Michael A. Howard a, Babak Mehrara b, * REVIEW. Introduction
|
|
|
- Jacob Cross
- 5 years ago
- Views:
Transcription
1 International Journal of Surgery (2005) 3, 53e60 REVIEW Emerging trends in microsurgical breast reconstruction: Deep inferior epigastric artery perforator (DIEP) and the superior gluteal artery perforator (SGAP) flaps Michael A. Howard a, Babak Mehrara b, * a The Division of Plastic Surgery, Evanston Northwestern Hospital, 2650 Ridge Avenue, Evanston, IL 60201, USA b The Plastic Surgery Service, Memorial Sloan-Kettering Cancer Center, 1275 York Avenue, 11th Floor, New York, NY 10021, USA KEYWORDS Breast reconstruction; Microsurgery; Deep inferior epigastric artery perforator flap; DIEP; Superior gluteal artery perforator flap; SGAP Abstract Breast reconstruction is an important adjunct in the treatment of breast cancer. Many reconstructive options exist, however autologous tissue remains the gold standard. One drawback to autologous reconstruction methods is the potential for flap donor site morbidity. Recent advances in microsurgical techniques include the development of perforator flaps, including the Deep Inferior Epigastric Artery Perforator flap (DIEP) and the Superior Gluteal Artery Perforator (SGAP) flaps. Harvest of these flaps attempt to minimize the impact on the donor site and thereby reduce the incidence of donor site complications. This article will review of the indications, advantages and drawbacks to the use of perforator flaps in breast reconstruction surgery. ª 2005 Surgical Associates Ltd. Published by Elsevier Ltd. All rights reserved. Introduction The incidence of breast cancer is rising. Nearly one in eight women in the USA will be diagnosed with * Corresponding author. Tel.: C ; fax: C address: mehrarab@mskcc.org (B. Mehrara). this disease at some point during their lifetime. According to the American Cancer Society, 211,300 new cases of invasive breast cancer were diagnosed in Although many women are treated with breast conservation, mastectomy remains an important treatment modality. Breast reconstruction has been shown to be an important adjunct in the treatment of women /$ - see front matter ª 2005 Surgical Associates Ltd. Published by Elsevier Ltd. All rights reserved. doi: /j.ijsu
2 54 M.A. Howard, B. Mehrara treated with mastectomy. 2 Numerous studies have demonstrated beneficial effects on quality of life and body image. 3,4 In addition, breast reconstruction serves as an important coping mechanism particularly in younger patients. 5,6 Traditionally, breast reconstruction has been performed using either autogenous tissues (excess fat from the abdomen or buttocks) or implants. The purpose of this manuscript is to review recent advancements in microsurgical autogenous tissue breast reconstruction. requiring mastectomy. Although tissue expander/ implant reconstruction is an excellent and expedient method for breast reconstruction, autogenous tissues remain the gold standard for a natural looking and natural feeling restoration of the female breast (Fig. 1). Autogenous tissue breast reconstruction can be divided into a number of categories based on the donor sites available and the methods used for tissue transfer. Background A number of reconstructive options ranging from simple procedures to complex microsurgical reconstructions are currently available for women Pedicled flaps Pedicled flaps refer to those that are transferred to the breast while the endogenous blood supply is kept intact. Examples of pedicled flaps include the Figure 1 (A and B) Pre-operative and (C and D) post-operative photographs of a woman treated with mastectomy and breast reconstruction using a deep inferior epigastric perforator flap.
3 Perforator flaps for breast reconstruction 55 pedicled transverse rectus abdominus myocutaneous flap (TRAM) and the latissimus dorsi myocutaneous flap. In general, pedicled flaps are transferred as a composite of muscle, fat, and skin and are then sculpted to re-create the missing breast. Most or all of the associated muscle is harvested in an effort to maintain the blood supply of the skin and overlying fat. Sacrifice of the rectus abdominus muscle may lead to significant abdominal wall morbidity including weakness, abdominal wall laxity, and abdominal wall hernia formation. 7e10 Often, synthetic mesh is required following flap harvest to repair the fascial defect. 11 The vascular supply of the pedicled TRAM flap is based on the superior epigastric vessels, which represents the secondary blood supply to the lower abdominal skin and subcutaneous tissues. Thus, these procedures may be associated with partial flap loss (7e31%). 12 Despite these shortcomings, pedicled flaps remain popular in many centers since they are relatively easy to perform and are, in general, associated with excellent outcomes. Perforator flaps Perforator flaps represent the logical extension of the microsurgical free flap. These flaps are designed to include the bare minimum of structures needed for reconstruction, while limiting the extraneous donor site tissues harvested with a flap. By reducing the amount of donor site tissue disturbance, one theoretically lowers the donor site morbidity. The development of these flaps arose from detailed anatomical description of the body s vascular supply to the skin and subcutaneous tissue. 18e22 Large, named vessels give off smaller branches that course superficially, or perforate through muscle and/or fascial planes to supply the overlying skin and subcutaneous tissue. These perforators are a neurovascular bundle consisting of an artery, vein, and nerve, and can be meticulously dissected through the muscle to their origin. This enables preservation of the myofibrils and their innervation, ultimately preserving the function of the underlying muscle. Two such perforator flaps have gained favor for autologous breast reconstruction. Microsurgical reconstruction The shortcomings of pedicled flaps have led to advancements in microsurgical breast reconstruction. In these procedures, small sections of the underlying muscle are dissected together with the dominant vascular pedicle and the blood supply of the tissue (flap) is temporarily disconnected and re-established in the breast pocket. Examples of free flaps include the free TRAM flap and gluteal flaps. The free TRAM flap theoretically decreases abdominal wall morbidity by preserving more innervated rectus muscle. In addition, the free TRAM and gluteal flaps are based on the dominant blood supply of the overlying skin, the deep inferior epigastric artery/vein (DIEA/V) and superior gluteal artery/vein (SGA/V), respectively, and are thus associated with decreased rates of partial flap loss or fat necrosis. Critics of the free TRAM flap procedure claim that overall abdominal complication rates remain high and comparable to pedicled TRAM flaps due to the alterations in muscle attachment and denervation. 13e16 They maintain that these alterations lead to weakness and atrophy of the remaining muscle with resultant abdominal wall function that is comparable to patients treated with pedicled TRAM flap harvest. 17 This concept remains contentious in the plastic surgery literature with a wide range of studies demonstrating various outcomes. Deep inferior epigastric artery perforator (DIEP) flap Rectus abdominus preservation Based on the TRAM flap concept, an abdominal skin and fat flap is dissected based on the perforating branches from the DIEA. 23e26 Unlike the pedicled or free TRAM flap harvest, however, the abdominal wall fascia and rectus muscle are not included with the flap. Preserving muscle vascularity and motor nerves in turn preserves the rectus muscle function. 27,28 Recent evidence suggests that preservation of the rectus muscle reduces donor site morbidity and results in lower rates of donor site complications such as site pain, abdominal wall laxity or hernia, back pain, and functional impairments. 29 These benefits are even more significant when bilateral reconstruction is performed. 30 DIEP anatomy/flap harvest Harvest of the DIEP flap is similar to thatof a standard free TRAM. The major differences lie in the meticulous dissection required to maintain the integrity of the rectus fibers and the continuity of the motor branches. Standard TRAM abdominal markings and incisions are utilized, giving consideration to pre-existing abdominal incisions. During initial flap
4 56 M.A. Howard, B. Mehrara Figure 2 (A) Identification of a single, dominate perforator entering abdominal flap (arrow); (B) DIEP flap has been harvested; single perforator entering central portion of the flap (arrow); (C) resulting donor site; note muscular viability and single incision of anterior rectus fascia that will be repaired with a simple running suture. For orientation, the patient s head is superior. elevation, perforators emerging from the anterior rectus sheath to the overlying flap are identified. A decision must be made as to which perforator(s) should be utilized, based on vessel size, quality, palpable pulse and location (Fig. 2AeC). Preferably, a single dominant perforator exists entering centrally on the flap. However, multiple perforators may be included if none appears dominant. The anterior rectus fascia is opened and the perforator is dissected along its course through the muscle to its origin from the deep inferior epigastric artery and vein. The vascular pedicle is further dissected until adequate length and caliber are achieved. Segmental sensory and motor nerves are encountered during dissection. The motor nerves are preserved to prevent de-innervation of the muscle. Sensory nerves that run with the perforator to the flap may be dissected for anastamosis in the chest for flap re-innervation. After flap harvest, a simple running or interrupted closure of the fascial incision is performed and the donor site is closed. The free flap is transferred to the mastectomy defect and microvascular anastamosis is performed to the internal mammary or thoracodorsal vessels. Neurotization is usually performed to medial branches of the 4th intercostals nerve. Further inset and shaping of the flap is then performed. DIEP patient selection Pre-operative considerations for the DIEP are similar to that of the free TRAM. They include the patient s breast size and volume, the amount and quality of abdominal tissue available, tobacco use, and coexisting medical conditions. 31 Obesity is a relative contraindication to the TRAM and DIEP flap due to increased rates of donor site complications, although some authors have argued that DIEP flaps may be safe in this setting as perforating vessels are often hypertrophied. 15,32 Pre-existing midline and Pfannenstiel incisions are of little consequence, however, midline incisions decrease the amount of tissue available for reconstruction as circulation to the contralateral flap is impeded by scar formation. Paramedian and ostomy incisions may have previously damaged the perforators and should be given particular consideration. A previous open cholecystectomy incision should not affect flap harvest; however, these incisions may diminish the blood supply of the anterior abdominal skin and result in wound healing complications. Intra-operatively, the decision to proceed with DIEP harvest is made based on the number, caliber, and location of the perforators, 31 and conversion to a standard free or pedicled TRAM necessary in
