Associations of clinical characteristics and interval between maintenance visits with peri-implant pathology
|
|
|
- Millicent Chase
- 5 years ago
- Views:
Transcription
1 143 Journal of Oral Science, Vol. 56, No. 2, , 2014 Original Associations of clinical characteristics and interval between maintenance visits with peri-implant pathology Miguel A. de Araújo Nobre 1,2), Paulo S. Maló 2), and Sílvia H. Oliveira 2) 1) Preventive Medicine Unit, Faculty of Medicine, University of Lisbon, Lisbon, Portugal 2) Malo Clinic, Lisbon, Portugal (Received January 7, 2014; Accepted April 21, 2014) Abstract: We investigated the effects of clinical characteristics and the interval between maintenance visits on incidence of peri-implant pathology in a sample of 1,350 patients treated with dental implants (270 cases of peri-implant pathology and 1,080 healthy controls). The chi-square test was used to evaluate differences between cases and controls in the presence of dental plaque, bleeding, peri-implant pockets >4 mm, bone level, and interval between maintenance visits (significance level, 5%). Crude odds ratios (ORs) and attributable fractions were calculated for variables that significantly differed between cases and controls. The variables identified as risk indicators were dental plaque (P < 0.001; OR = 5.2), bleeding (P < 0.001; OR = 5.0), peri-implant pockets >4 mm (P < 0.001; OR = 17.2), bone level (P < 0.001; middle third, OR = 8.4; apical third, OR = 8.6), and interval between maintenance visits (P < 0.001; 1-3 months, OR = 2.9; 3-5 months, OR = 2.1). Attributable fractions revealed a potential reduction in peri-implant pathology of 53-94% after removing exposures to dental plaque (81%), bleeding (80%), peri-implant pockets >4 mm (94%), bone level (88%), and interval between maintenance visits (53-66%). Selected clinical characteristics and the interval between maintenance visits were significantly associated with the incidence of peri-implant pathology. (J Oral Sci 56, , 2014) Correspondence to Dr. Miguel de Araújo Nobre, Malo Clinic, Avenida dos Combatentes, 43, Andar 5 A, , Lisbon, Portugal Fax: miguelnobre@fm.ul.pt & mnobre@maloclinics.com doi.org/ /josnusd DN/JST.JSTAGE/josnusd/ Keywords: peri-implant pathology; dental implants; risk indicators; dental plaque; bleeding; periimplant pockets. Introduction Peri-implant pathology is a term used to describe inflammatory reactions with loss of supporting bone tissue surrounding the dental implant (1). Its pathogenesis has been classified as classical (soft tissue apical to the bone) and retrograde (bone to soft tissue). The classical pathway of peri-implant pathology is caused by exposure to dental plaque (DP) and subsequent reversible mucositis, which can result in bone loss and, ultimately, implant loss (2,3). In the retrograde pathway, bone loss occurs at the bone crest and results from microfractures caused by overloading, premature loading, or lateral forces (4-6). These pathways sometimes overlap (7). The reported prevalence of peri-implant pathology ranges from 12-43% (8). However, only a few studies have focused on the pathology and risk factors for periimplant pathology (9-20). Several clinical characteristics are evaluated in an implant maintenance follow-up examination: bone level (BL) near the implant, peri-implant pockets, DP, and the condition of the superficial peri-implant complex, as assessed by means of the modified bleeding index (21) (which differs from bleeding on probing). Maintenance of adequate bone is vital for implant health and is regularly assessed in evaluations of dental implant systems. In the most widely used criterion for evaluating implant success, Albrektsson et al. (22) proposed that implants were successful if average marginal bone resorption after the first year of function was <0.2 mm annually. However, this criterion has been questioned by several
2 144 authors, principally due to uncertainty as to whether annual bone loss could be clearly ascertained. This reservation was supported by the results of clinical studies, which found that bone resorption greater than the above limit stabilized after 2-3 years. This evidence led to a recommendation that implants should only be considered failed when BL reached the apical third of the implant (23-25). The findings of a biomechanical study indicated that stability diminished as BL reached the apical third of the implant (26), as did the capacity to support occlusal forces. These biomechanical factors increased the risk of peri-implant pathology. Nevertheless, diminished BL is not always indicative of a pathological condition (22). It might instead be caused by impaired conditions at the implant site at the time of treatment, to implant length, or to physiologically marginal bone remodeling. The research community continues to debate the usefulness of probing the peri-implant sulcus/pocket. Some view such assessment as a highly sensitive diagnostic tool for monitoring peri-implant conditions (27). Others regard it with some distrust because of the large number of variables that influence such measurement, such as probing force and angulation, probe tip diameter, roughness of the implant and root surface, the inflammatory state of the periodontium, the firmness of marginal tissues, and access limitations (28). The issue of probing force is particularly important in the measurement of peri-implant pocket depth, as this procedure is more sensitive to variations in force (27,29). Absolute values for probing pocket depth should thus be interpreted with caution, due to variability in surgical implant positioning, e.g., the context of a submucosal implant placement in an esthetic anterior region differs from that of a conventional implant placement in a posterior non-esthetic region (28). It is important to establish a baseline value for probing pocket depth, as a peri-implant sulcus may develop until a pocket is formed as a result of inflammation. Thus, an increase from baseline probing pocket depth values should be seen as a sign of peri-implant pathology (30,31). The microbiological environments of periimplant pockets and periodontal pockets are comparable, as both facilitate colonization by gram-negative bacteria (32). However, some conditions mimic peri-implant pockets but are not evidence of pathological conditions (pseudopockets). These conditions are caused by a thicker mucosal biotype or loss of the osseous scallop at the interproximal aspect of the implant, in conjunction with the presence of a gingival scallop maintained by bone support from adjacent teeth (33). Furthermore, pocket probing alone is not sufficient to differentiate mucositis from peri-implant pathology (34). Bleeding at the peri-implant complex (as assessed by the modified bleeding index) (21) can be evaluated during assessment of superficial peri-implant conditions and can be used as an alternative to bleeding on probing (35). Indeed, some researchers believe this method to be the best technique for examining the health of peri-implant mucosa (21). Although this assessment technique permits differentiation between healthy and unhealthy tissues, it cannot identify incipient implant failure and its usefulness is limited in smokers (35). Potentially periodontopathogenic bacteria can colonize implants soon after insertion (36), and accumulation of DP induces an inflammatory response (37) characterized by inflammation signs such as edema, redness of soft tissue, and bleeding on probing, as confirmed in animal and human studies (38,39). Oral hygiene has a substantial impact on bone stability around osseointegrated implants, even in edentulous patients, and deficient oral hygiene is associated with greater bone resorption (40). A maintenance protocol is important for implantsupported restorations. An effective preventive regimen allows for maintenance of the health of peri-implant tissues and rapid intervention after diagnosis of a pathological condition (41). Maintenance is necessary for long-term implant success and in the prevention and early diagnosis of peri-implant pathology (42-44). Kourtis et al. (45) highlighted the necessity of a strict recall program for patients treated with implants. We investigated the associations of clinical characteristics and the interval between maintenance visits (IMV) with incidence of peri-implant pathology. Materials and Methods This report complies with the STROBE (strengthening the reporting of observational studies in epidemiology) guidelines (46). The study was approved by the National Commission of Data Protection (Portugal) and the Ethical Board of the Faculty of Medicine of the University of Lisbon (1976/2009). This study is a complement to a series of studies on risk factors for peri-implant pathology (20). The study population was men and women who underwent fixed prosthetic reconstruction supported by dental implants (Nobel Biocare AB, Gothenburg, Sweden) at a private clinic (Malo Clinic) in Lisbon, Portugal. To investigate the effects of clinical variables on the incidence of periimplant pathology, this matched case-control study used a hospital-based methodology (patients were selected from the same population treated at a private practice). The cases were patients who were treated with fixed
3 145 prosthetic implant-supported prostheses and later developed peri-implant pathology. The controls were patients who received fixed prosthetic implant-supported prostheses at the same private clinic but did not develop chronic peri-implant pathology. Peri-implant pathology was defined as the presence of peri-implant pockets 5 mm, as determined using a plastic periodontal probe calibrated to 0.25 N (Click- Probe, KerrHawe S. A., Bioggio Svizzera, Switzerland) (47); bleeding on probing (47); bone loss on periapical radiographs (32); and clinical attachment loss 2 mm (48). To be included in the study, the patients had to be treated and followed for at least 1 year at the private clinic and to have provided informed consent for participation and review of their medical charts. Patients were excluded from the study if they were younger than 18 years, if they declined or were unable to provide informed consent, if they had been followedup for less than 1 year, if their medical records were incomplete or missing, or if they were receiving immunosuppressive therapy. Data collection took place from January through July The control patients were matched to cases for sex (19), age (±2 years) (49), and duration of follow-up (±2 months). The decision to match for these variables was based on the possibility of a correlation between increased duration of follow-up (corresponding to increased exposure time) and incidence of peri-implant pathology (50). A case: control ratio of 1:4 was established to optimize the number of available cases. From among an initial 1,763 eligible adults (346 cases; 1,417 controls) retrieved from a list of patients treated with implants, 383 patients (66 cases and 317 controls) were