by the AO Foundation. Table of Contents Introduction
SYNPOR HD FACIAL SHAPE SYSTEM SURGICAL TECHNIQUE. For the augmentation or reconstruction of the craniomaxillofacial skeleton
 SYNPOR HD FACIAL SHAPE SYSTEM For the augmentation or reconstruction of the craniomaxillofacial skeleton SURGICAL TECHNIQUE Table of Contents Introduction SynPOR HD Facial Shape System 2 Indications and
SYNPOR HD FACIAL SHAPE SYSTEM For the augmentation or reconstruction of the craniomaxillofacial skeleton SURGICAL TECHNIQUE Table of Contents Introduction SynPOR HD Facial Shape System 2 Indications and
LCP Periarticular Proximal Humerus Plate 3.5. The anatomic fixation system with anterolateral shaft placement.
 LCP Periarticular Proximal Humerus Plate 3.5. The anatomic fixation system with anterolateral shaft placement. Surgical Technique This publication is not intended for distribution in the USA. Instruments
LCP Periarticular Proximal Humerus Plate 3.5. The anatomic fixation system with anterolateral shaft placement. Surgical Technique This publication is not intended for distribution in the USA. Instruments
TELEFIX SURGICAL TECHNIQUE. Implant system for the anterior stabilization of the thoracolumbar spine
 TELEFIX Implant system for the anterior stabilization of the thoracolumbar spine Instruments and implants approved by the AO Foundation. This publication is not intended for distribution in the USA. SURGICAL
TELEFIX Implant system for the anterior stabilization of the thoracolumbar spine Instruments and implants approved by the AO Foundation. This publication is not intended for distribution in the USA. SURGICAL
SYNPOR POROUS POLYETHYLENE IMPLANTS. For craniofacial and orbital augmentation and reconstruction
 SYNPOR POROUS POLYETHYLENE IMPLANTS For craniofacial and orbital augmentation and reconstruction SURGICAL TECHNIQUE TABLE OF CONTENTS INTRODUCTION SYNPOR Porous Polyethylene Implants 2 Indications and
SYNPOR POROUS POLYETHYLENE IMPLANTS For craniofacial and orbital augmentation and reconstruction SURGICAL TECHNIQUE TABLE OF CONTENTS INTRODUCTION SYNPOR Porous Polyethylene Implants 2 Indications and
Medium External Fixator Humeral Shaft Frame. Modular frame for upper extremity use.
 Medium External Fixator Humeral Shaft Frame. Modular frame for upper extremity use. Technique Guide Part of the Medium External Fixation System MRI Information Synthes Medium External Fixation devices
Medium External Fixator Humeral Shaft Frame. Modular frame for upper extremity use. Technique Guide Part of the Medium External Fixation System MRI Information Synthes Medium External Fixation devices
LCP Medial Distal Tibia Plate, without Tab. The Low Profile Anatomic Fixation System with Angular Stability and Optimal Screw Orientation.
 LCP Medial Distal Tibia Plate, without Tab. The Low Profile Anatomic Fixation System with Angular Stability and Optimal Screw Orientation. Technique Guide LCP Small Fragment System Table of Contents Introduction
LCP Medial Distal Tibia Plate, without Tab. The Low Profile Anatomic Fixation System with Angular Stability and Optimal Screw Orientation. Technique Guide LCP Small Fragment System Table of Contents Introduction
Cannulated Pediatric Osteotomy System (CAPOS). A single system of osteotomy blade plates and cannulated instrumentation.
 Cannulated Pediatric Osteotomy System (CAPOS). A single system of osteotomy blade plates and cannulated instrumentation. Surgical Technique This publication is not intended for distribution in the USA.
Cannulated Pediatric Osteotomy System (CAPOS). A single system of osteotomy blade plates and cannulated instrumentation. Surgical Technique This publication is not intended for distribution in the USA.