5 Perforator flaps for breast reconstruction 57 cases where adequate perforators are not identified. 16 Ideally, one dominant perforator is present which is usually able to supply the majority of the flap. Presence of several, smaller perforators may imply a less robust, though adequate, blood supply. In one series 20% of flaps were based on a single perforator, 50% on two perforators, and 30% on three or more. 16 In our experience, the majority of DIEP flaps are based on one or two large perforating vessels. Advantages of DIEP flap The DIEP flap is the preferred choice for many surgeons for delayed and immediate autologous breast reconstruction, particularly when performing bilateral breast reconstruction (Fig. 2A, B). 33 The DIEP is a reliable flap, with published success rates of 95e99.5% 15,16,31,32 and partial flap loss rate of 2.5%. 16 The fat necrosis rate (i.e., any amount of significant flap firmness post-operatively) ranges from 6 to 12.9%, 10,16,32,34 comparing favorably to that of the free or pedicled TRAM. 12,35,36 Use of the DIEP flap results in less impact on the abdominal donor site and therefore reduced donor site morbidity. 13,17,29 The reported abdominal hernia rate following DIEP harvest is 0.7% 16 and 2.1% in bilateral cases. 33 This compares favorably to the hernia rate of up to 15% following TRAM flap. 37 In the immediate setting, DIEP patients may experience less donor site pain 38 and ambulate sooner. 15 Also, the use of synthetic mesh is not required for fascial closure following DIEP harvest, while it may be needed following TRAM, harvest, particularly in bilateral flap harvest. 30 Drawbacks Use of the DIEP for reconstruction requires microsurgical proficiency and a hospital setting that provides competent care for microsurgical patients. In a surgeon s early experience with the DIEP flap, there may be an increased length of operative time due to perforator dissection. However, with experience, the operative times are rarely much longer than a free TRAM and the procedure has been shown to be a cost effective method of reconstruction. 39 Venous congestion may be problematic in the DIEP flap; therefore careful dissection of the superficial inferior epigastric vein for additional venous drainage may be necessary in some cases. 30,31,40,41 The DIEP flap has reduced, but not completely eliminated donor site complications. Gill et al. 16 reported that in a series of 758 DIEP flaps over 10 years, the overall donor site complication rate was 13.6%. While most of these complications consisted of delayed abdominal wound healing, the abdominal hernia rate was 0.7%. The incidence of complications is also significantly elevated among patients who actively smoke, suffer from hypertension, or who undergo post-operative XRT. 16,30,42 For this reason, many recommend avoiding flaps in active smokers and delaying flap reconstruction until after completion of XRT. 15,42 Gluteal artery perforator flaps General The gluteal donor sites provide another autologous option for those women who do not have adequate abdominal tissue, whose abdomen is not an option due to pre-existing scars, or those who prefer to avoid an abdominal donor site. The use of gluteal flaps, however, has been limited by the associated donor site scarring, difficult dissection, and short pedicle. 43e46 The superior gluteal artery perforator (SGAP) flap 47 and the inferior gluteal artery perforator (IGAP) flap 48 address these issues by avoiding gluteus muscle sacrifice and increasing pedicle length. Patient selection/indications Gluteal flaps are autologous reconstruction options for a select patient population who are not TRAM or DIEP flap candidates and who wish to avoid use of an implant or in whom an implant is not an option (i.e. poor chest skin quality following XRT). In addition, these flaps may be considered in patients who wish to avoid the abdominal donor site. Gluteal artery perforator flaps are also best suited to match a moderate-sized, non-ptotic, contralateral breast (Fig. 3). Gluteal flap anatomy/harvest Two different flaps may be harvested from the gluteal donor site. At the superior aspect of the buttock, a perforator emerges from the gluteus maximus one-third the distance between the posterior iliac spine and the greater trochanter. A flap up to 12! 32 cm in size may be designed over this perforator (Fig. 4). Harvest of the SGAP is performed from the ipsilateral buttock in the lateral decubitus position. The patient s torso may be corkscrewed to allow two-team approach.
6 58 M.A. Howard, B. Mehrara Figure 3 (A) Donor site from bilateral abdominal flap harvest, left TRAM (solid arrow) and right DIEP (empty arrow); (B) harvested flaps with vessels entering hemi-tram (solid arrow) and single perforator entering central portion of the DIEP flap (empty arrow). Note the lack of muscle harvested with DIEP flap. For orientation, the patient s head is superior. The flap elevated from lateral to medial until the perforator(s) is/are identified. The perforator is traced and dissected through the gluteus maximus to the level of anterior gluteal fascia, preserving the gluteal fibers. Dissection may be complete at this point if there is adequate vessel length and diameter or the fascia may be opened and dissection continued toward the superior gluteal artery. Use of the internal mammary vessels is preferred as the final pedicle length is often insufficient to reach the axilla. 27 If sensory re-innervation is planned, the nerves from T12-L2 entering the flap superiorly above muscle fascia layer should be identified at the outset of flap harvest. These fibers can be traced superiorly and included. 49,50 A second perforator flap may be designed on the lower buttock crease based on perforating vessels originating from the inferior gluteal artery (IGAP flap). Design of the flap places the inferior flap border and final closure in the gluteal crease. A flap 12e13 cm in vertical dimension can be harvested in a similar fashion to the SGAP flap. Care must be taken to prevent the resulting scar from extending to the anterior thigh and avoid damage to the sciatic and posterior cutaneous nerve that lie lateral to the inferior gluteal artery. Advantages The SGAP and IGAP flaps offer several advantages in autologous reconstruction. There is an Figure 4 (A) SGAP flap donor site markings; (B) harvested SGAP flap; (C) SGAP donor site; (D) healed donor site.
7 Perforator flaps for breast reconstruction 59 abundance of adipose tissue in gluteal region, even in thin patients, flap harvest results in a wellhidden scar, and the integrity of the gluteus maximus muscle is preserved. Due to the quality of the buttock tissue, the resulting flap has excellent projection of the reconstructed breast as compared to TRAM and DIEP without the need for folding the flap, which may affect flap circulation. This flap is an autologous option if the TRAM has been utilized previously. It also may be used in staged, bilateral breast reconstruction, whereas the TRAM offers a single-use opportunity. Advantages of the IGAP include the well-hidden donor site in the gluteal crease and a longer vascular pedicle than the SGAP that can reach the axilla. 51 Drawbacks The gluteal flaps are not widely taught in training programs, therefore, overall patient and physician comfort lags behind that of other alternatives. Like the DIEP flap, use of the gluteal flaps requires microsurgical experience and comfort with perforator dissection. In addition, patient positioning and operative logistics can be somewhat difficult, although in most instances simultaneous two-team work is possible. Bilateral reconstruction poses a particular challenge due to the long length of the surgical procedure and patient repositioning such that most surgeons choose to stage reconstruction. The gluteal donor site is thicker and more fibrous than the abdominal donor site tissue and less overall skin is available. These factors may limit the ability to achieve ptosis of the reconstructed breast and overall contouring to match the contralateral breast. This may also limit the flap s use in delayed reconstruction where the skin requirements are increased. SGAP flap harvest may result in a depressed scar particularly if more than 10 cm of skin is taken in the vertical dimension 51 or if significant undermining is performed to increase flap volume during harvest. This may result in difficulties with asymmetry an unsightly scarring. The IGAP donor site in the gluteal crease may affect sitting and ambulating in the short term, but this rarely persists. 48 Conclusions The DIEP flap is a reliable flap, results in fewer abdominal complications, and has minimal increase in surgical time as compared to traditional abdominal flaps used for breast reconstruction. Craigie et al. 30 point out that the initial arguments against use of the DIEP flap (i.e., long operative time and high failure rates) are no longer valid. The SGAP and the IGAP flaps are also excellent autologous tissue alternatives for breast reconstruction. The benefits of the flap reliability and inconspicuous donor site outweigh the slight increase in operative complexity due to the position change required intra-operatively. The DIEP, SGAP and IGAP flaps are reconstructive options available to appropriately selected patients undergoing autologous breast reconstruction. Familiarity with these options will enhance the care of the breast reconstruction patient. References 1. American Cancer Society, Inc.! Brandberg Y, Malm M, Blomqvist L. A prospective and randomized study, SVEA, comparing effects of three methods for delayed breast reconstruction on quality of life, patient-defined problem areas of life, and cosmetic result. Plastic and Reconstructive Surgery 2000;105(1): Edsander-Nord A, Brandberg Y, Wickman M. Quality of life, patients satisfaction, and aesthetic outcome after pedicled or free TRAM flap breast surgery. Plastic and Reconstructive Surgery 2001;107(5):1142e5. 4. Girotto JA, Schreiber J, Nahabedian MY. Breast reconstruction in the elderly: preserving excellent quality of life. Annals of Plastic Surgery 2003;50(6):572e8. 5. Pusic A, Thompson TA, Kerrigan CL, Sargeant R, Slezak S, Chang BW, et al. Surgical options for the early-stage breast cancer: factors associated with patient choice and postoperative quality of life. Plastic and Reconstructive Surgery 1999;104(5):1325e Schover LR. Sexuality and body image in younger women with breast cancer. [Review] [58 refs]. Journal of the National Cancer Institute 1994;16:177e182 [Monographs]. 7. Kroll SS, Schusterman MA, Reece GP, Miller MF, Robb G, Evans G. Abdominal wall strength, bulging, and hernia after TRAM flap breast reconstruction. Plastic and Reconstructive Surgery 1995;96(3):616e9. 8. Mizgala CL, Hartrampf Jr CR, Bennett GK. Abdominal function after pedicled TRAM flap surgery. Clinics in Plastic Surgery 1994;21(2):255e Hartrampf Jr CR. Abdominal wall competence in transverse abdominal island flap operations. Annals of Plastic Surgery 1984;12(2):139e Keller A. The deep inferior epigastric perforator free flap for breast reconstruction. Annals of Plastic Surgery 2001; 46(5):474e Zienowicz RJ, May Jr JW. Hernia prevention and aesthetic contouring of the abdomen following TRAM flap breast reconstruction by the use of polypropylene mesh. Plastic and Reconstructive Surgery 1995;96(6):1346e Hartrampf Jr CR. The transverse abdominal island flap for breast reconstruction. A 7-year experience. Clinics in Plastic Surgery 1988;15(4):703e Futter CM, Webster MH, Hagen S, Mitchell SL. A retrospective comparison of abdominal muscle strength following