excluded from the study: 202 (54 cases and 148 controls) declined to participate and 181 (12 cases and 169 controls) had incomplete medical records that did not permit accurate diagnosis. Thirty patients (10 cases and 20 controls) were randomly selected for a pilot study to test procedures for data collection and analysis and were excluded from the present study. Ultimately, a sample of 1,350 patients (270 cases and 1,080 controls) of both sexes was evaluated. The age range of the sample was years (average [SD], 55.8 [10.2] years); 62.7% of the patients were women. In total, 566 patients (102 cases and 464 controls) presented with systemic compromise, and 364 patients (104 cases and 260 controls) were smokers. The patients were treated with dental implants (296 machined-surface implants and 1,054 implants with a moderately rough surface; Nobel Biocare AB) during the period from February 1998 through November Peri-implant pathology was diagnosed after an average follow-up time of 3 years. Data were collected by means of indirect documentation using a digital form, after consulting patient records. The variables evaluated in cases and controls were DP (presence, absence), bleeding (B) at the peri-implant complex (presence, absence); peri-implant pockets (PIP) >4 mm (present, absent); BL (coronal, middle, or apical third of implants); IMV during the previous year (1-3 months, 4-5 months, 6 months, >6 months). Statistical analysis Using descriptive statistics, we characterized cases and controls with regard to the variables of interest. Inferential statistics were used to evaluate differences in the distributions of variables between cases and controls. For nominal independent variables, the chi-square test was used when appropriate, otherwise the Fisher exact test was used in conjunction with supplemental measurement of Cramer s V statistic or the contingency coefficient. The effect of independent variables that were significant in the analysis was estimated using crude odds ratios (ORs) with 95% confidence intervals (CIs). The percentage of cases that could be prevented by removing the exposure to a risk indicator was estimated using the attributable fraction (AF) equation (51) according to the OR for the exposure, as follows: A1+ OR 1 AF = M1+ OR where AF corresponds to the attributable fraction, A1+ represents disease prevalence among exposed individuals, and M1+ represents disease prevalence (20). Results The descriptive statistics are shown in Tables 1a-1c. Most cases and controls had no DP or B when evaluated (Table 1a). The percentage of implants with PIP >4 mm was 9.3%, while BL was usually at the coronal third of implants (88.4%) (Table 1b). The IMV during the previous year was >6 months in most patients (Table 1c). All investigated variables namely, DP, B, PIP >4 mm, BL, and FVM significantly differed between cases and controls (P < for all comparisons) (Table 2). The proportions of smokers among cases (38.5%) and controls (24%) also significantly differed (difference, 14%; P < 0.001). DP, B, PIP >4 mm, and BL around the middle or apical third of the implant were risk indicators for the incidence of peri-implant pathology. The OR for peri-implant pathology associated with PIP >4 mm was 17.21, and DP and B were associated with ORs for peri-implant
4 146 Table 1a Presence of dental plaque and bleeding in cases and controls Dental plaque Bleeding Absent Present Total Absent Present Total Cases, No % of cases 73.0% 27% 100% 74.1% 25.9% 100% % of total sample 14.6% 5.4% 20% 14.8% 5.2% 20% Controls, No. 1, ,080 1, ,080 % of controls 93.3% 6.7% 100% 93.4% 6.6% 100% % of total sample 74.7% 5.3% 80% 74.7% 5.3% 80% Total, No. 1, ,350 1, ,350 % of total sample 89.3% 10.7% 100% 89.6% 10.4% 100% Table 1b Presence of peri-implant pockets >4 mm and bone level around implants in cases and controls Peri-implant pockets >4 mm Absent Present Total Coronal third Middle third Bone level Apical third Cases, No % of cases 65.6% 34.4% 100% 65.2% 31.5% 3.3% 100% % of total sample 13.1% 6.9% 20% 13.0% 6.3% 0.7% 20% Controls, No. 1, ,080 1, ,080 % of controls 97.0% 3.0% 100% 94.2% 5.2% 0.6% 100% % of total sample 77.6% 2.4% 80% 75.3% 4.1% 0.5% 80% Total, No. 1, ,350 1, ,350 % of total sample 90.7% 9.3% 100% 88.4% 10.4% 1.2% 100% Total Table 1c Interval between maintenance visits during previous year in cases and controls Interval between maintenance visits 1-3 months 4-5 months 6 months >6 months Total Cases, No % of cases 8.1% 19.3% 32.2% 40.4% 100% % of total sample 1.6% 3.9% 6.4% 8.1% 20% Controls, No ,080 % of controls 3.0% 10.1% 38.7% 48.2% 100% % of total sample 2.4% 8.1% 31.0% 38.6% 80% Total, No ,350 % of total sample 4.0% 11.9% 37.4% 46.7% 100% pathology of approximately 5.0. Patients with BL around the middle and apical thirds of implants had ORs for peri-implant pathology of 8.4 and 8.6, respectively, and patients with a shorter IMV during the previous year had ORs of 2.9 (interval, 1-3 months) and 2.1 (4-5 months) (Table 3). AFS indicated that the number of cases with periimplant pathology could be decreased if exposures to the risk indicators DP, B, PIP >4 mm, BL (middle and apical thirds of the implant), and FVM (interval, 1-3 months and 3-5 months) were reduced (Table 3). Discussion The presence of DP, B, PIP >4 mm, and BL around the middle or apical thirds of implants significantly differed between cases and controls, and these variables are thus risk indicators for the incidence of peri-implant pathology. DP has known deleterious effects and is therefore considered a principal risk factor (52). Pontoriero et al. (2) attempted to replicate the conditions of an experimental gingivitis model in their study of 20 partially edentulous patients who were treated with implants and subsequently refrained from oral hygiene for a period of
5 147 Table 2 Inferential statistics for dental plaque, bleeding index, peri-implant pockets >4 mm, bone level, and interval between maintenance visits Cases, relative frequency (95% CI proportion) Presence of dental plaque around implant Controls, relative frequency (95% CI proportion) Absolute frequency (95% CI proportion) Yes 73/270 = 0.27 (0.22 ; 0.32) 72/1,080 = 0.07 (0.05 ; 0.08) 145/1,350 = 0.11 (0.09 ; 0.12) No 197/270 = 0.73 (0.68 ; 0.78) 1,008/1,080 = 0.93 (0.92 ; 0.95) 1,205/1,350 = 0.89 (0.88 ; 0.91) P value Presence of bleeding around implant Yes 70/270 = 0.26 (0.21 ; 0.31) 71/1,080 = 0.07 (0.05 ; 0.08) 141/1,350 = 0.10 (0.09 ; 0.12) No 200/270 = 0.74 (0.69 ; 0.79) 1,009/1,080 = 0.93 (0.92 ; 0.95) 1,209/1,350 = 0.90 (0.88 ; 0.91) Presence of peri-implant pockets >4 mm Yes 93/270 = 0.34 (0.29 ; 0.40) 32/1,080 = 0.03 (0.02 ; 0.04) 125/1,350 = 0.09 (0.08 ; 0.11) No 177/270 = 0.66 (0.60 ; 0.71) 1,048/1,080 = 0.97 (0.96 ; 0.98) 1,225/1,350 = 0.91 (0.89 ; 0.92) Bone level c1/3* 176/270 = 0.65 (0.60 ; 0.71) 1,017/1,080 = 0.94 (0.93 ; 0.96) 1,193/1,350 = 0.88 (0.87 ; 0.90) m1/3 π 85/270 = 0.31 (0.26 ; 0.37) 56/1,080 = 0.05 (0.04 ; 0.07) 141/1,350 = 0.10 (0.09 ; 0.12) a1/3 9/270 = 0.03 (0.01 ; 0.05) 7/1,080 = 0.01 (0.00 ; 0.01) 16/1,350 = 0.01 (0.01 ; 0.02) Interval between maintenance visits 1-3 m α 22/270 = 0.08 (0.05 ; 0.11) 32/1,080 = 0.03 (0.02 ; 0.04) 54/1,350 = 0.04 (0.03 ; 0.05) m φ 52/270 = 0.19 (0.15 ; 0.24) 109/1,080 = 0.10 (0.08 ; 0.12) 161/1,350 = 0.12 (0.10 ; 0.14) 6 m ψ 87/270 = 0.32 (0.27 ; 0.38) 418/1,080 = 0.39 (0.36 ; 0.42) 505/1,350 = 0.37 (0.35 ; 0.40) >6 m ϖ 109/270 = 0.40 (0.35 ; 0.46) 521/1,080 = 0.48 (0.45 ; 0.51) 630/1,350 = 0.47 (0.44 ; 0.49) * c1/3: coronal third of implant; π m1/3: middle third of implant; a1/3: apical third of implant; α 1-3 m: 1-3 months; φ 4-5 m: 4-5 months; ψ 6 m: 6 months; ϖ >6 m: >6 months Table 3 Crude odds ratios (ORs) and attributable fractions for peri-implant pathology associated with dental plaque, bleeding, peri-implant pockets >4 mm, bone level, and interval between maintenance visits during the previous year OR 95% Confidence interval Attributable fraction Presence of dental plaque around implant Absent 0.19 [0.14 ; 0.28] Present 5.19 [3.62 ; 7.43] 0.81 Presence of bleeding around implant Absent 0.20 [0.14 ; 0.29] Present 4.97 [3.46 ; 7.15] 0.80 Presence of peri-implant pockets >4 mm Absent 0.06 [0.04 ; 0.09] Present [11.17 ; 26.51] 0.94 Bone level Coronal 1/ [0.08 ; 0.17] Middle 1/ [5.79 ; 12.19] 0.88 Apical 1/ [3.15 ; 23.33] 0.88 Interval between maintenance visits 1-3 months 2.91 [1.66 ; 5.09] 0.66 during the previous year 4-5 months 2.13 [1.48 ; 3.05] months 0.75 [0.57 ; 1.00] >6 months 0.73 [0.55 ; 0.95] 3 weeks. They observed an increase in mucositis severity, including inflammation of the soft tissues and an increase of ±1 mm in peri-implant pockets. These findings confirm the causal relation between DP accumulation and periimplant health, i.e., the classical pathway of peri-implant pathology. The effect of B on the incidence of peri-implant pathology is likely due to its association with DP and consequent PIP. This represents the classical clinical manifestation of peri-implant pathology, namely, DP accumulation, followed by B resulting from gingival inflammation and PIP formation. This finding was previously reported (2,53,54). The type of mucosa (keratinized vs. non-keratinized) might also be important in disease
6 148 incidence and development; however, our study did not investigate mucosa type, and thus the effect of this variable is unknown. Presence of PIP >4 mm was more frequent in patients with peri-implant pathology. In our study, a 0.25-N calibrated plastic probe was used to measure PIP, in conjunction with routine tri-annual calibrations between clinicians, which aimed to increase measurement reproducibility and accuracy (55). This diagnostic tool has high sensitivity for monitoring peri-implant conditions, despite the number of variables that affect such measurements (28). As a result of inflammation, a peri-implant sulcus may develop until a pocket is formed, and this increase should be regarded as a sign of peri-implant pathology, as noted in previous reports (30,31). The microbiological characteristics of peri-implant pockets are comparable to those of periodontal pockets: both are associated with colonization of gram-negative bacteria (32). Therefore, evaluation for PIP is important for identifying peri-implant pathology. Nevertheless, increased probing depths around implants may not indicate the presence of pathology (33); thus, probing depth should be used in conjunction with other diagnostic tools (34). The inclusion of BL as a possible risk indicator for peri-implant pathology is a subject of discussion. If BL in cases reflects pathology (due to the presence of marginal bone resorption), BL in the controls (i.e., in the absence of PIP >4 mm, B, or marginal bone resorption) refers to the location of bone around a given implant and is influenced by bone quantity and quality available at the time of treatment, by implant length, and by physiological marginal bone resorption during follow-up (22). This