Jaw resection JAMES S BROWN. Contents. Resection of the mandible and maxilla. General principles. Applied anatomy
|
|
|
- Milton Horton
- 5 years ago
- Views:
Transcription
1 39 Jaw resection JAMES S BROWN Contents Resection of the mandible and maxilla 391 General principles 391 Applied anatomy 391 Mandible 391 Maxilla 392 Mandibular resection for oral squamous cell carcinoma 392 Patterns of invasion and routes of tumour entry 392 Pre-operative assessment 392 Methods of mandibular resection 393 Marginal or rim resection 393 Segmental resection of the mandible 395 Maintaining the occlusion in mandibular resection 396 Resecting the ramus and condyle 396 Resecting the maxilla 397 Pathology and pre-operative imaging 397 Class I (alveolectomy) 397 Class II (low-level maxillectomy) 397 Class III (high-level maxillectomy maintaining the orbit) 397 Class IV (radical maxillectomy with orbital exenteration) 399 References 399 Resection of the mandible and maxilla General principles This chapter concentrates on the resection of squamous cell carcinoma arising in the oral cavity or the midface. A similar approach is required for the resection of bone invaded by malignant salivary tumours but the points on the patterns of tumour invasion and entry may be different. The principles of the resection techniques may be appropriate to the management of odontogenic tumours especially if these are recurrent. Resection of the jaws for osteoradionecrosis or osteonecrosis is more of a debridement requiring the resection of bone back to a bleeding base prior to reconstruction. Bone resection for osteosarcoma or primary intraosseous carcinoma requires a more radical removal of bone as the tumour will invade the bone preferentially. Applied anatomy Mandible The mandible provides a bony framework to hold the teeth and sensation to the lip and chin is provided by the inferior alveolar nerve which enters at the mandibular foramen and exits at the mental foramen. Although there are often attempts to preserve this nerve in the treatment of benign disease, the loss of sensation to the lip and chin is an acceptable morbidity for most patients. The relationship of the teeth to the bone varies with patients and the molars run from a buccal position to a more lingual 391
2 392 Jaw resection position posteriorly. The temporomandibular joint articulates with the skull base and in some cases the condylar head may require resection. The loss of teeth results in the loss of the supporting alveolar bone. The inferior alveolar nerve will come to lie on the alveolar ridge and the relationship of the floor of mouth muscle insertions will alter with the loss of bone (Figure 39.1 and 39.2). Maxilla The maxilla is a complex structure which provides bone for the upper dental arch supports the alar base and facial curtain as well as providing the orbital floor, malar buttress and lateral nasal wall. The articulation with the rest of the skeleton is important to understand in tumour resection. Medially, the lateral nasal wall is the least important structure, but care is required in maintaining the lacrimal system. The frontal process of the maxilla and the nasal bones articulate with the frontal bone and immediately behind these structures is the ethmoid sinus and then the sphenoid sinus. The cranium lies directly above these bones and experience in skull base resections is required to safely resect these structures. The lamina papyracea of the medial wall often requires resection and care must be taken to identify the anterior ethmoidal artery in particular. The maxilla provides much of the orbital floor as far as the inferior orbital fissure, and more laterally the lateral wall is made up of the greater wing of the sphenoid and the malar. Mandibular resection for oral squamous cell carcinoma Marginal resection Segmental resection Figure 39.1 A rim or marginal resection maintains the lower border and a segmental resection requires the full thickness of the mandible to be resected. Patterns of invasion and routes of tumour entry Early or shallow invasion of the mandible from the oral cavity will often show an erosive pattern with a pushing front and a connective tissue layer separating the bone from the tumour. The more infiltrative pattern is related to deeper invasion in which the connective tissue layer is lost and separate islands of tumour infiltrate in a less favourable manner. 1 3 It is not possible to predict the pattern of invasion so the judgment on how much bone to resect remains clinical and based on imaging. Various theories of the route of tumour entry to the mandible have been suggested but it seems most likely that the tumour enters the mandible at the point of contact. In the dentate mandible, this tends to be at the junction of the attached and reflected mucosa and in the edentulous mandible, this is more likely at the crest of the ridge due to the lowering of the floor of the mouth due to the loss of teeth. 2,4 These are important issues if a marginal or more conservative resection of the mandible is being considered. Pre-operative assessment Saw cut Figure 39.2 The commonest form of rim resection is coronal. This figure illustrates the method used to enter the floor of the mouth deep to the tumour to obtain a clear margin even though the bone is not invaded. There are multiple papers looking at the accuracy of preoperative imaging techniques and their accuracy in predicting the presence of tumour invasion of the mandible. A recent review article has summarized the findings which are included in Table A widely accepted standard is to use a magnetic resonance imaging scan (MRI) as a standard image of the primary tumour and the neck nodes. This will usually provide 5-mm slices and will include T1, T2 and fat suppression sequences as well as gadolinium enhancement. The fat suppression sequence is the most sensitive in indicating tumour invasion of the mandible. The only additional image would be an orthopantomogram (OPG) if there is
3 Mandibular resection for oral squamous cell carcinoma 393 clear invasion of the mandible or in which the mandible is unlikely to be invaded. For tumours in which it is unclear if the mandible is invaded a single photon emission computerized tomography (SPECT) scan is included to get a further sensitive imaging of the mandible. The combination of an image with a high specificity with one with a high sensitivity can provide a reasonably accurate prediction of the extent of mandibular invasion and therefore the most appropriate method of resection. Cawood and Howell published a widely accepted classification of the mandible following the loss of teeth and it is clear that in Class V and VI mandibles (Figure 39.2) there is insufficient height of bone to safely perform a marginal resection for malignant disease. As a result, a guide to mandibular resection has been published which relates to the size of the mandible and the results of the investigations predicting bone invasion (Table 39.2). Methods of mandibular resection In the past, the commando operation in which the body of the mandible was sacrificed to remove potential lymphatics containing tumour and to facilitate the soft tissue reconstruction has now been discontinued and yet there are series published in which only 29% of the resected mandibles were invaded by tumour. 6 As in all oncological surgery, the aim is to cure the patient of disease through Table 39.1 Summary and comparison of the imaging techniques and clinical examination. Imaging technique No of reports Specificity (mean) Sensitivity (mean) Clinical examination Plain radiography Bone scintigraphy SPECT Computed tomography DentaScan 3 Magnetic resonance imaging Ultrasound Abbreviation: SPECT, single photo emission computed tomography. adequate resection. At the same time, the skilled surgeon should be trying to reduce the morbidity of the operation to a minimum and maintain the best possible function. Good functional results for patients depend more on the tissue left behind than the method of reconstruction. There are two basic methods of mandibular resection. In the marginal or rim resection, the integrity of the lower or upper border of the mandible is kept intact (Figures 39.1 and 39.2). In the full or segmental resection of the mandible, both the upper and lower border are included in the resection so that there is a loss of continuity of the mandible. There is clear evidence to show that functional and aesthetic results are poor if the continuity of the mandible is not restored. 7 The need to reconstruct the mandible to achieve the best functional and aesthetic result will often involve composite-free tissue transfers for malignant disease which will add to the donor site morbidity and increase the risk of flap failure. 8,9 Marginal or rim resection A marginal resection of the mandible can be performed in the coronal or the sagittal plane. In the majority of cases, a coronal marginal resection is used (Figure 39.2). This is the standard method for tumours in which a margin of normal bone is required. It can be used for smaller odontogenic tumours in which there is sufficient residual bone to maintain the lower border. A sagittal marginal resection cannot be used for bone pathology as preserving any kind of margin is not possible. It has been used for floor of mouth squamous cell carcinomas to obtain a clear margin when tumour is abutting the mandible but not obviously invading. This is a high-risk strategy as any invasion through the cortex will be reported as an involved margin. In addition, the angle of the mandible in the body region is difficult to judge (Figure 39.3). In this situation, it is a safer oncological approach to perform a segmental resection of the mandible. Rim resections that involve the ramus of the mandible can only be done in the coronal plane as the ramus is too thin to split for oncological reasons, and it is best to include the coronoid process as this may reduce trismus post-operatively. If the lower border of the mandible is to be preserved then 10 mm of the depth of bone will be necessary for jaw continuity to be reliably maintained. Table 39.2 Results of the investigations predicting bone invasion. Mandible classification OPG, MRI, BS No invasion/periosteal invasion OPG MRI or BS+ early invasion (<5 mm) OPG+, MRI+, BS+ late invasion (>5 mm) 1 2 (dentate) Rim Rim Rim/segment 3 4 (>20 mm mandibular Rim Rim/segment Segment height) 5 6 (<20 mm mandibular height) Rim/segment Segment Segment Abbreviations: BS, bone scan; MRI, magnetic resonance imaging; OPG, orthopantomogram.
