Review Article Diagnosis & Management of Temporomandibular Joint Disorders - What the Medical and Dental practitioners should know
|
|
|
- Tobias Peters
- 5 years ago
- Views:
Transcription
1 Chettinad Health City Medical Journal Diagnosis & Management of Temporomandibular Joint Disorders - What the Medical and Dental DrSVenkateswaran*, DrSaravanakumar**, DrAnnamalai**, DrDivya***, DrYamini*** *HOD & Professor, **Reader, ***Lecturer, Department of Orthodontics & Dentofacial Orthopedics, Chettinad Dental College & Research Institute, Chennai DrSVenkateswaran Graduated from the prestigious Madras Dental College and acquired his Masters in Orthodontics from the same Institution He is a Diplomat of National Board as well as Diplomate of the Indian Board of Orthodontics He is also a Member of National Academy of Medical sciences He has several national as well as international publications and presentations to his credit He underwent training in Roth - William center for Functional Occlusion USA for treating TMJ disorders Dr Venkateswaran s Research interests include Management of Tempero Mandibular Joint disorders and Micro implant anchorage in Orthodontics Corresponding author - Dr S Venkateswaran (venkatdental@gmailcom) Chettinad Health City Medical Journal 2014; 2(2): Abstract Temporomandibular disorders (TMD) are one of the most common causes of facial pain after odontogenic origin The temporomandibular disorders (TMD) are of multifactorial etiology and characterized by multiplicity of clinical signs and symptoms, making its diagnosis and management very difficult for the clinician TMD should be considered in the differential diagnosis of headache and orofacial pain in the absence of specific attributable organic cause Scientific evidence shows that noninvasive methods are preferred in the management of TMD These include occlusal, behavioral, physical and pharmacological treatment Practitioners of medicine and dentistry have the responsibility of diagnosing and managing people with TMD or refer them to an appropriate health care professional based on the nature and etiology of the problem Key words : TMD, Temporomandibular disorders, headache, facial pain, diagnosis 52 Introduction Historically, dentistry has been geared primarily to the diagnosis and treatment of odontogenic pain (pulpal and periodontal) However dentists come across orofacial pain originating from various other structures such as sinuses, ear, muscles, bones, nerves(neuralgia), blood vessels(migraine headaches) and temporomandibular joint(tmj), which may be referred to dental structures and vice versa It can stem from simple causes to life-threatening diseases and it can cause great suffering for patients Apart from the odontogenic causes, temporomandibular joint disorders are one of the most common causes of orofacial pain 1 The temporomandibular joint has a close anatomical and functional association with the structures of the head, neck and face and any disturbance in the joints, can produce symptoms which may be referred to any of these structures It can be from dental and non-dental source of origin including psycho-somatic disorders and therefore it is important that dentists, physicians, ophthalmologist, oto-laryngologist, surgeons, orthopedicians, psychologists and neurologists possess a fundamental knowledge of the TMJ disorders and consider it in the differential diagnosis of orofacial pain The diagnostic process for temporomandibular disorders (TMD) is complicated by the multifactorial etiology and multiplicity of clinical signs and symptoms characterizing such disorders However, proper diagnosis and management or referral of patients with these disorders as speedily as possible to the appropriate therapist is an important aspect of the quality of care provided by health care professionals The purpose of this article is to review the basic anatomy, function and disturbances of the temporomandibular joint, its diagnosis, differential diagnosis and clinical management The Temporo-Mandibular Joint The temporomandibular joint commonly called TMJ is an important joint that connects the mandible to the skull and regulates mandibular movement It is one of the most complex joint in the body, performing multiple vital functions It lets the mandible move up and down, side to side, forward and backward as a person does wondrous things as speaking, biting, chewing, swallowing, smiling, laughing, and frowning It is a bicondylar joint in which the condyles, located at the two ends of the mandible, function at the same time 2 The joint Anatomy The normal human skull possesses 2 temporomandibular joints (TMJs) that connect the skull to the lower jaw bone (the mandible) so as to allow the mouth to open and close The TMJ is a gliding joint, formed by the condyle of the mandible and the squamous portion of the temporal bone The articular surface of the temporal bone
2 consists of a convex articular eminence anteriorly and a concave articular fossa posterior The articular surface of the mandible is formed by the superior surface of the condyle Articular surfaces of the mandible and temporal bone are separated by an articular disc, which divides the joint cavity into 2 small spaces Design of the Masticatory System Articular Disc The articular disc, also known as the meniscus, is a biconcave, fibrocartilaginous structure, which provides the gliding surface for the mandibular condyle, resulting in smooth joint movement The articular disc has 3 parts a thick anterior band, a thin intermediate zone, and a thick posterior band When the mouth closed, the condyle is separated from the articular fossa of the temporal bone by the thick posterior band When the mouth is open, the condyle is separated from the articular eminence of the temporal bone by the thin intermediate zone The articular disc distributes the heavy masticatory forces to the condyle, articular eminence and the fossa The lateral ligament, sphenomandibular ligament and stylomandibular ligaments restricts the movements of the mandible and protects the joint The various movements of the mandible are brought about by the muscles of mastication and the supra-hyoid group of muscles All these structures including the dentition form an integral part of the masticatory system Uniqueness of the TM Joint The TMJs are 2 joints, formed by 3 bones and their functions are interdependent The articulating surfaces of the TMJ are covered by a fibrous connective tissue; this avascular and non-innervated structure has a greater capacity to resist degenerative change and regenerate itself than the hyaline cartilage of other synovial joints They are synovial joints with both rotatory and translatory movements possible The articular disc completely divides the joint space into separate upper and lower joint compartments The functions of the joints are not only influenced by the muscles and ligaments, but also by the teeth and their alignment The mandible is connected to the maxilla, cranium, clavicle, hyoid and spinal column through trapezius, Sterno-cleido-mastoid, suprahyoid group of muscles including digastric muscle, muscles of mastication and various ligaments The design and functioning of the masticatory system is a complex one and requires a balanced function of muscles, ligaments, bones and teeth Each movement is precisely co-ordinated, programmed and orchestrated 3,4 Relationship to Adjacent Structures All organs in the head-shoulder region are strongly networked via muscles and nerves by a complex biological feed-back mechanism Organs in the head-shoulder region: Masticatory organ ( teeth, mandibular joints, chewing muscles) Organs of swallowing ( swallowing muscles) Alveolar organ, Periodontium (Mechano -sensors) Organ of speech ( speech muscles) Hearing organ ( ears) Organ of sight (eyes) Olfactory organ ( nose) Central nervous system ( brain, impulse network via sensors an The temporo mandibular joint has a close anatomical and functional association with these structuresd nerves) The Temporomandibular Joint Disorder In the past, many physicians addressed this condition as TMJ disease or TMJ syndrome TMD was also previously known under the eponymous title of Costen syndrome, after Dr James Costen, an oto-laryngologist, who elucidated many aspects of the syndrome as it relates to dental malocclusion Today, a much more comprehensive view of this condition exists, and the term temporomandibular disorder (TMD) is the preferred term according to the 53
3 54 American Academy of Orofacial Pain (AAOP) which defines TMD as a collective term embracing a number of clinical problems that involve the masticatory musculature, Temporomandibular joint and associated structures or both As a group these conditions have no common etiology or biological explanation and comprise of a heterogeneous group of health problems whose signs and symptoms overlap Most often, these 2 types often coexist in one patient, making diagnosis and treatment more challenging Myogenous type is a more common form of TMD and in its pure form lacks apparent destructive changes of the TMJ on radiograph The causes of the symptoms (ie, pain, tenderness, and spasm of masticatory muscles) are muscular hyperactivity and dysfunction due to multiple etiologies such as bruxism and daytime jaw clenching and malocclusion of varying degree and duration Psychological factors may also play a role Arthrogenous TMD can be further specified as disk displacement disorder (more common), chronic recurrent dislocations, degenerative joint disorders, systemic arthritic conditions, ankylosis, infections, and neoplasia Etiology AAOP Classification of TMD (Based on anatomical structure involved) Myogenous/ TMD secondary to myofascial pain and dysfunction - Muscle-related TMD - Articular disorders include the articular surface, intra-articular disk, or articulating bones Arthrogenous/ TMD secondary to true articular disease - Joint-related TMD - Masticatory muscle disorders are problems within the muscles surrounding the TMJ The etiology of TMJ disorders remains unclear, but it is likely multifactorial Capsule inflammation or damage and muscle pain or spasm may be caused by abnormal occlusion, parafunctional habits (eg, bruxism [teeth grinding], teeth clenching, lip biting), stress, anxiety, or abnormalities of the intra-articular disk In recent years, many of the theories about the development of TMJ disorders have been questioned Abnormal dental occlusion appears to be equally common in persons with and without TMJ symptoms and occlusal correction does not reliably improve the symptoms or signs of TMJ disorders Parafunctional habits have been thought to cause TMJ microtrauma or masticatory muscle hyperactivity; however, these habits are also common in asymptomatic patients Although parafunctional habits may play a role in initiating or perpetuating symptoms in some patients, the cause-and-effect relationship remains uncertain 4,5 There is some evidence to suggest that anxiety, stress, and other emotional disturbances may exacerbate TMJ disorders, especially in patients who experience chronic pain As many as 75 percent of patients with TMJ disorders have a significant psychological abnormality Recognition and treatment of concomitant mental illness is important in the overall approach to management of chronic pain, including pain caused by TMJ disorders 5,6 Genetic variations in the gene coding for catecholamine-o-methyltransferase (COMT), a gene that relates in to some aspects of pain sensitivity has also been implicated 6 The other classifications of Etiology of TMD are I Dental and Non-Dental causes II Predisposing factors, Initiating factors, Perpetuating factors Predisposing factors factors that increase the risk of developing TMD Eg Systematic factors( degenerative, endocrine, infectious, metabolic, neoplastic, neurological,vascular and rheumatological diseases) Psychological factors (Anxiety, depression) Structural factors (change in synovial fluid viscosity, increased intra-articular pressure) Genetic factors Initiating factors factors that cause onset of the disorder Eg Trauma, parafunctional habits such as bruxism, clenching Perpetuating factors factors that interfere with healing and complicate management of the disorder Eg Mechanical and Muscular stress, metabolic problems Epidemiology Sex Predilection Temporomandibular disorder primarily affects women with a male-to-female ratio of 1:4 This could possibly be due to the presence of estrogen receptors in the TM joint 7,8,9 Age Even though it is common in adults and adolescents, the highest incidence is among young adults; especially women aged years In epidemiologic studies, up to 75 percent of adults show at least one sign of joint dysfunction on examination and as many as one third have at least one symptom However, only 5 percent of adults with TMJ