means that BL around a given implant represents the end result, which is due to bone loss (in the presence of periimplant pathology) or other non-pathological conditions. A BL around the middle or apical third of implants was identified as a risk indicator (OR = 8.4 and 8.6, respectively). As mentioned above, this can represent either a symptom or a cause of disease: as BL progresses toward the implant apex, implant support decreases, thereby reducing stability (26) and the ability to support occlusal forces, which increases the probability of disease due to biomechanical factors. This is particularly important when BL is such that more than two or three threads of the implant are exposed (the area of engagement of the abutment screw), as such conditions increase the risk of implant fracture due to bending overload (56). Our finding that a shorter IMV is a risk factor should be interpreted with caution. A possible explanation for this finding is that patients with shorter IMVs were considered to be at high risk at the start of therapy (e.g., patients with a history of periodontitis, mucositis, smokers, and those with low compliance to oral hygiene instructions) and were therefore scheduled for more frequent followup. This possibility was not investigated in this study, and the question remains open. Another possible explanation is the strong possibility of a confounder effect from DP and smoking. Among the 270 patients with peri-implant pathology, 196 had an IMV of 6 months during the previous year. Among these patients, 75 (38%) had DP accumulation. In contrast, among the 74 patients with peri-implant pathology and an IMV of <6 months during the previous year, 38 (51%) had DP accumulation. Similarly, the proportion of smokers was 14% higher among cases than among controls (38.5% vs. 24%, respectively), which was a significant difference. In consideration of these results and the important effects of DP and smoking on outcomes of dental implant treatment, this confounder effect is likely the main reason that shorter IMVs were found to be a risk indicator in our study. If so, the odds ratio for peri-implant pathology associated with shorter IMV is probably an overestimate. We do not mean to suggest that maintenance has a deleterious effect on implant outcome. Rather, other variables, such as good oral hygiene, likely have a stronger effect than implant maintenance on IMV. A recent prospective study (52) confirmed the importance of preventive maintenance: the incidence of peri-implantitis at 5 years of followup was 25% higher among patients without preventive maintenance than in those who had received preventive maintenance. Reduction of exposures to DP, B, PIP, and BL could reduce the number of exposed individuals by at least 80%. This suggests that prevention of DP accumulation in the present population could potentially result in an 81% decrease in the number of patients who develop disease (51). Moreover, in the clinical setting, one should consider the cumulative effect of reduced exposure to DP on the overall number of cases, as reduced exposure to DP would directly influence exposures to B, PIP, and BL, thus ceasing the chain of events leading to disease. B would be prevented because it occurs in response to plaque accumulation. PIP would potentially be partially prevented due to the absence of DP accumulation and consequent prevention of mucositis. Lower BL due to marginal bone resorption would also be substantially prevented. This further highlights the importance of controlling DP accumulation around implants and the consequent importance of maintenance. This study had the following limitations: a retrospective design, lack of control for possible confounders, and lack of control for the presence of other variables such as
7 149 systemic compromise (38% of cases and 43% of controls) and smoking habit (38% of cases and 24% of controls). The effect of variables on the incidence of peri-implant pathology should be investigated in prospective studies using multivariable analysis to control for confounding relationships between variables and the presence of other variables of interest. In conclusion, we found that DP, B, PIP >4 mm, BL in the middle or apical third of implants, and shorter IMVs were risk indicators for peri-implant pathology. Our findings suggest that DP has a direct effect on the other clinical characteristics investigated in this study. Reduced exposure to these variables could substantially reduce the number of affected individuals. Acknowledgments This study was supported by a grant from Nobel Biocare Services AG (grant ). Professor Maló is currently a consultant for Nobel Biocare. References 1. Albrektsson T, Isidor F (1994) Consensus report of session IV. In: Proceedings of the first European workshop on periodontology 1994, Lang NP, Karring T eds, Quintessence, London, Pontoriero R, Tonelli MP, Carnevale G, Mombelli A, Nyman SR, Lang NP (1994) Experimentally induced peri-implant mucositis. A clinical study in humans. Clin Oral Implants Res 5, Mombelli A (1999) In vitro models of biological responses to implant microbiological models. Adv Dent Res 13, Meffert RM (1990) Research in implantology at Louisiana State University School of Dentistry. Int J Oral Implantol 6, el Askary AS, Meffert RM, Griffin T (1998) Why do dental implants fail? Part II. Implant Dent 8, Ayangco L, Sheridan PJ (2001) Development and treatment of retrograde peri-implantitis involving a site with a history of failed endodontic and apicoectomy procedures: a series of reports. Int J Oral Maxillofac Implants 16, Esposito M, Hirsch JM, Lekholm U, Thomsen P (1998) Biological factors contributing to failures of osseointegrated oral implants. (II). Etiopathogenesis. Eur J Oral Sci 106, Zitzmann NU, Berglundh T (2008) Definition and prevalence of peri-implant diseases. J Clin Periodontol 35, Suppl, Haas R, Haimböck W, Mailath G, Watzek G (1996) The relationship of smoking on peri-implant tissue: a retrospective study. J Prosthet Dent 76, Rutar A, Lang NP, Buser D, Bürgin W, Mombelli A (2001) Retrospective assessment of clinical and microbiological factors affecting periimplant tissue conditions. Clin Oral Implants Res 12, Rosenberg ES, Cho SC, Elian N, Jalbout ZN, Froum S, Evian CI (2004) A comparison of characteristics of implant failure and survival in periodontally compromised and periodontally healthy patients: a clinical report. Int J Oral Maxillofac Implants 19, Karoussis IK, Müller S, Salvi GE, Heitz-Mayfield LJ, Brägger U, Lang NP (2004) Association between periodontal and peri-implant conditions: a 10-year prospective study. Clin Oral Implants Res 15, Quirynen M, Vogels R, Alsaadi G, Naert I, Jacobs R, van Steenberghe D (2005) Predisposing conditions for retrograde peri-implantitis, and treatment suggestions. Clin Oral Implants Res 16, Roos-Jansäker AM, Renvert H, Lindahl C, Renvert S (2006) Nine- to fourteen-year follow-up of implant treatment. Part III: factors associated with peri-implant lesions. J Clin Periodontol 33, Ferreira SD, Silva GL, Cortelli JR, Costa JE, Costa FO (2006) Prevalence and risk variables for peri-implant disease in Brazilian subjects. J Clin Periodontol 33, Máximo MB, de Mendonça AC, Alves JF, Cortelli SC, Peruzzo DC, Duarte PM (2008) Peri-implant diseases may be associated with increased time loading and generalized periodontal bone loss: preliminary results. J Oral Implantol 34, Serino G, Ström C (2009) Peri-implantitis in partially edentulous patients: association with inadequate plaque control. Clin Oral Implants Res 20, Zhou W, Han C, Li D, Li Y, Song Y, Zhao Y (2009) Endondontic treatment of teeth induces retrograde peri-implantitis. Clin Oral Implant Res 20, Aloufi F, Bissada N, Ficara A, Faddoul F, Al-Zahrani MS (2009) Clinical assessment of peri-implant tissues in patients with varying severity of chronic periodontitis. Clin Implant Dent Relat Res 11, de Araújo Nobre MA, Maló P (2014) The influence of rehabilitation characteristics in the incidence of peri-implant pathology: a case-control study. J Prosthodont 23, Buser D, Weber HP, Lang NP (1990) Tissue integration of non-submerged implants. 1-year results of a prospective study with 100 ITI hollow-cylinder and hollow-screw implants. Clin Oral Implants Res 1, Albrektsson T, Zarb G, Worthington P, Eriksson AR (1986) The long-term efficacy of currently used dental implants: a review and proposed criteria of success. Int J Oral Maxillofac Implants 1, Quirynen M, Naert I, van Steenberghe D, Schepers E, Calberson L, Theuniers G et al. (1991) The cumulative failure rate of the Brånemark system in the overdenture, the fixed partial, and the fixed full prostheses design: a prospective study on 1273 fixtures. J Head Neck Pathol 10, Quirynen M, Naert I, van Steenberghe D, Dekeyser C, Callens A (1992) Periodontal aspects of osseointegrated fixtures supporting a partial bridge. An up to 6-years retrospective
8 150 study. J Clin Periodontol 19, Lekholm U, van Steenberghe D, Herrmann I, Bolender C, Folmer T, Gunne J et al. (1994) Osseointegrated implants in the treatment of partially edentulous jaws: a prospective 5-year multicenter study. Int J Oral Maxillofac Implants 9, Chong L, Khocht A, Suzuki JB, Gaughan J (2009) Effect of implant design on initial stability of tapered implants. J Oral Implantol 35, Gerber JA, Tan WC, Balmer TE, Salvi GE, Lang NP (2009) Bleeding on probing and pocket probing depth in relation to probing pressure and mucosal health around oral implants. Clin Oral Implants Res 20, Salvi GE, Lang NP (2004) Diagnostic parameters for monitoring peri-implant conditions. Int J Oral Maxillofac Implants 19, S Mombelli A, Mühle T, Brägger U, Lang NP, Bürgin WB (1997) Comparison of periodontal and peri-implant probing by depth-force pattern analysis. Clin Oral Implants Res 8, Mombelli A, Lang NP (1994) Clinical parameters for the evaluation of dental implants. Periodontol , Lang NP, Berglundh T, Heitz-Mayfield LJ, Pjetursson BE, Salvi GE, Sanz M (2004) Consensus statements and recommended clinical procedures regarding implant survival and complications. Int J Oral Maxillofac Implants 19, S Quirynen M, De Soete M, van Steenberghe D (2002) Infectious risks for oral implants: a review of the literature. Clin Oral Implants Res 13, Kan JY, Rungcharassaeng K, Umezu K, Kois JC (2003) Dimensions of peri-implant mucosa: an evaluation of maxillary anterior single implants in humans. J Periodontol 74, Meyle J (2012) Mechanical, chemical and laser treatments of the implant surface in the presence of marginal bone loss around implants. Eur J Oral Implantol 5, S Esposito M, Hirsch JM, Lekholm U, Thomsen P (1998) Biological factors contributing to failures of osseointegrated oral implants. (I). Success criteria and epidemiology. Eur J Oral Sci 106, Nakou M, Mikx FH, Oosterwaal PJ, Kruijsen JC (1987) Early microbial colonization of permucosal implants in edentulous patients. J Dent Res 66, Zitzmann NU, Berglundh T, Marinello CP, Lindhe J (2001) Experimental