4 394 Jaw resection Figure 39.3 This is a partial sagittal rim resection but this diagram illustrates the angle of the body of the mandible from medial to lateral if the full sagittal rim is required. Figure 39.4 (Continued) For marginal resections involving malignant disease (all osteosarcomas and primary intraosseous carcinomas require segments), it is possible to assess the extent of tumour invasion into the mandible from the surrounding soft tissues and estimate the extent of the resection required. This technique is illustrated through Figure Note that periosteal stripping to assess the presence of mandibular invasion and its extent has been used. The use of periosteal striping is an essential part of the technique in the decision-making process for mandibular resection. It has been shown to be a reliable technique3 and in a large series from the unit in Liverpool our involved bone margin rate is very low compared to the soft tissue margin rate.10 (a) (b) (c) (d) (e) (f)
5 Mandibular resection for oral squamous cell carcinoma (g) (h) (i) (j) 395 Figure 39.4 (a d) Pre-operative clinical photograph, OPG, SPECT scan and MRI scan showing early tumour invasion of the mandible. (e) The resection of the buccal side of the mandible. (f) Completion of the planned coronal rim resection. (g) Turning the bone over to inspect the lingual side of the rim resection and ensure clearance of invaded mandible. (h) The resulting defect post resection. (i) The specimen with lingual periosteal stripping to confirm clearance of resection. (j) and (k) Post-operative OPG and clinical photograph of anterolateral thigh flap reconstruction. (k) Segmental resection of the mandible This is a basic procedure in the management of malignant disease once the decision has been made not to preserve any part of the involved mandible. The decision as to where the bone cuts are made will depend on the assessment of mandibular invasion and the entry and exit points of the inferior alveolar nerve. In benign disease, it is often possible to keep the nerve intact and allow it to lie in the soft tissues overlying the reconstructed bone. Periosteal stripping is also an important factor in the segmental resection of the mandible in malignant disease. Periosteum can be striped back from the undamaged bone until it becomes adherent, or the tumour is seen entering the bone. Once this is established, the margin can be decided and the bone cuts planned. It is also important to examine the specimen to ensure that the bone margins are clear of disease by direct inspection (Figure 39.5). This is much less reliable in a malignant tumour arising in bone such as a primary intraosseous carcinoma or an osteosarcoma. In these cases, the periosteum and the cortex of the bone may look clear of invasion as the tumour spreads along the marrow space. As a result, it is necessary to be much more aggressive in mandibular resection and frozen sections should be performed if possible. It may be necessary to excise the overlying skin in mandibular resection. In most cases, it is possible to preserve the skin cover but care must be taken in the buccal aspect of the resection to take sufficient tissue. It is seldom necessary to use an access procedure with segmental mandibular resection. The overlying skin is raised or excised depending on the needs of the oncological ablation and once the bone cuts have been made the mandible can be delivered into the neck and any further resection lingual
6 396 Jaw resection (a) (a) (b) Figure 39.5 (a and b) Periosteal stripping postresection to ensure that the buccal and lingual surfaces are clear of tumour in the distal part of the resection in the region of the lower right canine. to the jaw can be undertaken as the last part of the resection prior to the delivery of the specimen (Figure 39.6). Maintaining the occlusion in mandibular resection There are various methods used to maintain the occlusion prior to mandibular reconstruction. Some surgeons will use a form of external fixation of the nonresected part of the mandible but this is very cumbersome and the device impedes accurate oncological resection. Templates have been devised using stereolithographic models but again these are often impractical in surgery for malignant disease. The simplest technique is to prebend a plate if the tumour does not involve the buccal aspect of the mandible. In this way, the harvested bone can be grafted into position with the plate already in place. I usually move the plate back by a screw-hole in the edentulous situation to take the pressure off the soft tissues and reduce the risk of dehiscence. If the use of a pre-bent plate is not possible then the condylar position can be fixed with a miniplate from the part of the ramus that does not require resection to the maxilla prior to the resection with the mandible in occlusion. Once the mandible has been resected, the position of the (b) Figure 39.6 (a b) There is no need for access surgery such as a lip split in segmental surgery as the tumour can be delivered into the neck to complete the resection. ipsilateral condyle remains fixed and the collateral mandible can be located with the residual occlusion. A plate can then be bent into position prior to the placement of the graft. This can be carried out bilaterally for extensive mandibular resections. The length of the plate may need to be estimated but at least the condyles will be in the correct position relative to each other. Resecting the ramus and condyle In most cases of squamous cell carcinoma, it is possible to maintain the condyle and the condylar neck sufficiently to maintain a plate so that this important part of the joint is left in function. The need to resect the condyle makes the subsequent reconstruction more difficult as the condyle cannot be fixed and it is not possible to prebend a plate. The resection of the condyle with the ramus and body of the mandible is relatively straight forward but care must be taken to protect or tieoff the maxillary artery and avoid damage to the facial nerve. The facial nerve can be damaged by inappropriate retraction in this region. It is often necessary to use some form of intermaxillary fixation if the patient is dentate to help the patient maintain a functioning occlusion in the post-operative period.
7 Resecting the maxilla 397 Resecting the maxilla Pathology and pre-operative imaging There is much less controversy over the more conservative approach to maxillary resection than the mandible. It is possible to preserve the bone of the maxilla with a limited resection of the palatal or alveolar mucosa and place a dressing plate and await the pathology report. If there is an involved or close margin then bone can be resected at a second procedure. This process is also possible in more extensive resections of the maxilla in which an obturator can be placed and again the margins checked and more tissue taken at the time of the obturator change. There is little discussion on the role of pathology either in terms of the pattern of spread in the bone or the pathway of entry. Most accept that the route of entry in the maxilla is at the point of contact and thus the maxillary resection is guided by the extent of the soft tissue mass. For the assessment of bone invasion in the maxilla, most prefer a computed tomography (CT) scan. In our practice, both MRI and CT scans are used to fully assess the tumour when there is concern over the involvement of the orbit, skull base or the infratemporal or pterygoid fossa. The CT scan is probably best for the skull base, and the MRI to assess the infratemporal fossa and both contribute equally to the invasion of the orbital contents. The methods of resection are based on the classification illustrated in Figure Class I (alveolectomy) For Class I defects (Figure 39.1), there is no need to use an access procedure, as the tumour can usually be visualized with ease. This classification includes a medial maxillectomy often used for inverted papillomas but resection for this pathology is not included in this chapter. Class II (low-level maxillectomy) In this situation, the orbital floor is not involved with the resection and if the lesion is below the level of the infraorbital nerve then no access procedure may be required. Either a lip-split combined with a lateral rhinotomy or a midfacial degloving procedure may be used for access with equal effect. 13,14 There are four osteotomies required to deliver the low-level maxilla in ablative surgery: 1. Vertical alveolar (Figure 39.9a) In the dentate maxilla, it is best to remove a tooth in the line of the osteotomy which is continued to the floor of the nose. Maintaining bone adjacent to the remaining tooth helps the stability of the adjacent tooth to the bone cut for obturated cases. Ensure there is sufficient soft tissue to cover the exposed bone. 2. Le fort 1 level A further osteotomy is required at the required height which may include the infraorbital nerve if required. This is carried through to the pterygoid plates. 3. Pterygoid plates If the tumour is contained in the antrum, the pterygoid plates can be split from the maxilla with a chisel. If the tumour is through the antrum posteriorly it is essential to make a bone cut through the pterygoid plates superior to the position of the tumour and then resect the through the pterygoid muscles to obtain a margin of resection. 4. Palatal The alveolar osteotomy is continued into the palate. If possible, the soft tissue incision should allow some of the redundant mucoperiosteum to cover the bone cut especially if obturation is the method of rehabilitation. Once these osteotomies have been carried out the hemimaxilla can be mobilized and any soft tissue attachments released. Class III (high-level maxillectomy maintaining the orbit) The midfacial degloving technique reaches its limit if the orbital floor requires resection or there is extension into the medial orbital region of the ethmoids. In this situation, the lip split and lateral rhinotomy may be sufficient or it may be necessary to extend the incision as a blepharoplasty incision or sub-ciliary incision (Weber-Fergusson). In most situations, it is possible to reach the lateral orbital wall and malar without this extension reducing the risk of ectropion. Class 1 Class 2 Class 3 Class 4 Class 1 a b Class 1 Figure 39.7 Classification of the maxillectomy defect. 11 The need for reconstructive options increases from Class 1 to 4.
8 398 Jaw resection 1 1 x x 7 (a) (b) Verrucous carcinoma Figure 39.8 An example of a Class 1 type of resection without causing an oroantral fistula. Healing by secondary intention with the use of a dressing plate may be all that is required. (a) This is the most complex resection because of the need to preserve the orbit and the lacrimal apparatus. A guide to the osteotomies is as follows (Figure 39.10): 1. Vertical alveolar and nasal The previously described vertical alveolar bone cut is extended to include the nasal piriform fossa and extended to the level of the lacrimal crest. Care must be taken to expose the lacrimal sac and to preserve this structure. 2. Orbital In this situation, the orbital floor is included as far as the inferior orbital fissure. This horizontal bone cut can be extended to the lateral orbital wall or the frontal process of the malar bone as required. 3. Malar The orbital bone cut is linked to the malar buttress cut which is made lateral to the position of the tumour. 4. Pterygoid plates This often requires the plates to be sectioned higher than in the low maxillectomy close to the skull base. A chisel can be used to fracture off the pterygoid plates with a tumour contained within the antrum. In these more extensive tumours, this part of the maxillectomy can be delivered intact. In most situations, there will be extension into the ethmoid sinuses or superior to the lacrimal sac which will make delivery of the en bloc specimen more difficult. It is still essential to attempt to deliver the main part of the maxillectomy intact and carry out further resection of the medial orbital wall and ethmoid and sphenoid sinuses as required. If it has not been possible to maintain the lacrimal system, the punctum is stented with a silastic tube and delivered into the nose and tied off. The silastic tube can be cut between the upper and lower punctum at about 3 weeks. It may be possible to repair parts of the lacrimal sac and duct at the time of the resection but the placement of silastic (b) Figure 39.9 (a) The vertical, Le fort 1 level and pterygoid plate resection is shown. (b) This shows the palatal bone cut. It is usually best to remain on one side or other of the nasal septum depending on the extent of resection required. It is also important to ensure there is sufficient redundant mucoperiosteum to cover the bone cuts for obturated cases. Figure Class III. This shows the higher bone cuts required if the orbital floor and/or medial orbital wall require resection.