4 symptoms require treatment and even fewer develop chronic or debilitating symptoms Symptoms of Temporo mandibular disorder Soreness of Muscles of mastication Attrition of teeth and sensitivity Hypermobility of teeth Pain in the joints Clicking in the joints Crepitation in the joints Difficulty in opening of mouth Open lock of the mandible Apart from these symptoms, If a person suffers from any of the following symptoms without any specific or organic cause, then the possibility of Tempo mandibular disorder could be considered Headaches in the temple region Pain in the area of forehead and eyes Pain in the back of the head, possibly extending to the shoulders and neck Fullness in the ears Tinnitus Pressure on the eyes, sensitivity to light Dizzy spells, vertigo, nausea Lack of concentration Temporomandibular disorders can cause these disturbances due to its anatomic proximity and functional associations to these structures The trigeminal nerve, which is one of the main nerve supply to the TMJ and facial region, is a complex cranial nerve that can cause headaches when over stimulated by the muscles surrounding it 10 Diagnosis Medical History A comprehensive, chronological medical and dental history of the patient is essential for diagnosis of the problem and to decide about further investigations and treatment plan Observation Forward head posture (this has been shown to displace the condyles posteriorly) Jaw malocclusion, abnormal dental wear, and poor dentition Visible clenching or spasm of the ipsilateral neck musculature Physical Examination Joint range of motion: Evaluation of jaw opening and closure as well as lateral deviation bilaterally Normal range of motion for opening is 5 cm and lateral mandibular movement is 1 cm Patients with TMD usually have reduced opening Palpation: The TMJ is best palpated laterally as a depression below the zygomatic arch and 1-2 cm anterior to the tragus The posterior aspect of the joint is palpated through the external auditory canal The joint should be palpated in both open and closed positions and also both laterally and posteriorly While palpating, the examiner should feel for muscle spasm, muscle or joint tenderness, and joint sound The muscles palpated as a part of complete TMJ examination are masseter, temporalis, medial pterygoid, lateral pterygoid, and sternocleidomastoid In isolated myofascial pain and dysfunction, joint tenderness and joint click are usually absent Diagnostic Classification An abbreviated version of the diagnostic classification system developed by the American Academy of Orofacial Pain is shown in Table 1 TMJ disorders are separated into two main categories based on the anatomic origin of the problem: articular disorders and masticatory muscle disorders Accurate recognition of the origin of pain, either intra-articular or muscular, may help the dentst recommend an initial therapy; however, it is not clear which noninvasive therapies work best and varies TABLE 1 Diagnostic Classification of TMJ Disorders 1 Ankylosis Articular disorders of the TMJ Congenital or developmental disorders Aplasia, hyperplasia, or hypoplasia of the cranial bones or mandible Neoplasia of the TMJ or associated structures Disk derangement disorders Articular disk displacement with or without reduction Fracture of the condylar process Inflammatory disorders like Synovitis, Capsulitis, Polyarthritides including the TMJ Osteoarthritis TMJ dislocation Differential Diagnosis Masticatory muscle disorders Local myalgia (unclassified) Myofascial pain Myofibrotic contracture Myositis Myospasm Neoplasia The differential diagnosis for orofacial pain is listed in Table 2 TMJ disorders can cause referred pain, particularly undifferentiated headache Some studies have shown that as many as 55 percent of patients with chronic headache who were referred to a neurologist were found to have significant signs or symptoms of TMJ disorders Educating patients on self-care techniques and referral for noninvasive treatment should be considered in patients with chronic undifferentiated headache or headache that is not responding to standard treatment 55
5 TABLE 2 Differential Diagnosis of Orofacial Pain Condition Symptoms Signs Dental pathology Tooth abscess Pain with chewing over affected tooth Visible tooth decay; fluctuance along gum line; pain with palpation over the tooth Wisdom tooth eruption Dull ache behind posterior molars Tenderness to palpation over emerging tooth Infection or inflammation Herpes zoster and postherpetic neuralgia Mastoiditis Otitis externa Otitis media Parotitis Sialadenitis Trigeminal neuralgia Cluster Headache Migraine Headache Tumors Prodrome of pain followed by vesicular rash Fever; otalgia Pruritus, pain, and tenderness of the external ear Fever; malaise; otalgia Fever; malaise; myalgia; pain over parotid gland Pain and swelling of involved salivary gland Paroxysmal, unilateral lancinating pains in trigeminal nerve distribution retro-orbital or sinus pain, Episode, last 6 to 8 weeks, long pain free Unilateral dull, throbbing pain Weight loss, History of cancer Vesicular rash in dermatomal distribution, not crossing midline Postauricular erythema and swelling tenderness over mastoid process Erythema and edema of external auditory canal Tympanic membrane dull, bulging, erythematous; loss of landmarks on tympanic membrane Tenderness and induration over parotid gland Tenderness, induration, and/or erythema of salivary gland; usually unilateral Examination generally normal Rhinorrhea, nasal congestion and lacrimation from the involved side Unrelieved by a diagnostic block Unusual response to treatment, pain may become diffuse or paresthesia can occur 56 Diagnostic Testing Diagnostic testing and radiologic imaging of the TMJ have uncertain usefulness and generally should only be used for the most severe or chronic symptoms Local anesthetic nerve blocking can be helpful in differentiating whether orofacial pain originates from the TMJ capsule or from associated muscular structures Sensory innervation of the TMJ is delivered primarily through the auriculotemporal branch of the third division of the trigeminal nerve Patients who do not experience pain relief from diagnostic nerve blocking should be evaluated for other causes of orofacial pain 11, 12 Laboratory Studies If a systemic illness is suspected to be the cause of temporomandibular disorder (TMD), lab work is required WBC count may be done if infection is suspected Rheumatoid factor (RF), ESR, antinuclear antibody (ANA), and other specific antibodies should be checked if rheumatoid arthritis, temporal arteritis, or a connective tissue disorder is suspected Uric acid should be checked for gout Arthrocentesis may be required to demonstrate specific crystals Imaging Studies Conventional radiography is the most utilized imaging study It is simple, evaluates bony structures, and in most cases it is sufficient It involves specific techniques and views such as modified Schuller views of each TMJ, both open mouth and closed mouth Radiographic findings in TMJ depend on the etiology of TMD; in cases like rheumatoid arthritis, plain films show erosions, osteophytes, subchondral bony sclerosis, and condylar-glenoid fossa remodeling 13, 14 Dynamic high-resolution ultrasonography allows for visualization of the morphological elements and the functions of the TMJ, articular disk, mandibular condyle, and lateral pterygoid muscle 15,16 CT scans can explore both bony structures and muscular soft tissues Of interest, there is utility with cone beam computed tomography (CBCT) The patient is scanned with the mouth open and closed Specifically, CBCT can aid in the diagnosis of osteoarthritis, rheumatoid arthritis, synovial chondromatosis, and neoplastic disorders
6 Magnetic resonance image (MRI) should be used as the study of choice if an articular or meniscal pathology is suspected and an endoscopic or surgical procedure is contemplated, or in the case of traumatic TMD17 A a b C Fig - CBCT and reconstructed image of condyles Fig: B b - shows erosion on condylar head Fig: A a - Shows normal condylar morphology, Other Tests Quantitative analysis of occlusal strain and stress can be helpful by using photoplastic phenomenon of some polymers Results of strain analysis can help harmonize static and kinematic occlusal patterns by detecting and eliminating prematurities and interferences Stress analysis helps to understand the temporomandibular mechanical relationship 17 Procedures Diagnostic arthroscopy is an invasive diagnostic approach and should be used mainly in patients suffering from internal TMJ derangements recalcitrant to conservative measures MRI is suggested to be obtained prior to arthroscopy 18 Treatment The signs and symptoms of TMD improve for most of the patients over time with or without treatment As much as 50 percent of the patients improve from TMD symptoms in one year and almost 85 percent improve completely in three years Interventions that change the anatomy of the joint, invade the integrity of the joint space, or manipulate the jaw have the potential to cause harm and have not been shown to improve symptoms Therefore, self-care and noninvasive treatments are good options and should be attempted before invasive or permanent therapies, such as orthodontics or surgery, are recommended 19,20 Self - Care There is little evidence to suggest that any TMJ disorder treatment modality is superior to any other, although it is generally accepted that self-care and behavioral interventions should be encouraged for all patients, regardless of which therapies are considered Providing a few simple exercises, behavioral instructions, and reassurance are important steps when treating the average patient with new or intermittent symptoms Noninvasive Therapy Many noninvasive therapies are commonly used for the treatment of TMJ disorders The disciplines of medicine, dentistry (occlusal splint therapy, replacement of missing teeth, correcting malocclusion), physical therapy, and psychology can provide effective treatment in different clinical situations Pharmacotherapy The indicated classes of pharmacologic agents include analgesics, anti-inflammatory agents, corticosteroids, anxiolytics, muscle relaxants and antidepressants Non-opiate analgesics are effective for mild to moderate acute pain associated with TMD, and opioid narcotics are considered for short-term use in only controlling acute severe pain Additionally, tricyclic antidepressants appear to be effective in the control of chronic orofacial pain of non-inflammatory origin, independent of their effects on mood, with daily doses smaller than those typically used in the treatment of depression 17 Several available therapies are listed in Table 3 Because most patients with TMJ disorders improve with or without treatment, these conservative therapies should be encouraged before invasive treatments are considered 21, 22, 23 TABLE 3 Noninvasive Therapies for TMJ Disorders Alternative therapies Acupressure Acupuncture Hypnosis Massage Dental procedures Occlusal splint therapy, replacement of missing teeth, correcting malocclusion, Occlusal adjustments 57