peri-implant mucositis in man. J Clin Periodontol 28, Lang NP, Mombelli A, Tonetti MS, Brägger U, Hämmerle CH (1997) Clinical trials on therapies for peri-implant infections. Ann Periodontol 2, Abrahamsson I, Berglundh T, Lindhe J (1998) Soft tissue response to plaque formation at different implant systems. A comparative study in the dog. Clin Oral Implants Res 9, Lindquist LW, Carlsson GE, Jemt T (1996) A prospective 15-year follow-up study of mandibular fixed prostheses supported by osseointegrated implants. Clinical results and marginal bone loss. Clin Oral Implants Res 7, Grusovin MG, Coulthard P, Jourabchian E, Worthington HV, Esposito MA (2008) Interventions for replacing missing teeth: maintaining and recovering soft tissue health around dental implants. Cochrane Database Syst Rev, CD Kozlovsky A, Mozes O, Nemcovsky CE, Artzi Z (2003) Differential diagnosis and treatment strategies for periimplant diseases. Refuat Hapeh Vehashinayim 20, Yeung SC (2008) Biological basis for soft tissue management in implant dentistry. Aust Dent J 53, S Schou S (2008) Implant treatment in periodontitis-susceptible patients: a systematic review. J Oral Rehabil 35, S Kourtis SG, Sotiriadou S, Voliotis S, Challas A (2004) Private practice results of dental implants. Part I: survival and evaluation of risk factors--part II: surgical and prosthetic complications. Implant Dent 13, von Elm E, Altman DG, Egger M, Pocock SJ, Gøtzsche PC, Vandenbroucke JP (2007) The strengthening the reporting of observational studies in epidemiology (STROBE) statement: guidelines for reporting observational studies. Epidemiology 18, De Araújo Nobre M, Capelas C, Alves A, Almeida T, Carvalho R, Antunes E et al. (2006) Non-surgical treatment of peri-implant pathology. Int J Dent Hyg 4, Fiorellini JP, Weber HP (1994) Clinical trials on the prognosis of dental implants. Periodontol , Moy PK, Medina D, Shetty V, Aghaloo TL (2005) Dental implant failure rates and associated risk factors. Int J Oral Maxillofac Implants 20, Tonetti MS (1999) Determination of the success and failure of root-form osseointegrated dental implants. Adv Dent Res 13, Rothman KJ, Greenland S (1998) Measures of effect and measures of association. In: Modern epidemiology 1998, 2nd ed, Lippincott-Raven, Philadelphia, Esposito M, Grusovin MG, Worthington HV (2012) Interventions for replacing missing teeth: treatment of peri-implantitis. Cochrane Database Syst, CD Kaptein ML, De Lange GL, Blijdorp PA (1999) Peri-implant tissue health in reconstructed atrophic maxillae--report of 88 patients and 470 implants. J Oral Rehabil 26, Costa FO, Takenaka-Martinez S, Cota LO, Ferreira SD, Silva GL, Costa JE (2012) Peri-implant disease in subjects with and without preventive maintenance: a 5-year follow-up. J Clin Periodontol 39, Christensen MM, Joss A, Lang NP (1997) Reproducibility of automated periodontal probing around teeth and osseointegrated oral implants. Clin Oral Implants Res 8, Rangert B, Krogh PH, Langer B, Van Roekel N (1995) Bending overload and implant fracture: a retrospective clinical analysis. Int J Oral Maxillofac Implants 10,
The International Journal of Periodontics & Restorative Dentistry
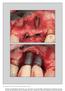 The International Journal of Periodontics & Restorative Dentistry 699 A Classification System for Peri-implant Diseases and Conditions Hector L. Sarmiento, DMD, MSc 1 Michael R. Norton, BDS, FDS, RCS(Ed)
The International Journal of Periodontics & Restorative Dentistry 699 A Classification System for Peri-implant Diseases and Conditions Hector L. Sarmiento, DMD, MSc 1 Michael R. Norton, BDS, FDS, RCS(Ed)
Evaluation of peri-implant tissue response according to the presence of keratinized mucosa Abstract Purpose: Materials and methods Results:
 Evaluation of peri-implant tissue response according to the presence of keratinized mucosa Bum-Soo Kim 1, Young-Kyun Kim 1, Pil-Young Yun 1, Yang-Jin Lee 2, Hyo-Jeong Lee 3, Su-Gwan Kim 4 1Department of
Evaluation of peri-implant tissue response according to the presence of keratinized mucosa Bum-Soo Kim 1, Young-Kyun Kim 1, Pil-Young Yun 1, Yang-Jin Lee 2, Hyo-Jeong Lee 3, Su-Gwan Kim 4 1Department of
Risk of Implant Failure and Marginal Bone Loss in Subjects with a History of Periodontitis: A Systematic Review and Meta-Analysis
 Risk of Implant Failure and Marginal Bone Loss in Subjects with a History of Periodontitis: A Systematic Review and Meta-Analysis Syarida H. Safii, DDS [Correction added after online publication 1 June
Risk of Implant Failure and Marginal Bone Loss in Subjects with a History of Periodontitis: A Systematic Review and Meta-Analysis Syarida H. Safii, DDS [Correction added after online publication 1 June
Creating emergence profiles in immediate implant dentistry
 Creating emergence profiles in immediate implant dentistry AUTHORS Dr. Daniel Capitán Maraver Dr. Manuel Fuentes Ortiz Visiting lecturers in the Master s Degree in Clinical Practice in Implantology and
Creating emergence profiles in immediate implant dentistry AUTHORS Dr. Daniel Capitán Maraver Dr. Manuel Fuentes Ortiz Visiting lecturers in the Master s Degree in Clinical Practice in Implantology and
Factors influencing severity of periimplantitis
 Martin Saaby Eva Karring Søren Schou Flemming Isidor Factors influencing severity of periimplantitis Authors affiliations: Martin Saaby, Søren Schou, Section for Oral and Maxillofacial Surgery and Oral
Martin Saaby Eva Karring Søren Schou Flemming Isidor Factors influencing severity of periimplantitis Authors affiliations: Martin Saaby, Søren Schou, Section for Oral and Maxillofacial Surgery and Oral
THE PERIODONTAL ASPECT OF IMPLANT THERAPY Prof. Dr. Windisch Péter
 THE PERIODONTAL ASPECT OF IMPLANT THERAPY Prof. Dr. Windisch Péter Periodontal aspects of implant therapy 1) Comprehensive perioprosthodontic treatment by utilizing implants on perio-patients. 2) Anatomical
THE PERIODONTAL ASPECT OF IMPLANT THERAPY Prof. Dr. Windisch Péter Periodontal aspects of implant therapy 1) Comprehensive perioprosthodontic treatment by utilizing implants on perio-patients. 2) Anatomical
Please visit the C.E. Pavilion to validate your course attendance Or If There s a Line Go cdapresents.com
 UCLA Innovations 2016 CDA Presents in Anaheim Tara Aghaloo, DDS, MD, PhD Dean Ho, MS, PhD Jay Jayanetti Eric C. Sung, DDS David T. W. Wong, DMD, DMSc Benjamin M. Wu, DDS, PhD Saturday, May 14, 2016 8:00
UCLA Innovations 2016 CDA Presents in Anaheim Tara Aghaloo, DDS, MD, PhD Dean Ho, MS, PhD Jay Jayanetti Eric C. Sung, DDS David T. W. Wong, DMD, DMSc Benjamin M. Wu, DDS, PhD Saturday, May 14, 2016 8:00
Mechanical and technical risks in implant therapy.
 Mechanical and technical risks in implant therapy. Salvi GE, Brägger U. Int J Oral Maxillofac Implants. 2009;24 Suppl:69-85. Department of Periodontology, School of Dental Medicine, University of Bern,
Mechanical and technical risks in implant therapy. Salvi GE, Brägger U. Int J Oral Maxillofac Implants. 2009;24 Suppl:69-85. Department of Periodontology, School of Dental Medicine, University of Bern,
Endosseous dental implants initially showed very
 Five-mm-Diameter Implants without a Smooth Surface Collar: Report on 98 Consecutive Placements Franck Renouard, DDS*/Jean-Pierre Arnoux, DDS**/David P. Sarment, DDS*** In recent years, indications for
Five-mm-Diameter Implants without a Smooth Surface Collar: Report on 98 Consecutive Placements Franck Renouard, DDS*/Jean-Pierre Arnoux, DDS**/David P. Sarment, DDS*** In recent years, indications for
The International Journal of Periodontics & Restorative Dentistry
 The International Journal of Periodontics & Restorative Dentistry 3 Influence of the 3-D Bone-to-Implant Relationship on Esthetics Ueli Grunder, DMD* Stefano Gracis, DMD** Matteo Capelli, DMD** There are
The International Journal of Periodontics & Restorative Dentistry 3 Influence of the 3-D Bone-to-Implant Relationship on Esthetics Ueli Grunder, DMD* Stefano Gracis, DMD** Matteo Capelli, DMD** There are
The Brånemark osseointegration method, using titanium dental implants (fixtures)
 Early Failures in 4,641 Consecutively Placed Brånemark Dental Implants: A Study From Stage 1 Surgery to the Connection of Completed Prostheses Bertil Friberg, DDS/Torsten Jemt, DDS, PhD/Ulf Lekholm, DDS,
Early Failures in 4,641 Consecutively Placed Brånemark Dental Implants: A Study From Stage 1 Surgery to the Connection of Completed Prostheses Bertil Friberg, DDS/Torsten Jemt, DDS, PhD/Ulf Lekholm, DDS,
A retrospective study on separate single-tooth implant restorations to replace two or more consecutive. maxillary posterior teeth up to 6 years.
 Original Article A retrospective study on separate single-tooth implant restorations to replace two or more consecutive maxillary posterior teeth up to 6 years follow up Myat Nyan Department of Prosthodontics,
Original Article A retrospective study on separate single-tooth implant restorations to replace two or more consecutive maxillary posterior teeth up to 6 years follow up Myat Nyan Department of Prosthodontics,
Areview of recent studies concerning molar. Single Molar Replacement with a Progressive Thread Design Implant System: A Retrospective Clinical Report
 Single Molar Replacement with a Progressive Thread Design Implant System: A Retrospective Clinical Report George E. Romanos, Dr med dent 1 /Georg H. Nentwig, Prof Dr med dent 2 Many clinical studies have
Single Molar Replacement with a Progressive Thread Design Implant System: A Retrospective Clinical Report George E. Romanos, Dr med dent 1 /Georg H. Nentwig, Prof Dr med dent 2 Many clinical studies have
Brånemark System Facts & Figures
 Brånemark System Facts & Figures Brånemark System is synonymous with the revolution in dental care by the introduction of safe and effective implants. Professor Brånemark, its inventor, always put the
Brånemark System Facts & Figures Brånemark System is synonymous with the revolution in dental care by the introduction of safe and effective implants. Professor Brånemark, its inventor, always put the
Brånemark System Facts & Figures
 Brånemark System Facts & Figures Brånemark System is synonymous with the revolution in dental care by the introduction of safe and effective implants. Professor Brånemark, its inventor, always put the
Brånemark System Facts & Figures Brånemark System is synonymous with the revolution in dental care by the introduction of safe and effective implants. Professor Brånemark, its inventor, always put the
Implant osseointegration and successful restoration
 Prosthodontic Complications in a Prospective Clinical Trial of Single-stage Implants at 36 Months Jacqueline P. Duncan, DMD, MDSc 1 /Elena Nazarova, DMD, PhD 2 /Theodora Vogiatzi, DDS 1 / Thomas D. Taylor,
Prosthodontic Complications in a Prospective Clinical Trial of Single-stage Implants at 36 Months Jacqueline P. Duncan, DMD, MDSc 1 /Elena Nazarova, DMD, PhD 2 /Theodora Vogiatzi, DDS 1 / Thomas D. Taylor,
Purpose: To assess the long term survival of sites treated by GTR.