8 60 M.A. Howard, B. Mehrara breast reconstruction with a free TRAM or DIEP flap. British Journal of Plastic Surgery 2000;53(7):578e Allen RJ. Discussion: breast reconstruction with superficial inferior epigastric artery flaps: a prospective comparison with TRAM and DIEP flaps. Plastic and Reconstructive Surgery 2004;114(5):1084e Allen RJ. DIEP versus TRAM for breast reconstruction. Plastic and Reconstructive Surgery 2003;111(7): Gill PS, Hunt JP, Guerra AB, Dellacroce FJ, Sullivan SK, Boraski J, et al. A 10-year retrospective review of 758 DIEP flaps for breast reconstruction. Plastic and Reconstructive Surgery 2004;113(4):1153e Futter CM. Abdominal donor site morbidity: Impact of the TRAM and DIEP flap on strength and function. Seminars in Plastic Surgery 2002;16(1):119e Taylor GI, Palmer JH. Angiosome theory. British Journal of Plastic Surgery 1992;45(4):327e Taylor GI, Palmer JH. The vascular territories (angiosomes) of the body: experimental study and clinical applications. British Journal of Plastic Surgery 1987;40(2):113e Taylor GI, Corlett RJ, Boyd JB. The versatile deep inferior epigastric (inferior rectus abdominis) flap. British Journal of Plastic Surgery 1984;37(3):330e Onishi K, Maruyama Y. Cutaneous and fascial vasculature around the rectus abdominis muscle: anatomic basis of abdominal fasciocutaneous flaps. Journal of Reconstructive Microsurgery 1986;2(4):247e Onishi K, Maruyama Y, Iwahira Y. Cutaneous and fascial vasculature of the leg: anatomic study of fasciocutaneous vessels. Journal of Reconstructive Microsurgery 1986;2(3): 181e Allen RJ, Treece P. Deep inferior epigastric perforator flap for breast reconstruction. Annals of Plastic Surgery 1994; 32(1):32e Blondeel PN, Boeckx WD. Refinements in free flap breast reconstruction: the free bilateral deep inferior epigastric perforator flap anastomosed to the internal mammary artery. British Journal of Plastic Surgery 1994;47(7):495e Koshima I, Moriguchi T, Soeda S, Tanaka H, Umeda N. Free thin paraumbilical perforator-based flaps. Annals of Plastic Surgery 1992;29(1):12e Koshima I, Soeda S. Inferior epigastric artery skin flaps without rectus abdominis muscle. British Journal of Plastic Surgery 1989;42(6):645e Blondeel PN, Van Landuyt K, Hamdi M, et al. Soft tissue reconstruction with the superior gluteal artery perforator flap. Clinics in Plastic Surgery 2003;30(3):371e Yap LH, Whiten SC, Forster A, Stevenson JH. The anatomical and neurophysiological basis of the sensate free TRAM and DIEP flaps. British Journal of Plastic Surgery 2002;55(1):35e Blondeel N, Vanderstraeten GG, Monstrey SJ, Van LanDuyt K, Tonnard P, Lysens R, et al. The donor site morbidity of free DIEP flaps and free TRAM flaps for breast reconstruction. British Journal of Plastic Surgery 1997; 50(5):322e Craigie JE, Allen RJ, Dellacroce FJ, Sullivan SK. Autogenous breast reconstruction with the deep inferior epigastric perforator flap. Clinics in Plastic Surgery 2003;30(3):359e Nahabedian MY, Momen B, Galdino G, Manson PN. Breast reconstruction with the free TRAM flap: patient selection, choice of flap, and outcome. Plastic and Reconstructive Surgery 2002;110(2):466e Blondeel PN. One hundred free DIEP flap breast reconstructions: a personal experience. British Journal of Plastic Surgery 1999;52(2):104e Guerra AB, Metzinger SE, Bidros RS, Rizzuto RP, Gill PS, Nguyen AH, et al. Bilateral breast reconstruction with the deep inferior epigastric perforator (DIEP) flap: an experience with 280 flaps. Annals of Plastic Surgery 2004;52(3): 246e Hamdi M, Weiler-Mithoff EM, Webster MH. Deep inferior epigastric perforator flap in breast reconstruction: experience with the first 50 flaps. Plastic and Reconstructive Surgery 1999;103(1):86e Kroll SS, Gherardini G, Martin JE, Reece GP, Miller MJ, Evans GR, et al. Fat necrosis in free and pedicled TRAM flaps. Plastic and Reconstructive Surgery 1998;102(5):1502e Hartrampf Jr CR, Bennett GK. Autogenous tissue reconstruction in the mastectomy patient. A critical review of 300 patients. Annals of Surgery 1987;205(5):508e Watterson PA, Bostwick III J, Hester Jr TR, Bried JT, Taylor GI. TRAM flap anatomy correlated with a 10-year clinical experience with 556 patients. Plastic and Reconstructive Surgery 1995;95(7):1185e Kroll SS, Sharma S, Koutz C, Langstein HN, Evans GRD, Robb GL, et al. Postoperative morphine requirements of free TRAM and DIEP flaps. Plastic and Reconstructive Surgery 2001;107(2):338e Kaplan JL, Allen RJ. Cost-based comparison between perforator flaps and TRAM flaps for breast reconstruction. Plastic and Reconstructive Surgery 2000;105(3):943e Blondeel PN, Arnstein M, Verstraete K, Depuydt K, Van Landuyt KG, Monstrey SJ, et al. Venous congestion and blood flow in free transverse rectus abdominis myocutaneous and deep inferior epigastric perforator flaps. Plastic and Reconstructive Surgery 2000;106(6):1295e Kroll SS. Fat necrosis in free transverse rectus abdominis myocutaneous and deep inferior epigastric perforator flaps. Plastic and Reconstructive Surgery 2000;106(3):576e Rogers NE, Allen RJ. Radiation effects on breast reconstruction with the deep inferior epigastric perforator flap. Plastic and Reconstructive Surgery 2002;109(6):1919e Fujino T, Harasina T, Aoyagi F. Reconstruction for aplasia of the breast and pectoral region by microvascular transfer of a free flap from the buttock. Plastic and Reconstructive Surgery 1975;56(2):178e Le Quang C. Two new free flaps developed from aesthetic surgery: the inferior gluteal flap. Aesthetic Plastic Surgery 1980;4147e Shaw WW. Breast reconstruction by superior gluteal microvascular free flaps without silicone implants. Plastic and Reconstructive Surgery 1983;72(4):490e Paletta CE, Bostwick III J, Nahai F. The inferior gluteal free flap in breast reconstruction. Plastic and Reconstructive Surgery 1989;84(6):875e Allen RJ, Tucker Jr C. Superior gluteal artery perforator free flap for breast reconstruction. Plastic and Reconstructive Surgery 1995;95(7):1207e Allen RJ. Perforator flaps in breast reconstruction: how to perform reliably. Philadelphia, PA: American Society of Plastic Surgeons; Blondeel PN. The sensate free superior gluteal artery perforator (S-GAP) flap: a valuable alternative in autologous breast reconstruction. British Journal of Plastic Surgery 1999;52(3):185e Blondeel PN, Demuynck M, Mete D, Monstrey SJ, Van Landuyt K, Matton G, et al. Sensory nerve repair in perforator flaps for autologous breast reconstruction: sensational or senseless? British Journal of Plastic Surgery 1999;52(1):37e Hidalgo DA. Superior gluteal free flap. In: Spear SL, Little JW, Lippman ME, et al., editors. Surgery of the breast: principles and art. Philadelphia: Lippincott-Raven Publishers; p. 627e35.
Breast Reconstruction with Superficial Inferior Epigastric Artery Flaps: A Prospective Comparison with TRAM and DIEP Flaps
 Breast Reconstruction with Superficial Inferior Epigastric Artery Flaps: A Prospective Comparison with TRAM and DIEP Flaps Pierre M. Chevray, M.D., Ph.D. Houston, Texas Breast reconstruction using the
Breast Reconstruction with Superficial Inferior Epigastric Artery Flaps: A Prospective Comparison with TRAM and DIEP Flaps Pierre M. Chevray, M.D., Ph.D. Houston, Texas Breast reconstruction using the
Anatomical Landmarks for Safe Elevation of the Deep Inferior Epigastric Perforator Flap: A Cadaveric Study
 Anatomical Landmarks for Safe Elevation of the Deep Inferior Epigastric Perforator Flap: A Cadaveric Study Saeed Chowdhry, MD, Ron Hazani, MD, Philip Collis, BS, and Bradon J. Wilhelmi, MD University of
Anatomical Landmarks for Safe Elevation of the Deep Inferior Epigastric Perforator Flap: A Cadaveric Study Saeed Chowdhry, MD, Ron Hazani, MD, Philip Collis, BS, and Bradon J. Wilhelmi, MD University of
Reconstruction of the Breast after Cancer An Overview of Procedures and Options by Karen M. Horton, MD, MSc, FRCSC
 Downloaded from Reconstruction of the Breast after Cancer An Overview of Procedures and Options by Karen M. Horton, MD, MSc, FRCSC What is Breast Reconstruction? Reconstruction of the breast involves recreating
Downloaded from Reconstruction of the Breast after Cancer An Overview of Procedures and Options by Karen M. Horton, MD, MSc, FRCSC What is Breast Reconstruction? Reconstruction of the breast involves recreating
Update on Breast Reconstruction Using Free TRAM, DIEP, and SIEA Flaps
 Update on Breast Reconstruction Using Free TRAM, DIEP, and SIEA Flaps Pierre M. Chevray, M.D., Ph.D. 1 ABSTRACT Breast reconstruction using autologous tissue is commonly accomplished using the transverse
Update on Breast Reconstruction Using Free TRAM, DIEP, and SIEA Flaps Pierre M. Chevray, M.D., Ph.D. 1 ABSTRACT Breast reconstruction using autologous tissue is commonly accomplished using the transverse
Breast Reconstruction Options
 Breast Reconstruction Options Natural reconstruction using your ABDOMINAL tissue: TRAM Flap (Transverse Rectus Abdominis Myocutaneous) There are various forms of TRAM flap reconstruction that are commonly
Breast Reconstruction Options Natural reconstruction using your ABDOMINAL tissue: TRAM Flap (Transverse Rectus Abdominis Myocutaneous) There are various forms of TRAM flap reconstruction that are commonly
Citation for published version (APA): Benditte-Klepetko, H. C. (2014). Breast surgery: A problem of beauty or health?
 UvA-DARE (Digital Academic Repository) Breast surgery: A problem of beauty or health? Benditte-Klepetko, H.C. Link to publication Citation for published version (APA): Benditte-Klepetko, H. C. (2014).
UvA-DARE (Digital Academic Repository) Breast surgery: A problem of beauty or health? Benditte-Klepetko, H.C. Link to publication Citation for published version (APA): Benditte-Klepetko, H. C. (2014).