9 References 399 tubes is still important to guide the tear flow as healing takes place. Class IV (radical maxillectomy with orbital exenteration) If the orbit requires resection with the maxilla then the approach includes the upper and lower lids if there is no attempt to reconstruct the defect with a prosthetic eye. This operation is much easier to perform as no orbital structures need to be preserved. In this operation, it is better to release the optic nerve after exenterating the superior part of the orbit after the access procedure. The same vertical bone cuts are made in the alveolus and nasal bones but no special attention is required regarding the medial canthal ligament and the lacrimal apparatus. The lateral bone cut is made from the inferior oblique fissure to the malar buttress prior to the release of the pterygoid plates. The palatal bone cuts link with the vertical alveolar and nasal cuts and at this stage the specimen can be mobilized. The soft tissue resection at the base of the orbit is completed and now it should be possible to deliver the specimen. Tumour extending into the skull base, the ethmoids and sphenoid sinuses require removal after the delivery of the main specimen. Tumours involving the skull base require a multidisciplinary team approach. In this situation, a coronal flap, craniotomy and frontal bar osteotomy may be required to obtain adequate access to the anterior skull base. Top tips Resection of the mandible Pre-operative imaging should include a sensitive (bone scan, MRI) and specific (OPG) technique. Pre-operative imaging, clinical examination and the use of perioperative periosteal stripping all help to decide the type and extent of resection. Remember that the tumour will invade the mandible at the point of contact which may be below the dental line or the crest of the ridge. Early invasion is more likely to be the erosive pattern and late invasion infiltrative, requiring a wider margin. The option of a rim resection decreases with the extent of mandibular resorption following the loss of teeth (Class V and VI). Resection of the maxilla Pre-operative imaging will include an OPG and a CT scan and often an additional MRI will be useful to assess the skull base. The main issues in maxillary resection involve the removal of the orbit and the extent of the disease into the infratemporal fossa. Using a saw to resect the pterygoid plates above the tumour will ensure a safer resection at the posterior maxilla. Close cooperation with the restorative dentist is essential in the planning of maxillary resection. References 1. Slootweg PJ and Muller H. Mandibular invasion by oral squamous cell carcinoma. J Cranio-Maxillo- Facial Surg. 1989; 17(2): Brown JS, Lowe D, Kalavrezos N, D souza J, Magennis P and Woolgar J. Patterns of invasion and routes of tumor entry into the mandible by oral squamous cell carcinoma. Head Neck. 2002; 24(4): Brown JS, Griffith JF, Phelps PD and Browne RM. A comparison of different imaging modalities and direct inspection after periosteal stripping in predicting the invasion of the mandible by oral squamous cell carcinoma. Br J Oral Maxillofac Surg. 1994; 32(6): McGregor AD and MacDonald DG. Routes of entry of squamous cell carcinoma to the mandible. Head Neck Surg. 1988; 10(5): Brown JS and Lewis-Jones H. Evidence for imaging the mandible in the management of oral squamous cell carcinoma: A review. Br J Oral Maxillofac Surg. 2001; 39(6): Brown JS, Kalavrezos N, D souza J, Lowe D, Magennis P and Woolgar JA. Factors that influence the method of mandibular resection in the management of oral squamous cell carcinoma. Br J Oral Maxillofac Surg. 2002; 40(4): Urken ML, Buchbinder D, Weinberg H, Vickery C, Sheiner A, Parker R et al. Functional evaluation following microvascular oromandibular reconstruction of the oral cancer patient: A comparative study of reconstructed and nonreconstructed patients. Laryngoscope. 1991; 101(9): Kroll SS, Schusterman MA, Reece GP, Miller MJ, Evans GR, Robb GL et al. Choice of flap and incidence of free flap success. Plast Reconstr Surg. 1996; 98(3): Brown JS, Magennis P, Rogers SN, Cawood JI, Howell R, Vaughan ED et al. Trends in head and neck microvascular reconstructive surgery in Liverpool ( ). Br J Oral Maxillofac Surg. 2006; 44(5): Shaw RJ, Brown JS, Woolgar JA, Lowe D, Rogers SN, Vaughan ED et al. The influence of the pattern of mandibular invasion on recurrence and survival in oral squamous cell carcinoma. Head Neck. 2004; 26(10): Marchetti C, Bianchi A, Mazzoni S, Cipriani R and Campobassi A. Oromandibular recosntruction using a fibula osteocutaneous free flap: Four different preplating methods. Plast Recosntr Surg. 2006; 118(3): Brown JS, Rogers SN, McNally DN and Boyle M. A modified classification for the maxillectomy defect. Head Neck. 2000; 22(1): Casson PR, Bonanno PC, Converse JM, Casson PR and Bonanno PC, Converse JM. The midface degloving procedure. Plastic Reconstr Surg. 1974; 53(1): Price JC, Holliday MJ, Johns ME, Kennedy DW, Richtsmeier WJ, Mattox DE et al. The versatile midface degloving approach. Laryngoscope. 1988; 98(3):
10
Considerations in Oncologic Resection (mandible & maxilla)
 Considerations in Oncologic Resection (mandible & maxilla) Jeeve Kanagalingam MA, FRCS (ORL-HNS), FAMS Consultant ENT / Head & Neck Surgeon Tan Tock Seng Hospital Assistant Professor Lee Kong Chian School
Considerations in Oncologic Resection (mandible & maxilla) Jeeve Kanagalingam MA, FRCS (ORL-HNS), FAMS Consultant ENT / Head & Neck Surgeon Tan Tock Seng Hospital Assistant Professor Lee Kong Chian School
Bones of the skull & face
 Bones of the skull & face Cranium= brain case or helmet Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display. The cranium is composed of eight bones : frontal Occipital
Bones of the skull & face Cranium= brain case or helmet Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display. The cranium is composed of eight bones : frontal Occipital
Anatomy and Physiology. Bones, Sutures, Teeth, Processes and Foramina of the Human Skull
 Anatomy and Physiology Chapter 6 DRO Bones, Sutures, Teeth, Processes and Foramina of the Human Skull Name: Period: Bones of the Human Skull Bones of the Cranium: Frontal bone: forms the forehead and the
Anatomy and Physiology Chapter 6 DRO Bones, Sutures, Teeth, Processes and Foramina of the Human Skull Name: Period: Bones of the Human Skull Bones of the Cranium: Frontal bone: forms the forehead and the
TRAUMA TO THE FACE AND MOUTH
 Dr.Yahya A. Ali 3/10/2012 F.I.C.M.S TRAUMA TO THE FACE AND MOUTH Bailey & Love s 25 th edition Injuries to the orofacial region are common, but the majority are relatively minor in nature. A few are major
Dr.Yahya A. Ali 3/10/2012 F.I.C.M.S TRAUMA TO THE FACE AND MOUTH Bailey & Love s 25 th edition Injuries to the orofacial region are common, but the majority are relatively minor in nature. A few are major
A Study of Classification Systems for Maxillectomy Defects
 A Study of Classification Systems for Maxillectomy Defects Zubair Durrani FFDRCS, FRCS, FRCS (OMFS)* Syed Ghazanfar Hassan FFDRCS** Shomaila Ameer Alam BDS*** * Associate Professor & Consultant Oral and
A Study of Classification Systems for Maxillectomy Defects Zubair Durrani FFDRCS, FRCS, FRCS (OMFS)* Syed Ghazanfar Hassan FFDRCS** Shomaila Ameer Alam BDS*** * Associate Professor & Consultant Oral and
Core Curriculum Syllabus Emergencies in Otolaryngology-Head and Neck Surgery FACIAL FRACTURES
 Core Curriculum Syllabus Emergencies in Otolaryngology-Head and Neck Surgery A. General Considerations FACIAL FRACTURES Look for other fractures like skull and/or cervical spine fractures Test function
Core Curriculum Syllabus Emergencies in Otolaryngology-Head and Neck Surgery A. General Considerations FACIAL FRACTURES Look for other fractures like skull and/or cervical spine fractures Test function
MALIGNANT TUMOURS OF THE JAWS
 MALIGNANT TUMOURS OF THE JAWS MALIGNANT TUMOURS OF THE JAWS Squamous cell carcinoma Osteogenic sarcoma Chondrosarcoma Fibrosarcoma Malignant lymphomas (incl. Burkitt s) Multiple myeloma Ameloblastoma Secondary
MALIGNANT TUMOURS OF THE JAWS MALIGNANT TUMOURS OF THE JAWS Squamous cell carcinoma Osteogenic sarcoma Chondrosarcoma Fibrosarcoma Malignant lymphomas (incl. Burkitt s) Multiple myeloma Ameloblastoma Secondary
Chapter 7 Part A The Skeleton
 Chapter 7 Part A The Skeleton Why This Matters Understanding the anatomy of the skeleton enables you to anticipate problems such as pelvic dimensions that may affect labor and delivery The Skeleton The
Chapter 7 Part A The Skeleton Why This Matters Understanding the anatomy of the skeleton enables you to anticipate problems such as pelvic dimensions that may affect labor and delivery The Skeleton The
Infratemporal fossa: Tikrit University college of Dentistry Dr.Ban I.S. head & neck Anatomy 2 nd y.