For the Attention of the Operating Surgeon: IMPORTANT INFORMATION ON THE MATRIXRIB FIXATION SYSTEM
 For the Attention of the Operating Surgeon: IMPORTANT INFORMATION ON THE MATRIXRIB FIXATION SYSTEM 10/16 GP2685-E-CAN DESCRIPTION The MatrixRIB Fixation System consists of locking plates, locking screws,
For the Attention of the Operating Surgeon: IMPORTANT INFORMATION ON THE MATRIXRIB FIXATION SYSTEM 10/16 GP2685-E-CAN DESCRIPTION The MatrixRIB Fixation System consists of locking plates, locking screws,
matrixwave tm mmf expand your possibilities A novel system that expands and compresses to achieve maxillomandibular fixation
 matrixwave tm mmf expand your possibilities A novel system that expands and compresses to achieve maxillomandibular fixation Designed for adaptability, versatility, and patient comfort MatrixWAVE TM MMF
matrixwave tm mmf expand your possibilities A novel system that expands and compresses to achieve maxillomandibular fixation Designed for adaptability, versatility, and patient comfort MatrixWAVE TM MMF
VA LCP MEDIAL COLUMN FUSION PLATES 3.5
 VA LCP MEDIAL COLUMN FUSION PLATES 3.5 Instruments and Implants approved by the AO Foundation. This publication is not intended for distribution in the USA. SURGICAL TECHNIQUE Image intensifier control
VA LCP MEDIAL COLUMN FUSION PLATES 3.5 Instruments and Implants approved by the AO Foundation. This publication is not intended for distribution in the USA. SURGICAL TECHNIQUE Image intensifier control
3.5 mm LCP Olecranon Plates
 Part of the DePuy Synthes Locking Compression Plate (LCP ) System 3.5 mm LCP Olecranon Plates Surgical Technique Table of Contents Introduction 3.5 mm LCP Olecranon Plates 2 AO Principles 3 Indications
Part of the DePuy Synthes Locking Compression Plate (LCP ) System 3.5 mm LCP Olecranon Plates Surgical Technique Table of Contents Introduction 3.5 mm LCP Olecranon Plates 2 AO Principles 3 Indications
LCP Proximal Tibial Plate 4.5/5.0 with Periarticular Aiming Arm Instruments
 LCP Proximal Tibial Plate 4.5/5.0 with Periarticular Aiming Arm Instruments Surgical Technique This publication is not intended for distribution in the USA. Instruments and implants approved by the AO
LCP Proximal Tibial Plate 4.5/5.0 with Periarticular Aiming Arm Instruments Surgical Technique This publication is not intended for distribution in the USA. Instruments and implants approved by the AO
DISTAL RADIUS. Instructions for Use
 DISTAL RADIUS Instructions for Use CAUTION: FEDERAL LAW RESTRICTS THESE DEVICES TO SALE BY OR ON THE ORDER OF A PHYSICIAN. Table of Contents 1. INTENDED USE... 3 2. DEVICE DESCRIPTION... 3 3. METHOD OF
DISTAL RADIUS Instructions for Use CAUTION: FEDERAL LAW RESTRICTS THESE DEVICES TO SALE BY OR ON THE ORDER OF A PHYSICIAN. Table of Contents 1. INTENDED USE... 3 2. DEVICE DESCRIPTION... 3 3. METHOD OF
Technique Guide. Titanium Wire with Barb and Needle. Surgical Technique Guide for Canthal Tendon Prodecures.
 Technique Guide Titanium Wire with Barb and Needle. Surgical Technique Guide for Canthal Tendon Prodecures. Indications/Features Indications The Synthes Titanium Wire with Barb and straight Needle is
Technique Guide Titanium Wire with Barb and Needle. Surgical Technique Guide for Canthal Tendon Prodecures. Indications/Features Indications The Synthes Titanium Wire with Barb and straight Needle is
MATrIxMANDIBLE. PrEFOrMED reconstruction PLATES. SUrgICAL TEChNIqUE
 MATrIxMANDIBLE PrEFOrMED reconstruction PLATES Preshaped ed to the mandibular anatomy SUrgICAL TEChNIqUE Table of Contents Introduction MatrixMANDIBLE Preformed Reconstruction Plates 2 AO Principles 5
MATrIxMANDIBLE PrEFOrMED reconstruction PLATES Preshaped ed to the mandibular anatomy SUrgICAL TEChNIqUE Table of Contents Introduction MatrixMANDIBLE Preformed Reconstruction Plates 2 AO Principles 5
Elbow Hinge Fixator. Guided Flexion/Extension for Unstable Elbow Fractures.