A multiple logistic regression analysis of complications following microsurgical breast reconstruction
 Original Article A multiple logistic regression analysis of complications following microsurgical breast reconstruction Samir Rao 1, Ellen C. Stolle 1, Sarah Sher 1, Chun-Wang Lin 1, Bahram Momen 2, Maurice
Original Article A multiple logistic regression analysis of complications following microsurgical breast reconstruction Samir Rao 1, Ellen C. Stolle 1, Sarah Sher 1, Chun-Wang Lin 1, Bahram Momen 2, Maurice
The dissection of the rectus abdominis myocutaneous flap with complete preservation of the anterior rectus sheath q
 The British Association of Plastic Surgeons (2003) 56, 395 400 The dissection of the rectus abdominis myocutaneous flap with complete preservation of the anterior rectus sheath q D. Erni*, Y.D. Harder
The British Association of Plastic Surgeons (2003) 56, 395 400 The dissection of the rectus abdominis myocutaneous flap with complete preservation of the anterior rectus sheath q D. Erni*, Y.D. Harder
The most common type of breast reconstruction
 BREAST Breast Reconstruction with Perforator Flaps Jay W. Granzow, M.D., M.P.H. Joshua L. Levine, M.D. Ernest S. Chiu, M.D. Maria M. LoTempio, M.D. Robert J. Allen, M.D. New Orleans, La.; Charleston, S.C.;
BREAST Breast Reconstruction with Perforator Flaps Jay W. Granzow, M.D., M.P.H. Joshua L. Levine, M.D. Ernest S. Chiu, M.D. Maria M. LoTempio, M.D. Robert J. Allen, M.D. New Orleans, La.; Charleston, S.C.;
Simultaneous Bilateral Breast Reconstruction With In-the-Crease Inferior Gluteal Artery Perforator Flaps
 BREAST SURGERY Simultaneous Bilateral Breast Reconstruction With In-the-Crease Inferior Gluteal Artery Perforator Flaps Joshua L. Levine, MD,* Quintessa Miller, MD, Julie Vasile, MD,* Kamran Khoobehi,
BREAST SURGERY Simultaneous Bilateral Breast Reconstruction With In-the-Crease Inferior Gluteal Artery Perforator Flaps Joshua L. Levine, MD,* Quintessa Miller, MD, Julie Vasile, MD,* Kamran Khoobehi,
Few would deny that lower abdominal tissue BREAST. An Intraoperative Algorithm for Use of the SIEA Flap for Breast Reconstruction.
 BREAST An Intraoperative Algorithm for Use of the SIEA Flap for Breast Reconstruction Aldona J. Spiegel, M.D. Farah N. Khan, M.D. Houston, Texas Background: The deep inferior epigastric perforator (DIEP)
BREAST An Intraoperative Algorithm for Use of the SIEA Flap for Breast Reconstruction Aldona J. Spiegel, M.D. Farah N. Khan, M.D. Houston, Texas Background: The deep inferior epigastric perforator (DIEP)
Breast reconstruction following mastectomy has
 Free full text on www.ijps.org Post-mastectomy breast reconstruction: Microsurgical methods Venkat Ramakrishnan, Makarand Tare St. Andrew s Centre for Burns and Plastic Surgery, BroomÞ eld Hospital, Chelmsford,
Free full text on www.ijps.org Post-mastectomy breast reconstruction: Microsurgical methods Venkat Ramakrishnan, Makarand Tare St. Andrew s Centre for Burns and Plastic Surgery, BroomÞ eld Hospital, Chelmsford,
JPRAS Open 3 (2015) 1e5. Contents lists available at ScienceDirect. JPRAS Open. journal homepage:
 JPRAS Open 3 (2015) 1e5 Contents lists available at ScienceDirect JPRAS Open journal homepage: http://www.journals.elsevier.com/ jpras-open Case report The pedicled transverse partial latissimus dorsi
JPRAS Open 3 (2015) 1e5 Contents lists available at ScienceDirect JPRAS Open journal homepage: http://www.journals.elsevier.com/ jpras-open Case report The pedicled transverse partial latissimus dorsi
Methods of autologous tissue breast reconstruction BREAST
 BREAST Comparison of Donor-Site Morbidity of SIEA, DIEP, and Muscle-Sparing TRAM Flaps for Breast Reconstruction Liza C. Wu, M.D. Anureet Bajaj, M.D. David W. Chang, M.D. Pierre M. Chevray, M.D., Ph.D.
BREAST Comparison of Donor-Site Morbidity of SIEA, DIEP, and Muscle-Sparing TRAM Flaps for Breast Reconstruction Liza C. Wu, M.D. Anureet Bajaj, M.D. David W. Chang, M.D. Pierre M. Chevray, M.D., Ph.D.
CASE REPORT An Innovative Solution to Complex Inguinal Defect: Deepithelialized SIEA Flap With Mini Abdominoplasty
 CASE REPORT An Innovative Solution to Complex Inguinal Defect: Deepithelialized SIEA Flap With Mini Abdominoplasty Augustine Reid Wilson, MS, Justin Daggett, MD, Michael Harrington, MD, MPH, and Deniz
CASE REPORT An Innovative Solution to Complex Inguinal Defect: Deepithelialized SIEA Flap With Mini Abdominoplasty Augustine Reid Wilson, MS, Justin Daggett, MD, Michael Harrington, MD, MPH, and Deniz
Selective salvage of zones 2 and 4 in the pedicled TRAM flap: a focus on reducing fat necrosis and improving aesthetic outcomes
 DOI 10.1186/s40064-016-1714-7 RESEARCH Open Access Selective salvage of zones 2 and 4 in the pedicled TRAM flap: a focus on reducing fat necrosis and improving aesthetic outcomes Chi Sun Yoon and Kyu Nam
DOI 10.1186/s40064-016-1714-7 RESEARCH Open Access Selective salvage of zones 2 and 4 in the pedicled TRAM flap: a focus on reducing fat necrosis and improving aesthetic outcomes Chi Sun Yoon and Kyu Nam
Soft tissue reconstruction with the superior gluteal artery perforator f lap
 Clin Plastic Surg 30 (2003) 371 382 Soft tissue reconstruction with the superior gluteal artery perforator f lap Phillip N. Blondeel, MD, PhD*, Koenraad Van Landuyt, MD, Moustapha Hamdi, MD, Stan J. Monstrey,
Clin Plastic Surg 30 (2003) 371 382 Soft tissue reconstruction with the superior gluteal artery perforator f lap Phillip N. Blondeel, MD, PhD*, Koenraad Van Landuyt, MD, Moustapha Hamdi, MD, Stan J. Monstrey,
Prophylactic Mastectomy & Reconstructive Implications
 Prophylactic Mastectomy & Reconstructive Implications Minas T Chrysopoulo, MD PRMA Center For Advanced Breast Reconstruction Prophylactic Mastectomy Surgical removal of one or both breasts to reduce the
Prophylactic Mastectomy & Reconstructive Implications Minas T Chrysopoulo, MD PRMA Center For Advanced Breast Reconstruction Prophylactic Mastectomy Surgical removal of one or both breasts to reduce the
Medical Journal of the Volume 20 Islamic Republic of Iran Number 3 Fall 1385 November Original Articles
 Medical Journal of the Volume 0 Islamic Republic of Iran Number 3 Fall 38 November 00 Original Articles ANATOMY OF THE SUPERFICIAL INFERIOR EPIGASTRIC ARTERY FLAP MAHDI FATHI, M.D., EBRAHIM HATAMIPOUR,
Medical Journal of the Volume 0 Islamic Republic of Iran Number 3 Fall 38 November 00 Original Articles ANATOMY OF THE SUPERFICIAL INFERIOR EPIGASTRIC ARTERY FLAP MAHDI FATHI, M.D., EBRAHIM HATAMIPOUR,
Tor Chiu. Deep Inferior Epigastric Artery Perforator Flap 161
 18 Deep Inferior Epigastric Artery Perforator Flap Tor Chiu Deep Inferior Epigastric Artery Perforator Flap 161 Deep Inferior Epigastric Artery Perforator Flap FLAP TERRITORY The deep inferior epigastric
18 Deep Inferior Epigastric Artery Perforator Flap Tor Chiu Deep Inferior Epigastric Artery Perforator Flap 161 Deep Inferior Epigastric Artery Perforator Flap FLAP TERRITORY The deep inferior epigastric
INTRODUCTION. Toshihiko Satake 1, Jun Sugawara 2, Kazunori Yasumura 1, Taro Mikami 2, Shinji Kobayashi 3, Jiro Maegawa 2. Idea and Innovation
 Mini-Flow-Through Deep Inferior Epigastric Perforator Flap for Breast Reconstruction with Preservation of Both Internal Mammary and Deep Inferior Epigastric Vessels Toshihiko Satake 1, Jun Sugawara 2,
Mini-Flow-Through Deep Inferior Epigastric Perforator Flap for Breast Reconstruction with Preservation of Both Internal Mammary and Deep Inferior Epigastric Vessels Toshihiko Satake 1, Jun Sugawara 2,
Breast reconstruction has an important role BREAST. A Two-Year Prospective Analysis of Trunk Function in TRAM Breast Reconstructions
 BREAST A Two-Year Prospective Analysis of Trunk Function in TRAM Breast Reconstructions Amy K. Alderman, M.D. William M. Kuzon, Jr., M.D., Ph.D. Edwin G. Wilkins, M.D. Ann Arbor, Mich. Background: Functional
BREAST A Two-Year Prospective Analysis of Trunk Function in TRAM Breast Reconstructions Amy K. Alderman, M.D. William M. Kuzon, Jr., M.D., Ph.D. Edwin G. Wilkins, M.D. Ann Arbor, Mich. Background: Functional
The lumbar artery perforator based island flap: anatomical study and case reports
 British Journal of Plastic Surgery (1999), 52, 541 546 1999 The British Association of Plastic Surgeons The lumbar artery perforator based island flap: anatomical study and case reports H. Kato*, M. Hasegawa,
British Journal of Plastic Surgery (1999), 52, 541 546 1999 The British Association of Plastic Surgeons The lumbar artery perforator based island flap: anatomical study and case reports H. Kato*, M. Hasegawa,
Breast Restoration Surgery After a mastectomy
 UW MEDICINE PATIENT EDUCATION Breast Restoration Surgery After a mastectomy This handout explains the most common procedures that are used at University of Washington Medical Center (UWMC) to restore a
UW MEDICINE PATIENT EDUCATION Breast Restoration Surgery After a mastectomy This handout explains the most common procedures that are used at University of Washington Medical Center (UWMC) to restore a
Achieving ideal donor site aesthetics with autologous breast reconstruction
 Review Article Achieving ideal donor site aesthetics with autologous breast reconstruction Maurice Y. Nahabedian Department of Plastic Surgery, Georgetown University, Washington, DC 20007, USA Correspondence
Review Article Achieving ideal donor site aesthetics with autologous breast reconstruction Maurice Y. Nahabedian Department of Plastic Surgery, Georgetown University, Washington, DC 20007, USA Correspondence