 Infratemporal fossa: This is a space lying beneath the base of the skull between the lateral wall of the pharynx and the ramus of the mandible. It is also referred to as the parapharyngeal or lateral pharyngeal
Infratemporal fossa: This is a space lying beneath the base of the skull between the lateral wall of the pharynx and the ramus of the mandible. It is also referred to as the parapharyngeal or lateral pharyngeal
3. The Jaw and Related Structures
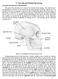 Overview and objectives of this dissection 3. The Jaw and Related Structures The goal of this dissection is to observe the muscles of jaw raising. You will also have the opportunity to observe several
Overview and objectives of this dissection 3. The Jaw and Related Structures The goal of this dissection is to observe the muscles of jaw raising. You will also have the opportunity to observe several
Techniques of local anesthesia in the mandible
 Techniques of local anesthesia in the mandible The technique of choice for anesthesia of the mandible is the block injection and this is attributed to the absence of the advantages which are present in
Techniques of local anesthesia in the mandible The technique of choice for anesthesia of the mandible is the block injection and this is attributed to the absence of the advantages which are present in
Temporal region. temporal & infratemporal fossae. Zhou Hong Ying Dept. of Anatomy
 Temporal region temporal & infratemporal fossae Zhou Hong Ying Dept. of Anatomy Temporal region is divided by zygomatic arch into temporal & infratemporal fossae. Temporal Fossa Infratemporal fossa Temporal
Temporal region temporal & infratemporal fossae Zhou Hong Ying Dept. of Anatomy Temporal region is divided by zygomatic arch into temporal & infratemporal fossae. Temporal Fossa Infratemporal fossa Temporal
CT of Maxillofacial Fracture Patterns. CT of Maxillofacial Fracture Patterns
 CT of Maxillofacial Fracture Patterns CT of Maxillofacial Fracture Patterns Stuart E. Mirvis, M.D., FACR Department of Radiology University of Maryland School of Medicine Viking 1 1976 MGS 2001 Technology
CT of Maxillofacial Fracture Patterns CT of Maxillofacial Fracture Patterns Stuart E. Mirvis, M.D., FACR Department of Radiology University of Maryland School of Medicine Viking 1 1976 MGS 2001 Technology
Screw hole-positioning guide and plate-positioning guide: A novel method to assist mandibular reconstruction
 Journal of Dental Sciences (2012) 7, 301e305 Available online at www.sciencedirect.com journal homepage: www.e-jds.com CASE REPORT Screw hole-positioning guide and plate-positioning guide: A novel method
Journal of Dental Sciences (2012) 7, 301e305 Available online at www.sciencedirect.com journal homepage: www.e-jds.com CASE REPORT Screw hole-positioning guide and plate-positioning guide: A novel method
Temporal fossa Infratemporal fossa Pterygopalatine fossa Terminal branches of external carotid artery Pterygoid venous plexus
 Outline of content Temporal fossa Infratemporal fossa Pterygopalatine fossa Terminal branches of external carotid artery Pterygoid venous plexus Boundary Content Communication Mandibular division of trigeminal
Outline of content Temporal fossa Infratemporal fossa Pterygopalatine fossa Terminal branches of external carotid artery Pterygoid venous plexus Boundary Content Communication Mandibular division of trigeminal
Upper arch. 1Prosthodontics. Dr.Bassam Ali Al-Turaihi. Basic anatomy & & landmark of denture & mouth
 1Prosthodontics Lecture 2 Dr.Bassam Ali Al-Turaihi Basic anatomy & & landmark of denture & mouth Upper arch Palatine process of maxilla: it form the anterior three quarter of the hard palate. Horizontal
1Prosthodontics Lecture 2 Dr.Bassam Ali Al-Turaihi Basic anatomy & & landmark of denture & mouth Upper arch Palatine process of maxilla: it form the anterior three quarter of the hard palate. Horizontal
OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY
 OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY INFERIOR MAXILLECTOMY Tumours of the hard palate and superior alveolus may be resected by inferior maxillectomy (Figure 1). A Le Fort
OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY INFERIOR MAXILLECTOMY Tumours of the hard palate and superior alveolus may be resected by inferior maxillectomy (Figure 1). A Le Fort
Anatomic Relations Summary. Done by: Sohayyla Yasin Dababseh
 Anatomic Relations Summary Done by: Sohayyla Yasin Dababseh Anatomic Relations Lecture 1 Part-1 - The medial wall of the nose is the septum. - The vestibule lies directly inside the nostrils (Nares). -
Anatomic Relations Summary Done by: Sohayyla Yasin Dababseh Anatomic Relations Lecture 1 Part-1 - The medial wall of the nose is the septum. - The vestibule lies directly inside the nostrils (Nares). -
CT of Maxillofacial Injuries
 CT of Maxillofacial Injuries Stuart E. Mirvis, M.D., FACR Department of Radiology University of Maryland School of Medicine Viking 1 1976 MGS 2001 Technology changes the diagnosis Technologic Evolution
CT of Maxillofacial Injuries Stuart E. Mirvis, M.D., FACR Department of Radiology University of Maryland School of Medicine Viking 1 1976 MGS 2001 Technology changes the diagnosis Technologic Evolution
Bones Ethmoid bone Inferior nasal concha Lacrimal bone Maxilla Nasal bone Palatine bone Vomer Zygomatic bone Mandible
 splanchnocranium - Consists of part of skull that is derived from branchial arches - The facial bones are the bones of the anterior and lower human skull Bones Ethmoid bone Inferior nasal concha Lacrimal
splanchnocranium - Consists of part of skull that is derived from branchial arches - The facial bones are the bones of the anterior and lower human skull Bones Ethmoid bone Inferior nasal concha Lacrimal
Cover Page. The handle holds various files of this Leiden University dissertation.
 Cover Page The handle http://hdl.handle.net/1887/31632 holds various files of this Leiden University dissertation. Author: Mensink, Gertjan Title: Bilateral sagittal split osteotomy by the splitter-separator
Cover Page The handle http://hdl.handle.net/1887/31632 holds various files of this Leiden University dissertation. Author: Mensink, Gertjan Title: Bilateral sagittal split osteotomy by the splitter-separator
King's College Hospital Dental School, London, S.E. 5.
 OSTECTOMY AT THE MANDIBULAR SYMPHYSIS J. H. SOWRAY, B.D.S., F.D.S.R.C.S. (Eng.), L.R.C.P., M.R.C.S. and R. HASKELL, M.B., B.S., F.D.S.R.C.S. (Eng.). King's College Hospital Dental School, London, S.E.
OSTECTOMY AT THE MANDIBULAR SYMPHYSIS J. H. SOWRAY, B.D.S., F.D.S.R.C.S. (Eng.), L.R.C.P., M.R.C.S. and R. HASKELL, M.B., B.S., F.D.S.R.C.S. (Eng.). King's College Hospital Dental School, London, S.E.
OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY
 OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY BUCCINATOR MYOMUCOSAL FLAP The Buccinator Myomucosal Flap is an axial flap, based on the facial and/or buccal arteries. It is a flexible
OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY BUCCINATOR MYOMUCOSAL FLAP The Buccinator Myomucosal Flap is an axial flap, based on the facial and/or buccal arteries. It is a flexible
The sebaceous glands (glands of Zeis) open directly into the eyelash follicles, ciliary glands (glands of Moll) are modified sweat glands that open
 The Orbital Region The orbits are a pair of bony cavities that contain the eyeballs; their associated muscles, nerves, vessels, and fat; and most of the lacrimal apparatus upper eyelid is larger and more
The Orbital Region The orbits are a pair of bony cavities that contain the eyeballs; their associated muscles, nerves, vessels, and fat; and most of the lacrimal apparatus upper eyelid is larger and more
Structure Location Function
 Frontal Bone Cranium forms the forehead and roof of the orbits Occipital Bone Cranium forms posterior and inferior portions of the cranium Temporal Bone Cranium inferior to the parietal bone forms the
Frontal Bone Cranium forms the forehead and roof of the orbits Occipital Bone Cranium forms posterior and inferior portions of the cranium Temporal Bone Cranium inferior to the parietal bone forms the
Cranium Facial bones. Sternum Rib
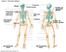 Figure 7.1 The human skeleton. Skull Thoracic cage (ribs and sternum) Cranium Facial bones Sternum Rib Bones of pectoral girdle Vertebral column Sacrum Vertebra Bones of pelvic girdle (a) Anterior view
Figure 7.1 The human skeleton. Skull Thoracic cage (ribs and sternum) Cranium Facial bones Sternum Rib Bones of pectoral girdle Vertebral column Sacrum Vertebra Bones of pelvic girdle (a) Anterior view
Oral cavity landmarks
 By: Dr. Ahmed Rabah Oral cavity landmarks The knowledge of oral anatomy and physiology will help the operator and provides enough landmarks to act as positive guide during denture construction. This subject
By: Dr. Ahmed Rabah Oral cavity landmarks The knowledge of oral anatomy and physiology will help the operator and provides enough landmarks to act as positive guide during denture construction. This subject
Skeletal System -Axial System. Chapter 7 Part A
 Skeletal System -Axial System Chapter 7 Part A Skeleton Learn: Names of the s. Identify specific landmarks that allow: Bones to fit into each other, Organs to fit into the cavities, Muscles to attach,
Skeletal System -Axial System Chapter 7 Part A Skeleton Learn: Names of the s. Identify specific landmarks that allow: Bones to fit into each other, Organs to fit into the cavities, Muscles to attach,
The orbit-1. Dr. Heba Kalbouneh Assistant Professor of Anatomy and Histology
 The orbit-1 Dr. Heba Kalbouneh Assistant Professor of Anatomy and Histology Orbital plate of frontal bone Orbital plate of ethmoid bone Lesser wing of sphenoid Greater wing of sphenoid Lacrimal bone Orbital
The orbit-1 Dr. Heba Kalbouneh Assistant Professor of Anatomy and Histology Orbital plate of frontal bone Orbital plate of ethmoid bone Lesser wing of sphenoid Greater wing of sphenoid Lacrimal bone Orbital
Oral cancer: Prognosis & Treatment. Dr. Hani Al Sheikh Radhi
 Oral cancer: Prognosis & Treatment Dr. Hani Al Sheikh Radhi Prognostic factors in Oral caner TNM staging T stage N stage M stage Site Histological Factors Vascular & Perineural Invasion Surgical Margins
Oral cancer: Prognosis & Treatment Dr. Hani Al Sheikh Radhi Prognostic factors in Oral caner TNM staging T stage N stage M stage Site Histological Factors Vascular & Perineural Invasion Surgical Margins
Chapter 7. Skeletal System
 Chapter 7 Skeletal System 1 Skull A. The skull is made up of 22 bones: 8 cranial bones, 13 facial bones, and the mandible. B. The Cranium encloses and protects the brain, provides attachments for muscles,
Chapter 7 Skeletal System 1 Skull A. The skull is made up of 22 bones: 8 cranial bones, 13 facial bones, and the mandible. B. The Cranium encloses and protects the brain, provides attachments for muscles,
Bony orbit Roof The orbital plate of the frontal bone Lateral wall: the zygomatic bone and the greater wing of the sphenoid
 Bony orbit Roof: Formed by: The orbital plate of the frontal bone, which separates the orbital cavity from the anterior cranial fossa and the frontal lobe of the cerebral hemisphere Lateral wall: Formed
Bony orbit Roof: Formed by: The orbital plate of the frontal bone, which separates the orbital cavity from the anterior cranial fossa and the frontal lobe of the cerebral hemisphere Lateral wall: Formed
PTERYGOPALATINE FOSSA
 PTERYGOPALATINE FOSSA Outline Anatomical Structure and Boundaries Foramina and Communications with other spaces and cavities Contents Pterygopalatine Ganglion Especial emphasis on certain arteries and
PTERYGOPALATINE FOSSA Outline Anatomical Structure and Boundaries Foramina and Communications with other spaces and cavities Contents Pterygopalatine Ganglion Especial emphasis on certain arteries and
Case Report. Orthognathic Correction of Class II Open Bite. Using the Piezoelectric System and MatrixORTHOGNATHIC Plating System.