 Cortellini P, Tonetti M. Long-term tooth survival following regenerative treatment of intrabony defects. J Periodontol 2004; 75:672-8. (28 Refs) Purpose: To assess the long term survival of sites treated
Cortellini P, Tonetti M. Long-term tooth survival following regenerative treatment of intrabony defects. J Periodontol 2004; 75:672-8. (28 Refs) Purpose: To assess the long term survival of sites treated
Consensus Statements and Recommended Clinical Procedures Regarding Loading Protocols
 Group 3 Consensus Statements Consensus Statements and Recommended Clinical Procedures Regarding Loading Protocols Hans-Peter Weber, DMD, Dr Med Dent 1 /Dean Morton, BDS, MS 2 /German O. Gallucci, DMD,
Group 3 Consensus Statements Consensus Statements and Recommended Clinical Procedures Regarding Loading Protocols Hans-Peter Weber, DMD, Dr Med Dent 1 /Dean Morton, BDS, MS 2 /German O. Gallucci, DMD,
The Importance of Implant Surface Characteristics in the Replacement of Failed Implants
 The Importance of Implant Surface Characteristics in the Replacement of Failed Implants Ghada Alsaadi, DDS, MSc 1 /Marc Quirynen, DDS, PhD 2 /Daniel van Steenberghe, MD, PhD, Dr hc 3 Purpose: The purpose
The Importance of Implant Surface Characteristics in the Replacement of Failed Implants Ghada Alsaadi, DDS, MSc 1 /Marc Quirynen, DDS, PhD 2 /Daniel van Steenberghe, MD, PhD, Dr hc 3 Purpose: The purpose
The Influence of Controlled Occlusal Overload on Peri-implant Tissue. Part 3: A Histologic Study in Monkeys
 The Influence of Controlled Occlusal Overload on Peri-implant Tissue. Part 3: A Histologic Study in Monkeys Takashi Miyata, DDS, DDSc 1 /Yukinao Kobayashi, DDS 2 /Hisao Araki, DDS, DDSc 3 / Takaichi Ohto,
The Influence of Controlled Occlusal Overload on Peri-implant Tissue. Part 3: A Histologic Study in Monkeys Takashi Miyata, DDS, DDSc 1 /Yukinao Kobayashi, DDS 2 /Hisao Araki, DDS, DDSc 3 / Takaichi Ohto,
Case study 2. A Retrospective Multi-Center Study on the Spiral Implant
 Case study 2 A Retrospective Multi-Center Study on the Spiral Implant Benny Karmon DMD, Jerry Kohen DMD, Ariel Lor DMD, Yiftach Gratciany DMD, Zvi Laster DMD, Gideon Hallel DMD MPA, Tsvia Karmon A Retrospective
Case study 2 A Retrospective Multi-Center Study on the Spiral Implant Benny Karmon DMD, Jerry Kohen DMD, Ariel Lor DMD, Yiftach Gratciany DMD, Zvi Laster DMD, Gideon Hallel DMD MPA, Tsvia Karmon A Retrospective
Straumann SmartOne. Stage 4 Af terc are and maintenance. Step 2 Maintenance visit
 Stage 4 Af terc are and maintenance Step 2 Maintenance visit Overview Assessment and treatment planning Step 1 Patient's expectations, history and examination Step 2 Treatment planning Step 3 Consultation
Stage 4 Af terc are and maintenance Step 2 Maintenance visit Overview Assessment and treatment planning Step 1 Patient's expectations, history and examination Step 2 Treatment planning Step 3 Consultation
Correlations between clinical parameters in implant maintenance patients: analysis among healthy and history-of-periodontitis groups
 Seki et al. International Journal of Implant Dentistry (2017) 3:45 DOI 10.1186/s40729-017-0108-0 International Journal of Implant Dentistry RESEARCH Correlations between clinical parameters in implant
Seki et al. International Journal of Implant Dentistry (2017) 3:45 DOI 10.1186/s40729-017-0108-0 International Journal of Implant Dentistry RESEARCH Correlations between clinical parameters in implant
Periodontal conditions in patients Title dental implant treatment. Ito, T; Yasuda, M; Norizuki, Y; Sas Author(s) S; Furuya, Y; Kato, T; Yajima, Y
 Periodontal conditions in patients Title dental implant treatment. Ito, T; Yasuda, M; Norizuki, Y; Sas Author(s) S; Furuya, Y; Kato, T; Yajima, Y Journal Bulletin of Tokyo Dental College, 5 URL http://hdl.handle.net/10130/2329
Periodontal conditions in patients Title dental implant treatment. Ito, T; Yasuda, M; Norizuki, Y; Sas Author(s) S; Furuya, Y; Kato, T; Yajima, Y Journal Bulletin of Tokyo Dental College, 5 URL http://hdl.handle.net/10130/2329
During the last 30 years, endosseous oral
 Influence of Variations in Implant Diameters: A 3- to 5-Year Retrospective Clinical Report Carl-Johan Ivanoff, DDS*/Kerstin Gröndahl, DDS, PhD**/Lars Sennerby, DDS, PhD***/ Christina Bergström, MSc****/Ulf
Influence of Variations in Implant Diameters: A 3- to 5-Year Retrospective Clinical Report Carl-Johan Ivanoff, DDS*/Kerstin Gröndahl, DDS, PhD**/Lars Sennerby, DDS, PhD***/ Christina Bergström, MSc****/Ulf
As an increasing number of
 LITERATURE REVIEWS Understanding Peri-implantitis: A Strategic Review Preetinder Singh, MDS* The high survival rate of osseointegrated dental implants is well documented, but it is becoming increasingly
LITERATURE REVIEWS Understanding Peri-implantitis: A Strategic Review Preetinder Singh, MDS* The high survival rate of osseointegrated dental implants is well documented, but it is becoming increasingly
Immediate implant placement in the Title central incisor region: a case repo. Journal Journal of prosthodontic research,
 Immediate implant placement in the Title central incisor region: a case repo Author(s) Sekine, H; Taguchi, T; Yamagami, M; Alternative Takanashi, T; Furuya, K Journal Journal of prosthodontic research,
Immediate implant placement in the Title central incisor region: a case repo Author(s) Sekine, H; Taguchi, T; Yamagami, M; Alternative Takanashi, T; Furuya, K Journal Journal of prosthodontic research,
Case Presentation. Overall Health. Oral Hygiene. Chief Complaint. I hate my upper denture. I can t taste food. I want an implant solution
 Case Presentation Medical History Age & Gender 62 years old female Peri-implant Osteitis Overall Health Good Hx of Smoking 5 cigarets per day (Peri-implantitis) Oral Hygiene Fair Systemic Disease Osteoarthritis
Case Presentation Medical History Age & Gender 62 years old female Peri-implant Osteitis Overall Health Good Hx of Smoking 5 cigarets per day (Peri-implantitis) Oral Hygiene Fair Systemic Disease Osteoarthritis
The International Journal of Periodontics & Restorative Dentistry
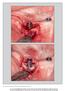 The International Journal of Periodontics & Restorative Dentistry 729 Resective Treatment of Peri-implantitis: Clinical and Radiographic Outcomes After 2 Years Emmanuel Englezos, DDS, MSc 1 Jan Cosyn,
The International Journal of Periodontics & Restorative Dentistry 729 Resective Treatment of Peri-implantitis: Clinical and Radiographic Outcomes After 2 Years Emmanuel Englezos, DDS, MSc 1 Jan Cosyn,
The majority of the early research concerning
 Gingival Recession Around Implants: A 1-Year Longitudinal Prospective Study Paula N. Small, DDS, MPH 1 /Dennis P. Tarnow, DDS 2 A longitudinal study was performed, which measured the soft tissue around
Gingival Recession Around Implants: A 1-Year Longitudinal Prospective Study Paula N. Small, DDS, MPH 1 /Dennis P. Tarnow, DDS 2 A longitudinal study was performed, which measured the soft tissue around
Osseointegrated dental implant treatment generally
 Placement of Dental Implants Without Flap Surgery: A Clinical Report Bader H. Al-Ansari, BDS, MScD*/Robert R. Morris, DMD** Traditionally, the procedure of implant placement requires a surgical periosteal
Placement of Dental Implants Without Flap Surgery: A Clinical Report Bader H. Al-Ansari, BDS, MScD*/Robert R. Morris, DMD** Traditionally, the procedure of implant placement requires a surgical periosteal
Outcome of dental implants in patients with a history of periodontitis
 Joint Degree Master Program of the International Medical College and the Universities Dresden, Essen, Saarland, Leipzig, Szeged and Bangkok Scientific director: Univ.-Prof. Dr. med. Dr. med. dent. Dr.
Joint Degree Master Program of the International Medical College and the Universities Dresden, Essen, Saarland, Leipzig, Szeged and Bangkok Scientific director: Univ.-Prof. Dr. med. Dr. med. dent. Dr.
Since the introduction of osseointegrated dental implants
 CLINICAL Papilla Formation in Response to Computer-Assisted Implant Surgery and Immediate Restoration Paul A. Schnitman, DDS, MSD 1 * Chie Hayashi, DDS, PhD, MMSc 2 This retrospective analysis was undertaken
CLINICAL Papilla Formation in Response to Computer-Assisted Implant Surgery and Immediate Restoration Paul A. Schnitman, DDS, MSD 1 * Chie Hayashi, DDS, PhD, MMSc 2 This retrospective analysis was undertaken
Since the early 1980s, when the concept of
 Retention of Teeth Versus Extraction and Implant Placement: Treatment Preferences of Dental Faculty and Dental Students Peter M. Di Fiore, D.D.S., M.S.; Lawrence Tam, D.D.S.; Ha T. Thai, D.D.S.; Eugene
Retention of Teeth Versus Extraction and Implant Placement: Treatment Preferences of Dental Faculty and Dental Students Peter M. Di Fiore, D.D.S., M.S.; Lawrence Tam, D.D.S.; Ha T. Thai, D.D.S.; Eugene
Peri-implant marginal bone loss: What is the current concensus? an academic controversy or a clinical challenge?