7 58 Medical interventions Intra-articular corticosteroid or anesthetic injection Myofascial trigger-point injection Pharmacologic treatment Acetaminophen Anxiolytics Benzodiazepines Muscle relaxants Nonsteroidal anti-inflammatory drugs Tricyclic antidepressants Physical therapy modalities Biofeedback Iontophoresis Superficial or deep heat Therapeutic exercise Lateral jaw movement Protrusive jaw movement Resisted closing Resisted opening Tongue-up exercise Transcutaneous electrical nerve stimulation Psychological interventions Cognitive behavior therapy Relaxation techniques Stress management Surgical treatment Surgery is indicated only in specific articular disorders, usually in cases that do not respond to conservative treatment, and when the patient s quality of life has been significantly affected 1,25,22 Surgical management may vary from closed surgical procedures, such as arthrocentesis and arthroscopy, to more complex open joint operations, such as arthrotomy, disk repositioning, diskectomy and condylotomy 24,25,26 Conclusion Medical and dental practitioners should consider temporomandibular Joint disorders as a possible cause in the diagnosis of oro-facial pain including headaches, shoulder and neck pain, vertigo and associated pain, blurring of vision, disorders of hearing, nausea, vomiting, and disturbances in concentration, in the absence of any specific, attributable or organic cause While orofacial pain and headache secondary to jaw muscle function and dental structures ideally be managed by dentists, pain in the head and neck region unrelated to it should be should be referred to an appropriate medical care specialists for management References 1) 2) 3) 4) 5) 6) 7) 8) 9) 10) 11) 12) Okeson JP, for the American Academy of Orofacial Pain Orofacial Pain: Guidelines for Assessment, Diagnosis, and Management Chicago, Ill: Quintessence Pub, 1996 Pertes RA, Gross SG Functional anatomy and biomechanics of the temporomandibular joint In: Pertes RA, Gross SG Clinical Management of Temporomandibular Disorders and Orofacial Pain Chicago, Ill: Quintessence Pub, 1995:1 12 F Luther Orthodontics and the temporomandibular joint: Where are we now? Part 2 Functional occlusion, malocclusion, and TMD The Angle Orthodontist Aug 1998, Vol 68, No 4 (August 1998) pp Badel T, Marotti M, Pavicin IS, Basić-Kes V Temporomandibular disorders and occlusion Acta Clin Croat 2012 Sep;51(3): Dawson PE, Functional occlusion-from TMJ to smile design: Mosby pub Wadhwa L, Utreja A, Tewari A A study of clinical signs and symptoms of temporomandibular dysfunction in subjects with normal occlusion, untreated, and treated malocclusions Am J Orthod Dentofacial Orthop 1993; 103:54-61 McNamara JA Jr, Seligman DA, Okeson JP Occlusion, orthodontic treatment, and temporomandibular disorders: a review J Orofac Pain 1995;9:73 90 Diatchenko, L, Slade, GD, Nackley, AG et al (2005) Genetic basis for individual variations in pain perception and the development of a chronic pain condition Human Molecular Genetics 14(1), Dworkin SF, Huggins KH, LeResche L, Von Korff M, Howard J, Truelove E, et al Epidemiology of signs and symptoms in temporomandibular disorders: clinical signs in cases and controls J Am Dent Assoc 1990; 120: Hentschel K, Capobianco DJ, Dodick DW Facial pain Neurologist 2005;11:244 9 Pertes RA, Bailey DR General concepts of diagnosis and treatment In: Pertes RA, Gross SG Clinical Management of Temporomandibular Disorders and Orofacial Pain Chicago, Ill: Quintessence Pub, 1995:59 68 De Boever, JA, Nilner, M, Orthlieb, J-D and Steenks, MH (2007) Recommendations for examination, diagnosis, management of patients with temporomandibular disorders and orofacial pain by the general dental practitioner European Academy of Craniomandibular Disorders
8 13) 14) 15) 16) 17) 18) 19) DuPont JS Jr Simplified anesthesia blocking of the temporomandibular joint Gen Dent 2004;52: American Academy of Oral and Maxillofacial Radiology Radiographic imaging of the temporomandibular joint Imaging of the TMJ, Oral Surg Oral Med Oral Pathol Oral Radiol Endod 83:609-18, (1997) Manfredini D Ultrasonography has an acceptable diagnostic efficacy for temporomandibular disc displacement Evid Based Dent 2012;13 (3):84-5 Manfredini D, Bonnini S, Stellini E, Salmaso L, Guarda-Nardini L Comparison of magnetic resonance imaging findings in temporomandibular joints of the two sides Clin Oral Investig 2013 May 3 Mannheimer JS Overview of physical therapy modalities and procedures In: Pertes RA, Gross SG Clinical Management of Temporomandibular Disorders and Orofacial Pain Chicago, Ill: Quintessence Pub, 1995: American Society of Temporomandibular Joint Surgeons Guidelines for diagnosis and management of disorders involving the temporomandibular joint and related musculoskeletal structures Cranio 2003;21:68 76 Al-Ani, MZ, Davies, SJ, Gray, RJM et al (2004)Stabilisation splint therapy for temporomandibular pain dysfunction syndrome (Cochrane Review) Issue 1 John Wiley & Sons, Ltd 20) 21) 22) 23) 24) 25) 26) Wassell RW, Adams N, Kelly PJ The treatment of temporomandibular disorders with stabilizing splints in general dental practice: one-year follow-up J Am Dent Assoc 2006;137: Pettengill CA & Reisner-Keller L; The use of tricyclic antidepressants for the control of chronic orofacial pain J Craniomand Pract 1997;15: Conti PC, dos Santos CN, Kogawa EM, de Castro Ferreira Conti AC, de Araujo Cdos R The treatment of painful temporomandibular joint clicking with oral splints: a randomized clinical trial J Am Dent Assoc 2006;137: Truelove E, Huggins KH, Mancl L, Dworkin SF The efficacy of traditional, low-cost and nonsplint therapies for temporomandibular disorder: a randomized controlled trial J Am Dent Assoc 2006;137: Shankland WE II Temporomandibular disorders: standard treatment options Gen Dent 2004;52: Dolwick MF;The role of temporomandibular joint surgery in the treatment of patients with internal derangement Oral Surg Oral Med Oral Pathol Oral Radiol Endod 1997;vol 83: McNeill C; Management of temporomandibular disorders: concept and controversies J Prosth Dent 1997; vol 77: Blueberries and Diabetes Results of three longitudinal cohort studies published in BMJ (BMJ 2013;347:f5001) appear to suggest that eating whole fruit is associated with reduced risk of developing type 2 diabetes But fruit juice does not appear to have similar effect The researchers took a look at the diets of more than 1,87,000 Americans Three servings per week of blueberries, grape, raisins, apples and pears significantly reduced the risk Replacing fruit juice with blueberries could reduce the risk of developing type 2 diabetes by 33%, with grapes and raisins by 19%, apples and pears by 13% and with any combination of whole fruit by 7% The beneficial effects are probably related to high levels anthocyanins in many of these fruits Besides, most fruits also have variable content of antioxidants, fibre, phytochemicals and other nutrients The UK government recommends eating five portions of fruit and vegetables every day - Dr K Ramesh Rao 59
TEMPORO-MANDIBULAR JOINT DISORDERS
 Disclaimer This movie is an educational resource only and should not be used to manage your dental health. All decisions about the management of TMJ Disorders must be made in conjunction with your Dental
Disclaimer This movie is an educational resource only and should not be used to manage your dental health. All decisions about the management of TMJ Disorders must be made in conjunction with your Dental
Temporomandibular Joint. Dr Noman ullah wazir
 Temporomandibular Joint Dr Noman ullah wazir Type of Joint TMJ is a Synovial joint between : The condylar head of the mandible. The mandibular fossa of squamous part of temporal bone. The joint cavity
Temporomandibular Joint Dr Noman ullah wazir Type of Joint TMJ is a Synovial joint between : The condylar head of the mandible. The mandibular fossa of squamous part of temporal bone. The joint cavity
Up Date on TMD WHAT IS TMD? Temporomandibular Disorders (TMD)*: Donald Nixdorf DDS, MS
 Up Date on TMD Donald Nixdorf DDS, MS Associate Professor Division of TMD and Orofacial Pain WHAT IS TMD? Temporomandibular Disorders (TMD)*: MUSCLE and JOINT DISORDERS * Temporomandibular Muscle and Joint
Up Date on TMD Donald Nixdorf DDS, MS Associate Professor Division of TMD and Orofacial Pain WHAT IS TMD? Temporomandibular Disorders (TMD)*: MUSCLE and JOINT DISORDERS * Temporomandibular Muscle and Joint
Temporomandibular Joint Disorders
 Temporomandibular Joint Disorders Introduction Temporomandibular joint disorders, or TMJ disorders, are a group of medical problems related to the jaw joint. TMJ disorders can cause headaches, ear pain,
Temporomandibular Joint Disorders Introduction Temporomandibular joint disorders, or TMJ disorders, are a group of medical problems related to the jaw joint. TMJ disorders can cause headaches, ear pain,
Initial Doctor Questionnaire
 Initial Doctor Questionnaire DO NOT enter the patient in this study: if your patient does not have a TMD pain diagnosis if your patient does not need treatment at this time if you are not going to treat
Initial Doctor Questionnaire DO NOT enter the patient in this study: if your patient does not have a TMD pain diagnosis if your patient does not need treatment at this time if you are not going to treat
The Skull and Temporomandibular joint II Prof. Abdulameer Al-Nuaimi. E. mail:
 The Skull and Temporomandibular joint II Prof. Abdulameer Al-Nuaimi E-mail: a.al-nuaimi@sheffield.ac.uk E. mail: abdulameerh@yahoo.com Temporal fossa The temporal fossa is a depression on the temporal
The Skull and Temporomandibular joint II Prof. Abdulameer Al-Nuaimi E-mail: a.al-nuaimi@sheffield.ac.uk E. mail: abdulameerh@yahoo.com Temporal fossa The temporal fossa is a depression on the temporal
Muscles of mastication [part 1]
![Muscles of mastication [part 1] Muscles of mastication [part 1]](/thumbs/76/73586850.jpg) Muscles of mastication [part 1] In this lecture well have the muscles of mastication, neuromuscular function, and its relationship to the occlusion morphology. The fourth determinant of occlusion is the
Muscles of mastication [part 1] In this lecture well have the muscles of mastication, neuromuscular function, and its relationship to the occlusion morphology. The fourth determinant of occlusion is the
Diagnosis and Treatment of Temporomandibular Disorders (TMD) By: Aman Bhojani. Background & Etiology
 Diagnosis and Treatment of Temporomandibular Disorders (TMD) By: Aman Bhojani Background & Etiology TMD affects approximately 10-15% of the population, but only 5% seek treatment. Incidence peaks from
Diagnosis and Treatment of Temporomandibular Disorders (TMD) By: Aman Bhojani Background & Etiology TMD affects approximately 10-15% of the population, but only 5% seek treatment. Incidence peaks from
Prof. Zvan Bojana, M.D., Ph.D., senior consultant, FESO University Medical Centre Ljubljana, Slovenia Clinical Department of Vascular Neurology
 TEPOROMANDIBULAR PAIN Prof. Zvan Bojana, M.D., Ph.D., senior consultant, FESO University Medical Centre Ljubljana, Slovenia Clinical Department of Vascular Neurology Facial pain TMJ pathology Other ethiology
TEPOROMANDIBULAR PAIN Prof. Zvan Bojana, M.D., Ph.D., senior consultant, FESO University Medical Centre Ljubljana, Slovenia Clinical Department of Vascular Neurology Facial pain TMJ pathology Other ethiology
Preface Introduction Initial Evaluation Patient Interview Review of the "Initial Patient Questionnaire" Clinical Examination Range of Motion TMJ
 Preface Introduction Initial Evaluation Patient Interview Review of the "Initial Patient Questionnaire" Clinical Examination Range of Motion TMJ Noise TMD Palpations Intraoral Examination Occlusal Changes
Preface Introduction Initial Evaluation Patient Interview Review of the "Initial Patient Questionnaire" Clinical Examination Range of Motion TMJ Noise TMD Palpations Intraoral Examination Occlusal Changes
TMJ UNDERSTANDING SYNDROME SPECIAL REPORT By Paul R. White, D.D.S. Special Report: Understanding TMJ Syndrome
 SPECIAL REPORT Special Report: Understanding TMJ Syndrome UNDERSTANDING TMJ SYNDROME By Paul R. White, D.D.S. 804.715.1647 www.smilerichmond.com 804.715.1647 www.smilerichmond.com 1 UNDERSTANDING TMJ SYNDROME
SPECIAL REPORT Special Report: Understanding TMJ Syndrome UNDERSTANDING TMJ SYNDROME By Paul R. White, D.D.S. 804.715.1647 www.smilerichmond.com 804.715.1647 www.smilerichmond.com 1 UNDERSTANDING TMJ SYNDROME
Classification of Tempromandibular Disorders
 Classification of Tempromandibular Disorders Defined as any disorder that affects or that is affected by deformity, disease, misalignment, or dysfunction of the tempromandibular articulation. This includes
Classification of Tempromandibular Disorders Defined as any disorder that affects or that is affected by deformity, disease, misalignment, or dysfunction of the tempromandibular articulation. This includes
Where is the Temporo-Mandibular Joint?