 Case Report Orthognathic Correction of Class II Open Bite. Using the Piezoelectric System and MatrixORTHOGNATHIC Plating System. Orthognathic Correction of Class II Open Bite. Using the Piezoelectric System
Case Report Orthognathic Correction of Class II Open Bite. Using the Piezoelectric System and MatrixORTHOGNATHIC Plating System. Orthognathic Correction of Class II Open Bite. Using the Piezoelectric System
The Skull and Temporomandibular joint II Prof. Abdulameer Al-Nuaimi. E. mail:
 The Skull and Temporomandibular joint II Prof. Abdulameer Al-Nuaimi E-mail: a.al-nuaimi@sheffield.ac.uk E. mail: abdulameerh@yahoo.com Temporal fossa The temporal fossa is a depression on the temporal
The Skull and Temporomandibular joint II Prof. Abdulameer Al-Nuaimi E-mail: a.al-nuaimi@sheffield.ac.uk E. mail: abdulameerh@yahoo.com Temporal fossa The temporal fossa is a depression on the temporal
Head & Neck Clinical Sub Group. Network Agreed Imaging Guidelines for UAT and Thyroid Cancer. Measure Nos: 11-1C-105i & 11-1C-106i
 Greater Manchester, Lancashire & South Cumbria Strategic Clinical Network & Senate Head & Neck Clinical Sub Group Network Agreed Imaging Guidelines for UAT and Thyroid Cancer Measure Nos: 11-1C-105i &
Greater Manchester, Lancashire & South Cumbria Strategic Clinical Network & Senate Head & Neck Clinical Sub Group Network Agreed Imaging Guidelines for UAT and Thyroid Cancer Measure Nos: 11-1C-105i &
Remember from the first year embryology Trilaminar disc has 3 layers: ectoderm, mesoderm, and endoderm
 Development of face Remember from the first year embryology Trilaminar disc has 3 layers: ectoderm, mesoderm, and endoderm The ectoderm forms the neural groove, then tube The neural tube lies in the mesoderm
Development of face Remember from the first year embryology Trilaminar disc has 3 layers: ectoderm, mesoderm, and endoderm The ectoderm forms the neural groove, then tube The neural tube lies in the mesoderm
Basic Anatomy and Physiology of the Lips and Oral Cavity. Dr. Faghih
 Basic Anatomy and Physiology of the Lips and Oral Cavity Dr. Faghih It is divided into seven specific subsites : 1. Lips 2. dentoalveolar ridges 3. oral tongue 4. retromolar trigone 5. floor of mouth 6.
Basic Anatomy and Physiology of the Lips and Oral Cavity Dr. Faghih It is divided into seven specific subsites : 1. Lips 2. dentoalveolar ridges 3. oral tongue 4. retromolar trigone 5. floor of mouth 6.
Imaging Orbit/Periorbital Injury
 Imaging Orbit/Periorbital Injury 9 th Nordic Trauma Radiology Course 2016 Stuart E. Mirvis, M.D., FACR Department of Radiology University of Maryland School of Medicine Fireworks Topics to Cover Struts
Imaging Orbit/Periorbital Injury 9 th Nordic Trauma Radiology Course 2016 Stuart E. Mirvis, M.D., FACR Department of Radiology University of Maryland School of Medicine Fireworks Topics to Cover Struts
Malignant growth Maxilla management an analysis
 ISSN: 2250-0359 Volume 3 Issue 2 2013 Malignant growth Maxilla management an analysis *Balasubramanian Thiagarajan *Geetha Ramamoorthy *Stanley Medical College Abstract: Malignant tumors involving maxilla
ISSN: 2250-0359 Volume 3 Issue 2 2013 Malignant growth Maxilla management an analysis *Balasubramanian Thiagarajan *Geetha Ramamoorthy *Stanley Medical College Abstract: Malignant tumors involving maxilla
OPERATIVE CORRECTION BY OSTEOTOMY OF RECESSED MALAR MAXILLARY COMPOUND IN A CASE OF OXYCEPHALY
 OPERATIVE CORRECTION BY OSTEOTOMY OF RECESSED MALAR MAXILLARY COMPOUND IN A CASE OF OXYCEPHALY By Sir HAROLD GILLIES, C.B.E., F.R.C.S., and STEWART H. HARRISON, F.R.C.S., L.D.S., R.C.S. From the Plastic
OPERATIVE CORRECTION BY OSTEOTOMY OF RECESSED MALAR MAXILLARY COMPOUND IN A CASE OF OXYCEPHALY By Sir HAROLD GILLIES, C.B.E., F.R.C.S., and STEWART H. HARRISON, F.R.C.S., L.D.S., R.C.S. From the Plastic
Elevators. elevators:- There are three major components of the elevator are:-
 Elevators Elevators:- Are exo-levers, instrument designed to elevate or luxate the teeth or roots from their bony socket in close or surgical method of extraction to force a tooth or root along the line
Elevators Elevators:- Are exo-levers, instrument designed to elevate or luxate the teeth or roots from their bony socket in close or surgical method of extraction to force a tooth or root along the line
Dr.Sepideh Falah-kooshki
 Dr.Sepideh Falah-kooshki MAXILLA Premaxillary/median palatal suture (radiolucent). Incisive fossa and foramen (radiolucent). Nasal passages (radiolucent). Nasal septum (radiopaque). Anterior nasal spine
Dr.Sepideh Falah-kooshki MAXILLA Premaxillary/median palatal suture (radiolucent). Incisive fossa and foramen (radiolucent). Nasal passages (radiolucent). Nasal septum (radiopaque). Anterior nasal spine
Dr. Sami Zaqout, IUG Medical School
 The skull The skull is composed of several separate bones united at immobile joints called sutures. Exceptions? Frontal bone Occipital bone Vault Cranium Sphenoid bone Zygomatic bones Base Ethmoid bone
The skull The skull is composed of several separate bones united at immobile joints called sutures. Exceptions? Frontal bone Occipital bone Vault Cranium Sphenoid bone Zygomatic bones Base Ethmoid bone
Maxilla, ORBIT and infratemporal fossa. Neophytos C Demetriades MD, DDS, MSc Associate professor European University of Cyprus School of Medicine
 Maxilla, ORBIT and infratemporal fossa Neophytos C Demetriades MD, DDS, MSc Associate professor European University of Cyprus School of Medicine MAXILLA Superior, middle, and inferior meatus Frontal sinus
Maxilla, ORBIT and infratemporal fossa Neophytos C Demetriades MD, DDS, MSc Associate professor European University of Cyprus School of Medicine MAXILLA Superior, middle, and inferior meatus Frontal sinus
Omran Saeed. Luma Taweel. Mohammad Almohtaseb. 1 P a g e
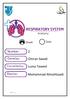 2 Omran Saeed Luma Taweel Mohammad Almohtaseb 1 P a g e I didn t include all the photos in this sheet in order to keep it as small as possible so if you need more clarification please refer to slides In
2 Omran Saeed Luma Taweel Mohammad Almohtaseb 1 P a g e I didn t include all the photos in this sheet in order to keep it as small as possible so if you need more clarification please refer to slides In
BUILDING A. Achieving total reconstruction in a single operation. 70 OCTOBER 2016 // dentaltown.com
 BUILDING A MANDI Achieving total reconstruction in a single operation by Dr. Fayette C. Williams Fayette C. Williams, DDS, MD, FACS, is clinical faculty at John Peter Smith Hospital in Fort Worth, Texas,
BUILDING A MANDI Achieving total reconstruction in a single operation by Dr. Fayette C. Williams Fayette C. Williams, DDS, MD, FACS, is clinical faculty at John Peter Smith Hospital in Fort Worth, Texas,
Reconstruction of a Mandibular Osteoradionecrotic Defect with a Fibula Osteocutaneous Flap.