The progress in microsurgical procedures has led
 Original Article Breast reconstruction with free anterolateral thigh flap Ranjit Raje, Ramesh Chepauk, Kanti Shetty, Rajendra Prasad J. S. Plastic & Reconstructive Services, Department of Surgical Oncology,
Original Article Breast reconstruction with free anterolateral thigh flap Ranjit Raje, Ramesh Chepauk, Kanti Shetty, Rajendra Prasad J. S. Plastic & Reconstructive Services, Department of Surgical Oncology,
Frederick J. Duffy, Jr., MD, FACS and Brice W. McKane, MD, FACS BREAST RECONSTRUCTION
 Frederick J. Duffy, Jr., MD, FACS and Brice W. McKane, MD, FACS BREAST RECONSTRUCTION BREAST RECONSTRUCTION: A WOMAN S DECISION Options and Information Our approach to breast reconstruction entails a very
Frederick J. Duffy, Jr., MD, FACS and Brice W. McKane, MD, FACS BREAST RECONSTRUCTION BREAST RECONSTRUCTION: A WOMAN S DECISION Options and Information Our approach to breast reconstruction entails a very
Immediate versus delayed free TRAM breast reconstruction: an analysis of perioperative factors and complications
 British Journal of Plastic Surgery (22), 55, l-6 9 22 The British Association of Plastic Surgeons doi:.54/bjps.22.3747 BRITISH JOURNAL OF / ~ ] PLASTIC SURGERY Immediate versus delayed free TRAM breast
British Journal of Plastic Surgery (22), 55, l-6 9 22 The British Association of Plastic Surgeons doi:.54/bjps.22.3747 BRITISH JOURNAL OF / ~ ] PLASTIC SURGERY Immediate versus delayed free TRAM breast
Four-flap Breast Reconstruction: Bilateral Stacked DIEP and PAP Flaps
 Original Article Breast Four-flap Breast Reconstruction: Bilateral Stacked DIEP and PAP Flaps James L. Mayo, MD Robert J. Allen, MD, FACS Alireza Sadeghi, MD, FACS Background: In cases of bilateral breast
Original Article Breast Four-flap Breast Reconstruction: Bilateral Stacked DIEP and PAP Flaps James L. Mayo, MD Robert J. Allen, MD, FACS Alireza Sadeghi, MD, FACS Background: In cases of bilateral breast
Breast Reconstruction
 Steven E. Copit, M.D. Chief- Division of Plastic Surgery Thomas Jefferson University Hospital Philadelphia, PA analysis of The Defect Skin Breast Volume Nipple Areola Complex analysis of The Defect the
Steven E. Copit, M.D. Chief- Division of Plastic Surgery Thomas Jefferson University Hospital Philadelphia, PA analysis of The Defect Skin Breast Volume Nipple Areola Complex analysis of The Defect the
Comparing the donor-site morbidity using DIEP, SIEA or MS-TRAM flaps for breast reconstructive surgery: A meta-analysis
 Journal of Plastic, Reconstructive & Aesthetic Surgery (2012) 65, 1474e1480 REVIEW Comparing the donor-site morbidity using DIEP, SIEA or MS-TRAM flaps for breast reconstructive surgery: A meta-analysis
Journal of Plastic, Reconstructive & Aesthetic Surgery (2012) 65, 1474e1480 REVIEW Comparing the donor-site morbidity using DIEP, SIEA or MS-TRAM flaps for breast reconstructive surgery: A meta-analysis
The Profunda Artery Perforator Flap: Investigating the Perforasome Using Three-Dimensional Computed Tomographic Angiography
 BREAST The Profunda Artery Perforator Flap: Investigating the Perforasome Using Three-Dimensional Computed Tomographic Angiography Corrine Wong, M.D. Purushottam Nagarkar, M.D. Sumeet Teotia, M.D. Nicholas
BREAST The Profunda Artery Perforator Flap: Investigating the Perforasome Using Three-Dimensional Computed Tomographic Angiography Corrine Wong, M.D. Purushottam Nagarkar, M.D. Sumeet Teotia, M.D. Nicholas
Anatomical relationship between arteries and veins in the paraumbilical region q
 The British Association of Plastic Surgeons (2003) 56, 552 556 Anatomical relationship between arteries and veins in the paraumbilical region q N. Imanishi a, *, H. Nakajima b, T. Minabe c, H. Chang d,
The British Association of Plastic Surgeons (2003) 56, 552 556 Anatomical relationship between arteries and veins in the paraumbilical region q N. Imanishi a, *, H. Nakajima b, T. Minabe c, H. Chang d,
Diagnosis and Treatment of Patients with Primary and Metastatic Breast Cancer. Oncoplastic and Reconstructive Surgery
 Diagnosis and Treatment of Patients with Primary and Metastatic Breast Cancer Oncoplastic and Reconstructive Surgery Plastic-reconstructive aspects after mastectomy Versions 2002 2017: Audretsch / Bauerfeind
Diagnosis and Treatment of Patients with Primary and Metastatic Breast Cancer Oncoplastic and Reconstructive Surgery Plastic-reconstructive aspects after mastectomy Versions 2002 2017: Audretsch / Bauerfeind
Current Strategies in Breast Reconstruction
 Current Strategies in Breast Reconstruction Hani Sbitany, MD Assistant Professor of Surgery University of California, San Francisco Division of Plastic and Reconstructive Surgery 12 th Annual School of
Current Strategies in Breast Reconstruction Hani Sbitany, MD Assistant Professor of Surgery University of California, San Francisco Division of Plastic and Reconstructive Surgery 12 th Annual School of
Algorithm for Autologous Breast Reconstruction for Partial Mastectomy Defects
 Algorithm for Autologous Breast Reconstruction for Partial Mastectomy Defects Joshua L. Levine, M.D., Nassif E. Soueid, M.D., and Robert J. Allen, M.D. New Orleans, La. Background: The use of lateral thoracic
Algorithm for Autologous Breast Reconstruction for Partial Mastectomy Defects Joshua L. Levine, M.D., Nassif E. Soueid, M.D., and Robert J. Allen, M.D. New Orleans, La. Background: The use of lateral thoracic
Breast Cancer Reconstruction
 Breast Cancer Jerome H. Liu, MD Tom S. Liu, MD Jerome H. Liu, MD Undergraduate: Brown University Medical School: University of California, Los Angeles Residency: UCLA Medical Center Fellowship:UCLA Medical
Breast Cancer Jerome H. Liu, MD Tom S. Liu, MD Jerome H. Liu, MD Undergraduate: Brown University Medical School: University of California, Los Angeles Residency: UCLA Medical Center Fellowship:UCLA Medical
Anatomical Background of the Perforator Flap Based on the Deep Branch of the Superficial Circumflex Iliac Artery (SCIP Flap): A Cadaveric Study
 Anatomical Background of the Perforator Flap Based on the Deep Branch of the Superficial Circumflex Iliac Artery (SCIP Flap): A Cadaveric Study Raphael Sinna, MD, a Hassene Hajji, MD, b Quentin Qassemyar,
Anatomical Background of the Perforator Flap Based on the Deep Branch of the Superficial Circumflex Iliac Artery (SCIP Flap): A Cadaveric Study Raphael Sinna, MD, a Hassene Hajji, MD, b Quentin Qassemyar,
Breast Reconstruction: Current Strategies and Future Opportunities
 Breast Reconstruction: Current Strategies and Future Opportunities Hani Sbitany, MD Assistant Professor of Surgery University of California, San Francisco Division of Plastic and Reconstructive Surgery
Breast Reconstruction: Current Strategies and Future Opportunities Hani Sbitany, MD Assistant Professor of Surgery University of California, San Francisco Division of Plastic and Reconstructive Surgery
Breast cancer reconstruction surgery (immediate and delayed) across Ontario: Patient indications and appropriate surgical options
 A Quality Initiative of the Program in Evidence-Based Care (PEBC), Cancer Care Ontario (CCO) Breast cancer reconstruction surgery (immediate and delayed) across Ontario: Patient indications and appropriate
A Quality Initiative of the Program in Evidence-Based Care (PEBC), Cancer Care Ontario (CCO) Breast cancer reconstruction surgery (immediate and delayed) across Ontario: Patient indications and appropriate
4/30/2010. Options for abdominal wall reconstruction. Scott L. Hansen, MD
 Components Separation Scott L. Hansen, MD University of California, San Francisco Chief, Plastic and Reconstructive Surgery San Francisco General Hospital Overview Options for abdominal wall reconstruction
Components Separation Scott L. Hansen, MD University of California, San Francisco Chief, Plastic and Reconstructive Surgery San Francisco General Hospital Overview Options for abdominal wall reconstruction
Breast conservation surgery and sentinal node biopsy: Dr R Botha Moderator: Dr E Osman
 Breast conservation surgery and sentinal node biopsy: Dr R Botha Moderator: Dr E Osman Breast anatomy: Breast conserving surgery: The aim of wide local excision is to remove all invasive and in situ
Breast conservation surgery and sentinal node biopsy: Dr R Botha Moderator: Dr E Osman Breast anatomy: Breast conserving surgery: The aim of wide local excision is to remove all invasive and in situ
Novel Interpositional Vein Grafting for Pedicle Extension of Island Pedicle Flaps
 e50 Case Report THIEME Novel Interpositional Vein Grafting for Pedicle Extension of Island Pedicle Flaps Shuhei Yoshida, MD 1 Isao Koshima, MD 1 Shogo Nagamatsu, MD 2 Kazunori Yokota, MD 2 Shuji Yamashita,
e50 Case Report THIEME Novel Interpositional Vein Grafting for Pedicle Extension of Island Pedicle Flaps Shuhei Yoshida, MD 1 Isao Koshima, MD 1 Shogo Nagamatsu, MD 2 Kazunori Yokota, MD 2 Shuji Yamashita,
Abdominal perforator vs. muscle sparing flaps for breast reconstruction
 Review Article Abdominal perforator vs. muscle sparing flaps for breast reconstruction Paris D. Butler, Liza C. Wu Division of Plastic Surgery, Department of Surgery, University of Pennsylvania Health
Review Article Abdominal perforator vs. muscle sparing flaps for breast reconstruction Paris D. Butler, Liza C. Wu Division of Plastic Surgery, Department of Surgery, University of Pennsylvania Health
Breast Reconstruction in Women Under 30: A 10-Year Experience