 TMJ Pain Open your jaw all the way and shut it. This simple movement would not be possible without the Temporo-Mandibular Joint (TMJ). It connects the temporal bone (the bone that forms the side of the
TMJ Pain Open your jaw all the way and shut it. This simple movement would not be possible without the Temporo-Mandibular Joint (TMJ). It connects the temporal bone (the bone that forms the side of the
Introduction to Occlusion and Mechanics of Mandibular Movement
 Introduction to Occlusion and Mechanics of Mandibular Movement Dr. Pauline Hayes Garrett Department of Endodontics, Prosthodontics, and Operative Dentistry University of Maryland, Baltimore Assigned reading
Introduction to Occlusion and Mechanics of Mandibular Movement Dr. Pauline Hayes Garrett Department of Endodontics, Prosthodontics, and Operative Dentistry University of Maryland, Baltimore Assigned reading
TMD: Epidemiology: Signs and Symptoms
 TMD: Epidemiology: Signs and Symptoms Mauno Könönen Prof., Dr. Odont. Dept. of Stomatognathic Physiology and Prosthetic Dentistry Institute of Dentistry University of Helsinki Finland Temporomandibular
TMD: Epidemiology: Signs and Symptoms Mauno Könönen Prof., Dr. Odont. Dept. of Stomatognathic Physiology and Prosthetic Dentistry Institute of Dentistry University of Helsinki Finland Temporomandibular
Original Research Article
 KNOWLEDGE ON TEMPOROMANDIBULAR JOINT DISORDERS AMONG DENTISTS IN CHENNAI, TAMILNADU K. Niraimathi 1, K. Ranjith 2, Vidya Albert Yen 3, Edward Nijesh 4, Shalini P 5, Preetha E. Chaly 6, Satheesh 7, Sathyanarayanan
KNOWLEDGE ON TEMPOROMANDIBULAR JOINT DISORDERS AMONG DENTISTS IN CHENNAI, TAMILNADU K. Niraimathi 1, K. Ranjith 2, Vidya Albert Yen 3, Edward Nijesh 4, Shalini P 5, Preetha E. Chaly 6, Satheesh 7, Sathyanarayanan
Temporomandibular Joint Disorders
 Temporomandibular Joint Disorders Temporomandibular Joint : Is a synovial joint located between the condyle (head of the mandible) and the glenoid fossa (inferior surface of the squamous part of Temporal
Temporomandibular Joint Disorders Temporomandibular Joint : Is a synovial joint located between the condyle (head of the mandible) and the glenoid fossa (inferior surface of the squamous part of Temporal
TMJ Parametro Classico
 TMJ Parametro Classico Total Temporomandibular Joint Prosthesis 2 Personalized total TMJ replacement system (Parametro Classic & Parametro Saddle ) Patient Information in English This patient information
TMJ Parametro Classico Total Temporomandibular Joint Prosthesis 2 Personalized total TMJ replacement system (Parametro Classic & Parametro Saddle ) Patient Information in English This patient information
Periodontal pain. Pulpal pain. Odontogenic Pain. Taking the pain out of diagnosis: a look at causes of non-odontogenic pain
 Taking the pain out of diagnosis: a look at causes of non-odontogenic pain 1. Pulpal pain 2. Periodontal pain Odontogenic Pain Dr. David Oliver Specialist in Oral Medicine BDSc (Melb), PGDipCD (Melb),
Taking the pain out of diagnosis: a look at causes of non-odontogenic pain 1. Pulpal pain 2. Periodontal pain Odontogenic Pain Dr. David Oliver Specialist in Oral Medicine BDSc (Melb), PGDipCD (Melb),
Index. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Alveolar osteitis (dry socket), periodontal pain due to, 436 Aphthous stomatitis, recurrent, mucosal pain due to, 439 440 Arthrocentesis/arthroscopy,
Index Note: Page numbers of article titles are in boldface type. A Alveolar osteitis (dry socket), periodontal pain due to, 436 Aphthous stomatitis, recurrent, mucosal pain due to, 439 440 Arthrocentesis/arthroscopy,
JAMSS Speed-to-Treat Protocol For treatment of jaw joint and muscle sprain/strain injuries
 JAMSS Speed-to-Treat Protocol For treatment of jaw joint and muscle sprain/strain injuries INTRODUCTION What is Jaw Joint and Muscle Sprain/Strain (JAMSS)? Jaw Joint and Muscle Sprain/Strain (JAMSS) is
JAMSS Speed-to-Treat Protocol For treatment of jaw joint and muscle sprain/strain injuries INTRODUCTION What is Jaw Joint and Muscle Sprain/Strain (JAMSS)? Jaw Joint and Muscle Sprain/Strain (JAMSS) is
Prosthetic Management of TMJ Disorders
 Prosthetic Management of TMJ Disorders Mohammed Alfarsi BDS, MDSc(Pros), PhD www.drmohdalfarsi.com com.+*()ا&%$ر"!. www Mohd@DrMohdAlfarsi.com @DrMohdAlfarsi DrMohdAlfarsi 056 224 2227 Overview Overview
Prosthetic Management of TMJ Disorders Mohammed Alfarsi BDS, MDSc(Pros), PhD www.drmohdalfarsi.com com.+*()ا&%$ر"!. www Mohd@DrMohdAlfarsi.com @DrMohdAlfarsi DrMohdAlfarsi 056 224 2227 Overview Overview
Toma este vals con la boca cerrada. Frederico Garcia Lorca: Pequeño vals vienés
 Toma este vals con la boca cerrada. Frederico Garcia Lorca: Pequeño vals vienés Toma este vals con la boca cerrada. Ay, Ay, Ay, Ay Take this waltz, take this waltz Take this waltz with the clamp on its
Toma este vals con la boca cerrada. Frederico Garcia Lorca: Pequeño vals vienés Toma este vals con la boca cerrada. Ay, Ay, Ay, Ay Take this waltz, take this waltz Take this waltz with the clamp on its
Anatomy and Physiology. Bones, Sutures, Teeth, Processes and Foramina of the Human Skull
 Anatomy and Physiology Chapter 6 DRO Bones, Sutures, Teeth, Processes and Foramina of the Human Skull Name: Period: Bones of the Human Skull Bones of the Cranium: Frontal bone: forms the forehead and the
Anatomy and Physiology Chapter 6 DRO Bones, Sutures, Teeth, Processes and Foramina of the Human Skull Name: Period: Bones of the Human Skull Bones of the Cranium: Frontal bone: forms the forehead and the
Temporomandibular Joint
 6 Temporomandibular Joint Most human bones are joined with one another. These connections of bones to each other are termed articulations or joints. Some joints are immovable as in the articulations of
6 Temporomandibular Joint Most human bones are joined with one another. These connections of bones to each other are termed articulations or joints. Some joints are immovable as in the articulations of
OCCLUSION: PHYSIOLOGIC vs. NON-PHYSIOLOGIC
 Oral Anatomy and Occlusion Prosthodontic Component OCCLUSION: PHYSIOLOGIC vs. NON-PHYSIOLOGIC By: Dr. Babak Shokati, DDS, MSc. MSc. Prosthodontics Definition of Masticatory System by The Academy of Prosthodontics
Oral Anatomy and Occlusion Prosthodontic Component OCCLUSION: PHYSIOLOGIC vs. NON-PHYSIOLOGIC By: Dr. Babak Shokati, DDS, MSc. MSc. Prosthodontics Definition of Masticatory System by The Academy of Prosthodontics
Arthrogenous disorders of the TMJ
 Arthrogenous disorders of the TMJ Seena Patel DMD, MPH Assistant Professor, Associate Director of Oral Medicine Arizona School of Dentistry & Oral Health, A.T. Still University, Mesa, AZ Southwest Orofacial
Arthrogenous disorders of the TMJ Seena Patel DMD, MPH Assistant Professor, Associate Director of Oral Medicine Arizona School of Dentistry & Oral Health, A.T. Still University, Mesa, AZ Southwest Orofacial
Index. Dent Clin N Am 51 (2007) Note: Page numbers of article titles are in boldface type.