 Case Report Reconstruction of a Mandibular Osteoradionecrotic Defect with a Fibula Osteocutaneous Flap. Using Synthes ProPlan CMF, Patient Specific Plate Contouring (PSPC) and the MatrixMANDIBLE Plating
Case Report Reconstruction of a Mandibular Osteoradionecrotic Defect with a Fibula Osteocutaneous Flap. Using Synthes ProPlan CMF, Patient Specific Plate Contouring (PSPC) and the MatrixMANDIBLE Plating
Case Study. Case # 1 Author: Dr. Suheil Boutros (USA) 2013 Zimmer Dental, Inc. All rights reserved. 6557, Rev. 03/13.
 Placement of a Zimmer Trabecular Metal Dental Implant with Simultaneous Ridge Augmentation and Immediate Non-Functional Loading Following Tooth Extraction and Orthodontic Treatment for Implant Site Development
Placement of a Zimmer Trabecular Metal Dental Implant with Simultaneous Ridge Augmentation and Immediate Non-Functional Loading Following Tooth Extraction and Orthodontic Treatment for Implant Site Development
Bisection of Head & Nasal Cavity 頭部對切以及鼻腔. 解剖學科馮琮涵副教授 分機
 Bisection of Head & Nasal Cavity 頭部對切以及鼻腔 解剖學科馮琮涵副教授 分機 3250 E-mail: thfong@tmu.edu.tw Outline: The structure of nose The concha and meatus in nasal cavity The openings of paranasal sinuses Canals, foramens
Bisection of Head & Nasal Cavity 頭部對切以及鼻腔 解剖學科馮琮涵副教授 分機 3250 E-mail: thfong@tmu.edu.tw Outline: The structure of nose The concha and meatus in nasal cavity The openings of paranasal sinuses Canals, foramens
Reconstruction of large mandibular defects
 Immediate Reconstruction of a Large Mandibular Defect of Locally Invasive Benign Lesions (A New Method) Gholamreza Shirani, OMFS, DDS, MS,* Mahnaz Arshad, DDS, 1 Farnoush Mohammadi, OMFS, DDS, MS* Tehran,
Immediate Reconstruction of a Large Mandibular Defect of Locally Invasive Benign Lesions (A New Method) Gholamreza Shirani, OMFS, DDS, MS,* Mahnaz Arshad, DDS, 1 Farnoush Mohammadi, OMFS, DDS, MS* Tehran,
A novel classification system for the evaluation and reconstruction of oral defects following oncological surgery
 ONCOLOGY LETTERS 14: 7049-7054, 2017 A novel classification system for the evaluation and reconstruction of oral defects following oncological surgery WEI WEI LIU, CHU YI ZHANG, JIAN YIN LI, MING FANG
ONCOLOGY LETTERS 14: 7049-7054, 2017 A novel classification system for the evaluation and reconstruction of oral defects following oncological surgery WEI WEI LIU, CHU YI ZHANG, JIAN YIN LI, MING FANG
Guided surgery as a way to simplify surgical implant treatment in complex cases
 52 STARGET 1 I 12 StraUMaNN CareS r ry vincenzo MiriSOLA Di TOrreSANTO AND LUCA COrDArO Guided surgery as a way to simplify surgical implant treatment in complex cases Background A 41-year-old woman with
52 STARGET 1 I 12 StraUMaNN CareS r ry vincenzo MiriSOLA Di TOrreSANTO AND LUCA COrDArO Guided surgery as a way to simplify surgical implant treatment in complex cases Background A 41-year-old woman with
CHAPTER 8 SECTION 1.4 ORAL SURGERY TRICARE/CHAMPUS POLICY MANUAL M DEC 1998 SPECIAL BENEFIT INFORMATION
 TRICARE/CHAMPUS POLICY MANUAL 6010.47-M DEC 1998 SPECIAL BENEFIT INFORMATION CHAPTER 8 SECTION 1.4 Issue Date: October 8, 1986 Authority: 32 CFR 199.4(e)(10) I. DESCRIPTION There are certain oral surgical
TRICARE/CHAMPUS POLICY MANUAL 6010.47-M DEC 1998 SPECIAL BENEFIT INFORMATION CHAPTER 8 SECTION 1.4 Issue Date: October 8, 1986 Authority: 32 CFR 199.4(e)(10) I. DESCRIPTION There are certain oral surgical
Trigeminal Nerve Worksheets, Distributions Page 1
 Trigeminal Nerve Worksheet #1 Distribution by Nerve Dr. Darren Hoffmann Dental Gross Anatomy, Spring 2013 We have drawn out each of the branches of CN V in lecture and you have an idea now for their basic
Trigeminal Nerve Worksheet #1 Distribution by Nerve Dr. Darren Hoffmann Dental Gross Anatomy, Spring 2013 We have drawn out each of the branches of CN V in lecture and you have an idea now for their basic
Mohammad Hisham Al-Mohtaseb. Lina Mansour. Reyad Jabiri. 0 P a g e
 2 Mohammad Hisham Al-Mohtaseb Lina Mansour Reyad Jabiri 0 P a g e This is only correction for the last year sheet according to our record. If you already studied this sheet just read the yellow notes which
2 Mohammad Hisham Al-Mohtaseb Lina Mansour Reyad Jabiri 0 P a g e This is only correction for the last year sheet according to our record. If you already studied this sheet just read the yellow notes which
Disclosures. The Expanding Role of Microvascular Reconstruction. Overview. Things they are a Changing. Surgical Advisory Board, Genentech Corp
 Disclosures Surgical Advisory Board, Genentech Corp The Expanding Role of Microvascular Reconstruction P. Daniel Knott, MD FACS Associate Professor Director, Facial Plastic and Reconstructive Surgery UCSF
Disclosures Surgical Advisory Board, Genentech Corp The Expanding Role of Microvascular Reconstruction P. Daniel Knott, MD FACS Associate Professor Director, Facial Plastic and Reconstructive Surgery UCSF
1 Eyelids. Lacrimal Apparatus. Orbital Region. 3 The Orbit. The Eye
 1 1 Eyelids Orbital Region 2 Lacrimal Apparatus 3 The Orbit 4 The Eye 2 Eyelids The eyelids protect the eye from injury and excessive light by their closure. The upper eyelid is larger and more mobile
1 1 Eyelids Orbital Region 2 Lacrimal Apparatus 3 The Orbit 4 The Eye 2 Eyelids The eyelids protect the eye from injury and excessive light by their closure. The upper eyelid is larger and more mobile
Human Anatomy and Physiology - Problem Drill 07: The Skeletal System Axial Skeleton
 Human Anatomy and Physiology - Problem Drill 07: The Skeletal System Axial Skeleton Question No. 1 of 10 Which of the following statements about the axial skeleton is correct? Question #01 A. The axial
Human Anatomy and Physiology - Problem Drill 07: The Skeletal System Axial Skeleton Question No. 1 of 10 Which of the following statements about the axial skeleton is correct? Question #01 A. The axial
University of Palestine. Midterm Exam 2013/2014 Total Grade:
 Course No: DNTS2208 Course Title: Head and Neck Anatomy Date: 09/11/2013 No. of Questions: (50) Time: 1hour Using Calculator (No) University of Palestine Midterm Exam 2013/2014 Total Grade: Instructor
Course No: DNTS2208 Course Title: Head and Neck Anatomy Date: 09/11/2013 No. of Questions: (50) Time: 1hour Using Calculator (No) University of Palestine Midterm Exam 2013/2014 Total Grade: Instructor
AXIAL SKELETON SKULL
 AXIAL SKELETON SKULL CRANIAL BONES (8 total flat bones w/ 2 paired) 1. Frontal forms forehead & upper portion of eyesocket (orbital) 2. Parietal paired bones; form superior & lateral walls of cranium 3.
AXIAL SKELETON SKULL CRANIAL BONES (8 total flat bones w/ 2 paired) 1. Frontal forms forehead & upper portion of eyesocket (orbital) 2. Parietal paired bones; form superior & lateral walls of cranium 3.
Oral Surgery. Basic Techniques of Dental Local Anesthesia. A variety of techniques used in administration and deposition of local anesthesia:
 Oral Surgery Lecture: 9 Dr. Saif Saadedeen Basic Techniques of Dental Local Anesthesia A variety of techniques used in administration and deposition of local anesthesia: 1. Topical anesthesia 2. Infiltration
Oral Surgery Lecture: 9 Dr. Saif Saadedeen Basic Techniques of Dental Local Anesthesia A variety of techniques used in administration and deposition of local anesthesia: 1. Topical anesthesia 2. Infiltration
Nasal region. cartilages: septal cartilage (l); lateral nasal cartilage (2); greater alar cartilages (2); lesser alar cartilages (?