 Elbow Hinge Fixator. Guided Flexion/Extension for Unstable Elbow Fractures. Surgical Technique MR Safe Radiolucent Table of Contents System Description 3 Indications and Contraindications 4 Fixation Components
Elbow Hinge Fixator. Guided Flexion/Extension for Unstable Elbow Fractures. Surgical Technique MR Safe Radiolucent Table of Contents System Description 3 Indications and Contraindications 4 Fixation Components
LCP Proximal Femoral Hook Plate 4.5/5.0. Part of the LCP Periarticular Plating System.
 LCP Proximal Femoral Hook Plate 4.5/5.0. Part of the LCP Periarticular Plating System. Surgical Technique This publication is not intended for distribution in the USA. Instruments and implants approved
LCP Proximal Femoral Hook Plate 4.5/5.0. Part of the LCP Periarticular Plating System. Surgical Technique This publication is not intended for distribution in the USA. Instruments and implants approved
LCP Medial Proximal Tibial Plate 4.5/5.0. Part of the Synthes LCP periarticular plating system.
 LCP Medial Proximal Tibial Plate 4.5/5.0. Part of the Synthes LCP periarticular plating system. Technique Guide This publication is not intended for distribution in the USA. Instruments and implants approved
LCP Medial Proximal Tibial Plate 4.5/5.0. Part of the Synthes LCP periarticular plating system. Technique Guide This publication is not intended for distribution in the USA. Instruments and implants approved
Cannulated Pediatric Osteotomy System (CAPOS). A single system of osteotomy blade plates and cannulated instrumentation.
 Cannulated Pediatric Osteotomy System (CAPOS). A single system of osteotomy blade plates and cannulated instrumentation. Surgical Technique This publication is not intended for distribution in the USA.
Cannulated Pediatric Osteotomy System (CAPOS). A single system of osteotomy blade plates and cannulated instrumentation. Surgical Technique This publication is not intended for distribution in the USA.
Cranial System. Neuro Plating and Screw System
 Cranial System Neuro Plating and Screw System Innovasis Cranial System INDICATIONS FOR USE The Innovasis Cranial System (ICS) is intended for use in selective trauma of cranial skeleton, cranial surgery
Cranial System Neuro Plating and Screw System Innovasis Cranial System INDICATIONS FOR USE The Innovasis Cranial System (ICS) is intended for use in selective trauma of cranial skeleton, cranial surgery
PROXIMAL FEMORAL NAIL REMOVAL SET
 PROXIMAL FEMORAL NAIL REMOVAL SET for PFN, TFN and PFNA/PFNA-II Instruments and Implants approved by the AO Foundation. This publication is not intended for distribution in the USA. SURGICAL TECHNIQUE
PROXIMAL FEMORAL NAIL REMOVAL SET for PFN, TFN and PFNA/PFNA-II Instruments and Implants approved by the AO Foundation. This publication is not intended for distribution in the USA. SURGICAL TECHNIQUE
3.5 mm LCP Extra-articular Distal Humerus Plate
 Part of the DePuy Synthes Locking Compression Plate (LCP ) System 3.5 mm LCP Extra-articular Distal Humerus Plate Surgical Technique Table of Contents Introduction 3.5 mm LCP Extra-articular Distal Humerus
Part of the DePuy Synthes Locking Compression Plate (LCP ) System 3.5 mm LCP Extra-articular Distal Humerus Plate Surgical Technique Table of Contents Introduction 3.5 mm LCP Extra-articular Distal Humerus
SYNEX The vertebral body replacement with ratchet mechanism
 SYNEX The vertebral body replacement with ratchet mechanism Instruments and implants approved by the AO Foundation. This publication is not intended for distribution in the USA. SURGICAL TECHNIQUE Image
SYNEX The vertebral body replacement with ratchet mechanism Instruments and implants approved by the AO Foundation. This publication is not intended for distribution in the USA. SURGICAL TECHNIQUE Image
Long Volar Plates for Diaphyseal-Metaphyseal Radius Fractures LCP. Dia-Meta Volar Distal Radius Plates. Surgical Technique
 Long Volar Plates for Diaphyseal-Metaphyseal Radius Fractures LCP Dia-Meta Volar Distal Radius Plates Surgical Technique Table of Contents Introduction LCP Dia-Meta Volar Distal Radius Plates 2 AO Principles
Long Volar Plates for Diaphyseal-Metaphyseal Radius Fractures LCP Dia-Meta Volar Distal Radius Plates Surgical Technique Table of Contents Introduction LCP Dia-Meta Volar Distal Radius Plates 2 AO Principles
RapidSorb Resorbable Tacks. Resorbable Fixation System.