 Dent Clin N Am 51 (2007) 275 279 Index Note: Page numbers of article titles are in boldface type. A Acupuncture, in persistent facial pain, 269 270 Analgesic systems, sex differences in, 6 8 Anticholinergic
Dent Clin N Am 51 (2007) 275 279 Index Note: Page numbers of article titles are in boldface type. A Acupuncture, in persistent facial pain, 269 270 Analgesic systems, sex differences in, 6 8 Anticholinergic
Parotid Gland, Temporomandibular Joint and Infratemporal Fossa
 M1 - Anatomy Parotid Gland, Temporomandibular Joint and Infratemporal Fossa Jeff Dupree Sanger 9-057 jldupree@vcu.edu Parotid gland: wraps around the mandible positioned between the mandible and the sphenoid
M1 - Anatomy Parotid Gland, Temporomandibular Joint and Infratemporal Fossa Jeff Dupree Sanger 9-057 jldupree@vcu.edu Parotid gland: wraps around the mandible positioned between the mandible and the sphenoid
Case Presentation #1 for the American Board of Craniofacial Pain July 2013
 Case Presentation #1 for the American Board of Craniofacial Pain July 2013 Case I Summary Presentation Pain in right temporomandibular joint with opening of mouth( 7 out of 10 ). Acute right non-reducing
Case Presentation #1 for the American Board of Craniofacial Pain July 2013 Case I Summary Presentation Pain in right temporomandibular joint with opening of mouth( 7 out of 10 ). Acute right non-reducing
Corporate Medical Policy
 Corporate Medical Policy Temporomandibular Joint Dysfunction (TMJD) File Name: Origination: Last CAP Review: Next CAP Review: Last Review: temporomandibular_joint_dysfunction_(tmjd) 1/1996 10/2017 10/2018
Corporate Medical Policy Temporomandibular Joint Dysfunction (TMJD) File Name: Origination: Last CAP Review: Next CAP Review: Last Review: temporomandibular_joint_dysfunction_(tmjd) 1/1996 10/2017 10/2018
U.S. DEPARTMENT OF HEALTH AND HUMAN SERVICES National Institutes of Health
 T M J D I S O R D E R S U.S. DEPARTMENT OF HEALTH AND HUMAN SERVICES National Institutes of Health CONTENTS 2 4 6 7 8 9 14 WHAT IS THE TEMPOROMANDIBULAR JOINT? WHAT ARE TMJ DISORDERS? WHAT CAUSES TMJ DISORDERS?
T M J D I S O R D E R S U.S. DEPARTMENT OF HEALTH AND HUMAN SERVICES National Institutes of Health CONTENTS 2 4 6 7 8 9 14 WHAT IS THE TEMPOROMANDIBULAR JOINT? WHAT ARE TMJ DISORDERS? WHAT CAUSES TMJ DISORDERS?
Anatomy and physiology of Temporomandibular Joint
 Anatomy and physiology of Temporomandibular Joint Temporomandibular joint (TMJ): It is the articulation of the condyle of the mandible, and the inter-articular disc; with the mandibular fossa (glenoid
Anatomy and physiology of Temporomandibular Joint Temporomandibular joint (TMJ): It is the articulation of the condyle of the mandible, and the inter-articular disc; with the mandibular fossa (glenoid
Principle of Occlusion
 Principle of Occlusion Mohammed Alfarsi BDS, MDSc(Pros), PhD www.drmohdalfarsi.com com.+*()ا&%$ر"!. www Overview Principle of Occlusion Overview Principle of Occlusion Point centric Long centric Freedom
Principle of Occlusion Mohammed Alfarsi BDS, MDSc(Pros), PhD www.drmohdalfarsi.com com.+*()ا&%$ر"!. www Overview Principle of Occlusion Overview Principle of Occlusion Point centric Long centric Freedom
TMJ Disorder & Sleep Conditions: The Effects on Your Body
 TMJ Disorder & Sleep Conditions: The Effects on Your Body TMJ Disorders: Temporomandibular Joint Disorders The mandible, or jaw, is the movable part of the head involving important functions of daily life,
TMJ Disorder & Sleep Conditions: The Effects on Your Body TMJ Disorders: Temporomandibular Joint Disorders The mandible, or jaw, is the movable part of the head involving important functions of daily life,
The Temporomandibular joint: Anatomy, Mechanics, Pathology. Aditya Bahel, DO
 The Temporomandibular joint: Anatomy, Mechanics, Pathology Aditya Bahel, DO Outline Anatomy Mechanics and function Indications for TMJ imaging MR Protocols and pitfalls Pathology Treatment options Anatomy
The Temporomandibular joint: Anatomy, Mechanics, Pathology Aditya Bahel, DO Outline Anatomy Mechanics and function Indications for TMJ imaging MR Protocols and pitfalls Pathology Treatment options Anatomy
Y. H. SHEN*, Y. K. CHEN & S. Y. CHUANG Departments of *Oral and Maxillofacial Surgery, Oral Pathology. Introduction. Case report
 Journal of Oral Rehabilitation 2005 32; 332 336 Condylar resorption during active orthodontic treatment and subsequent therapy: report of a special case dealing with iatrogenic TMD possibly related to
Journal of Oral Rehabilitation 2005 32; 332 336 Condylar resorption during active orthodontic treatment and subsequent therapy: report of a special case dealing with iatrogenic TMD possibly related to
A Look at Two Syndromes: TEMPOROMANDIBULAR JOINT & CERVICOCRANIAL DYSFUNCTION IN THE EDS PATIENT. John Mitakides D.D.S., FAACP
 TEMPOROMANDIBULAR JOINT & CERVICOCRANIAL DYSFUNCTION IN THE EDS PATIENT John Mitakides D.D.S., FAACP A Look at Two Syndromes: How TMJ and CCD impact the EDS patient as they occur separately or together
TEMPOROMANDIBULAR JOINT & CERVICOCRANIAL DYSFUNCTION IN THE EDS PATIENT John Mitakides D.D.S., FAACP A Look at Two Syndromes: How TMJ and CCD impact the EDS patient as they occur separately or together
Parotid Gland. Parotid Gland. Largest of 3 paired salivary glands (submandibular; sublingual) Ramus of Mandible. Medial pterygoid.
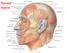 Parotid region Parotid Gland Largest of 3 paired salivary glands (submandibular; sublingual) Ramus of Mandible Medial pterygoid Cross section of mandible Masseter D S SCM Parotid Gland Mastoid Process
Parotid region Parotid Gland Largest of 3 paired salivary glands (submandibular; sublingual) Ramus of Mandible Medial pterygoid Cross section of mandible Masseter D S SCM Parotid Gland Mastoid Process
Total Prosthetic Replacement of the Temporomandibular Joint (TMJ)
 Total Prosthetic Replacement of the Temporomandibular Joint (TMJ) VERSION CONTROL Version: 2.0 Ratified by: Governing Body Date ratified: 13 November 2013 Name of originator/author: Name of responsible
Total Prosthetic Replacement of the Temporomandibular Joint (TMJ) VERSION CONTROL Version: 2.0 Ratified by: Governing Body Date ratified: 13 November 2013 Name of originator/author: Name of responsible
Muscle Pain. Muscle Pain. Muscle Pain. Management considerations for Temporomandibular Disorders. Classification of Temporomandibular Disorders
 Management considerations for Temporomandibular Disorders by Jeffrey P Okeson, DMD Director, Orofacial Pain Program Chief, Division of Orofacial Pain Provost's Distinguished Service Professor University
Management considerations for Temporomandibular Disorders by Jeffrey P Okeson, DMD Director, Orofacial Pain Program Chief, Division of Orofacial Pain Provost's Distinguished Service Professor University
Temporal region. temporal & infratemporal fossae. Zhou Hong Ying Dept. of Anatomy
 Temporal region temporal & infratemporal fossae Zhou Hong Ying Dept. of Anatomy Temporal region is divided by zygomatic arch into temporal & infratemporal fossae. Temporal Fossa Infratemporal fossa Temporal
Temporal region temporal & infratemporal fossae Zhou Hong Ying Dept. of Anatomy Temporal region is divided by zygomatic arch into temporal & infratemporal fossae. Temporal Fossa Infratemporal fossa Temporal
Dr. Sami Zaqout Faculty of Medicine IUG
 Auricle External Ear External auditory meatus The Ear Middle Ear (Tympanic Cavity) Auditory ossicles Internal Ear (Labyrinth) Bony labyrinth Membranous labyrinth External Ear Auricle External auditory
Auricle External Ear External auditory meatus The Ear Middle Ear (Tympanic Cavity) Auditory ossicles Internal Ear (Labyrinth) Bony labyrinth Membranous labyrinth External Ear Auricle External auditory
TMJ Joint Replacement System
 TMJ Joint Replacement System Patient Information What is the Temporomandibular Joint (TMJ)? The Temporomandibular Joint is one of the body s most complex joints. It is similar to a ball and socket, but
TMJ Joint Replacement System Patient Information What is the Temporomandibular Joint (TMJ)? The Temporomandibular Joint is one of the body s most complex joints. It is similar to a ball and socket, but