 Peri-implant marginal bone loss; What is the current concensus? Bjorn.Klinge@mah.se Peri-implant marginal bone loss: an academic controversy or a clinical challenge? Björn Klinge Eur J Oral Implantol 2012;5
Peri-implant marginal bone loss; What is the current concensus? Bjorn.Klinge@mah.se Peri-implant marginal bone loss: an academic controversy or a clinical challenge? Björn Klinge Eur J Oral Implantol 2012;5
The 2B-3D rule for implant planning, placement and restoration
 IJOI 27 INTERDISCIPLINARY TREATMENT The 2B-3D rule for implant planning, placement and restoration 1. What is biologic width? Is there a golden rule for implant planning, placement and restoration as the
IJOI 27 INTERDISCIPLINARY TREATMENT The 2B-3D rule for implant planning, placement and restoration 1. What is biologic width? Is there a golden rule for implant planning, placement and restoration as the
G03: Complications 12/7/2013 8:00AM 4:30PM
 American Association of Oral and Maxillofacial Surgeons 2013 Dental Implant Conference December 5 7, 2013 Sheraton Chicago Hotel & Towers G03: Complications 12/7/2013 8:00AM 4:30PM Prosthetic Complications
American Association of Oral and Maxillofacial Surgeons 2013 Dental Implant Conference December 5 7, 2013 Sheraton Chicago Hotel & Towers G03: Complications 12/7/2013 8:00AM 4:30PM Prosthetic Complications
Influence of Patient Age on the Success Rate of Dental Implants Supporting an Overdenture in an Edentulous Mandible: A 3-year Prospective Study
 Influence of Patient Age on the Success Rate of Dental Implants Supporting an Overdenture in an Edentulous Mandible: A 3-year Prospective Study Henny J. A. Meijer, DDS, PhD 1 /Rutger H. K. Batenburg, DDS,
Influence of Patient Age on the Success Rate of Dental Implants Supporting an Overdenture in an Edentulous Mandible: A 3-year Prospective Study Henny J. A. Meijer, DDS, PhD 1 /Rutger H. K. Batenburg, DDS,
Placement of osseointegrated implants is an increasingly
 Dental Implants in the Elderly Population: A Long-Term Follow-up Sharon M. Compton, PhD 1 /Danielle Clark, BSc 2 /Stephanie Chan, BSc 3 / Iris Kuc, DDS 4 /Berhanu A. Wubie, MSc 5 /Liran Levin, DMD 6 Purpose:
Dental Implants in the Elderly Population: A Long-Term Follow-up Sharon M. Compton, PhD 1 /Danielle Clark, BSc 2 /Stephanie Chan, BSc 3 / Iris Kuc, DDS 4 /Berhanu A. Wubie, MSc 5 /Liran Levin, DMD 6 Purpose:
Developing Keratinized Mucosa Around Nonsubmerged Dental Implants. Part I: The Use of Vascularized Flaps
 CLINICAL AND RESEARCH REPORTS Developing Keratinized Mucosa Around Nonsubmerged Dental Implants. Part I: The Use of Vascularized Flaps Jay R. Beagle Despite the continued debate regarding the need for
CLINICAL AND RESEARCH REPORTS Developing Keratinized Mucosa Around Nonsubmerged Dental Implants. Part I: The Use of Vascularized Flaps Jay R. Beagle Despite the continued debate regarding the need for
The effect of peri-implant bone exposure on soft tissue healing and bone loss in two adjacent implants
 Research Article J Periodontal Implant Sci 2012;42:20-24 http://dx.doi.org/10.5051/jpis.2012.42.1.20 on soft tissue healing and bone loss in two adjacent implants Seung-Yun Shin 1, Seung-Boem Kye 1, Jongrak
Research Article J Periodontal Implant Sci 2012;42:20-24 http://dx.doi.org/10.5051/jpis.2012.42.1.20 on soft tissue healing and bone loss in two adjacent implants Seung-Yun Shin 1, Seung-Boem Kye 1, Jongrak
The Endodontic / Implant Controversy
 The Endodontic / Implant Controversy Innovations in Endodontics Series Robert Handysides DDS Associate Professor and Chair Department of Endodontics Loma Linda University School of Dentistry Endodontic
The Endodontic / Implant Controversy Innovations in Endodontics Series Robert Handysides DDS Associate Professor and Chair Department of Endodontics Loma Linda University School of Dentistry Endodontic
The restoration of partially and completely
 CLINICAL MANAGEMENT OF DENTAL IMPLANT FRACTURES. ACASE HISTORY Firas A. M. AL Quran, PhD, MSc Med; Bashar A. Rashan, MS; Ziad N. AL-Dwairi, PhD The widespread use of endosseous osseointegrated implants
CLINICAL MANAGEMENT OF DENTAL IMPLANT FRACTURES. ACASE HISTORY Firas A. M. AL Quran, PhD, MSc Med; Bashar A. Rashan, MS; Ziad N. AL-Dwairi, PhD The widespread use of endosseous osseointegrated implants
Consensus Statements and Recommended Clinical Procedures Regarding Risk Factors in Implant Therapy
 Consensus Statements and Recommended Clinical Procedures Regarding Risk Factors in Implant Therapy David L. Cochran, DDS, MS, PhD, MMSci 1 /Søren Schou, DDS, PhD, Dr Odont 2 / Lisa J. A. Heitz-Mayfield,
Consensus Statements and Recommended Clinical Procedures Regarding Risk Factors in Implant Therapy David L. Cochran, DDS, MS, PhD, MMSci 1 /Søren Schou, DDS, PhD, Dr Odont 2 / Lisa J. A. Heitz-Mayfield,
Fixed full-arch implant-supported acrylic resin prostheses
 Tooth Fractures in Fixed Full-Arch Implant-Supported Acrylic Resin Prostheses: A Retrospective Clinical Study Javier Ventura, PhD, DMD 1 /Emilio Jiménez-Castellanos, PhD, DMD 2 / José Romero, PhD, DMD
Tooth Fractures in Fixed Full-Arch Implant-Supported Acrylic Resin Prostheses: A Retrospective Clinical Study Javier Ventura, PhD, DMD 1 /Emilio Jiménez-Castellanos, PhD, DMD 2 / José Romero, PhD, DMD
Peri-implant health and disease. A systematic review of current epidemiology
 J Clin Periodontol 2015; 42 (Suppl. 16): S158 S171 doi: 10.1111/jcpe.12334 Peri-implant health and disease. A systematic review of current epidemiology Jan Derks and Cristiano Tomasi Department of Periodontology,
J Clin Periodontol 2015; 42 (Suppl. 16): S158 S171 doi: 10.1111/jcpe.12334 Peri-implant health and disease. A systematic review of current epidemiology Jan Derks and Cristiano Tomasi Department of Periodontology,
The Effects of Anti-infective Preventive Measures on the Occurrence of Biologic Implant Complications and Implant Loss: A Systematic Review
 The Effects of Anti-infective Preventive Measures on the Occurrence of Biologic Implant Complications and Implant Loss: A Systematic Review Giovanni E. Salvi, DMD, Prof Dr Med Dent 1 /Nicola U. Zitzmann,
The Effects of Anti-infective Preventive Measures on the Occurrence of Biologic Implant Complications and Implant Loss: A Systematic Review Giovanni E. Salvi, DMD, Prof Dr Med Dent 1 /Nicola U. Zitzmann,
The Self-tapping and ICE 3i Implants: A Prospective 3-Year Multicenter Evaluation
 The Self-tapping and ICE 3i Implants: A Prospective 3-Year Multicenter Evaluation Mithridade Davarpanah, MD, DDS 1 /Henry Martinez, DDS 2 /Jean-François Tecucianu, MD, DDS 3 / Gil Alcoforado, DDS 4 /Daniel
The Self-tapping and ICE 3i Implants: A Prospective 3-Year Multicenter Evaluation Mithridade Davarpanah, MD, DDS 1 /Henry Martinez, DDS 2 /Jean-François Tecucianu, MD, DDS 3 / Gil Alcoforado, DDS 4 /Daniel
Is peri-implant maintenance therapy (PIMT) important for preventing peri-implant disease?
 C L I N I C A L Is peri-implant maintenance therapy (PIMT) important for preventing peri-implant disease? Johan Hartshorne 1 A critical appraisal of a systematic review: A. Monje, L. Aranda, K.T. Diaz,
C L I N I C A L Is peri-implant maintenance therapy (PIMT) important for preventing peri-implant disease? Johan Hartshorne 1 A critical appraisal of a systematic review: A. Monje, L. Aranda, K.T. Diaz,
Review Article Complications in Implants
 Review Article Complications in Implants 1 2 3 4 5 6 Dr Navjot Kaur, Dr Yashbir Raghav, Dr Amarpreet Kaur, Dinesh Duhan, Dr. Sumit Katoch, Dr. Apurva Sharma Kaur N, Raghav Y, Kaur A, Duhan D, Katoch S,
Review Article Complications in Implants 1 2 3 4 5 6 Dr Navjot Kaur, Dr Yashbir Raghav, Dr Amarpreet Kaur, Dinesh Duhan, Dr. Sumit Katoch, Dr. Apurva Sharma Kaur N, Raghav Y, Kaur A, Duhan D, Katoch S,
Retrospective Cohort Study of the Clinical Performance of 1-Stage Dental Implants
 Retrospective Cohort Study of the Clinical Performance of 1-Stage Dental Implants Alan B. Carr, DMD, MS 1 /Yong-Geun Choi, DDS, MPH, MPH 2 / Steven E. Eckert, DDS, MS 1 /Ronald P. Desjardins, DMD, MS 3
Retrospective Cohort Study of the Clinical Performance of 1-Stage Dental Implants Alan B. Carr, DMD, MS 1 /Yong-Geun Choi, DDS, MPH, MPH 2 / Steven E. Eckert, DDS, MS 1 /Ronald P. Desjardins, DMD, MS 3
Failures in Endosseous Dental Implants A Literature review
 Eswaran Arumugam et al/ International Journal of Biomedical Research 2015; 6(10): 756-762. 756 International Journal of Biomedical Research ISSN: 0976-9633 (Online); 2455-0566 (Print) Journal DOI: 10.7439/ijbr
Eswaran Arumugam et al/ International Journal of Biomedical Research 2015; 6(10): 756-762. 756 International Journal of Biomedical Research ISSN: 0976-9633 (Online); 2455-0566 (Print) Journal DOI: 10.7439/ijbr
BIOMECHANICS AND OVERDENTURES
 Proceedings of the 6th International Conference on Mechanics and Materials in Design, Editors: J.F. Silva Gomes & S.A. Meguid, P.Delgada/Azores, 26-30 July 2015 PAPER REF: 5734 BIOMECHANICS AND OVERDENTURES
Proceedings of the 6th International Conference on Mechanics and Materials in Design, Editors: J.F. Silva Gomes & S.A. Meguid, P.Delgada/Azores, 26-30 July 2015 PAPER REF: 5734 BIOMECHANICS AND OVERDENTURES
Importance of existence of keratinized gingival on the health of tissue around over dentures supporting implants: a case report
 Importance of existence of keratinized gingival on the health of tissue around over dentures supporting implants: a case report Maliheh Hamedi Jahroumi 1, Majid Vatankhah 2, Maryam Voosooghi shashkolati
Importance of existence of keratinized gingival on the health of tissue around over dentures supporting implants: a case report Maliheh Hamedi Jahroumi 1, Majid Vatankhah 2, Maryam Voosooghi shashkolati
Primary prevention of periimplantitis: peri-implant mucositis S152
 J Clin Periodontol 2015; 42 (Suppl. 16): S152 S157 doi: 10.1111/jcpe.12369 Primary prevention of periimplantitis: Managing peri-implant mucositis Jepsen S, Berglundh T, Genco R, Aass AM, Demirel K, Derks
J Clin Periodontol 2015; 42 (Suppl. 16): S152 S157 doi: 10.1111/jcpe.12369 Primary prevention of periimplantitis: Managing peri-implant mucositis Jepsen S, Berglundh T, Genco R, Aass AM, Demirel K, Derks
The notable success of dental implants. Relationship Between Smoking and Bleeding on Probing RESEARCH
 RESEARCH Relationship Between Smoking and Bleeding on Probing João Gustavo Oliveira de Souza 1 Marco Aurélio Bianchini, PhD, MSc 2 Cimara Fortes Ferreira, PhD, MSc 3 * The objective of this study was to
RESEARCH Relationship Between Smoking and Bleeding on Probing João Gustavo Oliveira de Souza 1 Marco Aurélio Bianchini, PhD, MSc 2 Cimara Fortes Ferreira, PhD, MSc 3 * The objective of this study was to
CEMENT-RETAINED PROSTHESES INCREASE RISK OF PERI-IMPLANTITIS WHEN COMPARED TO SCREW- RETAINED PROSTHESES
 Braz J Periodontol - September 2014 - volume 24 - issue 03 CEMENT-RETAINED PROSTHESES INCREASE RISK OF PERI-IMPLANTITIS WHEN COMPARED TO SCREW- RETAINED PROSTHESES Rachel de Queiroz Ferreira Rodrigues
Braz J Periodontol - September 2014 - volume 24 - issue 03 CEMENT-RETAINED PROSTHESES INCREASE RISK OF PERI-IMPLANTITIS WHEN COMPARED TO SCREW- RETAINED PROSTHESES Rachel de Queiroz Ferreira Rodrigues
JOMI on CD-ROM, 1990 Mar ( ): The Applicability of Osseointegrated Oral Imp