 ORIGINAL ARTICLE Breast Reconstruction in Women Under 30: A 10-Year Experience Warren A. Ellsworth, MD,* Barbara L. Bass, MD, FACS, Roman J. Skoracki, MD, à and Lior Heller, MD* *Division of Plastic Surgery,
ORIGINAL ARTICLE Breast Reconstruction in Women Under 30: A 10-Year Experience Warren A. Ellsworth, MD,* Barbara L. Bass, MD, FACS, Roman J. Skoracki, MD, à and Lior Heller, MD* *Division of Plastic Surgery,
Figure 1. Anatomy of the breast
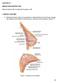 CHAPTER 12 BREAST RECONSTRUCTION Mihaela Rapolti, MD and Michelle Roughton, MD I. BREAST ANATOMY A. Mastering breast anatomy is essential for understanding how the breast changes with aging and principles
CHAPTER 12 BREAST RECONSTRUCTION Mihaela Rapolti, MD and Michelle Roughton, MD I. BREAST ANATOMY A. Mastering breast anatomy is essential for understanding how the breast changes with aging and principles
Essential Anatomy for oncoplastic surgery. Omar Z. Youssef M.D Professor of surgical oncology NCI- Cairo University
 Essential Anatomy for oncoplastic surgery Omar Z. Youssef M.D Professor of surgical oncology NCI- Cairo University Introduction Rationale for anatomical basis for OPS Anatomical considerations: 1. Surface
Essential Anatomy for oncoplastic surgery Omar Z. Youssef M.D Professor of surgical oncology NCI- Cairo University Introduction Rationale for anatomical basis for OPS Anatomical considerations: 1. Surface
Interesting Case Series. Scalp Reconstruction With Free Latissimus Dorsi Muscle
 Interesting Case Series Scalp Reconstruction With Free Latissimus Dorsi Muscle Danielle H. Rochlin, BA, Justin M. Broyles, MD, and Justin M. Sacks, MD Department of Plastic and Reconstructive Surgery,
Interesting Case Series Scalp Reconstruction With Free Latissimus Dorsi Muscle Danielle H. Rochlin, BA, Justin M. Broyles, MD, and Justin M. Sacks, MD Department of Plastic and Reconstructive Surgery,
The gluteal perforator-based flap in repair of pressure sores
 The British Association of Plastic Surgeons (2004) 57, 342 347 CASE REPORTS The gluteal perforator-based flap in repair of pressure sores Çilingir Meltem*, Çelik Esra, Fındık Hasan, Duman Ali Department
The British Association of Plastic Surgeons (2004) 57, 342 347 CASE REPORTS The gluteal perforator-based flap in repair of pressure sores Çilingir Meltem*, Çelik Esra, Fındık Hasan, Duman Ali Department
Scapular & Parascapular flap FLAP TERRITORY ANATOMY. is normally accompanied by two venae comitantes.
 Scapular & Parascapular flap FLAP TERRITORY This is a composite flap that is situated over the scapula with various incisional arrangements. It can be harvested as a skin and subcutaneous tissue flap,
Scapular & Parascapular flap FLAP TERRITORY This is a composite flap that is situated over the scapula with various incisional arrangements. It can be harvested as a skin and subcutaneous tissue flap,
Chest wall reconstruction using a combined musculocutaneous anterolateral anteromedial thigh flap
 Free full text on www.ijps.org Case Report DOI: 10.4103/0970-0358.63966 Chest wall reconstruction using a combined musculocutaneous anterolateral anteromedial thigh flap Pearlie W. W. Tan, Chin-Ho Wong,
Free full text on www.ijps.org Case Report DOI: 10.4103/0970-0358.63966 Chest wall reconstruction using a combined musculocutaneous anterolateral anteromedial thigh flap Pearlie W. W. Tan, Chin-Ho Wong,
BREAST RECONSTRUCTION POST MASTECTOMY
 UnitedHealthcare Commercial Coverage Determination Guideline BREAST RECONSTRUCTION POST MASTECTOMY Guideline Number: SUR057 Effective Date: January 1, 2019 Table of Contents Page INSTRUCTIONS FOR USE...
UnitedHealthcare Commercial Coverage Determination Guideline BREAST RECONSTRUCTION POST MASTECTOMY Guideline Number: SUR057 Effective Date: January 1, 2019 Table of Contents Page INSTRUCTIONS FOR USE...
Endoscopic assisted harvest of the pedicled pectoralis major muscle flap
 British Journal of Plastic Surgery (2005) 58, 170 174 Endoscopic assisted harvest of the pedicled pectoralis major muscle flap Arif Turkmen*, A. Graeme B. Perks Plastic Surgery Department, Nottingham City
British Journal of Plastic Surgery (2005) 58, 170 174 Endoscopic assisted harvest of the pedicled pectoralis major muscle flap Arif Turkmen*, A. Graeme B. Perks Plastic Surgery Department, Nottingham City
FREE DIEP-FLAP RECONSTRUCTION OF TUMOUR RELATED DEFECTS IN HEAD AND NECK
 JOURNAL OF PHYSIOLOGY AND PHARMACOLOGY 2008, 59, Suppl 5, 59 67 www.jpp.krakow.pl H. LEONHARDT 1, R. MAI 1, W. PRADEL 1, J. MARKWARDT 1, T. PINZER 2, A. SPASSOV 3, G. LAUER 1 FREE DIEP-FLAP RECONSTRUCTION
JOURNAL OF PHYSIOLOGY AND PHARMACOLOGY 2008, 59, Suppl 5, 59 67 www.jpp.krakow.pl H. LEONHARDT 1, R. MAI 1, W. PRADEL 1, J. MARKWARDT 1, T. PINZER 2, A. SPASSOV 3, G. LAUER 1 FREE DIEP-FLAP RECONSTRUCTION
BREAST RECONSTRUCTION/REMOVAL AND REPLACEMENT OF IMPLANTS
 Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices and drugs are dependent upon
Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices and drugs are dependent upon
BREAST RECONSTRUCTION POST MASTECTOMY
 UnitedHealthcare Commercial Coverage Determination Guideline BREAST RECONSTRUCTION POST MASTECTOMY Guideline Number: SUR057 Effective Date: February 1, 2018 Table of Contents Page INSTRUCTIONS FOR USE...
UnitedHealthcare Commercial Coverage Determination Guideline BREAST RECONSTRUCTION POST MASTECTOMY Guideline Number: SUR057 Effective Date: February 1, 2018 Table of Contents Page INSTRUCTIONS FOR USE...
The earlier clinic experience of the reverse-flow anterolateral thigh island flap
 British Journal of Plastic Surgery (2005) 58, 160 164 The earlier clinic experience of the reverse-flow anterolateral thigh island flap Gang Zhou, Qi-Xu Zhang*, Guang-Yu Chen Scar Multiple Treatment Centre,
British Journal of Plastic Surgery (2005) 58, 160 164 The earlier clinic experience of the reverse-flow anterolateral thigh island flap Gang Zhou, Qi-Xu Zhang*, Guang-Yu Chen Scar Multiple Treatment Centre,
Goals of Care. Restore shape and function after cancer
 Goals of Care Restore shape and function after cancer Aid in physiological and psychological benefit Relationship with significant other Self esteem and positive body image Feeling of a whole body Avoid
Goals of Care Restore shape and function after cancer Aid in physiological and psychological benefit Relationship with significant other Self esteem and positive body image Feeling of a whole body Avoid
The free thoracodorsal artery perforator flap in head and neck reconstruction
 European Annals of Otorhinolaryngology, Head and Neck diseases (2012) 129, 167 171 Available online at www.sciencedirect.com TECHNICAL NOTE The free thoracodorsal artery perforator flap in head and neck
European Annals of Otorhinolaryngology, Head and Neck diseases (2012) 129, 167 171 Available online at www.sciencedirect.com TECHNICAL NOTE The free thoracodorsal artery perforator flap in head and neck
Radial Artery Pedicle Flap To Cover Exposed Mesh After Abdominal Wound Dehiscence-An Easy Solution To A Difficult Problem
 ISPUB.COM The Internet Journal of Plastic Surgery Volume 6 Number 1 Radial Artery Pedicle Flap To Cover Exposed Mesh After Abdominal Wound Dehiscence-An Easy Solution To A Difficult Problem S Tripathy,
ISPUB.COM The Internet Journal of Plastic Surgery Volume 6 Number 1 Radial Artery Pedicle Flap To Cover Exposed Mesh After Abdominal Wound Dehiscence-An Easy Solution To A Difficult Problem S Tripathy,
Anterolateral Thigh Flap for Postmastectomy Breast Reconstruction
 Anterolateral Thigh Flap for Postmastectomy Breast Reconstruction Fu-chan Wei, M.D., Sinikka Suominen, M.D., Ph.D., Ming-huei Cheng, M.D., Naci Celik, M.D., and Yung-lung Lai, M.D. Taipei, Taiwan Most
Anterolateral Thigh Flap for Postmastectomy Breast Reconstruction Fu-chan Wei, M.D., Sinikka Suominen, M.D., Ph.D., Ming-huei Cheng, M.D., Naci Celik, M.D., and Yung-lung Lai, M.D. Taipei, Taiwan Most
Breast Reconstruction. Westmead Breast Cancer Institute
 Breast Reconstruction Westmead Breast Cancer Institute What is breast reconstruction? Breast reconstruction is a surgical procedure that creates a shape on the chest wall following a mastectomy. Occasionally,
Breast Reconstruction Westmead Breast Cancer Institute What is breast reconstruction? Breast reconstruction is a surgical procedure that creates a shape on the chest wall following a mastectomy. Occasionally,
The superior gluteal artery perforator flap: an additional tool in the treatment of sacral pressure sores
 ritish Journal of Plastic Surgery (1999), 52, 385 391 1999 The ritish ssociation of Plastic Surgeons The superior gluteal artery perforator flap: an additional tool in the treatment of sacral pressure
ritish Journal of Plastic Surgery (1999), 52, 385 391 1999 The ritish ssociation of Plastic Surgeons The superior gluteal artery perforator flap: an additional tool in the treatment of sacral pressure
Deep Inferior Epigastric Perforator Flap for Successful Simultaneous Breast and Chest Wall Reconstruction in a Poland Anomaly Patient
 CASE REPORT Deep Inferior Epigastric Perforator Flap for Successful Simultaneous Breast and Chest Wall Reconstruction in a Poland Anomaly Patient Han-Tsung Liao, MD, Ming-Huei Cheng, MD, Betul Gozel Ulusal,
CASE REPORT Deep Inferior Epigastric Perforator Flap for Successful Simultaneous Breast and Chest Wall Reconstruction in a Poland Anomaly Patient Han-Tsung Liao, MD, Ming-Huei Cheng, MD, Betul Gozel Ulusal,
Deep inferior epigastric artery perforated rectus abdominis free flap for head and neck reconstruction