Temporomandibular Joint Clicking Noises Caused by a Multilocular Bone Cyst: A Case Report
 Temporomandibular Joint Clicking Noises Caused by a Multilocular Bone Cyst: A Case Report Abstract When diagnosing patients with temporomandibular disorder (TMD) symptoms, the possibility of unusual causes
Temporomandibular Joint Clicking Noises Caused by a Multilocular Bone Cyst: A Case Report Abstract When diagnosing patients with temporomandibular disorder (TMD) symptoms, the possibility of unusual causes
 Research Confirms TMJ-Tinnitus Tinnitus Connection http://home.earthlink.net/~dhmorgan/research.html The connection between temporomandibular joint disorder (TMJ) and ear dysfunction was first researched
Research Confirms TMJ-Tinnitus Tinnitus Connection http://home.earthlink.net/~dhmorgan/research.html The connection between temporomandibular joint disorder (TMJ) and ear dysfunction was first researched
Appropriate Management of Temporomandibular Disorders in the Elderly
 Arthritis Appropriate Management of in the Elderly Benjamin R. Davis, BSc, DDS, FRCD(C), Department of Oral and Maxillofacial Surgery, Queen Elizabeth II Health Sciences Centre, Halifax, NS. Temporomandibular
Arthritis Appropriate Management of in the Elderly Benjamin R. Davis, BSc, DDS, FRCD(C), Department of Oral and Maxillofacial Surgery, Queen Elizabeth II Health Sciences Centre, Halifax, NS. Temporomandibular
PREVALENCE OF DISK DISPLACEMENT DISORDERS OF TMJ AMONG DENTAL STUDENTS
 International Journal of Research in Social Sciences Vol. 7 Issue 7, July 2017, ISSN: 2249-2496 Impact Factor: 7.081 Journal Homepage: Double-Blind Peer Reviewed Refereed Open Access International Journal
International Journal of Research in Social Sciences Vol. 7 Issue 7, July 2017, ISSN: 2249-2496 Impact Factor: 7.081 Journal Homepage: Double-Blind Peer Reviewed Refereed Open Access International Journal
Temporomandibular Disorders and their Management
 American Journal of Health Research 2015; 3(3-2): 1-5 Published online September 6, 2015 (http://www.sciencepublishinggroup.com/j/ajhr) doi: 10.11648/j.ajhr.s.2015030302.11 ISSN: 2330-8788 (Print); ISSN:
American Journal of Health Research 2015; 3(3-2): 1-5 Published online September 6, 2015 (http://www.sciencepublishinggroup.com/j/ajhr) doi: 10.11648/j.ajhr.s.2015030302.11 ISSN: 2330-8788 (Print); ISSN:
Establish a Healthy TMJ
 TW TMJ Establish a Healthy TMJ Prior to Restorative, Orthodontic or Prosthetic Treatment Dr. Brock Rondeau, D.D.S., I.B.O., D.A.B.C.P. Author: Dr. Brock Rondeau is one of North America s most sought after
TW TMJ Establish a Healthy TMJ Prior to Restorative, Orthodontic or Prosthetic Treatment Dr. Brock Rondeau, D.D.S., I.B.O., D.A.B.C.P. Author: Dr. Brock Rondeau is one of North America s most sought after
Artigo Original / Original Article
 Artigo Original / Original Article IJD ISSN:1806-146X Mandibular condyle morphology on panoramic radiographs of asymptomatic temporomandibular joints Christiano Oliveira 1 Renata Tarnoschi Bernardo 2 Ana
Artigo Original / Original Article IJD ISSN:1806-146X Mandibular condyle morphology on panoramic radiographs of asymptomatic temporomandibular joints Christiano Oliveira 1 Renata Tarnoschi Bernardo 2 Ana
Conventional radiograph verses CT for evaluation of sagittal fracture of mandibular condyle
 Case Report: Conventional radiograph verses CT for evaluation of sagittal fracture of mandibular condyle Dr Anjali Wadhwa, Dr Gaurav Shah, Dr Shweta Sharma, Dr Anand Bhatnagar, Dr Pallavi Malaviya NIMS
Case Report: Conventional radiograph verses CT for evaluation of sagittal fracture of mandibular condyle Dr Anjali Wadhwa, Dr Gaurav Shah, Dr Shweta Sharma, Dr Anand Bhatnagar, Dr Pallavi Malaviya NIMS
Diagnosis and Management of Temporomandibular Disorders
 Chapter 32 Diagnosis and Management of Temporomandibular Disorders Fina Navi, Mohammad Hosein Kalantar Motamedi, Koroush Taheri Talesh, Esshagh Lasemi and Zahra Nematollahi Additional information is available
Chapter 32 Diagnosis and Management of Temporomandibular Disorders Fina Navi, Mohammad Hosein Kalantar Motamedi, Koroush Taheri Talesh, Esshagh Lasemi and Zahra Nematollahi Additional information is available
SYLLABUS OF ORAL AND MAXILLOFACIAL SURGERY
 MEDICAL UNIVERSITY OF VARNA FACULTY OF DENTAL MEDICINE DEPARTMENT OF ORAL AND MAXILLOFACIAL SURGERY AND SID SYLLABUS OF ORAL AND MAXILLOFACIAL SURGERY (State examination) ACADEMIC YEAR 2015 2016 1. Asepsis
MEDICAL UNIVERSITY OF VARNA FACULTY OF DENTAL MEDICINE DEPARTMENT OF ORAL AND MAXILLOFACIAL SURGERY AND SID SYLLABUS OF ORAL AND MAXILLOFACIAL SURGERY (State examination) ACADEMIC YEAR 2015 2016 1. Asepsis
Transcutaneous Electrical Nerve Stimulation Therapy in Temporomandibular Disorder: A Clinical Study
 10.5005/jp-journals-10011-1090 Ganapathi ORIGINAL Moger ARTICLE et al Transcutaneous Electrical Nerve Stimulation Therapy in Temporomandibular Disorder: A Clinical Study 1 Ganapathi Moger, 2 MC Shashikanth,
10.5005/jp-journals-10011-1090 Ganapathi ORIGINAL Moger ARTICLE et al Transcutaneous Electrical Nerve Stimulation Therapy in Temporomandibular Disorder: A Clinical Study 1 Ganapathi Moger, 2 MC Shashikanth,
STRAIGHT TALK about CROOKED TEETH: Key #4, Healthy TMJ Function
 STRAIGHT TALK about CROOKED TEETH: Key #4, Healthy TMJ Function This is fourth in a series of articles by Derek Mahony, BDS, MDSc and S. Kent Lauson, DDS, MS (Orthodontists) Their book was written with
STRAIGHT TALK about CROOKED TEETH: Key #4, Healthy TMJ Function This is fourth in a series of articles by Derek Mahony, BDS, MDSc and S. Kent Lauson, DDS, MS (Orthodontists) Their book was written with
Dr Mohammed Alfarsi Page 1 9 December Principles of Occlusion
 Dr Mohammed Alfarsi Page 1 9 December 2013 Principles of Occlusion Overview: The occlusion is a very large, yet easy to manage once properly understood, topic. Thus, no one handout is enough to fully understand
Dr Mohammed Alfarsi Page 1 9 December 2013 Principles of Occlusion Overview: The occlusion is a very large, yet easy to manage once properly understood, topic. Thus, no one handout is enough to fully understand
Lec [8]: Mandibular nerve:
![Lec [8]: Mandibular nerve: Lec [8]: Mandibular nerve:](/thumbs/94/121295776.jpg) Lec [8]: Mandibular nerve: The mandibular branch from the trigeminal ganglion lies in the middle cranial fossa lateral to the cavernous sinus. With the motor root of the trigeminal nerve [motor roots lies
Lec [8]: Mandibular nerve: The mandibular branch from the trigeminal ganglion lies in the middle cranial fossa lateral to the cavernous sinus. With the motor root of the trigeminal nerve [motor roots lies
DR. PETER DAWSON S PHILOSOPHY OF FUNCTIONAL OCCLUSION
 DR. PETER DAWSON S PHILOSOPHY OF FUNCTIONAL OCCLUSION WHO IS PETER DAWSON? WHO IS PETER DAWSON? Peter Dawson is a dentist that specializes in the treatment of the exposed exterior surfaces of the teeth.
DR. PETER DAWSON S PHILOSOPHY OF FUNCTIONAL OCCLUSION WHO IS PETER DAWSON? WHO IS PETER DAWSON? Peter Dawson is a dentist that specializes in the treatment of the exposed exterior surfaces of the teeth.
Tempromandibular joint (TMJ) problems
 What is the tempromandibular joint (TMJ)? The tempromandibular joint (TMJ) is the jaw joint between the lower jaw (mandible) and the skull (in the temporal bone). There is one on each side of your face,
What is the tempromandibular joint (TMJ)? The tempromandibular joint (TMJ) is the jaw joint between the lower jaw (mandible) and the skull (in the temporal bone). There is one on each side of your face,
CBCT Specific Guidelines for South African Practice as Indicated by Current Literature:
 CBCT Specific Guidelines for South African Practice as Indicated by Current Literature: CF Hoogendijk Maxillo- facial and Oral surgery: Trauma: 1. Facial trauma for the confirmation or exclusion of fractures
CBCT Specific Guidelines for South African Practice as Indicated by Current Literature: CF Hoogendijk Maxillo- facial and Oral surgery: Trauma: 1. Facial trauma for the confirmation or exclusion of fractures
Infratemporal fossa: Tikrit University college of Dentistry Dr.Ban I.S. head & neck Anatomy 2 nd y.