 The Applicability of Osseointegrated Oral Implants in the Rehabilitation of Partial Edentulism: A Prospective Multicenter Study on 558 Fixtures Daniel van Steenberghe, MD, PhD/Ulf Lekholm, DDS, PhD/Charles
The Applicability of Osseointegrated Oral Implants in the Rehabilitation of Partial Edentulism: A Prospective Multicenter Study on 558 Fixtures Daniel van Steenberghe, MD, PhD/Ulf Lekholm, DDS, PhD/Charles
A Long-term Retrospective Analysis of Survival Rates of Implants in the Mandible
 A Long-term Retrospective Analysis of Survival Rates of Implants in the Mandible Thomas J. Balshi, DDS, PhD, FACP 1 /Glenn J. Wolfinger, DMD, FACP 2 / Brett E. Stein 3 /Stephen F. Balshi, MBE 4 Purpose:
A Long-term Retrospective Analysis of Survival Rates of Implants in the Mandible Thomas J. Balshi, DDS, PhD, FACP 1 /Glenn J. Wolfinger, DMD, FACP 2 / Brett E. Stein 3 /Stephen F. Balshi, MBE 4 Purpose:
Interproximal Papilla Levels Following Early Versus Delayed Placement of Single-Tooth Implants: A Controlled Clinical Trial
 Interproximal Papilla Levels Following Early Versus Delayed Placement of Single-Tooth Implants: A Controlled Clinical Trial Lars Schropp, DDS, PhD /Flemming Isidor, DDS, PhD, Dr Odont /Lambros Kostopoulos,
Interproximal Papilla Levels Following Early Versus Delayed Placement of Single-Tooth Implants: A Controlled Clinical Trial Lars Schropp, DDS, PhD /Flemming Isidor, DDS, PhD, Dr Odont /Lambros Kostopoulos,
The impact of smoking and previous periodontal disease on peri-implant microbiota and health: a retrospective study up to 7-year follow-up
 Original article The impact of smoking and previous periodontal disease on peri-implant microbiota and health: a retrospective study up to 7-year follow-up Alessandro Quaranta, DDS, PhD 1 Bartolomeo Assenza,
Original article The impact of smoking and previous periodontal disease on peri-implant microbiota and health: a retrospective study up to 7-year follow-up Alessandro Quaranta, DDS, PhD 1 Bartolomeo Assenza,
Etiology, risk factors and management of implant fractures
 Journal section: Oral Surgery Publication Types: Review doi:10.4317/medoral.15.e504 Etiology, risk factors and management of implant fractures Arturo Sánchez-Pérez 1, Mª José Moya-Villaescusa 1, Alfonso
Journal section: Oral Surgery Publication Types: Review doi:10.4317/medoral.15.e504 Etiology, risk factors and management of implant fractures Arturo Sánchez-Pérez 1, Mª José Moya-Villaescusa 1, Alfonso
ABSTRACT INTRODUCTION
 ABSTRACT Purpose: Evaluation of stress distribution maxilla under parafunctional loading on short dental implant using 3-dimensional (3D) finite element models. Material and method: 3D maxillary and mandibular
ABSTRACT Purpose: Evaluation of stress distribution maxilla under parafunctional loading on short dental implant using 3-dimensional (3D) finite element models. Material and method: 3D maxillary and mandibular
Many of the problems reported by conventional
 Maxillary Overdentures Retained by Splinted and Unsplinted Implants: A Retrospective Study Timo O. Närhi, DDS, PhD 1 /Miluska Hevinga, DDS 2 / Ralph A. C. A. Voorsmit, DDS, PhD 3 /Warner Kalk, DDS, PhD
Maxillary Overdentures Retained by Splinted and Unsplinted Implants: A Retrospective Study Timo O. Närhi, DDS, PhD 1 /Miluska Hevinga, DDS 2 / Ralph A. C. A. Voorsmit, DDS, PhD 3 /Warner Kalk, DDS, PhD
Persson GR, Salvi GE, Heitz-Mayfield LJA et al. Antimicrobial therapy using a local drug delivery system (Arestin) in the treatment of
 Persson GR, Salvi GE, Heitz-Mayfield LJA et al. Antimicrobial therapy using a local drug delivery system (Arestin) in the treatment of peri-implantitis I: microbiological outcomes. Clin Oral Imp Res 2006;
Persson GR, Salvi GE, Heitz-Mayfield LJA et al. Antimicrobial therapy using a local drug delivery system (Arestin) in the treatment of peri-implantitis I: microbiological outcomes. Clin Oral Imp Res 2006;
There is overwhelming evidence that implant-retained
 CLINICAL Two-Year Success Rate of Implant-Retained Mandibular Overdentures by Novice General Dentistry Residents Hans Malmstrom, DDS 1 * Jin Xiao, DDS, MS, PhD 1 Georgios Romanos, DDS, PhD 1,2 Yan-Fang
CLINICAL Two-Year Success Rate of Implant-Retained Mandibular Overdentures by Novice General Dentistry Residents Hans Malmstrom, DDS 1 * Jin Xiao, DDS, MS, PhD 1 Georgios Romanos, DDS, PhD 1,2 Yan-Fang
A Multicenter Report on 1,022 Consecutively Placed ITI Implants: A 7-Year Longitudinal Study
 A Multicenter Report on 1,022 Consecutively Placed ITI Implants: A 7-Year Longitudinal Study Daniel Brocard, DCD, DSO 1 /Pierre Barthet, DCD, DSO 2 /Eric Baysse, DCD 1 / Jean François Duffort, DCD, DSO
A Multicenter Report on 1,022 Consecutively Placed ITI Implants: A 7-Year Longitudinal Study Daniel Brocard, DCD, DSO 1 /Pierre Barthet, DCD, DSO 2 /Eric Baysse, DCD 1 / Jean François Duffort, DCD, DSO
The surgical placement of dental implants has
 Flapless Implant Surgery: A 10-year Clinical Retrospective Analysis Luis Dominguez Campelo, DDS 1 /Jose R. Dominguez Camara, MD, DDS 2 Purpose: This article is a retrospective clinical analysis of implants
Flapless Implant Surgery: A 10-year Clinical Retrospective Analysis Luis Dominguez Campelo, DDS 1 /Jose R. Dominguez Camara, MD, DDS 2 Purpose: This article is a retrospective clinical analysis of implants
Labial and lingual/palatal bone thickness of maxillary and mandibular anteriors in human cadavers in Koreans
 Research Article J Periodontal Implant Sci 2011;41:60-66 doi: 10.5051/jpis.2011.41.2.60 Labial and lingual/palatal bone thickness of maxillary and mandibular anteriors in human cadavers in Koreans Ji Young
Research Article J Periodontal Implant Sci 2011;41:60-66 doi: 10.5051/jpis.2011.41.2.60 Labial and lingual/palatal bone thickness of maxillary and mandibular anteriors in human cadavers in Koreans Ji Young
A 10-year prospective study of ITI dental implants placed in the posterior region I: Clinical and radiographic results
 Rafael Juan Blanes Jean Pierre Bernard Zulema Maria Blanes Urs Christoph Belser A 10-year prospective study of ITI dental implants placed in the posterior region I: Clinical and radiographic results Authors
Rafael Juan Blanes Jean Pierre Bernard Zulema Maria Blanes Urs Christoph Belser A 10-year prospective study of ITI dental implants placed in the posterior region I: Clinical and radiographic results Authors
The International Journal of Periodontics & Restorative Dentistry
 The International Journal of Periodontics & Restorative Dentistry 827 Thirty-Two Year Success of Dental Implants in Periodontally Compromised Dentition Thomas J. Balshi, DDS, PhD, FACP 1 Glenn J. Wolfinger,
The International Journal of Periodontics & Restorative Dentistry 827 Thirty-Two Year Success of Dental Implants in Periodontally Compromised Dentition Thomas J. Balshi, DDS, PhD, FACP 1 Glenn J. Wolfinger,
Planning for esthetics Part II: adjacent implant restorations
 C L I N I C A L Planning for esthetics Part II: adjacent implant restorations William C Martin, 1 Emma Lewis, 2 Dean Morton 3 1 DMD, MS, Associate Professor & Clinical Director, Center for Implant Dentistry,
C L I N I C A L Planning for esthetics Part II: adjacent implant restorations William C Martin, 1 Emma Lewis, 2 Dean Morton 3 1 DMD, MS, Associate Professor & Clinical Director, Center for Implant Dentistry,
The International Journal of Periodontics & Restorative Dentistry
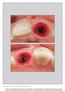 The International Journal of Periodontics & Restorative Dentistry 47 Provisional Restorations Used in Immediate Implant Placement Provide a Platform to Promote Peri-implant Soft Tissue Healing: A Pilot
The International Journal of Periodontics & Restorative Dentistry 47 Provisional Restorations Used in Immediate Implant Placement Provide a Platform to Promote Peri-implant Soft Tissue Healing: A Pilot
Mandibular implant-supported hybrid prostheses
 Occlusal Contacts of Edentulous Patients with Mandibular Hybrid Dentures Opposing Maxillary Complete Dentures Tetsuya Suzuki, DDS, PhD*/Hiroshi Kumagai, DDS, PhD**/ Nobuyuki Yoshitomi, DDS, PhD***/Edwin
Occlusal Contacts of Edentulous Patients with Mandibular Hybrid Dentures Opposing Maxillary Complete Dentures Tetsuya Suzuki, DDS, PhD*/Hiroshi Kumagai, DDS, PhD**/ Nobuyuki Yoshitomi, DDS, PhD***/Edwin
CHAPTER 1. General Introduction
 CHAPTER 1 General Introduction Chapter 1 The loss of remaining natural teeth and provision of artificial removable dentition is a major and irreversible procedure for the patient. The main limitations
CHAPTER 1 General Introduction Chapter 1 The loss of remaining natural teeth and provision of artificial removable dentition is a major and irreversible procedure for the patient. The main limitations
Peri-Implant Mucositis and Peri-Implantitis: A Current Understanding of Their Diagnoses and Clinical Implications*
 Volume 84 Number 4 Peri-Implant Mucositis and Peri-Implantitis: A Current Understanding of Their Diagnoses and Clinical Implications* The American Academy of Periodontology (AAP) periodically publishes
Volume 84 Number 4 Peri-Implant Mucositis and Peri-Implantitis: A Current Understanding of Their Diagnoses and Clinical Implications* The American Academy of Periodontology (AAP) periodically publishes
John P. Zarb, BA, DDS George A. Zarb, BChD, DDS, MS, MS, FRCD(C)
 C L I N I C A L P R A C T I C E Implant Prosthodontic Management of Anterior Partial Edentulism: Long-Term Follow-Up of a Prospective Study John P. Zarb, BA, DDS George A. Zarb, BChD, DDS, MS, MS, FRCD(C)
C L I N I C A L P R A C T I C E Implant Prosthodontic Management of Anterior Partial Edentulism: Long-Term Follow-Up of a Prospective Study John P. Zarb, BA, DDS George A. Zarb, BChD, DDS, MS, MS, FRCD(C)
Implant treatment in patients with severely
 Rehabilitation of Patients with Severely Resorbed Maxillae by Means of Implants With or Without Bone Grafts: A 3- to 5-Year Follow-up Clinical Report Göran Widmark, LDS, Odont Dr 1 /Bernt Andersson, LDS,
Rehabilitation of Patients with Severely Resorbed Maxillae by Means of Implants With or Without Bone Grafts: A 3- to 5-Year Follow-up Clinical Report Göran Widmark, LDS, Odont Dr 1 /Bernt Andersson, LDS,
High Crown to Implant Ratio as Stress Factor in Short Implants Therapy
 10.1515/bjdm-2016-0015 BALKAN JOURNAL OF DENTAL MEDICINE ISSN 2335-0245 STOMATOLOGICAL SOCIETY High Crown to Implant Ratio as Stress Factor in Short Implants Therapy SUMMARY Background/Aim: The purpose
10.1515/bjdm-2016-0015 BALKAN JOURNAL OF DENTAL MEDICINE ISSN 2335-0245 STOMATOLOGICAL SOCIETY High Crown to Implant Ratio as Stress Factor in Short Implants Therapy SUMMARY Background/Aim: The purpose
Effect of thread size on the implant neck area: preliminary results at 1 year of function
 Young-Il Kang* Dong-Won Lee* Kwang-Ho Park Ik-Sang Moon Effect of thread size on the implant neck area: preliminary results at 1 year of function Authors affiliations: Young-Il Kang*, Dong-Won Lee*, Ik-Sang
Young-Il Kang* Dong-Won Lee* Kwang-Ho Park Ik-Sang Moon Effect of thread size on the implant neck area: preliminary results at 1 year of function Authors affiliations: Young-Il Kang*, Dong-Won Lee*, Ik-Sang
Platform switching for marginal bone preservation around dental implants: a systematic review and meta-analysis.