 Eur Arch Otorhinolaryngol (2012) 269:1219 1224 DOI 10.1007/s00405-011-1749-x HEAD AND NECK Deep inferior epigastric artery perforated rectus abdominis free flap for head and neck reconstruction Johnny
Eur Arch Otorhinolaryngol (2012) 269:1219 1224 DOI 10.1007/s00405-011-1749-x HEAD AND NECK Deep inferior epigastric artery perforated rectus abdominis free flap for head and neck reconstruction Johnny
Neil J. Zemmel, MD, FACS Steven J. Montante, MD Megan J. Russell, PA-C. Your Guide To BREAST RECONSTRUCTION
 Neil J. Zemmel, MD, FACS Steven J. Montante, MD Megan J. Russell, PA-C Your Guide To BREAST RECONSTRUCTION Introduction The diagnosis of breast cancer begins a journey of making many informed decisions
Neil J. Zemmel, MD, FACS Steven J. Montante, MD Megan J. Russell, PA-C Your Guide To BREAST RECONSTRUCTION Introduction The diagnosis of breast cancer begins a journey of making many informed decisions
OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY
 OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY RECTUS ABDOMINIS FLAP FOR HEAD & NECK RECONSTRUCTION Patrik Pipkorn, Brian Nussenbaum The rectus abdominis flap is based on the deep inferior
OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY RECTUS ABDOMINIS FLAP FOR HEAD & NECK RECONSTRUCTION Patrik Pipkorn, Brian Nussenbaum The rectus abdominis flap is based on the deep inferior
INFORMED CONSENT-BREAST RECONSTRUCTION WITH TRAM ABDOMINAL MUSCLE FLAP
 INFORMED CONSENT-BREAST RECONSTRUCTION WITH TRAM ABDOMINAL MUSCLE FLAP 2000 American Society of Plastic Surgeons. Purchasers of the Patient Consultation Resource Book are given a limited license to modify
INFORMED CONSENT-BREAST RECONSTRUCTION WITH TRAM ABDOMINAL MUSCLE FLAP 2000 American Society of Plastic Surgeons. Purchasers of the Patient Consultation Resource Book are given a limited license to modify
In a second stage or a second operation that tissue expander is removed through the same incision and the implant is placed within the chest pocket.
 Hello, I m Summer Hanson. I m an assistant professor in the Department of Plastics & Reconstructive Surgery at The University of Texas MD Anderson Cancer Center and today I m going to talk about the role
Hello, I m Summer Hanson. I m an assistant professor in the Department of Plastics & Reconstructive Surgery at The University of Texas MD Anderson Cancer Center and today I m going to talk about the role
Do Preexisting Abdominal Scars Threaten Wound Healing in Abdominoplasty?
 Do Preexisting Abdominal Scars Threaten Wound Healing in Abdominoplasty? Michele A. Shermak, MD, Jessie Mallalieu, PA-C, and David Chang, PhD, MPH, MBA The Johns Hopkins Medical Institutions, Division
Do Preexisting Abdominal Scars Threaten Wound Healing in Abdominoplasty? Michele A. Shermak, MD, Jessie Mallalieu, PA-C, and David Chang, PhD, MPH, MBA The Johns Hopkins Medical Institutions, Division
ABDOMINAL WALL & RECTUS SHEATH
 ABDOMINAL WALL & RECTUS SHEATH Learning Objectives Describe the anatomy, innervation and functions of the muscles of the anterior, lateral and posterior abdominal walls. Discuss their functional relations
ABDOMINAL WALL & RECTUS SHEATH Learning Objectives Describe the anatomy, innervation and functions of the muscles of the anterior, lateral and posterior abdominal walls. Discuss their functional relations
Samer Saour, Guido Libondi, Venkat Ramakrishnan. Introduction
 Original Article Microsurgical refinements with the use of internal mammary (IM) perforators as recipient vessels in transverse upper gracilis (TUG) autologous breast reconstruction Samer Saour, Guido
Original Article Microsurgical refinements with the use of internal mammary (IM) perforators as recipient vessels in transverse upper gracilis (TUG) autologous breast reconstruction Samer Saour, Guido
Modified Radical Mastectomy
 Modified Radical Mastectomy Valerie L. Staradub, MD, and Monica Morrow, MD S urgical management options for breast cancer include modified radical mastectomy (MRM), MRM with immediate reconstruction, and
Modified Radical Mastectomy Valerie L. Staradub, MD, and Monica Morrow, MD S urgical management options for breast cancer include modified radical mastectomy (MRM), MRM with immediate reconstruction, and
Outcomes Evaluation Following Bilateral Breast Reconstruction Using Latissimus Dorsi Myocutaneous Flaps
 BREAST SURGERY Outcomes Evaluation Following Bilateral Breast Reconstruction Using Latissimus Dorsi Myocutaneous Flaps Albert Losken, MD, FACS, Claire S. Nicholas, MD, Ximena A. inell, MD, and Grant W.
BREAST SURGERY Outcomes Evaluation Following Bilateral Breast Reconstruction Using Latissimus Dorsi Myocutaneous Flaps Albert Losken, MD, FACS, Claire S. Nicholas, MD, Ximena A. inell, MD, and Grant W.
The Superficial Inferior Epigastric Artery (SIEA) Flap and Its Applications in Breast Reconstruction
 The Superficial Inferior Epigastric Artery (SIEA) Flap and Its Applications in Breast Reconstruction Zachary Menn and Aldona Spiegel Weill Cornell Medical College, The Methodist Hospital, Houston, Texas,
The Superficial Inferior Epigastric Artery (SIEA) Flap and Its Applications in Breast Reconstruction Zachary Menn and Aldona Spiegel Weill Cornell Medical College, The Methodist Hospital, Houston, Texas,
Advances and Innovations in Breast Reconstruction and Brest Surgery Presented by PCMC plastic surgeons
 Advances and Innovations in Breast Reconstruction and Brest Surgery Presented by PCMC plastic surgeons Options for reconstruction after mastectomy Implants Autologous tissue = from your own body: skin
Advances and Innovations in Breast Reconstruction and Brest Surgery Presented by PCMC plastic surgeons Options for reconstruction after mastectomy Implants Autologous tissue = from your own body: skin
-primarily by apposition of the anterior rectus
 2 Component separation Cop HARVEY CHIM, KAREN KIM EVANS, AND SAMIR MARDINI Mater al Introduction 7 Preoperative markings 7 Intraoperative details 9 Technique modification: Component separation with preservation
2 Component separation Cop HARVEY CHIM, KAREN KIM EVANS, AND SAMIR MARDINI Mater al Introduction 7 Preoperative markings 7 Intraoperative details 9 Technique modification: Component separation with preservation
A Clinical Anatomic Study of Internal Mammary Perforators as Recipient Vessels for Breast Reconstruction
 A Clinical Anatomic Study of Internal Mammary Perforators as Recipient Vessels for Breast Reconstruction In-Soo Baek 1, Jae-Pil You 1, Sung-Mi Rhee 1, Gil-Su Son 2, Deok-Woo Kim 1, Eun-Sang Dhong 1, Seung-Ha
A Clinical Anatomic Study of Internal Mammary Perforators as Recipient Vessels for Breast Reconstruction In-Soo Baek 1, Jae-Pil You 1, Sung-Mi Rhee 1, Gil-Su Son 2, Deok-Woo Kim 1, Eun-Sang Dhong 1, Seung-Ha
The decision to repair a partial mastectomy CME. State of the Art and Science in Postmastectomy Breast Reconstruction.
 CME State of the Art and Science in Postmastectomy Breast Reconstruction Steven J. Kronowitz, M.D. Houston, Texas Learning Objectives: After reading this article, the participant should be able to: 1.
CME State of the Art and Science in Postmastectomy Breast Reconstruction Steven J. Kronowitz, M.D. Houston, Texas Learning Objectives: After reading this article, the participant should be able to: 1.
Breast Reconstruction Surgery
 Breast Reconstruction Surgery I. Policy University Health Alliance (UHA) will reimburse for Breast Reconstruction Surgery when it is determined to be medically necessary and when it meets the medical criteria
Breast Reconstruction Surgery I. Policy University Health Alliance (UHA) will reimburse for Breast Reconstruction Surgery when it is determined to be medically necessary and when it meets the medical criteria
Advances in Breast Surgery. Catherine Campo, D.O. Breast Surgeon Meridian Health System April 17, 2015
 Advances in Breast Surgery Catherine Campo, D.O. Breast Surgeon Meridian Health System April 17, 2015 Objectives Understand the surgical treatment of breast cancer Be able to determine when a lumpectomy
Advances in Breast Surgery Catherine Campo, D.O. Breast Surgeon Meridian Health System April 17, 2015 Objectives Understand the surgical treatment of breast cancer Be able to determine when a lumpectomy
AESTHETIC SURGERY OF THE BREAST: MASTOPEXY, AUGMENTATION & REDUCTION
 CHAPTER 18 AESTHETIC SURGERY OF THE BREAST: MASTOPEXY, AUGMENTATION & REDUCTION Ali A. Qureshi, MD and Smita R. Ramanadham, MD Aesthetic surgery of the breast aims to either correct ptosis with a mastopexy,
CHAPTER 18 AESTHETIC SURGERY OF THE BREAST: MASTOPEXY, AUGMENTATION & REDUCTION Ali A. Qureshi, MD and Smita R. Ramanadham, MD Aesthetic surgery of the breast aims to either correct ptosis with a mastopexy,
SIMPOSIO Ricostruzione mammaria ed implicazioni radioterapiche Indicazioni
 SIMPOSIO Ricostruzione mammaria ed implicazioni radioterapiche Indicazioni Icro Meattini, MD Radiation Oncology Department - University of Florence Azienda Ospedaliero Universitaria Careggi Firenze Breast
SIMPOSIO Ricostruzione mammaria ed implicazioni radioterapiche Indicazioni Icro Meattini, MD Radiation Oncology Department - University of Florence Azienda Ospedaliero Universitaria Careggi Firenze Breast
Increasing options in autologous microsurgical breast reconstruction: four free flaps for stacked bilateral breast reconstruction
 Case Report Increasing options in autologous microsurgical breast reconstruction: four free flaps for stacked bilateral breast reconstruction Warren Matthew Rozen 1,2, Nakul Gamanlal Patel 1, Venkat V.