 Infratemporal fossa: This is a space lying beneath the base of the skull between the lateral wall of the pharynx and the ramus of the mandible. It is also referred to as the parapharyngeal or lateral pharyngeal
Infratemporal fossa: This is a space lying beneath the base of the skull between the lateral wall of the pharynx and the ramus of the mandible. It is also referred to as the parapharyngeal or lateral pharyngeal
MYOFASCIAL PAIN DYSFUNCTION SYNDROME - A CLINICAL STUDY
 SINGAPORE MEDICAL JOURNAL MYOFASCIAL PAIN DYSFUNCTION SYNDROME - A CLINICAL STUDY S B Keng SYNOPSIS Facial pain originating from the Temporomandibular Joint areas and jaw muscles is a condition which faces
SINGAPORE MEDICAL JOURNAL MYOFASCIAL PAIN DYSFUNCTION SYNDROME - A CLINICAL STUDY S B Keng SYNOPSIS Facial pain originating from the Temporomandibular Joint areas and jaw muscles is a condition which faces
Temporomandibular disorders and the need for stomatognathic treatment in orthodontically treated and untreated girls
 European Journal of Orthodontics 22 (2000) 283 292 2000 European Orthodontic Society Temporomandibular disorders and the need for stomatognathic treatment in orthodontically treated and untreated girls
European Journal of Orthodontics 22 (2000) 283 292 2000 European Orthodontic Society Temporomandibular disorders and the need for stomatognathic treatment in orthodontically treated and untreated girls
Screening orthodontic patients for temporomandibular disorders
 Clin Dent Rev (2017) 1:8 https://doi.org/10.1007/s41894-017-0007-z DIAGNOSIS Screening orthodontic patients for temporomandibular disorders Gary Klasser 1 Charles Greene 2 Received: 5 April 2017 / Accepted:
Clin Dent Rev (2017) 1:8 https://doi.org/10.1007/s41894-017-0007-z DIAGNOSIS Screening orthodontic patients for temporomandibular disorders Gary Klasser 1 Charles Greene 2 Received: 5 April 2017 / Accepted:
ALASKA CHIROPRACTIC SOCIETY TMJ. DR. MITCH MALLY International Speaker 10 th Degree Black Belt in Extremity Adjusting. Presents
 ALASKA CHIROPRACTIC SOCIETY Presents DR. MITCH MALLY International Speaker 10 th Degree Black Belt in Extremity Adjusting TMJ Temporomandibular Joint Syndrome Diagnostician s Dilemma Source: J-Med; 1991
ALASKA CHIROPRACTIC SOCIETY Presents DR. MITCH MALLY International Speaker 10 th Degree Black Belt in Extremity Adjusting TMJ Temporomandibular Joint Syndrome Diagnostician s Dilemma Source: J-Med; 1991
CHAPTER 3. OTALGIA 1. HISTORY. Professor Bruce Black MD Dr Jane Black PhD
 CHAPTER 3. OTALGIA Pain felt in the ear is a common problem, but not all earache originates in the ear. Pain can arise from structures near the ear, or alternatively from sites more distant in the head
CHAPTER 3. OTALGIA Pain felt in the ear is a common problem, but not all earache originates in the ear. Pain can arise from structures near the ear, or alternatively from sites more distant in the head
DENTAL CLINICS OF NORTH AMERICA. Tem poromandi bu lar Disorders and Orofacial Pain. GUEST EDITOR Henry A. Gremillion, DDS
 DENTAL CLINICS OF NORTH AMERICA Tem poromandi bu lar Disorders and Orofacial Pain GUEST EDITOR Henry A. Gremillion, DDS "EMFOROMANDIBULaR DISORDERS AND OROFACIAL PAIN Preface Henry A. Gremillion xi Overview
DENTAL CLINICS OF NORTH AMERICA Tem poromandi bu lar Disorders and Orofacial Pain GUEST EDITOR Henry A. Gremillion, DDS "EMFOROMANDIBULaR DISORDERS AND OROFACIAL PAIN Preface Henry A. Gremillion xi Overview
Conventional Radiographic Assessment of Temporomandibular Joint Disorders in Young Saudi Patients: A Retrospective and Prospective Radiographic Study
 10.5005/jp-journals-10029-1045 Sultan Mohammed Kaleem et al RESEARCH ARTICLE Conventional Radiographic Assessment of Temporomandibular Joint Disorders in Young Saudi Patients: A Retrospective and Prospective
10.5005/jp-journals-10029-1045 Sultan Mohammed Kaleem et al RESEARCH ARTICLE Conventional Radiographic Assessment of Temporomandibular Joint Disorders in Young Saudi Patients: A Retrospective and Prospective
Structure Location Function
 Frontal Bone Cranium forms the forehead and roof of the orbits Occipital Bone Cranium forms posterior and inferior portions of the cranium Temporal Bone Cranium inferior to the parietal bone forms the
Frontal Bone Cranium forms the forehead and roof of the orbits Occipital Bone Cranium forms posterior and inferior portions of the cranium Temporal Bone Cranium inferior to the parietal bone forms the
A Rare Case of Cheerleader Syndrome, Case Report
 47 A Rare Case of Cheerleader Syndrome, Case Report Dr. Ayad AL mudarris, FIBMS (1) and Dr. Shifaa Hussain, MSc (2) (1)Head of Maxillofacial Surgical Department. Al Imamain Al Kadhemain Medical City; (2)
47 A Rare Case of Cheerleader Syndrome, Case Report Dr. Ayad AL mudarris, FIBMS (1) and Dr. Shifaa Hussain, MSc (2) (1)Head of Maxillofacial Surgical Department. Al Imamain Al Kadhemain Medical City; (2)
TEMPOROMANDIBULAR DISORDERS
 10 TEMPOROMANDIBULAR DISORDERS BRUCE BLASBERG, DMD, FRCD(C) MARTIN S. GREENBERG, DDS FUNCTIONAL ANATOMY Temporomandibular Joint Muscles Associated with Mandibular Movement and Function Vascular Supply
10 TEMPOROMANDIBULAR DISORDERS BRUCE BLASBERG, DMD, FRCD(C) MARTIN S. GREENBERG, DDS FUNCTIONAL ANATOMY Temporomandibular Joint Muscles Associated with Mandibular Movement and Function Vascular Supply
Clinical details: Details of scan: CONE BEAM CT REPORT: Name: H. B. Gender: Reason for referral: Referred by:
 Name: H. B. Gender: Male DOB: 11/12/1950 Age: 64 Date taken: 16/11/2015 Date reported: 19/11/2015 Clinical details: Reason for referral: Referred by: Investigate symptoms related to left TMJ. Reconstructed
Name: H. B. Gender: Male DOB: 11/12/1950 Age: 64 Date taken: 16/11/2015 Date reported: 19/11/2015 Clinical details: Reason for referral: Referred by: Investigate symptoms related to left TMJ. Reconstructed
A Study on Temporomandibular Joint Disorders Among Nepalese Preclinical Students Studying at KMCTH
 Original article A Study on Temporomandibular Joint Disorders Among Nepalese Preclinical Students Studying at KMCTH Tiwari Nripendra 1, Budhathoki Deepesh 1, Kharel Sushil 2, Karki Prabin Kumar 2, Malla
Original article A Study on Temporomandibular Joint Disorders Among Nepalese Preclinical Students Studying at KMCTH Tiwari Nripendra 1, Budhathoki Deepesh 1, Kharel Sushil 2, Karki Prabin Kumar 2, Malla
Chapter 79: Temporomandibular Joint Disorders. Daniel M. Laskin
 Chapter 79: Temporomandibular Joint Disorders Daniel M. Laskin It has been estimated that as many as 10 million people in the USA suffer from disorders of the temporomandibular joint and such disorders
Chapter 79: Temporomandibular Joint Disorders Daniel M. Laskin It has been estimated that as many as 10 million people in the USA suffer from disorders of the temporomandibular joint and such disorders
For the following questions, indicate the letter that corresponds to the SINGLE MOST APPROPRIATE ANSWER
 GROSS ANATOMY EXAMINATION May 15, 2000 For the following questions, indicate the letter that corresponds to the SINGLE MOST APPROPRIATE ANSWER 1. Pain associated with an infection limited to the middle
GROSS ANATOMY EXAMINATION May 15, 2000 For the following questions, indicate the letter that corresponds to the SINGLE MOST APPROPRIATE ANSWER 1. Pain associated with an infection limited to the middle
pc oral surgery international
 pc oral surgery international Evidence-based TMJ Surgery 2013 Professor Paul Coulthard BDS FGDP(UK) MDS FDSRCS FDSRCS(OS) PhD evidence-based practice? - the integration of best research evidence with clinical
pc oral surgery international Evidence-based TMJ Surgery 2013 Professor Paul Coulthard BDS FGDP(UK) MDS FDSRCS FDSRCS(OS) PhD evidence-based practice? - the integration of best research evidence with clinical
Definition and History of Orthodontics
 In the name of GOD Definition and History of Orthodontics Presented by: Dr Somayeh Heidari Orthodontist Reference: Contemporary Orthodontics Chapter 1 William R. Proffit, Henry W. Fields, David M.Sarver.
In the name of GOD Definition and History of Orthodontics Presented by: Dr Somayeh Heidari Orthodontist Reference: Contemporary Orthodontics Chapter 1 William R. Proffit, Henry W. Fields, David M.Sarver.