 Platform switching for marginal bone preservation around dental implants: a systematic review and meta-analysis. Atieh MA, Ibrahim HM, Atieh AH. J Periodontol. 2010 Oct;81(10):1350-66. BACKGROUND: Platform
Platform switching for marginal bone preservation around dental implants: a systematic review and meta-analysis. Atieh MA, Ibrahim HM, Atieh AH. J Periodontol. 2010 Oct;81(10):1350-66. BACKGROUND: Platform
2017 WORLD WORKSHOP. Received: 20 December 2017 Revised: 6 February 2018 Accepted: 1 March DOI: /jcpe.12957
 Received: 20 December 2017 Revised: 6 February 2018 Accepted: 1 March 2018 DOI: 10.1111/jcpe.12957 2017 WORLD WORKSHOP Peri implant diseases and conditions: Consensus report of workgroup 4 of the 2017
Received: 20 December 2017 Revised: 6 February 2018 Accepted: 1 March 2018 DOI: 10.1111/jcpe.12957 2017 WORLD WORKSHOP Peri implant diseases and conditions: Consensus report of workgroup 4 of the 2017
The evaluation of long-term treatment results for
 Long-Term Results After Placement of Dental Implants: Longitudinal Study of 1,964 Implants over 16 Years Nicole Noack, MD*/Jürgen Willer, DMD**/Jürgen Hoffmann, MD, DMD*** In a retrospective study, Kaplan-Meier
Long-Term Results After Placement of Dental Implants: Longitudinal Study of 1,964 Implants over 16 Years Nicole Noack, MD*/Jürgen Willer, DMD**/Jürgen Hoffmann, MD, DMD*** In a retrospective study, Kaplan-Meier
Replacement of a congenitally missing lateral incisor in the maxillary anterior aesthetic zone using a narrow diameter implant: A case report
 C A S E R E P O R T Replacement of a congenitally missing lateral incisor in the maxillary anterior aesthetic zone using a narrow diameter implant: A case report Rhoodie Garrana 1 and Govindrau Mohangi
C A S E R E P O R T Replacement of a congenitally missing lateral incisor in the maxillary anterior aesthetic zone using a narrow diameter implant: A case report Rhoodie Garrana 1 and Govindrau Mohangi
Case Report Immediate, Early, and Conventional Implant Placement in a Patient with History of Periodontitis
 Case Reports in Dentistry Volume 2015, Article ID 217895, 10 pages http://dx.doi.org/10.1155/2015/217895 Case Report Immediate, Early, and Conventional Implant Placement in a Patient with History of Periodontitis
Case Reports in Dentistry Volume 2015, Article ID 217895, 10 pages http://dx.doi.org/10.1155/2015/217895 Case Report Immediate, Early, and Conventional Implant Placement in a Patient with History of Periodontitis
Periimplant diseases: where are we now? Consensus of the Seventh European Workshop on Periodontology
 Article Periimplant diseases: where are we now? Consensus of the Seventh European Workshop on Periodontology LANG, Niklaus P, BERGLUNDH, Tord, MOMBELLI, Andrea Abstract Peri-implant diseases present in
Article Periimplant diseases: where are we now? Consensus of the Seventh European Workshop on Periodontology LANG, Niklaus P, BERGLUNDH, Tord, MOMBELLI, Andrea Abstract Peri-implant diseases present in
Multidisciplinary treatment planning for patients with severe periodontal disease
 Clinical Multidisciplinary treatment planning for patients with severe periodontal disease Josselin Lethuillier, 1 Sébastien Felenc, 2 Philippe Bousquet 3 Abstract Periodontally compromised patients usually
Clinical Multidisciplinary treatment planning for patients with severe periodontal disease Josselin Lethuillier, 1 Sébastien Felenc, 2 Philippe Bousquet 3 Abstract Periodontally compromised patients usually
Supportive periodontal therapy and periodontal biotype as prognostic factors in implants placed in patients with a history of periodontitis
 Journal section: Periodontology Publication Types: Research doi:10.4317/medoral.19136 http://dx.doi.org/doi:10.4317/medoral.19136 Supportive periodontal therapy and periodontal biotype as prognostic factors
Journal section: Periodontology Publication Types: Research doi:10.4317/medoral.19136 http://dx.doi.org/doi:10.4317/medoral.19136 Supportive periodontal therapy and periodontal biotype as prognostic factors
A systematic review of survival of single implants as presented in longitudinal studies with a follow-up of at least 10 years
 REVIEW S155 Lars Hjalmarsson, Maryam Gheisarifar, Torsten Jemt A systematic review of survival of single implants as presented in longitudinal studies with a follow-up of at least 10 years Key words 10-year
REVIEW S155 Lars Hjalmarsson, Maryam Gheisarifar, Torsten Jemt A systematic review of survival of single implants as presented in longitudinal studies with a follow-up of at least 10 years Key words 10-year
Complex Rehabilitation of Advanced Periodontitis Subject with a Staged Approach; Implant Supported Fixed Detachable Prosthesis
 International Journal of Dental Sciences and Research, 2016, Vol. 4, No. 1, 5-9 Available online at http://pubs.sciepub.com/ijdsr/4/1/2 Science and Education Publishing DOI:10.12691/ijdsr-4-1-2 Complex
International Journal of Dental Sciences and Research, 2016, Vol. 4, No. 1, 5-9 Available online at http://pubs.sciepub.com/ijdsr/4/1/2 Science and Education Publishing DOI:10.12691/ijdsr-4-1-2 Complex
Evaluation of supported overdenture by implant and magnet
 * * 26 Evaluation of supported overdenture by implant and magnet Arab H.R * Assistant Professor, Dep. Of Periodontics, School of Dentistry, Mashhad University of Medical Sciences, Mashhad, Iran. Tamizi
* * 26 Evaluation of supported overdenture by implant and magnet Arab H.R * Assistant Professor, Dep. Of Periodontics, School of Dentistry, Mashhad University of Medical Sciences, Mashhad, Iran. Tamizi
Evaluation of Patient and Implant Characteristics as Potential Prognostic Factors for Oral Implant Failures
 220_Herrmann 3/18/05 12:59 PM Page 220 Evaluation of Patient and Implant Characteristics as Potential Prognostic Factors for Oral Implant Failures Irene Herrmann, LDS, Odont Lic 1 /Ulf Lekholm, LDS, Odont
220_Herrmann 3/18/05 12:59 PM Page 220 Evaluation of Patient and Implant Characteristics as Potential Prognostic Factors for Oral Implant Failures Irene Herrmann, LDS, Odont Lic 1 /Ulf Lekholm, LDS, Odont
Over the last decades, the use
 LITERATURE REVIEW Splinting Osseointegrated Implants and Natural Teeth in Partially Edentulous Patients: A Systematic Review of the Literature Anastasios Mamalis, DDS, MBA, MSc, PhD 1 Kleopatra Markopoulou,
LITERATURE REVIEW Splinting Osseointegrated Implants and Natural Teeth in Partially Edentulous Patients: A Systematic Review of the Literature Anastasios Mamalis, DDS, MBA, MSc, PhD 1 Kleopatra Markopoulou,
A 1-year prospective clinical study of soft tissue conditions and marginal bone changes around dental implants after flapless implant surgery
 A 1-year prospective clinical study of soft tissue conditions and marginal bone changes around dental implants after flapless implant surgery Seung-Mi Jeong, DDS, PhD, a Byung-Ho Choi, DDS, PhD, b Jihun
A 1-year prospective clinical study of soft tissue conditions and marginal bone changes around dental implants after flapless implant surgery Seung-Mi Jeong, DDS, PhD, a Byung-Ho Choi, DDS, PhD, b Jihun
Implants- immediate restoration of postextraction edentation both esthetically and functionally
 Implants- immediate restoration of postextraction edentation both esthetically and functionally Otilia Stana (Gag), LileIoana Elena, Freiman Paul, Mugur Popescu, Elisei Gabriela, Sebesan Voicu, Vincze
Implants- immediate restoration of postextraction edentation both esthetically and functionally Otilia Stana (Gag), LileIoana Elena, Freiman Paul, Mugur Popescu, Elisei Gabriela, Sebesan Voicu, Vincze
Dent Clin N Am 49 (2005) Peri-implantitis
 Dent Clin N Am 49 (2005) 661 676 Peri-implantitis Bjo rn Klinge, DDS, Odont Dr a, *, Margareta Hultin, DDS, Odont Dr a, Tord Berglundh, DDS, Odont Dr b a Karolinska Institutet, Institute of Odontology,
Dent Clin N Am 49 (2005) 661 676 Peri-implantitis Bjo rn Klinge, DDS, Odont Dr a, *, Margareta Hultin, DDS, Odont Dr a, Tord Berglundh, DDS, Odont Dr b a Karolinska Institutet, Institute of Odontology,
Citation for published version (APA): Hoeksema, A. (2016). Oral health in frail elderly [Groningen]: Rijksuniversiteit Groningen
![Citation for published version (APA): Hoeksema, A. (2016). Oral health in frail elderly [Groningen]: Rijksuniversiteit Groningen Citation for published version (APA): Hoeksema, A. (2016). Oral health in frail elderly [Groningen]: Rijksuniversiteit Groningen](/thumbs/87/96311633.jpg) University of Groningen Oral health in frail elderly Hoeksema, Albert IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check the
University of Groningen Oral health in frail elderly Hoeksema, Albert IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check the
The International Journal of Periodontics & Restorative Dentistry
 The International Journal of Periodontics & Restorative Dentistry 2011 BY QUINTESSENCE PUBLISHING CO, INC. PRINTING OF THIS DOCUMENT IS RESTRICTED TO PERSONAL USE ONLY.. 255 Multicenter Retrospective Analysis
The International Journal of Periodontics & Restorative Dentistry 2011 BY QUINTESSENCE PUBLISHING CO, INC. PRINTING OF THIS DOCUMENT IS RESTRICTED TO PERSONAL USE ONLY.. 255 Multicenter Retrospective Analysis
Prosthetic Options in Implant Dentistry. Hakimeh Siadat, DDS, MSc Associate Professor
 Prosthetic Options in Dentistry Hakimeh Siadat, DDS, MSc Associate Professor Dental Research Center, Department of Prosthodontics & Dental s Faculty of Dentistry, Tehran University of Medical Sciences
Prosthetic Options in Dentistry Hakimeh Siadat, DDS, MSc Associate Professor Dental Research Center, Department of Prosthodontics & Dental s Faculty of Dentistry, Tehran University of Medical Sciences