 Nasal region skull bones: nasal and frontal processes of maxilla cartilages: septal cartilage (l); lateral nasal cartilage (2); greater alar cartilages (2); lesser alar cartilages (?) 1 Nasal cavity Roof
Nasal region skull bones: nasal and frontal processes of maxilla cartilages: septal cartilage (l); lateral nasal cartilage (2); greater alar cartilages (2); lesser alar cartilages (?) 1 Nasal cavity Roof
TOTAL MAXILLECTOMY, ORBITAL EXENTERATION
 TOTAL MAXILLECTOMY, ORBITAL EXENTERATION CC-BY-NC 3.0 Johan Fagan Total maxillectomy refers to surgical resection of the entire maxilla. Resection includes the floor and medial wall of the orbit and the
TOTAL MAXILLECTOMY, ORBITAL EXENTERATION CC-BY-NC 3.0 Johan Fagan Total maxillectomy refers to surgical resection of the entire maxilla. Resection includes the floor and medial wall of the orbit and the
Parotid Gland. Parotid Gland. Largest of 3 paired salivary glands (submandibular; sublingual) Ramus of Mandible. Medial pterygoid.
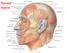 Parotid region Parotid Gland Largest of 3 paired salivary glands (submandibular; sublingual) Ramus of Mandible Medial pterygoid Cross section of mandible Masseter D S SCM Parotid Gland Mastoid Process
Parotid region Parotid Gland Largest of 3 paired salivary glands (submandibular; sublingual) Ramus of Mandible Medial pterygoid Cross section of mandible Masseter D S SCM Parotid Gland Mastoid Process
Dental Implants: A Predictable Solution for Tooth Loss. Reena Talwar, DDS PhD FRCD(C) Oral & Maxillofacial Surgeon Associate Clinical Professor
 Dental Implants: A Predictable Solution for Tooth Loss Reena Talwar, DDS PhD FRCD(C) Oral & Maxillofacial Surgeon Associate Clinical Professor What are Dental Implants? Titanium posts used to replace missing
Dental Implants: A Predictable Solution for Tooth Loss Reena Talwar, DDS PhD FRCD(C) Oral & Maxillofacial Surgeon Associate Clinical Professor What are Dental Implants? Titanium posts used to replace missing
J. 0. AKINOSI, B.D.s., F.D.S.R.C.S.
 British Journal of Oral Surgery 15 (1977-78) 83-87 A NEW APPROACH TO THE MANDIBULAR NERVE BLOCK J. 0. AKINOSI, B.D.s., F.D.S.R.C.S. Department of Oral Surgery and Pathology, College of Medicine, Lagos
British Journal of Oral Surgery 15 (1977-78) 83-87 A NEW APPROACH TO THE MANDIBULAR NERVE BLOCK J. 0. AKINOSI, B.D.s., F.D.S.R.C.S. Department of Oral Surgery and Pathology, College of Medicine, Lagos
Tikrit University collage of dentistry Dr.Ban I.S. head & neck anatomy 2 nd y. Lec [5] / Temporal fossa :
![Tikrit University collage of dentistry Dr.Ban I.S. head & neck anatomy 2 nd y. Lec [5] / Temporal fossa : Tikrit University collage of dentistry Dr.Ban I.S. head & neck anatomy 2 nd y. Lec [5] / Temporal fossa :](/thumbs/88/115294566.jpg) Lec [5] / Temporal fossa : Borders of the Temporal Fossa: Superior: Superior temporal line. Inferior: gap between zygomatic arch and infratemporal crest of sphenoid bone. Anterior: Frontal process of the
Lec [5] / Temporal fossa : Borders of the Temporal Fossa: Superior: Superior temporal line. Inferior: gap between zygomatic arch and infratemporal crest of sphenoid bone. Anterior: Frontal process of the
ANATOMY & PHYSIOLOGY I Laboratory Version B Name Section. REVIEW SHEET Exercise 10 Axial Skeleton
 ANATOMY & PHYSIOLOGY I Laboratory Version B Name Section REVIEW SHEET Exercise 10 Axial Skeleton 1 POINT EACH. THE SKULL MULTIPLE CHOICE 1. The major components of the axial skeleton include the 7. The
ANATOMY & PHYSIOLOGY I Laboratory Version B Name Section REVIEW SHEET Exercise 10 Axial Skeleton 1 POINT EACH. THE SKULL MULTIPLE CHOICE 1. The major components of the axial skeleton include the 7. The
Face. Definition: The area between the two ears and from the chin to the eye brows. The muscles of the face
 Face Definition: The area between the two ears and from the chin to the eye brows. The muscles of the face The muscle of facial expression (include the muscle of the face and the scalp). All are derived
Face Definition: The area between the two ears and from the chin to the eye brows. The muscles of the face The muscle of facial expression (include the muscle of the face and the scalp). All are derived
Maxillofacial Injuries Practical Tips
 Saturday, October 29, 2016 Maxillofacial Injuries Practical Tips Suyash Mohan MD, PDCC THE ROOTS OF PENN RADIOLOGY RADIOLOGICAL Assistant Professor of Radiology Assistant Professor of Neurosurgery Neuroradiology
Saturday, October 29, 2016 Maxillofacial Injuries Practical Tips Suyash Mohan MD, PDCC THE ROOTS OF PENN RADIOLOGY RADIOLOGICAL Assistant Professor of Radiology Assistant Professor of Neurosurgery Neuroradiology
Dr.Ban I.S. head & neck anatomy 2 nd y جامعة تكريت كلية طب االسنان مادة التشريح املرحلة الثانية أ.م.د. بان امساعيل صديق 6102/6102
 جامعة تكريت كلية طب االسنان مادة التشريح املرحلة الثانية أ.م.د. بان امساعيل صديق 6102/6102 Pterygopalatine fossa: The pterygopalatine fossa is a cone-shaped depression, It is located between the maxilla,
جامعة تكريت كلية طب االسنان مادة التشريح املرحلة الثانية أ.م.د. بان امساعيل صديق 6102/6102 Pterygopalatine fossa: The pterygopalatine fossa is a cone-shaped depression, It is located between the maxilla,
Parotid Gland, Temporomandibular Joint and Infratemporal Fossa
 M1 - Anatomy Parotid Gland, Temporomandibular Joint and Infratemporal Fossa Jeff Dupree Sanger 9-057 jldupree@vcu.edu Parotid gland: wraps around the mandible positioned between the mandible and the sphenoid
M1 - Anatomy Parotid Gland, Temporomandibular Joint and Infratemporal Fossa Jeff Dupree Sanger 9-057 jldupree@vcu.edu Parotid gland: wraps around the mandible positioned between the mandible and the sphenoid
Trigeminal Nerve (V)
 Trigeminal Nerve (V) Lecture Objectives Discuss briefly how the face is developed. Follow up the course of trigeminal nerve from its point of central connections, exit and down to its target areas. Describe
Trigeminal Nerve (V) Lecture Objectives Discuss briefly how the face is developed. Follow up the course of trigeminal nerve from its point of central connections, exit and down to its target areas. Describe
Skull-2. Norma Basalis Interna Norma Basalis Externa. Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology
 Skull-2 Norma Basalis Interna Norma Basalis Externa Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology Norma basalis interna Base of the skull- superior view The interior of the base of the
Skull-2 Norma Basalis Interna Norma Basalis Externa Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology Norma basalis interna Base of the skull- superior view The interior of the base of the
Total Maxillectomy. A review. Dr T Balasubramanian
 Total Maxillectomy A review Dr T Balasubramanian Maxillectomy a review Introduction: The concept of maxillectomy was first described by Lazars in 1826. After this description it took nearly three years
Total Maxillectomy A review Dr T Balasubramanian Maxillectomy a review Introduction: The concept of maxillectomy was first described by Lazars in 1826. After this description it took nearly three years
Radiological anatomy of frontal sinus By drtbalu
 2009 Radiological anatomy of frontal sinus By drtbalu Anatomy of frontal sinus is highly variable. Precise understanding of these variables will help a surgeon to avoid unnecessary complications during
2009 Radiological anatomy of frontal sinus By drtbalu Anatomy of frontal sinus is highly variable. Precise understanding of these variables will help a surgeon to avoid unnecessary complications during
Biology 218 Human Anatomy. Adapted from Martini Human Anatomy 7th ed. Chapter 6 The Skeletal System: Axial Division
 Adapted from Martini Human Anatomy 7th ed. Chapter 6 The Skeletal System: Axial Division Introduction The axial skeleton: Composed of bones along the central axis of the body Divided into three regions:
Adapted from Martini Human Anatomy 7th ed. Chapter 6 The Skeletal System: Axial Division Introduction The axial skeleton: Composed of bones along the central axis of the body Divided into three regions:
Introduction to Occlusion and Mechanics of Mandibular Movement
 Introduction to Occlusion and Mechanics of Mandibular Movement Dr. Pauline Hayes Garrett Department of Endodontics, Prosthodontics, and Operative Dentistry University of Maryland, Baltimore Assigned reading
Introduction to Occlusion and Mechanics of Mandibular Movement Dr. Pauline Hayes Garrett Department of Endodontics, Prosthodontics, and Operative Dentistry University of Maryland, Baltimore Assigned reading
Muscles of mastication [part 1]
![Muscles of mastication [part 1] Muscles of mastication [part 1]](/thumbs/76/73586850.jpg) Muscles of mastication [part 1] In this lecture well have the muscles of mastication, neuromuscular function, and its relationship to the occlusion morphology. The fourth determinant of occlusion is the
Muscles of mastication [part 1] In this lecture well have the muscles of mastication, neuromuscular function, and its relationship to the occlusion morphology. The fourth determinant of occlusion is the
APPENDICULAR SKELETON 126 AXIAL SKELETON SKELETAL SYSTEM. Cranium. Skull. Face. Skull and associated bones. Auditory ossicles. Associated bones.