 RapidSorb Resorbable Tacks. Resorbable Fixation System. Fast Safe Resorbable Drill Press Fixed Table of Contents Introduction Overview 2 Indications and Contraindications 4 RapidSorb 5 Surgical Technique
RapidSorb Resorbable Tacks. Resorbable Fixation System. Fast Safe Resorbable Drill Press Fixed Table of Contents Introduction Overview 2 Indications and Contraindications 4 RapidSorb 5 Surgical Technique
PERFORATED CLICK X Augmentable pedicle screws for osteoporotic bone
 PERFORATED CLICK X Augmentable pedicle screws for osteoporotic bone Instruments and implants approved by the AO Foundation. This publication is not intended for distribution in the USA. SURGICAL TECHNIQUE
PERFORATED CLICK X Augmentable pedicle screws for osteoporotic bone Instruments and implants approved by the AO Foundation. This publication is not intended for distribution in the USA. SURGICAL TECHNIQUE
Interbody fusion cage for the transforaminal approach. Travios. Surgical Technique
 Interbody fusion cage for the transforaminal approach Travios Surgical Technique Image intensifier control This description alone does not provide sufficient background for direct use of DePuy Synthes
Interbody fusion cage for the transforaminal approach Travios Surgical Technique Image intensifier control This description alone does not provide sufficient background for direct use of DePuy Synthes
Surgical technique. IMF Screw Set. For temporary, peri opera tive stabilisation of the occlusion in adults.
 Surgical technique IMF Screw Set. For temporary, peri opera tive stabilisation of the occlusion in adults. Table of contents Features and benefits 2 Indications and contraindications 3 Surgical technique
Surgical technique IMF Screw Set. For temporary, peri opera tive stabilisation of the occlusion in adults. Table of contents Features and benefits 2 Indications and contraindications 3 Surgical technique
LCP Anterolateral Distal Tibia Plate 3.5. The low profile anatomic fixation system with optimal plate placement and angular stability.
 LCP Anterolateral Distal Tibia Plate 3.5. The low profile anatomic fixation system with optimal plate placement and angular stability. Surgical Technique LCP Small Fragment System This publication is not
LCP Anterolateral Distal Tibia Plate 3.5. The low profile anatomic fixation system with optimal plate placement and angular stability. Surgical Technique LCP Small Fragment System This publication is not
Part of the DePuy Synthes Locking Compression Plate (LCP ) System. 3.5 mm LCP Medial Proximal Tibia Plates
 Part of the DePuy Synthes Locking Compression Plate (LCP ) System 3.5 mm LCP Medial Proximal Tibia Plates Surgical Technique Table of Contents Introduction 3.5 mm LCP Medial Proximal Tibia Plates 2 AO
Part of the DePuy Synthes Locking Compression Plate (LCP ) System 3.5 mm LCP Medial Proximal Tibia Plates Surgical Technique Table of Contents Introduction 3.5 mm LCP Medial Proximal Tibia Plates 2 AO