Case Report. A Novel Treatment of Recurrent Temporomandibular Joint Dislocation with Intermaxillary Fixation Using Microimplant: A Case Report
 JOMP Journal of Oral Medicine and Pain Case Report pissn 2288-9272 eissn 2383-8493 J Oral Med Pain 2014;39(4):156-162 http://dx.doi.org/10.14476/jomp.2014.39.4.156 A Novel Treatment of Recurrent Temporomandibular
JOMP Journal of Oral Medicine and Pain Case Report pissn 2288-9272 eissn 2383-8493 J Oral Med Pain 2014;39(4):156-162 http://dx.doi.org/10.14476/jomp.2014.39.4.156 A Novel Treatment of Recurrent Temporomandibular
By : Prof Saeed Abuel Makarem & Dr.Sanaa Alshaarawi
 By : Prof Saeed Abuel Makarem & Dr.Sanaa Alshaarawi OBJECTIVES By the end of the lecture, students shouldbe able to: List the nuclei of the deep origin of the trigeminal and facial nerves in the brain
By : Prof Saeed Abuel Makarem & Dr.Sanaa Alshaarawi OBJECTIVES By the end of the lecture, students shouldbe able to: List the nuclei of the deep origin of the trigeminal and facial nerves in the brain
Temporomandibular Joint Treatment
 Temporomandibular Joint Treatment Preamble As stated in the AAMT Position Statement, the Code of Ethics and Standards of Practice governing massage therapy apply to treating the Temporomandibular Joint
Temporomandibular Joint Treatment Preamble As stated in the AAMT Position Statement, the Code of Ethics and Standards of Practice governing massage therapy apply to treating the Temporomandibular Joint
TMD: CONSERVATIVE TREATMENT AND PHYSICAL THERAPY OPTIONS
 TMD: CONSERVATIVE TREATMENT AND PHYSICAL THERAPY OPTIONS Massage: The temporalis on the side of the head is easy to locate. Press on it looking for painful nodules, massaging gently. Opening and closing
TMD: CONSERVATIVE TREATMENT AND PHYSICAL THERAPY OPTIONS Massage: The temporalis on the side of the head is easy to locate. Press on it looking for painful nodules, massaging gently. Opening and closing
TitleTemporomandibular joint ankylosis: Mitarashi, S; Abe, S; Watanabe, H; Author(s) Hashimoto, M; Ide, Y
 TitleTemporomandibular joint ankylosis: Mitarashi, S; Abe, S; Watanabe, H; Author(s) Hashimoto, M; Ide, Y Cranio : the journal of craniomandi Journal 20(1): 67-71 URL http://hdl.handle.net/10130/1098 Right
TitleTemporomandibular joint ankylosis: Mitarashi, S; Abe, S; Watanabe, H; Author(s) Hashimoto, M; Ide, Y Cranio : the journal of craniomandi Journal 20(1): 67-71 URL http://hdl.handle.net/10130/1098 Right
3. The Jaw and Related Structures
 Overview and objectives of this dissection 3. The Jaw and Related Structures The goal of this dissection is to observe the muscles of jaw raising. You will also have the opportunity to observe several
Overview and objectives of this dissection 3. The Jaw and Related Structures The goal of this dissection is to observe the muscles of jaw raising. You will also have the opportunity to observe several
Review Article A 5 Year Retrospective Study on the Clinical Outcomes of Performing Arthrocentesis in Basildon Hospital
 Cronicon OPEN ACCESS Nikhil Gogna* and Jamal Siddiqi Department of Oral & Maxillofacial Surgery, Basildon Hospital, United Kingdom Received: July 17, 2015; Published: July 23, 2015. DENTAL SCIENCE Review
Cronicon OPEN ACCESS Nikhil Gogna* and Jamal Siddiqi Department of Oral & Maxillofacial Surgery, Basildon Hospital, United Kingdom Received: July 17, 2015; Published: July 23, 2015. DENTAL SCIENCE Review
Basic Functional Anatomy of the Gnathostomatic System and its Clinical Implications. Eugene Santucci DDS, MA, FACD
 Basic Functional Anatomy of the Gnathostomatic System and its Clinical Implications Eugene Santucci DDS, MA, FACD NOTHING IS MORE FUNDAMENTAL TO TREATING PATIENTS THAN KNOWING ANATOMY Jeffery P. Okeson
Basic Functional Anatomy of the Gnathostomatic System and its Clinical Implications Eugene Santucci DDS, MA, FACD NOTHING IS MORE FUNDAMENTAL TO TREATING PATIENTS THAN KNOWING ANATOMY Jeffery P. Okeson
Eastman Dental Hospital. Temporomandibular disorder. Facial Pain Team
 Eastman Dental Hospital Temporomandibular disorder Facial Pain Team If you would like this document in another language or format or if you require the services of an interpreter contact us on 020 3456
Eastman Dental Hospital Temporomandibular disorder Facial Pain Team If you would like this document in another language or format or if you require the services of an interpreter contact us on 020 3456
FOR CMS (MEDICARE) MEMBERS ONLY NATIONAL COVERAGE DETERMINATION (NCD) FOR MAGNETIC RESONANCE IMAGING:
 National Imaging Associates, Inc. Clinical guidelines TEMPOROMANDIBULAR JOINT (TMJ) MRI Original Date: May 23, 2003 Page 1 of 5 CPT Code: 70336 Last Review Date: May 2016 NCD 220.2 MRI Last Effective Date:
National Imaging Associates, Inc. Clinical guidelines TEMPOROMANDIBULAR JOINT (TMJ) MRI Original Date: May 23, 2003 Page 1 of 5 CPT Code: 70336 Last Review Date: May 2016 NCD 220.2 MRI Last Effective Date:
ChiroCredit.com Anatomy 226 INSTRUCTIONS/ASSIGNMENT FOR ANATOMICAL DISSECTION:
 ChiroCredit.com Anatomy 226 INSTRUCTIONS/ASSIGNMENT FOR ANATOMICAL DISSECTION: Once you click on the link to open the dissection module, the first thing you need to do is to be sure you can see all the
ChiroCredit.com Anatomy 226 INSTRUCTIONS/ASSIGNMENT FOR ANATOMICAL DISSECTION: Once you click on the link to open the dissection module, the first thing you need to do is to be sure you can see all the
Teeth and supporting tissues, e.g. dental. Maxillary sinus, salivary gland
 MJDF Facial Pain. Patricia Thomson Always start with SOCRATES S site O onset C character R radiation A associated features T timing E exacerbating/relieving factors S severity Examine the cranial nerves
MJDF Facial Pain. Patricia Thomson Always start with SOCRATES S site O onset C character R radiation A associated features T timing E exacerbating/relieving factors S severity Examine the cranial nerves
Protocol. Temporomandibular Joint Dysfunction
 Protocol Temporomandibular Joint Dysfunction (20121) Medical Benefit Effective Date: 01/01/17 Next Review Date: 05/18 Preauthorization No Review Dates: 09/07, 09/08, 09/09, 09/10, 09/11, 09/12, 09/13,
Protocol Temporomandibular Joint Dysfunction (20121) Medical Benefit Effective Date: 01/01/17 Next Review Date: 05/18 Preauthorization No Review Dates: 09/07, 09/08, 09/09, 09/10, 09/11, 09/12, 09/13,
A case report of TMJ closed lock reduced with occlusal splint therapy with MRI evidence
 Case Report DOI: 10.18231/2455-6750.2017.0022 A case report of TMJ closed lock reduced with occlusal splint therapy with MRI evidence Shruti Sambyal 1,*, Ajit D. Dinkar 2, Bhanu Pratap Singh 3, Atul Chauhan
Case Report DOI: 10.18231/2455-6750.2017.0022 A case report of TMJ closed lock reduced with occlusal splint therapy with MRI evidence Shruti Sambyal 1,*, Ajit D. Dinkar 2, Bhanu Pratap Singh 3, Atul Chauhan
INTRODUCTION: ANATOMY UNDERLYING CLINICAL TESTS OF CRANIAL NERVES
 INTRODUCTION: ANATOMY UNDERLYING CLINICAL TESTS OF CRANIAL NERVES CRANIAL NERVE I - OLFACTORY I - OLFACTORY NERVE - SMELL TEST: SMELL ODORS (note: not ammonia; pain in nasal cavity CN5 DAMAGE: LOSS OF
INTRODUCTION: ANATOMY UNDERLYING CLINICAL TESTS OF CRANIAL NERVES CRANIAL NERVE I - OLFACTORY I - OLFACTORY NERVE - SMELL TEST: SMELL ODORS (note: not ammonia; pain in nasal cavity CN5 DAMAGE: LOSS OF
MRI imaging of the temporo-mandibular joint (TMJ) with regard to degeneration and disk displacement.
 MRI imaging of the temporo-mandibular joint (TMJ) with regard to degeneration and disk displacement. Poster No.: P-0023 Congress: ESSR 2015 Type: Educational Poster Authors: A. Hagenkord; Basel/CH Keywords:
MRI imaging of the temporo-mandibular joint (TMJ) with regard to degeneration and disk displacement. Poster No.: P-0023 Congress: ESSR 2015 Type: Educational Poster Authors: A. Hagenkord; Basel/CH Keywords:
Temporomandibular Joint Remodeling for the Treatment of Temporomandibular Joint Disorders - A Clinical Case Study
 The Open Rehabilitation Journal, 2009, 2, 43-49 43 Open Access Temporomandibular Joint Remodeling for the Treatment of Temporomandibular Joint Disorders - A Clinical Case Study Rosita Wurgaft 1 and Ricky
The Open Rehabilitation Journal, 2009, 2, 43-49 43 Open Access Temporomandibular Joint Remodeling for the Treatment of Temporomandibular Joint Disorders - A Clinical Case Study Rosita Wurgaft 1 and Ricky
CRANIAL NERVES. Dr. Amani A. Elfaki Associate Professor Department of Anatomy
 CRANIAL NERVES Dr. Amani A. Elfaki Associate Professor Department of Anatomy LEARNING OBJECTIVES Named the cranial nerves Identify the funcunal component of each cranial nerve Identify the effect of each
CRANIAL NERVES Dr. Amani A. Elfaki Associate Professor Department of Anatomy LEARNING OBJECTIVES Named the cranial nerves Identify the funcunal component of each cranial nerve Identify the effect of each
Facet Joint Syndrome / Arthritis
 Facet Joint Syndrome / Arthritis Overview Facet joint syndrome is an arthritis-like condition of the spine that can be a significant source of back and neck pain. It is caused by degenerative changes to
Facet Joint Syndrome / Arthritis Overview Facet joint syndrome is an arthritis-like condition of the spine that can be a significant source of back and neck pain. It is caused by degenerative changes to
Prosthodontic Management of Temporomandibular Disorders
 J Indian Prosthodont Soc (Oct-Dec 2013) 13(4):400 405 DOI 10.1007/s13191-012-0229-3 REVIEW ARTICLE Prosthodontic Management of Temporomandibular Disorders Harsimran Kaur Kusum Datta Received: 25 October
J Indian Prosthodont Soc (Oct-Dec 2013) 13(4):400 405 DOI 10.1007/s13191-012-0229-3 REVIEW ARTICLE Prosthodontic Management of Temporomandibular Disorders Harsimran Kaur Kusum Datta Received: 25 October
PhD in Oral Surgery (50 Credit Hours)
 PhD in Oral Surgery (50 Credit Hours) First Semester (9 Credit Hours) OSRG 701 Oral Surgery I 1 OSRG 791 Oral Surgery Clinics I 2 OSRG 706 Applied Surgical Anatomy 1 OSRG 707 Pain and Anxiety Control 1
PhD in Oral Surgery (50 Credit Hours) First Semester (9 Credit Hours) OSRG 701 Oral Surgery I 1 OSRG 791 Oral Surgery Clinics I 2 OSRG 706 Applied Surgical Anatomy 1 OSRG 707 Pain and Anxiety Control 1
Ibelieve the time has come for the general dentists to
 EARLY ORTHODONTIC TREATMENT Brock Rondeau, D.D.S. I.B.O., D.A.B.C.P., D-A.C.S.D.D., D.A.B.D.S.M., D.A.B.C.D.S.M. Ibelieve the time has come for the general dentists to get serious and educated in an effort
EARLY ORTHODONTIC TREATMENT Brock Rondeau, D.D.S. I.B.O., D.A.B.C.P., D-A.C.S.D.D., D.A.B.D.S.M., D.A.B.C.D.S.M. Ibelieve the time has come for the general dentists to get serious and educated in an effort