 SKELETAL SYSTEM 206 AXIAL SKELETON 80 APPENDICULAR SKELETON 26 Skull Skull and associated s 29 Cranium Face Auditory ossicles 8 4 6 Associated s Hyoid Thoracic cage 25 Sternum Ribs 24 Vertebrae 24 column
SKELETAL SYSTEM 206 AXIAL SKELETON 80 APPENDICULAR SKELETON 26 Skull Skull and associated s 29 Cranium Face Auditory ossicles 8 4 6 Associated s Hyoid Thoracic cage 25 Sternum Ribs 24 Vertebrae 24 column
Alexander C Vlantis. Selective Neck Dissection 33
 05 Modified Radical Neck Dissection Type II Alexander C Vlantis Selective Neck Dissection 33 Modified Radical Neck Dissection Type II INCISION Various incisions can be used for a neck dissection. The incision
05 Modified Radical Neck Dissection Type II Alexander C Vlantis Selective Neck Dissection 33 Modified Radical Neck Dissection Type II INCISION Various incisions can be used for a neck dissection. The incision
It has been proposed that partially edentulous maxillectomy
 CLASSICAL ARTICLE Basic principles of obturator design for partially edentulous patients. Part II: Design principles Mohamed A. Aramany, DMD, MS* Eye and Ear Hospital of Pittsburgh and University of Pittsburgh,
CLASSICAL ARTICLE Basic principles of obturator design for partially edentulous patients. Part II: Design principles Mohamed A. Aramany, DMD, MS* Eye and Ear Hospital of Pittsburgh and University of Pittsburgh,
Prosthetic Options in Implant Dentistry. Hakimeh Siadat, DDS, MSc Associate Professor
 Prosthetic Options in Dentistry Hakimeh Siadat, DDS, MSc Associate Professor Dental Research Center, Department of Prosthodontics & Dental s Faculty of Dentistry, Tehran University of Medical Sciences
Prosthetic Options in Dentistry Hakimeh Siadat, DDS, MSc Associate Professor Dental Research Center, Department of Prosthodontics & Dental s Faculty of Dentistry, Tehran University of Medical Sciences
Case Report Mid Facial Degloving Procedure: Managing A Case of Multiple Mid Face Fractures with Significant External Deformity
 55 Bangladesh J Otorhinolaryngol 2015; 21(1): 51-56 Case Report Mid Facial Degloving Procedure: Managing A Case of Multiple Mid Face Fractures with Significant External Deformity Akhil Chndra Biswas 1,
55 Bangladesh J Otorhinolaryngol 2015; 21(1): 51-56 Case Report Mid Facial Degloving Procedure: Managing A Case of Multiple Mid Face Fractures with Significant External Deformity Akhil Chndra Biswas 1,
Musculoskeletal System (Part A-1) Module 7 -Chapter 10 Overview. Functions
 Musculoskeletal System (Part A-1) Module 7 -Chapter 10 Overview Susie Turner, M.D. 1/8/13 Muscles Attachments Bones Bone types Surface features of bones Divisions of the skeletal system Joints or Articulations
Musculoskeletal System (Part A-1) Module 7 -Chapter 10 Overview Susie Turner, M.D. 1/8/13 Muscles Attachments Bones Bone types Surface features of bones Divisions of the skeletal system Joints or Articulations
Conventional radiograph verses CT for evaluation of sagittal fracture of mandibular condyle
 Case Report: Conventional radiograph verses CT for evaluation of sagittal fracture of mandibular condyle Dr Anjali Wadhwa, Dr Gaurav Shah, Dr Shweta Sharma, Dr Anand Bhatnagar, Dr Pallavi Malaviya NIMS
Case Report: Conventional radiograph verses CT for evaluation of sagittal fracture of mandibular condyle Dr Anjali Wadhwa, Dr Gaurav Shah, Dr Shweta Sharma, Dr Anand Bhatnagar, Dr Pallavi Malaviya NIMS
(loco-regional disease)
 (loco-regional disease) (oral cavity) (circumvillae papillae) (subsite) A (upper & lower lips) B (buccal membrane) C (mouth floor) D (upper & lower gingiva) E (hard palate) F (tongue -- anterior 2/3 rds
(loco-regional disease) (oral cavity) (circumvillae papillae) (subsite) A (upper & lower lips) B (buccal membrane) C (mouth floor) D (upper & lower gingiva) E (hard palate) F (tongue -- anterior 2/3 rds
Research report for MSc Dent. University of Witwatersrand. Faculty of health science. Dr J Beukes. Student number: h
 Research report for MSc Dent University of Witwatersrand Faculty of health science Dr J Beukes Student number: 9507510h Supervisor: Prof JP Reyneke October 2011 1 1. Title 2. Aim 3. Introduction 4. Objectives
Research report for MSc Dent University of Witwatersrand Faculty of health science Dr J Beukes Student number: 9507510h Supervisor: Prof JP Reyneke October 2011 1 1. Title 2. Aim 3. Introduction 4. Objectives
Figure (2-6): Labial frenum and labial notch.
 The anatomy of the edentulous ridge in the maxilla and mandible is very important for the design of a complete denture. The consistency of the mucosa and architecture of the underlying bone is different
The anatomy of the edentulous ridge in the maxilla and mandible is very important for the design of a complete denture. The consistency of the mucosa and architecture of the underlying bone is different
INTERNATIONAL MEDICAL COLLEGE
 INTERNATIONAL MEDICAL COLLEGE Joint Degree Master Program: Implantology and Dental Surgery (M.Sc.) Specialized Modules: List of individual modules Specialized Module 1 Basic principles of implantology
INTERNATIONAL MEDICAL COLLEGE Joint Degree Master Program: Implantology and Dental Surgery (M.Sc.) Specialized Modules: List of individual modules Specialized Module 1 Basic principles of implantology
PALATAL POSITIONING OF IMPLANTS IN SEVERELY RESORBED POSTERIOR MAXILLAE F. Atamni, M.Atamni, M.Atamna, Private Practice Tel-aviv Israel
 PALATAL POSITIONING OF IMPLANTS IN SEVERELY RESORBED POSTERIOR MAXILLAE F. Atamni, M.Atamni, M.Atamna, Private Practice Tel-aviv Israel Abstract: Objectives: To evaluate an alternative treatment for rehabilitation
PALATAL POSITIONING OF IMPLANTS IN SEVERELY RESORBED POSTERIOR MAXILLAE F. Atamni, M.Atamni, M.Atamna, Private Practice Tel-aviv Israel Abstract: Objectives: To evaluate an alternative treatment for rehabilitation
CASE REPORT. CBCT-Assisted Treatment of the Failing Long Span Bridge with Staged and Immediate Load Implant Restoration
 Computer Aided Implantology Academy Newsletter - Newsletter 20 - July 2009 CASE REPORT CBCT-Assisted Treatment of the Failing Long Span Bridge with Staged and Immediate Load Implant Restoration Case Report
Computer Aided Implantology Academy Newsletter - Newsletter 20 - July 2009 CASE REPORT CBCT-Assisted Treatment of the Failing Long Span Bridge with Staged and Immediate Load Implant Restoration Case Report
By JOHN MARQUIS CONVERSE, M.D., and DAUBERT TELSEY, D.D.S.
 THE TRIPARTITE OSTEOTOMY OF THE MID-FACE FOR ORBITAL EXPANSION AND CORRECTION OF THE DEFORMITY IN CRANIOSTENOSIS By JOHN MARQUIS CONVERSE, M.D., and DAUBERT TELSEY, D.D.S. Center for Craniofacial Anomalies
THE TRIPARTITE OSTEOTOMY OF THE MID-FACE FOR ORBITAL EXPANSION AND CORRECTION OF THE DEFORMITY IN CRANIOSTENOSIS By JOHN MARQUIS CONVERSE, M.D., and DAUBERT TELSEY, D.D.S. Center for Craniofacial Anomalies
MAXILLOFACIAL TRAUMA. The on-call maxillofacial surgeons can be contacted through the switchboard at the Southern General Hospital
 MAXILLOFACIAL TRAUMA The on-call maxillofacial surgeons can be contacted through the switchboard at the Southern General Hospital Mandibular Injuries Mechanism of injury Assault, falls, RTA-Direct trauma
MAXILLOFACIAL TRAUMA The on-call maxillofacial surgeons can be contacted through the switchboard at the Southern General Hospital Mandibular Injuries Mechanism of injury Assault, falls, RTA-Direct trauma
Skull basic structures. Neurocranium
 Assoc. Prof. Květuše Lovásová, M.V.D., PhD. Skull basic structures Skull consists of two groups of bones: neurocranium (bones forming the brain box) splanchnocranium (bones forming the facial skeleton)
Assoc. Prof. Květuše Lovásová, M.V.D., PhD. Skull basic structures Skull consists of two groups of bones: neurocranium (bones forming the brain box) splanchnocranium (bones forming the facial skeleton)
Extraoral radiography Introduction: Extraoral radiographs (outside the mouth) are taken when large areas of the skull or jaw must be examined or when
 Extraoral radiography Introduction: Extraoral radiographs (outside the mouth) are taken when large areas of the skull or jaw must be examined or when patients are unable to open their mouths for film placement.
Extraoral radiography Introduction: Extraoral radiographs (outside the mouth) are taken when large areas of the skull or jaw must be examined or when patients are unable to open their mouths for film placement.