Case Report Increasing options in autologous microsurgical breast reconstruction: four free flaps for stacked bilateral breast reconstruction Warren Matthew Rozen 1,2, Nakul Gamanlal Patel 1, Venkat V.
Abdominal Wall Reconstruction With the Free Tensor Fascia Lata Musculofasciocutaneous Flap Using Intraperitoneal Gastroepiploic Recipient Vessels
 Abdominal Wall Reconstruction With the Free Tensor Fascia Lata Musculofasciocutaneous Flap Using Intraperitoneal Gastroepiploic Recipient Vessels Pierre M. Chevray, MD, PhD* Navin K. Singh, MD The authors
Abdominal Wall Reconstruction With the Free Tensor Fascia Lata Musculofasciocutaneous Flap Using Intraperitoneal Gastroepiploic Recipient Vessels Pierre M. Chevray, MD, PhD* Navin K. Singh, MD The authors
Plastic surgery of the breast includes; augmentation, reduction, Plastic Surgery of the Breast. Abstract. Continuing Education Column
 Plastic Surgery of the Breast Keuk Shun Shin, M.D. Keuk SHUN SHIN s Asthetic Plastic Surgery E mail: drsks@drsks.co.kr Abstract Plastic surgery of the breast includes; augmentation, reduction, reconstruction
Plastic Surgery of the Breast Keuk Shun Shin, M.D. Keuk SHUN SHIN s Asthetic Plastic Surgery E mail: drsks@drsks.co.kr Abstract Plastic surgery of the breast includes; augmentation, reduction, reconstruction
Donor-site morbidity of the segmental rectus abdominis muscle flap
 British Journal of Plastic Surgery (1998), 51,603607 9 1998 The British Association of Plastic Surgeons BRITISH JOURNAL OF ~ PLASTIC SURGERY Donorsite morbidity of the segmental rectus abdominis muscle
British Journal of Plastic Surgery (1998), 51,603607 9 1998 The British Association of Plastic Surgeons BRITISH JOURNAL OF ~ PLASTIC SURGERY Donorsite morbidity of the segmental rectus abdominis muscle
Versatility of Reverse Sural Artery Flap for Heel Reconstruction
 ORIGINAL ARTICLE Introduction: The heel has two parts, weight bearing and non-weight bearing part. Soft tissue heel reconstruction has been a challenge due to its complex nature of anatomy, weight bearing
ORIGINAL ARTICLE Introduction: The heel has two parts, weight bearing and non-weight bearing part. Soft tissue heel reconstruction has been a challenge due to its complex nature of anatomy, weight bearing
can see several late effects. Asymmetry is probably the most common and the thing that patients notice the most. We can also see implant wrinkling or
 Hello, I am Summer Hanson. I m an assistant professor with the Department of Plastic and Reconstructive Surgery at the University of Texas MD Anderson Cancer Center. And today I m going to talk to you
Hello, I am Summer Hanson. I m an assistant professor with the Department of Plastic and Reconstructive Surgery at the University of Texas MD Anderson Cancer Center. And today I m going to talk to you
Gastrocnemius Myocutaneous Flap: A Versatile Option to Cover the Defect of Upper and Middle Third Leg
 Downloaded from wjps.ir at 22:25 +0330 on Sunday November 18th 28 314 Gastrocnemius flap for coverage of leg defects Original Article Gastrocnemius Myocutaneous Flap: A Versatile Option to Cover the Defect
Downloaded from wjps.ir at 22:25 +0330 on Sunday November 18th 28 314 Gastrocnemius flap for coverage of leg defects Original Article Gastrocnemius Myocutaneous Flap: A Versatile Option to Cover the Defect
Reconstruction with autologous tissue remains a
 Original Article Increased Flap Weight and Decreased Perforator Number Predict Fat Necrosis in DIEP Breast Reconstruction Carolyn L. Mulvey, BS* Carisa M. Cooney, MPH* Francis F. Daily, BS* Elizabeth Colantuoni,
Original Article Increased Flap Weight and Decreased Perforator Number Predict Fat Necrosis in DIEP Breast Reconstruction Carolyn L. Mulvey, BS* Carisa M. Cooney, MPH* Francis F. Daily, BS* Elizabeth Colantuoni,
Flaps vs Grafts. Ronen Avram, MD MSc FRCSC
 Flaps vs Grafts Ronen Avram, MD MSc FRCSC POS Keratoacanthoma is not a malignant tumor! Methods of Reconstruction Reconstructive Ladder Primary closure Primary Delayed Secondary Intention Skin Graft Pedicled
Flaps vs Grafts Ronen Avram, MD MSc FRCSC POS Keratoacanthoma is not a malignant tumor! Methods of Reconstruction Reconstructive Ladder Primary closure Primary Delayed Secondary Intention Skin Graft Pedicled
Post-mastectomy breast reconstruction
 Follow the link from the online version of this article to obtain certified continuing medical education credits Post-mastectomy breast reconstruction Paul T R Thiruchelvam, 1 Fiona McNeill, 2 Navid Jallali,
Follow the link from the online version of this article to obtain certified continuing medical education credits Post-mastectomy breast reconstruction Paul T R Thiruchelvam, 1 Fiona McNeill, 2 Navid Jallali,
The Influence of Pfannenstiel Incision Scarring on Deep Inferior Epigastric Perforator
 The Influence of Pfannenstiel Incision Scarring on Deep Inferior Epigastric Perforator Young Jin Park, Eun Key Kim, Ji Young Yun, Jin Sup Eom, Taik Jong Lee Department of Plastic Surgery, Asan Medical
The Influence of Pfannenstiel Incision Scarring on Deep Inferior Epigastric Perforator Young Jin Park, Eun Key Kim, Ji Young Yun, Jin Sup Eom, Taik Jong Lee Department of Plastic Surgery, Asan Medical
Breast Reconstruction: Patient Information Document
 breastreconstructioncanada.ca Breast Reconstruction: Patient Information Document By Dr. Nicolas Guay Dr. Haemi Lee STANDARDIZED BREAST RECONSTRUCTION PATIENT INFORMATION TABLE OF CONTENTS Glossary...
breastreconstructioncanada.ca Breast Reconstruction: Patient Information Document By Dr. Nicolas Guay Dr. Haemi Lee STANDARDIZED BREAST RECONSTRUCTION PATIENT INFORMATION TABLE OF CONTENTS Glossary...
Anatomical Study of the Superior Gluteal Artery Perforator (S-GAP) for Free Flap Harvesting
 Anatomical Study of the Superior Gluteal Artery Perforator (S-GAP) for Free Flap Harvesting Tanvaa Tansatit MD*, Prayuth Chokrungyaranont MD**, Pasinee Sanguansit MSc*, Samang Wanidchaphloi MSc* * Department
Anatomical Study of the Superior Gluteal Artery Perforator (S-GAP) for Free Flap Harvesting Tanvaa Tansatit MD*, Prayuth Chokrungyaranont MD**, Pasinee Sanguansit MSc*, Samang Wanidchaphloi MSc* * Department
Anatomical study. Clinical study. R. Ogawa, H. Hyakusoku, M. Murakami, R. Aoki, K. Tanuma* and D. G. Pennington?
 British Journal of Plastic Surgery (2002) 55, 396-40 I 9 2002 The British Association of Plastic Surgeons doi: 10.1054/bjps.2002.3877 PLASTIC SURGERY An anatomical and clinical study of the dorsal intercostal
British Journal of Plastic Surgery (2002) 55, 396-40 I 9 2002 The British Association of Plastic Surgeons doi: 10.1054/bjps.2002.3877 PLASTIC SURGERY An anatomical and clinical study of the dorsal intercostal
Factors Associated with Anastomotic Failure after Microvascular Reconstruction of the Breast
 Factors Associated with Anastomotic Failure after Microvascular Reconstruction of the Breast Maurice Y. Nahabedian, M.D., Bahram Momen, Ph.D., and Paul N. Manson, M.D. Baltimore and College Park, Md. The
Factors Associated with Anastomotic Failure after Microvascular Reconstruction of the Breast Maurice Y. Nahabedian, M.D., Bahram Momen, Ph.D., and Paul N. Manson, M.D. Baltimore and College Park, Md. The
B11 Breast Reconstruction with Abdominal Tissue Flap
 B11 Breast Reconstruction with Abdominal Tissue Flap Issued March 2011 You can get more information about this procedure from www.aboutmyhealth.org Tell us how useful you found this document at www.patientfeedback.org
B11 Breast Reconstruction with Abdominal Tissue Flap Issued March 2011 You can get more information about this procedure from www.aboutmyhealth.org Tell us how useful you found this document at www.patientfeedback.org
How many procedures to make a breast?
 British Journal of Plastic Surgery (00 ), 5, 7-3 9 00 The British Association of Plastic Surgeons doi: 0.05/bjps.000.3538 BRITISH JOURNAL OF PLASTIC SURGERY How many procedures to make a breast? A. D.
British Journal of Plastic Surgery (00 ), 5, 7-3 9 00 The British Association of Plastic Surgeons doi: 0.05/bjps.000.3538 BRITISH JOURNAL OF PLASTIC SURGERY How many procedures to make a breast? A. D.
